PD-L1 blockade enhances response of pancreatic ductal adenocarcinoma to radiotherapy
|
|
|
- Barnard Osborne
- 6 years ago
- Views:
Transcription
1 Research Article PD-L1 blockade enhances response of pancreatic ductal adenocarcinoma to radiotherapy Abul Azad 1,, Su Yin Lim 1,, Zenobia D Costa 1, Keaton Jones 1, Angela Diana 1, Owen J Sansom 2, Philipp Kruger 3, Stanley Liu 4, W Gillies McKenna 1, Omer Dushek 3, Ruth J Muschel 1 & Emmanouil Fokas 1,,,,* Abstract Pancreatic ductal adenocarcinoma (PDAC) is considered a nonimmunogenic tumor, and immune checkpoint inhibitor monotherapy lacks efficacy in this disease. Radiotherapy (RT) can stimulate the immune system. Here, we show that treatment of KPC and Pan02 murine PDAC cells with RT and gemcitabine upregulated PD-L1 expression in a JAK/Stat1-dependent manner. In vitro, PD-L1 inhibition did not alter radio- and chemosensitivity. In vivo, addition of anti-pd-l1 to high (12, 5 3, 20 Gy) but not low (6, 5 2 Gy) RT doses significantly improved tumor response in KPC and Pan02 allografts. Radiosensitization after PD-L1 blockade was associated with reduced CD11b + Gr1 + myeloid cell infiltration and enhanced CD45 + CD8 + T-cell infiltration with concomitant upregulation of T-cell activation markers including CD69, CD44, and FasL, and increased CD8:Treg ratio. Depletion of CD8 + T cells abrogated radiosensitization by anti-pd-l1. Blockade of PD-L1 further augmented the effect of high RT doses (12 Gy) in preventing development of liver metastases. Exploring multiple mathematical models reveals a mechanism able to explain the observed synergy between RT and anti-pd-l1 therapy. Our findings provide a rationale for testing the use of immune checkpoint inhibitors with RT in PDAC. Keywords liver metastases; mathematical modeling; pancreatic cancer; PD-L1 immune checkpoint; radiosensitization Subject Categories Cancer; Digestive System; Immunology DOI /emmm Received 6 June 2016 Revised 26 October 2016 Accepted 28 October 2016 Introduction Pancreatic ductal adenocarcinoma (PDAC) is a deadly malignancy with a 5-year survival rate of 5% (Hidalgo, 2010). Surgery is the only curative option, but the majority of patients are diagnosed at an advanced or metastatic stage. Also, PDAC is refractory to radiotherapy (RT) and chemotherapy (Ryan et al, 2014). Therefore, new therapeutic strategies are urgently required to improve survival in PDAC. The immune checkpoint programmed death 1 (PD-1) receptor and its ligand PD-L1 (Iwai et al, 2002) are often activated in cancer and play an important role in mediating escape from immune control by inhibiting cytotoxic T-cell function (Tolaney et al, 2015). Inhibition of the PD-1/PD-L1 axis has produced impressive response rates in various malignancies, such as melanoma, renal and non-small cell lung cancer (Iwai et al, 2002; Topalian et al, 2012; Hamid et al, 2013). However, although PD-L1 is expressed in human PDAC samples (Spivak-Kroizman et al, 2013; Hutcheson et al, 2016), monotherapy with PD-L1 inhibitors lacked efficacy in this disease (Brahmer, 2012). This can be attributed to the fact that PDAC is a non-immunogenic tumor characterized by low mutational burden (Liu et al, 2011), lack of CD8 + T-cell infiltration (Ino et al, 2013), and the presence of immunosuppressive myeloid cell populations (Dunn et al, 2002; Stromnes et al, 2015). Radiotherapy can activate the immune system to trigger an antitumor immune response following cytotoxic death and release of immunostimulating signals that can increase trafficking of T cells to the tumor (Burnette & Weichselbaum, 2013; Formenti & Demaria, 2013). Although studies have proposed the use of immunomodulators to enhance response to RT in various tumor types (Sharabi et al, 2015a), the efficacy of this concept in PDAC remains unexplored. Because PDAC is considered non-immunogenic (Hiraoka et al, 2006; Lutz et al, 2014) and thus less responsive to immunotherapies alone, we hypothesized that RT and anti-pd-l1 might have synergistic roles in the treatment of this disease. Here, we demonstrate that blockade of PD-L1 significantly improves tumor response to high but not low radiation doses in different tumor microenvironments by shifting the balance toward a more favorable anti-tumorigenic phenotype. We have also generated a 1 Department of Oncology, CRUK/MRC Oxford Institute for Radiation Oncology, University of Oxford, Oxford, UK 2 CRUK Beatson Cancer Institute, University of Glasgow, Glasgow, UK 3 Sir William Dunn School of Pathology, University of Oxford, Oxford, UK 4 Department of Radiation Oncology, Sunnybrook Research Institute, Sunnybrook Health Sciences Centre, University of Toronto, Toronto, ON, Canada *Corresponding author. Tel: ; Fax: ; emmanouil.fokas@oncology.ox.ac.uk These authors contributed equally to this work Present address: Department of Radiotherapy and Oncology, Goethe University Frankfurt, Frankfurt, Germany Present address: German Cancer Research Center (DKFZ), Heidelberg, Germany Present address: German Cancer Consortium (DKTK) (Partner Site), Frankfurt, Germany ª 2016 The Authors. Published under the terms of the CC BY 4.0 license EMBO Molecular Medicine 1
2 EMBO Molecular Medicine PD-L1 blockade radiosenitizes PDAC Abul Azad et al mathematical model to explain the mechanism of action of PD-L1 blockade when combined with RT. Results PD-L1 expression is upregulated after radiotherapy and chemotherapy in PDAC cells We analyzed PD-L1 expression by flow cytometry in murine PDAC cell lines 24 h after RT and gemcitabine treatment (Fig 1A and B, and Appendix Fig S1A and B). Both mean fluorescence intensity (MFI) and percentage of PD-L1 + cells significantly increased in the KPC and Pan02 cell lines compared to the DMSO-treated controls. Similarly, we observed PD-L1 upregulation in the human pancreatic cancer PSN-1 cells upon RT and gemcitabine treatment (Appendix Fig S1C). However, conditioned medium (CM) obtained from KPC and PSN-1 cells 24 h after RT and chemotherapy did not alter PD-L1 expression (Appendix Fig S1D and E). The signal transducer and activator of transcription (Stat) is an important mediator of PD-L1 signaling (Mowen & David, 2000). Hence, we investigated the effect of JAK/Stat signaling on PD-L1 expression in both KPC and Pan02 cell lines (Fig 1C and D). Consistent with our flow cytometry results, we observed upregulation of PD-L1 following RT and gemcitabine treatment by Western blotting. Upon inhibition of the JAK/Stat using AG490, RT- and gemcitabine-mediated upregulation of PD-L1 was completely abolished (Fig 1C and D). Because AG490 can block both Stat1 and Stat3, we inhibited Stat1 and Stat3 by sirna and confirmed their downregulation by Western blot (Appendix Fig S1F and G). Subsequent flow cytometry analysis of PD-L1 after treatment showed that inhibition of Stat1 (Fig 1E and F) but not Stat3 (Appendix Fig S1H) decreased PD-L1 expression after RT and gemcitabine treatment in PDAC cells. IFNc has been shown to stimulate PD-L1 expression downstream of Stat1 in several cancer cells (Dovedi et al, 2014; Kharma et al, 2014). Hence, we examined whether IFNc expression in KPC and Pan02 cells were affected by treatments (Appendix Fig S2A). Gemcitabine stimulated a small but significant increase in MFI and percentage of IFNc-expressing cells compared to controls, but RT had no effect. Moreover, IFNc expression was not altered following Stat1 and Stat3 inhibition in PDAC cells after RT and gemcitabine treatment (Appendix Fig S2B and C). We next asked whether IL-6 affects PD-L1 and IFNc expression in PDAC cells as IL-6 also signals via the JAK/Stat pathway. Addition of recombinant murine IL-6 did not alter the percentage of PD-L1 + cells (Appendix Fig S3A) or IFNc expression (Appendix Fig S3B) compared to untreated PDAC cells. These results indicate that RT and gemcitabine treatments can induce PD-L1 expression in PDAC cells in vitro in a JAK/Stat1 but not Stat3-dependent manner and that blockade of JAK/Stat1 signaling can abrogate PD-L1 induction. Efficacy of PD-L1 blockade in radiosensitizing PDAC tumor to low radiation doses Next, we investigated the effect of anti-pd-l1 on tumor cell growth in vitro. Treatment with anti-pd-l1 did not sensitize KPC or Pan02 tumor cells to RT or gemcitabine (Appendix Fig S4A and B). In vivo, KPC syngeneic tumor-bearing mice were treated with either RT alone (6 Gy or 5 2 Gy), anti-pd-l1 alone, or their combination (Fig 2A). Treatment with anti-pd-l1 alone had no significant effect on tumor growth, whereas RT radiosensitized tumors compared to untreated controls. Addition of anti-pd-l1 to either RT schedule failed to significantly enhance tumor response to RT (Fig 2A). Similar to the KPC syngeneic tumor model, treatment of Pan02 allografts with either RT (6 Gy or 5 2 Gy), anti-pd-l1, or their combination failed to show significant growth delay compared to the untreated control group (data not shown). We conducted flow cytometry analysis of immune effector CD45 + CD8 + T cells, CD45 + CD4 + T cells, and CD11b + Gr1 + myeloid cells in the tumor 5 days after completion of the above treatments. We failed to detect any significant changes in any of the immune cell populations in the tumor after the different treatments (Fig 2B and Appendix Fig S5). Treatment was well tolerated with no weight loss observed in any of the mice throughout the experiment. Thus, PD-L1 blockade did not significantly sensitize PDAC tumors to low RT doses (6 Gy or 5 2 Gy). Although a trend toward radiosensitization was observed, it is important to note that low RT doses did not increase cytotoxic CD8 + T-cell numbers in the tumor microenvironment. PD-L1 blockade sensitizes pancreatic allografts to high RT doses Because anti-pd-l1 treatment failed to enhance tumor response to relatively low RT doses, we then asked whether combination with higher RT doses could induce a better response to PD-L1 blockade. We first tested the efficacy of high RT doses with anti-pd-l1 in the Pan02 allograft tumor model (Fig 3A). Both high RT doses (12 Gy or 5 3 Gy) resulted in significant tumor growth delay, whereas anti-pd-l1 alone did not affect tumor growth. However, PD-L1 blockade significantly enhanced response to both RT schedules. The in vivo experiment had to be terminated at around days because the extensive regression seen in several tumors in both combination groups resulted in large wounds that could compromise animal welfare. Flow cytometry analysis revealed significantly increased CD45 + CD8 + and CD45 + CD4 + T-cell infiltration in irradiated tumors compared to controls; these numbers were additionally significantly increased upon blockade of PD-L1 (Fig 3B and Appendix Fig S6). Compared to the control, CD11b + Gr1 + myeloid cell numbers only decreased significantly after 12 Gy + PD-L1 blockade. Similar to Pan02, mice bearing KPC tumors were treated with either 12 Gy, 5 3 Gy, anti-pd-l1, or the combinations (Fig 4A and B). Both RT doses resulted in increased tumor growth delay that was further enhanced after administration of anti-pd-l1. In parallel, we determined the effect of CD8 + T-cell depletion using anti-cd8 antibodies on the radiosensitization potential of PD-L1 blockade in the KPC model (Fig 4A and B). Of note, the control, the anti-pd-l1 and anti-cd8 alone group are the same in both Fig 4A and B. Treatment with anti-cd8 did not alter KPC tumor growth in either unirradiated or irradiated mice. However, addition of anti-cd8 reversed the radiosensitizing effect of PD-L1 blockade (Fig 4A and B), underscoring the importance of CD8 + T cells in mediating the radiosensitizing effect of PD-L1 blockade in PDAC. As in the Pan02 syngeneic models, CD45 + CD8 + and CD45 + CD4 + T-cell infiltration significantly increased after irradiation and was further enhanced after 2 EMBO Molecular Medicine ª 2016 The Authors
3 Abul Azad et al PD-L1 blockade radiosenitizes PDAC EMBO Molecular Medicine A B C D E F Figure 1. RT and chemotherapy alter PD-L1 expression in PDAC cells. A, B Flow cytometric analysis of PD-L1 expression in (A) KPC and (B) Pan02 cells following treatment with gemcitabine and RT. Gemcitabine was diluted in DMSO (vehicle) and DMSO was used for the untreated control group (mean SD, n = 3, one-way ANOVA, Bonferroni test). MFI, mean fluorescence index. C, D Western blot analysis of the indicated proteins in both KPC (C) and Pan02 (D) cells following radiation and chemotherapy AG490, a JAK/Stat kinase inhibitor. Actin represents loading control. E, F Flow cytometric analysis of PD-L1 after gemcitabine and RT (as described above) in KPC (E) and Pan02 (F) following Stat1 downregulation by sirna (mean SD, n = 3, Student s t-test). Source data are available online for this figure. ª 2016 The Authors EMBO Molecular Medicine 3
4 EMBO Molecular Medicine PD-L1 blockade radiosenitizes PDAC Abul Azad et al A B Figure 2. PD-L1 blockade does not significantly sensitize PDAC to low RT doses (6 Gy or 5 2 Gy; initiated at day 0) in the syngeneic KPC tumor allograft model. A Tumor growth delay was measured in the different groups, as indicated (n = 6 mice per group). Anti-PD-L1 was given at days 0, 3, 6, and 9 (black arrows). The average time (days) for tumors to reach a volume of 400 mm 3 from day 0 is shown (means SD, n = 1, one-way ANOVA, Bonferroni test). No weight loss was observed in the in vivo experiment. B Quantitative data on the percentage of gated cells are shown (n = 5 per group; means SD, n = 1, one-way ANOVA, Bonferroni test). PD-L1 blockade (data not shown). Additionally, we assessed the activation status of the CD45 + CD8 + T cells based on IFNc expression and found increased activated CD8 + T cells following combination of high RT doses and PD-L1 blockade (described in Appendix Results and Appendix Fig S7). We next compared simultaneous combination of 12 Gy with anti-pd-l1 to administration of anti-pd-l1 1 week after RT (Fig 4C). In contrast to the simultaneous combination, sequential administration of anti-pd-l1 1 week post-rt did not radiosensitize KPC tumor allografts. Moreover, we analyzed the effect of PD-L1 blockade after a very high single RT dose (20 Gy) in the KPC model. PD-L1 blockade significantly radiosensitized tumors after 20 Gy, but mice in both the RT alone and the RT + anti-pd-l1 groups developed grade 2 radiation dermatitis that forced termination of the experiment at approximately day 35 (Appendix Fig S9A). Taken together, anti-pd- L1 treatment resulted in significant tumor growth delay after high RT doses that correlated with enhanced tumor infiltration of CD8 + T cells and decreased CD11b + Gr1 + myeloid cells. Changes in cytokine profiles after RT and PD-L1 blockade We examined expression of several inflammatory cytokines in sera of mice after treatment with anti-pd-l1 and/or RT (Appendix Fig S8A). Levels of stromal derived factor 1 (SDF-1) and IL-1 receptor agonist (ra) decreased slightly after anti-pd-l1 and RT treatments in the cytokine array (Appendix Fig S8B). SDF-1 levels were 4 EMBO Molecular Medicine ª 2016 The Authors
