Estimates of Glomerular Filtration Rate From MR Renography and Tracer Kinetic Models
|
|
|
- Arlene Lloyd
- 6 years ago
- Views:
Transcription
1 JOURNAL OF MAGNETIC RESONANCE IMAGING 29: (29) Original Research Estimates of Glomerular Filtration Rate From MR Renography and Tracer Kinetic Models Louisa Bokacheva, PhD,* Henry Rusinek, PhD, Jeff L. Zhang, PhD, Qun Chen, PhD, and Vivian S. Lee, MD, PhD Purpose: To compare six methods for calculating the single-kidney glomerular filtration rate (GFR) from T 1 - weighted magnetic resonance (MR) renography (MRR) against reference radionuclide measurements. Materials and Methods: In 1 patients, GFR was determined using six published methods: the Baumann Rudin model (BR), the Patlak Rutland method (PR), the two-compartment model without bolus dispersion (2C) and with dispersion (2CD), the three-compartment model (3CD), and the distributed parameter model (3C-IRF). Reference single-kidney GFRs were measured by radionuclide renography. The coefficient of variation of GFR (CV) was determined for each method by Monte Carlo analyses for one healthy and one dysfunctional kidney at a noise level ( n )of 2%, 5%, and 1%. Results: GFR estimates in patients varied from 6% overestimation (BR) to 5% underestimation (PR and 2CD applied to cortical data). Correlations with reference GFRs ranged from R.74 (2CD, cortical data) to R.85 (BR). In simulations, the lowest CV was produced by 3C-IRF in healthy kidney (1.7 n ) and by PR in diseased kidney (( ) n ). In both kidneys the highest CV was obtained with 2CD (( ) n ) and with 3CD in diseased kidney (8.9 n at n 1%). Conclusion: GFR estimates depend on the renal model and type of data used. Two- and three-compartment models produce comparable GFR correlations. Key Words: renal function; glomerular filtration rate; MR renography; tracer kinetics; gadolinium chelates; compartmental modeling J. Magn. Reson. Imaging 29;29: Wiley-Liss, Inc. QUANTITATIVE DYNAMIC contrast-enhanced T 1 - weighted magnetic resonance imaging (MRI) of the kidneys, or MR renography (MRR) (1 3), has emerged as a promising radiological measure of renal function. MRR Department of Radiology, New York University School of Medicine, New York, NY. *Address reprint requests to: L.B., NYU School of Medicine, Department of Radiology, 66 First Ave., New York, NY louisa.bokacheva@med.nyu.edu. Received March 1, 28; Accepted September 3, 28. DOI 1.12/jmri Published online in Wiley InterScience ( provides high spatial and temporal resolution and can be performed in conjunction with anatomic imaging and angiography (4). Assessment of renal function with MRR is based on visualizing the passage of gadolinium contrast through the kidney and subsequent analysis of the contrast concentration in renal tissues. Determining renal functional parameters from MRR data requires several steps, which include image postprocessing, such as motion correction of dynamic images and segmentation of renal tissues, quantification of contrast concentration from MR signal intensity, and tracer kinetic modeling. A variety of techniques for deriving the functional parameters from MRR data have been recently published (5 1), including several methods for estimating the glomerular filtration rate (GFR) (11 17) (Table 1). These models represent the kidney as a combination of a vascular and one or more tubular compartments, although the details of these compartments and the required input data vary among models. Simpler methods describe only the inflow of contrast from the renal vasculature into the tubules (11 13), while more advanced models account for both tubular inflow and outflow (14 17). Some models take into account the dispersion of the bolus during its passage from the abdominal aorta into the renal arteries and arterioles (14,16), whereas other models ignore this effect (13,15). While some models require both cortical and medullary enhancement curves (11,16,17), others can be applied to either cortical or whole kidney data (13 15). All but one (11) require the aortic enhancement curves as input function. Applied to the analysis of computed tomography (CT) and MR renography data, these methods yield moderate to high correlation with reference GFR measurements and GFR estimates that vary from strong underestimation to strong overestimation (8,11 18). The direct comparison of model performance is difficult because of the discrepancies in acquisition and analysis techniques used by different groups. Annet et al (14), Buckley et al (15), and Sourbron et al (19) compared the Patlak Rutland method against two-compartment models with tubular outflow; however, more extensive comparison of existing renal models has not been undertaken. The purpose of this study was to compare GFR estimates using six renal models (11 17) applied 29 Wiley-Liss, Inc. 371
2 372 Bokacheva et al. Table 1 Tracer Kinetic Renal Models Model Compartments No Vascular Tubular Input data No of parameters Baumann-Rudin (BR) (11,12) 1 ND I Cx and Med 1 Patlak-Rutland (PR) (13-15) 2 ND I Ao and K (or Cx) 2 2C (15) 2 ND IO Ao and K (or Cx) 3 2CD (14) 2 D IO Ao and K (or Cx) 5 3CD (16) 3 D IO Ao, Cx, and Med 6 3C-IRF (17) 3 D I-IO Ao, Cx, and Med 7* 2C and 3C, two- and three-compartment models; IRF, impulse residue function-based model; ND, no dispersion; D, dispersion; I, inflow; IO, inflow and outflow; I-IO, inflow only followed by inflow-outflow; Ao, aorta; Cx, cortex; Med, medulla; K, whole kidney parenchyma. *In 3C-IRF model (17), the number of adjustable parameters was reduced from 9 to 7, by fixing two parameters. to the same MRR data against the reference GFR measured by the same-day 99m Tc-DTPA renography. Monte Carlo simulations were used to evaluate the reliability of each method in the presence of data noise. Renal Models Six methods for calculating GFR from MRR data were studied: the Baumann Rudin model (BR) (11,12), the Patlak Rutland method (PR) (13 15,2), a two-compartment model with bolus dispersion (2CD) (14) and without dispersion (2C) (15), a three-compartment model with dispersion (3CD) (16), and a similar model based on impulse retention function (IRF) approach (3C-IRF) (17) (Fig. 1). These models have been developed for analysis of the gadolinium concentration versus time curves measured in renal tissues after an intravenous bolus injection of contrast agent. All models describe the kidney as a combination of a prefiltration (vascular) compartment and one or more postfiltration (tubular) compartment(s). GFR is identified with the flow from the prefiltration to postfiltration compartments. All but the 3C-IRF model assume instantaneous Figure 1. Renal models: (a) Baumann Rudin (BR), (b) Patlak Rutland (PR), (c) 2C and 2CD, (d) 3CD and 3C-IRF. RPF is renal plasma flow; GFR is glomerular filtration rate. Ao p is the contrast concentration in aortic plasma; Cx and Med are the cortical and medullary concentrations; A is the vascular concentration; and T, P, L are the concentrations in all tubules, proximal tubules, and loops of Henle, respectively. In BR (a), k cl is the clearance index related to GFR. In PR (b) and 2C (c), A Ao p. Solid arrows indicate the flow of contrast and dashed arrows show the reabsorption of water in the tubular compartments. mixing of contrast within each compartment. The leakage of contrast into the interstitial space is neglected, and the venous compartment is also ignored. All concentrations are expressed per unit volume of plasma, unless stated otherwise. Each model is briefly described below and the mathematical details are given in the Appendix. Baumann Rudin Model The model proposed by Baumann and Rudin (BR; Fig. 1a) describes the initial inflow of contrast from the cortex, which is identified with the vascular compartment, into the medulla (11,12). The outflow from the medulla is neglected. A single free parameter, the clearance index k cl, defined as the rate constant for unidirectional flow from cortex to medulla, was shown to correlate with GFR (12). An example of BR fit is given in Fig. 2a. Patlak Rutland Method The Patlak Rutland method (PR) is based on a twocompartment model (Fig. 1b), in which the outflow of contrast from the tubular compartment is neglected (13 15). The dispersion of the bolus in renal vasculature is also ignored, and the vascular concentration is approximated by the plasma concentration in the aorta. The model yields two parameters, vascular volume fraction and GFR. The latter is found as the flow from the vascular to tubular compartment during the tubular uptake. To ensure the no-outflow condition in the renal tubules, the PR method is often applied to the wholekidney data (13,15,18). However, in animal MR and CT studies, significant correlations with the reference GFRs were obtained only from analyses of the cortical data (8,14). We evaluated both whole-kidney and cortical data fitting (PR-Kidney and PR-Cortex, respectively) (Fig. 2b,c). Two-Compartment Models With Tubular Outflow The two-compartment models that account for the outflow of contrast from the renal tubules are valid beyond the tubular uptake interval. Buckley et al (15) analyzed the whole-kidney human data with a two-compartment
3 Estimates of Glomerular Filtration Rate 373 Figure 2. Model fits for a kidney with radionuclide GFR 8.1 ml/min: (a) BR, (b) PR-Kidney and (c) PR-Cortex, (d) 2C-Kidney and (e) 2C-Cortex, (f) 2CD-Kidney and (g) 2CD-Cortex, (h) 3CD, (i) 3C-IRF model. model (2C) which, similar to the PR model, neglects the bolus dispersion and yields three parameters: vascular volume, GFR, and tubular outflow rate (Fig. 1c). A similar, five-parameter model with bolus dispersion and delay (2CD) had been previously proposed by Annet et al (14) and applied to cortical data in rabbits (Fig. 1c). We considered both implementations of the two-compartment models and applied them to the whole-kidney and cortical data (2C-Kidney, 2C-Cortex, 2CD-Kidney, and 2CD-Cortex) (Fig. 2d g).
