Sudden loss of vision
|
|
|
- Joy Moody
- 5 years ago
- Views:
Transcription
1 Sudden loss of vision Abstract Du Toit N, MBChB, DipOphth(SA), FRCS(Ed), FCOphth(SA), MMed, Senior Lecturer University of Cape Town; Groote Schuur Hospital, Cape Town Correspondence to: Nagib du Toit, Keywords: sudden loss of vision, transient visual loss, retinal vascular occlusion, vitreous haemorrhage, retinal detachment Sudden loss of vision, which causes consternation for both the patient and clinician, is a clinical problem that is encountered fairly regularly in most primary healthcare settings. Sudden visual loss or obscuration which is transient may simply be a symptom of a dry eye or a migraine, but it may also be the onset of irreversible visual loss or a stroke. Most cases of sudden loss of vision are serious, require referral and have an associated underlying systemic disease. Visual loss is usually unilateral, but may be bilateral. This clinical problem may present a diagnostic challenge. No cause may be found in some instances. However, it is important to remember that the more sinister causes of sudden visual loss, such as temporal arteritis, carotid or cardiac emboli that cause retinal vascular occlusion, retinal detachment, vitreous haemorrhage and orbital masses, need to be identified early. Using the duration of the visual loss as the primary differentiating factor, with associated symptoms and signs as supplementary factors, the causes can be narrowed down. A thorough history, goal-directed examination, proper investigation and appropriate referral should enable early diagnosis and adequate management. This will prevent further ocular morbidity, and even patient mortality. Peer reviewed. (Submitted: Accepted: ) Medpharm ;55(3): Introduction A sudden loss of vision causes consternation for both the patient and clinician. Sudden visual loss or obscuration which is transient may simply be a symptom of a dry eye, or it may be the onset of irreversible visual loss or a stroke. 1 Most cases of sudden loss of vision are serious, require referral and have an associated underlying systemic disease. Associated symptoms provide important clues to the cause. The need for an update in the field of primary healthcare eye care knowledge became apparent in a recent study that was carried out among general practitioners. 2 This article is the second in a series which attempts to address this issue. Approach to the patient A goal-directed assessment of a patient who presents with sudden loss of vision is required. A history of the duration of visual loss is critical. As pointed out by Goold et al, 1 it is important to distinguish between true sudden visual loss and the sudden realisation that vision has been lost. Spontaneous loss of vision when both eyes are open is probably acute, while gradual monocular loss of vision may appear to be acute when the normal eye is temporarily obscured or closed, thus revealing poor vision in the other eye. Sudden visual loss is usually unilateral, but may occasionally be bilateral. An examination should focus on visual acuity (VA), confrontation visual field testing, pupil testing for the presence of an afferent pupil defect (APD), assessment of the red reflex and fundoscopy. Many of the conditions discussed below will initially cause temporary visual loss, but several may become permanent if not promptly managed. 3 The more common conditions that cause sudden loss of vision can be divided into two groups, based on the duration of the visual loss. The conditions in these two categories are listed in Table I. Some of these will be discussed later. Trauma as a cause of visual loss is not discussed here. Table I: The more common clinical conditions that cause sudden loss of vision Transient visual loss Amaurosis fugax Migraines Papilloedema Tear film disturbance Functional visual loss Visual loss of longer or permanent duration Central retinal artery occlusion Central retinal vein occlusion Vitreous haemorrhage Ischaemic optic neuropathy Optic neuritis Retinal detachment It is important to establish whether the visual loss is unilateral or bilateral, as a bilateral visual disturbance rarely indicates 235 Vol 55 No 3
2 Sudden loss of vision Duration lasting seconds to minutes, and no APD Duration lasting minutes to an indefinite period Obscuration lasting a few seconds: Check for associated headaches, nausea and disc swelling - Papilloedema If absent, check for: Clearing of vision with blinking - Tear-film abnormalities Less than 10 minutes: Associated cardiovascular risk factors - Amaurosis fugax Also check for: Associated headaches, jaw claudication, scalp tenderness, and constitutional systoms - Giant cell arteritis (Transient loss may precede permanent visual loss which occurs when ischaemia causes infarction of the optic nerve head) Headache, duration ~20 mins and zigzag lines: - A migraine APD present: Cardiovascular risk factors - Central retinal artery occlusion - Central retinal vein occlusion - Ischaemic optic neuropathy Pain on eye movement - Optic neuritis Preceded by flashes and floaters - Retinal detachment Absent red reflex: - Vitreous haemorrhage APD: afferent pupillary defect Figure 1: Flow chart for the primary care assessment of patients with a sudden loss of vision bilateral ocular or optic nerve disease, but more commonly is a sign of disease posterior to the optic chiasm, including the optic tract and cerebral cortex. It may indicate impaired posterior cerebral circulation or even a migraine. 1 Transient loss of vision, particularly in patients with significant cardiovascular risk factors, may be owing to amaurosis fugax, resulting from atherosclerosis. These patients require further investigation. A floating, mobile scotoma is consistent with vitreous pathology, as the vitreous undulates relative to the retina when the globe moves. 1 Testing visual fields to confrontation is of importance in cases where history points to a retinal or neurological cause of the loss of vision. Keeping in mind that normal pupil reactions require normal oculomotor and optic nerve functioning, it is important to assess the direct, as well as consensual, pupillary responses in each eye. Subtle differences between the two optic nerves may be detected by carrying out the swinging flashlight test for a relative APD. It is important to assess the red reflex in each eye. This may be obscured by media opacities, such as vitreous haemorrhage, as well as intraocular pathology, for example, retinal detachment. 4 Fundoscopy should be performed after pupil dilation if acute angle closure glaucoma is not suspected. An examination of the cranial nerves may also help to diagnose orbital disease. In any setting, papilloedema requires prompt imaging. 1 Loss of vision may be associated with migraine. Usually, the visual aura of a migraine presents as zigzag lights or shimmering colours and precedes the headache. Atypical cases should be referred to a neurologist. Using the duration of the visual loss as the primary differentiating factor, with associated symptoms and signs as secondary factors, the causes can be narrowed down, as indicated in Figure 1. Clinical conditions Central retinal artery occlusion Blood cannot get into the eye, usually as a result of embolic (e.g. patients with endocarditis) or thrombotic (e.g. patients with atherosclerosis), occlusion of the retinal artery. Arteritic occlusion, as a result of giant cell arteritis (GCA), is less common. Usually, patients present with the VA of fingercounting or worse. An APD is present and the retina Figure 2: Non-perfused, thread-like arteries that are partly obscured by the retinal oedema are apparent 236 Vol 55 No 3