5 Abul Azad et al PD-L1 blockade radiosenitizes PDAC EMBO Molecular Medicine A B Figure 3. RT combined with blockade of PD-L1 amplifies anti-tumor effects in Pan02 tumor allograft. A Tumor growth delay was measured by treating tumors with RT (12 Gy or 5 3 Gy daily; initiated at day 0) and anti-pd-l1 alone or combination of RT (n = 6 mice per group). Anti-PD-L1 was given at days 0, 3, 6, and 9. The radiosensitizing effect of anti-pd-l1 after 12 and 5 3 Gy was assessed as shown by the capped lines (means SD, n = 1, one-way ANOVA, Bonferroni test). No weight loss was observed in the in vivo experiment. B Quantitative data on the percentage of gated cells are shown (n = 5 per group; means SD, n = 1, one-way ANOVA, Bonferroni test). significantly downregulated following RT and combination anti-pd-l1 + RT compared to controls as shown by ELISA (Appendix Fig S8C). PD-L1 blockade improves both response to chemoradiotherapy and radiation We examined PD-L1 expression in the syngeneic KPC tumor allografts after RT and gemcitabine treatment. PD-L1 was induced 5 days after treatment with gemcitabine, 12 Gy, 20 Gy, and 5 3 Gy (Appendix Fig S9B). Similarly, PD-L1 was upregulated 24 h (short term) as well as 3 7 weeks (long term) after completion of gemcitabine in the transgenic KPC mice compared to control (Appendix Fig S9C). Hence, similar to the in vitro conditions, RT and gemcitabine can upregulate PD-L1 in PDAC in vivo. We then assessed the impact of anti-pd-l1 when combined with gemcitabine and RT (Fig 5A). Neither gemcitabine alone, nor anti-pd-l1 alone affected tumor growth compared to control. The combination of anti-pd-l1 with gemcitabine produced a marginally significant tumor growth delay, whereas gemcitabine and RT had a more pronounced effect. Consistent with our previous findings, anti-pd-l1 significantly enhanced the RT-induced tumor growth delay. Compared to the double combinations, the ª 2016 The Authors EMBO Molecular Medicine 5
6 EMBO Molecular Medicine PD-L1 blockade radiosenitizes PDAC Abul Azad et al Figure 4. CD8 + T cells are required for efficacy of RT and anti-pd-l1 treatment. A KPC tumor growth delay after treatment with either 12 Gy (day 0), anti-pd-l1 (days 0, 3, 6, and 9; black arrows), anti-cd8 alone (days 0, 3, 6, and 9) or their combinations, as indicated. B KPC tumor growth delay after treatment with either 5 3 Gy (days 0 4), anti-pd-l1 alone (days 0, 3, 6, and 9; black arrows), anti-cd8 alone (days 0, 3, 6, and 9) or their combinations, as indicated. Of note, the control, the anti-pd-l1 and anti-cd8 alone groups are the same as in (A). C KPC tumor growth delay after either simultaneous (days 0, 3, 6, and 9; black arrows, upper row) or sequential (days 6, 9, 12, and 15; black arrows, lower row) addition of anti-pd-l1 to RT (day 0). Data information: The average time (days) for tumors to reach a volume of 400 mm 3 from day 0 is also shown in the graphs on the right (means SD, n = 1, one-way ANOVA, Bonferroni test). No weight loss was observed in the in vivo experiments. Source data are available online for this figure. 6 EMBO Molecular Medicine ª 2016 The Authors
7 Abul Azad et al PD-L1 blockade radiosenitizes PDAC EMBO Molecular Medicine A B C Figure 5. Impact of triple combination of gemcitabine-based chemoirradiation with anti-pd-l1 in the KPC tumor allograft. A Mice were treated with either gemcitabine (days 0, 3), anti-pd-l1 (days 4, 7, 10, and 13), 12 Gy (day 4) alone, or in combinations, as indicated (n = 8 mice per group). The average time (days) for tumors to reach a volume of 400 mm 3 from day 0 is shown (means SD, n = 1, one-way ANOVA, Bonferroni test). No weight loss was observed in the in vivo experiment. B, C RT plus anti-pd-l1 reverses T-cell exhaustion (B) and increases CD8:Treg ratio (C). Bar graphs show quantitation of T-cell activation markers and CD8:Treg ratio in tumor samples based on flow cytometry analysis, as indicated (n = 5 per group; means SD, n = 1, one-way ANOVA, Bonferroni test). triple combination significantly enhanced tumor growth delay, albeit the effect of gemcitabine appeared to be additive rather than synergistic (Fig 5A). It has been previously reported that T cells become exhausted in cancers and chronic infections (Virgin et al, 2009; Herbst et al, 2014). Because PD-L1 was upregulated in PDAC cells in vitro and in vivo following RT and gemcitabine treatment and could potentially suppress T-cell activation, we examined the expression of T-cell activation markers CD69, FasL, and CD44 on intratumoral CD8 + T cells after treatment with RT, gemcitabine, and/or anti-pd- L1. We did not detect any significant difference in T-cell activation markers after single-agent treatment (Fig 5B). However, addition of anti-pd-l1 to RT and gemcitabine + RT significantly increased numbers of CD69 + and CD44 + FasL + CD8 T cells compared to controls. Additionally, treatment with anti-pd-l1 alone, or anti-pd-l1 in combination with RT and RT + gemcitabine increased the CD8/Treg ratio compared to control or treatment with RT alone and RT + gemcitabine, respectively (Fig 5C). These data provide evidence on the potential of PD-L1 blockade to promote T-cell activation in RT, gemcitabine, and combined RT plus gemcitabine. Anti-PD-L1 enhances the anti-metastatic effect of RT We asked whether anti-pd-l1 could enhance the cytotoxic effect of RT in a microenvironment other than the tumor allografts. For that purpose, we assessed the effect of PD-L1 blockade in liver metastasis. Mice were injected intrasplenically with either naïve or pre-irradiated (12 Gy) KPC cells, then treated ª 2016 The Authors EMBO Molecular Medicine 7
8 EMBO Molecular Medicine PD-L1 blockade radiosenitizes PDAC Abul Azad et al with anti-pd-l1 every 3 days. After 14 days, livers were harvested and weighted. Compared to control, prior treatment with 12 Gy reduced metastatic tumor burden that was further enhanced by anti-pd-l1 treatment (Fig 6A). Combination of 12 Gy + anti-pd-l1 also increased CD8 + T-cell infiltration, while CD11b + Gr1 + myeloid cell and CD4 + CD25 + FOXP3 + Treg numbers were significantly reduced compared to controls (Fig 6B and Appendix Fig S10). Hence, the combination of RT and PD-L1 can enhance the cytotoxic effect of RT in an environment different from the primary tumor, further supporting the use of this therapeutic strategy. Mathematical modeling of immune cells interacting with tumor cells Finally, we used mathematical modeling (Dushek et al, 2011; Lever et al, 2014) to provide additional insight into the tumor growth behavior and underlying mechanism of synergy between RT and anti-pd-l1 (Appendix Fig S11A). For that purpose, we simulated populations of tumor cells, immune cells, and the effects of RT and anti-pd-l1 in different ways (i.e., assuming different mechanisms of action) and compared the overall tumor growth predicted by these different models to our experimental data. Experimentally, we observed that RT slowed overall tumor growth for up to 4 weeks, but our initial simulations failed to reproduce this long-term effect if we modeled RT as directly killing tumor cells (Appendix Fig S11B) or reducing their overall growth rate (i.e., permanently decreasing division rate or increasing cell death rate, Appendix Fig S11C). Given that RT is known to induce immune cell infiltration (Burnette & Weichselbaum, 2013), we generated a model where irradiated tumor cells became susceptible to killing by external factors (immune cells) that increase over time. Tumor growth simulations from this model can reproduce the effects of RT observed in our experiments (Appendix Fig S11D). Building on this model for RT, we next simulated the tumor growth curves for different mechanisms of PD-L1 blockade. We found that two different models can reproduce the synergistic effects observed in our experiments: Anti-PD-L1 increases CD8 + T-cell recruitment (Appendix Fig S11E) or CD8 + T-cell killing efficiency (Appendix Fig S11F). Both mechanisms are supported by our experiments (Figs 3 5) and therefore it is likely that both contribute to tumor control. A B Figure 6. Blockade of PD-L1 enhances the anti-metastatic effect of RT. A Representative images of livers from the different treatment groups, as indicated. The corresponding liver weights are shown on the right (n = 6 mice per group; means SD, n = 2, one-way ANOVA, Bonferroni test). B Flow cytometry analysis of CD45 + CD8 +,CD11b + Gr1 +, and CD4 + CD25 + FOXP3 + cell populations in the livers of the mice from the different treatment groups, as indicated (n = 5 mice per group; means SD, n = 1, one-way ANOVA, Bonferroni test). 8 EMBO Molecular Medicine ª 2016 The Authors
9 Abul Azad et al PD-L1 blockade radiosenitizes PDAC EMBO Molecular Medicine Lastly, we observed that radiosensitization was completely abolished when anti-pd-l1 was administered 7 days after RT (Fig 4C). The model could reproduce this result if it included suppressive microenvironment factors established earlier than 7 days (Appendix Fig S11G). The administration of anti-pd-l1 early but not late shifts the balance to a more inflammatory environment by preventing the establishment of factors that suppress the ability of CD8 + T cells to kill tumor cells (Appendix Fig S11G and E). This is in line with our findings of reduced CD11b + Gr1 + and Treg numbers in tumors treated with anti-pd-l1 and RT (Figs 3 6). In summary, we find that the synergy between RT and anti-pd- L1 observed in our experimental tumor growth curves can be explained by a model where (i) RT induces a large population of tumor cells to become susceptible to immune cell killing and (ii) anti-pd-l1 increases the recruitment and killing ability of CD8 T cells and, importantly, prevents the establishment of suppressive microenvironment factors (Appendix Fig S11A and G). Discussion PD-L1 plays a central role in permitting cancer evasion, mainly by interfering with T-cell functions, and inhibitors of the PD-1/PD-L1 axis have changed the paradigm in the management of melanoma patients (Clark et al, 2007). However, PDAC is characterized by a highly immunosuppressive stroma (Hiraoka et al, 2006; Lutz et al, 2014; Beatty et al, 2015; Diana et al, 2016b; Zhang et al, 2016) and immune checkpoint inhibitors alone were ineffective in the clinical setting (Royal et al, 2010; Brahmer et al, 2012). Evidence indicates potentially complementary roles for immunotherapy and RT (Sharabi et al, 2015a), but this combination has not been explored in PDAC. Here, we show that blockade of PD-L1 strongly enhanced tumor response to high (12, 5 3, and 20 Gy) but not low (6 and 5 2 Gy) RT doses, albeit a trend was noted for low doses. In addition to sensitizing tumors to RT, anti-pd-l1 improved response after gemcitabine-based chemoradiation. This is, to our knowledge, the first preclinical study to examine in detail the impact of this therapeutic strategy in PDAC. Our findings support and build on previous preclinical reports demonstrating enhanced radiosensitization using CTLA-4 and/or PD-1/PD-L1 immune checkpoint inhibitors in melanoma, breast, and colorectal cancer, and glioblastoma multiforme (Demaria et al, 2005; Deng et al, 2014; Dovedi et al, 2014; Sharabi et al, 2015b; Twyman-Saint Victor et al, 2015; Rodriguez-Ruiz et al, 2016). Although our observations with higher RT doses are in agreement with the majority of reports showing strong radiosensitization with PD-1/PD-L1 (Demaria et al, 2005; Deng et al, 2014; Dovedi et al, 2014; Sharabi et al, 2015b; Rodriguez-Ruiz et al, 2016) and CTLA-4 blockade (Twyman-Saint Victor et al, 2015), some suggestions that the effects of immunity could be overcome were noted; despite the significant growth delay after combination RT + anti-pd-l1, tumors eventually regrew in the KPC model. Unfortunately, the in vivo experiment using the Pan02 model had to be terminated early due to the profound tumor regression that led to the formation of extensive open wounds and hence tumor regrowth could not be monitored in this model. Also, 20 Gy treatment in KPC allografts resulted in RTinduced dermatitis (also in the RT alone group) that made tumor rechallenge impossible as the experiment had to be terminated. Interestingly, PD-L1 exerted a radiosensitizing effect only with higher RT doses in our models. In contrast, Dovedi et al demonstrated that PD-L1 inhibition in combination with lower RT doses (5 2 Gy) was sufficient to delay tumor growth in colorectal and triple-negative breast cancers (Dovedi et al, 2014). These differences could be attributed to the cell line behavior, such as higher intrinsic radiosensitivity compared to PDAC cells (Liu et al, 2011; Tolaney et al, 2015) that could render these cells more vulnerable to recognition and cytotoxic killing by T cells. PD-L1 expression is upregulated by either oncogenic signaling, such as PI3K/AKT activation (innate resistance) or inflammatory processes via IFNc (adaptive resistance) (Parsa et al, 2007; Kharma et al, 2014). In accordance with other groups (Spivak-Kroizman et al, 2013; Deng et al, 2014; Dovedi et al, 2014; Peng et al, 2015), we showed that both RT and gemcitabine induced PD-L1 expression in PDAC both in vitro and in vivo. Upregulation of PD-L1 by RT and gemcitabine lends support to coupling PD-L1 blockade with these conventional treatments to enhance anti-tumor response. Furthermore, PD-L1 expression can be suppressed by depletion of Stat1 (Kharma et al, 2014) and we found that the JAK/Stat kinase inhibitor AG490 abrogated baseline PD-L1 expression and upregulation after conventional treatments in our series. Because AG490 can inhibit both Stat1 and Stat3, we also used sirna to