The effects of angiotensin II on blood perfusion in the rat renal papilla
|
|
|
- Robert Randall
- 5 years ago
- Views:
Transcription
1 9325 Journal of Physiology (1999), 519.1, pp The effects of angiotensin II on blood perfusion in the rat renal papilla L. L. Walker, A. A. J. Rajaratne, J. R. Blair-West and P. J. Harris Department of Physiology, The University of Melbourne, Parkville, Victoria 3052, Australia (Received 2 March 1999; accepted after revision 25 May 1999) 1. Systemic infusion of angiotensin II (AII) increased papillary blood perfusion (PBP) measured by laser-doppler flowmetry in rats, aged about 5 weeks. 2. The mechanisms involved in this response were determined by infusion of AII in the presence of systemic doses of losartan (a type 1 AII receptor antagonist), HOE_140 (a bradykinin Bµ receptor antagonist), and an inhibitor of NO production N ù -nitro- _arginine (NOLA). 3. Mean arterial blood pressure (MAP) and PBP increased in a dose-dependent manner in response to intravenous infusions of AII. Infusion of losartan abolished these responses to AII but HOE_140 was without effect. Infusion of NOLA abolished the increase in PBP but did not affect the pressor response to AII. Systemic infusion of sodium nitroprusside restored the response to AII in experiments with NOLA infusion. 4. The results indicate that the increase in PBP caused by AII is mediated via angiotensin AT1 receptors and does not involve bradykinin Bµ receptors. The AII-induced increase in PBP is dependent upon the presence of NO, thus providing a mechanism for maintenance of papillary perfusion in the face of generalized renal vasoconstriction due to AII. Regional variations in blood flow in the kidney are related to zonal differences in function, ranging from glomerular filtration with solute and water reabsorption in the cortex to maximal osmotic concentration of urine at the papilla. The wide distribution of angiotensin II (AII) binding sites in the kidney (Mendelsohn et al. 1986) is consistent with a number of specific influences on these renal functions through effects on zonal blood flow, inter alia. Intense interest has been shown in studying mechanisms of regulation of renal medullary and papillary blood flow in view of their role in the maintenance of countercurrent exchange and the corticomedullary osmotic gradient, and thus in sodium and water metabolism (Jamison & Kriz, 1982). The contribution of AII to the regulation of papillary blood flow and the role that renomedullary interstitial cells (RMICs) may play in the mediating mechanism are not yet clear. However, experiments by colleagues (Zhou et al. 1992, 1998) have shown that the primary AII binding sites in the renal medulla of rats were found not in the inner medulla but in the inner stripe of the outer medulla and specifically in the RMICs, which may react to peptides and so exert paracrine influences on the medullary microcirculation. We have reported that systemic infusion of AII increases the rate of papillary blood perfusion (PBP) in young Sprague Dawley rats, as measured by laser-doppler flowmetry (LDF) (Nobes et al. 1991). The result differs from others (Faubert et al. 1987; Huang et al. 1991; Lu et al. 1993), which may be due to differences in species, age of rats, dose of AII, state of consciousness, or location of LDF probe in the inner medulla. The increase in PBP induced by systemic infusion of AII with our experimental procedure was shown to be independent of the increase in renal perfusion pressure by using an aortic clamp to maintain constant renal perfusion pressure (Nobes et al. 1991). In addition, equimolar infusion of angiotensin III (AIII) and AII caused similar increases in PBP despite the less potent systemic pressor effect of AIII (Nobes et al. 1991). A very recent study (Ortiz et al. 1998) concluded that pressor doses of AII that reduced renal blood flow increased PBP in a modest way. There is considerable evidence that the renal inner medulla, and probably the RMICs located there (Tobian et al. 1969), contain and release a number of vasodilator substances such as prostaglandins, kinins, and lipids including medullipin (Muirhead et al. 1970, 1972; Muirhead & Pitcock, 1985). Later studies suggest that endogenously formed kinins influence PBP (Roman et al. 1988) and that the PBP increase due to systemic AII may be mediated by kinins (Nobes et al. 1991). A more recent study (Mattson & Cowley, 1993) showed that the increase in PBP caused by renal medullary interstitial infusion of bradykinin was mediated by a mechanism involving nitric oxide. The involvement of prostaglandins was raised again by the finding that intravenous infusion of AII did not influence medullary blood
2 274 L. L. Walker, A. A. J. Rajaratne, J. R. Blair-West and P. J. Harris J. Physiol flow (Parekh et al. 1996) because prostaglandin production in the medulla antagonized the effect of some pressor hormones including AII (Parekh & Zou, 1996). Finally, a study (Ortiz et al. 1998) published since the brief reports of our results (Walker et al. 1996; Blair-West et al. 1997) indicated that the elevation of papillary blood flow caused by AII was greatly dependent on an increased production of NO, perhaps via the local release of kinins. We have examined further the mechanisms involved in the increase in PBP caused by systemic infusion of AII in young rats (Nobes et al. 1991). The procedures used here were the same as those used in that previous study. AII was infused in the presence of (i) losartan, the type 1 AII receptor antagonist; (ii) HOE_140, the bradykinin Bµ receptor antagonist; and (iii) an inhibitor of NO production. METHODS Experiments were performed on Sprague Dawley rats (body weight, g), approximately 5 weeks of age. Animals were allowed food (GR2 Rat and Mouse Breeder Cubes, Barastoc, Australia; 0 25 % sodium) and water ad libitum before experimentation. The rats were anaesthetized with Inactin (110 mg (kg body wt), i.p.) and placed on a heated table controlled via feedback from a rectal thermistor to maintain body temperature at 38 C. A tracheostomy was performed and polyethylene catheters were inserted into the jugular and femoral veins for intravenous infusions, and into the carotid artery for the recording of continuous pulsatile blood pressure. The left kidney was exposed by a flank incision and separated from the perineal attachments; the kidney capsule was left intact. The kidney was then immobilized in a stainless steel cup. The papilla was exposed by opening up the ureter to the cortical margin. Papillary blood perfusion (PBP) was recorded using a1mm diameter fibre-optic probe attached to a PeriFlux PF3 laser-doppler perfusion monitor. The laser output was directed through a fibre-optic bundle to the probe, which was placed on the tip of the papilla of the left kidney. Arterial blood pressure was measured and recorded continuously on a Grass 7D polygraph connected to a Gould P23 ID pressure transducer. Blood pressure measurements are presented as mean arterial pressure (MAP). PBP was recorded continuously through a second channel. The value of PBP was calculated as perfusion units (PU) from the trace, after calibrating the scale of the trace so that the Periflux PF3 internal standard (100 PU) was set at 100 divisions, and the external PF 1001 motility standard (250 PU) was set at 250 divisions. By this arrangement, the scale for PBP values was direct reading. After surgical preparation, baseline arterial blood pressure and PBP were recorded for at least 10 min. AII (Auspep, Melbourne, Australia) was then infused, with a 10 min interval between doses. Specific antagonists were then administered by intravenous injectionïinfusion into a femoral vein. After suitable delays (see experiments 1 4, below), the AII infusions were repeated during ongoing infusion or after bolus injections of antagonists. Antagonists used were losartan (Merck Research Laboratories, Rahway, NJ, USA), HOE_140 (Hoechst, Germany), N ù -nitro- _arginine (NOLA; Sigma) and sodium nitroprusside (SNP; Sigma). All infusion solutions were prepared in 0 9 % NaCl. After completion of the experiment the rat was killed by an intravenous injection of saturated potassium chloride. All experimental procedures were approved by the Institutional Animal Ethics Committee according to guidelines produced by the National Health and Medical Research Council of Australia and adopted by State Legislature. Experiment 1 (n =8) In these initial experiments, a solution of AII was infused into the jugular vein for 4 min periods at three doses, 150, 300 and 600 ng kg min, by increasing the rate of infusion from 0 75 to 1 5 and 3 0 ml h, respectively. The intermediate dose of 300 ng kg min was given routinely in all experiments and was used as the basis of comparisons in Results. Experiment 2 (n =7) Losartan was injected into the femoral vein as a bolus dose of 1 mg kg in 0 05 ml saline followed by an infusion of 50 ng kg min at 1 5 ml h. After waiting 45 min the AII infusions were repeated (Zhou et al. 1992). Experiment 3 (n =8) HOE_140 was infused at 120 mg kg min into a femoral vein at 1 5 ml h. After 10 min the AII infusions were restarted. The effectiveness of the HOE_140 dose was confirmed by blockade of the reduction in MAP and increase in PBP caused by intravenous bradykinin (1250 ng kg ). Experiment 4 (n =8) NOLA was administered as two doses of 10 mg kg in 0 05 ml saline at 5 min intervals. After 10 min the AII infusions were recommenced. SNP was then infused at 1 mg kg min into a femoral vein at 1 5 ml h for a period of 10 min and then the AII infusions were repeated. Statistical analysis Results are quoted as means ± s.e.m. Effects of treatments were evaluated by the application of Student s paired t tests to the control and treatment results in individual preparations. The effects on MAP and PBP were tested for dose dependency by one-way analysis of variance. Figure 1. Efect of i.v. infusion of AII at doses of 150, 300 and 600 ng kg min Top, mean arterial pressure (MAP). Bottom, renal papillary blood perfusion (PBP) expressed in perfusion units (PU). Results are means ± s.e.m., n =8. * P < compared with initial control value.
