By: Lec 7 Date:20 /11/2017
|
|
|
- Neal Dalton
- 5 years ago
- Views:
Transcription
1 By: Lec 7 Date:20 /11/2017 I include the slide within sheet with bold
2 From the previous lecture slide 29 **The respiratory center is divided into three major groups: dorsal, ventral and potine group which made up of two areas the pneuomtaxic centre and the apneustic centre Regulation of respiration Other factors affecting respiration: 1- voluntary control : for short period of times You can perform hypoventilation or hyperventilation voluntary, these are voluntary movements which can regulate the performance of respiration for a short period 2- irritant receptors: stimulated by many incidents coughing & sneezing when Irritation occurs to the mucus membrane of respiratory system 3- J receptor in alveolar walls lead to edema where the patient has dyspnea These receptors are sensory to the change of inflation so they are mostly involved in stimulation of edema where the patient has dyspnea 4- brain edema causes res. centre depression Brain edema when there is a concussion (may be caused by a trauma on the patient's head )which in turn causes depression of res. centre. And we can treat them by using hypertonic solution to remove excess fluid developed in the brain 5- anesthesia & narcotic overdose depresses res. centre (halothane, morphine, pentobarbital) Anesthesia regulatation of anesthesia during surgery is arranged into 4 stages : Stage 1: patient is still feeling Stage 2: patient is still feeling with strong stimulus, here the surgeon can not work Stage 3 : comatose patient, surgeon can work Stage 4: we lose the patient, the patient is die (overdose of anesthesia) Slide 30 Periodic Chyne-Stokes breathing : person over-breathes [O2], [CO2] after seconds these [ ] are sensed by the resp. centre inhibition of excess ventilation opposite cycle begins [O2], [CO2] after seconds these [ ] are sensed by the resp. centre the person is again over-breathing Periodic or chyne stokes breathing is a sort of breathing in which that increase in breathing and then decreased or stopped. Increase in breathing when there is a reduction of blood flow to the brain or reduction of O2 to the brain, then there is a hyperventilation Wash out of the co2 then the respiration will be decreased. Then co2 will accumulate more, increased the hyperventilation. This mainly developed in severe heart failure in which the ejection fraction is will be reduced, so the BF to the brain significantly reduced so oxygen will be reduced and co2 will be accumulated. When the co2 accumulate, it will stimulate the respiratory center. So it will increase the breathing. Washing Co2 then the breathing will be reduced. So this is the periodic or chyne stokes breathing in which the breathing increased or decreased and this is mainly not developed in normal people, but it mainly develops in patients with severe heart failure. And it is related to level of oxygen and carbon dioxide. Slide 31
3 Slide 32 Periodic Chyne-Stokes breathing : this cycle doesn t occur normally but can be seen in these conditions: 1- increased neg. feedback gain in resp. control areas change in [CO2], [H+] causes further great change in ventilation brain-damage 2- long delay in transporting blood from the lungs to the brain severe or chronic heart failure, Slide 33 Sleep apnea: episodes of apnea lasting for 10 secs. Or more, occurring times/night Obstructive sleep apnea: during sleep the pharynx is relaxed, in some individuals this may lead to complete closure snoring & labored breathing apnea O2, CO2 stimulation of resp. center sudden snorts and gasps Sleep apnea: it means cessation of breathing develops frequently during night. Most of us develop apnea during sleeping and this is developed frequently by relaxing of the glottis and then the airway will be closed so the subject will be snoring (شخير) and develops a difficulty in breathing and suddenly he wake up for few seconds and then start breathing again. Slide 34 Sleep apnea usually develops in 1- elderly, obese, nasal ostruction, large tongue, enlarged tonsils Elderly people, obese, and people with enlarged adenoid tissue or the tonsils. And mainly these patients do not sleep quite enough and they will be tired in the next day particularly if they are drivers which in turn increase the risk of accidents. 2- Sudden infant death syndrome (SIDS): exaggerated case of sleep apnea, premature baby, smoker pregnant mother Also In sudden infant death syndrome there is an exaggerated case of sleep apnea develops in premature baby and smoker pregnant mothers.most premature babies do not have enough surfactant. Slide 35 Treatment of obstructive sleep apnea 1- Surgery uvulopalatopharyngoplasty (remove excess fat at back of throat, tonsils, tracheostomy) Surgery to remove excess adipose tissue at back of throat, tonsils or tracheostomy which is an operative procedure that creates a surgical airway. It is most often performed in patients who have had difficulty weaning off a ventilator or positive breathing by special equipment during sleeping. 2- Continous positive airway pressure CPAP Or by CPAP which applies mild air pressure on a continuous basis to keep the airways continuously open in people who are able to breathe spontaneously on their own.
4 Now let s start with pathophysiology Pathophysiology: means the functional the RS when there are some types of disease Slide 2 Reduction of Pulmonary Function 1. Inadequate blood flow to the lungs hypoperfusion 2. Inadequate air flow to the alveoli - hypoventilation Before we continue you have to know that there is 3 main symptoms for pulmonary disease 1- Cough 2- dyspnea 3- chest pain Slide 3-5 Signs and Symptoms of Pulmonary Disease Dyspnea subjective sensation of uncomfortable breathing, feeling short of breath Ranges from mild discomfort after exertion to extreme difficulty breathing at rest. Usually caused by diffuse and extensive rather than focal pulmonary disease. Due to: Airway obstruction Greater force needed to provide adequate ventilation Wheezing sound due to air being forced through airways narrowed due to constriction or fluid accumulation Decreased compliance of lung tissue Signs of dyspnea: Flaring nostrils Use of accessory muscles in breathing Retraction (pulling back) of intercostal spaces Dyspnea: related to the exertion and its classification depends on when the dyspnea develops: Grade 1 at the level of high exercise Grade 2 at the level of moderate exercise Grade 3 mild exercise Grade 4 minimal exercise And sometimes the patient experience dyspnea when he goes to the bathroom Slide 6-9 The common complaint of patient in respiratory disease is cough Cough Attempt to clear the lower respiratory passages by abrupt and forceful expulsion of air Most common when fluid accumulates in lower airways Cough may result from:
5 Inflammation of lung tissue Increased secretion in response to mucosal irritation Inhalation of irritants Intrinsic source of mucosal disruption such as tumor invasion of bronchial wall Excessive blood hydrostatic pressure in pulmonary capillaries Pulmonary edema excess fluid passes into airways When cough can raise fluid into pharynx, the cough is described as a productive cough, and the fluid is sputum. Production of bloody sputum is called hemoptysis Usually involves only a small amount of blood loss Not threatening, but can indicate a serious pulmonary disease Tuberculosis, lung abscess, cancer, pulmonary infarction. If sputum is purulent, and infection of lung or airway is indicated. Cough that does not produce sputum is called a dry, nonproductive or hacking cough. Acute cough is one that resolves in 2-3 weeks from onset of illness or treatment of underlying condition. Us. caused by URT infections, allergic rhinitis, acute bronchitis, pneumonia, congestive heart failure, pulmonary embolus, or aspiration. Cough (commonest) ; which can be from URT or LRT ; depends on the time ( is it at early morning?, is it late night? ), is it productive or dry?, is there a blood in the sputum or not!.. So all these give possibilities of cause. In here, we listen to the patient in order to reach the diagnosis. Slide 10 A chronic cough is one that persists for more than 3 weeks. In nonsmokers, almost always due to postnasal drainage syndrome, asthma, or gastroesophageal reflux disease In smokers, chronic bronchitis is the most common cause, although lung cancer should be considered. Chronic cough means that is continuous. Periodic cough means that it develops at night or early morning and so on. (Periodically) The patient who develops cough with little or no sputum at the early morning is mainly a patient of COPD. Slide Cyanosis When blood contains a large amount of unoxygenated hemoglobin, it has a dark red-blue color which gives skin a characteristic bluish appearance. Most cases arise as a result of peripheral vasoconstriction result is reduced blood flow, which allows hemoglobin to give up more of its oxygen to tissues- peripheral cyanosis. Best seen in nail beds
