RESEARCH ARTICLE ABSTRACT
|
|
|
- Vivian Taylor
- 5 years ago
- Views:
Transcription
1 RESEARCH ARTICLE Evaluating the Impact of Implementing a Clinical Practice Guideline for Febrile Infants With Positive Respiratory Syncytial Virus or Enterovirus Testing Adrienne DePorre, MD, a David D. Williams, MPH, b Jennifer Schuster, MD, a Jason Newland, MD, a Jacqueline Bartlett, PhD, RN, c Rangaraj Selvarangan, PhD, d Keith Mann, MD, a,c Russell McCulloh, MD a ABSTRACT OBJECTIVES: To evaluate clinical practice patterns and patient outcomes among febrile low-risk infants with respiratory syncytial virus (RSV) infection or enterovirus (EV) meningitis after implementing a clinical practice guideline (CPG) that provides recommendations for managing febrile infants with RSV infection and EV meningitis. METHODS: Our institution implemented a CPG for febrile infants, which gives explicit recommendations for managing both RSV-positive and EV-positive infants in We retrospectively analyzed medical records of febrile infants #60 days old from June 2008 to January Among 134 low-risk RSV-positive infants, we compared the proportion of infants who underwent lumbar puncture (LP), the proportion of infants who received antibiotics, antibiotic hours of therapy (HOT), and length of stay (LOS) pre- and post-cpg implementation. Among 274 low-risk infants with EV meningitis, we compared HOT and LOS pre- and post-cpg implementation. RESULTS: Among low-risk RSV-positive patients, the proportion of infants undergoing LP, the proportion of infants receiving antibiotics, HOT, and LOS were unchanged post-cpg. Among low-risk infants with EV meningitis, HOT (79 hours pre-cpg implementation versus 46 hours post-cpg implementation, P,.001) and LOS (47 hours pre-cpg implementation versus 43 hours post-cpg implementation, P 5.01) both decreased post-cpg. CONCLUSIONS: CPG implementation is associated with decreased antibiotic exposure and hospital LOS among low-risk infants with EV meningitis; however, there were no associated changes in the proportion of infants undergoing LP, antibiotic exposure, or LOS among low-risk infants with RSV. Further studies are needed to determine specific barriers and facilitators to effectively incorporate diagnostic viral testing into medical decision-making for these infants. a Department of Pediatrics, Children s Mercy Kansas City, University of Missouri- Kansas City School of Medicine, Kansas City, Missouri; and Departments of b Health Services and Outcomes Research, d Pathology and Laboratory Medicine, and c Center for Clinical Effectiveness, Children s Mercy Kansas City, Kansas City, Missouri DOI: Copyright 2017 by the American Academy of Pediatrics Address correspondence to Adrienne DePorre, MD, Division of Hospital Medicine, Department of Pediatrics, Children s Mercy Hospital, 2401 Gillham Rd, Kansas City, MO adeporre@cmh.edu HOSPITAL PEDIATRICS (ISSN Numbers: Print, ; Online, ). FINANCIAL DISCLOSURE: The authors have indicated they have no financial relationships relevant to this article to disclose. FUNDING: No external funding. POTENTIAL CONFLICT OF INTEREST: The authors have indicated they have no potential conflicts of interest to disclose. Dr Newland s current affiliation is Department of Pediatrics, Washington University School of Medicine, St Louis, MO. Drs DePorre and McCulloh contributed to the concept and design of the study, performed data collection, drafted the initial manuscript, and coordinated all edits of the manuscript; Mr Williams contributed to the concept and design of the study, performed the statistical analyses for the study, and edited the manuscript; Dr Schuster contributed to study design and data analysis, helped draft the initial manuscript, and edited the manuscript; Drs Newland, Bartlett, Selvarangan, and Mann contributed to the concept and design of the study, crafted the clinical practice guideline, performed data collection, and edited the manuscript; and all authors approved the final version of the manuscript as submitted. HOSPITAL PEDIATRICS Volume 7, Issue 10, October
2 Medical decision-making for febrile infants #60 days of age can be challenging because it is often difficult to differentiate infants with a benign self-limiting illness from those with a more serious illness that could progress to sepsis, permanent disability, or death if left untreated. In addition, the lack of standardized national guidelines for the testing and empirical treatment of febrile infants can lead to variability and uncertainty in the management of febrile infants, especially among those with positive viral test results. 1 Infants with respiratory syncytial virus (RSV) infection and infants with enterovirus (EV) meningitis both have a relatively low rate of concomitant bacterial infection, 2 10 and recommendations for RSV and EV testing have been incorporated into local and regional practice guidelines for febrile infant management. 11 In previous work, Byington et al 11 described patient outcomes and cost after implementation of a care practice model that provided explicit guidelines regarding the care of both RSV-positive and EV-positive infants. The implementation of their care practice model was associated with overall increased rates of EV testing, decreased hospital length of stay (LOS), and decreased duration of antibiotics among all febrile infants. 11 However, clinical practice patterns and health outcomes specifically among RSV-positive and EV-positive febrile infants, 2 populations likely highly impacted by clinical practice guideline (CPG) implementation, are unknown. Our objectives in this study were to determine the impact of implementing a febrile infant CPG that gives explicit management recommendations for infants with RSV or EV has on the following outcomes: (1) proportion of lumbar punctures (LPs) performed, antibiotic exposure, and hospital LOS among low-risk RSV-positive infants, and (2) antibiotic exposure and LOS among low-risk infants with EV meningitis. METHODS CPG Creation On February 1, 2011, at our institution, we implemented a CPG for febrile infants #60 days of age that recommended RSV testing of infants with clinical signs of bronchiolitis and EV testing of cerebrospinal fluid (CSF) from infants evaluated for meningitis. Among low-risk RSV-positive infants, avoidance of both LPs and antibiotics was recommended (Fig 1). For low-risk RSV-positive infants #28 days old, hospital admission for observation (without antibiotics) was recommended; for low-risk RSV-positive infants.29 days old, discharge from the hospital with close follow-up was recommended. Among low-risk infants with EV meningitis, discontinuation of antibiotics and consideration of discharge was recommended (Fig 2). This was our institution s first febrile infant CPG, and no revisions were made to the CPG after initial implementation. This CPG was developed to address variability in the care of febrile infants, and it was created and implemented by a team consisting of physician and nurse representatives from the clinical areas most impacted by the guideline, physician and nurse informatics experts, experts in literature review, and a family member asked to represent the voice of the family. The quality of evidence was assessed by using the Grading of Recommendations Assessment, Development and Education approach. 12 The febrile infant CPG was completed in January 2011 and implemented in the Children s Mercy Hospital emergency departments (EDs), urgent care centers, and hospital in February An electronic order set guiding practice was developed for febrile infants #28 days old and for febrile infants 29 to 60 days old (Supplemental Figures 1 and 2, respectively). The guideline in both written and algorithmic format was placed on the Children s Mercy Hospital Evidence- Based Practice Web site. In addition, a supporting app with decision support was developed. Academic detailing with the ED, urgent care, hospital medicine, and general pediatric groups was completed. Study Design, Setting, and Population A retrospective study was performed at Children s Mercy Kansas City (CMKC), a pediatric health system that includes a tertiary-care freestanding children s hospital, a community-based suburban freestanding children s hospital (with its own ED), and 3 urgent care centers. Infants #60 days of life who presented to our health care system with caregiver report of fever or documented temperature $38.0 C ($100.4 F) between June 25, 2008 and January 31, 2013 were identified from medical records for inclusion by using both the International Classification of Diseases, Ninth Revision discharge diagnosis codes of (fever, unspecified) and (fever presenting with conditions classified elsewhere), and through query of our electronic health record (EHR). EHR query was done by using Business Objects software (Web Intelligence version 3.3; SAP Business Objects, San Jose, CA), which identified any of the following in medical provider notes: reason for visit being fever, documented temperature $38 C, or discharge diagnosis of fever. Qualifying charts were manually reviewed to ensure the presence of a fever. Febrile infants found to be RSV-positive or to have EV meningitis were divided into 2 separate low-risk cohorts. A subset of infants #28 days old were analyzed separately in each low-risk cohort. RSV-positive infants were included in the low-risk RSV cohort if they met our CPG s criteria for infants at low risk for serious bacterial infection on the basis of risk factors for herpes simplex virus, urinalysis, and/or clinical examination (Fig 1). For purposes of the study, ill-appearing infants included any infant described in the EHR by a health care provider as irritable, illappearing, lethargic, in moderate-severe respiratory distress, or in any distress not specified as respiratory. Of note, infant age was not a factor in determining which infants met low-risk criteria for RSV-positive infants. Infants diagnosed with EV meningitis were categorized as low-risk by our CPG if they were afebrile, well-appearing,.7 days of age, and had negative bacterial culture results at 24 hours of incubation (Fig 2). Infants #7 days old were considered to be at higher risk because of the risk of disseminated EV among young infants. Because of limitations in manual chart review, neither time to fever resolution nor 588 DEPORRE et al
3 FIGURE 1 RSV test interpretation algorithm. CBC, complete blood cell count; CBC-D, CBC with differential; Cx, culture; HPF, high-power field; UA, urinalysis; UAM, urinalysis with microscopic examination; WBC, white blood cell. culture results at 24 hours of incubation could be captured; thus, only infants #7 days were excluded from the low-risk EV cohort. Data Collected Data were collected on patient demographics, initial clinical presentation, diagnostic tests and results, medications administered, and the following patient outcomes: hospital admission, hospital LOS, subsequent ED visit, and subsequent hospital readmission. Positive bacterial cultures were independently reviewed by 2 authors (A.D. and R.M.) to assess growth of a true pathogen versus a contaminant based on bacteria isolated and urine colony counts. Definitions A positive urinalysis was defined by our febrile infant CPG as having.5 white blood cells per high-power field or positive nitrites. Urinary tract infection was defined by $ colony-forming units of a single species of bacterium isolated from a urinary catheter obtained specimen. Bacteremia and bacterial meningitis were defined by isolation of pathogenic bacteria in the blood or CSF. Presence of coagulasenegative Staphylococcus in the blood or CSF was determined to be a contaminant and was not considered a true infection unless multiple blood cultures grew isolates of coagulase-negative Staphylococcus with identical speciation and antimicrobial susceptibility. Hours of therapy (HOT) was defined as the aggregate number of hours of antibiotic exposure. The HOT for a patient on multiple antibiotics is the sum of the hours each antibiotic was administered to the patient. HOSPITAL PEDIATRICS Volume 7, Issue 10, October