3 J. Physiol Papillary blood perfusion in rats 275 RESULTS Effect of angiotensin II (Fig. 1) The infusions of AII caused dose-dependent increases in MAP and PBP. Doses of 150, 300 and 600 ng kg min increased MAP from an initial value of 93 ± 4 mmhg to 112±5 (P < 0 001), 117 ± 4 (P < 0 001) and 123 ± 4 mmhg (P < 0 001), respectively (comparison of individual increases by ANOVA; P < 0 001). PBP increased from220 ± 20 to 252 ± 22 PU with 150 ng kg min AII (P < 0 001), 269 ± 18 PU with 300 ng kg min AII (P < 0 001) and 277 ± 20 PU with 600 ng kg min AII (P < 0 001). The increase in PBP with 300 ng kg min was significantly greaterthanwiththelowerdose(p < 0 01, paired t test). Comparison of the increases in PBP for the two higher doses of AII showed that these were not significantly different. These data indicate that the change in PBP during graded AII infusions was dose dependent, tending to plateau at around 300 ng kg min. The dose of 300 ng kg min was therefore chosen as the routine dose in all subsequent experiments. Effect of losartan (Fig. 2) The initial values for MAP and PBP were 93 ± 4 mmhg and 217 ± 18 PU. Infusion of AII increased MAP to 115±6mmHg and PBP to 270 ± 18 PU (both P < 0 001). Infusion of losartan reduced MAP to 68 ± 6 mmhg (P < 0 001) but PBP was unchanged. Subsequent infusion of AII did not alter either MAP or PBP. Effect of HOE-140 (Fig. 3) Treatment with HOE-140 reduced MAP from its initial valueof85±5to68±5mmhg (P < 0 001) whereas PBP was not significantly altered. Infusion of AII increased MAP and PBP both before and after treatment with HOE_140. PBP increased from 180 ± 5 to 223 ± 8 PU in the control experiment and from 169 ± 9 to 219 ± 11 PU after HOE_140 infusion (both P < 0 001). Effect of NOLA and SNP (Fig. 4) Infusion of AII increased MAP and PBP as in previous control experiments (P < 0 001). Treatment with NOLA increased MAP from 78 ± 6 to 103 ± 6 mmhg (P < 0 001) and PBP was reduced from 219 ± 17 to 164 ± 24 PU (P < 0 001). Subsequent AII infusion increased MAP to 121 ± 4 mmhg (P < 0 01) but PBP was steady at 168 ± 23 PU. Further treatment with SNP reduced initial MAP to 51±6mmHg (P < 0 001) but initial PBP was unchanged at 166 ± 27 PU. Subsequent infusion of AII increased MAP to 74±7mmHg (P < 0 01) and PBP to 196 ± 23 PU (P < 0 01). DISCUSSION The major finding from these experiments was that the increase in PBP caused by intravenous infusion of AII was mediated through type 1 AII (ATÔ) receptors via a vasodilatory mechanism that probably involves the production of NO. Treatment with an inhibitor of NO production, NOLA, did not significantly affect the pressor response to intravenous infusion of AII, but it did reduce PBP and it abolished the PBP increase evoked by AII infusion. The ability of the NO donor SNP to reinstate the PBP response to AII provides further evidence that the vasodilatory mechanism evoked by intravenous AII depends on the presenceofno. Figure 2. Effect of i.v. infusion of losartan (1 mg kg bolus, 50 ng kg min ) on responses to i.v. infusion of AII at 300 ng kg min Top, MAP. Bottom, renal PBP. Results are means ± s.e.m., n =7. * P < compared with initial control value. Figure 3. Effect of i.v. infusion of HOE-140 (120 mg kg min ) on responses to i.v. infusion of AII at 300 ng kg min Top, MAP. Bottom, renal PBP. Results are means ± s.e.m., n =8. * P < compared with initial control value; P < compared with initial HOE-140 value.
4 276 L. L. Walker, A. A. J. Rajaratne, J. R. Blair-West and P. J. Harris J. Physiol This result and proposal are in agreement with the results of Ortiz et al. (1998). These authors observed that chronic NO deficiency in rats caused arterial hypertension, renal vasoconstriction and reduced papillary blood flow partly due to the effects of AII, acting via AT1 receptors. They suggested that the reduction in papillary blood flow was due to the disappearance of the tonic release of NO into the medullary environment. They also showed that AII infusion elevated papillary blood flow dependent on increased production of NO and suggested that NO may be an important antagonist of AII in the papillary circulation where it may maintain blood flow despite a reduction in cortical blood flow. Another important finding was that treatment with the bradykinin Bµ receptor blocker HOE_140, which completely inhibited responses to a large intravenous dose (1250 ng kg ) of bradykinin, did not significantly affect the pressor response to AII, nor did it modulate the associated increase in PBP. This result is important because previous work with the same preparation (Nobes et al. 1991) found that PBP did not increase when AII was infused during aprotinin administration, indicating that kinin release may be the cause of the increase of PBP by AII. That study (Nobes et al. 1991) also showed that the increase of PBP by AII did not appear to be mediated by prostaglandins, although such a mechanism has been indicated by other experiments in vivo (Parekh et al. 1996) and in vitro (Grenier et al. 1981). Our results raise the possibility that a kinin other than bradykinin is implicated or that the aprotinin-induced inhibition of the AII response (Nobes et al. 1991) was due to an action other than its inhibition of kallikrein. A possible Figure 4. Effect of i.v. infusion of NOLA (2 doses of 10 mg kg with 5 min interval) and SNP on responses to i.v. infusion of AII at 300 ng kg min Top, MAP. Bottom, renal PBP. Results are means ± s.e.m., n =8. * P < compared with initial control value; P < 0 01 compared with initial NOLA value; P< 0 01 compared with initial SNP value. explanation for the decrease in MAP during HOE_140 experiments in this preparation could be the longer than usual period of time before returning to AII infusion. During this period an effective dose of bradykinin was established and the effectiveness of the HOE_140 blockade was proved. It has been established that endogenously formed kinins may influence renal inner medullary blood flow in the rat. For example, intravenous infusion of an inhibitor of neutral endopeptidase, the major kininase in the rat kidney, increased inner medullary blood flow and this effect was blocked by a kinin receptor antagonist (Roman et al. 1988). Also, blockade of endogenous kinin degradation by intravenous enalaprilat (Roman et al. 1988) or by interstitial infusion of captopril (Mattson & Cowley, 1993) increased papillary blood flow. In addition, pretreatment with NOLA abolished the increases in papillary blood flow due to interstitial administration of either bradykinin or captopril (Mattson & Cowley, 1993). These data and our present findings support the proposition that the increase in PBP observed with intravenous AII may be NO dependent. The evidence presented in this paper indicates that the graded PBP response to AII might be dependent on the presence, but not the graded production, of NO and raises the possibility that some other regulatory pathway may be involved. Taken together, our earlier experiments (Nobes et al. 1991), the results of the HOE_140 experiments from the present study, and the studies mentioned above suggest that the release of a kinin other than bradykinin could be a contributory factor in the graded modulation of the response to AII. Our proposal that the increase of PBP caused by intravenous AII is independent of the systemic vascular response to AII is based on evidence (Nobes et al. 1991) that similar PBP responses were observed with intravenous angiotensin III (AIII) infusion and that PBP increased despite aortic clamping to maintain constant renal perfusion pressure during AII infusion. These observations suggest that the changes in initial MAP caused by various treatments in the present experiments, e. g. HOE_140, NOLA and SNP, none of which modified the MAP response to AII, did not contribute to the associated response of PBP to AII. Furthermore, treatment with NOLA increased initial MAP and lowered initial PBP with abolition of the PBP response to AII. Subsequent treatment with SNP (Fig. 4) did not restore the initial PBP to control levels but it did restore the increase in PBP caused by infusion of AII. In this context it is pertinent that MAP increased in a graded manner with increasing infusion of AII. In contrast, PBP increased significantly when the effects of the two lower rates of infusion were compared, but reached a plateau with the intermediate dose. This provides evidence for dissociation of PBP and arterial blood pressure and indicates autoregulation of PBP at higher perfusion pressures. The consistent and dose-dependent PBP responses to doses of intravenous AII in the range ng kg min confirm
