Protocol for the Examination of Resection Specimens From Patients With Ductal Carcinoma In Situ (DCIS) of the Breast
|
|
|
- Barnaby Terry
- 5 years ago
- Views:
Transcription
1 Protocol for the Examination of Specimens From Patients With Ductal Carcinoma In Situ (DCIS) of the Breast Version: Breast DCIS Protocol Posting Date: February 2019 CAP Laboratory Accreditation Program Protocol Required Use Date: November 2019 Includes ptnm requirements from the 8 th Edition, AJCC Staging Manual For accreditation purposes, this protocol should be used for the following procedures AND tumor types: Procedure Description Excision less than total Includes specimens designated excision, segmental resection, mastectomy lumpectomy, quadrantectomy and segmental or partial mastectomy, with or without axillary contents Total Mastectomy Includes skin-sparing and nipple-sparing mastectomy, with or without axillary contents Tumor Type Description Ductal carcinoma in situ without invasive carcinoma or microinvasion Paget disease of the nipple not associated with invasive breast carcinoma Encapsulated papillary carcinoma without invasive carcinoma Solid papillary carcinoma without invasive carcinoma This protocol is NOT required for accreditation purposes for the following: Procedure Needle or skin biopsies (consider Breast DCIS Biopsy protocol) Primary resection specimen with no residual cancer (eg, following neoadjuvant therapy) Additional excision performed after the definitive resection (eg, re-excision of surgical margins) Cytologic specimens The following tumor types should NOT be reported using this protocol Tumor Type Any tumor with invasive carcinoma, including DCIS with microinvasion only (consider Breast Invasive Carcinoma protocol) Authors Patrick L. Fitzgibbons, MD*; James L. Connolly, MD*; Shikha Bose, MD; Yunn-Yi Chen, MD, PhD; Monica E. de Baca, MD; Mary Edgerton, MD; Daniel F. Hayes, MD; Kalisha A. Hill, MD; Susan C. Lester, MD, PhD; Jean F. Simpson, MD; Ross Simpson, MD; Barbara L. Smith, MD, PhD; Lee K. Tan, MD; Donald L. Weaver, MD. With guidance from the CAP Cancer and CAP Pathology Electronic Reporting Committees. * Denotes primary author. All other contributing authors are listed alphabetically College of American Pathologists (CAP). All rights reserved. For Terms of Use please visit
2 Breast DCIS Accreditation Requirements This protocol can be utilized for a variety of procedures and tumor types for clinical care purposes. For accreditation purposes, only the definitive primary cancer resection specimen is required to have the core and conditional data elements reported in a synoptic format. Core data elements are required in reports to adequately describe appropriate malignancies. For accreditation purposes, essential data elements must be reported in all instances, even if the response is not applicable or cannot be determined. Conditional data elements are only required to be reported if applicable as delineated in the protocol. For instance, the total number of lymph nodes examined must be reported, but only if nodes are present in the specimen. Optional data elements are identified with + and although not required for CAP accreditation purposes, may be considered for reporting as determined by local practice standards. The use of this protocol is not required for recurrent tumors or for metastatic tumors that are resected at a different time than the primary tumor. Use of this protocol is also not required for pathology reviews performed at a second institution (ie, secondary consultation, second opinion, or review of outside case at second institution). Synoptic Reporting All core and conditionally required data elements outlined on the surgical case summary from this cancer protocol must be displayed in synoptic report format. Synoptic format is defined as: Data element: followed by its answer (response), outline format without the paired "Data element: Response" format is NOT considered synoptic. The data element should be represented in the report as it is listed in the case summary. The response for any data element may be modified from those listed in the case summary, including Cannot be determined if appropriate. Each diagnostic parameter pair (Data element: Response) is listed on a separate line or in a tabular format to achieve visual separation. The following exceptions are allowed to be listed on one line: o Anatomic site or specimen, laterality, and procedure o Pathologic Stage Classification (ptnm) elements o Negative margins, as long as all negative margins are specifically enumerated where applicable The synoptic portion of the report can appear in the diagnosis section of the pathology report, at the end of the report or in a separate section, but all Data element: Responses must be listed together in one location Organizations and pathologists may choose to list the required elements in any order, use additional methods in order to enhance or achieve visual separation, or add optional items within the synoptic report. The report may have required elements in a summary format elsewhere in the report IN ADDITION TO but not as replacement for the synoptic report ie, all required elements must be in the synoptic portion of the report in the format defined above. CAP Breast DCIS Protocol Summary of Changes v The following data elements were modified: Margins Added options for reporting distance from closest uninvolved margin Added distances from other uninvolved margins Modified responses for positive margins ENE is now a core element 2
3 CAP Approved Breast DCIS Surgical Pathology Cancer Case Summary Protocol posting date: February 2019 DCIS OF THE BREAST: Select a single response unless otherwise indicated. Procedure, Laterality, and Site may be listed separately or on 1 line. Procedure (Note A) Excision (less than total mastectomy) Total mastectomy (including nipple-sparing and skin-sparing mastectomy) Other (specify): Not specified Specimen Laterality Right Left Not specified + Tumor Site (select all that apply) + Upper outer quadrant + Lower outer quadrant + Upper inner quadrant + Lower inner quadrant + Central + Nipple + Clock position (specify): o clock + Distance from nipple (centimeters): cm + Other (specify): + Not specified Size (Extent) of DCIS (Note C) (select all that apply) Estimated size (extent) of DCIS is at least (millimeters) mm + Additional dimensions (millimeters): x mm + Number of blocks with DCIS: + Number of blocks examined: Note: The size (extent) of DCIS (greatest dimension using gross and microscopic evaluation) is an estimation of the volume of breast tissue occupied by DCIS. Histologic Type (Note D) Ductal carcinoma in situ Paget disease Encapsulated papillary carcinoma without invasive carcinoma Solid papillary carcinoma without invasive carcinoma + Architectural Patterns (select all that apply) (Note E) + Comedo + Paget disease (DCIS involving nipple skin) + Cribriform + Micropapillary + Papillary + Solid + Other (specify: ) + Data elements preceded by this symbol are not required for accreditation purposes. These optional elements may be clinically important but are not yet validated or regularly used in patient management. 3
4 CAP Approved Breast DCIS Nuclear Grade (Note F) Grade I (low) Grade II (intermediate) Grade III (high) Necrosis (Note G) Not identified Present, focal (small foci or single cell necrosis) Present, central (expansive comedo necrosis) Margins (Note H) Cannot be assessed Uninvolved by DCIS Distance from closest margin (millimeters): Specify mm Less than mm Greater than mm Cannot be determined (explain): Specify closest margin (required only if <10mm): Cannot be determined (explain): + Distance from other margins (specify millimeter distance including greater than if appropriate): + Anterior: mm + Posterior: mm + Superior: mm + Inferior: mm + Medial: mm + Lateral: mm + Other (specify margin): mm Positive for DCIS (select all that apply): Anterior + Extent (specify): Posterior + Extent (specify): Superior + Extent (specify): Inferior + Extent (specify): Medial + Extent (specify): Lateral + Extent (specify): Other (specify margin): + Extent (specify): Cannot be determined (explain): Note: Margin status is listed as positive if there is ink on DCIS (ie, the distance is 0 mm). If the margin is not positive, then a distance from the margin may be listed. Distances can be specific measurements or expressed as greater than or less than a measurement. Extent may be specified as unifocal, multifocal, or extensive. + Data elements preceded by this symbol are not required for accreditation purposes. These optional elements may be clinically important but are not yet validated or regularly used in patient management. 4
5 CAP Approved Breast DCIS Regional Lymph Nodes (Notes B, J) No lymph nodes submitted or found Uninvolved by tumor cells Number of Lymph Nodes Examined: Number of Sentinel Nodes Examined (if applicable): Involved by tumor cells Number of Lymph Nodes with Macrometastases (>2 mm): Number of Lymph Nodes with Micrometastases (>0.2 mm to 2 mm and/or >200 cells): Number of Lymph Nodes with Isolated Tumor Cells ( 0.2 mm or 200 cells) # : # Reporting the number of lymph nodes with isolated tumor cells is required only in the absence of macrometastasis or micrometastasis in other lymph nodes. + Size of Largest Metastatic Deposit (millimeters): mm Extranodal Extension: Not identified Present Cannot be determined Number of Lymph Nodes Examined: Number of Sentinel Nodes Examined (if applicable): Pathologic Stage Classification (ptnm, AJCC 8 th Edition) (Note K) Note: Reporting of pt, pn, and (when applicable) pm categories is based on information available to the pathologist at the time the report is issued. Only the applicable T, N, or M category is required for reporting; their definitions need not be included in the report. The categories (with modifiers when applicable) can be listed on 1 line or more than 1 line. TNM Descriptors (required only if applicable) r (recurrent) Primary Tumor (pt) ptis (DCIS): Ductal carcinoma in situ ptis (Paget): Paget disease of the nipple not associated with invasive carcinoma and/or DCIS in the underlying breast parenchyma # Note: Paget disease with underlying DCIS is classified as Tis (DCIS). Encapsulated and solid papillary carcinomas without conventional invasive carcinoma are staged as ptis (DCIS). If there has been a prior core needle biopsy, the pathologic findings from the core, if available, should be incorporated in the T classification. If invasive carcinoma or microinvasion were present on the core, the protocol for invasive carcinomas of the breast should be used and should incorporate this information. # Note: Lobular carcinoma in situ (LCIS) is removed from TNM staging in the AJCC Cancer Staging Manual, 8th Edition. Regional Lymph Nodes (pn) (choose a category if lymph nodes received with the specimen; immunohistochemistry and/or molecular studies are not required) Modifier (required only if applicable) (sn): Sentinel node(s) evaluated. If 6 or more nodes (sentinel or nonsentinel) are removed, this modifier should not be used. (f): Nodal metastasis confirmed by fine needle aspiration or core needle biopsy. Note: The (sn) modifier is added to the N category when a sentinel node biopsy is performed (using either dye or tracer) and fewer than six lymph nodes are removed (sentinel and nonsentinel). The (f) modifier is added to the N category to denote confirmation of metastasis by fine needle aspiration/core needle biopsy with NO further resection of nodes. + Data elements preceded by this symbol are not required for accreditation purposes. These optional elements may be clinically important but are not yet validated or regularly used in patient management. 5