3 Figure 3: Central rentinal artery occlusion with cilioretinal sparing appears pale (infarcted). Non-perfused, thread-like arteries that are partly obscured by the retinal oedema are apparent (Figure 2). A cherry-red spot at the macula, because of the visibility of the underlying intact choroidal circulation, is a classic sign. [Note: The macula is supplied by an artery from the ciliary circulation in approximately 20% of people. In these cases, central retinal artery occlusion (CRAO) (Figure 3) results in a perfused macula in a sea of infarcted retina.] Hemiretinal artery occlusions, where only half of the retina is affected, may also occur. 4 Branch retinal artery occlusions create a more limited scotoma, while cilioretinal artery occlusions may only reduce the central vision. 3 If embolus or thrombosis is suspected, patients need an age-appropriate stroke workup and appropriate management. The following measures to prevent permanent retinal damage and possible dislodgement of the embolus 5 can be taken in these patients, if they are seen within four hours of the event: digital massage of the globe and oral acetazolamide to reduce intraocular pressure. Breathing into a paper bag (the patient) which causes an increase in partial pressure of carbon dioxide and vasodilatation. If symptoms suggest GCA, an elevated erythrocyte sedimentation rate (ESR) and platelet count will confirm the diagnosis. Highdose oral steroids should be started before referral to an ophthalmologist. Central retinal vein occlusion Blood cannot get out of the eye, usually secondary to poorly controlled hypertension or diabetes. Central retinal vein occlusion (CRVO) can also be caused by raised intraocular pressure, as well as hypercoaguable states, including systemic malignancy. 4 Hypertension-related CRVO and branch vein occlusions are usually caused by sclerotic changes in the artery which contribute to compression of the vein. At presentation, VA is decreased to somewhere between 6/18 and finger-counting. Dilated, tortuous veins are visible on fundoscopy. Cottonwool spots, Figure 4: Cottonwool spots and retinal haemorrhages occur in all four quadrants in central retinal vein occlusion Figure 5: Cottonwool spots and retinal haemorrhages occur only in affected quadrants in branch vein occlusions retinal haemorrhages [which occur in all four quadrants in CRVO (Figure 4), and only in affected quadrants in branch vein occlusions (Figure 5)], as well as disc swelling, are pathognomonic. If there is very severe ischaemia, a blood and thunder retinal appearance is evident with VA of fingercounting, or worse. Vein and artery occlusions both cause sudden loss of vision and the resultant chronic ischaemia can also lead to neovascularisation of the disc, retina and iris; vitreous haemorrhage; and neovascular glaucoma. Patients should have their blood pressure and blood glucose checked to exclude hypertension and diabetes before referral to an ophthalmologist. 4 Vitreous haemorrhage Painless sudden loss of vision in a patient with diabetes or hypertension may suggest vitreous haemorrhage, which is often described as being heralded by a shower of black dots. Subhyaloid (Figure 6), retinal or subretinal haemorrhages are more discrete, less mobile, and may 237 Vol 55 No 3
4 Figure 6: Subhyaloid retinal or subretinal haemorrhages are more discrete, less mobile, and may initially appear as a red, brown or black scotomata initially appear as a red, brown or black scotomata. 1 Bleeding into the vitreous cavity results from any disease that causes retinal ischaemia (e.g. diabetes, CRVO and CRAO). These can stimulate the production of angiogenic factors with resultant new vessel formation. Haemorrhage occurs from these friable vessels into the vitreous gel. Nonischaemic causes of vitreous haemorrhage include trauma, bleeding disorders, tumours and retinal tears (with or without detachment). Patients experience floaters in the affected eye, followed by loss of vision. After major haemorrhage, the red reflex is lost. 4 Vitreous haemorrhage of any cause must be referred to an ophthalmologist for assessment. Ischaemic optic neuropathy Ischaemia, due to occlusion of the short posterior ciliary arteries, results in infarction of the optic nerve head and leads to ischaemic optic neuropathy. 4 Causes may be arteritic (GCA) or nonarteritic (arteriosclerotic). The physician should always consider GCA if the patient is older than 60 years of age. Patients with GCA often have malaise, myalgia, jaw claudication, weight loss and scalp tenderness. Neuropathy causes severe loss of vision and often affects the superior half of the optic disc, with a resultant inferior altitudinal field defect, which can be picked up on confrontation visual field testing. The affected part of the disc is pale and swollen on fundoscopy (Figure 7). Elevated ESR and C-reactive protein (CRP) should be assessed if GCA is suspected. The ESR may be normal in 17% of patients with GCA. The sensitivity of ESR alone for the diagnosis of GCA is 84.9%, the sensitivity of CRP alone is 97.5%, while the sensitivity of raised ESR and CRP is 99.2%. 6 The platelet count is also important as GCA is six times more probable in a patient with thrombocytosis, than in a patient with a normal platelet count. 6 If GCA is Figure 7: The affected part of the disc is pale and swollen on fundoscopy in ischaemic optic neuropathy diagnosed, oral prednisone of at least 1 mg/kg is needed and immediate referral required, as the other eye may also become affected if treatment is not started urgently. 4 The patient needs a temporal artery biopsy to confirm the diagnosis and will have to go on long-term steroid therapy, the aim of which is to further limit vision loss, as well as to protect the fellow eye. There is no immediate treatment for the nonarteritic type of ischaemic optic neuropathy. 1 All patients should be referred for further management. Retinal detachment The retina stays attached to the wall of the eye by fastening to the retinal pigment epithelium (RPE), which, in turn, is connected to the uveal tract and the sclera. There is an embryological potential space, analogous to the ventricles of the brain, between the neurosensory retina and the RPE, which stays closed by a pump mechanism in the RPE. If a hole develops in the retina, fluid leaks into this potential space and the retina detaches. In other words, the neurosensory retina separates from the RPE. Detachment may be rhegmatogenous (secondary to a retinal tear), tractional (involving scar tissue, e.g. with trauma, and in proliferative diabetic retinopathy) or exudative (e.g. with uveitis, tumours and severe hypertension). Signs and symptoms of the rhegmatogenous type include flashing lights (photopsia) and floaters ( dancing flies ) because of the development of posterior vitreous detachment. These are followed by showers of dots or tadpoles as vitreous haemorrhage ensues. A grey curtain or shadow that comes over the field of vision from the periphery indicates detachment of the retina. The differential diagnosis of these symptoms includes scintillating scotomata/fortification spectrum of a migraine for the flashes, and amaurosis fugax for the curtain. Both of these cause intermittent loss of vision and require 238 Vol 55 No 3
5 Figure 8: Cytomegalovirus retinitis primary care management. Loss of vision or part of the visual field only, if the macula is still attached, follows. The clinician should be particularly aware of detachment in patients with a history of cataract surgery, high myopia, recent eye trauma and a personal or family history of retinal detachment. 1 Loss of the red reflex, the presence of APD and an elevated, detached retina on fundoscopy, complete the spectrum of signs. Referral for urgent surgery is necessary if the vision is still good and if the detachment is of recent onset (within the last few days). Optic neuritis Optic neuritis refers to inflammation of the optic nerve owing to demyelination or infective, immune and infiltrative causes. 1 Compressive lesions in the orbit need to be eliminated as they may have a similar appearance, but also have associated proptosis and cranial nerve palsies. 3 The common causes are multiple sclerosis, syphilis, human immunodeficiency virus, sarcoidosis and idiopathy. Optic neuritis occurs in 70% of patients with known multiple sclerosis and may be the first sign of demyelinating disease. 1 Loss of vision varies from mild to profound. A central scotoma, APD and loss of colour vision, are usually present. Patients may have pain on eye movement in typical cases. The optic disc may be swollen or normal, if the inflammation is retrobulbar. Repeated attacks are not uncommon and the other eye may become affected as well, especially with demyelination. Usually, visual recovery is good after a single attack. Pallor of the temporal part of the disc may develop following repeated attacks. Referral for treatment is essential. Retinitis and choroiditis Inflammation of the retina and/or choroid, which may be infective, immune-mediated or idiopathic, may result in sudden loss of vision. More common causes include tuberculosis, syphilis, cytomegalovirus retinitis (Figure 8) Figure 9: Melanoma appears as a solid elevated lesion in tumours and toxoplasma chorioretinitis. 4 In toxoplasmosis, old pigmented scar tissue is seen, surrounded by sheathed vessels and vitreous haze. In viral, bacterial or protozoal retinitis, vision may be minimally affected until the fovea or optic nerve is affected. 7 There may be a poor red reflex. Sudden loss of vision means that referral should be urgent in order to save the other eye. Tumours Certain ocular tumours can cause sudden loss of vision. Choroidal metastases, usually from the breast or lung, choroidal malignant melanoma, as well as cancer and melanoma-associated retinopathy may be causative. 