Vasoconstriction if BP goes up. Vasodilation BP goes down. blood.. Vasodilation wastes detected, to move them away. None
|
|
|
- Moris Berry
- 5 years ago
- Views:
Transcription
1 Shuster s A&P Notes Series Blood Vessels,, Perfusion & Capillary Dynamics 15 Summary of Controls on Perfusion and Systemic BP (short version): 1. Autoregulation of perfusion Control Category Short Term Short Term Outcomes Longg Term Long Term Outcomes Autoregulation: Methods the tissues have to control their own available blood flow (Perfusion). In general, act to protect the tissues from high or low BP. High BP causes many problems; low BP causes wastes to build up and tissue death. Myogenic: Smooth muscle surrounding local arterioles dilate/contract to increase flow/decrease flow, depending on blood pressure. Local Metabolites: Presence of nutrients/wastes causes the precapillary sphincters to open or close, depending on need of tissues. Vasoconstriction if BP goes up. Vasodilation if BP goes down Vasodilation if wastes detected, to move them away. Vasoconstriction not discussed. Angiogenesis: Tissues can causee new blood vessels to grow, bring them more blood.. None Diverts blood flow to organ or tissue. Cancerous tumors mimic this, stealing blood from healthy tissues.
2 Anatomy & Physiology II Note Series 2. Nervous Controls of Systemic BP (Also see summary image at end of this section) CJ Shuster 16 Control Category Short Term Short Term Outcomes Long Term Long Term Outcomes Nervous System: Extrinsic control from the nervous system. In general, this is Systemic Control of BP - acts to protect the whole body, including the brain, from high or low BP. Often, opposite effects of the Autoregulation Control Methods. Only short-term (acute). Sympathetic control only! There seemss to be little influence from the parasympathetic system, allowing local controls (autoregulation) to determine blood flow. Baroreflexes mediated by pressure in the aorta & carotid bodies. Unfortunately, thesee homeostatic controls seem to be ignored in the case of chronic hypertension. That is, they tend to adapt, so blood pressure is not lowered properly. Vasodilate if need nutrients/get of wastes. rid No Vasoconstriction discussed. None Chemoreflexes Not discussed. None Monitor changes in ph and oxygen and carbon dioxide levels of the blood. Higher Brain influences, especially under stress/anxiety. Not discussed. None
3 Shuster s A&P Notes Series Blood Vessels,, Perfusion & Capillary Dynamics 17 Summary Image for Neural Control of BP, including effects on CO: NOTE TO STUDENT: Everything talked about up to this point concerns a relatively normal cardiovascular system, meaning an average person at sea level. There are a number of changes that occur due to abnormal circumstances that are NOT pathological, such as responses to exercise and living at a higher elevation. We will not go through this in this series. Rather, if it is offered, it will come as an addendum.
4 Anatomy & Physiology II Note Series CJ Shuster Endocrine Controls of Systemic BP Control Category Short Term Short Term Outcomes Long Term Long Term Outcomes Endocrine system: Extrinsic control from via hormones In general, this is Systemic Control of BP - acts to protect the whole body, including the brain, from high or low BP. Often, opposite effects of the Autoregulation Control Methods. Slower than the neural methods, but longer lasting. We only discussed short term (acute) methods. If BP goes down, 3 hormones discussed: Renin & Angiotensin II hormonal complex Antidiuretic Hormone (ADH) Adrenal medulla hormones: Epinephrine & Norepinephrine (Epi & NE) Raises BP if it drops (in a lot of ways, including generalized vasoconstriction) Raises BP if it drops (increases blood volume by lowering urine production) Raises BP if it drops (in a lot of ways, including generalized vasoconstriction) If BP goes up, 1 hormone discussed; short-term effect only: Atrial Natriuretic Lowers BP, Peptide generalized vasodilationn (among other things) Exist, but we didn t discuss them.
5 Shuster s A&P Notes Series Blood Vessels, Perfusion & Capillary Dynamics 19 - For exam, know/define the following: Autoregulation, & what happens to vasoconstriction/dilation if BP drops or rises Define Myogenic Define Local metabolites Define Angiogenesis Neural Systemic Control, & what happens to vasoconstriction/dilation if BP drops or rises Sympathetic response Define chemoreceptors and baroreceptors Hormonal Systemic Control, & what happens to vasoconstriction/dilation if BP drops or rises Define Renin, Angiotensin, and ACE. Where are they produced? What does Renin do to angiotensin I? What does angiotensin II do to blood vessels? What do the adrenal medulla hormones do to BP, in general, and under what circumstance? What does ANF do to BP, and under what circumstance?
6 Anatomy & Physiology II Note Series CJ Shuster 20 D) CAPILLARY EXCHANGE & HOMEOSTASIS OF THE VOLUME OF BLOOD (Capillary Dynamics) 1) Exchange with the interstitial tissues: Microcirculation. - What are the forces driving the nutrients & wastes in/out of the capillaries? Movement in/out of capillaries, over the endothelial surface or between cells: 1. Passive means: (i) Diffusion & osmosis the vast majority! (ii) Filtration ( bulk flow ): Areas where filtration is important have lots of intracellular clefts. Special capillaries are called "Fenestrated capillaries". * Kidneys, intestines, etc. * Fenestrations. 2. Active means: exocytosis, endocytosis, pinocytosis. We will not be dealing with the active means, however. - For the most part: move water via filtration or osmosis, and let ions/dissolves substances follow! This is what we will be talking about here. * Filtration: moving substancess out of the bloodstream. * Reabsorption: moving substances back into the bloodstream. Later, we will be seeing important places where these processes are active: The digestive & urinary tracks But for most of the tissues, the cardiovascular system uses passive means. - Important Terms: Ischemia: insufficient blood flow. Hemorrhage: blood loss due to a broken vessel.
7 Shuster s A&P Notes Series Blood Vessels,, Perfusion & Capillary Dynamics 21 - The process depends on the difference of gradients between the interstitium and blood, with molecules moving to low concentrated spaces from high concentrated ones. Wastes (such as CO2) move out of interstitial fluids into blood, nutrients such as glucose, amino acids, oxygen (O2) move opposite direction. Concentration gradients must be maintained, which is why blood flow is so important. * Diffusion through the capillary walls depends on the permeability of the wall to which exchange materials: 1. If charged, they need to be small. 2. Lipid-soluble molecules move freely (which is why lipid soluble toxins are so dangerous!). 2) Homeostasis of water movement between compartments (blood, interstitial fluids, intracellular fluids) - Since we wall. are dependent (mostly) on diffusion & osmosis, we must maintain concentration gradients across capillary - To maintain homeostasis of water levels in the bloodstream (Blood Volume): * Local Control: Some chemicals increase/decrease permeability of capillary walls. More about this as we use them during the semester! * Systemic Control: Lymphatics return water to the veins. More on this in the Lymphatics Chapter. - Homeostatic imbalances: 1. Increase movement of ions, water into tissues = edema. And, low BP. 2. Increase movement of ions/ /water into capillaries = dehydration (of the tissues). And, raises BP.
8 Anatomy & Physiology II Note Series - Detail of Capillary Dynamics - There are 4 pressures: 2 Hydrostatic and 2 Osmotic (Colloidal) Pressures There are two hydrostatic and two osmotic pressures that affect transcapillary fluid exchange. (but, only 2 are important under normal circumstances): 1. Capillary (plasma) hydrostatic pressure IMPORTANT pressure! An outward pressure. This is mostly due to blood pressure; therefore, Cardiac Output. This is filtration pressure. 2. Capillary (plasma) osmotic ( colloidal ) pressure IMPORTANT pressure! An inward pressure. Blood is hypertonic to the extracellular fluid. This pressure is principally determined by plasma proteins that are relatively impermeable. Thus, the term colloidal. Albumin generates about 70% of this pressure. 3. Tissue (interstitial) hydrostatic pressure. An inward pressure. Normally = zero! CJ Shuster Tissue (interstitial) osmotic ( colloidal ) pressure. An outward pressure. Water moves into tissues, due to thee presence of some large proteins. Only important in some pathologies. - We are going to ignore #3 & #4. So, from now on, Blood hydrostatic pressure ( filtration pressure ) and Blood colloidal pressure ( osmotic pressure ) are our only concerns.
