Mitigation of pain and anaesthetic drugs
|
|
|
- Lucinda Carr
- 6 years ago
- Views:
Transcription
1 Pharmacology Competing interests: None declared. Conflict of interests: None declared. Mitigation of pain and anaesthetic drugs S Kumar 1, R Gupta 2, A M Kaleem 3, A K Pandey 1* Page 1 of 5 Abstract Inroduction Anaesthetics are used for pain management in patient surgery. They may interact with different levels of pain transmission in the body and by doing so anaesthetics encounter with the immune system. Due to this, alterations in immune response occurs which may lead to complications in patients after surgery. This review discusses the mitigation of pain and anaesthetic drugs. Discussion Literature search revealed that there are four elements of pain transmission viz. transduction, transmission, modulation and perception. The nociceptive pathway is involved in the experience of pain and is modified by both psychosocial factors and damage/ or inflammation within tissues. There are different types of anaesthetics used by the clinicians which have an effect on one or more elements of pain transmission. Use of anaesthetics during preoperative treatment has an impact on immune elements which results in other ailments in patients post operatively. Conclusion Anaesthetics manage pain using various mechanisms. There is a need to explore and use multi modal techniques of anesthetics that have minimum post operative side effects. Inroduction The international association for the study of pain (IASP) defined pain as an unpleasant sensory and emotional experience associated with actual or potential tissue damage or described *Corresponding author akpandey23@rediffmail.com 1 University of Allahabad, Allahabad, India 2 King George s Medical University, Lucknow, India 3 King George s Medical University, Lucknow, India in terms of such damage. Several broad processes associated with pain viz., nociception, pain perception and a number of secondary consequences such as suffering as well as pain behavior may be useful in clinical settings. Nociception is the process which involves the detection of noxious stimuli and subsequent transmission of encoded information to the brain. On the other hand pain is a perceptual process that arises in response to such activity (Figure 1) 1. Primary afferent neurons in cutaneous and deep somatic tissues synapse with second order neurons in the dorsal horn of the spinal cord. They have three functions with respect to their role in nociception: 1- Detection of noxious or damaging stimuli. 2- Passage of the resulting sensory input from peripheral terminals to the spinal cord. 3- Synaptic transfer of this input to neurons within specific laminae of the dorsal horn. Information from the noxious stimuli in the form of sensory information is then relayed to supraspinal structures including the thalamus and brainstem. In descending modulatory systems powerful internal controls are present at all levels which exemplify the signal 2. Nociceptors are unspecialized, free, unmyelinated nerve endings that convert (transduce) a variety of stimuli into nerve impulses to produce the sensation of pain. The nerve cell bodies are located in the dorsal root ganglia or for the trigeminal nerve in the trigeminal ganglion, and they send one nerve fibre branch to the periphery and another into the spinal cord or brainstem 2. The nociceptors are distributed in the somatic and visceral structures. They are exposed to noxious stimuli when tissue damage and inflammation occurs. The nerve fibre of the nociceptor is of two types i.e., C fibres and A delta fibres. C fibres have a small diameter, unmyelinated nerves and conduct nerve impulse slowly (2m/sec) while A-delta fibres have a large diameter, lightly myelinated nerves and conduct nerve impulse faster (20m/sec). The C fibre and A-delta fibres are associated with different qualities of pain viz. diffuse/well-localised, dull/sharp, burning/stinging, and aching/pricking, respectively (Figure 1). Nowadays, in the fields of immunology and anaesthesia rapid developments have taken place. It has been proposed by anaesthesiologists that anaesthesia dysregulate or suppress the immune system during the perioperative period which may provoke postoperative complications, e.g., wound-healing disturbances and infections leading to sepsis, followed by multiple organ failure and death 3. The immunological effects of surgery and anaesthetics affect the long-term outcomes of patients after surgery. Therefore, awareness of these immunological properties is helpful for daily anaesthetic management. The aim of this review was to discuss mitigation of pain and anaesthetic drugs. Discussion Pain and its processing Acute pain has been defined as the normal, predicted, physiological response to an adverse chemical, thermal, or mechanical stimulus 4. Acute pain-induced change in the central nervous system is known as neuronal plasticity. In the nervous system neuroplastic changes occur due to tissue injury, which results in peripheral and central sensitization 5. The four elements of pain processing include transduction, transmission, modulation, and perception.
2 Page 2 of 5 Transduction of pain In brief, transduction of pain is the event whereby noxious chemical, thermal, or mechanical stimuli are converted into an action potential 6. It begins when the free nerve endings (nociceptors) of C fibres and A-delta fibres of primary afferent neurons respond to noxious stimuli. Externally or internally stimulated noxious stimuli (mechanical, thermal or chemical) causes a release of chemical mediators from the damaged cells such as prostaglandin, bradykinin, serotonin, substance P, potassium, and histamine. These chemical mediators activate and/or sensitize the nociceptors to the noxious stimuli. In order for a pain impulse to be generated, an exchange of sodium and potassium ions (depolarization and re-polarization) occurs in nerve cell membranes. This results in an action potential and generation of a pain impulse 2. Transmission of pain It occurs when the action potential is conducted through the nervous system via the first, second, and thirdorder neurons, which have cell bodies located in the dorsal root ganglion, dorsal horn, and thalamus, respectively. The transmission of pain impulses occur in three stages: - From the site of transduction along the nociceptor fibres to the dorsal horn in the spinal cord - From the spinal cord to the brain stem - From brain stem to the thalamus, cortex and higher levels of the brain. The C fibre and A-delta fibres terminate in the dorsal horn of the spinal cord. There is a synaptic cleft between the terminal ends of these fibres and the nociceptive dorsal horn neurones (NDHN). Excitatory neurotransmitters (adenosine triphosphate, glutamate, calcitonin gene-related peptide, bradykinin, nitrous oxide, and substance P) are released in order to transmit the pain impulse across the Figure 1: Different processes of pain: Experience of pain by the activity of nociceptive pathways can be stimulated/modified by both exogenous (psychosocial factors) and endogenous (damage/or inflammation within tissues) stress. The resultant pain behaviours and suffering can be measured and provide useful parameters for clinical assessment. Figure 2: Structure of some anaesthetics. synaptic cleft 6 to the NDHN, excitatory neurotransmitters bind to specific receptors in the NDHN. The pain impulse is then transmitted from the spinal cord to the brain stem and thalamus mainly via spinothalamic and spinoparabrachial nociceptive ascending pathways. When impulses arrive in the thalamus they are directed to multiple areas in the brain for processing. Modulation of pain Modulation of pain transmission involves altering afferent neural transmission along the pain pathway. The dorsal horn of the spinal cord is the most common site for modulation of
3 Page 3 of 5 the pain pathway, and modulation can involve either inhibition or augmentation of the pain signals 7. The multiple, complex pathways involved in the modulation of pain are referred to as the descending modulatory pain pathways (DMPP). Descending inhibition involves the release of inhibitory neurotransmitters (e.g., endogenous opioids, serotonin, norepinephirine, gamma-aminobutyric acid, neurotensin, acetylcholine, and oxytocin) that block or partially block the transmission of pain impulses, and therefore produce analgesia 7. Perception of pain Perception of pain is the final common pathway, which results from the integration of painful input into the somatosensory and limbic cortices. Generally speaking, traditional analgesic therapies have only targeted pain perception. A multimodal approach to pain therapy should target all four elements of the pain processing pathway. The multidimensional experience of pain has affective-motivational, sensory-discriminative, emotional and behavioural components. When the painful stimuli are transmitted to the brain stem and thalamus, multiple cortical areas are activated and responses are elicited. These areas are the reticular, somatosensory cortex and limbic systems. The reticular system is responsible for the autonomic and motor response to pain and for warning the individual to do something. The somatosensory cortex is involved with the perception and interpretation of sensations. The limbic system is responsible for the emotional and behavioural responses to pain. Anaesthetics and their mode of action Anaesthesia is a controlled, reversible intoxication of the nervous system and anaesthetics are the moieties which eliminates patient s pain by altering physiology of the patient. The main types of anaesthesia are local, Figure 3: Elements of pain and their blockage by different agents. regional, and general. Regional anaesthesia numbs a larger area of the body than local anaesthesia and may be used for many operations below the waist. Major types of regional anaesthesia are spinal, epidural and peripheral nerve block. General anaesthesia relaxes the muscles, puts in sleep, and keeps patients from feeling pain. The anaesthetic may be given through a vein (IV), or as a gas breathed in through a mask. Local anaesthesia numbs the part of the body where surgery has to be done. Local anaesthetics are a group of drugs with the ability to prevent sodium entry into axons, thereby preventing the generation of propagated action potentials in axons. They also have other actions, however, such as prevention of axonal sprouting and effects on G-proteincoupled receptors, and on conductance of ions in addition to sodium that might be important in the management of pain. Local anaesthetics are used in a wide range of clinical situations to prevent acute pain and to stop or ameliorate pain produced by cancer or pain associated with chronic painful conditions 8. They may act to produce a desired anaesthetic or analgesic effect at any part of the nervous system i.e. from the periphery to the brain (Figure 2). Bupivacaine It is an amide type local anaesthetic mainly used for surgical, obstetric, acute and chronic pain therapy. Most local anaesthetics, including the amide type anaesthetics, are described as state dependent Na + channel pore blockers. Nilsson et al. 9 suggests that anaesthetic action of bupivacaine in myelinated axons is primarily due to inhibition of the Na + channels. Important clinical properties of bupivacaine are a relatively high potency and a capacity to block sensory and motor fibres differently. It has been widely used extradurally for both obstetric and surgical procedures and post operative pain relief. Bupivacaine is more potent than other local anaesthetics such as lidocaine, procaine and benzocaine 9. Ketamine Ketamine produces dose-related unconsciousness and analgesia. The ketamine-anaesthetized patients have profound analgesia but keep their eyes open and maintain many reflexes. It selectively depresses neuronal function in the cortex and thalamus while simultaneously stimulates parts of the limbic system. It is reported that
