Techniques of Exposure, Hilar Dissection, and Parenchymal Division in Hepatic Surgery
|
|
|
- Dylan Shields
- 6 years ago
- Views:
Transcription
1 Techniques of Exposure, Hilar Dissection, and Parenchymal Division in Hepatic Surgery William C. Chapman, MD, J. Kelly Wright, MD, Paul E. Wise, MD, and C. Wright Pinson, MD, MBA A number of methods for hepatic parenchymal transection facilitate ligation and division of hepatic vessels and biliary ducts in the plane of resection. Each represents a tool available to the liver surgeon, depending on training, experience, and personal preference. Although each method may have slight advantages in specific circumstances, experienced liver surgeons can usually successfully complete the parenchymal transection using various techniques. SURGICAL TECHNIQUE Exposure Proper exposure is crucial to the safety, ease, and efficiency of any operative procedure. This is no less true for hepatobiliary procedures because of the size and location of the liver and its proximity to major vascular structures. Surgeons have developed numerous abdominal and thoracic incisions to provide adequate access to the entire surface of the liver. In addi- tion, by using self-retaining retractor systems, the surgeon can obtain and maintain adequate exposure without depending on fatigable and nonstationary assistants. Performing complete dissection of the liver's ligamentous attachments can then provide even better exposure by achieving increased mobility of the organ and the surrounding viscera. From the Division of Hepatobiliary Surgery and Liver Transplantation, Department of Surgery, Vanderbilt University Medical Center, Nashville, TN. Address reprint requests to C. Wright Pinson, M.D., M.B.A., F.A.C.S, Department of Surgery, Division of Hepatobiliary Surge D, and Liver Transplantation, Oxtord House, Suite 801, Vanderbilt University Medical Center, Nashville, TN ~-753. Copyright 2002, Elsevier Science (USA). All rig)its reserved X/02/ /0 doi: /otgn Operative Techniques in General Surgery, Vol 4, No 1 (March), 2002: pp
2 1
3 Exposure, Hilar Dissection, and Parenchymal Division ] 5 extension ;tension Thoracic exter Subcos f~ :ii!!!!i!i!!!~ii~ 84 2 The surgeon can choose from a number of incisions based on the planned procedure. Little literature has been dedicated to the choice of incision when performing hepatobiliary procedures.l'2"3 Thus, most surgeons' preferences are based on their training. The upper midline incision has been favored by most surgeons for traumatic liver injuries 4 and by some surgeons for elective cases on the biliary tract and left lobe of the liver. This incision provides limited access to the right side of the liver, may provide limited exposure in obese patients or those with a short distance between the xiphoid and the umbilicus, and has a significant incidence of ventral herniation postoperatively. ~ Paramedian, Kocher, and interneural right upper quadrant incisions have also been popular for some biliary procedures, but they have only limited usefulness because of the limited exposure of the liver that they afford. The bilateral subcostal incision is the most popular incision among hepatobiliary surgeons. 5'6 This incision allows for exposure of the supra-, retro-, and infrahepatic vena cava, excellent exposure of the porta hepatis, and room for complete mobilization of the liver if necessary. Beginning any right upper quadrant procedure with an 8 to 10-cm incision approximately 3-4 cm (two fingerbreadths) inferior to the right costal margin allows for quick and easy assessment of the upper abdomen for the presence of metastases, the extent of local pathology, resectability, and any anomalous anatomy. The incision can then be extended to the right and left subcostal regions as needed to provide improved exposure. Alternatively, laparoscopy may allow a quick, minimally invasive assessment of peritoneal metastases and can be combined with laparoscopic ultrasonography to provide more detail as to the number and location of hepatic tumors and their resectability.
4 , 16 Chapman et al Rectus sheath 2 (continued) A perpendicular midline extension to the xiphoid also improves mobilization of the thoracic and anterior abdominal walls, especially in patients with narrow costal angles. Excision of the xiphoid may prove useful (B). A thoracic extension of the right subcostal incision into the sixth or seventh intercostal space provides excellent exposure of the right suprahepatic and posterior liver but increases morbidity from postoperative pulmonary complications. 3,r We have found that appropriate use of the bilateral subcostal incisions with the midline extension and adequate retraction makes the thoracic extension unnecessary. 8 Some authors have also suggested turning the midline xiphoid extension into a full sternotomy to further increase suprahepatic exposure, 9 but this is seldom necessary unless the heart or supradiaphragmatic vena cava must be exposed. Once the initial celiotomy is complete, the ligamentum teres hepatis (round ligament) within the falciform ligament can be ligated and divided. This allows for complete opening of the wound and placement of the surgeon's choice of self-retaining retractor. Surgical assistants with hand-held retractors are not always available in all operating facilities in sufficient numbers (two or three may be needed), are fatigable, and may find it difficult to remain steady. In addition, the number of assistants needed to retract often restricts the surgeon at an overcrowded operating table. For these reasons, we encourage the use of a self-retaining retraction system. Different retractor systems are available, each with its individual advantages and disadvantages ,12
5 Exposure, Hilar Dissection, and Parenchymal Division 17 3 We have chosen the split-ring Bookwaher self-retaining retractor because of its ease of assembly and adjustment and have found it quite effective in providing adequate traction and countertraction when performing hepatobiliary procedures. 8 To use this system, a table post with a 30 to 45-degree extension bar is fixed over the drapes to the right siderail of the table at the patient's nipple line. A rod is suspended from this apparatus to hold the segmented ring, which is centered over the liver and tilted at 45 degrees.
6 18 Chapman et al A 4 The tilt in the ring allows for elevated cephalad retraction of the thorax along with caudal retraction of the other viscera. This is performed with a Balfour blade with a tilting ratchet in the upper midline along with three or more right-angle blades (depending on the incision size) on the costal margins to elevate the thorax and flatten the diaphragm. This is usually sufficient to provide access to the diaphragm and suprahepatic cava when caudal retraction on the liver is applied (A).
7 Exposure, Hilar Dissection, and Parenchymal Division 19 Falciform ligament divided '\. 3.,.84, J i /- J! Portal triad r < 3 9 iii'., h'>- ""... ~Jf B =! 4 (continued) Malleable retractors placed on the inferior portion of the ring can be used to retract the stomach and duodenum to the left and the hepatic flexure of the colon caudally and to the right out of the operative field, providing excellent exposure of the porta hepatis (B).
8 20 Chapman et al / Falciform ligament m / Right riangular ligament A Bare area (A, B) Once the retractor is in place, the liver can be further mobilized with division of the ligamentous attachments superiorly and posteriorly (Shown here from above and looking caudally). These suspensory ligaments, including the left and right triangular ligaments and the anterior and posterior coronary ligaments, form a triangular or diamond-shaped area along the posterior aspect of the liver that corresponds to the bare area of the liver and contains the retrohepatic inferior vena cava and hepatic veins.
9 Exposure, Hilar Dissection, and Parenchymal Division 21 IVC & hepatic veins Anterior coronary ligament Left triangular ligament., Falciform ligament Tissue corresponding to bare area of liver Right triangular ligament \ Portal triad B Posterior coronary ligament (continued)
10 22 Chapman et al Right hepatic vein Adrenal ve Adrenal gla 6 Careful division of these ligaments allows for elevation and rotation of the liver to provide access to the posterior right lobe of the liver, the retrohepatic cava, the right adrenal gland, and the right adrenal vein. Easy visualization and access to these structures provides a safe means of achieving sufficient vascular control before any resection. Access to and control of lesser hepatic veins emptying into the retrohepatic interior verla cava can be achieved. But hepatic rotation must be carefully performed, not only because the liver can be damaged with compression against any of the sharp retractor blades, but also because the liver might fracture, especially in patients with a friable or fatty liver.
11 Exposure, Hilar Dissection, and Parenchymal Division 23 7 Laparoscopy is increasingly used in hepatic resections of segments II- VI. 13'14 The subject and controversies of laparoscopic-assisted liver resections are discussed in detail in other articles in this issue, but obtaining adequate exposure is no less important in laparoscopic liver procedures than in those performed in an open fashion. Again, the process begins with proper positioning, depending on the area of liver in focus. For resections of segments 11, III, IVa, and V, the patient is placed supine with the legs separated so that the surgeon may stand between the legs (A). For resections of segment VI, the patient is best placed in the left lateral decubitus position (B). Twenty degrees of reverse Trendelenburg position can improve the exposure for laparoscopic resections by causing the free abdominal viscera to mobilize toward the pelvis. Exposure is further augmented with excision of the falciform and left triangular ligaments to the inferior vena cava for resections of segments II-IVa. Partial excision of the right triangular and posterior coronary ligaments facilitates the resection of segments V or VI.
