Anatomic repair of complex transposition with en bloc rotation of the truncus arteriosus: 10-year experience
|
|
|
- Angela Perry
- 5 years ago
- Views:
Transcription
1 European Journal of Cardio-Thoracic Surgery 49 (2016) doi: /ejcts/ezv056 Advance Access publication 19 February 2015 ORIGINAL ARTICLE Cite this article as: Mair R, Sames-Dolzer E, Innerhuber M, Tulzer A, Grohmann E, Tulzer G. Anatomic repair of complex transposition with en bloc rotation of the truncus arteriosus: 10-year experience. Eur J Cardiothorac Surg 2016;49: Anatomic repair of complex transposition with en bloc rotation of the truncus arteriosus: 10-year experience Rudolf Mair*, Eva Sames-Dolzer, Michaela Innerhuber, Andreas Tulzer, Eva Grohmann and Gerald Tulzer Children s Heart Center Linz, Linz, Austria * Corresponding author. Children s Heart Center Linz, Krankenhausstr. 9, 4020 Linz, Austria. Tel: ; fax: ; rudolf.mair@akh.linz.at (R. Mair). Received 20 September 2014; received in revised form 13 January 2015; accepted 19 January 2015 Abstract OBJECTIVES: Transposition of the great arteries, ventricular septal defect and left ventricular outflow tract obstruction are commonly called complex transposition. The traditional method of repair is the Rastelli procedure. Aortic translocation (Nikaidoh 1984) provides a more anatomic repair of this malformation. En bloc rotation of the truncus arteriosus (double root translocation, half turn truncal switch procedure) was introduced in 2003 (Yamagishi), and offers a complete anatomic repair with growth potential in all tubular structures. The aim of this study was to analyse our general experience with this method and the mid-term results concerning growth of the tubular structures as well as the function of the semilunar valves, if preserved. METHODS: Nineteen patients with transposition of the great arteries, ventricular septal defect and left ventricular outflow tract obstruction or similar cases of double outlet right ventricle (DORV) have been treated by an en bloc rotation of the truncus arteriosus in our centre since Patient age ranged between 4 days and 6.46 years. The median age was 0.39 [0.1; 2.25] years. Weight ranged between 3.1 and 18.8 kg. Median weight was 5.6 [3.6; 9] kg. Five patients had received between 1 and 4 palliative procedures prior to the definitive repair. The pulmonary valve could be preserved in 15 cases, whereas a transannular patch was necessary in 4 cases. RESULTS: One patient died of chronic left ventricular failure during the hospital stay. One patient acquired a severe cerebral haemorrhage 3 weeks after the operation. She was discharged and died 6 months later. One patient is not in a follow-up programme. Sixteen patients are now followed over a period of 153 days to 9.96 years. Aortic and pulmonary valves showed proportional growth during the follow-up period. The preserved pulmonary valves were small for age, but kept their competence satisfactorily. Three patients required a reoperation: one aortic valve repair, 1 permanent pacemaker, VSD closure. CONCLUSIONS: Up to now, reoperations had been caused by technical issues. The reoperation rate can be kept low, by understanding some important features of this procedure and avoiding these problems. Complete anatomic repair with growth potential and satisfactory preserved pulmonary valve function is possible. Keywords: Complex transposition Left ventricular outflow tract obstruction En bloc rotation Rastelli procedure INTRODUCTION Transposition of the great arteries (TGA), ventricular septal defect (VSD) and left ventricular outflow tract obstruction (LVOTO) and similar cases of DORV are commonly treated with the Rastelli procedure [1]. In this procedure, the systemic blood flow is directed from the systemic ventricle through the VSD into the aorta by an intracardiac baffle. This tunnel might be long, and could lead to subaortic obstruction later in life depending on the anatomic situation (length of the conus septum, size of the pulmonary root, distance of the VSD to the aortic root). Furthermore, a right ventricle to pulmonary artery (RV-PA) conduit is necessary [2 5]. Presented at the 28th Annual Meeting of the European Association for Cardio- Thoracic Surgery, Milan, Italy, October The Réparation à l étage ventriculaire (REV procedure) avoids the RV-PA conduit by using a Lecompte manoeuvre, and a direct anastomosis of the PA with the RV. Resection of the conus septum is also part of this procedure. In this case, the intracardiac tunnel should be somewhat shorter and wider than in a classic Rastelli operation [5 7]. The aortic translocation (Nikaidoh-Bex) brings the aorta directly over the LVOT to its original anatomic position. Pulmonary root and valve are sacrificed in this procedure [8]. In en bloc rotation of the truncus arteriosus (half turn truncal switch procedure Yamagishi, double root translocation etc.) the aorta is brought over the LVOT and the pulmonary root comes over the right ventricular outflow tract (RVOT). The pulmonary valve, not suitable for aortic position, may work properly in pulmonary position and growth potential should be preserved in all The Author Published by Oxford University Press on behalf of the European Association for Cardio-Thoracic Surgery. All rights reserved.
2 R. Mair et al. / European Journal of Cardio-Thoracic Surgery 177 tubular structures. With this procedure, a complete anatomic repair of this malformation should be achieved [9 11]. The aim of this retrospective study is to analyse our experience, as well as the mid-term outcome of this procedure. The study wanted to see whether, and how, the tubular structures grow and also to investigate whether the semilunar valve function can be preserved. PATIENTS AND METHODS Patients Nineteen patients with either TGA/VSD/LVOTO or similar forms of DORV underwent a complete repair by en bloc rotation of the truncus arteriosus from April 2003 to November 2013 (Table 1). Patient age ranged from 4 days to 6.46 years. Median age was 0.39 [0.1; 2.25] years, median weight 5.6 [3.6; 9] kg ( kg). Anatomy Thirteen patients were classified as TGA, 6 patients as similar forms of DORV. All patients had well-balanced ventricles. The VSD was sub-pulmonary in all cases. In 9 patients, the pulmonary valve was bicuspid: 6 of them were symmetric and hypoplastic; 3 were asymmetric and dysplastic. In 10 patients, the pulmonary valve was tricuspid: in 9 patients, it was symmetric and simply hypoplastic; in 1 patient, it was asymmetric and dysplastic. The LVOT obstruction was short in 8 patients; 11 patients had a tunnel type stenosis of the LVOT. Indication, decision making We regarded en bloc rotation as the procedure of choice in this malformation over the last 10 years. If there was no ductus dependency, the operation was planned electively as a primary repair at an age between 6 weeks and 3 months. The majority of patients however presented later in our centre. All of our patients would have otherwise been candidates for either a Rastelli procedure or other forms of repair of this type of malformation. An arterial switch operation was not possible in any of these cases. A Rastelli procedure was performed, if additional complex cardiac lesions were present. This was the case in 2 patients with additional complete atrioventricular (AV)-canal, one of them with heterotaxy syndrome. Initially, we restricted en bloc rotation of the truncus arteriosus to patients with a normal coronary anatomy for transposition. This means that the left coronary artery (RCA) arises from the left anterior facing sinus, the right coronary artery from the right posterior facing sinus (Yacoub type A). An intraoperative switch to a Rastelli procedure due to unfavourable coronary anatomy was performed in 7 cases during this period (e.g. circumflex artery from the RCA; RCA from the left anterior descending artery (LAD) or single coronary ostium). By gaining more and more experience, we were gradually able to extend the indication regarding coronary anatomy. Based on our present experience, 3 of these 7 patients would still be refused an en bloc rotation of the truncus arteriosus. However, patients with a circumflex artery coming from the right coronary artery and the posterior facing sinus, and patients with a right coronary artery arising from an LAD and crossing the RVOT have undergone an en bloc rotation successfully in the latter part of our series. Univentricular palliation is used only if biventricular repair is precluded either by severely unbalanced ventricles, by unbalanced or CONGENITAL Table 1: Patients and preoperative palliative procedures Patient number Sex Age (years) Weight (kg) Anatomy Palliations number Type of palliations Indication for palliation 1 m DORV, TGA, LVOTO 4 BT shunt + atrioseptectomy, shunt banding, Cyanosis bidirectional Glenn, right class. Glenn 2 f DORV, TGA, LVOTO 3 m TGA/VSD/LVOTO 4 f TGA, VSD, LVOTO 5 f DORV, TGA, LVOTO 6 m TGA/VSD/LVOTO 7 f TGA, VSD, LVOTO 8 m DORV, TGA, VSD, LVOTO 9 f TGA/VSD/LVOTO 10 f TGA/VSD/LVOTO 1 BT shunt + atrioseptectomy Lost stent 11 f TGA/VSDLVOTO 12 f TGA/VSD/LVOTO 13 m DORV, TGA, LVOTO 14 f DORV, TGA, VSD, LVOTO, 2 BT shunt, bidirectional Glenn Cyanosis 15 f TGA/VSD/LVOTO 16 m TGA/VSD/LVOTO 17 f TGA, VSD, LVOTO 2 BT shunt, central shunt Cyanosis 18 m TGA/VSD/LVOTO 1 BT shunt + atrioseptectomy Desperate condition after transport 19 m TGA/VSD/LVOTO F: female; m: male.
