CASE OF THE WEEK PROFESSOR YASSER METWALLY
|
|
|
- Gabriel Stone
- 5 years ago
- Views:
Transcription
1 CLINICAL PICTURE CLINICAL PICTURE A 40 Years old female patient, known to be suffering from multiple sclerosis, was presented clinically with painful diminution of vision in the right aye and mild weakness of the left upper limb. RADIOLOGICAL FINDINGS RADIOLOGICAL FINDINGS CASE OF THE WEEK PROFESSOR YASSER METWALLY Figure 1. A case of chronic multiple sclerosis. MRI T1 precontrast images showing multiple periventricular oval or rounded plaques. The plaques are well-defined, hypointense to markedly hypointense (black holes) with mild central atrophy. Some plaques are perpendicular to the ventricular surface (Dawson fingers). Tl hypointensities serve as a surrogate marker of disability in multiple sclerosis because they are specific for matrix destruction and axonal loss. Development of Tl hypointensities implies not only focal damage to axons within lesions, but also more widespread tissue loss, leading to generalized atrophy of the brain.
2 Figure 2. Postcontrast MRI T1 images showing contrast enhancement of multiple sclerosis plaques. Two patterns are seen. Diffuse contrast enhancement (A) and ring enhancement (either complete ring enhancement or incomplete ring enhancement, both patterns are seen in this patient) (B,C). Enhanced plaques are active plaques and is a manifestation of disease exacerbation even when not associated with clinical manifestations. Ring enhancement demonstrates how MRI can show dissemination in time as well as place. Plaques with ring enhancement are plaques with different ages. The central unenhanced parts are older than the peripherally enhanced parts. Reactivation of old plaques takes place at the periphery of plaques and that explains ring enhancement. Plaques with ring enhancement represent dissemination in time. Non enhanced plaques are plaques in remission while enhanced plaques are plaques in exacerbation. Plaques with ring enhancement are plaques which contain central parts in remission and peripheral parts in exacerbation. The open, incomplete, ring enhancement that is seen in the cerebellum in this patient (B) is more indicative of an MS lesion than metastatic disease or infection which almost always has a complete, fully enclosed ring of enhancement. Figure 3. A case of chronic multiple sclerosis. MRI T2 (A,B) and MRI FLAIR (C) images showing multiple periventricular oval or rounded plaques. The plaques are well-defined and hyperintense. Some plaques are perpendicular to the ventricular surface (Dawson fingers).
3 USING MRI CRITERIA, THE DIAGNOSIS OF THE CASE IS CHRONIC MULTIPLE SCLEROSIS BECAUSE OF 87 The existence of dissemination in place: MRI plaques that are widespread within the brain, in the periventricular regions, Some plaques are perpendicular to the ventricular surface (Dawson fingers). In particular Dawson fingers are rarely seen in other white matter diseases. The existence of dissemination in time: As manifested by some plaques showing contrast enhancement (active plaques) and other are not enhanced (chronic inactive plaques). Ring enhancement in a single plaque is also a sign of dissemination in time. Multiple sclerosis is characterized by dissemination in time and place. Dissemination in time and place (either clinically or by MRI) is not seen in other white matter diseases. While commenting on a neuroimaging study for a multiple sclerosis patient, four parameters must be commented upon. The anatomical distribution of the lesions, The presence or absence of brain atrophy, T2 and FLAIR appearance of the lesions and the appearance of the lesions on the pre and postcontrast T1 images. Parameter Anatomy Atrophy Comment Usually, MS lesions extend along medullary veins that drain into the subependymal veins lining the lateral ventricle at the callososeptal interface. MS lesions are characteristically oriented along the fibers of the corpus callosum (although the veins themselves are not visible on routine MR imaging) paralleling these veins. This appearance corresponds to the so-called Dawson's finger identified at pathology, and is well demonstrated on MR imaging. With an extensive lesion burden, marked atrophy may be present. The corpus callosum may be severely thinned throughout. 9, 67 To what extent the atrophy represents primary white matter disease or secondary loss due to Wallerian degeneration is not clear. T2, FLAIR Increased water content of tissue leads to an increase in the tissue T2 relaxation time. This results in hyperintense signal on FLAIR, PD- and T2-weighted imaging. Because most pathologic processes lead to increased tissue water, initially through edema and inflammation, and later through gliosis and frank replacement of tissue with fluid, T2 imaging is a sensitive but not particularly specific indicator of pathology. T1 pre and postcontrast Initially, MS lesions are isointense to mildly hypointense on T1-weighted imaging. With time, the mild hypointensity may progress to develop into a so-called T1 hole or black hole in which the lesion has completely been replaced by CSF. Alternatively, the lesion may remain stable in intensity. In many cases, there is a slightly hyperintense rim surrounding a lesion. This hyperintensity is typically ascribed to the presence of free radicals in the surrounding inflammatory tissue, but paramagnetic effects from petechial hemorrhage and fat signal from myelin breakdown also may contribute to this phenomenon. 58 Tl hypointensities serve as a surrogate marker of disability in multiple sclerosis because they are specific for matrix destruction and axonal loss. Development of Tl hypointensities implies not only focal damage to axons within lesions, but also more widespread tissue loss, leading to generalized atrophy of the brain. Contrast enhancement represents a disruption in the blood-brain barrier that allows for the leakage of gadolinium-chelates. The presence of enhancement can play an important role in the evaluation of MS, depending on the clinical context. Enhancement results from a local breakdown of the blood-brain barrier, and indicates the presence of an active inflammatory process; therefore, enhancement identifies "active lesions," which often correlate with the acute symptomatology. 2,71 These active lesions also may be clinically silent and are frequently seen on serial imaging performed as part of research protocols. Because nonenhancing lesions identified on T2-weighted images are thought to be chronic lesions, the simultaneous presence of enhancing and nonenhancing lesions is strong evidence to indicate that these are "multiple
4 lesions separated in time," supporting a putative diagnosis of MS at the time of initial presentation. The presence of ring-enhancement suggests the reactivation of an old lesion-the central nonenhancing portion of the lesion representing the "burnt out" portion of the lesion. An incomplete or open ring of enhancement is more indicative of an MS lesion than metastatic disease or infection, which almost always has a complete, fully enclosed ring of enhancement. 37 DIAGNOSIS: DIAGNOSIS: A CASE WITH CHRONIC MULTIPLE SCLEROSIS IN EXACERBATION BY CLINICAL AND MRI CRITERIA DISCUSSION DISCUSSION Multiple sclerosis (MS) is a histopathologic diagnosis manifesting clinically as neurologic signs and symptoms disseminated in time and space. 64 The Poser et al criteria established the important role of paraclinical tests in establishing the diagnosis of MS. 56 Magnetic resonance (MR) imaging has proven to be the dominant paraclinical test in establishing the diagnosis of MS, showing multiple white matter hyperintensities on T2-weighted images in more than 90% of patients. 49,66 The sensitivity of MR imaging is emphasized by longitudinal studies that demonstrate five to ten times more lesions than might be expected from overt clinical relapses. 32, 38, 84 Because MR imaging can be used to survey the entire neuraxis, it is able to identify these clinically silent lesions, thus establishing the presence of multiple lesions in space. Furthermore, as lesions enhance only when they are relatively acute, (typically < 2 months), enhancement or lack thereof dates a lesion 2, 71, 81; hence, the presence of enhancement provides temporal and anatomical information. That is, a single MR image with enhancing and nonenhancing lesions may be interpreted as having lesions separated in time. Thus, MR imaging is uniquely suited to provide information on white matter lesions distributed in time and space. Not to be overlooked is the strength of MR imaging in establishing or ruling out other diagnoses at the time of initial presentation. Although MR imaging is a sensitive technique for detecting lesions, it is hampered by its lack of specificity. Most insults to the brain, demyelinating disease included, increase water content because of edema and gliosis, prolonging tissue T2 relaxation time. Thus, lesions are hyperintense on sequences sensitized to the T2 relaxation time, namely, proton density (PD)-weighted, T2-weighted, and fluid attenuated inversion-recovery (FLAIR) sequences, both in their conventional spin- echo (CSE) and fast spin-echo (FSE) implementations. Because of this lack of specificity, arriving at a correct clinical diagnosis depends to a great extent on characterizing the anatomic configuration of the injury in the white matter, and the correlation of these findings with clinical data. MR IMAGING APPEARANCE OF MS LESIONS Anatomic Distribution MS lesions are typically nodular or ovoid in appearance, and range in size from several millimeters to more than 1 centimeter. 30 The lesions have a propensity for large white matter tracts, particularly the corpus callosum, but involvement of white matter tracts in the brainstem (e.g., the medial longitudinal fasciculus and the middle cerebellar peduncle) is also characteristically observed in MS patients. In addition, juxtacortical lesions involving the U-fiber system are found, and these may extend into the gray matter of the cortex. Usually, MS lesions extend along medullary veins that drain into the subependymal veins lining the lateral ventricle at the callososeptal interface. MS lesions are characteristically oriented along the fibers of the corpus callosum (although the veins themselves are not visible on routine MR imaging) paralleling these veins. This appearance corresponds to the so-called Dawson's finger identified at pathology (Fig. 4b), and is well demonstrated on MR imaging (Fig. 4a). Whereas the typical MS lesion is pericallosal or periventricular in location, they may involve any portion of the white matter, and can extend into the involved gray matter as well.
5 Figure 4a. Classic ovoid nodular MS plaques in a Dawson's finger configuration oriented parallel to the while matter tracts. Note the black hole appearance of many of the plaques on the T1 MRI image and the thin rim of T2 hyperintensity. A=spin-echo (SE)T-1 B =proton density, C=T2 weighted SE Figure 4b. MS lesions are characteristically oriented along the fibers of the corpus callosum (although the veins themselves are not visible on routine MR imaging) paralleling these veins. This appearance corresponds to the socalled Dawson's finger identified at pathology Identification of lesions at the callososeptal interface is, therefore, thought to represent a characteristic finding in MS, having high sensitivity and specificity (93% and 96%, respectively). This may be seen as "notching" on the undersurface of the corpus callosum on sagittal Tl-weighted imaging. 19 Recently, a subtler "subcallosal striation" has been described using thin-section (2 mm) sagittal FLAIR sequences. 26 These subtler lesions may be similarly sensitive (94%), although not as specific (84%). 51 These striations are thin white lines radiating away from the callososeptal interface, presumably representing the earliest manifestations of MS in this location (Fig. 5). In contrast to small vessel ischemic changes, MS lesions tend to be more discrete and well defined, becoming confluent only with severe disease progression. Occasionally, MS lesions present as large lesions with mass effect (tumefactive MS) and vasogenic edema, indistinguishable from a brain tumor by MR imaging. Even a small lesion with enhancement may appear identical to a tumor, metastasis, or abscess. 20 Other Imaging Findings in MS
6 With an extensive lesion burden, marked atrophy may be present (Fig. 6). The corpus callosum may be severely thinned throughout. 9, 67 To what extent the atrophy represents primary white matter disease or secondary loss due to Wallerian degeneration is not clear. Diffuse white matter abnormality also may be present. This occasionally appears on routine MR imaging as "dirty white matter," which has diffusely increased T2 signal throughout (Fig. 7). This may be difficult to distinguish from normal variation of myelination, and familiarity with the appearance of white matter on the particular scanner is essential to confidently identify this appearance. Figure 5. Thin section (2 mm) sagittal fluid attenuated inversion-recovery (FLAIR) images from lateral to medial (A-C) in a patient with a diagnosis of optic neuritis. The presence of subcallosal striations can be seen as thin hyperintense bands radiating from the undersurface of the callosum. This sign is highly predictive of developing clinical MS. Figure 6. Atrophy in a 26-year-old woman with MS. Note the marked thinning of the corpus callosum on the midline sagittal Tl-weighted image (A). Relatively confluent white matter disease is present. B, FLAIR image shows the frontal horns in particular are enlarged.