12 24 Chapman et al Hilar Dissection Extrahepatic dissection and control of the porta hepatis vessels and bile ducts will facilitate major hepatic resections by limiting bleeding and ensuring that the remaining liver is fully vascularized and has ade- quate biliary drainage. These major resections include lobectomies, extended lobectomies, and those liver resections of lesions situated in close apposition to hilar structures. 8 A full understanding of the relational anatomy of the structures in the hepatoduodenal ligament and hepatic hilum is imperative for safe liver resection. In general, the bile duct occupies the anterior right porta hepatis. At the inferior liver edge is a confluence of a transversely oriented left hepatic duct and a more axially oriented right hepatic duct, which descends as the common hepatic duct (CHD) to join the cystic duct at the inferior border of the triangle of Calot and become the common bile duct (CBD). The proper hepatic artery generally approaches the liver in the left anterior porta hepatis and branches into right and left hepatic arteries in the hepatic hilum. The right hepatic artery usually passes posterior to the CHD (85%) before entering the liver. The portal vein lies in the posterior porta hepatis, and its primary bifurcation is at the inferior edge of segment IV. 15
13 Exposure, Hilar Dissection, and Parenchymal Division 25 Left Replaced righl artery artery a~ Right artery.~ry artery 9 A significant variability exists in the arterial and biliary anatomy that needs to be anticipated and defined during dissection of the porta hepatis. A replaced right hepatic artery may arise from the superior mesenteric artery and ascend in the right posterior porta behind the CHD and CBD in 20% of patients. With similar frequency, a replaced left hepatic artery may arise from the left gastric artery and cross the gastrohepatic ligament to enter the left liver outside the porta hepatis. Wide variation in the locations of sectoral bile ducts and their confluences may be seen; for example, major sectoral ducts of the right liver may join the left hepatic duct peripheral to the primary bifurcation or may descend in the porta to join the CHD or CBD distally. 16'17
14 26 Chapman et al I-I Principal plane 10 Further variability of the anatomy of the porta hepatis can arise if the liver has undergone sectoral or lobar atrophy and/or hypertrophy. Rotational distortion of the relational anatomy of the hepatoduodenal ligament can hinder exposure of the hepatic hilum. as (Shown here as left-sided hypertrophy) In patients with adhesions and scarring from previous surgery in the porta hepatis, dissection of the hepatoduodenal ligament can be tedious. Careful division of the adhesions between the hepatic flexure of the colon and the liver, mobilization of the duodenum, and intermittent palpation of the region of the porta hepatis to identify hepatic artery pulses can facilitate approaching the hepatoduodenal ligament from the right in anticipation of exposing the CBD as an initial landmark.
15 Exposure, Hilar Dissection, and Parenchymal Division 27 Gall Hepatic artery ~ry Portal vein Bile duct 1 1 Hilar dissection for liver resection generally begins with cholecystectomy and exposure of the triangle of Calot to facilitate early identification of the CHD-CBD junction. Further incision across the peritoneum of the porta hepatis allows for progressive exposure and isolation of the primary branches of the hepatic artery and hepatic duct at the hilum of the liver. At times, exposure of the hilar structures is improved by the incision of Glisson's capsule and elevation of segment IV (quadrate lobe). This dissection within the hilar plate can be carried out peripherally to gain control of segmental vascular and bilary branches as necessary for the anticipated parenchymal resection. Lobar or sectoral divisions of the portal triads, enveloped in a sheath of fibrous tissue originating from Glisson's capsule, can be defined during parencymal dissection and ligated en masse. ~9 Exposure and control of portal vein branches may be easier after bile duct and hepatic artery branch ligation and division. Additionally, portal vein isolation is facilitated by full mobilization of the liver and rotation of the liver to the left to better expose the right posterior aspect of the porta hepatis.
16 28 Chapman et al 12 Occasionally, liver resection is part of the management of a proximal bile duct tumor. Because of the close proximity of the hilar biliary tumor and the hepatic artery, the portal vein, and their branches, exposure of these vascular structures can be difficult. Circumferential dissection and division of the CBD distally allows for the anterior reflection of the CBD and CHD with adjacent neural and lymphatic tissues to skeletonize the hepatic artery and portal vein cephalad towards the hilum of the liver. 19
17 Exposure, Hilar Dissection, and Parenchymal Division 29 artery Portal vein 13 Alternatives to extensive hilar dissection for liver resection include extrahepatic occlusion of the hepatoduodenal ligament (Pringle maneuver) (A) and total vascular isolation (B).
18 30 Chapman et al Parenchymal Division A 14 After abdominal exploration and exposure of the liver and hilar dissection, the final phase of liver resection is completed with parenchymal division. There are a number of techniques that have been developed to facilitate this portion of the procedure. Because of the extensive vascular and bile duct network within the liver, the goal of parenchymal division is to expediently dissect and ligate hepatic vessels and bile ducts in the plane of transection with minimal blood loss. 21 Portal venous tributaries are enveloped by Glisson's capsule, making them somewhat resistant to traumatic injury during the parenchymal transection. In contrast, hepatic venous branches may be thin walled and can be more easily avulsed during manipulation. The specific techniques used to dissect hepatic tissue away from vessels and bile ducts depend on the surgeon's preference and experience and by available technology within the surgeon's hospital setting. Temporary hepatic inflow occlusion (Pringle clamping) or complete vascular isolation are other techniques that may be used selectively to lessen blood loss during parenchymal division. 22'23 (A) Finger fracture (digitoclasia) parenchymal division has been the most widely used and is perhaps the simplest technique for parenchymal division in liver resection. 24 This technique is performed by initially incising the liver capsule along the planned resection plane, usually with electrocautery. After the liver capsule has been incised, the dissection is initiated with a blunt instrument (e.g., scissor tip or blunt clamp) by working through the parenchymal tissue. Vessels and bile ducts can be individually identified, encircled, and either suture ligated or divided with surgical clips. Many surgeons prefer to suture ligate ducts and larger vessels on the remnant liver side of the division and use surgical clips only on the specimen side, because clips may become dislodged during liver manipulation as the resection proceeds. Finger fracture techniques can also be combined with other methods of parenchymal division. The advantages of the finger fracture dissection technique are its simplicity and speed. This technique does not require sophisticated instrumentation that may be unavailable in some operative centers. The disadvantage of the finger fracture technique is the potential decrease in operative precision. Some authors have reported an increased blood loss using finger fracture compared with other methods, including ultrasonic dissection 25 (see below). However, one of the only reported randomized, prospective controlled trials comparing finger fracture dissection with ultrasonic dissection found no differences in operative blood loss, and the authors claimed that operative precisionwas actually improved with the finger fracture technique. 24