4 Melanoma of the choroid is the most common primary intraocular malignancy in adults. On fundoscopy, the majority of observed pigmented choroidal lesions are benign naevi. Choroidal malignant melanoma can present with flashing lights or visual loss, which may occur when fluid exudation or a solid tumour detach the fovea. Melanoma appears as a solid elevated lesion (Figure 9), often with greyish pigmentation. With metastases, vision is usually normal or distorted until a secondary exudative retinal detachment suddenly detaches the macula. Cancer and melanoma-associated retinopathy can cause sudden, bilateral blindness with no retinal findings. The blindness is permanent, on an autoimmune basis. Referral for investigation and treatment is needed in these cases. Homonymous hemianopia This refers to loss of the same half of the visual field of each eye and may appear as loss of vision in one eye only to the patient. A stroke is by far the most common cause. 4 Lesions that affect the visual pathway unilaterally, and anywhere from the optic tract to the occipital lobe, will result in a homonymous hemianopia, with varying degrees of congruency. Occipital lobe infarction is most likely if there are no other prominent neurological symptoms. 239 Vol 55 No 3
6 When taking a history, it should always be established whether or not the patient means one eye or one side of the world. The VA and pupil reactions are usually normal. Visual field testing by confrontation will reveal the hemianopia. Management includes immediate referral to a physician, neurologist or stroke unit if the lesion is less than 3-6 hours old. Otherwise, it should be discussed with a physician and referred as recommended. Functional visual loss Loss of vision, in the absence of organic disease, is referred to as functional. The diagnosis and management of this condition may present considerable problems. 4 Hysteria may be a cause or sometimes the patient may be malingering. 8 Detailed assessment by an ophthalmologist is required. Conclusion Patients with transient or sudden changes in vision may present a diagnostic challenge. In some cases, no cause may be found. Occasionally, tear film abnormalities, and less commonly, migraines, may be causative. 1 However, it is important to remember that more sinister causes of loss of vision exist. These include GCA, carotid or cardiac emboli, retinal detachment, vitreous haemorrhage, orbital tumours and other vascular events. A thorough history, goal-directed examination, proper investigation and appropriate referral will enable early diagnosis and adequate management, thus preventing further ocular morbidity, and even patient mortality. In many cases, follow-up monitoring by the ophthalmologist should be coupled with management of the patient s underlying systemic disease by the primary care physician. 9 Acknowledgements We acknowledge the Division of Ophthalmology, University of Cape Town, for permission to use the clinical photographs. Conflicts of interest The authors have no conflict of interest to declare. References 1. Goold L, Durkin S, Crompton J. Sudden loss of vision: history and examination. Aust Fam Phys. 2009;38(10): Van Zyl LM, Fernandes N, Rogers G, et al. Primary health eye knowledge among general practitioners in the Cape Town metropole. S Afr Fam Pract. 2011;53(1): Goold L, Durkin S, Crompton J. Sudden loss of vision: investigation and management. Aust Fam Phys. 2009;38(10): Du Toit N, Cook C. Sudden loss of vision. Cape Town: Juta, 2009; p Khan J, Chong V. Sudden visual loss. Lancet. 2007;370(9587): Danesh-Meyer HV, Savino PJ. Giant cell arteritis. Curr Opin Ophthalmol. 2007;18(6): Vortmann M, Schneider JI. Acute monocular visual loss. Emerg Med Clin North Am. 2008;26(1): Beran DI, Murphy-Lavoie H. Acute, painless vision loss. J La State Med Soc. 2009;161(4): Paulman A, Paulman P. Sudden loss of vision. J Fam Prac. 2004;53(4): Vol 55 No 3
Professor Helen Danesh-Meyer. Eye Institute Auckland
 Professor Helen Danesh-Meyer Eye Institute Auckland Bitten by Ophthalmology Emergencies Helen Danesh-Meyer, MBChB, MD, FRANZCO Sir William and Lady Stevenson Professor of Ophthalmology Head of Glaucoma
Professor Helen Danesh-Meyer Eye Institute Auckland Bitten by Ophthalmology Emergencies Helen Danesh-Meyer, MBChB, MD, FRANZCO Sir William and Lady Stevenson Professor of Ophthalmology Head of Glaucoma
Sudden loss of vision History and examination
 THEME vision at risk Lucy Goold MBBS, MMed(OphthSc), is ophthalmology resident and Associate Clinical Lecturer, South Australian Institute of Ophthalmology, Royal Adelaide Hospital, South Australia. lgoold@med.usyd.edu.au
THEME vision at risk Lucy Goold MBBS, MMed(OphthSc), is ophthalmology resident and Associate Clinical Lecturer, South Australian Institute of Ophthalmology, Royal Adelaide Hospital, South Australia. lgoold@med.usyd.edu.au
IMAGE OF THE MOMENT PRACTICAL NEUROLOGY
 178 PRACTICAL NEUROLOGY IMAGE OF THE MOMENT Gawn G. McIlwaine*, James H. Vallance* and Christian J. Lueck *Princess Alexandra Eye Pavilion, Chalmers Street, Edinburgh UK; The Canberra Hospital, P.O. Box
178 PRACTICAL NEUROLOGY IMAGE OF THE MOMENT Gawn G. McIlwaine*, James H. Vallance* and Christian J. Lueck *Princess Alexandra Eye Pavilion, Chalmers Street, Edinburgh UK; The Canberra Hospital, P.O. Box
Neuro-Ocular Grand Rounds
 Neuro-Ocular Grand Rounds Anthony B. Litwak,OD, FAAO VA Medical Center Baltimore, Maryland Dr. Litwak is on the speaker and advisory boards for Alcon and Zeiss Meditek COMMON OPTIC NEUROPATHIES THAT CAN
Neuro-Ocular Grand Rounds Anthony B. Litwak,OD, FAAO VA Medical Center Baltimore, Maryland Dr. Litwak is on the speaker and advisory boards for Alcon and Zeiss Meditek COMMON OPTIC NEUROPATHIES THAT CAN
Mild NPDR. Moderate NPDR. Severe NPDR
 Diabetic retinopathy Diabetic retinopathy is the most common cause of blindness in adults aged 35-65 years-old. Hyperglycaemia is thought to cause increased retinal blood flow and abnormal metabolism in
Diabetic retinopathy Diabetic retinopathy is the most common cause of blindness in adults aged 35-65 years-old. Hyperglycaemia is thought to cause increased retinal blood flow and abnormal metabolism in
Neuro-Ocular Grand Rounds Anthony B. Litwak,OD, FAAO VA Medical Center Baltimore, Maryland
 Neuro-Ocular Grand Rounds Anthony B. Litwak,OD, FAAO VA Medical Center Baltimore, Maryland Dr. Litwak is on the speaker and advisory boards for Alcon and Zeiss Meditek COMMON OPTIC NEUROPATHIES THAT CAN
Neuro-Ocular Grand Rounds Anthony B. Litwak,OD, FAAO VA Medical Center Baltimore, Maryland Dr. Litwak is on the speaker and advisory boards for Alcon and Zeiss Meditek COMMON OPTIC NEUROPATHIES THAT CAN
LECTURE # 7 EYECARE REVIEW: PART III
 LECTURE # 7 EYECARE REVIEW: PART III HOW TO TRIAGE EYE EMERGENCIES STEVE BUTZON, O.D. EYECARE REVIEW: HOW TO TRIAGE EYE EMERGENCIES FOR PRIMARY CARE PHYSICIANS Steve Butzon, O.D. Member Director IDOC President
LECTURE # 7 EYECARE REVIEW: PART III HOW TO TRIAGE EYE EMERGENCIES STEVE BUTZON, O.D. EYECARE REVIEW: HOW TO TRIAGE EYE EMERGENCIES FOR PRIMARY CARE PHYSICIANS Steve Butzon, O.D. Member Director IDOC President
10 EYE EMERGENCIES. Who goes, who you better not send! Brant Slomovic, MD, FRCPC University Health Network
 10 EYE EMERGENCIES Who goes, who you better not send! Brant Slomovic, MD, FRCPC University Health Network DISCLOSURES I have none PVD CASE 1 WHAT IS A PVD? a process of aging (45-55) liquefaction of vitreous
10 EYE EMERGENCIES Who goes, who you better not send! Brant Slomovic, MD, FRCPC University Health Network DISCLOSURES I have none PVD CASE 1 WHAT IS A PVD? a process of aging (45-55) liquefaction of vitreous
Sudden Vision Loss. Brendan Girschek, MD, FRCSC, FACS Vitreoretinal Surgery Cedar Valley Medical Specialists
 Sudden Vision Loss Brendan Girschek, MD, FRCSC, FACS Vitreoretinal Surgery Cedar Valley Medical Specialists My Credentials -Residency in Ophthalmology at the LSU Eye Center in New Orleans, LA -Fellowship
Sudden Vision Loss Brendan Girschek, MD, FRCSC, FACS Vitreoretinal Surgery Cedar Valley Medical Specialists My Credentials -Residency in Ophthalmology at the LSU Eye Center in New Orleans, LA -Fellowship
Course # Flashes and Floaters and Curtains, Oh My!
 Course # 132 Flashes and Floaters and Curtains, Oh My! FLASHES and FLOATERS and CURTAINS, OH MY!!! FLASHES OF LIGHT Vitreous is the villain Retinal traction Retinal hole Retinal tear Migraine Classic migraine
Course # 132 Flashes and Floaters and Curtains, Oh My! FLASHES and FLOATERS and CURTAINS, OH MY!!! FLASHES OF LIGHT Vitreous is the villain Retinal traction Retinal hole Retinal tear Migraine Classic migraine
Course # Flashes and Floaters and Curtains, Oh My!
