Severe cutaneous adverse reactions: an evidence based approach
|
|
|
- Shawn Craig
- 5 years ago
- Views:
Transcription
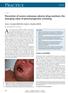
1 Original Article 21 Severe cutaneous adverse reactions: an evidence based approach D.P. Shrestha, D. Gurung, A. Kumar Department of Dermatology and Venereology, Maharagunj Campus, Institute of Medicine, Tribhuvan University Teaching Hospital, Kathmandu, Nepal. Correspondence to: Dr. D. P. Shrestha, Dept. of Dermatology, TU Teaching Hospital Maharajgung, Kathmandu, Nepal Background: Severe cutaneous adverse reactions (SCAR), comprising mainly Stevens-Johnson syndrome (SJS) and Toxic Epidermal Necrolysis (TEN), although rare, constitute a severe entity with life-threatening consequences. The aetiology is multifactorial but drugs have been implicated in the majority of cases. Depending on the severity of the reaction, it has a wide spectrum of clinical presentations and there is still confusion regarding its classification. Reliable information on the incidence of drug reactions has been difficult to obtain due to lack of standardised systems for data collection and reporting. The situation is poorer in developing countries where specific epidemiological studies have not been published, largely due to the lack of a reporting system and awareness of drug reaction patterns among medical professionals and patients alike. Method: We have reviewed available literature regarding SJS and TEN, and the hospital admission records of such patients at Tribhuvan University teaching hospital. A comparative study was done. Results: Drugs, mainly sulfonamides and anticonvulsants have been the aetiological factors in majority of the cases, and the presentation in the patients have ranged from mild to fatal reactions. In the TU teaching hospital, in almost all cases, steroids have been used in the management. Conclusion: Though a self-limiting disorder, patients with SCAR have a multisystem involvement, and a multi-disciplinary approach is necessary for its management. The need for intensive supportive care and the controversial role of steroids makes its management even more challenging. Thus, it is essential to develop a protocol/guidelines for the management of these disorders appropriate to our context. Introduction An adverse drug reaction (ADR) may be defined as an undesirable clinical manifestation resulting from administration of a particular drug, which includes reactions due to overdose, predictable side-effects and unanticipated adverse manifestations. 1 It has also been defined as an appreciably harmful or unpleasant reaction, resulting from an intervention related to the use of a medicinal product, which predicts hazard from future administration and warrants prevention or specific treatment, or alteration of the dosage regimen, or withdrawl of the product. 2 The criteria for assessment of potential drug reactions include recurrence on challenge; existence of a pharmacological basis for the reactions; the occurrence of immediate acute or local reactions with a new route of administration, or of repeated rare reactions; and the presence of immunological abnormalities. 3,4 With atleast 90 million courses of drug treatment given yearly in the USA, the incidence of adverse drug reactions varies from 6 % to 30 %. 5,6 The reported incidence of EM (Erythema Multiforme), SJS and TEN varies widely among different countries. A study from France estimated the incidence of TEN at 1.2 cases per million per year. 7 Another US study estimated the incidence of EM, SJS and TEN at 1.8 cases per million person years for patients between 20
2 22 D. P. Shrestha, D. Gurung, A. Kumar and 64 years. 8 Various population studies in the west have reported the incidence rate of TEN between 0.4 to 1.2 cases per million annually. 9 Reliable information on the incidence of drug reactions has been difficult to obtain due to lack of standardised systems for data collection and reporting. The situation is poorer in developing countries where specific epidemiological studies have not been published, largely due to the lack of a reporting system and awareness of drug reaction patterns among medical professionals and patients alike. It is possible that the frequency of such reactions in these countries could be much higher considering the fact that the main aetiologic agent, i.e, drugs such as antibiotics, anticonvulsants and non-steroidal anti-inflammatory drugs (NSAIDs) are easily available over the counter. 10 Drug reactions may arise as a result of non-immunological mechanisms, such as those caused by non-immune mediated degranulation of mast cells and basophils or immunological allergy directed against the drug itself, a reactive metabolite or some contaminant of the drug. About 80% of drug reactions are predictable non-immunological reactions, which includes overdosage, side-effects, cumulation, drug interactions, metabolic alterations, etc. 1 The more serious reactions, also known as SCAR, comprises EM, SJS and TEN. Bateman in 1814, described the target lesion. Bazin first recognised mucosal involvement and cutaneous symptoms attributed to drugs in In 1866, Ferdinand Von Hebra described Erythema exudativum multiforme and recognised these disorders as a single entity. Stevens and Johnson in 1922 first described the SJS and Lyell A in 1956 described TEN, also called Lyell s syndrome. 11,12 TEN represents the most severe form among all Types of SCAR. Cutaneous reactions to drugs may present with varied clinical patterns of eruption. Although certain drugs are commonly associated with a specific reaction, most drugs are capable of causing several different Types of eruptions. The most frequent Type of all cutaneous reactions to drugs are the exanthematic (erythematous maculo-papular) eruptions. Other Types of clinical presentations include purpura, annular erythema, pityriasis-rosea like eruption, psoriasiform eruptions, exfoliative dermatitis, anaphylaxis, urticaria, serum sickness, drug hypersensitivity syndrome, fixed eruptions, lichenoid eruptions, photosensitivity, pigmentation reactions, acneiform and pustular eruptions, eczematous eruptions, bullous eruptions, vasculitis, lupus erythematous-like syndrome, erythema nodosum, anticonvulsant hypersensitivity syndrome, hair changes like alopecia and hirsutism and various patterns of nail changes and onycholysis. 1 It is the rare but serious reactions like SJS and TEN which contribute to significant mortality. SJS involves an illness usually of sudden onset, associated with marked constitutional symptoms of high fever, malaise, myalgia, arthralgia with skin blisters and erosions covering less than 10 % of the body surface area. Significant involvement of the mucous membranes is present including the eyes, ano-genital mucosae and mucosa of the respiratory tract. 13 TEN is characterised by typical sheetlike erosions of the skin involving more than 30% of the body surface area with widespread purpuric macules or flat atypical target lesions and severe involvement of the conjunctival, corneal, irideal, buccal, labial and genital mucous membranes Objectives To determine the clinico-epidemiological pattern of patients with SCAR, admitted to the TU Teaching Hospital. To analyse the possible aetiology and the modalities of management in these patients. Methodology All available literature and texts regarding SJS and TEN were reviewed along with a review of the hospital admission records of patients admitted under various specialities of TU teaching hospital with these illnesses, between b.s 2056 and 2060, for a period of 4 yrs. The data regarding the clinical Types, age and sex distribution, the possible causes implicated and the various modalities of management were analysed and a comparative evaluation was done. Results A total of 33 patients (male-11: female-22) with varying severity of SCAR had been admitted to the departments of dermatology, internal medicine and ophthalmology in a period of 4 years. The patients were in the age range of 4-65 years (mean 34.5 years). Among them 6 had EM, had SJS and 2 had TEN (Fig. 1). No. of patients Fig. 1. Clinical types of SCAR 6 Types of SCAR Fig. 1. Clinical types of SCAR 2 EM SJS TEN
3 Severe cutaneous adverse reactions 23 The duration of their hospital stay ranged from 4-19 days (mean-11.5 days). Drugs were the cause in most of the patients, usually with history of antibiotic intake prior to the onset of the eruption. Reactions in 15 patients appeared to be due to antibiotics (sulfonamides, penicillins, quinolones), in 10 patients due to anticonvulsants (carbamazepine-5; phenytoin-4; phenobarbitone-1), in 4 patients due to NSAIDs, and in 4 patients no possible cause could be ascertained (Fig. 2). Types Fig. 2. Types of SCAR Fig. 2. Types of SCAR 10 No. of patients 15 Antibiotics Anticonvulsants NSAIDs Unknown All patients were treated with antibiotics and 29 of these patients had received steroids. Discussion The clinical picture of the SCAR spectrum appears to be a reaction pattern to many different triggering factors having an immunological basis, but the exact pathogenesis still remains largely unknown. Immune complexes have been demonstrated both in the skin and circulation and antibodies against epithelial cells and desmosomal plaque proteins desmoplakin I and II have been demonstrated in patients with EM Numerous evidence suggests the important role of T cells in the pathogenesis of SCAR, and the cytotoxic lymphocyte-mediated immune reaction (CTL) aimed at the destruction of the keratinocytes expressing foreign antigens seems to be the widely accepted view. 10 More recently it has been discovered that Fas-Fas ligand interactions may be directly responsible for apoptotic death of keratinocytes in TEN patients. Activated lymphocytes might induce apoptosis via an interaction between Fas antigen (CD 95), expressed by keratinocytes after exposure to IFN-gamma, and its ligand Fas-ligand(Fas L), expressed on the surface of and secreted by lymphocytes. 20 Drugs have been implicated as the possible aetiology in majority of the cases of SCAR, with % of cases of TEN and more than 50 % of cases of SJS.A wide range of drugs have been suspected to be causal, but the most frequently implicated are sulfa drugs (co-trimoxazole and other sulfonamides), anticonvulsants (phenytoin, carbamazepine, phenobarbital, valproic acid), NSAIDs (butazone, oxicam derivatives), allopurinol, anti-tubercular drugs (thiacetazone, isoniazid) and antibiotics (penicillins, quinolones). 21 Immunisation with DPT, measles, poliomyelitis and influenza vaccines have been recorded as a cause of TEN. 22,23 The latter has also been described with graft versus host disease. 