Physiology Chapter 14 Key Blood Flow and Blood Pressure, Plus Fun Review Study Guide
|
|
|
- Gary Pearson
- 6 years ago
- Views:
Transcription
1 Physiology Chapter 14 Key Blood Flow and Blood Pressure, Plus Fun Review Study Guide 1 Main Idea: The function of the circulatory system is to maintain adequate blood flow to all tissues. Clinical Application Questions 1. A patient was found to have a blood pressure recording of 125/77: a. What is the systolic pressure? 125 mm Hg b. What is the diastolic pressure? 77 mm Hg c. What is the pulse pressure? 48 mm Hg ( = 48 mm Hg) d. What is the mean arterial pressure? 93 mm Hg [77 + 1/3(48) = = 93 mm Hg] e. Would any sound be heard when the pressure in an external cuff around the arm was 130 mm Hg? No; no blood would be able to get through the brachial artery, so no sound would be heard. f. Would any sound be heard when cuff pressure was 118 mm Hg? Yes g. Would any sound be heard when cuff pressure was 75 mm Hg? No; blood would flow continuously through the brachial artery in smooth, laminar fashion, so no sound would be heard. 2. A classmate who has been standing still for several hours working on a laboratory experiment suddenly faints. What is the probable explanation? What would you do if the person next to him tried to get him up? The classmate apparently fainted because of insufficient blood flow to the brain as a result of pooling of blood in the lower extremities brought about by standing still for a prolonged time. When a person faints and assumes a horizontal position, the pooled blood will quickly be returned to the heart, improving cardiac output and blood flow to his brain. Trying to get the person up would be counter productive, so the classmate trying to get him up should be advised to let him remain lying down until he recovers on his own. 3. In a person that has a sudden decrease in blood pressure, describe the short-term mechanisms that will be activated in response to a sudden decrease in blood pressure. A sudden decrease in blood pressure is detected by baroreceptors in the carotid sinus and aortic arch. Baroreceptors decrease their rate of impulses that are being sent to the medulla oblongata.the medulla oblongata responds by : a. Decreased parasympathetic activity (vagus nerve). b. Increased sympathetic activity which: i. Increases heart rate and force of contraction - higher cardiac output ii. Causes vasoconstriction of arterioles. iii. Stimulates adrenal glands to release the hormones epinephrine and norepinephrine which enhances heart rate, contractility, and vasoconstriction. The result is an increase of blood pressure to normal levels.
2 4. Ima Fan loves to go to movies. After sitting in a movie for several hours she often develops edema in her legs and feet. Explain how this occurs (Hint: recall from your study of osmosis that a column of liquid has weight). 2 The weight of the blood produces pressure that increases the blood pressure in her lower limbs. Consequently, more fluid moves out of capillaries because of increased blood pressure than moves back into the capillaries by osmosis. The fluid accumulates in tissues as edema. In addition, because she is sitting, skeletal muscles cannot assist in moving (pumping) blood out of her legs. 5. After a long leisurely lunch at a restaurant, sometimes elderly people faint when they stand up to leave the restaurant. Explain how this happens (Hint: assume that a homeostatic mechanism is not working as well as when they we younger). Sitting has resulted in a shift of fluid from the elderly person s blood into the tissues because of the increased blood pressure in her legs. This causes a reduction in blood volume and blood pressure. Also, because of the demands o digestion, blood is rerouted to the digestive organs. Consequently, there is reduced blood flow toward the brain. When the elderly person stands up, there is an even greater tendency for blood to remain in the lower limbs because of gravity. Venous return decreases, which causes cardiac output to decrease (Frank-Starling law). Decreased cardiac output results in a decrease in blood pressure. Normally, the baroreceptor reflexes correct the decrease in blood pressure by increasing heart rate and stroke volume. However, if this mechanism does not respond rapidly enough as can happen in the elderly, blood pressure does not increase, blood delivery to the brain is impaired, and the person faints. 6. Buster Hart has a myocardial infarct (heart attack) and his blood pressure drops. Explain why his blood pressure drops and describe the neural mechanisms that would attempt to compensate for the decreased blood pressure. In Buster s case, his blood pressure was abnormally low following the myocardial infarct. Gradually (within a few days), however, it returned to normal. Explain how the long term mechanisms would compensate for this. Hint think about hormonal effects. The myocardial infarct damages the heart and reduces its ability to pump blood and thus will have a drop in blood pressure. With a decrease in cardiac output there is a decrease in blood pressure and blood oxygen and an increase in carbon dioxide levels. Neural mechanisms: The baroreceptor reflexes and the chemoreceptor reflexes compensate by increasing heart rate, stroke volume, and vasoconstriction (peripheral resistance), all of which increase blood pressure. Hormonal effects: In the days following the myocardial infarct, long term mechanisms compensate for the still low blood pressure. The rennin-angiotensin-aldosterone mechanism increases vasoconstriction and reduces fluid loss in the kidneys. With an increase in blood volume, blood pressure increases. 7. Explain the effect of respiratory activity on venous return to the heart. As a result of respiratory activity, particularly inhalation, the pressure within the chest cavity averages 5 mm Hg less than atmospheric pressure. As the venous system returns blood to the heart from the lower regions of the body, it travels through the chest cavity, where it is exposed to the subatmospheric pressure. This pressure differences squeezes blood from the lower veins to the chest veins, promoting increased venous return. This mechanism of facilitating
3 venous return in called the respiratory pump and greatly enhances venous return during exercise Explain the effect of cardiac vacuum ( suction ) on venous return to the heart. The extent of cardiac filling does not depend entirely on factors affecting the veins. The heart plays a role in its own filling. During ventricular relaxation, the AV valves are drawn downward, enlarging the atrial cavities. As a result, the atrial pressure transiently drops (creates a vacuum) below 0 mmhg, thus increasing the vein-to-atria pressure gradient so that venous return in enhanced. In addition, the rapid expansion of the ventricular chambers during ventricular relaxation creates a transient negative pressure (vacuum) in the ventricles so that blood is pushed in from the atria and veins; that is, the negative ventricular pressure increases vein-to-atria-to-ventricle pressure gradient, further enhancing venous return. Thus, the heart functions as a vacuum ( suction ) pump to facilitate cardiac filling. 9. Explain the effect of skeletal muscle activity on venous return to the heart. Many of the large veins in the extremities lie between skeletal muscles, so muscle contraction compresses the veins. This external venous compression increases venous pressure, in effect squeezing fluid in the veins forward toward the heart. This pumping action, known as the skeletal muscle pump, is one way the blood in veins is returned to the heart during exercise. Increased muscular activity pushes more blood out of the veins and into the heart. Veins contain one way valves that prevent blood from being squeezed away from the heart. Increased sympathetic activity that accompanies exercise causes venous vasoconstriction further enhancing venous return to the heart. 10. Explain how each of the following antihypertensive drugs would lower arterial blood pressure: Note, for this section you are not expected to remember the drug names in parenthesis, but instead, you are expected to know how the antihypertensive drugs work given the following descriptions. a. Drugs that block α1-adrenergic receptors (for example, phentolamine). Because activation of α1-adrenergic receptors in vascular smooth muscle brings about vasoconstriction, blockage of α1-adrenergic receptors reduces vasoconstrictor activity, thereby lowering the total peripheral resistance and arterial blood pressure. b. Drugs that block β1-adrenergic receptors (for example, metoprolol). Because activation of β1-adrenergic receptors, which are found primarily in the heart, increase the rate and strength of cardiac contraction, drugs that block β1-adrenergic receptors reduce cardiac output and thus arterial blood pressure by decreasing the rate and strength of the heartbeat. c. Drugs that directly relax arteriolar smooth muscle (for example, hydralazine). Drugs that directly relax arteriolar smooth muscle by decreasing the phosphorylation of smooth muscle myosin light chain thereby lower arterial blood pressure by promoting arteriolar vasodilation and reducing total peripheral resistance.
