Joint Theater Trauma System Clinical Practice Guideline
|
|
|
- Hugo Hubert Conley
- 5 years ago
- Views:
Transcription
1 Page 1 of 11 COMPARTMENT SYNDROME (CS) AND THE ROLE OF FASCIOTOMY IN EXTREMITY WAR WOUNDS Original Release/Approval 30 Apr 09 Note: This CPG requires an annual review. Reviewed: Feb 2012 Approved: 9 Mar 2012 Supersedes:, 30 Apr 2009 Minor Changes (or) Changes are substantial and require a thorough reading of this CPG (or) Significant Changes: System PI monitoring plan added; common reasons for incomplete fasciotomy added 1. Goal. Provide an overview of compartment syndrome (CS) and present a standardized approach to guide providers in the evaluation and treatment of patients with extremity war wounds, including the role of prophylactic and therapeutic fasciotomy. 2. Background. CS is a common, controversial, and disabling problem in extremity war injuries. Recent research indicates proper detection of compartment syndrome is lifesaving and delay in diagnosis can be lethal. 1 The operational definition of compartment syndrome is a clinical syndrome wherein high pressure within a myofascial space reduces perfusion and decreases tissue viability. Therapeutic fasciotomy is indicated for established compartment syndrome, and prophylactic fasciotomy is indicated for risk of compartment syndrome. 2-4 Fasciotomy during the lag phase between injury and syndrome onset is prophylactic. Early detection is challenging, so prophylactic fasciotomy should be routine when compartment syndrome is likely.. Prophylactic fasciotomy is most commonly indicated in patients with certain at risk fractures and in patients with prolonged ischemia or following limb reperfusion. Injury, treatment, and casualty variables affect risk (Tables 1 and 2) and may be interrelated. 1-7 The main factors are limb injury severity (particularly vessel injuries) and overall casualty injury severity (particularly shock) with a lesser factor being overresuscitation (particularly >5 liters of crystalloid). Tissue edema and subsequent swelling due to injury maximizes in 1 to 2 days. Additional swelling from post-injury ischemiareperfusion (e.g., revascularization, shock, and tourniquet use) appears to delay the maximal time of limb swelling further; perhaps to 2 to 5 days post injury. High altitude (including normal AE aircraft cabin pressure), in and of itself, is not a contributor to compartment syndrome (Ritenour, et al). Compartment syndrome can lead to significant morbidity and mortality (Table 3). Surveys indicate surgeons with more training and experience are more willing to perform fasciotomy. Once the decision is made to perform a prophylactic or therapeutic fasciotomy, a complete fasciotomy must be performed. There is evidence to support complete compartment release by full-length skin and fascial incisions is superior to limited fasciotomy. Incomplete fasciotomy, a clearly preventable problem, risks worsened patient morbidity, mortality and functional outcome. 3. Evaluation and Treatment. a. The signs and symptoms of CS are the classic 5 P s which include: pain on passive stretch of muscle often out of proportion to that of the injury as expected by the provider; palpably tense muscle compartments; paralysis; paresthesias or sensory deficit; pulselessness. 2 Pain is sensitive and early given a cooperative casualty, but it is not specific. Palpably tense muscle is specific but not sensitive, and usually there is some
2 Page 2 of 11 swelling.. Paralysis and paresthesias are generally late and least helpful acutely. Pulselessness is seen virtually never in civilian compartment syndrome, but occurs rarely in war, sometimes within minutes of an arterial injury or an expanding hematoma. b. The most common compartment syndrome is in the anterior leg. 1-2 About 45% of all compartment syndromes are caused by tibia fracture. Open fractures, even with traumatic fasciotomy, have higher CS rates than closed fractures because they are more severe, with more swelling and more often injured arteries. The most commonly missed compartment syndromes are in the anterior and deep posterior compartments of the leg. The most commonly incompletely released compartments are also in the leg. 1 The common reasons for incomplete calf fasciotomy are: 1) Improper identification of the septum dividing the anterior and lateral compartments. This can be avoided by making an initial transverse incision in the fascia overlying the septum, then deliberately opening the anterior and lateral compartments separately, creating a so called H incision. 2) Incomplete development of the deep posterior compartment release by not deliberately taking the the soleus muscle fibers off the posterior tibia. If performed correctly, the neuro-vascular bundle should be exposed in a fully decompressed deep posterior compartment. 3) Fascial incisions are too short and do not cover the entire extent of the fascial compartment either at the knee or ankle levels. c. Passive stretch pain (e.g., ankle dorsiflexion) and palpation of muscles for tenseness combined with an index of suspicion makes up the mainstay for clinical evaluation. Pressure monitoring by manometer does not reliably diagnose CS in theater, so the diagnosis remains clinical. Since there is currently no sensitive or specific technique for establishing the diagnosis of compartment syndrome, a fasciotomy should be considered in a patient with significant mechanism of injury and clinical findings suspicious for compartment syndrome. d. When monitoring patients for the development of CS, serial clinical examinations are repeated hourly when risk is high and less frequently when low. Provider experience and training improve detection. Documentation is important for later providers and performance improvement. The optimal methods of manometric monitoring of compartments and the clinically significant thresholds to identify compartment syndrome are, at present, not known. e. In one study, burns sustained in combat have been associated with an increased fasciotomy rate. 1 In the absence of crush injury, fracture, multiple trauma, overresuscitation, electrical injury or similar indications, prophylactic fasciotomies on burned extremities may increase morbidity and mortality and are not indicated. (For additional information on escharotomy and fasciotomy in the management of patients with extremity burns, see Burn Care JTTS CENTCOM CPG). f. Treatment of Compartment Syndrome of Prolonged Duration (>12 hours): Occasionally casualties present with a compartment syndrome of prolonged duration (> 12 hours) due to evacuation issues. This situation is associated with markedly increased risk of
3 complications including death and infection 6. These casualties may be best treated with appropriate resuscitation, urine alkalinization, mannitol use, and intensive support. Such conservative care has led to better outcomes than fasciotomy in casualties with closed injuries with mechanically crushed muscle (see Figure 1 and Reis & Better, 2005). Therefore, compartment syndromes with greater than 12 hours of warm ischemia with nonviable muscle should not routinely undergo fasciotomy. The role of amputation is currently unclear in this situation. 4. Performance Improvement (PI) Monitoring. a. Intent (Expected Outcomes). 1) When fasciotomy is performed, all compartments are completely released through full skin and fascial incisions 2) When indicated, fasciotomy is performed at the time of re-vascularizaton of an ischemic extremity. b. Performance/Adherence Measures. 1) When fasciotomy was performed, there was complete release of all compartments through full skin and fascial incisions 2) When indicated in patients with ischemic extremities, fasciotomy was performed at the time of re-vascularization c. Data Source. 1) Patient Record 2) Joint Theater Trauma Registry (JTTR) d. System Reporting & Frequency. The above constitutes the minimum criteria for PI monitoring of this CPG. System reporting will be performed annually; additional PI monitoring and system reporting may be performed as needed. The system review and data analysis will be performed by the Joint Theater Trauma System (JTTS) Director, JTTS Program Manager, and the Joint Trauma System (JTS) Performance Improvement Branch. 5. Responsibilities. It is the trauma team leader s responsibility to ensure familiarity, appropriate compliance and PI monitoring at the local level with this CPG. 6. References Ritenour AE, Dorlac WC, Fang R, et al. Complications after fasciotomy revision and delayed compartment release in combat patients. J Trauma. 2008;64(2 Suppl):S153-61; discussion S Landstuhl cohort. Inadequate fasciotomy risks mortality. Surgeons should have this. Mubarak SJ, Hargens AR. Compartment Syndromes and Volkmann s Contracture. Saunders, Philadelphia, First book on compartment syndrome, a dated classic. Page 3 of 11