24 Infections with Mycoplasma and Klebsiella pneumoniae have also been attributed as a cause of SJS and TEN. Among SCAR patients admitted to the TU teaching hospital, drugs were the cause in majority, usually with history of antibiotic intake prior to the onset of the eruption. The antibiotics commonly implicated were sulfonamides, penicillins and quinolones). In other patients, anticonvulsants (carbamazepine, phenytoin, phenobarbitone) and NSAIDs appeared to be the cause while in some no possible cause could be ascertained. Severe cutaneous adverse reactions traditionally comprise EM, SJS and TEN. EM involves macular, papular or urticarial lesions, and the classical target or iris lesions, distributed preferentially over the distal extremities. Lesions may involve the palms or trunk as well as the oral and genital mucosa with erosions. EM is most often related to Herpes simplex virus infections and occasionally to drugs. EM major usually effects younger males, frequently recurs, and has less fever and milder mucosal lesions. SJS involves skin blisters and erosions covering less than 10 % of the body surface area. TEN is characterised by detachment of the epidermis in typical sheet-like erosions involving more than 30 % of the body surface area and patients having features of both the groups who cannot be classified into either group comprise the SJS-TEN overlap syndrome. Significant differences exist between countries in the classification of SCAR, and seeing the need for precise definitions, the term acute disseminated epidermal necrosis (ADEN) has been proposed. ADEN Type 1 corresponds to SJS, Type 2 to transitional SJS-TEN with epidermal detachment between % and Type 3 to full-blown TEN. It has also been advocated by Lyell that the term exanthematic necrolysis should replace TEN. 26 Withdrawal of the potential causative drug/drugs should be the initial and immediate step in the management of patients with SCAR. They are an acute emergency and are life threatening if not treated promptly. Due to its unclear pathophysiology, rapid and intensive supportive care are essential for a favourable outcome. 10 This involves environmental temperature control, fluid and electrolyte balance and the use of broad spectrum antibiotics since patients are at an increased risk of death due to hypothermia, dehydration, electrolyte disturbances and septicaemia. Numerous reports have demonstrated a highly improved prognosis when TEN patients were treated through a multidisciplinary management in a burn center It is now
4 24 D. P. Shrestha, D. Gurung, A. Kumar standard treatment to admit TEN patients to a burn unit, whenever possible. If not available, then patients should be treated in an intensive care unit with reverse-isolation nursing techniques. All patients admitted to the TU teaching hospital were treated with antibiotics and 29 of these patients had received steroids. The role of corticosteroids in the management of SCAR remains controversial. Many recent studies have described prolonged wound healing and higher rate of mortality and morbidity associated with the use of corticosteroids. 31 Cases of TEN have occurred in patients already on high doses of steroids for other illnesses, suggesting no role of steroids in preventing TEN. 32 In a SCAR study, corticosteroids appeared to be an important risk factor for TEN, suggesting that epidemiologically, corticosteroids behave just as do other responsible drugs. 33 Many authorities, therefore, no longer routinely recommend corticosteroid therapy for patients with TEN. Infact, in the first international symposium on EM and Lyell s syndrome (TEN) in Creteil, France in 1985, attended by most of the world s authorities on this disease including Lyell himself, it was unanimously concluded that corticosteroids were of no particular value in the management of TEN and they condemned its use once the disease has progressed to more than 20% body surface area. 34 However, many authorities all over the world still use corticosteroids for the management of SJS/TEN in the early course of the disease. Besides steroids and supportive care, many other therapies have been attempted in recent times to treat TEN patients. Immunosuppressants including cyclosporine 35,36 and cyclophosphamide 37,38 have been claimed to prevent progression of disease in a small number of patients. However, it must be remembered that these treatments have the potential to promote infection, the main cause of death in TEN. Infusions of anti-tumor necrolysis factor-alfa and anti-interleukin-2 monoclonal antibodies have been used in patients with graft vs host disease related TEN. Use of recombinant granulocyte colony-stimulating factor and granulocyte-macrophage colony-stimulating factor and hyperbaric oxygen has been reported to enhance epidermal regrowth. 10 Plamapheresis has also been used to remove the offending drug or its metabolites. Unfortunately, the efficacies of these treatments have not been tested in larger cohorts and are thus not available for universal use. 10 Most recently, naturally occurring anti-fas immunoglobulin has been used intravenously ( gm/kg/day) as specific therapy to treat patients with TEN. Naturally occurring immunoglobulin in intravenous immunoglobulin preparations, which is pooled from plasma of healthy donors, may have little or no adverse effect compared to systemic corticosteroids or other immunosuppresants and it is hoped that this therapy should have tremendous potential to improve the outcome of TEN patients in the future. 39 Conclusion Major developments have been made in recent years in the management of SCAR and the morbidity and mortality of patients have decreased significantly. Care of patients in a burn center or a suitable ICU involving a multi-disciplinary approach, focussing the therapeutic goal towards promotion of wound healing, aggressive correction of fluid, electrolyte and protein balance, provision of pulmonary and eye care and prevention of sepsis is essential to achieve a favourable outcome. The controversy of corticosteroid use remain but the general consensus is that steroids may be most beneficial, if the body surface area involvement is less than or equal to 20%, if started very early in the course of illness (within the first hours), given at a relatively high dose (equivalent to 1-2 mg per kg body weight of oral prednisolone or intravenous methylprednisolone), for a brief period (not more than 3-5 days) and stopped or tapered off 40, 41 rapidly. In developing nations, the easy availability of potential drugs over the counter significantly increases the risk of SCAR, while the lack of standardised reporting systems and lack of awareness of SCAR contribute to the difficulty in research and formulating appropriate guidelines regarding management. Socio-economic factors and lack of or inaccessibility to healthcare facilities may also be responsible for hurdles in seeking healthcare. It is, therefore, necessary to develop guidelines/protocol for the identification, data collection and management of SCAR, appropriate to our context. References 1. S.M.Breathnach, Drug Reactions. In Burns T, Breathnach S, Cox N, Griffiths C, eds. Rook s textbook of Dermatology.Vol.4, Seventh edition, Blackwell Publishing, 2004; 73 : Meyboom RH, Lindquist M, Flygare AK et al. The value of reporting therapeutic ineffectiveness as an adverse drug reaction. Drug Saf 2000; 23: Venning GR. Validity of anecdotal reports of suspected adverse drug reactions: the problem of false alarms. Br Med J 1982; 284: Stern RS, Wintroub BU. Adverse drug reactions: reporting and evaluating cutaneous reactions. Adv Dermatol 1987; 2: Deswarte RD. Drug allergy: problems and strategies. J Allergy Clin Immunol 1984; 74: Jick H. Adverse drug reactions: the magnitude of the problem. J Allergy Clin Immunol 1984; 74: RoujeauJC, GuillaumeJC, Fabre JD etal, Toxic Epidermal Necrolysis(Lyell syndrome): incidence and drug aetiology in France, Arch Dermatol 1990; 126: Chan HL, Stern RS, Arndt KA et al. The incidence of
5 Severe cutaneous adverse reactions Erythema multiforme, Stevens-Johnson syndrome and Toxic Epidermal Necrolysis: a population based study with particular reference to reactions caused by drugs among out-patients. Arch Dematol 1990; 126 : Revuz JE, Ronjen JC, Toxic Epidermal Necrolysis. Cutaneous Medicine and Surgery. WB Saunders Press.1995; Saha K, Gupta AK. Toxic Epidermal Necrolysis: Current concepts in pathogenesis and treatment. Ind J Dermatol Venerol Leprol. 11. Fritsch PO, Maldonado RR. Erythema Multiforme, Stevens-Johnson Syndrome, and Toxic Epidermal Necrolysis. In: Freedberg IM, Eisen AZ, Wolff K, eds. Fitzpatrick s Dermatology in General Medicine.Vol 1,Sixth edition. McGraw Hill, 2003; Lyell A: Toxic epidermal necrolysis: An eruption resemblingscaldingoftheskin.brjdematol1956;68: Ashby DW, Lazar T. Erythema multiforme exudativum major (Stevens-Johnson syndrome). Lancet 1951; I: Bastuji-garin S, Rzany B, Stern RS et al. A clinical classification of cases of toxic epidermal necrolysis, Stevens-Johnson syndrome, and erythema multiforme. Arch Dermatol 1993; 129: Roujeau JC. The spectrum of Stevens-Johnson syndrome and toxic epidermal necrolysis: a clinical classification. J Invest Dermatol 1994; 102: 28S-30S. 16. Roujeau JC. Stevens-Johnson syndrome and toxic epidermal necrolysis are severity variants of the same disease which differs from erythema multiforme. J Dermatol 1997; 24: Bushkell LL, Mackel SE, Jordan RE. Erythema multiforme: direct immunoflourescence studies and detection of circulating immune complexes. J Invest Dermatol1980;74: Matsuoka LY,Wortsmann J,Stanley JR. Epidermal autoantibodies in erythema multiforme. J Am Acad Dermatol 1989;21; Foedinger d,sterickzy B,Elbe A et al. Autoantibodies against desmoplakin I and II define a subset of patients with erythema multiforme major. J Invest Dermatol1996;106: Aberer W.Stingl g,wolff K. Stevens-Johnson syndrome und toxische epidermale Nekrolyse nach Sulfonamideinahme. Hautarzt 1982;33: Roujeau et al: Medication use and the risk of SJS or TEN.N Eng J of Med, Shoss RG,Rayhanzadeh S. Toxic epidermal necrolysis following measles vaccination. Arch Dermatol 1974;110: Ball R,Ball LK,Wise RP et al. Stevens-Johnson syndrome and toxic epidermal necrolysis after vaccination: reports to the vaccine adverse event reporting system. Pediatr Infect Dis J2001;20: Peck GL,Herzig GP,Elias PM. Toxic epidermal necrolysis in a patient with graft-vs-host reaction. Arch Dermatol 1972;105: Ruiz-Maldonado R. Acute disseminated epidermal necrolysis Types 1,2, and 3:study of 60 cases. J Am Acad