JOPE. Abstract. Introduction /jp-journals
|
|
|
- Victoria Dixon
- 6 years ago
- Views:
Transcription
1 Bahareh Khatibi, Nav Parkash Sandhu Review Article /jp-journals Bahareh Khatibi, 2 Nav Parkash Sandhu Abstract The axillary vein has been shown to be a safe and effective cannulation site for patients requiring central venous access. Compared to subclavian vein cannulation, axillary vein cannulation may reduce the rate of pneumothorax and hemothorax. Long-term complications, including the rate of infection or deep vein thrombosis, are comparable to internal jugular vein cannulation. The use of ultrasound for cannulation at traditional central vein sites, such as the internal jugular and femoral veins has been shown to aid in successful cannulation and potentially reduce complications. For axillary vein cannulation, however, when ultrasound is used only for localization of the axillary vein precannulation, it has not been shown to improve successful cannulation or decrease the rate of arterial puncture. Real-time ultrasound-guided axillary vein cannulation has been described and may increase the rate of successful cannulation and decrease complications. Various techniques of real-time ultrasound-guided axillary vein cannulation have been studied over the past decade. They differ in various characteristics including technique for needle imaging (in-plane vs out-of-plane) and upper extremity positioning (neutral vs abducted). The in-plane technique, which images the axillary vein in longitudinal view and allows the needle to be visualized at all times, has been found to result in greater first-attempt success and easier overall placement than the transverse view technique. As for upper extremity positioning, 90º abduction may result a decreased risk of catheter misplacement after proximal axillary vein cannulation. Ultrasound-guided axillary vein cannulation has many emerging uses, including use in oncology, cardiology, and nephrology. Keywords: Axillary vein, Central venous access, Ultrasound. How to cite this article: Khatibi B, Sandhu NP. Real-time Ultrasound-guided Axillary Vein Cannulation. J Perioper Echocardiogr 2015;3(2): Source of support: Nil Conflict of interest: None Introduction Given the potential complications of subclavian vein cannulation, 1 including pneumothorax and mediastinal 42 1 Assistant Clinical Professor, 2 Professor 1,2 Department of Anesthesiology, University of California San Diego, CA, USA Corresponding Author: Bahareh Khatibi, Assistant Clinical Professor, Department of Anesthesiology, University of California, San Diego, 200 W Arbor Dr, 8770, San Diego CA 92103, USA, bkhatibi@ucsd.edu hematoma, axillary vein cannulation techniques, have been described as an alternative The use of ultrasound for axillary vein localization was first described in critical care patients for which the landmark-based technique was deemed suboptimal. 7,8 Real-time ultrasound-guided axillary vein cannulation was first described over a decade ago. 9 Since then, it has been studied in a wide range of patients, including critically ill patients In this article, we will review axillary vein cannulation, including techniques for placement with real-time ultrasound-guidance, benefits, risks and emerging uses. Axillary Vein Anatomy A thorough understanding of anatomy is essential to appreciate the potential benefits of cannulation of the axillary vein. The axillary vein is the continuation of the basilic and brachial veins and extends from the outer margin of teres major to the lateral border of the first rib, at which point it becomes the subclavian vein. Along its course, it receives tributaries from the cephalic, subscapular, circumflex humeral, lateral thoracic and thoracoacromial veins. The vein is accompanied by the axillary artery, which lies slightly superior and posterior to the vein. When a vein is to be punctured for cannulation, the structures posterior to the vein are of great importance. The medial portion of the axillary vein, like the subclavian vein, is bordered posteriorly by the ribs and lung. More laterally, the anterior chest wall moves posteriorly, resulting in a larger distance between the vein and lung. At the most lateral aspect of the axillary vein, there are no clinically significant posterior structures that may be inadvertently injured during cannulation. History of Axillary Vein Catheterization Multiple landmark-based approaches to axillary vein access have been described. 2-6 Studies using these techniques found axillary vein catheterization to be equally effective and safe as cannulation at other central vein sites. The reported failure rate ranged from 4 to 11%. Of the complications, the most frequent of was arterial puncture. 6 The first described use of ultrasound in axillary vein cannulation was for vein localization only. 7 The investigators used ultrasound to locate and mark the axillary vein prior to cannulation attempt. Although
2 Fig. 1: In-plane technique: The position of ultrasound transducer to obtain a longitudinal image of axillary vein and the needle is advanced in plane to reach the vein to puncture it (AV: Axillary vein; C: Clavicle) the use of ultrasound for cannulation of other central veins has been found to aid in accurate cannulation and potentially reduce complications, 17,18 ultrasound used only for vein localization did not have these benefits. Cannulation failure rate was 14% 12 and rate of complications including arterial puncture remained. 7 Real-time needle ultrasound guidance may have avoided some of these complications. Real-time Ultrasound-guidance Over a decade ago, axillary vein cannulation under continuous ultrasound guidance was first described in a series of five patients. 9 In this technique, the patient s arm is abducted 90 and a 4 to 7 MHz Sonosite 180 C 11 probe (Sonosite, Bothell, WA) is used to distinguish the axillary vein from the artery in the short-axis view. The axillary vein is centered in the ultrasound view and the probe is rotated 90. With the axillary vein viewed in long-axis, the needle is positioned under the middle of the probe so as to view the needle in-plane (Fig. 1). Care should be taken to select a vein puncture site a few inches lateral to the rib cage to minimize the risk of pneumothorax. The introducer needle is advanced with care taken to avoid the axillary artery and the surrounding nerves. Once the needle contacts the anterior surface of the vein, a short, jabbing motion is used to puncture the anterior vein wall (Fig. 2). After venous puncture is confirmed, the catheter is then inserted using the standard Seldinger technique. It is noted that the needle should enter the vein at an acute angle to minimize the risk of a soft catheter kinking once the dilator is removed. This technique was successful in all five patients with no adverse effects. It was suggested that this technique and real-time imaging might offer several advantages Fig. 2: In-plane technique: Ultrasound image with a curvilinear probe. The arrows point to needle. The needle tip has just made contact with anterior wall of vein (Pec maj: Pectoralis major muscle; Pec min: Pectoralis minor muscle; AV: Axillary vein). A venous valve is seen just lateral to 2nd rib. Guide wire tip may monitored across the venous valves when they are visible or resistance to guide wire advance is encountered over traditional techniques including decreasing the rate of arterial puncture and aiding in troubleshooting potential difficulties with catheter placement. For example, if excessive resistance is met with guidewire advancement, real-time ultrasound imaging can be used to identify wire malposition in the pectoral muscles or wire coiling at a venous valve. The longitudinal view of the vein allows for continuous imaging of the needle and lines during all maneuvers. Shortly thereafter, Sharma et al described another ultrasound-guided technique for axillary vein cannulation in a prospective series of 200 patients. 10 Patients were positioned in 15 of Trendelenburg with their arms at their sides. The axillary vein was visualized in all patients with either a Site Rite 7.5 MHz probe (Dymax/ Bard, Pittsburgh, PA, USA) or a SonoSite ilook with a 5/10 MHz probe (SonoSite, Biggleswade, UK). The vein and artery were imaged in short-axis with the chest wall visible. Unlike the original technique, the introducer needle was advanced at a steep angle out-of-plane (Fig. 3). The needle was visualized as a moving hyperechoic spot associated with tissue distortion. Gentle movements were used to identify the needle tip position. The needle was advanced into the vein or, if the needle had also penetrated the posterior wall, was withdrawn until blood could be aspirated freely. A guidewire was threaded and a catheter was tunneled subcutaneously from an exit site on the anterior chest wall to the puncture site. Of the 200 patients enrolled, four patients were deemed unsuitable for axillary vein cannulation secondary to narrow or thrombosed axillary veins. Catheterization was successful in 194 patients and on the first, second, and Journal of Perioperative Echocardiography, July-December 2015;3(2):