4 US Army, Medical Research and Materiel Command. Compartment Syndrome: Diagnosis and Surgical Management DVD, minutes, how to do surgery. Office of The US Army Surgeon General, Health Policy and Services (HP&S) Directorate, All Army Action Order, Complications after fasciotomy revision and delayed compartment release in combat patients. 15 May Ritenour message. Klenerman L. The Tourniquet Manual. London: Springer; The only book on tourniquets which increase the risk of compartment syndrome somewhat especially if used incorrectly such as a venous tourniquet. Reis ND. Better OS. Mechanical muscle-crush injury and acute muscle-crush compartment syndrome : with special reference to earthquake casualties. J Bone Joint Surg Br. 87(4) :450-3, Late fasciotomy risks infection and mortality. Walters TJ, Kragh JF, Kauvar DS, Baer DG. The combined influence of hemorrhage and tourniquet application on the recovery of muscle function in rats. J Orthop Trauma. 22(1) :47-51, Risk factors are interrelated. Ritenour AE, Christy RJ, Roe JL, Baer DG, Dubick MA, Wade CE, Holcomb JB, Walters TJ. The effect of a hypobaric, hypoxic environment on acute skeletal muscle edema after ischemia-reperfusion injury in rats. J Surg Res May 15;160(2): Approved by CENTCOM JTTS Director, JTS Director and CENTCOM SG Opinions, interpretations, conclusions, and recommendations are those of the authors and are not necessarily endorsed by the Services or DoD. Page 4 of 11
5 Decreased Compartment Volume Increased Compartment Contents APPENDIX A TABLES and FIGURES Table 1 Risks for Acute Traumatic Compartment Syndrome* Tight cast or dressing, closure of prior fasciotomy, excess traction External limb compression or crush particularly in obtunded or incapacitated casualty Frostbite, burns or electric injury (may include escharotomy) Edema accumulation: embolism, intravascular thrombosis, replantation, venous tourniquet, injections, extravasation, infiltration, ergotamine ingestion, ischemia-reperfusion, swelling, artery injury or spasm, revascularization procedures, prolonged arterial tourniquet use, shock hypoperfusion, angiography and catheterization, limbs positioned well above heart, mal-positioned joints (ankle dorsiflexion,) or stretched muscles Prolonged immobilization and limb compression particularly with obtunded or drugged casualty, some surgical positioning Hemorrhage, hemophilia, coagulopathy, anticoagulation, vessel injury *Modified from reference 2 Fractures particularly tibia fractures in adults, supracondylar humerus fractures in children displaced, comminuted, or open fractures increase hemorrhage, swelling, and CS risk Popliteal cyst, long leg brace Page 5 of 11
6 Figure 1 Algorithm for Clinical Decision Making on Compartment Syndrome in a Deployed Setting Risk assessment for extremity compartment syndrome (Risk variables are listed in Table 1) Established compartment syndrome? Yes Warm ischemia duration >12 hours? No Yes Therapeutic fasciotomy No Capacity to closely monitor over time? Yes Close monitoring: Periodic reassessments No Prophylactic fasciotomy Limb Fasciotomy Detection Clinical Practice Guideline 2008 Page 6 of 11 Table 2 Healthcare Record Data in the Setting of Compartment Syndrome During War Was the fasciotomy prophylactic (compartment syndrome absent) or therapeutic (compartment syndrome present)? When was the fasciotomy indicated and when was the injury? When was the procedure (to determine treatment lag)? Was the casualty able to be followed closely? If so, what was the clinical course? Was the casualty alert, intubated, or head injured? Was there a nerve injury or nerve block/regional anesthetic? What was the injury or risk factors, e.g., ischemia-reperfusion, that indicated the procedure? What are the sources of ischemia-reperfusion in the injury and care of this case? Associated injuries altering risk of compartment syndrome: shock, occult hypoperfusion, hypoxia, nerve dysfunction, impaired, obtunded, or uncooperative casualty, arterial injury or ischemia, fractures with soft tissue injury, over-resuscitation syndrome, coagulopathies (including hemophilia, etc.), hematoma formation, crush injury, capillary leak syndrome, and prolonged compression.
7 Table 2 Healthcare Record Data in the Setting of Compartment Syndrome During War What were the surgical findings and muscle compartment response to the procedure? What was the technique (dermotomy, fasciotomy, surgical approach, length of fasciotomy)? Was there retinaculotomy or epimysiotomy? List names of all compartments released. What delimited the fasciotomy extent, e.g., anterior leg fascia goes from the proximal tibial crest near Gerdy s tubercle to the anterior ankle extensor retinaculum (crural ligament)? List associated procedures: debridement, irrigation, fracture fixation, etc. Planned care: staged? Closure, repeat debridement, delayed primary, skin graft, or flap Table 3 Morbidity Risk and Sequelae of Compartment Syndrome and Fasciotomy Potential Morbidity: Compartment Syndrome and Early Fasciotomy Potential Sequelae List: Compartment Syndrome with Late or Incomplete Fasciotomy skin scar, scaly skin, ulceration, tethered tendons postoperative arterial or graft thrombosis, thromboembolic disease wound infection, nonhealing fasciotomy wounds limb swelling or chronic edema, shape change of limb, muscle hernia pain, paresis or paralysis, paresthesia coverage challenge: primary closure, delayed primary closure, skin graft, flap possible repair of arterial injury worsening ischemia-reperfusion injury mortality, sepsis, multi-organ failure, acute kidney failure, myonecrosis, myoglobinemia, myoglobinuria, or rhabdomyolysis paresis or paralysis stiffness or contracture limb amputation, tissue loss, e.g., muscle debridement Page 7 of 11
8 Table 4 Data Sheet: Compartment Names, Main Muscles, and Diagnosis and Procedure Codes Compartment Deltoid Arm, Anterior Arm, Posterior Forearm, volar Forearm, dorsal Forearm, mobile wad Hand, interossei Hand, central palmar Hand, hypothenar Hand, thenar Gluteus maximus Gluteus medius Tensor fascia lata Thigh, anterior Page 8 of 11 Main muscle(s) deltoid biceps, brachialis triceps flexors extensors brachioradialis interossei flexors digiti minimi thumb muscles gluteus maximus other glutei tensor quadriceps Left or Right Wound Notes, Compartment Syndrome (CS), Diagnoses, Indications, & Findings : traumatic CS of upper extremity : traumatic CS of lower extremity : traumatic CS of other sites : CS, unspecified Prophylactic (CS absent) or therapeutic (CS present). Artery, vein, clot, & hematoma findings in compartment on exploration Procedure(s) and Tissue Response to Procedure 83.12: fasciotomy of hand 83.14: fasciotomy, division of fascia 83.09: incision of fascia 86.09: escharotomy dermotomy, epimysiotomy Response: muscles bulged through fasciotomy, no bulge, pulse returned after absence
9 Table 4 Data Sheet: Compartment Names, Main Muscles, and Diagnosis and Procedure Codes Compartment Thigh, posterior Thigh, adductor Leg, anterior Leg, lateral Leg, deep posterior Leg, superficial posterior Foot, interossei Foot, central Foot, lateral Foot, medial Iliacus Main muscle(s) hamstrings adductors tibialis anterior peronei tibialis posterior gastrocnemius interossei flexors digiti minimi great toe muscles iliacus, psoas Left or Right Wound Notes, Compartment Syndrome (CS), Diagnoses, Indications, & Findings Procedure(s) and Tissue Response to Procedure Table 5 Operative Note Template for Dictation, Surgical Planning, or Data Collection 1. Patient 2. Surgeon 3. Date of Surgery 4. Anesthesia 5. EBL: 6. Tubes 7. Specimens 8. Complications 9. Implants, Devices 10. Indication for operation: a. established compartment syndrome (therapeutic) b. risk of compartment syndrome developing (prophylactic) 11. Preoperative wound appearance: a. size (volume of damaged tissue: large surgeon hand ~500ml) b. depth, location, contamination material or matter Page 9 of 11
10 Table 5 Operative Note Template for Dictation, Surgical Planning, or Data Collection 12. Preoperative imaging findings: a. soft tissue injury seen & fracture 13. Examination under anesthesia, fluoroscopy, and surgical exploration findings: a. distal pulse status b. wound size, depth, location, contamination, materials or matter; burn eschar location and depth c. vessel status, pulse, limb perfusion, capillary refill, congestion, edema, color of skin, warmth d. clot presence, intravascular or extra vascular site, size (volume), location e. hematoma presence f. compartment hardness: soft, hard i. epimysiotomy (if done by muscle name or compartment if known) ii. retinaculotomy (if done by name, e.g., partial proximal ankle extensor iii. retinaculotomy extended from anterior leg compartment fasciotomy iv. result of fasciotomy and procedure (distal perfusion and pulse; gap in fasciotomy edges on release in cm; bulging out of muscles in compartment) v. compartments soft or hard vi. muscle color, consistency, contractility, capacity to bleed 14. Patient condition, status, disposition and plan: 15. Key note for air evacuation: Patient has been monitored for X hours after injury/surgery and has not had progression of signs or symptoms of compartment syndrome. Page 10 of 11
