The antrum serves important hormonal and motor
|
|
|
- Domenic Goodwin
- 6 years ago
- Views:
Transcription
1 Daniel T. Dempsey, MD, and Abhijit Pathak, MD The antrum serves important hormonal and motor functions. The antral mucosa is the primary source of gastrin, a major stimulus for acid production by the parietal cells. Antral gastrin production is shut off by lumenal acid. When doing an antrectomy, it is particularly important to be certain that all antral tissue is removed distally when planning a Billroth II or Roux reconstruction. In these situations, antral tissue left on the duodenal stump will secrete gastrin unremittingly because it will no longer be exposed to acid. This syndrome of retained antrum is an important cause of hypergastrinemia and acid hypersecretion in the remaining stomach. Recurrent or marginal ulceration may result. The antrum also plays a major role in the trituration and subsequent gastric emptying of solid foods. Antral resection is generally associated with accelerated gastric emptying of liquids, and may be associated with delayed emptying of solids. Symptoms of dumping may or may not be present. Antrectomy refers to the resection of the antrum and the pylorus and usually involves removing at least 30% of the stomach. Distal or hemigastrectomy generally refers to resection of about 50% of the caudal stomach, including the antrum and pylorus. These operations are functionally identical, except in the latter in which the proximal margin of resection is extended cephalad. PATIENT SELECTION The most common benign indications for antrectomy or distal gastrectomy are duodenal ulcer, gastric ulcer, and large benign gastric tumors (leiomyoma, lipoma). Other indications include perforation or stricture from trauma or caustic ingestion. Relative contraindications include cirrhosis, extensive scarring of the proximal duodenum (obligating a difficult or tenuous duodenal closure), and previous operation on the proximal duodenum (eg, choledochoduodenostomy). DUODENAL ULCER In selected patients, antrectomy is still a good operation for intractable or obstructing duodenal ulcer disease. A From the Department of Surgery, Temple University, Philadelphia, PA. Address reprint requests to Dr. Daniel T. Dempsey, 301 South 8 th Street, Philadelphia, PA Elsevier Inc. All rights reserved X/03/ $30.00/0 doi: /otgn truncal or selective vagotomy is added. The advantage of the latter is that the extragastric visceral innervation is preserved and long term side effects such as gallstones and postvagotomy diarrhea may be less. It must be recognized that operative intervention for intractable duodenal ulcer disease should be very unusual nowadays, since over 95% of duodenal ulcers are known to be associated with Heliobacter pylori infection, NSAIDs, or gastrinoma. If these causes have been excluded or treated appropriately, the surgeon should be wary of the patient referred for intractable duodenal ulcer. This patient may be quite different from the large number of patients in the surgical literature who are known to have done well with vagotomy and antrectomy in the era before effective pharmacologic acid suppression (eg, cimetidine) and before recognition of the role of H. pylori. We feel strongly that if vagotomy and antrectomy are applied indiscriminately today as the operation of choice for intractable duodenal ulcer, the incidence of poor surgical outcomes (Visick 3 and 4) will be much higher than predicted in the existing literature. Medical therapy has healed all the easy patients, and the ones who are referred for elective surgery for intractable or nonhealing duodenal ulcer currently are the difficult patients who may not do well with gastric resection; in this population, nonresective procedures should be strongly considered. Most patients hospitalized today for gastric outlet obstruction from duodenal ulcer disease have H. pylori infection that should be treated. Nonetheless, most such patients will require some invasive treatment for their obstruction. In the low-risk surgical patient with obstructing duodenal ulcer disease, antrectomy and selective vagotomy is a good operation. This is especially true in the noncompliant patient population in whom eradication of H. pylori and chronic treatment with antisecretory medication (if necessary for recurrent ulcer) is less likely to be successful. Results of highly selective vagotomy and drainage for obstructing duodenal ulcer have been good, but recurrent or marginal ulceration is more common than after antrectomy. GASTRIC ULCER Distal gastrectomy (which also includes proximal resection) to include the gastric ulcer remains the elective operation of choice for gastric ulcer. The same admonitions discussed above regarding intractability apply. But 86 Operative Techniques in General Surgery, Vol 5, No 2 (June), 2003: pp
2 unlike duodenal ulcer, with a nonhealing gastric ulcer, the specter of malignancy lurks and makes long-term nonsurgical management less appealing. Resection is also an attractive option in many patients with a stable gastric ulcer who require urgent operation for bleeding or perforation; gastrectomy gets rid of the ulcer, which may be malignant in 5 to 10% of such patients. In contrast, resection is less commonly done today in the emergency setting for perforation or bleeding from duodenal ulcer. BENIGN TUMORS Wedge resection with negative margins is adequate treatment for benign gastric tumors such as leiomyoma (stromal tumors), lipoma, or adenoma. But when these benign neoplasms are large and located in the antrum or prepyloric region, formal distal gastrectomy is often more practical, because it avoids excessive lumenal narrowing. Frozen section should always be obtained to assure negative margins and benignity. 87 OPERATIVE TECHNIQUE 1 (A) We routinely use an upper midline incision and a mechanical retractor. An extended right subcostal incision also gives good exposure. (B) A minimal access laparoscopic approach usually requires at least 4 ports. Initially these may all be 5-mm ports with a 5-mm 30 degree scope in the umbilical site (a) and the 5-mm harmonic scalpel and 5 mm grasper in the paramedian ports (b,c). A 5-mm liver retractor can be placed through the 5-mm subxiphoid port (d) or through a right flank port (e). Once laparoscopic resection is deemed feasible, usually two sites are changed to 12-mm ports to accommodate the laparoscopic stapler. One of these sites can be enlarged eventually to remove the specimen.
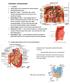
3 88 Dempsey and Pathak 2 The antrum includes at least the distal 30% of the stomach. Its proximal border is usually thought of as an imaginary line from the angularis incisura (a) on the lesser curvature side over to intersect at right angles with the greater curvature side (b); however, a tongue of antral mucosa usually extends 2 to 3 cm proximally up the lesser curvature. Proximal to this line is the parietal cell-containing body of the stomach, and distal to the line is the gastrin secreting G-cell containing antral mucosa. Anatomically, the distal border of the antrum is the pyloric ring usually marked by the vein of Mayo. When done for peptic ulcer disease, the pylorus should always be resected as part of an antrectomy, defined as resection of the stomach distal to line a-b. Resection from line c-d is termed distal gastric resection or hemigastrectomy, and from line e-f subtotal gastrectomy.
4 89 3 On entering the abdomen, exploration is done. The stomach is decompressed with a nasogastric tube. The nasogastric tube is then pulled back into the proximal stomach so that it will not be caught in the stapling instruments used to transect the stomach. It is important to reassess the original plan for antrectomy based on the findings at operation. A high juxta-cardiac gastric ulcer or marked duodenal inflammation might be better treated with nonresective procedures. In these situations, resection of the ulcer itself, without a vagotomy, is the procedure of choice. Note the presence of a large aberrant replaced left hepatic artery originating from the left gastric artery as occurs in 10% to 20% of patients.
5 90 Dempsey and Pathak 4 The avascular gastrohepatic ligament (lesser omentum) is opened and the lesser sac entered at about the level of the incisura angularis. If the posterior stomach is free, the fingers of the operator s left hand can push up on the greater curvature attachments, facilitating entry into the lesser sac from this side of the stomach. Alternatively, if the lesser sac is obliterated or if the lesser curvature is thickened or inflamed, the lesser sac is entered initially from the greater curvature side of the stomach, usually below the spleen at about the midpoint of the lesser curvature. The right gastroepiploic vessels are divided and ligated here, and a Penrose drain or catheter passed around the mid-stomach for manipulation. It is often easier to free the greater gastric curvature down toward the pylorus by staying just outside the right gastroepiploic vessels in the gastrocolic ligament, ligating small omental branches (x). Often, the lesser curvature dissection can be facilitated by palpating the plane between the lesser curvature and the liver with the aid of the surgeon s nondominant hand in the lesser sac, as introduced from the greater curvature side. Occasionally such an approach will render the omentum ischemic, necessitating resection. The surgeon should pay attention to the location of the middle colic vessels during this dissection, because inflammation and scarring especially in the obese patient may predispose these vessels to injury. Alternatively, the distal greater curvature may be mobilized by staying inside the gastroepiploic arcade, ligating the multiple small branches to the stomach (o).
6 91 5 (A) As the distal greater curvature is freed, the stomach is elevated and the antrum freed from the pancreas and mesocolon. The right gastric artery is identified and ligated usually cephalad and to the right of the pylorus. The pylorus is gently dissected off the capsule of the pancreas. Several small vessels may require ligation. If the pylorus can be freed only with great difficulty, and if cancer has clearly been ruled out, a nonresective operation should be considered. Generally it is necessary to free 1 or 2 cm of proximal duodenum distal to the muscular pyloric ring to perform an adequate resection and duodenal closure; this also assures total resection of antral mucosa distally. The right gastroepiploic pedicle is doubly ligated near its origin. We have also used a linear gastrointestinal stapler with a vascular load for this maneuver. Clips are avoided because they may foil the smooth firing of the stapler used to divide the duodenum. Losing control of the right gastroepiploic vein near its origin can result in troublesome bleeding and/or an impressive mesenteric hematoma, because it usually drains into the superior mesenteric vein (SMV). Alternatively the gastroepiploic artery and vein can be divided on the distal stomach and dissected away from the pylorus and duodenal bulb. (B) The proximal duodenum is transected with the stapler, and the duodenal staple line inspected for integrity and hemostasis. At the proposed proximal line of resection, the neurovascular bundle on the lesser curvature is encircled, divided and ligated. In the obese patient or if there is inflammation, a stapler with a vascular load may be useful here. A linear stapler with the 4.8 mm staples ( green cartridge ) is often most appropriate to transect the stomach. The specimen is removed, opened and marked, and sent to pathology. We usually request frozen section confirmation that the distal margin is indeed duodenum.