Dermatol 1985;13: Lyell A. Requim for toxic epidermal necrolysis. Br J Dermatol 1990;122: Bradley T,Brown RE,Kucan JO,et al. Toxic epidermal necrolysis: A review and report of the successful use of Biobrance for nearly wound coverage. Ann Plast Surg.1995;35: Barillo DJ,Goodwin CW. Dermatologists and the Burn center. Dermatologic clinic 1999;17: Kelemen JJ,Coiffi WG,Mc Mannus WF,et al. Burn center care for patients with toxic epidermal necrolysis. J Am Coll Surg 1995;180: Yarbrough DR. Treatment of toxic epidermal necrolysis in a Burn center. J South Carol Med Assoc 1997;1: Fine JD. Management of acquired bullous skin diseases. N Eng J Med 1995;333: Rzany B,Schmitt H,Schopf E. Toxic epidermal necrolysis in patients recieving glucocorticoids. Acta Derm Vener1991;71: Kelly JP,Aquier A,Razany B,et al. An international collaborative case-control study of severe cutaneous adverse reactions(scar).designs and methods. J Clin Epidemiol 1995;48; Revuz J,Roujeau JC,Guillaume,et al. Treatment of toxic epidermal necrolysis:creteil s experience. Arch Dermatol1987;123: Paquet P,Pierard GE. Would cyclosporin A be beneficial to mitigate drug induced toxic epidermal necrolysis. Dermatology 1999;198: Hewitt J,Ormerod AD. Toxic epidermal necrolysis treated with cyclosporine. Clin Exp Dermatol 1992;17: Heng MC,Allen SG. Efficacy of cyclophosphamide in Toxic epidermal necrolysis:clinical and pathological aspects. J Am Acad Dermatol 1991;: Frangogiannis NC,Boridy I,Mazhar M,et al. Cyclophosphamide in the treatment of Toxic epidermal necrolysis. South Med J 1996;89: Viard I,Wehrli P,Bullani R,et al. Inhibition of toxic epidermal necrolysis by blockage of CD95 with human intravenous immunoglobulin. Science 1998;282: Fine JD. Management of acquired bullous skin diseases. N Eng J Med 1995;333: Parischa JS,Khaitan BK,Shantharaman R,et al. Toxic epidermal necrolysis. Int J Dermatol 1996;35:
Skin Manifestations of Drug Reactions
 Skin Manifestations of Drug Reactions Dr Carol Hlela, Division of Dermatology Department of Medicine, University of Cape Town and Red Cross Children s Hospital What are the Skin Manifestations of Drug
Skin Manifestations of Drug Reactions Dr Carol Hlela, Division of Dermatology Department of Medicine, University of Cape Town and Red Cross Children s Hospital What are the Skin Manifestations of Drug
Emergency Dermatology Dr Melissa Barkham
 Emergency Dermatology Dr Melissa Barkham Spotlight Seminar 30 th September 2010 Why is this important? Urgent recognition and treatment of dermatologic emergencies can be life saving and prevent long term
Emergency Dermatology Dr Melissa Barkham Spotlight Seminar 30 th September 2010 Why is this important? Urgent recognition and treatment of dermatologic emergencies can be life saving and prevent long term
Drug Allergy A Guide to Diagnosis and Management
 Drug Allergy A Guide to Diagnosis and Management (Version 1 April 2015 updated April 2018) Author: Jed Hewitt Chief Pharmacist, Governance & Professional Practice Date of Preparation: April 2015 Updated:
Drug Allergy A Guide to Diagnosis and Management (Version 1 April 2015 updated April 2018) Author: Jed Hewitt Chief Pharmacist, Governance & Professional Practice Date of Preparation: April 2015 Updated:
Pediatric Dermatology
 Pediatric Dermatology --------- Emergencies & Urgencies Nicholas V. Nguyen, M.D. Director, Pediatric Dermatology Disclosures In the past 12 months, I have had the following financial relationships with
Pediatric Dermatology --------- Emergencies & Urgencies Nicholas V. Nguyen, M.D. Director, Pediatric Dermatology Disclosures In the past 12 months, I have had the following financial relationships with
A Case Report on Amoxicillin Induced Stevens- Johnson Syndrome
 Open Journal of Clinical & Medical Case Reports Volume 2 (2016) Issue 11 A Case Report on Amoxicillin Induced Stevens- Johnson Syndrome Rajendra Singh Airee*; Aastha Rawal; Binu Mathew; H. Doddayya Abstract
Open Journal of Clinical & Medical Case Reports Volume 2 (2016) Issue 11 A Case Report on Amoxicillin Induced Stevens- Johnson Syndrome Rajendra Singh Airee*; Aastha Rawal; Binu Mathew; H. Doddayya Abstract
They are updated regularly as new NICE guidance is published. To view the latest version of this NICE Pathway see:
 bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
Cutaneous Drug Reactions
 Cutaneous Drug Reactions Andrei Metelitsa, MD, FRCPC, FAAD Co-Director, Institute for Skin Advancement Clinical Associate Professor, Dermatology University of Calgary, Canada Copyright 2017 by Sea Courses
Cutaneous Drug Reactions Andrei Metelitsa, MD, FRCPC, FAAD Co-Director, Institute for Skin Advancement Clinical Associate Professor, Dermatology University of Calgary, Canada Copyright 2017 by Sea Courses
Future of Pediatrics: Blisters, Hives and Other Tales from the Emergency Room June 14 th, 2016
 A. Yasmine Kirkorian MD Assistant Professor of Dermatology & Pediatrics Children s National Health System George Washington University School of Medicine & Health Sciences Future of Pediatrics: Blisters,
A. Yasmine Kirkorian MD Assistant Professor of Dermatology & Pediatrics Children s National Health System George Washington University School of Medicine & Health Sciences Future of Pediatrics: Blisters,
Cutaneous Adverse Drug Reactions in Domestic Animals. Katherine Doerr, DVM, Dip. ACVD. Veterinary Dermatology Center
 Cutaneous Adverse Drug Reactions in Domestic Animals Katherine Doerr, DVM, Dip. ACVD Veterinary Dermatology Center Maitland, Rockledge, Waterford Lakes, FL Not highly studied in veterinary medicine Unknown
Cutaneous Adverse Drug Reactions in Domestic Animals Katherine Doerr, DVM, Dip. ACVD Veterinary Dermatology Center Maitland, Rockledge, Waterford Lakes, FL Not highly studied in veterinary medicine Unknown
Dilantin (phenytoin) ROBERT A. SCHWARTZ
 Dilantin (phenytoin) ROBERT A. SCHWARTZ Bailey & Galyen Attorney in Charge, Mass Tort Litigation Managing Attorney, Houston 18333 Egret Bay Blvd., Suite 120 Houston, Texas 77058 Toll Free: (866) 715-1529
Dilantin (phenytoin) ROBERT A. SCHWARTZ Bailey & Galyen Attorney in Charge, Mass Tort Litigation Managing Attorney, Houston 18333 Egret Bay Blvd., Suite 120 Houston, Texas 77058 Toll Free: (866) 715-1529
allergy Asia Pacific Stevens-Johnson syndrome and toxic epidermal necrolysis in Dr. Hasan Sadikin General Hospital Bandung, Indonesia from
 pissn -876 eissn -868 Original Article Asia Pac Allergy 6;6:-7 Stevens-Johnson syndrome and toxic epidermal necrolysis in Dr. Hasan Sadikin General Hospital Bandung, Indonesia from 9 Oki Suwarsa *, Wulan
pissn -876 eissn -868 Original Article Asia Pac Allergy 6;6:-7 Stevens-Johnson syndrome and toxic epidermal necrolysis in Dr. Hasan Sadikin General Hospital Bandung, Indonesia from 9 Oki Suwarsa *, Wulan
REGISTRY OF SEVERE CUTANEOUS ADVERSE REACTIONS TO DRUGS AND COLLECTION OF BIOLOGICAL SAMPLES. R e g i S C A R PATIENT'S DATA. Age country of birth
 REGISTRY OF SEVERE CUTANEOUS ADVERSE REACTIONS TO DRUGS AND COLLECTION OF BIOLOGICAL SAMPLES R e g i S C A R PATIENT'S DATA Initials of the patient date of birth Age country of birth Gender male female
REGISTRY OF SEVERE CUTANEOUS ADVERSE REACTIONS TO DRUGS AND COLLECTION OF BIOLOGICAL SAMPLES R e g i S C A R PATIENT'S DATA Initials of the patient date of birth Age country of birth Gender male female
CARBAMAZEPINE INDUCED STEVENS JOHNSON SYNDROME- A CASE STUDY
 WORLD JOURNAL OF PHARMACY AND PHARMACEUTICAL SCIENCES Ragesh SJIF Impact Factor 2.786 Volume 3, Issue 6, 1599-1604. Case Study ISSN 2278 4357 CARBAMAZEPINE INDUCED STEVENS JOHNSON SYNDROME- A CASE STUDY
WORLD JOURNAL OF PHARMACY AND PHARMACEUTICAL SCIENCES Ragesh SJIF Impact Factor 2.786 Volume 3, Issue 6, 1599-1604. Case Study ISSN 2278 4357 CARBAMAZEPINE INDUCED STEVENS JOHNSON SYNDROME- A CASE STUDY
Cutaneous Conditions Associated with Systemic Disease
 Cutaneous Conditions Associated with Systemic Disease Johnnie M Woodson, M.D., F.A.A.D. Assistant Professor of Dermatology University of Nevada School of Medicine Director of J. Woodson Dermatology & Associates,
Cutaneous Conditions Associated with Systemic Disease Johnnie M Woodson, M.D., F.A.A.D. Assistant Professor of Dermatology University of Nevada School of Medicine Director of J. Woodson Dermatology & Associates,
PedsCases Podcast Scripts
 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Drug Allergy. These podcasts are designed to give medical students an overview of key topics in pediatrics. The audio
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Drug Allergy. These podcasts are designed to give medical students an overview of key topics in pediatrics. The audio
A Retrospective Study of Spectrum of Nevirapine Induced Cutaneous Drug Reactions in HIV Positive Patients
 Journal of US-China Medical Science 12 (2015) 85-89 doi: 10.17265/1548-6648/2015.02.008 D DAVID PUBLISHING A Retrospective Study of Spectrum of Nevirapine Induced Cutaneous Drug Reactions in HIV Positive
Journal of US-China Medical Science 12 (2015) 85-89 doi: 10.17265/1548-6648/2015.02.008 D DAVID PUBLISHING A Retrospective Study of Spectrum of Nevirapine Induced Cutaneous Drug Reactions in HIV Positive
OXCARBAZEPINE-INDUCED STEVENS-JOHNSON SYNDROME: A CASE REPORT
 OXCARBAZEPINE-INDUCED STEVENS-JOHNSON SYNDROME: A CASE REPORT Lung-Chang Lin, 1,2 Ping-Chin Lai, 3 Sheau-Fang Yang, 4 and Rei-Cheng Yang 1,5 Departments of 1 Pediatrics and 4 Pathology, Kaohsiung Medical
OXCARBAZEPINE-INDUCED STEVENS-JOHNSON SYNDROME: A CASE REPORT Lung-Chang Lin, 1,2 Ping-Chin Lai, 3 Sheau-Fang Yang, 4 and Rei-Cheng Yang 1,5 Departments of 1 Pediatrics and 4 Pathology, Kaohsiung Medical
Emergency Dermatology. Emergency Dermatology
 Emergency Dermatology These are rapidly progressive skin conditions and some are potentially lifethreatening. Early recognition is important to implement prompt supportive care and therapy. Some are drug
Emergency Dermatology These are rapidly progressive skin conditions and some are potentially lifethreatening. Early recognition is important to implement prompt supportive care and therapy. Some are drug
Stevens Johnson Syndrome: How Diagnosis Impacts Disease Course
 Southern Adventist Univeristy KnowledgeExchange@Southern Graduate Research Projects Nursing 12-4-2015 Stevens Johnson Syndrome: How Diagnosis Impacts Disease Course Sharon K. Hart Southern Adventist University,
Southern Adventist Univeristy KnowledgeExchange@Southern Graduate Research Projects Nursing 12-4-2015 Stevens Johnson Syndrome: How Diagnosis Impacts Disease Course Sharon K. Hart Southern Adventist University,
Herbal and homeopathic products, often considered natural and non-toxic, can also cause adverse drug reactions.
