FEMALE REPRODUCTUVE SYSTEM
|
|
|
- Brenda Warren
- 6 years ago
- Views:
Transcription
1 FEMALE REPRODUCTUVE SYSTEM
2 Female reproductive organs Figure 81-1
3 Internal structures of the uterus, ovary and a Fallopian tube Figure 81-2
4 Fundamental reproductive unit = single ovarian follicle, composed of one germ cell (oocyte), surrounded by endocrine cells. Oogenesis : A developing egg (Oocyte) becomes Mature egg (Ovum) through series of steps.
5 Oogenesis: Oogonia produced by mitotic division (max # = 7 mil), Then during the last part (5 th month) of fetal life, prophase of 1 st meiosis starts but do not complete becomes primary oocyte (they contain diploid number of chromosomes 46 but do not separate). The primary oocytes stay in this meiotic arrest for years until prepare for ovulation. Number of primary oocytes decreases throughout childhood from 1-2 mil to 400,000 just before puberty. Before birth each oocyte surrounded by single layer of granulosa cells -- called primordial follicle -- complete about 6 mos after birth
6
7 Female hormonal system 1. Hypothalamic releasing hormone, gonadotropin releasing hormone GnRH 2. Anterior pituitary sex hormones,fst and LH 3. Ovarian hormones, estrogen and progesterone secreted in response to pituitary hormones 4. These hormones secreted at different rate during different parts of the female monthly sexual cycle.
8
9
10 Prior to birth first meiosis stops in prophase Pre-puberty MENARCHE 400,000 primary oocytes left 6-12 follicles develop One dominant follicle matures Ovulation -- end 1 st meiosis -- start 2 nd meiosis in fallopian tubes Figure 81-4
11
12 Differences between spermatogenesis and oogenesis 1. In females, mitotic proliferation of oogonia occurs prior to birth. In males, spermatogonia proliferate only after puberty. 2. In females, meiotic divisions of oocyte produces only one mature ovum. In males, meiotic divisions of primary spermatocyte produces 4 mature spermatozoa 3. In females, second meiotic division is completed only upon fertilization. In males, the products of meiosis (spermatids) undergo substantial differentiation in the maturing process.
13 The Basics Gametogenesis
14 Female sexual cycle: Menstrual cycle -- controlled by gonadotropins, gonadal hormones Ovarian cycle-- follicular phase -- avg 15 d (range, 9-23 days) ovulatory phase d -- culminates with ovulation luteal phase 13 d -- less variable than follicular Endometrial cycle -- menstruation, proliferative and secretory phases
15 OVARIAN CYCLE In female child each ovum is surrounded by single granulosa cells sheath called primordial follicle. Granulosa cells provide nourishment to the ovum and secrete oocyte maturation inhibition factor that keep the ovum in suspended in its primordial state. After puberty LH and FSH increase and cause growth of the follicle to becomes primary follicle.
16 Some spindle cells derived from ovary interstitium Collect in several layers outside granulosa giving rise to mass of cells outside granulosa cells called theca cells. 1- Theca interna secrete estrogen and progesterone 2-Theca externa form capsule of the developing follicle
17 After expulsion of the ovum from the follicle the remaining granulosa and theca interna cells change into lutein cells and growth to form corpus luteum. Now 1-Granulosa cells form progesterone and estrogen 2-Theca cells form androgen androstenedion and testosterone which are change by aromatase enzyme in the granulosa cells to estrogen
18
19 Introduction: Ovarian cycle is a series of monthly repetitive physiological and developmental changes in the ovaries, which prepare the ovaries for ovulation and subsequent development of a C.L whose hormones will assist in regulating the uterine cycle and, if the implantation of a developing embryo occurs, assist in regulating the pregnancy. It is regulated by FSH and LH from the anterior pit.
20 The changes that occur in the ovary during each cycle can be divided into three phases: 1) Follicular phase (day 1-13 ) 2) Ovulatory phase (day 13-15) 3) The luteal phase (day 15-28). These phases run in parallel with the phases of the uterine cycle and together comprise the menstrual cycle.
21 1) The follicular phase: Starts from the first day of menstruation until ovulation. The primary goal: to develop a viable follicle capable of undergoing ovulation. The early events initiated by in FSH levels at the first day of the cycle To a in P and E levels at the end of the previous cycle and the subsequent removal of inhibition of FSH by these ovarian hormones Stages: A- Primordial follicle C- Antral follicle B- Primary follicle D- Vesicular follicle
22 1) Follicular Phase of the ovarian cycle A.Primordial follicle (7 millions): ovum with granulosa cell (GC)sheath (nourisment & oocyte maturation-inhibiting substance). B. Primary Follicle: after puberty 2-3 fold increase, several layers of GC. 300,000 follicles C.Antral Follicle: FSH causes proliferation of GC, development of theca interna & theca externa, GC secrete follicular fluid rich in estrogen leading to antrum formation.
23 1) Follicular Phase, cont D. Vesicular Follicle: Estrogen makes GC more sensitive to FSH, FSH & Estrogen promote LH R, LH & Estrogen cause proliferation & secretion. On the 6 th day one follicle becomes dominant F, while others regress, forming atretic follicles. High level of estrogen acts on hypothalamus to decrease FSH by ant. Pit. Only one Graafian F (mature F with cm diameter) is formed each month.
24 A)Approximately 500 oocytes are ovulated over the course of a lifetime. B) At ovulation: The follicle ruptures releasing the secondary oocyte and corona radiata into the peritoneal cavity to be taken up by the oviduct. The zona granulosa and thecal cells remain in the ovary. Discharge of the ovum occur (with part of the cumulus) of the mature Graafian follicle from the surface of ovary at the middle of the cycle (14+2 days before the subsequent menstruation).
25 Chemical mechanics of ovulation: LH surge prostaglandin endoperoxide synthase in granulosa cells (sets up pseudoinflammatory response) FSH (some LH) stimulates release of plasminogen activator from granulosa cells (converts plasminogen to plasmin) Prostaglandins E and F release lysosomal enzymes that digest follicular wall -- not completely understood Stigma -- forms on surface of follicle, balloons out, forms vesicle and ruptures -- oocyte expelled Process facilitated by intrafollicular pressure and contraction of smooth muscle in theca
26
27 Corpus luteum (CL): Occur after ovulation, Morphological changes occur in the remaining part of the follicle within the next 2-3 days converting it to CL. Formed from: The zona granulosa granulosa lutein Theca cells theca lutein cells & some capilaries & c.t. } Cells become cuboidal with central nucleus
28 Corpus leutum 1-Granulosa cells secrete mainly progesterone and estrogen 2- Theca cells form androgen,androstenedione and testosterone and these converted by enzyme aromatase in the granulosa cells into estrogen 3-Local hormone in the follicular fluid called luteinization- inhibiting factor hold luteinization until after ovulation
29 3) Luteal phase (cont) corpus luteum (cont.) CL produces Progesterone if pregnancy occur promote required progesterone until formation of the placenta Some estrogen. NB: resulting in secretory endometrium in preparation for reception of fertilized ovum Corpus luteum life span In the absence of fertilization, 14 days apoptosis Corpus albicans. If pregnancy occur, The chorionic gonadotrophin having LH like action causes further growth of CL ( and its hormonal production ) CL of pregnancy (support the early embryo until placenta takes over the function of E & P production).
30 Involution of CL 1-Estrogen and progesterone inhibit the secretion Of ant Pit FSH & LH cause degeneration of CL 2- Lutein cells secrete small amount of inhibin hormone which inhibit FSH secretion cause degeneration of CL
31
32
33 H-P-O axis 1. Positive feedback Sex hormones (E) GnRH or LH/FSH E peak ( 200pg/ml) LH/FSH peak During ovulation only. 2. Negative feedback Sex hormones (E) GnRH or LH/FSH Follicular phase: E FSH Luteal phase: E P LH/FSH (formation) E P LH/FSH (regrescospyrigihto 201n1 by Sa)unders, an imprint of Elsevier Inc.
34 Indicators of ovulation: i. Mid-abdominal pain (irritation of the peritoneum). ii. elasticity of cervical mucus iii. Cervical mucus dries in Arborizing form iv. Cornified cells in the vaginal mucosa v. Basal body temperature ( 0.5 o C) vi. Urinary E, and pregnanediol or plasma progesterone level during luteal phase(day 21) Absolute proof of ovulation is pregnancy.