9 Shuster s A&P Notes Series Blood Vessels,, Perfusion & Capillary Dynamics 23 - In what direction will fluid move? Filtration versus Reabsorption 1. Capillary hydrostatic pressure on the capillary walls moves it out at the beginning of the capillary. Due to blood pressure. Theree is more pressure on the arteriole side because of friction in the capillary lowers P by the time it gets to the venule side. In a well-functioning cardiovascular system: on average, it is about +35 mmhg, giving us an outward pressure of about +10 mmhg, leading to filtration of waterr and any small ions and electrolytes dissolved in it. 2. Osmotic pressure moves it out at the end of the capillary. This pressure is also not constant throughoutt the capillary. This increasess as we get to the end of the capillary (venulee end), as we have moved water out of the capillary at the arterial end (making the blood more hypertonic). This pressure is typically mmhg, givingg us an average inward pressure of -7 to -10 mmhg, leading to the reabsorption of the water.
10 Anatomy & Physiology II Note Series CJ Shuster 24 Homeostasis of blood volume & pressure: Arteriole-end hydrostaticc pressure and venule-end osmotic pressure are equal. Imbalances: * If hydrostatic pressure (blood pressure) > osmotic pressure, we have edema. * If hydrostatic pressure (blood pressure) < osmotic pressure, we have dehydration. Congestive Heart Failure: Occurs when the heart is unable too provide sufficient pumpp action to maintain blood flow to meet the needs of the body. The term Congestive refers to fluid buildup in lungs. D) CIRCULATORY SHOCK - inadequate blood flow to tissuess causes series of events that leads to death. - Usually due to a loss of blood pressure. - There are many types, depending how BP was lost. Here are some common examples: 1. Hypovolemic Shock - loss of blood volume. * It may be due to Hemorrhage (blood loss due to a broken vessel) ), extreme dehydration, etc. 2. Cardiogenic shock - inadequate circulation due to insufficient heart contraction. This may be the result of heart attack or ectopic focus.
11 Shuster s A&P Notes Series Blood Vessels,, Perfusion & Capillary Dynamics Distributive shock - shock due to uncontrolled vasodilation, in response to some chemical/toxin present. The chemicals are called vasodilators. - Distributive shock: when a vasodilator ends up in the entire bloodstream, causing this local vasodilation to occur throughout thee body, dropping BP. There are several causes of distributive shock: 1. Septic shock - vasodilation in response to chemicals/metabolites released by an infecting agent (usually a bacterium). Sepsis or Septicemia infection of the blood Recall that certain metabolites produced normally lead to vasodilation (seee Perfusion section); this is an unfortunate consequence. 2. Anaphylactic shock - reaction to an allergen, antigen, drug or foreign protein causing the release of histamine which causes widespread vasodilation. 3. Neurogenic shock - Caused by any traumatic injuries withh immense pain. Recall that epinephrine also causes vasodilation, for example. ** There are other types of shock, all with different causes of loss of BP
12 Anatomy & Physiology II Note Series CJ Shuster 26 - Pathophysiology How this kills: The patient enters a positive feedback loop that results in death. Example: Often, shock occurs when there is a conflict between perfusion needs of local tissues, and systemic needs to maintain BP: A heart attack kills enough cardiac tissue to lessen blood flow due to a lowered BP. The body's tissues become hypoxic (low oxygen), which results in local vasodilation. That leads to a further lowering of systemic BP. The cardiovascular system responds by trying to increase BP via all the mechanism described earlier. There is a sympathetic nervous response, but the damaged cardiac tissue cannot keep it up. This causes vasoconstriction in some places, but vasodilation in others. - Patient goes through several stages of shock: The first stage is called Compensated Shock: the patient's body is employing physiological mechanisms, including neural, hormonal and local chemical mechanisms in an attempt to reverse the condition. The symptoms are rapid heart rate, anxiousness, and other signs of Sympathetic output. Life can be saved during Compensated Shock. We will not name the other stages of shock in this series. Eventually, the tissues become acidic, and the cells starve from lack of oxygen and glucose. This includes the cardiac cells (lowering CO further), and the pre-capillary sphincter muscles (causing more blood to pool up). Blood pools up, tissues die, organs fail.
13 Shuster s A&P Notes Series Blood Vessels,, Perfusion & Capillary Dynamics 27 E) MONITORING CIRCULATORY EFFICIENCY - VITAL SIGNS - circulatory + respiratory + body temperature. 1) PULSE - Put pressure against artery to feel pulse put out by each heartbeat. Must be an artery, as veins are not pulsatile. Also, arteries = large & close to the surface. * RADIAL - Most common. * Also act as PRESSURE POINTS to stop bleeding. * Normal = beats/min; but varies between lying down & sitting up, emotional states, etc. 2) BLOOD PRESSURE - AUSCULATORY METHOD - checking systemic BP using a Sphygmomanometer and a pressure cuff wrapped around arm.
14 Anatomy & Physiology II Note Series CJ Shuster Add air until P(cuff )> systolic pressure, at which point the artery is compressed and no blood can pass through. 2. Then, release air in cuff while listening to artery w/ a STETHESCOPE. When P(cuff) = P(systole), blood just barely can pass through artery. Can hear SOUNDS OF KOROTKOFF = blood squeezing through artery = SYSTOLIC PRESSURE = HIGHEST PRESSURE. 3. Keep releasing air until P(cuff) = P(diastole) - blood flows unobstructed through artery. SOUNDS OF KOROTKOFF disappear = DIASTOLIC PRESSURE = LOWEST PRESSURE OF SYSTEM. BP measured as SYSTOLE / DIASTOLE Normal = ( mmhg) / (75-80 mmhg). But, depends on age, race, weight, socioeconomic class, mood, physical activity, posture.