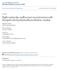
3 178 R. Mair et al. / European Journal of Cardio-Thoracic Surgery straddling AV-valves or by other situations making biventricular reconstruction impossible. Nevertheless, 5 patients had between 1 and 4 palliative procedures prior to en bloc rotation of the truncus arteriosus (Table 1). Three palliated patients came from other centres, where complete repair was not offered or possible (Table 1,patients 1,14 and 17). Two newborn patients received a primary palliation in our centre due to emergencies (Table 1, patients 10 and 18). Operative technique The operation is done on cardiopulmonary bypass (CPB) in moderate hypothermia with double venous cannulation. Cold crystalloid cardioplegia is used, and usually repeated at hourly intervals. Both PAs are extensively mobilized. After cross-clamping the aorta and instillation of cardioplegia, the aorta and PA are cut transversely at the same level. Marking stitches are placed at the most anterior aspect of the aortic root and at the most posterior aspect of the pulmonary root. The coronaries are excised and mobilized in the same fashion as an arterial switch procedure. The complete truncus arteriosus (aortic and pulmonary root together) is excised (Fig. 1). The conus septum is either totally resected together with the aortic and pulmonary root, or partially resected and divided. The incision of the conus septum is made leftwards to the papillary muscle of the conus (Fig. 2). The truncus arteriosus is rotated by 180 and reimplanted, so that the aorta comes over the LVOT and the pulmonary root comes over the RVOT. After implanting the posterior part of the aortic root, the LVOT is completed by closing the VSD with a patch. The LVOT is thereby enlarged to its appropriate size. It is important to carry out the suture line to both ends of the divided or resected conus septum at this level (Fig. 2). By doing so, the residual circumference of the aortic root can determine the exact width of the VSD patch. The next step is to reconnect the coronaries to their contralateral orifices, which are located anteriorly after rotation. A Lecompte manoeuvre is performed and the anastomosis between the aortic root and ascending aorta is made. Pulmonary root and RV are then anastomosed. Finally, the pulmonary root and PA are reconnected [10]. The pulmonary valve could be preserved in 15 patients. Commissurotomy, subannular and supravalvular patch enlargement was used in most of these cases. A transannular patch was necessary on 4 patients. All patches were of autologous pericardium, fixated in glutaraldehyde. Operative data The median CPB time was 289 min [263; 357] ranging from 213 to 419 min. Median aortic cross-clamp time was 157 min [142; 171] ranging from 128 to 190 min. Delayed chest closure was performed on 5 patients. Follow-up One patient, who was referred by an aid programme, does not have a fixed address, and we were therefore unable to get data from her. Four patients were referred by aid organizations from foreign countries. They are being followed by hospitals in their home countries. We have reliable echocardiographic reports and clinical follow-up examinations on all 4 patients. Seven patients are being followed in our centre and 5 patients are in the follow-up programmes coordinated with our centre, providing complete echocardiographic and clinical data. Data analysis Routine echocardiographic data of the LVOT and RVOT were analysed. To assess growth, the diameter of the aortic valve and the diameter of the pulmonary valve in the first postoperative echo were compared with the diameter at the last follow-up. To see whether growth in the two vessels was proportional, we compared the z-scores of the aortic valve and pulmonary valve diameter in the first postoperative echo with those in the last follow-up. These data, diameter and z-scores were only available in patients followed by our own centre and related clinics (n = 12). Figure 1: Aorta and pulmonary artery are cut transversely, coronaries are mobilized, the line of excision of the truncus arteriosus is depicted by the dashed lined. Figure 2: Truncus arteriosus is excised, rotated by 180, reimplantation started posteriorly, conus septum transected leftward to the papillary muscle of the conus.
4 R. Mair et al. / European Journal of Cardio-Thoracic Surgery 179 Statistical analysis Basic data are described as median and quartiles. For the comparison of z-scores, a paired t-test was applied. A Kaplan Meier plot was drawn for freedom from reoperation and reintervention. RESULTS Perioperative results Mortality. One patient, a 3-year-old child referred from a foreign centre, died due to chronic left ventricular failure during her hospital stay. She had a single ventricle palliation at the stage of a bidirectional Glenn. She was severely cyanotic due to multiple veno-venous fistulas to the coronary sinus. For this reason, we decided not to do a Fontan procedure, but to go for biventricular repair. After the operation, the patient suffered from left ventricular failure, and we had to take her on extracorporeal membrane oxygenation (ECMO). She could be weaned, but remained in chronic pulmonary congestion. She needed another ECMO support 6 weeks later, suffering from symptoms similar to an acute respiratory distress syndrome. She could be weaned again, but she died 8 weeks after the operation in our intensive care unit. There were no signs of ischaemic myocardial lesions. Although the left ventricle was used to systemic pressure, it was obviously too small to support systemic circulation without the help of the right ventricle. Morbidity. One patient acquired cerebral bleeding 3 weeks after the operation when she was already completely mobilized. This was presumably caused by cerebral arterio venous malformations. She was our oldest patient and she was extremely cyanotic prior to the operation. She could be discharged with a severe neurological deficit. Residual lesions One patient had a residual VSD. One patient had an intermittent AV block II. Perioperative results: left ventricular outflow tract None of the patients showed a gradient in the LVOT. Six patients showed some minor degree of aortic valve regurgitation of <II. One patient demonstrated mild-to-moderate aortic valve insufficiency (II +). Almost all patients had an increased aortic valve diameter in the first postoperative echo: median z-score of the aortic valve diameter in the first postoperative echocardiography was 3.97 [2.74; 4.32]. Perioperative results: right ventricular outflow tract Four patients had extremely hypoplastic pulmonary valves, such that a transannular patch was necessary. The pulmonary valve could be preserved in 15 patients. Subcommissural patchplasty and supra-annular patch enlargement of the pulmonary root had to be performed on some of these however. The pulmonary valves or roots of these patients were still small in the first postoperative echo. Median z-score was 0.66 [ 0.9; 0.29]. The pulmonary valve remained competent in 14 patients, and showed trivial regurgitation in 1 patient. One patient demonstrated a significant gradient (4 m/s) in the RVOT. This was due to a residual VSD (see: residual lesions, reoperations and reinterventions). Four other patients showed flow velocities up to 3 m/s. Flow velocities were <2.7 m/s for 14 patients, which is equivalent to a gradient of <30 mmhg. At discharge, all patients showed good ventricular function in both ventricles in the postoperative echocardiographic examinations. No serious AV-valve incompetence (>I ) could be detected. According to our protocol for patients after repair of complex cardiac malformations (prolonged CPB time, prolonged cross-clamp time), all patients were on a combination of angiotensin converting enzyme inhibitors and diuretics for 3 6 months postoperatively. Aside from the patient with the severe cerebral haemorrhage, no further patient presented any new neurological abnormalities. Two patients received seizure medication for a seizure disease that existed before admission. Follow-up, mid-term and late results Mortality. One patient, who was discharged with a severe neurological deficit, died after 6 months due to aspiration. Sixteen patients were followed either by our own unit or by their referral centres. The follow-up period ranged from 153 days to 9.96 years. The median follow-up was 3.95 years [1.49; 6.45]. Reoperations and reinterventions Three patients needed reoperations. One patient needed a pacemaker for AV block II 3 months after en bloc rotation (Patient 6). One patient had a residual VSD and was reoperated on after 8.7 months (Patient 11). One patient had aortic valve regurgitation, which was mild to moderate immediately after the operation and deteriorated to moderate to severe over the next few years. She required reoperation after 4 years. The valve could be repaired by a subcommissural annuloplasty (Patient 5). One patient had a catheter intervention for supravalvular PA stenosis and kinking of the left PA 6 months postoperatively (Patient 6). Pictures of this catheterization are shown in Figs 3 and 4. Freedom from reoperation and reintervention is expressed in a Kaplan Meier curve (Fig. 5). All patients are presently in New York Heart Association class I. Left ventricular outflow tract None of the patients developed a gradient in the LVOT. Six patients kept their minor degree of aortic valve regurgitation of <II. The moderate aortic valve insufficiency (II +) in the initial postoperative echo of 1 patient deteriorated throughout the follow-up and needed reoperation (see reoperations and reinterventions). Growth of the aortic valve could be demonstrated in absolute metric values throughout the follow-up (Fig. 6). Median z-score at the last follow-up was 3.62 [0.76; 4.58]. Although the z-score of the aortic valve decreased in some patients, this did not reach significance (P = 0.22 paired t-test). This means, that in most children the aortic valve is still too big for their age and size. Right ventricular outflow tract During the follow-up period, growth of the pulmonary valve or root could be shown in all patients (Fig. 7). However, the z-score CONGENITAL
5 180 R. Mair et al. / European Journal of Cardio-Thoracic Surgery Figure 5: Kaplan Meier curve for freedom from reoperation and reintervention: two reinterventions occurred in 1 patient (Patient 6). The second reintervention (118 days after the first one) cannot be displayed in a Kaplan Meier curve. Figure 3: Ventriculography of the left ventricle 6 months after en bloc rotation of the truncus arteriosus. Figure 6: Aortic valve growth after en bloc rotation of the truncus arteriosus. Figure 4: Ventriculography of the right ventricle 6 months after en bloc rotation of the truncus arteriosus and subcommisural patch plasty in the right ventricular outflow tract. in the whole group did not change significantly: median z-score at the last follow-up examination was 0.26 [ 1.82; 0.45] (P = 0.49). Significant flow accelerations of >3 m/s in the pulmonary root could be demonstrated by Doppler echocardiography in 2 patients. In both patients, the flow accelerations appeared supravalvar, at the site of the anatomosis to the pulmonary bifurcation. One patient had a flow velocity of 3.7 m/s (calculated gradient: 57 mmhg), and had a catheter intervention after 6 months (see reoperations and reinterventions). Figure 7: Pulmonary valve growth after en bloc rotation of the truncus arteriosus. The other patient has a peak velocity of 4 m/s now after 9.16 years (calculated gradient of 60 mmhg). A catheterization is planned. All other patients showed either normal flow patterns or minor flow velocity accelerations with calculated gradients between 10 and 31 mmhg, remaining constant up to now. A free pulmonary regurgitation has been seen in 3 patients with a transannular patch, the fourth patient died after 6 months due to aspiration. The pulmonary valve was competent in 5 patients. Trivial incompetence (I ) was found in 4 patients. A mild insufficiency (II ) was seen in 4 patients.
