Orbit and Sellar Region
|
|
|
- Georgina Osborne
- 5 years ago
- Views:
Transcription
1 Orbit and Sellar Region 2 Francisco de Asís Bravo-Rodríguez and Rocío Díaz-Aguilera Contents Case 1 Choroidal Melanoma Case 2 Grave s Ophthalmopathy Case 3 Inflammatory Pseudotumor of the Orbit Case 4 Orbital Hemangioma Case 5 Orbital Lymphoma Case 6 Optic Nerve Sheath Meningioma Case 7 Craniopharyngioma Case 8 Hypothalamic Hamartoma Case 9 Pituitary Adenoma Case 10 Rathke s Cleft Cyst F. de Asís Bravo-Rodríguez et al. (eds.), Learning Neuroimaging, Learning Imaging, DOI / _2, Springer-Verlag Berlin Heidelberg 2012
2 24 Francisco de Asís Bravo-Rodríguez and Rocío Díaz-Aguilera Case 1 History A 51-year-old man presented with a several-month history of progressive visual loss in the right eye. On ophthalmologic examination, an intraocular mass was found. Choroidal Melanoma a Comments Malignant melanomas are the most common primary intraocular tumors in adults. Nevertheless, these lesions are infrequent. The tumor arises from melanocytes within the choroid. Choroidal melanoma have race predominance, and most often affect white people while incidence among blacks is extremely rare. Median age is 55 years. Choroidal melanomas may have variable coloration, ranging from amelanotic to darkly pigmented, and are typically circumscribed, domed-shaped masses that grow to the vitreous cavity. Choroidal melanoma may metastasize before diagnosis. The tumor can spread hematogenously to the liver, lung, bone, skin, and the central nervous system (CNS). b c d Fig. 2.1
3 Orbit and Sellar Region 25 Choroidal melanomas usually remain asymptomatic for long time and the diagnosis is made incidentally during a routine ophthalmologic examination. In general, the more anterior their origin, the longer the delay of any symptoms. As the tumor grows, it may become symptomatic. The most common clinical presentation is painless visual loss with decreased visual acuity and visual field defects. Because of their anatomic location, choroidal tumors are not accessible to biopsy without intraocular surgery. Consequently, the diagnosis must be made on the basis of clinical examination in conjunction with different diagnostic modalities such as ultrasound, computed tomography (CT), magnetic resonance imaging (MRI), and angiography. Lesions more than 3 mm in size are usually well detected on CT and MRI, whereas smaller lesions are better evaluated with ultrasound. The accurate technique to diagnose the tumor and to determine its size is ultrasound. On B-scan mode, intraocular melanoma appears as a rounded or mushroom-shaped hypoechoic mass that produces excavation of underlying uveal tissue and shadowing of subjacent soft tissues. A thin hyperechoic rim is sometimes seen and represents a combination of elevated retina and peripheral blood vessels. These tumors are very vascular lesions. Color Doppler ultrasound allows evaluating the tumor vascularization both internally and in the periphery. This tumor characteristic is useful to differentiate choroidal melanoma from other non-neoplastic entities such as subretinal hemorrhage. Ultrasound may also detect some complications of the tumor as retinal elevation and vitreous hemorrhage. CT scan is more useful than ultrasound to evaluate extraocular extension and may help differentiate between choroidal or retinal detachment and a solid tumor. After contrast material administration, choroidal melanoma shows moderate enhancement. CT scan also is sensitive in detecting calcium, a feature of some tumors different from uveal melanomas (characteristically choroidal osteoma). On MRI, most choroidal melanomas appear as areas of high signal intensity on T1- and proton density-weighted MR images, due to the paramagnetic property of melanin, and moderately low signal intensity on T2-WI. The tumor demonstrates moderate enhancement after intravenous gadolinium injection. Documented growth of a lesion on serial examinations is the most important clinical feature favoring the diagnosis of a choroidal melanoma. Differential diagnosis must be made with retinal detachment, choroidal detachment, choroidal metastasis, choroidal hemangioma, and large choroidal nevus. Treatment depends on several factors such as visual acuity, size of tumor, age of the patient, and presence of metastases. Small tumors can be managed by periodic observation. In cases of tumor growth and in large and/or complicated tumors which compromise visual function, enucleation is indicated. Nevertheless, enucleation does not prevent metastasis. MRI study demonstrates a lobulated mass located in nasal aspect of the right ocular globe. The lesion appears slightly hyperintense to vitreous humor on axial T1-weighted image (Fig. 2.1a ) and hypointense on coronal STIR sequence (Fig. 2.1b ). A hyperintense rim surrounded the mass can be seen on T1-WI, which represents a retinal detachment ( arrow in Fig. 2.1a ). Contrast-enhanced fat-saturation T1-weighted image (Fig. 2.1c ) and contrastenhanced spin-echo T1-WI (Fig. 2.1d ) show homogeneous enhancement of the lesion. Imaging Findings
4 26 Francisco de Asís Bravo-Rodríguez and Rocío Díaz-Aguilera Case 2 Grave s Ophthalmopathy History A 57-year-old man presented with bilateral exophthalmos and eyelid swelling. On ophthalmologic examination, diplopia, visual acuity loss on the right eye, and right papilledema were found. a c b Fig. 2.2
5 Orbit and Sellar Region 27 Grave s ophthalmopathy (GO) is a thyroid-associated orbitopathy that represents a part of Grave s disease, an autoimmune process that can affect the orbital and periorbital tissue, the thyroid gland, and, rarely, the pretibial skin or digits (thyroid acropachy). Eye involvement in Grave s disease is clinically evident in 25 50% of patients. GO may precede, coincide, or follow the systemic complications of dysthyroidism. The underlying pathophysiology of GO is thought to be an antibody-mediated reaction against the TSH receptors present in retrobulbar tissue. There is a lymphocytic infiltration of the orbital tissue that causes edema in the extraocular muscles and transformation of preadipocyte fibroblasts into adipocytes. The enlargement of extraocular muscles in conjunction with the orbital fat accumulation produce an increase in orbital volume causing exophthalmos and, occasionally, optic nerve compression at the narrow posterior apex of the orbit. The edema results in tissue damage and fibrosis, with restriction in extraocular motility and lagophthalmos. GO is the most common cause of unilateral and bilateral proptosis in adults. GO usually occurs in patients aged years and is much more common in females, although severe cases occur more often in males. The ocular manifestations of GO include eyelid swelling or retraction, chemosis, tearing, corneal erosions or ulcerations, abnormal eye motility, exophthalmos, and periorbital edema. Although most cases of GO do not result in visual loss, GO can cause visionthreatening exposure keratopathy, troublesome diplopia, and compressive optic neuropathy. In typical cases, the diagnosis can be established clinically and imaging studies are not necessary. Orbital imaging is recommended in cases of very asymmetrical clinical picture and in cases of clinical suspicion of optic nerve involvement. Imaging techniques include ultrasound, CT, and MRI. Orbital ultrasound can quickly confirm if the patient has thickened muscles or an enlarged superior ophthalmic vein. CT and MRI, with both axial and coronal views, usually reveal thick muscles with tendon sparing. The inferior rectus muscle and the medial rectus muscle are usually involved. Bilateral muscle enlargement is common; unilateral cases usually represent asymmetric involvement rather than normality of the less involved side. The superior ophthalmic vein may be dilated. CT scan provides excellent views of the bony anatomy of the orbit, which is important in cases that orbital decompression is required. MRI is better to evaluate the orbital contents including the optic nerve, orbital fat, and extraocular muscles. Regarding treatment, the main goal is to achieve and maintain a euthyroid state. These measures alone are sufficient in many cases, because the majority of patients with GO present a favorable and often spontaneous self-limiting clinical course, although it may be prolonged over one or more years. Patients who suffer from severe forms of GO can be treated with systemic corticosteroids or orbital irradiation. Comments Orbital MRI study demonstrates diffuse orbital fat involvement in both sides and fusiform thickening of the extraocular muscles with tendon sparing (Fig. 2.2a ). On axial and coronal STIR sequence (Fig. 2.2b, c ), the extraocular muscles present high signal intensity consistent with inflammatory component. Note the optic nerve encasement in the apex of the orbit due to muscles enlargement ( arrow in Fig. 2.2b ). Imaging Findings
6 28 Francisco de Asís Bravo-Rodríguez and Rocío Díaz-Aguilera Case 3 History Inflammatory Pseudotumor of the Orbit A 28-year-old woman presented with a mass located in superolateral aspect of the left orbit of 6 months duration. The patient also complained of vague symptoms of tearing, limited motility of the left eye, and episodes of orbital inflammation since the last 2 weeks. a b c d Fig. 2.3
7 Orbit and Sellar Region 29 An inflammatory pseudotumor of the orbit represents a clinical and pathologic condition of unknown etiology that is characterized by the presence of a mass within the orbit that may mimic malignancy and that is composed of inflammatory cells and variable amounts of fibrosis. It constitutes about 9% of all orbital mass lesions. Inflammatory pseudotumors are most often confined to the orbit and frequently involve the lacrimal gland and the muscular cone. The extension of the lesion beyond the orbit or even intracranially is quite rare but it may occur in cases of extensive and chronic orbital inflammation. Orbital pseudotumor has no gender or race predominance and can appear in individuals of any age, although it most frequently occurs in middle-aged patients. It is usually unilateral, and the presence of bilateral masses suggests an underlying systemic disease. The symptoms of idiopathic pseudotumors depend on the inflammatory response (acute, subacute, or chronic) and the location of the inflammatory tissue. Clinical manifestations include exophthalmos, reduced ocular motility, diplopia, ptosis, and chemosis. In fact, inflammatory pseudotumors are a common cause of unilateral proptosis in adults. The radiological findings in a pseudotumor are characterized by inflammatory changes in the different intraorbital components, such as the globe, the lacrimal glands, the extraocular muscles, the orbital fat, and the optic nerve. On CT, inflammatory pseudotumors appear as an abnormal intraorbital mass of soft-tissue density, which varies widely in shape, location, and size. The presence of bony changes, reflected by hyperostosis or erosion and sclerotic change, indicates a long-standing benign process. Inflammatory pseudotumors of the orbit are frequently accompanied by edema or fat infiltration. On MRI, the lesions are hypointense on both T1- and T2-weighted images (possibly related to the fibrotic changes) with strong enhancement after gadolinium administration. Fat suppression techniques clearly show intraorbital inflammation. Orbital pseudotumor is diagnosed by exclusion, on the basis of the patient s history, clinical course, response to steroid therapy, laboratory test, and radiological and biopsy findings. The diagnosis becomes even more difficult in subacute and chronic forms. Sometimes, a chronic idiopathic inflammatory pseudotumor can simulate lymphoma, particularly when there is no history of an acute onset. Corticosteroids are the mainstay of treatment and are administered for several months to ensure remission. Radiotherapy may be used in patients who fail to respond to steroids or who have a rapidly progressive course. For those patients who are refractory to both corticosteroids and radiotherapy, anecdotal reports have suggested the use of chemotherapeutic agents such as cyclophosphamide, methotrexate, and cyclosporine. Comments Orbital coronal CT scan (Fig. 2.3a ) demonstrates an extraconal tumor in the theoretical location of left lacrimal gland. The tumor wraps around and displaces caudal and medially the ocular globe. On coronal STIR MR image (Fig. 2.3b ), the lesion presents high signal intensity due to the inflammatory component. On coronal and sagittal gadoliniumenhanced fat-suppressed T1-weighted images (Fig. 2.3c, d ), the tumor shows intense enhancement. Observe that the lesion is clearly depicted between orbital roof and superior rectus muscle in the sagittal plane. Imaging Findings