 Idiosyncratic and potentially serious cutaneous adverse drug reactions (CADRs), although relatively rare, account for significant morbidity and mortality. RANNAKOE J LEHLOENYA, BSc, MB ChB, FCDerm (SA)
Idiosyncratic and potentially serious cutaneous adverse drug reactions (CADRs), although relatively rare, account for significant morbidity and mortality. RANNAKOE J LEHLOENYA, BSc, MB ChB, FCDerm (SA)
Adverse cutaneous drug reactions: Clinical pattern and causative agents in a tertiary care center in South India
 Study Adverse cutaneous drug reactions: Clinical pattern and causative agents in a tertiary care center in South India David Pudukadan, Devinder Mohan Thappa Department of Dermatology and STD, Jawaharlal
Study Adverse cutaneous drug reactions: Clinical pattern and causative agents in a tertiary care center in South India David Pudukadan, Devinder Mohan Thappa Department of Dermatology and STD, Jawaharlal
Stevens-Johnson s Syndrome / Toxic Epidermal Necrolysis: An update
 Stevens-Johnson s Syndrome / Toxic Epidermal Necrolysis: An update Robert G. Micheletti, MD Assistant Professor of Dermatology and Medicine Director, Cutaneous Vasculitis Clinic, Penn Vasculitis Center
Stevens-Johnson s Syndrome / Toxic Epidermal Necrolysis: An update Robert G. Micheletti, MD Assistant Professor of Dermatology and Medicine Director, Cutaneous Vasculitis Clinic, Penn Vasculitis Center
Correspondence should be addressed to Wanjarus Roongpisuthipong; rr
 Dermatology Research and Practice, Article ID 237821, 5 pages http://dx.doi.org/10.1155/2014/237821 Research Article Retrospective Analysis of Corticosteroid Treatment in Stevens-Johnson Syndrome and/or
Dermatology Research and Practice, Article ID 237821, 5 pages http://dx.doi.org/10.1155/2014/237821 Research Article Retrospective Analysis of Corticosteroid Treatment in Stevens-Johnson Syndrome and/or
Prevalence and pattern of adverse cutaneous drug reactions presenting to a tertiary care hospital
 International Journal of Research in Dermatology Janardhan B et al. Int J Res Dermatol. 2017 Mar;3(1):74-78 http://www.ijord.com Original Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4529.intjresdermatol20164248
International Journal of Research in Dermatology Janardhan B et al. Int J Res Dermatol. 2017 Mar;3(1):74-78 http://www.ijord.com Original Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4529.intjresdermatol20164248
Toxic Epidermal Necrolysis and SJS : Case Reports & Brief Review
 Case Report Toxic Epidermal Necrolysis and SJS : Case Reports & Brief Review Deepali P. Mohite*, Satyajitraje Tekade*, Amol Gadbail*, M. S. Chaudhary** Abstract : Toxic epidermal necrolysis (TEN) and Stevens
Case Report Toxic Epidermal Necrolysis and SJS : Case Reports & Brief Review Deepali P. Mohite*, Satyajitraje Tekade*, Amol Gadbail*, M. S. Chaudhary** Abstract : Toxic epidermal necrolysis (TEN) and Stevens
CUTANEOUS DRUG REACTIONS OR I WOULDN T HAVE SEEN IT, IF I HADN T BELIEVED IT Edmund J. Rosser Jr., DVM, DACVD
 CUTANEOUS DRUG REACTIONS OR I WOULDN T HAVE SEEN IT, IF I HADN T BELIEVED IT Edmund J. Rosser Jr., DVM, DACVD DERMATOLOGY Pathogenesis Immunologic: can involve Type I, II, III, IV hypersensitivity reactions.
CUTANEOUS DRUG REACTIONS OR I WOULDN T HAVE SEEN IT, IF I HADN T BELIEVED IT Edmund J. Rosser Jr., DVM, DACVD DERMATOLOGY Pathogenesis Immunologic: can involve Type I, II, III, IV hypersensitivity reactions.
Adverse Drug Reactions (ADRs) Outline
 Adverse Drug Reactions (ADRs) Outline 1. What are Adverse Drug Reactions (ADRs)? WHAT WHY HOW 2. How important are ADRs and are they preventable? 3. What are the classifications and mechanisms of ADRs?
Adverse Drug Reactions (ADRs) Outline 1. What are Adverse Drug Reactions (ADRs)? WHAT WHY HOW 2. How important are ADRs and are they preventable? 3. What are the classifications and mechanisms of ADRs?
A Clinical Study of Stevens-Johnson Syndrome and Toxic Epidermal Necrolysis: Efficacy of Treatment in Burn Intensive Care Unit
 J Korean Surg Soc 0;:133-139 DOI:.414/jkss.0..3.133 원 저 A Clinical Study of Stevens-Johnson Syndrome and Toxic Epidermal Necrolysis: Efficacy of Treatment in Burn Intensive Care Unit Departments of Surgery
J Korean Surg Soc 0;:133-139 DOI:.414/jkss.0..3.133 원 저 A Clinical Study of Stevens-Johnson Syndrome and Toxic Epidermal Necrolysis: Efficacy of Treatment in Burn Intensive Care Unit Departments of Surgery
A. Erythema multiforme and related diseases
 Go Back to the Top To Order, Visit the Purchasing Page for Details Chapter Erythema, Erythroderma (Exfoliative Dermatitis) Erythema is caused by telangiectasia or hyperemia in the papillary and reticular
Go Back to the Top To Order, Visit the Purchasing Page for Details Chapter Erythema, Erythroderma (Exfoliative Dermatitis) Erythema is caused by telangiectasia or hyperemia in the papillary and reticular
SKIN REACTIONS WITH PSYCHOTROPICS: A SYSTEMATIC REVIEW
 SKIN REACTIONS WITH PSYCHOTROPICS: A SYSTEMATIC REVIEW *Anderson Isaac, PharmD Candidate, 2019 Pooja Patel, PharmD Candidate, 2019 Katelyn Thomasson, PharmD Candidate, 2019 Erika Tillery, PharmD, BCPP,
SKIN REACTIONS WITH PSYCHOTROPICS: A SYSTEMATIC REVIEW *Anderson Isaac, PharmD Candidate, 2019 Pooja Patel, PharmD Candidate, 2019 Katelyn Thomasson, PharmD Candidate, 2019 Erika Tillery, PharmD, BCPP,
Skin Disease in the Elderly
 Special Issue Skin Disease in the Elderly DoWon Kim, M.D. Department of Dermatology Kyungpook National University School of Medicine & Hospital Email : kimdw@knu.ac.kr Abstract With the advance of socioeconomy
Special Issue Skin Disease in the Elderly DoWon Kim, M.D. Department of Dermatology Kyungpook National University School of Medicine & Hospital Email : kimdw@knu.ac.kr Abstract With the advance of socioeconomy
AOU Ospedali Riuniti - Ancona
 AOU Ospedali Riuniti - Ancona Ospedale Materno-Infantile di Alta Specializzazione G. Salesi UOC Pediatria Allergia a farmaci e infezioni: tra coesistenza e casualità fabrizio franceschini Drug Hypersensitivity