6 R. Mair et al. / European Journal of Cardio-Thoracic Surgery 181 DISCUSSION The classic repair for TGA/VSD/LVOTO is the Rastelli procedure. Its long-term problems are well documented. A long intracardiac tunnel has an inherent tendency to obstruct. This might be one reason for the substantial late mortality [2, 5]. An RV-PA conduit leads to multiple reoperations or at least reinterventions. Kreutzer et al. [2] published a series of 101 Rastelli procedures over a period of 25 years. They reported 17 late deaths, 11 reoperations for LVOT obstruction, 44 conduit reoperations and 28 conduit reinterventions. The REV procedure does not need an RV-PA conduit, but it has no valve in the RVOT. By resection of the conus septum, the intracardiac tunnel is shortened. However, it is still not an anatomic repair regarding the LVOT. This procedure showed better results in the multicentre study by Hazekamp et al. [5] than the Rastelli procedure. In en bloc rotation of the truncus arteriosus, the aortic root comes over the left ventricle and the pulmonary root over the right ventricle. Due to the shorter follow-up period and the small number of patients, a comparison of our study to the above-mentioned studies is not justified. However, the incidence of reoperations and reinterventions for LVOT or RVOT obstruction is low. Most of our reoperations were due to either technical reasons or are not procedure specific. To avoid any possible LVOT obstruction, we used oversized VSD patches on our first patients. This led to central aortic valve regurgitation in some of them. We were able to solve this problem upon reoperation using plicating sutures in the subcommissural area in 1 patient, thereby narrowing the proximal valve annulus to its appropriate size. Since we use the implantation technique described above, carrying out the proximal suture line of the aortic root up to the remnants of the conus septum, thereby determining the width of the patch exactly, we did not have those aortic valve problems. We regard this as a technical problem, which can be avoided by following this principle of implantation and avoiding oversized patches in an oversized aortic root. The aortic annulus usually remains unchanged by this kind of operation. The pulmonary annulus however might be enlarged if subcommissural and supravalvular or transannular patches are used. We therefore used the first postoperative echocardiographic measurements for comparison with the follow-up examinations. Both the aortic and pulmonary valve showed growth. Almost all patients with this malformation started with an oversized aorta. This is explained by the preoperative flow patterns, which are similar to those in tetralogy of Fallot. Although blood flow normalized after the operation, as there were no shunts anymore, the aortic valve remained big and the z-score did not decrease significantly during the follow-up. On the RV-side, these patients started with a hypoplastic pulmonary root, which was still small after a valve sparing operation despite enlargement plasties. Growth was clearly demonstrated for the pulmonary valve and annulus; however, they remained small for the size and age of the patient. Z-scores did not show significant change. This discrepancy in size of the great arteries after the long follow-up periods might be explained by the fact that despite flow being normalized and equal in both vessels, wall tension is higher in bigger vessels according to the law of Laplace. This may increase growth. Although z-scores are usually not normalized during the followup, an occurrence of a significant stenosis, which required treatment, was rare in this series. It was predominantly supravalvular at the site of the anastomosis when it occurred, which is similar to the findings recorded after an arterial switch procedure. Therefore, this might be a result of scar formation, and not an effect of growth deficit. As we demonstrated in our series, the pulmonary valve, though dysplastic and not usable as an aortic valve, can function well in the pulmonary position in many cases. Most of the preserved pulmonary valves acceptably kept their competence and up to now no patient has required reoperation for a pulmonary valve problem. The virtual axis of rotation of the truncus arteriosus is either on the right side of the infundibular septum or slightly within posterior part of the aortic root. Therefore the coronary ostia, which are located in the posterior aspect of the aortic root, are in the anterior aspect afterwards, but almost at the same level. The shift of the coronary arteries is therefore minimal [9, 10]. The procedure itself can generally be described as invasive. Cross-clamp periods and CPB periods are long and myocardial protection has to be done thoroughly. It is technically demanding and the process of en bloc excision of the truncus arteriosus requires excellent anatomic orientation. For these reasons, we did not extend the indication for en bloc rotation to patients with additional malformations, as was mentioned in the patients and methods section. Concerning coronary anatomy, the indication was extended during the final years. Despite this there are still problems, which we have been unable to solve. For example, we had to switch to a Rastelli procedure in 2013 for a patient with a single coronary artery arising close to the commissure between the two facing sinuses and an anterior intramural course, despite this patient being an otherwise an excellent candidate for en bloc rotation. This is only one example and there will be more, due to the wide variation in coronary anatomy of this malformation. Due to its complexity and its dependency on the coronary anatomy, en bloc rotation of the truncus arteriosus is not currently as universally applicable to these malformations as the Rastelli procedure or the REV procedure. SUMMARY En bloc rotation of the truncus arteriosus is definitely an option of complete anatomic repair of transposition with VSD and left ventricular outflow tract obstruction or similar forms of DORV. It is important to understand and to follow a number of technical principles in reimplantation of the truncus arteriosus and sizing of the VSD patch to avoid problems with the aortic valve. It is an invasive procedure and it is technically demanding. Its late effects are similar to those found after repair of tetralogy of Fallot and the arterial switch procedure. Limitations The small number of patients limits the study. ACKNOWLEDGEMENTS We thank Wolfgang Schimetta for his statistical support. Conflict of interest: none declared. CONGENITAL
7 182 R. Mair et al. / European Journal of Cardio-Thoracic Surgery REFERENCES [1] Rastelli GC, Wallace RB, Ongley PA. Complete repair of transposition of the great arteries with pulmonary stenosis. Circulation 1969;39: [2] Kreutzer C, De Vive J, Oppido G, Kreutzer J, Gauvreau K, Freed M et al. Twenty-five-year experience with rastelli repair for transposition of the great arteries. J Thorac Cardiovasc Surg 2000;120: [3] Emani SM, Beroukhim R, Zurakowski D, Pigula FA, Mayer JE, del Nido PJ et al. Outcomes after anatomic repair for d-transposition of the great arteries with left ventricular outflow tract obstruction. Circulation 2009;120:S53 8. [4] Hörer J, Schreiber C, Dworak E, Cleuziou J, Prodan Z, Vogt M et al. Long-term results after the Rastelli repair for transposition of the great arteries. Ann Thorac Surg 2007;84: [5] Hazekamp MG, Gomez AA, Koolbergen DR, Hraska V, Metras DR, Mattila IP et al. European Congenital Heart Surgeons Association. Surgery for transposition of the great arteries, ventricular septal defect and left ventricular outflow tract obstruction: European Congenital Heart Surgeons Association multicenter study. Eur J Cardiothorac Surg 2010;38: [6] Lecompte Y, Neveux JY, Leca F, Zannini L, Tu TV, Dubois Y et al. Reconstruction of the pulmonary outflow tract without prosthetic conduit. J Thorac Cardiovasc Surg 1982;84: [7] Vouhe PR, Tamisier D, Leca F, Ouaknine R, Vernant F, Neveux JY. Transposition of the great arteries, ventricular septal defect and pulmonary outflow tract obstruction. Rastelli or Lecompte procedure? J Thorac Cardiovasc Surg 1992;103: [8] Nikaidoh H. Aortic translocation and biventricular outflow tract reconstruction. J Thorac Cardiovasc Surg 1984;88: [9] Yamagishi M, Shuntoh K, Matsushita T, Fujiwara K, Shinkawa T, Miyazaki T et al. Half- turned truncal switch operation for complete transposition of the great arteries with ventricular septal defect and pulmonary stenosis. J Thorac Cardiovasc Surg 2003;125: [10] Mair R, Sames-Dolzer E, Vondrys D, Lechner E, Tulzer G. En bloc rotation of the truncus arteriosus-an option for anatomic repair of transposition of the great arteries, ventricular septal defect and left ventricular outflow tract obstruction. J Thorac Cardiovasc Surg 2006;131: [11] Hu S, Xie Y, Li S, Wang X, Yan F, Li Y et al. Double root translocation, for double outlet right ventricle with noncommitted ventricular septal defect or double outlet right ventricle with subpulmonary ventricular septal defect and associated subpulmonary stenosis: an optimized solution. Ann Thorac Surg 2010;89: APPENDIX. CONFERENCE DISCUSSION Scan to your mobile or go to to search for the presentation on the EACTS library Dr V. Hraska (Sankt Augustin, Germany): The optimal therapeutic approach to complex transposition remains challenging and controversial, particularly in patients with non-committed/restrictive VSD, complex AV valve anatomy, borderline right ventricle, and left ventricular outflow tract obstruction. Under these circumstances, usually intraventricular rerouting using the REV or Rastelli operation is suboptimal and consideration is given either to conversion to the Fontan or to posterior translocation of the aorta or eventually to en bloc rotation of truncus arteriosus, as was demonstrated. That leads to the first question. Is en bloc rotation the method of choice even in patients with committed VSD to the aorta who are the perfect candidates for intraventricular rerouting in your institution? In other words, what are the contraindications for en bloc rotation? Dr Mair: We used this method for all patients with transposition of the great arteries or similar forms of DROV who otherwise would have needed a Rastelli procedure or a REV procedure. We restricted it in our initial series to forms with normal coronary anatomy for transposition. That means if the left coronary artery arises from the left coronary sinus and the right one from the right posterior coronary sinus. But with more and more experience we got more courageous and we are now doing it in almost all coronary anatomies. Dr Hraska: So, in other words, it is a method of choice in your institution? Dr Mair: Yes, the method of choice. Dr Hraska: The major advantage of Nikaidoh or en bloc rotation is creation of straight alignment of both outflows. However, in comparison with posterior aortic translocation, en bloc rotation should provide a functioning neopulmonary valve. That is basically the reason why the rotation is done. The question is, what is the functional performance of the pulmonary valve, which is very frequently stenotic and dysplastic in this group of patients? Dr Mair: The pulmonary valve was, of course, dysplastic, because this is one part of the indication of the operation, but you can do a lot to the pulmonary valve, even to a dysplastic pulmonary valve. If you think of tetralogy, you can also do a lot of things to the pulmonary valve that works in this more or less low pressure system. You can use subvalvular patches; you can use supravalvular patch plasty, and so on. As I said, the gradient which was found in most patients was between 10 and 31 mmhg and completely constant over the years, and in the patients in whom the valve was kept intact, we did not find any pulmonary valve incompetence of more than mild. Dr Hraska: Unfortunately data regarding pulmonary valve function has not been provided. I think this is very important information, because this is the reason why the en bloc rotation, in comparison with Nikaidoh, should be done. Dr Mair: This may be one reason. One other reason is maybe the coronary arteries, because the axis of rotation is about in the plane of the coronary arteries. So you don t have to mobilize them as far as in the Nikaidoh procedure. Dr Hraska: But if the Nikaidoh procedure is done correctly, there is no need for that. Dr P. Vouhe (Paris, France): You said that there is no contraindication related to coronary arteries. Is it true also with an artery crossing in front of the aorta, and in this case how do you deal with it? Dr Mair: When the coronaries cross in front of the aorta, when the right coronary comes in front of the aorta, you have to mobilize the coronary artery very extensively, but it works. The only contraindication we found in the last years was a single intramural coronary artery which came out of the posterior facing sinus.
