May 2017 Imaging Case of the Month. Prasad M. Panse, MD and Michael B. Gotway, MD. Department of Radiology Mayo Clinic Arizona Scottsdale, Arizona USA
|
|
|
- Meagan Evans
- 5 years ago
- Views:
Transcription
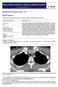
1 May 2017 Imaging Case of the Month Prasad M. Panse, MD and Michael B. Gotway, MD Department of Radiology Mayo Clinic Arizona Scottsdale, Arizona USA Clinical History: A 32-year-old man presented for routine physical examination. His past medical history is unremarkable and the physical examination and basic laboratory data were within normal limits. A frontal chest radiograph (Figure 1) was performed. Figure 1: Frontal (A) and lateral (B) chest radiography. Which of the following statements regarding the chest radiograph is most accurate? 1. The frontal chest radiograph shows an abnormal mediastinal contour 2. The frontal chest radiograph shows basal predominant fibrotic abnormalities 3. The frontal chest radiograph shows large lung volumes with a cystic appearance 4. The frontal chest radiograph shows multifocal small pulmonary nodules 5. The frontal chest radiograph shows no abnormal findings Southwest Journal of Pulmonary and Critical Care/2017/Volume
2 1. The frontal chest radiograph shows an abnormal mediastinal contour The frontal chest radiograph shows normal lung volumes and clear lungs; no pleural abnormality is present. There is no evidence of cystic lung disease or basal fibrotic abnormalities. An abnormal mediastinal contour is present on both the frontal and lateral chest radiographic projections (Figure 2). Figure 2. Frontal (A) and lateral (B) chest radiography shows an abnormal mediastinal contour creating a convex bulge in the ayzgoesophageal recess (arrows, A). The abnormal mediastinal contour is clearly visible in the infrahilar window region on the lateral chest radiograph (arrows, B). Regarding the frontal chest radiograph (Figure 1) abnormality, which of the following statements regarding the chest radiograph is most accurate? 1. The abnormal mediastinal contour affects the aorto-pulmonary window 2. The abnormal mediastinal contour affects the ayzgoesophageal recess 3. The abnormal mediastinal contour affects the pre-aortic space 4. The abnormal mediastinal contour affects the right para-aortic stripe 5. The abnormal mediastinal contour affects the right paratracheal stripe Southwest Journal of Pulmonary and Critical Care/2017/Volume
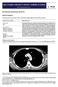
3 2. The abnormal mediastinal contour affects the ayzgoesophageal recess The frontal chest radiograph (Figure 1A) shows an abnormal mediastinal contour bulge that causes an outward convexity of along the mid-portion of the ayzgoesophageal recess. Normally the ayzgoesophageal recess is a mediastinal interface created by contact of the medial right lung with the right mediastinum extending cranially from the arch of the azygos vein caudally to the diaphragm. The mediastinum in this location typically contains the azygos vein, esophagus, small lymph nodes, and mediastinal fat, the former two contributing to the name of the ayzgoesophageal recess, with the azygos vein (and pleural covering the thoracic spine) often creating the posterior border, and the esophagus the medial border, of the ayzgoesophageal recess, although the anatomy may vary substantially from patient to patient. Typically the ayzgoesophageal recess describes a concave configuration with the adjacent right lung, or often a gentle S -shaped curve may be seen (Figure 3). Figure 3. Frontal chest radiographs in 2 separate patients showing the normal interface created between the medial right lung and the medial right mediastinal region, referred to as the ayzgoesophageal recess. In these patients, the ayzgoesophageal recess describes a gentle, S -shaped curve. Abnormalities of the ayzgoesophageal recess present as outward, convex bulges of this line, which may be noticeably focal in some circumstances. The right paratracheal stripe and right para-aortic stripe both appear normal in this patient. The aortopulmonary window and pre-aortic spaces also both appear normal and both are leftsided structures. Which of the following is the most appropriate next management step for this patient? FDG PET scan 2. Contrast enhanced thoracic CT 3. Echocardiography 4. Lateral decubitus chest radiography 5. Ventilation perfusion scintigraphy Southwest Journal of Pulmonary and Critical Care/2017/Volume
4 2. Contrast enhanced thoracic CT Contrast-enhanced thoracic CT is the most appropriate selection among the choices listed above. The injection of intravenous contrast, as opposed to an unenhanced thoracic CT, is generally preferred when the indication for thoracic CT is for evaluation of a mediastinal mass. Intravenous contrast is essential if the mass due to vascular abnormality, and when masses do not arise from vascular structures, intravenous contrast is nevertheless still very useful because intravenous contrast administration allows for optimal assessment of the relation of the mass to surrounding vascular structures, which is important both for pre-operative assessment and determining the biologic behavior of the lesion. 18 FDG PET scan could prove useful for evaluation of the mass, but generally 18 FDG PET scan is most rewarding when obtained for further characterization of indeterminate findings at thoracic CT, rather than immediately following chest radiography. Lateral decubitus chest radiography is useful for assessment of possible pleural effusion (for evaluation of the dependent thorax), or for assessment of pneumothorax (when attention is focused on the non-dependent thorax); neither situations are relevant here. Ventilation perfusion scintigraphy is most commonly employed for the assessment of acute or chronic thromboembolic disease, or occasionally for determination of differential pulmonary perfusion prior to thoracic surgery or for assessment of systemic shunting; none of these conditions are relevant to this outpatient with an incidentally detected, incompletely evaluated mediastinal mass. Echocardiography could potentially visualize the lesion and provide some characterization of the mediastinal mass, but it is likely that this lesion resides outside the heart and would not be the focus of an echocardiogram and probably would be incompletely visualized. The patient subsequently underwent unenhanced thoracic CT (Figure 4). Figure 4. Representative images from unenhanced axial (A-F) and sagittal (G-H) CT. Southwest Journal of Pulmonary and Critical Care/2017/Volume
5 Regarding this examination, which of the following is correct? 1. The thoracic CT shows a destructive chest wall mass 2. The thoracic CT shows a mass arising from the pleura 3. The thoracic CT shows a mildly hyperattenuating mass in the subcarinal region extending inferiorly into the azygoesophageal recess 4. The thoracic CT shows enlargement of the right pulmonary artery 5. The thoracic CT shows multifocal mediastinal and peribronchial lymph node enlargement Southwest Journal of Pulmonary and Critical Care/2017/Volume
6 6. The thoracic CT shows a mildly hyperattenuating mass in the subcarinal region extending inferiorly into the azygoesophageal recess The thoracic CT shows normal pleural surfaces and the chest wall appears normal; no evidence of bone destruction or chest wall mass is present. A mediastinal mass, representing the lesion seen at chest radiography, is present, located in the subcarinal region. There is no evidence of either peribronchial or mediastinal lymph node enlargement outside the subcarinal region. The right pulmonary artery is normal in size, but is displaced laterally by the azygoesophageal mass. The thoracic CT was inadvertently protocoled as an unenhanced examination, and therefore characterization of the lesion was incomplete. Attenuation measurements of the lesion shows that the lesion ranged in density from HU, which is consistent with complex fluid within a cyst, but could potentially be seen with a solid mass (Figure 5). Figure 5. Axial unenhanced (A) and enhanced (B) thoracic CT in a patient with esophageal leiomyoma shows a lesion just posterior to the carina that is mildly hyperattenuating on the unenhanced image (A); attenuation coefficients measured about 45 HU. Following contrast administration (B), the lesion shows enhancement, confirming its solid nature. Axial enhanced image in a different patient (C) with surgically-proven esophageal leiomyoma shows a homogeneous mass that measures only 52 HU following intravenous contrast administration; a previous unenhanced study (not shown) revealed that this lesion measured about 32 HU prior to intravenous contrast administration. These cases underscore the need for unenhanced and enhanced imaging for proper characterization of some mediastinal masses. Southwest Journal of Pulmonary and Critical Care/2017/Volume
7 Which of the following is the most appropriate next step for the management of this patient? FDG PET scan 2. Endoscopic ultrasound with biopsy 3. Follow up enhanced thoracic CT in 3 months 4. Repeat unenhanced and enhanced thoracic CT 5. Unenhanced and enhanced thoracic MR Southwest Journal of Pulmonary and Critical Care/2017/Volume
