Vascular Injuries. Chapter 25
|
|
|
- Lucinda Sparks
- 6 years ago
- Views:
Transcription
1 Vascular Injuries Chapter 25 Vascular Injuries Introduction History. o World War II: Popliteal artery injuries were routinely ligated and associated with a 73% amputation rate. o Korean War: Formal repair of peripheral arterial injuries instituted. o Vietnam War: Further refinements in arterial repair; amputation rate for popliteal artery injuries is reduced to 32%. o Iraq and Afghanistan: Forward Role 2 care refines use of temporary vascular shunts, and Joint Theater Trauma System (JTTS) advances recoding of injury. There are various types of wounds seen in combat. o Low-velocity missile/fragment damages a blood vessel lying directly in its path. o High-velocity missile/fragment wounds with blast causes widespread damage, including vascular injury at a distance (remote injury). o Blunt trauma, often resulting from sudden deceleration in motor vehicle accidents, falls, and rail and air disasters. o Popliteal artery injury associated with posterior knee dislocations. Epidemiology of Vascular Injury 1 in 5 (20%) battle injuries (nonreturn to duty) is coded with hemorrhage control not otherwise specified. Rate of vascular injury in modern combat is 12%, which is higher than the 1% 3% reported in World War II, Korea, and Vietnam. Rate of operative vascular injury is 9%, with half being ligations and half requiring repair. 357
2 Emergency War Surgery Extremity vessels account for 70% 80% of vascular injuries, whereas 10% 15% are in the cervical region and 5% 10% are in the torso. Roles of Care and the Management of Vascular Injury Each role has unique approaches to the management of vascular injury: Role 1. o Hemorrhage control (direct pressure, tourniquet, or topical hemostatic agent) and other life-saving interventions/ evacuation. Role 2. o Operations at forward operating locations are abbreviated (preferably <1 hour). o Intervention on extremity vascular injury is important and may make the difference in meaningful limb salvage. o Primary amputation or ligation is also an acceptable damage control technique when other life-threatening injuries are present. o If limb salvage is to be attempted, tourniquet removal, exploration and control of vascular injury, thrombectomy, and administration of heparinized saline through the inflow and outflow vessels are recommended. o Restoration of flow can then be established using a temporary vascular shunt followed by fasciotomy and MEDEVAC (medical evacuation). Definitive repair at this level can be considered with caution, depending on available equipment and the tactical situation. Role 3. o Removal of tourniquet(s) and temporary vascular shunts placed as forward locations followed by definitive vascular repair. o Saphenous vein is preferred as a conduit for extremity vascular injuries. o Extremity evaluation will be difficult during AIR EVAC (air evacuation) out of theater, and Role 3 must ensure adequacy of perfusion, fasciotomy, and debridement. 358
3 Vascular Injuries o Primary amputation or ligation is acceptable damage control technique when other life-threatening injuries are present. Role 4 (Safe Haven). o Surveillance of repair, including an assessment of soft-tissue wounds and tissue coverage prior to continuing AIR EVAC. Role 4 (CONUS). o Surveillance of vascular repair with duplex or CTA (computed tomography angiography) and assessment of soft-tissue wounds and adequacy of tissue coverage. o Revision of repairs with stenosis or inadequate tissue coverage leaving them prone to infection and blowout. o Delayed revascularization of viable, but poorly perfused, extremities in which ligation was chosen as the initial method of care. Evaluation and Diagnosis Hard signs. o Active hemorrhage or expanding hematoma. o Bruit or thrill. o Ischemia defined as the absence of Doppler signal in the extremity on multiple attempts over time after resuscitation warming, and reduction of fractures. o Hard signs require management in the operating room with wide exposure and exploration of the injury (ie, control of vascular injury). Unlike civilian vascular trauma, there can be multiple injuries in a single vessel. o There is limited need for other diagnostic tests (ie, CTA or angiography) that take time and often provide unclear findings. Soft signs. o Proximity to vessel, fracture/injury pattern (eg, knee dislocation), hematoma, or question regarding palpable pulse. o Often require another diagnostic test, such as continuous wave Doppler with or without calculation of the injured extremity index. o CTA or angiography is useful as a diagnostic adjunct in the presence of soft signs of vascular injury. 359
4 Emergency War Surgery The injured extremity index. o Similar to the ankle brachial index and is calculated using a manual blood pressure cuff and a continuous wave Doppler. o First step is to determine the pressure at which the arterial Doppler signal occludes in the injured extremity (numerator). o Cuff and Doppler moved to uninjured extremity and occlusion pressure of Doppler signal recorded (denominator). o Injured extremity index >0.90 is normal and has a high specificity for excluding extremity vascular injury in the absence of hard signs. Angiography. o Limited utility in the diagnosis of wartime extremity vascular injury and, in the presence of hard signs, preference is given to incision and exposure of segment in question. o Limitations related to the availability and quality of imaging technology in austere environments. o Extremity vasoconstriction with shock and hypothermia in young troops may lead to confusing or false-positive findings. o Angiography has the greatest utility in the setting of multiple penetrating wounds at various levels of the same extremity. o Angiography may be done via cut down using a small gauge needle or catheter to inject contrast minimizing complications. o Advantage to angio is its low volume of contrast, especially useful in patients at risk for renal failure. CTA. o Increasingly available in a mature theater of war and has the greatest utility in the diagnosis and triage of torso and neck wounds. o CTA is often used as a screening tool for suspected vascular injury. o This modality takes additional time, contrast, and technical experience to provide accurate and meaningful images. 360
5 Vascular Injuries Management Aspects: Extremity Vascular Injury Upper Extremity Consider prophylactic distal fasciotomies in all patients with prolonged ischemia times. Subclavian artery. o Recommendations: Shunt or ligate as damage control, or definitive repair. o Utility of temporary shunt: High, but difficult due to technical difficulty of exposure and placement. o Method/conduit: Interposition graft/6 8 mm eptfe (expanded polytetrafluoroethylene) or Dacron. Proximal subclavian vessels and innominate are approached through a median sternotomy. Alternatively, a proximal left subclavian artery can be approached using a high (third intercostal space) anterolateral thoracotomy supraclavicular approach through the clavicular head of the sternocleidomastoid, sternothyroid/hyoid muscles to the scalene fat pad with retraction of the phrenic nerve, and division of the anterior scalene; may resect the clavicular head. The mid- and distal subclavian arteries on both sides can be exposed through combination supra- and infraclavicular incisions. Avoid injury to the phrenic nerve, internal mammary, thyrocervical, and vertebral arteries. Axillary artery. o Recommendations: Shunt or ligate as damage control, or definitive repair. o Utility of temporary shunt: High. o Method/conduit: Interposition graft/reversed saphenous vein. Supra- and infraclavicular incisions allow proximal control and distal exposure. 361
6 Emergency War Surgery Prep axilla, arm, and hand into operative field. Infraclavicular exposure includes division of the clavipectoral fascia and the pectoralis major muscle. The proximal axillary artery is then visible under the pectoralis minor muscle, which can be retracted laterally or divided. Avoid the brachial plexus, which will be deep or lateral to the axillary artery. Brachial artery. o Recommendations: Shunt or ligate as damage control, or definitive repair. o Utility of temporary shunt: High. o Method/conduit: Interposition graft/reversed saphenous vein. Medial approach; adjacent to the median nerve in brachial sheath in biceps/triceps groove. Elastic artery with redundancy; flex arm slightly for interposition grafts to avoid kinking. Ligation may be tolerated if collaterals are intact. Radial/ulnar arteries. o Recommendations: Selective repair (maintain at least one vessel flow to hand). o Utility of temporary shunt: Low patency rate. o Method/conduit: Ligation or interposition graft/reversed saphenous vein. Perfusion to the hand should be assessed with Doppler before and after occlusion or ligation. The presence of an arterial Doppler signal in the hand obviates the need for arterial repair. Repair with saphenous vein in instances where there is persistent absence of an arterial signal. The majority of individuals have ulnar-dominant perfusion; when possible, repair/reconstruct the ulnar artery. Lower Extremity Consider prophylactic distal fasciotomies in all injuries with prolonged ischemia times. 362
7 Vascular Injuries Common femoral artery. o Recommendations: Shunt as damage control or definitive repair. o Utility of temporary shunt: High. o Method/conduit: Interposition graft/saphenous vein or 6 8 mm prosthetic. Injury to the common femoral artery is often fatal because hemorrhage control in the field is difficult. Expose artery at the inguinal ligament for proximal control (2 3 cm lateral to the pubic tubercle) (Fig. 25-1). Inguinal Ligament External Iliac Artery Rectus Femoris Sartorius Common Femoral Artery Saphenous Vein Fig Inguinal anatomy. Proximal control can be obtained in the retroperitoneum (ie, external iliac) through the proximal extension of this groin incision or by using an incision in the lower abdomen. Attempt to maintain flow in the profunda femorus artery. Cover with tissue (femoral sheath), the sartorius muscle, or the rectus flap (Role 4). Profunda femorus artery. o Recommendations: Selective repair. o Utility of temporary shunts: Low due to difficult exposure. 363
