Real-Time Three-Dimensional Transesophageal Echocardiography in Transcutaneous, Catheter-Based Procedures for Repair of Structural Heart Diseases
|
|
|
- Andrew Ray
- 6 years ago
- Views:
Transcription
1 Real-Time Three-Dimensional Transesophageal Echocardiography in Transcutaneous, Catheter-Based Procedures for Repair of Structural Heart Diseases Gila Perk, MD, Carlos Ruiz, MD, PhD, Muhamed Saric, MD, PhD, and Itzhak Kronzon, MD Corresponding author Itzhak Kronzon, MD Noninvasive Cardiology Laboratory, New York University Medical Center, 560 First Avenue, New York, NY 10016, USA. Current Cardiovascular Imaging Reports 2009, 2:xx xx Current Medicine Group LLC ISSN Copyright 2009 by Current Medicine Group LLC We review the use of real-time three-dimensional transesophageal echocardiography (RT3D-TEE) in guiding percutaneous catheter-based procedures to repair structural heart defects. The utility of this novel imaging technique in percutaneous mitral valve repair and valvuloplasty, aortic valve insertion, device closure of atrial and ventricular septal defects, obliteration of the left atrial appendage, and pulmonary vein ablation is described. The main advantages of RT3D-TEE lie in its ability to visualize the entire length of intracardiac devices, including their tips, and to demonstrate their relationship to cardiac structures, to provide en face views of cardiac structures (such as the interatrial septum and the mitral valve) that are unobtainable in real time by any other imaging technique, and to allow for continuous monitoring during the procedure. It is likely that RT3D-TEE will become the standard of care for guidance of percutaneous, catheter-based procedures. Introduction Transcutaneous, catheter-based repair of congenital or acquired cardiovascular defects has been challenging the invasive cardiology community for the past half century. Although the most obvious advances were achieved in percutaneous coronary intervention and angioplasty of other arteries, there have been many recent attempts to repair structural heart defects. In the beginning, this attempt was led by pediatric cardiologists, who used interatrial balloon septostomy as the initial treatment in newborns with transposition of the great vessels [1]. Later, improvements in catheters, devices, and technical skills resulted in a plethora of transcatheter procedures that could successfully replace open-heart surgery and provide similar or even better results without the pain and risk of thoracotomy and cardiopulmonary bypass. These procedures also decreased the length and the costs of hospitalization. Some of them (eg, mitral balloon valvuloplasty for mitral stenosis or closure of secundum atrial septal defect [ASD]) have already become the standard of care. Others (eg, transcutaneous aortic valve replacement for aortic stenosis or transcatheter mitral annuloplasty and mitral clipping for mitral regurgitation) are still considered experimental. However, the state of the art is moving rapidly, fueled by clinical needs, imagination, ingenuity, courage, and by industrial and economic drives. Imaging has always been an essential part of any transcatheter procedure. Historically, cardiac catheterizations under fluoroscopy and contrast angiography were considered the gold standard in the diagnosis of structural heart defects and in the catheter guidance to the site of lesion. Although this radiologic technology is still in routine use, it suffers from poor depth resolution and inability to differentiate between various soft tissues. It frequently requires the use of toxic radio opaque contrast and exposes the patient to ionizing radiation. Several modalities of echocardiographic images have been added to the imaging armamentarium of transcatheter procedures. Two-dimensional (2D) modalities include transthoracic echocardiography (TTE), intracardiac echocardiography (ICE), and transesophageal echocardiography (TEE). Although TTE is totally noninvasive,
2 364 I Echocardiography Figure 1. Two-dimensional (2D) transesophageal echocardiogram (TEE) obtained during mitral valve clipping. Although in reality the guiding catheter enters the left atrium across the interatrial septum and traverses the mitral valve, on this 2D-TEE, the most distal portion of the catheter and its tip are barely visible. the image quality is frequently suboptimal, especially during catheterization procedures that do not allow a change in patient position for image optimization. ICE is invasive. The 2D transducer is mounted on an 8- to 10-F catheter, which is advanced intravenously to the right heart to provide images of selected cardiac structures. The procedure is well tolerated by patients and does not require additional sedation. Although the image quality is good, ICE catheters are monoplane transducers that provide only a limited number of imaging planes. Furthermore, the transducers are disposable and are quite expensive (over $2000). 2D-TEE has been used extensively during transcatheter procedures. The imaging planes are unlimited, and the image quality is good. However, the esophageal intubation and the presence of the transducer in the esophagus are frequently unpleasant, and require extra sedation or even general anesthesia. Although all the 2D modalities have improved our ability to visualize the details of cardiac anatomy and to evaluate intracardiac blood flow by Doppler techniques, they suffer from a limitation that interferes with imaging during transcatheter procedures. This limitation is related to the tomographic nature of the 2D images. Intracardiac catheters move in a three-dimensional (3D) environment, and frequently their course takes them away from the imaging plane. Therefore, the course of the catheters and particularly their tips may not be accurately assessed (Fig. 1). In addition, 2D echocardiography frequently does not show an en face view of a structure, the way it is seen by anatomists or surgeons. Real-time 3D (RT3D) echocardiography is a recently developed technique and is being increasingly used in echocardiography and cardiac catheterization laboratories [2 ]. Over the past several years, improvements in transducer technologies have led to the development of a full-matrix array transducer that acquires pyramidal-shaped datasets. These datasets can be processed online and offline to allow accurate evaluation of cardiac structures, volumes, and mass. More recently, a transesophageal transducer with RT3D capabilities has been developed; it is capable of acquiring high-quality RT3D-TEE images. The full-matrix array transducers are capable of three different types of data acquisition: 1. Narrow-angle acquisition, which generates realtime images at frame rates of 10 to 26 Hz. This acquisition mode is suitable for visualization of structures that are in the far zone of the ultrasound beam (eg, vegetations on right atrial pacemaker wires). Images are displayed in real time and can be rotated in all directions to allow visualization of the cardiac structures from many angles. However, this mode does not allow color Doppler imaging. 2. 3D zoom mode, in which a truncated pyramidal dataset is generated. The dimensions of this sector can be manually adjusted to display the region of interest. The image can then be rotated in all three axes, allowing visualization of the imaged structure from all angles and views. In this mode, the frame rate usually is low (< 10 Hz), thus lowering temporal resolution. This mode is suitable for structures that are in the near zone of the ultrasound beam and can be imaged at a near-perpendicular angle to the ultrasound beam. Examples include the mitral valve, the interatrial septum, and the orifice of the left atrial appendage (LAA). This mode does not support color Doppler imaging. 3. Wide -angle acquisition full-volume mode, in which a larger dataset is acquired in a pyramidal block, allowing larger volumes of cardiac structures to be displayed. This mode requires electrocardiographic gating, and data acquisition is performed over four to seven cardiac cycles. Of note, in this mode, lateral resolution deteriorates when compared with the narrow-angle acquisition mode. However, the temporal resolution is higher compared with the narrow-angle mode (up to Hz). The full-volume dataset is amenable to further processing (online or offline) with cropping along any plane, thus allowing for visualization of all structures captured in the pyramidal dataset. This mode is suitable for structures that are in either the far zone or the near zone of the ultrasound beam. It is also capable of color Doppler imaging; a full-volume acquisition over seven cardiac cycles is required. The temporal resolution in color Doppler mode is up to 25 Hz. These three different imaging modes make detailed anatomic evaluation as well as accurate volumetric assessment of cardiac structures and chambers possible. Use of RT3D-TEE allows for acquisition of high-resolution 3D
3 RT3D-TEE in Transcutaneous, Catheter-Based Procedures for Structural Heart Diseases I Perk et al. I 365 Figure 2. Mitral valve clipping. A, Real-time three-dimensional (RT3D) transesophageal echocardiography (TEE) zoom image from the left atrial perspective clearly demonstrates the delivery catheter as it enters the left atrium through the interatrial septum and bends toward the mitral valve orifice prior to clip deployment. B, RT3D zoom image demonstrates proper orientation of the clip perpendicular to the mitral closure line. C, On the two-dimensional TEE image, the relative relationship between the mitral clip and the mitral closure line is extremely difficult to ascertain. (From Perk et al. [2 ]; with permission.) images of intracardiac structures. It also permits visualization of structures en face and from other angles that cannot be obtained by 2D echocardiographic modalities. More importantly, real-time images of the entire intracardiac course of the catheters can be monitored throughout transcatheter procedures. The accurate anatomic relations between the catheter and the device it carries and the target cardiac structure can be assessed continuously. The interventionalist can use 3D images to guide a transcatheter procedure and evaluate its results [3]. This review describes the use of RT3D-TEE in selected transcatheter procedures. Valvular Heart Disease Mitral valve clipping Mitral valve clipping (MVC) is an experimental catheterbased approach for the treatment of mitral regurgitation. It entails placement of a clip at the tips of the mitral valve leaflets and creation of an edge-to-edge repair, resulting in a double-orifice mitral valve [4]. MVC offers a treatment alternative to patients who are considered high risk for standard surgical repair [5]. The procedure is performed via a central venous approach and a transseptal puncture. Where the trans-septal puncture is performed is very important because proper location of transseptal puncture increases the likelihood of successful clip deployment at the mitral valve leaflet tips. The clip is deployed through the guiding catheter (Fig. 2A) and positioned in such a way that the clip arms are perpendicular to the mitral valve closure line (Fig. 2B). The mitral leaflets are then grasped, and the severity of mitral regurgitation is assessed prior to final deployment of the clip. RT3D-TEE provides a detailed anatomy of the mitral valve, including individual scallops of both valve leaflets [6 ]. 3D zoom mode is particularly valuable because it provides an en face view of the mitral valve from the left atrial perspective
4 366 I Echocardiography Figure 3. Mitral valve clipping using two clips. A, Real-time three-dimensional (RT3D) zoom image from the left atrial perspective demonstrates that clip 1 has already been deployed. The mitral inlet now consists of two orifices: O 1 and O 2. A delivery catheter carrying clip 2 is seen over the orifice O 2. B, RT3D zoom image obtained after the deployment of the second clip. Now the mitral valve has three orifices: O 1, O 2, and O 3. C, Two-dimensional color Doppler transesophageal echocardiography image demonstrates mitral regurgitation (MR) before clipping (left) and after placement of the second clip (right). (From Perk et al. [2 ]; with permission.) (the so-called surgical view ). Such a view cannot be obtained by any other imaging technique. When compared with 2D imaging, RT3D-TEE provides better visualization of all the catheters, guides, and device assemblies, as well as the clip itself. Because in RT3D imaging the entire length of the guiding catheters and devices is continuously monitored, their optimal positioning is enhanced. The position of the catheters and devices relative to pertinent cardiac structures (such as the LAA and mitral valve annulus) can be shown in a single frame, which permits precise guidance to the interventionalist in proper placement of the clip. It is much easier to ascertain that the clip is placed perpendicular to the closure line of the mitral valve by RT3D than by 2D imaging techniques (Fig. 2B and Fig. 2C). On 2D-TEE, clip orientation relative to mitral valve closure line usually requires transgastric views, which on occasion are difficult to obtain. Occasionally, placement of a second clip may be required if echocardiography reveals significant residual mitral regurgitation. RT3D imaging provides simultaneous visualization of the already deployed clip and facilitates accurate placement of the second clip (Fig. 3). Mitral balloon valvuloplasty for mitral stenosis Percutaneous mitral balloon valvuloplasty (PMBV) is considered the technique of choice for the treatment of selected patients with mitral stenosis [7]. 2D-TTE and TEE have been used prior to and during the procedure to accurately assess the severity of the stenosis [8]. It was also used to assess the mitral valve score and the feasibility of valvuloplasty (high scores are associated with lower success rates) [9]. TEE has also been used to evaluate the possibility of left atrial clots, which are considered a contraindication for PMBV [10]. 3D-TTE is now considered the noninvasive modality of choice for the assessment of mitral stenosis severity (Fig. 4A). In patients with mitral stenosis, the shape of the left ventricular inflow resembles a funnel, which has its narrowest orifice area at its left ventricular end. Using 3D echocardiography, one can select the narrowest orifice and accurately measure its area. PMBV is performed via a central venous approach and a transseptal puncture. A balloon is introduced through a guiding catheter into the mitral valve orifice and then inflated in an attempt to create a controlled commissural tear. 2D-TEE is often used to help guide this procedure [11]. This imaging technique is used to guide the transseptal puncture and the positioning of the balloon between the mitral valve leaflet tips prior to balloon inflation. This modality is useful to assess the presence of complications and severity of mitral regurgitation post-inflation that can be created by mitral valve tear. Doppler echocardiography can provide information about the transvalvular gradient and grade mitral regurgitation (if any). Guiding of the transseptal puncture can be optimized by using RT3D-TEE [12]. Visualization of the transseptal puncture needle tip provides better selection of the puncture site. After the puncture, the entire length of the left atrial portion of the guiding catheter can be visualized. This allows clear delineation of the spatial orientation of