6 Due to cold environment, anxiety, etc. Central cyanosis can be due to : Abnormalities of the respiratory membrane Mismatch between air flow and blood flow Expressed as a ratio of change in ventilation (V) to perfusion (Q) : V/Q ratio Pulmonary thromboembolus - reduced blood flow Airway obstruction reduced ventilation In persons with dark skin can be seen in the whites of the eyes and mucous membranes. The other possible symptoms of the patient : Cyanosis is the bluish of the skin and nails when there is a reduction of oxygenation of the blood ( which is a type of peripheral cyanosis ) or we can see -- on the tongue or mucus membrane - (which is a type of central cyanosis) Pain Originates in pleurae, airways or chest wall Inflammation of the parietal pleura causes sharp or stabbing pain when pleura stretches during inspiration Usually localized to an area of the chest wall, where a pleural friction rub can be heard Laughing or coughing makes pain worse Common with pulmonary infarction due to embolism The res. pain is mostly lateral and is related to respiration whereas the cardiac pain is central. ** So we listen to the patient, see the patient, examine the patient and one of the important signs that we can see clearly is the cyanosis, we can hear the sounds of breathing ( there is a prolonged expiration which results in increased sound ), restriction in inflation or harsh breathing. The patient with pleural effusion has a sort of crackles, congestion of the heart failure, when there is air or fluid in the alveoli, when you take a breath, the air gets in the fluid ( in bubbles ) so you will hear crepitation because of the air get In the fluid. This is a sign of pul. Edema. So this is one is a sign that we can examine it, see it or hear it. ( clinical finding). Tests of Pulmonary Function Slide 15 Chest radiographs are among the most common examinations of the pulmonary system. Chest x-ray Heart size Lung mass Pleural effusion Fibrosis Pneumonia Pneumothorax This will also give us an idea about the, inflation, any consolidation, any cyst... etc
7 Pneumothorax>> is the presence of air in the pleural cavity and this will lead to collapse of the lung or blockage of the lung according to the volume of the air that present in pleural cavity. The treatment simply, is by putting a chest tube in the pleural space and connect the tube with a water, and this will absorb the air, we need the tube for 2 days and we then repeat the chest X-ray to find out the lung badly inflated or no. When there is a normal inflation of the lung we remove the test tube and we make a suture for the cut. Slide 16 CT SCAN Sometimes we do the CT scan االشعة الطبقية) ) to find out how there is a good inflation in the lungs. Slide Spirometry The diagnosis of COPD is confirmed by spirometry, a test that measures breathing. Spirometry measures the forced expiratory volume in one second (FEV 1 ) which is the greatest volume of air that can be breathed out in the first second of a large breath and the forced vital capacity (FVC) which is the greatest volume of air that can be breathed out in a whole large breath. Normally at least 70% of the FVC comes out in the first second (i.e. the FEV 1 /FVC ratio is >70%). In COPD, this ratio is less than normal, (i.e. FEV 1 /FVC ratio is <70%) even after a bronchodilator medication has been given. Spirometry can help to determine the severity of COPD. The FEV 1 (measured post-bronchodilator) is expressed as a percent of a predicted "normal" value based on a person's age, gender, height and weight: We can ask for lung function test / lung volumes. Here, the specific test of investigation for the diagnosis of the pul. disease is FEV1/FVC ratio which is normally more than 70% When the ratio is less, there is an indication that there is obstructive pul. disease and it can be mild, moderate or severe according to the ratio. The more the reduction of FEV1/FVC ratio, the more the severity of the disease. These patients mostly complain dyspnea with severe disease, and here we ask the patient how long you walk? Or how much effort that you can exerted? You can assess the severity of dyspnea of the disease that is of the patient which is in a relation with the degree of the limitation of the effort. Slide 19 The doctor modifies the table as the following: Severity of COPD Mild FEV 1 % predicted 80 Normal: >= 80 Mild: Moderate: Severe: less than 30 Moderate Severe Very severe <30 or Chronic respiratory failure symptoms
8 **In bronchial asthma, we treat patients by bronchodilators. And in severe bronchial asthma, the patients do not respond to bronchodilators, and it is called status asthmatics and here we take the patient and put him on a respirator. Otherwise we lose the patient Slide 20 From the figure we can see the difference between normal and airway obstruction states **from this figure we can see 1) level (maximum inspiration) 2) the expiration prolonged **as we see in the airway obstruction its take more time to expire the air (prolonged),reduction in the maximum inspiration and need more (extra) muscle to expire the air (abdominal muscle) in attempt to expire as much as possible **so the obstruction lung disease cause difficulty in expiration because of obstruction in the airway and the obstruction may be 1) constriction of the bronchioles and bronchi 2) fibrosis of the elastic tissue of the bronchioles because of inflammation, infection or fibrosis and this will lead to reduction of the elasticity of the tissue of the bronchioles so its not easy to distended **90% of the COPD is due to smoke as major risk factor **as COPD develop we can t treat the disease and the treatment aim to alleviate the symptoms (can t cure the patient) as the disease affect the life style of the patient **other causes of COPD are pollutions ether indoor or outdoor like factor that contain aspis and other chemical substance Slide 21 Ventilation/perfusion ratio (or V/Q ratio) : It is defined as: the ratio of the amount of air reaching the alveoli to the amount of blood reaching the alveoli. "V" - ventilation - the air which reaches the alveoli "Q" - perfusion - the blood which reaches the alveoli These two variables constitute the main determinants of the blood oxygen concentration. In fact since V determines the quantity of oxygen mass reaching the alveoli per minute (g/min) and Q expresses the flow of blood in the lungs (l/min), the V/Q ratio refers to a concentration (g/l). Nuclear study Sometimes we do the V/P ratio ; with a special technique we can find out how much ventilation and how much perfusion. And accordingly we can know if there is a problem in ventilation or in perfusion. Slide 22 Pathophysiology A lower V/Q ratio usually seen in chronic bronchitis, asthma and acute pulmonary edema.
9 A high V/Q ratio increases pao2 and decreases paco2. This finding is typically associated with pulmonary embolism (where blood circulation is impaired by an embolus). And this ratio is mainly increased in pul. Embolism جلطة رئوية) ) that means parts of the lungs are completely blocked, no blood supply but there is ventilation. And here we may be lose the patient if the diagnosis was late. So V/p ratio is increased in pulmonary Embolism but not in asthma, emphysema and so on. slide 23 We also can make some diagnosis like: Pulmonary angiography Laryngoscopy >> is for the larynx Bronchoscopy >> is for the bronchioles If we can t reach the diagnosis we can use the bronchoscopy which we use it to find out if there is any tumors or we take a biopsy (small peace used to examination under the microscope to find if there is a fibrosis, infection) *usually we use the microscopy for reach the diagnosis if the other ways and methods don t give valuable information Slide 24 Skin test (TB) Microbiological (Sputum,Pleural fluid,throat swab) Histopathological and cytological Skin test give us an idea about patient If have TB or not This is type of tuberculin we inject it under the skin and we watch it for a day or two >> as a result if the positive it appear as swelling (flam up) and redness Slide 25 Sputum : It is usually in air passages in diseased lungs, bronchi, pneumonia It can be associate with blood (hemoptysis) if a chronic cough is present, possibly from severe cases of tuberculosis. We can examine the sputum: if the patients complain of productive cough (sputum or mucus) we take the sputum for 1)direct microscopic examination 2)or sent for culture (and this mainly done in case of TB infection) Slide 26 ABG Arterial blood gas analysis commonly performed for individuals with suggested or diagnosed pulmonary disease. Provides valuable information about an individual s gas exchange & acid-base status. We perform the ABG to find the oxygenation of the blood and the blood sample is taken from artery not from vein (any blood from any artery)>> and this will give us a good information about oxygenation, function of the lung, saturation and Po2 Slide 27 Inflammation of trachea or bronchi produce a central chest pain that is pronounced after coughing Must be differentiated from cardiac pain High blood pressure in the pulmonary circulation can cause pain during exercise that often mistaken for cardiac pain (angina pectoris)