8 Emergency War Surgery o Method/conduit: Ligation or interposition graft/saphenous vein. Exposure of proximal profunda is the same (distal extension) as the common femoral. If superficial femoral is injured, repair of the profunda is necessary to heal amputations. If superficial femoral is patent, ligation of mid- to distal profunda injuries is acceptable. Proximal profunda injuries should be repaired with reversed saphenous vein interposition. Superficial femoral artery. o Recommendations: Shunt as damage control or definitive repair. o Utility of temporary shunts: High. o Method/conduit: Interposition graft/reversed saphenous vein. Medial incision with bump under calf. Exposure of the proximal 1/3 below the sartorius and distal 1/3 above the sartorius. Be wary of the adjacent vein (may be adherent to artery) and geniculate branches at the distal artery (Hunter s canal). Popliteal artery. o Recommendations: Shunt as damage control or definitive repair. o Utility of temporary vascular shunts: High. o Conduit: Reversed saphenous vein. Medial incision with bump under calf for above knee and under thigh for below knee. Natural dissection planes exist in exposing the aboveknee popliteal artery (ie, popliteal space) with the exception of the need to divide the fibers of the adductor magnus that envelopes the distal superficial femoral artery (Hunter s canal) (Fig. 25-2). To completely expose the popliteal space, the medial attachments of the sartorius, semitendinosis, semimembrinosis, and gracilis to the medial condyle 364
9 Vascular Injuries a Vastus Medialis Adductor Magnus Femoral Vein Medial Head Gastrocnemius b Femoral Artery Sartorius Fig Exposure of distal femoral and popliteal vessels. of the tibia can be divided. Distal exposure by division of the gastrocnemius and soleus from the tibia allows dissection to the anterior tibial origin and the tibialperoneal trunk. Extraanatomical bypass can also be performed without the need to expose the injured segment (Figs and 25-4). Insertions of Sartorius, Gracilis, Semitendinosus Femoral Vein Femoral Artery Medial Head Gastrocnemius Fig Medial approach to popliteal vessels. 365
10 Emergency War Surgery Semimembranosus Semitendinosus Biceps Femoris Popliteal Artery Popliteal Vein Lesser Saphenous Vein Medial Head Lateral Head Gastrocnemius Fig Posterior approach to popliteal vessels. Tibial arteries. o Recommendations: Selective repair. o Utility of temporary vascular shunts: Low due to difficult exposure, small caliber, and low patency rates. o Method/conduit: Ligation or interposition graft with saphenous vein. If a Doppler signal is present at the ankle, indicating that one or more tibial arteries are patent, there is no need for additional tests or repair. Doppler exam should be repeated as patient is resuscitated and warmed. Exposure of the posterior tibial artery in the deep compartment of the leg is through a medial incision with a lift or bump under the knee or thigh. Repair with vein if three tibial arteries are injured and an absence of a Doppler signal persists. 366
11 Vascular Injuries Extremity venous injury. o Recommendations: Selective repair. o Utility of temporary vascular shunts: Moderate for large vessels. o Method/conduit: Ligation, repair, or saphenous interposition graft. Repair of proximal veins is indicated to reduce venous hypertension and congestion. Shunts in proximal veins will usually remain patent until formal repair can be performed. Techniques of lateral venorrhaphy are acceptable, although patch angioplasty or an interposition graft using saphenous vein from the uninjured limb is often necessary. Consider removing thrombus from the distal venous segments with compression (eg, ACE wrap or Esmark bandage) prior to repair. Pneumatic compression device on distal extremity to augment venous flow after repair. Limb salvage benefit of vein repair compared with ligation has been shown 2 years after injury. Repair of extremity venous injury should only be considered in stable patients. Management Aspects: Torso Vascular Injury Aorta. With small penetrating injuries to the aorta of the chest or abdomen, primary repair can be attempted. When not amenable to repair, a shunt can be placed (eg, chest tube). Recognize that penetrating injury may involve entrance and exit wounds to the aorta that may not be obvious. Management of penetrating injury to the aorta is very rare, given the prehospital lethality of this injury. Management of blunt injury to the thoracic aorta (partial transection or pseudoaneurysm) is rare. 367
12 Emergency War Surgery Most survivors can be managed medically with control of heart rate and blood pressure using beta-blockers and permissive hypotension. Endovascular repair can be attempted at some Role 3 facilities. Vena cava. Establish resuscitation lines above the diaphragm for abdominal vena cava injuries. Vena cava injuries should be exposed using the Cattell- Braasch and Kocher maneuvers. Lateral repair is acceptable, understanding that the lumen may be comprised. If occlusion of the cava results in hypotension, clamp aorta to support central perfusion. Retrohepatic and retroperitoneal hematomas should not be disturbed if not actively bleeding or expanding. Attempt to identify large lumbar veins feeding the injured segment that can bleed profusely. Patch angioplasty or resection and interposition graft using eptfe are reconstructive options. Ligation of the cava is acceptable as a damage control maneuver. If air transport is going to be utilized, then prophylactic bilateral lower extremity fasciotomies should be performed. Portal vein and hepatic artery. Pringle maneuver should precede exploration of the portal triad. Ligation of hepatic artery injuries is acceptable, if the portal vein is patent. Lateral venorrhaphy is preferred. Damage control ligation of the portal vein is an option; it results in hepatic ischemia, splanchnic congestion, and systemic hypervolemia. Cholangiography through the gallbladder or with a small butterfly needle in the common bile duct should be considered in order to look for associated injuries of the extrahepatic biliary system. 368
13 Vascular Injuries Mesenteric arteries. Present as supramesocolic zone I hematoma. Repair proximal mesenteric artery and vein injuries, including portal vein. Repair options: primary pledgeted repair, vein patch angioplasty, or replacement of the injured segment with interposition saphenous vein graft. Ligation can be performed for distal artery and vein injuries or as damage control. Renal arteries. Explore zone II expanding hematomas from penetrating injury; 90% of explored kidneys result in nephrectomy. Establish status of contralateral kidney by contrast study or manual palpation prior to nephrectomy. Damage control may require early nephrectomy. Devascularized kidney that is not bleeding may be left in situ. Iliac arteries. o Recommendations: Ligate or shunt as damage control, or definitive repair. o Utility of temporary vascular shunts: High. o Method/conduit: Interposition graft/eptfe or Dacron or saphenous vein. Explore zone III hematoma from penetrating wound after establishing aortic control. Distal control is obtained at the inguinal ligament (for external iliac arteries). If there is primary injury to, or back bleeding from the internal iliac artery (hypogastric), it may be ligated. Try to avoid ligating both internal iliacs due to risk of gluteal ischemia/necrosis. Management Aspects: Cervical Vascular Injury Carotid artery. o Recommendations: Ligate or shunt as damage control, or definitive repair. 369
14 Emergency War Surgery o Utility of temporary vascular shunts: High. o Method/conduit: Vein patch or vein interposition graft. Zone I injuries best approached with median sternotomy for ample proximal exposure. Early control of common carotid. 3 Fr Fogarty catheter with three-way stopcock is useful to occlude internal carotid back bleeding. During carotid repair consider temporary shunt and augmentation of mean arterial pressure. CTA aids in the triage for urgent operation, improves operative planning, and images the brain as a baseline. A selective approach to exploration of zone II neck wounds is acceptable in a patient without hard signs of vascular injury or aerodigestive involvement. Penetrating neck wounds that are not selected for exploration should undergo CTA to further evaluate for vascular, tracheal, or esophageal injury. Exposure of the carotid artery is through a standard anterior sternocleidomastoid neck incision. Vertebral artery. o Recommendations: Ligate. o Utility of temporary vascular shunts: None. o Method/conduit: Not applicable. Bleeding vertebral artery injuries are ligated with no role for reconstruction in theater. Vertebral artery occlusions are managed with anticoagulation, if it is not contraindicated. Endovascular embolization is an option if injury is not accessible by standard exposure. Exposure usually requires rongeur to open vertebral foramen; temporary occlusion with bone wax can be helpful. Jugular vein. o Recommendations: Ligation or selective repair. o Utility of temporary vascular shunts: None. o Method/conduit: Lateral venorrhaphy, vein patch, or saphenous vein. 370