4 FIGURE 2 EV test interpretation algorithm. a infants,1 week of age with EV are at risk for significant multisystem disease. An infectious disease consult is recommended. For example, the HOT for an infant who received 24 hours of ampicillin and 24 hours of cefotaxime is 48 hours. HOT is derived from antibiotic days of therapy, a well-described method to measure antibiotic exposure and stewardship Our data set provided sufficient detail to determine antibiotic exposure at the level of HOT based on the date and time antibiotics were administered. We defined a subsequent visit and readmission as presenting or being admitted to our health care system because of a febrile illness within 14 days of discharge. Hospital LOS was defined as the hours between the infant s admission time and date and the infant s discharge time and date as recorded in our health system s EMR. Time spent outside of an inpatient unit, including time spent in the ED or urgent care among those infants discharged from the hospital from EDs or urgent cares, was not included in LOS calculations. Virology Testing RSV testing during the study period was performed either as part of a multiplex polymerase chain reaction (PCR) panel (Biofire FilmArray or Luminex xtag RVP) or by rapid antigen testing (BD Veritor System, BD Directigen EZ RSV, or Binax NOW RSV). Turn-around time for RSV testing ranged from 1 to 15 hours depending on which testing modality was used and from which CMKC location the sample was collected. EV testing during the study period was performed via real-time reverse transcription PCR, by an Cepheid Enterovirus analyte-specific reagent assay (Cepheid, Sunnyvale, CA), an Enterovirus R-gene (bio-mérieux, Marcy-l Étoile, France), or via an in-house assay as described previously, 16 with the exception that during the nonpeak EV incidence months of 2008 to 2010, EV testing was performed at a reference laboratory. Reference laboratory EV testing time to results ranged from 24 to 48 hours. In-house EV testing time to results ranged from 8 to 43 hours depending at which CMKC location the specimen was collected and on the time of year. Data Analysis Primary outcomes among low-risk RSVpositive infants included the proportion of infants undergoing LPs, the proportion of infants who received antibiotics, and HOT and LOS pre- versus post-cpg implementation. Primary outcomes among low-risk infants with EV meningitis included HOT and LOS pre- versus post-cpg implementation. A subanalysis of low-risk infants with EV meningitis that excluded those who had testing performed at a reference laboratory, which had a longer turn-around-time of 24 to 48 hours, was conducted to assess whether observed differences in LOS and HOT were attributable to this subset of infants. Secondary outcomes among both cohorts included the proportion of subsequent ED visits and hospital readmissions pre- versus post-cpg implementation. We also determined the rates of positive blood, urine, and CSF bacterial cultures among both cohorts. Fisher s exact or x 2 tests were used for categorical variables and 2-sample Wilcoxon rank (Mann Whitney U test) tests were performed for continuous variables, as appropriate. Statistical significance was regarded at P,.05 (2-sided). Statistical analyses were performed by using Stata 13.0 (StataCorp, College Station, TX). The hospital s institutional review board approved the study. RESULTS Demographic and clinical outcome data collected from a total of 2036 febrile infants are presented in Table 1. A flow diagram depicting the included 134 low-risk RSV-positive infants, of whom 131 were diagnosed with RSV through rapid antigen testing, and the 274 low-risk infants with EV meningitis is presented in Fig 3. Primary Outcomes In the low-risk RSV cohort, the proportion of LPs performed, the proportion of infants receiving antibiotics, HOT, and LOS were unchanged post-cpg implementation (Table 2). In the low-risk EV cohort, HOT (median 79 hours pre-cpg versus median 46 hours post-cpg, P,.001) and LOS 590 DEPORRE et al
5 TABLE 1 Febrile Infant Patient Demographics and Microbiology Results (median 47 hours pre-cpg versus median 43 hours post-cpg, P 5.01) both decreased post-cpg implementation (Table 2). Among infants #28 days old included in the low-risk EV cohort, HOT decreased (median 90 hours pre-cpg versus median 75 hours post-cpg, P 5.03) and LOS was unchanged (Table 2). A subanalysis of infants with EV meningitis that excluded 27 infants whose EV testing was performed at a reference laboratory showed a similarly significant decrease TABLE 2 Patient Management and Outcomes Pre- Versus Post-CPG Implementation Pre-CPG Post-CPG P Low-risk RSV-positive infants N 5 61 N 5 73 LP performed, n (%) 17 (28) 19 (26).81 Infants #28 d old, LP performed, frequency (%) 7/11 (64) 8/12 (67).999 Received antibiotics, n (%) 18 (30) 15 (21).23 Infants #28 d old, received antibiotics, 7/11 (64) 7/12 (58).999 frequency (%) LOS in h, median (IQR) 41 (10 68) 36 (4 86).79 Infants #28d old, LOS in h, median (IQR) 46 (38 201) 56.5 ( ).78 HOT, median (IQR) 89 (54 94) 74 (16 106).59 Infants #28 d old, HOT, median (IQR) 92 (62 94) 98 (80 110).06 Subsequent ED visits, n (%) 5 (8.2) 9 (12.3).57 Subsequent readmission, n (%) 3 (4.9) 7 (9.6).35 Low-risk EV-positive infants N N 5 66 HOT, median (IQR) 79 (48 96) 46 (27 74),.0001 Infants #28 d old, HOT, median (IQR) 90 (75 103) 75 (53 95).03 LOS in h, median (IQR) 47 ( ) 42.5 (25 51).01 Infants #28 d old, LOS in h, median (IQR) 49 ( ) 48 (42 63).76 Subsequent ED visits, n (%) 6 (2.9) 0 (0).34 Subsequent readmission, n (%) 2 (1.0) 1 (1.5).56, not applicable. Low-risk RSV-positive (n 5 134) Low-risk EV-positive Meningitis (n 5 274) Admitted Febrile Infants (n ) All Febrile Infants (N ) Female, n (%) 58 (43) 135 (49) 734 (47) 929 (46) Public insurance, n (%) 81 (60) 154 (56) 937 (60) 1235 (61) (n ) Age #28 d old, n (%) 23 (17) 120 (44) 564 (36) 595 (29) Admitted to hospital, n (%) 100 (75) 267 (97) 1554 (100) 1554 (76) Temperature ( C) on arrival, mean 6 SD Positive urinalysis results, a 0/102 (0) 8/255 (3.1) 165/1408 (11.7) 177/1724 (10.3) frequency (%) Positive urine culture results, a 0/102 (0) 3/261 (1.2) 143/1428 (9.9) 151/1757 (8.6) frequency (%) Positive blood culture results, b 0/86 (0) 0/266 (0) 32/1444 (2.2) 33/1739 (1.9) frequency (%) Positive CSF culture results, frequency (%) 0/36 (0) 0/270 (0) 3/1288 (0.2) 3/1395 (0.2) a Infants with a positive urinalysis were excluded from the low-risk RSV-positive cohort. b With or without positive urine culture. in both LOS and HOT post-cpg implementation. Secondary Outcomes There were no differences in subsequent ED visits or hospitalizations post-cpg implementation in either cohort. In the low-risk RSV cohort, 8.2% of pre-cpg versus 12.3% of post-cpg (P 5.57) infants had subsequent ED visits, and 4.9% of pre-cpg versus 9.6% of post-cpg (P 5.35) infants had subsequent hospital readmissions. All revisits or readmissions were because of symptoms related to bronchiolitis, and there were no positive results for blood, urine, or CSF bacterial cultures noted on subsequent ED visits or readmissions. In the low-risk EV cohort, 2.9% of pre-cpg versus 0% of post-cpg (P 5.34) infants had subsequent ED visits and 1% of pre-cpg versus 1.5% of post-cpg (P 5.56) infants had subsequent hospital readmission. All revisits or readmissions were because of recurrence of fever, and there were no positive results for blood, urine, or CSF bacterial cultures noted on subsequent ED visits or readmissions. No cases of bacterial meningitis or bacteremia were diagnosed in either lowrisk RSV-positive infants or in low-risk infant with EV meningitis. Urine culture results were positive in 0% of low-risk RSV-positive infants and in 1.2% of low-risk infants with EV meningitis. As mentioned above, infants were excluded from our low-risk RSV cohort if they had a urinalysis that contained nitrites or.5 white blood cells per highpower field. We noted significant differences in patient outcomes when comparing low-risk RSVpositive infants and low-risk infants with EV meningitis evaluated pre-cpg to all other febrile infants evaluated pre-cpg. Specifically, compared with all other febrile infants evaluated pre-cpg, low-risk RSVpositive infants evaluated pre-cpg were observed to have a decreased proportion of both LP obtainment (29% of RSV-positive infants versus 70% of all other febrile infants, P,.001), and antibiotic administration (31% of RSV-positive infants versus 70% of all other febrile infants, P,.001). Compared with all other febrile infants evaluated pre-cpg, low-risk infants HOSPITAL PEDIATRICS Volume 7, Issue 10, October
6 FIGURE 3 Flow diagram of included low-risk RSV and low-risk EV infants. ALT, alanine aminotransferase; AST, aspartate aminotransferase; UA, urinalysis. a 1 RSV-positive infant was described as both seizing and ill appearing. with EV meningitis evaluated pre-cpg had decreased HOT (79 hours [interquartile range (IQR) 48 96] versus 90 hours [IQR ], P 5.001) and LOS (47 hours [IQR ] versus 48 hours [IQR 41 63], P 5.03). DISCUSSION We found that implementing a febrile infant CPG that gives explicit management recommendations based on RSV and EV test results was associated with no changes in the proportion of infants undergoing LP, antibiotic exposure, or LOS among low-risk RSV-positive infants but that HOT and LOS decreased among low-risk infants with EV meningitis. We also found a low rate of concomitant bacterial infections in both cohorts. CPG implementation was not associated with adverse patient outcomes, suggesting that adjusting clinical management of a well-defined low-risk subset of febrile infants based on RSV and EV test results is reasonably safe. The lack of observed changes among lowrisk RSV infants is likely multifactorial, but it could be attributed to preexisting clinician knowledge and skill in incorporating RSV testing into febrile infant management. Compared with all other febrile infants evaluated pre-cpg at our institution, lowrisk RSV-positive infants evaluated pre-cpg were observed to have a decreased proportion of both LP obtainment and antibiotic administration. Thus, on the basis of these observations, we speculate that CPG recommendations did not reflect a novel way of managing these patients in our health system, and that clinicians may have already been incorporating RSV testing and interpretation into their management practices. LOS was unchanged among lowrisk RSV-positive infants. This in our view is not surprising, given that RSV-positive infants likely had many confounding factors contributing to LOS, particularly symptoms of bronchiolitis. Additionally, although our CPG provided explicit discharge criteria for patients with EV, no similar criteria for discharge for RSV-positive infants were provided. No changes in management or outcomes were observed among low-risk RSV-positive infants #28 days of life, a population expected to be more conservatively managed pre-guidelines. This lack of change may be because of small sample size in this subset of infants, or health care providers may still have had uncertainty regarding optimal management of these young infants even after CPG implementation. Our study highlights the positive role that EV testing, when combined with explicit management recommendations for infants with EV meningitis, can play in medical decision-making. We build on previous research performed at both our institution and elsewhere that describes an associated reduction in hospital LOS and antibiotics received among febrile infants with positive EV testing. 17,18 Although EV testing had been available at our institution for more than a decade and had been associated with substantial reductions in antibiotic exposure and LOS, 17 we observed even further decreases in both post-cpg implementation. Specifically, compared with all other febrile infants evaluated pre-cpg, low-risk infants with EV meningitis had decreased HOT and LOS. Post-CPG implementation, we observed even further decreases in HOT and LOS for low-risk infants with EV meningitis (Table 2). Thus, we propose that guidelines that give explicit management recommendations based on test results are likely needed to optimize 592 DEPORRE et al
