Biological Considerations Related To Osseointegration
|
|
|
- Angelica Osborne
- 5 years ago
- Views:
Transcription
1 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: , p-issn: Volume 14, Issue 9 Ver. II (Sep. 2015), PP Biological Considerations Related To Osseointegration k.vinathi reddy Abstract: The innovation by P.I Branemark that bone tissue can adhere permanently to implant surface was a clinical breakthrough in oral rehabilitation. There are several reports by most of the authors which demonstrate the success of implants. The mean age of the implants is increasing in day today life. There are certain factors to be considered in maintaining the success rate of implants through process of osseointegration.this article explains about different biological aspects which are to be considered to increase the rate osseointegration in turn leading to success of implants. Key words: Implants,Osseointegration,Bone. I. Introduction Bone is a special form of connective tissue which makes up the maxilla and mandible. Knowledge about its structure and metabolism is essential in the process of osseointegration.[1] II. Types Of Bone 1. Mature (I) Compact (II) Cancellous (Trabecular, spongy) 2. Immature 3. Bundle Composition The bone is composed of both organic and inorganic constituents They are, Inorganic - 65% organic - 35% Collagen - 88% - 89% Noncollagen -11%-12% Glycoprotein s - 6.5% Proteoglycans - 0.8% Sialoproteins % Lipids - 0.4% Jaw Bones Can Be Classified Into:[1,2] Alveolar Process 1. Alveolar bone proper 2. Supporting bone a. Cortical plates (i) Buccal (ii) Lingual b. Spongy (Cancellous), between cortical plates and alveolar bone proper. Alveolar process is that part of the jaws which supports and attaches the teeth. [1,2] It consists of two parts. 1. Alveolar bone proper, which forms the socket wall and gives attachment to the PDL. 2. Supporting bone, consisting of buccal and lingual cortical plates and the cancellous bone in between the plates and socket walls. In many regions only one part of the bone is present. even this plate may be deficient and show perforations. the socket wall is also known as the cribriform plate because of the presence of numerous holes produced by blood vessels. The alveolar process is dependent on the presence of teeth and is formed after the teeth erupt into the oral cavity, it is reabsorbed after the teeth are lost. The presence of basal bone is independent of teeth. [2] III. The Cortical Plate The cortical plate of alveolar process is continuous with conical plate of basal bone. These are mature lamellate bone. It consists of dense lamellated, haversian systems. At the crest of the tooth sockets the surface cortical bone is continuous with the alveolar bone proper. The thickness varies in different aspect of the buccal DOI: / Page
2 or lingual arch. In general it is thicker in the lingual aspect than labial. The labial aspect of the plates in maxilla shows numerous Volkman s canals for the entry of vessels and nerves. In mandible these canals are large but less frequent. [2] The Spongiosa The Cancellous bone lies between the cortical plates and alveolar bone proper. It contains marrow spaces and is continuous with the spongiosa of the body of the jaws. The maxilla has more Cancellous bone than mandible. The spongiosa is more on the lingual aspect than on the buccal. It is frequently absent in the anterior region. The amount of cancellous bone increase posteriorly. The spongy bone transmits the masticatory forces from alveolar bone proper to cortical plates. These septae transmit blood vessels and the radiolucent lines of these on radiographs are called Hirschfield s canals. The spongy bone of alveolus contains fatty marrows. Red marrow may be seen in maxillary tuberosity and mandibular posterior region. The trabeculae tend to be arranged in a horizontal plane near the alveolar bone and are nearly perpendicular in the interradicular area. By this arrangement it Supports the tooth and resists vertical pressure. [1,2] The Cribriform Plate It is that layer of compact bone which forms the bony wall of the tooth socket. It appears radiopaque in radiograph and is called lamina dura.it transmits various blood vessels and nerves and is called cribriform plate. It consists of bundle bone and lamellated bone and gives attachment to Sharpey s fibers. Because of constant mesial and occulsal movement of the teeth this bone is remodeled constantly. These small openings of blood vessels, veins, nerves, lymph vessels, Open through nutrient canals. The interdental and interradicular septae contain perforating canals of Zuckerkandi and Hirschfield (Nutrient Canals).[2,3] Bone is a connective tissue derived from the multipotential embryonic mesenchymal cells. It consists of the following. [2,3] 1. Cell: osteoblast, osteocyte and osteoclasts. 2. Intercellular substances a. Collagen fibrils b. ground substance (mucopolysaccharide) Osteoblast (Fig.1) - Primarily connected with bone formation - Forms collagen fibrils and ground substance - Also takes part in calcification - Produce a homogenous intercellular substance called primary osteoid tissue. [2,3] Osteocyte Some osteoblasts become entrapped in osteoid (osseous matrix mineralization) tissue during its formation and are termed osteocytes. They occupy a space called lacunae and anastomose with each other by means of processes contained in Canaliculi. They are essential for the maintenance of bone. The process of osteocytes communicates with each other and with the central canal of a Haversian system. [2,3] OSTEOCLASTS Osteoclasts are large multinucleated connective tissue cells, active in bone resorption. They reside in irregular scalloped surface of bone known as Howship lacunae and exert its action with the help of proteolytic enzymes. However other theories state that osteoclasts are foreign body giant cells clearing up the debris after the removal of inorganic salts. They may also appear as clusters of osteocytes after the minerals have been removed. [2,3] 1. Mature Bone 2. Immature Bone 3. Bundle Bone IV. Types Of Bone Tissue Mature Bone Show incremental lines or lamellae and are called lamellated bone - Can be compact or spongy - Compact bone is thick and solid. The lamellae are arranged in the form of concentric cylinders surrounding a narrow canal. DOI: / Page
3 Each canal is surrounded by 5-20 lamellae. This whole unit is called Haversian system and the central canal is called a haversian canal. Haversian canals of adjacent units are connected with each other by finer canal called Volkman s canals. Osteocyte, through their Canaliculi also forms a communication with the Haversian canals.[2,3][fig:2] Immature Bone - Contains more osteocyte than lamellated bone - Cells are arranged haphazardly - Collagen fibrils are not arranged in orderly fashion and it is not lamellated - Fibrils are coarser and more in number. - Contains less ground substance and are less calcified. - Always arranged in a trabecular pattern. [2,3] Bundle Bone - Contains less collagen fibrils - Sharpey s fibers are embedded in it. - More ground substance and is more calcified - This type is restricted to alveolar bone proper. - Lamellae are less conspicuous because the fibrils are oriented in the same plane perpendicular to the surface function. Jaws are susceptible to metabolic attack when mechanical protection is compromised by an atrophic, mutilated dentition.[4] Bone physiology is controlled by an interaction of mechanical and metabolic factors. The Biochemical mediators of calcium metabolism (parathyroid, estrogen and vitamin D) predominate in controlling the process. [2,3] Bone Classification Schemes (Related To Implant Dentistry) The appreciation of bone density and its relation to oral implantology have existed for more than 25 years. Linkow, in 1970, classified bone density into three categories: [4] Class I bone structure: This ideal bone type consists of evenly placed trabeculae with small cancellated spaces. Class II bone structure: The bone has slightly larger cancellated spaces with less uniformity of the osseous pattern. Class III bone structure: Large marrow filled spaces exists between bone trabeculae. [4] MISCH CLASSIFICATION:[Fig:4] Dl-Dense cortical bone. D2-Thick dense to porous cortical bone on crest and coarse trabecular bone within. D3-Thin porous cortical bone on crest and fine trabecular bone within. D4 Fine trabecular bone D5 Immature, nonmineralized bone [4] These four macroscopic differences of bone may be arranged from the densest to the least dense, as first described by Frost Dense cortical Coarse trabecular Fine trabecular The macroscopic description of the Branemark bone density classification of Dl bone is primarily dense cortical bone. D2 bone has dense-to-thick porous cortical bone on the crest and within coarse trabecular bone. D3 has a thinner porous cortical crest and fine trabecular bone. D4 bone has almost Porous cortical no crestal cortical bone.[fig:3] The fine trabecular bone composes almost all of the total volume of bone next to the implant. A very soft bone, with incomplete mineralization, may be addressed as D5 bone. [4] V. Biologic Parameters For Implant Acceptance Ten years ago, one of the authors proposed six factors that needed to be more or less simultaneously controlled for osseointegration of an inserted implant to result. The authors' current viewpoints on these six factors, with particular emphasis on recent observations, are summarized here.[5-10] 1. Material Biocompatibility Comparative investigations have demonstrated a higher degree of bone-to-metal contact with commercially pure (CP) titanium than with stainless steel, cobalt-chromium alloy, and Ti-6AI-4V alloys. Hydroxyapatite is likewise known to be a most biocompatible material, and in short-term followup studies, there DOI: / Page
