Thirty-Day In-Vivo Performance of a Wearable Artificial Pump-Lung for Ambulatory Respiratory Support
|
|
|
- June Jacobs
- 5 years ago
- Views:
Transcription
1 Thirty-Day In-Vivo Performance of a Wearable Artificial Pump-Lung for Ambulatory Respiratory Support Zhongjun J. Wu, PhD, Tao Zhang, PhD, Giacomo Bianchi, MD, Xufeng Wei, MD, PhD, Ho-Sung Son, MD, PhD, Kang Zhou, MD, Pablo G. Sanchez, MD, PhD, Jose Garcia, MD, and Bartley P. Griffith, MD Artificial Organs Laboratory, Department of Surgery, University of Maryland School of Medicine, Baltimore, Maryland; Ospedale del Cuore G. Pasquinucci, Fondazione Toscana Gabriele Monasterio CNR, Massa, Italy; and Department of Thoracic and Cardiovascular Surgery, College of Medicine, Korea University, Seoul, Republic of Korea Background. The purpose of this study was to evaluate the long-term in-vivo hemodynamics, gas transfer, and biocompatibility of an integrated artificial pump-lung (APL) developed for ambulatory respiratory support. Methods. The study was conducted in an ovine model by surgically placing the APL between the right atrium and pulmonary artery. Nine sheep were implanted. Heparin was infused as an anticoagulant. The device flow, gas transfer, and plasma free hemoglobin were measured daily. Hematologic data, platelet activation, and blood biochemistry were assessed twice a week. After 30 days, the sheep were euthanized for postmortem examination. The explanted devices were examined for gross thrombosis. Results. Five sheep survived for 29 to 31 days and were electively terminated. Four sheep died or were terminated early owing to mechanical failure of intravenous lines or device. The APL devices in the 5 long-term animals were capable of delivering an oxygen transfer rate of ml/min at a flow rate of L/min with blood oxygen saturation of 96.7% 1.3%. The device flow and oxygen transfer were stable over 30 days. The animals had normal end-organ functions except for surgery-related transient alteration in kidney function, liver function, and cell and tissue injury. There was no hemolysis. The device flow path and membrane surface were free of gross thrombus. Conclusions. The APL exhibited the capability of providing respiratory support with excellent biocompatibility, long-term reliability, and the potential for bridging to lung transplant. (Ann Thorac Surg 2012;93:274 81) 2012 by The Society of Thoracic Surgeons Mechanical ventilation and extracorporeal membrane oxygenation (ECMO) are often used to provide respiratory support for patients suffering from adult respiratory distress syndrome/acute lung injury and as a bridge to lung transplantation [1]. Mechanical ventilation is effective as short-term support, yet the sustained and prolonged tidal volumes and airway pressures often damage the lungs through barotrauma, volutrauma, and other iatrogenic injuries [2]. Extracorporeal membrane oxygenation is attractive because it closely simulates physiological gas exchange, but can only be used for short term support. Extended ECMO support may be possible, but in practice, these systems are limited by the complexity of their operation, increased risk of bleeding, and reduced patient mobility. Patients are often bedridden, resulting in muscular atrophy and wasting syndrome that may affect patients survival. Recently, ambulatory ECMO support has been implemented in a number of centers using available pumps Accepted for publication Aug 29, Address correspondence to Dr Wu, Department of Surgery, University of Maryland School of Medicine, 10 S Pine St, MTSF-436, Baltimore, MD 21201; zuw@smail.umaryland.edu. and oxygenators [3-5], allowing patients to walk, eat, and exercise. This is a significant improvement because it allows patients to be ambulatory, to keep muscles from atrophying, and to participate in physical rehabilitation that ultimately leads to a better clinical course to full recovery or better status at the time of heart/lung transplantation. The systems currently available are very bulky, and multiple exchanges of oxygenators are required for long-term support. Based on the successful utilization of paracorporeal ventricular assist devices in heart failure patients [6], we envision that a paracorporeal artificial lung device may impact quality of life for respiratory failure patients and may open options for more aggressive medical therapies, which might extend survival as well, just as with mechanical circulatory support in time. We believe that the paracorporeal artificial lung might be reasonably introduced clinically as a temporary short- or long-term bridge to transplantation and as a short-term therapy for acute respiratory distress syndrome and related diseases. To this end, we have developed a paracorporeal artificial pump-lung (APL) for ambulatory respiratory or cardiopulmonary support. The APL is an ultracompact pump by The Society of Thoracic Surgeons /$36.00 Published by Elsevier Inc doi: /j.athoracsur
2 Ann Thorac Surg WU ET AL 2012;93: EVALUATION OF A WEARABLE PUMP-LUNG 275 oxygenator consisting of a uniquely designed hollow fiber membrane (HFM) bundle integrated with a magnetically levitated centrifugal impeller pump. The overall size of the APL is comparable to a 12-ounce soda can. It can function either as a respiratory support device or partial cardiopulmonary support device with maximal flexibility of application in the broad spectrum of heart/ lung diseases. The objective of this study was to evaluate the longterm in vivo hemodynamics, oxygen transfer, and biocompatibility performances of the APL for respiratory support in an ovine model. Material and Methods Device Description The APL is an ultracompact, low prime volume, low hemolytic device for ambulatory respiratory assistance or cardiopulmonary support. It is designed to be capable of providing respiratory support (partial to full) or cardiac support for adult patients who have respiratory failure or cardiopulmonary collapse. The following are the APL design specifications: (1) blood flow of 3.5 L/min; (2) oxygen delivery rate of 180 ml/min; (3) pressure head of 120 mm Hg; (4) 0.80 m 2 surface area of membranes for gas exchange; (5) minimal red blood cell injury/hemolysis and platelet activation; and (6) support duration of up to 30 days and exchangeable. The APL is suitable for either central (ie, right atrium to main pulmonary artery) or peripheral cannulation (ie, internal jugular vein to carotid artery or femoral vein to femoral artery). In both configurations, the device itself, controller, oxygen source, drive line, and power supply can be worn by the patients so that the patients can be ambulatory. Figure 1A illustrates the APL system with its surgical implantation to a human patient. Figure 1B shows the disposable APL device, the motor drive, and controller. The APL device is 117 mm in length and 89 mm in diameter. The priming volume of the device is approximately 115 ml. The combined weight of the APL device and the motor/controller unit is only approximately 0.54 kg. Figure 2 shows the sectional view of the flow path inside the APL. Venous blood is drawn from the patient into the APL pump chamber from a central cylindrical tube through a drainage cannula. Driven by a magnetically levitated rotating centrifugal pump impeller, the blood is propelled through the diffuser section and flows toward the space between the outer housing and the polymethylpentene HFM (Oxyplus; Membrana, Wuppertal, Germany) bundle. Owing to the increased hydrodynamic pressure by the impeller pump, the blood penetrates the HFM bundle in the radial direction. While the blood passes through the HFM bundle, the oxygen is transferred from the fiber lumen to the blood and the carbon dioxide is removed from the blood. The oxygenated blood is collected at the space between the HFM bundle and the center tube and returned back to the patient through the return cannula. The sweep gas enters the lumens of individual hollow fibers of the potted HFM bundle from the top and exits the device at the bottom through the channels imbedded in the diffuser fins. A vent port on the upper side of the outer housing wall (Fig 1B) can be used to remove the gas bubbles that may get into the device accidently. In addition, as a safety measure, an arterial filter may be added to the system to further reduce the risk of gas embolism. Surgical Procedure Nine Dorset hybrid sheep (45 kg to 65 kg) bred for laboratory research (Thomas Morris, Reisterstown, MD) were used. All the surgical procedures and postoperative care were carried out according to the approved protocol by the Institutional Animal Care and Use Committee of the University of Maryland School of Medicine. During the course of the animal experiments, all animals received humane care in accordance with the Guide for Care and Use of Laboratory Animals (NIH publication 86-23, revised 1996). Fig 1. (A) Typical implementation of the artificial pump lung (APL) for a human patient. (B) The APL system: magnetically levitated pump-oxygenator and controller-motor drive assembly, (top) disposable device, (bottom) controller and motor drive.
3 276 WU ET AL Ann Thorac Surg EVALUATION OF A WEARABLE PUMP-LUNG 2012;93: oxygen was used as the sweep gas. Thus, a mixture of oxygen (95%) and carbon dioxide (5%) was used as the sweep gas at a flow rate of approximately 1.0 L/min to maintain PCO 2 of the animal s venous blood within the physiologic range (40 to 50 mm Hg). At the conclusion of the study, each animal underwent postmortem examination and device explantation. A careful examination for thrombus formation, graft patency, and cannula position was performed. The internal organs and explanted device were examined grossly and microscopically for evidence of thromboembolism. Fig 2. Cross-sectional view of the artificial pump-lung and flow path. The sheep was induced and vital signs were monitored as previously described [7]. The APL device was surgically implanted between the right atrium and pulmonary artery through a left thoracotomy. After the sheep was given heparin to achieve an activated clotting time (ACT) of 250 s, the Dacron graft of an arterial cannula (Abiomed, Danvers, MA) was anastomosed end to side to the distal pulmonary artery. A 32F venous drain cannula (DLP, Medtronic, Minneapolis, MN) was placed in the right atrium through the right atrial appendage using the double pursestring suture technique. After the inflow and outflow cannulas were deaired using saline, clamped and tunneled out of the chest to exit the skin on the upper left lateral chest wall, the APL device primed with heparinized saline was connected to the inflow and outflow cannulas and deaired. The APL operation was then initiated for the in vivo evaluation. A flow probe (Transonic System, Ithaca, NY) was placed around the outflow tubing to measure the device-generated flow. The incision was closed, and the animals were allowed to recover. Once the animals became conscious and could breathe on their own, the animals were extubated and transported into the specially designed cage for recovery. Postoperative Care The sheep were monitored daily until the study endpoint. Pain was alleviated by giving flunixin meglumine at a loading dose of 2.2 mg/kg initially and thereafter 1.1 mg/kg (intravenously, twice daily) for 5 days. Buprenorphine would be used (0.005 to 0.01 mg/kg intramuscularly or intravenously) to relieve pain associated with the surgical procedure if the flunixin was not sufficient. Enrofloxacin was given every 12 hours for 5 days. Heparin was continuously infused to maintain a targeted ACT of 150 s by adjusting the infused heparin rate daily. The APL was operated to produce a blood flow of approximately 3.0 L/min. From our early experiments, we found that the partial pressure of carbon dioxide (PCO 2 )ofthe animals venous blood was low (35 to 40 mm Hg) if pure Device Function Evaluation The device-generated flow at a fixed operating speed was measured daily. The pressure drop across the fiber bundle was measured at the start and end of the study. Blood samples at the inlet and outlet of the APL were collected daily for blood gas analysis using a blood gas analyzer (Stat Profile Phox Plus L; Nova Biomedical, Waltham, MA). The oxygen transfer rate was calculated according to the published method [8]. Because 95% oxygen mixed with 5% carbon dioxide was used as the sweep gas, the carbon dioxide transfer rate could not be reliably evaluated and was not presented. Blood Chemistry, Hematologic, and Biocompatibility Measurements Blood samples were collected at baseline, after implantation, and twice a week for determination of complete metabolic panel, complete blood count, plasma free hemoglobin (PFH), lactic acid dehydrogenase, and platelet activation markers (percentage of P-selectin positive platelets and plasma soluble P-selectin). Collected blood samples were sent to an outside laboratory (Antech Diagnostics, Lake Success, NY) for complete metabolic panel, complete blood count, and lactic acid dehydrogenase determination. The PFH was measured using a modified cyanomethemoglobin method. Expression of P-selectin (CD62p) on platelets was quantified with flow cytometry. Plasma soluble P-selectin levels were measured by enzyme-linked immunosorbent assay developed in our laboratory specifically for ovine [9]. Statistical Analysis Data are presented as mean SE. Data collected daily over the 30-day study period were averaged every 5 days. Comparisons between the measured data at baseline (preimplant or initiation of device operation) and at subsequent times were performed using a mixed model with the sheep number as the subject variable and the data collection time as the fixed, repeated measure variable (SPSS Statistics 18; SPSS, Chicago, IL). Post hoc analysis using the least significant difference (LSD) corrected confidence interval was used to compare all the postoperatively measured variables with the baseline data to examine the changes with time.
