Terminal and nonterminal myelocystoceles
|
|
|
- Cleopatra Carr
- 5 years ago
- Views:
Transcription
1 See the corresponding editorial in this issue, pp J Neurosurg (2 Suppl Pediatrics) 107:87 97, 2007 Terminal and nonterminal myelocystoceles NATARAJAN MUTHUKUMAR, M.CH. Department of Neurosurgery, Madurai Medical College, Madurai, India Object. The purpose of this study was to report the author s experience with 14 cases of terminal and nine cases of nonterminal myelocystoceles and to highlight the differences between these two groups in regard to the embryological origins, clinical presentation, operative findings, results on neuroimaging studies, and prognosis for these lesions. Methods. This is a retrospective analysis of 14 cases of terminal and nine of nonterminal myelocystoceles treated between January 1998 and January All patients underwent neurological examination, plain x-ray films of the spine, computed tomography scans of the brain, and magnetic resonance (MR) imaging of the spine. In seven of these cases, MR imaging included three-dimensional constructive interference in steady-state sequences, and in four cases MR myelography was also done. Follow-up duration ranged from 3 months to 4 years. Results. All of the patients with terminal myelocystocele presented with swelling in the low back and varying degrees of neurological deficits, except four who had normal results on neurological tests. The MR images revealed classic features of terminal myelocystoceles in all patients. In each case, patients underwent excision of the meningocele sac and drainage of the syringocele with untethering of the spinal cord. During the last follow-up visit, there was no change in the neurological status of these children. In the nonterminal myelocystocele group, one lesion was cervical, six were thoracic, and two were lumbar lesions. All except one patient presented without neurological deficits; that patient had paraplegia with incontinence. Admission MR images revealed Rossi Type I nonterminal myelocystocele in six and Rossi Type II nonterminal myelocystocele in three patients. Children with Type I lesions underwent excision of the fibroneurovascular stalk and excision of the meningocele sac, whereas those with Type II lesions underwent drainage of the syringocele, untethering of the cord, and excision of the meningocele sac. There was no change in the neurological status postoperatively. During the follow-up period no patient in either group presented with retethering. Conclusions. Myelocystoceles, both terminal and nonterminal, are different from other skin-covered masses in the back. A proper imaging evaluation is required to differentiate myelocystoceles from other skin-covered masses in this area, because the surgical treatment and prognosis are different for this subset of patients with occult spinal dysraphism. Terminal myelocystoceles are different from nonterminal ones embryologically, clinically, radiologically, surgically, and prognostically. These differences are discussed. (DOI: /PED-07/08/087) KEY WORDS magnetic resonance myelography meningocele myelocystocele pediatric neurosurgery spina bifida spinal dysraphism tethered spinal cord three-dimensional constructive interference in steady-state imaging T ERMINAL myelocystoceles constitute approximately 5% of skin-covered lumbosacral masses and are characterized pathologically by the following features: 1) a skin-covered lumbosacral spina bifida; 2) an arachnoidlined meningocele that is directly continuous with the spinal subarachnoid space; and 3) a low-lying hydromyelic spinal cord that traverses the meningocele and then expands into a large terminal cyst. 16 This terminal cyst does not communicate with the subarachnoid space and is lined by ependyma and dysplastic glia. Terminal myelocystoceles are common in patients with cloacal exstrophy. 4,7,11,16 Nonterminal myelocystocele is a very rare type of closed Abbreviations used in this paper: CM-II = Chiari malformation Type II; CSF = cerebrospinal fluid; MR = magnetic resonance; OEIS = omphalocele, cloacal exstrophy, imperforate anus, spinal dysraphism; 3D-CISS = three-dimensional constructive interference in steady state. spinal dysraphism characterized by a skin-covered mass in the midline posteriorly, a narrow posterior spina bifida, a CSF-filled cyst, an expanded dural sheath (meningocele), and varying amounts of dorsal fat that are continuous with the subcutaneous fat of the back and skin. 22 Nonterminal myelocystoceles are much less common than terminal myelocystoceles and are frequently misdiagnosed as meningoceles. Rossi and colleagues 22 have classified nonterminal myelocystoceles into two types, as follows: Type I, a forme fruste type (myelocystocele manqué), in which the meningocele sac is traversed by a fibroneurovascular stalk that is attached to the dome of the sac; and Type II, a complete form in which there is a focal hydromyelia that has displaced the posterior wall of the spinal cord into the meningocele sac. The aim of the present study is to compare the clinical, radiological, surgical, and prognostic differences between terminal and nonterminal myelocystoceles treated by a single surgeon during a period of 8 years. 87
2 N. Muthukumar Clinical Material and Methods This was a retrospective analysis of all cases of myelocystoceles treated by a single surgeon between January 1998 and January This study included two patients reported earlier. 18 All patients underwent standard neurological evaluation, plain x-ray films of the spine, computed tomography scans of the brain (if MR imaging had not included brain screening), and MR imaging of the spine. The MR evaluation included standard sequences; MR myelography (TR 2800 msec, TE 1110 msec) and 3D-CISS imaging (TR 12 msec, TE 6 msec) sequences were performed in patients who underwent MR evaluation at our institution, whereas this was not available for patients referred from outside institutions who had undergone MR imaging at the referring hospital. Patient Population Fourteen patients with terminal myelocystoceles were treated during the study period. The clinical, neuroimaging, and outcome data in these patients are summarized in Table 1. Briefly, their ages ranged from newborn to 7 years, and there were 11 girls and three boys. During the same study period, nine cases of nonterminal myelocystoceles were treated (Table 2). The ages of these patients ranged from 10 days to 3 months, and all were girls. All patients underwent excision of the sac with untethering of the spinal cord. Neurological outcome during the last follow-up evaluation was recorded. Results Terminal Myelocystoceles There was no positive prenatal history of myelocystoceles in this group of children. All of them presented with a swelling in the low back; the size of the swellings ranged from 3 to 15 cm in diameter. In nine of the patients the swelling had normal skin at the base and the sides, whereas the dome of the swelling was covered by dystrophic skin. None of the sacs leaked CSF or showed signs of impending CSF leakage. Ten patients exhibited varying degrees of neurological deficits, whereas four had none. Among the children in whom neurological evaluations yielded normal results, the four patients ages were 7 and 4 years, 1 month, and 19 days. Associated abnormalities included aqueductal stenosis in four patients and tonsillar ectopia and CM-II in two each. No patient in the study group had OEIS complex or vertebral, anal, tracheoesophageal, renal, and radial anomalies syndrome. Neuroimaging. Plain x-ray films revealed spina bifida in the lumbosacral levels, and MR imaging revealed classic features of terminal myelocystoceles in all patients studied (Figs. 1A, 1B, and 2). There was evidence of posterior spina bifida, with a low-lying hydromyelic cord that herniated into a lumbosacral meningocele. The 3D-CISS images clearly delineated the nature of the lesion (Fig. 2C). Coronal T2- weighted MR sequences of the sac were found to be useful to delineate the hydromyelic cord within the meningocele sac, as shown by the presence of the target sign (Fig. 3). Eleven patients had low-lying conus at the L5 S1 level, and in three patients the conus ended at the L-4 level. Surgery. All patients underwent excision with untethering; the sac was dissected up to its neck. The first lamina immediately rostral to the defect was removed. The dura mater was opened from the normal area and then the incision was extended to the dome of the meningocele sac. Arachnoidal adhesions and meningocele manqué were encountered in most of the cases, although the degree of adhesions varied from case to case. Nerve roots were often found passing anteriorly from the myelocystocele. The distended cord was detached from the sac, which often resulted in the TABLE 1 Features of terminal myelocystoceles in 14 patients* Case Age, Associated Outcome No. Sex Location Neuro Status Anomalies Neuroimaging Findings (last FU) 1 7 yrs, M lumbosacral normal none conus at L5 S1, lipomyelocysto- normal (4 yrs) cele 2 1 yr, M lumbosacral incontinence aqueductal stenosis conus at L5 S1, myelocystocele incontinence improved (18 mos) 3 4 yrs, M lumbosacral normal tonsillar ectopia conus at L5 S1, myelocystocele normal (6 mos) 4 5 mos, F lumbosacral incontinence, CTEV none conus at L5 S1, myelocystocele status quo (1 yr) 5 1 mo, F sacral; off the normal none conus at L5 S1, myelocystocele normal (6 mos) midline 6 19 days, F lumbosacral normal none conus at L5 S1, myelocystocele normal (1 yr) 7 3 days, F lumbosacral incontinence, bilat aqueductal stenosis conus at L5 S1, myelocystocele status quo (6 mos) CTEV 8 18 days, F lumbosacral incontinence, lower hydrocephalus, conus at L5 S1, myelocystocele status quo (5 mos) limb weakness CM-II 9 5 days, F lumbosacral incontinence, lower CM-II conus at L5 S1, myelocystocele status quo (3 mos) limb weakness 10 6 mos, F lumbosacral incontinence tonsillar ectopia conus at S-1 status quo (4 mos) 11 2 yrs, F lumbosacral incontinence none conus at L-4 status quo (1 yr) 12 4 days, F lumbosacral incontinence, CTEV none conus at L-4 status quo (3 mos) 13 3 wks, F lumbosacral CTEV aqueductal stenosis conus at L-4 status quo (5 mos) 14 1 mo, F lumbosacral lower limb weakness, aqueductal stenosis conus at L5 S1 status quo (4 mos) incontinence * Treatment consisted of excision of the sac with untethering of the spinal cord in all patients. Abbreviations: CTEV = congenital talipes equinovarus; FU = follow-up; neuro = neurological. 88
