Ultrasound-Guided Infraclavicular Axillary Vein Cannulation
|
|
|
- Morgan Richard
- 5 years ago
- Views:
Transcription
1 International Journal of Clinical Medicine, 2017, 8, ISSN Online: ISSN Print: X Ultrasound-Guided Infraclavicular Axillary Vein Cannulation Miguel A. García-Díaz, Manuel Ruiz-Castro Department of Anesthesia, University Hospital Príncipe de Asturias, Madrid, Spain How to cite this paper: García-Díaz, M.A. and Ruiz-Castro, M. (2017) Ultrasound- Guided Infraclavicular Axillary Vein Cannulation. International Journal of Clinical Medicine, 8, Received: January 24, 2017 Accepted: April 27, 2017 Published: April 30, 2017 Copyright 2017 by authors and Scientific Research Publishing Inc. This work is licensed under the Creative Commons Attribution International License (CC BY 4.0). Open Access Abstract Background and Objective: Percutaneous central venous cannulation is a common invasive procedure. In comparison with an external landmark technique, the advantages of ultrasound-guided venous access include direct visualization of the anatomy and in vivo visualization of venous cannulation. Methods: We evaluated an ultrasound-guided technique for infraclavicular axillary vein cannulation, focusing on its ease of use, success rate and complications rate. One hundred and twenty patients who submitted to central venous catheter placement were punctured using our technique. The patients were positioned so that their ipsilateral upper limb was abducted at 90 to the longitudinal axis, which makes it possible to visualize the infraclavicular vessels due to the elevation of the clavicle, thereby improving accessibility. Results: Cannulation was successful in all patients. The median time from the start of the first puncture (of the skin) until the aspiration of blood was 15 s (range s). Both infraclavicular axillary veins were cannulated, and the vein was punctured successfully at the first attempt in 95% of the patients, without complications during the procedure. Conclusion: We propose an ultrasound-guided infraclavicular approach of the axillary vein, with a high success rate and no complications in the present cohort. Keywords Ultrasonography, Catheterization, Central Venous, Central Venous Catheter, Ultrasound-Guided Technique, Infraclavicular Axillary Vein 1. Introduction Central venous catheterization (CVC) is a common invasive procedure. Complications associated with CVC are often related to blind passage of the needle, and include bleeding, arterial puncture, pneumothorax, nerve damage, pain and DOI: /ijcm April 30, 2017
2 other less common complications. Most authors [1] [2] [3] [4] [5], currently recommend the use of ultrasound (US) for placing catheters in adults. In comparison with the use of superficial anatomical landmarks, the advantages of US-guided venous access include direct visualization of the anatomy and the in vivo visualization of venous cannulation [6] [7]. The use of real-time US technology to guide needle insertion has improved success rates and reduced the incidence of complications [1] [2]. It has recently been shown that US is beneficial for catheterizing the internal jugular vein (IJV), as well as the axillary and mid-arm basilica and cephalic veins. The IJV is more popular due to the easier access and perceived lower risk of complications, however, subclavian vein (SCV) catheter placement is associated with a lower incidence of infection and thrombosis [8] [9] [10]. Most authors contend that infraclavicular approaches are difficult to visualize with US due to the SCV being located under the clavicle and the inability to place the linear array probe in a position that allows the vessel to be visualized. For this reason, US-guided SCV access is often described using a supraclavicular [8], or a distal approach. We have developed an US-guided infraclavicular approach for axillary catheter placement using a standard high-frequency linear probe. The location of the axillary vein approach is very proximal, close to, or even over the lip of the first rib, where the SCV is renamed, and hence this approach could be comparable to the approach of the SCV. 2. Method Ethical approval for this prospective study (protocol number: PI/422010), was provided by the Ethical Committee of the Príncipe de Asturias University Hospital, Alcalá de Henares, Madrid, Spain (chairperson: Prof. Elvira Poves Martínez) on 25 November Written informed consent to participate was obtained from each patient. A GE Healthcare Venue 40 devices and a GE 12L-SC multifrequency linear transducer at 5-13 MHz (GE Healthcare, a division of General Electric Company, Piscataway, New Jersey, USA) were used. Both authors performed this procedure in sixty patients each. The patients were assigned to the study in a consecutive way. The objective of this work was to make a purely descriptive study, so it was not considered to perform the comparison with the conventional technique without ultrasonography, given the high success rate in the US-guided puncture. Therefore, the size of the sample was intended to be representative, although we did not perform a calculation of the sample size when not having to observe differences with a control group. The position of the patient and the anesthesiologist varies depending upon the standard external-anatomical-landmark-guided catheterization technique. The patient should be positioned so that the ipsilateral upper limb is abducted at 90 to the longitudinal axis, which makes it possible to visualize the infraclavicular vessels due to the elevation of the clavicle, thereby improving accessibility. This 228
3 improves the US visualization of the infraclavicular axillary vein (IAV), making almost its entire length visible. If the probe is moved laterally, it is possible to visualize the course of the axillary vein, while if the probe is moved medially with a slight cranial angulation, it is possible to visualize SCV. Moreover, placing the patient in the Trendelenburg position increases venous engorgement and ease of viewing. The anesthesiologist puts the patient s head and locates the sterile field and the equipment needed for the cannulation cephalad to the patient s arm or beside it, allowing intraoperative puncture. The anesthesiologist s non-dominant hand holds the US probe, while the dominant hand performs the cannulation. Initial exploration of the area with US is essential for placing the probe infraclavicularly, parallel and in close contact with the bottom edge of the clavicle, in the infraclavicular fossa, just lateral to the clavicular head of the sternocleidomastoid muscle Figure 1. A slight cranial angulation of the probe will facilitate the visualization of the infraclavicular vessels, which will be visible as long as the probe is moving parallel to the clavicle, medially and laterally. The vessels on the left side are caudal to those on the right side and the required degree of cranial angulation of the US probe is lower on the left side. The image obtained from the IAV is medial and superficial to the infraclavicular axillary artery (IAA), and has an elongated shape, close to the long axis view Figure 2. Furthermore, the pressure of the US probe on the patient can partially collapse the vein. In US imaging, the IAA is normally viewed in cross section, and it appears rounded, pulsatile, and incompressible under the pressure of the US probe. In-plane venipuncture is achieved from the lateral end of the probe, in the same plane as the US beam, which displays the progress of the needle as it moves Figure 1. Artistic drawing of the location and placement of the linear array probe (LP) and the needle (N) during the infraclavicular ultrasound-guided approach to cannulation of the right axillary vein. 229
4 (a) (b) Figure 2. Ultrasonographic image obtained at the infraclavicular level. (a) Blank image. (b) Labelled image. SCT, subcutaneous cellular tissue; PM, pectoralis major muscle; SM, subclavian muscle; SCV, subclavian vein; SCA, subclavian artery; Arrowheads, first rib. into the lumen of the vein. It is of paramount importance that the operator observes the needle advancement in real time. To improve visualization of the puncture needle, it is helpful to exert a slight pressure on the inner edge of the US probe so that the angle between the US beams and the needle is as close as possible to 90. While inserting the needle, mild aspiration is performed with the syringe, so 230
5 that blood is observed entering the syringe when the tip of the needle reaches the vessel lumen. Real-time visualization of the extent of the venous lumen demonstrates that the needle tip is at the correct location. The venous wall is more elastic in younger patients, and so the tip of the needle can be pushed against the wall without perforating it. Aspiration of blood will be necessary to show that the needle tip has reached the vein lumen, as the progress of the needle tip will be visible on the US image. Only minimal further progression from this point will cause the needle tip to enter the lumen without piercing the posterior venous wall. The usual Seldinger procedure is then performed. The no dominant hand releases the US probe and holds the needle. The guide wire is introduced into the venous lumen without a real-time US view. Once the guide wire is in the vein, its position is rechecked with the probe, and the supraclavicular area is scanned to detect possible migration of the guide wire into the IJV Figure 3. Early possible complications such as pneumothorax or hematoma, as well as catheter-tip position are checked after CVC positioning in every patient by means of a chest x-ray. 3. Results For a one year period, 120 patients who submitted to CVC were punctured using our technique. In all except one case the IAVs could be easily visualized from the infraclavicular level, so no patients were excluded from the study. The demographic data of the patients are listed in Table 1. A single attempt was required in 95% of the cases (114 patients). A second attempt was needed in three cases, two of them because although the IAV was catheterized at the first attempt, the vein was lost during guide-wire manipulation, thus requiring a second IAV puncture. In another case a chest x-ray revealed that the catheter had migrated distally to the distal axillary vein, which made it necessary to remove the catheter and puncture again on the other side. In one IAV the venous lumen on the left side could not be seen because it was thrombosed, but it could be catheterized on the other side. Another guide wire that migrated into the IJV could be repositioned without a new puncture, partially removing the guide wire, and reintroducing it under US guidance. The mean number of attempts per patient was More than two attempts at venipuncture, which is known to increase the incidence of complications, were not needed in the present cohort. Venous hematomas due to multiple failed attempts to catheterize the vein were thus not seen in this series. These results are comparable with those achieved using US-guided techniques for IJV puncture. The right IAV was the most frequently cannulated vein (55%), with most of the cannulations carried out during surgery, but no more attempts were needed when the left IAV was punctured. The median time from the start of puncture to aspiration of blood was 15 s (range s). We experienced no arterial puncture and no pneumothorax in this series, even though this cohort represented 231