4 Page 4 of 5 ketamine occupies opiate receptors in the brain and spinal cord, which could account for its analgesic effects. Analgesic effect in the spinal cord may be due to inhibition of the dorsal horn vide dynamic range neuronal activity 6. Paracetamol It is also known as acetaminophen and remains the most popular analgesic. Despite its popularity the mechanism by which paracetamol achieves its effects on pain is still debated. It has been assumed that paracetamol probably acts through the cyclooxygenase (COX) pathway. Alternative proposed mechanisms include reinforcement of descending inhibitory serotonergic pain pathways, inhibition of the L-argininenitric oxide (NO) pathway mediated through substance P, and active paracetamol metabolites that have an effect on cannabinoid (CB) receptors 10. One of the active metabolites of paracetamol (the fatty acid amide N- arachidonoylphenolamine) shares the ability of the cannabinoid receptor to display analgesic activity and to lower body temperature 11 (Figure 3). Dextromethorphan It is the dextrorotatory enantiomer of the methyl ether of levorphanol, an opioid analgesic but it does not act through opioid receptors. It is quickly absorbed in the gastrointestinal tract after oral administration, after that via the bloodstream it crosses the bloodbrain barrier and reaches the cerebral spinal fluid 12. As a noncompetitive N-methyl D- aspartate (NMDA) antagonist, dextromethorphan decreases glutamate activity. This attribute suggests a potential neuroprotective role for conditions such as amyotrophic lateral sclerosis, methotrexate neurotoxicity or a reduction of pain sensation by reducing the excitatory transmission of the primary afferent pathways along the spinothalamic tract 6. Anaesthetics and immune response Rapid development has taken place during recent decades, in the fields of anaesthesia and immunology. It is a well established fact among anaesthesiologists that dysregulation/suppression of the immune system during the perioperative period provokes postoperative complications which includes wound-healing disturbances and infections leading to sepsis, followed by multiple organ failure and death 3. In cancer patients after surgery, the development of residual cancer cells and the establishment of new metastases are accelerated by immunosuppression. The immunological effects of aanesthetics and surgery affect the long-term outcomes of patients after surgery. Awareness of these immunological properties may be helpful for pain management 13. Surgical stress induces release of hormones such as adrenocorticotropic hormone (ACTH), catecholamines, and cortisol, via the autonomic nervous system. The hypothalamic pituitary adrenal axis mediates inhibitory effects on immune functions, because monocytes, macrophages and T cells have both β2-adrenoreceptors and glucocorticoid receptors, which promote cellular signalling to inhibit the production of representative Th1 (helper-t-cell 1) cytokines such as interleukin-12 (IL-12) and interferonγ (IFN-γ), and to produce Th2 cytokines, the so-called antiinflammatory cytokines, such as IL-4 and IL Although these Th2 cytokines act intrinsically to limit the exaggerated inflammatory responses induced by surgical trauma, the excessive or uncontrolled secretion of Th2 cytokines engenders immunosuppression. Proinflammatory cytokines such as IL- 1, IL-6, and tumour necrosis factor (TNF-α) from monocytes and macrophages and lymphocytes activated by surgical stress can stimulate the hypothalamic-pituitaryadrenal (HPA) axis 3. Therefore, the neuroendocrine system, and proinflammatory cytokines and antiinflammatory cytokines, synergistically augment their suppressive effects in the perioperative immune system. Indeed, this immunosuppressive network manifested by the activated neuroendocrine system and hypercytokinemia during the perioperative period may adversely affect long-term clinical outcomes. Many studies have revealed the concentration and time dependent immunosuppressive effects of anaesthetics on various immune cells such as neutrophil, natural killer cell, monocyte, macrophage, and lymphocyte. Several studies confirmed that anaesthetics (halothane, enflurane, isoflurane, and sevoflurane) inhibit reactive oxygen soecies production by activated neutrophils. It is believed that the mechanism behind this process involves either a direct NADPH oxidase inhibiton or an inhibitory effect at some site in its regulatory signal transduction pathway, such as protein kinase C inhibition 14. NK cells can kill certain tumour cells and virus-infected cells naturally without prior sensitization or MHC restriction. These cells function as surveillance in the early tumour developmental stage and killing tumour cells. By producing IFN-γ they also help in the priming process of antigen processing cells, tumour-specific Tc cells, and Th1 cells 15. Due to blood transfusion or the activation of the neuroendocrine system, antiinflammatory cytokines are produced by immune cells. These cytokines (IL-4 and IL-10 i.e., Th2 cytokines) are known to suppress NK cell mediated tumour immunity. It has been found that anaesthetics (halothane and enflurane) can reversibly inhibit NK cell activity in a concentration dependent manner. An in vivo study indicated that the tumour metastases increase by the halothane induced suppression of NK cell activity 3,16. Inhibitory effects of anaesthetics on lymphocyte proliferation and cytokine
5 Page 5 of 5 release in peripheral blood mononuclear cells have been shown in various studies. These effects on lymphocytes may reduce their immunocapacity against microorganisms and tumour cells 3. The mechanisms by which anaesthetics inhibit lymphocyte function remain unclear. It is believed that the release of cytochrome C from the mitochondria, decrease of mitochondrial membrane potential, and interference with the MAPK cascade are the possible mechanisms for anaesthetic induced inhibitory or anti-inflammatory effects on lymphocytes 17,18. Conclusion Changes in the sensitivity of nociceptive neurons underly the development of the tissue hypersensitivity associated with inflammation. Recent advances in molecular neuroscience continue to provide tremendous opportunities for understanding the molecular actions of general anaesthetics on their targets. There is a need to develop anaesthetics that have multiple targets and lower side effects on the immune system after surgery. This may help in the management of pain as well as to get better outcomes of anaesthetics. References 1. Loeser JD, Melzack R. Pain: an overview. Lancet. 1999; 353: BL Kidd, LA Urban. Mechanisms of inflammatory pain. British J Anaesthesia. 2001; 87: Kurosawa S, Kato M. Anesthetics, immune cells, and immune responses. J Anesth. 2008; 22: Carr DB, Goudas LC. Acute pain. Lancet. 1999; 353: Wilder-Smith OH. Arendt-Nielsen L. Postoperative hyperalgesia: its clinical importance and relevance. Anesthesiology. 2006; 104(3): Barash P, Cullen B, Stoelting R, Cahalan M, Stock M. editors. Clinical Anesthesia (6th ed), Philadelphia, Lippincott Williams & Wilkins Raja SN, Dougherty PM. Anatomy and physiology of somatosensory and pain processing. In: Essentials of pain medicine and regional anesthesia, 2nd edition. Edited by Benzon HT, Raja SN, Molloy RE et al. Philadelphia, Elsevier, Churchill Livingstone, Heavner JE. Local anesthetics. Curr Opin Anaesthesiol. 2007; 20: Nilsson J, Elinder F, Arhem P. Mechanisms of bupivacaine action on Na+ and K channels in myelinated axons of Xenopus laevis. European J Pharmacol. 1998; 360: Anderson BJ. Paracetamol (Acetaminophen): mechanisms of action. Pediatric Anesthesia. 2008; 18: Guhring H, Hamza M, Sergejeva M. A role for endocannabinoids in indomethacin-induced spinal antinociception. Eur J Pharmacol. 2002; 454: Hollander D, Pradas J, Kaplan R, McLeod HL, Evans WE, Munsat TL. High-dose dextromethorphan in amyotrophic lateral sclerosis: phase I safety and pharmacokinetic studies. Ann Neurol. 1994; 36(6): Vallejo R, Hord ED, Barna SA, Santiago-Palma J, Ahmed S. Perioperative immunosuppression in cancer patients. J Environ Pathol Toxicol Oncol. 2003; 22: Nakagawara M, Takeshige K, Takamatsu J, Takahashi S, Yoshitake J, Minakami S. Inhibition of superoxide production and Ca2+ mobilization in human neutrophils by halothane, enflurane, and isoflurane. Anesthesiology. 1986; 64: Kurosawa S, Matsuzaki G, Harada M, Ando Takashi, Nomoto K. Early appearance and activation of natural killer cells in tumor-infiltrating lymphoid cells during tumor development. Eur J Immunol. 1993; 23: Melamed R, Bar-Yosef S, Shakhar G, Shakhar K, Ben-Eliyahu S. Suppression of natural killer cell activity and promotion of tumor metastasis by ketamine, thiopental, and halothane, but not by propofol: mediating mechanisms and prophylactic measures. Anesth Analg. 2003; 97: Green DR. Overview: apoptotic signaling pathway in the immune system. Immunol Rev. 2003; 193: Gwinn M, Vallyathan V. Respiration burst: role in signal transduction in alveolar macrophages. J Toxicol Environ Health Part B. 2006; 9:27 39.