7 Figure 7. Extensive confluent white matter involvement in MS. Extent of dirty white matter appearance is seen to greater advantage on FLAIR (A) than on fast spin-echo (FSE) T2-weighted sequence (B). Discrete nodular lesions are clearly seen against the background white matter abnormality on FSE PD weighted images (C) but are not seen as well on FLAIR or FSE T2-weighted images. No black holes are identified on SE Tl-weighted images (D), but numerous punctate enhancing lesions are seen following contrast administration (E). The enhancement must be evaluated against a background of hyperintense white matter when magnetization transfer is used after contrast (F). With progression of disease, non-heme iron deposition in the basal ganglia is greater than that seen in the normal populations This deposition of ferritin in the basal ganglia is not specific to MS but may be found in a number of degenerative processes in the brain. Signal Intensity Characteristics of MS Lesions Proton Density and T2-Weighted Signals Increased water content of tissue leads to an increase in the tissue T2 relaxation time. This results in hyperintense signal on FLAIR, PD- and T2-weighted imaging. Because most pathologic processes lead to increased tissue water, initially through edema and inflammation, and later through gliosis and frank replacement of tissue with fluid, T2 imaging is a sensitive but not particularly specific indicator of pathology. Conventional SE PD- and T2-weighted images were initially demonstrated to be highly sensitive for MS. 49, 62 In the last decade, FSE techniques have largely replaced CSE techniques, largely because of shorter acquisition times. Image contrast is similar between FSE and CSE techniques, with similar sensitivities for lesion detection. 72 Consistent with pathologic observations, the classic MR imaging appearance of MS is one of multiple hyperintense white matter lesions with periventricular predominance. An important limitation of MR imaging is the low pathologic specificity of these hyperintense lesions. MS plaques are readily seen on PD and T2-weighted sequences because they have a higher proton density and longer T2 relaxation times than
8 normal white matter; however this is equally the case for other pathologies whether infarcts, infections, other inflammatory conditions, and tumors. Furthermore any of the main pathologic features of the MS plaque itself may result in a similar hyperintense appearance. It occurs in new lesions because of the inflammatory edema associated with blood-brain barrier (BBB) breakdown. In chronic lesions, it may be the result of an increase in extracellular fluid associated with demyelination and axonal loss or to gliosis (fibrous astrogliosis) that may increase intracellular water content. Demyelination itself, with the breakdown of the fatty myelin sheaths within the MS lesion, probably does not contribute significantly to the prolonged T2 relaxation changes. The amount of lipid lost is not large enough to cause the magnitude of change demonstrated on MR imaging because the lipids related to myelin breakdown have an extremely short T2 relaxation time and are effectively invisible on conventional MR imaging. The loss of myelin lipid does, however, result in a more hydrophilic environment, and this increase in water content leads to the observed increases in proton density, Tl, and T2 relaxation times. Gliosis (fibrous astrogliosis) is important for the T2 signal in chronic lesions and the neutral fat resulting from demyelination per se is unlikely to make a contribution to the MR signal, whereas presumably the water that replaced the lipid lost by demyelination did. The T2 signal in acute lesions is likely caused by edema. Fluid Attenuated Inversion-Recovery Inversion-recovery techniques Suppress signal by placing an inversion pulse a certain time interval before image acquisitions Tissues with a Tl approximately 1.5 times this inversion time will have their signal suppressed. Short inversion times will suppress fat, and long inversion times will suppress water. The FLAIR technique uses inversion times on the order of 2 seconds to suppress signal from free fluid, namely, cerebrospinal fluid (CSF). The inversion is followed by a T2-weighted imaging sequence. The resulting image is heavily T2-weighted, with signal from free fluid (i.e., CSF) nulled. By suppressing CSF signal from the ventricles and subarachnoid spaces, the conspicuity of T2 hyperintense white matter lesions is markedly enhanced, particularly in the periventricular regions where MS lesions are most characteristically seen. In its original implementation, FLAIR imaging was time consuming. Fast FLAIR uses FSE techniques to achieve clinically reasonable imaging times. 63 Using this sequence, the conspicuity of lesions near CSF, namely, periventricular and juxtacortical lesions, is markedly enhanced resulting in identification of many more lesions than on CSE or FSE techniques. 77 Because of this, FLAIR is the sequence of choice in identifying supratentorial white matter lesions. Unfortunately, FLAIR has proven to be less sensitive than PD- and T2- weighted imaging in the infratentorial compartment (Fig. 8). 45,77 Because FLAIR uses inversion recovery, some Tl effects are present, and it may be that these Tl effects counter the T2 effects in the brainstem and cerebellum. Because of these different TI relaxation times, it is possible that a modification of the standard inversion times used for FLAIR may be necessary. Similar findings have been shown in the spinal cord, where FLAIR also is relatively insensitive. 28 Thus, in many situations, it may be prudent to use FLAIR, PD, and T2 sequences to fully evaluate the intracranial compartment. T1 Properties Initially, MS lesions are isointense to mildly hypointense on T1-weighted imaging. With time, the mild hypointensity may progress to develop into a so-called T1 hole or black hole in which the lesion has completely been replaced by CSF (Fig. 9). 75 Alternatively, the lesion may remain stable in intensity. In many cases, there is a slightly hyperintense rim surrounding a lesion. This hyperintensity is typically ascribed to the presence of free radicals in the surrounding inflammatory tissue, but paramagnetic effects from petechial hemorrhage and fat signal from myelin breakdown also may contribute to this phenomenon. 58 The appearance of a TI hyperintense ring around a Tl hypointense lesion is fairly characteristic of MS but may be seen with any inflammatory process, such as abscess formation. 22 Tl hypointensities serve as a surrogate marker of disability in multiple sclerosis because they are specific for matrix destruction and axonal loss. Development of Tl hypointensities implies not only focal damage to axons within lesions, but also more widespread tissue loss, leading to generalized atrophy of the brain.
9 A TI hypointensity is defined as an area on a conventional SE (short TR/short TE) Tl- weighted image that is hypointense compared with surrounding white matter (in this case referred to as normalappearing white matter [NAWMI) and cortex, and is accompanied by an equivalent hyperintense area on a T2-weighted image Hypointense lesions usually begin as focal enhancements on postcontrast Tl- weighted images (with accompanying hyperintensity on T2-weighted images) and most will be hypointense in the acute stage on precontrast Tl-weighted images. Later, they can resolve and become isointense on precontrast Tlweighted images or remain hypointense (but always stay hyperintense on T2- weighted images). These changes in appearance take place in the first 2 months of lesion evolution and remain unchanged thereafter. Sequence of events in the development of a black hole. After a lesion has enhanced on Tl-weighted imaging, it frequently goes through a transient hypointensity stage (seen on precontrast Tl -weighted MR imaging), which may be determined only by temporary edema in and around the lesion area. The subsequent course of the hypointensity is unknown at this starting point; it might develop into a permanent hypointensity (chronic black hole), or it might recover partially (remyelination and axonal survival), and become a gray lesion. In the best-case scenario, it will resolve completely and become isointense to surrounding white matter (temporary black hole). This does not apply for T2-weighted images; they will remain bright. Tl hypointensities should not be thought of simply as the sole areas of destruction, but rather as indicators of an underlying destructive process TI hypointensities is a marker of severe tissue damage and axonal loss, even early in the disease course. Although it is unlikely that axonal loss per se contributes to the appearance of the lesions on TI-weighted images, it is indeed an invariably associated finding. Most probably axonal loss is connected to the development of hypointensity through the accompanying increase in extracellular fluid. Four lesion stages were distinguished according to neuropathologic criteria and matched to the Tlweighted images: early active lesions, which appeared isointense or slightly hypointense on Tl- weighted images and with extensive gadolinium (Gd) enhancement; late active lesions, which were weakly hypointense or severely hypointense on Tl-weighted images and with variable Gd enhancement; demyelinated lesions, which were clearly hypointense on Tl- weighted images and with variable Gd enhancement; and remyelinating lesions, which emerged as weakly hypointense on Tl- weighted images with variable Gd enhancement. All lesion types except early active were hyperintense on T2-weighted images. The degree of axonal loss was correlated with the degree of lesion hypointensity. MS lesions on T2-weighted images are nonspecific for the neuropathologic substrate, and could represent old lesions that are demyelinated, partly or highly remyelinated, new lesions, gliosis, and axonal loss. Therefore T2-weighted lesions are bound to have a poor correlation with the expanded disability status scale (EDSS). Since hypointensity on TI-weighted imaging is a marker of axonal loss, one would expect a better correlation with disability. Indeed, cross-sectional studies show higher correlation compared with T2- weighted images. The occurrence of Tl hypointensities can be used to differentiate small vessel ischemic lesions from MS. The occurrence of Tl hypointensities is typical for MS but not for ischemic white matter lesions. Unfortunately, the number of Tl hypointensities at first presentation is low, indicating that the high specificity of this finding in the very early phases of the disease is offset by a low sensitivity.
10 Figure 8. Infratentorial lesion in the left pons is visualized best on the FSE PD-weighted sequence (A). FSE T2- weighted (B) and FLAIR images (C) show poorer lesion-to-background contrast. Figure 9. Juxtacortical Tl black hole, with rim of hyperintensity on TI-weighted image (A), with otherwise typical findings on FSE PD-weighted (B), FSE T2- weighted (C) and FLAIR (D) images. Note that incidental white matter lesions are virtually always isointense on Tl-weighted images. Contrast Enhancement Contrast enhancement represents a disruption in the blood-brain barrier that allows for the leakage of gadoliniumchelates. The presence of enhancement can play an important role in the evaluation of MS, depending on the clinical context. Enhancement results from a local breakdown of the blood-brain barrier, and indicates the presence of an active inflammatory process; therefore, enhancement identifies "active lesions," which often correlate with the acute symptomatology. 2,71 These active lesions also may be clinically silent and are frequently seen on serial imaging performed as part of research protocols. Because nonenhancing lesions identified on T2-weighted images are thought to be chronic lesions, the simultaneous presence of enhancing and nonenhancing lesions is strong evidence to indicate that these are "multiple lesions separated in time," supporting a putative diagnosis of MS at the time of initial presentation. The presence of ring-enhancement suggests the reactivation of an old lesion-the central nonenhancing portion of the lesion representing the "burnt out" portion of the lesion. An incomplete or open ring of enhancement is more indicative of an MS lesion than metastatic disease or infection, which almost always has a complete, fully enclosed ring of enhancement. 37 Detection of enhancing lesions may be increased by a number of techniques, including decreasing slice thickness, use