7 92 Dempsey and Pathak 6 If it is easy to free an additional 1 to 2 cm of proximal duodenum from the pancreas, and if a generous Kocher maneuver easily brings this proximal duodenum to the midline, a Billroth I gastroduodenostomy may be contemplated. We generally do this as a two-layer, end-to-end anastomosis to the transected stomach on the greater curvature side (A). But if this does not lay right, we do not hesitate to use any part of the transected stomach for the anastomosis. That part of the transected stomach not included in the anastomosis is oversewn with interrupted silk seromuscular Lembert sutures (B). The tip of the nasogastric tube is positioned 3 to 4 cm proximal to the anastomosis (C).
8 93 6 (continued).
9 94 Dempsey and Pathak 7 More commonly, we perform a 2-layer antecolic isoperistaltic Billroth II gastrojejunal anastomosis to the greater curvature aspect of the transected stomach (Hofmeister modification) (A). The lesser curvature end of stomach not included in the gastrojejunostomy is oversewn with Lembert sutures. Alternatively, the entire end of the stomach can be anastomosed to the side of antecolic jejunum (Polya reconstruction) (B). We usually cut additional holes in the nasogastric tube, and position the tip several cm past the anastomosis into the afferent limb (ie, toward the duodenum). The additional holes ensure that there is both gastric and afferent limb decompression.). We do not use a Roux-en-Y limb as primary reconstruction after distal gastrectomy unless the gastric remnant is 30% or less. However, small gastric remnants predispose to bile reflux esophagitis when reconstructed with a loop-type gastrojejunostomy, and Roux reconstruction is then most appropriate.
10 95 7 (continued)
11 96 Dempsey and Pathak 8 The duodenal stump is inspected again and the staple line gently wiped with a sponge to ensure hemostasis. If necessary, gentle cautery or a discreet suture may be placed distal to the staples. We do not routinely oversew the duodenal staple line or turn in the staple line with a second layer of sutures. The closed end of the transected duodenum is covered with well-vascularized, tension-free omentum or pericolic fat held in place with two or three carefully placed sutures. A closed suction drain is placed in Morrison s pouch (i.e. not near the staple or suture lines).
12 97 9 If possible, the surgeon should avoid distal gastric resection if it looks like the duodenum will be difficult to close. But when faced with a difficult duodenal stump, the surgeon should be guided by the principles of closure, decompression, and drainage. 1. Closure: If the proximal end of the duodenum is problematic, a gastroduodenostomy (Billroth I) is contraindicated. A single application of a linear stapler is adequate closure of the duodenal stump. This stump is buttressed with a vascularized omental flap. Inversion or imbrication is unnecessary and in our opinion mettlesome. If it is not possible to free the posterior wall of the duodenum from the pancreas, then the anterior duodenal wall is carefully preserved and its lip can be sutured to the posterior duodenal wall in situ (a to b). The location of the common bile duct and its entrance to the duodenum should be ascertained in this situation. If a posterior ulcer has destroyed the posterior wall of the proximal duodenum and scarified the pancreatic capsule, then the anterior lip of the duodenal wall can be sutured to this posterior scar with interrupted suture (a and b). Seromuscular bites anteriorly will dunk the mucosa. In our opinion, if the duodenal stump can be sutured to a Roux-en-Y limb, then it can be closed primarily and this more complex option avoided. Closure of the stump around a large drainage tube is an undesirable last resort that usually leaks. 2. Decompression of the duodenum should be considered if the duodenal stump closure is worrisome. This maneuver can be effected by lateral tube duodenostomy, by a transjejunal retrograde tube duodenostomy, by G-J tube with passage of the J part into the afferent limb and into the duodenum, or by similar passage of an NG tube into the afferent limb and into the duodenum. In the latter instance, a soft tube should be used, and although it can be sutured to the nose, this is less than ideal for long-term decompression because it is uncomfortable. For a lateral duodenostomy, we prefer a large t-tube or Malecot catheter (18F) placed through a small duodenotomy and secured with an absorbable pursestring and Lembert sutures. An extensive Kocher maneuver should be attempted to bring the duodenostomy site to the abdominal wall where it is sutured around the tube. As mentioned, we avoid placement of a tube through the end of the duodenal stump. The omentum can be wrapped around the tube between the exit site in the duodenum and the exit site in the peritoneum if the duodenum does not reach the abdominal wall. 3. Drainage: Closed suction drains are placed in the vicinity of (but not in contact with) the duodenal stump closure and tube duodenostomy and remain for at least 10 days.
13 98 Dempsey and Pathak 10 While we recognize that an intraluminal circular stapler may be used to fashion a Billroth I anastomosis (A) and that either a linear or circular stapling technique may be used to create a Billroth II anastomosis (B), we generally do not prefer staplers for reconstruction after antrectomy for the following reasons: 1. It is our clinical impression that anastomotic bleeding is more common after stapled gastrojejunostomy. 2. A circular stapler technique for Billroth I anastomosis requires more proximal duodenal mobilization than a hand sewn one. If the first attempt at a stapled anastomosis fails, there may be a critical loss of length in the proximal duodenum. 3. Gastroduodenostomy and gastrojejunostomy are great anastomoses for teaching residents proper surgical technique. 4. There are no data that stapled anastomosis are safer. SUMMARY Laparoscopic staplers with interchangeable gastrointestinal and vascular cartridges, and the ultrasonic shears have made laparoscopic antrectomy a more attractive surgical option. A periumbilical camera port and three or four working ports are used. A 30 degree angled laparoscope is essential, and it should be moved to other ports as necessary for optimal visualization. Although the important parts of the operation are the same whether it is done open or laparoscopically, there are some important differences in the conduct of the procedure: 1. The stomach is decompressed and then the NG tube is pulled way back to avoid stapling, since it is virtually impossible to palpate laparoscopically. 2. The proximal gastric margin is usually transected early. This maneuver facilitates elevation of the antrum off the pancreas and mesocolon. An endoscopic stapler with a vascular load can be used on the neurovascular bundle on the greater and lesser curvature, and a gastrointestinal cartridge with either 3.2 or preferably 4.8 mm staples on the stomach. 3. Just proximal to the pylorus, the right gastroepiploic vessels may be divided with clips or the vascular stapler, and then dissected away from the pylorus and proximal duodenum with the harmonic scalpel. 4. The proximal duodenum is divided with the laparoscopic stapler, and then the right gastric pedicle is divided. 5. A double staple technique is used for reconstruction with an antecolic Billroth II gastrojejunostomy. The NG tube is gently reintroduced with the tip only a few cm past the gastroesophageal junction ( 3 lines showing at the nose ), and position confirmed with x-ray in the recovery room. No attempt is made to put the tube through the anastomosis, and the tip should be proximal enough in the stomach that it is not near the anastomosis. Intraoperative Complications Antrectomy for benign disease is usually a straightforward operation. However intraoperative problems can arise, and the prudent surgeon will anticipate and avoid these. Significant bleeding is usually the result of venous injury from blunt dissection or excessive traction. Two potential trouble spots are the gastroepiploic vein at its
14 junction with the superior mesenteric vein, and the left gastric vein (coronary vein) near its junction usually with the portal vein. It is important not to make the injury worse by hasty or rough dissection in an attempt to expose the source of bleeding. Gentle pressure will control the hemorrhage indefinitely, and discreet controlled dissection will reveal the venous defect that can be repaired readily with a 5 0 polypropylene suture. Bleeding from the splenic capsule can usually be controlled with cautery and topical hemostatic agents. If staplers with a vascular load are used during gastrectomy, the staple lines should always be irrigated and gently abraded to check the adequacy of hemostasis. It is not uncommon that additional maneuvers are required. We avoid placing hemo-clips in proximity to where we plan to transect or anastomose with staplers. The difficult duodenal stump, more often talked about than seen nowadays, is best avoided by not doing an antrectomy in the face of significant scarring and/or inflammation in the proximal duodenum (see Fig 9). Injury to other organs during antrectomy should be unusual. Dissection is distal to the spleen, making injury to this organ infrequent. Injudicious traction on the omentum can occasionally cause a capsular tear, but splenectomy is rarely necessary. If pancreatic injury is suspected, drainage is mandatory. Before drain removal, the effluent is analyzed for amylase content. Adhesions from previous operation or gastroduodenal inflammation or scarring may predispose the colon to injury. Rarely the transverse colon can be rendered ischemic by injury to the middle colic artery and partial colectomy may be necessary. For these reasons, preoperative mechanical bowel preparation may be prudent when planning gastric resection in selected patients. Postoperative management and complications Early ambulation, incentive spirometry, antisecretory medications, and prophylactic, perioperative antibiotics are routine. The