A STUDY OF THE ACTION OF ANGIOTENSIN II ON PERFUSION THROUGH THE CORTEX AND PAPILLA OF THE RAT KIDNEY
|
|
|
- Kerry Flynn
- 5 years ago
- Views:
Transcription
1 Experimental Physiology (1991) 76, Printed in Great Britain A STUDY OF THE ACTION OF ANGIOTENSIN II ON PERFUSION THROUGH THE CORTEX AND PAPILLA OF THE RAT KIDNEY CHUNLONG HUANG*, GERARD DAVIS AND EDWARD J. JOHNS Department of Physiology, The Medical School, Birmingham B15 2TT (MANUSCRIPT RECEIVED 31 JANUARY 1991, ACCEPTED 18 MARCH 1991) SUMMARY The effect of angiotensin IL on blood pressure and perfusion of blood through the cortex and papilla regions of the kidney was determined in pentobarbitone-anaesthetized rats which were subjected to laser-doppler flowmetry to estimate regional renal haemodynamics. Angiotensin II was infused at 10, 45 and 150 ng (kg body weight-1 min-m) which caused dose-related increases in blood pressure of 3, 12 and 24 %, respectively, and decreases in cortical perfusion of 9, 15 and 24 %, respectively. Papillary perfusion did not change at any dose of angiotensin II. This pattern and magnitude of responses to angiotensin II in blood pressure, cortical and papillary perfusions was essentially unaffected (a) following blockade of cyclo-oxygenase activity with indomethacin (1 3 mg kg-' plus 2 mg kg-' h-1), (b) during infusion of a bradykinin antagonist, at 1 3 ug minm, (c) when renal perfusion pressure was regulated at control levels and (d) following Methylene Blue administration to inhibit potential endothelial-derived relaxing factor production. By contrast, infusion of phenylephrine at 5, 10 and 20,ug kg-1 min-' caused dose-related increases in blood pressure and decreases in both cortical and papillary perfusions reaching some 28, 7 and 17 % respectively at the highest dose of phenylephrine used. These results showed that both cortex and papilla were sensitive to vasoconstrictor agents. They are compatible with the suggestion that angiotensin II regulates cortical but not papillary perfusion in the kidney, and that these responses do not depend on prostaglandin, bradykinin, renal perfusion pressure or endothelium-derived relaxing factor. INTRODUCTION The vasculature of the kidney varies markedly in anatomy and architecture between cortex, medulla and papilla and as a result may be differentially regulated by neural and humoral factors. The major proportion of total renal blood flow perfuses the cortex, where filtration, bulk reabsorption and secretion occur. Some % of blood flow reaches the deeper regions of the medulla and passes into the papilla and this appears to be involved in the maintenance of the high osmotic gradients necessary for the concentration of urine (Jamison & Kriz, 1982). At the middle and outer cortical glomeruli, the efferent arterioles quickly break up into the peritubular capillaries surrounding the convoluted tubular portions of the nephron (Zimmerhackl, Robertson & Jamison, 1985). The situation is different at the juxtamedullary glomeruli, in so far as the wide muscular efferent arteriole immediately turns and enters the medulla where it divides to form up to thirty descending vasa recta. These vasa recta vessels penetrate to varying levels within the medulla with only a few of the larger diameter descending to reach the tip of the papilla (Pallone, Robertson & Jamison, 1990). Measurement of regional blood flow in the cortex, medulla and papillary regions of the kidney is notoriously difficult and each approach is open to criticism (Chou, Porush & * Present address: Biology Department, Tianjin Normal University, Tianjin, People's Republic of China.
2 788 C. HUANG, G. DAVIS AND E. J. JOHNS Faubert, 1990). The techniques that have been applied are an accumulation of radiolabelled markers, which only offer an estimate of perfusion, and the videomicroscopic approach which analyses in detail flow through individual vasa recta vessels in the papilla. Recently, laser-doppler flowmeters have been developed and applied to the measurement of regional haemodynamics in the kidney, and Smits, Roman & Lombard (1986) and Roman & Smits (1986) have validated its use against conventional methodologies in both the renal cortex and papilla. One factor which is importantly involved in the regulation of renal haemodynamics is angiotensin II. At the whole-kidney level angiotensin II can reduce total renal blood flow, but it is also involved in a subtle way in the regulation of glomerular filtration rate by means of a differential effect on pre- and post-glomerular resistances (Johns, 1989). There is a general consensus that under normal conditions angiotensin II exerts a tonic influence on perfusion of the medulla and papilla, as when its action is blocked by converting enzyme inhibitors or receptor blockers perfusion in these regions increases (Pallone et al. 1990). By contrast, a preliminary report by Davis & Johns (1990) demonstrated that although systemically administered angiotensin II reduced perfusion of the cortex it had no effect on papillary perfusion. This phenomenon was examined further by assessing the potential role of other systems which are active within the kidney at the level of the microvasculature. METHODS Young male Wistar rats, weighing g (mean +s.e.m.), were anaesthetized (60 mg kg-' sodium pentobarbitone i.p. plus 6 mg kg-1 h-' i.v.) and cannulae were placed in the left jugular vein, for infusion of normal saline and drugs, and the right carotid artery, for blood pressure measurements (Statham P231D linked to a Grass model 7 polygraph). In group IV, (see below) blood pressure was measured from a femoral arterial cannula. The left kidney was exposed via an abdominal incision, cleared of peripheral fat, its artery, vein and ureter freed, and placed in a plastic holder to expose its dorsal surface. The ureter was sectioned and dissected towards the renal hilus to expose the papilla. Laser-Doppler perfusion was measured using a Perimed PF3 (Stockholm, Sweden) and a PF303 probe (Stockholm, Sweden) of 1 mm diameter. The laser-doppler flowmeter was calibrated such that one perfusion unit was equivalent to 10 mv. Perfusion measured in this way represents the product of the velocity of moving blood cells and the concentration of moving blood cells (CMBC) in the volume of tissue under the probe. Thus, the velocity is measured as the magnitude of the frequency shift whilst the intensity of the signal is proportional to the number of red cells moving within the tissue being illuminated. CMBC approximates to the haematocrit beneath the probe and with the PF3 flowmeter this component can be extracted from the perfusion signal and is expressed as volts (Nilsson, 1990). Six to eight measurements of 1-2 min duration were made at different sites over the cortex and one or two measurements were made over the papilla, and the average values were calculated. An intravenous infusion of normal saline was started at a rate of 2 ml h-' immediately after the venous cannula had been inserted, and was continued throughout the experiment. The initial measurements began 1 h after exposure of the papilla. One of the following experimental protocols was then conducted. Protocols Group I (n = 7): angiotensin II alone. In this group of animals baseline measurements of cortical and papillary perfusion were taken before and after an infusion of angiotensin II (Sigma, Dorset) at 10, 45 and 150 ng kg-1 min-1 i.v. in random order. Experimental measurements of regional flows were taken once they had stabilized at the new levels induced by angiotensin II, which took approximately 15 min. Group II (n = 8): angiotensin II during indomethacin infusion. The initial measurements of cortical
3 ANGIOTENSIN II ANO RENAL HAEMODYNAMICS 789 Table 1. The effect of angiotensin II (ng kg-1 min- ) on blood pressure and renal cortical and papillaril haemodynamics [Angiotensin II] A (n = 7) Systemic blood pressure (mmhg) Cortical perfusion Papillary perfusion Cortical CMBC (V) Papillary CMBC (V) Saline * ** 115+3*** * 160+9** 144+9*** ( * l1 * Indomethacin (1 3 mg kg-'+ 2 mg kg-' h-') [Angiotensin II] B (n= 8) Saline Control Systemic blood pressure (mmhg) Cortical perfusion Papillary perfusion Cortical CMBC (V) Papillary CMBC (V) * * *** *** *** *** * * [Angiotensin II] C (n = 7) Saline 45 Renal Perfusion pressure (mmhg) Cortical perfusion Papillary perfusion Cortical CMBC (V) Papillary CMBC (V) Control RPP 150 Uncontrolled RPP *** ** *** 120+8** * ** n = number of animals tested. * P < 0 05; P < 001; *** P < RPP = renal perfusion pressure. and papillary perfusion were taken to establish basal levels, and an intravenous infusion of the cyclooxygenase inhibitor indomethacin (Sigma, Dorset) was continued to the end of the experiment. Indomethacin (I mg ml-') was placed in normal saline and sodium bicarbonate (1-5 mg) was added slowly until the indomethacin dissolved. A bolus dose of 1 3 mg kg-1 in a volume of 0-25 ml was given followed by a steady infusion of 2 mg kg-' h-1, and the experiment was begun 30 min later. Measurements of cortical and papillary perfusion were taken before, during and after an infusion of angiotensin II at 10, 45 and 150 ng kg-1 min' given in random order. Group III (n = 4): angiotensin II during bradykinin antagonist infusion. After measurement of basal levels of renal haemodynamics the bradykinin antagonist (D-Arg, Hyp3, Thi5 8, D-Phe')-bradykinin