4 Ann Thorac Surg WU ET AL 2012;93: EVALUATION OF A WEARABLE PUMP-LUNG 277 Results Study Summary The APL was successfully implanted on 9 sheep. All of the animals recovered from the surgery and were able to stand, drink, and eat within 24 hours. The results of the 9 in vivo animal experiments are summarized in Table 1. Five sheep survived for 29 to 31 days and were electively terminated. One sheep was terminated early when leaking from the device was observed at day 4. Three animals died of bleeding: 1 device related and 2 not device related. Of the 2 incidents not device related, 1 animal chewed the heparin infusion line, and in the other animal, the heparin infusion line used was unexpectedly dislodged at the glued joint between the tube and luer adapter. All the devices in the animals that survived to the study endpoint functioned normally. The data from these animals are presented in the following sections. Anticoagulation The heparin dose and attained ACT over the 30-day period are listed in Table 2. Escalating heparin infusion dosage was required initially to maintain the targeted ACT. However, the required dosage became stabilized after the second week. The similar anticoagulation requirement was observed in the juvenile sheep implanted with the child-size pediatric Jarvik 2000 heart [9]. Device Pumping Function and Oxygen Transfer Performance The device flow and oxygen transfer performance of the APL in the 5 animals over the 30-day period are shown in Figure 3. Owing to the slight differences in each sheep s hemodynamic responses to the surgery, cannula position, and the device placement, the operating speed of the APL was adjusted between 5,000 rpm and 6,000 rpm so that a device flow of approximately 3.25 L/min was generated at the beginning. Thereafter, the operation speed remained the same. The device flow decreased slightly in the first few days, remained stable in the first 2 weeks, and gradually decreased after the first 2 weeks. The change in the flow rate after the first 2 weeks reached statistical significance (p 0.05). After an examination of the factors affecting the device pumping function, it was noticed that this change corresponded well to the increase in hematocrit (See Table 2). Since the blood viscosity increases with hematocrit, the increase would cause the reduction of the flow rate under the same hemodynamic pressure head. It is expected that the flow generated by the APL would decrease owing to the increase in the hematocrit even without any device performance deterioration. The device flow was reanalyzed by factoring the effect of hematocrit (viscosity) of the blood at all the timepoints. There is no statistical difference in the hematocrit adjusted device flow from the baseline over the 30-day duration (p 0.25, baseline versus all timepoints). The oxygen transfer rate in individual animals varied depending on the animals hematologic conditions and device flows. The highest oxygen transfer rate reached ml/min at a device flow of 3.1 L/min at one timepoint in 1 animal while the animal had a very low oxygen partial pressure (PO 2 ) in the venous blood (PO mm Hg, SO %, hematocrit 32%). The overall oxygen transfer rate remained stable over the 30-day period. There was no statistical difference between the oxygen transfer rates at the baseline and at the subsequent timepoints over the 30-day period (p 0.29). In spite of the variation of the animals venous blood, the oxygen saturation at the APL outlet was stable over the 30-day period, and the normal physiologic arterial blood condition ( 95%) was achieved (see Table 2). Hematology and End-Organ Function Hematologic data (hematocrit, platelet, and white blood cell) counts) are summarized in Table 2. There was a drop in hematocrit from the presurgical value of 32.3% to 27% after the surgery. Postoperative hemodilution could be attributed to blood loss and fluid infusion during the surgery. Two weeks after the surgery, the hematocrit returned to the baseline level and gradually increased to 35.5% at the study endpoint. In 1 sheep, there was an unexplained drop in hematocrit on day 5 although there was no hemolysis or other abnormalities; 900 ml of blood was transfused to this sheep on day 6. The sudden drop of hematocrit in this particular sheep resulted in the lowest hematocrit at day 6 for the whole group. Although there is no statistical difference between the baseline hematocrit and the values at the subsequent timepoints Table 1. Summary of Nine In Vivo Animal Experiments Sheep No. Weight (kg) Duration (Days) Blood Flow (L/min) O 2 Transfer (ml/min) Termination Summary Elective Early termination Died because of IV line broken Elective Elective Elective Died because of device leaking Elective Died because of IV line broken IV intravenous; O 2 oxygen.
5 278 WU ET AL Ann Thorac Surg EVALUATION OF A WEARABLE PUMP-LUNG 2012;93: Table 2. Summary of Measurements During 30-Day In Vivo Study (n 5) Measurements POD 0 POD 1 5 POD 6 10 POD POD POD POD Heparin, U/h 1, , , , , , , Heparin, U/kg/h ACT, s SO 2, inlet, % SO 2, outlet, % Hematocrit, % Platelets, / L WBC, 10 3 / L Creatinine, mg/dl BUN, mg/dl ALT, U/L AST, U/L CPK, U/L , LDH, U/L PFH, mg/dl SurPsel, % SoPsel, ng/ L ACT activated clotting time; ALT alanine aminotransferase; AST aspartate aminotransferase; BUN blood urea nitrogen; CPK creatine phosphokinase; LDH lactate dehydrogenase; PFH plasma free hemoglobin; POD postoperative day; SO 2 oxygen saturation; SoPsel plasma soluble P-selectin; SurPsel surface expressed P-selectin; WBC white blood cells. Fig 3. The device-generated blood flow (squares) and oxygen transfer rate (circles) over the 30-day study period. Data were averaged every 5 days. (p 0.10), the difference between the hematocrits at days 6 to 10 and days 15 to 30 were significantly different (p 0.036). The platelet count also had a similar initial drop from its respective presurgical value after the surgery. The decrease in the platelet count was significant compared with the presurgical baseline value (p 0.05). However, the platelet count increased thereafter, and returned to the normal range after the first week. The white blood cell count varied slightly, but remained in the normal range. The variations in the white blood cell count at the postoperative timepoints did not reach statistical significance compared with their presurgical baseline value (p 0.19). Selected laboratory tests for kidney function (creatinine, blood urea nitrogen), liver function (alanine transaminase, aspartate aminotransferase), and cell and tissue injury (creatine phosphokinase, lactic dehydrogenase) are presented in Table 2. Among the 5 sheep, the creatinine and blood urea nitrogen values in three sheep remained in the normal range throughout the study. The creatinine and blood urea nitrogen values in the other 2 sheep had an acute elevation at days 1 to 6, returned to the normal range at day 9, and remained stable thereafter. This unusual elevation in 2 sheep may be attributed to the transient acute kidney insufficiency probably induced by low flow state or blood loss, or both, during the surgery. The device was not the cause of this problem as the kidneys from these 2 sheep were found to be normal without infarcts during the postmortem examination. Alanine transaminase, aspartate aminotransferase, creatine phosphokinase, and lactic dehydrogenase were all significantly elevated in the first week and returned to the normal ranges at days 6 to 15, and remained stable throughout the study. Similar trends for the respective laboratory tests were reported by others [10]. Biocompatibility The PFH and platelet activation markers over the 30-day period are shown in Table 2. The PFH fluctuated daily but remained in the normal range. The percentage of CD62p-positive platelets was less than 10%. There was no statistical difference between the percentages of
6 Ann Thorac Surg WU ET AL 2012;93: EVALUATION OF A WEARABLE PUMP-LUNG 279 CD62p-positive platelets at the postoperative timepoints and the baseline level. The soluble P-selectin concentration initially peaked significantly at 6 hours immediately after the surgery, indicating a significant rise in platelet activation state at this time ( ng/ml versus ng/ml, p 0.05). After peaking during the first 24 hours, the soluble P-selectin concentration decreased from the peak, but remained slightly elevated compared with the baseline concentration. Postmortem Findings and Examination of Explanted Devices Both the left thoracotomy incision and cannula exit sites healed well without any evidence of infection. The hearts from the animals were normal in size and shape without evidence of infarction, thrombi formation, or infective vegetations (Fig 4A). Localized endocardial bruising to the right atrium by the inflow cannula tip was found in 1 animal. The left lungs were normal at the gross appearance, with a limited area of atelectasis. The right lungs were fully expanded and of normal appearance. At gross examination, no lesion was found, and no clots were present in the major vessels and branches of the lungs (Fig 4A). The left kidney from 1 animal had a4mm 4 mm infarct whereas the right kidney was free of infarcts. The kidney function of this animal was completely normal over the course of the study. The kidneys from the other 4 animals were normal and free of any infarct. One of the 4 animals with the kidneys of normal appearance had elevated creatinine and blood urea nitrogen labora- Fig 4. (A) Photographs of (left) dissected pulmonary artery and branches of one explanted lung and (right) inflow cannula tip in the right atrium of the heart. (B) Photographs of two explanted artificial pump-lung (APL) devices (left: device 1; right: device 2). (C) Photographs of disassembled hollow fiber membrane sheets from one explanted APL device (left: all the fiber membranes; right: enlarged view of fiber membranes).