15 Shuster s A&P Notes Series Blood Vessels,, Perfusion & Capillary Dynamics 29 - Systolic and Diastolic blood pressure readings are variable in an individual,, and althoughh useful, are limited in their diagnostic use. Therefore, we use other measures of arterial efficiency: Pulse pressure is the difference between the systolic and diastolic pressure readings. It is measured in i millimeters of mercury (mmhg). It represents the force that the heart generates each time it contracts. If resting blood pressure is 120/80 mmhg, pulse pressure is 40. Mean arterial pressure (MAP) is a term used to describe an average blood pressure in an individual. It is defined as the average arterial pressure during a single cardiac cycle. Do not worry about how to figure MAP pressure for this series. But, it is the number we use in the rest of this chapter while talking about the pressure of blood as it enters the arterioles & capillaries. Lower MAP results in ischemia, or insufficient blood flow. 3) ALTERATIONS IN BP (i) HYPOTENSION - low BP; systolic < 90 mmhg. Not common. Low blood pressuree can be caused by low blood volume, hormonal changes, widening of blood vessels, medicine side effects, anemia,, heart problems or endocrine problems. (a) ORTHOSTATIC HYPOTENSION - head rush or dizzy spell, person's blood pressure suddenly falls when standing up or stretching. Common in elderly people; lessened sympathetic nervous response leads to blood pooling in lower limbs, leads to fainting spellss when rising from bed. Cure: slow postural changes before rising. (b) CHRONIC HYPOTENSION Condition last more than a year or two. Most common reason: Heart problems. Another example: bad nutrition leads to anemia leads to low blood protein leads to low viscosity leads to low PR leads to low BP. Hypothyroidism also causes it. (c) ACUTE HYPOTENSION usually blood loss. (ii) HYPERTENSION - Strains the heart and vessels. Big range for systolic pressures, as it is age and sex related. Heree is a simplified chart that most
16 Anatomy & Physiology II Note Series medical peoplee use: CJ Shuster 30 Not curable; often = a symptom. Death from stroke, heart attack, renal failure. (a) PRIMARY HYPERTENSION: No identifiable cause. Most common (90-95%). Complex; due to many factors. * Diet, obesity, age, race, heredity, stress, smoking. 30% of all people over 50. (b) SECONDARY HYPERTENS SION: Identifiable cause. Kidney disease most common cause (we ll look at the kidney s role in blood volume in the Kidney Chapter). (c) ORTHOSTATIC HYPERTENSION: person's blood pressure suddenly rises when standing up or stretching. Common in elderly people; breakdown in normal sympathetic nervous response. Heart palpitations
Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide
 Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide Main Idea: The function of the circulatory system is to maintain adequate blood flow to all tissues. Clinical
Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide Main Idea: The function of the circulatory system is to maintain adequate blood flow to all tissues. Clinical
Physiology of Circulation
 Physiology of Circulation Dr. Ali Ebneshahidi Blood vessels Arteries: Blood vessels that carry blood away from the heart to the lungs and tissues. Arterioles are small arteries that deliver blood to the
Physiology of Circulation Dr. Ali Ebneshahidi Blood vessels Arteries: Blood vessels that carry blood away from the heart to the lungs and tissues. Arterioles are small arteries that deliver blood to the
Blood Pressure. a change in any of these could cause a corresponding change in blood pressure
 Blood Pressure measured as mmhg Main factors affecting blood pressure: 1. cardiac output 2. peripheral resistance 3. blood volume a change in any of these could cause a corresponding change in blood pressure
Blood Pressure measured as mmhg Main factors affecting blood pressure: 1. cardiac output 2. peripheral resistance 3. blood volume a change in any of these could cause a corresponding change in blood pressure
Cardiovascular System. Blood Vessel anatomy Physiology & regulation
 Cardiovascular System Blood Vessel anatomy Physiology & regulation Path of blood flow Aorta Arteries Arterioles Capillaries Venules Veins Vena cava Vessel anatomy: 3 layers Tunica externa (adventitia):
Cardiovascular System Blood Vessel anatomy Physiology & regulation Path of blood flow Aorta Arteries Arterioles Capillaries Venules Veins Vena cava Vessel anatomy: 3 layers Tunica externa (adventitia):
The Cardiovascular System. The Structure of Blood Vessels. The Structure of Blood Vessels. The Blood Vessels. Blood Vessel Review
 The Cardiovascular System The Blood Vessels The Structure of Blood Vessels Blood Vessel Review Arteries carry blood away from the heart Pulmonary trunk to lungs Aorta to everything else Microcirculation
The Cardiovascular System The Blood Vessels The Structure of Blood Vessels Blood Vessel Review Arteries carry blood away from the heart Pulmonary trunk to lungs Aorta to everything else Microcirculation
Cardiovascular system: Blood vessels, blood flow. Latha Rajendra Kumar, MD
 Cardiovascular system: Blood vessels, blood flow Latha Rajendra Kumar, MD Outline 1- Physical laws governing blood flow and blood pressure 2- Overview of vasculature 3- Arteries 4. Capillaries and venules
Cardiovascular system: Blood vessels, blood flow Latha Rajendra Kumar, MD Outline 1- Physical laws governing blood flow and blood pressure 2- Overview of vasculature 3- Arteries 4. Capillaries and venules
Chapter 14 Blood Vessels, Blood Flow and Pressure Exam Study Questions
 Chapter 14 Blood Vessels, Blood Flow and Pressure Exam Study Questions 14.1 Physical Law Governing Blood Flow and Blood Pressure 1. How do you calculate flow rate? 2. What is the driving force of blood
Chapter 14 Blood Vessels, Blood Flow and Pressure Exam Study Questions 14.1 Physical Law Governing Blood Flow and Blood Pressure 1. How do you calculate flow rate? 2. What is the driving force of blood
Cardiovascular System: Vessels and Circulation (Chapter 21)
 Cardiovascular System: Vessels and Circulation (Chapter 21) Lecture Materials for Amy Warenda Czura, Ph.D. Suffolk County Community College Eastern Campus Primary Sources for figures and content: Marieb,
Cardiovascular System: Vessels and Circulation (Chapter 21) Lecture Materials for Amy Warenda Czura, Ph.D. Suffolk County Community College Eastern Campus Primary Sources for figures and content: Marieb,
BIOL 219 Spring Chapters 14&15 Cardiovascular System
 1 BIOL 219 Spring 2013 Chapters 14&15 Cardiovascular System Outline: Components of the CV system Heart anatomy Layers of the heart wall Pericardium Heart chambers, valves, blood vessels, septum Atrioventricular
1 BIOL 219 Spring 2013 Chapters 14&15 Cardiovascular System Outline: Components of the CV system Heart anatomy Layers of the heart wall Pericardium Heart chambers, valves, blood vessels, septum Atrioventricular
Blood Pressure Fox Chapter 14 part 2
 Vert Phys PCB3743 Blood Pressure Fox Chapter 14 part 2 T. Houpt, Ph.D. 1 Cardiac Output and Blood Pressure How to Measure Blood Pressure Contribution of vascular resistance to blood pressure Cardiovascular
Vert Phys PCB3743 Blood Pressure Fox Chapter 14 part 2 T. Houpt, Ph.D. 1 Cardiac Output and Blood Pressure How to Measure Blood Pressure Contribution of vascular resistance to blood pressure Cardiovascular
Six main classes of blood vessels (on handout) Wall structure of arteries and veins (on handout) Comparison: Arteries vs. Veins (on handout)
 Cardiovascular System: Vessels and Circulation (Chapter 21) Lecture Materials for Amy Warenda Czura, Ph.D. Suffolk County Community College Eastern Campus Six main classes of blood vessels Primary Sources
Cardiovascular System: Vessels and Circulation (Chapter 21) Lecture Materials for Amy Warenda Czura, Ph.D. Suffolk County Community College Eastern Campus Six main classes of blood vessels Primary Sources
Veins. VENOUS RETURN = PRELOAD = End Diastolic Volume= Blood returning to heart per cardiac cycle (EDV) or per minute (Venous Return)
 Veins Venous system transports blood back to heart (VENOUS RETURN) Capillaries drain into venules Venules converge to form small veins that exit organs Smaller veins merge to form larger vessels Veins
Veins Venous system transports blood back to heart (VENOUS RETURN) Capillaries drain into venules Venules converge to form small veins that exit organs Smaller veins merge to form larger vessels Veins
I. Cardiac Output Chapter 14
 10/24/11 I. Cardiac Output Chapter 14 Cardiac Output, Blood Flow, and Blood Pressure Lecture PowerPoint Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Cardiac
10/24/11 I. Cardiac Output Chapter 14 Cardiac Output, Blood Flow, and Blood Pressure Lecture PowerPoint Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Cardiac