AOU Ospedali Riuniti - Ancona Ospedale Materno-Infantile di Alta Specializzazione G. Salesi UOC Pediatria Allergia a farmaci e infezioni: tra coesistenza e casualità fabrizio franceschini Drug Hypersensitivity
Diagnosis and Management of Drug-induced Stevens-Johnson Syndrome: Report of Two Cases
 10.5005/jp-journals-10011-1189 CASE REPORT JIAOMR Diagnosis and Management of Drug-induced Stevens-Johnson Syndrome: Report of Two Cases 1 M Venkateshwarlu, 2 B Radhika 1 Professor and Head, Department
10.5005/jp-journals-10011-1189 CASE REPORT JIAOMR Diagnosis and Management of Drug-induced Stevens-Johnson Syndrome: Report of Two Cases 1 M Venkateshwarlu, 2 B Radhika 1 Professor and Head, Department
To update the use of IVIG and CORTICOIDS IN management of SJS/ TEN To remind Doctors being careful when giving
 Present : Dr Pham Thi Minh Rang Internal Department No2-Hospital for children No2 AIMS To update the use of IVIG and CORTICOIDS IN management of SJS/ TEN To remind Doctors being careful when giving To
Present : Dr Pham Thi Minh Rang Internal Department No2-Hospital for children No2 AIMS To update the use of IVIG and CORTICOIDS IN management of SJS/ TEN To remind Doctors being careful when giving To
Erythema Multiforme with Reference to Atypical Presentation in an HIV-Positive Patient Following Antiretroviral Therapy Discontinuation
 2009;17(1):9-15 CLINICAL ARTICLE Erythema Multiforme with Reference to Atypical Presentation in an HIV-Positive Patient Following Antiretroviral Therapy Discontinuation Liborija Lugović Mihić, Marija Buljan,
2009;17(1):9-15 CLINICAL ARTICLE Erythema Multiforme with Reference to Atypical Presentation in an HIV-Positive Patient Following Antiretroviral Therapy Discontinuation Liborija Lugović Mihić, Marija Buljan,
DERMATOLOGICAL EMERGENCIES. DR. Ian Hoyle MBBS DIP IMC RCS (Ed), DA (UK),FRACGP,FACRRM,DIP DERM(Wales) TASMANIAN SKIN AND BODY CENTRE
 DERMATOLOGICAL EMERGENCIES DR. Ian Hoyle MBBS DIP IMC RCS (Ed), DA (UK),FRACGP,FACRRM,DIP DERM(Wales) TASMANIAN SKIN AND BODY CENTRE Dermatological Emergencies INFECTIONS ERYTHRODERMA DRUG ERUPTIONS STEVENS-JOHNSON
DERMATOLOGICAL EMERGENCIES DR. Ian Hoyle MBBS DIP IMC RCS (Ed), DA (UK),FRACGP,FACRRM,DIP DERM(Wales) TASMANIAN SKIN AND BODY CENTRE Dermatological Emergencies INFECTIONS ERYTHRODERMA DRUG ERUPTIONS STEVENS-JOHNSON
CASE REPORT ATYPICAL BULLOUS PYODERMA GANGRENOSUM WITH EARLY LESIONS MIMICKING CHICKEN POX
 ATYPICAL BULLOUS PYODERMA GANGRENOSUM WITH EARLY LESIONS MIMICKING CHICKEN POX Ramesh M 1, Kavya Raju Nayak 2, M.G. Gopal 3, Sharath Kumar B.C 4, Nandini A.S 5 HOW TO CITE THIS ARTICLE: Ramesh M, Kavya
ATYPICAL BULLOUS PYODERMA GANGRENOSUM WITH EARLY LESIONS MIMICKING CHICKEN POX Ramesh M 1, Kavya Raju Nayak 2, M.G. Gopal 3, Sharath Kumar B.C 4, Nandini A.S 5 HOW TO CITE THIS ARTICLE: Ramesh M, Kavya
Egyptian Dermatology Online Journal Vol. 6 No 1: 14, June 2010
 Wells Syndrome H. Gammaz, H. Amer, A. Adly and S. Mahmoud Egyptian Dermatology Online Journal 6 (1): 14 Al-Haud Al-Marsoud Hospital, Cairo, Egypt e-mail: hananderma@hotmail.com Submitted: April 15, 2010
Wells Syndrome H. Gammaz, H. Amer, A. Adly and S. Mahmoud Egyptian Dermatology Online Journal 6 (1): 14 Al-Haud Al-Marsoud Hospital, Cairo, Egypt e-mail: hananderma@hotmail.com Submitted: April 15, 2010
EM minor EM major SJS SJS-TEN TEN
 North American study of pediatric SJS and TEN: Setting diagnostic criteria, systematic review and retrospective cohort analysis comparing outcomes of common treatments Michele Ramien, MDCM, FRCPC Dermatology,
North American study of pediatric SJS and TEN: Setting diagnostic criteria, systematic review and retrospective cohort analysis comparing outcomes of common treatments Michele Ramien, MDCM, FRCPC Dermatology,
Department of Dermatology, Christian Medical College and Hospital, Ludhiana, Punjab, India.
 Bullous pemphigoid mimicking granulomatous inflammation Abhilasha Williams, Emy Abi Thomas. Department of Dermatology, Christian Medical College and Hospital, Ludhiana, Punjab, India. Egyptian Dermatology
Bullous pemphigoid mimicking granulomatous inflammation Abhilasha Williams, Emy Abi Thomas. Department of Dermatology, Christian Medical College and Hospital, Ludhiana, Punjab, India. Egyptian Dermatology
Stevens-Johnson Syndrome in patients receiving cranial irradiation and concomitant diphenylhydantoin
 Turkish Journal of Cancer Vol. 32/ No. 4/2002 Stevens-Johnson Syndrome in patients receiving cranial irradiation and concomitant diphenylhydantoin ERKAN TOPKAN, FARUK ZORLU, MURAT GÜRKAYNAK Hacettepe University
Turkish Journal of Cancer Vol. 32/ No. 4/2002 Stevens-Johnson Syndrome in patients receiving cranial irradiation and concomitant diphenylhydantoin ERKAN TOPKAN, FARUK ZORLU, MURAT GÜRKAYNAK Hacettepe University
GOOD MORNING! AUGUST 5, 2014
 GOOD MORNING! AUGUST 5, 2014 PREP QUESTION During the health supervision visit of a term newborn boy, his mother relates that a cousins child died at age 4 months from sudden infant death syndrome. She
GOOD MORNING! AUGUST 5, 2014 PREP QUESTION During the health supervision visit of a term newborn boy, his mother relates that a cousins child died at age 4 months from sudden infant death syndrome. She
Case Report Cephazolin-Induced Toxic Epidermal Necrolysis Treated with Intravenous Immunoglobulin and N-Acetylcysteine
 Case Reports in Immunology Volume 2012, Article ID 931528, 4 pages doi:10.1155/2012/931528 Case Report Cephazolin-Induced Toxic Epidermal Necrolysis Treated with Intravenous Immunoglobulin and N-Acetylcysteine
Case Reports in Immunology Volume 2012, Article ID 931528, 4 pages doi:10.1155/2012/931528 Case Report Cephazolin-Induced Toxic Epidermal Necrolysis Treated with Intravenous Immunoglobulin and N-Acetylcysteine
Bugs and Drugs: What s New in Hypersensitivity Reactions?