4 374 Bokacheva et al. Three-Compartment Model The three-compartment model (3CD) proposed by Lee et al (16) describes the cortex and medulla as combinations of three serially connected compartments: vascular compartment, shared by cortex and medulla, proximal tubules, contained only in the cortex, and loops of Henle, contained only in the medulla (Fig. 1d). Simultaneous fitting of cortical and medullary concentrations yields five parameters including RPF, GFR, cortical and medullary vascular volumes, and water reabsorption fraction in proximal tubules and loops of Henle (Fig. 2h). Three-Compartment IRF-Based Model The model of Zhang et al (17) (3C-IRF) has the same structure as the 3CD model, but assumes that due to a distribution of pathways, the contrast takes a minimum transit time to traverse each compartment before emerging at the outlet (Fig. 1d). Until the minimum transit time, each compartment behaves like a no-outflow system and becomes an inflow outflow system afterwards (Fig. 2i). While the 3C-IRF model includes nine parameters: RPF, GFR, cortical vascular volume fraction, minimum transit times, and outflow constants for each of the three compartments, only six parameters can be reliably identified: RPF, GFR, cortical vascular volume fraction, and mean transit times in three compartments. MATERIALS AND METHODS Patients The study protocol was approved by the Institutional Review Board, and written informed consent was obtained from all subjects. Ten patients (five female, five male, mean age 69.8 years, range 38 9 years), all diagnosed with hypertension and one also with chronic renal failure, were referred for suspected renovascular disease. Serum creatinine levels ranged from.6 to 3 mg/dl. All patients underwent Gd-DTPA-enhanced, T 1 - weighted MRR. Reference GFRs were measured by the same-day radionuclide clearance and gamma camera renography. Reference GFR Measurements GFR values were measured using standard 99m Tc- DTPA clearance and gamma camera renography methods (21,22). Radionuclide renography was performed 1 3 hours prior to MRR. Patients were manually injected with 1 mci (37 MBq) of 99m Tc-DTPA and 2 ml saline flush. Coronal images with pixel size of 4.3 mm 4.3 mm were acquired every 3 seconds for the first 1.5 minutes and every 6 seconds afterwards for 1 hour maximum. The total GFR was determined from plasma clearance of 99m Tc-DTPA from two blood samples collected 1 hour and 3 hours after the injection. GFR was calculated by multiplying the total GFR by the fractional uptake by each kidney determined from imaging. MR Imaging MR imaging was performed at 1.5 T (Avanto; Siemens Medical Solutions, Erlangen, Germany) and included T 1 -mapping (23) and Gd-DTPA-enhanced T 1 -weighted low-dose MRR using oblique coronal 3D spoiled gradient echo sequence: TR 2.84 msec, TE 1.5 msec, flip angle 12, bandwidth 65 Hz/pixel, field of view mm 3, interpolated matrix , parallel imaging acceleration factor of 3, GRAPPA reconstruction with 24 central reference lines, and acquisition time 3 seconds. A bolus of 4 ml of Gd-DTPA (Magnevist; Berlex Laboratories, Wayne, NJ) and a 2-mL saline flush were both injected at a rate of 2 ml/sec with an automated injector (Spectris; Medrad, Indianola, PA). Five precontrast images were acquired to determine the baseline signal. Acquisition was started at 8 seconds after injection and repeated during separate breath-holds every 3 seconds up to.5 minutes, every 15 seconds between.5 and 1.5 minutes, 3 seconds at minutes, and 6 seconds at 5 1 minutes. Image and Data Analysis Coregistration and segmentation of serial images was performed using a semiautomatic algorithm (24). After motion correction, kidney parenchyma (excluding the collecting system and renal pelvis) was segmented from the surrounding tissue, and afterwards cortex was segmented from medulla. Aortic signal was sampled in the abdominal aorta at the level of renal arteries. For each region, the average signal intensity (SI) was computed at each timepoint. SI data were converted into gadolinium concentrations using previously validated phantom-based method (5,25). Precontrast parenchymal, cortical, and medullary T 1 values required for conversion were determined from T 1 maps (23); T 1 of 12 msec was assumed for aortic blood (26). Nonlinear least squares fitting with Levenberg Marquardt algorithm was performed in MatLab (Math- Works; Natick, MA). For curve fit models, the match between the fitted curves and data was assessed by the fit residual (root-mean-square (RMS) error) and expressed as percentage of the mean measured concentration. For three-compartment models the residual was calculated with equal weights for cortical and medullary RMS. The fitted interval for BR model was selected between the trough after the vascular peak and the maximum of the tubular peak in the medullary concentration. To obtain GFR, the BR clearance index k cl was multiplied by the volume of medulla. The PR method was implemented as a nonlinear curve fit (15). A fixed interval between and 12 seconds was selected for fitting the whole-kidney data and to 9 seconds was chosen for fitting the cortical data. To account for bolus arrival into the kidney in models without dispersion, PR and 2C, the arterial input function was shifted forward by 3 seconds, which was the smallest sampling interval in our protocol. In 2CD, bolus delay was adjusted by minimizing the fit residual while shifting the time axis of the aortic curve. The fit residuals were compared using two-sample paired Wilcoxon signed-rank test. The correlation between the model-derived and reference GFR was char-
5 Estimates of Glomerular Filtration Rate 375 Table 2 Average Fit Residuals Expressed as Percentages of Average Renal Concentration and Median Relative Differences GFR (GFR MR GFR Nuc )/GFR Nuc Between Model-Derived GFRs (GFR MR ) and Radionuclide GFRs (GFR Nuc ) Model Residual (%) GFR (%) BR 6. PR-Kidney PR-Cortex C-Kidney C-Cortex CD-Kidney CD-Cortex CD C-IRF acterized by linear regression and Pearson s correlation coefficient R. Variability Due to Data Noise The robustness of the models to data noise was evaluated by Monte Carlo analyses. Two representative experimental MRR datasets were assessed: one from a kidney with a normal reference GFR 8.1 ml/min and the other from kidney with abnormally low GFR 18.2 ml/min. Measured aortic curves were used as input functions. Aortic and renal data were perturbed by adding normally distributed noise with zero mean and standard deviation of n 2%, 5%, and 1% of the precontrast whole-kidney signal (for PR, 2C, 2CD models) or cortical signal (BR, 3CD, 3C-IRF). The signal curves were then converted into concentration (25) and fitted with each model. The coefficient of variation of GFR (CV(GFR)), or the ratio of the standard deviation to the mean value, was calculated from N 1 trials. RESULTS GFR Estimates With Six Renal Models All 2 MRR datasets were analyzed with six renal models. Examples of model fits are shown in Fig. 2 and fit residuals are given in Table 2. The PR method produced the highest residuals that reached 3% over the fitted interval. The inclusion of outflow in 2C decreased the residuals by half (14.9% for 2C-Kidney and 17.5% for 2C-Cortex) and accounting for dispersion resulted in another 2-fold decrease in residual (8.3% for 2CD-Kidney and 9.1% and 2CD-Cortex). For 2C model, the residuals were significantly lower for whole-kidney data than for cortical data (P.1); however, in PR and 2CD models this difference did not reach significance (P.5). The 3C-IRF model yielded significantly lower residuals than the 3CD model (11.6% vs. 15.5%, P.6). The residuals did not show any apparent trends in relation to GFR. The model-estimated vascular and tubular compartmental contributions are illustrated in detail for twoand three-compartment models (Figs. 3 and 4, respectively). In models without dispersion (PR, 2C; Fig. 3a,d), the vascular contribution shows a narrow first-pass peak followed by a low washout tail. A considerable part of the renal vascular peak and most of the tubular peak are attributed to the tubular compartment. In 2CD, the vascular contribution is broader and has a higher tail, and the tubular contribution is lower than in 2C. In 2C-Kidney (Fig. 3c), the area under the curve (AUC) of the vascular contribution between and 9 seconds accounts for 26% of the area under the renal concentration curve. In contrast, in 2CD-Kidney (Fig. 3e) the vascular AUC over the same time interval is 57% of the renal AUC. The fits to cortical data (Fig. 3d,f) show larger vascular and smaller tubular contributions than the corresponding whole-kidney fits (Fig. 3c,e). The 3CD model fits (Fig. 4a) are similar to the 2CD fits, with broadened vascular contributions. In 3C-IRF (Fig. 4b), the shapes of the vascular and tubular contributions appear to be intermediate between models with and without dispersion. Radionuclide single-kidney GFRs ranged from ml/min. The magnitude of model-derived GFRs varied among models from weak overestimation to strong underestimation (Table 2). The highest GFRs were obtained from the BR model, which produced the median 6% overestimation. All other models underestimated GFR by different amounts that varied from 2.5% for 2CD-Kidney to over 5% for the PR-Cortex and 2CD- Cortex models. GFRs derived using two-compartment models applied to cortical data were significantly lower than GFRs obtained using the same methods from whole-kidney data (P.1 in PR, 2C, and 2CD models). The correlations between the model-derived and radionuclide GFRs (Fig. 5) were significant in all cases (P.4) with the correlation coefficients ranging from R.74 for 2CD-Cx to R.85 for the BR model. There was one outlier kidney (radionuclide GFR 89.4 ml/min). Variability Due to Data Noise CV(GFR) estimated by Monte Carlo analyses in representative healthy and diseased kidneys shows that all models amplified data noise to different degrees (Fig. 6). Two-compartment models with two to three parameters (PR and 2C) amplified noise by factors of 2. to 3.6 in both functional and dysfunctional kidneys. The BR model produced higher errors ( n ). The 2CD model amplified noise more strongly, with CV(GFR) reaching on average 5.9 n (2CD-Kidney) and 8.2 n (2CD-Cortex) in both kidneys. The 3CD model yielded 2.7 times noise amplification in healthy kidney, but performed poorly in diseased kidney at 1% noise (CV 8.9 n ). In contrast, the 3C-IRF provided the lowest CV(GFR) among all models in healthy kidney (1.7 n ) and consistent CV(GFR) values in diseased kidney at all noise levels (3.1 n ). DISCUSSION We studied six models for calculating GFR from MRR data. As expected, the best fits (or the lowest fit residuals) were obtained using the most flexible model, the seven-parameter 3C-IRF model, and the worst fits (the highest residuals) were produced by the PR method and 2C model. Cortical data fitted with the 2C model tended
6 376 Bokacheva et al. Figure 3. Two-compartment model fits (solid black lines) and vascular (solid red lines) and tubular (dashed blue lines) compartmental contributions for MRR data (symbols and dotted lines) of a kidney with radionuclide GFR 8.1 ml/ min: (a) PR-Kidney, (b) PR-Cortex, (c) 2C-Kidney, (d) 2C-Cortex, (e) 2CD-Kidney, (f) 2CD- Cortex. The vascular and tubular contributions are labeled w a A and w T T, respectively, where A and T are concentrations and w a and w T are volume fractions (see Appendix). In no-dispersion models (PR and 2C, top and middle row), w a A is narrower and lower and w T T is higher than in 2CD (bottom row). Figure 4. Three-compartment model fits (solid black lines) with vascular (solid red line) and tubular (dashed blue and dash-dotted green lines) compartmental contributions for MRR data (symbols and dotted lines) of kidney with reference GFR 8.1 ml/min. (a) 3CD and (b) 3C-IRF fits. Cortical fits are shown in the left panels and medullary fits in the right panels. In 3CD (a) the modelderived vascular contribution is labeled w a A and the contributions of proximal tubules and loops of Henle are labeled w P P and w L L, where A, P, and L are concentrations in vasculature, proximal tubules, and loops, respectively, and w a, w P, and w L are the corresponding volume fractions. In 3C-IRF the concentrations are denoted the same way, but the volume fraction v acx is defined as the fraction of vascular compartment residing in the cortex (see Appendix).
7 Estimates of Glomerular Filtration Rate 377 to result in lower quality fits than whole-kidney data. We believe that this occurs because of the difficulty of describing the cortical curve, which contains features of the proximal and distal tubules, using a single tubular compartment in addition to vascular compartment. In the whole-kidney curve, all tubular features are lumped together and enveloped by the loop of Henle/ collecting ducts peak in medulla, and thus a two-compartment description is more suitable. The correlations between the model-derived and reference GFRs ranged from R.74 (2CD-Cortex) to R.85 (BR) and were not necessarily better for more sophisticated models. The magnitude of GFR estimates varied greatly across models, even when the same data were used (eg, among PR-Kidney, 2C-Kidney, and 2CD- Kidney), and were lower for cortical data than for wholekidney data. Large variations of GFRs obtained from the same data are likely caused by the models. We believe that the primary source of these variations is the uncertainty in determination of the relative magnitude of the vascular and tubular contributions to the net renal concentration. This uncertainty is caused by the unfeasibility of direct measurements of arterial contrast concentration immediately at the filtration site, ie, at the glomerulus. Instead, the arterial concentration is usually measured in the abdominal aorta and the concentration in the renal vasculature is inferred from it using model-specific assumptions. We noticed that accounting for bolus dispersion results in lower GFRs. For example, the 2CD model produced significantly lower GFRs than the 2C model. When dispersion is ignored, as in 2C (Fig. 3c,d), the vascular contribution is equated to the aortic concentration scaled by the vascular volume fraction (see Appendix) and the amplitude of this contribution is set almost exclusively by the height of the renal vascular peak. As a result, the vascular volume fraction is forced to be quite low to scale the aortic first-pass peak down to a less prominent renal vascular peak. Consequently, the vascular contribution has a narrow peak followed by a low tail, and the rest of the renal curve is attributed to the tubular component. In contrast, in models with dispersion, such as in 2CD and 3CD (Figs. 3e,f and 4a,b) the vascular volume fraction adjusts both the height and width of the vascular contribution to match the renal vascular peak. This results in a vascular curve with a broadened first-pass peak and higher tail and a lower tubular component than in the no-dispersion case. Larger vascular and lower tubular contributions in models with dispersion suggest that GFR obtained using these models is expected to be lower than in no-dispersion models applied to the same data. The description of the tubular compartment also affects GFR magnitude. Annet et al (14) first noticed that the PR method underestimated GFR relative to 2CD model and attributed this underestimation to neglecting the tubular outflow in the PR method. Similar observations were reported by Buckley et al for 2C (15) and by Sourbron et al for the 2CD model (19). Our results showed a similar trend: PR GFRs were lower than both 2C and 2CD GFRs applied to the same data. This observation is supported by the model solutions (see Appendix). In PR, GFR is multiplied by a monotonically increasing integral of the aortic concentration and is forced to be lower to compensate for this increase. In a similar 2C model, the aortic integral is reduced by the outflow term, and when applied to the same data this model yields higher GFR than PR method (Eq. [A4] vs. Eq. [A5]). Another problem in the no-outflow models arises from the uncertainty of defining the uptake interval, the choice of which strongly affects GFR values. Hackstein et al (2) observed that PR GFR decreased considerably as the fitted interval was shifted toward later times. We observed the same trend in our PR analyses; however, we did not attempt to optimize the fitted PR interval. Hackstein et al (2) obtained the highest correlations of PR GFR with the reference from fitting 4 11 seconds interval after the aortic rise; the same interval was used by Sourbron et al (19). We implemented the PR method as a nonlinear curve fit, following Buckley et al (15), to take advantage of the initial portions of the kidney data that are discarded in the graphical implementation, and used the interval from seconds to 12 seconds in whole-kidney data and seconds to 9 seconds in cortical data. In healthy kidneys, as the ones studied in Refs. (19) and (2), the interval of 4 11 seconds corresponds mainly to the medullary uptake. In dysfunctional kidneys, as in some of our patients, this interval may be extended or shifted toward later times. We suspect that even with the fitted interval ending at seconds the no-outflow condition is not fulfilled, especially in the cortical data, where the outflow from proximal tubules probably occurs before 6 75 seconds. The initial, inflow-only part of the tubular contribution is buried under the vascular peak, and the PR method relies on the exposed slope of the renal concentration instead. The methods proposed by Krier et al (27), Daghini et al (8), and Hermoye et al (5), which use gamma variate functions to estimate the upslope of the proximal tubular enhancement, may offer more accurate modeling. For our experimental protocol, the PR method may be suboptimal. Lower temporal resolution of our breathholding protocol results in few data points measured during the uptake interval. Furthermore, it has been shown that the PR results improve at higher injected doses of contrast (13), whereas in our study a low dose (4 ml, or.25 mmol/kg) of Gd-DTPA was used. Lower amounts of contrast minimize the signal loss associated with concentrated contrast (T 2 * effects) and may also be advantageous given the association of high doses of gadolinium chelates with the development of the nephrogenic systemic fibrosis (NSF) (28,29). Using cortical data for GFR estimates seems to be preferable because glomerular filtration occurs predominantly in the cortex. However, in addition to vascular and proximal tubular features, cortical enhancement also contains overlapping features of the distal tubules, which the contrast enters after passing through the medulla, and therefore the cortical concentration may not be a more direct indicator of filtration. In PR analysis of animal data, only cortical data yielded significant GFR correlations with the reference, but not the whole-kidney data (8,14). In human studies, whole-kidney enhancement is often
8 Figure 5. Model-derived GFR versus nuclear medicine GFR: (a) BR, (b) PR- Kidney, (c) PR-Cortex, (d) 2C-Kidney, (e) 2C-Cortex, (f) 2CD-Kidney, (g) 2CD-Cortex, (h) 3CD, (i) 3C-IRF models. Linear regressions are indicated by dotted lines and equations; identity lines are shown by solid lines.