11 of triple-dose gadolinium, application of magnetization transfer (MT), and acquiring delayed images 3, 18, 61, 85. The clinical value of these techniques must be weighed against the additional costs of contrast material, imaging time, and false-positive findings. Magnetization Transfer MT is used in combination with Tl- weighted imaging to suppress signal from bound protons. This combination suppresses signal from white matter to a greater degree than gray matter and thus reduces gray-white contrast. Signals from MS lesions suppress less than normal white matter with MT and therefore are somewhat hyperintense on Tl-weighted imaging. In the context of MS, the detection of a new enhancing lesion is an indicator of disease activity. In standard TIweighted imaging, chronic lesions usually are isointense to hypointense, relative to the background of white matter. Therefore, a new enhancing lesion is relatively easy to detect, because of the high contrast between new and old lesions. With MT, chronic lesions and the abnormal white matter background become hyperintense. Detection of enhancement requires careful comparison of pre- and postcontrast images to avoid over-interpreting hyperintensity as contrast enhancement. Thus although MT clearly plays a research role in the quantification of white matter disease, the ability to detect a new solitary lesion may be performed best by standard Tl-weighted imaging. Diffusion- Weighted Imaging Diffusion-weighted imaging has revolutionized MR imaging of stroke by acutely demonstrating cytotoxic edema. Diffusion- weighted sequences reliably differentiate vasogenic and cytotoxic edema. Recent explorations of diffusionweighted imaging in MS show that subtle vasogenic edema can be identified before the development of an enhancing lesion. 83 Temporal Characteristics Evolving MS lesions have a characteristic temporal profile demonstrable on T2-weighted sequences. 84 They reach a maximum size in approximately 4 weeks, before gradually shrinking, usually leaving a small residual abnormality indistinguishable from chronic MS lesions. The course of contrast enhancement is similar. 39, 41 Only 25% of enhancing lesions are found to enhance 1 month after initial identification. Six months later, essentially no lesions enhance. Retrospective analysis of serially imaged patients suggests that subtle MT 15, 27, 55 and diffusion 83 abnormalities precede the development of new lesions. This indicates that breakdown of the blood-brain barrier precedes the development of the inflammatory plaque. It is unclear what factors result in axonal loss and the formation of a Tl black hole. The extent of enhancement at the initial presentation of a lesion correlates poorly with eventual Tl and T2 lesion burden. 82 The burden of Tl hypointensity correlates with disability to a much higher degree than the T2 lesion load, indicating that the axonal loss or destruction is more directly related to neural dysfunction than demyelination alone. 75 Because MR imaging can be used to survey the entire neuraxis, it is able to identify these clinically silent lesions, thus establishing the presence of multiple lesions in space. Furthermore, as lesions enhance only when they are relatively acute, (typically < 2 months), enhancement or lack thereof dates a lesion ; hence, the presence of enhancement provides temporal and anatomical information. That is, a single MR image with enhancing and nonenhancing lesions may be interpreted as having lesions separated in time. MS lesions are typically nodular or ovoid in appearance, and range in size from several millimeters to more than 1 centimeter. 30 The lesions have a propensity for large white matter tracts, particularly the corpus callosum, but involvement of white matter tracts in the brainstem (e.g., the medial longitudinal fasciculus and the middle cerebellar peduncle) is also characteristically observed in MS patients. In addition, juxtacortical lesions involving the U-fiber system are found, and these may extend into the gray matter of the cortex. Usually, MS lesions extend along medullary veins that drain into the subependymal veins lining the lateral ventricle at the callososeptal interface. MS lesions are characteristically oriented along the fibers
12 of the corpus callosum (although the veins themselves are not visible on routine MR imaging) paralleling these veins. This appearance corresponds to the so-called Dawson's finger identified at pathology, and is well demonstrated on MR imaging Identification of lesions at the callososeptal interface is, therefore, thought to represent a characteristic finding in MS, having high sensitivity and specificity (93% and 96%, respectively). This may be seen as "notching" on the undersurface of the corpus callosum on sagittal Tl-weighted imaging. In contrast to small vessel ischemic changes, MS lesions tend to be more discrete and well defined, becoming confluent only with severe disease progression. Occasionally, MS lesions present as large lesions with mass effect (tumefactive MS) and vasogenic edema, indistinguishable from a brain tumor by MR imaging. Even a small lesion with enhancement may appear identical to a tumor, metastasis, or abscess. With an extensive lesion burden, marked atrophy may be present. The corpus callosum may be severely thinned throughout. To what extent the atrophy represents primary white matter disease or secondary loss due to Wallerian degeneration is not clear. Increased water content of tissue leads to an increase in the tissue T2 relaxation time. This results in hyperintense signal on PD- and T2-weighted imaging. Because most pathologic processes lead to increased tissue water, initially through edema and inflammation, and later through gliosis and frank replacement of tissue with fluid, T2 imaging is a sensitive but not particularly specific indicator of pathology. The FLAIR technique uses inversion times on the order of 2 seconds to suppress signal from free fluid, namely, cerebrospinal fluid (CSF). The inversion is followed by a T2-weighted imaging sequence. The resulting image is heavily T2-weighted, with signal from free fluid (i.e., CSF) nulled. By suppressing CSF signal from the ventricles and subarachnoid spaces, the conspicuity of T2 hyperintense white matter lesions is markedly enhanced, particularly in the periventricular regions where MS lesions are most characteristically seen. Because of this, FLAIR is the sequence of choice in identifying supratentorial white matter lesions. Unfortunately, FLAIR has proven to be less sensitive than PD- and T2- weighted imaging in the infratentorial compartment. Infratentorial lesions are more specific to multiple sclerosis than supratentorial lesions. The simultaneous presence of enhancing and nonenhancing lesions is strong evidence to indicate that these are "multiple lesions separated in time," supporting a putative diagnosis of MS at the time of initial presentation. The presence of ring-enhancement suggests the reactivation of an old lesion-the central nonenhancing portion of the lesion representing the "burnt out" portion of the lesion. An incomplete or open ring of enhancement is more indicative of an MS lesion than metastatic disease or infection, which almost always has a complete, fully enclosed ring of enhancement. TECHNIQUES FOR EXAMINING WHITE MATTER MR Imaging Sequences for Routine Clinical Examination Most MR imaging centers use a standard battery of sequences consisting of a sagittal Tl, an axial FSE T2, and an axial fast FLAIR or FSE PD. Although the FLAIR sequence is attractive for many reasons, its inconsistency in evaluating the infratentorial compartment and the potential superiority of PD-weighted imaging may support the inclusion of FLAIR and FSE PD-weighted imaging in the evaluation. This is particularly true because infratentorial lesions, although less common than supratentorial lesions, are more specific for MS. The presence of an enhancing lesion can strongly support the diagnosis, if other findings are equivocal; therefore, the use of contrast is strongly recommended. 13 Although MT can increase the detection of contrast enhancing lesions, MS lesions will be bright on precontrast images as well, making interpretation difficult without careful attention to the precontrast MT images. Similarly, triple doses of a contrast agent can improve the detection of contrast-enhancing lesions, but at a significant increase in cost. DIFFERENTIAL DIAGNOSIS OF WHITE MATTER DISEASE Normal Variation and Small Vessel lschemic Changes Virchow-Robin Spaces
13 Perivascular Virchow-Robin (VR) spaces represent extentions of subarachnoid space into the brain parenchyma along perforant vessels. These spaces are most often below the resolution of MR imaging, but they may be large enough to be confused with parenchymal lesions. VR spaces often are found along the path of the lenticulostriate arteries that penetrate the basal ganglia through the anterior perforated substance in the neighborhood of the anterior commissure. These dilated spaces may be as much as 2 centimeters in diameter, at which point they often are confused with lacunar infarcts. 26, 35 VR spaces also may extend along the path of perforant medullary arteries traversing gray and white matter in the high convexities. Dilations of these spaces greater than 2 millimeters may be found in 8% of patients; here they are more likely to be confused with MS lesions. 2, 27 As VR spaces are extensions of the subarachnoid space, their signal follows that of CSF on all sequences. Careful attention to CSF signal may be necessary to distinguish a VR space from a true T2 hyperintensity. In particular, there is no halo of high signal gliosis on a FLAIR sequence around the dark CSF, as might be seen in a lacunae or a chronic MS lesion (Fig. 10). 44 Ependymitis Granularis Ependymitis granularis refers to the patchy loss of ependyma along the frontal horns with astrocytic gliosis, a nearly ubiquitous finding in MR imaging, and particularly noticeable on FLAIR sequences. The presence of high signal anterior to the frontal horns, and extending as a thin line along the bodies of the lateral ventricles, should not be misconstrued as pathology (Fig. 11). 70 In particular, the more globular and continuous appearance of ependymitis granularis should not be confused with subcallosal striations. 51 Incidental Hyperintensities and Small Vessel Ischemic Changes Punctate foci of T2 prolongation are seen in the white matter in otherwise healthy individuals. The incidence of these lesions increases with advancing age, so that by age 50, approximately 50% of the normal population will have such lesions with advancing age. 80 These hyperintensities rarely enhance. They tend to be found more in the subcortical and periventricular white matter. juxtacortical white matter and the callososeptal areas are relatively spared, whereas the arterial watershed in the centrum semiovale is more directly affected 79; furthermore, small vessel ischemic changes are rarely hypointense on Tl- weighted images (Fig. 12). Infratentorial lesions are seen in the pons but rarely elsewhere. It is largely the presence of these incidental findings that reduces the specificity of MR imaging in establishing the diagnosis of MS. Migraine Migraine is associated in some series with a higher incidence of T2 hyperintensities than in the normal population, with T2 hyperintense foci present in 40% to 45% of migraineurs. 31, 68 This is thought to be related to the abnormal vasoreactivity of cerebral vessels. Presumably, the same vascular hyperreactivity that is responsible for the migraine aura can lead to ischemia, resulting in foci of white matter gliosis. Other series, however, show no such elevation in the incidence of MR imaging hyperintensities. 50
14 Figure 10. Prominent Virchow-Robin space in the left parietal lobe. Note the isointensity to CSF on all sequences (A, FSE T2-weighted; B, FSE PD weighted; C, FLAIR; and D, SE Tl-weighted images). Vasculopathies Immune-Mediated Vasculopathies As small vessel ischemia results in foci of white matter infarction, immune, nonimmune, and drug-induced vasculopathies can result in findings that mimic those of MS. The immune-mediated small vessel necrotizing vasculitides (e.g., Wegener's granulomatosis, micro polyangiitis, and polyarteritis nodosa) have been associated with central nervous system (CNS) findings. 59 Collagen vascular diseases, particularly systemic lupus erythematosus and Behcet's disease, may manifest with white matter lesions. In lupus, large vessel infarctions are not uncommon. Behcet's disease is remarkable in the preponderance of brainstem abnormalities when CNS involvement occurs. 36 Nonimmune Vasculopathies Nonimmune vasculopathies with a Mendelian inheritance pattern can give rise to small vessel ischemic changes. Examples of these entities include cerebral autosomal dominant arteriopathy with subcortical infarcts and leukoencephalopathy (CADASIL) and Fabry's disease. CADASIL is a nonatherosclerotic, nonamyloid angiopathy affecting mainly the small penetrating arteries of the subcortical white matter and basal ganglia. In contrast to MS, basal ganglia involvement is greater and cortical U fibers are spared. 5 Figure 11. Ependymitis granularis outlining the lateral ventricles in a 71-year-old man. Incidental, scattered foci of T2 prolongation are present. Cerebrospinal fluid suppression renders these findings more conspicuously on the