The Rastelli procedure has been traditionally used for repair
 En-bloc Rotation of the Truncus Arteriosus A Technique for Complete Anatomic Repair of Transposition of the Great Arteries/Ventricular Septal Defect/Left Ventricular Outflow Tract Obstruction or Double
En-bloc Rotation of the Truncus Arteriosus A Technique for Complete Anatomic Repair of Transposition of the Great Arteries/Ventricular Septal Defect/Left Ventricular Outflow Tract Obstruction or Double
In 1980, Bex and associates 1 first introduced the initial
 Technique of Aortic Translocation for the Management of Transposition of the Great Arteries with a Ventricular Septal Defect and Pulmonary Stenosis Victor O. Morell, MD, and Peter D. Wearden, MD, PhD In
Technique of Aortic Translocation for the Management of Transposition of the Great Arteries with a Ventricular Septal Defect and Pulmonary Stenosis Victor O. Morell, MD, and Peter D. Wearden, MD, PhD In
Surgical Treatment for Double Outlet Right Ventricle. Masakazu Nakao Consultant, Paediatric Cardiothoracic Surgery
 for Double Outlet Right Ventricle Masakazu Nakao Consultant, Paediatric Cardiothoracic Surgery 1 History Intraventricular tunnel (Kawashima) First repair of Taussig-Bing anomaly (Kirklin) Taussig-Bing
for Double Outlet Right Ventricle Masakazu Nakao Consultant, Paediatric Cardiothoracic Surgery 1 History Intraventricular tunnel (Kawashima) First repair of Taussig-Bing anomaly (Kirklin) Taussig-Bing
"Giancarlo Rastelli Lecture"
 "Giancarlo Rastelli Lecture" Surgical treatment of Malpositions of the Great Arteries Pascal Vouhé Giancarlo Rastelli (1933 1970) Cliquez pour modifier les styles du texte du masque Deuxième niveau Troisième
"Giancarlo Rastelli Lecture" Surgical treatment of Malpositions of the Great Arteries Pascal Vouhé Giancarlo Rastelli (1933 1970) Cliquez pour modifier les styles du texte du masque Deuxième niveau Troisième
The Double Switch Using Bidirectional Glenn and Hemi-Mustard. Frank Hanley
 The Double Switch Using Bidirectional Glenn and Hemi-Mustard Frank Hanley No relationships to disclose CCTGA Interesting Points for Discussion What to do when. associated defects must be addressed surgically:
The Double Switch Using Bidirectional Glenn and Hemi-Mustard Frank Hanley No relationships to disclose CCTGA Interesting Points for Discussion What to do when. associated defects must be addressed surgically:
Double outlet right ventricle: navigation of surgeon to chose best treatment strategy
 Double outlet right ventricle: navigation of surgeon to chose best treatment strategy Jan Marek Great Ormond Street Hospital & Institute of Cardiovascular Sciences, University College London Double outlet
Double outlet right ventricle: navigation of surgeon to chose best treatment strategy Jan Marek Great Ormond Street Hospital & Institute of Cardiovascular Sciences, University College London Double outlet
The arterial switch operation has been the accepted procedure
 The Arterial Switch Procedure: Closed Coronary Artery Transfer Edward L. Bove, MD The arterial switch operation has been the accepted procedure for the repair of transposition of the great arteries (TGA)
The Arterial Switch Procedure: Closed Coronary Artery Transfer Edward L. Bove, MD The arterial switch operation has been the accepted procedure for the repair of transposition of the great arteries (TGA)
TGA, VSD, and LVOTO. Cheul Lee, MD. Department of Thoracic and Cardiovascular Surgery Sejong General Hospital
 Surgical Management of TGA, VSD, and LVOTO Cheul Lee, MD Department of Thoracic and Cardiovascular Surgery Sejong General Hospital TGA, VSD, and LVOTO Incidence : 0.7% of all CHD 20% of TGA with VSD 4%
Surgical Management of TGA, VSD, and LVOTO Cheul Lee, MD Department of Thoracic and Cardiovascular Surgery Sejong General Hospital TGA, VSD, and LVOTO Incidence : 0.7% of all CHD 20% of TGA with VSD 4%
Long-Term Results After the Rastelli Repair for Transposition of the Great Arteries
 PEDIATRIC CARDIAC SURGERY: The Annals of Thoracic Surgery CME Program is located online at http://cme.ctsnetjournals.org. To take the CME activity related to this article, you must have either an STS member
PEDIATRIC CARDIAC SURGERY: The Annals of Thoracic Surgery CME Program is located online at http://cme.ctsnetjournals.org. To take the CME activity related to this article, you must have either an STS member
Complete Transposition of the Great Arteries
 1 Complete Transposition of the Great Arteries Contents Introduction 2 Anatomy 3 Complete Transposition of the Great Arteries, with or without Ventricular Septal Defect 5 Indication for Surgery 5 Approach
1 Complete Transposition of the Great Arteries Contents Introduction 2 Anatomy 3 Complete Transposition of the Great Arteries, with or without Ventricular Septal Defect 5 Indication for Surgery 5 Approach
Appendix A.1: Tier 1 Surgical Procedure Terms and Definitions
 Appendix A.1: Tier 1 Surgical Procedure Terms and Definitions Tier 1 surgeries AV Canal Atrioventricular Septal Repair, Complete Repair of complete AV canal (AVSD) using one- or two-patch or other technique,
Appendix A.1: Tier 1 Surgical Procedure Terms and Definitions Tier 1 surgeries AV Canal Atrioventricular Septal Repair, Complete Repair of complete AV canal (AVSD) using one- or two-patch or other technique,
TGA Surgical techniques: tips & tricks (Arterial switch operation)
 TGA Surgical techniques: tips & tricks (Arterial switch operation) Seoul National University Children s Hospital Woong-Han Kim Surgical History 1951 Blalock and Hanlon, atrial septectomy 1954 Mustard et
TGA Surgical techniques: tips & tricks (Arterial switch operation) Seoul National University Children s Hospital Woong-Han Kim Surgical History 1951 Blalock and Hanlon, atrial septectomy 1954 Mustard et
LEFT VENTRICULAR OUTFLOW OBSTRUCTION WITH A VSD: OPTIONS FOR SURGICAL MANAGEMENT
 LEFT VENTRICULAR OUTFLOW OBSTRUCTION WITH A VSD: OPTIONS FOR SURGICAL MANAGEMENT 10-13 March 2017 Ritz Carlton, Riyadh, Saudi Arabia Zohair AlHalees, MD Consultant, Cardiac Surgery Heart Centre LEFT VENTRICULAR
LEFT VENTRICULAR OUTFLOW OBSTRUCTION WITH A VSD: OPTIONS FOR SURGICAL MANAGEMENT 10-13 March 2017 Ritz Carlton, Riyadh, Saudi Arabia Zohair AlHalees, MD Consultant, Cardiac Surgery Heart Centre LEFT VENTRICULAR
14 Valvular Stenosis
 14 Valvular Stenosis 14-1. Valvular Stenosis unicuspid valve FIGUE 14-1. This photograph shows severe valvular stenosis as it occurs in a newborn. There is a unicuspid, horseshoe-shaped leaflet with a
14 Valvular Stenosis 14-1. Valvular Stenosis unicuspid valve FIGUE 14-1. This photograph shows severe valvular stenosis as it occurs in a newborn. There is a unicuspid, horseshoe-shaped leaflet with a
Since first successfully performed by Jatene et al, the
 Long-Term Predictors of Aortic Root Dilation and Aortic Regurgitation After Arterial Switch Operation Marcy L. Schwartz, MD; Kimberlee Gauvreau, ScD; Pedro del Nido, MD; John E. Mayer, MD; Steven D. Colan,
Long-Term Predictors of Aortic Root Dilation and Aortic Regurgitation After Arterial Switch Operation Marcy L. Schwartz, MD; Kimberlee Gauvreau, ScD; Pedro del Nido, MD; John E. Mayer, MD; Steven D. Colan,
The need for right ventricular outflow tract reconstruction
 Polytetrafluoroethylene Bicuspid Pulmonary Valve Implantation James A. Quintessenza, MD The need for right ventricular outflow tract reconstruction and pulmonary valve replacement is increasing for many
Polytetrafluoroethylene Bicuspid Pulmonary Valve Implantation James A. Quintessenza, MD The need for right ventricular outflow tract reconstruction and pulmonary valve replacement is increasing for many
Surgery for Congenital Heart Disease. The aortic translocation (Nikaidoh) procedure: Midterm results superior to the Rastelli procedure
 The aortic translocation (Nikaidoh) procedure: Midterm results superior to the Rastelli procedure Thomas Yeh Jr, MD, PhD, Claudio Ramaciotti, MD, Steven R. Leonard, MD, Lonnie Roy, PhD, and Hisashi Nikaidoh,
The aortic translocation (Nikaidoh) procedure: Midterm results superior to the Rastelli procedure Thomas Yeh Jr, MD, PhD, Claudio Ramaciotti, MD, Steven R. Leonard, MD, Lonnie Roy, PhD, and Hisashi Nikaidoh,
TGA atrial vs arterial switch what do we need to look for and how to react
 TGA atrial vs arterial switch what do we need to look for and how to react Folkert Meijboom, MD, PhD, FES Dept ardiology University Medical entre Utrecht The Netherlands TGA + atrial switch: Follow-up
TGA atrial vs arterial switch what do we need to look for and how to react Folkert Meijboom, MD, PhD, FES Dept ardiology University Medical entre Utrecht The Netherlands TGA + atrial switch: Follow-up
Surgical options for tetralogy of Fallot
 Surgical options for tetralogy of Fallot Serban Stoica FRCS(CTh) MD ACHD study day, 19 September 2017 Anatomy Physiology Children Adults Complications Follow up Anatomy Etienne Fallot (1850-1911) VSD Overriding
Surgical options for tetralogy of Fallot Serban Stoica FRCS(CTh) MD ACHD study day, 19 September 2017 Anatomy Physiology Children Adults Complications Follow up Anatomy Etienne Fallot (1850-1911) VSD Overriding
The modified Konno procedure, or subaortic ventriculoplasty,
 Modified Konno Procedure for Left Ventricular Outflow Tract Obstruction David P. Bichell, MD The modified Konno procedure, or subaortic ventriculoplasty, first described by Cooley and Garrett in1986, 1
Modified Konno Procedure for Left Ventricular Outflow Tract Obstruction David P. Bichell, MD The modified Konno procedure, or subaortic ventriculoplasty, first described by Cooley and Garrett in1986, 1
