Nothing to declare. Probable causes for the change
|
|
|
- Nathan Joseph
- 6 years ago
- Views:
Transcription
1 acute pancreatitis March 25, 2017 C. S PITCHUMONI. MD,MACP,MACG,MPH.FRCP (c) Adjunct Professor of Medicine New York Medical College Professor of Medicine Rutgers university Nothing to declare Lesser sac? Fluid can track down the planes The annual incidence of AP ranges from 13 to 45/100,000 persons, The Epidemiology of Pancreatitis and Pancreatic Cancer D. Yadav and A B. Lowenfels Gastroenterology. 2013; 144: Probable causes for the change 1. Increase in obesity 2. increase in gallstones 3. Increased testing amylase/lipase 4. increased use of CT scan abdomen Diagnosis of Acute pancreatitis Two out of the three features 1.Typical pain of pancreatitis. 2.Elevated ( >3 times) levels of Serum amylase/ lipase. 3.In selected cases imaging study such as contrast enhanced CT scan of abdomen. In delayed presentation, A/L may be normal, When history is difficult to obtain as in demented, disoriented patients. Pain is not typical of pancreatitis Classification of acute pancreatitis 2012: Gut 2013;62:
2 The above clinical classification recognizes the importance of pancreatic necrosis, but overlooks intermediary forms of disease with fluid collections. Bradley.E., International symposium on Acute Pancreatitis. Atlanta Terms used in new classification based on CECT Interstitial edematous pancreatitis: inflammation or stranding in the (peri)pancreatic tissues without tissue necrosis Pancreatic parenchyma enhances,iv contrast Lack of peripancreatic necrosis Necrotizing pancreatitis: Pancreatic parenchymal necrosis and/or peripancreatic necrosis Pancreatic parenchyma areas without enhancement by intravenous contrast and/or Peripancreatic necrosis Acute peripancreatic fluid collection: Peripancreatic fluid occurring in the setting of interstitial edematous pancreatitis; this peripancreatic fluid occurs within the first 4 weeks of interstitial edematous pancreatitis CECT criteria Homongenous fluid adjacent to pancreas confined by peripancreatic fascial planes No recognizable wall CECT contrast enhanced computed tomography The objectives of this presentation ; Management of Severe AP 1. NPO how long? 2. Early feeding, how early, 3. Fluid administration when? how aggressive? what kind? 4. Antibiotics needed or not? 5. Surgery in biliary pancreatitis. Early late, how early? 6. Fluid collection in acute pancreatitis natural history, when to intervene and when not to?. 7. Pancreatic necrosis a. Sterile necrosis conservative Vs Interventional b. Infected 8. Endoscopic interventions in acute complicated pancreatitis. Scope, indications, opportunities, future Initial management 1. Assess hemodynamic status, start resuscitative measures. 2. Risk assessment. 3. Patients with organ failure should be admitted to ICU Prognostic Markers in Acute Pancreatitis: Use anyone Too many: Ransons Imrie BISAP Harmless AP score APACHE II Balthazar CT based Single markers Procalcitonin C Reactive protein Interleukins BISAP (Bed Side Index of Severity) Score BUN > 25 Impaired mental status SIRS 2 or more of the following variables Fever of > 38 C (100.4 F) or < 36 C (96.8 F) Heart rate of > 90 beats per minute Respiratory rate > 20 bpm or arterial carbon dioxide tension (PaCO2) of < 32mm Hg Abnormal white blood cell count (>12,000/µL or < 4,000/µL or >10% immature [band] forms) Age > 60 years Pleural effusions 3 predict pancreatic necrosis And organ failure Mortality prediction similar to APACHE II 2
3 Indications for ICU ( too restrictive) Patients with severe acute pancreatitis Patients with AP and one or more of the following Pulse<40 or >150 BP systolic <80 or mean arterial pressure <60 RR. >35 Serum Na <110 or >170 Serum K <2.0 or >7 PaO2 <50 S.Glucose >800 S. Ca..>15 Anuria, Coma UpToDate 2016 SS Vege Abdominal imaging 1. Routine CECT is unwarranted,the CT may not be helpful, costly,may even delay treatment. 2.If a patient fails to improve after 48 hour or if fever, persistent pain CECT. 3. CECT and MRI equal sensitivity and specificity. 4. MRI/MRCP advantage in estimating CBD size, excluding CBD stone. 5. MRI is helpful in patients with allergy to contrast and renal insufficiency (without gadolinium). Tenner S. et al. American College of Gastroenterology Guideline:management of acute pancreatitis. Am.J.gastroenterol. 2013;108:1400 Initial management of AP.Critical issues during the first 72 hours Preventing severe disease: vigorous IV hydration. Golden period first hours. Aggressive hydration ml per hour of isotonic crystalloid solution,most beneficial in first hour ml/kg If severe depletion (Hypotension and tachycardia)bolus /more rapid infusion. Reassess fluid requirement frequently. Lactated Ringer's solution reduces systemic inflammation compared with saline in patients with acute pancreatitis One liter of Ringer's lactate solution contains: 130 meq of sodium ion = 130 mmol/l 109 meq of chloride ion = 109 mmol/l 28 meq of lactate = 28 mmol/l 4 meq of potassium ion = 4 mmol/l 3 meq of calcium ion = 1.5 mmol/l Ringer's lactate has an osmolarity of 273 mosm/l.the lactate is metabolized into bicarbonate by the liver, which can help correct metabolic acidosis. Ringer lactate may be preferred, ( may be contraindicated in rare hypercalcemic pancreatitis. Contains 3mEq/L calcium). Ringer lactate may reduce incidence of SIRS compared to NS Pain control./ monitoring Opioids are safe and effective. IV opiates. Fentanyl is being increasingly used. ( caution may depress respiratory function ) Patient controlled analgesia Note Morphine does not cause an increase in SOD, or worsen AP. Vital signs Urine output Electrolytes Serum Glucose levels EKG Abdominal compartment syndrome Feedings. NPO,NG,NJ,Oral,IV,TPN?. Or other Early oral feedings when the patient is hungry, pain free. Presence of bowel sounds, Usually 24 to 48 hours. Low residue, low fat, soft diet. Rationale?. If no ileus,nausea or vomiting Enteral feeding rather than parenteral. EF helps to maintain intestinal barrier and prevent translocation of bacteria. EN significantly reduces mortality, multiple organ failure systemic infections, and the need for surgery compared to those who get TPN. Petrow Ms et al. Systematic review Nutritional support in acute pancreatitis. Aliment Pharmacol and Ther. 2008;28:704. Mark PE et al. Meta analysis of parenteral versus enteral nutrition in patients with acute pancreatitis. BMJ.2004;328:
4 Several tests can help differentiate biliary pancreatitis from other causes of AP. Specificity of ALT > 150 IU/L for gallstone AP is 96%. Sensitivity only 48%; a normal ALT does not exclude gallstones as a cause. AST and ALT may be normal in about 11% of patients CT finding of CBD stones sensitivity as high as 80%, CT is often less sensitive than trans abdominal ultrasound. MRCP. EUS. ERCP. Treatment of biliary etiology. EUS/ERCP in early AP. Concurrent acute cholangitis and persistent jaundice and elevated AST?ALT. Suspected biliary etiology with SAP?. MRCP followed by EUS?ERCP Direct EUS followed by ERCP advantages Direct ERCP, sphincterotomy, stent placement. Stone extraction. Endoscopic therapies in AP 1. Endoscopic biliary sphincterotomy. Associated with several risks. Post ERCP pancreatitis, bleeding, infection, peroration. 2. Endoscopic papillary balloon dilatation. Patients with limited number of small stones (<1cm) and minimally dilated bile ducts are ideal candidates. 3. Lithotrypsy. For stones that are difficult to remove because of impaction or large size (typically 10 15MM). Copelan and Kapoor. Choledocholithiasis; diagnosis and management.techniques in vascular and interventional radiology. 2016;18:244 Role of antibiotics in severe acute pancreatitis (SAP). Generally not recommended Aim to prevent superinfection. Not preventive in SAP. Cochrane metaanalysis. Prophylactic antibiotics not indicated in AP regardless of interstitial or necrotizing or disease severity (mild,moderately severe or SAP). Opposing view. JPN guidelines. Tenner et al. Am. Coll. Gastroenterol. Guideline. 2013;108:1400 Acute pancreatitis is a systemic disease with major complications CT scan- Day 1 and Day 10 Patient clinically was worse on day 1 Local Fluid collections pseudocyst Necrosis, sterile and infected Ascites Erosion of adjacent blood vessels GI bleeding Colonic necrosis Abdominal compartment syndrome Systemic Pulmonary Cardiac Renal Multi organ dysfunction CNS, Puertscher s retinopathy Rhabdomyolysis TTP,DIC Arthralgia,bone necrosis Metabolic Hypocalcemia Hypoalbuminemia DKA 4