11 APPENDIX B ADDITIONAL INFORMATION REGARDING OFF-LABEL USES IN CPGs 1. Purpose. The purpose of this Appendix is to ensure an understanding of DoD policy and practice regarding inclusion in CPGs of off-label uses of U.S. Food and Drug Administration (FDA) approved products. This applies to off-label uses with patients who are armed forces members. 2. Background. Unapproved (i.e., off-label ) uses of FDA-approved products are extremely common in American medicine and are usually not subject to any special regulations. However, under Federal law, in some circumstances, unapproved uses of approved drugs are subject to FDA regulations governing investigational new drugs. These circumstances include such uses as part of clinical trials, and in the military context, command required, unapproved uses. Some command requested unapproved uses may also be subject to special regulations. 3. Additional Information Regarding Off-Label Uses in CPGs. The inclusion in CPGs of off-label uses is not a clinical trial, nor is it a command request or requirement. Further, it does not imply that the Military Health System requires that use by DoD health care practitioners or considers it to be the standard of care. Rather, the inclusion in CPGs of off-label uses is to inform the clinical judgment of the responsible health care practitioner by providing information regarding potential risks and benefits of treatment alternatives. The decision is for the clinical judgment of the responsible health care practitioner within the practitioner-patient relationship. 4. Additional Procedures. a. Balanced Discussion. Consistent with this purpose, CPG discussions of off-label uses specifically state that they are uses not approved by the FDA. Further, such discussions are balanced in the presentation of appropriate clinical study data, including any such data that suggest caution in the use of the product and specifically including any FDAissued warnings. b. Quality Assurance Monitoring. With respect to such off-label uses, DoD procedure is to maintain a regular system of quality assurance monitoring of outcomes and known potential adverse events. For this reason, the importance of accurate clinical records is underscored. c. Information to Patients. Good clinical practice includes the provision of appropriate information to patients. Each CPG discussing an unusual off-label use will address the issue of information to patients. When practicable, consideration will be given to including in an appendix an appropriate information sheet for distribution to patients, whether before or after use of the product. Information to patients should address in plain language: a) that the use is not approved by the FDA; b) the reasons why a DoD health care practitioner would decide to use the product for this purpose; and c) the potential risks associated with such use. Page 11 of 11
Compartment Syndrome
 Compartment Syndrome Chapter 34 Compartment Syndrome Introduction Compartment syndrome may occur with an injury to any fascial compartment. The fascial defect caused by the injury may not be adequate to
Compartment Syndrome Chapter 34 Compartment Syndrome Introduction Compartment syndrome may occur with an injury to any fascial compartment. The fascial defect caused by the injury may not be adequate to
Topic 4: Fractures and External Fixation
 Topic 4: Fractures and External Fixation Acute Compartment Syndrome Prof. Dr. Andreas Platz Stadtspital Triemli, Zürich Demographics Incidence: Men 7.3/100,000 Women 0.7/100,000 69% due to trauma 36% fx
Topic 4: Fractures and External Fixation Acute Compartment Syndrome Prof. Dr. Andreas Platz Stadtspital Triemli, Zürich Demographics Incidence: Men 7.3/100,000 Women 0.7/100,000 69% due to trauma 36% fx
Injuries to the Hands and Feet
 Injuries to the Hands and Feet Chapter 26 Injuries to the Hands and Feet Introduction Combat injuries to the hands and feet differ from those of the arms and legs in terms of mortality and morbidity. Death
Injuries to the Hands and Feet Chapter 26 Injuries to the Hands and Feet Introduction Combat injuries to the hands and feet differ from those of the arms and legs in terms of mortality and morbidity. Death
Compartment Syndrome
 Compartment Syndrome Andrew H. Schmidt, M.D. Professor, Dept. of Orthopedic Surgery, Univ. of Minnesota Chief, Department of Orthopaedic Surgery Hennepin County Medical Center April 2016 Disclosure Information
Compartment Syndrome Andrew H. Schmidt, M.D. Professor, Dept. of Orthopedic Surgery, Univ. of Minnesota Chief, Department of Orthopaedic Surgery Hennepin County Medical Center April 2016 Disclosure Information
This presentation is the intellectual property of the author. Contact them for permission to reprint and/or distribute.
 Introduction Compartment Syndromes of the Leg Related to Athletic Activity Mark M. Casillas, M.D. Consequences of a misdiagnosis persistence of a performance limitation loss of function/compartment loss
Introduction Compartment Syndromes of the Leg Related to Athletic Activity Mark M. Casillas, M.D. Consequences of a misdiagnosis persistence of a performance limitation loss of function/compartment loss
Combat Extremity Vascular Trauma
 Combat Extremity Vascular Trauma Training teams to be a TEAM Chatt A. Johnson LTC, MC, USA 08 March 2010 US Army Trauma Training Center Core Discussion Series Outline: Combat Vascular Injury Physiologic
Combat Extremity Vascular Trauma Training teams to be a TEAM Chatt A. Johnson LTC, MC, USA 08 March 2010 US Army Trauma Training Center Core Discussion Series Outline: Combat Vascular Injury Physiologic
Injuries to the Hands and Feet
 Injuries to the Hands and Feet Chapter 24 Injuries to the Hands and Feet Introduction Combat injuries to the hands and feet differ from those of the arms and legs in terms of mortality and morbidity. The
Injuries to the Hands and Feet Chapter 24 Injuries to the Hands and Feet Introduction Combat injuries to the hands and feet differ from those of the arms and legs in terms of mortality and morbidity. The
Joint Theater Trauma System Clinical Practice Guideline
 Page 1 of 7 Joint Theater Trauma System Clinical Practice Guideline TRAUMA AIRWAY MANAGEMENT Original Release/Approval 18 Dec 2004 Note: This CPG requires an annual review. Reviewed: May 2012 Approved:
Page 1 of 7 Joint Theater Trauma System Clinical Practice Guideline TRAUMA AIRWAY MANAGEMENT Original Release/Approval 18 Dec 2004 Note: This CPG requires an annual review. Reviewed: May 2012 Approved:
Rio Grande Trauma Conference December 1 st and 2 nd, 2016
 Rio Grande Trauma Conference December 1 st and 2 nd, 2016 Why is Acute Compartment Syndrome Important? It s a clinical emergency If left untreated, it can lead to severe morbidity and mortality. It triples
Rio Grande Trauma Conference December 1 st and 2 nd, 2016 Why is Acute Compartment Syndrome Important? It s a clinical emergency If left untreated, it can lead to severe morbidity and mortality. It triples
Joint Theater Trauma System Clinical Practice Guideline
 POST-SPLENECTOMY VACCINATION Original Release/Approval 30 Mar 2008 Note: This CPG requires an annual review. Reviewed: Jan 2012 Approved: 6 Mar 2012 Supersedes: Post Splenectomy Vaccination, 30 Jun 2010
POST-SPLENECTOMY VACCINATION Original Release/Approval 30 Mar 2008 Note: This CPG requires an annual review. Reviewed: Jan 2012 Approved: 6 Mar 2012 Supersedes: Post Splenectomy Vaccination, 30 Jun 2010
The Lower Limb VI: The Leg. Anatomy RHS 241 Lecture 6 Dr. Einas Al-Eisa
 The Lower Limb VI: The Leg Anatomy RHS 241 Lecture 6 Dr. Einas Al-Eisa Muscles of the leg Posterior compartment (superficial & deep): primary plantar flexors of the foot flexors of the toes Anterior compartment:
The Lower Limb VI: The Leg Anatomy RHS 241 Lecture 6 Dr. Einas Al-Eisa Muscles of the leg Posterior compartment (superficial & deep): primary plantar flexors of the foot flexors of the toes Anterior compartment:
Contributors. LCDR Charles Osier, MC, USN LCDR Chris Smith, MC, USN MAJ Daniel Stinner, MC, USA MAJ Jessica Rivera, MC, USA
 JOINT TRAUMA SYSTEM CLINICAL PRACTIC E GUIDELINE (JTS CPG ) Orthopaedic Trauma: Extremity Fractures (CPG ID: 56) To describe the initial non-surgical and surgical management of extremity fractures and
JOINT TRAUMA SYSTEM CLINICAL PRACTIC E GUIDELINE (JTS CPG ) Orthopaedic Trauma: Extremity Fractures (CPG ID: 56) To describe the initial non-surgical and surgical management of extremity fractures and
musculoskeletal system anatomy nerves of the lower limb 2 done by: Dina sawadha & mohammad abukabeer
 musculoskeletal system anatomy nerves of the lower limb 2 done by: Dina sawadha & mohammad abukabeer #Sacral plexus : emerges from the ventral rami of the spinal segments L4 - S4 and provides motor and
musculoskeletal system anatomy nerves of the lower limb 2 done by: Dina sawadha & mohammad abukabeer #Sacral plexus : emerges from the ventral rami of the spinal segments L4 - S4 and provides motor and
The Muscular System. Chapter 10 Part D. PowerPoint Lecture Slides prepared by Karen Dunbar Kareiva Ivy Tech Community College
 Chapter 10 Part D The Muscular System Annie Leibovitz/Contact Press Images PowerPoint Lecture Slides prepared by Karen Dunbar Kareiva Ivy Tech Community College Table 10.14: Muscles Crossing the Hip and
Chapter 10 Part D The Muscular System Annie Leibovitz/Contact Press Images PowerPoint Lecture Slides prepared by Karen Dunbar Kareiva Ivy Tech Community College Table 10.14: Muscles Crossing the Hip and
Peripheral Nervous System: Lower Body
 Peripheral Nervous System: Lower Body MSTN121 - Neurophysiology Session 11 Department of Myotherapy Lumbar Plexus Iliohypogastric nerve (T12-L1) Motor: Transverse abdominis and internal obliques Sensory:
Peripheral Nervous System: Lower Body MSTN121 - Neurophysiology Session 11 Department of Myotherapy Lumbar Plexus Iliohypogastric nerve (T12-L1) Motor: Transverse abdominis and internal obliques Sensory:
Where should you palpate the pulse of different arteries in the lower limb?