4 is convincing evidence of a more rapid bone response than seen with CP titanium. Gottlander compared several types of HA-coated implants to CP titanium controls and, with respect to long-term observations, found no indications of a stronger bone response to the HA-coated screws. Another advantage claimed for the hydroxyapatite coating - that it will protect against potentially toxic metal ion leakage - was not confirmed by Ducheyne and coworkers, who even reported an in vitro increase in the leakage of aluminum with HA-coated titanium alloy implants. The authors feel that hydroxyapatite-coated implants have been introduced too rapidly as clinical routine products. There has been a relative lack of adequate followup of clinical materials to motivate their present abundant use. [11,12,13] 2. Implant Design There is no doubt that several different types of implant designs may show primary osseointegration. The question is whether there are stability advantages of screw-type designs compared to cylinders with respect to maintenance of the bony anchorage. [14] 3. Implant Surface It has been known for some time that a certain implant roughness is advantageous for implant acceptance. However, there have been methodologic problems in identifying the "ideal surface" topography. With a newly developed threedimensional approach, for the first time it has been possible to describe the surface roughness of screw-shaped implants and then insert the same for quantified analyses of the importance of the surface topography for implant incorporation. It seems likely that when the surface is too rough, ion leakage will increase with potential disturbance of the interfacial response. At least one group of investigators has found no less than 1,600 ppm of titanium outside plasma-sprayed titanium implants and even suggested titanium leakage from such surfaces to be a potential drawback. [12] 4. State Of The Host Site A host site-related parameter is the proportion of cortical and cancellous bone. There is one negative characteristic of the cancellous bone bed: its relatively limited capability of carrying the load. It is known from numerous experiments that the cancellous bone bed is most suitable for implant placement and, provided overload does not occur, it will remodel and become condensed into more compact bone. The load-bearing capability of the host bone must be individually evaluated and, in host sites of an assumed poor stability, a prolonged time between first- and second-stage surgeries is recommended to allow the bone to condense around the implant. [16] 5. Surgical Technique Previous investigations have demonstrated the importance of controlling surgical trauma by not overheating or overstressing the bone. [17] 6. Loading Conditions This topics is, of course, of a particular interest to the prosthodontist. More research is needed on the specific loading conditions that exist around an osseointegrated oral implant. The issue may be viewed from biologic as well as a biomechanical standpoint. For the biologist it is evident that the same mother cell may differentiate into a bone forming osteoblast or soft tissue-forming fibroblast, depending on environmental influences, premature loading leads to implant movements that in turn will shift the ehaling response to predominant soft tissue repair. The two stage implantation procedure has been recommended to allow incorporation of the implant under relatively stable conditions whereafter loading is allowed. It has been advocated that it is clinically advantageous to allow no extension of a maxillary fixed prosthesis during the first few months of loading to await proper bone remodeling and condensation in accordance with Wolff s law. [22] 7. Fixture Site Positions The most important principle is to achieve good initial stability and full coverage of the fixtures in well-vascularized, highly osteogenic bone. Bicortical initial stabilization should be the goal. If this is not possible, one must resort to at least monocortical fixation. The additional stability that can be achieved by engaging the lingual cortical plate of the mandible should be used whenever possible. [17] For adequate load distribution to the bone and the fixtures themselves, the latter should be spread well apart and placed along a curve or any arrangement other than a straight line. The center and the ends of the tentative superstructure should be well supported. However, the final design and extension should await the experience of bone quality from fixture and abutment surgeries. No figure for any optimal interfixture distance can be given because this depends on the vitality and mechanical capacity of both the fixture sites and the interfixture bone and may vary from one area to another. A clinical rule of thumb is, however, that the DOI: / Page
5 interfixture distance should not be less than one fixture diameter. This approach also facilitates later hygiene efforts between abutments.[11] The anterior loop of the mandibular canal and the nasopalatine duct should be avoided so as not to interfere with nerve function and osseointegration.[11] 8. Number Of Fixture Sites The available bone volume in different areas can be reasonably well assessed preoperatively by palpation and, especially, by tomographic radiographs. The same is not true for bone quality, which can be adequately determined only after some drilling has been performed. One may find, for example, that areas planned as fixture sites are totally unsuitable due to the presence of empty or fatty marrow compartments. Consequently, the number and position of fixtures cannot be finally decided upon until the preoperative period. Within the jaws it is generally advisable to start drilling for fixture sites close to the midline and then prepare the next ones as far posteriorly as possible, because the central and posterior sites strongly influence the outcome of the entire treatment. Only then can decisions be made on any interpositional fixtures to be placed. [19,20] In the totally edentulous mandible, placement of fixtures from one molar area to the other (if the position of the mandibular canal allows) is not a recommended procedure. The mandible flexes somewhat during chewing, and rigid connection of such fixtures to a stiff bridge may cause micro fractures in the perifixtural bone during mandibular flexing. For oral purposes, one fixture can carry one crown only, two fixtures provide minimal support for a bridge in partial edentulism, and four fixtures are the minimum for a full-arch bridge, provided they are spaced well apart along a curve. Unpublished data from the Goteborg team showed no significant differences in 5- to 12-year survival rates for maxillary and mandibular bridges supported by four or six fixtures. 9. Inclination Of Fixture Sites The inclinations of the fixture sites depend on; [9] 1. Local bone anatomy:the dominant principle is still that the fixtures should be totally embedded in bone. This may call for lingual or buccal positioning or a tilting of a fixture site to avoid concavities in the bone. If no bone grafts are placed into the floor of the maxillary sinus, distal tilting of the marginal parts of fixture sites may also be needed in the first premolar region to avoid penetration into the maxillary sinus. Moreover, such an inclination frequently allows advantage to be taken of the canine eminence. 2. Jaw relationships: Unless orthognathic surgery is performed before or possibly in combination with bone grafting at fixture installation, pseudoprognathism due to resorption generally calls for buccal inclination of maxillary and lingual tilting of mandibular fixture sites in total edentulism. 3. Design of the suprastructure: With proper inclination of fixture sites, penetration of bridge screw canals through buccal facings can be avoided. An overly palatal inclination may, on the other hand, result in a bulky bridge that interferes with phonation. 4. Desire for parallelism: If parallel fixture sites are prepared, the construction of the suprastructure may be facilitated.[9] 10. Lengths Of Fixtures The lengths of the fixtures should be determined only after all "high-speed" drilling has been finished. In particular, marginal countersinking may reduce the depth of a fixture site, and then fixtures shorter than originally anticipated must be chosen. The depth of a fixture site should be measured with a graded (ball-point) explorer to the lowest marginal bone edge. [20,21] Major extra bony protrusions of the apical parts of fixtures (e.g., into the maxillary sinus or the nasal cavities) are not justified. Experience with surgical displacement of the inferior alveolar nerve to gain bicortical fixation in mandibular molar areas is thus far limited.[20,21] 11. Load-Bearing Capacity The net effect of all the considerations discussed above governs what dynamic load the fixtures are able to bear. It is the quality of all perifixtural bone and the total interface surface of all fixtures that determine the load-bearing capacity. Consequently, four 15-mm-long fixtures may be capable of carrying the same load as six 10-mm-long ones, provided all are strategically well placed. [14,15] The long-term fixture survival rate is slightly smaller for the maxillae than for the mandible. These results are likely to reflect, differences in the load-bearing capacity between the jaws. Such difference could theoretically require a greater fixture/bone interface in the maxillae for adequate load distribution, that is, more or possibly longer fixtures than in the mandible.[14.15] DOI: / Page