7 changes in practice patterns. We do note the discrepancy in the number of low-risk infants with EV meningitis evaluated pre-cpg versus post-cpg implementation. Because testing patterns were unchanged pre-cpg versus post-cpg (Fig 3), we attribute this discrepancy to natural temporal fluctuations that occur with EV. 19 Our study has several limitations. This review was performed at a single pediatric health system and was not a multicenter review, decreasing its generalizability. Febrile infant encounters may have been misclassified by using our case identification strategy; however, this risk was reduced through manual confirmation of patient encounter eligibility. Because HOT is based on the aggregate number of antibiotics given, the use of HOT as a marker of antibiotic exposure could confound results if infants presenting post-cpg received a different number of antibiotics than infants evaluated pre-cpg. We find this unlikely to affect our results because there were no significant differences in the number of antibiotics given to either lowrisk RSV-positive infants or low-risk infants with EV meningitis pre-cpg versus post-cpg. A subanalysis of infants within each low-risk cohort broken down by age #28 or.29 days similarly revealed no significant change in number of antibiotics given pre-cpg versus post- CPG. We cannot fully assess the impact that variations in test turnaround time could have had on clinical course or patient outcomes. Because of the retrospective nature of this study, changes seen in clinical practice patterns and patient outcomes cannot be attributed to CPG implementation with certainty. However, clinicians did use an electronic order set, which was linked to and based on the CPG in 80% of febrile infant encounters, suggesting that elements of the CPG were at least reviewed in most clinical encounters. Finally, patient and provider characteristics that may have driven viral testing were not analyzed. There may be a selection bias among infants who underwent viral testing, which we were unable to account for in a retrospective study. Specifically, although the proportion of infants tested for EV was unchanged, it is unknown if inherent clinical differences among infants tested for EV pre- versus post-cpg affected our results. CONCLUSIONS Integrating testing and clinical management recommendations for RSV and EV into CPGs for febrile infants may enhance medical decision-making and poses a minimal risk of missing concomitant bacterial infections. However, merely including recommendations regarding test interpretation into a CPG may be insufficient. Further studies are needed to determine specific barriers and facilitators to effectively incorporate diagnostic viral testing into medical decision-making for these infants. REFERENCES 1. Burstein B, Dubrovsky AS, Greene AW, Quach C. National survey on the impact of viral testing for the ED and inpatient management of febrile young infants. Hosp Pediatr. 2016;6(4): Greenes DS, Harper MB. Low risk of bacteremia in febrile children with recognizable viral syndromes. Pediatr Infect Dis J. 1999;18(3): Melendez E, Harper MB. Utility of sepsis evaluation in infants 90 days of age or younger with fever and clinical bronchiolitis. Pediatr Infect Dis J. 2003; 22(12): Purcell K, Fergie J. Concurrent serious bacterial infections in 912 infants and children hospitalized for treatment of respiratory syncytial virus lower respiratory tract infection. Pediatr Infect Dis J. 2004;23(3): Rittichier KR, Bryan PA, Bassett KE, et al. Diagnosis and outcomes of enterovirus infections in young infants. Pediatr Infect Dis J. 2005;24(6): Levine DA, Platt SL, Dayan PS, et al; Multicenter RSV-SBI Study Group of the Pediatric Emergency Medicine Collaborative Research Committee of the American Academy of Pediatrics. Risk of serious bacterial infection in young febrile infants with respiratory syncytial virus infections. Pediatrics. 2004;113(6): Byington CL, Enriquez FR, Hoff C, et al. Serious bacterial infections in febrile infants 1 to 90 days old with and without viral infections. Pediatrics. 2004;113(6): Antonow JA, Byington CL. Use of respiratory syncytial virus testing could safely eliminate many sepsis evaluations. Arch Pediatr Adolesc Med. 1999;153(12): Randolph AG, Reder L, Englund JA. Risk of bacterial infection in previously healthy respiratory syncytial virusinfected young children admitted to the intensive care unit. Pediatr Infect Dis J. 2004;23(11): Ralston S, Hill V, Waters A. Occult serious bacterial infection in infants younger than 60 to 90 days with bronchiolitis: a systematic review. Arch Pediatr Adolesc Med. 2011;165(10): Byington CL, Reynolds CC, Korgenski K, et al. Costs and infant outcomes after implementation of a care process model for febrile infants. Pediatrics. 2012; 130(1). Available at: cgi/content/full/130/1/e Guyatt GH, Oxman AD, Vist GE, et al; GRADE Working Group. GRADE: an emerging consensus on rating quality of evidence and strength of recommendations. BMJ. 2008;336(7650): Polk RE, Fox C, Mahoney A, Letcavage J, MacDougall C. Measurement of adult antibacterial drug use in 130 US hospitals: comparison of defined daily dose and days of therapy. Clin Infect Dis. 2007;44(5): Pakyz AL, MacDougall C, Oinonen M, Polk RE. Trends in antibacterial use in US academic health centers: 2002 to Arch Intern Med. 2008;168(20): Morris AM. Antimicrobial stewardship programs: appropriate measures and metrics to study their impact. Curr Treat Options Infect Dis. 2014;6(2): Selvaraju SB, Nix WA, Oberste MS, Selvarangan R. Optimization of a combined human parechovirusenterovirus real-time reverse HOSPITAL PEDIATRICS Volume 7, Issue 10, October
8 transcription-pcr assay and evaluation of a new parechovirus 3-specific assay for cerebrospinal fluid specimen testing. J Clin Microbiol. 2013;51(2): Hamilton MS, Jackson MA, Abel D. Clinical utility of polymerase chain reaction testing for enteroviral meningitis. Pediatr Infect Dis J. 1999; 18(6): King RL, Lorch SA, Cohen DM, Hodinka RL, Cohn KA, Shah SS. Routine cerebrospinal fluid enterovirus polymerase chain reaction testing reduces hospitalization and antibiotic use for infants 90 days of age or younger. Pediatrics. 2007;120(3): Khetsuriani N, Lamonte-Fowlkes A, Oberst S, Pallansch MA; Centers for Disease Control and Prevention. Enterovirus surveillance United States, MMWR Surveill Summ. 2006;55(8): DEPORRE et al
9 Evaluating the Impact of Implementing a Clinical Practice Guideline for Febrile Infants With Positive Respiratory Syncytial Virus or Enterovirus Testing Adrienne DePorre, David D. Williams, Jennifer Schuster, Jason Newland, Jacqueline Bartlett, Rangaraj Selvarangan, Keith Mann and Russell McCulloh Hospital Pediatrics 2017;7;587 DOI: /hpeds originally published online September 21, 2017; Updated Information & Services Supplementary Material References Permissions & Licensing Reprints including high resolution figures, can be found at: Supplementary material can be found at: 87.DCSupplemental This article cites 18 articles, 6 of which you can access for free at: Information about reproducing this article in parts (figures, tables) or in its entirety can be found online at: Information about ordering reprints can be found online:
10 Evaluating the Impact of Implementing a Clinical Practice Guideline for Febrile Infants With Positive Respiratory Syncytial Virus or Enterovirus Testing Adrienne DePorre, David D. Williams, Jennifer Schuster, Jason Newland, Jacqueline Bartlett, Rangaraj Selvarangan, Keith Mann and Russell McCulloh Hospital Pediatrics 2017;7;587 DOI: /hpeds originally published online September 21, 2017; The online version of this article, along with updated information and services, is located on the World Wide Web at: Hospital Pediatrics is the official journal of the American Academy of Pediatrics. A monthly publication, it has been published continuously since Hospital Pediatrics is owned, published, and trademarked by the American Academy of Pediatrics, 345 Park Avenue, Itasca, Illinois, Copyright 2017 by the American Academy of Pediatrics. All rights reserved. Print ISSN:
Beyond the Reflex Arc: An Evidence-Based Discussion of the Management of Febrile Infants
 Beyond the Reflex Arc: An Evidence-Based Discussion of the Management of Febrile Infants Cole Condra, MD MSc Division of Emergency Medical Services Children s Mercy Hospital October 1, 2011 Disclosure
Beyond the Reflex Arc: An Evidence-Based Discussion of the Management of Febrile Infants Cole Condra, MD MSc Division of Emergency Medical Services Children s Mercy Hospital October 1, 2011 Disclosure
Disclosures. Background. Definitions. Why Worry about these Infants? Goals. Bacterial infection in the neonate and young infant: a review
 Disclosures Bacterial infection in the neonate and young infant: a review Russell J. McCulloh, MD Med-Peds Infectious Diseases August 8, 2017 I have no financial interests to disclose Funding: Eva and
Disclosures Bacterial infection in the neonate and young infant: a review Russell J. McCulloh, MD Med-Peds Infectious Diseases August 8, 2017 I have no financial interests to disclose Funding: Eva and
Fever in neonates (age 0 to 28 days)
 Fever in neonates (age 0 to 28 days) INCLUSION CRITERIA Infant 28 days of life Temperature 38 C (100.4 F) by any route/parental report EXCLUSION CRITERIA Infants with RSV Febrile Infant 28 days old Ill
Fever in neonates (age 0 to 28 days) INCLUSION CRITERIA Infant 28 days of life Temperature 38 C (100.4 F) by any route/parental report EXCLUSION CRITERIA Infants with RSV Febrile Infant 28 days old Ill
REVIEW ARTICLE. Occult Serious Bacterial Infection in Infants Younger Than 60 to 90 Days With Bronchiolitis
 REVIEW ARTICLE Occult Serious Bacterial Infection in Infants Younger Than 60 to 90 Days With A Systematic Review Shawn Ralston, MD; Vanessa Hill, MD; Ami Waters, MD Objective: To summarize the risk of
REVIEW ARTICLE Occult Serious Bacterial Infection in Infants Younger Than 60 to 90 Days With A Systematic Review Shawn Ralston, MD; Vanessa Hill, MD; Ami Waters, MD Objective: To summarize the risk of
4/14/2010. Theoretical purpose of fever? Andrea Marmor, MD, MSEd Assistant Clinical Professor, Pediatrics UCSF April 13, 2010
 Andrea Marmor, MD, MSEd Assistant Clinical Professor, Pediatrics UCSF April 13, 2010 Parental touch? Absence of fever more reliable than presence. Axillary and tympanic Vulnerable to environmental and
Andrea Marmor, MD, MSEd Assistant Clinical Professor, Pediatrics UCSF April 13, 2010 Parental touch? Absence of fever more reliable than presence. Axillary and tympanic Vulnerable to environmental and
Disclosures. Objectives. Epidemiology. Enterovirus 68. Enterovirus species 9/24/2015. Enterovirus D68: Lessons Learned from the Frontline
 Enterovirus D68: Lessons Learned from the Frontline Disclosures Jennifer Schuster, MD MSCI Children s Mercy Hospital Pediatric Infectious Diseases September 16, 2015 I have nothing to disclose I do not
Enterovirus D68: Lessons Learned from the Frontline Disclosures Jennifer Schuster, MD MSCI Children s Mercy Hospital Pediatric Infectious Diseases September 16, 2015 I have nothing to disclose I do not
greater than 10 will be considered ill appearing; a score of 10 or less will be considered well appearing.