 Bugs and Drugs: What s New in Hypersensitivity Reactions? Erin Mathes, MD Associate Professor of Dermatology and Pediatrics University of California, San Francisco DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY
Bugs and Drugs: What s New in Hypersensitivity Reactions? Erin Mathes, MD Associate Professor of Dermatology and Pediatrics University of California, San Francisco DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY
PHENYTION, CARBAMAZEPINE, SODIUM VALPROATE AND LAMOTRIGINE INDUCED CUTANEOUS REACTIONS
 PHENYTION, CARBAMAZEPINE, SODIUM VALPROATE AND LAMOTRIGINE INDUCED CUTANEOUS REACTIONS M. Ghaffarpour *, S. S. Hejazie, M. H. Harirchian and H. Pourmahmoodian Department of Neurology, Imam Khomeini Hospital,
PHENYTION, CARBAMAZEPINE, SODIUM VALPROATE AND LAMOTRIGINE INDUCED CUTANEOUS REACTIONS M. Ghaffarpour *, S. S. Hejazie, M. H. Harirchian and H. Pourmahmoodian Department of Neurology, Imam Khomeini Hospital,
EFAVIRENZ ASSOCIATED STEVENS-JOHNSON SYNDROME
 EFAVIRENZ ASSOCIATED STEVENS-JOHNSON SYNDROME To the Editor: Persons with human immunodeficiency virus (HIV) infection are highly susceptible to adverse dermatological reactions to specific medications
EFAVIRENZ ASSOCIATED STEVENS-JOHNSON SYNDROME To the Editor: Persons with human immunodeficiency virus (HIV) infection are highly susceptible to adverse dermatological reactions to specific medications
Severe cutaneous adverse reactions due to isoniazid in a HIV Positive patient
 Indian J Lepr 202, 84 : 227-232 Hind Kusht Nivaran Sangh, New Delhi http://www.ijl.org.in Case Report Severe cutaneous adverse reactions due to isoniazid in a HIV Positive patient BK Viswanath, P Ranka,
Indian J Lepr 202, 84 : 227-232 Hind Kusht Nivaran Sangh, New Delhi http://www.ijl.org.in Case Report Severe cutaneous adverse reactions due to isoniazid in a HIV Positive patient BK Viswanath, P Ranka,
Clinical profile of skin diseases in accident and emergency department attenders
 Hong Kong J. Dermatol. Venereol. (2007) 15, 4-9 Original Article Clinical profile of skin diseases in accident and emergency department attenders CY Chan, KL Kam, CA Graham, TH Rainer, NM Luk Skin problems
Hong Kong J. Dermatol. Venereol. (2007) 15, 4-9 Original Article Clinical profile of skin diseases in accident and emergency department attenders CY Chan, KL Kam, CA Graham, TH Rainer, NM Luk Skin problems
PHM142 Autoimmune Disorders + Idiosyncratic Drug Reactions
 PHM142 Autoimmune Disorders + Idiosyncratic Drug Reactions 1 Autoimmune Disorders Auto-reactivity: low physiological levels (e.g. tolerance) vs. pathogenic levels 80+ types of autoimmune diseases affect
PHM142 Autoimmune Disorders + Idiosyncratic Drug Reactions 1 Autoimmune Disorders Auto-reactivity: low physiological levels (e.g. tolerance) vs. pathogenic levels 80+ types of autoimmune diseases affect
In the past few years, beta-lactam-resistant gram-positive
 Early Diagnosis Is Key in Vancomycin-Induced Linear IgA Bullous Dermatosis and Stevens-Johnson Syndrome Douglas H. Jones, MS Michael Todd, MD Timothy J. Craig, DO Background: With the emergence of highly
Early Diagnosis Is Key in Vancomycin-Induced Linear IgA Bullous Dermatosis and Stevens-Johnson Syndrome Douglas H. Jones, MS Michael Todd, MD Timothy J. Craig, DO Background: With the emergence of highly
Five things not to miss in Dermatology. Dr Judy Wismer Associate Clinical Professor Michael G DeGroote School of Medicine
 Five things not to miss in Dermatology Dr Judy Wismer Associate Clinical Professor Michael G DeGroote School of Medicine Key Descriptives Fever, skin pain Purpura, necrosis Bullae, Mucosal, Skin sloughing
Five things not to miss in Dermatology Dr Judy Wismer Associate Clinical Professor Michael G DeGroote School of Medicine Key Descriptives Fever, skin pain Purpura, necrosis Bullae, Mucosal, Skin sloughing
DERMATOLOGIC EMERGENCIES. Mary Evers D.O., F.A.O.C.D. Georgetown, Texas
 DERMATOLOGIC EMERGENCIES Mary Evers D.O., F.A.O.C.D. Georgetown, Texas SKIN EMERGENCIES??? Subclassifications: Autoimmune (Anaphylaxis, Vasculitis, Pemphigus) Erythroderma (AGEP, DRESS, SJS, TEN) Infectious
DERMATOLOGIC EMERGENCIES Mary Evers D.O., F.A.O.C.D. Georgetown, Texas SKIN EMERGENCIES??? Subclassifications: Autoimmune (Anaphylaxis, Vasculitis, Pemphigus) Erythroderma (AGEP, DRESS, SJS, TEN) Infectious
cipro loxacin; stevens-johnson syndrome; urinary tract infection; adverse drug reaction
 Open Journal of Clinical & Medical Case Reports Volume 3 (2017) Issue 7 ISSN 2379-1039 Cipro loxacin induced Stevens Johnson syndrome: A case report on Dermatology department P Mohammed Sha i*; K Narotham
Open Journal of Clinical & Medical Case Reports Volume 3 (2017) Issue 7 ISSN 2379-1039 Cipro loxacin induced Stevens Johnson syndrome: A case report on Dermatology department P Mohammed Sha i*; K Narotham
SEVERE CUTANEOUS ADVERSE DRUG REACTIONS: STEVENS-JOHNSON SYNDROME AND TOXIC EPIDERMAL NECROLYSISA, A REPORT OF 4 CASES SEEN AT UMMC
 SEVERE CUTANEOUS ADVERSE DRUG REACTIONS: STEVENS-JOHNSON SYNDROME AND TOXIC EPIDERMAL NECROLYSISA, A REPORT OF 4 CASES SEEN AT UMMC Shasha Khairullah, Rokiah Che Ismail Department of Medicine, Faculty
SEVERE CUTANEOUS ADVERSE DRUG REACTIONS: STEVENS-JOHNSON SYNDROME AND TOXIC EPIDERMAL NECROLYSISA, A REPORT OF 4 CASES SEEN AT UMMC Shasha Khairullah, Rokiah Che Ismail Department of Medicine, Faculty
Prevalence of pruritus in psoriatic skin lesions and its relations to different variables
 Original Article Prevalence of pruritus in psoriatic skin lesions and its relations to different variables Satyendra Kumar Singh Department of Dermatology & Venereology, Institute of Medical Sciences,
Original Article Prevalence of pruritus in psoriatic skin lesions and its relations to different variables Satyendra Kumar Singh Department of Dermatology & Venereology, Institute of Medical Sciences,
Drug eruptions and hepatic involvement: a study
 International Journal of Research in Dermatology http://www.ijord.com Original Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4529.intjresdermatol20183819 Drug eruptions and hepatic involvement:
International Journal of Research in Dermatology http://www.ijord.com Original Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4529.intjresdermatol20183819 Drug eruptions and hepatic involvement:
Warfarin-induced toxic epidermal necrolysis in combination therapy of Henoch- Schönlein purpura nephritis: a case report
 Kasahara et al. BMC Nephrology (2017) 18:237 DOI 10.1186/s12882-017-0648-9 CASE REPORT Open Access Warfarin-induced toxic epidermal necrolysis in combination therapy of Henoch- Schönlein purpura nephritis:
Kasahara et al. BMC Nephrology (2017) 18:237 DOI 10.1186/s12882-017-0648-9 CASE REPORT Open Access Warfarin-induced toxic epidermal necrolysis in combination therapy of Henoch- Schönlein purpura nephritis:
8/8/2016. Overview. Back to Basics: Immunology. Adverse Reactions to Drugs: Dispelling Myths
 Adverse Reactions to Drugs: Dispelling Myths Allison Ramsey, MD NPA Annual Conference September 30, 2016 Overview Review of types of hypersensitivity reactions Penicillin allergy IV contrast allergy Local
Adverse Reactions to Drugs: Dispelling Myths Allison Ramsey, MD NPA Annual Conference September 30, 2016 Overview Review of types of hypersensitivity reactions Penicillin allergy IV contrast allergy Local
=ﻰﻤاﻤﺤﻠا ﺔﻴﻘﻠﺤﻠا ﺔذﺒاﻨﻠا
 1 / 15 Erythema Annulare Centrifugum and Other Figurate Erythemas The figurate erythemas include a variety of eruptions characterized by annular and polycyclic lesions. Classification of this group has
1 / 15 Erythema Annulare Centrifugum and Other Figurate Erythemas The figurate erythemas include a variety of eruptions characterized by annular and polycyclic lesions. Classification of this group has
1 Introduction. Kenneth Irungu 1 David Nyamu
 Drugs - Real World Outcomes (2017) 4:79 85 DOI 10.1007/s40801-017-0105-x ORIGINAL RESEARCH ARTICLE Characterization of Stevens Johnson Syndrome and Toxic Epidermal Necrolysis Among Patients Admitted to
Drugs - Real World Outcomes (2017) 4:79 85 DOI 10.1007/s40801-017-0105-x ORIGINAL RESEARCH ARTICLE Characterization of Stevens Johnson Syndrome and Toxic Epidermal Necrolysis Among Patients Admitted to
Skin Manifestations of Systemic Disease. Approach to Dermatalogic Diagnosis 9/6/2016. Go Ahead---Judge a Book by its Cover!
 Go Ahead---Judge a Book by its Cover! Skin Manifestations of Systemic Disease Amelie Hollier, DNP, FNP-BC, FAANP Lafayette, LA President, APEA Objectives Compare diseases of the skin with reactions of
Go Ahead---Judge a Book by its Cover! Skin Manifestations of Systemic Disease Amelie Hollier, DNP, FNP-BC, FAANP Lafayette, LA President, APEA Objectives Compare diseases of the skin with reactions of
New product information wording Extracts from PRAC recommendations on signals
 12 October 2017 EMA/PRAC/610988/2017 Pharmacovigilance Risk Assessment Committee (PRAC) New product information wording Extracts from PRAC recommendations on signals Adopted at the 25-29 September 2017
12 October 2017 EMA/PRAC/610988/2017 Pharmacovigilance Risk Assessment Committee (PRAC) New product information wording Extracts from PRAC recommendations on signals Adopted at the 25-29 September 2017
Cutaneous manifestations of Systemic Lupus Erythematosus
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 5 Ver. 11 (May. 2018), PP 01-08 www.iosrjournals.org Cutaneous manifestations of Systemic Lupus
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 5 Ver. 11 (May. 2018), PP 01-08 www.iosrjournals.org Cutaneous manifestations of Systemic Lupus
Fluconazole erythema multiforme
 Fluconazole erythema multiforme Search 1. Eur J Dermatol. 2012 Sep-Oct;22(5):693-4. doi: 10.1684/ejd.2012.1806. Fluconazoleinduced fixed drug eruption imitating herpes labialis with erythema multiforme.
Fluconazole erythema multiforme Search 1. Eur J Dermatol. 2012 Sep-Oct;22(5):693-4. doi: 10.1684/ejd.2012.1806. Fluconazoleinduced fixed drug eruption imitating herpes labialis with erythema multiforme.
Dermatology GP Referral Guidelines
 Austin Health Dermatology Department holds 5 Clinic sessions to discuss and plan the treatment of with Dermatology conditions. Department of Health clinical urgency categories for specialist clinics Urgent:
Austin Health Dermatology Department holds 5 Clinic sessions to discuss and plan the treatment of with Dermatology conditions. Department of Health clinical urgency categories for specialist clinics Urgent:
Title: Cutaneous Adverse Drug Reactions in Indian population: A systematic review
 Title: Cutaneous Adverse Drug Reactions in Indian population: A systematic review Review question(s) To carry out a systematic review of the published evidence of the cutaneous adverse drug reactions in
Title: Cutaneous Adverse Drug Reactions in Indian population: A systematic review Review question(s) To carry out a systematic review of the published evidence of the cutaneous adverse drug reactions in
Dexamethasone Pulse Therapy for Stevens-Johnson Syndrome/ Toxic Epidermal Necrolysis
 Acta Derm Venereol 2007; 87: 144 148 CLINICAL REPORT Dexamethasone Pulse Therapy for Stevens-Johnson Syndrome/ Toxic Epidermal Necrolysis Sylvia H. Kardaun and Marcel F. Jonkman Center for Blistering Diseases,
Acta Derm Venereol 2007; 87: 144 148 CLINICAL REPORT Dexamethasone Pulse Therapy for Stevens-Johnson Syndrome/ Toxic Epidermal Necrolysis Sylvia H. Kardaun and Marcel F. Jonkman Center for Blistering Diseases,
Endocarditis. By : Mehrnoush. dianatkhah
 Endocarditis By : Mehrnoush. dianatkhah Case 5.31, 31 years old woman CC : Fever, dyspnea, 3 days postpartum PMH : Mitral prolapse Fever 38.5 WBC : 8900 ESR : 84 CRP : 10.4 Cr : 0.6 NT Pro BNP: 5469 Physical
Endocarditis By : Mehrnoush. dianatkhah Case 5.31, 31 years old woman CC : Fever, dyspnea, 3 days postpartum PMH : Mitral prolapse Fever 38.5 WBC : 8900 ESR : 84 CRP : 10.4 Cr : 0.6 NT Pro BNP: 5469 Physical
New product information wording Extracts from PRAC recommendations on signals
 20 July 2017 EMA/PRAC/406976/2017 Pharmacovigilance Risk Assessment Committee (PRAC) New product information wording Extracts from PRAC recommendations on signals Adopted at the 3-6 July 2017 PRAC The
20 July 2017 EMA/PRAC/406976/2017 Pharmacovigilance Risk Assessment Committee (PRAC) New product information wording Extracts from PRAC recommendations on signals Adopted at the 3-6 July 2017 PRAC The
The Role of Plasmacytoid Dendritic Cells in Psoriasis
 6 ème Journée du Groupe de Recherche sur le Psoriasis Paris, 9 novembre 2012 The Role of Plasmacytoid Dendritic Cells in Psoriasis Dr Curdin Conrad, PD & MER Department of Dermatology Psoriasis: Clinical
6 ème Journée du Groupe de Recherche sur le Psoriasis Paris, 9 novembre 2012 The Role of Plasmacytoid Dendritic Cells in Psoriasis Dr Curdin Conrad, PD & MER Department of Dermatology Psoriasis: Clinical
Clozapine Induced Skin Rash a report of two cases
 Jambulkar et al. : Clozapine induced skin rash 405 Case Report Clozapine Induced Skin Rash a report of two cases Reena Jambulkar 1, Sagar Karia 2, Akshay Chordia 3, Avinash De Sousa 4, Nilesh Shah 5 1,3
Jambulkar et al. : Clozapine induced skin rash 405 Case Report Clozapine Induced Skin Rash a report of two cases Reena Jambulkar 1, Sagar Karia 2, Akshay Chordia 3, Avinash De Sousa 4, Nilesh Shah 5 1,3
Syndrome de Lyell Approche diagnostique. seminaires iris. Veronique del Marmol Alexandre Chamoun Service de Dermatologie Hôpital Erasme.
 Syndrome de Lyell Approche diagnostique Veronique del Marmol Alexandre Chamoun Service de Dermatologie Hôpital Erasme Serge Jennes Hôpital Militaire Rash benign Pustulose exanthematique Aigue et généralisée
Syndrome de Lyell Approche diagnostique Veronique del Marmol Alexandre Chamoun Service de Dermatologie Hôpital Erasme Serge Jennes Hôpital Militaire Rash benign Pustulose exanthematique Aigue et généralisée
Study No.: Title: Rationale: Phase: Study Period: Study Design: Centers: Indication: Treatment: Objectives: Primary Outcome/Efficacy Variable:
 The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
Risk Factors and Management of Mood Stabilizer-associated Stevens-Johnson Syndrome/Toxic Epidermal Necrolysis: A Mini-review
 140 Taiwanese Journal of Psychiatry (Taipei) Vol. 25 No. 3 2011 Overview Risk Factors and Management of Mood Stabilizer-associated Stevens-Johnson Syndrome/Toxic Epidermal Necrolysis: A Mini-review Gen-Tang
140 Taiwanese Journal of Psychiatry (Taipei) Vol. 25 No. 3 2011 Overview Risk Factors and Management of Mood Stabilizer-associated Stevens-Johnson Syndrome/Toxic Epidermal Necrolysis: A Mini-review Gen-Tang
Address for correspondence: Dr. Patel Raksha M. R-3, Doctor s Quarters, Jail Road, Vadodara- 01, Gujarat, India.
 Clinical study of cutaneous drug eruptions in 200 patients Raksha M. Patel, Y. S. Marfatia Department of Skin and V.D, Medical College, Vadodara, Gujarat, India Address for correspondence: Dr. Patel Raksha
Clinical study of cutaneous drug eruptions in 200 patients Raksha M. Patel, Y. S. Marfatia Department of Skin and V.D, Medical College, Vadodara, Gujarat, India Address for correspondence: Dr. Patel Raksha
SEVERE CUTANEUS ADVERSE DRUGS EFFECTS MANIFESTED AS TOXIC EPIDERMAL NECROLYSIS (TEN) DUE TO ORAL ANTITUBERCULOSIS DRUGS AND REVIEW OF THE LITERATURE
 SEVERE CUTANEUS ADVERSE DRUGS EFFECTS MANIFESTED AS TOXIC EPIDERMAL NECROLYSIS (TEN) DUE TO ORAL ANTITUBERCULOSIS DRUGS AND REVIEW OF THE LITERATURE * HM Nataprawira, ** M Soepriadi * Respirology Division,
SEVERE CUTANEUS ADVERSE DRUGS EFFECTS MANIFESTED AS TOXIC EPIDERMAL NECROLYSIS (TEN) DUE TO ORAL ANTITUBERCULOSIS DRUGS AND REVIEW OF THE LITERATURE * HM Nataprawira, ** M Soepriadi * Respirology Division,
Subject Outline: Dermatology II
 Subject Outline: Dermatology II Course: Master of Dermatology (Coursework) Subject: Dermatology II (An introduction to clinical dermatology) Credit Points: 3 Year/Semester Delivered: 1/2 Subject Outline:
Subject Outline: Dermatology II Course: Master of Dermatology (Coursework) Subject: Dermatology II (An introduction to clinical dermatology) Credit Points: 3 Year/Semester Delivered: 1/2 Subject Outline:
DESCRIPTIONS FOR MED 3 ROTATIONS Dermatology A3S
 Regardless of your future field of practice, you will be exposed to a considerable amount of dermatology and this rotation provides you the chance to see a range of skin diseases. You will have the opportunity
Regardless of your future field of practice, you will be exposed to a considerable amount of dermatology and this rotation provides you the chance to see a range of skin diseases. You will have the opportunity
MabThera. SC. The wait is over. MabThera delivered in just 5 minutes. SC= subcutaneous injection
 MabThera SC. The wait is over. MabThera delivered in just 5 minutes Abbreviated Prescribing Information MabThera 1400 mg solution for subcutaneous (SC) injection (Rituximab) Indications: Indicated in adults
MabThera SC. The wait is over. MabThera delivered in just 5 minutes Abbreviated Prescribing Information MabThera 1400 mg solution for subcutaneous (SC) injection (Rituximab) Indications: Indicated in adults
COPYRIGHTED MATERIAL. Introduction CHAPTER 1. Introduction
 CHAPTER 1 Introduction OVERVIEW The clinical features of skin lesions are related to the underlying pathological processes. Broadly skin conditions fall into three clinical groups: (a) those with a well-defined
CHAPTER 1 Introduction OVERVIEW The clinical features of skin lesions are related to the underlying pathological processes. Broadly skin conditions fall into three clinical groups: (a) those with a well-defined
Egyptian Dermatology Online Journal Vol. 5 No 2:16, December Squamous Cell Carcinoma Arising on Extensive and Chronic Lupus Vulgaris
 Squamous Cell Carcinoma Arising on Extensive and Chronic Lupus Vulgaris Pathak D.* and Thapa A** Egyptian Dermatology Online Journal 5 (2): 16 * Consultant Dermatologist, Delhi Dermatology Group Kubba,
Squamous Cell Carcinoma Arising on Extensive and Chronic Lupus Vulgaris Pathak D.* and Thapa A** Egyptian Dermatology Online Journal 5 (2): 16 * Consultant Dermatologist, Delhi Dermatology Group Kubba,
HEMORRHAGIC BULLOUS HENOCH- SCHONLEIN PURPURA: A CASE REPORT
 HEMORRHAGIC BULLOUS HENOCH- SCHONLEIN PURPURA: A CASE REPORT Nirmala Ponnuthurai, Sabeera Begum, Lee Bang Rom Paediatric Dermatology Unit, Institute of Paediatric, Hospital Kuala Lumpur, Malaysia Abstract
HEMORRHAGIC BULLOUS HENOCH- SCHONLEIN PURPURA: A CASE REPORT Nirmala Ponnuthurai, Sabeera Begum, Lee Bang Rom Paediatric Dermatology Unit, Institute of Paediatric, Hospital Kuala Lumpur, Malaysia Abstract
TOXIC EPIDERMAL NECROLYSIS AND CLARITHROMYCIN
 TOXIC EPIDERMAL NECROLYSIS AND CLARITHROMYCIN Nadia Khaldi 1, Alain Miras 1, Sophie Gromb 1,2 1 Forensic Science Laboratory, Pellegrin Hospital, University Teaching Hospital Bordeaux, France, 2 Forensic
TOXIC EPIDERMAL NECROLYSIS AND CLARITHROMYCIN Nadia Khaldi 1, Alain Miras 1, Sophie Gromb 1,2 1 Forensic Science Laboratory, Pellegrin Hospital, University Teaching Hospital Bordeaux, France, 2 Forensic
REVIEW ARTICLES ADVERSE DRUG REACTION: A COMMON DERMATOLOGICAL EMERGENCY
 REVIEW ARTICLES ADVERSE DRUG REACTION: A COMMON DERMATOLOGICAL EMERGENCY LUBNA KHONDKER 1, MD ABDUL WAHAB 2, MD SHIRAJUL ISLAM KHAN 3. Abstract In the evaluation of patients with a history of adverse cutaneous
REVIEW ARTICLES ADVERSE DRUG REACTION: A COMMON DERMATOLOGICAL EMERGENCY LUBNA KHONDKER 1, MD ABDUL WAHAB 2, MD SHIRAJUL ISLAM KHAN 3. Abstract In the evaluation of patients with a history of adverse cutaneous
ACUTE ANNULAR URTICARIA IN A CHILD
 The West London Medical Journal 2013 Vol 5 No 2 pp 1-5 ACUTE ANNULAR URTICARIA IN A CHILD Aaron Yon Dayse Fernandes Michelle Pike Jodi Newcombe Colin Michie 1. ABSTRACT Urticarial skin rashes have a range
The West London Medical Journal 2013 Vol 5 No 2 pp 1-5 ACUTE ANNULAR URTICARIA IN A CHILD Aaron Yon Dayse Fernandes Michelle Pike Jodi Newcombe Colin Michie 1. ABSTRACT Urticarial skin rashes have a range
CLINICAL GUIDELINES. Summary of Literature and Recommendations Concerning Immunization and Steroid Injections Thomas J. Gilbert M.D., M.P.P.
 CLINICAL GUIDELINES Summary of Literature and Recommendations Concerning Immunization and Steroid Injections Thomas J. Gilbert M.D., M.P.P. 11/2/15 Several practices routinely delay steroid injections
CLINICAL GUIDELINES Summary of Literature and Recommendations Concerning Immunization and Steroid Injections Thomas J. Gilbert M.D., M.P.P. 11/2/15 Several practices routinely delay steroid injections
Drug induced allergy and hypersensitivity
 Drug induced allergy and hypersensitivity Yunita Sari Pane, Aznan Lelo Dept. Pharmacology & Therapeutic School of Medicine Universitas Sumatera Utara 13 Mei 2009, KBK-FK USU, Medan Drug Allergy Adverse
Drug induced allergy and hypersensitivity Yunita Sari Pane, Aznan Lelo Dept. Pharmacology & Therapeutic School of Medicine Universitas Sumatera Utara 13 Mei 2009, KBK-FK USU, Medan Drug Allergy Adverse
Prevention of severe cutaneous adverse drug reactions: the emerging value of pharmacogenetic screening
 CMAJ Cases Prevention of severe cutaneous adverse drug reactions: the emerging value of pharmacogenetic screening Suran L. Fernando MB BS PhD, Andrew J. Broadfoot MB BS Previously published at www.cmaj.ca
CMAJ Cases Prevention of severe cutaneous adverse drug reactions: the emerging value of pharmacogenetic screening Suran L. Fernando MB BS PhD, Andrew J. Broadfoot MB BS Previously published at www.cmaj.ca
A Middle-Aged Man with Newly Diagnosed HIV Infection and Rash
 CLINICAL CASE OF THE MONTH A Middle-Aged Man with Newly Diagnosed HIV Infection and Rash Patrick Njoku, MD; Temeka Tate, MD; Sousan Zadeh, MD; Erin Hauck, MD; Anila Chaudhry, MD; Betty Lo-Blais, MD; Lee
CLINICAL CASE OF THE MONTH A Middle-Aged Man with Newly Diagnosed HIV Infection and Rash Patrick Njoku, MD; Temeka Tate, MD; Sousan Zadeh, MD; Erin Hauck, MD; Anila Chaudhry, MD; Betty Lo-Blais, MD; Lee
Cutaneous drug reactions
 Maintenance of Certification clinical management series Series editor: James T. Li, MD, PhD Cutaneous drug reactions David A. Khan, MD Dallas, Tex INSTRUCTIONS Credit can now be obtained, free for a limited
Maintenance of Certification clinical management series Series editor: James T. Li, MD, PhD Cutaneous drug reactions David A. Khan, MD Dallas, Tex INSTRUCTIONS Credit can now be obtained, free for a limited
Undergraduate Dermatology Curriculum July 2016
 Undergraduate Dermatology Curriculum July 2016 British Association of Dermatologists Introduction This document is the 2016 revised dermatology undergraduate curriculum (UK) from the British Association
Undergraduate Dermatology Curriculum July 2016 British Association of Dermatologists Introduction This document is the 2016 revised dermatology undergraduate curriculum (UK) from the British Association
Stevens - Johnson syndrome (SJS) and Toxic Epidermal Necrolysis (TEN) In Sarawak: A Four Years Review
 Stevens - Johnson syndrome (SJS) and Toxic Epidermal Necrolysis (TEN) In Sarawak: A Four Years Review Yap FBB, MRCP; Wahiduzzaman M, MBBS; Pubalan M, MRCP. Egyptian Dermatology Online Journal 4 (1): 1,
Stevens - Johnson syndrome (SJS) and Toxic Epidermal Necrolysis (TEN) In Sarawak: A Four Years Review Yap FBB, MRCP; Wahiduzzaman M, MBBS; Pubalan M, MRCP. Egyptian Dermatology Online Journal 4 (1): 1,
JMSCR Vol 05 Issue 10 Page October 2017
 www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i10.125 Histomorphological Study of Lichen Planus
www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i10.125 Histomorphological Study of Lichen Planus
Cutaneous adverse drug reactions in a tertiary care hospital
 Available online at www.scholarsresearchlibrary.com Scholars Research Library Der Pharmacia Lettre, 202, 4 (2):408-43 (http://scholarsresearchlibrary.com/archive.html) ISSN 0975-507 USA CODEN: DPLEB4 Cutaneous
Available online at www.scholarsresearchlibrary.com Scholars Research Library Der Pharmacia Lettre, 202, 4 (2):408-43 (http://scholarsresearchlibrary.com/archive.html) ISSN 0975-507 USA CODEN: DPLEB4 Cutaneous
Clinico Pathological Test SCPA605-Essential Pathology
 Clinico Pathological Test SCPA605-Essential Pathology Somphong Narkpinit, M.D. Department of Pathogbiology, Faculty of Science, Mahidol University e-mail : somphong.nar@mahidol.ac.th Pathogenesis of allergic
Clinico Pathological Test SCPA605-Essential Pathology Somphong Narkpinit, M.D. Department of Pathogbiology, Faculty of Science, Mahidol University e-mail : somphong.nar@mahidol.ac.th Pathogenesis of allergic
An unpredictable, dose-independent adverse drug reaction which is immunologically or IgEmediated.
 R H E U M A T I S M D I S O R D E R S A N D A L L E R G I E S APPROACH TO DRUG ALLERGY Dr Bernard Thong DEFINITION OF DRUG ALLERGY An unpredictable, dose-independent adverse drug reaction which is immunologically
R H E U M A T I S M D I S O R D E R S A N D A L L E R G I E S APPROACH TO DRUG ALLERGY Dr Bernard Thong DEFINITION OF DRUG ALLERGY An unpredictable, dose-independent adverse drug reaction which is immunologically
What's New in Oncodermatopathology: Immunotherapy Reactions
 What's New in Oncodermatopathology: Immunotherapy Reactions Emily Y. Chu, M.D., Ph.D. Assistant Professor of Dermatology & Pathology and Laboratory Medicine Hospital of the University of Pennsylvania March
What's New in Oncodermatopathology: Immunotherapy Reactions Emily Y. Chu, M.D., Ph.D. Assistant Professor of Dermatology & Pathology and Laboratory Medicine Hospital of the University of Pennsylvania March
University Journal of Pre and Para Clinical Sciences
 ISSN 2455 2879 Volume 2 Issue 4 2016 CASE REPORT- A RARE CASE OF DAPSONE HYPERSENSITIVITY SYNDROME VINOTH KUMAR CHITTARANJAN Department of Pharmacology, MADRAS MEDICAL COLLEGE AND GOVERNMENT GENERAL HOSPITAL
ISSN 2455 2879 Volume 2 Issue 4 2016 CASE REPORT- A RARE CASE OF DAPSONE HYPERSENSITIVITY SYNDROME VINOTH KUMAR CHITTARANJAN Department of Pharmacology, MADRAS MEDICAL COLLEGE AND GOVERNMENT GENERAL HOSPITAL
If a drug trigger is suspected, stop the offending drug as this may reduce the risk of relapse.
 There is so much we don't know in medicine that could make a difference, and often we focus on the big things, and the little things get forgotten. To highlight some smaller but important issues, we've
There is so much we don't know in medicine that could make a difference, and often we focus on the big things, and the little things get forgotten. To highlight some smaller but important issues, we've
STEVENS-JOHNSON SYNDROME AND TOXIC EPIDERMAL NECROLYSIS IN CHILDREN: A LITERATURE REVIEW OF CURRENT TREATMENTS
 STEVENS-JOHNSON SYNDROME AND TOXIC EPIDERMAL NECROLYSIS IN CHILDREN: A LITERATURE REVIEW OF CURRENT TREATMENTS *Blanca R. Del Pozzo-Magaña, 1 Alejandro Lazo-Langner 2,3 1. Department of Pediatrics, University
STEVENS-JOHNSON SYNDROME AND TOXIC EPIDERMAL NECROLYSIS IN CHILDREN: A LITERATURE REVIEW OF CURRENT TREATMENTS *Blanca R. Del Pozzo-Magaña, 1 Alejandro Lazo-Langner 2,3 1. Department of Pediatrics, University