demonstrate that inhibition of Stat1 but not Stat3 decreased PD-L1 expression at baseline, and after RT and gemcitabine treatment in PDAC cells. Interestingly, IL-6 had marginal effects on PD-L1 expression in the PDAC cells despite activating the JAK/Stat pathway and its previous implication in PD-L1-mediated immunosuppression (Spary et al, 2014; Chen et al, 2016). PD-L1 upregulation can induce dysfunction in T cells leading to their exhaustion and impaired activation and immune surveillance (Wherry, 2011). Because both RT and gemcitabine upregulated PD- L1 in PDAC, we assessed whether this suppressed CD8 + T-cell activation. Addition of anti-pd-l1 to RT and RT + gemcitabine increased the proportion of intratumoral CD8 + T cells expressing the activation markers CD69, CD44, and FasL (Smith-Garvin et al, 2009; Wherry, 2011; Twyman-Saint Victor et al, 2015). These data suggest that despite inducing PD-L1 expression in PDAC, addition of anti-pd-l1 to RT and gemcitabine can overcome T-cell suppression and enhance T-cell activation. Radiotherapy can modulate the immune system to promote CD8 + T cells to attack tumor cells through multiple mechanisms (Burnette & Weichselbaum, 2013; Sharabi et al, 2015a) including the release of stimulatory cytokines such as IFNc. We only observed upregulation of IFNc expression in PDAC cells after treatment with gemcitabine but not with RT. IFNc can activate Jak/Stat resulting in PD-L1 upregulation (Bellucci et al, 2015), which could explain PD- L1 upregulation in PDAC cells after gemcitabine treatment. In an attempt to uncover other cytokines involved in the RT-mediated immune response, we examined the serum cytokine profiles of mice after treatment. RT alone or in combination with anti-pd-l1 significantly decreased SDF-1 expression. Interestingly, SDF-1 has been previously implicated in immunosuppression and tumor progression in PDAC (Feig et al, 2013) and downregulation of SDF-1 may contribute to the therapeutic effect of RT + anti-pd-l1 in reversing the immunosuppressive phenotype. The positive prognostic role of high CD8 + T-cell infiltration has been demonstrated consistently in the clinical setting in several ª 2016 The Authors EMBO Molecular Medicine 9
10 EMBO Molecular Medicine PD-L1 blockade radiosenitizes PDAC Abul Azad et al malignancies, including PDAC (Fridman et al, 2012; Ino et al, 2013; Diana et al, 2016a). We observed increased CD8 + T-cell infiltration in tumors after high RT doses that was further enhanced by inhibition of PD-L1. Anti-PD-L1 alone and in combination with RT significantly increased the CD8/Treg ratio, an important metric of anti-tumor response to treatment (Byrne et al, 2011; Amedei et al, 2013; Diana et al, 2016a). Furthermore, blockade of CD8 abrogated the radiosensitizing effect of anti-pd-l1 in PDAC cells in vivo, in agreement with other reports (Deng et al, 2014; Dovedi et al, 2014; Twyman-Saint Victor et al, 2015; Rodriguez-Ruiz et al, 2016). Addition of anti-pd-l1 to RT also caused a reduction in CD11b + Gr1 + myeloid cells in vivo. Infiltration of myeloid cells is a key feature of cancer inflammation in PDAC and CD11b + Gr1 + cells characteristic of myeloid-derived suppressor cells (MDSCs) are known to suppress antigen-specific T cells (Song et al, 2005). The reduction in CD11b + Gr1 + cells appears to be mutually exclusive from CD8 + T-cell infiltration (Clark et al, 2007). Deng et al revealed that addition of anti-pd-l1 to RT eliminated MDSCs from the tumor microenvironment (Deng et al, 2014). Consistent with this, we found reduced CD11b + Gr1 + cells following anti-pd-l1 and RT treatments. We additionally assessed whether anti-pd-l1 could enhance radiosensitization of PDAC cells in an environment other than the syngeneic allograft model. For that purpose, we intrasplenically injected untreated or previously irradiated (12 Gy) PDAC cells and assessed the impact of systemic PD-L1 blockade (i.p.) in the development of liver metastasis. Both RT alone and anti-pd-l1 alone reduced metastatic colonization compared to untreated controls, but addition of anti-pd-l1 significantly enhanced the anti-metastatic effect of RT. Recruitment of immune cells to the liver is known to precede development of liver metastases (Engblom et al, 2016). We found significant infiltration of CD8 + T cells after RT and anti-pd- L1 treatments compared to control. RT in combination with the anti-pd-l1 also significantly reduced infiltration of CD4 + CD25 + FOXP3 + T regulatory cells (Byrne et al, 2011), further supporting the notion that PD-L1 checkpoint inhibition together with RT can counteract the immunosuppressive tumor environment. Our observations are in line with a previous report showing decreased lung metastases after RT and CTLA-4 blockade in a mouse model of breast cancer (Demaria et al, 2005). Also, albeit in a different setting, combination of local RT with immune checkpoint blockade has demonstrated the so-called abscopal effect, that is, regression of metastatic lesions located outside the radiation field in melanoma patients due to the development of immune surveillance (Postow et al, 2012). Finally, we developed a minimal model of immune cell interactions with tumor cells that can explain the tumor growth behavior under treatment conditions. Importantly, we found that the synergistic effect of anti-pd-l1 treatment with RT cannot be explained solely with increased CD8 + T-cell recruitment or activation. An additional effect of anti-pd-l1 on the immunosuppressive microenvironment had to be invoked to explain the delayed tumor growth. Our model indicates that radiation + anti-pd-l1 combination therapy is only effective in patients with pre-existing CD8 T cells in the tumor microenvironment and that anti-pd-l1 should be administered early, in conjunction with RT for maximal anti-tumor responses. The mathematical model provides validation that anti-pd-l1 additionally targets the immunosuppressive cells, whereas radiotherapy alone may only stimulate immune cell recruitment. These findings are important for the design of future therapeutic strategies as they underscore the clinical value of combination therapy involving PD-1/PD-L1 blockade to target the immunosuppressive microenvironment. In summary, PD-L1 blockade can improve PDAC response to RT and chemoradiation and can enhance the effect of RT in preventing formation of liver metastases. Altogether, these findings indicate that RT combined with PD-L1 checkpoint inhibition can shift the balance toward a more favorable immune phenotype. Our data add important insight on the potential of immune checkpoint inhibitors to radiosensitize PDAC, a tumor that is traditionally considered as non-immunogenic. These findings provide a rationale for exploring the therapeutic potential of PD-L1 blockade in combination with RT in PDAC and should be explored in future clinical studies in patients with PDAC. Materials and Methods Cell culture and reagents The murine PDAC cell lines KPC and Pan02 were cultured in DMEM supplemented with 10% FBS and 1% penicillin/streptomycin. KPC cells were derived from KrasLSL G12D /+; p53 R172H /+; Pdx1-Cretg/+ (KPC) tumors. Murine Pan02 pancreatic adenocarcinoma cells were obtained from the NCI DCTD Tumor Repository, Maryland, USA. Gemcitabine was purchased from Eli Lilly and Company Ltd, UK. Murine anti-pd-l1 antibody (Clone 10F.9G2) was purchased from BioXCell. Clonogenic survival assay Both KPC and Pan02 cells were seeded into 6-well plates. Anti- PD-L1 antibody was added to the culture 1 h before irradiation with single dose of 2, 4, and 6 Gy. Similarly, cells were also treated with gemcitabine (0, 10, 20, and 50 nm). Gemcitabine was diluted in DMSO (vehicle), and hence, we used DMSO for the untreated control group. Twenty-four hours after treatment, cells were washed with PBS and replaced with fresh medium. The clonogenic survival of cells was assessed as described previously (Prevo et al, 2008). Syngeneic mouse models C57BL/6 mice were injected subcutaneously (s.c.) with KPC and Pan02 cells ( cells/100 ll in serum-free medium). Tumor size was measured with caliper using the formula Volume = (a b 2 )/2, in which a and b are the largest and the smallest perpendicular diameters, respectively. Mice were randomized into different groups when tumors reached 100 mm 3 and treatment was initiated (day 0) as described previously (Fokas et al, 2012). RT was initiated at day 0 (with the exception of the triple combination experiment where it was initiated at day 4) and was administered at a dose of either 6 Gy, 12 Gy, 20 Gy, 5 3 Gy, or 5 2 Gy given daily using the Gulmay 320 irradiator under inhalational anesthesia with isoflurane (2%). Only the tumor was irradiated, whereas the 10 EMBO Molecular Medicine ª 2016 The Authors
11 Abul Azad et al PD-L1 blockade radiosenitizes PDAC EMBO Molecular Medicine rest of the body was sealed to avoid unwanted side effects (Fokas et al, 2012). Gemcitabine (100 mg/kg) was given by intraperitoneal (i.p.) injection at days 0 and 3. Anti-PD-L1 antibody (clone 10F.9G2, BioXCell, UK) was administered at a dose of 10 mg/kg by i.p. injection at days 0, 3, 6, and 9 when combined with RT, or at days 4, 7, 10, and 13 in the triple combination experiment (gemcitabine + anti-pd-l1 + RT). For the combination doses, anti- PD-L1 was administered immediately after RT. The anti-cd8 (clone 2.43, BioXCell, UK) to deplete CD8 + T cells was given by i.p. injection at dose of 250 lg at days 0 (immediately post-rt), 3, 6, and 9. We assessed the time it took for the tumors to grow to 400 mm 3, starting from the beginning of treatment (day 0) to ensure that our experiments were according to the UK Home Office guidelines for animal welfare. Liver metastasis mouse model To generate liver metastasis, KPC cells ( cells/100 ll in PBS) were injected intrasplenically into C57BL/6 mice that are either naïve or pre-irradiated with 12 Gy 1 h before intrasplenic injection, as previously described (Lim et al, 2015). Spleen was removed 1 min following intrasplenic injection to avoid tumor growth in the spleen. Similar to the allograft experiments, anti-pd-l1 antibody was given at days 0, 3, 6, and 9 by i.p. injection at a dose of 10 mg/ kg. Livers were harvested and weighed at day 14. KPC transgenic mice The KPC transgenic mouse model has been described previously (Hingorani et al, 2005). When mice reached an age of weeks, monitoring for tumor was initiated using palpation twice per week and sonography (Ultrasound-Vevo 700). Treatment with gemcitabine (100 mg/kg) by i.p. injection for a total of three doses every 4 days was started when tumor reached mm 3. We assessed the impact of chemotherapy either short term (24 h) or long term (3 7 weeks, based on tumor size and deterioration of health status including weight loss > 20% and lethargy) after completion of treatment with gemcitabine. Tumors were harvested and analyzed for PD-L1 expression by flow cytometry as described below. All animal experiments were performed according to the regulations of the University of Oxford and the Home office, UK (Scientific Procedure Act, 1986; Project License Number 30/2922 issued by the Home Office). All protocols were approved by the Committee on the Ethics of Animal Experiments of the University of Oxford. Flow cytometry analysis KPC and Pan02 cells were seeded in 6-well plate. After 24 h, cells were treated with either 6, 4 2 Gy fractionated radiation given daily using cesium-137 irradiators, or 20 nm gemcitabine. Gemcitabine was diluted in DMSO (vehicle), and hence, we used DMSO for the untreated control group and the radiation groups as well. Cells were harvested 24 h post-treatment and washed with cold PBS. Cells were stained with mouse PE-PD-L1 and APC-IFNc. All the antibodies were purchased from ebiosciences. We also examined expression of PD-L1 following blockade of either Stat1 or Stat3 using sirna. For that purpose, cells were transfected with 50 nm negative control sirna (catalog number , Qiagen), 50 and 100 nm Stat1 (J , DermaFECT), or 50 nm Stat3 sirna (J , DermaFECT) using Lipofectamine 2000 (Invitrogen) reagent. After 48 h, proteins were isolated and knockdown was confirmed by Western blotting. For flow cytometry analysis of PD-L1 and IFNc, sirna-transfected cells were either irradiated with 6 Gy or treated with gemcitabine and PD-L1 expression examined as above. PD-L1 expression was also assessed following addition of recombinant mouse IL-6 (50 ng/ml; Pepro- Tech) for 1 h and subsequent treatments with 6 Gy and gemcitabine for 24 h. For flow cytometry analysis of mouse tissue samples, tumor, liver, and spleen were cut into small pieces and only liver samples were digested with 0.05% collagenase/dispase (Roche) for 15 min at 37 C in the presence of 0.01% trypsin inhibitor. Bone marrow was collected by flushing both femur and tibia with PBS using a 25-G syringe. All cells were washed with cold PBS. Cells were then filtered through 70-lm nylon strainer followed by red blood cell (RBC) lysis for 3 min at room temperature. Single-cell suspensions were then stained with the following antibodies: FITC-CD45, FITC- CD8, PeCy7-CD4, PeCy7-CD11b, PE-Gr1, PE-Ly6G and APC-IFNc, PE-CD25, APC-FOXP3, CD69-PE, APC-CD44, and PeCy7-FasL. Blood samples were collected in 40 mm EDTA and mixed with equal volume of PBS. Diluted blood was layered onto an equal volume of Histopaque (Sigma) and centrifuged at 400 g for 20 min at RT to isolate leukocyte population. The cells were washed with cold PBS and stained with FITC-CD8, PeCy7-CD4, and PE-PD-1. Flow cytometry was performed using a FACSCalibur (Becton Dickinson) and analyzed using FlowJo software (FlowJo, LLC, USA). All the antibodies were purchased from ebiosciences, UK. Western blotting Cells were first treated with 20 lm of JAK kinase inhibitor (AG490, Tocris) 1 h before RT (6 Gy) or addition of 20 nm gemcitabine. Following 24 h post-rt and gemcitabine, cell lysates were prepared in RIPA buffer containing protease inhibitor cocktail (Roche) and phosphatase inhibitor cocktail (Roche). In total, 30 lg of proteins were separated on SDS PAGE (Invitrogen) and transferred to Hybond-C membranes (Amersham Biosciences). Standard procedures were applied for Western blotting. The following antibodies were used: Stat1, phospho-stat1 (Y701), Stat3, mouse PD-L1 (all from R&D Systems), actin (Cell Signaling). Cytokine profile and SDF-1 ELISA in KPC allografts Serum was obtained from the KPC allograft-bearing mice 5 days after treatment with either vehicle (control), 12 Gy, anti-pd-l1, or 12 Gy + anti-pd-l1. Serum was assessed for expression of cytokines using a standard Cytokine Profiler kit and SDF-1 ELISA kit (both from R&D Systems) according to the manufacturer instructions. Array spot intensities were quantified using a Matlab software as reported (Zhao et al, 2013). Mathematical modeling We and others have previously used mathematical modeling to describe T-cell activation and antigen potency (Dushek et al, 2011; ª 2016 The Authors EMBO Molecular Medicine 11