8 5. Unenhanced and enhanced thoracic MR Unenhanced and enhanced imaging is integral to characterization of a number of mediastinal lesions, particularly mediastinal cysts, which are among the more common causes of mediastinal masses, particularly when incidentally detected in younger patients. In this patient, unenhanced followed by enhanced MR provides the unique ability to characterize this lesion without the use of ionizing radiation, and therefore obviates the need for repeat unenhanced and enhanced thoracic CT. 18 FDG PET scan could prove useful for evaluation of the mass, but the lesion should be further characterized with unenhanced and enhanced imaging without further exposure of this young patient to ionizing radiation. Follow up thoracic CT is occasionally useful for characterization of small, indeterminate pulmonary opacities, particularly when malignancy is considered, but would not play a reasonable role for the assessment of a nearly 6 cm mediastinal mass. Endoscopic ultrasound could prove useful for characterizing this lesion given its proximity to the esophagus (or using endobronchial ultrasound, given the proximity of the lesion to the tracheal carina), but biopsy should be avoided- if the lesion is indeed a cyst, endoscopy with biopsy could result in spillage of the cyst contents into the mediastinum and also runs the risk of introducing infection into a previously closed space. To further characterize the lesion discovered at CT scanning, the patient was underwent thoracic MR (Figure 6). Figure 6. Representative images from thoracic MRI. T1-weighted axial (A and B) and coronal (C) images. Axial T2-weighted imaging with fat saturation (a fluid-sensitive sequence; D and E). Axial unenhanced (F) and enhanced (G) gradient echo imaging. Southwest Journal of Pulmonary and Critical Care/2017/Volume
9 Which of the following regarding this MR examination is correct? 1. The thoracic MR reveals additional sites of abnormality, suggesting a systemic process 2. The thoracic MR shows that the lesion contains fat 3. The thoracic MR shows that the lesion does not enhance significantly 4. The thoracic MR shows that the lesion is solid 5. The thoracic MR shows the same mass at CT, but adds little additional information to that already available with CT Southwest Journal of Pulmonary and Critical Care/2017/Volume
10 3. The thoracic MR shows that the lesion does not enhance significantly The thoracic MR shows the same azygoesophageal recess mass seen at CT, but adds additional information regarding the azygoesophageal recess lesion s tissue components. The azygoesophageal recess lesion does show increased signal intensity on the T1-weighted images, which is common with fat [note the hyperintense signal of subcutaneous fat on these images]; however, the lesion continues to show hyperintense signal on T2-weighted MR sequencing employing fat saturation, indicating that the internal hyperintensity of the lesion is not due to fat (see Figures 6D and E). Fat saturation refers to MR techniques designed to eliminate signal from fat. When a lesion shows high signal on T1-weighted imaging, suggesting the possibility of intralesional fat, if that signal disappears when using fat-saturation techniques, then one can be relatively certain that the hyperintensity of the lesion on T1-weighted imaging is not due to the presence of intralesional fat; rather, the increased signal could be due to other causes of hyperattenuation on T1-weighted imaging, particularly hemorrhage or proteinaceous fluid. The increased signal on the fluid-sensitive images suggests the possibility of a cyst, but some solid lesions can display this behavior as well, so the lesion cannot be characterized as a cyst on this sequence alone. However, the images obtained before and after intravenous contrast administration, which show no evidence of enhancement, combined with the fluid signal on the fluid-sensitive T2-weighted sequences, are consistent with a cystic mediastinal lesion in the azygoesophageal recess l. The thoracic MR study shows no other sites of abnormality. Which of the following represents the next most appropriate step for the evaluation of this patient? FDG-PET Ga-citrate scintigraphy 3. Mediastinoscopy 4. Offer surgical excision 5. Percutaneous transthoracic fine needle aspiration biopsy Southwest Journal of Pulmonary and Critical Care/2017/Volume
11 4. Offer surgical excision The imaging features are consistent with a particular diagnosis, and invasive testing is not necessary. Therefore, percutaneous transthoracic fine needle aspiration biopsy and mediastinoscopy are not the correct answers. The risk of spillage of the cystic content during percutaneous transthoracic fine needle aspiration biopsy is unacceptably high whereas the likelihood of obtaining a histopathological diagnosis is low for this cystic, isolated, indolent-appearing, and incidentally detected lesion. The lesion may also be too caudally located in the subcarinal space to be reached via mediastinoscopy. While 18 FDG-PET could potentially be a useful procedure for the evaluation of mediastinal lesions, as it has the ability to assess for metabolic activity within the lesion as well as the ability to detect potential sites of disease elsewhere within and outside the thorax, the lesion has already been well-characterized by cross sectional imaging. The lack of tracer utilization within the lesion would simply reinforce the impression of a benign abnormality, whereas increased tracer utilization would most likely prompt incorrect consideration of an aggressive process for this lesion. 68 Ga-citrate scintigraphy would not provide addition useful information in this patient. Among the choices listed, offering surgical resection is reasonable. The lesion could be observed, given that the patient apparently is not exhibiting symptoms related to the presence of the lesion, but the sheer size of the lesion mandates some consideration for surgical resection. Based on the data thus far, which of the following represents the most likely diagnosis for this patient? 1. Bronchogenic / foregut duplication cyst 2. Isolated azygoesophageal recess metastasis 3. Müllerian duct (Hattori) cyst 4. Pericardial cyst 5. Thoracic duct cyst Southwest Journal of Pulmonary and Critical Care/2017/Volume
12 1. Bronchogenic / foregut duplication cyst As noted previously, the cross sectional imaging findings indicate an indolentappearing, incidentally discovered cyst in the ayzgoesophageal recess. Occasionally some malignancies, such as renal cell malignancies and squamous cell carcinomas, can occasionally appear necrotic, even cystic, and can manifest as isolated mediastinal lesions. However, this patient has no active or previous malignancy, and even prominently cystic or necrotic carcinoma metastases usually show some solid, enhancing areas; the latter are lacking in this patient. The lesion s location is unusual for pericardial cysts (typically anteriorly located in the right > left cardiophrenic angle), Müllerian duct (aka Hattori) cysts (typically posterior- superior mediastinum in women), and thoracic duct cysts (posterior mediastinum, connected to the thoracic duct). However, the lesion s location in the azygoesophageal recess, near the carina, is a common location for a bronchogenic / foregut duplication cyst, which also is the most common cause of a cystic middle mediastinal lesion. Further questioning disclosed that the patient had undergone a right thoracotomy (see Figure 1; note the thoracotomy defect manifesting as irregularity of the right posterior 6 th rib on the frontal radiograph) at least 8 years earlier for a right lung cyst, which was reportedly benign but incompletely resected due to close contact with the pericardium posteriorly, but no further information was available. Diagnosis: Bronchogenic cyst, recurrent, due to incomplete previous resection References 1. Shin KE, Yi CA, Kim TS, Lee HY, Choi YS, Kim HK, Kim J. Diffusion-weighted MRI for distinguishing non-neoplastic cysts from solid masses in the mediastinum: problem-solving in mediastinal masses of indeterminate internal characteristics on CT. Eur Radiol Mar;24(3): [CrossRef] [PubMed] 2. Jain A, Anand K, Singla S, Kumar A. Congenital cystic lung diseases. J Clin Imaging Sci Jan 30;3:5. [CrossRef] [PubMed] 3. Ballouhey Q, Galinier P, Abbo O, Andrieu G, Baunin C, Sartor A, Rittié JL, Léobon B. The surgical management and outcome of congenital mediastinal malformations. Interact Cardiovasc Thorac Surg Jun;14(6): [CrossRef] [PubMed] 4. Laberge JM, Puligandla P, Flageole H. Asymptomatic congenital lung malformations. Semin Pediatr Surg Feb;14(1): [CrossRef] [PubMed] 5. Berrocal T, Madrid C, Novo S, Gutiérrez J, Arjonilla A, Gómez-León N. Congenital anomalies of the tracheobronchial tree, lung, and mediastinum: embryology, radiology, and pathology. Radiographics Jan-Feb;24(1):e17. [CrossRef] [PubMed] Southwest Journal of Pulmonary and Critical Care/2017/Volume
September 2014 Imaging Case of the Month. Michael B. Gotway, MD. Department of Radiology Mayo Clinic Arizona Scottsdale, AZ
 September 2014 Imaging Case of the Month Michael B. Gotway, MD Department of Radiology Mayo Clinic Arizona Scottsdale, AZ Clinical History: A 57-year-old non-smoking woman presented to her physician as
September 2014 Imaging Case of the Month Michael B. Gotway, MD Department of Radiology Mayo Clinic Arizona Scottsdale, AZ Clinical History: A 57-year-old non-smoking woman presented to her physician as
Do you want to be an excellent Radiologist? - Focus on the thoracic aorta on lateral chest image!!!