4 790 C. HUANG, G. DAVIS AND E. J. JOHNS (Peninsula Laboratories Europe Ltd, Merseyside) was infused at a dose of 1 39,tg min-' and continued to the end of the experiment. Measurements of cortical and papillary perfusion were taken 30 min after the start of antagonist infusion, and during an infusion of angiotensin II at 45 and 150 ng kg-' min-m. Bradykinin (Peninsula Laboratories Europe Ltd, Merseyside) was given as an intravenous bolus of 333 ng in a volume of 0 2 ml before the antagonist infusion, and at the end of the experiment whilst the antagonist was still being infused. Group IV (n = 7): angiotensin II during controlled renal perfusion pressure. In this group of animals, the arterial cannula was placed in the right femoral artery and a silk ligature was loosely placed around the aorta rostral to the left renal artery and attached to a screw device such that the aorta could be constricted, thereby reducing pressure at the kidney (Davis & Johns, 1991). After the initial measurements, angiotensin II was infused at 45 and then at 150 ng kg-' min-', and as blood pressure began to rise under the influence of angiotensin II, the suture around the aorta was tightened such that perfusion pressure was returned to its value immediately prior to administration of the drug, and was kept at that level for the duration of the angiotensin infusion. The ligature was then released during angiotensin II infusion at 150 ng kg-1 min-' to allow perfusion pressure to rise, and measurements were then taken at the higher pressure. The infusion of angiotensin II was stopped and baseline measurements were taken once blood pressure had stabilized. Group V (n = 4): angiotensin II and Methylene Blue. In this group, angiotensin II was only infused at 150 ng kg-1 min-'. Initially the renal haemodynamic responses to angiotensin II were obtained. Methylene Blue (Sigma Chemical Company, Dorset), an inhibitor of the endothelium-dependent relaxing factor, was given intravenously as a bolus of 1 15 x 10-3 M in 0-2 ml and measurements were taken 20 min later. Two further doses of Methylene Blue (1-15 x 10-3 M in 0-2 ml) were given i.v. with measurements being taken 20 min after each dose. Group VI (n = 7): phenylephrine administration. The infusion and measurement protocol in this group was similar to that in group I. Phenylephrine hydrochloride (Boots Company plc, Nottingham), an ax1-adrenergic receptor agonist, was infused at 5, 10 or 20,ug kg-1 min-1 for 20 min at increasing doses and once a stable blood pressure had been achieved, papillary and cortical perfusion measurements were undertaken. Statistics The mean values+ standard errors of the means are presented and the absolute and percentage changes quoted are the means of individual values obtained from each group. The effect of indomethacin, bradykinin or Methylene Blue on baseline levels was calculated as the difference between the value obtained immediately before application of the compound and that obtained after its administration. The response to angiotensin II and phenylephrine was taken as the difference between the mean values recorded before and after administration with that obtained during administration of these vasoactive agents. Regression analysis was carried out to give the gradient and correlation values. Differences were taken as significant at the 5 % level using Student's t test and analysis of variance (Fastat Software and Apple Macintosh) as appropriate. RESULTS The initial study was undertaken to define the blood pressure and renal haemodynamic responses to angiotensin II given intravenously (Table 1 A). Angiotensin II caused doserelated increases in blood pressure with a gradient of mmhg (ng angiotensin II (kg body weight)-' min-')-' (P < 0 001). This was associated with a graded reduction in perfusion within the cortex which reached 24% at the highest dose of angiotensin II, with a gradient of PU (ng angiotensin II kg-' min-m') (P < 0 001). Cortical CMBC was only slightly, but significantly (P < 0 05) reduced at the two highest rates of infusion. By contrast, angiotensin II had no effect on papillary perfusion or CMBC. The potential role of prostaglandins in these responses was determined by blocking their production with the cyclo-oxygenase inhibitor indomethacin, and the results are presented
5 ANGIOTENSIN II AND RENAL HAEMODYNAMICS Change in systemic 30 blood pressure (mmhg) 20 Lg [Angiotensin II] (ng kg-1 min-1) -20-Vx Change in cortical perfusion IVA Change in papillary l'v ' 1 perfusion -lo0l &Irj Fig. 1. The absolute responses in systemic blood pressure, cortical and papillary perfusion (expressed as perfusion units, PU) in two groups of rats given increasing doses of angiotensin II (10, 45 and 150 ng kg-1 min-') in the absence (C1; group I rats) and presence of indomethacin (1 3 mg kg-1 plus 2 0 mg kg-1 h-i; 0; group II rats). Error bars show S.E.M. in Table 1 B. Administration of indomethacin (I 3 mg kg-' plus 2 mg kg-1 h-1) had no effect on blood pressure or cortical perfusion but caused a significant (P < 0O05) reduction in papillary perfusion of PU. Neither cortical nor papillary CMBC were affected. Under these conditions, angiotensin II infusion caused graded increases in blood pressure, with a gradient of mmhg (ng angiotensin II kg-' min-')-' (P < ), reaching mmhg at the highest dose, and decreases in cortical perfusion, having a gradient of PU (ng angiotensin II kg-' min-')-' (P < 0-001) with a maximum decrease of 29 %. The gradient of cortical perfusion to the angiotensin II in the presence of indomethacin was significantly (P < 005) greater than that obtained when indomethacin was not present. However, papillary perfusion was not changed by any dose of angiotensin II. Infusion of angiotensin II decreased cortical and increased papillary CMBC (P < 0 05) only when given at the highest dose. A comparison of the absolute changes in blood pressure, cortical and papillary perfusions in the absence and in the presence of indomethacin is given in Fig. 1. A second small study was performed in which a bradykinin antagonist was given intravenously, and the data are presented in Table 2A. A bolus dose of bradykinin (333 ng) was given and this caused a transient fall in blood pressure with a peak response of mmhg. A similar dose of bradykinin given at the end of the period of bradykinin antagonist application decreased blood pressure by only mmhg, an almost 50 % inhibition of the response. Administration of the bradykinin antagonist had no effect on
6 792 Table 2. C. HUANG. G. DAVIS AND E. J. JOHNS The effect ofangiotensin II (ng kg-1 min- ) and phenylephrine on bloodpressure and renal cortical and papillary haemodynamics Bradykinin antagonist (1 39 pg min-1) [Angiotensin II] A (n = 7) Saline Control Systemic blood pressure (mmhg) Cortical perfusion Papillary perfusion Cortical CMBC (V) Papillary CMBC (V) B (n = 4) Systemic blood pressure (mmhg) Cortical perfusion Papillary perfusion Cortical CMBC (V) Papillary CMBC (V) Saline ** 138+4** ** ** * * Methylene Blue 3-45 x 10-3 M [Angiotensin II] ** Phenylephrine (aug kg-1 min-1) C (n = 7) Saline * * Systemic blood pressure (mmhg) Cortical perfusion Papillary perfusion Cortical CMBC (V) Papillary CMBC (V) ** 117+6** 127+7** * ** ** * ** Abbreviations, see Table 1. blood pressure, cortical perfusion or cortical or papillary CMBC, but caused a significant (P < 0 05) reduction in papillary perfusion of PU. Only two doses of angiotensin II were given, 45 and 150 ng kg-1 min-1, and these increased blood pressure significantly (both P < 001) by and 28+3 mmhg respectively, and significantly (both P < 0-01) decreased cortical perfusion by 12 % and 15 %/o respectively, while papillary perfusion was not changed. Under these conditions angiotensin II had no effect on the CMBC of either cortex or papilla. The blood pressure and renal haemodynamic responses in the absence and presence of bradykinin is given in Fig. 2. A further potential complicating factor was the rise in blood pressure during angiotensin II adminstration. Therefore, a study was undertaken in which perfusion pressure at the
7 ANGIOTENSIN II AND RENAL HAEMODYNAMICS 793 Change in systemic 30 - blood pressure (mmhg) ~~~~~~~~~ [Angiotensin II] (ng kg-1 min-) -10 Change in cortical t - perfusion _30 _ _1 10 Change in papillary perfusion 0 _10L Fig. 2. The absolute changes in systemic blood pressure, cortical and papillary perfusion (expressed as perfusion units, PU) in two groups of rats given two doses of angiotensin II, 45 and 150 ng kg-' min-m in the absence (D-; group I rats) and in the presence of bradykinin antagonist (1 39 lug min-';1; group III rats). kidney was regulated at constant levels, and the results are shown in Table 1 C. In this group of animals blood pressure was effectively regulated during both the 45 and 150 ng kg-1 min-1 angiotensin II infusions, but there were significant reductions in cortical perfusion of 13 and respectively, while papillary perfusion was not changed at either dose of angiotensin II. Papillary CMBC was not changed following administration of either dose of angiotensin II, although there was a significant reduction in cortical CMBC at the higher dose. When perfusion pressure at the kidney was allowed to rise to prevailing levels (from 96+4 to mmhg) by loosening the aortic constriction, cortical perfusion remained at its depressed level and there was a small, but not significant, increase in papillary perfusion, while cortical and papillary CMBC remained unchanged. These responses are illustrated in Fig. 3. The effect of blocking the effects of potential EDRF formation with Methylene Blue was studied in a small group of animals and the results are given in Table 2B. Only one dose of angiotensin II was given, 150 ng kg-1 min-'. Angiotensin II at 150 ng kg-1 min-1 increased blood pressure by mmhg (P < 0-05) and decreased cortical perfusion by 20 % (P < 0 01) but had no effect on either papillary perfusion or CMBC in either cortex or papilla. The average responses over each of the three doses of Methylene Blue were calculated. Administration of Methylene Blue itself had no effect on the basal levels of any of the measured variables and while the average responses over the three doses of
8 794 C. HUANG, G. DAVIS AND E. J. JOHNS Change in systemic 15 - blood pressure (mmhg) [Angiotensin II] (ng kg-l min-') C Change in cortical perfusion Change in papillary 0 perfusion _ L Fig. 3. The absolute changes in systemic blood pressure, cortical and papillary perfusion (expressed as perfusion units, PU) during angiotensin II infusion at 45 and 150 ng kg-' min-' during controlled renal perfusion pressure (O; group IV rats) and when renal perfusion pressure was allowed to rise to systemic levels during 150 ng kg-' min-m angiotensin II infusion (3). Methylene Blue for blood pressure were not significantly different from that obtained before the compound was given, the fall in cortical perfusion was significantly (P < 0 01) attenuated. In the presence of Methylene Blue, angiotensin II had no effect on papillary perfusion or CMBC in either cortex or papilla. A dose-response curve to phenylephrine was drawn up for blood pressure and renal haemodynamics and the results are presented in Table 2C. Phenylephrine, 5, 10 and 20,ug kg-1 min-', caused increases in blood pressure, giving a gradient of f13 mmhg (phenylephrine jtg kg-1 min-1)-1 (P < 0 01) with a rise of mmhg at the highest dose, and decreases in cortical perfusion with a gradient of PU (,ug phenylephrine kg-' min-1)-' (P < 0 01) with a maximum reduction of 7 %. It also caused a reduction in papillary perfusion, with a gradient of PU (,ug phenylephrine kg-' min-1)-' (P < 0 05) with a fall of 17 % at the highest dose of phenylephrine. Neither cortical nor papillary CMBC changed during the phenylephrine infusion. Figure 4 shows the absolute responses of these variables to phenylephrine.
