Experimental posterior penetrating eye injury in the rabbit. II. Histology of wound, vitreous, and retina
|
|
|
- Ilene Allison
- 6 years ago
- Views:
Transcription
1 British Journal of Ophthalmology, 1979, 63, Experimental posterior penetrating eye injury in the rabbit. II. Histology of wound, vitreous, and retina PHILIP E. CLEARY AND STEPHEN J. RYAN From the Department of Ophthalmology, University of Southern California, and Estelle Doheny Eye Foundation, Los Angeles, California, USA SUMMARY The histological findings of the wound, the vitreous, and the retina in the rabbit eye with experimental posterior penetrating injury are described. Wound healing had just begun at 3 days after injury and was well established by 9 to 12 days. It involved proliferation of cells from the episclera and from the choroid. The progression to a fibrous ingrowth from the wound occurred only in eyes with blood in the vitreous. The intravitreal fibroblastic proliferation had begun at 6 days after injury and seemed to be derived from the choroid, the nonpigmented ciliary epithelium and, posteriorly, from the optic nervehead. During the development of retinal detachment the configuration of the peripheral and posterior retina, together with the orientation of vitreous strands, suggested the presence of vitreous traction. We postulate that the presence of contractile fibroblasts (myofibroblasts) in the vitreous may provide the mechanism for vitreous traction. The retinal detachments were also characterised by epiretinal and subretinal membranes, but these were not prominent. The end-stage appearance of a soft, shrunken eye with cyclitic membrane formation and retinal detachment resembles the outcome in many human eyes after severe penetrating injuries. Severe penetrating injuries in human eyes are characterised histologically by intraocular fibrosis with cyclitic membrane formation and traction retinal detachment (Hogan and Zimmerman, 1962; Coles and Haik, 1972). In fact, traction retinal detachment is the main reason for loss of vision in those injuries which are confined to the posterior segment (Eagling, 1975). It has been shown in the preceding paper (Cleary and Ryan, 1979) that the experimental model of a posterior penetrating injury in the rabbit eye results in cyclitic membrane formation and in traction retinal detachment. In the present paper we describe the sequence of histological changes. Materials and methods As previously described, rabbit eyes were injured by a standard wound which was 8 mm long through the pars plana, avoiding the lens and the peripheral retina. Prolapsed vitreous was abscissed and the wound carefully closed by microsurgical techniques with interrupted sutures of 8-0 silk. After wound Address for reprints: Mr Philip E. Cleary, FRCS, Ardkeen Hospital, Waterford, Ireland closure the fundus was inspected by indirect ophthalmoscopy and the area of the wound and the peripheral retina examined by scleral indentation. In some eyes autologus blood and in others balanced salt solution was injected through a 25-gauge needle inserted through the wound and under ophthalmoscopic control into the mid-vitreous, with avoidance of the lens and the retina. The eyes were enucleated at 3-day intervals for the first 3 weeks after injury as well as at 2 and 3 months after injury. Each group consisted of a minimum of 3 eyes. The eyes were fixed in Bouin's fixative for 24 hours and were then sectioned through the optic nerve and midpoint of the wound for gross examination. Each half eye was examined under the dissecting microscope, and drawings and photographs were made. The eyes were then slowly dehydrated in alcohol and embedded in paraffin. Vertical serial sections of 5 Fm thickness were made through the wound, through the retina, and through the optic disc. The sections were stained with haematoxylin-eosin, periodic acid Schiff, and trichrome after Masson. Controls included 7 normal eyes and 15 eyes with a standard injury but without blood injection. 312