19 Exposure, Hilar Dissection, and Parenchymal Division (continued) (B) The ultrasonic aspirator is a popular method among many liver surgeons for parenchymal transection. This device uses an ultrasonic dissector to lyse hepatic parenchyma while preserving the integrity of vascular and biliary structures within the substance of the liver. This technique is intended to allow precise visualization and dissection of portal venous and hepatic venous branches, which can then be individually ligated and divided. Available systems can incorporate electrocautery as a component in the ultrasonic dissection, facilitating division of small vessels and bile ducts during liver transection. Disadvantages of these systems include the relatively high system purchase cost ($60,000-$100,000) and the cost of disposables required on a per case basis ($500- $1,000). Moreover, parenchymal transection using ultrasonic dissection is usually slower than finger fracture transection or the use of other mechanical devices. Surgical staplers have been used during open and laparoscopic liver resections. 26 Vascular staplers
20 32 Chapman et al REFERENCES 1. Bluestone L, Freed JS, Szuchmacher PH: The interneural incision for biliary tract operations. Surg Gynecol Obstet 147:21-24, Thierry B, Morel P, Huber O, et al: Combined midline-transverse surgical approach for severe blunt injuries to the right liver. J Trauma 48: , Sato H, Sugawara Y, Yamasaki S, et al: Thoracoabdominal approaches versus inverted T incision for posterior segmentectomy in hepatocellular carcinoma. Hepatogastroenterology 47: , Feliciano DV: Surgery for liver trauma, Surg Clin North Am 69: , Huguet C, Addario-Chieco P, Gavelli A, et al: Technique of hepatic vascular exclusion for extensive liver resection. Am J Surg 163: , Meyers WC, Callery MP, Scaffer BK, et al: Staging, resection, and ablation of liver tumors, in Townsend CM (ed): Sabiston Textbook of Surgery, ed 16 Philadelphia: WB Saunders, 2001, p Foster JH: Liver resection techniques. Surg Clin North Am 69: , Pinson CW, Drougas JG, Lalikos JI: Optimal exposure for hepatobiliary operations using the Bookwalter retractor. Am Surg 61: , Jones RS: Atlas of Liver and Bjliary Surgery. Chicago, IL, Year Book, 1990, pp Stieber AC: Hepatic transplantation with the aid of the iron intern retractor. AmJ Surg 160: , Ong G, Nakayama F: New abdominal retractor for exposure of subphrenic region. Surg Gynecol Obstet 166:75-76, Dorton HE: New self-retaining retractor holder to facilitate surgical exposure. AmJ Surg 141: , Descottes B, Lachachi F, Sodji M, et al: Early experience with laparoscopic approach for solid liver tumors: Initial 16 cases. Ann Surg 232: , Cherqui D, Husson E, Hammound R, et ah Laparoscopic liver resections: a feasibility study in 30 patients. Ann Surg 232: , HealeyJE: A Synopsis of Clinical Anatomy. Philadelphia, PA WB Saunders, 1969, p Henderson, JM, Rikkers LE: Atlas of liver surgery, in Bell RH, Rikkers LF, Mulholland MW (eds): Digestive Tract Surgery: A Text and Atlas. Philadelphia, PA: Lippincott-Raven, 1996, pp Skandalakis LJ, Colborn GL, Gray SW, et al: Surgical Anatomy of the Liver and Extrahepatic Biliary Tract. In Nyhus LM, Baker RJ: Mastery of Surgery, ed 2 Boston, MA, Little, Brown 1992, pp Blumgart LH: Hilar and intrahepatic bilary enteric anastomosis. Surg Clin North Am 74: , Pinson CW, Rossi RL: Extended right hepatic lobectomy, left hepatic lobectomy and skeletonization resection for proximal bile duct cancer. WorldJ Surg 12:52-59, Launois B,Jamieson GG: The importance of Glisson's capsule and its sheaths in the intrahepatic approach to resection of the liver. Surg Gynecol Obstet 174:7-10, Rees M, Plant G, Wells J, et ah One hundred and fifty hepatic resections: Evolution of technique towards bloodless surgery. BrJ Surg 83: , Belghitti J, Noun R, Malafosse R., et al: Continuous versus intermittent portal triad clamping for liver resection: a controlled study. Ann Surg 229: , Elias D. Lasser P, Debaene B, et al: Intermittent vascular exclusion of the liver (without vena cava clamping) during major hepatectomy. BrJ Surg: 82: , Takayama T, Makuuchi M, Kubota K, et al: Randomized comparison of ultrasonic vs. clamp transection of the liver. Arch Surg 136: , Fan ST, Lai ES, Lo CM, et al: Hepatectomy with an ultrasonic dissector for hepatocellular carcinoma. BrJ Surg 83: , Fong Y, Blumgart LH: Useful stapling techniques in liver surgery. J Am Coll Surg 185:93-100, 1997
Accessory Glands of Digestive System
 Accessory Glands of Digestive System The liver The liver is soft and pliable and occupies the upper part of the abdominal cavity just beneath the diaphragm. The greater part of the liver is situated under
Accessory Glands of Digestive System The liver The liver is soft and pliable and occupies the upper part of the abdominal cavity just beneath the diaphragm. The greater part of the liver is situated under
Lecture 02 Anatomy of the LIVER
 Lecture 02 Anatomy of the LIVER BY Dr Farooq Khan Aurakzai Dated: 02.01.2018 Introduction to Liver Largest gland in the body. 2 nd largest organ of the body. Weight approximately 1500 gm, and is roughly
Lecture 02 Anatomy of the LIVER BY Dr Farooq Khan Aurakzai Dated: 02.01.2018 Introduction to Liver Largest gland in the body. 2 nd largest organ of the body. Weight approximately 1500 gm, and is roughly
Surgical anatomy of the biliary tract
 HPB, 2008; 10: 7276 REVIEW ARTICLE Surgical anatomy of the biliary tract DENIS CASTAING Centre hépato-biliaire, Hôpital Paul Brousse, Assistance Publique- Hôpitaux de Paris, Université Paris XI, Paris,
HPB, 2008; 10: 7276 REVIEW ARTICLE Surgical anatomy of the biliary tract DENIS CASTAING Centre hépato-biliaire, Hôpital Paul Brousse, Assistance Publique- Hôpitaux de Paris, Université Paris XI, Paris,
The Whipple Operation Illustrations
 The Whipple Operation Illustrations Fig. 1. Illustration of the sixstep pancreaticoduodenectomy (Whipple operation) as described in a number of recent text books by Dr. Evans. The operation is divided
The Whipple Operation Illustrations Fig. 1. Illustration of the sixstep pancreaticoduodenectomy (Whipple operation) as described in a number of recent text books by Dr. Evans. The operation is divided
Pancreas & Biliary System. Dr. Vohra & Dr. Jamila
 Pancreas & Biliary System Dr. Vohra & Dr. Jamila 1 Objectives At the end of the lecture, the student should be able to describe the: Location, surface anatomy, parts, relations & peritoneal reflection
Pancreas & Biliary System Dr. Vohra & Dr. Jamila 1 Objectives At the end of the lecture, the student should be able to describe the: Location, surface anatomy, parts, relations & peritoneal reflection
Surface Anatomy. Location Shape Weight Role of Five Surfaces Borders Fissures Lobes Peritoneal Lig
 The Liver Functions Bile production and secretion Detoxification Storage of glycogen Protein synthesis Production of heparin and bile pigments Erythropoiesis (in fetus) Surface Anatomy Location Shape Weight
The Liver Functions Bile production and secretion Detoxification Storage of glycogen Protein synthesis Production of heparin and bile pigments Erythropoiesis (in fetus) Surface Anatomy Location Shape Weight
Exploring Anatomy: the Human Abdomen
 Exploring Anatomy: the Human Abdomen PERITONEUM AND PERITONEAL CAVITY PERITONEUM The peritoneum is a thin serous membrane that lines the abdominal cavity and covers, in variable amounts, the viscera within
Exploring Anatomy: the Human Abdomen PERITONEUM AND PERITONEAL CAVITY PERITONEUM The peritoneum is a thin serous membrane that lines the abdominal cavity and covers, in variable amounts, the viscera within
Block 3: DISSECTION 2 CELIAC TRUNK, JEJUNUM/ILEUM, LARGE INTESTINE, DUODENUM, PANCREAS, PORTAL VEIN; MOBILIZATION OF THE LIVER
 1 Block 3: DISSECTION 2 CELIAC TRUNK, JEJUNUM/ILEUM, LARGE INTESTINE, DUODENUM, PANCREAS, PORTAL VEIN; MOBILIZATION OF THE LIVER Attempt to complete as much as you can of the dissection explained in the
1 Block 3: DISSECTION 2 CELIAC TRUNK, JEJUNUM/ILEUM, LARGE INTESTINE, DUODENUM, PANCREAS, PORTAL VEIN; MOBILIZATION OF THE LIVER Attempt to complete as much as you can of the dissection explained in the
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
To describe the liver. To list main structures in porta hepatis.