 1 Use the Yale Observation Scale to assess whether the patient is ill or well appearing. A score greater than 10 will be considered ill appearing; a score of 10 or less will be considered well appearing.
1 Use the Yale Observation Scale to assess whether the patient is ill or well appearing. A score greater than 10 will be considered ill appearing; a score of 10 or less will be considered well appearing.
Fever Without a Source Age: 0-28 Day Pathway - Emergency Department Evidence Based Outcome Center
 Age: 0-28 Day Pathway - Emergency Department EXCLUSION CRITERIA Toxic appearing No fever Born < 37 weeks gestational age INCLUSION CRITERIA Non-toxic with temperature > 38 C (100.4 F) < 36 C (96.5 F) measured
Age: 0-28 Day Pathway - Emergency Department EXCLUSION CRITERIA Toxic appearing No fever Born < 37 weeks gestational age INCLUSION CRITERIA Non-toxic with temperature > 38 C (100.4 F) < 36 C (96.5 F) measured
The Febrile Infant. SJRH ED Rounds Dec By: Robin Clouston
 1 The Febrile Infant SJRH ED Rounds Dec 11 2018 By: Robin Clouston 2 Objectives Discuss the risk of serious bacterial infection (SBI) in the neonate or young infant (
1 The Febrile Infant SJRH ED Rounds Dec 11 2018 By: Robin Clouston 2 Objectives Discuss the risk of serious bacterial infection (SBI) in the neonate or young infant (
Fever in Infants: Pediatric Dilemmas in Antibiotherapy
 Fever in Infants: Pediatric Dilemmas in Antibiotherapy Jahzel M. Gonzalez Pagan, MD, FAAP Pediatric Emergency Medicine Associate Professor, UPH Medical Advisor, SJCH June 9 th, 2017 S Objectives S Review
Fever in Infants: Pediatric Dilemmas in Antibiotherapy Jahzel M. Gonzalez Pagan, MD, FAAP Pediatric Emergency Medicine Associate Professor, UPH Medical Advisor, SJCH June 9 th, 2017 S Objectives S Review
Evidence-based Management of Fever in Infants and Young Children
 Evidence-based Management of Fever in Infants and Young Children Shabnam Jain, MD, MPH Associate Professor of Pediatrics Emory University Medical Director for Clinical Effectiveness Objectives Understand
Evidence-based Management of Fever in Infants and Young Children Shabnam Jain, MD, MPH Associate Professor of Pediatrics Emory University Medical Director for Clinical Effectiveness Objectives Understand
Faculty Disclosure. Stephen I. Pelton, MD. Dr. Pelton has listed no financial interest/arrangement that would be considered a conflict of interest.
 Faculty Disclosure Stephen I. Pelton, MD Dr. Pelton has listed no financial interest/arrangement that would be considered a conflict of interest. Advances in the management of fever in infants 0 to 3 and
Faculty Disclosure Stephen I. Pelton, MD Dr. Pelton has listed no financial interest/arrangement that would be considered a conflict of interest. Advances in the management of fever in infants 0 to 3 and
Sample Selection- Vignettes
 Sample Selection- Vignettes Rangaraj Selvarangan, BVSc, PhD, D(ABMM) Professor, UMKC School of Medicine Director, Microbiology, Virology and Molecular Infectious Diseases Laboratory Director, Laboratory
Sample Selection- Vignettes Rangaraj Selvarangan, BVSc, PhD, D(ABMM) Professor, UMKC School of Medicine Director, Microbiology, Virology and Molecular Infectious Diseases Laboratory Director, Laboratory
Fever in the Newborn Period
 Fever in the Newborn Period 1. Definitions 1 2. Overview 1 3. History and Physical Examination 2 4. Fever in Infants Less than 3 Months Old 2 a. Table 1: Rochester criteria for low risk infants 3 5. Fever
Fever in the Newborn Period 1. Definitions 1 2. Overview 1 3. History and Physical Examination 2 4. Fever in Infants Less than 3 Months Old 2 a. Table 1: Rochester criteria for low risk infants 3 5. Fever
Low prevalence of invasive bacterial infection in febrile infants under 3 months of age with enterovirus infection
 ORIGINAL ARTICLE INFECTIOUS DISEASES Low prevalence of invasive bacterial infection in febrile infants under 3 months of age with enterovirus infection A. Martínez Planas 1, C. Muñoz Almagro 2, C. Luaces
ORIGINAL ARTICLE INFECTIOUS DISEASES Low prevalence of invasive bacterial infection in febrile infants under 3 months of age with enterovirus infection A. Martínez Planas 1, C. Muñoz Almagro 2, C. Luaces
Bronchiolitis Management Before and After the AAP Guidelines
 ARTICLE Bronchiolitis Management Before and After the AAP Guidelines AUTHORS: Kavita Parikh, MD, a Matthew Hall, PhD, b and Stephen J. Teach, MD, MPH c a Division of Hospitalist Medicine, and c Division
ARTICLE Bronchiolitis Management Before and After the AAP Guidelines AUTHORS: Kavita Parikh, MD, a Matthew Hall, PhD, b and Stephen J. Teach, MD, MPH c a Division of Hospitalist Medicine, and c Division
Rhinovirus in Febrile Infants and Risk of Bacterial Infection
 Sign up for Insight Alerts highlighting editor-chosen studies with the greatest impact on clinical care. Get Involved! Journal editorial boards are seeking candidates. Due to the popularity of the AAP
Sign up for Insight Alerts highlighting editor-chosen studies with the greatest impact on clinical care. Get Involved! Journal editorial boards are seeking candidates. Due to the popularity of the AAP
Estimating RSV Disease Burden in the United States
 Estimating RSV Disease Burden in the United States Brian Rha, MD, MSPH Medical Epidemiologist, Division of Viral Diseases Centers for Disease Control and Prevention Severe Acute Respiratory Infection Surveillance
Estimating RSV Disease Burden in the United States Brian Rha, MD, MSPH Medical Epidemiologist, Division of Viral Diseases Centers for Disease Control and Prevention Severe Acute Respiratory Infection Surveillance
Fever in Young Infants 7 90 days of age
 Fever in Young Infants 7 90 days of age Derek Zhorne, MD Clinical Assistant Professor of Pediatrics Pediatric Hospitalist Disclosures I have no actual or potential conflicts in relation to this presentation.
Fever in Young Infants 7 90 days of age Derek Zhorne, MD Clinical Assistant Professor of Pediatrics Pediatric Hospitalist Disclosures I have no actual or potential conflicts in relation to this presentation.