2 Experimental posterior penetrating eye injury in the rabbit. II. Histology of wound, vitreous, and retina 313 Fig. 1 At 3 days after injury. The wound has been artifactually separated during processing (arrow). The striking features are the evidence ofproliferation from the episcleral tissues into the wound, and the incarceration of vitreous with vitreous strands radiating from the wound (double arrow) (H and E, x 28) Results STANDARD INCISION.7 AND BLOOD INJECTION Early phase (O to 3 days) At 3 days after injury the wound and vitreous in the inner aspect of the wound were infiltrated with leucocytes and macrophages (Fig. 1). The edges of the scleral wound remained clearly defined, and there was some early evidence of wound healing with proliferation from the episclera (Fig. 1). Vitreous was incarcerated in the wound, and strands of vitreous radiated from the wound to the posterior retina and also to the peripheral retina in the area of the vitreous base (both directly posterior to the wound and at 180 degrees from the wound). At this stage intravitreal fibroblastic proliferation was not seen. In these eyes the retina was attached, and the configuration of the peripheral retina resembled that of the normal control eyes and did not suggest the presence of vitreous traction. Intermediate phase (6 to 15 days) From 6 to 15 days after injury cellular proliferation occurred and became progressively more prominent at the wound and within the vitreous. In most of these eyes the retina was detached. During this phase the blood clot became more diffuse and showed signs of absorption, but it remained loculated within the vitreous. The vitreous did not separate posteriorly from the retina. Haemosiderin-containing macrophages were present within the vitreous and in the inner retina. Wound healing involved proliferation of cells from the episclera initially, but in the inner aspect of the wound fibroblastic proliferation occurred from the uvea and also from proliferation of the nonpigmented ciliary epithelium. Even with good wound apposition fibroblastic ingrowth was already present at 6 days after injury and was prominent by 12 days (Figs. 2 and 3). The fibroblasts permeated the blood clot and lined up along the vitreous strands, which were incarcerated in the wound (Figs. 2 and 3). Fibroblastic proliferation into the vitreous also occurred posteriorly from the optic nervehead, where the fibroblasts were also lined up along the vitreous strands (Figs 2 and 3). During the development of retinal detachment the configuration of the peripheral and posterior retina, together with the orientation of vitreous strands, suggested the presence of vitreous traction (Figs. 4, 5, 6). At 6 days after injury, but more prominently at 9 and 12 days, the peripheral retina assumed a characteristic appearance of being dragged or rolled forward on to the pars plana, not only directly posterior to the wound but also at 180 degrees from the wound (Figs. 5 and 6). In fact, this rolling forward of the peripheral retina was present throughout its entire circumference. Vitreous strands were attached to these areas of peripheral retina, and the vitreous was lined up between the retina and the wound (Figs. 5 and 6). Detachment of the posterior retina occurred typically at 12 days after injury, with a similar appearance of lining up of vitreous strands between the wound and the detached posterior retina. Late phase (18 days to 3 months) Eyes examined between 18 days and 3 months after injury showed progression from the initial stages of
3 314 Fig. 3 The same eye as Fig. 24 at 12 days after injury. This photograph shows the attachments S. of the vitreous over the optic nerve head. The blood vessels which are normally present on the surface of the nerve are apparent (arrow). Vitreous strands are attached to the surface of the optic nerve head, and the ; remarkable feature is the organisation offibroblasts with their long spindle-shaped nuclei along the vitreous strands (double arrow). (Hand E, x 60) retinal detachment to the advanced stage of total retinal detachment, with the retina drawn up into the wound, with cyclitic membrane formation (Figs. 7 and 8), ciliary body and choroidal detachments, and finally the development of an atrophic shrunken eye Ṗroliferations on the surface of the retina with the formation of epiretinal membranes were identified occasionally at 18 and 21 days after injury. However, when the retinal detachments became total and the retina was convoluted and drawn up into the wound, it was not possible to identify discrete epiretinal or subretinal membranes. gm, Philip E. Cleary and Stephen J. Ryan Fig. 2 At 12 days ajter injury. Note the marked fibrous proliferation extending inward from the wound. The ciliary processes are drawn up to the wound. There is a proliferation of the nonpigmented ciliary epithelium (arrow). The fibroblastic proliferation has invaded the blood clot and is extending posteriorly along the vitreous condensation. In the rabbit eye after injury the vitreous