4 d. Diuretic drugs that increase urinary output (for example, furosemide). 4 Diuretic drugs reduce the plasma volume, thereby lowering arterial blood pressure, by increasing urinary output. Salt and water that normally would have been retained in the plasma are excreted in the urine. e. Drugs that block release of norepinephrine from sympathetic endings (for example, guanethidine). Because sympathetic activity promotes generalized arteriolar vasoconstriction, thereby increasing total peripheral resistance and arterial blood pressure, drugs that block the release of norepinephrine from sympathetic endings lower blood pressure by preventing this vasoconstrictor effect. f. Drugs that act on the brain to reduce sympathetic output (for example, clonidine). Similarly, drugs that act on the brain to reduce sympathetic output lower blood pressue by preventing the effect of sympathetic activity on promoting arteriolar vasoconstriction and the resultant increase in total peripheral resistance and arterial blood pressure. g. Drugs that block calcium channels of smooth muscle cells in blood vessels (for example, verapamil). Drugs that block calcium channels reduce the entry of calcium into the vascular smooth muscle cells from the ECF in response to excitatory input. Because the level of contractile activity in vascular smooth muscle cells depends on their cytosolic calcium concentration, drugs that block calcium channels reduce the contractile activity of these cells by reducing calcium entry and lowering their cytosolic calcium concentration. Total peripheral resistance and, accordingly, arterial blood pressure are decreased as a result of reduced arteriolar contractile activity. h. Drugs that interfere with the production of angiotensin II (for example captopril, an ACE inhibitor). Angiotensin converting enzyme (ACE) inhibitors interfere with the production of angiotensin II and blocks activation of the hormonal pathway that releases aldosterone which promotes salt and water conservation via the rennin-angiotensin-aldosterone system. As a result, more salt and water are lost in the urine, and less fluid is retained in the plasma. The resultant reduction in plasma volume lowers the arterial blood pressure. Angiotensin II is a powerful vasoconstrictor of arterioles which increases total peripheral resistance and increases arterial BP. It also stimulates ADH release and activates the body s thirst center within the hypothalamus. i. Drugs that block angiotensin II receptors (for example, losartan). Drugs that block angiotensinii receptors prevent angiotensin II from causing arteriolar vasoconstriction, thereby decreasing total peripheral resistance, and also reduce the action of the salt- and water-conserving rennin-angiotensin-aldosterone system, thereby decreasing plasma volume. Blocks the angiostensin II stimulation of ADH release. Together these effects lower blood pressure.
5 Part I 1. increased; decreased; pre; after; increases; increases 2. kidney; blood; blood; hydrostatic; colloid osmotic 3. lymph; lymphatic; edema 4. antidiuretic; aldosterone; cortex; retention 5. Poiseuille s; sympathetic; aerobically 6. aerobically; high; intrinsic 7. decreased; increased; stroke; output 8. constrict; dilation; sympathetic; anastomoses; constrict 9. carotid sinus; aortic arch; medulla oblongata; rate; resistance; autonomic 10. laminar; turbulent; korotkoff ; 90; primary; secondary 12. oxygen; venous 13. B 14. C 15. False; Replace capillaries with arterioles 16. True 17. True 18. False; Replace pons with medulla oblongata 19. True 20. True 21. True 22. False; Replace diastole with systole 23. False; MAP = 1/3 pulse pressure + diastolic pressure 24. C 25. D 26. True 27. True 28. False; Replace greater with less 29. True 30. True 31. False; Osmoreceptors would stop firing ADH levels would decrease 32. True 33. True 34. False: replace increase with decrease 35. B 36. C 37. E 38. B 39. D 40. C 41. B 42. C 43. A 5
6 6 Part II 1. A and B antigens; AB; People with type AB blood lack both Anti-A and Anti-B antibodies 2. +; + 3. neither Rh group 4. - ; ; +; +; hemolytic disease of the newborn or erythroblastosis fetalis; Anti-Rh antibody therapy (Rhogam) is given to the mother to bind to any fetal Rh antigens, destroying them. Therefore the Rh- mother will not produce antibodies that would attack antigens of a future Rh+ fetus. 6. oxyhemoglobin; 1.5% 7. iron; HbO2; saturated; increase 8. E 9. C 10. True 11. True 12. False; replace type I (IDDM) with Type II (NIDDM) 13. False; replace obesity with exercise 14. False; replace high with low and lowered with raised 15. True 16. True 17. Through the metarteriole-thoroughfare channel 18. A 19. capillary blood 20. capillary hydrostatic (blood) pressure 21. blood pressure 22. capillary colloid osmotic pressure 23. albumin 24. at the arteriole end 25. It is picked up by lymphatic vessels for return to the blood stream 26. D 27. I 28. I 29. I 30. I 31. D 32. D 33. I 34. D 35. D 36. D 37. I 38. I Part III 1. A 2. A 3. B 4. A 5. B 6. A 7. Hypertension 8. Orthostatic hypotension 9. Cardiogenic 10. Hypovolemic 11. Varicose veins 12. Baroreceptors
7 Part IV 1. B 2. A 3. B 4. A 5. A 6. A 7. B 8. A 9. B 10. A 11. B 12. A 13. A 14. E 7 Part V, A 1. Blood pressure 2. Systolic pressure 3. Diastolic pressure 4. Auscultatory 5. Korotkoff sounds 6. Systolic pressure 7. Diastolic pressure Part V, B 1. Pulse pressure 2. Increases 3. Increase 4. Increases 5. Pulse 6. Decreases 7. Increases Part V, C 1. Diffusion 2. Blood pressure 3. Osmosis 4. Blood pressure 5. Osmosis 6. Lymphatic capillaries 7. Edema Part V, D Local and Nervous Control of Blood Vessels 1. Local control 4. Vasomotor center 2. Relaxation 5. Vasomotor tone 3. Nervous control 6. Nervous control 7. Local control Part V, E Baroreceptor Reflexes 1. Baroreceptors 2. Vasoconstrict 3. Increases 4. Increase 5. Increase 6. Increase 7. Increase Part V, F Chemoreceptor Reflexes 1. Chemoreceptors 3. Increases 2. Vasoconstrict 4. Increase 5. Increase 6. Increases Part V, G Hormonal Mechanisms 1. Epinephrine 2. Renin 3. Angiotensin II 4. Angiotensin II 5. Aldosterone 6. Antidiuretic hormone 7. Atrial natriuretic hormone
Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide
 Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide Main Idea: The function of the circulatory system is to maintain adequate blood flow to all tissues. Clinical
Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide Main Idea: The function of the circulatory system is to maintain adequate blood flow to all tissues. Clinical
Blood Pressure Regulation. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation Faisal I. Mohammed, MD,PhD 1 Objectives Outline the short term and long term regulators of BP Know how baroreceptors and chemoreceptors work Know function of the atrial reflex.
Blood Pressure Regulation Faisal I. Mohammed, MD,PhD 1 Objectives Outline the short term and long term regulators of BP Know how baroreceptors and chemoreceptors work Know function of the atrial reflex.