1. Introduction Algorithm: Infant with Fever 0-28 Days Algorithm: Infant with Fever Days...3
 These guidelines are designed to assist clinicians and are not intended to supplant good clinical judgement or to establish a protocol for all patients with this condition. MANAGEMENT OF FEVER 38 C (100.4F)
These guidelines are designed to assist clinicians and are not intended to supplant good clinical judgement or to establish a protocol for all patients with this condition. MANAGEMENT OF FEVER 38 C (100.4F)
Use of High-Dose Oral Valacyclovir During an Intravenous Acyclovir Shortage: A Retrospective Analysis of Tolerability and Drug Shortage Management
 Infect Dis Ther (2017) 6:259 264 DOI 10.1007/s40121-017-0157-y BRIEF REPORT Use of High-Dose Oral Valacyclovir During an Intravenous Acyclovir Shortage: A Retrospective Analysis of Tolerability and Drug
Infect Dis Ther (2017) 6:259 264 DOI 10.1007/s40121-017-0157-y BRIEF REPORT Use of High-Dose Oral Valacyclovir During an Intravenous Acyclovir Shortage: A Retrospective Analysis of Tolerability and Drug
National Survey on the Impact of Viral Testing for the ED and Inpatient Management of Febrile Young Infants
 RESEARCH ARTICLE National Survey on the Impact of Viral Testing for the ED and Inpatient Management of Febrile Young Infants Brett Burstein, MD CM, PhD, a Alexander Sasha Dubrovsky, MD CM, MSc, a Andrew
RESEARCH ARTICLE National Survey on the Impact of Viral Testing for the ED and Inpatient Management of Febrile Young Infants Brett Burstein, MD CM, PhD, a Alexander Sasha Dubrovsky, MD CM, MSc, a Andrew
Association of Clinical Practice Guidelines With Emergency Department Management of Febrile Infants 56 Days of Age
 ORIGINAL RESEARCH Association of Clinical Practice Guidelines With Emergency Department Management of Febrile Infants 56 Days of Age Paul L. Aronson, MD 1 *, Cary Thurm, PhD 2, Derek J. Williams, MD, MPH
ORIGINAL RESEARCH Association of Clinical Practice Guidelines With Emergency Department Management of Febrile Infants 56 Days of Age Paul L. Aronson, MD 1 *, Cary Thurm, PhD 2, Derek J. Williams, MD, MPH
Fevers and Seizures in Infants and Young Children
 Fevers and Seizures in Infants and Young Children Kellie Holtmeier, PharmD Pediatric Clinical Pharmacist University of New Mexico Hospital Disclosure I have no conflicts of interest 1 Pharmacist Objectives
Fevers and Seizures in Infants and Young Children Kellie Holtmeier, PharmD Pediatric Clinical Pharmacist University of New Mexico Hospital Disclosure I have no conflicts of interest 1 Pharmacist Objectives
Fever is one of the most frequent reasons for consultation in
 ORIGINAL STUDIES Impact of Rapid Viral Testing for Influenza A and B Viruses on Management of Febrile Infants Without Signs of Focal Infection Javier Benito-Fernández, MD, Miguel A. Vázquez-Ronco, MD,
ORIGINAL STUDIES Impact of Rapid Viral Testing for Influenza A and B Viruses on Management of Febrile Infants Without Signs of Focal Infection Javier Benito-Fernández, MD, Miguel A. Vázquez-Ronco, MD,
Facing the ongoing challenge of the febrile young infant
 DePorre et al. Critical Care (2017) 21:68 DOI 10.1186/s13054-017-1646-9 REVIEW Facing the ongoing challenge of the febrile young infant Adrienne G. DePorre 1,2*, Paul L. Aronson 3 and Russell J. McCulloh
DePorre et al. Critical Care (2017) 21:68 DOI 10.1186/s13054-017-1646-9 REVIEW Facing the ongoing challenge of the febrile young infant Adrienne G. DePorre 1,2*, Paul L. Aronson 3 and Russell J. McCulloh
Rational Evaluation of the Febrile Infant
 Disclosures Rational Evaluation of the Febrile Infant Samir S. Shah, MD, MSCE Professor, Department of Pediatrics University of Cincinnati College of Medicine Director, Division of Hospital Medicine Attending
Disclosures Rational Evaluation of the Febrile Infant Samir S. Shah, MD, MSCE Professor, Department of Pediatrics University of Cincinnati College of Medicine Director, Division of Hospital Medicine Attending
IP Lab Webinar 8/23/2012
 2 What Infection Preventionists need to know about the Laboratory Anne Maher, MS, M(ASCP), CIC Richard VanEnk PhD, CIC 1 Objectives Describe what the laboratory can do for you; common laboratory tests
2 What Infection Preventionists need to know about the Laboratory Anne Maher, MS, M(ASCP), CIC Richard VanEnk PhD, CIC 1 Objectives Describe what the laboratory can do for you; common laboratory tests
Fever Interval before Diagnosis, Prior Antibiotic Treatment, and Clinical Outcome for Young Children with Bacterial Meningitis
 MAJOR ARTICLE Fever Interval before Diagnosis, Prior Antibiotic Treatment, and Clinical Outcome for Young Children with Bacterial Meningitis Bema K. Bonsu 1 and Marvin B. Harper 2 1 Department of Medicine,
MAJOR ARTICLE Fever Interval before Diagnosis, Prior Antibiotic Treatment, and Clinical Outcome for Young Children with Bacterial Meningitis Bema K. Bonsu 1 and Marvin B. Harper 2 1 Department of Medicine,
PCR Is Not Always the Answer
 PCR Is Not Always the Answer Nicholas M. Moore, PhD(c), MS, MLS(ASCP) CM Assistant Director, Division of Clinical Microbiology Assistant Professor Rush University Medical Center Disclosures Contracted
PCR Is Not Always the Answer Nicholas M. Moore, PhD(c), MS, MLS(ASCP) CM Assistant Director, Division of Clinical Microbiology Assistant Professor Rush University Medical Center Disclosures Contracted
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES
 DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
Downloaded from:
 Granerod, J; Davison, KL; Ramsay, ME; Crowcroft, NS (26) Investigating the aetiology of and evaluating the impact of the Men C vaccination programme on probable meningococcal disease in England and Wales.
Granerod, J; Davison, KL; Ramsay, ME; Crowcroft, NS (26) Investigating the aetiology of and evaluating the impact of the Men C vaccination programme on probable meningococcal disease in England and Wales.
Time to Detection of Bacterial Cultures in Infants Aged 0 to 90 Days
 RESEARCH ARTICLE Time to Detection of Bacterial Cultures in Infants Aged 0 to 90 Days AUTHORS Rianna C. Evans, MD, Bryan R. Fine, MD, MPH Division of Pediatric Hospital Medicine, Department of Pediatrics,
RESEARCH ARTICLE Time to Detection of Bacterial Cultures in Infants Aged 0 to 90 Days AUTHORS Rianna C. Evans, MD, Bryan R. Fine, MD, MPH Division of Pediatric Hospital Medicine, Department of Pediatrics,
Fever in Babies. Too much testing or not enough testing? Martin E. Weisse, M.D. Pediatric Infectious Diseases
 Fever in Babies Too much testing or not enough testing? Martin E. Weisse, M.D. Pediatric Infectious Diseases Disclosures I have nothing to disclose Learning Objectives At the end of the talk, participants
Fever in Babies Too much testing or not enough testing? Martin E. Weisse, M.D. Pediatric Infectious Diseases Disclosures I have nothing to disclose Learning Objectives At the end of the talk, participants
PDFlib PLOP: PDF Linearization, Optimization, Protection. Page inserted by evaluation version
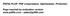 PDFlib PLOP: PDF Linearization, Optimization, Protection Page inserted by evaluation version www.pdflib.com sales@pdflib.com ACAD EMERG MED d December 2004, Vol. 11, No. 12 d www.aemj.org 1297 A Low Peripheral
PDFlib PLOP: PDF Linearization, Optimization, Protection Page inserted by evaluation version www.pdflib.com sales@pdflib.com ACAD EMERG MED d December 2004, Vol. 11, No. 12 d www.aemj.org 1297 A Low Peripheral
UTI Update: Have We Been Led Astray? Disclosure. Objectives
 UTI Update: Have We Been Led Astray? KAAP Sept 28, 2012 Robert Wittler, MD 1 Disclosure Neither I nor any member of my immediate family has a financial relationship or interest with any entity related
UTI Update: Have We Been Led Astray? KAAP Sept 28, 2012 Robert Wittler, MD 1 Disclosure Neither I nor any member of my immediate family has a financial relationship or interest with any entity related
Good Morning! Welcome Applicants! FRIDAY, N OVEMBER, 7 TH 2014
 Good Morning! Welcome Applicants! FRIDAY, N OVEMBER, 7 TH 2014 Prep Question You are camping with a group of boys at a rural campground in the southeastern Unites States when one of the campers is bitten
Good Morning! Welcome Applicants! FRIDAY, N OVEMBER, 7 TH 2014 Prep Question You are camping with a group of boys at a rural campground in the southeastern Unites States when one of the campers is bitten
ARTICLE. Cerebrospinal Fluid Enterovirus Testing in Infants 56 Days or Younger
 ARTICLE Cerebrospinal Fluid Enterovirus Testing in Infants 56 Days or Younger Maya Dewan, MD, MPH; Joseph J. Zorc, MD, MSCE; Richard L. Hodinka, PhD; Samir S. Shah, MD, MSCE Objective: To determine whether
ARTICLE Cerebrospinal Fluid Enterovirus Testing in Infants 56 Days or Younger Maya Dewan, MD, MPH; Joseph J. Zorc, MD, MSCE; Richard L. Hodinka, PhD; Samir S. Shah, MD, MSCE Objective: To determine whether
The Role of POCT in Management of Infectious Disease in the Critical Care Setting
 The Role of POCT in Management of Infectious Disease in the Critical Care Setting Nathan A Ledeboer Associate Professor of Pathology Medical College of Wisconsin Medical Director, Microbiology and Molecular
The Role of POCT in Management of Infectious Disease in the Critical Care Setting Nathan A Ledeboer Associate Professor of Pathology Medical College of Wisconsin Medical Director, Microbiology and Molecular
EPG Clinical Guidelines
 Guidelines for the Management of Febrile Young Children Neonate age 7 days Temperature > 38 C, documented at home or in the ED Complete blood count with manual differential (CBCD), urinalysis (UA), urine
Guidelines for the Management of Febrile Young Children Neonate age 7 days Temperature > 38 C, documented at home or in the ED Complete blood count with manual differential (CBCD), urinalysis (UA), urine
RSV Surveillance in the U.S.