7 280 WU ET AL Ann Thorac Surg EVALUATION OF A WEARABLE PUMP-LUNG 2012;93: tory test values in days 1 to 6. The other organs (liver, spleen, gastrointestinal tract, brain) were of normal shape and appearance. The inflow and outflow cannulas were free of thrombus. There was a thin layer of intima inside the Dacron graft section of the outflow cannula. The graft section in 1 animal was slightly kinked at the fused interface between the Dacron graft and polyurethane tube. There was an adherent clot in the kinked site. Rings of thrombus were also found at some of the transition steps between the cannula and connectors. All of the APL devices explanted from the 5 sheep were clean and without structural failure (Fig 4B). There were no massive occlusive clots or deposited materials in the fiber bundle as commonly observed in the explanted oxygenators used in cardiopulmonary bypass or respiratory support [10-12]. Three of the five explanted devices were free of gross thrombotic formation in the fiber bundle and flow path. The other two had isolated clots in the space between the outer housing and the outer layer of the fiber bundle. There were scattered microthrombi ( 1 mm) in some areas of the fiber bundle and flow path (Fig 4C). The microscopic examination showed that these microthrombi mainly formed on the wefts of the fiber sheets and at the crevices of the blood contacting surfaces. Comment Various concepts for integrated pump-oxygenator devices have been presented before. The pumping function can be achieved by mating a blood pump to an oxygenator or rotating either an impeller within a fiber bundle or rotating the fiber bundle itself [13-19]. The integrated pump-oxygenator in the demised Cardiovention CORx system represents the strategy of serially connected pump-oxygenator [20]. The CORx system has only been used for cardiopulmonary bypass during cardiac surgical procedures, and not as an ambulatory respiratory system. The rotational component in these devices is usually supported by a mechanical shaft (with or without seal) and bearing, whereby many problems may arise, such as leaking, part failure, heat generation, hemolysis, platelet activation, and thrombosis formation. In our new design, the utilization of the magnetically levitated rotor/ impeller with a uniquely configured flow path across the fiber bundle helped mitigate the thromboembolic phenomenon and biocompatibility problem. The only moving component within the APL is a magnetically levitated rotor/impeller. This feature greatly reduces the risk of hemolysis, thrombus formation, and mechanical failure. The unique uniform radial flow path across the HFM bundle eliminates the flow stagnation. This feature ensures that the fiber membranes are effectively and uniformly perfused to achieve maximum gas exchange efficiency, and there are no deleterious stagnant flow or high shear stress areas. The early transient changes in hematocrit, complete blood count, platelet activation, creatine phosphokinase, lactic dehydrogenase, and liver transaminases were most likely to be surgery related since they all returned to their respective normal ranges after 2 weeks. Thus, it is reasonable to make the assumption that the blood chemistry data collected after recovery from the surgical trauma should be true indicators of biocompatibility. If an implanted device causes blood cell damage, end-organ dysfunction, and detrimental biologic responses, laboratory tests for these indications or functions should remain at abnormal levels. Both the surface-expressed p-selectin and soluble p-selectin also exhibited a similar trend. These observations indicate that the newly developed APL is biocompatible. Although isolated clots were observed in some of the devices, they did not impair the device functionality. During the experiments, both the pump function and oxygen transfer rate over the 30-day period were stable. It is interesting to notice that the clots (approximately 1 mm) were only observed in the flow path before fiber bundle. Because we observed the rings of thrombus in the transition steps between the tubing and connectors, some of them might have embolized and were entrapped by the fiber bundle. The fibers might have acted as a clot filter if clots had formed upstream. The existence of the kidney infarct in 1 of the study animals might not be related to the thrombosis in the implanted APL. If there were clots dislodged from the APL, the clots would have been trapped in the natural lungs and could not reach the kidneys because the APL was implanted in the right side of the heart. We have seen kidney infarcts in sheep without any surgical intervention. Therefore, we believe this infarct may have been a preexisting condition. The newly developed APL is an integrated pump oxygenator system that can provide both respiratory and cardiopulmonary support. Overall, the results from the animal studies are excellent, showing paracorporeal placement, partial to complete respiratory support, excellent gas transfer efficiency, excellent biocompatibility, and long-term reliability. The performance was stable for at least 30 days during the five long-term animal experiments. Compared with the conventional system, the prime volume and foreign surface area of the system are greatly reduced; therefore, the risks of systemic inflammatory reaction and hemodilution can be minimized. The new compact system reduces the complexity of operation and is suitable for ambulatory respiratory support. The extracorporeal placement enables easy exchange and permits sustained longterm (several months) respiratory support for bridge to lung transplant. The authors thank Ms Yanan Ding and Dr Jingping Hu for assistance with the hematologic measurements of blood samples. This work was supported by National Institutes of Health grants (R01HL082631, R42 HL084807, and R01HL088100). References 1. Bartlett RH. Extracorporeal life support: history and new directions. Semin Perinatol 2005;29: Weinacker AB, Vaszar LT. Acute respiratory distress syndrome: physiology and new management strategies. Annu Rev Med 2001;52:
8 Ann Thorac Surg WU ET AL 2012;93: EVALUATION OF A WEARABLE PUMP-LUNG Mangi AA, Mason DP, Yun JJ, Murthy SC, Pettersson GB. Bridge to lung transplantation using short-term ambulatory extracorporeal membrane oxygenation. J Thorac Cardiovasc Surg 2010;140: Garcia. JP, Iacono A, Kon ZN, Griffith BP. Ambulatory extracorporeal membrane oxygenation: a new approach for bridge-to-lung transplantation. J Thorac Cardiovasc Surg 2010;139:e Broomé M, Palmér K, Scherstén H, Frenckner B, Nilsson F. Prolonged extracorporeal membrane oxygenation and circulatory support as bridge to lung transplant. Ann Thorac Surg 2008;86: Potapov EV, Loforte A, Weng Y, et al. Experience with over 1000 implanted ventricular assist devices. J Card Surg 2008; 23: Zhang T, Cheng G, Koert A, et al. Functional and biocompatibility performances of an integrated Maglev pumpoxygenator. Artif Organs 2009;33: Dierickx PW, De Wachter DS, De Somer F, Van Nooten G, Verdonck PR. Mass transfer characteristics of artificial lungs. ASAIO J 2001;47: Gibber M, Wu ZJ, Chang WB, et al. In vivo experience of the child-size pediatric Jarvik 2000 heart: update. ASAIO J 2010; Sato H, Hall CM, Lafayette NG, et al. Thirty-day in-parallel artificial lung testing in sheep. Ann Thorac Surg 2007;84: Snyder TA, Eash HJ, Litwak KN, et al. Blood biocompatibility assessment of an intravenous gas exchange device. Artif Organs 2006;30: Lehle K, Philipp A, Gleich O, et al. Efficiency in extracorporeal membrane oxygenation-cellular deposits on polymethylpentene membranes increase resistance to blood flow and reduce gas exchange capacity. ASAIO J 2008;54: Wu ZJ, Gartner M, Litwak KN, Griffith BP. Progress toward an ambulatory pump-lung. J Thorac Cardiovasc Surg 2005; 130: Svitek RG, Frankowski BJ, Federspiel WJ. Evaluation of a pumping assist lung that uses a rotating fiber bundle. ASAIO J 2005;51: Tatsumi E, Takano H, Taenaka Y, et al. Development of an ultracompact integrated heart-lung assist device. Artif Organs 1999;23: von Segesser LK, Tozzi P, Mallbiabrrena I, Jegger D, Horisberger J, Corno A. Miniaturization in cardiopulmonary bypass. Perfusion 2003;18: Arens J, Schnoering H, Pfennig M, et al. The Aachen MiniHLM a miniaturized heartlung machine for neonates with an integrated rotary blood pump. Artif Organs 2010;34: Pantalos GM, Horrell T, Merkley T, et al. In vitro characterization and performance testing of the Ension pediatric cardiopulmonary assist system. ASAIO J 2009;55: Kopp R, Bensberg R, Arens J, et al. A miniaturized extracorporeal membrane oxygenator with integrated rotary blood pump: preclinical in vivo testing. ASAIO J 2011;57: Asakawa Y, Funakubo A, Fukunaga K, et al. Development of an implantable oxygenator with cross-flow pump. ASAIO J 2006;52: INVITED COMMENTARY Serious pulmonary disease represents a major health problem. At present more than 4,000 patients in the United States are on the waiting list for lung transplantation and nearly 300 die each year without receiving an organ. Others with severe acute pulmonary injury that is potentially reversible are not saved even with the best available mechanical ventilation techniques. In addition, a significant proportion of patients who receive a lung transplant experience severe early graft dysfunction that is potentially reversible if a period of intensive respiratory support is provided. In this article, Wu and associates [1] report the results of an experimental study evaluating hemodynamics, gas transfer, and biocompatibility of a novel integrated artificial pump lung, which was implanted between the right atrium and the pulmonary artery in 9 sheep. Although 4 animals died because of mechanical failure in some component, the survivors were found to have stable device flow and oxygen transfer that maintained good blood oxygen saturation. No end-organ dysfunction was identified and hemolysis was not detected. As such, this artificial pump lung may provide an option for intensive respiratory support in patients awaiting lung transplantation or for acute short-term therapy for patients with reversible pulmonary injury. This is an important first step in the path toward reliable and effective mechanical pulmonary support, but more work is needed. Further evaluation of carbon dioxide removal efficiency would be instructive. Examination of hemodynamic sequelae of this form of support, particularly in patients with impaired cardiac function or with pulmonary hypertension, is needed. In addition, analysis of safety measures, particularly the risk of gas embolism, and further studies in diseased lung models are needed before this novel technology can progress to clinical trials and ultimately to clinical acceptance. This study represents a first step toward improved support for patients with the most serious forms of pulmonary disease and provides an encouraging picture of the potential for progress in this field in the near future. Michael E. Jessen, MD Department of Cardiovascular and Thoracic Surgery University of Texas Southwestern Medical Center at Dallas 5323 Harry Hines Blvd Dallas, TX michael.jessen@utsouthwestern.edu Reference 1. Wu ZJ, Zhang T, Bianchi G, et al. Thirty-day in-vivo performance of a wearable artificial pump-lung for ambulatory respiratory support. Ann Thorac Surg 2012;93: by The Society of Thoracic Surgeons /$36.00 Published by Elsevier Inc doi: /j.athoracsur
Safety Evaluation of the Pericardial HeartWare MVAD System
 Safety Evaluation of the Pericardial HeartWare MVAD System Edwin C. McGee, Jr. M.D. Surgical Director, Heart Failure, Heart Transplantation, and Mechanical Assistance Bluhm Cardiovascular Institute, Northwestern
Safety Evaluation of the Pericardial HeartWare MVAD System Edwin C. McGee, Jr. M.D. Surgical Director, Heart Failure, Heart Transplantation, and Mechanical Assistance Bluhm Cardiovascular Institute, Northwestern
ECMO as a bridge to durable LVAD therapy. Jonathan Haft, MD Department of Cardiac Surgery University of Michigan
 ECMO as a bridge to durable LVAD therapy Jonathan Haft, MD Department of Cardiac Surgery University of Michigan Systolic Heart Failure Prevalence 4.8 million U.S. 287,000 deaths per year $39 billion spent
ECMO as a bridge to durable LVAD therapy Jonathan Haft, MD Department of Cardiac Surgery University of Michigan Systolic Heart Failure Prevalence 4.8 million U.S. 287,000 deaths per year $39 billion spent
Initial Experience With Single Cannulation for Venovenous Extracorporeal Oxygenation in Adults
 Initial Experience With Single Cannulation for Venovenous Extracorporeal Oxygenation in Adults Christian A. Bermudez, MD, Rodolfo V. Rocha, MD, Penny L. Sappington, MD, Yoshiya Toyoda, MD, PhD, Holt N.
