Contrast-Enhanced MR of the Facial Nerve in Patients with Posttraumatic Peripheral Facial Nerve Palsy
|
|
|
- Joel Palmer
- 5 years ago
- Views:
Transcription
1 Contrast-Enhanced MR of the Facial Nerve in Patients with Posttraumatic Peripheral Facial Nerve Palsy Sabine Sartoretti-Schefer, Martin Scherler, Werner Wichmann, and Anton Valavanis PURPOSE: To estimate the value of noncontrast and contrast-enhanced T1-weighted MR imaging in detecting the underlying mechanisms of injury and regeneration in immediate- or delayed-onset posttraumatic peripheral facial nerve palsy. METHODS: Twenty-four patients with posttraumatic peripheral facial nerve palsy were examined on a 1.5-T MR imaging unit with precontrast and postcontrast T1-weighted spin-echo and gradient-echo sequences. RESULTS: Abnormal enhancement of the distal intrameatal nerve segment was visible in 92% of the patients up to 2 years after their initial trauma. A hematoma within the geniculate ganglion was seen in 33% of the patients with a longitudinal fracture. The greater superficial petrosal nerve (in 32% of patients) and the geniculate ganglion (in 48% of patients) were thick and intensely enhancing. Hematoma within the cochlea/vestibule or enhancement of the cochlea/vestibule and the vestibulocochlear (eighth) nerve was observed in transverse fractures. CONCLUSION: MR images can show long-lasting abnormal nerve enhancement, especially in the distal intrameatal nerve segment, related to the long-lasting breakdown of the blood/peripheral nerve barrier associated with nerve degeneration and regeneration after traumatic stretching of the greater superficial petrosal nerve. Additionally, intraoperatively observed perineural and intraneural scar formation leads to thickening and intense enhancement of the affected nerve segments on MR images. A hematoma in the region of the geniculate ganglion can be seen in some but not all patients. Associated damage of the inner ear structures in patients with transverse fractures is also visible on MR images. Index terms: Nerves, facial (VII); Nerves, magnetic resonance AJNR Am J Neuroradiol 18: , June 1997 Received September 4, 1996; accepted after revision January 2, From the Institute of Neuroradiology (S.S-S., W.W., A.V.) and ENT (M.S.), University Hospital of Zürich (Switzerland). Address reprint requests to Sabine Sartoretti-Schefer, MD, Institut für Neuroradiologie, Universitätsspital Zürich, Frauenklinikstrasse 10, CH Zürich, Switzerland. AJNR 18: , Jun /97/ American Society of Neuroradiology 1115 A posttraumatic peripheral facial nerve palsy can develop after either longitudinal or transverse fracture of the temporal bone (1 5). Diagnosis of temporal bone fracture can be accurately established with computed tomography (CT) (6 10). Axial and coronal CT scans can show the exact course of the fracture line in relation to the bony facial nerve canal as well as associated injuries (ie, disruption of the ossicular chain, hematotympanun, the site of leakage of cerebrospinal fluid in patients with otorhinoliquorrhea, and injury of the temporomandibular joint) (6 10). In patients with posttraumatic peripheral facial nerve palsy, CT may correctly show the course of the fracture line through the bony facial nerve canal. It occasionally depicts hematoma in the region of the geniculate ganglion and compression of the facial nerve by an adjacent bony fragment (7), but the facial nerve itself is not visible, and therefore CT only indirectly delineates the nerve lesion. Magnetic resonance (MR) imaging, however, allows direct visibility of the injured peripheral facial nerve in patients with posttraumatic facial nerve palsy. Several intraoperative investigations have established different mechanisms for posttraumatic facial nerve damage (2, 3, 11). First, the nerve can be transected. Second, adjacent bony fragments and/or hematoma can compress the nerve. Third, an intraneural hematoma can develop as a result of traction of the greater su-
2 1116 SARTORETTI-SCHEFER AJNR: 18, June 1997 perficial petrosal nerve (GSPN) associated with formation of intraneural edema that extends in a retrograde direction. This leads to compression of the facial nerve at the meatal foramen with secondary ischemia, nerve degeneration, and, occasionally, regeneration via a pathogenic mechanism similar to that described in inflammatory palsy (2, 3, 12 16). Histologic examination of facial nerve biopsy specimens in patients who have had surgery for posttraumatic peripheral facial nerve palsy reveals simultaneous degeneration and regeneration processes with intraneural scar formation within the facial nerve (17). In our retrospective study, we tried to estimate the value of noncontrast and contrastenhanced MR imaging in patients with posttraumatic peripheral facial nerve palsy in terms of its ability to identify the location of the nerve injury, the underlying mechanism of injury (ie, intraneural hematoma/edema, nerve compression by bony fragment, or hematoma and nerve transection) (2, 3, 17), and the regeneration processes as known from histologic examinations. The intraoperative findings in eight patients who had surgery were correlated with the preoperative MR abnormalities to identify the fracture line and its course as well as to determine associated injuries of the inner ear structures in patients with transverse fractures. Materials and Methods We retrospectively evaluated the pathologic and radiologic findings in 24 patients (16 male, eight female; mean age, 38 years; range, 13 to 79 years) with posttraumatic peripheral facial nerve palsy. All patients were examined on a 1.5-T MR unit using a 5-inch surface coil centered over the external ear. Noncontrast and contrast-enhanced T1-weighted spin-echo sequences were performed in all patients, and fast T2- weighted spin-echo images were obtained in 12 patients. A standard MR protocol with T1-weighted spin-echo sequences ( /15 21/2 3 [precontrast] or 4 [postcontrast], [repetition time/echo time/excitations]), overlapped 2- to 3-mm-thick sections, and a 160- to 170-mm field of view (FOV) was used in all patients. In two patients, a gradient-echo three-dimensional T1-weighted (fast fieldecho) sequence (19/8.4/4) with a flip angle of 35, section thickness of 0.9 mm, 30 sections, and FOV of 160 mm was added. T2-weighted images were acquired with parameters of /80 120/4 and a section thickness of 2 to 3 mm. Sections were obtained in the axial (precontrast and postcontrast T1- and T2-weighted) and coronal (postcontrast T1-weighted) planes as well as occasionally in an oblique sagittal plane (postcontrast T1-weighted) along the axis of the tympanic segment (in four patients). Contrast material was injected intravenously using a bolus of 0.5 mmol/kg body weight (a high-dose protocol, used routinely in our department). MR imaging was performed immediately after injection of the contrast agent. Axial and coronal CT studies of the affected ear were obtained with a section thickness/table feed of 1 mm/460 ma in all patients to ascertain the presence or absence of an associated transverse or longitudinal fracture of the temporal bone. On CT scans, a longitudinal fracture of the temporal bone was diagnosed in 17 patients, a unilateral fracture was present in 14 patients, and a bilateral fracture in three patients. Only in one patient with bilateral longitudinal fracture was a bilateral MR examination done. In the other two patients with bilateral longitudinal fractures and bilateral facial nerve palsy, only the more severely affected side was examined with MR imaging. Therefore, 18 MR studies of longitudinal fractures and associated peripheral facial nerve palsies were evaluated. A transverse fracture of the temporal bone was visible on CT scans in three patients. In four patients, no fracture was identified at CT. A total of 25 posttraumatically paretic peripheral facial nerves were examined on MR images. The peripheral facial nerve palsy was of immediate onset (occurring within 24 hours after the trauma) in 16 facial nerves; these were associated with a transverse fracture in three patients, a longitudinal fracture in 12 patients, and with no fracture (at CT) in one patient. A palsy of delayed onset (occurring more than 24 hours after the trauma) was diagnosed in nine facial nerves; these were associated with a longitudinal fracture in six patients and with no visible fracture (at CT) in three patients. In three patients with transverse fractures, an additional loss of inner ear function was demonstrated by auditory and vestibular function tests. In 23 patients, single MR examinations were performed. In another patient, the first examination was on the 38th day after trauma and the second was on the 65th day after trauma. The earliest MR examination was obtained 7 days after trauma; the latest, 2 years after trauma. The mean interval between trauma and MR examination was 75.5 days. Table 1 shows the delay in days between the MR examination and the trauma itself and correlates the maximal percentage of nerve fiber degeneration on electroneurography with day of MR examination. The intensity of the contrast enhancement within the distal intrameatal, labyrinthine, geniculate ganglion, proximal tympanic, distal tympanic, and mastoid segments was evaluated. Evaluation consisted of visual inspection and classification of the degree of contrast enhancement into one of three grades: intense, moderate, or minimal. The region-of-interest method for objectively measuring the signal intensity of the facial nerve could not be applied owing to the small dimensions of the bony facial nerve canal (1.02 mm in the labyrinthine segment, 1.53 mm in the proximal tympanic/distal tympanic segments, and
3 AJNR: 18, June 1997 FACIAL NERVE PALSY 1117 TABLE 1: Delay between MR examination and trauma and correlation with maximal percentage of nerve fiber degeneration at electroneurography Days between MR and trauma No. of patients Percentage of nerve degeneration at electroneurography TABLE 2: Intensity of contrast enhancement of the various facial nerve segments in patients with posttraumatic peripheral facial nerve palsy Degree of Enhancement Facial Nerve Segment (25 Nerves) DIS LS GG PTS DTS MS Intense Moderate Minimal Not visible Note. Bold numbers indicate abnormally intense enhancement not observed in normal facial nerves. According to our previous study (13), in normal facial nerves a normal enhancement pattern can be seen in different nerve segments. Usually, the geniculate ganglion shows a moderate enhancement and the PTS, DTS, and MS a moderate or minimal enhancement. Therefore, the numbers in italics remind the reader that these enhancement intensities are also normally seen in healthy nerves and do not indicate an abnormal enhancement pattern. DIS indicates distal intrameatal segment; LS, labyrinthine segment; GG, geniculate ganglion; PTS, proximal tympanic segment; DTS, distal tympanic segment; and MS, mastoid segment mm in the mastoid segment) and of the smallness of the facial nerve itself (0.85 mm in the labyrinthine segment, 1.12 mm in the proximal tympanic/distal tympanic segments, and 0.94 mm in the mastoid segment) as compared with the smallest region of interest available (16, 18). Other possible abnormalities of the temporal bone evaluated on MR images were as follows: 1) visibility of the fracture line itself and the course of the fracture line in relation to the different facial nerve segments; 2) presence of an associated hematoma within the bony facial nerve canal or within the facial nerve itself, especially in or adjacent to the geniculate ganglion; 3) presence of a transection or compression of the facial nerve by an adjacent bony fragment; 4) presence of dural enhancement along the anterior border of the petrous bone or within the internal auditory canal as a possible indirect sign of an osseous microfracture or macrofracture, even if the fracture line could not be identified radiologically; 5) presence on late posttraumatic MR images of a thick and intensely enhancing GSPN and of a thick and intensely enhancing geniculate ganglion (both over 1 mm in diameter) (18, 19), related to scar formation as proved by facial nerve biopsy samples (17); and 6) presence of a hematoma within the inner ear spaces (cochlea and vestibule) or of abnormal contrast enhancement of the inner ear spaces or of the vestibulocochlear (eighth) nerve in patients with transverse fractures. Eight patients had surgery for immediate-onset posttraumatic facial nerve palsy. Two patients had a transverse fracture (operated on 49 and 1095 days, respectively, after the trauma); five patients had a longitudinal fracture (operated on 53, 62, 72, 85, and 480 days, respectively, TABLE 3: Visibility and course of fracture line on MR images in longitudinal and transverse fractures of the temporal bone Longitudinal Fracture (n 18) Transverse Fracture (n 3) Fracture line visible on MR 12 3 Course of the fracture line through: Internal auditory canal... 2 Vestibule... 1 GG 5... Slightly lateral to GG with extension to GSPN 5... PTS/DTS 2 1 Note. GG indicates geniculate ganglion; GSPN, greater superficial petrosal nerve; PTS, proximal tympanic segment; and DTS, distal tympanic segment. after the trauma); and one patient had no radiologically visible fracture (operated on 9 days after the trauma). The intraoperative findings were compared with the preoperative abnormal findings on MR images. Results Tables 2 through 5 present the pathologic findings in our 24 patients with posttraumatic peripheral facial nerve palsy. In 23 paretic nerves (92% of patients) with a mean interval between trauma and MR examination of 88 days, abnormal contrast enhance-