8 30 Francisco de Asís Bravo-Rodríguez and Rocío Díaz-Aguilera Case 4 Orbital Hemangioma a b c Fig. 2.4
9 Orbit and Sellar Region 31 A 57-year-old woman presented with a soft mass located in superomedial portion of the left orbit that had been slowly growing for the last three years. History Cavernous hemangioma is the most common primary benign tumor of the orbit in adults. It is a slow-growing, vascular tumor, which is considered as developmental hamartoma. The tumor is characteristically unilateral and solitary; bilateral or multiple hemangiomas are quite rare. Most cavernous hemangiomas are located within the intraconal retrobulbar region. These tumors usually present in the fifth decade of life with female gender predominance. Pregnancy may accelerate the growth of the tumor. The most common clinical presentation is a unilateral, painless, progressive proptosis. Other manifestations such as visual acuity compromise, diplopia, and extraocular muscle or pupillary dysfunction may occur as a result of compression of intraorbital contents by the tumor. The diagnosis can be made by imaging studies. Ultrasound typically shows a lesion with good sound transmission with moderate high-echogenity on A-scan secondary to the septae within the tumor. Doppler flow study may reveal subdued blood flow within the hemangioma. On CT scan, the tumor appears as an oval- or round-shaped, well-defined, homogeneous intraconal mass, which enhanced with intravenous contrast. The enhancing pattern can be homogenous or nonhomogenous. On MRI, hemangiomas are well-defined oval masses, homogeneous, isointense relative to muscle on T1-weighted images and hyperintense on T2-weighted images. On dynamic MRI after gadolinium administration, progressive and total homogeneous filling up of the mass can be seen. This enhancement pattern is considered a typical feature of a cavernous hemangioma of the orbit, and is similar to hepatic cavernous hemangiomas. The typical contrast-enhancement spread pattern of hemangiomas can be used to distinguish this tumor from others lesions such as schwannomas. Most hemangiomas remain stable throughout a patient s life and cause no visual impairment, therefore, the majority of patients require no interventions and can be observed clinically. In cases of symptomatic tumors, surgical excision is the treatment of choice. Comments MRI study reveals a mass located in superomedial aspect of the left orbit, hyperintense on STIR (Fig. 2.4a ), and T2-weighted (Fig. 2.4b ) MR images and hypointense on T1-weighted image (Fig. 2.4c ). The lesion presents well-defined lobulated margins and hypointense round images within it consistent with calcifications (phebolites) ( arrows ). Imaging Findings
10 32 Francisco de Asís Bravo-Rodríguez and Rocío Díaz-Aguilera Case 5 Orbital Lymphoma a b c d Fig. 2.5
11 Orbit and Sellar Region 33 A 65-year-old male presented with bilateral eyelid swelling, moderate exophthalmos, and orbital discomfort. History Lymphomas are the most frequent orbital malignant tumors. According to recent publications, these tumors account for 11% of all orbital masses and 55% of all malignant tumors. Orbital lymphomas are predominantly low-grade, small, B-cell types, and are associated with systemic disease, occurring either sequentially or concurrently, in about one-third of the cases. Hence, a patient diagnosed with orbital lymphoma must be examined to rule out systemic disease. Normal orbital lymphoid tissue is located on conjunctivae and lacrimal glands, therefore, these are the most common locations of orbital lymphomas. Lymphoid tumors of the orbit are considered a disease spectrum that includes benign lymphoid hyperplasia, atypical lymphoid hyperplasia, and malignant lymphoma. There are no clinical or laboratory or imaging tests that permit to distinguish between benign and malignant lymphoid lesions. Orbital lymphomas usually occur in older people, the average age for occurrence is the sixth decade of life and there is a slight female predominance. Clinically, lymphoma of the orbit generally presents with symptoms secondary to gradually increasing mass effect on surrounding structures. Clinical features include progressive painless proptosis with or without motility impairment, diplopia, ptosis, and, rarely, visual loss. Proptosis and visible conjunctival mass are the most common modes of presentation. Most lesions are unilateral although bilateral orbital involvement is seen in about 10 25% of the patients. Ultrasound, CT, and MRI are different imaging techniques to diagnose orbital lymphoma. CT and MRI findings are unspecified and should be evaluated in conjunction with clinical signs and symptoms. On CT, orbital lymphomas appear as hyperdense, homogeneous well-defined masses usually located on the retrobulbar region or on the superior orbital compartment. The tumor is molded to the adjacent structures without eroding the bone or expanding the orbit. After contrast administration, the lesion shows mild enhancement. Biopsy is always mandatory for stage grouping of lymphomas. On MRI, malignant lymphoma lesions are hyperintense compared to the extraocular muscles on both precontrast and postcontrast T1-weighted images. When the lacrimal duct is involved or there is bilateral disease, it is more likely to be malignant lymphoma. Therapeutic options for orbital lymphoma include surgical excision, radiation therapy, and chemotherapy. The prognosis depends on the histologic type and stage of lymphoma and therapy. In general, with modern treatment of patients with NHL, the overall survival rate at 5 years is approximately 60%. Comments Coronal un-enhanced CT-scan (Fig. 2.5a ) demonstrates bilateral, solid, homogeneous, and soft-tissue attenuation masses that molded to the adjacent ocular globe. Lacrimal glands are involved and appear enlarged. On axial T1-weighted MR image (Fig. 2.5b ), the lesions present the same signal intensity than extraocular muscles. On axial gadolinium-enhanced T1-WI (Fig. 2.5c ) and sagittal contrast-enhanced fat-saturated T1-WI (Fig. 2.5d ), the masses show homogeneous and intense enhancement. Imaging Findings
12 34 Francisco de Asís Bravo-Rodríguez and Rocío Díaz-Aguilera Case 6 Optic Nerve Sheath Meningioma History A 40-year-old female presented with progressive visual acuity loss in the left eye with self-limited episodes of mild ocular pain in this eye. On physical examination, slight proptosis and mild unilateral papilledema were found. a b c d Fig. 2.6
13 Orbit and Sellar Region 35 Optic nerve sheath meningioma (ONSM) is a rare, benign tumor that arises from the cap cells of the arachnoid that surround the intraorbital or intracanalicular optic nerve. The tumor can develop anywhere along the course of the optic nerve. ONSM represents about 1 2% of all meningiomas, 2% of all orbital tumors, and about 10% of optic nerve lesions. The majority of cases occur in middle-aged females, with a 2:1 female-to-male ratio. The tumor may be unilateral, bilateral, or multifocal with the latter two subgroups occurring most commonly in patients with type 2 neurofibromatosis. The clinical presentation of optic nerve sheath meningioma depends on whether they arise from the orbit, within the optic canal or intracranially. The tumor typically grows slowly causing gradually compression of the optic nerve with progressive visual loss in the affected eye. The classic triad, known as the Hoyt Spencer triad, includes loss of vision, optic atrophy, and optociliary shunt vessels. These enlarged blood vessels indicated that the tumor has disrupted the natural circulation through the optic nerve to the retina and choroid. Other clinical manifestations are color vision disturbance, visual field defect, proptosis, optic disc edema, and motility impairment. The diagnosis of ONSM relies heavily on imaging findings. MRI currently remains the method of choice for diagnosis of ONSM, although it is less sensitive than CT in the detection of calcification. ONSMs are typically isointense or slightly hypointense to brain and optic nerve tissue on T1-weighted images and hyperintense (may also be hypointense) on T2-weighted images. They present a homogeneous intense enhancement after gadolinium administration often suggesting in appearance a tram track around the hypointense optic nerve in axial sequences. Intracranial extension is rare and, when present, it is restricted in a short distance along the prechiasmatic optic nerve sheath. Contrastenhanced CT is another useful imaging technique for evaluation of optic nerve sheath meningioma. On CT, the tumor usually appears as a fusiform thickening of the optic nerve. This enlargement may appear as localized or as an eccentric expansion of the optic nerve and occurs most commonly at the orbital apex. After intravenous contrast injection, ONSMs usually shows an intense homogeneous enhancement. Linear, diffuse, or patchy calcifications within or along an optic nerve mass are commonly detected. The differential diagnosis includes optic glioma, orbital pseudotumor, and lymphoma. ONSM management is variable and depends on several factors. In cases of mild or no visual impairment with evidence of no intracranial extension, follow-up is recommended. If loss of vision occurs and progresses, radiation therapy is the treatment of choice either primarily or following surgery. Radiotherapy can improve vision in some patients or preserve it in others. Chemotherapy is reserved for patients with unresectable, recurrent, or previously irradiated meningiomas. Comments Axial T1-weighted MR image of the orbits (Fig. 2.6a ) demonstrates a fusiform lesion that surrounds the left optic nerve, isointense to extraocular muscles. After contrast material administration (Fig. 2.6c, d ), the lesion shows intense and homogeneous enhancement. On both T1-weighted MR image (Fig. 2.6b ) and contrast-enhanced fat-suppression T1-weighted MR images (Fig. 2.6c ), the optic nerve can be clearly depicted. It appears thinner than contralateral optic nerve and encased by the lesion ( arrow in Fig. 2.6c ). Imaging Findings
14 36 Francisco de Asís Bravo-Rodríguez and Rocío Díaz-Aguilera Case 7 Craniopharyngioma a b c d Fig. 2.7