3 Terminal and nonterminal myelocystoceles TABLE 2 Features of NT myelocystoceles in nine patients* Case Age, Associated Surgery Outcome No. Sex Location Neuro Status Anomalies Neuroimaging Findings (intraop findings) (last FU) 1 3 mos, F lower thoracic paraplegia; aqueductal stenosis; hydromyelic dilation of SC from excision & repair w/ un- no change in incontinence CM-II lower cervical; hydromyelic SC tethering (Rossi Type II neuro status expanded into funnel-shaped NT myelocystocele) (5 mos) structure w/in meningocele sac 2 2 mos, F upper thoracic normal split cord malfor- split cord malformation w/ hydro- exicision of meningocele, no change in mation myelia of the lt hemicord, which sectioning of the CSF- neuro status communicated through a stalk- containing stalk; excision (8 mos) like structure to thedorsal me- of septum btwn heminingocele cords (Rossi Type I NT myelocystocele) 3 45 days, F upper thoracic normal none upper thoracic meningocele; exten- excision of sac; untethering normal (7 mos) sion of hydromyelic SC into (Rossi Type II NT mymeningocele sac elocystocele) 4 2 mos, F upper thoracic normal none upper thoracic meningocele; exten- excision of sac; untethering normal (13 mos) sion of hydromyelic SC into (Rossi Type II NT mymeningocele sac elocystocele) 5 18 days, F lower thoracic normal none lower thoracic meningocele w/ excision of sac & untether- normal (3 mos) stalk extending into the sac; ing (Rossi Type I NT conus at L-4 myelocystocele) 6 10 days, F lower thoracic normal none lower thoracic meningocele w/ excision & untethering normal (18 mos) stalk extending from dorsal SC into meningocele sac; conus at L days, F cervical normal none cervical meningocele w/ a stalklike excision & untethering normal (3 mos) structure extending from dorsal (Rossi Type I NT myelosurface of the SC into the me- cystocele) ningocele & attached to the sac dome 8 3 mos, F lumbosacral normal none lumbosacral meningocele; SC teth- excision of fibroneurovas- normal (6 mos) ered at sacral level; a fibroneu- cular stalk; untethering rovascular stalk extended from of SC by filum terminale dorsal aspect of low-lying SC to sectioning; excision & the sac dome (Rossi Type I NT repair of meningocele sac myelocystocele) 9 10 days, F lumbosacral normal none lumbosacral meningocele; SC teth- excision of fibroneurovas- normal (3 mos) ered at sacral level; a fibroneu- cular stalk; untethering rovascular stalk extended from of SC by filum terminale dorsal aspect of the SC to me- sectioning; excision & ningocele sac dome repair of sac *NT = nonterminal; SC = spinal cord. egress of CSF from the dilated central canal (Figs. 1C, 2D, and 2E). The amount of CSF egress varied from case to case. After the outflow of CSF, the trumpetlike spinal cord collapsed. No attempt was made to reconstruct the conus by using pial sutures as has been done in some of the earlier studies; 7,10,16 I believe that leaving the central canal open permits free communication of the dilated central canal with the subarachnoid space, and that this may reduce the chances of FIG. 1. A: Sagittal T1-weighted MR image demonstrating a dilated central canal in a low-lying spinal cord herniating into a meningocele sac. B: Axial T2-weighted MR image demonstrating the dilated central canal surrounded by the meningocele sac. C: Intraoperative photograph showing the trumpetlike flaring of the hydromyelic cord (double arrows) and the meningocele sac (single arrow). 89
4 N. Muthukumar FIG. 2. Sagittal T1- (A) and T2-weighted (B) MR images demonstrating the hydromyelic cord herniating into a lumbar meningocele sac. Sagittal 3D-CISS image (C) delineating the nature of the lesion in a terminal myelocystocele. Intraoperative photographs showing the dilated hydromyelic cord (D) and the opened syringocele with the probe inside the lesion s cavity (E). Postoperative sagittal T1- (F) and T2-weighted (G) MR images obtained 7 months after surgery, demonstrating complete disappearance of the syringocele. Postoperative 3D-CISS image (H) obtained 7 months after surgery demonstrating absence of the syringocele. recurrence of syringocele. In one patient a teratoma was encountered in the sac and was excised. Five of these children required plastic surgery repair in the form of rotation flaps to cover the defect left behind by sac excision because these children had significant areas of dystrophic skin, which precluded tension-free closure of the skin. Postoperatively, patients were maintained in the prone position with the foot end of the bed elevated until the sutures were removed. Postoperatively, CSF leaks were encountered in five patients. All CSF leaks were treated conservatively by placing the patient prone, elevating the foot end of the bed, and applying compressive dressings. None of the children with CSF leaks had untreated hydrocephalus. Three children experienced flap necrosis. There was no change in the neurological deficits in any of these patients during the follow-up period. Six of the 14 patients were old enough during the last follow-up visit for their ambulatory status to be assessed, and all six were found to be ambulatory without support. No child with preoperative incontinence achieved complete sphincter control. No patient has presented with retethering so far. Nonterminal Myelocystoceles All the children presented with swelling in the back; the base and sides of the swelling were covered by normal skin, whereas varying extents of the dome of the swelling were covered by dystrophic skin. None of the sacs leaked CSF. Except for one child who presented with paraplegia, 90
5 Terminal and nonterminal myelocystoceles FIG. 3. Coronal T2-weighted MR sequences through the meningocele sac demonstrating the target sign (arrows) produced by the hydromyelic cord within the meningocele sac. all the others were neurologically normal. The paraplegic child also had macrocephaly due to aqueductal stenosis. Neuroimaging. Plain x-ray films of the spine were obtained in all children, and MR examinations of the spine and brain were performed as well. Three of these children also underwent 3D-CISS imaging and MR myelography. The MR imaging revealed Rossi Type I nonterminal myelocystoceles in six patients and Rossi Type II nonterminal myelocystoceles in the remaining three (Figs. 4A D and 5A and B). 18 The 3D-CISS images and MR myelograms were very useful in the evaluation of the nature of these rare malformations (Figs. 4E, 5C, and 6). Associated anomalies included split cord malformation in one patient with a thoracic myelocystocele, and a low-lying conus due to a thickened filum terminale in two patients with lumbosacral nonterminal myelocystoceles. The patient with the split cord malformation had a hydromyelic hemicord that communicated with the dorsal meningocele. 18 Surgery. The surgical procedure varied with the type of nonterminal myelocystocele. In the three patients with Type II lesions, the meningocele sac was opened and the dilated cord with syringocele was detached from the sac, the syringocele was drained, and the meningocele sac was excised (Fig. 4F and G). In Type I nonterminal myelocystoceles, the sac was opened and the neurofibrovascular stalk extending from the spinal cord to the dome of the sac was cut close to the cord surface, and the sac was then excised (Fig. 5D). In the only patient with associated split cord malformation, excision of the septum was then done. In the two patients who had lumbosacral nonterminal myelocystoceles with a lowlying conus due to a thickened filum terminale, the filum terminale was identified and sectioned. There was no change in the neurological status in this group of patients. In one patient with Type I nonterminal myelocystocele and associated split cord malformation, a transient CSF leak developed, which subsided with conservative treatment. There was no change in the neurological status during the followup period, which ranged from 3 to 18 months. No patient with nonterminal myelocystocele has presented with retethering so far. Discussion The term myelocystocele was originally used by Lassman et al. 13 to designate a relatively severe form of spina bifida cystica and lumbar hydromyelia in which the dilation of the central canal is so excessive that the cyst may project through the laminal defect and occupy the major portion of the sac. 16 These authors used the term myelocystomeningocele to designate a relatively milder form of spina bifida cystica and lumbar hydromyelia in which only the thinned and stretched dorsal wall of the cyst will enter the main protrusion of the meninges to a limited extent. Myelocystoceles can occur at any level of the spine. 16 They are classified into terminal and nonterminal lesions depending on their location and postsurgical pathological findings. 1,2,7 9,22 27 The term nonterminal myelocystocele was introduced recently in the literature by Rossi and colleagues. 22 Nevertheless, the existence of this entity has been recognized for many years, although by different names. 1,2,8, 9,24 27 Doran and Guthkelch 8 analyzed a series of 308 patients with spina bifida cystica and noted the existence of a lesion accompanied by hydromyelia of the cord and a cystic lesion at the level of the bone defect at the cervical or thoracic level, which they called a syringocele Even though 91
6 N. Muthukumar FIG. 4. Images demonstrating a Type II nonterminal myelocystocele. A: Sagittal T1-weighted MR image demonstrating a portion of the spinal cord with the dilated central canal herniating into the meningocele sac. B: Sagittal T2-weighted image demonstrating the presence of CSF in the portion of the cord herniating into the meningocele sac. C: Axial T1-weighted image demonstrating a portion of the cord with the central canal herniating into the meningocele sac. D: Axial T2-weighted image demonstrating a portion of the CSF-containing cord within the meningocele sac. E: A 3D-CISS image clearly delineating the nature of the lesion in the Type II nonterminal myelocystocele. F: Intraoperative photograph showing the hydromyelic cord (arrow) attached to the dome of the meningocele sac. G: Intraoperative photograph showing the untethered cord with the probe in the opening of the syringocele cavity. Barson 2 had reported similar lesions earlier, it was Friede 9 who used the term myelocystoceles to refer to these lesions in the cervical and thoracic regions. Subsequently, several authors have indicated that many so-called cervical and thoracic meningoceles are in fact myelocystoceles. 1,14, 19,20,24 27 The true incidence of this abnormality is not known because many of the lesions are erroneously diagnosed as meningoceles. There has been a spike in the reports of nonterminal myelocystoceles since the advent of MR imaging. 1,18,22,24 26 The following discussion highlights the differences between these two entities in embryological features, clinical presentation, results on neuroimaging studies, surgical findings, and prognosis. The differences between terminal and nonterminal myelocystoceles are summarized in Table 3. Embryological Differences Terminal Myelocystoceles. These lesions develop from abnormalities of the caudal cell mass (Fig. 7). McLone and Naidich 16 proposed the following theory for the mechanisms involved in the pathogenesis of terminal myelocystoceles: 1) for unknown reasons, CSF is unable to exit from the early neural tube; 2) this CSF vents into the terminal ventricle after canalization of the tail bud occurs; 3) the terminal ventricle dilates; 4) the expanding terminal ventricle bulges into and disrupts the dorsal mesenchyme but not the superficial ectoderm; 5) as a result, the posterior elements of the spine fail to develop (spina bifida), but the lesion remains deep beneath an intact skin cover; 6) as the terminal ventricle balloons into a cyst, it distends the arachnoid lining of the distal spinal cord, forming a meningocele; 7) the bulk of the cyst prevents the ascent of the cord, producing a tethered cord; 8) after formation of arachnoid, progressive distension of the distalmost cord causes it to bulge caudally below the end of the meningocele into the extraarachnoid space, where it is covered by fat; 9) the cyst also bulges cephalically to expand the distal cord; and 10) disruption of the caudal motor segments produces symptoms that may be present at birth or may appear later and be progressive. The intimate association of the caudal cell mass to the progenitors of the hindgut and urogenital system is responsible for the frequent occurrence of abnormalities of these systems in patients with terminal myelocystoceles. Nonterminal Myelocystoceles. The embryology of nonterminal myelocystoceles can be explained by the limited dorsal myeloschisis theory of Pang and Dias 19 (Fig. 8). In limited dorsal myeloschisis, neurulation proceeds normally in all areas except in the area of the abnormality, where final fusion of the opposed neural folds does not occur. Basic configuration of the neural tube has been achieved, however, except for a thin slip in the dorsal midline. Here, disjunction between cutaneous ectoderm and neuroectoderm never 92
