A genetic model defines the importance of the atrial natriuretic peptide receptor (guanylyl cyclase-a) in the regulation of kidney function
|
|
|
- Samuel Doyle
- 6 years ago
- Views:
Transcription
1 A genetic model defines the importance of the atrial natriuretic peptide receptor (guanylyl cyclase-a) in the regulation of kidney function Susan K. Dubois*, Ichiro Kishimoto, Terence O. Lillis*, and David L. Garbers ** Cecil H. and Ida Green Center for Reproductive Biology Sciences, Department of Pharmacology, and Howard Hughes Medical Institute, University of Texas Southwestern Medical Center, 5323 Harry Hines Boulevard, Dallas, TX ; and *Department of Medicine, University of West Virginia Medical School, Morgantown, WV, Contributed by David L. Garbers, December 30, 1999 Disruption of the atrial natriuretic peptide (ANP) receptor [guanylyl cyclase-a (GC-A)] gene yields mice with a salt-resistant form of hypertension, raising fundamental questions on the role of ANP in acute regulation of the kidney. Here, we show that water intake, food consumption, stool weight, urine volume, and sodium excretion are not significantly different between wild-type and GC-A null mice on standard rodent chow (0.7% NaCl) or a high-salt diet (8% NaCl). In conscious mice with an indwelling catheter, the infusion of a physiological saline solution containing 4% BSA resulted in a marked natriuresis diuresis in wild-type mice but no response in GC-A null animals. When physiological saline was given by gavage, however, the kidney response of wild-type and null mice was equivalent, raising the possibility that the gastrointestinal tract can directly regulate kidney function. However, administration of 0.9% saline through an intraperitoneal route also resulted in equal kidney responses in wild-type and null mice. When 0.9% NaCl lacking protein was infused i.v., wild-type and null mice both responded at the kidney level. Thus, GC-A appears dispensable for regulation of sodium water excretion in response to changes in dietary sodium concentration, but likely becomes critical in volume expansions where the isooncotic pressure remains constant, such as head-out immersion or the initial and correctable stages of congestive heart failure. Atrial natriuretic peptide (ANP) and B type natriuretic peptide are signaling molecules that can be released by the endocrine heart to stimulate natriuresis diuresis in the kidney. The receptor for both peptides appears to be guanylyl cyclase-a (GC-A; natriuretic peptide receptor-a) based on binding affinities and disruption of the GC-A gene (1). At least three prominent phenotypes are evident in GC-A null mice: elevated basal blood pressure, resistance to dietary saltassociated increases in blood pressure, and marked cardiac hypertrophy (2, 3). The salt-resistant elevation in blood pressure mimics the phenotype of at least 20 million Americans with essential hypertension (4 6) and suggests that GC-A is not a critical regulator of kidney function under chronic high- or low-salt diets. Yet, previous studies suggest that GC-A is essential for acute natriuresis associated with intravascular volume expansion (7). In those studies, when anesthetized mice were infused with a Lactated Ringer s solution containing 4% BSA, wild-type mice elevated sodium excretion and urine output by 5-fold, whereas no natriuretic response occurred in the GC-A null mice (7). One possible explanation for this disparity in response to dietary compared with i.v. salt would be direct communication between the gastrointestinal tract and the kidney, resulting in natriuresis during high dietary salt. Indeed, several laboratories have demonstrated a greater natriuresis in response to enteral or portal saline administration when compared with peripheral i.v. saline loading (8 13). Furthermore, one family of peptides (guanylin, uroguanylin) found in the intestine, and suggested to regulate the kidney, binds to another guanylyl cyclase receptor, GC-C (14), which, at least in some animals, is expressed in the kidney (15). Here, we show that GC-A appears unnecessary in the acute regulation of kidney function unless intravascular volume is increased at a constant protein concentration. Materials and Methods The generation of GC-A-deficient mice has been described previously (2). Studies were carried out in adult mice that had been backcrossed for three to six generations into the C57BL6 strain. The Animal Care and Use Committee of West Virginia University and the University of Texas Southwestern Medical Center approved all studies. Metabolic and Blood Pressure Responses to Dietary Salt. Mice were acclimated to metabolic cages (Mouse Diuresis Cage; Nalge) for 2 days before data collection. They received a standard, powdered rodent chow (0.7% NaCl; Harlan Teklad, Madison, WI) and water ad libitum for the first 4 days of measurements and then were subsequently switched to the 8% NaCl diet (Harlan Teklad). Urine was collected every 24 hr for measurement of sodium (Beckman Astra, Richardson, TX) and cgmp (RIA). Blood pressure was measured by tail cuff (Softron, Tokyo) each afternoon as described previously (2). Acute Saline Loading by Gavage or Intraperitoneal Injection. Animals were trained in the metabolic cages for 2 hr per day for 2 days before data collection. In addition, for gavage studies, mice received 2 days of sham gavage followed by 1 day of tap water gavage before data collection. After the training period, mice were given two 1-ml boluses of 0.9% sodium chloride separated by 1 hr, either by gavage or i.p. injection. Urine was collected in metabolic cages for a total period of 6 hr. Urine volume was recorded and then cages were rinsed with deionized water to maximize sodium recovery. Sodium was measured by flame photometry. Acute Saline Loading Through a Chronic Indwelling Jugular Catheter. Mice were anesthetized with ketamine xylazine. The jugular vein was cannulated with Micro-Renathane tubing (Braintree Scientific), and the tubing was exteriorized between the scapulae. Mice were allowed 2 days recovery before training. Chronically catheterized mice were trained in holders for 2 days. Beginning on the fifth postoperative day, mice received either Abbreviations: GC-A, guanylyl cyclase-a; ANP, atrial natriuretic peptide. S.K.D. and I.K. contributed equally to this work. Present address: Department of Medicine and Clinical Science, Kyoto University Graduate School of Medicine, 54 Kawahara-cho, Shogoin Sakyo-ku, Kyoto, Japan, **To whom reprint requests should be addressed. dgarbe@mednet.swmed.edu. The publication costs of this article were defrayed in part by page charge payment. This article must therefore be hereby marked advertisement in accordance with 18 U.S.C solely to indicate this fact. PHARMACOLOGY PNAS April 11, 2000 vol. 97 no
2 Fig. 1. Daily water intake, food consumption, stool weight, urine output (UO), and sodium excretion (UNaV) of wild-type and GC-A null mice on a 0.7% NaCl diet (A) or 8% NaCl diet (B). Data are presented as means SE; n 5 for each genotype. No significant differences were noted between the genotypes for any of the parameters. 0.9% NaCl or 0.9% NaCl plus 4% BSA (Sigma) as two 1-ml i.v. boluses given over 15 min each and separated by 1 hr. Urine was collected in metabolic cages for the 6-hr time period as described above. Urinary cgmp. Urine was collected from metabolic cages, centrifuged promptly to remove sediment, and stored at 80 C. cgmp was measured by ELISA (Assay Designs, Ann Arbor, MI). Plasma ANP. Under methoxyflurane anesthesia, 50 l of blood was collected from tails before or at 0.5, 2, and 4 hr after gavage with 0.9% NaCl. EDTA (1 mg ml) and aprotinin (500 kallikrein inhibitor units ml) were added to the samples before centrifugation and storage at 80 C. ANP was measured by RIA (Peninsula Laboratories). Statistical Analyses. Data are presented as the average of means SEM. Data analyses involving all three genotypes were performed by one-way ANOVA (GraphPad, San Diego) or by ANOVA with repeated measures where indicated. Individual groups then were compared by using Tukey s method. Wild-type vs. null animals were compared by use of an unpaired, two-tailed t test. Results and Discussion To determine whether the absence of GC-A modified eating or drinking behavior, we measured water intake, food consumption, stool weight, urine volume, and sodium excretion on standard rodent chow (0.7% NaCl) and on a high-salt diet (8% NaCl). There were no significant differences between genotypes with respect to the measured parameters on either diet (Fig. 1). Systolic blood pressure of the GC-A null mice was significantly higher compared with wild-type mice on the standard diet (129 2mmHgfor vs mmHgfor ; P ), but no increase in blood pressure in either genotype occurred on the high-salt diet (129 4mmHgfor vs mmHgfor ) (Fig. 2). Urine output was higher on the high-salt diet, but no difference between the genotypes with regard to sodium excretion was apparent (Fig. 3 A and B). Wild-type mice showed significant elevations in cgmp in response to high dietary salt (Fig. 3C), suggesting that the ANP GC-A-signaling pathway was activated by high salt. Several papers have suggested that ANP in the brain plays an important role in the central control of drinking behavior. Intracerebroventricular administration of synthetic ANP decreases the water intake of dehydrated rats (16 18), and neutralization of ANP with anti-anp antiserum potentates water intake induced by water deprivation or angiotensin II injection (16, 19). These findings suggest that endogenous ANP in rat brain antagonizes the action of angiotensin and plays an important role in the maintenance of drinking behavior. Because there was no apparent difference between GC-A null mice and wild-type mice with respect to drinking behavior, the ANP- GC-A pathway appears to have little, if any, effect on drinking behavior when body fluid volume is not reduced. To study further the gastrointestinal response to salt and to avoid the expected increase in serum osmolarity associated with the 8% NaCl diet, we administered isotonic 0.9% NaCl by gavage. Wild-type and GC-A heterozygous or null mice displayed similar urine output and sodium excretion in response to two 1-ml saline boluses given 1 hr apart (Fig. 4). Urinary cgmp was 2- to 3-fold higher in wild-type than null mice (data not shown). We next explored the consequences of sodium loading through an i.p. injection, thus bypassing the interaction of saline with the intestinal epithelium. Again, there was no difference between urine volume or sodium excretion between the genotypes (Fig. 5). Previous studies from our laboratory revealed marked differences in urine output and sodium excretion between anesthetized wild-type and GC-A null mice infused with a bolus of 3% body weight of an isotonic, isooncotic solution (7). To remove confounding factors associated with anesthesia, in the present study we used conscious animals with an indwelling jugular catheter and expanded the cardiovascular volume with 0.9% NaCl containing 4% BSA (isooncotic). Whereas the wild-type Fig. 2. Effect of dietary salt on systemic blood pressure of wild-type and GC-A null mice. Animals were fed normal chow (0.7% NaCl) on days 1 4 and then switched to a high-salt (8%) diet on day Dubois et al.