15 Orbit and Sellar Region 37 A 61-year-old woman was referred to ophthalmologist for visual loss and progressive headache. On physical examination, right temporal hemianopsia was found. Neuroimaging studies were performed next. History Craniopharyngioma is a benign, slow-growing, extra-axial, epithelial, calcified cystic tumor arising from squamous cell rests along the involuted hypophyseal Rathke s cleft. For this reason they occur exclusively in the region of the sella turcica and suprasellar cistern. Craniopharyngiomas account for 3 5% of all primary intracranial brain tumors. The prevalence of craniopharyngiomas peaks between 10 and 14 years of age, with a second peak occurring in the fourth to sixth decades of life. There is no gender predilection. The most common presenting symptoms are headache, visual disturbances, and endocrine dysfunction. Although craniopharyngiomas exhibit no hormonal activity, endocrine symptoms can occur due to compression of the hypothalamus, pituitary stalk, and pituitary gland. Imaging studies strongly suggest the diagnosis. The radiologic hallmark of a craniopharyngioma is the appearance of a suprasellar calcified and cystic mass. About 80 87% of craniopharyngiomas are calcified and 70 75% are cystic. Calcifications are more common in children (90%) than in adults (50%). CT scan is the most sensitive technique to demonstrate calcifications. It is useful in defining both calcified and cystic components. Cyst content usually has the same attenuation as cerebrospinal fluid (CSF); contrast administration better defines the enhancing cyst capsule. On MRI, craniopharyngiomas present a heterogeneous spectrum. The most common pattern is a cyst that is hypointense on T1WI and hyperintense on T2WI. Sometimes, craniopharyngiomas are hyperintense on T1WI due to high protein concentration, blood degradation products, or both. After gadolinium administration, the tumor enhances strongly and heterogeneously. MRI is the imaging modality used to plan the surgical approach. Differential diagnosis includes the following entities: Rathke s cleft cyst, necrotic pituitary adenoma, suprasellar dermoid, teratoma, thrombosed aneurysm, and cystic suprasellar hypothalamic and chiasmatic glioma. Surgical removal is the treatment of choice for tumor eradication. Nevertheless, craniopharyngiomas tend to recur after surgery. Therefore, postoperative follow-up with gadolinium-enhanced MRI is mandatory. Comments Un-enhanced CT scan (Fig. 2.7a ) demonstrates a sellar and suprasellar mass, hypoattenuating to brain parenchyma, with calcifications. On MRI, the lesion appears hypointense on T1-weighted image (Fig. 2.7b ) and hyperintense on T2-WI (Fig. 2.7c ), which is consistent with a predominantly cystic component. After gadolinium administration (Fig. 2.7d ), the tumor shows intense and heterogeneous enhancement and solid and necrotic or cystic components are better differentiated. Note encasement of left internal carotid artery by tumor ( arrow in Fig. 2.7c ). Imaging Findings
16 38 Francisco de Asís Bravo-Rodríguez and Rocío Díaz-Aguilera Case 8 Hypothalamic Hamartoma a b c Fig. 2.8
17 Orbit and Sellar Region 39 A 28-year-old woman underwent an urgent unenhanced CT-scan for cranial trauma after traffic accident. A small lesion located in interpeduncular cistern was incidentally found on CT. The patient referred a past medical history of epilepsy treatment long time ago. History Hypothalamic hamartoma, also called tuber cinereum hamartoma, is a relative rare congenital non-neoplastic heterotopia. It represents a midline dysraphic syndrome and presents as an ectopic cerebral gray matter, comprising a mass of normal neuronal tissue. Most of these lesions are small with a diameter of a few millimeters to 1.5 cm. They lie between the infundibular stalk anteriorly and the mamillary bodies posteriorly. These lesions have been divided into two main clinicoanatomic types: para-hypothalamic hamartomas and intra-hypothalamic hamartomas. Parahypothalamic hamartomas are pedunculated masses that are attached to the floor of the hypothalamus by a narrow stalk. These lesions seem more likely to be associated with isosexual precocious puberty. Intrahypothalamic hamartomas are sessile masses with a broad attachment to the hypothalamus. These lesions seem to be associated more often with gelastic seizures, intellectual impairment, and psychiatric disturbances than with precocious puberty. These clinical features are noted commonly in early life and may occur as early as in the neonatal period. On MR imaging, hamartomas appear as well-defined pedunculated or sessile lesions at the tuber cinereum and are isointense or mildly hypointense on T1-weighted images and iso- to hyperintense on T2-weighted images. Hamartomas neither calcify nor exhibit enhancement following contrast administration. Surgery, radiosurgery, and medical treatment are the different therapeutic options. The choice of treatment must be individualized depending on the age and clinical circumstances of the patient and the size and anatomic relationships of the hamartoma. The absence of any long-term change in the size, shape, or signal intensity of the lesion strongly supports the diagnosis of hypothalamic hamartoma. Comments Axial T1-weighted MR image (Fig. 2.8a ) reveals a mass in interpenducular cistern ( arrow ), isointense to brain parenchyma. Sagittal T1-weighted MR images, before (Fig. 2.8b ) and after (Fig. 2.8c ) intravenous gadolinium administration, show a lesion that lies between the infundibular stalk anteriorly and the mamillary bodies posteriorly ( arrows ). The mass presents the same signal intensity as the brain parenchyma and does not enhance with the contrast material. Imaging Findings
18 40 Francisco de Asís Bravo-Rodríguez and Rocío Díaz-Aguilera History Case 9 Pituitary Adenoma Comments A 18-year-old boy was referred to the emergency department with a three-day history of right periorbital headache, blurred vision, and diplopia. On physical examination, right temporal hemianopsia was found. Pituitary adenomas are benign, slow-growing tumors that arise from cells in the pituitary gland. Pituitary adenomas are relatively common, accounting for approximately 15% of primary brain tumors. These tumors occur in individuals of years of age and do not show gender predilection. Based on size, pituitary tumors can be divided into microadenomas (<1 cm in diameter) and macroadenomas (>1 cm in diameter). Microadenomas typically present with endocrine disturbances (according to the hormone secreted by the tumor), a b c d Fig. 2.9
19 Orbit and Sellar Region 41 whereas macroadenomas usually manifest with symptoms due to the local mass effect on the optic chiasm or with pituitary failure. Lateral extension of the tumor may involve cavernous sinus and may affect the III, IV, and VI cranial nerves causing ocular motility impairment. Pituitary adenomas are usually solid capsulated tumors that may contain internal areas of necrosis, cyst formation, or hemorrhage. Calcifications are rare. According to the hormone secreted by the tumor, adenomas can be divided into two categories: (1) hormoneinactive (nonfunctional) pituitary adenomas, which typically cause problems related to the size of the tumor compressing adjacent brain structures and (2) hormone-producing pituitary adenomas. The three most common are prolactin-secreting pituitary adenoma (prolactinoma), growth hormone-secreting pituitary adenoma, and ACTH-secreting pituitary adenoma. Other hormone producing pituitary tumors are very rare. Pituitary adenomas, with a few exceptions, are not under the control of hypothalamic releasing factors. Clinical manifestations are due to the local effect of the mass and distant endocrine manifestations that can affect a variety of organ systems. The diagnosis of a pituitary adenoma is made based on a combination of pituitary function testing (blood hormone levels) and pituitary imaging. Conventional singlesection CT has a limited role in pituitary imaging, with a sensitivity of 17 22% in detecting microadenomas. Multidetector-row CT with 64 channels may have a role, especially in patients unable to undergo MRI. CT is best for visualizing bony detail and calcification. On CT, microadenomas appear as a focal hypodense area within the pituitary gland. MRI is generally preferred over CT for the diagnosis of pituitary adenomas because of its superior definition of small lesions in the pituitary sella and its improved anatomic definition before surgery. MRI is also preferred for postsurgical surveillance. On MRI, microadenomas are sometimes difficult to detect unless dynamic techniques are used. Microadenomas enhance less rapidly than normal pituitary tissue and therefore appear relatively hypointense on rapid-sequence contrast-enhanced T1-WI. Uncomplicated macroadenomas show the same signal intensity than gray matter on all imaging sequences. Enhancement after gadolinium injection is typically intense but is often heterogeneous. The optimal treatment of a pituitary adenoma depends on multiple factors including the hormone production by the tumor (if present), size of the tumor, how invasive the tumor is into surrounding structures, and the age and health of the patient. Treatment options include surgery (performed in more than 99% of cases via a transphenoidal route), radiotherapy, and medical treatment. On urgent noncontrast CT scan (Fig. 2.9a ), a sellar and suprasellar hyperattenuating mass was found. On MRI study, the lesion is well-circumscribed and appears isointense to brain parenchyma on T1-weighted image (Fig. 2.9b ). After intravenous gadolinium administration (Fig. 2.9c, d ), the mass shows intense and homogeneous enhancement. A small cystic component can be seen in the superior aspect of the lesion ( arrow in Fig. 2.9c ). The large suprasellar component of the tumor causes optic chiasm compression. This structure cannot be identified. Imaging Findings
20 42 Francisco de Asís Bravo-Rodríguez and Rocío Díaz-Aguilera Case 10 Rathke s Cleft Cyst a b c d Fig. 2.10
21 Orbit and Sellar Region 43 A 38-year-old woman presented with tension-type headache. She underwent a cerebral MRI study that demonstrated an incidental pituitary tumor. History Rathke s cleft cysts (RCCs) are benign cystic lesions that originate from the failure of obliteration of lumen of the Rathke pouch. RCCs commonly appear as single, unilocated, well-defined, intra/suprasellar cyst without calcification. Forty percent of these cysts are completely intrasellar and the remaining 60% have suprasellar extension. They commonly measure between 5 and 15 mm but can occasionally become very large. Cyst contents vary from serous to mucoid. Most lesions are detected in middle-aged adults with female gender predominance. The vast majority of RCCs are asymptomatic and they are found incidentally on imaging studies. Symptomatic RCCs are rare, but cysts can enlarge and produce symptoms as pituitary dysfunction, visual disturbances, and/or headache. On CT, RCCs appear as well-delineated, round, hypodense, intra/suprasellar mass without enhancement after contrast administration. MRI findings depend on the cyst content. On T1-weighted image, two-thirds are hyperintense to brain and one-third show low signal intensity similar to CSF. On T2 WI, half are hyperintense, 25% are isointense, and 25% are hypointense. RCCs typically do not show enhancement following gadolinium administration, although an enhancing rim of compressed pituitary gland surrounding the cyst is sometimes present. The differential diagnosis includes arachnoid cyst, cystic pituitary adenoma, cystic craniopharyngioma, and inflammatory cyst. Asymptomatic RCCs are treated conservatively. In symptomatic cases, drainage or partial excision of the cyst wall ( marsupialization ) may be done. The recurrence rate varies from 19 to 28%. Comments Axial and sagittal T1-weighted MR images (Fig. 2.10a, b ) and fluid-attenuated inversion recovery (FLAIR) MR image (Fig. 2.10c ) reveal a hyperintense nodular lesion located in the pituitary gland. On sagittal contrast-enhanced T1-weighted MR image (Fig. 2.10d ), the lesion does not show enhancement and can be clearly differentiated from hypophysis. Imaging Findings