9 ANGIOTENSIN II AND RENAL HAEMODYNAMICS Change in systemic 30 blood pressure (mmhg) 20 []T Fig Change in cortical -10 perfusion Change in papillary -20 perfusion _ [Phenylephrine] (ug kg-' min--) 0 - The absolute changes in systemic blood pressure, cortical and papillary perfusion (expressed as perfusion units, PU) during phenylephrine infusion at 5, 10 and 20,tg kg-1 min-1 (group VI rats). DISCUSSION In a previous report (Davis & Johns, 1990) we observed that vasopressin at doses which increased blood pressure decreased perfusion at both cortex and papilla, whereas angiotensin II, which caused similar dose-dependent increases in blood pressure, decreased cortical perfusion but had no effect on perfusion through the papilla. The intention of the present study was to explore potential mechanisms for this differential action of angiotensin II on regional haemodynamics. A laser-doppler flowmeter was used, as its applicability for use in the kidney has been rigorously validated at the renal cortex by Smits et al. (1986) using electromagnetic flowmeter measurements, and at the renal papilla by Roman & Smits (1986) using 51Cr-labelled erythrocyte accumulation in this region. The control levels for cortical and papillary perfusions in the various groups of animals reported herein are closely comparable to those obtained in previous work by ourselves (Davis & Johns, 1990; Huang, Davis & Johns, 1991) and others (Roman, Cowley, Garcia-Estan & Lombard, 1988). The experimental design was such that angiotensin II was given systemically at rates which caused small to modest (approximately 25 mmhg), increases in blood pressure. There were concomitant dose-related decreases in cortical perfusion, reaching a maximum of about 25 % with the largest dose of angiotensin II, which was very similar to the
10 796 C. HUANG, G. DAVIS AND E. J. JOHNS magnitude and pattern of that reported previously (Davis & Johns, 1990). The most striking observation was that, over the whole of this dose range of angiotensin II, papillary perfusion did not change. Comparable observations were reported by Cupples, Sakai & Marsh, (1988), using dual slit videomicroscopy in the rat, who found that systemic infusion of angiotensin II at doses which reduced total renal blood flow by 25 % (equivalent to 63 ng kg-1 min-1) did not alter vasa recta red cell velocity, and a preliminary report by Mathson, Raff & Roman (1988) using laser-doppler flowmetry found that angiotensin II infusion into the rat at 20 ng kg-1 min-1 failed to affect papillary perfusion. Together these two reports, one of which used a different methodology, provide supportive evidence for our own findings that angiotensin II has a minimal effect on perfusion of blood through the papilla, at least in the rat. By contrast, Faubert, Chou & Porush (1987), using the dog, found that direct intra-renal perfusion of angiotensin II, which had no effect on total renal blood flow or glomerular filtration rate, decreased [125I]albumin accumulation by 66%, while Carmines & Navar (1989), using videomicroscopic measurements in the rat with topical application of angiotensin II, demonstrated both afferent and efferent arteriolar constriction of juxtamedullary glomeruli. The reason for these conflicting responses is not clear but may reside in the different nature of the experimental measurements employed and the high local concentrations of angiotensin II achieved by these workers. An attempt has been made to define the mechanism(s) which could underlie the inability of angiotensin II to influence papillary haemodynamics, possibly by the generation of a vasodilator compound locally. Cortical constriction could have generated prostaglandin production (Cooper, Shaffer & Malik, 1985), could have stimulated renal bradykinin production (Chou et al. 1990) or involved the production of endothelium-derived relaxing factor (Furchgott & Vanhoutte, 1989), each of which could have acted on vessels regulating papillary perfusion to overcome any potential vasoconstrictor action of angiotensin II. Administration of blocking doses of indomethacin (Roman, Kauker, Terragno & Wong, 1978), a bradykinin antagonist (Roman, Kaldunski, Scicli & Carretero, 1988) or Methylene Blue (Martin, Villani, Jothianandan & Furchgott, 1985) caused small reductions or no change, respectively, in basal levels of papillary perfusion, but had no effect on either the cortical or papillary perfusion responses to angiotensin II. The conclusion from these studies was that neither prostaglandins, bradykinin nor endothelium-derived relaxing factors were involved in mediating the angiotensin II responses in perfusion at the cortex and papilla. Administration of angiotensin II was associated with rises in blood pressure which itself would have called into play autoregulatory myogenic responses of the renal vasculature which could have overridden a potential vasoconstrictor action to decrease papillary perfusion. However, the magnitude of the angiotensin II-induced decreases in cortical perfusion when renal perfusion pressure was servo controlled was identical to that observed in the group in which renal perfusion pressure rose with systemic pressure. Further, cortical perfusion remained unchanged when the aortic constriction was released and the pressure at the kidney was allowed to increase to systemic levels during infusion of the highest dose of angiotensin II. Once more, papillary perfusion was unaffected by angiotensin II and was in no way dependent upon whether perfusion pressure at the kidney was controlled at preangiotensin II levels or allowed to rise to the elevated systemic pressure. A final study was undertaken to investigate whether papillary perfusion was sensitive to other vasoconstrictor agents. The a1-adrenoceptor agonist phenylephrine was used, as this is known to cause vasoconstriction in many vascular beds. Phenylephrine induced doserelated increases in blood pressure and decreases in both cortical and papillary perfusions.
11 ANGIOTENSIN II AND RENAL HAEMODYNAMICS 797 These responses clearly demonstrated that these two regions of the kidney vasculature were sensitive to vasoconstrictor peptides. Indeed, this supports our previous observation with another peptide vasoconstrictor, vasopressin (Huang et al. 1991) in which both cortical and papillary perfusions were sensitive to and decreased by vasopressin. This study aimed to describe the action of vasopressor doses of angiotensin II on perfusion in the renal cortex and papilla. Whereas angiotensin II caused dose-related reductions in cortical perfusion, papillary perfusion did not change. This selective pattern of renal responses to angiotensin II did not appear to depend on the generation of prostaglandins, bradykinin or endothelium-derived relaxing factor or the level of renal perfusion pressure. This pattern of haemodynamic changes appeared to be a characteristic of angiotensin II, as vasoactive agents such as phenylephrine and vasopressin appeared equally effective at both cortex and papilla. The mechanisms underlying this selective action of angiotensin II on renal haemodynamics remains to be elucidated. The financial support of Roche Products Limited is gratefully acknowledged. C. H. is a scholar funded by the Chinese Education Commission. REFERENCES CARMINES, P. K. & NAVAR, L. G. (1989). Disparate effects of Ca channel blockade on afferent and efferent arteriolar responses to angiotensin II. American Journal of Physiology 256, F CHOU, S.-Y., PORUSH, J. G. & FAUBERT, P. F. (1990). Renal medullary circulation: hormonal control. Kidney International 37, COOPER, C. L., SHAFFER, J. E. & MALIK, K. U. (1985). Mechanism of action of angiotensin II and bradykinin on prostaglandin synthesis and vascular tone in the isolated rat kidney. Effect of Ca++ antagonists and calmodulin inhibitors. Circulation Research 56, CUPPLES, W. A., SAKAI, T. & MARSH, D. J. (1988). Angiotensin II and prostaglandins in control of vasa recta blood flow. American Journal of Physiology 254, F DAVIS, G. & JoHNs, E. J. (1990). The effects of angiotensin II and vasopressin on renal haemodynamics. Journal of Medical Engineering and Technology 14, DAVIS, G. & JOHNs, E. J. (1991). Effect of somatic nerve stimulation on the kidney in intact, vagotomized and carotid sinus-denervated rats. Journal of Physiology 432, FAUBERT, P. F., CHOU, S.-Y. & PORUSH, J. G. (1987). Regulation of papillary plasma flow by angiotensin II. Kidney International 32, FURCHGOTT, R. F. & VANHOUTTE, P. M. (1989). Endothelium derived relaxing and contracting factors. FASEB Journal 3, HUANG, C., DAVIS, G. & JOHNs, E. J. (1991). An investigation into the influence of vasopressin on perfusion of the cortex and papilla of the rat kidney. Journal of Experimental Physiology 76, JAMISON, R. L. & KRIZ, W. (1982). Urinary Concentrating Mechanism: Structure and Function. Oxford University Press, New York and Oxford. JOHNS, E. J. (1989). Role of angiotensin and the sympathetic nervous system in the control of renal function. Journal of Hypertension 7, MARTIN, W., VILLANI, G. M., JOTHIANANDAN, D. & FURCHGOTT, R. F. (1985). Selective blockade of endothelium-dependent and glyceryl trinitrate-induced relaxation by haemoglobin and by methylene blue in the rabbit aorta. Journal of Pharmacology and Experimental Therapeutics 232, MATHSON, D. L., RAFF, H. & ROMAN, R. J. (1988). Effect of captopril and angiotensin II (AII) on cortical and papillary blood flow in rats. FASEB Journal 2, A5674. NILSSON, G. E. (1990). Perimed's LDV flowmeter. In Laser-Doppler Blood Flowmetry, chap. 4, ed. SHEPHERD, A. P. & OBERG, T. A., pp Kluwer Academic Publishers, Boston, Dordrecht & London. PALLONE, T. L., ROBERTSON, C. R. & JAMISON, R. L. (1990). Renal medullary microcirculation. Physiological Reviews 70, EPH 76 28E8 7
