INTRODUCTION. Getting the best scan. Choosing a probe. Choosing the frequency
|
|
|
- Christine Lester
- 5 years ago
- Views:
Transcription
1 Getting the best scan Choosing a probe Select the most appropriate probe for the particular scan required. s vary in their: operating frequency range higher ultrasound frequencies provide better discrimination of fine detail but have lower penetration because of increased attenuation by the tissues. physical size the smaller the probe, the smaller its footprint when placed on the patient. the width of the tissue field scanned an ultrasound probe scans a slice of tissue approximately 1 3 mm thick, with a width dependent on the size of the probe. Common types of probe available (Fig. 1) are: Linear These probes have a flat face and give a parallel-sided scan field approximately 1 mm thick. Linear probes operate at frequencies typically between 5 and 18 MHz. They come in different widths, between 20 and 40 mm, with correspondingly different lengths of probe footprint. These are the best general-purpose probes. Hockey-stick These are small probes that can be held with a fountain-pen grip. They are appropriate for small or paediatric patients. They are also useful for awkward areas such as close to the clavicle or posterior to the medial malleolus, where the physical size of the wider probes may make it difficult to manipulate the probe or obtain good skin contact. The less the width of the probe, the smaller its footprint, but the narrower the field covered in the scan and the more difficult it is to identify the anatomy in the scan. Curvilinear These probes have a curved face giving a fan-shaped scan field. The field is diverging, with Linear probe Hockey-stick probe Fig 1 Three common types of ultrasound probe curvilinear distortion in the horizontal direction analogous to that seen with a fish-eye lens in photography. more panoramic view is therefore obtained in the scan, which can make identification of the local anatomy easier. Curvilinear probes generally operate at relatively lower frequencies (typically 2 5 MHz), giving greater depths of penetration but with coarser discrimination. Choosing the frequency Curvilinear probe The frequency of ultrasound can significantly alter the appearance of the scan obtained. The frequency will determine both the depth of penetration and the discrimination of detail in the scan. Unfortunately there is a trade-off between depth of penetration and discrimination of detail. The higher the frequency the better the resolution of detail in the scan, but the lower the penetration of tissues. Typically a linear probe operating at 10 MHz gives good resolution of detail but only provides good penetration to depths of 2 3 cm. Targets beyond this range are more difficult to visualize (Fig. 2). curvilinear probe working at 2 5 MHz can penetrate soft tissues reasonably well up to 4 10 cm, but the discrimination of detail is coarser (Fig. 3). 1 in this web service
2 0 cm cm SN Suprascapular notch 2 SN Suprascapular notch 3 3 SN 4 SN Fig 2 High resolution but low penetration: a high-resolution scan of the suprascapular notch, using a linear probe at 10 MHz Fig 3 High penetration but low resolution: a low-resolution scan of the suprascapular notch, using a curvilinear probe at 4 MHz Gain control This control is equivalent to the brightness control, and it may make targets easier to see in the scan (Fig. 4). It changes the overall appearance of the scan from dark (black) to bright (white). It will not necessarily make targets easier to distinguish or identify. More sophisticated machines can increase the gain at a selected depth, known as time gain compensation (TGC). This feature can be useful when trying to visualize more distal targets at depths where the penetration of the ultrasound is poor. Depth Use the depth control to place the target area at approximately two-thirds of the total depth of the scan. Focus Some machines have a focus control which enhances image quality at a chosen level. This should be set just deep to the target area. Identifying the anatomy in a scan Gross anatomy Orientation in an ultrasound scan is predominantly a process of pattern recognition. Knowledge of the anatomy in the region being scanned is essential in interpreting and identifying structures in the scan. Using the surface anatomy to aid accurate and consistent placement of the probe helps to obtain a scan with a familiar pattern. Fig 4 scan of the carotid artery and internal jugular vein: with the gain adjusted too low; with the scan gain increased 2 in this web service
3 0 cm 1 R Brachial plexus Subclavian artery First rib 2 R Fig 5 Vascular and bony landmarks in an ultrasound scan: locating the brachial plexus 3 Scan landmarks Use vascular and bony landmarks to orientate in a scan. For example, use the subclavian artery and first rib to orientate in a supraclavicular scan of the brachial plexus (Fig. 5). Tracking In some patients it may prove difficult to identify a target structure in a scan with the probe at a particular location. This can often be solved by identifying the structure at an alternative location where it is easy to see, and then tracking it back to the desired location. For example, if it is proving difficult to find the ulnar nerve at mid forearm level, first find the nerve at the wrist, where it can easily be located between the ulnar artery and the flexor carpi ulnaris tendon. Then track it proximally to forearm level by slowly sliding the probe up the forearm while taking care to keep the ulnar nerve in view (Fig. 6). s the nerve and artery are tracked proximally it can be seen that although the nerve starts adjacent to the artery in the wrist its course diverges from the artery in the proximal forearm, where it can be blocked with reduced risk of arterial puncture. nisotropy Slight adjustments of the probe about its long axis (tilting the probe) when at the scan position can greatly improve the view of a target or even reveal its presence when previously unseen (Fig. 7). This is a result of altering the angle at which the ultrasound waves strike the target and thus optimizing the reflections received by the probe. This effect is referred to as anisotropy. Fig. 8 compares two views of the median nerve obtained with the probe in exactly the same position on the forearm. The only difference between the two scans is a slight change of the probe angle about its long axis, to maximize and minimize the anisotropic effect. Recognizing different tissues in an ultrasound scan The use of ultrasound when scanning body tissues demonstrates some differences between tissues. Detail in the scans is dependent on the wavelength, which is inversely dependent on frequency. The production of targets (bright reflections) in a scan relies on reflection of ultrasound, the reflected waves having to pass back to the probe in order to be 3 in this web service
4 N N N Ulnar nerve Ulnar artery N Ulnar nerve N N Ulnar nerve Ulnar artery Fig 6 Tracking the ulnar nerve from wrist to forearm Slight tilting movement of probe minimizes anisotropy effect Ultrasound beam Fig 7 Tilting the probe to minimize anisotropy received. This means that the visibility of a target relies on reflection and can be attenuated by scattering. Reflection at a boundary between different tissues is determined by the differences in acoustic impedances of the tissues. The best-defined targets have boundaries (surfaces) which separate media with the greatest mismatch of acoustic impedances for example, between soft tissue and air, soft tissue and bone, soft tissue and fluid. Some representative acoustic impedances are shown in Table 1. Modern machines have tissue harmonic imaging, which uses harmonics of the ultrasound beam to reduce the effects of scattering and improve tissue resolution. Nerves Peripheral nerves have a granular appearance in crosssection due to the echogenicity of the endoneurium tissue around the nerve fascicles (Fig. 9). They appear less echogenic when viewed more centrally. In longitudinal section the fascicles are visible as parallel streaks within the nerve. Tendons Tendons may easily be confused with nerves, but usually the granularity in cross-section and the streaking in longitudinal section are finer, and the appearance is more homogeneous (Fig. 10). Distinguish between nerves and tendons in a scan by tracking. Track nerves from areas where they are 4 in this web service
5 Fig 8 Two views of the median nerve: poor and good probe adjustment to reduce anisotropy effect View with poor probe adjustment tilted for best view of nerve more easily identifiable, or track tendons to the muscles they are attached to. lternatively, ask the patient to make appropriate movements, which cause the tendons to move in the scan while the nerves remain relatively stationary. Muscle Muscle is coarsely speckled in cross-section, with more dense connective tissue outlining the fascicles. Table 1 Values of acoustic impedance for different tissues Tissue Velocity of sound (m s 1 ) Gas Fat Blood Muscle Bone coustic impedance (kg m 2 s 1 ) 10 6 In longitudinal section the fascicles produce coarse irregular striations (Fig. 11). Bone Bone can only be visualized in a scan by the proximal surface that is exposed to the incident ultrasound. Since the ultrasound waves do not penetrate this proximal boundary (as they do in the case of soft tissue structures such as blood vessels and nerves), the proximal surface of a bone in the scan leaves a dark region or drop-out shadow distally. Therefore bones do not appear in an ultrasound scan as a two-dimensional structure or cross-section. Instead, bones are recognized as hyperechoic (bright) profiles proximal to a dark drop-out shadow (Fig. 12). Fig 9 Ultrasound appearance of nerve fascicular pattern Cross-section of nerve Longitudinal section of nerve 5 in this web service
6 Fig 10 Ultrasound appearance of tendon fibrillar pattern Cross-section of tendon Longitudinal section of tendon Fig 11 Ultrasound appearance of muscle Cross-section of muscle Longitudinal section of muscle Fig 12 Bone profiles and drop-out shadows in an ultrasound scan Spinous process Ulna Ulnar shadow at the wrist Shadow of lumbar spinous process Blood vessels rteries and veins are readily recognized because of the low echogenicity of the blood they contain. rteries retain their circular cross-section and pulsate even when pressure is applied to the probe, unlike accompanying veins, which are of greater cross-sectional area but with a more irregular cross-section and a tendency to collapse when pressure is applied to the probe (Fig. 13). Occasionally a valve may be seen in the lumen of a large central vein as a pulsatile intraluminal echo. 6 in this web service