12 EMBO Molecular Medicine PD-L1 blockade radiosenitizes PDAC Abul Azad et al The paper explained Problem Pancreatic ductal adenocarcinoma is characterized by a dismal prognosis and it is refractory to conventional treatment, such as radiotherapy and chemotherapy, and immune checkpoint inhibitor monotherapy. In contrast to the notion that all patients with PDAC die of metastatic disease, at least 20% suffer and die of local recurrence. Hence, there is a need to improve radiotherapy efficacy to enhance local control and clinical outcome. Evidence indicates potentially complementary roles for immunotherapy and radiotherapy, but this combination has not been explored in PDAC. Results Here, we show that radiation and gemcitabine chemotherapy have substantial immunomodulatory effects, including upregulation of PD-L1 in vitro and in vivo. Inhibition of PD-L1 strongly enhanced tumor response to high (12 Gy, 5 3 Gy, 20 Gy) but not low (6 Gy, 5 2 Gy) RT doses, and to gemcitabine-based chemoradiotherapy in different mouse models of PDAC. The increased tumor response to radiation observed upon PD-L1 blockade correlated with increased intratumoral T-cell numbers and activation and reduced myeloid cell infiltration, whereas depletion of CD8 + T cells abrogated the radiosensitization by anti-pd-l1. Additionally, inhibition of PD-L1 enhanced the impact of radiotherapy in preventing development of liver metastases. We generated a novel mathematical model that explains the synergistic effect of radiation and PD-L1. Impact In the present work, we provide a strong rationale for testing the use of PD-L1 immune checkpoint inhibition with radiotherapy in PDAC in the clinical setting that could lead to improved outcome in patients with this disease. Prism version 5 (GraphPad software, USA). P-values lower than 0.05 were considered statistically significant. Error bars represent standard deviation. Expanded View for this article is available online. Acknowledgements This work was funded by CRUK, the Marie Curie Innovative Training Network and the Kidani Memorial Trust. This work was partly funded by a Sir Henry Dale Fellowship jointly funded by the Wellcome Trust and Royal Society (grant ). We thank Dr. Ana Gomez, Mick Woodcock, and Graham Brown for the technical support. Author contributions AA, SYL, and EF designed the experimental strategy. AA, SYL, ZD C, and EF organized the experiments and collected and analyzed the data. AD and SYL provided assistance with the experimental methodology. AA, SYL, and EF prepared the protocols for mouse radiotherapy. OJS, WGM, and RJM provided experimental advice. PK and OD generated the mathematical modeling. AA, SYL, and EF wrote the manuscript with advice from OJS, WGM, OD, and RJM. KJ assisted with the in vivo studies. SL helped with the manuscript preparation. All authors discussed and approved the manuscript. Conflict of interest Part of this work was presented at the ESTRO 35 and the NCRI 2015 conference. The authors declare that they have no conflict of interest. For more information Lever et al, 2014; Tolaney et al, 2015). Here, we used the same principles to model the efficacy of anti-pd-l1 and RT in the different experiments. The mathematical model consists of a system of ordinary differential equations (ODEs), which are often used to describe the interactions among cellular populations in immunology and = = = = = φ (resistant tumor cells) (susceptible tumor cells) (CD8 effector T cells) (other immune cells) (microenvironment factors) where: k = 0.19, c = 0.025, b = 0.16, e2 = , M 1, K 1, tumor volume V = T1 + T2, and under the different treatment conditions: no treatment: e1 = 0.002, φ = 3, T1 day 0 = 100, T2 day 0 = 0; radiation: e1 = 0.002, φ = 3, T1 day 0 = 0.4, T2 day 0 = 99.6; radiation + anti-pd-l1 (day 0): e1 = 0.02, φ = 0.2, T1 day 0 = 0.4, T2 day 0 = 99.6; radiation + anti-pd-l1 (day 6): e1 day 0 = 0.002, e1 day 6 = 0.02, φ day 0 = 3, φ day 6 = 0.2, T1 day 0 = 0.4, T2 day 0 = The ODEs were integrated in Matlab (Mathworks, MA, USA) using ode45. Statistical analyses Differences between groups were determined using Student s paired t-test and one-way ANOVA (Bonferroni test) with the GraphPad References Amedei A, Niccolai E, Benagiano M, Della Bella C, Cianchi F, Bechi P, Taddei A, Bencini L, Farsi M, Cappello P et al (2013) Ex vivo analysis of pancreatic cancer-infiltrating T lymphocytes reveals that ENO-specific Tregs accumulate in tumor tissue and inhibit Th1/Th17 effector cell functions. Cancer Immunol Immunother 62: Beatty GL, Winograd R, Evans RA, Long KB, Luque SL, Lee JW, Clendenin C, Gladney WL, Knoblock DM, Guirnalda PD et al (2015) Exclusion of T cells from pancreatic carcinomas in mice is regulated by Ly6C(low) F4/80(+) extratumoral macrophages. Gastroenterology 149: Bellucci R, Martin A, Bommarito D, Wang K, Hansen SH, Freeman GJ, Ritz J (2015) Interferon-gamma-induced activation of JAK1 and JAK2 suppresses tumor cell susceptibility to NK cells through upregulation of PD-L1 expression. Oncoimmunology 4: e Brahmer JR (2012) PD-1-targeted immunotherapy: recent clinical findings. Clin Adv Hematol Oncol 10: Brahmer JR, Tykodi SS, Chow LQ, Hwu WJ, Topalian SL, Hwu P, Drake CG, Camacho LH, Kauh J, Odunsi K et al (2012) Safety and activity of anti-pd-l1 antibody in patients with advanced cancer. N Engl J Med 366: Burnette B, Weichselbaum RR (2013) Radiation as an immune modulator. Semin Radiat Oncol 23: Byrne WL, Mills KH, Lederer JA, O Sullivan GC (2011) Targeting regulatory T cells in cancer. Cancer Res 71: EMBO Molecular Medicine ª 2016 The Authors
13 Abul Azad et al PD-L1 blockade radiosenitizes PDAC EMBO Molecular Medicine Chen MF, Chen PT, Chen WC, Lu MS, Lin PY, Lee KD (2016) The role of PD-L1 in the radiation response and prognosis for esophageal squamous cell carcinoma related to IL-6 and T-cell immunosuppression. Oncotarget 7: Clark CE, Hingorani SR, Mick R, Combs C, Tuveson DA, Vonderheide RH (2007) Dynamics of the immune reaction to pancreatic cancer from inception to invasion. Cancer Res 67: Demaria S, Kawashima N, Yang AM, Devitt ML, Babb JS, Allison JP, Formenti SC (2005) Immune-mediated inhibition of metastases after treatment with local radiation and CTLA-4 blockade in a mouse model of breast cancer. Clin Cancer Res 11: Deng L, Liang H, Burnette B, Beckett M, Darga T, Weichselbaum RR, Fu YX (2014) Irradiation and anti-pd-l1 treatment synergistically promote antitumor immunity in mice. J Clin Invest 124: Diana A, Wang LM, D Costa Z, Allen P, Azad A, Silva MA, Soonawalla Z, Liu S, McKenna WG, Muschel RJ et al (2016a) Prognostic value, localization and correlation of PD-1/PD-L1, CD8 and FOXP3 with the desmoplastic stroma in pancreatic ductal adenocarcinoma. Oncotarget 7: Diana A, Wang LM, D Costa Z, Azad A, Silva MA, Soonawalla Z, Allen P, Liu S, McKenna WG, Muschel RJ et al (2016b) Prognostic role and correlation of CA9, CD31, CD68 and CD20 with the desmoplastic stroma in pancreatic ductal adenocarcinoma. Oncotarget doi: /oncotarget Dovedi SJ, Adlard AL, Lipowska-Bhalla G, McKenna C, Jones S, Cheadle EJ, Stratford IJ, Poon E, Morrow M, Stewart R et al (2014) Acquired resistance to fractionated radiotherapy can be overcome by concurrent PD-L1 blockade. Cancer Res 74: Dunn GP, Bruce AT, Ikeda H, Old LJ, Schreiber RD (2002) Cancer immunoediting: from immunosurveillance to tumor escape. Nat Immunol 3: Dushek O, Aleksic M, Wheeler RJ, Zhang H, Cordoba SP, Peng YC, Chen JL, Cerundolo V, Dong T, Coombs D et al (2011) Antigen potency and maximal efficacy reveal a mechanism of efficient T cell activation. Sci Signal 4: ra39 Engblom C, Pfirschke C, Pittet MJ (2016) The role of myeloid cells in cancer therapies. Nat Rev Cancer 16: Feig C, Jones JO, Kraman M, Wells RJ, Deonarine A, Chan DS, Connell CM, Roberts EW, Zhao Q, Caballero OL et al (2013) Targeting CXCL12 from FAP-expressing carcinoma-associated fibroblasts synergizes with anti-pd- L1 immunotherapy in pancreatic cancer. Proc Natl Acad Sci USA 110: Fokas E, Im JH, Hill S, Yameen S, Stratford M, Beech J, Hackl W, Maira SM, Bernhard EJ, McKenna WG et al (2012) Dual inhibition of the PI3K/mTOR pathway increases tumor radiosensitivity by normalizing tumor vasculature. Cancer Res 72: Formenti SC, Demaria S (2013) Combining radiotherapy and cancer immunotherapy: a paradigm shift. J Natl Cancer Inst 105: Fridman WH, Pages F, Sautes-Fridman C, Galon J (2012) The immune contexture in human tumours: impact on clinical outcome. Nat Rev Cancer 12: Hamid O, Robert C, Daud A, Hodi FS, Hwu WJ, Kefford R, Wolchok JD, Hersey P, Joseph RW, Weber JS et al (2013) Safety and tumor responses with lambrolizumab (anti-pd-1) in melanoma. N Engl J Med 369: Herbst RS, Soria JC, Kowanetz M, Fine GD, Hamid O, Gordon MS, Sosman JA, McDermott DF, Powderly JD, Gettinger SN et al (2014) Predictive correlates of response to the anti-pd-l1 antibody MPDL3280A in cancer patients. Nature 515: Hidalgo M (2010) Pancreatic cancer. N Engl J Med 362: Hingorani SR, Wang L, Multani AS, Combs C, Deramaudt TB, Hruban RH, Rustgi AK, Chang S, Tuveson DA (2005) Trp53R172H and KrasG12D cooperate to promote chromosomal instability and widely metastatic pancreatic ductal adenocarcinoma in mice. Cancer Cell 7: Hiraoka N, Onozato K, Kosuge T, Hirohashi S (2006)PrevalenceofFOXP3 + regulatory T cells increases during the progression of pancreatic ductal adenocarcinoma and its premalignant lesions. Clin Cancer Res 12: Hutcheson J, Balaji U, Porembka MR, Wachsmann M, McCue PA, Knudsen E, Witkiewicz AK (2016) Immunological and metabolic features of pancreatic ductal adenocarcinoma define prognostic subtypes of disease. Clin Cancer Res 22: Ino Y, Yamazaki-Itoh R, Shimada K, Iwasaki M, Kosuge T, Kanai Y, Hiraoka N (2013) Immune cell infiltration as an indicator of the immune microenvironment of pancreatic cancer. Br J Cancer 108: Iwai Y, Ishida M, Tanaka Y, Okazaki T, Honjo T, Minato N (2002) Involvement of PD-L1 on tumor cells in the escape from host immune system and tumor immunotherapy by PD-L1 blockade. Proc Natl Acad Sci USA 99: Kharma B, Baba T, Matsumura N, Kang HS, Hamanishi J, Murakami R, McConechy MM, Leung S, Yamaguchi K, Hosoe Y et al (2014) STAT1 drives tumor progression in serous papillary endometrial cancer. Cancer Res 74: Lever M, Maini PK, van der Merwe PA, Dushek O (2014) Phenotypic models of T cell activation. Nat Rev Immunol 14: Lim SY, Gordon-Weeks A, Allen D, Kersemans V, Beech J, Smart S, Muschel RJ (2015) Cd11b(+) myeloid cells support hepatic metastasis through downregulation of angiopoietin-like 7 in cancer cells. Hepatology 62: Liu J, Liao S, Huang Y, Samuel R, Shi T, Naxerova K, Huang P, Kamoun W, Jain RK, Fukumura D et al (2011) PDGF-D improves drug delivery and efficacy via vascular normalization, but promotes lymphatic metastasis by activating CXCR4 in breast cancer. Clin Cancer Res 17: Lutz ER, Wu AA, Bigelow E, Sharma R, Mo G, Soares K, Solt S, Dorman A, Wamwea A, Yager A et al (2014) Immunotherapy converts nonimmunogenic pancreatic tumors into immunogenic foci of immune regulation. Cancer Immunol Res 2: Mowen K, David M (2000) Regulation of STAT1 nuclear export by Jak1. Mol Cell Biol 20: Parsa AT, Waldron JS, Panner A, Crane CA, Parney IF, Barry JJ, Cachola KE, Murray JC, Tihan T, Jensen MC et al (2007) Loss of tumor suppressor PTEN function increases B7-H1 expression and immunoresistance in glioma. Nat Med 13: Peng J, Hamanishi J, Matsumura N, Abiko K, Murat K, Baba T, Yamaguchi K, Horikawa N, Hosoe Y, Murphy SK et al (2015) Chemotherapy induces programmed cell death-ligand 1 overexpression via the nuclear factorkappab to foster an immunosuppressive tumor microenvironment in ovarian cancer. Cancer Res 75: Postow MA, Callahan MK, Barker CA, Yamada Y, Yuan J, Kitano S, Mu Z, Rasalan T, Adamow M, Ritter E et al (2012) Immunologic correlates of the abscopal effect in a patient with melanoma. N Engl J Med 366: Prevo R, Deutsch E, Sampson O, Diplexcito J, Cengel K, Harper J, O Neill P, McKenna WG, Patel S, Bernhard EJ (2008) Class I PI3 kinase inhibition by the pyridinylfuranopyrimidine inhibitor PI-103 enhances tumor radiosensitivity. Cancer Res 68: Rodriguez-Ruiz ME, Rodriguez I, Garasa S, Barbes B, Solorzano JL, Perez- Gracia JL, Labiano S, Sanmamed MF, Azpilikueta A, Bolanos E et al (2016) Abscopal effects of radiotherapy are enhanced by combined immunostimulatory mabs and are dependent on CD8 T cells and crosspriming. Cancer Res 76: Royal RE, Levy C, Turner K, Mathur A, Hughes M, Kammula US, Sherry RM, Topalian SL, Yang JC, Lowy I et al (2010) Phase 2 trial of single agent ª 2016 The Authors EMBO Molecular Medicine 13
Appendix Figure S1 A B C D E F G H
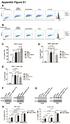 ppendix Figure S1 C D E F G H ppendix Figure S1. RT and chemotherapy alter PD-L1 expression in PDC cells. Flow cytometric analysis of PD-L1 expression in () KPC and () Pan02 cells following treatment with
ppendix Figure S1 C D E F G H ppendix Figure S1. RT and chemotherapy alter PD-L1 expression in PDC cells. Flow cytometric analysis of PD-L1 expression in () KPC and () Pan02 cells following treatment with
Radiation Therapy as an Immunomodulator
 Radiation Therapy as an Immunomodulator Yvonne Mowery, MD, PhD February 20, 2017 Tumor/Immune System Balance Kalbasi, JCI 2013 UNC-Duke-NC State-Wake Forest Spring 2017 2 RT Can Shift Balance Toward Elimination
Radiation Therapy as an Immunomodulator Yvonne Mowery, MD, PhD February 20, 2017 Tumor/Immune System Balance Kalbasi, JCI 2013 UNC-Duke-NC State-Wake Forest Spring 2017 2 RT Can Shift Balance Toward Elimination
Supplementary Figure 1. Deletion of Smad3 prevents B16F10 melanoma invasion and metastasis in a mouse s.c. tumor model.