6 Bibliography [1]. Orbans; Book on Oral Anatomy, Histology and Embryology; 10th Edition; CBS Publishers and distributors 1990: [2]. W.EugeneRoberts, LawrenceP.Garetto.Bone physiology and metabolism;contemporary Implant Dentistry; 2 nd Edition; Elsevier publishers: [3]. Robert A James, Ralph V.Mc Kinney,Jr.Roland M. Meffert;Tissues surrounding dental implants, ContemporaryImplantDentistry,2ndedition,QuintessencePublishers, [4]. Carl Misch;Contemporary Implant Dentistry; Bone Density; A Key Determinant for Treatment Planning; Elsevier publishers: [5]. Deborah F Rigsby,Martha Warren Bidez,Carl E.Misch;Bone response to mechanical loads. Contemporary Implant Dentistry; 2 nd edition; Elsevier publishers: [6]. Natalie Leow;University Of Sydney;Osseointegration ;The Implant Bone Interface:1-11. [7]. Per-Ingvar BraneMark,Albertsson, Zarb et al;introduction To Osseointegration; Chapter 1, Tissue Integrated Prosthesis, Elsevier publishers; [8]. Per Ingvar BraneMark;Book on Osseointegration;Elsevier publishers.chapter-3; [9]. Carl J.Drago;Rates of Osseointegration of Dental Implants With Regard To Anatomical Location; J Prothod.19921; 1: [10]. Tomas O. Alberktsson,CarinaB.Johansson and Lars Sennerby ;Biological Aspects of Implants Dentistry: Osseointegration. Periodontology ; 4: [11]. Samuel G.Steinemann. Titanium the Material of Choice.Periodontology ; 17:7-21. [12]. Jan Eirik Ellingsen;Surface Configuration of Dental Implants.Periodontology ; 17: [13]. T.ogawa;Titanium nanodular technology on Osseo integration of dental implants. clin oral implants research : [14]. David M.Davis;The Shift in the Therapeutic Paradigm; Osseointegration. J Prothet Dent. 1998; 79: [15]. Robert K.Schenk and Daniel Buser;Osseointegration; A Reality.Periodontology ; 17: [16]. Gerald A. Niznick;Achieving Osseointegration in Soft Bone; the Search for Improved Results. Oral Health. 2000: [17]. Marco Esposito,Jan Hirsch, Ulf Lekholm and Peter Thomsen;Difference Diagnosis and Treatment Strategies for Biologic Complications and Failing Oral Implants; A Review Of Literature. Int J Oral Maxillofac Implants.1999; 14: [18]. Richard Skalak;Aspects of Biomechanical Considerations; Osseointegration in Clinical Dentistry; Tissue Integrated Prosthesis: Elsevier publishers: Clin Oral Impl Res.2000; 11:1-11. [19]. Niklaus P.Lang, Wilson TG, Corbert EF;Biological complications with dental implants;their prevention diagnosis and treatment.clin Oral Impl Res.2000;11: [20]. Wim Teughels,Nel Van Assche,Isabelle Sliepen,Marc Qurynen;Effect of Material Characteristics and/or Surface Topography On Biofilm Development. Clin Oral Implant Research. 2006; 17: [21]. Bjorn Klinge,Joerg Meyle;Soft Tissue Integration Of Implants, Consensus Report Of Working Group 2.Clin.Oral Impl. Res.2006; 17: [22]. Ferreira. C.F,R.S.Magini and P.T.Sharpe;Biological Tooth Replacement and Repair; Journal of Oral Rehabilitation. 2007; 34: Fig.1: High Resolution Scanning Electron Micrograph of an Osteoblast Fig.2: Tissue components of bone marrow DOI: / Page
7 Fig.3: Bone quality as categorized by Branemark Fig.4: Macroscopic description of the four Misch densities DOI: / Page
Oral Histology. Alveolar bone or process: Functions of alveolar bone: Chemical composition: Development of the alveolar process: Dr.
 Oral Histology Lec.12 Alveolar bone or process: Dr. Nada Al-Ghaban Alveolar bone is a specialized part of the mandibular and maxillary bones that forms the primary support structure for teeth. Although
Oral Histology Lec.12 Alveolar bone or process: Dr. Nada Al-Ghaban Alveolar bone is a specialized part of the mandibular and maxillary bones that forms the primary support structure for teeth. Although
ANATOMY OF THE PERIODONTIUM. Dr. Fatin Awartani
 ANATOMY OF THE PERIODONTIUM Part II Cementum and Alveolar bone Associate Professor Periodontal division King Saud university Cementum Calcified mesenchymal tissue that forms the outer covering of the anatomic
ANATOMY OF THE PERIODONTIUM Part II Cementum and Alveolar bone Associate Professor Periodontal division King Saud university Cementum Calcified mesenchymal tissue that forms the outer covering of the anatomic
BONE TISSUE. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 BONE TISSUE Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology BONE FUNCTION Support Protection (protect internal organs) Movement (provide leverage system for skeletal muscles, tendons, ligaments
BONE TISSUE Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology BONE FUNCTION Support Protection (protect internal organs) Movement (provide leverage system for skeletal muscles, tendons, ligaments
Prosthetic Options in Implant Dentistry. Hakimeh Siadat, DDS, MSc Associate Professor
 Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Biology. Dr. Khalida Ibrahim
 Biology Dr. Khalida Ibrahim BONE TISSUE Bone tissue is a specialized form of connective tissue and is the main element of the skeletal tissues. It is composed of cells and an extracellular matrix in which
Biology Dr. Khalida Ibrahim BONE TISSUE Bone tissue is a specialized form of connective tissue and is the main element of the skeletal tissues. It is composed of cells and an extracellular matrix in which
Contemporary Implant Dentistry
 Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
Dental Implants: A Predictable Solution for Tooth Loss. Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor
 Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Osseointegrated dental implant treatment generally
 Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
What are the parts of the skeletal system? Chapter 6- Part I Bones and Skeletal Tissues. Growth of Cartilage. Bones come in many shapes
 Chapter 6- Part I Bones and Skeletal Tissues Components of the skeletal system Classification of Bone (bone shapes) Functions of bone Bone structure Microscopic structure of bone and bone cells What are
Chapter 6- Part I Bones and Skeletal Tissues Components of the skeletal system Classification of Bone (bone shapes) Functions of bone Bone structure Microscopic structure of bone and bone cells What are
Chapter 6: Skeletal System: Bones and Bone Tissue
 Chapter 6: Skeletal System: Bones and Bone Tissue I. Functions A. List and describe the five major functions of the skeletal system: 1. 2. 3.. 4. 5.. II. Cartilage A. What do chondroblasts do? B. When
Chapter 6: Skeletal System: Bones and Bone Tissue I. Functions A. List and describe the five major functions of the skeletal system: 1. 2. 3.. 4. 5.. II. Cartilage A. What do chondroblasts do? B. When
PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel
 PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel Abstract: Objectives: To evaluate an alternative treatment for rehabilitation
PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel Abstract: Objectives: To evaluate an alternative treatment for rehabilitation
CASE REPORT. CBCT-Assisted Treatment of the Failing Long Span Bridge with Staged and Immediate Load Implant Restoration
 Computer Aided Implantology Academy Newsletter - Newsletter 20 - July 2009 CASE REPORT CBCT-Assisted Treatment of the Failing Long Span Bridge with Staged and Immediate Load Implant Restoration Case Report
Computer Aided Implantology Academy Newsletter - Newsletter 20 - July 2009 CASE REPORT CBCT-Assisted Treatment of the Failing Long Span Bridge with Staged and Immediate Load Implant Restoration Case Report
CHAPTER 6 LECTURE OUTLINE
 CHAPTER 6 LECTURE OUTLINE I. INTRODUCTION A. Bone is made up of several different tissues working together: bone, cartilage, dense connective tissue, epithelium, various blood forming tissues, adipose
CHAPTER 6 LECTURE OUTLINE I. INTRODUCTION A. Bone is made up of several different tissues working together: bone, cartilage, dense connective tissue, epithelium, various blood forming tissues, adipose
6. Timing for orthodontic force
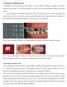 6. Timing for orthodontic force Orthodontic force is generally less than 300gm, so early mechanical stability is enough for immediate orthodontic force. There is no actually difference in success rate
6. Timing for orthodontic force Orthodontic force is generally less than 300gm, so early mechanical stability is enough for immediate orthodontic force. There is no actually difference in success rate
Functions of the Skeletal System. Chapter 6: Osseous Tissue and Bone Structure. Classification of Bones. Bone Shapes
 Chapter 6: Osseous Tissue and Bone Structure Functions of the Skeletal System 1. Support 2. Storage of minerals (calcium) 3. Storage of lipids (yellow marrow) 4. Blood cell production (red marrow) 5. Protection
Chapter 6: Osseous Tissue and Bone Structure Functions of the Skeletal System 1. Support 2. Storage of minerals (calcium) 3. Storage of lipids (yellow marrow) 4. Blood cell production (red marrow) 5. Protection
Osteology. Dr. Carmen E. Rexach Anatomy 35 Mt San Antonio College
 Osteology Dr. Carmen E. Rexach Anatomy 35 Mt San Antonio College Functions of the Skeletal System: Support Movement Protection Hemopoiesis Electrolyte balance (Ca ++ /PO -3 4 ) Acid-base balance Storage
Osteology Dr. Carmen E. Rexach Anatomy 35 Mt San Antonio College Functions of the Skeletal System: Support Movement Protection Hemopoiesis Electrolyte balance (Ca ++ /PO -3 4 ) Acid-base balance Storage
Module 2:! Functional Musculoskeletal Anatomy A! Semester 1! !!! !!!! Hard Tissues, Distal Upper Limb & Neurovascular Supply of Upper Limb!