does not separate from the posterior retina, and vitreous becomes condensed and lined up between the wound and the posterior retina. (H and E, x 30) Hyperplasia of the retinal pigment epithelium was frequent, with sheets of flattened pigmented cells and plaques of spindle-shaped cells (Fig. 9). In addition, these eyes were characterised histologically by a focal nongranulomatous inflammatory infiltration of the choroid. STANDARD INCISION AND INJECTION OF BALANCED SALT SOLUTION These eyes demonstrated uncomplicated healing of the wound, which had started at 3 days after injury and was well established by 21 days. Proliferation from the episclera appeared as the initial response
4 Experimental posterior penetrating eye injury in the rabbit. IL Histology of wound, vitreous, and retina 315 Fig. 4 At 12 days after injury. The fibrous proliferation from the wound is quite prominent. The fibrous ingrowth appears to be derived from the uvea and also firom the scleral wound. Note the lining up of the condensed vitreous fibrils which extend from the wound to the posterior retina (arrows). There are a number of inflammatory cells in the vitreous, and overlying the vitreous is the blood clot which is in the process of Iysis and organisation. (H and E, x23) 3, Fig. 6 The same eye as Fig. S at 12 days after injury. At 180 degrees from the wound the peripheral retina has also rolled forward on to the nonpigmented ciliary epithelium. The condensation of vitreous over the peripheral retina and vitreous base is quite striking. Note again the lining-up of vitreous fibrils and the organisation of inflammatory cells within this matrix. The nonpigmented ciliary epithelium shows a suggestion of early proliferation (arrow). (H and E, x 37) Fig. 5 At 12 days after injury. The lens has been lost during processing. The wound in this animal illustrates a less luxuriant fibrous proliferation. None the less the incarceration of vitreous in the wound and the proliferation offibroblasts along the anterior vitreous are quite apparent (arrow). The vitreous is condensed in the region of the vitrous base, and strands of vitreous extend between the wound and the Deripheral retina (double arrow). The peripheral retina has rolled forward on to the nonpigmented ciliary epithelium. There is a real retinal detachment in the periphery as evidenced by serous fluid beneath the sensory retina (broad arrow). (H and E, x 28)
5 Philip E. Cleary and Stephen J. Ryan Fig. 8 Another eye showing the Y end stage appearance at 4 weeks "'u after injury. The wound is organised and has blood vessels U- and scattered pigment in the new fibrous tissue (arrows). A marked fibrous proliferation extends inwards from the wound, and, >., swirls of fibrous tissue form a " plaque on the surface of the retina. In this animal the entire retina is drawn up into the region of the wound and fibrous proliferation. (H and E, x 56) Fig. 7 At 21 days after injury. The lens has been lost during processing. Fibrous proliferation from the wound appears to be derived mainly from the uveal tract. The retina has been thrown into folds and is drawn up to the wound by this fibrous proliferation. The fibrous tissue in the process offorming a cyclitic membrane extends along the surface of the Z detached retina. (H and E,,20) Br J Ophthalmol: first published as /bjo on 1 May Downloaded from in wound healing, but fibroblastic proliferation from the choroid, together with proliferation of the nonpigmented ciliary epithelium, was also present. Some cellular proliferation occurred on the inner vitreal aspect of the wound, but it did not show progression, and fibroblastic proliferation within the vitreous was not seen (Fig. 10). Vitreous strands were incarcerated in the wound, and they were also attached to the posterior retina and to the peripheral retina in the region of the vitreous base. The configuration of the retina, however, did not suggest evidence of vitreous traction (Fig. 10). Eyes examined at 3 months after injury showed a healed and remodeled scar, an attached retina, and the absence of fibrous ingrowth. Some eyes showed proliferation of the nonpigmented ciliary epithelium just posterior to the wound. STANDARD INCISION WITH INJURY TO THE RETINA Typically, wound healing was uncomplicated, and, although vitreous was incarcerated in the wound, neither a fibrous ingrowth from the wound nor intravitreal fibrous proliferations were seen. The detached retina showed the usual associated on 30 June 2018 by guest. Protected by copyright.