Initial Experience With Single Cannulation for Venovenous Extracorporeal Oxygenation in Adults Christian A. Bermudez, MD, Rodolfo V. Rocha, MD, Penny L. Sappington, MD, Yoshiya Toyoda, MD, PhD, Holt N.
Extracorporeal life support (ECLS) supplements the
 CARDIOPULMONARY SUPPORT AND PHYSIOLOGY A PROSPECTIVE COMPARISON OF ATRIO-FEMORAL AND FEMORO-ATRIAL FLOW IN ADULT VENOVENOUS EXTRACORPOREAL LIFE SUPPORT Preston B. Rich, MD Samir S. Awad, MD Stefania Crotti,
CARDIOPULMONARY SUPPORT AND PHYSIOLOGY A PROSPECTIVE COMPARISON OF ATRIO-FEMORAL AND FEMORO-ATRIAL FLOW IN ADULT VENOVENOUS EXTRACORPOREAL LIFE SUPPORT Preston B. Rich, MD Samir S. Awad, MD Stefania Crotti,
Case scenario V AV ECMO. Dr Pranay Oza
 Case scenario V AV ECMO Dr Pranay Oza Case Summary 53 y/m, k/c/o MVP with myxomatous mitral valve with severe Mitral regurgitation underwent Mitral valve replacement with mini thoracotomy Pump time nearly
Case scenario V AV ECMO Dr Pranay Oza Case Summary 53 y/m, k/c/o MVP with myxomatous mitral valve with severe Mitral regurgitation underwent Mitral valve replacement with mini thoracotomy Pump time nearly
Cite this article as:
 doi: 10.21037/acs.2018.08.06 Cite this article as: Loforte A, Baiocchi M, Gliozzi G, Coppola G, Di Bartolomeo R, Lorusso R. Percutaneous pulmonary artery venting via jugular vein while on peripheral extracorporeal
doi: 10.21037/acs.2018.08.06 Cite this article as: Loforte A, Baiocchi M, Gliozzi G, Coppola G, Di Bartolomeo R, Lorusso R. Percutaneous pulmonary artery venting via jugular vein while on peripheral extracorporeal
ECMO BASICS CHLOE STEINSHOUER, MD PULMONARY AND SLEEP CONSULTANTS OF KANSAS
 ECMO BASICS CHLOE STEINSHOUER, MD PULMONARY AND SLEEP CONSULTANTS OF KANSAS DISCLOSURES No financial disclosures or conflicts of interest OBJECTIVES Define ECMO/ECLS and be able to identify the main types
ECMO BASICS CHLOE STEINSHOUER, MD PULMONARY AND SLEEP CONSULTANTS OF KANSAS DISCLOSURES No financial disclosures or conflicts of interest OBJECTIVES Define ECMO/ECLS and be able to identify the main types
Cardiovascular Institute
 Allegheny Health Network Cardiovascular Institute Extracorporeal Membrane Oxygenation (ECMO) Program Our patient survival rate is higher than the national average. ECMO experts. Multidisciplinary team.
Allegheny Health Network Cardiovascular Institute Extracorporeal Membrane Oxygenation (ECMO) Program Our patient survival rate is higher than the national average. ECMO experts. Multidisciplinary team.
Innovative ECMO Configurations in Adults
 Innovative ECMO Configurations in Adults Practice at a Single Center with Platinum Level ELSO Award for Excellence in Life Support Monika Tukacs, BSN, RN, CCRN Columbia University Irving Medical Center,
Innovative ECMO Configurations in Adults Practice at a Single Center with Platinum Level ELSO Award for Excellence in Life Support Monika Tukacs, BSN, RN, CCRN Columbia University Irving Medical Center,
Prolonged Extracorporeal Membrane Oxygenation Support for Acute Respiratory Distress Syndrome
 CASE REPORT Prolonged Extracorporeal Membrane Oxygenation Support for Acute Respiratory Distress Syndrome Wen-Je Ko,* Hsao-Hsun Hsu, Pi-Ru Tsai When all conventional treatments for respiratory failure
CASE REPORT Prolonged Extracorporeal Membrane Oxygenation Support for Acute Respiratory Distress Syndrome Wen-Je Ko,* Hsao-Hsun Hsu, Pi-Ru Tsai When all conventional treatments for respiratory failure
Kevin K. Nunnink Extracorporeal Membrane Oxygenation Program
 PATIE NT I N FO R M ATI O N Kevin K. Nunnink Extracorporeal Membrane Oxygenation Program A family s guide to understanding this specialized treatment for cardiac and pulmonary complications Saint Luke
PATIE NT I N FO R M ATI O N Kevin K. Nunnink Extracorporeal Membrane Oxygenation Program A family s guide to understanding this specialized treatment for cardiac and pulmonary complications Saint Luke
In-Parallel Artificial Lung Attachment at High Flows in Normal and Pulmonary Hypertension Models
 In-Parallel Artificial Lung Attachment at High Flows in Normal and Pulmonary Hypertension Models Begum Akay, MD, Junewai L. Reoma, MD, Daniele Camboni, MD, Joshua R. Pohlmann, MS, John M. Albert, BS, Ayushi
In-Parallel Artificial Lung Attachment at High Flows in Normal and Pulmonary Hypertension Models Begum Akay, MD, Junewai L. Reoma, MD, Daniele Camboni, MD, Joshua R. Pohlmann, MS, John M. Albert, BS, Ayushi
Extra Corporeal Life Support for Acute Heart failure
 Extra Corporeal Life Support for Acute Heart failure Benjamin Medalion, MD Director Heart and Lung Transplantation Department of Cardiothoracic Surgery Rabin Medical Center, Beilinson Campus, Israel Mechanical
Extra Corporeal Life Support for Acute Heart failure Benjamin Medalion, MD Director Heart and Lung Transplantation Department of Cardiothoracic Surgery Rabin Medical Center, Beilinson Campus, Israel Mechanical
Circulatory, Respiratory, and Excretory Systems
 34 Circulatory, Respiratory, and Excretory Systems section 1 Circulatory System Before You Read Press the tips of two fingers to the inside of your wrist, at a point just below your thumb. Can you feel
34 Circulatory, Respiratory, and Excretory Systems section 1 Circulatory System Before You Read Press the tips of two fingers to the inside of your wrist, at a point just below your thumb. Can you feel
Clinical Performance of Microporous Polypropylene Hollow-Fiber Oxygenator
 Clinical Performance of Microporous Polypropylene Hollow-Fiber Oxygenator Kozo Suma, M.D., Takayuki Tsuji, M.D., Yasuo Takeuchi, M.D., Kenji Inoue, M.D., Kenji Shiroma, M.D., Tetsuo Yoshikawa, M.D., and
Clinical Performance of Microporous Polypropylene Hollow-Fiber Oxygenator Kozo Suma, M.D., Takayuki Tsuji, M.D., Yasuo Takeuchi, M.D., Kenji Inoue, M.D., Kenji Shiroma, M.D., Tetsuo Yoshikawa, M.D., and
Preclinical Test of an Electro-Mechanical Implantable Left Ventricular Assist System
 ORIGINAL ARTICLE Korean Circ J 2008;38:7-11 Print ISSN 1738-5520 / On-line ISSN 1738-5555 Copyright 2008 The Korean Society of Cardiology Preclinical Test of an Electro-Mechanical Implantable Left Ventricular
ORIGINAL ARTICLE Korean Circ J 2008;38:7-11 Print ISSN 1738-5520 / On-line ISSN 1738-5555 Copyright 2008 The Korean Society of Cardiology Preclinical Test of an Electro-Mechanical Implantable Left Ventricular
FOCUS CONFERENCE 2018
 FOCUS CONFERENCE 2018 Current Practice in Pediatric and Neonatal Extracorporeal Life Support Daniel W. Chipman, RRT Assistant Director of Respiratory Care Massachusetts General Hospital Boston, Massachusetts
FOCUS CONFERENCE 2018 Current Practice in Pediatric and Neonatal Extracorporeal Life Support Daniel W. Chipman, RRT Assistant Director of Respiratory Care Massachusetts General Hospital Boston, Massachusetts
ECMO Extracorporeal Membrane Oxygenation
 ECMO Extracorporeal Membrane Oxygenation patienteducation.osumc.edu ECMO Table of Contents ECMO: Extracorporeal Membrane Oxygenation... 3 ECMO Treatment... 5 Care Team... 7 Discontinuing ECMO... 8 Notes,
ECMO Extracorporeal Membrane Oxygenation patienteducation.osumc.edu ECMO Table of Contents ECMO: Extracorporeal Membrane Oxygenation... 3 ECMO Treatment... 5 Care Team... 7 Discontinuing ECMO... 8 Notes,
Systemic inflammatory response syndrome (SIRS) after extracorporeal membrane oxygenation (ECMO): Incidence, risks and survivals.