7 Fig 13 Scans of an artery and a vein, showing collapse of vein with pressure applied to probe Vein Vein rtery rtery rtery and uncollapsed vein rtery and collapsed vein due to probe pressue Post-cystic enhancement Often a bright area can be seen distal to a fluid-filled cyst or vessel (Fig. 14). This is the combined result of (1) low attenuation of ultrasound waves as they pass through the vessel, (2) refraction and (3) edge shadows. The edge shadows are caused by scattering of the incident ultrasound waves from the edges of the vessel. Uses of ultrasound in procedures Guiding the needle in regional anaesthesia Use of ultrasound enables real-time guidance of the needle in regional anaesthesia. The ultrasound beam is only approximately 1 mm in thickness. In order to guide the needle it is necessary to obtain the best possible view of the needle and needle tip. Obtaining a good view of the needle good view of the needle in the scan requires the needle to be in the plane of the ultrasound beam. In addition, the angle between the needle and the face of the probe should be as small as possible in order to maximize the reflection of ultrasound waves back to the probe (Fig. 15). When the angle between the needle and probe face is greater than 45 degrees poor visibility of the needle results, since the ultrasound is reflected from the needle at an angle rather than back to the probe (highvisibility needles can improve this poor visibility). Ideally, try to maintain an angle of less than 30 degrees between needle and probe face. The best view of the needle is obtained when the needle is parallel to the face of the probe. Keeping the bevel of the needle tip facing the probe improves needle tip visualization. In-plane and out-of-plane needling techniques In-plane needling refers to needle insertion parallel to the ultrasound beam, keeping the needle within the plane of the beam, so that the length of the needle and its tip are visualized during insertion. Out-of-plane needle insertion is performed with the needle perpendicular to the ultrasound beam. In this case the needle is only visualized as a hyperechoic spot where it crosses the plane of the ultrasound beam. In-plane needling s long as the whole needle, and in particular its tip, lies in the plane of the ultrasound beam, it can be observed as it passes along its track, and puncturing unwanted structures such as blood vessels and pleura can be avoided (Fig. 16). However, because the ultrasound beam is only 1 3 mm thick, it is easy to only obtain a partial view of the needle, leaving the tip invisible because it is out of the plane of the ultrasound beam (Fig. 16B). In such a case the puncture of unwanted structures is more likely. Therefore in-plane needling is the safest technique to use, provided good alignment of the needle is maintained. 7 in this web service
8 Incident ultrasound scattered from edges of artery Fig 14 Post-cystic enhancement S S PCE S S PCE rtery PCE Post-cystic enhancement S Edge shadows Reflected ultrasound 45 o Needle Optimum reflection of ultrasound back to probe Needle Fig 15 The effect of different angles between needle and probe: poor visibility with a steep angle; good visibility when the needle is parallel to the probe Out-of-plane needling Often gives an advantage in identifying surrounding anatomy but does increase the risks of puncturing unwanted structures, since the needle tip is out of plane and not visible. hyperechoic dot in the scan marks the point at which the needle crosses the plane of the ultrasound beam. The position of the needle tip can be located by sliding the probe along the needle axis until this hyperechoic dot disappears. In this position, tilting the probe about its long axis causes the needle tip to appear and disappear, confirming its position in the ultrasound beam. Out-of-plane needling may be used for practical reasons such as passing a catheter for continuous infusion blockade. In such a case the catheter needs to be inserted parallel to a nerve, and needling out of plane can make this significantly easier (Fig. 17). The track of the needle in out-of-plane needling is observed indirectly on an ultrasound scan by looking for the movement of tissue in the scan caused by the passage of the needle. Observation of local anaesthetic spread When performing regional anaesthetic blocks, the distribution or spread of the injected local anaesthetic can determine whether or not an 8 in this web service
9 Needle - good alignment in plane Needle - poor alignment in plane Ultrasound beam Ultrasound beam Fig 16 In-plane needling with good and poor alignment (needle tip out of plane) Needle inserted out of plane Fig 17 Out-of-plane needling Point at which needle passes through beam produces bright spot in scan Ultrasound beam effective block is obtained. Thus when using ultrasound guidance for regional anaesthesia it is useful to observe the spread of local anaesthetic as it is injected. Fig. 18 shows how the local anaesthetic in a femoral nerve block can spread away from the nerve rather than around the nerve. This might occur even in the presence of good muscle twitches if a nerve stimulator is used. Good spread of local anaesthetic in a regional block can be observed in real time as the local anaesthetic, which is echolucent, can be seen to surround the target nerves as injection takes place. Fig. 19 shows an ultrasound scan of the supraclavicular brachial plexus, with local anaesthetic surrounding the trunks of the plexus. Checking perineural catheter placement Insertion of a perineural catheter can be used in cases where continuous infusion blockade is required (Fig. 20). Insertion of a catheter to lie alongside the nerve being blocked can sometimes be difficult, as the track of the catheter may not stay close to the nerve. Needling out of plane can facilitate passing the catheter. The final catheter position can be checked using ultrasound, but the catheter usually appears only intermittently as bright dots in the scan. Injection of a small quantity of air under ultrasound observation can also help confirm placement. 9 in this web service
10 IF N FN L IF L N FN Fig 18 Good spread and poor spread of local anaesthetic in a femoral nerve block, depending on whether the needle penetrates the iliopectineal fascia L Local anaesthetic FN Femoral nerve N Needle IF Iliopectineal fascia L L Fig 19 Spread of local anaesthetic in brachial plexus block, showing local anaesthetic surrounding the divisions of the plexus SM SM Brachial plexus L Local anaesthetic Subclavian artery SM Scalenus medius muscle Guiding intravascular cannulation Intravascular cannulation can be guided by ultrasound, either for central venous cannulation or for peripheral vessel cannulation in cases where peripheral vessels are not easily visualized. Ultrasound can be used to detect an appropriate vessel, check entry of a guide wire into the vessel and check final placement of the cannula into the vessel. Fig. 21 shows the stages in cannulation of an internal jugular vein, using an in-plane technique. 10 in this web service
Brachial plexus blockade within the interscalene groove involves local anesthetic
 Interscalene Brachial Plexus Block- How I do it. Part 1 of a 2 part discussion on technique. Stuart Grant Professor of Anesthesiology Duke University Medical Center Durham NC Brachial plexus blockade within
Interscalene Brachial Plexus Block- How I do it. Part 1 of a 2 part discussion on technique. Stuart Grant Professor of Anesthesiology Duke University Medical Center Durham NC Brachial plexus blockade within
Principles of Ultrasound. Cara C. Prideaux, M.D. University of Utah PM&R Sports Medicine Fellow March 14, 2012
 Principles of Ultrasound Cara C. Prideaux, M.D. University of Utah PM&R Sports Medicine Fellow March 14, 2012 None Disclosures Outline Introduction Benefits and Limitations of US Ultrasound (US) Physics
Principles of Ultrasound Cara C. Prideaux, M.D. University of Utah PM&R Sports Medicine Fellow March 14, 2012 None Disclosures Outline Introduction Benefits and Limitations of US Ultrasound (US) Physics
Background & Indications Probe Selection
 Teresa S. Wu, MD, FACEP Director, EM Ultrasound Program & Fellowship Co-Director, Simulation Based Training Program & Fellowship Associate Program Director, EM Residency Program Maricopa Medical Center
Teresa S. Wu, MD, FACEP Director, EM Ultrasound Program & Fellowship Co-Director, Simulation Based Training Program & Fellowship Associate Program Director, EM Residency Program Maricopa Medical Center
Terminology Tissue Appearance
 By Marc Nielsen, MD Advantages/Disadvantages Generation of Image Ultrasound Machine/Transducer selection Modes of Ultrasound Terminology Tissue Appearance Scanning Technique Real-time Portable No ionizing
By Marc Nielsen, MD Advantages/Disadvantages Generation of Image Ultrasound Machine/Transducer selection Modes of Ultrasound Terminology Tissue Appearance Scanning Technique Real-time Portable No ionizing
Basics of US Regional Anaesthesia. November 2008
 Basics of US Regional Anaesthesia November 2008 Essential Physics HIGH frequency = great resolution but poor penetration LOW frequency = poor resolution but great penetration Potential Advantages of US
Basics of US Regional Anaesthesia November 2008 Essential Physics HIGH frequency = great resolution but poor penetration LOW frequency = poor resolution but great penetration Potential Advantages of US
Basic Physics of Ultrasound and Knobology
 WELCOME TO UTMB Basic Physics of Ultrasound and Knobology By Daneshvari Solanki, FRCA Laura B. McDaniel Distinguished Professor Anesthesiology and Pain Medicine University of Texas Medical Branch Galveston,
WELCOME TO UTMB Basic Physics of Ultrasound and Knobology By Daneshvari Solanki, FRCA Laura B. McDaniel Distinguished Professor Anesthesiology and Pain Medicine University of Texas Medical Branch Galveston,
Needle visualization with ZONARE ultrasound systems
 Needle visualization with ZONARE ultrasound systems This material provides a general overview of ultrasound guided needle imaging and techniques and is not intended to replace formal training or education
Needle visualization with ZONARE ultrasound systems This material provides a general overview of ultrasound guided needle imaging and techniques and is not intended to replace formal training or education
Introduction to Ultrasound Guided Region Anesthesia
 Introduction to Ultrasound Guided Region Anesthesia Brian D. Sites, MD Dept of Anesthesiology Dartmouth-Hitchcock Medical Center INTRODUCTION Welcome to Introduction to Ultrasound Guided Regional Anesthesia.