15 FLAIR images (B and D) than on the FSE T2-weighted (A and C) images. Figure 12. Small vessel ischemic changes in a 79-year-old woman. Note that the larger lesions in the parietal white matter are not nodular or discrete. Ependymitis granularis is present, capping the frontal horns. (A, FSE T2- weighted; B, FLAIR; C, SE Tl-weighted images.) Fabry's disease is an X-linked recessive disorder of lipid metabolism, resulting from alpha-galactosidase A deficiency. Progressive accumulation of ceramidetrihexoside within the intima and media of cerebral blood vessels results in a typical small vessel ischemic pattern (Fig. 13). 7 Figure 13. Fabry's disease. Adjacent FLAIR images through the corpus callosum demonstrate patchy lesions resulting from small vessel ischemia. Note the linear band of hyperintensity extending across the corpus callosum (B). Lesions here are atypical for small vessel ischemia, and may in this case represent Wallerian degeneration. Many drugs of abuse have vasoactive effects that can lead to large or small vessel infarcts. Small vessel ischemia may be seen commonly with vasculitis related to cocaine and amphetamine addiction. 17 Infectious and Inflammatory Causes Neuroborreleosis Lyme disease typically presents as an encephalopathy, which may be associated with a normal brain MR image; however, it can present as an MS-like illness with lesions indistinguishable from those of MS, so that differentiating between MS and Lyme disease cannot be based on imaging findings (Fig. 14). 23 Neurosarcoidosis
16 Neurosarcoidosis has protean manifestations and as such may present in a manner mimicking that of MS; however, more typical presentations of CNS sarcoid effectively exclude MS. Densely enhancing basilar meningitis is a common presentation, often involving the neurohypophysis and cranial nerves. 65 Acute Disseminated Encephalomyelitis ADEM results from the cross-reaction of antibodies with myelin basic protein following a vaccination or viral infection. The pathophysiology is similar to that of MS, although ADEM is monophasic in course. No new lesions should develop several months after the initial ictus. Although multiple enhancing lesions may be seen at presentation, the lesions will follow the same time course of enhancement and should not enhance on subsequent MR scans. 36 Progressive Multifocal Leukoencephalopathy PML is a fatal papovavirus infection seen in the immunocompromised host. PML may present as a solitary lesion, although multifocal nonenhancing white matter lesions are more typically seen. Gray matter involvement and mass effect are unusual. The presence of mass effect is associated with a poor prognosis. The lack of enhancement was once considered a diagnostic requirement, but the presence of peripheral enhancement has been reported (Fig. 15). 57 Figure 14. Lyme disease. FSE PD-weighted (A), FSE T2-weighted (B), and FLAIR (C) images demonstrate ovoid periventricular lesions mimicking those of MS. A juxtacortical left frontal lesion is seen clearly only on the FLAIR sequence (C). Figure 15. lmmunocompromised patient with biopsy-proven progressive multifocal leukoencephalopathy. Hyperintense lesion is seen in the left middle cerebellar pedun- cle on FLAIR (A) and T2-weighted (B) images. No
17 enhancement is seen following contrast administration (C and D). There is a suggestion of slight mass effect on the fourth ventricle, a poor prognostic sign. Note that these images were obtained after biopsy. Human Immunodeficiency Virus HIV encephalopathy develops in up to 60% of HIV patients. T2 prolongation is found diffusely throughout the white matter. The abnormality is confluent, symmetric, and relatively homogeneous. Gray matter is spared, and enhancement is not seen. Atrophy develops in concordance with the white matter changes. Focal lesions are not seen, and it is not likely to be confused with MS (Fig. 16). 73 Figure 16. Spin-echo PD weighted (A) and SE T2-weighted (B) images showing diffuse, ill-defined, relatively symmetrical hyperintensity throughout the white matter in a patient with longstanding HIV, beginning to manifest dementia, presumably representing HIV encephalopathy. Metabolic and Toxic White Matter Diseases Reversible Posterior (Leuko)Encephalopathy Syndrome This entity refers to a fairly consistent clinical syndrome often seen with the development of acute hypertension, such as in eclampsia. It also is seen in the context of chemotherapy (typically with the use of cyclosporin), in transplantation or transfusion, with hypertension not clearly demonstrated. Clinically, seizures and visual disturbances are common presentations. The abnormalities may reverse with normalization of blood pressure and may or may not require discontinuation of the offending agent. 27 MR imaging demonstrates patchy regions of T2 prolongation in the periventricular and subcortical white matter in posterior parts of the brain, characteristically involving the white matter of the occipital and parietal lobes, but the cerebellum also may be involved (Fig. 20). Petechial hemorrhage may be seen on T2*-weighted imaging. The high signal primarily represents vasogenic edema and so is hypointense on diffusion-weighted imaging. Small foci of enhancement may be seen, and these may show high signal on diffusion-weighted imaging, indicating regions of irreversible damage. 54 Radiation-Induced White Matter Disease Neuropathologic consequences of therapeutic radiation include demyelination, microvascular occlusion, and bloodbrain barrier breakdown. In a dose-dependent manner, white matter signal changes from patchy foci of T2 prolongation to confluence and finally to coagulative necrosis with blood-brain barrier breakdown. The posterior fossa, basal ganglia, and internal capsules are relatively spared (Fig. 21). 6, 76 Osmotic Myelinolysis Demyelination of white matter tracts in the pons may be seen following overly aggressive correction of severe hyponatremia. Although classically this is restricted to the central pons, sparing the periphery, the demyelination
18 may extend into the midbrain, thalamus, and basal ganglia. Occasionally, only these extrapontine sites are involved; hence, the entity is no longer referred to as central Pontine myelinolysis. Initially, high signal edema is seen. Although some of the abnormality is reversible, progression to frank cavitation also occurs. 29, 69 (Fig. 17,18,19) Figure 17. T2-weighted MRI scan of the brain demonstrating patchy areas of signal change within the pons that are consistent with demyelination or central pontine myelinolysis Figure 18. T1-weighted MRI scan of the brain demonstrating patchy areas of signal change within the pons that are consistent with demyelination or central pontine myelinolysis
19 Figure 19. A post mortem section through the pons showing central pontine myelinolysis Figure 20. Posterior reversible leukoencephalopathy in a posttransplant patient receiving cyclosporin and presenting with visual disturbances. Confluent white matter signal abnormalities extend throughout the parietal and occipital white matter. (A, FLAIR; B, FSE T2-weighted; C, SE Tl-weighted; D, SE Tl-weighted with contrasted Figure 21. White matter changes after radiotherapy. Edema and gliosis are seen as hyperintensity on FLAIR (A) and T2-weighted (B) images, and as hypointensity on Tl -weighted images postcontrast (C). Note the normal variant venous angioma (C). Leukodystrophies Leukodystrophies are dysmyelinating disorders that represent defects in the formation or maintenance of myelin. Whereas most leukodystrophies present in childhood, metachromatic leukodystrophy and adrenomyeloneuropathy
20 have an adult onset and may enter into the clinical differential of MS. In the adult variant of metachromatic leukodystrophy, symmetric diffuse involvement of white matter, sparing the subcortical U fibers, is seen. 60 Figure 22. Adrenoleukodystrophy Lesions in adrenomyeloneuropathy initially involve the pyramidal tracts, usually in the posterior limbs of the internal capsules. With progression of disease, the symmetric posterior parietal white matter involvement of adrenoleukodystrophy may be seen. Female carriers of X-linked adrenoleukodystrophy present with a late-onset neurologic dysfunction, as in adrenomyeloneuropathy. 78 OPTIC NEURITIS AND MS Acute monosymptomatic optic neuritis (ON) is a common manifestation of MS, and the reported risk for developing MS varies widely. A small, long-term 8-year follow-up study demonstrated that 50% of patients develop clinically definite MS. 11 A larger study of 388 patients by the Optic Neuritis Study Group demonstrated that 30% of patients with ON progress to clinically definite MS within 5 years. 46 The risk of progression to clinically definite MS correlated highly with the number of lesions seen at MR imaging. A normal brain MR image at presentation did not preclude the development of MS in the future, with 16% of patients developing MS. One half (51%) of those with three or more MR imaging lesions went on to develop MS. 46 As with MS plaques in the brain, enhancement may be seen in the optic nerves during the acute phase, resolving over weeks to months (Fig. 23). 86 MR imaging of the brain is used to evaluate for lesions suggestive of MS, which are found at presentation in 57% of patients. 33 Although ON is most often associated with typical MS lesions in the brain, Devic's neuromyelitis optica is a syndrome in which a severe myelopathy is associated with the neuropathy. Brain lesions are absent. It has been regarded as a form of MS or as a separate neurologic syndrome. Recent MR imaging evidence suggests that it may in fact be distinct from MS, because the MT ratio of white matter in these patients is similar to that of a healthy cohort. 16 Another cause of ON, Leber's hereditary optic neuropathy, is a mitochondrial disorder, which in females can manifest in a manner identical to MS. 24 BRAINSTEM SYNDROMES, TRANSVERSE MYELITIS AND MS Progression to clinically definite MS is seen in nearly half of patients presenting with transverse myelitis (42%) and nearly two thirds of those presenting with a brain stem syndrome. 39, 48 MR IMAGING IN THE DIAGNOSIS OF MS: PREDICTIVE VALUE IN THE CLINICALLY ISOLATED SYNDROME MS typically presents as an acute, reversible episode of neurologic dysfunction-the clinically isolated syndrome (CIS). Spinal cord, optic nerve, or brain stem involvement accounts for most cases. Poser et al set forth criteria to establish a definitive diagnosis of MS. 56 Clinically definite MS (CDMS) requires clinical evidence of two lesions
21 separated in time and space. A positive MR image can establish the diagnosis of CDMS in patients who have had two attacks but have clinical evidence of only one lesion. Furthermore, Poser and colleagues defined a category of laboratory-definite MS (LDMS) in patients with oligoclonal bands in the CSF and positive MR imaging findings, but without satisfying the more stringent criteria of clinical evidence. Figure 23. Optic neuritis in a patient with MS. Sagittal (A) coronal (B) and axial (C) SE Tl - weighted images through the optic chiasm demonstrate extensive enhancement of the optic nerves, tracts, and chiasm. Axial FLAIR image shows typical MS plaques. The Poser criteria reflected the fact that when a patient presents with a CIS, the condition may progress to CDMS, or it may be a solitary event with no subsequent attacks. These criteria recognized that MR imaging and other paraclinical tests have an important role in predicting the development of MS. CSF oligoclonal bands, according to some authors, have a higher positive predictive value than MR imaging 34,52; however, recent studies have established the predictive power of MR imaging. O'Riordan et al have shown a strong correlation between the baseline T2-weighted MR image appearance and the probability of progression to CDMS in a 10-year follow-up study. 47 Two thirds of their patient population had lesions at baseline, and 83% of these patients progressed to CDMS at 10 years. Of the one third with normal MR images, only 11% progressed to CDMS. Furthermore, the number of lesions at baseline correlated with the probability of progression to MS and with the disability scores 5 and 10 years lateral 14,42, 47 Specificity may be improved by the presence of an enhancing lesion at the expense of sensitivity, as these lesions are found in approximately one third of patients undergoing MR imaging. 71 A higher incidence of abnormal MR images at initial presentation is found using thin sections (3 mm) and higher field strength (1.5 Tesla). 4 Attempts to increase the diagnostic accuracy of MR imaging by using fixed criteria have been proposed (Table 1). Initially, these attempts were based solely on CSE, PD, and T2 imaging. The Paty et al, 53 criteria used four or more lesions (Paty A) or three lesions with one bordering a ventricle (Paty B) as strongly suggestive of MS. Fazekas et al, 13 developed criteria similar to Paty for using MR imaging to predict the development of MS. Three or more lesions were required, with two of the following features: found to be larger than 5 mm, and in a periventricular or infratentorial location. These criteria reflect the lesser weight given to lesions in the centrum semiovale, which are commonly found incidentally and with small vessel ischemia. These criteria led to a further improvement in specificity (96%) at the expense of a decrease in sensitivity (81 %). 43 Table 1. MR IMAGING CRITERIA FOR CLINICAL PROGRESSION TO MS Paty et al, 53, lesions > 3 lesions, including 1 periventricular lesion