 RSV Surveillance in the U.S. Susan I. Gerber, MD Respiratory Virus Program Division of Viral Diseases National Center for Immunization and Respiratory Diseases Centers for Disease Control and Prevention
RSV Surveillance in the U.S. Susan I. Gerber, MD Respiratory Virus Program Division of Viral Diseases National Center for Immunization and Respiratory Diseases Centers for Disease Control and Prevention
Critical Review Form Clinical Prediction or Decision Rule
 Critical Review Form Clinical Prediction or Decision Rule Development and Validation of a Multivariable Predictive Model to Distinguish Bacterial from Aseptic Meningitis in Children, Pediatrics 2002; 110:
Critical Review Form Clinical Prediction or Decision Rule Development and Validation of a Multivariable Predictive Model to Distinguish Bacterial from Aseptic Meningitis in Children, Pediatrics 2002; 110:
Guideline for the Management of Fever and Neutropenia in Children with Cancer and/or Undergoing Hematopoietic Stem-Cell Transplantation
 Guideline for the Management of Fever Neutropenia in Children with Cancer /or Undergoing Hematopoietic Stem-Cell Transplantation COG Supportive Care Endorsed Guidelines Click here to see all the COG Supportive
Guideline for the Management of Fever Neutropenia in Children with Cancer /or Undergoing Hematopoietic Stem-Cell Transplantation COG Supportive Care Endorsed Guidelines Click here to see all the COG Supportive
Progress in the Control of Childhood Obesity
 William H. Dietz, MD, PhD a, Christina D. Economos, PhD b Two recent reports from the Centers for Disease Control and Prevention and reports from a number of states and municipalities suggest that we are
William H. Dietz, MD, PhD a, Christina D. Economos, PhD b Two recent reports from the Centers for Disease Control and Prevention and reports from a number of states and municipalities suggest that we are
Catheter-Associated Urinary Tract Infection (CAUTI) Event
 Catheter-Associated Urinary Tract Infection () Event Introduction: The urinary tract is the most common site of healthcare-associated infection, accounting for more than 30% of infections reported by acute
Catheter-Associated Urinary Tract Infection () Event Introduction: The urinary tract is the most common site of healthcare-associated infection, accounting for more than 30% of infections reported by acute
Corporate Medical Policy
 Corporate Medical Policy Identification of Microorganisms Using Nucleic Acid Probes File Name: Origination: Last CAP Review: Next CAP Review: Last Review: identification_of_microorganisms_using_nucleic_acid_probes
Corporate Medical Policy Identification of Microorganisms Using Nucleic Acid Probes File Name: Origination: Last CAP Review: Next CAP Review: Last Review: identification_of_microorganisms_using_nucleic_acid_probes
Cerebrospinal Fluid Glucose and Protein in Disposition and Treatment Decisions
 298 BRIEF REPORTS Givens et al. CSF GLUCOSE AND PROTEIN Cerebrospinal Fluid Glucose and Protein in Disposition and Treatment Decisions Routine laboratory analysis performed when bacterial meningitis is
298 BRIEF REPORTS Givens et al. CSF GLUCOSE AND PROTEIN Cerebrospinal Fluid Glucose and Protein in Disposition and Treatment Decisions Routine laboratory analysis performed when bacterial meningitis is
PEDIATRIC INFECTIOUS DISEASES UPDATE. Neonatal HSV. Recognition, Diagnosis, and Management Coleen Cunningham MD
 Neonatal HSV Recognition, Diagnosis, and Management Coleen Cunningham MD Important questions Who is at risk? When do you test? What tests do you perform? When do you treat? What is appropriate therapy?
Neonatal HSV Recognition, Diagnosis, and Management Coleen Cunningham MD Important questions Who is at risk? When do you test? What tests do you perform? When do you treat? What is appropriate therapy?
Ancillary Testing in Children with Rotavirus Gastroenteritis
 ORIGINAL RESEARCH Ancillary Testing in Children with Rotavirus Gastroenteritis Peter A. Rowinsky, MD 1,2 Andrew P. Steenhoff, MBBCh, DCH (UK), FCP (SA) Paed 3,4,5,6,7 Shiang-Ju Kung, MBBCh, DCH (SA) 8
ORIGINAL RESEARCH Ancillary Testing in Children with Rotavirus Gastroenteritis Peter A. Rowinsky, MD 1,2 Andrew P. Steenhoff, MBBCh, DCH (UK), FCP (SA) Paed 3,4,5,6,7 Shiang-Ju Kung, MBBCh, DCH (SA) 8
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A AAP. See American Academy of Pediatrics (AAP) Acyclovir dosing in infants, 185 187 American Academy of Pediatrics (AAP) COFN of, 199 204 Amphotericin
Note: Page numbers of article titles are in boldface type. A AAP. See American Academy of Pediatrics (AAP) Acyclovir dosing in infants, 185 187 American Academy of Pediatrics (AAP) COFN of, 199 204 Amphotericin
Redefine Performance. BD Veritor. System Revolutionizes Testing at the Point of Care. Fast. Streamlined Workflow Requires minimal hands-on time
 CLIA WAIVED Redefine Performance System BD Veritor System Revolutionizes Testing at the Point of Care Accurate The first CLIA-waived Digital Immunoassay (DIA), a new category of diagnostic tests where
CLIA WAIVED Redefine Performance System BD Veritor System Revolutionizes Testing at the Point of Care Accurate The first CLIA-waived Digital Immunoassay (DIA), a new category of diagnostic tests where
The Child with HIV and a Fever 1
 The Child with HIV and a Fever 1 Author: Andrew Riordan Amanda Williams Date of preparation: August 2003 Date reviewed: February 2012 Next review date: February 2014 Contents 1. Introduction 2. HIV disease
The Child with HIV and a Fever 1 Author: Andrew Riordan Amanda Williams Date of preparation: August 2003 Date reviewed: February 2012 Next review date: February 2014 Contents 1. Introduction 2. HIV disease
Clinical Guidelines And Primary Care
 Clinical Guidelines And Primary Care Alfred O. Berg, MD, MPH, Series Editor Management Of Infants And Children 0 To 36 Months Of Age With Fever Without Source Nancy S. Gmbb, MD, Sarah Lyle, MD, MPH, jeffrey
Clinical Guidelines And Primary Care Alfred O. Berg, MD, MPH, Series Editor Management Of Infants And Children 0 To 36 Months Of Age With Fever Without Source Nancy S. Gmbb, MD, Sarah Lyle, MD, MPH, jeffrey
abstract ARTICLE BACKGROUND: There is considerable variation in the approach to infants presenting to the
 Management and Outcomes of Previously Healthy, Full-Term, Febrile Infants Ages 7 to 90 Days Tara L. Greenhow, MD, a Yun-Yi Hung, PhD, b Robert H. Pantell, MD c BACKGROUND: There is considerable variation
Management and Outcomes of Previously Healthy, Full-Term, Febrile Infants Ages 7 to 90 Days Tara L. Greenhow, MD, a Yun-Yi Hung, PhD, b Robert H. Pantell, MD c BACKGROUND: There is considerable variation
Surveillance report Published: 7 July 2016 nice.org.uk. NICE All rights reserved.
 Surveillance report 2016 Urinary tract infection in under 16s: diagnosis and management (2007) NICE guideline CG54 Surveillance report Published: 7 July 2016 nice.org.uk NICE 2016. All rights reserved.
Surveillance report 2016 Urinary tract infection in under 16s: diagnosis and management (2007) NICE guideline CG54 Surveillance report Published: 7 July 2016 nice.org.uk NICE 2016. All rights reserved.