 Where should you palpate the pulse of different arteries in the lower limb? The femoral artery In the femoral triangle, its pulse is easily felt just inferior to the inguinal ligament midway between the
Where should you palpate the pulse of different arteries in the lower limb? The femoral artery In the femoral triangle, its pulse is easily felt just inferior to the inguinal ligament midway between the
Year 2004 Paper one: Questions supplied by Megan
 QUESTION 47 A 58yo man is noted to have a right foot drop three days following a right total hip replacement. On examination there is weakness of right ankle dorsiflexion and toe extension (grade 4/5).
QUESTION 47 A 58yo man is noted to have a right foot drop three days following a right total hip replacement. On examination there is weakness of right ankle dorsiflexion and toe extension (grade 4/5).
Joint Theater Trauma System Clinical Practice Guideline
 CERVICAL SPINE EVALUATION & N-SURGICAL MANAGEMENT Original Release/Approval: 1 March 2010 Note: This CPG requires an annual review Reviewed: Feb 2012 Approved: 19 Mar 2012 Supersedes: Cervical Spine Evaluation,
CERVICAL SPINE EVALUATION & N-SURGICAL MANAGEMENT Original Release/Approval: 1 March 2010 Note: This CPG requires an annual review Reviewed: Feb 2012 Approved: 19 Mar 2012 Supersedes: Cervical Spine Evaluation,
lesser trochanter of femur lesser trochanter of femur iliotibial tract (connective tissue) medial surface of proximal tibia
 LOWER LIMB MUSCLES OF THE APPENDICULAR SKELETON The muscles that act on the lower limb fall into three groups: those that move the thigh, those that move the lower leg, and those that move the ankle, foot,
LOWER LIMB MUSCLES OF THE APPENDICULAR SKELETON The muscles that act on the lower limb fall into three groups: those that move the thigh, those that move the lower leg, and those that move the ankle, foot,
Lumbar Plexus. Ventral rami L1 L4 Supplies: Major nerves.. Abdominal wall External genitalia Anteromedial thigh
 Lower Limb Nerves Lectures Objectives Describe the structure and relationships of the plexuses of the lower limb. Describe the course, relationships and structures supplied for the major nerves of the
Lower Limb Nerves Lectures Objectives Describe the structure and relationships of the plexuses of the lower limb. Describe the course, relationships and structures supplied for the major nerves of the
Lower Limb Nerves. Clinical Anatomy
 Lower Limb Nerves Clinical Anatomy Lumbar Plexus Ventral rami L1 L4 Supplies: Abdominal wall External genitalia Anteromedial thigh Major nerves.. Lumbar Plexus Nerves relation to psoas m. : Obturator n.
Lower Limb Nerves Clinical Anatomy Lumbar Plexus Ventral rami L1 L4 Supplies: Abdominal wall External genitalia Anteromedial thigh Major nerves.. Lumbar Plexus Nerves relation to psoas m. : Obturator n.
CHAPTER 16 LOWER EXTREMITY. Amanda K Silva, MD and Warren Ellsworth, MD, FACS
 CHAPTER 16 LOWER EXTREMITY Amanda K Silva, MD and Warren Ellsworth, MD, FACS The plastic and reconstructive surgeon is often called upon to treat many wound problems of the lower extremity. These include
CHAPTER 16 LOWER EXTREMITY Amanda K Silva, MD and Warren Ellsworth, MD, FACS The plastic and reconstructive surgeon is often called upon to treat many wound problems of the lower extremity. These include
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 18 Orthopedic Trauma Key Points 2 18.1 Upper Extremity Injuries Clavicle Fractures Diagnose fractures from the history and by physical examination Treat with a
Surgical Care at the District Hospital 1 18 Orthopedic Trauma Key Points 2 18.1 Upper Extremity Injuries Clavicle Fractures Diagnose fractures from the history and by physical examination Treat with a
CASE REPORT Compartment Syndrome of the Hand: Beware of Innocuous Radius Fractures
 CASE REPORT Compartment Syndrome of the Hand: Beware of Innocuous Radius Fractures Francesco Maria Egro, MBChB, BSc (Hons), MRCS, MSc, Matthew Robert Frederick Jaring, MBBS, BSc (Hons), and Asif Zafar
CASE REPORT Compartment Syndrome of the Hand: Beware of Innocuous Radius Fractures Francesco Maria Egro, MBChB, BSc (Hons), MRCS, MSc, Matthew Robert Frederick Jaring, MBBS, BSc (Hons), and Asif Zafar
OBJECTIVES: Define basic assessments skills needed to identify orthopedic injuries. Differentiate when an orthopedic injury is a medical emergency
 1 2 How to Triage Orthopaedic Care David W. Gray, M.D. OBJECTIVES: Define basic assessments skills needed to identify orthopedic injuries Differentiate when an orthopedic injury is a medical emergency
1 2 How to Triage Orthopaedic Care David W. Gray, M.D. OBJECTIVES: Define basic assessments skills needed to identify orthopedic injuries Differentiate when an orthopedic injury is a medical emergency
Nursing Management: Musculoskeletal Trauma and Orthopedic Surgery. By: Aun Lauriz E. Macuja SAC_SN4
 Nursing Management: Musculoskeletal Trauma and Orthopedic Surgery By: Aun Lauriz E. Macuja SAC_SN4 The most common cause of musculoskeletal injuries is a traumatic event resulting in fracture, dislocation,
Nursing Management: Musculoskeletal Trauma and Orthopedic Surgery By: Aun Lauriz E. Macuja SAC_SN4 The most common cause of musculoskeletal injuries is a traumatic event resulting in fracture, dislocation,
Versatility of Reverse Sural Artery Flap for Heel Reconstruction
 ORIGINAL ARTICLE Introduction: The heel has two parts, weight bearing and non-weight bearing part. Soft tissue heel reconstruction has been a challenge due to its complex nature of anatomy, weight bearing
ORIGINAL ARTICLE Introduction: The heel has two parts, weight bearing and non-weight bearing part. Soft tissue heel reconstruction has been a challenge due to its complex nature of anatomy, weight bearing
Anatomy MCQs Week 13
 Anatomy MCQs Week 13 1. Posterior to the medial malleolus of the ankle: The neurovascular bundle lies between Tibialis Posterior and Flexor Digitorum Longus The tendon of Tibialis Posterior inserts into
Anatomy MCQs Week 13 1. Posterior to the medial malleolus of the ankle: The neurovascular bundle lies between Tibialis Posterior and Flexor Digitorum Longus The tendon of Tibialis Posterior inserts into
Vascular Injuries. Chapter 27
 Vascular Injuries Chapter 27 Vascular Injuries Introduction History. ο World War II: Popliteal artery injuries were routinely ligated with a 73% amputation rate. ο Korean War: Formal repair of peripheral
Vascular Injuries Chapter 27 Vascular Injuries Introduction History. ο World War II: Popliteal artery injuries were routinely ligated with a 73% amputation rate. ο Korean War: Formal repair of peripheral
Organization of the Lower Limb
 Organization of the Lower Limb Limb Development Lower limb develops in an aterolateral position at the level of the L2 to S3 trunk segments Great toe positioned cephalic direction with the soles of the
Organization of the Lower Limb Limb Development Lower limb develops in an aterolateral position at the level of the L2 to S3 trunk segments Great toe positioned cephalic direction with the soles of the
Basic Care of Common Fractures Utku Kandemir, MD
 Basic Care of Common Fractures Utku Kandemir, MD Assistant Clinical Professor Trauma & Sports Medicine Dept. of Orthopaedic Surgery UCSF / SFGH History Physical Exam Radiology Treatment History Acute trauma
Basic Care of Common Fractures Utku Kandemir, MD Assistant Clinical Professor Trauma & Sports Medicine Dept. of Orthopaedic Surgery UCSF / SFGH History Physical Exam Radiology Treatment History Acute trauma
Contributors. LtCol Wade Gordon, MC, USAF CDR Luke Balsamo, MC, USN LtCol Max Talbot, RCMS, CF LCDR Charles Osier, MC, USN
 JOINT TRAUMA SYSTEM CLINICAL PRACTIC E GUIDELINE (JTS CPG ) Amputation: Evaluation and Treatment (CPG 07) To provide standardization of optimal care for the performance of wound management and life-saving
JOINT TRAUMA SYSTEM CLINICAL PRACTIC E GUIDELINE (JTS CPG ) Amputation: Evaluation and Treatment (CPG 07) To provide standardization of optimal care for the performance of wound management and life-saving
Presented at 2015 TQIP conference. Developed by a panel of experts. Evidence based with expert opinion as needed
 Presented at 2015 TQIP conference Developed by a panel of experts Evidence based with expert opinion as needed Orthopaedic Trauma Best Practice Guidelines (BPG) Goals Offer guidance on what is practical
Presented at 2015 TQIP conference Developed by a panel of experts Evidence based with expert opinion as needed Orthopaedic Trauma Best Practice Guidelines (BPG) Goals Offer guidance on what is practical
Injuries to the Pelvis and Extremities
 Injuries to the Pelvis and Extremities Presley Regional Trauma Center Department of Surgery University of Tennessee Health Science Center Memphis, Tennessee General Common occur in 85% of blunt trauma
Injuries to the Pelvis and Extremities Presley Regional Trauma Center Department of Surgery University of Tennessee Health Science Center Memphis, Tennessee General Common occur in 85% of blunt trauma
Amputations. Chapter 23
 Amputations Chapter 23 Amputations Introduction Battle casualties who sustain amputations have the most severe extremity injuries. Historically, 1 in 3 patients with a major amputation (proximal to the
Amputations Chapter 23 Amputations Introduction Battle casualties who sustain amputations have the most severe extremity injuries. Historically, 1 in 3 patients with a major amputation (proximal to the
Muscles of the Gluteal Region
 Muscles of the Gluteal Region 1 Some of the most powerful in the body Extend the thigh during forceful extension Stabilize the iliotibial band and thoracolumbar fascia Related to shoulders and arms because
Muscles of the Gluteal Region 1 Some of the most powerful in the body Extend the thigh during forceful extension Stabilize the iliotibial band and thoracolumbar fascia Related to shoulders and arms because
Due in Lab weeks because of Thanksgiving Prelab #10. Homework #8. Both sides! Both sides!