Introduction to Ultrasound Guided Region Anesthesia Brian D. Sites, MD Dept of Anesthesiology Dartmouth-Hitchcock Medical Center INTRODUCTION Welcome to Introduction to Ultrasound Guided Regional Anesthesia.
Ultrasound Guidance Needle Techniques
 Ultrasound Guidance Needle Techniques Dr TANG Ho-ming AED/UCH USG Guidance Needle Techniques Commonly used in EM 1. Vessel cannulation-peripheral & central 2. Foreign body removal 3. Peripheral nerve/plexus
Ultrasound Guidance Needle Techniques Dr TANG Ho-ming AED/UCH USG Guidance Needle Techniques Commonly used in EM 1. Vessel cannulation-peripheral & central 2. Foreign body removal 3. Peripheral nerve/plexus
Ultrasound Guided Injections
 Ultrasound Guided Injection Technique More accurate injections Better Results! 1 Benefits: Increased Level of Certainty ie : really know how accurate PRP/Prolotherapy Avoid damage to articular cartilage
Ultrasound Guided Injection Technique More accurate injections Better Results! 1 Benefits: Increased Level of Certainty ie : really know how accurate PRP/Prolotherapy Avoid damage to articular cartilage
Ultrasound Physics and Knobology Alan Macfarlane. Consultant Anaesthetist Glasgow Royal Infirmary
 Ultrasound Physics and Knobology Alan Macfarlane Consultant Anaesthetist Glasgow Royal Infirmary RAPM 2009; 34: 40-46 Ultrasound Proficiency Understanding US image generation and device operation Image
Ultrasound Physics and Knobology Alan Macfarlane Consultant Anaesthetist Glasgow Royal Infirmary RAPM 2009; 34: 40-46 Ultrasound Proficiency Understanding US image generation and device operation Image
The Essentials Tissue Characterization and Knobology
 The Essentials Tissue Characterization and Knobology Randy E. Moore, DC, RDMS RMSK No relevant financial relationships Ultrasound The New Standard of Care Musculoskeletal sonography has become the standard
The Essentials Tissue Characterization and Knobology Randy E. Moore, DC, RDMS RMSK No relevant financial relationships Ultrasound The New Standard of Care Musculoskeletal sonography has become the standard
3/20/2017. Disclosures. Ultrasound Fundamentals. Ultrasound Fundamentals. Bone Anatomy. Tissue Characteristics
 Disclosures Images of ultrasound equipment in this presentation are not an endorsement Fundamentals of Musculoskeletal Ultrasound Physics and Knobology Shane A. Shapiro, M.D. Assistant Professor Orthopedic
Disclosures Images of ultrasound equipment in this presentation are not an endorsement Fundamentals of Musculoskeletal Ultrasound Physics and Knobology Shane A. Shapiro, M.D. Assistant Professor Orthopedic
Ultrasound Guided Peripheral Intravenous Access
 Ultrasound Guided Peripheral Intravenous Access J. Christian Fox, MD, RDMS, FACEP, FAAEM, FAIUM Professor and Interim Chair of Emergency Medicine Director of Instructional Ultrasound University of California,
Ultrasound Guided Peripheral Intravenous Access J. Christian Fox, MD, RDMS, FACEP, FAAEM, FAIUM Professor and Interim Chair of Emergency Medicine Director of Instructional Ultrasound University of California,
1 Fundamentals. Basic Definitions and Physics Principles. Fundamentals
 1 To become versed in the language of ultrasonography, it is necessary to review some of the basic principles of physics. The wave physics principles of ordinary (i.e., audible) sound apply to ultrasound
1 To become versed in the language of ultrasonography, it is necessary to review some of the basic principles of physics. The wave physics principles of ordinary (i.e., audible) sound apply to ultrasound
Diana Mathioudakis DEAA EDIC AFRCA. consultant paediatric cardiac anaesthetist Intensivist(D/NL) emergency physician(d)
 & Diana Mathioudakis DEAA EDIC AFRCA consultant paediatric cardiac anaesthetist Intensivist(D/NL) emergency physician(d) Anatomy Probe handling Sonoanatomy Tips and Tricks Literature For ultrasound guided
& Diana Mathioudakis DEAA EDIC AFRCA consultant paediatric cardiac anaesthetist Intensivist(D/NL) emergency physician(d) Anatomy Probe handling Sonoanatomy Tips and Tricks Literature For ultrasound guided
Ultrasonography of Peripheral Nerve -upper extremity
 Ultrasonography of Peripheral Nerve -upper extremity Department of Physical Medicine and Rehabilitation Korea University Guro Hospital Korea University College of Medicine Yoon Joon Shik Normal median
Ultrasonography of Peripheral Nerve -upper extremity Department of Physical Medicine and Rehabilitation Korea University Guro Hospital Korea University College of Medicine Yoon Joon Shik Normal median
Ultrasound Guided Lower Extremity Blocks
 Ultrasound Guided Lower Extremity Blocks CONTENTS: 1. Femoral Nerve Block 2. Popliteal Nerve Block Updated December 2017 1 1. Femoral Nerve Block Indications Surgery involving the knee, anterior thigh,
Ultrasound Guided Lower Extremity Blocks CONTENTS: 1. Femoral Nerve Block 2. Popliteal Nerve Block Updated December 2017 1 1. Femoral Nerve Block Indications Surgery involving the knee, anterior thigh,
Basic of Ultrasound Physics E FAST & Renal Examination. Dr Muhammad Umer Ihsan MBBS,MD, DCH CCPU,DDU1,FACEM
 Basic of Ultrasound Physics E FAST & Renal Examination Dr Muhammad Umer Ihsan MBBS,MD, DCH CCPU,DDU1,FACEM What is Sound? Sound is Mechanical pressure waves What is Ultrasound? Ultrasounds are sound waves
Basic of Ultrasound Physics E FAST & Renal Examination Dr Muhammad Umer Ihsan MBBS,MD, DCH CCPU,DDU1,FACEM What is Sound? Sound is Mechanical pressure waves What is Ultrasound? Ultrasounds are sound waves
Preamble (disclaimer)
 Preamble (disclaimer) PHYSICS AND PRINCIPLES OF HEAD/NECK ULTRASOUND Joseph C. Sniezek, MD FACS LTC, MC, USA Otolaryngology/H&N Surgery Tripler Army Medical Center 1. I am not a physicist 2. ACS has recommended
Preamble (disclaimer) PHYSICS AND PRINCIPLES OF HEAD/NECK ULTRASOUND Joseph C. Sniezek, MD FACS LTC, MC, USA Otolaryngology/H&N Surgery Tripler Army Medical Center 1. I am not a physicist 2. ACS has recommended
Clinical Protocols of the Anesthesiology Department at the Dartmouth-Hitchcock Medical Center: Techniques for lower extremity nerve blocks.