choice of prophylactic antibiotic depends on whether you expect the presence of gastric outlet obstruction or achlorhydria; in these situations, coverage of anaerobic organisms is also wise. Oral liquids are started when there is clinical evidence that gastrointestinal function has returned, usually on postoperative day 3 to 5 as heralded by bowel sounds, decreased NG drainage, and passage of flatus. First we often obtain a limited upper GI study with water-soluble contrast to confirm emptying of the gastric remnant and to rule out leak. Then liquids may be started with the NG tube in place and residuals checked, or the tube may be discontinued. Patients are advised to start oral intake slowly for the first day or two in an effort to avoid distention of the gastric remnant. Careful reinsertion of the NG tube should be considered for persistent vomiting, distention, or hiccups. Common postoperative complications include atelectasis, pneumonia, wound infection, ileus (including gastric stasis), and electrolyte abnormalities. Delayed gastric emptying during the first postoperative month is by itself almost never an indication for reoperation. Erythromycin may be useful in ameliorating this problem; metoclopramide, as a kinetic, is not effective when the antrum has been removed. Less common complications include intraabdominal hemorrhage, suture line bleeding (ie, GI bleed), duodenal stump leak, anastomotic leak, pancreatitis, intraabdominal abscess and internal hernia. Duodenal stump leak may be managed nonoperatively only if the patient continues to do well and there is radiologic evidence of adequate drainage and no intraabdominal collection. Otherwise early reoperation to effect the following is wise: close or intubate the leak; buttress this closure with omentum; decompress the duodenum; drain adequately; and place a feeding jejunostomy to allow long-term postduodenal enteral feeding and the ability to reinfuse duodenal drainage. Outcomes The overall operative mortality rate for antrectomy is around 2% but is higher in patients with critical organ dysfunction, insulin-dependent diabetes, or immunosuppression. Eighty percent of patients do well (Visick 1 or 2), while up to 20% of patients develop some form of postgastrectomy and/or postvagotomy complications (Visick 3 or 4). Problems in this latter group include recurrent ulcer, dumping, diarrhea, gastric stasis, bile reflux gastritis, bowel obstruction and chronic abdominal pain. If antrectomy is performed judiciously for benign disease only when necessary, the incidence of poor outcomes will not increase in our modern era. SUGGESTED READING Adkins RB Jr., DeLozier JB 3 rd, Scott HW Jr, Sawyers JL: The management of gastric ulcers. A current review. Ann Surg. 201: , Behrns KE, Sarr MG: Diagnosis and management of gastric emptying disorders. Adv Surg 27: , Csendes A, Maluenda F, Braghetto I, et al: Prospective randomized study comparing three surgical techniques for the treatment of gastric outlet obstruction secondary to duodenal ulcer. Am J Surg 166:45 49, Delcore R, Cheung LY: Surgical options in postgastrectomy syndromes. Surg Clin No Amer 71:57 75, De Vries BC, Schattenkerk ME, Smith EE, et al: Prospective randomized multicentre trial of proximal gastric vagotomy or truncal vagotomy and antrectomy for chronic duodenal ulcer: results after 5 7 years. Br J Surg 70: , Donahue PE: Parietal cell vagotomy versus vagotomy-antrectomy: ulcer surgery in the modern era. World J Surg. 24: , Eagon JC, Miedema BW, Kelly KA: Postgastrectomy syndromes. Surg Clin No Amer 72: , Gibril F, Lindeman RJ, Abou-Saif A, et al: Retained gastric antrum syndrome: a forgotten, treatable cause of refractory peptic ulcer disease. Dig Dis Sci 46: , 2001
15 100 Dempsey and Pathak 9. Goligher JC, Feather DB, Hall R, et al: Several standard elective operations for duodenal ulcer: Ten to 16 year clinical results. Ann Surg 189:18 24, Herrington JL Jr: Gastroduodenal ulcer. Overview of 150 papers presented before the Southern Surgical Association Ann Surg 207: , Jordan PH Jr, Thornby J: Twenty years after parietal cell vagotomy or selective vagotomy antrectomy for treatment of duodenal ulcer. Final report. Ann Surg 220: , Kaneko K, Kondo H, Saito D, et al: Early gastric stump cancer following distal gastrectomy. Gut 43: , Kendall BJ, Chakravarti A, Kendall E, et al: The effect of intravenous erythromycin on solid meal gastric emptying in patients with chronic symptomatic post-vagotomy-antrectomy gastroparesis. Aliment Pharm Therap 11: , Koo J, Lam SK, Chan P, et al: Proximal gastric vagotomy, truncal vagotomy with drainage, and truncal vagotomy with antrectomy for chronic duodenal ulcer. A prospective, randomized controlled trial. Ann Surg. 197: , Mayers TM, Orebaugh MG: Totally laparoscopic Billroth I gastrectomy. J Amer Coll Surg 186: , McConnell DB, Baba GC, Deveney CW: Changes in surgical treatment of peptic ulcer disease within a veterans hospital in the 1970s and the 1980s. Arch Surg 124: , McFadden DW, Zinner MJ: Reoperation for recurrent peptic ulcer disease. Surg Clin No Amer 71:77 92, Millat B, Fingerhut A, Borie F: Surgical treatment of complicated duodenal ulcers: controlled trials. World J Surg 24: , Paimela H, Tuompo PK, Perakyla T, et al: Peptic ulcer surgery during the H2-receptor antagonist era: a population-based epidemiological study of ulcer surgery in Helsinki from 1972 to Br J Surg 78:28 31, Ramirez B, Eaker EY, Drane WE, et al: Erythromycin enhances gastric emptying in patients with gastroparesis after vagotomy and antrectomy. Dig Dis Sci 39: , So JB, Yam A, Cheah WK, et al: Risk factors related to operative mortality and morbidity in patients undergoing emergency gastrectomy. Br J Surg 87: , Xynos E, Vassilakis JS, Fountos A, et al: Enterogastric reflux after various types of antiulcer gastric surgery: Quantitation by 99mTC- HIDA scintigraphy. Gastroenterology 101: , 1991
OPERATIVE TREATMENT OF ULCER DISEASE
 Página 1 de 8 Copyright 2001 Lippincott Williams & Wilkins Greenfield, Lazar J., Mulholland, Michael W., Oldham, Keith T., Zelenock, Gerald B., Lillemoe, Keith D. Surgery: Scientific Principles & Practice,
Página 1 de 8 Copyright 2001 Lippincott Williams & Wilkins Greenfield, Lazar J., Mulholland, Michael W., Oldham, Keith T., Zelenock, Gerald B., Lillemoe, Keith D. Surgery: Scientific Principles & Practice,
The Whipple Operation Illustrations
 The Whipple Operation Illustrations Fig. 1. Illustration of the sixstep pancreaticoduodenectomy (Whipple operation) as described in a number of recent text books by Dr. Evans. The operation is divided
The Whipple Operation Illustrations Fig. 1. Illustration of the sixstep pancreaticoduodenectomy (Whipple operation) as described in a number of recent text books by Dr. Evans. The operation is divided
Surgery for Complications of Peptic Ulcer Disease (Definitive Treatment)
 Surgery for Complications of Peptic Ulcer Disease (Definitive Treatment) Amid Keshavarzi, MD UCHSC Grand Round 3/20/2006 Department of Surgery Introduction Epidemiology Pathophysiology Clinical manifestation
Surgery for Complications of Peptic Ulcer Disease (Definitive Treatment) Amid Keshavarzi, MD UCHSC Grand Round 3/20/2006 Department of Surgery Introduction Epidemiology Pathophysiology Clinical manifestation
Perforated peptic ulcers. Dr V. Roudnitsky KCH
 Perforated peptic ulcers Dr V. Roudnitsky KCH Peptic ulcer disease Peptic ulcers are focal defects in the gastric or duodenal mucosa that extend into the submucosa or deeper Caused by an imbalance between
Perforated peptic ulcers Dr V. Roudnitsky KCH Peptic ulcer disease Peptic ulcers are focal defects in the gastric or duodenal mucosa that extend into the submucosa or deeper Caused by an imbalance between
By incision of the pyloric muscle and plastic reconstruction
 Pyloroplasty Jon Arne Söreide, MD, PhD, FACS and Kjetil Söreide, MD By incision of the pyloric muscle and plastic reconstruction of the pyloric channel, pyloroplasty facilitates gastric emptying when the
Pyloroplasty Jon Arne Söreide, MD, PhD, FACS and Kjetil Söreide, MD By incision of the pyloric muscle and plastic reconstruction of the pyloric channel, pyloroplasty facilitates gastric emptying when the
Minimally Invasive Esophagectomy
 American Association of Thoracic Surgery (AATS) 95 th Annual Meeting Seattle, WA April 29, 2015 General Thoracic Masters of Surgery Video Session Minimally Invasive Esophagectomy James D. Luketich MD,
American Association of Thoracic Surgery (AATS) 95 th Annual Meeting Seattle, WA April 29, 2015 General Thoracic Masters of Surgery Video Session Minimally Invasive Esophagectomy James D. Luketich MD,
Postgastrectomy Syndromes
 Postgastrectomy Syndromes Postgastrectomy syndromes are iatrogenic conditions that may arise from partial gastrectomies, independent of whether the gastric surgery was initially performed for peptic ulcer
Postgastrectomy Syndromes Postgastrectomy syndromes are iatrogenic conditions that may arise from partial gastrectomies, independent of whether the gastric surgery was initially performed for peptic ulcer
STOMACH and DUODENUM DISEASE
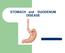 STOMACH and DUODENUM DISEASE STOMACH ANATOMY In the living and upright posture, the stomach is a j-shaped. It has two surfaces, two curvatures and two openings. Esophagus Fundus cardia Pylorus B o d y
STOMACH and DUODENUM DISEASE STOMACH ANATOMY In the living and upright posture, the stomach is a j-shaped. It has two surfaces, two curvatures and two openings. Esophagus Fundus cardia Pylorus B o d y
JOHN M UECKER, MD, FACS COMPLEX PANCREATICODUODENAL INJURIES
 JOHN M UECKER, MD, FACS COMPLEX PANCREATICODUODENAL INJURIES THE PROBLEM DUODENAL / PANCREATIC INJURIES Difficult to diagnose Not very common Anatomic and physiologic challenges 90% rate of associated
JOHN M UECKER, MD, FACS COMPLEX PANCREATICODUODENAL INJURIES THE PROBLEM DUODENAL / PANCREATIC INJURIES Difficult to diagnose Not very common Anatomic and physiologic challenges 90% rate of associated
AATS Focus on Thoracic Surgery: Minimally Invasive Esophagectomy: Are We Still Getting Better in 2017?