9 Estimates of Glomerular Filtration Rate 379 Figure 6. Coefficient of variation of GFR CV(GFR) at 2%, 5%, and 1% data noise for two kidneys: (a) functioning kidney (GFR 8.1 ml/min), and (b) dysfunctional kidney (GFR 18.2 ml/min). The two-compartment models with two or three parameters (PR and 2C) produce lower CV than the five-parameter model (2CD) or BR model. The 3CD model performs well in a normal kidney, yet fails at 1% noise in dysfunctional kidney. In contrast, the 3C-IRF produces the lowest CV(GFR) in healthy kidney and performs comparably with more rigid PR and 2C models in dysfunctional kidney. used (13,15,18). In our study, both cortical and whole-kidney data provided similar correlations, but cortical GFRs were lower than GFRs obtained from whole-kidney data. We believe that this occurs because the inclusion of the medulla into whole-kidney enhancement alters the relative contributions of vascular and tubular components in favor of the tubules. In the whole-kidney curve the vascular peak is lower (because of lower vascular content in medulla) and the tubular peak is higher (mainly due to contrast in loops of Henle and collecting ducts) than in the cortical curve (Fig. 2d,e), which results in higher wholekidney GFRs. Higher tubular enhancement in medulla also accounts for the higher GFR values obtained with the BR model. Both three-compartment models provide good curve fits, especially the 3C-IRF model. GFR correlations provided by the three-compartment models were on par with the two-compartment models. Among the studied models, the BR model is the only one that does not require measurements of the aortic input function (AIF). The use of the cortical data as an approximation of AIF is both a flaw and an advantage. Unlike other models, the BR model does not compute GFR directly, but only an index k cl that is proportional to GFR. The BR model ignores both the nonvascular contributions to cortical concentration and the vascular contribution in the medulla. This may be an appropriate assumption in animal studies (2), but not in human kidneys (Fig. 2). On the other hand, the BR model eliminates potentially large errors associated with AIF measurements, which can be unreliable due to flow artifacts and inadequate temporal sampling of the arterial peak. For our patient group, the BR model gave a good correlation with the reference GFR values, suggesting that AIF errors may be the dominant sources of GFR errors. For methods that require arterial input function, variations of the aortic enhancement have a strong impact on the modeling results and are a major source of uncertainty in GFR. Aortic signal, particularly in a tortuous aorta, can be distorted by the inflow artifacts. In our study, this problem was reduced by imaging in coronal direction and sampling the abdominal aorta signal at the level of the renal arteries. Other methods of reducing errors in AIF, such as postprocessing corrections and population-averaged AIF curves, may also be helpful (3). The stability of computed parameters in the presence of noise is always a concern, especially for more complex models. Our simulations show that curve-fit models with three or fewer parameters (PR and 2C) amplify noise by a factor of 2 to 3.6. In contrast, the five-parameter 2CD model amplifies noise 6 8-fold. The 3CD produces CV(GFR) 89.% in diseased kidney at 1% noise, which agrees with our routine experience with this model. On the other hand, due to its ability to capture correctly both the uptake and the washout portions of the data, the more complex 3C-IRF model amplifies noise by a factor of 1.7 in a healthy kidney and 3-fold in a dysfunctional kidney. The models considered here share assumptions that may be sources of error. The distribution of parameters was considered homogeneous within a given tissue. In all but the 3C-IRF model, complete instantaneous mixing within each compartment was assumed, and concentration gradients in the renal tubules were ignored. Each kidney region (parenchyma, cortex, and medulla) was described by no more than two compartments (vascular and tubular), which is a gross oversimplification. The distribution of contrast agent over the interstitial space was also neglected. In normal kidneys, interstitial space occupies only about 1% of parenchymal volume; however, in patients with inflammatory renal disease, the interstitial space may be increased, and ignoring it was shown to cause overestimation of GFR (18). In the patients studied here, renal volumes were not obviously increased ( ml), and therefore neglecting the interstitial space was justified in the first approximation. Our study suffered from the following limitations. First, the number of studied cases was small. Second, we explored only a single type of MRR protocol, and the influence of acquisition details on GFR results should
10 38 Bokacheva et al. be studied further. Third, we considered the PR method with an empirically selected fitted interval which was the same for all cases and not systematically optimized. Fourth, we used a fixed bolus delay in the no-dispersion models. Although this delay does not change the trends in GFR results, the best method for treating the bolus delay needs to be determined. Additionally, our Monte Carlo simulations were performed for only two sets of representative kidney parameters and did not explore a range of renal states. Finally, the reference radionuclide GFRs are imperfect and may contain about 1% errors (31). Many other methods have been used to estimate renal functional parameters from MR and CT renography. Some investigators have used fast T 1 -measurements and phase contrast flow quantification to determine GFR from renal extraction fraction of gadolinium chelates (9,1); however, these methods require high spatial and temporal resolution. Other approaches, such as reported by Boss et al (6), are based on gadolinium clearance principles, similar to radionuclide clearance methods, and fit the exponential washout of gadobutrol contrast from the renal cortex. Unlike the models studied here, this method relies on estimates of extracellular fluid volume determined from patient height and weight to convert the washout constant into the total GFR. In conclusion, compartmental models provide means for calculating GFR and other parameters from MRR data. The choice of renal model is determined by the parameters that need to be measured, availability and accuracy of tissue segmentation, quality of dynamic images, and patient s kidney condition. It is important to know the biases and error propagation associated with each model, as these properties may strongly influence the resulting parameters. The three-parameter two-compartment model without dispersion enables calculation of GFR when either whole-kidney or cortical data are available. The four-parameter (with dispersion only) or five-parameter (with dispersion and delay) versions of this model also provide RPF, but should be used with caution, preferably in experiments with high signal-to-noise ratio (SNR), because of their lower stability. The three-compartment models require more involved image processing (24,32), but provide GFR, RPF, and other parameters and can characterize cortex and medulla separately. The distributed-parameter 3C-IRF model offers excellent curve fits and parameter stability and GFR estimates on par with other models. Reliable determination of aortic signal is crucial for models that require arterial input functions. APPENDIX Baumann Rudin Model (11,12) The clearance index k cl related to GFR is found from cortical and medullary concentrations, Cx(t) and Med(t): dmed t k dt cl Cx t [A1] Patlak Rutland Model (13 15) The contrast concentration in renal tissue K(t) is found as a combination of vascular and tubular concentrations, A(t) and T(t), respectively: K t w a A t w t T t, [A2] where w a V a /V, w t V t /V, and V a and V t are the compartmental volumes and V is the renal tissue volume. A(t) is equated to the plasma concentration in aorta, Ao p (t), which can be found from whole-blood concentration Ao(t) and hematocrit Hct: A t Ao p t Ao t / 1 Hct [A3] During uptake of contrast by renal tubules, the PR model solution can be fitted to the renal data with two free parameters, vascular volume fraction w a and GFR: K t w a Ao p t GFR V t Ao p u du. [A4] In traditional implementation of the PR method, Eq. [A4] is divided by Ao p (t), and GFR and w a are found, respectively, from the slope and intercept of linear regression between y K(t)/Ao p (t) and normalized time t t Ao p u du/ao p t. 2C and 2CD models (14,15) In 2C and 2CD models, the kidney concentration K(t) has the form of Eq. [A2] and the model solution is given by: K t w a A t GFR V t A u e kout t u du, [A5] where k out is the tubular outflow rate constant. In the 2C model, A(t) Ao p (t). In the 2CD model, it is expressed as follows: A t RPF V a t Ao p u e RPF t u V a du, [A6] where RPF is the renal plasma flow. 2C has three free parameters: w a, GFR, k out ; and 2CD has an additional parameter, RPF. Fitted bolus delay was introduced in 2CD according to the original implementation of the model (14): Ao p (t) 3 Ao p (t ).