7 Terminal and nonterminal myelocystoceles FIG. 5. Type I nonterminal myelocystocele in the lumbosacral region. A: Sagittal T1-weighted MR image demonstrating the spinal cord extending up to the sacral region, with a fibroneurovascular stalk extending from the posterior aspect of the low-lying cord to the dome of the meningocele sac. B: Sagittal T2-weighted MR image demonstrating the spinal cord (arrowheads) extending to the sacral region. The long arrow points to the syringocele cavity within the lowlying cord, and the short arrow points to the fibroneurovascular stalk extending into the meningocele sac. C: Preoperative 3D-CISS images showing the nature of the lesion in a nonterminal myelocystocele. Double arrows point to the syringocele cavity within the low-lying cord, and the single arrow points to the bleb of CSF within the fibroneurovascular stalk in the meningocele sac. D: Intraoperative photograph showing the fibroneurovascular stalk (double arrows), which is attached to the low-lying spinal cord (single arrow). truly occurs, but the midline gap between the converging cutaneous ectoderm and dorsal sclerotomes from the opposite sides of the embryo remains very narrow. Further development of the full-thickness dorsal myofascial tissues (except for the narrow slip in the midline) progressively sets the integument farther away from the neural tube, which ultimately retains its intraspinal location. A dorsal median stalk exists between the neural tube and the cutaneous ectoderm. The CSF from the central canal dissects through the median stalk and ultimately distends into a sac to form the nonterminal myelocystocele. The attachment of the dorsal median stalk tents the cord posteriorly. Even though this theory of limited dorsal myeloschisis was originally proposed by Pang and Dias 19 for the pathogenesis of what they termed cervical myelomeningoceles, as pointed out by McComb 14 and Parent, 20 some of the cases described by Pang and Dias are in reality cervical myelocystoceles, and therefore this theory is applicable to all nonterminal myelocystoceles. By using 3D-CISS imaging we have shown that the fibroneurovascular stalk in nonterminal myelocystoceles occasionally contains a bleb of CSF (Fig. 5C), thereby proving the limited dorsal myeloschisis theory of Pang and Dias. Clinical Differences Terminal Myelocystoceles. Patients with terminal myelocystoceles usually present with a lumbosacral mass at birth; the size of the mass is variable. 16 The skin overlying the mass may be normal or may exhibit a hemangioma, nevus, or hypertrichosis. In our series, however, nine of 14 patients had dystrophic skin covering the dome of the sac. Even though patients with terminal myelocystoceles usually present with lumbosacral masses, recently Cartmill et al. 5 reported on a patient who did not have a lumbosacral mass, and in whom this led to a delay in the diagnosis. Early reports of patients with this condition mentioned the absence of neurological deficits at birth as a prominent feature. With experience, however, it is now more evident that many of these children present with a neurological deficit at birth. The presence of neurological deficits at birth is understandable because, as pointed out by McLone and Naidich 16 in their theories on the pathogenesis of terminal myelocystoceles, the distension of the terminal ventricle might disrupt the developing caudal motor segments. Sim et al. 23 have reported on a patient with this condition who presented with saddle anesthesia and incontinence. All four children with terminal myelocystoceles reported by Cohen 7 had neurological deficits, as did 47% of patients reported by Gupta and Mahapatra 10 and five of the eight patients reported by James and Lubinsky. 11 In the present study, 10 of the 14 children had varying degrees of neurological deficits. Associated Anomalies. In early reports of terminal myelocystoceles, a disproportionately high incidence of abdominal wall defects and OEIS complex was noted in children with these lesions. 7,16,21 With the widespread availability of MR imaging, however, recent reports do not indicate such 93
8 N. Muthukumar TABLE 3 Differences between terminal and NT myelocystoceles Feature Terminal Myelocystocele NT Myelocystocele embryology abnormality of caudal cell mass limited dorsal myelo- (abnormality of secondary schisis (abnormality neurulation) of primary neurulation) neuro deficits common rare associated common rare anomalies radiology homogeneous two types findings op drainage of syringocele, unteth- varies w/ the type of NT ering of the SC, & excision myelocystocele of meningocele sac prognosis less favorable more favorable FIG. 6. Preoperative sagittal MR myelogram of a Type II nonterminal myelocystocele clearly delineating the nature of the lesion. a high association, 10,12 with the exception of the report by James and Lubinsky. 11 In the present study, no patient had associated OEIS complex. The importance of coexisting cloacal exstrophy in the outcome of patients with this condition will be discussed subsequently. The incidence of CM-II in patients with myelocystoceles has been the subject of much discussion. 15,17 Midrio et al. 17 reported on a patient in whom a prenatal diagnosis of terminal myelocystocele was made on the basis of the absence of CM-II on prenatal ultrasound and MR imaging studies, and based on negative alpha fetoprotein levels in the amniotic fluid. Midrio et al. depended on the absence of CM-II to diagnose terminal myelocystocele and thus avoided prenatal surgery. As pointed out by McLone, 15 and as shown by the present study, in which two of the 14 patients had CM-II, the incidence of CM-II is low when compared with open forms of spinal dysraphism, but its mere presence does not exclude the diagnosis of terminal myelocystocele. This gains importance in the era of prenatal surgery, when proper prenatal diagnosis is necessary to differentiate myelomeningocele from terminal myelocystocele. Nonterminal Myelocystoceles. Nonterminal myelocystoceles have frequently been reported in the cervical, cervicothoracic, and thoracic regions, 1,18,24 27 but rarely in the lumbar region. 22 Among the six patients with nonterminal myelocystoceles reported by Rossi et al., 22 only one had a lesion with a lumbar location, three had lesions in the cervical area, and two had lesions in the thoracic region. However, in our series there were six patients with thoracic, two with lumbar, and one with cervical myelocystoceles. As was common in the series of Rossi et al., most of these patients presented with masses that had good skin coverage over the base and sides, but with dystrophic epithelium over the dome of the swelling. The clinical features of nonterminal myelocystoceles are quite variable. In their recent series of nonterminal myelocystoceles, Rossi et al. 22 reported on six patients, all of whom were neurologically normal at presentation. Nevertheless, earlier reports of this condition indicate that some of these patients have neurological deficits at presentation. Steinbok and Cochrane 26 presented a series of patients with cervicothoracic midline cutaneous mass lesions. Among these patients, there were three with myelocystoceles, two of whom had neurological deficits at presentation. In the present study also, among the nine patients with nonterminal myelocystoceles, one patient presented with paraplegia and incontinence. Thus, when compared with terminal myelocystoceles, a higher proportion of patients with nonterminal lesions are neurologically better preserved at presentation. Associated Anomalies. In the series of cervical myelocystoceles reported by Steinbok and Cochrane, 26 all three patients had associated hydrocephalus. In a series of six patients with nonterminal myelocystoceles published by Rossi et al., 22 five of the patients had associated malformations as follows: three with CM-II and one each with a neurenteric cyst, hydrocephalus, and filar lipoma. In the present series, two had thickened filum terminale, one had a split cord malformation, and one had aqueductal stenosis and a CM-II. Thus, associated anomalies are not uncommon in nonterminal myelocystoceles. Nevertheless, in all patients with nonterminal myelocystoceles reported to date, associated anomalies were confined to the nervous system, unlike terminal myelocystoceles, for which there is a disproportionately high association with abdominal wall defects. Neuroimaging Differences Terminal Myelocystoceles. The neuroimaging features of terminal myelocystoceles have been described adequately in earlier studies. 3,4,7,16,21 In the present series, all patients had the classic features of terminal myelocystoceles, which are characterized by low-lying hydromyelic cord herniating 94
9 Terminal and nonterminal myelocystoceles FIG. 7. Schematic representations of the embryogenesis of terminal myelocystoceles. A: During secondary neurulation, vacuoles (arrowhead) develop in the cell mass caudal to the primary neural tube formed by primary neurulation (arrow). B: Vacuoles coalesce to form the secondary neural tube (arrowhead). C: The secondary neural tube (arrowhead) fuses with the primary neural tube (arrow). D: The small arrow points to the mesoderm, and the large arrow points to the terminal ventricle; because the CSF is unable to exit the terminal ventricle, the terminal ventricle bulges into and disrupts the dorsal mesenchyme but not the cutaneous ectoderm. through a posterior spina bifida into a meningocele sac. In my experience, it is necessary to study the sagittal, axial, and coronal images carefully to make a diagnosis of myelocystocele. Relying on images obtained only in one plane (especially sagittal images) will lead to an erroneous diagnosis of meningocele. The axial and coronal images need to be studied in great detail to identify the true nature of the underlying entity. We found the 3D-CISS MR sequences to be useful in the evaluation of patients with terminal myelocystoceles. Sagittal images of the 3D-CISS sequence often show the syringocele within the cord, which might not be visible on the conventional MR images. Coronal T2- weighted images of the sac often show the relationship of the syringocele to the meningocele sac ( target sign ), and thus these images are very helpful in establishing the diagnosis. Nonterminal Myelocystoceles. Recently, Rossi and coauthors 22 described the neuroimaging findings in patients with nonterminal myelocystoceles. They divided nonterminal myelocystoceles into two types depending on the neuroimaging findings, as follows: Type I, which is a forme fruste myelocystocele in which the meningocele sac is traversed by a fibroneurovascular stalk extending from the spinal cord to the dome of the meningocele sac (this forme fruste type was also termed myelocystocele manqué ); and Type 2, which is a complete form in which the major component of the CSF-filled cyst is a focal hydromyelia that has displaced into the meningocele. In their series, they had three Type I and three Type II nonterminal myelocystoceles. In my series, however, there were six patients with Type I nonterminal myelocystoceles and three with Type II nonterminal myelocystoceles. In both types, the cord appears tented posteriorly at the site of the abnormality. This differentiation of nonterminal myelocystoceles into two types based on neuroimaging results is of surgical importance, as will be discussed subsequently. My experience has shown that MR myelography and 3D-CISS sequences are very helpful in delineating the nature of the underlying entity in this rare form of occult spinal dysraphism. I recommend inclusion of 3D-CISS sequences and MR myelography in the routine evaluation of all skin-covered masses in the back. In this study, it has been shown for the first time on 3D-CISS imaging the presence of CSF loculation within the fibroneurovascular stalk of nonterminal myelocystoceles. Surgical Differences Terminal Myelocystoceles. Surgery for terminal myelocystoceles differs from surgery for meningoceles due to the fact that the spinal cord herniates into the meningocele sac to which it is attached. As a consequence, it is mandatory to expose the lamina immediately proximal to the defect and remove it. The dural opening should start from the normal dura mater and then be extended toward the meningocele. This will prevent inadvertent cord injury, which might occur if the sac were to be opened directly at the dome of the meningocele. In most cases, the trumpetlike flaring of the hydromyelic cord was visible on opening of the sac, with the nerve roots passing back into the spinal canal from the cord. In addition, arachnoidal adhesions and meningocele manqué were frequently encountered. After detaching the hydromyelic cord from the sac, there was egress of CSF from the central canal. The amount of CSF outflow was variable and was not profuse. In all cases, the fluid was clear and colorless, unlike in certain reports in which it was found to be xanthochromic or even purulent. 