Congenital Heart Defects
 Normal Heart Congenital Heart Defects 1. Patent Ductus Arteriosus The ductus arteriosus connects the main pulmonary artery to the aorta. In utero, it allows the blood leaving the right ventricle to bypass
Normal Heart Congenital Heart Defects 1. Patent Ductus Arteriosus The ductus arteriosus connects the main pulmonary artery to the aorta. In utero, it allows the blood leaving the right ventricle to bypass
The Edge-to-Edge Technique f For Barlow's Disease
 The Edge-to-Edge Technique f For Barlow's Disease Ottavio Alfieri, Michele De Bonis, Elisabetta Lapenna, Francesco Maisano, Lucia Torracca, Giovanni La Canna. Department of Cardiac Surgery, San Raffaele
The Edge-to-Edge Technique f For Barlow's Disease Ottavio Alfieri, Michele De Bonis, Elisabetta Lapenna, Francesco Maisano, Lucia Torracca, Giovanni La Canna. Department of Cardiac Surgery, San Raffaele
Recent technical advances and increasing experience
 Pediatric Open Heart Operations Without Diagnostic Cardiac Catheterization Jean-Pierre Pfammatter, MD, Pascal A. Berdat, MD, Thierry P. Carrel, MD, and Franco P. Stocker, MD Division of Pediatric Cardiology,
Pediatric Open Heart Operations Without Diagnostic Cardiac Catheterization Jean-Pierre Pfammatter, MD, Pascal A. Berdat, MD, Thierry P. Carrel, MD, and Franco P. Stocker, MD Division of Pediatric Cardiology,
Adult Congenital Heart Disease: What All Echocardiographers Should Know Sharon L. Roble, MD, FACC Echo Hawaii 2016
 1 Adult Congenital Heart Disease: What All Echocardiographers Should Know Sharon L. Roble, MD, FACC Echo Hawaii 2016 DISCLOSURES I have no disclosures relevant to today s talk 2 Why should all echocardiographers
1 Adult Congenital Heart Disease: What All Echocardiographers Should Know Sharon L. Roble, MD, FACC Echo Hawaii 2016 DISCLOSURES I have no disclosures relevant to today s talk 2 Why should all echocardiographers
Tetralogy of Fallot (TOF) with atrioventricular (AV)
 Tetralogy of Fallot with Atrioventricular Canal Defect: Two Patch Repair Sitaram M. Emani, MD, and Pedro J. del Nido, MD Tetralogy of Fallot (TOF) with atrioventricular (AV) canal defect is classified
Tetralogy of Fallot with Atrioventricular Canal Defect: Two Patch Repair Sitaram M. Emani, MD, and Pedro J. del Nido, MD Tetralogy of Fallot (TOF) with atrioventricular (AV) canal defect is classified
Surgical Management of TOF in Adults. Dr Flora Tsang Associate Consultant Department of Cardiothoracic Surgery Queen Mary Hospital
 Surgical Management of TOF in Adults Dr Flora Tsang Associate Consultant Department of Cardiothoracic Surgery Queen Mary Hospital Tetralogy of Fallot (TOF) in Adults Most common cyanotic congenital heart
Surgical Management of TOF in Adults Dr Flora Tsang Associate Consultant Department of Cardiothoracic Surgery Queen Mary Hospital Tetralogy of Fallot (TOF) in Adults Most common cyanotic congenital heart
Congenital Heart Disease An Approach for Simple and Complex Anomalies
 Congenital Heart Disease An Approach for Simple and Complex Anomalies Michael D. Pettersen, MD Director, Echocardiography Rocky Mountain Hospital for Children Denver, CO None Disclosures 1 ASCeXAM Contains
Congenital Heart Disease An Approach for Simple and Complex Anomalies Michael D. Pettersen, MD Director, Echocardiography Rocky Mountain Hospital for Children Denver, CO None Disclosures 1 ASCeXAM Contains
Appendix A.2: Tier 2 Surgical Procedure Terms and Definitions
 Appendix A.2: Tier 2 Surgical Procedure Terms and Definitions Tier 2 surgeries Anomalous Systemic Venous Connection Anomalous Systemic Venous Connection Repair Repair includes a range of surgical approaches,
Appendix A.2: Tier 2 Surgical Procedure Terms and Definitions Tier 2 surgeries Anomalous Systemic Venous Connection Anomalous Systemic Venous Connection Repair Repair includes a range of surgical approaches,
Surgical Results in Patients With Double Outlet Right Ventricle: A 20-Year Experience
 Surgical Results in Patients With Double Outlet Right Ventricle: A 20-Year Experience John W. Brown, MD, Mark Ruzmetov, MD, Yuji Okada, MD, Palaniswamy Vijay, PhD, MPH, and Mark W. Turrentine, MD Section
Surgical Results in Patients With Double Outlet Right Ventricle: A 20-Year Experience John W. Brown, MD, Mark Ruzmetov, MD, Yuji Okada, MD, Palaniswamy Vijay, PhD, MPH, and Mark W. Turrentine, MD Section
3/14/2011 MANAGEMENT OF NEWBORNS CARDIAC INTENSIVE CARE CONFERENCE FOR HEALTH PROFESSIONALS IRVINE, CA. MARCH 7, 2011 WITH HEART DEFECTS
 CONFERENCE FOR HEALTH PROFESSIONALS IRVINE, CA. MARCH 7, 2011 MANAGEMENT OF NEWBORNS WITH HEART DEFECTS A NTHONY C. CHANG, MD, MBA, MPH M E D I C AL D I RE C T OR, HEART I N S T I T U T E C H I LDRE N
CONFERENCE FOR HEALTH PROFESSIONALS IRVINE, CA. MARCH 7, 2011 MANAGEMENT OF NEWBORNS WITH HEART DEFECTS A NTHONY C. CHANG, MD, MBA, MPH M E D I C AL D I RE C T OR, HEART I N S T I T U T E C H I LDRE N
Cardiac Catheterization Cases Primary Cardiac Diagnoses Facility 12 month period from to PRIMARY DIAGNOSES (one per patient)
 PRIMARY DIAGNOSES (one per patient) Septal Defects ASD (Atrial Septal Defect) PFO (Patent Foramen Ovale) ASD, Secundum ASD, Sinus venosus ASD, Coronary sinus ASD, Common atrium (single atrium) VSD (Ventricular
PRIMARY DIAGNOSES (one per patient) Septal Defects ASD (Atrial Septal Defect) PFO (Patent Foramen Ovale) ASD, Secundum ASD, Sinus venosus ASD, Coronary sinus ASD, Common atrium (single atrium) VSD (Ventricular
Perioperative Management of DORV Case
 Perioperative Management of DORV Case James P. Spaeth, MD Department of Anesthesia Cincinnati Children s Hospital Medical Center University of Cincinnati Objectives: 1. Discuss considerations regarding
Perioperative Management of DORV Case James P. Spaeth, MD Department of Anesthesia Cincinnati Children s Hospital Medical Center University of Cincinnati Objectives: 1. Discuss considerations regarding
Surgical Treatment for Atrioventricular Septal Defect. Masakazu Nakao Consultant, Paediatric Cardiothoracic Surgery
 Surgical Treatment for Atrioventricular Septal Defect Masakazu Nakao Consultant, Paediatric Cardiothoracic Surgery 1 History Rastelli classification (Rastelli) Pulmonary artery banding (Muller & Dammann)
Surgical Treatment for Atrioventricular Septal Defect Masakazu Nakao Consultant, Paediatric Cardiothoracic Surgery 1 History Rastelli classification (Rastelli) Pulmonary artery banding (Muller & Dammann)
Anatomy determines the close vicinity of the sinuses of
 Aortic Valve Reimplantation According to the David Type I Technique Matthias Karck, MD, and Axel Haverich, MD Department of Thoracic and Cardiovascular Surgery, Hannover Medical School, Hannover, Germany.
Aortic Valve Reimplantation According to the David Type I Technique Matthias Karck, MD, and Axel Haverich, MD Department of Thoracic and Cardiovascular Surgery, Hannover Medical School, Hannover, Germany.
Children with Single Ventricle Physiology: The Possibilities
 Children with Single Ventricle Physiology: The Possibilities William I. Douglas, M.D. Pediatric Cardiovascular Surgery Children s Memorial Hermann Hospital The University of Texas Health Science Center
Children with Single Ventricle Physiology: The Possibilities William I. Douglas, M.D. Pediatric Cardiovascular Surgery Children s Memorial Hermann Hospital The University of Texas Health Science Center
Anatomy of the coronary arteries in transposition
 Thorax, 1978, 33, 418-424 Anatomy of the coronary arteries in transposition of the great arteries and methods for their transfer in anatomical correction MAGDI H YACOUB AND ROSEMARY RADLEY-SMITH From Harefield
Thorax, 1978, 33, 418-424 Anatomy of the coronary arteries in transposition of the great arteries and methods for their transfer in anatomical correction MAGDI H YACOUB AND ROSEMARY RADLEY-SMITH From Harefield
An anterior aortoventriculoplasty, known as the Konno-
 The Konno-Rastan Procedure for Anterior Aortic Annular Enlargement Mark E. Roeser, MD An anterior aortoventriculoplasty, known as the Konno-Rastan procedure, is a useful tool for the cardiac surgeon. Originally,
The Konno-Rastan Procedure for Anterior Aortic Annular Enlargement Mark E. Roeser, MD An anterior aortoventriculoplasty, known as the Konno-Rastan procedure, is a useful tool for the cardiac surgeon. Originally,
Aortic valve repair is an accepted option for aortic valve
 Complex Aortic Valve Disease in Children Christopher W. Baird, MD,* and Pedro J. del Nido, MD Aortic valve repair is an accepted option for aortic valve pathologic conditions in children and young adults.
Complex Aortic Valve Disease in Children Christopher W. Baird, MD,* and Pedro J. del Nido, MD Aortic valve repair is an accepted option for aortic valve pathologic conditions in children and young adults.
Current Technique of the Arterial Switch Procedure for Transposition of the Great Arteries
 Current Technique of the Arterial Switch Procedure for Transposition of the Great Arteries EDWARD L. BOVE, M.D. Section of Thoracic Surgev, C.S. Mott Children's Hospital, The University of Michigan Medical
Current Technique of the Arterial Switch Procedure for Transposition of the Great Arteries EDWARD L. BOVE, M.D. Section of Thoracic Surgev, C.S. Mott Children's Hospital, The University of Michigan Medical
Common Defects With Expected Adult Survival:
 Common Defects With Expected Adult Survival: Bicuspid aortic valve :Acyanotic Mitral valve prolapse Coarctation of aorta Pulmonary valve stenosis Atrial septal defect Patent ductus arteriosus (V.S.D.)