15 Table Vessels Amenable to Ligation Veins That Can Be Ligated Routinely Vascular Injuries Significant jugular vein injuries can be ligated without adverse effects. Repair of jugular injuries should be considered in the setting of traumatic brain injury with elevated intracranial pressure. Large vein injuries. Initial control can be accomplished by one or more fingers on the bleeding segment. Use of clamps for control may injure the vein further. Avoid too small of a needle and suture, which are difficult to maneuver in blood. 4-0 PROLENE on an SHtapered needle is a substantive suture on a needle large enough to see. Manual direct pressure can be replaced with a small sponge stick or Kittner. Hemorrhage control with ligation is preferable to patency with death from exsanguination. Be wary of risk of air embolism with large vein injuries. Ligation of vessels. Acceptable damage control maneuver, especially for small, more distal arteries and veins (Table 25-1). Internal/external jugular Brachiocephalic Infrarenal inferior vena cava Left renal Internal iliac Subclavian Mesenteric Tibialis Arteries That Can Be Ligated Routinely Digital Radial or ulnar, but not both; preserve ulnar when possible External carotid Brachial distal to profundi and adequate wrist; Doppler signal Subclavian branches Internal iliacs Profunda femoris Hepatic 371
16 Emergency War Surgery Temporary vascular shunting to restore perfusion should be considered before ligation. Continuous wave Doppler should be checked before arterial ligation to judge perfusion/viability. Fogarty thrombectomy catheters. Sized at 2 7 Fr catheters; maximum balloon diameter of the 2 and 3 Fr catheters is 4 and 5 mm, respectively. Inflate with saline using a 1 cc tuberculin syringe ( cc) while withdrawing from the vessel. Goal is clot, not intima, removal; so, do not overinflate or drag too much. May be used to control bleeding with use of a three-way stopcock to maintain inflation. Proximal and distal thrombectomies should be performed prior to performing repair. Temporary vascular shunts. Inline shunts rest in the vessel ( in situ ), whereas long external shunts are designed to loop. Inline Argyl shunts come in a cylinder container with sizes 8, 10, 12, and 14 Fr Fogarty catheters. Inline Javid shunts are longer and individually packaged. Sundt shunts are designed with short (15 cm; inline) and long (30 cm; external) profiles. Equal success has been had with Argyl, Javid, and Sundt shunts without systemic anticoagulation. Secured with silk ligatures and patent for up to 6 hours; reports of longer duration exist. Shunts should be removed with formal repair in-theater prior to AIR EVAC to Role 4. Temporary vascular shunts are effective and should be considered in the management of nearly all extremity vascular injury patterns, including proximal venous injuries. Their main advantage is provision of early restoration of flow and mitigation of the damaging effects of arterial ischemia and venous hypertension. As an abbreviated procedure, compared with formal vascular repair, shunting extends the window of opportunity for limb salvage 372
17 Vascular Injuries in some patterns of vascular injury. Although the patency at 3 4 hours is higher in larger, more proximal vessels (axillary/brachial and femoral/popliteal), shunts have been used effectively in smaller (distal brachial/forearm and tibial) vessels. Outcomes of extremity vascular injury managed with temporary shunts have been recorded, demonstrating no adverse effect of this technique and a limb salvage advantage in the most severely injured limbs (Mangled Extremity Severity Score [MESS] 8). Consider distal fasciotomies. Pediatric vascular injuries. Less than 10 years old: intervention should be avoided in those given a propensity for spasm. Ligation is more well tolerated in infants and toddlers, given the ability to recruit collaterals. Perform interrupted suture lines (6-0 PROLENE) to allow expansion with growth of the child Endovascular capability and inferior vena cava filters. Techniques should be used in a small subset of injuries and directed in consultation with a trauma surgeon. Placement of vena cava filters should be considered in patients who have contraindications for anticoagulation. Use of prosthetic graft material. eptfe (GORE-TEX) or Dacron used for central torso vascular injuries (aorta, great vessels). Prosthetic conduit acceptable as a last resort in extremities when vein cannot be harvested. If prosthetic used in extremity injury, notify higher levels of care to facilitate surveillance. Harvesting and use of autologous vein. If possible, use reversed greater saphenous vein from the uninjured extremity. Expose at saphenofemoral junction or anterior to medial malleolus (consistent locations). Be sure to mark anatomically distal end as inflow, ensuring reversal of vein conduit. 373
18 Emergency War Surgery Introduce 18-gauge plastic vein or metallic olive tip cannula to distend with heparin saline. Nearly always in the setting of trauma, the vein appears in situ as too small or not adequate due to vasoconstriction or spasm. Best assessed after hydrodistention. Soft-tissue coverage and anastomotic disruption. Cover vascular repairs with available, viable local tissue (muscle and adipose). If no soft tissue to cover, route grafts out of the zone of injury. Poorly covered vascular anastamosis can blow out. Avoid direct placement of negative pressure wound therapy sponge on vascular structures. If no tissue is available to cover the vascular repair, route an interposition graft out of the zone of injury through another myocutaneous or even subcutaneous path. Anticoagulation. Heparin saline is typically 1,000 U/1 L, although other mixtures with or without papaverine (60 mg/1 L) are acceptable. Systemic anticoagulation is achieved with 50 U/kg of IV heparin with 1,000 units repeated at 1 hour. Repeat doses are not recommended, given the propensity for bleeding in wartime injury. Regional anticoagulation is the use of heparin saline flush in the inflow/outflow vessels. Post-op care. o Palpable pulses obtained in the operating room should remain palpable post-op. o Pulse changes, even if Doppler signals remain, may indicate graft thrombosis and should be investigated. o Consider low-dose heparin as deep vein thrombosis prophylaxis. 374
19 Vascular Injuries o Use with caution in multiply injured and head-injured patients. o Slight elevation of injured extremity improves post-op edema. For Clinical Practice Guidelines, go to guidelines.html 375
20 Emergency War Surgery 376
Vascular Injuries. Chapter 27
 Vascular Injuries Chapter 27 Vascular Injuries Introduction History. ο World War II: Popliteal artery injuries were routinely ligated with a 73% amputation rate. ο Korean War: Formal repair of peripheral
Vascular Injuries Chapter 27 Vascular Injuries Introduction History. ο World War II: Popliteal artery injuries were routinely ligated with a 73% amputation rate. ο Korean War: Formal repair of peripheral
Combat Extremity Vascular Trauma
 Combat Extremity Vascular Trauma Training teams to be a TEAM Chatt A. Johnson LTC, MC, USA 08 March 2010 US Army Trauma Training Center Core Discussion Series Outline: Combat Vascular Injury Physiologic
Combat Extremity Vascular Trauma Training teams to be a TEAM Chatt A. Johnson LTC, MC, USA 08 March 2010 US Army Trauma Training Center Core Discussion Series Outline: Combat Vascular Injury Physiologic
Joint Theater Trauma System Clinical Practice Guideline
 WARTIME VASCULAR INJURY Original Release/Approval 18 Dec 004 Note: This CPG requires an annual review. Reviewed: May 01 Approved: 7 Jun 01 Supersedes: Vascular Injury, 7 Nov 008 Minor Changes (or) Significant
WARTIME VASCULAR INJURY Original Release/Approval 18 Dec 004 Note: This CPG requires an annual review. Reviewed: May 01 Approved: 7 Jun 01 Supersedes: Vascular Injury, 7 Nov 008 Minor Changes (or) Significant
EAST MULTICENTER STUDY DATA DICTIONARY. Temporary Intravascular Shunt Study Data Dictionary
 EAST MULTICENTER STUDY DATA DICTIONARY Temporary Intravascular Shunt Study Data Dictionary Data Entry Points and appropriate definitions / clarifications: Entry space Definition / Instructions 1. Specific
EAST MULTICENTER STUDY DATA DICTIONARY Temporary Intravascular Shunt Study Data Dictionary Data Entry Points and appropriate definitions / clarifications: Entry space Definition / Instructions 1. Specific
Contributors. First Publication Date: 18 Dec 2004 Publication Date: 12 Aug 2016 Supersedes CPG dated 07 Jun 2012
 JOINT TRAUMA SYS TEM CLINICAL PRACTIC E GUIDELINE (JTS CPG ) Vascular Injury (CPG ID: 46) The CPG provides guidance on the diagnosis, treatment and surgical management of vascular injuries sustained by
JOINT TRAUMA SYS TEM CLINICAL PRACTIC E GUIDELINE (JTS CPG ) Vascular Injury (CPG ID: 46) The CPG provides guidance on the diagnosis, treatment and surgical management of vascular injuries sustained by
Hemorrhage Control. Chapter 6
 Chapter 6 The hemorrhage that take[s] place when a main artery is divided is usually so rapid and so copious that the wounded man dies before help can reach him. Colonel H. M. Gray, 1919 Stop the Bleeding!
Chapter 6 The hemorrhage that take[s] place when a main artery is divided is usually so rapid and so copious that the wounded man dies before help can reach him. Colonel H. M. Gray, 1919 Stop the Bleeding!
Schedule of Benefits. for Professional Fees Vascular Procedures
 Schedule of Benefits for Professional Fees 2018 Vascular Procedures ANASTOMOSIS RULES 820 Arteriovenous anastomosis in arm 1453 Arteriovenous anastomosis, open by basilic vein transposition 1465 Splenorenal
Schedule of Benefits for Professional Fees 2018 Vascular Procedures ANASTOMOSIS RULES 820 Arteriovenous anastomosis in arm 1453 Arteriovenous anastomosis, open by basilic vein transposition 1465 Splenorenal
Sample page. POWER UP YOUR CODING with Optum360, your trusted coding partner for 32 years. Visit optum360coding.com.