11 Estimates of Glomerular Filtration Rate 381 3C model (16) Cortical and medullary concentrations, Cx(t) and Med(t), are expressed as combinations of concentrations in vasculature, A, proximal tubules, P, and loops of Henle L: Cx t w acx A t w p P t, Med t w amed A t w l L t, RPF A t V acx V amed Ao p u e P t GFR V p t t L t GFR 1 f p V l RPF V t u acx V amed du, [A7a] [A7b] [A8a] A u e GFR 1 fp V p t u du, [A8b] t P u e GFR 1 fp fl V l t u du, [A8c] where w acx V acx /V Cx,w amed V amed /V Med, and V acx and V amed are cortical and medullary vascular volumes, V Cx and V Med are tissue volumes, and f p and f l are water reabsorption fractions in P and L. The volume fractions of P in the cortex, w p, and L in medulla, w l were found to be fully correlated with f p and f l and were fixed at constant values: w p V p /V Cx.3, w l V l /V Med.5. The model yields six parameters: RPF, GFR, w acx, w amed, f p, and f l. Only a sum f p f l can be reliably identified, thus reducing the number of parameters to five. 3C-IRF model (17) The cortical and medullary contrast residues (in mass units), M Cx and M Med are expressed through compartmental IRFs, Rˆ A, Rˆ P, and Rˆ L, convolved with aortic concentration Ao p (t): M Cx t RPF Ao p v acx Rˆ A Rˆ P, M Med t RPF Ao p 1 v acx Rˆ A Rˆ L. [A9a] [A9b] Here v acx is the fraction of vascular compartment in the cortex. Inherited IRFs (i A, P, L) correspond to an ideal delta-function bolus applied to the entrance of the whole system and can be found as follows: Rˆ A R A. Rˆ P GFR RPF O A R P, [A1a] [A1b] R i t 1 Rˆ L O P R L, t t i e ki t ti t t i, O i I i drˆ i dt, [A1c] [A1d] [A1e] where R i is a native IRF in response to an ideal bolus applied at the entrance of i-th compartment, t i is the minimum transit time (mintt), and I i and O i are the compartmental input and output fluxes of contrast (mass per unit time). The input to the first compartment, A, is equal to the ideal bolus applied to the whole system, ie, I A (t). The model yields nine parameters: RPF, GFR, v acx, mintts t A, t P, t L, and outflow constants k A, k P, k L. To improve the stability of the model, two parameters were fixed: t P seconds and t L 1/k L. Although k A could not be identified reliably, mean transit times MTT A t A 1/k A was shown to be robust. REFERENCES 1. Prasad PV. Functional MRI of the kidney: tools for translational studies of pathophysiology of renal disease. Am J Physiol Renal Physiol 26;29:F958 F Huang AJ, Lee VS, Rusinek H. Functional renal MR imaging. Magn Reson Imaging Clin N Am 24;12: Michoux N, Vallée J-P, Pechère-Bertschi A, Montet X, Buehler L, Van Beers BE. Analysis of contrast-enhanced MR images to assess renal function. MAGMA 26;19: Lee VS, Rusinek H, Noz M, Lee P, Raghavan M, Kramer EL. Dynamic three-dimensional MR renography for the measurement of single kidney function: Initial experience. Radiology 23;227: Hermoye L, Annet L, Lemmerling P, et al. Calculation of the renal perfusion and glomerular filtration rate from the renal impulse response obtained with MRI. Magn Reson Med 24;51: Boss A, Martirosian P, Gehrmann M, et al. Quantitative assessment of glomerular filtration rate with MR gadolinium slope clearance measurements. Radiology 27;242: Michaely HJ, Schoenberg SO, Oesingmann N, et al. Renal artery stenosis: Functional assessment with dynamic MR perfusion measurements feasibility study. Radiology 26;238: Daghini E, Julliard L, Haas JA, Krier JD, Romero JC, Lerman LO. Comparison of mathematic models of assessment of glomerular filtration rate in electron-beam CT in pigs. Radiology 27;242: Coulam CH, Lee JH, Wedding KL, et al. Noninvasive measurement of extraction fraction and single-kidney glomerular filtration rate with MR imaging in swine with surgically created renal arterial stenosis. Radiology 22;223: Niendorf ER, Grist TM, Lee FT Jr, Brazy PC, Santyr GE. Rapid in vivo measurement of single-kidney extraction fraction and glomerular filtration rate with MR imaging. Radiology 1998;26: Baumann D, Rudin M. Quantitative assessment of rat kidney function by measuring the clearance of the contrast agent Gd(DOTA) using dynamic MRI. Magn Reson Imaging 2;18: Laurent D, Poirier K, Wasvary J, Rudin M. Effect of essential hypertension on kidney function as measured in rat by dynamic MRI. Magn Reson Med 24;47: Hackstein N, Heckrodt J, Rau WS. Measurement of single-kidney glomerular filtration rate using a contrast-enhanced dynamic gradient-echo sequence and the Rutland-Patlak plot technique. J Magn Reson Imaging 23;18: Annet L, Hermoye L, Peeters F, Jamar F, Dehoux J-P, Van Beers BE. Glomerular filtration rate: assessment with dynamic contrastenhanced MRI and a cortical-compartment model in the rabbit kidney. J Magn Reson Imaging 24;2: Buckley DL, Shurrab A, Cheung CM, Jones AP, Mamtora H, Kalra PA. Measurement of single kidney function using dynamic contrast-enhanced MRI: comparison of two models in human subjects. J Magn Reson Imaging 26;24:
12 382 Bokacheva et al. 16. Lee VS, Rusinek H, Bokacheva L, et al. Renal function measurements from MR renography and a simplified multicompartmental model. Am J Physiol Renal Physiol 27;292:F Zhang JL, Rusinek H, Bokacheva L, et al. Functional assessment of the kidney from MR and CT renography: impulse retention approach to a multi-compartment model. Magn Reson Med 28;59: Hackstein N, Bauer J, Hauck EW, Ludwig M, Kramer H-J, Rau WS. Measuring single-kidney glomerular filtration rate on single-detector helical CT using a two-point Patlak plot technique in patients with increased interstitial space. AJR Am J Roentgenol 23;181: Sourbron SP, Michaely HJ, Reiser MF, Schoenberg SO. MRI-measurement of perfusion and glomerular filtration in the human kidney with a separable compartment model. Invest Radiol 28;43: Hackstein N, Kooijman H, Tomaselli S, Rau WS. Glomerular filtration rate measured using the Patlak plot technique and contrastenhanced dynamic MRI with different amounts of gadolinium- DTPA. J Magn Reson Imaging 25;22: Rowell KL, Kontzen FN, Stutzman ME, et al. Technical aspects of a new technique for estimating glomerular filtration rate using technetium-99m-dtpa. J Nucl Med Technol 1986;14: Russell CD, Rowell K, Scott JW. Quality control of technetium-99m DTPA: correlation of analytic tests with in vivo protein binding in man. J Nucl Med 1986;27: Bokacheva L, Huang AJ, Chen Q, et al. Single breath-hold T1 measurement using low flip angle TrueFISP. Magn Reson Med 26;55: Rusinek H, Boykov Y, Kaur M, et al. Performance of an automated segmentation algorithm for 3D MR renography. Magn Reson Med 27;57: Bokacheva L, Rusinek H, Chen Q, et al. Quantitative determination of Gd-DTPA concentration in T1-weighted MR renography studies. Magn Reson Med 27;57: Parker DL, Tsuruda JS, Goodrich KC, Alexander AL, Buswell HR. Contrast-enhanced magnetic resonance angiography of cerebral arteries. Invest Radiol 1998;33: Krier JD, Ritman EL, Bajzer Z, Romero JC, Lerman A, Lerman LO. Noninvasive measurement of concurrent single-kidney perfusion, glomerular filtration, and tubular function. Am J Physiol Renal Physiol 21;281:F63 F Kuo PH. Gadolinium-containing MRI contrast agents: important variations on a theme for NSF. J Am Coll Radiol 28;5: Sadowski EA, Bennett LK, Chan MR, et al. Nephrogenic systemic fibrosis: risk factors and incidence estimation. Radiology 27; 243: Parker GJ, Roberts C, Macdonald A, et al. Experimentally-derived functional form for a population-averaged high-temporal-resolution arterial input function for dynamic contrast-enhanced MRI. Magn Reson Med 26;56: Moonen M, Jacobsson L. Effect of administered activity on precision in the assessment of renal function using gamma camera renography. Nucl Med Commun 1997;18: de Priester JA, den Boer JA, Giele ELW, et al. MR renography: an algorithm for calculation and correction of cortical volume averaging in medullary renographs. J Magn Reson Imaging 2;12:
Renal function measurements from MR renography and a simplified multicompartmental model
 Am J Physiol Renal Physiol 292: F1548 F1559, 2007. First published January 9, 2007; doi:10.1152/ajprenal.00347.2006. Renal function measurements from MR renography and a simplified multicompartmental model
Am J Physiol Renal Physiol 292: F1548 F1559, 2007. First published January 9, 2007; doi:10.1152/ajprenal.00347.2006. Renal function measurements from MR renography and a simplified multicompartmental model
Functional Assessment of the Kidney From Magnetic Resonance and Computed Tomography Renography: Impulse Retention Approach to a Multicompartment Model
 Magnetic Resonance in Medicine 59:278 288 (2008) Functional Assessment of the Kidney From Magnetic Resonance and Computed Tomography Renography: Impulse Retention Approach to a Multicompartment Model Jeff
Magnetic Resonance in Medicine 59:278 288 (2008) Functional Assessment of the Kidney From Magnetic Resonance and Computed Tomography Renography: Impulse Retention Approach to a Multicompartment Model Jeff
Assessment of Renal Function with Dynamic Contrast-Enhanced MR Imaging
 Assessment of Renal Function with Dynamic Contrast-Enhanced MR Imaging Louisa Bokacheva, PhD a, *,HenryRusinek,PhD a, Jeff L. Zhang, PhD a,vivian S. Lee, MD,PhD,MBA b KEYWORDS Dynamic contrast-enhanced
Assessment of Renal Function with Dynamic Contrast-Enhanced MR Imaging Louisa Bokacheva, PhD a, *,HenryRusinek,PhD a, Jeff L. Zhang, PhD a,vivian S. Lee, MD,PhD,MBA b KEYWORDS Dynamic contrast-enhanced
Measurement of glomerular filtration rate by dynamic contrast-enhanced magnetic resonance imaging using a subject-specific two-compartment model
 ORIGINAL RESEARCH Physiological Reports ISSN 2051-817X Measurement of glomerular filtration rate by dynamic contrast-enhanced magnetic resonance imaging using a subject-specific two-compartment model Aaryani
ORIGINAL RESEARCH Physiological Reports ISSN 2051-817X Measurement of glomerular filtration rate by dynamic contrast-enhanced magnetic resonance imaging using a subject-specific two-compartment model Aaryani
Quantitative Estimation of Renal Function with Dynamic Contrast-Enhanced MRI Using a Modified Two-Compartment Model
 Quantitative Estimation of Renal Function with Dynamic Contrast-Enhanced MRI Using a Modified Two-Compartment Model Bin Chen 1, Yudong Zhang 2, Xiaojian Song 1,3, Xiaoying Wang 1,2 *, Jue Zhang 1,4 *,
Quantitative Estimation of Renal Function with Dynamic Contrast-Enhanced MRI Using a Modified Two-Compartment Model Bin Chen 1, Yudong Zhang 2, Xiaojian Song 1,3, Xiaoying Wang 1,2 *, Jue Zhang 1,4 *,
Pediatric* MR Urography
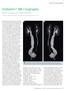 Abdominal Imaging Clinical Pediatric* MR Urography Richard A. Jones; Stephen Little; J. Damien Grattan-Smith Children s Healthcare of Atlanta, Department of Radiology, Atlanta, GA, USA MR urography represents
Abdominal Imaging Clinical Pediatric* MR Urography Richard A. Jones; Stephen Little; J. Damien Grattan-Smith Children s Healthcare of Atlanta, Department of Radiology, Atlanta, GA, USA MR urography represents
Angiotensin-Converting Enzyme Inhibitor-Enhanced MR Renography: Repeated Measures of GFR and RPF in Hypertensive Patients
 Articles in PresS. Am J Physiol Renal Physiol (January 21, 2009). doi:10.1152/ajprenal.90648.2008 1 Angiotensin-Converting Enzyme Inhibitor-Enhanced MR Renography: Repeated Measures of GFR and RPF in Hypertensive
Articles in PresS. Am J Physiol Renal Physiol (January 21, 2009). doi:10.1152/ajprenal.90648.2008 1 Angiotensin-Converting Enzyme Inhibitor-Enhanced MR Renography: Repeated Measures of GFR and RPF in Hypertensive
Angiotensin-converting enzyme inhibitor-enhanced MR renography: repeated measures of GFR and RPF in hypertensive patients
 Am J Physiol Renal Physiol 296: F884 F891, 2009. First published January 21, 2009; doi:10.1152/ajprenal.90648.2008. Angiotensin-converting enzyme inhibitor-enhanced MR renography: repeated measures of
Am J Physiol Renal Physiol 296: F884 F891, 2009. First published January 21, 2009; doi:10.1152/ajprenal.90648.2008. Angiotensin-converting enzyme inhibitor-enhanced MR renography: repeated measures of