 Course # 132 Flashes and Floaters and Curtains, Oh My! FLASHES and FLOATERS and CURTAINS, OH MY!!! FLASHES OF LIGHT Vitreous is the villain Retinal traction Retinal hole Retinal tear Migraine Classic migraine
Course # 132 Flashes and Floaters and Curtains, Oh My! FLASHES and FLOATERS and CURTAINS, OH MY!!! FLASHES OF LIGHT Vitreous is the villain Retinal traction Retinal hole Retinal tear Migraine Classic migraine
Rapid Visual Loss. Dr Michael Johnson PhD FCOptom DipOrth DipGlauc DipTp(IP) Independent Prescribing Optometrist
 Rapid Visual Loss Dr Michael Johnson PhD FCOptom DipOrth DipGlauc DipTp(IP) Independent Prescribing Optometrist Outline Pathophysiology Differential diagnosis. Patient scenarios in community practice:
Rapid Visual Loss Dr Michael Johnson PhD FCOptom DipOrth DipGlauc DipTp(IP) Independent Prescribing Optometrist Outline Pathophysiology Differential diagnosis. Patient scenarios in community practice:
3/16/2018. Optic Nerve Examination. Hassan Eisa Swify FRCS Ed (Ophthalmology) Air Force Hospital
 Optic Nerve Examination Hassan Eisa Swify FRCS Ed (Ophthalmology) Air Force Hospital 1 Examination Structure ( optic disc) Function Examination of the optic disc The only cranial nerve (brain tract) which
Optic Nerve Examination Hassan Eisa Swify FRCS Ed (Ophthalmology) Air Force Hospital 1 Examination Structure ( optic disc) Function Examination of the optic disc The only cranial nerve (brain tract) which
NANOS Patient Brochure
 NANOS Patient Brochure Transient Visual Loss Copyright 2016. North American Neuro-Ophthalmology Society. All rights reserved. These brochures are produced and made available as is without warranty and
NANOS Patient Brochure Transient Visual Loss Copyright 2016. North American Neuro-Ophthalmology Society. All rights reserved. These brochures are produced and made available as is without warranty and
OCCLUSIVE VASCULAR DISORDERS OF THE RETINA
 OCCLUSIVE VASCULAR DISORDERS OF THE RETINA Learning outcomes By the end of this lecture the students would be able to Classify occlusive vascular disorders (OVD) of the retina. Correlate the clinical features
OCCLUSIVE VASCULAR DISORDERS OF THE RETINA Learning outcomes By the end of this lecture the students would be able to Classify occlusive vascular disorders (OVD) of the retina. Correlate the clinical features
Alan G. Kabat, OD, FAAO (901)
 THE SWOLLEN OPTIC DISC: EMERGENCY OR ANOMALY? Alan G. Kabat, OD, FAAO (901) 252-3691 Memphis, Tennessee alan.kabat@alankabat.com Course description: The swollen disc presents a diagnostic dilemma. While
THE SWOLLEN OPTIC DISC: EMERGENCY OR ANOMALY? Alan G. Kabat, OD, FAAO (901) 252-3691 Memphis, Tennessee alan.kabat@alankabat.com Course description: The swollen disc presents a diagnostic dilemma. While
Ophthalmology. Juliette Stenz, MD
 Ophthalmology Juliette Stenz, MD Required Slide Disclosures NO SIGNIFICANT FINANCIAL, GENERAL, OR OBLIGATION INTERESTS TO REPORT Required Slide At the end of this session, students will be able to: 1.
Ophthalmology Juliette Stenz, MD Required Slide Disclosures NO SIGNIFICANT FINANCIAL, GENERAL, OR OBLIGATION INTERESTS TO REPORT Required Slide At the end of this session, students will be able to: 1.
Optic neuritis. * Young women. * Pain on moving eye. * Central scotoma
 ABC of Eyes ACUTE VSUAL DSTURBANCE A R Elkington, P T Khaw Symptoms and signs Retinal detachment *Flashing lights * Shadow Optic neuritis * Young women * Pain on moving eye * Central scotoma Migraine *
ABC of Eyes ACUTE VSUAL DSTURBANCE A R Elkington, P T Khaw Symptoms and signs Retinal detachment *Flashing lights * Shadow Optic neuritis * Young women * Pain on moving eye * Central scotoma Migraine *
For details on measurement and recording of visual acuity, refer to Annex 1. VISION INTERPRETING RESULTS ABSTRACT
 management update on functional decline in older adults 2012 Unit No. 5 VISION Dr Au Eong Kah Guan, Ms Yulianti, Ms Fifiana ABSTRACT Among Singaporean adults of Chinese origin aged 40 to 79 years old,
management update on functional decline in older adults 2012 Unit No. 5 VISION Dr Au Eong Kah Guan, Ms Yulianti, Ms Fifiana ABSTRACT Among Singaporean adults of Chinese origin aged 40 to 79 years old,
Central venous occlusion
 Central venous occlusion Central venous occlusion (right eye) There are dark haemorrhages at the macula and all over the retina. Choroidal haemangioma A choroidal haemangioma has salmon pink colour. There
Central venous occlusion Central venous occlusion (right eye) There are dark haemorrhages at the macula and all over the retina. Choroidal haemangioma A choroidal haemangioma has salmon pink colour. There
Sahand Ensafi PA, CCPA, B.H.Sc.,Department of Emergency Medicine, University Health Network
 Sahand Ensafi PA, CCPA, B.H.Sc.,Department of Emergency Medicine, University Health Network No Disclosures Definitions Ophthalmologic Blindness Practical definition? WHO V/A less than 3/60 (snellen)
Sahand Ensafi PA, CCPA, B.H.Sc.,Department of Emergency Medicine, University Health Network No Disclosures Definitions Ophthalmologic Blindness Practical definition? WHO V/A less than 3/60 (snellen)
Case Follow Up. Sepi Jooniani PGY-1
 Case Follow Up Sepi Jooniani PGY-1 Triage 54 year old M Pt presents to prelim states noticed today he had reddness to eyes, states worse in R eye. Pt denies any pain or itching. No further complaints.
Case Follow Up Sepi Jooniani PGY-1 Triage 54 year old M Pt presents to prelim states noticed today he had reddness to eyes, states worse in R eye. Pt denies any pain or itching. No further complaints.
Rafik Girgis. Consultant Ophthalmic Surgeon ( Cataract & Primary Care)
 Rafik Girgis Consultant Ophthalmic Surgeon ( Cataract & Primary Care) Blepharitis Is a very common condition which usually bilateral & symmetrical. The main types are: Anterior, posterior or mixed Complications:
Rafik Girgis Consultant Ophthalmic Surgeon ( Cataract & Primary Care) Blepharitis Is a very common condition which usually bilateral & symmetrical. The main types are: Anterior, posterior or mixed Complications:
UNDERSTAND MORE ABOUT UVEITIS UVEITIS
 UNDERSTAND MORE ABOUT UVEITIS UVEITIS Uveitis What is uveitis? Uveitis is inflammation of the uvea, the middle layer of your eye. The eye is shaped much like a tennis ball, with three different layers
UNDERSTAND MORE ABOUT UVEITIS UVEITIS Uveitis What is uveitis? Uveitis is inflammation of the uvea, the middle layer of your eye. The eye is shaped much like a tennis ball, with three different layers
OPHTHALMOLOGY REFERRAL GUIDE FOR GPS
 OPHTHALMOLOGY REFERRAL GUIDE FOR GPS A guidebook to support general practitioners in the management and referral of a range of common eye problems. Contents 3 Introduction 4 Ophthalmic Workup 6 Acute Visual
OPHTHALMOLOGY REFERRAL GUIDE FOR GPS A guidebook to support general practitioners in the management and referral of a range of common eye problems. Contents 3 Introduction 4 Ophthalmic Workup 6 Acute Visual
Anterior Ischemic Optic Neuropathy (AION)
 Anterior Ischemic Optic Neuropathy (AION) Your doctor thinks you have suffered an episode of anterior ischemic optic neuropathy (AION). This is the most common cause of sudden decreased vision in patients
Anterior Ischemic Optic Neuropathy (AION) Your doctor thinks you have suffered an episode of anterior ischemic optic neuropathy (AION). This is the most common cause of sudden decreased vision in patients
EYE TRAUMA: INCIDENCE
 Introduction EYE TRAUMA: INCIDENCE 2.5 million eye injuries per year in U.S. 40,000 60,000 of eye injuries lead to visual loss Introduction Final visual outcome of many ocular emergencies depends on prompt,
Introduction EYE TRAUMA: INCIDENCE 2.5 million eye injuries per year in U.S. 40,000 60,000 of eye injuries lead to visual loss Introduction Final visual outcome of many ocular emergencies depends on prompt,
Year 2 MBChB Clinical Skills Session Ophthalmoscopy. Reviewed & ratified by: Mr M Batterbury Consultant Ophthalmologist
 Year 2 MBChB Clinical Skills Session Ophthalmoscopy Reviewed & ratified by: o Mr M Batterbury Consultant Ophthalmologist Learning objectives o To understand the anatomy and physiology of the external and
Year 2 MBChB Clinical Skills Session Ophthalmoscopy Reviewed & ratified by: o Mr M Batterbury Consultant Ophthalmologist Learning objectives o To understand the anatomy and physiology of the external and
Patient with Daily Headache NTERNATIONAL CLASSIFICATION HEADACHE DISORDERS. R. Allan Purdy, MD, FRCPC,FACP. Professor of Medicine (Neurology)
 Patient with Daily Headache NTERNATIONAL CLASSIFICATION of R. Allan Purdy, MD, FRCPC,FACP HEADACHE DISORDERS Professor of Medicine (Neurology) 2nd edition (ICHD-II) Learning Issues Headaches in the elderly
Patient with Daily Headache NTERNATIONAL CLASSIFICATION of R. Allan Purdy, MD, FRCPC,FACP HEADACHE DISORDERS Professor of Medicine (Neurology) 2nd edition (ICHD-II) Learning Issues Headaches in the elderly
Objectives. Unexplained Vision Loss: Where Do I Go From Here. History. History. Drug Induced Vision Loss
 Objectives Unexplained Vision Loss: Where Do I Go From Here Denise Goodwin, OD, FAAO Coordinator, Neuro-ophthalmic Disease Clinic Pacific University College of Optometry goodwin@pacificu.edu Know the importance
Objectives Unexplained Vision Loss: Where Do I Go From Here Denise Goodwin, OD, FAAO Coordinator, Neuro-ophthalmic Disease Clinic Pacific University College of Optometry goodwin@pacificu.edu Know the importance
Moncef Khairallah, MD
 Moncef Khairallah, MD Department of Ophthalmology, Fattouma Bourguiba University Hospital Faculty of Medicine, University of Monastir Monastir, Tunisia INTRODUCTION IU: anatomic form of uveitis involving
Moncef Khairallah, MD Department of Ophthalmology, Fattouma Bourguiba University Hospital Faculty of Medicine, University of Monastir Monastir, Tunisia INTRODUCTION IU: anatomic form of uveitis involving
Amber Priority. Image Library
 Amber Priority Image Library Amber flag Diabetic Maculopathy (M1) Pre-proliferative Diabetic Retinopathy (R2) Old, treated and now inactive DR (R1/M0/P1or R0/M0/P1) Where only partial or incomplete images
Amber Priority Image Library Amber flag Diabetic Maculopathy (M1) Pre-proliferative Diabetic Retinopathy (R2) Old, treated and now inactive DR (R1/M0/P1or R0/M0/P1) Where only partial or incomplete images
Step 4: Ask permission to turn off lights or draw the curtains
 STEPS OF EYE EXAMINATION - FUNDUS Step 1: Approach the patient Read the instructions carefully for clues Shake hands, introduce yourself Ask permission to examine him I would like to examine your eyes,
STEPS OF EYE EXAMINATION - FUNDUS Step 1: Approach the patient Read the instructions carefully for clues Shake hands, introduce yourself Ask permission to examine him I would like to examine your eyes,
CENTRAL MERSEY LOCAL OPTICAL COMMITTEE
 CENTRAL MERSEY LOCAL OPTICAL COMMITTEE OPTOMETRIC REFERRAL GUIDELINES The ocular conditions listed in this document are intended to reflect those that might be encountered in optometric practice and this
CENTRAL MERSEY LOCAL OPTICAL COMMITTEE OPTOMETRIC REFERRAL GUIDELINES The ocular conditions listed in this document are intended to reflect those that might be encountered in optometric practice and this
Identify the choice that best completes the statement or answers the question.
 Chapter 5. The Eye Multiple Choice Identify the choice that best completes the statement or answers the question. 1. The most common type of eye disorder is: A. Refractive errors B. Macular conditions
Chapter 5. The Eye Multiple Choice Identify the choice that best completes the statement or answers the question. 1. The most common type of eye disorder is: A. Refractive errors B. Macular conditions
5/2/2016 EYE EMERGENCIES. Nathaniel Pelsor, O.D., FAAO Talley Medical-Surgical Eye Care Associates. Anatomy. Tools
 EYE EMERGENCIES Nathaniel Pelsor, O.D., FAAO Talley Medical-Surgical Eye Care Associates Anatomy Tools 1 Contact dermatitis Blepharitis HSV Preseptal Cellulitis Anterior Chamber Subconjunctival hemorrhage
EYE EMERGENCIES Nathaniel Pelsor, O.D., FAAO Talley Medical-Surgical Eye Care Associates Anatomy Tools 1 Contact dermatitis Blepharitis HSV Preseptal Cellulitis Anterior Chamber Subconjunctival hemorrhage
Optic Nerve Disorders: Structure and Function and Causes
 Optic Nerve Disorders: Structure and Function and Causes Using Visual Fields, OCT and B-scan Ultrasound to Diagnose and Follow Optic Nerve Visual Losses Ohio Ophthalmological Society and Ophthalmic Tech
Optic Nerve Disorders: Structure and Function and Causes Using Visual Fields, OCT and B-scan Ultrasound to Diagnose and Follow Optic Nerve Visual Losses Ohio Ophthalmological Society and Ophthalmic Tech
VASCULAR DISEASE IN OPTOMETRIC PRACTICE
 VASCULAR DISEASE IN OPTOMETRIC PRACTICE Outline notes to accompany City University 3 rd year undergraduate Clinical Practice course lecture Introduction Dr PhD BSc FCOptom FAAO DCLP Optometrists in the
VASCULAR DISEASE IN OPTOMETRIC PRACTICE Outline notes to accompany City University 3 rd year undergraduate Clinical Practice course lecture Introduction Dr PhD BSc FCOptom FAAO DCLP Optometrists in the
Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (CSC)
 HPTER 12 Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (S) linical Features VKH disease is a bilateral granulomatous panuveitis often associated with exudative
HPTER 12 Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (S) linical Features VKH disease is a bilateral granulomatous panuveitis often associated with exudative
Dr Jo-Anne Pon. Consultant Ophthalmologist and Oculoplastic Surgeon Southern Eye Specialists Christchurch
 Dr Jo-Anne Pon Consultant Ophthalmologist and Oculoplastic Surgeon Southern Eye Specialists Christchurch 12:15-12:30 Visual Migraines to be Worried About Visual Migraines To Be Worried About Jo-Anne Pon
Dr Jo-Anne Pon Consultant Ophthalmologist and Oculoplastic Surgeon Southern Eye Specialists Christchurch 12:15-12:30 Visual Migraines to be Worried About Visual Migraines To Be Worried About Jo-Anne Pon
Sudden loss of vision: a GP's guide to the many causes
 MODERN MEDICINE CPD ARTICLE NUMBER THREE: 1 point Sudden loss of vision: a GP's guide to the many causes JOHN KING, MD, FRACP ^ Sudden loss of vision at any age is an alarming symptom that usually results
MODERN MEDICINE CPD ARTICLE NUMBER THREE: 1 point Sudden loss of vision: a GP's guide to the many causes JOHN KING, MD, FRACP ^ Sudden loss of vision at any age is an alarming symptom that usually results
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Acetazolamide, in idiopathic intracranial hypertension, 49 52, 60 Angiography, computed tomography, in cranial nerve palsy, 103 107 digital
Index Note: Page numbers of article titles are in boldface type. A Acetazolamide, in idiopathic intracranial hypertension, 49 52, 60 Angiography, computed tomography, in cranial nerve palsy, 103 107 digital
Ocular Lecture. Sue Bednar NP Ali Atwater PA-C
 Ocular Lecture Sue Bednar NP Ali Atwater PA-C Triaging Ocular Complaints Painful Eye/Red eye +/-blurry vision +/-visual loss +/-floaters +/-fevers If any of the above findings exist, pt is likely to have
Ocular Lecture Sue Bednar NP Ali Atwater PA-C Triaging Ocular Complaints Painful Eye/Red eye +/-blurry vision +/-visual loss +/-floaters +/-fevers If any of the above findings exist, pt is likely to have
Handbook for Medical Students Learning Ophthalmology
 International Council of Ophthalmology Handbook for Medical Students Learning Ophthalmology 2009 Compiled by the Task Force on Undergraduate Teaching in Ophthalmology of the International Council of Ophthalmology
International Council of Ophthalmology Handbook for Medical Students Learning Ophthalmology 2009 Compiled by the Task Force on Undergraduate Teaching in Ophthalmology of the International Council of Ophthalmology
Faculty Financial Disclosure. Learning Objectives: Office Ophthalmology. Basic Eye Exam: What s in your pocket/office? Office Ophthalmology
 Faculty Financial Disclosure Office Ophthalmology Lynn K. Gordon, MD, PhD, has no financial relationships to disclose. Lynn K. Gordon, MD, PhD Professor and Vernon O Underwood Family Chair Department of
Faculty Financial Disclosure Office Ophthalmology Lynn K. Gordon, MD, PhD, has no financial relationships to disclose. Lynn K. Gordon, MD, PhD Professor and Vernon O Underwood Family Chair Department of
Neovascular Glaucoma Associated with Cilioretinal Artery Occlusion Combined with Perfused Central Retinal Vein Occlusion
 Neovascular Glaucoma Associated with Cilioretinal Artery Occlusion Combined with Perfused Central Retinal Vein Occlusion Man-Seong Seo,* Jae-Moon Woo* and Jeong-Jin Seo *Department of Ophthalmology, Chonnam
Neovascular Glaucoma Associated with Cilioretinal Artery Occlusion Combined with Perfused Central Retinal Vein Occlusion Man-Seong Seo,* Jae-Moon Woo* and Jeong-Jin Seo *Department of Ophthalmology, Chonnam
OCULAR HEMORRHAGES. ROSCOE J. KENNEDY, M.D. Department of Ophthalmology
 OCULAR HEMORRHAGES ROSCOE J. KENNEDY, M.D. Department of Ophthalmology Ocular hemorrhages are important not only because they produce visual loss but also because they usually indicate a disorder elsewhere
OCULAR HEMORRHAGES ROSCOE J. KENNEDY, M.D. Department of Ophthalmology Ocular hemorrhages are important not only because they produce visual loss but also because they usually indicate a disorder elsewhere
Temporal arteritis. Occurrence of ocular complications 7 years after diagnosis. University of Edinburgh, and Royal Infirmary of Edinburgh
 Brit. J. Ophthal. (I 972) 56, 584 Temporal arteritis Occurrence of ocular complications 7 years after diagnosis JAMES F. CULLEN Department of Ophthalmology, University of Edinburgh, and Royal Infirmary
Brit. J. Ophthal. (I 972) 56, 584 Temporal arteritis Occurrence of ocular complications 7 years after diagnosis JAMES F. CULLEN Department of Ophthalmology, University of Edinburgh, and Royal Infirmary
Ischaemic optic neuropathy: the Singapore scene
 O r i g i n a l A r t i c l e Singapore Med J 2007; 48 (4) : 281 Ischaemic optic neuropathy: the Singapore scene Cullen J F, Por Y M Abstract The commonest cause of an optic neuropathy in Singapore is
O r i g i n a l A r t i c l e Singapore Med J 2007; 48 (4) : 281 Ischaemic optic neuropathy: the Singapore scene Cullen J F, Por Y M Abstract The commonest cause of an optic neuropathy in Singapore is
9/11/11. Temporal Arteritis. Background. Background. Richard E. Castillo, OD, DO NORTHEASTERN STATE UNIVERSITY Director, Ophthalmic Surgery Service
 Temporal Arteritis Richard E. Castillo, OD, DO NORTHEASTERN STATE UNIVERSITY Director, Ophthalmic Surgery Service 1 Background Giant Cell Arteritis Temporal Arteritis Cranial Arteritis Granulomatous Arteritis
Temporal Arteritis Richard E. Castillo, OD, DO NORTHEASTERN STATE UNIVERSITY Director, Ophthalmic Surgery Service 1 Background Giant Cell Arteritis Temporal Arteritis Cranial Arteritis Granulomatous Arteritis
A Patient s Guide to Diabetic Retinopathy
 Diabetic Retinopathy A Patient s Guide to Diabetic Retinopathy 840 Walnut Street, Philadelphia PA 19107 www.willseye.org Diabetic Retinopathy 1. Definition Diabetic retinopathy is a complication of diabetes
Diabetic Retinopathy A Patient s Guide to Diabetic Retinopathy 840 Walnut Street, Philadelphia PA 19107 www.willseye.org Diabetic Retinopathy 1. Definition Diabetic retinopathy is a complication of diabetes
Speaker Disclosure Statement. " Dr. Tim Maillet and Dr. Vladimir Kozousek have no conflicts of interest to disclose.