4 1118 SARTORETTI-SCHEFER AJNR: 18, June 1997 TABLE 4: Abnormal MR findings in patients with posttraumatic peripheral facial nerve palsy with or without temporal bone fracture Longitudinal Fracture (n 18) Transverse Fracture (n 3) No Fracture (n 4) Hematoma within GG (hyperintense on T1-weighted images; subacute stage) Hematoma lateral to GG Transection of seventh cranial nerve Compression of seventh cranial nerve by adjacent bony fragment Enhanced and thickened GSPN Enhanced and thickened GG Thickened PTS 1 2 Enhancing scar in IAC Dural enhancement along anterior border of temporal bone * Questionable. Note. GG indicates geniculate ganglion; GSPN, greater superficial petrosal nerve; PTS, proximal tympanic segment; and IAC, internal auditory canal. TABLE 5: No. of associated abnormalities of the inner ear spaces/eighth cranial nerve after transverse fracture of the temporal bone Hematoma Abnormal Contrast Enhancement Fracture Line through the Inner Ear Yes No Yes No Cochlea 1 3 Vestibule/semicircular canals Eighth cranial nerve 2 ment with variable intensity was seen in the distal intrameatal segment (Figs 1 8). This enhancement was visible even up to 2 years after the trauma. In two patients with longitudinal fractures, with an interval between trauma and MR examination of 36 and 457 days, respectively, no pathologic enhancement of the distal intrameatal segment could be identified, despite complete peripheral facial nerve palsy (Fig 9). In the other nerve segments, abnormally intense contrast enhancement was observed in the labyrinthine segment in 96% of affected nerves (Figs 1, 3, and 4), in the geniculate ganglion in 72% (Figs 1, 2, 4, and 9), in the proximal tympanic segment in 40% (Figs 1, 2, 4, 8, and 9), in the distal tympanic segment in 32% (Fig 4), and in the mastoid segment in 28%, as compared with normal facial nerves (13). No correlation could be established between the degree of enhancement of the nerve segment and the maximal percentage of nerve degeneration at electroneurography (Table 1). The fracture line itself was visible in 100% of the patients with transverse fractures (Figs 7 and 8) and in 66% of the patients with longitudinal fractures (Figs 2, 5, 6, and 9). Usually, the fracture line coursed either through the geniculate ganglion or slightly lateral to the geniculate ganglion with extension through the GSPN (Figs 2, 5, and 6) or through the proximal tympanic segment (Fig 9) in longitudinal fractures and through the internal auditory canal (Fig 7) or the inner ear (Fig 8) and possibly through the proximal tympanic segment (Fig 8) in transverse fractures. A hematoma within the geniculate ganglion was observed in 33% of the patients with longitudinal fractures (Fig 6), but compression of the nerve by an adjacent bony fragment was never established (Table 4). Transection of the nerve was suspected in one patient (case 7); nerve enhancement stopped at the transition from the proximal to the distal tympanic segments, and no enhancement was visible in the distal tympanic and mastoid segments (Fig 9). In the second patient with intraoperatively proved nerve transection, the transection was not demonstrable on MR images (Tables 6 and 7). The GSPN appeared as an intensely enhancing and thickened nerve in eight (32%) of the patients (Fig 2). A thickened geniculate ganglion (Figs 1, 2, 4, and 9) was visible in 12 patients (48%). In patients with transverse fractures of the temporal bone, an associated hematoma within the inner ear (Fig 7) and/or abnormal enhancement of the inner ear spaces (Figs 7 and 8) and of the eighth cranial nerve (as a result of nerve damage) (Fig 7) could be seen.
5 AJNR: 18, June 1997 FACIAL NERVE PALSY 1119 Fig 1. Contrast-enhanced transverse T1-weighted (560/16/4) MR image 142 days after delayed posttraumatic peripheral facial nerve palsy shows no visible fracture line. Minimal enhancement of the distal intrameatal segment (1), moderate enhancement of the labyrinthine segment (2), and intense enhancement and thickening of the geniculate ganglion (3) and proximal tympanic segment (4) are related to long-lasting damage of the blood/ peripheral nerve barrier and formation of perineural fibrosis in the region of the geniculate ganglion. Fig 2. Case 3: Contrast-enhanced transverse T1-weighted (600/20/4) MR image 45 days after longitudinal fracture of the petrous bone and immediate-onset peripheral facial nerve palsy shows intense enhancement and thickening of the geniculate ganglion (3) and GSPN (5). The proximal tympanic segment is intensely enhanced (4). The longitudinal fracture line (6) courses through the geniculate ganglion and GSPN. The distal intrameatal segment (1) is moderately enhanced. Minimal dural enhancement is seen along the rostral border of the temporal bone (arrowheads). Fig 3. Noncontrast (500/15/2) (A) and contrast-enhanced (600/20/4) (B) transverse and coronal (C) T1-weighted MR images in a patient with delayed posttraumatic peripheral facial nerve palsy without associated fracture of the temporal bone, obtained 7 days after trauma, show moderate enhancement of the distal intrameatal segment (1) and minimal enhancement of the labyrinthine segment (2). The geniculate ganglion (3) and proximal tympanic segment (4) are normally enhanced. Intense dural enhancement is seen along the rostral border of the temporal bone, indicating possible microtrauma of both the temporal bone and the adjacent dura (arrowheads). Dural enhancement along the rostral border of the temporal bone was observed in 68% of patients either with or without a visible fracture line (Figs 2 4). Tables 6 through 8 compare intraoperative and preoperative MR findings in the eight patients who had surgery for posttraumatic peripheral facial nerve palsy. In patients with intraoperatively proved scar formation, especially of the GSPN and geniculate ganglion, the preoperative MR examination showed a correspondingly thickened and intensely enhancing nerve segment. Discussion The facial nerve is the only cranial motor nerve commonly affected by trauma to the head. A fracture of the temporal bone must be assumed in patients with posttraumatic facial nerve palsy even when a fracture cannot be identified radiologically (1). The commonly observed dural enhancement along the rostral border of the temporal bone on MR images in patients with or without temporal bone fracture may prove to be radiologically
6 1120 SARTORETTI-SCHEFER AJNR: 18, June 1997 Fig 4. Contrast-enhanced transverse (A) and coronal (B) T1-weighted (640/ 21/4) MR images, obtained 195 days after longitudinal fracture of the temporal bone and immediate-onset peripheral facial nerve palsy, show intense enhancement of the distal intrameatal (1), proximal tympanic (4), and distal tympanic (7) segments and of the thick geniculate ganglion (3) and the thick GSPN (5). The labyrinthine segment (2) is moderately enhanced. Dural enhancement is seen within the fundus of the internal auditory canal (arrowheads) that blends with the enhancement of the distal intrameatal nerve segment. Fig 5. Case 5: Contrast-enhanced transverse fast field-echo (gradient-echo) T1- weighted (19/8.4/4, 35 ) MR image, obtained 71 days after longitudinal fracture and immediate-onset facial nerve palsy, shows the longitudinal fracture line (6) coursing through the geniculate ganglion (3). The distal intrameatal segment (1) and the GSPN (5) are abnormally moderately enhanced. Fig 6. Noncontrast (500/15/2) (A) and contrast-enhanced (640/21/4) (B) transverse T1-weighted images, obtained 44 days after longitudinal fracture and immediateonset palsy, show subacute hyperintense hematoma (8) within the geniculate ganglion, an enhancing broad longitudinal fracture line (6), and abnormal enhancement of the distal intrameatal (1) and labyrinthine (2) segments. Note associated subdural hematoma (arrowheads). invisible microfractures of the temporal bone associated with microtears of the adjacent dura. Fractures of the temporal bone are subdivided into longitudinal (80% to 90%, with associated peripheral facial nerve palsy in 10% to 20% of the patients) and transverse (10% to 20%, with secondary loss of inner ear function and associated peripheral facial nerve palsy in 38% to 50%, depending on the course of the fracture line through the temporal bone) fractures (1 5). Posttraumatic partial or complete peripheral facial nerve palsy can be classified as either immediate onset (occurring within 24 hours after the trauma and often caused by nerve transection) or delayed onset (occurring more than 24 hours after the trauma, caused by intraneural hematoma/edema after stretching of the GSPN, with or without associated fracture, or by nerve compression) (1, 2, 20). Surgically verified posttraumatic facial nerve lesions associated with a longitudinal fracture are located in the region of the geniculate ganglion in 64% of patients, in the GSPN in 25%, in the distal tympanic/mastoid segment in 7%, and in the labyrinthine segment in 4% (2). In transverse fractures, the nerve lesion is located within the internal auditory canal in 10% of patients, within the labyrinthine segment in 80%,
7 AJNR: 18, June 1997 FACIAL NERVE PALSY 1121 Fig 7. Noncontrast transverse (500/15/2) (A) and contrast-enhanced coronal (600/20/4) (B and C) T1-weighted images, obtained 38 (A) and 65 (B and C) days after transverse fracture, show a fracture line (6) coursing through the internal auditory canal and associated palsy of immediate onset. A hyperintense hematoma within the cochlea (9) and vestibule (10) was seen 38 days after trauma (A). Sixty-five days after trauma, the distal intrameatal segment (1) and superoinferior vestibulocochlear nerve (11) within the internal auditory canal show intense enhancement. The cochlea (9) and vestibule/semicircular canals (10) are also intensely enhanced. (The noncontrast images, not depicted, no longer showed the hyperintense hematoma within the cochlea/vestibule.) Note intense enhancement of the labyrinthine (2) and proximal tympanic (4) segments. Fig 8. Noncontrast transverse (500/15/2) (A) and contrast-enhanced transverse (B) and coronal (C) T1-weighted (640/21/4) images, obtained 45 days after transverse fracture and immediate-onset palsy, show abnormal enhancement in the distal intrameatal segment (1). The contrast-enhancing fracture line (6) crosses the vestibule and the thickened proximal tympanic segment (4) of the facial nerve. The cochlea (9) and vestibule (10) show moderate enhancement. The geniculate ganglion (3) is thickened and enhanced. and in the region in or around the geniculate ganglion in 10% (2), corresponding to the results obtained in our study (Table 3). Different mechanisms of injury to the peripheral facial nerve are possible and can be observed intraoperatively. In longitudinal fractures, most commonly an intraneural hematoma at the level of the geniculate ganglion is present (in about 50% of the patients) (3). A bony fragment compressing the adjacent nerve is visible in 17% to 20% of the patients, and a transection of the nerve occurs in 26% to 30% of the patients (3). In a few patients, no definite injury can be identified intraoperatively (2, 3, 17). Severe traction and stretching of the GSPN are present in all patients, and lead to the formation of an intraneural hematoma and secondary edema that extends in a retrograde direction along the proximal nerve (3, 14). Facial nerve injury sustained after stretching of the facial nerve during cerebellopontine angle operations is said to result from movements of the nerve within its immobile sheath in the preganglionic segment, subsequent rupture of