Common Defects With Expected Adult Survival: Bicuspid aortic valve :Acyanotic Mitral valve prolapse Coarctation of aorta Pulmonary valve stenosis Atrial septal defect Patent ductus arteriosus (V.S.D.)
Tetralogy of Fallot (TOF) with absent pulmonary valve
 Repair of Tetralogy of Fallot with Absent Pulmonary Valve Syndrome Karl F. Welke, MD, and Ross M. Ungerleider, MD, MBA Tetralogy of Fallot (TOF) with absent pulmonary valve syndrome (APVS) occurs in 5%
Repair of Tetralogy of Fallot with Absent Pulmonary Valve Syndrome Karl F. Welke, MD, and Ross M. Ungerleider, MD, MBA Tetralogy of Fallot (TOF) with absent pulmonary valve syndrome (APVS) occurs in 5%
SURGICAL TREATMENT AND OUTCOME OF CONGENITAL HEART DISEASE
 SURGICAL TREATMENT AND OUTCOME OF CONGENITAL HEART DISEASE Mr. W. Brawn Birmingham Children s Hospital. Aims of surgery The aim of surgery in congenital heart disease is to correct or palliate the heart
SURGICAL TREATMENT AND OUTCOME OF CONGENITAL HEART DISEASE Mr. W. Brawn Birmingham Children s Hospital. Aims of surgery The aim of surgery in congenital heart disease is to correct or palliate the heart
Indications and Outcomes of the Double Switch in cctga. David Barron Birmingham, UK
 Indications and Outcomes of the Double Switch in cctga David Barron Birmingham, UK No Disclosures cctga: The Problem cctga does not fit into neat, clincially discrete sub-groups Atrial Situs Wide range
Indications and Outcomes of the Double Switch in cctga David Barron Birmingham, UK No Disclosures cctga: The Problem cctga does not fit into neat, clincially discrete sub-groups Atrial Situs Wide range
Pediatric Echocardiography Examination Content Outline
 Pediatric Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 Anatomy and Physiology Normal Anatomy and Physiology 10% 2 Abnormal Pathology and Pathophysiology
Pediatric Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 Anatomy and Physiology Normal Anatomy and Physiology 10% 2 Abnormal Pathology and Pathophysiology
Introduction. Study Design. Background. Operative Procedure-I
 Risk Factors for Mortality After the Norwood Procedure Using Right Ventricle to Pulmonary Artery Shunt Ann Thorac Surg 2009;87:178 86 86 Addressor: R1 胡祐寧 2009/3/4 AM7:30 SICU 討論室 Introduction Hypoplastic
Risk Factors for Mortality After the Norwood Procedure Using Right Ventricle to Pulmonary Artery Shunt Ann Thorac Surg 2009;87:178 86 86 Addressor: R1 胡祐寧 2009/3/4 AM7:30 SICU 討論室 Introduction Hypoplastic
Heart and Lungs. LUNG Coronal section demonstrates relationship of pulmonary parenchyma to heart and chest wall.
 Heart and Lungs Normal Sonographic Anatomy THORAX Axial and coronal sections demonstrate integrity of thorax, fetal breathing movements, and overall size and shape. LUNG Coronal section demonstrates relationship
Heart and Lungs Normal Sonographic Anatomy THORAX Axial and coronal sections demonstrate integrity of thorax, fetal breathing movements, and overall size and shape. LUNG Coronal section demonstrates relationship
Repair of Complete Atrioventricular Septal Defects Single Patch Technique
 Repair of Complete Atrioventricular Septal Defects Single Patch Technique Fred A. Crawford, Jr., MD The first repair of a complete atrioventricular septal defect was performed in 1954 by Lillehei using
Repair of Complete Atrioventricular Septal Defects Single Patch Technique Fred A. Crawford, Jr., MD The first repair of a complete atrioventricular septal defect was performed in 1954 by Lillehei using
Right ventricular outflow tract reconstruction with bicuspid valved polytetrafluoroethylene conduit.
 Carnegie Mellon University Research Showcase @ CMU Department of Biomedical Engineering Carnegie Institute of Technology 4-1-2011 Right ventricular outflow tract reconstruction with bicuspid valved polytetrafluoroethylene
Carnegie Mellon University Research Showcase @ CMU Department of Biomedical Engineering Carnegie Institute of Technology 4-1-2011 Right ventricular outflow tract reconstruction with bicuspid valved polytetrafluoroethylene
The vast majority of patients, especially children, who
 Technique of Mechanical Pulmonary Valve Replacement John M. Stulak, MD, and Joseph A. Dearani, MD The vast majority of patients, especially children, who require pulmonary valve replacement (PVR), obtain
Technique of Mechanical Pulmonary Valve Replacement John M. Stulak, MD, and Joseph A. Dearani, MD The vast majority of patients, especially children, who require pulmonary valve replacement (PVR), obtain
Repair of very severe tricuspid regurgitation following detachment of the tricuspid valve
 OPEN ACCESS Images in cardiology Repair of very severe tricuspid regurgitation following detachment of the tricuspid valve Ahmed Mahgoub 1, Hassan Kamel 2, Walid Simry 1, Hatem Hosny 1, * 1 Aswan Heart
OPEN ACCESS Images in cardiology Repair of very severe tricuspid regurgitation following detachment of the tricuspid valve Ahmed Mahgoub 1, Hassan Kamel 2, Walid Simry 1, Hatem Hosny 1, * 1 Aswan Heart
Damus-Kaye-Stansel Procedure: Midterm Follow-up and Technical Considerations
 Damus-Kaye-Stansel Procedure: Midterm Follow-up and Technical Considerations Thomas L. Carter, MD, Richard D. Mainwaring, MD, and John J. Lamberti, MD Division of Cardiac Surgery, Children's Hospital and
Damus-Kaye-Stansel Procedure: Midterm Follow-up and Technical Considerations Thomas L. Carter, MD, Richard D. Mainwaring, MD, and John J. Lamberti, MD Division of Cardiac Surgery, Children's Hospital and
Pulmonary Valve Replacement
 Pulmonary Valve Replacement Christian Kreutzer MD Hospital Nacional Alejandro Posadas Hospital Universitario Austral (No disclosures) Scope of the problem. CHD with PS or PA require a RVOT procedure. Tetralogy
Pulmonary Valve Replacement Christian Kreutzer MD Hospital Nacional Alejandro Posadas Hospital Universitario Austral (No disclosures) Scope of the problem. CHD with PS or PA require a RVOT procedure. Tetralogy
ADULT CONGENITAL HEART DISEASE. Stuart Lilley
 ADULT CONGENITAL HEART DISEASE Stuart Lilley More adults than children have congenital heart disease Huge variety of congenital lesions from minor to major Heart failure, re-operation and arrhythmia are
ADULT CONGENITAL HEART DISEASE Stuart Lilley More adults than children have congenital heart disease Huge variety of congenital lesions from minor to major Heart failure, re-operation and arrhythmia are
Echocardiographic assessment in Adult Patients with Congenital Heart Diseases
 Echocardiographic assessment in Adult Patients with Congenital Heart Diseases Athanasios Koutsakis Cardiologist, Cl. Research Fellow George Giannakoulas Ass. Professor in Cardiology 1st Cardiology Department,
Echocardiographic assessment in Adult Patients with Congenital Heart Diseases Athanasios Koutsakis Cardiologist, Cl. Research Fellow George Giannakoulas Ass. Professor in Cardiology 1st Cardiology Department,
Patrick O. Myers, MD, 1,2 Pedro J. del Nido, MD, 1 Sitaram M. Emani, MD, 1 Gerald R. Marx, MD, 3 Christopher W. Baird, MD 1
 Valve-Sparing Aortic Root Replacement and Remodeling with Complex Aortic Valve Reconstruction in Children and Young Adults with Moderate or Severe Aortic Regurgitation Patrick O. Myers, MD, 1,2 Pedro J.
Valve-Sparing Aortic Root Replacement and Remodeling with Complex Aortic Valve Reconstruction in Children and Young Adults with Moderate or Severe Aortic Regurgitation Patrick O. Myers, MD, 1,2 Pedro J.