35
36 C.Luteal phase a. Interval between ovulation and menstrual flow (15 th - 28 th day). b. Duration is κ: 14±2d (t½ = corpus luteum). c. Day of ovulation = Length of the menstrual cycle - 14d d. Predominant Hormone: Progesterone nc.
37 Corpus luteum Provides necessary hormones for implantation of blastocyst and maintenance of zygote until placenta can take over 80% granulosa cells, 20% thecal cells If not fertilization, will regress in about 14 d Avascular scar = corpus albicans
38 .
39 Ovarian Cycle: follicular phase luteal phase ovulation (FORMAT FOR NEXT FEW SLIDES) Endometrial 1 Cycle: 4 14 menstrual proliferative phase (11 d) secretory phase (12d) 28
40 Ovarian Cycle:follicular phase LH surge ovulation FSH and LH in the Follicular phase LH surge lasts 48 h Inc GnRH bursts FSH LH Endometrial Cycle: menstrual proliferative phase (11 d) secretory phase (12d) 28
41 Ovarian Cycle: follicular phase LH surge ovulation Increase in estradiol to stimulate LH surge. Then estradiol has negative feedback on GnRH to reduce LH, FSH. estradiol FSH LH Endometrial Cycle: Proliferative phase neg feedback--g nrh Secretory phase (12d) 28
42 Ovarian Cycle: follicular phase Changes in activin and inhibin in follicular phase. ovulation + FSH _ Granulosa cells Activin inhibin FSH activin inhibin Endometrial Proliferative phase Cycle: menstrual Secretory phase (12d)28 activin inhibin
43 Ovarian Cycle: follicular phase ovulation Changes in progesterone in follicular phase. progesterone activin progesterone 1 Endometrial Cycle:menstrual 4 14 Proliferative phase (11 d) 28 inhibin
44 The uterine cycle and normal menstruation: Because of the monthly cyclic production of estrogens and progesterone, the endometrial lining of the uterus passes into three phases. They are; Proliferative phase, Secretory (or luteal phase), and menstrual phase.
45
46 1-Proliferative phase It is about 9-11 days in duration. Estrogen secreted in increasing quantities by the developing follicle causes proliferation of the epithelial cells left after endometrial desquamation. Endothelial re-epithelialization occurs within 4-7 days after the beginning of menstruation (when bleeding ceases). The next 7-10 days the endometrial thickness increases greatly to about 3-5 mm (formation of new endometrial glands and blood vessels). The mucus strings secreted by the endometrial glands (especially these of the cervix), align in the cervical canal, forming channels that guide sperm in the proper direction from vagina into the uterus.
47 2. The secretory phase (progesterone phase, luteal phase) The length of this phase is remarkably constant at about 14 days. Occurs after ovulation (the second half of the cycle). Estrogens cause slight additional cellular proliferation, whereas progesterone causes marked swelling and secretory development with further increase in blood supply to the endometrium. Both blood vessels and glands become highly tortuous. Lipid and glycogen deposit greatly in the stromal cells. The peak of the secretory phase is about 1 week after ovulation. At this time, the endometrial thickness reaches to 5-6 mm. During the secretory phase, the endometrium provides appropriate conditions for implantation of a fertilized ovum. The fertilized ovum needs 3-4 days to enter the uterine cavity from fallopian tube and another 4-5 days for implantation. During this intervals uterine secretions (uterine milk) provide nutrition for the early dividing ovum. Once the ovum implants, trophoblastic cells of the blastocyst begin to digest the endometrium.
48 3. Normal menstruation Occurs when fertilization fails to occur during the secretory phase (involution of corpus luteum). The usual duration of the menstrual flow is 3-5 days (1-8 days range). Blood loss reaches up to 80 ml (average ml). Bleeding can increase because of medications and diseases that affect the clotting mechanism. 24 hours before menstruation blood vessels leading to the mucosal layers become vasospastic, presumably because of vasoconstrictor types of prostaglandins. The vasospasm + nutrients + hormonal stimulation endometrial necrosis Hemorrhage + Sloughing of outer layers of the endometrium Prostaglandins and desquamated tissues initiate uterine contractions that expel the uterine contents. The menstrual fluid is normally non-clotting because of released fibrinolysin. Clots presence may indicate uterine pathology. Menstrual flow is rich in leukocytes. This outflow of leukocytes may explain the resistance of uterus to infection during menstruation despite the denuded endothelial surface.
49 Normal menstruation
50 The standard classification of abnormal bleeding for patterns (1)Menorrhagia (hypermenorrhea) is heavy or prolonged menstrual flow during regular period. The presence of clots may not be abnormal but may signify excessive bleeding. (2)Hypomenorrhea (cryptomenorrhea) is unusually light menstrual flow, sometimes only spotting, during regular period. An obstruction such as hymenal or cervical stenosis may be the cause.
51 (3) Metrorrhagia (intermenstrual bleeding) is bleeding that occurs at any time between menstrual periods. (4) Polymenorrhea describes periods that occur too frequently, usually associated with anovulation and rarely with a shortened luteal phase in the menstrual cycle. (5)Oligomenorrhea describes menstrual periods that occur more than 35 days apart. Bleeding usually is decreased in amount and associated with anovulation, either from endocrine causes (eg, pregnancy, pituitary-hypothalamic causes, menopause) or systemic causes (eg, excessive weight loss).
52 Cyclic changes in Cervix, vagina & breasts: 1-Cervix 2-Vagina 3-Breasts Estrogen:make mucus Thinner,more alkaline If spread on slide dries in fern like manner Estrogen:cornification of vaginal epithelium Estrogen:Proliferation of breasts ducts Progesterone:make mucus thick,tenaciuous,more cellular,if spread on slide doesn t fern Progesterone:thick mucus secretion,proliferation of vaginal epithelium and leucocytes infiltration Progesterone:growth of breast lobules & alveoli
53 2011 by Saunders, an imprint of Elsevier Inc.
54 H-P-O axis 1. Positive feedback Sex hormones (E) GnRH or LH/FSH E peak ( 200pg/ml) LH/FSH peak During ovulation only. 2. Negative feedback Sex hormones (E) GnRH or LH/FSH Follicular phase: E FSH Luteal phase: E P LH/FSH (formation) E P LH/FSH (regrescospyrigihto 201n1 by Sa)unders, an
55 Ovarian Cycle: ovulation + Corpus albicans Luteal phase + FSH _ Granulosa cells Activin inhibin FSH activin inhibin 1 Endometrial Cycle: 4 14 Proliferative phase menstrual (11 d) Secretory phase (12d) 28
56 Ovarian Cycle: + Luteal phase Corpus albicans ovulation Levels of estradiol in luteal phase + FSH _ Granulosa cells Activin inhibin estradiol Endometrial Cycle: proliferative phase FSH secretory phase 28 inhibin
57 Ovarian Cycle: follicular phase ovulation Corpus luteum + _ Luteal phase Corpus albicans Changes in estradiol And progesterone in luteal phase. + Produces inhib GnRH _ progesterone estradiol 1 4 mens Endometrial proliferative phase Cycle: 14 secretory phase 28
58
59 Functions of estradiol Fat deposition: more subcutaneous fat in women than men Estrogens: hips and thighs fat deposition (prior to menopause) then more abdominal (Men: androgens: abdominal fat deposition) Skin: increase vascularization of skin, smooth and soft. Bones: estrogen inhibits osteoclastic activity, so height increases after puberty,but epiphyses and shafts of bones unite early and growth stops
60 Functions of estradiol External female sex organs: at puberty, increase in size of fallopian tubes, uterus and vagina, external genitalia deposition of fat in mons pubis change vaginal epithelia from cuboidal to stratified type endometrium: proliferation of cells and endometrial glands (important in nutrition of fertilized ovum) Breasts: fat deposition, development of stromal cells, ducts (progesterone, prolactin important in milk production)
61
62
63 Functions of estrogen and Progesterone: Estrogen Progesterone 1-Facilitate growth of follicles 1-Causes secretory phase of menstrual cycle 2-growth of ovaries, fallopian tubes, uterus, vagina and female external genitalia,breasts duct system and deposit of fat in the breast. 3-Produce female 2ry sex characters,body configuration,fat distribution & increase libido 4-Produce proliferative phase of Menstrual cycle,++uterine blood flow,musculature and make it more sensitive to oxytocin 5-produce cyclic changes in cervix & vagina 6-Control FSH&LH secretion & causes the LH surge at midcycle 7-Has metabolic anabolic effects, cause epiphyseal closure of bones(also ++bone density),decrease serum cholesterol level,++angiotensinogen secretion from liver,increase HDL,--LDL(Cardioprotective) Produce salt & water retention. Increase metabolism and fat deposition, slight increase protein deposition. 2-Stimulate developmentof breast lobules & alveoli 3-Essentia for maitenance of pregnancy and increase secretion of fallopian tubes essential for nutient of fertilized ovum. 4-Decrease sensitivity of uterus to oxytocin 5-Produce cyclic changes in cervix & vagina 6-Inhibit LH secretion during pregnancy (producing amenorrhea) 7-Thermogenic effect(++body temperature by 0.5 C at ovulation) ++respiratory rate Produce natriuresis No anabolic functions ---alveolar CO2
64 Female sexual act 1-Stimulation of female sexual act : Thinking lead to sexual desire and this desire change during the cycle reaching the peak near ovulation because of high estrogen. Physical stimulation as in male ( perineal region). Same nerve signals. 2-Female erection and lubrication (clitoris): as the penis control by parasympathetic nerves, same mechanism as in male 3-Female orgasm (female climax):analog to emission and ejaculation in male.