 Functional Musculoskeletal Anatomy A Module 2: Hard Tissues, Distal Upper Limb & Neurovascular Supply of Upper Limb Semester 1 1 18. Bone Tissue & Growth of Bones 18.1 Describe the structure of bone tissue
Functional Musculoskeletal Anatomy A Module 2: Hard Tissues, Distal Upper Limb & Neurovascular Supply of Upper Limb Semester 1 1 18. Bone Tissue & Growth of Bones 18.1 Describe the structure of bone tissue
Case Study. Case # 1 Author: Dr. Suheil Boutros (USA) 2013 Zimmer Dental, Inc. All rights reserved. 6557, Rev. 03/13.
 Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
In-Silico approach on Offset placement of implant-supported bridges placed in bone of different density in Orthodontics.
 In-Silico approach on Offset placement of implant-supported bridges placed in bone of different density in Orthodontics. Chandrasenan.P 1, Vishnu.G 2, Akshay K Nair 3 1M Tech student, Department of Mechanical
In-Silico approach on Offset placement of implant-supported bridges placed in bone of different density in Orthodontics. Chandrasenan.P 1, Vishnu.G 2, Akshay K Nair 3 1M Tech student, Department of Mechanical
Dr.Sepideh Falah-kooshki
 Dr.Sepideh Falah-kooshki MAXILLA Premaxillary/median palatal suture (radiolucent). Incisive fossa and foramen (radiolucent). Nasal passages (radiolucent). Nasal septum (radiopaque). Anterior nasal spine
Dr.Sepideh Falah-kooshki MAXILLA Premaxillary/median palatal suture (radiolucent). Incisive fossa and foramen (radiolucent). Nasal passages (radiolucent). Nasal septum (radiopaque). Anterior nasal spine
OpenStax-CNX module: m Bone Structure * Ildar Yakhin. Based on Bone Structure by OpenStax. Abstract
 OpenStax-CNX module: m63474 1 Bone Structure * Ildar Yakhin Based on Bone Structure by OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 4.0 By
OpenStax-CNX module: m63474 1 Bone Structure * Ildar Yakhin Based on Bone Structure by OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 4.0 By
Human Biology Chapter 15.3: Bone Structure *
 OpenStax-CNX module: m58082 1 Human Biology Chapter 15.3: Bone Structure * Willy Cushwa Based on Bone Structure by OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons
OpenStax-CNX module: m58082 1 Human Biology Chapter 15.3: Bone Structure * Willy Cushwa Based on Bone Structure by OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons
Derived copy of Bone *
 OpenStax-CNX module: m57739 1 Derived copy of Bone * Shannon McDermott Based on Bone by OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 4.0 By
OpenStax-CNX module: m57739 1 Derived copy of Bone * Shannon McDermott Based on Bone by OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 4.0 By
Immediate implant placement in the Title central incisor region: a case repo. Journal Journal of prosthodontic research,
 Immediate implant placement in the Title central incisor region: a case repo Author(s) Sekine, H; Taguchi, T; Yamagami, M; Alternative Takanashi, T; Furuya, K Journal Journal of prosthodontic research,
Immediate implant placement in the Title central incisor region: a case repo Author(s) Sekine, H; Taguchi, T; Yamagami, M; Alternative Takanashi, T; Furuya, K Journal Journal of prosthodontic research,
The Skeletal System:Bone Tissue
 The Skeletal System:Bone Tissue Dynamic and ever-changing throughout life Skeleton composed of many different tissues cartilage, bone tissue, epithelium, nerve, blood forming tissue, adipose, and dense
The Skeletal System:Bone Tissue Dynamic and ever-changing throughout life Skeleton composed of many different tissues cartilage, bone tissue, epithelium, nerve, blood forming tissue, adipose, and dense
EFFECTIVE DATE: 04/24/14 REVISED DATE: 04/23/15, 04/28/16, 06/22/17, 06/28/18 POLICY NUMBER: CATEGORY: Dental
 MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
OSSEOUS TISSUE & BONE STRUCTURE PART I: OVERVIEW & COMPONENTS
 OSSEOUS TISSUE & BONE STRUCTURE PART I: OVERVIEW & COMPONENTS The Skeletal System Skeletal system includes: bones of the skeleton, cartilages, ligaments, and connective tissues What are the functions of
OSSEOUS TISSUE & BONE STRUCTURE PART I: OVERVIEW & COMPONENTS The Skeletal System Skeletal system includes: bones of the skeleton, cartilages, ligaments, and connective tissues What are the functions of
SKELETAL TISSUES CHAPTER 7 INTRODUCTION TO THE SKELETAL SYSTEM TYPES OF BONES
 SKELETAL TISSUES CHAPTER 7 By John McGill Supplement Outlines: Beth Wyatt Original PowerPoint: Jack Bagwell INTRODUCTION TO THE SKELETAL SYSTEM STRUCTURE Organs: Bones Related Tissues: Cartilage and Ligaments
SKELETAL TISSUES CHAPTER 7 By John McGill Supplement Outlines: Beth Wyatt Original PowerPoint: Jack Bagwell INTRODUCTION TO THE SKELETAL SYSTEM STRUCTURE Organs: Bones Related Tissues: Cartilage and Ligaments
Upper arch. 1Prosthodontics. Dr.Bassam Ali Al-Turaihi. Basic anatomy & & landmark of denture & mouth
 1Prosthodontics Lecture 2 Dr.Bassam Ali Al-Turaihi Basic anatomy & & landmark of denture & mouth Upper arch Palatine process of maxilla: it form the anterior three quarter of the hard palate. Horizontal
1Prosthodontics Lecture 2 Dr.Bassam Ali Al-Turaihi Basic anatomy & & landmark of denture & mouth Upper arch Palatine process of maxilla: it form the anterior three quarter of the hard palate. Horizontal
Placement of Posterior Mandibular and Maxillary Implants in Patients with Severe Bone Deficiency: A Clinical Report of Procedure
 Placement of Posterior Mandibular and Maxillary Implants in Patients with Severe Bone Deficiency: A Clinical Report of Procedure Leonard Krekmanov, DDS, PhD 1 The purpose of this investigation was to modify
Placement of Posterior Mandibular and Maxillary Implants in Patients with Severe Bone Deficiency: A Clinical Report of Procedure Leonard Krekmanov, DDS, PhD 1 The purpose of this investigation was to modify
Cartilage & bone. Red: important. Black: in male female slides. Gray: notes extra. Editing File
 Cartilage & bone Red: important. Black: in male female slides. Gray: notes extra. Editing File OBJECTIVES describe the microscopic structure, distribution and growth of the different types of Cartilage
Cartilage & bone Red: important. Black: in male female slides. Gray: notes extra. Editing File OBJECTIVES describe the microscopic structure, distribution and growth of the different types of Cartilage
FORMATION OF BONE. Intramembranous Ossification. Bone-Lec-10-Prof.Dr.Adnan Albideri
 FORMATION OF BONE All bones are of mesodermal origin. The process of bone formation is called ossification. We have seen that formation of most bones is preceded by the formation of a cartilaginous model,
FORMATION OF BONE All bones are of mesodermal origin. The process of bone formation is called ossification. We have seen that formation of most bones is preceded by the formation of a cartilaginous model,
Due in Lab. Due next week in lab - Scientific America Article Select one article to read and complete article summary
 Due in Lab 1. Skeletal System 33-34 2. Skeletal System 26 3. PreLab 6 Due next week in lab - Scientific America Article Select one article to read and complete article summary Cell Defenses and the Sunshine
Due in Lab 1. Skeletal System 33-34 2. Skeletal System 26 3. PreLab 6 Due next week in lab - Scientific America Article Select one article to read and complete article summary Cell Defenses and the Sunshine
The Brånemark osseointegration method, using titanium dental implants (fixtures)
 Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
Chapter 6: SKELETAL SYSTEM
 Chapter 6: SKELETAL SYSTEM I. FUNCTIONS A. Support B. Protection C. Movement D. Mineral storage E. Lipid storage (Fig. 6.8b) F. Blood cell production (Fig. 6.4) II. COMPONENTS A. Cartilage 1. Hyaline 2.