 Lab 8 MUSCLES Due in Lab 10 2 weeks because of Thanksgiving Prelab #10 Both sides! Homework #8 Both sides! Refer to Muscles 22-23 Naming of muscles Origin Site of muscle attachment that doesn t move during
Lab 8 MUSCLES Due in Lab 10 2 weeks because of Thanksgiving Prelab #10 Both sides! Homework #8 Both sides! Refer to Muscles 22-23 Naming of muscles Origin Site of muscle attachment that doesn t move during
Mohammad Ashraf. Abdulrahman Al-Hanbali. Ahmad Salman. 1 P a g e
 - 7 Mohammad Ashraf Abdulrahman Al-Hanbali Ahmad Salman 1 P a g e Structures under the cover of Gluteus Maximus: 1-Bones: Ileum, Femur (Head, greater trochanter and gluteal tuberosity), Ischium (ischial
- 7 Mohammad Ashraf Abdulrahman Al-Hanbali Ahmad Salman 1 P a g e Structures under the cover of Gluteus Maximus: 1-Bones: Ileum, Femur (Head, greater trochanter and gluteal tuberosity), Ischium (ischial
Knee Disarticulation Amputation
 Knee Disarticulation Amputation Pre-Op 64 year old man, previous spinal cord injury, diabetes, renal failure, and a history of spasticity with dynamic knee flexion contracture. He had an open left ankle
Knee Disarticulation Amputation Pre-Op 64 year old man, previous spinal cord injury, diabetes, renal failure, and a history of spasticity with dynamic knee flexion contracture. He had an open left ankle
The Leg. Prof. Oluwadiya KS
 The Leg Prof. Oluwadiya KS www.oluwadiya.sitesled.com Compartments of the leg 4 Four Compartments: 1. Anterior compartment Deep fibular nerve Dorsiflexes the foot and toes 2. Lateral Compartment Superficial
The Leg Prof. Oluwadiya KS www.oluwadiya.sitesled.com Compartments of the leg 4 Four Compartments: 1. Anterior compartment Deep fibular nerve Dorsiflexes the foot and toes 2. Lateral Compartment Superficial
DISSECTION SCHEDULE. Session I - Hip (Front) & Thigh (Superficial)
 DISSECTION SCHEDULE Session I - Hip (Front) & Thigh (Superficial) Surface anatomy Inguinal region Gluteal region Thigh Leg Foot bones Hip bone Femur Superficial fascia Great saphenous vein Superficial
DISSECTION SCHEDULE Session I - Hip (Front) & Thigh (Superficial) Surface anatomy Inguinal region Gluteal region Thigh Leg Foot bones Hip bone Femur Superficial fascia Great saphenous vein Superficial
Minor Surgical Procedures. Thomas W. White, MD, FACS, CNSC. Mark R. Michael, ANCP
 Minor Surgical Procedures Thomas W. White, MD, FACS, CNSC Trauma Surgery/Critical Care, Medical Director Nutrition Support Service, Shock Trauma ICU Attending, Intermountain Medical Center; Clinical Professor
Minor Surgical Procedures Thomas W. White, MD, FACS, CNSC Trauma Surgery/Critical Care, Medical Director Nutrition Support Service, Shock Trauma ICU Attending, Intermountain Medical Center; Clinical Professor
1/3/2008. Karen Burke Priscilla LeMone Elaine Mohn-Brown. Medical-Surgical Nursing Care, 2e Karen Burke, Priscilla LeMone, and Elaine Mohn-Brown
 Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 42 Caring for Clients with Musculoskeletal Trauma Musculoskeletal Trauma Tissue is subjected to more
Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 42 Caring for Clients with Musculoskeletal Trauma Musculoskeletal Trauma Tissue is subjected to more
How to Triage Orthopaedic Care. David W. Gray, M.D.
 How to Triage Orthopaedic Care David W. Gray, M.D. OBJECTIVES: Define basic assessments skills needed to identify orthopedic injuries Differentiate when an orthopedic injury is a medical emergency Determine
How to Triage Orthopaedic Care David W. Gray, M.D. OBJECTIVES: Define basic assessments skills needed to identify orthopedic injuries Differentiate when an orthopedic injury is a medical emergency Determine
HUMAN BODY COURSE LOWER LIMB NERVES AND VESSELS
 HUMAN BODY COURSE LOWER LIMB NERVES AND VESSELS October 22, 2010 D. LOWER LIMB MUSCLES 2. Lower limb compartments ANTERIOR THIGH COMPARTMENT General lfunction: Hip flexion, knee extension, other motions
HUMAN BODY COURSE LOWER LIMB NERVES AND VESSELS October 22, 2010 D. LOWER LIMB MUSCLES 2. Lower limb compartments ANTERIOR THIGH COMPARTMENT General lfunction: Hip flexion, knee extension, other motions
Tibial and Common Peroneal Nerve Compression in The Popliteal Fossa: A Case Report and Literature Review
 ISPUB.COM The Internet Journal of Plastic Surgery Volume 2 Number 1 Tibial and Common Peroneal Nerve Compression in The Popliteal Fossa: A Case Report and Literature D Reichner, G Evans Citation D Reichner,
ISPUB.COM The Internet Journal of Plastic Surgery Volume 2 Number 1 Tibial and Common Peroneal Nerve Compression in The Popliteal Fossa: A Case Report and Literature D Reichner, G Evans Citation D Reichner,
REPLANTATION OF POST-TRAUMATIC LOWER LIMB AMPUTATION
 Int. J. Pharm. Med. & Bio. Sc. 2014 Sanjitsingh R Sulhyan et al., 2014 Research Paper ISSN 2278 5221 www.ijpmbs.com Vol. 3, No. 1, January 2014 2014 IJPMBS. All Rights Reserved REPLANTATION OF POST-TRAUMATIC
Int. J. Pharm. Med. & Bio. Sc. 2014 Sanjitsingh R Sulhyan et al., 2014 Research Paper ISSN 2278 5221 www.ijpmbs.com Vol. 3, No. 1, January 2014 2014 IJPMBS. All Rights Reserved REPLANTATION OF POST-TRAUMATIC
Gluteal Compartment Syndrome
 Gluteal Compartment Syndrome AND other common compartment syndromes Erlanger Trauma Symposium June 1, 2017 Hunter Rooks, MD Philip W. Smith, MD Nicholas Ballay, MD; John Huggins, MD; Timothy Stevens, MD;
Gluteal Compartment Syndrome AND other common compartment syndromes Erlanger Trauma Symposium June 1, 2017 Hunter Rooks, MD Philip W. Smith, MD Nicholas Ballay, MD; John Huggins, MD; Timothy Stevens, MD;
Surgical Complications
 Surgical Complications Complications are common even with ideal management. Recently, Bashyal performed a retrospective review of 622 patients treated for supracondylar fractures and evaluated the complications
Surgical Complications Complications are common even with ideal management. Recently, Bashyal performed a retrospective review of 622 patients treated for supracondylar fractures and evaluated the complications
MUSCLES OF THE LOWER LIMBS
 MUSCLES OF THE LOWER LIMBS Naming, location and general function Dr. Nabil khouri ROLES THAT SHOULD NOT BE FORGOTTEN Most anterior compartment muscles of the hip and thigh Flexor of the femur at the hip
MUSCLES OF THE LOWER LIMBS Naming, location and general function Dr. Nabil khouri ROLES THAT SHOULD NOT BE FORGOTTEN Most anterior compartment muscles of the hip and thigh Flexor of the femur at the hip
Leg. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 Leg Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Skin of the Leg Cutaneous Nerves Medially: The saphenous nerve, a branch of the femoral nerve supplies the skin on the medial surface
Leg Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Skin of the Leg Cutaneous Nerves Medially: The saphenous nerve, a branch of the femoral nerve supplies the skin on the medial surface
Sussex Trauma Network Guidelines for: The Management of Compartment Syndrome
 Sussex Trauma Network Guidelines for: The Management of Compartment Syndrome Management of Compartment Syndrome Control Page Version: 1 Category number: Approved by: Date approved: Name of author: and
Sussex Trauma Network Guidelines for: The Management of Compartment Syndrome Management of Compartment Syndrome Control Page Version: 1 Category number: Approved by: Date approved: Name of author: and
KNEE DISLOCATION. The most common injury will be an anterior dislocation, and this usually results from a hyperextension mechanism.