5 Pancreatic and Peripancreatic Fluid Collections Incidence, location, natural history Pancreatic Fluid Collections Natural History and management options In both acute Interstitial (edematous) and Necrotizing pancreatitis: Nearly 40% of hospitalized patients will have fluid collection. Located pancreatic and or peripancreatic In > 50% of cases fluid collections regress. No explanation for the regression. Regression cannot be predicted Bradley E. Acute Pancreatitis,Principles and Practice *Bollen etal. Br J Surg 2008:95;6-21 ** Cannon etal. Am Coll Surg 2009: 209; Acute Fluid Collection in AP FNA is not required for all peripancreatic fluid collections 1. Fluid collections that lack a discrete capsule Vary in size and shape 2. Occur in 30-50% of patients 3. Resolve spontaneously in 50% 4. Located within the lesser sac or anterior pararenal space Less commonly track into other regions Bradley EL III. Arch Surg 1993;128: Case 4. A 32 year old physician with acute pancreatitis, day 5 after onset of pancreatitis. No abdominal pain. Two months later fluid completely resolved. Ten years later asymptomatic. Localization of fluid collections Lesser Sac Anterior pararenal space Posterior pararenal space In and around the left lobe of liver Spleen Persistence of fluid collection means a pancreatic fistula has developed with a duct. 5
6 Pancreatic Pseudocysts Become defined after 4 weeks of onset of AP. Well circumscribed, round or oval homogenous fluid collection Well defined wall No associated tissue necrosis Cyst fluid usually shows increased amylase-lipase Pseudocyst formation may seal off spontaneous regression >50% Presence or absence of ductal communication- (important to know for Transpapillary drainage) Pseudocysts: When to intervene? > 6 cm in size is no longer the threshold for intervention Total resolution is documented in cysts > 6cm in size Logic dictates that larger the pseudocysts, longer the duration the less likely spontaneous resolution will occur. Pseudocysts (with underlying chronic pancreatitis), PC with thicker wall or known communication with a duct needs intervention Recommendation : close clinical and radiological follow up, action be taken when PC increases in size, becomes symptomatic or complications are suspected. To be differentiated from cystic neoplasms Pre-drainage evaluation of a pseudocyst 1. Exclude a cystic neoplasm. 2. R/O IPMN or a pancreatic cancer. 3. Exclude solid content in a pseudocyst. 4. Delineate the relationship with stomach or duodenum. 5. Exclude vascular structures in the route of approach to the cyst.( Important in patients with portal hypertension). 6. Trans papillary approach is possible only when there is a communication with a pancreatic duct. ERCP/ MRCP needed. Barthet etal Gastrointest Endosc 2008:67; Varadarajulu etal Gastro intest Endoscopy 2007:66; Hookey etal Gastrointest Endosc 2006:63; Pseudocyst Drainage: Role of EUS Baron. J gastrointest Surg 2008:12;369 Baron.Gastro endoscc Clin NA 2007:17;559 Ahlawat etal JOP 2006:7;616 Localizes cyst Determines distance from stomach wall Detects vascular structures 6
7 Necrotizing Pancreatitis Challenges and solutions An overview of current approaches Pancreatic Necrosis Approximately 15% of patients with AP. Focal or diffuse regions of non-viable pancreatic tissue On CECT necrosis is characterized by areas of pancreatic tissue with absent or poor contrast media enhancement (hypoperfusion) or lack of enhancement of the entire gland Infected necrosis generally occurs within 3 weeks of onset of AP. Note mortality in infected pancreatic necrosis is double that of pancreatic abscess. Acute Pancreatitis Timing of Pancreatic Infections % Cases < 7 days 7-14 days days > 21 days Adapted from H. Beger et al., Gastroenterology 1986; 91:433 Case 7:A 78 year old Mexican Lady admitted with Biliary pancreatitis 3 weeks in the hospital Fever, shock, anuria, Follow up CT scan 7
8 How should pancreatic necrosis be managed?. Managed conservatively. Intervention rarely needed in Sterile necrosis Intervention needed only rarely as in multiorgan dysfunction not improving despite maximal therapy in ICU. In infected necrosis delayed necrosectomy and catheter drainage Santvoort et al. A conservative and minimally invasive approach to necrotizing pancreatitis improves outcome. Gastroenterology. 2011:142:1254. Pezelli et al. Practical Guide lines for acute pancreatitis. Pancreatology 2010;10:523. Is necrosectomy obsolete for IPN? A paradigm shift needed? 1960s Explorative laparotomy to total pancreatectomy. 1990s. 100% mortality if IPN is not operated immediately severe IPN benefit from delayed surgical necrosectomy and drainage minimally invasive techniques. Percutaneous catheter, endoscopic transluminal drainage. Followed by video assisted retroperitoneal or endoscopic drainage. Improved outcome over open necrosectomy. Chang Y. WJG. 2014;20:16925 Rosenberg Surg Infect 2015 Walled off Pancreatic necrosis Abdominal Compartment syndrome in acute pancreatitis. (Mentula P et al Arch.Surg. 2010;145: ) intraabdominal pressure results in new onset organ failure A large low-attenuation fluid collection replaces almost entire pancreatic parenchyma. Pancreatic head and tail are markedly displaced by the fluid collection. Destructive pathway similar to compartment syndrome of extremities Occurs when increased Surgical decompression Opening the abdominal wall and abdominal fascia. Early surgical decompression is associated With reduced mortality. 8
9 Learning points 1. An early evaluation of severity of acute pancreatitis should be made clinically and by one of the scoring systems on admission. 2. Initial management. Pain control, adequate,timely, fluid administration. 3. Oral feeding or enteral feeding, seldom TPN. 4. Routine antibiotics not advocated 3. Assessment of Complications. Complicated acute pancreatitis. 1.Fluid collections Most of them resolve,do not needle. 2.Pancreatic pseudocyst if symptomatic, enlarging, Infected, compressing adjacent organs need intervention. 3. Pancreatic necrosis. If sterile usually does not require intervention 4. Pancreatic necrosis if infected intervention endoscopic or surgical. Delay if not avoid surgery. THANK YOU 9
ACG Clinical Guideline: Management of Acute Pancreatitis
 ACG Clinical Guideline: Management of Acute Pancreatitis Scott Tenner, MD, MPH, FACG 1, John Baillie, MB, ChB, FRCP, FACG 2, John DeWitt, MD, FACG 3 and Santhi Swaroop Vege, MD, FACG 4 1 State University
ACG Clinical Guideline: Management of Acute Pancreatitis Scott Tenner, MD, MPH, FACG 1, John Baillie, MB, ChB, FRCP, FACG 2, John DeWitt, MD, FACG 3 and Santhi Swaroop Vege, MD, FACG 4 1 State University
Severe necrotizing pancreatitis. ICU Fellowship Training Radboudumc
 Severe necrotizing pancreatitis ICU Fellowship Training Radboudumc Acute pancreatitis Patients with acute pancreatitis van Dijk SM. Gut 2017;66:2024-2032 Diagnosis Revised Atlanta classification Abdominal
Severe necrotizing pancreatitis ICU Fellowship Training Radboudumc Acute pancreatitis Patients with acute pancreatitis van Dijk SM. Gut 2017;66:2024-2032 Diagnosis Revised Atlanta classification Abdominal
Endoscopic Management of Acute Pancreatitis. Theo Doukides, MD Gastroenterology and Therapeutic Endoscopy February 13, 2018
 Endoscopic Management of Acute Pancreatitis Theo Doukides, MD Gastroenterology and Therapeutic Endoscopy February 13, 2018 Objectives Assessment of acute pancreatitis Early management Who needs an ERCP