12 798 C. HUANG, G. DAVIS AND E. J. JOHNS ROMAN, R. G., COWLEY, A. W., GARCIA-ESTAN, J. & LOMBARD, J. H. (1988). Pressure diuresis in volume expanded rats. Hypertension 12, ROMAN, R. J., KALDUNSKI, M. L., SCICLI, A. G. & CARRETERO, 0. A. (1988). Influence of kinins and angiotensin II on the regulation of papillary blood flow. Anmerican Journal of Phy'siologv 255, F ROMAN, R. J., KAUKER, M. L., TERRAGNO, N. A. & WONG, P. Y.-K. (1978). Inhibition of renal prostaglandin synthesis and metabolism by indomethacin in rats. Proceedings of the Society for Experimental Biology and Medicine 159, ROMAN, R. J. & SMITS, G. J. (1986). Laser-Doppler determination of papillary blood flow in young and adult rats. American Journal of Physiology 251, F SMITS, G. J., ROMAN, R. J. & LOMBARD, J. H. (1986). Evaluation of laser-doppler flowmetry as a measure of tissue blood flow. Journal of Applied Physiology 61, ZIMMERHACKL, B., ROBERTSON, C. R. & JAMISON, R. L. (1985). The microcirculation of the renal medulla. Circulation Research 57,
The effects of angiotensin II on blood perfusion in the rat renal papilla
 9325 Journal of Physiology (1999), 519.1, pp. 273 278 273 The effects of angiotensin II on blood perfusion in the rat renal papilla L. L. Walker, A. A. J. Rajaratne, J. R. Blair-West and P. J. Harris Department
9325 Journal of Physiology (1999), 519.1, pp. 273 278 273 The effects of angiotensin II on blood perfusion in the rat renal papilla L. L. Walker, A. A. J. Rajaratne, J. R. Blair-West and P. J. Harris Department
Chapter 23. The Nephron. (functional unit of the kidney
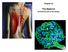 Chapter 23 The Nephron (functional unit of the kidney Renal capsule The Nephron Renal cortex Nephron Collecting duct Efferent arteriole Afferent arteriole (a) Renal corpuscle: Glomerular capsule Glomerulus
Chapter 23 The Nephron (functional unit of the kidney Renal capsule The Nephron Renal cortex Nephron Collecting duct Efferent arteriole Afferent arteriole (a) Renal corpuscle: Glomerular capsule Glomerulus
Outline the functional anatomy, and the physiological factors, that determine oxygen delivery to the renal medulla.
 2011-2-21 Outline the functional anatomy, and the physiological factors, that determine oxygen delivery to the renal medulla. Oxygen delivery = Blood flow CaO 2 Where Blood flow determined by (arterial
2011-2-21 Outline the functional anatomy, and the physiological factors, that determine oxygen delivery to the renal medulla. Oxygen delivery = Blood flow CaO 2 Where Blood flow determined by (arterial
Excretory Lecture Test Questions Set 1
 Excretory Lecture Test Questions Set 1 1. The separation and ejection of metabolic wastes, usually in aqueous solution, is: a. reabsorption b. secretion c. filtration d. excretion e. endocrinology 2. Besides
Excretory Lecture Test Questions Set 1 1. The separation and ejection of metabolic wastes, usually in aqueous solution, is: a. reabsorption b. secretion c. filtration d. excretion e. endocrinology 2. Besides
RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015
 RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015 1. In which abdominal cavity do the kidneys lie? a) Peritoneum. b) Anteperitoneal. c) Retroperitoneal. d) Parietal peritoneal 2. What is the
RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015 1. In which abdominal cavity do the kidneys lie? a) Peritoneum. b) Anteperitoneal. c) Retroperitoneal. d) Parietal peritoneal 2. What is the
Lab Activity 31. Anatomy of the Urinary System. Portland Community College BI 233
 Lab Activity 31 Anatomy of the Urinary System Portland Community College BI 233 Urinary System Organs Kidneys Urinary bladder: provides a temporary storage reservoir for urine Paired ureters: transport
Lab Activity 31 Anatomy of the Urinary System Portland Community College BI 233 Urinary System Organs Kidneys Urinary bladder: provides a temporary storage reservoir for urine Paired ureters: transport
Figure 26.1 An Introduction to the Urinary System
 Chapter 26 Figure 26.1 An Introduction to the Urinary System Components of the Urinary System Kidney Produces urine Ureter Transports urine toward the urinary bladder Urinary Bladder Temporarily stores
Chapter 26 Figure 26.1 An Introduction to the Urinary System Components of the Urinary System Kidney Produces urine Ureter Transports urine toward the urinary bladder Urinary Bladder Temporarily stores
19. RENAL PHYSIOLOGY ROLE OF THE URINARY SYSTEM THE URINARY SYSTEM. Components and function. V BS 122 Physiology II 151 Class of 2011
 19. RENAL PHYSIOLOGY THE URINARY SYSTEM Components and function The urinary system is composed of two kidneys, the functionally filtering apparatus, which connect through two tubular structures called
19. RENAL PHYSIOLOGY THE URINARY SYSTEM Components and function The urinary system is composed of two kidneys, the functionally filtering apparatus, which connect through two tubular structures called
Human Urogenital System 26-1
 Human Urogenital System 26-1 Urogenital System Functions Filtering of blood, Removal of wastes and metabolites Regulation of blood volume and composition concentration of blood solutes ph of extracellular
Human Urogenital System 26-1 Urogenital System Functions Filtering of blood, Removal of wastes and metabolites Regulation of blood volume and composition concentration of blood solutes ph of extracellular
Kidney Functions Removal of toxins, metabolic wastes, and excess ions from the blood Regulation of blood volume, chemical composition, and ph
 The Urinary System Urinary System Organs Kidneys are major excretory organs Urinary bladder is the temporary storage reservoir for urine Ureters transport urine from the kidneys to the bladder Urethra
The Urinary System Urinary System Organs Kidneys are major excretory organs Urinary bladder is the temporary storage reservoir for urine Ureters transport urine from the kidneys to the bladder Urethra
modulating the tubuloglomerular feed-back mechanism in the canine kidney; Sciences Center, 4200 East Ninth Avenue, Denver, CO 80262, U.S.A.
 J. Physiol. (1986), 380, pp. 35-43 35 With 3 text-figures Printed in Great Britain RENAL VASOCONSTRICTOR RESPONSE TO HYPERTONIC SALINE IN THE DOG: EFFECTS OF PROSTAGLANDINS, INDOMETHACIN AND THEOPHYLLINE
J. Physiol. (1986), 380, pp. 35-43 35 With 3 text-figures Printed in Great Britain RENAL VASOCONSTRICTOR RESPONSE TO HYPERTONIC SALINE IN THE DOG: EFFECTS OF PROSTAGLANDINS, INDOMETHACIN AND THEOPHYLLINE
MAJOR FUNCTIONS OF THE KIDNEY
 MAJOR FUNCTIONS OF THE KIDNEY REGULATION OF BODY FLUID VOLUME REGULATION OF OSMOTIC BALANCE REGULATION OF ELECTROLYTE COMPOSITION REGULATION OF ACID-BASE BALANCE REGULATION OF BLOOD PRESSURE ERYTHROPOIESIS
MAJOR FUNCTIONS OF THE KIDNEY REGULATION OF BODY FLUID VOLUME REGULATION OF OSMOTIC BALANCE REGULATION OF ELECTROLYTE COMPOSITION REGULATION OF ACID-BASE BALANCE REGULATION OF BLOOD PRESSURE ERYTHROPOIESIS
Urinary System Organization. Urinary System Organization. The Kidneys. The Components of the Urinary System
 Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion.
 The Kidney Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion. The kidney has 6 roles in the maintenance of homeostasis. 6 Main Functions 1. Ion Balance
The Kidney Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion. The kidney has 6 roles in the maintenance of homeostasis. 6 Main Functions 1. Ion Balance
Urinary System and Fluid Balance. Urine Production
 Urinary System and Fluid Balance Name Pd Date Urine Production The three processes critical to the formation of urine are filtration, reabsorption, and secretion. Match these terms with the correct statement
Urinary System and Fluid Balance Name Pd Date Urine Production The three processes critical to the formation of urine are filtration, reabsorption, and secretion. Match these terms with the correct statement
A. Incorrect! The urinary system is involved in the regulation of blood ph. B. Correct! The urinary system is involved in the synthesis of vitamin D.