6 CAP Approved Breast DCIS Category (pn) pnx: Regional lymph nodes cannot be assessed (eg, not removed for pathological study or previously removed) pn0: No regional lymph node metastasis identified or ITCs only # pn0 (i+): ITCs only (malignant cell clusters no larger than 0.2 mm) in regional lymph node(s) pn0 (mol+): Positive molecular findings (RT-PCR), but no ITCs detected pn1mi: Micrometastases (approximately 200 cells, larger than 0.2 mm, but none larger than 2.0 mm) pn1a: Metastases in 1 to 3 axillary lymph nodes, at least 1 metastasis larger than 2.0 mm ## pn1b: Metastases in ipsilateral internal mammary sentinel nodes, excluding ITCs pn1c: pn1a and pn1b combined pn2a: Metastases in 4 to 9 axillary lymph nodes (at least 1 tumor deposit larger than 2.0 mm) ## pn2b: Metastases in clinically detected internal mammary lymph nodes with or without microscopic confirmation; with pathologically negative axillary nodes pn3a: Metastases in 10 or more axillary lymph nodes (at least 1 tumor deposit larger than 2.0 mm) ## pn3b: pn3c: or metastases to the infraclavicular (Level III axillary lymph) nodes pn1a or pn2a in the presence of cn2b (positive internal mammary nodes by imaging); or pn2a in the presence of pn1b Metastases in ipsilateral supraclavicular lymph nodes # Isolated tumor cells (ITCs) are defined as small clusters of cells not larger than 0.2 mm or single tumor cells, or a cluster of fewer than 200 cells in a single histologic cross-section. ITCs may be detected by routine histology or by immunohistochemical (IHC) methods. Nodes containing only ITCs are excluded from the total positive node count for purposes of N classification but should be included in the total number of nodes evaluated. ## Approximately 1000 tumor cells are contained in a 3-dimensional 0.2-mm cluster. Thus, if more than 200 individual tumor cells are identified as single dispersed tumor cells or as a nearly confluent elliptical or spherical focus in a single histologic section of a lymph node, there is a high probability that more than 1000 cells are present in the lymph node. In these situations, the node should be classified as containing a micrometastasis (pn1mi). Cells in different lymph node cross-sections or longitudinal sections or levels of the block are not added together; the 200 cells must be in a single node profile even if the node has been thinly sectioned into multiple slices. It is recognized that there is substantial overlap between the upper limit of the ITC and the lower limit of the micrometastasis categories due to inherent limitations in pathologic nodal evaluation and detection of minimal tumor burden in lymph nodes. Thus, the threshold of 200 cells in a single cross-section is a guideline to help pathologists distinguish between these 2 categories. The pathologist should use judgment regarding whether it is likely that the cluster of cells represents a true micrometastasis or is simply a small group of isolated tumor cells. Distant Metastasis (pm) (required only if confirmed pathologically in this case) pm1: Histologically proven metastases larger than 0.2 mm Specify site, if known + Specify report ID (if from a separate procedure) Note: The presence of distant metastases in a case of DCIS would be very unusual. Additional sampling to identify invasive carcinoma in the breast or additional history to document a prior or synchronous invasive carcinoma is advised in the evaluation of such cases. + Additional Pathologic Findings (Note L) + Specify: + Ancillary Studies Note: For hormone receptor reporting for this specimen, the CAP Breast Biomarker Template should be used. Pending biomarker studies should be listed in the Comments section of this report. + Breast Biomarker Testing Performed on Previous Biopsy + Estrogen Receptor (ER) + Positive % + Negative + Cannot be determined (indeterminate) + Data elements preceded by this symbol are not required for accreditation purposes. These optional elements may be clinically important but are not yet validated or regularly used in patient management. 6
7 CAP Approved Breast DCIS Progesterone Receptor (PgR) + Positive % + Negative + Cannot be determined (indeterminate) + Testing Performed on Case Number: + Microcalcifications (select all that apply) (Note M) + Not identified + Present in DCIS + Present in nonneoplastic tissue + Other (specify): + Clinical History (select all that apply) Note: The current clinical/radiologic breast findings for which this surgery is performed include: + Palpable mass + Nipple discharge + Other (specify): + Prior history of breast cancer + Specify site, diagnosis, and prior treatment: + Radiologic Finding (select all that apply) + Mass or architectural distortion + Calcifications + Other (specify): + Comment(s) + Data elements preceded by this symbol are not required for accreditation purposes. These optional elements may be clinically important but are not yet validated or regularly used in patient management. 7
8 Explanatory Notes A. Breast Specimens and Breast Procedures Breast Specimens The following types of breast specimens and procedures may be reported with the case summary: Excisions. Removal of breast tissue without the intent of removing the entire breast. The nipple is only rarely removed with excisions. Excisions include specimens designated biopsies, partial mastectomies, lumpectomies, and quadrantectomies. Total Mastectomy. Removal of all breast tissue, including the nipple and areola. Simple mastectomy: This procedure consists of a total mastectomy without removal of axillary lymph nodes. Skin-sparing mastectomy: This is a total mastectomy with removal of the nipple and only a narrow surrounding rim of skin. Modified radical mastectomy: This procedure consists of a total mastectomy and an axillary dissection. In the case summary, the breast and lymph node specimens are documented separately. Radical mastectomy: This procedure consists of a total mastectomy, axillary contents, and removal of the pectoralis muscles and currently is performed only rarely. This type of specimen and procedure can be indicated on the case summary as Other. The following types of specimens should not be reported using this protocol: Very small incisional biopsies (including core needle biopsies). Excisions containing only DCIS after a core needle biopsy or other specimen showing invasive carcinoma or DCIS with microinvasion (invasion measuring 1 mm). This type of case should be reported by using the protocol for invasive carcinoma of the breast, 1 and the report should incorporate information from the prior needle biopsy. Specimen Sampling Specimen sampling for specimens with DCIS has the following goals: 2-5 The clinical or radiologic lesion for which the surgery was performed must be examined microscopically. If the lesion is a nonpalpable imaging finding, the specimen radiograph and/or additional radiologic studies may be necessary to identify the lesion. When practical, the entire specimen should be submitted in a sequential fashion for histologic examination. If this is not possible, at least the entire region of the targeted lesion should be examined microscopically. If DCIS, lobular carcinoma in situ (LCIS), or atypical hyperplasia is identified, all fibrous tissue should be examined. 2 All other gross lesions noted in the specimen must be sampled. The margins must be evaluated for involvement by DCIS. If the specimen is received sectioned or fragmented, this should be noted, as this will limit the ability to evaluate the size of the lesion and the status of margins. If the specimen is an incisional biopsy, margins need not be evaluated. For specimens with a known diagnosis of DCIS (eg, by prior core needle biopsy) it is recommended that the entire specimen be examined, if practical, using serial sequential sampling to exclude the possibility of invasion, to completely evaluate the margins, and to aid in determining extent. 6-8 If an entire excisional specimen or grossly evident lesion is not examined microscopically, it is helpful to note the approximate percentage of the specimen or lesion that has been examined. Carcinomas present in excisions removed for lesions seen best by MRI studies are generally not grossly evident and not seen on specimen radiography. Recording the specimen size is important, as the volume of tissue excised has been associated with the likelihood of recurrence. 9 Tissue may be taken for research studies or assays that do not involve the histologic examination of the tissue (eg, reverse transcriptase polymerase chain reaction [RT-PCR]) only when taken in such a way to be able to 8
9 evaluate the tissue for small areas of invasion. For example, a thin slice of tissue taken for research studies should be matched with an adjacent slice of tissue that will be examined microscopically. 1. Fitzgibbons PL, Bose S, Chen Y, et al. Protocol for the Examination of Specimens From Patients with Invasive Carcinoma of the Breast. 2019; 2. Owings DV, Hann L, Schnitt SJ, How thoroughly should needle localization breast biopsies be sampled for microscopic examination? A prospective mammographic/pathologic correlative study. Am J Surg Pathol. 1990;14: Schwartz GF, Lagios MD, Carter D, et al. Consensus conference on the classification of ductal carcinoma in situ. Cancer. 1997;80: Silverstein MJ, Lagios MD, Recht A, et al. Image-detected breast cancer: state of the art diagnosis and treatment. J Am Coll Surg. 2005;201: Lester SC. Manual of Surgical Pathology. 2nd ed. New York: Elsevier; Silverstein MJ, Poller D, Craig P, et al. A prognostic index for ductal carcinoma in situ of the breast. Cancer. 1996;77: Grin A, Horne G, Ennis M, O Malley FP. Measuring extent of DCIS in breast excision specimens: a comparison of four methods. Arch Pathol Lab Med. 2009;133: Dadmanesh F, Fan X, Dastane A, Amin MB, Bose S. Comparative analysis of size estimation by mapping and counting number of blocks with DCIS in breast excision specimens. Arch Pathol Lab Med. 2009;133: Vicini FA, Kestin LL, Goldstein NS, Baglan KL, Pettinga JE, Martinez AA. Relationship between excision volume, margin status, and tumor size with the development of local recurrence in patients with ductal carcinoma-in-situ treated with breast-conserving therapy. J Surg Oncol. 2001;76: B. Lymph Node Sampling Patients with DCIS may have lymph nodes sampled in the following situations: Extensive DCIS: Patients with extensive DCIS are more likely to have areas of invasion and it may be difficult or impractical to examine all involved areas of the breast microscopically. 1-3 A lymph node with a metastasis would indicate an occult area of invasion. Pathologic findings on a prior needle biopsy or excision raising concern for invasion or microinvasion (invasion measuring 1 mm in size): If invasion has been documented, the protocol for invasive carcinoma of the breast 4 should be used. Imaging findings (eg, an irregular mass) or clinical findings (eg, a large palpable mass) that increase the likelihood that stromal invasion is present. 2 Planned mastectomy: The additional sampling of low lymph nodes or a sentinel lymph node does not result in increased morbidity. If the node or nodes are negative, and invasive cancer is found, another surgical procedure for node sampling can be avoided. Most tumor cells in lymph nodes of patients with DCIS would be classified as isolated tumor cells. 5,6 Artifactual displacement of epithelium within a lymph node can occur following a core needle biopsy; this finding should not be considered isolated tumor cells or a micrometastasis. 7,8 If a larger nodal metastasis is found and the breast tissue has not been entirely submitted for microscopic examination, additional sampling should be considered to attempt to identify invasive carcinoma. 1,3 Grossly uninvolved nodes should be submitted in their entirety for histologic examination, whereas a representative section of a grossly positive node may be submitted. Small nodes (eg, 2 to 3 mm) may be submitted intact, but larger nodes should be thinly sectioned. An accurate assessment of the number of positive lymph nodes is a critical prognostic indicator. Sentinel lymph nodes are identified as such by the surgeon, generally by uptake of radiotracer or dye. 1. Lagios MD, Westdahl PR, Margolin FR, et al. Duct carcinoma in situ: relationship of extent of noninvasive disease to the frequency of occult invasion, multicentricity, lymph node metastasis, and short-term treatment failures. Cancer. 1982;50:
10 2. Maffuz A, Barroso-Bravo S, Najera I, Zarco G, Alvarado-Cabrero I, Rogriguez-Cuevas SI. Tumor size as predictor of microinvasion, invasion, and axillary metastasis in ductal carcinoma in situ. J Exp Clin Cancer Res. 2006;25: Moore KH, Sweeney KJ, Wilson ME, et al. Outcomes for women with ductal carcinoma-in-situ and a positive sentinel lymph node: a multi-institutional audit. Ann Surg Oncol. 2007;14: Fitzgibbons PL, Bose S, Chen Y, et al. Protocol for the Examination of Specimens From Patients with Invasive Carcinoma of the Breast. 2017; 5. Broekhuizen LN, Wijsman JH, Peterse JL, Rutgers EJT. The incidence and significance of micrometastases in lymph nodes of patients with ductal carcinoma in situ and T1a carcinoma of the breast. Eur J Surg Oncol. 2006; 32: Lara JF, Young SM, Velilla RE, Santoro EJ, Templeton SF. The relevance of occult axillary micrometastasis in DCIS: a clinicopathologic study with long-term follow-up. Cancer. 2003;98: Carter BA, Jensen RA, Simpson JF, Page DL. Benign transport of breast epithelium into axillary lymph nodes after biopsy. Am J Clin Pathol. 2000;113: Bleiweiss IJ, Nagi CS, Jaffer S. Axillary sentinal lymph nodes can be falsely positive due to iatrogenic displacement and transport of benign epithelial cells in patients with breast carcinoma. J Clin Oncol. 2006;24: C. Size (Extent) of DCIS Although not required for pt classification or stage assignment, the size (extent) of DCIS is an important factor in patient management. 1,2 Extent (as determined by a number of different methods) is correlated with the likelihood of residual disease after re-excision, 3-6 close or positive margins, 3,6 local recurrence, 7-9 and the possibility of missed areas of invasion Extent is not as important for predicting local recurrence when wide margins are obtained. 7,8,12 Extent is an estimation of the volume of breast tissue involved by DCIS. Mammographic assessment of DCIS, usually based on distribution of calcifications, frequently underestimates, and sometimes overestimates, the extent of DCIS. Precise measurement of extent is generally difficult or impossible for the following reasons: 13 DCIS involves the ductal system in a complex 3-dimensional branching pattern that is usually only apparent by microscopic examination. When gross findings are present (eg, areas of tissue thickening and/or punctate necrosis), they often do not correspond to the entire area of involvement. The ductal system and surrounding tissue is highly compressible. Specimens may be distorted during surgery or specimen processing or compressed during specimen radiography. 14,15 Diagnostic gaps in ductal involvement may be present (particularly for low-grade DCIS. DCIS is often not removed in 1 excision and may be present in multiple specimens from 1 surgical procedure or in multiple specimens from multiple procedures. This is more likely in cases of large areas of involvement. The mean or median extent of DCIS is 14 mm to 27 mm 3,6,16,17 but ranges from 1 mm to extensive involvement of all 4 quadrants of the breast. Although a precise measurement is often not possible, an estimate of the extent of DCIS is clinically important (Table 1). Table 1. Extent of Ductal Carcinoma In Situ (DCIS) and Clinical Significance Size Extent Up to 20 mm Breast conservation with wide negative margins can be achieved in most women. Microscopic examination of the entire area involved by DCIS is recommended and should be possible in most cases. This will require complete microscopic examination of smaller biopsies, or sampling of large excisions or mastectomies to include all areas likely to contain DCIS (eg, tissue with radiologic calcifications or grossly abnormal tissue). >20-40 mm Wide negative margins may be difficult to achieve in some women with breast-conserving surgery. Microscopic examination of the entire area involved by DCIS is recommended but may be difficult to achieve in some cases. This will require complete microscopic examination of smaller biopsies or sampling of large excisions or mastectomies to include all areas likely to contain DCIS (eg, tissue with radiologic calcifications or grossly abnormal tissue). >40 mm Breast conservation with wide negative margins may be impossible to achieve in some women. Microscopic examination of the entire area involved by DCIS is recommended but may be impractical in some cases. This will require complete microscopic examination of smaller biopsies or selective sampling of large excisions or mastectomies to include areas likely to contain DCIS (eg, tissue with radiologic calcifications or grossly abnormal tissue). There is a possibility of undetected areas of invasion if the area involved by DCIS is not completely examined. Lymph node sampling may be recommended. 10
11 There are multiple methods for estimating the extent of DCIS (see Figure): DCIS in 1 block: The area involved by DCIS can be measured from a single slide, if DCIS is present in only 1 block. If separate foci are present, the largest distance between foci should be reported. This method will underestimate the extent of DCIS when multiple blocks are involved and should not be used in such cases. 16 Serial sequential sampling: The entire specimen is blocked out in such a way that the location of each block can be determined. The extent of the DCIS can be calculated by using a diagram of the specimen, the thickness of the slices, and the location of the involved blocks This method is recommended for all excisions likely to harbor DCIS or with previously diagnosed DCIS (eg, by diagnosis on a prior core needle biopsy). Nonsequential sampling: The number of blocks involved by DCIS is correlated with the extent of DCIS up to 40 mm. 16 Multiplying the number of blocks involved by DCIS by the approximate width of a tissue section gives an estimate of the extent. In 2 studies, multiplying by 3 mm underestimated the extent of DCIS, and multiplying by 5 mm may overestimate the extent. 16,17 Therefore, multiplying by 4 mm is recommended unless there is additional information that a different number would yield a more accurate result. This method may underestimate extent if not all areas of DCIS are sampled. Therefore, it is recommended that all tissue likely to be involved by DCIS be sampled (eg, all grossly abnormal tissue and all tissue with radiologically suspicious calcifications). When feasible, the entire specimen should be examined microscopically. This method may result in a larger estimation of extent than the serial sequential sampling method when DCIS is present in a large volume of tissue in 3 dimensions rather than in a predominantly linear 11
12 distribution. The best estimate for correlation with outcomes (eg, residual disease or recurrence) will require further studies. This method can be applied to any specimen and will give a better estimation of extent than measuring extent on a single slide when multiple blocks contain DCIS. Margins: If DCIS involves or is close to 2 opposing margins, the distance between the margins can be used as the extent of the DCIS within the specimen. Gross lesions: In some cases of high-grade DCIS, there may be a gross lesion that can be measured. Confirmation of the gross size must be confirmed by microscopic evaluation. The largest estimate obtained using any of these methods should be used to report the estimated size (extent) of the DCIS. 1. Silverstein MJ, Lagios MD, Recht A, et al. Image-detected breast cancer: state of the art diagnosis and treatment. J Am Coll Surg. 2005;201: O Sullivan MJ, Morrow M. Ductal carcinoma in situ: current management. Surg Clin North Am. 2007;87: , viii. 3. Dillon MF, McDermott EW, O Doherty A, et al. Factors effecting successful breast conservation for ductal carcinoma in situ. Ann Surg Oncol. 2007:14: Sigal-Zafrani B, Lewis JS, Clough KB, et al; on behalf of the Institut Curie Breast Study Group. Histologic margin assessment for breast ductal carcinoma in situ: precision and implications. Mod Pathol. 2004;17: Neuschatz AC, DiPetrillo T, Steinhoff M, et al. The value of breast lumpectomy margin assessment as a predictor of residual tumor burden in ductal carcinoma in situ of the breast. Cancer. 2002;94: Cheng L, Al-Kaisi NK, Gordon NH, Liu AY, Gebrail F, Shenk RR. Relationship between the size and margin status of ductal carcinoma in situ of the breast and residual disease. J Natl Cancer Inst. 1997;89: Di Saverio S, Catena F, Santini D, et al. 259 patients with DCIS of the breast applying USC/Van Nuys prognostic index: a retrospective review with long term follow up. Breast Cancer Res Treat. 2008;109: MacDonald HR, Silverstein MJ, Mabry H, et al. Local control in ductal carcinoma in situ treated by excision alone: incremental benefit of larger margins. Am J Surg. 2005;190: Asjoe FT, Altintas S, Huizing MT, et al. The value of the Van Nuys Prognostic Index in ductal carcinoma in situ of the breast: a retrospective analysis. Breast J. 2007;13: Maffuz A, Barroso-Bravo S, Najera I, Zarco G, Alvarado-Cabrero I, Rogriguez-Cuevas SI. Tumor size as predictor of microinvasion, invasion, and axillary metastasis in ductal carcinoma in situ. J Exp Clin Cancer Res. 2006;25: Moore KH, Sweeney KJ, Wilson ME, et al. Outcomes for women with ductal carcinoma-in-situ and a positive sentinel lymph node: a multi-institutional audit. Ann Surg Oncol. 2007;14: MacDonald HR, Silverstein MJ, Lee LA, et al. Margin width as the sole determinant of local recurrence after breast conservation in patients with ductal carcinoma in situ of the breast. Am J Surg. 2006;192: Saqi A, Osborne MP, Rosenblatt R, Shin SJ, Hoda SA, Quantifying mammary duct carcinoma in situ: a wild-goose chase? Am J Clin Pathol. 2000;113(suppl 1):S30-S Clingan R, Griffen M, Phillips J, et al. Potential margin distortion in breast tissue by specimen mammography. Arch Surg. 2003;138: Graham RA, Homer MJ, Katz J, et al. The pancake phenomenon contributes to the inaccuracy of margin assessment in patients with breast cancer. Am J Surg. 2002;184: Grin A, Horne G, Ennis M, O Malley FP. Measuring extent of DCIS in breast excision specimens: a comparison of four methods. Arch Pathol Lab Med. 2009;133: Dadmanesh F, Fan X, Dastane A, Amin MB, Bose S. Comparative analysis of size estimation by mapping and counting number of blocks with DCIS in breast excision specimens. Arch Pathol Lab Med. 2009;133: Silverstein MJ, Poller D, Craig P, et al. A prognostic index for ductal carcinoma in situ of the breast. Cancer. 1996;77:
13 D. Histologic Type This protocol applies only to cases of DCIS. The protocol for invasive carcinoma of the breast 1 applies if invasion or microinvasion (less than or equal to 1 mm) is present. Pleomorphic lobular carcinoma in situ (LCIS) has overlapping features with DCIS and may be treated similarly, but at present there is insufficient evidence to establish definitive recommendations for treatment. Thus, pleomorphic LCIS is not currently included in the ptis classification. When DCIS involves nipple skin only, without underlying invasive carcinoma or DCIS, the classification is DCIS (ie, Tis [Paget]). The majority of these cases are strongly positive for HER2. 1. Fitzgibbons PL, Bose S, Chen Y, et al. Protocol for the Examination of Specimens From Patients with Invasive Carcinoma of the Breast. 2017; E. Architectural Pattern The architectural pattern has been reported traditionally for DCIS. 1-2 However, nuclear grade and the presence of necrosis are more predictive of clinical outcome. 1. Schwartz GF, Lagios MD, Carter D, et al. Consensus conference on the classification of ductal carcinoma in situ. Cancer. 1997;80: Silverstein MJ, Lagios MD, Recht A, et al. Image-detected breast cancer: state of the art diagnosis and treatment. J Am Coll Surg. 2005;201: F. Nuclear Grade The nuclear grade of DCIS is determined using 6 morphologic features (Table 2). 1,2 Table 2. Nuclear Grade of Ductal Carcinoma In Situ Grade I Grade II Grade III Feature (Low) (Intermediate) (High) Pleomorphism Monotonous (monomorphic) Intermediate Markedly pleomorphic Size 1.5 to 2 x the size of a normal RBC or a normal duct epithelial cell nucleus Intermediate >2.5 x the size of a normal RBC or a normal duct epithelial cell nucleus Chromatin Usually diffuse, finely dispersed chromatin Intermediate Usually vesicular with irregular chromatin distribution Nucleoli Only occasional Prominent, often multiple Mitoses Only occasional Intermediate May be frequent Orientation Polarized toward luminal spaces Intermediate Usually not polarized toward the luminal space Definition: RBC, red blood cell. 1. Schwartz GF, Lagios MD, Carter D, et al. Consensus conference on the classification of ductal carcinoma in situ. Cancer. 1997;80: Radiation Therapy Oncology Group (RTOG). Evaluation of Breast Specimens Removed by Needle Localization Technique. Available at: Accessed 20 Feb 2019 G. Necrosis 1 The presence of necrosis is correlated with the finding of mammographic calcifications (ie, most areas of necrosis will calcify). DCIS that presents as mammographic calcifications often recurs as calcifications. Necrosis can be classified as follows: Central ( comedo ): The central portion of an involved ductal space is replaced by an area of expansive necrosis that is easily detected at low magnification. Ghost cells and karyorrhectic debris are generally 13