1 MS Lesions in T2-Weighted Images
 1 MS Lesions in T2-Weighted Images M.A. Sahraian, E.-W. Radue 1.1 Introduction Multiple hyperintense lesions on T2- and PDweighted sequences are the characteristic magnetic resonance imaging (MRI) appearance
1 MS Lesions in T2-Weighted Images M.A. Sahraian, E.-W. Radue 1.1 Introduction Multiple hyperintense lesions on T2- and PDweighted sequences are the characteristic magnetic resonance imaging (MRI) appearance
MRI and differential diagnosis in patients suspected of having MS
 Andrea Falini Italy MRI and differential diagnosis in patients suspected of having MS IMPROVING THE PATIENT S LIFE THROUGH MEDICAL EDUCATION www.excemed.org Outline of presentation - Diagnostic criteria
Andrea Falini Italy MRI and differential diagnosis in patients suspected of having MS IMPROVING THE PATIENT S LIFE THROUGH MEDICAL EDUCATION www.excemed.org Outline of presentation - Diagnostic criteria
Interactive Cases: Demyelinating Diseases and Mimics. Disclosures. Case 1 25 yo F with nystagmus; look for tumor 4/14/2017
 Interactive Cases: Demyelinating Diseases and Mimics Disclosures None Brad Wright, MD 27 March 2017 Case 1 25 yo F with nystagmus; look for tumor What do you suspect? A. Demyelinating disease B. Malignancy
Interactive Cases: Demyelinating Diseases and Mimics Disclosures None Brad Wright, MD 27 March 2017 Case 1 25 yo F with nystagmus; look for tumor What do you suspect? A. Demyelinating disease B. Malignancy
Demyelinating Diseases of the Brain
 Department of Radiology University of California San Diego Demyelinating Diseases of the Brain John R. Hesselink, M.D. T1-Weighted Images Normal White Matter Contents Axons with envelope of myelin Neuroglia
Department of Radiology University of California San Diego Demyelinating Diseases of the Brain John R. Hesselink, M.D. T1-Weighted Images Normal White Matter Contents Axons with envelope of myelin Neuroglia
Radiologic-Pathologic Correlation of White Matter Disease
 The Neuroradiology Journal 22 (Suppl. 1): 26-32, 2009 www. centauro. it Radiologic-Pathologic Correlation of White Matter Disease J.G. SMIRNIOTOPOULOS 1,2,3,.. SMITH 1,2, E. RUSHING 2,4, F.M. MURPHY 2,
The Neuroradiology Journal 22 (Suppl. 1): 26-32, 2009 www. centauro. it Radiologic-Pathologic Correlation of White Matter Disease J.G. SMIRNIOTOPOULOS 1,2,3,.. SMITH 1,2, E. RUSHING 2,4, F.M. MURPHY 2,
Essentials of Clinical MR, 2 nd edition. 14. Ischemia and Infarction II
 14. Ischemia and Infarction II Lacunar infarcts are small deep parenchymal lesions involving the basal ganglia, internal capsule, thalamus, and brainstem. The vascular supply of these areas includes the
14. Ischemia and Infarction II Lacunar infarcts are small deep parenchymal lesions involving the basal ganglia, internal capsule, thalamus, and brainstem. The vascular supply of these areas includes the
Helpful Information for evaluation of new neurological symptoms in patients receiving TYSABRI
 Helpful Information for evaluation of new neurological symptoms in patients receiving TYSABRI This information is provided as an educational resource for healthcare providers and should be considered current
Helpful Information for evaluation of new neurological symptoms in patients receiving TYSABRI This information is provided as an educational resource for healthcare providers and should be considered current
White matter diseases affecting the corpus callosum; demyelinating and metabolic diseases
 White matter diseases affecting the corpus callosum; demyelinating and metabolic diseases Poster No.: C-0199 Congress: ECR 2011 Type: Educational Exhibit Authors: J. H. Yoo; Seoul/KR Keywords: Neuroradiology
White matter diseases affecting the corpus callosum; demyelinating and metabolic diseases Poster No.: C-0199 Congress: ECR 2011 Type: Educational Exhibit Authors: J. H. Yoo; Seoul/KR Keywords: Neuroradiology
Magnetic resonance imaging in multiple sclerosis
 APRIL 2002 103 Magnetic resonance imaging in multiple sclerosis Beside the ability to detect the Olga Ciccarelli and David H. Miller NMR Unit, Institute of Neurology, University College London, Queen Square,
APRIL 2002 103 Magnetic resonance imaging in multiple sclerosis Beside the ability to detect the Olga Ciccarelli and David H. Miller NMR Unit, Institute of Neurology, University College London, Queen Square,
Patologie infiammatorie encefaliche e midollari
 Patologie infiammatorie encefaliche e midollari Maria Laura Stromillo Department of Medicine, Surgery and Neuroscience Inflammatory disorders of the CNS NMOSD ADEM Multiple Sclerosis Neuro-Myelitis Optica
Patologie infiammatorie encefaliche e midollari Maria Laura Stromillo Department of Medicine, Surgery and Neuroscience Inflammatory disorders of the CNS NMOSD ADEM Multiple Sclerosis Neuro-Myelitis Optica
A pictorial review of neurological complications of systemic lupus erythematosus and antiphospholipid syndrome
 A pictorial review of neurological complications of systemic lupus erythematosus and antiphospholipid syndrome Poster No.: C-2780 Congress: ECR 2010 Type: Educational Exhibit Topic: Neuro Authors: E. Tavernaraki,
A pictorial review of neurological complications of systemic lupus erythematosus and antiphospholipid syndrome Poster No.: C-2780 Congress: ECR 2010 Type: Educational Exhibit Topic: Neuro Authors: E. Tavernaraki,
MRI in Differential Diagnosis. CMSC, June 2, Jill Conway, MD, MA, MSCE
 MRI in Differential Diagnosis CMSC, June 2, 2016 Jill Conway, MD, MA, MSCE Director, Carolinas MS Center Clerkship Director, UNCSOM-Charlotte Campus Charlotte, NC Disclosures Speaking, consulting, and/or
MRI in Differential Diagnosis CMSC, June 2, 2016 Jill Conway, MD, MA, MSCE Director, Carolinas MS Center Clerkship Director, UNCSOM-Charlotte Campus Charlotte, NC Disclosures Speaking, consulting, and/or
Disclosure. + Outline. Case-based approach to neurological emergencies that might present to the ED
 Kathleen R. Fink, MD University of Washington 5 th Nordic Emergency Radiology Course May 21, 2015 Disclosure My spouse receives research salary support from: Bracco BayerHealthcare Guerbet Outline Case-based
Kathleen R. Fink, MD University of Washington 5 th Nordic Emergency Radiology Course May 21, 2015 Disclosure My spouse receives research salary support from: Bracco BayerHealthcare Guerbet Outline Case-based
Neuroradiological, clinical and genetic characterization of new forms of hereditary leukoencephalopathies
 Neuroradiological, clinical and genetic characterization of new forms of hereditary leukoencephalopathies Principal Investigator: Dr. Donatella Tampieri, MD, FRCPC, Department of Neuroradiology, Montreal
Neuroradiological, clinical and genetic characterization of new forms of hereditary leukoencephalopathies Principal Investigator: Dr. Donatella Tampieri, MD, FRCPC, Department of Neuroradiology, Montreal
The Role of MRI in Multiple Sclerosis
 September 2006 The Role of MRI in Multiple Sclerosis David Cochran, Harvard Medical School Year IV Meet our patient WM 49yoF presents to Multiple Sclerosis Clinic for follow-up regarding worsening symptoms
September 2006 The Role of MRI in Multiple Sclerosis David Cochran, Harvard Medical School Year IV Meet our patient WM 49yoF presents to Multiple Sclerosis Clinic for follow-up regarding worsening symptoms
HYPERTENSIVE ENCEPHALOPATHY
 HYPERTENSIVE ENCEPHALOPATHY Reversible posterior leukoencephalopathy syndrome Cause Renal disease Pheochromocytoma Disseminated vasculitis Eclampsia Acute toxemia Medications & illicit drugs (cocaine)
HYPERTENSIVE ENCEPHALOPATHY Reversible posterior leukoencephalopathy syndrome Cause Renal disease Pheochromocytoma Disseminated vasculitis Eclampsia Acute toxemia Medications & illicit drugs (cocaine)
brain MRI for neuropsychiatrists: what do you need to know
 brain MRI for neuropsychiatrists: what do you need to know Christoforos Stoupis, MD, PhD Department of Radiology, Spital Maennedorf, Zurich & Inselspital, University of Bern, Switzerland c.stoupis@spitalmaennedorf.ch
brain MRI for neuropsychiatrists: what do you need to know Christoforos Stoupis, MD, PhD Department of Radiology, Spital Maennedorf, Zurich & Inselspital, University of Bern, Switzerland c.stoupis@spitalmaennedorf.ch
SHORTLY AFTER ITS FIRST DEpiction
 OBSERVATION Seven-Tesla Magnetic Resonance Imaging New Vision of Microvascular Abnormalities in Multiple Sclerosis Yulin Ge, MD; Vahe M. Zohrabian, MD; Robert I. Grossman, MD Background: Although the role
OBSERVATION Seven-Tesla Magnetic Resonance Imaging New Vision of Microvascular Abnormalities in Multiple Sclerosis Yulin Ge, MD; Vahe M. Zohrabian, MD; Robert I. Grossman, MD Background: Although the role
COPYRIGHT 2012 THE TRANSVERSE MYELITIS ASSOCIATION. ALL RIGHTS RESERVED
 The Transverse Myelitis Association...advocating for those with acute disseminated encephalomyelitis, neuromyelitis optica, optic neuritis and transverse myelitis ACUTE DISSEMINATED ENCEPHALOMYELITIS (ADEM)
The Transverse Myelitis Association...advocating for those with acute disseminated encephalomyelitis, neuromyelitis optica, optic neuritis and transverse myelitis ACUTE DISSEMINATED ENCEPHALOMYELITIS (ADEM)
New Insights on Optic Neuritis in Young People
 Cronicon OPEN ACCESS EC OPHTHALMOLOGY Case Study New Insights on Optic Neuritis in Young People Sergio Carmona 1, Sandra Barbosa 1 and Maria Laura Ortube 2 * 1 Department of Neuro-ophthalmology, Hospital
Cronicon OPEN ACCESS EC OPHTHALMOLOGY Case Study New Insights on Optic Neuritis in Young People Sergio Carmona 1, Sandra Barbosa 1 and Maria Laura Ortube 2 * 1 Department of Neuro-ophthalmology, Hospital
SWI including phase and magnitude images
 On-line Table: MRI imaging recommendation and summary of key features Sequence Pathologies Visible Key Features T1 volumetric high-resolution whole-brain reformatted in axial, coronal, and sagittal planes
On-line Table: MRI imaging recommendation and summary of key features Sequence Pathologies Visible Key Features T1 volumetric high-resolution whole-brain reformatted in axial, coronal, and sagittal planes
CT and MR findings of systemic lupus erythematosus involving the brain: Differential diagnosis based on lesion distribution
 CT and MR findings of systemic lupus erythematosus involving the brain: Differential diagnosis based on lesion distribution Poster No.: C-2723 Congress: ECR 2010 Type: Educational Exhibit Topic: Neuro
CT and MR findings of systemic lupus erythematosus involving the brain: Differential diagnosis based on lesion distribution Poster No.: C-2723 Congress: ECR 2010 Type: Educational Exhibit Topic: Neuro
Idiopathic Inflammatory Demyelinating Diseases of the Brainstem
 Idiopathic Inflammatory Demyelinating Diseases of the Brainstem 1 A. Rovira-Cañellas, 2 A. Rovira-Gols, 1 J. Sastre-Garriga, 1 C. Auger, 1 J. Munuera, 1 X. Montalban 1 Hospital Vall d Hebron, Barcelona.
Idiopathic Inflammatory Demyelinating Diseases of the Brainstem 1 A. Rovira-Cañellas, 2 A. Rovira-Gols, 1 J. Sastre-Garriga, 1 C. Auger, 1 J. Munuera, 1 X. Montalban 1 Hospital Vall d Hebron, Barcelona.
The central nervous system
 Sectc.qxd 29/06/99 09:42 Page 81 Section C The central nervous system CNS haemorrhage Subarachnoid haemorrhage Cerebral infarction Brain atrophy Ring enhancing lesions MRI of the pituitary Multiple sclerosis
Sectc.qxd 29/06/99 09:42 Page 81 Section C The central nervous system CNS haemorrhage Subarachnoid haemorrhage Cerebral infarction Brain atrophy Ring enhancing lesions MRI of the pituitary Multiple sclerosis
Structural and functional imaging for the characterization of CNS lymphomas
 Structural and functional imaging for the characterization of CNS lymphomas Cristina Besada Introduction A few decades ago, Primary Central Nervous System Lymphoma (PCNSL) was considered as an extremely
Structural and functional imaging for the characterization of CNS lymphomas Cristina Besada Introduction A few decades ago, Primary Central Nervous System Lymphoma (PCNSL) was considered as an extremely
NIH Public Access Author Manuscript Arch Neurol. Author manuscript; available in PMC 2008 November 5.