5 J. Physiol Papillary blood perfusion in rats 277 our earlier report of an enhancement of PBP by AII in the systemic circulation (Nobes et al. 1991). This observation appears to conflict with various other findings (Faubert et al. 1987; Huang et al. 1991; Lu et al. 1993) but there are a number of possible reasons for this including differences in methods, doses of AII and species. The data in dogs (Faubert et al. 1987) involve (i) a different method and site of measurement of PBP, (ii) AII application by renal arterial infusion at 0 5 ng kg min and (iii) a possible species difference in responsiveness. The experiments of Huang et al. (1991) involved young Wistar rats anaesthetized with sodium pentobarbitone. Those workers also used LDF to measure PBP but their intravenous doses of AII were without effect on PBP. Their highest dose, 150 ng kg min, was equal to the smallest dose used in the present experiments, and in our hands this dose often produced small or even doubtful responses so that higher doses were routinely used. The study of Lu et al. (1993) was performed with adult Sprague Dawley rats, and measured cortical and medullary blood flow using chronically implanted fibre-optic probes in conscious animals. Bolus intravenous injections of 12 5 ng of AII reduced blood flow in both regions. Amongst other differences, that study did not relate specifically to blood perfusion in the renal papilla. An important issue here is the siting of the fibre-optic probe for optimal measurement of PBP. The young (100 g) Sprague Dawley rat has a prominent renal papilla that extends into the ureter. In our experiments, the fibre-optic probe was positioned towards the tip of the papilla so that the 1 mm tip of the probe was still in full and intimate contact with the tissue surface. This position was therefore the last possible position before the probe tip lost full contact with the papilla. Moving the tip of the probe towards the outer medulla offered a number of options for positioning. This lack of certainty was always avoided in our experiments as our method provided assurance that the probe was placed in a unique, reproducible position. This precise procedure for placement of the probe has not been used by other workers reporting measurements of PBP or medullary blood flow. It should be noted that the initial MAP in these young rats tended to be lower than would be expected for adult rats with similar anaesthesia and surgical preparation. The lowest initial MAP was in the NOLA experiments, but this value was not significantly less than the values in the other sets of experiments. In summary, intravenous infusion of AII causes an increase in PBP. This response is mediated through AT1 receptors but does not involve bradykinin Bµ receptors. Further, it is concluded that the AII-induced increase in PBP depends on the presence of endogenous NO. This mechanism would provide a basis for the maintenance of papillary perfusion during renal vasoconstriction as a consequence of elevated systemic or intrarenal levels of AII. Blair-West, J. R., Walker, L. L., Rajaratne, A. A. J. & Harris, P. J. (1997). Nitric oxide modulates the effects of angiotensin II on blood perfusion in the rat renal papilla. Proceedings of the XXXIII International Congress of Physiological Sciences, St Petersburg, P Faubert, P. F., Chou, S. Y. & Porush, J. G. (1987). Regulation of papillary plasma flow by angiotensin II. Kidney International 32, Grenier, F. C., Rollins, T. E. & Smith, W. L. (1981). Kinin-induced prostaglandin synthesis by renal papillary collecting tubule cells in culture. American Journal of Physiology 241, F Huang, C. L., Davis, G. & Johns, E. J. (1991).Astudyoftheactionof angiotensin II on perfusion through the cortex and papilla of the rat kidney. Experimental Physiology 76, Jamison, R. L. & Kriz, W. (1982). Urinary Concentrating Mechanism, pp Oxford University Press, New York. Lu, S., Mattson, D. L., Roman, R. J., Becker, C. G. & Cowley, A. W. Jr (1993). Assessment of changes in intrarenal blood flow in conscious rats using laser-doppler flowmetry. American Journal of Physiology 264, F Mattson, D. L. & Cowley, A. W. Jr (1993). Kinin actions on renal papillary blood flow and sodium excretion. Hypertension 21, Mendelsohn, F. A. O., Dunbar, M., Allen, A., Chou, S. T., Millan, M. A., Aguilera, G. & Catt, K. J. (1986). Angiotensin II receptors in the kidney. Federation Proceedings 45, Muirhead, E. E., Brown, G. B., Germain, G. S. & Leach, B. E. (1970). The renal medulla as an antihypertensive organ. Journal of Laboratory and Clinical Medicine 76, Muirhead, E. E., Germain, G., Leach, B. E., Pitcock, J. A., Stephenson, P., Brooks, B., Brosius, W. L., Daniels, E. G. & Hinman, J. W. (1972). Production of renomedullary prostaglandins by renomedullary interstitial cells grown in tissue culture. Circulation Research 31, suppl. 2, Muirhead, E. E. & Pitcock, J. A. (1985). The renal antihypertensive hormone. Journal of Hypertension 3, 1 8. Nobes, M. S., Harris, P. J., Yamada, H. & Mendelsohn, F. A. O. (1991). Effects of angiotensin on renal cortical and papillary blood flows measured by laser-doppler flowmetry. American Journal of Physiology 261, F Ortiz, M. C., Fortepiani, L. A., Ruis-Marcos, F. M., Atucha, N. M. & Garcia-Estan, J. (1998). Role of AT1 receptors in the renal papillary effects of acute and chronic nitric oxide inhibition. American Journal of Physiology 274, R Parekh, N., Dobrowolski, L., Zou, A. P. & Steinhausen, M. (1996). Nitric oxide modulates angiotensin II- and norepinephrinedependent vasoconstriction in rat kidney. American Journal of Physiology 270, R Parekh, N. & Zou, A. P. (1996). Role of prostaglandins in renal medullary circulation: response to different vasoconstrictors. American Journal of Physiology 271, F Roman, R. J., Kaldunski, M. L., Scicli, A. G. & Carretero, O. A. (1988). Influence of kinins and angiotensin II on the regulation of papillary blood flow. American Journal of Physiology 255, F Tobian, L., Ishii, M. & Duke, M. (1969). Relationship of cytoplasmic granules in renal papillary interstitial cells to postsalt hypertension. Journal of Laboratory and Clinical Medicine 73, Walker, L. L., Rajaratne, A. A. J., Blair-West, J. R. & Harris, P. J. (1996). Modulation of effects of angiotensin on rat papillary blood flow by nitric oxide. Proceedings of the Australian Physiological and Pharmacological Society 27, 210P.
6 278 L. L. Walker, A. A. J. Rajaratne, J. R. Blair-West and P. J. Harris J. Physiol Zhou, J., Alcorn, D., Allen, A. M. & Mendelsohn, F. A. O. (1992). High resolution localization of angiotensin II receptors in the rat renal medulla. Kidney International 42, Zhou, J., Dean, R., Maric, C., Aldred, P. G., Harris, P., Alcorn, D. & Mendelsohn, F. A. O. (1998). Localization and interactions of vasoactive peptide receptors in renomedullary interstial cells of the kidney. Kidney International 54, suppl. 67, S22 S28. Zhou, J., Thomas, D., Harris, P. J. & Skinner, S. L. (1992). The role of endogenous angiotensin II in the regulation of renal haemodynamics and proximal fluid reabsorption in the rat. Journal of Physiology 435, Acknowledgements This project was funded by a grant from the National Health and Medical Research Council of Australia. A. A. J. Rajaratne received a travel grant from The University of Melbourne. Corresponding author P. J. Harris: Department of Physiology, The University of Melbourne, Parkville, Victoria 3052, Australia. p.harris@physiology.unimelb.edu.au
A STUDY OF THE ACTION OF ANGIOTENSIN II ON PERFUSION THROUGH THE CORTEX AND PAPILLA OF THE RAT KIDNEY
 Experimental Physiology (1991) 76, 787-798 Printed in Great Britain A STUDY OF THE ACTION OF ANGIOTENSIN II ON PERFUSION THROUGH THE CORTEX AND PAPILLA OF THE RAT KIDNEY CHUNLONG HUANG*, GERARD DAVIS AND
Experimental Physiology (1991) 76, 787-798 Printed in Great Britain A STUDY OF THE ACTION OF ANGIOTENSIN II ON PERFUSION THROUGH THE CORTEX AND PAPILLA OF THE RAT KIDNEY CHUNLONG HUANG*, GERARD DAVIS AND
Differential effect of angiotensin II on blood circulation in the renal medulla and cortex of anaesthetised rats
 Journal of Physiology (2002), 538.1, pp. 159 166 DOI: 10.1013/jphysiol.2001.012921 The Physiological Society 2002 www.jphysiol.org Differential effect of angiotensin II on blood circulation in the renal
Journal of Physiology (2002), 538.1, pp. 159 166 DOI: 10.1013/jphysiol.2001.012921 The Physiological Society 2002 www.jphysiol.org Differential effect of angiotensin II on blood circulation in the renal
It is well recognized that the kidney plays a fundamental
 337 Renal Medullary Captopril Delivery Lowers Blood Pressure in Spontaneously Hypertensive Rats Shanhong Lu, David L. Mattson, Allen W. Cowley, Jr Abstract We examined the contribution of renal medullary
337 Renal Medullary Captopril Delivery Lowers Blood Pressure in Spontaneously Hypertensive Rats Shanhong Lu, David L. Mattson, Allen W. Cowley, Jr Abstract We examined the contribution of renal medullary
The ability of the kidneys to regulate extracellular fluid volume by altering sodium
 REGULATION OF EXTRACELLULAR FLUID VOLUME BY INTEGRATED CONTROL OF SODIUM EXCRETION Joey P. Granger Department of Physiology and Biophysics, University of Mississippi Medical Center, Jackson, Mississippi
REGULATION OF EXTRACELLULAR FLUID VOLUME BY INTEGRATED CONTROL OF SODIUM EXCRETION Joey P. Granger Department of Physiology and Biophysics, University of Mississippi Medical Center, Jackson, Mississippi
Outline the functional anatomy, and the physiological factors, that determine oxygen delivery to the renal medulla.