3 PHARMACOLOGY Fig. 4. Urine volume (A) and sodium excretion (B) in wild-type, heterozygous, and GC-A null mice in response to gavage with two 1-ml boluses of 0.9% NaCl separated by 1 hr. There was no significant difference between wild-type and GC-A null mice with respect to urine. Urinary cgmp levels were significantly less for null mice than for wild-type mice (P 0.001; data not shown). Fig. 3. Effect of high-salt diet on urine volume (A), urine sodium excretion (B), and urinary cgmp levels (C) in wild-type and GC-A null mice. Data are presented as means SE; n 5 for each genotype. On days 1 4, mice were fed standard chow (0.7% NaCl) and then the diet was changed to 8% NaCl on day 5. Urine volume and sodium excretion increased in both genotypes in response to the high-salt diet (P , two-way ANOVA). Urine volume was significantly higher in wild-type mice compared with null (P 0.05, two-way ANOVA), but there was no significant difference between the genotypes with respect to urine sodium excretion (P 0.39, two-way ANOVA). Only wild-type mice showed significant elevations of urinary cyclic GMP in response to the high-salt diet (P 0.05, repeated-measures ANOVA), and urinary cgmp levels were significantly higher in wild-type mice compared with null mice (P , unpaired t test). mice had a marked increase in sodium excretion and urine volume in response to the infusion, heterozygote animals had about one-half the response and homozygous nulls failed to respond (Fig. 6). Thus, under conditions of an isooncotic volume expansion, the endocrine heart appears to be required for renal sodium excretion, and this regulation proceeds through the GC-A-signaling pathway. Isooncotic volume expansion is observed in some clinical settings such as congestive heart failure, renal failure, and liver cirrhosis with ascites (20). Studies in an experimental model of congestive heart failure have demonstrated that inhibition of ANP by either specific antibodies (21) or the ANP receptor antagonist, HS (22), causes decreased urine flow or sodium excretion. These results together with our previous findings (7) demonstrate that GC-A plays a prominent role in natriuresis diuresis after isooncotic volume expansion and, thus, suggests that activation of GC-A could provide a therapeutic remedy for the disease. When 0.9% NaCl lacking protein was used for the volume expansion of wild-type and null mice, natriuresis diuresis in the null animals now exceeded that of the wild-type mice (Fig. 6). That GC-A null mice displayed increased sodium excretion under conditions of low protein volume expansion is consistent with data from many laboratories demonstrating exaggerated natriuresis in both animals and humans with hypertension (23 27). Various hypotheses for enhanced natriuresis have included an augmented effect of ANP on the kidney (25, 28). We have shown previously that ANP infusion does not cause natri- Dubois et al. PNAS April 11, 2000 vol. 97 no
4 Fig. 6. Urine volume (A) and sodium excretion (B) in response to i.v. infusion of two 1-ml boluses of either an isotonic saline solution (IV) or an isooncotic saline solution (0.9% NaCl, 4% BSA; IV BSA). The GC-A null mice that were infused with the isooncotic solution showed significantly lower urine output and sodium excretion than either wild-type or heterozygous mice. The null mice also had a significantly elevated sodium excretion relative to wild-type animals. Fig. 5. Urine volume (A) and sodium excretion (B) in wild-type and GC-A null mice in response to i.p. injection of two 1-ml boluses of 0.9% NaCl separated by 1 hr. There was no significant difference between the genotypes with respect to urine volume or sodium excretion. uresis in GC-A null mice, suggesting that ANP does not signal through another receptor for sodium excretion (7). Thus, other mechanisms must lead to exaggerated natriuresis in GC-A null mice. Although GC-A did not seem necessary for excretion of sodium after saline gavage or i.v. infusion of saline, urinary cgmp nevertheless was elevated in wild-type mice, and, therefore, GC-A could be responsible for some part of the natriuretic response to oral sodium ingestion in normal animals although clearly was not required. Plasma ANP levels, used as a measure of intravascular volume expansion, rise by 5-fold in wild-type mice after i.v. administration of an isotonic, isooncotic fluid (7). Here, ANP levels did not change significantly, however, in the wild-type mice after gavage with 0.9% NaCl (Fig. 7). The most striking finding of this study is that the ANP GC- A-signaling pathway appears critical for regulation of acute kidney function in the case of an i.v. isotonic, isooncotic volume expansion, but not for volume expansions where the oncotic pressure is altered. Various investigators have reported that proximal tubule reabsorption of sodium varies directly with protein concentration of infusate and, thus, capillary oncotic pressure (29 32). Ott et al. (32) demonstrated that protein concentration affected proximal sodium reabsorption in dogs only in the presence of extracellular volume expansion. We hypothesize that in the absence of GC-A, the mouse is unable to overcome the effect of increased proximal tubule sodium reabsorption that occurs under conditions of isooncotic volume expansion. In humans, Loon et al. (33) examined filtration dynamics and the natriuretic response to volume expansion with either 5% albumin in 0.9% NaCl or 0.9% NaCl alone. Subjects had a significantly higher sodium excretion rate during the saline infusion than the infusion containing 5% albumin. Patients were followed for 4 hr after the infusion and showed delayed sodium excretion such that subjects tended to return toward sodium balance with time. We did not measure sodium excretion in the days after the bolus, but would expect them to compensate with late natriuresis to avoid the sequelae of marked volume expansion such as uncompensated congestive heart failure or edema, neither of which was clinically evident. Fig. 7. Plasma ANP levels before and 0.5, 2, and 4 hr after gavage with two 1-ml boluses of 0.9% NaCl. There was a significant effect of genotype (twoway ANOVA, P 0.003), but not time, on plasma ANP levels Dubois et al.