5 RT3D-TEE in Transcutaneous, Catheter-Based Procedures for Structural Heart Diseases I Perk et al. I 367 Figure 4. Percutaneous mitral balloon valvuloplasty (PMBV). All images represent real-time three-dimensional (RT3D) zoom view ( surgical view ) from the left atrial perspective. A, RT3D zoom view demonstrates the shape of the stenosed mitral orifice prior to PMBV. B, Deflated valvuloplasty balloon is seen being positioned inside the stenosed mitral orifice. C, Inflated valvuloplasty balloon (arrow) stretches the mitral orifice. D, After PMBV, the orifice of the mitral valve has increased in size. the catheter and the balloon in the left atrium, and their relation to the mitral valve orifice. Localization of the balloon in the mitral valve orifice can be achieved using the 3D zoom mode (Fig. 4B). The narrow portion of the balloon is placed through the tips of the mitral valve leaflets. The location is then confirmed by examining the balloon position from several angles by rotating the image, thus obviating the need for changing the imaging angles or adjusting the probe position. Immediately following balloon inflation (Fig. 4C), the mitral valve is inspected to determine if commissural splitting has been achieved, and to assess the increment in the mitral orifice area (Fig. 4D). RT3D imaging can also provide information about potential complications (eg, leaflet tear that, unlike commissural splitting, is perpendicular to the long axis of the mitral orifice). Post-PMBV, mitral regurgitation is a known potential complication. Its mechanism, site, and severity can be assessed by full-volume 3D-TEE. Percutaneous closure of prosthetic valve dehiscence Prosthetic valve dehiscence is a common complication of valve replacement surgery. It is estimated that 30% of all prosthetic valve regurgitations are associated with dehiscence. Prosthetic valve dehiscence results in paravalvular regurgitation, which may be severe and can result in heart failure symptoms and hemolysis. The latter can complicate even a very small paravalvular leak. Until recently, this complication has been treated by repeat open heart surgery to repair the leak, and not infrequently, re-replacement of the prosthetic valve. These reoperations carry a significant risk and suffering to the patient. A novel percutaneous approach has been attempted to correct these complications [13]. It involves implantation of an occlusion device in the dehisced portion of the mitral or aortic prosthetic valve [14]. In mitral valve dehiscence, the catheter approach to the dehiscence site in most cases is antegrade, using transseptal puncture. Occasionally, the
6 368 I Echocardiography Figure 5. Percutaneous closure of prosthetic valve dehiscence. A, Real-time three-dimensional (RT3D) transesophageal echocardiography zoom view from the left atrial perspective demonstrates the precise location and shape of the dehisced segment. B, Full-volume color RT3D image shows paravalvular mitral regurgitation due to prosthetic valve dehiscence. C, RT3D zoom imaging from the left atrial perspective is used to guide the catheter to the dehisced segment. D, RT3D zoom image demonstrates the atrial side of the closure device plugging the dehisced segment. retrograde approach is preferred, and the dehiscence site is reached via the left ventricle using arterial puncture or even direct percutaneous left ventricular apical puncture. 2D echocardiography can demonstrate paravalvular regurgitation, but usually cannot demonstrate its exact location, size, and shape. This information is essential for the closure procedure. Using the 3D zoom mode, a surgical view of the mitral prosthesis can be obtained (Fig. 5A), with clear definition of the location, shape, size, and extent of the dehisced portion [15 ]. Full-volume 3D imaging with color Doppler flow imaging (Fig. 5B) enables accurate assessment of valvular regurgitation (paravalvular, transvalvular, or both). This allows identification of patients with suitable anatomy for percutaneous closure
7 RT3D-TEE in Transcutaneous, Catheter-Based Procedures for Structural Heart Diseases I Perk et al. I 369 Figure 6. Percutaneous closure of atrial septal defect (ASD). A, Full-volume threedimensional (3D) image with an en face view of a secundum ASD from the left atrial perspective. B, Real-time (RT) 3D zoom image is used to guide the catheter used in percutaneous ASD closure. C, RT3D zoom image shows that ASD closure device is in place. In the left panel, there is a side view of the ASD closure device; the right atrium is to the left of the ASD device. In the right panel, the ASD closure device is seen en face from the left atrial perspective. procedure. Use of RT3D imaging during the closure procedure allows verification of catheter placement through the dehisced segment, avoiding the mitral valve orifice (Fig. 5C). It also enables real-time assessment of the success of the occlusion procedure (Fig. 5D). Occasionally, more than one closure device is required. Catheter-based aortic valve implantation In patients with severe aortic stenosis who are not candidates for surgical valve replacement, percutaneous, catheter-based aortic valve implantation (PAVI) is a promising alternative [16]. PAVI is in its infancy, and the issues pertaining to its safety and long-term durability are yet to be determined. PAVI is performed either transfemorally or transapically. As with other percutaneous procedures, RT3D-TEE is used in both patient selection and intraprocedural guidance. Before the procedure, RT3D imaging allows for precise assessment of the aortic annulus size and the aortic valve morphology. Intraprocedurally, one can use RT3D imaging to continually monitor placement of catheters and devices used in PAVI. Following PAVI, RT3D-TEE is used to evaluate the outcomes of the procedure. It is important to confirm that the orifice of the left main coronary artery remains patent after the aortic valve is deployed. Cardiac Septal Defects ASD and patent foramen ovale closure In suitable patients, percutaneous closure of secundum ASD and patent foramen ovale (PFO) is replacing open-heart surgery as the preferred repair method. Both short- and long-term success rates of percutaneous ASD [17] and PFO [18] closures in such patients are excellent. Appropriate patient selection for percutaneous device closure is of utmost importance for the procedure s success [19]. RT3D-TEE allows for accurate measurement of the size of the septal defect and the size of the tissue rim that surrounds the defect, as well as for evaluation of the spatial relation between the defect and the aortic valve. These three parameters are crucial in determining if the patient is a candidate for percutaneous ASD or PFO closure, and for choosing the size of the closure device in suitable candidates. Using the RT3D zoom mode, either the secundum atrial defect or the region of the fossa ovalis can be visualized en face revealing the defect s true size and morphology (Fig. 6A). RT3D-TEE images often demonstrate that the secundum defect is not perfectly round. It may also show fenestrations, tissue strips, and partial membranes within the defect [20]. 2D imaging may underestimate the defect s size because the apparent diameters measured on 2D images are often geometric chords rather than true diameters. In contrast, RT3D-TEE imaging, with its ability to measure true diameters of the ASD, helps avoid inappropriate patient selection for percutaneous ASD or PFO closure. After the septal defect is sized and deemed amenable to percutaneous repair, a collapsed closure device is deployed via the guiding catheter (Fig. 6B). RT3D-TEE allows for continuous visualization of the tip of the guiding catheter, as well as of the closure device as it is being delivered.
8 370 I Echocardiography Figure 7. Ventricular septal defect (VSD). A, Color Doppler two-dimensional transthoracic echocardiogram in the parasternal long-axis view demonstrates a postinfarction VSD in the apical portion of the interatrial septum. B, Continuous-wave Doppler tracing demonstrates a high-velocity flow across the VSD in systole and a lower-velocity flow in diastole. The flow is from the left ventricle into the right ventricle (left-to-right shunt). C, Transthoracic three-dimensional (3D) image in the apical four-chamber view shows the location of the postinfarction VSD. D, Reconstructed full-volume transthoracic 3D image demonstrates an en face view of the VSD from the left ventricular perspective. LA left atrium; LV left ventricle; RA right atrium; RV right ventricle. (From Halpern et al. [21]; with permission.) Once the closure device has been expanded and deployed, RT3D imaging is used to ascertain its proper positioning (Fig. 6C). Both the left atrial and the right atrial plate of the device are easily visualized. In addition, RT3D-TEE helps determine if sufficient tissue rim is caught in between the two plates of the device. In case of device malpositioning, RT3D-TEE can be used to guide repositioning of the device. After the device is fully deployed, RT3D-TEE color Doppler imaging is used to verify that no residual blood flow across the device is present. Percutaneous closure of ventricular septal defect Traditionally, closure of congenital or acquired ventricular septal defect (VSD) was performed surgically. This operation requires cardiopulmonary bypass and carries a significant risk to the patient. The risk is particularly high in patients with post myocardial infarction VSD. These patients are frequently hemodynamically unstable. In addition, such a VSD is surrounded by ischemic, friable tissue, which does not permit effective suturing. Recently, percutaneous, catheter-based closure of VSD has become a nonsurgical option in selected patients [21]. After arterial puncture, a catheter is delivered retrogradely through the aortic valve and into the left ventricle close to the VSD. A separate catheter is advanced to the right ventricle using a central venous approach. This venous catheter is used to snare the arterial catheter. A closure device is then advanced to close the defect [22]. 2D echocardiography is frequently used to diagnose the site of the defect (Fig. 7A) and to assess its hemodynamics (Fig. 7B). However, this modality is unable to provide en face view of the defect and therefore cannot demonstrate its exact shape and size. RT3D echocardiography allows accurate visualization of the defect location, size, and shape (Fig. 7C and Fig. 7D). The information thus obtained is important for a decision about the feasibility of device closure, and aids in
9 RT3D-TEE in Transcutaneous, Catheter-Based Procedures for Structural Heart Diseases I Perk et al. I 371 Figure 8. Percutaneous closure of ventricular septal defect (VSD). A, Real-time three-dimensional (RT3D) transesophageal echocardiography (TEE) image shows a postinfarction VSD. In addition, the arterial catheter enters the left ventricle (LV) across the aortic valve and crosses the VSD. B, RT3D-TEE image rotated toward the right ventricle (RV) demonstrates the venous catheter in the RV used to snare the arterial catheter. C, Deployed Amplatzer VSD closure device (AGA Medical Corporation, Plymouth, MN) is seen on RT3D-TEE image. (From Halpern et al. [21]; with permission.) selecting the proper size of the closure device. RT3D-TEE is capable of imaging the entire length of the intracardiac portion of the arterial (Fig. 8A) and venous (Fig. 8B) catheters, and is therefore used to direct the catheters into the defect. It can also guide the accurate positioning and alignment of the closure device and provide immediate assessment of procedural results (Fig. 8C). LAA Obliteration The LAA is the most common site of thrombus formation in patients with nonvalvular atrial fibrillation. In addition, LAA clots are commonly seen in patients with mitral stenosis. Anticoagulation is the standard of care for the treatment and prevention of LAA thrombi. In patients who cannot receive anticoagulation, LAA occlusion may be considered as an alternative approach in reducing the embolic risk in such patients. LAA obliteration can be achieved either surgically (by oversewing the mouth of the LAA, for instance) [23] or percutaneously using a closure device [24]. Despite several studies, percutaneous LAA closure continues to be an experimental procedure. Percutaneous LAA closure is performed via a central venous approach. After transseptal puncture, an introducer is advanced across the interatrial septum and its tip is placed inside the left atrium. In the next step, a pigtail catheter is passed through the introducer and advanced into the LAA. Using the pigtail catheter as a guide, the introducer is then carefully advanced into the LAA. The pigtail catheter is then removed, and a collapsed LAA closure device assembly is passed through the introducer. When the assembly reaches the LAA, the closure device is expanded in order to obliterate the LAA orifice. As in PMBV, RT3D-TEE in used for both patient selection and procedure guidance. RT3D imaging can be used to accurately visualize the LAA prior to the procedure (Fig. 9A), to demonstrate the intracardiac trajectory of the catheters and introducers, to direct the transseptal puncture, and to guide the placement of the closure device (Fig. 9B).