3 Bahareh Khatibi, Nav Parkash Sandhu Fig. 3: Out-of-plane technique: The position of transducer in relation to needle (C: Clavicle; SVC: Superior vena cava) third needle pass in 76, 16, and 6% of cases respectively. Complications included arterial puncture in three (1.5%) patients, which was treated with 5 minutes of manual compression as well as transient neuralgia during guidewire or dilator insertion in two (1%) patients. This out-of-plane technique with real-time ultrasound guidance for vessel puncture resulted in successful axillary vein cannulation in 96% of patients. Through and through puncture of the vein was known to have occurred in 54 (28%) cases. This is likely attributable to the out-of-plane needle imaging that was employed in this technique. With the out-of-plane technique, it may be difficult to confirm that the tip of the needle is being visualized and the authors relied distortion of tissue to help localize the needle advancement. The out-of-plane technique may have also attributed to the 5.4% of cases in which the needle was inadvertently advanced even more posteriorly and contacted the rib cage. Even though there were no cases of pneumothorax, lung injury does appear possible with this technique. This may be because the chest wall was visible in the ultrasound view in which venous puncture was attempted. A more lateral crosssection would have allowed the anterior chest wall to move more posteriorly, and perhaps, completely out of view. Finally, ultrasound was only used until aspiration of blood was confirmed. The authors note that the rate of arterial puncture and transient neuralgia might have been decreased with the use of dynamic ultrasound guidance during the rest of the procedure. Clinical Use Since the description of these two techniques, real-time ultrasound-guided axillary vein cannulation has been described in a wide range of patients The first reported case in which this technique was reproduced was in an emergency department patient who had septic shock and dementia. 11 The patient had difficulty remaining stationary for a traditional central venous cannulation. To minimize the risk of injury to structures in the thorax and neck, the authors chose to approach central venous access via the more distal axillary vein. The arm was abducted 120 and secured with a soft restraint. The axillary vein and artery were visualized in the axilla with a high frequency linear ultrasound probe. An 18-gauge catheter was inserted in the skin 2 centimeters distal to this site. After presence of venous blood was confirmed, a triplelumen catheter was threaded using Seldinger technique. Radiography confirmed that the tip of the catheter was in the superior vena cava. The authors also describe having used this approach in patients with severe coagulopathy to allow for central venous access through a compressible peripheral site. The authors did not specify whether the procedure was performed with the axillary vein viewed in short-axis or long-axis. Real-time ultrasound-guided axillary vein catheterization was also described in a retrospective review of six neurosurgical intensive care patients. 12 The authors stated that the axillary vessel anatomy was confirmed using combined transverse, longitudinal, and Doppler color flow images, but that the procedure itself was performed using the in-plane technique, presumably with a longitudinal view of the axillary vein. The catheter was inserted using the Seldinger technique and chest radiograph was obtained after the procedure. Five of the six central lines were inserted easily without complication. One central line was inserted without complications but more proximally because of difficulty in visualizing the axillary vein secondary to the patient s morbid obesity and severe hypovolemia. The authors noted that the technique of real-time ultrasound-guided axillary vein cannulation requires minimal additional training and is reasonable option for many critically ill patients in whom other central venous catheter approaches may not be ideal. Large-scale clinical studies on have also been conducted based on the real-time ultrasound-based technique. In a prospective study of mechanically ventilated intensive care patients, 13 the placement of ultrasoundguided axillary catheters was evaluated. All catheters were inserted using real-time ultrasound guidance with an out-of-plane technique. One hundred and twenty-five consecutive procedures occurred in 119 patients. Successful line placement was achieved in 94% of procedures. Complications consisted of one arterial puncture and four procedures that required repeating due to catheter malposition. The authors concluded that the technique of ultrasound-guided axillary vein cannulation could be undertaken successfully in ventilated intensive care 44
4 patients, even in challenging circumstances. Given the utility and safety of this technique, they suggested that it be adopted more widely in the intensive care population. In a large analysis of ultrasound-guided tunneled axillary vein catheterizations, 14 cannulation was successful in 99.5% of 1923 patients. The vein and the axillary artery were first imaged in short axis to determine the depth from the skin. The probe was then rotated to perform a long-axis examination to identify other structures, such as branches of the axillary artery, which can cross the axillary vein. The probe was then returned to the shortaxis and the introducer needle was advanced out-of-plane at a steep angle toward the vein until the tip was seen to indent the vein wall. Vein puncture was identified by free aspiration of nonpulsatile blood. Guidewire was seen by fluoroscopy to ensure that the tip was in a satisfactory position in the superior vena cava or right atrium. Cannulation was successful on the first attempt in 94% of patients. The authors reported that patients undergoing axillary vein cannulation demonstrated a low rate of complications. Arterial puncture occurred in eight cases (0.004%), one in which a 6.6 French sheath was inserted then withdrawn immediately. The superior vena cava was punctured by the guidewire in one patient and was identified by fluoroscopy, however, there were no issues after guidewire removal. Additionally, the authors noted four cases of pneumothorax and one case in which a pre-existing pleural effusion was aspirated. These specific complications may have resulted from utilizing the technique of directing the needle steeply in short-axis in which the needle itself is not seen at all times. Given the high success rate and low complication rate, the authors concluded that the axillary vein route of access appears to be a safe and effective alternative to the internal jugular vein. Procedural Factors The clinical descriptions of real-time ultrasound-guided axillary vein cannulation differ in regards to several factors, including needle visualization (in-plane vs out-ofplane technique) and arm position (abducted or neutral). In terms of needle visualization, both techniques have been endorsed clinically, one study 15 sought to determine whether the longitudinal (in-plane) or transverse (outof-plane) view of the axillary vein during cannulation is advantageous. In this prospective study, 57 emergency medicine physicians were asked to cannulate the axillary vein in an anatomically correct torso phantom model using each technique. The investigators compared the two techniques in regard to the rate of successful cannulations on first skin puncture, the number of needle redirections, the number of complications, and the time to successful cannulation. The investigators found that the longitudinal method of visualizing the axillary vein is associated with greater first-attempt success, fewer needle redirections, fewer skin punctures and a trend of fewer arterial punctures compared with the transverse orientation. For successful attempts, the time spent for the longitudinal method was less than for the transverse method. Although this was a single-center study, it is surprising to note that the physicians at this center historically favor and more often perform a transverse approach to central venous access. Another study 16 investigated the influence of arm position during proximal axillary vein cannulation on catheter placement and complications. Four hundred and eighty-one patients undergoing real-time ultrasoundguided infraclavicular proximal axillary cannulation were randomized to either the neutral group (n = 240) or the 90 abduction group (n = 241). After cannulation was performed, misplacement of the catheter and complications were evaluated with ultrasound and chest radiography. The success rate of catheterization before evaluation with ultrasound or radiography was high in both groups and not statistically significant (97.1 vs 98.8%). The rate of arterial puncture was also not statistically different (1.7 vs 0%, p = 0.061). However, the incidence of catheter misplacement was higher in the neutral group than in the abduction group (3.9 vs 0.4%, p = 0.01). Most of the misplaced catheters were located in the right internal jugular vein. Only one catheter was located in the left subclavian vein, which occurred in the neutral group. The investigators concluded that 90 arm abduction might minimize the risk of misplacement of the catheter during real-time ultrasound-guided proximal axillary vein cannulation. Long-term Safety Studies of the long-term safety of axillary vein cannulation have all been performed on the landmark-based technique and have found similar complication rates as with other central venous catheterization. A prospective study 19 of 141 axillary vein catheters found that catheter-related infection was similar to that observed after internal jugular vein catheterization. When performed in critically ill patients, the chance of developing catheter-related sepsis was less than 10% with either route. A prospective study 20 of 60 patients found that axillary vein cannulation was associated with an 11.6% rate of upper-extremity deep vein thrombosis. This rate of thrombosis is similar to that observed after subclavian or internal jugular vein catheterization. Because, thrombosis is rare or absent in catheterizations lasting less than 15 days, the authors Journal of Perioperative Echocardiography, July-December 2015;3(2):