12 Many earlier authors have recommended closing the decompressed hydromyelic conus with pial sutures to reconstruct the spinal cord. 7,10,16 In this series this was not done because I believe that leaving the central canal open allows free communication between the dilated central canal and the subarachnoid space, and thereby theoretically reduces the chance of recurrence of syringocele, even though such a recurrence has not been reported to date. Nonterminal Myelocystoceles. Surgical techniques in non- 95
10 N. Muthukumar FIG. 8. Schematic representations of the limited dorsal myeloschisis theory of Pang and Dias as applied to the embryogenesis of nonterminal myelocystoceles. A: Incomplete fusion of the neural folds is shown; the neural tube retains an attachment to the cutaneous ectoderm. B: Growth of the mesenchyme pushes the neural tube ventrally; the connection with the cutaneous ectoderm remains as a neural stalk. C: A Type I nonterminal myelocystocele; CSF dissects around the neural stalk and forms a subcutaneous meningocele under the intact skin. D: The dilated central canal of the spinal cord herniates into the meningocele sac to form a Type II nonterminal myelocystocele. terminal myelocystoceles are dependent on the recognition of the two subtypes of these entities. In Type I, in which there is a fibroneurovascular stalk extending from the spinal cord to the dome of the meningocele sac, the surgical technique consists of untethering the cord by sectioning the stalk flush with the cord and then excising the meningocele sac. Failure to untether the cord by this method will lead to delayed deterioration, as reported by Pang and Dias. 19 On the other hand, in Type II nonterminal myelocystoceles, the procedure consists of opening the meningocele sac, untethering the cord from its attachment to the sac, and opening the syringocele to drain the CSF, followed by excision and repair of the meningocele sac. The cord with the collapsed syringocele is easily contained within the spinal canal because of the existence of the posterior spina bifida. Failure to untether the cord and/or to drain the syringocele might lead to progressive neurological deterioration. Pang and Dias reported on nine patients with cervical myelomeningoceles, six of whom underwent simple sac excision without untethering of the cord. Five of the six patients exhibited late neurological deterioration after a mean follow-up duration of 3.6 years. A second surgical procedure to untether the cord resulted in neurological improvement. This shows the importance of untethering the cord. Prognostic Differences Outcome in Terminal Myelocystoceles. The outcome in children with terminal myelocystoceles is variable. Initial studies of terminal myelocystoceles reported a favorable outcome. McLone and Naidich 16 reported that patients with terminal myelocystoceles were born without neurological deficits. However, subsequent reports have shown that many of these children had disabling neurological deficits. 6,7,10,11 Choi and McComb 6 reported on nine patients with a mean follow-up duration of 63 months. In their series, all patients had associated OEIS complex, and all had sphincter disturbances and were significantly neurologically impaired. Cohen 7 reported on five patients with cloacal exstrophy, four of whom had terminal myelocystocele, and the fifth had lipomyelomeningocele. All four children with terminal myelo- 96
11 Terminal and nonterminal myelocystoceles cystoceles had significant neurological deficits, and after surgery one did not ambulate, two ambulated independently, and one ambulated with orthoses. Recently, James and Lubinsky 11 reported on a unique series of patients with terminal myelocystoceles with and without abdominal wall defects. Among the eight patients in their series, four had abdominal wall defects and four did not. Those without abdominal wall defects were able to ambulate with the aid of orthotic devices, whereas those with associated abdominal wall defects were not able to ambulate independently. Recently, Gupta and Mahapatra 10 reported on 17 patients with terminal myelocystoceles, of whom eight experienced varying degrees of neurological deficits, including two patients with complete paraplegia. In the present study, 10 of the 14 patients had neurological deficits. The neurological status remained stable in all patients during the follow-up period. From my experience and based on a review of the literature, it is evident that patients with terminal myelocystoceles do not constitute a single homogeneous group. Those with associated cloacal exstrophy generally have severe neurological deficits, require multiple surgical procedures, and their prognosis is less favorable. On the other hand, in those without cloacal exstrophy, the outcome is directly related to the neurological status at presentation; those who are well preserved neurologically improve and maintain their improvement, in contrast to those with neurological deficits at presentation whose improvement is less favorable. Surprisingly, in all the series reported to date, including the present study, there was no report of retethering. Outcome in Nonterminal Myelocystoceles. The outcome in these entities is generally more favorable than the outcome in terminal myelocystoceles. In this series, eight of the nine children with a nonterminal myelocystocele presented without neurological deficits, and they maintained the same neurological status during the follow-up period. In comparison, 10 of the 14 patients with terminal myelocystoceles presented with neurological deficits, and their neurological status did not improve significantly during the follow-up period. In the series published by Rossi et al., 22 follow-up assessments were available for four of the six patients, and in all of these there was no evidence of neurological deterioration. Overall, the outcome in nonterminal myelocystoceles is likely to be better than in terminal myelocystoceles, probably because nonterminal myelocystoceles are not associated with abnormalities in other systems (such as cloacal exstrophy), which contribute significantly to the overall handicap of these patients. 11 Conclusions Terminal and nonterminal myelocystoceles differ from one another embryologically, clinically, radiologically, surgically, and prognostically. With the widespread availability of MR imaging, many cases of terminal and nonterminal myelocystoceles are likely to be recognized. A proper understanding of these rarer subtypes of occult spinal dysraphism is necessary for providing optimal care to these patients. References 1. Arts MP, de Jong TH: Thoracic meningocele, meningomyelocele or myelocystocele? Diagnostic difficulties, consequent implications and treatment. Pediatr Neurosurg 40:75 79, Barson AJ: Spina bifida: the significance of the level and extent of the defect to the morphogenesis. Dev Med Child Neurol 12: , Byrd SE, Harvey C, Darling CF: MR of terminal myelocystoceles. Eur J Radiol 20: , Byrd SE, Harvey C, McLone DG, Darling CF: Imaging of terminal myelocystoceles. J Natl Med Assoc 88: , Cartmill M, Jaspan T, Punt J: Terminal myelocystocele: an unusual presentation. Pediatr Neurosurg 32:83 85, Choi S, McComb JG: Long-term outcome of terminal myelocystocele patients. Pediatr Neurosurg 32:86 91, Cohen AR: The mermaid malformation: cloacal exstrophy and occult spinal dysraphism. Neurosurgery 28: , Doran PA, Guthkelch AN: Studies in spina bifida cystica. I. General survey and reassessment of the problem. J Neurol Neurosurg Psychiatry 24: , Friede RL: Developmental Neuropathology. New York: Springer-Verlag, 1975, pp Gupta DK, Mahapatra AK: Terminal myelocystoceles: a series of 17 cases. J Neurosurg 103 (4 Suppl): , James HE, Lubinsky G: Terminal myelocystocele. J Neurosurg 103 (5 Suppl): , Kumar R, Chandra A: Terminal myelocystocele. Indian J Pediatr 69: , Lassman LP, James CC, Foster JB: Hydromyelia. J Neurol Sci 7: , McComb JG: Cervical myelomeningoceles. Neurosurgery 33: 365, 1993 (Comment) 15. McLone DG: Prenatal diagnosis of terminal myelocystocele in the fetal surgery era. Neurosurgery 50:1155, 2002 (Comment) 16. McLone DG, Naidich TP: Terminal myelocystocele. Neurosurgery 16:36 43, Midrio P, Silberstein H, Bilaniuk L, Adzick NS, Sutton LN: Prenatal diagnosis of terminal myelocystocele in the fetal surgery era: case report. Neurosurgery 50: , Muthukumar N: Thoracic myelocystoceles two variants. Acta Neurochir (Wien) 148: , Pang D, Dias MS: Cervical myelomeningoceles. Neurosurgery 33: , Parent AD: Cervical myelomeningoceles. Neurosurgery 33: 365, 1993 (Comment) 21. Peacock WJ, Murovic JA: Magnetic resonance imaging in myelocystoceles. Report of two cases. J Neurosurg 70: , Rossi A, Piatelli G, Gondolfo C, Pavanello M, Hoffman C, Van Goetherm JW, et al: Spectrum of nonterminal myelocystoceles. Neurosurgery 58: , Sim KB, Wang KC, Cho BK: Terminal myelocystocele case report. J Korean Med Sci 11: , Steinbok P: Dysraphic lesions of the cervical spinal cord. Neurosurg Clin N Am 6: , Steinbok P, Cochrane DD: Cervical meningoceles and myelocystoceles: a unifying hypothesis. Pediatr Neurosurg 23: , Steinbok P, Cochrane DD: The nature of congenital posterior cervical or cervicothoracic midline cutaneous mass lesions. Report of eight cases. J Neurosurg 75: , Suneson A, Kalimo H: Myelocystocele with cerebellar heterotopia. Case report. J Neurosurg 51: , 1979 Manuscript submitted March 4, Accepted May 2, Address reprint requests to: Natarajan Muthukumar, M.Ch., Muruganagam, 138, Anna Nagar, Madurai , Tamil Nadu, India. prasan86@eth.net. 97
Persistent Terminal Ventricle
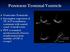 Persistent Terminal Ventricle Ventriculus Terminalis Incomplete regression of TV of 2 neurulation, continuity with central canal small cavity PTV vs terminal myelocystocele (?severe manifestation from
Persistent Terminal Ventricle Ventriculus Terminalis Incomplete regression of TV of 2 neurulation, continuity with central canal small cavity PTV vs terminal myelocystocele (?severe manifestation from
Long segment composite split cord malformation with double bony spur