Chapter 6: SKELETAL SYSTEM I. FUNCTIONS A. Support B. Protection C. Movement D. Mineral storage E. Lipid storage (Fig. 6.8b) F. Blood cell production (Fig. 6.4) II. COMPONENTS A. Cartilage 1. Hyaline 2.
in compact bone, large vertical canals carrying blood vessels and nerves. in compact bone, large horizontal canals carrying blood vessels and nerves.
 Carl Christensen, PhD Skeletal System (Bones`) Bio. 2304 Human Anatomy 1. Identify a term for each of the following: shaft of a long bone ends of a long bone ossified remnant of the "growth plate" connective
Carl Christensen, PhD Skeletal System (Bones`) Bio. 2304 Human Anatomy 1. Identify a term for each of the following: shaft of a long bone ends of a long bone ossified remnant of the "growth plate" connective
Pre op Failed endodontic treatment with sinus involvement.
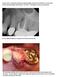 Case #1 of 10 consecutive extraction sockets grafted with Socket Graft Putty, covered with Socket Seal and sealed with Periacryl. I D # HEU This patient is a 66 year old female. Pre op Failed endodontic
Case #1 of 10 consecutive extraction sockets grafted with Socket Graft Putty, covered with Socket Seal and sealed with Periacryl. I D # HEU This patient is a 66 year old female. Pre op Failed endodontic
It has been proposed that partially edentulous maxillectomy
 CLASSICAL ARTICLE Basic principles of obturator design for partially edentulous patients. Part II: Design principles Mohamed A. Aramany, DMD, MS* Eye and Ear Hospital of Pittsburgh and University of Pittsburgh,
CLASSICAL ARTICLE Basic principles of obturator design for partially edentulous patients. Part II: Design principles Mohamed A. Aramany, DMD, MS* Eye and Ear Hospital of Pittsburgh and University of Pittsburgh,
BIOL 2457 CHAPTER 6 SI 1. irregular ectopic: sutural (Wormian) The is between the shaft and end. It contains cartilage that is
 BIOL 2457 CHAPTER 6 SI 1 1. List 5 functions of bones: 2. Classify bones according to shape: give descriptions and examples: long short flat irregular ectopic: sutural (Wormian) ectopic: sesamoid 3. The
BIOL 2457 CHAPTER 6 SI 1 1. List 5 functions of bones: 2. Classify bones according to shape: give descriptions and examples: long short flat irregular ectopic: sutural (Wormian) ectopic: sesamoid 3. The
Human Anatomy and Physiology I Laboratory
 Human Anatomy and Physiology I Laboratory Skeletal Tissue: Cartilage and Bone This lab involves study of the laboratory exercise Overview of the Skeleton, Classification and Structure of Bones and Cartilages,
Human Anatomy and Physiology I Laboratory Skeletal Tissue: Cartilage and Bone This lab involves study of the laboratory exercise Overview of the Skeleton, Classification and Structure of Bones and Cartilages,
THE NEW STANDARD OF EXCELLENCE IN BIOMATERIALS. Collagenated heterologous cortico-cancellous bone mix + TSV Gel GTO I N S P I R E D B Y N A T U R E
 GTO THE NEW STANDARD OF EXCELLENCE IN BIOMATERIALS Collagenated heterologous cortico-cancellous bone mix + TSV Gel R E G E N E R A T I O N S C I E N C E I N S P I R E D B Y N A T U R E A unique biotechnology
GTO THE NEW STANDARD OF EXCELLENCE IN BIOMATERIALS Collagenated heterologous cortico-cancellous bone mix + TSV Gel R E G E N E R A T I O N S C I E N C E I N S P I R E D B Y N A T U R E A unique biotechnology
MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION
 Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
The Skeletal System:Bone Tissue
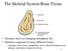 The Skeletal System:Bone Tissue Dynamic and ever-changing throughout life Skeleton composed of many different tissues cartilage, bone tissue, epithelium, nerve, blood forming tissue, adipose, and dense
The Skeletal System:Bone Tissue Dynamic and ever-changing throughout life Skeleton composed of many different tissues cartilage, bone tissue, epithelium, nerve, blood forming tissue, adipose, and dense
Dental Anatomy and Occlusion
 CHAPTER 53 Dental Anatomy and Occlusion Ma Lou C. Sabino DDS, and Emily G. Smythe, DDS What numerical system is used most commonly in the United States for designating the adult dentition? Pediatric dentition?
CHAPTER 53 Dental Anatomy and Occlusion Ma Lou C. Sabino DDS, and Emily G. Smythe, DDS What numerical system is used most commonly in the United States for designating the adult dentition? Pediatric dentition?