 2011-2-21 Outline the functional anatomy, and the physiological factors, that determine oxygen delivery to the renal medulla. Oxygen delivery = Blood flow CaO 2 Where Blood flow determined by (arterial
2011-2-21 Outline the functional anatomy, and the physiological factors, that determine oxygen delivery to the renal medulla. Oxygen delivery = Blood flow CaO 2 Where Blood flow determined by (arterial
Questions? Homework due in lab 6. PreLab #6 HW 15 & 16 (follow directions, 6 points!)
 Questions? Homework due in lab 6 PreLab #6 HW 15 & 16 (follow directions, 6 points!) Part 3 Variations in Urine Formation Composition varies Fluid volume Solute concentration Variations in Urine Formation
Questions? Homework due in lab 6 PreLab #6 HW 15 & 16 (follow directions, 6 points!) Part 3 Variations in Urine Formation Composition varies Fluid volume Solute concentration Variations in Urine Formation
Sunday, July 17, 2011 URINARY SYSTEM
 URINARY SYSTEM URINARY SYSTEM Let s take a look at the anatomy first! KIDNEYS: are complex reprocessing centers where blood is filtered through and waste products are removed. Wastes and extra water become
URINARY SYSTEM URINARY SYSTEM Let s take a look at the anatomy first! KIDNEYS: are complex reprocessing centers where blood is filtered through and waste products are removed. Wastes and extra water become
modulating the tubuloglomerular feed-back mechanism in the canine kidney; Sciences Center, 4200 East Ninth Avenue, Denver, CO 80262, U.S.A.
 J. Physiol. (1986), 380, pp. 35-43 35 With 3 text-figures Printed in Great Britain RENAL VASOCONSTRICTOR RESPONSE TO HYPERTONIC SALINE IN THE DOG: EFFECTS OF PROSTAGLANDINS, INDOMETHACIN AND THEOPHYLLINE
J. Physiol. (1986), 380, pp. 35-43 35 With 3 text-figures Printed in Great Britain RENAL VASOCONSTRICTOR RESPONSE TO HYPERTONIC SALINE IN THE DOG: EFFECTS OF PROSTAGLANDINS, INDOMETHACIN AND THEOPHYLLINE
Chapter 23. The Nephron. (functional unit of the kidney
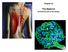 Chapter 23 The Nephron (functional unit of the kidney Renal capsule The Nephron Renal cortex Nephron Collecting duct Efferent arteriole Afferent arteriole (a) Renal corpuscle: Glomerular capsule Glomerulus
Chapter 23 The Nephron (functional unit of the kidney Renal capsule The Nephron Renal cortex Nephron Collecting duct Efferent arteriole Afferent arteriole (a) Renal corpuscle: Glomerular capsule Glomerulus
Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion.
 The Kidney Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion. The kidney has 6 roles in the maintenance of homeostasis. 6 Main Functions 1. Ion Balance
The Kidney Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion. The kidney has 6 roles in the maintenance of homeostasis. 6 Main Functions 1. Ion Balance
CONTROLLING THE INTERNAL ENVIRONMENT
 AP BIOLOGY ANIMAL FORM & FUNCTION ACTIVITY #5 NAME DATE HOUR CONTROLLING THE INTERNAL ENVIRONMENT KIDNEY AND NEPHRON NEPHRON FUNCTIONS Animal Form & Function Activity #5 page 1 NEPHRON STRUCTURE NEPHRON
AP BIOLOGY ANIMAL FORM & FUNCTION ACTIVITY #5 NAME DATE HOUR CONTROLLING THE INTERNAL ENVIRONMENT KIDNEY AND NEPHRON NEPHRON FUNCTIONS Animal Form & Function Activity #5 page 1 NEPHRON STRUCTURE NEPHRON
Impairment of pressure-natriuresis and renal autoregulation in ANG II-infused hypertensive rats
 Am J Physiol Renal Physiol 279: F319 F325, 2000. Impairment of pressure-natriuresis and renal autoregulation in ANG II-infused hypertensive rats CHI-TARNG WANG, SO YEON CHIN, AND L. GABRIEL NAVAR Department
Am J Physiol Renal Physiol 279: F319 F325, 2000. Impairment of pressure-natriuresis and renal autoregulation in ANG II-infused hypertensive rats CHI-TARNG WANG, SO YEON CHIN, AND L. GABRIEL NAVAR Department
Chapter 25 The Urinary System
 Chapter 25 The Urinary System 10/30/2013 MDufilho 1 Kidney Functions Removal of toxins, metabolic wastes, and excess ions from the blood Regulation of blood volume, chemical composition, and ph Gluconeogenesis
Chapter 25 The Urinary System 10/30/2013 MDufilho 1 Kidney Functions Removal of toxins, metabolic wastes, and excess ions from the blood Regulation of blood volume, chemical composition, and ph Gluconeogenesis
3/10/2009 VESSELS PHYSIOLOGY D.HAMMOUDI.MD. Palpated Pulse. Figure 19.11
 VESSELS PHYSIOLOGY D.HAMMOUDI.MD Palpated Pulse Figure 19.11 1 shows the common sites where the pulse is felt. 1. Temporal artery at the temple above and to the outer side of the eye 2. External maxillary
VESSELS PHYSIOLOGY D.HAMMOUDI.MD Palpated Pulse Figure 19.11 1 shows the common sites where the pulse is felt. 1. Temporal artery at the temple above and to the outer side of the eye 2. External maxillary
Chapter 1 RENAL HAEMODYNAMICS AND GLOMERULAR FILTRATION
 3 Chapter 1 RENAL HAEMODYNAMICS AND GLOMERULAR FILTRATION David Shirley, Giovambattista Capasso and Robert Unwin The kidney has three homeostatic functions that can broadly be described as excretory, regulatory
3 Chapter 1 RENAL HAEMODYNAMICS AND GLOMERULAR FILTRATION David Shirley, Giovambattista Capasso and Robert Unwin The kidney has three homeostatic functions that can broadly be described as excretory, regulatory
Relaxation responses of aortic rings from salt-loaded high calcium fed rats to potassium chloride, calcium chloride and magnesium sulphate
 Pathophysiology 4 (1998) 275 280 Relaxation responses of aortic rings from salt-loaded high calcium fed rats to potassium chloride, calcium chloride and magnesium sulphate B.J. Adegunloye, O.A. Sofola
Pathophysiology 4 (1998) 275 280 Relaxation responses of aortic rings from salt-loaded high calcium fed rats to potassium chloride, calcium chloride and magnesium sulphate B.J. Adegunloye, O.A. Sofola
Mechanisms responsible for postmenopausal hypertension in a rat model: Roles of the renal sympathetic nervous system and the renin angiotensin system
 ORIGINAL RESEARCH Physiological Reports ISSN 2051-817X Mechanisms responsible for postmenopausal hypertension in a rat model: Roles of the renal sympathetic nervous system and the renin angiotensin system
ORIGINAL RESEARCH Physiological Reports ISSN 2051-817X Mechanisms responsible for postmenopausal hypertension in a rat model: Roles of the renal sympathetic nervous system and the renin angiotensin system
The principal functions of the kidneys
 Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Interactions between neural and hormonal mediators of renal vascular tone in anaesthetized rabbits
 Interactions between neural and hormonal mediators of renal vascular tone in anaesthetized rabbits Sarah-Jane Guild *, Carolyn J. Barrett, Roger G. Evans and Simon C. Malpas Circulatory Control Laboratory,
Interactions between neural and hormonal mediators of renal vascular tone in anaesthetized rabbits Sarah-Jane Guild *, Carolyn J. Barrett, Roger G. Evans and Simon C. Malpas Circulatory Control Laboratory,
Physiology Lecture 2. What controls GFR?