 AATS Focus on Thoracic Surgery: Mastering Surgical Innovation Las Vegas, NV October 28, 2017 Session VIII: Video Session Minimally Invasive Esophagectomy: Are We Still Getting Better in 2017? James D.
AATS Focus on Thoracic Surgery: Mastering Surgical Innovation Las Vegas, NV October 28, 2017 Session VIII: Video Session Minimally Invasive Esophagectomy: Are We Still Getting Better in 2017? James D.
Laparoscopy-assisted D2 radical distal subtotal gastrectomy
 Masters of Gastrointestinal Surgery Laparoscopy-assisted D2 radical distal subtotal gastrectomy Xiaogeng Chen, Weihua Li, Jinsi Wang, Changshun Yang Department of Tumor Surgery, Fujian Provincial Hospital,
Masters of Gastrointestinal Surgery Laparoscopy-assisted D2 radical distal subtotal gastrectomy Xiaogeng Chen, Weihua Li, Jinsi Wang, Changshun Yang Department of Tumor Surgery, Fujian Provincial Hospital,
Intraabdominal Roux-en-Y reconstruction with a novel stapling technique after laparoscopic distal gastrectomy
 Gastric Cancer (2009) 12: 164 169 DOI 10.1007/s10120-009-0520-0 Technical note 2009 by International and Japanese Gastric Cancer Associations Intraabdominal Roux-en-Y reconstruction with a novel stapling
Gastric Cancer (2009) 12: 164 169 DOI 10.1007/s10120-009-0520-0 Technical note 2009 by International and Japanese Gastric Cancer Associations Intraabdominal Roux-en-Y reconstruction with a novel stapling
Limited en bloc Resection of the Gastroesophageal Junction with Isoperistaltic Jejunal Interposition
 22 Limited en bloc Resection of the Gastroesophageal Junction with Isoperistaltic Jejunal Interposition J.R. Izbicki, W.T. Knoefel, D. C. Broering ] Indications Severe dysplasia in the distal esophagus
22 Limited en bloc Resection of the Gastroesophageal Junction with Isoperistaltic Jejunal Interposition J.R. Izbicki, W.T. Knoefel, D. C. Broering ] Indications Severe dysplasia in the distal esophagus
Proximal Gastric Vagotomy Without Drainage for Treatment of Perforated Duodenal Ulcer
 GASTROENTEROLOGY 1982;179-83 Proximal Gastric Vagotomy Without Drainage for Treatment of Perforated Duodenal Ulcer PAUL H. JORDAN, Jr. Surgical Services of the Cora and Webb Mading Department of Surgery,
GASTROENTEROLOGY 1982;179-83 Proximal Gastric Vagotomy Without Drainage for Treatment of Perforated Duodenal Ulcer PAUL H. JORDAN, Jr. Surgical Services of the Cora and Webb Mading Department of Surgery,
The abdominal Esophagus, Stomach and the Duodenum. Prof. Oluwadiya KS
 The abdominal Esophagus, Stomach and the Duodenum Prof. Oluwadiya KS www.oluwadiya.com Viscera of the abdomen Abdominal esophagus: Terminal part of the esophagus The stomach Intestines: Small and Large
The abdominal Esophagus, Stomach and the Duodenum Prof. Oluwadiya KS www.oluwadiya.com Viscera of the abdomen Abdominal esophagus: Terminal part of the esophagus The stomach Intestines: Small and Large
Bariatric Surgery Risk Education Packet Walter J. Chlysta MD, FACS
 Date: Patient Name: Height: Weight: Ideal Body Weight: Excess Weight: Realistic Gastric Bypass Weight Goal (77 % Excess weight loss): Realistic Sleeve Gastrectomy Weight Goal (70 % Excess weight loss):
Date: Patient Name: Height: Weight: Ideal Body Weight: Excess Weight: Realistic Gastric Bypass Weight Goal (77 % Excess weight loss): Realistic Sleeve Gastrectomy Weight Goal (70 % Excess weight loss):
Stomach. R.B. Kolachalam, MD
 Stomach R.B. Kolachalam, MD Relevent Anatomy 1.four regions: Cardia, Fundus, Body, and the Pylorus 2. fixed in two locations- at the GEJ and the duodenum Gastric Anatomy body of the stomach: site of mechanical
Stomach R.B. Kolachalam, MD Relevent Anatomy 1.four regions: Cardia, Fundus, Body, and the Pylorus 2. fixed in two locations- at the GEJ and the duodenum Gastric Anatomy body of the stomach: site of mechanical
د. عصام طارق. Objectives:
 GI anatomy Lecture: 5 د. عصام طارق Objectives: To describe anatomy of stomach, duodenum & pancreas. To list their main relations. To define their blood & nerve supply. To list their lymph drainage. To
GI anatomy Lecture: 5 د. عصام طارق Objectives: To describe anatomy of stomach, duodenum & pancreas. To list their main relations. To define their blood & nerve supply. To list their lymph drainage. To
Perforated peptic ulcer
 Perforated peptic ulcer - Despite the widespread use of gastric anti-secretory agents and eradication therapy, the incidence of perforated peptic ulcer has changed little, age limits increase NSAIDs elderly
Perforated peptic ulcer - Despite the widespread use of gastric anti-secretory agents and eradication therapy, the incidence of perforated peptic ulcer has changed little, age limits increase NSAIDs elderly
RECTAL INJURY IN UROLOGIC SURGERY. Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences.
 RECTAL INJURY IN 27 UROLOGIC SURGERY Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences. With good mechanical bowel preparation plus antibiotic
RECTAL INJURY IN 27 UROLOGIC SURGERY Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences. With good mechanical bowel preparation plus antibiotic
Anatomy of laparoscopy-assisted distal D2 radical gastrectomy for gastric cancer
 Masters of Gastrointestinal Surgery Anatomy of laparoscopy-assisted distal D2 radical gastrectomy for gastric cancer Da-Guang Wang, Liang He, Yang Zhang, Jing-Hai Yu, Yan Chen, Ming-Jie Xia, Jian Suo Department
Masters of Gastrointestinal Surgery Anatomy of laparoscopy-assisted distal D2 radical gastrectomy for gastric cancer Da-Guang Wang, Liang He, Yang Zhang, Jing-Hai Yu, Yan Chen, Ming-Jie Xia, Jian Suo Department
Laparoscopic and Thoracoscopic Ivor Lewis Esophagectomy With Colonic Interposition
 HOW TO DO IT Laparoscopic and Thoracoscopic Ivor Lewis Esophagectomy With Colonic Interposition Ninh T. Nguyen, MD, FACS, Marcelo Hinojosa, MD, Christine Fayad, BS, James Gray, BS, Zuri Murrell, MD, and
HOW TO DO IT Laparoscopic and Thoracoscopic Ivor Lewis Esophagectomy With Colonic Interposition Ninh T. Nguyen, MD, FACS, Marcelo Hinojosa, MD, Christine Fayad, BS, James Gray, BS, Zuri Murrell, MD, and
duodenal ulcer by vagotomy and gastric drainage operation
 Gut, 1961, 2,158 A clinical appraisal of the treatment of chronic duodenal ulcer by vagotomy and gastric drainage operation W. GERALD AUSTEN' AND HAROLD C. EDWARDS From King's College Hospital, London
Gut, 1961, 2,158 A clinical appraisal of the treatment of chronic duodenal ulcer by vagotomy and gastric drainage operation W. GERALD AUSTEN' AND HAROLD C. EDWARDS From King's College Hospital, London
Unusual manifestations of peptic
 Unusual manifestations of peptic ulcer disease William M. Thompson, M.D. George Norton, M.D.* Frederick M. Kelvin, F.R.C.R., M.R.C.P. R. Kristina Gedgaudas, M.D. Robert A. Halvorsen, M.D. Reed P. Rice,
Unusual manifestations of peptic ulcer disease William M. Thompson, M.D. George Norton, M.D.* Frederick M. Kelvin, F.R.C.R., M.R.C.P. R. Kristina Gedgaudas, M.D. Robert A. Halvorsen, M.D. Reed P. Rice,
Pancreatico-Duodenal Trauma: Drain, Debride, Divert, Despair BACKGROUND EPIDEMIOLOGY 9/11/2018
 Pancreatico-Duodenal Trauma: Drain, Debride, Divert, Despair Rochelle A. Dicker, M.D. Professor of Surgery and Anesthesia UCLA BACKGROUND Lancet 1827: Travers, B Rupture of the Pancreas British Journal
Pancreatico-Duodenal Trauma: Drain, Debride, Divert, Despair Rochelle A. Dicker, M.D. Professor of Surgery and Anesthesia UCLA BACKGROUND Lancet 1827: Travers, B Rupture of the Pancreas British Journal
Clinical benefit of Totally Laparoscopic over Laparoscopically Assisted Distal Gastrectomy with Roux-en-Y Reconstruction for Early Gastric Cancer
 Med. Bull. Fukuoka Univ. 39 3/4 251 256 2012 Clinical benefit of Totally Laparoscopic over Laparoscopically Assisted Distal Gastrectomy with Roux-en-Y Reconstruction for Early Gastric Cancer Tatsuya HASHIMOTO,
Med. Bull. Fukuoka Univ. 39 3/4 251 256 2012 Clinical benefit of Totally Laparoscopic over Laparoscopically Assisted Distal Gastrectomy with Roux-en-Y Reconstruction for Early Gastric Cancer Tatsuya HASHIMOTO,
Placing PEG and Jejunostomy Tubes in Dogs and Cats
 Placing PEG and Jejunostomy Tubes in Dogs and Cats I. Gastrostomy tube A. Percutaneous Endoscopic Gastrostomy (PEG) tube placement Supplies for PEG tube placement: Supplies and equipment for general anesthesia
Placing PEG and Jejunostomy Tubes in Dogs and Cats I. Gastrostomy tube A. Percutaneous Endoscopic Gastrostomy (PEG) tube placement Supplies for PEG tube placement: Supplies and equipment for general anesthesia
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Adenocarcinoma, pancreatic ductal, laparoscopic distal pancreatectomy for, 61 Adrenal cortical carcinoma, laparoscopic adrenalectomy for, 114
Note: Page numbers of article titles are in boldface type. A Adenocarcinoma, pancreatic ductal, laparoscopic distal pancreatectomy for, 61 Adrenal cortical carcinoma, laparoscopic adrenalectomy for, 114
Laparoscopy-assisted radical total gastrectomy plus D2 lymph node dissection
 Masters of Gastrointestinal Surgery Laparoscopy-assisted radical total gastrectomy plus D2 lymph node dissection Chaohui Zheng, Changming Huang, Ping Li, Jianwei Xie, Jiabin Wang, Jianxian Lin, Jun Lu
Masters of Gastrointestinal Surgery Laparoscopy-assisted radical total gastrectomy plus D2 lymph node dissection Chaohui Zheng, Changming Huang, Ping Li, Jianwei Xie, Jiabin Wang, Jianxian Lin, Jun Lu
Totally laparoscopic distal gastrectomy reconstructed by Rouxen-Y with D2 lymphadenectomy and needle catheter jejunostomy for gastric cancer