14 present. Although central necrosis is generally associated with high-grade nuclei (ie, comedo DCIS), it can also occur with DCIS of low or intermediate nuclear grade. This type of necrosis often correlates with a linear and/or branching pattern of calcifications on mammography. Focal (punctate): Small foci, indistinct at low magnification, or single cell necrosis. Necrosis should be distinguished from secretory material, which can also be associated with calcifications, cytoplasmic blebs, and histiocytes, but does not include nuclear debris. 1. Schwartz GF, Lagios MD, Carter D, et al. Consensus conference on the classification of ductal carcinoma in situ. Cancer. 1997;80: H. Margins Whenever feasible, the specimen should be oriented in order to identify specific margins. Margins may be identified by sutures or clips placed on the specimen surface or by other means of communication between surgeon and pathologist and should be documented in the pathology report. Margins can be identified microscopically in several ways, including the use of multiple colored inks, by submitting the margins in specific cassettes, or by the surgeon submitting each margin as a separately excised specimen. Inks should be applied to the surface of the specimen, taking care to avoid penetration into the specimen. If margins are sampled with perpendicular sections, the pathologist should report the distance from the DCIS to the closest margin, when possible. Due to the growth pattern of DCIS in the ductal system, a negative but close margin does not ensure the absence of DCIS in the adjacent tissue. A positive margin requires ink on DCIS. If the specimen is oriented, the specific site(s) of involvement (eg, superior margin) should also be reported. The deep margin may be at muscle fascia. If so, the likelihood of additional breast tissue beyond this margin (and therefore possible involvement by DCIS) is extremely small. A deep muscle fascial margin (eg, on a mastectomy specimen) is unlikely to have clinical significance. A superficial (generally anterior) margin may be immediately below the skin, and there may not be additional breast tissue beyond this margin. However, some breast tissue can be left in skin flaps, and the likelihood of residual breast tissue is related to the thickness of the flap. 1 Specimen radiography is important to assess the adequacy of excision. Compression of the specimen should be minimized, as it can severely compromise the ability to assess the distance of the DCIS from the surgical margin. 2 Mechanical compression devices should be used with caution and preferably reserved for nonpalpable lesions that require this technique for imaging (eg, microcalcifications). If DCIS is present at the margin, the extent of margin involvement is associated with the likelihood of residual disease 3,4 : Focal: DCIS at the margin in a <1 mm area in 1 block Minimal/moderate: between focal and extensive Extensive: DCIS at the margin in an area 15 mm or in 5 or more low-power fields and/or in 8 or more blocks) 1. Torresan RZ, dos Santos CC, Okamura H, Alvarenga M. Evaluation of glandular tissue after skin-sparing mastectomies. Ann Surg Oncol. 2005;12: Saqi A, Osborne MP, Rosenblatt R, Shin SJ, Hoda SA, Quantifying mammary duct carcinoma in situ: a wild-goose chase? Am J Clin Pathol. 2000;113(suppl 1):S30-S Dillon MF, McDermott EW, O Doherty A, et al. Factors effecting successful breast conservation for ductal carcinoma in situ. Ann Surg Oncol. 2007:14:
15 4. Sigal-Zafrani B, Lewis JS, Clough KB, et al; on behalf of the Institut Curie Breast Study Group. Histologic margin assessment for breast ductal carcinoma in situ: precision and implications. Mod Pathol. 2004;17: I. Neoadjuvant Therapy Patients may be treated with endocrine therapy, chemotherapy, or HER2-targeted therapy prior to surgical excision, as part of treatment of a contralateral carcinoma. It has been observed after treatment of women with invasive carcinoma that the invasive carcinoma may respond to a greater extent than the accompanying DCIS. The histologic changes occurring in DCIS after treatment have not been well described and will likely vary with the specific agents used. Comparison to a pretreatment specimen is necessary to attribute histologic changes to the effects of treatment. The significance of histologic changes in DCIS is unknown. If the patient had invasive carcinoma prior to treatment, but only DCIS after treatment, additional classification systems are available to evaluate residual carcinoma in the breast and lymph nodes Gralow JR, Burstein HJ, Wood W, et al. Preoperative therapy in invasive breast cancer: pathologic assessment and systemic therapy issues in operable disease. J Clin Oncol. 2008;26: J. Lymph Nodes Reporting Lymph Nodes The pathology report should state the total number of lymph nodes examined (including the number of sentinel nodes), the number of nodes with metastases, and the greatest dimension of the largest metastatic focus. If a patient has at least 1 macrometastasis, only nodes with micro and macrometastases are included for the total number of involved nodes for N classification. 1 Nodes with isolated tumor cells are not included in this count. At least 1 node with presence or absence of cancer documented by pathologic examination is required for pathologic N classification The (sn) modifier indicates that nodal categorization is based on less than an axillary dissection. When the combination of sentinel and nonsentinel nodes removed is less than a standard low axillary dissection (fewer than six nodes), the (sn) modifier is used, eg, pn0(i+)(sn). The (sn) modifier is not used if 6 or more lymph nodes are examined (including sentinel and nonsentinel lymph nodes). Isolated tumor cells (ITCs) are defined as single tumor cells or small cell clusters not greater than 0.2 mm and numbering less than 200 cells. 2-5 They may be detected by routine histologic examination or by immunohistochemical (IHC) or molecular methods. ITCs do not usually show evidence of malignant activity (eg, proliferation or stromal reaction), but micrometastases may show these changes. Almost all tumor cells present in lymph nodes of patients with DCIS are isolated tumor cells or the cells may be artifactually displaced from a previous procedure. 6,7 Isolated tumor cells detected in cases of DCIS have not been shown to have prognostic importance. 8,9 If a larger metastasis is found, additional tissue sampling and review of slides are helpful to determine if an area of invasion is present Amin MB, Edge SB, Greene FL, et al, eds. AJCC Cancer Staging Manual. 8th ed. New York, NY: Springer; Fitzgibbons PL, Bose S, Chen Y, et al. Protocol for the Examination of Specimens From Patients with Invasive Carcinoma of the Breast. 2019; 3. Connolly JL. Changes and problematic areas in interpretation of the AJCC Cancer Staging Manual, 6 th Edition, for breast cancer. Arch Pathol Lab Med. 2006;130: Singletary SE, Connolly JL, Breast cancer staging: working with the sixth edition of the AJCC Cancer Staging Manual. CA Cancer J Clin. 2006;56: Singletary SE, Greene FL, Sobin LH. Classification of isolated tumor cells: clarification of the 6 th edition of the American Joint Committee on Cancer Staging Manual. Cancer. 2003;90: Carter BA, Jensen RA, Simpson JF, Page DL. Benign transport of breast epithelium into axillary lymph nodes after biopsy. Am J Clin Pathol. 2000;113:
16 7. Bleiweiss IJ, Nagi CS, Jaffer S. Axillary sentinal lymph nodes can be falsely positive due to iatrogenic displacement and transport of benign epithelial cells in patients with breast carcinoma. J Clin Oncol. 2006;24: Broekhuizen LN, Wijsman JH, Peterse JL, Rutgers EJT. The incidence and significance of micrometastases in lymph nodes of patients with ductal carcinoma in situ and T1a carcinoma of the breast. Eur J Surg Oncol. 2006; 32: Lara JF, Young SM, Velilla RE, Santoro EJ, Templeton SF. The relevance of occult axillary micrometastasis in DCIS: a clinicopathologic study with long-term follow-up. Cancer. 2003;98: Moore KH, Sweeney KJ, Wilson ME, et al. Outcomes for women with ductal carcinoma-in-situ and a positive sentinel lymph node: a multi-institutional audit. Ann Surg Oncol. 2007;14: K. Pathologic Stage Classification The tumor-node-metastasis (TNM) staging system maintained collaboratively by the American Joint Committee on Cancer (AJCC) and the International Union Against Cancer (UICC) is recommended. 1-5 Pathologic Classification The pathologic classification of a cancer is based on information acquired before treatment supplemented and modified by the additional evidence acquired during and from surgery, particularly from pathologic examination of resected tissues. The pathologic classification provides additional precise and objective data. Classification of T, N, and M by pathologic means is denoted by use of a lower case p prefix (pt, pn, pm). Pathologic T. Tumor size should be recorded in whole millimeters. If the size is reported in smaller units such as a tenth or hundredth of a millimeter, it should be rounded to the nearest whole millimeter for reporting stage. Rounding is performed as follows: one through four are rounded down, and five through nine are rounded up. For example, a breast tumor reported as 4.2 mm in size should be recorded for staging as a 4-mm tumor, and a 4.7- mm tumor should be recorded as a 5-mm tumor. If the tumor is not resected, but a biopsy of the primary tumor is performed that is adequate to evaluate the highest pt category, the pt classification is assigned. Some disease sites have specific rules to guide assignment of pt category in such cases. On rare occasions, the tumor size is obtained from a previous core needle biopsy specimen, as the tumor in the core may be larger than the tumor in the excision specimen. Pathologic N. At least one node with presence or absence of cancer documented by pathologic examination is required for pathologic N classification. A tumor nodule with a smooth contour in a regional node area is classified as a positive node. The size of the metastasis, not the size of the node, is used for the criterion for the N category. Specialized pathologic techniques such as immunohistochemistry or molecular techniques may identify limited metastases in lymph nodes that may not have been identified without the use of the special diagnostic techniques. Single tumor cells or small clusters of cells are classified as isolated tumor cells (ITCs). The standard definition for ITC is a cluster of cells not more than 0.2 mm in greatest diameter. Cases with ITC only in lymph nodes are classified as pn0. This rule also generally applies to cases with findings of tumor cells or their components by nonmorphologic techniques such as flow cytometry or DNA analysis. Pathologic M. The pathologic assignment of the presence of metastases (pm1) requires a biopsy positive for cancer at the metastatic site. Pathologic M0 is an undefined concept and the category pm0 may not be used. Pathologic classification of the absence of distant metastases can only be made at autopsy. It would be extremely rare to have distant metastasis in examples of DCIS, and would surely indicate an unsampled area of invasive carcinoma. Posttherapy or Postneoadjuvant Therapy Classification (ytnm). Cases where systemic and/or radiation therapy are given before surgery (neoadjuvant) or where no surgery is performed may have the extent of disease assessed at the conclusion of the therapy by clinical or pathologic means (if resection performed). This classification is useful to clinicians because the extent of response to therapy may provide important prognostic information to patients and help direct the extent of surgery or subsequent systemic and/or radiation therapy. T and N are classified by using the same categories as for clinical or pathologic staging for the disease type, and the findings are recorded by using the prefix designator y (eg, yct; ycn; ypt; ypn). The yc prefix is used for the clinical stage after therapy, and the yp prefix is used for the pathologic stage for those cases that have surgical 16
Protocol for the Examination of Specimens From Patients With Ductal Carcinoma In Situ (DCIS) of the Breast
 Protocol for the Examination of Specimens From Patients With Ductal Carcinoma In Situ (DCIS) of the Breast Version: Protocol Posting Date: June 2017 Includes ptnm requirements from the 8 th Edition, AJCC
Protocol for the Examination of Specimens From Patients With Ductal Carcinoma In Situ (DCIS) of the Breast Version: Protocol Posting Date: June 2017 Includes ptnm requirements from the 8 th Edition, AJCC
Descriptor Definition Author s notes TNM descriptors Required only if applicable; select all that apply multiple foci of invasive carcinoma
 S5.01 The tumour stage and stage grouping must be recorded to the extent possible, based on the AJCC Cancer Staging Manual (7 th Edition). 11 (See Tables S5.01a and S5.01b below.) Table S5.01a AJCC breast
S5.01 The tumour stage and stage grouping must be recorded to the extent possible, based on the AJCC Cancer Staging Manual (7 th Edition). 11 (See Tables S5.01a and S5.01b below.) Table S5.01a AJCC breast
Protocol for the Examination of Specimens From Patients With Invasive Carcinoma of the Breast
 Protocol for the Examination of Specimens From Patients With Invasive Carcinoma of the Breast Version: Protocol Posting Date: June 2017 Includes ptnm requirements from the 8 th Edition, AJCC Staging Manual
Protocol for the Examination of Specimens From Patients With Invasive Carcinoma of the Breast Version: Protocol Posting Date: June 2017 Includes ptnm requirements from the 8 th Edition, AJCC Staging Manual
Protocol for the Examination of Resection Specimens From Patients With Invasive Carcinoma of the Breast
 Protocol for the Examination of Specimens From Patients With Invasive Carcinoma of the Breast Version: Breast Invasive 4.2.0.0 Protocol Posting Date: February 2019 CAP Laboratory Accreditation Program
Protocol for the Examination of Specimens From Patients With Invasive Carcinoma of the Breast Version: Breast Invasive 4.2.0.0 Protocol Posting Date: February 2019 CAP Laboratory Accreditation Program
ACRIN 6666 Therapeutic Surgery Form
 S1 ACRIN 6666 Therapeutic Surgery Form 6666 Instructions: Complete a separate S1 form for each separate area of each breast excised with the intent to treat a cancer (e.g. each lumpectomy or mastectomy).
S1 ACRIN 6666 Therapeutic Surgery Form 6666 Instructions: Complete a separate S1 form for each separate area of each breast excised with the intent to treat a cancer (e.g. each lumpectomy or mastectomy).