Endoscopic Management of Acute Pancreatitis Theo Doukides, MD Gastroenterology and Therapeutic Endoscopy February 13, 2018 Objectives Assessment of acute pancreatitis Early management Who needs an ERCP
Pancreatic Benign April 27, 2016
 Department of Surgery Pancreatic Benign April 27, 2016 James Choi Dr. Hernandez Objectives Medical Expert: 1. Anatomy and congenital anomalies of the pancreas and pancreatic duct (divisum, annular pancreas
Department of Surgery Pancreatic Benign April 27, 2016 James Choi Dr. Hernandez Objectives Medical Expert: 1. Anatomy and congenital anomalies of the pancreas and pancreatic duct (divisum, annular pancreas
Disclosures. Extra-hepatic Biliary Disease and the Pancreas. Objectives. Pancreatitis 10/3/2018. No relevant financial disclosures to report
 Extra-hepatic Biliary Disease and the Pancreas Disclosures No relevant financial disclosures to report Jeffrey Coughenour MD FACS Clinical Associate Professor of Surgery and Emergency Medicine Division
Extra-hepatic Biliary Disease and the Pancreas Disclosures No relevant financial disclosures to report Jeffrey Coughenour MD FACS Clinical Associate Professor of Surgery and Emergency Medicine Division
U Nordic Forum - Trauma & Emergency Radiology. Lecture Objectives. MDCT in Acute Pancreatitis. Acute Pancreatitis: Etiologies
 Nordic Forum - Trauma & Emergency Radiology Lecture Objectives MDCT in Acute Pancreatitis Borut Marincek Institute of Diagnostic Radiology niversity Hospital Zurich, Switzerland To describe the role of
Nordic Forum - Trauma & Emergency Radiology Lecture Objectives MDCT in Acute Pancreatitis Borut Marincek Institute of Diagnostic Radiology niversity Hospital Zurich, Switzerland To describe the role of
Management of Acute Pancreatitis and its Complications Aspirus Grand Rounds June 6, 2017 Eric A. Johnson MD
 Management of Acute Pancreatitis and its Complications Aspirus Grand Rounds June 6, 2017 Eric A. Johnson MD Disclosure: None In accordance with the Standards of the Wisconsin Medical Society, all those
Management of Acute Pancreatitis and its Complications Aspirus Grand Rounds June 6, 2017 Eric A. Johnson MD Disclosure: None In accordance with the Standards of the Wisconsin Medical Society, all those
PANCREATIC PSEUDOCYSTS. Madhuri Rao MD PGY-5 Kings County Hospital Center
 PANCREATIC PSEUDOCYSTS Madhuri Rao MD PGY-5 Kings County Hospital Center 34 yo M Case Presentation PMH: Chronic pancreatitis (ETOH related) PSH: Nil Meds: Nil NKDA www.downstatesurgery.org Symptoms o Chronic
PANCREATIC PSEUDOCYSTS Madhuri Rao MD PGY-5 Kings County Hospital Center 34 yo M Case Presentation PMH: Chronic pancreatitis (ETOH related) PSH: Nil Meds: Nil NKDA www.downstatesurgery.org Symptoms o Chronic
Acute Pancreatitis:
 American College of Gastroenterology 2014 Acute Pancreatitis Scott Tenner, MD, MPH, FACG Clinical Professor of Medicine State University of New York Health Sciences Center Director, Brooklyn Gastroenterology
American College of Gastroenterology 2014 Acute Pancreatitis Scott Tenner, MD, MPH, FACG Clinical Professor of Medicine State University of New York Health Sciences Center Director, Brooklyn Gastroenterology
The Bile Duct (and Pancreas) and the Physician
 The Bile Duct (and Pancreas) and the Physician Javaid Iqbal Consultant in Gastroenterology and Pancreato-biliary Medicine University Hospital South Manchester Not so common?! Two weeks 38 ERCP s 20 15
The Bile Duct (and Pancreas) and the Physician Javaid Iqbal Consultant in Gastroenterology and Pancreato-biliary Medicine University Hospital South Manchester Not so common?! Two weeks 38 ERCP s 20 15
Acute Pancreatitis. Falk Symposium 161 Dresden
 Acute Pancreatitis Falk Symposium 161 Dresden 12.10.2007 Incidence of Acute Pancreatitis (Malmö) Lindkvist B, et al Clin Gastroenterol Hepatol 2004;2:831-837 Gallstones Alcohol AGA Medical Position Statement
Acute Pancreatitis Falk Symposium 161 Dresden 12.10.2007 Incidence of Acute Pancreatitis (Malmö) Lindkvist B, et al Clin Gastroenterol Hepatol 2004;2:831-837 Gallstones Alcohol AGA Medical Position Statement
ACUTE PANCREATITIS: NEW CLASSIFICATION OF AN OLD FOE. T Barrow, A Nasrullah, S Liong, V Rudralingam, S A Sukumar
 ACUTE PANCREATITIS: NEW CLASSIFICATION OF AN OLD FOE T Barrow, A Nasrullah, S Liong, V Rudralingam, S A Sukumar LEARNING OBJECTIVES q Through a series of cases illustrate the updated Atlanta symposium
ACUTE PANCREATITIS: NEW CLASSIFICATION OF AN OLD FOE T Barrow, A Nasrullah, S Liong, V Rudralingam, S A Sukumar LEARNING OBJECTIVES q Through a series of cases illustrate the updated Atlanta symposium
PANCREATIC PSEUDOCYST DRAINAGE: ENDOSCOPIC APPROACHES & THE NURSING ROLE. PRESENTED BY: Susan DePasquale, CGRN, MSN
 PANCREATIC PSEUDOCYST DRAINAGE: ENDOSCOPIC APPROACHES & THE NURSING ROLE PRESENTED BY: Susan DePasquale, CGRN, MSN Pancreatic Fluid Collection (PFC) A result of pancreatic duct (PD) and side branch disruption,
PANCREATIC PSEUDOCYST DRAINAGE: ENDOSCOPIC APPROACHES & THE NURSING ROLE PRESENTED BY: Susan DePasquale, CGRN, MSN Pancreatic Fluid Collection (PFC) A result of pancreatic duct (PD) and side branch disruption,
Management of Pancreatic Fistulae
 Management of Pancreatic Fistulae Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Fistula definition A Fistula is a permanent abnormal passageway between two organs (epithelial
Management of Pancreatic Fistulae Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Fistula definition A Fistula is a permanent abnormal passageway between two organs (epithelial
LOKUN! I got stomach ache!
 LOKUN! I got stomach ache! Mr L is a 67year old Chinese gentleman who is a non smoker, social drinker. He has a medical history significant for Hypertension, Hyperlipidemia, Type 2 Diabetes Mellitus, Chronic
LOKUN! I got stomach ache! Mr L is a 67year old Chinese gentleman who is a non smoker, social drinker. He has a medical history significant for Hypertension, Hyperlipidemia, Type 2 Diabetes Mellitus, Chronic
Case Scenario 1. Discharge Summary
 Case Scenario 1 Discharge Summary A 69-year-old woman was on vacation and noted that she was becoming jaundiced. Two months prior to leaving on that trip, she had had a workup that included an abdominal
Case Scenario 1 Discharge Summary A 69-year-old woman was on vacation and noted that she was becoming jaundiced. Two months prior to leaving on that trip, she had had a workup that included an abdominal
Does it matter what we drain?
 Endoscopic Management of Pancreatic Fluid Collections Shyam Varadarajulu, MD Medical Director Center for Interventional Endoscopy Florida Hospital, Orlando Does it matter what we drain? Makes all the difference!
Endoscopic Management of Pancreatic Fluid Collections Shyam Varadarajulu, MD Medical Director Center for Interventional Endoscopy Florida Hospital, Orlando Does it matter what we drain? Makes all the difference!
Emergency Surgery Course Graz, March ACUTE PANCREATITIS. Carlos Mesquita Coimbra
 ACUTE PANCREATITIS Carlos Mesquita Coimbra ESSENTIALS (1) AP occurs when digestive enzymes become activated while still in the pancreas, causing inflammation repeated bouts of AP can lead to chronic pancreatitis
ACUTE PANCREATITIS Carlos Mesquita Coimbra ESSENTIALS (1) AP occurs when digestive enzymes become activated while still in the pancreas, causing inflammation repeated bouts of AP can lead to chronic pancreatitis
Siddharth Gosavi, Vydehi Institute of Medical Sciences & Research Centre, India Under the guidance of Gillian Lieberman, MD
 Under the guidance of Gillian Lieberman, MD March 2016 RADIOLOGICAL HALLMARKS OF NECROTIZING PANCREATITIS Siddharth Gosavi, Vydehi Institute of Medical Sciences & Research Centre, India Under the guidance
Under the guidance of Gillian Lieberman, MD March 2016 RADIOLOGICAL HALLMARKS OF NECROTIZING PANCREATITIS Siddharth Gosavi, Vydehi Institute of Medical Sciences & Research Centre, India Under the guidance
Acute Pancreatitis. Encourage You to Read!