 GI anatomy Lecture: 6 د. عصام طارق Objectives: To describe the liver. To list main structures in porta hepatis. To define portal system & portosystemic anastomosis. To list parts of biliary system. To
GI anatomy Lecture: 6 د. عصام طارق Objectives: To describe the liver. To list main structures in porta hepatis. To define portal system & portosystemic anastomosis. To list parts of biliary system. To
pitfall Table 1 4 disorientation pitfall pitfall Table 1 Tel:
 11 687 692 2002 pitfall 1078 29 17 9 1 2 3 dislocation outflow block 11 1 2 3 9 1 2 3 4 disorientation pitfall 11 687 692 2002 Tel: 075-751-3606 606-8507 54 2001 8 27 2002 10 31 29 4 pitfall 16 1078 Table
11 687 692 2002 pitfall 1078 29 17 9 1 2 3 dislocation outflow block 11 1 2 3 9 1 2 3 4 disorientation pitfall 11 687 692 2002 Tel: 075-751-3606 606-8507 54 2001 8 27 2002 10 31 29 4 pitfall 16 1078 Table
EFSUMB Course Book, 2 nd Edition
 Ultrasound of the liver. 11.04.2018 10:01 1 EFSUMB Course Book, 2 nd Edition Editor: Christoph F. Dietrich Ultrasound of the liver Christoph F. Dietrich, Carla Serra 2, Maciej Jedrzejczyk 3 1 Caritas-Krankenhaus
Ultrasound of the liver. 11.04.2018 10:01 1 EFSUMB Course Book, 2 nd Edition Editor: Christoph F. Dietrich Ultrasound of the liver Christoph F. Dietrich, Carla Serra 2, Maciej Jedrzejczyk 3 1 Caritas-Krankenhaus
Step-by-step isolated resection of segment 1 of the liver using the hanging maneuver
 The American Journal of Surgery (2009) 198, e42 e48 HowIDoIt Step-by-step isolated resection of segment 1 of the liver using the hanging maneuver Rafael López-Andújar, Ph.D.*, Eva Montalvá, Ph.D., Marcos
The American Journal of Surgery (2009) 198, e42 e48 HowIDoIt Step-by-step isolated resection of segment 1 of the liver using the hanging maneuver Rafael López-Andújar, Ph.D.*, Eva Montalvá, Ph.D., Marcos
The abdominal Esophagus, Stomach and the Duodenum. Prof. Oluwadiya KS
 The abdominal Esophagus, Stomach and the Duodenum Prof. Oluwadiya KS www.oluwadiya.com Viscera of the abdomen Abdominal esophagus: Terminal part of the esophagus The stomach Intestines: Small and Large
The abdominal Esophagus, Stomach and the Duodenum Prof. Oluwadiya KS www.oluwadiya.com Viscera of the abdomen Abdominal esophagus: Terminal part of the esophagus The stomach Intestines: Small and Large
Duodenum retroperitoneal
 Duodenum retroperitoneal C shaped Initial region out of stomach into small intestine RETROperitoneal viscus Superior 1 st part duodenal cap ; moves upwards and backwards to lie on the R crura medial to
Duodenum retroperitoneal C shaped Initial region out of stomach into small intestine RETROperitoneal viscus Superior 1 st part duodenal cap ; moves upwards and backwards to lie on the R crura medial to
HOW I DO IT Feasibility of Bisegmentectomy 7 8 is Independent of the Presence of a Large Inferior Right Hepatic Vein
 Journal of Surgical Oncology 2006;93:338 342 HOW I DO IT Feasibility of Bisegmentectomy 7 8 is Independent of the Presence of a Large Inferior Right Hepatic Vein MARCEL AUTRAN C. MACHADO, MD, 1,2 * PAULO
Journal of Surgical Oncology 2006;93:338 342 HOW I DO IT Feasibility of Bisegmentectomy 7 8 is Independent of the Presence of a Large Inferior Right Hepatic Vein MARCEL AUTRAN C. MACHADO, MD, 1,2 * PAULO
RPLND: Tips and Tricks
 RPLND: Tips and Tricks Andrew J. Stephenson, MD FACS FRCS(C) Director, Center for Urologic Oncology Glickman Urological & Kidney Institute Cleveland Clinic, Cleveland, OH RPLND: Keys to success Knowledge
RPLND: Tips and Tricks Andrew J. Stephenson, MD FACS FRCS(C) Director, Center for Urologic Oncology Glickman Urological & Kidney Institute Cleveland Clinic, Cleveland, OH RPLND: Keys to success Knowledge
The Thoracic wall including the diaphragm. Prof Oluwadiya KS
 The Thoracic wall including the diaphragm Prof Oluwadiya KS www.oluwadiya.com Components of the thoracic wall Skin Superficial fascia Chest wall muscles (see upper limb slides) Skeletal framework Intercostal
The Thoracic wall including the diaphragm Prof Oluwadiya KS www.oluwadiya.com Components of the thoracic wall Skin Superficial fascia Chest wall muscles (see upper limb slides) Skeletal framework Intercostal
Parenchyma-sparing lung resections are a potential therapeutic
 Lung Segmentectomy for Patients with Peripheral T1 Lesions Bryan A. Whitson, MD, Rafael S. Andrade, MD, and Michael A. Maddaus, MD Parenchyma-sparing lung resections are a potential therapeutic option
Lung Segmentectomy for Patients with Peripheral T1 Lesions Bryan A. Whitson, MD, Rafael S. Andrade, MD, and Michael A. Maddaus, MD Parenchyma-sparing lung resections are a potential therapeutic option
Case Report Formation of a Tunnel under the Major Hepatic Vein Mouths during Removal of IVC Tumor Thrombus
 Case Reports in Urology Volume 2013, Article ID 129632, 4 pages http://dx.doi.org/10.1155/2013/129632 Case Report Formation of a Tunnel under the Major Hepatic Vein Mouths during Removal of IVC Tumor Thrombus
Case Reports in Urology Volume 2013, Article ID 129632, 4 pages http://dx.doi.org/10.1155/2013/129632 Case Report Formation of a Tunnel under the Major Hepatic Vein Mouths during Removal of IVC Tumor Thrombus
Pancreas and Biliary System
 Pancreas and Biliary System Please view our Editing File before studying this lecture to check for any changes. Color Code Important Doctors Notes Notes/Extra explanation Objectives At the end of the lecture,
Pancreas and Biliary System Please view our Editing File before studying this lecture to check for any changes. Color Code Important Doctors Notes Notes/Extra explanation Objectives At the end of the lecture,
Lecture 01 Internal surface of anterolateral abdominal wall. BY Dr Farooq Khan Aurakzai
 Lecture 01 Internal surface of anterolateral abdominal wall BY Dr Farooq Khan Aurakzai Dated: 21.12.2017 Internal surface of the anterolateral abdominal wall The internal ( posterior ) surface of the anterolateral
Lecture 01 Internal surface of anterolateral abdominal wall BY Dr Farooq Khan Aurakzai Dated: 21.12.2017 Internal surface of the anterolateral abdominal wall The internal ( posterior ) surface of the anterolateral
Basic Abdominal Sonography
 24S Basic Abdominal Sonography Procedural Overview JOHN FATCHETT II, RDMS is provided. Patient preparation (i.e., fasting) scanning techniques, spleen, transducer. evaluation of abdominal anatomy in the
24S Basic Abdominal Sonography Procedural Overview JOHN FATCHETT II, RDMS is provided. Patient preparation (i.e., fasting) scanning techniques, spleen, transducer. evaluation of abdominal anatomy in the
Thoracoscopic left upper lobectomy with systematic lymph nodes dissection under left pulmonary artery clamping
 GCTAB Column Thoracoscopic left upper lobectomy with systematic lymph nodes dissection under left pulmonary artery clamping Yi-Nan Dong, Nan Sun, Yi Ren, Liang Zhang, Ji-Jia Li, Yong-Yu Liu Department
GCTAB Column Thoracoscopic left upper lobectomy with systematic lymph nodes dissection under left pulmonary artery clamping Yi-Nan Dong, Nan Sun, Yi Ren, Liang Zhang, Ji-Jia Li, Yong-Yu Liu Department
Alexander C Vlantis. Selective Neck Dissection 33
 05 Modified Radical Neck Dissection Type II Alexander C Vlantis Selective Neck Dissection 33 Modified Radical Neck Dissection Type II INCISION Various incisions can be used for a neck dissection. The incision
05 Modified Radical Neck Dissection Type II Alexander C Vlantis Selective Neck Dissection 33 Modified Radical Neck Dissection Type II INCISION Various incisions can be used for a neck dissection. The incision
Variations in portal and hepatic vein branching of the liver
 Yamagata Med J (ISSN 0288-030X)2015;33(2):115-121 DOI 10.15022/00003476 Variations in portal and hepatic vein branching of the liver Wataru Kimura, Tsuyoshi Fukumoto, Toshihiro Watanabe, Ichiro Hirai First
Yamagata Med J (ISSN 0288-030X)2015;33(2):115-121 DOI 10.15022/00003476 Variations in portal and hepatic vein branching of the liver Wataru Kimura, Tsuyoshi Fukumoto, Toshihiro Watanabe, Ichiro Hirai First
Minimally invasive lobectomy and thoracic lymph node
 Minimally Invasive Segmentectomy Joshua R. Sonett, MD, FACS Minimally invasive lobectomy and thoracic lymph node dissection is now widely established as a safe, anatomic, and oncologically sound procedure
Minimally Invasive Segmentectomy Joshua R. Sonett, MD, FACS Minimally invasive lobectomy and thoracic lymph node dissection is now widely established as a safe, anatomic, and oncologically sound procedure
The peritoneum. Prof. Oluwadiya KS, MBBS, FMCS(Orthop) Website:
 The peritoneum Prof. Oluwadiya KS, MBBS, FMCS(Orthop) Website: http://oluwadiya.com The peritoneum Serous membrane that lines the abdominopelvic cavity and invests the viscera The largest serous membrane
The peritoneum Prof. Oluwadiya KS, MBBS, FMCS(Orthop) Website: http://oluwadiya.com The peritoneum Serous membrane that lines the abdominopelvic cavity and invests the viscera The largest serous membrane
Peritoneum: Def. : It is a thin serous membrane that lines the walls of the abdominal and pelvic cavities and clothes the viscera.
 Peritoneum: Def. : It is a thin serous membrane that lines the walls of the abdominal and pelvic cavities and clothes the viscera. Layers of the peritoneum: 1. Outer Layer ( Parietal Peritoneum) : lines
Peritoneum: Def. : It is a thin serous membrane that lines the walls of the abdominal and pelvic cavities and clothes the viscera. Layers of the peritoneum: 1. Outer Layer ( Parietal Peritoneum) : lines
Mousa Salah. Dr. Mohammad Al. Mohtasib. 1 P a g e
 8 Mousa Salah Dr. Mohammad Al. Mohtasib 1 P a g e In the previous lecture we talked about the peritoneum, and we said that the peritonium is a serous sac, and it consists of two layers, visceral and parietal.