5 Several lines of evidence have suggested that resistance to ANP explains in part the maintenance of volume expansion in congestive heart failure, nephrotic syndrome, and cirrhosis. Patients with sodium-retaining disorders are resistant to the effects of ANP infusion or to endogenously released ANP during head-out immersion (28, 34, 35). It is reasonable to suggest that humans with GC-A deficiency are more vulnerable to volume expansion in such pathological conditions. Increased ANP levels also have been reported in patients with essential hypertension (36) and cardiac hypertrophy (35 37). Sodium excretion was similar in wild-type and heterozygous mice after gavage, i.p., or i.v. bolus and was increased in the GC-A null mice after i.v. bolus compared with enteral saline, making it unlikely that an intestinal factor was responsible for natriuresis in absence of GC-A. Urinary cgmp excretion also was significantly less in GC-A null mice after saline gavage, again suggesting that a cgmp-dependent pathway (e.g., guanylin, uroguanylin) was not responsible for natriuresis in response to enteral saline. Finally, the data also suggest that ANP B type natriuretic peptide may activate GC-A in wild-type mice in response to high-salt diets, but GC-A activation is not an essential event, because the failure to elevate cgmp in null mice had no effect on normal kidney function. In summary, the GC-A-deficient mouse demonstrates that the ANP GC-A-signaling pathway is essential for acute natriuresis in response to an isooncotic saline volume expansion. Thus, in situations such as head-out immersion, or the initial and correctable phases of congestive heart failure, the endocrine heart coupled to signaling through GC-A is likely essential for natriuresis and, perhaps, survival. Yet, under conditions that are not isooncotic (administration of physiological saline by gavage, i.p. injection, or i.v. infusion), GC-A is not required for normal kidney function. This work was supported by the Howard Hughes Medical Institute and by the Cecil H. and Ida Green Center for Reproductive Biology Sciences. 1. Garbers, D. L. & Wedel, B. (1999) Trends Endocrinol. Metab. 9, Lopez, M. J., Kishimoto, I., Mach, V., Garbers, D. L., Wong, S. K., Dubois, S., Friesen, J. & Beuve, A. (1995) Nature (London) 378, Oliver, P. M., Fox, J. E., Kim, R., Rockman, H. A., Kim, H. S., Reddick, R. L., Pandey, K. N., Milgram, S. L., Smithies, O. & Maeda, N. (1997) Proc. Natl. Acad. Sci. USA 94, Sullivan, J. M. (1991) Hypertension 17, Suppl. I, I-61 I The Sixth Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure (1997) Arch. Intern. Med. 157, Dubois, S. K. & Garbers, D. L. (1999) Annu. Rev. Biochem. 6, Kishimoto, I., Dubois, S. K. & Garbers, D. L. (1996) Proc. Natl. Acad. Sci. USA 93, Hansson, G. C., Mu, J. Y. & Lundgren, O. (1995) Blood Press. 4, Carey, R. M. (1978) Circ. Res. 43, Monita, H., Matsuda, F., Furuya, F., Khanchowdhury, M. R. & Hosomi, H. (1993) Circ. Res. 72, Passo, S. S., Thornborough, J. R. & Rothballer, A. B. (1973) Am. J. Physiol. 224, Daly, J. J., Roe, J. W. & Horrocks, P. (1967) Clin. Sci. Mol. Med. 33, Fonteles, M. C., Greenberg, R. N., Monteiro, H. S., Currie, M. G. & Forte, L. R. (1998) Am. J. Physiol. 275, F191 F Schulz, S., Green, C. K., Yuen, P. S. & Garbers, D. L. (1990) Cell 63, London, R. M., Eber, S. L., Visweswariah, S. S., Krause, W. J. & Forte, L. R. (1999) Am. J. Physiol. 276, F882 F Katsuura, G., Nakamura, M., Inouye, K., Kono, M., Nakao, K. & Imura, H. (1986) Eur. J. Pharmacol. 121, Weisinger, R. S., Blair-West, J. R., Denton, D. A. & Tarjan, E. (1992) Brain Res. 579, Antunes-Rodrigues, J., McCann, S. M., Rogers, L. C. & Samson, W. K. (1985) Proc. Natl. Acad. Sci. USA 82, Ehrlich, K. J. & Fitts, D. A. (1990) Behav. Neurosci. 104, Winavier, J., Abassi, Z., Green, J. & Skorecki, K. L. (2000) in The Kidney Sixth Edition, ed. Brenner, B. M. (Saunders, Philadelphia), pp Awazu, M., Imada, T., Kon, V., Inagami, T. & Ichikawa, I. (1989) Am. J. Physiol. 257, R Wada, A., Tsutamoto, T., Matsuda, Y. & Kinoshita, M. (1994) Circulation 89, Willassen, Y. & Ofstad, J. (1980) Hypertension 2, Mimran, A., Nussberger, J., Ribstein, J., Waeber, B. & Brunner, H. R. (1988) Am. J. Physiol. 255, F1085 F Weinberger, M. H., Smith, J. B., Fineberg, N. S. & Luft, F. C. (1989) Hypertension 13, Luft, F. C., Fineberg, N. S. & Weinberger, M. H. (1992) Am. J. Hypertens. 5, Widecka, K., Celibala, R., Gozdzik, J., Syrenicz, A., Ciechanowski, K. & Czekalski, S. (1993) Transplant 8, Koepke, J. P. & DiBona, G. F. (1987) Am. J. Physiol. 252, F865 F Brenner, B. M., Falchuk, K., Keimowitz, R. & Berliner, R. (1969) J. Clin. Invest. 48, Spitzer, A. & Windhager, E. E. (1970) Am. J. Physiol. 218, Weinman, E. J., Kashgarian, M. & Hayslett, J. P. (1971) Am. J. Physiol. 221, Ott, C. E., Haas, J. A. Cuche, J. L. & Knox, F. G. (1975) J. Clin. Invest. 55, Loon, N., Chagnac, A., Parra, L., Schmidt, K., Deen, W. M. & Myers, B. D. (1992) Am. J. Physiol. 263, F284 F Wong, F., Tobe, S., Legault, L., Logaon, A. G., Skorecki, K. & Blendis, L. M. (1993) Hepatology 18, Gerbes, A. L., Wernze, H., Arendt, R. M., Riedel, A., Sauerbruch, T. & Paumgartner, G. (1989) Hepatology 9, Hollister, A. S. & Inagami, T. (1991) Am. J. Hypertens. 4, Nishikimi, T., Yoshihara, F., Morimoto, A., Ishikawa, K., Ishimitsu, T., Saito, Y., Kangawa, K., Matsuo, H., Omae, T. & Matsuoka, H. (1996) Hypertension 28, PHARMACOLOGY Dubois et al. PNAS April 11, 2000 vol. 97 no
J Jpn Coll Angiol, 2009, 49:
 Online publication October 6, 2009 48 2 20 J Jpn Coll Angiol, 2009, 49: 293 297 atrial natriuretic peptide, brain natriuretic peptide, guanylyl cyclase-a receptor, cardiac remodeling, cardiac hypertrophy
Online publication October 6, 2009 48 2 20 J Jpn Coll Angiol, 2009, 49: 293 297 atrial natriuretic peptide, brain natriuretic peptide, guanylyl cyclase-a receptor, cardiac remodeling, cardiac hypertrophy
The Guanylyl Cyclase-deficient Mouse Defines Differential Pathways of Natriuretic Peptide Signaling*
 THE JOURNAL OF BIOLOGICAL CHEMISTRY Vol. 272, No. 37, Issue of September 12, pp. 23064 23068, 1997 1997 by The American Society for Biochemistry and Molecular Biology, Inc. Printed in U.S.A. The Guanylyl
THE JOURNAL OF BIOLOGICAL CHEMISTRY Vol. 272, No. 37, Issue of September 12, pp. 23064 23068, 1997 1997 by The American Society for Biochemistry and Molecular Biology, Inc. Printed in U.S.A. The Guanylyl
had no effect on the production of aldosterone, corticosterone, or cortisol after
 INHIBITION OF THE EFFECTS OF ANGIOTENSIN II ON ADRENAL STEROID PRODUCTION BY DIETARY SODIUM BY WARREN W. DAVIS,* LAWRENCE R. BURWELL,t AND FREDERIC C. BARTTERt ENDOCRINOLOGY BRANCH, NATIONAL HEART INSTITUTE,
INHIBITION OF THE EFFECTS OF ANGIOTENSIN II ON ADRENAL STEROID PRODUCTION BY DIETARY SODIUM BY WARREN W. DAVIS,* LAWRENCE R. BURWELL,t AND FREDERIC C. BARTTERt ENDOCRINOLOGY BRANCH, NATIONAL HEART INSTITUTE,
Patterns of Sodium Excretion During Sympathetic Nervous System Arousal. Gregory A. Harshfield, Derrick A. Pulliam, and Bruce S.
 1156 Patterns of Sodium Excretion During Sympathetic Nervous System Arousal Gregory A. Harshfield, Derrick A. Pulliam, and Bruce S. Alpert The purpose of this study was to examine Na + handling and regulation
1156 Patterns of Sodium Excretion During Sympathetic Nervous System Arousal Gregory A. Harshfield, Derrick A. Pulliam, and Bruce S. Alpert The purpose of this study was to examine Na + handling and regulation
Paul M McKie, Alessandro Cataliotti, Guido Boerrigter, Horng C Chen, Fernando L Martin, and John C Burnett Jr
 Cardiorenal Enhancing and Aldosterone Suppressing Actions of a Novel Designer Natriuretic Peptide in Experimental Hypertension with Ventricular Pressure Overload Paul M McKie, Alessandro Cataliotti, Guido
Cardiorenal Enhancing and Aldosterone Suppressing Actions of a Novel Designer Natriuretic Peptide in Experimental Hypertension with Ventricular Pressure Overload Paul M McKie, Alessandro Cataliotti, Guido
Guanylin peptides: cyclic GMP signaling mechanisms
 Brazilian Journal of Medical and Biological Research (1999) 32: 1329-1336 Guanylin peptides and cgmp ISSN 0100-879X 1329 Guanylin peptides: cyclic GMP signaling mechanisms L.R. Forte 1,2, R.H. Freeman
Brazilian Journal of Medical and Biological Research (1999) 32: 1329-1336 Guanylin peptides and cgmp ISSN 0100-879X 1329 Guanylin peptides: cyclic GMP signaling mechanisms L.R. Forte 1,2, R.H. Freeman
Renal Quiz - June 22, 21001
 Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
neurally derived AII could be involved in induction of drinking (2). In contrast, atrial natriuretic peptide (ANP) has been
 Proc. Nati. Acad. Sci. USA Vol. 6, pp. 2952-2956, April 199 Physiological Sciences Water intake in rats subjected to hypothalamic immunoneutralization of angiotensin II, atrial natauretic peptide, vasopressin,
Proc. Nati. Acad. Sci. USA Vol. 6, pp. 2952-2956, April 199 Physiological Sciences Water intake in rats subjected to hypothalamic immunoneutralization of angiotensin II, atrial natauretic peptide, vasopressin,
Body Water Content Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are
 Fluid, Electrolyte, and Acid-Base Balance Body Water Content Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are about 60%
Fluid, Electrolyte, and Acid-Base Balance Body Water Content Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are about 60%
Sodium balance and blood pressure response to salt ingestion in uninephrectomized rats
 Kidney International, Vol. 54, Suppl. 67 (1998), pp. S-245 S-249 Sodium balance and blood pressure response to salt ingestion in uninephrectomized rats TAKUYUKI ISE, KEN-ICHI KOBAYASHI, WOLFGANG BILLER,
Kidney International, Vol. 54, Suppl. 67 (1998), pp. S-245 S-249 Sodium balance and blood pressure response to salt ingestion in uninephrectomized rats TAKUYUKI ISE, KEN-ICHI KOBAYASHI, WOLFGANG BILLER,
Salt Sensitivity: Mechanisms, Diagnosis, and Clinical Relevance
 Salt Sensitivity: Mechanisms, Diagnosis, and Clinical Relevance Matthew R. Weir, MD Professor and Director Division of Nephrology University of Maryland School of Medicine Overview Introduction Mechanisms
Salt Sensitivity: Mechanisms, Diagnosis, and Clinical Relevance Matthew R. Weir, MD Professor and Director Division of Nephrology University of Maryland School of Medicine Overview Introduction Mechanisms
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1
 BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
IV Fluids. I.V. Fluid Osmolarity Composition 0.9% NaCL (Normal Saline Solution, NSS) Uses/Clinical Considerations
 IV Fluids When administering IV fluids, the type and amount of fluid may influence patient outcomes. Make sure to understand the differences between fluid products and their effects. Crystalloids Crystalloid
IV Fluids When administering IV fluids, the type and amount of fluid may influence patient outcomes. Make sure to understand the differences between fluid products and their effects. Crystalloids Crystalloid
The Art and Science of Diuretic therapy
 The Art and Science of Diuretic therapy Dr. Fayez EL Shaer Associate Professour of cardiology Consultant cardiologist MD, MSc, PhD, CBNC, NBE FESC, ACCP, FASNC,HFA KKUH, KFCC Heart failure: fluid overload
The Art and Science of Diuretic therapy Dr. Fayez EL Shaer Associate Professour of cardiology Consultant cardiologist MD, MSc, PhD, CBNC, NBE FESC, ACCP, FASNC,HFA KKUH, KFCC Heart failure: fluid overload
BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1
 BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1 1. a. Proximal tubule. b. Proximal tubule. c. Glomerular endothelial fenestrae, filtration slits between podocytes of Bowman's capsule.
BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1 1. a. Proximal tubule. b. Proximal tubule. c. Glomerular endothelial fenestrae, filtration slits between podocytes of Bowman's capsule.
Blood Pressure Fox Chapter 14 part 2
 Vert Phys PCB3743 Blood Pressure Fox Chapter 14 part 2 T. Houpt, Ph.D. 1 Cardiac Output and Blood Pressure How to Measure Blood Pressure Contribution of vascular resistance to blood pressure Cardiovascular
Vert Phys PCB3743 Blood Pressure Fox Chapter 14 part 2 T. Houpt, Ph.D. 1 Cardiac Output and Blood Pressure How to Measure Blood Pressure Contribution of vascular resistance to blood pressure Cardiovascular
BODY FLUID. Outline. Functions of body fluid Water distribution in the body Maintenance of body fluid. Regulation of fluid homeostasis
 BODY FLUID Nutritional Biochemistry Yue-Hwa Chen Dec 13, 2007 Chen 1 Outline Functions of body fluid Water distribution in the body Maintenance of body fluid Intake vs output Regulation of body fluid Fluid
BODY FLUID Nutritional Biochemistry Yue-Hwa Chen Dec 13, 2007 Chen 1 Outline Functions of body fluid Water distribution in the body Maintenance of body fluid Intake vs output Regulation of body fluid Fluid
20 Barton et al. Fourteen female mongrel dogs, weighing between 10 to 20 kg, were studied. Light pentobarbital anesthesia
 20 Barton et al. critical determinant of the occurrence and magnitude of natriuresis. It is possible that volume expansion suppresses sodium reabsorption in the loop, and that in the absence of this inhibitory
20 Barton et al. critical determinant of the occurrence and magnitude of natriuresis. It is possible that volume expansion suppresses sodium reabsorption in the loop, and that in the absence of this inhibitory
Renal Regulation of Sodium and Volume. Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM
 Renal Regulation of Sodium and Volume Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM Maintaining Volume Plasma water and sodium (Na + ) are regulated independently - you are already familiar
Renal Regulation of Sodium and Volume Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM Maintaining Volume Plasma water and sodium (Na + ) are regulated independently - you are already familiar
Regulation of Arterial Blood Pressure 2 George D. Ford, Ph.D.
 Regulation of Arterial Blood Pressure 2 George D. Ford, Ph.D. OBJECTIVES: 1. Describe the Central Nervous System Ischemic Response. 2. Describe chemical sensitivities of arterial and cardiopulmonary chemoreceptors,
Regulation of Arterial Blood Pressure 2 George D. Ford, Ph.D. OBJECTIVES: 1. Describe the Central Nervous System Ischemic Response. 2. Describe chemical sensitivities of arterial and cardiopulmonary chemoreceptors,
Fal Fal P h y s i o l o g y 6 1 1, S a n F r a n c i s c o S t a t e U n i v e r s i t y
 Fall 12 OSMOTIC REGULATION OF THE RENAL SYSTEM: Effects of fasting and ingestion of water, coke, or Gatorade on urine flow rate and specific gravity Dorette Franks The purpose of the physiology experiment
Fall 12 OSMOTIC REGULATION OF THE RENAL SYSTEM: Effects of fasting and ingestion of water, coke, or Gatorade on urine flow rate and specific gravity Dorette Franks The purpose of the physiology experiment
In the name of GOD. Animal models of cardiovascular diseases: myocardial infarction & hypertension
 In the name of GOD Animal models of cardiovascular diseases: myocardial infarction & hypertension 44 Presentation outline: Cardiovascular diseases Acute myocardial infarction Animal models for myocardial
In the name of GOD Animal models of cardiovascular diseases: myocardial infarction & hypertension 44 Presentation outline: Cardiovascular diseases Acute myocardial infarction Animal models for myocardial
7/31/2009. G.Y. Prince Used Cars 10 am Los Angelos, CA Mullholland Drive..later that day. Would you buy a car without taking it for a spin first?
 7/31/29 My Anna will love it! Who needs a test drive? Or a Warranty? It looked great in the lot! Do mean to say that you never actually test drove the car? G.Y. Prince Used Cars 1 am Los Angelos, CA Mullholland
7/31/29 My Anna will love it! Who needs a test drive? Or a Warranty? It looked great in the lot! Do mean to say that you never actually test drove the car? G.Y. Prince Used Cars 1 am Los Angelos, CA Mullholland
DIAGNOSIS AND MANAGEMENT OF DIURETIC RESISTANCE. Jules B. Puschett, M.D.