Cardiovascular System B L O O D V E S S E L S 2
 Cardiovascular System B L O O D V E S S E L S 2 Blood Pressure Main factors influencing blood pressure: Cardiac output (CO) Peripheral resistance (PR) Blood volume Peripheral resistance is a major factor
Cardiovascular System B L O O D V E S S E L S 2 Blood Pressure Main factors influencing blood pressure: Cardiac output (CO) Peripheral resistance (PR) Blood volume Peripheral resistance is a major factor
The Cardiovascular system: physiology of circulation
 Chapter 21 The Cardiovascular system: physiology of circulation blood vessel structure and function physiology of circulation: blood flow, blood pressure, and resistance blood flow the amount of blood
Chapter 21 The Cardiovascular system: physiology of circulation blood vessel structure and function physiology of circulation: blood flow, blood pressure, and resistance blood flow the amount of blood
Physiology Chapter 14 Key Blood Flow and Blood Pressure, Plus Fun Review Study Guide
 Physiology Chapter 14 Key Blood Flow and Blood Pressure, Plus Fun Review Study Guide 1 Main Idea: The function of the circulatory system is to maintain adequate blood flow to all tissues. Clinical Application
Physiology Chapter 14 Key Blood Flow and Blood Pressure, Plus Fun Review Study Guide 1 Main Idea: The function of the circulatory system is to maintain adequate blood flow to all tissues. Clinical Application
Blood Flow, Blood Pressure, Cardiac Output. Blood Vessels
 Blood Flow, Blood Pressure, Cardiac Output Blood Vessels Blood Vessels Made of smooth muscle, elastic and fibrous connective tissue Cells are not electrically coupled Blood Vessels Arteries arterioles
Blood Flow, Blood Pressure, Cardiac Output Blood Vessels Blood Vessels Made of smooth muscle, elastic and fibrous connective tissue Cells are not electrically coupled Blood Vessels Arteries arterioles
BIPN100 F15 Human Physiol I (Kristan) Lecture 14 Cardiovascular control mechanisms p. 1
 BIPN100 F15 Human Physiol I (Kristan) Lecture 14 Cardiovascular control mechanisms p. 1 Terms you should understand: hemorrhage, intrinsic and extrinsic mechanisms, anoxia, myocardial contractility, residual
BIPN100 F15 Human Physiol I (Kristan) Lecture 14 Cardiovascular control mechanisms p. 1 Terms you should understand: hemorrhage, intrinsic and extrinsic mechanisms, anoxia, myocardial contractility, residual
Heart. Large lymphatic vessels Lymph node. Lymphatic. system Arteriovenous anastomosis. (exchange vessels)
 Venous system Large veins (capacitance vessels) Small veins (capacitance vessels) Postcapillary venule Thoroughfare channel Heart Large lymphatic vessels Lymph node Lymphatic system Arteriovenous anastomosis
Venous system Large veins (capacitance vessels) Small veins (capacitance vessels) Postcapillary venule Thoroughfare channel Heart Large lymphatic vessels Lymph node Lymphatic system Arteriovenous anastomosis
Blood Pressure Regulation. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation Faisal I. Mohammed, MD,PhD 1 Objectives Outline the short term and long term regulators of BP Know how baroreceptors and chemoreceptors work Know function of the atrial reflex.
Blood Pressure Regulation Faisal I. Mohammed, MD,PhD 1 Objectives Outline the short term and long term regulators of BP Know how baroreceptors and chemoreceptors work Know function of the atrial reflex.
Structure and organization of blood vessels
 The cardiovascular system Structure of the heart The cardiac cycle Structure and organization of blood vessels What is the cardiovascular system? The heart is a double pump heart arteries arterioles veins
The cardiovascular system Structure of the heart The cardiac cycle Structure and organization of blood vessels What is the cardiovascular system? The heart is a double pump heart arteries arterioles veins
Physiology of Circulation. Dr. Hiwa Shafiq 16/12/2018
 Physiology of Circulation Dr. Hiwa Shafiq 16/12/2018 Overview of the circulation The function of the circulation is to: 1. transport nutrients to the body tissues 2. transport waste products away 3. conduct
Physiology of Circulation Dr. Hiwa Shafiq 16/12/2018 Overview of the circulation The function of the circulation is to: 1. transport nutrients to the body tissues 2. transport waste products away 3. conduct
Cardiovascular System B L O O D V E S S E L S 3
 Cardiovascular System B L O O D V E S S E L S 3 Fluid Shifts Between Capillaries and Tissue Permeable capillaries allow plasma and solutes to pass into interstitial space interstitial or extracellular
Cardiovascular System B L O O D V E S S E L S 3 Fluid Shifts Between Capillaries and Tissue Permeable capillaries allow plasma and solutes to pass into interstitial space interstitial or extracellular
Chapter 9. Body Fluid Compartments. Body Fluid Compartments. Blood Volume. Blood Volume. Viscosity. Circulatory Adaptations to Exercise Part 4
 Body Fluid Compartments Chapter 9 Circulatory Adaptations to Exercise Part 4 Total body fluids (40 L) Intracellular fluid (ICF) 25 L Fluid of each cell (75 trillion) Constituents inside cell vary Extracellular
Body Fluid Compartments Chapter 9 Circulatory Adaptations to Exercise Part 4 Total body fluids (40 L) Intracellular fluid (ICF) 25 L Fluid of each cell (75 trillion) Constituents inside cell vary Extracellular
d) Cardiovascular System Higher Human Biology
 d) Cardiovascular System Higher Human Biology What can your remember about the heart and blood vessels? What is the Cardiovascular System? The cardiovascular system, also known as the circulatory system,
d) Cardiovascular System Higher Human Biology What can your remember about the heart and blood vessels? What is the Cardiovascular System? The cardiovascular system, also known as the circulatory system,
1. Distinguish among the types of blood vessels on the basis of their structure and function.
 Blood Vessels and Circulation Objectives This chapter describes the structure and functions of the blood vessels Additional subjects contained in Chapter 13 include cardiovascular physiology, regulation,
Blood Vessels and Circulation Objectives This chapter describes the structure and functions of the blood vessels Additional subjects contained in Chapter 13 include cardiovascular physiology, regulation,
3/10/2009 VESSELS PHYSIOLOGY D.HAMMOUDI.MD. Palpated Pulse. Figure 19.11
 VESSELS PHYSIOLOGY D.HAMMOUDI.MD Palpated Pulse Figure 19.11 1 shows the common sites where the pulse is felt. 1. Temporal artery at the temple above and to the outer side of the eye 2. External maxillary
VESSELS PHYSIOLOGY D.HAMMOUDI.MD Palpated Pulse Figure 19.11 1 shows the common sites where the pulse is felt. 1. Temporal artery at the temple above and to the outer side of the eye 2. External maxillary
Blood Pressure Regulation -1
 CVS Physiology Lecture 18 Blood Pressure Regulation -1 Please study the previous sheet before studying this one, even if the first part in this sheet is revision. In the previous lecture we were talking
CVS Physiology Lecture 18 Blood Pressure Regulation -1 Please study the previous sheet before studying this one, even if the first part in this sheet is revision. In the previous lecture we were talking
Presenter: Tom Mulvey
 Slides are from Level 3 Biology Course Content Day, 7 th November 2012 Presenter: Tom Mulvey Teachers are free to use these for teaching purposes with appropriate acknowledgement Blood Pressure Ways of
Slides are from Level 3 Biology Course Content Day, 7 th November 2012 Presenter: Tom Mulvey Teachers are free to use these for teaching purposes with appropriate acknowledgement Blood Pressure Ways of
Physiology lecture 15 Hemodynamic
 Physiology lecture 15 Hemodynamic Dispensability (D) : proportional change in volume per unit change in pressure D = V/ P*V It is proportional (divided by the original volume). Compliance (C) : total change
Physiology lecture 15 Hemodynamic Dispensability (D) : proportional change in volume per unit change in pressure D = V/ P*V It is proportional (divided by the original volume). Compliance (C) : total change
Any of these questions could be asked as open question or lab question, thus study them well
 Any of these questions could be asked as open question or lab question, thus study them well describe the factors which regulate cardiac output describe the sympathetic and parasympathetic control of heart
Any of these questions could be asked as open question or lab question, thus study them well describe the factors which regulate cardiac output describe the sympathetic and parasympathetic control of heart
Mechanism: 1- waterretention from the last part of the nephron which increases blood volume, venous return EDV, stroke volume and cardiac output.
