Vascular and Nonvascular Mimics of the CT Angiography Spot Sign in Patients With Secondary Intracerebral Hemorrhage
|
|
|
- Lewis Goodwin
- 5 years ago
- Views:
Transcription
1 Vascular and Nonvascular Mimics of the CT Angiography Spot Sign in Patients With Secondary Intracerebral Hemorrhage Steve Gazzola, MD; Richard I. Aviv, MBChB, FRCR; David J. Gladstone, MD, FRCPC; Gabriella Mallia, BSc(C); Vivian Li, BA(C); Allan J. Fox, MD, FRCPC; Sean P. Symons, MD, MSc, FRCPC Background and Purpose The newly-described computed tomography angiography (CTA) Spot Sign is present in about one third of patients with acute primary intracerebral hemorrhage (PICH) and predicts hematoma expansion. This sign has not been systematically evaluated in patients with secondary causes of ICH, and mimics have not been characterized. The purpose of this study was to assess for the presence of the Spot Sign in secondary ICH and to document potential mimics of the Spot Sign and their distinguishing features. Methods We performed a retrospective chart review of consecutive patients presenting with ICH to our regional stroke center between January 2002 and May Ninety-six ICH patients underwent a CT stroke protocol including CTA. CTA documented a secondary cause for hemorrhage in 30 patients (31%). Each patient was assessed for the presence or absence of the CTA Spot Sign or a mimic by 2 blinded neuroradiologists. Clinical and radiological features of PICH and secondary ICH were compared. Results No patients with secondary ICH had a true CTA Spot Sign, but several Spot Sign mimics were identified including: micro AVM, posterior communicating artery aneurysm, Moya Moya, and neoplasm-associated calcification. The secondary ICH group was younger (P ) and less likely to be hypertensive at presentation (P ). Significant hematoma expansion ( 33% increase from baseline volume) occurred in 20% of secondary ICH patients and 28% of PICH patients (P ). Conclusion This study describes mimics of the CTA Spot Sign and classifies them as vascular (microavm, aneurysm, Moya Moya) or nonvascular (tumor and choroid plexus calcification). Evaluation of the noncontrast CT together with the CTA source images is an essential part of the evaluation for the Spot Sign. Vessels entering the hematoma from the periphery are indicative of an underlying vascular lesion. Our findings suggest that the Spot Sign may be rare in secondary ICH and most specific for PICH. (Stroke. 2008;39: ) Key Words: computed tomography angiography intracerebral hemorrhage hematoma expansion Spot Sign secondary ICH factor VIIa The Computed Tomography Angiography (CTA) Spot Sign has recently been shown to predict hematoma expansion in patients presenting acutely with primary intracerebral hemorrhage (PICH). 1 The ability to accurately predict which patients will undergo hematoma expansion is of major clinical importance, not only to predict morbidity and mortality well known to be associated with hematoma size and expansion, 1 5 but also to potentially guide acute therapy. However, the prevalence of the sign in the context of secondary causes of intracerebral hemorrhage is unknown. Accurate identification of the Spot Sign and distinction from potential mimics is essential for the success of studies that may use this sign to stratify or select patients for treatment interventions. In this study, we assess the prevalence of the CTA Spot Sign in secondary ICH patients and report on several spot mimics. We hypothesize that the CTA Spot Sign is specific for PICH and may be less common in SICH. Patients and Methods Study Group A retrospective chart review of consecutive patients presenting with ICH between January 2002 and May 2007 was performed. Ninetysix patients investigated with a CT stroke protocol including CTA were reviewed. Six patients with only subarachnoid blood were excluded. Fifty-nine patients with PICH and 31 patients with CTA documented secondary cause for ICH formed the patient cohort. One Received July 16, 2007; final revision received August 23, 2007; accepted August 30, From the Division of Neuroradiology (R.A., S.S., A.J.F., V.L., G.M.), Department of Medical Imaging (S.G.), and Regional Stroke Centre (D.G.), Sunnybrook Health Sciences Centre, University of Toronto, Ontario, Canada. Correspondence to Dr R. Aviv, MBChB, Department of Medical Imaging, Division of Neuroradiology, Room AG 31, Sunnybrook Health Sciences Centre, 2075 Bayview Avenue, Toronto, Ontario, M4N 3M5, Canada. Richard.aviv@sunnybrook.ca 2008 American Heart Association, Inc. Stroke is available at DOI: /STROKEAHA
2 1178 Stroke April 2008 Table 1. Demographic Characteristics of Patients With PICH and SICH Primary ICH Secondary ICH P Value Median age, y 64 (31 86) 45.5 (16 82) Male gender 26 (44.1%) 16 (53%) No. of patients with CTA under 6 hours 6 (20%) 39 (100%) Volume of hematoma at presentation 33.5 (32.75) 20.9 (19.43) Volume of hematoma at follow-up, mean (SD) 36.7 (34.42) 22.3 (18.30) No. with expansion 11 (18.6%) 20 (20%) ICH location: lobar 34 (58.6%) 18 (60%) ICH location: basal ganglia 22 (37.2%) 6 (20%) ICH location: cerebellar 3 (5.1%) 6 (20%) Presentation mean arterial pressure, mean (SD) (17.16) (21.75) MAP (25.4%) 4 (13.3%) History of hypertension 18 (30.1%) 5 (16.7%) Anticoagulation at presentation 11 (18.6%) 1 (3.3%) Presentation INR, mean (SD) 1.3 (0.59) 1.07 (0.19) Presentation APTT, mean (SD) 30.2 (7.27) 28.4 (3.18) Presentation Glucose, mean (SD) 8 (3.13) 7.7 (2.28) Glucose 8.3 mmol/l at presentation 10 (16.9%) 8 (26.6%) Median mrs at 3 months 3 (0 6) 2.5 (0 6) Presence of hydrocephalus 5 (8.5%) 17 (62.9%) Median hospital length of stay 11 (2 76) 10 (3 210) All values represent No. of patients (percent) unless otherwise indicated. SICH patient was excluded because of surgical decompression before CTA. Thirty SICH patients were therefore available for review. The study was institutional review board approved. Materials/Image Acquisition A hemorrhagic stroke protocol was performed on a 4-slice ( ) or a 64-slice ( ) CT (GE Lightspeed plus and VCT; GE). Noncontrast head imaging is followed by a CTA study and a postcontrast study 1 to 2 minutes after contrast injection. Pre- and postcontrast head imaging is acquired from the skull base to the vertex with the following parameters: 120 kvp; 340mA; 4 5 mm collimation; 1 second/rotation; and a table speed of 15 mm/rotation. CTA studies are obtained from the level of the C6 vertebra to the vertex in the helical HS mode. CTA parameters are 0.7 ml/kg contrast (to a maximum of 90 ml through an antecubital vein via at least an 18 or 20 gauge angiocatheter); 5 to 10 second delay; 120 kvp; 270 ma; 1 second/rotation; 1.25 mm slice thickness reconstructed to mm. Table speed 3.75 mm/rotation. CT technologists perform all postprocessing including multiplanar reformats at the CT operator s console. Coronal and sagittal multiplanar reformat images are created as 10.0-mm-thick images, spaced by 3 mm. Bilateral rotational multiplanar reformat images are created at each carotid terminus with a thickness of 7 mm and a spacing of 3 mm. All images are viewed on AGFA Impax 4.5 PACS workstation. Cerebral digital subtraction angiography (DSA) was used as the reference standard for confirmation of vascular lesion presence where the diagnosis was in doubt or occasionally to confirm a diagnosis or before therapeutic intervention. DSA was performed on a Phillips uniplane neuroangiographic unit. Selective angiography was performed for confirmation of CTA-detected lesions or for therapeutic procedures. Four vessel angiography was performed where no abnormality was detected on CTA. Imaging Analysis/Interpretation All studies were prospectively evaluated by 2 neuroradiologists for the presence or absence of the CTA spot sign. The sign was defined as a 1- to 2-mm focus of enhancement within a hematoma on the CT angiographic axial source and multiplanar reformatted (MPR) images as assessed by simple visual inspection. 6 Presence of potential CTA spot sign mimics was recorded. The modality securing the final diagnosis was recorded. The location and size of hematoma was noted. Hematoma volume at presentation and follow-up study was calculated using the previously validated ABC/2 method. 7 Intraventricular extension was graded as mild, moderate, or severe. Mild IVH constituted a small amount of dependant blood in any ventricle. Moderate IVH was scored when more than one ventricle contained blood. Blood filling all ventricles was considered severe IVH. An increase in hematoma volume of 33% was considered significant. 8 Statistical Methods For each patient baseline data that was collected included: the presence of the CTA Spot Sign or mimic, time to CTA from presentation to first ER, time to CTA from symptom onset, age at presentation, sex, anticoagulant/antiplatelet use, history of hypertension, blood pressure, clotting profile, and glucose at presentation. The size of the hematoma at presentation and on follow-up was documented. Thresholds of glucose 8.3 mmol/l and mean arterial pressure (MAP) 120 mm Hg were selected based on previous studies. 2,3 Modified Rankin scores at 3 months were recorded. The primary and secondary ICH groups were compared for age, gender, MAP, glucose, hematoma volume at presentation and follow-up, and clinical outcome. The Student t test and Fisher test were used for group comparisons for continuous and categorical data, respectively. Data were analyzed using SPSS for Windows (Version 14; SPSS Inc). A probability value 0.05 is considered significant. Results A secondary cause of ICH was present in 31 patients, representing 34% of consecutive ICHs presenting to our institution investigated with CT angiography. One patient was excluded because of surgical decompression before CTA. Cerebral angiography was performed in 25/31 patients (80%). Patients who did not undergo angiography included 4
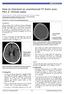
3 Gazzola et al CTA Spot Sign in Secondary Intracranial Hemorrhage 1179 Table 2. Summary of Cases Demonstrating CTA Spot Sign Mimics Classified by Etiology, Mimic Type, and Presence of Expansion Patient Actual Diagnosis Type of Mimic Explanation Expansion 1 Tumoral hemorrhage Nonvascular Left thalamic hematoma calcifications in a patient yes with metastasis 2 Tumoral hemorrhage Nonvascular Right frontal lobe hematoma calcification in a no patient with oligodendroglioma 3 Tumoral hemorrhage Nonvascular Choroid plexus calcification no 4 Moya Moya Vascular Pseudoaneurysm arising from lenticulostriate no artery 5 Micro AVM Vascular Micro AVM draining to a cortical vein no 6 Micro AVM Vascular Micro AVM with pseudoaneurysm draining to no lateral ventricular vein 7 PCOM aneurysm Vascular Partially thrombosed PCOM aneurysm yes patients with tumor and 2 patients with large CTA identified aneurysms which were surgically treated. Characteristics of patients with primary and secondary ICH are presented in Table 1. Patients with secondary ICH were younger (P ) with a median age of 45 years (range, 16 to 82 years). There was a trend for initial and follow-up hematoma volumes to be smaller than PICH patients (P ). There was a trend to more posterior fossa lesions in the secondary ICH patients (P ). History of hypertension, MAP, and number of patients with MAP elevation 120 were lower (P , P , P , respectively). Fewer patients were on anticoagulants (P ), and there was a trend to a lower mean INR (P ). Hydrocephalus was more often seen in SICH than PICH (P ). Secondary causes of ICH in the study patients were: arteriovenous malformation (AVM) (n 12), dural arteriovenous fistula (AVF) (n 2), tumor (n 6), aneurysm (n 9), and Moya Moya (n 1). Sixty-three percent of SICH patients presented between the 4th to 6th decades. Aneurysms and tumor were more common beyond the 4th decade, and AVMs presented predominately in the first 4 decades. Sixteen percent of patients over 60 had a secondary cause for ICH. CTA revealed a secondary cause for basal ganglia bleeds in 18% of cases. Hemorrhage from aneurysm and AVM accounted for the majority of causes and greatest severity of hydrocephalus. Significant hematoma expansion occurred in 6/30 (20%) SICH and 11/59 (19%) of PICH patients, respectively. One patient taken to surgery emergently for hematoma evacuation because of sudden clinical deterioration without interval scan was included. This patient s initial CTA, done at 3.7 hours from symptom onset, showed no hydrocephalus or intraventricular extension of a temporal lobe hematoma secondary to a dural AVF. The median time from presentation to CTA was 7 hours (0.5 to 116 hours). Eighty-four percent (26/31) of SICH patients had CTA within 48 hours of symptom onset and 77% (24/31) within 24 hours. Twenty percent presented within 6 hours. All SICH expansion occurred within 24 hours of symptom onset, half occurring within 12 hours. The CTA Spot Sign was not present on any study, but several mimics were identified. We divided the causes into nonvascular and vascular (Table 2). Nonvascular causes were attributable to punctuate calcification that simulated contrast on a postcontrast study. Distinction may not have been possible without the presence of a noncontrast study for comparison (Figure 1). In 2 cases punctuate perihematoma calcification was present. Hematoma induced compressed, irregularly calcified, choroid plexus accounted for the other mimic. Three vascular mimics were seen Figure year-old male with a right frontal oligodendroglioma (patient 2, Table 2). A, NCCT demonstrates punctuate peripheral calcification, (white arrow) within the hematoma (white asterisk). B, Hyperdensity apparent on CTA axial source images and post contrast CT images.