 2018 Complete Guide for Interventional Radiology An in-depth guide to interventional radiology coding, billing, and reimbursement for facilities and physicians POWER UP YOUR CODING with Optum360, your
2018 Complete Guide for Interventional Radiology An in-depth guide to interventional radiology coding, billing, and reimbursement for facilities and physicians POWER UP YOUR CODING with Optum360, your
inerve Guide to Nerves 2009
 inerve Guide to Nerves 2009 A guide to self learning and self assessment Context: The following guide is intended to help interpret the sono-anatomy and follow a systematic stepwise approach to the practice
inerve Guide to Nerves 2009 A guide to self learning and self assessment Context: The following guide is intended to help interpret the sono-anatomy and follow a systematic stepwise approach to the practice
Amputations. Chapter 23
 Amputations Chapter 23 Amputations Introduction Battle casualties who sustain amputations have the most severe extremity injuries. Historically, 1 in 3 patients with a major amputation (proximal to the
Amputations Chapter 23 Amputations Introduction Battle casualties who sustain amputations have the most severe extremity injuries. Historically, 1 in 3 patients with a major amputation (proximal to the
Evaluation & Management of Penetrating Wounds to the NECK
 Evaluation & Management of Penetrating Wounds to the NECK Goal Effectively identify patients with a high probability of injury requiring surgical intervention Define the role of diagnostic tests in assessing
Evaluation & Management of Penetrating Wounds to the NECK Goal Effectively identify patients with a high probability of injury requiring surgical intervention Define the role of diagnostic tests in assessing
2017 Cardiology Survival Guide
 2017 Cardiology Survival Guide Chapter 2: Angioplasty/Atherectomy/Stent The term angioplasty literally means "blood vessel repair." During an angioplasty procedure, the physician inserts a catheter, with
2017 Cardiology Survival Guide Chapter 2: Angioplasty/Atherectomy/Stent The term angioplasty literally means "blood vessel repair." During an angioplasty procedure, the physician inserts a catheter, with
Arterial Map of the Thorax, Abdomen and Pelvis 2017 Edition
 Arterial Map of the Thorax, Abdomen and Pelvis Angiography 75605 (-26) Aortography, thoracic 75625 (-26) Aortography, abdominal by serialography 75630 (-26) Aortography, abdominal + bilat iliofemoral 75705
Arterial Map of the Thorax, Abdomen and Pelvis Angiography 75605 (-26) Aortography, thoracic 75625 (-26) Aortography, abdominal by serialography 75630 (-26) Aortography, abdominal + bilat iliofemoral 75705
3 Circulatory Pathways
 40 Chapter 3 Circulatory Pathways Systemic Arteries -Arteries carry blood away from the heart to the various organs of the body. -The aorta is the longest artery in the body; it branches to give rise to
40 Chapter 3 Circulatory Pathways Systemic Arteries -Arteries carry blood away from the heart to the various organs of the body. -The aorta is the longest artery in the body; it branches to give rise to
Cat Dissection. Muscular Labs
 Cat Dissection Muscular Labs Tibialis anterior External oblique Pectroalis minor Gastrocnemius Sartorius Pectoralis major Gastrocnemius Semitendinosis Sartorius External oblique Trapezius Latissimus dorsi
Cat Dissection Muscular Labs Tibialis anterior External oblique Pectroalis minor Gastrocnemius Sartorius Pectoralis major Gastrocnemius Semitendinosis Sartorius External oblique Trapezius Latissimus dorsi
Chapter 48 Vascular Trauma
 Chapter 48 Vascular Trauma Episode Overview: 1. List three types/mechanisms of occlusive and four types of non-occlusive vascular injuries. 2. What are the hard and soft signs of peripheral vascular injury?
Chapter 48 Vascular Trauma Episode Overview: 1. List three types/mechanisms of occlusive and four types of non-occlusive vascular injuries. 2. What are the hard and soft signs of peripheral vascular injury?
Artery 1 Head and Thoracic Arteries. Arrange the parts in the order blood flows through them.
 Artery 1 Head and Thoracic Arteries 1. Given the following parts of the aorta: 1. abdominal aorta 2. aortic arch 3. ascending aorta 4. thoracic aorta Arrange the parts in the order blood flows through
Artery 1 Head and Thoracic Arteries 1. Given the following parts of the aorta: 1. abdominal aorta 2. aortic arch 3. ascending aorta 4. thoracic aorta Arrange the parts in the order blood flows through
RadRx Your Prescription for Accurate Coding & Reimbursement Copyright All Rights Reserved.
 Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of November 19, 2018 Abdominal Aortogram, Bilateral Runoff
Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of November 19, 2018 Abdominal Aortogram, Bilateral Runoff
Appendix. Vascular Anastomosis Workshop PURPOSE DESCRIPTION WORKSHOP TOOLS
 Appendix Vascular Anastomosis Workshop PURPOSE The purpose of this workshop is to expose the participant to commonly used basic vascular reconstructions. The participant is expected to learn new skills
Appendix Vascular Anastomosis Workshop PURPOSE The purpose of this workshop is to expose the participant to commonly used basic vascular reconstructions. The participant is expected to learn new skills
YOU MUST BRING GLOVES FOR THIS ACTIVITY
 ACTIVITY 10: VESSELS AND CIRCULATION OBJECTIVES: 1) How to get ready: Read Chapter 23, McKinley et al., Human Anatomy, 5e. All text references are for this textbook. 2) Observe and sketch histology slide
ACTIVITY 10: VESSELS AND CIRCULATION OBJECTIVES: 1) How to get ready: Read Chapter 23, McKinley et al., Human Anatomy, 5e. All text references are for this textbook. 2) Observe and sketch histology slide
VESSELS: GROSS ANATOMY
 ACTIVITY 10: VESSELS AND CIRCULATION OBJECTIVES: 1) How to get ready: Read Chapter 23, McKinley et al., Human Anatomy, 4e. All text references are for this textbook. 2) Observe and sketch histology slide
ACTIVITY 10: VESSELS AND CIRCULATION OBJECTIVES: 1) How to get ready: Read Chapter 23, McKinley et al., Human Anatomy, 4e. All text references are for this textbook. 2) Observe and sketch histology slide
Biology 323 Human Anatomy for Biology Majors Lecture 11 Dr. Stuart S. Sumida. Peripheral Circulation
 Biology 323 Human Anatomy for Biology Majors Lecture 11 Dr. Stuart S. Sumida Peripheral Circulation Structures of the Splanchnopleure: receive unpaired vessels of the abdominal aorta. Structures of the
Biology 323 Human Anatomy for Biology Majors Lecture 11 Dr. Stuart S. Sumida Peripheral Circulation Structures of the Splanchnopleure: receive unpaired vessels of the abdominal aorta. Structures of the
Compartment Syndrome
 Compartment Syndrome Chapter 34 Compartment Syndrome Introduction Compartment syndrome may occur with an injury to any fascial compartment. The fascial defect caused by the injury may not be adequate to
Compartment Syndrome Chapter 34 Compartment Syndrome Introduction Compartment syndrome may occur with an injury to any fascial compartment. The fascial defect caused by the injury may not be adequate to
Day 5 Respiratory & Cardiovascular: Respiratory System
 Day 5 Respiratory & Cardiovascular: Respiratory System Be very careful not to damage the heart and lungs while separating the ribs! Analysis Questions-Respiratory & Cardiovascular Log into QUIA using your
Day 5 Respiratory & Cardiovascular: Respiratory System Be very careful not to damage the heart and lungs while separating the ribs! Analysis Questions-Respiratory & Cardiovascular Log into QUIA using your
2 Aortic Arch Debranching UCSF Vascular Symposium /14/16. J Endovasc Ther 2002;9:suppl 2; II98 105
 How I Do It: Aortic Arch Debranching Exposures, Tunnels and Techniques Warren Gasper MD Assistant Professor of Surgery UCSF Vascular Surgery No disclosures 2 Aortic Arch Debranching UCSF Vascular Symposium
How I Do It: Aortic Arch Debranching Exposures, Tunnels and Techniques Warren Gasper MD Assistant Professor of Surgery UCSF Vascular Surgery No disclosures 2 Aortic Arch Debranching UCSF Vascular Symposium
Surgical Privileges Form: Vascular Surgery
 Surgical Form: Vascular Surgery Clinical Request Applicant s Name:. License No. (If Any):... Date:... Scope of Practice:. Facility:.. Place of Work:. CATEGORY I: GENERAL PRIVILEGES 1. Admitting privileges
Surgical Form: Vascular Surgery Clinical Request Applicant s Name:. License No. (If Any):... Date:... Scope of Practice:. Facility:.. Place of Work:. CATEGORY I: GENERAL PRIVILEGES 1. Admitting privileges
Adductor canal (Subsartorial) or Hunter s canal
 Adductor canal (Subsartorial) or Hunter s canal John Hunter described the exposure and ligation of the femoral artery in this canal for aneurysm of the popliteal artery; this method has the advantage that
Adductor canal (Subsartorial) or Hunter s canal John Hunter described the exposure and ligation of the femoral artery in this canal for aneurysm of the popliteal artery; this method has the advantage that
Surgical Options for revascularisation P E T E R S U B R A M A N I A M
 Surgical Options for revascularisation P E T E R S U B R A M A N I A M The goal Treat pain Heal ulcer Preserve limb Preserve life The options Conservative Endovascular Surgical bypass Primary amputation
Surgical Options for revascularisation P E T E R S U B R A M A N I A M The goal Treat pain Heal ulcer Preserve limb Preserve life The options Conservative Endovascular Surgical bypass Primary amputation
PUT YOUR BEST FOOT FORWARD
 PUT YOUR BEST FOOT FORWARD Bala Ramanan, MBBS 1 st year vascular surgery fellow Introduction The epidemic of diabetes and ageing of our population ensures critical limb ischemia will continue to grow.