Structure and organization of blood vessels
 The cardiovascular system Structure of the heart The cardiac cycle Structure and organization of blood vessels What is the cardiovascular system? The heart is a double pump heart arteries arterioles veins
The cardiovascular system Structure of the heart The cardiac cycle Structure and organization of blood vessels What is the cardiovascular system? The heart is a double pump heart arteries arterioles veins
Veins. VENOUS RETURN = PRELOAD = End Diastolic Volume= Blood returning to heart per cardiac cycle (EDV) or per minute (Venous Return)
 Veins Venous system transports blood back to heart (VENOUS RETURN) Capillaries drain into venules Venules converge to form small veins that exit organs Smaller veins merge to form larger vessels Veins
Veins Venous system transports blood back to heart (VENOUS RETURN) Capillaries drain into venules Venules converge to form small veins that exit organs Smaller veins merge to form larger vessels Veins
Heart. Large lymphatic vessels Lymph node. Lymphatic. system Arteriovenous anastomosis. (exchange vessels)
 Venous system Large veins (capacitance vessels) Small veins (capacitance vessels) Postcapillary venule Thoroughfare channel Heart Large lymphatic vessels Lymph node Lymphatic system Arteriovenous anastomosis
Venous system Large veins (capacitance vessels) Small veins (capacitance vessels) Postcapillary venule Thoroughfare channel Heart Large lymphatic vessels Lymph node Lymphatic system Arteriovenous anastomosis
Therefore MAP=CO x TPR = HR x SV x TPR
 Regulation of MAP Flow = pressure gradient resistance CO = MAP TPR Therefore MAP=CO x TPR = HR x SV x TPR TPR is the total peripheral resistance: this is the combined resistance of all blood vessels (remember
Regulation of MAP Flow = pressure gradient resistance CO = MAP TPR Therefore MAP=CO x TPR = HR x SV x TPR TPR is the total peripheral resistance: this is the combined resistance of all blood vessels (remember
Blood Pressure Fox Chapter 14 part 2
 Vert Phys PCB3743 Blood Pressure Fox Chapter 14 part 2 T. Houpt, Ph.D. 1 Cardiac Output and Blood Pressure How to Measure Blood Pressure Contribution of vascular resistance to blood pressure Cardiovascular
Vert Phys PCB3743 Blood Pressure Fox Chapter 14 part 2 T. Houpt, Ph.D. 1 Cardiac Output and Blood Pressure How to Measure Blood Pressure Contribution of vascular resistance to blood pressure Cardiovascular
I. Cardiac Output Chapter 14
 10/24/11 I. Cardiac Output Chapter 14 Cardiac Output, Blood Flow, and Blood Pressure Lecture PowerPoint Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Cardiac
10/24/11 I. Cardiac Output Chapter 14 Cardiac Output, Blood Flow, and Blood Pressure Lecture PowerPoint Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Cardiac
BIPN100 F15 Human Physiol I (Kristan) Lecture 14 Cardiovascular control mechanisms p. 1
 BIPN100 F15 Human Physiol I (Kristan) Lecture 14 Cardiovascular control mechanisms p. 1 Terms you should understand: hemorrhage, intrinsic and extrinsic mechanisms, anoxia, myocardial contractility, residual
BIPN100 F15 Human Physiol I (Kristan) Lecture 14 Cardiovascular control mechanisms p. 1 Terms you should understand: hemorrhage, intrinsic and extrinsic mechanisms, anoxia, myocardial contractility, residual
BIOL 219 Spring Chapters 14&15 Cardiovascular System
 1 BIOL 219 Spring 2013 Chapters 14&15 Cardiovascular System Outline: Components of the CV system Heart anatomy Layers of the heart wall Pericardium Heart chambers, valves, blood vessels, septum Atrioventricular
1 BIOL 219 Spring 2013 Chapters 14&15 Cardiovascular System Outline: Components of the CV system Heart anatomy Layers of the heart wall Pericardium Heart chambers, valves, blood vessels, septum Atrioventricular
Blood Pressure Regulation. Slides 9-12 Mean Arterial Pressure (MAP) = 1/3 systolic pressure + 2/3 diastolic pressure
 Sheet physiology(18) Sunday 24-November Blood Pressure Regulation Slides 9-12 Mean Arterial Pressure (MAP) = 1/3 systolic pressure + 2/3 diastolic pressure MAP= Diastolic Pressure+1/3 Pulse Pressure CO=MAP/TPR
Sheet physiology(18) Sunday 24-November Blood Pressure Regulation Slides 9-12 Mean Arterial Pressure (MAP) = 1/3 systolic pressure + 2/3 diastolic pressure MAP= Diastolic Pressure+1/3 Pulse Pressure CO=MAP/TPR
Physiology lecture 15 Hemodynamic
 Physiology lecture 15 Hemodynamic Dispensability (D) : proportional change in volume per unit change in pressure D = V/ P*V It is proportional (divided by the original volume). Compliance (C) : total change
Physiology lecture 15 Hemodynamic Dispensability (D) : proportional change in volume per unit change in pressure D = V/ P*V It is proportional (divided by the original volume). Compliance (C) : total change
Cardiovascular System. Heart
 Cardiovascular System Heart Electrocardiogram A device that records the electrical activity of the heart. Measuring the relative electrical activity of one heart cycle. A complete contraction and relaxation.
Cardiovascular System Heart Electrocardiogram A device that records the electrical activity of the heart. Measuring the relative electrical activity of one heart cycle. A complete contraction and relaxation.
Presenter: Tom Mulvey
 Slides are from Level 3 Biology Course Content Day, 7 th November 2012 Presenter: Tom Mulvey Teachers are free to use these for teaching purposes with appropriate acknowledgement Blood Pressure Ways of
Slides are from Level 3 Biology Course Content Day, 7 th November 2012 Presenter: Tom Mulvey Teachers are free to use these for teaching purposes with appropriate acknowledgement Blood Pressure Ways of
Blood pressure. Formation of the blood pressure: Blood pressure. Formation of the blood pressure 5/1/12
 Blood pressure Blood pressure Dr Badri Paudel www.badripaudel.com Ø Blood pressure means the force exerted by the blood against the vessel wall Ø ( or the force exerted by the blood against any unit area
Blood pressure Blood pressure Dr Badri Paudel www.badripaudel.com Ø Blood pressure means the force exerted by the blood against the vessel wall Ø ( or the force exerted by the blood against any unit area
Cardiovascular system: Blood vessels, blood flow. Latha Rajendra Kumar, MD
 Cardiovascular system: Blood vessels, blood flow Latha Rajendra Kumar, MD Outline 1- Physical laws governing blood flow and blood pressure 2- Overview of vasculature 3- Arteries 4. Capillaries and venules
Cardiovascular system: Blood vessels, blood flow Latha Rajendra Kumar, MD Outline 1- Physical laws governing blood flow and blood pressure 2- Overview of vasculature 3- Arteries 4. Capillaries and venules
Blood Pressure. a change in any of these could cause a corresponding change in blood pressure
 Blood Pressure measured as mmhg Main factors affecting blood pressure: 1. cardiac output 2. peripheral resistance 3. blood volume a change in any of these could cause a corresponding change in blood pressure
Blood Pressure measured as mmhg Main factors affecting blood pressure: 1. cardiac output 2. peripheral resistance 3. blood volume a change in any of these could cause a corresponding change in blood pressure
Physiology of Circulation
 Physiology of Circulation Dr. Ali Ebneshahidi Blood vessels Arteries: Blood vessels that carry blood away from the heart to the lungs and tissues. Arterioles are small arteries that deliver blood to the
Physiology of Circulation Dr. Ali Ebneshahidi Blood vessels Arteries: Blood vessels that carry blood away from the heart to the lungs and tissues. Arterioles are small arteries that deliver blood to the
The Cardiovascular System. The Structure of Blood Vessels. The Structure of Blood Vessels. The Blood Vessels. Blood Vessel Review
 The Cardiovascular System The Blood Vessels The Structure of Blood Vessels Blood Vessel Review Arteries carry blood away from the heart Pulmonary trunk to lungs Aorta to everything else Microcirculation
The Cardiovascular System The Blood Vessels The Structure of Blood Vessels Blood Vessel Review Arteries carry blood away from the heart Pulmonary trunk to lungs Aorta to everything else Microcirculation
Chapter 24 Vital Signs. Copyright 2011 Wolters Kluwer Health Lippincott Williams & Wilkins
 Chapter 24 Vital Signs Vital Signs Temperature Pulse Respiration Blood pressure When to Assess Vital Signs Upon admission to any healthcare agency Based on agency institutional policy and procedures Anytime
Chapter 24 Vital Signs Vital Signs Temperature Pulse Respiration Blood pressure When to Assess Vital Signs Upon admission to any healthcare agency Based on agency institutional policy and procedures Anytime
Cardiovascular System. Blood Vessel anatomy Physiology & regulation
 Cardiovascular System Blood Vessel anatomy Physiology & regulation Path of blood flow Aorta Arteries Arterioles Capillaries Venules Veins Vena cava Vessel anatomy: 3 layers Tunica externa (adventitia):
Cardiovascular System Blood Vessel anatomy Physiology & regulation Path of blood flow Aorta Arteries Arterioles Capillaries Venules Veins Vena cava Vessel anatomy: 3 layers Tunica externa (adventitia):
Circulation. Blood Pressure and Antihypertensive Medications. Venous Return. Arterial flow. Regulation of Cardiac Output.