 Acute Pancreatitis Laith H. Jamil, MD, FACG Associate Director of Interventional Endoscopy Cedars Sinai Medical Center Los Angeles, CA Encourage You to Read! Copyright 2015 American College of Gastroenterology
Acute Pancreatitis Laith H. Jamil, MD, FACG Associate Director of Interventional Endoscopy Cedars Sinai Medical Center Los Angeles, CA Encourage You to Read! Copyright 2015 American College of Gastroenterology
Surgical Management of Acute Pancreatitis
 Surgical Management of Acute Pancreatitis Steven J. Hughes, MD, FACS Cracchiolo Family Professor of Surgery and Chief, General Surgery Overview Biliary pancreatitis a cost effective algorithm Key concepts
Surgical Management of Acute Pancreatitis Steven J. Hughes, MD, FACS Cracchiolo Family Professor of Surgery and Chief, General Surgery Overview Biliary pancreatitis a cost effective algorithm Key concepts
Mild. Moderate. Severe
 2012 Revised Atlanta Classification Acute pancreatitis Classified based on absence or presence of local and/or systemic complications Mild Acute Pancreatits Moderate Severe P. A. Banks, T. L. Bollen, C.
2012 Revised Atlanta Classification Acute pancreatitis Classified based on absence or presence of local and/or systemic complications Mild Acute Pancreatits Moderate Severe P. A. Banks, T. L. Bollen, C.
Management of Acute Pancreatitis
 Management of Acute Pancreatitis A Clinical Practice Guideline developed by the University of Toronto s Best Practice in Surgery JA Greenberg, M Bawazeer, J Hsu, J Marshall, JO Friedrich, A Nathens, N
Management of Acute Pancreatitis A Clinical Practice Guideline developed by the University of Toronto s Best Practice in Surgery JA Greenberg, M Bawazeer, J Hsu, J Marshall, JO Friedrich, A Nathens, N
Multidetector CT evaluation of acute pancreatitis and its complications and its correlation with clinical outcome
 INTERNATIONAL JOURNAL OF CURRENT RESEARCH IN BIOLOGY AND MEDICINE ISSN: 2455-944X www.darshanpublishers.com DOI:10.22192/ijcrbm Volume 3, Issue 1-2018 Original Research Article Multidetector CT evaluation
INTERNATIONAL JOURNAL OF CURRENT RESEARCH IN BIOLOGY AND MEDICINE ISSN: 2455-944X www.darshanpublishers.com DOI:10.22192/ijcrbm Volume 3, Issue 1-2018 Original Research Article Multidetector CT evaluation
Role of Imaging Methods in Diagnosis of Acute Pancreatitis. Válek V. Radiologická klinika, FN Brno a LF MU v Brně
 Role of Imaging Methods in Diagnosis of Acute Pancreatitis Válek V. Radiologická klinika, FN Brno a LF MU v Brně New Classification: Acute Pancreatitis 2007 revision of Atlanta classification and definitions
Role of Imaging Methods in Diagnosis of Acute Pancreatitis Válek V. Radiologická klinika, FN Brno a LF MU v Brně New Classification: Acute Pancreatitis 2007 revision of Atlanta classification and definitions
PANCREATIC PSEUDOCYSTS: Optimal therapeutic strategies. Jacques DEVIERE, MD, PhD Erasme University Hospital Brussels
 PANCREATIC PSEUDOCYSTS: Optimal therapeutic strategies Jacques DEVIERE, MD, PhD Erasme University Hospital Brussels 1. Diagnosis. 2. Multidisciplinary approach. 3. Therapeutic planning. 4. How? 5. Follow-up
PANCREATIC PSEUDOCYSTS: Optimal therapeutic strategies Jacques DEVIERE, MD, PhD Erasme University Hospital Brussels 1. Diagnosis. 2. Multidisciplinary approach. 3. Therapeutic planning. 4. How? 5. Follow-up
Exocrine functions: secretion of digestive enzymes (eg. lipase, amylase,
 Chapter 91 Pancreas Episode Overview: 1. List 10 differential diagnoses for acute pancreatitis 2. List 10 causes of pancreatitis. Which are most common in adults? Which one is most common in pediatrics?
Chapter 91 Pancreas Episode Overview: 1. List 10 differential diagnoses for acute pancreatitis 2. List 10 causes of pancreatitis. Which are most common in adults? Which one is most common in pediatrics?
Resident Teaching Conference 10/16/09 Rondi Kauffmann Resident presenter William Nealon Faculty presenter
 Resident Teaching Conference 10/16/09 Rondi Kauffmann Resident presenter William Nealon Faculty presenter KC 59 year old male Referred to Surgery clinic for incidentally discovered 5cm x 3cm pancreatic
Resident Teaching Conference 10/16/09 Rondi Kauffmann Resident presenter William Nealon Faculty presenter KC 59 year old male Referred to Surgery clinic for incidentally discovered 5cm x 3cm pancreatic
ERCP / PTC Surgical Laparoscopic vs open Timing and order of approach
 Choledocholithiasis Which Approach and When? Lygia Stewart, MD University of California, San Francisco 2010 Naffziger Post-Graduate Course Clinical Manifestations of Choledocholithiasis Asymptomatic (no
Choledocholithiasis Which Approach and When? Lygia Stewart, MD University of California, San Francisco 2010 Naffziger Post-Graduate Course Clinical Manifestations of Choledocholithiasis Asymptomatic (no
Disclosures. Overview. Case 1. Common Bile Duct Sizes 10/14/2016. General GI + Advanced Endoscopy: NAFLD/Stones/Pancreatitis
 Disclosures General GI + Advanced Endoscopy: NAFLD/Stones/Pancreatitis 123 Blank Blank, LLC Aldo Maspons, MD Assistant Professor Director of Endoscopy Department of Pediatrics Texas Tech University Health
Disclosures General GI + Advanced Endoscopy: NAFLD/Stones/Pancreatitis 123 Blank Blank, LLC Aldo Maspons, MD Assistant Professor Director of Endoscopy Department of Pediatrics Texas Tech University Health
ESPEN Congress Brussels 2005
 ESPEN Congress Brussels 2005 Therapeutic endoscopy of pancreatic diseases. How endoscopy may improve nutrition? Myriam Delhaye Therapeutic endoscopy of pancreatic diseases. How endoscopy may improve nutrition?
ESPEN Congress Brussels 2005 Therapeutic endoscopy of pancreatic diseases. How endoscopy may improve nutrition? Myriam Delhaye Therapeutic endoscopy of pancreatic diseases. How endoscopy may improve nutrition?
American College of Gastroenterology Guideline: Management of Acute Pancreatitis
 PRACTICE GUIDELINES nature publishing group 1 American College of Gastroenterology Guideline: Management of Acute Pancreatitis Scott Tenner, MD, MPH, FACG1, John Baillie, MB, ChB, FRCP, FACG 2, Joh n D
PRACTICE GUIDELINES nature publishing group 1 American College of Gastroenterology Guideline: Management of Acute Pancreatitis Scott Tenner, MD, MPH, FACG1, John Baillie, MB, ChB, FRCP, FACG 2, Joh n D
A Prospective Study of Bedside Index for Severity in Acute Pancreatitis Score in Acute Pancreatitis
 Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2018/210 A Prospective Study of Bedside Index for Severity in Acute Pancreatitis Score in Acute Pancreatitis S Kasturi Bai
Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2018/210 A Prospective Study of Bedside Index for Severity in Acute Pancreatitis Score in Acute Pancreatitis S Kasturi Bai
Imaging of liver and pancreas
 Imaging of liver and pancreas.. Disease of the liver Focal liver disease Diffusion liver disease Focal liver disease Benign Cyst Abscess Hemangioma FNH Hepatic adenoma HCC Malignant Fibrolamellar carcinoma
Imaging of liver and pancreas.. Disease of the liver Focal liver disease Diffusion liver disease Focal liver disease Benign Cyst Abscess Hemangioma FNH Hepatic adenoma HCC Malignant Fibrolamellar carcinoma
ERCP and EUS: What s New and What Should We Do?