 Blood pressure regulators: 1- Short term regulation:nervous system Occurs Within secondsof the change in BP (they are short term because after a while (2-3 days) they adapt/reset the new blood pressure
Blood pressure regulators: 1- Short term regulation:nervous system Occurs Within secondsof the change in BP (they are short term because after a while (2-3 days) they adapt/reset the new blood pressure
Vascular System Part One
 Vascular System Part One Objectives Trace the route taken by blood as it leaves, and then returns to the heart. Describe the structure of the walls of arteries and veins. Discuss the structure and function
Vascular System Part One Objectives Trace the route taken by blood as it leaves, and then returns to the heart. Describe the structure of the walls of arteries and veins. Discuss the structure and function
Chapter 21! Chapter 21 Blood Vessels and Circulation! Blood Vessels and Circulation!
 Chapter 21! Blood Vessels and Circulation! SECTION 21-1! Blood vessels differ in size, structure, and functional properties! 2 Major Vessel Types! Arteries - carry blood away from the heart Higher pressure
Chapter 21! Blood Vessels and Circulation! SECTION 21-1! Blood vessels differ in size, structure, and functional properties! 2 Major Vessel Types! Arteries - carry blood away from the heart Higher pressure
Chapter 21! Blood Vessels and Circulation! SECTION 21-1! Blood vessels differ in size, structure, and functional properties!
 Chapter 21! Blood Vessels and Circulation! SECTION 21-1! Blood vessels differ in size, structure, and functional properties! 2 1! Major Vessel Types! Arteries - carry blood away from the heart Higher pressure
Chapter 21! Blood Vessels and Circulation! SECTION 21-1! Blood vessels differ in size, structure, and functional properties! 2 1! Major Vessel Types! Arteries - carry blood away from the heart Higher pressure
Cardiovascular system
 Cardiovascular system L-4 Blood pressure & special circulation Dr Than Kyaw 27 February 2012 Blood Pressure (BP) Pressure generation and flow Blood is under pressure within its closed system. Pressure
Cardiovascular system L-4 Blood pressure & special circulation Dr Than Kyaw 27 February 2012 Blood Pressure (BP) Pressure generation and flow Blood is under pressure within its closed system. Pressure
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1
 BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
Chapter 25 The Urinary System
 Chapter 25 The Urinary System 10/30/2013 MDufilho 1 Kidney Functions Removal of toxins, metabolic wastes, and excess ions from the blood Regulation of blood volume, chemical composition, and ph Gluconeogenesis
Chapter 25 The Urinary System 10/30/2013 MDufilho 1 Kidney Functions Removal of toxins, metabolic wastes, and excess ions from the blood Regulation of blood volume, chemical composition, and ph Gluconeogenesis
Types of Blood Vessels
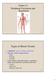 Chapter 21 Peripheral Circulation and Regulation 21-1 Types of Blood Vessels Capillaries: site of exchange with tissue Arteries in dif. Types & sizes Elastic Muscular Arterioles Veins: thinner walls than
Chapter 21 Peripheral Circulation and Regulation 21-1 Types of Blood Vessels Capillaries: site of exchange with tissue Arteries in dif. Types & sizes Elastic Muscular Arterioles Veins: thinner walls than
Sunday, July 17, 2011 URINARY SYSTEM
 URINARY SYSTEM URINARY SYSTEM Let s take a look at the anatomy first! KIDNEYS: are complex reprocessing centers where blood is filtered through and waste products are removed. Wastes and extra water become
URINARY SYSTEM URINARY SYSTEM Let s take a look at the anatomy first! KIDNEYS: are complex reprocessing centers where blood is filtered through and waste products are removed. Wastes and extra water become
Blood Vessels. Over view. We have about 60,000 miles of blood vessels!
 Blood Vessels Over view 3 types of blood vessels arteries - carry blood away from heart "branch", "diverge", and "fork" veins - carry blood toward heart "join", "merge", and "converge" capillaries - site
Blood Vessels Over view 3 types of blood vessels arteries - carry blood away from heart "branch", "diverge", and "fork" veins - carry blood toward heart "join", "merge", and "converge" capillaries - site
Glomerular Capillary Blood Pressure
 Glomerular Capillary Blood Pressure Fluid pressure exerted by blood within glomerular capillaries Depends on Contraction of the heart Resistance to blood flow offered by afferent and efferent arterioles
Glomerular Capillary Blood Pressure Fluid pressure exerted by blood within glomerular capillaries Depends on Contraction of the heart Resistance to blood flow offered by afferent and efferent arterioles
CHAPTER 21 LECTURE OUTLINE
 CHAPTER 21 LECTURE OUTLINE I. INTRODUCTION A. One main focus of this chapter considers hemodynamics, the means by which blood flow is altered and distributed and by which blood pressure is regulated. B.
CHAPTER 21 LECTURE OUTLINE I. INTRODUCTION A. One main focus of this chapter considers hemodynamics, the means by which blood flow is altered and distributed and by which blood pressure is regulated. B.
Chapter 24 Vital Signs. Copyright 2011 Wolters Kluwer Health Lippincott Williams & Wilkins
 Chapter 24 Vital Signs Vital Signs Temperature Pulse Respiration Blood pressure When to Assess Vital Signs Upon admission to any healthcare agency Based on agency institutional policy and procedures Anytime
Chapter 24 Vital Signs Vital Signs Temperature Pulse Respiration Blood pressure When to Assess Vital Signs Upon admission to any healthcare agency Based on agency institutional policy and procedures Anytime
P215 SPRING 2019: CIRCULATORY SYSTEM Chaps 13, 14 & 15: pp , , , I. Major Functions of the Circulatory System
 P215 SPRING 2019: CIRCULATORY SYSTEM Chaps 13, 14 & 15: pp 360-390, 395-404, 410-428 433-438, 441-445 I. Major Functions of the Circulatory System 1. 2. 3. 4. II. Structure of the Heart 1. atria 2. ventricles
P215 SPRING 2019: CIRCULATORY SYSTEM Chaps 13, 14 & 15: pp 360-390, 395-404, 410-428 433-438, 441-445 I. Major Functions of the Circulatory System 1. 2. 3. 4. II. Structure of the Heart 1. atria 2. ventricles
AS OCR PHYSICAL EDUCATION The Vascular System
 AS OCR PHYSICAL EDUCATION The Vascular System Learning Objectives: - Distribution of Cardiac output at rest and during exercise - Role of the Vasomotor centre, arterioles and pre-capillary sphincters -
AS OCR PHYSICAL EDUCATION The Vascular System Learning Objectives: - Distribution of Cardiac output at rest and during exercise - Role of the Vasomotor centre, arterioles and pre-capillary sphincters -
Blood Pressure and its Regulation
 Blood Pressure and its Regulation Blood pressure in your blood vessels is closely monitored by baroreceptors; they send messages to the cardio regulatory center of your medulla oblongata to regulate your
Blood Pressure and its Regulation Blood pressure in your blood vessels is closely monitored by baroreceptors; they send messages to the cardio regulatory center of your medulla oblongata to regulate your
Microcirculation and Edema. Faisal I. Mohammed MD, PhD.