Measurement of Glomerular Filtration Rate With Magnetic Resonance Imaging: Principles, Limitations, and Expectations
 Measurement of Glomerular Filtration Rate With Magnetic Resonance Imaging: Principles, Limitations, and Expectations Nicolas Grenier, Iosif Mendichovszky, Baudouin Denis de Senneville, Sébastien Roujol,
Measurement of Glomerular Filtration Rate With Magnetic Resonance Imaging: Principles, Limitations, and Expectations Nicolas Grenier, Iosif Mendichovszky, Baudouin Denis de Senneville, Sébastien Roujol,
MR Renographic Measurement of Renal Function in Patients Undergoing Partial Nephrectomy
 Genitourinary Imaging Review Kang et al. MR Renography and Partial Nephrectomy Genitourinary Imaging Review FOCUS ON: Stella K. Kang 1,2 William C. Huang 3 Vivian S. Lee 4 Hersh Chandarana 1 Kang SK, Huang
Genitourinary Imaging Review Kang et al. MR Renography and Partial Nephrectomy Genitourinary Imaging Review FOCUS ON: Stella K. Kang 1,2 William C. Huang 3 Vivian S. Lee 4 Hersh Chandarana 1 Kang SK, Huang
Use of Cardiac Output to Improve Measurement of Input Function in Quantitative Dynamic Contrast- Enhanced MRI
 JOURNAL OF MAGNETIC RESONANCE IMAGING 30:656 665 (2009) Original Research Use of Cardiac Output to Improve Measurement of Input Function in Quantitative Dynamic Contrast- Enhanced MRI Jeff L. Zhang, PhD,*
JOURNAL OF MAGNETIC RESONANCE IMAGING 30:656 665 (2009) Original Research Use of Cardiac Output to Improve Measurement of Input Function in Quantitative Dynamic Contrast- Enhanced MRI Jeff L. Zhang, PhD,*
Diffusion weighted MRI in evaluation of transplanted kidney: Preliminary clinical experience
 African Journal of Nephrology (2009) 13: 26-30 Original Article AJN Diffusion weighted MRI in evaluation of transplanted kidney: Preliminary clinical experience Mohamed Abou El-Ghar; M.D, Huda Refaie;
African Journal of Nephrology (2009) 13: 26-30 Original Article AJN Diffusion weighted MRI in evaluation of transplanted kidney: Preliminary clinical experience Mohamed Abou El-Ghar; M.D, Huda Refaie;
Magnetic Resonance Angiography
 Magnetic Resonance Angiography 1 Magnetic Resonance Angiography exploits flow enhancement of GR sequences saturation of venous flow allows arterial visualization saturation of arterial flow allows venous
Magnetic Resonance Angiography 1 Magnetic Resonance Angiography exploits flow enhancement of GR sequences saturation of venous flow allows arterial visualization saturation of arterial flow allows venous
Non Contrast MRA. Mayil Krishnam. Director, Cardiovascular and Thoracic Imaging University of California, Irvine
 Non Contrast MRA Mayil Krishnam Director, Cardiovascular and Thoracic Imaging University of California, Irvine No disclosures Non contrast MRA-Why? Limitations of CTA Radiation exposure Iodinated contrast
Non Contrast MRA Mayil Krishnam Director, Cardiovascular and Thoracic Imaging University of California, Irvine No disclosures Non contrast MRA-Why? Limitations of CTA Radiation exposure Iodinated contrast
1Pulse sequences for non CE MRA
 MRI: Principles and Applications, Friday, 8.30 9.20 am Pulse sequences for non CE MRA S. I. Gonçalves, PhD Radiology Department University Hospital Coimbra Autumn Semester, 2011 1 Magnetic resonance angiography
MRI: Principles and Applications, Friday, 8.30 9.20 am Pulse sequences for non CE MRA S. I. Gonçalves, PhD Radiology Department University Hospital Coimbra Autumn Semester, 2011 1 Magnetic resonance angiography
Dynamic Contrast-Enhanced MR Urography in the Evaluation of Pediatric Hydronephrosis: Part 1, Functional Assessment
 Jones et al. MR Urography of Pediatric Hydronephr osis Pediatric Imaging Original Research Richard A. Jones 1,2 Kirk Easley 3 Stephen B. Little 2 Hal Scherz 4,5 Andrew J. Kirsch 4,5 J. Damien Grattan-Smith
Jones et al. MR Urography of Pediatric Hydronephr osis Pediatric Imaging Original Research Richard A. Jones 1,2 Kirk Easley 3 Stephen B. Little 2 Hal Scherz 4,5 Andrew J. Kirsch 4,5 J. Damien Grattan-Smith
PERFUSION MRI CONTRAST BASED TECHNIQUES
 PERFUSION MRI CONTRAST BASED TECHNIQUES by Kenny K Israni Mar 28, 2006 PERFUSION - MRI Dynamic Susceptibility contrast Dynamic Relaxivity contrast STEADY-STATE STATE TECHNIQUES Steady-state Susceptibility
PERFUSION MRI CONTRAST BASED TECHNIQUES by Kenny K Israni Mar 28, 2006 PERFUSION - MRI Dynamic Susceptibility contrast Dynamic Relaxivity contrast STEADY-STATE STATE TECHNIQUES Steady-state Susceptibility
Perfusion Physics. ICMRI2018 March 29-31, 2018 Grand Hilton Hotel, Seoul, Korea. Asian Forum Ⅱ: Perfusion MRI SY24-1.
 SY24-1 Perfusion Physics Hiroyuki Kabasawa MR Collaborations and Development, GE Healthcare, Tokyo, Japan Perfusion is referred as the blood supply to micro capillary in tissue. Perfusion parameter such
SY24-1 Perfusion Physics Hiroyuki Kabasawa MR Collaborations and Development, GE Healthcare, Tokyo, Japan Perfusion is referred as the blood supply to micro capillary in tissue. Perfusion parameter such
Whole brain CT perfusion maps with paradoxical low mean transit time to predict infarct core
 Whole brain CT perfusion maps with paradoxical low mean transit time to predict infarct core Poster No.: B-292 Congress: ECR 2011 Type: Scientific Paper Topic: Neuro Authors: S. Chakraborty, M. E. Ahmad,
Whole brain CT perfusion maps with paradoxical low mean transit time to predict infarct core Poster No.: B-292 Congress: ECR 2011 Type: Scientific Paper Topic: Neuro Authors: S. Chakraborty, M. E. Ahmad,
MR Advance Techniques. Vascular Imaging. Class II
 MR Advance Techniques Vascular Imaging Class II 1 Vascular Imaging There are several methods that can be used to evaluate the cardiovascular systems with the use of MRI. MRI will aloud to evaluate morphology
MR Advance Techniques Vascular Imaging Class II 1 Vascular Imaging There are several methods that can be used to evaluate the cardiovascular systems with the use of MRI. MRI will aloud to evaluate morphology
Liver Fat Quantification
 Liver Fat Quantification Jie Deng, PhD, DABMP Department of Medical Imaging May 18 th, 2017 Disclosure Research agreement with Siemens Medical Solutions 2 Background Non-alcoholic fatty liver diseases
Liver Fat Quantification Jie Deng, PhD, DABMP Department of Medical Imaging May 18 th, 2017 Disclosure Research agreement with Siemens Medical Solutions 2 Background Non-alcoholic fatty liver diseases
Cardiovascular magnetic resonance in acute myocardial infarction
 European Society of Cardiology Paris, France 2011 Session: Myocardial oedema - a new diagnostic target? Cardiovascular magnetic resonance in acute myocardial infarction Andrew E. Arai, MD National Heart,
European Society of Cardiology Paris, France 2011 Session: Myocardial oedema - a new diagnostic target? Cardiovascular magnetic resonance in acute myocardial infarction Andrew E. Arai, MD National Heart,
Quantitation of Cerebral Glucose Utilization using the Arterial Input Function or the Standardized Uptake Value (SUV)
 Quantitation of Cerebral Glucose Utilization using the Arterial Input Function or the Standardized Uptake Value (SUV) Brian R. Moyer BRMoyer & Associates, LLC, Amherst, NH 03031 http://www.brmassocllc-org.com/
Quantitation of Cerebral Glucose Utilization using the Arterial Input Function or the Standardized Uptake Value (SUV) Brian R. Moyer BRMoyer & Associates, LLC, Amherst, NH 03031 http://www.brmassocllc-org.com/
Measurement of Single-Kidney Glomerular Filtration Rate Using a Contrast-Enhanced Dynamic Gradient-Echo Sequence and the Rutland-Patlak Plot Technique
 JOURNAL OF MAGNETIC RESONANCE IMAGING 18:714 725 (2003) Original Research Measurement of Single-Kidney Glomerular Filtration Rate Using a Contrast-Enhanced Dynamic Gradient-Echo Sequence and the Rutland-Patlak
JOURNAL OF MAGNETIC RESONANCE IMAGING 18:714 725 (2003) Original Research Measurement of Single-Kidney Glomerular Filtration Rate Using a Contrast-Enhanced Dynamic Gradient-Echo Sequence and the Rutland-Patlak
Anatomical and Functional MRI of the Pancreas
 Anatomical and Functional MRI of the Pancreas MA Bali, MD, T Metens, PhD Erasme Hospital Free University of Brussels Belgium mbali@ulb.ac.be Introduction The use of MRI to investigate the pancreas has
Anatomical and Functional MRI of the Pancreas MA Bali, MD, T Metens, PhD Erasme Hospital Free University of Brussels Belgium mbali@ulb.ac.be Introduction The use of MRI to investigate the pancreas has
Non-Invasive MR-based Evaluation of Kidney Function without Exogenous Contrast Agent. Xiang He, PhD Department of Radiology University of Pittsburgh
 Non-Invasive MR-based Evaluation of Kidney Function without Exogenous Contrast Agent Xiang He, PhD Department of Radiology University of Pittsburgh Contents MR-based non-invasive estimation of single kidney
Non-Invasive MR-based Evaluation of Kidney Function without Exogenous Contrast Agent Xiang He, PhD Department of Radiology University of Pittsburgh Contents MR-based non-invasive estimation of single kidney
Influence of Velocity Encoding and Position of Image Plane in Patients with Aortic Valve Insufficiency Using 2D Phase Contrast MRI
 Influence of Velocity Encoding and Position of Image Plane in Patients with Aortic Valve Insufficiency Using 2D Phase Contrast MRI M. Sc. Thesis Frida Svensson gussvefrh@student.gu.se Supervisors: Kerstin
Influence of Velocity Encoding and Position of Image Plane in Patients with Aortic Valve Insufficiency Using 2D Phase Contrast MRI M. Sc. Thesis Frida Svensson gussvefrh@student.gu.se Supervisors: Kerstin
Flow Quantification from 2D Phase Contrast MRI in Renal Arteries using Clustering
 Flow Quantification from 2D Phase Contrast MRI in Renal Arteries using Clustering Frank G. Zöllner 1,2, Jan Ankar Monnsen 1, Arvid Lundervold 2, Jarle Rørvik 1 1 Department for Radiology, University of
Flow Quantification from 2D Phase Contrast MRI in Renal Arteries using Clustering Frank G. Zöllner 1,2, Jan Ankar Monnsen 1, Arvid Lundervold 2, Jarle Rørvik 1 1 Department for Radiology, University of
Biases affecting tumor uptake measurements in FDG-PET
 Biases affecting tumor uptake measurements in FDG-PET M. Soret, C. Riddell, S. Hapdey, and I. Buvat Abstract-- The influence of tumor diameter, tumor-tobackground activity ratio, attenuation, spatial resolution,
Biases affecting tumor uptake measurements in FDG-PET M. Soret, C. Riddell, S. Hapdey, and I. Buvat Abstract-- The influence of tumor diameter, tumor-tobackground activity ratio, attenuation, spatial resolution,
How I do it: Non Contrast-Enhanced MR Angiography (syngo NATIVE)
 Clinical How-I-do-it Cardiovascular How I do it: Non Contrast-Enhanced MR Angiography (syngo NATIVE) Manuela Rick, Nina Kaarmann, Peter Weale, Peter Schmitt Siemens Healthcare, Erlangen, Germany Introduction
Clinical How-I-do-it Cardiovascular How I do it: Non Contrast-Enhanced MR Angiography (syngo NATIVE) Manuela Rick, Nina Kaarmann, Peter Weale, Peter Schmitt Siemens Healthcare, Erlangen, Germany Introduction
PHA5128 Dose Optimization II Case Study I Spring 2013
 Silsamicin is an investigational compound being evaluated for its antimicrobial effect. The route of administration for this drug is via intravenous bolus. Approximately 99.9% of this drug is eliminated
Silsamicin is an investigational compound being evaluated for its antimicrobial effect. The route of administration for this drug is via intravenous bolus. Approximately 99.9% of this drug is eliminated
Combined Anatomical and Functional Imaging with Revolution * CT
 GE Healthcare Case studies Combined Anatomical and Functional Imaging with Revolution * CT Jean-Louis Sablayrolles, M.D. Centre Cardiologique du Nord, Saint-Denis, France Case 1 Whole Brain Perfusion and
GE Healthcare Case studies Combined Anatomical and Functional Imaging with Revolution * CT Jean-Louis Sablayrolles, M.D. Centre Cardiologique du Nord, Saint-Denis, France Case 1 Whole Brain Perfusion and
DIRECT RENIN INHIBITOR (DRI) EFFECT ON GFR AND USE IN RENAL ARTERY STENOSIS SCREENING
 DIRECT RENIN INHIBITOR (DRI) EFFECT ON GFR AND USE IN RENAL ARTERY STENOSIS SCREENING Harold Thomas Pretorius, MD, PhD, Nichole Richards, and Michael Harrell Abstract Objective: A new method using a nuclear