Chapter 2 Staging of Breast Cancer
 Chapter 2 Staging of Breast Cancer Zeynep Ozsaran and Senem Demirci Alanyalı 2.1 Introduction Five decades ago, Denoix et al. proposed classification system (tumor node metastasis [TNM]) based on the dissemination
Chapter 2 Staging of Breast Cancer Zeynep Ozsaran and Senem Demirci Alanyalı 2.1 Introduction Five decades ago, Denoix et al. proposed classification system (tumor node metastasis [TNM]) based on the dissemination
Evaluation of Breast Specimens Removed by Needle Localization Technique
 Evaluation of Breast Specimens Removed by Needle Localization Technique Specimen Handling: The breast specimen when received should be measured and grossly inspected for any orientation designated by the
Evaluation of Breast Specimens Removed by Needle Localization Technique Specimen Handling: The breast specimen when received should be measured and grossly inspected for any orientation designated by the
STAGE CATEGORY DEFINITIONS
 CLINICAL Extent of disease before any treatment y clinical staging completed after neoadjuvant therapy but before subsequent surgery TX Tis Tis (DCIS) Tis (LCIS) Tis (Paget s) T1 T1mi T1a T1b T1c a b c
CLINICAL Extent of disease before any treatment y clinical staging completed after neoadjuvant therapy but before subsequent surgery TX Tis Tis (DCIS) Tis (LCIS) Tis (Paget s) T1 T1mi T1a T1b T1c a b c
Protocol for the Examination of Specimens from Patients with Invasive Carcinoma of the Breast
 Protocol for the Examination of Specimens from Patients with Invasive Carcinoma of the Breast Protocol applies to all invasive carcinomas of the breast, including ductal carcinoma in situ (DCIS) with microinvasion.
Protocol for the Examination of Specimens from Patients with Invasive Carcinoma of the Breast Protocol applies to all invasive carcinomas of the breast, including ductal carcinoma in situ (DCIS) with microinvasion.
Protocol for the Examination of Biopsy Specimens From Patients With Invasive Carcinoma of the Breast
 Protocol for the Examination of Specimens From Patients With Invasive Carcinoma of the Breast Version: BreastInvasive 1.0.0.0 Protocol Posting Date: February 2019 Accreditation Requirements The use of
Protocol for the Examination of Specimens From Patients With Invasive Carcinoma of the Breast Version: BreastInvasive 1.0.0.0 Protocol Posting Date: February 2019 Accreditation Requirements The use of
Overview of AJCC 8 th Staging in Pathologic Aspects
 Overview of AJCC 8 th Staging in Pathologic Aspects Jee Yeon KIM, M.D.,Ph.D. Department of Pathology, Pusan National University, College of Medicine, Pusan National University Yangsan Hospital, KOREA Major
Overview of AJCC 8 th Staging in Pathologic Aspects Jee Yeon KIM, M.D.,Ph.D. Department of Pathology, Pusan National University, College of Medicine, Pusan National University Yangsan Hospital, KOREA Major
Recurrence following Treatment of Ductal Carcinoma in Situ with Skin-Sparing Mastectomy and Immediate Breast Reconstruction
 Recurrence following Treatment of Ductal Carcinoma in Situ with Skin-Sparing Mastectomy and Immediate Breast Reconstruction Aldona J. Spiegel, M.D., and Charles E. Butler, M.D. Houston, Texas Skin-sparing
Recurrence following Treatment of Ductal Carcinoma in Situ with Skin-Sparing Mastectomy and Immediate Breast Reconstruction Aldona J. Spiegel, M.D., and Charles E. Butler, M.D. Houston, Texas Skin-sparing
Case Scenario 1 History and Physical 3/15/13 Imaging Pathology
 Case Scenario 1 History and Physical 3/15/13 The patient is an 84 year old white female who presented with an abnormal mammogram. The patient has a five year history of refractory anemia with ringed sideroblasts
Case Scenario 1 History and Physical 3/15/13 The patient is an 84 year old white female who presented with an abnormal mammogram. The patient has a five year history of refractory anemia with ringed sideroblasts
Completing the Puzzle AJCC TNM Staging Breast. Nicole Catlett, CTR 2017 Kentucky Cancer Registry Fall Conference, September 21 & 22, 2017
 Completing the Puzzle AJCC TNM Staging Breast Nicole Catlett, CTR 2017 Kentucky Cancer Registry Fall Conference, September 21 & 22, 2017 OBJECTIVES Understanding of Breast TNM staging Identify clinical
Completing the Puzzle AJCC TNM Staging Breast Nicole Catlett, CTR 2017 Kentucky Cancer Registry Fall Conference, September 21 & 22, 2017 OBJECTIVES Understanding of Breast TNM staging Identify clinical
Case Scenario 1: This case has been slightly modified from the case presented during the live session to add clarity.
 Case Scenario 1: This case has been slightly modified from the case presented during the live session to add clarity. Background: 46 year old married premenopausal female with dense breasts has noticed
Case Scenario 1: This case has been slightly modified from the case presented during the live session to add clarity. Background: 46 year old married premenopausal female with dense breasts has noticed
Definition of Synoptic Reporting
 Definition of Synoptic Reporting The CAP has developed this list of specific features that define synoptic reporting formatting: 1. All required cancer data from an applicable cancer protocol that are
Definition of Synoptic Reporting The CAP has developed this list of specific features that define synoptic reporting formatting: 1. All required cancer data from an applicable cancer protocol that are
Breast Cancer. Most common cancer among women in the US. 2nd leading cause of death in women. Mortality rates though have declined
 Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women Mortality rates though have declined 1 in 8 women will develop breast cancer Breast Cancer Breast cancer increases
Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women Mortality rates though have declined 1 in 8 women will develop breast cancer Breast Cancer Breast cancer increases
Handout for Dr Allison s Lectures on Grossing Breast Specimens:
 Handout for Dr Allison s Lectures on Grossing Breast Specimens: Dr. Kimberly H. Allison Director of Breast Pathology and Breast Pathology Fellowship Director of Residency Training in Pathology Stanford
Handout for Dr Allison s Lectures on Grossing Breast Specimens: Dr. Kimberly H. Allison Director of Breast Pathology and Breast Pathology Fellowship Director of Residency Training in Pathology Stanford
A712(18)- Test slide, Breast cancer tissues with corresponding normal tissues
 A712(18)- Test slide, Breast cancer tissues with corresponding normal tissues (formalin fixed) For research use only Specifications: No. of cases: 12 Tissue type: Breast cancer tissues with corresponding
A712(18)- Test slide, Breast cancer tissues with corresponding normal tissues (formalin fixed) For research use only Specifications: No. of cases: 12 Tissue type: Breast cancer tissues with corresponding
Breast Cancer. Saima Saeed MD
 Breast Cancer Saima Saeed MD Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women 1 in 8 women will develop breast cancer Incidence/mortality rates have declined Breast
Breast Cancer Saima Saeed MD Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women 1 in 8 women will develop breast cancer Incidence/mortality rates have declined Breast
3/23/2017. Disclosure of Relevant Financial Relationships. Pathologic Staging Updates in Breast Cancer. Pathologic Staging Updates Breast Cancer
 Pathologic Staging Updates in Breast Cancer Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position to influence or control the content of CME
Pathologic Staging Updates in Breast Cancer Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position to influence or control the content of CME
Case Scenario 1: This case has been slightly modified from the case presented during the live session to add clarity.
 Case Scenario 1: This case has been slightly modified from the case presented during the live session to add clarity. Background: 46 year old married premenopausal female with dense breasts has noticed
Case Scenario 1: This case has been slightly modified from the case presented during the live session to add clarity. Background: 46 year old married premenopausal female with dense breasts has noticed
B REAST STAGING FORM. PATHOLOGIC Extent of disease through completion of definitive surgery. CLINICAL Extent of disease before any treatment
 B REAST STAGING FORM CLINICAL Extent of disease before any treatment y clinical staging completed after neoadjuvant therapy but before subsequent surgery (DCIS) (LCIS) (Paget s) mi c a b c d TUMOR SIZE:
B REAST STAGING FORM CLINICAL Extent of disease before any treatment y clinical staging completed after neoadjuvant therapy but before subsequent surgery (DCIS) (LCIS) (Paget s) mi c a b c d TUMOR SIZE:
B REAST STAGING FORM. PATHOLOGIC Extent of disease through completion of definitive surgery. CLINICAL Extent of disease before any treatment
 B REAST STAGING FORM Extent of disease before any treatment y clinical staging completed after neoadjuvant therapy but before subsequent surgery (DCIS) (LCIS) (Paget s) mi a b c a b c d TUMOR SIZE: S TAGE
B REAST STAGING FORM Extent of disease before any treatment y clinical staging completed after neoadjuvant therapy but before subsequent surgery (DCIS) (LCIS) (Paget s) mi a b c a b c d TUMOR SIZE: S TAGE
BREAST PATHOLOGY GROSSING GUIDELINES
 THINGS TO CONSIDER: A. Please review ALL imaging and previous biopsies PRIOR to grossing any breast case. a. It may be helpful to draw out your own guide to assist when grossing B. Faxitron your breast
THINGS TO CONSIDER: A. Please review ALL imaging and previous biopsies PRIOR to grossing any breast case. a. It may be helpful to draw out your own guide to assist when grossing B. Faxitron your breast
Sentinel nodes. Location: Location: S1.04 Principal clinician. G1.01 Record other relevant information. S2.01 Number of specimens submitted
 Invasive Breast Cancer Histopathology Reporting Proforma Mandatory questions (i.e. protocol standards) are in bold (e.g. S1.01). S1.01 Identification Family name Given name(s) Date of birth DD MM YYYY
Invasive Breast Cancer Histopathology Reporting Proforma Mandatory questions (i.e. protocol standards) are in bold (e.g. S1.01). S1.01 Identification Family name Given name(s) Date of birth DD MM YYYY
Case Scenario 1. 2/15/2011 The patient received IMRT 45 Gy at 1.8 Gy per fraction for 25 fractions.