Bone Tissue- Chapter 5 5-1
 Bone Tissue- Chapter 5 5-1 Bone Functions Support Protection Assistance in movement Mineral storage and release Blood cell production Triglyceride storage 5-2 Bone Chemistry Water (25%) Organic Constituent
Bone Tissue- Chapter 5 5-1 Bone Functions Support Protection Assistance in movement Mineral storage and release Blood cell production Triglyceride storage 5-2 Bone Chemistry Water (25%) Organic Constituent
Techniques of local anesthesia in the mandible
 Techniques of local anesthesia in the mandible The technique of choice for anesthesia of the mandible is the block injection and this is attributed to the absence of the advantages which are present in
Techniques of local anesthesia in the mandible The technique of choice for anesthesia of the mandible is the block injection and this is attributed to the absence of the advantages which are present in
Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis
 CASE REPORT Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis Dr Ashish Yadav 1, Dr Aratee Gupta 2, Dr Archana Singh 3, 1,3-
CASE REPORT Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis Dr Ashish Yadav 1, Dr Aratee Gupta 2, Dr Archana Singh 3, 1,3-
An Introduction to the Skeletal System Skeletal system includes Bones of the skeleton Cartilages, ligaments, and connective tissues
 An Introduction to the Skeletal System Skeletal system includes Bones of the skeleton Cartilages, ligaments, and connective tissues Functions of the Skeletal System Support Storage of minerals (calcium)
An Introduction to the Skeletal System Skeletal system includes Bones of the skeleton Cartilages, ligaments, and connective tissues Functions of the Skeletal System Support Storage of minerals (calcium)
Chapter 6 Bones and Bone Tissue Chapter Outline
 Chapter 6 Bones and Bone Tissue Chapter Outline Module 6.1: Introduction to Bones as Organs (Figures 6.1, 6.2, 6.3, 6.4) A. The skeletal system includes the bones, joints, and their associated supporting
Chapter 6 Bones and Bone Tissue Chapter Outline Module 6.1: Introduction to Bones as Organs (Figures 6.1, 6.2, 6.3, 6.4) A. The skeletal system includes the bones, joints, and their associated supporting
Dental Implants. From the beginning up to now. By: Dr Arash Khojasteh
 Dental Implants From the beginning up to now By: Dr Arash Khojasteh WHAT IS A DENTAL IMPLANT? Dental implant is an artificial fixture which is placed surgically into the jaw bone to substitute for a missing
Dental Implants From the beginning up to now By: Dr Arash Khojasteh WHAT IS A DENTAL IMPLANT? Dental implant is an artificial fixture which is placed surgically into the jaw bone to substitute for a missing
Periodontal ligament
 Periodontal ligament The periodontium The periodontium includes: The gingiva Cementum Periodontal ligament Alveolar bone Def: The periodontal ligament is the dense fibrous connective tissue that occupies
Periodontal ligament The periodontium The periodontium includes: The gingiva Cementum Periodontal ligament Alveolar bone Def: The periodontal ligament is the dense fibrous connective tissue that occupies
The Skeletal System PART A. PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College
 PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Skeletal System 5 PART A The Skeletal System Parts of the skeletal system Bones (skeleton) Joints
PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Skeletal System 5 PART A The Skeletal System Parts of the skeletal system Bones (skeleton) Joints
Implant Site Development Part I
 REVIEW ARTICLE Implant Site Development Part I 1 Umang Nayar, 2 Shankar Iyer IJCID Implant Site Development Part I 1 Consultant, Dental Surgeon and Periodontist at Max Health Care, New Delhi, Professor
REVIEW ARTICLE Implant Site Development Part I 1 Umang Nayar, 2 Shankar Iyer IJCID Implant Site Development Part I 1 Consultant, Dental Surgeon and Periodontist at Max Health Care, New Delhi, Professor
Osseous Tissue and Bone Structure
 C h a p t e r 6 Osseous Tissue and Bone Structure PowerPoint Lecture Slides prepared by Jason LaPres Lone Star College - North Harris Copyright 2009 Pearson Education, Inc., publishing as Pearson Benjamin
C h a p t e r 6 Osseous Tissue and Bone Structure PowerPoint Lecture Slides prepared by Jason LaPres Lone Star College - North Harris Copyright 2009 Pearson Education, Inc., publishing as Pearson Benjamin
Elevators. elevators:- There are three major components of the elevator are:-
 Elevators Elevators:- Are exo-levers, instrument designed to elevate or luxate the teeth or roots from their bony socket in close or surgical method of extraction to force a tooth or root along the line
Elevators Elevators:- Are exo-levers, instrument designed to elevate or luxate the teeth or roots from their bony socket in close or surgical method of extraction to force a tooth or root along the line
Samantha W. Chou, D.M.D N. Southport Ave. Chicago, Illinois Phone: Fax:
 Samantha W. Chou, D.M.D. 2325 N. Southport Ave. Chicago, Illinois 60614 Phone: 312-608-6881 Fax: 773-296-0601 Samanthawchou@gmail.com What is our role as the dentist? "We live in a culture in which people
Samantha W. Chou, D.M.D. 2325 N. Southport Ave. Chicago, Illinois 60614 Phone: 312-608-6881 Fax: 773-296-0601 Samanthawchou@gmail.com What is our role as the dentist? "We live in a culture in which people
BONE AUGMENTATION AND GRAFTING
 1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
Mini implants for Stabilization of partial dentures
 Systematically to the goal Mini implants for Stabilization of partial dentures Winfried Walzer Prostheses are still considered by many to be aesthetically pleasing, cost-effective, but often associated
Systematically to the goal Mini implants for Stabilization of partial dentures Winfried Walzer Prostheses are still considered by many to be aesthetically pleasing, cost-effective, but often associated
Periodontal Disease. Radiology of Periodontal Disease. Periodontal Disease. The Role of Radiology in Assessment of Periodontal Disease
 Radiology of Periodontal Disease Steven R. Singer, DDS srs2@columbia.edu 212.305.5674 Periodontal Disease! Includes several disorders of the periodontium! Gingivitis! Marginal Periodontitis! Localized
Radiology of Periodontal Disease Steven R. Singer, DDS srs2@columbia.edu 212.305.5674 Periodontal Disease! Includes several disorders of the periodontium! Gingivitis! Marginal Periodontitis! Localized
Chapter 4. Cartilage and Bone. Li Shu-Lei instructor. Dept. Histology and Embryology, School of Basic Medical Sciences, Jilin University
 Chapter 4 Cartilage and Bone Li Shu-Lei instructor Dept. Histology and Embryology, School of Basic Medical Sciences, Jilin University I Cartilage a specialized connective tissue Characterizers: Cartilage
Chapter 4 Cartilage and Bone Li Shu-Lei instructor Dept. Histology and Embryology, School of Basic Medical Sciences, Jilin University I Cartilage a specialized connective tissue Characterizers: Cartilage
Unusual transmigration of canines report of two cases in a family
 ISSN: Electronic version: 1984-5685 RSBO. 2014 Jan-Mar;11(1):88-92 Case Report Article Unusual transmigration of canines report of two cases in a family Sulabha A. Narsapur 1 Sameer Choudhari 2 Shrishal
ISSN: Electronic version: 1984-5685 RSBO. 2014 Jan-Mar;11(1):88-92 Case Report Article Unusual transmigration of canines report of two cases in a family Sulabha A. Narsapur 1 Sameer Choudhari 2 Shrishal
ANATOMY & PHYSIOLOGY - CLUTCH CH. 8 - BONE AND CARTILAGE.
 !! www.clutchprep.com CONCEPT: BONE CLASSIFICATIONS There are four classifications of bones based on their 1. Long bones are greater in length than in width - Found in the upper and lower limbs (ex: arm,
!! www.clutchprep.com CONCEPT: BONE CLASSIFICATIONS There are four classifications of bones based on their 1. Long bones are greater in length than in width - Found in the upper and lower limbs (ex: arm,
Young-Jin Park, DDS,* and Sung-Am Cho, DDS, MS, PhD
 J Oral Maxillofac Surg 68:1338-1344, 2010 Retrospective Chart Analysis on Survival Rate of Fixtures Installed at the Tuberosity Bone for Cases With Missing Unilateral Upper Molars: A Study of 7 Cases Young-Jin
J Oral Maxillofac Surg 68:1338-1344, 2010 Retrospective Chart Analysis on Survival Rate of Fixtures Installed at the Tuberosity Bone for Cases With Missing Unilateral Upper Molars: A Study of 7 Cases Young-Jin
Arrangement of the artificial teeth:
 Lecture Prosthodontic Dr. Osama Arrangement of the artificial teeth: It s the placement of the teeth on a denture with definite objective in mind or it s the setting of teeth on temporary bases. Rules
Lecture Prosthodontic Dr. Osama Arrangement of the artificial teeth: It s the placement of the teeth on a denture with definite objective in mind or it s the setting of teeth on temporary bases. Rules
Osseointegrated implant-supported
 CLINICAL SCREWLESS FIXED DETACHABLE PARTIAL OVERDENTURE TREATMENT FOR ATROPHIC PARTIAL EDENTULISM OF THE ANTERIOR MAXILLA Dennis Flanagan, DDS This is a case report of the restoration of a partially edentulous
CLINICAL SCREWLESS FIXED DETACHABLE PARTIAL OVERDENTURE TREATMENT FOR ATROPHIC PARTIAL EDENTULISM OF THE ANTERIOR MAXILLA Dennis Flanagan, DDS This is a case report of the restoration of a partially edentulous
World Journal of Pharmaceutical and Life Sciences WJPLS
 INTRODUCTION Awareness over the years in Dental Implants has increased. Research on newer materials and invention of newer techniques has certainly widened the scope of dental implants. However there are
INTRODUCTION Awareness over the years in Dental Implants has increased. Research on newer materials and invention of newer techniques has certainly widened the scope of dental implants. However there are
A retrospective study on separate single-tooth implant restorations to replace two or more consecutive. maxillary posterior teeth up to 6 years.
 Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
Skeletal System Module 4: Bone Structure
 Connexions module: m47981 1 Skeletal System Module 4: Bone Structure Donna Browne Based on Bone Structure by OpenStax College This work is produced by The Connexions Project and licensed under the Creative
Connexions module: m47981 1 Skeletal System Module 4: Bone Structure Donna Browne Based on Bone Structure by OpenStax College This work is produced by The Connexions Project and licensed under the Creative
BIOH111. o Cell Module o Tissue Module o Integumentary system o Skeletal system o Muscle system o Nervous system o Endocrine system
 BIOH111 o Cell Module o Tissue Module o Integumentary system o Skeletal system o Muscle system o Nervous system o Endocrine system Endeavour College of Natural Health endeavour.edu.au 1 TEXTBOOK AND REQUIRED/RECOMMENDED
BIOH111 o Cell Module o Tissue Module o Integumentary system o Skeletal system o Muscle system o Nervous system o Endocrine system Endeavour College of Natural Health endeavour.edu.au 1 TEXTBOOK AND REQUIRED/RECOMMENDED
Human Anatomy & Physiology
 PowerPoint Lecture Slides prepared by Barbara Heard, Atlantic Cape Community College Ninth Edition Human Anatomy & Physiology C H A P T E R 6 Annie Leibovitz/Contact Press Images 2013 Pearson Education,
PowerPoint Lecture Slides prepared by Barbara Heard, Atlantic Cape Community College Ninth Edition Human Anatomy & Physiology C H A P T E R 6 Annie Leibovitz/Contact Press Images 2013 Pearson Education,
Case Report. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
 Case Report RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
Case Report RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol. RapidSorb Rapid Resorbable Fixation System. Ridge augmentation in a one-step surgical protocol.
SPACE MAINTAINER. Multimedia Health Education. Disclaimer
 Disclaimer This movie is an educational resource only and should not be used to manage your health. All decisions about the management of premature loss of primary teeth and use of space maintainers must
Disclaimer This movie is an educational resource only and should not be used to manage your health. All decisions about the management of premature loss of primary teeth and use of space maintainers must
Socket preservation in the daily practice: A clinical case report
 Clinical Socket preservation in the daily practice: A clinical case report Rabih Abi Nader 1 and Carine Tabarani 2 Abstract Soft tissue contour depends on the underlying bone anatomy. Following tooth extraction,
Clinical Socket preservation in the daily practice: A clinical case report Rabih Abi Nader 1 and Carine Tabarani 2 Abstract Soft tissue contour depends on the underlying bone anatomy. Following tooth extraction,
Skeletal System. The skeletal System... Components
 Skeletal System The skeletal System... What are the general components of the skeletal system? What does the skeletal system do for you & how does it achieve these functions? Components The skeletal system
Skeletal System The skeletal System... What are the general components of the skeletal system? What does the skeletal system do for you & how does it achieve these functions? Components The skeletal system
BONE LABORATORY DEMONSTRATIONS. These demonstrations are found on the bulletin boards outside the MCO Bookstore.
 BONE LABORATORY DEMONSTRATIONS These demonstrations are found on the bulletin boards outside the MCO Bookstore. COMPACT & TRABECULAR BONE - LM When viewed under the polarizing light microscope, the layering
BONE LABORATORY DEMONSTRATIONS These demonstrations are found on the bulletin boards outside the MCO Bookstore. COMPACT & TRABECULAR BONE - LM When viewed under the polarizing light microscope, the layering
Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report
 Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
The Application of Cone Beam CT Image Analysis for the Mandibular Ramus Bone Harvesting
 44 The Application of Cone Beam CT Image Analysis for the Mandibular Ramus Bone Harvesting LivingWell Institute of Dental Research Lee, Jang-yeol, Youn, Pil-sang, Kim, Hyoun-chull, Lee Sang-chull Ⅰ. Introduction
44 The Application of Cone Beam CT Image Analysis for the Mandibular Ramus Bone Harvesting LivingWell Institute of Dental Research Lee, Jang-yeol, Youn, Pil-sang, Kim, Hyoun-chull, Lee Sang-chull Ⅰ. Introduction
Concepts of occlusion Balanced occlusion. Monoplane occlusion. Lingualized occlusion. Figure (10-1)
 Any contact between teeth of opposing dental arches; usually, referring to contact between the occlusal surface. The static relationship between the incising or masticatory surfaces of the maxillary or
Any contact between teeth of opposing dental arches; usually, referring to contact between the occlusal surface. The static relationship between the incising or masticatory surfaces of the maxillary or
Oral Embryology and Histology
 Oral Embryology and Histology Chapter 8 Copyright 2018, Elsevier Inc. All Rights Reserved. 1 Learning Objectives Lesson 8.1: Oral Embryology 1. Pronounce, define, and spell the key terms. 2. Define embryology
Oral Embryology and Histology Chapter 8 Copyright 2018, Elsevier Inc. All Rights Reserved. 1 Learning Objectives Lesson 8.1: Oral Embryology 1. Pronounce, define, and spell the key terms. 2. Define embryology
1- Implant-supported vs. implant retained distal extension mandibular partial overdentures and residual ridge resorption. Abstract Purpose: This
 1- Implant-supported vs. implant retained distal extension mandibular partial overdentures and residual ridge resorption. Abstract Purpose: This retrospective study in male patients sought to examine posterior
1- Implant-supported vs. implant retained distal extension mandibular partial overdentures and residual ridge resorption. Abstract Purpose: This retrospective study in male patients sought to examine posterior
Immediate Implant Placement:
 Immediate Implant Placement: Parameters Influencing Tissue Remodeling Bernard Touati, DDS and Mario Groisman, DDS In esthetic implant therapy, the patient s objective is to obtain an imperceptible, natural-looking
Immediate Implant Placement: Parameters Influencing Tissue Remodeling Bernard Touati, DDS and Mario Groisman, DDS In esthetic implant therapy, the patient s objective is to obtain an imperceptible, natural-looking
KEY CONCEPTS Unit 6 THE SKELETAL SYSTEM
 ANATOMY & PHYSIOLOGY 1 (101-805 - AB) PAUL ANDERSON 2011 KEY CONCEPTS Unit 6 THE SKELETAL SYSTEM A Overview of The Skeletal System 1. Definition: Anatomically the SKELETAL SYSTEM consists of bones, cartilages,
ANATOMY & PHYSIOLOGY 1 (101-805 - AB) PAUL ANDERSON 2011 KEY CONCEPTS Unit 6 THE SKELETAL SYSTEM A Overview of The Skeletal System 1. Definition: Anatomically the SKELETAL SYSTEM consists of bones, cartilages,
b. Adult bones produce 2.5 million RBCs each second.
 Ch 6 Skeletal System I. Functions of the Skeletal System A. The skeletal system consists of: 1. bones, cartilage, tendons and ligaments B. Living bone is not Gr. dried up 1. It is dynamic and adaptable
Ch 6 Skeletal System I. Functions of the Skeletal System A. The skeletal system consists of: 1. bones, cartilage, tendons and ligaments B. Living bone is not Gr. dried up 1. It is dynamic and adaptable
Failures in implant therapy. Biological and mechanical complications. Their prevention management. Dr. Katalin Csurgay Dr.