22 44 Francisco de Asís Bravo-Rodríguez and Rocío Díaz-Aguilera Further Reading Arita K, Ikawa F, Kurisu K et al (1999) The relationship between magnetic resonance imaging findings and clinical manifestations of hypothalamic hamartoma. J Neurosurg 91: Augsburger JJ, Peyster RG, Markoe AM et al (1987) Computed tomography of posterior uveal melanomas. Arch Ophthalmol 105(11): Barkovich AJ (2005) Intracranial, orbital, and neck masses of childhood. In: Barkovich AJ (ed) Pediatric neuroimaging, 4th edn. Lippincott Williams & Wilkins, Philadelphia, pp Bartalena L, Baldeschi L, Dickinson A, Eckstein A, Kendall- Taylor P, Marcocci C (2008) Consensus statement of the European Group on Graves orbitopathy (EUGOGO) on management of GO. Eur J Endocrinol 158(3): Bilaniuk L (1999) Orbital vascular lesions: role of imaging. Radiol Clin North Am 37: Billeci D, Marton E, Tripodi M et al (2004) Symptomatic Rathke s cleft cysts: a radiological, surgical and pathological review. Pituitary 7(3): Bonneville JF, Cattin F, Bonneville F (2009) Imaging of pituitary adenomas. Presse Med 38(1):84 91 Boyko OB, Curnes JT, Oakes WJ, Burger PC (1991) Hamartomas of the tuber cinereum: CT, MR, and pathologic findings. AJNR Am J Neuroradiol 12: Bunin GR, Surawicz TS, Witman PA et al (1998) The descriptive epidemiology of craniopharyngioma. J Neurosurg 89(4): Cham MC, Pavlin CJ (2000) Ultrasound detection of posterior scleral bowing in young patients with choroidal melanoma. Can J Ophthalmol 35(5): Chanson P, Salenave S (2004) Diagnosis and treatment of pituitary adenomas. Minerva Endocrinol 29(4): Dodds NI, Atcha AW, Birchall D, Jackson A (2009) Use of highresolution MRI of the optic nerve in Graves ophthalmopathy. Br J Radiol 82(979): Gupta DK, Ojha BK, Sarkar C, Mahapatra AK, Mehta VS (2006) Recurrence in craniopharyngiomas: analysis of clinical and histological features. J Clin Neurosci 13(4): Hagiwara A, Inoue Y, Wakasa K et al (2003) Comparison of growth hormone-producing and non-growth hormone-producing pituitary adenomas: imaging characteristics and pathologic correlation. Radiology 228(2): Harold Lee HB, Garrity JA, Cameron JD, Strianese D, Bonavolontà G, Patrinely JR (2008) Primary optic nerve sheath meningioma in children. Surv Ophthalmol 53(6): Ing E, Abuhaleeqa K (2007) Graves ophthalmopathy (thyroidassociated orbitopathy). Clin Surg Ophthalmol 25: Jacobs D, Galetta S (2002) Diagnosis and management of orbital pseudotumor. Curr Opin Ophthalmol 13(6): Jung WS, Ahn KJ, Park MR et al (2007) The radiological spectrum of orbital pathologies that involve the lacrimal gland and the lacrimal fossa. Korean J Radiol 8(4): Lee EJ et al (2005) MR Imaging of orbital inflammatory pseudotumors with extraorbital extension. Korean J Radiol 6(2):82 88 Mafee MF et al (2005) Anatomy and pathology of the eye: role of MR imaging and CT. Neuroimaging Clin N Am 15:23 47 Meredith TA (1998) Choroidal melanoma: diagnosis and management. Am J Ophthalmol 125(6): Nishioka H, Haraoka J, Izawa H, Ikeda Y (2006) Magnetic resonance imaging, clinical manifestations, and management of Rathke s cleft cyst. Clin Endocrinol (Oxf) 64(2): Noth D, Gebauer M, Müller B et al (2001) Graves ophthalmopathy: natural history and treatment outcomes. Swiss Med Wkly 131: Ohtsuka K, Hashimoto M, Akiba H (1997) Serial dynamic magnetic resonance imaging of orbital cavernous hemangioma. Am J Ophthalmol 123: Osborn A (1994) Diagnostic neuroradiology. Mosby, London, pp Park SB, Lee JH, Weon YC (2009) Imaging findings of head and neck inflammatory pseudotumor. AJR Am J Roentgenol 193(4): ; Review Rey-Porca C, Pérez-Encinas M, González F (2008) Orbital lymphomas. Presentation of nine cases. Arch Soc Esp Oftalmol 83(2): Saeed P, Rootman J, Nugent RA, White VA, Mackenzie IR, Koornneef L (2003) Optic nerve sheath meningiomas. Ophthalmology 110(10): Saeki N, Sunami K, Sugaya Y, Yamaura A (1999) MRI findings and clinical manifestations in Rathke s cleft cyst. Acta Neurochir (Wien) 141: Sharma RR (1987) Hamartoma of the hypothalamus and tuber cinereum: a brief review of the literature. J Postgrad Med 33:1 13 Sibony PA, Krauss HR, Kennerdell JS, Maroon JC, Slamovits TL (1984) Optic nerve sheath meningiomas. Clinical manifestations. Ophthalmology 91(11): Som PM, Curtin HD (2003) Head and neck imaging, 4th edn. Mosby, St Louis, pp Tanaka A, Mihara F, Yoshiura T et al (2004) Differentiation of cavernous hemangioma from schwannoma of the orbit: a dynamic MRI study. AJR 183: Thorn-Kany M, Arrue P, Delisle MB, Lacroix F, Lagarrigue J, Manelfe C (1999) Cavernous hemangiomas of the orbit: MR imaging. J Neuroradiol 26:79 86 Tominaga JY, Higano S, Takahashi S (2003) Characteristics of Rathke s cleft cyst in MR imaging. Magn Reson Med Sci 2(1):1 8 Turbin RE, Pokorny K (2004) Diagnosis and treatment of orbital optic nerve sheath meningioma. Cancer Control 11(5): Weber AL, Romo LV, Sabates NR (1999) Pseudotumor of the orbit. Clinical, pathologic, and radiologic evaluation. Radiol Clin North Am 37: Yadav BS, Sharma SC (2009) Orbital lymphoma: role of radiation. Indian J Ophthalmol 57(2):91 97
23
PITUITARY PARASELLAR LESIONS. Kim Learned, MD
 PITUITARY PARASELLAR LESIONS Kim Learned, MD DIFFERENTIALS Pituitary Sella Clivus, Sphenoid Sinus Suprasellar Optic chiasm, Hypothalamus, Circle of Willis Parasellar Cavernous Sinus Case 1 17 YEAR-OLD
PITUITARY PARASELLAR LESIONS Kim Learned, MD DIFFERENTIALS Pituitary Sella Clivus, Sphenoid Sinus Suprasellar Optic chiasm, Hypothalamus, Circle of Willis Parasellar Cavernous Sinus Case 1 17 YEAR-OLD
Metastasis. 57 year old with progressive Headache and Right Sided Visual Loss
 Metastasis 1% of sellar/parasellar masses Usually occurs with known primary Can involve third ventricle, hypothalamus, infundibular stalk May be both supra-, intrasellar 57 year old with progressive Headache
Metastasis 1% of sellar/parasellar masses Usually occurs with known primary Can involve third ventricle, hypothalamus, infundibular stalk May be both supra-, intrasellar 57 year old with progressive Headache
Imaging The Turkish Saddle. Russell Goodman, HMS III Dr. Gillian Lieberman
 Imaging The Turkish Saddle Russell Goodman, HMS III Dr. Gillian Lieberman Learning Objectives Review the anatomy of the sellar region Discuss the differential diagnosis of sellar masses Discuss typical
Imaging The Turkish Saddle Russell Goodman, HMS III Dr. Gillian Lieberman Learning Objectives Review the anatomy of the sellar region Discuss the differential diagnosis of sellar masses Discuss typical
Laurie A. Loevner, MD
 Laurie A. Loevner, MD Chief, Division of Neuroradiology UPHS Professor of Radiology, Otorhinolaryngology: Head & Neck Surgery, Neurosurgery, and Ophthalmology University of Pennsylvania Health System Disclosures
Laurie A. Loevner, MD Chief, Division of Neuroradiology UPHS Professor of Radiology, Otorhinolaryngology: Head & Neck Surgery, Neurosurgery, and Ophthalmology University of Pennsylvania Health System Disclosures
EXPERT DIFFERENTIAL DIAGNOSIS:
 EXPERT DIFFERENTIAL DIAGNOSIS: Sellar Region Anne G. Osborn, M.D. DISCLOSURE: Published RSNA 2008 SELLA, PITUITARY: Normal Gross, 3T Anatomy SELLA, PITUITARY: Anatomically-Based Differential Diagnoses
EXPERT DIFFERENTIAL DIAGNOSIS: Sellar Region Anne G. Osborn, M.D. DISCLOSURE: Published RSNA 2008 SELLA, PITUITARY: Normal Gross, 3T Anatomy SELLA, PITUITARY: Anatomically-Based Differential Diagnoses
TABLES. Imaging Modalities Evidence Tables Table 1 Computed Tomography (CT) Imaging. Conclusions. Author (Year) Classification Process/Evid ence Class
 TABLES Imaging Modalities Evidence Tables Table 1 Computed Tomography (CT) Imaging Author Clark (1986) 9 Reformatted sagittal images in the differential diagnosis meningiomas and adenomas with suprasellar
TABLES Imaging Modalities Evidence Tables Table 1 Computed Tomography (CT) Imaging Author Clark (1986) 9 Reformatted sagittal images in the differential diagnosis meningiomas and adenomas with suprasellar
A Case of Carotid-Cavernous Fistula
 A Case of Carotid-Cavernous Fistula By : Mohamed Elkhawaga 2 nd Year Resident of Ophthalmology Alexandria University A 19 year old male patient came to our outpatient clinic, complaining of : -Severe conjunctival
A Case of Carotid-Cavernous Fistula By : Mohamed Elkhawaga 2 nd Year Resident of Ophthalmology Alexandria University A 19 year old male patient came to our outpatient clinic, complaining of : -Severe conjunctival
Orbital facia. Periororbital facia Orbital septum Bulbar facia Muscular facia
 Anatomy Orbital facia Periororbital facia Orbital septum Bulbar facia Muscular facia Physiology of symptoms 1) Proptosis ( exophthalmos) Pseudoproptosis Axial Non axial Pulsating Positional Intermittent
Anatomy Orbital facia Periororbital facia Orbital septum Bulbar facia Muscular facia Physiology of symptoms 1) Proptosis ( exophthalmos) Pseudoproptosis Axial Non axial Pulsating Positional Intermittent
Where Has My Vision Gone? Evaluation of Sellar Lesions. Caleb Stowell,, HMS III Gillian Lieberman, MD November 2008
 Where Has My Vision Gone? Evaluation of Sellar Lesions Caleb Stowell,, HMS III Gillian Lieberman, MD November 2008 Objectives Present a case highlighting the clinical presentation and evaluation of a sellar
Where Has My Vision Gone? Evaluation of Sellar Lesions Caleb Stowell,, HMS III Gillian Lieberman, MD November 2008 Objectives Present a case highlighting the clinical presentation and evaluation of a sellar
RADIOANATOMY OF SELLA TURCICA
 RADIOANATOMY OF SELLA TURCICA O.BAKKACHA, H.MALAJATI, M.RHISSASSI, H. BENCHAABOUNE, N.CHAKIR, My R. EL HASSANI,M.JIDDANE Department of Neuroradiology specialties Hospital. Rabat Objective: New imaging
RADIOANATOMY OF SELLA TURCICA O.BAKKACHA, H.MALAJATI, M.RHISSASSI, H. BENCHAABOUNE, N.CHAKIR, My R. EL HASSANI,M.JIDDANE Department of Neuroradiology specialties Hospital. Rabat Objective: New imaging
Imaging pituitary gland tumors
 November 2005 Imaging pituitary gland tumors Neel Varshney,, Harvard Medical School Year IV Two categories of presenting signs of a pituitary mass Functional tumors present with symptoms due to excess
November 2005 Imaging pituitary gland tumors Neel Varshney,, Harvard Medical School Year IV Two categories of presenting signs of a pituitary mass Functional tumors present with symptoms due to excess
Pediatric Ocular Sonography
 Pediatric Ocular Sonography Cicero J Torres A Silva, MD Associate Professor of Radiology 2016 SPR Pediatric Ultrasound Course Yale University School of Medicine None Disclosures Objectives of Presentation
Pediatric Ocular Sonography Cicero J Torres A Silva, MD Associate Professor of Radiology 2016 SPR Pediatric Ultrasound Course Yale University School of Medicine None Disclosures Objectives of Presentation
Visual pathways in the chiasm
 Visual pathways in the chiasm Intracranial relationships of the optic nerve Fixation of the chiasm Chiasmatic pathologies The function of the optic chiasm may be altered by the presence of : 4) Artero
Visual pathways in the chiasm Intracranial relationships of the optic nerve Fixation of the chiasm Chiasmatic pathologies The function of the optic chiasm may be altered by the presence of : 4) Artero
13/02/1440 بسم ا هلل ا لرحمن ا لر حيم
 بسم ا هلل ا لرحمن ا لر حيم 1 Slowly progressive versus rapidly progressive proptosis by Ali M ISMAIL professor of ophthalmology @SOHAG U H Occuloplastic fellow @NNUH Occuloplastic fellow @Cambridge UH
بسم ا هلل ا لرحمن ا لر حيم 1 Slowly progressive versus rapidly progressive proptosis by Ali M ISMAIL professor of ophthalmology @SOHAG U H Occuloplastic fellow @NNUH Occuloplastic fellow @Cambridge UH
Orbital Tumors - A Clinico Pathological Study
 Orbital Tumors - A Clinico Pathological Study Radha. J. DO, Ani Sreedhar. MS. Little Flower Hospital, Angamaly, Kerala ORIGINAL ARTICLES Abstract: Aim. To study the clinical and histopathological profiles
Orbital Tumors - A Clinico Pathological Study Radha. J. DO, Ani Sreedhar. MS. Little Flower Hospital, Angamaly, Kerala ORIGINAL ARTICLES Abstract: Aim. To study the clinical and histopathological profiles
CLINICAL ASSESSMENT OF PATIENTS WITH GRAVES ORBITOPATHY
 44 MEDICINSKI GLASNIK / str. 44-48 Biljana Nedeljković-Beleslin 1 CLINICAL ASSESSMENT OF PATIENTS WITH GRAVES ORBITOPATHY Abstract: Clinical examination is the basis of a good assessment of a patient with
44 MEDICINSKI GLASNIK / str. 44-48 Biljana Nedeljković-Beleslin 1 CLINICAL ASSESSMENT OF PATIENTS WITH GRAVES ORBITOPATHY Abstract: Clinical examination is the basis of a good assessment of a patient with
In some patients with pituitary macroadenoma, visual acuity
 ORIGINAL RESEARCH A.M. Tokumaru I. Sakata H. Terada S. Kosuda H. Nawashiro M. Yoshii Optic Nerve Hyperintensity on T2-Weighted Images among Patients with Pituitary Macroadenoma: Correlation with Visual
ORIGINAL RESEARCH A.M. Tokumaru I. Sakata H. Terada S. Kosuda H. Nawashiro M. Yoshii Optic Nerve Hyperintensity on T2-Weighted Images among Patients with Pituitary Macroadenoma: Correlation with Visual
! Women greater than men (4:1)» Typical of other autoimmune diseases
 1 2 3 4 : Overview and Diagnosis Suzanne K. Freitag, M.D. Director, Ophthalmic Plastic Surgery Massachusetts Eye and Ear Infirmary Harvard Medical School! I have no financial disclosures. Learning Objectives!