 The lateral chest radiograph: Challenging area around the thoracic aorta!!! Do you want to be an excellent Radiologist? - Focus on the thoracic aorta on lateral chest image!!! Dong Yoon Han 1, So Youn
The lateral chest radiograph: Challenging area around the thoracic aorta!!! Do you want to be an excellent Radiologist? - Focus on the thoracic aorta on lateral chest image!!! Dong Yoon Han 1, So Youn
October 2012 Imaging Case of the Month. Michael B. Gotway, MD Associate Editor Imaging. Department of Radiology Mayo Clinic Arizona Scottsdale, AZ
 October 2012 Imaging Case of the Month Michael B. Gotway, MD Associate Editor Imaging Department of Radiology Mayo Clinic Arizona Scottsdale, AZ Clinical History: A 65-year-old non-smoking woman presented
October 2012 Imaging Case of the Month Michael B. Gotway, MD Associate Editor Imaging Department of Radiology Mayo Clinic Arizona Scottsdale, AZ Clinical History: A 65-year-old non-smoking woman presented
Basic Data. Sex:Male 31 years old Occupation: 搬家工人
 Basic Data Sex:Male 31 years old Occupation: 搬家工人 Chief Complaint Intermittent chest pain with shortness of breath for 2-3 months. Present Illness 4 months ago, he started having occasional chest pain
Basic Data Sex:Male 31 years old Occupation: 搬家工人 Chief Complaint Intermittent chest pain with shortness of breath for 2-3 months. Present Illness 4 months ago, he started having occasional chest pain
August 2018 Imaging Case of the Month: Dyspnea in a 55-Year-Old Smoker. Michael B. Gotway, MD
 August 2018 Imaging Case of the Month: Dyspnea in a 55-Year-Old Smoker Michael B. Gotway, MD Department of Radiology Mayo Clinic Arizona Scottsdale, AZ USA Clinical History: A 55 year old woman presented
August 2018 Imaging Case of the Month: Dyspnea in a 55-Year-Old Smoker Michael B. Gotway, MD Department of Radiology Mayo Clinic Arizona Scottsdale, AZ USA Clinical History: A 55 year old woman presented
Lung sequestration and Scimitar syndrome
 Lung sequestration and Scimitar syndrome Imaging approaches M. Mearadji International Foundation for Pediatric Imaging Aid Rotterdam, The Netherlands Pulmonary sequestration Pulmonary sequestration (PS)
Lung sequestration and Scimitar syndrome Imaging approaches M. Mearadji International Foundation for Pediatric Imaging Aid Rotterdam, The Netherlands Pulmonary sequestration Pulmonary sequestration (PS)
Sectional Anatomy Quiz - III
 Sectional Anatomy - III Rashid Hashmi * Rural Clinical School, University of New South Wales (UNSW), Wagga Wagga, NSW, Australia A R T I C L E I N F O Article type: Article history: Received: 30 Jun 2018
Sectional Anatomy - III Rashid Hashmi * Rural Clinical School, University of New South Wales (UNSW), Wagga Wagga, NSW, Australia A R T I C L E I N F O Article type: Article history: Received: 30 Jun 2018
MEDIASTINAL STAGING surgical pro
 MEDIASTINAL STAGING surgical pro Paul E. Van Schil, MD, PhD Department of Thoracic and Vascular Surgery University of Antwerp, Belgium Mediastinal staging Invasive techniques lymph node mapping cervical
MEDIASTINAL STAGING surgical pro Paul E. Van Schil, MD, PhD Department of Thoracic and Vascular Surgery University of Antwerp, Belgium Mediastinal staging Invasive techniques lymph node mapping cervical
Adam J. Hansen, MD UHC Thoracic Surgery
 Adam J. Hansen, MD UHC Thoracic Surgery Sometimes seen on Chest X-ray (CXR) Common incidental findings on computed tomography (CT) chest and abdomen done for other reasons Most lung cancers discovered
Adam J. Hansen, MD UHC Thoracic Surgery Sometimes seen on Chest X-ray (CXR) Common incidental findings on computed tomography (CT) chest and abdomen done for other reasons Most lung cancers discovered
Signs in Chest Radiology
 Signs in Chest Radiology Jonathan H. Chung, MD Disclosures No pertinent disclosures Jonathan H. Chung, MD Assistant Professor Institute t of fadvanced d Biomedical Imaging National Jewish Health Denver,
Signs in Chest Radiology Jonathan H. Chung, MD Disclosures No pertinent disclosures Jonathan H. Chung, MD Assistant Professor Institute t of fadvanced d Biomedical Imaging National Jewish Health Denver,
Role of imaging in RCC. Ultrasonography. Solid lesion. Cystic RCC. Solid RCC 31/08/60. From Diagnosis to Treatment: the Radiologist Perspective
 Role of imaging in RCC From Diagnosis to Treatment: the Radiologist Perspective Diagnosis Staging Follow up Imaging modalities Limitations and pitfalls Duangkamon Prapruttam, MD Department of Therapeutic
Role of imaging in RCC From Diagnosis to Treatment: the Radiologist Perspective Diagnosis Staging Follow up Imaging modalities Limitations and pitfalls Duangkamon Prapruttam, MD Department of Therapeutic
10/17/2016. Nuts and Bolts of Thoracic Radiology. Objectives. Techniques
 Nuts and Bolts of Thoracic Radiology October 20, 2016 Carleen Risaliti Objectives Understand the basics of chest radiograph Develop a system for interpreting chest radiographs Correctly identify thoracic
Nuts and Bolts of Thoracic Radiology October 20, 2016 Carleen Risaliti Objectives Understand the basics of chest radiograph Develop a system for interpreting chest radiographs Correctly identify thoracic
Mediastinal lines, stripes and interfaces on PA chest radiograph with CT correlations
 Mediastinal lines, stripes and interfaces on PA chest radiograph with CT correlations Award: Certificate of Merit Poster No.: C-0442 Congress: ECR 2013 Type: Educational Exhibit Authors: N. Bystrická,
Mediastinal lines, stripes and interfaces on PA chest radiograph with CT correlations Award: Certificate of Merit Poster No.: C-0442 Congress: ECR 2013 Type: Educational Exhibit Authors: N. Bystrická,
Mediastinal Tumors: Imaging
 Mediastinal Tumors: Imaging References Imaging in Oncology, Husband and Reznek Computed Tomography and Magnetic Resonance of the thorax, Naidich, Zerhouni, Siegelman, Mediastinal compartments Anterior:
Mediastinal Tumors: Imaging References Imaging in Oncology, Husband and Reznek Computed Tomography and Magnetic Resonance of the thorax, Naidich, Zerhouni, Siegelman, Mediastinal compartments Anterior:
SETTING Fudan University Shanghai Cancer Center. RESPONSIBLE PARTY Haiquan Chen MD.
 OFFICIAL TITLE A Phase Ⅲ Study of Left Side Thoracotomy Approach (SweetProcedure) Versus Right Side Thoracotomy Plus Midline Laparotomy Approach (Ivor-Lewis Procedure) Esophagectomy in Middle or Lower
OFFICIAL TITLE A Phase Ⅲ Study of Left Side Thoracotomy Approach (SweetProcedure) Versus Right Side Thoracotomy Plus Midline Laparotomy Approach (Ivor-Lewis Procedure) Esophagectomy in Middle or Lower
Bronchogenic Carcinoma
 A 55-year-old construction worker has smoked 2 packs of ciggarettes daily for the past 25 years. He notes swelling in his upper extremity & face, along with dilated veins in this region. What is the most
A 55-year-old construction worker has smoked 2 packs of ciggarettes daily for the past 25 years. He notes swelling in his upper extremity & face, along with dilated veins in this region. What is the most
24. An infant with recurrent pneumonia underwent a frontal chest radiograph (Fig 24-A) followed by
 24. An infant with recurrent pneumonia underwent a frontal chest radiograph (Fig 24-A) followed by diagnosis? ndings, what is the most likely A. Pulmonary sequestration B. Congenital pulmonary airway malformation
24. An infant with recurrent pneumonia underwent a frontal chest radiograph (Fig 24-A) followed by diagnosis? ndings, what is the most likely A. Pulmonary sequestration B. Congenital pulmonary airway malformation
FDG PET/CT in Lung Cancer Read with the experts. Homer A. Macapinlac, M.D.