Receptors and Neurotransmitters: It Sounds Greek to Me. Agenda. What We Know About Pain 9/7/2012
 Receptors and Neurotransmitters: It Sounds Greek to Me Cathy Carlson, PhD, RN Northern Illinois University Agenda We will be going through this lecture on basic pain physiology using analogies, mnemonics,
Receptors and Neurotransmitters: It Sounds Greek to Me Cathy Carlson, PhD, RN Northern Illinois University Agenda We will be going through this lecture on basic pain physiology using analogies, mnemonics,
Pain Pathways. Dr Sameer Gupta Consultant in Anaesthesia and Pain Management, NGH
 Pain Pathways Dr Sameer Gupta Consultant in Anaesthesia and Pain Management, NGH Objective To give you a simplistic and basic concepts of pain pathways to help understand the complex issue of pain Pain
Pain Pathways Dr Sameer Gupta Consultant in Anaesthesia and Pain Management, NGH Objective To give you a simplistic and basic concepts of pain pathways to help understand the complex issue of pain Pain
211MDS Pain theories
 211MDS Pain theories Definition In 1986, the International Association for the Study of Pain (IASP) defined pain as a sensory and emotional experience associated with real or potential injuries, or described
211MDS Pain theories Definition In 1986, the International Association for the Study of Pain (IASP) defined pain as a sensory and emotional experience associated with real or potential injuries, or described
Pharmacology of Pain Transmission and Modulation
 Pharmacology of Pain Transmission and Modulation 2 Jürg Schliessbach and Konrad Maurer Nociceptive Nerve Fibers Pain is transmitted to the central nervous system via thinly myelinated Aδ and unmyelinated
Pharmacology of Pain Transmission and Modulation 2 Jürg Schliessbach and Konrad Maurer Nociceptive Nerve Fibers Pain is transmitted to the central nervous system via thinly myelinated Aδ and unmyelinated
Pain. Pain. Pain: One definition. Pain: One definition. Pain: One definition. Pain: One definition. Psyc 2906: Sensation--Introduction 9/27/2006
 Pain Pain Pain: One Definition Classic Paths A new Theory Pain and Drugs According to the international Association for the Study (Merskey & Bogduk, 1994), Pain is an unpleasant sensory and emotional experience
Pain Pain Pain: One Definition Classic Paths A new Theory Pain and Drugs According to the international Association for the Study (Merskey & Bogduk, 1994), Pain is an unpleasant sensory and emotional experience
Chapter 16. Sense of Pain
 Chapter 16 Sense of Pain Pain Discomfort caused by tissue injury or noxious stimulation, and typically leading to evasive action important /// helps to protect us lost of pain in diabetes mellitus = diabetic
Chapter 16 Sense of Pain Pain Discomfort caused by tissue injury or noxious stimulation, and typically leading to evasive action important /// helps to protect us lost of pain in diabetes mellitus = diabetic
CHAPTER 4 PAIN AND ITS MANAGEMENT
 CHAPTER 4 PAIN AND ITS MANAGEMENT Pain Definition: An unpleasant sensory and emotional experience associated with actual or potential tissue damage, or described in terms of such damage. Types of Pain
CHAPTER 4 PAIN AND ITS MANAGEMENT Pain Definition: An unpleasant sensory and emotional experience associated with actual or potential tissue damage, or described in terms of such damage. Types of Pain
Pain and impulse conduction
 1 Pain and impulse conduction L.H.D.J. Booij According to the World Health Organisation pain is defined as an unpleasant sensation that occurs from imminent tissue damage. From a physiological perspective,
1 Pain and impulse conduction L.H.D.J. Booij According to the World Health Organisation pain is defined as an unpleasant sensation that occurs from imminent tissue damage. From a physiological perspective,
Neural Basis of Motor Control
 Neural Basis of Motor Control Central Nervous System Skeletal muscles are controlled by the CNS which consists of the brain and spinal cord. Determines which muscles will contract When How fast To what
Neural Basis of Motor Control Central Nervous System Skeletal muscles are controlled by the CNS which consists of the brain and spinal cord. Determines which muscles will contract When How fast To what
What is Pain? An unpleasant sensory and emotional experience associated with actual or potential tissue damage. Pain is always subjective
 Pain & Acupuncture What is Pain? An unpleasant sensory and emotional experience associated with actual or potential tissue damage. NOCICEPTION( the neural processes of encoding and processing noxious stimuli.)
Pain & Acupuncture What is Pain? An unpleasant sensory and emotional experience associated with actual or potential tissue damage. NOCICEPTION( the neural processes of encoding and processing noxious stimuli.)