1 2 3 4 : Overview and Diagnosis Suzanne K. Freitag, M.D. Director, Ophthalmic Plastic Surgery Massachusetts Eye and Ear Infirmary Harvard Medical School! I have no financial disclosures. Learning Objectives!
RADIOLOGY TEACHING CONFERENCE
 RADIOLOGY TEACHING CONFERENCE John Athas, MD Monica Tadros, MD Columbia University, College of Physicians & Surgeons Department of Otolaryngology- Head & Neck Surgery September 27, 2007 CT SCAN IMAGING
RADIOLOGY TEACHING CONFERENCE John Athas, MD Monica Tadros, MD Columbia University, College of Physicians & Surgeons Department of Otolaryngology- Head & Neck Surgery September 27, 2007 CT SCAN IMAGING
Case 7391 Intraventricular Lesion
 Case 7391 Intraventricular Lesion Bastos Lima P1, Marques C1, Cabrita F2, Barbosa M2, Rebelo O3, Rio F1. 1Neuroradiology, 2Neurosurgery, 3Neuropathology, Coimbra University Hospitals, Portugal. University
Case 7391 Intraventricular Lesion Bastos Lima P1, Marques C1, Cabrita F2, Barbosa M2, Rebelo O3, Rio F1. 1Neuroradiology, 2Neurosurgery, 3Neuropathology, Coimbra University Hospitals, Portugal. University
The many faces of extranodal lymphoma
 The many faces of extranodal lymphoma Frank Pameijer Departments of Radiology and Radiation Oncology University Medical Center Utrecht Special thanks to Ilona M Schmalfuss, MD University of Florida Gainesville,
The many faces of extranodal lymphoma Frank Pameijer Departments of Radiology and Radiation Oncology University Medical Center Utrecht Special thanks to Ilona M Schmalfuss, MD University of Florida Gainesville,
Part II - Revising the sellar and parasellar region: differential diagnosis of a sellar region mass
 Part II - Revising the sellar and parasellar region: differential diagnosis of a sellar region mass Poster No.: C-1390 Congress: ECR 2015 Type: Educational Exhibit Authors: I. Candelaria, C. Figueira,
Part II - Revising the sellar and parasellar region: differential diagnosis of a sellar region mass Poster No.: C-1390 Congress: ECR 2015 Type: Educational Exhibit Authors: I. Candelaria, C. Figueira,
DISCLOSURES LEARNING OBJECTIVES WE WILL NOT DISCUSS. CSB: Birdseye View MESSAGE NAVIGATING THE SELLA AND CENTRAL SKULL BASE
 NAVIGATING THE SELLA AND CENTRAL SKULL BASE Christopher P. Hess, M.D., Ph.D. DISCLOSURES Research Support, General Electric SLIDES: http://www.radiology.ucsf.edu/research/meetings/rsna LEARNING OBJECTIVES
NAVIGATING THE SELLA AND CENTRAL SKULL BASE Christopher P. Hess, M.D., Ph.D. DISCLOSURES Research Support, General Electric SLIDES: http://www.radiology.ucsf.edu/research/meetings/rsna LEARNING OBJECTIVES
Is there a role of CT in the evaluation of Proptosis
 International Journal of scientific research and management (IJSRM) Volume 3 Issue 4 Pages 2662-2666 2015 \ Website: www.ijsrm.in ISSN (e): 2321-3418 Is there a role of CT in the evaluation of Proptosis
International Journal of scientific research and management (IJSRM) Volume 3 Issue 4 Pages 2662-2666 2015 \ Website: www.ijsrm.in ISSN (e): 2321-3418 Is there a role of CT in the evaluation of Proptosis
C. Douglas Phillips MD FACR Director of Head and Neck Imaging Weill Cornell Medical College/NewYork-Presbyterian Hospital
 C. Douglas Phillips MD FACR Director of Head and Neck Imaging Weill Cornell Medical College/NewYork-Presbyterian Hospital Disclosures Neither I nor any family members have any pertinent financial relations
C. Douglas Phillips MD FACR Director of Head and Neck Imaging Weill Cornell Medical College/NewYork-Presbyterian Hospital Disclosures Neither I nor any family members have any pertinent financial relations
Intrasphenoidal Rathke's Cleft Cyst: Case presentation and review of the literature
 Romanian Neurosurgery Volume XXX Number 4 2016 October - December Article Intrasphenoidal Rathke's Cleft Cyst: Case presentation and review of the literature Umit Kocaman, Muhammet Bahadir Yilmaz, Hakan
Romanian Neurosurgery Volume XXX Number 4 2016 October - December Article Intrasphenoidal Rathke's Cleft Cyst: Case presentation and review of the literature Umit Kocaman, Muhammet Bahadir Yilmaz, Hakan
Neuro-Ocular Grand Rounds
 Neuro-Ocular Grand Rounds Anthony B. Litwak,OD, FAAO VA Medical Center Baltimore, Maryland Dr. Litwak is on the speaker and advisory boards for Alcon and Zeiss Meditek COMMON OPTIC NEUROPATHIES THAT CAN
Neuro-Ocular Grand Rounds Anthony B. Litwak,OD, FAAO VA Medical Center Baltimore, Maryland Dr. Litwak is on the speaker and advisory boards for Alcon and Zeiss Meditek COMMON OPTIC NEUROPATHIES THAT CAN
Pleomorphic adenoma head and neck
 Pleomorphic adenoma head and neck Poster No.: C-1042 Congress: ECR 2015 Type: Educational Exhibit Authors: M. E. Pérez Montilla, I. Bravo Rey, E. Roldán Romero, F. BravoRodríguez; Cordoba/ES Keywords:
Pleomorphic adenoma head and neck Poster No.: C-1042 Congress: ECR 2015 Type: Educational Exhibit Authors: M. E. Pérez Montilla, I. Bravo Rey, E. Roldán Romero, F. BravoRodríguez; Cordoba/ES Keywords:
Optic Pathway Gliomas, Germinomas, Spinal Cord Tumours. Colin Kennedy March 2015
 Optic Pathway Gliomas, Germinomas, Spinal Cord Tumours Colin Kennedy March 2015 Glioma of the optic chiasm. T1-weighted MRI with gadolinium enhancement, showing intense irregular uptake of contrast. The
Optic Pathway Gliomas, Germinomas, Spinal Cord Tumours Colin Kennedy March 2015 Glioma of the optic chiasm. T1-weighted MRI with gadolinium enhancement, showing intense irregular uptake of contrast. The
Graves Ophthalmopathy Overview. Graves Disease Hyperthyroidism TSIgs (anti-tsh-receptor-abs) Graves Disease 10/22/2010
 Graves Disease Robert Graves Graves Ophthalmopathy Overview Robert C. Kersten Dept. of Ophthalmology UCSF Triad Hyperthyroidism Eye findings Pretibial Myxedema (phalangeal acropachy-1%) Most common auto-immune
Graves Disease Robert Graves Graves Ophthalmopathy Overview Robert C. Kersten Dept. of Ophthalmology UCSF Triad Hyperthyroidism Eye findings Pretibial Myxedema (phalangeal acropachy-1%) Most common auto-immune
Characteristic Ultrasonographic Findings of Choroidal Tumors
 Characteristic Ultrasonographic Findings of Choroidal Tumors Tsung-Jen Wang, Chang-Hao Yang, Shu-Lang Liao, Tzyy-Chang Ho, Jen-Shang Huang, Chang-Ping Lin, Chung-May Yang, Muh-Shy Chen and Luke Long-Kuang
Characteristic Ultrasonographic Findings of Choroidal Tumors Tsung-Jen Wang, Chang-Hao Yang, Shu-Lang Liao, Tzyy-Chang Ho, Jen-Shang Huang, Chang-Ping Lin, Chung-May Yang, Muh-Shy Chen and Luke Long-Kuang
Case Studies In the Orbit
 Case Studies In the Orbit Ethan Neufeld MD Department of Radiology and Imaging Sciences University of Utah Health Sciences Center Salt Lake City, Utah, USA Case Studies In the Orbit Learning objectives:
Case Studies In the Orbit Ethan Neufeld MD Department of Radiology and Imaging Sciences University of Utah Health Sciences Center Salt Lake City, Utah, USA Case Studies In the Orbit Learning objectives:
Outline. Brief history and principles of ophthalmic ultrasound. Types of ocular ultrasound. Examination techniques. Types of Ultrasound
 Ultrasound and Intraocular Tumors 2015 Ophthalmic Photographers' Society Mid-Year Program Cagri G. Besirli MD, PhD Kellogg Eye Center University of Michigan Outline Brief history and principles of ophthalmic
Ultrasound and Intraocular Tumors 2015 Ophthalmic Photographers' Society Mid-Year Program Cagri G. Besirli MD, PhD Kellogg Eye Center University of Michigan Outline Brief history and principles of ophthalmic
CT and MRI Imaging Spectrum of Orbital Masses: A Pictorial Essay.
 CT and MRI Imaging Spectrum of Orbital Masses: A Pictorial Essay. Poster No.: C-1556 Congress: ECR 2014 Type: Educational Exhibit Authors: I. Chouchene, S. MAJDOUB, A. Achour, H. Zaghouani, M. 1 1 1 1
CT and MRI Imaging Spectrum of Orbital Masses: A Pictorial Essay. Poster No.: C-1556 Congress: ECR 2014 Type: Educational Exhibit Authors: I. Chouchene, S. MAJDOUB, A. Achour, H. Zaghouani, M. 1 1 1 1
A CASE OF A Huge Submandibular Pleomorphic Adenoma
 ISPUB.COM The Internet Journal of Head and Neck Surgery Volume 4 Number 2 S VERMA Citation S VERMA.. The Internet Journal of Head and Neck Surgery. 2009 Volume 4 Number 2. Abstract Pleomorphic adenoma
ISPUB.COM The Internet Journal of Head and Neck Surgery Volume 4 Number 2 S VERMA Citation S VERMA.. The Internet Journal of Head and Neck Surgery. 2009 Volume 4 Number 2. Abstract Pleomorphic adenoma
Year 2003 Paper two: Questions supplied by Tricia
 question 43 A 42-year-old man presents with a two-year history of increasing right facial numbness. He has a history of intermittent unsteadiness, mild hearing loss and vertigo but has otherwise been well.
question 43 A 42-year-old man presents with a two-year history of increasing right facial numbness. He has a history of intermittent unsteadiness, mild hearing loss and vertigo but has otherwise been well.