8 1122 SARTORETTI-SCHEFER AJNR: 18, June 1997 Fig 9. Case 7: Transverse noncontrast (500/15/2) (A) and contrast-enhanced (600/20/4) (B) T1-weighted spin-echo images, obtained 457 days after longitudinal petrous bone fracture and immediateonset palsy, show nerve transection (proved intraoperatively). The contrastenhancing fracture line (6) courses through the tympanic segment (7). The intensely enhanced and thickened geniculate ganglion (3) and proximal tympanic segment (4) may be attributed to possible scar formation. The distal tympanic and mastoid segments are not depicted reliably. The very proximal GSPN is minimally thickened (5). The labyrinthine segment is abnormally enhanced (2). TABLE 6: Preoperative MR findings Case Delay between Trauma and MR, d Abnormal Enhancement of Seventh Cranial Nerve Segments Thickened Seventh Nerve Segment Hematoma in GG Seventh Nerve Transection Abnormal Enhancement DIS LS GG PTS GSPN GG V/C Eighth Nerve *... * * Questionable enhancement in PTS. Note. Cases 1 and 2 had surgery for transverse fracture, cases 3 through 7 had surgery for longitudinal fracture, case 8 had no radiologically visible fracture. indicates intense enhancement;, moderate enhancement;, minimal enhancement; DIS, distal intrameatal segment; LS, labyrinthine segment; GG, geniculate ganglion; PTS, proximal tympanic segment; GSPN, greater superficial petrosal nerve; and V/C, vestibule and cochlea. the supplying blood vessels to the facial nerve, and formation of intraneural hemorrhage and edema (21). The swollen facial nerve is secondarily compressed and damaged at the meatal foramen (this is the canalicular entrance of the facial nerve into the bony labyrinthine segment). An identical mechanism (namely, compression of the edematous nerve) is also responsible for the development of facial nerve palsy in inflammatory palsy (ie, Bell palsy or herpetic palsy) (12, 13). Therefore, identical enhancement patterns of the different facial nerve segments can be assumed in patients with inflammatory (13) and posttraumatic peripheral facial nerve palsy; and identical enhancement patterns are observed independent of the exact site of the nerve injury along the course of the facial nerve in posttraumatic palsy. Abnormal nerve enhancement is always or nearly always observed in the distal intrameatal segment and is commonly seen in the labyrinthine segment and the proximal tympanic segment as well as in the geniculate ganglion. The distal tympanic and mastoid segments more rarely show abnormally intense enhancement as compared with a normal facial nerve (13). In our series, only two patients with posttraumatic peripheral facial nerve palsy (imaged 36 and 457 days, respectively, after trauma) did not have the commonly observed abnormal enhancement of the distal intrameatal segment, indicating damage to the nerve itself (13, 32), on contrast-enhanced MR images, despite clinical persistence of the palsy. In both patients, however, abnormally intense enhancement of the geniculate ganglion and proximal tympanic segment was observed. We have no reasonable explanation for the absence of
9 AJNR: 18, June 1997 FACIAL NERVE PALSY 1123 TABLE 7: Intraoperative findings in eight patients Case Delay between Trauma and Surgery, d Nerve Transection Fresh or Organized Hematoma/Scar in Different Nerve Segments LS GG PTS GSPN V/C Bone within Fallopian Canal Other Findings Seventh nerve atrophy GG 5 72 (PTS) * * GG (PTS) Traction of GSPN, retrograde edema, compression at meatal foramen Note. Cases 1 and 2 had transverse fracture, cases 3 through 7 had longitudinal fractures, and case 8 had no radiologically visible fracture. See Table 6 for abbreviations. TABLE 8: Comparison between preoperative MR findings and intraoperative findings Finding Preoperative MR Imaging Surgery Hematoma within GG 1 6 Bony fragment in GG... 2 Nerve transection 1* 2 Thickened GSPN (scar) 4 4 Thickened GG (scar) 7 6 * Questionable. Note. GG indicates geniculate ganglion; GSPN, greater superficial petrosal nerve. nerve enhancement in the distal intrameatal segment in these two patients. Further examinations are probably necessary to accumulate more information on the pathophysiology of posttraumatic nerve palsy. Additionally, no correlation can be established between nerve enhancement and maximal percentage of nerve fiber degeneration at electroneurography (Table 1); a circumstance that has already been described in connection with inflammatory nerve palsy (32). In our retrospective study, a hematoma in or around the region of the geniculate ganglion was seen on MR images in six (33%) of 18 patients with longitudinal fractures of the temporal bone. In the eight patients who had surgery, seven had intraoperative findings of a hematoma in the geniculate ganglion. However, only in one patient was this hematoma identified correctly on the preoperative MR study. Therefore, it must be assumed that MR imaging is not able to show the hematoma in the geniculate ganglion in all affected patients. In two patients (cases 5 and 7), a transection of the nerve was identified intraoperatively in the proximal/middle tympanic segment. Despite the transection, continuous enhancement of the facial nerve was seen on MR images in case 5; in case 7, however, the discontinuity of the nerve was only suspected on MR images, since the very distal tympanic and mastoid segments of the nerve were not identified reliably. All the same, it must be assumed that detection of a nerve transection with the help of MR imaging is either impossible or very difficult, since nerve transection was suspected in only one (5%) of our patients with longitudinal fractures, whereas from previous surgical studies (3) it is known that intraoperatively proved nerve transection occurs in up to 30% of patients with such fractures (3). The same difficulties were encountered in cases of transverse fractures. Intraoperatively, a transection of the nerve was seen within the internal auditory canal or the labyrinthine segment in all patients (2, 17); however, it was not seen on the MR images, because in all three patients with transverse fractures, continuous enhancement of the facial nerve was observed. Similarly, a second, more distal, facial nerve injury that is not visible on MR images often may be proved intraoperatively in patients with either longitudinal or transverse fractures (17). Histologic examination of facial nerve biopsy specimens, obtained intraoperatively in patients who have surgery for posttraumatic peripheral facial nerve palsy after longitudinal fracture (17), reveal intense retrograde degeneration of myelinated fibers in the facial nerve proximal to the geniculate ganglion and proximal to the site of the nerve injury related to stretching of the nerve after traumatically induced deformation of the bone. This nerve fiber degeneration is accompanied by a simultaneous regeneration
10 1124 SARTORETTI-SCHEFER AJNR: 18, June 1997 in the proximal nerve segments. The phase of nerve fiber regeneration may persist up to 48 months after the trauma (17, 22). Additionally, endoneural and perineural fibrosis of variable extent, partly seen as thick scar surrounding the regenerating axons, especially in the distal labyrinthine segment or in the proximal tympanic segment, is seen both early and late after injury, but fibrosis formation starts as early as 5 weeks after the trauma. In accordance with these histologic findings, the thickening (defined as a specific nerve segment with a diameter of more than 1 mm on contrast-enhanced MR images compared with a neuronal diameter of less than 1 mm seen in healthy volunteers [13, 18, 19]) and intense enhancement of the GSPN and/or the geniculate ganglion on contrast-enhanced T1- weighted MR images result from this posttraumatic endoneural and perineural fibrosis (as proved in several of the patients in our study who had surgery [Tables 6 8]). The long-lasting abnormal contrast enhancement of various facial nerve segments (especially the distal intrameatal segment, the labyrinthine segment, the proximal tympanic segment, and the geniculate ganglion) observed on MR images in several patients up to 2 years after trauma can be explained by long-lasting damage to the blood/ peripheral nerve barrier (23 31). According to experimental studies in animals, the complex process of degeneration and regeneration following nerve injury is accompanied by a vasogenic response associated with a two-phase breakdown in the blood/peripheral nerve barrier formed by endoneurium and perineurium (23 26, 28, 29, 32). The first phase occurs during wallerian degeneration. It is early, rapid, and associated with a breakdown of the endoneural barrier, leading secondarily to macrophage infiltration and removal of debris. The second phase occurs during nerve regeneration. It is late in onset but lasts for months. It is associated with a breakdown of the perineural barrier and provides for the increased transfer of metabolic substrates to the regenerating nerves. These experimental observations can also be applied to the facial nerve, since this nerve behaves histologically and electrophysiologically as a peripheral nerve. Therefore, long-lasting damage to the blood/peripheral nerve barrier related to degeneration and regeneration of nerve fibers as well as to formation of perineural fibrosis has to be suspected as the underlying pathophysiologic mechanism that explains the long-lasting contrast enhancement of the facial nerve observed in our study (24 29, 32). In summary, intraoperative findings show that posttraumatic peripheral facial nerve palsy results from nerve transection, from compression by a bony fragment/hematoma, or from formation of an intraneural hematoma/edema after stretching of the GSPN with secondary compression of the swollen nerve within the bony facial nerve canal. MR images show longlasting abnormal nerve enhancement, especially in the distal intrameatal segment but often also in the labyrinthine and proximal tympanic segments and in the geniculate ganglion related to the long-lasting breakdown of the blood/peripheral nerve barrier associated with nerve degeneration and regeneration after injury. Intraoperatively observed perineural and intraneural scar formation leads to thickening and intense enhancement of the affected nerve segments on MR images. MR imaging is able to show the hematoma in or around the region of the geniculate ganglion in some but not all patients, but it is not able to depict nerve compression reliably by an adjacent bony fragment or the nerve transection itself. Most associated injuries of the inner ear and of the eighth cranial nerve as well as the course of the fracture line are visible on MR images. References 1. Harker LA, McCabe BF. Temporal bone fractures and facial nerve injury. Otolaryngol Clin North Am 1974;2: Fisch U. Facial paralysis in fractures of the petrous bone. Laryngoscope 1974;84: Fisch U. Management of intratemporal facial nerve injuries. J Laryngol Otol 1980;94: McCabe BF. Injuries to the facial nerve: symposium on trauma in otolaryngology. Laryngoscope 1972;82: McGovern FH. Facial nerve injuries in skull fractures. Arch Otolaryngol 1968;88: Yamaki T, Yoshino E, Higuchi T, Horikawa Y, Hirakawa K. Value of high-resolution computed tomography in diagnosis of petrous bone fracture. Surg Neurol 1991;26: Schubiger O, Valavanis A, Stuckmann G, Antonucci F. Temporal bone fractures and their complications: examination with high resolution CT. Neuroradiology 1986;28: Valavanis A, Schubiger O, Stuckmann G, Antonucci F. CT-Diagnostik traumatischer Läsionen des Felsenbeines. Radiologe 1986; 26: Dolan KD. Temporal bone fractures. Semin Ultrasound CT MR 1989;10: Holland BA, Brant-Zawadzi M. High-resolution CT of temporal bone trauma. AJR Am J Roentgenol 1984;143:
11 AJNR: 18, June 1997 FACIAL NERVE PALSY Murakami M, Ohtani I, Aikawa T, Anzai. Temporal bone findings in two cases of head injury. J Laryngol Otol 1990;104: Fisch U, Felix H. On the pathogenesis of Bell s palsy. Acta Otolaryngol 1983;95: Sartoretti-Schefer S, Wichmann W, Valavanis A. Gadolinium-enhanced MR in patients with idiopathic, herpetic and HIV-associated facial nerve palsies: abnormal enhancement patterns compared with normal individuals. AJNR Am J Neuroradiol 1994;15: Anderson J, Awad IA, Hahn JF. Delayed facial nerve palsy after temporal lobectomy for epilepsy: report of four cases and discussion of possible mechanisms. Neurosurgery 1991;28: Morello G, Bianchi M, Migliavacca F. Combined extra-intradural temporal rhizotomy for the treatment of trigeminal neuralgia: results in 409 patients. J Neurosurg 1971;34: Fisch U. Surgery for Bell s palsy. Arch Otolaryngol 19891;107: Felix H, Eby TL, Fisch U. New aspects of facial nerve pathology in temporal bone fractures. Acta Otolaryngol (Stockh) 1991;111: Miehlke A, Fisch U. Fazialislähmungen im labyrinthären, meatalen und intrakraniellen Bereich. In: Berendes J, Link R, Zöllner F, eds. Hals-Nasen-Ohrenheilkunde in Praxis und Klinik. Stuttgart, Germany: Thieme; 1979: Gulya AJ, Schuknecht HF. Neuroanatomy: the facial nerve. In: Gulya AJ, Schuknecht HF, eds. Anatomy of the Temporal Bone with Surgical Implications. New York, NY: Parthenon; 1995: Potter JM. Facial palsy following head injury. J Laryngol Otol 1964;78: Sekiya T, Iwabuchi T, Okabe S. Occurrence of vestibular and facial nerve injury following cerebellopontine angle operations. Acta Neurochir (Wien) 1990;102: Ylikoski J, Brackmann DE, Savolainen S. Facial nerve abnormalities after acoustic tumor removal: morphological and clinical study of seven patients with postoperative facial paralysis. Arch Otolaryngol 1982;108: Mellick RS, Cavanagh JB. Changes in blood vessel permeability during degeneration and regeneration in peripheral nerves. Brain 1968;91: Bush MS, Reid AR, Allt G. Blood-nerve barrier: ultrastructural and endothelial surface charge alterations following nerve crush. Neuropathol Appl Neurobiol 1993;19: Podhajsky RJ, Myers RR. The vascular response to nerve crush: relationship to wallerian degeneration and regeneration. Brain Res 1993;623: Weerasuriya A, Hockman CH. Perineurial permeability to sodium during wallerian degeneration in rat sciatic nerve. Brain Res 1992; 581: Latker CH, Wadhwani KC, Balbo A, Rapoport SI. Blood-nerve barrier in the frog during wallerian degeneration: are axons necessary for maintenance of barrier function? J Comp Neurol 1991; 309: West NR, Collins GH. Relationship of wallerian degeneration to regrowing axons. J Neuropathol Exp Neurol 1991;50: Sparrow JR, Kiernan JA. Endoneurial vascular permeability in degenerating and regenerating peripheral nerves. Acta Neuropathol 1981;53: Bradbury M. The Concept of the Blood-Brain-Barrier. New York, NY: Wiley; 1979: , Lundborg G. Structure and function of the intraneural microvessels as related to trauma, edema formation and nerve function. J Bone Joint Surg Am 1975;57-A: Sartoretti-Schefer S, Brändle P, Wichmann W, Valavanis A. Intensity of MR-contrast enhancement does not correspond to clinical and electroneurographic findings in acute inflammatory facial nerve palsy. AJNR Am J Neuroradiol 1996;17:
Intensity of MR Contrast Enhancement Does Not Correspond to Clinical and Electroneurographic Findings in Acute Inflammatory Facial Nerve Palsy
 Intensity of MR Contrast Enhancement Does Not Correspond to Clinical and Electroneurographic Findings in Acute Inflammatory Facial Nerve Palsy Sabine Sartoretti-Schefer, Peter Brändle, Werner Wichmann,
Intensity of MR Contrast Enhancement Does Not Correspond to Clinical and Electroneurographic Findings in Acute Inflammatory Facial Nerve Palsy Sabine Sartoretti-Schefer, Peter Brändle, Werner Wichmann,
Spatial Relationship between Vestibular Schwannoma and Facial Nerve on Three-dimensional T2-weighted Fast Spin-echo MR Images
 AJNR Am J Neuroradiol 21:810 816, May 2000 Spatial Relationship between Vestibular Schwannoma and Facial Nerve on Three-dimensional T2-weighted Fast Spin-echo MR Images Sabine Sartoretti-Schefer, Spyros
AJNR Am J Neuroradiol 21:810 816, May 2000 Spatial Relationship between Vestibular Schwannoma and Facial Nerve on Three-dimensional T2-weighted Fast Spin-echo MR Images Sabine Sartoretti-Schefer, Spyros
Idiopathic, Herpetic, and HIV -Associated Facial Nerve Palsies: Abnormal MR Enhancement Patterns
 Idiopathic, Herpetic, and HIV -ssociated Facial Nerve Palsies: bnormal MR Enhancement Patterns Sabine Sartoretti-Schefer, Werner Wichmann, and nton Valavanis PURPOSE: To determine specific criteria that
Idiopathic, Herpetic, and HIV -ssociated Facial Nerve Palsies: bnormal MR Enhancement Patterns Sabine Sartoretti-Schefer, Werner Wichmann, and nton Valavanis PURPOSE: To determine specific criteria that
ORIGINAL ARTICLE. Temporal Lobe Injury in Temporal Bone Fractures. imaging (MRI) to evaluate lesions of the temporal
 ORIGINAL ARTICLE Temporal Lobe Injury in Temporal Bone Fractures Richard M. Jones, MD; Michael I. Rothman, MD; William C. Gray, MD; Gregg H. Zoarski, MD; Douglas E. Mattox, MD Objective: To determine the
ORIGINAL ARTICLE Temporal Lobe Injury in Temporal Bone Fractures Richard M. Jones, MD; Michael I. Rothman, MD; William C. Gray, MD; Gregg H. Zoarski, MD; Douglas E. Mattox, MD Objective: To determine the
Via Transmastoid Approach. Mitul Chaitan Bhatt. Maharashtra University Miraj India
 ISSN: 2250-0359 Volume 6 Issue 1 2016 Evaluation Of Patients Of Traumatic Facial Palsy Treated By Facial Nerve Decompression Via Transmastoid Approach Mitul Chaitan Bhatt Maharashtra University Miraj India
ISSN: 2250-0359 Volume 6 Issue 1 2016 Evaluation Of Patients Of Traumatic Facial Palsy Treated By Facial Nerve Decompression Via Transmastoid Approach Mitul Chaitan Bhatt Maharashtra University Miraj India
POST TRAUMATIC FACIAL PARALYSIS - A REVIEW
 POST TRAUMATIC FACIAL PARALYSIS - A REVIEW Pages with reference to book, From 105 To 107 Naresh K. Panda, Y. N. Mehra, S.B.S. Mann, Satish K. Mehta ( Deptt. of Otolaryngology, Postgraduate Institute of
POST TRAUMATIC FACIAL PARALYSIS - A REVIEW Pages with reference to book, From 105 To 107 Naresh K. Panda, Y. N. Mehra, S.B.S. Mann, Satish K. Mehta ( Deptt. of Otolaryngology, Postgraduate Institute of
RADIOLOGY TEACHING CONFERENCE
 RADIOLOGY TEACHING CONFERENCE John Athas, MD Monica Tadros, MD Columbia University, College of Physicians & Surgeons Department of Otolaryngology- Head & Neck Surgery September 27, 2007 CT SCAN IMAGING
RADIOLOGY TEACHING CONFERENCE John Athas, MD Monica Tadros, MD Columbia University, College of Physicians & Surgeons Department of Otolaryngology- Head & Neck Surgery September 27, 2007 CT SCAN IMAGING
Dr. T. Venkat Kishan Asst. Prof Department of Radiodiagnosis
 Dr. T. Venkat Kishan Asst. Prof Department of Radiodiagnosis Schwannomas (also called neurinomas or neurilemmomas) constitute the most common primary cranial nerve tumors. They are benign slow-growing
Dr. T. Venkat Kishan Asst. Prof Department of Radiodiagnosis Schwannomas (also called neurinomas or neurilemmomas) constitute the most common primary cranial nerve tumors. They are benign slow-growing
ARTICLE. Imaging the cranial nerves in cancer
 Cancer Imaging (2004) 4, S1 S5 DOI: 10.1102/1470-7330.2004.0006 CI ARTICLE Vincent Chong Department of Diagnostic Radiology, Singapore General Hospital, Outram Road, Singapore 169608, Singapore Corresponding
Cancer Imaging (2004) 4, S1 S5 DOI: 10.1102/1470-7330.2004.0006 CI ARTICLE Vincent Chong Department of Diagnostic Radiology, Singapore General Hospital, Outram Road, Singapore 169608, Singapore Corresponding
Differences in the Diameter of Facial Nerve and Facial Canal in Bell s PalsyVA 3-Dimensional Temporal Bone Study
 Otology & Neurotology 35:514Y518 Ó 2014, Otology & Neurotology, Inc. Differences in the Diameter of Facial Nerve and Facial Canal in Bell s PalsyVA 3-Dimensional Temporal Bone Study * Melissa Vianna, *Meredith
Otology & Neurotology 35:514Y518 Ó 2014, Otology & Neurotology, Inc. Differences in the Diameter of Facial Nerve and Facial Canal in Bell s PalsyVA 3-Dimensional Temporal Bone Study * Melissa Vianna, *Meredith
Abnormal direction of internal auditory canal and vestibulocochlear nerve
 Medicine Otorhinolaryngology fields Okayama University Year 2004 Abnormal direction of internal auditory canal and vestibulocochlear nerve Shin Kariya kazunori Nishizaki Hirofumi Akagi Michael M. Paparella
Medicine Otorhinolaryngology fields Okayama University Year 2004 Abnormal direction of internal auditory canal and vestibulocochlear nerve Shin Kariya kazunori Nishizaki Hirofumi Akagi Michael M. Paparella
Neurovascular elements of the PCF
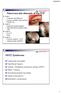 Level I: Neurovascular elements of the PCF Trigeminal and Abducent Superior cerebellar artery and vein Dandy s vein Level II: Facial and Cochleovestibular AICA and internal auditory artery, veins Level
Level I: Neurovascular elements of the PCF Trigeminal and Abducent Superior cerebellar artery and vein Dandy s vein Level II: Facial and Cochleovestibular AICA and internal auditory artery, veins Level
The Usefulness of MR Imaging of the Temporal Bone in the Evaluation of Patients with Facial and Audiovestibular Dysfunction
 The Usefulness of MR Imaging of the Temporal Bone in the Evaluation of Patients with Facial and Audiovestibular Dysfunction Sang Uk Park, MD 1 Hyung-Jin Kim, MD 1 Young Kuk Cho, MD 1 Myung Kwan Lim, MD
The Usefulness of MR Imaging of the Temporal Bone in the Evaluation of Patients with Facial and Audiovestibular Dysfunction Sang Uk Park, MD 1 Hyung-Jin Kim, MD 1 Young Kuk Cho, MD 1 Myung Kwan Lim, MD
Meniere s disease and Sudden Sensorineural Hearing Loss
 Meniere s disease and Sudden Sensorineural Hearing Loss Tsutomu Nakashima 1,2 1 Ichinomiya Medical Treatment & Habilitation Center, Ichinomiya, Japan 2 Department of Otorhinolaryngology, Nagoya University,
Meniere s disease and Sudden Sensorineural Hearing Loss Tsutomu Nakashima 1,2 1 Ichinomiya Medical Treatment & Habilitation Center, Ichinomiya, Japan 2 Department of Otorhinolaryngology, Nagoya University,
MR imaging of patients with facial neuritis is usually not
 Published December 29, 2011 as 10.3174/ajnr.A2851 ORIGINAL RESEARCH H.K. Lim J.H. Lee D. Hyun J.W. Park J.L. Kim H.Y. Lee S. Park J.H. Ahn J.H. Baek C.G. Choi MR Diagnosis of Facial Neuritis: Diagnostic
Published December 29, 2011 as 10.3174/ajnr.A2851 ORIGINAL RESEARCH H.K. Lim J.H. Lee D. Hyun J.W. Park J.L. Kim H.Y. Lee S. Park J.H. Ahn J.H. Baek C.G. Choi MR Diagnosis of Facial Neuritis: Diagnostic
Contrast-Enhanced MR Imaging of the Facial Nerve in 11 Patients with Bell's Palsy
 735 Contrast-Enhanced MR Imaging of the Facial Nerve in 11 Patients with Bell's Palsy Robert Tien 1 2 William P. Dillon 1 Robert K. Jackler Contrast-enhanced MR images (at 1.5 T) were obtained in 11 patients
735 Contrast-Enhanced MR Imaging of the Facial Nerve in 11 Patients with Bell's Palsy Robert Tien 1 2 William P. Dillon 1 Robert K. Jackler Contrast-enhanced MR images (at 1.5 T) were obtained in 11 patients
High Signal from the Otic Labyrinth on Onenhanced Magnetic Resonance Imaging
 High Signal from the Otic Labyrinth on Onenhanced Magnetic Resonance Imaging JaneL. Weissman, 1 Hugh D. Curtin, 1 3 Barry E. Hirsch, 2 and William L. Hirsch, Jr. 1 Summary: High signal from the otic labyrinth
High Signal from the Otic Labyrinth on Onenhanced Magnetic Resonance Imaging JaneL. Weissman, 1 Hugh D. Curtin, 1 3 Barry E. Hirsch, 2 and William L. Hirsch, Jr. 1 Summary: High signal from the otic labyrinth
Internal Auditory Canal Involvement of Acoustic Neuromas: Surgical Correlates to Magnetic Resonance Imaging Findings
 Otology & Neurotology 22:92 96 200, Otology & Neurotology, Inc. Internal Auditory Canal Involvement of Acoustic Neuromas: Surgical Correlates to Magnetic Resonance Imaging Findings * Samuel H. Selesnick,
Otology & Neurotology 22:92 96 200, Otology & Neurotology, Inc. Internal Auditory Canal Involvement of Acoustic Neuromas: Surgical Correlates to Magnetic Resonance Imaging Findings * Samuel H. Selesnick,
Title. Author(s) Takahashi, Haruo. Issue Date Right.