biological psychology, p. 40 The study of the nervous system, especially the brain. neuroscience, p. 40
 biological psychology, p. 40 The specialized branch of psychology that studies the relationship between behavior and bodily processes and system; also called biopsychology or psychobiology. neuroscience,
biological psychology, p. 40 The specialized branch of psychology that studies the relationship between behavior and bodily processes and system; also called biopsychology or psychobiology. neuroscience,
San Francisco Chronicle, June 2001
 PAIN San Francisco Chronicle, June 2001 CONGENITAL INSENSITIVITY TO PAIN PAIN IS A SUBJECTIVE EXPERIENCE: It is not a stimulus MAJOR FEATURES OF THE PAIN EXPERIENCE: Sensory discriminative Affective (emotional)
PAIN San Francisco Chronicle, June 2001 CONGENITAL INSENSITIVITY TO PAIN PAIN IS A SUBJECTIVE EXPERIENCE: It is not a stimulus MAJOR FEATURES OF THE PAIN EXPERIENCE: Sensory discriminative Affective (emotional)
Pain Mechanisms. Prof Michael G Irwin MD, FRCA, FANZCA FHKAM Head Department of Anaesthesiology University of Hong Kong. The Somatosensory System
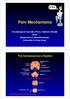 ain Mechanisms rof Michael G Irwin MD, FRCA, FANZCA FHKAM Head Department of Anaesthesiology University of Hong Kong The Somatosensory System Frontal cortex Descending pathway eriaqueductal gray matter
ain Mechanisms rof Michael G Irwin MD, FRCA, FANZCA FHKAM Head Department of Anaesthesiology University of Hong Kong The Somatosensory System Frontal cortex Descending pathway eriaqueductal gray matter
PAIN IS A SUBJECTIVE EXPERIENCE: It is not a stimulus. MAJOR FEATURES OF THE PAIN EXPERIENCE: Sensory discriminative Affective (emotional) Cognitive
 PAIN PAIN IS A SUBJECTIVE EXPERIENCE: It is not a stimulus MAJOR FEATURES OF THE PAIN EXPERIENCE: Sensory discriminative Affective (emotional) Cognitive MEASUREMENT OF PAIN: A BIG PROBLEM Worst pain ever
PAIN PAIN IS A SUBJECTIVE EXPERIENCE: It is not a stimulus MAJOR FEATURES OF THE PAIN EXPERIENCE: Sensory discriminative Affective (emotional) Cognitive MEASUREMENT OF PAIN: A BIG PROBLEM Worst pain ever
The anatomy and physiology of pain
 The anatomy and physiology of pain Charlotte E Steeds Abstract Pain is an unpleasant experience that results from both physical and psychological responses to injury. A complex set of pathways transmits
The anatomy and physiology of pain Charlotte E Steeds Abstract Pain is an unpleasant experience that results from both physical and psychological responses to injury. A complex set of pathways transmits
Proceedings of the World Small Animal Veterinary Association Sydney, Australia 2007
 Proceedings of the World Small Animal Sydney, Australia 2007 Hosted by: Next WSAVA Congress REDUCING THE PAIN FACTOR AN UPDATE ON PERI-OPERATIVE ANALGESIA Sandra Forysth, BVSc DipACVA Institute of Veterinary,
Proceedings of the World Small Animal Sydney, Australia 2007 Hosted by: Next WSAVA Congress REDUCING THE PAIN FACTOR AN UPDATE ON PERI-OPERATIVE ANALGESIA Sandra Forysth, BVSc DipACVA Institute of Veterinary,
By the end of this lecture the students will be able to:
 UNIT VII: PAIN Objectives: By the end of this lecture the students will be able to: Review the concept of somatosensory pathway. Describe the function of Nociceptors in response to pain information. Describe
UNIT VII: PAIN Objectives: By the end of this lecture the students will be able to: Review the concept of somatosensory pathway. Describe the function of Nociceptors in response to pain information. Describe
Spinal Cord Injury Pain. Michael Massey, DO CentraCare Health St Cloud, MN 11/07/2018
 Spinal Cord Injury Pain Michael Massey, DO CentraCare Health St Cloud, MN 11/07/2018 Objectives At the conclusion of this session, participants should be able to: 1. Understand the difference between nociceptive
Spinal Cord Injury Pain Michael Massey, DO CentraCare Health St Cloud, MN 11/07/2018 Objectives At the conclusion of this session, participants should be able to: 1. Understand the difference between nociceptive
Sensory coding and somatosensory system
 Sensory coding and somatosensory system Sensation and perception Perception is the internal construction of sensation. Perception depends on the individual experience. Three common steps in all senses
Sensory coding and somatosensory system Sensation and perception Perception is the internal construction of sensation. Perception depends on the individual experience. Three common steps in all senses
Somatosensory Physiology (Pain And Temperature) Richard M. Costanzo, Ph.D.
 Somatosensory Physiology (Pain And Temperature) Richard M. Costanzo, Ph.D. OBJECTIVES After studying the material of this lecture the student should be familiar with: 1. The relationship between nociception
Somatosensory Physiology (Pain And Temperature) Richard M. Costanzo, Ph.D. OBJECTIVES After studying the material of this lecture the student should be familiar with: 1. The relationship between nociception
Visualizing Psychology
 Visualizing Psychology by Siri Carpenter & Karen Huffman PowerPoint Lecture Notes Presentation Chapter 2: Neuroscience and Biological Foundations Siri Carpenter, Yale University Karen Huffman, Palomar
Visualizing Psychology by Siri Carpenter & Karen Huffman PowerPoint Lecture Notes Presentation Chapter 2: Neuroscience and Biological Foundations Siri Carpenter, Yale University Karen Huffman, Palomar
Virtually everyone has experienced pain in one
 Transfer of Advances in Sciences into Dental Education Recent Insights into Brainstem Mechanisms Underlying Craniofacial Pain Barry J. Sessle, B.D.S., M.D.S., B.Sc., Ph.D., F.R.S.C., D.Sc. (honorary) Abstract:
Transfer of Advances in Sciences into Dental Education Recent Insights into Brainstem Mechanisms Underlying Craniofacial Pain Barry J. Sessle, B.D.S., M.D.S., B.Sc., Ph.D., F.R.S.C., D.Sc. (honorary) Abstract:
Basic Neuroscience. Sally Curtis
 The Physiology of Pain Basic Neuroscience Sally Curtis sac3@soton.ac.uk The behaviour of humans is a result of the actions of nerves. Nerves form the basis of Thoughts, sensations and actions both reflex
The Physiology of Pain Basic Neuroscience Sally Curtis sac3@soton.ac.uk The behaviour of humans is a result of the actions of nerves. Nerves form the basis of Thoughts, sensations and actions both reflex
Somatic Sensation (MCB160 Lecture by Mu-ming Poo, Friday March 9, 2007)
 Somatic Sensation (MCB160 Lecture by Mu-ming Poo, Friday March 9, 2007) Introduction Adrian s work on sensory coding Spinal cord and dorsal root ganglia Four somatic sense modalities Touch Mechanoreceptors
Somatic Sensation (MCB160 Lecture by Mu-ming Poo, Friday March 9, 2007) Introduction Adrian s work on sensory coding Spinal cord and dorsal root ganglia Four somatic sense modalities Touch Mechanoreceptors
Objectives 9/7/2012. Optimizing Analgesia to Enhance the Recovery After Surgery CME FACULTY DISCLOSURE
 Optimizing Analgesia to Enhance the Recovery After Surgery Francesco Carli, M.D.. McGill University, Montreal, QC, Canada. ASPMN, Baltimore, 2012 CME FACULTY DISCLOSURE Francesco Carli has no affiliation
Optimizing Analgesia to Enhance the Recovery After Surgery Francesco Carli, M.D.. McGill University, Montreal, QC, Canada. ASPMN, Baltimore, 2012 CME FACULTY DISCLOSURE Francesco Carli has no affiliation
What it Takes to be a Pain
 What it Takes to be a Pain Pain Pathways and the Neurophysiology of pain Dennis S. Pacl, MD, FACP, FAChPM Austin Palliative Care/ Hospice Austin A Definition of Pain complex constellation of unpleasant
What it Takes to be a Pain Pain Pathways and the Neurophysiology of pain Dennis S. Pacl, MD, FACP, FAChPM Austin Palliative Care/ Hospice Austin A Definition of Pain complex constellation of unpleasant
ANALGESIA and LOCAL ANAESTHESIA. Professor Donald G. MacLellan Executive Director Health Education & Management Innovations
 ANALGESIA and LOCAL ANAESTHESIA Professor Donald G. MacLellan Executive Director Health Education & Management Innovations Definition of Pain Pain is an unpleasant sensory and emotional experience with
ANALGESIA and LOCAL ANAESTHESIA Professor Donald G. MacLellan Executive Director Health Education & Management Innovations Definition of Pain Pain is an unpleasant sensory and emotional experience with
PAIN MANAGEMENT in the CANINE PATIENT
 PAIN MANAGEMENT in the CANINE PATIENT Laurie Edge-Hughes, BScPT, MAnimSt (Animal Physio), CAFCI, CCRT Part 1: Laurie Edge-Hughes, BScPT, MAnimSt (Animal Physio), CAFCI, CCRT 1 Pain is the most common reason
PAIN MANAGEMENT in the CANINE PATIENT Laurie Edge-Hughes, BScPT, MAnimSt (Animal Physio), CAFCI, CCRT Part 1: Laurie Edge-Hughes, BScPT, MAnimSt (Animal Physio), CAFCI, CCRT 1 Pain is the most common reason
Prof Wayne Derman MBChB,BSc (Med)(Hons) PhD, FFIMS. Pain Management in the Elite Athlete: The 2017 IOC Consensus Statement
 Prof Wayne Derman MBChB,BSc (Med)(Hons) PhD, FFIMS Pain Management in the Elite Athlete: The 2017 IOC Consensus Statement 2 as 20 Experts published and leaders in their respective field 12 month lead in
Prof Wayne Derman MBChB,BSc (Med)(Hons) PhD, FFIMS Pain Management in the Elite Athlete: The 2017 IOC Consensus Statement 2 as 20 Experts published and leaders in their respective field 12 month lead in
Chapter 17. Nervous System Nervous systems receive sensory input, interpret it, and send out appropriate commands. !