6 Experimental posterior penetrating eye injury in the rabbit. II. Histology of wound, vitreous, and retina 317 Fig. 9 At 2 months after injury. Hyperplasia of the retinal pigment epithelium has occurred. Note the tubular proliferation of the retinal pigment epithelium cells (arrow). Note the overlying plaque ofpartially depigmented spindle cells (double arrows), presumably laid down by the pigment epithelium during its proliferation into the subretinal space. (H and E, x 22) nlr'~:00, Fig. 10 At 3 months after injury and injection of balanced salt solution. The wound has healed and is remodelled. There 4 4 ~~is a limited fibrous proliferation at the site of/penetration of'the pars plana and ciliary body (arrow). There has been a sliding forward of the nonpigmented ciliary epithelium in the region of the wound. More importantly, the retina is noted to be in a normal position without detachment (double arrows). This view of the peripheral retina is also noteworthy in that the same means offixation as well as histopathological techniques were employed as for all other eyes. Thus we can feel confident that the rolling forward of the peripheral retina on to the pars plana ciliary epithelium observed in eyes with a standard injury and blood injection is not an artifact due to processing. (H and E, x 26) degenerative changes, with loss of photoreceptors and intraretinal cystoid swelling. In some areas the retina was thrown into folds, which could be related to the presence of epiretinal membranes. However, the configuration of the retinal detachment remained funnel shaped, and the retina was not drawn up into the wound. As early as 21 days after injury epiretinal membranes were found, which in some eyes were connected to the underlying retina by a small bridge of.;ox.--.a tissue and which contained cells with abundant cytoplasm and oval-to-spindle-shaped nuclei. In other eyes the epiretinal membranes may have originated from the prepapillary blood vessels (Fig. 11). The epiretinal membranes also contained pigmented cells which stained positive with Prussian blue for iron. These cells had the appearance of haemosiderin-laden macrophages. Subretinal membranes lying outside the external limiting membrane could also be found as early as
7 days after injury, but were very uncommon and were confined to retinal folds (Fig. 12). Within retinal folds it was more common to observe a proliferation in the outer retina, of irregularly arranged cells with abundant cytoplasm and oval or spindle-shaped nuclei, but lying within the external limiting membrane (Fig. 12). These cells had displaced the outer retinal layers from the external limiting membrane to the inner nuclear layer. When the retina was detached, proliferation of the retinal pigment epithelial cells was common and was observed as early as 15 days after injury. Both diffuse hyperplasia with sheets of flattened pigmented cells and plaques of partially depigmented, closely packed, spindle-shaped cells were seen (Fig. 9). When the retinal detachment extended anteriorly to the ora, the pigment epithelium proliferated in the area of the detached pars plana epithelium, becoming 2 or 3 layers thick with irregularly arranged depigmented cells. Two additional eyes that suffered spontaneous choroidal and subretinal haemorrhage during the injury were enucleated immediately after wound closure. These eyes had a choroidal vascular bed that was engorged with blood. Discussion In experimental posterior penetrating injury in the rabbit eye we observed intraocular fibrous proliferation, the formation of cyclitic membranes, and the development of traction retinal detachment. Human eyes suffer the same sequelae after severe posterior penetrating injuries, although the time course is Philip E. Cleary and Stephen J. Ryan Fig. 11 At 2 months after injury. Full-thickness retinal folds are present. The medullated and nerve fibre layers have been pulled close to each other and approximated in one region (arrow). The epiretinal membrane consists of cells with abundant cytoplasm and oval nuclei which may be glial in origin, and also contains pigmented haemosiderinladen macrophages. In addition the epiretinal membrane has continuity with the blood vessels which are normally present on the surface of the medullary rays in the rabbit eye (double arrows). (H and E, x 45) quite different (Coles and Haik, 1972; Eagling, 1975; Winthrop et al., 1978). The evolution of the pathological process can be conveniently divided into 2 stages. (1) FIBROUS INGROWTH AND INTRAVITREAL FIBROUS PROLIFERATION The process of wound healing and repair with proliferation from the episclera and choroid had just begun at 3 days after injury and was well advanced by 9 days, which accords with previous observations (Duke-Elder, 1965). However, the presence of blood in the vitreous