Stroke on the acute medical take
|
|
|
- Erica Jacobs
- 5 years ago
- Views:
Transcription
1 Clinical Medicine 2010, Vol 10, No 1: Stroke on the acute medical take T Hughes, consultant neurologist, University Hospital of Wales, Cardiff This article is based on the excellent recent stroke guideline from the Royal College of Physicians (RCP) which is comprehensive, evidence based and easy both to read and to use. 1 From the perspective of the physician on-take, the approach to stroke medicine is changing because thrombolysis is now considered best practice if given within three hours of onset of symptoms. 2 Time is now in short supply and on the side of the stroke mimics. Diagnosis Triage A Face Arm Speech Test (FAST) 3 should be used outside hospital as a screening test for stroke and transient ischaemic attack (TIA), and the Recognition of Stroke in the Emergency Room (ROSIER) test 4 by hospital healthcare staff. Stroke patients can be difficult to prioritise on a busy medical take which may include: patients unable to recognise their new disability (anosagnosia) due to their right parietal infarct people with a mild or recovering limb weakness in whom a dense quadrantanopia (of interest to the DVLA) may pass unsuspected, and people dramatically unwell with a branch vertebral artery occlusion. The lack of a close or reliable relationship between the severity and nature of the vascular pathology within the nervous system and the drama of its clinical presentation, coupled with the tendency for ischaemic symptoms to be negative rather than positive, militates against all patients with ischaemic stroke being recognised as in need of urgent attention. When compared to bleeding, pain or breathlessness, the symptoms and signs of ischaemic cerebrovascular disease do not lend themselves to the triage process. Stroke patients do not do autotriage. Differential diagnosis The arrival of a door-to-needle type mentality amongst frontline staff may lead to more incorrect diagnoses of stroke. The acute non-neurological causes of disability, including fractures of upper and lower limb bones, tendon ruptures, dislocations and joint effusions have already triggered concerns in our department following triage-type, snapshot assessments. It seems entirely reasonable for ischaemic vascular disease to be part of a clinician s differential diagnosis when faced for the first time with patients who subsequently will be shown to have (to name just a few): localised cerebral malignancy or infection myasthenia gravis Wernicke s encephalopathy Miler Fisher syndrome and other partial forms of Guillain-Barré syndrome benign positional paroxysmal vertigo (BPPV) Ménière s disease subdural haematoma (Fig 1) hypo- and hyperglycaemia, or compressive cervical cord lesions (particularly when presenting with asymmetric weakness). Key Points Fig 1. Computed tomography head scan showing large subdural haematoma. The patient had been treated with antiplatelet therapy for symptoms thought to be due to transient cerebral ischaemia. He required a craniectomy and a prolonged period of neurorehabilitation. The causes of episodic weakness (eg migraine, channelopathies and epilepsy (post-ictally)) will also cause some diagnostic problems when presenting for the first time. Although demyelination typically affects the optic nerve, the spinal cord and the cerebellar peduncles, it can present with a hemiparesis or hemisensory loss, and rarely with cortical type deficits due to lesions in the thalamus. Vascular causes of ischaemia not attributable to in situ arterial thrombosis or arterial emboli will also produce the clinical picture of ischaemic stroke and, if diagnosed, raise questions about the The immaturity of some clinical signs can make the diagnosis of acute ischaemic stroke difficult in the first few hours after symptom onset Thrombolysis for ischaemic stroke is licensed for use in the first three hours after symptom onset All clinicians need to be aware of the inclusion and exclusion criteria for thrombolysis Prompt initiation of secondary prevention following a transient ischaemic attack dramatically reduces the incidence of further events KEY WORDS: clinical signs, stroke, thrombolysis, transient ischaemic attack 68 Royal College of Physicians, All rights reserved.
2 appropriateness of thrombolysis, for example: venous infarction related to venous sinus thrombosis low flow states with associated infarction due to bilateral critical carotid stenosis large artery dissection causing hypoperfusion rather than embolic complications cerebral vasculitis, and profound hypotension or hypoxia. History There are familiar and useful pointers in the story even though the patient or their relatives may not have had a chance to work out what it is they can and cannot do. The symptoms which make ischaemic cerebrovascular disease less likely include: severe headache (although some headache may be present, particularly in posterior circulation large artery events, with or without dissection) loss of consciousness at an early stage, with the exception of infarcts of the paramedian thalamus which can present with coma pain in the affected limb at presentation the discomfort of hypertonia, the musculoskeletal complications of the upper motor neurone syndrome and central post-stroke pain, usually come weeks or months later lone vertigo, usually due to BPPV or viral labyrinthitis. Vague symptoms such as slurred speech, transiently blurred vision, unsteadiness, dizziness and clumsiness are anatomically unhelpful but do not exclude a focal ischaemic event. Some constellations of symptoms (and signs) described during the course of a telephone referral may not at first suggest a single lesion, for example: medullary infarcts causing weakness of one arm and the opposite leg (the so-called cruciate hemiparesis) bilateral ptosis with unilateral third nerve nucleus infarcts Table 1. Clinical deficits associated with different vascular territories of the brain. Anatomical location left frontal lobe infarcts causing a right hemiparesis with a (sympathetic) apraxia of the left hand a Bell s palsy with an ipsilateral gaze palsy and a contralateral hemiparesis (Foville s syndrome due to a pontine infarct), and selective involvement of the face, hand and foot in the cheiro-oralpedal syndrome. The sudden onset of the more familiar problems listed in Table 1 makes for easier telephone triage. Examination If the problem is thought to be vascular, a detailed general medical examination Common neurological deficits Left middle cerebral artery Right-sided weakness involving face and arm leg with expressive, receptive or mixed dysphasia Right middle cerebral artery Left-sided weakness, face and arm leg, visual and/or sensory neglect or inattention of left side, denial of disability (anosognosia) Lateral medulla (posterior Ipsilateral Horner s syndrome, Xth nerve palsy (due inferior cerebellar artery and/or to infarction of nucleus ambiguus), facial sensory loss parent vertebral artery) (trigeminal nerve), limb ataxia with contralateral spinothalamic sensory loss. Typically, patients are vertiginous and unable to feed by mouth due (mainly) to failure of laryngeal closure during swallowing and ineffective coughing. Cervical radiculopathies may occur due to involvement of radicular branches of the vertebral artery Posterior cerebral artery Homonymous hemianopia with variable additional deficits due to involvement of parietal and/or temporal lobe Internal capsule Motor, sensory or sensorimotor loss involving face, arm and leg to a roughly similar extent. There may be profound dysarthria due to involvement of corticobulbar fibres but the patient should not be dysphasic or have other cortical type deficits such as dyslexia or dysgraphia Bilateral paramedian thalamus Coma or disturbed vigilance at presentation, (30% of the population have ophthalmoplegia (internal and/or external), ataxia and a single common arterial stem memory impairment. Some patients require ventilation supplying the medial aspect of both thalami) Carotid artery dissection Ipsilateral Horner s syndrome due to compression of the sympathetic plexus around the carotid artery; the same process can also affect the lower cranial nerves (Xth and XIIth most obvious clinically) in the carotid sheath, or the VIth nerve in the cavernous sinus. If ipsilateral cerebral infarction follows (due to hypoperfusion or embolisation) the clinical picture can mimic a brain stem event; in this way, carotid artery dissection can mimic vertebral artery dissection can be of more immediate relevance than a detailed neurological examination. Neurological examination There are limitations to neurological examination in acute medicine. In the first few hours after an event some of the normally reliable upper motor neurone signs (spasticity, brisk reflexes, cocontraction, flexor or extensor spasms in response to noxious or proprioceptive stimuli) are immature or absent, making anatomical localisation difficult. Some deficits produce anatomically helpful clinical signs, but eliciting them requires considerable time, effort and cooperation between patient and doctor. This is Royal College of Physicians, All rights reserved. 69