PUT YOUR BEST FOOT FORWARD Bala Ramanan, MBBS 1 st year vascular surgery fellow Introduction The epidemic of diabetes and ageing of our population ensures critical limb ischemia will continue to grow.
Non-invasive examination
 Non-invasive examination Segmental pressure and Ankle-Brachial Index (ABI) The segmental blood pressure (SBP) examination is a simple, noninvasive method for diagnosing and localizing arterial disease.
Non-invasive examination Segmental pressure and Ankle-Brachial Index (ABI) The segmental blood pressure (SBP) examination is a simple, noninvasive method for diagnosing and localizing arterial disease.
Intro: Slide 1. Slide 2. Slide 3. Basic understanding of interventional radiology. Gain knowledge of key terms and phrases
 Slide 1 Intro: PRESENTED BY: Selena M. Moore, AAS, CCS, CPC HIMS Physician Liaison Coder This is a modified/updated presentation that was originally written by: Rosemary Waligorski, RHIT, CCS, RCC and
Slide 1 Intro: PRESENTED BY: Selena M. Moore, AAS, CCS, CPC HIMS Physician Liaison Coder This is a modified/updated presentation that was originally written by: Rosemary Waligorski, RHIT, CCS, RCC and
Morbidity Audit and Logbook Tool SNOMED Board Reporting Terms for SET and IMG Vascular Surgery AMPUTATION AORTA
 SNOMED s for SET and IMG Vascular Surgery AMPUTATION Amputation above-knee Amputation of leg through tibia and fibula Amputation of the foot Amputation of toe Through knee amputation Ray amputation of
SNOMED s for SET and IMG Vascular Surgery AMPUTATION Amputation above-knee Amputation of leg through tibia and fibula Amputation of the foot Amputation of toe Through knee amputation Ray amputation of
RadRx Your Prescription for Accurate Coding & Reimbursement Copyright All Rights Reserved.
 Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of June 4, 2018 Thrombolysis, Thrombectomy & Angioplasty
Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of June 4, 2018 Thrombolysis, Thrombectomy & Angioplasty
Peripheral Arterial Disease: A Practical Approach
 Peripheral Arterial Disease: A Practical Approach Sanjoy Kundu BSc, MD, FRCPC, DABR, FASA, FCIRSE, FSIR The Scarborough Hospital Toronto Endovascular Centre The Vein Institute of Toronto Scarborough Vascular
Peripheral Arterial Disease: A Practical Approach Sanjoy Kundu BSc, MD, FRCPC, DABR, FASA, FCIRSE, FSIR The Scarborough Hospital Toronto Endovascular Centre The Vein Institute of Toronto Scarborough Vascular
Knee Disarticulation Amputation
 Knee Disarticulation Amputation Pre-Op 64 year old man, previous spinal cord injury, diabetes, renal failure, and a history of spasticity with dynamic knee flexion contracture. He had an open left ankle
Knee Disarticulation Amputation Pre-Op 64 year old man, previous spinal cord injury, diabetes, renal failure, and a history of spasticity with dynamic knee flexion contracture. He had an open left ankle
HUMAN BODY COURSE LOWER LIMB NERVES AND VESSELS
 HUMAN BODY COURSE LOWER LIMB NERVES AND VESSELS October 22, 2010 D. LOWER LIMB MUSCLES 2. Lower limb compartments ANTERIOR THIGH COMPARTMENT General lfunction: Hip flexion, knee extension, other motions
HUMAN BODY COURSE LOWER LIMB NERVES AND VESSELS October 22, 2010 D. LOWER LIMB MUSCLES 2. Lower limb compartments ANTERIOR THIGH COMPARTMENT General lfunction: Hip flexion, knee extension, other motions
Transfemoral Amputation
 Transfemoral Amputation Pre-Op: 42 year old male who sustained severe injuries in a motorcycle accident. Note: he is a previous renal transplant recipient and is on immunosuppressive treatments. His injuries
Transfemoral Amputation Pre-Op: 42 year old male who sustained severe injuries in a motorcycle accident. Note: he is a previous renal transplant recipient and is on immunosuppressive treatments. His injuries
Misc Anatomy. Upper Limb! 2. Lower Limb! 5. Venous Drainage! Head & neck! 8
 Misc Anatomy Upper Limb! 2 Arteries!... 2 Veins!... 2 Spaces!... 4 Lower Limb! 5 Arteries!... 5 Venous Drainage!... 6 Spaces!... 7 Head & neck! 8 Artery!... 8 Ultrasound View for IJ CVL!... 8 Arteries
Misc Anatomy Upper Limb! 2 Arteries!... 2 Veins!... 2 Spaces!... 4 Lower Limb! 5 Arteries!... 5 Venous Drainage!... 6 Spaces!... 7 Head & neck! 8 Artery!... 8 Ultrasound View for IJ CVL!... 8 Arteries
Interventional Radiology in Trauma. Vikash Prasad, MD, FRCPC Vascular and Interventional Radiology The Moncton Hospital
 Interventional Radiology in Trauma Vikash Prasad, MD, FRCPC Vascular and Interventional Radiology The Moncton Hospital Disclosures None relevant to this presentation Shareholder Johnson and Johnson Goal
Interventional Radiology in Trauma Vikash Prasad, MD, FRCPC Vascular and Interventional Radiology The Moncton Hospital Disclosures None relevant to this presentation Shareholder Johnson and Johnson Goal
SAMPLE EDITION PELVIC AND LOWER EXTREMITY ARTERIES WITH ENDOVASCULAR REVASCULARIZATION. Cardiovascular Illustrations and Guidelines
 Cardiovascular Illustrations and Guidelines PELVIC AND LOWER EXTREMITY ARTERIES WITH ENDOVASCULAR REVASCULARIZATION ANGIOPLASTY INTRAVASCULAR STENT PLACEMENT ATHERECTOMY For Fem-Pop Territory Angioplasty
Cardiovascular Illustrations and Guidelines PELVIC AND LOWER EXTREMITY ARTERIES WITH ENDOVASCULAR REVASCULARIZATION ANGIOPLASTY INTRAVASCULAR STENT PLACEMENT ATHERECTOMY For Fem-Pop Territory Angioplasty
Primary to non-coronary IVUS
 codes 2018 2018 codes Primary to non-coronary IVUS Page 2 All coding, coverage, billing and payment information provided herein by Philips is gathered from third-party sources and is subject to change.
codes 2018 2018 codes Primary to non-coronary IVUS Page 2 All coding, coverage, billing and payment information provided herein by Philips is gathered from third-party sources and is subject to change.