Diagnostic Imaging in Patients with Orbital Cellulitis and Inflammatory Pseudotumor. Fumiyuki Uehara, M.D. Norio Ohba, M.D.
 Diagnostic Imaging in Patients with Orbital Cellulitis and Inflammatory Pseudotumor Fumiyuki Uehara, M.D. Norio Ohba, M.D. We have had the opportunity, at an eye clinic, to examine and treat a patient
Diagnostic Imaging in Patients with Orbital Cellulitis and Inflammatory Pseudotumor Fumiyuki Uehara, M.D. Norio Ohba, M.D. We have had the opportunity, at an eye clinic, to examine and treat a patient
Results of Transmedial-Canthal Ethmoidal Decompression for Severe Dysthyroid Optic Neuropathy
 Results of Transmedial-Canthal Ethmoidal Decompression for Severe Dysthyroid Optic Neuropathy Kenji Ohtsuka and Yasushi Nakamura Department of Ophthalmology, Sapporo Medical University School of Medicine,
Results of Transmedial-Canthal Ethmoidal Decompression for Severe Dysthyroid Optic Neuropathy Kenji Ohtsuka and Yasushi Nakamura Department of Ophthalmology, Sapporo Medical University School of Medicine,
Solitary Orbital Metastasis Presenting as Extraocular Muscle Mass in Lung Cancer Patient: A Case Report 외안근비대의형태로나타난폐암환자의고립성안와전이 : 증례보고
 Case Report pissn 1738-2637 / eissn 2288-2928 https://doi.org/10.3348/jksr.2017.77.3.143 Solitary Orbital Metastasis Presenting as Extraocular Muscle Mass in Lung Cancer Patient: A Case Report 외안근비대의형태로나타난폐암환자의고립성안와전이
Case Report pissn 1738-2637 / eissn 2288-2928 https://doi.org/10.3348/jksr.2017.77.3.143 Solitary Orbital Metastasis Presenting as Extraocular Muscle Mass in Lung Cancer Patient: A Case Report 외안근비대의형태로나타난폐암환자의고립성안와전이
Role of imaging in RCC. Ultrasonography. Solid lesion. Cystic RCC. Solid RCC 31/08/60. From Diagnosis to Treatment: the Radiologist Perspective
 Role of imaging in RCC From Diagnosis to Treatment: the Radiologist Perspective Diagnosis Staging Follow up Imaging modalities Limitations and pitfalls Duangkamon Prapruttam, MD Department of Therapeutic
Role of imaging in RCC From Diagnosis to Treatment: the Radiologist Perspective Diagnosis Staging Follow up Imaging modalities Limitations and pitfalls Duangkamon Prapruttam, MD Department of Therapeutic
Neuro-Ocular Grand Rounds Anthony B. Litwak,OD, FAAO VA Medical Center Baltimore, Maryland
 Neuro-Ocular Grand Rounds Anthony B. Litwak,OD, FAAO VA Medical Center Baltimore, Maryland Dr. Litwak is on the speaker and advisory boards for Alcon and Zeiss Meditek COMMON OPTIC NEUROPATHIES THAT CAN
Neuro-Ocular Grand Rounds Anthony B. Litwak,OD, FAAO VA Medical Center Baltimore, Maryland Dr. Litwak is on the speaker and advisory boards for Alcon and Zeiss Meditek COMMON OPTIC NEUROPATHIES THAT CAN
Orbital and Ocular Adnexal Disorders with Red Eyes
 Orbital and Ocular Adnexal Disorders with Red Eyes Jason Lee Associate Consultant Department of Ophthalmology and Visual Sciences Practical Ophthalmology for the Family Physician 21 Jan 2017 No financial
Orbital and Ocular Adnexal Disorders with Red Eyes Jason Lee Associate Consultant Department of Ophthalmology and Visual Sciences Practical Ophthalmology for the Family Physician 21 Jan 2017 No financial
Pituitary Apoplexy: Early Detection with Diffusion-Weighted MR Imaging
 AJNR Am J Neuroradiol 23:1240 1245, August 2002 Case Report Pituitary Apoplexy: Early Detection with Diffusion-Weighted MR Imaging Jeffrey M. Rogg, Glenn A. Tung, Gordon Anderson, and Selina Cortez Summary:
AJNR Am J Neuroradiol 23:1240 1245, August 2002 Case Report Pituitary Apoplexy: Early Detection with Diffusion-Weighted MR Imaging Jeffrey M. Rogg, Glenn A. Tung, Gordon Anderson, and Selina Cortez Summary:
Advances In Orbital Neuropathology
 Advances In Orbital Neuropathology Charles G. Eberhart, MD PhD Associate Professor of Pathology, Ophthalmology and Oncology Johns Hopkins University School of Medicine Overview Non-neoplastic lesions Microphthalmos/pseudoglioma
Advances In Orbital Neuropathology Charles G. Eberhart, MD PhD Associate Professor of Pathology, Ophthalmology and Oncology Johns Hopkins University School of Medicine Overview Non-neoplastic lesions Microphthalmos/pseudoglioma
Cross sectional imaging of Intracranial cystic lesions Abdel Razek A
 Cross sectional imaging of Intracranial cystic lesions Abdel Razek A Department of Radiology. Mansoura Faculty of Medicine, Mansoura. Egypt. arazek@mans.edu.eg Introduction Intracranial cystic lesions
Cross sectional imaging of Intracranial cystic lesions Abdel Razek A Department of Radiology. Mansoura Faculty of Medicine, Mansoura. Egypt. arazek@mans.edu.eg Introduction Intracranial cystic lesions
Case Studies in Sella/Parasellar Region. Child thirsty, increased urination. Imaging. Suprasellar Germ Cell Tumor (Germinoma) No Disclosures
 Case Studies in Sella/Parasellar Region No Disclosures 2018 Head and Neck Imaging Conference Child thirsty, increased urination Suprasellar Germ Cell Tumor (Germinoma) Midline Pineal >> Suprasellar > Other
Case Studies in Sella/Parasellar Region No Disclosures 2018 Head and Neck Imaging Conference Child thirsty, increased urination Suprasellar Germ Cell Tumor (Germinoma) Midline Pineal >> Suprasellar > Other
CT & MRI Evaluation of Brain Tumour & Tumour like Conditions
 CT & MRI Evaluation of Brain Tumour & Tumour like Conditions Dr. Anjana Trivedi 1, Dr. Jay Thakkar 2, Dr. Maulik Jethva 3, Dr. Ishita Virda 4 1 M.D. Radiology, Professor and Head, P.D.U. Medical College
CT & MRI Evaluation of Brain Tumour & Tumour like Conditions Dr. Anjana Trivedi 1, Dr. Jay Thakkar 2, Dr. Maulik Jethva 3, Dr. Ishita Virda 4 1 M.D. Radiology, Professor and Head, P.D.U. Medical College
Anatomy: There are 6 muscles that move your eye.
 Thyroid Eye Disease Your doctor thinks you have thyroid orbitopathy. This is an autoimmune condition where your body's immune system is producing factors that stimulate enlargement of the muscles that
Thyroid Eye Disease Your doctor thinks you have thyroid orbitopathy. This is an autoimmune condition where your body's immune system is producing factors that stimulate enlargement of the muscles that
Craniopharyngioma. Michael Gottschalk, MD,PhD University of California San Diego Rady Children s Hospital
 Craniopharyngioma Michael Gottschalk, MD,PhD University of California San Diego Rady Children s Hospital Objectives Incidence Clinical Presentation Treatment Options Perioperative concerns Long-term endocrine
Craniopharyngioma Michael Gottschalk, MD,PhD University of California San Diego Rady Children s Hospital Objectives Incidence Clinical Presentation Treatment Options Perioperative concerns Long-term endocrine
Pediatric CNS Tumors. Disclosures. Acknowledgements. Introduction. Introduction. Posterior Fossa Tumors. Whitney Finke, MD
 Pediatric CNS Tumors Disclosures Whitney Finke, MD Neuroradiology Fellow PGY-6 University of Utah Health Sciences Center Salt Lake City, Utah None Acknowledgements Introduction Nicholas A. Koontz, MD Luke
Pediatric CNS Tumors Disclosures Whitney Finke, MD Neuroradiology Fellow PGY-6 University of Utah Health Sciences Center Salt Lake City, Utah None Acknowledgements Introduction Nicholas A. Koontz, MD Luke
CLINICAL PEARLS IN OCULAR ONCOLOGY
 CLINICAL PEARLS IN OCULAR ONCOLOGY IRIS NEVUS - Two kinds circumscribed and diffuse - Photodocumentation important to monitor growth - Risk Factors for iris nevus growth to melanoma (ABCDEF) A Age (young),
CLINICAL PEARLS IN OCULAR ONCOLOGY IRIS NEVUS - Two kinds circumscribed and diffuse - Photodocumentation important to monitor growth - Risk Factors for iris nevus growth to melanoma (ABCDEF) A Age (young),
Imaging of Hearing Loss
 Contemporary Imaging of Sensorineural Hearing Loss Imaging of Hearing Loss Discussion Outline (SNHL) Imaging Approaches Anatomic Relationships Lesions: SNHL KL Salzman, MD University of Utah School of
Contemporary Imaging of Sensorineural Hearing Loss Imaging of Hearing Loss Discussion Outline (SNHL) Imaging Approaches Anatomic Relationships Lesions: SNHL KL Salzman, MD University of Utah School of
Neuro - imaging. Sella. ssregypt.com
 Neuro - imaging Sella ssregypt.com Bony Sella AP diameter Depth Contents 16mm 14mm Pituitary gland, part of infundibular stalk, CSF CT Technique 5 mm slices Axial and coronal Contrast injection Bone and
Neuro - imaging Sella ssregypt.com Bony Sella AP diameter Depth Contents 16mm 14mm Pituitary gland, part of infundibular stalk, CSF CT Technique 5 mm slices Axial and coronal Contrast injection Bone and
Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (CSC)
 HPTER 12 Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (S) linical Features VKH disease is a bilateral granulomatous panuveitis often associated with exudative
HPTER 12 Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (S) linical Features VKH disease is a bilateral granulomatous panuveitis often associated with exudative
Hypothalamic glioma masquerading as craniopharyngioma
 1 di 7 24/01/2014 18.58 J Neurosci Rural Pract. 2013 Jul-Sep; 4(3): 323 325. doi: 10.4103/0976-3147.118790 PMCID: PMC3821425 Hypothalamic glioma masquerading as craniopharyngioma Sameer Vyas, Nidhi Prabhakar,
1 di 7 24/01/2014 18.58 J Neurosci Rural Pract. 2013 Jul-Sep; 4(3): 323 325. doi: 10.4103/0976-3147.118790 PMCID: PMC3821425 Hypothalamic glioma masquerading as craniopharyngioma Sameer Vyas, Nidhi Prabhakar,
No Financial Interest
 Pituitary Apoplexy Michael Vaphiades, D.O. Professor Department of Ophthalmology, Neurology, Neurosurgery University of Alabama at Birmingham, Birmingham, AL No Financial Interest N E U R O L O G I C
Pituitary Apoplexy Michael Vaphiades, D.O. Professor Department of Ophthalmology, Neurology, Neurosurgery University of Alabama at Birmingham, Birmingham, AL No Financial Interest N E U R O L O G I C
Cryptogenic Enlargement Of Bilateral Superior Ophthalmic Veins
 ISPUB.COM The Internet Journal of Radiology Volume 18 Number 1 Cryptogenic Enlargement Of Bilateral Superior Ophthalmic Veins K Kragha Citation K Kragha. Cryptogenic Enlargement Of Bilateral Superior Ophthalmic
ISPUB.COM The Internet Journal of Radiology Volume 18 Number 1 Cryptogenic Enlargement Of Bilateral Superior Ophthalmic Veins K Kragha Citation K Kragha. Cryptogenic Enlargement Of Bilateral Superior Ophthalmic
Carotid Cavernous Fistula
 Chief Complaint: Double vision. Carotid Cavernous Fistula Alex W. Cohen, MD, PhD; Richard Allen, MD, PhD May 14, 2010 History of Present Illness: A 46 year old female patient presented to the Oculoplastics
Chief Complaint: Double vision. Carotid Cavernous Fistula Alex W. Cohen, MD, PhD; Richard Allen, MD, PhD May 14, 2010 History of Present Illness: A 46 year old female patient presented to the Oculoplastics
What was going on. Thyroid Related Orbitopathy. Pathophysiology. Definition GALLO EYE AND FACIAL PLASTIC SURGERY 3/16/2017
 GALLO EYE AND FACIAL PLASTIC SURGERY What was going on A. She found out the increase to her Premium and Deductible for employee health care next year B. She is getting an over agressive Physical Exam by
GALLO EYE AND FACIAL PLASTIC SURGERY What was going on A. She found out the increase to her Premium and Deductible for employee health care next year B. She is getting an over agressive Physical Exam by
Orbital Tumors And Pseudotumors
 Orbital Tumors And Pseudotumors Poster No.: C-2412 Congress: ECR 2015 Type: Educational Exhibit Authors: M. Limeme, N. Benzina, A. BelKhiria, H. Zaghouani, S. Majdoub, N. Mallat, H. Amara, D. Bakir, C.