 Chapter 17 Sensory receptor Sensory input Integration Nervous System Motor output Brain and spinal cord Effector cells Peripheral nervous system (PNS) Central nervous system (CNS) 28.1 Nervous systems
Chapter 17 Sensory receptor Sensory input Integration Nervous System Motor output Brain and spinal cord Effector cells Peripheral nervous system (PNS) Central nervous system (CNS) 28.1 Nervous systems
Shift 1, 8 July 2018, 09:30-13:00
 Shift 1, 8 July 2018, 09:30-13:00 CNS patterning A001-A014 Stem cells: basic biology and postnatal neurogenesis - part I Development of neural systems: Molecular and genetic characterisationa Epigenetic
Shift 1, 8 July 2018, 09:30-13:00 CNS patterning A001-A014 Stem cells: basic biology and postnatal neurogenesis - part I Development of neural systems: Molecular and genetic characterisationa Epigenetic
1 The Physiology of Pain
 1 The Physiology of Pain Rohit Juneja and Siân Jaggar Introduction Definitions Key Messages Pain is still underdiagnosed and undertreated. Pain is a subjective experience and may even be present in the
1 The Physiology of Pain Rohit Juneja and Siân Jaggar Introduction Definitions Key Messages Pain is still underdiagnosed and undertreated. Pain is a subjective experience and may even be present in the
Acute Pain Management in the Opioid Tolerant Patient. Objectives. Opioids. The participant will be able to define opioid tolerance
 Acute Pain Management in the Opioid Tolerant Patient Kathleen M. Colfer, MSN, RN-BC Clinical Nurse Specialist Acute Pain Management Service Department of Anesthesiology Thomas Jefferson University Hospital
Acute Pain Management in the Opioid Tolerant Patient Kathleen M. Colfer, MSN, RN-BC Clinical Nurse Specialist Acute Pain Management Service Department of Anesthesiology Thomas Jefferson University Hospital
CHAPTER 10 THE SOMATOSENSORY SYSTEM
 CHAPTER 10 THE SOMATOSENSORY SYSTEM 10.1. SOMATOSENSORY MODALITIES "Somatosensory" is really a catch-all term to designate senses other than vision, hearing, balance, taste and smell. Receptors that could
CHAPTER 10 THE SOMATOSENSORY SYSTEM 10.1. SOMATOSENSORY MODALITIES "Somatosensory" is really a catch-all term to designate senses other than vision, hearing, balance, taste and smell. Receptors that could
Multimodal analgesic therapy has gained widespread
 TOPICAL REVIEW Analgesia for Anesthetized Patients Kip A. Lemke, DVM, MSc, Dipl. ACVA, and Catherine M. Creighton, DVM Many perioperative pain management protocols for cats and dogs are overly complex,
TOPICAL REVIEW Analgesia for Anesthetized Patients Kip A. Lemke, DVM, MSc, Dipl. ACVA, and Catherine M. Creighton, DVM Many perioperative pain management protocols for cats and dogs are overly complex,
Pathophysiology of Pain. Ramon Go MD Assistant Professor Anesthesiology and Pain medicine NYP-CUMC
 Pathophysiology of Pain Ramon Go MD Assistant Professor Anesthesiology and Pain medicine NYP-CUMC Learning Objectives Anatomic pathway of nociception Discuss the multiple target sites of pharmacological
Pathophysiology of Pain Ramon Go MD Assistant Professor Anesthesiology and Pain medicine NYP-CUMC Learning Objectives Anatomic pathway of nociception Discuss the multiple target sites of pharmacological
PAIN. Physiology of pain relating to pain management
 PAIN Physiology of pain relating to pain management What is pain? An unpleasant sensory and emotional experience associated with actual or potential tissue damage. (Melzac and Wall) The generation of pain
PAIN Physiology of pain relating to pain management What is pain? An unpleasant sensory and emotional experience associated with actual or potential tissue damage. (Melzac and Wall) The generation of pain
Mechanism of Pain Production
 Mechanism of Pain Production Pain conducting nerve fibers are small myelinated (A-delta) or unmyelinated nerve fibers (C-fibers). Cell bodies are in the dorsal root ganglia (DRG) or sensory ganglia of
Mechanism of Pain Production Pain conducting nerve fibers are small myelinated (A-delta) or unmyelinated nerve fibers (C-fibers). Cell bodies are in the dorsal root ganglia (DRG) or sensory ganglia of
PAIN & ANALGESIA. often accompanied by clinical depression. fibromyalgia, chronic fatigue, etc. COX 1, COX 2, and COX 3 (a variant of COX 1)
 Pain - subjective experience associated with detection of tissue damage ( nociception ) acute - serves as a warning chronic - nociception gone bad often accompanied by clinical depression fibromyalgia,
Pain - subjective experience associated with detection of tissue damage ( nociception ) acute - serves as a warning chronic - nociception gone bad often accompanied by clinical depression fibromyalgia,
Anaesthesia and Pain Management for Endo Exo Femoral Prosthesis (EEFP) Bridging the Gap from Surgery to Rehabilitation
 Anaesthesia and Pain Management for Endo Exo Femoral Prosthesis (EEFP) Bridging the Gap from Surgery to Rehabilitation Dr Ajay Kumar Senior Lecturer Macquarie and Melbourne University Introduction Amputee
Anaesthesia and Pain Management for Endo Exo Femoral Prosthesis (EEFP) Bridging the Gap from Surgery to Rehabilitation Dr Ajay Kumar Senior Lecturer Macquarie and Melbourne University Introduction Amputee
Unit 3: The Biological Bases of Behaviour
 Unit 3: The Biological Bases of Behaviour Section 1: Communication in the Nervous System Section 2: Organization in the Nervous System Section 3: Researching the Brain Section 4: The Brain Section 5: Cerebral
Unit 3: The Biological Bases of Behaviour Section 1: Communication in the Nervous System Section 2: Organization in the Nervous System Section 3: Researching the Brain Section 4: The Brain Section 5: Cerebral
Chapter 11 Introduction to the Nervous System and Nervous Tissue Chapter Outline
 Chapter 11 Introduction to the Nervous System and Nervous Tissue Chapter Outline Module 11.1 Overview of the Nervous System (Figures 11.1-11.3) A. The nervous system controls our perception and experience
Chapter 11 Introduction to the Nervous System and Nervous Tissue Chapter Outline Module 11.1 Overview of the Nervous System (Figures 11.1-11.3) A. The nervous system controls our perception and experience
Thermoreceptors (hot & cold fibers) Temperature gated Na+ channels. Adaptation in thermoreceptors
 Thermoreceptors (hot & cold fibers) Temperature gated Na+ channels Adaptation in thermoreceptors Response of a cold receptor Drugs can mimic sensory stimuli Response of taste nerve to cold water or menthol
Thermoreceptors (hot & cold fibers) Temperature gated Na+ channels Adaptation in thermoreceptors Response of a cold receptor Drugs can mimic sensory stimuli Response of taste nerve to cold water or menthol
Primary Functions. Monitor changes. Integrate input. Initiate a response. External / internal. Process, interpret, make decisions, store information
 NERVOUS SYSTEM Monitor changes External / internal Integrate input Primary Functions Process, interpret, make decisions, store information Initiate a response E.g., movement, hormone release, stimulate/inhibit
NERVOUS SYSTEM Monitor changes External / internal Integrate input Primary Functions Process, interpret, make decisions, store information Initiate a response E.g., movement, hormone release, stimulate/inhibit
Fundamentals of the Nervous System and Nervous Tissue: Part C
 PowerPoint Lecture Slides prepared by Janice Meeking, Mount Royal College C H A P T E R 11 Fundamentals of the Nervous System and Nervous Tissue: Part C Warm Up What is a neurotransmitter? What is the
PowerPoint Lecture Slides prepared by Janice Meeking, Mount Royal College C H A P T E R 11 Fundamentals of the Nervous System and Nervous Tissue: Part C Warm Up What is a neurotransmitter? What is the
Psychophysical laws. Legge di Fechner: I=K*log(S/S 0 )
 Psychophysical laws Legge di Weber: ΔS=K*S Legge di Fechner: I=K*log(S/S 0 ) Sensory receptors Vision Smell Taste Touch Thermal senses Pain Hearing Balance Proprioception Sensory receptors Table 21-1 Classification
Psychophysical laws Legge di Weber: ΔS=K*S Legge di Fechner: I=K*log(S/S 0 ) Sensory receptors Vision Smell Taste Touch Thermal senses Pain Hearing Balance Proprioception Sensory receptors Table 21-1 Classification
Acetylcholine (ACh) Action potential. Agonists. Drugs that enhance the actions of neurotransmitters.