 DIAGNOSIS AND MANAGEMENT OF DIURETIC RESISTANCE Jules B. Puschett, M.D. Diuretic Resistance A clinical circumstance in which patients do not respond to a combination of salt restriction and even large
DIAGNOSIS AND MANAGEMENT OF DIURETIC RESISTANCE Jules B. Puschett, M.D. Diuretic Resistance A clinical circumstance in which patients do not respond to a combination of salt restriction and even large
Body fluids. Lecture 13:
 Lecture 13: Body fluids Body fluids are distributed in compartments: A. Intracellular compartment: inside the cells of the body (two thirds) B. Extracellular compartment: (one third) it is divided into
Lecture 13: Body fluids Body fluids are distributed in compartments: A. Intracellular compartment: inside the cells of the body (two thirds) B. Extracellular compartment: (one third) it is divided into
Fluids and electrolytes
 Body Water Content Fluids and electrolytes Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are about 60% water; healthy females
Body Water Content Fluids and electrolytes Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are about 60% water; healthy females
Hyperglycemia: Type I Diabetes Mellitus
 296 PHYSIOLOGY CASES AND PROBLEMS Case 53 Hyperglycemia: Type I Diabetes Mellitus David Mandel was diagnosed with type I (insulin-dependent) diabetes mellitus when he was 12 years old (see Cases 30 and
296 PHYSIOLOGY CASES AND PROBLEMS Case 53 Hyperglycemia: Type I Diabetes Mellitus David Mandel was diagnosed with type I (insulin-dependent) diabetes mellitus when he was 12 years old (see Cases 30 and
Figure S1 Genetic or pharmacologic COX-2 inhibition led to increased kidney
 SUPPLEMENTAL FIGURE LEGENDS Figure S1 Genetic or pharmacologic COX-2 inhibition led to increased kidney macrophage infiltration. Wild type or COX-2 -/- mice (2 months old, C57/Bl6 background) were treated
SUPPLEMENTAL FIGURE LEGENDS Figure S1 Genetic or pharmacologic COX-2 inhibition led to increased kidney macrophage infiltration. Wild type or COX-2 -/- mice (2 months old, C57/Bl6 background) were treated
The ability of the kidneys to regulate extracellular fluid volume by altering sodium
 REGULATION OF EXTRACELLULAR FLUID VOLUME BY INTEGRATED CONTROL OF SODIUM EXCRETION Joey P. Granger Department of Physiology and Biophysics, University of Mississippi Medical Center, Jackson, Mississippi
REGULATION OF EXTRACELLULAR FLUID VOLUME BY INTEGRATED CONTROL OF SODIUM EXCRETION Joey P. Granger Department of Physiology and Biophysics, University of Mississippi Medical Center, Jackson, Mississippi
Monday, 17 April 2017 BODY FLUID HOMEOSTASIS
 Monday, 17 April 2017 BODY FLUID HOMEOSTASIS Phenomenon: shipwrecked sailor on raft in ocean ("water, water everywhere but not a drop to drink") Why are the sailors thirsty? (What stimulated thirst?) Why
Monday, 17 April 2017 BODY FLUID HOMEOSTASIS Phenomenon: shipwrecked sailor on raft in ocean ("water, water everywhere but not a drop to drink") Why are the sailors thirsty? (What stimulated thirst?) Why
Introduction to the kidney: regulation of sodium & glucose. Dr Nick Ashton Senior Lecturer in Renal Physiology Faculty of Biology, Medicine & Health
 Introduction to the kidney: regulation of sodium & glucose Dr Nick Ashton Senior Lecturer in Renal Physiology Faculty of Biology, Medicine & Health Objectives Overview of kidney structure & function Glomerular
Introduction to the kidney: regulation of sodium & glucose Dr Nick Ashton Senior Lecturer in Renal Physiology Faculty of Biology, Medicine & Health Objectives Overview of kidney structure & function Glomerular
Regulation of fluid and electrolytes balance
 Regulation of fluid and electrolytes balance Three Compartment Fluid Compartments Intracellular = Cytoplasmic (inside cells) Extracellular compartment is subdivided into Interstitial = Intercellular +
Regulation of fluid and electrolytes balance Three Compartment Fluid Compartments Intracellular = Cytoplasmic (inside cells) Extracellular compartment is subdivided into Interstitial = Intercellular +
(Received 22 July 1957) It is now generally accepted that the unequal distribution of ions between cells
 190 J. Physiol. (I958) I40, I90-200 THE EFFECT OF ALTERATIONS OF PLASMA SODIUM ON THE SODIUM AND POTASSIUM CONTENT OF MUSCLE IN THE RAT By F. 0. DOSEKUN AND D. MENDEL From the Department of Physiology,
190 J. Physiol. (I958) I40, I90-200 THE EFFECT OF ALTERATIONS OF PLASMA SODIUM ON THE SODIUM AND POTASSIUM CONTENT OF MUSCLE IN THE RAT By F. 0. DOSEKUN AND D. MENDEL From the Department of Physiology,
venous blood samples were drawn. The plasma was separated rapidly by centrifugation and assayed within one
 THE ANTIDIURETIC ACTIVITY OF PLASMA OF PATIENTS WITH HEPATIC CIRRHOSIS, CONGESTIVE HEART FAIL- URE, HYPERTENSION AND OTHER CLINICAL DISORDERS' By MARVIN STEIN,2 ROBERT SCHWARTZ, AND I. ARTHUR MIRSKY (From
THE ANTIDIURETIC ACTIVITY OF PLASMA OF PATIENTS WITH HEPATIC CIRRHOSIS, CONGESTIVE HEART FAIL- URE, HYPERTENSION AND OTHER CLINICAL DISORDERS' By MARVIN STEIN,2 ROBERT SCHWARTZ, AND I. ARTHUR MIRSKY (From
Regulation of Body Fluids: Na + and Water Linda Costanzo, Ph.D.
 Regulation of Body Fluids: Na + and Water Linda Costanzo, Ph.D. OBJECTIVES: After studying this lecture, the student should understand: 1. Why body sodium content determines ECF volume and the relationships
Regulation of Body Fluids: Na + and Water Linda Costanzo, Ph.D. OBJECTIVES: After studying this lecture, the student should understand: 1. Why body sodium content determines ECF volume and the relationships
Blood Pressure Regulation 2. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
After studying this lecture, you should be able to...
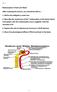 Reabsorption of Salt and Water After studying this lecture, you should be able to... 1. Define the obligatory water loss. 2. Describe the mechanism of Na ++ reabsorption in the distal tubule and explain
Reabsorption of Salt and Water After studying this lecture, you should be able to... 1. Define the obligatory water loss. 2. Describe the mechanism of Na ++ reabsorption in the distal tubule and explain
Differences in the Fate of Methylmercury between Mice with and without Hair
 450 Journal of Health Science, 52(4) 450 454 (2006) Differences in the Fate of Methylmercury between Mice with and without Hair Tatsumi Adachi*, a, b and Takashi Kuwana a, c a Department of Basic Medical
450 Journal of Health Science, 52(4) 450 454 (2006) Differences in the Fate of Methylmercury between Mice with and without Hair Tatsumi Adachi*, a, b and Takashi Kuwana a, c a Department of Basic Medical
Urinary Kallikrein Excretion in Hypertensive Man
 Urinary Kallikrein Excretion in Hypertensive Man RELATIONSHIPS TO SODIUM INTAKE AND SODIUM-RETAINING STEROIDS By Harry S. Margolius, David Horwttz, John J. Pisano, and Harry R. Kelser ABSTRACT Urinary
Urinary Kallikrein Excretion in Hypertensive Man RELATIONSHIPS TO SODIUM INTAKE AND SODIUM-RETAINING STEROIDS By Harry S. Margolius, David Horwttz, John J. Pisano, and Harry R. Kelser ABSTRACT Urinary
Chapter 27: WATER, ELECTROLYTES, AND ACID-BASE BALANCE
 Chapter 27: WATER, ELECTROLYTES, AND ACID-BASE BALANCE I. RELATED TOPICS Integumentary system Cerebrospinal fluid Aqueous humor Digestive juices Feces Capillary dynamics Lymph circulation Edema Osmosis
Chapter 27: WATER, ELECTROLYTES, AND ACID-BASE BALANCE I. RELATED TOPICS Integumentary system Cerebrospinal fluid Aqueous humor Digestive juices Feces Capillary dynamics Lymph circulation Edema Osmosis
DIURETICS-4 Dr. Shariq Syed
 DIURETICS-4 Dr. Shariq Syed AIKTC - Knowledge Resources & Relay Center 1 Pop Quiz!! Loop diuretics act on which transporter PKCC NKCC2 AIKTCC I Don t know AIKTC - Knowledge Resources & Relay Center 2 Pop
DIURETICS-4 Dr. Shariq Syed AIKTC - Knowledge Resources & Relay Center 1 Pop Quiz!! Loop diuretics act on which transporter PKCC NKCC2 AIKTCC I Don t know AIKTC - Knowledge Resources & Relay Center 2 Pop
AJH 1998;11: by the American Journal of Hypertension, Ltd /98/$19.00
 AJH 1998;11:8 13 Acute Effects of Intravenous Sodium Chloride Load on Calcium Metabolism and on Parathyroid Function in Patients With Primary Aldosteronism Compared With Subjects With Essential Hypertension
AJH 1998;11:8 13 Acute Effects of Intravenous Sodium Chloride Load on Calcium Metabolism and on Parathyroid Function in Patients With Primary Aldosteronism Compared With Subjects With Essential Hypertension
Abnormalities in serum sodium. David Metz Paediatric Nephrology
 Abnormalities in serum sodium David Metz Paediatric Nephrology Basics Total body sodium regulated by aldosterone and ANP Mediated by intravascular volume (not sodium) RAAS and intrarenal determines Na
Abnormalities in serum sodium David Metz Paediatric Nephrology Basics Total body sodium regulated by aldosterone and ANP Mediated by intravascular volume (not sodium) RAAS and intrarenal determines Na