 Long segment composite split cord malformation with double bony spur Anand Sharma, Achal Sharma, R.S. Mittal SMS Medical College, Jaipur, India Abstract: A composite type of SCM is very rare and only a
Long segment composite split cord malformation with double bony spur Anand Sharma, Achal Sharma, R.S. Mittal SMS Medical College, Jaipur, India Abstract: A composite type of SCM is very rare and only a
Wound healing in trophic ulcers in spina bifida patients
 J Neurosurg 82:000 000, 1995 Wound healing in trophic ulcers in spina bifida patients VINOD KUMAR SRIVASTAVA, M.B.B.S, M.CH. Neurosurgical Unit, J. N. Medical College, Aligarh Muslim University, Aligarh,
J Neurosurg 82:000 000, 1995 Wound healing in trophic ulcers in spina bifida patients VINOD KUMAR SRIVASTAVA, M.B.B.S, M.CH. Neurosurgical Unit, J. N. Medical College, Aligarh Muslim University, Aligarh,
Asymptomatic posterior cervical myelomeningocele with tethered cord in an adolescent: a rare form of spinal dysraphism with rare presentation
 Romanian Neurosurgery (2016) XXX 1: 113-117 113 Asymptomatic posterior cervical myelomeningocele with tethered cord in an adolescent: a rare form of spinal dysraphism with rare presentation Gangesh Gunjan,
Romanian Neurosurgery (2016) XXX 1: 113-117 113 Asymptomatic posterior cervical myelomeningocele with tethered cord in an adolescent: a rare form of spinal dysraphism with rare presentation Gangesh Gunjan,
SPLIT NOTOCHORD SYNDROME ASSOCIATION. DR. Hasan Nugud Consultant Paediatric Surgeon
 SPLIT NOTOCHORD SYNDROME ASSOCIATION DR. Hasan Nugud Consultant Paediatric Surgeon CASE PRESENTATION :- New born baby, boy, referred to the paediatric surgical team at the age of 14 hours. Birth History
SPLIT NOTOCHORD SYNDROME ASSOCIATION DR. Hasan Nugud Consultant Paediatric Surgeon CASE PRESENTATION :- New born baby, boy, referred to the paediatric surgical team at the age of 14 hours. Birth History
Pediatric Spinal Anomalies
 Department of Radiology University of California San Diego Pediatric Spinal Anomalies John R. Hesselink, M.D. Spine Embryogenesis 1. Primitive streak 2. Proliferation of cells at primitive pit (Hensen's
Department of Radiology University of California San Diego Pediatric Spinal Anomalies John R. Hesselink, M.D. Spine Embryogenesis 1. Primitive streak 2. Proliferation of cells at primitive pit (Hensen's
University Journal of Surgery and Surgical Specialties
 University Journal of Surgery and Surgical Specialties ISSN 2455-2860 Volume 2 Issue 1 2016 TWO RARE CASES OF DIASTEMATOMYELIA MUTHURAMAN P Department of Neuro Surgery, THANJAVUR MEDICAL COLLEGE Abstract
University Journal of Surgery and Surgical Specialties ISSN 2455-2860 Volume 2 Issue 1 2016 TWO RARE CASES OF DIASTEMATOMYELIA MUTHURAMAN P Department of Neuro Surgery, THANJAVUR MEDICAL COLLEGE Abstract
Development of Spinal Cord & Vertebral Column. Dr. Sanaa Alshaarawi & Prof. Ahmed Fathalla
 Development of Spinal Cord & Vertebral Column Dr. Sanaa Alshaarawi & Prof. Ahmed Fathalla OBJECTIVES At the end of the lecture, students should be able to: q Describe the development of the spinal cord
Development of Spinal Cord & Vertebral Column Dr. Sanaa Alshaarawi & Prof. Ahmed Fathalla OBJECTIVES At the end of the lecture, students should be able to: q Describe the development of the spinal cord
Role of helical CT and MRI in the evaluation of spinal dysraphism
 International Journal of Advances in Medicine Kumaran SK et al. Int J Adv Med. 2017 Feb;4(1):124-132 http://www.ijmedicine.com pissn 2349-3925 eissn 2349-3933 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20170095
International Journal of Advances in Medicine Kumaran SK et al. Int J Adv Med. 2017 Feb;4(1):124-132 http://www.ijmedicine.com pissn 2349-3925 eissn 2349-3933 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20170095
Sonography of the Neonatal Spine: Part 2, Spinal Disorders
 Neonatal Spine Sonography Pediatric Imaging Pictorial Essay Downloaded from www.ajronline.org by 148.251.232.83 on 04/11/18 from IP address 148.251.232.83. Copyright RRS. For personal use only; all rights
Neonatal Spine Sonography Pediatric Imaging Pictorial Essay Downloaded from www.ajronline.org by 148.251.232.83 on 04/11/18 from IP address 148.251.232.83. Copyright RRS. For personal use only; all rights
Congenital Spinal Lipoma: analyzing the perplexed nomenclature and our management
 Congenital Spinal Lipoma: analyzing the perplexed nomenclature and our management Nidal Khasawneh MD *, Rami Alqroom MD *, Firas Sha'ban MD *, Rafeed Al Drous MD *, Rima Nserat **, Amer Al Shurbaji MD
Congenital Spinal Lipoma: analyzing the perplexed nomenclature and our management Nidal Khasawneh MD *, Rami Alqroom MD *, Firas Sha'ban MD *, Rafeed Al Drous MD *, Rima Nserat **, Amer Al Shurbaji MD
Symptomatic Multiple Level Lateral Meningoceles with Intraspinal Meningocele: A Case Study and Its Surgical Management
 THIEME Original Article 15 Symptomatic Multiple Level Lateral Meningoceles with Intraspinal Meningocele: A Case Study and Its Surgical Management Vernon Velho 1 Sachin Guthe 1 Pravin Survashe 1 Poonam
THIEME Original Article 15 Symptomatic Multiple Level Lateral Meningoceles with Intraspinal Meningocele: A Case Study and Its Surgical Management Vernon Velho 1 Sachin Guthe 1 Pravin Survashe 1 Poonam
Diastematomyelia: A Case with Familial Aggregation of Neural Tube Defects
 Case Study TheScientificWorldJOURNAL (2004) 4, 847 852 ISSN 1537-744X; DOI 10.1100/tsw.2004.140 Diastematomyelia: A Case with Familial Aggregation of Neural Tube Defects Nuray Öksüz Kanbur 1, *, Pınar
Case Study TheScientificWorldJOURNAL (2004) 4, 847 852 ISSN 1537-744X; DOI 10.1100/tsw.2004.140 Diastematomyelia: A Case with Familial Aggregation of Neural Tube Defects Nuray Öksüz Kanbur 1, *, Pınar
A Retrospective Analysis of Clinical Profile and Surgical Outcome in Patients with Spinal Dysraphism at Tertiary Care Center
 Original Research Article A Retrospective Analysis of Clinical Profile and Surgical Outcome in Patients with Spinal Dysraphism at Tertiary Care Center Premlal KV * Assistant Professor, Department of Neurosurgery,
Original Research Article A Retrospective Analysis of Clinical Profile and Surgical Outcome in Patients with Spinal Dysraphism at Tertiary Care Center Premlal KV * Assistant Professor, Department of Neurosurgery,
University Journal of Surgery and Surgical Specialties
 University Journal of Surgery and Surgical Specialties ISSN 2455-2860 Volume 2 Issue 1 2016 Profile of paediatric patients with split cord malformation MANORANJITHAKUMARI M Department of Neuro Surgery,
University Journal of Surgery and Surgical Specialties ISSN 2455-2860 Volume 2 Issue 1 2016 Profile of paediatric patients with split cord malformation MANORANJITHAKUMARI M Department of Neuro Surgery,
Congenital Spine and Spinal Cord Malformations Pictorial Review
 JR Integrative Imaging LIFELONG LERNING FOR RDIOLOGY ongenital Spine and Spinal ord Malformations Pictorial Review Stephanie L. Rufener 1,2, Mohannad Ibrahim 2, harles. Raybaud 3, Hemant. Parmar 2 Downloaded
JR Integrative Imaging LIFELONG LERNING FOR RDIOLOGY ongenital Spine and Spinal ord Malformations Pictorial Review Stephanie L. Rufener 1,2, Mohannad Ibrahim 2, harles. Raybaud 3, Hemant. Parmar 2 Downloaded
Neuroanatomy. Assistant Professor of Anatomy Faculty of Medicine The University of Jordan Dr Maha ELBeltagy
 Neuroanatomy Dr. Maha ELBeltagy Assistant Professor of Anatomy Faculty of Medicine The University of Jordan 2018 Development of the Central Nervous System Development of the nervous system Development
Neuroanatomy Dr. Maha ELBeltagy Assistant Professor of Anatomy Faculty of Medicine The University of Jordan 2018 Development of the Central Nervous System Development of the nervous system Development
Spinal congenital dermal sinus with dual ostia
 J Neurosurg Pediatrics 3:000 000, 3:407 411, 2009 Spinal congenital dermal sinus with dual ostia Clinical article Ch a n g Su b Le e, M.D., 1 Ji Ho o n Ph i, M.D., 2 Se u n g -Ki Kim, M.D., Ph.D., 2 By
J Neurosurg Pediatrics 3:000 000, 3:407 411, 2009 Spinal congenital dermal sinus with dual ostia Clinical article Ch a n g Su b Le e, M.D., 1 Ji Ho o n Ph i, M.D., 2 Se u n g -Ki Kim, M.D., Ph.D., 2 By
MRI of chronic spinal cord injury
 The British Journal of Radiology, 76 (2003), 347 352 DOI: 10.1259/bjr/11881183 E 2003 The British Institute of Radiology Pictorial review MRI of chronic spinal cord injury 1 K POTTER, FRCR and 1 A SAIFUDDIN,
The British Journal of Radiology, 76 (2003), 347 352 DOI: 10.1259/bjr/11881183 E 2003 The British Institute of Radiology Pictorial review MRI of chronic spinal cord injury 1 K POTTER, FRCR and 1 A SAIFUDDIN,
Synovial cyst of spinal facet
 Case report CHUN C. KAO, M.D., STEFAN S. WINKLER, M.D., AND J. H. TURNER, M.D. Sections of Neurosurgery, Radiology, and Pathology, Madison Veterans Administration Hospital, and University of Wisconsin,
Case report CHUN C. KAO, M.D., STEFAN S. WINKLER, M.D., AND J. H. TURNER, M.D. Sections of Neurosurgery, Radiology, and Pathology, Madison Veterans Administration Hospital, and University of Wisconsin,
What Every Spine Surgeon Should Know About Neurosurgical Issues
 What Every Spine Surgeon Should Know About Neurosurgical Issues Amer Samdani, MD Chief of Surgery Shriners Hospitals for Children Philadelphia, PA Objectives Main intraspinal lesions Chiari malformation
What Every Spine Surgeon Should Know About Neurosurgical Issues Amer Samdani, MD Chief of Surgery Shriners Hospitals for Children Philadelphia, PA Objectives Main intraspinal lesions Chiari malformation
Chapter IV: Percutaneous Puncture of Spinal Cord Cysts
 Acta Radiologica: Diagnosis ISSN: 0567-8056 (Print) (Online) Journal homepage: http://www.tandfonline.com/loi/iard19 Chapter IV: Percutaneous Puncture of Spinal Cord Cysts To cite this article: (1966)
Acta Radiologica: Diagnosis ISSN: 0567-8056 (Print) (Online) Journal homepage: http://www.tandfonline.com/loi/iard19 Chapter IV: Percutaneous Puncture of Spinal Cord Cysts To cite this article: (1966)
Chapter 8. Pediatric Surgery
 Chapter 8 Pediatric Surgery 8.1 Hydrocephalus Hydrocephalus is a congenital disorder. There may be difficulties during normal vaginal delivery due large size of the head. In 1970s, when these pictures
Chapter 8 Pediatric Surgery 8.1 Hydrocephalus Hydrocephalus is a congenital disorder. There may be difficulties during normal vaginal delivery due large size of the head. In 1970s, when these pictures
1 Normal Anatomy and Variants
 1 Normal Anatomy and Variants 1.1 Normal Anatomy MR Technique. e standard MR protocol for a routine evaluation of the spine always comprises imaging in sagittal and axial planes, while coronal images are
1 Normal Anatomy and Variants 1.1 Normal Anatomy MR Technique. e standard MR protocol for a routine evaluation of the spine always comprises imaging in sagittal and axial planes, while coronal images are
CAUDAL REGRESSION SYNDROME
 CAUDAL REGRESSION SYNDROME *Prateek Gehlot 1 and Jagdish Mandliya 2 1 Department of Radio-Diagnosis, R.D.Gardi Medical College,, Ujjain (MP). 2 Department of Pediatrics, R.D.Gardi Medical College, Ujjain
CAUDAL REGRESSION SYNDROME *Prateek Gehlot 1 and Jagdish Mandliya 2 1 Department of Radio-Diagnosis, R.D.Gardi Medical College,, Ujjain (MP). 2 Department of Pediatrics, R.D.Gardi Medical College, Ujjain
Neurosurgery Clinic, University of Wisconsin Hospitals and Clinics, Madison, WI 53792, USA 3
 Case Reports in Neurological Medicine Volume 2012, Article ID 635029, 4 pages doi:10.1155/2012/635029 Case Report Tethered Cord Syndrome Secondary to the Unusual Constellation of a Split Cord Malformation,