 Masters of Gastrointestinal Surgery Totally laparoscopic distal gastrectomy reconstructed by Rouxen-Y with D2 lymphadenectomy and needle catheter jejunostomy for gastric cancer Xin Ye, Jian-Chun Yu, Wei-Ming
Masters of Gastrointestinal Surgery Totally laparoscopic distal gastrectomy reconstructed by Rouxen-Y with D2 lymphadenectomy and needle catheter jejunostomy for gastric cancer Xin Ye, Jian-Chun Yu, Wei-Ming
It passes through the diaphragm at the level of the 10th thoracic vertebra to join the stomach
 The esophagus is a tubular structure (muscular, collapsible tube ) about 10 in. (25 cm) long that is continuous above with the laryngeal part of the pharynx opposite the sixth cervical vertebra The esophagus
The esophagus is a tubular structure (muscular, collapsible tube ) about 10 in. (25 cm) long that is continuous above with the laryngeal part of the pharynx opposite the sixth cervical vertebra The esophagus
General'Surgery'Service'
 General'Surgery'Service' Patient Care Goals and Objectives 1)! Stomach/Duodenum and Bariatric 2)! Interpret the results of clinical evaluations (history, physical examination) performed on patients being
General'Surgery'Service' Patient Care Goals and Objectives 1)! Stomach/Duodenum and Bariatric 2)! Interpret the results of clinical evaluations (history, physical examination) performed on patients being
Pylorus Preserving Pancreaticoduodenectomy
 REVIEW Pylorus Preserving Pancreaticoduodenectomy Jacqueline M. Garonzik-Wang, M. B. Majella Doyle Pancreaticoduodenectomy (PD) has become the standard of care for resectable pancreatic cancer and premalignant
REVIEW Pylorus Preserving Pancreaticoduodenectomy Jacqueline M. Garonzik-Wang, M. B. Majella Doyle Pancreaticoduodenectomy (PD) has become the standard of care for resectable pancreatic cancer and premalignant
Surgical Treatment of Localized Gastric Cancer
 13 Surgical Treatment of Localized Gastric Cancer JOHN I. LEW, MD MITCHELL C. POSNER, MD Theodor Billroth performed the first successful gastric resection (a distal subtotal gastrectomy for stomach cancer)
13 Surgical Treatment of Localized Gastric Cancer JOHN I. LEW, MD MITCHELL C. POSNER, MD Theodor Billroth performed the first successful gastric resection (a distal subtotal gastrectomy for stomach cancer)
Surgical Management of CBD Injury Jin Seok Heo
 Surgical Management of CBD Injury Jin Seok Heo Department of Surgery, Samsung Medical Center Sungkyunkwan University School of Medicine, Seoul, Republic of Korea Bile duct injury (BDI) Introduction Incidence
Surgical Management of CBD Injury Jin Seok Heo Department of Surgery, Samsung Medical Center Sungkyunkwan University School of Medicine, Seoul, Republic of Korea Bile duct injury (BDI) Introduction Incidence
Combined Collis-Nissen Reconstruction. of the esophagogastric junction at. Mark B. Orringer, M.D., and Herbert Sloan, M.D.
 Combined Collis-Nissen Reconstruction of the Esophagogastric Junction Mark B. Orringer, M.D., and Herbert Sloan, M.D. ABSTRACT Recent reports have indicated that combined Collis-Belsey reconstruction of
Combined Collis-Nissen Reconstruction of the Esophagogastric Junction Mark B. Orringer, M.D., and Herbert Sloan, M.D. ABSTRACT Recent reports have indicated that combined Collis-Belsey reconstruction of
Tools of the Gastroenterologist: Introduction to GI Endoscopy
 Tools of the Gastroenterologist: Introduction to GI Endoscopy Objectives Endoscopy Upper endoscopy Colonoscopy Endoscopic retrograde cholangiopancreatography (ERCP) Endoscopic ultrasound (EUS) Endoscopic
Tools of the Gastroenterologist: Introduction to GI Endoscopy Objectives Endoscopy Upper endoscopy Colonoscopy Endoscopic retrograde cholangiopancreatography (ERCP) Endoscopic ultrasound (EUS) Endoscopic
Esophageal Perforation
 Esophageal Perforation Dr. Carmine Simone Thoracic Surgeon, Division of General Surgery Head, Division of Critical Care May 15, 2006 Overview Case presentation Radiology Pre-operative management Operative
Esophageal Perforation Dr. Carmine Simone Thoracic Surgeon, Division of General Surgery Head, Division of Critical Care May 15, 2006 Overview Case presentation Radiology Pre-operative management Operative
Esophageal anastomotic techniques
 Esophageal anastomotic techniques Raphael Bueno, MD, Brigham and Women s Hospital Slide 1 Good afternoon, I would like thank the association and Dr and Dr for inviting me to speak today. Slide 2 I am trying
Esophageal anastomotic techniques Raphael Bueno, MD, Brigham and Women s Hospital Slide 1 Good afternoon, I would like thank the association and Dr and Dr for inviting me to speak today. Slide 2 I am trying
Done by: Dina Sawadha & Mohammad Abukabeer
 Done by: Dina Sawadha & Mohammad Abukabeer The stomach *the stomach is a dilated part of the gastro intestinal tract, it's "J" shape. *the lower surface of the stomach ( the greater curvature ) reaches
Done by: Dina Sawadha & Mohammad Abukabeer The stomach *the stomach is a dilated part of the gastro intestinal tract, it's "J" shape. *the lower surface of the stomach ( the greater curvature ) reaches
DIAGNOSIS AND MANAGEMENT OF BENIGN GASTRIC AND DUODENAL DISEASE
 gastrointestinal tract and abdomen DIAGNOSIS AND MANAGEMENT OF BENIGN GASTRIC AND DUODENAL DISEASE Gentian Kristo, MD, and Thomas E. Clancy, MD* The treatment of benign gastric and duodenal disease has
gastrointestinal tract and abdomen DIAGNOSIS AND MANAGEMENT OF BENIGN GASTRIC AND DUODENAL DISEASE Gentian Kristo, MD, and Thomas E. Clancy, MD* The treatment of benign gastric and duodenal disease has
Gastrectomy procedure and its complications: Findings at TC multi-detector 64 row.
 Gastrectomy procedure and its complications: Findings at TC multi-detector 64 row. Poster No.: C-2184 Congress: ECR 2012 Type: Educational Exhibit Authors: M. M. Mendigana Ramos, A. Burguete, A. Sáez de
Gastrectomy procedure and its complications: Findings at TC multi-detector 64 row. Poster No.: C-2184 Congress: ECR 2012 Type: Educational Exhibit Authors: M. M. Mendigana Ramos, A. Burguete, A. Sáez de
Tornado Roux-en-Y anastomosis in laparoscopy-assisted distal gastrectomy
 Gastric Cancer (2008) 11: 181 185 DOI 10.1007/s10120-008-0474-7 Technical note 2008 by International and Japanese Gastric Cancer Associations Tornado Roux-en-Y anastomosis in laparoscopy-assisted distal
Gastric Cancer (2008) 11: 181 185 DOI 10.1007/s10120-008-0474-7 Technical note 2008 by International and Japanese Gastric Cancer Associations Tornado Roux-en-Y anastomosis in laparoscopy-assisted distal
Here are some types of gastric bypass surgery:
 Gastric Bypass- Definition By Mayo Clinic staff Weight-loss (bariatric) surgeries change your digestive system, often limiting the amount of food you can eat. These surgeries help you lose weight and can
Gastric Bypass- Definition By Mayo Clinic staff Weight-loss (bariatric) surgeries change your digestive system, often limiting the amount of food you can eat. These surgeries help you lose weight and can
Peptic ulcer disease. Nomin-Erdene. D SOM-531
 Peptic ulcer disease Nomin-Erdene. D SOM-531 Learning objectives Stomach gross anatomy PUD Epidemiology Pathogenesis Clinical manifestation Diagnosing Treatment Complicated ulcer disease Surgical procedures
Peptic ulcer disease Nomin-Erdene. D SOM-531 Learning objectives Stomach gross anatomy PUD Epidemiology Pathogenesis Clinical manifestation Diagnosing Treatment Complicated ulcer disease Surgical procedures
Emergency Operations for Bleeding Duodenal Ulcer:A simple option to consider Case Report Abstract Key words Case Report
 Vtáx exñéüà :A simple option to consider: Case Report Gamal E H A El Shallaly, Eltayeb A Ali, Suzan Salih Abstract We report a 46 years-old man who had severe bleeding from a posterior duodenal ulcer (DU)
Vtáx exñéüà :A simple option to consider: Case Report Gamal E H A El Shallaly, Eltayeb A Ali, Suzan Salih Abstract We report a 46 years-old man who had severe bleeding from a posterior duodenal ulcer (DU)
Gastrointestinal Tract. Anatomy of GI Tract. Anatomy of GI Tract. (Effective February 2007) (1%-5%)
 Gastrointestinal Tract (Effective February 2007) (1%-5%) Anatomy of GI Tract Esophagus bulls-eye or target EG junction seen on sagittal scan posterior to left lobe of liver and anterior to aorta Anatomy
Gastrointestinal Tract (Effective February 2007) (1%-5%) Anatomy of GI Tract Esophagus bulls-eye or target EG junction seen on sagittal scan posterior to left lobe of liver and anterior to aorta Anatomy
Chapter 14: Training in Radiology. DDSEP Chapter 1: Question 12
 DDSEP Chapter 1: Question 12 A 52-year-old white male presents for evaluation of sudden onset of abdominal pain and shoulder pain. His past medical history is notable for a history of coronary artery disease,
DDSEP Chapter 1: Question 12 A 52-year-old white male presents for evaluation of sudden onset of abdominal pain and shoulder pain. His past medical history is notable for a history of coronary artery disease,
Anastomotic Complications after Esophagectomy. Bryan Meyers, MD MPH Thoracic Surgery Washington University School of Medicine
 Anastomotic Complications after Esophagectomy Bryan Meyers, MD MPH Thoracic Surgery Washington University School of Medicine Use of Stomach as Conduit Simplest choice after esophagectomy Single anastomosis
Anastomotic Complications after Esophagectomy Bryan Meyers, MD MPH Thoracic Surgery Washington University School of Medicine Use of Stomach as Conduit Simplest choice after esophagectomy Single anastomosis
Gastric and duodenal diseases. Important. Notes (Doctors'/students') 431 SURGERY TEAM. Ahmed Aloqayli. Hayfa AlAbdulkareem.