5 Bahareh Khatibi, Nav Parkash Sandhu suggest that axillary catheters should be withdrawn after a maximum of 2 weeks. Emerging Uses Ultrasound-guided axillary vein access has been described for use outside the realm of traditional vascular cannulation. It has been used in placing totally implantable venous access devices, 21 venous access for permanent pacemakers and defibrillators 22 and cannulation for renal replacement therapy in the critical care unit. 23 Authors of these descriptions cite several potential advantages of ultrasound-guided axillary vein techniques. For example, when used for permanent pacemaker or implantable cardioverter defibrillator placement, the ultrasound-guided axillary vein approach may be a favorable site when compared with the classical subclavian approach. It may reduce the rate of complications from venous access and device implantation as well as reduce the incidence of lead crush and the risk of damage to chronic leads when upgrading devices. In a study of 26 patients requiring pacemakers or defibrillators in which ultrasound-guided axillary approach was used, 22 there were no instances of lead failure or lead damage. The authors also noted that there was no difficulty in advancing the guidewire and 7F sheath attributable to the relatively steeper angle of entry of the needle into the vein. The authors concluded that ultrasound guidance provides a safe and rapid technique for axillary vein lead placement. Summary Since real-time ultrasound-guided axillary vein cannulation was first described, it has been used in a wide range of patients. It has been shown to be safe, require minimal training, and have low rates of complications. Compared to subclavian vein cannulation, it has a decreased risk of pneumothorax or hemothorax. Long-term studies on axillary vein cannulation show comparable rates of infection and deep vein thrombosis to internal jugular catheterization. The in-plane ultrasound technique, in which the axillary vein is seen longitudinally and the needle is completely visualized, may potentially be superior to the out-of plane technique. Although the rate of pneumothorax using the out-of-plane technique is extremely low, there have been no reports of pneumothorax with the in-plane technique. In a center where the physicians typically favor an out-of-plane view when performing central venous access, the in-plane technique to axillary vein cannulation was found to be preferable in terms of rate of success and a trend toward fewer complications. Large-scale studies of the in-plane technique in the clinical setting would need to be performed to confirm whether the in-plane technique would result in more successful placement or decreased complications. Real-time ultrasound-guided axillary vein cannulation has been shown to be safe and effective in a diverse patient population, including those that are critically ill. More recently, this technique has been used for more than simple cannulation, including placement of totally implantable venous access devices, venous access for permanent pacemakers and defibrillators and cannulation for renal replacement therapy. References 1. Mansfield PF, Hohn DC, Fornage BD, et al. Complications and failures of subclavian vein catheterization. N Engl J Med 1994;331(26): Spracklen FHN, Niesche F, Lord PW, Betterman EMM. Percutaneous catheterization of axillary vein. Cardiovasc Res 1967;1(3): Ayiem EN. Percutaneous catheterization of axillary and proximal basilic vein. Anaesthesia 1977;32(8): Gouin F, Martin C, Saux P. Central venous and pulmonary artery catheterization via axillary vein. Acta Anaesthesiol Scand 1985;29(s81): Nickalls RWD. A new percutaneous infraclavicular approach to axillary vein. Anaesthesia 1987;42(2): Taylor BL, Yellowlees I. Central venous cannulation using infraclavicular axillary vein. Anesthesiology 1990;72(1): Schregel W, Höer H, Radtke J, Cunitz G. Ultrasonic guided cannulation of the axillary vein in intensive care patients. Anaesthesist 1994;43(10): Galloway S, Bodenham A. Ultrasound imaging of the axillary vein: anatomical basis for central venous access. Br J Anaesth 2003;90(5): Sandhu NS. Transpectoral ultrasound-guided catheterization of the axillary vein: an alternative to standard catheterization of the subclavian vein. Anesth Analg 2004;99(1): Sharma A, Bodenham AR, Mallick A. Ultrasound-guided infraclavicular axillary vein cannulation for central venous access. Br J Anaesth 2004;93(2): Bentley SK, Seethala R, Weingart SD. Ultrasound-guided axillary vein approach to the subclavian vein for central venous access. Ann Emerg Med 2008;52(4): Uhlenkott MC, Sathishkumar S, Murray WB, McQuillan PM, Das Adhikary S. Real-time multimodal axillary vein imaging enhances the safety and efficacy of axillary vein catheterization in neurosurgical intensive care patients. J Neurosurg Anesthesiol 2013;25(1): Glen H, Lang I, Christie L. Infraclavicular axillary vein cannulation using ultrasound in a mechanically ventilated general intensive care population. Anaesth Intensive Care 2015;43(5): O Leary R, Ahmed SM, McLure H, Oram J, Mallick A, Bhambra B, Bodenham AR. Ultrasound-guided infraclavicular axillary vein cannulation: a useful alternative to the internal jugular vein. Br J Anaesth 2012;109(5): Sommerkamp SK, Romaniuk VM, Witting MD, Ford DR, Allison MG, Euerle BD. A comparison of longitudinal and transverse approaches to ultrasound-guided axillary vein cannulation. Am J Emerg Med 2013;31(3):
6 16. Ahn JH, Kim IS, Shin KM, Kang SS, Hong SJ, Park JH, Kim HJ, Lee SH, Kim DY, Jung JH. Influence of arm position on catheter placement during real-time ultrasound-guided right infraclavicular proximal axillary venous catheterization. Br J Anaesth 2015 Oct Denys BG, Uretsky BF, Reddy PS. Ultrasound assisted cannulation of the internal jugular vein: a prospective comparison to the external landmark-guided technique. Circulation 1993;87(5): Kwon TH, Kim YL, Cho DK. Ultrasound-guided cannulation of the femoral vein for acute haemodialysis access. Nephrol Dial Transplant 1997;12(5): Martin C, Bruder N, Papazian L, Saux P, Gouin F. Catheterrelated infections following axillary vein caheterization. Acta Anaesthesiol Scand 1998;42(1): Martin C, Viviand X, Saux P, Gouin F. Upper-extremity deep vein thrombosis after central venous catheterization via the axillary vein. Crit Care Med 1999 Dec;27(12): Lin CP, Wang YC, Lin FS, Huang CH, Sun WZ. Ultrasoundassisted percutaneous catheterization of the axillary vein for totally implantable venous access device. Eur J Surg Oncol 2011;37(5): Seto AH, Jolly A, Salcedo J. Ultrasound-guided venous access for pacemakers and defibrillators. J Cardiovasc Electrophysiol 2013;24(3): Czarnik T, Gawda R, Nowotarski J. Real-time, ultrasoundguided infraclavicular axillary vein cannulation for renal replacement therapy in the critical care unit: a prospective intervention study. J Crit Care 2015;30(3): Journal of Perioperative Echocardiography, July-December 2015;3(2):
Ultrasound-guided infraclavicular axillary vein cannulation for central venous access {
 British Journal of Anaesthesia 93 (2): 188 92 DOI: 10.1093/bja/aeh187 Advance Access publication June 25, 2004 Ultrasound-guided infraclavicular axillary vein cannulation for central venous access { A.
British Journal of Anaesthesia 93 (2): 188 92 DOI: 10.1093/bja/aeh187 Advance Access publication June 25, 2004 Ultrasound-guided infraclavicular axillary vein cannulation for central venous access { A.
Background & Indications Probe Selection
 Teresa S. Wu, MD, FACEP Director, EM Ultrasound Program & Fellowship Co-Director, Simulation Based Training Program & Fellowship Associate Program Director, EM Residency Program Maricopa Medical Center
Teresa S. Wu, MD, FACEP Director, EM Ultrasound Program & Fellowship Co-Director, Simulation Based Training Program & Fellowship Associate Program Director, EM Residency Program Maricopa Medical Center
Dr. prakruthi Dept. of anaesthesiology, Rrmch, bangalore
 CENTRAL VENOUS CATHETERIZATION Dr. prakruthi Dept. of anaesthesiology, Rrmch, bangalore OBJECTIVES Introduction Indications and Contraindications Complications Technique Basic principles Specifics by Site
CENTRAL VENOUS CATHETERIZATION Dr. prakruthi Dept. of anaesthesiology, Rrmch, bangalore OBJECTIVES Introduction Indications and Contraindications Complications Technique Basic principles Specifics by Site
Ultrasound Guidance Needle Techniques
 Ultrasound Guidance Needle Techniques Dr TANG Ho-ming AED/UCH USG Guidance Needle Techniques Commonly used in EM 1. Vessel cannulation-peripheral & central 2. Foreign body removal 3. Peripheral nerve/plexus
Ultrasound Guidance Needle Techniques Dr TANG Ho-ming AED/UCH USG Guidance Needle Techniques Commonly used in EM 1. Vessel cannulation-peripheral & central 2. Foreign body removal 3. Peripheral nerve/plexus
Ultrasound Guided Vascular Access. 7/25/2016
 Ultrasound Guided Vascular Access 7/25/2016 www.ezono.com 1 Objectives Indications for insertion of central and peripheral lines Complications associated with procedures Role of ultrasound in vascular
Ultrasound Guided Vascular Access 7/25/2016 www.ezono.com 1 Objectives Indications for insertion of central and peripheral lines Complications associated with procedures Role of ultrasound in vascular
Needle tip visualization during ultrasound-guided vascular access: short-axis vs long-axis approach
 American Journal of Emergency Medicine (2010) 28, 343 347 www.elsevier.com/locate/ajem Brief Report Needle tip visualization during ultrasound-guided vascular access: short-axis vs long-axis approach Michael
American Journal of Emergency Medicine (2010) 28, 343 347 www.elsevier.com/locate/ajem Brief Report Needle tip visualization during ultrasound-guided vascular access: short-axis vs long-axis approach Michael
Peel-Apart Percutaneous Introducer Kits for
 Bard Access Systems Peel-Apart Percutaneous Introducer Kits for Table of Contents Contents Page Bard Implanted Ports Hickman*, Leonard*, Broviac*, Tenckhoff*, and Groshong* Catheters Introduction....................................
Bard Access Systems Peel-Apart Percutaneous Introducer Kits for Table of Contents Contents Page Bard Implanted Ports Hickman*, Leonard*, Broviac*, Tenckhoff*, and Groshong* Catheters Introduction....................................
Troubleshooting Technique for Hemodialysis Catheter Insertion
 Troubleshooting Technique for Hemodialysis Catheter Insertion Withoon Ungkitphaiboon Assistant Professor, Department of Surgery, Maha Chakri Sirindhorn Medical Center Srinakharinwirot University Present
Troubleshooting Technique for Hemodialysis Catheter Insertion Withoon Ungkitphaiboon Assistant Professor, Department of Surgery, Maha Chakri Sirindhorn Medical Center Srinakharinwirot University Present
Lines and tubes. 1 Nasogastric tubes Endotracheal tubes Central lines Permanent pacemakers Chest drains...
 Lines and tubes 1 Nasogastric tubes... 15 2 Endotracheal tubes.... 19 3 Central lines... 21 4 Permanent pacemakers.... 25 5 Chest drains... 30 This page intentionally left blank 1 Nasogastric tubes Background
Lines and tubes 1 Nasogastric tubes... 15 2 Endotracheal tubes.... 19 3 Central lines... 21 4 Permanent pacemakers.... 25 5 Chest drains... 30 This page intentionally left blank 1 Nasogastric tubes Background
Research Article Can we predict the Position of Central Venous Catheter Tip Following Cannulation of Internal Jugular Vein?