DIRECT RENIN INHIBITOR (DRI) EFFECT ON GFR AND USE IN RENAL ARTERY STENOSIS SCREENING Harold Thomas Pretorius, MD, PhD, Nichole Richards, and Michael Harrell Abstract Objective: A new method using a nuclear
Genitourinary Imaging Original Research
 Genitourinary Imaging Original Research Eikefjord et al. Renal 3D DCE-MRI Using FLASH and KWIC Genitourinary Imaging Original Research Eli Eikefjord 1,2 Erling Andersen 1,3 Erlend Hodneland 4 Frank Zöllner
Genitourinary Imaging Original Research Eikefjord et al. Renal 3D DCE-MRI Using FLASH and KWIC Genitourinary Imaging Original Research Eli Eikefjord 1,2 Erling Andersen 1,3 Erlend Hodneland 4 Frank Zöllner
Essentials of Clinical MR, 2 nd edition. 99. MRA Principles and Carotid MRA
 99. MRA Principles and Carotid MRA As described in Chapter 12, time of flight (TOF) magnetic resonance angiography (MRA) is commonly utilized in the evaluation of the circle of Willis. TOF MRA allows depiction
99. MRA Principles and Carotid MRA As described in Chapter 12, time of flight (TOF) magnetic resonance angiography (MRA) is commonly utilized in the evaluation of the circle of Willis. TOF MRA allows depiction
Method Comparison for Interrater Reliability of an Image Processing Technique in Epilepsy Subjects
 22nd International Congress on Modelling and Simulation, Hobart, Tasmania, Australia, 3 to 8 December 2017 mssanz.org.au/modsim2017 Method Comparison for Interrater Reliability of an Image Processing Technique
22nd International Congress on Modelling and Simulation, Hobart, Tasmania, Australia, 3 to 8 December 2017 mssanz.org.au/modsim2017 Method Comparison for Interrater Reliability of an Image Processing Technique
Perfusion MRI. Youngkyoo Jung, PhD Associate Professor Radiology, Biomedical Engineering, and Clinical & Translational Science Institute
 Perfusion MRI Youngkyoo Jung, PhD Associate Professor Radiology, Biomedical Engineering, and Clinical & Translational Science Institute Perfusion The delivery of blood to a capillary bed in tissue Perfusion
Perfusion MRI Youngkyoo Jung, PhD Associate Professor Radiology, Biomedical Engineering, and Clinical & Translational Science Institute Perfusion The delivery of blood to a capillary bed in tissue Perfusion
Sum of Neurally Distinct Stimulus- and Task-Related Components.
 SUPPLEMENTARY MATERIAL for Cardoso et al. 22 The Neuroimaging Signal is a Linear Sum of Neurally Distinct Stimulus- and Task-Related Components. : Appendix: Homogeneous Linear ( Null ) and Modified Linear
SUPPLEMENTARY MATERIAL for Cardoso et al. 22 The Neuroimaging Signal is a Linear Sum of Neurally Distinct Stimulus- and Task-Related Components. : Appendix: Homogeneous Linear ( Null ) and Modified Linear
Renal-Related Questions
 Renal-Related Questions 1) List the major segments of the nephron and for each segment describe in a single sentence what happens to sodium there. (10 points). 2) a) Describe the handling by the nephron
Renal-Related Questions 1) List the major segments of the nephron and for each segment describe in a single sentence what happens to sodium there. (10 points). 2) a) Describe the handling by the nephron
Cardiac Imaging Tests
 Cardiac Imaging Tests http://www.medpagetoday.com/upload/2010/11/15/23347.jpg Standard imaging tests include echocardiography, chest x-ray, CT, MRI, and various radionuclide techniques. Standard CT and
Cardiac Imaging Tests http://www.medpagetoday.com/upload/2010/11/15/23347.jpg Standard imaging tests include echocardiography, chest x-ray, CT, MRI, and various radionuclide techniques. Standard CT and
Myocardial Blood Flow from Dynamic PET using Independent Component Analysis
 2012 IEEE Nuclear Science Symposium and Medical Imaging Conference Record (NSSIMIC) M07-4 Myocardial Blood Flow from Dynamic PET using Independent Component Analysis Alexander Karpikov, Hemant Tagare,
2012 IEEE Nuclear Science Symposium and Medical Imaging Conference Record (NSSIMIC) M07-4 Myocardial Blood Flow from Dynamic PET using Independent Component Analysis Alexander Karpikov, Hemant Tagare,
Early Learning vs Early Variability 1.5 r = p = Early Learning r = p = e 005. Early Learning 0.
 The temporal structure of motor variability is dynamically regulated and predicts individual differences in motor learning ability Howard Wu *, Yohsuke Miyamoto *, Luis Nicolas Gonzales-Castro, Bence P.
The temporal structure of motor variability is dynamically regulated and predicts individual differences in motor learning ability Howard Wu *, Yohsuke Miyamoto *, Luis Nicolas Gonzales-Castro, Bence P.
Conditional spectrum-based ground motion selection. Part II: Intensity-based assessments and evaluation of alternative target spectra
 EARTHQUAKE ENGINEERING & STRUCTURAL DYNAMICS Published online 9 May 203 in Wiley Online Library (wileyonlinelibrary.com)..2303 Conditional spectrum-based ground motion selection. Part II: Intensity-based
EARTHQUAKE ENGINEERING & STRUCTURAL DYNAMICS Published online 9 May 203 in Wiley Online Library (wileyonlinelibrary.com)..2303 Conditional spectrum-based ground motion selection. Part II: Intensity-based
Computer aided detection of acute renal allograft dysfunction using dynamic contrast enhanced MRI
 The Egyptian Journal of Radiology and Nuclear Medicine (2011) 42, 443 449 Egyptian Society of Radiology and Nuclear Medicine The Egyptian Journal of Radiology and Nuclear Medicine www.elsevier.com/locate/ejrnm
The Egyptian Journal of Radiology and Nuclear Medicine (2011) 42, 443 449 Egyptian Society of Radiology and Nuclear Medicine The Egyptian Journal of Radiology and Nuclear Medicine www.elsevier.com/locate/ejrnm
CT angiography techniques. Boot camp
 CT angiography techniques Boot camp Overview Basic concepts Contrast administration arterial opacification Time scan acquisition during the arterial phase Protocol examples Helical non-gated CTA Pulmonary
CT angiography techniques Boot camp Overview Basic concepts Contrast administration arterial opacification Time scan acquisition during the arterial phase Protocol examples Helical non-gated CTA Pulmonary
Modifi ed CT perfusion contrast injection protocols for improved CBF quantifi cation with lower temporal sampling
 Investigations and research Modifi ed CT perfusion contrast injection protocols for improved CBF quantifi cation with lower temporal sampling J. Wang Z. Ying V. Yao L. Ciancibello S. Premraj S. Pohlman
Investigations and research Modifi ed CT perfusion contrast injection protocols for improved CBF quantifi cation with lower temporal sampling J. Wang Z. Ying V. Yao L. Ciancibello S. Premraj S. Pohlman
CT Versus MR for the Runoff
 CT Versus MR for the Runoff Robert R. Edelman, M.D. Dept. of Radiology NorthShore University HealthSystem Feinberg School of Medicine, Northwestern University Magnetic Resonance Computed Tomography Radio
CT Versus MR for the Runoff Robert R. Edelman, M.D. Dept. of Radiology NorthShore University HealthSystem Feinberg School of Medicine, Northwestern University Magnetic Resonance Computed Tomography Radio
Renal artery disease: MR Techniques and Interpretation
 Renal artery disease: MR Techniques and Interpretation Prof. Dr. Stefan O. Schoenberg Professor and Chairman of Radiology Department of Clinical Radiology and Nuclear Medicine University Medicine Mannheim
Renal artery disease: MR Techniques and Interpretation Prof. Dr. Stefan O. Schoenberg Professor and Chairman of Radiology Department of Clinical Radiology and Nuclear Medicine University Medicine Mannheim
Dynamic susceptibility contrast MR imaging was performed to determine the local cerebral blood flow and blood volume.
 RSNA, 2016 10.1148/radiol.2016152244 Appendix E1 Neuropsychological Tests All patients underwent a battery of neuropsychological tests. This included the Rey auditory verbal learning test (34), the digit
RSNA, 2016 10.1148/radiol.2016152244 Appendix E1 Neuropsychological Tests All patients underwent a battery of neuropsychological tests. This included the Rey auditory verbal learning test (34), the digit
On the feasibility of speckle reduction in echocardiography using strain compounding
 Title On the feasibility of speckle reduction in echocardiography using strain compounding Author(s) Guo, Y; Lee, W Citation The 2014 IEEE International Ultrasonics Symposium (IUS 2014), Chicago, IL.,
Title On the feasibility of speckle reduction in echocardiography using strain compounding Author(s) Guo, Y; Lee, W Citation The 2014 IEEE International Ultrasonics Symposium (IUS 2014), Chicago, IL.,
A quality control program for MR-guided focused ultrasound ablation therapy
 JOURNAL OF APPLIED CLINICAL MEDICAL PHYSICS, VOLUME 3, NUMBER 2, SPRING 2002 A quality control program for MR-guided focused ultrasound ablation therapy Tao Wu* and Joel P. Felmlee Department of Radiology,
JOURNAL OF APPLIED CLINICAL MEDICAL PHYSICS, VOLUME 3, NUMBER 2, SPRING 2002 A quality control program for MR-guided focused ultrasound ablation therapy Tao Wu* and Joel P. Felmlee Department of Radiology,
Group-Wise FMRI Activation Detection on Corresponding Cortical Landmarks
 Group-Wise FMRI Activation Detection on Corresponding Cortical Landmarks Jinglei Lv 1,2, Dajiang Zhu 2, Xintao Hu 1, Xin Zhang 1,2, Tuo Zhang 1,2, Junwei Han 1, Lei Guo 1,2, and Tianming Liu 2 1 School
Group-Wise FMRI Activation Detection on Corresponding Cortical Landmarks Jinglei Lv 1,2, Dajiang Zhu 2, Xintao Hu 1, Xin Zhang 1,2, Tuo Zhang 1,2, Junwei Han 1, Lei Guo 1,2, and Tianming Liu 2 1 School
Research Article Kidney Modelling for FDG Excretion with PET
 Biomedical Imaging Volume 2007, Article ID 63234, 4 pages doi:10.1155/2007/63234 Research Article Kidney Modelling for FDG Excretion with PET Huiting Qiao, 1 Jing Bai, 1 Yingmao Chen, 2 and Jiahe Tian
Biomedical Imaging Volume 2007, Article ID 63234, 4 pages doi:10.1155/2007/63234 Research Article Kidney Modelling for FDG Excretion with PET Huiting Qiao, 1 Jing Bai, 1 Yingmao Chen, 2 and Jiahe Tian
ORIGINAL ARTICLE. Jack A Wells 1, Bernard Siow 1,2, Mark F Lythgoe 1,4 and David L Thomas 3,4
 Journal of Cerebral Blood Flow & Metabolism (2013) 33, 215 224 & 2013 ISCBFM All rights reserved 0271-678X/13 $32.00 www.jcbfm.com ORIGINAL ARTICLE Measuring biexponential transverse relaxation of the
Journal of Cerebral Blood Flow & Metabolism (2013) 33, 215 224 & 2013 ISCBFM All rights reserved 0271-678X/13 $32.00 www.jcbfm.com ORIGINAL ARTICLE Measuring biexponential transverse relaxation of the
Quantification of myocardial perfusion by cardiovascular magnetic resonance
 REVIEW Open Access Quantification of myocardial perfusion by cardiovascular magnetic resonance Michael Jerosch-Herold Abstract The potential of contrast-enhanced cardiovascular magnetic resonance (CMR)
REVIEW Open Access Quantification of myocardial perfusion by cardiovascular magnetic resonance Michael Jerosch-Herold Abstract The potential of contrast-enhanced cardiovascular magnetic resonance (CMR)
SUPPLEMENTAL MATERIAL
 1 SUPPLEMENTAL MATERIAL Response time and signal detection time distributions SM Fig. 1. Correct response time (thick solid green curve) and error response time densities (dashed red curve), averaged across
1 SUPPLEMENTAL MATERIAL Response time and signal detection time distributions SM Fig. 1. Correct response time (thick solid green curve) and error response time densities (dashed red curve), averaged across
C OBJECTIVES. Basic Pharmacokinetics LESSON. After completing Lesson 2, you should be able to:
 LESSON 2 Basic Pharmacokinetics C OBJECTIVES After completing Lesson 2, you should be able to: 1. Define the concept of apparent volume of distribution and use an appropriate mathematical equation to calculate
LESSON 2 Basic Pharmacokinetics C OBJECTIVES After completing Lesson 2, you should be able to: 1. Define the concept of apparent volume of distribution and use an appropriate mathematical equation to calculate
Evaluation of the Cockroft Gault, Jelliffe and Wright formulae in estimating renal function in elderly cancer patients
 Original article Annals of Oncology 15: 291 295, 2004 DOI: 10.1093/annonc/mdh079 Evaluation of the Cockroft Gault, Jelliffe and Wright formulae in estimating renal function in elderly cancer patients G.