 NIH Public Access Author Manuscript Published in final edited form as: Arch Neurol. 2008 June ; 65(6): 812 816. doi:10.1001/archneur.65.6.812. 7T MRI: New Vision of Microvascular Abnormalities in Multiple
NIH Public Access Author Manuscript Published in final edited form as: Arch Neurol. 2008 June ; 65(6): 812 816. doi:10.1001/archneur.65.6.812. 7T MRI: New Vision of Microvascular Abnormalities in Multiple
Once a vessel is torn, blood accumulating under arterial pressure can dissect the tightly applied dura away from the inner skull surface producing a
 Once a vessel is torn, blood accumulating under arterial pressure can dissect the tightly applied dura away from the inner skull surface producing a hematoma that compresses the brain surface. - Clinically,
Once a vessel is torn, blood accumulating under arterial pressure can dissect the tightly applied dura away from the inner skull surface producing a hematoma that compresses the brain surface. - Clinically,
MRI in MS. MRI in multiple sclerosis. MS T2 Lesions: Pathology. Brain lesions Morphology Matters. Sagittal FLAIR Morphology Matters
 MRI in multiple sclerosis MRI in MS Rohit Bakshi, MD, MA Breakstone Professor of Neurology & Radiology Director, Laboratory for Neuroimaging Research Senior Neurologist, MS Center Brigham & Women s Hospital
MRI in multiple sclerosis MRI in MS Rohit Bakshi, MD, MA Breakstone Professor of Neurology & Radiology Director, Laboratory for Neuroimaging Research Senior Neurologist, MS Center Brigham & Women s Hospital
Actualização no diagnóstico e tratamento das doenças desmielinizantes na infância. Silvia Tenembaum
 Actualização no diagnóstico e tratamento das doenças desmielinizantes na infância Silvia Tenembaum Acquired CNS inflammatory/demyelinating disorders: Background information More frequent in children than
Actualização no diagnóstico e tratamento das doenças desmielinizantes na infância Silvia Tenembaum Acquired CNS inflammatory/demyelinating disorders: Background information More frequent in children than
PRIMARY DISEASES OF MYELIN. By: Shifaa Al Qa qa
 PRIMARY DISEASES OF MYELIN By: Shifaa Al Qa qa Most diseases of myelin are primarily white matter disorders??? Myelinated axons most diseases of CNS myelin do not involve the peripheral nerves to any significant
PRIMARY DISEASES OF MYELIN By: Shifaa Al Qa qa Most diseases of myelin are primarily white matter disorders??? Myelinated axons most diseases of CNS myelin do not involve the peripheral nerves to any significant
The Neurology of HIV Infection. Carolyn Barley Britton, MD, MS Associate Professor of Clinical Neurology Columbia University
 The Neurology of HIV Infection Carolyn Barley Britton, MD, MS Associate Professor of Clinical Neurology Columbia University HIV/AIDS Epidemiology World-wide pandemic, 40 million affected U.S.- Disproportionate
The Neurology of HIV Infection Carolyn Barley Britton, MD, MS Associate Professor of Clinical Neurology Columbia University HIV/AIDS Epidemiology World-wide pandemic, 40 million affected U.S.- Disproportionate
Cerebro-vascular stroke
 Cerebro-vascular stroke CT Terminology Hypodense lesion = lesion of lower density than the normal brain tissue Hyperdense lesion = lesion of higher density than normal brain tissue Isodense lesion = lesion
Cerebro-vascular stroke CT Terminology Hypodense lesion = lesion of lower density than the normal brain tissue Hyperdense lesion = lesion of higher density than normal brain tissue Isodense lesion = lesion
Pearls and Pitfalls in Neuroradiology of Cerebrovascular Disease The Essentials with MR and CT
 Pearls and Pitfalls in Neuroradiology of Cerebrovascular Disease The Essentials with MR and CT Val M. Runge, MD Wendy R. K. Smoker, MD Anton Valavanis, MD Control # 823 Purpose The focus of this educational
Pearls and Pitfalls in Neuroradiology of Cerebrovascular Disease The Essentials with MR and CT Val M. Runge, MD Wendy R. K. Smoker, MD Anton Valavanis, MD Control # 823 Purpose The focus of this educational
Essentials of Clinical MR, 2 nd edition. 51. Primary Neoplasms
 51. Primary Neoplasms As with spinal central canal neoplasms in other regions, those of the lumbar spine may be classified as extradural, intradural extramedullary, and medullary. If an extradural lesion
51. Primary Neoplasms As with spinal central canal neoplasms in other regions, those of the lumbar spine may be classified as extradural, intradural extramedullary, and medullary. If an extradural lesion
Osmotic Demyelination Syndrome Case Report POPOVA RD, KALCHEV EB, VALCHEV GN, KALOYANOVA DV, TENEVA TG, BALEV BD
 Osmotic Demyelination Syndrome Case Report POPOVA RD, KALCHEV EB, VALCHEV GN, KALOYANOVA DV, TENEVA TG, BALEV BD Once upon a time on a Saturday shift u An emergency head CT scan was ordered from the ICU
Osmotic Demyelination Syndrome Case Report POPOVA RD, KALCHEV EB, VALCHEV GN, KALOYANOVA DV, TENEVA TG, BALEV BD Once upon a time on a Saturday shift u An emergency head CT scan was ordered from the ICU
Disease of Myelin. Reid R. Heffner, MD Distinguished Teaching Professor Emeritus Department of Pathology and Anatomy January 9, 2019
 Disease of Myelin Reid R. Heffner, MD Distinguished Teaching Professor Emeritus Department of Pathology and Anatomy January 9, 2019 1 I HAVE NO CONFLICTS OF INTEREST OR DISCLOSURES TO DECLARE. I HAVE NO
Disease of Myelin Reid R. Heffner, MD Distinguished Teaching Professor Emeritus Department of Pathology and Anatomy January 9, 2019 1 I HAVE NO CONFLICTS OF INTEREST OR DISCLOSURES TO DECLARE. I HAVE NO
CADASIL: structural MR imaging changes and apolipoprotein E genotype S E V E N
 CADASIL: structural MR imaging changes and apolipoprotein E genotype S E V E N CADASIL: structural MR imaging changes and apolipoprotein E genotype R. van den Boom S.A.J. Lesnik Oberstein A.A. van den
CADASIL: structural MR imaging changes and apolipoprotein E genotype S E V E N CADASIL: structural MR imaging changes and apolipoprotein E genotype R. van den Boom S.A.J. Lesnik Oberstein A.A. van den
MRI OF THE THALAMUS. Mohammed J. Zafar, MD, FAAN Kalamazoo, MI
 1 MRI OF THE THALAMUS Mohammed J. Zafar, MD, FAAN Kalamazoo, MI Objectives: The thalamic nuclei can be involved in a wide variety of conditions. A systematic imaging approach would be useful for narrowing
1 MRI OF THE THALAMUS Mohammed J. Zafar, MD, FAAN Kalamazoo, MI Objectives: The thalamic nuclei can be involved in a wide variety of conditions. A systematic imaging approach would be useful for narrowing
Dean Shibata, M.D. Department of Radiology, University of Washington. White Matter, Metabolic, and Degenerative Disease.
 White Matter, Metabolic, and Degenerative Disease UW Radiology Review 2015 Dean Shibata, M.D Neuroradiology Department of Radiology, University of Washington MS (Multiple Sclerosis) ADEM (Acute Disseminated
White Matter, Metabolic, and Degenerative Disease UW Radiology Review 2015 Dean Shibata, M.D Neuroradiology Department of Radiology, University of Washington MS (Multiple Sclerosis) ADEM (Acute Disseminated
myelin in the CNS Multiple axons are oligodendrocyte
 Pathologic classification of white matter disorders d Demyelinating - loss of normal myelin autoimmune/inflammatory component Dysmyelinating - loss of chemically abnormal myelin Hypomyelinating - paucity
Pathologic classification of white matter disorders d Demyelinating - loss of normal myelin autoimmune/inflammatory component Dysmyelinating - loss of chemically abnormal myelin Hypomyelinating - paucity
Cerebral malaria: MR imaging spectrum
 Cerebral malaria: MR imaging spectrum Poster No.: C-2705 Congress: ECR 2010 Type: Educational Exhibit Topic: Neuro Authors: P. S. Naphade, M. D. Agrawal, S. S. Sankhe, K. M. Siva, B. K. Jain; Mumbai/IN
Cerebral malaria: MR imaging spectrum Poster No.: C-2705 Congress: ECR 2010 Type: Educational Exhibit Topic: Neuro Authors: P. S. Naphade, M. D. Agrawal, S. S. Sankhe, K. M. Siva, B. K. Jain; Mumbai/IN
Attenuation value in HU From -500 To HU From -10 To HU From 60 To 90 HU. From 200 HU and above
 Brain Imaging Common CT attenuation values Structure Air Fat Water Brain tissue Recent hematoma Calcifications Bone Brain edema and infarction Normal liver parenchyma Attenuation value in HU From -500
Brain Imaging Common CT attenuation values Structure Air Fat Water Brain tissue Recent hematoma Calcifications Bone Brain edema and infarction Normal liver parenchyma Attenuation value in HU From -500
Pediatric MS MRI Study Methodology
 General Pediatric MS MRI Study Methodology SCAN PREPARATION axial T2-weighted scans and/or axial FLAIR scans were obtained for all subjects when available, both T2 and FLAIR scans were scored. In order
General Pediatric MS MRI Study Methodology SCAN PREPARATION axial T2-weighted scans and/or axial FLAIR scans were obtained for all subjects when available, both T2 and FLAIR scans were scored. In order
Characteristic features of CNS pathology. By: Shifaa AlQa qa
 Characteristic features of CNS pathology By: Shifaa AlQa qa Normal brain: - The neocortex (gray matter): six layers: outer plexiform, outer granular, outer pyramidal, inner granular, inner pyramidal, polymorphous
Characteristic features of CNS pathology By: Shifaa AlQa qa Normal brain: - The neocortex (gray matter): six layers: outer plexiform, outer granular, outer pyramidal, inner granular, inner pyramidal, polymorphous
Masses of the Corpus Callosum
 Masses of the Corpus Callosum Kesav Raghavan, HMS Year III Dr. Agenda Corpus Callosum Development and Anatomy Our Patient: Clinical Presentation Differential Diagnosis of Masses in the Corpus Callosum
Masses of the Corpus Callosum Kesav Raghavan, HMS Year III Dr. Agenda Corpus Callosum Development and Anatomy Our Patient: Clinical Presentation Differential Diagnosis of Masses in the Corpus Callosum
Index. aneurysm, 92 carotid occlusion, 94 ICA stenosis, 95 intracranial, 92 MCA, 94
 A ADC. See Apparent diffusion coefficient (ADC) Aneurysm cerebral artery aneurysm, 93 CT scan, 93 gadolinium, 93 Angiography, 13 Anoxic brain injury, 25 Apparent diffusion coefficient (ADC), 7 Arachnoid
A ADC. See Apparent diffusion coefficient (ADC) Aneurysm cerebral artery aneurysm, 93 CT scan, 93 gadolinium, 93 Angiography, 13 Anoxic brain injury, 25 Apparent diffusion coefficient (ADC), 7 Arachnoid
Benign brain lesions
 Benign brain lesions Diagnostic and Interventional Radiology Hung-Wen Kao Department of Radiology, Tri-Service General Hospital, National Defense Medical Center Computed tomography Hounsfield unit (HU)
Benign brain lesions Diagnostic and Interventional Radiology Hung-Wen Kao Department of Radiology, Tri-Service General Hospital, National Defense Medical Center Computed tomography Hounsfield unit (HU)
Role of MRI in acute disseminated encephalomyelitis
 Original Research Article Role of MRI in acute disseminated encephalomyelitis Shashvat Modiya 1*, Jayesh Shah 2, C. Raychaudhuri 3 1 1 st year resident, 2 Associate Professor, 3 HOD and Professor Department
Original Research Article Role of MRI in acute disseminated encephalomyelitis Shashvat Modiya 1*, Jayesh Shah 2, C. Raychaudhuri 3 1 1 st year resident, 2 Associate Professor, 3 HOD and Professor Department
Diffusion-Weighted and Conventional MR Imaging Findings of Neuroaxonal Dystrophy
 AJNR Am J Neuroradiol 25:1269 1273, August 2004 Diffusion-Weighted and Conventional MR Imaging Findings of Neuroaxonal Dystrophy R. Nuri Sener BACKGROUND AND PURPOSE: Neuroaxonal dystrophy is a rare progressive
AJNR Am J Neuroradiol 25:1269 1273, August 2004 Diffusion-Weighted and Conventional MR Imaging Findings of Neuroaxonal Dystrophy R. Nuri Sener BACKGROUND AND PURPOSE: Neuroaxonal dystrophy is a rare progressive
MULTIPLE SCLEROSIS Update
 MULTIPLE SCLEROSIS Update E. Torage Shivapour, M.D. Clinical Professor Department of Neurology University of Iowa Hospitals & Clinics Disclosures I do not have any disclosures. Multiple Sclerosis Most