6 (a) (b) Figure 3. Puncture technique. (a) The needle punctures the IAV and progresses under direct vision to the lumen of the vein. Arrows, needle. (b) The guide-wire is inserted after removing the needle. Arrowheads, guide-wire. Table 1. Demographic distribution of patients undergoing US-guided infraclavicular axillary vein cannulation. Mean Age Weight Height Body Mass Index years Kg cm Kg/cm 2 Standard Deviation years Kg 8.60 cm 3.12 Kg/m 2 *Total number of cases 120: 68 females and 52 males. 232
7 our learning curve for this technique. 4. Discussion US-guided venous access has been described and widely recommended for IJV cannulation [11]. However, few studies have investigated US-guided SCV puncture, most of which have focused on paediatric venous cannulation [6] [7]. One paper reports the use of US to puncture the SCV via a supraclavicular approach with an endocavitary probe with good results [8], but we describe here a technique that uses a standard linear array probe to puncture the IAV, in close proximity to the SCV. The boundary between the two is defined by the edge of the first rib, so we believe that there are no clinically significant differences. In previous studies, the venous approach was performed more laterally, even at the level of the mid-axillary vein, where mobility is greater, but fixation of the catheter is worse. Only a few articles [12] [13] have reported on US-guided for axillary vein puncture. Two studies imaged both the vein and the needle transversely, which offers poorer needle visualization. Another paper [14] describes a more lateral approach to the axillary vein, where longitudinal visualization of both the vein and needle was possible. Our longitudinal in-line puncture technique offers a clear view of both the needle and the vein, which should produce consistently good results. The risk of accidental puncture of pleura or other structures (e.g., arteries) is lower, regardless of how deep the needle is, since the advancement of the needle, the vessel, and the surrounding structures can all be viewed in real time. Moreover, the place where the SCV passes over the first rib has been defined as a safe spot for its cannulation, since at this location, the first rib protects the lung from accidental puncture and the direction of the subclavian artery differs from that of the SCV, passing behind the anterior scalene muscle whereas the vein passes in front of it. Abduction of the upper limb and the clavicle with it provides a US view of the infraclavicular vessels at this level, allowing safe puncture and cannulation. Puncture time was measured in this study. The preparation time is known to be longer with US-guided techniques than with landmark-guided techniques. With experience, anatomical screening, and appropriate equipment preparation, the time should not exceed 5 min. Because the anatomical (vein position) and pathological (vein thrombosis) variations are now diagnosed by US, the time from skin puncture to guide-wire placement is reduced. Furthermore, the very time-consuming vicious circle of multiple attempts, venous or arterial hematoma, failed puncture, and need to change to another central venous insertion site is probably minimized by US guidance. The entire procedure is likely to be completed faster than when using the anatomical-landmark-based technique. It should also be noted that the procedure can be carried out during surgery because the abducted position of the upper extremities is common in the operating room, thus further reducing the time required. This is a clear advantage over the traditional external landmark technique where the adducted position of the upper extremity is required and forces the anesthesi- 233
8 ologist to cannulate the IJV in the operating setting, associated with a higher incidence of infection and thrombosis [8] [9] [10]. Another advantage of US is the early detection of incorrect guide-wire catheterization or migration of the guide wire into the IJV. In our study, we experienced a single case of misplacement of the guide-wire, perhaps because the abduction of the upper limb directs the IAV toward the territory of the superior vena cava. In a completely sterile setting, the assistance of a third hand is usually not needed because the probe can be left in the sterile field during maneuvers that require two hands, such as clavicle palpation for needle insertion or guide-wire advancement. The use of US not only provides needle guidance but also makes it easy to check the patency of the IAV, regardless of whether the cases are hypovolemic patients whose veins have little filler, or are well hydrated (e.g., with engorged veins). Lumen vein in hypovolemic patients is very narrow, being very difficult to place the tip of the needle inside. When it is closed to the venous wall, a Valsalva maneuver can distend the vein and facilitate the puncture. The learning curve of this approach, as for every US-guided technique, will probably be highly operator-dependant. Prior to the start of the study, each of the anaesthesiologists cannulated at least three IAV with this US-guided technique, to familiarize themselves with it. Then, during the study, each of the anesthesiologists performed this procedure in sixty patients. Both of them had previous experience in US-guided puncture techniques (regional anesthesia and CVC) and in IJV and SCV anatomical-landmark-based cannulation. We consider that it takes a minimum of five cases to perform the procedure safely, with many more being needed in the absence of prior experience in managing US. For inexperienced clinicians, residents, or fellows, the US-guided IAV cannulation should be considered an advanced technique given the complexity and risk of complications with this approach. In conclusion US-guided IAV cannulation can be performed by using a linear-array probe and ipsilaterally abducting the patient s upper limb at 90. We propose an infraclavicular approach when performing this technique, since it was associated with a high success rate and no complications in this the present cohort. This procedure is safe and easy to learn for CVC, and we recommend this technique even in an early learning stage. Moreover, the procedure can be performed in an intraoperative setting. Acknowledgements We thank M. Sanz, MD, F. Barrios and M. Ayuso for their assistance with the study. This work was supported by the Department of Anesthesiology, University Hospital Príncipe de Asturias, Alcalá de Henares, Madrid, Spain. References [1] Waldman, C.S. (2001) Use of Central Venous Catheters (CVC) An Algorithm. 234
9 Care of the Critically Ill, 17, [2] Randolph, A.G., Cook, D.J., Gonzales, C.A. and Pribble, C.G. (1996) Ultrasound Guidance for Placement of Central Venous Catheters: A Meta-Analysis of the Literature. Critical Care Medicine, 24, [3] Maslove, D. and Mihm, F. (2010) Ultrasound-Guided Internal Jugular Vein Cannulation. The New England Journal of Medicine, 363, [4] Levitov, A.B., Aziz, S. and Slonim, A.D. (2009) Before We Go Too Far: Ultrasound-Guided Central Catheter Placement. Critical Care Medicine, 37, [5] Barash, P. (2009) Ultrasound-Guided Central Venous Access. F1000 Medicine Reports, 1, [6] Hind, D., Calvert, N., McWilliams, R., et al. (2003) Ultrasonic Locating Devices for Central Venous Cannulation: Meta-Analysis. BMJ, 327, [7] Theodoro, D., Bausano, B., Lewis, L., Evanoff, B. and Kollef. M. (2010) A Descriptive Comparison of Ultrasound-Guided Central Venous Cannulation of the Internal Jugular Vein to Landmark-Based Subclavian Vein Cannulation. Academic Emergency Medicine, 17, [8] Mallin, M., Louis, H. and Madsen, T. (2010) A Novel Technique for Ultrasound-Guided Supraclavicular Subclavian Cannulation. American Journal of Emergency Medicine, 28, [9] McGee, D.C. and Gould, M.K. (2003) Preventing Complications of Central Venous Catheterization. The New England Journal of Medicine, 348, [10] Stone, M.B., Moon, C., Sutijono, D. and Blaivas, M. (2010) Needle Tip Visualization during Ultrasound-Guided Vascular Access: Short-Axis vs. Long-Axis Approach. American Journal of Emergency Medicine, 28, [11] Gualtieri, E., Deppe, S.A., Sipperly, M.E., et al. (1995) Subclavian Venous Catheterization: Greater Success Rate for Less Experienced Operators Using Ultrasound Guidance. Critical Care Medicine, 23, [12] Sharma, A., Bodenham, A.R. and Mallick, A. (2004) Ultrasound-Guided Infraclavicular Axillary Vein Cannulation for Central Venous Access. British Journal of Anaesthesia, 93, [13] Sandhu, N.S. (2004) Transpectoral Ultrasound-Guided Catheterization of the Axillary Vein: An Alternative of Standard Catheterization of the Subclavian Vein. Anesthesia & Analgesia, 99, [14] Stone, M.B., Nagdev, A., Murphy, M.C. and Sisson, C.A. (2010) Ultrasound Detection of Guidewire Position during Central Venous Catheterization. American Journal of Emergency Medicine, 28,
10 Submit or recommend next manuscript to SCIRP and we will provide best service for you: Accepting pre-submission inquiries through , Facebook, LinkedIn, Twitter, etc. A wide selection of journals (inclusive of 9 subjects, more than 200 journals) Providing 24-hour high-quality service User-friendly online submission system Fair and swift peer-review system Efficient typesetting and proofreading procedure Display of the result of downloads and visits, as well as the number of cited articles Maximum dissemination of your research work Submit your manuscript at: Or contact ijcm@scirp.org
Background & Indications Probe Selection
 Teresa S. Wu, MD, FACEP Director, EM Ultrasound Program & Fellowship Co-Director, Simulation Based Training Program & Fellowship Associate Program Director, EM Residency Program Maricopa Medical Center
Teresa S. Wu, MD, FACEP Director, EM Ultrasound Program & Fellowship Co-Director, Simulation Based Training Program & Fellowship Associate Program Director, EM Residency Program Maricopa Medical Center
Ultrasound Guidance Needle Techniques
 Ultrasound Guidance Needle Techniques Dr TANG Ho-ming AED/UCH USG Guidance Needle Techniques Commonly used in EM 1. Vessel cannulation-peripheral & central 2. Foreign body removal 3. Peripheral nerve/plexus
Ultrasound Guidance Needle Techniques Dr TANG Ho-ming AED/UCH USG Guidance Needle Techniques Commonly used in EM 1. Vessel cannulation-peripheral & central 2. Foreign body removal 3. Peripheral nerve/plexus
Ultrasound-guided infraclavicular axillary vein cannulation for central venous access {
 British Journal of Anaesthesia 93 (2): 188 92 DOI: 10.1093/bja/aeh187 Advance Access publication June 25, 2004 Ultrasound-guided infraclavicular axillary vein cannulation for central venous access { A.