 Gastric and duodenal diseases Important Notes (Doctors'/students') 431 SURGERY TEAM Done By: Ahmed Aloqayli Revised By: Hayfa AlAbdulkareem Abeer Al-Suwailem Leaders Mohammed Alshammari The duodenum is
Gastric and duodenal diseases Important Notes (Doctors'/students') 431 SURGERY TEAM Done By: Ahmed Aloqayli Revised By: Hayfa AlAbdulkareem Abeer Al-Suwailem Leaders Mohammed Alshammari The duodenum is
Pancreas & Biliary System. Dr. Vohra & Dr. Jamila
 Pancreas & Biliary System Dr. Vohra & Dr. Jamila 1 Objectives At the end of the lecture, the student should be able to describe the: Location, surface anatomy, parts, relations & peritoneal reflection
Pancreas & Biliary System Dr. Vohra & Dr. Jamila 1 Objectives At the end of the lecture, the student should be able to describe the: Location, surface anatomy, parts, relations & peritoneal reflection
THE SURGEON S LIBRARY
 THE SURGEON S LIBRARY THE HISTORY AND SURGICAL ANATOMY OF THE VAGUS NERVE Lee J. Skandalakis, M.D., Chicago, Illinois, Stephen W. Gray, PH.D., and John E. Skandalakis, M.D., PH.D., F.A.C.S., Atlanta, Georgia
THE SURGEON S LIBRARY THE HISTORY AND SURGICAL ANATOMY OF THE VAGUS NERVE Lee J. Skandalakis, M.D., Chicago, Illinois, Stephen W. Gray, PH.D., and John E. Skandalakis, M.D., PH.D., F.A.C.S., Atlanta, Georgia
Exploring Anatomy: the Human Abdomen
 Exploring Anatomy: the Human Abdomen PERITONEUM AND PERITONEAL CAVITY PERITONEUM The peritoneum is a thin serous membrane that lines the abdominal cavity and covers, in variable amounts, the viscera within
Exploring Anatomy: the Human Abdomen PERITONEUM AND PERITONEAL CAVITY PERITONEUM The peritoneum is a thin serous membrane that lines the abdominal cavity and covers, in variable amounts, the viscera within
Preview from Notesale.co.uk Page 1 of 34
 Abdominal viscera and digestive tract Digestive tract Abdominal viscera comprise majority of the alimentary system o Terminal oesophagus, stomach, pancreas, spleen, liver, gallbladder, kidneys, suprarenal
Abdominal viscera and digestive tract Digestive tract Abdominal viscera comprise majority of the alimentary system o Terminal oesophagus, stomach, pancreas, spleen, liver, gallbladder, kidneys, suprarenal
Endoscopic Treatment of Luminal Perforations and Leaks
 Endoscopic Treatment of Luminal Perforations and Leaks Ali A. Siddiqui, MD Professor of Medicine Director of Interventional Endoscopy Jefferson Medical College Philadelphia, PA When Do You Suspect a Luminal
Endoscopic Treatment of Luminal Perforations and Leaks Ali A. Siddiqui, MD Professor of Medicine Director of Interventional Endoscopy Jefferson Medical College Philadelphia, PA When Do You Suspect a Luminal
Laparoscopic Right Colectomy
 Laparoscopic Right Colectomy Shawnee Mission Medical Center February 22, 2011 Hi, and welcome to the program. My name is Dr. Sanjay Thekkeurumbil, and I m a colorectal surgeon at Shawnee Mission Medical
Laparoscopic Right Colectomy Shawnee Mission Medical Center February 22, 2011 Hi, and welcome to the program. My name is Dr. Sanjay Thekkeurumbil, and I m a colorectal surgeon at Shawnee Mission Medical
Block 3: DISSECTION 2 CELIAC TRUNK, JEJUNUM/ILEUM, LARGE INTESTINE, DUODENUM, PANCREAS, PORTAL VEIN; MOBILIZATION OF THE LIVER
 1 Block 3: DISSECTION 2 CELIAC TRUNK, JEJUNUM/ILEUM, LARGE INTESTINE, DUODENUM, PANCREAS, PORTAL VEIN; MOBILIZATION OF THE LIVER Attempt to complete as much as you can of the dissection explained in the
1 Block 3: DISSECTION 2 CELIAC TRUNK, JEJUNUM/ILEUM, LARGE INTESTINE, DUODENUM, PANCREAS, PORTAL VEIN; MOBILIZATION OF THE LIVER Attempt to complete as much as you can of the dissection explained in the
Laparoscopic Subtotal Gastrectomy for Gastric Cancer
 SCIENTIFIC PAPER Laparoscopic Subtotal Gastrectomy for Gastric Cancer Danny Rosin, MD, Yuri Goldes, MD, Barak Bar Zakai, MD, Moshe Shabtai, MD, Amram Ayalon, MD, Oded Zmora, MD ABSTRACT Background: The
SCIENTIFIC PAPER Laparoscopic Subtotal Gastrectomy for Gastric Cancer Danny Rosin, MD, Yuri Goldes, MD, Barak Bar Zakai, MD, Moshe Shabtai, MD, Amram Ayalon, MD, Oded Zmora, MD ABSTRACT Background: The
LOOKING FOR AIR IN ALL THE WRONG PLACES Richard M. Gore, MD North Shore University Health System University of Chicago Evanston, IL
 SIGNIFICANCE OF EXTRALUMINAL ABDOMINAL GAS: LOOKING FOR AIR IN ALL THE WRONG PLACES Richard M. Gore, MD North Shore University Health System University of Chicago Evanston, IL SCBT/MR 2012 October 26,
SIGNIFICANCE OF EXTRALUMINAL ABDOMINAL GAS: LOOKING FOR AIR IN ALL THE WRONG PLACES Richard M. Gore, MD North Shore University Health System University of Chicago Evanston, IL SCBT/MR 2012 October 26,
FIG The inferior and posterior peritoneal reflection is easily
 PSOAS HITCH, BOARI FLAP, AND COMBINATION OF PSOAS 7 HITCH AND BOARI FLAP The psoas hitch procedure, Boari flap, and transureteroureterostomy are useful operative procedures for reestablishing continuity
PSOAS HITCH, BOARI FLAP, AND COMBINATION OF PSOAS 7 HITCH AND BOARI FLAP The psoas hitch procedure, Boari flap, and transureteroureterostomy are useful operative procedures for reestablishing continuity
Bariatric Surgery: How complex is this? Pradeep Pallati, MD, FACS, FASMBS
 Bariatric Surgery: How complex is this? Pradeep Pallati, MD, FACS, FASMBS Nothing to Disclose Types of Bariatric Surgery Restrictive Malabsorptive Combination Restrictive and Malabsorptive Newer Endoluminal
Bariatric Surgery: How complex is this? Pradeep Pallati, MD, FACS, FASMBS Nothing to Disclose Types of Bariatric Surgery Restrictive Malabsorptive Combination Restrictive and Malabsorptive Newer Endoluminal
7/11/17. The Surgeon s Operative Report: Tools and Tips to Enhance Abstraction. Stopwoundinfection.com. Impact to Healthcare
 1. Scott, R. Douglas. The Direct Medical Costs of Healthcare-Associated Infections in U.S. Hospitals and the Benefits of Prevention. March 2009. http://www.cdc.gov/hai/pdfs/hai/scott_costpaper.pdf. 2.
1. Scott, R. Douglas. The Direct Medical Costs of Healthcare-Associated Infections in U.S. Hospitals and the Benefits of Prevention. March 2009. http://www.cdc.gov/hai/pdfs/hai/scott_costpaper.pdf. 2.