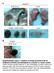 A B16F1 s.c. Lung LN Distant lymph nodes Colon B B16F1 s.c. Supplementary Figure 1. Deletion of Smad3 prevents B16F1 melanoma invasion and metastasis in a mouse s.c. tumor model. Highly invasive growth
A B16F1 s.c. Lung LN Distant lymph nodes Colon B B16F1 s.c. Supplementary Figure 1. Deletion of Smad3 prevents B16F1 melanoma invasion and metastasis in a mouse s.c. tumor model. Highly invasive growth
SUPPLEMENTARY INFORMATION
 Table S1: Combination Immunotherapy: Small Molecules that Boost Immune Response in Combination with Other Agents Target Compound (MOA) NLG919 and indoximod 1- MT Combination Model Observation Reference
Table S1: Combination Immunotherapy: Small Molecules that Boost Immune Response in Combination with Other Agents Target Compound (MOA) NLG919 and indoximod 1- MT Combination Model Observation Reference
Immunotherapy Concept Turned Reality
 Authored by: Jennifer Dolan Fox, PhD VirtualScopics Inc. jennifer_fox@virtualscopics.com +1 585 249 6231 Immunotherapy Concept Turned Reality Introduction While using the body s own immune system as a
Authored by: Jennifer Dolan Fox, PhD VirtualScopics Inc. jennifer_fox@virtualscopics.com +1 585 249 6231 Immunotherapy Concept Turned Reality Introduction While using the body s own immune system as a
Checkpoint Regulators Cancer Immunotherapy takes centre stage. Dr Oliver Klein Department of Medical Oncology 02 May 2015
 Checkpoint Regulators Cancer Immunotherapy takes centre stage Dr Oliver Klein Department of Medical Oncology 02 May 2015 Adjuvant chemotherapy improves outcome in early breast cancer FDA approval of Imatinib
Checkpoint Regulators Cancer Immunotherapy takes centre stage Dr Oliver Klein Department of Medical Oncology 02 May 2015 Adjuvant chemotherapy improves outcome in early breast cancer FDA approval of Imatinib
WIN 2015 Symposium Radiation and immunology: a new therapeutic partnership
 WIN 215 Symposium Radiation and immunology: a new therapeutic partnership Dr. Ralph Weichselbaum Conflict of Interest Nothing to Disclose Limitations of Radiotherapy Radiotherapy cannot be given in high
WIN 215 Symposium Radiation and immunology: a new therapeutic partnership Dr. Ralph Weichselbaum Conflict of Interest Nothing to Disclose Limitations of Radiotherapy Radiotherapy cannot be given in high
Targeting tumour associated macrophages in anti-cancer therapies. Annamaria Gal Seminar Series on Drug Discovery Budapest 5 January 2018
 Targeting tumour associated macrophages in anti-cancer therapies Annamaria Gal Seminar Series on Drug Discovery Budapest 5 January 2018 Macrophages: Professional phagocytes of the myeloid lineage APC,
Targeting tumour associated macrophages in anti-cancer therapies Annamaria Gal Seminar Series on Drug Discovery Budapest 5 January 2018 Macrophages: Professional phagocytes of the myeloid lineage APC,
Blocking antibodies and peptides. Rat anti-mouse PD-1 (29F.1A12, rat IgG2a, k), PD-
 Supplementary Methods Blocking antibodies and peptides. Rat anti-mouse PD-1 (29F.1A12, rat IgG2a, k), PD- L1 (10F.9G2, rat IgG2b, k), and PD-L2 (3.2, mouse IgG1) have been described (24). Anti-CTLA-4 (clone
Supplementary Methods Blocking antibodies and peptides. Rat anti-mouse PD-1 (29F.1A12, rat IgG2a, k), PD- L1 (10F.9G2, rat IgG2b, k), and PD-L2 (3.2, mouse IgG1) have been described (24). Anti-CTLA-4 (clone
Focused Ultrasound and Cancer Immunotherapy
 Focused Ultrasound and Cancer Immunotherapy Overview A number of therapeutic modalities including radiation, radiofrequency and laser-induced heating, cryoablation, and focused ultrasound have been shown
Focused Ultrasound and Cancer Immunotherapy Overview A number of therapeutic modalities including radiation, radiofrequency and laser-induced heating, cryoablation, and focused ultrasound have been shown
NKTR-214 plus NKTR-262, a Scientifically-Guided Rational Combination Approach for Immune Oncology
 plus NKTR-262, a Scientifically-Guided Rational Combination Approach for Immune Oncology Jonathan Zalevsky SVP, Biology and Preclinical Development Nektar Therapeutics World Preclinical Congress, 2017
plus NKTR-262, a Scientifically-Guided Rational Combination Approach for Immune Oncology Jonathan Zalevsky SVP, Biology and Preclinical Development Nektar Therapeutics World Preclinical Congress, 2017
L1 on PyMT tumor cells but Py117 cells are more responsive to IFN-γ. (A) Flow
 A MHCI B PD-L1 Fold expression 8 6 4 2 Fold expression 3 2 1 No tx 1Gy 2Gy IFN Py117 Py117 Supplementary Figure 1. Radiation and IFN-γ enhance MHCI expression and PD- L1 on PyMT tumor cells but Py117 cells
A MHCI B PD-L1 Fold expression 8 6 4 2 Fold expression 3 2 1 No tx 1Gy 2Gy IFN Py117 Py117 Supplementary Figure 1. Radiation and IFN-γ enhance MHCI expression and PD- L1 on PyMT tumor cells but Py117 cells
NKTR-255: Accessing IL-15 Therapeutic Potential through Robust and Sustained Engagement of Innate and Adaptive Immunity
 NKTR-255: Accessing IL-15 Therapeutic Potential through Robust and Sustained Engagement of Innate and Adaptive Immunity Peiwen Kuo Scientist, Research Biology Nektar Therapeutics August 31 st, 2018 Emerging
NKTR-255: Accessing IL-15 Therapeutic Potential through Robust and Sustained Engagement of Innate and Adaptive Immunity Peiwen Kuo Scientist, Research Biology Nektar Therapeutics August 31 st, 2018 Emerging
Combining ADCs with Immuno-Oncology Agents
 Combining ADCs with Immuno-Oncology Agents Chad May, PhD Senior Director Targeted Immunotherapy Oncology Research Unit, Pfizer 7 th Annual World ADC October 10, 2016 Cancer-Immunity Cycle Innate Immunity
Combining ADCs with Immuno-Oncology Agents Chad May, PhD Senior Director Targeted Immunotherapy Oncology Research Unit, Pfizer 7 th Annual World ADC October 10, 2016 Cancer-Immunity Cycle Innate Immunity
Cytokine Arrays Reveal Black Ops Tactics of Tumor-induced Immunosuppression
 Cytokine Arrays Reveal Black Ops Tactics of Tumor-induced Immunosuppression Jarad J Wilson, Ph.D. Technical Support & Marketing Specialist Ruo-Pan Huang, MD, Ph.D. Founder and CEO What are Antibody Arrays?
Cytokine Arrays Reveal Black Ops Tactics of Tumor-induced Immunosuppression Jarad J Wilson, Ph.D. Technical Support & Marketing Specialist Ruo-Pan Huang, MD, Ph.D. Founder and CEO What are Antibody Arrays?
NKTR-255: Accessing The Immunotherapeutic Potential Of IL-15 for NK Cell Therapies
 NKTR-255: Accessing The Immunotherapeutic Potential Of IL-15 for NK Cell Therapies Saul Kivimäe Senior Scientist, Research Biology Nektar Therapeutics NK Cell-Based Cancer Immunotherapy, September 26-27,
NKTR-255: Accessing The Immunotherapeutic Potential Of IL-15 for NK Cell Therapies Saul Kivimäe Senior Scientist, Research Biology Nektar Therapeutics NK Cell-Based Cancer Immunotherapy, September 26-27,
Darwinian selection and Newtonian physics wrapped up in systems biology
 Darwinian selection and Newtonian physics wrapped up in systems biology Concept published in 1957* by Macfarland Burnet (1960 Nobel Laureate for the theory of induced immune tolerance, leading to solid
Darwinian selection and Newtonian physics wrapped up in systems biology Concept published in 1957* by Macfarland Burnet (1960 Nobel Laureate for the theory of induced immune tolerance, leading to solid
Posters and Presentations
 Posters and Presentations June 2017: American Society of Clinical Oncology (ASCO) Annual - Preliminary Correlative Analysis of PD-L1 expression from the SUNRISE Study. View April 2017: American Association
Posters and Presentations June 2017: American Society of Clinical Oncology (ASCO) Annual - Preliminary Correlative Analysis of PD-L1 expression from the SUNRISE Study. View April 2017: American Association
Reviewers' comments: Reviewer #1 (Remarks to the Author):
 Reviewers' comments: Reviewer #1 (Remarks to the Author): In the manuscript Rational Combination of CXCL11-Expressing Oncolytic Virus and PD-L1 Blockade Works Synergistically to Enhance Therapeutic Efficacy
Reviewers' comments: Reviewer #1 (Remarks to the Author): In the manuscript Rational Combination of CXCL11-Expressing Oncolytic Virus and PD-L1 Blockade Works Synergistically to Enhance Therapeutic Efficacy
Priming the Immune System to Kill Cancer and Reverse Tolerance. Dr. Diwakar Davar Assistant Professor, Melanoma and Phase I Therapeutics
 Priming the Immune System to Kill Cancer and Reverse Tolerance Dr. Diwakar Davar Assistant Professor, Melanoma and Phase I Therapeutics Learning Objectives Describe the role of the immune system in cancer
Priming the Immune System to Kill Cancer and Reverse Tolerance Dr. Diwakar Davar Assistant Professor, Melanoma and Phase I Therapeutics Learning Objectives Describe the role of the immune system in cancer
VENTANA PD-L1 (SP142) Assay Guiding immunotherapy
 VENTANA PD-L1 (SP142) Assay Guiding immunotherapy Hiker s path: VENTANA PD-L1 (SP142) Assay on urothelial carcinoma tissue Location: Point Conception, CA VENTANA PD-L1 (SP142) Assay Identify patients most
VENTANA PD-L1 (SP142) Assay Guiding immunotherapy Hiker s path: VENTANA PD-L1 (SP142) Assay on urothelial carcinoma tissue Location: Point Conception, CA VENTANA PD-L1 (SP142) Assay Identify patients most
VENTANA PD-L1 (SP142) Assay
 VENTANA (SP142) Assay Guiding immunotherapy Hiker s path: VENTANA (SP142) Assay on urothelial carcinoma tissue Location: Point Conception, CA VENTANA (SP142) Assay Assess UC patient benefit from TECENTRIQ
VENTANA (SP142) Assay Guiding immunotherapy Hiker s path: VENTANA (SP142) Assay on urothelial carcinoma tissue Location: Point Conception, CA VENTANA (SP142) Assay Assess UC patient benefit from TECENTRIQ
Immunologic Effects of Clinical Stage FAK & PI3K-Delta/Gamma Inhibitors
 1 Immunologic Effects of Clinical Stage FAK & PI3K-Delta/Gamma Inhibitors Jonathan Pachter, Ph.D - Chief Scientific Officer 3rd Annual Immuno-Oncology Congress, May 24, 2018 Disclosures 2 I am an employee
1 Immunologic Effects of Clinical Stage FAK & PI3K-Delta/Gamma Inhibitors Jonathan Pachter, Ph.D - Chief Scientific Officer 3rd Annual Immuno-Oncology Congress, May 24, 2018 Disclosures 2 I am an employee
Supplementary Figure 1. Immune profiles of untreated and PD-1 blockade resistant EGFR and Kras mouse lung tumors (a) Total lung weight of untreated
 1 Supplementary Figure 1. Immune profiles of untreated and PD-1 blockade resistant EGFR and Kras mouse lung tumors (a) Total lung weight of untreated (U) EGFR TL mice (n=7), Kras mice (n=7), PD-1 blockade
1 Supplementary Figure 1. Immune profiles of untreated and PD-1 blockade resistant EGFR and Kras mouse lung tumors (a) Total lung weight of untreated (U) EGFR TL mice (n=7), Kras mice (n=7), PD-1 blockade
Releasing the Brakes on Tumor Immunity: Immune Checkpoint Blockade Strategies
 Releasing the Brakes on Tumor Immunity: Immune Checkpoint Blockade Strategies Jason Muhitch, PhD MIR 509 October 1 st, 2014 Email: jason.muhitch@roswellpark.org 0 Holy Grail of Tumor Immunity Exquisite
Releasing the Brakes on Tumor Immunity: Immune Checkpoint Blockade Strategies Jason Muhitch, PhD MIR 509 October 1 st, 2014 Email: jason.muhitch@roswellpark.org 0 Holy Grail of Tumor Immunity Exquisite
Immune Checkpoint Inhibitors: The New Breakout Stars in Cancer Treatment
 Immune Checkpoint Inhibitors: The New Breakout Stars in Cancer Treatment 1 Introductions Peter Langecker, MD, PhD Executive Medical Director, Global Oncology Clinipace Worldwide Mark Shapiro Vice President
Immune Checkpoint Inhibitors: The New Breakout Stars in Cancer Treatment 1 Introductions Peter Langecker, MD, PhD Executive Medical Director, Global Oncology Clinipace Worldwide Mark Shapiro Vice President
A Versatile Tool to Study Immune Checkpoint Therapeutics: Syngeneic Tumor Mouse Models in vivo
 The Solution Provider for Drug Discovery in Oncology A Versatile Tool to Study Immune Checkpoint Therapeutics: Syngeneic Tumor Mouse Models in vivo Holger Weber - 1 - Drug discovery platform for oncology
The Solution Provider for Drug Discovery in Oncology A Versatile Tool to Study Immune Checkpoint Therapeutics: Syngeneic Tumor Mouse Models in vivo Holger Weber - 1 - Drug discovery platform for oncology
Novel RCC Targets from Immuno-Oncology and Antibody-Drug Conjugates
 Novel RCC Targets from Immuno-Oncology and Antibody-Drug Conjugates Christopher Turner, MD Vice President, Clinical Science 04 November 2016 Uveal Melanoma Celldex Pipeline CANDIDATE INDICATION Preclinical
Novel RCC Targets from Immuno-Oncology and Antibody-Drug Conjugates Christopher Turner, MD Vice President, Clinical Science 04 November 2016 Uveal Melanoma Celldex Pipeline CANDIDATE INDICATION Preclinical
Future Perspectives in mpca. Michel Ducreux, MD, PhD Gustave Roussy Villejuif, France
 Future Perspectives in mpca Michel Ducreux, MD, PhD Gustave Roussy Villejuif, France Number of Novel Therapies and Targets in Pancreatic Cancer Are Expanding Garrido-Laguna I, et al. Nat Rev Clin Oncol.