 KNEE DISLOCATION Introduction Dislocation of the knee is a severe injury associated with major soft tissue injury and a high incidence of damage to the popliteal artery. There is displacement of the tibia
KNEE DISLOCATION Introduction Dislocation of the knee is a severe injury associated with major soft tissue injury and a high incidence of damage to the popliteal artery. There is displacement of the tibia
Muscles of the Hip 1. Tensor Fasciae Latae O: iliac crest I: lateral femoral condyle Action: abducts the thigh Nerve: gluteal nerve
 Muscles of the Hip 1. Tensor Fasciae Latae O: iliac crest I: lateral femoral condyle Action: abducts the thigh Nerve: gluteal nerve 2. Gluteus Maximus O: ilium I: femur Action: abduct the thigh Nerve:
Muscles of the Hip 1. Tensor Fasciae Latae O: iliac crest I: lateral femoral condyle Action: abducts the thigh Nerve: gluteal nerve 2. Gluteus Maximus O: ilium I: femur Action: abduct the thigh Nerve:
Organization of the Lower Limb
 Organization of the Lower Limb Most illustrations from: Thieme Atlas of Anatomy: Musculoskeletal System. M Schuenke, et al, 2006. Anatomy: A Regional Atlas of the Human Body. Carmine Clemente, 4th edition.
Organization of the Lower Limb Most illustrations from: Thieme Atlas of Anatomy: Musculoskeletal System. M Schuenke, et al, 2006. Anatomy: A Regional Atlas of the Human Body. Carmine Clemente, 4th edition.
موسى صالح عبد الرحمن الحنبلي أحمد سلمان
 8 موسى صالح عبد الرحمن الحنبلي أحمد سلمان 1 P a g e Today we will talk about a new region, which is the leg. And as always, we will start with studying the sensory innervation of the leg. What is the importance
8 موسى صالح عبد الرحمن الحنبلي أحمد سلمان 1 P a g e Today we will talk about a new region, which is the leg. And as always, we will start with studying the sensory innervation of the leg. What is the importance
Hemorrhage Control. Chapter 6
 Chapter 6 The hemorrhage that take[s] place when a main artery is divided is usually so rapid and so copious that the wounded man dies before help can reach him. Colonel H. M. Gray, 1919 Stop the Bleeding!
Chapter 6 The hemorrhage that take[s] place when a main artery is divided is usually so rapid and so copious that the wounded man dies before help can reach him. Colonel H. M. Gray, 1919 Stop the Bleeding!
Muscles of the lower extremities. Dr. Nabil khouri MD, MSc, Ph.D
 Muscles of the lower extremities Dr. Nabil khouri MD, MSc, Ph.D Posterior leg Popliteal fossa Boundaries Biceps femoris (superior-lateral) Semitendinosis and semimembranosis (superior-medial) Gastrocnemius
Muscles of the lower extremities Dr. Nabil khouri MD, MSc, Ph.D Posterior leg Popliteal fossa Boundaries Biceps femoris (superior-lateral) Semitendinosis and semimembranosis (superior-medial) Gastrocnemius
ANATYOMY OF The thigh
 ANATYOMY OF The thigh 1- Lateral cutaneous nerve of the thigh Ι) Skin of the thigh Anterior view 2- Femoral branch of the genitofemoral nerve 5- Intermediate cutaneous nerve of the thigh 1, 2 and 3 are
ANATYOMY OF The thigh 1- Lateral cutaneous nerve of the thigh Ι) Skin of the thigh Anterior view 2- Femoral branch of the genitofemoral nerve 5- Intermediate cutaneous nerve of the thigh 1, 2 and 3 are
Muscle Anatomy Review Chart
 Muscle Anatomy Review Chart BACK Superficial (5) Trapezius Transverse cervical a. Latissimus dorsi Thoracodorsal a. Rhomboideus major Dorsal scapular a. Rhomboideus minor Levator scapulae Intermediate
Muscle Anatomy Review Chart BACK Superficial (5) Trapezius Transverse cervical a. Latissimus dorsi Thoracodorsal a. Rhomboideus major Dorsal scapular a. Rhomboideus minor Levator scapulae Intermediate
Split Hemianterior Tibialis Turndown Muscle Flap for Coverage of Distal Leg Wounds With Preservation of Function
 Split Hemianterior Tibialis Turndown Muscle Flap for Coverage of Distal Leg Wounds With Preservation of Function Vinay Gundlapalli, MD, a John W. Gillespie III, MD, b and Chris D. Tzarnas, MD, FACS c a
Split Hemianterior Tibialis Turndown Muscle Flap for Coverage of Distal Leg Wounds With Preservation of Function Vinay Gundlapalli, MD, a John W. Gillespie III, MD, b and Chris D. Tzarnas, MD, FACS c a
Lower limb summary. Anterior compartment of the thigh. Done By: Laith Qashou. Doctor_2016
 Lower limb summary Done By: Laith Qashou Doctor_2016 Anterior compartment of the thigh Sartorius Anterior superior iliac spine Upper medial surface of shaft of tibia 1. Flexes, abducts, laterally rotates
Lower limb summary Done By: Laith Qashou Doctor_2016 Anterior compartment of the thigh Sartorius Anterior superior iliac spine Upper medial surface of shaft of tibia 1. Flexes, abducts, laterally rotates
Transfemoral Amputation
 Transfemoral Amputation Preop This 26 year old male sustained a gunshot wound to the left thigh. He was treated emergently with revascularization and fasciotomies. He was transferred to our regional trauma
Transfemoral Amputation Preop This 26 year old male sustained a gunshot wound to the left thigh. He was treated emergently with revascularization and fasciotomies. He was transferred to our regional trauma
MUSCULOSKELETAL LOWER LIMB
 MUSCULOSKELETAL LOWER LIMB Spinal Cord Lumbar and Sacral Regions Spinal cord Dorsal root ganglion Conus medullaris Cauda equina Dorsal root ganglion of the fifth lumbar nerve End of subarachnoid space
MUSCULOSKELETAL LOWER LIMB Spinal Cord Lumbar and Sacral Regions Spinal cord Dorsal root ganglion Conus medullaris Cauda equina Dorsal root ganglion of the fifth lumbar nerve End of subarachnoid space
57b Deep Tissue: Technique Demo and Practice - Anterior Lower Body!