 NAOSITE: Nagasaki University's Ac Title Author(s) Citation A case with posterior fossa epiderm symptoms caused by insufficiency of usefulness of free DICOM image view Takasaki, Kenji; Kumagami, Hidetaka
NAOSITE: Nagasaki University's Ac Title Author(s) Citation A case with posterior fossa epiderm symptoms caused by insufficiency of usefulness of free DICOM image view Takasaki, Kenji; Kumagami, Hidetaka
Schriftenreihe Neurologie
 Schriftenreihe Neurologie 18 Neurology Series Herausgeber H.I Bauer, Gottingen. H. Ganshirt, Heidelberg P. Vogel, Heidelberg Beirat H.Caspers, Munster H.Hager, GieBen M.Mumenthaler, Bern A. Pentschew,
Schriftenreihe Neurologie 18 Neurology Series Herausgeber H.I Bauer, Gottingen. H. Ganshirt, Heidelberg P. Vogel, Heidelberg Beirat H.Caspers, Munster H.Hager, GieBen M.Mumenthaler, Bern A. Pentschew,
Major Anatomic Components of the Orbit
 Major Anatomic Components of the Orbit 1. Osseous Framework 2. Globe 3. Optic nerve and sheath 4. Extraocular muscles Bony Orbit Seven Bones Frontal bone Zygomatic bone Maxillary bone Ethmoid bone Sphenoid
Major Anatomic Components of the Orbit 1. Osseous Framework 2. Globe 3. Optic nerve and sheath 4. Extraocular muscles Bony Orbit Seven Bones Frontal bone Zygomatic bone Maxillary bone Ethmoid bone Sphenoid
Cranial Nerve VII - Facial Nerve. The facial nerve has 3 main components with distinct functions
 Cranial Nerve VII - Facial Nerve The facial nerve has 3 main components with distinct functions Somatic motor efferent Supplies the muscles of facial expression; posterior belly of digastric muscle; stylohyoid,
Cranial Nerve VII - Facial Nerve The facial nerve has 3 main components with distinct functions Somatic motor efferent Supplies the muscles of facial expression; posterior belly of digastric muscle; stylohyoid,
Anatomy of Peripheral Nerve 가톨릭대학교 재활의학과 김재민
 Anatomy of Peripheral Nerve 가톨릭대학교 재활의학과 김재민 Contents US appearance of nerves Scanning technique Peripheral nerve pathology Nerves of arm Nerves of leg US Appearance of Nerve Multiple longitudinal hypoechoic
Anatomy of Peripheral Nerve 가톨릭대학교 재활의학과 김재민 Contents US appearance of nerves Scanning technique Peripheral nerve pathology Nerves of arm Nerves of leg US Appearance of Nerve Multiple longitudinal hypoechoic
Radiologic Evaluation of Petrous Apex Masses. Pavan Kavali, MS-IV Morehouse School of Medicine November 16, 2009
 Radiologic Evaluation of Petrous Apex Masses Pavan Kavali, MS-IV Morehouse School of Medicine November 16, 2009 Roadmap Petrous Apex Anatomy Patient D.S.: Clinical Presentation Differential diagnosis of
Radiologic Evaluation of Petrous Apex Masses Pavan Kavali, MS-IV Morehouse School of Medicine November 16, 2009 Roadmap Petrous Apex Anatomy Patient D.S.: Clinical Presentation Differential diagnosis of
Role of High-resolution Computed Tomography in the Evaluation of Temporal Bone Fracture
 Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/147 Role of High-resolution Computed Tomography in the Evaluation of Temporal Bone Fracture R Manimaran 1, K Sivakumar
Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/147 Role of High-resolution Computed Tomography in the Evaluation of Temporal Bone Fracture R Manimaran 1, K Sivakumar
Relationship of the Optic Nerve to the Posterior Paranasal Sinuses: A CT Anatomic Study
 Relationship of the Optic Nerve to the Posterior Paranasal Sinuses: A CT Anatomic Study Mark C. DeLano, F. Y. Fun, and S. James Zinreich PURPOSE: To delineate the relationship between the optic nerves
Relationship of the Optic Nerve to the Posterior Paranasal Sinuses: A CT Anatomic Study Mark C. DeLano, F. Y. Fun, and S. James Zinreich PURPOSE: To delineate the relationship between the optic nerves
diagnosis Temporal bone fractures: a clinical
 Archives of Emergency Medicine, 1988, 5, 146-150 Temporal bone fractures: a clinical diagnosis J. WALDRON & S. E. J. HURLEY Department of Ear Nose and Throat Surgery, St Mary's Hospital, London, England
Archives of Emergency Medicine, 1988, 5, 146-150 Temporal bone fractures: a clinical diagnosis J. WALDRON & S. E. J. HURLEY Department of Ear Nose and Throat Surgery, St Mary's Hospital, London, England
Quantitative Analysis of the Facial Nerve Using Contrast-Enhanced Three Dimensional FLAIR-VISTA Imaging in Pediatric Bell s Palsy
 pissn 2384-1095 eissn 2384-1109 imri 2015;19:162-167 http://dx.doi.org/10.13104/imri.2015.19.3.162 Quantitative Analysis of the Facial Nerve Using Contrast-Enhanced Three Dimensional FLAIR-VISTA Imaging
pissn 2384-1095 eissn 2384-1109 imri 2015;19:162-167 http://dx.doi.org/10.13104/imri.2015.19.3.162 Quantitative Analysis of the Facial Nerve Using Contrast-Enhanced Three Dimensional FLAIR-VISTA Imaging
Middle Fossa Approach
 aijoc AIJOC surgical technique (reprint) 1 JJ Waterval, 2 RJ Stokroos, 3 J Dings INTRODUCTION A middle fossa approach is an operation technique that offers surgical access to the lateral skull base including
aijoc AIJOC surgical technique (reprint) 1 JJ Waterval, 2 RJ Stokroos, 3 J Dings INTRODUCTION A middle fossa approach is an operation technique that offers surgical access to the lateral skull base including
1. Axial view, left temporal bone. Plane through the upper antrum (A), superior semicircular canal (SSC) and IAC.
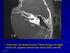 PA IAC SSC A 1. Axial view, left temporal bone. Plane through the upper antrum (A), superior semicircular canal (SSC) and IAC. IAC VII M I LSC Plane through the IAC, malleus head and incus and the lateral
PA IAC SSC A 1. Axial view, left temporal bone. Plane through the upper antrum (A), superior semicircular canal (SSC) and IAC. IAC VII M I LSC Plane through the IAC, malleus head and incus and the lateral
Enhancement Pattern of the Normal Facial Nerve on Three - Dimensional (3D) - Fluid Attenuated Inversion Recovery (FLAIR) Sequence at 3.
 www.ksmrm.org JKSMRM 16(1) : 25-30, 2012 Print ISSN 1226-9751 Original Article Enhancement Pattern of the Normal Facial Nerve on Three - Dimensional (3D) - Fluid Attenuated Inversion Recovery (FLAIR) Sequence
www.ksmrm.org JKSMRM 16(1) : 25-30, 2012 Print ISSN 1226-9751 Original Article Enhancement Pattern of the Normal Facial Nerve on Three - Dimensional (3D) - Fluid Attenuated Inversion Recovery (FLAIR) Sequence
Magnetic Resonance Imaging. Basics of MRI in practice. Generation of MR signal. Generation of MR signal. Spin echo imaging. Generation of MR signal
 Magnetic Resonance Imaging Protons aligned with B0 magnetic filed Longitudinal magnetization - T1 relaxation Transverse magnetization - T2 relaxation Signal measured in the transverse plane Basics of MRI
Magnetic Resonance Imaging Protons aligned with B0 magnetic filed Longitudinal magnetization - T1 relaxation Transverse magnetization - T2 relaxation Signal measured in the transverse plane Basics of MRI
From Targeted Fascicular Biopsy of Major Nerve to Targeted Cutaneous Nerve Biopsy: Implementing Clinical Anatomy Can Catalyze a Paradigm Shift
 Clinical Anatomy 31:616 621 (2018) EDITORIAL From Targeted Fascicular Biopsy of Major Nerve to Targeted Cutaneous Nerve Biopsy: Implementing Clinical Anatomy Can Catalyze a Paradigm Shift TOMAS MAREK,
Clinical Anatomy 31:616 621 (2018) EDITORIAL From Targeted Fascicular Biopsy of Major Nerve to Targeted Cutaneous Nerve Biopsy: Implementing Clinical Anatomy Can Catalyze a Paradigm Shift TOMAS MAREK,
Post Traumatic Delayed Bilateral simultaneous symmetrical facial palsy-a rare presentation
 ISSN 2250-0359 Volume 2 Issue 1 2012 Post Traumatic Delayed Bilateral simultaneous symmetrical facial palsy-a rare presentation Prof.Dr.R.Muthukumar MS DLO DNB Post graduate Dr.S.Raghukumaran DLO Madras
ISSN 2250-0359 Volume 2 Issue 1 2012 Post Traumatic Delayed Bilateral simultaneous symmetrical facial palsy-a rare presentation Prof.Dr.R.Muthukumar MS DLO DNB Post graduate Dr.S.Raghukumaran DLO Madras
External carotid blood supply to acoustic neurinomas
 External carotid blood supply to acoustic neurinomas Report of two cases HARVEY L. LEVINE, M.D., ERNEST J. FERmS, M.D., AND EDWARD L. SPATZ, M.D. Departments of Radiology, Neurology, and Neurosurgery,
External carotid blood supply to acoustic neurinomas Report of two cases HARVEY L. LEVINE, M.D., ERNEST J. FERmS, M.D., AND EDWARD L. SPATZ, M.D. Departments of Radiology, Neurology, and Neurosurgery,
Paragangliomas of the Jugular Bulb and Carotid Body: MR Imaging
 83 Paragangliomas of the Jugular Bulb and Carotid Body: MR Imaging with Short Sequences and Gd-DTPA Enhancement T. Vogl 1 R. Bruning 1 H. Schedel 1 K. Kang 1 G. Grevers D. Hahn 1 J. Lissner 1 Twenty-six
83 Paragangliomas of the Jugular Bulb and Carotid Body: MR Imaging with Short Sequences and Gd-DTPA Enhancement T. Vogl 1 R. Bruning 1 H. Schedel 1 K. Kang 1 G. Grevers D. Hahn 1 J. Lissner 1 Twenty-six
Methods. Yahya Paksoy, Bülent Oğuz Genç, and Emine Genç. AJNR Am J Neuroradiol 24: , August 2003
 AJNR Am J Neuroradiol 24:1364 1368, August 2003 Retrograde Flow in the Left Inferior Petrosal Sinus and Blood Steal of the Cavernous Sinus Associated with Central Vein Stenosis: MR Angiographic Findings