SURGICAL MANAGEMENT OF MORBID OBESITY
 Página 1 de 9 Copyright 2001 Lippincott Williams & Wilkins Greenfield, Lazar J., Mulholland, Michael W., Oldham, Keith T., Zelenock, Gerald B., Lillemoe, Keith D. Surgery: Scientific Principles & Practice,
Página 1 de 9 Copyright 2001 Lippincott Williams & Wilkins Greenfield, Lazar J., Mulholland, Michael W., Oldham, Keith T., Zelenock, Gerald B., Lillemoe, Keith D. Surgery: Scientific Principles & Practice,
Conservative Management of Anastomotic Leaks after 557 Open Gastric Bypasses
 Obesity Surgery, 15, 1252-1256 Conservative Management of Anastomotic Leaks after 557 Open Gastric Bypasses Attila Csendes, MD, FACS (Hon); Patricio Burdiles, MD, FACS; Ana Maria Burgos, MD; Fernando Maluenda,
Obesity Surgery, 15, 1252-1256 Conservative Management of Anastomotic Leaks after 557 Open Gastric Bypasses Attila Csendes, MD, FACS (Hon); Patricio Burdiles, MD, FACS; Ana Maria Burgos, MD; Fernando Maluenda,
An Innovative Option for Venous Reconstruction After Pancreaticoduodenectomy: the Left Renal Vein
 J Gastrointest Surg (2007) 11:425 431 DOI 10.1007/s11605-007-0131-1 An Innovative Option for Venous Reconstruction After Pancreaticoduodenectomy: the Left Renal Vein Rory L. Smoot & John D. Christein &
J Gastrointest Surg (2007) 11:425 431 DOI 10.1007/s11605-007-0131-1 An Innovative Option for Venous Reconstruction After Pancreaticoduodenectomy: the Left Renal Vein Rory L. Smoot & John D. Christein &
Dr. Zahiri. In the name of God
 Dr. Zahiri In the name of God small intestine = small bowel is the part of the gastrointestinal tract Boundaries: Pylorus Ileosecal junction Function: digestion and absorption of food It receives bile
Dr. Zahiri In the name of God small intestine = small bowel is the part of the gastrointestinal tract Boundaries: Pylorus Ileosecal junction Function: digestion and absorption of food It receives bile
Laparoscopic Gastric Bypass Information
 1441 Constitution Boulevard, Salinas, CA 93906 (831) 783-2556 www.natividad.com/weight-loss (Roux-en-Y Gastric Bypass) What is gastric bypass surgery? Gastric bypass surgery, a type of bariatric surgery
1441 Constitution Boulevard, Salinas, CA 93906 (831) 783-2556 www.natividad.com/weight-loss (Roux-en-Y Gastric Bypass) What is gastric bypass surgery? Gastric bypass surgery, a type of bariatric surgery
GASTROINTESTINAL SYSTEM
 GASTROINTESTINAL SYSTEM Topographic Anatomy of the Abdomen Surface Landmarks Xiphoid process T9/T10 Inferior costal margin L2/L3 Iliac Crest L4 level ASIS L5/S1 level Pubic symphysis level of greater trochanter
GASTROINTESTINAL SYSTEM Topographic Anatomy of the Abdomen Surface Landmarks Xiphoid process T9/T10 Inferior costal margin L2/L3 Iliac Crest L4 level ASIS L5/S1 level Pubic symphysis level of greater trochanter
Cover Page. The following handle holds various files of this Leiden University dissertation:
 Cover Page The following handle holds various files of this Leiden University dissertation: http://hdl.handle.net/1887/6119 Author: Spruit, E.N. Title: Increasing the efficiency of laparoscopic surgical
Cover Page The following handle holds various files of this Leiden University dissertation: http://hdl.handle.net/1887/6119 Author: Spruit, E.N. Title: Increasing the efficiency of laparoscopic surgical
Pancreaticoduodenectomy the anatomy and the surgical approaches
 Pancreaticoduodenectomy the anatomy and the surgical approaches Paul BS LAI Division of Hepato biliary and Pancreatic Surgery Department of Surgery The Chinese Univesity of Hong Kong Whipple s operation
Pancreaticoduodenectomy the anatomy and the surgical approaches Paul BS LAI Division of Hepato biliary and Pancreatic Surgery Department of Surgery The Chinese Univesity of Hong Kong Whipple s operation
Nutritional Management in Enterocutaneous fistula Dr Deepak Govil
 Nutritional Management in Enterocutaneous fistula Dr Deepak Govil MS, PhD (GI Surgery) Senior Consultant Surgical Gastroenterology Indraprastha Apollo Hospital New Delhi What is enterocutaneous fistula
Nutritional Management in Enterocutaneous fistula Dr Deepak Govil MS, PhD (GI Surgery) Senior Consultant Surgical Gastroenterology Indraprastha Apollo Hospital New Delhi What is enterocutaneous fistula
ADVANCED LAPAROSCOPIC PANCREAS SURGERY A HANDS-ON WORKSHOP
 ADVANCED LAPAROSCOPIC PANCREAS SURGERY A HANDS-ON WORKSHOP 3-4 November 2017 at the AMC in Amsterdam Organizing committee: Mo Abu Hilal, Professor of Surgery at Southampton University Marc Besselink, Professor
ADVANCED LAPAROSCOPIC PANCREAS SURGERY A HANDS-ON WORKSHOP 3-4 November 2017 at the AMC in Amsterdam Organizing committee: Mo Abu Hilal, Professor of Surgery at Southampton University Marc Besselink, Professor
Geoffrey Axiak M.Sc. Nursing (Manch.), B.Sc. Nursing, P.G. Dip. Nutrition & Dietetics Clinical Nutrition Practice Nurse
 The Percutaneous Endoscopic Gastrostomy Geoffrey Axiak M.Sc. Nursing (Manch.), B.Sc. Nursing, P.G. Dip. Nutrition & Dietetics Clinical Nutrition Practice Nurse What is a P.E.G.? Percutaneous Endoscopic
The Percutaneous Endoscopic Gastrostomy Geoffrey Axiak M.Sc. Nursing (Manch.), B.Sc. Nursing, P.G. Dip. Nutrition & Dietetics Clinical Nutrition Practice Nurse What is a P.E.G.? Percutaneous Endoscopic
Penetrating Injuries to the Stomach, Duodenum, and Small Bowel
 Curr Trauma Rep (2015) 1:107 112 DOI 10.1007/s40719-015-0010-2 PENETRATING INJURIES TO HOLLOW ABDOMINAL VISCERA (K INABA, SECTION EDITOR) Penetrating Injuries to the Stomach, Duodenum, and Small Bowel
Curr Trauma Rep (2015) 1:107 112 DOI 10.1007/s40719-015-0010-2 PENETRATING INJURIES TO HOLLOW ABDOMINAL VISCERA (K INABA, SECTION EDITOR) Penetrating Injuries to the Stomach, Duodenum, and Small Bowel
1. Epidemiology of Esophageal Cancer 2. Operative Strategies 3. Minimally Invasive Esophagectomy 4. Video
 Minimally Invasive Esophagectomy Guilherme M Campos, MD, FACS Assistant Professor of Surgery Director G.I. Motility Center Director Bariatric Surgery Program University of California San Francisco ESOPHAGEAL
Minimally Invasive Esophagectomy Guilherme M Campos, MD, FACS Assistant Professor of Surgery Director G.I. Motility Center Director Bariatric Surgery Program University of California San Francisco ESOPHAGEAL
-12. -Renad Habahbeh. -Dr Mohammad mohtasib
 -12 -Renad Habahbeh - -Dr Mohammad mohtasib The Gallbladder -The gallbladder has a body, a fundus (a rounded end), a neck, Hartmann s pouch before the neck and a cystic duct that meets the common hepatic
-12 -Renad Habahbeh - -Dr Mohammad mohtasib The Gallbladder -The gallbladder has a body, a fundus (a rounded end), a neck, Hartmann s pouch before the neck and a cystic duct that meets the common hepatic
Citation Hepato-Gastroenterology, 55(86-87),
 NAOSITE: Nagasaki University's Ac Title Author(s) Combined pancreatic resection and p multiple lesions of the pancreas: i of the pancreas concomitant with du Kuroki, Tamotsu; Tajima, Yoshitsugu Tomohiko;
NAOSITE: Nagasaki University's Ac Title Author(s) Combined pancreatic resection and p multiple lesions of the pancreas: i of the pancreas concomitant with du Kuroki, Tamotsu; Tajima, Yoshitsugu Tomohiko;
Left-sided approach for suprapancreatic lymph node dissection in laparoscopy-assisted distal gastrectomy without duodenal transection
 Gastric Cancer (2009) 12: 106 112 DOI 10.1007/s10120-009-0508-9 Technical note 2009 by International and Japanese Gastric Cancer Associations Left-sided approach for suprapancreatic lymph node dissection
Gastric Cancer (2009) 12: 106 112 DOI 10.1007/s10120-009-0508-9 Technical note 2009 by International and Japanese Gastric Cancer Associations Left-sided approach for suprapancreatic lymph node dissection
The peritoneum. Prof. Oluwadiya KS, MBBS, FMCS(Orthop) Website:
 The peritoneum Prof. Oluwadiya KS, MBBS, FMCS(Orthop) Website: http://oluwadiya.com The peritoneum Serous membrane that lines the abdominopelvic cavity and invests the viscera The largest serous membrane
The peritoneum Prof. Oluwadiya KS, MBBS, FMCS(Orthop) Website: http://oluwadiya.com The peritoneum Serous membrane that lines the abdominopelvic cavity and invests the viscera The largest serous membrane
Adipocytes, Obesity, Bariatric Surgery and its Complications
 Adipocytes, Obesity, Bariatric Surgery and its Complications Daniel C. Morris, MD, FACEP, FAHA Senior Staff Physician Department of Emergency Medicine Objectives Basic science of adipocyte Adipocyte tissue
Adipocytes, Obesity, Bariatric Surgery and its Complications Daniel C. Morris, MD, FACEP, FAHA Senior Staff Physician Department of Emergency Medicine Objectives Basic science of adipocyte Adipocyte tissue
BY DR NOMAN ULLAH WAZIR
 BY DR NOMAN ULLAH WAZIR The stomach (from ancient Greek word stomachos, stoma means mouth) is a muscular, hollow and the most dilated part of the GIT. It starts from the point where esophagus ends. It