 57b Deep Tissue: Technique Demo and Practice - Anterior Lower Body! 57b Deep Tissue: Technique Demo and Practice - Anterior Lower Body! Class Outline" 5 minutes" "Attendance, Breath of Arrival, and Reminders
57b Deep Tissue: Technique Demo and Practice - Anterior Lower Body! 57b Deep Tissue: Technique Demo and Practice - Anterior Lower Body! Class Outline" 5 minutes" "Attendance, Breath of Arrival, and Reminders
Peripheral Vascular Examination. Dr. Gary Mumaugh Western Physical Assessment
 Peripheral Vascular Examination Dr. Gary Mumaugh Western Physical Assessment Competencies 1. Inspection of upper extremity for: size symmetry swelling venous pattern color Texture nail beds Competencies
Peripheral Vascular Examination Dr. Gary Mumaugh Western Physical Assessment Competencies 1. Inspection of upper extremity for: size symmetry swelling venous pattern color Texture nail beds Competencies
Compartmental Syndromes: When the Pressure Gets Too Great
 FREDERICK A. MATSEN III, M.D. PROFESSOR AND CHAIRMAN UNIVERSITY OF WASHINGTON MEDICAL CENTER SHOULDER AND ELBOW WWW.ORTHOP.WASHINGTON.EDU/FACULTY/MATSEN Compartmental Syndromes: When the Pressure Gets
FREDERICK A. MATSEN III, M.D. PROFESSOR AND CHAIRMAN UNIVERSITY OF WASHINGTON MEDICAL CENTER SHOULDER AND ELBOW WWW.ORTHOP.WASHINGTON.EDU/FACULTY/MATSEN Compartmental Syndromes: When the Pressure Gets
ANATYOMY OF The thigh
 ANATYOMY OF The thigh 1- Lateral cutaneous nerve of the thigh Ι) Skin of the thigh Anterior view 2- Femoral branch of the genitofemoral nerve 5- Intermediate cutaneous nerve of the thigh 1, 2 and 3 are
ANATYOMY OF The thigh 1- Lateral cutaneous nerve of the thigh Ι) Skin of the thigh Anterior view 2- Femoral branch of the genitofemoral nerve 5- Intermediate cutaneous nerve of the thigh 1, 2 and 3 are
Primary Care Office Orthopedic Emergencies/ Urgencies
 Primary Care Office Orthopedic Emergencies/ Urgencies Joshua Crum M.D. Hill Country Sports Medicine San Marcos, TX Goals Define what constitutes and orthopedic emergency/urgency Know what conditions need
Primary Care Office Orthopedic Emergencies/ Urgencies Joshua Crum M.D. Hill Country Sports Medicine San Marcos, TX Goals Define what constitutes and orthopedic emergency/urgency Know what conditions need
Tibial Shaft Fractures
 Tibial Shaft Fractures Mr Krishna Vemulapalli Consultant Orthopaedics Surgeon Queens & King George Hospitals Queens Hospital 14/03/2018 Google Maps Map data 2018 Google 10 km Orthopaedics Department Covers
Tibial Shaft Fractures Mr Krishna Vemulapalli Consultant Orthopaedics Surgeon Queens & King George Hospitals Queens Hospital 14/03/2018 Google Maps Map data 2018 Google 10 km Orthopaedics Department Covers
Will it heal? How to assess the probability of wound healing
 Will it heal? How to assess the probability of wound healing Richard F. Neville, M.D. Professor of Surgery Chief, Division of Vascular Surgery George Washington University Limb center case 69 yr old male
Will it heal? How to assess the probability of wound healing Richard F. Neville, M.D. Professor of Surgery Chief, Division of Vascular Surgery George Washington University Limb center case 69 yr old male
Joint Theater Trauma System Clinical Practice Guideline
 INITIAL MANAGEMENT OF WAR WOUNDS: Wound Debridement and Irrigation Original Release/Approval: 2 Oct 2006 Note: This CPG requires an annual review Reviewed: Mar 2012 Approved: 24 Apr 2012 Supersedes: Extremity
INITIAL MANAGEMENT OF WAR WOUNDS: Wound Debridement and Irrigation Original Release/Approval: 2 Oct 2006 Note: This CPG requires an annual review Reviewed: Mar 2012 Approved: 24 Apr 2012 Supersedes: Extremity
Muscle fiber (cell) Blood vessel. Perimysium. Epimysium. Fascicle (wrapped by perimysium) Endomysium (between fibers) Tendon. Bone
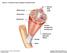 Figure 6.1 Connective tissue wrappings of skeletal muscle. Blood vessel Muscle fiber (cell) Perimysium Epimysium Fascicle (wrapped by perimysium) Tendon Endomysium (between fibers) Bone Figure 6.15 Superficial
Figure 6.1 Connective tissue wrappings of skeletal muscle. Blood vessel Muscle fiber (cell) Perimysium Epimysium Fascicle (wrapped by perimysium) Tendon Endomysium (between fibers) Bone Figure 6.15 Superficial
Arthroplasty after previous surgery: previous vascular problems
 Arthroplasty after previous surgery: previous vascular problems Jacques Menetrey & Victoria B. Duthon Centre de médecine de l appareil locomoteur et du sport Swiss Olympic medical Center Unité d Orthopédie
Arthroplasty after previous surgery: previous vascular problems Jacques Menetrey & Victoria B. Duthon Centre de médecine de l appareil locomoteur et du sport Swiss Olympic medical Center Unité d Orthopédie
In which arm muscle are intramuscular injections most often given? (not in text)
 AP1 Lab 9 - Muscles of the Arms and Legs Locate the following muscles on the models and on yourself. Recall anatomical position. Directional terms such as anterior, posterior, lateral, etc. all assume
AP1 Lab 9 - Muscles of the Arms and Legs Locate the following muscles on the models and on yourself. Recall anatomical position. Directional terms such as anterior, posterior, lateral, etc. all assume
.org. Tibia (Shinbone) Shaft Fractures. Anatomy. Types of Tibial Shaft Fractures
 Tibia (Shinbone) Shaft Fractures Page ( 1 ) The tibia, or shinbone, is the most common fractured long bone in your body. The long bones include the femur, humerus, tibia, and fibula. A tibial shaft fracture
Tibia (Shinbone) Shaft Fractures Page ( 1 ) The tibia, or shinbone, is the most common fractured long bone in your body. The long bones include the femur, humerus, tibia, and fibula. A tibial shaft fracture
17 FibulA FlAP Tor Chiu fibula flap 153
 17 Fibula Flap Tor Chiu Fibula Flap 153 Fibula Flap FLAP TERRITORY This flap includes a segment of the fibular bone with or without the overlying skin island on the peroneal/ lateral aspect of the calf.
17 Fibula Flap Tor Chiu Fibula Flap 153 Fibula Flap FLAP TERRITORY This flap includes a segment of the fibular bone with or without the overlying skin island on the peroneal/ lateral aspect of the calf.
Case report. Your Diagnosis?
 Case report 18 year Male Panel beater referred with a tibial shin syndrome with pain of 6 months. Pain over the anterolateral aspect of leg, bilateral and is precipitated walking 10 minutes. Your Diagnosis?
Case report 18 year Male Panel beater referred with a tibial shin syndrome with pain of 6 months. Pain over the anterolateral aspect of leg, bilateral and is precipitated walking 10 minutes. Your Diagnosis?