Entresto Development of sacubitril/valsartan (LCZ696) for the treatment of heart failure with reduced ejection fraction
 Cardio-Metabolic Franchise Entresto Development of sacubitril/valsartan (LCZ696) for the treatment of heart failure with reduced ejection fraction Randy L Webb, PhD Rutgers Workshop October 21, 2016 Heart
Cardio-Metabolic Franchise Entresto Development of sacubitril/valsartan (LCZ696) for the treatment of heart failure with reduced ejection fraction Randy L Webb, PhD Rutgers Workshop October 21, 2016 Heart
Counter-Current System Regulation of Renal Functions
 Counter-Current System Regulation of Renal Functions Assoc. Prof. MUDr. Markéta Bébarová, Ph.D. Department of Physiology Faculty of Medicine, Masaryk University This presentation includes only the most
Counter-Current System Regulation of Renal Functions Assoc. Prof. MUDr. Markéta Bébarová, Ph.D. Department of Physiology Faculty of Medicine, Masaryk University This presentation includes only the most
Adrenocorticotropin Responses to Corticotropin Releasing Factor and Vasopressin in Spontaneously Hypertensive Rats
 Laboratory Studies Adrenocorticotropin Responses to Corticotropin Releasing Factor and Vasopressin in Spontaneously Hypertensive Rats TERUHIKO HATTORI, KOZO HASHIMOTO, AND ZENSUKE OTA SUMMARY The effects
Laboratory Studies Adrenocorticotropin Responses to Corticotropin Releasing Factor and Vasopressin in Spontaneously Hypertensive Rats TERUHIKO HATTORI, KOZO HASHIMOTO, AND ZENSUKE OTA SUMMARY The effects
BIPN100 F12 FINAL EXAM ANSWERS Name Answer Key PID p. 1
 BIPN100 F12 FINAL EXAM ANSWERS Name Answer Key PID p. 1 READ THIS PAGE BEFORE YOU BEGIN THE EXAM. 1. Write your name on every page, in both packets of stapled-together pages. (5 points off for EACH unnamed
BIPN100 F12 FINAL EXAM ANSWERS Name Answer Key PID p. 1 READ THIS PAGE BEFORE YOU BEGIN THE EXAM. 1. Write your name on every page, in both packets of stapled-together pages. (5 points off for EACH unnamed
Basic Fluid and Electrolytes
 Basic Fluid and Electrolytes Chapter 22 Basic Fluid and Electrolytes Introduction Infants and young children have a greater need for water and are more vulnerable to alterations in fluid and electrolyte
Basic Fluid and Electrolytes Chapter 22 Basic Fluid and Electrolytes Introduction Infants and young children have a greater need for water and are more vulnerable to alterations in fluid and electrolyte
Lund, 1948), the effect of which was to produce glomerular lesions without. relationship between increased protein loads and the tubular reabsorption
 544 J. Phy8iol. (1961), 156, pp. 544-554 With 5 text-ftgure8 Printed in Great Britain TUBULAR REABSORPTION OF PROTEIN IN RATS WITH EXPERIMENTAL PROTEINURIA BY D. MENDEL* From the Department of Physiology,
544 J. Phy8iol. (1961), 156, pp. 544-554 With 5 text-ftgure8 Printed in Great Britain TUBULAR REABSORPTION OF PROTEIN IN RATS WITH EXPERIMENTAL PROTEINURIA BY D. MENDEL* From the Department of Physiology,
Excretory System 1. a)label the parts indicated above and give one function for structures Y and Z
 Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- X- Y- Z- b) Which of the following is not a function of the organ shown? A. to produce
Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- X- Y- Z- b) Which of the following is not a function of the organ shown? A. to produce
Sunday, July 17, 2011 URINARY SYSTEM
 URINARY SYSTEM URINARY SYSTEM Let s take a look at the anatomy first! KIDNEYS: are complex reprocessing centers where blood is filtered through and waste products are removed. Wastes and extra water become
URINARY SYSTEM URINARY SYSTEM Let s take a look at the anatomy first! KIDNEYS: are complex reprocessing centers where blood is filtered through and waste products are removed. Wastes and extra water become
The kidneys are excretory and regulatory organs. By
 exercise 9 Renal System Physiology Objectives 1. To define nephron, renal corpuscle, renal tubule, afferent arteriole, glomerular filtration, efferent arteriole, aldosterone, ADH, and reabsorption 2. To
exercise 9 Renal System Physiology Objectives 1. To define nephron, renal corpuscle, renal tubule, afferent arteriole, glomerular filtration, efferent arteriole, aldosterone, ADH, and reabsorption 2. To
IN RESPONSE to arginine vasopressin (AVP), concentrated
 0021-972X/97/$03.00/0 Vol. 82, No. 6 Journal of Clinical Endocrinology and Metabolism Printed in U.S.A. Copyright 1997 by The Endocrine Society Urinary Excretion of Aquaporin-2 in the Diagnosis of Central
0021-972X/97/$03.00/0 Vol. 82, No. 6 Journal of Clinical Endocrinology and Metabolism Printed in U.S.A. Copyright 1997 by The Endocrine Society Urinary Excretion of Aquaporin-2 in the Diagnosis of Central
Renal Pharmacology. Diuretics: Carbonic Anhydrase Inhibitors Thiazides Loop Diuretics Potassium-sparing Diuretics BIMM118
 Diuretics: Carbonic Anhydrase Inhibitors Thiazides Loop Diuretics Potassium-sparing Diuretics Renal Pharmacology Kidneys: Represent 0.5% of total body weight, but receive ~25% of the total arterial blood
Diuretics: Carbonic Anhydrase Inhibitors Thiazides Loop Diuretics Potassium-sparing Diuretics Renal Pharmacology Kidneys: Represent 0.5% of total body weight, but receive ~25% of the total arterial blood
Moderate (20%) fructose-enriched diet stimulates saltsensitive hypertension with increased salt retention and decreased renal nitric oxide
 ORIGINAL RESEARCH Physiological Reports ISSN 2051-817X Moderate (20%) fructose-enriched diet stimulates saltsensitive hypertension with increased salt retention and decreased renal nitric oxide Kevin L.
ORIGINAL RESEARCH Physiological Reports ISSN 2051-817X Moderate (20%) fructose-enriched diet stimulates saltsensitive hypertension with increased salt retention and decreased renal nitric oxide Kevin L.
Impaired sodium excretion and salt-sensitive hypertension in corin-deficient mice
 original article http://www.kidney-international.org & International Society of Nephrology see commentary on page 7 Impaired sodium excretion and salt-sensitive hypertension in corin-deficient mice Wei
original article http://www.kidney-international.org & International Society of Nephrology see commentary on page 7 Impaired sodium excretion and salt-sensitive hypertension in corin-deficient mice Wei
Cholecystokinin antagonist, proglumide, stimulates growth hormone release in the rat
 J. Biosci., Vol. 15, Number 1, March 1990, pp. 17 21. Printed in India. Cholecystokinin antagonist, proglumide, stimulates growth hormone release in the rat E. VIJAYAN* and S. M. McCANN Department of Physiology,
J. Biosci., Vol. 15, Number 1, March 1990, pp. 17 21. Printed in India. Cholecystokinin antagonist, proglumide, stimulates growth hormone release in the rat E. VIJAYAN* and S. M. McCANN Department of Physiology,
Tiny Jaarsma Linköping University No conflict of interest
 Detrimental effects of sodium in heart failure - Tiny Jaarsma Linköping University No conflict of interest Sodium restriction in Heart Failure Why? Prevention of heart failure Blood pressure treatment
Detrimental effects of sodium in heart failure - Tiny Jaarsma Linköping University No conflict of interest Sodium restriction in Heart Failure Why? Prevention of heart failure Blood pressure treatment
Osmoregulation and Renal Function
 1 Bio 236 Lab: Osmoregulation and Renal Function Fig. 1: Kidney Anatomy Fig. 2: Renal Nephron The kidneys are paired structures that lie within the posterior abdominal cavity close to the spine. Each kidney
1 Bio 236 Lab: Osmoregulation and Renal Function Fig. 1: Kidney Anatomy Fig. 2: Renal Nephron The kidneys are paired structures that lie within the posterior abdominal cavity close to the spine. Each kidney
CONCERNING THE EFFECTS OF MAGNESIUM SULFATE ON RENAL FUNCTION, ELECTROLYTE EXCRETION, AND CLEARANCE OF MAGNESIUM
 CONCERNING THE EFFECTS OF MAGNESIUM SULFATE ON RENAL FUNCTION, ELECTROLYTE EXCRETION, AND CLEARANCE OF MAGNESIUM B. I. Heller,, J. F. Hammarsten, F. L. Stutzman J Clin Invest. 1953;32(9):858-861. https://doi.org/10.1172/jci102803.
CONCERNING THE EFFECTS OF MAGNESIUM SULFATE ON RENAL FUNCTION, ELECTROLYTE EXCRETION, AND CLEARANCE OF MAGNESIUM B. I. Heller,, J. F. Hammarsten, F. L. Stutzman J Clin Invest. 1953;32(9):858-861. https://doi.org/10.1172/jci102803.
Renal Function in Mice: Effects of Volume Expansion and Angiotensin II
 J Am Soc Nephrol 10: 2631 2636, 1999 Renal Function in Mice: Effects of Volume Expansion and Angiotensin II LUDEK CERVENKA,* KENNETH D. MITCHELL, and L. GABRIEL NAVAR *Department of Experimental Medicine,
J Am Soc Nephrol 10: 2631 2636, 1999 Renal Function in Mice: Effects of Volume Expansion and Angiotensin II LUDEK CERVENKA,* KENNETH D. MITCHELL, and L. GABRIEL NAVAR *Department of Experimental Medicine,
(ethanol) suggests that it is similar to the diuresis following ingestion of water.