 Case Scenario 1 1/3/11 A 57 year old white female presents for her annual mammogram and is found to have a suspicious area of calcification, spread out over at least 4 centimeters. She is scheduled to
Case Scenario 1 1/3/11 A 57 year old white female presents for her annual mammogram and is found to have a suspicious area of calcification, spread out over at least 4 centimeters. She is scheduled to
Seventh Edition Staging 2017 Breast
 Seventh Edition Staging 2017 Breast Donna M. Gress, RHIT, CTR Validating science. Improving patient care. No materials in this presentation may be repurposed in print or online without the express written
Seventh Edition Staging 2017 Breast Donna M. Gress, RHIT, CTR Validating science. Improving patient care. No materials in this presentation may be repurposed in print or online without the express written
Surgical Therapy: Sentinel Node Biopsy and Breast Conservation
 Surgical Therapy: Sentinel Node Biopsy and Breast Conservation Stephen B. Edge, MD Professor of Surgery and Oncology Roswell Park Cancer Institute University at Buffalo Dr. Roswell Park: Tradition in Cancer
Surgical Therapy: Sentinel Node Biopsy and Breast Conservation Stephen B. Edge, MD Professor of Surgery and Oncology Roswell Park Cancer Institute University at Buffalo Dr. Roswell Park: Tradition in Cancer
Lesion Imaging Characteristics Mass, Favoring Benign Circumscribed Margins Intramammary Lymph Node
 Lesion Imaging Characteristics Mass, Favoring Benign Circumscribed Margins Intramammary Lymph Node Oil Cyst Mass, Intermediate Concern Microlobulated Margins Obscured Margins Mass, Favoring Malignant Indistinct
Lesion Imaging Characteristics Mass, Favoring Benign Circumscribed Margins Intramammary Lymph Node Oil Cyst Mass, Intermediate Concern Microlobulated Margins Obscured Margins Mass, Favoring Malignant Indistinct
Q&A. Fabulous Prizes. Collecting Cancer Data: Breast 4/4/13. NAACCR Webinar Series Collecting Cancer Data Breast
 Collecting Cancer Data Breast NAACCR 2012 2013 Webinar Series Q&A Please submit all questions concerning webinar content through the Q&A panel. Reminder: If you have participants watching this webinar
Collecting Cancer Data Breast NAACCR 2012 2013 Webinar Series Q&A Please submit all questions concerning webinar content through the Q&A panel. Reminder: If you have participants watching this webinar
Case study 1. Rie Horii, M.D., Ph.D. Division of Pathology Cancer Institute Hospital, Japanese Foundation for Cancer Research
 NCCN/JCCNB Seminar in Japan April 15, 2012 Case study 1 Rie Horii, M.D., Ph.D. Division of Pathology Cancer Institute Hospital, Japanese Foundation for Cancer Research Present illness: A 50y.o.premenopausal
NCCN/JCCNB Seminar in Japan April 15, 2012 Case study 1 Rie Horii, M.D., Ph.D. Division of Pathology Cancer Institute Hospital, Japanese Foundation for Cancer Research Present illness: A 50y.o.premenopausal
Post Neoadjuvant therapy: issues in interpretation
 Post Neoadjuvant therapy: issues in interpretation Disclosure: Overview D Prognostic features in assessment of post treatment specimens: Tumor size Cellularity Grade Receptors LN Neoadjuvant chemotherapy:
Post Neoadjuvant therapy: issues in interpretation Disclosure: Overview D Prognostic features in assessment of post treatment specimens: Tumor size Cellularity Grade Receptors LN Neoadjuvant chemotherapy:
Imaging in breast cancer. Mammography and Ultrasound Donya Farrokh.MD Radiologist Mashhad University of Medical Since
 Imaging in breast cancer Mammography and Ultrasound Donya Farrokh.MD Radiologist Mashhad University of Medical Since A mammogram report is a key component of the breast cancer diagnostic process. A mammogram
Imaging in breast cancer Mammography and Ultrasound Donya Farrokh.MD Radiologist Mashhad University of Medical Since A mammogram report is a key component of the breast cancer diagnostic process. A mammogram
Savitri Krishnamurthy, MD 1
 EVOLVING TRENDS IN PATHOLOGIC EVALUATION OF AXILLARY LYMPH NODES IN BREAST CANCER Savitri Krishnamurthy, M.D. Professor Department of Pathology University of Texas M. D. Anderson Cancer Center AXILLARY
EVOLVING TRENDS IN PATHOLOGIC EVALUATION OF AXILLARY LYMPH NODES IN BREAST CANCER Savitri Krishnamurthy, M.D. Professor Department of Pathology University of Texas M. D. Anderson Cancer Center AXILLARY
Papillary Lesions of the Breast: WHO Update
 Papillary Lesions of the Breast: WHO Update Stuart J. Schnitt, M.D. Department of Pathology Beth Israel Deaconess Medical Center and Harvard Medical School Boston, MA, USA Papillary Lesions of the Breast
Papillary Lesions of the Breast: WHO Update Stuart J. Schnitt, M.D. Department of Pathology Beth Israel Deaconess Medical Center and Harvard Medical School Boston, MA, USA Papillary Lesions of the Breast
Breast Imaging: Multidisciplinary Approach. Madelene Lewis, MD Assistant Professor Associate Program Director Medical University of South Carolina
 Breast Imaging: Multidisciplinary Approach Madelene Lewis, MD Assistant Professor Associate Program Director Medical University of South Carolina No Disclosures Objectives Discuss a multidisciplinary breast
Breast Imaging: Multidisciplinary Approach Madelene Lewis, MD Assistant Professor Associate Program Director Medical University of South Carolina No Disclosures Objectives Discuss a multidisciplinary breast
Proliferative Breast Disease: implications of core biopsy diagnosis. Proliferative Breast Disease
 Proliferative Breast Disease: implications of core biopsy diagnosis Jean F. Simpson, M.D. Breast Pathology Consultants, Inc. Nashville, TN Proliferative Breast Disease Must be interpreted in clinical and
Proliferative Breast Disease: implications of core biopsy diagnosis Jean F. Simpson, M.D. Breast Pathology Consultants, Inc. Nashville, TN Proliferative Breast Disease Must be interpreted in clinical and
Image guided core biopsies:
 Recommendations on the Surgical, Radiologic and Pathologic Approaches to Breast Disease: Using best practices based on multidisciplinary methodologies developed through the Allina Breast Committee. Image
Recommendations on the Surgical, Radiologic and Pathologic Approaches to Breast Disease: Using best practices based on multidisciplinary methodologies developed through the Allina Breast Committee. Image
Invasive Papillary Breast Carcinoma
 410 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the
410 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the
Collaborative Stage for TNM 7 - Revised 12/02/2009 [ Schema ]
![Collaborative Stage for TNM 7 - Revised 12/02/2009 [ Schema ] Collaborative Stage for TNM 7 - Revised 12/02/2009 [ Schema ]](/thumbs/82/86783199.jpg) CS Tumor Size Collaborative Stage for TNM 7 - Revised 12/02/2009 [ Schema ] Note: the specific tumor size as documented in the medical record. If the ONLY information regarding tumor size is the physician's
CS Tumor Size Collaborative Stage for TNM 7 - Revised 12/02/2009 [ Schema ] Note: the specific tumor size as documented in the medical record. If the ONLY information regarding tumor size is the physician's
Problems in staging breast carcinoma
 Problems in staging breast carcinoma Primary systemic therapy (PST) of breast carcinoma pathologists tasks Dr. Janina Kulka, 2nd Department of Pathology, Semmelweis University Budapest Austro-Hungarian
Problems in staging breast carcinoma Primary systemic therapy (PST) of breast carcinoma pathologists tasks Dr. Janina Kulka, 2nd Department of Pathology, Semmelweis University Budapest Austro-Hungarian
Ductal Carcinoma in Situ. Laura C. Collins, M.D. Department of Pathology Beth Israel Deaconess Medical Center and Harvard Medical School Boston, MA
 Ductal Carcinoma in Situ Laura C. Collins, M.D. Department of Pathology Beth Israel Deaconess Medical Center and Harvard Medical School Boston, MA Definition of DCIS WHO 2012 A neoplastic proliferation
Ductal Carcinoma in Situ Laura C. Collins, M.D. Department of Pathology Beth Israel Deaconess Medical Center and Harvard Medical School Boston, MA Definition of DCIS WHO 2012 A neoplastic proliferation
In Situ Breast Carcinoma. James L. Connolly, M.D Beth Israel Deaconess Medical Center Professor of Pathology Harvard Medical School Boston, MA
 In Situ Breast Carcinoma James L. Connolly, M.D Beth Israel Deaconess Medical Center Professor of Pathology Harvard Medical School Boston, MA Content In Situ Ductal Carcinoma In Situ Lobular Carcinoma
In Situ Breast Carcinoma James L. Connolly, M.D Beth Israel Deaconess Medical Center Professor of Pathology Harvard Medical School Boston, MA Content In Situ Ductal Carcinoma In Situ Lobular Carcinoma
PART VII Breast. Breast 345
 PART VII Breast Breast 345 3 2 Breast At-A-Glance SUMMARY OF CHANGES Tumor (T) Identified specific imaging modalities that can be used to estimate clinical tumor size, including mammography, ultrasound,
PART VII Breast Breast 345 3 2 Breast At-A-Glance SUMMARY OF CHANGES Tumor (T) Identified specific imaging modalities that can be used to estimate clinical tumor size, including mammography, ultrasound,
A712(19)- Test slide, Breast cancer tissues with corresponding normal tissues
 A712(19)- Test slide, Breast cancer tissues with corresponding normal tissues (formalin fixed) For research use only Specifications: No. of cases: 12 Tissue type: Breast cancer tissues with corresponding
A712(19)- Test slide, Breast cancer tissues with corresponding normal tissues (formalin fixed) For research use only Specifications: No. of cases: 12 Tissue type: Breast cancer tissues with corresponding
Pathology Report Patient Companion Guide
 Pathology Report Patient Companion Guide Breast Cancer - Understanding Your Pathology Report Pathology Reports can be overwhelming. They contain scientific terms that are unfamiliar and might be a bit
Pathology Report Patient Companion Guide Breast Cancer - Understanding Your Pathology Report Pathology Reports can be overwhelming. They contain scientific terms that are unfamiliar and might be a bit
Cytyc Corporation - Case Presentation Archive - March 2002
 FirstCyte Ductal Lavage History: 68 Year Old Female Gail Index: Unknown Clinical History: Negative Mammogram in 1995 6 yrs. later presents with bloody nipple discharge Subsequent suspicious mammogram Suspicious
FirstCyte Ductal Lavage History: 68 Year Old Female Gail Index: Unknown Clinical History: Negative Mammogram in 1995 6 yrs. later presents with bloody nipple discharge Subsequent suspicious mammogram Suspicious
Papillary Lesions of the Breast A Practical Approach to Diagnosis. (Arch Pathol Lab Med. 2016;140: ; doi: /arpa.
 Papillary Lesions of the Breast A Practical Approach to Diagnosis (Arch Pathol Lab Med. 2016;140:1052 1059; doi: 10.5858/arpa.2016-0219-RA) Papillary lesions of the breast Span the spectrum of benign,
Papillary Lesions of the Breast A Practical Approach to Diagnosis (Arch Pathol Lab Med. 2016;140:1052 1059; doi: 10.5858/arpa.2016-0219-RA) Papillary lesions of the breast Span the spectrum of benign,
Surgical Pathology Issues of Practical Importance
 Surgical Pathology Issues of Practical Importance Anne Moore, MD Medical Oncology Syed Hoda, MD Surgical Pathology The pathologist is central to the team approach needed to manage the patient with breast
Surgical Pathology Issues of Practical Importance Anne Moore, MD Medical Oncology Syed Hoda, MD Surgical Pathology The pathologist is central to the team approach needed to manage the patient with breast
How to Use MRI Following Neoadjuvant Chemotherapy (NAC) in Locally Advanced Breast Cancer
 Global Breast Cancer Conference 2016 & 5 th International Breast Cancer Symposium April 29 th 2016, 09:40-10:50 How to Use MRI Following Neoadjuvant Chemotherapy (NAC) in Locally Advanced Breast Cancer
Global Breast Cancer Conference 2016 & 5 th International Breast Cancer Symposium April 29 th 2016, 09:40-10:50 How to Use MRI Following Neoadjuvant Chemotherapy (NAC) in Locally Advanced Breast Cancer
Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer. Pathology. AGO e. V. in der DGGG e.v. sowie in der DKG e.v.
 Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer Pathology Pathology Versions 2004 2017: Blohmer / Costa / Fehm / Friedrichs / Huober / Kreipe / Lück / Schneeweis / Sinn /
Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer Pathology Pathology Versions 2004 2017: Blohmer / Costa / Fehm / Friedrichs / Huober / Kreipe / Lück / Schneeweis / Sinn /
Collecting Cancer Data: Breast. Prizes! Collecting Cancer Data: Breast 8/4/ NAACCR Webinar Series 1. NAACCR Webinar Series
 Collecting Cancer Data: Breast NAACCR 2008 2009 Webinar Series Prizes! Question of the Month! The participant that submits the best question of the session will receive a fbl fabulous Pi Prize! Shannon
Collecting Cancer Data: Breast NAACCR 2008 2009 Webinar Series Prizes! Question of the Month! The participant that submits the best question of the session will receive a fbl fabulous Pi Prize! Shannon
Mammographic imaging of nonpalpable breast lesions. Malai Muttarak, MD Department of Radiology Chiang Mai University Chiang Mai, Thailand
 Mammographic imaging of nonpalpable breast lesions Malai Muttarak, MD Department of Radiology Chiang Mai University Chiang Mai, Thailand Introduction Contents Mammographic signs of nonpalpable breast cancer
Mammographic imaging of nonpalpable breast lesions Malai Muttarak, MD Department of Radiology Chiang Mai University Chiang Mai, Thailand Introduction Contents Mammographic signs of nonpalpable breast cancer
Evaluation of Pathologic Response in Breast Cancer Treated with Primary Systemic Therapy
 Evaluation of Pathologic Response in Breast Cancer Treated with Primary Systemic Therapy Eun Yoon Cho, MD, PhD Department of Pathology and Translational Genomics Samsung Medical Center Sungkyunkwan University
Evaluation of Pathologic Response in Breast Cancer Treated with Primary Systemic Therapy Eun Yoon Cho, MD, PhD Department of Pathology and Translational Genomics Samsung Medical Center Sungkyunkwan University
Kidney Case 1 SURGICAL PATHOLOGY REPORT
 Kidney Case 1 Surgical Pathology Report February 9, 2007 Clinical History: This 45 year old woman was found to have a left renal mass. CT urography with reconstruction revealed a 2 cm medial mass which
Kidney Case 1 Surgical Pathology Report February 9, 2007 Clinical History: This 45 year old woman was found to have a left renal mass. CT urography with reconstruction revealed a 2 cm medial mass which
Ductal carcinoma in situ with microinvasion
 ORIGINAL ARTICLE Microinvasive Breast Cancer and the Role of Sentinel Node Biopsy: An Institutional Experience and Review of the Literature Amber A. Guth, MD,* Cecilia Mercado, MD, Daniel F. Roses, MD,*
ORIGINAL ARTICLE Microinvasive Breast Cancer and the Role of Sentinel Node Biopsy: An Institutional Experience and Review of the Literature Amber A. Guth, MD,* Cecilia Mercado, MD, Daniel F. Roses, MD,*
Consensus Guideline on Image-Guided Percutaneous Biopsy of Palpable and Nonpalpable Breast Lesions
 Consensus Guideline on Image-Guided Percutaneous Biopsy of Palpable and Nonpalpable Breast Lesions Purpose: To outline the use of minimally invasive biopsy techniques (MIBT) for palpable and nonpalpable
Consensus Guideline on Image-Guided Percutaneous Biopsy of Palpable and Nonpalpable Breast Lesions Purpose: To outline the use of minimally invasive biopsy techniques (MIBT) for palpable and nonpalpable
04/10/2018. Intraductal Papillary Neoplasms Of Breast INTRADUCTAL PAPILLOMA
 Intraductal Papillary Neoplasms Of Breast Savitri Krishnamurthy MD Professor of Pathology Deputy Division Head The University of Texas MD Anderson Cancer Center 25 th Annual Seminar in Pathology Pittsburgh,
Intraductal Papillary Neoplasms Of Breast Savitri Krishnamurthy MD Professor of Pathology Deputy Division Head The University of Texas MD Anderson Cancer Center 25 th Annual Seminar in Pathology Pittsburgh,
3/23/2017. Disclaimer. Common Changes in TNM Staging. Overview. Overview. Understanding Terminology. Overview
 Common Changes in TNM Staging Understanding the General Rules of Cancer Staging Thomas P. Baker, MD FCAP March 5, 2017 Disclaimer The identification of specific products or scientific instrumentation is
Common Changes in TNM Staging Understanding the General Rules of Cancer Staging Thomas P. Baker, MD FCAP March 5, 2017 Disclaimer The identification of specific products or scientific instrumentation is
ANNEX 1 OBJECTIVES. At the completion of the training period, the fellow should be able to:
 1 ANNEX 1 OBJECTIVES At the completion of the training period, the fellow should be able to: 1. Breast Surgery Evaluate and manage common benign and malignant breast conditions. Assess the indications
1 ANNEX 1 OBJECTIVES At the completion of the training period, the fellow should be able to: 1. Breast Surgery Evaluate and manage common benign and malignant breast conditions. Assess the indications
PROTOCOL SENTINEL NODE BIOPSY (NON OPERATIVE) BREAST CANCER - PATHOLOGY ASSESSMENT
 PROTOCOL SENTINEL NODE BIOPSY (NON OPERATIVE) BREAST CANCER - PATHOLOGY ASSESSMENT Author: Dr Sally Ann Hales On behalf of the Breast and pathology CNGs Written: March 2005 Reviewed by CNG: June 2009 &
PROTOCOL SENTINEL NODE BIOPSY (NON OPERATIVE) BREAST CANCER - PATHOLOGY ASSESSMENT Author: Dr Sally Ann Hales On behalf of the Breast and pathology CNGs Written: March 2005 Reviewed by CNG: June 2009 &
CLINICAL SIGNIFICANCE OF BENIGN EPITHELIAL CHANGES
 Papillomas. Papillomas are composed of multiple branching fibrovascular cores, each having a connective tissue axis lined by luminal and myoepithelial cells ( Fig. 23-11 ). Growth occurs within a dilated
Papillomas. Papillomas are composed of multiple branching fibrovascular cores, each having a connective tissue axis lined by luminal and myoepithelial cells ( Fig. 23-11 ). Growth occurs within a dilated
Basement membrane in lobule.
 Bahram Memar, MD Basement membrane in lobule. Normal lobule-luteal phase Normal lobule-follicular phase Lactating breast Greater than 95% are adenocarcinomas in situ carcinomas and invasive carcinomas.
Bahram Memar, MD Basement membrane in lobule. Normal lobule-luteal phase Normal lobule-follicular phase Lactating breast Greater than 95% are adenocarcinomas in situ carcinomas and invasive carcinomas.
Papillary Lesions of the Breast
 Papillary Lesions of the Breast Laura C. Collins, M.D. Associate Professor of Pathology Associate Director, Division of Anatomic Pathology Beth Israel Deaconess Medical Center and Harvard Medical School
Papillary Lesions of the Breast Laura C. Collins, M.D. Associate Professor of Pathology Associate Director, Division of Anatomic Pathology Beth Israel Deaconess Medical Center and Harvard Medical School
Ductal Carcinoma-in-Situ: New Concepts and Controversies
 Ductal Carcinoma-in-Situ: New Concepts and Controversies James J. Stark, MD, FACP Medical Director, Cancer Program and Palliative Care Maryview Medical Center Professor of Medicine, EVMS Case Presentation
Ductal Carcinoma-in-Situ: New Concepts and Controversies James J. Stark, MD, FACP Medical Director, Cancer Program and Palliative Care Maryview Medical Center Professor of Medicine, EVMS Case Presentation
Management of Ductal Carcinoma In Situ
 Management of Ductal Carcinoma In Situ Stella Hetelekidis, MD Stuart J. Schnitt, MD Monica Morrow, MD Jay R. Harris, MD Introduction Ductal carcinoma in situ (DCIS), also known as intraductal carcinoma,
Management of Ductal Carcinoma In Situ Stella Hetelekidis, MD Stuart J. Schnitt, MD Monica Morrow, MD Jay R. Harris, MD Introduction Ductal carcinoma in situ (DCIS), also known as intraductal carcinoma,
Interpretation of Breast Pathology in the Era of Minimally Invasive Procedures
 Shahla Masood, M.D. Professor and Chair Department of Pathology and Laboratory Medicine University of Florida College of Medicine Jacksonville Medical Director, UF Health Breast Center Chief of Pathology
Shahla Masood, M.D. Professor and Chair Department of Pathology and Laboratory Medicine University of Florida College of Medicine Jacksonville Medical Director, UF Health Breast Center Chief of Pathology
VULVAR CARCINOMA. Page 1 of 5
 VULVAR CARCINOMA EXAMPLE OF A VULVAR CARCINOMA USING PROPOSED TEMPLATE Case: Invasive squamous cell carcinoma arising in D-VIN Tumor in left labia major Left partial vaginectomy and sentinel lymph node
VULVAR CARCINOMA EXAMPLE OF A VULVAR CARCINOMA USING PROPOSED TEMPLATE Case: Invasive squamous cell carcinoma arising in D-VIN Tumor in left labia major Left partial vaginectomy and sentinel lymph node
Epithelial Columnar Breast Lesions: Histopathology and Molecular Markers
 29th Annual International Conference Advances in the Application of Monoclonal Antibodies in Clinical Oncology and Symposium on Cancer Stem Cells 25 th -27t h June, 2012, Mykonos, Greece Epithelial Columnar
29th Annual International Conference Advances in the Application of Monoclonal Antibodies in Clinical Oncology and Symposium on Cancer Stem Cells 25 th -27t h June, 2012, Mykonos, Greece Epithelial Columnar
ACRIN 6666 IM Additional Evaluation: Additional Views/Targeted US
 Additional Evaluation: Additional Views/Targeted US For revised or corrected form check box and fax to 215-717-0936. Instructions: The form is completed based on recommendations (from ID form) for additional
Additional Evaluation: Additional Views/Targeted US For revised or corrected form check box and fax to 215-717-0936. Instructions: The form is completed based on recommendations (from ID form) for additional
Lobular Carcinoma In Situ Variants in Breast Cores
 Lobular Carcinoma In Situ Variants in Breast Cores Potential for Misdiagnosis, Upgrade Rates at Surgical Excision, and Practical Implications Megan E. Sullivan, MD; Seema A. Khan, MD; Yurdanur Sullu, MD;
Lobular Carcinoma In Situ Variants in Breast Cores Potential for Misdiagnosis, Upgrade Rates at Surgical Excision, and Practical Implications Megan E. Sullivan, MD; Seema A. Khan, MD; Yurdanur Sullu, MD;
Papillary Lesions of the breast
 Papillary Lesions of the breast Emad Rakha Professor of Breast Pathology The University of Nottingham Papillary lesions of the breast are a heterogeneous group of disease, which are characterised by neoplastic
Papillary Lesions of the breast Emad Rakha Professor of Breast Pathology The University of Nottingham Papillary lesions of the breast are a heterogeneous group of disease, which are characterised by neoplastic
Advances in Breast Surgery. Catherine Campo, D.O. Breast Surgeon Meridian Health System April 17, 2015
 Advances in Breast Surgery Catherine Campo, D.O. Breast Surgeon Meridian Health System April 17, 2015 Objectives Understand the surgical treatment of breast cancer Be able to determine when a lumpectomy
Advances in Breast Surgery Catherine Campo, D.O. Breast Surgeon Meridian Health System April 17, 2015 Objectives Understand the surgical treatment of breast cancer Be able to determine when a lumpectomy
Breast pathology. 2nd Department of Pathology Semmelweis University
 Breast pathology 2nd Department of Pathology Semmelweis University Breast pathology - Summary - Benign lesions - Acute mastitis - Plasma cell mastitis / duct ectasia - Fat necrosis - Fibrocystic change/
Breast pathology 2nd Department of Pathology Semmelweis University Breast pathology - Summary - Benign lesions - Acute mastitis - Plasma cell mastitis / duct ectasia - Fat necrosis - Fibrocystic change/
Balancing Evidence and Clinical Practice in the Treatment of Localized Breast Cancer May 5, 2006
 Balancing Evidence and Clinical Practice in the Treatment of Localized Breast Cancer May 5, 2006 Deborah Hamolsky MS, RN : DCIS Carol Franc Buck Breast Care Center UCSF Comprehensive Cancer Center Jane
Balancing Evidence and Clinical Practice in the Treatment of Localized Breast Cancer May 5, 2006 Deborah Hamolsky MS, RN : DCIS Carol Franc Buck Breast Care Center UCSF Comprehensive Cancer Center Jane
Purposes and Principles of Cancer Staging
 Purposes and Principles of Cancer Staging INTRODUCTION AND OVERVIEW The extent or stage of cancer at the time of diagnosis is a key factor that defines prognosis and is a critical element in determining
Purposes and Principles of Cancer Staging INTRODUCTION AND OVERVIEW The extent or stage of cancer at the time of diagnosis is a key factor that defines prognosis and is a critical element in determining
Concordance with Breast Cancer Pathology Reporting Practice Guidelines
 Concordance with Breast Cancer Pathology Reporting Practice Guidelines Neal W Wilkinson, MD, FACS, Azin Shahryarinejad, MD, Janet S Winston, MD, Nancy Watroba, MPA, Stephen B Edge, MD, FACS BACKGROUND:
Concordance with Breast Cancer Pathology Reporting Practice Guidelines Neal W Wilkinson, MD, FACS, Azin Shahryarinejad, MD, Janet S Winston, MD, Nancy Watroba, MPA, Stephen B Edge, MD, FACS BACKGROUND:
S1.04 Principal clinician. G1.01 Comments. G2.01 *Specimen dimensions (prostate) S2.02 *Seminal vesicles
 Prostate Cancer Histopathology Reporting Proforma (Radical Prostatectomy) Includes the International Collaboration on Cancer reporting dataset denoted by * Family name Given name(s) Date of birth Sex Male
Prostate Cancer Histopathology Reporting Proforma (Radical Prostatectomy) Includes the International Collaboration on Cancer reporting dataset denoted by * Family name Given name(s) Date of birth Sex Male
Good afternoon everyone. First of all many thanks to Dr. Bonaventura and Dr. Arn for inviting
 PATHOLOGY IN-SITU CARCINOMA, ROHIT BHARGAVA, MD 1 Good afternoon everyone. First of all many thanks to Dr. Bonaventura and Dr. Arn for inviting me here, it s great to be here and I m going to talk about
PATHOLOGY IN-SITU CARCINOMA, ROHIT BHARGAVA, MD 1 Good afternoon everyone. First of all many thanks to Dr. Bonaventura and Dr. Arn for inviting me here, it s great to be here and I m going to talk about
Breast Imaging Lexicon
 9//201 200 BI RADS th Edition 201 BI RADS th Edition Breast Imaging Lexicon Mammographic Pathology and Assessment Categories Deborah Thames, R.T.(R)(M)(QM) The Advanced Health Education Center Nonmember:
9//201 200 BI RADS th Edition 201 BI RADS th Edition Breast Imaging Lexicon Mammographic Pathology and Assessment Categories Deborah Thames, R.T.(R)(M)(QM) The Advanced Health Education Center Nonmember:
COPE Library Sample
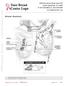 Breast Anatomy LOBULE LOBE ACINI (MILK PRODUCING UNITS) NIPPLE AREOLA COMPLEX ENLARGEMENT OF DUCT AND LOBE LOBULE SUPRACLAVICULAR NODES INFRACLAVICULAR NODES DUCT DUCT ACINI (MILK PRODUCING UNITS) 8420
Breast Anatomy LOBULE LOBE ACINI (MILK PRODUCING UNITS) NIPPLE AREOLA COMPLEX ENLARGEMENT OF DUCT AND LOBE LOBULE SUPRACLAVICULAR NODES INFRACLAVICULAR NODES DUCT DUCT ACINI (MILK PRODUCING UNITS) 8420
1 Purposes and Principles of Cancer Staging
 Purposes and Principles of Cancer Staging INTRODUCTION AND OVERVIEW The extent or stage of cancer at the time of diagnosis is a key factor that defines prognosis and is a critical element in determining
Purposes and Principles of Cancer Staging INTRODUCTION AND OVERVIEW The extent or stage of cancer at the time of diagnosis is a key factor that defines prognosis and is a critical element in determining
Clinical Trials of Proton Therapy for Breast Cancer. Andrew L. Chang, MD 張維安 Study Chair
 Clinical Trials of Proton Therapy for Breast Cancer Andrew L. Chang, MD 張維安 Study Chair AndrewLChangMD@gmail.com Disclosure Proton Center Development Corporation Scripps San Diego Proton Therapy Center
Clinical Trials of Proton Therapy for Breast Cancer Andrew L. Chang, MD 張維安 Study Chair AndrewLChangMD@gmail.com Disclosure Proton Center Development Corporation Scripps San Diego Proton Therapy Center
Case #1: 75 y/o Male (treated and followed by prostate cancer oncology specialist ).