 Human Anatomy - Problem Drill 22: The Urinary System Question No. 1 of 10 1. Which of the following statements about the functions of the urinary system is not correct? Question #01 (A) The urinary system
Human Anatomy - Problem Drill 22: The Urinary System Question No. 1 of 10 1. Which of the following statements about the functions of the urinary system is not correct? Question #01 (A) The urinary system
CHAPTER 25 URINARY. Urinary system. Kidneys 2 Ureters 2 Urinary Bladder 1 Urethra 1. functions
 CHAPTER 25 URINARY Kidneys 2 Ureters 2 Urinary Bladder 1 Urethra 1 fluid waste elimination secretion of wastes control blood volume and BP control blood ph electrolyte levels RBC levels hormone production
CHAPTER 25 URINARY Kidneys 2 Ureters 2 Urinary Bladder 1 Urethra 1 fluid waste elimination secretion of wastes control blood volume and BP control blood ph electrolyte levels RBC levels hormone production
Urinary System. consists of the kidneys, ureters, urinary bladder and urethra
 Urinary System 1 Urinary System consists of the kidneys, ureters, urinary bladder and urethra 2 Location of Kidneys The kidneys which are positioned retroperitoneally lie on either side of the vertebral
Urinary System 1 Urinary System consists of the kidneys, ureters, urinary bladder and urethra 2 Location of Kidneys The kidneys which are positioned retroperitoneally lie on either side of the vertebral
Basic Functions of the Kidneys
 Dr. Adelina Vlad Basic Functions of the Kidneys Eliminate plasma METABOLIC WASTE PRODUCTS and FOREIGN COMPOUNDS The kidney are the primary means for eliminating metabolic waste products (urea, creatinine,
Dr. Adelina Vlad Basic Functions of the Kidneys Eliminate plasma METABOLIC WASTE PRODUCTS and FOREIGN COMPOUNDS The kidney are the primary means for eliminating metabolic waste products (urea, creatinine,
Chapter 25 The Urinary System
 Chapter 25 The Urinary System 10/30/2013 MDufilho 1 Kidney Functions Removal of toxins, metabolic wastes, and excess ions from the blood Regulation of blood volume, chemical composition, and ph Gluconeogenesis
Chapter 25 The Urinary System 10/30/2013 MDufilho 1 Kidney Functions Removal of toxins, metabolic wastes, and excess ions from the blood Regulation of blood volume, chemical composition, and ph Gluconeogenesis
Chapter 14 Blood Vessels, Blood Flow and Pressure Exam Study Questions
 Chapter 14 Blood Vessels, Blood Flow and Pressure Exam Study Questions 14.1 Physical Law Governing Blood Flow and Blood Pressure 1. How do you calculate flow rate? 2. What is the driving force of blood
Chapter 14 Blood Vessels, Blood Flow and Pressure Exam Study Questions 14.1 Physical Law Governing Blood Flow and Blood Pressure 1. How do you calculate flow rate? 2. What is the driving force of blood
The ability of the kidneys to regulate extracellular fluid volume by altering sodium
 REGULATION OF EXTRACELLULAR FLUID VOLUME BY INTEGRATED CONTROL OF SODIUM EXCRETION Joey P. Granger Department of Physiology and Biophysics, University of Mississippi Medical Center, Jackson, Mississippi
REGULATION OF EXTRACELLULAR FLUID VOLUME BY INTEGRATED CONTROL OF SODIUM EXCRETION Joey P. Granger Department of Physiology and Biophysics, University of Mississippi Medical Center, Jackson, Mississippi
Human Anatomy and Physiology - Problem Drill 23: The Urinary System, Fluid, Electrolyte and Acid-Base Balance
 Human Anatomy and Physiology - Problem Drill 23: The Urinary System, Fluid, Electrolyte and Acid-Base Balance Question No. 1 of 10 Which of the following statements about the functions of the urinary system
Human Anatomy and Physiology - Problem Drill 23: The Urinary System, Fluid, Electrolyte and Acid-Base Balance Question No. 1 of 10 Which of the following statements about the functions of the urinary system
Body fluid volume is small (~5L (blood + serum)) Composition can change rapidly e.g. due to increase in metabolic rate
 Renal physiology The kidneys Allow us to live on dry land. Body fluid volume is small (~5L (blood + serum)) Composition can change rapidly e.g. due to increase in metabolic rate Kidneys maintain composition
Renal physiology The kidneys Allow us to live on dry land. Body fluid volume is small (~5L (blood + serum)) Composition can change rapidly e.g. due to increase in metabolic rate Kidneys maintain composition
describe the location of the kidneys relative to the vertebral column:
 Basic A & P II Dr. L. Bacha Chapter Outline (Martini & Nath 2010) list the three major functions of the urinary system: by examining Fig. 24-1, list the organs of the urinary system: describe the location
Basic A & P II Dr. L. Bacha Chapter Outline (Martini & Nath 2010) list the three major functions of the urinary system: by examining Fig. 24-1, list the organs of the urinary system: describe the location
RENAL PHYSIOLOGY DR.CHARUSHILA RUKADIKAR ASSISTANT PROFESSOR PHYSIOLOGY
 RENAL PHYSIOLOGY DR.CHARUSHILA RUKADIKAR ASSISTANT PROFESSOR PHYSIOLOGY GROSS ANATOMY Location *Bean-shaped *Retroperitoneal *At level of T12 L1 vertebrae. *The right kidney lies slightly inferior to left
RENAL PHYSIOLOGY DR.CHARUSHILA RUKADIKAR ASSISTANT PROFESSOR PHYSIOLOGY GROSS ANATOMY Location *Bean-shaped *Retroperitoneal *At level of T12 L1 vertebrae. *The right kidney lies slightly inferior to left
Sunday, July 17, 2011 URINARY SYSTEM
 URINARY SYSTEM URINARY SYSTEM Let s take a look at the anatomy first! KIDNEYS: are complex reprocessing centers where blood is filtered through and waste products are removed. Wastes and extra water become
URINARY SYSTEM URINARY SYSTEM Let s take a look at the anatomy first! KIDNEYS: are complex reprocessing centers where blood is filtered through and waste products are removed. Wastes and extra water become
Urinary System. BSC 2086 A & P 2 Professor Tcherina Duncombe Palm Beach State College
 Urinary System BSC 2086 A & P 2 Professor Tcherina Duncombe Palm Beach State College Filter plasma, separate and eliminate wastes Functions Regulate blood volume and pressure Regulate osmolarity of body
Urinary System BSC 2086 A & P 2 Professor Tcherina Duncombe Palm Beach State College Filter plasma, separate and eliminate wastes Functions Regulate blood volume and pressure Regulate osmolarity of body
Urinary system. Urinary system
 INTRODUCTION. Several organs system Produce urine and excrete it from the body Maintenance of homeostasis. Components. two kidneys, produce urine; two ureters, carry urine to single urinary bladder for
INTRODUCTION. Several organs system Produce urine and excrete it from the body Maintenance of homeostasis. Components. two kidneys, produce urine; two ureters, carry urine to single urinary bladder for
Urinary System Laboratory
 Urinary System Laboratory 1 Adrenal gland Organs of The Urinary System Renal artery and vein Kidney Ureter Urinary bladder Figure 26.1 2 Urethra Functions of the urinary system organs: Urethra expels urine
Urinary System Laboratory 1 Adrenal gland Organs of The Urinary System Renal artery and vein Kidney Ureter Urinary bladder Figure 26.1 2 Urethra Functions of the urinary system organs: Urethra expels urine
Chapter 1 RENAL HAEMODYNAMICS AND GLOMERULAR FILTRATION
 3 Chapter 1 RENAL HAEMODYNAMICS AND GLOMERULAR FILTRATION David Shirley, Giovambattista Capasso and Robert Unwin The kidney has three homeostatic functions that can broadly be described as excretory, regulatory
3 Chapter 1 RENAL HAEMODYNAMICS AND GLOMERULAR FILTRATION David Shirley, Giovambattista Capasso and Robert Unwin The kidney has three homeostatic functions that can broadly be described as excretory, regulatory
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1
 BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
Regulation of Arterial Blood Pressure 2 George D. Ford, Ph.D.