Management of Complex Avulsion Injuries of the Dorsum of the Foot and Ankle in Pediatric Patients by Using Local Delayed Flaps and Skin Grafts
 Management of Complex Avulsion Injuries of the Dorsum of the Foot and Ankle in Pediatric Patients by Using Local Delayed Flaps and Skin Grafts Ahmed Elshahat, MD Plastic Surgery Department, Ain Shams University,
Management of Complex Avulsion Injuries of the Dorsum of the Foot and Ankle in Pediatric Patients by Using Local Delayed Flaps and Skin Grafts Ahmed Elshahat, MD Plastic Surgery Department, Ain Shams University,
Lecture 09. Popliteal Fossa. BY Dr Farooq Khan Aurakzai
 Lecture 09 Popliteal Fossa BY Dr Farooq Khan Aurakzai Dated: 14.02.2018 What is popliteus? Introduction Anything relating to, or near the part of the leg behind the knee. From New Latin popliteus the muscle
Lecture 09 Popliteal Fossa BY Dr Farooq Khan Aurakzai Dated: 14.02.2018 What is popliteus? Introduction Anything relating to, or near the part of the leg behind the knee. From New Latin popliteus the muscle
Surgery Under Regional Anesthesia
 Surgery Under Regional Anesthesia Jean Daniel Eloy, MD Assistant Professor Residency Program Director Rutgers-New Jersey Medical School Rutgers The State University of New Jersey Peripheral Nerve Block
Surgery Under Regional Anesthesia Jean Daniel Eloy, MD Assistant Professor Residency Program Director Rutgers-New Jersey Medical School Rutgers The State University of New Jersey Peripheral Nerve Block
Muscles of the Cat. N Deltoid MUSCLES OF THE CHEST. Pectoralis major. (This muscle is superior to Pectoralis minor) MUSCLES OF THE CHEST
 MUSCLES OF THE CHEST Pectoralis major (This muscle is superior to Pectoralis minor) 1. MUSCLES OF THE CHEST Pectoralis minor (This muscle is inferior to Pectoralis major) 2. MUSCLES OF THE ARM Deltoid
MUSCLES OF THE CHEST Pectoralis major (This muscle is superior to Pectoralis minor) 1. MUSCLES OF THE CHEST Pectoralis minor (This muscle is inferior to Pectoralis major) 2. MUSCLES OF THE ARM Deltoid
OVERVIEW OF THE SIX FLEXIBILITY HIGHWAYS
 A P P E N D I X O N E OVERVIEW OF THE SIX FLEXIBILITY HIGHWAYS THE ANTERIOR FLEXIBILITY HIGHWAY STRETCHING THE ANTERIOR FLEXIBILITY HIGHWAY LEVEL 1 LEVEL 2 PHOTO A1.1A AND B STRETCHING THE ANTERIOR FLEXIBILITY
A P P E N D I X O N E OVERVIEW OF THE SIX FLEXIBILITY HIGHWAYS THE ANTERIOR FLEXIBILITY HIGHWAY STRETCHING THE ANTERIOR FLEXIBILITY HIGHWAY LEVEL 1 LEVEL 2 PHOTO A1.1A AND B STRETCHING THE ANTERIOR FLEXIBILITY
North of England Bone and Soft Tissue Tumour Service
 North of England Bone and Soft Tissue Tumour Service Guidelines for rehabilitation after proximal tibial replacement Proximal tibial replacement surgery is usually carried out as part of treatment for
North of England Bone and Soft Tissue Tumour Service Guidelines for rehabilitation after proximal tibial replacement Proximal tibial replacement surgery is usually carried out as part of treatment for
1. A worker falls from a height and lands on his feet. Radiographs reveal a fracture of the sustentaculum tali. The muscle passing immediately
 1. A worker falls from a height and lands on his feet. Radiographs reveal a fracture of the sustentaculum tali. The muscle passing immediately beneath it that would be adversely affected is the: fibularis
1. A worker falls from a height and lands on his feet. Radiographs reveal a fracture of the sustentaculum tali. The muscle passing immediately beneath it that would be adversely affected is the: fibularis
The Muscular System. Chapter 10 Part C. PowerPoint Lecture Slides prepared by Karen Dunbar Kareiva Ivy Tech Community College
 Chapter 10 Part C The Muscular System Annie Leibovitz/Contact Press Images PowerPoint Lecture Slides prepared by Karen Dunbar Kareiva Ivy Tech Community College Table 10.9: Muscles Crossing the Shoulder
Chapter 10 Part C The Muscular System Annie Leibovitz/Contact Press Images PowerPoint Lecture Slides prepared by Karen Dunbar Kareiva Ivy Tech Community College Table 10.9: Muscles Crossing the Shoulder
VENOUS DRAINAGE OF THE LOWER LIMB
 Anatomy of the lower limb Superficial veins & nerve injuries Dr. Hayder VENOUS DRAINAGE OF THE LOWER LIMB The venous drainage of the lower limb is of huge clinical & surgical importance. Since the venous
Anatomy of the lower limb Superficial veins & nerve injuries Dr. Hayder VENOUS DRAINAGE OF THE LOWER LIMB The venous drainage of the lower limb is of huge clinical & surgical importance. Since the venous
Toe walking gives rise to parental concern. Therefore, toe-walkers are often referred at the 3 years of age.
 IDIOPATHIC TOE WALKING Toe walking is a common feature in immature gait and is considered normal up to 3 years of age. As walking ability improves, initial contact is made with the heel. Toe walking gives
IDIOPATHIC TOE WALKING Toe walking is a common feature in immature gait and is considered normal up to 3 years of age. As walking ability improves, initial contact is made with the heel. Toe walking gives
RN(EC) ENC(C) GNC(C) MN ACNP *** MECHANISM OF INJURY.. MOST IMPORTANT ***
 HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age of patient - Certain conditions are more prevalent in particular age groups (Hip pain in children may refer to the knee from Legg-Calve-Perthes
HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age of patient - Certain conditions are more prevalent in particular age groups (Hip pain in children may refer to the knee from Legg-Calve-Perthes
REFERENCE DIAGRAMS OF UPPER LIMB MUSCLES: NAMES, LOCATIONS, ATTACHMENTS, FUNCTIONS MUSCLES CONNECTING THE UPPER LIMB TO THE AXIAL SKELETON
 REFERENCE DIAGRAMS OF UPPER LIMB MUSCLES: NAMES, LOCATIONS, ATTACHMENTS, FUNCTIONS MUSCLES CONNECTING THE UPPER LIMB TO THE AXIAL SKELETON A25LAB EXERCISES: UPPER LIMB MUSCLES Page 1 MUSCLES CONNECTING
REFERENCE DIAGRAMS OF UPPER LIMB MUSCLES: NAMES, LOCATIONS, ATTACHMENTS, FUNCTIONS MUSCLES CONNECTING THE UPPER LIMB TO THE AXIAL SKELETON A25LAB EXERCISES: UPPER LIMB MUSCLES Page 1 MUSCLES CONNECTING
Section Three: The Leg, Ankle, and Foot Lecture: Review of Clinical Anatomy, Patterns of Dysfunction and Injury, and
 Section Three: The Leg, Ankle, and Foot Lecture: Review of Clinical Anatomy, Patterns of Dysfunction and Injury, and Treatment Implications for the Leg, Ankle, and Foot Levels I and II Demonstration and
Section Three: The Leg, Ankle, and Foot Lecture: Review of Clinical Anatomy, Patterns of Dysfunction and Injury, and Treatment Implications for the Leg, Ankle, and Foot Levels I and II Demonstration and
11/15/2018. Temporalis Elevates & retracts mandible. Masseter = Prime mover of jaw closure. Levator scapulae Supraspinatus Clavicle.
 Due in Lab 10 Lab 8 MUSCLES 2 weeks because of Thanksgiving Prelab #10 Both sides! Homework #8 Both sides! Refer to Muscles 22-23 Examples of Origin & Insertion Naming of muscles Origin Site of muscle
Due in Lab 10 Lab 8 MUSCLES 2 weeks because of Thanksgiving Prelab #10 Both sides! Homework #8 Both sides! Refer to Muscles 22-23 Examples of Origin & Insertion Naming of muscles Origin Site of muscle
The Hip (Iliofemoral) Joint. Presented by: Rob, Rachel, Alina and Lisa
 The Hip (Iliofemoral) Joint Presented by: Rob, Rachel, Alina and Lisa Surface Anatomy: Posterior Surface Anatomy: Anterior Bones: Os Coxae Consists of 3 Portions: Ilium Ischium Pubis Bones: Pubis Portion
The Hip (Iliofemoral) Joint Presented by: Rob, Rachel, Alina and Lisa Surface Anatomy: Posterior Surface Anatomy: Anterior Bones: Os Coxae Consists of 3 Portions: Ilium Ischium Pubis Bones: Pubis Portion
Acute arterial embolism
 Acute arterial embolism Definition Thrombus come from heart or blood vessel or other embolus such as tumor,air gas or fat flow with blood stream and occlude distal limb or visceral arteries which causes
Acute arterial embolism Definition Thrombus come from heart or blood vessel or other embolus such as tumor,air gas or fat flow with blood stream and occlude distal limb or visceral arteries which causes
Civilian versus Military Trauma Management
 Western University From the SelectedWorks of Vivian C. McAlister November, 2010 Civilian versus Military Trauma Management Vivian C. McAlister Available at: https://works.bepress.com/vivianmcalister/151/
Western University From the SelectedWorks of Vivian C. McAlister November, 2010 Civilian versus Military Trauma Management Vivian C. McAlister Available at: https://works.bepress.com/vivianmcalister/151/
Initial management of war wounds with fractures
 Initial management of war wounds with fractures Presented by Paul Ley ICRC orthopedic surgeon Beirut, Lebanon May 12, 2017 BONE FRACTURES CANNOT BE CONSIDERED AS AN ISOLATED LESION SURROUNDING SOFT TISSUES
Initial management of war wounds with fractures Presented by Paul Ley ICRC orthopedic surgeon Beirut, Lebanon May 12, 2017 BONE FRACTURES CANNOT BE CONSIDERED AS AN ISOLATED LESION SURROUNDING SOFT TISSUES
EndoBlade Soft Tissue Release System
 Surgical Technique Endoscopic Gastroc Recession Endoscopic Plantar Fascia Release EndoBlade Soft Tissue Release System Endoscopic Gastroc Recession Arthrex has developed a comprehensive, completely disposable
Surgical Technique Endoscopic Gastroc Recession Endoscopic Plantar Fascia Release EndoBlade Soft Tissue Release System Endoscopic Gastroc Recession Arthrex has developed a comprehensive, completely disposable
Management of Brachial Plexus & Peripheral Nerves Blast Injuries. First Global Conflict Medicine Congress
 Management of Brachial Plexus & Peripheral Nerves Blast Injuries Joseph BAKHACH First Global Conflict Medicine Congress Hand & Microsurgery Department American University of Beirut Medical Centre Brachial
Management of Brachial Plexus & Peripheral Nerves Blast Injuries Joseph BAKHACH First Global Conflict Medicine Congress Hand & Microsurgery Department American University of Beirut Medical Centre Brachial