8 Mousa Salah Dr. Mohammad Al. Mohtasib 1 P a g e In the previous lecture we talked about the peritoneum, and we said that the peritonium is a serous sac, and it consists of two layers, visceral and parietal.
Pancreaticoduodenectomy the anatomy and the surgical approaches
 Pancreaticoduodenectomy the anatomy and the surgical approaches Paul BS LAI Division of Hepato biliary and Pancreatic Surgery Department of Surgery The Chinese Univesity of Hong Kong Whipple s operation
Pancreaticoduodenectomy the anatomy and the surgical approaches Paul BS LAI Division of Hepato biliary and Pancreatic Surgery Department of Surgery The Chinese Univesity of Hong Kong Whipple s operation
In the name ofgod. Abdomen 3. Dr. Zahiri
 In the name ofgod Abdomen 3 Dr. Zahiri Peritoneum Peritoneum It is the serous membrane(a type of loose connective tissue and is covered by mesothelium) that lines the abdominal cavity. Extensions of the
In the name ofgod Abdomen 3 Dr. Zahiri Peritoneum Peritoneum It is the serous membrane(a type of loose connective tissue and is covered by mesothelium) that lines the abdominal cavity. Extensions of the
Original article: new surgical approaches to the Klatskin tumour
 Alimentary Pharmacology & Therapeutics Original article: new surgical approaches to the Klatskin tumour T. M. VAN GULIK*, S. DINANT*, O. R. C. BUSCH*, E. A. J. RAUWS, H. OBERTOP* & D. J. GOUMA Departments
Alimentary Pharmacology & Therapeutics Original article: new surgical approaches to the Klatskin tumour T. M. VAN GULIK*, S. DINANT*, O. R. C. BUSCH*, E. A. J. RAUWS, H. OBERTOP* & D. J. GOUMA Departments
Cholecystectomy. Sarah Forsyth
 Cholecystectomy Sarah Forsyth History of Cholecystectomy First open cholecystectomy 1882 by Carl Langenbuch in Germany First lap cholecystectomy 1987, Philip Mouret (Gynaecologist) in Lyon, France 1990,
Cholecystectomy Sarah Forsyth History of Cholecystectomy First open cholecystectomy 1882 by Carl Langenbuch in Germany First lap cholecystectomy 1987, Philip Mouret (Gynaecologist) in Lyon, France 1990,
Preview from Notesale.co.uk Page 1 of 34
 Abdominal viscera and digestive tract Digestive tract Abdominal viscera comprise majority of the alimentary system o Terminal oesophagus, stomach, pancreas, spleen, liver, gallbladder, kidneys, suprarenal
Abdominal viscera and digestive tract Digestive tract Abdominal viscera comprise majority of the alimentary system o Terminal oesophagus, stomach, pancreas, spleen, liver, gallbladder, kidneys, suprarenal
THE SURGEON S LIBRARY
 THE SURGEON S LIBRARY THE HISTORY AND SURGICAL ANATOMY OF THE VAGUS NERVE Lee J. Skandalakis, M.D., Chicago, Illinois, Stephen W. Gray, PH.D., and John E. Skandalakis, M.D., PH.D., F.A.C.S., Atlanta, Georgia
THE SURGEON S LIBRARY THE HISTORY AND SURGICAL ANATOMY OF THE VAGUS NERVE Lee J. Skandalakis, M.D., Chicago, Illinois, Stephen W. Gray, PH.D., and John E. Skandalakis, M.D., PH.D., F.A.C.S., Atlanta, Georgia
BLOCK IV: OFFICIAL BODY PARTS LIST FOR ANTERIOR ABDOMINAL WALL AND ABDOMINAL CONTENTS
 BLOCK IV: OFFICIAL BODY PARTS LIST FOR ANTERIOR ABDOMINAL WALL AND ABDOMINAL CONTENTS External oblique muscle Muscular portion Aponeurotic portion Superficial inguinal ring Lateral (inferior) crus Medial
BLOCK IV: OFFICIAL BODY PARTS LIST FOR ANTERIOR ABDOMINAL WALL AND ABDOMINAL CONTENTS External oblique muscle Muscular portion Aponeurotic portion Superficial inguinal ring Lateral (inferior) crus Medial
Anatomy: Know Your Abdomen
 Anatomy: Know Your Abdomen Glossary Abdomen - part of the body below the thorax (chest cavity); separated by the diaphragm. Anterior - towards the front of the body. For example, the umbilicus is anterior
Anatomy: Know Your Abdomen Glossary Abdomen - part of the body below the thorax (chest cavity); separated by the diaphragm. Anterior - towards the front of the body. For example, the umbilicus is anterior
My Patient Has Abdominal Pain PoCUS of the Biliary Tract and the Urinary Tract
 My Patient Has Abdominal Pain PoCUS of the Biliary Tract and the Urinary Tract Objectives PoCUS for Biliary Disease PoCUS for Renal Colic PoCUS for Urinary Retention Biliary Disease A patient presents
My Patient Has Abdominal Pain PoCUS of the Biliary Tract and the Urinary Tract Objectives PoCUS for Biliary Disease PoCUS for Renal Colic PoCUS for Urinary Retention Biliary Disease A patient presents
Thoracoscopic anterior segmentectomy of the right upper lobe (S 3 )
 Surgical Technique on Thoracic Surgery Page 1 of 6 Thoracoscopic anterior segmentectomy of the right upper lobe (S 3 ) Jon Lutz 1,2, Agathe Seguin-Givelet 1,3, Dominique Gossot 1 1 ; 2 Division of General
Surgical Technique on Thoracic Surgery Page 1 of 6 Thoracoscopic anterior segmentectomy of the right upper lobe (S 3 ) Jon Lutz 1,2, Agathe Seguin-Givelet 1,3, Dominique Gossot 1 1 ; 2 Division of General
2 Adrenal Disease. Open Surgery. Andrew C. Novick SURGICAL ANATOMY
 Preface More than 125 years have passed since the basic contributions of John Hunter, Crawford Long, and Lord Lister transformed surgery into a sound science as well as a delicate art. Several great surgeons
Preface More than 125 years have passed since the basic contributions of John Hunter, Crawford Long, and Lord Lister transformed surgery into a sound science as well as a delicate art. Several great surgeons
Partial Nephrectomy Techniques for Renal Preservation: Historical and Modern Approaches
 Partial Nephrectomy Techniques for Renal Preservation: Historical and Modern Approaches Cary N Robertson MD FACS Associate Professor Division of Urology Associate Director Urologic Oncology Duke Cancer
Partial Nephrectomy Techniques for Renal Preservation: Historical and Modern Approaches Cary N Robertson MD FACS Associate Professor Division of Urology Associate Director Urologic Oncology Duke Cancer
Large veins of the thorax Brachiocephalic veins
 Large veins of the thorax Brachiocephalic veins Right brachiocephalic vein: formed at the root of the neck by the union of the right subclavian & the right internal jugular veins. Left brachiocephalic
Large veins of the thorax Brachiocephalic veins Right brachiocephalic vein: formed at the root of the neck by the union of the right subclavian & the right internal jugular veins. Left brachiocephalic
Anatomy of the SMALL INTESTINE. Dr. Noman Ullah Wazir PMC
 Anatomy of the SMALL INTESTINE Dr. Noman Ullah Wazir PMC SMALL INTESTINE The small intestine, consists of the duodenum, jejunum, and illium. It extends from the pylorus to the ileocecal junction were the
Anatomy of the SMALL INTESTINE Dr. Noman Ullah Wazir PMC SMALL INTESTINE The small intestine, consists of the duodenum, jejunum, and illium. It extends from the pylorus to the ileocecal junction were the
Cover Page. The following handle holds various files of this Leiden University dissertation:
 Cover Page The following handle holds various files of this Leiden University dissertation: http://hdl.handle.net/1887/6119 Author: Spruit, E.N. Title: Increasing the efficiency of laparoscopic surgical
Cover Page The following handle holds various files of this Leiden University dissertation: http://hdl.handle.net/1887/6119 Author: Spruit, E.N. Title: Increasing the efficiency of laparoscopic surgical
This presentation will discuss the anatomy of the anterior abdominal wall as it pertains to gynaecological and obstetric surgery.