Original article Annals of Oncology 15: 291 295, 2004 DOI: 10.1093/annonc/mdh079 Evaluation of the Cockroft Gault, Jelliffe and Wright formulae in estimating renal function in elderly cancer patients G.
Photon Attenuation Correction in Misregistered Cardiac PET/CT
 Photon Attenuation Correction in Misregistered Cardiac PET/CT A. Martinez-Möller 1,2, N. Navab 2, M. Schwaiger 1, S. G. Nekolla 1 1 Nuklearmedizinische Klinik der TU München 2 Computer Assisted Medical
Photon Attenuation Correction in Misregistered Cardiac PET/CT A. Martinez-Möller 1,2, N. Navab 2, M. Schwaiger 1, S. G. Nekolla 1 1 Nuklearmedizinische Klinik der TU München 2 Computer Assisted Medical
Lecture-2 Review of the previous lecture:
 Lecture-2 Review of the previous lecture: -Kidney s function is to clean the blood by the removing of the waste plus adding some valuable substances -kidney failure will lead to death for many reasons,
Lecture-2 Review of the previous lecture: -Kidney s function is to clean the blood by the removing of the waste plus adding some valuable substances -kidney failure will lead to death for many reasons,
Free-Breathing 3D Liver Perfusion Quantification Using a Dual-Input Two-Compartment Model
 www.nature.com/scientificreports Received: 18 August 2017 Accepted: 23 November 2017 Published: xx xx xxxx OPEN Free-Breathing 3D Liver Perfusion Quantification Using a Dual-Input Two-Compartment Model
www.nature.com/scientificreports Received: 18 August 2017 Accepted: 23 November 2017 Published: xx xx xxxx OPEN Free-Breathing 3D Liver Perfusion Quantification Using a Dual-Input Two-Compartment Model
Using lesion washout volume fraction as a biomarker to improve suspicious breast lesion characterization
 JOURNAL OF APPLIED CLINICAL MEDICAL PHYSICS, VOLUME 16, NUMBER 5, 2015 Using lesion washout volume fraction as a biomarker to improve suspicious breast lesion characterization Jie Huang, a Sarah M. Schafer,
JOURNAL OF APPLIED CLINICAL MEDICAL PHYSICS, VOLUME 16, NUMBER 5, 2015 Using lesion washout volume fraction as a biomarker to improve suspicious breast lesion characterization Jie Huang, a Sarah M. Schafer,
Index. mri.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Angiogenesis, and cancer of prostate, 689 690 Angiography, MR. See MR angiography. Apoptosis, MR imaging of, 637 Apparent diffusion coefficient,
Index Note: Page numbers of article titles are in boldface type. A Angiogenesis, and cancer of prostate, 689 690 Angiography, MR. See MR angiography. Apoptosis, MR imaging of, 637 Apparent diffusion coefficient,
RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D.
 RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D. Learning Objectives 1. Identify the region of the renal tubule in which reabsorption and secretion occur. 2. Describe the cellular
RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D. Learning Objectives 1. Identify the region of the renal tubule in which reabsorption and secretion occur. 2. Describe the cellular
B-Flow, Power Doppler and Color Doppler Ultrasound in the Assessment of Carotid Stenosis: Comparison with 64-MD-CT Angiography
 Med. J. Cairo Univ., Vol. 85, No. 2, March: 805-809, 2017 www.medicaljournalofcairouniversity.net B-Flow, Power Doppler and Color Doppler Ultrasound in the Assessment of Carotid Stenosis: Comparison with
Med. J. Cairo Univ., Vol. 85, No. 2, March: 805-809, 2017 www.medicaljournalofcairouniversity.net B-Flow, Power Doppler and Color Doppler Ultrasound in the Assessment of Carotid Stenosis: Comparison with
Animals. Male C57Bl/6 mice (n=27) were obtained from Charles River (Sulzfeld, Germany) and
 Supplemental Methods Animals. Male C57Bl/6 mice (n=27) were obtained from Charles River (Sulzfeld, Germany) and housed in groups of 5-10 in individually ventilated BCU cages within a temperature controlled
Supplemental Methods Animals. Male C57Bl/6 mice (n=27) were obtained from Charles River (Sulzfeld, Germany) and housed in groups of 5-10 in individually ventilated BCU cages within a temperature controlled
T2, T2*, ute. Yeo Ju Kim. Radiology, Inha University Hospital, Incheon, Korea
 SY28-1 T2, T2*, ute Yeo Ju Kim Radiology, Inha University Hospital, Incheon, Korea T2 relaxation times relate to the rate of transverse magnetization decay, caused by the loss of phase coherence induced
SY28-1 T2, T2*, ute Yeo Ju Kim Radiology, Inha University Hospital, Incheon, Korea T2 relaxation times relate to the rate of transverse magnetization decay, caused by the loss of phase coherence induced
BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1
 BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1 1. a. Proximal tubule. b. Proximal tubule. c. Glomerular endothelial fenestrae, filtration slits between podocytes of Bowman's capsule.
BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1 1. a. Proximal tubule. b. Proximal tubule. c. Glomerular endothelial fenestrae, filtration slits between podocytes of Bowman's capsule.
Protocol for iv. iodine and gadolinium contrast studies
 Protocol for iv. iodine and gadolinium contrast studies Royal College of Radiologists Standard The individual administering the contrast agent must ensure that the patient understands that it is to be
Protocol for iv. iodine and gadolinium contrast studies Royal College of Radiologists Standard The individual administering the contrast agent must ensure that the patient understands that it is to be
Basic Pharmacokinetics and Pharmacodynamics: An Integrated Textbook with Computer Simulations
 Basic Pharmacokinetics and Pharmacodynamics: An Integrated Textbook with Computer Simulations Rosenbaum, Sara E. ISBN-13: 9780470569061 Table of Contents 1 Introduction to Pharmacokinetics and Pharmacodynamics.
Basic Pharmacokinetics and Pharmacodynamics: An Integrated Textbook with Computer Simulations Rosenbaum, Sara E. ISBN-13: 9780470569061 Table of Contents 1 Introduction to Pharmacokinetics and Pharmacodynamics.
Objectives 8/17/2011. Challenges in Cardiac Imaging. Challenges in Cardiac Imaging. Basic Cardiac MRI Sequences
 8/17/2011 Traditional Protocol Model for Tomographic Imaging Cardiac MRI Sequences and Protocols Frandics Chan, M.D., Ph.D. Stanford University Medical Center Interpretation Lucile Packard Children s Hospital
8/17/2011 Traditional Protocol Model for Tomographic Imaging Cardiac MRI Sequences and Protocols Frandics Chan, M.D., Ph.D. Stanford University Medical Center Interpretation Lucile Packard Children s Hospital
A Magnetic Resonance Imaging Method for
 Journal of Cardiovascular Magnetic Resonance, 1(1), 59-64 (1999) INVITED PAPER Use of MRI in ASD Asessment A Magnetic Resonance Imaging Method for Evaluating Atrial Septa1 Defects Godtfred Holmvang Cardiac
Journal of Cardiovascular Magnetic Resonance, 1(1), 59-64 (1999) INVITED PAPER Use of MRI in ASD Asessment A Magnetic Resonance Imaging Method for Evaluating Atrial Septa1 Defects Godtfred Holmvang Cardiac
Fully-Automatic Determination of the Arterial Input Function for Dynamic Contrast-Enhanced Pulmonary MR Imaging (DCE-pMRI)
 Fully-Automatic Determination of the Arterial Input Function for Dynamic Contrast-Enhanced Pulmonary MR Imaging (DCE-pMRI) Kohlmann P. 1, Laue H. 1, Anjorin A. 2, Wolf U. 3, Terekhov M. 3, Krass S. 1,
Fully-Automatic Determination of the Arterial Input Function for Dynamic Contrast-Enhanced Pulmonary MR Imaging (DCE-pMRI) Kohlmann P. 1, Laue H. 1, Anjorin A. 2, Wolf U. 3, Terekhov M. 3, Krass S. 1,
Introduction to the kidney: regulation of sodium & glucose. Dr Nick Ashton Senior Lecturer in Renal Physiology Faculty of Biology, Medicine & Health
 Introduction to the kidney: regulation of sodium & glucose Dr Nick Ashton Senior Lecturer in Renal Physiology Faculty of Biology, Medicine & Health Objectives Overview of kidney structure & function Glomerular
Introduction to the kidney: regulation of sodium & glucose Dr Nick Ashton Senior Lecturer in Renal Physiology Faculty of Biology, Medicine & Health Objectives Overview of kidney structure & function Glomerular
Assessment of Adipose Tissue from Whole Body 3T MRI Scans
 Assessment of Adipose Tissue from Whole Body 3T MRI Scans Ting Song 1, Jing An 2, Qun Chen 2, Vivian Lee 2, Andrew Laine 1 1 Department of Biomedical Engineering, Columbia University, New York, NY, USA
Assessment of Adipose Tissue from Whole Body 3T MRI Scans Ting Song 1, Jing An 2, Qun Chen 2, Vivian Lee 2, Andrew Laine 1 1 Department of Biomedical Engineering, Columbia University, New York, NY, USA
MRI qbold Based Evaluation. Renal Oxidative Metabolism. Department of Radiology and Hernando Gomez, MD Critical Care Medicine
 MRI qbold Based Evaluation of Renal Oxidative Metabolism Xiang He, PhD Department of Radiology and Hernando Gomez, MD Critical Care Medicine Background High oxygen-demand and lower medullary blood flow
MRI qbold Based Evaluation of Renal Oxidative Metabolism Xiang He, PhD Department of Radiology and Hernando Gomez, MD Critical Care Medicine Background High oxygen-demand and lower medullary blood flow
Chapter 23. The Nephron. (functional unit of the kidney
 Chapter 23 The Nephron (functional unit of the kidney Renal capsule The Nephron Renal cortex Nephron Collecting duct Efferent arteriole Afferent arteriole (a) Renal corpuscle: Glomerular capsule Glomerulus
Chapter 23 The Nephron (functional unit of the kidney Renal capsule The Nephron Renal cortex Nephron Collecting duct Efferent arteriole Afferent arteriole (a) Renal corpuscle: Glomerular capsule Glomerulus
University of Groningen. Quantitative CT myocardial perfusion Pelgrim, Gert
 University of Groningen Quantitative CT myocardial perfusion Pelgrim, Gert IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check
University of Groningen Quantitative CT myocardial perfusion Pelgrim, Gert IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check
--Manuscript Draft-- University of Saskatchewan Royal University Hospital Saskatoon, Saskatchewan CANADA. Gary R Conrad, M.D.