 Clinical Protocols of the Anesthesiology Department at the Dartmouth-Hitchcock Medical Center: Techniques for lower extremity nerve blocks. Authors from DHMC: Brian D. Sites, MD. Assistant Professor of
Clinical Protocols of the Anesthesiology Department at the Dartmouth-Hitchcock Medical Center: Techniques for lower extremity nerve blocks. Authors from DHMC: Brian D. Sites, MD. Assistant Professor of
Ultrasound Physics & Terminology
 Ultrasound Physics & Terminology This module includes the following: Basic physics terms Basic principles of ultrasound Ultrasound terminology and terms Common artifacts seen Doppler principles Terms for
Ultrasound Physics & Terminology This module includes the following: Basic physics terms Basic principles of ultrasound Ultrasound terminology and terms Common artifacts seen Doppler principles Terms for
The Elbow 3/5/2015. The Elbow Scanning Sequence. * Anterior Joint (The anterior Pyramid ) * Lateral Epicondyle * Medial Epicondyle * Posterior Joint
 Scanning Sequence * Anterior Joint (The anterior Pyramid ) * Lateral Epicondyle * Medial Epicondyle * Posterior Joint Anterior Elbow Pyramid Courtesy of Jay Smith, MD. Vice chair PMR Mayo Clinic Rochester,
Scanning Sequence * Anterior Joint (The anterior Pyramid ) * Lateral Epicondyle * Medial Epicondyle * Posterior Joint Anterior Elbow Pyramid Courtesy of Jay Smith, MD. Vice chair PMR Mayo Clinic Rochester,
Ultrasound Use in Anaesthesia
 Trainee Name: 1 Ultrasound Use in Anaesthesia Assessments to accompany Workbook for anaesthetic trainees in North Queensland 2010 Authors: Mark Fairley, Emile Kurukchi, Andrew Potter 2 Trainee Name: Ultrasound
Trainee Name: 1 Ultrasound Use in Anaesthesia Assessments to accompany Workbook for anaesthetic trainees in North Queensland 2010 Authors: Mark Fairley, Emile Kurukchi, Andrew Potter 2 Trainee Name: Ultrasound
inerve Guide to Nerves 2009
 inerve Guide to Nerves 2009 A guide to self learning and self assessment Context: The following guide is intended to help interpret the sono-anatomy and follow a systematic stepwise approach to the practice
inerve Guide to Nerves 2009 A guide to self learning and self assessment Context: The following guide is intended to help interpret the sono-anatomy and follow a systematic stepwise approach to the practice
Certificate in Clinician Performed Ultrasound (CCPU) Syllabus. Vascular Access (venous (peripheral and central) and arterial)
 Certificate in Clinician Performed Ultrasound (CCPU) Syllabus Vascular Access (venous (peripheral and central) and arterial) Page 1 of 8 04/16 Vascular Access (venous (peripheral and central) and arterial)
Certificate in Clinician Performed Ultrasound (CCPU) Syllabus Vascular Access (venous (peripheral and central) and arterial) Page 1 of 8 04/16 Vascular Access (venous (peripheral and central) and arterial)
The Physics of Ultrasound. The Physics of Ultrasound. Claus G. Roehrborn. Professor and Chairman. Ultrasound Physics
 The Physics of Ultrasound Pipe Organ 10-8000 Emission Dog 452-1080 Man 85-1100 Spectrum Bat 10,000-120,000 Porpoise 7000-120,000 Claus G. Roehrborn Professor and Chairman 10 20 Cycles per second Reception
The Physics of Ultrasound Pipe Organ 10-8000 Emission Dog 452-1080 Man 85-1100 Spectrum Bat 10,000-120,000 Porpoise 7000-120,000 Claus G. Roehrborn Professor and Chairman 10 20 Cycles per second Reception
What is Ultrasound? Resolution Image production Attenuation Imaging modes Ultrasound artifacts... 7
 What is Ultrasound?... 1 Resolution... 3 Image production... 3 Attenuation... 4 Imaging modes... 5 Ultrasound artifacts... 7 0 What is Ultrasound? High frequency sound of frequencies 2-50 MHz is used in
What is Ultrasound?... 1 Resolution... 3 Image production... 3 Attenuation... 4 Imaging modes... 5 Ultrasound artifacts... 7 0 What is Ultrasound? High frequency sound of frequencies 2-50 MHz is used in
WELCOME! Introduction to Bedside Ultrasound
 WELCOME! Introduction to Bedside Ultrasound TEACHERS University of California-Irvine School of Medicine Nathan Molina nathan.d.molina@gmail.com Trevor Plescia taplescia90@gmail.com Jack Silva jpsilva42@gmail.com
WELCOME! Introduction to Bedside Ultrasound TEACHERS University of California-Irvine School of Medicine Nathan Molina nathan.d.molina@gmail.com Trevor Plescia taplescia90@gmail.com Jack Silva jpsilva42@gmail.com
Ultrasound-guided supraclavicular block
 THE JOURNAL OF NEW YORK SCHOOL J u l y 2009 V o l u m e OF REGIONAL ANESTHESIA 1 3 Ultrasound-guided supraclavicular block Arthur Atchabahian, MD Department of Anesthesiology, St. Vincent Medical Center,
THE JOURNAL OF NEW YORK SCHOOL J u l y 2009 V o l u m e OF REGIONAL ANESTHESIA 1 3 Ultrasound-guided supraclavicular block Arthur Atchabahian, MD Department of Anesthesiology, St. Vincent Medical Center,
Ultrasound. Principles of Medical Imaging. Contents. Prof. Dr. Philippe Cattin. MIAC, University of Basel. Oct 17th, 2016
 Ultrasound Principles of Medical Imaging Prof. Dr. Philippe Cattin MIAC, University of Basel Contents Abstract 1 Image Generation Echography A-Mode B-Mode M-Mode 2.5D Ultrasound 3D Ultrasound 4D Ultrasound
Ultrasound Principles of Medical Imaging Prof. Dr. Philippe Cattin MIAC, University of Basel Contents Abstract 1 Image Generation Echography A-Mode B-Mode M-Mode 2.5D Ultrasound 3D Ultrasound 4D Ultrasound
Dr Emma Chung. Safety first - Physical principles for excellent imaging
 Safety first - Physical principles for excellent imaging Dr Emma Chung Lecturer in Medical Physics, University of Leicester Clinical Scientist, University Hospitals of Leicester NHS Trust Thanks to Caroline
Safety first - Physical principles for excellent imaging Dr Emma Chung Lecturer in Medical Physics, University of Leicester Clinical Scientist, University Hospitals of Leicester NHS Trust Thanks to Caroline
Ultrasonography of the Neck as an Adjunct to FNA. Nicole Massoll M.D.
 Ultrasonography of the Neck as an Adjunct to FNA Nicole Massoll M.D. Basic Features of Head and Neck Ultrasound and Anatomy Nicole Massoll M.D. University of Arkansas for Medical Sciences, Little Rock
Ultrasonography of the Neck as an Adjunct to FNA Nicole Massoll M.D. Basic Features of Head and Neck Ultrasound and Anatomy Nicole Massoll M.D. University of Arkansas for Medical Sciences, Little Rock
Image optimization for critical care US
 Image optimization for critical care US 1 Although we assume you are already familiar with focused US in the ED, it might not hurt to revise the basics: Machines & transducers US appearance of normal tissues
Image optimization for critical care US 1 Although we assume you are already familiar with focused US in the ED, it might not hurt to revise the basics: Machines & transducers US appearance of normal tissues
Ultrasound Physics & Doppler
 Ultrasound Physics & Doppler Endocrine University 2018 Mark Lupo, MD, FACE, ECNU Objectives Review the essential components of ultrasound physics in neck sonography Demonstrate the importance of ultrasound
Ultrasound Physics & Doppler Endocrine University 2018 Mark Lupo, MD, FACE, ECNU Objectives Review the essential components of ultrasound physics in neck sonography Demonstrate the importance of ultrasound
Diagnostic Ultrasound. Sutiporn Khampunnip, M.D.