 Microcirculation and Edema Faisal I. Mohammed MD, PhD. Objectives: Point out the structure and function of the microcirculation. Describe how solutes and fluids are exchang in capillaries. Outline what
Microcirculation and Edema Faisal I. Mohammed MD, PhD. Objectives: Point out the structure and function of the microcirculation. Describe how solutes and fluids are exchang in capillaries. Outline what
Contents. Page 1. Homework 11 Chapter Blood Vessels Due: Week 6 Lec 11
 Page 1 Homework 11 Chapter 18-19 Blood Vessels Due: Week 6 Lec 11 Contents When printing, make sure that you specify the page range that you want to print out! Learning objectives for Lecture 11:...pg
Page 1 Homework 11 Chapter 18-19 Blood Vessels Due: Week 6 Lec 11 Contents When printing, make sure that you specify the page range that you want to print out! Learning objectives for Lecture 11:...pg
Chapter 21. Blood Vessels and Circulation
 Chapter 21 Blood Vessels and Circulation INTRODUCTION A. One main focus of this chapter considers hemodynamics, the means by which blood flow is altered and distributed and by which blood pressure is regulated.
Chapter 21 Blood Vessels and Circulation INTRODUCTION A. One main focus of this chapter considers hemodynamics, the means by which blood flow is altered and distributed and by which blood pressure is regulated.
Blood Pressure Regulation. Slides 9-12 Mean Arterial Pressure (MAP) = 1/3 systolic pressure + 2/3 diastolic pressure
 Sheet physiology(18) Sunday 24-November Blood Pressure Regulation Slides 9-12 Mean Arterial Pressure (MAP) = 1/3 systolic pressure + 2/3 diastolic pressure MAP= Diastolic Pressure+1/3 Pulse Pressure CO=MAP/TPR
Sheet physiology(18) Sunday 24-November Blood Pressure Regulation Slides 9-12 Mean Arterial Pressure (MAP) = 1/3 systolic pressure + 2/3 diastolic pressure MAP= Diastolic Pressure+1/3 Pulse Pressure CO=MAP/TPR
Chapter 21 Peripheral circulation and Regulation
 Chapter 21 Peripheral circulation and Regulation I. Blood vessel structure A. Blood flows from large arteries to small capillaries 1. Large arteries contain large amounts of elastic tissue and little smooth
Chapter 21 Peripheral circulation and Regulation I. Blood vessel structure A. Blood flows from large arteries to small capillaries 1. Large arteries contain large amounts of elastic tissue and little smooth
Fluids and electrolytes
 Body Water Content Fluids and electrolytes Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are about 60% water; healthy females
Body Water Content Fluids and electrolytes Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are about 60% water; healthy females
Blood Vessels. Chapter 20
 Blood Vessels Chapter 20 Summary of the Characteristics of Arteries and Veins Characteristic Artery Vein Wall thickness thick thin Shape in cross section round flattened Thickest tunic media externa Collagen
Blood Vessels Chapter 20 Summary of the Characteristics of Arteries and Veins Characteristic Artery Vein Wall thickness thick thin Shape in cross section round flattened Thickest tunic media externa Collagen
Chapter 19 The Urinary System Fluid and Electrolyte Balance
 Chapter 19 The Urinary System Fluid and Electrolyte Balance Chapter Outline The Concept of Balance Water Balance Sodium Balance Potassium Balance Calcium Balance Interactions between Fluid and Electrolyte
Chapter 19 The Urinary System Fluid and Electrolyte Balance Chapter Outline The Concept of Balance Water Balance Sodium Balance Potassium Balance Calcium Balance Interactions between Fluid and Electrolyte
The Excretory System. Biology 20
 The Excretory System Biology 20 Introduction Follow along on page 376 What dangers exist if your body is unable to regulate the fluid balance of your tissues? What challenged would the body have to respond
The Excretory System Biology 20 Introduction Follow along on page 376 What dangers exist if your body is unable to regulate the fluid balance of your tissues? What challenged would the body have to respond
Capillary vessel. A) permeability which can vary between tissues, within tissues at different times and along the capillary
 I. Capillary bed structure Single layer of endothelium supports diffusion MedSoc Teaching CRH Session 2 Capillary circualtion Chanel Tobinska Arteriole Capillary vessel Venules BLOOD Blood flow velocity
I. Capillary bed structure Single layer of endothelium supports diffusion MedSoc Teaching CRH Session 2 Capillary circualtion Chanel Tobinska Arteriole Capillary vessel Venules BLOOD Blood flow velocity
(D) (E) (F) 6. The extrasystolic beat would produce (A) increased pulse pressure because contractility. is increased. increased
 Review Test 1. A 53-year-old woman is found, by arteriography, to have 5% narrowing of her left renal artery. What is the expected change in blood flow through the stenotic artery? Decrease to 1 2 Decrease
Review Test 1. A 53-year-old woman is found, by arteriography, to have 5% narrowing of her left renal artery. What is the expected change in blood flow through the stenotic artery? Decrease to 1 2 Decrease
Microcirculation and Edema- L1 L2
 Microcirculation and Edema- L1 L2 Faisal I. Mohammed MD, PhD. University of Jordan 1 Objectives: Point out the structure and function of the microcirculation. Describe how solutes and fluids are exchanged
Microcirculation and Edema- L1 L2 Faisal I. Mohammed MD, PhD. University of Jordan 1 Objectives: Point out the structure and function of the microcirculation. Describe how solutes and fluids are exchanged
Physiology Unit 3 CARDIOVASCULAR PHYSIOLOGY: THE VASCULAR SYSTEM
 Physiology Unit 3 CARDIOVASCULAR PHYSIOLOGY: THE VASCULAR SYSTEM In Physiology Today Hemodynamics F = ΔP/R Blood flow (F) High to low pressure Rate = L/min Pressure (P) Hydrostatic pressure Pressure exerted
Physiology Unit 3 CARDIOVASCULAR PHYSIOLOGY: THE VASCULAR SYSTEM In Physiology Today Hemodynamics F = ΔP/R Blood flow (F) High to low pressure Rate = L/min Pressure (P) Hydrostatic pressure Pressure exerted
Therefore MAP=CO x TPR = HR x SV x TPR
 Regulation of MAP Flow = pressure gradient resistance CO = MAP TPR Therefore MAP=CO x TPR = HR x SV x TPR TPR is the total peripheral resistance: this is the combined resistance of all blood vessels (remember
Regulation of MAP Flow = pressure gradient resistance CO = MAP TPR Therefore MAP=CO x TPR = HR x SV x TPR TPR is the total peripheral resistance: this is the combined resistance of all blood vessels (remember
describe the location of the kidneys relative to the vertebral column:
 Basic A & P II Dr. L. Bacha Chapter Outline (Martini & Nath 2010) list the three major functions of the urinary system: by examining Fig. 24-1, list the organs of the urinary system: describe the location
Basic A & P II Dr. L. Bacha Chapter Outline (Martini & Nath 2010) list the three major functions of the urinary system: by examining Fig. 24-1, list the organs of the urinary system: describe the location
BIOL 2402 Fluid/Electrolyte Regulation
 Dr. Chris Doumen Collin County Community College BIOL 2402 Fluid/Electrolyte Regulation 1 Body Water Content On average, we are 50-60 % water For a 70 kg male = 40 liters water This water is divided into
Dr. Chris Doumen Collin County Community College BIOL 2402 Fluid/Electrolyte Regulation 1 Body Water Content On average, we are 50-60 % water For a 70 kg male = 40 liters water This water is divided into
REGULATION OF CARDIOVASCULAR SYSTEM
 REGULATION OF CARDIOVASCULAR SYSTEM Jonas Addae Medical Sciences, UWI REGULATION OF CARDIOVASCULAR SYSTEM Intrinsic Coupling of cardiac and vascular functions - Autoregulation of vessel diameter Extrinsic
REGULATION OF CARDIOVASCULAR SYSTEM Jonas Addae Medical Sciences, UWI REGULATION OF CARDIOVASCULAR SYSTEM Intrinsic Coupling of cardiac and vascular functions - Autoregulation of vessel diameter Extrinsic
PHYSIOLOGY WEEK 9. vascular physiology - ED Primary Exam Teaching
 PHYSIOLOGY WEEK 9 vascular physiology - ED Primary Exam Teaching CONCEPTS OF BLOOD FLOW Vascular distensibility - when pressure in the arterioles is increased, this dilates the arterioles and therefore
PHYSIOLOGY WEEK 9 vascular physiology - ED Primary Exam Teaching CONCEPTS OF BLOOD FLOW Vascular distensibility - when pressure in the arterioles is increased, this dilates the arterioles and therefore
Chapter 21: Cardiovascular System: Peripheral Circulation and Regulation
 Chapter 21: Cardiovascular System: Peripheral Circulation and Regulation I. General Features of Blood Vessel Structure A. General Pattern of Circulation 1. Ventricles pump blood into 2. These arteries
Chapter 21: Cardiovascular System: Peripheral Circulation and Regulation I. General Features of Blood Vessel Structure A. General Pattern of Circulation 1. Ventricles pump blood into 2. These arteries
The Cardiovascular System: Vessels and Routes. Pulmonary Circulation H E A R T. Systemic Circulation
 The Cardiovascular System: Vessels and Routes 1. Overview of Blood Circulation A. Pulmonary Circulation Lung Arterioles Pulmonary Artery Capillaries Pulmonary Circulation Venules Pulmonary Veins H E A
The Cardiovascular System: Vessels and Routes 1. Overview of Blood Circulation A. Pulmonary Circulation Lung Arterioles Pulmonary Artery Capillaries Pulmonary Circulation Venules Pulmonary Veins H E A
Chapter 15 Fluid and Acid-Base Balance
 Chapter 15 Fluid and Acid-Base Balance by Dr. Jay M. Templin Brooks/Cole - Thomson Learning Fluid Balance Water constitutes ~60% of body weight. All cells and tissues are surrounded by an aqueous environment.