10 **can detect by bronchoscopy and take biopsy Slide 28 Respiratory Failure The inability of the lungs to adequately oxygenate the blood and to clear it of carbon dioxide. Can be acute: ARDS or pulmonary embolism Direct injury to the lungs, airways or chest wall Indirect due to injury of another body system, such as the brain or spinal cord. Some time with accident If the chest injury in one side then the pneumothorax develop in one side and the patient still breathing from the other side but some time the injury developed in both side and this is an emergency situation because both lung can be collapsed and if we can t reach the hospital within short period we will lose the patient **in some cases the chest wall is injured and become flexible (pliable) >> in this case we take breathing but you can t expire it so this will collapsing (make pressure) on the lung >> this called flial pneumothorax >> in this case the chest wall moving but appleing pressure so the lung can t be inflated >> this is one of the life threatening situation Slide >> as from slides Chronic respiratory failure Due to progressive hypoventilation from airway obstruction or restrictive disease Respiratory failure always presents a serious threat Dysnpea always present, but may be difficult to detect a change in a chronic patient Since nervous tissue it highly oxygen-dependent, see CNS signs and symptoms Memory loss, visual impairment, drowsiness Headache due to increased intracranial pressure due to cerebral vasodilation Obstructive Pulmonary Disease Characterized by airway obstruction that is worse with expiration. More force is required to expire a given volume of air, or emptying of lungs is slowed, or both. The most common obstructive diseases are asthma, chronic bronchitis, and emphysema. Many people have both chronic bronchitis and emphysema, and together these are often called chronic obstructive pulmonary disease COPD COPD Major symptom of obstructive pulmonary disease is dyspnea, and the unifying sign is wheezing. Individuals have increased work of breathing, V/Q mismatching, and a decreased forced expiratory volume. Pathological changes that cause reduced expiratory air flow
11 Does not change markedly over time Slide 34 Does not show major reversibility in response to pharmacological agents Progressive Associated with abnormal inflammatory response of the lungs to noxious particles or gases. Fourth leading cause of death in U.S. Increasing in incidence over the past 30 years Primary cause is cigarette smoking Both active and passive smoking have been implicated Other risks are occupational exposures and air pollution Genetic susceptibilities identified the upper respiratory tract infection mainly mean the infection of the trachea, bronchi and bronchioles but the lower respiratory tract infection mean the infection of the tissue and include (2,3,4,5) from the following points Infection of respiratory system 1-Upper resp tract inf >>we usually called it common cold 2-Pneumonia 3-TB 4-Fungal inf 5-Tumour and carcinoma **the other possibility of the sign and symptoms is plural effusion **plural effusion: the accumulations of the fluid in the plural cavity which may apply force/pressure in the lung depend on the amount of the fluid The plural effusion can develop from 1)local cause when there is an infection on the plural membrane or infection or problem in the lung as case of TB or pneumonia or from 2)systemic disease(systemic cause) as in case of heart failure, renal failure and liver cirrhosis Good luck *-*
Pulmonary Pathophysiology
 Pulmonary Pathophysiology 1 Reduction of Pulmonary Function 1. Inadequate blood flow to the lungs hypoperfusion 2. Inadequate air flow to the alveoli - hypoventilation 2 Signs and Symptoms of Pulmonary
Pulmonary Pathophysiology 1 Reduction of Pulmonary Function 1. Inadequate blood flow to the lungs hypoperfusion 2. Inadequate air flow to the alveoli - hypoventilation 2 Signs and Symptoms of Pulmonary
Respiratory Diseases and Disorders
 Chapter 9 Respiratory Diseases and Disorders Anatomy and Physiology Chest, lungs, and conducting airways Two parts: Upper respiratory system consists of nose, mouth, sinuses, pharynx, and larynx Lower
Chapter 9 Respiratory Diseases and Disorders Anatomy and Physiology Chest, lungs, and conducting airways Two parts: Upper respiratory system consists of nose, mouth, sinuses, pharynx, and larynx Lower
Unconscious exchange of air between lungs and the external environment Breathing
 Respiration Unconscious exchange of air between lungs and the external environment Breathing Two types External Exchange of carbon dioxide and oxygen between the environment and the organism Internal Exchange
Respiration Unconscious exchange of air between lungs and the external environment Breathing Two types External Exchange of carbon dioxide and oxygen between the environment and the organism Internal Exchange
Respiratory Disease. Dr Amal Damrah consultant Neonatologist and Paediatrician
 Respiratory Disease Dr Amal Damrah consultant Neonatologist and Paediatrician Signs and Symptoms of Respiratory Diseases Cardinal Symptoms Cough Sputum Hemoptysis Dyspnea Wheezes Chest pain Signs and Symptoms
Respiratory Disease Dr Amal Damrah consultant Neonatologist and Paediatrician Signs and Symptoms of Respiratory Diseases Cardinal Symptoms Cough Sputum Hemoptysis Dyspnea Wheezes Chest pain Signs and Symptoms
Function of the Respiratory System. Exchange CO2 (on expiration) for O2 (on inspiration)
 Function of the Respiratory System Exchange CO2 (on expiration) for O2 (on inspiration) Upper Respiratory Tract Includes: Nose Mouth Pharynx Larynx Function: Warms and humidifies the inspired air Filters
Function of the Respiratory System Exchange CO2 (on expiration) for O2 (on inspiration) Upper Respiratory Tract Includes: Nose Mouth Pharynx Larynx Function: Warms and humidifies the inspired air Filters
Phases of Respiration
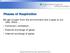 Phases of Respiration We get oxygen from the environment and it goes to our cells, there. Pulmonary ventilation External exchange of gases Internal exchange of gases Overview of respiration. In ventilation,
Phases of Respiration We get oxygen from the environment and it goes to our cells, there. Pulmonary ventilation External exchange of gases Internal exchange of gases Overview of respiration. In ventilation,
The Respiratory System
 The Respiratory System By Mr. Danilo Villar Rogayan Jr. Instructor I, Department of Natural Sciences RMTU San Marcelino Introduction Function Move air in an out of lungs (ventilation) Delivers oxygen (O
The Respiratory System By Mr. Danilo Villar Rogayan Jr. Instructor I, Department of Natural Sciences RMTU San Marcelino Introduction Function Move air in an out of lungs (ventilation) Delivers oxygen (O
Chapter 10 The Respiratory System
 Chapter 10 The Respiratory System Biology 2201 Why do we breathe? Cells carry out the reactions of cellular respiration in order to produce ATP. ATP is used by the cells for energy. All organisms need
Chapter 10 The Respiratory System Biology 2201 Why do we breathe? Cells carry out the reactions of cellular respiration in order to produce ATP. ATP is used by the cells for energy. All organisms need
CHAPTER 7.1 STRUCTURES OF THE RESPIRATORY SYSTEM
 CHAPTER 7.1 STRUCTURES OF THE RESPIRATORY SYSTEM Pages 244-247 DO NOW What structures, do you think, are active participating in the breathing process? 2 WHAT ARE WE DOING IN TODAY S CLASS Finishing Digestion
CHAPTER 7.1 STRUCTURES OF THE RESPIRATORY SYSTEM Pages 244-247 DO NOW What structures, do you think, are active participating in the breathing process? 2 WHAT ARE WE DOING IN TODAY S CLASS Finishing Digestion
Chronic obstructive pulmonary disease
 Chronic obstructive pulmonary disease By: Dr. Fatima Makee AL-Hakak () University of kerbala College of nursing Out lines What is the? Overview Causes of Symptoms of What's the difference between and asthma?
Chronic obstructive pulmonary disease By: Dr. Fatima Makee AL-Hakak () University of kerbala College of nursing Out lines What is the? Overview Causes of Symptoms of What's the difference between and asthma?
Chronic obstructive lung disease. Dr/Rehab F.Gwada
 Chronic obstructive lung disease Dr/Rehab F.Gwada Obstructive lung diseases Problem is in the expiratory phase Lung disease Restrictive lung disease Restriction may be with, or within the chest wall Problem
Chronic obstructive lung disease Dr/Rehab F.Gwada Obstructive lung diseases Problem is in the expiratory phase Lung disease Restrictive lung disease Restriction may be with, or within the chest wall Problem
The Respiratory System
 130 20 The Respiratory System 1. Define important words in this chapter 2. Explain the structure and function of the respiratory system 3. Discuss changes in the respiratory system due to aging 4. Discuss
130 20 The Respiratory System 1. Define important words in this chapter 2. Explain the structure and function of the respiratory system 3. Discuss changes in the respiratory system due to aging 4. Discuss
Chapter 10. The Respiratory System Exchange of Gases. Copyright 2009 Pearson Education, Inc.