 Regulation of Arterial Blood Pressure 2 George D. Ford, Ph.D. OBJECTIVES: 1. Describe the Central Nervous System Ischemic Response. 2. Describe chemical sensitivities of arterial and cardiopulmonary chemoreceptors,
Regulation of Arterial Blood Pressure 2 George D. Ford, Ph.D. OBJECTIVES: 1. Describe the Central Nervous System Ischemic Response. 2. Describe chemical sensitivities of arterial and cardiopulmonary chemoreceptors,
Glomerular Capillary Blood Pressure
 Glomerular Capillary Blood Pressure Fluid pressure exerted by blood within glomerular capillaries Depends on Contraction of the heart Resistance to blood flow offered by afferent and efferent arterioles
Glomerular Capillary Blood Pressure Fluid pressure exerted by blood within glomerular capillaries Depends on Contraction of the heart Resistance to blood flow offered by afferent and efferent arterioles
CONTROLLING THE INTERNAL ENVIRONMENT
 AP BIOLOGY ANIMAL FORM & FUNCTION ACTIVITY #5 NAME DATE HOUR CONTROLLING THE INTERNAL ENVIRONMENT KIDNEY AND NEPHRON NEPHRON FUNCTIONS Animal Form & Function Activity #5 page 1 NEPHRON STRUCTURE NEPHRON
AP BIOLOGY ANIMAL FORM & FUNCTION ACTIVITY #5 NAME DATE HOUR CONTROLLING THE INTERNAL ENVIRONMENT KIDNEY AND NEPHRON NEPHRON FUNCTIONS Animal Form & Function Activity #5 page 1 NEPHRON STRUCTURE NEPHRON
Copyright 2009 Pearson Education, Inc. Copyright 2009 Pearson Education, Inc. Figure 19-1c. Efferent arteriole. Juxtaglomerular apparatus
 /6/0 About this Chapter Functions of the Kidneys Anatomy of the urinary system Overview of kidney function Secretion Micturition Regulation of extracellular fluid volume and blood pressure Regulation of
/6/0 About this Chapter Functions of the Kidneys Anatomy of the urinary system Overview of kidney function Secretion Micturition Regulation of extracellular fluid volume and blood pressure Regulation of
Functions of the kidney
 Physiology of Urinary tract Kidney, Ureter, Urinary bladder Urethra Kidney function Excretion Physiology of volume regulation Functions of the kidney Excretion of dangerous substances endogenous (metabolites):
Physiology of Urinary tract Kidney, Ureter, Urinary bladder Urethra Kidney function Excretion Physiology of volume regulation Functions of the kidney Excretion of dangerous substances endogenous (metabolites):
BCH 450 Biochemistry of Specialized Tissues
 BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
Gonzalez, 1971; Mitchell, Kaufman & Iwamoto, 1983), resulting in an increased
 Journal of Physiology (1991), 432, pp. 573-584 573 With 2 figures Printed in Great Britain EFFECT OF SOMATIC NERVE STIMULATION ON THE KIDNEY IN INTACT, VAGOTOMIZED AND CAROTID SINUS-DENERVATED RATS BY
Journal of Physiology (1991), 432, pp. 573-584 573 With 2 figures Printed in Great Britain EFFECT OF SOMATIC NERVE STIMULATION ON THE KIDNEY IN INTACT, VAGOTOMIZED AND CAROTID SINUS-DENERVATED RATS BY
The Urinary System 15PART A. PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College
 PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Urinary System 15PART A Functions of the Urinary System Elimination of waste products Nitrogenous
PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Urinary System 15PART A Functions of the Urinary System Elimination of waste products Nitrogenous
Kidney and urine formation
 Kidney and urine formation Renal structure & function Urine formation Urinary y concentration and dilution Regulation of urine formation 1 Kidney and urine formation 1.Renal structure & function 1)General
Kidney and urine formation Renal structure & function Urine formation Urinary y concentration and dilution Regulation of urine formation 1 Kidney and urine formation 1.Renal structure & function 1)General
Cardiovascular Physiology
 Cardiovascular Physiology Lecture 1 objectives Explain the basic anatomy of the heart and its arrangement into 4 chambers. Appreciate that blood flows in series through the systemic and pulmonary circulations.
Cardiovascular Physiology Lecture 1 objectives Explain the basic anatomy of the heart and its arrangement into 4 chambers. Appreciate that blood flows in series through the systemic and pulmonary circulations.
Differential effect of angiotensin II on blood circulation in the renal medulla and cortex of anaesthetised rats
 Journal of Physiology (2002), 538.1, pp. 159 166 DOI: 10.1013/jphysiol.2001.012921 The Physiological Society 2002 www.jphysiol.org Differential effect of angiotensin II on blood circulation in the renal
Journal of Physiology (2002), 538.1, pp. 159 166 DOI: 10.1013/jphysiol.2001.012921 The Physiological Society 2002 www.jphysiol.org Differential effect of angiotensin II on blood circulation in the renal
BIOH122 Human Biological Science 2
 BIOH122 Human Biological Science 2 Session 16 Urinary System 1 The Kidneys Bioscience Department Endeavour College of Natural Health endeavour.edu.au Session Plan o Functions of Urinary system o The Kidneys:
BIOH122 Human Biological Science 2 Session 16 Urinary System 1 The Kidneys Bioscience Department Endeavour College of Natural Health endeavour.edu.au Session Plan o Functions of Urinary system o The Kidneys:
Chapter 17: Urinary System
 Introduction Chapter 17: Urinary System Organs of the Urinary System REFERENCE FIGURE 17.1 2 kidneys filters the blood 2 ureters transport urine from the kidneys to the urinary bladder Urinary bladder
Introduction Chapter 17: Urinary System Organs of the Urinary System REFERENCE FIGURE 17.1 2 kidneys filters the blood 2 ureters transport urine from the kidneys to the urinary bladder Urinary bladder
Urine Formation by the Kidneys: I. Glomerular Filtration, Renal Blood Flow and Their Control.
 Urine Formation by the Kidneys: I. Glomerular Filtration, Renal Blood Flow and Their Control. Chapter 26 Yanal A Shafagoj. MD. PhD Lecture-1 Introduction 31/3/2015 1 University of Jordan Faculty of Medicine
Urine Formation by the Kidneys: I. Glomerular Filtration, Renal Blood Flow and Their Control. Chapter 26 Yanal A Shafagoj. MD. PhD Lecture-1 Introduction 31/3/2015 1 University of Jordan Faculty of Medicine
General Anatomy of Urinary System
 General Anatomy of Urinary System URINARY SYSTEM ORGANS Kidneys (2) Ureters (2) Urinary bladder Urethra KIDNEY FUNCTIONS Control blood volume and composition KIDNEY FUNCTIONS Filter blood plasma, eliminate
General Anatomy of Urinary System URINARY SYSTEM ORGANS Kidneys (2) Ureters (2) Urinary bladder Urethra KIDNEY FUNCTIONS Control blood volume and composition KIDNEY FUNCTIONS Filter blood plasma, eliminate
The Urinary System Pearson Education, Inc.
 26 The Urinary System Introduction The urinary system does more than just get rid of liquid waste. It also: Regulates plasma ion concentrations Regulates blood volume and blood pressure Stabilizes blood
26 The Urinary System Introduction The urinary system does more than just get rid of liquid waste. It also: Regulates plasma ion concentrations Regulates blood volume and blood pressure Stabilizes blood
2) This is a Point and Click question. You must click on the required structure.
 Class: A&P2-1 Description: Test: Excretory Test Points: 144 Test Number: 28379 Printed: 31-March-10 12:03 1) This is a Point and Click question. You must click on the required structure. Click on the Bowman's
Class: A&P2-1 Description: Test: Excretory Test Points: 144 Test Number: 28379 Printed: 31-March-10 12:03 1) This is a Point and Click question. You must click on the required structure. Click on the Bowman's
BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1
 BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1 1. a. Proximal tubule. b. Proximal tubule. c. Glomerular endothelial fenestrae, filtration slits between podocytes of Bowman's capsule.
BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1 1. a. Proximal tubule. b. Proximal tubule. c. Glomerular endothelial fenestrae, filtration slits between podocytes of Bowman's capsule.
Pharmacology - Problem Drill 11: Vasoactive Agents
 Pharmacology - Problem Drill 11: Vasoactive Agents Question No. 1 of 10 1. Vascular smooth muscle contraction is triggered by a rise in. Question #01 (A) Luminal calcium (B) Extracellular calcium (C) Intracellular
Pharmacology - Problem Drill 11: Vasoactive Agents Question No. 1 of 10 1. Vascular smooth muscle contraction is triggered by a rise in. Question #01 (A) Luminal calcium (B) Extracellular calcium (C) Intracellular
Lab 19 The Urinary System
 Lab 19 The Urinary System Laboratory Objectives Identify and describe the micro- and macroscopic anatomy of the kidney. Track the blood flow in and out of the kidney. Compare blood, glomerular filtrate,
Lab 19 The Urinary System Laboratory Objectives Identify and describe the micro- and macroscopic anatomy of the kidney. Track the blood flow in and out of the kidney. Compare blood, glomerular filtrate,
RENAL PHYSIOLOGY WESTMEAD PRIMARY EXAM
 RENAL PHYSIOLOGY WESTMEAD PRIMARY EXAM RENAL PHYSIOLOGY - ANATOMY Glomerulus + renal tubule Each kidney has 1.3 million nephrons Cortical nephrons (85%) have shorter Loop of Henle than Juxtamedullary nephrons
RENAL PHYSIOLOGY WESTMEAD PRIMARY EXAM RENAL PHYSIOLOGY - ANATOMY Glomerulus + renal tubule Each kidney has 1.3 million nephrons Cortical nephrons (85%) have shorter Loop of Henle than Juxtamedullary nephrons
BIOL2030 Human A & P II -- Exam 6
 BIOL2030 Human A & P II -- Exam 6 Name: 1. The kidney functions in A. preventing blood loss. C. synthesis of vitamin E. E. making ADH. B. white blood cell production. D. excretion of metabolic wastes.
BIOL2030 Human A & P II -- Exam 6 Name: 1. The kidney functions in A. preventing blood loss. C. synthesis of vitamin E. E. making ADH. B. white blood cell production. D. excretion of metabolic wastes.