 Diagnostic Ultrasound Sutiporn Khampunnip, M.D. Definition of Ultrasound Ultrasound is simply sound waves, like audible sound. High-frequency sound and refers to mechanical vibrations above 20 khz. Human
Diagnostic Ultrasound Sutiporn Khampunnip, M.D. Definition of Ultrasound Ultrasound is simply sound waves, like audible sound. High-frequency sound and refers to mechanical vibrations above 20 khz. Human
TG-128: Quality Assurance for Prostate Brachytherapy Ultrasound
 TG-128: Quality Assurance for Prostate Brachytherapy Ultrasound STEVEN SUTLIEF DOUG PFEIFFER (HEATHER PIERCE, WENGZHENG FENG, JIM KOFLER) AAPM ANNUAL MEETING 2010 Educational Objectives To describe the
TG-128: Quality Assurance for Prostate Brachytherapy Ultrasound STEVEN SUTLIEF DOUG PFEIFFER (HEATHER PIERCE, WENGZHENG FENG, JIM KOFLER) AAPM ANNUAL MEETING 2010 Educational Objectives To describe the
Point-of-Care Ultrasound: An Introduction
 Point-of-Care Ultrasound: An Introduction Delegation Teaching Package for Registered Respiratory Therapists and Anesthesia Assistants Developed by: Rob Bryan RRT, AA Edited by: Kelly Hassall RRT, FCSRT,
Point-of-Care Ultrasound: An Introduction Delegation Teaching Package for Registered Respiratory Therapists and Anesthesia Assistants Developed by: Rob Bryan RRT, AA Edited by: Kelly Hassall RRT, FCSRT,
ULTRASOUND GUIDED NERVE BLOCKS
 2 ULTRASOUND GUIDED NERVE BLOCKS Elizabeth Kwan, MD UCSF High Risk Emergency Medicine 2014 1 Instructors Kristin Berona Reza Danesh Sally Graglia Daniel Kievlan Starr Knight Allison Mulcahy Carmen Partida
2 ULTRASOUND GUIDED NERVE BLOCKS Elizabeth Kwan, MD UCSF High Risk Emergency Medicine 2014 1 Instructors Kristin Berona Reza Danesh Sally Graglia Daniel Kievlan Starr Knight Allison Mulcahy Carmen Partida
Chapter 2 Pitfalls in Musculoskeletal Ultrasound
 Chapter 2 Pitfalls in Musculoskeletal Ultrasound Violeta Maria Vlad MD, PhD Introduction Taking a good ultrasound (US) picture is an art. Interpreting it is a science. This is in fact everything US is
Chapter 2 Pitfalls in Musculoskeletal Ultrasound Violeta Maria Vlad MD, PhD Introduction Taking a good ultrasound (US) picture is an art. Interpreting it is a science. This is in fact everything US is
Ultrasound in Peripheral Nerve Interventions
 Ultrasound in Peripheral Nerve Interventions John L. Lin, M.D. Shepherd Center Assistant Clinical Professor Emory University, School of Medicine Outline Ultrasound basics Nerve blocks in physiatric setting
Ultrasound in Peripheral Nerve Interventions John L. Lin, M.D. Shepherd Center Assistant Clinical Professor Emory University, School of Medicine Outline Ultrasound basics Nerve blocks in physiatric setting
Ultrasound Principles cycle Frequency Wavelength Period Velocity
 ! Teresa S. Wu, MD, FACEP Director, EM Ultrasound Program & Fellowship Co-Director, Simulation Based Training Program & Fellowship Associate Program Director, EM Residency Program Maricopa Medical Center
! Teresa S. Wu, MD, FACEP Director, EM Ultrasound Program & Fellowship Co-Director, Simulation Based Training Program & Fellowship Associate Program Director, EM Residency Program Maricopa Medical Center
Candidate s instructions Look at this cross-section taken at the level of C5. Answer the following questions.
 Section 1 Anatomy Chapter 1. Trachea 1 Candidate s instructions Look at this cross-section taken at the level of C5. Answer the following questions. Pretracheal fascia 1 2 5 3 4 Questions 1. Label the
Section 1 Anatomy Chapter 1. Trachea 1 Candidate s instructions Look at this cross-section taken at the level of C5. Answer the following questions. Pretracheal fascia 1 2 5 3 4 Questions 1. Label the
Abdominal Ultrasound
 Abdominal Ultrasound Imaging Control Buttons Depth The organ imaged should take up 3/4 of the screen Frequency = Penetration Use high frequencies (harmonics) for fluid filled and superficial structures
Abdominal Ultrasound Imaging Control Buttons Depth The organ imaged should take up 3/4 of the screen Frequency = Penetration Use high frequencies (harmonics) for fluid filled and superficial structures
Ultrasound Knobology
 Ultrasound Knobology Raj Dasgupta MD, FACP, FCCP, FASSM Assistant Professor of Clinical Medicine Pulmonary / Critical Care / Sleep Medicine University of Southern California (USC) Objectives Physics of
Ultrasound Knobology Raj Dasgupta MD, FACP, FCCP, FASSM Assistant Professor of Clinical Medicine Pulmonary / Critical Care / Sleep Medicine University of Southern California (USC) Objectives Physics of
Sign up to receive ATOTW weekly -
 1 SUBCLAVIAN PERIVASCULAR BRACHIAL PLEXUS BLOCK ANAESTHESIA TUTORIAL OF THE WEEK 156 19 th OCTOBER 2009 Dr. Martin Herrick Department of Anaesthesia, Addenbrooke s Hospital, Cambridge, U.K. Correspondence
1 SUBCLAVIAN PERIVASCULAR BRACHIAL PLEXUS BLOCK ANAESTHESIA TUTORIAL OF THE WEEK 156 19 th OCTOBER 2009 Dr. Martin Herrick Department of Anaesthesia, Addenbrooke s Hospital, Cambridge, U.K. Correspondence
Physical Principles of Ultrasound
 Physical Principles of Ultrasound Grateful appreciation to Richard A. Lopchinsky, MD, FACS and Nancy H. Van Name, RDMS, RTR, and MarleneKattaron, RDMS 2000 UIC All Rights Reserved. Course Objectives Identify
Physical Principles of Ultrasound Grateful appreciation to Richard A. Lopchinsky, MD, FACS and Nancy H. Van Name, RDMS, RTR, and MarleneKattaron, RDMS 2000 UIC All Rights Reserved. Course Objectives Identify
Focused Assessment Sonography of Trauma (FAST) Scanning Protocol
 Focused Assessment Sonography of Trauma (FAST) Scanning Protocol Romolo Gaspari CHAPTER 3 GOAL OF THE FAST EXAM Demonstrate free fluid in abdomen, pleural space, or pericardial space. EMERGENCY ULTRASOUND
Focused Assessment Sonography of Trauma (FAST) Scanning Protocol Romolo Gaspari CHAPTER 3 GOAL OF THE FAST EXAM Demonstrate free fluid in abdomen, pleural space, or pericardial space. EMERGENCY ULTRASOUND
Needle tip visualization during ultrasound-guided vascular access: short-axis vs long-axis approach
 American Journal of Emergency Medicine (2010) 28, 343 347 www.elsevier.com/locate/ajem Brief Report Needle tip visualization during ultrasound-guided vascular access: short-axis vs long-axis approach Michael
American Journal of Emergency Medicine (2010) 28, 343 347 www.elsevier.com/locate/ajem Brief Report Needle tip visualization during ultrasound-guided vascular access: short-axis vs long-axis approach Michael
What is Ultrasound? What is Ultrasound? B A. Basic Principles of Ultrasound. Basic Principles of Ultrasound. Basic Principles of Ultrasound
 Introduction to Ultrasound Principles Mani Montazemi, RDMS Baylor College of Medicine Division of Maternal-Fetal Medicine Department of Obstetrics and Gynecology Manager, Maternal Fetal Center Imaging
Introduction to Ultrasound Principles Mani Montazemi, RDMS Baylor College of Medicine Division of Maternal-Fetal Medicine Department of Obstetrics and Gynecology Manager, Maternal Fetal Center Imaging
Ultrasound User Demonstration
 Ultrasound User Demonstration Disclaimer: This presentation is intended to be used as a demonstration educational device to showcase Terumo products. It is NOT intended to be used as a diagnostic device
Ultrasound User Demonstration Disclaimer: This presentation is intended to be used as a demonstration educational device to showcase Terumo products. It is NOT intended to be used as a diagnostic device
Ultrasound in Anesthesia: Applying Scientific Principles to Clinical Practice
 AANA Journal Course Update for Nurse Anesthetists 3 6 CE Credits* Ultrasound in Anesthesia: Applying Scientific Principles to Clinical Practice Christian R. Falyar, CRNA, DNAP The use of ultrasound as
AANA Journal Course Update for Nurse Anesthetists 3 6 CE Credits* Ultrasound in Anesthesia: Applying Scientific Principles to Clinical Practice Christian R. Falyar, CRNA, DNAP The use of ultrasound as
CONTENTS. Test Number cpd Tanya Reynolds (Nat. Dip. Diag. Rad., B. Tech. Diag. Rad., B. Tech. Ultrasound)
 CONTENTS page 1-15 page 16 BASIC 2-DIMENSIONAL ULTRASOUND PRINCIPLES Multiple Choice Test Test Number cpd 41640 Tanya Reynolds (Nat. Dip. Diag. Rad., B. Tech. Diag. Rad., B. Tech. Ultrasound) Tanya is
CONTENTS page 1-15 page 16 BASIC 2-DIMENSIONAL ULTRASOUND PRINCIPLES Multiple Choice Test Test Number cpd 41640 Tanya Reynolds (Nat. Dip. Diag. Rad., B. Tech. Diag. Rad., B. Tech. Ultrasound) Tanya is
Carotid Doppler: Doppler wave forms obtained from the common, external and internal carotid arteries. As well as the vertebral and subclavian
 Competency Carotid Doppler: Doppler wave forms obtained from the common, external and internal carotid arteries. As well as the vertebral and subclavian arteries. Preferred angle is 60 degrees or less.