65 Female sexual response -- process is similar in males and females: 1) Excitement phase:caused by psychological or physical stimulation; engorgement and erection of clitoris, vaginal congestion -- due to NO, secreted by parasympathetic nerves 2) Plateau phase:intensification of these responses, increased HR, BP, respiratory rate, muscle tension 3) Orgasmic phase:culmination of sexual excitement, intense physical pleasure 4) Resolution phase:returns genitalia and body systems to pre-arousal state
66 Male and female sexual response Differences: Women don t require refractory time before beginning excitation again No ejaculation in the female
67 Female sexual dysfunction may be as high as 45% in women aged yrs mechanisms: psychological illness unknown
68 Menopause Defn:obsolescence of ovaries, no estradiol production, ova only occasional secondary follicle, few primary follicles Occurs at 51.4 yr of age (average) Due to reduction in estrogen, low levels of inhibin, no negative feedback of LH and FSH; therefore, high levels LH and FSH Can occur naturally, due to surgery or as a result of chemotherapy
69 Women s Health Initiative Increased risk of CHD, stroke, pulm embolis (3x), breast cancer HRT regimen should not be initiated or continued for primary prevention of CHD JAMA 2002
70 pppp Physiological changes in the body during menopause 1-Hot flushes 2-Irritability 3-Anxiety 4- Fatigue 5- Psychic dyspnea 6-Decrease strength of the bones 7-Vaginal dryness 8-Gradual atrophy of genital organs Small dose of estrogen reverse these symptoms
71 Polycystic ovary syndrome Affects 10% of reproductive age women Characteristics: hyperandrogenemia oligomenorrhea obesity hirsutism infertility enlarged cystic ovaries Rx: metformin, anti-androgens?
72 Abnormal secretion of the ovaries: 1-Hypogonadism reduce secretion A- Before puberty cause infantile sexual organs, no secondary sexual character and tall female B- After puberty cause infantile sexual organs include the uterus, small vagina, breast atrophy C-Irregularity of menses and amenorrhea. 2-hypersecretion rare (granulosa cell tumor) and mainly cause irregular bleeding.
73 Female fertility: 1-Fertile period of each cycle (4-5 days), before ovulation 2-Rhythm method for contraceptive (75%). 3- Hormonal suppression of fertility (the pills) : use of estrogen or progesterone in the first half of the cycle prevent ovulation by prevent preovulatory surge of LH secretion by pituitary gland (90%). 4- Female sterility : A-Failure of ovulation mainly reduce gonadotropin hormone B-Endometriosis, salpingitis,
Female reproductive system II Enas Omar. Notes are in green
 Female reproductive system II Enas Omar Notes are in green C.Luteal phase a. Interval between ovulation and menstrual flow (15 th - 28 th day.( b. Duration is κ: 2± 14d (t½ = corpus luteum.( c. Day of
Female reproductive system II Enas Omar Notes are in green C.Luteal phase a. Interval between ovulation and menstrual flow (15 th - 28 th day.( b. Duration is κ: 2± 14d (t½ = corpus luteum.( c. Day of
Reproductive System. Testes. Accessory reproductive organs. gametogenesis hormones. Reproductive tract & Glands
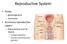 Reproductive System Testes gametogenesis hormones Accessory reproductive organs Reproductive tract & Glands transport gametes provide nourishment for gametes Hormonal regulation in men Hypothalamus - puberty
Reproductive System Testes gametogenesis hormones Accessory reproductive organs Reproductive tract & Glands transport gametes provide nourishment for gametes Hormonal regulation in men Hypothalamus - puberty
The reproductive lifespan
 The reproductive lifespan Reproductive potential Ovarian cycles Pregnancy Lactation Male Female Puberty Menopause Age Menstruation is an external indicator of ovarian events controlled by the hypothalamicpituitary
The reproductive lifespan Reproductive potential Ovarian cycles Pregnancy Lactation Male Female Puberty Menopause Age Menstruation is an external indicator of ovarian events controlled by the hypothalamicpituitary
Chapter 27 The Reproductive System. MDufilho
 Chapter 27 The Reproductive System 1 Figure 27.19 Events of oogenesis. Before birth Meiotic events 2n Oogonium (stem cell) Mitosis Follicle development in ovary Follicle cells Oocyte 2n Primary oocyte
Chapter 27 The Reproductive System 1 Figure 27.19 Events of oogenesis. Before birth Meiotic events 2n Oogonium (stem cell) Mitosis Follicle development in ovary Follicle cells Oocyte 2n Primary oocyte
Outline. Male Reproductive System Testes and Sperm Hormonal Regulation
 Outline Male Reproductive System Testes and Sperm Hormonal Regulation Female Reproductive System Genital Tract Hormonal Levels Uterine Cycle Fertilization and Pregnancy Control of Reproduction Infertility
Outline Male Reproductive System Testes and Sperm Hormonal Regulation Female Reproductive System Genital Tract Hormonal Levels Uterine Cycle Fertilization and Pregnancy Control of Reproduction Infertility
Chapter 28: REPRODUCTIVE SYSTEM: MALE
 Chapter 28: REPRODUCTIVE SYSTEM: MALE I. FUNCTIONAL ANATOMY (Fig. 28.1) A. Testes: glands which produce male gametes, as well as glands producing testosterone 2. Seminiferous tubules (Fig.28.3; 28.5) a.
Chapter 28: REPRODUCTIVE SYSTEM: MALE I. FUNCTIONAL ANATOMY (Fig. 28.1) A. Testes: glands which produce male gametes, as well as glands producing testosterone 2. Seminiferous tubules (Fig.28.3; 28.5) a.
9.4 Regulating the Reproductive System
 9.4 Regulating the Reproductive System The Reproductive System to unite a single reproductive cell from a female with a single reproductive cell from a male Both male and female reproductive systems include
9.4 Regulating the Reproductive System The Reproductive System to unite a single reproductive cell from a female with a single reproductive cell from a male Both male and female reproductive systems include
CASE 41. What is the pathophysiologic cause of her amenorrhea? Which cells in the ovary secrete estrogen?
 CASE 41 A 19-year-old woman presents to her gynecologist with complaints of not having had a period for 6 months. She reports having normal periods since menarche at age 12. She denies sexual activity,
CASE 41 A 19-year-old woman presents to her gynecologist with complaints of not having had a period for 6 months. She reports having normal periods since menarche at age 12. She denies sexual activity,
Testes (male gonads) -Produce sperm -Produce sex hormones -Found in a sac called the scrotum -Suspended outside of the body cavity for temperature
 REPRODUCTION Testes (male gonads) -Produce sperm -Produce sex hormones -Found in a sac called the scrotum -Suspended outside of the body cavity for temperature reduction -Testes wall made of fibrous connective
REPRODUCTION Testes (male gonads) -Produce sperm -Produce sex hormones -Found in a sac called the scrotum -Suspended outside of the body cavity for temperature reduction -Testes wall made of fibrous connective
REPRODUCCIÓN. La idea fija. Copyright 2004 Pearson Education, Inc., publishing as Benjamin Cummings
 REPRODUCCIÓN La idea fija How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development, birth
REPRODUCCIÓN La idea fija How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development, birth
Functions of male Reproductive System: produce gametes deliver gametes protect and support gametes
 Functions of male Reproductive System: produce gametes deliver gametes protect and support gametes Spermatogenesis occurs in the testes after puberty. From the testes they are deposited into the epididymas
Functions of male Reproductive System: produce gametes deliver gametes protect and support gametes Spermatogenesis occurs in the testes after puberty. From the testes they are deposited into the epididymas
Physiology of Male Reproductive System
 Physiology of Male Reproductive System the anterior pituitary gland serves as the primary control of reproductive function at puberty Ant Pituitary secretes FSH & large amounts of LH (ICSH) FSH & LH cause
Physiology of Male Reproductive System the anterior pituitary gland serves as the primary control of reproductive function at puberty Ant Pituitary secretes FSH & large amounts of LH (ICSH) FSH & LH cause
SISTEMA REPRODUCTOR (LA IDEA FIJA) Copyright 2004 Pearson Education, Inc., publishing as Benjamin Cummings
 SISTEMA REPRODUCTOR (LA IDEA FIJA) How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development,
SISTEMA REPRODUCTOR (LA IDEA FIJA) How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development,
MULTIPLE CHOICE: match the term(s) or description with the appropriate letter of the structure.