Chapter 24: The Urinary System
 Chapter 24: The Urinary System Overview of kidney functions n Regulation of blood ionic composition n Regulation of blood ph n Regulation of blood volume n Regulation of blood pressure n Maintenance of
Chapter 24: The Urinary System Overview of kidney functions n Regulation of blood ionic composition n Regulation of blood ph n Regulation of blood volume n Regulation of blood pressure n Maintenance of
The Urinary System PART A
 15 The Urinary System PART A PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB Functions of the Urinary
15 The Urinary System PART A PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB Functions of the Urinary
PHYSIOLOGY WEEK 9. vascular physiology - ED Primary Exam Teaching
 PHYSIOLOGY WEEK 9 vascular physiology - ED Primary Exam Teaching CONCEPTS OF BLOOD FLOW Vascular distensibility - when pressure in the arterioles is increased, this dilates the arterioles and therefore
PHYSIOLOGY WEEK 9 vascular physiology - ED Primary Exam Teaching CONCEPTS OF BLOOD FLOW Vascular distensibility - when pressure in the arterioles is increased, this dilates the arterioles and therefore
CARDIOVASCULAR SYSTEM
 CARDIOVASCULAR SYSTEM 1. Resting membrane potential of the ventricular myocardium is: A. -55 to-65mv B. --65 to-75mv C. -75 to-85mv D. -85 to-95 mv E. -95 to-105mv 2. Regarding myocardial contraction:
CARDIOVASCULAR SYSTEM 1. Resting membrane potential of the ventricular myocardium is: A. -55 to-65mv B. --65 to-75mv C. -75 to-85mv D. -85 to-95 mv E. -95 to-105mv 2. Regarding myocardial contraction:
Blood Pressure Regulation. Slides 9-12 Mean Arterial Pressure (MAP) = 1/3 systolic pressure + 2/3 diastolic pressure
 Sheet physiology(18) Sunday 24-November Blood Pressure Regulation Slides 9-12 Mean Arterial Pressure (MAP) = 1/3 systolic pressure + 2/3 diastolic pressure MAP= Diastolic Pressure+1/3 Pulse Pressure CO=MAP/TPR
Sheet physiology(18) Sunday 24-November Blood Pressure Regulation Slides 9-12 Mean Arterial Pressure (MAP) = 1/3 systolic pressure + 2/3 diastolic pressure MAP= Diastolic Pressure+1/3 Pulse Pressure CO=MAP/TPR
It is well recognized that the kidney plays a fundamental
 337 Renal Medullary Captopril Delivery Lowers Blood Pressure in Spontaneously Hypertensive Rats Shanhong Lu, David L. Mattson, Allen W. Cowley, Jr Abstract We examined the contribution of renal medullary
337 Renal Medullary Captopril Delivery Lowers Blood Pressure in Spontaneously Hypertensive Rats Shanhong Lu, David L. Mattson, Allen W. Cowley, Jr Abstract We examined the contribution of renal medullary
The Excretory System. Biology 20
 The Excretory System Biology 20 Introduction Follow along on page 376 What dangers exist if your body is unable to regulate the fluid balance of your tissues? What challenged would the body have to respond
The Excretory System Biology 20 Introduction Follow along on page 376 What dangers exist if your body is unable to regulate the fluid balance of your tissues? What challenged would the body have to respond
Chapter 25: Urinary System
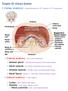 Chapter 25: Urinary System I. Kidney anatomy: retroperitoneal from 12 th thoracic to 3 rd lumbar area A. External anatomy: hilus is the indentation 1. Adrenal gland: in the fat at the superior end of each
Chapter 25: Urinary System I. Kidney anatomy: retroperitoneal from 12 th thoracic to 3 rd lumbar area A. External anatomy: hilus is the indentation 1. Adrenal gland: in the fat at the superior end of each
Angiotensin II and prostaglandins in control of vasa recta blood flow
 Angiotensin II and prostaglandins in control of vasa recta blood flow W. A. CUPPLES, T. SAKAI, AND D. J. MARSH Department of Physiology and Biophysics, University of Southern California, Los Angeles, California
Angiotensin II and prostaglandins in control of vasa recta blood flow W. A. CUPPLES, T. SAKAI, AND D. J. MARSH Department of Physiology and Biophysics, University of Southern California, Los Angeles, California
Urinary Physiology. Chapter 17 Outline. Kidney Function. Chapter 17
 Urinary Physiology Chapter 17 Chapter 17 Outline Structure and Function of the Kidney Glomerular Filtration Reabsorption of Salt and Water Renal Plasma Clearance Renal Control of Electrolyte and Acid-Base
Urinary Physiology Chapter 17 Chapter 17 Outline Structure and Function of the Kidney Glomerular Filtration Reabsorption of Salt and Water Renal Plasma Clearance Renal Control of Electrolyte and Acid-Base
SHORT ANSWER. Write the word or phrase that best completes each statement or answers the question.
 Exam Name SHORT ANSWER. Write the word or phrase that best completes each statement or answers the question. Figure 25.1 Using Figure 25.1, match the following: 1) Glomerulus. 2) Afferent arteriole. 3)
Exam Name SHORT ANSWER. Write the word or phrase that best completes each statement or answers the question. Figure 25.1 Using Figure 25.1, match the following: 1) Glomerulus. 2) Afferent arteriole. 3)
Renal Quiz - June 22, 21001
 Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
1. Urinary System, General
 S T U D Y G U I D E 16 1. Urinary System, General a. Label the figure by placing the numbers of the structures in the spaces by the correct labels. 7 Aorta 6 Kidney 8 Ureter 2 Inferior vena cava 4 Renal
S T U D Y G U I D E 16 1. Urinary System, General a. Label the figure by placing the numbers of the structures in the spaces by the correct labels. 7 Aorta 6 Kidney 8 Ureter 2 Inferior vena cava 4 Renal
Class XI Chapter 19 Excretory Products and their Elimination Biology
 Class XI Chapter 19 Excretory Products and their Elimination Biology Question 1: Define Glomerular Filtration Rate (GFR) Glomerular filtration rate is the amount of glomerular filtrate formed in all the
Class XI Chapter 19 Excretory Products and their Elimination Biology Question 1: Define Glomerular Filtration Rate (GFR) Glomerular filtration rate is the amount of glomerular filtrate formed in all the
Outline Urinary System. Urinary System and Excretion. Urine. Urinary System. I. Function II. Organs of the urinary system
 Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
A&P 2 CANALE T H E U R I N A R Y S Y S T E M
 A&P 2 CANALE T H E U R I N A R Y S Y S T E M URINARY SYSTEM CONTRIBUTION TO HOMEOSTASIS Regulates body water levels Excess water taken in is excreted Output varies from 2-1/2 liter/day to 1 liter/hour
A&P 2 CANALE T H E U R I N A R Y S Y S T E M URINARY SYSTEM CONTRIBUTION TO HOMEOSTASIS Regulates body water levels Excess water taken in is excreted Output varies from 2-1/2 liter/day to 1 liter/hour
Kidney Structure. Renal Lobe = renal pyramid & overlying cortex. Renal Lobule = medullary ray & surrounding cortical labryinth.
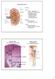 Kidney Structure Capsule Hilum ureter renal pelvis major and minor calyxes renal and vein segmental arteries interlobar arteries arcuate arteries interlobular arteries Medulla renal pyramids cortical/renal
Kidney Structure Capsule Hilum ureter renal pelvis major and minor calyxes renal and vein segmental arteries interlobar arteries arcuate arteries interlobular arteries Medulla renal pyramids cortical/renal
Osmotic Regulation and the Urinary System. Chapter 50
 Osmotic Regulation and the Urinary System Chapter 50 Challenge Questions Indicate the areas of the nephron that the following hormones target, and describe when and how the hormones elicit their actions.
Osmotic Regulation and the Urinary System Chapter 50 Challenge Questions Indicate the areas of the nephron that the following hormones target, and describe when and how the hormones elicit their actions.
Copyright 2010 Pearson Education, Inc. Urinary System
 Urinary System What are the organs that comprise the urinary system? Urinary System Organs Kidneys Urinary bladder Ureters Urethra Hepatic veins (cut) Esophagus (cut) Inferior vena cava Adrenal gland Aorta
Urinary System What are the organs that comprise the urinary system? Urinary System Organs Kidneys Urinary bladder Ureters Urethra Hepatic veins (cut) Esophagus (cut) Inferior vena cava Adrenal gland Aorta
Blood pressure. Formation of the blood pressure: Blood pressure. Formation of the blood pressure 5/1/12
 Blood pressure Blood pressure Dr Badri Paudel www.badripaudel.com Ø Blood pressure means the force exerted by the blood against the vessel wall Ø ( or the force exerted by the blood against any unit area
Blood pressure Blood pressure Dr Badri Paudel www.badripaudel.com Ø Blood pressure means the force exerted by the blood against the vessel wall Ø ( or the force exerted by the blood against any unit area
Histology Urinary system
 Histology Urinary system Urinary system Composed of two kidneys, two ureters, the urinary bladder, and the urethra, the urinary system plays a critical role in: 1- Blood filtration,(filtration of cellular
Histology Urinary system Urinary system Composed of two kidneys, two ureters, the urinary bladder, and the urethra, the urinary system plays a critical role in: 1- Blood filtration,(filtration of cellular
Blood Pressure Regulation 2. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Urinary System kidneys, ureters, bladder & urethra
 Urinary System kidneys, ureters, bladder & urethra Kidney Function Filters blood removes waste products conserves salts, glucose, proteins, nutrients and water Produces urine Endocrine functions regulates
Urinary System kidneys, ureters, bladder & urethra Kidney Function Filters blood removes waste products conserves salts, glucose, proteins, nutrients and water Produces urine Endocrine functions regulates
Chapter 26: Urinary System By: Eddie Tribiana and Piers Frieden
 Chapter 26: Urinary System By: Eddie Tribiana and Piers Frieden The urinary system is important because it performs vital excretory functions Takes blood from renal arteries into the kidney to filtrate
Chapter 26: Urinary System By: Eddie Tribiana and Piers Frieden The urinary system is important because it performs vital excretory functions Takes blood from renal arteries into the kidney to filtrate
AP2, Lab 7 - THE URINARY SYSTEM
 AP2, Lab 7 - THE URINARY SYSTEM I. SYSTEM COMPONENTS (Figs. 25.1 25.4) KIDNEYS Each kidney contains approx. 1,000,000 tubular NEPHRONS which produce FILTRATE from the plasma and then add to or take from
AP2, Lab 7 - THE URINARY SYSTEM I. SYSTEM COMPONENTS (Figs. 25.1 25.4) KIDNEYS Each kidney contains approx. 1,000,000 tubular NEPHRONS which produce FILTRATE from the plasma and then add to or take from
Running head: NEPHRON 1. The nephron the functional unit of the kidney. [Student Name] [Name of Institute] Author Note
![Running head: NEPHRON 1. The nephron the functional unit of the kidney. [Student Name] [Name of Institute] Author Note Running head: NEPHRON 1. The nephron the functional unit of the kidney. [Student Name] [Name of Institute] Author Note](/thumbs/77/75431210.jpg) Running head: NEPHRON 1 The nephron the functional unit of the kidney [Student Name] [Name of Institute] Author Note NEPHRON 2 The nephron the functional unit of the kidney The kidney is an important excretory
Running head: NEPHRON 1 The nephron the functional unit of the kidney [Student Name] [Name of Institute] Author Note NEPHRON 2 The nephron the functional unit of the kidney The kidney is an important excretory
RENAL PHYSIOLOGY. Physiology Unit 4
 RENAL PHYSIOLOGY Physiology Unit 4 Renal Functions Primary Function is to regulate the chemistry of plasma through urine formation Additional Functions Regulate concentration of waste products Regulate
RENAL PHYSIOLOGY Physiology Unit 4 Renal Functions Primary Function is to regulate the chemistry of plasma through urine formation Additional Functions Regulate concentration of waste products Regulate
URINARY SYSTEM CHAPTER 28 I ANATOMY OF THE URINARY SYSTEM. Student Name
 Student Name CHAPTER 28 URINARY SYSTEM L iving produces wastes. Wherever people live or work or play, wastes accumulate. To keep these areas healthy, there must be a method of disposing of these wastes
Student Name CHAPTER 28 URINARY SYSTEM L iving produces wastes. Wherever people live or work or play, wastes accumulate. To keep these areas healthy, there must be a method of disposing of these wastes
The Urinary System. Medical Assisting Third Edition. Booth, Whicker, Wyman, Pugh, Thompson The McGraw-Hill Companies, Inc. All rights reserved
 The Urinary System PowerPoint presentation to accompany: Medical Assisting Third Edition Booth, Whicker, Wyman, Pugh, Thompson 30-2 Learning Outcomes 30.1 Describe the structure, location, and functions
The Urinary System PowerPoint presentation to accompany: Medical Assisting Third Edition Booth, Whicker, Wyman, Pugh, Thompson 30-2 Learning Outcomes 30.1 Describe the structure, location, and functions
Diagram of the inner portions of the kidney
 Excretory and Endocrine functions of the kidney The kidneys are the main excretory organs which eliminate in the urine, most metabolites primarily those containing nitrogen such as ammonia, urea and creatinine.