 ERCP and EUS: What s New and What Should We Do? Rajesh N. Keswani, MD Associate Professor of Medicine Division of Gastroenterology Northwestern University Feinberg School of Medicine EUS/ERCP in 2015 THE
ERCP and EUS: What s New and What Should We Do? Rajesh N. Keswani, MD Associate Professor of Medicine Division of Gastroenterology Northwestern University Feinberg School of Medicine EUS/ERCP in 2015 THE
Prophylactic Antibiotics in Severe Acute Pancreatitis: Antibiotics are good. Karen Lo R 3 University of Colorado Oct 11, 2010
 Prophylactic Antibiotics in Severe Acute Pancreatitis: Antibiotics are good Karen Lo R 3 University of Colorado Oct 11, 2010 Overview Pancreas: The History Pancreas: The Organ The Disease Pathogenesis
Prophylactic Antibiotics in Severe Acute Pancreatitis: Antibiotics are good Karen Lo R 3 University of Colorado Oct 11, 2010 Overview Pancreas: The History Pancreas: The Organ The Disease Pathogenesis
Correspondence should be addressed to Justin Cochrane;
 Case Reports in Gastrointestinal Medicine Volume 2015, Article ID 794282, 4 pages http://dx.doi.org/10.1155/2015/794282 Case Report Acute on Chronic Pancreatitis Causing a Highway to the Colon with Subsequent
Case Reports in Gastrointestinal Medicine Volume 2015, Article ID 794282, 4 pages http://dx.doi.org/10.1155/2015/794282 Case Report Acute on Chronic Pancreatitis Causing a Highway to the Colon with Subsequent
JOHN M UECKER, MD, FACS COMPLEX PANCREATICODUODENAL INJURIES
 JOHN M UECKER, MD, FACS COMPLEX PANCREATICODUODENAL INJURIES THE PROBLEM DUODENAL / PANCREATIC INJURIES Difficult to diagnose Not very common Anatomic and physiologic challenges 90% rate of associated
JOHN M UECKER, MD, FACS COMPLEX PANCREATICODUODENAL INJURIES THE PROBLEM DUODENAL / PANCREATIC INJURIES Difficult to diagnose Not very common Anatomic and physiologic challenges 90% rate of associated
JMSCR Vol 05 Issue 06 Page June 2017
 www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i6.76 A Comparative Study of Assessment of Different
www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i6.76 A Comparative Study of Assessment of Different
Endoscopic pancreatic necrosectomy in 2017
 Endoscopic pancreatic necrosectomy in 2017 Mouen Khashab, MD Associate Professor of Medicine Director of Therapeutic Endoscopy The Johns Hopkins Hospital Revised Atlanta Classification Entity Acute fluid
Endoscopic pancreatic necrosectomy in 2017 Mouen Khashab, MD Associate Professor of Medicine Director of Therapeutic Endoscopy The Johns Hopkins Hospital Revised Atlanta Classification Entity Acute fluid
COMPUTED TOMOGRAPHY FINDINGS IN ACUTE PANCREATITIS
 ORIGINAL ARTICLE COMPUTED TOMOGRAPHY FINDINGS IN ACUTE PANCREATITIS Noorul Hadi, Kalsoom Nawab, Ayesha Amin Department Of Radiology, Post Graduate Medical Institute, Hayatabad Medical Complex, Peshawar
ORIGINAL ARTICLE COMPUTED TOMOGRAPHY FINDINGS IN ACUTE PANCREATITIS Noorul Hadi, Kalsoom Nawab, Ayesha Amin Department Of Radiology, Post Graduate Medical Institute, Hayatabad Medical Complex, Peshawar
The Pancreas. Basic Anatomy. Endocrine pancreas. Exocrine pancreas. Pancreas vasculature. Islets of Langerhans. Acinar cells Ductal System
 SGNA: Back to Basics Rogelio G. Silva, MD Assistant Clinical Professor of Medicine University of Illinois at Chicago Department of Medicine Division of Gastroenterology Advocate Christ Medical Center GI
SGNA: Back to Basics Rogelio G. Silva, MD Assistant Clinical Professor of Medicine University of Illinois at Chicago Department of Medicine Division of Gastroenterology Advocate Christ Medical Center GI
CT 101 :Pancreas and Spleen
 CT 101 :Pancreas and Spleen Shikha Khullar,, MD, MPH Division of Radiology University of South Alabama The Pancreas Normal Pancreas 3 Phase Pancreatic CT Non contrast Arterial phase : 30-35 35 second
CT 101 :Pancreas and Spleen Shikha Khullar,, MD, MPH Division of Radiology University of South Alabama The Pancreas Normal Pancreas 3 Phase Pancreatic CT Non contrast Arterial phase : 30-35 35 second
Comprehensive Study of Acute Pancreatitis (Diagnosis, Disease Course, and Clinical Management): A Retrospective and Prospective Study
 Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/449 Comprehensive Study of Acute Pancreatitis (Diagnosis, Disease Course, and Clinical Management): A Retrospective
Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/449 Comprehensive Study of Acute Pancreatitis (Diagnosis, Disease Course, and Clinical Management): A Retrospective
IMAGING OF ACUTE AND CHRONIC PANCREATITIS, INCLUDING EXOCRINE FUNCTION
 IMAGING OF ACUTE AND CHRONIC PANCREATITIS, INCLUDING EXOCRINE FUNCTION Andrew T. Trout, MD @AndrewTroutMD Disclosures Grant support National Pancreas Foundation In-kind support - ChiRhoClin modified from:
IMAGING OF ACUTE AND CHRONIC PANCREATITIS, INCLUDING EXOCRINE FUNCTION Andrew T. Trout, MD @AndrewTroutMD Disclosures Grant support National Pancreas Foundation In-kind support - ChiRhoClin modified from:
Pathophysiology ACUTE PANCREATITIS
 Pancreatitis Pathophysiology ACUTE PANCREATITIS BILIARY OBSTRUCTION Duct obstruction in the bile duct, pancreatic duct, or both. Increasing pressure Unregulated activation of digestive enzymes. Inflammation
Pancreatitis Pathophysiology ACUTE PANCREATITIS BILIARY OBSTRUCTION Duct obstruction in the bile duct, pancreatic duct, or both. Increasing pressure Unregulated activation of digestive enzymes. Inflammation
ERCP complications and challenges in their diagnosis and management.
 ERCP complications and challenges in their diagnosis and management. Sandie R Thomson Chair of the Division of Gastroenterology, University of Cape Town ERCP Do I have a good Indication? . Algorithm for
ERCP complications and challenges in their diagnosis and management. Sandie R Thomson Chair of the Division of Gastroenterology, University of Cape Town ERCP Do I have a good Indication? . Algorithm for
Updated Imaging Nomenclature for Acute Pancreatitis
 Residents Section Structured Review Murphy et al. Imaging Nomenclature for Acute Pancreatitis Residents Section Structured Review Residents inradiology Kevin P. Murphy 1,2 Owen J. O Connor 1,2 Michael
Residents Section Structured Review Murphy et al. Imaging Nomenclature for Acute Pancreatitis Residents Section Structured Review Residents inradiology Kevin P. Murphy 1,2 Owen J. O Connor 1,2 Michael
Joint Trust Management of Acute Severe Pancreatitis in Adults
 A clinical guideline recommended for use For Use in: By: For: Division responsible for document: All clinical areas (as a reference for screening) ITU/HDU (for definitive care) All medical staff likely
A clinical guideline recommended for use For Use in: By: For: Division responsible for document: All clinical areas (as a reference for screening) ITU/HDU (for definitive care) All medical staff likely
ESPEN Congress The Hague 2017
 ESPEN Congress The Hague 2017 Meeting nutritional needs of acute care patients Feeding acute pancreatitis patients J. Luttikhold (NL) FEEDING ACUTE PANCREATITIS PATIENTS Joanna Luttikhold, MD PhD Registrar