Judith Klein, MD 2011 FEVER IN THE FIRST 36 MONTHS OF LIFE
 Judith Klein, MD 2011 FEVER IN THE FIRST 36 MONTHS OF LIFE Objectives A short history of the kiddie fever business Vaccinations Rapid viral testing Biomarkers Month-by-month approach to fevers in these
Judith Klein, MD 2011 FEVER IN THE FIRST 36 MONTHS OF LIFE Objectives A short history of the kiddie fever business Vaccinations Rapid viral testing Biomarkers Month-by-month approach to fevers in these
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Edwards KM, Zhu Y, Griffin MR, et al. Burden of human metapneumovirus
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Edwards KM, Zhu Y, Griffin MR, et al. Burden of human metapneumovirus
 Fever Phobia and the ED Doc Ran Goldman, MD (rgoldman@cw.bc.ca) BC Children s Hospital, Professor, University of British Columbia SLIDES ON : www.clinicalpeds.com/whistler Define Fever 38.0 o Doesn t
Fever Phobia and the ED Doc Ran Goldman, MD (rgoldman@cw.bc.ca) BC Children s Hospital, Professor, University of British Columbia SLIDES ON : www.clinicalpeds.com/whistler Define Fever 38.0 o Doesn t
Microbiology Laboratory Directors, Infection Preventionists, Primary Care Providers, Emergency Department Directors, Infectious Disease Physicians
 MEMORANDUM DATE: October 1, 2009 TO: FROM: SUBJECT: Microbiology Laboratory Directors, Infection Preventionists, Primary Care Providers, Emergency Department Directors, Infectious Disease Physicians Michael
MEMORANDUM DATE: October 1, 2009 TO: FROM: SUBJECT: Microbiology Laboratory Directors, Infection Preventionists, Primary Care Providers, Emergency Department Directors, Infectious Disease Physicians Michael
Evaluating Fever in Infants. Derek Zhorne, MD Clinical Assistant Professor of Pediatrics Pediatric Hospitalist
 Evaluating Fever in Infants Derek Zhorne, MD Clinical Assistant Professor of Pediatrics Pediatric Hospitalist Disclosures I have no actual or potential conflicts in relation to this presentation. I will
Evaluating Fever in Infants Derek Zhorne, MD Clinical Assistant Professor of Pediatrics Pediatric Hospitalist Disclosures I have no actual or potential conflicts in relation to this presentation. I will
Syncytial Virus. Surveillance: A. Respiratory (RSV) New Initiative for NM
 Respiratory Syncytial Virus (RSV) Surveillance: A New Initiative for NM Sarah Shrum, MPH EIP Surveillance Officer, NMDOH EIP Day Conference September 23 rd, 2016 Objectives 1. Describe basic virology,
Respiratory Syncytial Virus (RSV) Surveillance: A New Initiative for NM Sarah Shrum, MPH EIP Surveillance Officer, NMDOH EIP Day Conference September 23 rd, 2016 Objectives 1. Describe basic virology,
Etiology and Resource Use of Fever of Unknown Origin in Hospitalized Children
 RESEARCH ARTICLE Etiology and Resource Use of Fever of Unknown Origin in Hospitalized Children James W. Antoon, MD, PhD, a David C. Peritz, MD, b Michael R. Parsons, MD, c Asheley C. Skinner, PhD, d Jacob
RESEARCH ARTICLE Etiology and Resource Use of Fever of Unknown Origin in Hospitalized Children James W. Antoon, MD, PhD, a David C. Peritz, MD, b Michael R. Parsons, MD, c Asheley C. Skinner, PhD, d Jacob
Emerging Pediatric Infectious Disease
 Emerging Pediatric Infectious Disease M A R Y K I N G M D, M P H P E D I A T R I C I N T E N S I V I S T H A R B O R V I E W A N D S E A T T L E C H I L D R E N S S E P T E M B E R 1 9, 2 0 1 4 P E D I
Emerging Pediatric Infectious Disease M A R Y K I N G M D, M P H P E D I A T R I C I N T E N S I V I S T H A R B O R V I E W A N D S E A T T L E C H I L D R E N S S E P T E M B E R 1 9, 2 0 1 4 P E D I
Enrichment culture of CSF is of limited value in the diagnosis of neonatal meningitis
 Enrichment culture of CSF is of limited value in the diagnosis of neonatal S. H. Chaudhry, D. Wagstaff, Anupam Gupta, I. C. Bowler, D. P. Webster To cite this version: S. H. Chaudhry, D. Wagstaff, Anupam
Enrichment culture of CSF is of limited value in the diagnosis of neonatal S. H. Chaudhry, D. Wagstaff, Anupam Gupta, I. C. Bowler, D. P. Webster To cite this version: S. H. Chaudhry, D. Wagstaff, Anupam
PCR Is Not Always the Answer
 PCR Is Not Always the Answer Nicholas M. Moore, PhD, MS, MLS(ASCP) CM Assistant Director, Division of Clinical Microbiology Assistant Professor Rush University Medical Center Disclosures Contracted research:
PCR Is Not Always the Answer Nicholas M. Moore, PhD, MS, MLS(ASCP) CM Assistant Director, Division of Clinical Microbiology Assistant Professor Rush University Medical Center Disclosures Contracted research:
Management of Febrile Neonates in US Pediatric Emergency Departments
 ARTICLE Management of Febrile Neonates in US Pediatric Emergency Departments AUTHORS: Shabnam Jain, MD, MPH, a John Cheng, MD, a Elizabeth R. Alpern, MD, MSCE, b Cary Thurm, PhD, c Lisa Schroeder, MD,
ARTICLE Management of Febrile Neonates in US Pediatric Emergency Departments AUTHORS: Shabnam Jain, MD, MPH, a John Cheng, MD, a Elizabeth R. Alpern, MD, MSCE, b Cary Thurm, PhD, c Lisa Schroeder, MD,
3.5. Background - CAP. Disclosure. Goal. Why Guidelines
 Disclosure The New PIDS-IDSA Community Acquired Pneumonia Guidelines Ricardo Quiñonez, MD, FAAP, FHM Section of Pediatric Hospital Medicine Baylor College of Medicine Texas Children s Hospital I have no
Disclosure The New PIDS-IDSA Community Acquired Pneumonia Guidelines Ricardo Quiñonez, MD, FAAP, FHM Section of Pediatric Hospital Medicine Baylor College of Medicine Texas Children s Hospital I have no
Appendix A: Disease-Specific Chapters
 Ministry of Health and Long-Term Care Infectious Diseases Protocol Appendix A: Disease-Specific Chapters Chapter: Haemophilus influenzae disease, all types, invasive Effective: May 2018 Haemophilus influenzae,
Ministry of Health and Long-Term Care Infectious Diseases Protocol Appendix A: Disease-Specific Chapters Chapter: Haemophilus influenzae disease, all types, invasive Effective: May 2018 Haemophilus influenzae,
Hospital-wide Impact of Mandatory Infectious Disease Consultation on Staphylococcus aureus Septicemia
 Hospital-wide Impact of Mandatory Infectious Disease Consultation on Staphylococcus aureus Septicemia Amanda Guth 1 Amy Slenker MD 1,2 1 Department of Infectious Diseases, Lehigh Valley Health Network
Hospital-wide Impact of Mandatory Infectious Disease Consultation on Staphylococcus aureus Septicemia Amanda Guth 1 Amy Slenker MD 1,2 1 Department of Infectious Diseases, Lehigh Valley Health Network
Variation in Diagnostic Testing and Hospitalization Rates in Children With Acute Gastroenteritis
 RESEARCH ARTICLE Variation in Diagnostic Testing and Hospitalization Rates in Children With Acute Gastroenteritis Carrie H. Lind, MD, a Matt Hall, PhD, b Donald H. Arnold, MD, MPH, c Whitney Browning,
RESEARCH ARTICLE Variation in Diagnostic Testing and Hospitalization Rates in Children With Acute Gastroenteritis Carrie H. Lind, MD, a Matt Hall, PhD, b Donald H. Arnold, MD, MPH, c Whitney Browning,
Dipstick Urinalysis as a Test for Microhematuria and Occult Bladder Cancer
 Bladder Cancer 3 (2017) 45 49 DOI 10.3233/BLC-160068 IOS Press Research Report 45 Dipstick Urinalysis as a Test for Microhematuria and Occult Bladder Cancer Richard S. Matulewicz a,b,, John Oliver DeLancey
Bladder Cancer 3 (2017) 45 49 DOI 10.3233/BLC-160068 IOS Press Research Report 45 Dipstick Urinalysis as a Test for Microhematuria and Occult Bladder Cancer Richard S. Matulewicz a,b,, John Oliver DeLancey
MICROBIOLOGICAL TESTING IN PICU
 MICROBIOLOGICAL TESTING IN PICU This is a guideline for the taking of microbiological samples in PICU to diagnose or exclude infection. The diagnosis of infection requires: Ruling out non-infectious causes
MICROBIOLOGICAL TESTING IN PICU This is a guideline for the taking of microbiological samples in PICU to diagnose or exclude infection. The diagnosis of infection requires: Ruling out non-infectious causes
Healthcare-associated infections acquired in intensive care units
 SURVEILLANCE REPORT Annual Epidemiological Report for 2015 Healthcare-associated infections acquired in intensive care units Key facts In 2015, 11 788 (8.3%) of patients staying in an intensive care unit
SURVEILLANCE REPORT Annual Epidemiological Report for 2015 Healthcare-associated infections acquired in intensive care units Key facts In 2015, 11 788 (8.3%) of patients staying in an intensive care unit
Syndromic Testing for Infectious Diseases
 Syndromic Testing for Infectious Diseases Part 3: Central Nervous System Infections HOT TOPIC / 2017 Presenter: Elitza S. Theel, Ph.D., D(ABMM) Director of Infectious Diseases Serology Department of Laboratory
Syndromic Testing for Infectious Diseases Part 3: Central Nervous System Infections HOT TOPIC / 2017 Presenter: Elitza S. Theel, Ph.D., D(ABMM) Director of Infectious Diseases Serology Department of Laboratory
ABSTRACT PURPOSE METHODS
 ABSTRACT PURPOSE The purpose of this study was to characterize the CDI population at this institution according to known risk factors and to examine the effect of appropriate evidence-based treatment selection
ABSTRACT PURPOSE The purpose of this study was to characterize the CDI population at this institution according to known risk factors and to examine the effect of appropriate evidence-based treatment selection
The Culture of Culturing: Laboratory Diagnostic Stewardship
 The Culture of Culturing: Laboratory Diagnostic Stewardship Isabella W. Martin, MD Medical Director of Clinical Microbiology Laboratory, Dartmouth-Hitchcock Medical Center Michael S. Calderwood, MD, MPH
The Culture of Culturing: Laboratory Diagnostic Stewardship Isabella W. Martin, MD Medical Director of Clinical Microbiology Laboratory, Dartmouth-Hitchcock Medical Center Michael S. Calderwood, MD, MPH
Quick Literature Searches
 Quick Literature Searches National Pediatric Nighttime Curriculum Written by Leticia Shanley, MD, FAAP Institution: University of Texas Southwestern Medical Center Case 1 It s 1:00am and you have just
Quick Literature Searches National Pediatric Nighttime Curriculum Written by Leticia Shanley, MD, FAAP Institution: University of Texas Southwestern Medical Center Case 1 It s 1:00am and you have just