 Chapter 10 The Respiratory System Exchange of Gases http://www.encognitive.com/images/respiratory-system.jpg Human Respiratory System UPPER RESPIRATORY TRACT LOWER RESPIRATORY TRACT Nose Passageway for
Chapter 10 The Respiratory System Exchange of Gases http://www.encognitive.com/images/respiratory-system.jpg Human Respiratory System UPPER RESPIRATORY TRACT LOWER RESPIRATORY TRACT Nose Passageway for
Anatomy. The respiratory system starts from the nose, mouth, larynx, trachea, and the two lungs.
 Respiratory System Anatomy The respiratory system starts from the nose, mouth, larynx, trachea, and the two lungs. Within the lungs, the bronchi transport air with oxygen to the alveoli on inspiration
Respiratory System Anatomy The respiratory system starts from the nose, mouth, larynx, trachea, and the two lungs. Within the lungs, the bronchi transport air with oxygen to the alveoli on inspiration
Phases of Respiration. Chapter 18: The Respiratory System. Structures of the Respiratory System. Structures of the Respiratory System
 Phases of Respiration Chapter 18: The Respiratory System Respiration Process of obtaining oxygen from environment and delivering it to cells Phases of Respiration 1. Pulmonary ventilation between air and
Phases of Respiration Chapter 18: The Respiratory System Respiration Process of obtaining oxygen from environment and delivering it to cells Phases of Respiration 1. Pulmonary ventilation between air and
RESPIRATORY PHYSIOLOGY Pre-Lab Guide
 RESPIRATORY PHYSIOLOGY Pre-Lab Guide NOTE: A very useful Study Guide! This Pre-lab guide takes you through the important concepts that where discussed in the lab videos. There will be some conceptual questions
RESPIRATORY PHYSIOLOGY Pre-Lab Guide NOTE: A very useful Study Guide! This Pre-lab guide takes you through the important concepts that where discussed in the lab videos. There will be some conceptual questions
Chapter 10 Respiration
 1 Chapter 10 Respiration Introduction/Importance of the Respiratory System All eukaryotic organisms need oxygen to perform cellular respiration (production of ATP), either aerobically or anaerobically.
1 Chapter 10 Respiration Introduction/Importance of the Respiratory System All eukaryotic organisms need oxygen to perform cellular respiration (production of ATP), either aerobically or anaerobically.
5/5/2013. The Respiratory System. Chapter 16 Notes. The Respiratory System. Nasal Cavity. Sinuses
 The Respiratory System Chapter 16 Notes The Respiratory System Objectives List the general functions of the respiratory system. Identify the organs of the respiratory system. Describe the functions of
The Respiratory System Chapter 16 Notes The Respiratory System Objectives List the general functions of the respiratory system. Identify the organs of the respiratory system. Describe the functions of
Unit 9. Respiratory System 16-1
 Unit 9 Respiratory System 16-1 Works together with the circulatory system Exchange of gases between atmosphere, blood, and cells If respiratory system and/or circulatory system fails, death will occur
Unit 9 Respiratory System 16-1 Works together with the circulatory system Exchange of gases between atmosphere, blood, and cells If respiratory system and/or circulatory system fails, death will occur
The Respiratory System. Dr. Ali Ebneshahidi
 The Respiratory System Dr. Ali Ebneshahidi Functions of The Respiratory System To allow gases from the environment to enter the bronchial tree through inspiration by expanding the thoracic volume. To allow
The Respiratory System Dr. Ali Ebneshahidi Functions of The Respiratory System To allow gases from the environment to enter the bronchial tree through inspiration by expanding the thoracic volume. To allow
Chapter 10. Respiratory System and Gas Exchange. Copyright 2005 Pearson Education, Inc. publishing as Benjamin Cummings
 Chapter 10 Respiratory System and Gas Exchange Function of the Respiratory System To obtain oxygen (O 2 ) for all cells in the body. To rid the cells of waste gas (CO 2 ). Oxygen (O 2 ) is vital chemical
Chapter 10 Respiratory System and Gas Exchange Function of the Respiratory System To obtain oxygen (O 2 ) for all cells in the body. To rid the cells of waste gas (CO 2 ). Oxygen (O 2 ) is vital chemical
Anatomy & Physiology 2 Canale. Respiratory System: Exchange of Gases
 Anatomy & Physiology 2 Canale Respiratory System: Exchange of Gases Why is it so hard to hold your breath for Discuss! : ) a long time? Every year carbon monoxide poisoning kills 500 people and sends another
Anatomy & Physiology 2 Canale Respiratory System: Exchange of Gases Why is it so hard to hold your breath for Discuss! : ) a long time? Every year carbon monoxide poisoning kills 500 people and sends another
Your Lungs and COPD. Patient Education Pulmonary Rehabilitation. A guide to how your lungs work and how COPD affects your lungs
 Patient Education Your Lungs and COPD A guide to how your lungs work and how COPD affects your lungs Your lungs are organs that process every breath you take. They provide oxygen (O 2 ) to the blood and
Patient Education Your Lungs and COPD A guide to how your lungs work and how COPD affects your lungs Your lungs are organs that process every breath you take. They provide oxygen (O 2 ) to the blood and
Chapter 10 Lecture Outline
 Chapter 10 Lecture Outline See separate PowerPoint slides for all figures and tables preinserted into PowerPoint without notes. Copyright 2016 McGraw-Hill Education. Permission required for reproduction
Chapter 10 Lecture Outline See separate PowerPoint slides for all figures and tables preinserted into PowerPoint without notes. Copyright 2016 McGraw-Hill Education. Permission required for reproduction
The RESPIRATORY System. Unit 3 Transportation Systems
 The RESPIRATORY System Unit 3 Transportation Systems The Respiratory System Functions of the Respiratory System Warms, moistens, and filters incoming air Nasal cavity Resonating chambers for speech and
The RESPIRATORY System Unit 3 Transportation Systems The Respiratory System Functions of the Respiratory System Warms, moistens, and filters incoming air Nasal cavity Resonating chambers for speech and
LUNGS. Requirements of a Respiratory System
 Respiratory System Requirements of a Respiratory System Gas exchange is the physical method that organisms use to obtain oxygen from their surroundings and remove carbon dioxide. Oxygen is needed for aerobic
Respiratory System Requirements of a Respiratory System Gas exchange is the physical method that organisms use to obtain oxygen from their surroundings and remove carbon dioxide. Oxygen is needed for aerobic
Chapter 16. The Respiratory System. Mosby items and derived items 2010, 2006, 2002, 1997, 1992 by Mosby, Inc., an affiliate of Elsevier Inc.
 Chapter 16 The Respiratory System Objectives Discuss the generalized functions of the respiratory system List the major organs of the respiratory system and describe the function of each Compare, contrast,
Chapter 16 The Respiratory System Objectives Discuss the generalized functions of the respiratory system List the major organs of the respiratory system and describe the function of each Compare, contrast,
Respiratory System. December 20, 2011
 Respiratory System December 20, 2011 Nasal Cavity: Contains cilia (hair cells) to prevent particles from entering the respiratory tract Mucus does the same, in addition to warming and moistening the air
Respiratory System December 20, 2011 Nasal Cavity: Contains cilia (hair cells) to prevent particles from entering the respiratory tract Mucus does the same, in addition to warming and moistening the air
The RESPIRATORY System. Unit 3 Transportation Systems
 The RESPIRATORY System Unit 3 Transportation Systems Functions of the Respiratory System Warm, moisten, and filter incoming air Resonating chambers for speech and sound production Oxygen and Carbon Dioxide
The RESPIRATORY System Unit 3 Transportation Systems Functions of the Respiratory System Warm, moisten, and filter incoming air Resonating chambers for speech and sound production Oxygen and Carbon Dioxide
Paramedic Rounds. Pre-Hospital Continuous Positive Airway Pressure (CPAP)
 Paramedic Rounds Pre-Hospital Continuous Positive Airway Pressure (CPAP) Morgan Hillier MD Class of 2011 Dr. Mike Peddle Assistant Medical Director SWORBHP Objectives Outline evidence for pre-hospital
Paramedic Rounds Pre-Hospital Continuous Positive Airway Pressure (CPAP) Morgan Hillier MD Class of 2011 Dr. Mike Peddle Assistant Medical Director SWORBHP Objectives Outline evidence for pre-hospital
Respiratory system. Applied Anatomy &Physiology
 Respiratory system Applied Anatomy &Physiology Anatomy The respiratory system consists of 1)The Upper airway : Nose, mouth and larynx 2)The Lower airways Trachea and the two lungs. Within the lungs,
Respiratory system Applied Anatomy &Physiology Anatomy The respiratory system consists of 1)The Upper airway : Nose, mouth and larynx 2)The Lower airways Trachea and the two lungs. Within the lungs,
11.3 RESPIRATORY SYSTEM DISORDERS
 11.3 RESPIRATORY SYSTEM DISORDERS TONSILLITIS Infection of the tonsils Bacterial or viral Symptoms: red and swollen tonsils, sore throat, fever, swollen glands Treatment: surgically removed Tonsils: in
11.3 RESPIRATORY SYSTEM DISORDERS TONSILLITIS Infection of the tonsils Bacterial or viral Symptoms: red and swollen tonsils, sore throat, fever, swollen glands Treatment: surgically removed Tonsils: in
People with asthma who smoke. The combination of asthma, a chronic airway disease, and smoking increases the risk of COPD even more.