 FDG PET/CT in Lung Cancer Read with the experts Homer A. Macapinlac, M.D. Patient with suspected lung cancer presents with left sided chest pain T3 What is the T stage of this patient? A) T2a B) T2b C)
FDG PET/CT in Lung Cancer Read with the experts Homer A. Macapinlac, M.D. Patient with suspected lung cancer presents with left sided chest pain T3 What is the T stage of this patient? A) T2a B) T2b C)
Mediastinal Staging. Samer Kanaan, M.D.
 Mediastinal Staging Samer Kanaan, M.D. Overview Importance of accurate nodal staging Accuracy of radiographic staging Mediastinoscopy EUS EBUS Staging TNM Definitions T Stage Size of the Primary Tumor
Mediastinal Staging Samer Kanaan, M.D. Overview Importance of accurate nodal staging Accuracy of radiographic staging Mediastinoscopy EUS EBUS Staging TNM Definitions T Stage Size of the Primary Tumor
Slide 1. Slide 2. Slide 3. Investigation and management of lung cancer Robert Rintoul. Epidemiology. Risk factors/aetiology
 Slide 1 Investigation and management of lung cancer Robert Rintoul Department of Thoracic Oncology Papworth Hospital Slide 2 Epidemiology Second most common cancer in the UK (after breast). 38 000 new
Slide 1 Investigation and management of lung cancer Robert Rintoul Department of Thoracic Oncology Papworth Hospital Slide 2 Epidemiology Second most common cancer in the UK (after breast). 38 000 new
Sectional Anatomy Quiz II
 Sectional Anatomy II Rashid Hashmi Rural Clinical School, University of New South Wales, Wagga Wagga, New South Wales, Australia A R T I C L E I N F O Article type: Article history: Received: 3 Aug 2017
Sectional Anatomy II Rashid Hashmi Rural Clinical School, University of New South Wales, Wagga Wagga, New South Wales, Australia A R T I C L E I N F O Article type: Article history: Received: 3 Aug 2017
Chest Radiology Interpretation: Findings of Tuberculosis
 Chest Radiology Interpretation: Findings of Tuberculosis Get out your laptops, smart phones or other devices pollev.com/chestradiology Case #1 1 Plombage Pneumonia Cancer 2 Reading the TB CXR Be systematic!
Chest Radiology Interpretation: Findings of Tuberculosis Get out your laptops, smart phones or other devices pollev.com/chestradiology Case #1 1 Plombage Pneumonia Cancer 2 Reading the TB CXR Be systematic!
PET/CT in lung cancer
 PET/CT in lung cancer Andrei Šamarin North Estonia Medical Centre 3 rd Baltic Congress of Radiology 08.10.2010 Imaging in lung cancer Why do we need PET/CT? CT is routine imaging modality for staging of
PET/CT in lung cancer Andrei Šamarin North Estonia Medical Centre 3 rd Baltic Congress of Radiology 08.10.2010 Imaging in lung cancer Why do we need PET/CT? CT is routine imaging modality for staging of
FDG PET/CT STAGING OF LUNG CANCER. Dr Shakher Ramdave
 FDG PET/CT STAGING OF LUNG CANCER Dr Shakher Ramdave FDG PET/CT STAGING OF LUNG CANCER FDG PET/CT is used in all patients with lung cancer who are considered for curative treatment to exclude occult disease.
FDG PET/CT STAGING OF LUNG CANCER Dr Shakher Ramdave FDG PET/CT STAGING OF LUNG CANCER FDG PET/CT is used in all patients with lung cancer who are considered for curative treatment to exclude occult disease.
Lung Cancer Imaging. Terence Z. Wong, MD,PhD. Department of Radiology Duke University Medical Center Durham, NC 9/9/09
 Lung Cancer Imaging Terence Z. Wong, MD,PhD Department of Radiology Duke University Medical Center Durham, NC 9/9/09 Acknowledgements Edward F. Patz, Jr., MD Jenny Hoang, MD Ellen L. Jones, MD, PhD Lung
Lung Cancer Imaging Terence Z. Wong, MD,PhD Department of Radiology Duke University Medical Center Durham, NC 9/9/09 Acknowledgements Edward F. Patz, Jr., MD Jenny Hoang, MD Ellen L. Jones, MD, PhD Lung
American College of Radiology ACR Appropriateness Criteria
 American College of Radiology ACR Criteria Radiologic Management of Thoracic Nodules and Masses Variant 1: Middle-aged patient (35 60 years old) with an incidental 1.5-cm lung nodule. The lesion was smooth.
American College of Radiology ACR Criteria Radiologic Management of Thoracic Nodules and Masses Variant 1: Middle-aged patient (35 60 years old) with an incidental 1.5-cm lung nodule. The lesion was smooth.
Case of the Day Chest
 Case of the Day Chest Darin White MDCM FRCPC Department of Radiology, Mayo Clinic 76 th Annual Scientific Meeting Canadian Association of Radiologists Montreal, QC April 26, 2013 2013 MFMER slide-1 Disclosures
Case of the Day Chest Darin White MDCM FRCPC Department of Radiology, Mayo Clinic 76 th Annual Scientific Meeting Canadian Association of Radiologists Montreal, QC April 26, 2013 2013 MFMER slide-1 Disclosures
Imaging of the cisterna chyli on PET-CT in patients with known malignancy: Report of two cases
 Imaging of the cisterna chyli on PET-CT in patients with known malignancy: Report of two cases Natalie Burns, B.S., Jason Barksdale, M.D., Linh Ho, M.D., and Patrick M. Colletti, M.D. Citation: Burns N,
Imaging of the cisterna chyli on PET-CT in patients with known malignancy: Report of two cases Natalie Burns, B.S., Jason Barksdale, M.D., Linh Ho, M.D., and Patrick M. Colletti, M.D. Citation: Burns N,
Radiological staging of lung cancer. Shukri Loutfi,MD,FRCR Consultant Thoracic Radiologist KAMC-Riyadh
 Radiological staging of lung cancer Shukri Loutfi,MD,FRCR Consultant Thoracic Radiologist KAMC-Riyadh Bronchogenic Carcinoma Accounts for 14% of new cancer diagnoses in 2012. Estimated to kill ~150,000
Radiological staging of lung cancer Shukri Loutfi,MD,FRCR Consultant Thoracic Radiologist KAMC-Riyadh Bronchogenic Carcinoma Accounts for 14% of new cancer diagnoses in 2012. Estimated to kill ~150,000
Dr. Pratik Mukherjee, MMed, FRCR Dr. Ashish Chawla, MD, ABR (USA) Khoo Teck Puat Hospital, Singapore
 Dr. Pratik Mukherjee, MMed, FRCR Dr. Ashish Chawla, MD, ABR (USA) Khoo Teck Puat Hospital, Singapore The authors declare no financial disclosures. To revisit the basics of approach to mediastinal masses
Dr. Pratik Mukherjee, MMed, FRCR Dr. Ashish Chawla, MD, ABR (USA) Khoo Teck Puat Hospital, Singapore The authors declare no financial disclosures. To revisit the basics of approach to mediastinal masses
TB Radiology for Nurses Garold O. Minns, MD
 TB Nurse Case Management Salina, Kansas March 31-April 1, 2010 TB Radiology for Nurses Garold O. Minns, MD April 1, 2010 TB Radiology for Nurses Highway Patrol Training Center Salina, KS April 1, 2010
TB Nurse Case Management Salina, Kansas March 31-April 1, 2010 TB Radiology for Nurses Garold O. Minns, MD April 1, 2010 TB Radiology for Nurses Highway Patrol Training Center Salina, KS April 1, 2010
GUIDELINES FOR CANCER IMAGING Lung Cancer
 GUIDELINES FOR CANCER IMAGING Lung Cancer Greater Manchester and Cheshire Cancer Network Cancer Imaging Cross-Cutting Group April 2010 1 INTRODUCTION This document is intended as a ready reference for
GUIDELINES FOR CANCER IMAGING Lung Cancer Greater Manchester and Cheshire Cancer Network Cancer Imaging Cross-Cutting Group April 2010 1 INTRODUCTION This document is intended as a ready reference for
Chest and cardiovascular
 Module 1 Chest and cardiovascular A. Doss and M. J. Bull 1. Regarding the imaging modalities of the chest: High resolution computed tomography (HRCT) uses a slice thickness of 4 6 mm to identify mass lesions
Module 1 Chest and cardiovascular A. Doss and M. J. Bull 1. Regarding the imaging modalities of the chest: High resolution computed tomography (HRCT) uses a slice thickness of 4 6 mm to identify mass lesions
B-I-2 CARDIAC AND VASCULAR RADIOLOGY
 (YEARS 1 3) CURRICULUM FOR RADIOLOGY 13 B-I-2 CARDIAC AND VASCULAR RADIOLOGY KNOWLEDGE To describe the normal anatomy of the heart and vessels including the lymphatic system as demonstrated by radiographs,
(YEARS 1 3) CURRICULUM FOR RADIOLOGY 13 B-I-2 CARDIAC AND VASCULAR RADIOLOGY KNOWLEDGE To describe the normal anatomy of the heart and vessels including the lymphatic system as demonstrated by radiographs,
AJCC-NCRA Education Needs Assessment Results
 AJCC-NCRA Education Needs Assessment Results Donna M. Gress, RHIT, CTR Survey Tool 1 Survey Development, Delivery, Analysis THANKS to NCRA for the following work Developed survey with input from partners
AJCC-NCRA Education Needs Assessment Results Donna M. Gress, RHIT, CTR Survey Tool 1 Survey Development, Delivery, Analysis THANKS to NCRA for the following work Developed survey with input from partners
Esophageal Cancer Staging Essentials: The New TNM Staging System (7th edition) and Clinicoradiologic Implications
 Esophageal Cancer Staging Essentials: The New TNM Staging System (7th edition) and Clinicoradiologic Implications Poster No.: E-0060 Congress: ESTI 2012 Type: Scientific Exhibit Authors: K. Lee, T. J.