Future Perspectives in mpca Michel Ducreux, MD, PhD Gustave Roussy Villejuif, France Number of Novel Therapies and Targets in Pancreatic Cancer Are Expanding Garrido-Laguna I, et al. Nat Rev Clin Oncol.
Approved for Public Release; Distribution Unlimited
 AD Award Number: W81XWH-04-1-0186 TITLE: A Novel Therapeutic System for the Treatment of Occult Prostate Cancer PRINCIPAL INVESTIGATOR: Shongyun Dong, M.D., Ph.D. CONTRACTING ORGANIZATION: University of
AD Award Number: W81XWH-04-1-0186 TITLE: A Novel Therapeutic System for the Treatment of Occult Prostate Cancer PRINCIPAL INVESTIGATOR: Shongyun Dong, M.D., Ph.D. CONTRACTING ORGANIZATION: University of
CB-1158 Inhibits the Immuno-oncology Target Arginase and Causes an Immune Mediated Anti-Tumor Response
 CB-1158 Inhibits the Immuno-oncology Target Arginase and Causes an Immune Mediated Anti-Tumor Response Francesco Parlati, Ph.D. Calithera Biosciences South San Francisco, CA Arginine Depletion by Arginase
CB-1158 Inhibits the Immuno-oncology Target Arginase and Causes an Immune Mediated Anti-Tumor Response Francesco Parlati, Ph.D. Calithera Biosciences South San Francisco, CA Arginine Depletion by Arginase
STATE OF THE ART 4: Combination Immune Therapy-Chemotherapy. Elizabeth M. Jaffee (JHU) James Yang (NCI) Jared Gollob (Duke) John Kirkwood (UPMI)
 STATE OF THE ART 4: Combination Immune Therapy-Chemotherapy Elizabeth M. Jaffee (JHU) James Yang (NCI) Jared Gollob (Duke) John Kirkwood (UPMI) Topics for Consideration What are the rules for integrating
STATE OF THE ART 4: Combination Immune Therapy-Chemotherapy Elizabeth M. Jaffee (JHU) James Yang (NCI) Jared Gollob (Duke) John Kirkwood (UPMI) Topics for Consideration What are the rules for integrating
Regulation of anti-tumor immunity through migration of immune cell subsets within the tumor microenvironment Thomas F. Gajewski, M.D., Ph.D.
 Regulation of anti-tumor immunity through migration of immune cell subsets within the tumor microenvironment Thomas F. Gajewski, M.D., Ph.D. Professor, Departments of Pathology and Medicine Program Leader,
Regulation of anti-tumor immunity through migration of immune cell subsets within the tumor microenvironment Thomas F. Gajewski, M.D., Ph.D. Professor, Departments of Pathology and Medicine Program Leader,
Supplementary Information
 Supplementary Information Methods Lymphocyte subsets analysis was performed on samples of 7 subjects by flow cytometry on blood samples collected in ethylenediaminetetraacetic acid (EDTA)-containing tubes
Supplementary Information Methods Lymphocyte subsets analysis was performed on samples of 7 subjects by flow cytometry on blood samples collected in ethylenediaminetetraacetic acid (EDTA)-containing tubes
PD-L1 and Immunotherapy of GI cancers: What do you need to know
 None. PD-L1 and Immunotherapy of GI cancers: What do you need to know Rondell P. Graham September 3, 2017 2017 MFMER slide-2 Disclosure No conflicts of interest to disclose 2017 MFMER slide-3 Objectives
None. PD-L1 and Immunotherapy of GI cancers: What do you need to know Rondell P. Graham September 3, 2017 2017 MFMER slide-2 Disclosure No conflicts of interest to disclose 2017 MFMER slide-3 Objectives
 Rath, N., and Olson, M. (2016) Regulation of pancreatic cancer aggressiveness by stromal stiffening. Nature Medicine, 22(5), pp. 462-463. There may be differences between this version and the published
Rath, N., and Olson, M. (2016) Regulation of pancreatic cancer aggressiveness by stromal stiffening. Nature Medicine, 22(5), pp. 462-463. There may be differences between this version and the published
Co-operative Radio-Immune-Stimulating Cancer Therapy by Bertil R.R. Persson PhD, MDh.c Professor emeritus of medical radiation physics at Lund
 Co-operative Radio-Immune-Stimulating Cancer Therapy by Bertil R.R. Persson PhD, MDh.c Professor emeritus of medical radiation physics at Lund University, 221 85 LUND Sweden. E-mail: bertil_r.persson@med.lu.se
Co-operative Radio-Immune-Stimulating Cancer Therapy by Bertil R.R. Persson PhD, MDh.c Professor emeritus of medical radiation physics at Lund University, 221 85 LUND Sweden. E-mail: bertil_r.persson@med.lu.se
Cancer Progress. The State of Play in Immuno-Oncology
 Cancer Progress The State of Play in Immuno-Oncology Axel Hoos, MD, PhD VP, Oncology R&D, Glaxo Smith Kline Co-Director, Cancer Immunotherapy Consortium Key Drivers in Immuno-Oncology Science Methods Combinations
Cancer Progress The State of Play in Immuno-Oncology Axel Hoos, MD, PhD VP, Oncology R&D, Glaxo Smith Kline Co-Director, Cancer Immunotherapy Consortium Key Drivers in Immuno-Oncology Science Methods Combinations
Interpreting Therapeutic Response on Immune Cell Number and Spatial Distribution within the Tumor Microenvironment. Lorcan Sherry, CSO OracleBio
 Interpreting Therapeutic Response on Immune Cell Number and Spatial Distribution within the Tumor Microenvironment Lorcan Sherry, CSO OracleBio Company Overview OracleBio is a specialised CRO providing
Interpreting Therapeutic Response on Immune Cell Number and Spatial Distribution within the Tumor Microenvironment Lorcan Sherry, CSO OracleBio Company Overview OracleBio is a specialised CRO providing
Supplementary Table 1
 Supplementary Table 1 Flow Cytometry Antibodies Antibody Fluorochrome Clone Vendor CD45 PE-cyanine 7 30-F11 D ioscience CD3 Pacific lue 17A2 iolegend (San Diego, CA) CD11b APC M1/70 iolegend (San Diego,
Supplementary Table 1 Flow Cytometry Antibodies Antibody Fluorochrome Clone Vendor CD45 PE-cyanine 7 30-F11 D ioscience CD3 Pacific lue 17A2 iolegend (San Diego, CA) CD11b APC M1/70 iolegend (San Diego,
International Society of Breast Pathology. Immune Targeting in Breast Cancer. USCAP 2017 Annual Meeting
 International Society of Breast Pathology USCAP 2017 Annual Meeting Immune Targeting in Breast Cancer Ashley Cimino-Mathews, MD Assistant Professor of Pathology and Oncology The Johns Hopkins Hospital
International Society of Breast Pathology USCAP 2017 Annual Meeting Immune Targeting in Breast Cancer Ashley Cimino-Mathews, MD Assistant Professor of Pathology and Oncology The Johns Hopkins Hospital
Letter to Editor Tissue micro arrays for immunohistochemical detection of inflammatory infiltrates in renal cell carcinoma
 Int J Clin Exp Med 2014;7(4):1175-1179 www.ijcem.com /ISSN:1940-5901/IJCEM0000102 Letter to Editor Tissue micro arrays for immunohistochemical detection of inflammatory infiltrates in renal cell carcinoma
Int J Clin Exp Med 2014;7(4):1175-1179 www.ijcem.com /ISSN:1940-5901/IJCEM0000102 Letter to Editor Tissue micro arrays for immunohistochemical detection of inflammatory infiltrates in renal cell carcinoma
Cancer immunity and immunotherapy. General principles
 1 Cancer immunity and immunotherapy Abul K. Abbas UCSF General principles 2 The immune system recognizes and reacts against cancers The immune response against tumors is often dominated by regulation or
1 Cancer immunity and immunotherapy Abul K. Abbas UCSF General principles 2 The immune system recognizes and reacts against cancers The immune response against tumors is often dominated by regulation or
Immune Checkpoints. PD Dr med. Alessandra Curioni-Fontecedro Department of Hematology and Oncology Cancer Center Zurich University Hospital Zurich
 Immune Checkpoints PD Dr med. Alessandra Curioni-Fontecedro Department of Hematology and Oncology Cancer Center Zurich University Hospital Zurich Activation of T cells requires co-stimulation Science 3
Immune Checkpoints PD Dr med. Alessandra Curioni-Fontecedro Department of Hematology and Oncology Cancer Center Zurich University Hospital Zurich Activation of T cells requires co-stimulation Science 3
The Immune System. Innate. Adaptive. - skin, mucosal barriers - complement - neutrophils, NK cells, mast cells, basophils, eosinophils
 Objectives - explain the rationale behind cellular adoptive immunotherapy - describe methods of improving cellular adoptive immunotherapy - identify mechanisms of tumor escape from cellular adoptive immunotherapy
Objectives - explain the rationale behind cellular adoptive immunotherapy - describe methods of improving cellular adoptive immunotherapy - identify mechanisms of tumor escape from cellular adoptive immunotherapy
COURSE: Medical Microbiology, PAMB 650/720 - Fall 2008 Lecture 16
 COURSE: Medical Microbiology, PAMB 650/720 - Fall 2008 Lecture 16 Tumor Immunology M. Nagarkatti Teaching Objectives: Introduction to Cancer Immunology Know the antigens expressed by cancer cells Understand
COURSE: Medical Microbiology, PAMB 650/720 - Fall 2008 Lecture 16 Tumor Immunology M. Nagarkatti Teaching Objectives: Introduction to Cancer Immunology Know the antigens expressed by cancer cells Understand
Circulating PD-L1 in NSCLC patients and the correlation between the level of PD-L1 expression and the clinical characteristics
 Thoracic Cancer ISSN 1759-7706 ORIGINAL ARTICLE Circulating PD-L1 in NSCLC patients and the correlation between the level of PD-L1 expression and the clinical characteristics Jie Zhang, Jing Gao, Yanyan
Thoracic Cancer ISSN 1759-7706 ORIGINAL ARTICLE Circulating PD-L1 in NSCLC patients and the correlation between the level of PD-L1 expression and the clinical characteristics Jie Zhang, Jing Gao, Yanyan
Enhanced Cancer Vaccine Effectiveness with NKTR-214, a CD122-Biased Cytokine
 Enhanced Cancer Vaccine Effectiveness with NKTR-214, a CD122-Biased Cytokine Jonathan Zalevsky SVP, Biology and Preclinical Development Nektar Therapeutics SMI Cancer Vaccines, September 2017 Nektar Therapeutics
Enhanced Cancer Vaccine Effectiveness with NKTR-214, a CD122-Biased Cytokine Jonathan Zalevsky SVP, Biology and Preclinical Development Nektar Therapeutics SMI Cancer Vaccines, September 2017 Nektar Therapeutics
Licia Rivoltini, MD Unit of Immunotherapy of Human Tumors
 Licia Rivoltini, MD Unit of Immunotherapy of Human Tumors The complex network of anti-tumor immunity Innate immunity First line defense Tumor cell Adaptive immunity Specificity & memory Kidd et al., Nature
Licia Rivoltini, MD Unit of Immunotherapy of Human Tumors The complex network of anti-tumor immunity Innate immunity First line defense Tumor cell Adaptive immunity Specificity & memory Kidd et al., Nature
Understanding Checkpoint Inhibitors: Approved Agents, Drugs in Development and Combination Strategies. Michael A. Curran, Ph.D.