British Journal of Anaesthesia 93 (2): 188 92 DOI: 10.1093/bja/aeh187 Advance Access publication June 25, 2004 Ultrasound-guided infraclavicular axillary vein cannulation for central venous access { A.
CATHETER MALPOSITION FOLLOWING SUPRACLAVICULAR APPROACH FOR SUBCLAVIAN VEIN CATHETERISATION
 CATHETER MALPOSITION FOLLOWING SUPRACLAVICULAR APPROACH FOR SUBCLAVIAN VEIN CATHETERISATION - Case Reports - Prem K Singh *, Zulfiquar Ali *, Girija P Rath ** and Hemanshu Prabhakar *** Abstract The supraclavicular
CATHETER MALPOSITION FOLLOWING SUPRACLAVICULAR APPROACH FOR SUBCLAVIAN VEIN CATHETERISATION - Case Reports - Prem K Singh *, Zulfiquar Ali *, Girija P Rath ** and Hemanshu Prabhakar *** Abstract The supraclavicular
Dr. prakruthi Dept. of anaesthesiology, Rrmch, bangalore
 CENTRAL VENOUS CATHETERIZATION Dr. prakruthi Dept. of anaesthesiology, Rrmch, bangalore OBJECTIVES Introduction Indications and Contraindications Complications Technique Basic principles Specifics by Site
CENTRAL VENOUS CATHETERIZATION Dr. prakruthi Dept. of anaesthesiology, Rrmch, bangalore OBJECTIVES Introduction Indications and Contraindications Complications Technique Basic principles Specifics by Site
Brachial plexus blockade within the interscalene groove involves local anesthetic
 Interscalene Brachial Plexus Block- How I do it. Part 1 of a 2 part discussion on technique. Stuart Grant Professor of Anesthesiology Duke University Medical Center Durham NC Brachial plexus blockade within
Interscalene Brachial Plexus Block- How I do it. Part 1 of a 2 part discussion on technique. Stuart Grant Professor of Anesthesiology Duke University Medical Center Durham NC Brachial plexus blockade within
Research Article Can we predict the Position of Central Venous Catheter Tip Following Cannulation of Internal Jugular Vein?
 Cronicon OPEN ACCESS ANAESTHESIA Research Article Can we predict the Position of Central Venous Catheter Tip Following Cannulation of Internal Jugular Vein? Pradeep Marur Venkategowda 1, Surath Manimala
Cronicon OPEN ACCESS ANAESTHESIA Research Article Can we predict the Position of Central Venous Catheter Tip Following Cannulation of Internal Jugular Vein? Pradeep Marur Venkategowda 1, Surath Manimala
Research Article Comparison of Ultrasound Guided Radial Artery Cannulation with Conventional Palpation Technique
 Cronicon OPEN ACCESS ANAESTHESIA Research Article Comparison of Ultrasound Guided Radial Artery Cannulation with Conventional Palpation Technique Amna 1 *, Saira Mehboob 2, Waqas Alam 3, Amna Gulraze 4
Cronicon OPEN ACCESS ANAESTHESIA Research Article Comparison of Ultrasound Guided Radial Artery Cannulation with Conventional Palpation Technique Amna 1 *, Saira Mehboob 2, Waqas Alam 3, Amna Gulraze 4
Central Venous Line Insertion
 Central Venous Line Insertion Understand the indications and risks of CVC insertion Understand and troubleshoot the seldinger technique Understand available sites and select the appropriate site for clinical
Central Venous Line Insertion Understand the indications and risks of CVC insertion Understand and troubleshoot the seldinger technique Understand available sites and select the appropriate site for clinical
INTRODUCTION. Getting the best scan. Choosing a probe. Choosing the frequency
 Getting the best scan Choosing a probe Select the most appropriate probe for the particular scan required. s vary in their: operating frequency range higher ultrasound frequencies provide better discrimination
Getting the best scan Choosing a probe Select the most appropriate probe for the particular scan required. s vary in their: operating frequency range higher ultrasound frequencies provide better discrimination
Troubleshooting Technique for Hemodialysis Catheter Insertion
 Troubleshooting Technique for Hemodialysis Catheter Insertion Withoon Ungkitphaiboon Assistant Professor, Department of Surgery, Maha Chakri Sirindhorn Medical Center Srinakharinwirot University Present
Troubleshooting Technique for Hemodialysis Catheter Insertion Withoon Ungkitphaiboon Assistant Professor, Department of Surgery, Maha Chakri Sirindhorn Medical Center Srinakharinwirot University Present
Kristin Wise, MD, FHM Division of General Internal Medicine and Geriatrics Hospital Medicine 2013
 Kristin Wise, MD, FHM Division of General Internal Medicine and Geriatrics Hospital Medicine 2013 Objectives for CVC Placement Understand the indications and contraindications Determine appropriate CVC
Kristin Wise, MD, FHM Division of General Internal Medicine and Geriatrics Hospital Medicine 2013 Objectives for CVC Placement Understand the indications and contraindications Determine appropriate CVC
JOPE. Abstract. Introduction /jp-journals
 Bahareh Khatibi, Nav Parkash Sandhu Review Article 10.5005/jp-journals-10034-1036 1 Bahareh Khatibi, 2 Nav Parkash Sandhu Abstract The axillary vein has been shown to be a safe and effective cannulation
Bahareh Khatibi, Nav Parkash Sandhu Review Article 10.5005/jp-journals-10034-1036 1 Bahareh Khatibi, 2 Nav Parkash Sandhu Abstract The axillary vein has been shown to be a safe and effective cannulation
Peel-Apart Percutaneous Introducer Kits for
 Bard Access Systems Peel-Apart Percutaneous Introducer Kits for Table of Contents Contents Page Bard Implanted Ports Hickman*, Leonard*, Broviac*, Tenckhoff*, and Groshong* Catheters Introduction....................................
Bard Access Systems Peel-Apart Percutaneous Introducer Kits for Table of Contents Contents Page Bard Implanted Ports Hickman*, Leonard*, Broviac*, Tenckhoff*, and Groshong* Catheters Introduction....................................
AIUM Practice Parameter for the Use of Ultrasound to Guide Vascular Access Procedures
 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 37 38 39 40 AIUM Practice Parameter for the Use of Ultrasound to Guide Vascular Access Procedures Parameter
1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 37 38 39 40 AIUM Practice Parameter for the Use of Ultrasound to Guide Vascular Access Procedures Parameter
Upper Extremity Venous Duplex. Michigan Sonographers Society Fall Ultrasound Symposium October 15, 2016
 Upper Extremity Venous Duplex Michigan Sonographers Society Fall Ultrasound Symposium October 15, 2016 Patricia A. (Tish) Poe, BA RVT FSVU Director of Quality Assurance Navix Diagnostix Patricia A. Poe
Upper Extremity Venous Duplex Michigan Sonographers Society Fall Ultrasound Symposium October 15, 2016 Patricia A. (Tish) Poe, BA RVT FSVU Director of Quality Assurance Navix Diagnostix Patricia A. Poe
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
Background: Bedside ultrasound is emerging as a useful tool in the assessment of
 Abstract: Background: Bedside ultrasound is emerging as a useful tool in the assessment of intravascular volume status by examining measurements of the inferior vena cava (IVC). Many previous studies do
Abstract: Background: Bedside ultrasound is emerging as a useful tool in the assessment of intravascular volume status by examining measurements of the inferior vena cava (IVC). Many previous studies do
Ultrasound Guided Vascular Access. 7/25/2016
 Ultrasound Guided Vascular Access 7/25/2016 www.ezono.com 1 Objectives Indications for insertion of central and peripheral lines Complications associated with procedures Role of ultrasound in vascular
Ultrasound Guided Vascular Access 7/25/2016 www.ezono.com 1 Objectives Indications for insertion of central and peripheral lines Complications associated with procedures Role of ultrasound in vascular
D.K. Baidya, M.K. Arora, B.R. Ray, V.K. Mohan, R.K. Anand, P. Khanna, S. Maitra
 (Acta Anaesth. Belg., 2018, 69, 107-112) Comparison between classic short-axis out-of-plane approach and novel medial-oblique in-plane approach to ultrasound guided right internal jugular vein cannulation:
(Acta Anaesth. Belg., 2018, 69, 107-112) Comparison between classic short-axis out-of-plane approach and novel medial-oblique in-plane approach to ultrasound guided right internal jugular vein cannulation:
Certificate in Clinician Performed Ultrasound (CCPU) Syllabus. Vascular Access (venous (peripheral and central) and arterial)
 Certificate in Clinician Performed Ultrasound (CCPU) Syllabus Vascular Access (venous (peripheral and central) and arterial) Page 1 of 8 04/16 Vascular Access (venous (peripheral and central) and arterial)
Certificate in Clinician Performed Ultrasound (CCPU) Syllabus Vascular Access (venous (peripheral and central) and arterial) Page 1 of 8 04/16 Vascular Access (venous (peripheral and central) and arterial)
Ultrasound (US) assistance for Central Venous Catheterization (CVC) and Peripherally Inserted Central Catheters (PICC)
 Ultrasound (US) assistance for Central Venous Catheterization (CVC) and Peripherally Inserted Central Catheters (PICC) Education - Training plan for Critical Care Nurses Pre-reading Objectives Comprehensive
Ultrasound (US) assistance for Central Venous Catheterization (CVC) and Peripherally Inserted Central Catheters (PICC) Education - Training plan for Critical Care Nurses Pre-reading Objectives Comprehensive
Needle tip visualization during ultrasound-guided vascular access: short-axis vs long-axis approach
 American Journal of Emergency Medicine (2010) 28, 343 347 www.elsevier.com/locate/ajem Brief Report Needle tip visualization during ultrasound-guided vascular access: short-axis vs long-axis approach Michael
American Journal of Emergency Medicine (2010) 28, 343 347 www.elsevier.com/locate/ajem Brief Report Needle tip visualization during ultrasound-guided vascular access: short-axis vs long-axis approach Michael
SPECIAL ARTICLE January 2012 Volume 114 Number 1
 Guidelines for Performing Ultrasound Guided Vascular Cannulation: Recommendations of the American Society of Echocardiography and the Society of Cardiovascular Anesthesiologists Christopher A. Troianos,
Guidelines for Performing Ultrasound Guided Vascular Cannulation: Recommendations of the American Society of Echocardiography and the Society of Cardiovascular Anesthesiologists Christopher A. Troianos,
A novel suture-traction method for right internal jugular vein catheterization in left-lateral position in anesthetized patients.
 Biomedical Research 2017; 28 (12): 5628-5632 ISSN 0970-938X www.biomedres.info A novel suture-traction method for right internal jugular vein catheterization in left-lateral position in anesthetized patients.
Biomedical Research 2017; 28 (12): 5628-5632 ISSN 0970-938X www.biomedres.info A novel suture-traction method for right internal jugular vein catheterization in left-lateral position in anesthetized patients.
Sterile Technique & IJ/Femoral Return Demonstration
 Sterile Technique & IJ/Femoral Return Demonstration Sterile Technique Description: This is a return demonstration checklist used to evaluate participants in the simulated hands on skills portions for certification
Sterile Technique & IJ/Femoral Return Demonstration Sterile Technique Description: This is a return demonstration checklist used to evaluate participants in the simulated hands on skills portions for certification
The role of ultrasound duplex in endovenous procedures
 The role of ultrasound duplex in endovenous procedures Neophytos A. Zambas MD, PhD Vascular Surgeon Polyclinic Ygia, Limassol, Cyprus ΚΕΑΕΧ ΚΥΠΡΙΑΚΗ ΕΤΑΙΡΕΙΑ ΑΓΓΕΙΑΚΗΣ ΚΑΙ ΕΝΔΑΓΓΕΙΑΚΗΣ ΧΕΙΡΟΥΡΓΙΚΗΣ Pre
The role of ultrasound duplex in endovenous procedures Neophytos A. Zambas MD, PhD Vascular Surgeon Polyclinic Ygia, Limassol, Cyprus ΚΕΑΕΧ ΚΥΠΡΙΑΚΗ ΕΤΑΙΡΕΙΑ ΑΓΓΕΙΑΚΗΣ ΚΑΙ ΕΝΔΑΓΓΕΙΑΚΗΣ ΧΕΙΡΟΥΡΓΙΚΗΣ Pre
Veins that are firm to
 Intravenous cannulation is a technique in which a cannula is placed inside a vein to provide venous access. Venous access allows sampling of blood as well as administration of fluids, medications, parenteral
Intravenous cannulation is a technique in which a cannula is placed inside a vein to provide venous access. Venous access allows sampling of blood as well as administration of fluids, medications, parenteral
Children s Acute Transport Service
 Children s Acute Transport Service Vascular Access Document Control Information Author Ramnarayan Author Position Consultant, CATS Document Owner Polke Document Owner Position CATS Co-ordinator Document
Children s Acute Transport Service Vascular Access Document Control Information Author Ramnarayan Author Position Consultant, CATS Document Owner Polke Document Owner Position CATS Co-ordinator Document
Advocate Christ Medical Center CVC Placement Certification Course
 Advocate Christ Medical Center CVC Placement Certification Course July 12th, 2012 Hannah Watts, MD Medical Simulation Director Modified August 10, 2017 Taajwar Khan, MD Chief Resident of Internal Medicine
Advocate Christ Medical Center CVC Placement Certification Course July 12th, 2012 Hannah Watts, MD Medical Simulation Director Modified August 10, 2017 Taajwar Khan, MD Chief Resident of Internal Medicine
How Safe Is the Ultrasonographically-Guided Peripheral Internal Jugular Line?
 GENERAL MEDICINE/BEST AVAILABLE EVIDENCE How Safe Is the Ultrasonographically-Guided Peripheral Internal Jugular Line? Michael Gottlieb, MD, RDMS*; Frances M. Russell, MD, RDMS *Corresponding Author. E-mail:
GENERAL MEDICINE/BEST AVAILABLE EVIDENCE How Safe Is the Ultrasonographically-Guided Peripheral Internal Jugular Line? Michael Gottlieb, MD, RDMS*; Frances M. Russell, MD, RDMS *Corresponding Author. E-mail:
Document No. BMB/IFU/40 Rev No. & Date 00 & 15/11/2017 Issue No & Date 01 & 15/11/2017
 Central Venous Catheter Device Description Multi-lumen catheters incorporate separate, non-communicating vascular access lumens within a single catheter body. Minipunctur Access Sets And Trays: Used for
Central Venous Catheter Device Description Multi-lumen catheters incorporate separate, non-communicating vascular access lumens within a single catheter body. Minipunctur Access Sets And Trays: Used for
Ultrasound Guided Regional Nerve Blocks
 Ultrasound Guided Regional Nerve Blocks In the country of the blind the one eyed man is King -Deciderius Erasmus (1466-1536) Objectives Benefits of Regional Anesthesia Benefits of US guidance Role of ultrasound
Ultrasound Guided Regional Nerve Blocks In the country of the blind the one eyed man is King -Deciderius Erasmus (1466-1536) Objectives Benefits of Regional Anesthesia Benefits of US guidance Role of ultrasound
Ultrasound Guidance for Central Venous Catheter Placement
 Clinical Review Article Ultrasound Guidance for Central Venous Catheter Placement Frantz J. Gibbs, MD, FACEP Michael C. Murphy, MD In 1952, Sven-Ivar Seldinger developed an innovative technique for the
Clinical Review Article Ultrasound Guidance for Central Venous Catheter Placement Frantz J. Gibbs, MD, FACEP Michael C. Murphy, MD In 1952, Sven-Ivar Seldinger developed an innovative technique for the
ANATOMICAL VARIATIONS OF THE INTERNAL JUGULAR VEIN IN RELATION TO COMMON CAROTID ARTERY IN LESSER SUPRA CLAVICULAR FOSSA A COLOUR DOPPLER STUDY
 Original Article ANATOMICAL VARIATIONS OF THE INTERNAL JUGULAR VEIN IN RELATION TO COMMON CAROTID ARTERY IN LESSER SUPRA CLAVICULAR FOSSA A COLOUR DOPPLER STUDY Shanta Chandrasekaran*, V.P.Chandrasekaran**
Original Article ANATOMICAL VARIATIONS OF THE INTERNAL JUGULAR VEIN IN RELATION TO COMMON CAROTID ARTERY IN LESSER SUPRA CLAVICULAR FOSSA A COLOUR DOPPLER STUDY Shanta Chandrasekaran*, V.P.Chandrasekaran**
Sonoanatomy Of The Brachial Plexus With Single Broad Band-High Frequency (L17-5 Mhz) Linear Transducer
 ISPUB.COM The Internet Journal of Anesthesiology Volume 11 Number 2 Sonoanatomy Of The Brachial Plexus With Single Broad Band-High Frequency (L17-5 Mhz) Linear A Thallaj Citation A Thallaj.. The Internet
ISPUB.COM The Internet Journal of Anesthesiology Volume 11 Number 2 Sonoanatomy Of The Brachial Plexus With Single Broad Band-High Frequency (L17-5 Mhz) Linear A Thallaj Citation A Thallaj.. The Internet
Neck Ultrasound. Faculty Info: Amy Kule, MD
 Neck Ultrasound Date: Friday, October 19, 2018 Time: 11:00 AM Location: SMALL GROUP LABORATORY SSOM L71 Watch: Ø Neck Ultrasound Scanning Protocol (4:00): https://www.youtube.com/watch?v=zozd2x2ll4q Faculty
Neck Ultrasound Date: Friday, October 19, 2018 Time: 11:00 AM Location: SMALL GROUP LABORATORY SSOM L71 Watch: Ø Neck Ultrasound Scanning Protocol (4:00): https://www.youtube.com/watch?v=zozd2x2ll4q Faculty
Candidate s instructions Look at this cross-section taken at the level of C5. Answer the following questions.
 Section 1 Anatomy Chapter 1. Trachea 1 Candidate s instructions Look at this cross-section taken at the level of C5. Answer the following questions. Pretracheal fascia 1 2 5 3 4 Questions 1. Label the
Section 1 Anatomy Chapter 1. Trachea 1 Candidate s instructions Look at this cross-section taken at the level of C5. Answer the following questions. Pretracheal fascia 1 2 5 3 4 Questions 1. Label the
Ultrasound Guided Injections
 Ultrasound Guided Injection Technique More accurate injections Better Results! 1 Benefits: Increased Level of Certainty ie : really know how accurate PRP/Prolotherapy Avoid damage to articular cartilage
Ultrasound Guided Injection Technique More accurate injections Better Results! 1 Benefits: Increased Level of Certainty ie : really know how accurate PRP/Prolotherapy Avoid damage to articular cartilage
anatomic relationship between the internal jugular vein and the carotid artery in children after laryngeal mask insertion. An ultrasonographic study.
 The anatomic relationship between the internal jugular vein and the carotid artery in children after laryngeal mask insertion. An ultrasonographic study. Ravi Gopal Nagaraja, Morven Wilson, Graham Wilson,
The anatomic relationship between the internal jugular vein and the carotid artery in children after laryngeal mask insertion. An ultrasonographic study. Ravi Gopal Nagaraja, Morven Wilson, Graham Wilson,
Ultrasound-guided supraclavicular block
 THE JOURNAL OF NEW YORK SCHOOL J u l y 2009 V o l u m e OF REGIONAL ANESTHESIA 1 3 Ultrasound-guided supraclavicular block Arthur Atchabahian, MD Department of Anesthesiology, St. Vincent Medical Center,
THE JOURNAL OF NEW YORK SCHOOL J u l y 2009 V o l u m e OF REGIONAL ANESTHESIA 1 3 Ultrasound-guided supraclavicular block Arthur Atchabahian, MD Department of Anesthesiology, St. Vincent Medical Center,
Ultrasound-guided oblique approach for peripheral venous access in a phantom model
 Tassone et al. Critical Ultrasound Journal 2012, 4:14 ORIGINAL ARTICLE Open Access Ultrasound-guided oblique approach for peripheral venous access in a phantom model Heather M Tassone 1,2, Vivek S Tayal
Tassone et al. Critical Ultrasound Journal 2012, 4:14 ORIGINAL ARTICLE Open Access Ultrasound-guided oblique approach for peripheral venous access in a phantom model Heather M Tassone 1,2, Vivek S Tayal
Basics of US Regional Anaesthesia. November 2008
 Basics of US Regional Anaesthesia November 2008 Essential Physics HIGH frequency = great resolution but poor penetration LOW frequency = poor resolution but great penetration Potential Advantages of US
Basics of US Regional Anaesthesia November 2008 Essential Physics HIGH frequency = great resolution but poor penetration LOW frequency = poor resolution but great penetration Potential Advantages of US
inerve Guide to Nerves 2009
 inerve Guide to Nerves 2009 A guide to self learning and self assessment Context: The following guide is intended to help interpret the sono-anatomy and follow a systematic stepwise approach to the practice
inerve Guide to Nerves 2009 A guide to self learning and self assessment Context: The following guide is intended to help interpret the sono-anatomy and follow a systematic stepwise approach to the practice
Background & Indications Probe Selection
 Teresa S. Wu, MD, FACEP Director, EM Ultrasound Program & Fellowship Co-Director, Simulation Based Training Program & Fellowship Associate Program Director, EM Residency Program Maricopa Medical Center
Teresa S. Wu, MD, FACEP Director, EM Ultrasound Program & Fellowship Co-Director, Simulation Based Training Program & Fellowship Associate Program Director, EM Residency Program Maricopa Medical Center
MODULE 9 ARTERIAL AND VENOUS CATHETERIZATION. Robert B. McLafferty M.D. Southern Illinois University
 MODULE 9 ARTERIAL AND VENOUS CATHETERIZATION Robert B. McLafferty M.D. Southern Illinois University I. OBJECTIVES By the end of this laboratory session the residents should be able to A. Identify the anatomic
MODULE 9 ARTERIAL AND VENOUS CATHETERIZATION Robert B. McLafferty M.D. Southern Illinois University I. OBJECTIVES By the end of this laboratory session the residents should be able to A. Identify the anatomic
Technique of the VenaSeal System
 Technique of the VenaSeal System Indication & Contraindications VenaSeal Indication: The Sapheon VenaSeal System is intended for the permantent, complete, endovascular adhesive closure of the great saphenous
Technique of the VenaSeal System Indication & Contraindications VenaSeal Indication: The Sapheon VenaSeal System is intended for the permantent, complete, endovascular adhesive closure of the great saphenous
Infraclavicular brachial plexus blocks have been designed
 The Supraclavicular Lateral Paravascular Approach for Brachial Plexus Regional Anesthesia: A Simulation Study Using Magnetic Resonance Imaging Øivind Klaastad, MD* and Örjan Smedby, Dr Med Sci *Department
The Supraclavicular Lateral Paravascular Approach for Brachial Plexus Regional Anesthesia: A Simulation Study Using Magnetic Resonance Imaging Øivind Klaastad, MD* and Örjan Smedby, Dr Med Sci *Department
Cordis EXOSEAL Vascular Closure Device
 to receive our latest news and key activities. Cordis EXOSEAL Vascular Closure Device A Guide to Good Access and Closure Transfemoral Access Closure Pocket Guide LinkedIn page Follow us on CORDIS EMEA
to receive our latest news and key activities. Cordis EXOSEAL Vascular Closure Device A Guide to Good Access and Closure Transfemoral Access Closure Pocket Guide LinkedIn page Follow us on CORDIS EMEA
The Language of Anatomy. (Anatomical Terminology)
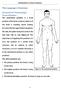 The Language of Anatomy (Anatomical Terminology) Terms of Position The anatomical position is a fixed position of the body (cadaver) taken as if the body is standing (erect) looking forward with the upper
The Language of Anatomy (Anatomical Terminology) Terms of Position The anatomical position is a fixed position of the body (cadaver) taken as if the body is standing (erect) looking forward with the upper
A Comparative Study Of Internal Jugular Vein Cannulation- Central Approach Versus Subclavian Vein Cannulation Infraclavicular Approach.
 DOI:.76/aimdr.6..3. Original Article ISSN (O):395-8; ISSN (P):395-84 A Comparative Study Of Internal Jugular Vein Cannulation- Central Approach Versus Subclavian Vein Cannulation Infraclavicular Approach.
DOI:.76/aimdr.6..3. Original Article ISSN (O):395-8; ISSN (P):395-84 A Comparative Study Of Internal Jugular Vein Cannulation- Central Approach Versus Subclavian Vein Cannulation Infraclavicular Approach.
Overview of CVADs. Type of device commonly used. Dwell time Flushing requirement Associated complications. lumens
 Source: Clinical Skills Management of Vascular Access Devices Pre-course handbook. Adapted with permission from NHS Lothian Employee and Education Development Team. Overview of CVADs Type of device Veins
Source: Clinical Skills Management of Vascular Access Devices Pre-course handbook. Adapted with permission from NHS Lothian Employee and Education Development Team. Overview of CVADs Type of device Veins
Randomized comparison of three transducer orientation approaches for ultrasound guided internal jugular venous cannulation
 British Journal of Anaesthesia, 116 (3): 370 6 (2016) doi: 10.1093/bja/aev399 Advance Access Publication Date: 24 December 2015 Clinical Practice Randomized comparison of three transducer orientation approaches
British Journal of Anaesthesia, 116 (3): 370 6 (2016) doi: 10.1093/bja/aev399 Advance Access Publication Date: 24 December 2015 Clinical Practice Randomized comparison of three transducer orientation approaches
Arterial Line Insertion Pre Reading
 PROCEDURE ACCREDITATION THE CANBERRA HOSPITAL EMERGENCY DEPARTMENT Arterial Line Insertion Pre Reading Indications Requirement for continuous blood pressure monitoring (all patients on pressors, inotropes,
PROCEDURE ACCREDITATION THE CANBERRA HOSPITAL EMERGENCY DEPARTMENT Arterial Line Insertion Pre Reading Indications Requirement for continuous blood pressure monitoring (all patients on pressors, inotropes,
Ultrasound Use in Anaesthesia
 Trainee Name: 1 Ultrasound Use in Anaesthesia Assessments to accompany Workbook for anaesthetic trainees in North Queensland 2010 Authors: Mark Fairley, Emile Kurukchi, Andrew Potter 2 Trainee Name: Ultrasound
Trainee Name: 1 Ultrasound Use in Anaesthesia Assessments to accompany Workbook for anaesthetic trainees in North Queensland 2010 Authors: Mark Fairley, Emile Kurukchi, Andrew Potter 2 Trainee Name: Ultrasound
Ultrasound Guidance in Anesthesia Practice
 Objectives Ultrasound Guidance in Anesthesia Practice Maria Hirsch, CRNA, DNAP Describe the basic principles of ultrasound Explore the various applications of ultrasound in anesthesia practice Discuss
Objectives Ultrasound Guidance in Anesthesia Practice Maria Hirsch, CRNA, DNAP Describe the basic principles of ultrasound Explore the various applications of ultrasound in anesthesia practice Discuss
Ultrasound Guided Peripheral Intravenous Access
 Ultrasound Guided Peripheral Intravenous Access J. Christian Fox, MD, RDMS, FACEP, FAAEM, FAIUM Professor and Interim Chair of Emergency Medicine Director of Instructional Ultrasound University of California,
Ultrasound Guided Peripheral Intravenous Access J. Christian Fox, MD, RDMS, FACEP, FAAEM, FAIUM Professor and Interim Chair of Emergency Medicine Director of Instructional Ultrasound University of California,
Mary Lou Garey MSN EMT-P MedFlight of Ohio
 Mary Lou Garey MSN EMT-P MedFlight of Ohio Function Prolonged and frequent access to venous circulation Allows for patient to carry on normal life; decrease number of needle sticks Medications, parenteral
Mary Lou Garey MSN EMT-P MedFlight of Ohio Function Prolonged and frequent access to venous circulation Allows for patient to carry on normal life; decrease number of needle sticks Medications, parenteral
Surface Anatomy and Sonoanatomy for the Occasional Regional Anesthesiologist
 Surface Anatomy and Sonoanatomy for the Occasional Regional Anesthesiologist Edward R. Mariano, M.D., M.A.S. Professor of Anesthesiology, Perioperative & Pain Medicine Stanford University School of Medicine
Surface Anatomy and Sonoanatomy for the Occasional Regional Anesthesiologist Edward R. Mariano, M.D., M.A.S. Professor of Anesthesiology, Perioperative & Pain Medicine Stanford University School of Medicine
Anatomical Anomalies of Femoral Vein are Not Observed in Indian Patients with Renal Failure: Ultrasound-based Study
 Brief Communication Anatomical Anomalies of Femoral Vein are Not Observed in Indian Patients with Renal Failure: Ultrasound-based Study Jai Prakash, Naveen Sharma, Rubina Vohra, Amit Dwivedi, Raja Ramachandran,
Brief Communication Anatomical Anomalies of Femoral Vein are Not Observed in Indian Patients with Renal Failure: Ultrasound-based Study Jai Prakash, Naveen Sharma, Rubina Vohra, Amit Dwivedi, Raja Ramachandran,
Depth of Central Venous Catheterization by Intracardiac ECG in Paediatric Patients
 Original Article Elmer Press Depth of Central Venous Catheterization by Intracardiac ECG in Paediatric Patients Prerana N. Shah a, b, Jithesh Appukutty a, Deepa Kane a Abstract Background: Central venous
Original Article Elmer Press Depth of Central Venous Catheterization by Intracardiac ECG in Paediatric Patients Prerana N. Shah a, b, Jithesh Appukutty a, Deepa Kane a Abstract Background: Central venous
Ultrasound User Demonstration
 Ultrasound User Demonstration Disclaimer: This presentation is intended to be used as a demonstration educational device to showcase Terumo products. It is NOT intended to be used as a diagnostic device
Ultrasound User Demonstration Disclaimer: This presentation is intended to be used as a demonstration educational device to showcase Terumo products. It is NOT intended to be used as a diagnostic device
Ultrasound Guidance for Common Procedures
 18-Levitov_CH18_p230-246.qxd 3/31/10 4:24 PM Page 230 CHAPTER 18 Ultrasound Guidance for Common Procedures Christian H. Butcher, MD, FCCP and Sameh Aziz, MD, FCCP, FACP INTRODUCTION The advent of high-quality,
18-Levitov_CH18_p230-246.qxd 3/31/10 4:24 PM Page 230 CHAPTER 18 Ultrasound Guidance for Common Procedures Christian H. Butcher, MD, FCCP and Sameh Aziz, MD, FCCP, FACP INTRODUCTION The advent of high-quality,
PEMSS PROTOCOLS INVASIVE PROCEDURES
 PEMSS PROTOCOLS INVASIVE PROCEDURES Panhandle Emergency Medical Services System SURGICAL AND NEEDLE CRICOTHYROTOMY Inability to intubate is the primary indication for creating an artificial airway. Care
PEMSS PROTOCOLS INVASIVE PROCEDURES Panhandle Emergency Medical Services System SURGICAL AND NEEDLE CRICOTHYROTOMY Inability to intubate is the primary indication for creating an artificial airway. Care
Surgery Under Regional Anesthesia
 Surgery Under Regional Anesthesia Jean Daniel Eloy, MD Assistant Professor Residency Program Director Rutgers-New Jersey Medical School Rutgers The State University of New Jersey Peripheral Nerve Block
Surgery Under Regional Anesthesia Jean Daniel Eloy, MD Assistant Professor Residency Program Director Rutgers-New Jersey Medical School Rutgers The State University of New Jersey Peripheral Nerve Block
Diana Mathioudakis DEAA EDIC AFRCA. consultant paediatric cardiac anaesthetist Intensivist(D/NL) emergency physician(d)
 & Diana Mathioudakis DEAA EDIC AFRCA consultant paediatric cardiac anaesthetist Intensivist(D/NL) emergency physician(d) Anatomy Probe handling Sonoanatomy Tips and Tricks Literature For ultrasound guided
& Diana Mathioudakis DEAA EDIC AFRCA consultant paediatric cardiac anaesthetist Intensivist(D/NL) emergency physician(d) Anatomy Probe handling Sonoanatomy Tips and Tricks Literature For ultrasound guided
Three-step method for ultrasound-guided central vein catheterization
 British Journal of naesthesia Page 1 of 6 doi:10.1093/bja/aes381 Three-step method for ultrasound-guided central vein catheterization J. Tokumine 1 *,. T. Lefor 4,. Yonei 5,. Kagaya 2, K. Iwasaki 2 and
British Journal of naesthesia Page 1 of 6 doi:10.1093/bja/aes381 Three-step method for ultrasound-guided central vein catheterization J. Tokumine 1 *,. T. Lefor 4,. Yonei 5,. Kagaya 2, K. Iwasaki 2 and
Jake Hutchins, M.D. Aaron Berg, D.O.
 Jake Hutchins, M.D. Aaron Berg, D.O. Jacob Hutchins is on the speaker s bureau, is a consultant, and has received research funding from Pacira Pharmaceuticals He also is a consultant for Insitu Biologics,
Jake Hutchins, M.D. Aaron Berg, D.O. Jacob Hutchins is on the speaker s bureau, is a consultant, and has received research funding from Pacira Pharmaceuticals He also is a consultant for Insitu Biologics,
Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman
 Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman Breast anatomy: Breast conserving surgery: The aim of wide local excision is to remove all invasive and in situ
Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman Breast anatomy: Breast conserving surgery: The aim of wide local excision is to remove all invasive and in situ
Ahsan Mustafa, Khaja Ali Hassan and Syed Abdur Rahman. Department of Anaesthesiology, Deccan College of Medical Sciences, Hyderabad, India
 International Journal of Advances in Health Sciences (IJHS) ISSN 2349-7033 Vol-3, Issue-1, 2016, pp54-59 http://www.ijhsonline.com Research Article Comparison of the rate of success and incidence of complications
International Journal of Advances in Health Sciences (IJHS) ISSN 2349-7033 Vol-3, Issue-1, 2016, pp54-59 http://www.ijhsonline.com Research Article Comparison of the rate of success and incidence of complications
Sign up to receive ATOTW weekly -
 1 SUBCLAVIAN PERIVASCULAR BRACHIAL PLEXUS BLOCK ANAESTHESIA TUTORIAL OF THE WEEK 156 19 th OCTOBER 2009 Dr. Martin Herrick Department of Anaesthesia, Addenbrooke s Hospital, Cambridge, U.K. Correspondence
1 SUBCLAVIAN PERIVASCULAR BRACHIAL PLEXUS BLOCK ANAESTHESIA TUTORIAL OF THE WEEK 156 19 th OCTOBER 2009 Dr. Martin Herrick Department of Anaesthesia, Addenbrooke s Hospital, Cambridge, U.K. Correspondence
10/14/2018 Dr. Shatarat
 2018 Objectives To discuss mediastina and its boundaries To discuss and explain the contents of the superior mediastinum To describe the great veins of the superior mediastinum To describe the Arch of
2018 Objectives To discuss mediastina and its boundaries To discuss and explain the contents of the superior mediastinum To describe the great veins of the superior mediastinum To describe the Arch of
Is finder needle necessary for internal jugular vein catheterization?
 Original Article Is finder needle necessary for internal jugular vein catheterization? Eisa Bilehjani, Amir Abbas Kianfar, Solmaz Fakhari From Department of Cardiovascular Anesthesiology, Madani Heart
Original Article Is finder needle necessary for internal jugular vein catheterization? Eisa Bilehjani, Amir Abbas Kianfar, Solmaz Fakhari From Department of Cardiovascular Anesthesiology, Madani Heart
The use of ultrasound during and after central venous catheter insertion versus conventional chest X-ray after insertion of a central venous catheter
 ORIGINAL ARTICLE The use of ultrasound during and after central venous catheter insertion versus conventional chest X-ray after insertion of a central venous catheter M.J. Blans 1 *, H. Endeman 2, F.H.
ORIGINAL ARTICLE The use of ultrasound during and after central venous catheter insertion versus conventional chest X-ray after insertion of a central venous catheter M.J. Blans 1 *, H. Endeman 2, F.H.
Arterial Access for Diagnosis and Intervention T-Woei Tan, MD, FACS
 Arterial Access for Diagnosis and Intervention T-Woei Tan, MD, FACS Assistant Professor of Surgery Vascular Endovascular Surgery Louisiana State University Health - Shreveport Disclosures None Objective
Arterial Access for Diagnosis and Intervention T-Woei Tan, MD, FACS Assistant Professor of Surgery Vascular Endovascular Surgery Louisiana State University Health - Shreveport Disclosures None Objective
As with any intervention, selection of an appropriate
 DVT: ccess Decisions for Interventions ssessing the advantages and disadvantages of venous access options is crucial for safe and successful DVT intervention. Y JOHN. KUFMN, MD, MS, FSIR, FH, FCIRSE, EIR
DVT: ccess Decisions for Interventions ssessing the advantages and disadvantages of venous access options is crucial for safe and successful DVT intervention. Y JOHN. KUFMN, MD, MS, FSIR, FH, FCIRSE, EIR
Central Line Care and Management
 Central Line Care and Management What is a Central Line/ CVAD? (central venous access device) A vascular infusion device that terminates at or close to the heart or in one of the great vessels (aorta,
Central Line Care and Management What is a Central Line/ CVAD? (central venous access device) A vascular infusion device that terminates at or close to the heart or in one of the great vessels (aorta,
Imbibe Bone marrow aspiration needle. Operative technique
 Imbibe Bone marrow aspiration needle Operative technique Imbibe Bone Marrow Aspiration Needle Imbibe Bone marrow aspiration needle Contents 1. Smart design... 3 2. Operative technique... 4 Posterior iliac
Imbibe Bone marrow aspiration needle Operative technique Imbibe Bone Marrow Aspiration Needle Imbibe Bone marrow aspiration needle Contents 1. Smart design... 3 2. Operative technique... 4 Posterior iliac
Peripherally Inserted Central Catheter & Midline Placement with ECG Confirmation of Tip Placement
 Title/Description: Peripherally Inserted Central Catheter & Midline Placement with ECG Confirmation of Tip Placement Department: Patient Care Services Personnel: Nursing Services Effective Date: April
Title/Description: Peripherally Inserted Central Catheter & Midline Placement with ECG Confirmation of Tip Placement Department: Patient Care Services Personnel: Nursing Services Effective Date: April
Catheter Fracture of a Totally Implantable Venous Device Due to Pinch Off Syndrome in Breast Cancer: A Case Report
 Kosin Medical Journal 2016;31:167-172. https://doi.org/10.7180/kmj.2016.31.2.167 KMJ Case Report Catheter Fracture of a Totally Implantable Venous Device Due to Pinch Off Syndrome in Breast Cancer: A Case
Kosin Medical Journal 2016;31:167-172. https://doi.org/10.7180/kmj.2016.31.2.167 KMJ Case Report Catheter Fracture of a Totally Implantable Venous Device Due to Pinch Off Syndrome in Breast Cancer: A Case
Effects of Tube Depth and Infusion Rate of Continuous Humidification by Endotracheal Intubation on Humidification Effect
 Open Journal of Nursing, 2017, 7, 123-127 http://www.scirp.org/journal/ojn ISSN Online: 2162-5344 ISSN Print: 2162-5336 Effects of Tube Depth and Infusion Rate of Continuous Humidification by Endotracheal
Open Journal of Nursing, 2017, 7, 123-127 http://www.scirp.org/journal/ojn ISSN Online: 2162-5344 ISSN Print: 2162-5336 Effects of Tube Depth and Infusion Rate of Continuous Humidification by Endotracheal
BEDSIDE ULTRASOUND BEDSIDE ULTRASOUND. Deep Vein Thrombosis. Probe used
 BEDSIDE ULTRASOUND Part 2 Diagnosis of deep vein thrombosis Kishore Kumar Pichamuthu, Professor, Department of Critical Care, CMC, Vellore Summary: Deep vein thrombosis (DVT) is a problem encountered in
BEDSIDE ULTRASOUND Part 2 Diagnosis of deep vein thrombosis Kishore Kumar Pichamuthu, Professor, Department of Critical Care, CMC, Vellore Summary: Deep vein thrombosis (DVT) is a problem encountered in
Over the Wire Technique vs. Modified Seldinger Technique in Insertion of PICC
 Over the Wire Technique vs. Modified Seldinger Technique in Insertion of PICC Deniz Kasikci Department of Radiology, Jena University Hospital Friedrich-Schiller-University, Jena, Germany Disclosure Speaker
Over the Wire Technique vs. Modified Seldinger Technique in Insertion of PICC Deniz Kasikci Department of Radiology, Jena University Hospital Friedrich-Schiller-University, Jena, Germany Disclosure Speaker
Focused Assessment Sonography of Trauma (FAST) Scanning Protocol
 Focused Assessment Sonography of Trauma (FAST) Scanning Protocol Romolo Gaspari CHAPTER 3 GOAL OF THE FAST EXAM Demonstrate free fluid in abdomen, pleural space, or pericardial space. EMERGENCY ULTRASOUND
Focused Assessment Sonography of Trauma (FAST) Scanning Protocol Romolo Gaspari CHAPTER 3 GOAL OF THE FAST EXAM Demonstrate free fluid in abdomen, pleural space, or pericardial space. EMERGENCY ULTRASOUND
UC Irvine Western Journal of Emergency Medicine: Integrating Emergency Care with Population Health
 UC Irvine Western Journal of Emergency Medicine: Integrating Emergency Care with Population Health Title Supraclavicular Subclavian Vein Catherization: The Forgotten Central Line Permalink https://escholarship.org/uc/item/8kf7q46w
UC Irvine Western Journal of Emergency Medicine: Integrating Emergency Care with Population Health Title Supraclavicular Subclavian Vein Catherization: The Forgotten Central Line Permalink https://escholarship.org/uc/item/8kf7q46w
Ultrasound Guided Lower Extremity Blocks
 Ultrasound Guided Lower Extremity Blocks CONTENTS: 1. Femoral Nerve Block 2. Popliteal Nerve Block Updated December 2017 1 1. Femoral Nerve Block Indications Surgery involving the knee, anterior thigh,
Ultrasound Guided Lower Extremity Blocks CONTENTS: 1. Femoral Nerve Block 2. Popliteal Nerve Block Updated December 2017 1 1. Femoral Nerve Block Indications Surgery involving the knee, anterior thigh,
Interscalene brachial plexus blocks in the management of shoulder dislocations
 Archives of Emergency Medicine, 1989, 6, 199-204 Interscalene brachial plexus blocks in the management of shoulder dislocations T. J. UNDERHILL, A. WAN & M. MORRICE Accident and Emergency Department, Derbyshire
Archives of Emergency Medicine, 1989, 6, 199-204 Interscalene brachial plexus blocks in the management of shoulder dislocations T. J. UNDERHILL, A. WAN & M. MORRICE Accident and Emergency Department, Derbyshire
Regional Anaesthesia
 Regional Anaesthesia Basic Sciences Anaesthetic Course Dr Vassilis ATHANASSOGLOU FRCA Consultant Anaesthetist and Lecturer in Medicine Oxford University Hospitals NHS Trust, UK Geneva, 5th June 2017 Faculty
Regional Anaesthesia Basic Sciences Anaesthetic Course Dr Vassilis ATHANASSOGLOU FRCA Consultant Anaesthetist and Lecturer in Medicine Oxford University Hospitals NHS Trust, UK Geneva, 5th June 2017 Faculty
RadRx Your Prescription for Accurate Coding & Reimbursement Copyright All Rights Reserved.
 Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of October 22, 2018 Paracentesis & Transjugular Liver Biopsy
Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of October 22, 2018 Paracentesis & Transjugular Liver Biopsy
USRA OF THE UPPER EXTREMITY
 USRA OF THE UPPER EXTREMITY Christian R. Falyar, DNAP, CRNA Department of Nurse Anesthesia Virginia Commonwealth University Disclosure Statement of Financial Interest I, Christian Falyar, DO NOT have a
USRA OF THE UPPER EXTREMITY Christian R. Falyar, DNAP, CRNA Department of Nurse Anesthesia Virginia Commonwealth University Disclosure Statement of Financial Interest I, Christian Falyar, DO NOT have a
Ultrasound technology has. Ultrasound-Guided Central Vein Cannulation: Current Recommendations and Guidelines
 PRINTER-FRIENDLY VERSION AT ANESTHESIOLOGYNEWS.COM Ultrasound-Guided Central Vein Cannulation: Current Recommendations and Guidelines JULIE A. GAYLE, MD Assistant Professor of Clinical Anesthesiology Louisiana
PRINTER-FRIENDLY VERSION AT ANESTHESIOLOGYNEWS.COM Ultrasound-Guided Central Vein Cannulation: Current Recommendations and Guidelines JULIE A. GAYLE, MD Assistant Professor of Clinical Anesthesiology Louisiana
Perioperative Ultrasonography Ehab Farag, MD, FRCA Hesham Elsharkawy David G. Anthony, M.D.
 Perioperative Ultrasonography Ehab Farag, MD, FRCA Hesham Elsharkawy David G. Anthony, M.D. Cleveland Clinic, Cleveland OH 1 Complications during central venous catheterization (CVC) occur 2% -15% of the
Perioperative Ultrasonography Ehab Farag, MD, FRCA Hesham Elsharkawy David G. Anthony, M.D. Cleveland Clinic, Cleveland OH 1 Complications during central venous catheterization (CVC) occur 2% -15% of the
Safety and efficacy of the oblique-axis plane in ultrasound-guided internal jugular vein puncture: A meta-analysis
 Clinical Research Report Safety and efficacy of the oblique-axis plane in ultrasound-guided internal jugular vein puncture: A meta-analysis Journal of International Medical Research 2018, Vol. 46(7) 2587
Clinical Research Report Safety and efficacy of the oblique-axis plane in ultrasound-guided internal jugular vein puncture: A meta-analysis Journal of International Medical Research 2018, Vol. 46(7) 2587
Home Health Foundation, Inc. To create more permanent IV access for patients undergoing long term IV therapy.
 PROCEDURE ORIGINAL DATE: 06/99 Revised Date: 09/02 Home Health Foundation, Inc. SUBJECT: PURPOSE: MIDLINE CATHETER INSERTION To create more permanent IV access for patients undergoing long term IV therapy.
PROCEDURE ORIGINAL DATE: 06/99 Revised Date: 09/02 Home Health Foundation, Inc. SUBJECT: PURPOSE: MIDLINE CATHETER INSERTION To create more permanent IV access for patients undergoing long term IV therapy.
Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi
 Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi For the purpose of anatomical description the neck is sub divided into two major triangles, the Anterior and the Posterior by muscle bellies
Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi For the purpose of anatomical description the neck is sub divided into two major triangles, the Anterior and the Posterior by muscle bellies
Large veins of the thorax Brachiocephalic veins
 Large veins of the thorax Brachiocephalic veins Right brachiocephalic vein: formed at the root of the neck by the union of the right subclavian & the right internal jugular veins. Left brachiocephalic
Large veins of the thorax Brachiocephalic veins Right brachiocephalic vein: formed at the root of the neck by the union of the right subclavian & the right internal jugular veins. Left brachiocephalic
Definition of Anatomy. Anatomy is the science of the structure of the body and the relation of its parts.
 Definition of Anatomy Anatomy is the science of the structure of the body and the relation of its parts. Basic Anatomical Terms Anatomical terms for describing positions: Anatomical position: Supine position:
Definition of Anatomy Anatomy is the science of the structure of the body and the relation of its parts. Basic Anatomical Terms Anatomical terms for describing positions: Anatomical position: Supine position:
Upper Extremity Venous Duplex Evaluation
 VASCULARTECHNOLOGY PROFESSIONAL PERFORMANCE GUIDELINES Upper Extremity Venous Duplex Evaluation This Guideline was prepared by the Professional Guidelines Subcommittee of the Society for Vascular Ultrasound
VASCULARTECHNOLOGY PROFESSIONAL PERFORMANCE GUIDELINES Upper Extremity Venous Duplex Evaluation This Guideline was prepared by the Professional Guidelines Subcommittee of the Society for Vascular Ultrasound
Introduction to Ultrasound Guided Region Anesthesia
 Introduction to Ultrasound Guided Region Anesthesia Brian D. Sites, MD Dept of Anesthesiology Dartmouth-Hitchcock Medical Center INTRODUCTION Welcome to Introduction to Ultrasound Guided Regional Anesthesia.
Introduction to Ultrasound Guided Region Anesthesia Brian D. Sites, MD Dept of Anesthesiology Dartmouth-Hitchcock Medical Center INTRODUCTION Welcome to Introduction to Ultrasound Guided Regional Anesthesia.