Competency Carotid Doppler: Doppler wave forms obtained from the common, external and internal carotid arteries. As well as the vertebral and subclavian arteries. Preferred angle is 60 degrees or less.
High resolution ultrasound scanner for skin imaging
 High resolution ultrasound scanner for skin imaging Christine Turlat Sales Director Atys medical 17 Parc d Arbora 69510 SOUCIEU EN JARREST Atys company Principle of ultrasound imaging DERMCUP Normal image
High resolution ultrasound scanner for skin imaging Christine Turlat Sales Director Atys medical 17 Parc d Arbora 69510 SOUCIEU EN JARREST Atys company Principle of ultrasound imaging DERMCUP Normal image
Central Venous Line Insertion
 Central Venous Line Insertion Understand the indications and risks of CVC insertion Understand and troubleshoot the seldinger technique Understand available sites and select the appropriate site for clinical
Central Venous Line Insertion Understand the indications and risks of CVC insertion Understand and troubleshoot the seldinger technique Understand available sites and select the appropriate site for clinical
ULTRASOUND IMAGING EE 472 F2018. Prof. Yasser Mostafa Kadah
 ULTRASOUND IMAGING EE 472 F2018 Prof. Yasser Mostafa Kadah www.k-space.org Recommended Textbook Diagnostic Ultrasound: Physics and Equipment, 2nd ed., by Peter R. Hoskins (Editor), Kevin Martin (Editor),
ULTRASOUND IMAGING EE 472 F2018 Prof. Yasser Mostafa Kadah www.k-space.org Recommended Textbook Diagnostic Ultrasound: Physics and Equipment, 2nd ed., by Peter R. Hoskins (Editor), Kevin Martin (Editor),
Background & Indications Probe Selection
 Teresa S. Wu, MD, FACEP Director, EM Ultrasound Program & Fellowship Co-Director, Simulation Based Training Program & Fellowship Associate Program Director, EM Residency Program Maricopa Medical Center
Teresa S. Wu, MD, FACEP Director, EM Ultrasound Program & Fellowship Co-Director, Simulation Based Training Program & Fellowship Associate Program Director, EM Residency Program Maricopa Medical Center
AIUM Practice Parameter for the Use of Ultrasound to Guide Vascular Access Procedures
 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 37 38 39 40 AIUM Practice Parameter for the Use of Ultrasound to Guide Vascular Access Procedures Parameter
1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 37 38 39 40 AIUM Practice Parameter for the Use of Ultrasound to Guide Vascular Access Procedures Parameter
Musculoskeletal Ultrasound: Basics, Utility, and Clinical Applications
 Musculoskeletal Ultrasound: Basics, Utility, and Clinical Applications Andrew Lavigne, MD, FRCPC Physical Medicine and Rehabilitation CSCN Diplomat (EMG) Dip Sport Medicine Eugene Maida, MD, PGY-4 Resident
Musculoskeletal Ultrasound: Basics, Utility, and Clinical Applications Andrew Lavigne, MD, FRCPC Physical Medicine and Rehabilitation CSCN Diplomat (EMG) Dip Sport Medicine Eugene Maida, MD, PGY-4 Resident
Dr. prakruthi Dept. of anaesthesiology, Rrmch, bangalore
 CENTRAL VENOUS CATHETERIZATION Dr. prakruthi Dept. of anaesthesiology, Rrmch, bangalore OBJECTIVES Introduction Indications and Contraindications Complications Technique Basic principles Specifics by Site
CENTRAL VENOUS CATHETERIZATION Dr. prakruthi Dept. of anaesthesiology, Rrmch, bangalore OBJECTIVES Introduction Indications and Contraindications Complications Technique Basic principles Specifics by Site
Carotid Abnormalities Coils, Kinks and Tortuosity David Lorelli M.D., RVT, FACS Michigan Vascular Association Conference Saturday, October 20, 2012
 Carotid Abnormalities Coils, Kinks and Tortuosity David Lorelli M.D., RVT, FACS Michigan Vascular Association Conference Saturday, October 20, 2012 Page 1 Table of Contents Carotid Anatomy Carotid Duplex
Carotid Abnormalities Coils, Kinks and Tortuosity David Lorelli M.D., RVT, FACS Michigan Vascular Association Conference Saturday, October 20, 2012 Page 1 Table of Contents Carotid Anatomy Carotid Duplex
Sterile Technique & IJ/Femoral Return Demonstration
 Sterile Technique & IJ/Femoral Return Demonstration Sterile Technique Description: This is a return demonstration checklist used to evaluate participants in the simulated hands on skills portions for certification
Sterile Technique & IJ/Femoral Return Demonstration Sterile Technique Description: This is a return demonstration checklist used to evaluate participants in the simulated hands on skills portions for certification
Underwater Acoustic Measurements in Megahertz Frequency Range.