 Chapter 27 Exam Due NLT Thursday, July 31, 2015 Name MULTIPLE CHOICE: match the term(s) or description with the appropriate letter of the structure. Figure 27.1 Using Figure 27.1, match the following:
Chapter 27 Exam Due NLT Thursday, July 31, 2015 Name MULTIPLE CHOICE: match the term(s) or description with the appropriate letter of the structure. Figure 27.1 Using Figure 27.1, match the following:
Reproductive physiology. About this Chapter. Case introduction. The brain directs reproduction 2010/6/29. The Male Reproductive System
 Section Ⅻ Reproductive physiology Ming-jie Wang E-Mail: mjwang@shmu.edu.cn About this Chapter The reproductive organs and how they work the major endocrine functions of sexual glands actions of sex hormones
Section Ⅻ Reproductive physiology Ming-jie Wang E-Mail: mjwang@shmu.edu.cn About this Chapter The reproductive organs and how they work the major endocrine functions of sexual glands actions of sex hormones
Female Reproductive System. Lesson 10
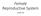 Female Reproductive System Lesson 10 Learning Goals 1. What are the five hormones involved in the female reproductive system? 2. Understand the four phases of the menstrual cycle. Human Reproductive System
Female Reproductive System Lesson 10 Learning Goals 1. What are the five hormones involved in the female reproductive system? 2. Understand the four phases of the menstrual cycle. Human Reproductive System
MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question.
 MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) Which of the following hormones controls the release of anterior pituitary gonadotropins? A) LH
MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) Which of the following hormones controls the release of anterior pituitary gonadotropins? A) LH
Male Reproduction Organs. 1. Testes 2. Epididymis 3. Vas deferens 4. Urethra 5. Penis 6. Prostate 7. Seminal vesicles 8. Bulbourethral glands
 Outline Terminology Human Reproduction Biol 105 Lecture Packet 21 Chapter 17 I. Male Reproduction A. Reproductive organs B. Sperm development II. Female Reproduction A. Reproductive organs B. Egg development
Outline Terminology Human Reproduction Biol 105 Lecture Packet 21 Chapter 17 I. Male Reproduction A. Reproductive organs B. Sperm development II. Female Reproduction A. Reproductive organs B. Egg development
10.7 The Reproductive Hormones
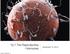 10.7 The Reproductive Hormones December 10, 2013. Website survey?? QUESTION: Who is more complicated: men or women? The Female Reproductive System ovaries: produce gametes (eggs) produce estrogen (steroid
10.7 The Reproductive Hormones December 10, 2013. Website survey?? QUESTION: Who is more complicated: men or women? The Female Reproductive System ovaries: produce gametes (eggs) produce estrogen (steroid
Embryology Lecture # 4
 1 Quick Review: Oogenesis : - Oogonia start appear in the ovary when the age of the fetus 1 is th (5 week). - Then the Oogonia transformed into 1ry Oocyte. - 1ry Oocyte is surrounded by a follicle (cover).
1 Quick Review: Oogenesis : - Oogonia start appear in the ovary when the age of the fetus 1 is th (5 week). - Then the Oogonia transformed into 1ry Oocyte. - 1ry Oocyte is surrounded by a follicle (cover).
Biology of Reproduction- Zool 346 Exam 2
 Biology of Reproduction- Zool 346 Exam 2 ANSWER ALL THE QUESTIONS ON THE ANSWER SHEET. THE ANSWER ON THE ANSWER SHEET IS YOUR OFFICIAL ANSWER. Some critical words are boldfaced. This exam is 7 pages long.
Biology of Reproduction- Zool 346 Exam 2 ANSWER ALL THE QUESTIONS ON THE ANSWER SHEET. THE ANSWER ON THE ANSWER SHEET IS YOUR OFFICIAL ANSWER. Some critical words are boldfaced. This exam is 7 pages long.
Sample Provincial exam Q s: Reproduction
 Sample Provincial exam Q s: Reproduction 11. Functions Testosterone Makes the male sex organs function normally, and also inhibits hypothalamus s release of GnRH and thus LH & FSH and thus testosterone
Sample Provincial exam Q s: Reproduction 11. Functions Testosterone Makes the male sex organs function normally, and also inhibits hypothalamus s release of GnRH and thus LH & FSH and thus testosterone
Chapter 14 Reproduction Review Assignment
 Date: Mark: _/45 Chapter 14 Reproduction Review Assignment Multiple Choice Identify the choice that best completes the statement or answers the question. 1. Use the diagram above to answer the next question.
Date: Mark: _/45 Chapter 14 Reproduction Review Assignment Multiple Choice Identify the choice that best completes the statement or answers the question. 1. Use the diagram above to answer the next question.
Sperm production. Sperm production. Meiosis. Mitosis. The cells of Leydig in testes secrete
 Sperm production Ductus deferens Epididymis The cells of Leydig in testes secrete Seminiferous testosterone (T) tubules T secreted at puberty produces 2 o sex characteristics, spermatogenesis, & maintain
Sperm production Ductus deferens Epididymis The cells of Leydig in testes secrete Seminiferous testosterone (T) tubules T secreted at puberty produces 2 o sex characteristics, spermatogenesis, & maintain
Sperm production. Sperm production. Controlling sperm production. Meiosis. Mitosis. The cells of Leydig in testes secrete
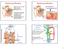 Ductus deferens Sperm production Epididymis The cells of Leydig in testes secrete Seminiferous testosterone (T) tubules T secreted at puberty produces 2 o sex characteristics, spermatogenesis, & maintain
Ductus deferens Sperm production Epididymis The cells of Leydig in testes secrete Seminiferous testosterone (T) tubules T secreted at puberty produces 2 o sex characteristics, spermatogenesis, & maintain
Reproductive System (Hormone Function) Physiology Department Medical School, University of Sumatera Utara
 Reproductive System (Hormone Function) Physiology Department Medical School, University of Sumatera Utara 1 Endocrine Control: Three Levels of Integration Hormones of the hypothalamic-anterior pituitary
Reproductive System (Hormone Function) Physiology Department Medical School, University of Sumatera Utara 1 Endocrine Control: Three Levels of Integration Hormones of the hypothalamic-anterior pituitary
Reproductive Hormones
 Reproductive Hormones Male gonads: testes produce male sex cells! sperm Female gonads: ovaries produce female sex cells! ovum The union of male and female sex cells during fertilization produces a zygote
Reproductive Hormones Male gonads: testes produce male sex cells! sperm Female gonads: ovaries produce female sex cells! ovum The union of male and female sex cells during fertilization produces a zygote
The Reproductive System
 Essentials of Anatomy & Physiology, 4th Edition Martini / Bartholomew The Reproductive System PowerPoint Lecture Outlines prepared by Alan Magid, Duke University Slides 1 to 84 Overview of Reproduction
Essentials of Anatomy & Physiology, 4th Edition Martini / Bartholomew The Reproductive System PowerPoint Lecture Outlines prepared by Alan Magid, Duke University Slides 1 to 84 Overview of Reproduction
Chapter 14 The Reproductive System
 Biology 12 Name: Reproductive System Per: Date: Chapter 14 The Reproductive System Complete using BC Biology 12, page 436-467 14. 1 Male Reproductive System pages 440-443 1. Distinguish between gametes
Biology 12 Name: Reproductive System Per: Date: Chapter 14 The Reproductive System Complete using BC Biology 12, page 436-467 14. 1 Male Reproductive System pages 440-443 1. Distinguish between gametes
Hormonal Control of Human Reproduction
 Hormonal Control of Human Reproduction Bởi: OpenStaxCollege The human male and female reproductive cycles are controlled by the interaction of hormones from the hypothalamus and anterior pituitary with
Hormonal Control of Human Reproduction Bởi: OpenStaxCollege The human male and female reproductive cycles are controlled by the interaction of hormones from the hypothalamus and anterior pituitary with
Reproduction and Development. Female Reproductive System
 Reproduction and Development Female Reproductive System Outcomes 5. Identify the structures in the human female reproductive system and describe their functions. Ovaries, Fallopian tubes, Uterus, Endometrium,
Reproduction and Development Female Reproductive System Outcomes 5. Identify the structures in the human female reproductive system and describe their functions. Ovaries, Fallopian tubes, Uterus, Endometrium,
a. the tail disappears b. they become spermatids c. they undergo capacitation d. they have been stored in the uterus for several days
 (2 points each) Multiple Choice. Read each question thoroughly before answering. From the choices available, choose the answer that is the most correct. Place all answers on the accompanying answer sheet.