 435 J. Physiol. (I946) I04, 435-442 6I2.464.I THE EFFECT OF ETHYL ALCOHOL AND SOME OTHER DIURETICS ON CHLORIDE EXCRETION IN MAN BY M. GRACE EGGLETON AND ISABEL G. SMITH, From the Physiology Department,
435 J. Physiol. (I946) I04, 435-442 6I2.464.I THE EFFECT OF ETHYL ALCOHOL AND SOME OTHER DIURETICS ON CHLORIDE EXCRETION IN MAN BY M. GRACE EGGLETON AND ISABEL G. SMITH, From the Physiology Department,
renal function and renin release in acute experimental heart failure
 LABORATORY INVESTIGATION ATRIAL NATRIURETIC PEPTIDE Effects of synthetic atrial natriuretic peptide on renal function and renin release in acute experimental heart failure TERRY A. SCRIVEN, B.A., AND JOHN
LABORATORY INVESTIGATION ATRIAL NATRIURETIC PEPTIDE Effects of synthetic atrial natriuretic peptide on renal function and renin release in acute experimental heart failure TERRY A. SCRIVEN, B.A., AND JOHN
A. Correct! Flushing acids from the system will assist in re-establishing the acid-base equilibrium in the blood.
 OAT Biology - Problem Drill 16: The Urinary System Question No. 1 of 10 1. Which of the following would solve a drop in blood ph? Question #01 (A) Decreased retention of acids. (B) Increased excretion
OAT Biology - Problem Drill 16: The Urinary System Question No. 1 of 10 1. Which of the following would solve a drop in blood ph? Question #01 (A) Decreased retention of acids. (B) Increased excretion
Hyperaldosteronism: Conn's Syndrome
 RENAL AND ACID-BASE PHYSIOLOGY 177 Case 31 Hyperaldosteronism: Conn's Syndrome Seymour Simon is a 54-year-old college physics professor who maintains a healthy lifestyle. He exercises regularly, doesn't
RENAL AND ACID-BASE PHYSIOLOGY 177 Case 31 Hyperaldosteronism: Conn's Syndrome Seymour Simon is a 54-year-old college physics professor who maintains a healthy lifestyle. He exercises regularly, doesn't
Renal System and Excretion
 Renal System and Excretion Biology 105 Lecture 19 Chapter 16 Outline Renal System I. Functions II. Organs of the renal system III. Kidneys 1. Structure 2. Function IV. Nephron 1. Structure 2. Function
Renal System and Excretion Biology 105 Lecture 19 Chapter 16 Outline Renal System I. Functions II. Organs of the renal system III. Kidneys 1. Structure 2. Function IV. Nephron 1. Structure 2. Function
Principles of Anatomy and Physiology
 Principles of Anatomy and Physiology 14 th Edition CHAPTER 27 Fluid, Electrolyte, and Acid Base Fluid Compartments and Fluid In adults, body fluids make up between 55% and 65% of total body mass. Body
Principles of Anatomy and Physiology 14 th Edition CHAPTER 27 Fluid, Electrolyte, and Acid Base Fluid Compartments and Fluid In adults, body fluids make up between 55% and 65% of total body mass. Body
CHAPTER 27 LECTURE OUTLINE
 CHAPTER 27 LECTURE OUTLINE I. INTRODUCTION A. Body fluid refers to body water and its dissolved substances. B. Regulatory mechanisms insure homeostasis of body fluids since their malfunction may seriously
CHAPTER 27 LECTURE OUTLINE I. INTRODUCTION A. Body fluid refers to body water and its dissolved substances. B. Regulatory mechanisms insure homeostasis of body fluids since their malfunction may seriously
Osmotic Regulation and the Urinary System. Chapter 50
 Osmotic Regulation and the Urinary System Chapter 50 Challenge Questions Indicate the areas of the nephron that the following hormones target, and describe when and how the hormones elicit their actions.
Osmotic Regulation and the Urinary System Chapter 50 Challenge Questions Indicate the areas of the nephron that the following hormones target, and describe when and how the hormones elicit their actions.
Water (Dysnatremia) & Sodium (Dysvolemia) Disorders Ahmad Raed Tarakji, MD, MSPH, PGCertMedEd, FRCPC, FACP, FASN, FNKF, FISQua
 Water (Dysnatremia) & Sodium (Dysvolemia) Disorders Ahmad Raed Tarakji, MD, MSPH, PGCertMedEd, FRCPC, FACP, FASN, FNKF, FISQua Assistant Professor Nephrology Unit, Department of Medicine College of Medicine,
Water (Dysnatremia) & Sodium (Dysvolemia) Disorders Ahmad Raed Tarakji, MD, MSPH, PGCertMedEd, FRCPC, FACP, FASN, FNKF, FISQua Assistant Professor Nephrology Unit, Department of Medicine College of Medicine,
OT Exam 3, August 19, 2002 Page 1 of 6. Occupational Therapy Physiology, Summer Examination 3. August 19, 2002
 Page 1 of 6 Occupational Therapy Physiology, Summer 2002 Examination 3 August 19, 2002 There are 20 questions and each question is worth 5 points for a total of 100 points. Dr. Heckman's section is questions
Page 1 of 6 Occupational Therapy Physiology, Summer 2002 Examination 3 August 19, 2002 There are 20 questions and each question is worth 5 points for a total of 100 points. Dr. Heckman's section is questions
NIH Public Access Author Manuscript Kidney Int. Author manuscript; available in PMC 2013 November 01.
 NIH Public Access Author Manuscript Published in final edited form as: Kidney Int. 2013 May ; 83(5): 779 782. doi:10.1038/ki.2012.468. Need to quickly excrete K +? Turn off NCC Alicia A. McDonough 1 and
NIH Public Access Author Manuscript Published in final edited form as: Kidney Int. 2013 May ; 83(5): 779 782. doi:10.1038/ki.2012.468. Need to quickly excrete K +? Turn off NCC Alicia A. McDonough 1 and
Relaxation responses of aortic rings from salt-loaded high calcium fed rats to potassium chloride, calcium chloride and magnesium sulphate
 Pathophysiology 4 (1998) 275 280 Relaxation responses of aortic rings from salt-loaded high calcium fed rats to potassium chloride, calcium chloride and magnesium sulphate B.J. Adegunloye, O.A. Sofola
Pathophysiology 4 (1998) 275 280 Relaxation responses of aortic rings from salt-loaded high calcium fed rats to potassium chloride, calcium chloride and magnesium sulphate B.J. Adegunloye, O.A. Sofola
WATER, SODIUM AND POTASSIUM
 WATER, SODIUM AND POTASSIUM Attila Miseta Tamás Kőszegi Department of Laboratory Medicine, 2016 1 Average daily water intake and output of a normal adult 2 Approximate contributions to plasma osmolality
WATER, SODIUM AND POTASSIUM Attila Miseta Tamás Kőszegi Department of Laboratory Medicine, 2016 1 Average daily water intake and output of a normal adult 2 Approximate contributions to plasma osmolality
Neonatal Fluid Therapy Not my mother s physiology!!
 Neonatal Fluid Therapy Not my mother s physiology!! Physiologic Approach to Neonatal Fluid Therapy General principles of fluid balance Fetal physiology of fluid balance Neonatal physiology of fluid balance
Neonatal Fluid Therapy Not my mother s physiology!! Physiologic Approach to Neonatal Fluid Therapy General principles of fluid balance Fetal physiology of fluid balance Neonatal physiology of fluid balance
Kidneys and Homeostasis
 16 The Urinary System The Urinary System OUTLINE: Eliminating Waste Components of the Urinary System Kidneys and Homeostasis Urination Urinary Tract Infections Eliminating Waste Excretion Elimination of
16 The Urinary System The Urinary System OUTLINE: Eliminating Waste Components of the Urinary System Kidneys and Homeostasis Urination Urinary Tract Infections Eliminating Waste Excretion Elimination of
IN this issue of Hypertension is an article by Kimura and his colleagues
 Hypertension Editorials Renal Function Curve A Key to Understanding the Pathogenesis of Hypertension IN this issue of Hypertension is an article by Kimura and his colleagues 1 entitled "Renal Function
Hypertension Editorials Renal Function Curve A Key to Understanding the Pathogenesis of Hypertension IN this issue of Hypertension is an article by Kimura and his colleagues 1 entitled "Renal Function
ARG-13 OF B-TYPE NATRIURETIC PEPTIDE RECIPROCALLY MODULATES BINDING TO GUANYLYL CYCLASE BUT NOT CLEARANCE RECEPTORS #
 Molecular Pharmacology This article has not Fast been Forward. copyedited and Published formatted. The on final June version 8, 2010 may differ as doi:10.1124/mol.110.066084 from this version. MOL #66084
Molecular Pharmacology This article has not Fast been Forward. copyedited and Published formatted. The on final June version 8, 2010 may differ as doi:10.1124/mol.110.066084 from this version. MOL #66084
HELMY M. SIRAGY*, TADASHI INAGAMI, TOSHIHIRO ICHIKI, AND ROBERT M. CAREY* METHODS
 Proc. Natl. Acad. Sci. USA Vol. 96, pp. 6506 6510, May 1999 Physiology Sustained hypersensitivity to angiotensin II and its mechanism in mice lacking the subtype-2 (AT 2 ) angiotensin receptor (blood pressure
Proc. Natl. Acad. Sci. USA Vol. 96, pp. 6506 6510, May 1999 Physiology Sustained hypersensitivity to angiotensin II and its mechanism in mice lacking the subtype-2 (AT 2 ) angiotensin receptor (blood pressure
Hypovolemic Shock: Regulation of Blood Pressure