Case Reports in Neurological Medicine Volume 2012, Article ID 635029, 4 pages doi:10.1155/2012/635029 Case Report Tethered Cord Syndrome Secondary to the Unusual Constellation of a Split Cord Malformation,
Split cord malformation in children undergoing neurosurgical intervetion in India: a descriptive study
 ORIGINAL ARTICLE Journal of Pediatric Neurology 2004; 2(1): 21-27 www.jpneurology.org in children undergoing neurosurgical intervetion in India: a descriptive study Raj Kumar 1, Vinita Singh 2, Satya Narayan
ORIGINAL ARTICLE Journal of Pediatric Neurology 2004; 2(1): 21-27 www.jpneurology.org in children undergoing neurosurgical intervetion in India: a descriptive study Raj Kumar 1, Vinita Singh 2, Satya Narayan
Using the sac membrane to close the flap donor site in large meningomyeloceles
 The British Association of Plastic Surgeons (2004) 57, 273 277 Using the sac membrane to close the flap donor site in large meningomyeloceles Cengiz Bozkurt a, Selçuk Akın a, *,Şeref Doğan b, Erkut Özdamar
The British Association of Plastic Surgeons (2004) 57, 273 277 Using the sac membrane to close the flap donor site in large meningomyeloceles Cengiz Bozkurt a, Selçuk Akın a, *,Şeref Doğan b, Erkut Özdamar
The spinal dermal-sinus-like stalk
 Childs Nerv Syst (2009) 25:191 197 DOI 10.1007/s00381-008-0669-6 ORIGINAL PAPER The spinal dermal-sinus-like stalk J. van Aalst & E. A. M. Beuls & E. M. J. Cornips & H. W. M. van Straaten & A. F. M. Boselie
Childs Nerv Syst (2009) 25:191 197 DOI 10.1007/s00381-008-0669-6 ORIGINAL PAPER The spinal dermal-sinus-like stalk J. van Aalst & E. A. M. Beuls & E. M. J. Cornips & H. W. M. van Straaten & A. F. M. Boselie
Iatrogenic lumbar Pseudomeningocele: A case report and review of literature
 Available online at Available online at: www.ijmrhs.com ISSN No: 2319-5886 International Journal of Medical Research & Health Sciences, 2016, 5, 1:153-157 Iatrogenic lumbar Pseudomeningocele: A case report
Available online at Available online at: www.ijmrhs.com ISSN No: 2319-5886 International Journal of Medical Research & Health Sciences, 2016, 5, 1:153-157 Iatrogenic lumbar Pseudomeningocele: A case report
Guidelines in the management of neural tube defects and hydrocephalus
 Guidelines in the management of neural tube defects and hydrocephalus Dominic Venne, MD, MSc, FRCSC, Division of Neurosurgery Sheikh Khalifa Medical City Abu Dhabi, UAE 1. Introduction: Neural tube defects
Guidelines in the management of neural tube defects and hydrocephalus Dominic Venne, MD, MSc, FRCSC, Division of Neurosurgery Sheikh Khalifa Medical City Abu Dhabi, UAE 1. Introduction: Neural tube defects
CNS Embryology 5th Menstrual Week (Dorsal View)
 Imaging of the Fetal Brain; Normal & Abnormal Alfred Abuhamad, M.D. Eastern Virginia Medical School CNS Embryology 5th Menstrual Week (Dorsal View) Day 20 from fertilization Neural plate formed in ectoderm
Imaging of the Fetal Brain; Normal & Abnormal Alfred Abuhamad, M.D. Eastern Virginia Medical School CNS Embryology 5th Menstrual Week (Dorsal View) Day 20 from fertilization Neural plate formed in ectoderm
Prospective Evaluation of Role of MRI in Suspected Spinal Dysraphism and Its Management
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 5 Ver. 1 (May. 2018), PP 21-28 www.iosrjournals.org Prospective Evaluation of Role of MRI in
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 5 Ver. 1 (May. 2018), PP 21-28 www.iosrjournals.org Prospective Evaluation of Role of MRI in
Anatomy of the Nervous System. Brain Components
 Anatomy of the Nervous System Brain Components NERVOUS SYSTEM INTRODUCTION Is the master system of human body, controlling the functions of rest of the body systems Nervous System CLASSIFICATION A. Anatomical
Anatomy of the Nervous System Brain Components NERVOUS SYSTEM INTRODUCTION Is the master system of human body, controlling the functions of rest of the body systems Nervous System CLASSIFICATION A. Anatomical
Johnson Rogers and colleagues- used Term LMM
 LIPOMENINGOMYELOCELE: CLASSIFICATION, MANAGEMENT AND CONTROVERSIES Definition : Lipomyelomeningocele is a form of OSD in which a subcutaneous fibrofatty mass traverses the lumbodorsal fascia, causes a
LIPOMENINGOMYELOCELE: CLASSIFICATION, MANAGEMENT AND CONTROVERSIES Definition : Lipomyelomeningocele is a form of OSD in which a subcutaneous fibrofatty mass traverses the lumbodorsal fascia, causes a
Skeletal System. Prof. Dr. Malak A. Al-yawer Department of Anatomy/Embryology Section
 Skeletal System Prof. Dr. Malak A. Al-yawer Department of Anatomy/Embryology Section Learning objectives At the end of this lecture, the medical student will be able to: State the embryonic origin of skeletal
Skeletal System Prof. Dr. Malak A. Al-yawer Department of Anatomy/Embryology Section Learning objectives At the end of this lecture, the medical student will be able to: State the embryonic origin of skeletal
A Very Unusual Case of a Dorsal Heteropagus Twin
 PRG A Very Unusual Case of a Dorsal Heteropagus Twin Nathan David P. Concepcion, MD 1, Bernard F. Laya, DO 1, Eduardo P. Manrique, MD 2 and Faith Caroline D. Bayabos, MD 1 1 Section of Pediatric Radiology,
PRG A Very Unusual Case of a Dorsal Heteropagus Twin Nathan David P. Concepcion, MD 1, Bernard F. Laya, DO 1, Eduardo P. Manrique, MD 2 and Faith Caroline D. Bayabos, MD 1 1 Section of Pediatric Radiology,
Midgut. Over its entire length the midgut is supplied by the superior mesenteric artery
 Gi Embryology 3 Midgut the midgut is suspended from the dorsal abdominal wall by a short mesentery and communicates with the yolk sac by way of the vitelline duct or yolk stalk Over its entire length the
Gi Embryology 3 Midgut the midgut is suspended from the dorsal abdominal wall by a short mesentery and communicates with the yolk sac by way of the vitelline duct or yolk stalk Over its entire length the
Ligaments of the vertebral column:
 In the last lecture we started talking about the joints in the vertebral column, and we said that there are two types of joints between adjacent vertebrae: 1. Between the bodies of the vertebrae; which
In the last lecture we started talking about the joints in the vertebral column, and we said that there are two types of joints between adjacent vertebrae: 1. Between the bodies of the vertebrae; which
ORIGINAL PAPER. Mehmet Selçuki & Ahmet Şükrü Umur & Yusuf Kurtulus Duransoy & Seymen Ozdemir & Deniz Selcuki
 DOI 10.1007/s00381-012-1713-0 ORIGINAL PAPER Inappropriate surgical interventions for midline fusion defects cause secondary tethered cord symptoms: implications for natural history report of four cases
DOI 10.1007/s00381-012-1713-0 ORIGINAL PAPER Inappropriate surgical interventions for midline fusion defects cause secondary tethered cord symptoms: implications for natural history report of four cases
Prenatal ultrasound evaluation of fetal diastematomyelia: two cases of type I split cord malformation
 Ultrasound Obstet Gynecol 2000; 15: 78 82. Prenatal ultrasound evaluation of fetal diastematomyelia: two cases of type I split cord malformation L.M. ALLEN and R.K. SILVERMAN Perinatal Center, SUNY Health
Ultrasound Obstet Gynecol 2000; 15: 78 82. Prenatal ultrasound evaluation of fetal diastematomyelia: two cases of type I split cord malformation L.M. ALLEN and R.K. SILVERMAN Perinatal Center, SUNY Health
Neurosurgical Techniques
 Neurosurgical Techniques Neurosurgical Techniques Laminectomy for the Removal of Spinal Cord Tumors J. GRAFTON LOVE, M.D. Section of Neurologic Surgery, Mayo Clinic and Mayo Foundation, Rochester, Minnesota
Neurosurgical Techniques Neurosurgical Techniques Laminectomy for the Removal of Spinal Cord Tumors J. GRAFTON LOVE, M.D. Section of Neurologic Surgery, Mayo Clinic and Mayo Foundation, Rochester, Minnesota
Chiari Malformations. Google. Objectives Seventh Annual NKY TBI Conference 3/22/13. Kerry R. Crone, M.D.
 Chiari Malformations Kerry R. Crone, M.D. Professor of Neurosurgery and Pediatrics University of Cincinnati College of Medicine University of Cincinnati Medical Center Cincinnati Children s Hospital Medical
Chiari Malformations Kerry R. Crone, M.D. Professor of Neurosurgery and Pediatrics University of Cincinnati College of Medicine University of Cincinnati Medical Center Cincinnati Children s Hospital Medical
Neonatal Spinal Ultrasound Imaging - A Pictorial Review from The Royal Liverpool Children Hospital, Alder Hey, Liverpool
 Neonatal Spinal Ultrasound Imaging - A Pictorial Review from The Royal Liverpool Children Hospital, Alder Hey, Liverpool Poster No.: C-0081 Congress: ECR 2012 Type: Educational Exhibit Authors: K. Chetcuti,
Neonatal Spinal Ultrasound Imaging - A Pictorial Review from The Royal Liverpool Children Hospital, Alder Hey, Liverpool Poster No.: C-0081 Congress: ECR 2012 Type: Educational Exhibit Authors: K. Chetcuti,
Case Based Urology Learning Program
 Case Based Urology Learning Program Resident s Corner: UROLOGY Case Number 23 CBULP 2011 077 Case Based Urology Learning Program Editor: Associate Editors: Manager: Case Contributors: Steven C. Campbell,
Case Based Urology Learning Program Resident s Corner: UROLOGY Case Number 23 CBULP 2011 077 Case Based Urology Learning Program Editor: Associate Editors: Manager: Case Contributors: Steven C. Campbell,
Dorsal dermal sinus in children
 Dorsal dermal sinus in children Poster No.: C-2581 Congress: ECR 2015 Type: Educational Exhibit Authors: J. Marjanovic, A. Paterson, P. C. McSherry, A. Nixon, A. 1 1 2 1 2 1 1 2 TRIPALO BATOS, T. Grmoja
Dorsal dermal sinus in children Poster No.: C-2581 Congress: ECR 2015 Type: Educational Exhibit Authors: J. Marjanovic, A. Paterson, P. C. McSherry, A. Nixon, A. 1 1 2 1 2 1 1 2 TRIPALO BATOS, T. Grmoja
A NOVEL CAUSE FOR CAUDA- EQUINA SYNDROME WITH A NEW RADIOLOGICAL SIGN
 A NOVEL CAUSE FOR CAUDA- EQUINA SYNDROME WITH A NEW RADIOLOGICAL SIGN W Singleton, D Ramnarine, N Patel, C Wigfield Department of Neurological Surgery, Frenchay Hospital, Bristol, UK Introduction We present
A NOVEL CAUSE FOR CAUDA- EQUINA SYNDROME WITH A NEW RADIOLOGICAL SIGN W Singleton, D Ramnarine, N Patel, C Wigfield Department of Neurological Surgery, Frenchay Hospital, Bristol, UK Introduction We present
Case Report Occult Spinal Dysraphism in the Presence of Rare Cutaneous Stigma in a Neonate: Importance of Ultrasound and Magnetic Resonance Imaging
 Case Reports in Medicine Volume 2013, Article ID 468376, 4 pages http://dx.doi.org/10.1155/2013/468376 Case Report Occult Spinal Dysraphism in the Presence of Rare Cutaneous Stigma in a Neonate: Importance
Case Reports in Medicine Volume 2013, Article ID 468376, 4 pages http://dx.doi.org/10.1155/2013/468376 Case Report Occult Spinal Dysraphism in the Presence of Rare Cutaneous Stigma in a Neonate: Importance
Purpose: To discuss the fatty filum terminale which is incidentally demonstrated on MRI concerning the causes of TCS
 ISPUB.COM The Internet Journal of Spine Surgery Volume 3 Number 1 T Iizuka Citation T Iizuka.. The Internet Journal of Spine Surgery. 2006 Volume 3 Number 1. Abstract Background: Fatty filum terminale
ISPUB.COM The Internet Journal of Spine Surgery Volume 3 Number 1 T Iizuka Citation T Iizuka.. The Internet Journal of Spine Surgery. 2006 Volume 3 Number 1. Abstract Background: Fatty filum terminale
Giant invasive spinal schwannomas: definition and surgical management
 J Neurosurg (Spine 2) 94:210 215, 2001 Giant invasive spinal schwannomas: definition and surgical management K. SRIDHAR, D.N.B. (NEUROSURG), RAVI RAMAMURTHI, M.S, F.R.C.S.ED. (SN), M. C. VASUDEVAN, M.D.,
J Neurosurg (Spine 2) 94:210 215, 2001 Giant invasive spinal schwannomas: definition and surgical management K. SRIDHAR, D.N.B. (NEUROSURG), RAVI RAMAMURTHI, M.S, F.R.C.S.ED. (SN), M. C. VASUDEVAN, M.D.,
Radiologic and pathologic features of spinal dysraphism. A pictorial review.