J of Evolution of Med and Dent Sci/ eissn , pissn / Vol. 4/ Issue 66/ Aug 17, 2015 Page 11432
 BLOOD CULTURE AND BACTEREMIA PREDICTORS IN INFANTS LESS THAN ONE YEAR OF AGE WITH FEVER WITHOUT SOURCE (FWS) Y. G. Sathish Kumar 1, A. Udayamaliny 2, S. Ankitha 3 HOW TO CITE THIS ARTICLE: Y. G. Sathish
BLOOD CULTURE AND BACTEREMIA PREDICTORS IN INFANTS LESS THAN ONE YEAR OF AGE WITH FEVER WITHOUT SOURCE (FWS) Y. G. Sathish Kumar 1, A. Udayamaliny 2, S. Ankitha 3 HOW TO CITE THIS ARTICLE: Y. G. Sathish
Advanced Pediatric Emergency Medicine Assembly
 (+)Joan Shook, MD, FACEP Professor of Pediatrics, Baylor College of Medicine; Chief Safety Officer and Chief Clinical Information Officer, Texas Children's Hospital Advanced Pediatric Emergency Medicine
(+)Joan Shook, MD, FACEP Professor of Pediatrics, Baylor College of Medicine; Chief Safety Officer and Chief Clinical Information Officer, Texas Children's Hospital Advanced Pediatric Emergency Medicine
Prospective audit and feedback of piperacillin-tazobactam use in a 1115 bed acute care hospital
 Prospective audit and feedback of piperacillin-tazobactam use in a 1115 bed acute care hospital Final Results Nathan Beahm, BSP, PharmD(student) September 10, 2016 Objectives Review background information
Prospective audit and feedback of piperacillin-tazobactam use in a 1115 bed acute care hospital Final Results Nathan Beahm, BSP, PharmD(student) September 10, 2016 Objectives Review background information
Community Acquired Pneumonia
 April 2014 References: 1. Bradley JS, Byington CL, Shah SS, Alverson B, Carter ER, Harrison C, Kaplan SL Mace SE, McCracken Jr. GH, Moor MR, St. Peter SD, Stockwell JA, and Swanson JT. The Management of
April 2014 References: 1. Bradley JS, Byington CL, Shah SS, Alverson B, Carter ER, Harrison C, Kaplan SL Mace SE, McCracken Jr. GH, Moor MR, St. Peter SD, Stockwell JA, and Swanson JT. The Management of
Age-Specific Reference Values for Cerebrospinal Fluid Protein Concentration in Neonates and Young Infants
 ORIGINAL RESEARCH Age-Specific Reference Values for Cerebrospinal Fluid Protein Concentration in Neonates and Young Infants Samir S. Shah, MD, MSCE 1,2,6,7 Jessica Ebberson, MD 1 Lori A. Kestenbaum, MD
ORIGINAL RESEARCH Age-Specific Reference Values for Cerebrospinal Fluid Protein Concentration in Neonates and Young Infants Samir S. Shah, MD, MSCE 1,2,6,7 Jessica Ebberson, MD 1 Lori A. Kestenbaum, MD
Hot Hot Tot:! The Hot Tot. Fever in KIds <90 Days 5/26/10
 Hot Hot Tot:! Fever in KIds
Hot Hot Tot:! Fever in KIds
Scott Williams, MD Pediatric Nephrology OLOL Children s Hospital September 29, Controversies in Urinary Tract Infections
 Scott Williams, MD Pediatric Nephrology OLOL Children s Hospital September 29, 2013 Controversies in Urinary Tract Infections Disclaimer I have no affiliations with any pharmaceutical or equipment company
Scott Williams, MD Pediatric Nephrology OLOL Children s Hospital September 29, 2013 Controversies in Urinary Tract Infections Disclaimer I have no affiliations with any pharmaceutical or equipment company
Group B Streptococcus
 Group B Streptococcus (Invasive Disease) Infants Younger than 90 Days Old DISEASE REPORTABLE WITHIN 24 HOURS OF DIAGNOSIS Per N.J.A.C. 8:57, healthcare providers and administrators shall report by mail
Group B Streptococcus (Invasive Disease) Infants Younger than 90 Days Old DISEASE REPORTABLE WITHIN 24 HOURS OF DIAGNOSIS Per N.J.A.C. 8:57, healthcare providers and administrators shall report by mail
Outpatient parenteral antibiotic therapy with daptomycin: insights from a patient registry
 doi: 10.1111/j.1742-1241.2008.01824.x ORIGINAL PAPER Outpatient parenteral antibiotic therapy with daptomycin: insights from a patient registry W. J. Martone, K. C. Lindfield, D. E. Katz OnlineOpen: This
doi: 10.1111/j.1742-1241.2008.01824.x ORIGINAL PAPER Outpatient parenteral antibiotic therapy with daptomycin: insights from a patient registry W. J. Martone, K. C. Lindfield, D. E. Katz OnlineOpen: This
FILMARRAY: CAN IT MAKE A DIFFERENCE FOR CSF TESTING L O U I S E O S U L L I V A N, M M U H O S U L L I V A N M A T E R. I E
 FILMARRAY: CAN IT MAKE A DIFFERENCE FOR CSF TESTING L O U I S E O S U L L I V A N, M M U H O S U L L I V A N L @ M A T E R. I E Level 4 teaching hospital based in Dublin s north inner city Over 600 in-patient
FILMARRAY: CAN IT MAKE A DIFFERENCE FOR CSF TESTING L O U I S E O S U L L I V A N, M M U H O S U L L I V A N L @ M A T E R. I E Level 4 teaching hospital based in Dublin s north inner city Over 600 in-patient
+ Objectives. n Define who is at risk for SBI. n Clarify risk stratification. n Provide treatment guidelines. n Bust some myths
 Objectives n Define wo is at risk for SBI n Clarify risk stratification n Provide treatment guidelines Neonatal Fever Benjamin B. Constance, MD, FAWM n Bust some myts Based on Case wat do you want to know?
Objectives n Define wo is at risk for SBI n Clarify risk stratification n Provide treatment guidelines Neonatal Fever Benjamin B. Constance, MD, FAWM n Bust some myts Based on Case wat do you want to know?
Urinary tract infection. Mohamed Ahmed Fouad Lecturer of pediatrics Jazan faculty of medicine
 Urinary tract infection Mohamed Ahmed Fouad Lecturer of pediatrics Jazan faculty of medicine Objectives To differentiate between types of urinary tract infections To recognize the epidemiology of UTI in
Urinary tract infection Mohamed Ahmed Fouad Lecturer of pediatrics Jazan faculty of medicine Objectives To differentiate between types of urinary tract infections To recognize the epidemiology of UTI in
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES
 DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
Multiplex Syndromic Testing s Effect on Public Health Molecular Testing & Emerging Technology WCLN Workshop April 28, 2016
 Multiplex Syndromic Testing s Effect on Public Health Molecular Testing & Emerging Technology- 2016 WCLN Workshop April 28, 2016 Objectives Learn what current multi-target testing activities are ongoing
Multiplex Syndromic Testing s Effect on Public Health Molecular Testing & Emerging Technology- 2016 WCLN Workshop April 28, 2016 Objectives Learn what current multi-target testing activities are ongoing
Pertussis Update 8/22/2014. Objectives. Pertussis. Pertussis. Pertussis: from Latin meaning intense cough. Pertussis Diagnosis
 Objectives Pertussis Update Jim Dunn, PhD, D(ABMM) Director, Medical Microbiology and Virology Texas Children s Hospital Describe the current epidemiology of pertussis infections in the U.S. Discuss the
Objectives Pertussis Update Jim Dunn, PhD, D(ABMM) Director, Medical Microbiology and Virology Texas Children s Hospital Describe the current epidemiology of pertussis infections in the U.S. Discuss the
New Antimicrobials and Rapid Diagnostics: Implications for Antibiotic Stewardship
 New Antimicrobials and Rapid Diagnostics: Implications for Antibiotic Stewardship Mia A. Taormina, DO, FACOI Chair, Department of Infectious Disease, DuPage Medical Group Disclosures While product trade
New Antimicrobials and Rapid Diagnostics: Implications for Antibiotic Stewardship Mia A. Taormina, DO, FACOI Chair, Department of Infectious Disease, DuPage Medical Group Disclosures While product trade
Does Extending Clostridium Difficile Treatment In Patients Who Are Receiving Concomitant Antibiotics Reduce The Rate Of Relapse?
 ISPUB.COM The Internet Journal of Infectious Diseases Volume 15 Number 1 Does Extending Clostridium Difficile Treatment In Patients Who Are Receiving Concomitant Antibiotics Reduce The Rate Of Relapse?
ISPUB.COM The Internet Journal of Infectious Diseases Volume 15 Number 1 Does Extending Clostridium Difficile Treatment In Patients Who Are Receiving Concomitant Antibiotics Reduce The Rate Of Relapse?
Does This Child Have a Urinary Tract Infection?
 EVIDENCE-BASED EMERGENCY MEDICINE/RATIONAL CLINICAL EXAMINATION ABSTRACT Does This Child Have a Urinary Tract Infection? EBEM Commentator Contact Rupinder Singh Sahsi, BSc, MD Christopher R. Carpenter,
EVIDENCE-BASED EMERGENCY MEDICINE/RATIONAL CLINICAL EXAMINATION ABSTRACT Does This Child Have a Urinary Tract Infection? EBEM Commentator Contact Rupinder Singh Sahsi, BSc, MD Christopher R. Carpenter,
Performance of a Rapid Influenza Test in Children During the H1N Influenza A Outbreak
 ARTICLES Performance of a Rapid Influenza Test in Children During the H1N1 2009 Influenza A Outbreak AUTHORS: Andrea T. Cruz, MD, MPH, a,b Gail J. Demmler- Harrison, MD, b,c,d A. Chantal Caviness, MD,
ARTICLES Performance of a Rapid Influenza Test in Children During the H1N1 2009 Influenza A Outbreak AUTHORS: Andrea T. Cruz, MD, MPH, a,b Gail J. Demmler- Harrison, MD, b,c,d A. Chantal Caviness, MD,
Catheter-Associated Urinary Tract Infection (CAUTI) Event
 Device-associated Events Catheter-Associated Urinary Tract Infection () Event Introduction: The urinary tract is the most common site of healthcare-associated infection, accounting for more than 30% of
Device-associated Events Catheter-Associated Urinary Tract Infection () Event Introduction: The urinary tract is the most common site of healthcare-associated infection, accounting for more than 30% of
Highlights. NEW YORK CITY DEPARTMENT OF HEALTH AND MENTAL HYGIENE Influenza Surveillance Report Week ending January 28, 2017 (Week 4)
 NEW YORK CITY DEPARTMENT OF HEALTH AND MENTAL HYGIENE Influenza Surveillance Report Week ending January 28, 2017 (Week 4) Highlights * Influenza surveillance activities for the 2016-2017 season began on
NEW YORK CITY DEPARTMENT OF HEALTH AND MENTAL HYGIENE Influenza Surveillance Report Week ending January 28, 2017 (Week 4) Highlights * Influenza surveillance activities for the 2016-2017 season began on
ASPIRES Urinary Tract Infection Algorithm
 ASPIRES Urinary Tract Infection Algorithm Dr. Jennifer Grant Dr. Tim Lau Donna Leung February 2013 VCH Antimicrobial Stewardship 1 Programme: Innovation, Research, Education & Safety KEY PRINCIPLES 1.
ASPIRES Urinary Tract Infection Algorithm Dr. Jennifer Grant Dr. Tim Lau Donna Leung February 2013 VCH Antimicrobial Stewardship 1 Programme: Innovation, Research, Education & Safety KEY PRINCIPLES 1.