 Cronicon OPEN ACCESS ANAESTHESIA Research Article Can we predict the Position of Central Venous Catheter Tip Following Cannulation of Internal Jugular Vein? Pradeep Marur Venkategowda 1, Surath Manimala
Cronicon OPEN ACCESS ANAESTHESIA Research Article Can we predict the Position of Central Venous Catheter Tip Following Cannulation of Internal Jugular Vein? Pradeep Marur Venkategowda 1, Surath Manimala
CATHETER MALPOSITION FOLLOWING SUPRACLAVICULAR APPROACH FOR SUBCLAVIAN VEIN CATHETERISATION
 CATHETER MALPOSITION FOLLOWING SUPRACLAVICULAR APPROACH FOR SUBCLAVIAN VEIN CATHETERISATION - Case Reports - Prem K Singh *, Zulfiquar Ali *, Girija P Rath ** and Hemanshu Prabhakar *** Abstract The supraclavicular
CATHETER MALPOSITION FOLLOWING SUPRACLAVICULAR APPROACH FOR SUBCLAVIAN VEIN CATHETERISATION - Case Reports - Prem K Singh *, Zulfiquar Ali *, Girija P Rath ** and Hemanshu Prabhakar *** Abstract The supraclavicular
Brachial plexus blockade within the interscalene groove involves local anesthetic
 Interscalene Brachial Plexus Block- How I do it. Part 1 of a 2 part discussion on technique. Stuart Grant Professor of Anesthesiology Duke University Medical Center Durham NC Brachial plexus blockade within
Interscalene Brachial Plexus Block- How I do it. Part 1 of a 2 part discussion on technique. Stuart Grant Professor of Anesthesiology Duke University Medical Center Durham NC Brachial plexus blockade within
Ultrasound (US) assistance for Central Venous Catheterization (CVC) and Peripherally Inserted Central Catheters (PICC)
 Ultrasound (US) assistance for Central Venous Catheterization (CVC) and Peripherally Inserted Central Catheters (PICC) Education - Training plan for Critical Care Nurses Pre-reading Objectives Comprehensive
Ultrasound (US) assistance for Central Venous Catheterization (CVC) and Peripherally Inserted Central Catheters (PICC) Education - Training plan for Critical Care Nurses Pre-reading Objectives Comprehensive
Ultrasound-Guided Infraclavicular Axillary Vein Cannulation
 International Journal of Clinical Medicine, 2017, 8, 227-235 http://www.scirp.org/journal/ijcm ISSN Online: 2158-2882 ISSN Print: 2158-284X Ultrasound-Guided Infraclavicular Axillary Vein Cannulation Miguel
International Journal of Clinical Medicine, 2017, 8, 227-235 http://www.scirp.org/journal/ijcm ISSN Online: 2158-2882 ISSN Print: 2158-284X Ultrasound-Guided Infraclavicular Axillary Vein Cannulation Miguel
Upper Extremity Venous Duplex. Michigan Sonographers Society Fall Ultrasound Symposium October 15, 2016
 Upper Extremity Venous Duplex Michigan Sonographers Society Fall Ultrasound Symposium October 15, 2016 Patricia A. (Tish) Poe, BA RVT FSVU Director of Quality Assurance Navix Diagnostix Patricia A. Poe
Upper Extremity Venous Duplex Michigan Sonographers Society Fall Ultrasound Symposium October 15, 2016 Patricia A. (Tish) Poe, BA RVT FSVU Director of Quality Assurance Navix Diagnostix Patricia A. Poe
Advocate Christ Medical Center CVC Placement Certification Course
 Advocate Christ Medical Center CVC Placement Certification Course July 12th, 2012 Hannah Watts, MD Medical Simulation Director Modified August 10, 2017 Taajwar Khan, MD Chief Resident of Internal Medicine
Advocate Christ Medical Center CVC Placement Certification Course July 12th, 2012 Hannah Watts, MD Medical Simulation Director Modified August 10, 2017 Taajwar Khan, MD Chief Resident of Internal Medicine
AIUM Practice Parameter for the Use of Ultrasound to Guide Vascular Access Procedures
 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 37 38 39 40 AIUM Practice Parameter for the Use of Ultrasound to Guide Vascular Access Procedures Parameter
1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 37 38 39 40 AIUM Practice Parameter for the Use of Ultrasound to Guide Vascular Access Procedures Parameter
INTRODUCTION. Getting the best scan. Choosing a probe. Choosing the frequency
 Getting the best scan Choosing a probe Select the most appropriate probe for the particular scan required. s vary in their: operating frequency range higher ultrasound frequencies provide better discrimination
Getting the best scan Choosing a probe Select the most appropriate probe for the particular scan required. s vary in their: operating frequency range higher ultrasound frequencies provide better discrimination
Certificate in Clinician Performed Ultrasound (CCPU) Syllabus. Vascular Access (venous (peripheral and central) and arterial)
 Certificate in Clinician Performed Ultrasound (CCPU) Syllabus Vascular Access (venous (peripheral and central) and arterial) Page 1 of 8 04/16 Vascular Access (venous (peripheral and central) and arterial)
Certificate in Clinician Performed Ultrasound (CCPU) Syllabus Vascular Access (venous (peripheral and central) and arterial) Page 1 of 8 04/16 Vascular Access (venous (peripheral and central) and arterial)
Influence of arm position during infraclavicular subclavian vein catheterization in coronary artery bypass graft surgery
 doi: 10.15171/jcvtr.2018.33 http://jcvtr.tbzmed.ac.ir TUOMS Publishing Group Original Article Influence of arm position during infraclavicular subclavian vein catheterization in coronary artery bypass
doi: 10.15171/jcvtr.2018.33 http://jcvtr.tbzmed.ac.ir TUOMS Publishing Group Original Article Influence of arm position during infraclavicular subclavian vein catheterization in coronary artery bypass
Document No. BMB/IFU/40 Rev No. & Date 00 & 15/11/2017 Issue No & Date 01 & 15/11/2017
 Central Venous Catheter Device Description Multi-lumen catheters incorporate separate, non-communicating vascular access lumens within a single catheter body. Minipunctur Access Sets And Trays: Used for
Central Venous Catheter Device Description Multi-lumen catheters incorporate separate, non-communicating vascular access lumens within a single catheter body. Minipunctur Access Sets And Trays: Used for
Basics of US Regional Anaesthesia. November 2008
 Basics of US Regional Anaesthesia November 2008 Essential Physics HIGH frequency = great resolution but poor penetration LOW frequency = poor resolution but great penetration Potential Advantages of US
Basics of US Regional Anaesthesia November 2008 Essential Physics HIGH frequency = great resolution but poor penetration LOW frequency = poor resolution but great penetration Potential Advantages of US
10/14/2018 Dr. Shatarat
 2018 Objectives To discuss mediastina and its boundaries To discuss and explain the contents of the superior mediastinum To describe the great veins of the superior mediastinum To describe the Arch of
2018 Objectives To discuss mediastina and its boundaries To discuss and explain the contents of the superior mediastinum To describe the great veins of the superior mediastinum To describe the Arch of
Sterile Technique & IJ/Femoral Return Demonstration
 Sterile Technique & IJ/Femoral Return Demonstration Sterile Technique Description: This is a return demonstration checklist used to evaluate participants in the simulated hands on skills portions for certification
Sterile Technique & IJ/Femoral Return Demonstration Sterile Technique Description: This is a return demonstration checklist used to evaluate participants in the simulated hands on skills portions for certification
Over the Wire Technique vs. Modified Seldinger Technique in Insertion of PICC
 Over the Wire Technique vs. Modified Seldinger Technique in Insertion of PICC Deniz Kasikci Department of Radiology, Jena University Hospital Friedrich-Schiller-University, Jena, Germany Disclosure Speaker
Over the Wire Technique vs. Modified Seldinger Technique in Insertion of PICC Deniz Kasikci Department of Radiology, Jena University Hospital Friedrich-Schiller-University, Jena, Germany Disclosure Speaker
Case #1. Case #1- Possible codes. Unraveling the -59 modifier. Principles of Interventional. CASE 1: Simple angioplasty
 Unraveling the -59 modifier Principles of Interventional Coding Donald Schon, MD, FACP Debra Lawson, CPC, PCS Distinct or independent from other services performed on the same day Normally not reported
Unraveling the -59 modifier Principles of Interventional Coding Donald Schon, MD, FACP Debra Lawson, CPC, PCS Distinct or independent from other services performed on the same day Normally not reported
Girish M Nair, Seeger Shen, Pablo B Nery, Calum J Redpath, David H Birnie
 268 Case Report Cardiac Resynchronization Therapy in a Patient with Persistent Left Superior Vena Cava Draining into the Coronary Sinus and Absent Innominate Vein: A Case Report and Review of Literature
268 Case Report Cardiac Resynchronization Therapy in a Patient with Persistent Left Superior Vena Cava Draining into the Coronary Sinus and Absent Innominate Vein: A Case Report and Review of Literature
Ultrasound Guided Peripheral Intravenous Access
 Ultrasound Guided Peripheral Intravenous Access J. Christian Fox, MD, RDMS, FACEP, FAAEM, FAIUM Professor and Interim Chair of Emergency Medicine Director of Instructional Ultrasound University of California,
Ultrasound Guided Peripheral Intravenous Access J. Christian Fox, MD, RDMS, FACEP, FAAEM, FAIUM Professor and Interim Chair of Emergency Medicine Director of Instructional Ultrasound University of California,
Background & Indications Probe Selection
 Teresa S. Wu, MD, FACEP Director, EM Ultrasound Program & Fellowship Co-Director, Simulation Based Training Program & Fellowship Associate Program Director, EM Residency Program Maricopa Medical Center
Teresa S. Wu, MD, FACEP Director, EM Ultrasound Program & Fellowship Co-Director, Simulation Based Training Program & Fellowship Associate Program Director, EM Residency Program Maricopa Medical Center
Central Venous Line Insertion
 Central Venous Line Insertion Understand the indications and risks of CVC insertion Understand and troubleshoot the seldinger technique Understand available sites and select the appropriate site for clinical
Central Venous Line Insertion Understand the indications and risks of CVC insertion Understand and troubleshoot the seldinger technique Understand available sites and select the appropriate site for clinical
Children s Acute Transport Service
 Children s Acute Transport Service Vascular Access Document Control Information Author Ramnarayan Author Position Consultant, CATS Document Owner Polke Document Owner Position CATS Co-ordinator Document
Children s Acute Transport Service Vascular Access Document Control Information Author Ramnarayan Author Position Consultant, CATS Document Owner Polke Document Owner Position CATS Co-ordinator Document
Mary Lou Garey MSN EMT-P MedFlight of Ohio
 Mary Lou Garey MSN EMT-P MedFlight of Ohio Function Prolonged and frequent access to venous circulation Allows for patient to carry on normal life; decrease number of needle sticks Medications, parenteral
Mary Lou Garey MSN EMT-P MedFlight of Ohio Function Prolonged and frequent access to venous circulation Allows for patient to carry on normal life; decrease number of needle sticks Medications, parenteral
Sample page. POWER UP YOUR CODING with Optum360, your trusted coding partner for 32 years. Visit optum360coding.com.
 2018 Complete Guide for Interventional Radiology An in-depth guide to interventional radiology coding, billing, and reimbursement for facilities and physicians POWER UP YOUR CODING with Optum360, your
2018 Complete Guide for Interventional Radiology An in-depth guide to interventional radiology coding, billing, and reimbursement for facilities and physicians POWER UP YOUR CODING with Optum360, your
Ultrasound-guided oblique approach for peripheral venous access in a phantom model
 Tassone et al. Critical Ultrasound Journal 2012, 4:14 ORIGINAL ARTICLE Open Access Ultrasound-guided oblique approach for peripheral venous access in a phantom model Heather M Tassone 1,2, Vivek S Tayal
Tassone et al. Critical Ultrasound Journal 2012, 4:14 ORIGINAL ARTICLE Open Access Ultrasound-guided oblique approach for peripheral venous access in a phantom model Heather M Tassone 1,2, Vivek S Tayal
Catheter Fracture of a Totally Implantable Venous Device Due to Pinch Off Syndrome in Breast Cancer: A Case Report
 Kosin Medical Journal 2016;31:167-172. https://doi.org/10.7180/kmj.2016.31.2.167 KMJ Case Report Catheter Fracture of a Totally Implantable Venous Device Due to Pinch Off Syndrome in Breast Cancer: A Case
Kosin Medical Journal 2016;31:167-172. https://doi.org/10.7180/kmj.2016.31.2.167 KMJ Case Report Catheter Fracture of a Totally Implantable Venous Device Due to Pinch Off Syndrome in Breast Cancer: A Case
Background: Bedside ultrasound is emerging as a useful tool in the assessment of
 Abstract: Background: Bedside ultrasound is emerging as a useful tool in the assessment of intravascular volume status by examining measurements of the inferior vena cava (IVC). Many previous studies do
Abstract: Background: Bedside ultrasound is emerging as a useful tool in the assessment of intravascular volume status by examining measurements of the inferior vena cava (IVC). Many previous studies do
PEMSS PROTOCOLS INVASIVE PROCEDURES
 PEMSS PROTOCOLS INVASIVE PROCEDURES Panhandle Emergency Medical Services System SURGICAL AND NEEDLE CRICOTHYROTOMY Inability to intubate is the primary indication for creating an artificial airway. Care
PEMSS PROTOCOLS INVASIVE PROCEDURES Panhandle Emergency Medical Services System SURGICAL AND NEEDLE CRICOTHYROTOMY Inability to intubate is the primary indication for creating an artificial airway. Care
Kristin Wise, MD, FHM Division of General Internal Medicine and Geriatrics Hospital Medicine 2013
 Kristin Wise, MD, FHM Division of General Internal Medicine and Geriatrics Hospital Medicine 2013 Objectives for CVC Placement Understand the indications and contraindications Determine appropriate CVC
Kristin Wise, MD, FHM Division of General Internal Medicine and Geriatrics Hospital Medicine 2013 Objectives for CVC Placement Understand the indications and contraindications Determine appropriate CVC
A novel suture-traction method for right internal jugular vein catheterization in left-lateral position in anesthetized patients.
 Biomedical Research 2017; 28 (12): 5628-5632 ISSN 0970-938X www.biomedres.info A novel suture-traction method for right internal jugular vein catheterization in left-lateral position in anesthetized patients.
Biomedical Research 2017; 28 (12): 5628-5632 ISSN 0970-938X www.biomedres.info A novel suture-traction method for right internal jugular vein catheterization in left-lateral position in anesthetized patients.
MODULE 9 ARTERIAL AND VENOUS CATHETERIZATION. Robert B. McLafferty M.D. Southern Illinois University
 MODULE 9 ARTERIAL AND VENOUS CATHETERIZATION Robert B. McLafferty M.D. Southern Illinois University I. OBJECTIVES By the end of this laboratory session the residents should be able to A. Identify the anatomic
MODULE 9 ARTERIAL AND VENOUS CATHETERIZATION Robert B. McLafferty M.D. Southern Illinois University I. OBJECTIVES By the end of this laboratory session the residents should be able to A. Identify the anatomic
Jake Hutchins, M.D. Aaron Berg, D.O.
 Jake Hutchins, M.D. Aaron Berg, D.O. Jacob Hutchins is on the speaker s bureau, is a consultant, and has received research funding from Pacira Pharmaceuticals He also is a consultant for Insitu Biologics,
Jake Hutchins, M.D. Aaron Berg, D.O. Jacob Hutchins is on the speaker s bureau, is a consultant, and has received research funding from Pacira Pharmaceuticals He also is a consultant for Insitu Biologics,
Perioperative Ultrasonography Ehab Farag, MD, FRCA Hesham Elsharkawy David G. Anthony, M.D.
 Perioperative Ultrasonography Ehab Farag, MD, FRCA Hesham Elsharkawy David G. Anthony, M.D. Cleveland Clinic, Cleveland OH 1 Complications during central venous catheterization (CVC) occur 2% -15% of the
Perioperative Ultrasonography Ehab Farag, MD, FRCA Hesham Elsharkawy David G. Anthony, M.D. Cleveland Clinic, Cleveland OH 1 Complications during central venous catheterization (CVC) occur 2% -15% of the
Radiology Department, Evangelismos University Hospital, Athens, Greece 2
 Hindawi Publishing Corporation Critical Care Research and Practice Volume 2012, Article ID 617149, 6 pages doi:10.1155/2012/617149 Research Article Optimization of Cannula Visibility during Ultrasound-Guided
Hindawi Publishing Corporation Critical Care Research and Practice Volume 2012, Article ID 617149, 6 pages doi:10.1155/2012/617149 Research Article Optimization of Cannula Visibility during Ultrasound-Guided
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
You have a what, inside you?
 Costal Emergency Medicine Conference You have a what, inside you? Less than mainstream medical devices encountered in the ED. Eric Ossmann, MD, FACEP Associate Professor Duke University Medical Center
Costal Emergency Medicine Conference You have a what, inside you? Less than mainstream medical devices encountered in the ED. Eric Ossmann, MD, FACEP Associate Professor Duke University Medical Center
You have a what, inside you?
 Costal Emergency Medicine Conference You have a what, inside you? Less than mainstream medical devices encountered in the ED. Eric Ossmann, MD, FACEP Associate Professor Duke University Medical Center
Costal Emergency Medicine Conference You have a what, inside you? Less than mainstream medical devices encountered in the ED. Eric Ossmann, MD, FACEP Associate Professor Duke University Medical Center
Surface Anatomy and Sonoanatomy for the Occasional Regional Anesthesiologist
 Surface Anatomy and Sonoanatomy for the Occasional Regional Anesthesiologist Edward R. Mariano, M.D., M.A.S. Professor of Anesthesiology, Perioperative & Pain Medicine Stanford University School of Medicine
Surface Anatomy and Sonoanatomy for the Occasional Regional Anesthesiologist Edward R. Mariano, M.D., M.A.S. Professor of Anesthesiology, Perioperative & Pain Medicine Stanford University School of Medicine
Veins that are firm to
 Intravenous cannulation is a technique in which a cannula is placed inside a vein to provide venous access. Venous access allows sampling of blood as well as administration of fluids, medications, parenteral
Intravenous cannulation is a technique in which a cannula is placed inside a vein to provide venous access. Venous access allows sampling of blood as well as administration of fluids, medications, parenteral
inerve Guide to Nerves 2009
 inerve Guide to Nerves 2009 A guide to self learning and self assessment Context: The following guide is intended to help interpret the sono-anatomy and follow a systematic stepwise approach to the practice
inerve Guide to Nerves 2009 A guide to self learning and self assessment Context: The following guide is intended to help interpret the sono-anatomy and follow a systematic stepwise approach to the practice
3 Mohammad Al-Mohtasib Areej Mosleh
 3 Mohammad Al-Mohtasib Areej Mosleh ***Muscles Connecting the Upper Limb to the Vertebral Column 1.Trapezius Muscle ***The first muscle on the back is trapezius muscle, it s called so according
3 Mohammad Al-Mohtasib Areej Mosleh ***Muscles Connecting the Upper Limb to the Vertebral Column 1.Trapezius Muscle ***The first muscle on the back is trapezius muscle, it s called so according
Large veins of the thorax Brachiocephalic veins
 Large veins of the thorax Brachiocephalic veins Right brachiocephalic vein: formed at the root of the neck by the union of the right subclavian & the right internal jugular veins. Left brachiocephalic
Large veins of the thorax Brachiocephalic veins Right brachiocephalic vein: formed at the root of the neck by the union of the right subclavian & the right internal jugular veins. Left brachiocephalic
Ultrasound Guidance for Common Procedures
 18-Levitov_CH18_p230-246.qxd 3/31/10 4:24 PM Page 230 CHAPTER 18 Ultrasound Guidance for Common Procedures Christian H. Butcher, MD, FCCP and Sameh Aziz, MD, FCCP, FACP INTRODUCTION The advent of high-quality,
18-Levitov_CH18_p230-246.qxd 3/31/10 4:24 PM Page 230 CHAPTER 18 Ultrasound Guidance for Common Procedures Christian H. Butcher, MD, FCCP and Sameh Aziz, MD, FCCP, FACP INTRODUCTION The advent of high-quality,
A Primer on Central Venous Access: Peripherally-Inserted Central Catheters, Tunneled Catheters, and Subcutaneous Ports
 Disclosures A Primer on Central Venous Access: Peripherally-Inserted Central Catheters, Tunneled Catheters, and Subcutaneous Ports No conflicts of interest relevant to this presentation Jason W. Pinchot,
Disclosures A Primer on Central Venous Access: Peripherally-Inserted Central Catheters, Tunneled Catheters, and Subcutaneous Ports No conflicts of interest relevant to this presentation Jason W. Pinchot,
Infraclavicular brachial plexus blocks aim at the
 REGIONAL ANESTHESIA AND PAIN MEDICINE SECTION EDITOR DENISE J. WEDEL A Magnetic Resonance Imaging Study of Modifications to the Infraclavicular Brachial Plexus Block Øivind Klaastad, MD*, Finn G. Lilleås,
REGIONAL ANESTHESIA AND PAIN MEDICINE SECTION EDITOR DENISE J. WEDEL A Magnetic Resonance Imaging Study of Modifications to the Infraclavicular Brachial Plexus Block Øivind Klaastad, MD*, Finn G. Lilleås,
RadRx Your Prescription for Accurate Coding & Reimbursement Copyright All Rights Reserved.
 Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of October 22, 2018 Paracentesis & Transjugular Liver Biopsy
Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of October 22, 2018 Paracentesis & Transjugular Liver Biopsy
Sectional Anatomy Quiz - III
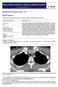 Sectional Anatomy - III Rashid Hashmi * Rural Clinical School, University of New South Wales (UNSW), Wagga Wagga, NSW, Australia A R T I C L E I N F O Article type: Article history: Received: 30 Jun 2018
Sectional Anatomy - III Rashid Hashmi * Rural Clinical School, University of New South Wales (UNSW), Wagga Wagga, NSW, Australia A R T I C L E I N F O Article type: Article history: Received: 30 Jun 2018
ANATOMICAL VARIATIONS OF THE INTERNAL JUGULAR VEIN IN RELATION TO COMMON CAROTID ARTERY IN LESSER SUPRA CLAVICULAR FOSSA A COLOUR DOPPLER STUDY
 Original Article ANATOMICAL VARIATIONS OF THE INTERNAL JUGULAR VEIN IN RELATION TO COMMON CAROTID ARTERY IN LESSER SUPRA CLAVICULAR FOSSA A COLOUR DOPPLER STUDY Shanta Chandrasekaran*, V.P.Chandrasekaran**
Original Article ANATOMICAL VARIATIONS OF THE INTERNAL JUGULAR VEIN IN RELATION TO COMMON CAROTID ARTERY IN LESSER SUPRA CLAVICULAR FOSSA A COLOUR DOPPLER STUDY Shanta Chandrasekaran*, V.P.Chandrasekaran**
Images in Medicine: Central Venous Misadventure
 Images in Medicine: Central Venous Misadventure Andrew Lui BSc 1, Steven M. Friedman MD MPH 2, Eran Hayeems MD 3 1 Medical Student, University of Toronto, Ontario, Canada 2 Assistant Professor, Faculty
Images in Medicine: Central Venous Misadventure Andrew Lui BSc 1, Steven M. Friedman MD MPH 2, Eran Hayeems MD 3 1 Medical Student, University of Toronto, Ontario, Canada 2 Assistant Professor, Faculty
Optimal Filter Placement
 Obtaining Optimal Filter Placement How imaging and technical skill ensure safe placement of an IVC filter. BY MARK W. BURKET, MD When compared to many other endovascular procedures, placement of an inferior
Obtaining Optimal Filter Placement How imaging and technical skill ensure safe placement of an IVC filter. BY MARK W. BURKET, MD When compared to many other endovascular procedures, placement of an inferior
Ultrasound Use in Anaesthesia
 Trainee Name: 1 Ultrasound Use in Anaesthesia Assessments to accompany Workbook for anaesthetic trainees in North Queensland 2010 Authors: Mark Fairley, Emile Kurukchi, Andrew Potter 2 Trainee Name: Ultrasound
Trainee Name: 1 Ultrasound Use in Anaesthesia Assessments to accompany Workbook for anaesthetic trainees in North Queensland 2010 Authors: Mark Fairley, Emile Kurukchi, Andrew Potter 2 Trainee Name: Ultrasound
SPECIAL ARTICLE January 2012 Volume 114 Number 1
 Guidelines for Performing Ultrasound Guided Vascular Cannulation: Recommendations of the American Society of Echocardiography and the Society of Cardiovascular Anesthesiologists Christopher A. Troianos,
Guidelines for Performing Ultrasound Guided Vascular Cannulation: Recommendations of the American Society of Echocardiography and the Society of Cardiovascular Anesthesiologists Christopher A. Troianos,
Arterial Access for Diagnosis and Intervention T-Woei Tan, MD, FACS
 Arterial Access for Diagnosis and Intervention T-Woei Tan, MD, FACS Assistant Professor of Surgery Vascular Endovascular Surgery Louisiana State University Health - Shreveport Disclosures None Objective
Arterial Access for Diagnosis and Intervention T-Woei Tan, MD, FACS Assistant Professor of Surgery Vascular Endovascular Surgery Louisiana State University Health - Shreveport Disclosures None Objective
Intro: Slide 1. Slide 2. Slide 3. Basic understanding of interventional radiology. Gain knowledge of key terms and phrases
 Slide 1 Intro: PRESENTED BY: Selena M. Moore, AAS, CCS, CPC HIMS Physician Liaison Coder This is a modified/updated presentation that was originally written by: Rosemary Waligorski, RHIT, CCS, RCC and
Slide 1 Intro: PRESENTED BY: Selena M. Moore, AAS, CCS, CPC HIMS Physician Liaison Coder This is a modified/updated presentation that was originally written by: Rosemary Waligorski, RHIT, CCS, RCC and
Candidate s instructions Look at this cross-section taken at the level of C5. Answer the following questions.
 Section 1 Anatomy Chapter 1. Trachea 1 Candidate s instructions Look at this cross-section taken at the level of C5. Answer the following questions. Pretracheal fascia 1 2 5 3 4 Questions 1. Label the
Section 1 Anatomy Chapter 1. Trachea 1 Candidate s instructions Look at this cross-section taken at the level of C5. Answer the following questions. Pretracheal fascia 1 2 5 3 4 Questions 1. Label the
Ultrasound User Demonstration
 Ultrasound User Demonstration Disclaimer: This presentation is intended to be used as a demonstration educational device to showcase Terumo products. It is NOT intended to be used as a diagnostic device
Ultrasound User Demonstration Disclaimer: This presentation is intended to be used as a demonstration educational device to showcase Terumo products. It is NOT intended to be used as a diagnostic device
VENOUS DRAINAGE O US F UPPER UPPER LIM B BY dr.fahad Ullah
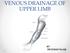 VENOUS DRAINAGE OF UPPER LIMB BY dr.fahad Ullah Venous drainage of the supper limb The venous system of the upper limb drains deoxygenated blood from the arm, forearm and hand It can anatomically be divided
VENOUS DRAINAGE OF UPPER LIMB BY dr.fahad Ullah Venous drainage of the supper limb The venous system of the upper limb drains deoxygenated blood from the arm, forearm and hand It can anatomically be divided
As with any intervention, selection of an appropriate
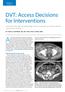 DVT: ccess Decisions for Interventions ssessing the advantages and disadvantages of venous access options is crucial for safe and successful DVT intervention. Y JOHN. KUFMN, MD, MS, FSIR, FH, FCIRSE, EIR
DVT: ccess Decisions for Interventions ssessing the advantages and disadvantages of venous access options is crucial for safe and successful DVT intervention. Y JOHN. KUFMN, MD, MS, FSIR, FH, FCIRSE, EIR
Establishing reliable vascular
 Randomized, controlled clinical trial of point-of-care limited ultrasonography assistance of central venous cannulation: The Third Sonography Outcomes Assessment Program (SOAP-3) Trial* Truman J. Milling,
Randomized, controlled clinical trial of point-of-care limited ultrasonography assistance of central venous cannulation: The Third Sonography Outcomes Assessment Program (SOAP-3) Trial* Truman J. Milling,
I Was Too Late With Device Placement
 SCAI SHOCK 2018 A Team-Based Course On Cardiogenic Shock General Session # 2 Saturday, October 13, 2018 8:39 8:51 AM Boston Park Plaza - Boston, MA I Was Too Late With Device Placement M Chadi Alraies,
SCAI SHOCK 2018 A Team-Based Course On Cardiogenic Shock General Session # 2 Saturday, October 13, 2018 8:39 8:51 AM Boston Park Plaza - Boston, MA I Was Too Late With Device Placement M Chadi Alraies,
Infraclavicular brachial plexus blocks have been designed
 The Supraclavicular Lateral Paravascular Approach for Brachial Plexus Regional Anesthesia: A Simulation Study Using Magnetic Resonance Imaging Øivind Klaastad, MD* and Örjan Smedby, Dr Med Sci *Department
The Supraclavicular Lateral Paravascular Approach for Brachial Plexus Regional Anesthesia: A Simulation Study Using Magnetic Resonance Imaging Øivind Klaastad, MD* and Örjan Smedby, Dr Med Sci *Department
Exceptional Performance and Ease of Placement
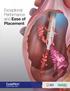 Exceptional Performance and Ease of Placement S IMU LATED FLO W PERFO RMANC E Higher Flow Rates Higher is Better GLIDEPATH catheters demonstrated on average in forward Precision catheters Lower Pressures
Exceptional Performance and Ease of Placement S IMU LATED FLO W PERFO RMANC E Higher Flow Rates Higher is Better GLIDEPATH catheters demonstrated on average in forward Precision catheters Lower Pressures
Three-step method for ultrasound-guided central vein catheterization
 British Journal of naesthesia Page 1 of 6 doi:10.1093/bja/aes381 Three-step method for ultrasound-guided central vein catheterization J. Tokumine 1 *,. T. Lefor 4,. Yonei 5,. Kagaya 2, K. Iwasaki 2 and
British Journal of naesthesia Page 1 of 6 doi:10.1093/bja/aes381 Three-step method for ultrasound-guided central vein catheterization J. Tokumine 1 *,. T. Lefor 4,. Yonei 5,. Kagaya 2, K. Iwasaki 2 and
Ultrasound Guidance versus the Landmark Technique for the Placement of Central Venous Catheters in the Emergency Department
 800 Miller et al. ULTRASOUND-GUIDED CENTRAL VENOUS ACCESS Ultrasound Guidance versus the Landmark Technique for the Placement of Central Venous Catheters in the Emergency Department Adam H. Miller, MD,
800 Miller et al. ULTRASOUND-GUIDED CENTRAL VENOUS ACCESS Ultrasound Guidance versus the Landmark Technique for the Placement of Central Venous Catheters in the Emergency Department Adam H. Miller, MD,
Stuck dialysis catheters. ANZSIN 2013 Michael Lam & Kendal Redmond
 Stuck dialysis catheters ANZSIN 2013 Michael Lam & Kendal Redmond NT 39 yr old CI Maori - ESKD 2 o to cortical necrosis HD August 2002 R IJ tunneled Tesio catheter Oct 2002 Failed L RC AVF Feb 2004 Failed
Stuck dialysis catheters ANZSIN 2013 Michael Lam & Kendal Redmond NT 39 yr old CI Maori - ESKD 2 o to cortical necrosis HD August 2002 R IJ tunneled Tesio catheter Oct 2002 Failed L RC AVF Feb 2004 Failed
Axilla and Brachial Region
 L 4 A B O R A T O R Y Axilla and Brachial Region BRACHIAL PLEXUS 5 Roots/Rami (ventral rami C5 T1) 3 Trunks Superior (C5, C6) Middle (C7) Inferior (C8, T1) 3 Cords Lateral Cord (Anterior Superior and Anterior
L 4 A B O R A T O R Y Axilla and Brachial Region BRACHIAL PLEXUS 5 Roots/Rami (ventral rami C5 T1) 3 Trunks Superior (C5, C6) Middle (C7) Inferior (C8, T1) 3 Cords Lateral Cord (Anterior Superior and Anterior
Safety of arteriovenous fistulae and grafts for continuous renal replacement therapy: The Michigan experience
 Hemodialysis International 2018; 22:50 55 Original Article Access Safety of arteriovenous fistulae and grafts for continuous renal replacement therapy: The Michigan experience Anas AL RIFAI, 1,2 Nidhi
Hemodialysis International 2018; 22:50 55 Original Article Access Safety of arteriovenous fistulae and grafts for continuous renal replacement therapy: The Michigan experience Anas AL RIFAI, 1,2 Nidhi
Intraosseous Vascular Access. Dr Merl & Dr Veera
 Intraosseous Vascular Access Dr Merl & Dr Veera INDICATIONS The EZ-IO can be used for adult and pediatric patients, Is indicated any time vascular access is difficult to obtain Can be in emergent, urgent,
Intraosseous Vascular Access Dr Merl & Dr Veera INDICATIONS The EZ-IO can be used for adult and pediatric patients, Is indicated any time vascular access is difficult to obtain Can be in emergent, urgent,
Saphenous Vein Autograft Replacement
 Saphenous Vein Autograft Replacement of Severe Segmental Coronary Artery Occlusion Operative Technique Rene G. Favaloro, M.D. D irect operation on the coronary artery has been performed in 180 patients
Saphenous Vein Autograft Replacement of Severe Segmental Coronary Artery Occlusion Operative Technique Rene G. Favaloro, M.D. D irect operation on the coronary artery has been performed in 180 patients
TUNNELLED PERIPHERALLY INSERTED CENTRAL CATHERER- HOW WE DO THEM
 TUNNELLED PERIPHERALLY INSERTED CENTRAL CATHERER- HOW WE DO THEM Vijaynanthan A 1, Nawawi O 1, Abdullah BJJ 1 1 Department of Biomedical Imaging, Faculty of Medicine, University of Malaya, 50603 Kuala
TUNNELLED PERIPHERALLY INSERTED CENTRAL CATHERER- HOW WE DO THEM Vijaynanthan A 1, Nawawi O 1, Abdullah BJJ 1 1 Department of Biomedical Imaging, Faculty of Medicine, University of Malaya, 50603 Kuala
How Safe Is the Ultrasonographically-Guided Peripheral Internal Jugular Line?
 GENERAL MEDICINE/BEST AVAILABLE EVIDENCE How Safe Is the Ultrasonographically-Guided Peripheral Internal Jugular Line? Michael Gottlieb, MD, RDMS*; Frances M. Russell, MD, RDMS *Corresponding Author. E-mail:
GENERAL MEDICINE/BEST AVAILABLE EVIDENCE How Safe Is the Ultrasonographically-Guided Peripheral Internal Jugular Line? Michael Gottlieb, MD, RDMS*; Frances M. Russell, MD, RDMS *Corresponding Author. E-mail:
Gateway to the upper limb. An area of transition between the neck and the arm.
 Gateway to the upper limb An area of transition between the neck and the arm. Pyramidal space inferior to shoulder @ junction of arm & thorax Distribution center for the neurovascular structures that serve
Gateway to the upper limb An area of transition between the neck and the arm. Pyramidal space inferior to shoulder @ junction of arm & thorax Distribution center for the neurovascular structures that serve
INDIANA HEALTH COVERAGE PROGRAMS
 INDIANA HEALTH COVERAGE PROGRAMS PROVIDER CODE TABLES Note: Due to possible changes in Indiana Health Coverage Programs (IHCP) policy or national coding updates, inclusion of a code on the code tables
INDIANA HEALTH COVERAGE PROGRAMS PROVIDER CODE TABLES Note: Due to possible changes in Indiana Health Coverage Programs (IHCP) policy or national coding updates, inclusion of a code on the code tables
Lecture 2: Clinical anatomy of thoracic cage and cavity II
 Lecture 2: Clinical anatomy of thoracic cage and cavity II Dr. Rehan Asad At the end of this session, the student should be able to: Identify and discuss clinical anatomy of mediastinum such as its deflection,
Lecture 2: Clinical anatomy of thoracic cage and cavity II Dr. Rehan Asad At the end of this session, the student should be able to: Identify and discuss clinical anatomy of mediastinum such as its deflection,
Dignity Dual Power Injectable Implantable Infusion Port INSTRUCTIONS FOR USE
 DESCRIPTION: Dignity Dual Power Injectable Implantable Infusion Port INSTRUCTIONS FOR USE The Dignity Dual power injectable implantable infusion port is an implantable access device designed to provide
DESCRIPTION: Dignity Dual Power Injectable Implantable Infusion Port INSTRUCTIONS FOR USE The Dignity Dual power injectable implantable infusion port is an implantable access device designed to provide
Safety and efficacy of the oblique-axis plane in ultrasound-guided internal jugular vein puncture: A meta-analysis
 Clinical Research Report Safety and efficacy of the oblique-axis plane in ultrasound-guided internal jugular vein puncture: A meta-analysis Journal of International Medical Research 2018, Vol. 46(7) 2587
Clinical Research Report Safety and efficacy of the oblique-axis plane in ultrasound-guided internal jugular vein puncture: A meta-analysis Journal of International Medical Research 2018, Vol. 46(7) 2587
ompanionport Speciality Medical Devices For The Veterinary Community Surgical Suggestions
 Speciality Medical Devices For The Veterinary Community suture holes Place the CompanionPort in the subcutaneous port pocket off to one side so that the septum of the port will not lie directly beneath
Speciality Medical Devices For The Veterinary Community suture holes Place the CompanionPort in the subcutaneous port pocket off to one side so that the septum of the port will not lie directly beneath
Central Line Care and Management
 Central Line Care and Management What is a Central Line/ CVAD? (central venous access device) A vascular infusion device that terminates at or close to the heart or in one of the great vessels (aorta,
Central Line Care and Management What is a Central Line/ CVAD? (central venous access device) A vascular infusion device that terminates at or close to the heart or in one of the great vessels (aorta,
Recanalization Techniques: Sharp Needle Recanalization. Recanalization Techniques: Sharp Needle Recanalization
 Recanalization of Occluded Central Veins When Conventional Methods Failed: Abigail Falk, MD, FSIR American Access Care New York, NY Conventional Methods of Recanalization Directional 0.035 and 0.018 Guidewires
Recanalization of Occluded Central Veins When Conventional Methods Failed: Abigail Falk, MD, FSIR American Access Care New York, NY Conventional Methods of Recanalization Directional 0.035 and 0.018 Guidewires
Appendix E: Overview of Vascular
 Appendix E: Overview of Vascular 56 Peripheral Short Catheter, less than 3 inches (7.5 cm) in length; over-the-needle catheter is most common. Inserted by percutaneous venipuncture, generally into a hand
Appendix E: Overview of Vascular 56 Peripheral Short Catheter, less than 3 inches (7.5 cm) in length; over-the-needle catheter is most common. Inserted by percutaneous venipuncture, generally into a hand
The University of Toledo Medical Center and its Medical Staff
 Name of Policy: Policy Number: Department: 3364-109-GEN-705 Infection Control Medical Staff Hospital Administration Approving Officer: Responsible Agent: Scope: Chair, Infection Control Committee Chief
Name of Policy: Policy Number: Department: 3364-109-GEN-705 Infection Control Medical Staff Hospital Administration Approving Officer: Responsible Agent: Scope: Chair, Infection Control Committee Chief
Ultrasound Guided Injections
 Ultrasound Guided Injection Technique More accurate injections Better Results! 1 Benefits: Increased Level of Certainty ie : really know how accurate PRP/Prolotherapy Avoid damage to articular cartilage
Ultrasound Guided Injection Technique More accurate injections Better Results! 1 Benefits: Increased Level of Certainty ie : really know how accurate PRP/Prolotherapy Avoid damage to articular cartilage
The Arm and Cubital Fossa
 The Arm and Cubital Fossa Dr. Andrew Gallagher School of Anatomical Sciences University of the Witwatersrand Introduction The ARM (BRACHIUM) is the most proximal segment of the upper limb musculoskeletal
The Arm and Cubital Fossa Dr. Andrew Gallagher School of Anatomical Sciences University of the Witwatersrand Introduction The ARM (BRACHIUM) is the most proximal segment of the upper limb musculoskeletal
Region of upper limb attachment to the trunk Proximal segment of limb overlaps parts of the trunk (thorax and back) and lower lateral neck.
 Region of upper limb attachment to the trunk Proximal segment of limb overlaps parts of the trunk (thorax and back) and lower lateral neck. includes Pectoral Scapular Deltoid regions of the upper limb
Region of upper limb attachment to the trunk Proximal segment of limb overlaps parts of the trunk (thorax and back) and lower lateral neck. includes Pectoral Scapular Deltoid regions of the upper limb
THE VESSELS OF BLOOD CIRCULATION
 THE VESSELS OF BLOOD CIRCULATION scientistcindy.com /the-vessels-of-blood-circulation.html NOTE: You should familiarize yourself with the anatomy of the heart and have a good understanding of the flow
THE VESSELS OF BLOOD CIRCULATION scientistcindy.com /the-vessels-of-blood-circulation.html NOTE: You should familiarize yourself with the anatomy of the heart and have a good understanding of the flow
Ahsan Mustafa, Khaja Ali Hassan and Syed Abdur Rahman. Department of Anaesthesiology, Deccan College of Medical Sciences, Hyderabad, India
 International Journal of Advances in Health Sciences (IJHS) ISSN 2349-7033 Vol-3, Issue-1, 2016, pp54-59 http://www.ijhsonline.com Research Article Comparison of the rate of success and incidence of complications
International Journal of Advances in Health Sciences (IJHS) ISSN 2349-7033 Vol-3, Issue-1, 2016, pp54-59 http://www.ijhsonline.com Research Article Comparison of the rate of success and incidence of complications
BEDSIDE ULTRASOUND BEDSIDE ULTRASOUND. Deep Vein Thrombosis. Probe used
 BEDSIDE ULTRASOUND Part 2 Diagnosis of deep vein thrombosis Kishore Kumar Pichamuthu, Professor, Department of Critical Care, CMC, Vellore Summary: Deep vein thrombosis (DVT) is a problem encountered in
BEDSIDE ULTRASOUND Part 2 Diagnosis of deep vein thrombosis Kishore Kumar Pichamuthu, Professor, Department of Critical Care, CMC, Vellore Summary: Deep vein thrombosis (DVT) is a problem encountered in
JKSS. Pinch-off syndrome INTRODUCTION CASE REPORTS
 CASE REPORT pissn 2233-7903 eissn 2093-0488 Journal of the Korean Surgical Society Pinch-off syndrome Jin-Beom Cho, Il-Young Park, Ki-Young Sung, Jong-Min Baek, Jun-Hyun Lee, Do-Sang Lee Department of
CASE REPORT pissn 2233-7903 eissn 2093-0488 Journal of the Korean Surgical Society Pinch-off syndrome Jin-Beom Cho, Il-Young Park, Ki-Young Sung, Jong-Min Baek, Jun-Hyun Lee, Do-Sang Lee Department of
The role of ultrasound duplex in endovenous procedures
 The role of ultrasound duplex in endovenous procedures Neophytos A. Zambas MD, PhD Vascular Surgeon Polyclinic Ygia, Limassol, Cyprus ΚΕΑΕΧ ΚΥΠΡΙΑΚΗ ΕΤΑΙΡΕΙΑ ΑΓΓΕΙΑΚΗΣ ΚΑΙ ΕΝΔΑΓΓΕΙΑΚΗΣ ΧΕΙΡΟΥΡΓΙΚΗΣ Pre
The role of ultrasound duplex in endovenous procedures Neophytos A. Zambas MD, PhD Vascular Surgeon Polyclinic Ygia, Limassol, Cyprus ΚΕΑΕΧ ΚΥΠΡΙΑΚΗ ΕΤΑΙΡΕΙΑ ΑΓΓΕΙΑΚΗΣ ΚΑΙ ΕΝΔΑΓΓΕΙΑΚΗΣ ΧΕΙΡΟΥΡΓΙΚΗΣ Pre
Central Venous Access Devices. Stephanie Cunningham Amy Waters
 Central Venous Access Devices Stephanie Cunningham Amy Waters 5 Must Know Facts About CVAD s 1) What are CVAD s? 2) What are CVAD s used for? 3) How are these devices put in? 4) What are the complications
Central Venous Access Devices Stephanie Cunningham Amy Waters 5 Must Know Facts About CVAD s 1) What are CVAD s? 2) What are CVAD s used for? 3) How are these devices put in? 4) What are the complications