 Underwater Acoustic Measurements in Megahertz Frequency Range. Current State and Prospects of Development in Russia Alexander M. Enyakov,, Many medical applications of underwater acoustic measurements
Underwater Acoustic Measurements in Megahertz Frequency Range. Current State and Prospects of Development in Russia Alexander M. Enyakov,, Many medical applications of underwater acoustic measurements
Regional Anaesthesia
 Regional Anaesthesia Basic Sciences Anaesthetic Course Dr Vassilis ATHANASSOGLOU FRCA Consultant Anaesthetist and Lecturer in Medicine Oxford University Hospitals NHS Trust, UK Geneva, 5th June 2017 Faculty
Regional Anaesthesia Basic Sciences Anaesthetic Course Dr Vassilis ATHANASSOGLOU FRCA Consultant Anaesthetist and Lecturer in Medicine Oxford University Hospitals NHS Trust, UK Geneva, 5th June 2017 Faculty
ULTRASOUND NOMENCLATURE
 Chapter 1: Ultrasound Nomenclature, Image Orientation, and Basic Instrumentation CYNTHIA SIKOWSKI Ultrasound waves are sound waves that have a frequency exceeding 20,000 Hz. When sound waves are transmitted
Chapter 1: Ultrasound Nomenclature, Image Orientation, and Basic Instrumentation CYNTHIA SIKOWSKI Ultrasound waves are sound waves that have a frequency exceeding 20,000 Hz. When sound waves are transmitted
Neck Ultrasound. Faculty Info: Amy Kule, MD
 Neck Ultrasound Date: Friday, October 19, 2018 Time: 11:00 AM Location: SMALL GROUP LABORATORY SSOM L71 Watch: Ø Neck Ultrasound Scanning Protocol (4:00): https://www.youtube.com/watch?v=zozd2x2ll4q Faculty
Neck Ultrasound Date: Friday, October 19, 2018 Time: 11:00 AM Location: SMALL GROUP LABORATORY SSOM L71 Watch: Ø Neck Ultrasound Scanning Protocol (4:00): https://www.youtube.com/watch?v=zozd2x2ll4q Faculty
Guide to Small Animal Vascular Imaging using the Vevo 770 Micro-Ultrasound System
 Guide to Small Animal Vascular Imaging using the Vevo 770 Micro-Ultrasound System January 2007 Objectives: After completion of this module, the participant will be able to accomplish the following: Understand
Guide to Small Animal Vascular Imaging using the Vevo 770 Micro-Ultrasound System January 2007 Objectives: After completion of this module, the participant will be able to accomplish the following: Understand
The Upper Limb III. The Brachial Plexus. Anatomy RHS 241 Lecture 12 Dr. Einas Al-Eisa
 The Upper Limb III The Brachial Plexus Anatomy RHS 241 Lecture 12 Dr. Einas Al-Eisa Brachial plexus Network of nerves supplying the upper limb Compression of the plexus results in motor & sensory changes
The Upper Limb III The Brachial Plexus Anatomy RHS 241 Lecture 12 Dr. Einas Al-Eisa Brachial plexus Network of nerves supplying the upper limb Compression of the plexus results in motor & sensory changes
Ultrasound Guided Regional Nerve Blocks
 Ultrasound Guided Regional Nerve Blocks In the country of the blind the one eyed man is King -Deciderius Erasmus (1466-1536) Objectives Benefits of Regional Anesthesia Benefits of US guidance Role of ultrasound
Ultrasound Guided Regional Nerve Blocks In the country of the blind the one eyed man is King -Deciderius Erasmus (1466-1536) Objectives Benefits of Regional Anesthesia Benefits of US guidance Role of ultrasound
ULTRASOUND. OB/Gyn (Core) Ultrasound PIEZOELECTRIC EFFECT. Principles of Ultrasound Physics and Instrumentation. Nathan Pinkney, BS, CDOS
 1 OB/Gyn (Core) Ultrasound Principles of Ultrasound Physics and Instrumentation Nathan Pinkney, BS, CDOS Philadelphia College of Osteopathic Medicine 2016 ULTRASOUND CATEGORIES OF SOUND INFRASOUND = below
1 OB/Gyn (Core) Ultrasound Principles of Ultrasound Physics and Instrumentation Nathan Pinkney, BS, CDOS Philadelphia College of Osteopathic Medicine 2016 ULTRASOUND CATEGORIES OF SOUND INFRASOUND = below
Surface Anatomy and Sonoanatomy for the Occasional Regional Anesthesiologist
 Surface Anatomy and Sonoanatomy for the Occasional Regional Anesthesiologist Edward R. Mariano, M.D., M.A.S. Professor of Anesthesiology, Perioperative & Pain Medicine Stanford University School of Medicine
Surface Anatomy and Sonoanatomy for the Occasional Regional Anesthesiologist Edward R. Mariano, M.D., M.A.S. Professor of Anesthesiology, Perioperative & Pain Medicine Stanford University School of Medicine
Diploma of Medical Ultrasonography (DMU) Physical Principles of Ultrasound and Instrumentation Syllabus
 Diploma of Medical Ultrasonography (DMU) Physical Principles of Ultrasound and Instrumentation Syllabus Page 1 of 7 11/18 Candidates are expected to cover all of the content of this syllabus when preparing
Diploma of Medical Ultrasonography (DMU) Physical Principles of Ultrasound and Instrumentation Syllabus Page 1 of 7 11/18 Candidates are expected to cover all of the content of this syllabus when preparing
Ultrasound Guided Vascular Access. 7/25/2016
 Ultrasound Guided Vascular Access 7/25/2016 www.ezono.com 1 Objectives Indications for insertion of central and peripheral lines Complications associated with procedures Role of ultrasound in vascular
Ultrasound Guided Vascular Access 7/25/2016 www.ezono.com 1 Objectives Indications for insertion of central and peripheral lines Complications associated with procedures Role of ultrasound in vascular
Arterial Line Insertion Pre Reading
 PROCEDURE ACCREDITATION THE CANBERRA HOSPITAL EMERGENCY DEPARTMENT Arterial Line Insertion Pre Reading Indications Requirement for continuous blood pressure monitoring (all patients on pressors, inotropes,
PROCEDURE ACCREDITATION THE CANBERRA HOSPITAL EMERGENCY DEPARTMENT Arterial Line Insertion Pre Reading Indications Requirement for continuous blood pressure monitoring (all patients on pressors, inotropes,
Flaw Assessment Using Shear wave Phased array Ultrasonic Transducer
 18th World Conference on Nondestructive Testing, 16-20 April 2012, Durban, South Africa Flaw Assessment Using Shear wave Phased array Ultrasonic Transducer Byungsik YOON AUTHOR 1, Hee-Jong LEE CO-AUTHOR
18th World Conference on Nondestructive Testing, 16-20 April 2012, Durban, South Africa Flaw Assessment Using Shear wave Phased array Ultrasonic Transducer Byungsik YOON AUTHOR 1, Hee-Jong LEE CO-AUTHOR
Levels of the anatomical cuts of the upper extremity RADIUS AND ULNA right
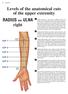 11 CHAPTER 2 Levels of the anatomical cuts of the upper extremity AND right CUT 1 CUT 4 1 2 3 4 5 6 Isolated fixation of the radius is difficult at this level because of the anterolateral vessels and the
11 CHAPTER 2 Levels of the anatomical cuts of the upper extremity AND right CUT 1 CUT 4 1 2 3 4 5 6 Isolated fixation of the radius is difficult at this level because of the anterolateral vessels and the
Ultrasound Applied Physics
 Ultrasound Applied Physics University of Toronto Department of Medical Imaging Applied Physics Mini-Course #3 2016 Ultrasound Laboratory Manual and Examination Booklet 1/21/2016 Ultrasound Applied Physics
Ultrasound Applied Physics University of Toronto Department of Medical Imaging Applied Physics Mini-Course #3 2016 Ultrasound Laboratory Manual and Examination Booklet 1/21/2016 Ultrasound Applied Physics
The Shoulder. Systematically scanning the shoulder provides extremely useful diagnostic information. The Shoulder
 1 ! The most ACCESSIBLE to sonographic exam! The most MOBILE and VULNERABLE extremity AND Systematically scanning the shoulder provides extremely useful diagnostic information! The Goal for this section
1 ! The most ACCESSIBLE to sonographic exam! The most MOBILE and VULNERABLE extremity AND Systematically scanning the shoulder provides extremely useful diagnostic information! The Goal for this section
Lesson 07: Ultrasound Transducers. This lesson contains 73 slides plus 16 multiple-choice questions.
 Lesson 07: Ultrasound Transducers This lesson contains 73 slides plus 16 multiple-choice questions. This lesson was derived from pages 33 through 42 in the textbook: Ultrasound Transducers Ultrasound Transducers
Lesson 07: Ultrasound Transducers This lesson contains 73 slides plus 16 multiple-choice questions. This lesson was derived from pages 33 through 42 in the textbook: Ultrasound Transducers Ultrasound Transducers
E-Cath according to Tsui
 E-Cath according to Tsui The revolutionary technique for continuous peripheral nerve blocks Nerve blocks Simple, safe, quick 1 Continuous peripheral regional anaesthesia with E-Cath E-Cath, a joint development
E-Cath according to Tsui The revolutionary technique for continuous peripheral nerve blocks Nerve blocks Simple, safe, quick 1 Continuous peripheral regional anaesthesia with E-Cath E-Cath, a joint development
Table of contents. Foreword. Preface. 1 Introduction Historical Perspective 00
 Table of contents Foreword Preface 1 Introduction 00 1.1 Historical Perspective 00 2 Fundamentals of musculoskeletal ultrasound 00 2.1 Frequency and wavelength 00 2.2 Generating ultrasound waves 00 2.3
Table of contents Foreword Preface 1 Introduction 00 1.1 Historical Perspective 00 2 Fundamentals of musculoskeletal ultrasound 00 2.1 Frequency and wavelength 00 2.2 Generating ultrasound waves 00 2.3
Knobology for Dummies
 Knobology for Dummies Power On/Off Preset button Patient Information Entry Choose preset Transducer probes Connect and disconnect transducer Approach to the patient (machine placement, comfort, draping,
Knobology for Dummies Power On/Off Preset button Patient Information Entry Choose preset Transducer probes Connect and disconnect transducer Approach to the patient (machine placement, comfort, draping,
Chest Ultrasound: Pneumothorax
 WINFOCUS BASIC ECHO (WBE) Chest Ultrasound: Pneumothorax Mark Hamlin, MD, MS Associate Professor of Anesthesiology and Surgery University of Vermont College of Medicine Co-Director of Surgical Critical
WINFOCUS BASIC ECHO (WBE) Chest Ultrasound: Pneumothorax Mark Hamlin, MD, MS Associate Professor of Anesthesiology and Surgery University of Vermont College of Medicine Co-Director of Surgical Critical
Regional Anaesthesia of the Thoracic Limb
 Regional Anaesthesia of the Thoracic Limb Trauma and inflammation cause sensitization of the peripheral nervous system and the subsequent barrage of nociceptive input (usually by surgery) produces sensitization
Regional Anaesthesia of the Thoracic Limb Trauma and inflammation cause sensitization of the peripheral nervous system and the subsequent barrage of nociceptive input (usually by surgery) produces sensitization
BEDSIDE ULTRASOUND BEDSIDE ULTRASOUND. Deep Vein Thrombosis. Probe used
 BEDSIDE ULTRASOUND Part 2 Diagnosis of deep vein thrombosis Kishore Kumar Pichamuthu, Professor, Department of Critical Care, CMC, Vellore Summary: Deep vein thrombosis (DVT) is a problem encountered in
BEDSIDE ULTRASOUND Part 2 Diagnosis of deep vein thrombosis Kishore Kumar Pichamuthu, Professor, Department of Critical Care, CMC, Vellore Summary: Deep vein thrombosis (DVT) is a problem encountered in
High-resolution ultrasound of the elbow - didactic approach.