 Understanding Checkpoint Inhibitors: Approved Agents, Drugs in Development and Combination Strategies Michael A. Curran, Ph.D. MD Anderson Cancer Center Department of Immunology Disclosures I have research
Understanding Checkpoint Inhibitors: Approved Agents, Drugs in Development and Combination Strategies Michael A. Curran, Ph.D. MD Anderson Cancer Center Department of Immunology Disclosures I have research
Tumor Microenvironment and Immune Suppression
 Tumor Microenvironment and Immune Suppression Hassane M. Zarour,, MD Department of Medicine, Division of Hematology-Oncology, University of Pittsburgh Cancer Institute Hallmarks of Cancer: The Next Generation
Tumor Microenvironment and Immune Suppression Hassane M. Zarour,, MD Department of Medicine, Division of Hematology-Oncology, University of Pittsburgh Cancer Institute Hallmarks of Cancer: The Next Generation
5% of patients with genetic immunodeficiency develop a cancer during their lifetime (200x)
 Immune surveillance 5% of patients with genetic immunodeficiency develop a cancer during their lifetime (200x) Transplanted patients following an immunosuppressor therapy are 80 times more likely to develop
Immune surveillance 5% of patients with genetic immunodeficiency develop a cancer during their lifetime (200x) Transplanted patients following an immunosuppressor therapy are 80 times more likely to develop
Synergistic combinations of targeted immunotherapy to combat cancer
 Synergistic combinations of targeted immunotherapy to combat cancer Myung Ah Lee, M.D., Ph. D Division of Medical Oncology, Hepato-biliary pancreatic cancer center Seoul St. Mary s hospital, The Catholic
Synergistic combinations of targeted immunotherapy to combat cancer Myung Ah Lee, M.D., Ph. D Division of Medical Oncology, Hepato-biliary pancreatic cancer center Seoul St. Mary s hospital, The Catholic
Immunotherapy versus targeted treatments in metastatic renal cell carcinoma: The return game?
 Immunotherapy versus targeted treatments in metastatic renal cell carcinoma: The return game? Sylvie NEGRIER MD, PhD Centre Léon Bérard, Lyon Université Lyon I IMMUNOTHERAPY: A LONG AND WIDING ROAD! WHERE
Immunotherapy versus targeted treatments in metastatic renal cell carcinoma: The return game? Sylvie NEGRIER MD, PhD Centre Léon Bérard, Lyon Université Lyon I IMMUNOTHERAPY: A LONG AND WIDING ROAD! WHERE
Immunotherapy for Breast Cancer. Aurelio B. Castrellon Medical Oncology Memorial Healthcare System
 Immunotherapy for Breast Cancer Aurelio B. Castrellon Medical Oncology Memorial Healthcare System Conflicts Research support : Cascadian therapeutics, Puma biotechnology, Odonate therapeutics, Pfizer,
Immunotherapy for Breast Cancer Aurelio B. Castrellon Medical Oncology Memorial Healthcare System Conflicts Research support : Cascadian therapeutics, Puma biotechnology, Odonate therapeutics, Pfizer,
A Prospective Phase II Trial of Deintensified Chemoradiation Therapy for Low Risk HPV Associated Oropharyngeal Squamous Cell Carcinoma
 A Prospective Phase II Trial of Deintensified Chemoradiation Therapy for Low Risk HPV Associated Oropharyngeal Squamous Cell Carcinoma B. S. Chera 1, R. J. Amdur 2, J. E. Tepper 3, B. Qaqish 4, R. Green
A Prospective Phase II Trial of Deintensified Chemoradiation Therapy for Low Risk HPV Associated Oropharyngeal Squamous Cell Carcinoma B. S. Chera 1, R. J. Amdur 2, J. E. Tepper 3, B. Qaqish 4, R. Green
Engineered Immune Cells for Cancer Therapy : Current Status and Prospects
 When Engineering Meets Immunology Engineered Immune Cells for Cancer Therapy : Current Status and Prospects Yong Taik Lim, Ph.D. Nanomedical Systems Laboratory (http://www.nanomedicalsystems.org) SKKU
When Engineering Meets Immunology Engineered Immune Cells for Cancer Therapy : Current Status and Prospects Yong Taik Lim, Ph.D. Nanomedical Systems Laboratory (http://www.nanomedicalsystems.org) SKKU
Supplemental Materials. Stromal Modulation Reverses Primary Resistance to Immune Checkpoint Blockade in. Pancreatic Cancer.
 Supplemental Materials Stromal Modulation Reverses Primary Resistance to Immune Checkpoint Blockade in Pancreatic Cancer Jun Zhao 1, Zhilan Xiao 2, 3, Tingting Li 1, 4, Huiqin Chen 5, Ying Yuan 5, Alan
Supplemental Materials Stromal Modulation Reverses Primary Resistance to Immune Checkpoint Blockade in Pancreatic Cancer Jun Zhao 1, Zhilan Xiao 2, 3, Tingting Li 1, 4, Huiqin Chen 5, Ying Yuan 5, Alan
Supplementary Figure 1. Double-staining immunofluorescence analysis of invasive colon and breast cancers. Specimens from invasive ductal breast
 Supplementary Figure 1. Double-staining immunofluorescence analysis of invasive colon and breast cancers. Specimens from invasive ductal breast carcinoma (a) and colon adenocarcinoma (b) were staining
Supplementary Figure 1. Double-staining immunofluorescence analysis of invasive colon and breast cancers. Specimens from invasive ductal breast carcinoma (a) and colon adenocarcinoma (b) were staining
Bihong Zhao, M.D, Ph.D Department of Pathology
 Bihong Zhao, M.D, Ph.D Department of Pathology 04-28-2009 Is tumor self or non-self? How are tumor antigens generated? What are they? How does immune system respond? Introduction Tumor Antigens/Categories
Bihong Zhao, M.D, Ph.D Department of Pathology 04-28-2009 Is tumor self or non-self? How are tumor antigens generated? What are they? How does immune system respond? Introduction Tumor Antigens/Categories
Synergistic effects of indoleamine 2,3-dioxygenase (IDO) inhibitor drugs and chemotherapy in melanoma.
 Synergistic effects of indoleamine 2,3-dioxygenase (IDO) inhibitor drugs and chemotherapy in melanoma. Madhav D. Sharma Cancer Immunology, Inflammation, and Tolerance Program, Department of Pediatrics,
Synergistic effects of indoleamine 2,3-dioxygenase (IDO) inhibitor drugs and chemotherapy in melanoma. Madhav D. Sharma Cancer Immunology, Inflammation, and Tolerance Program, Department of Pediatrics,
Oncolytic Immunotherapy: A Local and Systemic Antitumor Approach
 Oncolytic Immunotherapy: A Local and Systemic Antitumor Approach Oncolytic immunotherapy Oncolytic immunotherapy the use of a genetically modified virus to attack tumors and induce a systemic immune response
Oncolytic Immunotherapy: A Local and Systemic Antitumor Approach Oncolytic immunotherapy Oncolytic immunotherapy the use of a genetically modified virus to attack tumors and induce a systemic immune response
IMMUNOTHERAPY FOR CANCER A NEW HORIZON. Ekaterini Boleti MD, PhD, FRCP Consultant in Medical Oncology Royal Free London NHS Foundation Trust
 IMMUNOTHERAPY FOR CANCER A NEW HORIZON Ekaterini Boleti MD, PhD, FRCP Consultant in Medical Oncology Royal Free London NHS Foundation Trust ASCO Names Advance of the Year: Cancer Immunotherapy No recent
IMMUNOTHERAPY FOR CANCER A NEW HORIZON Ekaterini Boleti MD, PhD, FRCP Consultant in Medical Oncology Royal Free London NHS Foundation Trust ASCO Names Advance of the Year: Cancer Immunotherapy No recent
VENTANA PD-L1 (SP142) Assay Guiding immunotherapy in NSCLC
 VENTANA (SP142) Assay Guiding immunotherapy in NSCLC Hiker s path: VENTANA (SP142) Assay on non-small cell lung cancer tissue Location: Point Conception, CA VENTANA (SP142) Assay Assess NSCLC patient benefit
VENTANA (SP142) Assay Guiding immunotherapy in NSCLC Hiker s path: VENTANA (SP142) Assay on non-small cell lung cancer tissue Location: Point Conception, CA VENTANA (SP142) Assay Assess NSCLC patient benefit
Exploring the PD-L1 Pathway
 Active Within the tumor microenvironment Steps 1-3: Initiating and propagating anticancer immunity 1 may inhibit T-cell activity in the tumor microenvironment Dendritic cells capture cancer and then prime
Active Within the tumor microenvironment Steps 1-3: Initiating and propagating anticancer immunity 1 may inhibit T-cell activity in the tumor microenvironment Dendritic cells capture cancer and then prime
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/23854 holds various files of this Leiden University dissertation. Author: Marel, Sander van der Title: Gene and cell therapy based treatment strategies
Cover Page The handle http://hdl.handle.net/1887/23854 holds various files of this Leiden University dissertation. Author: Marel, Sander van der Title: Gene and cell therapy based treatment strategies
Innovation in Prevention, Early Detection & Diagnosis of Colorectal Cancer Heidelberg Workshop Session VI, Oncology Pipeline June 6, 2014
 Innovation in Prevention, Early Detection & Diagnosis of Colorectal Cancer Heidelberg Workshop Session VI, Oncology Pipeline June 6, 2014 Bernd Mueller MSD Sharp & Dohme, Germany Normal Immune Surveillance:
Innovation in Prevention, Early Detection & Diagnosis of Colorectal Cancer Heidelberg Workshop Session VI, Oncology Pipeline June 6, 2014 Bernd Mueller MSD Sharp & Dohme, Germany Normal Immune Surveillance:
Molecular mechanisms of the T cellinflamed tumor microenvironment: Implications for cancer immunotherapy
 Molecular mechanisms of the T cellinflamed tumor microenvironment: Implications for cancer immunotherapy Thomas F. Gajewski, M.D., Ph.D. Professor, Departments of Pathology and Medicine Program Leader,
Molecular mechanisms of the T cellinflamed tumor microenvironment: Implications for cancer immunotherapy Thomas F. Gajewski, M.D., Ph.D. Professor, Departments of Pathology and Medicine Program Leader,
Supplementary Figure S1. Flow cytometric analysis of the expression of Thy1 in NH cells. Flow cytometric analysis of the expression of T1/ST2 and
 Supplementary Figure S1. Flow cytometric analysis of the expression of Thy1 in NH cells. Flow cytometric analysis of the expression of T1/ST2 and Thy1 in NH cells derived from the lungs of naïve mice.
Supplementary Figure S1. Flow cytometric analysis of the expression of Thy1 in NH cells. Flow cytometric analysis of the expression of T1/ST2 and Thy1 in NH cells derived from the lungs of naïve mice.
VISTA, a novel immune checkpoint protein ligand that suppresses anti-tumor tumor T cell responses. Li Wang. Dartmouth Medical School
 VISTA, a novel immune checkpoint protein ligand that suppresses anti-tumor tumor T cell responses Li Wang Dartmouth Medical School The B7 Immunoglobulin Super-Family immune regulators APC T cell Co-stimulatory:
VISTA, a novel immune checkpoint protein ligand that suppresses anti-tumor tumor T cell responses Li Wang Dartmouth Medical School The B7 Immunoglobulin Super-Family immune regulators APC T cell Co-stimulatory:
Supplementary Materials for
 www.sciencetranslationalmedicine.org/cgi/content/full/8/352/352ra110/dc1 Supplementary Materials for Spatially selective depletion of tumor-associated regulatory T cells with near-infrared photoimmunotherapy
www.sciencetranslationalmedicine.org/cgi/content/full/8/352/352ra110/dc1 Supplementary Materials for Spatially selective depletion of tumor-associated regulatory T cells with near-infrared photoimmunotherapy
Chapter 7 Conclusions
 VII-1 Chapter 7 Conclusions VII-2 The development of cell-based therapies ranging from well-established practices such as bone marrow transplant to next-generation strategies such as adoptive T-cell therapy
VII-1 Chapter 7 Conclusions VII-2 The development of cell-based therapies ranging from well-established practices such as bone marrow transplant to next-generation strategies such as adoptive T-cell therapy
Basic Principles of Tumor Immunotherapy and Mechanisms of Tumor Immune Suppression. Bryon Johnson, PhD
 Basic Principles of Tumor Immunotherapy and Mechanisms of Tumor Immune Suppression Bryon Johnson, PhD Disclosures There will be discussion about the use of products for non-fda indications in this presentation.
Basic Principles of Tumor Immunotherapy and Mechanisms of Tumor Immune Suppression Bryon Johnson, PhD Disclosures There will be discussion about the use of products for non-fda indications in this presentation.