 Acetylcholine (ACh) The neurotransmitter responsible for motor control at the junction between nerves and muscles; also involved in mental processes such as learning, memory, sleeping, and dreaming. (See
Acetylcholine (ACh) The neurotransmitter responsible for motor control at the junction between nerves and muscles; also involved in mental processes such as learning, memory, sleeping, and dreaming. (See
General Anesthesia. Mohamed A. Yaseen
 General Anesthesia Mohamed A. Yaseen M.S,c Surgery Before Anesthesia General Anesthesia ( GA ) Drug induced absence of perception of all sensation allowing surgery or other painful procedure to be carried
General Anesthesia Mohamed A. Yaseen M.S,c Surgery Before Anesthesia General Anesthesia ( GA ) Drug induced absence of perception of all sensation allowing surgery or other painful procedure to be carried
number Done by Corrected by Doctor
 number 13 Done by Tamara Wahbeh Corrected by Doctor Omar Shaheen In this sheet the following concepts will be covered: 1. Divisions of the nervous system 2. Anatomy of the ANS. 3. ANS innervations. 4.
number 13 Done by Tamara Wahbeh Corrected by Doctor Omar Shaheen In this sheet the following concepts will be covered: 1. Divisions of the nervous system 2. Anatomy of the ANS. 3. ANS innervations. 4.
The Nervous System. Chapter 4. Neuron 3/9/ Components of the Nervous System
 Chapter 4 The Nervous System 1. Components of the Nervous System a. Nerve cells (neurons) Analyze and transmit information Over 100 billion neurons in system Four defined regions Cell body Dendrites Axon
Chapter 4 The Nervous System 1. Components of the Nervous System a. Nerve cells (neurons) Analyze and transmit information Over 100 billion neurons in system Four defined regions Cell body Dendrites Axon
Chapter 9. Nervous System
 Chapter 9 Nervous System Central Nervous System (CNS) vs. Peripheral Nervous System(PNS) CNS Brain Spinal cord PNS Peripheral nerves connecting CNS to the body Cranial nerves Spinal nerves Neurons transmit
Chapter 9 Nervous System Central Nervous System (CNS) vs. Peripheral Nervous System(PNS) CNS Brain Spinal cord PNS Peripheral nerves connecting CNS to the body Cranial nerves Spinal nerves Neurons transmit
Neural Communication. Central Nervous System Peripheral Nervous System. Communication in the Nervous System. 4 Common Components of a Neuron
 Neural Communication Overview of CNS / PNS Electrical Signaling Chemical Signaling Central Nervous System Peripheral Nervous System Somatic = sensory & motor Autonomic = arousal state Parasympathetic =
Neural Communication Overview of CNS / PNS Electrical Signaling Chemical Signaling Central Nervous System Peripheral Nervous System Somatic = sensory & motor Autonomic = arousal state Parasympathetic =
Nervous System. Master controlling and communicating system of the body. Secrete chemicals called neurotransmitters
 Nervous System Master controlling and communicating system of the body Interacts with the endocrine system to control and coordinate the body s responses to changes in its environment, as well as growth,
Nervous System Master controlling and communicating system of the body Interacts with the endocrine system to control and coordinate the body s responses to changes in its environment, as well as growth,
The Nervous System. Anatomy of a Neuron
 The Nervous System Chapter 38.1-38.5 Anatomy of a Neuron I. Dendrites II. Cell Body III. Axon Synaptic terminal 1 Neuron Connections dendrites cell body terminal cell body cell body terminals dendrites
The Nervous System Chapter 38.1-38.5 Anatomy of a Neuron I. Dendrites II. Cell Body III. Axon Synaptic terminal 1 Neuron Connections dendrites cell body terminal cell body cell body terminals dendrites
ANAT2010. Concepts of Neuroanatomy (II) S2 2018
 ANAT2010 Concepts of Neuroanatomy (II) S2 2018 Table of Contents Lecture 13: Pain and perception... 3 Lecture 14: Sensory systems and visual pathways... 11 Lecture 15: Techniques in Neuroanatomy I in vivo
ANAT2010 Concepts of Neuroanatomy (II) S2 2018 Table of Contents Lecture 13: Pain and perception... 3 Lecture 14: Sensory systems and visual pathways... 11 Lecture 15: Techniques in Neuroanatomy I in vivo
Axon Nerve impulse. Axoplasm Receptor. Axomembrane Stimuli. Schwann cell Effector. Myelin Cell body
 Nervous System Review 1. Explain a reflex arc. 2. Know the structure, function and location of a sensory neuron, interneuron, and motor neuron 3. What is (a) Neuron Axon Nerve impulse Axoplasm Receptor
Nervous System Review 1. Explain a reflex arc. 2. Know the structure, function and location of a sensory neuron, interneuron, and motor neuron 3. What is (a) Neuron Axon Nerve impulse Axoplasm Receptor
Neuroimmunology. Innervation of lymphoid organs. Neurotransmitters. Neuroendocrine hormones. Cytokines. Autoimmunity
 Neuroimmunology Innervation of lymphoid organs Neurotransmitters Neuroendocrine hormones Cytokines Autoimmunity CNS has two ways of contacting and regulating structures in the periphery Autonomic
Neuroimmunology Innervation of lymphoid organs Neurotransmitters Neuroendocrine hormones Cytokines Autoimmunity CNS has two ways of contacting and regulating structures in the periphery Autonomic
Chapter 45: Synapses Transmission of Nerve Impulses Between Neurons. Chad Smurthwaite & Jordan Shellmire
 Chapter 45: Synapses Transmission of Nerve Impulses Between Neurons Chad Smurthwaite & Jordan Shellmire The Chemical Synapse The most common type of synapse used for signal transmission in the central
Chapter 45: Synapses Transmission of Nerve Impulses Between Neurons Chad Smurthwaite & Jordan Shellmire The Chemical Synapse The most common type of synapse used for signal transmission in the central
What are the 6 types of neuroglia and their functions?!
 Warm Up! Take out your 11C Notes What are the 6 types of neuroglia and their functions?! Astrocytes Microglia Ependymal Cells Satellite Cells Schwann Cells Oligodendrocytes Support, brace, & nutrient transfer
Warm Up! Take out your 11C Notes What are the 6 types of neuroglia and their functions?! Astrocytes Microglia Ependymal Cells Satellite Cells Schwann Cells Oligodendrocytes Support, brace, & nutrient transfer
Lesson 14. The Nervous System. Introduction to Life Processes - SCI 102 1
 Lesson 14 The Nervous System Introduction to Life Processes - SCI 102 1 Structures and Functions of Nerve Cells The nervous system has two principal cell types: Neurons (nerve cells) Glia The functions
Lesson 14 The Nervous System Introduction to Life Processes - SCI 102 1 Structures and Functions of Nerve Cells The nervous system has two principal cell types: Neurons (nerve cells) Glia The functions
Guided Reading Activities
 Name Period Chapter 28: Nervous Systems Guided Reading Activities Big idea: Nervous system structure and function Answer the following questions as you read modules 28.1 28.2: 1. Your taste receptors for
Name Period Chapter 28: Nervous Systems Guided Reading Activities Big idea: Nervous system structure and function Answer the following questions as you read modules 28.1 28.2: 1. Your taste receptors for
Pre-Emptive Analgesia for Reduction of Postoperative Pain
 REDUCTION THE IRAQI POSTGRADUATE OF POSTOPERATIVE MEDICAL JOURNAL PAIN Pre-Emptive Analgesia for Reduction of Postoperative Pain Ali Abdul Hammed, Khulood Salih Al-Ani ABSTRACT: BACKGROUND: Pre-emptive
REDUCTION THE IRAQI POSTGRADUATE OF POSTOPERATIVE MEDICAL JOURNAL PAIN Pre-Emptive Analgesia for Reduction of Postoperative Pain Ali Abdul Hammed, Khulood Salih Al-Ani ABSTRACT: BACKGROUND: Pre-emptive
SOMATOSENSORY SYSTEMS AND PAIN
 SOMATOSENSORY SYSTEMS AND PAIN A 21 year old man presented with a stab wound of the right side of the neck (Panel A). Neurological examination revealed right hemiplegia and complete right-sided loss of
SOMATOSENSORY SYSTEMS AND PAIN A 21 year old man presented with a stab wound of the right side of the neck (Panel A). Neurological examination revealed right hemiplegia and complete right-sided loss of
Lesson 33. Objectives: References: Chapter 16: Reading for Next Lesson: Chapter 16:
 Lesson 33 Lesson Outline: Nervous System Structure and Function Neuronal Tissue Supporting Cells Neurons Nerves Functional Classification of Neuronal Tissue Organization of the Nervous System Peripheral
Lesson 33 Lesson Outline: Nervous System Structure and Function Neuronal Tissue Supporting Cells Neurons Nerves Functional Classification of Neuronal Tissue Organization of the Nervous System Peripheral