 Physiology Lecture 2 Too much blood is received by the glomerular capillaries, this blood contains plasma, once this plasma enters the glomerular capillaries it will be filtered to bowman s space. The
Physiology Lecture 2 Too much blood is received by the glomerular capillaries, this blood contains plasma, once this plasma enters the glomerular capillaries it will be filtered to bowman s space. The
A. Correct! Flushing acids from the system will assist in re-establishing the acid-base equilibrium in the blood.
 OAT Biology - Problem Drill 16: The Urinary System Question No. 1 of 10 1. Which of the following would solve a drop in blood ph? Question #01 (A) Decreased retention of acids. (B) Increased excretion
OAT Biology - Problem Drill 16: The Urinary System Question No. 1 of 10 1. Which of the following would solve a drop in blood ph? Question #01 (A) Decreased retention of acids. (B) Increased excretion
Septic Acute Kidney Injury (AKI) Rinaldo Bellomo Australian and New Zealand Intensive Care Research Centre (ANZIC-RC) Melbourne Australia
 Septic Acute Kidney Injury (AKI) Rinaldo Bellomo Australian and New Zealand Intensive Care Research Centre (ANZIC-RC) Melbourne Australia Things we really, honestly know about septic AKI AKI is common
Septic Acute Kidney Injury (AKI) Rinaldo Bellomo Australian and New Zealand Intensive Care Research Centre (ANZIC-RC) Melbourne Australia Things we really, honestly know about septic AKI AKI is common
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1
 BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
Blood Pressure Regulation 2. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Acute Kidney Injury. APSN JSN CME for Nephrology Trainees May Professor Robert Walker
 Acute Kidney Injury APSN JSN CME for Nephrology Trainees May 2017 Professor Robert Walker Kidney International (2017) 91, 1033 1046; http://dx.doi.org/10.1016/ j.kint.2016.09.051 Case for discussion 55year
Acute Kidney Injury APSN JSN CME for Nephrology Trainees May 2017 Professor Robert Walker Kidney International (2017) 91, 1033 1046; http://dx.doi.org/10.1016/ j.kint.2016.09.051 Case for discussion 55year
BIOL2030 Human A & P II -- Exam 6
 BIOL2030 Human A & P II -- Exam 6 Name: 1. The kidney functions in A. preventing blood loss. C. synthesis of vitamin E. E. making ADH. B. white blood cell production. D. excretion of metabolic wastes.
BIOL2030 Human A & P II -- Exam 6 Name: 1. The kidney functions in A. preventing blood loss. C. synthesis of vitamin E. E. making ADH. B. white blood cell production. D. excretion of metabolic wastes.
Human Urogenital System 26-1
 Human Urogenital System 26-1 Urogenital System Functions Filtering of blood, Removal of wastes and metabolites Regulation of blood volume and composition concentration of blood solutes ph of extracellular
Human Urogenital System 26-1 Urogenital System Functions Filtering of blood, Removal of wastes and metabolites Regulation of blood volume and composition concentration of blood solutes ph of extracellular
Body fluid volume is small (~5L (blood + serum)) Composition can change rapidly e.g. due to increase in metabolic rate
 Renal physiology The kidneys Allow us to live on dry land. Body fluid volume is small (~5L (blood + serum)) Composition can change rapidly e.g. due to increase in metabolic rate Kidneys maintain composition
Renal physiology The kidneys Allow us to live on dry land. Body fluid volume is small (~5L (blood + serum)) Composition can change rapidly e.g. due to increase in metabolic rate Kidneys maintain composition
A&P 2 CANALE T H E U R I N A R Y S Y S T E M
 A&P 2 CANALE T H E U R I N A R Y S Y S T E M URINARY SYSTEM CONTRIBUTION TO HOMEOSTASIS Regulates body water levels Excess water taken in is excreted Output varies from 2-1/2 liter/day to 1 liter/hour
A&P 2 CANALE T H E U R I N A R Y S Y S T E M URINARY SYSTEM CONTRIBUTION TO HOMEOSTASIS Regulates body water levels Excess water taken in is excreted Output varies from 2-1/2 liter/day to 1 liter/hour
Preparation of Animals for Live Animal Imaging
 Preparation of Animals for Live Animal Imaging George A. Tanner, Ph.D. Department of Cellular and Integrative Physiology Indiana University School of Medicine Ideal Condition of Rats during Experiments:
Preparation of Animals for Live Animal Imaging George A. Tanner, Ph.D. Department of Cellular and Integrative Physiology Indiana University School of Medicine Ideal Condition of Rats during Experiments:
Nephron Structure inside Kidney:
 In-Depth on Kidney Nephron Structure inside Kidney: - Each nephron has two capillary regions in close proximity to the nephron tubule, the first capillary bed for fluid exchange is called the glomerulus,
In-Depth on Kidney Nephron Structure inside Kidney: - Each nephron has two capillary regions in close proximity to the nephron tubule, the first capillary bed for fluid exchange is called the glomerulus,
MAJOR FUNCTIONS OF THE KIDNEY
 MAJOR FUNCTIONS OF THE KIDNEY REGULATION OF BODY FLUID VOLUME REGULATION OF OSMOTIC BALANCE REGULATION OF ELECTROLYTE COMPOSITION REGULATION OF ACID-BASE BALANCE REGULATION OF BLOOD PRESSURE ERYTHROPOIESIS
MAJOR FUNCTIONS OF THE KIDNEY REGULATION OF BODY FLUID VOLUME REGULATION OF OSMOTIC BALANCE REGULATION OF ELECTROLYTE COMPOSITION REGULATION OF ACID-BASE BALANCE REGULATION OF BLOOD PRESSURE ERYTHROPOIESIS
Excretory System 1. a)label the parts indicated above and give one function for structures Y and Z
 Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- X- Y- Z- b) Which of the following is not a function of the organ shown? A. to produce
Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- X- Y- Z- b) Which of the following is not a function of the organ shown? A. to produce
Pressure Diuresis 9 Sample Student Essays
 Pressure Diuresis 9 Sample Student Essays Below please find assembled consecutively in one document the brief analyses submitted by nine students in Mammalian Physiology 08 to the Teach Yourself Pressure
Pressure Diuresis 9 Sample Student Essays Below please find assembled consecutively in one document the brief analyses submitted by nine students in Mammalian Physiology 08 to the Teach Yourself Pressure
Glomerular Capillary Blood Pressure
 Glomerular Capillary Blood Pressure Fluid pressure exerted by blood within glomerular capillaries Depends on Contraction of the heart Resistance to blood flow offered by afferent and efferent arterioles
Glomerular Capillary Blood Pressure Fluid pressure exerted by blood within glomerular capillaries Depends on Contraction of the heart Resistance to blood flow offered by afferent and efferent arterioles
Dominance of pressure natriuresis in acute depressor responses to increased renal artery pressure in rabbits and rats
 Journal of Physiology (2002), 538.3, pp. 901 910 DOI: 10.1013/jphysiol.2001.013280 The Physiological Society 2002 www.jphysiol.org Dominance of pressure natriuresis in acute depressor responses to increased
Journal of Physiology (2002), 538.3, pp. 901 910 DOI: 10.1013/jphysiol.2001.013280 The Physiological Society 2002 www.jphysiol.org Dominance of pressure natriuresis in acute depressor responses to increased
The kidneys are excretory and regulatory organs. By
 exercise 9 Renal System Physiology Objectives 1. To define nephron, renal corpuscle, renal tubule, afferent arteriole, glomerular filtration, efferent arteriole, aldosterone, ADH, and reabsorption 2. To
exercise 9 Renal System Physiology Objectives 1. To define nephron, renal corpuscle, renal tubule, afferent arteriole, glomerular filtration, efferent arteriole, aldosterone, ADH, and reabsorption 2. To
RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015
 RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015 1. In which abdominal cavity do the kidneys lie? a) Peritoneum. b) Anteperitoneal. c) Retroperitoneal. d) Parietal peritoneal 2. What is the
RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015 1. In which abdominal cavity do the kidneys lie? a) Peritoneum. b) Anteperitoneal. c) Retroperitoneal. d) Parietal peritoneal 2. What is the
Renal Quiz - June 22, 21001
 Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
had no effect on the production of aldosterone, corticosterone, or cortisol after
 INHIBITION OF THE EFFECTS OF ANGIOTENSIN II ON ADRENAL STEROID PRODUCTION BY DIETARY SODIUM BY WARREN W. DAVIS,* LAWRENCE R. BURWELL,t AND FREDERIC C. BARTTERt ENDOCRINOLOGY BRANCH, NATIONAL HEART INSTITUTE,
INHIBITION OF THE EFFECTS OF ANGIOTENSIN II ON ADRENAL STEROID PRODUCTION BY DIETARY SODIUM BY WARREN W. DAVIS,* LAWRENCE R. BURWELL,t AND FREDERIC C. BARTTERt ENDOCRINOLOGY BRANCH, NATIONAL HEART INSTITUTE,
flux study and SD rats ( g) for microdissection study were obtained from SLC
 Supplemental Methods Experimental Animals. Male Sprague-Dawley (SD) rats (280 370 g) for regional renal blood flux study and SD rats (200-250 g) for microdissection study were obtained from SLC (Shizuoka,
Supplemental Methods Experimental Animals. Male Sprague-Dawley (SD) rats (280 370 g) for regional renal blood flux study and SD rats (200-250 g) for microdissection study were obtained from SLC (Shizuoka,
RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D.
 RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D. Learning Objectives 1. Identify the region of the renal tubule in which reabsorption and secretion occur. 2. Describe the cellular
RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D. Learning Objectives 1. Identify the region of the renal tubule in which reabsorption and secretion occur. 2. Describe the cellular
Kidney and urine formation
 Kidney and urine formation Renal structure & function Urine formation Urinary y concentration and dilution Regulation of urine formation 1 Kidney and urine formation 1.Renal structure & function 1)General
Kidney and urine formation Renal structure & function Urine formation Urinary y concentration and dilution Regulation of urine formation 1 Kidney and urine formation 1.Renal structure & function 1)General
PARTS OF THE URINARY SYSTEM
 EXCRETORY SYSTEM Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid-base concentrations and metabolite concentrations 1 ORGANS OF EXCRETION Skin and
EXCRETORY SYSTEM Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid-base concentrations and metabolite concentrations 1 ORGANS OF EXCRETION Skin and
Chapter 19 The Urinary System Fluid and Electrolyte Balance
 Chapter 19 The Urinary System Fluid and Electrolyte Balance Chapter Outline The Concept of Balance Water Balance Sodium Balance Potassium Balance Calcium Balance Interactions between Fluid and Electrolyte
Chapter 19 The Urinary System Fluid and Electrolyte Balance Chapter Outline The Concept of Balance Water Balance Sodium Balance Potassium Balance Calcium Balance Interactions between Fluid and Electrolyte
Angiotensin II and prostaglandins in control of vasa recta blood flow
 Angiotensin II and prostaglandins in control of vasa recta blood flow W. A. CUPPLES, T. SAKAI, AND D. J. MARSH Department of Physiology and Biophysics, University of Southern California, Los Angeles, California
Angiotensin II and prostaglandins in control of vasa recta blood flow W. A. CUPPLES, T. SAKAI, AND D. J. MARSH Department of Physiology and Biophysics, University of Southern California, Los Angeles, California
Osmotic Regulation and the Urinary System. Chapter 50
 Osmotic Regulation and the Urinary System Chapter 50 Challenge Questions Indicate the areas of the nephron that the following hormones target, and describe when and how the hormones elicit their actions.
Osmotic Regulation and the Urinary System Chapter 50 Challenge Questions Indicate the areas of the nephron that the following hormones target, and describe when and how the hormones elicit their actions.
Physiology of Excretory Systems
 Physiology of Excretory Systems Fig 12-2 (a) Urea is formed by the ornithine-urea cycle in most vertebrates. Because ATP is required for the first step, nitrogen excretion in ureotelic animals is more
Physiology of Excretory Systems Fig 12-2 (a) Urea is formed by the ornithine-urea cycle in most vertebrates. Because ATP is required for the first step, nitrogen excretion in ureotelic animals is more
Cornerstone: A Collection of Scholarly and Creative Works for Minnesota State University, Mankato. Minnesota State University, Mankato
 Minnesota State University, Mankato Cornerstone: A Collection of Scholarly and Creative Works for Minnesota State University, Mankato Theses, Dissertations, and Other Capstone Projects 2009 The Increase
Minnesota State University, Mankato Cornerstone: A Collection of Scholarly and Creative Works for Minnesota State University, Mankato Theses, Dissertations, and Other Capstone Projects 2009 The Increase
014 Chapter 14 Created: 9:25:14 PM CST
 014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
Actions of prostaglandin F20 on the splenic vascular and capsular smooth muscle in the dog
 Br. J. Pharmac. (1971), 41, 1-7 Actions of prostaglandin F20 on the splenic vascular and capsular smooth muscle in the dog B. N. DAVIES ADi P. G. WITHRINGTON Department of Physiology, Medical College of
Br. J. Pharmac. (1971), 41, 1-7 Actions of prostaglandin F20 on the splenic vascular and capsular smooth muscle in the dog B. N. DAVIES ADi P. G. WITHRINGTON Department of Physiology, Medical College of
Renal physiology D.HAMMOUDI.MD
 Renal physiology D.HAMMOUDI.MD Functions Regulating blood ionic composition Regulating blood ph Regulating blood volume Regulating blood pressure Produce calcitrol and erythropoietin Regulating blood glucose
Renal physiology D.HAMMOUDI.MD Functions Regulating blood ionic composition Regulating blood ph Regulating blood volume Regulating blood pressure Produce calcitrol and erythropoietin Regulating blood glucose
LABORATORY EXERCISES FOR THE URINARY SYSTEM
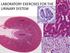 LABORATORY EXERCISES FOR THE URINARY SYSTEM cortex Medulla DEMO SLIDE BOX 172 (450-E001-H-76). Kidney, horse. the inner medulla medullary rays, Uriniferous tubules expand both the cortex and medulla corticomedullary
LABORATORY EXERCISES FOR THE URINARY SYSTEM cortex Medulla DEMO SLIDE BOX 172 (450-E001-H-76). Kidney, horse. the inner medulla medullary rays, Uriniferous tubules expand both the cortex and medulla corticomedullary
Copyright 2009 Pearson Education, Inc. Copyright 2009 Pearson Education, Inc. Figure 19-1c. Efferent arteriole. Juxtaglomerular apparatus
 /6/0 About this Chapter Functions of the Kidneys Anatomy of the urinary system Overview of kidney function Secretion Micturition Regulation of extracellular fluid volume and blood pressure Regulation of
/6/0 About this Chapter Functions of the Kidneys Anatomy of the urinary system Overview of kidney function Secretion Micturition Regulation of extracellular fluid volume and blood pressure Regulation of
A. Incorrect! The urinary system is involved in the regulation of blood ph. B. Correct! The urinary system is involved in the synthesis of vitamin D.
 Human Anatomy - Problem Drill 22: The Urinary System Question No. 1 of 10 1. Which of the following statements about the functions of the urinary system is not correct? Question #01 (A) The urinary system
Human Anatomy - Problem Drill 22: The Urinary System Question No. 1 of 10 1. Which of the following statements about the functions of the urinary system is not correct? Question #01 (A) The urinary system
Functions of the kidney
 Physiology of Urinary tract Kidney, Ureter, Urinary bladder Urethra Kidney function Excretion Physiology of volume regulation Functions of the kidney Excretion of dangerous substances endogenous (metabolites):
Physiology of Urinary tract Kidney, Ureter, Urinary bladder Urethra Kidney function Excretion Physiology of volume regulation Functions of the kidney Excretion of dangerous substances endogenous (metabolites):
Ch 17 Physiology of the Kidneys
 Ch 17 Physiology of the Kidneys Review Anatomy on your own SLOs List and describe the 4 major functions of the kidneys. List and explain the 4 processes of the urinary system. Diagram the filtration barriers
Ch 17 Physiology of the Kidneys Review Anatomy on your own SLOs List and describe the 4 major functions of the kidneys. List and explain the 4 processes of the urinary system. Diagram the filtration barriers
Urinary Physiology. Chapter 17 Outline. Kidney Function. Chapter 17
 Urinary Physiology Chapter 17 Chapter 17 Outline Structure and Function of the Kidney Glomerular Filtration Reabsorption of Salt and Water Renal Plasma Clearance Renal Control of Electrolyte and Acid-Base
Urinary Physiology Chapter 17 Chapter 17 Outline Structure and Function of the Kidney Glomerular Filtration Reabsorption of Salt and Water Renal Plasma Clearance Renal Control of Electrolyte and Acid-Base
Use the following diagram to answer the next question. 1. In the diagram above, pressure filtration occurs in a. W b. X c. Y d. Z
 Part A: Multiple Choice Questions Value: 32 Marks Suggested time: 40 minutes Instructions: For each question select the best answer and record your choice on the Scantron card provided. Using an HB pencil,
Part A: Multiple Choice Questions Value: 32 Marks Suggested time: 40 minutes Instructions: For each question select the best answer and record your choice on the Scantron card provided. Using an HB pencil,
41B. Metabolism produces wastes that must be eliminated from the body. This. Renal System Physiology: Computer Simulation
 41B E X E R C I S E Renal System Physiology: Computer Simulation O B J E C T I V E S 1. To define the following terms: glomerulus, glomerular capsule, renal corpuscle, renal tubule, nephron, proximal convoluted
41B E X E R C I S E Renal System Physiology: Computer Simulation O B J E C T I V E S 1. To define the following terms: glomerulus, glomerular capsule, renal corpuscle, renal tubule, nephron, proximal convoluted
1. a)label the parts indicated above and give one function for structures Y and Z
 Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- renal cortex - X- renal medulla Y- renal pelvis collecting center of urine and then
Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- renal cortex - X- renal medulla Y- renal pelvis collecting center of urine and then
Basic Functions of the Kidneys
 Dr. Adelina Vlad Basic Functions of the Kidneys Eliminate plasma METABOLIC WASTE PRODUCTS and FOREIGN COMPOUNDS The kidney are the primary means for eliminating metabolic waste products (urea, creatinine,
Dr. Adelina Vlad Basic Functions of the Kidneys Eliminate plasma METABOLIC WASTE PRODUCTS and FOREIGN COMPOUNDS The kidney are the primary means for eliminating metabolic waste products (urea, creatinine,