had a major effect in the development of a fibrous ingrowth from the wound. In eyes without blood in the vitreous healing of the scleral wound was rapid and the resultant scar was inconspicuous. By contrast, in the eyes with blood in the vitreous, the progression to an intraocular fibrous ingrowth from the wound was a constant feature. Other factors are recognised as important in the development of a fibrous ingrowth, such as incarceration of tissues and poor wound apposition (Duke-Elder, 1965). Yet in these experiments despite good wound apposition a prominent fibrous ingrowth was typical. During intravitreal fibrous proliferation the cells appeared to line up along vitreous strands as a scaffolding. Cellular proliferation into the vitreous from the wound appeared to be derived not only from the episclera and choroid, but also from the non-pigmented ciliary epithelium (Fig. 14). These cells hypertrophy and become elongated and may proliferate along the vitreous strands to which they are attached. The normal nonpigmented ciliary
8 Experimental posterior penetrating eye injury in the rabbit. II. Histology of wound, vitreous, and retina 319 Fig. 12 At 3 months after injury. Note the external limiting membrane delimits the outer retina. An intraretinal glial proliferation has occurred, containing irregularly arranged cells with abundant cytoplasm and oval-to-spindle-shaped nuclei. Inflammatory cells, macrophages, and polymorphonuclear leucocytes are present in the subretinal space. (H and E, x 123) -... Fig. 13 At 3 weeks after injury. 4 1 Note the absence of the external * > limiting membrane. There is a ;a] - 2 proliferation of glial cells extending from the outer aspect p ; e S, of, S, oneiretinal fold to another (arrows). These cells contain s RS R abundant cytoplasm and long processes and oval-to-spindleshaped nuclei. (H and E, x 154) Br J Ophthalmol: first published as /bjo on 1 May Downloaded from epithelium may give rise to collagen fibrils in the vitreous (Fine and Zimmerman, 1963), and hyperplasia of these cells is recognised in a variety of conditions, including injury and inflammation (Hogan and Zimmerman, 1962). Intravitreal fibrous proliferation from the optic nervehead has been observed previously in rabbit eyes after injection of autogenous blood or saccharated iron oxide (Cibis and Yamashita, 1959). This proliferation may be derived from epipapillary glial tissue or, more likely, from the prepapillary blood vessels. The eyes which contained blood also contained monocytes and macrophages; and it is possible that fibroblasts may be derived from haematogenous cells, particularly monocytes and macrophages (Ailgower and Hullinger, 1960), although most of the experimental evidence now supports the view that fibroblasts involved in wound healing are derived locally (Grubl, 1964). It is also possible that cells which originated in the pigment epithelium in the area of the wound may have contributed to the fibrous ingrowth, and we observed some spindleshaped cells with pigment other than haemosiderin in their cytoplasm. Certainly, 'fibrous metaplasia' of pigment epithelium is not uncommon (Hogan and on 30 June 2018 by guest. Protected by copyright.
9 320 Zimmerman, 1962; Freyer, 1966; Wallow and Tso, 1972; Tso, 1973; Machemer and Laqua, 1975), but recognition of the epithelial characteristics of these 'fibrocyte-like' cells can be demonstrated only by electron microscopy (Wallow and Tso, 1972; Machemer and Laqua, 1975). (2) TRACTION RETINAL DETACHMENT In the rabbit eyes, with experimental posterior penetrating injury and blood in the vitreous, we have suggested that the development of retinal detachment may be related to vitreous traction. We interpreted the characteristic configuration of the peripheral retina and elevation of the posterior retina, which was confined initially to the medullary rays, as evidence of vitreoretinal traction (Figs. 4, 5, 6). The lining up of vitreous strands between the wound and posterior retina and between the wound and peripheral retina in the region of the vitreous base suggests a mechanism by which traction is effected. Certainly in the rabbit eye it is apparent during vitrectomy that the vitreous is tightly attached not only over the peripheral retina in the vitreous base but also over the posterior retina in the region of the medullary rays. The onset of traction retinal detachment at about 12 days after injury coincides with the presence of significant intravitreal fibroblastic proliferation. In fact fibrous proliferation within the vitreous was present at 6 days after injury but showed a significant progression by 9 to 12 days. Although we have implicated vitreous traction in the development of retinal detachment, the mechanism for traction is obscure but is perhaps related to changes in vitreous Philip E. Cleary and Stephen