AJNR Am J Neuroradiol 24:1364 1368, August 2003 Retrograde Flow in the Left Inferior Petrosal Sinus and Blood Steal of the Cavernous Sinus Associated with Central Vein Stenosis: MR Angiographic Findings
MR Signal Intensity of the Optic Radiation
 MR Signal Intensity of the Optic Radiation Mika Kitajima, Yukunori Korogi, Mutsumasa Takahashi, and Komyo Eto PURPOSE: To determine whether a hyperintense layer adjacent to the lateral ventricle on T2-
MR Signal Intensity of the Optic Radiation Mika Kitajima, Yukunori Korogi, Mutsumasa Takahashi, and Komyo Eto PURPOSE: To determine whether a hyperintense layer adjacent to the lateral ventricle on T2-
12 Anatomy and Physiology of Peripheral Nerves
 12 Anatomy and Physiology of Peripheral Nerves Introduction Anatomy Classification of Peripheral Nerves Sensory Nerves Motor Nerves Pathologies of Nerves Focal Injuries Regeneration of Injured Nerves Signs
12 Anatomy and Physiology of Peripheral Nerves Introduction Anatomy Classification of Peripheral Nerves Sensory Nerves Motor Nerves Pathologies of Nerves Focal Injuries Regeneration of Injured Nerves Signs
The Best Candidates for Nerve-Sparing Stripping Surgery for Facial Nerve Schwannoma
 The Laryngoscope VC 2014 The American Laryngological, Rhinological and Otological Society, Inc. The Best Candidates for Nerve-Sparing Stripping Surgery for Facial Nerve Schwannoma Soon H. Park, MD; Jin
The Laryngoscope VC 2014 The American Laryngological, Rhinological and Otological Society, Inc. The Best Candidates for Nerve-Sparing Stripping Surgery for Facial Nerve Schwannoma Soon H. Park, MD; Jin
4/30/2009 FN PARALYSIS HEMIFACIAL SPASM
 FN PARALYSIS HEMIFACIAL SPASM 1 Hemifacial spasm (Involuntary twitches) Etiology: Vascular loop compressing the FN at the root exit zone in the CPA = Neuro-vascular conflict Diagnosis: CT & MRI, Electrophysiology
FN PARALYSIS HEMIFACIAL SPASM 1 Hemifacial spasm (Involuntary twitches) Etiology: Vascular loop compressing the FN at the root exit zone in the CPA = Neuro-vascular conflict Diagnosis: CT & MRI, Electrophysiology
Case Report Bilateral Facial Paralysis Caused by Bilateral Temporal Bone Fracture: A Case Report and a Literature Review
 Case Reports in Otolaryngology Volume 2015, Article ID 306950, 4 pages http://dx.doi.org/10.1155/2015/306950 Case Report Bilateral Facial Paralysis Caused by Bilateral Temporal Bone Fracture: A Case Report
Case Reports in Otolaryngology Volume 2015, Article ID 306950, 4 pages http://dx.doi.org/10.1155/2015/306950 Case Report Bilateral Facial Paralysis Caused by Bilateral Temporal Bone Fracture: A Case Report
SHORTLY AFTER ITS FIRST DEpiction
 OBSERVATION Seven-Tesla Magnetic Resonance Imaging New Vision of Microvascular Abnormalities in Multiple Sclerosis Yulin Ge, MD; Vahe M. Zohrabian, MD; Robert I. Grossman, MD Background: Although the role
OBSERVATION Seven-Tesla Magnetic Resonance Imaging New Vision of Microvascular Abnormalities in Multiple Sclerosis Yulin Ge, MD; Vahe M. Zohrabian, MD; Robert I. Grossman, MD Background: Although the role
Anomalous Facial Nerve Canal with Cochlear Malformations
 AJNR Am J Neuroradiol 22:838 844, May 2001 Anomalous Facial Nerve Canal with Cochlear Malformations Laura Vitale Romo and Hugh D. Curtin BACKGROUND AND PURPOSE: Anteromedial migration of the first segment
AJNR Am J Neuroradiol 22:838 844, May 2001 Anomalous Facial Nerve Canal with Cochlear Malformations Laura Vitale Romo and Hugh D. Curtin BACKGROUND AND PURPOSE: Anteromedial migration of the first segment
Bilateral temporal bone fractures: a case report
 International Journal of Otorhinolaryngology and Head and Neck Surgery Natarajan K et al. Int J Otorhinolaryngol Head Neck Surg. 2018 Jan;4(1):271-275 http://www.ijorl.com pissn 2454-5929 eissn 2454-5937
International Journal of Otorhinolaryngology and Head and Neck Surgery Natarajan K et al. Int J Otorhinolaryngol Head Neck Surg. 2018 Jan;4(1):271-275 http://www.ijorl.com pissn 2454-5929 eissn 2454-5937
Indications and contra-indications of auditory brainstem implants. Systematic review and illustrative cases
 Manuscript: Authors: Journal: Indications and contra-indications of auditory brainstem implants. Systematic review and illustrative cases Merkus P (p.merkus@vumc.nl), Di Lella F, Di Trapani G, Pasanisi
Manuscript: Authors: Journal: Indications and contra-indications of auditory brainstem implants. Systematic review and illustrative cases Merkus P (p.merkus@vumc.nl), Di Lella F, Di Trapani G, Pasanisi
Congenital aural atresia (CAA) is a rare disorder of the temporal
 Published July 3, 2014 as 10.3174/ajnr.A4022 CLINICAL REPORT HEAD & NECK The Boomerang Malleus-Incus Complex in Congenital Aural Atresia S. Mukherjee, B.W. Kesser, and P. Raghavan ABSTRACT SUMMARY: Boomerang
Published July 3, 2014 as 10.3174/ajnr.A4022 CLINICAL REPORT HEAD & NECK The Boomerang Malleus-Incus Complex in Congenital Aural Atresia S. Mukherjee, B.W. Kesser, and P. Raghavan ABSTRACT SUMMARY: Boomerang
Dumbbell Shaped Thoracic Spine Cavernous Hemangioma: A Case Report and Review of the Literature
 ISPUB.COM The Internet Journal of Neurosurgery Volume 3 Number 1 Dumbbell Shaped Thoracic Spine Cavernous Hemangioma: A Case Report and Review of the Literature J Gonzalez-Cruz, A Nanda Citation J Gonzalez-Cruz,
ISPUB.COM The Internet Journal of Neurosurgery Volume 3 Number 1 Dumbbell Shaped Thoracic Spine Cavernous Hemangioma: A Case Report and Review of the Literature J Gonzalez-Cruz, A Nanda Citation J Gonzalez-Cruz,
Hideyuki Mitsuoka, Akira Tsunoda, Osamu Okuda, Kiyoshi Sato, and Junichi Makita
 AJNR Am J Neuroradiol 19:1823 1829, November 1998 Delineation of Small Nerves and Blood Vessels with Three-dimensional Fast Spin-Echo MR Imaging: Comparison of Presurgical and Surgical Findings in Patients
AJNR Am J Neuroradiol 19:1823 1829, November 1998 Delineation of Small Nerves and Blood Vessels with Three-dimensional Fast Spin-Echo MR Imaging: Comparison of Presurgical and Surgical Findings in Patients
The Temporal Bone Anatomy & Pathology
 Department of Radiology University of California San Diego The Temporal Bone Anatomy & Pathology John R. Hesselink, M.D. Temporal Bone Axial View Temporal Bone Coronal View Longitudinal Fracture The Temporal
Department of Radiology University of California San Diego The Temporal Bone Anatomy & Pathology John R. Hesselink, M.D. Temporal Bone Axial View Temporal Bone Coronal View Longitudinal Fracture The Temporal
Cochlear Implant Failure: Imaging Evaluation of the Electrode Course
 Clinical Radiology (2003) 58: 288 293 doi:10.1016/s0009-9260(02)00523-8, available online at www.sciencedirect.com Pictorial Review Cochlear Implant Failure: Imaging Evaluation of the Electrode Course
Clinical Radiology (2003) 58: 288 293 doi:10.1016/s0009-9260(02)00523-8, available online at www.sciencedirect.com Pictorial Review Cochlear Implant Failure: Imaging Evaluation of the Electrode Course
Fracture of the Temporal Bone: A Tomographic V/S Autopsy Study
 Fracture of the Temporal Bone: A Tomographic V/S Autopsy Study * Dr. Mukesh Kumar Goel, ** Dr. Rashmi Goel, *** Dr. Shiv R Kochar, **** Dr. M. R. Goel, *Asst Proff, Department of Forensic Medicine, People,s
Fracture of the Temporal Bone: A Tomographic V/S Autopsy Study * Dr. Mukesh Kumar Goel, ** Dr. Rashmi Goel, *** Dr. Shiv R Kochar, **** Dr. M. R. Goel, *Asst Proff, Department of Forensic Medicine, People,s
Expand The Scope of Temporal Bone Reporting: Why, What and Where to Look For.
 Expand The Scope of Temporal Bone Reporting: Why, What and Where to Look For. Award: Certificate of Merit Poster No.: C-1521 Congress: ECR 2014 Type: Educational Exhibit Authors: P. Mundada, B. S. Purohit,
Expand The Scope of Temporal Bone Reporting: Why, What and Where to Look For. Award: Certificate of Merit Poster No.: C-1521 Congress: ECR 2014 Type: Educational Exhibit Authors: P. Mundada, B. S. Purohit,
3D high-resolution MR imaging can provide reliable information
 Published April 11, 2013 as 10.3174/ajnr.A3472 ORIGINAL RESEARCH HEAD & NECK High-Resolution MRI of the Intraparotid Facial Nerve Based on a Microsurface Coil and a 3D Reversed Fast Imaging with Steady-State
Published April 11, 2013 as 10.3174/ajnr.A3472 ORIGINAL RESEARCH HEAD & NECK High-Resolution MRI of the Intraparotid Facial Nerve Based on a Microsurface Coil and a 3D Reversed Fast Imaging with Steady-State
Temporal Lobe Cystic Collection and Associated Oedema: A Rare Complication of Translabyrinthine Resection of Vestibular Schwannoma
 Open Access Case Report DOI: 10.7759/cureus.2217 Temporal Lobe Cystic Collection and Associated Oedema: A Rare Complication of Translabyrinthine Resection of Vestibular Schwannoma Abdurrahman Raeiq 1 1.
Open Access Case Report DOI: 10.7759/cureus.2217 Temporal Lobe Cystic Collection and Associated Oedema: A Rare Complication of Translabyrinthine Resection of Vestibular Schwannoma Abdurrahman Raeiq 1 1.