(2 points each) Multiple Choice. Read each question thoroughly before answering. From the choices available, choose the answer that is the most correct. Place all answers on the accompanying answer sheet.
Unit 15 ~ Learning Guide
 Unit 15 ~ Learning Guide Name: INSTRUCTIONS Complete the following notes and questions as you work through the related lessons. You are required to have this package completed BEFORE you write your unit
Unit 15 ~ Learning Guide Name: INSTRUCTIONS Complete the following notes and questions as you work through the related lessons. You are required to have this package completed BEFORE you write your unit
Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor)
 Indifferent ducts of embryo Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor) Y chromosome present Y chromosome absent Phenotypic sex is depends on development of external
Indifferent ducts of embryo Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor) Y chromosome present Y chromosome absent Phenotypic sex is depends on development of external
Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor)
 Indifferent ducts of embryo Y chromosome present Y chromosome absent Male Female penis ovary uterus vagina testis Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor) Phenotypic
Indifferent ducts of embryo Y chromosome present Y chromosome absent Male Female penis ovary uterus vagina testis Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor) Phenotypic
Chapter 46 ~ Animal Reproduction
 Chapter 46 ~ Animal Reproduction Overview Asexual (one parent) fission (parent separation) budding (corals) fragmentation & regeneration (inverts) parthenogenesis Sexual (fusion of haploid gametes) gametes
Chapter 46 ~ Animal Reproduction Overview Asexual (one parent) fission (parent separation) budding (corals) fragmentation & regeneration (inverts) parthenogenesis Sexual (fusion of haploid gametes) gametes
Chapter 22 The Reproductive System (I)
 Chapter 22 The Reproductive System (I) An Overview of Reproductive Physiology o The Male Reproductive System o The Female Reproductive System 22.1 Reproductive System Overview Reproductive system = all
Chapter 22 The Reproductive System (I) An Overview of Reproductive Physiology o The Male Reproductive System o The Female Reproductive System 22.1 Reproductive System Overview Reproductive system = all
Reproductive physiology
 Reproductive physiology Sex hormones: Androgens Estrogens Gestagens Learning objectives 86 (also 90) Sex Genetic sex Gonadal sex Phenotypic sex XY - XX chromosomes testes - ovaries external features Tha
Reproductive physiology Sex hormones: Androgens Estrogens Gestagens Learning objectives 86 (also 90) Sex Genetic sex Gonadal sex Phenotypic sex XY - XX chromosomes testes - ovaries external features Tha
Web Activity: Simulation Structures of the Female Reproductive System
 differentiate. The epididymis is a coiled tube found along the outer edge of the testis where the sperm mature. 3. Testosterone is a male sex hormone produced in the interstitial cells of the testes. It
differentiate. The epididymis is a coiled tube found along the outer edge of the testis where the sperm mature. 3. Testosterone is a male sex hormone produced in the interstitial cells of the testes. It
Human Reproductive System
 Human Reproductive System I. The male reproductive anatomy is a delivery system for sperm. A. The male s external reproductive organs consist of the scrotum and penis. 1. The penis is the external organ
Human Reproductive System I. The male reproductive anatomy is a delivery system for sperm. A. The male s external reproductive organs consist of the scrotum and penis. 1. The penis is the external organ
Mohammad. Renad zakaria ---
 13 Mohammad Renad zakaria --- Before we start: - I didn t follow the record order, for organizing purposes. - I added extra information from our text box which is Guyton 12 th edition, pages 987-997, actually
13 Mohammad Renad zakaria --- Before we start: - I didn t follow the record order, for organizing purposes. - I added extra information from our text box which is Guyton 12 th edition, pages 987-997, actually
Chapter 26: Reproductive Systems. Male 11/29/2015. Male reproductive system is composed of... BIO 218 Fall Gonads (testes)
 Chapter 26: Reproductive Systems BIO 218 Fall 2015 Male Male reproductive system is composed of... Gonads (testes) Duct system (epididymis, ductus deferens, ejaculatory ducts, urethra) Accessory sex glands
Chapter 26: Reproductive Systems BIO 218 Fall 2015 Male Male reproductive system is composed of... Gonads (testes) Duct system (epididymis, ductus deferens, ejaculatory ducts, urethra) Accessory sex glands
STRUCTURE AND FUNCTION OF THE FEMALE REPRODUCTIVE SYSTEM
 Unit 7B STRUCTURE AND FUNCTION OF THE FEMALE REPRODUCTIVE SYSTEM LEARNING OBJECTIVES 1. Learn the structures of the female reproductive tract. 2. Learn the functions of the female reproductive tract. 3.
Unit 7B STRUCTURE AND FUNCTION OF THE FEMALE REPRODUCTIVE SYSTEM LEARNING OBJECTIVES 1. Learn the structures of the female reproductive tract. 2. Learn the functions of the female reproductive tract. 3.
Female reproductive cycle: A Comprehensive Review Rachel Ledden Paper for Bachelors in Science January 20, 2018
 Running head: 1 Female reproductive cycle: A Comprehensive Review Rachel Ledden Paper for Bachelors in Science January 20, 2018 Female reproductive cycle: A Comprehensive Review 2 The reproductive cycle
Running head: 1 Female reproductive cycle: A Comprehensive Review Rachel Ledden Paper for Bachelors in Science January 20, 2018 Female reproductive cycle: A Comprehensive Review 2 The reproductive cycle
Reproductive Endocrinology. Isabel Hwang Department of Physiology Faculty of Medicine University of Hong Kong Hong Kong May2007
 Reproductive Endocrinology Isabel Hwang Department of Physiology Faculty of Medicine University of Hong Kong Hong Kong May2007 isabelss@hkucc.hku.hk A 3-hormone chain of command controls reproduction with
Reproductive Endocrinology Isabel Hwang Department of Physiology Faculty of Medicine University of Hong Kong Hong Kong May2007 isabelss@hkucc.hku.hk A 3-hormone chain of command controls reproduction with
TRHC.UEMEE Ph P y h si s o i logy l of fmen M str st u r at a i t on i
 . TRHCUEMEE Physiology of Menstruation Learning objectives: By the end of this lecture the students should be able to: Define menstruation. List the Characters of normal menstruation Enumerate Components
. TRHCUEMEE Physiology of Menstruation Learning objectives: By the end of this lecture the students should be able to: Define menstruation. List the Characters of normal menstruation Enumerate Components
Reproductive Systems. BIOLOGY OF HUMANS Concepts, Applications, and Issues. Judith Goodenough Betty McGuire
 BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 17 Reproductive Systems Lecture Presentation Anne Gasc Hawaii Pacific University and University of Hawaii
BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 17 Reproductive Systems Lecture Presentation Anne Gasc Hawaii Pacific University and University of Hawaii
Female Reproductive System
 21 Female Reproductive System I. Introduction to the Female Reproductive System Concept: The female reproductive system produces ova, secretes sex hormones, receives spermatozoa from the male, and provides
21 Female Reproductive System I. Introduction to the Female Reproductive System Concept: The female reproductive system produces ova, secretes sex hormones, receives spermatozoa from the male, and provides
Objectives: 1. Review male & female reproductive anatomy 2. Gametogenesis & steroidogenesis 3. Reproductive problems
 CH. 15 - REPRODUCTIVE SYSTEM Objectives: 1. Review male & female reproductive anatomy 2. Gametogenesis & steroidogenesis 3. Reproductive problems 3. Male Reproductive anatomy and physiology. Testes = paired