 COPD Chronic obstructive pulmonary disease (COPD) is a chronic inflammatory lung disease that causes obstructed airflow from the lungs. Symptoms include breathing difficulty, cough, sputum (phlegm) production
COPD Chronic obstructive pulmonary disease (COPD) is a chronic inflammatory lung disease that causes obstructed airflow from the lungs. Symptoms include breathing difficulty, cough, sputum (phlegm) production
Respiratory Emergencies. Chapter 11
 Respiratory Emergencies Chapter 11 Respiratory System Anatomy and Function of the Lung Characteristics of Adequate Breathing Normal rate and depth Regular breathing pattern Good breath sounds on both sides
Respiratory Emergencies Chapter 11 Respiratory System Anatomy and Function of the Lung Characteristics of Adequate Breathing Normal rate and depth Regular breathing pattern Good breath sounds on both sides
The Respiratory System
 The Respiratory System Respiratory Anatomy Upper respiratory tract Nose Nasal passages Pharynx Larynx Respiratory Anatomy Functions of the upper respiratory tract: Provide entry for inhaled air Respiratory
The Respiratory System Respiratory Anatomy Upper respiratory tract Nose Nasal passages Pharynx Larynx Respiratory Anatomy Functions of the upper respiratory tract: Provide entry for inhaled air Respiratory
Why do you breathe? What is oxygen used for? Where does CO2 come from?
 RESPIRATORY SYSTEM How You Breathe Why do you breathe? What is oxygen used for? Where does CO2 come from? Respiration: exchange of gases between air & your body cells 1. Outside air (O2) lungs metabolism
RESPIRATORY SYSTEM How You Breathe Why do you breathe? What is oxygen used for? Where does CO2 come from? Respiration: exchange of gases between air & your body cells 1. Outside air (O2) lungs metabolism
The Respiratory System
 Elaine N. Marieb Katja Hoehn Human Anatomy & Physiology SEVENTH EDITION C H A P T E R PowerPoint Lecture Slides prepared by Vince Austin, Bluegrass Technical and Community College 22P A R T B The Respiratory
Elaine N. Marieb Katja Hoehn Human Anatomy & Physiology SEVENTH EDITION C H A P T E R PowerPoint Lecture Slides prepared by Vince Austin, Bluegrass Technical and Community College 22P A R T B The Respiratory
B Unit III Notes 6, 7 and 8
 The Respiratory System Why do we breathe? B. 2201 Unit III Notes 6, 7 and 8 Respiratory System We know that our cells respire to produce ATP (energy). All organisms need energy to live, so that s why we
The Respiratory System Why do we breathe? B. 2201 Unit III Notes 6, 7 and 8 Respiratory System We know that our cells respire to produce ATP (energy). All organisms need energy to live, so that s why we
Tuesday, December 13, 16. Respiratory System
 Respiratory System Trivia Time... What is the fastest sneeze speed? What is the surface area of the lungs? (hint... think of how large the small intestine was) How many breaths does the average person
Respiratory System Trivia Time... What is the fastest sneeze speed? What is the surface area of the lungs? (hint... think of how large the small intestine was) How many breaths does the average person
Lecture Notes. Chapter 3: Asthma
 Lecture Notes Chapter 3: Asthma Objectives Define asthma and status asthmaticus List the potential causes of asthma attacks Describe the effect of asthma attacks on lung function List the clinical features
Lecture Notes Chapter 3: Asthma Objectives Define asthma and status asthmaticus List the potential causes of asthma attacks Describe the effect of asthma attacks on lung function List the clinical features
Respiratory System. Chapter 9
 Respiratory System Chapter 9 Air Intake Air in the atmosphere is mostly Nitrogen (78%) Only ~21% oxygen Carbon dioxide is less than 0.04% Air Intake Oxygen is required for Aerobic Cellular Respiration
Respiratory System Chapter 9 Air Intake Air in the atmosphere is mostly Nitrogen (78%) Only ~21% oxygen Carbon dioxide is less than 0.04% Air Intake Oxygen is required for Aerobic Cellular Respiration
Pulmonary Pearls. Medical Pearls. Case 1: Case 1 (cont.): Case 1: What is the Most Likely Diagnosis? Case 1 (cont.):
 Pulmonary Pearls Christopher H. Fanta, MD Pulmonary and Critical Care Division Brigham and Women s Hospital Partners Asthma Center Harvard Medical School Medical Pearls Definition: Medical fact that is
Pulmonary Pearls Christopher H. Fanta, MD Pulmonary and Critical Care Division Brigham and Women s Hospital Partners Asthma Center Harvard Medical School Medical Pearls Definition: Medical fact that is
GOALS AND INSTRUCTIONAL OBJECTIVES
 October 4-7, 2004 Respiratory GOALS: GOALS AND INSTRUCTIONAL OBJECTIVES By the end of the week, the first quarter student will have an in-depth understanding of the diagnoses listed under Primary Diagnoses
October 4-7, 2004 Respiratory GOALS: GOALS AND INSTRUCTIONAL OBJECTIVES By the end of the week, the first quarter student will have an in-depth understanding of the diagnoses listed under Primary Diagnoses
ADVANCED ASSESSMENT Respiratory System
 ONTARIO BASE HOSPITAL GROUP QUIT ADVANCED ASSESSMENT Respiratory System 2007 Ontario Base Hospital Group ADVANCED ASSESSMENT Respiratory System AUTHOR(S) Mike Muir AEMCA, ACP, BHSc Paramedic Program Manager
ONTARIO BASE HOSPITAL GROUP QUIT ADVANCED ASSESSMENT Respiratory System 2007 Ontario Base Hospital Group ADVANCED ASSESSMENT Respiratory System AUTHOR(S) Mike Muir AEMCA, ACP, BHSc Paramedic Program Manager
Basic mechanisms disturbing lung function and gas exchange
 Basic mechanisms disturbing lung function and gas exchange Blagoi Marinov, MD, PhD Pathophysiology Department, Medical University of Plovdiv Respiratory system 1 Control of breathing Structure of the lungs
Basic mechanisms disturbing lung function and gas exchange Blagoi Marinov, MD, PhD Pathophysiology Department, Medical University of Plovdiv Respiratory system 1 Control of breathing Structure of the lungs
CARDIOVASCULAR AND RESPIRATORY SYSTEMS
 CARDIOVASCULAR AND RESPIRATORY SYSTEMS KEY TERMS: Cardiovascular System, cardio, vascular, blood vessels, valves, arteries, capillaries, veins, systemic circulation, pulmonary circulation Your Cardiovascular
CARDIOVASCULAR AND RESPIRATORY SYSTEMS KEY TERMS: Cardiovascular System, cardio, vascular, blood vessels, valves, arteries, capillaries, veins, systemic circulation, pulmonary circulation Your Cardiovascular
Cardiovascular and Respiratory Disorders
 Cardiovascular and Respiratory Disorders Blood Pressure Normal blood pressure is 120/80 mmhg (millimeters of mercury) Hypertension is when the resting blood pressure is too high Systolic BP is 140 mmhg
Cardiovascular and Respiratory Disorders Blood Pressure Normal blood pressure is 120/80 mmhg (millimeters of mercury) Hypertension is when the resting blood pressure is too high Systolic BP is 140 mmhg
Respiratory Anesthetic Emergencies in Oral and Maxillofacial Surgery. By: Lillian Han
 Respiratory Anesthetic Emergencies in Oral and Maxillofacial Surgery By: Lillian Han Background: Respiratory anesthetic emergencies are the most common complications during the administration of anesthesia
Respiratory Anesthetic Emergencies in Oral and Maxillofacial Surgery By: Lillian Han Background: Respiratory anesthetic emergencies are the most common complications during the administration of anesthesia
BELLWORK page 343. Apnea Dyspnea Hypoxia pneumo pulmonary Remember the structures of the respiratory system 1
 BELLWORK page 343 Apnea Dyspnea Hypoxia pneumo pulmonary respiratory system 1 STANDARDS 42) Review case studies that involve persons with respiratory disorders, diseases, or syndromes. Citing information
BELLWORK page 343 Apnea Dyspnea Hypoxia pneumo pulmonary respiratory system 1 STANDARDS 42) Review case studies that involve persons with respiratory disorders, diseases, or syndromes. Citing information
HASPI Medical Anatomy & Physiology 14b Lab Activity
 HASPI Medical Anatomy & Physiology 14b Lab Activity Name(s): Period: Date: Respiratory Distress Respiratory distress is a broad medical term that applies to any type of breathing difficulty and the associated
HASPI Medical Anatomy & Physiology 14b Lab Activity Name(s): Period: Date: Respiratory Distress Respiratory distress is a broad medical term that applies to any type of breathing difficulty and the associated
Unit 14: The Respiratory System
 Unit 14: The Respiratory System See what you already know! 1. Fill in the diagram on your own 2. Collaborate with your partner The Respiratory System The major function of the respiratory system is gas
Unit 14: The Respiratory System See what you already know! 1. Fill in the diagram on your own 2. Collaborate with your partner The Respiratory System The major function of the respiratory system is gas
Questions 1-3 refer to the following diagram. Indicate the plane labeled by the corresponding question number.