10 372 I Echocardiography Figure 9. Percutaneous left atrial appendage obliteration. A, Real-time three-dimensional (RT3D) transesophageal echocardiography (TEE) en face zoom image of the orifice of the left atrial appendage from the left atrial perspective. B, RT3D-TEE image demonstrates proper placement of the pigtail catheter in the left atrial appendage. C, 3D-TEE image of a deployed left atrial appendage occluder device; full-volume 3D acquisition is shown on the left, and 3D zoom view on the right. The success of device deployment can be assessed in RT3D zoom mode with en face imaging of the closure device at the orifice of the LAA (Fig. 9C). The device is properly placed when its long axis is parallel to the long axis of the LAA. Improper (off-angle) positions of the device are much easier to demonstrate by RT3D than by 2D techniques. RT3D-TEE color Doppler imaging is crucial for ascertaining that no residual communication between the LAA and the left atrium persists after closure device placement. Incomplete obliteration of the LAA orifice has been shown to actually increase the embolic risk. In case of improper device placement, RT3D-TEE is also used to guide recapture and redeployment of the device. Pulmonary Vein Ablation In selected patients with either paroxysmal or chronic atrial fibrillation, percutaneous pulmonary vein ablation may offer symptomatic relief and may even obviate the need for long-term anticoagulation [25]. The procedure is performed under fluoroscopic guidance and with the aid of a 3D electrical map of the left atrium superimposed on previously acquired CT or MRI. Neither CT nor MRI images are truly live at the time of pulmonary vein ablation. In addition, both techniques have shortcomings: CT exposes the patient to radiation and potentially toxic iodinated contrast agents; and MRI is time consuming, expensive, and contraindicated in claustrophobic patients and patients with pacemakers or defibrillators. In some electrophysiology laboratories, ICE is used for additional guidance. However, as noted earlier, ICE is both invasive and expensive. RT3D-TEE is emerging as an alternative to ICE. Utilizing the RT3D zoom mode, one can obtain en face images of the ridge between the LAA and the left-sided pulmonary veins, an area that is important in pulmonary vein ablation procedures [26], and to guide the placement of the radiofrequency catheter in that region. Other Procedures RT3D imaging may be useful in monitoring myocardial biopsies and alcohol septal ablation for hypertrophic cardiomyopathy (HCM). During myocardial biopsy, RT3D-TEE may help define the anatomy and guide the deployment of the bioptome tip to the desired region of the heart. This in turn may increase the safety of the procedure and increase the yield for the tissue diagnosis of cardiac rejection, cardiomyopathy, or cardiac tumors. In HCM, RT3D images may provide the exact location of the septal-leaflet contact, which often is not central but rather displaced medially or laterally within the left ventricular outflow tract. However, RT3D imaging is limited in HCM by the fact that the outcome of alcohol septal ablation may not be evident at the time of the procedure. Conclusions RT3D imaging has several advantages over other imaging techniques in guiding percutaneous catheter-based
11 RT3D-TEE in Transcutaneous, Catheter-Based Procedures for Structural Heart Diseases I Perk et al. I 373 procedures to repair structural heart defects. The primary advantage of RT3D imaging lies in its ability to visualize the entire length of intracardiac devices, including the tips of various catheters, introducers, balloons, and other devices, as well as their relationship to cardiac structures. Another advantage of RT3D imaging is its ability to provide the en face views of cardiac structures of interest to the interventionalist, including the interatrial septum and the mitral valve. Currently, no other real-time imaging technique is capable of such views. Furthermore, 3D rendering of cardiac structures appears more intuitive and more easily understood than multiplane 2D tomographic imaging. Despite a few limitations (eg, reduced temporal resolution, occasional drop-outs masquerading as cardiac defects), RT3D imaging provides remarkable new insights into cardiac anatomy and pathophysiology. In summary, we believe that RT3D-TEE will become the technique of choice and the standard of care for guidance of percutaneous, catheter-based procedures. RT3D imaging will likely lead to safer percutaneous procedures because its use may lead to shorter procedure time, and decreased radiation and contrast exposure. Disclosure Dr. Kronzon has received grant support from GE Healthcare and has served on the speakers bureau for Philips. No other potential conflicts of interest relevant to this article were reported. References and Recommended Reading Papers of particular interest, published recently, have been highlighted as: Of importance Of major importance 1. Rashkind WJ: Palliative procedures for transposition of the great arteries. Br Heart J 1971, 33(Suppl): Perk G, Lang RM, Garcia-Fernandez MA, et al.: Use of real time three-dimensional transesophageal echocardiography in intracardiac catheter based interventions. J Am Soc Echocardiogr 2009, 22: This article represents one of the largest compendiums of cases in which RT3D-TEE was used to monitor catheter-based procedures to repair heart defects. It is based on the experience from several medical centers in the United States and Europe. 3. Balzer J, Kelm M, Kühl H: Real-time three-dimensional transoesophageal echocardiography for guidance of noncoronary interventions in the catheter laboratory. Eur J Echocardiogr 2009, 10: Feldman T, Wasserman HS, Herrmann HC, et al.: Percutaneous mitral valve repair using the edge-to-edge technique: six-month results of the EVEREST Phase I Clinical Trial. J Am Coll Cardiol 2005, 46: Herrmann HC, Rohatgi S, Wasserman HS, et al.: Mitral valve hemodynamic effects of percutaneous edge-to-edge repair with the MitraClip device for mitral regurgitation. Catheter Cardiovasc Interv 2006, 68: Sugeng L, Shernan SK, Weinert L, et al.: Real-time threedimensional transesophageal echocardiography in valve disease: comparison with surgical findings and evaluation of prosthetic valves. J Am Soc Echocardiogr 2008, 21: In this article, the authors provide an in-depth comparison between mitral valve anatomy seen on RT3D-TEE and in vivo findings at time of mitral valve surgery. They conclude that this novel imaging technique provides excellent imaging and accurate presurgical evaluation of native mitral valve pathology and mitral prostheses. 7. Arora R, Kalra GS, Singh S, et al.: Percutaneous transvenous mitral commissurotomy: immediate and long-term follow-up results. Catheter Cardiovasc Interv 2002, 55: Goldstein SA, Campbell A, Mintz GS, et al.: Feasibility of on-line transesophageal echocardiography during balloon mitral valvulotomy: experience with 93 patients. J Heart Valve Dis 1994, 3: Wilkins GT, Weyman AE, Abascal VM, et al.: Percutaneous balloon dilatation of the mitral valve: an analysis of echocardiographic variables related to outcome and the mechanism of dilatation. Br Heart J 1988, 60: Kronzon I, Tunick PA, Glassman E, et al.: Transesophageal echocardiography to detect atrial clots in candidates for percutaneous transseptal mitral balloon valvuloplasty. J Am Coll Cardiol 1990, 16: Kronzon I, Tunick PA, Schwinger ME, et al.: Transesophageal echocardiography during percutaneous mitral valvuloplasty. J Am Soc Echocardiogr 1989, 2: Applebaum RM, Kasliwal RR, Kanojia A, et al.: Utility of three-dimensional echocardiography during balloon mitral valvuloplasty. J Am Coll Cardiol 1998, 32: Kim MS, Casserly IP, Garcia JA, et al.: Percutaneous transcatheter closure of prosthetic mitral paravalvular leaks. Are we there yet? J Am Coll Cardiol Intv 2009, 2: Lasorda DM, Mohsin JC: Percutaneous closure of perivalvular mitral regurgitation with an Amplatzer occluder device in a patient with both prosthetic mitral and aortic valves. J Interv Cardiol 2008, 21: Kronzon I, Sugeng L, Perk G, et al.: Real-time 3-dimensional transesophageal echocardiography in the evaluation of post-operative mitral annuloplasty ring and prosthetic valve dehiscence. J Am Coll Cardiol 2009, 53: In this article, the authors describe the use of one or more closure devices to repair dehisced segments of prosthetic valves. This repair is extremely difficult to perform unless monitored by RT3D-TEE. 16. Bleiziffer S, Ruge H, Mazzitelli D, et al.: Valve implantation on the beating heart: catheter-assisted surgery for aortic stenosis. Dtsch Arztebl Int 2009, 106: Masura J, Gavora P, Pondar T: Long-term outcome of transcatheter secundum-type atrial septal defect closure using Amplatzer septal occluders. J Am Coll Cardiol 2005, 45: Luermans JG, Post MC, Schräder R, et al.: Outcome after percutaneous closure of a patent foramen ovale using the Intrasept device: a multi-centre study. Catheter Cardiovasc Interv 2008, 71: Podnar T, Martanovic P, Gavora P, Masura J: Morphological variations of secundum-type atrial septal defects: feasibility for percutaneous closure using Amplatzer septal occluders. Catheter Cardiovasc Interv 2001, 53: Acar P, Saliba Z, Bonhoeffer P, et al.: Influence of atrial septal defect anatomy in patient selection and assessment of closure with the Cardioseal device; a three-dimensional transoesophageal echocardiographic reconstruction. Eur Heart J 2000, 21: Halpern DG, Perk G, Ruiz C, et al.: Percutaneous closure of a post-myocardial infarction ventricular septal defect guided by real-time three-dimensional echocardiography. Eur J Echocardiogr 2009, 10: Holzer R, Balzer D, Amin Z, et al.: Transcatheter closure of postinfarction ventricular septal defects using the new Amplatzer muscular VSD occluder: results of a U.S. registry. Catheter Cardiovasc Interv 2004, 61:
12 374 I Echocardiography 23. Crystal E, Lamy A, Connolly SJ, et al.: Left Atrial Appendage Occlusion Study (LAAOS): A randomized clinical trial of left atrial appendage occlusion during routine coronary artery bypass graft surgery for long-term stroke prevention. Am Heart J 2003, 145: Möbius-Winkler S, Schuler GC, Sick PB: Interventional treatments for stroke prevention in atrial fibrillation with emphasis upon the WATCHMAN device. Curr Opin Neurol 2008, 21: Pappone C, Rosanio S, Oreto G, et al.: Circumferential radiofrequency ablation of pulmonary vein ostia: a new anatomic approach for curing atrial fibrillation. Circulation 2000, 102: Shah SJ, Bardo DM, Sugeng L, et al.: Real-time threedimensional transesophageal echocardiography of the left atrial appendage: initial experience in the clinical setting. J Am Soc Echocardiogr 2008, 21:
Revealing new insights. irotate electronic rotation and xplane adjustable biplane imaging. Ultrasound cardiology. irotate and xplane
 Ultrasound cardiology irotate and xplane Revealing new insights irotate electronic rotation and xplane adjustable biplane imaging Annemien van den Bosch and Jackie McGhie Department of Cardiology, Erasmus
Ultrasound cardiology irotate and xplane Revealing new insights irotate electronic rotation and xplane adjustable biplane imaging Annemien van den Bosch and Jackie McGhie Department of Cardiology, Erasmus
ATRIAL SEPTAL CLOSURE AND LEFT ATRIAL APPENDAGE OCCLUSION: INDICATIONS AND GUIDANCE ECHOCARDIOGRAPHY IN INTERVENTIONAL CARDIOLOGY
 ATRIAL SEPTAL CLOSURE AND LEFT ATRIAL APPENDAGE OCCLUSION: INDICATIONS AND GUIDANCE Aristides G. Panlilio, MD, FPCP, FPCC,FPSE, FASE Philippine Heart Center Chinese General Hospital and Medical Center
ATRIAL SEPTAL CLOSURE AND LEFT ATRIAL APPENDAGE OCCLUSION: INDICATIONS AND GUIDANCE Aristides G. Panlilio, MD, FPCP, FPCC,FPSE, FASE Philippine Heart Center Chinese General Hospital and Medical Center
Case Report Hemostasis of Left Atrial Appendage Bleed With Lariat Device
 273 Case Report Hemostasis of Left Atrial Appendage Bleed With Lariat Device Amena Hussain MD, Muhamed Saric MD, Scott Bernstein MD, Douglas Holmes MD, Larry Chinitz MD NYU Langone Medical Center, United
273 Case Report Hemostasis of Left Atrial Appendage Bleed With Lariat Device Amena Hussain MD, Muhamed Saric MD, Scott Bernstein MD, Douglas Holmes MD, Larry Chinitz MD NYU Langone Medical Center, United
When Does 3D Echo Make A Difference?