 Thomas Jefferson University Jefferson Digital Commons Department of Surgery Faculty Papers Department of Surgery 9-1-2016 Systemic inflammatory response syndrome (SIRS) after extracorporeal membrane oxygenation
Thomas Jefferson University Jefferson Digital Commons Department of Surgery Faculty Papers Department of Surgery 9-1-2016 Systemic inflammatory response syndrome (SIRS) after extracorporeal membrane oxygenation
CIE Biology GCSE. 9: Transport in animals. Notes.
 CIE Biology GCSE 9: Transport in animals Notes The circulatory system acts as the main transport system in animals. It is made up of blood vessels such as arteries, veins and capillaries, in which blood
CIE Biology GCSE 9: Transport in animals Notes The circulatory system acts as the main transport system in animals. It is made up of blood vessels such as arteries, veins and capillaries, in which blood
Artificial Lung: A New Inspiration
 Artificial Lung: A New Inspiration Joseph B. Zwischenberger MD Johnston-Wright Professor and Chairman: Department of Surgery j.zwische@uky.edu The University of Kentucky Lexington, Kentucky Presenter Disclosure
Artificial Lung: A New Inspiration Joseph B. Zwischenberger MD Johnston-Wright Professor and Chairman: Department of Surgery j.zwische@uky.edu The University of Kentucky Lexington, Kentucky Presenter Disclosure
Temporary circulatory support in the form of extracorporeal
 Preliminary In Vivo Testing of a Novel Pump for Short-Term Extracorporeal Life Support David J. Spurlock, MD, Kelly Koch, BS, Daniel E. Mazur, BS, Emilia M. Fracz, ME, Robert H. Bartlett, MD, and Jonathan
Preliminary In Vivo Testing of a Novel Pump for Short-Term Extracorporeal Life Support David J. Spurlock, MD, Kelly Koch, BS, Daniel E. Mazur, BS, Emilia M. Fracz, ME, Robert H. Bartlett, MD, and Jonathan
Indications. The AngioVac cannula is intended for use as a venous drainage cannula and for the removal of fresh, soft thrombi or emboli
 Indications Straight Cannula or Cannula with 20 O Angle 17F Working Channel The AngioVac cannula is intended for use as a venous drainage cannula and for the removal of fresh, soft thrombi or emboli Radiopaque
Indications Straight Cannula or Cannula with 20 O Angle 17F Working Channel The AngioVac cannula is intended for use as a venous drainage cannula and for the removal of fresh, soft thrombi or emboli Radiopaque
Adverse Event. Adverse Event Status. Please enter the date of the event you are reporting: Please enter a label describing this event:
 Adverse Event Adverse Event Status Please enter the date of the event you are reporting: Please enter a label describing this event: 1 of 17 Adverse Event Infection Was there a major infection? Date of
Adverse Event Adverse Event Status Please enter the date of the event you are reporting: Please enter a label describing this event: 1 of 17 Adverse Event Infection Was there a major infection? Date of
Echo assessment of patients with an ECMO device
 Echo assessment of patients with an ECMO device Evangelos Leontiadis Cardiologist 1st Cardiology Dept. Onassis Cardiac Surgery Center Athens, Greece Gibbon HLM 1953 Goldstein DJ et al, NEJM 1998; 339:1522
Echo assessment of patients with an ECMO device Evangelos Leontiadis Cardiologist 1st Cardiology Dept. Onassis Cardiac Surgery Center Athens, Greece Gibbon HLM 1953 Goldstein DJ et al, NEJM 1998; 339:1522
ECLS as Bridge to Transplant
 ECLS as Bridge to Transplant Marcelo Cypel MD, MSc Assistant Professor of Surgery Division of Thoracic Surgery Toronto General Hospital University of Toronto Application of ECLS Bridge to lung recovery
ECLS as Bridge to Transplant Marcelo Cypel MD, MSc Assistant Professor of Surgery Division of Thoracic Surgery Toronto General Hospital University of Toronto Application of ECLS Bridge to lung recovery
First Experiences With the HeartWare Ventricular Assist System in Children
 First Experiences With the HeartWare Ventricular Assist System in Children Oliver Miera, MD, Evgenij V. Potapov, MD, PhD, Matthias Redlin, MD, Alexander Stepanenko, MD, Felix Berger, MD, PhD, Roland Hetzer,
First Experiences With the HeartWare Ventricular Assist System in Children Oliver Miera, MD, Evgenij V. Potapov, MD, PhD, Matthias Redlin, MD, Alexander Stepanenko, MD, Felix Berger, MD, PhD, Roland Hetzer,
PROVEN. TRUSTED. COMMITTED. HeartWare HVAD System
 PROVEN. TRUSTED. COMMITTED. HeartWare HVAD System PROVEN. TRUSTED. COMMITTED. 42% of all heart transplant patients worldwide are bridge to transplant with a VAD. 1 Our commitment to advance the treatment
PROVEN. TRUSTED. COMMITTED. HeartWare HVAD System PROVEN. TRUSTED. COMMITTED. 42% of all heart transplant patients worldwide are bridge to transplant with a VAD. 1 Our commitment to advance the treatment
Circulation And Blood. Circulation And Blood. Circulation And Blood. Circulation And Blood. Blood 10/22/2012
 Cells in our body build their own membranes and organelles Make their own ATP Assemble their own enzymes and other proteins And may manufacture substances used elsewhere in the body To do these things,
Cells in our body build their own membranes and organelles Make their own ATP Assemble their own enzymes and other proteins And may manufacture substances used elsewhere in the body To do these things,
Planned, Short-Term RVAD During Durable LVAD Implant: Indications and Management
 Planned, Short-Term RVAD During Durable LVAD Implant: Indications and Management Yoshifumi Naka, MD, PhD Columbia University Medical Center New York, NY Disclosure Abbott/St. Jude Med./Thoratec Consultant
Planned, Short-Term RVAD During Durable LVAD Implant: Indications and Management Yoshifumi Naka, MD, PhD Columbia University Medical Center New York, NY Disclosure Abbott/St. Jude Med./Thoratec Consultant
ECLS. The Basics. Jeannine Hermens Intensive Care Center UMC Utrecht
 ECLS The Basics Jeannine Hermens Intensive Care Center UMC Utrecht Conflict of interest None Terminology ECMO - ExtraCorporeal Membrane Oxygenation ECLS - ExtraCorporeal Life Support PLS - Veno-venous
ECLS The Basics Jeannine Hermens Intensive Care Center UMC Utrecht Conflict of interest None Terminology ECMO - ExtraCorporeal Membrane Oxygenation ECLS - ExtraCorporeal Life Support PLS - Veno-venous
Extracorporeal Life Support Organization (ELSO) Guidelines for Pediatric Respiratory Failure
 Extracorporeal Life Support Organization (ELSO) Guidelines for Pediatric Respiratory Failure Introduction This pediatric respiratory failure guideline is a supplement to ELSO s General Guidelines for all
Extracorporeal Life Support Organization (ELSO) Guidelines for Pediatric Respiratory Failure Introduction This pediatric respiratory failure guideline is a supplement to ELSO s General Guidelines for all
To ECMO Or Not To ECMO Challenges of venous arterial ECMO. Dr Emily Granger St Vincent s Hospital Darlinghurst NSW
 To ECMO Or Not To ECMO Challenges of venous arterial ECMO Dr Emily Granger St Vincent s Hospital Darlinghurst NSW The Start: 1972 St Vincent s Hospital The Turning Point ECMO program restarted in 2004
To ECMO Or Not To ECMO Challenges of venous arterial ECMO Dr Emily Granger St Vincent s Hospital Darlinghurst NSW The Start: 1972 St Vincent s Hospital The Turning Point ECMO program restarted in 2004
Ambulatory Oxygenator Right Ventricular Assist Device for Total Right Heart and Respiratory Support
 Ambulatory Oxygenator Right Ventricular Assist Device for Total Right Heart and Respiratory Support Dongfang Wang, MD, Scott D. Lick, MD, Xiaoqin Zhou, MD, Xiaojun Liu, MD, Robert J. Benkowski, MD, and
Ambulatory Oxygenator Right Ventricular Assist Device for Total Right Heart and Respiratory Support Dongfang Wang, MD, Scott D. Lick, MD, Xiaoqin Zhou, MD, Xiaojun Liu, MD, Robert J. Benkowski, MD, and
Mary Lou Garey MSN EMT-P MedFlight of Ohio
 Mary Lou Garey MSN EMT-P MedFlight of Ohio Function Prolonged and frequent access to venous circulation Allows for patient to carry on normal life; decrease number of needle sticks Medications, parenteral
Mary Lou Garey MSN EMT-P MedFlight of Ohio Function Prolonged and frequent access to venous circulation Allows for patient to carry on normal life; decrease number of needle sticks Medications, parenteral
Hemodynamic Monitoring and Circulatory Assist Devices
 Hemodynamic Monitoring and Circulatory Assist Devices Speaker: Jana Ogden Learning Unit 2: Hemodynamic Monitoring and Circulatory Assist Devices Hemodynamic monitoring refers to the measurement of pressure,
Hemodynamic Monitoring and Circulatory Assist Devices Speaker: Jana Ogden Learning Unit 2: Hemodynamic Monitoring and Circulatory Assist Devices Hemodynamic monitoring refers to the measurement of pressure,
The Role of ECMO in Thoracic Surgery. Matthew Hartwig, MD
 The Role of ECMO in Thoracic Surgery Matthew Hartwig, MD Disclosure Slide Consultant for Mallincrodkt and Quark Pharmaceuticals Case #1 28 y.o. female with tracheal mass No previous medical or surgical
The Role of ECMO in Thoracic Surgery Matthew Hartwig, MD Disclosure Slide Consultant for Mallincrodkt and Quark Pharmaceuticals Case #1 28 y.o. female with tracheal mass No previous medical or surgical
Mechanical Bleeding Complications During Heart Surgery
 Mechanical Bleeding Complications During Heart Surgery Arthur C. Beall, Jr., M.D., Kenneth L. Mattox, M.D., Mary Martin, R.N., C.C.P., Bonnie Cromack, C.C.P., and Gary Cornelius, C.C.P. * Potential for
Mechanical Bleeding Complications During Heart Surgery Arthur C. Beall, Jr., M.D., Kenneth L. Mattox, M.D., Mary Martin, R.N., C.C.P., Bonnie Cromack, C.C.P., and Gary Cornelius, C.C.P. * Potential for
1 Description. 2 Indications. 3 Warnings ASPIRATION CATHETER
 Page 1 of 5 ASPIRATION CATHETER Carefully read all instructions prior to use, observe all warnings and precautions noted throughout these instructions. Failure to do so may result in complications. STERILE.