Excretory and Endocrine functions of the kidney The kidneys are the main excretory organs which eliminate in the urine, most metabolites primarily those containing nitrogen such as ammonia, urea and creatinine.
The functions of the kidney:
 The functions of the kidney: After reading this lecture you should be able to.. 1. List the main functions of the kidney. 2. Know the basic physiological anatomy of the kidney and the nephron 3. Describe
The functions of the kidney: After reading this lecture you should be able to.. 1. List the main functions of the kidney. 2. Know the basic physiological anatomy of the kidney and the nephron 3. Describe
Impairment of pressure-natriuresis and renal autoregulation in ANG II-infused hypertensive rats
 Am J Physiol Renal Physiol 279: F319 F325, 2000. Impairment of pressure-natriuresis and renal autoregulation in ANG II-infused hypertensive rats CHI-TARNG WANG, SO YEON CHIN, AND L. GABRIEL NAVAR Department
Am J Physiol Renal Physiol 279: F319 F325, 2000. Impairment of pressure-natriuresis and renal autoregulation in ANG II-infused hypertensive rats CHI-TARNG WANG, SO YEON CHIN, AND L. GABRIEL NAVAR Department
Circulation. Blood Pressure and Antihypertensive Medications. Venous Return. Arterial flow. Regulation of Cardiac Output.
 Circulation Blood Pressure and Antihypertensive Medications Two systems Pulmonary (low pressure) Systemic (high pressure) Aorta 120 mmhg Large arteries 110 mmhg Arterioles 40 mmhg Arteriolar capillaries
Circulation Blood Pressure and Antihypertensive Medications Two systems Pulmonary (low pressure) Systemic (high pressure) Aorta 120 mmhg Large arteries 110 mmhg Arterioles 40 mmhg Arteriolar capillaries
Collin College. BIOL Anatomy & Physiology WEEK 12. Urinary System INTRODUCTION. Main functions of the kidneys are
 Collin College BIOL. 2402 Anatomy & Physiology WEEK 12 Urinary System 1 INTRODUCTION Main functions of the kidneys are regulate blood volume, water content regulate blood composition e..g. Na, Cl, K, ph
Collin College BIOL. 2402 Anatomy & Physiology WEEK 12 Urinary System 1 INTRODUCTION Main functions of the kidneys are regulate blood volume, water content regulate blood composition e..g. Na, Cl, K, ph
Blood Pressure Regulation -1
 CVS Physiology Lecture 18 Blood Pressure Regulation -1 Please study the previous sheet before studying this one, even if the first part in this sheet is revision. In the previous lecture we were talking
CVS Physiology Lecture 18 Blood Pressure Regulation -1 Please study the previous sheet before studying this one, even if the first part in this sheet is revision. In the previous lecture we were talking
URINARY SYSTEM. These organs lie posterior or inferior to the. (membrane).
 URINARY SYSTEM I. INTRODUCTION Each kidney is made up of about a million tiny tubules called nephrons. Each nephron individually filters the blood and makes urine and it does the job completely, from start
URINARY SYSTEM I. INTRODUCTION Each kidney is made up of about a million tiny tubules called nephrons. Each nephron individually filters the blood and makes urine and it does the job completely, from start
Cardiovascular System B L O O D V E S S E L S 2
 Cardiovascular System B L O O D V E S S E L S 2 Blood Pressure Main factors influencing blood pressure: Cardiac output (CO) Peripheral resistance (PR) Blood volume Peripheral resistance is a major factor
Cardiovascular System B L O O D V E S S E L S 2 Blood Pressure Main factors influencing blood pressure: Cardiac output (CO) Peripheral resistance (PR) Blood volume Peripheral resistance is a major factor
BIOH122 Human Biological Science 2
 BIOH122 Human Biological Science 2 Session 17 Urinary System 2 Glomerular Filtration Bioscience Department Endeavour College of Natural Health endeavour.edu.au Session Plan o Overview of Renal Physiology
BIOH122 Human Biological Science 2 Session 17 Urinary System 2 Glomerular Filtration Bioscience Department Endeavour College of Natural Health endeavour.edu.au Session Plan o Overview of Renal Physiology
Urinary System. Chapter 17 7/19/11. Introduction
 7/19/11 Chapter 17 Urinary System Introduction A. The urinary system consists of two kidneys that filter the blood, two ureters, a urinary bladder, and a urethra to convey waste substances to the outside.
7/19/11 Chapter 17 Urinary System Introduction A. The urinary system consists of two kidneys that filter the blood, two ureters, a urinary bladder, and a urethra to convey waste substances to the outside.
QUIZ/TEST REVIEW NOTES SECTION 1 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19 CHAPTER 19
![QUIZ/TEST REVIEW NOTES SECTION 1 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19 CHAPTER 19 QUIZ/TEST REVIEW NOTES SECTION 1 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19 CHAPTER 19](/thumbs/77/74887026.jpg) QUIZ/TEST REVIEW NOTES SECTION 1 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19 CHAPTER 19 Learning Objectives: Differentiate the following processes: filtration, reabsorption, secretion,
QUIZ/TEST REVIEW NOTES SECTION 1 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19 CHAPTER 19 Learning Objectives: Differentiate the following processes: filtration, reabsorption, secretion,
P215 Spring 2018: Renal Physiology Chapter 18: pp , Chapter 19: pp ,
 P215 Spring 2018: Renal Physiology Chapter 18: pp. 504-520, 525-527 Chapter 19: pp. 532-548, 553-560 I. Main Components of the Renal System 1. kidneys 2. ureters 3. urinary bladder 4. urethra 4 Major Functions
P215 Spring 2018: Renal Physiology Chapter 18: pp. 504-520, 525-527 Chapter 19: pp. 532-548, 553-560 I. Main Components of the Renal System 1. kidneys 2. ureters 3. urinary bladder 4. urethra 4 Major Functions
1. a)label the parts indicated above and give one function for structures Y and Z
 Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- renal cortex - X- renal medulla Y- renal pelvis collecting center of urine and then
Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- renal cortex - X- renal medulla Y- renal pelvis collecting center of urine and then
Nephron Function and Urine Formation. Ms. Kula December 1, 2014 Biology 30S
 Nephron Function and Urine Formation Ms. Kula December 1, 2014 Biology 30S The Role of the Nephron In order for the body to properly function and maintain homeostasis, the amount of dissolved substances
Nephron Function and Urine Formation Ms. Kula December 1, 2014 Biology 30S The Role of the Nephron In order for the body to properly function and maintain homeostasis, the amount of dissolved substances
Urinary System kidneys, ureters, bladder & urethra
 Urinary System kidneys, ureters, bladder & urethra Filters blood removes waste products conserves salts, glucose, proteins, nutrients and water Produces urine Kidney Function Endocrine functions regulates
Urinary System kidneys, ureters, bladder & urethra Filters blood removes waste products conserves salts, glucose, proteins, nutrients and water Produces urine Kidney Function Endocrine functions regulates