ESPEN Congress The Hague 2017 Meeting nutritional needs of acute care patients Feeding acute pancreatitis patients J. Luttikhold (NL) FEEDING ACUTE PANCREATITIS PATIENTS Joanna Luttikhold, MD PhD Registrar
The role of ERCP in chronic pancreatitis
 The role of ERCP in chronic pancreatitis Marianna Arvanitakis Erasme University Hospital, ULB, Brussels, Belgium 10 th Nottingham Endoscopy Masterclass SPEAKER DECLARATIONS This presenter has the following
The role of ERCP in chronic pancreatitis Marianna Arvanitakis Erasme University Hospital, ULB, Brussels, Belgium 10 th Nottingham Endoscopy Masterclass SPEAKER DECLARATIONS This presenter has the following
Pancreatic Lesions. Valerie Jefford Pediatric Surgery Rounds June 6, 2003
 Pancreatic Lesions Valerie Jefford Pediatric Surgery Rounds June 6, 2003 Embryology 4 th week 2 buds of endodermal origin from caudal foregut Dorsal and ventral bud Ventral migrates dorsally with CBD (below/behind
Pancreatic Lesions Valerie Jefford Pediatric Surgery Rounds June 6, 2003 Embryology 4 th week 2 buds of endodermal origin from caudal foregut Dorsal and ventral bud Ventral migrates dorsally with CBD (below/behind
Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds
 Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds Imaging in jaundice and 2ww pathway Image protocol Staging Limitations Pancreatic cancer 1.2.4 Refer people using a suspected
Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds Imaging in jaundice and 2ww pathway Image protocol Staging Limitations Pancreatic cancer 1.2.4 Refer people using a suspected
Prognostic Indicator in Severe Acute Pancreatitis
 Open Access Journal Research Article DOI: 10.23958/ijirms/vol03-i05/10 Prognostic Indicator in Severe Acute Pancreatitis Dr. Ajay Khanolkar 1, Dr. Manish Khare *2 1 Associate Professor, 2 Assistant Professor
Open Access Journal Research Article DOI: 10.23958/ijirms/vol03-i05/10 Prognostic Indicator in Severe Acute Pancreatitis Dr. Ajay Khanolkar 1, Dr. Manish Khare *2 1 Associate Professor, 2 Assistant Professor
CLINICAL CASE OF THE MONTH. A 35 Year Old Woman with Abdominal Pain
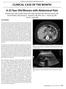 CASE REPORT JOURNAL OF THE LOUISIANA STATE MEDICAL SOCIETY CLINICAL CASE OF THE MONTH A 35 Year Old Woman with Abdominal Pain Melissa Spera, MD, Camille Thelin, MD, Abby Gandolfi, MD, Nicholas Clayton,
CASE REPORT JOURNAL OF THE LOUISIANA STATE MEDICAL SOCIETY CLINICAL CASE OF THE MONTH A 35 Year Old Woman with Abdominal Pain Melissa Spera, MD, Camille Thelin, MD, Abby Gandolfi, MD, Nicholas Clayton,
Anatomical and Functional MRI of the Pancreas
 Anatomical and Functional MRI of the Pancreas MA Bali, MD, T Metens, PhD Erasme Hospital Free University of Brussels Belgium mbali@ulb.ac.be Introduction The use of MRI to investigate the pancreas has
Anatomical and Functional MRI of the Pancreas MA Bali, MD, T Metens, PhD Erasme Hospital Free University of Brussels Belgium mbali@ulb.ac.be Introduction The use of MRI to investigate the pancreas has
Acute pancreatitis complications and a method to improve the outcome
 Acute pancreatitis complications and a method to improve the outcome Poster No.: C-2959 Congress: ECR 2017 Type: Authors: Keywords: DOI: Scientific Exhibit B. Angheloiu, A. Leandru; Brasov/RO Abdomen,
Acute pancreatitis complications and a method to improve the outcome Poster No.: C-2959 Congress: ECR 2017 Type: Authors: Keywords: DOI: Scientific Exhibit B. Angheloiu, A. Leandru; Brasov/RO Abdomen,
Chronic Pancreatitis: When to Scope? Gregory A. Cote, MD, MS Assistant Professor of Medicine Indiana University School of Medicine
 Chronic Pancreatitis: When to Scope? Gregory A. Cote, MD, MS Assistant Professor of Medicine Indiana University School of Medicine Endoscopy & Chronic Pancreatitis Diagnosis EUS ERCP Exocrine Function
Chronic Pancreatitis: When to Scope? Gregory A. Cote, MD, MS Assistant Professor of Medicine Indiana University School of Medicine Endoscopy & Chronic Pancreatitis Diagnosis EUS ERCP Exocrine Function
Morning Report. Allison Haden, MD October 1, 2002
 Morning Report Allison Haden, MD October 1, 2002 68 yo WM with N/V and abdominal pain Became ill about 2 weeks ago, per pt. intermittent nausea: worse w/eating vomiting within 30min of eating, nonbilious,
Morning Report Allison Haden, MD October 1, 2002 68 yo WM with N/V and abdominal pain Became ill about 2 weeks ago, per pt. intermittent nausea: worse w/eating vomiting within 30min of eating, nonbilious,
Imaging Techniques for Acute Necrotizing Pancreatitis: Multidetector Computed Tomography
 AISP - 29 th National Congress. Bologna (Italy). September 15-17, 2005. Imaging Techniques for Acute Necrotizing Pancreatitis: Multidetector Computed Tomography Lucia Calculli 1, Raffaele Pezzilli 2, Riccardo
AISP - 29 th National Congress. Bologna (Italy). September 15-17, 2005. Imaging Techniques for Acute Necrotizing Pancreatitis: Multidetector Computed Tomography Lucia Calculli 1, Raffaele Pezzilli 2, Riccardo
Chronic Pancreatitis
 Gastro Foundation Fellows Weekend 2017 Chronic Pancreatitis Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Aetiology in SA Alcohol (up to 80%) Idiopathic Tropical Obstruction Autoimmune
Gastro Foundation Fellows Weekend 2017 Chronic Pancreatitis Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Aetiology in SA Alcohol (up to 80%) Idiopathic Tropical Obstruction Autoimmune
CLINICAL MANIFESTATIONS AND DIAGNOSIS OF ACUTE PANCREATITIS. Raed Abu Sham a, M.D
 CLINICAL MANIFESTATIONS AND DIAGNOSIS OF ACUTE PANCREATITIS Raed Abu Sham a, M.D ACUTE PANCREATITIS Acute inflammatory process of the pancreas that resolves both clinically and histologically. It is usually
CLINICAL MANIFESTATIONS AND DIAGNOSIS OF ACUTE PANCREATITIS Raed Abu Sham a, M.D ACUTE PANCREATITIS Acute inflammatory process of the pancreas that resolves both clinically and histologically. It is usually
Radiology of hepatobiliary diseases
 GI cycle - Lecture 14 436 Teams Radiology of hepatobiliary diseases Objectives 1. To Interpret plan x-ray radiograph of abdomen with common pathologies. 2. To know the common pathologies presentation.
GI cycle - Lecture 14 436 Teams Radiology of hepatobiliary diseases Objectives 1. To Interpret plan x-ray radiograph of abdomen with common pathologies. 2. To know the common pathologies presentation.
Surgical Management of Chronic Pancreatitis VERENA LIU, MD KINGS COUNTY HOSPITAL CENTER SURGERY GRAND ROUNDS 4/1/2013
 Surgical Management of Chronic Pancreatitis VERENA LIU, MD KINGS COUNTY HOSPITAL CENTER SURGERY GRAND ROUNDS 4/1/2013 Case Report 42F with h/o chronic pancreatitis due to alcohol use with chronic upper
Surgical Management of Chronic Pancreatitis VERENA LIU, MD KINGS COUNTY HOSPITAL CENTER SURGERY GRAND ROUNDS 4/1/2013 Case Report 42F with h/o chronic pancreatitis due to alcohol use with chronic upper
Int. Med J Vol. 6 No 1 June 2007 Enteral Nutrition In Intensive Care: Tiger Tube For Small Bowel Feeding In Acute Pancreatitis.