 This presentation will discuss the anatomy of the anterior abdominal wall as it pertains to gynaecological and obstetric surgery. 1 The border of the anterior abdominal wall is defined superiorly by the
This presentation will discuss the anatomy of the anterior abdominal wall as it pertains to gynaecological and obstetric surgery. 1 The border of the anterior abdominal wall is defined superiorly by the
Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman
 Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman Breast anatomy: Breast conserving surgery: The aim of wide local excision is to remove all invasive and in situ
Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman Breast anatomy: Breast conserving surgery: The aim of wide local excision is to remove all invasive and in situ
Guide to Small Animal Vascular Imaging using the Vevo 770 Micro-Ultrasound System
 Guide to Small Animal Vascular Imaging using the Vevo 770 Micro-Ultrasound System January 2007 Objectives: After completion of this module, the participant will be able to accomplish the following: Understand
Guide to Small Animal Vascular Imaging using the Vevo 770 Micro-Ultrasound System January 2007 Objectives: After completion of this module, the participant will be able to accomplish the following: Understand
د. عصام طارق. Objectives:
 GI anatomy Lecture: 5 د. عصام طارق Objectives: To describe anatomy of stomach, duodenum & pancreas. To list their main relations. To define their blood & nerve supply. To list their lymph drainage. To
GI anatomy Lecture: 5 د. عصام طارق Objectives: To describe anatomy of stomach, duodenum & pancreas. To list their main relations. To define their blood & nerve supply. To list their lymph drainage. To
The posterior abdominal wall. Prof. Oluwadiya KS
 The posterior abdominal wall Prof. Oluwadiya KS www.oluwadiya.sitesled.com Posterior Abdominal Wall Lumbar vertebrae and discs. Muscles opsoas, quadratus lumborum, iliacus, transverse, abdominal wall
The posterior abdominal wall Prof. Oluwadiya KS www.oluwadiya.sitesled.com Posterior Abdominal Wall Lumbar vertebrae and discs. Muscles opsoas, quadratus lumborum, iliacus, transverse, abdominal wall
An Innovative Option for Venous Reconstruction After Pancreaticoduodenectomy: the Left Renal Vein
 J Gastrointest Surg (2007) 11:425 431 DOI 10.1007/s11605-007-0131-1 An Innovative Option for Venous Reconstruction After Pancreaticoduodenectomy: the Left Renal Vein Rory L. Smoot & John D. Christein &
J Gastrointest Surg (2007) 11:425 431 DOI 10.1007/s11605-007-0131-1 An Innovative Option for Venous Reconstruction After Pancreaticoduodenectomy: the Left Renal Vein Rory L. Smoot & John D. Christein &
BY DR NOMAN ULLAH WAZIR
 BY DR NOMAN ULLAH WAZIR The stomach (from ancient Greek word stomachos, stoma means mouth) is a muscular, hollow and the most dilated part of the GIT. It starts from the point where esophagus ends. It
BY DR NOMAN ULLAH WAZIR The stomach (from ancient Greek word stomachos, stoma means mouth) is a muscular, hollow and the most dilated part of the GIT. It starts from the point where esophagus ends. It
Laparoscopic Right Colectomy
 Laparoscopic Right Colectomy Shawnee Mission Medical Center February 22, 2011 Hi, and welcome to the program. My name is Dr. Sanjay Thekkeurumbil, and I m a colorectal surgeon at Shawnee Mission Medical
Laparoscopic Right Colectomy Shawnee Mission Medical Center February 22, 2011 Hi, and welcome to the program. My name is Dr. Sanjay Thekkeurumbil, and I m a colorectal surgeon at Shawnee Mission Medical
Borders of the Abdomen
 Abdominal wall Borders of the Abdomen Abdomen is the region of the trunk that lies between the diaphragm above and the inlet of the pelvis below Borders Superior: Costal cartilages 7-12. Xiphoid process:
Abdominal wall Borders of the Abdomen Abdomen is the region of the trunk that lies between the diaphragm above and the inlet of the pelvis below Borders Superior: Costal cartilages 7-12. Xiphoid process:
Chapter 2. Simple Nephrectomy. Please Give Three Tips for Laparoscopic Simple Nephrectomy. Dr. de la Rosette
 Chapter 2 Simple Nephrectomy Please Give Three Tips for Laparoscopic Simple Nephrectomy............. 39 How Does One Find the Renal Hilum during Transperitoneal Laparoscopic Nephrectomy?.................
Chapter 2 Simple Nephrectomy Please Give Three Tips for Laparoscopic Simple Nephrectomy............. 39 How Does One Find the Renal Hilum during Transperitoneal Laparoscopic Nephrectomy?.................
Dr. Weyrich G07: Superior and Posterior Mediastina. Reading: 1. Gray s Anatomy for Students, chapter 3
 Dr. Weyrich G07: Superior and Posterior Mediastina Reading: 1. Gray s Anatomy for Students, chapter 3 Objectives: 1. Subdivisions of mediastinum 2. Structures in Superior mediastinum 3. Structures in Posterior
Dr. Weyrich G07: Superior and Posterior Mediastina Reading: 1. Gray s Anatomy for Students, chapter 3 Objectives: 1. Subdivisions of mediastinum 2. Structures in Superior mediastinum 3. Structures in Posterior
Liver o The liver is the largest gland in the body and has a wide variety of functions. - It s an accessory organ of GIT
 بسم رلاهللا You don t need to refer to the slides, we included everything here In this lecture we will talk about Liver & Gallbladder Liver o The liver is the largest gland in the body and has a wide variety
بسم رلاهللا You don t need to refer to the slides, we included everything here In this lecture we will talk about Liver & Gallbladder Liver o The liver is the largest gland in the body and has a wide variety
Normal Sonographic Anatomy
 hapter 2:The Liver DUNSTAN ABRAHAM Normal Sonographic Anatomy Homogeneous, echogenic texture (Figure 2-1) Measures approximately 15 cm in length and 10 12.5 cm anterior to posterior; measurement taken
hapter 2:The Liver DUNSTAN ABRAHAM Normal Sonographic Anatomy Homogeneous, echogenic texture (Figure 2-1) Measures approximately 15 cm in length and 10 12.5 cm anterior to posterior; measurement taken
Anatomy of thoracic wall
 Anatomy of thoracic wall Topographic Anatomy of the Thorax 1 Bones of Thoracic wall ribs 1-7"true" ribs -those which attach directly to the sternum true ribs actually attach to the sternum by means of
Anatomy of thoracic wall Topographic Anatomy of the Thorax 1 Bones of Thoracic wall ribs 1-7"true" ribs -those which attach directly to the sternum true ribs actually attach to the sternum by means of
Topography and distribution of ostia venae hepatica in the retrohepatic inferior vena cava
 Original Article Topography and distribution of ostia venae hepatica in the retrohepatic inferior vena cava P.K. Bundi, BSc. (Anat). 4 th year Medical Student, University of Nairobi, J.A. Ogeng o, BSc.
Original Article Topography and distribution of ostia venae hepatica in the retrohepatic inferior vena cava P.K. Bundi, BSc. (Anat). 4 th year Medical Student, University of Nairobi, J.A. Ogeng o, BSc.