 Name: Grade: ANATOMY TEST Questions 1-3 refer to the following diagram. Indicate the plane labeled by the corresponding question number. 1. Plane #1 is the... 2. Plane #2 is the... 3. Plane #3 is the...
Name: Grade: ANATOMY TEST Questions 1-3 refer to the following diagram. Indicate the plane labeled by the corresponding question number. 1. Plane #1 is the... 2. Plane #2 is the... 3. Plane #3 is the...
Anatomy Review. Anatomy Review. Respiratory Emergencies CHAPTER 16
 CHAPTER 16 Respiratory Emergencies Anatomy Review Anatomy Review 1 Pediatric Anatomy Airway structure differences Proportionally larger tongue Smaller, more flexible trachea Abdominal breathers Reasons
CHAPTER 16 Respiratory Emergencies Anatomy Review Anatomy Review 1 Pediatric Anatomy Airway structure differences Proportionally larger tongue Smaller, more flexible trachea Abdominal breathers Reasons
The primary function of the respiratory system is to supply the blood with oxygen in order for the blood to deliver oxygen to all parts of the body.
 Respiratory System The primary function of the respiratory system is to supply the blood with oxygen in order for the blood to deliver oxygen to all parts of the body. The respiratory system does this
Respiratory System The primary function of the respiratory system is to supply the blood with oxygen in order for the blood to deliver oxygen to all parts of the body. The respiratory system does this
Respiratory System. Introduction. Atmosphere. Some Properties of Gases. Human Respiratory System. Introduction
 Introduction Respiratory System Energy that we consume in our food is temporarily stored in the bonds of ATP (adenosine triphosphate) before being used by the cell. Cells use ATP for movement and to drive
Introduction Respiratory System Energy that we consume in our food is temporarily stored in the bonds of ATP (adenosine triphosphate) before being used by the cell. Cells use ATP for movement and to drive
Respiratory Emergencies
 CHAPTER 16 Respiratory Emergencies Anatomy Review Anatomy Review Pediatric Anatomy Airway structure differences Proportionally larger tongue Smaller, more flexible trachea Abdominal breathers Reasons for
CHAPTER 16 Respiratory Emergencies Anatomy Review Anatomy Review Pediatric Anatomy Airway structure differences Proportionally larger tongue Smaller, more flexible trachea Abdominal breathers Reasons for
Respiratory System Mechanics
 M56_MARI0000_00_SE_EX07.qxd 8/22/11 3:02 PM Page 389 7 E X E R C I S E Respiratory System Mechanics Advance Preparation/Comments 1. Demonstrate the mechanics of the lungs during respiration if a bell jar
M56_MARI0000_00_SE_EX07.qxd 8/22/11 3:02 PM Page 389 7 E X E R C I S E Respiratory System Mechanics Advance Preparation/Comments 1. Demonstrate the mechanics of the lungs during respiration if a bell jar
Chronic inflammation of the airways Hyperactive bronchi Shortness of breath Tightness in chest Coughing Wheezing
 Chronic inflammation of the airways Hyperactive bronchi Shortness of breath Tightness in chest Coughing Wheezing Components of the respiratory system Nasal cavity Pharynx Trachea Bronchi Bronchioles Lungs
Chronic inflammation of the airways Hyperactive bronchi Shortness of breath Tightness in chest Coughing Wheezing Components of the respiratory system Nasal cavity Pharynx Trachea Bronchi Bronchioles Lungs
1 Chapter 13 Respiratory Emergencies 2 Respiratory Distress Patients often complain about. Shortness of breath Symptom of many different Cause can be
 1 Chapter 13 Respiratory Emergencies 2 Respiratory Distress Patients often complain about. Shortness of breath Symptom of many different Cause can be difficult to determine. Even for physician in hospital
1 Chapter 13 Respiratory Emergencies 2 Respiratory Distress Patients often complain about. Shortness of breath Symptom of many different Cause can be difficult to determine. Even for physician in hospital
Chapter 11 The Respiratory System
 Biology 12 Name: Respiratory System Per: Date: Chapter 11 The Respiratory System Complete using BC Biology 12, page 342-371 11.1 The Respiratory System pages 346-350 1. Distinguish between A. ventilation:
Biology 12 Name: Respiratory System Per: Date: Chapter 11 The Respiratory System Complete using BC Biology 12, page 342-371 11.1 The Respiratory System pages 346-350 1. Distinguish between A. ventilation:
The Respiratory System Structures of the Respiratory System Structures of the Respiratory System Structures of the Respiratory System Nose Sinuses
 CH 14 D.E. Human Biology The Respiratory System The Respiratory System OUTLINE: Mechanism of Breathing Transport of Gases between the Lungs and the Cells Respiratory Centers in the Brain Function Provides
CH 14 D.E. Human Biology The Respiratory System The Respiratory System OUTLINE: Mechanism of Breathing Transport of Gases between the Lungs and the Cells Respiratory Centers in the Brain Function Provides
The Respiratory System
 BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 14 The Respiratory System Lecture Presentation Anne Gasc Hawaii Pacific University and University of Hawaii
BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 14 The Respiratory System Lecture Presentation Anne Gasc Hawaii Pacific University and University of Hawaii
Semiology of respiratory system in children Simple choice 1. Mark the intrauterine age of lung development onset from the gut: a) 1 week b) 24 days
 Semiology of respiratory system in children Simple choice 1. Mark the intrauterine age of lung development onset from the gut: a) 1 week b) 24 days c) 6 weeks d) 12 weeks e) 35 weeks 2. Stridor is not
Semiology of respiratory system in children Simple choice 1. Mark the intrauterine age of lung development onset from the gut: a) 1 week b) 24 days c) 6 weeks d) 12 weeks e) 35 weeks 2. Stridor is not
Overview of COPD INTRODUCTION
 Overview of COPD INTRODUCTION Chronic obstructive pulmonary disease (COPD) is a common lung disease that affects millions of people, and it is the fourth leading cause of death in the United States. It
Overview of COPD INTRODUCTION Chronic obstructive pulmonary disease (COPD) is a common lung disease that affects millions of people, and it is the fourth leading cause of death in the United States. It
Collin County Community College
 Collin County Community College BIOL. 2402 Anatomy & Physiology WEEK 10 Respiratory System Carbon Dioxide Transport Carbon dioxide is transported in the blood in three forms Dissolved in plasma 7 to 10%
Collin County Community College BIOL. 2402 Anatomy & Physiology WEEK 10 Respiratory System Carbon Dioxide Transport Carbon dioxide is transported in the blood in three forms Dissolved in plasma 7 to 10%
CPAP. Pre-Hospital Treatment Using The Respironics Whisperflow CPAP Device. Charlottesville Albemarle Rescue Squad - CPAP
 CPAP Pre-Hospital Treatment Using The Respironics Whisperflow CPAP Device CPAP What Is It? C ontinuous P ositive A irway P ressure Anatomy Review Anatomy Review Anatomy Review Alveoli Anatomy Review Chest
CPAP Pre-Hospital Treatment Using The Respironics Whisperflow CPAP Device CPAP What Is It? C ontinuous P ositive A irway P ressure Anatomy Review Anatomy Review Anatomy Review Alveoli Anatomy Review Chest
About the Respiratory System. Respiratory System. Human Respiratory System. Cellular Respiration. Nostrils. Label diagram
 Respiratory System Human Respiratory System A system to deliver oxygen (O2) to body cells & get rid of carbon dioxide (CO2) as a waste through cellular respiration. Two systems involved: Respiratory &
Respiratory System Human Respiratory System A system to deliver oxygen (O2) to body cells & get rid of carbon dioxide (CO2) as a waste through cellular respiration. Two systems involved: Respiratory &
THE RESPIRATORY SYSTEM. Pages and
 THE RESPIRATORY SYSTEM Pages 103-105 and 146-150 1 When the respiratory system is mentioned, people generally think of breathing, but breathing is only one of the activities of the respiratory system.