3 particularly true for cortical cognitive deficits which are not readily apparent during conversation, for example: apraxia (dominant parietal lobe) visual and sensory inattention (nondominant parietal lobe) alexia and agraphia (left angular gyrus), and visual agnosias (non-dominant parieto-occipital cortex). Visual field defects Visual field defects are very helpful in anatomical localisation, particularly the superior and inferior quadrantinopias of temporal and parietal lobe lesions, respectively, and the hemianopia of an optic tract or occipital cortex lesion. In a cerebral lesion the speed and amplitude of saccadic eye movement to the contralateral side (ie the weak side) is often reduced,whereas the gaze palsy of a pontine lesion is to the side of the lesion (so called wrong way eyes ). Cranial nerve palsies Infarction of the nucleus or the fascicle of the nerve within the brain stem is usually the cause of the cranial nerve palsies of stroke syndromes. In conjunction with the associated motor and sensory signs, this is anatomically very helpful in localising the lesion, with the possible exception of the third nerve nucleus as mentioned above. Transient symptoms and signs The RCP guideline recommends that any person seen in hospital or the community after a short-lived acute transient event that could be due to a cerebrovascular disturbance is given aspirin 300 mg daily and referred to a specialist service. If their age, blood pressure, clinical features, duration of symptoms and diabetes (ABCD2) score is 4 or above (or if they have crescendo TIAs, defined as more than two in a week) they should have specialist assessment and investigation within 24 hours of symptom onset and within one week for those with lower ABCD2 scores. The EXPRESS study has shown how important it is to make the diagnosis of TIA, particularly in those patients at high risk of further events. 5 The incidence of such events is significantly reduced in those patients seen and treated urgently using conventional proven therapies. The risks of stroke after a TIA according to the score are listed in Table 2. Treatment Carotid endarterectomy When the diagnosis of a TIA has been confirmed, carotid Dopplers are indicated to detect those who might benefit from carotid endarterectomy. This should be 50 99% or 70 99% stenosis according to the North American Symptomatic Carotid Endarterectomy Trial (NASCET) criteria 6 and the European Carotid Surgery Trialists (ECST) Collaborative Group, 7 respectively. Suitable patients should undergo surgery within a maximum of two weeks of symptom onset. Medical therapy The RCP guideline is clear about best medical therapy. It should include giving advice and information relating to smoking, exercise, diet, weight loss, salt intake and alcohol. Blood pressure (BP) should also be controlled, ideally at 130/80 mmhg unless there are bilateral severe ( 70%) stenoses when a systolic BP of around 150 mmhg may be appropriate. If BP needs treating, for patients aged over 55 years or black patients of any age the first choice should be either a calcium-channel blocker or a thiazide-type diuretic. In hypertensive patients below 55 years the first choice should be an angiotensinconverting enzyme inhibitor (ACEI) or an angiotensin-ii receptor antagonist if an ACEI is not tolerated. Cholesterol. If total cholesterol is above 3.5 mmol/l or the low-density lipoprotein cholesterol is above 2.5 mmol/l statin therapy is recommended. Anti-platelet therapy should comprise aspirin mg per day and dipyridamole (modified release) 200 mg bd. If dipyridamole cannot be tolerated, aspirin alone is sufficient. If aspirin is not tolerated, clopidogrel 75 mg daily is a suitable alternative. The combination of aspirin and clopidogrel is not recommended. 8,9 Anticoagulants or antiplatelet therapy is recommended for people with arterial dissection, preferably as part of a randomised controlled trial (RCT) (eg CADISS 10 ). Table 2. ABCD2 risk of stroke after a transient ischaemic attack. Age Blood pressure Clinical Symptom Diabetes Score (years) (mmhg) features duration (min) mellitus /90 Other neurological deficit 10 No 1 60 Systolic 140 Speech disturbance Yes or diastolic without weakness 90 or both 2 Unilateral weakness 60 Two-day risk of stroke: Score 6 7: high risk (8.1%) 4 5: medium risk (4.1%) 0 3: low risk (1.0%) 70 Royal College of Physicians, All rights reserved.
4 Table 3. Inclusion and exclusion criteria used in the SITS-MOST study of particular relevance to the on-call general physician. 11 Inclusion Exclusion Male or female aged years Clinical diagnosis of ischaemic stroke Onset of symptoms within 3 hours of predicted initiation of thrombolysis Stroke symptoms present for at least 30 min without significant improvement before commencement of therapy Evidence of ICH on the CT scan Duration of symptoms 3 hours from likely time of initiation of tpa infusion or unknown time of symptom onset Minor neurological symptoms or symptoms rapidly improving Severe stroke, as assessed clinically or by appropriate imaging techniques Seizure at stroke onset Symptoms suggestive of SAH even if the CT scan is normal Administration of heparin within the previous 48 hours and thromboplastin time above the upper limit of normal Past history of stroke and concomitant diabetes Previous stroke within last 3 months Known platelet count 100,000/mm 3 Systolic BP 185 mmhg or diastolic 110 mmhg or the need to treat aggressively with iv medication to achieve these levels Blood glucose 50 or 400 mg/l Known haemorrhagic diathesis Warfarin therapy (although considered appropriate if INR 1.4) Recent or current bleeding Known history of or suspected ICH Presenting symptoms and signs or disability, likely to be due to recent or past SAH Known CNS disease (eg neoplasm, aneurysm, past intracranial or spinal surgery) Haemorrhagic retinopathy Recent ( 10 days) traumatic external heart massage, childbirth, puncture of a non-compressible blood vessel (eg subclavian vein) Known bacterial endocarditis, pericarditis Acute pancreatitis Documented ulcerative GI disease during the last 3 months or oesophageal varices Neoplasm with increased bleeding risk Severe liver disease Major surgery or significant trauma in last 3 months Fig 2. Computed tomography head scan showing middle cerebral artery occlusion with associated cerebral infarction and oedema 24 hours after symptom onset. Thrombolysis had been given 2 hours 40 min after presentation, without benefit. BP blood pressure; CNS central nervous system; CT computed tomography; GI gastrointestinal; ICH intracranial haemorrhage; INR international normalised ratio; iv intravenous; SAH subarachnoid haemorrhage; tpa tissue plasminogen activator. Warfarin is recommended for patients with persistent or paroxysmal atrial fibrillation, heparin and then warfarin for patients with cerebral venous sinus thrombosis (including those with secondary cerebral haemorrhage). Recommendations for stroke Thrombolysis The RCP guideline emphasises the need for thrombolysis to be given by physicians trained and experienced in the management of acute stroke, within a well organised stroke service with appropriate protocols for giving thrombolysis and managing the post-thrombolysis complications. The SITS-MOST study 11 compared the results of symptomatic intracerebral haemorrhage and death (primary end-points) and independence (secondary end-point) for stroke patients treated with recombinant tissue plasminogen activator (rt-pa) in routine clinical settings with those from corresponding rt-pa treated patients in RCTs. This observational study confirmed that intravenous alteplase is safe and effective in routine clinical use Fig 3. Computed tomography head scan showing changes following craniectomy. The patient survived and now does standing transfers independently six months after surgery. when given within three hours of stroke onset, even in centres with little previous experience of thrombolytic therapy for acute stroke. For those centres not involved in thrombolysis, the Third International Stroke Trial is an excellent way to start. 12 The inclusion and exclusion criteria used in the SITS-MOST study protocol serve as a guide for the on-call physician regarding the suitability of patients for referral to a thrombolysis service (Table 3). Royal College of Physicians, All rights reserved. 71
5 Decompressive craniectomy Decompressive craniectomy can be a lifesaving intervention for people with raised intracranial pressure occurring as a result of infarct-related cerebral oedema (Figs 2 and 3). Patients should be referred within 24 hours of symptom onset and treated within 48 hours. Patients under 60 years who have a middle cerebral artery infarct involving at least 50% of the middle cerebral artery territory on computed tomography scan and a depressed conscious level are potential candidates. Conclusions The clinical horizon has changed for physicians faced with a patient with symptoms and/or signs which could be due to vascular disease of the brain. If the potential of thrombolysis is to be realised, an accurate diagnosis is required within three hours in all patients who present with an acute problem that could be an ischaemic cerebral event. For patients with TIAs, an urgent diagnosis and initiation of secondary preventive measures dramatically reduce the risk of further events. Acknowledgements I am grateful to Dr Margaret Hourihan and Dr Shawn Halpin for their help in the preparation of this article. References 1 Royal College of Physicians Intercollegiate Stroke Working Party. National clinical guideline for stroke, 3rd edn. London: RCP, National Institute for Health and Clinical Excellence. Alteplase for the treatment of acute ischaemic stroke, TA122.London: NICE, Nor AM, McAllister C, Louw SJ et al. Agreement between ambulance paramedicand physician-recorded neurological signs with Face Arm Speech Test (FAST) in acute stroke patients. Stroke 2004;35: Nor AM, Davis J, Sen B et al.the Recognition of Stroke in the Emergency Room (ROSIER) scale: development and validation of a stroke recognition instrument. Lancet Neurol 2005;4: Rothwell PM, Giles M, Chandrathevea A et al. Effect of urgent treatment of transient ischaemic attack and minor stroke on early recurrent stroke (EXPRESS study): a prospective population-based sequential comparison. Lancet 2007;370: Barnett HJ, Taylor DW, Eliasziw M et al. Benefit of carotid endarterectomy in patients with symptomatic moderate or severe stenosis. North American Symptomatic Carotid Endarterectomy Trial Collaborators. N Engl J Med 1998;339: Randomised trial of endarterectomy for recently symptomatic carotid stenosis: final results of the MRCS European Carotid Surgery Trial. Lancet 1998;351: Bhatt DL, Fox KA, Hacke W et al; CHARISMA Investigators. Clopidogrel and aspirin versus aspirin alone for the prevention of atherothrombotic events. N Engl J Med 2006;354: Diener HC, Bogousslavsky J, Brass LM et al; MATCH investigators. Aspirin and clopidogrel compared with clopidogrel alone after recent ischaemic stroke or transient ischaemic attack in high-risk patients (MATCH): randomised, double-blind, placebo-controlled trial. Lancet 2004;364: Cervical Artery Dissection in Stroke Study Trial Investigators. Antiplatelet therapy vs. anticoagulation in cervical artery dissection: rationale and design of the Cervical Artery Dissection in Stroke Study (CADISS). Int J Stroke 2007;2: Wahlgren N, Ahmed N, Dávalos A et al; SITS-MOST investigators. Thrombolysis with alteplase for acute ischaemic stroke in the Safe Implementation of Thrombolysis in Stroke-Monitoring Study (SITS-MOST): an observational study. Lancet 2007;369: ist3@skull.dcn.ed.ac.uk Address for correspondence: Dr T Hughes, University of Wales, Cardiff CF14 4XN. tom.hughes@cardiffandvale. wales.nhs.uk 72 Royal College of Physicians, All rights reserved.
Stroke in the ED. Dr. William Whiteley. Scottish Senior Clinical Fellow University of Edinburgh Consultant Neurologist NHS Lothian
 Stroke in the ED Dr. William Whiteley Scottish Senior Clinical Fellow University of Edinburgh Consultant Neurologist NHS Lothian 2016 RCP Guideline for Stroke RCP guidelines for acute ischaemic stroke
Stroke in the ED Dr. William Whiteley Scottish Senior Clinical Fellow University of Edinburgh Consultant Neurologist NHS Lothian 2016 RCP Guideline for Stroke RCP guidelines for acute ischaemic stroke
Appendix 2C - Stroke Services in Fife
 Appendix 2C - Stroke Services in Fife Stroke and TIA Management Guidance for GPs The aim of this document is to; Inform GPs of acute stroke services in Fife Summarise who to admit and describe acute management
Appendix 2C - Stroke Services in Fife Stroke and TIA Management Guidance for GPs The aim of this document is to; Inform GPs of acute stroke services in Fife Summarise who to admit and describe acute management
TIA AND STROKE. Topics/Order of the day 1. Topics/Order of the day 2 01/08/2012
 Charles Ashton Medical Director TIA AND STROKE Topics/Order of the day 1 What Works? Clinical features of TIA inc the difference between Carotid and Vertebral territories When is a TIA not a TIA TIA management
Charles Ashton Medical Director TIA AND STROKE Topics/Order of the day 1 What Works? Clinical features of TIA inc the difference between Carotid and Vertebral territories When is a TIA not a TIA TIA management
Dr Ben Turner. Consultant Neurologist and Honorary Senior Lecturer Barts and The London NHS Trust London Bridge Hospital
 Stroke Management Dr Ben Turner Consultant Neurologist and Honorary Senior Lecturer Barts and The London NHS Trust London Bridge Hospital Introduction Stroke is the major cause of disability in the developed
Stroke Management Dr Ben Turner Consultant Neurologist and Honorary Senior Lecturer Barts and The London NHS Trust London Bridge Hospital Introduction Stroke is the major cause of disability in the developed
Alan Barber. Professor of Clinical Neurology University of Auckland
 Alan Barber Professor of Clinical Neurology University of Auckland Presented with Non-fluent dysphasia R facial weakness Background Ischaemic heart disease Hypertension Hyperlipidemia L MCA branch
Alan Barber Professor of Clinical Neurology University of Auckland Presented with Non-fluent dysphasia R facial weakness Background Ischaemic heart disease Hypertension Hyperlipidemia L MCA branch
Thrombolysis for acute ischaemic stroke Rapid Assessment Protocol NORTHERN IRELAND Regional Protocol (Version 002 July 08)
 Thrombolysis for acute ischaemic stroke Rapid Assessment Protocol NORTHERN IRELAND Regional Protocol (Version 002 July 08) Patient Details Time of onset? Capillary Blood glucose 2.8-22.2 mmol/l? Blood
Thrombolysis for acute ischaemic stroke Rapid Assessment Protocol NORTHERN IRELAND Regional Protocol (Version 002 July 08) Patient Details Time of onset? Capillary Blood glucose 2.8-22.2 mmol/l? Blood
CEREBRO VASCULAR ACCIDENTS
 CEREBRO VASCULAR S MICHAEL OPONG-KUSI, DO MBA MORTON CLINIC, TULSA, OK, USA 8/9/2012 1 Cerebrovascular Accident Third Leading cause of deaths (USA) 750,000 strokes in USA per year. 150,000 deaths in USA
CEREBRO VASCULAR S MICHAEL OPONG-KUSI, DO MBA MORTON CLINIC, TULSA, OK, USA 8/9/2012 1 Cerebrovascular Accident Third Leading cause of deaths (USA) 750,000 strokes in USA per year. 150,000 deaths in USA
Stroke/TIA. Tom Bedwell
 Stroke/TIA Tom Bedwell tab1g11@soton.ac.uk The Plan Definitions Anatomy Recap Aetiology Pathology Syndromes Brocas / Wernickes Investigations Management Prevention & Prognosis TIAs Key Definitions Transient
Stroke/TIA Tom Bedwell tab1g11@soton.ac.uk The Plan Definitions Anatomy Recap Aetiology Pathology Syndromes Brocas / Wernickes Investigations Management Prevention & Prognosis TIAs Key Definitions Transient
Nicolas Bianchi M.D. May 15th, 2012
 Nicolas Bianchi M.D. May 15th, 2012 New concepts in TIA Differential Diagnosis Stroke Syndromes To learn the new definitions and concepts on TIA as a condition of high risk for stroke. To recognize the
Nicolas Bianchi M.D. May 15th, 2012 New concepts in TIA Differential Diagnosis Stroke Syndromes To learn the new definitions and concepts on TIA as a condition of high risk for stroke. To recognize the
The NIHSS score is 4 (considering 2 pts for the ataxia involving upper and lower limbs.
 Neuroscience case 5 1. Speech comprehension, ability to speak, and word use were normal in Mr. Washburn, indicating that aphasia (cortical language problem) was not involved. However, he did have a problem
Neuroscience case 5 1. Speech comprehension, ability to speak, and word use were normal in Mr. Washburn, indicating that aphasia (cortical language problem) was not involved. However, he did have a problem
Alan Barber. Professor of Clinical Neurology University of Auckland
 Alan Barber Professor of Clinical Neurology University of Auckland Presented with L numbness & slurred speech 2 episodes; 10 mins & 2 hrs Hypertension Type II DM Examination pulse 80/min reg, BP 160/95
Alan Barber Professor of Clinical Neurology University of Auckland Presented with L numbness & slurred speech 2 episodes; 10 mins & 2 hrs Hypertension Type II DM Examination pulse 80/min reg, BP 160/95
TIA Transient Ischaemic Attack?
 TIA Transient Ischaemic Attack? OR Transient loss of function (TLOF) Tal Anjum Consultant Stroke Physician, Morriston Hospital Training & education lead, WASP (Welsh Association of Stroke Physicians) Qs.
TIA Transient Ischaemic Attack? OR Transient loss of function (TLOF) Tal Anjum Consultant Stroke Physician, Morriston Hospital Training & education lead, WASP (Welsh Association of Stroke Physicians) Qs.
STROKE UPDATE ANTHEA PARRY MAY 2010
 STROKE UPDATE ANTHEA PARRY MAY 2010 Delivery of stroke care Clinical presentations Management Health Care for London plan 8 HASU (hyperacute) units 20 stroke units TIA services Hyperacute stroke units
STROKE UPDATE ANTHEA PARRY MAY 2010 Delivery of stroke care Clinical presentations Management Health Care for London plan 8 HASU (hyperacute) units 20 stroke units TIA services Hyperacute stroke units
Stroke: clinical presentations, symptoms and signs
 Stroke: clinical presentations, symptoms and signs Professor Peter Sandercock University of Edinburgh EAN teaching course Burkina Faso 8 th November 2017 Clinical diagnosis is important to Ensure stroke
Stroke: clinical presentations, symptoms and signs Professor Peter Sandercock University of Edinburgh EAN teaching course Burkina Faso 8 th November 2017 Clinical diagnosis is important to Ensure stroke
Pharmacy STROKE. Anne Kinnear Lead Pharmacist NHS Lothian. Educational Solutions for Workforce Development
 STROKE Anne Kinnear Lead Pharmacist NHS Lothian Aim To update pharmacists on Stroke: the disease and its management and explore ways to implement pharmaceutical care for this patient group as part of normal
STROKE Anne Kinnear Lead Pharmacist NHS Lothian Aim To update pharmacists on Stroke: the disease and its management and explore ways to implement pharmaceutical care for this patient group as part of normal
Stroke School for Internists Part 1
 Stroke School for Internists Part 1 November 4, 2017 Dr. Albert Jin Dr. Gurpreet Jaswal Disclosures I receive a stipend for my role as Medical Director of the Stroke Network of SEO I have no commercial
Stroke School for Internists Part 1 November 4, 2017 Dr. Albert Jin Dr. Gurpreet Jaswal Disclosures I receive a stipend for my role as Medical Director of the Stroke Network of SEO I have no commercial
Alan Barber. Professor of Clinical Neurology University of Auckland
 Alan Barber Professor of Clinical Neurology University of Auckland Presented with L numbness & slurred speech 2 episodes; 10 mins & 2 hrs Hypertension Type II DM Examination P 80/min reg, BP 160/95, normal
Alan Barber Professor of Clinical Neurology University of Auckland Presented with L numbness & slurred speech 2 episodes; 10 mins & 2 hrs Hypertension Type II DM Examination P 80/min reg, BP 160/95, normal
CONCISE GUIDE National Clinical Guidelines for Stroke 2nd Edition
 CONCISE GUIDE 2004 National for Stroke 2nd Edition This concise guide summarises the recommendations, graded according to the evidence, from the National 2nd edition. As critical aspects of care are not
CONCISE GUIDE 2004 National for Stroke 2nd Edition This concise guide summarises the recommendations, graded according to the evidence, from the National 2nd edition. As critical aspects of care are not
Stroke and transient ischaemic attack -
 Stroke and transient ischaemic attack Stroke and transient ischaemic attack - cerebrovascular accident unspecified G66) I60-I64, G45 (Clinical term: Stroke and Presenting complaints Usually sudden on-set
Stroke and transient ischaemic attack Stroke and transient ischaemic attack - cerebrovascular accident unspecified G66) I60-I64, G45 (Clinical term: Stroke and Presenting complaints Usually sudden on-set
Stroke & the Emergency Department. Dr. Barry Moynihan, March 2 nd, 2012
 Stroke & the Emergency Department Dr. Barry Moynihan, March 2 nd, 2012 Outline Primer Stroke anatomy & clinical syndromes Diagnosing stroke Anterior / Posterior Thrombolysis Haemorrhage The London model
Stroke & the Emergency Department Dr. Barry Moynihan, March 2 nd, 2012 Outline Primer Stroke anatomy & clinical syndromes Diagnosing stroke Anterior / Posterior Thrombolysis Haemorrhage The London model
New Zealand Guideline for the Assessment and Management of Transient Ischaemic Attack (TIA) User Guide
 New Zealand Guideline for the Assessment and Management of Transient Ischaemic Attack (TIA) User Guide Acknowledgements The generous voluntary contribution of time and expertise by writers, consumers and
New Zealand Guideline for the Assessment and Management of Transient Ischaemic Attack (TIA) User Guide Acknowledgements The generous voluntary contribution of time and expertise by writers, consumers and
Management of TIA. Dr Ali Ali Consultant Stroke and Geriatrics Royal Hallamshire Hospital
 Management of TIA Dr Ali Ali Consultant Stroke and Geriatrics Royal Hallamshire Hospital Objectives Definition TIA and stroke TIA: Diagnosis & mimics Risk assessment Referral and emergency management Secondary
Management of TIA Dr Ali Ali Consultant Stroke and Geriatrics Royal Hallamshire Hospital Objectives Definition TIA and stroke TIA: Diagnosis & mimics Risk assessment Referral and emergency management Secondary
CVA. Alison Atwater PA-C
 CVA Alison Atwater PA-C Types of CVAs Ischemic strokes 80% of strokes 2/3 are thrombotic 1/3 are embolic emboli from the heart or arteries feeding the brain such as carotids, vertebral and basilar etc
CVA Alison Atwater PA-C Types of CVAs Ischemic strokes 80% of strokes 2/3 are thrombotic 1/3 are embolic emboli from the heart or arteries feeding the brain such as carotids, vertebral and basilar etc
Acute stroke. Ischaemic stroke. Characteristics. Temporal classification. Clinical features. Interpretation of Emergency Head CT
 Ischaemic stroke Characteristics Stroke is the third most common cause of death in the UK, and the leading cause of disability. 80% of strokes are ischaemic Large vessel occlusive atheromatous disease
Ischaemic stroke Characteristics Stroke is the third most common cause of death in the UK, and the leading cause of disability. 80% of strokes are ischaemic Large vessel occlusive atheromatous disease
Guideline scope Stroke and transient ischaemic attack in over 16s: diagnosis and initial management (update)
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Guideline scope Stroke and transient ischaemic attack in over s: diagnosis and initial management (update) 0 0 This will update the NICE on stroke and
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Guideline scope Stroke and transient ischaemic attack in over s: diagnosis and initial management (update) 0 0 This will update the NICE on stroke and
Emergency Room Procedure The first few hours in hospital...
 Emergency Room Procedure The first few hours in hospital... ER 5 level Emergency Severity Index SOP s for Stroke Stroke = Level 2 Target Time = 1 Hour 10 min from door 2 Doctor 25 min from door 2 CT 60
Emergency Room Procedure The first few hours in hospital... ER 5 level Emergency Severity Index SOP s for Stroke Stroke = Level 2 Target Time = 1 Hour 10 min from door 2 Doctor 25 min from door 2 CT 60
Thrombolysis administration
 Thrombolysis administration Liz Mackey Stroke Nurse Practitioner Western Health Sunshine & Footscray Hospital, Melbourne Thanks ASNEN committee members Skye Coote, Acute Stroke Nurse, Eastern Health (slide
Thrombolysis administration Liz Mackey Stroke Nurse Practitioner Western Health Sunshine & Footscray Hospital, Melbourne Thanks ASNEN committee members Skye Coote, Acute Stroke Nurse, Eastern Health (slide
TIAs and posterior circulation problems
 TIAs and posterior circulation problems A/Professor Helen Dewey Head, Stroke Service Austin Health Austin Health How many strokes and TIAs are out there? depends on the definition! ~60,000 strokes in
TIAs and posterior circulation problems A/Professor Helen Dewey Head, Stroke Service Austin Health Austin Health How many strokes and TIAs are out there? depends on the definition! ~60,000 strokes in
Thrombolysis Assessment
 Thrombolysis Assessment Brief Clinical Summary of symptom onset of arrival of patient of assessment BP GCS BM If BM
Thrombolysis Assessment Brief Clinical Summary of symptom onset of arrival of patient of assessment BP GCS BM If BM
/ / / / / / Hospital Abstraction: Stroke/TIA. Participant ID: Hospital Code: Multi-Ethnic Study of Atherosclerosis
 Multi-Ethnic Study of Atherosclerosis Participant ID: Hospital Code: Hospital Abstraction: Stroke/TIA History and Hospital Record 1. Was the participant hospitalized as an immediate consequence of this
Multi-Ethnic Study of Atherosclerosis Participant ID: Hospital Code: Hospital Abstraction: Stroke/TIA History and Hospital Record 1. Was the participant hospitalized as an immediate consequence of this
ACCESS CENTER:
 ACCESS CENTER: 1-877-367-8855 Emergency Specialty Services: BRAIN ATTACK Criteria: Stroke symptom onset time less than 6 hours Referring Emergency Department Patient Information Data: Time last known normal:
ACCESS CENTER: 1-877-367-8855 Emergency Specialty Services: BRAIN ATTACK Criteria: Stroke symptom onset time less than 6 hours Referring Emergency Department Patient Information Data: Time last known normal:
Neuroanatomy of a Stroke. Joni Clark, MD Professor of Neurology Barrow Neurologic Institute
 Neuroanatomy of a Stroke Joni Clark, MD Professor of Neurology Barrow Neurologic Institute No disclosures Stroke case presentations Review signs and symptoms Review pertinent exam findings Identify the
Neuroanatomy of a Stroke Joni Clark, MD Professor of Neurology Barrow Neurologic Institute No disclosures Stroke case presentations Review signs and symptoms Review pertinent exam findings Identify the
Canadian Best Practice Recommendations for Stroke Care. (Updated 2008) Section # 3 Section # 3 Hyperacute Stroke Management
 Canadian Best Practice Recommendations for Stroke Care (Updated 2008) Section # 3 Section # 3 Hyperacute Stroke Management Reorganization of Recommendations 2008 2006 RECOMMENDATIONS: 2008 RECOMMENDATIONS:
Canadian Best Practice Recommendations for Stroke Care (Updated 2008) Section # 3 Section # 3 Hyperacute Stroke Management Reorganization of Recommendations 2008 2006 RECOMMENDATIONS: 2008 RECOMMENDATIONS:
AGWS Stroke Thrombolysis Clinical Profoma
 AGWS Stroke Thrombolysis Clinical Profoma Incorporating Salisbury NHS Foundation Trust guidance Date: On Arrival: Affix patient label here) GCS NIHSS Score: Pulse SaO on Air Give O only if < 95 % on Air
AGWS Stroke Thrombolysis Clinical Profoma Incorporating Salisbury NHS Foundation Trust guidance Date: On Arrival: Affix patient label here) GCS NIHSS Score: Pulse SaO on Air Give O only if < 95 % on Air
Heart of England Foundation Trust ACUTE STROKE PATHWAY EMERGENCY DEPARTMENT ATTACHMENTS
 STROKE Name: PID: DOB: Consultant: Heart of England Foundation Trust ACUTE STROKE PATHWAY EMERGENCY DEPARTMENT ATTACHMENTS November 2010 TIME IS BRAIN SUSPECTED STROKE Onset Within 6 Hours? (FAST TEST
STROKE Name: PID: DOB: Consultant: Heart of England Foundation Trust ACUTE STROKE PATHWAY EMERGENCY DEPARTMENT ATTACHMENTS November 2010 TIME IS BRAIN SUSPECTED STROKE Onset Within 6 Hours? (FAST TEST
Journal Club. 1. Develop a PICO (Population, Intervention, Comparison, Outcome) question for this study
 Journal Club Articles for Discussion Tissue plasminogen activator for acute ischemic stroke. The National Institute of Neurological Disorders and Stroke rt-pa Stroke Study Group. N Engl J Med. 1995 Dec
Journal Club Articles for Discussion Tissue plasminogen activator for acute ischemic stroke. The National Institute of Neurological Disorders and Stroke rt-pa Stroke Study Group. N Engl J Med. 1995 Dec
It s Always a Stroke; Except For When It s Not..
 It s Always a Stroke; Except For When It s Not.. TREVOR PHINNEY, D.O. Disclosures No Relevant Disclosures 1 Objectives Discuss variables of differential diagnosis for stroke Review when to TPA and when
It s Always a Stroke; Except For When It s Not.. TREVOR PHINNEY, D.O. Disclosures No Relevant Disclosures 1 Objectives Discuss variables of differential diagnosis for stroke Review when to TPA and when
Shawke A. Soueidan, MD. Riverside Neurology & Sleep Specialists
 Shawke A. Soueidan, MD Riverside Neurology & Sleep Specialists 757-221-0110 Epidemiology of stroke 2018 Affects nearly 800,000 people in the US annually Approximately 600000 first-ever strokes and 185000
Shawke A. Soueidan, MD Riverside Neurology & Sleep Specialists 757-221-0110 Epidemiology of stroke 2018 Affects nearly 800,000 people in the US annually Approximately 600000 first-ever strokes and 185000
Vascular Disorders. Nervous System Disorders (Part B-1) Module 8 -Chapter 14. Cerebrovascular disease S/S 1/9/2013
 Nervous System Disorders (Part B-1) Module 8 -Chapter 14 Overview ACUTE NEUROLOGIC DISORDERS Vascular Disorders Infections/Inflammation/Toxins Metabolic, Endocrinologic, Nutritional, Toxic Neoplastic Traumatic
Nervous System Disorders (Part B-1) Module 8 -Chapter 14 Overview ACUTE NEUROLOGIC DISORDERS Vascular Disorders Infections/Inflammation/Toxins Metabolic, Endocrinologic, Nutritional, Toxic Neoplastic Traumatic
Initial symptom or syndrome: (1) FOCAL WEAKNESS OR NUMBNESS
 View the referenced DVD patient cases, especially if few hospital or clinic patients are encountered for any one symptom or syndrome. The DVD patient cases are referenced by initial symptom or syndrome
View the referenced DVD patient cases, especially if few hospital or clinic patients are encountered for any one symptom or syndrome. The DVD patient cases are referenced by initial symptom or syndrome
Primary Stroke Center Quality & Performance Measures
 Primary Stroke Center Quality & Performance Measures This section of the manual contains information related to the quality performance of Primary Stroke Centers. Brain Attack Coalition Definitions Recognition
Primary Stroke Center Quality & Performance Measures This section of the manual contains information related to the quality performance of Primary Stroke Centers. Brain Attack Coalition Definitions Recognition
Stroke Mimics. Paul Guyler
 Stroke Mimics Paul Guyler Consultant Stroke Physician at Southend University Hospital Clinical Lead for Acute Stroke Essex Cardiac and Stroke Network Aims Why worry? Stroke Recognition Tools History, Examination
Stroke Mimics Paul Guyler Consultant Stroke Physician at Southend University Hospital Clinical Lead for Acute Stroke Essex Cardiac and Stroke Network Aims Why worry? Stroke Recognition Tools History, Examination
Assessing the Stroke Patient. Arlene Boudreaux, MSN, RN, CCRN, CNRN
 Assessing the Stroke Patient Arlene Boudreaux, MSN, RN, CCRN, CNRN Cincinnati Pre-Hospital Stroke Scale May be done by EMS o One of many o F facial droop on one side o A arm drift (hold a pizza box, close
Assessing the Stroke Patient Arlene Boudreaux, MSN, RN, CCRN, CNRN Cincinnati Pre-Hospital Stroke Scale May be done by EMS o One of many o F facial droop on one side o A arm drift (hold a pizza box, close
Unclogging The Pipes. Zahraa Rabeeah MD Chief Resident February 9,2018
 Unclogging The Pipes Zahraa Rabeeah MD Chief Resident February 9,2018 Please join Polleverywhere by texting: ZRABEEAH894 to 37607 Disclosures None Objectives Delineate the differences between TPA vs thrombectomy
Unclogging The Pipes Zahraa Rabeeah MD Chief Resident February 9,2018 Please join Polleverywhere by texting: ZRABEEAH894 to 37607 Disclosures None Objectives Delineate the differences between TPA vs thrombectomy
Department Specific Guideline
 Department Specific Guideline Stroke/TIA Management ED Applicable to: Nursing/Medical staff caring Authorised by: Stroke services team for Acute stroke/tia patients Contact person: Clinical nurse manager,
Department Specific Guideline Stroke/TIA Management ED Applicable to: Nursing/Medical staff caring Authorised by: Stroke services team for Acute stroke/tia patients Contact person: Clinical nurse manager,
Overview of Stroke: Etiologies, Demographics, Syndromes, and Outcomes. Alex Abou-Chebl, MD, FSVIN Medical Director, Stroke Baptist Health Louisville
 Overview of Stroke: Etiologies, Demographics, Syndromes, and Outcomes Alex Abou-Chebl, MD, FSVIN Medical Director, Stroke Baptist Health Louisville Disclosure Statement of Financial Interest Within the
Overview of Stroke: Etiologies, Demographics, Syndromes, and Outcomes Alex Abou-Chebl, MD, FSVIN Medical Director, Stroke Baptist Health Louisville Disclosure Statement of Financial Interest Within the
CMS Limitations Guide - Radiology Services
 CMS Limitations Guide - Radiology Services Starting October 1, 2015, CMS will update their existing medical necessity limitations on tests and procedures to correspond to ICD-10 codes. This limitations
CMS Limitations Guide - Radiology Services Starting October 1, 2015, CMS will update their existing medical necessity limitations on tests and procedures to correspond to ICD-10 codes. This limitations
IDPH EMS Region Five. Stroke Education
 IDPH EMS Region Five Stroke Education Time is Brain!!!!! Time is Brain!!!! Stroke refers to any spontaneous damage to the brain caused by an abnormality of the blood supply by means of a clot or bleed.
IDPH EMS Region Five Stroke Education Time is Brain!!!!! Time is Brain!!!! Stroke refers to any spontaneous damage to the brain caused by an abnormality of the blood supply by means of a clot or bleed.
Posterior Circulation Stroke
 Posterior Circulation Stroke Brett Kissela, MD, MS Professor and Chair Department of Neurology and Rehabilitation Medicine Senior Associate Dean of Clinical Research University of Cincinnati College of
Posterior Circulation Stroke Brett Kissela, MD, MS Professor and Chair Department of Neurology and Rehabilitation Medicine Senior Associate Dean of Clinical Research University of Cincinnati College of
Key Clinical Concepts
 Cerebrovascular Review and General Vascular Syndromes, Including Those That Impact Dizziness Key Clinical Concepts Basic Review of Cerebrovascular Circulation Circulation to the brain is divided into anterior
Cerebrovascular Review and General Vascular Syndromes, Including Those That Impact Dizziness Key Clinical Concepts Basic Review of Cerebrovascular Circulation Circulation to the brain is divided into anterior
Michael Horowitz, MD Pittsburgh, PA
 Michael Horowitz, MD Pittsburgh, PA Introduction Cervical Artery Dissection occurs by a rupture within the arterial wall leading to an intra-mural Hematoma. A possible consequence is an acute occlusion
Michael Horowitz, MD Pittsburgh, PA Introduction Cervical Artery Dissection occurs by a rupture within the arterial wall leading to an intra-mural Hematoma. A possible consequence is an acute occlusion
o Unenhanced Head CT
 Drip & Ship Protocol Acute Stroke Ready Hospital (ASRH) Duluth Area Primary Stroke Center (St. Luke s & St. Mary s Essentia) PATIENT LABEL Patient displays strokelike symptoms EMS/ED CSS > 0 Glucose >
Drip & Ship Protocol Acute Stroke Ready Hospital (ASRH) Duluth Area Primary Stroke Center (St. Luke s & St. Mary s Essentia) PATIENT LABEL Patient displays strokelike symptoms EMS/ED CSS > 0 Glucose >
Inside Your Patient s Brain Michelle Peterson, APRN, CNP Centracare Stroke and Vascular Neurology
 Inside Your Patient s Brain Michelle Peterson, APRN, CNP Centracare Stroke and Vascular Neurology Activity Everyone stand up, raise your right hand, tell your neighbors your name 1 What part of the brain
Inside Your Patient s Brain Michelle Peterson, APRN, CNP Centracare Stroke and Vascular Neurology Activity Everyone stand up, raise your right hand, tell your neighbors your name 1 What part of the brain
[(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD]
![[(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD] [(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD]](/thumbs/89/98619893.jpg) 2015 PHYSICIAN SIGN-OFF (1) STUDY NO (PHY-1) CASE, PER PHYSICIAN REVIEW 1=yes 2=no [strictly meets case definition] (PHY-1a) CASE, IN PHYSICIAN S OPINION 1=yes 2=no (PHY-2) (PHY-3) [based on all available
2015 PHYSICIAN SIGN-OFF (1) STUDY NO (PHY-1) CASE, PER PHYSICIAN REVIEW 1=yes 2=no [strictly meets case definition] (PHY-1a) CASE, IN PHYSICIAN S OPINION 1=yes 2=no (PHY-2) (PHY-3) [based on all available
Stroke Awareness. Presented by: Duane Anderson, MD Snoqualmie Valley Hospital Emergency Department Medical Director
 Stroke Awareness Presented by: Duane Anderson, MD Snoqualmie Valley Hospital Emergency Department Medical Director What is a stroke? Stroke can happen to anyone. Stroke is the fourth leading cause of death
Stroke Awareness Presented by: Duane Anderson, MD Snoqualmie Valley Hospital Emergency Department Medical Director What is a stroke? Stroke can happen to anyone. Stroke is the fourth leading cause of death
Updated Ischemic Stroke Guidelines นพ.ส ชาต หาญไชยพ บ ลย ก ล นายแพทย ทรงค ณว ฒ สาขาประสาทว ทยา สถาบ นประสาทว ทยา กรมการแพทย กระทรวงสาธารณส ข
 Updated Ischemic Stroke Guidelines นพ.ส ชาต หาญไชยพ บ ลย ก ล นายแพทย ทรงค ณว ฒ สาขาประสาทว ทยา สถาบ นประสาทว ทยา กรมการแพทย กระทรวงสาธารณส ข Emergency start at community level: Prehospital care Acute stroke
Updated Ischemic Stroke Guidelines นพ.ส ชาต หาญไชยพ บ ลย ก ล นายแพทย ทรงค ณว ฒ สาขาประสาทว ทยา สถาบ นประสาทว ทยา กรมการแพทย กระทรวงสาธารณส ข Emergency start at community level: Prehospital care Acute stroke
Principles Arteries & Veins of the CNS LO14
 Principles Arteries & Veins of the CNS LO14 14. Identify (on cadaver specimens, models and diagrams) and name the principal arteries and veins of the CNS: Why is it important to understand blood supply
Principles Arteries & Veins of the CNS LO14 14. Identify (on cadaver specimens, models and diagrams) and name the principal arteries and veins of the CNS: Why is it important to understand blood supply
University Journal of Medicine and Medical Sciences
 ISSN 2455-2852 Volume 2 Issue 5 2016 Case report -Opalski's syndrome A rare variant of lateral medullary syndrome in TAKAYASUS ARTERITIS SHANKAR GANESH N NAINAR Department of Neurology, MADRAS MEDICAL
ISSN 2455-2852 Volume 2 Issue 5 2016 Case report -Opalski's syndrome A rare variant of lateral medullary syndrome in TAKAYASUS ARTERITIS SHANKAR GANESH N NAINAR Department of Neurology, MADRAS MEDICAL
Stroke in the Emergency Room: What do we need to know?
 Stroke in the Emergency Room: What do we need to know? Salah G. Keyrouz, MD, FAHA March 10, 2012 Stroke in the Emergency Room: What do we need to know? Disclosure: None 2 1 Outline Definition Introduction
Stroke in the Emergency Room: What do we need to know? Salah G. Keyrouz, MD, FAHA March 10, 2012 Stroke in the Emergency Room: What do we need to know? Disclosure: None 2 1 Outline Definition Introduction
Cerebrovascular Disease
 Cerebrovascular Disease I. INTRODUCTION Cerebrovascular disease (CVD) includes all disorders in which an area of the brain is transiently or permanently affected by ischemia or bleeding and one or more
Cerebrovascular Disease I. INTRODUCTION Cerebrovascular disease (CVD) includes all disorders in which an area of the brain is transiently or permanently affected by ischemia or bleeding and one or more
2015 Update in Diagnosis and Management of Stroke
 2015 Update in Diagnosis and Management of Stroke S. Andrew Josephson MD Carmen Castro Franceschi and Gladyne K. Mitchell Neurohospitalist Distinguished Professor Senior Executive Vice Chair, Department
2015 Update in Diagnosis and Management of Stroke S. Andrew Josephson MD Carmen Castro Franceschi and Gladyne K. Mitchell Neurohospitalist Distinguished Professor Senior Executive Vice Chair, Department
ACUTE ISCHEMIC STROKE. Current Treatment Approaches for Acute Ischemic Stroke
 ACUTE ISCHEMIC STROKE Current Treatment Approaches for Acute Ischemic Stroke EARLY MANAGEMENT OF ACUTE ISCHEMIC STROKE Rapid identification of a stroke Immediate EMS transport to nearest stroke center
ACUTE ISCHEMIC STROKE Current Treatment Approaches for Acute Ischemic Stroke EARLY MANAGEMENT OF ACUTE ISCHEMIC STROKE Rapid identification of a stroke Immediate EMS transport to nearest stroke center
Primary Stroke Center Acute Stroke Transfer Guidelines When to Consider a Transfer:
 When to Consider a Transfer: Hemorrhagic Stroke Large volume intracerebral hematoma greater than 5cm on CT Concern for expanding hematoma Rapidly declining mental status, especially requiring intubation
When to Consider a Transfer: Hemorrhagic Stroke Large volume intracerebral hematoma greater than 5cm on CT Concern for expanding hematoma Rapidly declining mental status, especially requiring intubation
BY: Ramon Medina EMT-LP/RN
 BY: Ramon Medina EMT-LP/RN Discuss types of strokes Discuss the physical and neurological assessment of stroke patients Discuss pertinent historical findings Discuss pre-hospital and emergency management
BY: Ramon Medina EMT-LP/RN Discuss types of strokes Discuss the physical and neurological assessment of stroke patients Discuss pertinent historical findings Discuss pre-hospital and emergency management
Antithrombotic therapy in patients with transient ischemic attack / stroke (acute phase <48h)
 Antithrombotic therapy in patients with transient ischemic attack / stroke (acute phase
Antithrombotic therapy in patients with transient ischemic attack / stroke (acute phase
Neurology. Hollie Wilson
 Neurology Hollie Wilson Objectives Anatomy Physiology: Functional centres of brain UMN lesion vs. LMN lesion Spinal cord Main tracts ascending and descending Nerve roots and peripheral nerves action potentials
Neurology Hollie Wilson Objectives Anatomy Physiology: Functional centres of brain UMN lesion vs. LMN lesion Spinal cord Main tracts ascending and descending Nerve roots and peripheral nerves action potentials
Strategies for Stroke
 Ischemic stroke is a complex disease, the management of which involves features of cardiology, internal medicine and rehabilitative medicine. Is there a thorough, yet simplified, approach to acute ischemic
Ischemic stroke is a complex disease, the management of which involves features of cardiology, internal medicine and rehabilitative medicine. Is there a thorough, yet simplified, approach to acute ischemic
CLINICAL GUIDELINES ID TAG
 Title: Author: Speciality/ Division: Directorate: Date Uploaded: Review Date: September 2019 CG ID TAG CG0423 CLINICAL GUIDELINES ID TAG Clinical Guideline for Alteplase in intra-arterial thrombolysis
Title: Author: Speciality/ Division: Directorate: Date Uploaded: Review Date: September 2019 CG ID TAG CG0423 CLINICAL GUIDELINES ID TAG Clinical Guideline for Alteplase in intra-arterial thrombolysis
Protocol for IV rtpa Treatment of Acute Ischemic Stroke
 Protocol for IV rtpa Treatment of Acute Ischemic Stroke Acute stroke management is progressing very rapidly. Our team offers several options for acute stroke therapy, including endovascular therapy and
Protocol for IV rtpa Treatment of Acute Ischemic Stroke Acute stroke management is progressing very rapidly. Our team offers several options for acute stroke therapy, including endovascular therapy and
Guideline Stroke and transient ischaemic attack in over 16s: diagnosis and initial management
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Guideline Stroke and transient ischaemic attack in over s: diagnosis and initial management Draft for consultation, November 0 This guideline covers interventions
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Guideline Stroke and transient ischaemic attack in over s: diagnosis and initial management Draft for consultation, November 0 This guideline covers interventions
Brain and Central Nervous System Cancers
 Brain and Central Nervous System Cancers NICE guidance link: https://www.nice.org.uk/guidance/ta121 Clinical presentation of brain tumours History and Examination Consider immediate referral Management
Brain and Central Nervous System Cancers NICE guidance link: https://www.nice.org.uk/guidance/ta121 Clinical presentation of brain tumours History and Examination Consider immediate referral Management
2018 Early Management of Acute Ischemic Stroke Guidelines Update
 2018 Early Management of Acute Ischemic Stroke Guidelines Update Brandi Bowman, PhC, Pharm.D. April 17, 2018 Pharmacist Objectives Describe the recommendations for emergency medical services and hospital
2018 Early Management of Acute Ischemic Stroke Guidelines Update Brandi Bowman, PhC, Pharm.D. April 17, 2018 Pharmacist Objectives Describe the recommendations for emergency medical services and hospital
Cerebral Vascular Diseases. Nabila Hamdi MD, PhD
 Cerebral Vascular Diseases Nabila Hamdi MD, PhD Outline I. Stroke statistics II. Cerebral circulation III. Clinical symptoms of stroke IV. Pathogenesis of cerebral infarcts (Stroke) 1. Ischemic - Thrombotic
Cerebral Vascular Diseases Nabila Hamdi MD, PhD Outline I. Stroke statistics II. Cerebral circulation III. Clinical symptoms of stroke IV. Pathogenesis of cerebral infarcts (Stroke) 1. Ischemic - Thrombotic
GOVERNANCE BOARD. 14th January Clinical Audit of Stroke Services. At Shrewsbury and Telford Hospitals NHS Trust
 GOVERNANCE BOARD 14th January 2014 Clinical Audit of Stroke Services At Shrewsbury and Telford Hospitals NHS Trust 1.0 Introduction A clinical review of cases recorded and coded as with a 0-1 day length
GOVERNANCE BOARD 14th January 2014 Clinical Audit of Stroke Services At Shrewsbury and Telford Hospitals NHS Trust 1.0 Introduction A clinical review of cases recorded and coded as with a 0-1 day length
Stroke Transfer Checklist
 Stroke Transfer Checklist When preparing to transfer an acute stroke patient to the UF Health Shands Comprehensive Stroke Center, please make every attempt to include the following information: Results
Stroke Transfer Checklist When preparing to transfer an acute stroke patient to the UF Health Shands Comprehensive Stroke Center, please make every attempt to include the following information: Results
Cerebrovascular Disorders. Blood, Brain, and Energy. Blood Supply to the Brain 2/14/11
 Cerebrovascular Disorders Blood, Brain, and Energy 20% of body s oxygen usage No oxygen/glucose reserves Hypoxia - reduced oxygen Anoxia - Absence of oxygen supply Cell death can occur in as little as
Cerebrovascular Disorders Blood, Brain, and Energy 20% of body s oxygen usage No oxygen/glucose reserves Hypoxia - reduced oxygen Anoxia - Absence of oxygen supply Cell death can occur in as little as
Pathophysiology of stroke
 A practical approach to acute stro ke Dr. Sanjith Aaron, M.D., D.M., Professor, Department of Neurosciences, CMC Vellore Stroke is characterized by an abrupt onset of neurological deficit lasting more
A practical approach to acute stro ke Dr. Sanjith Aaron, M.D., D.M., Professor, Department of Neurosciences, CMC Vellore Stroke is characterized by an abrupt onset of neurological deficit lasting more
Standard NICE (CG ) RCP (2016)
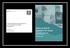 Standard NICE (CG68 2008) RCP (2016) Stroke Unit Adults presenting at an A&E department with suspected stroke are admitted to a specialist stroke unit within 4 hours direct admission of patients with acute
Standard NICE (CG68 2008) RCP (2016) Stroke Unit Adults presenting at an A&E department with suspected stroke are admitted to a specialist stroke unit within 4 hours direct admission of patients with acute
The central nervous system
 Sectc.qxd 29/06/99 09:42 Page 81 Section C The central nervous system CNS haemorrhage Subarachnoid haemorrhage Cerebral infarction Brain atrophy Ring enhancing lesions MRI of the pituitary Multiple sclerosis
Sectc.qxd 29/06/99 09:42 Page 81 Section C The central nervous system CNS haemorrhage Subarachnoid haemorrhage Cerebral infarction Brain atrophy Ring enhancing lesions MRI of the pituitary Multiple sclerosis
Vivek R. Deshmukh, MD Director, Cerebrovascular and Endovascular Neurosurgery Chairman, Department of Neurosurgery Providence Brain and Spine
 Vivek R. Deshmukh, MD Director, Cerebrovascular and Endovascular Neurosurgery Chairman, Department of Neurosurgery Providence Brain and Spine Institute The Oregon Clinic Disclosure I declare that neither
Vivek R. Deshmukh, MD Director, Cerebrovascular and Endovascular Neurosurgery Chairman, Department of Neurosurgery Providence Brain and Spine Institute The Oregon Clinic Disclosure I declare that neither
Traumatic brain injuries are caused by external mechanical forces such as: - Falls - Transport-related accidents - Assault
 PP2231 Brain injury Cerebrum consists of frontal, parietal, occipital and temporal lobes Diencephalon consists of thalamus, hypothalamus Cerbellum Brain stem consists of midbrain, pons, medulla Central
PP2231 Brain injury Cerebrum consists of frontal, parietal, occipital and temporal lobes Diencephalon consists of thalamus, hypothalamus Cerbellum Brain stem consists of midbrain, pons, medulla Central
Vague Neurological Conditions
 Vague Neurological Conditions Dr. John Lefebre, MD, FRCPC Chief Regional Medical Director Europe, India, South Africa, Middle East and Turkey Canada 2014 2 3 4 Agenda Dr. John Lefebre, M.D., FRCPC 1. TIA
Vague Neurological Conditions Dr. John Lefebre, MD, FRCPC Chief Regional Medical Director Europe, India, South Africa, Middle East and Turkey Canada 2014 2 3 4 Agenda Dr. John Lefebre, M.D., FRCPC 1. TIA
What Do You Think of My Posterior?
 What Do You Think of My Posterior? Posterior Stroke and Stroke Mimics Peter Panagos, MD, FACEP, FAHA Associate Professor Emergency Medicine and Neurology Washington University School of Medicine Disclosures
What Do You Think of My Posterior? Posterior Stroke and Stroke Mimics Peter Panagos, MD, FACEP, FAHA Associate Professor Emergency Medicine and Neurology Washington University School of Medicine Disclosures
Dr Julia Hopyan Stroke Neurologist Sunnybrook Health Sciences Centre
 Dr Julia Hopyan Stroke Neurologist Sunnybrook Health Sciences Centre Objectives To learn what s new in stroke care 2010-11 1) Acute stroke management Carotid artery stenting versus surgery for symptomatic
Dr Julia Hopyan Stroke Neurologist Sunnybrook Health Sciences Centre Objectives To learn what s new in stroke care 2010-11 1) Acute stroke management Carotid artery stenting versus surgery for symptomatic
2014 Update in Diagnosis and Management of Stroke
 2014 Update in Diagnosis and Management of Stroke S. Andrew Josephson MD Carmen Castro Franceschi and Gladyne K. Mitchell Neurohospitalist Distinguished Professor Acting Chairman, Department of Neurology
2014 Update in Diagnosis and Management of Stroke S. Andrew Josephson MD Carmen Castro Franceschi and Gladyne K. Mitchell Neurohospitalist Distinguished Professor Acting Chairman, Department of Neurology
Patient characteristics. Intervention Comparison Length of followup. Outcome measures. Number of patients. Evidence level.
 5.0 Rapid recognition of symptoms and diagnosis 5.1. Pre-hospital health professional checklists for the prompt recognition of symptoms of TIA and stroke Evidence Tables ASM1: What is the accuracy of a
5.0 Rapid recognition of symptoms and diagnosis 5.1. Pre-hospital health professional checklists for the prompt recognition of symptoms of TIA and stroke Evidence Tables ASM1: What is the accuracy of a
Karl Meisel, MD MA Director of Stroke Clinic University of California San Francisco
 Karl Meisel, MD MA Director of Stroke Clinic University of California San Francisco I have no financial disclosures 1 Hospital Management Thrombolytic and Thrombectomy Blood pressure Stroke in the Young
Karl Meisel, MD MA Director of Stroke Clinic University of California San Francisco I have no financial disclosures 1 Hospital Management Thrombolytic and Thrombectomy Blood pressure Stroke in the Young
Cerebrovascular Disease
 Neuropathology lecture series Cerebrovascular Disease Physiology of cerebral blood flow Brain makes up only 2% of body weight Percentage of cardiac output: 15-20% Percentage of O 2 consumption (resting):
Neuropathology lecture series Cerebrovascular Disease Physiology of cerebral blood flow Brain makes up only 2% of body weight Percentage of cardiac output: 15-20% Percentage of O 2 consumption (resting):
Stroke 101. Maine Cardiovascular Health Summit. Eileen Hawkins, RN, MSN, CNRN Pen Bay Stroke Program Coordinator November 7, 2013
 Stroke 101 Maine Cardiovascular Health Summit Eileen Hawkins, RN, MSN, CNRN Pen Bay Stroke Program Coordinator November 7, 2013 Stroke Statistics Definition of stroke Risk factors Warning signs Treatment
Stroke 101 Maine Cardiovascular Health Summit Eileen Hawkins, RN, MSN, CNRN Pen Bay Stroke Program Coordinator November 7, 2013 Stroke Statistics Definition of stroke Risk factors Warning signs Treatment
Referral Guideline for Patients with TIA
 DERBYSHIRE COUNTY PCT & NHS DERBY CITY Clinical Effectiveness & Guidelines Group Referral Guideline for Patients with TIA Key Messages This is a revised guideline for patients referred to the TIA service
DERBYSHIRE COUNTY PCT & NHS DERBY CITY Clinical Effectiveness & Guidelines Group Referral Guideline for Patients with TIA Key Messages This is a revised guideline for patients referred to the TIA service
NEURORADIOLOGY DIL part 4
 NEURORADIOLOGY DIL part 4 Strokes and infarcts K. Agyem MD, G. Hall MD, D. Palathinkal MD, Alexandre Menard March/April 2015 OVERVIEW Introduction to Neuroimaging - DIL part 1 Basic Brain Anatomy - DIL
NEURORADIOLOGY DIL part 4 Strokes and infarcts K. Agyem MD, G. Hall MD, D. Palathinkal MD, Alexandre Menard March/April 2015 OVERVIEW Introduction to Neuroimaging - DIL part 1 Basic Brain Anatomy - DIL
Stroke. Understanding. Professor Richard Iain Lindley
 Understanding Stroke Professor Richard Iain Lindley Published by Family Doctor Publications Limited in association with the British Medical Association IMPORTANT This book is intended not as a substitute
Understanding Stroke Professor Richard Iain Lindley Published by Family Doctor Publications Limited in association with the British Medical Association IMPORTANT This book is intended not as a substitute
Marc Norman, Ph.D. - Do Not Use without Permission 1. Cerebrovascular Accidents. Marc Norman, Ph.D. Department of Psychiatry
 Cerebrovascular Accidents Marc Norman, Ph.D. Department of Psychiatry Neuropsychiatry and Behavioral Medicine Neuropsychology Clinical Training Seminar 1 5 http://www.nlm.nih.gov/medlineplus/ency/images/ency/fullsize/18009.jpg
Cerebrovascular Accidents Marc Norman, Ph.D. Department of Psychiatry Neuropsychiatry and Behavioral Medicine Neuropsychology Clinical Training Seminar 1 5 http://www.nlm.nih.gov/medlineplus/ency/images/ency/fullsize/18009.jpg
Suspected neurological conditions: clinical questions
 Suspected neurological clinical questions For questions on signs and symptoms, the committee wanted to consider any studies that determine whether a certain sign or symptom accompanying a main presenting
Suspected neurological clinical questions For questions on signs and symptoms, the committee wanted to consider any studies that determine whether a certain sign or symptom accompanying a main presenting
Medical Review Guidelines Magnetic Resonance Angiography
 Medical Review Guidelines Magnetic Resonance Angiography Medical Guideline Number: MRG2001-05 Effective Date: 2/13/01 Revised Date: 2/14/2006 OHCA Reference OAC 317:30-5-24. Radiology. (f) Magnetic Resonance
Medical Review Guidelines Magnetic Resonance Angiography Medical Guideline Number: MRG2001-05 Effective Date: 2/13/01 Revised Date: 2/14/2006 OHCA Reference OAC 317:30-5-24. Radiology. (f) Magnetic Resonance
Carotid Artery Dissection Causing an Isolated Hypoglossal. Nerve Palsy
 Archives of Clinical and Medical Case Reports doi: 10.26502/acmcr.96550035 Volume 2, Issue 5 Case Report Carotid Artery Dissection Causing an Isolated Hypoglossal Muzzammil Ali*, Yatin Sardana Nerve Palsy
Archives of Clinical and Medical Case Reports doi: 10.26502/acmcr.96550035 Volume 2, Issue 5 Case Report Carotid Artery Dissection Causing an Isolated Hypoglossal Muzzammil Ali*, Yatin Sardana Nerve Palsy
How to Think like a Neurologist Review of Exam Process and Assessment Findings
 Lehigh Valley Health Network LVHN Scholarly Works Neurology Update for the Non-Neurologist 2013 Neurology Update for the Non-Neurologist Feb 20th, 5:10 PM - 5:40 PM How to Think like a Neurologist Review
Lehigh Valley Health Network LVHN Scholarly Works Neurology Update for the Non-Neurologist 2013 Neurology Update for the Non-Neurologist Feb 20th, 5:10 PM - 5:40 PM How to Think like a Neurologist Review
Stroke - Intracranial hemorrhage. Dr. Amitesh Aggarwal Associate Professor Department of Medicine
 Stroke - Intracranial hemorrhage Dr. Amitesh Aggarwal Associate Professor Department of Medicine Etiology and pathogenesis ICH accounts for ~10% of all strokes 30 day mortality - 35 45% Incidence rates
Stroke - Intracranial hemorrhage Dr. Amitesh Aggarwal Associate Professor Department of Medicine Etiology and pathogenesis ICH accounts for ~10% of all strokes 30 day mortality - 35 45% Incidence rates