Orbital Tumors And Pseudotumors Poster No.: C-2412 Congress: ECR 2015 Type: Educational Exhibit Authors: M. Limeme, N. Benzina, A. BelKhiria, H. Zaghouani, S. Majdoub, N. Mallat, H. Amara, D. Bakir, C.
Dr. T. Venkat Kishan Asst. Prof Department of Radiodiagnosis
 Dr. T. Venkat Kishan Asst. Prof Department of Radiodiagnosis Schwannomas (also called neurinomas or neurilemmomas) constitute the most common primary cranial nerve tumors. They are benign slow-growing
Dr. T. Venkat Kishan Asst. Prof Department of Radiodiagnosis Schwannomas (also called neurinomas or neurilemmomas) constitute the most common primary cranial nerve tumors. They are benign slow-growing
Ranbir Singh Sandhu Gillian Lieberman, MD. Orbital Lymphoma. Ranbir Singh Sandhu, University College London Medical School Gillian Lieberman MD, BIDMC
 Orbital Lymphoma Ranbir Singh Sandhu, University College London Medical School Gillian Lieberman MD, BIDMC 1 Our Patient Clinical Picture This topic will be presented in the context of our patient. She
Orbital Lymphoma Ranbir Singh Sandhu, University College London Medical School Gillian Lieberman MD, BIDMC 1 Our Patient Clinical Picture This topic will be presented in the context of our patient. She
Pituitary Macroadenoma with Superior Orbital Fissure Syndrome
 1 CASE REPORT OPEN ACCESS Pituitary Macroadenoma with Superior Orbital Fissure Syndrome Tapan Nagpal, Ankit Singhania ABSTRACT Introduction: Pituitary adenomas are benign tumours which arise within the
1 CASE REPORT OPEN ACCESS Pituitary Macroadenoma with Superior Orbital Fissure Syndrome Tapan Nagpal, Ankit Singhania ABSTRACT Introduction: Pituitary adenomas are benign tumours which arise within the
Case Fibrothecoma of the ovary
 Case 10646 Fibrothecoma of the ovary Elisa Melo Abreu, Teresa Margarida Cunha Section: Genital (Female) Imaging Published: 2015, Jan. 2 Patient: 70 year(s), female Authors' Institution Department of Radiology,
Case 10646 Fibrothecoma of the ovary Elisa Melo Abreu, Teresa Margarida Cunha Section: Genital (Female) Imaging Published: 2015, Jan. 2 Patient: 70 year(s), female Authors' Institution Department of Radiology,
Essentials of Clinical MR, 2 nd edition. 65. Benign Hepatic Masses
 65. Benign Hepatic Masses Pulse sequences acquired for abdominal MRI typically consist of fast acquisition schemes such as single-shot turbo spin echo (i.e. HASTE) and gradient echo schemes such as FLASH
65. Benign Hepatic Masses Pulse sequences acquired for abdominal MRI typically consist of fast acquisition schemes such as single-shot turbo spin echo (i.e. HASTE) and gradient echo schemes such as FLASH
The central nervous system
 Sectc.qxd 29/06/99 09:42 Page 81 Section C The central nervous system CNS haemorrhage Subarachnoid haemorrhage Cerebral infarction Brain atrophy Ring enhancing lesions MRI of the pituitary Multiple sclerosis
Sectc.qxd 29/06/99 09:42 Page 81 Section C The central nervous system CNS haemorrhage Subarachnoid haemorrhage Cerebral infarction Brain atrophy Ring enhancing lesions MRI of the pituitary Multiple sclerosis
CNS TUMORS. D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria)
 CNS TUMORS D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria) CNS TUMORS The annual incidence of intracranial tumors of the CNS ISmore than intraspinal tumors May be Primary or Secondary
CNS TUMORS D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria) CNS TUMORS The annual incidence of intracranial tumors of the CNS ISmore than intraspinal tumors May be Primary or Secondary
Orbit Deformities in Craniofacial Neurofibromatosis Type 1
 AJNR Am J Neuroradiol 24:1678 1682, September 2003 Orbit Deformities in Craniofacial Neurofibromatosis Type 1 Claude Jacquemin, Thomas M. Bosley, and Helena Svedberg BACKGROUND AND PURPOSE: The possible
AJNR Am J Neuroradiol 24:1678 1682, September 2003 Orbit Deformities in Craniofacial Neurofibromatosis Type 1 Claude Jacquemin, Thomas M. Bosley, and Helena Svedberg BACKGROUND AND PURPOSE: The possible
Imaging Orbit/Periorbital Injury
 Imaging Orbit/Periorbital Injury 9 th Nordic Trauma Radiology Course 2016 Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Fireworks Topics to Cover Struts
Imaging Orbit/Periorbital Injury 9 th Nordic Trauma Radiology Course 2016 Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Fireworks Topics to Cover Struts
Renal masses - the role of diagnostic imaging
 Renal masses - the role of diagnostic imaging Poster No.: C-2471 Congress: ECR 2015 Type: Educational Exhibit Authors: V. Rai#; Bjelovar/HR Keywords: Cysts, Cancer, Structured reporting, Ultrasound, MR,
Renal masses - the role of diagnostic imaging Poster No.: C-2471 Congress: ECR 2015 Type: Educational Exhibit Authors: V. Rai#; Bjelovar/HR Keywords: Cysts, Cancer, Structured reporting, Ultrasound, MR,
Coexisting Rathke Cleft Cyst and Pituitary Adenoma Presenting with Pituitary Apoplexy: Report of Two Cases
 Coexisting Rathke Cleft Cyst and Pituitary Adenoma Presenting with Pituitary Apoplexy: Report of Two Cases Florian Gessler, M.D., 1,* Valerie C. Coon, M.D., 1,* Steven S. Chin, M.D., Ph.D., 2 and William
Coexisting Rathke Cleft Cyst and Pituitary Adenoma Presenting with Pituitary Apoplexy: Report of Two Cases Florian Gessler, M.D., 1,* Valerie C. Coon, M.D., 1,* Steven S. Chin, M.D., Ph.D., 2 and William
MR Imaging of Orbital and Ocular Disease
 259 MR Imaging of Orbital and Ocular Disease David F. Sobel 1 William Kelly 1 Bent O. Kjos1 Devron Char 2 Michael Brant-Zawadzki1 David Norman 1 Magnetic resonance (MR) images of 27 patients with ocular
259 MR Imaging of Orbital and Ocular Disease David F. Sobel 1 William Kelly 1 Bent O. Kjos1 Devron Char 2 Michael Brant-Zawadzki1 David Norman 1 Magnetic resonance (MR) images of 27 patients with ocular
Benign brain lesions
 Benign brain lesions Diagnostic and Interventional Radiology Hung-Wen Kao Department of Radiology, Tri-Service General Hospital, National Defense Medical Center Computed tomography Hounsfield unit (HU)
Benign brain lesions Diagnostic and Interventional Radiology Hung-Wen Kao Department of Radiology, Tri-Service General Hospital, National Defense Medical Center Computed tomography Hounsfield unit (HU)
Supplementary Appendix
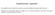 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Vernooij MW, Ikram MA, Tanghe HL, et al. Incidental findings
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Vernooij MW, Ikram MA, Tanghe HL, et al. Incidental findings
Diagnostic Role of CT in the Evaluation of Proptosis
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 4 Ver. IX (Apr. 2015), PP 25-31 www.iosrjournals.org Diagnostic Role of CT in the Evaluation
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 4 Ver. IX (Apr. 2015), PP 25-31 www.iosrjournals.org Diagnostic Role of CT in the Evaluation
NANOS Patient Brochure
 NANOS Patient Brochure Pituitary Tumor Copyright 2015. North American Neuro-Ophthalmology Society. All rights reserved. These brochures are produced and made available as is without warranty and for informational
NANOS Patient Brochure Pituitary Tumor Copyright 2015. North American Neuro-Ophthalmology Society. All rights reserved. These brochures are produced and made available as is without warranty and for informational
Intracranial Lesions: MRI Signs for Localization
 Intracranial Lesions: MRI Signs for Localization Poster No.: C-1574 Congress: ECR 2017 Type: Educational Exhibit Authors: M. Cucos, A. Puiu, S. Manole ; Cluj-Napoca/RO, Cluj napoca/ RO Keywords: Cerebrospinal
Intracranial Lesions: MRI Signs for Localization Poster No.: C-1574 Congress: ECR 2017 Type: Educational Exhibit Authors: M. Cucos, A. Puiu, S. Manole ; Cluj-Napoca/RO, Cluj napoca/ RO Keywords: Cerebrospinal
Retina Center of Oklahoma Sam S. Dahr, M.D. Adult Intraocular Tumors
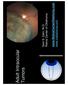 Adult Intraocular Tumors Sam S. Dahr, M.D. Retina Center of Oklahoma www.retinacenteroklahoma.com www.rcoklahoma.com Table of Contents Posterior uveal malignant melanoma Uveal metastasis Uveal melanoma
Adult Intraocular Tumors Sam S. Dahr, M.D. Retina Center of Oklahoma www.retinacenteroklahoma.com www.rcoklahoma.com Table of Contents Posterior uveal malignant melanoma Uveal metastasis Uveal melanoma
Anatomy of the orbit. Lay-out. Imaging technique. 3 x 3. brief overview of the basic anatomy of the orbit and its structures
 Anatomy of the orbit Prof. Pia C Sundgren MD, PhD Department of Diagnostic Radiology, Clinical Sciences, Lund University, Sweden Lay-out brief overview of the basic anatomy of the orbit and its structures
Anatomy of the orbit Prof. Pia C Sundgren MD, PhD Department of Diagnostic Radiology, Clinical Sciences, Lund University, Sweden Lay-out brief overview of the basic anatomy of the orbit and its structures
Diseases of pituitary gland
 Diseases of pituitary gland A brief introduction Anterior lobe = adenohypophysis Posterior lobe = neurohypophysis The production of most pituitary hormones is controlled in large part by positively and
Diseases of pituitary gland A brief introduction Anterior lobe = adenohypophysis Posterior lobe = neurohypophysis The production of most pituitary hormones is controlled in large part by positively and
Case Studies in the Skull Base
 Case Studies in the Skull Base Amy C Tsai, MD Neuroradiology Fellow Department of Radiology and Imaging Sciences University of Utah Health Sciences Center Salt Lake City, Utah, USA No disclosures related