Page 1 of 5 ASPIRATION CATHETER Carefully read all instructions prior to use, observe all warnings and precautions noted throughout these instructions. Failure to do so may result in complications. STERILE.
Extracorporeal Membrane Oxygenation (ECMO)
 Extracorporeal Membrane Oxygenation (ECMO) Policy Number: Original Effective Date: MM.12.006 05/16/2006 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 01/01/2017 Section: Other/Miscellaneous
Extracorporeal Membrane Oxygenation (ECMO) Policy Number: Original Effective Date: MM.12.006 05/16/2006 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 01/01/2017 Section: Other/Miscellaneous
Transfusion and Blood Conservation
 Transfusion and Blood Conservation Kenneth G. Shann, CCP Assistant Director, Perfusion Services Senior Advisor, Performance Improvement Department of Cardiovascular and Thoracic Surgery Montefiore Medical
Transfusion and Blood Conservation Kenneth G. Shann, CCP Assistant Director, Perfusion Services Senior Advisor, Performance Improvement Department of Cardiovascular and Thoracic Surgery Montefiore Medical
ECLS Registry Form Extracorporeal Life Support Organization (ELSO)
 ECLS Registry Form Extracorporeal Life Support Organization (ELSO) Center ID: Center name: Run No (for this patient) Unique ID: Birth Date/Time Sex: (M, F) Race: (Asian, Black, Hispanic, White, Other)
ECLS Registry Form Extracorporeal Life Support Organization (ELSO) Center ID: Center name: Run No (for this patient) Unique ID: Birth Date/Time Sex: (M, F) Race: (Asian, Black, Hispanic, White, Other)
Low Dose versus High Dose Heparinization during Post Cardiotomy ECMO: A Case Control Study Disclosures Introduction
 Low Dose versus High Dose Heparinization during Post Cardiotomy ECMO: A Case Control Study Vanessa Arnold, BS Mindy M Blackwell, MS, CCP Perfusion Technology Program College of Health Sciences Rush University
Low Dose versus High Dose Heparinization during Post Cardiotomy ECMO: A Case Control Study Vanessa Arnold, BS Mindy M Blackwell, MS, CCP Perfusion Technology Program College of Health Sciences Rush University
HeartWare ADVANCE Bridge to Transplant Trial and Continued Access Protocol Update
 HeartWare ADVANCE Bridge to Transplant Trial and Continued Access Protocol Update Mark S. Slaughter, MD University of Louisville, KY, USA HeartWare Users Meeting 29 October 2012 Barcelona, Spain HEARTWARE,
HeartWare ADVANCE Bridge to Transplant Trial and Continued Access Protocol Update Mark S. Slaughter, MD University of Louisville, KY, USA HeartWare Users Meeting 29 October 2012 Barcelona, Spain HEARTWARE,
Chapter 42: Circulation / Gas Exchange. d = t 2
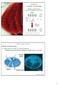 Chapter 42: Circulation / Gas Exchange Transport systems connect organs of exchange with body cells Diffusion Lung Blood 100 m 1 s 1 mm 100 s 1 cm 10000 s d = t 2 Bulk Flow (Pressure) Blood Cells Methods
Chapter 42: Circulation / Gas Exchange Transport systems connect organs of exchange with body cells Diffusion Lung Blood 100 m 1 s 1 mm 100 s 1 cm 10000 s d = t 2 Bulk Flow (Pressure) Blood Cells Methods
Mechanical Cardiac Support in Acute Heart Failure. Michael Felker, MD, MHS Associate Professor of Medicine Director of Heart Failure Research
 Mechanical Cardiac Support in Acute Heart Failure Michael Felker, MD, MHS Associate Professor of Medicine Director of Heart Failure Research Disclosures Research Support and/or Consulting NHLBI Amgen Cytokinetics
Mechanical Cardiac Support in Acute Heart Failure Michael Felker, MD, MHS Associate Professor of Medicine Director of Heart Failure Research Disclosures Research Support and/or Consulting NHLBI Amgen Cytokinetics
Disclosures. No disclosures to report
 Disclosures No disclosures to report Update on MOMENTUM 3 Trial: The Final Word? Francis D. Pagani MD PhD Otto Gago MD Professor of Cardiac Surgery University of Michigan Ann Arbor, Michigan, USA LVAD
Disclosures No disclosures to report Update on MOMENTUM 3 Trial: The Final Word? Francis D. Pagani MD PhD Otto Gago MD Professor of Cardiac Surgery University of Michigan Ann Arbor, Michigan, USA LVAD
Perfusion for Repair of Aneurysms of the Transverse Aortic Arch
 technique This new section is open for technicians to explore the unusual, the difficult, the innovative methods by which perfusion meets the challenge of the hour and produces the ultimate goal - a life
technique This new section is open for technicians to explore the unusual, the difficult, the innovative methods by which perfusion meets the challenge of the hour and produces the ultimate goal - a life
Extracorporeal membrane oxygenators (ECMO) provide
 Case Report Interhospital Transport of the ECMO Patients in Bangkok Hospital Abstract An extracorporeal membrane oxygenator (ECMO) is used to support the heart and lungs in patients with severe cardiogenic
Case Report Interhospital Transport of the ECMO Patients in Bangkok Hospital Abstract An extracorporeal membrane oxygenator (ECMO) is used to support the heart and lungs in patients with severe cardiogenic
Understanding Blood Tests
 PATIENT EDUCATION patienteducation.osumc.edu Your heart pumps the blood in your body through a system of blood vessels. Blood delivers oxygen and nutrients to all parts of the body. It also carries away
PATIENT EDUCATION patienteducation.osumc.edu Your heart pumps the blood in your body through a system of blood vessels. Blood delivers oxygen and nutrients to all parts of the body. It also carries away
Veno-Venous ECMO Support. Chris Cropsey, MD Sept. 21, 2015
 Veno-Venous ECMO Support Chris Cropsey, MD Sept. 21, 2015 Objectives List indications and contraindications for ECMO Describe hemodynamics and oxygenation on ECMO Discuss evidence for ECMO outcomes Identify
Veno-Venous ECMO Support Chris Cropsey, MD Sept. 21, 2015 Objectives List indications and contraindications for ECMO Describe hemodynamics and oxygenation on ECMO Discuss evidence for ECMO outcomes Identify
Circulatory System Notes
 Circulatory System Notes Functions of Circulatory System A. Transports B. Transports C. Transports D. Transports E. of fluids F. G. Regulate temperature H. Blood clotting Characteristics of various blood
Circulatory System Notes Functions of Circulatory System A. Transports B. Transports C. Transports D. Transports E. of fluids F. G. Regulate temperature H. Blood clotting Characteristics of various blood
7.L.1.4 Circulatory System Guided Study Notes. Circulation
 1 7.L.1.4 Circulatory System Guided Study Notes Circulation Sect. 1: The Body s Transport System Sect. 2: A Closer Look at Blood Vessels Sect. 3: Blood and Lymph Sect. 4: Cardiovascular Health Sect. 1:
1 7.L.1.4 Circulatory System Guided Study Notes Circulation Sect. 1: The Body s Transport System Sect. 2: A Closer Look at Blood Vessels Sect. 3: Blood and Lymph Sect. 4: Cardiovascular Health Sect. 1:
37 1 The Circulatory System
 H T H E E A R T 37 1 The Circulatory System The circulatory system and respiratory system work together to supply cells with the nutrients and oxygen they need to stay alive. a) The respiratory system:
H T H E E A R T 37 1 The Circulatory System The circulatory system and respiratory system work together to supply cells with the nutrients and oxygen they need to stay alive. a) The respiratory system:
Complications of ECLS. Rajasekhar Malyala, MD Assistant Professor, Surgery University of Kentucky
 Complications of ECLS Rajasekhar Malyala, MD Assistant Professor, Surgery University of Kentucky Faculty Disclosure No financial Disclosures Education Need/Practice Gap Recommendations and guidelines regarding
Complications of ECLS Rajasekhar Malyala, MD Assistant Professor, Surgery University of Kentucky Faculty Disclosure No financial Disclosures Education Need/Practice Gap Recommendations and guidelines regarding
ECMO for cardiac arrest patients: Update 2017
 ECMO for cardiac arrest patients: Update 2017 Lim Swee Han MBBS (NUS), FRCS Ed (A&E), FRCP (Edin), FAMS Senior Consultant, Department of Emergency Medicine, Singapore General Hospital Adjunct Associate
ECMO for cardiac arrest patients: Update 2017 Lim Swee Han MBBS (NUS), FRCS Ed (A&E), FRCP (Edin), FAMS Senior Consultant, Department of Emergency Medicine, Singapore General Hospital Adjunct Associate
ORIGINAL ARTICLE. Alexander M. Bernhardt a, *, Theo M.M.H. De By b, Hermann Reichenspurner a and Tobias Deuse a. Abstract INTRODUCTION
 European Journal of Cardio-Thoracic Surgery 48 (2015) 158 162 doi:10.1093/ejcts/ezu406 Advance Access publication 29 October 2014 ORIGINAL ARTICLE Cite this article as: Bernhardt AM, De By TMMH, Reichenspurner
European Journal of Cardio-Thoracic Surgery 48 (2015) 158 162 doi:10.1093/ejcts/ezu406 Advance Access publication 29 October 2014 ORIGINAL ARTICLE Cite this article as: Bernhardt AM, De By TMMH, Reichenspurner
Pro 01: Development and In Vitro Evaluation of a Hydraulic System for a Mini axial Flow Blood Pump
 Pro 01: Development and In Vitro Evaluation of a Hydraulic System for a Mini axial Flow Blood Pump Background: Fully implantable rotary blood pumps are used for mechanical circulatory support of heart
Pro 01: Development and In Vitro Evaluation of a Hydraulic System for a Mini axial Flow Blood Pump Background: Fully implantable rotary blood pumps are used for mechanical circulatory support of heart