Study Guide Answer Key Nervous System
 Biology 12 Human Biology Textbook: BC Biology 12 Study Guide Answer Key Nervous System 1. Draw a neuron, label 3 parts and give the function of those parts. Dendrite: carry signals to the cell body Cell
Biology 12 Human Biology Textbook: BC Biology 12 Study Guide Answer Key Nervous System 1. Draw a neuron, label 3 parts and give the function of those parts. Dendrite: carry signals to the cell body Cell
THE CENTRAL NERVOUS SYSTE M
 THE CENTRAL NERVOUS SYSTE M Structure and Functio n THIRD EDITIO N PER BRODAL A Brief Survey, x i Studying the Structures and Function of the Nervous System, xii i Animal Experiments Crucial for Progress,
THE CENTRAL NERVOUS SYSTE M Structure and Functio n THIRD EDITIO N PER BRODAL A Brief Survey, x i Studying the Structures and Function of the Nervous System, xii i Animal Experiments Crucial for Progress,
CHAPTER 4 PAIN AND ITS MANAGEMENT
 CHAPTER 4 PAIN AND ITS MANAGEMENT Pain Definition: An unpleasant sensory and emotional experience associated with actual or potential tissue damage, or described in terms of such damage. Types of Pain
CHAPTER 4 PAIN AND ITS MANAGEMENT Pain Definition: An unpleasant sensory and emotional experience associated with actual or potential tissue damage, or described in terms of such damage. Types of Pain
Function of the Nervous System
 Nervous System Function of the Nervous System Receive sensory information, interpret it, and send out appropriate commands to form a response Composed of neurons (functional unit of the nervous system)
Nervous System Function of the Nervous System Receive sensory information, interpret it, and send out appropriate commands to form a response Composed of neurons (functional unit of the nervous system)
Brain and behaviour (Wk 6 + 7)
 Brain and behaviour (Wk 6 + 7) What is a neuron? What is the cell body? What is the axon? The basic building block of the nervous system, the individual nerve cell that receives, processes and transmits
Brain and behaviour (Wk 6 + 7) What is a neuron? What is the cell body? What is the axon? The basic building block of the nervous system, the individual nerve cell that receives, processes and transmits
CHAPTER 48: NERVOUS SYSTEMS
 CHAPTER 48: NERVOUS SYSTEMS Name I. AN OVERVIEW OF NERVOUS SYSTEMS A. Nervous systems perform the three overlapping functions of sensory input, integration, and motor output B. Networks of neurons with
CHAPTER 48: NERVOUS SYSTEMS Name I. AN OVERVIEW OF NERVOUS SYSTEMS A. Nervous systems perform the three overlapping functions of sensory input, integration, and motor output B. Networks of neurons with
Module H NERVOUS SYSTEM
 Module H NERVOUS SYSTEM Topic from General functions of the nervous system Organization of the nervous system from both anatomical & functional perspectives Gross & microscopic anatomy of nervous tissue
Module H NERVOUS SYSTEM Topic from General functions of the nervous system Organization of the nervous system from both anatomical & functional perspectives Gross & microscopic anatomy of nervous tissue
Biology 12 Human Biology - The Nervous System Name. Main reference: Biology Concepts and Connects Sixth edition Chapter 28
 Biology 12 Human Biology - The Nervous System Name Main reference: Biology Concepts and Connects Sixth edition Chapter 28 Vocabulary acetylcholine (ACh), acetylcholinesterase (AChE), action potential,
Biology 12 Human Biology - The Nervous System Name Main reference: Biology Concepts and Connects Sixth edition Chapter 28 Vocabulary acetylcholine (ACh), acetylcholinesterase (AChE), action potential,
NERVOUS SYSTEM C H A P T E R 2 8
 NERVOUS SYSTEM C H A P T E R 2 8 CAN AN INJURED SPINAL CORD BE FIXED? Injuries to the spinal cord disrupt communication between the central nervous system (brain and spinal cord) and the rest of the body
NERVOUS SYSTEM C H A P T E R 2 8 CAN AN INJURED SPINAL CORD BE FIXED? Injuries to the spinal cord disrupt communication between the central nervous system (brain and spinal cord) and the rest of the body
The Nervous System 7PART A. PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College
 PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Nervous System 7PART A Functions of the Nervous System Sensory input gathering information To monitor
PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Nervous System 7PART A Functions of the Nervous System Sensory input gathering information To monitor
ANAT2010. Concepts of Neuroanatomy (II) S2 2018
 ANAT2010 Concepts of Neuroanatomy (II) S2 2018 Table of Contents Lecture 13: Pain and perception... 3 Lecture 14: Sensory systems and visual pathways... 11 Lecture 15: Techniques in Neuroanatomy I in vivo
ANAT2010 Concepts of Neuroanatomy (II) S2 2018 Table of Contents Lecture 13: Pain and perception... 3 Lecture 14: Sensory systems and visual pathways... 11 Lecture 15: Techniques in Neuroanatomy I in vivo
Neural Basis of Motor Control. Chapter 4
 Neural Basis of Motor Control Chapter 4 Neurological Perspective A basic understanding of the physiology underlying the control of voluntary movement establishes a more comprehensive appreciation and awareness
Neural Basis of Motor Control Chapter 4 Neurological Perspective A basic understanding of the physiology underlying the control of voluntary movement establishes a more comprehensive appreciation and awareness
Action Potentials and Synaptic Transmission. BIO 219 Napa Valley College Dr. Adam Ross
 Action Potentials and Synaptic Transmission BIO 219 Napa Valley College Dr. Adam Ross Review of action potentials Nodes of Ranvier Nucleus Dendrites Cell body In saltatory conduction, the nerve impulses
Action Potentials and Synaptic Transmission BIO 219 Napa Valley College Dr. Adam Ross Review of action potentials Nodes of Ranvier Nucleus Dendrites Cell body In saltatory conduction, the nerve impulses
Nervous System. 2. Receives information from the environment from CNS to organs and glands. 1. Relays messages, processes info, analyzes data
 Nervous System 1. Relays messages, processes info, analyzes data 2. Receives information from the environment from CNS to organs and glands 3. Transmits impulses from CNS to muscles and glands 4. Transmits
Nervous System 1. Relays messages, processes info, analyzes data 2. Receives information from the environment from CNS to organs and glands 3. Transmits impulses from CNS to muscles and glands 4. Transmits
Dendrites Receive impulse from the axon of other neurons through synaptic connection. Conduct impulse towards the cell body Axon
 Dendrites Receive impulse from the axon of other neurons through synaptic connection. Conduct impulse towards the cell body Axon Page 22 of 237 Conduct impulses away from cell body Impulses arise from
Dendrites Receive impulse from the axon of other neurons through synaptic connection. Conduct impulse towards the cell body Axon Page 22 of 237 Conduct impulses away from cell body Impulses arise from
Name: Period: Test Review: Chapter 2
 Name: Period: Test Review: Chapter 2 1. The function of dendrites is to A) receive incoming signals from other neurons. B) release neurotransmitters into the spatial junctions between neurons. C) coordinate
Name: Period: Test Review: Chapter 2 1. The function of dendrites is to A) receive incoming signals from other neurons. B) release neurotransmitters into the spatial junctions between neurons. C) coordinate
AKA a painful lecture by Colleen Blanchfield, MD Full Circle Neuropsychiatric Wellness Center
 A lecture on PAIN AKA a painful lecture by Colleen Blanchfield, MD Full Circle Neuropsychiatric Wellness Center 1 Overview of the lecture Anatomy of the Pain Tract How a painful stimulus travels from the
A lecture on PAIN AKA a painful lecture by Colleen Blanchfield, MD Full Circle Neuropsychiatric Wellness Center 1 Overview of the lecture Anatomy of the Pain Tract How a painful stimulus travels from the
Pathophysiology of Pain
 Pathophysiology of Pain Wound Inflammatory response Chemical mediators Activity in Pain Path PAIN http://neuroscience.uth.tmc.edu/s2/chapter08.html Chris Cohan, Ph.D. Dept. of Pathology/Anat Sci University
Pathophysiology of Pain Wound Inflammatory response Chemical mediators Activity in Pain Path PAIN http://neuroscience.uth.tmc.edu/s2/chapter08.html Chris Cohan, Ph.D. Dept. of Pathology/Anat Sci University
Name: Period: Chapter 2 Reading Guide The Biology of Mind
 Name: Period: Chapter 2 Reading Guide The Biology of Mind The Nervous System (pp. 55-58) 1. What are nerves? 2. Complete the diagram below with definitions of each part of the nervous system. Nervous System