Case Studies in the Skull Base Amy C Tsai, MD Neuroradiology Fellow Department of Radiology and Imaging Sciences University of Utah Health Sciences Center Salt Lake City, Utah, USA No disclosures related
Neuroradiology Case of the Day
 Neuroradiology Case of the Day 76 th CAR Annual Meeting, Montreal, Quebec April 27, 2013 Eugene Yu, MD Assistant Professor of Radiology and Otolaryngology-Head and Neck Surgery Head and Neck Imaging Princess
Neuroradiology Case of the Day 76 th CAR Annual Meeting, Montreal, Quebec April 27, 2013 Eugene Yu, MD Assistant Professor of Radiology and Otolaryngology-Head and Neck Surgery Head and Neck Imaging Princess
Interesting Cases from Liver Tumor Board. Jeffrey C. Weinreb, M.D.,FACR Yale University School of Medicine
 Interesting Cases from Liver Tumor Board Jeffrey C. Weinreb, M.D.,FACR Yale University School of Medicine jeffrey.weinreb@yale.edu Common Liver Diseases Hemangioma Cyst FNH Focal Fat/Sparing THID Non-Cirrhotic
Interesting Cases from Liver Tumor Board Jeffrey C. Weinreb, M.D.,FACR Yale University School of Medicine jeffrey.weinreb@yale.edu Common Liver Diseases Hemangioma Cyst FNH Focal Fat/Sparing THID Non-Cirrhotic
Bilateral Retinoblastoma Joseph Junewick, MD FACR
 Bilateral Retinoblastoma Joseph Junewick, MD FACR 06/11/2010 History 17 month old adopted female with proptosis. Diagnosis Bilateral Retinoblastoma Discussion Retinoblastoma is the most common pediatric
Bilateral Retinoblastoma Joseph Junewick, MD FACR 06/11/2010 History 17 month old adopted female with proptosis. Diagnosis Bilateral Retinoblastoma Discussion Retinoblastoma is the most common pediatric
A Patient Presenting with Ptosis, Ophthalmoplegia, and Decreased Periorbital Sensations and Facial Droop in Tolosa-Hunt Syndrome
 A Patient Presenting with Ptosis, Ophthalmoplegia, and Decreased Periorbital Sensations and Facial Droop in Tolosa-Hunt Syndrome medicine2.missouri.edu/jahm/patient-presenting-ptosis-ophthalmoplegia-decreased-periorbital-sensations-facial-drooptolosa-hunt-syndrome/
A Patient Presenting with Ptosis, Ophthalmoplegia, and Decreased Periorbital Sensations and Facial Droop in Tolosa-Hunt Syndrome medicine2.missouri.edu/jahm/patient-presenting-ptosis-ophthalmoplegia-decreased-periorbital-sensations-facial-drooptolosa-hunt-syndrome/
MRI Dynamic Color Mapping: a new quantitative technique for imaging soft tissue motion in the orbit
 MRI DYNAMIC COLOR MAPPING: A NEW QUANTITATIVE TECHNIQUE FOR IMAGING SOFT TISSUE MOTION IN THE ORBIT 79 6 MRI Dynamic Color Mapping: a new quantitative technique for imaging soft tissue motion in the orbit
MRI DYNAMIC COLOR MAPPING: A NEW QUANTITATIVE TECHNIQUE FOR IMAGING SOFT TISSUE MOTION IN THE ORBIT 79 6 MRI Dynamic Color Mapping: a new quantitative technique for imaging soft tissue motion in the orbit
Case Conference: Neuroradiology. Case 1: Tumor Case 1: 22yo F w/ HA and prior Seizures
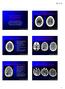 Case Conference: Neuroradiology Case 1: 22yo F w/ HA and prior Seizures David E. Rex, MD, PhD Stanford University Hospital Department of Radiology Case 1: Tumor Most likely gangiloglioma, oligodendroglioma,
Case Conference: Neuroradiology Case 1: 22yo F w/ HA and prior Seizures David E. Rex, MD, PhD Stanford University Hospital Department of Radiology Case 1: Tumor Most likely gangiloglioma, oligodendroglioma,
Radiology of hypothalamic lesions: A pictorial essay depicting characteristic hypothalamic pathologies
 Radiology of hypothalamic lesions: A pictorial essay depicting characteristic hypothalamic pathologies Poster No.: C-2713 Congress: ECR 2010 Type: Scientific Exhibit Topic: Neuro Authors: A. J. B. Baxi,
Radiology of hypothalamic lesions: A pictorial essay depicting characteristic hypothalamic pathologies Poster No.: C-2713 Congress: ECR 2010 Type: Scientific Exhibit Topic: Neuro Authors: A. J. B. Baxi,
Pediatric Retroperitoneal Masses Radiologic-Pathologic Correlation
 Acta Radiológica Portuguesa, Vol.XVIII, nº 70, pág. 61-70, Abr.-Jun., 2006 Pediatric Retroperitoneal Masses Radiologic-Pathologic Correlation Marilyn J. Siegel Mallinckrodt Institute of Radiology, Washington
Acta Radiológica Portuguesa, Vol.XVIII, nº 70, pág. 61-70, Abr.-Jun., 2006 Pediatric Retroperitoneal Masses Radiologic-Pathologic Correlation Marilyn J. Siegel Mallinckrodt Institute of Radiology, Washington
Neckmasses in infancy and childhood: Clinical and radiological classification and imaging approaches M. Mearadji
 Neckmasses in infancy and childhood: Clinical and radiological classification and imaging approaches M. Mearadji International Foundation for Pediatric Imaging Aid Introduction Neck masses are a frequent
Neckmasses in infancy and childhood: Clinical and radiological classification and imaging approaches M. Mearadji International Foundation for Pediatric Imaging Aid Introduction Neck masses are a frequent
Criteria of Malignancy. Evaluation Score
 30 5 Diagnostic Criteria Criteria of Malignancy Table 5.2 lists criteria in contrast-enhancing MR mammography that strongly indicate the presence of malignancy or are unspecific. Unifactorial evaluation
30 5 Diagnostic Criteria Criteria of Malignancy Table 5.2 lists criteria in contrast-enhancing MR mammography that strongly indicate the presence of malignancy or are unspecific. Unifactorial evaluation
Methods. Yahya Paksoy, Bülent Oğuz Genç, and Emine Genç. AJNR Am J Neuroradiol 24: , August 2003
 AJNR Am J Neuroradiol 24:1364 1368, August 2003 Retrograde Flow in the Left Inferior Petrosal Sinus and Blood Steal of the Cavernous Sinus Associated with Central Vein Stenosis: MR Angiographic Findings
AJNR Am J Neuroradiol 24:1364 1368, August 2003 Retrograde Flow in the Left Inferior Petrosal Sinus and Blood Steal of the Cavernous Sinus Associated with Central Vein Stenosis: MR Angiographic Findings
Index. radiologic.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A ACC. See Adrenal cortical carcinoma. Acromegaly and the pituitary gland, 551 Acute suppurative thyroiditis, 405, 406 Addison, Thomas and
Index Note: Page numbers of article titles are in boldface type. A ACC. See Adrenal cortical carcinoma. Acromegaly and the pituitary gland, 551 Acute suppurative thyroiditis, 405, 406 Addison, Thomas and
JMSCR Vol 3 Issue 11 Page November 2015
 www.jmscr.igmpublication.org Impact Factor 3.79 Index Copernicus Value: 5.88 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: http://dx.doi.org/10.18535/jmscr/v3i11.37 Accuracy of CT in Diagnosis of Orbital
www.jmscr.igmpublication.org Impact Factor 3.79 Index Copernicus Value: 5.88 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: http://dx.doi.org/10.18535/jmscr/v3i11.37 Accuracy of CT in Diagnosis of Orbital
Radiological Appearance of Extra-axial CNS Hemangioma
 Chin J Radiol 2002; 27: 183-190 183 Radiological Appearance of Extra-axial CNS Hemangioma MING-SHIANG YANG CLAYTON CHI-CHANG CHEN WEN-HSIEN CHEN HAO-CHUN HUNG SAN-KAN LEE Department of Radiology, Taichung
Chin J Radiol 2002; 27: 183-190 183 Radiological Appearance of Extra-axial CNS Hemangioma MING-SHIANG YANG CLAYTON CHI-CHANG CHEN WEN-HSIEN CHEN HAO-CHUN HUNG SAN-KAN LEE Department of Radiology, Taichung
IMAGING OF A CASE OF SPINAL MENINGIOMA- A CASE REPORT
 IMAGING OF A CASE OF SPINAL MENINGIOMA- A CASE REPORT Ramneet Wadi 1, Anil Kumar Shukla 2, Seetha Pramila V. V 3, Sabyasachi Basu 4, Sonam Sanjay 5 1Postgraduate Student, Department of Radiodiagnosis,
IMAGING OF A CASE OF SPINAL MENINGIOMA- A CASE REPORT Ramneet Wadi 1, Anil Kumar Shukla 2, Seetha Pramila V. V 3, Sabyasachi Basu 4, Sonam Sanjay 5 1Postgraduate Student, Department of Radiodiagnosis,
Essentials of Clinical MR, 2 nd edition. 51. Primary Neoplasms
 51. Primary Neoplasms As with spinal central canal neoplasms in other regions, those of the lumbar spine may be classified as extradural, intradural extramedullary, and medullary. If an extradural lesion
51. Primary Neoplasms As with spinal central canal neoplasms in other regions, those of the lumbar spine may be classified as extradural, intradural extramedullary, and medullary. If an extradural lesion
Typical idiopathic intracranial hypertension Optic nerve appearance and brain MRI findings. Jonathan A. Micieli, MD Valérie Biousse, MD
 Typical idiopathic intracranial hypertension Optic nerve appearance and brain MRI findings Jonathan A. Micieli, MD Valérie Biousse, MD A 24 year old African American woman is referred for bilateral optic
Typical idiopathic intracranial hypertension Optic nerve appearance and brain MRI findings Jonathan A. Micieli, MD Valérie Biousse, MD A 24 year old African American woman is referred for bilateral optic
The Radiological Spectrum of Orbital Pathologies that Involve the Lacrimal Gland and the Lacrimal Fossa
 The Radiological Spectrum of Orbital Pathologies that Involve the Lacrimal Gland and the Lacrimal Fossa Won Sang Jung, MD 1 Kook Jin Ahn, MD 1 Mi Ra Park, MD 2 Ji Young Kim, MD 1 Jae Jeong Choi, MD 1 Bum
The Radiological Spectrum of Orbital Pathologies that Involve the Lacrimal Gland and the Lacrimal Fossa Won Sang Jung, MD 1 Kook Jin Ahn, MD 1 Mi Ra Park, MD 2 Ji Young Kim, MD 1 Jae Jeong Choi, MD 1 Bum
Rethinking Orbital Imaging
 Rethinking Orbital Imaging Establishing Guidelines for Interpreting Orbital Imaging Studies and Evaluating Their Predictive Value in Patients with Orbital Tumors Guy J. Ben Simon, MD, 1 Christine C. Annunziata,
Rethinking Orbital Imaging Establishing Guidelines for Interpreting Orbital Imaging Studies and Evaluating Their Predictive Value in Patients with Orbital Tumors Guy J. Ben Simon, MD, 1 Christine C. Annunziata,