 Circulation Blood Pressure and Antihypertensive Medications Two systems Pulmonary (low pressure) Systemic (high pressure) Aorta 120 mmhg Large arteries 110 mmhg Arterioles 40 mmhg Arteriolar capillaries
Circulation Blood Pressure and Antihypertensive Medications Two systems Pulmonary (low pressure) Systemic (high pressure) Aorta 120 mmhg Large arteries 110 mmhg Arterioles 40 mmhg Arteriolar capillaries
Cardiovascular System B L O O D V E S S E L S 2
 Cardiovascular System B L O O D V E S S E L S 2 Blood Pressure Main factors influencing blood pressure: Cardiac output (CO) Peripheral resistance (PR) Blood volume Peripheral resistance is a major factor
Cardiovascular System B L O O D V E S S E L S 2 Blood Pressure Main factors influencing blood pressure: Cardiac output (CO) Peripheral resistance (PR) Blood volume Peripheral resistance is a major factor
Physiology of Circulation. Dr. Hiwa Shafiq 16/12/2018
 Physiology of Circulation Dr. Hiwa Shafiq 16/12/2018 Overview of the circulation The function of the circulation is to: 1. transport nutrients to the body tissues 2. transport waste products away 3. conduct
Physiology of Circulation Dr. Hiwa Shafiq 16/12/2018 Overview of the circulation The function of the circulation is to: 1. transport nutrients to the body tissues 2. transport waste products away 3. conduct
BIOH122 Session 6 Vascular Regulation
 BIOH122 Session 6 Vascular Regulation To complete this worksheet, select: Module: Distribution Title: Vascular Regulation Introduction 1. a. How do Mean Arterial Blood Pressure (MABP) and Systemic Vascular
BIOH122 Session 6 Vascular Regulation To complete this worksheet, select: Module: Distribution Title: Vascular Regulation Introduction 1. a. How do Mean Arterial Blood Pressure (MABP) and Systemic Vascular
Cardiac Output 1 Fox Chapter 14 part 1
 Vert Phys PCB3743 Cardiac Output 1 Fox Chapter 14 part 1 T. Houpt, Ph.D. Regulation of Heart & Blood Pressure Keep Blood Pressure constant if too low, not enough blood (oxygen, glucose) reaches tissues
Vert Phys PCB3743 Cardiac Output 1 Fox Chapter 14 part 1 T. Houpt, Ph.D. Regulation of Heart & Blood Pressure Keep Blood Pressure constant if too low, not enough blood (oxygen, glucose) reaches tissues
(D) (E) (F) 6. The extrasystolic beat would produce (A) increased pulse pressure because contractility. is increased. increased
 Review Test 1. A 53-year-old woman is found, by arteriography, to have 5% narrowing of her left renal artery. What is the expected change in blood flow through the stenotic artery? Decrease to 1 2 Decrease
Review Test 1. A 53-year-old woman is found, by arteriography, to have 5% narrowing of her left renal artery. What is the expected change in blood flow through the stenotic artery? Decrease to 1 2 Decrease
During exercise the heart rate is 190 bpm and the stroke volume is 115 ml/beat. What is the cardiac output?
 The Cardiovascular System Part III: Heart Outline of class lecture After studying part I of this chapter you should be able to: 1. Be able to calculate cardiac output (CO) be able to define heart rate
The Cardiovascular System Part III: Heart Outline of class lecture After studying part I of this chapter you should be able to: 1. Be able to calculate cardiac output (CO) be able to define heart rate
Collage of medicine Cardiovascular Physiology 3- Arterial and venous blood Pressure.
 University of Babylon Collage of medicine Dr. Ghafil Seyhood Hassan Al-Shujiari Cardiovascular Physiology 3- Arterial and venous blood Pressure. UArterial blood pressureu: Arterial pressure = COP X Peripheral
University of Babylon Collage of medicine Dr. Ghafil Seyhood Hassan Al-Shujiari Cardiovascular Physiology 3- Arterial and venous blood Pressure. UArterial blood pressureu: Arterial pressure = COP X Peripheral
The Cardiovascular system: physiology of circulation
 Chapter 21 The Cardiovascular system: physiology of circulation blood vessel structure and function physiology of circulation: blood flow, blood pressure, and resistance blood flow the amount of blood
Chapter 21 The Cardiovascular system: physiology of circulation blood vessel structure and function physiology of circulation: blood flow, blood pressure, and resistance blood flow the amount of blood
Chapter 14 Blood Vessels, Blood Flow and Pressure Exam Study Questions
 Chapter 14 Blood Vessels, Blood Flow and Pressure Exam Study Questions 14.1 Physical Law Governing Blood Flow and Blood Pressure 1. How do you calculate flow rate? 2. What is the driving force of blood
Chapter 14 Blood Vessels, Blood Flow and Pressure Exam Study Questions 14.1 Physical Law Governing Blood Flow and Blood Pressure 1. How do you calculate flow rate? 2. What is the driving force of blood
Chapter 21: Cardiovascular System: Peripheral Circulation and Regulation
 Chapter 21: Cardiovascular System: Peripheral Circulation and Regulation I. General Features of Blood Vessel Structure A. General Pattern of Circulation 1. Ventricles pump blood into 2. These arteries
Chapter 21: Cardiovascular System: Peripheral Circulation and Regulation I. General Features of Blood Vessel Structure A. General Pattern of Circulation 1. Ventricles pump blood into 2. These arteries
Blood Pressure Regulation Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.