MULTIPLE SCLEROSIS Update E. Torage Shivapour, M.D. Clinical Professor Department of Neurology University of Iowa Hospitals & Clinics Disclosures I do not have any disclosures. Multiple Sclerosis Most
Head CT Scan Interpretation: A Five-Step Approach to Seeing Inside the Head Lawrence B. Stack, MD
 Head CT Scan Interpretation: A Five-Step Approach to Seeing Inside the Head Lawrence B. Stack, MD Five Step Approach 1. Adequate study 2. Bone windows 3. Ventricles 4. Quadrigeminal cistern 5. Parenchyma
Head CT Scan Interpretation: A Five-Step Approach to Seeing Inside the Head Lawrence B. Stack, MD Five Step Approach 1. Adequate study 2. Bone windows 3. Ventricles 4. Quadrigeminal cistern 5. Parenchyma
Detection of Leptomeningeal CNS Metastases in Children
 Detection of Leptomeningeal CNS Metastases in Children Noah D. Sabin, M.D. Julie H. Harreld M.D. Kathleen J. Helton M.D. Zoltan Patay M.D., Ph.D. St. Jude Children s Research Hospital Memphis, TN Leptomeningeal
Detection of Leptomeningeal CNS Metastases in Children Noah D. Sabin, M.D. Julie H. Harreld M.D. Kathleen J. Helton M.D. Zoltan Patay M.D., Ph.D. St. Jude Children s Research Hospital Memphis, TN Leptomeningeal
Neuroradiology of AIDS
 Neuroradiology of AIDS Frank Minja,, HMS IV Gillian Lieberman MD September 2002 AIDS 90% of HIV patients have CNS involvement 1 10% of AIDS patients present first with neurological symptoms 2 73-80% of
Neuroradiology of AIDS Frank Minja,, HMS IV Gillian Lieberman MD September 2002 AIDS 90% of HIV patients have CNS involvement 1 10% of AIDS patients present first with neurological symptoms 2 73-80% of
2. Subarachnoid Hemorrhage
 Causes: 2. Subarachnoid Hemorrhage A. Saccular (berry) aneurysm - Is the most frequent cause of clinically significant subarachnoid hemorrhage is rupture of a saccular (berry) aneurysm. B. Vascular malformation
Causes: 2. Subarachnoid Hemorrhage A. Saccular (berry) aneurysm - Is the most frequent cause of clinically significant subarachnoid hemorrhage is rupture of a saccular (berry) aneurysm. B. Vascular malformation
NEURO IMAGING OF ACUTE STROKE
 1 1 NEURO IMAGING OF ACUTE STROKE ALICIA RICHARDSON, MSN, RN, ACCNS-AG, ANVP-BC WENDY SMITH, MA, RN, MBA, SCRN, FAHA LYNN HUNDLEY, APRN, CNRN, CCNS, ANVP-BC 2 2 1 DISCLOSURES Alicia Richardson: Stryker
1 1 NEURO IMAGING OF ACUTE STROKE ALICIA RICHARDSON, MSN, RN, ACCNS-AG, ANVP-BC WENDY SMITH, MA, RN, MBA, SCRN, FAHA LYNN HUNDLEY, APRN, CNRN, CCNS, ANVP-BC 2 2 1 DISCLOSURES Alicia Richardson: Stryker
Acute Disseminated Encephalomyelitis Presenting as Rhombencephalitis: An Atypical Case Presentation
 pissn 2384-1095 eissn 2384-1109 imri 2015;19:186-190 http://dx.doi.org/10.13104/imri.2015.19.3.186 Acute Disseminated Encephalomyelitis Presenting as Rhombencephalitis: An Atypical Case Presentation Joonseok
pissn 2384-1095 eissn 2384-1109 imri 2015;19:186-190 http://dx.doi.org/10.13104/imri.2015.19.3.186 Acute Disseminated Encephalomyelitis Presenting as Rhombencephalitis: An Atypical Case Presentation Joonseok
1 Normal Anatomy and Variants
 1 Normal Anatomy and Variants 1.1 Normal Anatomy MR Technique. e standard MR protocol for a routine evaluation of the spine always comprises imaging in sagittal and axial planes, while coronal images are
1 Normal Anatomy and Variants 1.1 Normal Anatomy MR Technique. e standard MR protocol for a routine evaluation of the spine always comprises imaging in sagittal and axial planes, while coronal images are
Demyelinating Diseases: Multiple Sclerosis January 10, 2018 Dr. Ostrow
 Demyelinating Diseases: Multiple Sclerosis January 10, 2018 Dr. Ostrow Reading: Robbins & Cotran, 9 th edition, pp 1283-1286 Robbins Basic Pathology, 9 th edition, 832-835 Overview: Grossly, myelin is
Demyelinating Diseases: Multiple Sclerosis January 10, 2018 Dr. Ostrow Reading: Robbins & Cotran, 9 th edition, pp 1283-1286 Robbins Basic Pathology, 9 th edition, 832-835 Overview: Grossly, myelin is
The Low Sensitivity of Fluid-Attenuated Inversion-Recovery MR in the Detection of Multiple Sclerosis of the Spinal Cord
 The Low Sensitivity of Fluid-Attenuated Inversion-Recovery MR in the Detection of Multiple Sclerosis of the Spinal Cord Mark D. Keiper, Robert I. Grossman, John C. Brunson, and Mitchell D. Schnall PURPOSE:
The Low Sensitivity of Fluid-Attenuated Inversion-Recovery MR in the Detection of Multiple Sclerosis of the Spinal Cord Mark D. Keiper, Robert I. Grossman, John C. Brunson, and Mitchell D. Schnall PURPOSE:
NEURO IMAGING 2. Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity
 NEURO IMAGING 2 Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity I. EPIDURAL HEMATOMA (EDH) LOCATION Seventy to seventy-five percent occur in temporoparietal region. CAUSE Most likely caused
NEURO IMAGING 2 Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity I. EPIDURAL HEMATOMA (EDH) LOCATION Seventy to seventy-five percent occur in temporoparietal region. CAUSE Most likely caused
Automated Identification of Neoplasia in Diagnostic Imaging text reports
 Automated Identification of Neoplasia in Diagnostic Imaging text reports "This work has been funded in whole or in part with Federal funds from the National Cancer Institute, National Institutes of Health,
Automated Identification of Neoplasia in Diagnostic Imaging text reports "This work has been funded in whole or in part with Federal funds from the National Cancer Institute, National Institutes of Health,
multiple sclerosis by magnetic resonance imaging
 Index terms: Computed tomography Magnetic resonance sequence optimization Multiple sclerosis The evaluation of multiple sclerosis by magnetic resonance imaging Val M. Runge, M.D.*1 4, Ann C. Price, M.D.*
Index terms: Computed tomography Magnetic resonance sequence optimization Multiple sclerosis The evaluation of multiple sclerosis by magnetic resonance imaging Val M. Runge, M.D.*1 4, Ann C. Price, M.D.*
MR neuroimaging of HIV infected patients : A pictorial review
 MR neuroimaging of HIV infected patients : A pictorial review Poster No.: R-0198 Congress: 2014 CSM Type: Scientific Exhibit Authors: P. F. Kwan, R. Thomas, A. Dixon; SOUTH YARRA/AU Keywords: Neuroradiology
MR neuroimaging of HIV infected patients : A pictorial review Poster No.: R-0198 Congress: 2014 CSM Type: Scientific Exhibit Authors: P. F. Kwan, R. Thomas, A. Dixon; SOUTH YARRA/AU Keywords: Neuroradiology
Toxins in Brain! Magnetic Resonance (MR) Imaging of Toxic Leukoencephalopathy A Pictorial Essay
 Signature: Pol J Radiol, 2017; 82: 311-319 DOI: 10.12659/PJR.901791 REVIEW ARTICLE Received: 2016.10.02 Accepted: 2016.10.11 Published: 2017.06.13 Authors Contribution: A Study Design B Data Collection
Signature: Pol J Radiol, 2017; 82: 311-319 DOI: 10.12659/PJR.901791 REVIEW ARTICLE Received: 2016.10.02 Accepted: 2016.10.11 Published: 2017.06.13 Authors Contribution: A Study Design B Data Collection
TOXIC AND NUTRITIONAL DISORDER MODULE
 TOXIC AND NUTRITIONAL DISORDER MODULE Objectives: For each of the following entities the student should be able to: 1. Describe the etiology/pathogenesis and/or pathophysiology, gross and microscopic morphology
TOXIC AND NUTRITIONAL DISORDER MODULE Objectives: For each of the following entities the student should be able to: 1. Describe the etiology/pathogenesis and/or pathophysiology, gross and microscopic morphology
RINGS N THINGS: Imaging Patterns in Differential Diagnosis. Anne G. Osborn, M.D.
 RINGS N THINGS: Imaging Patterns in Differential Diagnosis Anne G. Osborn, M.D. ExpDDxs: Intra-axial (Parenchymal) Lesions Ring-enhancing lesions, solitary 1 Ring-enhancing lesion crossing corpus callosum
RINGS N THINGS: Imaging Patterns in Differential Diagnosis Anne G. Osborn, M.D. ExpDDxs: Intra-axial (Parenchymal) Lesions Ring-enhancing lesions, solitary 1 Ring-enhancing lesion crossing corpus callosum
Keep Imaging Simple: An Introduction To Neuroimaging
 Keep Imaging Simple: An Introduction To Neuroimaging Meghan Elkins, OD, FAAO Please silence all mobile devices and remove items from chairs so others can sit. Unauthorized recording of this session is
Keep Imaging Simple: An Introduction To Neuroimaging Meghan Elkins, OD, FAAO Please silence all mobile devices and remove items from chairs so others can sit. Unauthorized recording of this session is
PRESERVE: How intensively should we treat blood pressure in established cerebral small vessel disease? Guide to assessing MRI scans
 PRESERVE: How intensively should we treat blood pressure in established cerebral small vessel disease? Guide to assessing MRI scans Inclusion Criteria Clinical syndrome Patients must have clinical evidence
PRESERVE: How intensively should we treat blood pressure in established cerebral small vessel disease? Guide to assessing MRI scans Inclusion Criteria Clinical syndrome Patients must have clinical evidence
Acute stroke. Ischaemic stroke. Characteristics. Temporal classification. Clinical features. Interpretation of Emergency Head CT
 Ischaemic stroke Characteristics Stroke is the third most common cause of death in the UK, and the leading cause of disability. 80% of strokes are ischaemic Large vessel occlusive atheromatous disease
Ischaemic stroke Characteristics Stroke is the third most common cause of death in the UK, and the leading cause of disability. 80% of strokes are ischaemic Large vessel occlusive atheromatous disease
RING ENCHANCING LESION BY M.S. HEMHNATH
 RING ENCHANCING LESION BY M.S. HEMHNATH A 21 YRS FEMALE CAME WITH H/O HEADACHE AND SEIZURE FOR THE PAST ONE MONTH. NO OTHER FOCAL NEUROLOGICAL DEFICIT. DIFFERENTIAL DIAGNOSIS For this case are Neurocysticerosis
RING ENCHANCING LESION BY M.S. HEMHNATH A 21 YRS FEMALE CAME WITH H/O HEADACHE AND SEIZURE FOR THE PAST ONE MONTH. NO OTHER FOCAL NEUROLOGICAL DEFICIT. DIFFERENTIAL DIAGNOSIS For this case are Neurocysticerosis
Gross Organization I The Brain. Reading: BCP Chapter 7
 Gross Organization I The Brain Reading: BCP Chapter 7 Layout of the Nervous System Central Nervous System (CNS) Located inside of bone Includes the brain (in the skull) and the spinal cord (in the backbone)
Gross Organization I The Brain Reading: BCP Chapter 7 Layout of the Nervous System Central Nervous System (CNS) Located inside of bone Includes the brain (in the skull) and the spinal cord (in the backbone)
Neuropathology lecture series. III. Neuropathology of Cerebrovascular Disease. Physiology of cerebral blood flow
 Neuropathology lecture series III. Neuropathology of Cerebrovascular Disease Physiology of cerebral blood flow Brain makes up only 2% of body weight Percentage of cardiac output: 15-20% Percentage of O
Neuropathology lecture series III. Neuropathology of Cerebrovascular Disease Physiology of cerebral blood flow Brain makes up only 2% of body weight Percentage of cardiac output: 15-20% Percentage of O
PRIMARY DISEASES OF MYELIN
 PRIMARY DISEASES OF MYELIN Acquired forms - Characterized by preferential damage to previously normal myelin with relative preservation of axons and include: 1. Immune-mediated injury, such as multiple
PRIMARY DISEASES OF MYELIN Acquired forms - Characterized by preferential damage to previously normal myelin with relative preservation of axons and include: 1. Immune-mediated injury, such as multiple
Imaging of Multiple Sclerosis: Role in Neurotherapeutics
 NeuroRx : The Journal of the American Society for Experimental NeuroTherapeutics Imaging of Multiple Sclerosis: Role in Neurotherapeutics Rohit Bakshi,* Alireza Minagar, Zeenat Jaisani,* and Jerry S. Wolinsky
NeuroRx : The Journal of the American Society for Experimental NeuroTherapeutics Imaging of Multiple Sclerosis: Role in Neurotherapeutics Rohit Bakshi,* Alireza Minagar, Zeenat Jaisani,* and Jerry S. Wolinsky