 Radiologic and pathologic features of spinal dysraphism. A pictorial review. Poster No.: C-0586 Congress: ECR 2011 Type: Educational Exhibit Authors: N. Arcalis, J. L. Ribó, J. Muchart, L. Riaza, J. Blanch
Radiologic and pathologic features of spinal dysraphism. A pictorial review. Poster No.: C-0586 Congress: ECR 2011 Type: Educational Exhibit Authors: N. Arcalis, J. L. Ribó, J. Muchart, L. Riaza, J. Blanch
Introduction to Neurosurgical Subspecialties:
 Introduction to Neurosurgical Subspecialties: Pediatric Neurosurgery Brian L. Hoh, MD 1 and Gregory J. Zipfel, MD 2 1 University of Florida, 2 Washington University Pediatric Neurosurgery Pediatric neurosurgeons
Introduction to Neurosurgical Subspecialties: Pediatric Neurosurgery Brian L. Hoh, MD 1 and Gregory J. Zipfel, MD 2 1 University of Florida, 2 Washington University Pediatric Neurosurgery Pediatric neurosurgeons
Neuroimaging. spine / spinal cord
 Neuroimaging spine / spinal cord Spine & spinal cord imaging methodology Plain x-ray of spine Computed tomography CT - traditional ( normal CT) - reconstructions - myelo-ct Magnetic resonance MR - standard
Neuroimaging spine / spinal cord Spine & spinal cord imaging methodology Plain x-ray of spine Computed tomography CT - traditional ( normal CT) - reconstructions - myelo-ct Magnetic resonance MR - standard
Efficacy of electromyography and nerve conduction velocity monitoring in surgical management of terminal lipoma in children
 Romanian Neurosurgery Volume XXXI Number 2 2017 April-June Article Efficacy of electromyography and nerve conduction velocity monitoring in surgical management of terminal lipoma in children Ashraf El
Romanian Neurosurgery Volume XXXI Number 2 2017 April-June Article Efficacy of electromyography and nerve conduction velocity monitoring in surgical management of terminal lipoma in children Ashraf El
Moderators Dr A Suri Dr Deepak Gupta. Presented by Dr A Bisht
 Moderators Dr A Suri Dr Deepak Gupta Presented by Dr A Bisht A distinct group of congenital anomalies characterized by a failure of midline structures of ecto- and mesodermal origin to fuse Nicolas Tulp
Moderators Dr A Suri Dr Deepak Gupta Presented by Dr A Bisht A distinct group of congenital anomalies characterized by a failure of midline structures of ecto- and mesodermal origin to fuse Nicolas Tulp
A Case of Naso-Ethmoidal Meningoencephalocele
 A Case of Naso-Ethmoidal Meningoencephalocele Divyanshu Dubey, Sonjjay Pande, Pradeep Dubey, Anshudha Sawhney Vol. 3 No. 8 (August 2011) International Journal of Collaborative Research on Internal Medicine
A Case of Naso-Ethmoidal Meningoencephalocele Divyanshu Dubey, Sonjjay Pande, Pradeep Dubey, Anshudha Sawhney Vol. 3 No. 8 (August 2011) International Journal of Collaborative Research on Internal Medicine
Anorectal Malformations
 CHAPTER Anorectal Malformations P. Stephen Almond Incidence The incidence of imperforate anus is one in every 5,000 live births, with cloaca malformations accounting for 10%. Males (58%) are more commonly
CHAPTER Anorectal Malformations P. Stephen Almond Incidence The incidence of imperforate anus is one in every 5,000 live births, with cloaca malformations accounting for 10%. Males (58%) are more commonly
disclosure Pediatric Tethered cord Syndrome Learning Objectives overview definiton Hoffman 1976 Pediatrics Grand Rounds 26 June 2015
 disclosure Pediatric Tethered cord Syndrome None Izabela, Tarasiewicz, MD,FRCS(C), has no relationships with commercial companies to disclose. Izabela Tarasiewicz MD. FRCS(C) Pediatric Neurosurgery overview
disclosure Pediatric Tethered cord Syndrome None Izabela, Tarasiewicz, MD,FRCS(C), has no relationships with commercial companies to disclose. Izabela Tarasiewicz MD. FRCS(C) Pediatric Neurosurgery overview
Surgical treatment of the retethered spinal cord after repair of lipomyelomeningocele
 J Neurosurg 74:709-714, 1991 Surgical treatment of the retethered spinal cord after repair of lipomyelomeningocele HIROAKI SAKAMOTO, M.D., AKIRA HAKUBA, M.D., KEN FUJITANI, M.D., AND SttURO NISHIMURA,
J Neurosurg 74:709-714, 1991 Surgical treatment of the retethered spinal cord after repair of lipomyelomeningocele HIROAKI SAKAMOTO, M.D., AKIRA HAKUBA, M.D., KEN FUJITANI, M.D., AND SttURO NISHIMURA,
Essentials of Clinical MR, 2 nd edition. 51. Primary Neoplasms
 51. Primary Neoplasms As with spinal central canal neoplasms in other regions, those of the lumbar spine may be classified as extradural, intradural extramedullary, and medullary. If an extradural lesion
51. Primary Neoplasms As with spinal central canal neoplasms in other regions, those of the lumbar spine may be classified as extradural, intradural extramedullary, and medullary. If an extradural lesion
Intraoperative Sonography in Spinal Dysraphism and Syringohydromyelia
 329 Intraoperative Sonography in Spinal Dysraphism and Syringohydromyelia Robert M. Quencerl erta M. Montalvo 2 Thomas P. Naidich 3 M. Judith Donovan Post 1 arth. Green 4 Larry K. Page 4 The use of intraoperative
329 Intraoperative Sonography in Spinal Dysraphism and Syringohydromyelia Robert M. Quencerl erta M. Montalvo 2 Thomas P. Naidich 3 M. Judith Donovan Post 1 arth. Green 4 Larry K. Page 4 The use of intraoperative
Case Report Surgical Treatment of a Patient with Human Tail and Multiple Abnormalities of the Spinal Cord and Column
 SAGE-Hindawi Access to Research Advances in Orthopedics Volume 2011, Article ID 153797, 4 pages doi:10.4061/2011/153797 Case Report Surgical Treatment of a Patient with Human Tail and Multiple Abnormalities
SAGE-Hindawi Access to Research Advances in Orthopedics Volume 2011, Article ID 153797, 4 pages doi:10.4061/2011/153797 Case Report Surgical Treatment of a Patient with Human Tail and Multiple Abnormalities
Stab wound of the neck: potential pitfalls in management
 Archives of Emergency Medicine, 1989, 6, 225-229 CASE REPORT Stab wound of the neck: potential pitfalls in management R.D. PAGE &R.H. LYE University Department of Neurosurgery, Manchester Royal Infirmary,
Archives of Emergency Medicine, 1989, 6, 225-229 CASE REPORT Stab wound of the neck: potential pitfalls in management R.D. PAGE &R.H. LYE University Department of Neurosurgery, Manchester Royal Infirmary,
Giant schwannoma with extensive scalloping of the lumbar vertebral body treated with one-stage posterior surgery: a case report
 Iizuka et al. Journal of Medical Case Reports 2014, 8:421 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Giant schwannoma with extensive scalloping of the lumbar vertebral body treated with one-stage
Iizuka et al. Journal of Medical Case Reports 2014, 8:421 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Giant schwannoma with extensive scalloping of the lumbar vertebral body treated with one-stage
Human Anatomy. Spinal Cord and Spinal Nerves
 Human Anatomy Spinal Cord and Spinal Nerves 1 The Spinal Cord Link between the brain and the body. Exhibits some functional independence from the brain. The spinal cord and spinal nerves serve two functions:
Human Anatomy Spinal Cord and Spinal Nerves 1 The Spinal Cord Link between the brain and the body. Exhibits some functional independence from the brain. The spinal cord and spinal nerves serve two functions:
Ventriculus Terminalis of the Conus Medullaris: MR Imaging in Four Patients with Congenital Dilatation
 733 Ventriculus Terminalis of the Conus Medullaris: MR Imaging in Four Patients with Congenital Dilatation Robert Sigal 1 2 Alban Denys 2 Philippe Halimi 2 Lorraine Shapeero 1 3 Dominique Doyon 2 Frank
733 Ventriculus Terminalis of the Conus Medullaris: MR Imaging in Four Patients with Congenital Dilatation Robert Sigal 1 2 Alban Denys 2 Philippe Halimi 2 Lorraine Shapeero 1 3 Dominique Doyon 2 Frank
Two-Stage Management of Mega Occipito Encephalocele
 Two-Stage Management of Mega Occipito Encephalocele CASE REPORT A I Mardzuki*, J Abdullah**, G Ghazaime*, A R Ariff!'*, M Ghazali* *Department of Neurosciences, **Department of Radiology, Hospital Universiti
Two-Stage Management of Mega Occipito Encephalocele CASE REPORT A I Mardzuki*, J Abdullah**, G Ghazaime*, A R Ariff!'*, M Ghazali* *Department of Neurosciences, **Department of Radiology, Hospital Universiti
Case Report Ipsilateral Hip Dysplasia in Patients with Sacral Hemiagenesis: A Report of Two Cases
 Case Reports in Orthopedics Volume 2015, Article ID 854151, 4 pages http://dx.doi.org/10.1155/2015/854151 Case Report Ipsilateral Hip Dysplasia in Patients with Sacral Hemiagenesis: A Report of Two Cases
Case Reports in Orthopedics Volume 2015, Article ID 854151, 4 pages http://dx.doi.org/10.1155/2015/854151 Case Report Ipsilateral Hip Dysplasia in Patients with Sacral Hemiagenesis: A Report of Two Cases
Development of the Digestive System. W.S. O The University of Hong Kong
 Development of the Digestive System W.S. O The University of Hong Kong Plan for the GI system Then GI system in the abdomen first develops as a tube suspended by dorsal and ventral mesenteries. Blood
Development of the Digestive System W.S. O The University of Hong Kong Plan for the GI system Then GI system in the abdomen first develops as a tube suspended by dorsal and ventral mesenteries. Blood
Congenital Tethered Spinal Cord Syndrome in Adults
 Page 1 of 7 http://www.medscape.com/ To Print: Click your browser's PRINT button. NOTE: To view the article with Web enhancements, go to: http://www.medscape.com/viewarticle/405679 Congenital Tethered
Page 1 of 7 http://www.medscape.com/ To Print: Click your browser's PRINT button. NOTE: To view the article with Web enhancements, go to: http://www.medscape.com/viewarticle/405679 Congenital Tethered
ISUOG Basic Training. Examining Fetal Anatomy from Longitudinal Sections Titia Cohen-Overbeek, The Netherlands
 ISUOG Basic Training Examining Fetal Anatomy from Longitudinal Sections Titia Cohen-Overbeek, The Netherlands Learning objectives 2 & 3 At the end of the lecture you will be able to: describe how to obtain
ISUOG Basic Training Examining Fetal Anatomy from Longitudinal Sections Titia Cohen-Overbeek, The Netherlands Learning objectives 2 & 3 At the end of the lecture you will be able to: describe how to obtain
Central Nervous System Congenital Abnormalities
 Central Nervous System Congenital Abnormalities Eva Brichtova, M.D., Ph.D., Department of Pediatric Sugery, Orthopaedics and Traumatology, University Hospital Brno Neural tube defects Dysraphism uncomplete
Central Nervous System Congenital Abnormalities Eva Brichtova, M.D., Ph.D., Department of Pediatric Sugery, Orthopaedics and Traumatology, University Hospital Brno Neural tube defects Dysraphism uncomplete
Early Development of Neural Tube Development of Medulla Spinalis and Peripheral Nervous System. Assoc.Prof. E.Elif Güzel, M.D.
 Early Development of Neural Tube Development of Medulla Spinalis and Peripheral Nervous System Assoc.Prof. E.Elif Güzel, M.D. Third week of Embryogenesis Primitive streak/pit appears on the epiblast (day
Early Development of Neural Tube Development of Medulla Spinalis and Peripheral Nervous System Assoc.Prof. E.Elif Güzel, M.D. Third week of Embryogenesis Primitive streak/pit appears on the epiblast (day
Neuropathic bladder and spinal dysraphism
 Archives of Disease in Childhood, 1981, 56, 176-180 Neuropathic bladder and spinal dysraphism MALGORZATA BORZYSKOWSKI AND B G R NEVILLE Evelina Children's Department, Guy's Hospital, London SUMMARY The
Archives of Disease in Childhood, 1981, 56, 176-180 Neuropathic bladder and spinal dysraphism MALGORZATA BORZYSKOWSKI AND B G R NEVILLE Evelina Children's Department, Guy's Hospital, London SUMMARY The
Congenital tethered spinal cord syndrome in adults
 Neurosurg Focus 10 (1):Article 7, 2001, Click here to return to Table of Contents Congenital tethered spinal cord syndrome in adults BERMANS J. ISKANDAR, M.D., BENJAMIN B. FULMER, M.D., MARK N. HADLEY,
Neurosurg Focus 10 (1):Article 7, 2001, Click here to return to Table of Contents Congenital tethered spinal cord syndrome in adults BERMANS J. ISKANDAR, M.D., BENJAMIN B. FULMER, M.D., MARK N. HADLEY,
Focal Anterior Displacement of the Thoracic Spinal Cord without Evidence of Spinal Cord Herniation or an Intradural Mass
 Original Article Musculoskeletal Imaging http://dx.doi.org/10.3348/kjr.2014.15.6.733 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2014;15(6):733-738 Focal Anterior Displacement of the Thoracic Spinal
Original Article Musculoskeletal Imaging http://dx.doi.org/10.3348/kjr.2014.15.6.733 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2014;15(6):733-738 Focal Anterior Displacement of the Thoracic Spinal
Development of the Digestive System. W.S. O School of Biomedical Sciences, University of Hong Kong.