Respiratory dialysis with an active-mixing extracorporeal carbon dioxide removal system in a chronic sheep study
 Intensive Care Med (2012) 38:1705 1711 DOI 10.1007/s00134-012-2651-8 EXPERIMENTAL Peter D. Wearden William J. Federspiel Scott W. Morley Meir Rosenberg Paul D. Bieniek Laura W. Lund Burt D. Ochs Respiratory
Intensive Care Med (2012) 38:1705 1711 DOI 10.1007/s00134-012-2651-8 EXPERIMENTAL Peter D. Wearden William J. Federspiel Scott W. Morley Meir Rosenberg Paul D. Bieniek Laura W. Lund Burt D. Ochs Respiratory
Jennifer A. Brown The Cleveland Clinic School of Perfusion Cleveland, Ohio
 Biventricular Heart Failure Advanced Treatment Options at The Cleveland Clinic Jennifer A. Brown The Cleveland Clinic School of Perfusion Cleveland, Ohio I have no disclosures. Examine respiratory and
Biventricular Heart Failure Advanced Treatment Options at The Cleveland Clinic Jennifer A. Brown The Cleveland Clinic School of Perfusion Cleveland, Ohio I have no disclosures. Examine respiratory and
ISPUB.COM. Concepts Of Neonatal ECMO. D Thakar, A Sinha, O Wenker HISTORY PATIENT SELECTION AND ECMO CRITERIA
 ISPUB.COM The Internet Journal of Emergency and Intensive Care Medicine Volume 5 Number 2 D Thakar, A Sinha, O Wenker Citation D Thakar, A Sinha, O Wenker.. The Internet Journal of Emergency and Intensive
ISPUB.COM The Internet Journal of Emergency and Intensive Care Medicine Volume 5 Number 2 D Thakar, A Sinha, O Wenker Citation D Thakar, A Sinha, O Wenker.. The Internet Journal of Emergency and Intensive
Cardioplegia Circuit Products { CARDIOPLEGIA ADAPTERS}
 Cardioplegia Circuit Products { CARDIOPLEGIA ADAPTERS} Cardioplegia adapters are designed to permit customization of the cardioplegia circuit. Medtronic adapters can be used to connect multiple cardioplegia
Cardioplegia Circuit Products { CARDIOPLEGIA ADAPTERS} Cardioplegia adapters are designed to permit customization of the cardioplegia circuit. Medtronic adapters can be used to connect multiple cardioplegia
2017 Cardiovascular Symposium CARDIAC SURGERY UPDATE: SMALLER INCISIONS AND LESS COUMADIN DAVID L. SAINT, MD
 2017 Cardiovascular Symposium CARDIAC SURGERY UPDATE: SMALLER INCISIONS AND LESS COUMADIN DAVID L. SAINT, MD David L Saint M.D. Tallahassee Memorial Hospital Southern Medical Group Division of Cardiothoracic
2017 Cardiovascular Symposium CARDIAC SURGERY UPDATE: SMALLER INCISIONS AND LESS COUMADIN DAVID L. SAINT, MD David L Saint M.D. Tallahassee Memorial Hospital Southern Medical Group Division of Cardiothoracic
BASIC CRITICAL CARE OF THE PATIENT. Hannelisa Callisen PA C February 2017
 BASIC CRITICAL CARE OF THE PATIENT Hannelisa Callisen PA C February 2017 Disclosures Industry: None ECMO is off label Objectives ECMO initiation selection, cannulation Physiology : Review of DO2 on ECMO
BASIC CRITICAL CARE OF THE PATIENT Hannelisa Callisen PA C February 2017 Disclosures Industry: None ECMO is off label Objectives ECMO initiation selection, cannulation Physiology : Review of DO2 on ECMO
ECMO CPR. Ravi R. Thiagarajan MBBS, MPH. Cardiac Intensive Care Unit
 ECMO CPR Ravi R. Thiagarajan MBBS, MPH Staff Intensivist Cardiac Intensive Care Unit Children s Hospital Boston PCICS 2008, Miami, FL No disclosures Disclosures Outline Outcomes for Pediatric in-hospital
ECMO CPR Ravi R. Thiagarajan MBBS, MPH Staff Intensivist Cardiac Intensive Care Unit Children s Hospital Boston PCICS 2008, Miami, FL No disclosures Disclosures Outline Outcomes for Pediatric in-hospital
The DuraHeart VAD, a Magnetically Levitated Centrifugal Pump
 Circ J 2006; 70: 1421 1425 The DuraHeart VAD, a Magnetically Levitated Centrifugal Pump The University of Vienna Bridgeto-Transplant Experience Tomohiro Nishinaka, MD; Heinrich Schima, PhD*; Wilfried Roethy,
Circ J 2006; 70: 1421 1425 The DuraHeart VAD, a Magnetically Levitated Centrifugal Pump The University of Vienna Bridgeto-Transplant Experience Tomohiro Nishinaka, MD; Heinrich Schima, PhD*; Wilfried Roethy,
HEARTMATE 3 LEFT VENTRICULAR ASSIST SYSTEM
 HEARTMATE 3 LEFT VENTRICULAR ASSIST SYSTEM A New Milestone in LVAD Therapy HeartMate 3 Left Ventricular Assist Device Introducing the new HEARTMATE 3 LVAD WITH FULL MAGLEV FLOW TECHNOLOGY HeartMate 3 LVAD
HEARTMATE 3 LEFT VENTRICULAR ASSIST SYSTEM A New Milestone in LVAD Therapy HeartMate 3 Left Ventricular Assist Device Introducing the new HEARTMATE 3 LVAD WITH FULL MAGLEV FLOW TECHNOLOGY HeartMate 3 LVAD
Patient Management Code Blue in the CT Suite
 Patient Management Code Blue in the CT Suite David Stultz, MD November 28, 2001 Case Presentation A 53-year-old woman experienced acute respiratory distress during an IV contrast enhanced CT scan of the
Patient Management Code Blue in the CT Suite David Stultz, MD November 28, 2001 Case Presentation A 53-year-old woman experienced acute respiratory distress during an IV contrast enhanced CT scan of the
Use of EKOS Catheter in the management of Venous Mr. Manoj Niverthi, Mr. Sarang Pujari, and Ms. Nupur Dandavate, The GTF Group
 Use of EKOS Catheter in the management of Venous Thromboembolism @ Mr. Manoj Niverthi, Mr. Sarang Pujari, and Ms. Nupur Dandavate, The GTF Group Introduction Georgia Thrombosis Forum (GTF, www.gtfonline.net)
Use of EKOS Catheter in the management of Venous Thromboembolism @ Mr. Manoj Niverthi, Mr. Sarang Pujari, and Ms. Nupur Dandavate, The GTF Group Introduction Georgia Thrombosis Forum (GTF, www.gtfonline.net)
Artificial Lungs: A New Inspiration
 Artificial Lungs: A New Inspiration Joseph B. Zwischenberger MD Johnston-Wright Professor and Chairman: Department of Surgery j.zwische@uky.edu The University of Kentucky Lexington, Kentucky Presenter
Artificial Lungs: A New Inspiration Joseph B. Zwischenberger MD Johnston-Wright Professor and Chairman: Department of Surgery j.zwische@uky.edu The University of Kentucky Lexington, Kentucky Presenter
Ultrasound-enhanced, catheter-directed thrombolysis for pulmonary embolism
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Ultrasound-enhanced, catheter-directed thrombolysis for pulmonary embolism A pulmonary embolism (PE) is
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Ultrasound-enhanced, catheter-directed thrombolysis for pulmonary embolism A pulmonary embolism (PE) is
3.4. The Circulatory System
 The Circulatory System The human circulatory system is made up of the blood, the heart, and the blood vessels. The function of the circulatory system is to transport substances around the body. It moves
The Circulatory System The human circulatory system is made up of the blood, the heart, and the blood vessels. The function of the circulatory system is to transport substances around the body. It moves
Understanding the Pediatric Ventricular Assist Device
 Understanding the Pediatric Ventricular Assist Device W. James Parks, MSc., MD Pediatric Cardiologist Assistant Professor of Pediatrics and Radiology Children s Healthcare of Atlanta Sibley Heart Center
Understanding the Pediatric Ventricular Assist Device W. James Parks, MSc., MD Pediatric Cardiologist Assistant Professor of Pediatrics and Radiology Children s Healthcare of Atlanta Sibley Heart Center
By Semih. The first system is about the respiratory system. It provides our body with the oxygen it needs and gets rid of carbon dioxide.
 By Semih Exercise is very important to our body. Exercise is an everyday activity and it keeps your body fit and healthy. There are 3 main systems involved are the respiratory system, the circulatory system
By Semih Exercise is very important to our body. Exercise is an everyday activity and it keeps your body fit and healthy. There are 3 main systems involved are the respiratory system, the circulatory system
CONVENTIONAL ADULT CANNULAE
 CONVENTIONAL ADULT CANNULAE Cannulae that can Comprehensive portfolio of aortic, venous and cardioplegia cannulae, vents, suction wands and sumps 1. Assmann et al. Artificial Organs 214; 39(3): 23-211
CONVENTIONAL ADULT CANNULAE Cannulae that can Comprehensive portfolio of aortic, venous and cardioplegia cannulae, vents, suction wands and sumps 1. Assmann et al. Artificial Organs 214; 39(3): 23-211
CONVENTIONAL ADULT CANNULAE
 CONVENTIONAL ADULT CANNULAE Cannulae that can Comprehensive portfolio of aortic, venous and cardioplegia cannulae, vents, suction wands and sumps CONVENTIONAL ADULT CANNULAE Conventional Adult Cannulae
CONVENTIONAL ADULT CANNULAE Cannulae that can Comprehensive portfolio of aortic, venous and cardioplegia cannulae, vents, suction wands and sumps CONVENTIONAL ADULT CANNULAE Conventional Adult Cannulae
Patient Information. Atrial Septal Defect (ASD) Repair
 Patient Information Atrial Septal Defect (ASD) Repair Table of Contents Overview................................. 4 Symptoms................................ 5 Causes..................................
Patient Information Atrial Septal Defect (ASD) Repair Table of Contents Overview................................. 4 Symptoms................................ 5 Causes..................................
1. Which of the following blood vessels has a thin elastic layer? A. Aorta. B. Pulmonary artery. C. Posterior vena cava. D. Mesenteric capillary.