CH. 15 - REPRODUCTIVE SYSTEM Objectives: 1. Review male & female reproductive anatomy 2. Gametogenesis & steroidogenesis 3. Reproductive problems 3. Male Reproductive anatomy and physiology. Testes = paired
Study Guide Answer Key Reproductive System
 Biology 12 Human Biology Textbook: BC Biology 12 Study Guide Answer Key Reproductive System 1. Distinguish between a gamete and a gonad using specific examples from the male and female systems. Gonads
Biology 12 Human Biology Textbook: BC Biology 12 Study Guide Answer Key Reproductive System 1. Distinguish between a gamete and a gonad using specific examples from the male and female systems. Gonads
Stage 4 - Ovarian Cancer Symptoms
 WELCOME Stage 4 - Ovarian Cancer Symptoms University of Baghdad College of Nursing Department of Basic Medical Sciences Overview of Anatomy and Physioloy II Second Year Students Asaad Ismail Ahmad,
WELCOME Stage 4 - Ovarian Cancer Symptoms University of Baghdad College of Nursing Department of Basic Medical Sciences Overview of Anatomy and Physioloy II Second Year Students Asaad Ismail Ahmad,
Human Reproductive System
 Human Reproductive System I. The male reproductive anatomy is a delivery system for sperm. A. The male=s external reproductive organs consist of the scrotum and penis. 1. The penis is the external organ
Human Reproductive System I. The male reproductive anatomy is a delivery system for sperm. A. The male=s external reproductive organs consist of the scrotum and penis. 1. The penis is the external organ
Female Reproductive System
 Female Reproductive System (Part A-1) Module 10 -Chapter 12 Overview Female reproductive organs Ovaries Fallopian tubes Uterus and vagina Mammary glands Menstrual cycle Pregnancy Labor and childbirth Menopause
Female Reproductive System (Part A-1) Module 10 -Chapter 12 Overview Female reproductive organs Ovaries Fallopian tubes Uterus and vagina Mammary glands Menstrual cycle Pregnancy Labor and childbirth Menopause
THE MENSTRUAL CYCLE INA S. IRABON, MD, FPOGS, FPSRM, FPSGE OBSTETRICS AND GYNECOLOGY REPRODUCTIVE ENDOCRINOLOGY AND INFERTILITY
 THE MENSTRUAL CYCLE INA S. IRABON, MD, FPOGS, FPSRM, FPSGE OBSTETRICS AND GYNECOLOGY REPRODUCTIVE ENDOCRINOLOGY AND INFERTILITY REFERENCE Comprehensive Gynecology 7 th edition, 2017 (Lobo RA, Gershenson
THE MENSTRUAL CYCLE INA S. IRABON, MD, FPOGS, FPSRM, FPSGE OBSTETRICS AND GYNECOLOGY REPRODUCTIVE ENDOCRINOLOGY AND INFERTILITY REFERENCE Comprehensive Gynecology 7 th edition, 2017 (Lobo RA, Gershenson
The beginning of puberty is marked by the progressive increase in the production of sex hormones.
 Puberty is characterized by the changes that prepare the human body for the ability to reproduce. This stage generally occurs between the ages of 10 and 14 years old. The beginning of puberty is marked
Puberty is characterized by the changes that prepare the human body for the ability to reproduce. This stage generally occurs between the ages of 10 and 14 years old. The beginning of puberty is marked
AP Biology Ch ANIMAL REPRODUCTION. Using only what you already know (you cannot look up anything) complete the chart below.
 AP Biology Ch. 46 - ANIMAL REPRODUCTION Using only what you already know (you cannot look up anything) complete the chart below. I. Overview of Animal Reproduction A. Both asexual and sexual reproduction
AP Biology Ch. 46 - ANIMAL REPRODUCTION Using only what you already know (you cannot look up anything) complete the chart below. I. Overview of Animal Reproduction A. Both asexual and sexual reproduction
Ch 20: Reproduction. Keypoints: Human Chromosomes Gametogenesis Fertilization Early development Parturition
 Ch 20: Reproduction Keypoints: Human Chromosomes Gametogenesis Fertilization Early development Parturition SLOs Contrast mitosis/meiosis, haploid/diploid, autosomes/sex chromosomes. Outline the hormonal
Ch 20: Reproduction Keypoints: Human Chromosomes Gametogenesis Fertilization Early development Parturition SLOs Contrast mitosis/meiosis, haploid/diploid, autosomes/sex chromosomes. Outline the hormonal
Female Reproductive Physiology. Dr Raelia Lew CREI, FRANZCOG, PhD, MMed, MBBS Fertility Specialist, Melbourne IVF
 Female Reproductive Physiology Dr Raelia Lew CREI, FRANZCOG, PhD, MMed, MBBS Fertility Specialist, Melbourne IVF REFERENCE Lew, R, Natural History of ovarian function including assessment of ovarian reserve
Female Reproductive Physiology Dr Raelia Lew CREI, FRANZCOG, PhD, MMed, MBBS Fertility Specialist, Melbourne IVF REFERENCE Lew, R, Natural History of ovarian function including assessment of ovarian reserve
Animal Reproductive Systems. Chapter 42
 Animal Reproductive Systems Chapter 42 Impacts, Issues Male or Female? Body or Genes? Body and genes don t always match male or female characteristics also depend on hormones mutations can result in intersex
Animal Reproductive Systems Chapter 42 Impacts, Issues Male or Female? Body or Genes? Body and genes don t always match male or female characteristics also depend on hormones mutations can result in intersex
The Female Reproductive System
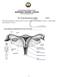 The Female Reproductive System STD X The female reproductive system consists of a pair of ovaries, a pair of oviducts, uterus, a vagina and the outermost part - the vulva. 1 1. Ovaries The ovaries are
The Female Reproductive System STD X The female reproductive system consists of a pair of ovaries, a pair of oviducts, uterus, a vagina and the outermost part - the vulva. 1 1. Ovaries The ovaries are
The Reproductive System
 The Reproductive System The Reproductive System Gonads primary sex organs Testes in males Ovaries in females Gonads produce gametes (sex cells) and secrete hormones Sperm male gametes Ova (eggs) female
The Reproductive System The Reproductive System Gonads primary sex organs Testes in males Ovaries in females Gonads produce gametes (sex cells) and secrete hormones Sperm male gametes Ova (eggs) female
AnS 214 SI Multiple Choice Set 4 Weeks 10/14-10/23
 AnS 214 SI Multiple Choice Set 4 Weeks 10/14-10/23 The following multiple choice questions pertain to material covered in the last two weeks' lecture sets. Answering the following questions will aid your
AnS 214 SI Multiple Choice Set 4 Weeks 10/14-10/23 The following multiple choice questions pertain to material covered in the last two weeks' lecture sets. Answering the following questions will aid your
The Human Menstrual Cycle
 The Human Menstrual Cycle Name: The female human s menstrual cycle is broken into two phases: the Follicular Phase and the Luteal Phase. These two phases are separated by an event called ovulation. (1)
The Human Menstrual Cycle Name: The female human s menstrual cycle is broken into two phases: the Follicular Phase and the Luteal Phase. These two phases are separated by an event called ovulation. (1)
Investigation: The Human Menstrual Cycle Research Question: How do hormones control the menstrual cycle?
 Investigation: The Human Menstrual Cycle Research Question: How do hormones control the menstrual cycle? Introduction: The menstrual cycle (changes within the uterus) is an approximately 28-day cycle that
Investigation: The Human Menstrual Cycle Research Question: How do hormones control the menstrual cycle? Introduction: The menstrual cycle (changes within the uterus) is an approximately 28-day cycle that
2 - male hormones/ female system
 2 - male hormones/ female system May 7, 2012 5:08 PM I) Testosterone: main androgen (male sex hormone) A) Intro to Testosterone: -steroid hormone produced by interstitial cells in testes -produced in response
2 - male hormones/ female system May 7, 2012 5:08 PM I) Testosterone: main androgen (male sex hormone) A) Intro to Testosterone: -steroid hormone produced by interstitial cells in testes -produced in response
6.7 IN. Continuity through Reproduction. What are the differences between male and female gametes? Discuss their formation and physical attributes.