THE RESPIRATORY SYSTEM Pages 103-105 and 146-150 1 When the respiratory system is mentioned, people generally think of breathing, but breathing is only one of the activities of the respiratory system.
Asthma Management Introduction, Anatomy and Physiology
 Asthma Management Introduction, Anatomy and Physiology University of Utah Center for Emergency Programs and The Utah Asthma Program Incidence, Impact and Goals of Asthma Management Prevalence, Morbidity
Asthma Management Introduction, Anatomy and Physiology University of Utah Center for Emergency Programs and The Utah Asthma Program Incidence, Impact and Goals of Asthma Management Prevalence, Morbidity
RESPIRATORY SYSTEM MODULE. Academic Year Study Guide
 RESPIRATORY SYSTEM MODULE Academic Year 2004-2005 Study Guide Respiratory Objectives By the end of this system, students should recognize the followings: 1. The respiratory passages and its classification
RESPIRATORY SYSTEM MODULE Academic Year 2004-2005 Study Guide Respiratory Objectives By the end of this system, students should recognize the followings: 1. The respiratory passages and its classification
Function: to supply blood with, and to rid the body of
 1 2 3 4 5 Bio 1102 Lec. 7 (guided): Chapter 10 The Respiratory System Respiratory System Function: to supply blood with, and to rid the body of Oxygen: needed by cells to break down food in cellular respiration
1 2 3 4 5 Bio 1102 Lec. 7 (guided): Chapter 10 The Respiratory System Respiratory System Function: to supply blood with, and to rid the body of Oxygen: needed by cells to break down food in cellular respiration
an inflammation of the bronchial tubes
 BRONCHITIS DEFINITION Bronchitis is an inflammation of the bronchial tubes (or bronchi), which are the air passages that extend from the trachea into the small airways and alveoli. Triggers may be infectious
BRONCHITIS DEFINITION Bronchitis is an inflammation of the bronchial tubes (or bronchi), which are the air passages that extend from the trachea into the small airways and alveoli. Triggers may be infectious
Overview. The Respiratory System. Chapter 18. Respiratory Emergencies 9/11/2012
 Chapter 18 Respiratory Emergencies Slide 1 Overview Respiratory System Review Anatomy Physiology Breathing Assessment Adequate Breathing Breathing Difficulty Focused History and Physical Examination Emergency
Chapter 18 Respiratory Emergencies Slide 1 Overview Respiratory System Review Anatomy Physiology Breathing Assessment Adequate Breathing Breathing Difficulty Focused History and Physical Examination Emergency
Chapter 13. Respiratory Emergencies
 Chapter 13 Respiratory Emergencies Introduction Patients often complain about dyspnea. Shortness of breath Symptom of many different conditions Cause can be difficult to determine. Even for physician in
Chapter 13 Respiratory Emergencies Introduction Patients often complain about dyspnea. Shortness of breath Symptom of many different conditions Cause can be difficult to determine. Even for physician in
Gas exchange Regulate blood ph Voice production Olfaction Innate immunity
 Respiration Functions Gas exchange: Grab O 2, eject CO 2 Regulate blood ph: Alters CO 2 levels Voice production: air movement past vocal cords Olfaction: in nasal cavity Innate immunity: physical protection
Respiration Functions Gas exchange: Grab O 2, eject CO 2 Regulate blood ph: Alters CO 2 levels Voice production: air movement past vocal cords Olfaction: in nasal cavity Innate immunity: physical protection
Tracheostomy and Ventilator Education Program Module 2: Respiratory Anatomy
 Tracheostomy and Ventilator Education Program Module 2: Respiratory Anatomy Disclaimer This material is intended for use by trained family members and caregivers of children with tracheostomies who are
Tracheostomy and Ventilator Education Program Module 2: Respiratory Anatomy Disclaimer This material is intended for use by trained family members and caregivers of children with tracheostomies who are
RESPIRATORY FAILURE. Michael Kelly, MD Division of Pediatric Critical Care Dept. of Pediatrics
 RESPIRATORY FAILURE Michael Kelly, MD Division of Pediatric Critical Care Dept. of Pediatrics What talk is he giving? DO2= CO * CaO2 CO = HR * SV CaO2 = (Hgb* SaO2 * 1.34) + (PaO2 * 0.003) Sound familiar??
RESPIRATORY FAILURE Michael Kelly, MD Division of Pediatric Critical Care Dept. of Pediatrics What talk is he giving? DO2= CO * CaO2 CO = HR * SV CaO2 = (Hgb* SaO2 * 1.34) + (PaO2 * 0.003) Sound familiar??
Competency Title: Continuous Positive Airway Pressure
 Competency Title: Continuous Positive Airway Pressure Trainee Name: ------------------------------------------------------------- Title: ---------------------------------------------------------------
Competency Title: Continuous Positive Airway Pressure Trainee Name: ------------------------------------------------------------- Title: ---------------------------------------------------------------
Respiratory Failure. Causes of Acute Respiratory Failure (ARF): a- Intrapulmonary:
 Respiratory failure exists whenever the exchange of O 2 for CO 2 in the lungs cannot keep up with the rate of O 2 consumption & CO 2 production in the cells of the body. This results in a fall in arterial
Respiratory failure exists whenever the exchange of O 2 for CO 2 in the lungs cannot keep up with the rate of O 2 consumption & CO 2 production in the cells of the body. This results in a fall in arterial
Care of the Patient with a Respiratory Disorder
 Care of the Patient with a Respiratory Disorder 1 Slide 1 Overview of Anatomy and Physiology External respiration Exchange of oxygen and carbon dioxide between the lung and the environment Internal respiration
Care of the Patient with a Respiratory Disorder 1 Slide 1 Overview of Anatomy and Physiology External respiration Exchange of oxygen and carbon dioxide between the lung and the environment Internal respiration
Respiration. Chapter 35
 Respiration Chapter 35 Respiration Respiration is the exchange of gasses between an organism and its environment Gas exchange occurs between the environment and blood at the lungs, and the blood and cells
Respiration Chapter 35 Respiration Respiration is the exchange of gasses between an organism and its environment Gas exchange occurs between the environment and blood at the lungs, and the blood and cells
Oxygenation. Chapter 45. Re'eda Almashagba 1
 Oxygenation Chapter 45 Re'eda Almashagba 1 Respiratory Physiology Structure and function Breathing: inspiration, expiration Lung volumes and capacities Pulmonary circulation Respiratory gas exchange: oxygen,
Oxygenation Chapter 45 Re'eda Almashagba 1 Respiratory Physiology Structure and function Breathing: inspiration, expiration Lung volumes and capacities Pulmonary circulation Respiratory gas exchange: oxygen,
Chapter 19 - Respiratory_Emergencies
 Introduction to Emergency Medical Care 1 OBJECTIVES 19.1 Define key terms introduced in this chapter. Slides 14 15, 41, 54 19.2 Describe the anatomy and physiology of respiration. Slides 13 15 19.3 Differentiate
Introduction to Emergency Medical Care 1 OBJECTIVES 19.1 Define key terms introduced in this chapter. Slides 14 15, 41, 54 19.2 Describe the anatomy and physiology of respiration. Slides 13 15 19.3 Differentiate
Anatomy and Physiology
 Anatomy and Physiology Respiratory Diagnostic Procedures 2004 Delmar Learning, a Division of Thomson Learning, Inc. Bell Work Complete cost of smoking exercise. We will go over this together! (Don t worry)!