Esophageal Cancer Staging Essentials: The New TNM Staging System (7th edition) and Clinicoradiologic Implications Poster No.: E-0060 Congress: ESTI 2012 Type: Scientific Exhibit Authors: K. Lee, T. J.
Large veins of the thorax Brachiocephalic veins
 Large veins of the thorax Brachiocephalic veins Right brachiocephalic vein: formed at the root of the neck by the union of the right subclavian & the right internal jugular veins. Left brachiocephalic
Large veins of the thorax Brachiocephalic veins Right brachiocephalic vein: formed at the root of the neck by the union of the right subclavian & the right internal jugular veins. Left brachiocephalic
performed to help sway the clinician in what the appropriate diagnosis is, which can substantially alter the treatment of management.
 Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 4/30/2011 Radiology Quiz of the Week # 18 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 4/30/2011 Radiology Quiz of the Week # 18 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
North of Scotland Cancer Network Clinical Management Guideline for Non Small Cell Lung Cancer
 THIS DOCUMENT IS North of Scotland Cancer Network Clinical Management Guideline for Non Small Cell Lung Cancer [Based on WOSCAN NSCLC CMG with further extensive consultation within NOSCAN] UNCONTROLLED
THIS DOCUMENT IS North of Scotland Cancer Network Clinical Management Guideline for Non Small Cell Lung Cancer [Based on WOSCAN NSCLC CMG with further extensive consultation within NOSCAN] UNCONTROLLED
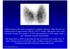
Dr. Weyrich G07: Superior and Posterior Mediastina. Reading: 1. Gray s Anatomy for Students, chapter 3
 Dr. Weyrich G07: Superior and Posterior Mediastina Reading: 1. Gray s Anatomy for Students, chapter 3 Objectives: 1. Subdivisions of mediastinum 2. Structures in Superior mediastinum 3. Structures in Posterior
Dr. Weyrich G07: Superior and Posterior Mediastina Reading: 1. Gray s Anatomy for Students, chapter 3 Objectives: 1. Subdivisions of mediastinum 2. Structures in Superior mediastinum 3. Structures in Posterior
Imaging of cardio-pulmonary treatment related damage. Radiotheraphy and Lung
 Imaging of cardio-pulmonary treatment related damage Dr. Andrea Borghesi Dr. Emanuele Gavazzi Department of Radiology 2 University of Brescia Radiotheraphy and Lung The goal of radiation therapy (RT) is
Imaging of cardio-pulmonary treatment related damage Dr. Andrea Borghesi Dr. Emanuele Gavazzi Department of Radiology 2 University of Brescia Radiotheraphy and Lung The goal of radiation therapy (RT) is
1/25/13 Right partial nephrectomy followed by completion right radical nephrectomy.
 History and Physical Case Scenario 1 45 year old white male presents with complaints of nausea, weight loss, and back pain. A CT of the chest, abdomen and pelvis was done on 12/8/12 that revealed a 12
History and Physical Case Scenario 1 45 year old white male presents with complaints of nausea, weight loss, and back pain. A CT of the chest, abdomen and pelvis was done on 12/8/12 that revealed a 12
Radiology Pathology Conference
 Radiology Pathology Conference Sharlin Johnykutty,, MD, Cytopathology Fellow Sara Majewski, MD, Radiology Resident Friday, August 28, 2009 Presentation material is for education purposes only. All rights
Radiology Pathology Conference Sharlin Johnykutty,, MD, Cytopathology Fellow Sara Majewski, MD, Radiology Resident Friday, August 28, 2009 Presentation material is for education purposes only. All rights
An Introduction to Radiology for TB Nurses
 An Introduction to Radiology for TB Nurses Garold O. Minns, MD September 14, 2017 TB Nurse Case Management September 12 14, 2017 EXCELLENCE EXPERTISE INNOVATION Garold O. Minns, MD has the following disclosures
An Introduction to Radiology for TB Nurses Garold O. Minns, MD September 14, 2017 TB Nurse Case Management September 12 14, 2017 EXCELLENCE EXPERTISE INNOVATION Garold O. Minns, MD has the following disclosures
Imaging Of Cystic Paravertebral Masses:
 Imaging Of Cystic Paravertebral Masses: Differential Diagnosis and Key Discriminators John P. Lichtenberger III, MD, Maj, USAF, MC Brent McCarragher, MD, CPT, USA John R. Dryden, MD, LT, USN P. Gabriel
Imaging Of Cystic Paravertebral Masses: Differential Diagnosis and Key Discriminators John P. Lichtenberger III, MD, Maj, USAF, MC Brent McCarragher, MD, CPT, USA John R. Dryden, MD, LT, USN P. Gabriel
Boot Camp Case Scenarios
 Boot Camp Case Scenarios Case Scenario 1 Patient is a 69-year-old white female. She presents with dyspnea on exertion, cough, and right rib pain. Patient is a smoker. 9/21/12 CT Chest FINDINGS: There is
Boot Camp Case Scenarios Case Scenario 1 Patient is a 69-year-old white female. She presents with dyspnea on exertion, cough, and right rib pain. Patient is a smoker. 9/21/12 CT Chest FINDINGS: There is
Surgical indications: Non-malignant pulmonary diseases. Punnarerk Thongcharoen
 Surgical indications: Non-malignant pulmonary diseases Punnarerk Thongcharoen Non-malignant Malignant as a pathological term: Cancer Non-malignant = not cancer Malignant as an adjective: Disposed to cause
Surgical indications: Non-malignant pulmonary diseases Punnarerk Thongcharoen Non-malignant Malignant as a pathological term: Cancer Non-malignant = not cancer Malignant as an adjective: Disposed to cause
Collaborative Stage. Site-Specific Instructions - LUNG
 Slide 1 Collaborative Stage Site-Specific Instructions - LUNG In this presentation, we are going to review the AJCC Cancer Staging criteria for the lung primary site. Slide 2 Reading Assignments As each
Slide 1 Collaborative Stage Site-Specific Instructions - LUNG In this presentation, we are going to review the AJCC Cancer Staging criteria for the lung primary site. Slide 2 Reading Assignments As each
Endobronchial Ultrasound in the Diagnosis & Staging of Lung Cancer
 Endobronchial Ultrasound in the Diagnosis & Staging of Lung Cancer Dr Richard Booton PhD FRCP Lead Lung Cancer Clinician, Consultant Respiratory Physician & Speciality Director Manchester University NHS
Endobronchial Ultrasound in the Diagnosis & Staging of Lung Cancer Dr Richard Booton PhD FRCP Lead Lung Cancer Clinician, Consultant Respiratory Physician & Speciality Director Manchester University NHS
REVIEW. Radiographic Features of Mediastinal Anatomy* RADIOGRAPHIC FEATURES OF MEDIAmNAl ANATOMY 609
 REVIEW Radiographic Features of Mediastinal Anatomy* Eric A.Hyson, M.D., andcarl E. Ravin, M.D., F.C.C.P. The increasing use of higher kilovoltage techniques and shorter exposure times in chest radiography
REVIEW Radiographic Features of Mediastinal Anatomy* Eric A.Hyson, M.D., andcarl E. Ravin, M.D., F.C.C.P. The increasing use of higher kilovoltage techniques and shorter exposure times in chest radiography
PET IMAGING (POSITRON EMISSION TOMOGRAPY) FACT SHEET
 Positron Emission Tomography (PET) When calling Anthem (1-800-533-1120) or using the Point of Care authorization system for a Health Service Review, the following clinical information may be needed to
Positron Emission Tomography (PET) When calling Anthem (1-800-533-1120) or using the Point of Care authorization system for a Health Service Review, the following clinical information may be needed to
Eun-Young Kang, M.D., Jae Wook Lee, M.D., Ji Yung Choo, M.D., Hwan Seok Yong, M.D., Ki Yeol Lee, M.D., Yu-Whan Oh, M.D.