 When Does 3D Echo Make A Difference? Wendy Tsang, MD, SM Assistant Professor, University of Toronto Toronto General Hospital, University Health Network 1 Practical Applications of 3D Echocardiography Recommended
When Does 3D Echo Make A Difference? Wendy Tsang, MD, SM Assistant Professor, University of Toronto Toronto General Hospital, University Health Network 1 Practical Applications of 3D Echocardiography Recommended
Francesco Fulvio Faletra Gila Perk Natesa G. Pandian Hans-Joachim Nesser Itzhak Kronzon. Real-Time 3D Interventional Echocardiography
 Francesco Fulvio Faletra Gila Perk Natesa G. Pandian Hans-Joachim Nesser Itzhak Kronzon Real-Time 3D Interventional Echocardiography 123 Real-Time 3D Interventional Echocardiography Francesco Fulvio Faletra
Francesco Fulvio Faletra Gila Perk Natesa G. Pandian Hans-Joachim Nesser Itzhak Kronzon Real-Time 3D Interventional Echocardiography 123 Real-Time 3D Interventional Echocardiography Francesco Fulvio Faletra
Percutaneous Therapy for Calcific Mitral Valve Disease
 31 st Annual State of the Art Echocardiography San Diego, CA February 18, 2018 5:00 5:15 PM 15 min Percutaneous Therapy for Calcific Mitral Valve Disease Muhamed Sarić MD, PhD, MPA Director of Noninvasive
31 st Annual State of the Art Echocardiography San Diego, CA February 18, 2018 5:00 5:15 PM 15 min Percutaneous Therapy for Calcific Mitral Valve Disease Muhamed Sarić MD, PhD, MPA Director of Noninvasive
Adult Echocardiography Examination Content Outline
 Adult Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 Anatomy and Physiology Pathology Clinical Care and Safety Measurement Techniques, Maneuvers,
Adult Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 Anatomy and Physiology Pathology Clinical Care and Safety Measurement Techniques, Maneuvers,
Conflict of Interests
 Introduction to Interventional Echocardiography Roberto M Lang, MD Tomtec Conflict of Interests Research Grants Philips Medical Imaging Research Grants Speakers bureau Advisory bureau 1 Structural Heart
Introduction to Interventional Echocardiography Roberto M Lang, MD Tomtec Conflict of Interests Research Grants Philips Medical Imaging Research Grants Speakers bureau Advisory bureau 1 Structural Heart
JOINT MEETING 2 Tricuspid club Chairpersons: G. Athanassopoulos, A. Avgeropoulou, M. Khoury, G. Stavridis
 JOINT MEETING 2 Tricuspid club Chairpersons: G. Athanassopoulos, A. Avgeropoulou, M. Khoury, G. Stavridis Similarities and differences in Tricuspid vs. Mitral Valve Anatomy and Imaging. Echo evaluation
JOINT MEETING 2 Tricuspid club Chairpersons: G. Athanassopoulos, A. Avgeropoulou, M. Khoury, G. Stavridis Similarities and differences in Tricuspid vs. Mitral Valve Anatomy and Imaging. Echo evaluation
2D/3D in Evaluation of Atrial Septum
 2D/3D in Evaluation of Atrial Septum Roberto M Lang, MD OSTIUM SECUNDUM ASD: 2D AND 3D TNSESOPHAGEAL ECHO 1 Biplane views 90 0 3D Acquisi on Acquire 3D volume Lang RM et al. JASE 2012;25:3 46. Right atrial
2D/3D in Evaluation of Atrial Septum Roberto M Lang, MD OSTIUM SECUNDUM ASD: 2D AND 3D TNSESOPHAGEAL ECHO 1 Biplane views 90 0 3D Acquisi on Acquire 3D volume Lang RM et al. JASE 2012;25:3 46. Right atrial
Clinical Value of 3D Echo: Volumes and Valves
 Clinical Value of 3D Echo: Volumes and Valves James D. Thomas, M.D., F.A.C.C. Cardiovascular Imaging Center Department of Cardiology Cleveland Clinic Foundation Cleveland, Ohio, USA Conflicts: None 3D2011:1
Clinical Value of 3D Echo: Volumes and Valves James D. Thomas, M.D., F.A.C.C. Cardiovascular Imaging Center Department of Cardiology Cleveland Clinic Foundation Cleveland, Ohio, USA Conflicts: None 3D2011:1
The variety and complexity of percutaneous
 Hellenic J Cardiol 2012; 53: 1-5 Editorial Real-Time 3-Dimensional Transoesophageal Echocardiography: n Indispensable Resident in the Catheter Laboratory Constantina ggeli 1, Michael ellamy 1, Nilesh Sutaria
Hellenic J Cardiol 2012; 53: 1-5 Editorial Real-Time 3-Dimensional Transoesophageal Echocardiography: n Indispensable Resident in the Catheter Laboratory Constantina ggeli 1, Michael ellamy 1, Nilesh Sutaria
TAVR: Echo Measurements Pre, Post And Intra Procedure
 2017 ASE Florida, Orlando, FL October 10, 2017 8:00 8:25 AM 25 min TAVR: Echo Measurements Pre, Post And Intra Procedure Muhamed Sarić MD, PhD, MPA Director of Noninvasive Cardiology Echo Lab Associate
2017 ASE Florida, Orlando, FL October 10, 2017 8:00 8:25 AM 25 min TAVR: Echo Measurements Pre, Post And Intra Procedure Muhamed Sarić MD, PhD, MPA Director of Noninvasive Cardiology Echo Lab Associate
Treatment of Inter-MitraClip Regurgitation Due to Posterior Leaflet Cleft by Use of The Amplatzer Vascular Plug II device
 Volume 1, Issue 3 Case Report ISSN: 2572-9292 Treatment of Inter-MitraClip Regurgitation Due to Posterior Leaflet Cleft by Use of The Amplatzer Vascular Plug II device Neha M. Mantri, Gagan D. Singh, Thomas
Volume 1, Issue 3 Case Report ISSN: 2572-9292 Treatment of Inter-MitraClip Regurgitation Due to Posterior Leaflet Cleft by Use of The Amplatzer Vascular Plug II device Neha M. Mantri, Gagan D. Singh, Thomas
INTEGRATING ECHOCARDIOGRAPHY WITH CATHETER INTERVENTIONS FOR CONGENITAL HEART DISEASE. Krishna Kumar SevenHills Hospital, Mumbai, India
 INTEGRATING ECHOCARDIOGRAPHY WITH CATHETER INTERVENTIONS FOR CONGENITAL HEART DISEASE Krishna Kumar SevenHills Hospital, Mumbai, India Why talk about it? What is the big deal? Are we not stating the obvious?
INTEGRATING ECHOCARDIOGRAPHY WITH CATHETER INTERVENTIONS FOR CONGENITAL HEART DISEASE Krishna Kumar SevenHills Hospital, Mumbai, India Why talk about it? What is the big deal? Are we not stating the obvious?