Imaging Findings in Schwannomas of the Jugular Foramen
 AJNR Am J Neuroradiol 21:1139 1144, June/July 2000 Imaging Findings in Schwannomas of the Jugular Foramen O. Petter Eldevik, Trygve O. Gabrielsen, and Eva A. Jacobsen BACKGROUND AND PURPOSE: Tumors of
AJNR Am J Neuroradiol 21:1139 1144, June/July 2000 Imaging Findings in Schwannomas of the Jugular Foramen O. Petter Eldevik, Trygve O. Gabrielsen, and Eva A. Jacobsen BACKGROUND AND PURPOSE: Tumors of
Chapter 7: Head & Neck
 Chapter 7: Head & Neck Osteology I. Overview A. Skull The cranium is composed of irregularly shaped bones that are fused together at unique joints called sutures The skull provides durable protection from
Chapter 7: Head & Neck Osteology I. Overview A. Skull The cranium is composed of irregularly shaped bones that are fused together at unique joints called sutures The skull provides durable protection from
The mandibular condyle fracture is a common mandibular
 ORIGINAL RESEARCH P. Wang J. Yang Q. Yu MR Imaging Assessment of Temporomandibular Joint Soft Tissue Injuries in Dislocated and Nondislocated Mandibular Condylar Fractures BACKGROUND AND PURPOSE: Evaluation
ORIGINAL RESEARCH P. Wang J. Yang Q. Yu MR Imaging Assessment of Temporomandibular Joint Soft Tissue Injuries in Dislocated and Nondislocated Mandibular Condylar Fractures BACKGROUND AND PURPOSE: Evaluation
Functional components
 Facial Nerve VII cranial nerve Emerges from Pons Two roots Functional components: 1. GSA (general somatic afferent) 2. SA (Somatic afferent) 3. GVE (general visceral efferent) 4. BE (Special visceral/branchial
Facial Nerve VII cranial nerve Emerges from Pons Two roots Functional components: 1. GSA (general somatic afferent) 2. SA (Somatic afferent) 3. GVE (general visceral efferent) 4. BE (Special visceral/branchial
The Asymmetric Mamillary Body: Association with Medial Temporal Lobe Disease Demonstrated with MR
 The Mamillary Body: Association with Medial Temporal Lobe Disease Demonstrated with MR Alexander C. Mamourian, Lawrence Rodichok, and Javad Towfighi PURPOSE: To determine whether mamillary body atrophy
The Mamillary Body: Association with Medial Temporal Lobe Disease Demonstrated with MR Alexander C. Mamourian, Lawrence Rodichok, and Javad Towfighi PURPOSE: To determine whether mamillary body atrophy
MR imaging at 3.0 tesla of glossopharyngeal neuralgia by neurovascular compression
 MR imaging at 3.0 tesla of glossopharyngeal neuralgia by neurovascular compression Poster No.: C-1281 Congress: ECR 2011 Type: Scientific Exhibit Authors: M. Nishihara 1, T. Noguchi 1, H. Irie 1, K. Sasaguri
MR imaging at 3.0 tesla of glossopharyngeal neuralgia by neurovascular compression Poster No.: C-1281 Congress: ECR 2011 Type: Scientific Exhibit Authors: M. Nishihara 1, T. Noguchi 1, H. Irie 1, K. Sasaguri
International Journal of Research and Review E-ISSN: ; P-ISSN:
 International Journal of Research and Review www.ijrrjournal.com E-ISSN: 2349-9788; P-ISSN: 2454-2237 Original Research Article Effectiveness of Facial Nerve Stimulation with Kabat Technique in Bell s
International Journal of Research and Review www.ijrrjournal.com E-ISSN: 2349-9788; P-ISSN: 2454-2237 Original Research Article Effectiveness of Facial Nerve Stimulation with Kabat Technique in Bell s
MRI of chronic spinal cord injury
 The British Journal of Radiology, 76 (2003), 347 352 DOI: 10.1259/bjr/11881183 E 2003 The British Institute of Radiology Pictorial review MRI of chronic spinal cord injury 1 K POTTER, FRCR and 1 A SAIFUDDIN,
The British Journal of Radiology, 76 (2003), 347 352 DOI: 10.1259/bjr/11881183 E 2003 The British Institute of Radiology Pictorial review MRI of chronic spinal cord injury 1 K POTTER, FRCR and 1 A SAIFUDDIN,
Ramsay Hunt syndrome a case report and review of literature
 From the SelectedWorks of Balasubramanian Thiagarajan January 1, 2013 Ramsay Hunt syndrome a case report and review of literature Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/27/
From the SelectedWorks of Balasubramanian Thiagarajan January 1, 2013 Ramsay Hunt syndrome a case report and review of literature Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/27/
Role of 3D T2 weighted imaging at 3T in evaluation of cranial nerve pathologies - An overview
 Role of 3D T2 weighted imaging at 3T in evaluation of cranial nerve pathologies - An overview Poster No.: C-1153 Congress: ECR 2013 Type: Educational Exhibit Authors: V. Kasi Arunachalam 1, R. Renganathan
Role of 3D T2 weighted imaging at 3T in evaluation of cranial nerve pathologies - An overview Poster No.: C-1153 Congress: ECR 2013 Type: Educational Exhibit Authors: V. Kasi Arunachalam 1, R. Renganathan
Editorial Manager(tm) for European Archives of Oto-Rhino-Laryngology and Head & Neck Manuscript Draft
 Editorial Manager(tm) for European Archives of Oto-Rhino-Laryngology and Head & Neck Manuscript Draft Manuscript Number: EAORL-D-07-00196 Title: Usefulness of CT scans in malignant external otitis: Effective
Editorial Manager(tm) for European Archives of Oto-Rhino-Laryngology and Head & Neck Manuscript Draft Manuscript Number: EAORL-D-07-00196 Title: Usefulness of CT scans in malignant external otitis: Effective
Evaluation and Management of Bell's Palsy January 2002
 TITLE: Evaluation and Management of Bell s Palsy SOURCE: Grand Rounds Presentation, UTMB, Dept. of Otolaryngology DATE: January 29, 2002 RESIDENT PHYSICIAN: Russell D. Briggs, MD FACULTY PHYSICIAN: Byron
TITLE: Evaluation and Management of Bell s Palsy SOURCE: Grand Rounds Presentation, UTMB, Dept. of Otolaryngology DATE: January 29, 2002 RESIDENT PHYSICIAN: Russell D. Briggs, MD FACULTY PHYSICIAN: Byron
CT and MRI of the temporal bone provide complementary
 ORIGINAL ARTICLE Registration and Fusion of CT and MRI of the Temporal Bone Soenke Heinrich Bartling, MD,* Kersten Peldschus, MD,* Thomas Rodt, MD, Florian Kral, MD, Herbert Matthies, PhD, Ron Kikinis,
ORIGINAL ARTICLE Registration and Fusion of CT and MRI of the Temporal Bone Soenke Heinrich Bartling, MD,* Kersten Peldschus, MD,* Thomas Rodt, MD, Florian Kral, MD, Herbert Matthies, PhD, Ron Kikinis,
ASSESSMENT AND TREATMENT OF FACIAL PALSY. Michael J. LaRouere, M.D. Michigan Ear Institute Farmington Hills, Michigan
 ASSESSMENT AND TREATMENT OF FACIAL PALSY Michael J. LaRouere, M.D. Michigan Ear Institute Farmington Hills, Michigan FACIAL PARALYSIS - ETIOLOGY Bells Palsy Ramsay Hunt Syndrome Infection (Acute/Chronic)
ASSESSMENT AND TREATMENT OF FACIAL PALSY Michael J. LaRouere, M.D. Michigan Ear Institute Farmington Hills, Michigan FACIAL PARALYSIS - ETIOLOGY Bells Palsy Ramsay Hunt Syndrome Infection (Acute/Chronic)
Evaluation of Variation in the Course of the Facial Nerve, Nerve Adhesion to Tumors, and Postoperative Facial Palsy in Acoustic Neuroma
 Original Article 39 Evaluation of Variation in the Course of the Facial Nerve, Nerve Adhesion to Tumors, and Postoperative Facial Palsy in Acoustic Neuroma Tetsuro Sameshima 1 Akio Morita 1 Rokuya Tanikawa
Original Article 39 Evaluation of Variation in the Course of the Facial Nerve, Nerve Adhesion to Tumors, and Postoperative Facial Palsy in Acoustic Neuroma Tetsuro Sameshima 1 Akio Morita 1 Rokuya Tanikawa
Research Journal of Pharmaceutical, Biological and Chemical Sciences
 Research Journal of Pharmaceutical, Biological and Chemical Sciences Morphometric Analysis of Internal Acoustic Meatus and Its Surgically Relevant Relations in Human Temporal Bones. Rajanigandha Vadagaonkar
Research Journal of Pharmaceutical, Biological and Chemical Sciences Morphometric Analysis of Internal Acoustic Meatus and Its Surgically Relevant Relations in Human Temporal Bones. Rajanigandha Vadagaonkar
imaging sequences obtained in brachial plexopathy with/without TOS MR Imaging Sequences Associated Anatomic Structures or Pathologic Conditions
 Brachial plexus imaging sequences obtained in brachial plexopathy with/without TOS MR Imaging Sequences Associated Anatomic Structures or Pathologic Conditions Sagittal TSE T2WI through cervical spine
Brachial plexus imaging sequences obtained in brachial plexopathy with/without TOS MR Imaging Sequences Associated Anatomic Structures or Pathologic Conditions Sagittal TSE T2WI through cervical spine
Case SCIWORA in patient with congenital block vertebra
 Case 15428 SCIWORA in patient with congenital block vertebra Lucas Walgrave 1, Charlotte Vanhoenacker 1-2, Thomas Golinvaux 3, Filip Vanhoenacker3-5 1: Leuven University Hospital, Department of Radiology,
Case 15428 SCIWORA in patient with congenital block vertebra Lucas Walgrave 1, Charlotte Vanhoenacker 1-2, Thomas Golinvaux 3, Filip Vanhoenacker3-5 1: Leuven University Hospital, Department of Radiology,
Correlation of HRCT mastoid with clinical presentation and operative findings in ear diseases
 International Journal of Otorhinolaryngology and Head and Neck Surgery Chintale SG et al. Int J Otorhinolaryngol Head Neck Surg. 2017 Jul;3(3):656-660 http://www.ijorl.com pissn 2454-5929 eissn 2454-5937
International Journal of Otorhinolaryngology and Head and Neck Surgery Chintale SG et al. Int J Otorhinolaryngol Head Neck Surg. 2017 Jul;3(3):656-660 http://www.ijorl.com pissn 2454-5929 eissn 2454-5937
High resolution computed tomography of temporal bone in the evaluation of otologic diseases
 International Journal of Otorhinolaryngology and Head and Neck Surgery Handi PS et al. Int J Otorhinolaryngol Head Neck Surg. 2018 Jan;4(1):87-92 http://www.ijorl.com pissn 2454-5929 eissn 2454-5937 Original
International Journal of Otorhinolaryngology and Head and Neck Surgery Handi PS et al. Int J Otorhinolaryngol Head Neck Surg. 2018 Jan;4(1):87-92 http://www.ijorl.com pissn 2454-5929 eissn 2454-5937 Original
Imaging of Hearing Loss
 Contemporary Imaging of Sensorineural Hearing Loss Imaging of Hearing Loss Discussion Outline (SNHL) Imaging Approaches Anatomic Relationships Lesions: SNHL KL Salzman, MD University of Utah School of
Contemporary Imaging of Sensorineural Hearing Loss Imaging of Hearing Loss Discussion Outline (SNHL) Imaging Approaches Anatomic Relationships Lesions: SNHL KL Salzman, MD University of Utah School of
A case of neurosarcoidosis with labyrinthine involvement.
 A case of neurosarcoidosis with labyrinthine involvement. Peter B. Johnson, University of the West Indies Roxanne Melbourne-Chambers, University of the West Indies Amit Saindane, Emory University Nilesh
A case of neurosarcoidosis with labyrinthine involvement. Peter B. Johnson, University of the West Indies Roxanne Melbourne-Chambers, University of the West Indies Amit Saindane, Emory University Nilesh
Partial Lesions on Intratemporal Segment of the Facial Nerve. Total Graft or Partial Reconstruction?