 Eun-Young Kang, M.D., Jae Wook Lee, M.D., Ji Yung Choo, M.D., Hwan Seok Yong, M.D., Ki Yeol Lee, M.D., Yu-Whan Oh, M.D. Department of Radiology, Korea University Guro Hospital, College of Medicine, Korea
Eun-Young Kang, M.D., Jae Wook Lee, M.D., Ji Yung Choo, M.D., Hwan Seok Yong, M.D., Ki Yeol Lee, M.D., Yu-Whan Oh, M.D. Department of Radiology, Korea University Guro Hospital, College of Medicine, Korea
The External Anatomy of the Lungs. Prof Oluwadiya KS
 The External Anatomy of the Lungs Prof Oluwadiya KS www.oluwadiya.com Introduction The lungs are the vital organs of respiration Their main function is to oxygenate the blood by bringing inspired air into
The External Anatomy of the Lungs Prof Oluwadiya KS www.oluwadiya.com Introduction The lungs are the vital organs of respiration Their main function is to oxygenate the blood by bringing inspired air into
Incidental Esophageal Findings on Chest CT. Amira Hussien, MD, Elliot Fishman, MD, Bouchra Younes, MD, Ahmed Hatw. Johns Hopkins Medical Institution
 Incidental Esophageal Findings on Chest CT Amira Hussien, MD, Elliot Fishman, MD, ouchra Younes, MD, Ahmed Hatw. Johns Hopkins Medical Institution I have nothing to disclose. DISCLOSURE INTRODUCTION Although
Incidental Esophageal Findings on Chest CT Amira Hussien, MD, Elliot Fishman, MD, ouchra Younes, MD, Ahmed Hatw. Johns Hopkins Medical Institution I have nothing to disclose. DISCLOSURE INTRODUCTION Although
Diffuse high-attenuation within mediastinal lymph nodes on non-enhanced CT scan: Usefulness in the prediction of benignancy
 Diffuse high-attenuation within mediastinal lymph nodes on non-enhanced CT scan: Usefulness in the prediction of benignancy Poster No.: C-1785 Congress: ECR 2012 Type: Authors: Keywords: DOI: Scientific
Diffuse high-attenuation within mediastinal lymph nodes on non-enhanced CT scan: Usefulness in the prediction of benignancy Poster No.: C-1785 Congress: ECR 2012 Type: Authors: Keywords: DOI: Scientific
Pulmonary Sequestration
 July 26, 2004 Pulmonary Sequestration Jonathan Shaw, Harvard Medical School Year IV What do these two patients have in common? Patient 1: 50 y.o. non-smoking female with several months cough and hemoptysis;
July 26, 2004 Pulmonary Sequestration Jonathan Shaw, Harvard Medical School Year IV What do these two patients have in common? Patient 1: 50 y.o. non-smoking female with several months cough and hemoptysis;
Undergraduate Teaching
 Prof. James F Meaney Undergraduate Teaching Chest X-Ray Understanding the normal anatomical by reference to cross sectional imaging Radiology? It s FUN! Cryptic puzzle Sudoku (Minecraft?) It s completely
Prof. James F Meaney Undergraduate Teaching Chest X-Ray Understanding the normal anatomical by reference to cross sectional imaging Radiology? It s FUN! Cryptic puzzle Sudoku (Minecraft?) It s completely
42 yr old male with h/o Graves disease and prior I 131 treatment presents with hyperthyroidism and undetectable TSH. 2 hr uptake 20%, 24 hr uptake 50%
 Pinhole images of the neck are acquired in multiple projections, 24hrs after the oral administration of approximately 200 µci of I123. Usually, 24hr uptake value if also calculated (normal 24 hr uptake
Pinhole images of the neck are acquired in multiple projections, 24hrs after the oral administration of approximately 200 µci of I123. Usually, 24hr uptake value if also calculated (normal 24 hr uptake
Imaging of Thoracic Trauma: Tips and Traps. Arun C. Nachiappan, MD Associate Professor of Clinical Radiology University of Pennsylvania
 Imaging of Thoracic Trauma: Tips and Traps Arun C. Nachiappan, MD Associate Professor of Clinical Radiology University of Pennsylvania None Disclosures Objectives Describe blunt and penetrating traumatic
Imaging of Thoracic Trauma: Tips and Traps Arun C. Nachiappan, MD Associate Professor of Clinical Radiology University of Pennsylvania None Disclosures Objectives Describe blunt and penetrating traumatic
Update on RECIST and Staging of Common Pediatric Tumors Ethan A. Smith, MD
 Update on RECIST and Staging of Common Pediatric Tumors Ethan A. Smith, MD Section of Pediatric Radiology C.S. Mott Children s Hospital University of Michigan ethans@med.umich.edu Disclosures No relevant
Update on RECIST and Staging of Common Pediatric Tumors Ethan A. Smith, MD Section of Pediatric Radiology C.S. Mott Children s Hospital University of Michigan ethans@med.umich.edu Disclosures No relevant
Two Cases of Incidentally Picked Up Adult Unilateral Pulmonary Artery Atresia with Variable Imaging Features
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 12 Ver. III (Dec. 2017), PP 45-49 www.iosrjournals.org Two Cases of Incidentally Picked Up
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 12 Ver. III (Dec. 2017), PP 45-49 www.iosrjournals.org Two Cases of Incidentally Picked Up
objectives Pitfalls and Pearls in PET/CT imaging Kevin Robinson, DO Assistant Professor Department of Radiology Michigan State University
 objectives Pitfalls and Pearls in PET/CT imaging Kevin Robinson, DO Assistant Professor Department of Radiology Michigan State University To determine the regions of physiologic activity To understand
objectives Pitfalls and Pearls in PET/CT imaging Kevin Robinson, DO Assistant Professor Department of Radiology Michigan State University To determine the regions of physiologic activity To understand
An Update: Lung Cancer
 An Update: Lung Cancer Andy Barlow Consultant in Respiratory Medicine Lead Clinician for Lung Cancer (West Herts Hospitals NHS Trust) Lead for EBUS-Harefield Hospital (RB&HFT) Summary Lung cancer epidemiology
An Update: Lung Cancer Andy Barlow Consultant in Respiratory Medicine Lead Clinician for Lung Cancer (West Herts Hospitals NHS Trust) Lead for EBUS-Harefield Hospital (RB&HFT) Summary Lung cancer epidemiology
Assignable revenue codes: Explanation of services:
 computed tomography Chest/Cardiac Assignable revenue codes: Explanation of services: 0350 CT Scan General Classification 0351 CT Scan Head Scan 0352 CT Scan Body Scan 0359 CT Scan Other CT Scans Known
computed tomography Chest/Cardiac Assignable revenue codes: Explanation of services: 0350 CT Scan General Classification 0351 CT Scan Head Scan 0352 CT Scan Body Scan 0359 CT Scan Other CT Scans Known
Hong Kong Society of Upper Gastrointestinal Surgeons CLINICAL MEETING 29 NOV 2012
 Hong Kong Society of Upper Gastrointestinal Surgeons CLINICAL MEETING 29 NOV 2012 Esophageal Leiomyoma Introduction Case presentation Operative video Discussion Esophageal Leiomyoma Benign tumors of the
Hong Kong Society of Upper Gastrointestinal Surgeons CLINICAL MEETING 29 NOV 2012 Esophageal Leiomyoma Introduction Case presentation Operative video Discussion Esophageal Leiomyoma Benign tumors of the
Non-Small Cell Lung Cancer: Disease Spectrum and Management in a Tertiary Care Hospital
 Non-Small Cell Lung Cancer: Disease Spectrum and Management in a Tertiary Care Hospital Muhammad Rizwan Khan,Sulaiman B. Hasan,Shahid A. Sami ( Department of Surgery, The Aga Khan University Hospital,