PEMSS PROTOCOLS INVASIVE PROCEDURES
 PEMSS PROTOCOLS INVASIVE PROCEDURES Panhandle Emergency Medical Services System SURGICAL AND NEEDLE CRICOTHYROTOMY Inability to intubate is the primary indication for creating an artificial airway. Care
PEMSS PROTOCOLS INVASIVE PROCEDURES Panhandle Emergency Medical Services System SURGICAL AND NEEDLE CRICOTHYROTOMY Inability to intubate is the primary indication for creating an artificial airway. Care
Breathing. Heart Rate
 Breathing Heart Rate Inspiration Expiration (Pressos not Stretched) Heart Rate increases with inspiration (Pressos Stretched) Heart Rate decreases with expiration Upside Down (Pressos Stretched) HR Decreases
Breathing Heart Rate Inspiration Expiration (Pressos not Stretched) Heart Rate increases with inspiration (Pressos Stretched) Heart Rate decreases with expiration Upside Down (Pressos Stretched) HR Decreases
Visceral aneurysm. Diagnosis and Interventions M.NEDEVSKA
 Visceral aneurysm Diagnosis and Interventions M.NEDEVSKA History 1953 De Bakeyand Cooley Visceral aneurysm VAAs rare, reported incidence of 0.01 to 0.2% on routine autopsies. Clinically important Potentially
Visceral aneurysm Diagnosis and Interventions M.NEDEVSKA History 1953 De Bakeyand Cooley Visceral aneurysm VAAs rare, reported incidence of 0.01 to 0.2% on routine autopsies. Clinically important Potentially
Georgia Vascular Society 6th Annual Scientific Sessions September 14 16, 2018 Ritz-Carlton Reynolds, Lake Oconee Greensboro, GA
 The Gamete of Pediatric Vascular Surgery: One Surgeon s Experience Georgia Vascular Society 6th Annual Scientific Sessions September 14 16, 2018 Ritz-Carlton Reynolds, Lake Oconee Greensboro, GA Mohammed
The Gamete of Pediatric Vascular Surgery: One Surgeon s Experience Georgia Vascular Society 6th Annual Scientific Sessions September 14 16, 2018 Ritz-Carlton Reynolds, Lake Oconee Greensboro, GA Mohammed
Lecture 2: Clinical anatomy of thoracic cage and cavity II
 Lecture 2: Clinical anatomy of thoracic cage and cavity II Dr. Rehan Asad At the end of this session, the student should be able to: Identify and discuss clinical anatomy of mediastinum such as its deflection,
Lecture 2: Clinical anatomy of thoracic cage and cavity II Dr. Rehan Asad At the end of this session, the student should be able to: Identify and discuss clinical anatomy of mediastinum such as its deflection,
Emergency Approach to the Subclavian and Innominate Vessels
 Emergency Approach to the Subclavian and Innominate Vessels Joseph J. Amato, M.D., Robert M. Vanecko, M.D., See Tao Yao, M.D., and Milton Weinberg, Jr., M.D. T he operative approach to an acutely injured
Emergency Approach to the Subclavian and Innominate Vessels Joseph J. Amato, M.D., Robert M. Vanecko, M.D., See Tao Yao, M.D., and Milton Weinberg, Jr., M.D. T he operative approach to an acutely injured
The thigh. Prof. Oluwadiya KS
 The thigh Prof. Oluwadiya KS www.oluwadiya.com The Thigh: Boundaries The thigh is the region of the lower limb that is approximately between the hip and knee joints Anteriorly, it is separated from the
The thigh Prof. Oluwadiya KS www.oluwadiya.com The Thigh: Boundaries The thigh is the region of the lower limb that is approximately between the hip and knee joints Anteriorly, it is separated from the
Recommendations for Follow-up After Vascular Surgery Arterial Procedures SVS Practice Guidelines
 Recommendations for Follow-up After Vascular Surgery Arterial Procedures 2018 SVS Practice Guidelines vsweb.org/svsguidelines About the guidelines Published in the July 2018 issue of Journal of Vascular
Recommendations for Follow-up After Vascular Surgery Arterial Procedures 2018 SVS Practice Guidelines vsweb.org/svsguidelines About the guidelines Published in the July 2018 issue of Journal of Vascular
2018 CPT CODING CHANGES
 17 2018 CPT coding changes by Samuel Smith, MD, FACS; Megan McNally, MD, FACS; and Jan Nagle, MS, RPh JAN 2018 BULLETIN American College of Surgeons 18 Significant changes in Current Procedural Terminology
17 2018 CPT coding changes by Samuel Smith, MD, FACS; Megan McNally, MD, FACS; and Jan Nagle, MS, RPh JAN 2018 BULLETIN American College of Surgeons 18 Significant changes in Current Procedural Terminology
Diagnosis & Management of Kidney Trauma. LAU - Urology Residency Program LOP Urology Residents Meeting
 Diagnosis & Management of Kidney Trauma LAU - Urology Residency Program LOP Urology Residents Meeting Outline Introduction Investigation Staging Treatment Introduction The kidneys are the most common genitourinary
Diagnosis & Management of Kidney Trauma LAU - Urology Residency Program LOP Urology Residents Meeting Outline Introduction Investigation Staging Treatment Introduction The kidneys are the most common genitourinary
Subclavian artery Stenting
 Subclavian artery Stenting Etiology Atherosclerosis Takayasu s arteritis Fibromuscular dysplasia Giant Cell Arteritis Radiation-induced Vascular Injury Thoracic Outlet Syndrome Neurofibromatosis Incidence
Subclavian artery Stenting Etiology Atherosclerosis Takayasu s arteritis Fibromuscular dysplasia Giant Cell Arteritis Radiation-induced Vascular Injury Thoracic Outlet Syndrome Neurofibromatosis Incidence
Physician s Vascular Interpretation Examination Content Outline
 Physician s Vascular Interpretation Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 6 Cerebrovascular Abdominal Peripheral Arterial - Duplex Imaging Peripheral Arterial
Physician s Vascular Interpretation Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 6 Cerebrovascular Abdominal Peripheral Arterial - Duplex Imaging Peripheral Arterial
Resident Teaching Conference 3/12/2010
 Resident Teaching Conference 3/12/2010 Goals Definition and Classification of Acute Limb Ischemia Clinical Assessment of the Vascular Patient History and Physical Diagnostic Modalities Management of Acute
Resident Teaching Conference 3/12/2010 Goals Definition and Classification of Acute Limb Ischemia Clinical Assessment of the Vascular Patient History and Physical Diagnostic Modalities Management of Acute
Trauma. Neck trauma zones. Neck Injuries 1/3/2018. Basic principles A ; Airway B ; Breathing C ; Circulation D ; Disability E ; Exposure
 Trauma 45 minutes highest points Ahmed Mahmoud, MD Basic principles A ; Airway B ; Breathing C ; Circulation D ; Disability E ; Exposure Neck trauma zones Airway ;Rapid sequence intubation Breathing ;Needle
Trauma 45 minutes highest points Ahmed Mahmoud, MD Basic principles A ; Airway B ; Breathing C ; Circulation D ; Disability E ; Exposure Neck trauma zones Airway ;Rapid sequence intubation Breathing ;Needle
Injuries to the Hands and Feet
 Injuries to the Hands and Feet Chapter 26 Injuries to the Hands and Feet Introduction Combat injuries to the hands and feet differ from those of the arms and legs in terms of mortality and morbidity. Death
Injuries to the Hands and Feet Chapter 26 Injuries to the Hands and Feet Introduction Combat injuries to the hands and feet differ from those of the arms and legs in terms of mortality and morbidity. Death
Overview of Surgical Resection of Space Sarcomas
 13282_ON-33.qxd 3/31/09 4:50 PM Page 1 Chapter 33 Overview of Surgical Resection of Space Sarcomas Amir Sternheim, Tamir Pritsch, and Martin M. Malawer BACKGROUND The three main extracompartmental spaces
13282_ON-33.qxd 3/31/09 4:50 PM Page 1 Chapter 33 Overview of Surgical Resection of Space Sarcomas Amir Sternheim, Tamir Pritsch, and Martin M. Malawer BACKGROUND The three main extracompartmental spaces
Arterial Access for Diagnosis and Intervention T-Woei Tan, MD, FACS
 Arterial Access for Diagnosis and Intervention T-Woei Tan, MD, FACS Assistant Professor of Surgery Vascular Endovascular Surgery Louisiana State University Health - Shreveport Disclosures None Objective
Arterial Access for Diagnosis and Intervention T-Woei Tan, MD, FACS Assistant Professor of Surgery Vascular Endovascular Surgery Louisiana State University Health - Shreveport Disclosures None Objective
Surgery Under Regional Anesthesia
 Surgery Under Regional Anesthesia Jean Daniel Eloy, MD Assistant Professor Residency Program Director Rutgers-New Jersey Medical School Rutgers The State University of New Jersey Peripheral Nerve Block
Surgery Under Regional Anesthesia Jean Daniel Eloy, MD Assistant Professor Residency Program Director Rutgers-New Jersey Medical School Rutgers The State University of New Jersey Peripheral Nerve Block
A A U
 PVD Venous AUC Rating Sheet 2nd Round 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 Median I NI MADM Rating Agree Disagree Upper Extremity Venous Evaluation Table 1. Venous Duplex of the Upper Extremities for Patency
PVD Venous AUC Rating Sheet 2nd Round 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 Median I NI MADM Rating Agree Disagree Upper Extremity Venous Evaluation Table 1. Venous Duplex of the Upper Extremities for Patency
Access (Antegrade, Retrograde, Pedal)
 Access (Antegrade, Retrograde, Pedal) ARCH St. Louis Craig M. Walker, MD, FACC, FACP Clinical Professor of Medicine Tulane University School of Medicine New Orleans, LA Clinical Professor of Medicine LSU
Access (Antegrade, Retrograde, Pedal) ARCH St. Louis Craig M. Walker, MD, FACC, FACP Clinical Professor of Medicine Tulane University School of Medicine New Orleans, LA Clinical Professor of Medicine LSU
Ali Yaghi. Omar Eyad. Ahmad Salman. 1 P a g e
 5 Ali Yaghi Omar Eyad Ahmad Salman 1 P a g e **There are two types of groin hernia; the femoral hernia and the inguinal hernia. But how can we differentiate between the inguinal hernia and the femoral
5 Ali Yaghi Omar Eyad Ahmad Salman 1 P a g e **There are two types of groin hernia; the femoral hernia and the inguinal hernia. But how can we differentiate between the inguinal hernia and the femoral
Tracheo-innominate artery fistula (TIF) is an uncommon
 Technique for Managing Tracheo-Innominate Artery Fistula Gorav Ailawadi, MD Tracheo-innominate artery fistula (TIF) is an uncommon complication (0.1-1%) following both open and percutaneous tracheostomy.
Technique for Managing Tracheo-Innominate Artery Fistula Gorav Ailawadi, MD Tracheo-innominate artery fistula (TIF) is an uncommon complication (0.1-1%) following both open and percutaneous tracheostomy.