Chapter 15 Fluid and Acid-Base Balance by Dr. Jay M. Templin Brooks/Cole - Thomson Learning Fluid Balance Water constitutes ~60% of body weight. All cells and tissues are surrounded by an aqueous environment.
Human Urogenital System 26-1
 Human Urogenital System 26-1 Urogenital System Functions Filtering of blood, Removal of wastes and metabolites Regulation of blood volume and composition concentration of blood solutes ph of extracellular
Human Urogenital System 26-1 Urogenital System Functions Filtering of blood, Removal of wastes and metabolites Regulation of blood volume and composition concentration of blood solutes ph of extracellular
Unit 1: Human Systems. The Circulatory System
 Unit 1: Human Systems The Circulatory System nourish all cells with oxygen, glucose, amino acids and other nutrients and carry away carbon dioxide, urea and other wastes Purposes Transport chemical messengers
Unit 1: Human Systems The Circulatory System nourish all cells with oxygen, glucose, amino acids and other nutrients and carry away carbon dioxide, urea and other wastes Purposes Transport chemical messengers
Questions? Homework due in lab 6. PreLab #6 HW 15 & 16 (follow directions, 6 points!)
 Questions? Homework due in lab 6 PreLab #6 HW 15 & 16 (follow directions, 6 points!) Part 3 Variations in Urine Formation Composition varies Fluid volume Solute concentration Variations in Urine Formation
Questions? Homework due in lab 6 PreLab #6 HW 15 & 16 (follow directions, 6 points!) Part 3 Variations in Urine Formation Composition varies Fluid volume Solute concentration Variations in Urine Formation
Physiological Response to Hypovolemic Shock Dr Khwaja Mohammed Amir MD Assistant Professor(Physiology) Objectives At the end of the session the
 Physiological Response to Hypovolemic Shock Dr Khwaja Mohammed Amir MD Assistant Professor(Physiology) Objectives At the end of the session the students should be able to: List causes of shock including
Physiological Response to Hypovolemic Shock Dr Khwaja Mohammed Amir MD Assistant Professor(Physiology) Objectives At the end of the session the students should be able to: List causes of shock including
UNIVERSITY OF MEDICAL SCIENCES, ONDO DEPARTMENT OF PHYSIOLOGY PHS 211 TRANSPORT MECHANISM LECTURER: MR A.O. AKINOLA
 UNIVERSITY OF MEDICAL SCIENCES, ONDO DEPARTMENT OF PHYSIOLOGY PHS 211 TRANSPORT MECHANISM LECTURER: MR A.O. AKINOLA OUTLINE Introduction Basic mechanisms Passive transport Active transport INTRODUCTION
UNIVERSITY OF MEDICAL SCIENCES, ONDO DEPARTMENT OF PHYSIOLOGY PHS 211 TRANSPORT MECHANISM LECTURER: MR A.O. AKINOLA OUTLINE Introduction Basic mechanisms Passive transport Active transport INTRODUCTION
Urine Formation. Urinary Physiology Urinary Section pages Urine Formation. Glomerular Filtration 4/24/2016
 Urine Formation Urinary Physiology Urinary Section pages 9-17 Filtrate Blood plasma minus most proteins Urine
Urine Formation Urinary Physiology Urinary Section pages 9-17 Filtrate Blood plasma minus most proteins Urine
Excretion and Waste Management. Biology 30S - Miss Paslawski
 Excretion and Waste Management Biology 30S - Miss Paslawski Lesson 1 Waste Products and Organs 2 3 Excretion Excretion: Process by which dissolved metabolic wastes are separated from body fluids and removed
Excretion and Waste Management Biology 30S - Miss Paslawski Lesson 1 Waste Products and Organs 2 3 Excretion Excretion: Process by which dissolved metabolic wastes are separated from body fluids and removed
Copyright 2009 Pearson Education, Inc. Copyright 2009 Pearson Education, Inc. Figure 19-1c. Efferent arteriole. Juxtaglomerular apparatus
 /6/0 About this Chapter Functions of the Kidneys Anatomy of the urinary system Overview of kidney function Secretion Micturition Regulation of extracellular fluid volume and blood pressure Regulation of
/6/0 About this Chapter Functions of the Kidneys Anatomy of the urinary system Overview of kidney function Secretion Micturition Regulation of extracellular fluid volume and blood pressure Regulation of
Collin County Community College RENAL PHYSIOLOGY
 Collin County Community College BIOL. 2402 Anatomy & Physiology WEEK 12 Urinary System 1 RENAL PHYSIOLOGY Glomerular Filtration Filtration process that occurs in Bowman s Capsule Blood is filtered and
Collin County Community College BIOL. 2402 Anatomy & Physiology WEEK 12 Urinary System 1 RENAL PHYSIOLOGY Glomerular Filtration Filtration process that occurs in Bowman s Capsule Blood is filtered and
Introduction to Emergency Medical Care 1
 Introduction to Emergency Medical Care 1 OBJECTIVES 6.1 Define key terms introduced in this chapter. Slides 11, 15, 17, 26, 27, 31, 33, 37, 40 42, 44, 45, 51, 58 6.2 Describe the basic roles and structures
Introduction to Emergency Medical Care 1 OBJECTIVES 6.1 Define key terms introduced in this chapter. Slides 11, 15, 17, 26, 27, 31, 33, 37, 40 42, 44, 45, 51, 58 6.2 Describe the basic roles and structures
Blood Pressure Regulation Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.
 Blood Pressure Regulation Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction There are two basic mechanisms for regulating
Blood Pressure Regulation Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction There are two basic mechanisms for regulating
12/1/2009. Chapter 19: Hemorrhage. Hemorrhage and Shock Occurs when there is a disruption or leak in the vascular system Internal hemorrhage
 Chapter 19: Hemorrhage Hemorrhage and Shock Occurs when there is a disruption or leak in the vascular system External hemorrhage Internal hemorrhage Associated with higher morbidity and mortality than
Chapter 19: Hemorrhage Hemorrhage and Shock Occurs when there is a disruption or leak in the vascular system External hemorrhage Internal hemorrhage Associated with higher morbidity and mortality than
Water compartments inside and outside cells maintain a balanced distribution of total body water.