Giovanni Di Salvo MD, PhD, FESC Second University of Naples Monaldi Hospital
 Giovanni Di Salvo MD, PhD, FESC Second University of Naples Monaldi Hospital VSD is one of the most common congenital cardiac abnormalities in the newborn. It can occur as an isolated finding or in combination
Giovanni Di Salvo MD, PhD, FESC Second University of Naples Monaldi Hospital VSD is one of the most common congenital cardiac abnormalities in the newborn. It can occur as an isolated finding or in combination
5.8 Congenital Heart Disease
 5.8 Congenital Heart Disease Congenital heart diseases (CHD) refer to structural or functional heart diseases, which are present at birth. Some of these lesions may be discovered later. prevalence of Chd
5.8 Congenital Heart Disease Congenital heart diseases (CHD) refer to structural or functional heart diseases, which are present at birth. Some of these lesions may be discovered later. prevalence of Chd
Techniques for repair of complete atrioventricular septal
 No Ventricular Septal Defect Patch Atrioventricular Septal Defect Repair Carl L. Backer, MD *, Osama Eltayeb, MD *, Michael C. Mongé, MD *, and John M. Costello, MD For the past 10 years, our center has
No Ventricular Septal Defect Patch Atrioventricular Septal Defect Repair Carl L. Backer, MD *, Osama Eltayeb, MD *, Michael C. Mongé, MD *, and John M. Costello, MD For the past 10 years, our center has
Bicuspid aortic root spared during ascending aorta surgery: an update of long-term results
 Short Communication Bicuspid aortic root spared during ascending aorta surgery: an update of long-term results Marco Russo, Guglielmo Saitto, Paolo Nardi, Fabio Bertoldo, Carlo Bassano, Antonio Scafuri,
Short Communication Bicuspid aortic root spared during ascending aorta surgery: an update of long-term results Marco Russo, Guglielmo Saitto, Paolo Nardi, Fabio Bertoldo, Carlo Bassano, Antonio Scafuri,
How to Assess and Treat Obstructive Lesions
 How to Assess and Treat Obstructive Lesions Erwin Oechslin, MD, FESC, FRCPC, Director, Congenital Cardiac Centre for Adults Peter Munk Cardiac Centre University Health Network/Toronto General Hospital
How to Assess and Treat Obstructive Lesions Erwin Oechslin, MD, FESC, FRCPC, Director, Congenital Cardiac Centre for Adults Peter Munk Cardiac Centre University Health Network/Toronto General Hospital
Congenital Heart Disease II: The Repaired Adult
 Congenital Heart Disease II: The Repaired Adult Doreen DeFaria Yeh, MD FACC Assistant Professor, Harvard Medical School MGH Adult Congenital Heart Disease Program Echocardiography Section, no disclosures
Congenital Heart Disease II: The Repaired Adult Doreen DeFaria Yeh, MD FACC Assistant Professor, Harvard Medical School MGH Adult Congenital Heart Disease Program Echocardiography Section, no disclosures
Although most patients with Ebstein s anomaly live
 Management of Neonatal Ebstein s Anomaly Christopher J. Knott-Craig, MD, FACS Although most patients with Ebstein s anomaly live through infancy, those who present clinically as neonates are a distinct
Management of Neonatal Ebstein s Anomaly Christopher J. Knott-Craig, MD, FACS Although most patients with Ebstein s anomaly live through infancy, those who present clinically as neonates are a distinct
Double Outlet Right Ventricle with Anterior and Left-Sided Aorta and Subpulmonary Ventricular Septal Defect
 Case Report Double Outlet Right Ventricle with Anterior and Left-Sided rta and Subpulmonary Ventricular Septal Defect Luciana Braz Peixoto, Samira Morhy Borges Leal, Carlos Eduardo Suaide Silva, Sandra
Case Report Double Outlet Right Ventricle with Anterior and Left-Sided rta and Subpulmonary Ventricular Septal Defect Luciana Braz Peixoto, Samira Morhy Borges Leal, Carlos Eduardo Suaide Silva, Sandra
Anomalous Systemic Venous Connection Systemic venous anomaly
 World Database for Pediatric and Congenital Heart Surgery Appendix B: Diagnosis (International Paediatric and Congenital Cardiac Codes (IPCCC) and definitions) Anomalous Systemic Venous Connection Systemic
World Database for Pediatric and Congenital Heart Surgery Appendix B: Diagnosis (International Paediatric and Congenital Cardiac Codes (IPCCC) and definitions) Anomalous Systemic Venous Connection Systemic
Management of Difficult Aortic Root, Old and New solutions
 Management of Difficult Aortic Root, Old and New solutions Hani K. Najm MD, Msc, FRCSC,, FACC, FESC Chairman, Pediatric and Congenital Heart Surgery Cleveland Clinic Conflict of Interest None Difficult
Management of Difficult Aortic Root, Old and New solutions Hani K. Najm MD, Msc, FRCSC,, FACC, FESC Chairman, Pediatric and Congenital Heart Surgery Cleveland Clinic Conflict of Interest None Difficult
Echocardiography in Adult Congenital Heart Disease
 Echocardiography in Adult Congenital Heart Disease Michael Vogel Kinderherz-Praxis München CHD missed in childhood Subsequent lesions after repaired CHD Follow-up of cyanotic heart disease CHD missed in
Echocardiography in Adult Congenital Heart Disease Michael Vogel Kinderherz-Praxis München CHD missed in childhood Subsequent lesions after repaired CHD Follow-up of cyanotic heart disease CHD missed in
Coronary Artery from the Wrong Sinus of Valsalva: A Physiologic Repair Strategy
 Coronary Artery from the Wrong Sinus of Valsalva: A Physiologic Repair Strategy Tom R. Karl, MS, MD he most commonly reported coronary artery malformation leading to sudden death in children and young
Coronary Artery from the Wrong Sinus of Valsalva: A Physiologic Repair Strategy Tom R. Karl, MS, MD he most commonly reported coronary artery malformation leading to sudden death in children and young
Indications for the Brock operation in current
 Thorax (1973), 28, 1. Indications for the Brock operation in current treatment of tetralogy of Fallot H. R. MATTHEWS and R. H. R. BELSEY Department of Thoracic Surgery, Frenchay Hospital, Bristol It is
Thorax (1973), 28, 1. Indications for the Brock operation in current treatment of tetralogy of Fallot H. R. MATTHEWS and R. H. R. BELSEY Department of Thoracic Surgery, Frenchay Hospital, Bristol It is
Long-term results (22 years) of the Ross Operation a single institutional experience
 Long-term results (22 years) of the Ross Operation a single institutional experience Authors: Costa FDA, Schnorr GM, Veloso M,Calixto A, Colatusso D, Balbi EM, Torres R, Ferreira ADA, Colatusso C Department
Long-term results (22 years) of the Ross Operation a single institutional experience Authors: Costa FDA, Schnorr GM, Veloso M,Calixto A, Colatusso D, Balbi EM, Torres R, Ferreira ADA, Colatusso C Department
World Database for Pediatric and Congenital Heart Surgery Appendix A: Surgical Procedure Terms and Definitions
 World Database for Pediatric and Congenital Heart Surgery Appendix A: Surgical Procedure Terms and Definitions All surgeries are Tier 2 surgeries unless otherwise noted. Anomalous Systemic Venous Connection
World Database for Pediatric and Congenital Heart Surgery Appendix A: Surgical Procedure Terms and Definitions All surgeries are Tier 2 surgeries unless otherwise noted. Anomalous Systemic Venous Connection
Atrioventricular valve repair: The limits of operability
 Atrioventricular valve repair: The limits of operability Francis Fynn-Thompson, MD Co-Director, Center for Airway Disorders Surgical Director, Pediatric Mechanical Support Program Surgical Director, Heart
Atrioventricular valve repair: The limits of operability Francis Fynn-Thompson, MD Co-Director, Center for Airway Disorders Surgical Director, Pediatric Mechanical Support Program Surgical Director, Heart
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/19123 holds various files of this Leiden University dissertation. Author: Hoohenkerk, Gerard Joannes Franciscus Title: Surgical correction of atrioventricular
Cover Page The handle http://hdl.handle.net/1887/19123 holds various files of this Leiden University dissertation. Author: Hoohenkerk, Gerard Joannes Franciscus Title: Surgical correction of atrioventricular
Annular Stabilization Techniques in the Context of Aortic Valve Repair
 Annular Stabilization Techniques in the Context of Aortic Valve Repair Prashanth Vallabhajosyula, MD MS University of Pennsylvania, Philadelphia, Pennsylvania 2 nd North American Aortic Valve Repair Symposium
Annular Stabilization Techniques in the Context of Aortic Valve Repair Prashanth Vallabhajosyula, MD MS University of Pennsylvania, Philadelphia, Pennsylvania 2 nd North American Aortic Valve Repair Symposium
Congenital Coronary Anomalies
 Chapter 50 Congenital Coronary Anomalies S. Adil Husain, Brett C. Sheridan, and Michael R. Mill Congenital coronary anomalies may have a significant impact on myocardial perfusion and secondary ischemia,
Chapter 50 Congenital Coronary Anomalies S. Adil Husain, Brett C. Sheridan, and Michael R. Mill Congenital coronary anomalies may have a significant impact on myocardial perfusion and secondary ischemia,
Will we face a big problem with the aortic valve/root after ASO?
 Will we face a big problem with the aortic valve/root after ASO? Laurence Iserin Unité médico-chirurgicale de Cardiologie Congénitale Adulte Hôpital Universitaire Européen Georges Pompidou APHP, Université
Will we face a big problem with the aortic valve/root after ASO? Laurence Iserin Unité médico-chirurgicale de Cardiologie Congénitale Adulte Hôpital Universitaire Européen Georges Pompidou APHP, Université
Adult Echocardiography Examination Content Outline
 Adult Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 Anatomy and Physiology Pathology Clinical Care and Safety Measurement Techniques, Maneuvers,
Adult Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 Anatomy and Physiology Pathology Clinical Care and Safety Measurement Techniques, Maneuvers,
Case. 15-year-old boy with bicuspid AV Severe AR with moderate AS. Ross vs. AVR (or AVP)
 Case 15-year-old boy with bicuspid AV Severe AR with moderate AS Ross vs. AVR (or AVP) AMC case 14-year-old boy with bicuspid AV Severe AS with mild AR Body size Bwt: 55 kg, Ht: 154 cm, BSA: 1.53 m 2 Echocardiography
Case 15-year-old boy with bicuspid AV Severe AR with moderate AS Ross vs. AVR (or AVP) AMC case 14-year-old boy with bicuspid AV Severe AS with mild AR Body size Bwt: 55 kg, Ht: 154 cm, BSA: 1.53 m 2 Echocardiography
SURGICAL APPROACHES FOR DOUBLE-OUTLET RIGHT VENTRICLE OR TRANSPOSITION OF THE GREAT ARTERIES ASSOCIATED WITH STRADDLING ATRIOVENTRICULAR VALVES
 SURGICAL APPROACHES FOR DOUBLE-OUTLET RIGHT VENTRICLE OR TRANSPOSITION OF THE GREAT ARTERIES ASSOCIATED WITH STRADDLING ATRIOVENTRICULAR VALVES Alain Serraf, MD ~ Tomohiro Nakamura, MD ~ Fran ois Lacour-Gayet,
SURGICAL APPROACHES FOR DOUBLE-OUTLET RIGHT VENTRICLE OR TRANSPOSITION OF THE GREAT ARTERIES ASSOCIATED WITH STRADDLING ATRIOVENTRICULAR VALVES Alain Serraf, MD ~ Tomohiro Nakamura, MD ~ Fran ois Lacour-Gayet,
The application of autologous pulmonary artery in surgical correction of complicated aortic arch anomaly
 Original Article The application of autologous pulmonary artery in surgical correction of complicated aortic arch anomaly Shusheng Wen, Jianzheng Cen, Jimei Chen, Gang Xu, Biaochuan He, Yun Teng, Jian
Original Article The application of autologous pulmonary artery in surgical correction of complicated aortic arch anomaly Shusheng Wen, Jianzheng Cen, Jimei Chen, Gang Xu, Biaochuan He, Yun Teng, Jian
Absent Pulmonary Valve Syndrome
 Absent Pulmonary Valve Syndrome Fact sheet on Absent Pulmonary Valve Syndrome In this condition, which has some similarities to Fallot's Tetralogy, there is a VSD with narrowing at the pulmonary valve.
Absent Pulmonary Valve Syndrome Fact sheet on Absent Pulmonary Valve Syndrome In this condition, which has some similarities to Fallot's Tetralogy, there is a VSD with narrowing at the pulmonary valve.