 Page 1 of 6 Int. Med J Vol. 6 No 1 June 2007 Enteral Nutrition In Intensive Care: Tiger Tube For Small Bowel Feeding In Acute Pancreatitis. Case Report Mohd Basri bin Mat Nor. Department of Anaesthesiology
Page 1 of 6 Int. Med J Vol. 6 No 1 June 2007 Enteral Nutrition In Intensive Care: Tiger Tube For Small Bowel Feeding In Acute Pancreatitis. Case Report Mohd Basri bin Mat Nor. Department of Anaesthesiology
IV Fluids. I.V. Fluid Osmolarity Composition 0.9% NaCL (Normal Saline Solution, NSS) Uses/Clinical Considerations
 IV Fluids When administering IV fluids, the type and amount of fluid may influence patient outcomes. Make sure to understand the differences between fluid products and their effects. Crystalloids Crystalloid
IV Fluids When administering IV fluids, the type and amount of fluid may influence patient outcomes. Make sure to understand the differences between fluid products and their effects. Crystalloids Crystalloid
Evidence based imaging of the pancreas
 Evidence based imaging of the pancreas D.Vanbeckevoort, D.Bielen, K.Op de beeck, R.Vanslembrouck Department of Radiology Chairman Prof. Dr. R.Oyen Non-invasive imaging tests available for the diagnosis
Evidence based imaging of the pancreas D.Vanbeckevoort, D.Bielen, K.Op de beeck, R.Vanslembrouck Department of Radiology Chairman Prof. Dr. R.Oyen Non-invasive imaging tests available for the diagnosis
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Abdominal pain, enteral therapy in acute pancreatitis and, 812 Abscess(es), pancreatic, nutritional support for, 814 815 Acute Physiology and
Note: Page numbers of article titles are in boldface type. A Abdominal pain, enteral therapy in acute pancreatitis and, 812 Abscess(es), pancreatic, nutritional support for, 814 815 Acute Physiology and
Management of Gallbladder Disease
 Management of Gallbladder Disease Steven B. Johnson, MD, FACS, FCCM Professor and Chairman, Department of Surgery Program Director, Phoenix Integrated Surgical Residency University of Arizona College of
Management of Gallbladder Disease Steven B. Johnson, MD, FACS, FCCM Professor and Chairman, Department of Surgery Program Director, Phoenix Integrated Surgical Residency University of Arizona College of
Pancreatitis. Acute Pancreatitis
 Pancreatitis Pancreatitis is an inflammation of the pancreas. The pancreas is a large gland behind the stomach and close to the duodenum. The duodenum is the upper part of the small intestine. The pancreas
Pancreatitis Pancreatitis is an inflammation of the pancreas. The pancreas is a large gland behind the stomach and close to the duodenum. The duodenum is the upper part of the small intestine. The pancreas
Overview. Doumit S. BouHaidar, MD ACG/VGS/ODSGNA Regional Postgraduate Course Copyright American College of Gastroenterology 1
 Doumit S. BouHaidar, MD Associate Professor of Medicine Director, Advanced Therapeutic Endoscopy Virginia Commonwealth University Overview Copyright American College of Gastroenterology 1 Incidence: 4
Doumit S. BouHaidar, MD Associate Professor of Medicine Director, Advanced Therapeutic Endoscopy Virginia Commonwealth University Overview Copyright American College of Gastroenterology 1 Incidence: 4
Endoscopic Ultrasonography Clinical Impact. Giancarlo Caletti. Gastroenterologia Università di Bologna. Caletti
 Clinical Impact Giancarlo Gastroenterologia Università di Bologna AUSL di Imola,, Castel S. Pietro Terme (BO) 1982 Indications Diagnosis of Submucosal Tumors (SMT) Staging of Neoplasms Evaluation of Pancreato-Biliary
Clinical Impact Giancarlo Gastroenterologia Università di Bologna AUSL di Imola,, Castel S. Pietro Terme (BO) 1982 Indications Diagnosis of Submucosal Tumors (SMT) Staging of Neoplasms Evaluation of Pancreato-Biliary
Lumen Apposing Metal Stents: Expanding the Role of the Interventional Endoscopist. Alireza Sedarat, MD UCLA Division of Digestive Diseases
 Lumen Apposing Metal Stents: Expanding the Role of the Interventional Endoscopist Alireza Sedarat, MD UCLA Division of Digestive Diseases Disclosures Consultant for Boston Scientific and Olympus Corporation
Lumen Apposing Metal Stents: Expanding the Role of the Interventional Endoscopist Alireza Sedarat, MD UCLA Division of Digestive Diseases Disclosures Consultant for Boston Scientific and Olympus Corporation
Original Article. Abstract. Introduction
 Original Article Role of Computed Tomography in Acute Pancreatitis and its Complications among Age Groups Ishtiaq Ahmed Chishty, Vaqar Bari, Sajida Pasha, Dawar Burhan, Zishan Haider, Zafar Rafique Radiology
Original Article Role of Computed Tomography in Acute Pancreatitis and its Complications among Age Groups Ishtiaq Ahmed Chishty, Vaqar Bari, Sajida Pasha, Dawar Burhan, Zishan Haider, Zafar Rafique Radiology
Comparison of Different Scoring System in Predicting the Severity and Prognosis of Acute Pancreatitis
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 5 Ver. 3 (May. 2018), PP 56-60 www.iosrjournals.org Comparison of Different Scoring System
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 5 Ver. 3 (May. 2018), PP 56-60 www.iosrjournals.org Comparison of Different Scoring System
Case Discussion Splenic Abscess
 Case Discussion Splenic Abscess Personal Data Gender: male Birth Date: 1928/Mar/06th Allergy: Mefenamic Smoking: 0.5 PPD for 55 years Alcohol: negative (?) 4 Months Ago Abdominal pain: epigastric area
Case Discussion Splenic Abscess Personal Data Gender: male Birth Date: 1928/Mar/06th Allergy: Mefenamic Smoking: 0.5 PPD for 55 years Alcohol: negative (?) 4 Months Ago Abdominal pain: epigastric area
ACG Clinical Guideline: Diagnosis and Management of Pancreatic Cysts
 ACG Clinical Guideline: Diagnosis and Management of Pancreatic Cysts Grace H. Elta, MD, FACG 1, Brintha K. Enestvedt, MD, MBA 2, Bryan G. Sauer, MD, MSc, FACG (GRADE Methodologist) 3 and Anne Marie Lennon,
ACG Clinical Guideline: Diagnosis and Management of Pancreatic Cysts Grace H. Elta, MD, FACG 1, Brintha K. Enestvedt, MD, MBA 2, Bryan G. Sauer, MD, MSc, FACG (GRADE Methodologist) 3 and Anne Marie Lennon,
A Retrospective & Prospective Comprehensive Study of Acute Pancreatitis (Diagnosis, Course & Managment)
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 5 Ver. X (May. 2016), PP 15-19 www.iosrjournals.org A Retrospective & Prospective Comprehensive
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 5 Ver. X (May. 2016), PP 15-19 www.iosrjournals.org A Retrospective & Prospective Comprehensive
Management of Gastroenterology Emergencies Tim Gardner, MD Director, Pancreatic Disorders Section of Gastroenterology and Hepatology
 Management of Gastroenterology Emergencies Tim Gardner, MD Director, Pancreatic Disorders Section of Gastroenterology and Hepatology DHMC CREST Symposium November 7, 2008 There are no financial disclosures
Management of Gastroenterology Emergencies Tim Gardner, MD Director, Pancreatic Disorders Section of Gastroenterology and Hepatology DHMC CREST Symposium November 7, 2008 There are no financial disclosures
Acute pancreatitis Case reports. Clinical problems. Use of antibiotics? (P 1 & 2) Surgical treatment of AP? (P 3 & 4)
 Case reports Clinical problems Use of antibiotics? (P 1 & 2) Surgical treatment of AP? (P 3 & 4) Case reports Case 1 Case 1 Patient KD History M, 63 y Obesity BMI 30.3 kg/m 2 Gallbladder stones No concomitant
Case reports Clinical problems Use of antibiotics? (P 1 & 2) Surgical treatment of AP? (P 3 & 4) Case reports Case 1 Case 1 Patient KD History M, 63 y Obesity BMI 30.3 kg/m 2 Gallbladder stones No concomitant
Randomized Controlled Trials in Pancreatic Diseases. James Buxbaum MD University of Southern California Los Angeles County Hospital
 Randomized Controlled Trials in Pancreatic Diseases James Buxbaum MD University of Southern California Los Angeles County Hospital Randomized Trials in Pancreatic Diseases Focus acute pancreatitis Challenges
Randomized Controlled Trials in Pancreatic Diseases James Buxbaum MD University of Southern California Los Angeles County Hospital Randomized Trials in Pancreatic Diseases Focus acute pancreatitis Challenges
Original Policy Date 12:2013
 MP 6.01.30 Magnetic Resonance Cholangiopancreatography Medical Policy Section Radiology Is12:2013sue 3:2005 Original Policy Date 12:2013 Last Review Status/Date 12:2013 Return to Medical Policy Index Disclaimer