 Chapter 9 Water Balance Chapter 9 Lesson 9.1 Key Concepts Water compartments inside and outside cells maintain a balanced distribution of total body water. The concentration of various solute particles
Chapter 9 Water Balance Chapter 9 Lesson 9.1 Key Concepts Water compartments inside and outside cells maintain a balanced distribution of total body water. The concentration of various solute particles
Levels of Organization. Chapter 19 6/11/2012. Homeostasis & Organization of the animal body. 4 Primary Tissues
 Levels of Organization Chapter 19 Homeostasis & Organization of the animal body Chemical Cellular Tissue Organs System Level Organismic 1-2 4 Primary Tissues 1. Epithelial Tissue: covers surfaces lines
Levels of Organization Chapter 19 Homeostasis & Organization of the animal body Chemical Cellular Tissue Organs System Level Organismic 1-2 4 Primary Tissues 1. Epithelial Tissue: covers surfaces lines
Blood Flow and Blood Pressure Regulation *
 OpenStax-CNX module: m44806 1 Blood Flow and Blood Pressure Regulation * OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 4.0 By the end of this
OpenStax-CNX module: m44806 1 Blood Flow and Blood Pressure Regulation * OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 4.0 By the end of this
Blood Pressure Regulation 2. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Vessel s Wall. heart. arteries. veins. all vessels in body = CONDUITS only! They 1. TUNICA. the heart. 2. TUNICA. of the lumen). 3.
 Blood Vessels, Perfusion & Capillary Dynamics 1 CARDIOVASCULAR SYSTEM: Blood Vessels Vessel Structure, Cardiovascular Dynamics, Perfusion & Capillary Dynamics I. OVERVIEW - Path of BLOOD FLOW: heart arteries
Blood Vessels, Perfusion & Capillary Dynamics 1 CARDIOVASCULAR SYSTEM: Blood Vessels Vessel Structure, Cardiovascular Dynamics, Perfusion & Capillary Dynamics I. OVERVIEW - Path of BLOOD FLOW: heart arteries
Arteries AWAY. Branch. Typically oxygenated.
 Arteries AWAY Branch Typically oxygenated. Capillaries Smallest. Most abundant. 10 billion. Huge surface area. Exchange Veins TOWARDS Converge. Typically deoxygenated. 3 Layers of the Vascular Wall Tunica
Arteries AWAY Branch Typically oxygenated. Capillaries Smallest. Most abundant. 10 billion. Huge surface area. Exchange Veins TOWARDS Converge. Typically deoxygenated. 3 Layers of the Vascular Wall Tunica
Urinary Physiology. Chapter 17 Outline. Kidney Function. Chapter 17
 Urinary Physiology Chapter 17 Chapter 17 Outline Structure and Function of the Kidney Glomerular Filtration Reabsorption of Salt and Water Renal Plasma Clearance Renal Control of Electrolyte and Acid-Base
Urinary Physiology Chapter 17 Chapter 17 Outline Structure and Function of the Kidney Glomerular Filtration Reabsorption of Salt and Water Renal Plasma Clearance Renal Control of Electrolyte and Acid-Base
Cardiac Output 1 Fox Chapter 14 part 1
 Vert Phys PCB3743 Cardiac Output 1 Fox Chapter 14 part 1 T. Houpt, Ph.D. Regulation of Heart & Blood Pressure Keep Blood Pressure constant if too low, not enough blood (oxygen, glucose) reaches tissues
Vert Phys PCB3743 Cardiac Output 1 Fox Chapter 14 part 1 T. Houpt, Ph.D. Regulation of Heart & Blood Pressure Keep Blood Pressure constant if too low, not enough blood (oxygen, glucose) reaches tissues
Physio 12 -Summer 02 - Renal Physiology - Page 1
 Physiology 12 Kidney and Fluid regulation Guyton Ch 20, 21,22,23 Roles of the Kidney Regulation of body fluid osmolarity and electrolytes Regulation of acid-base balance (ph) Excretion of natural wastes
Physiology 12 Kidney and Fluid regulation Guyton Ch 20, 21,22,23 Roles of the Kidney Regulation of body fluid osmolarity and electrolytes Regulation of acid-base balance (ph) Excretion of natural wastes
Biology 1442 Supplemental Instruction Worksheet Cardiovascular System Jacaruso - 1 -
 Biology 1442 Supplemental Instruction Worksheet Cardiovascular System Jacaruso - 1-2. Organs of a closed circulatory system: A. Have valves a. Arteriole B. Regulate blood flow b. Artery C. Lead to heart
Biology 1442 Supplemental Instruction Worksheet Cardiovascular System Jacaruso - 1-2. Organs of a closed circulatory system: A. Have valves a. Arteriole B. Regulate blood flow b. Artery C. Lead to heart
Collage of medicine Cardiovascular Physiology 3- Arterial and venous blood Pressure.
 University of Babylon Collage of medicine Dr. Ghafil Seyhood Hassan Al-Shujiari Cardiovascular Physiology 3- Arterial and venous blood Pressure. UArterial blood pressureu: Arterial pressure = COP X Peripheral
University of Babylon Collage of medicine Dr. Ghafil Seyhood Hassan Al-Shujiari Cardiovascular Physiology 3- Arterial and venous blood Pressure. UArterial blood pressureu: Arterial pressure = COP X Peripheral
Homeostatic Regulation of the Vascular System *
 OpenStax-CNX module: m46603 1 Homeostatic Regulation of the Vascular System * OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 3.0 By the end of
OpenStax-CNX module: m46603 1 Homeostatic Regulation of the Vascular System * OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 3.0 By the end of
Circulatory System Review
 Circulatory System Review 1. Know the diagrams of the heart, internal and external. a) What is the pericardium? What is myocardium? What is the septum? b) Explain the 4 valves of the heart. What is their
Circulatory System Review 1. Know the diagrams of the heart, internal and external. a) What is the pericardium? What is myocardium? What is the septum? b) Explain the 4 valves of the heart. What is their
Body fluid volume is small (~5L (blood + serum)) Composition can change rapidly e.g. due to increase in metabolic rate
 Renal physiology The kidneys Allow us to live on dry land. Body fluid volume is small (~5L (blood + serum)) Composition can change rapidly e.g. due to increase in metabolic rate Kidneys maintain composition
Renal physiology The kidneys Allow us to live on dry land. Body fluid volume is small (~5L (blood + serum)) Composition can change rapidly e.g. due to increase in metabolic rate Kidneys maintain composition
Osmotic Regulation and the Urinary System. Chapter 50
 Osmotic Regulation and the Urinary System Chapter 50 Challenge Questions Indicate the areas of the nephron that the following hormones target, and describe when and how the hormones elicit their actions.
Osmotic Regulation and the Urinary System Chapter 50 Challenge Questions Indicate the areas of the nephron that the following hormones target, and describe when and how the hormones elicit their actions.
Peripheral Circulation and Regulation
 Peripheral Circulation and Regulation Functions of Peripheral Circulation 1. Contain the blood 2. Exchange nutrients, waste products, and gases with tissues 3. Transport 4. Regulate blood pressure, along
Peripheral Circulation and Regulation Functions of Peripheral Circulation 1. Contain the blood 2. Exchange nutrients, waste products, and gases with tissues 3. Transport 4. Regulate blood pressure, along
Glomerular Filtration Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.
 Glomerular Filtration Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction Formation of urine by the kidney involves
Glomerular Filtration Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction Formation of urine by the kidney involves
1. a)label the parts indicated above and give one function for structures Y and Z
 Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- renal cortex - X- renal medulla Y- renal pelvis collecting center of urine and then
Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- renal cortex - X- renal medulla Y- renal pelvis collecting center of urine and then