 High-resolution ultrasound of the elbow - didactic approach. Poster No.: C-2358 Congress: ECR 2014 Type: Educational Exhibit Authors: C. M. Olchowy, M. Lasecki, U. Zaleska-Dorobisz; Wroclaw/PL Keywords:
High-resolution ultrasound of the elbow - didactic approach. Poster No.: C-2358 Congress: ECR 2014 Type: Educational Exhibit Authors: C. M. Olchowy, M. Lasecki, U. Zaleska-Dorobisz; Wroclaw/PL Keywords:
Introduction to Musculoskeletal Ultrasound. Disclosures. Evidence Based Medicine Key References 8/30/2017
 Introduction to Musculoskeletal Ultrasound Johannes Roth MD, PhD, FRCPC, RhMSUS Professor of Pediatrics University of Ottawa Gurjit S Kaeley MBBS, MRCP, RhMSUS Professor of Medicine Division Chief Director
Introduction to Musculoskeletal Ultrasound Johannes Roth MD, PhD, FRCPC, RhMSUS Professor of Pediatrics University of Ottawa Gurjit S Kaeley MBBS, MRCP, RhMSUS Professor of Medicine Division Chief Director
Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi
 Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi For the purpose of anatomical description the neck is sub divided into two major triangles, the Anterior and the Posterior by muscle bellies
Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi For the purpose of anatomical description the neck is sub divided into two major triangles, the Anterior and the Posterior by muscle bellies
Fascia Iliaca Compartment Block for Proximal Femur Fracture in the Emergency Department
 IAEM Clinical Guideline Fascia Iliaca Compartment Block for Proximal Femur Fracture in the Emergency Department Version 1 November 2018 Author: Ronan Murphy Guideline lead: Dr Vicky Meighan, in collaboration
IAEM Clinical Guideline Fascia Iliaca Compartment Block for Proximal Femur Fracture in the Emergency Department Version 1 November 2018 Author: Ronan Murphy Guideline lead: Dr Vicky Meighan, in collaboration
Abdominal Ultrasound : Aorta, Kidneys, Bladder
 Abdominal Ultrasound : Aorta, Kidneys, Bladder Nilam J. Soni, MD, MSc Associate Professor of Medicine Divisions of Hospital Medicine and Pulmonary/Critical Care Medicine Department of Medicine University
Abdominal Ultrasound : Aorta, Kidneys, Bladder Nilam J. Soni, MD, MSc Associate Professor of Medicine Divisions of Hospital Medicine and Pulmonary/Critical Care Medicine Department of Medicine University
This appendix was part of the submitted manuscript and has been peer reviewed. It is posted as supplied by the authors.
 This appendix was part of the submitted manuscript and has been peer reviewed. It is posted as supplied by the authors. - Figure S1: The four quadrant approach lung ultrasound at the bedside. * The anterolateral
This appendix was part of the submitted manuscript and has been peer reviewed. It is posted as supplied by the authors. - Figure S1: The four quadrant approach lung ultrasound at the bedside. * The anterolateral
Bony Thorax. Anatomy and Procedures of the Bony Thorax Edited by M. Rhodes
 Bony Thorax Anatomy and Procedures of the Bony Thorax 10-526-191 Edited by M. Rhodes Anatomy Review Bony Thorax Formed by Sternum 12 pairs of ribs 12 thoracic vertebrae Conical in shape Narrow at top Posterior
Bony Thorax Anatomy and Procedures of the Bony Thorax 10-526-191 Edited by M. Rhodes Anatomy Review Bony Thorax Formed by Sternum 12 pairs of ribs 12 thoracic vertebrae Conical in shape Narrow at top Posterior
Ultrasound-guided Sciatic Nerve Blocks: Higher and Popliteal Approaches
 10.5005/jp-journals-10027-1026 K Kondov, S Fransis REVIEW ARTICLE Ultrasound-guided Sciatic Nerve Blocks: Higher and Popliteal Approaches K Kondov, S Fransis ABSTRACT Background and objective: In modern
10.5005/jp-journals-10027-1026 K Kondov, S Fransis REVIEW ARTICLE Ultrasound-guided Sciatic Nerve Blocks: Higher and Popliteal Approaches K Kondov, S Fransis ABSTRACT Background and objective: In modern
Chapter 14. Imaging Artifacts
 Chapter 14 Image Artifacts The complex physical interactions that occur between an ultrasound beam and human anatomy and the intricate and sophisticated technological components of a sonographic imaging
Chapter 14 Image Artifacts The complex physical interactions that occur between an ultrasound beam and human anatomy and the intricate and sophisticated technological components of a sonographic imaging
Surgery Under Regional Anesthesia
 Surgery Under Regional Anesthesia Jean Daniel Eloy, MD Assistant Professor Residency Program Director Rutgers-New Jersey Medical School Rutgers The State University of New Jersey Peripheral Nerve Block
Surgery Under Regional Anesthesia Jean Daniel Eloy, MD Assistant Professor Residency Program Director Rutgers-New Jersey Medical School Rutgers The State University of New Jersey Peripheral Nerve Block
NEW PRODUCT INSIDE. E-Cath/E-Cath Plus. Echogenic Catheter over Needle CNB System. Nerve Blocks
 E-Cath/E-Cath Plus NEW PRODUCT INSIDE Nerve Blocks The Nerve Block Catheter Challenge Is your traditional catheter system giving you headaches? LEAKAGE MISSING 3RD HAND DIFFICULT TO PLACE DISLOCATION TOO
E-Cath/E-Cath Plus NEW PRODUCT INSIDE Nerve Blocks The Nerve Block Catheter Challenge Is your traditional catheter system giving you headaches? LEAKAGE MISSING 3RD HAND DIFFICULT TO PLACE DISLOCATION TOO
FHS Appendicitis US Protocol
 FHS Appendicitis US Protocol Reviewed By: Shireen Khan, MD; Sarah Farley, MD; Anna Ellermeier, MD Last Reviewed: May 2018 Contact: (866) 761-4200 **NOTE for all examinations: 1. If documenting possible
FHS Appendicitis US Protocol Reviewed By: Shireen Khan, MD; Sarah Farley, MD; Anna Ellermeier, MD Last Reviewed: May 2018 Contact: (866) 761-4200 **NOTE for all examinations: 1. If documenting possible
Muscle-Tendon Mechanics Dr. Ted Milner (KIN 416)
 Muscle-Tendon Mechanics Dr. Ted Milner (KIN 416) Muscle Fiber Geometry Muscle fibers are linked together by collagenous connective tissue. Endomysium surrounds individual fibers, perimysium collects bundles
Muscle-Tendon Mechanics Dr. Ted Milner (KIN 416) Muscle Fiber Geometry Muscle fibers are linked together by collagenous connective tissue. Endomysium surrounds individual fibers, perimysium collects bundles
My Patient Has Abdominal Pain PoCUS of the Biliary Tract and the Urinary Tract
 My Patient Has Abdominal Pain PoCUS of the Biliary Tract and the Urinary Tract Objectives PoCUS for Biliary Disease PoCUS for Renal Colic PoCUS for Urinary Retention Biliary Disease A patient presents
My Patient Has Abdominal Pain PoCUS of the Biliary Tract and the Urinary Tract Objectives PoCUS for Biliary Disease PoCUS for Renal Colic PoCUS for Urinary Retention Biliary Disease A patient presents