Proceedings of the 34th World Small Animal Veterinary Congress WSAVA 2009
 www.ivis.org Proceedings of the 34th World Small Animal Veterinary Congress WSAVA 2009 São Paulo, Brazil - 2009 Next WSAVA Congress : Reprinted in IVIS with the permission of the Congress Organizers PROTEINURIA
www.ivis.org Proceedings of the 34th World Small Animal Veterinary Congress WSAVA 2009 São Paulo, Brazil - 2009 Next WSAVA Congress : Reprinted in IVIS with the permission of the Congress Organizers PROTEINURIA
COMPLETE INHIBITION OF RENAL RESERVE IN CHRONIC RENAL FAILURE BY A COMBINATION OF ACEI AND ARB
 COMPLETE INHIBITION OF RENAL RESERVE IN CHRONIC RENAL FAILURE BY A COMBINATION OF ACEI AND ARB CG Musso ¹, J Reynaldi¹, N Imperiali ¹, L Algranati ¹, DG Oreopoulos ² Nephrology Department Hospital Italiano
COMPLETE INHIBITION OF RENAL RESERVE IN CHRONIC RENAL FAILURE BY A COMBINATION OF ACEI AND ARB CG Musso ¹, J Reynaldi¹, N Imperiali ¹, L Algranati ¹, DG Oreopoulos ² Nephrology Department Hospital Italiano
Kidney Physiology. Mechanisms of Urine Formation TUBULAR SECRETION Eunise A. Foster Shalonda Reed
 Kidney Physiology Mechanisms of Urine Formation TUBULAR SECRETION Eunise A. Foster Shalonda Reed The purpose of tubular secrection To dispose of certain substances that are bound to plasma proteins. To
Kidney Physiology Mechanisms of Urine Formation TUBULAR SECRETION Eunise A. Foster Shalonda Reed The purpose of tubular secrection To dispose of certain substances that are bound to plasma proteins. To
General Anatomy of Urinary System
 General Anatomy of Urinary System URINARY SYSTEM ORGANS Kidneys (2) Ureters (2) Urinary bladder Urethra KIDNEY FUNCTIONS Control blood volume and composition KIDNEY FUNCTIONS Filter blood plasma, eliminate
General Anatomy of Urinary System URINARY SYSTEM ORGANS Kidneys (2) Ureters (2) Urinary bladder Urethra KIDNEY FUNCTIONS Control blood volume and composition KIDNEY FUNCTIONS Filter blood plasma, eliminate
Cardiovascular System B L O O D V E S S E L S 2
 Cardiovascular System B L O O D V E S S E L S 2 Blood Pressure Main factors influencing blood pressure: Cardiac output (CO) Peripheral resistance (PR) Blood volume Peripheral resistance is a major factor
Cardiovascular System B L O O D V E S S E L S 2 Blood Pressure Main factors influencing blood pressure: Cardiac output (CO) Peripheral resistance (PR) Blood volume Peripheral resistance is a major factor
Nephron Anatomy Nephron Anatomy
 Kidney Functions: (Eckert 14-17) Mammalian Kidney -Paired -1% body mass -20% blood flow (Eckert 14-17) -Osmoregulation -Blood volume regulation -Maintain proper ion concentrations -Dispose of metabolic
Kidney Functions: (Eckert 14-17) Mammalian Kidney -Paired -1% body mass -20% blood flow (Eckert 14-17) -Osmoregulation -Blood volume regulation -Maintain proper ion concentrations -Dispose of metabolic
2) This is a Point and Click question. You must click on the required structure.
 Class: A&P2-1 Description: Test: Excretory Test Points: 144 Test Number: 28379 Printed: 31-March-10 12:03 1) This is a Point and Click question. You must click on the required structure. Click on the Bowman's
Class: A&P2-1 Description: Test: Excretory Test Points: 144 Test Number: 28379 Printed: 31-March-10 12:03 1) This is a Point and Click question. You must click on the required structure. Click on the Bowman's
Responsiveness vs. basal activity of plasma ANG II as a determinant of arterial pressure salt sensitivity
 Am J Physiol Heart Circ Physiol 285: H2142 H2149, 2003. First published July 24, 2003; 10.1152/ajpheart.00200.2003. Responsiveness vs. basal activity of plasma ANG II as a determinant of arterial pressure
Am J Physiol Heart Circ Physiol 285: H2142 H2149, 2003. First published July 24, 2003; 10.1152/ajpheart.00200.2003. Responsiveness vs. basal activity of plasma ANG II as a determinant of arterial pressure
(Received 22 July 1957) It is now generally accepted that the unequal distribution of ions between cells
 190 J. Physiol. (I958) I40, I90-200 THE EFFECT OF ALTERATIONS OF PLASMA SODIUM ON THE SODIUM AND POTASSIUM CONTENT OF MUSCLE IN THE RAT By F. 0. DOSEKUN AND D. MENDEL From the Department of Physiology,
190 J. Physiol. (I958) I40, I90-200 THE EFFECT OF ALTERATIONS OF PLASMA SODIUM ON THE SODIUM AND POTASSIUM CONTENT OF MUSCLE IN THE RAT By F. 0. DOSEKUN AND D. MENDEL From the Department of Physiology,
Salt Sensitivity: Mechanisms, Diagnosis, and Clinical Relevance
 Salt Sensitivity: Mechanisms, Diagnosis, and Clinical Relevance Matthew R. Weir, MD Professor and Director Division of Nephrology University of Maryland School of Medicine Overview Introduction Mechanisms
Salt Sensitivity: Mechanisms, Diagnosis, and Clinical Relevance Matthew R. Weir, MD Professor and Director Division of Nephrology University of Maryland School of Medicine Overview Introduction Mechanisms
Osmoregulation and Renal Function
 1 Bio 236 Lab: Osmoregulation and Renal Function Fig. 1: Kidney Anatomy Fig. 2: Renal Nephron The kidneys are paired structures that lie within the posterior abdominal cavity close to the spine. Each kidney
1 Bio 236 Lab: Osmoregulation and Renal Function Fig. 1: Kidney Anatomy Fig. 2: Renal Nephron The kidneys are paired structures that lie within the posterior abdominal cavity close to the spine. Each kidney
RENAL PHYSIOLOGY. Physiology Unit 4
 RENAL PHYSIOLOGY Physiology Unit 4 Renal Functions Primary Function is to regulate the chemistry of plasma through urine formation Additional Functions Regulate concentration of waste products Regulate
RENAL PHYSIOLOGY Physiology Unit 4 Renal Functions Primary Function is to regulate the chemistry of plasma through urine formation Additional Functions Regulate concentration of waste products Regulate
Principles of Renal Physiology. 4th Edition
 Principles of Renal Physiology 4th Edition Principles of Renal Physiology 4th Edition Chris Lote Professor of Experimental Nephrology, University of Birmingham, UK SPRINGER SCIENCE+BUSINESS MEDIA, B.V.
Principles of Renal Physiology 4th Edition Principles of Renal Physiology 4th Edition Chris Lote Professor of Experimental Nephrology, University of Birmingham, UK SPRINGER SCIENCE+BUSINESS MEDIA, B.V.
Chapter 14 Blood Vessels, Blood Flow and Pressure Exam Study Questions
 Chapter 14 Blood Vessels, Blood Flow and Pressure Exam Study Questions 14.1 Physical Law Governing Blood Flow and Blood Pressure 1. How do you calculate flow rate? 2. What is the driving force of blood
Chapter 14 Blood Vessels, Blood Flow and Pressure Exam Study Questions 14.1 Physical Law Governing Blood Flow and Blood Pressure 1. How do you calculate flow rate? 2. What is the driving force of blood
Urinary System Organization. Urinary System Organization. The Kidneys. The Components of the Urinary System
 Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
Regulation of Body Fluids: Na + and Water Linda Costanzo, Ph.D.
 Regulation of Body Fluids: Na + and Water Linda Costanzo, Ph.D. OBJECTIVES: After studying this lecture, the student should understand: 1. Why body sodium content determines ECF volume and the relationships
Regulation of Body Fluids: Na + and Water Linda Costanzo, Ph.D. OBJECTIVES: After studying this lecture, the student should understand: 1. Why body sodium content determines ECF volume and the relationships
Regulation of fluid and electrolytes balance
 Regulation of fluid and electrolytes balance Three Compartment Fluid Compartments Intracellular = Cytoplasmic (inside cells) Extracellular compartment is subdivided into Interstitial = Intercellular +
Regulation of fluid and electrolytes balance Three Compartment Fluid Compartments Intracellular = Cytoplasmic (inside cells) Extracellular compartment is subdivided into Interstitial = Intercellular +
Question 1: Solution 1: Question 2: Question 3: Question 4: Class X The Excretory System Biology
 A. MULTIPLE CHOICE TYPE: (select the most appropriate option in each case) Book Name: Selina Concise Question 1: Excretion primarily involves (a) removal of all byproducts during catabolism (b) removal
A. MULTIPLE CHOICE TYPE: (select the most appropriate option in each case) Book Name: Selina Concise Question 1: Excretion primarily involves (a) removal of all byproducts during catabolism (b) removal
describe the location of the kidneys relative to the vertebral column:
 Basic A & P II Dr. L. Bacha Chapter Outline (Martini & Nath 2010) list the three major functions of the urinary system: by examining Fig. 24-1, list the organs of the urinary system: describe the location
Basic A & P II Dr. L. Bacha Chapter Outline (Martini & Nath 2010) list the three major functions of the urinary system: by examining Fig. 24-1, list the organs of the urinary system: describe the location
Urinary System. consists of the kidneys, ureters, urinary bladder and urethra
 Urinary System 1 Urinary System consists of the kidneys, ureters, urinary bladder and urethra 2 Location of Kidneys The kidneys which are positioned retroperitoneally lie on either side of the vertebral
Urinary System 1 Urinary System consists of the kidneys, ureters, urinary bladder and urethra 2 Location of Kidneys The kidneys which are positioned retroperitoneally lie on either side of the vertebral
BIOLOGY - CLUTCH CH.44 - OSMOREGULATION AND EXCRETION.