Atrial Septal Defects
 Supplementary ACHD Echo Acquisition Protocol for Atrial Septal Defects The following protocol for echo in adult patients with atrial septal defects (ASDs) is a guide for performing a comprehensive assessment
Supplementary ACHD Echo Acquisition Protocol for Atrial Septal Defects The following protocol for echo in adult patients with atrial septal defects (ASDs) is a guide for performing a comprehensive assessment
8/31/2016. Mitraclip in Matthew Johnson, MD
 Mitraclip in 2016 Matthew Johnson, MD 1 Abnormal Valve Function Valve Stenosis Obstruction to valve flow during that phase of the cardiac cycle when the valve is normally open. Hemodynamic hallmark - pressure
Mitraclip in 2016 Matthew Johnson, MD 1 Abnormal Valve Function Valve Stenosis Obstruction to valve flow during that phase of the cardiac cycle when the valve is normally open. Hemodynamic hallmark - pressure
PART II ECHOCARDIOGRAPHY LABORATORY OPERATIONS ADULT TRANSTHORACIC ECHOCARDIOGRAPHY TESTING
 PART II ECHOCARDIOGRAPHY LABORATORY OPERATIONS ADULT TRANSTHORACIC ECHOCARDIOGRAPHY TESTING STANDARD - Primary Instrumentation 1.1 Cardiac Ultrasound Systems SECTION 1 Instrumentation Ultrasound instruments
PART II ECHOCARDIOGRAPHY LABORATORY OPERATIONS ADULT TRANSTHORACIC ECHOCARDIOGRAPHY TESTING STANDARD - Primary Instrumentation 1.1 Cardiac Ultrasound Systems SECTION 1 Instrumentation Ultrasound instruments
Index. interventional.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Ablation, of mitral leaflets, 80 Accucinch Annuloplasty system, for mitral regurgitation, 79, 94 95 Accutrak delivery system, for CoreValve
Index Note: Page numbers of article titles are in boldface type. A Ablation, of mitral leaflets, 80 Accucinch Annuloplasty system, for mitral regurgitation, 79, 94 95 Accutrak delivery system, for CoreValve
National Imaging Associates, Inc. Clinical guidelines CARDIAC CATHETERIZATION -LEFT HEART CATHETERIZATION. Original Date: October 2015 Page 1 of 5
 National Imaging Associates, Inc. Clinical guidelines CARDIAC CATHETERIZATION -LEFT HEART CATHETERIZATION CPT Codes: 93451, 93452, 93453, 93454, 93455, 93456, 93457, 93458, 93459, 93460, 93461 LCD ID Number:
National Imaging Associates, Inc. Clinical guidelines CARDIAC CATHETERIZATION -LEFT HEART CATHETERIZATION CPT Codes: 93451, 93452, 93453, 93454, 93455, 93456, 93457, 93458, 93459, 93460, 93461 LCD ID Number:
The earliest application of intracardiac imaging
 Intracardiac Echocardiography for Structural Heart Defects A review of ICE innovations, devices, and techniques. BY ZAHID AMIN, MD; QI-LING CAO, MD; AND ZIYAD M. HIJAZI, MD The earliest application of
Intracardiac Echocardiography for Structural Heart Defects A review of ICE innovations, devices, and techniques. BY ZAHID AMIN, MD; QI-LING CAO, MD; AND ZIYAD M. HIJAZI, MD The earliest application of
1. CARDIOLOGY. These listings cannot be correctly interpreted without reference to the Preamble. Anes. $ Level
 1. CARDIOLOGY These listings cannot be correctly interpreted without reference to the Preamble. Anes. Referred Cases 33010 Consultation: To consist of examination, review of history, laboratory, X-ray
1. CARDIOLOGY These listings cannot be correctly interpreted without reference to the Preamble. Anes. Referred Cases 33010 Consultation: To consist of examination, review of history, laboratory, X-ray
Index. interventional.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Alagille syndrome, pulmonary artery stenosis in, 143 145, 148 149 Amplatz devices for atrial septal defect closure, 42 46 for coronary
Index Note: Page numbers of article titles are in boldface type. A Alagille syndrome, pulmonary artery stenosis in, 143 145, 148 149 Amplatz devices for atrial septal defect closure, 42 46 for coronary
For Personal Use. Copyright HMP 2013
 Case Report J INVASIVE CARDIOL 2013;25(2):E42-E44 Percutaneous Closure of Iatrogenic Ventricular Septal Defect Following Surgical Aortic Valve Replacement Using Two Different Approaches Takashi Matsumoto,
Case Report J INVASIVE CARDIOL 2013;25(2):E42-E44 Percutaneous Closure of Iatrogenic Ventricular Septal Defect Following Surgical Aortic Valve Replacement Using Two Different Approaches Takashi Matsumoto,
Structural Heart Disease: Setting the Stage for Success
 Structural Heart Disease: Setting the Stage for Success Brenda McCulloch, RN MSN RCIS Cardiovascular Clinical Nurse Specialist, Interventional & Medical Cardiology Sutter Medical Center, Sacramento mccullb@sutterhealth.org
Structural Heart Disease: Setting the Stage for Success Brenda McCulloch, RN MSN RCIS Cardiovascular Clinical Nurse Specialist, Interventional & Medical Cardiology Sutter Medical Center, Sacramento mccullb@sutterhealth.org
Original Date: October 2009 TRANSESOPHAGEAL (TEE) ECHO Page 1 of 6
 National Imaging Associates, Inc. Clinical guideline Original Date: October 2009 TRANSESOPHAGEAL (TEE) ECHO Page 1 of 6 CPT codes: 93312, 93313, 93314, 93315, Last Review Date: September 2017 93316, 93317,
National Imaging Associates, Inc. Clinical guideline Original Date: October 2009 TRANSESOPHAGEAL (TEE) ECHO Page 1 of 6 CPT codes: 93312, 93313, 93314, 93315, Last Review Date: September 2017 93316, 93317,
A Magnetic Resonance Imaging Method for
 Journal of Cardiovascular Magnetic Resonance, 1(1), 59-64 (1999) INVITED PAPER Use of MRI in ASD Asessment A Magnetic Resonance Imaging Method for Evaluating Atrial Septa1 Defects Godtfred Holmvang Cardiac
Journal of Cardiovascular Magnetic Resonance, 1(1), 59-64 (1999) INVITED PAPER Use of MRI in ASD Asessment A Magnetic Resonance Imaging Method for Evaluating Atrial Septa1 Defects Godtfred Holmvang Cardiac
Successful Percutaneous Closure of Mitral Bioprosthetic Paravalvular Leak Using Figulla ASD Occluder
 Hans R. Figulla, M.D., PhD ; Ali Hamadanchi, M.D. Medicine, Pneumology Universitity Hospital, Jena, Germany Successful Percutaneous Closure of Mitral Bioprosthetic Paravalvular Leak Using Figulla ASD Occluder
Hans R. Figulla, M.D., PhD ; Ali Hamadanchi, M.D. Medicine, Pneumology Universitity Hospital, Jena, Germany Successful Percutaneous Closure of Mitral Bioprosthetic Paravalvular Leak Using Figulla ASD Occluder
TEE Essential in Paravalvular Leak Closure and Pseudoaneurysm Repair. Gerard T Wilkins
 TEE Essential in Paravalvular Leak Closure and Pseudoaneurysm Repair. Gerard T Wilkins Assoc Prof Medicine Consultant Cardiologist Dunedin Hospital Structural Heart Disease: short history Rubio-Alvares
TEE Essential in Paravalvular Leak Closure and Pseudoaneurysm Repair. Gerard T Wilkins Assoc Prof Medicine Consultant Cardiologist Dunedin Hospital Structural Heart Disease: short history Rubio-Alvares
Congenital Absence of the Left Atrial Appendage Visualized by 3D Echocardiography in Two Adult Patients
 DOI: 10.1111/echo.12882 2015, Wiley Periodicals, Inc. Echocardiography CASE REPORT Congenital Absence of the Left Atrial Appendage Visualized by 3D Echocardiography in Two Adult Patients Mona Saleh, B.A.,*
DOI: 10.1111/echo.12882 2015, Wiley Periodicals, Inc. Echocardiography CASE REPORT Congenital Absence of the Left Atrial Appendage Visualized by 3D Echocardiography in Two Adult Patients Mona Saleh, B.A.,*
Hybrid Muscular VSD Closure in Small Weight Children
 Hybrid Muscular VSD Closure in Small Weight Children Shakeel A Qureshi, on behalf of: John P. Cheatham, MD George H. Dunlap Endowed Chair in Interventional Cardiology Director Cardiac Catheterization &
Hybrid Muscular VSD Closure in Small Weight Children Shakeel A Qureshi, on behalf of: John P. Cheatham, MD George H. Dunlap Endowed Chair in Interventional Cardiology Director Cardiac Catheterization &
Cigna - Prior Authorization Procedure List Cardiology
 Cigna - Prior Authorization Procedure List Cardiology Category CPT Code CPT Code Description 33206 Insertion of new or replacement of permanent pacemaker with transvenous electrode(s); atrial 33207 Insertion
Cigna - Prior Authorization Procedure List Cardiology Category CPT Code CPT Code Description 33206 Insertion of new or replacement of permanent pacemaker with transvenous electrode(s); atrial 33207 Insertion
ICE: Echo Core Lab-CRF
 APPENDIX 1 ICE: Echo Core Lab-CRF Study #: - Pt Initials: 1. Date of study: / / D D M M M Y Y Y Y 2. Type of Study: TTE TEE 3. Quality of Study: Poor Moderate Excellent Ejection Fraction 4. Ejection Fraction
APPENDIX 1 ICE: Echo Core Lab-CRF Study #: - Pt Initials: 1. Date of study: / / D D M M M Y Y Y Y 2. Type of Study: TTE TEE 3. Quality of Study: Poor Moderate Excellent Ejection Fraction 4. Ejection Fraction
Uncommon Doppler Echocardiographic Findings of Severe Pulmonic Insufficiency
 Uncommon Doppler Echocardiographic Findings of Severe Pulmonic Insufficiency Rahul R. Jhaveri, MD, Muhamed Saric, MD, PhD, FASE, and Itzhak Kronzon, MD, FASE, New York, New York Background: Two-dimensional
Uncommon Doppler Echocardiographic Findings of Severe Pulmonic Insufficiency Rahul R. Jhaveri, MD, Muhamed Saric, MD, PhD, FASE, and Itzhak Kronzon, MD, FASE, New York, New York Background: Two-dimensional
How to manage device embolization?
 How to manage device embolization? Swiss Fellow Course Interventional Cardiology Amir-Ali Fassa Hôpital de La Tour Meyrin, Geneva Coronary interventions: Definitions Stent loss: stent dislodgment from
How to manage device embolization? Swiss Fellow Course Interventional Cardiology Amir-Ali Fassa Hôpital de La Tour Meyrin, Geneva Coronary interventions: Definitions Stent loss: stent dislodgment from
Transseptal catheterization is an established
 Site-Specific Transseptal Puncture for Emerging Structural Heart Interventions Imaging-assisted techniques for accurate access. By Michael J. Rinaldi, MD, FACC, FSCAI; Markus Scherer, MD, FACC, FSCCT;
Site-Specific Transseptal Puncture for Emerging Structural Heart Interventions Imaging-assisted techniques for accurate access. By Michael J. Rinaldi, MD, FACC, FSCAI; Markus Scherer, MD, FACC, FSCCT;
Successful Transfemoral Edwards Sapien Aortic. Valve Implantation in a Patient with Previous. Mitral Valve Replacement
 Advanced Studies in Medical Sciences, Vol. 2, 2014, no. 1, 37-45 HIKARI Ltd, www.m-hikari.com http://dx.doi.org/10.12988/asms.2014.31213 Successful Transfemoral Edwards Sapien Aortic Valve Implantation
Advanced Studies in Medical Sciences, Vol. 2, 2014, no. 1, 37-45 HIKARI Ltd, www.m-hikari.com http://dx.doi.org/10.12988/asms.2014.31213 Successful Transfemoral Edwards Sapien Aortic Valve Implantation
MITRAL STENOSIS. Joanne Cusack
 MITRAL STENOSIS Joanne Cusack BSE Breakdown Recognition of rheumatic mitral stenosis Qualitative description of valve and sub-valve calcification and fibrosis Measurement of orifice area by planimetry
MITRAL STENOSIS Joanne Cusack BSE Breakdown Recognition of rheumatic mitral stenosis Qualitative description of valve and sub-valve calcification and fibrosis Measurement of orifice area by planimetry
Tayyar Gökdeniz, Emre Ertürk, M. Ali Astarcıoğlu, Sabahattin Gündüz, A. Çağrı Aykan, A. Emrah Oğuz, Zübeyde Bayram, Mustafa Yıldız, N.