 6.7 IN What are the differences between male and female gametes? Discuss their formation and physical attributes. Males - 4 sperm per parent cell; Females - 1 ovum per parent cell Sperm - motile (tail);
6.7 IN What are the differences between male and female gametes? Discuss their formation and physical attributes. Males - 4 sperm per parent cell; Females - 1 ovum per parent cell Sperm - motile (tail);
BIOL 2402 Reproductive Systems!
 Dr. Chris Doumen! Female Reproductive Anatomy BIOL 2402 Reproductive Systems! Establishing the Ovarian Cycle During childhood, until puberty Ovaries grow and secrete small amounts of estrogens Estrogen
Dr. Chris Doumen! Female Reproductive Anatomy BIOL 2402 Reproductive Systems! Establishing the Ovarian Cycle During childhood, until puberty Ovaries grow and secrete small amounts of estrogens Estrogen
Two important cells in female are the theca cells and the granulose cells. Granulosa cells are affected by the two gonadotropin hormones; FSH and LH.
 1 UGS physiology sheet #13 lecture 3 Dr.Saleem Khresha. Now we will start discussing the female reproductive system Ovarian Steroids Two important cells in female are the theca cells and the granulose
1 UGS physiology sheet #13 lecture 3 Dr.Saleem Khresha. Now we will start discussing the female reproductive system Ovarian Steroids Two important cells in female are the theca cells and the granulose
Urinary System Chapter 16
 Urinary System Chapter 16 1 Urology- the branch of medicine that treats male and female urinary systems as well as the male reproductive system. Nephrology- the scientific study of the anatomy, physiology,
Urinary System Chapter 16 1 Urology- the branch of medicine that treats male and female urinary systems as well as the male reproductive system. Nephrology- the scientific study of the anatomy, physiology,
BIOH122 Human Biological Science 2
 BIOH122 Human Biological Science 2 Session 22 Female Reproductive System 2 The Reproductive Cycle Bioscience Department Endeavour College of Natural Health endeavour.edu.au Session Plan o The female reproductive
BIOH122 Human Biological Science 2 Session 22 Female Reproductive System 2 The Reproductive Cycle Bioscience Department Endeavour College of Natural Health endeavour.edu.au Session Plan o The female reproductive
Physiology Unit 4 REPRODUCTIVE PHSYIOLOGY
 Physiology Unit 4 REPRODUCTIVE PHSYIOLOGY Gonads Gonads have 2 func7ons Gametogenesis Spermatogenesis Oogenesis Secrete steroid hormones Testosterone Estrogens (3 forms) Estradiol, produced by ovaries,
Physiology Unit 4 REPRODUCTIVE PHSYIOLOGY Gonads Gonads have 2 func7ons Gametogenesis Spermatogenesis Oogenesis Secrete steroid hormones Testosterone Estrogens (3 forms) Estradiol, produced by ovaries,
OVARY The surface of the ovary is covered with surface epithelium
 OVARY Cow The ovary, or female gonad, is: 1. an exocrine gland, producing oocytes 2. an endocrine gland, secreting hormones, i.e., estrogen and progesterone OVARY OVARY The surface of the ovary is covered
OVARY Cow The ovary, or female gonad, is: 1. an exocrine gland, producing oocytes 2. an endocrine gland, secreting hormones, i.e., estrogen and progesterone OVARY OVARY The surface of the ovary is covered
Chapter 36 Active Reading Guide Reproduction and Development
 Name: AP Biology Mr. Croft Chapter 36 Active Reading Guide Reproduction and Development Section 1 1. Distinguish between sexual reproduction and asexual reproduction. 2. Which form of reproduction: a.
Name: AP Biology Mr. Croft Chapter 36 Active Reading Guide Reproduction and Development Section 1 1. Distinguish between sexual reproduction and asexual reproduction. 2. Which form of reproduction: a.
Animal Science 434! Tonic and Preovulatory Surge of GnRH! Tonic and Preovulatory Surge of GnRH! Lecture 11: The Follicular Phase of the Estrous Cycle!
 Tonic and Preovulatory Surge of GnRH! Animal Science 434! Lecture 11: The Follicular Phase of the Estrous Cycle!! (-)! Hypothalamus! GnRH! Estradiol! (-)! Tonic and Preovulatory Surge of GnRH! Anterior!
Tonic and Preovulatory Surge of GnRH! Animal Science 434! Lecture 11: The Follicular Phase of the Estrous Cycle!! (-)! Hypothalamus! GnRH! Estradiol! (-)! Tonic and Preovulatory Surge of GnRH! Anterior!
1. During the follicular phase of the ovarian cycle, the hypothalamus releases GnRH.
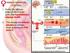 1. During the follicular phase of the ovarian cycle, the hypothalamus releases GnRH. 2. This causes the anterior pituitary to secrete small quantities of FSH and LH. 3. At this time, the follicles in the
1. During the follicular phase of the ovarian cycle, the hypothalamus releases GnRH. 2. This causes the anterior pituitary to secrete small quantities of FSH and LH. 3. At this time, the follicles in the
Reproduction Lecture Spring 2009
 Reproduction Lecture Spring 2009 Slide #2: The term gonads refer to the sex organs. In the male, these are the testes, and the in the female, the ovary. The produce sex cells, or gametes. The male gamete
Reproduction Lecture Spring 2009 Slide #2: The term gonads refer to the sex organs. In the male, these are the testes, and the in the female, the ovary. The produce sex cells, or gametes. The male gamete
to ensure the. Sexual reproduction requires the (from the mother) by a (from the father). Fertilization is the fusion of.
 The Reproductive System Fill-In Notes Purpose of life: to ensure the. Stages of Human Development Sexual reproduction requires the (from the mother) by a (from the father). Fertilization is the fusion
The Reproductive System Fill-In Notes Purpose of life: to ensure the. Stages of Human Development Sexual reproduction requires the (from the mother) by a (from the father). Fertilization is the fusion
Human Sexuality - Ch. 2 Sexual Anatomy (Hock)
 Human Sexuality - Ch. 2 Sexual Anatomy (Hock) penis penile glans corona frenulum penile shaft erection foreskin circumcision corpora cavernosa corpus spongiosum urethra scrotum spermatic cords testicles
Human Sexuality - Ch. 2 Sexual Anatomy (Hock) penis penile glans corona frenulum penile shaft erection foreskin circumcision corpora cavernosa corpus spongiosum urethra scrotum spermatic cords testicles
Female Reproduction 1 and 2: The Menstrual Cycle R.J. Witorsch, Ph.D.