Name: Period: Chapter 2 Reading Guide The Biology of Mind The Nervous System (pp. 55-58) 1. What are nerves? 2. Complete the diagram below with definitions of each part of the nervous system. Nervous System
Chapter 17 Nervous System
 Chapter 17 Nervous System 1 The Nervous System Two Anatomical Divisions Central Nervous System (CNS) Brain and Spinal Cord Peripheral Nervous System (PNS) Two Types of Cells Neurons Transmit nerve impulses
Chapter 17 Nervous System 1 The Nervous System Two Anatomical Divisions Central Nervous System (CNS) Brain and Spinal Cord Peripheral Nervous System (PNS) Two Types of Cells Neurons Transmit nerve impulses
MOLECULAR AND CELLULAR NEUROSCIENCE
 MOLECULAR AND CELLULAR NEUROSCIENCE BMP-218 November 4, 2014 DIVISIONS OF THE NERVOUS SYSTEM The nervous system is composed of two primary divisions: 1. CNS - Central Nervous System (Brain + Spinal Cord)
MOLECULAR AND CELLULAR NEUROSCIENCE BMP-218 November 4, 2014 DIVISIONS OF THE NERVOUS SYSTEM The nervous system is composed of two primary divisions: 1. CNS - Central Nervous System (Brain + Spinal Cord)
Hole s Human Anatomy and Physiology Tenth Edition. Chapter 10
 PowerPoint Lecture Outlines to accompany Hole s Human Anatomy and Physiology Tenth Edition Shier Butler Lewis Chapter 10 Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or
PowerPoint Lecture Outlines to accompany Hole s Human Anatomy and Physiology Tenth Edition Shier Butler Lewis Chapter 10 Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or
The nervous system regulates most body systems using direct connections called nerves. It enables you to sense and respond to stimuli
 The nervous system regulates most body systems using direct connections called nerves. It enables you to sense and respond to stimuli The basic function of nervous system are: Receive sensory input internal
The nervous system regulates most body systems using direct connections called nerves. It enables you to sense and respond to stimuli The basic function of nervous system are: Receive sensory input internal
Understanding the experience and physiology of pain
 If you would like to contribute to the art and science section contact: Gwen Clarke, art and science editor, Nursing Standard, The Heights, 59-65 Lowlands Road, Harrow-on-the-Hill, Middlesex HA1 3AW. email:
If you would like to contribute to the art and science section contact: Gwen Clarke, art and science editor, Nursing Standard, The Heights, 59-65 Lowlands Road, Harrow-on-the-Hill, Middlesex HA1 3AW. email:
Warm-Up. Label the parts of the neuron below.
 Warm-Up Label the parts of the neuron below. A B C D E F G Warm-Up 1. One neuron transmits a nerve impulse at 40 m/s. Another conducts at the rate of 1 m/s. Which neuron has a myelinated axon? 2. List
Warm-Up Label the parts of the neuron below. A B C D E F G Warm-Up 1. One neuron transmits a nerve impulse at 40 m/s. Another conducts at the rate of 1 m/s. Which neuron has a myelinated axon? 2. List
PAIN MANAGEMENT. It is important to know as much about the man who has pain as it is to know about pain the man has Quote by Macnab et al
 PAIN MANAGEMENT It is important to know as much about the man who has pain as it is to know about pain the man has Quote by Macnab et al DEFINATION OF PAIN International Association for the study of pain
PAIN MANAGEMENT It is important to know as much about the man who has pain as it is to know about pain the man has Quote by Macnab et al DEFINATION OF PAIN International Association for the study of pain
ANATOMY & PHYSIOLOGY: ( Division B) Boyceville Invite Dec. 3, 2016 (50pts.)
 ANATOMY & PHYSIOLOGY: ( Division B) Boyceville Invite Dec. 3, 2016 (50pts.) Multiple Choice Identify the choice that best completes the statement or answers the question. 1. Which of the following statements
ANATOMY & PHYSIOLOGY: ( Division B) Boyceville Invite Dec. 3, 2016 (50pts.) Multiple Choice Identify the choice that best completes the statement or answers the question. 1. Which of the following statements
*Anteriolateral spinothalamic tract (STT) : a sensory pathway that is positioned anteriorly and laterally in the spinal cord.
 *somatic sensations : PAIN *Anteriolateral spinothalamic tract (STT) : a sensory pathway that is positioned anteriorly and laterally in the spinal cord. *This pathway carries a variety of sensory modalities:
*somatic sensations : PAIN *Anteriolateral spinothalamic tract (STT) : a sensory pathway that is positioned anteriorly and laterally in the spinal cord. *This pathway carries a variety of sensory modalities:
Chapter 2. An Integrative Approach to Psychopathology
 Page 1 Chapter 2 An Integrative Approach to Psychopathology One-Dimensional vs. Multidimensional Models One-Dimensional Models Could mean a paradigm, school, or conceptual approach Could mean an emphasis
Page 1 Chapter 2 An Integrative Approach to Psychopathology One-Dimensional vs. Multidimensional Models One-Dimensional Models Could mean a paradigm, school, or conceptual approach Could mean an emphasis
Neurobiology of Pain Adjuvant analgesia
 Neurobiology of Pain Adjuvant analgesia Jason Brooks Consultant Anaesthesia and Pain Management BCH March 2017 The Brief A broad overview of the abnormal and normal anatomy and physiology of pain pathways
Neurobiology of Pain Adjuvant analgesia Jason Brooks Consultant Anaesthesia and Pain Management BCH March 2017 The Brief A broad overview of the abnormal and normal anatomy and physiology of pain pathways
Chapter 7. Objectives
 Chapter 7 The Nervous System: Structure and Control of Movement Objectives Discuss the general organization of the nervous system Describe the structure & function of a nerve Draw and label the pathways
Chapter 7 The Nervous System: Structure and Control of Movement Objectives Discuss the general organization of the nervous system Describe the structure & function of a nerve Draw and label the pathways
Somatosensation. Recording somatosensory responses. Receptive field response to pressure
 Somatosensation Mechanoreceptors that respond to touch/pressure on the surface of the body. Sensory nerve responds propotional to pressure 4 types of mechanoreceptors: Meissner corpuscles & Merkel discs
Somatosensation Mechanoreceptors that respond to touch/pressure on the surface of the body. Sensory nerve responds propotional to pressure 4 types of mechanoreceptors: Meissner corpuscles & Merkel discs
BIOLOGY 12 NERVOUS SYSTEM PRACTICE
 1 Name: BIOLOGY 12 NERVOUS SYSTEM PRACTICE Date: 1) Identify structures X, Y and Z and give one function of each. 2) Which processes are involved in the movement of molecule Y from point X to point Z?
1 Name: BIOLOGY 12 NERVOUS SYSTEM PRACTICE Date: 1) Identify structures X, Y and Z and give one function of each. 2) Which processes are involved in the movement of molecule Y from point X to point Z?
Nervous Tissue Nervous tissue is the term for groups of organized cells in the nervous system, which is the organ system that controls the body s
 Nervous Tissue Nervous tissue is the term for groups of organized cells in the nervous system, which is the organ system that controls the body s movements, sends and carries signals to and from the different
Nervous Tissue Nervous tissue is the term for groups of organized cells in the nervous system, which is the organ system that controls the body s movements, sends and carries signals to and from the different
The Nervous System: Neural Tissue Pearson Education, Inc.
 13 The Nervous System: Neural Tissue Introduction Nervous System Characteristics Controls and adjust the activity of the body Provides swift but brief responses The nervous system includes: Central Nervous
13 The Nervous System: Neural Tissue Introduction Nervous System Characteristics Controls and adjust the activity of the body Provides swift but brief responses The nervous system includes: Central Nervous
Page 1. Neurons Transmit Signal via Action Potentials: neuron At rest, neurons maintain an electrical difference across
 Chapter 33: The Nervous System and the Senses Neurons: Specialized excitable cells that allow for communication throughout the body via electrical impulses Neuron Anatomy / Function: 1) Dendrites: Receive
Chapter 33: The Nervous System and the Senses Neurons: Specialized excitable cells that allow for communication throughout the body via electrical impulses Neuron Anatomy / Function: 1) Dendrites: Receive