 European Journal of Nuclear Medicine and Molecular Imaging A simple method for determining split renal function from dynamic mtc-mag scintigraphic data --Manuscript Draft-- Manuscript Number: Full Title:
European Journal of Nuclear Medicine and Molecular Imaging A simple method for determining split renal function from dynamic mtc-mag scintigraphic data --Manuscript Draft-- Manuscript Number: Full Title:
Calculation methods in Hermes Medical Solutions dosimetry software
 Calculation methods in Hermes Medical Solutions dosimetry software Helena McMeekin MSc. Clinical Applications Scientist, Hermes Medical Solutions MRTDosimetry Scientific Workshop The Principals and Clinical
Calculation methods in Hermes Medical Solutions dosimetry software Helena McMeekin MSc. Clinical Applications Scientist, Hermes Medical Solutions MRTDosimetry Scientific Workshop The Principals and Clinical
Controversies around antenatally detected PUJ syndrom. Amy Piepsz, CHU St Pierre, Brussels, Belgium
 Controversies around antenatally detected PUJ syndrom Amy Piepsz, CHU St Pierre, Brussels, Belgium Editors : Anthony Caldamone, USA Pierre Mouriquand, France Newborn boy History of prenatally diagnosed
Controversies around antenatally detected PUJ syndrom Amy Piepsz, CHU St Pierre, Brussels, Belgium Editors : Anthony Caldamone, USA Pierre Mouriquand, France Newborn boy History of prenatally diagnosed
PHYSICS OF MRI ACQUISITION. Alternatives to BOLD for fmri
 PHYSICS OF MRI ACQUISITION Quick Review for fmri HST-583, Fall 2002 HST.583: Functional Magnetic Resonance Imaging: Data Acquisition and Analysis Harvard-MIT Division of Health Sciences and Technology
PHYSICS OF MRI ACQUISITION Quick Review for fmri HST-583, Fall 2002 HST.583: Functional Magnetic Resonance Imaging: Data Acquisition and Analysis Harvard-MIT Division of Health Sciences and Technology
Nephron Function and Urine Formation. Ms. Kula December 1, 2014 Biology 30S
 Nephron Function and Urine Formation Ms. Kula December 1, 2014 Biology 30S The Role of the Nephron In order for the body to properly function and maintain homeostasis, the amount of dissolved substances
Nephron Function and Urine Formation Ms. Kula December 1, 2014 Biology 30S The Role of the Nephron In order for the body to properly function and maintain homeostasis, the amount of dissolved substances
Comparison of T2-weighted MRCP before and after injection of Gd-EOB-DTPA in patients with primary sclerosing cholangitis (PSC)
 Comparison of T2-weighted MRCP before and after injection of Gd-EOB-DTPA in patients with primary sclerosing cholangitis (PSC) Poster No.: C-0051 Congress: ECR 2010 Type: Scientific Exhibit Topic: Abdominal
Comparison of T2-weighted MRCP before and after injection of Gd-EOB-DTPA in patients with primary sclerosing cholangitis (PSC) Poster No.: C-0051 Congress: ECR 2010 Type: Scientific Exhibit Topic: Abdominal
BASIC PHARMACOKINETICS
 BASIC PHARMACOKINETICS MOHSEN A. HEDAYA CRC Press Taylor & Francis Croup Boca Raton London New York CRC Press is an imprint of the Taylor & Francis Group, an informa business Table of Contents Chapter
BASIC PHARMACOKINETICS MOHSEN A. HEDAYA CRC Press Taylor & Francis Croup Boca Raton London New York CRC Press is an imprint of the Taylor & Francis Group, an informa business Table of Contents Chapter
Chapter 1. Introduction
 Chapter 1 Introduction 1.1 Motivation and Goals The increasing availability and decreasing cost of high-throughput (HT) technologies coupled with the availability of computational tools and data form a
Chapter 1 Introduction 1.1 Motivation and Goals The increasing availability and decreasing cost of high-throughput (HT) technologies coupled with the availability of computational tools and data form a
Renal. Prof John Buscombe
 Renal Prof John Buscombe Renal nuclear Medicine Only consistent test of kidney func7on Many good tests for renal anatomy Ultrasound good looking at cysts and renal pelvis CT can look at perfusion, size
Renal Prof John Buscombe Renal nuclear Medicine Only consistent test of kidney func7on Many good tests for renal anatomy Ultrasound good looking at cysts and renal pelvis CT can look at perfusion, size
Methods of MR Fat Quantification and their Pros and Cons
 Methods of MR Fat Quantification and their Pros and Cons Michael Middleton, MD PhD UCSD Department of Radiology International Workshop on NASH Biomarkers Washington, DC April 29-30, 2016 1 Disclosures
Methods of MR Fat Quantification and their Pros and Cons Michael Middleton, MD PhD UCSD Department of Radiology International Workshop on NASH Biomarkers Washington, DC April 29-30, 2016 1 Disclosures
Estimating the number of components with defects post-release that showed no defects in testing
 SOFTWARE TESTING, VERIFICATION AND RELIABILITY Softw. Test. Verif. Reliab. 2002; 12:93 122 (DOI: 10.1002/stvr.235) Estimating the number of components with defects post-release that showed no defects in
SOFTWARE TESTING, VERIFICATION AND RELIABILITY Softw. Test. Verif. Reliab. 2002; 12:93 122 (DOI: 10.1002/stvr.235) Estimating the number of components with defects post-release that showed no defects in
A mathematical model of tumor dynamics during stereotactic body radiation therapy for non-small cell lung cancer
 A mathematical model of tumor dynamics during stereotactic body radiation therapy for non-small cell lung cancer Russell Injerd, Emma Turian Abstract Image guided radiotherapy allows tumor volume dynamics
A mathematical model of tumor dynamics during stereotactic body radiation therapy for non-small cell lung cancer Russell Injerd, Emma Turian Abstract Image guided radiotherapy allows tumor volume dynamics
Annex III. Amendments to relevant sections of the product information
 Annex III Amendments to relevant sections of the product information Note: These amendments to the relevant sections of the product information are the outcome of the referral procedure. The product information
Annex III Amendments to relevant sections of the product information Note: These amendments to the relevant sections of the product information are the outcome of the referral procedure. The product information
RECENT ADVANCES IN CLINICAL MR OF ARTICULAR CARTILAGE
 In Practice RECENT ADVANCES IN CLINICAL MR OF ARTICULAR CARTILAGE By Atsuya Watanabe, MD, PhD, Director, Advanced Diagnostic Imaging Center and Associate Professor, Department of Orthopedic Surgery, Teikyo
In Practice RECENT ADVANCES IN CLINICAL MR OF ARTICULAR CARTILAGE By Atsuya Watanabe, MD, PhD, Director, Advanced Diagnostic Imaging Center and Associate Professor, Department of Orthopedic Surgery, Teikyo
New magnetic resonance imaging methods in nephrology
 http://www.kidney-international.org & 2013 International Society of Nephrology New magnetic resonance imaging methods in nephrology Jeff L. Zhang 1, Glen Morrell 1, Henry Rusinek 2, Eric E. Sigmund 2,
http://www.kidney-international.org & 2013 International Society of Nephrology New magnetic resonance imaging methods in nephrology Jeff L. Zhang 1, Glen Morrell 1, Henry Rusinek 2, Eric E. Sigmund 2,
Original Research JOURNAL OF MAGNETIC RESONANCE IMAGING 22: (2005)
 JOURNAL OF MAGNETIC RESONANCE IMAGING 22:788 793 (2005) Original Research STIR vs. T1-Weighted Fat-Suppressed Gadolinium- Enhanced MRI of Bone Marrow Edema of the Knee: Computer-Assisted Quantitative Comparison
JOURNAL OF MAGNETIC RESONANCE IMAGING 22:788 793 (2005) Original Research STIR vs. T1-Weighted Fat-Suppressed Gadolinium- Enhanced MRI of Bone Marrow Edema of the Knee: Computer-Assisted Quantitative Comparison
Department of Radiology, Division of MRI, University of Michigan, 1500 E. Medical Center Drive, Ann Arbor, MI , USA
 Abdom Imaging 23:469 484 (1998) Abdominal Imaging Springer-Verlag New York Inc. 1998 Contrast-enhanced MR angiography J. H. Maki, T. L. Chenevert, M. R. Prince Department of Radiology, Division of MRI,
Abdom Imaging 23:469 484 (1998) Abdominal Imaging Springer-Verlag New York Inc. 1998 Contrast-enhanced MR angiography J. H. Maki, T. L. Chenevert, M. R. Prince Department of Radiology, Division of MRI,
Copyright 2008 Society of Photo Optical Instrumentation Engineers. This paper was published in Proceedings of SPIE, vol. 6915, Medical Imaging 2008:
 Copyright 2008 Society of Photo Optical Instrumentation Engineers. This paper was published in Proceedings of SPIE, vol. 6915, Medical Imaging 2008: Computer Aided Diagnosis and is made available as an
Copyright 2008 Society of Photo Optical Instrumentation Engineers. This paper was published in Proceedings of SPIE, vol. 6915, Medical Imaging 2008: Computer Aided Diagnosis and is made available as an
Hyperaldosteronism: Conn's Syndrome
 RENAL AND ACID-BASE PHYSIOLOGY 177 Case 31 Hyperaldosteronism: Conn's Syndrome Seymour Simon is a 54-year-old college physics professor who maintains a healthy lifestyle. He exercises regularly, doesn't
RENAL AND ACID-BASE PHYSIOLOGY 177 Case 31 Hyperaldosteronism: Conn's Syndrome Seymour Simon is a 54-year-old college physics professor who maintains a healthy lifestyle. He exercises regularly, doesn't
RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015
 RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015 1. In which abdominal cavity do the kidneys lie? a) Peritoneum. b) Anteperitoneal. c) Retroperitoneal. d) Parietal peritoneal 2. What is the
RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015 1. In which abdominal cavity do the kidneys lie? a) Peritoneum. b) Anteperitoneal. c) Retroperitoneal. d) Parietal peritoneal 2. What is the
Supplementary Information Methods Subjects The study was comprised of 84 chronic pain patients with either chronic back pain (CBP) or osteoarthritis
 Supplementary Information Methods Subjects The study was comprised of 84 chronic pain patients with either chronic back pain (CBP) or osteoarthritis (OA). All subjects provided informed consent to procedures
Supplementary Information Methods Subjects The study was comprised of 84 chronic pain patients with either chronic back pain (CBP) or osteoarthritis (OA). All subjects provided informed consent to procedures
Classification and Statistical Analysis of Auditory FMRI Data Using Linear Discriminative Analysis and Quadratic Discriminative Analysis
 International Journal of Innovative Research in Computer Science & Technology (IJIRCST) ISSN: 2347-5552, Volume-2, Issue-6, November-2014 Classification and Statistical Analysis of Auditory FMRI Data Using
International Journal of Innovative Research in Computer Science & Technology (IJIRCST) ISSN: 2347-5552, Volume-2, Issue-6, November-2014 Classification and Statistical Analysis of Auditory FMRI Data Using