 Female Reproduction 1 and 2: The Menstrual Cycle R.J. Witorsch, Ph.D. OBJECTIVES: At the end of this block of lectures, the student should be able to: 1. Describe the functional anatomy of ovary with particular
Female Reproduction 1 and 2: The Menstrual Cycle R.J. Witorsch, Ph.D. OBJECTIVES: At the end of this block of lectures, the student should be able to: 1. Describe the functional anatomy of ovary with particular
Embryology 3. Spermatogenesis:
 Embryology 3 Spermatogenesis: The 2 testis in males are each divided into lobes and lobules by connective tissue septa forming 250 lobule and in each lobule there are 1 to 4 seminefrous tubule ( so almost
Embryology 3 Spermatogenesis: The 2 testis in males are each divided into lobes and lobules by connective tissue septa forming 250 lobule and in each lobule there are 1 to 4 seminefrous tubule ( so almost
Ch 28 Lecture Study Guide
 Ch 28 Lecture Study Guide 1. List the characteristics of the reproductive system. Only organ system not essential to life Ensures continued existence of human species Produces, stores, nourishes, and transports
Ch 28 Lecture Study Guide 1. List the characteristics of the reproductive system. Only organ system not essential to life Ensures continued existence of human species Produces, stores, nourishes, and transports
Bio 12- Ch. 21: Reproductive System
 Bio 12- Ch. 21: Reproductive System 21.1- Male Reproductive System o Male anatomy o Testes and how they relate to sperm production and male sex hormones o Hormone regulation in males 21.2- Female Reproductive
Bio 12- Ch. 21: Reproductive System 21.1- Male Reproductive System o Male anatomy o Testes and how they relate to sperm production and male sex hormones o Hormone regulation in males 21.2- Female Reproductive
Bio 322 Human Anatomy Objectives for the laboratory exercise Female Reproductive System
 Bio 322 Human Anatomy Objectives for the laboratory exercise Female Reproductive System Required reading before beginning this lab: Saladin, KS: Human Anatomy 5 th ed (2017) Chapter 26 For this lab you
Bio 322 Human Anatomy Objectives for the laboratory exercise Female Reproductive System Required reading before beginning this lab: Saladin, KS: Human Anatomy 5 th ed (2017) Chapter 26 For this lab you
Objectives: 1. Review male & female reproductive anatomy 2. Gametogenesis & steroidogenesis 3. Reproductive problems
 CH. 15 - REPRODUCTIVE SYSTEM Objectives: 1. Review male & female reproductive anatomy 2. Gametogenesis & steroidogenesis 3. Reproductive problems Review of Male Reproductive Anatomy Fig 15.9 Vas deferens
CH. 15 - REPRODUCTIVE SYSTEM Objectives: 1. Review male & female reproductive anatomy 2. Gametogenesis & steroidogenesis 3. Reproductive problems Review of Male Reproductive Anatomy Fig 15.9 Vas deferens
Human Reproductive Anatomy The female anatomy first just the reproductive parts:
 Human Reproduction: Structures, Functions, and Hormones Human reproduction differs from the mechanisms in lower vertebrates and many invertebrates. We depend on internal fertilization sperm are deposited
Human Reproduction: Structures, Functions, and Hormones Human reproduction differs from the mechanisms in lower vertebrates and many invertebrates. We depend on internal fertilization sperm are deposited
 MOCK TEST I (HUMAN REPRODUCTION) 1. In human transfer of sperms into female genital tract is called as 1) Fertilization 2) Implantation 3) Insemination 4) Gestation 2. In male human scrotum maintains the
MOCK TEST I (HUMAN REPRODUCTION) 1. In human transfer of sperms into female genital tract is called as 1) Fertilization 2) Implantation 3) Insemination 4) Gestation 2. In male human scrotum maintains the
BIOLOGY. Animal Reproduction CAMPBELL. Reece Urry Cain Wasserman Minorsky Jackson. Lecture Presentation by Nicole Tunbridge and Kathleen Fitzpatrick
 CAMPBELL BIOLOGY TENTH EDITION Reece Urry Cain Wasserman Minorsky Jackson 46 Animal Reproduction Lecture Presentation by Nicole Tunbridge and Kathleen Fitzpatrick 1. Asexual vs Sexual Reproduction Both
CAMPBELL BIOLOGY TENTH EDITION Reece Urry Cain Wasserman Minorsky Jackson 46 Animal Reproduction Lecture Presentation by Nicole Tunbridge and Kathleen Fitzpatrick 1. Asexual vs Sexual Reproduction Both
Grade 9 Science - Human Reproduction
 Grade 9 Science - Human Reproduction The human reproductive system is a series of organs that work together for one purpose: reproduction (creating new humans). Each part has a specific role in the reproductive
Grade 9 Science - Human Reproduction The human reproductive system is a series of organs that work together for one purpose: reproduction (creating new humans). Each part has a specific role in the reproductive
Endocrine and Reproductive Systems. Chapter 39: Biology II
 Endocrine and Reproductive Systems Chapter 39: Biology II The Endocrine System Made up of glands that release their products into the bloodstream These products broadcast messages throughout the body Chemicals
Endocrine and Reproductive Systems Chapter 39: Biology II The Endocrine System Made up of glands that release their products into the bloodstream These products broadcast messages throughout the body Chemicals
Phases of the Ovarian Cycle
 OVARIAN CYCLE An ovary contains many follicles, and each one contains an immature egg called an oocyte. A female is born with as many as 2 million follicles, but the number is reduced to 300,000 to 400,000
OVARIAN CYCLE An ovary contains many follicles, and each one contains an immature egg called an oocyte. A female is born with as many as 2 million follicles, but the number is reduced to 300,000 to 400,000
1. Be able to characterize the menstrual cycle from the perspective of the ovary a. Follicular phase b. Luteal phase
 Human Sexuality Exam II Review Material Gametogenesis: Oogenesis 1. Be able to characterize the menstrual cycle from the perspective of the ovary a. Follicular phase b. Luteal phase 2. Know the relative
Human Sexuality Exam II Review Material Gametogenesis: Oogenesis 1. Be able to characterize the menstrual cycle from the perspective of the ovary a. Follicular phase b. Luteal phase 2. Know the relative
REPRODUCTIVE SYSTEM OBJECTIVES
 REPRODUCTIVE SYSTEM OBJECTIVES OBJECTIVES: 1. List the organs and functions of the reproductive system. Female Organs Male Organs Functions 1 OVARIES 1 TESTES 1 Produce gametes 2 fallopian tubes 2 scrotum
REPRODUCTIVE SYSTEM OBJECTIVES OBJECTIVES: 1. List the organs and functions of the reproductive system. Female Organs Male Organs Functions 1 OVARIES 1 TESTES 1 Produce gametes 2 fallopian tubes 2 scrotum
SHORT ANSWER. Write the word or phrase that best completes each statement or answers the question.
 Exam Name SHORT ANSWER. Write the word or phrase that best completes each statement or answers the question. Figure 27.3 Using Figure 27.3, match the following: 1) The stage called ovulation. 2) Corpus
Exam Name SHORT ANSWER. Write the word or phrase that best completes each statement or answers the question. Figure 27.3 Using Figure 27.3, match the following: 1) The stage called ovulation. 2) Corpus
1. Both asexual and sexual reproduction occur in the animal kingdom
 1. Both asexual and sexual reproduction occur in the animal kingdom Asexual reproduction involves the formation of individuals whose genes all come from one parent. There is no fusion of sperm and egg.
1. Both asexual and sexual reproduction occur in the animal kingdom Asexual reproduction involves the formation of individuals whose genes all come from one parent. There is no fusion of sperm and egg.
Lecture 28, The Reproductive System
 Fundamentals of Anatomy & Physiology Lecture 28, The Reproductive System SIXTH EDITION Frederic H. Martini Lecturer: Dr. Barjis Room: P313 Phone: (718) 260-5285 E-Mail: ibarjis@citytech.cuny.edu Copyright
Fundamentals of Anatomy & Physiology Lecture 28, The Reproductive System SIXTH EDITION Frederic H. Martini Lecturer: Dr. Barjis Room: P313 Phone: (718) 260-5285 E-Mail: ibarjis@citytech.cuny.edu Copyright
The Sex Hormones & Reproductive Systems (6)
 The Sex Hormones & Reproductive Systems (6) The Male Reproductive System The male reproductive system Lumen) Sperm Scrotum ~300 lobules Sertoli cell Leydig cell Testosterone Testes : - produce sperm cells
The Sex Hormones & Reproductive Systems (6) The Male Reproductive System The male reproductive system Lumen) Sperm Scrotum ~300 lobules Sertoli cell Leydig cell Testosterone Testes : - produce sperm cells
The Male Reproductive System
 The Male Reproductive System Male Reproductive System The male sex cell is a sperm cell The whole purpose is to produce and deliver sperm to the egg Structure of a Human Sperm Cell Streamlined, built to
The Male Reproductive System Male Reproductive System The male sex cell is a sperm cell The whole purpose is to produce and deliver sperm to the egg Structure of a Human Sperm Cell Streamlined, built to
The menstrual cycle. François Pralong
 The menstrual cycle François Pralong Services d Endocrinologie, Diabétologie et Métabolisme, Hôpitaux Universitaires de Genève et Lausanne Centre des Maladies CardioVasculaires et Métaboliques, Lausanne
The menstrual cycle François Pralong Services d Endocrinologie, Diabétologie et Métabolisme, Hôpitaux Universitaires de Genève et Lausanne Centre des Maladies CardioVasculaires et Métaboliques, Lausanne
The menstrual Cycle. François Pralong
 The menstrual Cycle François Pralong Services d Endocrinologie, Diabétologie et Métabolisme, Hôpitaux Universitaires de Genève et Lausanne Centre des Maladies CardioVasculaires et Métaboliques, Lausanne
The menstrual Cycle François Pralong Services d Endocrinologie, Diabétologie et Métabolisme, Hôpitaux Universitaires de Genève et Lausanne Centre des Maladies CardioVasculaires et Métaboliques, Lausanne
What are the main functions of the male reproductive system? 1. Produce sperm 2. Deposit sperm into the female 3. Provide a pathway for the removal
 What are the main functions of the male reproductive system? 1. Produce sperm 2. Deposit sperm into the female 3. Provide a pathway for the removal of urine Where is sperm produced? -In the 2 testes What
What are the main functions of the male reproductive system? 1. Produce sperm 2. Deposit sperm into the female 3. Provide a pathway for the removal of urine Where is sperm produced? -In the 2 testes What