BY DR NOMAN ULLAH WAZIR The stomach (from ancient Greek word stomachos, stoma means mouth) is a muscular, hollow and the most dilated part of the GIT. It starts from the point where esophagus ends. It
Accessory Glands of Digestive System
 Accessory Glands of Digestive System The liver The liver is soft and pliable and occupies the upper part of the abdominal cavity just beneath the diaphragm. The greater part of the liver is situated under
Accessory Glands of Digestive System The liver The liver is soft and pliable and occupies the upper part of the abdominal cavity just beneath the diaphragm. The greater part of the liver is situated under
Totally laparoscopic total gastrectomy for locally advanced middle-upper-third gastric cancer
 Original Article on Gastrointestinal Surgery Totally laparoscopic total gastrectomy for locally advanced middle-upper-third gastric cancer Mi Lin, Chang-Ming Huang, Chao-Hui Zheng, Ping Li, Jian-Wei Xie,
Original Article on Gastrointestinal Surgery Totally laparoscopic total gastrectomy for locally advanced middle-upper-third gastric cancer Mi Lin, Chang-Ming Huang, Chao-Hui Zheng, Ping Li, Jian-Wei Xie,
Peptic ulcer disease Disorders of the esophagus
 Peptic ulcer disease Disorders of the esophagus Peptic ulcer disease Burning epigastric pain Exacerbated by fasting Improved with meals Ulcer: disruption of mucosal integrity >5 mm in size, with depth
Peptic ulcer disease Disorders of the esophagus Peptic ulcer disease Burning epigastric pain Exacerbated by fasting Improved with meals Ulcer: disruption of mucosal integrity >5 mm in size, with depth
Classification and Management of Leaks after Gastric Bypass for Patients with Morbid Obesity: A Prospective Study of 60 Patients
 OBES SURG (2012) 22:855 862 DOI 10.1007/s11695-011-0519-6 CLINICAL REPORT Classification and Management of Leaks after Gastric Bypass for Patients with Morbid Obesity: A Prospective Study of 60 Patients
OBES SURG (2012) 22:855 862 DOI 10.1007/s11695-011-0519-6 CLINICAL REPORT Classification and Management of Leaks after Gastric Bypass for Patients with Morbid Obesity: A Prospective Study of 60 Patients
Traditionally, surgical antireflux therapy has been
 Laparoscopic Fundoplication Mary Maish, MD and Jeffrey A. Hagen, MD Traditionally, surgical antireflux therapy has been reserved for patients with complicated gastroesophageal reflux disease. The introduction
Laparoscopic Fundoplication Mary Maish, MD and Jeffrey A. Hagen, MD Traditionally, surgical antireflux therapy has been reserved for patients with complicated gastroesophageal reflux disease. The introduction
Cattell-Braasch maneuver combined with superior mesenteric artery first approach for resection of borderline resectable pancreatic cancer
 Masters of Surgery Page 1 of 5 Cattell-Braasch maneuver combined with superior mesenteric artery first approach for resection of borderline resectable pancreatic cancer Tingsong Yang 1, Fairweather Mark
Masters of Surgery Page 1 of 5 Cattell-Braasch maneuver combined with superior mesenteric artery first approach for resection of borderline resectable pancreatic cancer Tingsong Yang 1, Fairweather Mark
Duodenum retroperitoneal
 Duodenum retroperitoneal C shaped Initial region out of stomach into small intestine RETROperitoneal viscus Superior 1 st part duodenal cap ; moves upwards and backwards to lie on the R crura medial to
Duodenum retroperitoneal C shaped Initial region out of stomach into small intestine RETROperitoneal viscus Superior 1 st part duodenal cap ; moves upwards and backwards to lie on the R crura medial to
Imaging Following Mini-Gastric Bypass and Sleeve Gastrectomy: what every radiologists need to know
 Imaging Following Mini-Gastric Bypass and Sleeve Gastrectomy: what every radiologists need to know Poster No.: C-1264 Congress: ECR 2016 Type: Educational Exhibit Authors: C. Yazgan, S. BALCI, T. Sahin,
Imaging Following Mini-Gastric Bypass and Sleeve Gastrectomy: what every radiologists need to know Poster No.: C-1264 Congress: ECR 2016 Type: Educational Exhibit Authors: C. Yazgan, S. BALCI, T. Sahin,
Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman
 Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman Breast anatomy: Breast conserving surgery: The aim of wide local excision is to remove all invasive and in situ
Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman Breast anatomy: Breast conserving surgery: The aim of wide local excision is to remove all invasive and in situ
While the gastric conduit has been the method of choice
 Colon Interposition for Staged Esophageal Reconstruction Andrew C. Chang, MD While the gastric conduit has been the method of choice for esophageal replacement for most surgeons, 1,2 the colon also is
Colon Interposition for Staged Esophageal Reconstruction Andrew C. Chang, MD While the gastric conduit has been the method of choice for esophageal replacement for most surgeons, 1,2 the colon also is
Pancreatic Benign April 27, 2016
 Department of Surgery Pancreatic Benign April 27, 2016 James Choi Dr. Hernandez Objectives Medical Expert: 1. Anatomy and congenital anomalies of the pancreas and pancreatic duct (divisum, annular pancreas
Department of Surgery Pancreatic Benign April 27, 2016 James Choi Dr. Hernandez Objectives Medical Expert: 1. Anatomy and congenital anomalies of the pancreas and pancreatic duct (divisum, annular pancreas
REFLUX ALKALINE GASTRITIS* SYRACUSE, NEW YORK
 VOL. 115, No. 2 REFLUX ALKALINE GASTRITIS* By SEUK KY KIM, M.D.,t LLOYD S. ROGERS, M.D.,t and ROBERT E. HEITZMAN, M.D. SYRACUSE, NEW YORK E ARLY physiologists thought that gastric acid was partly controlled
VOL. 115, No. 2 REFLUX ALKALINE GASTRITIS* By SEUK KY KIM, M.D.,t LLOYD S. ROGERS, M.D.,t and ROBERT E. HEITZMAN, M.D. SYRACUSE, NEW YORK E ARLY physiologists thought that gastric acid was partly controlled
C.Y. Lin, B.Y. Lin, and P.L. Kang Aortic aneurysm Figure 1. Preoperative computerized tomography shows a 6.8 cm infrarenal abdominal aortic aneurysm.
 DUODENAL OBSTRUCTION AFTER ELECTIVE ABDOMINAL AORTIC ANEURYSM REPAIR: A CASE REPORT Chun-Yao Lin, Bor-Yen Lin, and Pei-Luen Kang Division of Cardiology, Department of Surgery, Kaohsiung Veterans General
DUODENAL OBSTRUCTION AFTER ELECTIVE ABDOMINAL AORTIC ANEURYSM REPAIR: A CASE REPORT Chun-Yao Lin, Bor-Yen Lin, and Pei-Luen Kang Division of Cardiology, Department of Surgery, Kaohsiung Veterans General
INFORMATION ON PANCREATIC HEAD AND PERIAMPULLARY CANCER
 INFORMATION ON PANCREATIC HEAD AND PERIAMPULLARY CANCER What is Pancreas? The pancreas is a gland located in the back of your abdomen behind the stomach. pancreas is divided into four parts: the head,
INFORMATION ON PANCREATIC HEAD AND PERIAMPULLARY CANCER What is Pancreas? The pancreas is a gland located in the back of your abdomen behind the stomach. pancreas is divided into four parts: the head,
Prevention Of Pancreaticojejunal Fistula After Whipple Procedure
 ISPUB.COM The Internet Journal of Surgery Volume 4 Number 2 Prevention Of Pancreaticojejunal Fistula After Whipple Procedure N Barbetakis, K Setsiz Citation N Barbetakis, K Setsiz. Prevention Of Pancreaticojejunal
ISPUB.COM The Internet Journal of Surgery Volume 4 Number 2 Prevention Of Pancreaticojejunal Fistula After Whipple Procedure N Barbetakis, K Setsiz Citation N Barbetakis, K Setsiz. Prevention Of Pancreaticojejunal
Catherine Kerschen DO, FACOI Michigan State University College of Osteopathic Medicine
 Catherine Kerschen DO, FACOI Michigan State University College of Osteopathic Medicine none none Reserved for pts: Complications from GERD Refractory esophagitis** Stricture Barrett s Persistent reflux
Catherine Kerschen DO, FACOI Michigan State University College of Osteopathic Medicine none none Reserved for pts: Complications from GERD Refractory esophagitis** Stricture Barrett s Persistent reflux
Surgical Management of Obesity. David A. Edelman, MD, MSHPEd, FACS Associate Professor of Surgery
 Surgical Management of Obesity David A. Edelman, MD, MSHPEd, FACS Associate Professor of Surgery Objectives Describe indications for surgical management of obesity Describe three types of bariatric surgery
Surgical Management of Obesity David A. Edelman, MD, MSHPEd, FACS Associate Professor of Surgery Objectives Describe indications for surgical management of obesity Describe three types of bariatric surgery
What can you expect after your ERCP?
 ERCP Explained and respond to bed rest, pain relief and fasting to rest the gut with the patient needing to stay in hospital for only a few days. Some patients develop severe pancreatitis and may require
ERCP Explained and respond to bed rest, pain relief and fasting to rest the gut with the patient needing to stay in hospital for only a few days. Some patients develop severe pancreatitis and may require