 Tayyar Gökdeniz, Emre Ertürk, M. Ali Astarcıoğlu, Sabahattin Gündüz, A. Çağrı Aykan, A. Emrah Oğuz, Zübeyde Bayram, Mustafa Yıldız, N. Ekşi Duran, Mehmet Özkan Introduction The incidence of development
Tayyar Gökdeniz, Emre Ertürk, M. Ali Astarcıoğlu, Sabahattin Gündüz, A. Çağrı Aykan, A. Emrah Oğuz, Zübeyde Bayram, Mustafa Yıldız, N. Ekşi Duran, Mehmet Özkan Introduction The incidence of development
Cardiac MRI in ACHD What We. ACHD Patients
 Cardiac MRI in ACHD What We Have Learned to Apply to ACHD Patients Faris Al Mousily, MBChB, FAAC, FACC Consultant, Pediatric Cardiology, KFSH&RC/Jeddah Adjunct Faculty, Division of Pediatric Cardiology
Cardiac MRI in ACHD What We Have Learned to Apply to ACHD Patients Faris Al Mousily, MBChB, FAAC, FACC Consultant, Pediatric Cardiology, KFSH&RC/Jeddah Adjunct Faculty, Division of Pediatric Cardiology
Part II: Fundamentals of 3D Echocardiography: Acquisition and Application
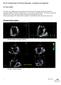 Part II: Fundamentals of 3D Echocardiography: Acquisition and Application Dr. Bruce Bollen 3D matrix array TEE probes provide options for both 2D and 3D imaging. Indeed, their utility in obtaining multiple
Part II: Fundamentals of 3D Echocardiography: Acquisition and Application Dr. Bruce Bollen 3D matrix array TEE probes provide options for both 2D and 3D imaging. Indeed, their utility in obtaining multiple
Case 47 Clinical Presentation
 93 Case 47 C Clinical Presentation 45-year-old man presents with chest pain and new onset of a murmur. Echocardiography shows severe aortic insufficiency. 94 RadCases Cardiac Imaging Imaging Findings C
93 Case 47 C Clinical Presentation 45-year-old man presents with chest pain and new onset of a murmur. Echocardiography shows severe aortic insufficiency. 94 RadCases Cardiac Imaging Imaging Findings C
Bogdan A. Popescu. University of Medicine and Pharmacy Bucharest, Romania. EAE Course, Bucharest, April 2010
 Bogdan A. Popescu University of Medicine and Pharmacy Bucharest, Romania EAE Course, Bucharest, April 2010 This is how it started Mitral stenosis at a glance 2D echo narrow diastolic opening of MV leaflets
Bogdan A. Popescu University of Medicine and Pharmacy Bucharest, Romania EAE Course, Bucharest, April 2010 This is how it started Mitral stenosis at a glance 2D echo narrow diastolic opening of MV leaflets
Absent Pulmonary Valve Syndrome
 Absent Pulmonary Valve Syndrome Fact sheet on Absent Pulmonary Valve Syndrome In this condition, which has some similarities to Fallot's Tetralogy, there is a VSD with narrowing at the pulmonary valve.
Absent Pulmonary Valve Syndrome Fact sheet on Absent Pulmonary Valve Syndrome In this condition, which has some similarities to Fallot's Tetralogy, there is a VSD with narrowing at the pulmonary valve.
Repair or Replacement
 Surgical intervention post MitraClip Device: Repair or Replacement Saudi Heart Association, February 21-24 Rüdiger Lange, MD, PhD Nicolo Piazza, MD, FRCPC, FESC German Heart Center, Munich, Germany Division
Surgical intervention post MitraClip Device: Repair or Replacement Saudi Heart Association, February 21-24 Rüdiger Lange, MD, PhD Nicolo Piazza, MD, FRCPC, FESC German Heart Center, Munich, Germany Division
10 ο ΣΥΝΕΔΡΙΟ ΕΠΕΜΒΑΤΙΚΗΣ ΚΑΡΔΙΟΛΟΓΙΑΣ ΚΑΙ ΗΛΕΚΤΡΟΦΥΣΙΟΛΟΓΙΑΣ Σεπτεμβρίου 2017 Electra Palace Θεσσαλονικη
 10 ο ΣΥΝΕΔΡΙΟ ΕΠΕΜΒΑΤΙΚΗΣ ΚΑΡΔΙΟΛΟΓΙΑΣ ΚΑΙ ΗΛΕΚΤΡΟΦΥΣΙΟΛΟΓΙΑΣ 14-16 Σεπτεμβρίου 2017 Electra Palace Θεσσαλονικη Ηχωκαρδιογραφία στην ένδειξη-προετοιμασία, διενέργεια, παρακολούθηση ασθενών που υποβάλλονται
10 ο ΣΥΝΕΔΡΙΟ ΕΠΕΜΒΑΤΙΚΗΣ ΚΑΡΔΙΟΛΟΓΙΑΣ ΚΑΙ ΗΛΕΚΤΡΟΦΥΣΙΟΛΟΓΙΑΣ 14-16 Σεπτεμβρίου 2017 Electra Palace Θεσσαλονικη Ηχωκαρδιογραφία στην ένδειξη-προετοιμασία, διενέργεια, παρακολούθηση ασθενών που υποβάλλονται
Transcatheter Aortic Valve Implantation Procedure (TAVI)
 Page 1 of 5 Procedure (TAVI) Introduction Aortic stenosis (AS) is a common heart valve problem associated with heart failure and death. Surgical valve repair or replacement is recommended if AS patients
Page 1 of 5 Procedure (TAVI) Introduction Aortic stenosis (AS) is a common heart valve problem associated with heart failure and death. Surgical valve repair or replacement is recommended if AS patients
Echocardiographic Guidance During Placement of the Buttoned Double-Disk Device for Atrial Septa1 Defect Closure
 Echocardiographic Guidance During Placement of the Buttoned Double-Disk Device for Atrial Septa1 Defect Closure L. LUANN MINICH, M.D., and A. REBECCA SNIDER, M.D. Department of Pediatrics, C.S. Mott Children
Echocardiographic Guidance During Placement of the Buttoned Double-Disk Device for Atrial Septa1 Defect Closure L. LUANN MINICH, M.D., and A. REBECCA SNIDER, M.D. Department of Pediatrics, C.S. Mott Children
Peripheral and Cardiology Coder 2018
 Peripheral and Cardiology Coder 2018 Cardiovascular Services and Procedures Prepared and Published By: MedLearn Publishing A Division of MedLearn Media, Inc. 445 Minnesota Street, Suite 514 St. Paul, MN
Peripheral and Cardiology Coder 2018 Cardiovascular Services and Procedures Prepared and Published By: MedLearn Publishing A Division of MedLearn Media, Inc. 445 Minnesota Street, Suite 514 St. Paul, MN
Left atrial function. Aliakbar Arvandi MD
 In the clinic Left atrial function Abstract The left atrium (LA) is a left posterior cardiac chamber which is located adjacent to the esophagus. It is separated from the right atrium by the inter-atrial
In the clinic Left atrial function Abstract The left atrium (LA) is a left posterior cardiac chamber which is located adjacent to the esophagus. It is separated from the right atrium by the inter-atrial
Index. B B-type natriuretic peptide (BNP), 76
 Index A ACCESS-EU registry, 158 159 Acute kidney injury (AKI), 76, 88 Annular enlargement, RV, 177 178 Annuloplasty chordal cutting, 113 complete ring, 99 etiology-specific ring, 100 evolution, 98 flexible
Index A ACCESS-EU registry, 158 159 Acute kidney injury (AKI), 76, 88 Annular enlargement, RV, 177 178 Annuloplasty chordal cutting, 113 complete ring, 99 etiology-specific ring, 100 evolution, 98 flexible
Mitral Regurgitation
 UW MEDICINE PATIENT EDUCATION Mitral Regurgitation Causes, symptoms, diagnosis, and treatment This handout describes mitral regurgitation, a disease of the mitral valve. It explains how this disease is
UW MEDICINE PATIENT EDUCATION Mitral Regurgitation Causes, symptoms, diagnosis, and treatment This handout describes mitral regurgitation, a disease of the mitral valve. It explains how this disease is
Pediatric Echocardiography Examination Content Outline
 Pediatric Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 Anatomy and Physiology Normal Anatomy and Physiology 10% 2 Abnormal Pathology and Pathophysiology
Pediatric Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 Anatomy and Physiology Normal Anatomy and Physiology 10% 2 Abnormal Pathology and Pathophysiology
Rotation: Echocardiography: Transthoracic Echocardiography (TTE)
 Rotation: Echocardiography: Transthoracic Echocardiography (TTE) Rotation Format and Responsibilities: Fellows rotate in the echocardiography laboratory in each clinical year. Rotations during the first
Rotation: Echocardiography: Transthoracic Echocardiography (TTE) Rotation Format and Responsibilities: Fellows rotate in the echocardiography laboratory in each clinical year. Rotations during the first
Copyright 2017 American College of Emergency Physicians. All rights reserved.
 POLICY Approved April 2017 Guidelines for the Use of Transesophageal Echocardiography (TEE) in the ED for Cardiac Arrest Approved by the ACEP Board of Directors April 2017 1. Introduction The American
POLICY Approved April 2017 Guidelines for the Use of Transesophageal Echocardiography (TEE) in the ED for Cardiac Arrest Approved by the ACEP Board of Directors April 2017 1. Introduction The American
EAE RECOMMENDATIONS FOR TRANSESOPHAGEAL ECHO. Cardiac Sources of Embolism. Luigi P. Badano, MD, FESC
 EAE RECOMMENDATIONS FOR TRANSESOPHAGEAL ECHO. Cardiac Sources of Embolism Luigi P. Badano, MD, FESC Background Stroke is the 3 cause of death in several industrial countries; Embolism accounts for 15-30%
EAE RECOMMENDATIONS FOR TRANSESOPHAGEAL ECHO. Cardiac Sources of Embolism Luigi P. Badano, MD, FESC Background Stroke is the 3 cause of death in several industrial countries; Embolism accounts for 15-30%
Update on Percutaneous Therapies for Structural Heart Disease. William Thomas MD Director of Structural Heart Program Tucson Medical Center
 Update on Percutaneous Therapies for Structural Heart Disease William Thomas MD Director of Structural Heart Program Tucson Medical Center NCVH 2014- Tucson Disclosure of Financial Interest Research: Stock
Update on Percutaneous Therapies for Structural Heart Disease William Thomas MD Director of Structural Heart Program Tucson Medical Center NCVH 2014- Tucson Disclosure of Financial Interest Research: Stock
Imaging Evaluation of the Ventricular Septum
 Imaging Evaluation of the Ventricular Septum Craig E Fleishman, MD FACC FASE The Heart Center at Arnold Palmer Hospital for Children, Orlando SCAI Fall Fellows Course 2013 Las Vegas Disclosure Information
Imaging Evaluation of the Ventricular Septum Craig E Fleishman, MD FACC FASE The Heart Center at Arnold Palmer Hospital for Children, Orlando SCAI Fall Fellows Course 2013 Las Vegas Disclosure Information
Catheter-based left atrial appendage occlusion procedure: role of echocardiography
 European Heart Journal Cardiovascular Imaging (2012) 13, 132 138 doi:10.1093/ejechocard/jer158 REVIEWS Catheter-based left atrial appendage occlusion procedure: role of echocardiography Gila Perk 1 *,
European Heart Journal Cardiovascular Imaging (2012) 13, 132 138 doi:10.1093/ejechocard/jer158 REVIEWS Catheter-based left atrial appendage occlusion procedure: role of echocardiography Gila Perk 1 *,
Feasibility of real-time three-dimensional transoesophageal echocardiography for guidance of percutaneous atrial septal defect closure
 European Journal of Echocardiography (2009) 10, 543 548 doi:10.1093/ejechocard/jen337 Feasibility of real-time three-dimensional transoesophageal echocardiography for guidance of percutaneous atrial septal
European Journal of Echocardiography (2009) 10, 543 548 doi:10.1093/ejechocard/jen337 Feasibility of real-time three-dimensional transoesophageal echocardiography for guidance of percutaneous atrial septal
Organic mitral regurgitation
 The best in heart valve disease Organic mitral regurgitation Ewa Szymczyk Department of Cardiology Medical University of Lodz, Poland I have nothing to declare Organic mitral regurgitation leaflet abnormality
The best in heart valve disease Organic mitral regurgitation Ewa Szymczyk Department of Cardiology Medical University of Lodz, Poland I have nothing to declare Organic mitral regurgitation leaflet abnormality
evicore cardiology procedures and services requiring prior authorization
 evicore cardiology procedures and services requiring prior authorization Moda Health Commercial Group and Individual Members* *Check EBT to verify member enrollment in evicore program Radiology Advanced
evicore cardiology procedures and services requiring prior authorization Moda Health Commercial Group and Individual Members* *Check EBT to verify member enrollment in evicore program Radiology Advanced
Assessment of Atrial Septal Defect Role of Real-Time 3D Color Doppler Echocardiography for Interventional Catheterization
 Original Article Chung-Hsien Su et al. Acta Cardiol Sin 2005;21:146 52 Pediatric Cardiology Assessment of Atrial Septal Defect Role of Real-Time 3D Color Doppler Echocardiography for Interventional Catheterization
Original Article Chung-Hsien Su et al. Acta Cardiol Sin 2005;21:146 52 Pediatric Cardiology Assessment of Atrial Septal Defect Role of Real-Time 3D Color Doppler Echocardiography for Interventional Catheterization
Atrial Septal Defect Closure. Stephen Brecker Director, Cardiac Catheterisation Labs
 Stephen Brecker Director, Cardiac Catheterisation Labs ADVANCED ANGIOPLASTY Incorporating The Left Main 5 Plus Course Conflicts of Interest The following companies have supported educational courses held
Stephen Brecker Director, Cardiac Catheterisation Labs ADVANCED ANGIOPLASTY Incorporating The Left Main 5 Plus Course Conflicts of Interest The following companies have supported educational courses held
New Cardiovascular Devices and Interventions: Non-Contrast MRI for TAVR Abhishek Chaturvedi Assistant Professor. Cardiothoracic Radiology
 New Cardiovascular Devices and Interventions: Non-Contrast MRI for TAVR Abhishek Chaturvedi Assistant Professor Cardiothoracic Radiology Disclosure I have no disclosure pertinent to this presentation.