MP 6.01.30 Magnetic Resonance Cholangiopancreatography Medical Policy Section Radiology Is12:2013sue 3:2005 Original Policy Date 12:2013 Last Review Status/Date 12:2013 Return to Medical Policy Index Disclaimer
GASTROENTEROLOGY ESSENTIALS
 GASTROENTEROLOGY ESSENTIALS Practical Gastroenterology 8/25/2018 Jahnavi Koppala, MBBS Abdullah Abdussalam, MD A 48-year-old male was evaluated for noncardiac chest pain. Treatment with PPI twice daily
GASTROENTEROLOGY ESSENTIALS Practical Gastroenterology 8/25/2018 Jahnavi Koppala, MBBS Abdullah Abdussalam, MD A 48-year-old male was evaluated for noncardiac chest pain. Treatment with PPI twice daily
Acute Pancreatitis: New Developments and Strategies for the Hospitalist
 REVIEWS Acute Pancreatitis: New Developments and Strategies for the Hospitalist John F. Dick, III, MD 1 *, Timothy B. Gardner, MD, MS 2, Edward J. Merrens, MD, MS 1 1 Geisel School of Medicine, Section
REVIEWS Acute Pancreatitis: New Developments and Strategies for the Hospitalist John F. Dick, III, MD 1 *, Timothy B. Gardner, MD, MS 2, Edward J. Merrens, MD, MS 1 1 Geisel School of Medicine, Section
Chronic pancreatitis mimicking intraductal papillary mucinous neoplasm of the pancreas; Report of tow cases
 Jichi Medical University Journal Chronic pancreatitis mimicking intraductal papillary mucinous neoplasm of the pancreas; Report of tow cases Noritoshi Mizuta, Hiroshi Noda, Nao Kakizawa, Nobuyuki Toyama,
Jichi Medical University Journal Chronic pancreatitis mimicking intraductal papillary mucinous neoplasm of the pancreas; Report of tow cases Noritoshi Mizuta, Hiroshi Noda, Nao Kakizawa, Nobuyuki Toyama,
Anubhav Harshit Kumar* and Mahavir Singh Griwan ORIGINAL ARTICLE. Abstract. Department of Surgery, Pt. B. D. Sharma PGIMS, Rohtak, India
 Gastroenterology Report, 2017, 1 5 doi: 10.1093/gastro/gox029 Original article ORIGINAL ARTICLE A comparison of APACHE II, BISAP, Ranson s score and modified CTSI in predicting the severity of acute pancreatitis
Gastroenterology Report, 2017, 1 5 doi: 10.1093/gastro/gox029 Original article ORIGINAL ARTICLE A comparison of APACHE II, BISAP, Ranson s score and modified CTSI in predicting the severity of acute pancreatitis
Correspondence should be addressed to Supot Pongprasobchai;
 Hindawi Gastroenterology Research and Practice Volume 2017, Article ID 3525349, 7 pages https://doi.org/10.1155/2017/3525349 Research Article Severity, Treatment, and Outcome of Acute Pancreatitis in Thailand:
Hindawi Gastroenterology Research and Practice Volume 2017, Article ID 3525349, 7 pages https://doi.org/10.1155/2017/3525349 Research Article Severity, Treatment, and Outcome of Acute Pancreatitis in Thailand:
General Surgery Service
 General Surgery Service Patient Care Goals and Objectives Stomach/Duodenum and Bariatric assessed for a) Obesity surgery b) Treatment of i) Adenocarcinoma of the stomach ii) GIST iii) Carcinoid 2) Optimize
General Surgery Service Patient Care Goals and Objectives Stomach/Duodenum and Bariatric assessed for a) Obesity surgery b) Treatment of i) Adenocarcinoma of the stomach ii) GIST iii) Carcinoid 2) Optimize
Prof. (DR.) MD. ISMAIL PATWARY. MBBS, FCPS, MD, FACP, FRCP(Glasgow, Edin) Professor, Dept. of Medicine, Sylhet women s Medical College, Sylhet
 Prof. (DR.) MD. ISMAIL PATWARY MBBS, FCPS, MD, FACP, FRCP(Glasgow, Edin) Professor, Dept. of Medicine, Sylhet women s Medical College, Sylhet CHRONIC PANCREATITIS Defined as a progressive inflammatory
Prof. (DR.) MD. ISMAIL PATWARY MBBS, FCPS, MD, FACP, FRCP(Glasgow, Edin) Professor, Dept. of Medicine, Sylhet women s Medical College, Sylhet CHRONIC PANCREATITIS Defined as a progressive inflammatory
Overview. The Pancreas Pancreatitis Signs + Symptoms Investigations Grading Systems Role of Surgery Management of Chronic Pancreatitis Summary
 James Bain May 2014 1. What are the grading systems for Pancreatitis? 2. What is the role of surgery in acute pancreatitis? 3. What the principles of managing chronic pancreatitis? Overview The Pancreas
James Bain May 2014 1. What are the grading systems for Pancreatitis? 2. What is the role of surgery in acute pancreatitis? 3. What the principles of managing chronic pancreatitis? Overview The Pancreas
Making ERCP Easy: Tips From A Master
 Making ERCP Easy: Tips From A Master Raj J. Shah, M.D., FASGE Associate Professor of Medicine University of Colorado School of Medicine Co-Director, Endoscopy Director, Pancreaticobiliary Endoscopy Services
Making ERCP Easy: Tips From A Master Raj J. Shah, M.D., FASGE Associate Professor of Medicine University of Colorado School of Medicine Co-Director, Endoscopy Director, Pancreaticobiliary Endoscopy Services
Acute Pancreatitis: Review of Updated Atlanta Classification and Its Advantages
 Acute Pancreatitis: Review of Updated Atlanta Classification and Its Advantages Poster No.: C-1880 Congress: ECR 2014 Type: Educational Exhibit Authors: U. Koç, B. De#irmenci, A. R. Aktas; Isparta/TR Keywords:
Acute Pancreatitis: Review of Updated Atlanta Classification and Its Advantages Poster No.: C-1880 Congress: ECR 2014 Type: Educational Exhibit Authors: U. Koç, B. De#irmenci, A. R. Aktas; Isparta/TR Keywords:
Original Article. Gastrointestinal bleeding in acute pancreatitis: etiology, clinical features, risk factors and outcome
 Tropical Gastroenterology 2015;36(1):31 35 Original Article Gastrointestinal bleeding in acute pancreatitis: etiology, clinical features, risk factors and outcome Surinder S Rana 1, Vishal Sharma 1, Deepak
Tropical Gastroenterology 2015;36(1):31 35 Original Article Gastrointestinal bleeding in acute pancreatitis: etiology, clinical features, risk factors and outcome Surinder S Rana 1, Vishal Sharma 1, Deepak
Acute Pancreatitis: Role of Imaging Modalities
 International Journal of Interdisciplinary and Multidisciplinary Studies (IJIMS), 2015, Vol 2, No.9,109-114. 109 Available online at http://www.ijims.com ISSN: 2348 0343 Abstract Acute Pancreatitis: Role
International Journal of Interdisciplinary and Multidisciplinary Studies (IJIMS), 2015, Vol 2, No.9,109-114. 109 Available online at http://www.ijims.com ISSN: 2348 0343 Abstract Acute Pancreatitis: Role
MRI Abdomen Protocol Pancreas/MRCP with Contrast
 MRI Abdomen Protocol Pancreas/MRCP with Contrast Reviewed By: Brett Mollard, MD; Anna Ellermeier, MD Last Reviewed: July 2018 Contact: (866) 761-4200 Standard uses: 1. Characterization of cystic and solid
MRI Abdomen Protocol Pancreas/MRCP with Contrast Reviewed By: Brett Mollard, MD; Anna Ellermeier, MD Last Reviewed: July 2018 Contact: (866) 761-4200 Standard uses: 1. Characterization of cystic and solid
Clinical profile, degree of severity and underlying factors of acute pancreatitis among a group of Bangladeshi patients
 Clinical profile, degree of severity and underlying factors of acute pancreatitis among a group of Bangladeshi patients Indrajit Kumar Datta 1, Md Nazmul Haque 1, Tareq M Bhuiyan 2 Original Article 1 Deaprtment
Clinical profile, degree of severity and underlying factors of acute pancreatitis among a group of Bangladeshi patients Indrajit Kumar Datta 1, Md Nazmul Haque 1, Tareq M Bhuiyan 2 Original Article 1 Deaprtment
A Comparative Study of Different Predictive Severity Scoring Systems for Acute Pancreatitis in Relation To Outcome A Prospective Study
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 12 Ver. 2 (December. 2018), PP 01-09 www.iosrjournals.org A Comparative Study of Different
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 12 Ver. 2 (December. 2018), PP 01-09 www.iosrjournals.org A Comparative Study of Different
Disclosure 6/13/2015. Acute Pancreatitis - Update. Causes of mortality DEATH
 Disclosure Acute Pancreatitis - Update Jamie S. Barkin, MD, MACP. MACP Professor of Medicine Division of Gastroenterology I do not have any relevant financial relationships with any commercial interests.
Disclosure Acute Pancreatitis - Update Jamie S. Barkin, MD, MACP. MACP Professor of Medicine Division of Gastroenterology I do not have any relevant financial relationships with any commercial interests.
Evaluation of Suspected Pancreatic Cancer
 Evaluation of Suspected Pancreatic Cancer October 15, 2015 If you experience technical difficulty during the presentation: Contact WebEx Technical Support directly at: US Toll Free: 1-866-779-3239 Toll
Evaluation of Suspected Pancreatic Cancer October 15, 2015 If you experience technical difficulty during the presentation: Contact WebEx Technical Support directly at: US Toll Free: 1-866-779-3239 Toll