CORONARY ARTERY BYPASS GRAFTING (CABG) (Part 1) Mark Shikhman, MD, Ph.D., CSA Andrea Scott, CST
 CORONARY ARTERY BYPASS GRAFTING (CABG) (Part 1) Mark Shikhman, MD, Ph.D., CSA Andrea Scott, CST I have constructed this lecture based on publications by leading cardiothoracic American surgeons: Timothy
CORONARY ARTERY BYPASS GRAFTING (CABG) (Part 1) Mark Shikhman, MD, Ph.D., CSA Andrea Scott, CST I have constructed this lecture based on publications by leading cardiothoracic American surgeons: Timothy
Femoral Artery. Its entrance to the thigh Position Midway between ASIS and pubic symphysis
 Lower Limb Vessels Lecture Objectives Describe the major arteries of the lower limb. Describe the deep and superficial veins of the lower limb. Describe the topographical relationships of the arteries
Lower Limb Vessels Lecture Objectives Describe the major arteries of the lower limb. Describe the deep and superficial veins of the lower limb. Describe the topographical relationships of the arteries
Guidelines, Policies and Statements D20 Statement on Peripheral Venous Ultrasound
 Guidelines, Policies and Statements D20 Statement on Peripheral Venous Ultrasound Disclaimer and Copyright The ASUM Standards of Practice Board have made every effort to ensure that this Guideline/Policy/Statement
Guidelines, Policies and Statements D20 Statement on Peripheral Venous Ultrasound Disclaimer and Copyright The ASUM Standards of Practice Board have made every effort to ensure that this Guideline/Policy/Statement
Vascular Technology Examination Content Outline
 Vascular Technology Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 Normal Anatomy, Perfusion, and Function Evaluate normal anatomy, perfusion, function 2 Pathology, Perfusion,
Vascular Technology Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 Normal Anatomy, Perfusion, and Function Evaluate normal anatomy, perfusion, function 2 Pathology, Perfusion,
ANATYOMY OF The thigh
 ANATYOMY OF The thigh 1- Lateral cutaneous nerve of the thigh Ι) Skin of the thigh Anterior view 2- Femoral branch of the genitofemoral nerve 5- Intermediate cutaneous nerve of the thigh 1, 2 and 3 are
ANATYOMY OF The thigh 1- Lateral cutaneous nerve of the thigh Ι) Skin of the thigh Anterior view 2- Femoral branch of the genitofemoral nerve 5- Intermediate cutaneous nerve of the thigh 1, 2 and 3 are
DISSECTION SCHEDULE. Session I - Hip (Front) & Thigh (Superficial)
 DISSECTION SCHEDULE Session I - Hip (Front) & Thigh (Superficial) Surface anatomy Inguinal region Gluteal region Thigh Leg Foot bones Hip bone Femur Superficial fascia Great saphenous vein Superficial
DISSECTION SCHEDULE Session I - Hip (Front) & Thigh (Superficial) Surface anatomy Inguinal region Gluteal region Thigh Leg Foot bones Hip bone Femur Superficial fascia Great saphenous vein Superficial
Bare Metal Stents vs Stent Grafts
 Bare Metal Stents vs Stent Grafts ASDIN 12th Annual Scientific Meeting Phoenix, AZ, February 20, 2016 Dirk Hentschel, MD Director, Interventional Nephrology Brigham and Women s Hospital Disclosure Consultant:
Bare Metal Stents vs Stent Grafts ASDIN 12th Annual Scientific Meeting Phoenix, AZ, February 20, 2016 Dirk Hentschel, MD Director, Interventional Nephrology Brigham and Women s Hospital Disclosure Consultant:
Lower Limb Nerves. Clinical Anatomy
 Lower Limb Nerves Clinical Anatomy Lumbar Plexus Ventral rami L1 L4 Supplies: Abdominal wall External genitalia Anteromedial thigh Major nerves.. Lumbar Plexus Nerves relation to psoas m. : Obturator n.
Lower Limb Nerves Clinical Anatomy Lumbar Plexus Ventral rami L1 L4 Supplies: Abdominal wall External genitalia Anteromedial thigh Major nerves.. Lumbar Plexus Nerves relation to psoas m. : Obturator n.
Surgical Options in Thrombectomy for Non-Surgeons
 Surgical Options in Thrombectomy for Non-Surgeons Shouwen Wang, MD, PhD, FASDIN AKDHC Ambulatory Surgery Center Arizona Kidney Disease and Hypertension Center Phoenix, Arizona Disclosure No relevant financial
Surgical Options in Thrombectomy for Non-Surgeons Shouwen Wang, MD, PhD, FASDIN AKDHC Ambulatory Surgery Center Arizona Kidney Disease and Hypertension Center Phoenix, Arizona Disclosure No relevant financial
Peripheral Vascular Examination. Dr. Gary Mumaugh Western Physical Assessment
 Peripheral Vascular Examination Dr. Gary Mumaugh Western Physical Assessment Competencies 1. Inspection of upper extremity for: size symmetry swelling venous pattern color Texture nail beds Competencies
Peripheral Vascular Examination Dr. Gary Mumaugh Western Physical Assessment Competencies 1. Inspection of upper extremity for: size symmetry swelling venous pattern color Texture nail beds Competencies
How to manage the left subclavian and left vertebral artery during TEVAR
 How to manage the left subclavian and left vertebral artery during TEVAR Jürg Schmidli Chief of Vascular Surgery Inselspital Hamburg 2017 Dept Cardiovascular Surgery, Bern, Switzerland Disclosure No Disclosures
How to manage the left subclavian and left vertebral artery during TEVAR Jürg Schmidli Chief of Vascular Surgery Inselspital Hamburg 2017 Dept Cardiovascular Surgery, Bern, Switzerland Disclosure No Disclosures
Clinical Examination of VASCULAR PATIENTS. Stephanie Hirst & Alexander Sunde
 Clinical Examination of VASCULAR PATIENTS Stephanie Hirst & Alexander Sunde Goals of Medical History To record the patient s symptoms at time of presentation. To organize the events which have lead to
Clinical Examination of VASCULAR PATIENTS Stephanie Hirst & Alexander Sunde Goals of Medical History To record the patient s symptoms at time of presentation. To organize the events which have lead to
Vascular Surgery Cases: Detours. Brian F. Stull, RDMS, RVT UNC REX Healthcare Vascular Specialists
 Vascular Surgery Cases: Detours Brian F. Stull, RDMS, RVT UNC REX Healthcare Vascular Specialists Brian.Stull@Unchealth.unc.edu Objectives Anatomy of a bypass graft Where does it connect, where does it
Vascular Surgery Cases: Detours Brian F. Stull, RDMS, RVT UNC REX Healthcare Vascular Specialists Brian.Stull@Unchealth.unc.edu Objectives Anatomy of a bypass graft Where does it connect, where does it
ANATYOMY OF The thigh
 ANATYOMY OF The thigh 1- Lateral cutaneous nerve of the thigh Ι) Skin of the thigh Anterior view 2- Femoral branch of the genitofemoral nerve 1, 2 and 3 are From the lumber plexus 5- Intermediate cutaneous
ANATYOMY OF The thigh 1- Lateral cutaneous nerve of the thigh Ι) Skin of the thigh Anterior view 2- Femoral branch of the genitofemoral nerve 1, 2 and 3 are From the lumber plexus 5- Intermediate cutaneous
Lung cancer or primary malignant tumors of the mediastinum
 Technique of Superior Vena Cava Resection for Lung Carcinomas David R. Jones, MD Division of Thoracic and Cardiovascular Surgery, Department of Surgery, University of Virginia School of Medicine, Charlottesville,
Technique of Superior Vena Cava Resection for Lung Carcinomas David R. Jones, MD Division of Thoracic and Cardiovascular Surgery, Department of Surgery, University of Virginia School of Medicine, Charlottesville,
The Cardiovascular System
 PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Cardiovascular System 11PART B The Heart: Cardiac Output Cardiac output (CO) Amount of blood pumped
PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Cardiovascular System 11PART B The Heart: Cardiac Output Cardiac output (CO) Amount of blood pumped
Lecture 09. Popliteal Fossa. BY Dr Farooq Khan Aurakzai
 Lecture 09 Popliteal Fossa BY Dr Farooq Khan Aurakzai Dated: 14.02.2018 What is popliteus? Introduction Anything relating to, or near the part of the leg behind the knee. From New Latin popliteus the muscle
Lecture 09 Popliteal Fossa BY Dr Farooq Khan Aurakzai Dated: 14.02.2018 What is popliteus? Introduction Anything relating to, or near the part of the leg behind the knee. From New Latin popliteus the muscle
Candidate s instructions Look at this cross-section taken at the level of C5. Answer the following questions.
 Section 1 Anatomy Chapter 1. Trachea 1 Candidate s instructions Look at this cross-section taken at the level of C5. Answer the following questions. Pretracheal fascia 1 2 5 3 4 Questions 1. Label the
Section 1 Anatomy Chapter 1. Trachea 1 Candidate s instructions Look at this cross-section taken at the level of C5. Answer the following questions. Pretracheal fascia 1 2 5 3 4 Questions 1. Label the
Year 2004 Paper one: Questions supplied by Megan
 QUESTION 47 A 58yo man is noted to have a right foot drop three days following a right total hip replacement. On examination there is weakness of right ankle dorsiflexion and toe extension (grade 4/5).
QUESTION 47 A 58yo man is noted to have a right foot drop three days following a right total hip replacement. On examination there is weakness of right ankle dorsiflexion and toe extension (grade 4/5).