Anatomy and Physiology Respiratory Diagnostic Procedures 2004 Delmar Learning, a Division of Thomson Learning, Inc. Bell Work Complete cost of smoking exercise. We will go over this together! (Don t worry)!
The Respiratory System
 13 PART A The Respiratory System PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB Organs of the Respiratory
13 PART A The Respiratory System PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB Organs of the Respiratory
RESPIRATORY DISORDERS
 RESPIRATORY DISORDERS INTRODUCTION Respiratory disorders refers to the medical term that include different pathological conditions affecting the organs and tissues of respiratory system which make gas
RESPIRATORY DISORDERS INTRODUCTION Respiratory disorders refers to the medical term that include different pathological conditions affecting the organs and tissues of respiratory system which make gas
Chronic Obstructive Pulmonary Disease (COPD) Copyright 2014 by Mosby, an imprint of Elsevier Inc.
 Chronic Obstructive Pulmonary Disease () 8.18.18 Copyright 2014 by Mosby, an imprint of Elsevier Inc. Description Airflow limitation not fully reversible progressive Abnormal inflammatory response of lungs
Chronic Obstructive Pulmonary Disease () 8.18.18 Copyright 2014 by Mosby, an imprint of Elsevier Inc. Description Airflow limitation not fully reversible progressive Abnormal inflammatory response of lungs
Foundation in Critical Care Nursing. Airway / Respiratory / Workbook
 Foundation in Critical Care Nursing Airway / Respiratory / Workbook Airway Anatomy: Please label the following: Tongue Larynx Epiglottis Pharynx Trachea Vertebrae Oesophagus Where is the ET (endotracheal)
Foundation in Critical Care Nursing Airway / Respiratory / Workbook Airway Anatomy: Please label the following: Tongue Larynx Epiglottis Pharynx Trachea Vertebrae Oesophagus Where is the ET (endotracheal)
The Respiratory System
 The Respiratory System Function of the Respiratory System Oversees gas exchanges (oxygen and carbon dioxide) between the blood and external environment Exchange of gasses takes place within the lungs in
The Respiratory System Function of the Respiratory System Oversees gas exchanges (oxygen and carbon dioxide) between the blood and external environment Exchange of gasses takes place within the lungs in
Restrictive Pulmonary Diseases
 Restrictive Pulmonary Diseases Causes: Acute alveolo-capillary sysfunction Interstitial disease Pleural disorders Chest wall disorders Neuromuscular disease Resistance Pathophysiology Reduced compliance
Restrictive Pulmonary Diseases Causes: Acute alveolo-capillary sysfunction Interstitial disease Pleural disorders Chest wall disorders Neuromuscular disease Resistance Pathophysiology Reduced compliance
The Respiratory System
 Essentials of Human Anatomy & Physiology Elaine N. Marieb Seventh Edition Chapter 13 The Respiratory System Slides 13.1 13.30 Lecture Slides in PowerPoint by Jerry L. Cook Copyright 2003 Pearson Education,
Essentials of Human Anatomy & Physiology Elaine N. Marieb Seventh Edition Chapter 13 The Respiratory System Slides 13.1 13.30 Lecture Slides in PowerPoint by Jerry L. Cook Copyright 2003 Pearson Education,
Respiratory System. Organization of the Respiratory System
 Respiratory System In addition to the provision of oxygen and elimination of carbon dioxide, the respiratory system serves other functions, as listed in (Table 15 1). Respiration has two quite different
Respiratory System In addition to the provision of oxygen and elimination of carbon dioxide, the respiratory system serves other functions, as listed in (Table 15 1). Respiration has two quite different
2. List seven functions performed by the respiratory system?
 The Respiratory System C23 Study Guide Tortora and Derrickson 1. In physiology we recognize that the word respiration has three meanings. What are the three different meanings of the word respiration as
The Respiratory System C23 Study Guide Tortora and Derrickson 1. In physiology we recognize that the word respiration has three meanings. What are the three different meanings of the word respiration as
Chapter 11: Respiratory Emergencies
 29698_CH11_ANS_p001_005 4/12/05 2:02 PM Page 1 Answer Key Chapter 11 1 Chapter 11: Respiratory Emergencies Matching 1. B (page 373) 8. E (page 370) 2. D (page 369) 9. M(page 389) 3. H (page 370) 10. A
29698_CH11_ANS_p001_005 4/12/05 2:02 PM Page 1 Answer Key Chapter 11 1 Chapter 11: Respiratory Emergencies Matching 1. B (page 373) 8. E (page 370) 2. D (page 369) 9. M(page 389) 3. H (page 370) 10. A
Known Allergies: Shellfish. Symptoms: abdominal pain, nausea, diarrhea, or vomiting. congestion, trouble breathing, or wheezing.
 CSTAR CASE STUDIES: BLOCK B Asthma or COPD? Setting: Walk in clinic. Dan: I havi g that cough thi g agai HPI: Dan is a 49-year-old male teacher who reports having had episodes of cough with mucus production
CSTAR CASE STUDIES: BLOCK B Asthma or COPD? Setting: Walk in clinic. Dan: I havi g that cough thi g agai HPI: Dan is a 49-year-old male teacher who reports having had episodes of cough with mucus production
COPD Management in LTC: Presented By: Jessica Denney RRT
 COPD Management in LTC: Presented By: Jessica Denney RRT Sponsored by Z & D Medical Services, Diamond Sponsor Seizing Opportunities to Provide Individualized Treatment and Device Selection for your COPD
COPD Management in LTC: Presented By: Jessica Denney RRT Sponsored by Z & D Medical Services, Diamond Sponsor Seizing Opportunities to Provide Individualized Treatment and Device Selection for your COPD
Respiratory Physiology
 Respiratory Physiology Dr. Aida Korish Associate Prof. Physiology KSU The main goal of respiration is to 1-Provide oxygen to tissues 2- Remove CO2 from the body. Respiratory system consists of: Passages
Respiratory Physiology Dr. Aida Korish Associate Prof. Physiology KSU The main goal of respiration is to 1-Provide oxygen to tissues 2- Remove CO2 from the body. Respiratory system consists of: Passages
Altered Ventilation and Diffusion
 Respiratory Structures Altered Ventilation and Diffusion Alveolar type 1: provide structure and air exchange Alveolar type 2: lubricant that coats the inner portion of the alveolus, promotes easy expansion,
Respiratory Structures Altered Ventilation and Diffusion Alveolar type 1: provide structure and air exchange Alveolar type 2: lubricant that coats the inner portion of the alveolus, promotes easy expansion,
COPD. Helen Suen & Lexi Smith
 COPD Helen Suen & Lexi Smith What is COPD? Chronic obstructive pulmonary disease: a non reversible, long term lung disease Characterized by progressively limited airflow and an inability to perform full
COPD Helen Suen & Lexi Smith What is COPD? Chronic obstructive pulmonary disease: a non reversible, long term lung disease Characterized by progressively limited airflow and an inability to perform full
Bronchitis. Anatomy of the Lungs The lungs allow us to fill our blood with oxygen. The oxygen we breathe is absorbed into our blood in the lungs.
 Bronchitis Introduction Bronchitis is an inflammation of the bronchial tubes, the airways that carry air to the lungs. It causes shortness of breath, wheezing and chest tightness as well as a cough that
Bronchitis Introduction Bronchitis is an inflammation of the bronchial tubes, the airways that carry air to the lungs. It causes shortness of breath, wheezing and chest tightness as well as a cough that