Guidelines, Policies and Statements D5 Statement on Abdominal Scanning
 Guidelines, Policies and Statements D5 Statement on Abdominal Scanning Disclaimer and Copyright The ASUM Standards of Practice Board have made every effort to ensure that this Guideline/Policy/Statement
Guidelines, Policies and Statements D5 Statement on Abdominal Scanning Disclaimer and Copyright The ASUM Standards of Practice Board have made every effort to ensure that this Guideline/Policy/Statement
East and Central African Journal of Surgery Volume 12 Number 1 - April 2007
 Gross Anatomical Variations and Congenital Anomalies of Surgical Importance in Hepatobiliary Surgery in Uganda. 93 C.B.R. Ibingira Senior Lecturer and Head of Department of Anatomy Faculty of Medicine
Gross Anatomical Variations and Congenital Anomalies of Surgical Importance in Hepatobiliary Surgery in Uganda. 93 C.B.R. Ibingira Senior Lecturer and Head of Department of Anatomy Faculty of Medicine
ABDOMEN - GI. Duodenum
 TALA SALEH ABDOMEN - GI Duodenum - Notice the shape of the duodenum, it looks like capital G shape tube which extends from the pyloroduodenal junction to the duodenojejunal junction. - It is 10 inches
TALA SALEH ABDOMEN - GI Duodenum - Notice the shape of the duodenum, it looks like capital G shape tube which extends from the pyloroduodenal junction to the duodenojejunal junction. - It is 10 inches
Anatomy of the spleen. Oluwadiya KS
 Anatomy of the spleen Oluwadiya KS www.oluwadiya.com Introduction The spleen is an ovoid, usually purplish, pulpy mass about the size and shape of one's fist. It is the largest lymphoid tissue in the body
Anatomy of the spleen Oluwadiya KS www.oluwadiya.com Introduction The spleen is an ovoid, usually purplish, pulpy mass about the size and shape of one's fist. It is the largest lymphoid tissue in the body
Diaphragm and intercostal muscles. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 Diaphragm and intercostal muscles Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Skeletal System Adult Human contains 206 Bones 2 parts: Axial skeleton (axis): Skull, Vertebral column,
Diaphragm and intercostal muscles Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Skeletal System Adult Human contains 206 Bones 2 parts: Axial skeleton (axis): Skull, Vertebral column,
Minimally Invasive Esophagectomy
 American Association of Thoracic Surgery (AATS) 95 th Annual Meeting Seattle, WA April 29, 2015 General Thoracic Masters of Surgery Video Session Minimally Invasive Esophagectomy James D. Luketich MD,
American Association of Thoracic Surgery (AATS) 95 th Annual Meeting Seattle, WA April 29, 2015 General Thoracic Masters of Surgery Video Session Minimally Invasive Esophagectomy James D. Luketich MD,
Internal Injury Documentation Guidelines
 Internal Injury Documentation Guidelines General Open Wound of Thorax Injury to Heart Identify episode of care Initial Subsequent Sequela Laterality Sequela of injury Place of occurrence of injury Activity
Internal Injury Documentation Guidelines General Open Wound of Thorax Injury to Heart Identify episode of care Initial Subsequent Sequela Laterality Sequela of injury Place of occurrence of injury Activity
STERNUM. Lies in the midline of the anterior chest wall It is a flat bone Divides into three parts:
 STERNUM Lies in the midline of the anterior chest wall It is a flat bone Divides into three parts: 1-Manubrium sterni 2-Body of the sternum 3- Xiphoid process The body of the sternum articulates above
STERNUM Lies in the midline of the anterior chest wall It is a flat bone Divides into three parts: 1-Manubrium sterni 2-Body of the sternum 3- Xiphoid process The body of the sternum articulates above
Netter's Anatomy Flash Cards Section 4 List 4 th Edition
 Netter's Anatomy Flash Cards Section 4 List 4 th Edition https://www.memrise.com/course/1577335/ Section 4 Abdomen (31 cards) Plate 4-1 Bony Framework of Abdomen 1.1 Costal cartilages 1.2 Iliac crest 1.3
Netter's Anatomy Flash Cards Section 4 List 4 th Edition https://www.memrise.com/course/1577335/ Section 4 Abdomen (31 cards) Plate 4-1 Bony Framework of Abdomen 1.1 Costal cartilages 1.2 Iliac crest 1.3
ANTERIOR CERVICAL TRIANGLE (Fig. 2.1 )
 2 Neck Anatomy ANTERIOR CERVICAL TRIANGLE (Fig. 2.1 ) The boundaries are: Lateral: sternocleidomastoid muscle Superior: inferior border of the mandible Medial: anterior midline of the neck This large triangle
2 Neck Anatomy ANTERIOR CERVICAL TRIANGLE (Fig. 2.1 ) The boundaries are: Lateral: sternocleidomastoid muscle Superior: inferior border of the mandible Medial: anterior midline of the neck This large triangle
TRANSPLANT A TION OF LIVER, PANCREAS, heart, heart/
 Rcpnmcd twill A:-':-'AL~ 01 ~LKlJt.K). I,lll J"~. I No.5. November 1983. Copyright. ~ 1983. by J. B. Lippincott Company. Printed in U.S.A. Principles of Multiple Organ Procurement from Cadaver Donors J.
Rcpnmcd twill A:-':-'AL~ 01 ~LKlJt.K). I,lll J"~. I No.5. November 1983. Copyright. ~ 1983. by J. B. Lippincott Company. Printed in U.S.A. Principles of Multiple Organ Procurement from Cadaver Donors J.
DESCRIPTION: This is the part of the trunk, which is located between the root of the neck and the superior border of the abdominal region.
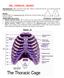 1 THE THORACIC REGION DESCRIPTION: This is the part of the trunk, which is located between the root of the neck and the superior border of the abdominal region. SHAPE : T It has the shape of a truncated
1 THE THORACIC REGION DESCRIPTION: This is the part of the trunk, which is located between the root of the neck and the superior border of the abdominal region. SHAPE : T It has the shape of a truncated
The pericardial sac is composed of the outer fibrous pericardium
 Pericardiectomy for Constrictive or Recurrent Inflammatory Pericarditis Mauricio A. Villavicencio, MD, Joseph A. Dearani, MD, and Thoralf M. Sundt, III, MD Anatomy and Preoperative Considerations The pericardial
Pericardiectomy for Constrictive or Recurrent Inflammatory Pericarditis Mauricio A. Villavicencio, MD, Joseph A. Dearani, MD, and Thoralf M. Sundt, III, MD Anatomy and Preoperative Considerations The pericardial
Citation Transplantation Proceedings, 47(3),
 NAOSITE: Nagasaki University's Ac Title Author(s) Hybrid Procedure in Living Donor Li Soyama, Akihiko; Takatsuki, Mitsuhi Tomohiko; Kitasato, Amane; Kinoshit Baimakhanov, Zhassulan; Kuroki, Tam Citation
NAOSITE: Nagasaki University's Ac Title Author(s) Hybrid Procedure in Living Donor Li Soyama, Akihiko; Takatsuki, Mitsuhi Tomohiko; Kitasato, Amane; Kinoshit Baimakhanov, Zhassulan; Kuroki, Tam Citation
Emergency Approach to the Subclavian and Innominate Vessels
 Emergency Approach to the Subclavian and Innominate Vessels Joseph J. Amato, M.D., Robert M. Vanecko, M.D., See Tao Yao, M.D., and Milton Weinberg, Jr., M.D. T he operative approach to an acutely injured
Emergency Approach to the Subclavian and Innominate Vessels Joseph J. Amato, M.D., Robert M. Vanecko, M.D., See Tao Yao, M.D., and Milton Weinberg, Jr., M.D. T he operative approach to an acutely injured
Radiofrequency Ablation of Liver Tumors
 Radiofrequency Ablation of Liver Tumors Michael M. Awad, Michael A. Choti Indications and Contraindications Indications Unresectable malignant tumors of the liver (e.g., hepatocellular carcinoma, colorectal
Radiofrequency Ablation of Liver Tumors Michael M. Awad, Michael A. Choti Indications and Contraindications Indications Unresectable malignant tumors of the liver (e.g., hepatocellular carcinoma, colorectal
Thyroidectomy. Siu Kwan Ng. Modified Radical Neck Dissection Type II 47
 06 Thyroidectomy Siu Kwan Ng Modified Radical Neck Dissection Type II 47 Thyroidectomy STEP 1. EXPOSING THE THYROID GLAND The collar incision Figure 1 (curvilinear skin crease incision) is made at 1.5-2
06 Thyroidectomy Siu Kwan Ng Modified Radical Neck Dissection Type II 47 Thyroidectomy STEP 1. EXPOSING THE THYROID GLAND The collar incision Figure 1 (curvilinear skin crease incision) is made at 1.5-2
OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function
 The root of the neck Jeff Dupree, Ph.D. e mail: jldupree@vcu.edu OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function READING ASSIGNMENT: Moore and
The root of the neck Jeff Dupree, Ph.D. e mail: jldupree@vcu.edu OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function READING ASSIGNMENT: Moore and
The Physician as Medical Illustrator
 The Physician as Medical Illustrator Francois Luks Arlet Kurkchubasche Division of Pediatric Surgery Wednesday, December 9, 2015 Week 5 A good picture is worth a 1,000 bad ones How to illustrate an operation
The Physician as Medical Illustrator Francois Luks Arlet Kurkchubasche Division of Pediatric Surgery Wednesday, December 9, 2015 Week 5 A good picture is worth a 1,000 bad ones How to illustrate an operation
Saphenous Vein Autograft Replacement
 Saphenous Vein Autograft Replacement of Severe Segmental Coronary Artery Occlusion Operative Technique Rene G. Favaloro, M.D. D irect operation on the coronary artery has been performed in 180 patients
Saphenous Vein Autograft Replacement of Severe Segmental Coronary Artery Occlusion Operative Technique Rene G. Favaloro, M.D. D irect operation on the coronary artery has been performed in 180 patients
Isolated complete caudate lobectomy for hepatic tumor of the anterior transhepatic approach: surgical approaches and perioperative outcomes
 Yang et al. World Journal of Surgical Oncology 2013, 11:197 WORLD JOURNAL OF SURGICAL ONCOLOGY CASE REPORT Open Access Isolated complete caudate lobectomy for hepatic tumor of the anterior transhepatic
Yang et al. World Journal of Surgical Oncology 2013, 11:197 WORLD JOURNAL OF SURGICAL ONCOLOGY CASE REPORT Open Access Isolated complete caudate lobectomy for hepatic tumor of the anterior transhepatic
CORONARY ARTERY BYPASS GRAFTING (CABG) (Part 1) Mark Shikhman, MD, Ph.D., CSA Andrea Scott, CST
 CORONARY ARTERY BYPASS GRAFTING (CABG) (Part 1) Mark Shikhman, MD, Ph.D., CSA Andrea Scott, CST I have constructed this lecture based on publications by leading cardiothoracic American surgeons: Timothy
CORONARY ARTERY BYPASS GRAFTING (CABG) (Part 1) Mark Shikhman, MD, Ph.D., CSA Andrea Scott, CST I have constructed this lecture based on publications by leading cardiothoracic American surgeons: Timothy
Lab 9 Abdomen MUSCLES
 Lab 9 Abdomen MUSCLES External abdominal oblique continuous with the external intercostal muscle; its fibers point in a caudal direction as it moves anteriorly until it inserts on the linea alba via its
Lab 9 Abdomen MUSCLES External abdominal oblique continuous with the external intercostal muscle; its fibers point in a caudal direction as it moves anteriorly until it inserts on the linea alba via its
UNIVERSITY DEVELOPMENT CENTER. Course Specification 2015/2016 For the Anatomy (first year) Medicine Anatomy and Embryology Department 29/12/2015
 Course Specification 2015/2016 For the Anatomy (first year) Faculty : Department : Medicine Anatomy and Embryology Department Course Specification: Programme (s) on which the course is given : M.B.B.Ch
Course Specification 2015/2016 For the Anatomy (first year) Faculty : Department : Medicine Anatomy and Embryology Department Course Specification: Programme (s) on which the course is given : M.B.B.Ch
Dissection Lab Manuals: Required Content
 Dissection Lab Manuals: Required Content 1. Introduction a. Basic terminology (directions) b. External features of the cat c. Adaptations to predatory niche d. How to skin a cat e. How to make the incisions
Dissection Lab Manuals: Required Content 1. Introduction a. Basic terminology (directions) b. External features of the cat c. Adaptations to predatory niche d. How to skin a cat e. How to make the incisions
LECTURE 11 & 12: ABDOMINAL VISCERA ABDOMINAL CONTENTS DIVISION. The location of abdominal viscera is divided into 4 quadrants:
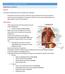 LECTURE 11 & 12: ABDOMINAL VISCERA ABDOMINAL CONTENTS DIVISION The location of abdominal viscera is divided into 4 quadrants: - horizontal line across the umbilicus divides the upper quadrants from the
LECTURE 11 & 12: ABDOMINAL VISCERA ABDOMINAL CONTENTS DIVISION The location of abdominal viscera is divided into 4 quadrants: - horizontal line across the umbilicus divides the upper quadrants from the
بسم هللا الرحمن الرحيم
 بسم هللا الرحمن الرحيم **As we remember from the last lecture: The arterial supply which comes from the single branches of the aorta drains in the portal vein (venous drainage of the gut = portal vein).