 SOLID TUMORS WORKSHOP Cases for review Prostate Cancer Case #1: 75 y/o Male (treated and followed by prostate cancer oncology specialist ). January 2009 PSA 4.4, 20% free; August 2009 PSA 5.2; Sept 2009
SOLID TUMORS WORKSHOP Cases for review Prostate Cancer Case #1: 75 y/o Male (treated and followed by prostate cancer oncology specialist ). January 2009 PSA 4.4, 20% free; August 2009 PSA 5.2; Sept 2009
Prostate cancer ~ diagnosis and impact of pathology on prognosis ESMO 2017
 Prostate cancer ~ diagnosis and impact of pathology on prognosis ESMO 2017 Dr Puay Hoon Tan Division of Pathology Singapore General Hospital Prostate cancer (acinar adenocarcinoma) Invasive carcinoma composed
Prostate cancer ~ diagnosis and impact of pathology on prognosis ESMO 2017 Dr Puay Hoon Tan Division of Pathology Singapore General Hospital Prostate cancer (acinar adenocarcinoma) Invasive carcinoma composed
Ana Sofia Preto 19/06/2013
 Ana Sofia Preto 19/06/2013 Understanding the underlying pathophysiologic processes leading to the various types of calcifications Description and illustration of the several types of calcifications, according
Ana Sofia Preto 19/06/2013 Understanding the underlying pathophysiologic processes leading to the various types of calcifications Description and illustration of the several types of calcifications, according
CAP Cancer Protocol and ecc Summary of Changes for August 2014 Thyroid Agile Release
 CAP Cancer Protocol and ecc Summary of Changes for August 2014 Thyroid Agile Release 2 REVISION HISTORY Date Author / Editor Comments 5/19/2014 Jaleh Mirza Created the document 8/12/2014 Samantha Spencer/Jaleh
CAP Cancer Protocol and ecc Summary of Changes for August 2014 Thyroid Agile Release 2 REVISION HISTORY Date Author / Editor Comments 5/19/2014 Jaleh Mirza Created the document 8/12/2014 Samantha Spencer/Jaleh
BREAST PATHOLOGY. Fibrocystic Changes
 BREAST PATHOLOGY Lesions of the breast are very common, and they present as palpable, sometimes painful, nodules or masses. Most of these lesions are benign. Breast cancer is the 2 nd most common cause
BREAST PATHOLOGY Lesions of the breast are very common, and they present as palpable, sometimes painful, nodules or masses. Most of these lesions are benign. Breast cancer is the 2 nd most common cause
Treatment options for the precancerous Atypical Breast lesions. Prof. YOUNG-JIN SUH The Catholic University of Korea
 Treatment options for the precancerous Atypical Breast lesions Prof. YOUNG-JIN SUH The Catholic University of Korea Not so benign lesions? Imaging abnormalities(10% recall) lead to diagnostic evaluation,
Treatment options for the precancerous Atypical Breast lesions Prof. YOUNG-JIN SUH The Catholic University of Korea Not so benign lesions? Imaging abnormalities(10% recall) lead to diagnostic evaluation,
Case Scenario 1: Thyroid
 Case Scenario 1: Thyroid History and Physical Patient is an otherwise healthy 80 year old female with the complaint of a neck mass first noticed two weeks ago. The mass has increased in size and is palpable.
Case Scenario 1: Thyroid History and Physical Patient is an otherwise healthy 80 year old female with the complaint of a neck mass first noticed two weeks ago. The mass has increased in size and is palpable.
Thyroid Gland. Protocol applies to all malignant tumors of the thyroid gland, except lymphomas.
 Thyroid Gland Protocol applies to all malignant tumors of the thyroid gland, except lymphomas. Procedures Cytology (No Accompanying Checklist) Partial Thyroidectomy Total Thyroidectomy With/Without Lymph
Thyroid Gland Protocol applies to all malignant tumors of the thyroid gland, except lymphomas. Procedures Cytology (No Accompanying Checklist) Partial Thyroidectomy Total Thyroidectomy With/Without Lymph
Resection Margins in Breast Conserving Surgery. Alberto Costa, MD Canton Ticino Breast Unit Lugano, Switzerland
 Resection Margins in Breast Conserving Surgery Alberto Costa, MD Canton Ticino Breast Unit Lugano, Switzerland Breast Conserving Surgery 1 Probably one of the most important innovation in cancer surgery
Resection Margins in Breast Conserving Surgery Alberto Costa, MD Canton Ticino Breast Unit Lugano, Switzerland Breast Conserving Surgery 1 Probably one of the most important innovation in cancer surgery
Staging for Residents, Nurses, and Multidisciplinary Health Care Team
 Staging for Residents, Nurses, and Multidisciplinary Health Care Team Donna M. Gress, RHIT, CTR Validating science. Improving patient care. Learning Objectives Introduce the concept and history of stage
Staging for Residents, Nurses, and Multidisciplinary Health Care Team Donna M. Gress, RHIT, CTR Validating science. Improving patient care. Learning Objectives Introduce the concept and history of stage
Breast Surgery When Less is More and More is Less. E MacIntosh, MD June 6, 2015
 Breast Surgery When Less is More and More is Less E MacIntosh, MD June 6, 2015 Presenter Disclosure Faculty: E. MacIntosh Relationships with commercial interests: None Mitigating Potential Bias Not applicable
Breast Surgery When Less is More and More is Less E MacIntosh, MD June 6, 2015 Presenter Disclosure Faculty: E. MacIntosh Relationships with commercial interests: None Mitigating Potential Bias Not applicable
Proliferative Epithelial lesions of the Breast. Sami Shousha, MD, FRCPath Charing Cross Hospital & Imperial College, London
 Proliferative Epithelial lesions of the Breast Sami Shousha, MD, FRCPath Charing Cross Hospital & Imperial College, London Amman, November2013 Proliferative Epithelial Lesions of the Breast Usual type
Proliferative Epithelial lesions of the Breast Sami Shousha, MD, FRCPath Charing Cross Hospital & Imperial College, London Amman, November2013 Proliferative Epithelial Lesions of the Breast Usual type
Protocol for the Examination of Specimens From Patients With Merkel Cell Carcinoma of the Skin
 Protocol for the Examination of Specimens From Patients With Merkel Cell Carcinoma of the Skin Version: Protocol Posting Date: June 2017 Includes ptnm requirements from the 8 th Edition, AJCC Staging Manual
Protocol for the Examination of Specimens From Patients With Merkel Cell Carcinoma of the Skin Version: Protocol Posting Date: June 2017 Includes ptnm requirements from the 8 th Edition, AJCC Staging Manual
RUTGERS CANCER INSTITUTE OF NEW JERSEY - ROBERT WOOD JOHNSON MEDICAL SCHOOL INTERDISCIPLINARY BREAST SURGERY FELLOWSHIP CORE EDUCATIONAL OBJECTIVES
 RUTGERS CANCER INSTITUTE OF NEW JERSEY - ROBERT WOOD JOHNSON MEDICAL SCHOOL INTERDISCIPLINARY BREAST SURGERY FELLOWSHIP CORE EDUCATIONAL OBJECTIVES At the completion of Breast Fellowship training, the
RUTGERS CANCER INSTITUTE OF NEW JERSEY - ROBERT WOOD JOHNSON MEDICAL SCHOOL INTERDISCIPLINARY BREAST SURGERY FELLOWSHIP CORE EDUCATIONAL OBJECTIVES At the completion of Breast Fellowship training, the
16/09/2015. ACOSOG Z011 changing practice. Presentation outline. Nodal mets #1 prognostic tool. Less surgery no change in oncologic outcomes
 ACOSOG Z011 changing practice The end of axillary US/FNA? Preoperative staging of the axilla in the era of Z011 Adena S Scheer MD MSc FRCSC Surgical Oncologist, St. Michael s Hospital Assistant Professor,
ACOSOG Z011 changing practice The end of axillary US/FNA? Preoperative staging of the axilla in the era of Z011 Adena S Scheer MD MSc FRCSC Surgical Oncologist, St. Michael s Hospital Assistant Professor,
Breast Specimen Processing and Reporting With an Emphasis on Margin Evaluation. A College of American Pathologists Survey of 866 Laboratories
 Breast Specimen Processing and Reporting With an Emphasis on Margin Evaluation A College of American Pathologists Survey of 866 Laboratories Anthony J. Guidi, MD; Joseph A. Tworek, MD; Daniel D. Mais,
Breast Specimen Processing and Reporting With an Emphasis on Margin Evaluation A College of American Pathologists Survey of 866 Laboratories Anthony J. Guidi, MD; Joseph A. Tworek, MD; Daniel D. Mais,