 !! www.clutchprep.com Osmoregulation regulation of solute balance and water loss to maintain homeostasis of water content Excretion process of eliminating waste from the body, like nitrogenous waste Kidney
!! www.clutchprep.com Osmoregulation regulation of solute balance and water loss to maintain homeostasis of water content Excretion process of eliminating waste from the body, like nitrogenous waste Kidney
April 08, biology 2201 ch 11.3 excretion.notebook. Biology The Excretory System. Apr 13 9:14 PM EXCRETORY SYSTEM.
 Biology 2201 11.3 The Excretory System EXCRETORY SYSTEM 1 Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid base concentrations and metabolite concentrations
Biology 2201 11.3 The Excretory System EXCRETORY SYSTEM 1 Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid base concentrations and metabolite concentrations
19. RENAL PHYSIOLOGY ROLE OF THE URINARY SYSTEM THE URINARY SYSTEM. Components and function. V BS 122 Physiology II 151 Class of 2011
 19. RENAL PHYSIOLOGY THE URINARY SYSTEM Components and function The urinary system is composed of two kidneys, the functionally filtering apparatus, which connect through two tubular structures called
19. RENAL PHYSIOLOGY THE URINARY SYSTEM Components and function The urinary system is composed of two kidneys, the functionally filtering apparatus, which connect through two tubular structures called
BCH 450 Biochemistry of Specialized Tissues
 BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
BBSG 503, 2009 Section 11: Systems Biology
 BBSG 503, 2009 Section 11: Systems Biology Section Director: W.K. Samson, Ph.D. Classes: April 6-May 1 Study Day: April 30 Progress Exam: May 1 Faculty: W.K. Samson, Ph.D. C-207A 977-8677 samsonwk@slu.edu
BBSG 503, 2009 Section 11: Systems Biology Section Director: W.K. Samson, Ph.D. Classes: April 6-May 1 Study Day: April 30 Progress Exam: May 1 Faculty: W.K. Samson, Ph.D. C-207A 977-8677 samsonwk@slu.edu
Studies on the Mechanism of Sodium Excretion during Drug-induced Vasodilatation in the Dog
 Studies on the Mechanism of Sodium Excretion during Drug-induced Vasodilatation in the Dog STEPHEN Z. FADEM, GUILLERMO HERNANDEZ-LLAMAS, RAM V. PATAK, STEVEN G. ROSENBLATT, MEYER D. LIFSCHITZ, and JAY
Studies on the Mechanism of Sodium Excretion during Drug-induced Vasodilatation in the Dog STEPHEN Z. FADEM, GUILLERMO HERNANDEZ-LLAMAS, RAM V. PATAK, STEVEN G. ROSENBLATT, MEYER D. LIFSCHITZ, and JAY
November 30, 2016 & URINE FORMATION
 & URINE FORMATION REVIEW! Urinary/Renal System 200 litres of blood are filtered daily by the kidneys Usable material: reabsorbed back into blood Waste: drained into the bladder away from the heart to the
& URINE FORMATION REVIEW! Urinary/Renal System 200 litres of blood are filtered daily by the kidneys Usable material: reabsorbed back into blood Waste: drained into the bladder away from the heart to the
Human Anatomy and Physiology - Problem Drill 23: The Urinary System, Fluid, Electrolyte and Acid-Base Balance
 Human Anatomy and Physiology - Problem Drill 23: The Urinary System, Fluid, Electrolyte and Acid-Base Balance Question No. 1 of 10 Which of the following statements about the functions of the urinary system
Human Anatomy and Physiology - Problem Drill 23: The Urinary System, Fluid, Electrolyte and Acid-Base Balance Question No. 1 of 10 Which of the following statements about the functions of the urinary system
Renal Regulation of Sodium and Volume. Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM
 Renal Regulation of Sodium and Volume Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM Maintaining Volume Plasma water and sodium (Na + ) are regulated independently - you are already familiar
Renal Regulation of Sodium and Volume Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM Maintaining Volume Plasma water and sodium (Na + ) are regulated independently - you are already familiar
1. Anatomy / Vascularisation. 2. Urine concentration. 3. Axial heterogeneity of some segments
 Lise BANKIR 1. Anatomy / Vascularisation 2. Urine concentration 3. Axial heterogeneity of some segments Rat kidney. Arterial filling with Microfil silicone rubber Alcian Blue staining Filling of arterial
Lise BANKIR 1. Anatomy / Vascularisation 2. Urine concentration 3. Axial heterogeneity of some segments Rat kidney. Arterial filling with Microfil silicone rubber Alcian Blue staining Filling of arterial
Mechanism: 1- waterretention from the last part of the nephron which increases blood volume, venous return EDV, stroke volume and cardiac output.
 Blood pressure regulators: 1- Short term regulation:nervous system Occurs Within secondsof the change in BP (they are short term because after a while (2-3 days) they adapt/reset the new blood pressure
Blood pressure regulators: 1- Short term regulation:nervous system Occurs Within secondsof the change in BP (they are short term because after a while (2-3 days) they adapt/reset the new blood pressure
renoprotection therapy goals 208, 209
 Subject Index Aldosterone, plasminogen activator inhibitor-1 induction 163, 164, 168 Aminopeptidases angiotensin II processing 64 66, 214 diabetic expression 214, 215 Angiotensin I intrarenal compartmentalization
Subject Index Aldosterone, plasminogen activator inhibitor-1 induction 163, 164, 168 Aminopeptidases angiotensin II processing 64 66, 214 diabetic expression 214, 215 Angiotensin I intrarenal compartmentalization
Chapter 44. Osmoregulation and Excretion
 Chapter 44 Osmoregulation and Excretion Overview: A Balancing Act Physiological systems of animals operate in a fluid environment Relative concentrations of water and solutes must be maintained within
Chapter 44 Osmoregulation and Excretion Overview: A Balancing Act Physiological systems of animals operate in a fluid environment Relative concentrations of water and solutes must be maintained within
RENAL PHYSIOLOGY DR.CHARUSHILA RUKADIKAR ASSISTANT PROFESSOR PHYSIOLOGY
 RENAL PHYSIOLOGY DR.CHARUSHILA RUKADIKAR ASSISTANT PROFESSOR PHYSIOLOGY GROSS ANATOMY Location *Bean-shaped *Retroperitoneal *At level of T12 L1 vertebrae. *The right kidney lies slightly inferior to left
RENAL PHYSIOLOGY DR.CHARUSHILA RUKADIKAR ASSISTANT PROFESSOR PHYSIOLOGY GROSS ANATOMY Location *Bean-shaped *Retroperitoneal *At level of T12 L1 vertebrae. *The right kidney lies slightly inferior to left
THE EFFECTS OF AN ANGIOTENSIN BLOCKER (SARALASIN) ON KIDNEY FUNCTION IN DEHYDRATED SHEEP
 Quarterly Journal of Experimental Physiology (1982) 67, 97-103 Printed in Great Britain THE EFFECTS OF AN ANGIOTENSIN BLOCKER (SARALASIN) ON KIDNEY FUNCTION IN DEHYDRATED SHEEP NANCY E. YESBERG, MYRNA
Quarterly Journal of Experimental Physiology (1982) 67, 97-103 Printed in Great Britain THE EFFECTS OF AN ANGIOTENSIN BLOCKER (SARALASIN) ON KIDNEY FUNCTION IN DEHYDRATED SHEEP NANCY E. YESBERG, MYRNA
28/04/2013 LEARNING OUTCOME C13 URINARY SYSTEM STUDENT ACHIEVEMENT INDICATORS STUDENT ACHIEVEMENT INDICATORS URINARY SYSTEM & EXCRETION
 LEARNING OUTCOME C13 Analyse the functional interrelationships of the structures of the urinary system Learning Outcome C13 URINARY SYSTEM STUDENT ACHIEVEMENT INDICATORS Students who have fully met this
LEARNING OUTCOME C13 Analyse the functional interrelationships of the structures of the urinary system Learning Outcome C13 URINARY SYSTEM STUDENT ACHIEVEMENT INDICATORS Students who have fully met this
Chapter 17: Urinary System
 Introduction Chapter 17: Urinary System Organs of the Urinary System REFERENCE FIGURE 17.1 2 kidneys filters the blood 2 ureters transport urine from the kidneys to the urinary bladder Urinary bladder
Introduction Chapter 17: Urinary System Organs of the Urinary System REFERENCE FIGURE 17.1 2 kidneys filters the blood 2 ureters transport urine from the kidneys to the urinary bladder Urinary bladder