Surgical Results of Arterial Switch Operation for Taussig-Bing Anomaly: Is Position of the Great Arteries a Risk Factor?
 Surgical Results of Arterial Switch Operation for Taussig-Bing Anomaly: Is Position of the Great Arteries a Risk Factor? Mark D. Rodefeld, MD, Mark Ruzmetov, MD, PhD, Palaniswamy Vijay, PhD, MPH, Andrew
Surgical Results of Arterial Switch Operation for Taussig-Bing Anomaly: Is Position of the Great Arteries a Risk Factor? Mark D. Rodefeld, MD, Mark Ruzmetov, MD, PhD, Palaniswamy Vijay, PhD, MPH, Andrew
Surgical Procedures. Direct suture of small ASDs Patch repair Transcatheter closure with a prosthetic device called occluder
 PEDIATRIC Review Surgical Procedures Atrial Septal Defect repair: Direct suture of small ASDs Patch repair Transcatheter closure with a prosthetic device called occluder Balloon atrial septostomy (Rashkind)
PEDIATRIC Review Surgical Procedures Atrial Septal Defect repair: Direct suture of small ASDs Patch repair Transcatheter closure with a prosthetic device called occluder Balloon atrial septostomy (Rashkind)
A Unique Milieu for Perioperative Care of Adult Congenital Heart Disease Patients at a Single Institution
 Original Article A Unique Milieu for Perioperative Care of Adult Congenital Heart Disease Patients at a Single Institution Ghassan Baslaim, MD, and Jill Bashore, RN Purpose: Adult patients with congenital
Original Article A Unique Milieu for Perioperative Care of Adult Congenital Heart Disease Patients at a Single Institution Ghassan Baslaim, MD, and Jill Bashore, RN Purpose: Adult patients with congenital
The background of the Cardiac Sonographer Network News masthead is a diagnostic image:
 Number 5 Welcome Number 5 Welcome to the newsletter created just for you: sonographers who perform pediatric echocardiograms in primarily adult echo labs. Each issue features tips on echocardiography of
Number 5 Welcome Number 5 Welcome to the newsletter created just for you: sonographers who perform pediatric echocardiograms in primarily adult echo labs. Each issue features tips on echocardiography of
Congenital heart disease: When to act and what to do?
 Leading Article Congenital heart disease: When to act and what to do? Duminda Samarasinghe 1 Sri Lanka Journal of Child Health, 2010; 39: 39-43 (Key words: Congenital heart disease) Congenital heart disease
Leading Article Congenital heart disease: When to act and what to do? Duminda Samarasinghe 1 Sri Lanka Journal of Child Health, 2010; 39: 39-43 (Key words: Congenital heart disease) Congenital heart disease
Outcomes of Mitral Valve Repair for Mitral Regurgitation Due to Degenerative Disease
 Outcomes of Mitral Valve Repair for Mitral Regurgitation Due to Degenerative Disease TIRONE E. DAVID, MD ; SEMIN THORAC CARDIOVASC SURG 19:116-120c 2007 ELSEVIER INC. PRESENTED BY INTERN 許士盟 Mitral valve
Outcomes of Mitral Valve Repair for Mitral Regurgitation Due to Degenerative Disease TIRONE E. DAVID, MD ; SEMIN THORAC CARDIOVASC SURG 19:116-120c 2007 ELSEVIER INC. PRESENTED BY INTERN 許士盟 Mitral valve
Patients with congenitally corrected transposition of the great arteries
 Surgery for Congenital Heart Disease Midterm results after restoration of the morphologically left ventricle to the systemic circulation in patients with congenitally corrected transposition of the great
Surgery for Congenital Heart Disease Midterm results after restoration of the morphologically left ventricle to the systemic circulation in patients with congenitally corrected transposition of the great
Adult Congenital Heart Disease T S U N ` A M I!
 Adult Congenital Heart Disease T S U N ` A M I! Erwin Oechslin, MD, FRCPC, FESC Director, Congenital Cardiac Centre for Adults University Health Network Peter Munk Cardiac Centre / Toronto General Hospital
Adult Congenital Heart Disease T S U N ` A M I! Erwin Oechslin, MD, FRCPC, FESC Director, Congenital Cardiac Centre for Adults University Health Network Peter Munk Cardiac Centre / Toronto General Hospital
World Database for Pediatric and Congenital Heart Surgery Appendix A: Surgical Procedure Terms and Definitions
 World Database for Pediatric and Congenital Heart Surgery Appendix A: Surgical Procedure Terms and Definitions All surgeries are Tier 2 surgeries unless otherwise noted. Anomalous Systemic Venous Connection
World Database for Pediatric and Congenital Heart Surgery Appendix A: Surgical Procedure Terms and Definitions All surgeries are Tier 2 surgeries unless otherwise noted. Anomalous Systemic Venous Connection
Commissural Malalignment of Aortic-Pulmonary Sinus in Complete Transposition of Great Arteries
 Commissural Malalignment of Aortic-Pulmonary Sinus in Complete Transposition of Great Arteries Soo-Jin Kim, MD, Woong-Han Kim, MD, Cheong Lim, MD, Sam Se Oh, MD, and Yang-Min Kim, MD Departments of Pediatric
Commissural Malalignment of Aortic-Pulmonary Sinus in Complete Transposition of Great Arteries Soo-Jin Kim, MD, Woong-Han Kim, MD, Cheong Lim, MD, Sam Se Oh, MD, and Yang-Min Kim, MD Departments of Pediatric
S. Bert Litwin, MD. Preface
 Preface Because of the wide variety of anomalies encountered in congenital heart surgery, a broad understanding of the pathologic anatomy of defects is vitally important to the surgeon. More than in many
Preface Because of the wide variety of anomalies encountered in congenital heart surgery, a broad understanding of the pathologic anatomy of defects is vitally important to the surgeon. More than in many
42yr Old Male with Severe AR Mild LV dysfunction s/p TOF -AV Replacement(tissue valve) or AoV plasty- Kyung-Hwan Kim
 42yr Old Male with Severe AR Mild LV dysfunction s/p TOF -AV Replacement(tissue valve) or AoV plasty- Kyung-Hwan Kim Current Guideline for AR s/p TOF Surgery is reasonable in adults with prior repair of
42yr Old Male with Severe AR Mild LV dysfunction s/p TOF -AV Replacement(tissue valve) or AoV plasty- Kyung-Hwan Kim Current Guideline for AR s/p TOF Surgery is reasonable in adults with prior repair of
Adult Congenital Heart Disease: A Growing Problem. Dr. Gary Webb Cincinnati Children s Hospital Heart Institute
 Adult Congenital Heart Disease: A Growing Problem Dr. Gary Webb Cincinnati Children s Hospital Heart Institute ACHD Resources in Ohio ACHAHEART.ORG Situations When We Might Help When you don t know a
Adult Congenital Heart Disease: A Growing Problem Dr. Gary Webb Cincinnati Children s Hospital Heart Institute ACHD Resources in Ohio ACHAHEART.ORG Situations When We Might Help When you don t know a
Perimembranous VSD: When Do We Ask For A Surgical Closure? LI Xin. Department of Cardiothoracic Surgery Queen Mary Hospital Hong Kong
 Perimembranous VSD: When Do We Ask For A Surgical Closure? LI Xin Department of Cardiothoracic Surgery Queen Mary Hospital Hong Kong Classification (by Kirklin) I. Subarterial (10%) Outlet, conal, supracristal,
Perimembranous VSD: When Do We Ask For A Surgical Closure? LI Xin Department of Cardiothoracic Surgery Queen Mary Hospital Hong Kong Classification (by Kirklin) I. Subarterial (10%) Outlet, conal, supracristal,
BIVENTRICULAR REPAIR FOR AORTIC ATRESIA OR HYPOPLASIA AND VENTRICULAR SEPTAL DEFECT
 BIVENTRICULAR REPAIR FOR AORTIC ATRESIA OR HYPOPLASIA AND VENTRICULAR SEPTAL DEFECT Richard G. Ohye, MD a Koji Kagisaki, MD a Lisa A. Lee, MD b Ralph S. Mosca, MD a Caren S. Goldberg, MD b Edward L. Bove,
BIVENTRICULAR REPAIR FOR AORTIC ATRESIA OR HYPOPLASIA AND VENTRICULAR SEPTAL DEFECT Richard G. Ohye, MD a Koji Kagisaki, MD a Lisa A. Lee, MD b Ralph S. Mosca, MD a Caren S. Goldberg, MD b Edward L. Bove,
Long-term results of a strategy of aortic valve repair in the paediatric population: Should we avoid cusp extension?
 Long-term results of a strategy of aortic valve repair in the paediatric population: Should we avoid cusp extension? Y d Udekem, J Siddiqui, C Seaman, I Konstantinov, J Galati, M Cheung, C Brizard Royal
Long-term results of a strategy of aortic valve repair in the paediatric population: Should we avoid cusp extension? Y d Udekem, J Siddiqui, C Seaman, I Konstantinov, J Galati, M Cheung, C Brizard Royal
Ebstein s anomaly is characterized by malformation of
 Fenestrated Right Ventricular Exclusion (Starnes Procedure) for Severe Neonatal Ebstein s Anomaly Brian L. Reemtsen, MD,* and Vaughn A. Starnes, MD*, Ebstein s anomaly is characterized by malformation
Fenestrated Right Ventricular Exclusion (Starnes Procedure) for Severe Neonatal Ebstein s Anomaly Brian L. Reemtsen, MD,* and Vaughn A. Starnes, MD*, Ebstein s anomaly is characterized by malformation
DIAGNOSIS, MANAGEMENT AND OUTCOME OF HEART DISEASE IN SUDANESE PATIENTS
 434 E AST AFRICAN MEDICAL JOURNAL September 2007 East African Medical Journal Vol. 84 No. 9 September 2007 DIAGNOSIS, MANAGEMENT AND OUTCOME OF CONGENITAL HEART DISEASE IN SUDANESE PATIENTS K.M.A. Sulafa,
434 E AST AFRICAN MEDICAL JOURNAL September 2007 East African Medical Journal Vol. 84 No. 9 September 2007 DIAGNOSIS, MANAGEMENT AND OUTCOME OF CONGENITAL HEART DISEASE IN SUDANESE PATIENTS K.M.A. Sulafa,