 Original Article Partial Lesions on Intratemporal Segment of the Facial Nerve. Total Graft or Partial Reconstruction? Ricardo Ferreira Bento*, Raquel Salomone**, Rubens Brito Neto***, Robinson Koiji Tsuji****,
Original Article Partial Lesions on Intratemporal Segment of the Facial Nerve. Total Graft or Partial Reconstruction? Ricardo Ferreira Bento*, Raquel Salomone**, Rubens Brito Neto***, Robinson Koiji Tsuji****,
Synovial cyst of spinal facet
 Case report CHUN C. KAO, M.D., STEFAN S. WINKLER, M.D., AND J. H. TURNER, M.D. Sections of Neurosurgery, Radiology, and Pathology, Madison Veterans Administration Hospital, and University of Wisconsin,
Case report CHUN C. KAO, M.D., STEFAN S. WINKLER, M.D., AND J. H. TURNER, M.D. Sections of Neurosurgery, Radiology, and Pathology, Madison Veterans Administration Hospital, and University of Wisconsin,
By : Prof Saeed Abuel Makarem & Dr.Sanaa Alshaarawi
 By : Prof Saeed Abuel Makarem & Dr.Sanaa Alshaarawi OBJECTIVES By the end of the lecture, students shouldbe able to: List the nuclei of the deep origin of the trigeminal and facial nerves in the brain
By : Prof Saeed Abuel Makarem & Dr.Sanaa Alshaarawi OBJECTIVES By the end of the lecture, students shouldbe able to: List the nuclei of the deep origin of the trigeminal and facial nerves in the brain
THE ROLE OF IMAGING IN DIAGNOSIS OF SUBDURAL HEMATOMA: REVIEW ARTICLE
 THE ROLE OF IMAGING IN DIAGNOSIS OF SUBDURAL HEMATOMA: REVIEW ARTICLE * Dr. Sumendra Raj Pandey, Prof. Dr. Liu Pei WU, Dr. Sohan Kumar Sah, Dr. Lalu Yadav, Md. Sadam Husen Haque and Rajan KR. Chaurasiya
THE ROLE OF IMAGING IN DIAGNOSIS OF SUBDURAL HEMATOMA: REVIEW ARTICLE * Dr. Sumendra Raj Pandey, Prof. Dr. Liu Pei WU, Dr. Sohan Kumar Sah, Dr. Lalu Yadav, Md. Sadam Husen Haque and Rajan KR. Chaurasiya
Pearls and Pitfalls in Neuroradiology of Cerebrovascular Disease The Essentials with MR and CT
 Pearls and Pitfalls in Neuroradiology of Cerebrovascular Disease The Essentials with MR and CT Val M. Runge, MD Wendy R. K. Smoker, MD Anton Valavanis, MD Control # 823 Purpose The focus of this educational
Pearls and Pitfalls in Neuroradiology of Cerebrovascular Disease The Essentials with MR and CT Val M. Runge, MD Wendy R. K. Smoker, MD Anton Valavanis, MD Control # 823 Purpose The focus of this educational
The Low Sensitivity of Fluid-Attenuated Inversion-Recovery MR in the Detection of Multiple Sclerosis of the Spinal Cord
 The Low Sensitivity of Fluid-Attenuated Inversion-Recovery MR in the Detection of Multiple Sclerosis of the Spinal Cord Mark D. Keiper, Robert I. Grossman, John C. Brunson, and Mitchell D. Schnall PURPOSE:
The Low Sensitivity of Fluid-Attenuated Inversion-Recovery MR in the Detection of Multiple Sclerosis of the Spinal Cord Mark D. Keiper, Robert I. Grossman, John C. Brunson, and Mitchell D. Schnall PURPOSE:
The cone tympanic membrane is 9-10 mm long, 8. Magnetic Resonance Imaging of the In-vivo Human Tympanic Membrane
 Original Article 166 Magnetic Resonance Imaging of the In-vivo Human Tympanic Membrane Tung-Yu Lin 1, MD; Jen-Fang Yu 2,3, PhD; Chin-Kuo Chen 1,3,4, MD Background: To obtain magnetic resonance images of
Original Article 166 Magnetic Resonance Imaging of the In-vivo Human Tympanic Membrane Tung-Yu Lin 1, MD; Jen-Fang Yu 2,3, PhD; Chin-Kuo Chen 1,3,4, MD Background: To obtain magnetic resonance images of
41 year old female with headache. Elena G. Violari MD and Leo Wolansky MD
 41 year old female with headache Elena G. Violari MD and Leo Wolansky MD ? Dural Venous Sinus Thrombosis with Hemorrhagic Venous Infarct Acute intraparenchymal hematoma measuring ~3 cm in diameter centered
41 year old female with headache Elena G. Violari MD and Leo Wolansky MD ? Dural Venous Sinus Thrombosis with Hemorrhagic Venous Infarct Acute intraparenchymal hematoma measuring ~3 cm in diameter centered
Neuroradiology MR Protocols
 Neuroradiology MR Protocols Brain protocols N 1: Brain MRI without contrast N 2: Pre- and post-contrast brain MRI N 3 is deleted N 4: Brain MRI without or pre-/post-contrast (seizure protocol) N 5: Pre-
Neuroradiology MR Protocols Brain protocols N 1: Brain MRI without contrast N 2: Pre- and post-contrast brain MRI N 3 is deleted N 4: Brain MRI without or pre-/post-contrast (seizure protocol) N 5: Pre-
Schwannoma of the intermediate nerve
 J Neurosurg 109:144 148, 2008 Schwannoma of the intermediate nerve Case report CHRISTIAN SCHELLER, M.D., 1 JENS RACHINGER, M.D., 1 JULIAN PRELL, M.D., 1 MALTE KORNHUBER, M.D., 2 AND CHRISTIAN STRAUSS,
J Neurosurg 109:144 148, 2008 Schwannoma of the intermediate nerve Case report CHRISTIAN SCHELLER, M.D., 1 JENS RACHINGER, M.D., 1 JULIAN PRELL, M.D., 1 MALTE KORNHUBER, M.D., 2 AND CHRISTIAN STRAUSS,
The Seventh Cranial Nerve The Facial By Prof. Dr. Muhammad Imran Qureshi
 The Seventh Cranial Nerve The Facial By Prof. Dr. Muhammad Imran Qureshi Functional Components: SVE: Fibers originate from nucleus of facial nerve, and supply facial muscles GVE: Fibers derived from superior
The Seventh Cranial Nerve The Facial By Prof. Dr. Muhammad Imran Qureshi Functional Components: SVE: Fibers originate from nucleus of facial nerve, and supply facial muscles GVE: Fibers derived from superior
MAST CELLS IN THE TYMPANIC PART OF THE FACIAL NERVE IN CHRONIC OTITIS MEDIA WITHOUT ASSOCIATED FACIAL PARALYSIS
 i Medical Journal of the Number 1,2 Bahar & Tabestan 1368 Spring & Summer 1989 Islamic Republic of Iran Volume 3 MAST CELLS IN THE TYMPANIC PART OF THE FACIAL NERVE IN CHRONIC OTITIS MEDIA WITHOUT ASSOCIATED
i Medical Journal of the Number 1,2 Bahar & Tabestan 1368 Spring & Summer 1989 Islamic Republic of Iran Volume 3 MAST CELLS IN THE TYMPANIC PART OF THE FACIAL NERVE IN CHRONIC OTITIS MEDIA WITHOUT ASSOCIATED
The Nervous System PART C. PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College
 PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Nervous System 7 PART C Protection of the Central Nervous System Scalp and skin Skull and vertebral
PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Nervous System 7 PART C Protection of the Central Nervous System Scalp and skin Skull and vertebral
Nerve Autografts, Allografts, Conduits, Wraps, and Glue. What Should I Do?
 Nerve Autografts, Allografts, Conduits, Wraps, and Glue. What Should I Do? David Kahan, MD Fellow, Hand & Upper Extremity Surgery Rothman Institute at Thomas Jefferson University Outline Wallerian Degeneration
Nerve Autografts, Allografts, Conduits, Wraps, and Glue. What Should I Do? David Kahan, MD Fellow, Hand & Upper Extremity Surgery Rothman Institute at Thomas Jefferson University Outline Wallerian Degeneration
Case Report An Unusual Case of Bilateral Agenesis of the Cochlear Nerves
 Case Reports in Neurological Medicine Volume 2012, rticle D 581920, 4 pages doi:10.1155/2012/581920 Case Report n Unusual Case of Bilateral genesis of the Cochlear Nerves Vítor Yamashiro Rocha oares, 1
Case Reports in Neurological Medicine Volume 2012, rticle D 581920, 4 pages doi:10.1155/2012/581920 Case Report n Unusual Case of Bilateral genesis of the Cochlear Nerves Vítor Yamashiro Rocha oares, 1
CLASSIFICATION OF CONGENITAL MIDDLE AND EXTERNAL EAR MALFORMATIONS: CT STUDY
 VolumeS Medicalloumal of the Islamic Republic of Iran Number 3,4 Payiz & Zemestan 1370 Fall & Winter 1991 CLASSIFICATION OF CONGENITAL MIDDLE AND EXTERNAL EAR MALFORMATIONS: CT STUDY D. SAYIC, MD, DMS:
VolumeS Medicalloumal of the Islamic Republic of Iran Number 3,4 Payiz & Zemestan 1370 Fall & Winter 1991 CLASSIFICATION OF CONGENITAL MIDDLE AND EXTERNAL EAR MALFORMATIONS: CT STUDY D. SAYIC, MD, DMS:
Skull Base Course. Dissection with fresh temporal bones and half heads
 Skull Base Course Dissection with fresh temporal bones and half heads 711 November 2016 Gruppo Otologico Via Emmanueli 42 Piacenza 29122 t +39 0523 754 362 fax +39 0523 453 708 www.gruppootologico.com
Skull Base Course Dissection with fresh temporal bones and half heads 711 November 2016 Gruppo Otologico Via Emmanueli 42 Piacenza 29122 t +39 0523 754 362 fax +39 0523 453 708 www.gruppootologico.com
Case Studies in CPA/IAC
 Outline Case Studies in CPA/IAC Atul K Mallik MD PhD Department of Radiology and Imaging Sciences University of Utah Health Sciences Center Salt Lake City, Utah, USA Case based review of cerebellopontine
Outline Case Studies in CPA/IAC Atul K Mallik MD PhD Department of Radiology and Imaging Sciences University of Utah Health Sciences Center Salt Lake City, Utah, USA Case based review of cerebellopontine
Radiological Appearance of Extra-axial CNS Hemangioma
 Chin J Radiol 2002; 27: 183-190 183 Radiological Appearance of Extra-axial CNS Hemangioma MING-SHIANG YANG CLAYTON CHI-CHANG CHEN WEN-HSIEN CHEN HAO-CHUN HUNG SAN-KAN LEE Department of Radiology, Taichung
Chin J Radiol 2002; 27: 183-190 183 Radiological Appearance of Extra-axial CNS Hemangioma MING-SHIANG YANG CLAYTON CHI-CHANG CHEN WEN-HSIEN CHEN HAO-CHUN HUNG SAN-KAN LEE Department of Radiology, Taichung
Neurotrauma. Béla Faludi Dept.. of Neurology University of PécsP
 Neurotrauma Béla Faludi Dept.. of Neurology University of PécsP Emergency!!! Why here? Opened cranial injury visible: neurosurgery Closed injuries sometimes diagnosed by neurologist Masking situation:
Neurotrauma Béla Faludi Dept.. of Neurology University of PécsP Emergency!!! Why here? Opened cranial injury visible: neurosurgery Closed injuries sometimes diagnosed by neurologist Masking situation:
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 11/24/2012 Radiology Quiz of the Week # 100 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 11/24/2012 Radiology Quiz of the Week # 100 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
102 Results RESULTS. Age Mean=S.D Range 42= years -84 years Number % <30 years years >50 years
 102 Results RESULTS A total of 50 cases were studied 39 males and 11females.Their age ranged between 16 years and 84 years (mean 42years). T1 and T2WI were acquired for all cases in sagittal and axial
102 Results RESULTS A total of 50 cases were studied 39 males and 11females.Their age ranged between 16 years and 84 years (mean 42years). T1 and T2WI were acquired for all cases in sagittal and axial
Endoscopically-assisted transmastoid approach to the geniculate ganglion and labyrinthine facial nerve
 Jufas and Bance Journal of Otolaryngology - Head and Neck Surgery (2017) 46:53 DOI 10.1186/s40463-017-0231-1 ORIGINAL RESEARCH ARTICLE Endoscopically-assisted transmastoid approach to the geniculate ganglion
Jufas and Bance Journal of Otolaryngology - Head and Neck Surgery (2017) 46:53 DOI 10.1186/s40463-017-0231-1 ORIGINAL RESEARCH ARTICLE Endoscopically-assisted transmastoid approach to the geniculate ganglion