New Cardiovascular Devices and Interventions: Non-Contrast MRI for TAVR Abhishek Chaturvedi Assistant Professor Cardiothoracic Radiology Disclosure I have no disclosure pertinent to this presentation.
Course Learning Objectives Sunday, February 17 Friday, February 22
 Course Learning Objectives Sunday, February 17 Friday, February 22 1. Define the physical principles of ultrasound technology and its applications for two and threedimensional (2D, 3D) imaging and use
Course Learning Objectives Sunday, February 17 Friday, February 22 1. Define the physical principles of ultrasound technology and its applications for two and threedimensional (2D, 3D) imaging and use
PROSTHETIC VALVE BOARD REVIEW
 PROSTHETIC VALVE BOARD REVIEW The correct answer D This two chamber view shows a porcine mitral prosthesis with the typical appearance of the struts although the leaflets are not well seen. The valve
PROSTHETIC VALVE BOARD REVIEW The correct answer D This two chamber view shows a porcine mitral prosthesis with the typical appearance of the struts although the leaflets are not well seen. The valve
ASCeXAM / ReASCE. Practice Board Exam Questions Monday Morning
 ASCeXAM / ReASCE Practice Board Exam Questions Monday Morning Ultrasound Physics Artifacts Doppler Physics Imaging, Knobology, and Artifacts Echocardiographic Evaluation of the RV Tricuspid and Pulmonary
ASCeXAM / ReASCE Practice Board Exam Questions Monday Morning Ultrasound Physics Artifacts Doppler Physics Imaging, Knobology, and Artifacts Echocardiographic Evaluation of the RV Tricuspid and Pulmonary
Cardiac Valve/Structural Therapies
 Property of Dr. Chad Rammohan Cardiac Valve/Structural Therapies Chad Rammohan, MD FACC Medical Director, El Camino Hospital Cardiac Catheterization Lab Director, Interventional and Structural Cardiology,
Property of Dr. Chad Rammohan Cardiac Valve/Structural Therapies Chad Rammohan, MD FACC Medical Director, El Camino Hospital Cardiac Catheterization Lab Director, Interventional and Structural Cardiology,
Pre-procedural CT angiography for Transcatheter Aortic Valve Implantation: What a Radiologist Needs to Know?
 Pre-procedural CT angiography for Transcatheter Aortic Valve Implantation: What a Radiologist Needs to Know? E O Dwyer, C O Brien, I Murphy, C Shortt, O Buckley Department of Radiology, AMNCH, Dublin,
Pre-procedural CT angiography for Transcatheter Aortic Valve Implantation: What a Radiologist Needs to Know? E O Dwyer, C O Brien, I Murphy, C Shortt, O Buckley Department of Radiology, AMNCH, Dublin,
CY2017 Hospital Outpatient: Vascular Procedure APCs and Complexity Adjustments
 CY2017 Hospital Outpatient: Vascular Procedure APCs and Complexity Adjustments Comprehensive Ambulatory Payment Classifications (c-apcs) In CY2015 and in an effort to help pay providers for quality, not
CY2017 Hospital Outpatient: Vascular Procedure APCs and Complexity Adjustments Comprehensive Ambulatory Payment Classifications (c-apcs) In CY2015 and in an effort to help pay providers for quality, not
Chapter 24: Diagnostic workup and evaluation: eligibility, risk assessment, FDA guidelines Ashwin Nathan, MD, Saif Anwaruddin, MD, FACC Penn Medicine
 Chapter 24: Diagnostic workup and evaluation: eligibility, risk assessment, FDA guidelines Ashwin Nathan, MD, Saif Anwaruddin, MD, FACC Penn Medicine Mitral regurgitation, regurgitant flow between the
Chapter 24: Diagnostic workup and evaluation: eligibility, risk assessment, FDA guidelines Ashwin Nathan, MD, Saif Anwaruddin, MD, FACC Penn Medicine Mitral regurgitation, regurgitant flow between the
Complicated Percutaneous Repair of a Paravalvular Mitral Leak. Dr. K Kam Resident Specialist Division of Cardiology, PWH M&T (Courtesy: Prof.
 Complicated Percutaneous Repair of a Paravalvular Mitral Leak Dr. K Kam Resident Specialist Division of Cardiology, PWH M&T (Courtesy: Prof. PW Lee) A new job for echo guy Interventional echocardiologist!
Complicated Percutaneous Repair of a Paravalvular Mitral Leak Dr. K Kam Resident Specialist Division of Cardiology, PWH M&T (Courtesy: Prof. PW Lee) A new job for echo guy Interventional echocardiologist!
Fabien Praz, Andreas Wahl, Sophie Beney, Stephan Windecker, Heinrich P. Mattle*, Bernhard Meier
 Procedural Outcome after Percutaneous Closure of Patent Foramen Ovale using the Amplatzer PFO Occluder Without Intra-Procedural Echocardiography in 1,000 Patients Fabien Praz, Andreas Wahl, Sophie Beney,
Procedural Outcome after Percutaneous Closure of Patent Foramen Ovale using the Amplatzer PFO Occluder Without Intra-Procedural Echocardiography in 1,000 Patients Fabien Praz, Andreas Wahl, Sophie Beney,
Intracardiac echocardiography: an ideal guiding tool for device closure of interatrial communications
 Eur J Echocardiography (2005) 6, 92e96 Intracardiac echocardiography: an ideal guiding tool for device closure of interatrial communications Thomas Bartel a, *, Thomas Konorza a, Ulrich Neudorf b, Tiko
Eur J Echocardiography (2005) 6, 92e96 Intracardiac echocardiography: an ideal guiding tool for device closure of interatrial communications Thomas Bartel a, *, Thomas Konorza a, Ulrich Neudorf b, Tiko
INTERNAL MEDICINE SUBSPECIALTY CARDIOLOGY
 KALEIDA HEALTH Name: Date: INTERNAL MEDICINE SUBSPECIALTY CARDIOLOGY PLEASE NOTE: Please check the box for each requested. Do not use an arrow or line to make selections. We will return applications that
KALEIDA HEALTH Name: Date: INTERNAL MEDICINE SUBSPECIALTY CARDIOLOGY PLEASE NOTE: Please check the box for each requested. Do not use an arrow or line to make selections. We will return applications that
Transcatheter Closures for Fistula Tract and Paravalvular Leak after Mitral Valve Replacement and Tricuspid Annuloplasty
 Case Report Print ISSN 1738-5520 On-line ISSN 1738-5555 Korean Circulation Journal Transcatheter Closures for Fistula Tract and Paravalvular Leak after Mitral Valve Replacement and Tricuspid nnuloplasty
Case Report Print ISSN 1738-5520 On-line ISSN 1738-5555 Korean Circulation Journal Transcatheter Closures for Fistula Tract and Paravalvular Leak after Mitral Valve Replacement and Tricuspid nnuloplasty
Echocardiographic evaluation of mitral stenosis
 Echocardiographic evaluation of mitral stenosis Euroecho 2011 Philippe Unger, MD, FESC Erasme Hospital, ULB, Brussels, Belgium I have nothing to declare EuroHeart Survey Etiology of single native left-sided
Echocardiographic evaluation of mitral stenosis Euroecho 2011 Philippe Unger, MD, FESC Erasme Hospital, ULB, Brussels, Belgium I have nothing to declare EuroHeart Survey Etiology of single native left-sided
Percutaneous Mitral Valve Repair
 Percutaneous Mitral Valve Repair MitraClip: Procedure, Data, Patient Selection Chad Rammohan, MD FACC Director, Cardiac Cath Lab El Camino Hospital Mountain View, California Mitral Regurgitation MitraClip
Percutaneous Mitral Valve Repair MitraClip: Procedure, Data, Patient Selection Chad Rammohan, MD FACC Director, Cardiac Cath Lab El Camino Hospital Mountain View, California Mitral Regurgitation MitraClip
How Do I Evaluate a Patient Being Considered for TAVR? Sunday, February 14, :00 11:25 PM 25 min
 2016 ASE State of the Art Echocardiography Course Tucson, AZ How Do I Evaluate a Patient Being Considered for TAVR? Sunday, February 14, 2016 11:00 11:25 PM 25 min 1 M U H A M E D S A R I Ć, M D, P H D
2016 ASE State of the Art Echocardiography Course Tucson, AZ How Do I Evaluate a Patient Being Considered for TAVR? Sunday, February 14, 2016 11:00 11:25 PM 25 min 1 M U H A M E D S A R I Ć, M D, P H D
UNMH Pediatric Cardiology Clinical Privileges. Name: Effective Dates: From To
 All new applicants must meet the following requirements as approved by the UNMH Board of Trustees, effective August 18, 2017: Initial Privileges (initial appointment) Renewal of Privileges (reappointment)
All new applicants must meet the following requirements as approved by the UNMH Board of Trustees, effective August 18, 2017: Initial Privileges (initial appointment) Renewal of Privileges (reappointment)
Percutaneous atrial septal defect closure with the Occlutech Figulla Flex ASD Occluder.