 CIRCULATORY SYSTEM 1. Which of the following blood vessels has a thin elastic layer? A. Aorta. B. Pulmonary artery. C. Posterior vena cava. D. Mesenteric capillary. 2. Capillary beds are equipped with
CIRCULATORY SYSTEM 1. Which of the following blood vessels has a thin elastic layer? A. Aorta. B. Pulmonary artery. C. Posterior vena cava. D. Mesenteric capillary. 2. Capillary beds are equipped with
Vessels by Design: Basic Vessel Anatomy. Student Information Page 3A
 Vessels by Design: Basic Vessel Anatomy Student Information Page 3A Activity Introduction: Once you get home from running around all day, your throat is probably a little dry. You go to your kitchen, get
Vessels by Design: Basic Vessel Anatomy Student Information Page 3A Activity Introduction: Once you get home from running around all day, your throat is probably a little dry. You go to your kitchen, get
Pearson's Comprehensive Medical Assisting Administrative and Clinical Competencies
 Pearson's Comprehensive Medical Assisting Administrative and Clinical Competencies THIRD EDITION CHAPTER 27 The Cardiovascular System Lesson 1: Overview of the Cardiovascular System Lesson Objectives Upon
Pearson's Comprehensive Medical Assisting Administrative and Clinical Competencies THIRD EDITION CHAPTER 27 The Cardiovascular System Lesson 1: Overview of the Cardiovascular System Lesson Objectives Upon
ECMO & Renal Failure Epidemeology Renal failure & effect on out come
 ECMO Induced Renal Issues Transient renal dysfunction Improvement in renal function ECMO & Renal Failure Epidemeology Renal failure & effect on out come With or Without RRT Renal replacement Therapy Utilizes
ECMO Induced Renal Issues Transient renal dysfunction Improvement in renal function ECMO & Renal Failure Epidemeology Renal failure & effect on out come With or Without RRT Renal replacement Therapy Utilizes
Left Ventricular Assist Devices (LVADs): Overview and Future Directions
 Left Ventricular Assist Devices (LVADs): Overview and Future Directions FATIMA KARAKI, M.D. PGY-3, DEPARTMENT OF MEDICINE WASHINGTON UNIVERSITY IN ST. LOUIS ST. LOUIS, MISSOURI, USA St. Louis, Missouri,
Left Ventricular Assist Devices (LVADs): Overview and Future Directions FATIMA KARAKI, M.D. PGY-3, DEPARTMENT OF MEDICINE WASHINGTON UNIVERSITY IN ST. LOUIS ST. LOUIS, MISSOURI, USA St. Louis, Missouri,
Extracorporeal support in acute respiratory failure. Dr Anthony Bastin Consultant in critical care Royal Brompton Hospital, London
 Extracorporeal support in acute respiratory failure Dr Anthony Bastin Consultant in critical care Royal Brompton Hospital, London Objectives By the end of this session, you will be able to: Describe different
Extracorporeal support in acute respiratory failure Dr Anthony Bastin Consultant in critical care Royal Brompton Hospital, London Objectives By the end of this session, you will be able to: Describe different
End Stage Heart Failure - Time to Bring the Hammer Down
 End Stage Heart Failure - Time to Bring the Hammer Down Eric R. Skipper, MD, FACS Chief, Adult Cardiovascular Surgery Surgical Director of Cardiac Transplantation and Mechanical Circulatory Support 2 3
End Stage Heart Failure - Time to Bring the Hammer Down Eric R. Skipper, MD, FACS Chief, Adult Cardiovascular Surgery Surgical Director of Cardiac Transplantation and Mechanical Circulatory Support 2 3
ORIGINAL ARTICLE. Abstract INTRODUCTION
 European Journal of Cardio-Thoracic Surgery 52 (2017) 1055 1061 doi:10.1093/ejcts/ezx189 Advance Access publication 22 June 2017 ORIGINAL ARTICLE Cite this article as: Takeda K, Garan AR, Ando M, Han J,
European Journal of Cardio-Thoracic Surgery 52 (2017) 1055 1061 doi:10.1093/ejcts/ezx189 Advance Access publication 22 June 2017 ORIGINAL ARTICLE Cite this article as: Takeda K, Garan AR, Ando M, Han J,
Use of Blood Lactate Measurements in the Critical Care Setting
 Use of Blood Lactate Measurements in the Critical Care Setting John G Toffaletti, PhD Director of Blood Gas and Clinical Pediatric Labs Professor of Pathology Duke University Medical Center Chief, VAMC
Use of Blood Lactate Measurements in the Critical Care Setting John G Toffaletti, PhD Director of Blood Gas and Clinical Pediatric Labs Professor of Pathology Duke University Medical Center Chief, VAMC
Adult Extracorporeal Life Support (ECLS)
 Adult Extracorporeal Life Support (ECLS) Steven Scott, M.D., F.A.C.S. Piedmont Heart Institute Cardiothoracic Surgery Disclosures None ECMO = ECLS A technique of life support that involves a continuous
Adult Extracorporeal Life Support (ECLS) Steven Scott, M.D., F.A.C.S. Piedmont Heart Institute Cardiothoracic Surgery Disclosures None ECMO = ECLS A technique of life support that involves a continuous
From Recovery to Transplant: One Patient's Journey
 From Recovery to Transplant: One Patient's Journey Tonya Elliott, RN, MSN Assist Device and Thoracic Transplant Coordinator Inova Transplant Center at Inova Fairfax Hospital Falls Church, VA Introduction
From Recovery to Transplant: One Patient's Journey Tonya Elliott, RN, MSN Assist Device and Thoracic Transplant Coordinator Inova Transplant Center at Inova Fairfax Hospital Falls Church, VA Introduction
Blood Functions. Blood and the Cardiovascular System. Blood. Plasma. Erythrocytes (RBCs) Erythrocytes (RBCs) 4/7/2017
 Blood Functions Blood and the Cardiovascular System Distribution Delivery of oxygen and nutrients to all body cells; Transport of wastes to lungs and excretory organs; Transport of hormones Regulation
Blood Functions Blood and the Cardiovascular System Distribution Delivery of oxygen and nutrients to all body cells; Transport of wastes to lungs and excretory organs; Transport of hormones Regulation
ECMO: a breakthrough in care for respiratory failure. PD Dr. Thomas Müller Regensburg no conflict of interest
 ECMO: a breakthrough in care for respiratory failure? PD Dr. Thomas Müller Regensburg no conflict of interest 1 Overview Mortality of severe ARDS Indication for ECMO PaO 2 /FiO 2 Efficiency of ECMO: gas
ECMO: a breakthrough in care for respiratory failure? PD Dr. Thomas Müller Regensburg no conflict of interest 1 Overview Mortality of severe ARDS Indication for ECMO PaO 2 /FiO 2 Efficiency of ECMO: gas
One system involved in exercising is the respiratory system. The respiratory system includes three main parts breathing, lungs and blood.
 By Andrea.K 2012 Grade 3 There are many different systems that help us exercise and the three main systems are the respiratory system which is about how we breathe, the circulatory system which is about
By Andrea.K 2012 Grade 3 There are many different systems that help us exercise and the three main systems are the respiratory system which is about how we breathe, the circulatory system which is about
University of Florida Department of Surgery. CardioThoracic Surgery VA Learning Objectives
 University of Florida Department of Surgery CardioThoracic Surgery VA Learning Objectives This service performs coronary revascularization, valve replacement and lung cancer resections. There are 2 faculty
University of Florida Department of Surgery CardioThoracic Surgery VA Learning Objectives This service performs coronary revascularization, valve replacement and lung cancer resections. There are 2 faculty
Transport in Animals (IGCSE Biology Syllabus )
 Transport in Animals (IGCSE Biology Syllabus 2016-2018) Blood o Red blood cells: heamoglobin and oxygen transport o White blood cells: phagocyte phagocytosis (engulf pathogen, vesicles fuse with vacuole,
Transport in Animals (IGCSE Biology Syllabus 2016-2018) Blood o Red blood cells: heamoglobin and oxygen transport o White blood cells: phagocyte phagocytosis (engulf pathogen, vesicles fuse with vacuole,
Case Report Reconstruction of Deep Posttraumatic Tracheal Stenosis while under Lung Assist
 IBIMA Publishing International Journal of Case Reports in Medicine http://www.ibimapublishing.com/journals/ijcrm/ijcrm.html Vol. 2013 (2013), Article ID 540350, 5 pages DOI: 10.5171/2013.540350 Case Report
IBIMA Publishing International Journal of Case Reports in Medicine http://www.ibimapublishing.com/journals/ijcrm/ijcrm.html Vol. 2013 (2013), Article ID 540350, 5 pages DOI: 10.5171/2013.540350 Case Report
ADULT OXYGENATORS CATALOGUE
 ADULT OXYGENATORS CATALOGUE A solution for every need Clinical flexibility Optimized priming High performance gas exchange Low contact surface Low GME activity Easy to set up and debubbling The path of
ADULT OXYGENATORS CATALOGUE A solution for every need Clinical flexibility Optimized priming High performance gas exchange Low contact surface Low GME activity Easy to set up and debubbling The path of
CRRT Fundamentals Pre- and Post- Test. AKI & CRRT Conference 2018
 CRRT Fundamentals Pre- and Post- Test AKI & CRRT Conference 2018 Question 1 Which ONE of the following statements regarding solute clearance in CRRT is MOST correct? A. Convective and diffusive solute
CRRT Fundamentals Pre- and Post- Test AKI & CRRT Conference 2018 Question 1 Which ONE of the following statements regarding solute clearance in CRRT is MOST correct? A. Convective and diffusive solute
Module 7 Your Blood Work
 Module 7 Your Blood Work Every month you will need to collect a sample of your blood just before you start dialysis, and depending on your doctor s recommendation, at the end of your dialysis treatment.
Module 7 Your Blood Work Every month you will need to collect a sample of your blood just before you start dialysis, and depending on your doctor s recommendation, at the end of your dialysis treatment.
Types of circulatory systems
 Types of circulatory systems Open system Mostly invertebrates Low pressure Haemocoel Suitable for small organisms Closed system Vertebrates High pressure Blood remains in blood vessels Separate tissue
Types of circulatory systems Open system Mostly invertebrates Low pressure Haemocoel Suitable for small organisms Closed system Vertebrates High pressure Blood remains in blood vessels Separate tissue
Diagnosis of Device Thrombosis
 Diagnosis of Device Thrombosis Andrew Civitello MD, FACC Medical Director, Heart Transplant Program Director, Fellowship Co-Director, Baylor St. Luke's Medical Center / Texas Heart Institute Trends in
Diagnosis of Device Thrombosis Andrew Civitello MD, FACC Medical Director, Heart Transplant Program Director, Fellowship Co-Director, Baylor St. Luke's Medical Center / Texas Heart Institute Trends in