 Failures in implant therapy. Biological and mechanical complications. Their prevention management. Dr. Katalin Csurgay Dr. Tatiana Shkolnik Complications could be: Doctor related Patient related Early
Failures in implant therapy. Biological and mechanical complications. Their prevention management. Dr. Katalin Csurgay Dr. Tatiana Shkolnik Complications could be: Doctor related Patient related Early
Guided surgery as a way to simplify surgical implant treatment in complex cases
 52 STARGET 1 I 12 StraUMaNN CareS r ry vincenzo MiriSOLA Di TOrreSANTO AND LUCA COrDArO Guided surgery as a way to simplify surgical implant treatment in complex cases Background A 41-year-old woman with
52 STARGET 1 I 12 StraUMaNN CareS r ry vincenzo MiriSOLA Di TOrreSANTO AND LUCA COrDArO Guided surgery as a way to simplify surgical implant treatment in complex cases Background A 41-year-old woman with
The Skeletal System PART A
 5 The Skeletal System PART A PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB The Skeletal System
5 The Skeletal System PART A PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB The Skeletal System
Component parts of Chrome Cobalt Removable Partial Denture
 Lec. 5 د.بسام الطريحي Component parts of Chrome Cobalt Removable Partial Denture Major connectors: Are either bars or plates, the difference between them is in the amount of tissue covers. Plates are broad
Lec. 5 د.بسام الطريحي Component parts of Chrome Cobalt Removable Partial Denture Major connectors: Are either bars or plates, the difference between them is in the amount of tissue covers. Plates are broad
Chapter 6: Osseous Tissue and Bone Structure
 Chapter 6: Osseous Tissue and Bone Structure I. An Introduction to the Skeletal System, p. 180 Objective: Describe the functions of the skeletal system The skeletal system includes: - bones of the skeleton
Chapter 6: Osseous Tissue and Bone Structure I. An Introduction to the Skeletal System, p. 180 Objective: Describe the functions of the skeletal system The skeletal system includes: - bones of the skeleton
Treatment planning in a case of restoration of the maxilla and mandible using osseointegrated implants with four types of bone graft
 227 Journal of Oral Science, Vol. 45, No. 4, 227-232, 2003 Case report Treatment planning in a case of restoration of the maxilla and mandible using osseointegrated implants with four types of bone graft
227 Journal of Oral Science, Vol. 45, No. 4, 227-232, 2003 Case report Treatment planning in a case of restoration of the maxilla and mandible using osseointegrated implants with four types of bone graft
Bones. The division of bones anatomically is : long, short, irregular, flat and sesamoid.
 Bones Osteocytes : Are responsible for maintenance of bones Present in lacunae, and send processes. Unable to divide. The division of bones anatomically is : long, short, irregular, flat and sesamoid.
Bones Osteocytes : Are responsible for maintenance of bones Present in lacunae, and send processes. Unable to divide. The division of bones anatomically is : long, short, irregular, flat and sesamoid.
CHAPTER. 1. Uncontrolled systemic disease 2. Retrognathic jaw relationship
 CHAPTER 7 Immediate Implant Supported Restoration of the Edentulous Arch Stephen G. Alfano and Robert M. Laughlin Department of Oral and Maxillofacial Surgery, Naval Medical Center San Diego, San Diego,
CHAPTER 7 Immediate Implant Supported Restoration of the Edentulous Arch Stephen G. Alfano and Robert M. Laughlin Department of Oral and Maxillofacial Surgery, Naval Medical Center San Diego, San Diego,
Prosthodontic Rehabilitation with Overdenture Using Modified Impression Technique: A Case Report
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 10 Ver.VII (Oct. 2015), PP 102-107 www.iosrjournals.org Prosthodontic Rehabilitation with Overdenture
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 10 Ver.VII (Oct. 2015), PP 102-107 www.iosrjournals.org Prosthodontic Rehabilitation with Overdenture
Fundamental & Preventive Curvatures of Teeth and Tooth Development. Lecture Three Chapter 15 Continued; Chapter 6 (parts) Dr. Margaret L.
 Fundamental & Preventive Curvatures of Teeth and Tooth Development Lecture Three Chapter 15 Continued; Chapter 6 (parts) Dr. Margaret L. Dennis Proximal contact areas Contact areas are on the mesial and
Fundamental & Preventive Curvatures of Teeth and Tooth Development Lecture Three Chapter 15 Continued; Chapter 6 (parts) Dr. Margaret L. Dennis Proximal contact areas Contact areas are on the mesial and
Fig Articular cartilage. Epiphysis. Red bone marrow Epiphyseal line. Marrow cavity. Yellow bone marrow. Periosteum. Nutrient foramen Diaphysis
 Fig. 7.1 Articular cartilage Epiphysis Red bone marrow Epiphyseal line Marrow cavity Yellow bone marrow Nutrient foramen Diaphysis Site of endosteum Compact bone Spongy bone Epiphyseal line Epiphysis Articular
Fig. 7.1 Articular cartilage Epiphysis Red bone marrow Epiphyseal line Marrow cavity Yellow bone marrow Nutrient foramen Diaphysis Site of endosteum Compact bone Spongy bone Epiphyseal line Epiphysis Articular
Utilizing Digital Treatment Planning and Guided Surgery in Conjunction with Narrow Body Implants. by Timothy F. Kosinski, DDS, MAGD
 Utilizing Digital Treatment Planning and Guided Surgery in Conjunction with Narrow Body Implants by Timothy F. Kosinski, DDS, MAGD Implant dentistry is undergoing some amazing transformations. With the
Utilizing Digital Treatment Planning and Guided Surgery in Conjunction with Narrow Body Implants by Timothy F. Kosinski, DDS, MAGD Implant dentistry is undergoing some amazing transformations. With the
Quiz 6. Cartilage and Bone
 Quiz 6 Cartilage and Bone MCQs X type (true or false): 1. Cartilage tissue: a. Has a rich blood supply. b. Develops from mesenchyme. c. Has ability for a quick regeneration. d. Has chondrocytes as precursor
Quiz 6 Cartilage and Bone MCQs X type (true or false): 1. Cartilage tissue: a. Has a rich blood supply. b. Develops from mesenchyme. c. Has ability for a quick regeneration. d. Has chondrocytes as precursor
PERIODONTAL REVIEW DENTALELLE TUTORING ANDREA TWAROWSKI
 PERIODONTAL REVIEW DENTALELLE TUTORING ANDREA TWAROWSKI Periodontics Questions 1. What is the periodontium composed of? 2. What type of mucosa is the gingiva composed of? 3. Is it normal to have melanin
PERIODONTAL REVIEW DENTALELLE TUTORING ANDREA TWAROWSKI Periodontics Questions 1. What is the periodontium composed of? 2. What type of mucosa is the gingiva composed of? 3. Is it normal to have melanin
LAB: The Skeletal System System
 WLHS/A&P/Oppelt Name LAB: The Skeletal System System Background: The skeletal system is primarily responsible for supporting the body and protecting vital organs. We are bone with more than 270 bones that
WLHS/A&P/Oppelt Name LAB: The Skeletal System System Background: The skeletal system is primarily responsible for supporting the body and protecting vital organs. We are bone with more than 270 bones that
Non-osseointegrated. What type of mini-implants? 3/27/2008. Require a tight fit to be effective Stability depends on the quality and.
 Non-osseointegrated What type of mini-implants? Require a tight fit to be effective Stability depends on the quality and quantity of cortical and trabecular bone. Osseointegrated Non-osseointegrated AbsoAnchor
Non-osseointegrated What type of mini-implants? Require a tight fit to be effective Stability depends on the quality and quantity of cortical and trabecular bone. Osseointegrated Non-osseointegrated AbsoAnchor
SKELETAL SYSTEM I NOTE: LAB ASSIGNMENTS for this topic will run over 3 Weeks. A SEPARATE WORKSHEET WILL BE PROVIDED.
 BIO 211; Anatomy and Physiology I REFERENCE: CHAPTER 07 1 Dr. Lawrence Altman Naugatuck Valley Community College LECTURE TOPICS OUTLINE SKELETAL SYSTEM I NOTE: LAB ASSIGNMENTS for this topic will run over
BIO 211; Anatomy and Physiology I REFERENCE: CHAPTER 07 1 Dr. Lawrence Altman Naugatuck Valley Community College LECTURE TOPICS OUTLINE SKELETAL SYSTEM I NOTE: LAB ASSIGNMENTS for this topic will run over