 Percutaneous atrial septal defect closure with the Occlutech Figulla Flex ASD Occluder. First case with a novel delivery system. Werner Budts, Md, PhD, FESC Congenital and Structural Cardiology University
Percutaneous atrial septal defect closure with the Occlutech Figulla Flex ASD Occluder. First case with a novel delivery system. Werner Budts, Md, PhD, FESC Congenital and Structural Cardiology University
Competency Training Requirements for the Area of Focused Competence in Adult Echocardiography
 Competency Training Requirements for the Area of Focused Competence in Adult Echocardiography 2013 VERSION 1.0 These training requirements apply to those who begin training on or after July 1 st, 2013.
Competency Training Requirements for the Area of Focused Competence in Adult Echocardiography 2013 VERSION 1.0 These training requirements apply to those who begin training on or after July 1 st, 2013.
Tissue Doppler Imaging in Congenital Heart Disease
 Tissue Doppler Imaging in Congenital Heart Disease L. Youngmin Eun, M.D. Department of Pediatrics, Division of Pediatric Cardiology, Kwandong University College of Medicine The potential advantage of ultrasound
Tissue Doppler Imaging in Congenital Heart Disease L. Youngmin Eun, M.D. Department of Pediatrics, Division of Pediatric Cardiology, Kwandong University College of Medicine The potential advantage of ultrasound
ΔΙΑΔΕΡΜΙΚΗ ΑΝΤΙΜΕΤΩΠΙΣΗ ΔΟΜΙΚΩΝ ΠΑΘΗΣΕΩΝ: Ο ΡΟΛΟΣ ΤΗΣ ΑΠΕΙΚΟΝΙΣΗΣ ΣΤΟ ΑΙΜΟΔΥΝΑΜΙΚΟ ΕΡΓΑΣΤΗΡΙΟ ΣΤΗΝ ΤΟΠΟΘΕΤΗΣΗ MITRACLIP
 ΔΙΑΔΕΡΜΙΚΗ ΑΝΤΙΜΕΤΩΠΙΣΗ ΔΟΜΙΚΩΝ ΠΑΘΗΣΕΩΝ: Ο ΡΟΛΟΣ ΤΗΣ ΑΠΕΙΚΟΝΙΣΗΣ ΣΤΟ ΑΙΜΟΔΥΝΑΜΙΚΟ ΕΡΓΑΣΤΗΡΙΟ ΣΤΗΝ ΤΟΠΟΘΕΤΗΣΗ MITRACLIP ΒΛΑΣΗΣ ΝΙΝΙΟΣ MD MRCP ΚΛΙΝΙΚΗ ΑΓΙΟΣ ΛΟΥΚΑΣ ΘΕΣΣΑΛΟΝΙΚΗ CONFLICT OF INTEREST PROCTOR
ΔΙΑΔΕΡΜΙΚΗ ΑΝΤΙΜΕΤΩΠΙΣΗ ΔΟΜΙΚΩΝ ΠΑΘΗΣΕΩΝ: Ο ΡΟΛΟΣ ΤΗΣ ΑΠΕΙΚΟΝΙΣΗΣ ΣΤΟ ΑΙΜΟΔΥΝΑΜΙΚΟ ΕΡΓΑΣΤΗΡΙΟ ΣΤΗΝ ΤΟΠΟΘΕΤΗΣΗ MITRACLIP ΒΛΑΣΗΣ ΝΙΝΙΟΣ MD MRCP ΚΛΙΝΙΚΗ ΑΓΙΟΣ ΛΟΥΚΑΣ ΘΕΣΣΑΛΟΝΙΚΗ CONFLICT OF INTEREST PROCTOR
Interventional procedures guidance Published: 26 September 2014 nice.org.uk/guidance/ipg504
 Transcatheter valve-in-valve e implantation for aortic bioprosthetic valve dysfunction Interventional procedures guidance Published: 26 September 2014 nice.org.uk/guidance/ipg504 Your responsibility This
Transcatheter valve-in-valve e implantation for aortic bioprosthetic valve dysfunction Interventional procedures guidance Published: 26 September 2014 nice.org.uk/guidance/ipg504 Your responsibility This
Diagnostic & Therapeutic Cardiac Catheterization Coder 2017
 Diagnostic & Therapeutic Cardiac Catheterization Coder 2017 Including peripheral and cardiovascular services and procedures Prepared and Published By: MedLearn Publishing A Division of Panacea Healthcare
Diagnostic & Therapeutic Cardiac Catheterization Coder 2017 Including peripheral and cardiovascular services and procedures Prepared and Published By: MedLearn Publishing A Division of Panacea Healthcare
Adult Congenital Heart Disease: What All Echocardiographers Should Know Sharon L. Roble, MD, FACC Echo Hawaii 2016
 1 Adult Congenital Heart Disease: What All Echocardiographers Should Know Sharon L. Roble, MD, FACC Echo Hawaii 2016 DISCLOSURES I have no disclosures relevant to today s talk 2 Why should all echocardiographers
1 Adult Congenital Heart Disease: What All Echocardiographers Should Know Sharon L. Roble, MD, FACC Echo Hawaii 2016 DISCLOSURES I have no disclosures relevant to today s talk 2 Why should all echocardiographers
Diagnostic approach to heart disease
 Diagnostic approach to heart disease Initial work up History Physical exam Chest radiographs ECG Special studies Echocardiography Cardiac catheterization Echocardiography principles Technique of producing
Diagnostic approach to heart disease Initial work up History Physical exam Chest radiographs ECG Special studies Echocardiography Cardiac catheterization Echocardiography principles Technique of producing
Mitral Valve Disease, When to Intervene
 Mitral Valve Disease, When to Intervene Swedish Heart and Vascular Institute Ming Zhang MD PhD Interventional Cardiology Structure Heart Disease Conflict of Interest None Current ACC/AHA guideline Stages
Mitral Valve Disease, When to Intervene Swedish Heart and Vascular Institute Ming Zhang MD PhD Interventional Cardiology Structure Heart Disease Conflict of Interest None Current ACC/AHA guideline Stages
7. Echocardiography Appropriate Use Criteria (by Indication)
 Criteria for Echocardiography 1133 7. Echocardiography Criteria (by ) Table 1. TTE for General Evaluation of Cardiac Structure and Function Suspected Cardiac Etiology General With TTE 1. Symptoms or conditions
Criteria for Echocardiography 1133 7. Echocardiography Criteria (by ) Table 1. TTE for General Evaluation of Cardiac Structure and Function Suspected Cardiac Etiology General With TTE 1. Symptoms or conditions
Disclosure Statement of Financial Interest Saibal Kar, MD, FACC
 MitraClip Therapy Saibal Kar, MD, FACC, FAHA, FSCAI Director of Interventional Cardiac Research Program Director, Interventional Cardiology Heart Institute, Cedars-Sinai Medical Center, Los Angeles, CA
MitraClip Therapy Saibal Kar, MD, FACC, FAHA, FSCAI Director of Interventional Cardiac Research Program Director, Interventional Cardiology Heart Institute, Cedars-Sinai Medical Center, Los Angeles, CA
(Ann Thorac Surg 2008;85:845 53)
 I Made Adi Parmana The utility of intraoperative TEE has become increasingly more evident as anesthesiologists, cardiologists, and surgeons continue to appreciate its potential application as an invaluable
I Made Adi Parmana The utility of intraoperative TEE has become increasingly more evident as anesthesiologists, cardiologists, and surgeons continue to appreciate its potential application as an invaluable
SUPPLEMENTAL MATERIAL
 SUPPLEMENTAL MATERIAL Table S1. Patient Selection Codes, CIED Generator Procedures Code Type Code Description ICD9 Proc 00.51 Implantation of cardiac resynchronization defibrillator, total system [CRT-D]
SUPPLEMENTAL MATERIAL Table S1. Patient Selection Codes, CIED Generator Procedures Code Type Code Description ICD9 Proc 00.51 Implantation of cardiac resynchronization defibrillator, total system [CRT-D]
Cardiology Fellowship Manual. Goals & Objectives -Cardiac Imaging- 1 P a g e
 Cardiology Fellowship Manual Goals & Objectives -Cardiac Imaging- 1 P a g e UNIV. OF NEBRASKA CHILDREN S HOSPITAL & MEDICAL CENTER DIVISION OF CARDIOLOGY FELLOWSHIP PROGRAM CARDIAC IMAGING ROTATION GOALS
Cardiology Fellowship Manual Goals & Objectives -Cardiac Imaging- 1 P a g e UNIV. OF NEBRASKA CHILDREN S HOSPITAL & MEDICAL CENTER DIVISION OF CARDIOLOGY FELLOWSHIP PROGRAM CARDIAC IMAGING ROTATION GOALS
Options for my no option Patients Treating Heart Conditions Via a Tiny Catheter
 Options for my no option Patients Treating Heart Conditions Via a Tiny Catheter Nirat Beohar, MD Associate Professor of Medicine Director Cardiac Catheterization Laboratory, Medical Director Structural
Options for my no option Patients Treating Heart Conditions Via a Tiny Catheter Nirat Beohar, MD Associate Professor of Medicine Director Cardiac Catheterization Laboratory, Medical Director Structural
Intracardiac EchoCardiography (ICE) Common Views
 Intracardiac EchoCardiography (ICE) Common Views Introduction What is ICE? Catheter with microscopic ultrasound transducer tip and doppler capabilities inserted into the heart via the IVC (typically) or
Intracardiac EchoCardiography (ICE) Common Views Introduction What is ICE? Catheter with microscopic ultrasound transducer tip and doppler capabilities inserted into the heart via the IVC (typically) or
The Normal Echocardiogram
 The Normal Echocardiogram Pravin V. Patil, MD FACC Lewis Katz School of Medicine at Temple University Acknowledgments Dr. Susan Wiegers Dr. Martin Keane Temple Cardiac Sonographers Disclosures No relevant
The Normal Echocardiogram Pravin V. Patil, MD FACC Lewis Katz School of Medicine at Temple University Acknowledgments Dr. Susan Wiegers Dr. Martin Keane Temple Cardiac Sonographers Disclosures No relevant
Outline. EuroScore II. Society of Thoracic Surgeons Score. EuroScore II
 SURGICAL RISK IN VALVULAR HEART DISEASE: WHAT 2D AND 3D ECHO CAN TELL YOU AND WHAT THEY CAN'T Ernesto E Salcedo, MD Professor of Medicine University of Colorado School of Medicine Director of Echocardiography
SURGICAL RISK IN VALVULAR HEART DISEASE: WHAT 2D AND 3D ECHO CAN TELL YOU AND WHAT THEY CAN'T Ernesto E Salcedo, MD Professor of Medicine University of Colorado School of Medicine Director of Echocardiography
Type Size AP/PS RP/RS Qp/Qs. Ia Resistive <0.3 < Ib Resistive <0.3 < IIa Resistive <0.5 >2
 Transcatheter closure of VSD using Duct Occluder device Nguyen Lan Hieu, MD, PhD Hanoi Medical University Vietnam Heart Institute Anatomy of VSD 1. Perimembranous VSD: Aneurysm septal membranous(tv or
Transcatheter closure of VSD using Duct Occluder device Nguyen Lan Hieu, MD, PhD Hanoi Medical University Vietnam Heart Institute Anatomy of VSD 1. Perimembranous VSD: Aneurysm septal membranous(tv or