 Blood Pressure Regulation Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction There are two basic mechanisms for regulating
Blood Pressure Regulation Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction There are two basic mechanisms for regulating
Responses to Changes in Posture QUESTIONS. Case PHYSIOLOGY CASES AND PROBLEMS
 64 PHYSIOLOGY CASES AND PROBLEMS Case 12 Responses to Changes in Posture Joslin Chambers is a 27-year-old assistant manager at a discount department store. One morning, she awakened from a deep sleep and
64 PHYSIOLOGY CASES AND PROBLEMS Case 12 Responses to Changes in Posture Joslin Chambers is a 27-year-old assistant manager at a discount department store. One morning, she awakened from a deep sleep and
Chapter 21 Peripheral circulation and Regulation
 Chapter 21 Peripheral circulation and Regulation I. Blood vessel structure A. Blood flows from large arteries to small capillaries 1. Large arteries contain large amounts of elastic tissue and little smooth
Chapter 21 Peripheral circulation and Regulation I. Blood vessel structure A. Blood flows from large arteries to small capillaries 1. Large arteries contain large amounts of elastic tissue and little smooth
Types of Blood Vessels
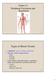 Chapter 21 Peripheral Circulation and Regulation 21-1 Types of Blood Vessels Capillaries: site of exchange with tissue Arteries in dif. Types & sizes Elastic Muscular Arterioles Veins: thinner walls than
Chapter 21 Peripheral Circulation and Regulation 21-1 Types of Blood Vessels Capillaries: site of exchange with tissue Arteries in dif. Types & sizes Elastic Muscular Arterioles Veins: thinner walls than
Blood Pressure Regulation -1
 CVS Physiology Lecture 18 Blood Pressure Regulation -1 Please study the previous sheet before studying this one, even if the first part in this sheet is revision. In the previous lecture we were talking
CVS Physiology Lecture 18 Blood Pressure Regulation -1 Please study the previous sheet before studying this one, even if the first part in this sheet is revision. In the previous lecture we were talking
CHAPTER 14 CARDIAC OUTPUT, BLOOD FLOW, AND BLOOD PRESSURE
 CHAPTER 14 CARDIAC OUTPUT, BLOOD FLOW, AND BLOOD PRESSURE CHAPTER SCOPE The last chapter introduced the blood, the structure and function of the heart and the blood vessels. Logically, this chapter follows
CHAPTER 14 CARDIAC OUTPUT, BLOOD FLOW, AND BLOOD PRESSURE CHAPTER SCOPE The last chapter introduced the blood, the structure and function of the heart and the blood vessels. Logically, this chapter follows
1. Which of the following blood vessels has a thin elastic layer? A. Aorta. B. Pulmonary artery. C. Posterior vena cava. D. Mesenteric capillary.
 CIRCULATORY SYSTEM 1. Which of the following blood vessels has a thin elastic layer? A. Aorta. B. Pulmonary artery. C. Posterior vena cava. D. Mesenteric capillary. 2. Capillary beds are equipped with
CIRCULATORY SYSTEM 1. Which of the following blood vessels has a thin elastic layer? A. Aorta. B. Pulmonary artery. C. Posterior vena cava. D. Mesenteric capillary. 2. Capillary beds are equipped with
Properties of Pressure
 OBJECTIVES Overview Relationship between pressure and flow Understand the differences between series and parallel circuits Cardiac output and its distribution Cardiac function Control of blood pressure
OBJECTIVES Overview Relationship between pressure and flow Understand the differences between series and parallel circuits Cardiac output and its distribution Cardiac function Control of blood pressure
CASE 13. What neural and humoral pathways regulate arterial pressure? What are two effects of angiotensin II?
 CASE 13 A 57-year-old man with long-standing diabetes mellitus and newly diagnosed hypertension presents to his primary care physician for follow-up. The patient has been trying to alter his dietary habits
CASE 13 A 57-year-old man with long-standing diabetes mellitus and newly diagnosed hypertension presents to his primary care physician for follow-up. The patient has been trying to alter his dietary habits
d) Cardiovascular System Higher Human Biology
 d) Cardiovascular System Higher Human Biology What can your remember about the heart and blood vessels? What is the Cardiovascular System? The cardiovascular system, also known as the circulatory system,
d) Cardiovascular System Higher Human Biology What can your remember about the heart and blood vessels? What is the Cardiovascular System? The cardiovascular system, also known as the circulatory system,
REGULATION OF CARDIOVASCULAR SYSTEM
 REGULATION OF CARDIOVASCULAR SYSTEM Jonas Addae Medical Sciences, UWI REGULATION OF CARDIOVASCULAR SYSTEM Intrinsic Coupling of cardiac and vascular functions - Autoregulation of vessel diameter Extrinsic
REGULATION OF CARDIOVASCULAR SYSTEM Jonas Addae Medical Sciences, UWI REGULATION OF CARDIOVASCULAR SYSTEM Intrinsic Coupling of cardiac and vascular functions - Autoregulation of vessel diameter Extrinsic
Circulatory System Review
 Circulatory System Review 1. Know the diagrams of the heart, internal and external. a) What is the pericardium? What is myocardium? What is the septum? b) Explain the 4 valves of the heart. What is their
Circulatory System Review 1. Know the diagrams of the heart, internal and external. a) What is the pericardium? What is myocardium? What is the septum? b) Explain the 4 valves of the heart. What is their
Blood Pressure and its Regulation
 Blood Pressure and its Regulation Blood pressure in your blood vessels is closely monitored by baroreceptors; they send messages to the cardio regulatory center of your medulla oblongata to regulate your
Blood Pressure and its Regulation Blood pressure in your blood vessels is closely monitored by baroreceptors; they send messages to the cardio regulatory center of your medulla oblongata to regulate your
10. Thick deposits of lipids on the walls of blood vessels, called, can lead to serious circulatory issues. A. aneurysm B. atherosclerosis C.
 Heart Student: 1. carry blood away from the heart. A. Arteries B. Veins C. Capillaries 2. What is the leading cause of heart attack and stroke in North America? A. alcohol B. smoking C. arteriosclerosis
Heart Student: 1. carry blood away from the heart. A. Arteries B. Veins C. Capillaries 2. What is the leading cause of heart attack and stroke in North America? A. alcohol B. smoking C. arteriosclerosis
Regulation of Arterial Blood Pressure 2 George D. Ford, Ph.D.
 Regulation of Arterial Blood Pressure 2 George D. Ford, Ph.D. OBJECTIVES: 1. Describe the Central Nervous System Ischemic Response. 2. Describe chemical sensitivities of arterial and cardiopulmonary chemoreceptors,
Regulation of Arterial Blood Pressure 2 George D. Ford, Ph.D. OBJECTIVES: 1. Describe the Central Nervous System Ischemic Response. 2. Describe chemical sensitivities of arterial and cardiopulmonary chemoreceptors,
Cardiovascular System B L O O D V E S S E L S 3
 Cardiovascular System B L O O D V E S S E L S 3 Fluid Shifts Between Capillaries and Tissue Permeable capillaries allow plasma and solutes to pass into interstitial space interstitial or extracellular
Cardiovascular System B L O O D V E S S E L S 3 Fluid Shifts Between Capillaries and Tissue Permeable capillaries allow plasma and solutes to pass into interstitial space interstitial or extracellular
1. Distinguish among the types of blood vessels on the basis of their structure and function.
 Blood Vessels and Circulation Objectives This chapter describes the structure and functions of the blood vessels Additional subjects contained in Chapter 13 include cardiovascular physiology, regulation,
Blood Vessels and Circulation Objectives This chapter describes the structure and functions of the blood vessels Additional subjects contained in Chapter 13 include cardiovascular physiology, regulation,
Blood pressure control Contin. Reflex Mechanisms. Dr. Hiwa Shafiq
 Blood pressure control Contin. Reflex Mechanisms Dr. Hiwa Shafiq 17-12-2018 A. Baroreceptor reflexes Baroreceptors (stretch receptors) located in the walls of several large systemic arteries( specially
Blood pressure control Contin. Reflex Mechanisms Dr. Hiwa Shafiq 17-12-2018 A. Baroreceptor reflexes Baroreceptors (stretch receptors) located in the walls of several large systemic arteries( specially
Chapter 21. Blood Vessels and Circulation
 Chapter 21 Blood Vessels and Circulation INTRODUCTION A. One main focus of this chapter considers hemodynamics, the means by which blood flow is altered and distributed and by which blood pressure is regulated.
Chapter 21 Blood Vessels and Circulation INTRODUCTION A. One main focus of this chapter considers hemodynamics, the means by which blood flow is altered and distributed and by which blood pressure is regulated.
CHAPTER 21 LECTURE OUTLINE
 CHAPTER 21 LECTURE OUTLINE I. INTRODUCTION A. One main focus of this chapter considers hemodynamics, the means by which blood flow is altered and distributed and by which blood pressure is regulated. B.
CHAPTER 21 LECTURE OUTLINE I. INTRODUCTION A. One main focus of this chapter considers hemodynamics, the means by which blood flow is altered and distributed and by which blood pressure is regulated. B.
Circulation. Sinoatrial (SA) Node. Atrioventricular (AV) Node. Cardiac Conduction System. Cardiac Conduction System. Linked to the nervous system
 Circulation Cardiac Conduction System AHS A H S Your body resembles a large roadmap. There are routes or arteries that take you downtown to the heart of the city and veins that take you to the outskirts
Circulation Cardiac Conduction System AHS A H S Your body resembles a large roadmap. There are routes or arteries that take you downtown to the heart of the city and veins that take you to the outskirts
The Circulatory System. Lesson Overview. Lesson Overview The Circulatory System
 33.1 THINK ABOUT IT More than one-third of the 1.2 million Americans who suffer a heart attack each year die. This grim evidence shows that the heart and the circulatory system it powers are vital to life.
33.1 THINK ABOUT IT More than one-third of the 1.2 million Americans who suffer a heart attack each year die. This grim evidence shows that the heart and the circulatory system it powers are vital to life.
3/10/2009 VESSELS PHYSIOLOGY D.HAMMOUDI.MD. Palpated Pulse. Figure 19.11
 VESSELS PHYSIOLOGY D.HAMMOUDI.MD Palpated Pulse Figure 19.11 1 shows the common sites where the pulse is felt. 1. Temporal artery at the temple above and to the outer side of the eye 2. External maxillary
VESSELS PHYSIOLOGY D.HAMMOUDI.MD Palpated Pulse Figure 19.11 1 shows the common sites where the pulse is felt. 1. Temporal artery at the temple above and to the outer side of the eye 2. External maxillary
Principles of Biomedical Systems & Devices. Lecture 8: Cardiovascular Dynamics Dr. Maria Tahamont
 Principles of Biomedical Systems & Devices Lecture 8: Cardiovascular Dynamics Dr. Maria Tahamont Review of Cardiac Anatomy Four chambers Two atria-receive blood from the vena cave and pulmonary veins Two
Principles of Biomedical Systems & Devices Lecture 8: Cardiovascular Dynamics Dr. Maria Tahamont Review of Cardiac Anatomy Four chambers Two atria-receive blood from the vena cave and pulmonary veins Two
Contents. Page 1. Homework 11 Chapter Blood Vessels Due: Week 6 Lec 11
 Page 1 Homework 11 Chapter 18-19 Blood Vessels Due: Week 6 Lec 11 Contents When printing, make sure that you specify the page range that you want to print out! Learning objectives for Lecture 11:...pg
Page 1 Homework 11 Chapter 18-19 Blood Vessels Due: Week 6 Lec 11 Contents When printing, make sure that you specify the page range that you want to print out! Learning objectives for Lecture 11:...pg
Mechanism: 1- waterretention from the last part of the nephron which increases blood volume, venous return EDV, stroke volume and cardiac output.
 Blood pressure regulators: 1- Short term regulation:nervous system Occurs Within secondsof the change in BP (they are short term because after a while (2-3 days) they adapt/reset the new blood pressure
Blood pressure regulators: 1- Short term regulation:nervous system Occurs Within secondsof the change in BP (they are short term because after a while (2-3 days) they adapt/reset the new blood pressure
Blood Flow, Blood Pressure, Cardiac Output. Blood Vessels
 Blood Flow, Blood Pressure, Cardiac Output Blood Vessels Blood Vessels Made of smooth muscle, elastic and fibrous connective tissue Cells are not electrically coupled Blood Vessels Arteries arterioles
Blood Flow, Blood Pressure, Cardiac Output Blood Vessels Blood Vessels Made of smooth muscle, elastic and fibrous connective tissue Cells are not electrically coupled Blood Vessels Arteries arterioles
HYPERTENSION: Sustained elevation of arterial blood pressure above normal o Systolic 140 mm Hg and/or o Diastolic 90 mm Hg
 Lecture 39 Anti-Hypertensives B-Rod BLOOD PRESSURE: Systolic / Diastolic NORMAL: 120/80 Systolic = measure of pressure as heart is beating Diastolic = measure of pressure while heart is at rest between
Lecture 39 Anti-Hypertensives B-Rod BLOOD PRESSURE: Systolic / Diastolic NORMAL: 120/80 Systolic = measure of pressure as heart is beating Diastolic = measure of pressure while heart is at rest between
Cardiac Output (C.O.) Regulation of Cardiac Output
 Cardiac Output (C.O.) Is the volume of the blood pumped by each ventricle per minute (5 Litre) Stroke volume: Is the volume of the blood pumped by each ventricle per beat. Stroke volume = End diastolic
Cardiac Output (C.O.) Is the volume of the blood pumped by each ventricle per minute (5 Litre) Stroke volume: Is the volume of the blood pumped by each ventricle per beat. Stroke volume = End diastolic
AS Level OCR Cardiovascular System
 AS Level OCR Cardiovascular System Learning Objectives The link between the Cardiac Cycle and the Conduction system of the heart. The relationship between Stroke volume, Heart rate and Cardiac Output.
AS Level OCR Cardiovascular System Learning Objectives The link between the Cardiac Cycle and the Conduction system of the heart. The relationship between Stroke volume, Heart rate and Cardiac Output.
1. Label the Diagram using the following terms: artery, arterioles, vein, venules, capillaries, valve, inner wall, middle wall, outer wall
 Bio 20 Ms. Nyboer Arteries, Veins, Capillaries, and the Heart Structure and Function Workbook Use your textbook (Ch. 10) and notes to fill in this workbook Part A: Arteries, Veins, Capillaries 1. Label
Bio 20 Ms. Nyboer Arteries, Veins, Capillaries, and the Heart Structure and Function Workbook Use your textbook (Ch. 10) and notes to fill in this workbook Part A: Arteries, Veins, Capillaries 1. Label
The Cardiovascular System
 The Cardiovascular System The Cardiovascular System A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function of
The Cardiovascular System The Cardiovascular System A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function of
This is a TRANSPORT system that allows every cell: i) uptake of nutrients ( ex. oxygen, glucose) ii) excretes wastes (ex C02, ammonia)
 Biology 20 Unit D This is a TRANSPORT system that allows every cell: i) uptake of nutrients ( ex. oxygen, glucose) ii) excretes wastes (ex C02, ammonia) requires action of: heart: muscular force to move
Biology 20 Unit D This is a TRANSPORT system that allows every cell: i) uptake of nutrients ( ex. oxygen, glucose) ii) excretes wastes (ex C02, ammonia) requires action of: heart: muscular force to move
Hypovolemic Shock: Regulation of Blood Pressure
 CARDIOVASCULAR PHYSIOLOGY 81 Case 15 Hypovolemic Shock: Regulation of Blood Pressure Mavis Byrne is a 78-year-old widow who was brought to the emergency room one evening by her sister. Early in the day,
CARDIOVASCULAR PHYSIOLOGY 81 Case 15 Hypovolemic Shock: Regulation of Blood Pressure Mavis Byrne is a 78-year-old widow who was brought to the emergency room one evening by her sister. Early in the day,
Cardiovascular Physiology. Heart Physiology. Introduction. The heart. Electrophysiology of the heart
 Cardiovascular Physiology Heart Physiology Introduction The cardiovascular system consists of the heart and two vascular systems, the systemic and pulmonary circulations. The heart pumps blood through
Cardiovascular Physiology Heart Physiology Introduction The cardiovascular system consists of the heart and two vascular systems, the systemic and pulmonary circulations. The heart pumps blood through
IP: Regulation of Cardiac Output
 ANP 1105D Winter 2013 Assignment 9: The Heart, part 2: Chap... Assignment 9: The Heart, part 2: Chapter 18 Signed in as Alex Sokolowski Help Close Resources Due: 11:59pm on Monday, March 25, 2013 Note:
ANP 1105D Winter 2013 Assignment 9: The Heart, part 2: Chap... Assignment 9: The Heart, part 2: Chapter 18 Signed in as Alex Sokolowski Help Close Resources Due: 11:59pm on Monday, March 25, 2013 Note:
Physiology Unit 3 CARDIOVASCULAR PHYSIOLOGY: THE VASCULAR SYSTEM
 Physiology Unit 3 CARDIOVASCULAR PHYSIOLOGY: THE VASCULAR SYSTEM In Physiology Today Hemodynamics F = ΔP/R Blood flow (F) High to low pressure Rate = L/min Pressure (P) Hydrostatic pressure Pressure exerted
Physiology Unit 3 CARDIOVASCULAR PHYSIOLOGY: THE VASCULAR SYSTEM In Physiology Today Hemodynamics F = ΔP/R Blood flow (F) High to low pressure Rate = L/min Pressure (P) Hydrostatic pressure Pressure exerted
Cardiovascular System: Vessels and Circulation (Chapter 21)
 Cardiovascular System: Vessels and Circulation (Chapter 21) Lecture Materials for Amy Warenda Czura, Ph.D. Suffolk County Community College Eastern Campus Primary Sources for figures and content: Marieb,
Cardiovascular System: Vessels and Circulation (Chapter 21) Lecture Materials for Amy Warenda Czura, Ph.D. Suffolk County Community College Eastern Campus Primary Sources for figures and content: Marieb,
Cardiovascular system
 BIO 301 Human Physiology Cardiovascular system The Cardiovascular System: consists of the heart plus all the blood vessels transports blood to all parts of the body in two 'circulations': pulmonary (lungs)
BIO 301 Human Physiology Cardiovascular system The Cardiovascular System: consists of the heart plus all the blood vessels transports blood to all parts of the body in two 'circulations': pulmonary (lungs)
Cardiovascular regulation. Neural and hormonal Regulation Dr Badri Paudel GMC. 1-Local factors (autoregulation) Control of Blood Flow
 Neural and hormonal Regulation Dr Badri Paudel GMC 1 Cardiovascular regulation Fa c t o r s i nvo l v e d i n t h e regulation of cardiovascular function include: 1- Autoregulation 2- Neural regulation
Neural and hormonal Regulation Dr Badri Paudel GMC 1 Cardiovascular regulation Fa c t o r s i nvo l v e d i n t h e regulation of cardiovascular function include: 1- Autoregulation 2- Neural regulation
Unit 1: Human Systems. The Circulatory System
 Unit 1: Human Systems The Circulatory System nourish all cells with oxygen, glucose, amino acids and other nutrients and carry away carbon dioxide, urea and other wastes Purposes Transport chemical messengers
Unit 1: Human Systems The Circulatory System nourish all cells with oxygen, glucose, amino acids and other nutrients and carry away carbon dioxide, urea and other wastes Purposes Transport chemical messengers
Blood flows away from the heart in arteries, to the capillaries and back to the heart in the veins
 Cardiovascular System Summary Notes The cardiovascular system includes: The heart, a muscular pump The blood, a fluid connective tissue The blood vessels, arteries, veins and capillaries Blood flows away
Cardiovascular System Summary Notes The cardiovascular system includes: The heart, a muscular pump The blood, a fluid connective tissue The blood vessels, arteries, veins and capillaries Blood flows away
Chapter 10 Worksheet Blood Pressure and Antithrombotic Agents
 Complete the following. 1. A layer of cells lines each vessel in the vascular system. This layer is a passive barrier that keeps cells and proteins from going into tissues; it also contains substances
Complete the following. 1. A layer of cells lines each vessel in the vascular system. This layer is a passive barrier that keeps cells and proteins from going into tissues; it also contains substances
Vascular System Part One
 Vascular System Part One Objectives Trace the route taken by blood as it leaves, and then returns to the heart. Describe the structure of the walls of arteries and veins. Discuss the structure and function
Vascular System Part One Objectives Trace the route taken by blood as it leaves, and then returns to the heart. Describe the structure of the walls of arteries and veins. Discuss the structure and function
Cardiovascular Responses to Exercise
 CARDIOVASCULAR PHYSIOLOGY 69 Case 13 Cardiovascular Responses to Exercise Cassandra Farias is a 34-year-old dietician at an academic medical center. She believes in the importance of a healthy lifestyle
CARDIOVASCULAR PHYSIOLOGY 69 Case 13 Cardiovascular Responses to Exercise Cassandra Farias is a 34-year-old dietician at an academic medical center. She believes in the importance of a healthy lifestyle
Blood Pressure Regulation 2. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
P215 SPRING 2019: CIRCULATORY SYSTEM Chaps 13, 14 & 15: pp , , , I. Major Functions of the Circulatory System
 P215 SPRING 2019: CIRCULATORY SYSTEM Chaps 13, 14 & 15: pp 360-390, 395-404, 410-428 433-438, 441-445 I. Major Functions of the Circulatory System 1. 2. 3. 4. II. Structure of the Heart 1. atria 2. ventricles
P215 SPRING 2019: CIRCULATORY SYSTEM Chaps 13, 14 & 15: pp 360-390, 395-404, 410-428 433-438, 441-445 I. Major Functions of the Circulatory System 1. 2. 3. 4. II. Structure of the Heart 1. atria 2. ventricles
Introductory Clinical Pharmacology Chapter 41 Antihypertensive Drugs
 Introductory Clinical Pharmacology Chapter 41 Antihypertensive Drugs Blood Pressure Normal = sys
Introductory Clinical Pharmacology Chapter 41 Antihypertensive Drugs Blood Pressure Normal = sys
Peripheral Circulation and Regulation
 Peripheral Circulation and Regulation Functions of Peripheral Circulation 1. Contain the blood 2. Exchange nutrients, waste products, and gases with tissues 3. Transport 4. Regulate blood pressure, along
Peripheral Circulation and Regulation Functions of Peripheral Circulation 1. Contain the blood 2. Exchange nutrients, waste products, and gases with tissues 3. Transport 4. Regulate blood pressure, along
Six main classes of blood vessels (on handout) Wall structure of arteries and veins (on handout) Comparison: Arteries vs. Veins (on handout)
 Cardiovascular System: Vessels and Circulation (Chapter 21) Lecture Materials for Amy Warenda Czura, Ph.D. Suffolk County Community College Eastern Campus Six main classes of blood vessels Primary Sources
Cardiovascular System: Vessels and Circulation (Chapter 21) Lecture Materials for Amy Warenda Czura, Ph.D. Suffolk County Community College Eastern Campus Six main classes of blood vessels Primary Sources
Chapter 21! Chapter 21 Blood Vessels and Circulation! Blood Vessels and Circulation!
 Chapter 21! Blood Vessels and Circulation! SECTION 21-1! Blood vessels differ in size, structure, and functional properties! 2 Major Vessel Types! Arteries - carry blood away from the heart Higher pressure
Chapter 21! Blood Vessels and Circulation! SECTION 21-1! Blood vessels differ in size, structure, and functional properties! 2 Major Vessel Types! Arteries - carry blood away from the heart Higher pressure
Chapter 21! Blood Vessels and Circulation! SECTION 21-1! Blood vessels differ in size, structure, and functional properties!
 Chapter 21! Blood Vessels and Circulation! SECTION 21-1! Blood vessels differ in size, structure, and functional properties! 2 1! Major Vessel Types! Arteries - carry blood away from the heart Higher pressure
Chapter 21! Blood Vessels and Circulation! SECTION 21-1! Blood vessels differ in size, structure, and functional properties! 2 1! Major Vessel Types! Arteries - carry blood away from the heart Higher pressure
Special circulations, Coronary, Pulmonary. Faisal I. Mohammed, MD,PhD
 Special circulations, Coronary, Pulmonary Faisal I. Mohammed, MD,PhD 1 Objectives Describe the control of blood flow to different circulations (Skeletal muscles, pulmonary and coronary) Point out special
Special circulations, Coronary, Pulmonary Faisal I. Mohammed, MD,PhD 1 Objectives Describe the control of blood flow to different circulations (Skeletal muscles, pulmonary and coronary) Point out special
30.1 Respiratory and Circulatory Functions. KEY CONCEPT The respiratory and circulatory systems bring oxygen and nutrients to the cells.
 30.1 Respiratory and Circulatory Functions KEY CONCEPT The respiratory and circulatory systems bring oxygen and nutrients to the cells. 30.1 Respiratory and Circulatory Functions The respiratory and circulatory
30.1 Respiratory and Circulatory Functions KEY CONCEPT The respiratory and circulatory systems bring oxygen and nutrients to the cells. 30.1 Respiratory and Circulatory Functions The respiratory and circulatory
Figure ) The specific chamber of the heart that is indicated by letter A is called the. Diff: 1 Page Ref: 364
 Essentials of Anatomy and Physiology, 9e (Marieb) Chapter 11 The Cardiovascular System Short Answer Figure 11.1 Using Figure 11.1, identify the following: 1) The Purkinje fibers are indicated by label.
Essentials of Anatomy and Physiology, 9e (Marieb) Chapter 11 The Cardiovascular System Short Answer Figure 11.1 Using Figure 11.1, identify the following: 1) The Purkinje fibers are indicated by label.
The ancient Babylonians, Egyptians, Indians and Chinese believed the heart was the centre of thinking and emotions
 The Concept of Mind The ancient Babylonians, Egyptians, Indians and Chinese believed the heart was the centre of thinking and emotions Hippocrates 460 BC 370 BC - Thoughts, ideas, and feelings come from
The Concept of Mind The ancient Babylonians, Egyptians, Indians and Chinese believed the heart was the centre of thinking and emotions Hippocrates 460 BC 370 BC - Thoughts, ideas, and feelings come from
Cardiovascular Physiology
 Cardiovascular Physiology Introduction The cardiovascular system consists of the heart and two vascular systems, the systemic and pulmonary circulations. The heart pumps blood through two vascular systems
Cardiovascular Physiology Introduction The cardiovascular system consists of the heart and two vascular systems, the systemic and pulmonary circulations. The heart pumps blood through two vascular systems
Chapters 9 & 10. Cardiorespiratory System. Cardiovascular Adjustments to Exercise. Cardiovascular Adjustments to Exercise. Nervous System Components
 Cardiorespiratory System Chapters 9 & 10 Cardiorespiratory Control Pulmonary ventilation Gas exchange Left heart Arterial system Tissues Right heart Lungs Pulmonary ventilation Cardiovascular Regulation-
Cardiorespiratory System Chapters 9 & 10 Cardiorespiratory Control Pulmonary ventilation Gas exchange Left heart Arterial system Tissues Right heart Lungs Pulmonary ventilation Cardiovascular Regulation-
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1
 BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
1. Antihypertensive agents 2. Vasodilators & treatment of angina 3. Drugs used in heart failure 4. Drugs used in arrhythmias
 1. Antihypertensive agents 2. Vasodilators & treatment of angina 3. Drugs used in heart failure 4. Drugs used in arrhythmias Only need to know drugs discussed in class At the end of this section you should
1. Antihypertensive agents 2. Vasodilators & treatment of angina 3. Drugs used in heart failure 4. Drugs used in arrhythmias Only need to know drugs discussed in class At the end of this section you should
Glomerular Capillary Blood Pressure
 Glomerular Capillary Blood Pressure Fluid pressure exerted by blood within glomerular capillaries Depends on Contraction of the heart Resistance to blood flow offered by afferent and efferent arterioles
Glomerular Capillary Blood Pressure Fluid pressure exerted by blood within glomerular capillaries Depends on Contraction of the heart Resistance to blood flow offered by afferent and efferent arterioles
Blood Vessels. Over view. We have about 60,000 miles of blood vessels!
 Blood Vessels Over view 3 types of blood vessels arteries - carry blood away from heart "branch", "diverge", and "fork" veins - carry blood toward heart "join", "merge", and "converge" capillaries - site
Blood Vessels Over view 3 types of blood vessels arteries - carry blood away from heart "branch", "diverge", and "fork" veins - carry blood toward heart "join", "merge", and "converge" capillaries - site
Renal Regulation of Sodium and Volume. Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM
 Renal Regulation of Sodium and Volume Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM Maintaining Volume Plasma water and sodium (Na + ) are regulated independently - you are already familiar
Renal Regulation of Sodium and Volume Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM Maintaining Volume Plasma water and sodium (Na + ) are regulated independently - you are already familiar
Physiological Response to Hypovolemic Shock Dr Khwaja Mohammed Amir MD Assistant Professor(Physiology) Objectives At the end of the session the
 Physiological Response to Hypovolemic Shock Dr Khwaja Mohammed Amir MD Assistant Professor(Physiology) Objectives At the end of the session the students should be able to: List causes of shock including
Physiological Response to Hypovolemic Shock Dr Khwaja Mohammed Amir MD Assistant Professor(Physiology) Objectives At the end of the session the students should be able to: List causes of shock including
PHYSIOLOGY MeQ'S (Morgan) All the following statements related to blood volume are correct except for: 5 A. Blood volume is about 5 litres. B.
 PHYSIOLOGY MeQ'S (Morgan) Chapter 5 All the following statements related to capillary Starling's forces are correct except for: 1 A. Hydrostatic pressure at arterial end is greater than at venous end.
PHYSIOLOGY MeQ'S (Morgan) Chapter 5 All the following statements related to capillary Starling's forces are correct except for: 1 A. Hydrostatic pressure at arterial end is greater than at venous end.
Blood Pressure Regulation 2. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
The Circulatory System
 The Circulatory System Key Questions What are the functions of the circulatory system? How does the heart pump blood through the body? What are three types of blood vessels? Vocabulary myocardium atrium
The Circulatory System Key Questions What are the functions of the circulatory system? How does the heart pump blood through the body? What are three types of blood vessels? Vocabulary myocardium atrium