بسم هللا الرحمن الرحيم **As we remember from the last lecture: The arterial supply which comes from the single branches of the aorta drains in the portal vein (venous drainage of the gut = portal vein).
Background & Indications Probe Selection
 Teresa S. Wu, MD, FACEP Director, EM Ultrasound Program & Fellowship Co-Director, Simulation Based Training Program & Fellowship Associate Program Director, EM Residency Program Maricopa Medical Center
Teresa S. Wu, MD, FACEP Director, EM Ultrasound Program & Fellowship Co-Director, Simulation Based Training Program & Fellowship Associate Program Director, EM Residency Program Maricopa Medical Center
3 Circulatory Pathways
 40 Chapter 3 Circulatory Pathways Systemic Arteries -Arteries carry blood away from the heart to the various organs of the body. -The aorta is the longest artery in the body; it branches to give rise to
40 Chapter 3 Circulatory Pathways Systemic Arteries -Arteries carry blood away from the heart to the various organs of the body. -The aorta is the longest artery in the body; it branches to give rise to
using the dorsally fixed liver-hang Terumitsu; Nagayasu, Takeshi
 NAOSITE: Nagasaki University's Ac Title Author(s) Left hepatectomy accompanied by a r using the dorsally fixed liver-hang Nanashima, Atsushi; Tobinaga, Syuui Terumitsu; Nagayasu, Takeshi Citation Surgery
NAOSITE: Nagasaki University's Ac Title Author(s) Left hepatectomy accompanied by a r using the dorsally fixed liver-hang Nanashima, Atsushi; Tobinaga, Syuui Terumitsu; Nagayasu, Takeshi Citation Surgery
Technique of Split-Liver Transplant for Two Adult Recipients
 F'UJIUWA H.EAL,THCAREi, INC. PRESENTS IMAGES mljk?zr 3TUiVU?MAZ7ON Technique of Split-Liver Transplant for Two Adult Recipients Abhinuv Humur, KhuLid Khwuju> Timothy D. SieLu$'John R. Luke, und WiLLium
F'UJIUWA H.EAL,THCAREi, INC. PRESENTS IMAGES mljk?zr 3TUiVU?MAZ7ON Technique of Split-Liver Transplant for Two Adult Recipients Abhinuv Humur, KhuLid Khwuju> Timothy D. SieLu$'John R. Luke, und WiLLium
Abdominal Ultrasound
 Abdominal Ultrasound Imaging Control Buttons Depth The organ imaged should take up 3/4 of the screen Frequency = Penetration Use high frequencies (harmonics) for fluid filled and superficial structures
Abdominal Ultrasound Imaging Control Buttons Depth The organ imaged should take up 3/4 of the screen Frequency = Penetration Use high frequencies (harmonics) for fluid filled and superficial structures
CT abdomen and pelvis
 CT abdomen and pelvis General indications: Assessment of vague abdominal symptoms (pain, colics,distenstion,...) Varifecation of a lesion discovered by other diagnostic modalities as US, barium,ivp, Staging
CT abdomen and pelvis General indications: Assessment of vague abdominal symptoms (pain, colics,distenstion,...) Varifecation of a lesion discovered by other diagnostic modalities as US, barium,ivp, Staging
Laparoscopy-assisted D2 radical distal subtotal gastrectomy
 Masters of Gastrointestinal Surgery Laparoscopy-assisted D2 radical distal subtotal gastrectomy Xiaogeng Chen, Weihua Li, Jinsi Wang, Changshun Yang Department of Tumor Surgery, Fujian Provincial Hospital,
Masters of Gastrointestinal Surgery Laparoscopy-assisted D2 radical distal subtotal gastrectomy Xiaogeng Chen, Weihua Li, Jinsi Wang, Changshun Yang Department of Tumor Surgery, Fujian Provincial Hospital,
INVITED REVIEW ARTICL.E BILIARY ATRESIA
 INVITED REVIEW ARTICL.E Nagoya J. Meel. Sci. 62. 107-114. 1999 A NEW OPERATION FOR NONCORRECTABLE BILIARY ATRESIA HISAMI ANDO Departrnent o{ Pediatric Surgery, Nagoya University Schoo! of Medicine ABSTRACT
INVITED REVIEW ARTICL.E Nagoya J. Meel. Sci. 62. 107-114. 1999 A NEW OPERATION FOR NONCORRECTABLE BILIARY ATRESIA HISAMI ANDO Departrnent o{ Pediatric Surgery, Nagoya University Schoo! of Medicine ABSTRACT
Intrahepatic ramifications of the portal vein in the horse
 Intrahepatic ramifications of the portal vein in the horse Tadjalli, M. 1* and Moslemy, H. R. 2 1 Department of Anatomical Sciences, School of Veterinary Medicine, University of Shiraz, Shiraz, Iran; 2
Intrahepatic ramifications of the portal vein in the horse Tadjalli, M. 1* and Moslemy, H. R. 2 1 Department of Anatomical Sciences, School of Veterinary Medicine, University of Shiraz, Shiraz, Iran; 2
REPAIR OF LARGE CYSTOCELE
 REPAIR OF LARGE CYSTOCELE WITH RAZ SUSPENSION 17 VAGINAL INCISION AND DISSECTION Premarin cream application to the anterior vagina daily for 1 month before cystocele repair enriches the vasculature and
REPAIR OF LARGE CYSTOCELE WITH RAZ SUSPENSION 17 VAGINAL INCISION AND DISSECTION Premarin cream application to the anterior vagina daily for 1 month before cystocele repair enriches the vasculature and
THE THORACIC WALL. Boundaries Posteriorly by the thoracic part of the vertebral column. Anteriorly by the sternum and costal cartilages
 THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces Superiorly by the suprapleural
THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces Superiorly by the suprapleural
AATS Focus on Thoracic Surgery: Minimally Invasive Esophagectomy: Are We Still Getting Better in 2017?
 AATS Focus on Thoracic Surgery: Mastering Surgical Innovation Las Vegas, NV October 28, 2017 Session VIII: Video Session Minimally Invasive Esophagectomy: Are We Still Getting Better in 2017? James D.
AATS Focus on Thoracic Surgery: Mastering Surgical Innovation Las Vegas, NV October 28, 2017 Session VIII: Video Session Minimally Invasive Esophagectomy: Are We Still Getting Better in 2017? James D.