4 1180 Stroke April 2008 Figure year-old female with a micro AVM (patient 6, Table 2). A, NCCT demonstrates centrum semiovale hematoma (white asterisk). B, A punctate focus of enhancement (white arrow) representing a pseudoaneurysm (white arrow) on CTA axial source images mimics a CTA spot sign. C, A vessel is clearly seen extending from the lateral ventricular surface to the hematoma periphery and communicates with the focal spot of enhancement on coronal MPR image (black arrow). D, AP Oblique conventional angiographic image demonstrates a micro AVM with pseudoaneurysm (black arrow) fed by branches of the anterior cerebral artery and draining to the lateral ventricular vein. in patients with micro AVM (Figure 2) and Moya Moya (Figure 3). These cases demonstrated pseudoaneurysms arising from discrete CTA discernable vessels. This differs from the CTA Spot Sign where contrast foci are suspended within the hematoma with no vascular connection to surrounding structures. The other mimic occurred in a patient with a partially thrombosed posterior communicating artery aneurysm (PCOM). However, in this unusual case the punctuate foci of enhancement occurred in the subarachnoid space and were slightly distanced from the hematoma edge (Figure 4). Discussion This is the first study to evaluate the CTA Spot Sign in secondary ICH cases and to describe spot sign mimics. The CTA Spot Sign is defined as 1 to 2 mm foci of enhancement within a parenchymal hematoma. 6 These densities may be spot-like or linear, single or multiple, and are only visualized on CT angiographic axial source and multiplanar reformatted images images. Previous studies suggest that the sign may have important implications for stratification of hematoma expansion risk. If the sign is to be used to select a target group Figure year-old male with moya moya (patient 4, Table 2). An enhancing focus is seen in the inferior Basal Ganglia/Nucleus accumbens consistent with a pseudoaneurysm (white arrow) arising from a lenticulostriate artery (white arrowhead) on (A) CTA source, (B) coronal MPR, and (C) saggital MPR images. The lenticulostriate vessel lies peripheral to the hematoma only contacting it at the site of pseudoaneurysm. Intraventricular hemorrhage and hydrocephalus incidentally noted.
5 Gazzola et al CTA Spot Sign in Secondary Intracranial Hemorrhage 1181 Figure year-old female with PCOM aneurysm (patient 7, Table 2). A punctuate enhancing focus (white arrow) is present slightly remote from a right PCOM aneurysm (white arrowhead). The focus lies outside of the mesial temporal hematoma (white asterisk) within the subarachnoid space seen on (A) CTA axial source and (B) saggital MPR images. C, Conventional angiographic images reveal filling of a right PCOM aneurysm (white arrow) in a loculated fashion attributable to partial thrombosis. D, Dependant contrast opacification is evident on delayed images consistent with the focal enhancement seen on CTA. for therapy, correct recognition of potential mimics is essential. It might be argued that patients with secondary causes may not be precluded from treatment with Factor Viia to prevent hematoma expansion. However, correct identification of these lesions is important to allow definitive treatment to prevent future hemorrhage risk. Importantly, enhancing densities are isolated within the hematoma and not connected to vascular structures peripheral to the hematoma. The presence of calcification should be excluded on noncontrast CT. We previously reported a prevalence of the Spot Sign in 30% of PICH patients presenting within 3 hours of stoke onset. 6 This study reported extravasation independent of the Spot Sign in half of spot positive cases. Extravasation was defined as an accumulation of contrast on a postcontrast CT. Other studies found contrast extravasation in 50% of ICH patients. 9 Extravasation was reported as late as 5 days after symptom onset. 3 Studies focusing on the hyperacute period (0 to 6 hours) 10,11 found similar rates of contrast extravasation. The CTA Spot Sign has been found to be an independent predictor of hematoma expansion with sensitivity, specificity, positive, and negative predictive value of 91, 89, 77, and 96%, respectively. 6 Contrast extravasation from aneurysms and other vascular lesions is recognized. 11 In our view the detection of extravasation is a later sign in the natural history of a spot-positive patient with less specificity for hematoma expansion. The absence of the Spot Sign in secondary ICH suggests specificity for PICH and reinforces our hypothesis that the Spot Sign may be the cause of PICH bleeding. The presence of multiple Spot Signs in a hematoma does not preclude this notion. Fisher described fibrin globes or pseudoaneurysms up to 600 in size. 12 These are masses of red cells in concentric rings of fibrin adjacent to an arteriolar defect. The lesions are frequently multiple, present at the hematoma margin, and seen in association with focal lipohyalinosis which reflects a more widespread vessel abnormality or fragility. Fisher proposed a domino effect whereby one or more lesions rupture and are responsible for the majority of hematoma growth. The expanding hematoma then results in secondary damage to already fragile vessels with ongoing albeit lesser bleeding. It is unknown what the individual contribution of the multiple lesions to hematoma growth is but we have certainly identified active extravasation from multiple spots on postcontrast CT. This hypothesis could explain the presence of multiple lesions with and without extravasation and an apparent specificity to PICH. Several mimics of the CTA Spot Sign were found in this study, classified as vascular or nonvascular. Nonvascular causes are attributable to calcific deposition. Review of the noncontrast CT before CTA confirmed the presence of calcification in all patients. Three patients had a peripheral hyperdense spot on CTA images. One lesion was deep, situated within the left thalamus, the other lobar, within the right frontal lobe. Both had underlying tumor; a metastasis and oligodendroglioma, respectively. The third had calcification in the choroid plexus, compressed by the hematoma. Although not encountered in this study IVH clot surrounding choroid may be difficult to distinguish from adjacent parenchymal hematoma. The hematoma then appears to engulf the calcification rather than displacing it mimicking the Spot Sign. Careful scrutiny of the choroid plexus on contiguous noncontrast CT slices is sufficient to avoid this pitfall. Physiological and postinfective/inflammatory calcification although not described in this study would similarly be expected to mimic the Spot Sign.