 Development of the Digestive System W.S. O School of Biomedical Sciences, University of Hong Kong. Organization of the GI tract: Foregut (abdominal part) supplied by coeliac trunk; derivatives include
Development of the Digestive System W.S. O School of Biomedical Sciences, University of Hong Kong. Organization of the GI tract: Foregut (abdominal part) supplied by coeliac trunk; derivatives include
Spectrum of Magnetic Resonance Imaging findings in infective intra spinal complications of dermal sinus and associated inclusion cysts
 Spectrum of Magnetic Resonance Imaging findings in infective intra spinal complications of dermal sinus and associated inclusion cysts Poster No.: C-1443 Congress: ECR 2015 Type: Educational Exhibit Authors:
Spectrum of Magnetic Resonance Imaging findings in infective intra spinal complications of dermal sinus and associated inclusion cysts Poster No.: C-1443 Congress: ECR 2015 Type: Educational Exhibit Authors:
Surgery for Spinal Cord Lipomas
 39 Original Article Surgery for Spinal Cord Lipomas Manish K. Kasliwal and Ashok K. Mahapatra Department of Neurosurgery, Neurosciences Centre, All India Institute of Medical Sciences, New Delhi, India
39 Original Article Surgery for Spinal Cord Lipomas Manish K. Kasliwal and Ashok K. Mahapatra Department of Neurosurgery, Neurosciences Centre, All India Institute of Medical Sciences, New Delhi, India
Utilizing real-time contrast medium to detect the fistula of giant spinal arachnoid cyst and treat with minimal invasive surgery
 Ying et al. BMC Surgery (2019) 19:11 https://doi.org/10.1186/s12893-019-0475-y CASE REPORT Open Access Utilizing real-time contrast medium to detect the fistula of giant spinal arachnoid cyst and treat
Ying et al. BMC Surgery (2019) 19:11 https://doi.org/10.1186/s12893-019-0475-y CASE REPORT Open Access Utilizing real-time contrast medium to detect the fistula of giant spinal arachnoid cyst and treat
Case Report. Case Report
 34 Case Report Multiple dysraphic anomalies with double thoracic meningocele and lumbosacral myelomeningocele, concurrent Chiari malformation Type I, diastematomyelia, lipomyelomeningocele and hydrocephalus:
34 Case Report Multiple dysraphic anomalies with double thoracic meningocele and lumbosacral myelomeningocele, concurrent Chiari malformation Type I, diastematomyelia, lipomyelomeningocele and hydrocephalus:
Sonography of the Neonatal Spine: Part 1, Normal Anatomy, Imaging Pitfalls, and Variations That May Simulate Disorders
 Sonography of Neonatal Spine Pediatric Imaging Pictorial Essay Downloaded from www.ajronline.org by 46.3.195.60 on 02/04/18 from IP address 46.3.195.60. Copyright RRS. For personal use only; all rights
Sonography of Neonatal Spine Pediatric Imaging Pictorial Essay Downloaded from www.ajronline.org by 46.3.195.60 on 02/04/18 from IP address 46.3.195.60. Copyright RRS. For personal use only; all rights
The "Keyhole": A Sign of
 473 The "Keyhole": A Sign of Herniation of a Trapped Fourth Ventricle and Other Posterior Fossa Cysts Barbara J. Wolfson' Eric N. Faerber' Raymond C. Truex, Jr. 2 When a cystic structure in the posterior
473 The "Keyhole": A Sign of Herniation of a Trapped Fourth Ventricle and Other Posterior Fossa Cysts Barbara J. Wolfson' Eric N. Faerber' Raymond C. Truex, Jr. 2 When a cystic structure in the posterior
Scoliosis and hydrocephalus in myelocele patients
 J Neurosurg 50:174-178, 1979 Scoliosis and hydrocephalus in myelocele patients The effects of ventricular shunting PETER HALL, M.B., B.S., RICHARD LINDSETH, M.D., ROBERT CAMPBELL, M.D., JOHN E. KALSBECK,
J Neurosurg 50:174-178, 1979 Scoliosis and hydrocephalus in myelocele patients The effects of ventricular shunting PETER HALL, M.B., B.S., RICHARD LINDSETH, M.D., ROBERT CAMPBELL, M.D., JOHN E. KALSBECK,
Brain Imaging. Bearbeitet von Klaus Sartor, Stefan Hähnel, Bodo Kress
 Brain Imaging Bearbeitet von Klaus Sartor, Stefan Hähnel, Bodo Kress 1. Auflage 2007. Taschenbuch. 312 S. Paperback ISBN 978 3 13 143961 1 Format (B x L): 12,5 x 19 cm Weitere Fachgebiete > Medizin > Sonstige
Brain Imaging Bearbeitet von Klaus Sartor, Stefan Hähnel, Bodo Kress 1. Auflage 2007. Taschenbuch. 312 S. Paperback ISBN 978 3 13 143961 1 Format (B x L): 12,5 x 19 cm Weitere Fachgebiete > Medizin > Sonstige
Spinal dysraphism: genetic relation to
 Journal of Medical Genetics (1976). 13, 343-350. Spinal dysraphism: genetic relation to neural tube malformations C. 0. CARTER, K. A. EVANS, and K. TILL* From MRC Clinical Genetics Unit, Institute of Child
Journal of Medical Genetics (1976). 13, 343-350. Spinal dysraphism: genetic relation to neural tube malformations C. 0. CARTER, K. A. EVANS, and K. TILL* From MRC Clinical Genetics Unit, Institute of Child
Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts
 Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts Exceptional healthcare, personally delivered Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts What is hydrocephalus? Hydrocephalus is the build up of an excess
Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts Exceptional healthcare, personally delivered Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts What is hydrocephalus? Hydrocephalus is the build up of an excess
Overview. Spinal Anatomy Spaces & Meninges Spinal Cord. Anatomy of the dura. Anatomy of the arachnoid. Anatomy of the spinal meninges
 European Course in Neuroradiology Module 1 - Anatomy and Embryology Dubrovnik, October 2018 Spinal Anatomy Spaces & Meninges Spinal Cord Johan Van Goethem Overview spinal meninges & spaces spinal cord
European Course in Neuroradiology Module 1 - Anatomy and Embryology Dubrovnik, October 2018 Spinal Anatomy Spaces & Meninges Spinal Cord Johan Van Goethem Overview spinal meninges & spaces spinal cord
Spinal Cord and Properties of Cerebrospinal Fluid: Options for Drug Delivery. SMA Foundation New York
 Spinal Cord and Properties of Cerebrospinal Fluid: Options for Drug Delivery New York Why Do We Need to Know about the Spinal Cord Anatomy and Properties of Cerebrospinal Fluid? SMA therapeutics need to
Spinal Cord and Properties of Cerebrospinal Fluid: Options for Drug Delivery New York Why Do We Need to Know about the Spinal Cord Anatomy and Properties of Cerebrospinal Fluid? SMA therapeutics need to
The Chiari malformation I (CM I) is a disorder that has been
 DOI: 10.5137/1019-5149.JTN.18349-16.1 Received: 31.05.2016 / Accepted: 01.07.2016 Published Online: 22.08.2016 Original Investigation Are Herniated Cerebellar Tonsils the Main Culprit of Chiari Malformation
DOI: 10.5137/1019-5149.JTN.18349-16.1 Received: 31.05.2016 / Accepted: 01.07.2016 Published Online: 22.08.2016 Original Investigation Are Herniated Cerebellar Tonsils the Main Culprit of Chiari Malformation
TUMOURS IN THE REGION OF FORAMEN MAGNUM
 TUMOURS IN THE REGION OF FORAMEN MAGNUM Abstract Pages with reference to book, From 119 To 122 Naim-ur-Rahman ( Department of Neurosurgery, Rawalpindi Medical College, Rawalpindi. ) A very unusual case
TUMOURS IN THE REGION OF FORAMEN MAGNUM Abstract Pages with reference to book, From 119 To 122 Naim-ur-Rahman ( Department of Neurosurgery, Rawalpindi Medical College, Rawalpindi. ) A very unusual case
Lumbar Disc Prolapse. Dr. Ahmed Salah Eldin Hassan. Professor of Neurosurgery & Consultant spinal surgeon
 Lumbar Disc Prolapse By Dr. Ahmed Salah Eldin Hassan Professor of Neurosurgery & Consultant spinal surgeon 1-What are the Functions of the Spine Structural support for upright posture Protection of Spinal
Lumbar Disc Prolapse By Dr. Ahmed Salah Eldin Hassan Professor of Neurosurgery & Consultant spinal surgeon 1-What are the Functions of the Spine Structural support for upright posture Protection of Spinal
SPINAL CORD AND PROPERTIES OF CEREBROSPINAL FLUID: OPTIONS FOR DRUG DELIVERY
 SPINAL CORD AND PROPERTIES OF CEREBROSPINAL FLUID: OPTIONS FOR DRUG DELIVERY WHY DO WE NEED TO KNOW ABOUT THE SPINAL CORD ANATOMY AND PROPERTIES OF CEREBROSPINAL FLUID? SMA therapeutics need to reach cells
SPINAL CORD AND PROPERTIES OF CEREBROSPINAL FLUID: OPTIONS FOR DRUG DELIVERY WHY DO WE NEED TO KNOW ABOUT THE SPINAL CORD ANATOMY AND PROPERTIES OF CEREBROSPINAL FLUID? SMA therapeutics need to reach cells
Malformations of the Nervous System November 10, Dr. Peter Ostrow
 Malformations of the Nervous System November 10, 2016 Dr. Peter Ostrow Malformations of the Nervous System 1. Abnormal closure of the neural tube 1. Disorders of forebrain formation 1. Cortical anomalies
Malformations of the Nervous System November 10, 2016 Dr. Peter Ostrow Malformations of the Nervous System 1. Abnormal closure of the neural tube 1. Disorders of forebrain formation 1. Cortical anomalies
intracranial anomalies
 Chapter 5: Fetal Central Nervous System 84 intracranial anomalies Hydrocephaly Dilatation of ventricular system secondary to an increase in the amount of CSF. Effects of hydrocephalus include flattening
Chapter 5: Fetal Central Nervous System 84 intracranial anomalies Hydrocephaly Dilatation of ventricular system secondary to an increase in the amount of CSF. Effects of hydrocephalus include flattening
Selective laminoplasty for cervical spondylotic myelopathy: a comparative study with a minimum 5-year follow-up
 Selective laminoplasty for cervical spondylotic myelopathy: a comparative study with a minimum 5-year follow-up Minori Kato*, Hiroaki Nakamura**, Koji Tamai**, Kazunori Hayashi**, Akira Matsumura**, Sadahiko
Selective laminoplasty for cervical spondylotic myelopathy: a comparative study with a minimum 5-year follow-up Minori Kato*, Hiroaki Nakamura**, Koji Tamai**, Kazunori Hayashi**, Akira Matsumura**, Sadahiko
Imaging in neurofibromatosis type 1: An original research article with focus on spinal lesions
 Original Research Article Imaging in neurofibromatosis type 1: An original research article with focus on spinal lesions Kalpesh Patel 1*, Siddharth Zala 2, C. Raychaudhuri 3 1 Assistant Professor, 2 1
Original Research Article Imaging in neurofibromatosis type 1: An original research article with focus on spinal lesions Kalpesh Patel 1*, Siddharth Zala 2, C. Raychaudhuri 3 1 Assistant Professor, 2 1
Decompression of the spinal subarachnoid space as a solution for syringomyelia without Chiari malformation
 (2002) 40, 501 ± 506 ã 2002 International Society All rights reserved 1362 ± 4393/02 $25.00 www.nature.com/sc Original Article Decompression of the spinal subarachnoid space as a solution for syringomyelia
(2002) 40, 501 ± 506 ã 2002 International Society All rights reserved 1362 ± 4393/02 $25.00 www.nature.com/sc Original Article Decompression of the spinal subarachnoid space as a solution for syringomyelia
Fetal Medicine. Case Presentations. Dr Ermos Nicolaou Fetal Medicine Unit Chris Hani Baragwanath Hospital. October 2003
 Case Presentations Dr Ermos Nicolaou Fetal Medicine Unit Chris Hani Baragwanath Hospital October 2003 Case 1 Ms A M 22year old P0 G1 Referred from Sebokeng Hospital at 36w for polyhydramnios On Ultrasound:
Case Presentations Dr Ermos Nicolaou Fetal Medicine Unit Chris Hani Baragwanath Hospital October 2003 Case 1 Ms A M 22year old P0 G1 Referred from Sebokeng Hospital at 36w for polyhydramnios On Ultrasound:
