Diagram of the inner portions of the kidney
|
|
|
- Kristin Rich
- 6 years ago
- Views:
Transcription
1 Excretory and Endocrine functions of the kidney The kidneys are the main excretory organs which eliminate in the urine, most metabolites primarily those containing nitrogen such as ammonia, urea and creatinine. The production and excretion of urine is termed diuresis. Therefore the major function of the kidney involves the elimination of degradable by products, toxic substance, excess water, salt and some drugs from the body. The kidney also maintains homeostasis by participating in the water-salt metabolism (eliminates excess salt & water) and also through osmoregulation. Hence, together with other mechanisms the kidney maintains the acid base balance of the body by modifying the rate of secretion of acid or alkaline phosphate when the blood becomes acidic or alkaline. The kidney also mediates the synthesis of a number of compounds and also eliminates these compound e.g. Hippuric acid which is a product of glycocol and benzoic acid and ammonia which is a product of deamination of amino acid. The kidney also functions in the secretion of the organic acids and bases including K + and H +. They are also involved in lipid protein, carbohydrate metabolism such as arginine metabolism, gluconeogenesis and peptide hydrolysis. The kidneys are also a source of hormones e.g. Angiotensin II, D hormones, prostaglandins and Erythropoietin. Erythropoietin, synthesized in the kidney, stimulates the production of red blood cells in the bone marrow and thus, regulates the oxygen carrying capacity of the blood. Therefore the kidney maintains relative homeostasis by regulating the osmotic pressure, acid base balance, synthesis, secretion and excretion of metabolic by products. Diagram of the inner portions of the kidney Summary of the functions of the kidney
2 Conservation of water, fixed cations, glucose and amino acids. This implies the return to the body fluids of the amount of the substances required by the body s needs, with the excesses being excreted in the urine. Elimination of nitrogenous end products of protein metabolism, primarily urea (uric acid in birds), creatinine and ammonia. Elimination of excess H + and the maintenance of physiological ph of body fluids. Elimination of complex organic compound both endogenous and exogenous. Secretion of endocrine substances e.g. erythropoietin which assumes a role in normal hematopoiesis, renin which is involved in the regulation of aldosterone secretion by the adrenal cortex. C.N.S. contribution to Renal Iintegration Maximum urine concentration requires the secretion of antidiuretic hormone (ADH) or vasopressin by the hypothalamo neurohypophyseal complex. Reflexes from peripheral receptors (e.g. the postulated volume receptors) may influence renal functions by central nervous integration through hypothalamus and autonomic nervous system. Hypothalamic mediation of the adenohypophyseal secretion represents another pathway through which the CNS may alter the output of hormones that modify renal functions. Thyroid hormones and adenohypophyseal growth hormone exerts tropic effect on the kidney. The hormones that assume major importance in kidney function regulation are steroid secretions of the adrenal cortex and the hormones of the parathyroid gland e.g. the permissive action of the cortisol-type steroids is essential for maximal rates of H 2 0 excretion, while aldosterone regulates transport of K + into urine and the retention of Na + within body fluids. The hormone of the parathyroid gland influences the rate of Calcium and Phosphate excretion into the urine. The normal kidney demonstrates considerable functional autonomy and is adequately perfused with blood. Just a smalll percentage decrease in any given process can be produced by removing a specific neuro-humoral or endocrine mediator. Volumes of fluids passing through the kidney each day are of such magnitude that small percentage decreases in any given function usually represents a major crisis in terms of maintaining the physiological integrity of the body fluid compartments. AnAtomy of the kidney
3 Nephrons, which are the functional units of kidney are of 2 types in mammals and are distinguished by: Locus of the origin i.e. the area of the cortex in which the glomeruli are found. The extent to which the loops of Henle penetrates the medulla. Types of Nephron (1) Cortical / corticomedullary nephrons: They arise from glomeruli located in the peripheral and central area of the kidney cortex with their loops of Henle extending into the corticomedullary junctional area and to variable levels of the outer medulla. (2) Juxtamedullary nephrons: They originate from glomeruli situated in the deeper portion of the cortex adjacent to the corticomedullary junctional area with their loop of Henle, particularly the thin segments extending into medullary substance. Many of the longer looped nephrons penetrate to the medullary crest or renal papilla. Schematic representation of cortical and juxtamedullary nephrons PrinciPal mechanism of nephron functions A. Nephron filters a large portion of plasma ( 1 / 5 ) from glomeruli blood throughout the glomerular membrane into the tubular system.
4 B. As filtered fluids pass through the tubular systems, unwanted substances are allowed to pass out into urine, while wanted substances are reabsorbed back into the plasma through the peritubular capillary network Functions of the renal tubules Filtration: An average of 21% of the blood pumped by the heart each minute flows through the kidneys. Of the total volume of blood plasma that flow through the glomerular capillaries, about 19% passes through the filtration membrane into the Bowman s capsule to become filtrate. In all of the nephrons of both kidneys, about 180lt of filtrate are produed each day but only about 1% or less of the filtate becomes urine. Filtration is the passage of plasma, aqueous, ionic and crystalloid components of blood across the filtrates membrane of the renal corpuscles (Bowman s capsule and glomerulus) into the Bowman s space. Erythrocytes and most of the plasma proteins {albumin, a blood protein with a diameter slightly less than the openings in the filtration barriers enters the filtrate in trace (small) amount} do not filter through the glomerular membrane. In other respects, the glomerular filtrate prior to its entrance into the proximal convolutions is almost identical in composition and osmolality to plasma. Diagram of the glomerulus and bowman s capsule
5 Diagram of the filtration membrane of the glomerulus and bowman s capsule Re-absorption: About 99% of the filtrate volume is reabsorbed and enters the peritubular capillaries. Reabsorption as used here means that a substances moves from the tubular lumen to the peritubular capillary and it is not allowed to get into the collecting duct. The reabsorbed filtrate flows through the renal vein to enter the general circulation. Excess ions and metabolic waste e.g. urea, uric acid and creatinine are not readily reabsorbed. Therefore the small volume of urine produced contains a high concentration of metabolic waste products. Tubular reabsorption may result from either passive back diffusion or active cellular transport. Secretion: Tubular secretion is similar to reabsorption except that substances enter the renal the renal tubules instead of leaving it. Tubular secretion can either be active or passive. e.g. NH 3 diffuses into the lumen of the nephron whereas H +, K +, creatinine, histamine & penicillin are actively transported into the nephrons. SPECIFIC FUNCTIONS OF NEPHRON The glomeruli and the proximal convoluted tubules: The glomeruli function primarily as filters. The glomeruli membrane is composed of the endothelium of the glomeruli capillaries, a basement membrane and the invaginations of the Bowman s capsule. The membrane is of differential permeability that permits the passage of aqueous, ionic and crystalloid components of blood into the Bowman s space. Erythrocytes and most of the plasma proteins do not filter through the membrane.
6 Proximal convoluted tubule is the primary site for reabsorbing solute and water. Tubular fluid near the end of the PCT is devoid of glucose and amino acids and most of the filtered proteins and has a fluid- plasma osmolal ratio of 1. Quantitative estimates indicate that only 20% of the original glomerular filtrate remains after its passage through the PCT. In summary, the primary function of the PCT is to return 70% of the glomerular filtrate into the peritubular blood and hence into the systemic circulation. When plasma glucose concentrations are normal, all of the filtered glucose is transported from the tubular fluid of the PCT into the plasma. Amino acids are almost entirely removed (reabsorbed) from the proximal tubular fluid. The major determinants of PCT reabsorption apparently are: 1. Active transport of Na against an electrochemical gradient, from the tubular fluid into the peritubular interstitial fluid and capillary blood. 2. H + -Na + exchange processes 3. Reabsorptions of glucose Chloride either diffuses along with Na + to maintain electrical neutrality or may also be transported by some carrier system. Other substances that are actively transported from the PCT includes proteins, Na +, K +, Ca 2+, HCO - 3, CL -. The PCT is permeable to water. As solute molecules are transported from the PCT to the peritubular capillaries, water moves by osmosis in the same direction. N.B: Difference between osmolality & osmolarity, active and passive transport. Consequently, 65% of the glomerular filtrate volume is reabsorbed from the PCT. Creatinine and urea which are other nitrogenous components of glomerular filtrate are differentially affected by events in the PCT. Creatinine which is not reabsorbed by the nephrons becomes more concentrated as reabsorption proceeds while urea on the other hand diffuses readily across most biological membranes. Approximately 30-40% of filtered urea is reabsorbed in the PCT. H + is actively secreted in the PCT. How? The epithelial cells secrete large quantities of H + across the wall of the nephrone into the filtrate. Loop of Henle: Tubular fluids in Henle s loops become increasingly hypertonic as it passes through the medulla. The descending limb of Henle s loop (DLH) is apparently permeable to the
7 passage of ions & crystalloids. Both NaCl and urea are added by passive diffusion to the tubular fluid in this segment from the medullary interstitium. Fluids from the tip of Henle s loop are almost equal in composition and the osmolality to the medullary interstitial fluid. The initial segment of the ascending limb of Henle s loop (ALH) may be less permeable than the descending, but some equilibration occur between tubular fluids and medullar interstitium. LH, therefore functions as a counter current diffusion system in concert/association with the vasa recta, as NaCl and urea diffuse circuitously from the ascending segment into the medullary interstitium and into the descending segment. The medullary segment of the thick ascending LH is relatively impermeable to water and it is the site of active transport system that translocates chloride (accompanied by sodium) against the significant concentration from the tubular fluid into the interstitial fluid into the interstitial fluid of the of the inner medulla. Since NaCl is reabsorbed at this site into the interstitial fluid, the tubular fluid becomes increasingly dilute. N.B.: Water excretion (elimination of dilute urine) is not a passive process solely related to the absence of ADH. The active transport of chloride (accompanied by sodium) from the relatively water impermeable ascending LH represents an essential energy dependent process in the formation of dilute urine. Active chloride transport from the thick ascending loop of Henle could supply NaCl to be carried into and sequestered within the counter current multiplier. NaCl and particularly urea apparently can be concentrated solely by passive diffusion within the counter current multiplier system of the thin portion of the LH and side by side the apposed descending and ascending vasa recta. The maintenance of the gradient is enhanced by the progressive decrease in medullary blood flow from the inner medulla to the medullary crest or papilla. N. B. the daily production of primary urine (glomerular filtrate) is about liters, but due to tubular reabsorption of H 2 0 and numerous substances from the primary urine, only liters of the secondary urine is excreted daily. concentrating mechanism of the kidney By the time the tubular fluid leaves the PCT, its volume has been considerably reduced and certain chemicals have been reabsorbed or excreted, but the osmotic concentration of the urine is still essentially the same as blood. Some additional reabsorption and excretion occurs in the
8 distal convoluted tubule (DCT) and in the collecting duct (CD), but concentration of urine primarily involves movements of CL -, Na + and water. A major function of the LH is to establish differences in osmotic concentration of NaCl in the fluid surrounding the collecting duct from the upper cortex down to the inner medulla of the kidney. Tubular fluid that enters the descending limb of the LH has an osmotic concentration similar to blood and the membrane of the descending LH is permeable to H 2 0 but not to NaCl. The membrane of the ascending limb of LH actively transports chloride from tubular fluid to interstitial fluid bathing the nephron. Sodium passively moves from tubular fluid to interstitial fluid but the membrane of the ascending LH is not permeable to H 2 0. As a result, NaCl accumulates in fluid surrounding the nephron in increasing concentration from the cortex down through the medulla. The descending LH serves to provide NaCl to be transported out the ascending limb. N.B.: Water is withdrawn from the tubular fluid in the descending limb. The LH is called a counter current multiplier. Counter current multiplier system in the loop of Henle for producing a hyperosmotic renal medulla Why? Fluid flow in the ascending limb of LH is counter current to the flow of the descending limb and the collecting duct. In addition energy is expended to produce concentration gradient along the loop and collecting duct. Each small section of membrane on the ascending limb transports a certain amount of NaCl against a particular difference in concentration. This
9 addition of small sections of membrane along the entire length of the ascending limb produces a multiplicative effect because multiplication is a series of successive addition of the same amount. When tubular fluid reaches the top of the ascending limb, it may be slightly less concentrated than blood plasma resulting in some H 2 0 movement by osmosis to blood and further reduction of urine volume. As fluid passes back down through the CD, water will move by osmosis out of urine if the CD membranes are permeable to water (i.e. in the presence of ADH). Because the concentration of fluids surrounding the collecting duct increases along their length, more and more water can be withdrawn by osmosis as the fluid move down the CD. The H 2 0 that moves from the descending limb of LH and the collecting duct must be removed from the fluid surrounding the nephron tubules; otherwise the gradient of NaCl concentration will be dilute. Water removal occurs with blood flow in the capillary loops called vasa recta. Counter current exchanger: Venous blood leaving the glomerulus gains NaCl by diffusion and looses water by osmosis on the descending limb of the vasa recta, but by looping back, the blood loses sodium by diffusion and gains water by osmosis on the ascending limb. Counter current exchanger system in the loop of Henle and Vasa recta for producing a hyperosmotic renal medulla Urea diffuses across all of the membranes in the nephron tubules and in the vasa recta. Urea is transported passively and becomes more concentrated in tubular fluid in CD as a consequence of
10 the movement of water out of the ducts and into blood. The permeability of the CD to water and urea is variable, depending upon the presence of ADH. Distal convoluted tubule and collecting duct: The distal CT receives a hypotonic fluid from the medullary region. Isoosmotic equilibration occurs in the 1 st 1 / rd 3 of the DCT (assuming that the kidney is elaborating a concentrated urine) as water leaves the tubular fluids in the direction of its concentration gradient. Further isoosmotic reabsorption occurs in the remaining portions of the DCT secondary to Na transport from tubular fluid into plasma. The osmolality of the fluid at the end of DCT is equal to the osmolality of plasma but quantitatively now represents approximately 5% of the original glomerular filtrate. N.B.: Isoosmotic equilibration of tublar fluid does not occur in the DCT of dog nephrons. Rather the tubular fluid at the end of DCT is still hypotonic to plasma. Some portions of the ascending LH in the dog kidney appear to be involved in the processes that regulate urine concentration and dilution. Fluid entering the DCT shows a fluid plasma osmolal ratio of when the dog is elaborating a concentrated urine. Under conditions of water diuresis, i.e. when the kidney excretes a hypotonic urine, the osmolal ratio may be as low as 0.2. Final concentration of urine takes place in the collecting duct as these terminal segments of the nephron system carry the urine through the medulla to the renal pelvis. The permeability of the collecting duct to water and urea is variable depending upon the presence of ADH. When the kidney is excreting concentrated urine i.e. in the presence of ADH, the collecting duct becomes
11 increasingly permeable to water and urea. Water, free of solute, then passes in the direction of its concentration, from the lumen of the collecting duct into the hypertonic medullary interstitium. As the fluid in the collecting duct becomes concentrated, urea concentration in the collecting duct fluid increases until it exceeds the urea concentration in the medulla. Urea then diffuses from the collecting duct fluid into the medullary interstitium, thus, obligating the reabsorption of H 2 0 from the collecting duct fluid. The collecting duct appears to be relatively impermeable to non-urea solute e.g. Na, K salts of chloride, sulphate, bi-carbonate and to creatinine, and these solutes becomes increasingly concentrated. The net result of these processes is the excretion of urine that may be 5-7 times the concentration of plasma. Dilute urine is excreted when the release of ADH is inhibited. The primary target organs of ADH are the collecting duct, but the DCT and ALH in the dog at least, share to some extent as sites of action of this hormone. In the absence of ADH, the DCT, CD and the ALH in the dog becomes relatively impermeable to water and urea. Na reabsorption still takes place from the fluid in DCT, but water movement is decreased; concurrently, water reabsorption in the CD is markedly inhibited. Therefore, the absence of ADH, results in water diuresis i.e. the excretion of large volume of urine hypotonc to plasma. The specialized morphology and metabolism of the medulla permits the mammalian kidney to concentrate urine and thereby conserve water. However, there is evidence that the hyperosmosity / hyperosmolatity may also be detrimental. It has been shown that chronic infectious diseases of the kidney may also be closely associated with the maintenance of the cortico-medullary osmotic gradient. Reasons are: The hyperosmotic environment of the medulla apparently inhibits the migration of leucocytes to the sites of infection, thus depriving the area of one of the primary defense mechanisms against bacteria. The relatively small medullary blood flow, will limit the amount of antimicrobial drugs that could be carried into the medulla. These 2 factors complicate the therapeutic management of renal infection.
12 The urine concentrating process functions most effectively when protein intake is sufficient to maintain positive nitrogen balance. Protein deficient diet results in impairment in the capacity of the kidney to conserve water. There may be subtle changes in the permeability characteristics as protein turnover in the kidney responds to unfavorable nitrogen equilibrium. Enzyme synthesis in the kidney may be similarly affected. Urea, however, assumes an important role in the renal responses to changes in protein intake. The urea component of the cortico-medullary osmotic gradient is virtually eliminated by protein deficiency and urea excretion falls to low levels. As urine is concentrated in the CD, there is a minimal reabsorption of urea and the amount of water reabsorption obligated by urea diffusion is greatly reduced. A decrease in the cortico-medullary osmotic gradient also occurs since the quantity of urea is decreased. Water conservation, therefore, depends to a large extent upon reabsorption and is decreased as the result of the decrease in the osmolality of the medullary interstitium.
BIOLOGY - CLUTCH CH.44 - OSMOREGULATION AND EXCRETION.
 !! www.clutchprep.com Osmoregulation regulation of solute balance and water loss to maintain homeostasis of water content Excretion process of eliminating waste from the body, like nitrogenous waste Kidney
!! www.clutchprep.com Osmoregulation regulation of solute balance and water loss to maintain homeostasis of water content Excretion process of eliminating waste from the body, like nitrogenous waste Kidney
Osmotic Regulation and the Urinary System. Chapter 50
 Osmotic Regulation and the Urinary System Chapter 50 Challenge Questions Indicate the areas of the nephron that the following hormones target, and describe when and how the hormones elicit their actions.
Osmotic Regulation and the Urinary System Chapter 50 Challenge Questions Indicate the areas of the nephron that the following hormones target, and describe when and how the hormones elicit their actions.
Nephron Structure inside Kidney:
 In-Depth on Kidney Nephron Structure inside Kidney: - Each nephron has two capillary regions in close proximity to the nephron tubule, the first capillary bed for fluid exchange is called the glomerulus,
In-Depth on Kidney Nephron Structure inside Kidney: - Each nephron has two capillary regions in close proximity to the nephron tubule, the first capillary bed for fluid exchange is called the glomerulus,
The principal functions of the kidneys
 Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
014 Chapter 14 Created: 9:25:14 PM CST
 014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
BCH 450 Biochemistry of Specialized Tissues
 BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
2) This is a Point and Click question. You must click on the required structure.
 Class: A&P2-1 Description: Test: Excretory Test Points: 144 Test Number: 28379 Printed: 31-March-10 12:03 1) This is a Point and Click question. You must click on the required structure. Click on the Bowman's
Class: A&P2-1 Description: Test: Excretory Test Points: 144 Test Number: 28379 Printed: 31-March-10 12:03 1) This is a Point and Click question. You must click on the required structure. Click on the Bowman's
1. a)label the parts indicated above and give one function for structures Y and Z
 Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- renal cortex - X- renal medulla Y- renal pelvis collecting center of urine and then
Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- renal cortex - X- renal medulla Y- renal pelvis collecting center of urine and then
I. Metabolic Wastes Metabolic Waste:
 I. Metabolic Wastes Metabolic Waste: a) Carbon Dioxide: by-product of cellular respiration. b) Water: by-product of cellular respiration & dehydration synthesis reactions. c) Inorganic Salts: by-product
I. Metabolic Wastes Metabolic Waste: a) Carbon Dioxide: by-product of cellular respiration. b) Water: by-product of cellular respiration & dehydration synthesis reactions. c) Inorganic Salts: by-product
Functions of Proximal Convoluted Tubules
 1. Proximal tubule Solute reabsorption in the proximal tubule is isosmotic (water follows solute osmotically and tubular fluid osmolality remains similar to that of plasma) 60-70% of water and solute reabsorption
1. Proximal tubule Solute reabsorption in the proximal tubule is isosmotic (water follows solute osmotically and tubular fluid osmolality remains similar to that of plasma) 60-70% of water and solute reabsorption
Urinary bladder provides a temporary storage reservoir for urine
 Urinary System Organs Kidney Filters blood, allowing toxins, metabolic wastes, and excess ions to leave the body in urine Urinary bladder provides a temporary storage reservoir for urine Paired ureters
Urinary System Organs Kidney Filters blood, allowing toxins, metabolic wastes, and excess ions to leave the body in urine Urinary bladder provides a temporary storage reservoir for urine Paired ureters
November 30, 2016 & URINE FORMATION
 & URINE FORMATION REVIEW! Urinary/Renal System 200 litres of blood are filtered daily by the kidneys Usable material: reabsorbed back into blood Waste: drained into the bladder away from the heart to the
& URINE FORMATION REVIEW! Urinary/Renal System 200 litres of blood are filtered daily by the kidneys Usable material: reabsorbed back into blood Waste: drained into the bladder away from the heart to the
Excretory Lecture Test Questions Set 1
 Excretory Lecture Test Questions Set 1 1. The separation and ejection of metabolic wastes, usually in aqueous solution, is: a. reabsorption b. secretion c. filtration d. excretion e. endocrinology 2. Besides
Excretory Lecture Test Questions Set 1 1. The separation and ejection of metabolic wastes, usually in aqueous solution, is: a. reabsorption b. secretion c. filtration d. excretion e. endocrinology 2. Besides
Excretory System 1. a)label the parts indicated above and give one function for structures Y and Z
 Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- X- Y- Z- b) Which of the following is not a function of the organ shown? A. to produce
Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- X- Y- Z- b) Which of the following is not a function of the organ shown? A. to produce
Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion.
 The Kidney Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion. The kidney has 6 roles in the maintenance of homeostasis. 6 Main Functions 1. Ion Balance
The Kidney Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion. The kidney has 6 roles in the maintenance of homeostasis. 6 Main Functions 1. Ion Balance
Osmoregulation regulates solute concentrations and balances the gain and loss of water
 Ch 44 Osmoregulation & Excretion Osmoregulation regulates solute concentrations and balances the gain and loss of water Freshwater animals show adaptations that reduce water uptake and conserve solutes
Ch 44 Osmoregulation & Excretion Osmoregulation regulates solute concentrations and balances the gain and loss of water Freshwater animals show adaptations that reduce water uptake and conserve solutes
One Minute Movies: Molecular Action at the Nephron Joy Killough / Westwood High School / Austin,TX
 One Minute Movies: Molecular Action at the Nephron Joy Killough / Westwood High School / Austin,TX To prepare your nephron model: ( A nephron is a tubule and the glomerulus. There are about a million of
One Minute Movies: Molecular Action at the Nephron Joy Killough / Westwood High School / Austin,TX To prepare your nephron model: ( A nephron is a tubule and the glomerulus. There are about a million of
Nephron Anatomy Nephron Anatomy
 Kidney Functions: (Eckert 14-17) Mammalian Kidney -Paired -1% body mass -20% blood flow (Eckert 14-17) -Osmoregulation -Blood volume regulation -Maintain proper ion concentrations -Dispose of metabolic
Kidney Functions: (Eckert 14-17) Mammalian Kidney -Paired -1% body mass -20% blood flow (Eckert 14-17) -Osmoregulation -Blood volume regulation -Maintain proper ion concentrations -Dispose of metabolic
Excretion Chapter 29. The Mammalian Excretory System consists of. The Kidney. The Nephron: the basic unit of the kidney.
 Excretion Chapter 29 The Mammalian Excretory System consists of The Kidney 1. Vertebrate kidneys perform A. Ion balance B. Osmotic balance C. Blood pressure D. ph balance E. Excretion F. Hormone production
Excretion Chapter 29 The Mammalian Excretory System consists of The Kidney 1. Vertebrate kidneys perform A. Ion balance B. Osmotic balance C. Blood pressure D. ph balance E. Excretion F. Hormone production
Renal System and Excretion
 Renal System and Excretion Biology 105 Lecture 19 Chapter 16 Outline Renal System I. Functions II. Organs of the renal system III. Kidneys 1. Structure 2. Function IV. Nephron 1. Structure 2. Function
Renal System and Excretion Biology 105 Lecture 19 Chapter 16 Outline Renal System I. Functions II. Organs of the renal system III. Kidneys 1. Structure 2. Function IV. Nephron 1. Structure 2. Function
PARTS OF THE URINARY SYSTEM
 EXCRETORY SYSTEM Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid-base concentrations and metabolite concentrations 1 ORGANS OF EXCRETION Skin and
EXCRETORY SYSTEM Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid-base concentrations and metabolite concentrations 1 ORGANS OF EXCRETION Skin and
Salt and Water Balance and Nitrogen Excretion
 Announcements Exam is in class on WEDNESDAY. Bring a #2 pencil and your UFID. You must come to your registered class section (except those with DRC accommodations). Office hours Mon 1-3 pm. Teaching evals:
Announcements Exam is in class on WEDNESDAY. Bring a #2 pencil and your UFID. You must come to your registered class section (except those with DRC accommodations). Office hours Mon 1-3 pm. Teaching evals:
Urinary System Organization. Urinary System Organization. The Kidneys. The Components of the Urinary System
 Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
Normal Renal Function
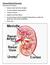 Normal Renal Function Functions of the Kidney: balances solute and water transport excretes metabolic waste products conserves nutrient regulates acid-base balance secretes hormones that help regulate
Normal Renal Function Functions of the Kidney: balances solute and water transport excretes metabolic waste products conserves nutrient regulates acid-base balance secretes hormones that help regulate
Osmoregulation and the Excretory System
 Honors Biology Study Guide Chapter 25.4 25.10 Name Osmoregulation and the Excretory System FUNCTIONS OF THE EXCRETORY SYSTEM OSMOREGULATION Freshwater: Marine: Land Animals: Sources of Nitrogenous Wastes?
Honors Biology Study Guide Chapter 25.4 25.10 Name Osmoregulation and the Excretory System FUNCTIONS OF THE EXCRETORY SYSTEM OSMOREGULATION Freshwater: Marine: Land Animals: Sources of Nitrogenous Wastes?
Outline Urinary System
 Urinary System and Excretion Bio105 Lecture Packet 20 Chapter 16 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure B. Urine formation 1. Hormonal regulation
Urinary System and Excretion Bio105 Lecture Packet 20 Chapter 16 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure B. Urine formation 1. Hormonal regulation
The Excretory System. Biology 20
 The Excretory System Biology 20 Introduction Follow along on page 376 What dangers exist if your body is unable to regulate the fluid balance of your tissues? What challenged would the body have to respond
The Excretory System Biology 20 Introduction Follow along on page 376 What dangers exist if your body is unable to regulate the fluid balance of your tissues? What challenged would the body have to respond
Chapter 44. Regulating the Internal Environment. AP Biology
 Chapter 44. Regulating the Internal Environment Homeostasis Living in the world organisms had a choice: regulate their internal environment maintain relatively constant internal conditions conform to the
Chapter 44. Regulating the Internal Environment Homeostasis Living in the world organisms had a choice: regulate their internal environment maintain relatively constant internal conditions conform to the
Nephron Function and Urine Formation. Ms. Kula December 1, 2014 Biology 30S
 Nephron Function and Urine Formation Ms. Kula December 1, 2014 Biology 30S The Role of the Nephron In order for the body to properly function and maintain homeostasis, the amount of dissolved substances
Nephron Function and Urine Formation Ms. Kula December 1, 2014 Biology 30S The Role of the Nephron In order for the body to properly function and maintain homeostasis, the amount of dissolved substances
Questions? Homework due in lab 6. PreLab #6 HW 15 & 16 (follow directions, 6 points!)
 Questions? Homework due in lab 6 PreLab #6 HW 15 & 16 (follow directions, 6 points!) Part 3 Variations in Urine Formation Composition varies Fluid volume Solute concentration Variations in Urine Formation
Questions? Homework due in lab 6 PreLab #6 HW 15 & 16 (follow directions, 6 points!) Part 3 Variations in Urine Formation Composition varies Fluid volume Solute concentration Variations in Urine Formation
Other Factors Affecting GFR. Chapter 25. After Filtration. Reabsorption and Secretion. 5 Functions of the PCT
 Other Factors Affecting GFR Chapter 25 Part 2. Renal Physiology Nitric oxide vasodilator produced by the vascular endothelium Adenosine vasoconstrictor of renal vasculature Endothelin a powerful vasoconstrictor
Other Factors Affecting GFR Chapter 25 Part 2. Renal Physiology Nitric oxide vasodilator produced by the vascular endothelium Adenosine vasoconstrictor of renal vasculature Endothelin a powerful vasoconstrictor
28/04/2013 LEARNING OUTCOME C13 URINARY SYSTEM STUDENT ACHIEVEMENT INDICATORS STUDENT ACHIEVEMENT INDICATORS URINARY SYSTEM & EXCRETION
 LEARNING OUTCOME C13 Analyse the functional interrelationships of the structures of the urinary system Learning Outcome C13 URINARY SYSTEM STUDENT ACHIEVEMENT INDICATORS Students who have fully met this
LEARNING OUTCOME C13 Analyse the functional interrelationships of the structures of the urinary system Learning Outcome C13 URINARY SYSTEM STUDENT ACHIEVEMENT INDICATORS Students who have fully met this
Osmoregulation and Renal Function
 1 Bio 236 Lab: Osmoregulation and Renal Function Fig. 1: Kidney Anatomy Fig. 2: Renal Nephron The kidneys are paired structures that lie within the posterior abdominal cavity close to the spine. Each kidney
1 Bio 236 Lab: Osmoregulation and Renal Function Fig. 1: Kidney Anatomy Fig. 2: Renal Nephron The kidneys are paired structures that lie within the posterior abdominal cavity close to the spine. Each kidney
RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015
 RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015 1. In which abdominal cavity do the kidneys lie? a) Peritoneum. b) Anteperitoneal. c) Retroperitoneal. d) Parietal peritoneal 2. What is the
RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015 1. In which abdominal cavity do the kidneys lie? a) Peritoneum. b) Anteperitoneal. c) Retroperitoneal. d) Parietal peritoneal 2. What is the
Urinary System and Excretion. Bio105 Lecture 20 Chapter 16
 Urinary System and Excretion Bio105 Lecture 20 Chapter 16 1 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of the urinary system
Urinary System and Excretion Bio105 Lecture 20 Chapter 16 1 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of the urinary system
Kidney Physiology. Mechanisms of Urine Formation TUBULAR SECRETION Eunise A. Foster Shalonda Reed
 Kidney Physiology Mechanisms of Urine Formation TUBULAR SECRETION Eunise A. Foster Shalonda Reed The purpose of tubular secrection To dispose of certain substances that are bound to plasma proteins. To
Kidney Physiology Mechanisms of Urine Formation TUBULAR SECRETION Eunise A. Foster Shalonda Reed The purpose of tubular secrection To dispose of certain substances that are bound to plasma proteins. To
NOTES: CH 44 Regulating the Internal Environment (Homeostasis & The Urinary System)
 NOTES: CH 44 Regulating the Internal Environment (Homeostasis & The Urinary System) HOMEOSTASIS **Recall HOMEOSTASIS is the steady-state physiological condition of the body. It includes: 1) Thermoregulation:
NOTES: CH 44 Regulating the Internal Environment (Homeostasis & The Urinary System) HOMEOSTASIS **Recall HOMEOSTASIS is the steady-state physiological condition of the body. It includes: 1) Thermoregulation:
1. Urinary System, General
 S T U D Y G U I D E 16 1. Urinary System, General a. Label the figure by placing the numbers of the structures in the spaces by the correct labels. 7 Aorta 6 Kidney 8 Ureter 2 Inferior vena cava 4 Renal
S T U D Y G U I D E 16 1. Urinary System, General a. Label the figure by placing the numbers of the structures in the spaces by the correct labels. 7 Aorta 6 Kidney 8 Ureter 2 Inferior vena cava 4 Renal
April 08, biology 2201 ch 11.3 excretion.notebook. Biology The Excretory System. Apr 13 9:14 PM EXCRETORY SYSTEM.
 Biology 2201 11.3 The Excretory System EXCRETORY SYSTEM 1 Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid base concentrations and metabolite concentrations
Biology 2201 11.3 The Excretory System EXCRETORY SYSTEM 1 Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid base concentrations and metabolite concentrations
Chapter 44. Osmoregulation and Excretion
 Chapter 44 Osmoregulation and Excretion Overview: A Balancing Act Physiological systems of animals operate in a fluid environment Relative concentrations of water and solutes must be maintained within
Chapter 44 Osmoregulation and Excretion Overview: A Balancing Act Physiological systems of animals operate in a fluid environment Relative concentrations of water and solutes must be maintained within
osmoregulation mechanisms in gills, salt glands, and kidneys
 Ionic & Osmotic Homeostasis osmoregulation mechanisms in gills, salt glands, and kidneys extracellular intracellular 22 23 Salt Secretion: recycle Figure in Box 26.2 Hill et al. 2004 active Down electrochemical
Ionic & Osmotic Homeostasis osmoregulation mechanisms in gills, salt glands, and kidneys extracellular intracellular 22 23 Salt Secretion: recycle Figure in Box 26.2 Hill et al. 2004 active Down electrochemical
Chapter 23. The Nephron. (functional unit of the kidney
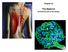 Chapter 23 The Nephron (functional unit of the kidney Renal capsule The Nephron Renal cortex Nephron Collecting duct Efferent arteriole Afferent arteriole (a) Renal corpuscle: Glomerular capsule Glomerulus
Chapter 23 The Nephron (functional unit of the kidney Renal capsule The Nephron Renal cortex Nephron Collecting duct Efferent arteriole Afferent arteriole (a) Renal corpuscle: Glomerular capsule Glomerulus
Regulating the Internal Environment. AP Biology
 Regulating the Internal Environment 2006-2007 Conformers vs. Regulators Two evolutionary paths for organisms regulate internal environment maintain relatively constant internal conditions conform to external
Regulating the Internal Environment 2006-2007 Conformers vs. Regulators Two evolutionary paths for organisms regulate internal environment maintain relatively constant internal conditions conform to external
describe the location of the kidneys relative to the vertebral column:
 Basic A & P II Dr. L. Bacha Chapter Outline (Martini & Nath 2010) list the three major functions of the urinary system: by examining Fig. 24-1, list the organs of the urinary system: describe the location
Basic A & P II Dr. L. Bacha Chapter Outline (Martini & Nath 2010) list the three major functions of the urinary system: by examining Fig. 24-1, list the organs of the urinary system: describe the location
Ch. 44 Regulating the Internal Environment
 Ch. 44 Regulating the Internal Environment 2006-2007 Conformers vs. Regulators Two evolutionary paths for organisms regulate internal environment maintain relatively constant internal conditions conform
Ch. 44 Regulating the Internal Environment 2006-2007 Conformers vs. Regulators Two evolutionary paths for organisms regulate internal environment maintain relatively constant internal conditions conform
Hill et al. 2004, Fig. 27.6
 Lecture 25, 15 November 2005 Osmoregulation (Chapters 25-28) Vertebrate Physiology ECOL 437 (aka MCB 437, VetSci 437) University of Arizona Fall 2005 1. Osmoregulation 2. Kidney Function Text: Chapters
Lecture 25, 15 November 2005 Osmoregulation (Chapters 25-28) Vertebrate Physiology ECOL 437 (aka MCB 437, VetSci 437) University of Arizona Fall 2005 1. Osmoregulation 2. Kidney Function Text: Chapters
Human Urogenital System 26-1
 Human Urogenital System 26-1 Urogenital System Functions Filtering of blood, Removal of wastes and metabolites Regulation of blood volume and composition concentration of blood solutes ph of extracellular
Human Urogenital System 26-1 Urogenital System Functions Filtering of blood, Removal of wastes and metabolites Regulation of blood volume and composition concentration of blood solutes ph of extracellular
Urinary Physiology. Chapter 17 Outline. Kidney Function. Chapter 17
 Urinary Physiology Chapter 17 Chapter 17 Outline Structure and Function of the Kidney Glomerular Filtration Reabsorption of Salt and Water Renal Plasma Clearance Renal Control of Electrolyte and Acid-Base
Urinary Physiology Chapter 17 Chapter 17 Outline Structure and Function of the Kidney Glomerular Filtration Reabsorption of Salt and Water Renal Plasma Clearance Renal Control of Electrolyte and Acid-Base
Urinary System BIO 250. Waste Products of Metabolism Urea Carbon dioxide Inorganic salts Water Heat. Routes of Waste Elimination
 Urinary System BIO 250 Waste Products of Metabolism Urea Carbon dioxide Inorganic salts Water Heat Routes of Waste Elimination Skin: Variable amounts of heat, salts, and water; small amounts of urea and
Urinary System BIO 250 Waste Products of Metabolism Urea Carbon dioxide Inorganic salts Water Heat Routes of Waste Elimination Skin: Variable amounts of heat, salts, and water; small amounts of urea and
1.&Glomerular/Pressure&Filtration&
 Urine&Formation& Overall&Process&! Urine gets rid of wastes (NH 3, urea, uric acid, creatinine) and other substances (vitamins, penicillin, histamines) found in excess in the blood!! blood is filtered
Urine&Formation& Overall&Process&! Urine gets rid of wastes (NH 3, urea, uric acid, creatinine) and other substances (vitamins, penicillin, histamines) found in excess in the blood!! blood is filtered
KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin
![KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin](/thumbs/87/96174332.jpg) Renal Physiology MCQ KD01 [Mar96] [Apr01] Renal blood flow is dependent on: A. Juxtaglomerular apparatus B. [Na+] at macula densa C. Afferent vasodilatation D. Arterial pressure (poorly worded/recalled
Renal Physiology MCQ KD01 [Mar96] [Apr01] Renal blood flow is dependent on: A. Juxtaglomerular apparatus B. [Na+] at macula densa C. Afferent vasodilatation D. Arterial pressure (poorly worded/recalled
Chapter 19 The Urinary System Fluid and Electrolyte Balance
 Chapter 19 The Urinary System Fluid and Electrolyte Balance Chapter Outline The Concept of Balance Water Balance Sodium Balance Potassium Balance Calcium Balance Interactions between Fluid and Electrolyte
Chapter 19 The Urinary System Fluid and Electrolyte Balance Chapter Outline The Concept of Balance Water Balance Sodium Balance Potassium Balance Calcium Balance Interactions between Fluid and Electrolyte
Sunday, July 17, 2011 URINARY SYSTEM
 URINARY SYSTEM URINARY SYSTEM Let s take a look at the anatomy first! KIDNEYS: are complex reprocessing centers where blood is filtered through and waste products are removed. Wastes and extra water become
URINARY SYSTEM URINARY SYSTEM Let s take a look at the anatomy first! KIDNEYS: are complex reprocessing centers where blood is filtered through and waste products are removed. Wastes and extra water become
A&P 2 CANALE T H E U R I N A R Y S Y S T E M
 A&P 2 CANALE T H E U R I N A R Y S Y S T E M URINARY SYSTEM CONTRIBUTION TO HOMEOSTASIS Regulates body water levels Excess water taken in is excreted Output varies from 2-1/2 liter/day to 1 liter/hour
A&P 2 CANALE T H E U R I N A R Y S Y S T E M URINARY SYSTEM CONTRIBUTION TO HOMEOSTASIS Regulates body water levels Excess water taken in is excreted Output varies from 2-1/2 liter/day to 1 liter/hour
Renal physiology D.HAMMOUDI.MD
 Renal physiology D.HAMMOUDI.MD Functions Regulating blood ionic composition Regulating blood ph Regulating blood volume Regulating blood pressure Produce calcitrol and erythropoietin Regulating blood glucose
Renal physiology D.HAMMOUDI.MD Functions Regulating blood ionic composition Regulating blood ph Regulating blood volume Regulating blood pressure Produce calcitrol and erythropoietin Regulating blood glucose
Use the following diagram to answer the next question. 1. In the diagram above, pressure filtration occurs in a. W b. X c. Y d. Z
 Part A: Multiple Choice Questions Value: 32 Marks Suggested time: 40 minutes Instructions: For each question select the best answer and record your choice on the Scantron card provided. Using an HB pencil,
Part A: Multiple Choice Questions Value: 32 Marks Suggested time: 40 minutes Instructions: For each question select the best answer and record your choice on the Scantron card provided. Using an HB pencil,
EXCRETION QUESTIONS. Use the following information to answer the next two questions.
 EXCRETION QUESTIONS Use the following information to answer the next two questions. 1. Filtration occurs at the area labeled A. V B. X C. Y D. Z 2. The antidiuretic hormone (vasopressin) acts on the area
EXCRETION QUESTIONS Use the following information to answer the next two questions. 1. Filtration occurs at the area labeled A. V B. X C. Y D. Z 2. The antidiuretic hormone (vasopressin) acts on the area
organs of the urinary system
 organs of the urinary system Kidneys (2) bean-shaped, fist-sized organ where urine is formed. Lie on either sides of the vertebral column, in a depression beneath peritoneum and protected by lower ribs
organs of the urinary system Kidneys (2) bean-shaped, fist-sized organ where urine is formed. Lie on either sides of the vertebral column, in a depression beneath peritoneum and protected by lower ribs
12/7/10. Excretory System. The basic function of the excretory system is to regulate the volume and composition of body fluids by:
 Excretory System The basic function of the excretory system is to regulate the volume and composition of body fluids by: o o removing wastes returning needed substances to the body for reuse Body systems
Excretory System The basic function of the excretory system is to regulate the volume and composition of body fluids by: o o removing wastes returning needed substances to the body for reuse Body systems
Outline Urinary System. Urinary System and Excretion. Urine. Urinary System. I. Function II. Organs of the urinary system
 Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
RENAL PHYSIOLOGY. Physiology Unit 4
 RENAL PHYSIOLOGY Physiology Unit 4 Renal Functions Primary Function is to regulate the chemistry of plasma through urine formation Additional Functions Regulate concentration of waste products Regulate
RENAL PHYSIOLOGY Physiology Unit 4 Renal Functions Primary Function is to regulate the chemistry of plasma through urine formation Additional Functions Regulate concentration of waste products Regulate
Chapter 44: Osmoregulation and Excretion
 Name Period The steady-state physiological condition that organisms must maintain is termed homeostasis. Osmoregulation and excretion are frequently cited examples of homeostasis and are the central ideas
Name Period The steady-state physiological condition that organisms must maintain is termed homeostasis. Osmoregulation and excretion are frequently cited examples of homeostasis and are the central ideas
Renal System Dr. Naim Kittana Department of Biomedical Sciences Faculty of Medicine & Health Sciences An-Najah National University
 Renal System Dr. Naim Kittana Department of Biomedical Sciences Faculty of Medicine & Health Sciences An-Najah National University Declaration The content and the figures of this seminar were directly
Renal System Dr. Naim Kittana Department of Biomedical Sciences Faculty of Medicine & Health Sciences An-Najah National University Declaration The content and the figures of this seminar were directly
Chapter 25: Urinary System
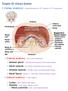 Chapter 25: Urinary System I. Kidney anatomy: retroperitoneal from 12 th thoracic to 3 rd lumbar area A. External anatomy: hilus is the indentation 1. Adrenal gland: in the fat at the superior end of each
Chapter 25: Urinary System I. Kidney anatomy: retroperitoneal from 12 th thoracic to 3 rd lumbar area A. External anatomy: hilus is the indentation 1. Adrenal gland: in the fat at the superior end of each
Urinary System. consists of the kidneys, ureters, urinary bladder and urethra
 Urinary System 1 Urinary System consists of the kidneys, ureters, urinary bladder and urethra 2 Location of Kidneys The kidneys which are positioned retroperitoneally lie on either side of the vertebral
Urinary System 1 Urinary System consists of the kidneys, ureters, urinary bladder and urethra 2 Location of Kidneys The kidneys which are positioned retroperitoneally lie on either side of the vertebral
Renal Quiz - June 22, 21001
 Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
Chapter 25 The Urinary System
 Chapter 25 The Urinary System 10/30/2013 MDufilho 1 Kidney Functions Removal of toxins, metabolic wastes, and excess ions from the blood Regulation of blood volume, chemical composition, and ph Gluconeogenesis
Chapter 25 The Urinary System 10/30/2013 MDufilho 1 Kidney Functions Removal of toxins, metabolic wastes, and excess ions from the blood Regulation of blood volume, chemical composition, and ph Gluconeogenesis
Glomerular Capillary Blood Pressure
 Glomerular Capillary Blood Pressure Fluid pressure exerted by blood within glomerular capillaries Depends on Contraction of the heart Resistance to blood flow offered by afferent and efferent arterioles
Glomerular Capillary Blood Pressure Fluid pressure exerted by blood within glomerular capillaries Depends on Contraction of the heart Resistance to blood flow offered by afferent and efferent arterioles
Homeostasis. Thermoregulation. Osmoregulation. Excretion. how organisms regulate their body temperature
 Homeostasis the steady-state physiological condition of the body Ability to regulate the internal environment important for proper functioning of cells Thermoregulation Homeostasis how organisms regulate
Homeostasis the steady-state physiological condition of the body Ability to regulate the internal environment important for proper functioning of cells Thermoregulation Homeostasis how organisms regulate
Class XI - Biology Excretory Products and their Elimination
 Class XI - Biology Excretory Products and their Elimination MULTIPLE CHOICE QUESTIONS 1. The following substances are the excretory products in animals. Choose the least toxic form among them? a. Urea
Class XI - Biology Excretory Products and their Elimination MULTIPLE CHOICE QUESTIONS 1. The following substances are the excretory products in animals. Choose the least toxic form among them? a. Urea
Homeostatic Regulation
 Homeostatic Regulation A hormone is :a Water-soluble hormones: Composed of amino acids and bind a receptor protein on the of the target cell. This starts a signal cascade inside the cell and the signal
Homeostatic Regulation A hormone is :a Water-soluble hormones: Composed of amino acids and bind a receptor protein on the of the target cell. This starts a signal cascade inside the cell and the signal
BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1
 BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1 1. a. Proximal tubule. b. Proximal tubule. c. Glomerular endothelial fenestrae, filtration slits between podocytes of Bowman's capsule.
BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1 1. a. Proximal tubule. b. Proximal tubule. c. Glomerular endothelial fenestrae, filtration slits between podocytes of Bowman's capsule.
BIOH122 Human Biological Science 2
 BIOH122 Human Biological Science 2 Session 18 Urinary System 3 Tubular Reabsorption and Secretion Bioscience Department Endeavour College of Natural Health endeavour.edu.au Session Plan o Principles of
BIOH122 Human Biological Science 2 Session 18 Urinary System 3 Tubular Reabsorption and Secretion Bioscience Department Endeavour College of Natural Health endeavour.edu.au Session Plan o Principles of
PHGY210 Renal Physiology
 PHGY210 Renal Physiology Tomoko Takano, MD, PhD *Associate Professor of Medicine and Physiology McGill University *Nephrologist, McGill University Health Centre Lecture plan Lecture 1: Anatomy, basics
PHGY210 Renal Physiology Tomoko Takano, MD, PhD *Associate Professor of Medicine and Physiology McGill University *Nephrologist, McGill University Health Centre Lecture plan Lecture 1: Anatomy, basics
Osmoregulation and Excretion
 Chapter 44 Osmoregulation and Excretion PowerPoint Lecture Presentations for Biology Eighth Edition Neil Campbell and Jane Reece Lectures by Chris Romero, updated by Erin Barley with contributions from
Chapter 44 Osmoregulation and Excretion PowerPoint Lecture Presentations for Biology Eighth Edition Neil Campbell and Jane Reece Lectures by Chris Romero, updated by Erin Barley with contributions from
CONTROLLING THE INTERNAL ENVIRONMENT
 AP BIOLOGY ANIMAL FORM & FUNCTION ACTIVITY #5 NAME DATE HOUR CONTROLLING THE INTERNAL ENVIRONMENT KIDNEY AND NEPHRON NEPHRON FUNCTIONS Animal Form & Function Activity #5 page 1 NEPHRON STRUCTURE NEPHRON
AP BIOLOGY ANIMAL FORM & FUNCTION ACTIVITY #5 NAME DATE HOUR CONTROLLING THE INTERNAL ENVIRONMENT KIDNEY AND NEPHRON NEPHRON FUNCTIONS Animal Form & Function Activity #5 page 1 NEPHRON STRUCTURE NEPHRON
Basic mechanisms of Kidney function
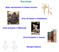 Excretion Basic mechanisms of Kidney function Urine formation in Amphibians Urine formation in Mammals Urine formation in Insects Nitrogen balance Kidneys The most fundamental function of kidneys) is to
Excretion Basic mechanisms of Kidney function Urine formation in Amphibians Urine formation in Mammals Urine formation in Insects Nitrogen balance Kidneys The most fundamental function of kidneys) is to
RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D.
 RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D. Learning Objectives 1. Identify the region of the renal tubule in which reabsorption and secretion occur. 2. Describe the cellular
RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D. Learning Objectives 1. Identify the region of the renal tubule in which reabsorption and secretion occur. 2. Describe the cellular
Kidney and urine formation
 Kidney and urine formation Renal structure & function Urine formation Urinary y concentration and dilution Regulation of urine formation 1 Kidney and urine formation 1.Renal structure & function 1)General
Kidney and urine formation Renal structure & function Urine formation Urinary y concentration and dilution Regulation of urine formation 1 Kidney and urine formation 1.Renal structure & function 1)General
Running head: NEPHRON 1. The nephron the functional unit of the kidney. [Student Name] [Name of Institute] Author Note
![Running head: NEPHRON 1. The nephron the functional unit of the kidney. [Student Name] [Name of Institute] Author Note Running head: NEPHRON 1. The nephron the functional unit of the kidney. [Student Name] [Name of Institute] Author Note](/thumbs/77/75431210.jpg) Running head: NEPHRON 1 The nephron the functional unit of the kidney [Student Name] [Name of Institute] Author Note NEPHRON 2 The nephron the functional unit of the kidney The kidney is an important excretory
Running head: NEPHRON 1 The nephron the functional unit of the kidney [Student Name] [Name of Institute] Author Note NEPHRON 2 The nephron the functional unit of the kidney The kidney is an important excretory
Class XI Chapter 19 Excretory Products and their Elimination Biology
 Class XI Chapter 19 Excretory Products and their Elimination Biology Question 1: Define Glomerular Filtration Rate (GFR) Glomerular filtration rate is the amount of glomerular filtrate formed in all the
Class XI Chapter 19 Excretory Products and their Elimination Biology Question 1: Define Glomerular Filtration Rate (GFR) Glomerular filtration rate is the amount of glomerular filtrate formed in all the
AP Biology. Homeostasis. Chapter 44. Regulating the Internal Environment. Homeostasis
 Chapter 44. Regulating the Internal Environment omeostasis Living in the world organisms had a choice: regulate their internal environment maintain relatively constant internal conditions conform to the
Chapter 44. Regulating the Internal Environment omeostasis Living in the world organisms had a choice: regulate their internal environment maintain relatively constant internal conditions conform to the
From Blood Filtrate to Urine: A Closer Look
 Blood Vessels Associated with the Nephrons Each nephron supplied with blood by an afferent arteriole branch of renal artery divides into glomerular capillaries capillaries converge as they leave glomerulus
Blood Vessels Associated with the Nephrons Each nephron supplied with blood by an afferent arteriole branch of renal artery divides into glomerular capillaries capillaries converge as they leave glomerulus
Refer to the figure below, a diagram of a renal tubule, to answer the following questions.
 1. The digestion and utilization of which nutrient creates the greatest need for osmoregulation by the kidneys? a. protein b. starch c. fat d. oil e. cellulose 2. Which of the following is true of urea?
1. The digestion and utilization of which nutrient creates the greatest need for osmoregulation by the kidneys? a. protein b. starch c. fat d. oil e. cellulose 2. Which of the following is true of urea?
Human Anatomy and Physiology - Problem Drill 23: The Urinary System, Fluid, Electrolyte and Acid-Base Balance
 Human Anatomy and Physiology - Problem Drill 23: The Urinary System, Fluid, Electrolyte and Acid-Base Balance Question No. 1 of 10 Which of the following statements about the functions of the urinary system
Human Anatomy and Physiology - Problem Drill 23: The Urinary System, Fluid, Electrolyte and Acid-Base Balance Question No. 1 of 10 Which of the following statements about the functions of the urinary system
Body fluid volume is small (~5L (blood + serum)) Composition can change rapidly e.g. due to increase in metabolic rate
 Renal physiology The kidneys Allow us to live on dry land. Body fluid volume is small (~5L (blood + serum)) Composition can change rapidly e.g. due to increase in metabolic rate Kidneys maintain composition
Renal physiology The kidneys Allow us to live on dry land. Body fluid volume is small (~5L (blood + serum)) Composition can change rapidly e.g. due to increase in metabolic rate Kidneys maintain composition
Excretion and Waste Management. Biology 30S - Miss Paslawski
 Excretion and Waste Management Biology 30S - Miss Paslawski Lesson 1 Waste Products and Organs 2 3 Excretion Excretion: Process by which dissolved metabolic wastes are separated from body fluids and removed
Excretion and Waste Management Biology 30S - Miss Paslawski Lesson 1 Waste Products and Organs 2 3 Excretion Excretion: Process by which dissolved metabolic wastes are separated from body fluids and removed
URINE CONCENTRATION AND REGULATION OF ECF OSMOLARITY
 URINE CONCENTRATION AND REGULATION OF ECF OSMOLARITY Dilute and concentrated urine 1-Dilute urine : Nephron function continuous reabsorption. Solutes while failing to reabsorbe water in distal tubule and
URINE CONCENTRATION AND REGULATION OF ECF OSMOLARITY Dilute and concentrated urine 1-Dilute urine : Nephron function continuous reabsorption. Solutes while failing to reabsorbe water in distal tubule and
Title: Oct 12 3:37 PM (1 of 39) Ch 44 Osmoregulation and Excretion
 Title: Oct 12 3:37 PM (1 of 39) Ch 44 Osmoregulation and Excretion Water Balance and Waste Disposal osmoregulation managing water content and solute composition based on movements of solutes excretion
Title: Oct 12 3:37 PM (1 of 39) Ch 44 Osmoregulation and Excretion Water Balance and Waste Disposal osmoregulation managing water content and solute composition based on movements of solutes excretion
UNIT II HUMAN ANATOMY AND PHYSIOLOGY
 UNIT II HUMAN ANATOMY AND PHYSIOLOGY II B--EXCRETORY PRODUCTS AND THEIR ELIMINATION Very Short Answer Questions 1. Name the blood vessels that enter and exit the kidney? A. Renal artery enters kidney and
UNIT II HUMAN ANATOMY AND PHYSIOLOGY II B--EXCRETORY PRODUCTS AND THEIR ELIMINATION Very Short Answer Questions 1. Name the blood vessels that enter and exit the kidney? A. Renal artery enters kidney and
Urine Formation. Urinary Physiology Urinary Section pages Urine Formation. Glomerular Filtration 4/24/2016
 Urine Formation Urinary Physiology Urinary Section pages 9-17 Filtrate Blood plasma minus most proteins Urine
Urine Formation Urinary Physiology Urinary Section pages 9-17 Filtrate Blood plasma minus most proteins Urine
OSMOREGULATION AND EXCRETION
 1 2 3 4 5 6 OSMOREGULATION AND EXCRETION OSMOREGULATION Process by which animals control their solute concentrations and balance water gain and loss Freshwater animals show adaptations that reduce water
1 2 3 4 5 6 OSMOREGULATION AND EXCRETION OSMOREGULATION Process by which animals control their solute concentrations and balance water gain and loss Freshwater animals show adaptations that reduce water
Points To Remember. The structural and functional unit of kidneys. Each kidney contains about one million of nephrons.
 Ammonotelism : Points To Remember The animals which excrete ammonia are called ammonotelic and excretion of ammonia is known as ammonotelism eg. Amoeba, sycon, hydra, liver fluke, tapeworm, Leech, Prawn,
Ammonotelism : Points To Remember The animals which excrete ammonia are called ammonotelic and excretion of ammonia is known as ammonotelism eg. Amoeba, sycon, hydra, liver fluke, tapeworm, Leech, Prawn,
19. RENAL PHYSIOLOGY ROLE OF THE URINARY SYSTEM THE URINARY SYSTEM. Components and function. V BS 122 Physiology II 151 Class of 2011
 19. RENAL PHYSIOLOGY THE URINARY SYSTEM Components and function The urinary system is composed of two kidneys, the functionally filtering apparatus, which connect through two tubular structures called
19. RENAL PHYSIOLOGY THE URINARY SYSTEM Components and function The urinary system is composed of two kidneys, the functionally filtering apparatus, which connect through two tubular structures called
Histology Urinary system
 Histology Urinary system Urinary system Composed of two kidneys, two ureters, the urinary bladder, and the urethra, the urinary system plays a critical role in: 1- Blood filtration,(filtration of cellular
Histology Urinary system Urinary system Composed of two kidneys, two ureters, the urinary bladder, and the urethra, the urinary system plays a critical role in: 1- Blood filtration,(filtration of cellular
A. Incorrect! The urinary system is involved in the regulation of blood ph. B. Correct! The urinary system is involved in the synthesis of vitamin D.
 Human Anatomy - Problem Drill 22: The Urinary System Question No. 1 of 10 1. Which of the following statements about the functions of the urinary system is not correct? Question #01 (A) The urinary system
Human Anatomy - Problem Drill 22: The Urinary System Question No. 1 of 10 1. Which of the following statements about the functions of the urinary system is not correct? Question #01 (A) The urinary system
URINARY SYSTEM. Primary functions. Major organs & structures
 URINARY SYSTEM Primary functions Excretion of metabolic wastes Regulation of water and ion balances Regulation of blood pressure Vitamin D activation Regulation of rbc s (erythropoietin) Gluconeogenesis
URINARY SYSTEM Primary functions Excretion of metabolic wastes Regulation of water and ion balances Regulation of blood pressure Vitamin D activation Regulation of rbc s (erythropoietin) Gluconeogenesis
BIOL2030 Human A & P II -- Exam 6
 BIOL2030 Human A & P II -- Exam 6 Name: 1. The kidney functions in A. preventing blood loss. C. synthesis of vitamin E. E. making ADH. B. white blood cell production. D. excretion of metabolic wastes.
BIOL2030 Human A & P II -- Exam 6 Name: 1. The kidney functions in A. preventing blood loss. C. synthesis of vitamin E. E. making ADH. B. white blood cell production. D. excretion of metabolic wastes.
11/05/1431. Urine Formation by the Kidneys Tubular Processing of the Glomerular Filtrate
 Urine Formation by the Kidneys Tubular Processing of the Glomerular Filtrate Chapter 27 pages 327 347 1 OBJECTIVES At the end of this lecture you should be able to describe: Absorptive Characteristics
Urine Formation by the Kidneys Tubular Processing of the Glomerular Filtrate Chapter 27 pages 327 347 1 OBJECTIVES At the end of this lecture you should be able to describe: Absorptive Characteristics