Non-Small Cell Lung Cancer: Disease Spectrum and Management in a Tertiary Care Hospital Muhammad Rizwan Khan,Sulaiman B. Hasan,Shahid A. Sami ( Department of Surgery, The Aga Khan University Hospital,
Imaging of Gastrointestinal Stromal Tumors (GIST) Amir Reza Radmard, MD Assistant Professor Shariati hospital Tehran University of Medical Sciences
 Imaging of Gastrointestinal Stromal Tumors (GIST) Amir Reza Radmard, MD Assistant Professor Shariati hospital Tehran University of Medical Sciences Describe the typical imaging findings of GIST at initial
Imaging of Gastrointestinal Stromal Tumors (GIST) Amir Reza Radmard, MD Assistant Professor Shariati hospital Tehran University of Medical Sciences Describe the typical imaging findings of GIST at initial
JMSCR Vol 05 Issue 06 Page June 2017
 www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i6.29 MRI in Clinically Suspected Uterine and
www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i6.29 MRI in Clinically Suspected Uterine and
Role of CT imaging to evaluate solitary pulmonary nodule with extrapulmonary neoplasms
 Original Research Article Role of CT imaging to evaluate solitary pulmonary nodule with extrapulmonary neoplasms Anand Vachhani 1, Shashvat Modia 1*, Varun Garasia 1, Deepak Bhimani 1, C. Raychaudhuri
Original Research Article Role of CT imaging to evaluate solitary pulmonary nodule with extrapulmonary neoplasms Anand Vachhani 1, Shashvat Modia 1*, Varun Garasia 1, Deepak Bhimani 1, C. Raychaudhuri
Disclosure. Acknowledgement. What is the Best Workup for Rectal Cancer Staging: US/MRI/PET? Rectal cancer imaging. None
 What is the Best Workup for Rectal Cancer Staging: US/MRI/PET? Zhen Jane Wang, MD Assistant Professor in Residence UC SF Department of Radiology Disclosure None Acknowledgement Hueylan Chern, MD, Department
What is the Best Workup for Rectal Cancer Staging: US/MRI/PET? Zhen Jane Wang, MD Assistant Professor in Residence UC SF Department of Radiology Disclosure None Acknowledgement Hueylan Chern, MD, Department
Looking Outside the Box: Incidental Extracardiac Finding in Echo
 Looking Outside the Box: Incidental Extracardiac Finding in Echo Dr. Aijaz Shah Head of Division, Adult Echocardiography Laboratory Prince Sultan Cardiac Centre Riyadh Case 1 17 year old boy presented
Looking Outside the Box: Incidental Extracardiac Finding in Echo Dr. Aijaz Shah Head of Division, Adult Echocardiography Laboratory Prince Sultan Cardiac Centre Riyadh Case 1 17 year old boy presented
Mediastinoscopy, Mediastinotomy And Thoracoscopy For Mediastinal Lesions. Alper Toker, MD
 Mediastinoscopy, Mediastinotomy And Thoracoscopy For Mediastinal Lesions Alper Toker, MD Istanbul University, Istanbul Medical School Department of Thoracic Surgery The mediastinum is a complex anatomic
Mediastinoscopy, Mediastinotomy And Thoracoscopy For Mediastinal Lesions Alper Toker, MD Istanbul University, Istanbul Medical School Department of Thoracic Surgery The mediastinum is a complex anatomic
Video-Mediastinoscopy Thoracoscopy (VATS)
 Surgical techniques Video-Mediastinoscopy Thoracoscopy (VATS) Gunda Leschber Department of Thoracic Surgery ELK Berlin Chest Hospital, Berlin, Germany Teaching Hospital of Charité Universitätsmedizin Berlin
Surgical techniques Video-Mediastinoscopy Thoracoscopy (VATS) Gunda Leschber Department of Thoracic Surgery ELK Berlin Chest Hospital, Berlin, Germany Teaching Hospital of Charité Universitätsmedizin Berlin
Chest X-ray (CXR) Interpretation Brent Burbridge, MD, FRCPC
 Chest X-ray (CXR) Interpretation Brent Burbridge, MD, FRCPC An approach to reviewing a chest x-ray will create a foundation that will facilitate the detection of abnormalities. You should create your own
Chest X-ray (CXR) Interpretation Brent Burbridge, MD, FRCPC An approach to reviewing a chest x-ray will create a foundation that will facilitate the detection of abnormalities. You should create your own
Lung. 10/24/13 Chest X-ray: 2.9 cm mass like density in the inferior lingular segment worrisome for neoplasm. Malignancy cannot be excluded.
 Lung Case Scenario 1 A 54 year white male presents with a recent abnormal CT of the chest. The patient has a history of melanoma, kidney, and prostate cancers. 10/24/13 Chest X-ray: 2.9 cm mass like density
Lung Case Scenario 1 A 54 year white male presents with a recent abnormal CT of the chest. The patient has a history of melanoma, kidney, and prostate cancers. 10/24/13 Chest X-ray: 2.9 cm mass like density
Heart and Lungs. LUNG Coronal section demonstrates relationship of pulmonary parenchyma to heart and chest wall.
 Heart and Lungs Normal Sonographic Anatomy THORAX Axial and coronal sections demonstrate integrity of thorax, fetal breathing movements, and overall size and shape. LUNG Coronal section demonstrates relationship
Heart and Lungs Normal Sonographic Anatomy THORAX Axial and coronal sections demonstrate integrity of thorax, fetal breathing movements, and overall size and shape. LUNG Coronal section demonstrates relationship
Understanding the Diagnostic and Prognostic Role of Imaging in the Evaluation of an Anterior Mediastinal Mass
 Understanding the Diagnostic and Prognostic Role of Imaging in the Evaluation of an Anterior Mediastinal Mass Daniel W. Kim, Harvard Medical School Year III Agenda Mediastinum Menu of tests Anatomy Normal
Understanding the Diagnostic and Prognostic Role of Imaging in the Evaluation of an Anterior Mediastinal Mass Daniel W. Kim, Harvard Medical School Year III Agenda Mediastinum Menu of tests Anatomy Normal
Case Based Fetal Lung Masses
 Case Based Fetal Lung Masses Advances in Fetal and Neonatal Imaging Course Orlando, Florida, January 28, 2017 Leann E. Linam, MD Associate Professor Radiology University of Arkansas for Medical Sciences/
Case Based Fetal Lung Masses Advances in Fetal and Neonatal Imaging Course Orlando, Florida, January 28, 2017 Leann E. Linam, MD Associate Professor Radiology University of Arkansas for Medical Sciences/
CT Chest. Verification of an opacity seen on the straight chest X ray
 CT Chest Indications: To assess equivocal plain x-ray findings Staging of lung neoplasm Merastatic workup of extra thoraces malignancies Diagnosis of diffuse lung diseases with HRCT Assessment of bronchietasis
CT Chest Indications: To assess equivocal plain x-ray findings Staging of lung neoplasm Merastatic workup of extra thoraces malignancies Diagnosis of diffuse lung diseases with HRCT Assessment of bronchietasis
Non-neoplastic Conditions in the Mediastinum
 2017 WCTI Non-neoplastic Conditions in the Mediastinum Mi Young Kim, MD, PhD Hyun Jung Koo, MD Jae Woo Song, MD, PhD Department of Radiology and Research Institute of Radiology Asan Medical Center, University
2017 WCTI Non-neoplastic Conditions in the Mediastinum Mi Young Kim, MD, PhD Hyun Jung Koo, MD Jae Woo Song, MD, PhD Department of Radiology and Research Institute of Radiology Asan Medical Center, University
A Case of Pediatric Plasma Cell Granuloma
 August 2001 A Case of Pediatric Plasma Cell Granuloma Nii Tetteh, Harvard Medical School Year IV Our Patient 8 year old male with history of recurrent left lower lobe and lingular pneumonias since 1994.