 Speaker Disclosure Statement Dr. Tim Maillet and Dr. Vladimir Kozousek have no conflicts of interest to disclose. Diabetes Morbidity Diabetes doubles the risk of stroke. Diabetes quadruples the risk of
Speaker Disclosure Statement Dr. Tim Maillet and Dr. Vladimir Kozousek have no conflicts of interest to disclose. Diabetes Morbidity Diabetes doubles the risk of stroke. Diabetes quadruples the risk of
FRANZCO, MD, MBBS. Royal Darwin Hospital
 Diabetes and Eye By Dr. Nishantha Wijesinghe FRANZCO, MD, MBBS Consultant Ophthalmologist Royal Darwin Hospital 98% of Diabetics do not need to suffer from severe visual loss Yet Diabetic eye disease is
Diabetes and Eye By Dr. Nishantha Wijesinghe FRANZCO, MD, MBBS Consultant Ophthalmologist Royal Darwin Hospital 98% of Diabetics do not need to suffer from severe visual loss Yet Diabetic eye disease is
THE 35 GOLDEN EYE RULES
 THE 35 GOLDEN EYE RULES The Sense of Sight, from La Dame a la Licorne, The Lady and the Unicorn Tapestries, Late 15th Century Flemish Tapestry in wool and silk, Musée Nationale du Moyen Age, Paris. 1.
THE 35 GOLDEN EYE RULES The Sense of Sight, from La Dame a la Licorne, The Lady and the Unicorn Tapestries, Late 15th Century Flemish Tapestry in wool and silk, Musée Nationale du Moyen Age, Paris. 1.
I have nothing to disclose but I
 OPTIC NEUROPATHIES Robert L. Tomsak MD PhD Professor of Ophthalmology and Neurology Wayne State t University it Sh School of Mdii Medicine I have nothing to disclose but I wish I did. dd Road map for this
OPTIC NEUROPATHIES Robert L. Tomsak MD PhD Professor of Ophthalmology and Neurology Wayne State t University it Sh School of Mdii Medicine I have nothing to disclose but I wish I did. dd Road map for this
Neurology Case Presentation. Rawan Albadareen, MD 12/20/13
 Neurology Case Presentation Rawan Albadareen, MD 12/20/13 Case presentation A 49 y.o. female presented to the ED after an episode of zigzagging w a jagged bright light crossing through her Rt visual field
Neurology Case Presentation Rawan Albadareen, MD 12/20/13 Case presentation A 49 y.o. female presented to the ED after an episode of zigzagging w a jagged bright light crossing through her Rt visual field
Blindness In An Elderly Woman
 Blindness In An Elderly Woman A 74 y/o woman with a chief complaint of: a cloud in front of my right eye and I can t t see through it Symptoms began 24 hours prior to examination. Visual loss was painless
Blindness In An Elderly Woman A 74 y/o woman with a chief complaint of: a cloud in front of my right eye and I can t t see through it Symptoms began 24 hours prior to examination. Visual loss was painless
Retinal Tear and Detachment
 Retinal Tear and Detachment Introduction The retina is the layer of tissue in the back of the eye that is responsible for vision. It is attached to the choroid tissue, which supplies the retina with blood.
Retinal Tear and Detachment Introduction The retina is the layer of tissue in the back of the eye that is responsible for vision. It is attached to the choroid tissue, which supplies the retina with blood.
A Case of Carotid-Cavernous Fistula
 A Case of Carotid-Cavernous Fistula By : Mohamed Elkhawaga 2 nd Year Resident of Ophthalmology Alexandria University A 19 year old male patient came to our outpatient clinic, complaining of : -Severe conjunctival
A Case of Carotid-Cavernous Fistula By : Mohamed Elkhawaga 2 nd Year Resident of Ophthalmology Alexandria University A 19 year old male patient came to our outpatient clinic, complaining of : -Severe conjunctival
Flashers and Floaters
 Flashers and Floaters Introduction Sometimes people see small, moving spots or specks in their field of vision. These sensations are called floaters. About 7 out of 10 people experience floaters at some
Flashers and Floaters Introduction Sometimes people see small, moving spots or specks in their field of vision. These sensations are called floaters. About 7 out of 10 people experience floaters at some
RETINAL CONDITIONS RETINAL CONDITIONS
 GENERAL INFORMATION RETINAL CONDITIONS RETINAL CONDITIONS WHAT ARE RETINAL CONDITIONS? Retinal conditions affect the light-sensitive tissue at the back of eye known as the retina. They include diseases
GENERAL INFORMATION RETINAL CONDITIONS RETINAL CONDITIONS WHAT ARE RETINAL CONDITIONS? Retinal conditions affect the light-sensitive tissue at the back of eye known as the retina. They include diseases
Grand Rounds Clinical Cases from Alex D. Gibberman, O.D. Harpers Point Eye Associates
 Grand Rounds Clinical Cases from 2016 Alex D. Gibberman, O.D. Harpers Point Eye Associates Relevant Financial Interests -none Case 1: 54 year old African American Female CC: Noticed a green line in
Grand Rounds Clinical Cases from 2016 Alex D. Gibberman, O.D. Harpers Point Eye Associates Relevant Financial Interests -none Case 1: 54 year old African American Female CC: Noticed a green line in
Role Of Various Factors In The Treatment Of Optic Neuritis----A Study Abstract Aim: Materials & Methods Discussion: Conclusion: Key words
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 9 Ver. X (September). 2016), PP 51-57 www.iosrjournals.org Role Of Various Factors In The Treatment
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 9 Ver. X (September). 2016), PP 51-57 www.iosrjournals.org Role Of Various Factors In The Treatment
Optical Coherence Tomography in Diabetic Retinopathy. Mrs Samantha Mann Consultant Ophthalmologist Clinical Lead of SEL-DESP
 Optical Coherence Tomography in Diabetic Retinopathy Mrs Samantha Mann Consultant Ophthalmologist Clinical Lead of SEL-DESP Content OCT imaging Retinal layers OCT features in Diabetes Some NON DR features
Optical Coherence Tomography in Diabetic Retinopathy Mrs Samantha Mann Consultant Ophthalmologist Clinical Lead of SEL-DESP Content OCT imaging Retinal layers OCT features in Diabetes Some NON DR features
Pearls, Pitfalls and Advances in Neuro-Ophthalmology
 Pearls, Pitfalls and Advances in Neuro-Ophthalmology Nancy J. Newman, MD Emory University Atlanta, GA Consultant for Gensight Biologics, Santhera Data Safety Monitoring Board for Quark AION Study Medical-legal
Pearls, Pitfalls and Advances in Neuro-Ophthalmology Nancy J. Newman, MD Emory University Atlanta, GA Consultant for Gensight Biologics, Santhera Data Safety Monitoring Board for Quark AION Study Medical-legal
Common eye disorders in the elderly a short review
 Common eye disorders in the elderly a short review Visser L, FCOphth(SA), MMed(Ophth) Acting Head of Department of Ophthalmology, Nelson R Mandela School of Medicine, University of KwaZulu-Natal Correspondence
Common eye disorders in the elderly a short review Visser L, FCOphth(SA), MMed(Ophth) Acting Head of Department of Ophthalmology, Nelson R Mandela School of Medicine, University of KwaZulu-Natal Correspondence
Eyes, ears, teeth and everything in between
 Eyes, ears, teeth and everything in between E M E R G E N C Y D E P A R T M E N T J U N I O R T E A C H created 14/11/10 by S.R. Bruijns, version 1.0 Objectives Eyes Ears Teeth Maxilla- facial EYES Approaching
Eyes, ears, teeth and everything in between E M E R G E N C Y D E P A R T M E N T J U N I O R T E A C H created 14/11/10 by S.R. Bruijns, version 1.0 Objectives Eyes Ears Teeth Maxilla- facial EYES Approaching
Ophthalmology Unit Referral Guidelines
 Ophthalmology Unit Referral Guidelines Austin Health Ophthalmology Unit holds sub-specialty sessions to discuss and plan the treatment of patients with specific ocular conditions. General including cataract
Ophthalmology Unit Referral Guidelines Austin Health Ophthalmology Unit holds sub-specialty sessions to discuss and plan the treatment of patients with specific ocular conditions. General including cataract
Fast Facts. Fast Facts: Ophthalmology. Peter Simcock and Andre Burger. Second edition
 Fast Facts Fast Facts: Ophthalmology Peter Simcock and Andre Burger Second edition A fantastic companion for all clinicians involved in primary eye care. Dr Amit Jinabhai, Lecturer in Optometry, University
Fast Facts Fast Facts: Ophthalmology Peter Simcock and Andre Burger Second edition A fantastic companion for all clinicians involved in primary eye care. Dr Amit Jinabhai, Lecturer in Optometry, University
Diabetic Eye Disease
 Manchester Royal Eye Hospital Medical Retinal Services Information for Patients Diabetic Eye Disease This leaflet sets out to answer some of your questions about diabetic eye disease. You may wish to discuss
Manchester Royal Eye Hospital Medical Retinal Services Information for Patients Diabetic Eye Disease This leaflet sets out to answer some of your questions about diabetic eye disease. You may wish to discuss
Chris Brown, M.D. Eye Specialty Group, PLC Continuing Education Series
 Chris Brown, M.D. Eye Specialty Group, PLC 2018 Continuing Education Series Disclaimer I have no financial interests in this lecture or any information discussed therein Objectives Fluorescein Angiogram
Chris Brown, M.D. Eye Specialty Group, PLC 2018 Continuing Education Series Disclaimer I have no financial interests in this lecture or any information discussed therein Objectives Fluorescein Angiogram
What the Primary Care Optometrist Should Never Miss
 What the Primary Care Optometrist Should Never Miss Ron Melton, OD, FAAO Randall Thomas, OD, FAAO www.eyeupdate.com Financial Disclosure Dr. Ron Melton and Dr. Randall Thomas are consultants to, on the
What the Primary Care Optometrist Should Never Miss Ron Melton, OD, FAAO Randall Thomas, OD, FAAO www.eyeupdate.com Financial Disclosure Dr. Ron Melton and Dr. Randall Thomas are consultants to, on the
ZEISS AngioPlex OCT Angiography. Clinical Case Reports
 Clinical Case Reports Proliferative Diabetic Retinopathy (PDR) Case Report 969 PROLIFERATIVE DIABETIC RETINOPATHY 1 1-year-old diabetic female presents for follow-up of proliferative diabetic retinopathy
Clinical Case Reports Proliferative Diabetic Retinopathy (PDR) Case Report 969 PROLIFERATIVE DIABETIC RETINOPATHY 1 1-year-old diabetic female presents for follow-up of proliferative diabetic retinopathy
Neuro-ophthalmologyophthalmology. Marek Michalec, MD.
 Neuro-ophthalmologyophthalmology Marek Michalec, MD. Neuro-ophthalmology Study integrating ophthalmology and neurology Disorders affecting parts of CNS devoted to vision or eye: Afferent system (visual
Neuro-ophthalmologyophthalmology Marek Michalec, MD. Neuro-ophthalmology Study integrating ophthalmology and neurology Disorders affecting parts of CNS devoted to vision or eye: Afferent system (visual
VITREOUS FLOATERS AND PHOTOPSIA AS PREDICTORS OF VITREORETINAL PATHOLOGY
 Basrah Journal Of Surgery VITREOUS FLOATERS AND PHOTOPSIA AS PREDICTORS OF VITREORETINAL PATHOLOGY Salah Zuhair Al-Asadi MB,ChB, FRCS, FIBMS, Lecturer of Ophthalmology, College of Medicine, University
Basrah Journal Of Surgery VITREOUS FLOATERS AND PHOTOPSIA AS PREDICTORS OF VITREORETINAL PATHOLOGY Salah Zuhair Al-Asadi MB,ChB, FRCS, FIBMS, Lecturer of Ophthalmology, College of Medicine, University
PREAMBLE TO MSC PAYMENT SCHEDULE: OPTOMETRY SERVICES
 PREAMBLE TO MSC PAYMENT SCHEDULE: OPTOMETRY SERVICES A. GENERAL PROVISIONS 1. Eye Examination Benefits Optometric benefits are services defined in Section 23 of the Medical and Health Care Services Regulations,
PREAMBLE TO MSC PAYMENT SCHEDULE: OPTOMETRY SERVICES A. GENERAL PROVISIONS 1. Eye Examination Benefits Optometric benefits are services defined in Section 23 of the Medical and Health Care Services Regulations,
NEPTUNE RED BANK BRICK
 NEPTUNE RED BANK BRICK Diabetes & The Eye Diabetics are more likely to develop Cataracts at a younger age. Diabetics are twice as likely to develop Glaucoma when compared to non-diabetics. The primary
NEPTUNE RED BANK BRICK Diabetes & The Eye Diabetics are more likely to develop Cataracts at a younger age. Diabetics are twice as likely to develop Glaucoma when compared to non-diabetics. The primary
GRADUAL LOSS OF VISION. Teresa Anthony Consultant Ophthalmologist Emersons Green NHS Treatment Centre Bristol
 GRADUAL LOSS OF VISION Teresa Anthony Consultant Ophthalmologist Emersons Green NHS Treatment Centre Bristol CVI Registration Low Vision: 6/60 Sight impaired: 3/60 Severe sight impaired:
GRADUAL LOSS OF VISION Teresa Anthony Consultant Ophthalmologist Emersons Green NHS Treatment Centre Bristol CVI Registration Low Vision: 6/60 Sight impaired: 3/60 Severe sight impaired:
TOP 5 EYE CONDITIONS NOT TO BE MISSED
 TOP 5 EYE CONDITIONS NOT TO BE MISSED Dr Kolin Foo Consultant Ophthalmologist Senior Lecturer in Ophthalmology Wellington Hospital Terrace Eye Centre Financial disclosure No financial interest in the products
TOP 5 EYE CONDITIONS NOT TO BE MISSED Dr Kolin Foo Consultant Ophthalmologist Senior Lecturer in Ophthalmology Wellington Hospital Terrace Eye Centre Financial disclosure No financial interest in the products
Test Bank for Medical Surgical Nursing An Integrated Approach 3rd Edition by White
 Test Bank for Medical Surgical Nursing An Integrated Approach 3rd Edition by White Link full download : http://testbankair.com/download/test-bank-for-medical-surgical-nursing-anintegrated-approach-3rd-edition-by-white/
Test Bank for Medical Surgical Nursing An Integrated Approach 3rd Edition by White Link full download : http://testbankair.com/download/test-bank-for-medical-surgical-nursing-anintegrated-approach-3rd-edition-by-white/
Preventing blindness: Ultrasound in Giant cell arteritis
 Preventing blindness: Ultrasound in Giant cell arteritis Elizabeth Jernberg, MD Associate Clinical Professor of Medicine Division of Rheumatology University of Washington Virginia Mason Medical Center
Preventing blindness: Ultrasound in Giant cell arteritis Elizabeth Jernberg, MD Associate Clinical Professor of Medicine Division of Rheumatology University of Washington Virginia Mason Medical Center
Preliminary report on effect of retinal panphotocoagulation on rubeosis iridis and
 British Journal of Ophthalmology, 1977, 61, 278-284 Preliminary report on effect of retinal panphotocoagulation on rubeosis iridis and neovascular glaucoma LEILA LAATIKAINEN From Moorfields Eye Hospital,
British Journal of Ophthalmology, 1977, 61, 278-284 Preliminary report on effect of retinal panphotocoagulation on rubeosis iridis and neovascular glaucoma LEILA LAATIKAINEN From Moorfields Eye Hospital,
Delayed Choroidal Perfusion in Giant Cell Arteritis
 Tournai of Clinical Neuro-ophthalmology 11(4): 221-227,1991. 1991 Raven Press, Ltd., New York Delayed Choroidal Perfusion in Giant Cell Arteritis H. G. Mack, B. Me SC., M.B.B.S., J. O'Day, F.R.A.C.P.,
Tournai of Clinical Neuro-ophthalmology 11(4): 221-227,1991. 1991 Raven Press, Ltd., New York Delayed Choroidal Perfusion in Giant Cell Arteritis H. G. Mack, B. Me SC., M.B.B.S., J. O'Day, F.R.A.C.P.,
World Sight Day Case Studies. Mark Frost Screening Manager South East London DESP
 World Sight Day 2015 Case Studies Mark Frost Screening Manager South East London DESP Introduction All of the following cases have been identified in our screening programme over the last 3 years. The
World Sight Day 2015 Case Studies Mark Frost Screening Manager South East London DESP Introduction All of the following cases have been identified in our screening programme over the last 3 years. The
The College of Optometrists - Learning outcomes for the Professional Certificate in Medical Retina
 Learning outcomes for the Professional Certificate in Medical Retina, incorporating diabetic retinopathy screening and age related macular degeneration The professional certificate is a prerequisite to
Learning outcomes for the Professional Certificate in Medical Retina, incorporating diabetic retinopathy screening and age related macular degeneration The professional certificate is a prerequisite to
 measure of your overall performance. An isolated glucose test is helpful to let you know what your sugar level is at one moment, but it doesn t tell you whether or not your diabetes is under adequate control
measure of your overall performance. An isolated glucose test is helpful to let you know what your sugar level is at one moment, but it doesn t tell you whether or not your diabetes is under adequate control
ISPUB.COM. An Atypical Presentation of Posterior Scleritis. A Ramanathan, A Gaur CASE REPORT
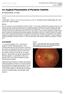 ISPUB.COM The Internet Journal of Ophthalmology and Visual Science Volume 8 Number 2 A Ramanathan, A Gaur Citation A Ramanathan, A Gaur.. The Internet Journal of Ophthalmology and Visual Science. 2009
ISPUB.COM The Internet Journal of Ophthalmology and Visual Science Volume 8 Number 2 A Ramanathan, A Gaur Citation A Ramanathan, A Gaur.. The Internet Journal of Ophthalmology and Visual Science. 2009
Recurrent transient visual loss in a middle aged woman
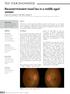 Recurrent transient visual loss in a middle aged woman Chow SY, Draman N, Teh WM, Azhany Y Chow SY, Draman N, Teh WM, et al. Recurrent transient visual loss in a middle aged woman. Malays Fam Physician.
Recurrent transient visual loss in a middle aged woman Chow SY, Draman N, Teh WM, Azhany Y Chow SY, Draman N, Teh WM, et al. Recurrent transient visual loss in a middle aged woman. Malays Fam Physician.
Questions to ponder today
 Questions to ponder today What clinical signs/symptoms help me identify a retinal artery occlusion (RAO)? Past RAO? What is my responsibility to patient when I diagnose a RAO? Lab test? Imaging? If my
Questions to ponder today What clinical signs/symptoms help me identify a retinal artery occlusion (RAO)? Past RAO? What is my responsibility to patient when I diagnose a RAO? Lab test? Imaging? If my
Shared embryology Eye and brain develop from neuro-ectoderm
 The Patient with Visual Loss: Localization of Neuropathologic Disease and Select Diseases of Neuropathologic Interest Steven A. Kane, M.D., Ph.D. The Edward S. Harkness Eye Institute Shared embryology
The Patient with Visual Loss: Localization of Neuropathologic Disease and Select Diseases of Neuropathologic Interest Steven A. Kane, M.D., Ph.D. The Edward S. Harkness Eye Institute Shared embryology
Non-arteritic anterior ischemic optic neuropathy (NAION) with segmental optic disc edema. Jonathan A. Micieli, MD Valérie Biousse, MD
 Non-arteritic anterior ischemic optic neuropathy (NAION) with segmental optic disc edema Jonathan A. Micieli, MD Valérie Biousse, MD A 75 year old white woman lost vision in the inferior part of her visual
Non-arteritic anterior ischemic optic neuropathy (NAION) with segmental optic disc edema Jonathan A. Micieli, MD Valérie Biousse, MD A 75 year old white woman lost vision in the inferior part of her visual
Uveitis. Pt Info Brochure. Q: What is Uvea?
 Pt Info Brochure Uveitis Q: What is Uvea? A: Uvea is the middle layer of the eye. It is the most vascular structure of the eye. It provides nutrition to the other parts of the eye. The uvea is made up
Pt Info Brochure Uveitis Q: What is Uvea? A: Uvea is the middle layer of the eye. It is the most vascular structure of the eye. It provides nutrition to the other parts of the eye. The uvea is made up
SUDDEN BLINDNESS IN CRANIAL ARTERITIS*
 Brit. J. Ophthal. (1959) 43, 204. SUDDEN BLINDNESS IN CRANIAL ARTERITIS* BY Western Ophthalmic Hospital (St. Mary's Hospital), London THAT vision may be affected during an attack of cranial arteritis is
Brit. J. Ophthal. (1959) 43, 204. SUDDEN BLINDNESS IN CRANIAL ARTERITIS* BY Western Ophthalmic Hospital (St. Mary's Hospital), London THAT vision may be affected during an attack of cranial arteritis is
Treatment of Retinal Vein Occlusion (RVO)
 Manchester Royal Eye Hospital Medical Retina Services Information for Patients Treatment of Retinal Vein Occlusion (RVO) What is a Retinal Vein Occlusion (RVO)? The retina is the light sensitive layer
Manchester Royal Eye Hospital Medical Retina Services Information for Patients Treatment of Retinal Vein Occlusion (RVO) What is a Retinal Vein Occlusion (RVO)? The retina is the light sensitive layer
Information for Patients. Retinal Detachment
 Information for Patients Retinal Detachment Manchester Royal Eye Hospital Retinal services Your eye doctor has told you that you have a retinal detachment. This leaflet will help you understand your condition
Information for Patients Retinal Detachment Manchester Royal Eye Hospital Retinal services Your eye doctor has told you that you have a retinal detachment. This leaflet will help you understand your condition
LOOKING AT BLINDNESS FROM NEUROLOGIST S PERSPECTIVE
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk LOOKING AT BLINDNESS FROM NEUROLOGIST S PERSPECTIVE Author : LAURENT S GAROSI Categories : Vets Date : June 23, 2008 LAURENT
Vet Times The website for the veterinary profession https://www.vettimes.co.uk LOOKING AT BLINDNESS FROM NEUROLOGIST S PERSPECTIVE Author : LAURENT S GAROSI Categories : Vets Date : June 23, 2008 LAURENT
UVEITIS IN GENERAL. Information for patients UVEITIS CLINIC WHAT IS UVEITIS? MAIN CATEGORIES OF UVEITIS
 Information for patients UVEITIS CLINIC UVEITIS IN GENERAL WHAT IS UVEITIS? The uvea is a name given to the pigmented layer of tissue inside the eye. When all or part of the uvea becomes inflamed, the
Information for patients UVEITIS CLINIC UVEITIS IN GENERAL WHAT IS UVEITIS? The uvea is a name given to the pigmented layer of tissue inside the eye. When all or part of the uvea becomes inflamed, the
Headache Assessment In Primary Eye Care
 Headache Assessment In Primary Eye Care Spencer Johnson, O.D., F.A.A.O. Northeastern State University Oklahoma College of Optometry johns137@nsuok.edu Course Objectives Review headache classification Understand
Headache Assessment In Primary Eye Care Spencer Johnson, O.D., F.A.A.O. Northeastern State University Oklahoma College of Optometry johns137@nsuok.edu Course Objectives Review headache classification Understand
Scrub In. What is the function of vitreous humor? What does the pupil do when exposed to bright light? a. Maintain eye shape and provide color vision
 Scrub In What is the function of vitreous humor? a. Maintain eye shape and provide color vision b. Maintain eye shape and refract light rays c. Provide night vision and color vision d. Provide night vision
Scrub In What is the function of vitreous humor? a. Maintain eye shape and provide color vision b. Maintain eye shape and refract light rays c. Provide night vision and color vision d. Provide night vision