6 1182 Stroke April 2008 Vascular mimics were a partially thrombosed posterior communicating aneurysm (PCOM), 2 micro AVMs and a patient with Moya Moya and lenticulostriate pseudoaneurysm. Careful inspection of the PCOM aneurysm case revealed enhancing densities external to the hematoma and brain parenchyma. The extra axial (subarachnoid) location precluded a diagnosis of the Spot Sign. DSA revealed loculated filling of the aneurysm attributable to partial thrombosis. Although not present in our series we speculate that, internal carotid artery terminus, anterior communicating, and middle cerebral artery bifurcation aneurysms that are closely applied to adjacent brain parenchyma may present similar difficulties. In our experience review of CT angiographic images usually confirm the extra axial nature of these vascular lesions. Both patients with micro-avm revealed a continuous linear density extending from vessels on the brain or ventricular surface into the depths of the hematoma. The Moya Moya case had a similar appearance with lenticulostriate vessel arising outside the hematoma and coursing through it to terminate as a pseudoaneurysm. Extension of linear densities beyond the hematoma margin is not seen in any case of CTA Spot Sign. Noncontrast CT (NCCT) has poor sensitivity and specificity for prediction of underlying vascular lesions in ICH patients. 13 Risk of neurological deficit limits the potential use of DSA in certain subgroups where the incidence of a known cause of ICH is low. The American Heart Association guidelines acknowledge that underlying etiology cannot reliably be predicted by hematoma location alone. 2 Apparently typical bleeds have an underlying vascular cause for ICH in 2% to 36%, 14,15 and the incidence of underlying vascular lesions in all ICH cases is 30%. 13,15 We believe that the low complication rates of CTA justify its use even in patients with typical hypertensive bleeds. This is especially so in the face of a potential CTA marker for hematoma expansion and treatment target. The accuracy of CTA for detection of underlying vascular lesions is 90% (Yeung R, unpublished data, 2007). CTA is rapid, accessible, and widely available. Therefore NCCT followed by CTA are the first line of investigation in ICH patients in our institution. DSA is used as a confirmatory test in abnormal cases and to confirm AVM angioarchitecture and drainage pattern. Younger patients without CTA abnormality would also progress to DSA according to the AHA guidelines. The main limitation of this study was that few patients were scanned ultraearly. The delayed onset-to-cta times may therefore have limited our ability to detect Spot Signs in this cohort. The longer delay from presentation to CTA in this study is largely a reflection of patient inclusion before the introduction of a citywide acute stroke prehospital bypass protocol. Our PICH cohort dates predominantly after the implementation of this protocol. We cannot exclude the possibility that a Spot Sign may have been present in some patients if they had been scanned earlier. In our experience, however, half of spot positive patients progress to extravasation. Other studies have confirmed extravasation in half of patients presenting with ICH investigated at a median time of 11 hours (13 to 33 hours) 9 and up to 5 days. 3 Furthermore, the median time to CTA in this and the study by Goldstein et al study is identical. 9 Another limitation of this study is that we did not capture all consecutive patients presenting with ICH. Before the introduction of routine CTA in acute stroke at our institution, the decision to perform a CTA was at the discretion of the referring clinician. This may have resulted in selection bias and resulted in the observed differences in the 2 groups. Larger prospective studies with patients scanned at earlier time points will be important to confirm and extend these findings. Conclusion The Spot Sign is a potentially promising sign for predicting hematoma expansion. This sign may play a role in patient selection for clinical trials of acute hemostatic therapy or surgical interventions aimed at minimizing hematoma growth. Correct recognition of the sign and exclusion of secondary ICH causes will be crucial to the success of such studies. Clinicians should be aware of the Spot Sign mimics, classified as either vascular or nonvascular. Nonvascular causes are easily distinguished with NCCT but may be misinterpreted as contrast density in its absence. The presence of a vessel extending from brain or ventricular surface into a hematoma strongly suggests the presence of underlying vascular malformation. A true CTA Spot Sign was not found in any of our patients with secondary ICH. The absence of a Spot Sign in secondary ICH, then, implies that this sign has greater specificity for primary ICH than for secondary ICH, although this will need to be confirmed in larger prospective studies. Acknowledgements We acknowledge our Tech staff without whose dedication and effort our imaging data would be deplete. Sources of Funding Dr Richard Aviv receives grant funding from the Canadian Stroke consortium. Dr Gladstone is supported by the Heart and Stroke Foundation of Ontario, the Heart and Stroke Foundation Centre for Stroke Recovery, and the Department of Medicine at Sunnybrook Health Sciences Centre and University of Toronto. None. Disclosures References 1. Kazui S, Naritomi H, Yamamoto H, Sawada T, Yamaguchi T. Enlargement of spontaneous intracerebral hemorrhage. Incidence and time course. Stroke. 1996;27: Broderick J, Connolly S, Feldmann E, Hanley D, Kase C, Krieger D, Mayberg M, Morgenstern L, Ogilvy CS, Vespa P, Zuccarello M. Guidelines for the management of spontaneous intracerebral hemorrhage in adults update. A guideline from the American Heart Association, American Stroke Association Stroke Council, High Blood Pressure Research Council, and the Quality Of Care And Outcomes In Research Interdisciplinary Working Group. Stroke. 2007;38: Becker KJ, Baxter AB, Bybee HM, Tirschwell DL, Abouelsaad T, Cohen WA. Extravasation of radiographic contrast is an independent predictor of death in primary intracerebral hemorrhage. Stroke. 1999;30: Mayer SA, Brun NC, Begtrup K, Broderick J, Davis S, Diringer MN, Skolnick BE, Steiner T. Recombinant activated factor vii for acute intracerebral hemorrhage. N Engl J Med. 2005;352:
7 Gazzola et al CTA Spot Sign in Secondary Intracranial Hemorrhage Fujii Y, Tanaka R, Takeuchi S, Koike T, Minakawa T, Sasaki O. Hematoma enlargement in spontaneous intracerebral hemorrhage. J Neurosurg. 1994; 80: Wada R, Aviv RI, Fox AJ, Sahlas DJ, Gladstone DJ, Tomlinson G, Symons SP. Ct angiography Spot sign Predicts hematoma expansion in acute intracerebral hemorrhage. Stroke. 2007;38: Kothari RU, Brott T, Broderick JP, Barsan WG, Sauerbeck LR, Zuccarello M, Khoury J. The abcs of measuring intracerebral hemorrhage volumes. Stroke. 1996;27: Brott T, Broderick J, Kothari R, Barsan W, Tomsick T, Sauerbeck L, Spilker J, Duldner J, Khoury J. Early hemorrhage growth in patients with intracerebral hemorrhage. Stroke. 1997;28: Goldstein JN, Fazen LE, Snider R, Schwab K, Greenberg SM, Smith EE, Lev MH, Rosand J. Contrast extravasation on ct angiography predicts hematoma expansion in intracerebral hemorrhage. Neurology. 2007;68: Yamaguchi K, Uemura K, Takahashi H, Kowada M, Kutsuzawa T. Intracerebral leakage of contrast medium in apoplexy. Br J Radiol. 1971;44: Murai Y, Takagi R, Ikeda Y, Yamamoto Y, Teramoto A. Threedimensional computerized tomography angiography in patients with hyperacute intracerebral hemorrhage. J Neurosurg. 1999;91: Fisher CM. Pathological observations in hypertensive cerebral hemorrhage. J Neuropathol Exp Neurol. 1971;30: Halpin SF, Britton JA, Byrne JV, Clifton A, Hart G, Moore A. Prospective evaluation of cerebral angiography and computed tomography in cerebral haematoma. J Neurol Neurosurg Psychiatry. 1994;57: McCormick WF, Rosenfield DB. Massive brain hemorrhage: A review of 144 cases and an examination of their causes. Stroke. 1973;4: Zhu XL, Chan MS, Poon WS. Spontaneous intracranial hemorrhage: Which patients need diagnostic cerebral angiography? A prospective study of 206 cases and review of the literature. Stroke. 1997;28:
Postcontrast CT Extravasation Is Associated With Hematoma Expansion in CTA Spot Negative Patients
 Postcontrast CT Extravasation Is Associated With Hematoma Expansion in CTA Spot Negative Patients Ashraf Ederies, MBChB; Andrew Demchuk, MD, FRCPC; Tze Chia, BSc; David J. Gladstone, MD, PhD, FRCPC; Dar
Postcontrast CT Extravasation Is Associated With Hematoma Expansion in CTA Spot Negative Patients Ashraf Ederies, MBChB; Andrew Demchuk, MD, FRCPC; Tze Chia, BSc; David J. Gladstone, MD, PhD, FRCPC; Dar
Primary intracerebral hemorrhage (ICH) is one of the most
 ORIGINAL RESEARCH J. Kim A. Smith J.C. Hemphill III W.S. Smith Y. Lu W.P. Dillon M. Wintermark Contrast Extravasation on CT Predicts Mortality in Primary Intracerebral Hemorrhage BACKGROUND AND PURPOSE:
ORIGINAL RESEARCH J. Kim A. Smith J.C. Hemphill III W.S. Smith Y. Lu W.P. Dillon M. Wintermark Contrast Extravasation on CT Predicts Mortality in Primary Intracerebral Hemorrhage BACKGROUND AND PURPOSE:
CT angiography and its role in the investigation of intracranial haemorrhage
 CT angiography and its role in the investigation of intracranial haemorrhage RD Magazine, 39, 458, 29-30 Dr M Igra Radiology SPR Leeds General Infirmary Dr I Djoukhadar Research fellow Wolfson Molecular
CT angiography and its role in the investigation of intracranial haemorrhage RD Magazine, 39, 458, 29-30 Dr M Igra Radiology SPR Leeds General Infirmary Dr I Djoukhadar Research fellow Wolfson Molecular
UPSTATE Comprehensive Stroke Center. Neurosurgical Interventions Satish Krishnamurthy MD, MCh
 UPSTATE Comprehensive Stroke Center Neurosurgical Interventions Satish Krishnamurthy MD, MCh Regional cerebral blood flow is important Some essential facts Neurons are obligatory glucose users Under anerobic
UPSTATE Comprehensive Stroke Center Neurosurgical Interventions Satish Krishnamurthy MD, MCh Regional cerebral blood flow is important Some essential facts Neurons are obligatory glucose users Under anerobic
Comparison of ABC/2 Estimation Technique to Computer-Assisted Planimetric Analysis in Warfarin-Related Intracerebral Parenchymal Hemorrhage
 Comparison of ABC/2 Estimation Technique to Computer-Assisted Planimetric Analysis in Warfarin-Related Intracerebral Parenchymal Hemorrhage Hagen B. Huttner, MD; Thorsten Steiner, MD; Marius Hartmann,
Comparison of ABC/2 Estimation Technique to Computer-Assisted Planimetric Analysis in Warfarin-Related Intracerebral Parenchymal Hemorrhage Hagen B. Huttner, MD; Thorsten Steiner, MD; Marius Hartmann,
Nontraumatic ICH accounts for 10% 15% of cases of acute
 ORIGINAL RESEARCH J.E. Delgado Almandoz P.W. Schaefer J.N. Goldstein J. Rosand M.H. Lev R.G. González J.M. Romero Practical Scoring System for the Identification of Patients with Intracerebral Hemorrhage
ORIGINAL RESEARCH J.E. Delgado Almandoz P.W. Schaefer J.N. Goldstein J. Rosand M.H. Lev R.G. González J.M. Romero Practical Scoring System for the Identification of Patients with Intracerebral Hemorrhage
Comparison of Spot Sign, Blend Sign and Black Hole Sign for Outcome Prediction in Patients with Intracerebral Hemorrhage
 Journal of Stroke 2017;19(3):333-339 Original Article Comparison of Spot Sign, Blend Sign and Black Hole Sign for Outcome Prediction in Patients with Intracerebral Hemorrhage Peter B. Sporns, a Michael
Journal of Stroke 2017;19(3):333-339 Original Article Comparison of Spot Sign, Blend Sign and Black Hole Sign for Outcome Prediction in Patients with Intracerebral Hemorrhage Peter B. Sporns, a Michael
Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage
 Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Spontaneous ICH accounts for 10% 15% of cases
 J Neurosurg 117:761 766, 2012 Computed tomography angiography: improving diagnostic yield and cost effectiveness in the initial evaluation of spontaneous nonsubarachnoid intracerebral hemorrhage Clinical
J Neurosurg 117:761 766, 2012 Computed tomography angiography: improving diagnostic yield and cost effectiveness in the initial evaluation of spontaneous nonsubarachnoid intracerebral hemorrhage Clinical
Angel J. Lacerda MD PhD, Daisy Abreu MD, Julio A. Díaz MD, Sandro Perez MD, Julio C Martin MD, Daiyan Martin MD.