August 2001 A Case of Pediatric Plasma Cell Granuloma Nii Tetteh, Harvard Medical School Year IV Our Patient 8 year old male with history of recurrent left lower lobe and lingular pneumonias since 1994.
Thoracostomy: An Update on Imaging Features and Current Surgical Practice
 Thoracostomy: An Update on Imaging Features and Current Surgical Practice Robert D. Ambrosini, MD, PhD, Christopher Gange, MD, Katherine Kaproth-Joslin, MD, PhD, Susan Hobbs, MD, PhD Department of Imaging
Thoracostomy: An Update on Imaging Features and Current Surgical Practice Robert D. Ambrosini, MD, PhD, Christopher Gange, MD, Katherine Kaproth-Joslin, MD, PhD, Susan Hobbs, MD, PhD Department of Imaging
Shadow because the air
 Thyroid Ultrasound Thyroid US examination needs: 1. high frequency transducer 2. extended patient's neck 3. check all the neck area because the swelling could be in areas other than the thyroid such as
Thyroid Ultrasound Thyroid US examination needs: 1. high frequency transducer 2. extended patient's neck 3. check all the neck area because the swelling could be in areas other than the thyroid such as
Mediastinum and pericardium
 Mediastinum and pericardium Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com The mediastinum: is the central compartment of the thoracic cavity surrounded by
Mediastinum and pericardium Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com The mediastinum: is the central compartment of the thoracic cavity surrounded by
Use of Integrated PET CT in the Clinical Staging of Non Small Cell Lung Cancer
 November 2010 Use of Integrated PET CT in the Clinical Staging of Non Small Cell Lung Cancer Laura Myers, Harvard Medical School, Year III Clinical Presentation 79yo woman with cough productive of green
November 2010 Use of Integrated PET CT in the Clinical Staging of Non Small Cell Lung Cancer Laura Myers, Harvard Medical School, Year III Clinical Presentation 79yo woman with cough productive of green
MEASUREMENT OF EFFECT SOLID TUMOR EXAMPLES
 MEASUREMENT OF EFFECT SOLID TUMOR EXAMPLES Although response is not the primary endpoint of this trial, subjects with measurable disease will be assessed by standard criteria. For the purposes of this
MEASUREMENT OF EFFECT SOLID TUMOR EXAMPLES Although response is not the primary endpoint of this trial, subjects with measurable disease will be assessed by standard criteria. For the purposes of this
Children are not small adults Children are Not Small Adults Anatomic considerations Pliable bony & cartilagenous structures - Significant thoracic inj
 PEDIATRIC CHEST TRAUMA Children are not small adults Role of imaging Spectrum of injury Children are not small adults Children are Not Small Adults Anatomic considerations Pliable bony & cartilagenous
PEDIATRIC CHEST TRAUMA Children are not small adults Role of imaging Spectrum of injury Children are not small adults Children are Not Small Adults Anatomic considerations Pliable bony & cartilagenous
MEDIASTINAL LYMPH NODE METASTASIS IN PATIENTS WITH CLINICAL STAGE I PERIPHERAL NON-SMALL-CELL LUNG CANCER
 MEDIASTINAL LYMPH NODE METASTASIS IN PATIENTS WITH CLINICAL STAGE I PERIPHERAL NON-SMALL-CELL LUNG CANCER Tsuneyo Takizawa, MD a Masanori Terashima, MD a Teruaki Koike, MD a Hideki Akamatsu, MD a Yuzo
MEDIASTINAL LYMPH NODE METASTASIS IN PATIENTS WITH CLINICAL STAGE I PERIPHERAL NON-SMALL-CELL LUNG CANCER Tsuneyo Takizawa, MD a Masanori Terashima, MD a Teruaki Koike, MD a Hideki Akamatsu, MD a Yuzo
Evaluation of Thyroid Nodules
 Evaluation of Thyroid Nodules Stephan Kowalyk, MD January 25 28, 2018 1 Primary goal Exclude malignancy Incidental thyroid nodules If found on CT, MRI, PET scan, carotid Doppler ULTRASOUND!! January 25
Evaluation of Thyroid Nodules Stephan Kowalyk, MD January 25 28, 2018 1 Primary goal Exclude malignancy Incidental thyroid nodules If found on CT, MRI, PET scan, carotid Doppler ULTRASOUND!! January 25
Radiology Pathology Conference
 Radiology Pathology Conference Nadia F. Yusaf, M.D. PGY-3 1/29/2010 Presentation material is for education purposes only. All rights reserved. 2010 URMC Radiology Page 1 of 90 Case 1 60 year- old man presents
Radiology Pathology Conference Nadia F. Yusaf, M.D. PGY-3 1/29/2010 Presentation material is for education purposes only. All rights reserved. 2010 URMC Radiology Page 1 of 90 Case 1 60 year- old man presents
Aliu Sanni MD SUNY Downstate Medical Center August 16, 2012
 Aliu Sanni MD SUNY Downstate Medical Center August 16, 2012 Case Presentation 60yr old AAF with PMH of CAD s/p PCI 1983, CVA, GERD, HTN presented with retrosternal chest pain on 06/12 Associated dysphagia
Aliu Sanni MD SUNY Downstate Medical Center August 16, 2012 Case Presentation 60yr old AAF with PMH of CAD s/p PCI 1983, CVA, GERD, HTN presented with retrosternal chest pain on 06/12 Associated dysphagia
Right lung. -fissures:
 -Right lung is shorter and wider because it is compressed by the right copula of the diaphragm by the live.. 2 fissure, 3 lobes.. hilum : 2 bronchi ( ep-arterial, hyp-arterial ), one artery mediastinal
-Right lung is shorter and wider because it is compressed by the right copula of the diaphragm by the live.. 2 fissure, 3 lobes.. hilum : 2 bronchi ( ep-arterial, hyp-arterial ), one artery mediastinal
A 64 y.o. man presents to the hospital with persistent cough and hemoptysis. Fernando Mut Montevideo - Uruguay
 A 64 y.o. man presents to the hospital with persistent cough and hemoptysis Fernando Mut Montevideo - Uruguay Teaching case Bone # 1 A 64 y.o. man presents to the hospital with persistent cough and hemoptysis.
A 64 y.o. man presents to the hospital with persistent cough and hemoptysis Fernando Mut Montevideo - Uruguay Teaching case Bone # 1 A 64 y.o. man presents to the hospital with persistent cough and hemoptysis.
RF Ablation: indication, technique and imaging follow-up
 RF Ablation: indication, technique and imaging follow-up Trongtum Tongdee, M.D. Radiology Department, Faculty of Medicine, Siriraj Hospital, Mahidol University, Bangkok, Thailand Objective Basic knowledge
RF Ablation: indication, technique and imaging follow-up Trongtum Tongdee, M.D. Radiology Department, Faculty of Medicine, Siriraj Hospital, Mahidol University, Bangkok, Thailand Objective Basic knowledge
The Various Methods to Biopsy the Lung PROF SHITRIT DAVID HEAD, PULMONARY DEPARTMENT MEIR MEDICAL CENTER, ISRAEL
 The Various Methods to Biopsy the Lung PROF SHITRIT DAVID HEAD, PULMONARY DEPARTMENT MEIR MEDICAL CENTER, ISRAEL Conflict of Interest This presentation is supported by AstraZeneca Two main steps before
The Various Methods to Biopsy the Lung PROF SHITRIT DAVID HEAD, PULMONARY DEPARTMENT MEIR MEDICAL CENTER, ISRAEL Conflict of Interest This presentation is supported by AstraZeneca Two main steps before
Lecture 2: Clinical anatomy of thoracic cage and cavity II
 Lecture 2: Clinical anatomy of thoracic cage and cavity II Dr. Rehan Asad At the end of this session, the student should be able to: Identify and discuss clinical anatomy of mediastinum such as its deflection,
Lecture 2: Clinical anatomy of thoracic cage and cavity II Dr. Rehan Asad At the end of this session, the student should be able to: Identify and discuss clinical anatomy of mediastinum such as its deflection,
Pulmonary vascular anatomy & anatomical variants
 Review Article Pulmonary vascular anatomy & anatomical variants Asha Kandathil, Murthy Chamarthy Department of Radiology, University of Texas Southwestern Medical Center, Dallas, TX, USA Contributions:
Review Article Pulmonary vascular anatomy & anatomical variants Asha Kandathil, Murthy Chamarthy Department of Radiology, University of Texas Southwestern Medical Center, Dallas, TX, USA Contributions:
