Clarifying Murky Waters: Head and Cervical Spine Injuries in Children
|
|
|
- Geoffrey Page
- 5 years ago
- Views:
Transcription
1 Clarifying Murky Waters: Head and Cervical Spine Injuries in Children Judith R. Klein, MD, FACEP Assistant Professor of Emergency Medicine UCSF-SFGH Emergency Services Case #1: Newborn Leo 2 month old dropped 4 feet onto sidewalk during removal from car seat Cried/fed since Physical exam: small frontal hematoma To image or not to image, that is the question 1 2 Ø Ø Objectives Whom to image? How to image? Skull films vs. CT Plain c-spine x-rays vs. CT Ø How to read those Rorschach tests called c- spine films? Ø Whom to admit? Ø How to manage injuries? Pediatric head trauma: what s the big deal? #1 cause of death age 1-14 years >7K deaths, 60K hospitalizations, >600K ED visits per year 3 to 6% incidence of TBI post minor head trauma Up to 20% of TBI pts < 2 years old asymptomatic! 3 4 1
2 Who gets imaged? GCS>14: To CT or not To CT?? 40-50% to ED get imaged!! Higher CT rates: white race older general vs pediatric hospital more emergent triage status attending treated Lifetime cancer risk from 1 head CT: 1:2000 (infant) to 1:5000 (older child) < 10% of CT s have TBI/0.5% with Reduce # of CT s performed Radiation Sedation $$$$ Identify all TBI or just CI TBI? NSU intervention Hospital >2 nights/intubation>24 hrs Death/long term neurological sequelae Identify TBI clinically important (CI) TBI 5 6 Cancer PECARN Minor Head Trauma Decision Rule Under 2 years old Derivation and validation study 42K kids GCS>14: >10K under 2 yrs <2 years: 100% NPV for CI TBI and all TBI >2 years: 99.9% NPV for CI TBI 98.4% NPV for all TBI CT by 20-25% 7 Why identify all TBI: implications for sports/other activities? Kuppermann et al. Lancet
3 Over 2 years old Severe Mechanism Why identify all TBI: implications for sports/other activities? MVA with ejection, rollover or death of another Ped or bike w/o helmet vs. car Fall >3 ft (<2 yr) or >5 ft (>2 yr) High impact object to head Kuppermann et al. Lancet Imaging? A good idea.. Back to Baby Leo Imaging for <3 months with scalp hematoma + >3 ft fall Thin skull easily fractured strong correlation with TBI Well, can I just do a skull x-ray? Skull film cons: Hard to read Not sensitive/specific enough If (+) still need to do CT CT cons: Radiation Cost Transport from ED Sedation Survey says: CT
4 Baby Leo gets a CT Case #2: Wild Bill How do I keep him still Swaddle/dextrose H 2 0 Acetaminophen CT shows a skull fracture Admit? YES Admit criteria skull fx: Very young bleeding Depressed Wide diastasis High energy High risk location Poor home situation month old rolls down 8 stairs Few seconds of LOC Cried. Ate. Physical Exam: GCS? Talk his language 3 cm temporal hematoma To CT or not to CT? 14 Wild Bill: CT or Observation? Keeping Bill Still CT or 6 hour obs for all < 2 yrs with non-frontal scalp hematoma Location, location : Temporal > parietooccipital > frontal Severe mechanism?: 8 stairs=fall>3 feet?? LOC too brief to count but... My call CT Sedation choices: Ketamine is OK Rectal methohexital IV/IM pentobarbital Etomidate Avoid versed CT (+) epidural: Admit Brutane
5 Case #3: The Car s a Mess... 5 year old helmeted bike vs low speed MV No LOC V x 3 en route Mild headache PE: Playing Small parietal scalp hematoma To CT or not to CT? Let s talk observation > 2 years Isolated vomiting Non-severe mechanism Mild headache Consider observation if parents comfortable Criteria: Normal MS Discharge home? Vomiting controlled No abuse suspected Responsible home/ reliable transportation Normal head CT* Holmes, Annals EM, Case #4: Tell me again what happened to Jane? 18 mo old BIB father Vomiting x 3 days Tripped at daycare 4 days ago PE: somnolent CT by criteria: +SAH! What do you do? Neurosurgery Admit Child Protective Services (CPS) 20 5
6 Epidemic: Non-accidental trauma (NAT) 6-10% of pediatric trauma: NAT #1 NAT mortality: head injury Suspect NAT: (+) CT: minor/no reported trauma Delayed presentation Changing history Other injuries inconsistent with reported mechanism Retinal hemorrhages* 21 Nutshell: Whom to CT after trauma? <2 years: AMS Sx skull fracture Non frontal scalp hematoma >5 seconds LOC Not acting ly per parent Severe mechanism > 2 years: AMS Sx basilar skull fracture Vomiting Severe HA LOC Severe mechanism 22 Nutshell (cont): Return to sports post concussion Whom to admit?: All TBI High risk skull fractures Depressed Wide diastasis Very young High energy mechanism High bleeding risk Poor social/transport situation Suspected abuse Neurosurgery discretion 23 Grading systems not useful Stepwise return to play based on sx: No activity Light aerobic Sports specific exercise Non contact drills Contact practice Return to play 24 6
7 Case #5: Do you have neck pain?? 6 month old rear carseat passenger MVArear-ended Car-seat/patient in place PE: VS nl. Happy, no signs of trauma How do I clear the c- spine? Some background on pediatric c-spine injuries Uncommon injury More common in older kids (> 8 years) Leading causes: MVA (<8 yrs) Sports (>8 yrs) PVA Kids aren t just little adults Unique anatomy: Large head high fulcrum Higher injuries more common in < 8 year old Horizontal facets slippage/dislocation More cartilage tough to read x-rays More pre-vertebral soft tissue > 8 years more like adult NEXUS: 3065 kids Clearing little c-spines 30 CS injuries: Only 4 injuries 2-8 years None < 2 years Criteria: (100% sens) No neck tenderness No focal neuro sx No distracting injury Normal MS No intoxication
8 Applying NEXUS criteria 187 kids with c-spine injury-->nexus rules applied: 32 kids < 8 yrs: 94% sensitivity 155 kids > 8 yrs: 100% sensitivity *Garton, Neurosurgery, PECARN: Risk factors for CSI 540 CSI cases/1060 controls Risk factors: AMS/focal neuro sx Neck pain/torticollis Significant torso injury High risk condition Diving/high risk MVA 98% sensitive CT use by 25% 29 Leonard, Annals EM, Modified NEXUS: Clearing younger c-spines Age appropriate MS/no LOC/no focal neuro sx No distracting injury/significant torso injury No neck tenderness or pain/muscle spasm Low force mechanism... Case # 6: Johnny Walker 5 yr old 20 mph PVA BIBA with (+) LOC Now awake/alert No c/o of neck pain or neurological sx Open leg fracture Image: YES LOC Distracting injury High force mechanism Let them look around
9 Pediatric Cervical Spine Clearance Bad CNS status yes Very positive history or physical Positive or inadequate plain films Full Cervical Spine CT Pediatric Cervical Spine Clearance Bad CNS status Very positive history or physical Positive or inadequate plain films yes Full Cervical Spine CT <3 years Attempt clinical clearance: -Age appropriate mental status -No history of LOC -No neck pain or tenderness -Normal neurological exam -No distracting injury -Low force mechanism THEN let them look around left/right/flex/extend 3-8 years: Use NEXUS criteria (as in >8 years) to clinically clear ab clinically clear >8 years Attempt clinical clearance with NEXUS criteria -Normal mental status/no intoxication -No neck pain or tenderness -Normal neurological exam -No distracting injury ab <8 years Attempt clinical clearance: -Age appropriate mental status -No history of LOC -No neck pain or tenderness -Normal neurological exam -No distracting injury -Low force mechanism THEN let them look around left/right/flex/extend >8 years Attempt clinical clearance with NEXUS criteria -Normal mental status/no intoxication -No neck pain or tenderness -Normal neurological exam -No distracting injury ab ab Start with 3 view plain X-rays clinically clear ab Start with 3 view plain X-rays clinically clear clinically clear Consider AP/Lat plain XR PLUS Occiput to C3 CT ab or inadequate clinically clear Consider AP/Lat plain XR PLUS Occiput to C3 CT ab or inadequate ab or inadequate attempt clinical clearance ab or inadequate attempt clinical clearance attempt clinical clearance Fails attempt clinical clearance Fails Fails Full cervical spine CT Fails Full cervical spine CT *Low force mechanism: -Fall <3-5 feet vertical -Lower speed MVA where patient/car-seat all stay in place MRI Persistent pain/tenderness/neuro sx *Low force mechanism: -Fall <3-5 feet vertical -Lower speed MVA where patient/car-seat all stay in place MRI Persistent pain/tenderness/neuro sx Rorschach tests: reading pediatric c-spine x-rays ABC S Alignment Bones Cartilage/Physes Spaces Pre-dental Child: < 4 mm Adolescent: < 2-3 mm Pre-C2 Child: < 7 mm Adolescent: < 5 mm Pre-C6 Child: < 14 mm Adolescent: < 21 mm 35 More on pediatric c-spine films Psuedo-subluxation: < 4-5 mm of C2 on C3 Up to 40% < 8 yrs C1-3 spinolaminar line alignment SCIWORA: Injury visible on MRI NL CT does not = clinical clearance If neuro sx/guarding/ pain and (-) CT get MRI/call neurosurgery 36 9
10 Final case: Suzy Q 8 year old diving from board Struck head on bottom of pool C/O neck pain and hand paresthesias BIBA in full C-spine precautions PE: tender, mild hand weakness Start with CT Suzy s got a fracture High pretest probability Vertebral burst C5 Image whole spine Management: Strict immobilization: highly unstable Steroids? No data on kids 30 mg/kg solumedrol bolus 5.4 mg/kg/hr x 24 to 48 hours Nutshell: Nutshell (cont): Whom to image? Neck pain or tenderness Focal neurological symptoms /signs Distracting injury/significant torso injury AMS/LOC/intoxication High force mechanism Unwilling to look around/ guarding neck 39 Try to avoid reflex CT in kids How to image? CT first if: Very positive history/pe Significant AMS Otherwise: Consider AP/Lat XR plus occiput to C3 CT if <8 yrs 3 view XR alone if >8 yrs If one fracture, image whole spine How to manage? Immobilization/NSU Steroids-your call 40 10
11 41 11
Clarifying Murky Waters: Head Injuries in Children
 Clarifying Murky Waters: Head Injuries in Children Judith R. Klein, MD, FACEP Assistant Professor of Emergency Medicine UCSF-SFGH Emergency Services 1 Case #1: Newborn Leo 2 month old dropped 4 feet onto
Clarifying Murky Waters: Head Injuries in Children Judith R. Klein, MD, FACEP Assistant Professor of Emergency Medicine UCSF-SFGH Emergency Services 1 Case #1: Newborn Leo 2 month old dropped 4 feet onto
Pediatric Trauma: Pearls of Management
 Pediatric Trauma: Pearls of Management Judith R. Klein, MD Assistant Professor UCSF-SFGH SFGH Department of Emergency Medicine Pediatric Trauma: The Problem Leading cause of M/M age 1-241 50% of all pediatric
Pediatric Trauma: Pearls of Management Judith R. Klein, MD Assistant Professor UCSF-SFGH SFGH Department of Emergency Medicine Pediatric Trauma: The Problem Leading cause of M/M age 1-241 50% of all pediatric
Head injury in children
 Head injury in children Michael Kim, MD Department of Emergency Medicine University of Wisconsin- Madison #1 cause of death and disability Bimodal distribution 62,000 hospitalization 564,000 ED visits
Head injury in children Michael Kim, MD Department of Emergency Medicine University of Wisconsin- Madison #1 cause of death and disability Bimodal distribution 62,000 hospitalization 564,000 ED visits
Pre-hospital Response to Trauma and Brain Injury. Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center
 Pre-hospital Response to Trauma and Brain Injury Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center Traumatic Brain Injury is Common 235,000 Americans hospitalized for non-fatal TBI
Pre-hospital Response to Trauma and Brain Injury Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center Traumatic Brain Injury is Common 235,000 Americans hospitalized for non-fatal TBI
SCIWORA Rozlyn McTeer BSN, RN, CEN Pediatric Trauma Coordinator Trauma Services OBJECTIVES DEFINITION 11/8/2017. Identify SCIWORA.
 SCIWORA Rozlyn McTeer BSN, RN, CEN Pediatric Trauma Coordinator Trauma Services Identify SCIWORA. OBJECTIVES Identify the population at risk. To identify anatomic and physiologic reasons for SCIWORA. To
SCIWORA Rozlyn McTeer BSN, RN, CEN Pediatric Trauma Coordinator Trauma Services Identify SCIWORA. OBJECTIVES Identify the population at risk. To identify anatomic and physiologic reasons for SCIWORA. To
Time Equals Neurons - Spinal Cord Injury Management in the first 4 Hours
 Time Equals Neurons - Spinal Cord Injury Management in the first 4 Hours William D. Whetstone M.D. Clinical Professor UCSF Department of Emergency Medicine SFGH ED Center for Neuro-Critical Emergencies
Time Equals Neurons - Spinal Cord Injury Management in the first 4 Hours William D. Whetstone M.D. Clinical Professor UCSF Department of Emergency Medicine SFGH ED Center for Neuro-Critical Emergencies
Disclosure Statement. Dr. Kadish has no relevant financial relationships with any commercial interests mentioned in this talk.
 Disclosure Statement Dr. Kadish has no relevant financial relationships with any commercial interests mentioned in this talk. Head Trauma Evaluation Primary and secondary injury Disposition Sports related
Disclosure Statement Dr. Kadish has no relevant financial relationships with any commercial interests mentioned in this talk. Head Trauma Evaluation Primary and secondary injury Disposition Sports related
Imaging in the Trauma Patient
 Imaging in the Trauma Patient David A. Spain, MD Department of Surgery Stanford University Pan Scan Instead of Clinical Exam? 1 Granted, some patients don t need CT scan Platinum Package Stanford Special
Imaging in the Trauma Patient David A. Spain, MD Department of Surgery Stanford University Pan Scan Instead of Clinical Exam? 1 Granted, some patients don t need CT scan Platinum Package Stanford Special
Shenandoah Co. Fire & Rescue. Injuries to. and Spine. December EMS Training Bill Streett Training Section Chief
 Shenandoah Co. Fire & Rescue Injuries to the Head and Spine December EMS Training Bill Streett Training Section Chief C.E. Card Information BLS Providers 2 Cards / Provider Category 1 Course # Blank Topic#
Shenandoah Co. Fire & Rescue Injuries to the Head and Spine December EMS Training Bill Streett Training Section Chief C.E. Card Information BLS Providers 2 Cards / Provider Category 1 Course # Blank Topic#
of Trauma Assembly 27 th Page 1
 Eastern Association for the Surgery of Trauma 27 th Annual Scientific Assembly Sunrise Session 08 To Scan or Not To Scan Thatt is the Question January 16, 2014 Waldorf Astoria Naples Naples, Floridaa Page
Eastern Association for the Surgery of Trauma 27 th Annual Scientific Assembly Sunrise Session 08 To Scan or Not To Scan Thatt is the Question January 16, 2014 Waldorf Astoria Naples Naples, Floridaa Page
Kristin s Head Trauma Board Questions 11/07/14
 Kristin s Head Trauma Board Questions { 11/07/14 A healthy 15 y/o boy was playing football at a park near his home with a group of friends when he tripped over a friend s leg while trying to catch a pass.
Kristin s Head Trauma Board Questions { 11/07/14 A healthy 15 y/o boy was playing football at a park near his home with a group of friends when he tripped over a friend s leg while trying to catch a pass.
Introduction. Objectives C-Spine: Where Are We Now? NAEMSP Medical Director Course 1/9/2013
 NAEMSP Medical Director Course 1/9/2013 Objectives C-Spine: Where Are We Now? Robert M. Domeier, MD EMS Medical Director Washtenaw/Livingston Medical Control Authority Department of Emergency Medicine
NAEMSP Medical Director Course 1/9/2013 Objectives C-Spine: Where Are We Now? Robert M. Domeier, MD EMS Medical Director Washtenaw/Livingston Medical Control Authority Department of Emergency Medicine
3/14/2014 USED TO BE SIMPLE.. TO IMMOBILIZE OR NOT TO IMMOBILIZE.THAT IS THE QUESTION THE PROBLEM OLD THINKING
 USED TO BE SIMPLE.. TO IMMOBILIZE OR NOT TO IMMOBILIZE.THAT IS THE QUESTION Immobilization following injury used to be a simple decision--but no one was thinking. Up to 5 million people per year receive
USED TO BE SIMPLE.. TO IMMOBILIZE OR NOT TO IMMOBILIZE.THAT IS THE QUESTION Immobilization following injury used to be a simple decision--but no one was thinking. Up to 5 million people per year receive
Pan Scan Instead of Clinical Exam? David A. Spain, MD
 Pan Scan Instead of Clinical Exam? David A. Spain, MD Granted, some patients don t t need CT scan Platinum Package Stanford Special CT Scan Head Neck Chest Abdomen Pelvis Takes about 20 minutes to do
Pan Scan Instead of Clinical Exam? David A. Spain, MD Granted, some patients don t t need CT scan Platinum Package Stanford Special CT Scan Head Neck Chest Abdomen Pelvis Takes about 20 minutes to do
Evaluation and Stabilization of the Athlete with Possible Spine Injury
 Evaluation and Stabilization of the Athlete with Possible Spine Injury Jeffrey H. Bohmer, MD, FACEP Emergency Physician Northwestern Medicine Central DuPage Hospital June 12, 2015 Introduction Goals: 1.
Evaluation and Stabilization of the Athlete with Possible Spine Injury Jeffrey H. Bohmer, MD, FACEP Emergency Physician Northwestern Medicine Central DuPage Hospital June 12, 2015 Introduction Goals: 1.
Trauma Echo PVA. Improving Spinal Cord Injury Acute Management
 Improving Spinal Cord Injury Acute Management William D. Whetstone M.D. Clinical Professor UCSF Department of Emergency Medicine SFGH ED Center for Neuro-Critical Emergencies Trauma Echo PVA 86 yo PVA
Improving Spinal Cord Injury Acute Management William D. Whetstone M.D. Clinical Professor UCSF Department of Emergency Medicine SFGH ED Center for Neuro-Critical Emergencies Trauma Echo PVA 86 yo PVA
Indications for cervical spine immobilisation: -
 Paediatric Trauma Cervical Spine Guidelines UHW Traumatic injuries of the cervical spine (C-spine) are uncommon in children. However, it is safer assume there is a cervical spine injury until examination
Paediatric Trauma Cervical Spine Guidelines UHW Traumatic injuries of the cervical spine (C-spine) are uncommon in children. However, it is safer assume there is a cervical spine injury until examination
Pediatric Procedural Sedation
 Pediatric Procedural Sedation Case 1: 2 year old complex facial laceration Judith R. Klein, MD, FACEP Assistant Professor of Emergency Medicine UCSF-SFGH Department of Emergency Medicine Objectives: The
Pediatric Procedural Sedation Case 1: 2 year old complex facial laceration Judith R. Klein, MD, FACEP Assistant Professor of Emergency Medicine UCSF-SFGH Department of Emergency Medicine Objectives: The
Pediatric Subdural Hematoma and Traumatic Brain Injury J. Charles Mace MD FACS Springfield Neurological Institute CoxHealth. Objectives 11/7/2017
 Pediatric Subdural Hematoma and Traumatic Brain Injury J. Charles Mace MD FACS Springfield Neurological Institute CoxHealth Objectives 1. Be able to discuss brain anatomy and physiology as it applies to
Pediatric Subdural Hematoma and Traumatic Brain Injury J. Charles Mace MD FACS Springfield Neurological Institute CoxHealth Objectives 1. Be able to discuss brain anatomy and physiology as it applies to
TALK TRAUMA Clearing the C-Spine. David Ouellette
 TALK TRAUMA 2011 Clearing the C-Spine David Ouellette Case #1 - Mother / Daughter MVC 34 y/o female Dangerous mechanism CHI Mumbling incoherently Femur # - distracting injury ETOH - 22 9 y/o female Dangerous
TALK TRAUMA 2011 Clearing the C-Spine David Ouellette Case #1 - Mother / Daughter MVC 34 y/o female Dangerous mechanism CHI Mumbling incoherently Femur # - distracting injury ETOH - 22 9 y/o female Dangerous
3/10/17 Spinal a Injury 1
 Spinal Injury 1 'Paralysed' Watmough vows he'll have the backbone for Game Two after treatment for neck injury Watmough will have cortisone injected into his spine this morning to speed up the recovery
Spinal Injury 1 'Paralysed' Watmough vows he'll have the backbone for Game Two after treatment for neck injury Watmough will have cortisone injected into his spine this morning to speed up the recovery
Injuries to the Head and Spine
 Injuries to the Head and Spine Anatomy Review Skull Protects the brain Made up of several bones with seam like sutures Regions of the scalp-frontal, occipital, parietal, temporal Bones of face Orbits Mandible
Injuries to the Head and Spine Anatomy Review Skull Protects the brain Made up of several bones with seam like sutures Regions of the scalp-frontal, occipital, parietal, temporal Bones of face Orbits Mandible
Chapter 32. Objectives. Objectives 01/09/2013. Spinal Column and Spinal Cord Trauma
 Chapter 32 Spinal Column and Spinal Cord Trauma Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1.
Chapter 32 Spinal Column and Spinal Cord Trauma Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1.
vel 2 Level 2 3,034 c-spine evaluations with CSR Level 3 detected injury only 53% of the time. Level 3 False (-) rate 47%
 Objectives Blunt and Penetrating Neck Trauma Julie Mayglothling, MD, FACEP Virginia Commonwealth University Richmond, VA Summit to Sound, May 20 th, 2011 Blunt Neck Trauma Evaluation of the low mechanism,
Objectives Blunt and Penetrating Neck Trauma Julie Mayglothling, MD, FACEP Virginia Commonwealth University Richmond, VA Summit to Sound, May 20 th, 2011 Blunt Neck Trauma Evaluation of the low mechanism,
Selective Spinal Immobilization
 Selective Spinal Immobilization Objectives Understand the background of spinal immobilization. Understand the rationale for developing a current selective spinal immobilization protocol. Review the data
Selective Spinal Immobilization Objectives Understand the background of spinal immobilization. Understand the rationale for developing a current selective spinal immobilization protocol. Review the data
CBT 445 Head & Spine Thoracic Scenario 1
 CBT 445 Head & Spine Thoracic Scenario 1 Evaluator s notes: Patient 36 year old male fall patient, Impaled branch, quick transport to ER. Dispatch/Description of the problem: You are dispatched to 36 year
CBT 445 Head & Spine Thoracic Scenario 1 Evaluator s notes: Patient 36 year old male fall patient, Impaled branch, quick transport to ER. Dispatch/Description of the problem: You are dispatched to 36 year
Reviewing the recent literature to answer clinical questions: Should I change my practice?
 Reviewing the recent literature to answer clinical questions: Should I change my practice? JILL MILLER, MD PEM ATTENDING CHKD ASSISTANT PROFESSOR PEDIATRICS, EVMS Objectives Review the literature to answer
Reviewing the recent literature to answer clinical questions: Should I change my practice? JILL MILLER, MD PEM ATTENDING CHKD ASSISTANT PROFESSOR PEDIATRICS, EVMS Objectives Review the literature to answer
Avoidable Imaging Learning Collaborative: 2008 Mild Traumatic Brain Injury Clinical Policy Success Story BWH Head and PE CTs with Clinical Decision
 Avoidable Imaging Learning Collaborative: 2008 Mild Traumatic Brain Injury Clinical Policy Success Story BWH Head and PE CTs with Clinical Decision Support Using the Canadian CT Head Rule to Reduce Unnecessary
Avoidable Imaging Learning Collaborative: 2008 Mild Traumatic Brain Injury Clinical Policy Success Story BWH Head and PE CTs with Clinical Decision Support Using the Canadian CT Head Rule to Reduce Unnecessary
Mild Traumatic Brain Injury. Timothy Johnson, MD, FACEP, FAAEM Fairview Southdale Emergency Department
 Mild Traumatic Brain Injury Timothy Johnson, MD, FACEP, FAAEM Fairview Southdale Emergency Department Objectives Review the epidemiology of mild TBI. Learn to appreciate the risks and benefits of CT imaging
Mild Traumatic Brain Injury Timothy Johnson, MD, FACEP, FAAEM Fairview Southdale Emergency Department Objectives Review the epidemiology of mild TBI. Learn to appreciate the risks and benefits of CT imaging
USE OF CT SCAN IN A CHILD WITH MTBI
 TO SCAN OR NOT TO SCAN USE OF CT SCAN IN A CHILD WITH MTBI LISA AYOUB-RODRIGUEZ MD PEDIATRIC HOSPITALIST MIKE LEE MD PEDIATRIC RESIDENT BERT JOHANSSON MD PEDIATRIC HOSPITALIST DISCLOSURES I M NOT A SURGEON
TO SCAN OR NOT TO SCAN USE OF CT SCAN IN A CHILD WITH MTBI LISA AYOUB-RODRIGUEZ MD PEDIATRIC HOSPITALIST MIKE LEE MD PEDIATRIC RESIDENT BERT JOHANSSON MD PEDIATRIC HOSPITALIST DISCLOSURES I M NOT A SURGEON
Cervical Spine Precautions A quick review. By Joseph Lewis, M.D. Medical Director, Honolulu EMS Board Certified in Emergency Medicine
 Cervical Spine Precautions A quick review By Joseph Lewis, M.D. Medical Director, Honolulu EMS Board Certified in Emergency Medicine 1 Goals of this Cervical Spine Immobilization In-service Learn Objectives:
Cervical Spine Precautions A quick review By Joseph Lewis, M.D. Medical Director, Honolulu EMS Board Certified in Emergency Medicine 1 Goals of this Cervical Spine Immobilization In-service Learn Objectives:
Evaluation of Children with Blunt Abdominal Trauma. James F. Holmes, MD, MPH UC Davis School of Medicine
 Evaluation of Children with Blunt Abdominal Trauma James F. Holmes, MD, MPH UC Davis School of Medicine Objectives Epidemiology of intra-abdominal injury (IAI) Physical examination findings with IAI Laboratory
Evaluation of Children with Blunt Abdominal Trauma James F. Holmes, MD, MPH UC Davis School of Medicine Objectives Epidemiology of intra-abdominal injury (IAI) Physical examination findings with IAI Laboratory
Use of CT in minor traumatic brain injury. Lisa Ayoub-Rodriguez, MD Bert Johansson, MD Michael Lee, MD
 Use of CT in minor traumatic brain injury Lisa Ayoub-Rodriguez, MD Bert Johansson, MD Michael Lee, MD No financial or other conflicts of interest Epidemiology of traumatic brain injury (TBI) Risks associated
Use of CT in minor traumatic brain injury Lisa Ayoub-Rodriguez, MD Bert Johansson, MD Michael Lee, MD No financial or other conflicts of interest Epidemiology of traumatic brain injury (TBI) Risks associated
The Crashing Pediatric Patient: Stopping the Fall
 The Crashing Pediatric Patient: Stopping the Fall I can t breathe... 4 year old BIBA from school with sudden severe resp distress Hx of asthma, food allergies Judith Klein, MD FACEP Assistant Professor
The Crashing Pediatric Patient: Stopping the Fall I can t breathe... 4 year old BIBA from school with sudden severe resp distress Hx of asthma, food allergies Judith Klein, MD FACEP Assistant Professor
Spine and Spinal Cord Injury in Children
 Spine and Spinal Cord Injury in Children S. Danielle Brown, MS, RN, CNRN, SCRN Director, Research Coordination and Education Barrow Neurological Institute at Phoenix Children s Hospital Introduction Trauma
Spine and Spinal Cord Injury in Children S. Danielle Brown, MS, RN, CNRN, SCRN Director, Research Coordination and Education Barrow Neurological Institute at Phoenix Children s Hospital Introduction Trauma
2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: CLAIMS, REGISTRY
 Measure #416: Emergency Medicine: Emergency Department Utilization of CT for Minor Blunt Head Trauma for Patients Aged 2 through 17 Years - National Quality Strategy Domain: Efficiency and Cost Reduction
Measure #416: Emergency Medicine: Emergency Department Utilization of CT for Minor Blunt Head Trauma for Patients Aged 2 through 17 Years - National Quality Strategy Domain: Efficiency and Cost Reduction
Restore adequate respiratory and circulatory conditions. Reduce pain
 Pre-hospital management of the trauma patient is best performed by an integrated team focused on minimizing the time from injury to definitive care at an appropriate trauma center. Dispatchers, first responders,
Pre-hospital management of the trauma patient is best performed by an integrated team focused on minimizing the time from injury to definitive care at an appropriate trauma center. Dispatchers, first responders,
Measuring Overuse and Underuse of Brain CTs in Pediatric Patients with mtbi in Two Canadian Emergency Departments
 Measuring Overuse and Underuse of Brain CTs in Pediatric Patients with mtbi in Two Canadian Emergency Departments Martin Gariépy, PhD Dr Patrick Archambault Dr Jocelyn Gravel 2017 Quebec City, Quebec,
Measuring Overuse and Underuse of Brain CTs in Pediatric Patients with mtbi in Two Canadian Emergency Departments Martin Gariépy, PhD Dr Patrick Archambault Dr Jocelyn Gravel 2017 Quebec City, Quebec,
2017 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Efficiency
 Measure #416: Emergency Medicine: Emergency Department Utilization of CT for Minor Blunt Head Trauma for Patients Aged 2 Through 17 Years - National Quality Strategy Domain: Efficiency and Cost Reduction
Measure #416: Emergency Medicine: Emergency Department Utilization of CT for Minor Blunt Head Trauma for Patients Aged 2 Through 17 Years - National Quality Strategy Domain: Efficiency and Cost Reduction
Head injuries in children. Dr Jason Hort Paediatrician Paediatric Emergency Physician, June 2017 Children s Hospital Westmead
 Head injuries in children Dr Jason Hort Paediatrician Paediatric Emergency Physician, June 2017 Children s Hospital Westmead Objectives Approach to minor head injury Child protection issues Concussion
Head injuries in children Dr Jason Hort Paediatrician Paediatric Emergency Physician, June 2017 Children s Hospital Westmead Objectives Approach to minor head injury Child protection issues Concussion
Chapter 39 Trauma in the Elderly
 Chapter 39 Trauma in the Elderly Episode Overview 1) 5 Risk Factors for falls in the elderly? 2) What anatomic and physiologic changes in the elderly patient are important for the management of trauma
Chapter 39 Trauma in the Elderly Episode Overview 1) 5 Risk Factors for falls in the elderly? 2) What anatomic and physiologic changes in the elderly patient are important for the management of trauma
Bilateral rib fractures 2 on right and 1 on left In different stages of healing, with left fracture older than right fractures
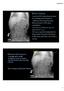 More history: Seen by PCP yesterday because of vomiting and fussinesss. Called by ED today because Mom presents with same complaints. ED found nothing but got an abdominal x ray. ED now wants kid admitted
More history: Seen by PCP yesterday because of vomiting and fussinesss. Called by ED today because Mom presents with same complaints. ED found nothing but got an abdominal x ray. ED now wants kid admitted
10/8/17. I have no disclosures. What are they? Upper extremity fractures Lower extremity fractures Non accidental trauma
 I have no disclosures Upper extremity fractures Lower extremity fractures Non accidental trauma What are they? Fractures of the radius, ulna and/or humerus Who gets them? Active children usually after
I have no disclosures Upper extremity fractures Lower extremity fractures Non accidental trauma What are they? Fractures of the radius, ulna and/or humerus Who gets them? Active children usually after
Pediatric Trauma Cases
 Pediatric Trauma Cases QPEM 2018 Barbara Blackie, MD, MEd, FRCPC DISCLOSURE I do not have any relevant financial relationship with commercial interest to disclose. Learning Objectives -Manage interactive
Pediatric Trauma Cases QPEM 2018 Barbara Blackie, MD, MEd, FRCPC DISCLOSURE I do not have any relevant financial relationship with commercial interest to disclose. Learning Objectives -Manage interactive
Author Manuscript. Received Date : 27-Oct Revised Date : 09-Jan-2017 Accepted Date : 31-Jan-2017
 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 Received Date : 27-Oct-2016 Revised Date : 09-Jan-2017 Accepted Date : 31-Jan-2017 Article type ABSTRACT : Original Contribution
1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 Received Date : 27-Oct-2016 Revised Date : 09-Jan-2017 Accepted Date : 31-Jan-2017 Article type ABSTRACT : Original Contribution
Cases from the Streets. Kelly Buchanan MD, ATC/L EMS Fellow December, 2011
 Cases from the Streets Kelly Buchanan MD, ATC/L EMS Fellow December, 2011 The Scene Car vs Light Pole, 35 mph, front right side damage 10 with no PCI + airbag deployment, starring on windshield Given the
Cases from the Streets Kelly Buchanan MD, ATC/L EMS Fellow December, 2011 The Scene Car vs Light Pole, 35 mph, front right side damage 10 with no PCI + airbag deployment, starring on windshield Given the
PedsCases Podcast Scripts
 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on the Approach to Pediatric Head Injury. These podcasts are designed to give medical students an overview of key topics
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on the Approach to Pediatric Head Injury. These podcasts are designed to give medical students an overview of key topics
SPINE EVALUATION AND CLEARANCE Basic Principles
 SPINE EVALUATION AND CLEARANCE Basic Principles General 1. Entire spine is immobilized during primary survey. 2. Radiographic clearance of the spine is not required before emergent surgical procedures.
SPINE EVALUATION AND CLEARANCE Basic Principles General 1. Entire spine is immobilized during primary survey. 2. Radiographic clearance of the spine is not required before emergent surgical procedures.
Overview. Overview. Chapter 30. Injuries to the Head and Spine 9/11/2012. Review of the Nervous and Skeletal Systems. Devices for Immobilization
 Chapter 30 Injuries to the Head and Spine Slide 1 Overview Review of the Nervous and Skeletal Systems The Nervous System The Skeletal System Devices for Immobilization Cervical Spine Short Backboards Long
Chapter 30 Injuries to the Head and Spine Slide 1 Overview Review of the Nervous and Skeletal Systems The Nervous System The Skeletal System Devices for Immobilization Cervical Spine Short Backboards Long
PRACTICE GUIDELINE. DEFINITIONS: Mild head injury: Glasgow Coma Scale* (GCS) score Moderate head injury: GCS 9-12 Severe head injury: GCS 3-8
 PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
MEDICAL CONTROL POLICY STATEMENT/ADVISORY. Re: Spinal Injury Assessment & Spinal Precautions Procedure
 MEDICAL CONTROL POLICY STATEMENT/ADVISORY No. 2015-01 Date: January 20, 2015 Re: Spinal Injury Assessment & Spinal Precautions Procedure Office of the Medical Director Noel Wagner, MD, NREMT-P 1000 Houghton
MEDICAL CONTROL POLICY STATEMENT/ADVISORY No. 2015-01 Date: January 20, 2015 Re: Spinal Injury Assessment & Spinal Precautions Procedure Office of the Medical Director Noel Wagner, MD, NREMT-P 1000 Houghton
Cervical Spine Injury Guidelines
 6/15/2018 Cervical Spine Injury Guidelines Benjamin Oshlag, MD, CAQSM Assistant Professor of Emergency Medicine Assistant Professor of Sports Medicine Columbia University Medical Center Nothing to Disclose
6/15/2018 Cervical Spine Injury Guidelines Benjamin Oshlag, MD, CAQSM Assistant Professor of Emergency Medicine Assistant Professor of Sports Medicine Columbia University Medical Center Nothing to Disclose
PEDIATRIC MILD TRAUMATIC HEAD INJURY
 PEDIATRIC MILD TRAUMATIC HEAD INJURY October 2011 Quality Improvement Resources Illinois Emergency Medical Services for Children is a collaborative program between the Illinois Department of Public Health
PEDIATRIC MILD TRAUMATIC HEAD INJURY October 2011 Quality Improvement Resources Illinois Emergency Medical Services for Children is a collaborative program between the Illinois Department of Public Health
8/29/2011. Brain Injury Incidence: 200/100,000. Prehospital Brain Injury Mortality Incidence: 20/100,000
 Traumatic Brain Injury Almario G. Jabson MD Section Of Neurosurgery Asian Hospital And Medical Center Brain Injury Incidence: 200/100,000 Prehospital Brain Injury Mortality Incidence: 20/100,000 Hospital
Traumatic Brain Injury Almario G. Jabson MD Section Of Neurosurgery Asian Hospital And Medical Center Brain Injury Incidence: 200/100,000 Prehospital Brain Injury Mortality Incidence: 20/100,000 Hospital
10/11/2017. AGENDA What you should expect. Complete Service. Structured Reporting: Reducing Failure to Observe TECHNOLOGY ENABLED RADIOLOGY SERVICES
 Web-based survey of 41 ED physicians Level 1 trauma center 38 responses (93%) Average years in practice 14.4 (range 2-35 years) Collectively group orders 100,000 exams / year 79% very satisfied or somewhat
Web-based survey of 41 ED physicians Level 1 trauma center 38 responses (93%) Average years in practice 14.4 (range 2-35 years) Collectively group orders 100,000 exams / year 79% very satisfied or somewhat
Traumatic Brain Injuries
 Traumatic Brain Injuries Scott P. Sherry, MS, PA-C, FCCM Assistant Professor Department of Surgery Division of Trauma, Critical Care and Acute Care Surgery DISCLOSURES Nothing to disclose Discussion of
Traumatic Brain Injuries Scott P. Sherry, MS, PA-C, FCCM Assistant Professor Department of Surgery Division of Trauma, Critical Care and Acute Care Surgery DISCLOSURES Nothing to disclose Discussion of
Coastal Carolina University Athletic Training Department Policy and Procedure Manual Concussion Management Revised/Reviewed 6/2012
 Coastal Carolina University Athletic Training Department Policy and Procedure Manual Concussion Management Revised/Reviewed 6/2012 INTRODUCTION: Concussion classification, management, and protocols have
Coastal Carolina University Athletic Training Department Policy and Procedure Manual Concussion Management Revised/Reviewed 6/2012 INTRODUCTION: Concussion classification, management, and protocols have
Spinal Cord Injuries: The Basics. Kadre Sneddon POS Rounds October 1, 2003
 Spinal Cord Injuries: The Basics Kadre Sneddon POS Rounds October 1, 2003 Anatomy Dorsal columntouch, vibration Corticospinal tract- UMN Anterior horn-lmn Spinothalamic tractpain, temperature (contralateral)
Spinal Cord Injuries: The Basics Kadre Sneddon POS Rounds October 1, 2003 Anatomy Dorsal columntouch, vibration Corticospinal tract- UMN Anterior horn-lmn Spinothalamic tractpain, temperature (contralateral)
Traumatic Brain Injury (1.2.3) Management of severe TBI ( ) Learning Objectives
 Traumatic Brain Injury (1.2.3) 1.2.3.1 Management of severe TBI 1.2.3.2 Management of concussions 1.2.3.3 Sideline management for team medics/physicians 1.4.2.3.10 Controlled hyperventilation for management
Traumatic Brain Injury (1.2.3) 1.2.3.1 Management of severe TBI 1.2.3.2 Management of concussions 1.2.3.3 Sideline management for team medics/physicians 1.4.2.3.10 Controlled hyperventilation for management
Pediatric Abusive Head Trauma
 Pediatric Abusive Head Trauma Rebecca Girardet Associate Professor of Pediatrics Director, Division of Child Protection Pediatrics McGovern Medical School at The University of Texas Health Science Center
Pediatric Abusive Head Trauma Rebecca Girardet Associate Professor of Pediatrics Director, Division of Child Protection Pediatrics McGovern Medical School at The University of Texas Health Science Center
Objective 1 Review Research on spine injuries and evaluation standards.
 To Backboard or Not To Backboard? Spinal Clearance Protocols Will Smith, MD, NREMT-P Medical Director, Jackson Hole Fire/EMS, Grand Teton National Park Wilderness and Emergency Medicine Consulting (WEMC),
To Backboard or Not To Backboard? Spinal Clearance Protocols Will Smith, MD, NREMT-P Medical Director, Jackson Hole Fire/EMS, Grand Teton National Park Wilderness and Emergency Medicine Consulting (WEMC),
To Backboard or Not To Backboard, That is the Question? Selective Spinal Immobilization
 To Backboard or Not To Backboard, That is the Question? Selective Spinal Immobilization Will Smith, MD, NREMT-P Medical Director, Jackson Hole Fire/EMS, Grand Teton National Park Emergency Medicine, St.
To Backboard or Not To Backboard, That is the Question? Selective Spinal Immobilization Will Smith, MD, NREMT-P Medical Director, Jackson Hole Fire/EMS, Grand Teton National Park Emergency Medicine, St.
SPINAL IMMOBILIZATION
 Spinal Immobilization Decision Assessment Recent studies have shown an increase in mortality for patients with isolated penetrating trauma who are spinally immobilized. Therefore spinal immobilization
Spinal Immobilization Decision Assessment Recent studies have shown an increase in mortality for patients with isolated penetrating trauma who are spinally immobilized. Therefore spinal immobilization
Outline. Epidemiology Indications for C-spine imaging Modalities Interpretation Types of fractures
 C-Spine Plain Films Outline Epidemiology Indications for C-spine imaging Modalities Interpretation Types of fractures Epidemiology 7000-10000 c-spine injuries treated each year Additional 5000 die at the
C-Spine Plain Films Outline Epidemiology Indications for C-spine imaging Modalities Interpretation Types of fractures Epidemiology 7000-10000 c-spine injuries treated each year Additional 5000 die at the
CLINICAL MANUAL. Trauma System Activation Trauma Code Criteria
 CLINICAL MANUAL Policy Number: CM T-28 Approved by: Nursing Congress, Management Forum Issue Date: 09/1999 Applies to: Downtown Value(s): Respect, Integrity, Innovation Page(s): 1 of 4 Trauma System Activation
CLINICAL MANUAL Policy Number: CM T-28 Approved by: Nursing Congress, Management Forum Issue Date: 09/1999 Applies to: Downtown Value(s): Respect, Integrity, Innovation Page(s): 1 of 4 Trauma System Activation
Injuries to the head and spine
 Injuries to the head and spine Aaron J. Katz, AEMT-P, CIC www.es26medic.net 2013 Nervous System Two sub-systems Central Nervous System ( CNS ) Brain and spinal cord Peripheral Nervous System 12 cranial
Injuries to the head and spine Aaron J. Katz, AEMT-P, CIC www.es26medic.net 2013 Nervous System Two sub-systems Central Nervous System ( CNS ) Brain and spinal cord Peripheral Nervous System 12 cranial
Overview of Abusive Head Trauma: What Everyone Needs to Know. 11 th Annual Keeping Children Safe Conference Boise, ID October 17, 2012
 Overview of Abusive Head Trauma: What Everyone Needs to Know 11 th Annual Keeping Children Safe Conference Boise, ID October 17, 2012 Deborah Lowen, MD Associate Professor Pediatrics Director, Child Abuse
Overview of Abusive Head Trauma: What Everyone Needs to Know 11 th Annual Keeping Children Safe Conference Boise, ID October 17, 2012 Deborah Lowen, MD Associate Professor Pediatrics Director, Child Abuse
Introduction to Neurosurgical Subspecialties:
 Introduction to Neurosurgical Subspecialties: Trauma and Critical Care Neurosurgery Brian L. Hoh, MD 1, Gregory J. Zipfel, MD 2 and Stacey Q. Wolfe, MD 3 1 University of Florida, 2 Washington University,
Introduction to Neurosurgical Subspecialties: Trauma and Critical Care Neurosurgery Brian L. Hoh, MD 1, Gregory J. Zipfel, MD 2 and Stacey Q. Wolfe, MD 3 1 University of Florida, 2 Washington University,
Spinal, or Suspected Spinal Injury
 Approved by: Spinal, or Suspected Spinal Injury Vice President and Chief Medical Officer; and Vice President and Chief Operating Officer Corporate Policy & Procedures Manual Number: VII-B-150 Date Approved
Approved by: Spinal, or Suspected Spinal Injury Vice President and Chief Medical Officer; and Vice President and Chief Operating Officer Corporate Policy & Procedures Manual Number: VII-B-150 Date Approved
Introduction to Emergency Medical Care 1
 Introduction to Emergency Medical Care 1 OBJECTIVES 31.1 Define key terms introduced in this chapter. Slides 13 15, 17, 19, 28 31.2 Describe the components and function of the nervous system and the anatomy
Introduction to Emergency Medical Care 1 OBJECTIVES 31.1 Define key terms introduced in this chapter. Slides 13 15, 17, 19, 28 31.2 Describe the components and function of the nervous system and the anatomy
Selective Spine Assessment & Spinal Motion Restriction
 Selective Spine Assessment & Spinal Motion Restriction Supersedes: 02-09-15 Effective: 10-20-15 Spinal cord injury may be the result of direct blunt and/or penetrating trauma, compression forces (axial
Selective Spine Assessment & Spinal Motion Restriction Supersedes: 02-09-15 Effective: 10-20-15 Spinal cord injury may be the result of direct blunt and/or penetrating trauma, compression forces (axial
Chapter 26 Head and Spine Trauma The Nervous System The nervous system controls virtually all of our body activities including reflex, voluntary and
 1 2 3 4 5 Chapter 26 Head and Spine Trauma The Nervous System The nervous system controls virtually all of our body activities including reflex, voluntary and involuntary activities Voluntary activities
1 2 3 4 5 Chapter 26 Head and Spine Trauma The Nervous System The nervous system controls virtually all of our body activities including reflex, voluntary and involuntary activities Voluntary activities
TRAUMATIC CAROTID &VERTEBRAL ARTERY INJURIES
 TRAUMATIC CAROTID &VERTEBRAL ARTERY INJURIES ALBERTO MAUD, MD ASSOCIATE PROFESSOR TEXAS TECH UNIVERSITY HEALTH SCIENCES CENTER EL PASO PAUL L. FOSTER SCHOOL OF MEDICINE 18TH ANNUAL RIO GRANDE TRAUMA 2017
TRAUMATIC CAROTID &VERTEBRAL ARTERY INJURIES ALBERTO MAUD, MD ASSOCIATE PROFESSOR TEXAS TECH UNIVERSITY HEALTH SCIENCES CENTER EL PASO PAUL L. FOSTER SCHOOL OF MEDICINE 18TH ANNUAL RIO GRANDE TRAUMA 2017
Review of: NATA Position Statement Management of Sport Concussion.
 Review of: NATA Position Statement Management of Sport Concussion www.csm-institute.com Topics: Education and Prevention Documentation and Legal Aspects Evaluation and RTP Other Considerations Strength
Review of: NATA Position Statement Management of Sport Concussion www.csm-institute.com Topics: Education and Prevention Documentation and Legal Aspects Evaluation and RTP Other Considerations Strength
IT S ALL IN YOUR HEAD!
 IT S ALL IN YOUR HEAD! CARING FOR CONCUSSIONS IN YOUR COMMUNITY Stephen K Stacey, DO CPT, MC, USA OUTLINE Definition Epidemiology Diagnosis Evaluation Recovery Sequelae Prevention Resources for providers
IT S ALL IN YOUR HEAD! CARING FOR CONCUSSIONS IN YOUR COMMUNITY Stephen K Stacey, DO CPT, MC, USA OUTLINE Definition Epidemiology Diagnosis Evaluation Recovery Sequelae Prevention Resources for providers
Pediatric head trauma: the evidence regarding indications for emergent neuroimaging
 DOI 10.1007/s00247-008-0996-5 ALARA: BUILDING BRIDGES BETWEEN RADIOLOGY AND EMERGENCY MEDICINE Pediatric head trauma: the evidence regarding indications for emergent neuroimaging Nathan Kuppermann Received:
DOI 10.1007/s00247-008-0996-5 ALARA: BUILDING BRIDGES BETWEEN RADIOLOGY AND EMERGENCY MEDICINE Pediatric head trauma: the evidence regarding indications for emergent neuroimaging Nathan Kuppermann Received:
Imaging of Cervical Spine Trauma
 Imaging of Cervical Spine Trauma C Craig Blackmore, MD, MPH Professor of Radiology and Adjunct Professor of Health Services University of Washington, Harborview Medical Center Salary support: AHRQ grant
Imaging of Cervical Spine Trauma C Craig Blackmore, MD, MPH Professor of Radiology and Adjunct Professor of Health Services University of Washington, Harborview Medical Center Salary support: AHRQ grant
Little Kids in Big Crashes The Bio-mechanics of Kids in Car Crashes. Lisa Schwing, RN Trauma Program Manager Dayton Children s
 Little Kids in Big Crashes The Bio-mechanics of Kids in Car Crashes Lisa Schwing, RN Trauma Program Manager Dayton Children s Very Little Research There has been very little research on the forces a crash
Little Kids in Big Crashes The Bio-mechanics of Kids in Car Crashes Lisa Schwing, RN Trauma Program Manager Dayton Children s Very Little Research There has been very little research on the forces a crash
Management of Severe Traumatic Brain Injury
 Guideline for North Bristol Trust Management of Severe Traumatic Brain Injury This guideline describes the following: Initial assessment and management of the patient with head injury Indications for CT
Guideline for North Bristol Trust Management of Severe Traumatic Brain Injury This guideline describes the following: Initial assessment and management of the patient with head injury Indications for CT
EMS Spinal Assessment and Precautions
 EMS Spinal Assessment and Precautions Adapted from a presentation prepared by Chelsea C. White IV, MD, NREMT-P Medical Director, Bernalillo County Fire Department Robert M. Domeier, MD, EMS Medical Director,
EMS Spinal Assessment and Precautions Adapted from a presentation prepared by Chelsea C. White IV, MD, NREMT-P Medical Director, Bernalillo County Fire Department Robert M. Domeier, MD, EMS Medical Director,
10O SPLINTING OF INJURIES ADULT & PEDIATRIC. 10Oa: Axial/Spine with Selective Spinal Motion Restriction Adult & Pediatric:
 10O SPLINTING OF INJURIES ADULT & PEDIATRIC EMERGENCY MEDICAL RESPONDER EMT EMT-INTERMEDIATE 85 ADVANCED EMT PARAMEDIC 10Oa: Axial/Spine with Selective Spinal Motion Restriction Adult & Pediatric: Many
10O SPLINTING OF INJURIES ADULT & PEDIATRIC EMERGENCY MEDICAL RESPONDER EMT EMT-INTERMEDIATE 85 ADVANCED EMT PARAMEDIC 10Oa: Axial/Spine with Selective Spinal Motion Restriction Adult & Pediatric: Many
Concussion Management and Update. Objectives
 Concussion Management and Update Ricardo Guirola MD M Ed Pediatric Rheumatology Primary Care Sports Medicine Objectives Review definition, signs and symptoms Discuss the initial evaluation of a patient
Concussion Management and Update Ricardo Guirola MD M Ed Pediatric Rheumatology Primary Care Sports Medicine Objectives Review definition, signs and symptoms Discuss the initial evaluation of a patient
Upper Cervical Spine - Occult Injury and Trigger for CT Exam
 Upper Cervical Spine - Occult Injury and Trigger for CT Exam Main Menu Introduction Clinical clearance of C-SpineC Radiographic evaluation Norms for C-spineC Triggers for CT exam: Odontoid Lateral view
Upper Cervical Spine - Occult Injury and Trigger for CT Exam Main Menu Introduction Clinical clearance of C-SpineC Radiographic evaluation Norms for C-spineC Triggers for CT exam: Odontoid Lateral view
6/23/2017. What do you see? skull fracture
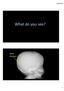 What do you see? skull fracture 1 Head CT On soft tissue windows, posterior soft tissues swelling and hemorrhage, no definite evidence of fracture Head CT On bone windows, fracture now seen subjacent to
What do you see? skull fracture 1 Head CT On soft tissue windows, posterior soft tissues swelling and hemorrhage, no definite evidence of fracture Head CT On bone windows, fracture now seen subjacent to
Sports Related Concussion. Joshua T. Williams, PT, DPT, OCS, SCS, CSCS
 Sports Related Concussion Joshua T. Williams, PT, DPT, OCS, SCS, CSCS Concussion & Traumatic Brain Injury Glasgow Coma Scale Minimal Mild Mod Severe? Sports concussion Severe GCS 8 Moderate GCS 9-12 Mild
Sports Related Concussion Joshua T. Williams, PT, DPT, OCS, SCS, CSCS Concussion & Traumatic Brain Injury Glasgow Coma Scale Minimal Mild Mod Severe? Sports concussion Severe GCS 8 Moderate GCS 9-12 Mild
Head trauma is a common chief complaint among children visiting
 Discussions in Surgery Validation of the Sainte-Justine Head Trauma Pathway for children younger than two years of age Sarah Spénard Serge Gouin, MDCM Marianne Beaudin, MD Jocelyn Gravel, MD, MSc Partial
Discussions in Surgery Validation of the Sainte-Justine Head Trauma Pathway for children younger than two years of age Sarah Spénard Serge Gouin, MDCM Marianne Beaudin, MD Jocelyn Gravel, MD, MSc Partial
Effects of Immobilization. N24 Pedi Musculoskeletal Spring 2012, Week 14. Cabrillo ADN/C. Madsen RN, MSN 1. Physical effects on other systems
 Common Orthopedic Problems of Children Congenital Acquired Bones Neuromuscular Physical effects on other systems Pulmonary Cardiac Skin integrity Elimination GI GU 1 4 General Nursing Considerations any
Common Orthopedic Problems of Children Congenital Acquired Bones Neuromuscular Physical effects on other systems Pulmonary Cardiac Skin integrity Elimination GI GU 1 4 General Nursing Considerations any
KIDS PUT THINGS IN THE CRAZIEST PLACES...
 KIDS PUT THINGS IN THE CRAZIEST PLACES... YOU CAN T MAKE ME EAT MY DINNER! 2 year old observed to stuff corn up right nostril Judith Klein, MD FACEP Assistant Professor of Emergency Medicine UCSF-SFGH
KIDS PUT THINGS IN THE CRAZIEST PLACES... YOU CAN T MAKE ME EAT MY DINNER! 2 year old observed to stuff corn up right nostril Judith Klein, MD FACEP Assistant Professor of Emergency Medicine UCSF-SFGH
Concussion in Children
 S306- Management of Concussion in Children John Kuluz, MD Neurorehabilitation Miami Children s Hospital Disclosure of Relevant Relationship Dr. Kuluz (or spouse/partner) has not had (in the past 12 months)
S306- Management of Concussion in Children John Kuluz, MD Neurorehabilitation Miami Children s Hospital Disclosure of Relevant Relationship Dr. Kuluz (or spouse/partner) has not had (in the past 12 months)
Form 1 ED Data Blunt Traumatic Brain Injury (TBI)
 Complete this form * Prior to reviewing CT or skull xray (if obtained) Data Source faculty physician, fellow or resident physician, NP or PA with faculty oversight Patient Study ID Number Faculty physician,
Complete this form * Prior to reviewing CT or skull xray (if obtained) Data Source faculty physician, fellow or resident physician, NP or PA with faculty oversight Patient Study ID Number Faculty physician,
Thicker than Water. Alisa McQueen MD, FAAP, FACEP Associate Professor of Pediatrics The University of Chicago
 Thicker than Water Alisa McQueen MD, FAAP, FACEP Associate Professor of Pediatrics The University of Chicago I have no relevant financial relationships to disclose. Who is bleeding? How much and what kind
Thicker than Water Alisa McQueen MD, FAAP, FACEP Associate Professor of Pediatrics The University of Chicago I have no relevant financial relationships to disclose. Who is bleeding? How much and what kind
TOPICS. Wheezing/Asthma THE BEST PEDIATRIC LITERATURE THAT STILL AFFECT YOUR PRACTICE
 THE BEST PEDIATRIC LITERATURE THAT STILL AFFECT YOUR PRACTICE Ghazala Q. Sharieff MD, MBA Wheezing/asthma Croup Immunizations and fever Appendicitis Complex febrile seizures Procedures Head Injury Zofran
THE BEST PEDIATRIC LITERATURE THAT STILL AFFECT YOUR PRACTICE Ghazala Q. Sharieff MD, MBA Wheezing/asthma Croup Immunizations and fever Appendicitis Complex febrile seizures Procedures Head Injury Zofran
Instructional Course #34. Review of Neuropharmacology in Pediatric Brain Injury. John Pelegano MD Jilda Vargus-Adams MD, MSc Micah Baird MD
 Instructional Course #34 Review of Neuropharmacology in Pediatric Brain Injury John Pelegano MD Jilda Vargus-Adams MD, MSc Micah Baird MD Outline of Course 1. Introduction John Pelegano MD 2. Neuropharmocologic
Instructional Course #34 Review of Neuropharmacology in Pediatric Brain Injury John Pelegano MD Jilda Vargus-Adams MD, MSc Micah Baird MD Outline of Course 1. Introduction John Pelegano MD 2. Neuropharmocologic
Controversies in Spinal Immobilization
 Controversies in Spinal Immobilization Ken Berumen, BSN, MD, FACEP Medical Director El Paso Fire Department Medical Director Emergency Services District #1 Network Director EM Sierra Providence Health
Controversies in Spinal Immobilization Ken Berumen, BSN, MD, FACEP Medical Director El Paso Fire Department Medical Director Emergency Services District #1 Network Director EM Sierra Providence Health
Acute spinal cord injury
 Acute spinal cord injury Thakul Oearsakul Songklanagarind hospital Hat Yai Songkhla Introduction New SCI 10000-12000 cases Approximately 4.0-5.3 per 100000 population Common causes of traumatic SCI :Motor
Acute spinal cord injury Thakul Oearsakul Songklanagarind hospital Hat Yai Songkhla Introduction New SCI 10000-12000 cases Approximately 4.0-5.3 per 100000 population Common causes of traumatic SCI :Motor
What Do You Think of My Posterior?
 What Do You Think of My Posterior? Posterior Stroke and Stroke Mimics Peter Panagos, MD, FACEP, FAHA Associate Professor Emergency Medicine and Neurology Washington University School of Medicine Disclosures
What Do You Think of My Posterior? Posterior Stroke and Stroke Mimics Peter Panagos, MD, FACEP, FAHA Associate Professor Emergency Medicine and Neurology Washington University School of Medicine Disclosures
Suspected Physical Abuse Clinical Practice Guideline
 Suspected Physical Abuse Clinical Practice Guideline WHEN TO CONSIDER ABUSE Consider abuse on the differential Injuries to multiple organ systems Injuries in different stages of healing Patterned injuries
Suspected Physical Abuse Clinical Practice Guideline WHEN TO CONSIDER ABUSE Consider abuse on the differential Injuries to multiple organ systems Injuries in different stages of healing Patterned injuries
School of Hard Knocks! Richard Beebe MS RN NRP MedicThink LLC
 School of Hard Knocks! Richard Beebe MS RN NRP MedicThink LLC Fall of a Teton How Bad is He Hurt? What REALLY happened inside Johnny s head? How common are these types of injuries? PONDER THIS What part
School of Hard Knocks! Richard Beebe MS RN NRP MedicThink LLC Fall of a Teton How Bad is He Hurt? What REALLY happened inside Johnny s head? How common are these types of injuries? PONDER THIS What part
Follow your protocols!
 By Will Dunn, BA, NRP, CCEMTP & Myles Sibley, BA, NREMT P Eagle County Paramedic Services, Eagle County, CO. FIELD ASSESSMENT AND TREATMENT OF CLOSED HEAD AND SPINAL INJURY Follow your protocols! Objectives
By Will Dunn, BA, NRP, CCEMTP & Myles Sibley, BA, NREMT P Eagle County Paramedic Services, Eagle County, CO. FIELD ASSESSMENT AND TREATMENT OF CLOSED HEAD AND SPINAL INJURY Follow your protocols! Objectives