 CARDIOVASCULAR PHYSIOLOGY 81 Case 15 Hypovolemic Shock: Regulation of Blood Pressure Mavis Byrne is a 78-year-old widow who was brought to the emergency room one evening by her sister. Early in the day,
CARDIOVASCULAR PHYSIOLOGY 81 Case 15 Hypovolemic Shock: Regulation of Blood Pressure Mavis Byrne is a 78-year-old widow who was brought to the emergency room one evening by her sister. Early in the day,
Effect of an Intravenous Sodium Chloride Load on Renal Hemodynamics and Electrolyte Excretion in Essential Hypertension
 Effect of an Intravenous Sodium Chloride Load on Renal Hemodynamics and Electrolyte Excretion in Essential Hypertension BY PAUL T. COTTIER, M.D., JOHN M. WELLER, M.D., AND SIBLEY W. HOOBLER, M.D. Excretion
Effect of an Intravenous Sodium Chloride Load on Renal Hemodynamics and Electrolyte Excretion in Essential Hypertension BY PAUL T. COTTIER, M.D., JOHN M. WELLER, M.D., AND SIBLEY W. HOOBLER, M.D. Excretion
SUMMARY OF PRODUCT CHARACTERISTICS 2. QUALITATIVE AND QUANTITATIVE COMPOSITION
 SUMMARY OF PRODUCT CHARACTERISTICS PRODUCT SUMMARY 1. NAME OF THE MEDICINAL PRODUCT Sterile Potassium Chloride Concentrate 15%. 2. QUALITATIVE AND QUANTITATIVE COMPOSITION 15% of Potassium Chloride in
SUMMARY OF PRODUCT CHARACTERISTICS PRODUCT SUMMARY 1. NAME OF THE MEDICINAL PRODUCT Sterile Potassium Chloride Concentrate 15%. 2. QUALITATIVE AND QUANTITATIVE COMPOSITION 15% of Potassium Chloride in
Amjad Bani Hani Ass.Prof. of Cardiac Surgery & Intensive Care FLUIDS AND ELECTROLYTES
 Amjad Bani Hani Ass.Prof. of Cardiac Surgery & Intensive Care FLUIDS AND ELECTROLYTES Body Water Content Water Balance: Normal 2500 2000 1500 1000 500 Metab Food Fluids Stool Breath Sweat Urine
Amjad Bani Hani Ass.Prof. of Cardiac Surgery & Intensive Care FLUIDS AND ELECTROLYTES Body Water Content Water Balance: Normal 2500 2000 1500 1000 500 Metab Food Fluids Stool Breath Sweat Urine
Relation Between Sodium Intake, Renal Function, and the Regulation of Arterial Pressure. Jeffrey L. Osborn
 1-91 Relation Between Sodium Intake, Renal Function, and the Regulation of Arterial Pressure Jeffrey L. Osborn The long-term regulation of arterial pressure requires the maintenance of a balance between
1-91 Relation Between Sodium Intake, Renal Function, and the Regulation of Arterial Pressure Jeffrey L. Osborn The long-term regulation of arterial pressure requires the maintenance of a balance between
Blood Pressure Regulation in ANF-Transgenic Mice: Role of Angiotensin and Vasopressin
 Physiol. Res. 43: 145-150, 1994 Blood Pressure Regulation in ANF-Transgenic Mice: Role of Angiotensin and Vasopressin B. LICHARDUS1, A.T. VERESS, L.J. FIELD2, H. SONNENBERG ' y Department of Physiology,
Physiol. Res. 43: 145-150, 1994 Blood Pressure Regulation in ANF-Transgenic Mice: Role of Angiotensin and Vasopressin B. LICHARDUS1, A.T. VERESS, L.J. FIELD2, H. SONNENBERG ' y Department of Physiology,
Role of Minerals in Hypertension
 Role of Minerals in Hypertension Lecture objectives By the end of the lecture students will be able to Define primary and secondary hypertention and their risk factors. Relate role of minerals with hypertention.
Role of Minerals in Hypertension Lecture objectives By the end of the lecture students will be able to Define primary and secondary hypertention and their risk factors. Relate role of minerals with hypertention.
Renal physiology D.HAMMOUDI.MD
 Renal physiology D.HAMMOUDI.MD Functions Regulating blood ionic composition Regulating blood ph Regulating blood volume Regulating blood pressure Produce calcitrol and erythropoietin Regulating blood glucose
Renal physiology D.HAMMOUDI.MD Functions Regulating blood ionic composition Regulating blood ph Regulating blood volume Regulating blood pressure Produce calcitrol and erythropoietin Regulating blood glucose
RENAL PHYSIOLOGY. Physiology Unit 4
 RENAL PHYSIOLOGY Physiology Unit 4 Renal Functions Primary Function is to regulate the chemistry of plasma through urine formation Additional Functions Regulate concentration of waste products Regulate
RENAL PHYSIOLOGY Physiology Unit 4 Renal Functions Primary Function is to regulate the chemistry of plasma through urine formation Additional Functions Regulate concentration of waste products Regulate
Studies on the Control of Sodium Excretion
 Studies on the Control of Sodium Excretion in Experimental Uremia RAYMOND G. SCHULTZE, HowARD S. SHAPIRo, and NEAL S. BRICKER From the Renal Division, Department of Internal Medicine, Washington University
Studies on the Control of Sodium Excretion in Experimental Uremia RAYMOND G. SCHULTZE, HowARD S. SHAPIRo, and NEAL S. BRICKER From the Renal Division, Department of Internal Medicine, Washington University
Hyponatremia as a Cardiovascular Biomarker
 Hyponatremia as a Cardiovascular Biomarker Uri Elkayam, MD Professor of Medicine University of Southern California Keck School of Medicine elkayam@usc.edu Disclosure Research grant from Otsuka for the
Hyponatremia as a Cardiovascular Biomarker Uri Elkayam, MD Professor of Medicine University of Southern California Keck School of Medicine elkayam@usc.edu Disclosure Research grant from Otsuka for the
Major intra and extracellular ions Lec: 1
 Major intra and extracellular ions Lec: 1 The body fluids are solutions of inorganic and organic solutes. The concentration balance of the various components is maintained in order for the cell and tissue
Major intra and extracellular ions Lec: 1 The body fluids are solutions of inorganic and organic solutes. The concentration balance of the various components is maintained in order for the cell and tissue
Proceedings of the 34th World Small Animal Veterinary Congress WSAVA 2009
 www.ivis.org Proceedings of the 34th World Small Animal Veterinary Congress WSAVA 2009 São Paulo, Brazil - 2009 Next WSAVA Congress : Reprinted in IVIS with the permission of the Congress Organizers PROTEINURIA
www.ivis.org Proceedings of the 34th World Small Animal Veterinary Congress WSAVA 2009 São Paulo, Brazil - 2009 Next WSAVA Congress : Reprinted in IVIS with the permission of the Congress Organizers PROTEINURIA
Outline Urinary System. Urinary System and Excretion. Urine. Urinary System. I. Function II. Organs of the urinary system
 Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
The Urinary S. (Chp. 10) & Excretion. What are the functions of the urinary system? Maintenance of water-salt and acidbase
 10.1 Urinary system The Urinary S. (Chp. 10) & Excretion 10.1 Urinary system What are the functions of the urinary system? 1. Excretion of metabolic wastes (urea, uric acid & creatinine) 1. Maintenance
10.1 Urinary system The Urinary S. (Chp. 10) & Excretion 10.1 Urinary system What are the functions of the urinary system? 1. Excretion of metabolic wastes (urea, uric acid & creatinine) 1. Maintenance
** TMP mean page 340 in 12 th edition. Questions 1 and 2 Use the following clinical laboratory test results for questions 1 and 2:
 QUESTION Questions 1 and 2 Use the following clinical laboratory test results for questions 1 and 2: Urine flow rate = 1 ml/min Urine inulin concentration = 100 mg/ml Plasma inulin concentration = 2 mg/ml
QUESTION Questions 1 and 2 Use the following clinical laboratory test results for questions 1 and 2: Urine flow rate = 1 ml/min Urine inulin concentration = 100 mg/ml Plasma inulin concentration = 2 mg/ml
Renal-Related Questions
 Renal-Related Questions 1) List the major segments of the nephron and for each segment describe in a single sentence what happens to sodium there. (10 points). 2) a) Describe the handling by the nephron
Renal-Related Questions 1) List the major segments of the nephron and for each segment describe in a single sentence what happens to sodium there. (10 points). 2) a) Describe the handling by the nephron
Enteral and parenteral nutrition in GI failure and short bowel syndrome
 Enteral and parenteral nutrition in GI failure and short bowel syndrome Alastair Forbes University College London Intestinal failure Inadequate functional intestine to allow health to be maintained by
Enteral and parenteral nutrition in GI failure and short bowel syndrome Alastair Forbes University College London Intestinal failure Inadequate functional intestine to allow health to be maintained by
Pharmacokinetics and Biological Actions of Subcutaneously Administered Human Brain Natriuretic Peptide
 0022-3565/98/2871-0067$03.00/0 THE JOURNAL OF PHARMACOLOGY AND EXPERIMENTAL THERAPEUTICS Vol. 287, No. 1 Copyright 1998 by The American Society for Pharmacology and Experimental Therapeutics Printed in
0022-3565/98/2871-0067$03.00/0 THE JOURNAL OF PHARMACOLOGY AND EXPERIMENTAL THERAPEUTICS Vol. 287, No. 1 Copyright 1998 by The American Society for Pharmacology and Experimental Therapeutics Printed in