SUPPORTING INFORMATIONS
 SUPPORTING INFORMATIONS Mice MT/ret RetCD3ε KO α-cd25 treated MT/ret Age 1 month 3 mnths 6 months 1 month 3 months 6 months 1 month 3 months 6 months 2/87 Survival 87/87 incidence of 17/87 1 ary tumor
SUPPORTING INFORMATIONS Mice MT/ret RetCD3ε KO α-cd25 treated MT/ret Age 1 month 3 mnths 6 months 1 month 3 months 6 months 1 month 3 months 6 months 2/87 Survival 87/87 incidence of 17/87 1 ary tumor
Pancreatic Adenocarcinoma: What`s hot
 Pancreatic Adenocarcinoma: What`s hot Eva Karamitopoulou-Diamantis Institute of Pathology University of Bern 11.09.2018, 30th ECP, Bilbao Pancreatic Cancer and the Microbiome The Pancreatic Cancer Microbiome
Pancreatic Adenocarcinoma: What`s hot Eva Karamitopoulou-Diamantis Institute of Pathology University of Bern 11.09.2018, 30th ECP, Bilbao Pancreatic Cancer and the Microbiome The Pancreatic Cancer Microbiome
AWARD NUMBER: W81XWH TITLE: An in Vivo shrna-drug Screen to Identify Novel Targeted Therapy Combinations for KRAS Mutant Cancers
 AWARD NUMBER: W81XWH-12-1-0420 TITLE: An in Vivo shrna-drug Screen to Identify Novel Targeted Therapy Combinations for KRAS Mutant Cancers PRINCIPAL INVESTIGATOR: Ryan B. Corcoran, M.D., Ph.D. CONTRACTING
AWARD NUMBER: W81XWH-12-1-0420 TITLE: An in Vivo shrna-drug Screen to Identify Novel Targeted Therapy Combinations for KRAS Mutant Cancers PRINCIPAL INVESTIGATOR: Ryan B. Corcoran, M.D., Ph.D. CONTRACTING
Immune Checkpoint Inhibitors Drug Combinations: Patients Relevance & Ways Forward
 March 25, 2015 Immune Checkpoint Inhibitors Drug Combinations: Patients Relevance & Ways Forward Dr. Alexandre Passioukov p 1 Therapeutic efficacy of agents targeting immune checkpoints Introduction Deep
March 25, 2015 Immune Checkpoint Inhibitors Drug Combinations: Patients Relevance & Ways Forward Dr. Alexandre Passioukov p 1 Therapeutic efficacy of agents targeting immune checkpoints Introduction Deep
Supplemental Table 1. Primer sequences for transcript analysis
 Supplemental Table 1. Primer sequences for transcript analysis Primer Sequence (5 3 ) Primer Sequence (5 3 ) Mmp2 Forward CCCGTGTGGCCCTC Mmp15 Forward CGGGGCTGGCT Reverse GCTCTCCCGGTTTC Reverse CCTGGTGTGCCTGCTC
Supplemental Table 1. Primer sequences for transcript analysis Primer Sequence (5 3 ) Primer Sequence (5 3 ) Mmp2 Forward CCCGTGTGGCCCTC Mmp15 Forward CGGGGCTGGCT Reverse GCTCTCCCGGTTTC Reverse CCTGGTGTGCCTGCTC
New insights into the anti-pd-l1 and anti-pd-1 reagents in cancer therapy
 626423EJI0010.1177/1721727X15626423European Journal of InflammationChen and Huang research-article2016 Letter to the editor New insights into the anti-pd-l1 and anti-pd-1 reagents in cancer therapy European
626423EJI0010.1177/1721727X15626423European Journal of InflammationChen and Huang research-article2016 Letter to the editor New insights into the anti-pd-l1 and anti-pd-1 reagents in cancer therapy European
Tumor Immunity and Immunotherapy. Andrew Lichtman M.D., Ph.D. Brigham and Women s Hospital Harvard Medical School
 Tumor Immunity and Immunotherapy Andrew Lichtman M.D., Ph.D. Brigham and Women s Hospital Harvard Medical School Lecture Outline Evidence for tumor immunity Types of tumor antigens Generation of anti-tumor
Tumor Immunity and Immunotherapy Andrew Lichtman M.D., Ph.D. Brigham and Women s Hospital Harvard Medical School Lecture Outline Evidence for tumor immunity Types of tumor antigens Generation of anti-tumor
IMMUNOTHERAPY IN THE TREATMENT OF CERVIX CANCER
 Gynecologic Cancer InterGroup Cervix Cancer Research Network IMMUNOTHERAPY IN THE TREATMENT OF CERVIX CANCER Linda Mileshkin, Medical Oncologist Peter MacCallum Cancer Centre, Melbourne Australia Cervix
Gynecologic Cancer InterGroup Cervix Cancer Research Network IMMUNOTHERAPY IN THE TREATMENT OF CERVIX CANCER Linda Mileshkin, Medical Oncologist Peter MacCallum Cancer Centre, Melbourne Australia Cervix
IMMUNOTARGET THERAPY: ASPETTI GENERALI
 IMMUNOTARGET THERAPY: ASPETTI GENERALI Alessandro Minisini Dipartimento di Oncologia Azienda Ospedaliero Universitaria Udine Verona, 19 settembre 2015 HALLMARKS OF CANCER Douglas Hanahan, Robert A. Weinberg,
IMMUNOTARGET THERAPY: ASPETTI GENERALI Alessandro Minisini Dipartimento di Oncologia Azienda Ospedaliero Universitaria Udine Verona, 19 settembre 2015 HALLMARKS OF CANCER Douglas Hanahan, Robert A. Weinberg,
08/02/59. Tumor Immunotherapy. Development of Tumor Vaccines. Types of Tumor Vaccines. Immunotherapy w/ Cytokine Gene-Transfected Tumor Cells
 Tumor Immunotherapy Autologous virus Inactivation Inactivated virus Lymphopheresis Culture? Monocyte s Dendritic cells Immunization Autologous vaccine Development of Tumor Vaccines Types of Tumor Vaccines
Tumor Immunotherapy Autologous virus Inactivation Inactivated virus Lymphopheresis Culture? Monocyte s Dendritic cells Immunization Autologous vaccine Development of Tumor Vaccines Types of Tumor Vaccines
Supplementary Information:
 Supplementary Information: Follicular regulatory T cells with Bcl6 expression suppress germinal center reactions by Yeonseok Chung, Shinya Tanaka, Fuliang Chu, Roza Nurieva, Gustavo J. Martinez, Seema
Supplementary Information: Follicular regulatory T cells with Bcl6 expression suppress germinal center reactions by Yeonseok Chung, Shinya Tanaka, Fuliang Chu, Roza Nurieva, Gustavo J. Martinez, Seema
Supporting Information
 Supporting Information lpek et al. 1.173/pnas.1121217 SI Materials and Methods Mice. cell knockout, inos / (Taconic arms), Rag1 /, INγR /, and IL-12p4 / mice (The Jackson Laboratory) were maintained and/or
Supporting Information lpek et al. 1.173/pnas.1121217 SI Materials and Methods Mice. cell knockout, inos / (Taconic arms), Rag1 /, INγR /, and IL-12p4 / mice (The Jackson Laboratory) were maintained and/or
The PD-1 pathway of T cell exhaustion
 The PD-1 pathway of T cell exhaustion SAMO 18.3.2016 Overview T cell exhaustion Biology of PD-1 Mechanism Ligands expressed on tumor cell and on non-tumor cells other receptor pairs Biomarkers for apd-1/pd-l1
The PD-1 pathway of T cell exhaustion SAMO 18.3.2016 Overview T cell exhaustion Biology of PD-1 Mechanism Ligands expressed on tumor cell and on non-tumor cells other receptor pairs Biomarkers for apd-1/pd-l1
Tumor Associated Macrophages as a Novel Target for Cancer Therapy
 Tumor mass Tumor Associated Macrophage Tumor Associated Macrophages as a Novel Target for Cancer Therapy This booklet contains forward-looking statements that are based on Amgen s current expectations
Tumor mass Tumor Associated Macrophage Tumor Associated Macrophages as a Novel Target for Cancer Therapy This booklet contains forward-looking statements that are based on Amgen s current expectations
Developing Novel Immunotherapeutic Cancer Treatments for Clinical Use
 Developing Novel Immunotherapeutic Cancer Treatments for Clinical Use Oncology for Scientists March 8 th, 2016 Jason Muhitch, PhD Assistant Professor Department of Urology Email: jason.muhitch@roswellpark.org
Developing Novel Immunotherapeutic Cancer Treatments for Clinical Use Oncology for Scientists March 8 th, 2016 Jason Muhitch, PhD Assistant Professor Department of Urology Email: jason.muhitch@roswellpark.org
B Cells Promote Pancreatic Tumorigenesis
 B Cells Promote Pancreatic Tumorigenesis The MIT Faculty has made this article openly available. Please share how this access benefits you. Your story matters. Citation As Published Publisher Roghanian,
B Cells Promote Pancreatic Tumorigenesis The MIT Faculty has made this article openly available. Please share how this access benefits you. Your story matters. Citation As Published Publisher Roghanian,
Camillo Porta S.C. di Oncologia Medica Università degli Studi di Pavia & I.R.C.C.S. Fondazione Policlinico San Matteo di Pavia
 Keynote Lecture: Immunotherapy in GU cancer: where are we, and where are we going? Camillo Porta S.C. di Oncologia Medica Università degli Studi di Pavia & I.R.C.C.S. Fondazione Policlinico San Matteo
Keynote Lecture: Immunotherapy in GU cancer: where are we, and where are we going? Camillo Porta S.C. di Oncologia Medica Università degli Studi di Pavia & I.R.C.C.S. Fondazione Policlinico San Matteo
Understanding the T cell response to tumors using transnuclear mouse models
 Understanding the T cell response to tumors using transnuclear mouse models Stephanie Dougan Dana-Farber Cancer Institute Boston, MA Presenter Disclosure Information Stephanie Dougan The following relationships
Understanding the T cell response to tumors using transnuclear mouse models Stephanie Dougan Dana-Farber Cancer Institute Boston, MA Presenter Disclosure Information Stephanie Dougan The following relationships
Radiation Therapy and Immunotherapy: New Frontiers
 Radiation Therapy and Immunotherapy: New Frontiers Nevada Oncology Society Fall Meeting November 16 th, 2017 Anshu K. Jain, MD Radiation Oncologist, Ashland Bellefonte Cancer Center Assistant Clinical
Radiation Therapy and Immunotherapy: New Frontiers Nevada Oncology Society Fall Meeting November 16 th, 2017 Anshu K. Jain, MD Radiation Oncologist, Ashland Bellefonte Cancer Center Assistant Clinical
Emerging Concepts of Cancer Immunotherapy
 Emerging Concepts of Cancer Immunotherapy Jeffrey Schlom, Ph.D. Laboratory of Tumor Immunology and Biology (LTIB) Center for Cancer Research National Cancer Institute, NIH Immune Cell Infiltrate in Primary
Emerging Concepts of Cancer Immunotherapy Jeffrey Schlom, Ph.D. Laboratory of Tumor Immunology and Biology (LTIB) Center for Cancer Research National Cancer Institute, NIH Immune Cell Infiltrate in Primary
The Promise of Adjuvant Epigenetic Therapy in Early Stage Esophageal Cancer. Zhihao Lu M.D. Peking University Cancer Hospital
 The Promise of Adjuvant Epigenetic Therapy in Early Stage Esophageal Cancer Zhihao Lu M.D. Peking University Cancer Hospital Current Treatment Strategies for Early Stage Esophageal Cancer Rate Prognosis
The Promise of Adjuvant Epigenetic Therapy in Early Stage Esophageal Cancer Zhihao Lu M.D. Peking University Cancer Hospital Current Treatment Strategies for Early Stage Esophageal Cancer Rate Prognosis
Manipulating the Tumor Environment
 Manipulating the Tumor Environment Vincenzo Bronte Verona University Hospital vincenzo.bronte@univr.it Escape from immune control can be viewed as one of the «Hallmarks of Cancer» D. Hanahan and R. A.
Manipulating the Tumor Environment Vincenzo Bronte Verona University Hospital vincenzo.bronte@univr.it Escape from immune control can be viewed as one of the «Hallmarks of Cancer» D. Hanahan and R. A.
Role of the Pathologist in Guiding Immuno-oncological Therapies. Scott Rodig MD, PhD
 Role of the Pathologist in Guiding Immuno-oncological Therapies Scott Rodig MD, PhD Department of Pathology, Brigham & Women s Hospital Center for Immuno-Oncology, Dana-Farber Cancer Institute Associate
Role of the Pathologist in Guiding Immuno-oncological Therapies Scott Rodig MD, PhD Department of Pathology, Brigham & Women s Hospital Center for Immuno-Oncology, Dana-Farber Cancer Institute Associate
IMMUNOTHERAPY IN THE TREATMENT OF CERVIX CANCER. Linda Mileshkin, Medical Oncologist Peter MacCallum Cancer Centre, Melbourne Australia
 IMMUNOTHERAPY IN THE TREATMENT OF CERVIX CANCER Linda Mileshkin, Medical Oncologist Peter MacCallum Cancer Centre, Melbourne Australia Distinguishing self from non-self T cells trained in the thymus as
IMMUNOTHERAPY IN THE TREATMENT OF CERVIX CANCER Linda Mileshkin, Medical Oncologist Peter MacCallum Cancer Centre, Melbourne Australia Distinguishing self from non-self T cells trained in the thymus as
ASSESSMENT OF IMMUNE STABILITY IN BREAST CANCER SUBJECTS
 ASSESSMENT OF IMMUNE STABILITY IN BREAST CANCER SUBJECTS Oluboyo, A.O Dr. Department of Medical Laboratory Science, Faculty of Health Sciences and Technology, College of Health Sciences, Nnamdi Azikiwe,
ASSESSMENT OF IMMUNE STABILITY IN BREAST CANCER SUBJECTS Oluboyo, A.O Dr. Department of Medical Laboratory Science, Faculty of Health Sciences and Technology, College of Health Sciences, Nnamdi Azikiwe,
Disclosure Information. Mary L. Disis
 Disclosure Information Mary L. Disis I have the following financial relationships to disclose: Consultant for: VentiRx, Celgene, Emergent, EMD Serono Speaker s Bureau for: N/A Grant/Research support from:
Disclosure Information Mary L. Disis I have the following financial relationships to disclose: Consultant for: VentiRx, Celgene, Emergent, EMD Serono Speaker s Bureau for: N/A Grant/Research support from:
A case report of using nivolumab for a malignant melanoma patient with rheumatoid arthritis
 Int Canc Conf J (6) 5:9 96 DOI.7/s369-6-56-8 CASE REPORT A case report of using nivolumab for a malignant melanoma patient with rheumatoid arthritis Shun-Ichiro Kageyama Shigeo Yamaguchi Shin Ito Yoshiyuki
Int Canc Conf J (6) 5:9 96 DOI.7/s369-6-56-8 CASE REPORT A case report of using nivolumab for a malignant melanoma patient with rheumatoid arthritis Shun-Ichiro Kageyama Shigeo Yamaguchi Shin Ito Yoshiyuki