Epidemiology. 16% incidence in knee. dislocation
 Epidemiology Highest risk group: Young male between 15 and 45 years (USA) Mortality Ratio after trauma : male/female: 7/1 Peripheral vascular injuries : 70%-80% of all cases of vascular trauma : Vascular
Epidemiology Highest risk group: Young male between 15 and 45 years (USA) Mortality Ratio after trauma : male/female: 7/1 Peripheral vascular injuries : 70%-80% of all cases of vascular trauma : Vascular
CARDIOVASCULAR DANIL HAMMOUDI.MD
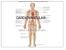 CARDIOVASCULAR DANIL HAMMOUDI.MD 18 Systemic Circulation Figure 19.19 Pulmonary Circulation Figure 19.18b 1. Thyroid gland 2. Trachea 3. Brachiocephalic 4. Common carotid 5. Internal jugular 6. Superior
CARDIOVASCULAR DANIL HAMMOUDI.MD 18 Systemic Circulation Figure 19.19 Pulmonary Circulation Figure 19.18b 1. Thyroid gland 2. Trachea 3. Brachiocephalic 4. Common carotid 5. Internal jugular 6. Superior
BC Vascular Day. Contents. November 3, Abdominal Aortic Aneurysm 2 3. Peripheral Arterial Disease 4 6. Deep Venous Thrombosis 7 8
 BC Vascular Day Contents Abdominal Aortic Aneurysm 2 3 November 3, 2018 Peripheral Arterial Disease 4 6 Deep Venous Thrombosis 7 8 Abdominal Aortic Aneurysm Conservative Management Risk factor modification
BC Vascular Day Contents Abdominal Aortic Aneurysm 2 3 November 3, 2018 Peripheral Arterial Disease 4 6 Deep Venous Thrombosis 7 8 Abdominal Aortic Aneurysm Conservative Management Risk factor modification
Curtiss T. Stinis, M.D., F.A.C.C., F.S.C.A.I. SCRIPPS CLINIC
 Avoiding and Managing Femoral Access Site Complications Curtiss T. Stinis, M.D., F.A.C.C., F.S.C.A.I. Director, Peripheral Interventions Program Director, Interventional Cardiology Fellowship Division
Avoiding and Managing Femoral Access Site Complications Curtiss T. Stinis, M.D., F.A.C.C., F.S.C.A.I. Director, Peripheral Interventions Program Director, Interventional Cardiology Fellowship Division
Distal Femoral Resection
 Distal Femoral Resection Annie Arteau, Bruno Fuchs Introduction This text is a general description of a distal femoral resection. Focus is on anatomical structures and muscle resection. Each femoral resection
Distal Femoral Resection Annie Arteau, Bruno Fuchs Introduction This text is a general description of a distal femoral resection. Focus is on anatomical structures and muscle resection. Each femoral resection
ANATYOMY OF The thigh
 ANATYOMY OF The thigh 1- Lateral cutaneous nerve of the thigh Ι) Skin of the thigh Anterior view 2- Femoral branch of the genitofemoral nerve 5- Intermediate cutaneous nerve of the thigh 1, 2 and 3 are
ANATYOMY OF The thigh 1- Lateral cutaneous nerve of the thigh Ι) Skin of the thigh Anterior view 2- Femoral branch of the genitofemoral nerve 5- Intermediate cutaneous nerve of the thigh 1, 2 and 3 are
Penetrating Neck Injuries. Jason Levine MD Lutheran Medical Center July 22, 2010
 Penetrating Neck Injuries Jason Levine MD Lutheran Medical Center July 22, 2010 CASE PRESENTATION 19 YO M 3 Stab Wounds Right zone I neck SW 2 SW anterior abdomen Left epigastrium anterior axillary line
Penetrating Neck Injuries Jason Levine MD Lutheran Medical Center July 22, 2010 CASE PRESENTATION 19 YO M 3 Stab Wounds Right zone I neck SW 2 SW anterior abdomen Left epigastrium anterior axillary line
The posterior abdominal wall. Prof. Oluwadiya KS
 The posterior abdominal wall Prof. Oluwadiya KS www.oluwadiya.sitesled.com Posterior Abdominal Wall Lumbar vertebrae and discs. Muscles opsoas, quadratus lumborum, iliacus, transverse, abdominal wall
The posterior abdominal wall Prof. Oluwadiya KS www.oluwadiya.sitesled.com Posterior Abdominal Wall Lumbar vertebrae and discs. Muscles opsoas, quadratus lumborum, iliacus, transverse, abdominal wall
Subclavian and Axillary Artery Aneurysms
 Subclavian and Axillary Artery Aneurysms April 2008 Francesco A Aiello, M.D. Assistant Professor of Surgery Division of Vascular Endovascular Surgery University of Massachusetts Medical School None DISCLOSURES
Subclavian and Axillary Artery Aneurysms April 2008 Francesco A Aiello, M.D. Assistant Professor of Surgery Division of Vascular Endovascular Surgery University of Massachusetts Medical School None DISCLOSURES
The Whipple Operation Illustrations
 The Whipple Operation Illustrations Fig. 1. Illustration of the sixstep pancreaticoduodenectomy (Whipple operation) as described in a number of recent text books by Dr. Evans. The operation is divided
The Whipple Operation Illustrations Fig. 1. Illustration of the sixstep pancreaticoduodenectomy (Whipple operation) as described in a number of recent text books by Dr. Evans. The operation is divided
musculoskeletal system anatomy nerves of the lower limb 1 done by: dina sawadha & mohammad abukabeer
 musculoskeletal system anatomy nerves of the lower limb 1 done by: dina sawadha & mohammad abukabeer What is the importance of plexuses? plexuses provides us the advantage of a phenomenon called convergence
musculoskeletal system anatomy nerves of the lower limb 1 done by: dina sawadha & mohammad abukabeer What is the importance of plexuses? plexuses provides us the advantage of a phenomenon called convergence
The Lower Limb II. Anatomy RHS 241 Lecture 3 Dr. Einas Al-Eisa
 The Lower Limb II Anatomy RHS 241 Lecture 3 Dr. Einas Al-Eisa Tibia The larger & medial bone of the leg Functions: Attachment of muscles Transfer of weight from femur to skeleton of the foot Articulations
The Lower Limb II Anatomy RHS 241 Lecture 3 Dr. Einas Al-Eisa Tibia The larger & medial bone of the leg Functions: Attachment of muscles Transfer of weight from femur to skeleton of the foot Articulations
Reimbursement Guide Zenith Fenestrated AAA Endovascular Graft
 MEDICAL Reimbursement Guide Zenith Fenestrated AAA Endovascular Graft Disclaimer: The information provided herein reflects Cook s understanding of the procedure(s) and/or device(s) from sources that may
MEDICAL Reimbursement Guide Zenith Fenestrated AAA Endovascular Graft Disclaimer: The information provided herein reflects Cook s understanding of the procedure(s) and/or device(s) from sources that may
Patient Brochure. Clearstream Technologies, Ltd. Moyne Upper Enniscorthy Co. Wexford, Ireland. PK Rev. 0 05/17
 Patient Brochure Clearstream Technologies, Ltd. Moyne Upper Enniscorthy Co. Wexford, Ireland PK1411100 Rev. 0 05/17 LIFESTREAM Patient Brochure If you or a member of your family has been diagnosed with
Patient Brochure Clearstream Technologies, Ltd. Moyne Upper Enniscorthy Co. Wexford, Ireland PK1411100 Rev. 0 05/17 LIFESTREAM Patient Brochure If you or a member of your family has been diagnosed with
CT Imaging of Blunt and Penetrating Vascular Trauma DENNIS FOLEY MEDICAL COLLEGE WISCONSIN
 CT Imaging of Blunt and Penetrating Vascular Trauma DENNIS FOLEY MEDICAL COLLEGE WISCONSIN THORACO ABDOMINAL TRAUMA 0 10 20 30 40 50 60 5 cc/sec 30 secs 1.25 mm/ 55 mm Z1.375 2.5 mm/ 55 mm Z 1.375 Grade
CT Imaging of Blunt and Penetrating Vascular Trauma DENNIS FOLEY MEDICAL COLLEGE WISCONSIN THORACO ABDOMINAL TRAUMA 0 10 20 30 40 50 60 5 cc/sec 30 secs 1.25 mm/ 55 mm Z1.375 2.5 mm/ 55 mm Z 1.375 Grade
Ultrasound Guided Lower Extremity Blocks
 Ultrasound Guided Lower Extremity Blocks CONTENTS: 1. Femoral Nerve Block 2. Popliteal Nerve Block Updated December 2017 1 1. Femoral Nerve Block Indications Surgery involving the knee, anterior thigh,
Ultrasound Guided Lower Extremity Blocks CONTENTS: 1. Femoral Nerve Block 2. Popliteal Nerve Block Updated December 2017 1 1. Femoral Nerve Block Indications Surgery involving the knee, anterior thigh,
Open fenestration for complicated acute aortic B dissection
 Art of Operative Techniques Open fenestration for complicated acute aortic B dissection Santi Trimarchi 1, Sara Segreti 1, Viviana Grassi 1, Chiara Lomazzi 1, Marta Cova 1, Gabriele Piffaretti 2, Vincenzo
Art of Operative Techniques Open fenestration for complicated acute aortic B dissection Santi Trimarchi 1, Sara Segreti 1, Viviana Grassi 1, Chiara Lomazzi 1, Marta Cova 1, Gabriele Piffaretti 2, Vincenzo