Tony Traboulsee, MD Associate Professor (Medicine/Neurology) Head, UBC MS and NMO Programs. MRI Diagnostic Red Flags
 Tony Traboulsee, MD Associate Professor (Medicine/Neurology) Head, UBC MS and NMO Programs MRI Diagnostic Red Flags UBC MS and NMO Research Programs LEARNING OBJECTIVES By the end of this presentation,
Tony Traboulsee, MD Associate Professor (Medicine/Neurology) Head, UBC MS and NMO Programs MRI Diagnostic Red Flags UBC MS and NMO Research Programs LEARNING OBJECTIVES By the end of this presentation,
CNS pathology Third year medical students. Dr Heyam Awad 2018 Lecture 4: Myelin diseases of the CNS
 CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 4: Myelin diseases of the CNS ILOS 1. to understand differences and similarities between diseases of myelin in CNS and PNS. 2. to understand
CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 4: Myelin diseases of the CNS ILOS 1. to understand differences and similarities between diseases of myelin in CNS and PNS. 2. to understand
Common and uncommon differential diagnosis of cerebral microhemorrhages
 Common and uncommon differential diagnosis of cerebral microhemorrhages Poster No.: C-0261 Congress: ECR 2014 Type: Educational Exhibit Authors: T. C. Rodrigues 1, S. B. Bergamaschi 1, C. F. R. B. Milito
Common and uncommon differential diagnosis of cerebral microhemorrhages Poster No.: C-0261 Congress: ECR 2014 Type: Educational Exhibit Authors: T. C. Rodrigues 1, S. B. Bergamaschi 1, C. F. R. B. Milito
Vascular Malformations of the Brain: A Review of Imaging Features and Risks
 Vascular Malformations of the Brain: A Review of Imaging Features and Risks Comprehensive Neuroradiology: Best Practices October 27-30, 2016 Sudhakar R. Satti, MD Associate Director Neurointerventional
Vascular Malformations of the Brain: A Review of Imaging Features and Risks Comprehensive Neuroradiology: Best Practices October 27-30, 2016 Sudhakar R. Satti, MD Associate Director Neurointerventional
Imaging in a confused patient: Infections and Inflammation
 American Society of Neuroimaging Imaging in a confused patient: Infections and Inflammation January 21, 2017 Los Angeles, California Joshua P. Klein, MD, PhD, FANA, FAAN, FASN Chief, Division of Hospital
American Society of Neuroimaging Imaging in a confused patient: Infections and Inflammation January 21, 2017 Los Angeles, California Joshua P. Klein, MD, PhD, FANA, FAAN, FASN Chief, Division of Hospital
The MRI Appearance of Tumefactive Demyelinating Lesions
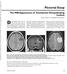 ownloaded from www.ajronline.org by 37.44.198.148 on 12/05/17 from IP address 37.44.198.148. opyright RRS. For personal use only; all rights reserved The MRI ppearance of Tumefactive emyelinating Lesions
ownloaded from www.ajronline.org by 37.44.198.148 on 12/05/17 from IP address 37.44.198.148. opyright RRS. For personal use only; all rights reserved The MRI ppearance of Tumefactive emyelinating Lesions
Cerebrovascular diseases-2
 Cerebrovascular diseases-2 Primary angiitis of CNS - Other causes of infarction i. Hypercoagulable states ii. Drug-abuse such as amphetamine, heroin and cocain Note - The venous side of the circulation
Cerebrovascular diseases-2 Primary angiitis of CNS - Other causes of infarction i. Hypercoagulable states ii. Drug-abuse such as amphetamine, heroin and cocain Note - The venous side of the circulation
Patient with vertigo, dizziness and depression
 Clinical Case - Test Yourself Neuro/Head and Neck Radiology Patient with vertigo, dizziness and depression Michael Mantatzis, Paraskevi Argyropoulou, Panos Prassopoulos Radiology Department, Democritus
Clinical Case - Test Yourself Neuro/Head and Neck Radiology Patient with vertigo, dizziness and depression Michael Mantatzis, Paraskevi Argyropoulou, Panos Prassopoulos Radiology Department, Democritus
ANATOMY & PHYSIOLOGY DISSECTION OF THE SHEEP BRAIN LAB GROUP:
 ANATOMY & PHYSIOLOGY DISSECTION OF THE SHEEP BRAIN LAB GROUP: Introduction The purpose of the sheep brain dissection is to familiarize you with the three dimensional structure of the brain and teach you
ANATOMY & PHYSIOLOGY DISSECTION OF THE SHEEP BRAIN LAB GROUP: Introduction The purpose of the sheep brain dissection is to familiarize you with the three dimensional structure of the brain and teach you
Pathologic Analysis of CNS Surgical Specimens
 2015 Kenneth M. Earle Memorial Neuropathology Review Pathologic Analysis of CNS Surgical Specimens Peter C. Burger, MD Interdisciplinary Quality Control Familiarity with entities Use of diagnostic algorithm
2015 Kenneth M. Earle Memorial Neuropathology Review Pathologic Analysis of CNS Surgical Specimens Peter C. Burger, MD Interdisciplinary Quality Control Familiarity with entities Use of diagnostic algorithm
Five Most Common Problems in Surgical Neuropathology
 Five Most Common Problems in Surgical Neuropathology If the brain were so simple that we could understand it, we would be so simple that we couldn t Emerson Pugh What is your greatest difficulty in neuropathology?
Five Most Common Problems in Surgical Neuropathology If the brain were so simple that we could understand it, we would be so simple that we couldn t Emerson Pugh What is your greatest difficulty in neuropathology?
RADIOLOGY TEACHING CONFERENCE
 RADIOLOGY TEACHING CONFERENCE John Athas, MD Monica Tadros, MD Columbia University, College of Physicians & Surgeons Department of Otolaryngology- Head & Neck Surgery September 27, 2007 CT SCAN IMAGING
RADIOLOGY TEACHING CONFERENCE John Athas, MD Monica Tadros, MD Columbia University, College of Physicians & Surgeons Department of Otolaryngology- Head & Neck Surgery September 27, 2007 CT SCAN IMAGING
Department of Cognitive Science UCSD
 Department of Cognitive Science UCSD Verse 1: Neocortex, frontal lobe, Brain stem, brain stem, Hippocampus, neural node, Right hemisphere, Pons and cortex visual, Brain stem, brain stem, Sylvian fissure,
Department of Cognitive Science UCSD Verse 1: Neocortex, frontal lobe, Brain stem, brain stem, Hippocampus, neural node, Right hemisphere, Pons and cortex visual, Brain stem, brain stem, Sylvian fissure,
MRI Atlas of MS Lesions
 MRI Atlas of MS Lesions M. A. Sahraian, E.-W. Radue MRI Atlas of MS Lesions With the collaboration of A. Gass, S. Haller, L. Kappos, J. Kesselring, J.-I. Kira, K. Weier 123 Prof. Dr. med. Mohammad Ali
MRI Atlas of MS Lesions M. A. Sahraian, E.-W. Radue MRI Atlas of MS Lesions With the collaboration of A. Gass, S. Haller, L. Kappos, J. Kesselring, J.-I. Kira, K. Weier 123 Prof. Dr. med. Mohammad Ali
CNS pathology Third year medical students. Dr Heyam Awad 2018 Lecture 7: Non traumatic brain haemorrhage
 CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 7: Non traumatic brain haemorrhage ILOS To list the causes of intracranial haemorrhage. To understand the pathogenesis of each cause.
CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 7: Non traumatic brain haemorrhage ILOS To list the causes of intracranial haemorrhage. To understand the pathogenesis of each cause.
CNS pathology Third year medical students. Dr Heyam Awad 2018 Lecture 5: disturbed fluid balance and increased intracranial pressure
 CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 5: disturbed fluid balance and increased intracranial pressure ILOs Understand causes and symptoms of increased intracranial pressure.
CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 5: disturbed fluid balance and increased intracranial pressure ILOs Understand causes and symptoms of increased intracranial pressure.
Magnetic Resonance Imaging and Spectroscopy: Insights into the Pathology and Pathophysiology of Multiple Sclerosis.
 Chapter 10 (pp 139-167) of Multiple Sclerosis 2 - Blue Books of Practical Neurology, vol. 27. J.H Noseworthy, W.I. McDonald (eds.). Elsevier Science (USA), 2003. Magnetic Resonance Imaging and Spectroscopy:
Chapter 10 (pp 139-167) of Multiple Sclerosis 2 - Blue Books of Practical Neurology, vol. 27. J.H Noseworthy, W.I. McDonald (eds.). Elsevier Science (USA), 2003. Magnetic Resonance Imaging and Spectroscopy:
MRI and CT of the CNS
 MRI and CT of the CNS Dr.Maha ELBeltagy Assistant Professor of Anatomy Faculty of Medicine The University of Jordan 2018 Computed Tomography CT is used for the detection of intracranial lesions. CT relies
MRI and CT of the CNS Dr.Maha ELBeltagy Assistant Professor of Anatomy Faculty of Medicine The University of Jordan 2018 Computed Tomography CT is used for the detection of intracranial lesions. CT relies
V. CENTRAL NERVOUS SYSTEM TRAUMA
 V. CENTRAL NERVOUS SYSTEM TRAUMA I. Concussion - Is a clinical syndrome of altered consiousness secondary to head injury - Brought by a change in the momentum of the head when a moving head suddenly arrested
V. CENTRAL NERVOUS SYSTEM TRAUMA I. Concussion - Is a clinical syndrome of altered consiousness secondary to head injury - Brought by a change in the momentum of the head when a moving head suddenly arrested
Peripheral neuropathies, neuromuscular junction disorders, & CNS myelin diseases
 Peripheral neuropathies, neuromuscular junction disorders, & CNS myelin diseases Peripheral neuropathies according to which part affected Axonal Demyelinating with axonal sparing Many times: mixed features
Peripheral neuropathies, neuromuscular junction disorders, & CNS myelin diseases Peripheral neuropathies according to which part affected Axonal Demyelinating with axonal sparing Many times: mixed features
Blood Supply of the CNS
 Blood Supply of the CNS Lecture Objectives Describe the four arteries supplying the CNS. Follow up each artery to its destination. Describe the circle of Willis and its branches. Discuss the principle
Blood Supply of the CNS Lecture Objectives Describe the four arteries supplying the CNS. Follow up each artery to its destination. Describe the circle of Willis and its branches. Discuss the principle
Histology of the CNS
 Histology of the CNS Lecture Objectives Describe the histology of the cerebral cortex layers. Describe the histological features of the cerebellum; layers and cells of cerebellar cortex. Describe the elements
Histology of the CNS Lecture Objectives Describe the histology of the cerebral cortex layers. Describe the histological features of the cerebellum; layers and cells of cerebellar cortex. Describe the elements
C. Douglas Phillips, MD FACR Director of Head and Neck Imaging Weill Cornell Medical College NewYork-Presbyterian Hospital
 C. Douglas Phillips, MD FACR Director of Head and Neck Imaging Weill Cornell Medical College NewYork-Presbyterian Hospital I have no financial disclosures Understand range of pathology that may present
C. Douglas Phillips, MD FACR Director of Head and Neck Imaging Weill Cornell Medical College NewYork-Presbyterian Hospital I have no financial disclosures Understand range of pathology that may present
Diffusion-weighted magnetic resonance imaging (MRI) allows for tissue
 MAGNETIC RESONANCE IMAGING / IMAGERIE PAR RÉSONANCE MAGNÉTIQUE Nonischemic causes of hyperintense signals on diffusion-weighted magnetic resonance images: a pictorial essay Jeffrey M. Hinman, MD; James
MAGNETIC RESONANCE IMAGING / IMAGERIE PAR RÉSONANCE MAGNÉTIQUE Nonischemic causes of hyperintense signals on diffusion-weighted magnetic resonance images: a pictorial essay Jeffrey M. Hinman, MD; James
Magnetic Resonance Imaging. Basics of MRI in practice. Generation of MR signal. Generation of MR signal. Spin echo imaging. Generation of MR signal
 Magnetic Resonance Imaging Protons aligned with B0 magnetic filed Longitudinal magnetization - T1 relaxation Transverse magnetization - T2 relaxation Signal measured in the transverse plane Basics of MRI
Magnetic Resonance Imaging Protons aligned with B0 magnetic filed Longitudinal magnetization - T1 relaxation Transverse magnetization - T2 relaxation Signal measured in the transverse plane Basics of MRI