 Angel J. Lacerda MD PhD, Daisy Abreu MD, Julio A. Díaz MD, Sandro Perez MD, Julio C Martin MD, Daiyan Martin MD. Introduction: Spontaneous intracerebral haemorrhage (SICH) represents one of the most severe
Angel J. Lacerda MD PhD, Daisy Abreu MD, Julio A. Díaz MD, Sandro Perez MD, Julio C Martin MD, Daiyan Martin MD. Introduction: Spontaneous intracerebral haemorrhage (SICH) represents one of the most severe
Intracranial spontaneous hemorrhage mechanisms, imaging and management
 Intracranial spontaneous hemorrhage mechanisms, imaging and management Dora Zlatareva Department of Diagnostic Imaging Medical University, Sofia, Bulgaria Intracranial hemorrhage (ICH) ICH 15% of strokes
Intracranial spontaneous hemorrhage mechanisms, imaging and management Dora Zlatareva Department of Diagnostic Imaging Medical University, Sofia, Bulgaria Intracranial hemorrhage (ICH) ICH 15% of strokes
A review: Prediction model for the incidence rate of intracerebral hemorrhage
 2nd Information Technology and Mechatronics Engineering Conference (ITOEC 2016) A review: Prediction model for the incidence rate of intracerebral hemorrhage Kaikai Yin1, a, Le Zhang1, b *, Hua Feng2,c,
2nd Information Technology and Mechatronics Engineering Conference (ITOEC 2016) A review: Prediction model for the incidence rate of intracerebral hemorrhage Kaikai Yin1, a, Le Zhang1, b *, Hua Feng2,c,
CLEAR III TRIAL : UPDATE ON SURGICAL MATTERS THAT MATTER
 CLEAR III TRIAL : UPDATE ON SURGICAL MATTERS THAT MATTER CLEAR Surgical Center Team July 2011 Trial Enrollment Status Updates Insert latest enrollment update chart from most recent CLEAR newsletter Imaging
CLEAR III TRIAL : UPDATE ON SURGICAL MATTERS THAT MATTER CLEAR Surgical Center Team July 2011 Trial Enrollment Status Updates Insert latest enrollment update chart from most recent CLEAR newsletter Imaging
Timing of Occurrence Is the Most Important Characteristic of Spot Sign
 Timing of Occurrence Is the Most Important Characteristic of Spot Sign Binli Wang, MM*; Shenqiang Yan, MD*; Mengjun Xu, MD; Sheng Zhang, PhD; Keqin Liu, MD; Haitao Hu, MD; Magdy Selim, MD, PhD; Min Lou,
Timing of Occurrence Is the Most Important Characteristic of Spot Sign Binli Wang, MM*; Shenqiang Yan, MD*; Mengjun Xu, MD; Sheng Zhang, PhD; Keqin Liu, MD; Haitao Hu, MD; Magdy Selim, MD, PhD; Min Lou,
Can a Subset of Intracerebral Hemorrhage Patients Benefit From Hemostatic Therapy With Recombinant Activated Factor VII?
 Can a Subset of Intracerebral Hemorrhage Patients Benefit From Hemostatic Therapy With Recombinant Activated Factor VII? Stephan A. Mayer, MD; Stephen M. Davis, MD; Brett E. Skolnick, PhD; Nikolai C. Brun,
Can a Subset of Intracerebral Hemorrhage Patients Benefit From Hemostatic Therapy With Recombinant Activated Factor VII? Stephan A. Mayer, MD; Stephen M. Davis, MD; Brett E. Skolnick, PhD; Nikolai C. Brun,
Lothian Audit of the Treatment of Cerebral Haemorrhage (LATCH)
 1. INTRODUCTION Stroke physicians, emergency department doctors, and neurologists are often unsure about which patients they should refer for neurosurgical intervention. Early neurosurgical evacuation
1. INTRODUCTION Stroke physicians, emergency department doctors, and neurologists are often unsure about which patients they should refer for neurosurgical intervention. Early neurosurgical evacuation
Pearls and Pitfalls in Neuroradiology of Cerebrovascular Disease The Essentials with MR and CT
 Pearls and Pitfalls in Neuroradiology of Cerebrovascular Disease The Essentials with MR and CT Val M. Runge, MD Wendy R. K. Smoker, MD Anton Valavanis, MD Control # 823 Purpose The focus of this educational
Pearls and Pitfalls in Neuroradiology of Cerebrovascular Disease The Essentials with MR and CT Val M. Runge, MD Wendy R. K. Smoker, MD Anton Valavanis, MD Control # 823 Purpose The focus of this educational
Swirls and spots: relationship between qualitative and quantitative hematoma heterogeneity, hematoma expansion, and the spot sign
 Connor et al. Neurovascular Imaging (2015) 1:8 DOI 10.1186/s40809-015-0010-1 RESEARCH ARTICLE Open Access Swirls and spots: relationship between qualitative and quantitative hematoma heterogeneity, hematoma
Connor et al. Neurovascular Imaging (2015) 1:8 DOI 10.1186/s40809-015-0010-1 RESEARCH ARTICLE Open Access Swirls and spots: relationship between qualitative and quantitative hematoma heterogeneity, hematoma
Cerebro-vascular stroke
 Cerebro-vascular stroke CT Terminology Hypodense lesion = lesion of lower density than the normal brain tissue Hyperdense lesion = lesion of higher density than normal brain tissue Isodense lesion = lesion
Cerebro-vascular stroke CT Terminology Hypodense lesion = lesion of lower density than the normal brain tissue Hyperdense lesion = lesion of higher density than normal brain tissue Isodense lesion = lesion
Brain Arteriovenous Malformations Endovascular Therapy and Associated Therapeutic Protocols Jorge Guedes Cabral de Campos
 Endovascular Therapy and Associated Therapeutic Protocols Jorge Guedes Cabral de Campos Neuroradiology Department Hospital de Santa Maria University of Lisbon CEREBRAL AVM CLINICAL / EPIDEMIOLOGY Brain
Endovascular Therapy and Associated Therapeutic Protocols Jorge Guedes Cabral de Campos Neuroradiology Department Hospital de Santa Maria University of Lisbon CEREBRAL AVM CLINICAL / EPIDEMIOLOGY Brain
HEAD AND NECK IMAGING. James Chen (MS IV)
 HEAD AND NECK IMAGING James Chen (MS IV) Anatomy Course Johns Hopkins School of Medicine Sept. 27, 2011 OBJECTIVES Introduce cross sectional imaging of head and neck Computed tomography (CT) Review head
HEAD AND NECK IMAGING James Chen (MS IV) Anatomy Course Johns Hopkins School of Medicine Sept. 27, 2011 OBJECTIVES Introduce cross sectional imaging of head and neck Computed tomography (CT) Review head
Supratentorial cerebral arteriovenous malformations : a clinical analysis
 Original article: Supratentorial cerebral arteriovenous malformations : a clinical analysis Dr. Rajneesh Gour 1, Dr. S. N. Ghosh 2, Dr. Sumit Deb 3 1Dept.Of Surgery,Chirayu Medical College & Research Centre,
Original article: Supratentorial cerebral arteriovenous malformations : a clinical analysis Dr. Rajneesh Gour 1, Dr. S. N. Ghosh 2, Dr. Sumit Deb 3 1Dept.Of Surgery,Chirayu Medical College & Research Centre,
Vascular Malformations of the Brain: A Review of Imaging Features and Risks
 Vascular Malformations of the Brain: A Review of Imaging Features and Risks Comprehensive Neuroradiology: Best Practices October 27-30, 2016 Sudhakar R. Satti, MD Associate Director Neurointerventional
Vascular Malformations of the Brain: A Review of Imaging Features and Risks Comprehensive Neuroradiology: Best Practices October 27-30, 2016 Sudhakar R. Satti, MD Associate Director Neurointerventional
Recombinant Factor VIIa for Intracerebral Hemorrhage
 Recombinant Factor VIIa for Intracerebral Hemorrhage January 24, 2006 Justin Lee Pharmacy Resident University Health Network Outline 1. Introduction to patient case 2. Overview of intracerebral hemorrhage
Recombinant Factor VIIa for Intracerebral Hemorrhage January 24, 2006 Justin Lee Pharmacy Resident University Health Network Outline 1. Introduction to patient case 2. Overview of intracerebral hemorrhage
NEURO IMAGING 2. Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity
 NEURO IMAGING 2 Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity I. EPIDURAL HEMATOMA (EDH) LOCATION Seventy to seventy-five percent occur in temporoparietal region. CAUSE Most likely caused
NEURO IMAGING 2 Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity I. EPIDURAL HEMATOMA (EDH) LOCATION Seventy to seventy-five percent occur in temporoparietal region. CAUSE Most likely caused
CT Angiography Spot Sign Predicts Hematoma Expansion in Acute Intracerebral Hemorrhage
 CT Angiography Spot Sign Predicts Hematoma Expansion in Acute Intracerebral Hemorrhage Ryan Wada, MD; Richard I. Aviv, MBChB; Allan J. Fox, MD; Demetrios J. Sahlas, MD; David J. Gladstone, MD; George Tomlinson,
CT Angiography Spot Sign Predicts Hematoma Expansion in Acute Intracerebral Hemorrhage Ryan Wada, MD; Richard I. Aviv, MBChB; Allan J. Fox, MD; Demetrios J. Sahlas, MD; David J. Gladstone, MD; George Tomlinson,
Essentials of Clinical MR, 2 nd edition. 14. Ischemia and Infarction II
 14. Ischemia and Infarction II Lacunar infarcts are small deep parenchymal lesions involving the basal ganglia, internal capsule, thalamus, and brainstem. The vascular supply of these areas includes the
14. Ischemia and Infarction II Lacunar infarcts are small deep parenchymal lesions involving the basal ganglia, internal capsule, thalamus, and brainstem. The vascular supply of these areas includes the
Case Report 1. CTA head. (c) Tele3D Advantage, LLC
 Case Report 1 CTA head 1 History 82 YEAR OLD woman with signs and symptoms of increased intra cranial pressure in setting of SAH. CT Brain was performed followed by CT Angiography of head. 2 CT brain Extensive
Case Report 1 CTA head 1 History 82 YEAR OLD woman with signs and symptoms of increased intra cranial pressure in setting of SAH. CT Brain was performed followed by CT Angiography of head. 2 CT brain Extensive
The management of ICH when to operate when not to?
 The management of ICH when to operate when not to? Intracranial Hemorrhage High Incidence o Accounts for 10-15% of all strokes 1,2,5 o 80,000 cases in US; 2 million WW 2,5 o Incidence doubles for African-
The management of ICH when to operate when not to? Intracranial Hemorrhage High Incidence o Accounts for 10-15% of all strokes 1,2,5 o 80,000 cases in US; 2 million WW 2,5 o Incidence doubles for African-
Traumatic brain injury is a major health and socioeconomic. Traumatic Intracranial Hematomas: Prognostic Value of Contrast Extravasation
 ORIGINAL RESEARCH BRAIN Traumatic Intracranial Hematomas: Prognostic Value of Contrast Extravasation L. Letourneau-Guillon, T. Huynh, R. Jakobovic, R. Milwid, S.P. Symons, and R.I. Aviv ABSTRACT BACKGROUND
ORIGINAL RESEARCH BRAIN Traumatic Intracranial Hematomas: Prognostic Value of Contrast Extravasation L. Letourneau-Guillon, T. Huynh, R. Jakobovic, R. Milwid, S.P. Symons, and R.I. Aviv ABSTRACT BACKGROUND
A Guide to the Radiologic Evaluation of Extra-Axial Hemorrhage
 July 2013 A Guide to the Radiologic Evaluation of Extra-Axial Hemorrhage John Dickson, Harvard Medical School Year III Agenda 1. Define extra-axial hemorrhage and introduce its subtypes 2. Review coup
July 2013 A Guide to the Radiologic Evaluation of Extra-Axial Hemorrhage John Dickson, Harvard Medical School Year III Agenda 1. Define extra-axial hemorrhage and introduce its subtypes 2. Review coup
Canadian Best Practice Recommendations for Stroke Care 3.7 Acute Intracerebral Hemorrhage
 Last Updated: May 21st, 2013 Canadian Best Practice Recommendations for Stroke Care 3.7 Acute Intracerebral Hemorrhage Canadian Best Practice Recommendations for Stroke Care 2012-2013 Update Contents Search
Last Updated: May 21st, 2013 Canadian Best Practice Recommendations for Stroke Care 3.7 Acute Intracerebral Hemorrhage Canadian Best Practice Recommendations for Stroke Care 2012-2013 Update Contents Search
There are many methods to quantify carotid stenosis. 1 With
 ORIGINAL RESEARCH E.S. Bartlett S.P. Symons A.J. Fox Correlation of Carotid Stenosis Diameter and Cross-Sectional Areas with CT Angiography PURPOSE: Carotid stenosis quantification traditionally uses measurements
ORIGINAL RESEARCH E.S. Bartlett S.P. Symons A.J. Fox Correlation of Carotid Stenosis Diameter and Cross-Sectional Areas with CT Angiography PURPOSE: Carotid stenosis quantification traditionally uses measurements
Pharmacological Deep Vein Thrombosis Prophylaxis Does Not Lead to Hematoma Expansion in Intracerebral Hemorrhage With Intraventricular Extension
 Pharmacological Deep Vein Thrombosis Prophylaxis Does Not Lead to Hematoma Expansion in Intracerebral Hemorrhage With Intraventricular Extension Tzu-Ching Wu, MD; Mallik Kasam, PhD; Nusrat Harun, MS; Hen
Pharmacological Deep Vein Thrombosis Prophylaxis Does Not Lead to Hematoma Expansion in Intracerebral Hemorrhage With Intraventricular Extension Tzu-Ching Wu, MD; Mallik Kasam, PhD; Nusrat Harun, MS; Hen
Short Communications. Alcoholic Intracerebral Hemorrhage
 Short Communications 1565 Alcoholic Intracerebral Hemorrhage Leon A. Weisberg, MD Six alcoholic patients developed extensive cerebral hemispheric hemorrhages with both intraventricular and subarachnoid
Short Communications 1565 Alcoholic Intracerebral Hemorrhage Leon A. Weisberg, MD Six alcoholic patients developed extensive cerebral hemispheric hemorrhages with both intraventricular and subarachnoid
The central nervous system
 Sectc.qxd 29/06/99 09:42 Page 81 Section C The central nervous system CNS haemorrhage Subarachnoid haemorrhage Cerebral infarction Brain atrophy Ring enhancing lesions MRI of the pituitary Multiple sclerosis
Sectc.qxd 29/06/99 09:42 Page 81 Section C The central nervous system CNS haemorrhage Subarachnoid haemorrhage Cerebral infarction Brain atrophy Ring enhancing lesions MRI of the pituitary Multiple sclerosis
Dural Arteriovenous Fistula of the Cavernous Sinus Presenting with Progressive Venous Congestion of the Pons and Cerebrum: Report of one case
 Dural Arteriovenous Fistula of the Cavernous Sinus Presenting with Progressive Venous Congestion of the Pons and Cerebrum: Report of one case Soo-Bin Yim, M.D., Jong-Sung Kim, M.D., Yang Kwon,M.D.*, Choong-Gon
Dural Arteriovenous Fistula of the Cavernous Sinus Presenting with Progressive Venous Congestion of the Pons and Cerebrum: Report of one case Soo-Bin Yim, M.D., Jong-Sung Kim, M.D., Yang Kwon,M.D.*, Choong-Gon
Detectability of unruptured intracranial aneurysms on thinslice non-contrast-enhanced CT
 Detectability of unruptured intracranial aneurysms on thinslice non-contrast-enhanced CT Poster No.: C-9 Congress: ECR 5 Type: Scientific Exhibit Authors: M. Nakadate, Y. Iwasa, M. Kishino, U. Tateishi;
Detectability of unruptured intracranial aneurysms on thinslice non-contrast-enhanced CT Poster No.: C-9 Congress: ECR 5 Type: Scientific Exhibit Authors: M. Nakadate, Y. Iwasa, M. Kishino, U. Tateishi;
Correlation between Intracerebral Hemorrhage Score and surgical outcome of spontaneous intracerebral hemorrhage
 Bangladesh Med Res Counc Bull 23; 39: -5 Correlation between Intracerebral Hemorrhage Score and surgical outcome of spontaneous intracerebral hemorrhage Rashid HU, Amin R, Rahman A, Islam MR, Hossain M,
Bangladesh Med Res Counc Bull 23; 39: -5 Correlation between Intracerebral Hemorrhage Score and surgical outcome of spontaneous intracerebral hemorrhage Rashid HU, Amin R, Rahman A, Islam MR, Hossain M,
Hypertensive Haemorrhagic Stroke. Dr Philip Lam Thuon Mine
 Hypertensive Haemorrhagic Stroke Dr Philip Lam Thuon Mine Intracerebral Haemorrhage Primary ICH Spontaneous rupture of small vessels damaged by HBP Basal ganglia, thalamus, pons and cerebellum Amyloid
Hypertensive Haemorrhagic Stroke Dr Philip Lam Thuon Mine Intracerebral Haemorrhage Primary ICH Spontaneous rupture of small vessels damaged by HBP Basal ganglia, thalamus, pons and cerebellum Amyloid
Neurosurgical decision making in structural lesions causing stroke. Dr Rakesh Ranjan MS, MCh, Dip NB (Neurosurgery)
 Neurosurgical decision making in structural lesions causing stroke Dr Rakesh Ranjan MS, MCh, Dip NB (Neurosurgery) Subarachnoid Hemorrhage Every year, an estimated 30,000 people in the United States experience
Neurosurgical decision making in structural lesions causing stroke Dr Rakesh Ranjan MS, MCh, Dip NB (Neurosurgery) Subarachnoid Hemorrhage Every year, an estimated 30,000 people in the United States experience
Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD
 Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD Boston Children s Hospital Harvard Medical School None Disclosures Conventional US Anterior fontanelle
Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD Boston Children s Hospital Harvard Medical School None Disclosures Conventional US Anterior fontanelle
Intracerebral hemorrhage (ICH) is the most fatal form of
 Hematoma Growth and Outcome in Treated Neurocritical Care Patients With Intracerebral Hemorrhage Related to Oral Anticoagulant Therapy Comparison of Acute Treatment Strategies Using Vitamin K, Fresh Frozen
Hematoma Growth and Outcome in Treated Neurocritical Care Patients With Intracerebral Hemorrhage Related to Oral Anticoagulant Therapy Comparison of Acute Treatment Strategies Using Vitamin K, Fresh Frozen
Vascular Malformations
 Vascular Malformations LTC Robert Shih Chief of Neuroradiology Walter Reed Medical Center Special thanks to LTC Alice Smith (retired) Disclosures: None. This presentation reflects the personal views of
Vascular Malformations LTC Robert Shih Chief of Neuroradiology Walter Reed Medical Center Special thanks to LTC Alice Smith (retired) Disclosures: None. This presentation reflects the personal views of
Cryptogenic Enlargement Of Bilateral Superior Ophthalmic Veins
 ISPUB.COM The Internet Journal of Radiology Volume 18 Number 1 Cryptogenic Enlargement Of Bilateral Superior Ophthalmic Veins K Kragha Citation K Kragha. Cryptogenic Enlargement Of Bilateral Superior Ophthalmic
ISPUB.COM The Internet Journal of Radiology Volume 18 Number 1 Cryptogenic Enlargement Of Bilateral Superior Ophthalmic Veins K Kragha Citation K Kragha. Cryptogenic Enlargement Of Bilateral Superior Ophthalmic
ORIGINAL ARTICLE COMPUTED TOMOGRAPHY EVALUATION OF SPONTANEOUS INTRACRANIAL HAEMORRHAGE
 Available online at www.journalijmrr.com INTERNATIONAL JOURNAL OF MODERN RESEARCH AND REVIEWS IJMRR ISSN: 2347-8314 Int. J. Modn. Res. Revs. Volume 3, Issue 4, pp 647-652, April, 2015 ORIGINAL ARTICLE
Available online at www.journalijmrr.com INTERNATIONAL JOURNAL OF MODERN RESEARCH AND REVIEWS IJMRR ISSN: 2347-8314 Int. J. Modn. Res. Revs. Volume 3, Issue 4, pp 647-652, April, 2015 ORIGINAL ARTICLE
Head CT Scan Interpretation: A Five-Step Approach to Seeing Inside the Head Lawrence B. Stack, MD
 Head CT Scan Interpretation: A Five-Step Approach to Seeing Inside the Head Lawrence B. Stack, MD Five Step Approach 1. Adequate study 2. Bone windows 3. Ventricles 4. Quadrigeminal cistern 5. Parenchyma
Head CT Scan Interpretation: A Five-Step Approach to Seeing Inside the Head Lawrence B. Stack, MD Five Step Approach 1. Adequate study 2. Bone windows 3. Ventricles 4. Quadrigeminal cistern 5. Parenchyma
Welcome to our MISTIE III Safety Forum September 12, 2016
 Welcome to our MISTIE III Safety Forum September 12, 2016 Agenda: Update from our Surgical Centers: Where we stand surgically Mario Zuccarello, MD, University of Cincinnati Revisiting the Importance of
Welcome to our MISTIE III Safety Forum September 12, 2016 Agenda: Update from our Surgical Centers: Where we stand surgically Mario Zuccarello, MD, University of Cincinnati Revisiting the Importance of
Insertion of an external ventricular drain (EVD) is a
 Short Communication Intracerebral Hemorrhage With Severe Ventricular Involvement Lumbar Drainage for Communicating Hydrocephalus Hagen B. Huttner, MD; Simon Nagel, MD; Elena Tognoni; Martin Köhrmann, MD;
Short Communication Intracerebral Hemorrhage With Severe Ventricular Involvement Lumbar Drainage for Communicating Hydrocephalus Hagen B. Huttner, MD; Simon Nagel, MD; Elena Tognoni; Martin Köhrmann, MD;
Decreased Perihematomal Edema in Thrombolysis-Related Intracerebral Hemorrhage Compared With Spontaneous Intracerebral Hemorrhage
 Decreased Perihematomal Edema in Thrombolysis-Related Intracerebral Hemorrhage Compared With Spontaneous Intracerebral Hemorrhage James M. Gebel, MD; Thomas G. Brott, MD; Cathy A. Sila, MD; Thomas A. Tomsick,
Decreased Perihematomal Edema in Thrombolysis-Related Intracerebral Hemorrhage Compared With Spontaneous Intracerebral Hemorrhage James M. Gebel, MD; Thomas G. Brott, MD; Cathy A. Sila, MD; Thomas A. Tomsick,
Microsurgery for ruptured cerebellar arteriovenous malformations
 European Review for Medical and Pharmacological Sciences Microsurgery for ruptured cerebellar arteriovenous malformations S.-F. GONG 1,2, X.-B. WANG 1,3, Y.-Q. LIAO 1,2, T.-P. JIANG 1,2, J.-B. HE 1,2,
European Review for Medical and Pharmacological Sciences Microsurgery for ruptured cerebellar arteriovenous malformations S.-F. GONG 1,2, X.-B. WANG 1,3, Y.-Q. LIAO 1,2, T.-P. JIANG 1,2, J.-B. HE 1,2,
Klinikum Frankfurt Höchst
 Blood pressure management in hemorrhagic stroke Blood pressure in acute ICH Do we need additional trials after INTERACT2 and ATTACH-II? Focus.de Department of Neurology,, Germany Department of Neurology,
Blood pressure management in hemorrhagic stroke Blood pressure in acute ICH Do we need additional trials after INTERACT2 and ATTACH-II? Focus.de Department of Neurology,, Germany Department of Neurology,
Independent predictors of short-term mortality (30 days)
 Regular Aspirin-Use Preceding the Onset of Primary Intracerebral Hemorrhage is an Independent Predictor for Death Pertti Saloheimo, MD; Mikko Ahonen, MD; Seppo Juvela, MD, PhD; Juhani Pyhtinen, MD, PhD;
Regular Aspirin-Use Preceding the Onset of Primary Intracerebral Hemorrhage is an Independent Predictor for Death Pertti Saloheimo, MD; Mikko Ahonen, MD; Seppo Juvela, MD, PhD; Juhani Pyhtinen, MD, PhD;
Diagnostic Cerebral Angiography in Spontaneous Intracranial Haemorrhage: A Guide for Developing Countries
 Original Article Diagnostic Cerebral Angiography in Spontaneous Intracranial Haemorrhage: A Guide for Developing Countries Ishak Abu Bakar, Ibrahim Lutfi Shuaib, Abdul Rahman Mohd Ariff, Nyi Nyi Naing
Original Article Diagnostic Cerebral Angiography in Spontaneous Intracranial Haemorrhage: A Guide for Developing Countries Ishak Abu Bakar, Ibrahim Lutfi Shuaib, Abdul Rahman Mohd Ariff, Nyi Nyi Naing
Epidemiology And Treatment Of Cerebral Aneurysms At An Australian Tertiary Level Hospital
 ISPUB.COM The Internet Journal of Neurosurgery Volume 9 Number 2 Epidemiology And Treatment Of Cerebral Aneurysms At An Australian Tertiary Level Hospital A Granger, R Laherty Citation A Granger, R Laherty.
ISPUB.COM The Internet Journal of Neurosurgery Volume 9 Number 2 Epidemiology And Treatment Of Cerebral Aneurysms At An Australian Tertiary Level Hospital A Granger, R Laherty Citation A Granger, R Laherty.
Benefit of cone-beam computed tomography angiography in acute management of angiographically undetectable ruptured arteriovenous malformations
 J Neurosurg 119:1015 1020, 2013 AANS, 2013 Benefit of cone-beam computed tomography angiography in acute management of angiographically undetectable ruptured arteriovenous malformations Clinical article
J Neurosurg 119:1015 1020, 2013 AANS, 2013 Benefit of cone-beam computed tomography angiography in acute management of angiographically undetectable ruptured arteriovenous malformations Clinical article
Blunt Carotid Injury- CT Angiography is Adequate For Screening. Kelly Knudson, M.D. UCHSC April 3, 2006
 Blunt Carotid Injury- CT Angiography is Adequate For Screening Kelly Knudson, M.D. UCHSC April 3, 2006 CT Angiography vs Digital Subtraction Angiography Blunt carotid injury screening is one of the very
Blunt Carotid Injury- CT Angiography is Adequate For Screening Kelly Knudson, M.D. UCHSC April 3, 2006 CT Angiography vs Digital Subtraction Angiography Blunt carotid injury screening is one of the very
Department of Neurosurgery, Medical Research Institute, Pusan National University College of Medicine and Hospital, Busan, Korea
 Journal of Cerebrovascular and Endovascular Neurosurgery pissn 2234-8565, eissn 2287-3139, http://dx.doi.org/10.7461/jcen.2015.17.1.20 Case Report Contrast Extravasation on Computed Tomography Angiography
Journal of Cerebrovascular and Endovascular Neurosurgery pissn 2234-8565, eissn 2287-3139, http://dx.doi.org/10.7461/jcen.2015.17.1.20 Case Report Contrast Extravasation on Computed Tomography Angiography
Case 37 Clinical Presentation
 Case 37 73 Clinical Presentation The patient is a 62-year-old woman with gastrointestinal (GI) bleeding. 74 RadCases Interventional Radiology Imaging Findings () Image from a selective digital subtraction
Case 37 73 Clinical Presentation The patient is a 62-year-old woman with gastrointestinal (GI) bleeding. 74 RadCases Interventional Radiology Imaging Findings () Image from a selective digital subtraction
How to interpret an unenhanced CT brain scan. Part 2: Clinical cases
 How to interpret an unenhanced CT brain scan. Part 2: Clinical cases Thomas Osborne a, Christine Tang a, Kivraj Sabarwal b and Vineet Prakash c a Radiology Registrar; b Radiology Foundation Year 1 Doctor;
How to interpret an unenhanced CT brain scan. Part 2: Clinical cases Thomas Osborne a, Christine Tang a, Kivraj Sabarwal b and Vineet Prakash c a Radiology Registrar; b Radiology Foundation Year 1 Doctor;
TRAUMATIC CAROTID &VERTEBRAL ARTERY INJURIES
 TRAUMATIC CAROTID &VERTEBRAL ARTERY INJURIES ALBERTO MAUD, MD ASSOCIATE PROFESSOR TEXAS TECH UNIVERSITY HEALTH SCIENCES CENTER EL PASO PAUL L. FOSTER SCHOOL OF MEDICINE 18TH ANNUAL RIO GRANDE TRAUMA 2017
TRAUMATIC CAROTID &VERTEBRAL ARTERY INJURIES ALBERTO MAUD, MD ASSOCIATE PROFESSOR TEXAS TECH UNIVERSITY HEALTH SCIENCES CENTER EL PASO PAUL L. FOSTER SCHOOL OF MEDICINE 18TH ANNUAL RIO GRANDE TRAUMA 2017
Intracerebral Hemorrhage
 Review of Primary Intracerebral Hemorrhage Réza Behrouz, DO Assistant Professor of Neurology University of South Florida College of Medicine STROKE 85% ISCHEMIC 15% HEMORRHAGIC HEMORRHAGIC STROKE 1/3 Subarachnoid
Review of Primary Intracerebral Hemorrhage Réza Behrouz, DO Assistant Professor of Neurology University of South Florida College of Medicine STROKE 85% ISCHEMIC 15% HEMORRHAGIC HEMORRHAGIC STROKE 1/3 Subarachnoid
Principles Arteries & Veins of the CNS LO14
 Principles Arteries & Veins of the CNS LO14 14. Identify (on cadaver specimens, models and diagrams) and name the principal arteries and veins of the CNS: Why is it important to understand blood supply
Principles Arteries & Veins of the CNS LO14 14. Identify (on cadaver specimens, models and diagrams) and name the principal arteries and veins of the CNS: Why is it important to understand blood supply
IMAGING IN ACUTE ISCHEMIC STROKE
 IMAGING IN ACUTE ISCHEMIC STROKE Timo Krings MD, PhD, FRCP (C) Professor of Radiology & Surgery Braley Chair of Neuroradiology, Chief and Program Director of Diagnostic and Interventional Neuroradiology;
IMAGING IN ACUTE ISCHEMIC STROKE Timo Krings MD, PhD, FRCP (C) Professor of Radiology & Surgery Braley Chair of Neuroradiology, Chief and Program Director of Diagnostic and Interventional Neuroradiology;
Assessment of Vasospasm and Delayed Cerebral Ischemia after Subarachnoid Hemorrhage: Current concepts and Value of CT Perfusion and CT Angiography
 Assessment of Vasospasm and Delayed Cerebral Ischemia after Subarachnoid Hemorrhage: Current concepts and Value of CT Perfusion and CT Angiography Poster No.: C-2563 Congress: ECR 2012 Type: Educational
Assessment of Vasospasm and Delayed Cerebral Ischemia after Subarachnoid Hemorrhage: Current concepts and Value of CT Perfusion and CT Angiography Poster No.: C-2563 Congress: ECR 2012 Type: Educational
A New Trend in Vascular Imaging: the Arterial Spin Labeling (ASL) Sequence
 A New Trend in Vascular Imaging: the Arterial Spin Labeling (ASL) Sequence Poster No.: C-1347 Congress: ECR 2013 Type: Educational Exhibit Authors: J. Hodel, A. GUILLONNET, M. Rodallec, S. GERBER, R. 1
A New Trend in Vascular Imaging: the Arterial Spin Labeling (ASL) Sequence Poster No.: C-1347 Congress: ECR 2013 Type: Educational Exhibit Authors: J. Hodel, A. GUILLONNET, M. Rodallec, S. GERBER, R. 1
Benign brain lesions
 Benign brain lesions Diagnostic and Interventional Radiology Hung-Wen Kao Department of Radiology, Tri-Service General Hospital, National Defense Medical Center Computed tomography Hounsfield unit (HU)
Benign brain lesions Diagnostic and Interventional Radiology Hung-Wen Kao Department of Radiology, Tri-Service General Hospital, National Defense Medical Center Computed tomography Hounsfield unit (HU)
Moyamoya Syndrome with contra lateral DACA aneurysm: First Case report with review of literature
 Romanian Neurosurgery Volume XXXI Number 3 2017 July-September Article Moyamoya Syndrome with contra lateral DACA aneurysm: First Case report with review of literature Ashish Kumar Dwivedi, Pradeep Kumar,
Romanian Neurosurgery Volume XXXI Number 3 2017 July-September Article Moyamoya Syndrome with contra lateral DACA aneurysm: First Case report with review of literature Ashish Kumar Dwivedi, Pradeep Kumar,
Case Report Endoport-Assisted Microsurgical Treatment of a Ruptured Periventricular Aneurysm
 Case Reports in Neurological Medicine Volume 2016, Article ID 8654262, 4 pages http://dx.doi.org/10.1155/2016/8654262 Case Report Endoport-Assisted Microsurgical Treatment of a Ruptured Periventricular
Case Reports in Neurological Medicine Volume 2016, Article ID 8654262, 4 pages http://dx.doi.org/10.1155/2016/8654262 Case Report Endoport-Assisted Microsurgical Treatment of a Ruptured Periventricular
Radiographic and statistical analysis of Brain Arteriovenous Malformations.
 Radiographic and statistical analysis of Brain Arteriovenous Malformations. Poster No.: C-0996 Congress: ECR 2017 Type: Educational Exhibit Authors: C. E. Rodriguez 1, A. Lopez Moreno 1, D. Sánchez Paré
Radiographic and statistical analysis of Brain Arteriovenous Malformations. Poster No.: C-0996 Congress: ECR 2017 Type: Educational Exhibit Authors: C. E. Rodriguez 1, A. Lopez Moreno 1, D. Sánchez Paré
Stroke - Intracranial hemorrhage. Dr. Amitesh Aggarwal Associate Professor Department of Medicine
 Stroke - Intracranial hemorrhage Dr. Amitesh Aggarwal Associate Professor Department of Medicine Etiology and pathogenesis ICH accounts for ~10% of all strokes 30 day mortality - 35 45% Incidence rates
Stroke - Intracranial hemorrhage Dr. Amitesh Aggarwal Associate Professor Department of Medicine Etiology and pathogenesis ICH accounts for ~10% of all strokes 30 day mortality - 35 45% Incidence rates
Sign up to receive ATOTW weekly -
 ANTICOAGULATION & INTRACRANIAL BLEEDS - MANAGEMENT OF THE ANTICOAGULATED PATIENT PRESENTING WITH INTRACRANIAL HAEMORRHAGE ANAESTHESIA TUTORIAL OF THE WEEK 82 12 th January 2008 Rebecca Appelboam, Exeter,
ANTICOAGULATION & INTRACRANIAL BLEEDS - MANAGEMENT OF THE ANTICOAGULATED PATIENT PRESENTING WITH INTRACRANIAL HAEMORRHAGE ANAESTHESIA TUTORIAL OF THE WEEK 82 12 th January 2008 Rebecca Appelboam, Exeter,
CT of the Head, Spine, and Cerebral Vessels
 CT of the Head, Spine, and Cerebral Vessels Objectives Determine specific imaging plane used to acquire or reformat CT scan, i.e. sagittal, coronal, transverse, and offaxis or oblique. Assess and evaluate
CT of the Head, Spine, and Cerebral Vessels Objectives Determine specific imaging plane used to acquire or reformat CT scan, i.e. sagittal, coronal, transverse, and offaxis or oblique. Assess and evaluate
The standard examination to evaluate for a source of subarachnoid
 Published April 11, 2013 as 10.3174/ajnr.A3478 ORIGINAL RESEARCH INTERVENTIONAL Use of CT Angiography and Digital Subtraction Angiography in Patients with Ruptured Cerebral Aneurysm: Evaluation of a Large
Published April 11, 2013 as 10.3174/ajnr.A3478 ORIGINAL RESEARCH INTERVENTIONAL Use of CT Angiography and Digital Subtraction Angiography in Patients with Ruptured Cerebral Aneurysm: Evaluation of a Large
Pediatric Neurointervention: Vein of Galen Malformations
 Pediatric Neurointervention: Vein of Galen Malformations Johanna T. Fifi, M.D. Assistant Professor of Neurology, Neurosurgery, and Radiology Icahn School of Medicine at Mount Sinai November 9 th, 2014
Pediatric Neurointervention: Vein of Galen Malformations Johanna T. Fifi, M.D. Assistant Professor of Neurology, Neurosurgery, and Radiology Icahn School of Medicine at Mount Sinai November 9 th, 2014
NEURORADIOLOGY Part I
 NEURORADIOLOGY Part I Vörös Erika University of Szeged Department of Radiology SZEGED BRAIN IMAGING METHODS Plain film radiography Ultrasonography (US) Computer tomography (CT) Magnetic resonance imaging
NEURORADIOLOGY Part I Vörös Erika University of Szeged Department of Radiology SZEGED BRAIN IMAGING METHODS Plain film radiography Ultrasonography (US) Computer tomography (CT) Magnetic resonance imaging
Multislice CT Angiography of Cerebral Aneurysms in Nontraumatic Subarachnoid and Intraparenchymal Haemorrhage
 Med. J. Cairo Univ., Vol. 80, No. 2, June: 173-178, 2012 www.medicaljournalofcairouniversity.com Multislice CT Angiography of Cerebral Aneurysms in Nontraumatic Subarachnoid and Intraparenchymal Haemorrhage
Med. J. Cairo Univ., Vol. 80, No. 2, June: 173-178, 2012 www.medicaljournalofcairouniversity.com Multislice CT Angiography of Cerebral Aneurysms in Nontraumatic Subarachnoid and Intraparenchymal Haemorrhage
Stroke School for Internists Part 1
 Stroke School for Internists Part 1 November 4, 2017 Dr. Albert Jin Dr. Gurpreet Jaswal Disclosures I receive a stipend for my role as Medical Director of the Stroke Network of SEO I have no commercial
Stroke School for Internists Part 1 November 4, 2017 Dr. Albert Jin Dr. Gurpreet Jaswal Disclosures I receive a stipend for my role as Medical Director of the Stroke Network of SEO I have no commercial
Subtraction CT Angiography with Controlled- Orbit Helical Scanning for Detection of Intracranial Aneurysms
 AJNR Am J Neuroradiol 19:291 295, February 1998 Subtraction CT Angiography with Controlled- Orbit Helical Scanning for Detection of Intracranial Aneurysms Satoshi Imakita, Yoshitaka Onishi, Tokihiro Hashimoto,
AJNR Am J Neuroradiol 19:291 295, February 1998 Subtraction CT Angiography with Controlled- Orbit Helical Scanning for Detection of Intracranial Aneurysms Satoshi Imakita, Yoshitaka Onishi, Tokihiro Hashimoto,
CT perfusion in Moyamoya disease
 CT perfusion in Moyamoya disease Poster No.: C-1726 Congress: ECR 2015 Type: Scientific Exhibit Authors: K. C. Lam, C. P. Tsang, K. K. Wong, R. LEE ; HK, Hong Kong/HK Keywords: Hemodynamics / Flow dynamics,
CT perfusion in Moyamoya disease Poster No.: C-1726 Congress: ECR 2015 Type: Scientific Exhibit Authors: K. C. Lam, C. P. Tsang, K. K. Wong, R. LEE ; HK, Hong Kong/HK Keywords: Hemodynamics / Flow dynamics,
Three-Dimensional Rotational Angiography of Neurovascular Lesions in Pediatric Patients
 ngiography of Neurovascular Lesions in Pediatric Patients Pediatric Imaging Pictorial Essay M E E N T U R I L I M G I N G JR 2006; 186:75 84 0361 803X/06/1861 75 merican Roentgen Ray Society Y O John M.
ngiography of Neurovascular Lesions in Pediatric Patients Pediatric Imaging Pictorial Essay M E E N T U R I L I M G I N G JR 2006; 186:75 84 0361 803X/06/1861 75 merican Roentgen Ray Society Y O John M.
Dilemma in Imaging Diagnosis, Endovascular Management and Complications
 Vascular anomaly at the craniocervical junction presenting with sub arachnoid hemorrhage: Dilemma in Imaging Diagnosis, Endovascular Management and Complications Ajeet 1* 1. Department of Radiology, St
Vascular anomaly at the craniocervical junction presenting with sub arachnoid hemorrhage: Dilemma in Imaging Diagnosis, Endovascular Management and Complications Ajeet 1* 1. Department of Radiology, St
Longitudinal anterior-to-posterior shift of collateral channels in patients with moyamoya disease: an implication for its hemorrhagic onset
 CLINICAL ARTICLE Longitudinal anterior-to-posterior shift of collateral channels in patients with moyamoya disease: an implication for its hemorrhagic onset Shusuke Yamamoto, MD, Satoshi Hori, MD, PhD,
CLINICAL ARTICLE Longitudinal anterior-to-posterior shift of collateral channels in patients with moyamoya disease: an implication for its hemorrhagic onset Shusuke Yamamoto, MD, Satoshi Hori, MD, PhD,
Applicable Neuroradiology
 For the Clinical Neurology Clerkship LSU Medical School New Orleans Amy W Voigt, MD Clerkship Director Introduction The field of Radiology first developed following the discovery of X-Rays by Wilhelm Roentgen
For the Clinical Neurology Clerkship LSU Medical School New Orleans Amy W Voigt, MD Clerkship Director Introduction The field of Radiology first developed following the discovery of X-Rays by Wilhelm Roentgen
CT - Brain Examination
 CT - Brain Examination Submitted by: Felemban 1 CT - Brain Examination The clinical indication of CT brain are: a) Chronic cases (e.g. headache - tumor - abscess) b) ER cases (e.g. trauma - RTA - child
CT - Brain Examination Submitted by: Felemban 1 CT - Brain Examination The clinical indication of CT brain are: a) Chronic cases (e.g. headache - tumor - abscess) b) ER cases (e.g. trauma - RTA - child
GUIDELINES FOR THE EARLY MANAGEMENT OF PATIENTS WITH ACUTE ISCHEMIC STROKE
 2018 UPDATE QUICK SHEET 2018 American Heart Association GUIDELINES FOR THE EARLY MANAGEMENT OF PATIENTS WITH ACUTE ISCHEMIC STROKE A Summary for Healthcare Professionals from the American Heart Association/American
2018 UPDATE QUICK SHEET 2018 American Heart Association GUIDELINES FOR THE EARLY MANAGEMENT OF PATIENTS WITH ACUTE ISCHEMIC STROKE A Summary for Healthcare Professionals from the American Heart Association/American
An Introduction to Imaging the Brain. Dr Amy Davis
 An Introduction to Imaging the Brain Dr Amy Davis Common reasons for imaging: Clinical scenarios: - Trauma (NICE guidelines) - Stroke - Tumours - Seizure - Neurological degeneration memory, motor dysfunction,
An Introduction to Imaging the Brain Dr Amy Davis Common reasons for imaging: Clinical scenarios: - Trauma (NICE guidelines) - Stroke - Tumours - Seizure - Neurological degeneration memory, motor dysfunction,
Importance of Hematoma Removal Ratio in Ruptured Middle Cerebral Artery Aneurysm Surgery with Intrasylvian Hematoma
 Journal of Cerebrovascular and Endovascular Neurosurgery pissn 2234-8565, eissn 2287-3139, http://dx.doi.org/10.7461/jcen.2017.19.1.5 Original Article Importance of Hematoma Removal Ratio in Ruptured Middle
Journal of Cerebrovascular and Endovascular Neurosurgery pissn 2234-8565, eissn 2287-3139, http://dx.doi.org/10.7461/jcen.2017.19.1.5 Original Article Importance of Hematoma Removal Ratio in Ruptured Middle
Acute abdominal venous thromboses- the hyperdense noncontrast CT sign
 Acute abdominal venous thromboses- the hyperdense noncontrast CT sign Poster No.: C-1095 Congress: ECR 2011 Type: Educational Exhibit Authors: M. Goldstein, K. Jhaveri; Toronto, ON/CA Keywords: Abdomen,
Acute abdominal venous thromboses- the hyperdense noncontrast CT sign Poster No.: C-1095 Congress: ECR 2011 Type: Educational Exhibit Authors: M. Goldstein, K. Jhaveri; Toronto, ON/CA Keywords: Abdomen,
ISCHEMIC STROKE IMAGING
 ISCHEMIC STROKE IMAGING ผศ.พญ พญ.จ ร ร ตน ธรรมโรจน ภาคว ชาร งส ว ทยา คณะแพทยศาสตร มหาว ทยาล ยขอนแก น A case of acute hemiplegia Which side is the abnormality, right or left? Early Right MCA infarction
ISCHEMIC STROKE IMAGING ผศ.พญ พญ.จ ร ร ตน ธรรมโรจน ภาคว ชาร งส ว ทยา คณะแพทยศาสตร มหาว ทยาล ยขอนแก น A case of acute hemiplegia Which side is the abnormality, right or left? Early Right MCA infarction
NEURORADIOLOGY DIL part 3
 NEURORADIOLOGY DIL part 3 Bleeds and hemorrhages K. Agyem MD, G. Hall MD, D. Palathinkal MD, Alexandre Menard March/April 2015 OVERVIEW Introduction to Neuroimaging - DIL part 1 Basic Brain Anatomy - DIL
NEURORADIOLOGY DIL part 3 Bleeds and hemorrhages K. Agyem MD, G. Hall MD, D. Palathinkal MD, Alexandre Menard March/April 2015 OVERVIEW Introduction to Neuroimaging - DIL part 1 Basic Brain Anatomy - DIL
Starting or Resuming Anticoagulation or Antiplatelet Therapy after ICH: A Neurology Perspective
 Starting or Resuming Anticoagulation or Antiplatelet Therapy after ICH: A Neurology Perspective Cathy Sila MD George M Humphrey II Professor and Vice Chair of Neurology Director, Comprehensive Stroke Center
Starting or Resuming Anticoagulation or Antiplatelet Therapy after ICH: A Neurology Perspective Cathy Sila MD George M Humphrey II Professor and Vice Chair of Neurology Director, Comprehensive Stroke Center
The "filling defect" sign helps localise the site of intracranial aneurysm rupture on an unenhanced CT
 The "filling defect" sign helps localise the site of intracranial aneurysm rupture on an unenhanced CT Poster No.: C-3380 Congress: ECR 2010 Type: Topic: Authors: Keywords: DOI: Educational Exhibit Neuro
The "filling defect" sign helps localise the site of intracranial aneurysm rupture on an unenhanced CT Poster No.: C-3380 Congress: ECR 2010 Type: Topic: Authors: Keywords: DOI: Educational Exhibit Neuro
ACUTE STROKE TREATMENT IN LARGE NIHSS PATIENTS. Justin Nolte, MD Assistant Profession Marshall University School of Medicine
 ACUTE STROKE TREATMENT IN LARGE NIHSS PATIENTS Justin Nolte, MD Assistant Profession Marshall University School of Medicine History of Presenting Illness 64 yo wf with PMHx of COPD, HTN, HLP who was in
ACUTE STROKE TREATMENT IN LARGE NIHSS PATIENTS Justin Nolte, MD Assistant Profession Marshall University School of Medicine History of Presenting Illness 64 yo wf with PMHx of COPD, HTN, HLP who was in
North Oaks Trauma Symposium Friday, November 3, 2017
 Traumatic Intracranial Hemorrhage Aaron C. Sigler, DO, MS Neurosurgery Tulane Neurosciences None Disclosures Overview Anatomy Epidural hematoma Subdural hematoma Cerebral contusions Outline Traumatic ICH
Traumatic Intracranial Hemorrhage Aaron C. Sigler, DO, MS Neurosurgery Tulane Neurosciences None Disclosures Overview Anatomy Epidural hematoma Subdural hematoma Cerebral contusions Outline Traumatic ICH
Neurosurgical Management of Stroke
 Overview Hemorrhagic Stroke Ischemic Stroke Aneurysmal Subarachnoid hemorrhage Neurosurgical Management of Stroke Jesse Liu, MD Instructor, Neurological Surgery Initial management In hospital management
Overview Hemorrhagic Stroke Ischemic Stroke Aneurysmal Subarachnoid hemorrhage Neurosurgical Management of Stroke Jesse Liu, MD Instructor, Neurological Surgery Initial management In hospital management
Treatment of Acute Hemorrhagic Stroke 5th QSVS Neurovascular Conference Dar Dowlatshahi MD PhD FRCPC Sept 14, 2012
 Treatment of Acute Hemorrhagic Stroke 5th QSVS Neurovascular Conference Dar Dowlatshahi MD PhD FRCPC Sept 14, 2012 Disclosure of potential conflicts of interest Quebec Society of Vascular Sciences presents
Treatment of Acute Hemorrhagic Stroke 5th QSVS Neurovascular Conference Dar Dowlatshahi MD PhD FRCPC Sept 14, 2012 Disclosure of potential conflicts of interest Quebec Society of Vascular Sciences presents
Overview of imaging modalities for cerebral aneurysms
 Overview of imaging modalities for cerebral aneurysms Soroush Zaghi BIDMC PCE: Radiology August 2008 (Images from BIDMC, PACS.) Our Patient: Presentation Our patient is a 57 y/o woman who reports blowing
Overview of imaging modalities for cerebral aneurysms Soroush Zaghi BIDMC PCE: Radiology August 2008 (Images from BIDMC, PACS.) Our Patient: Presentation Our patient is a 57 y/o woman who reports blowing
T HE blood supply of cerebral arteriovenous malformations is often extensive
 NOVEMBER, 1974 ROENTGENOGRAPHIC ANALYSIS OF ARTERIOVENOUS MALFORMATIONS OF THE OCCIPITAL LOBE* By B. TODD TROOST, M.D.,t and THOMAS H. NEWTON, M.D4 T HE blood supply of cerebral arteriovenous malformations
NOVEMBER, 1974 ROENTGENOGRAPHIC ANALYSIS OF ARTERIOVENOUS MALFORMATIONS OF THE OCCIPITAL LOBE* By B. TODD TROOST, M.D.,t and THOMAS H. NEWTON, M.D4 T HE blood supply of cerebral arteriovenous malformations