J. Ryan Fig. 14 At 21 days after injury the appearance of the ciliary body at 180 degrees from the wound in an eye with a subtotal retinal detachment. This photograph shows proliferation of the nonpigmented ciliary epithelium. The appearance cannot be explained on the basis of tangential cutting alone, which is apparent in I ciliary process. The number of cells and their nuclei suggest a real proliferation of the nonpigmented ciliary epithelium cells. (H and E, x 50) collagen, such as reorientation of collagen fibrils as a result of changes in cross-linkage between the native vitreous collagen and the new collagen laid down by fibroblasts. On the other hand it has been shown that wound contraction occurs independently of collagen formation (Abercrombie et al., 1956) and is mediated by fibroblasts with characteristics typical of smooth muscle cells-myofibroblasts (Gabbiani et al., 1972). The presence of such contractile fibroblasts in the vitreous could provide a mechanism for vitreous traction. Furthermore, the development of vitreous traction leading to traction retinal detachment in the rabbit eye at about 12 days after injury coincides with the rapid increase in the percentage of myofibroblasts observed at between 1 and 2 weeks in experimental full-thickness skin wounds (Rudolph et al., 1977). Although we have not performed electron microscopy on the injured rabbit eyes, we have observed typical myofibroblasts in rhesus monkey eyes after an experimental posterior penetrating injury. Epiretinal and subretinal membrane formation complicates many posterior penetrating injuries in human eyes (Winthrop et al., 1978). In some contraction of epiretinal membranes at the macula results in macular pucker, while in others massive periretinal proliferation leads to inoperable retinal detachment (Hutton et al., 1976; Benson and Machemer, 1976; Faulborn et al., 1977; Winthrop et al., 1978). In the rabbit eye epiretinal membranes were not common and were probably glial in origin, as indicated by the bridges connecting the epiretinal fibrous tissue and the retina. In human eyes the
10 Experimental posterior penetrating eye injury in the rabbit. II. Histology of wound, vitreous, and retina 321 development of epiretinal fibrosis and surface wrinkling retinopathy has been linked with detachment of the posterior vitreous (Roth and Foos, 1971; Wise, 1975; Gass, 1977), though the relationship is far from clear (Foos, 1977). It is of interest, therefore, that in the rabbit eye posterior vitreous detachment does not occur, and we have commented on the tight attachment between the vitreous and posterior retina over the medullary rays. It is recognised that subretinal membrane in both human and monkey eyes can have their origin in the retinal pigment epithelium (Machemer and Laqua, 1975; Machemer et al., 1978). In the rabbit we noted that proliferation of pigment epithelial cells was common in eyes in which the retina was detached. Nonetheless we found subretinal membranes infrequently in the rabbit eyes, while their appearance and continuity with the retina and a total lack of pigmentation suggested a glial cell rather than pigment epithelium cell origin. The rabbit eyes enucleated at 3 months after a standard injury and blood injection were soft, the anterior chamber was frequently absent, the lens was often cataractous, the retina was detached, and a cyclitic membrane was present. This end-stage appearance resembles the atrophy and shrinkage seen in many human eyes enucleated after severe ocular trauma (Hogan and Zimmerman, 1962). We thank Ms K. Borkowski for technical assistance for this paper. References Abercrombie, M., Flint, M. H., and James, D. W. (1956). Wound contraction in relation to collagen formation in scorbutic guinea pigs. Journal of Embryology and Experimental Morphology, 4, Allgower, M., and Hullinger, L. (1960). Origin of fibroblasts from mononuclear blood cells: A study of in vitro formation of the collagen precursor, hydroxproline, in buffy-coat cultures. Surgery, 47, Benson, W. E., and Machemer, R. (1976). Severe perforating injuries treated with pars plana vitrectomy. American Journal of Ophthalmology, 76, Cibis, D., and Yamashita, T. (1959). Experimental aspects of ocular siderosis and hemosiderosis. American Journal of Ophthalmology, 48, Cleary, P. E., and Ryan, S. J. (1979). Experimental posterior penetrating eye injury in the rabbit. I. Method of production and natural history. British Journal of Ophthalmology, 63, Coles, W. H., and Haik, G. M. (1972). Vitrectomy in intraocular trauma. Archives of Ophthalmology, 87, Duke-Elder, S. (1965). Diseases of the Outer Eye, Part 2, Vol. 8. Mosby: St Louis, Missouri. Eagling E. M. (1975). Perforating injuries involving the posterior segment. Transactions of the Ophthalmological Societies of the United Kingdom, 95, Faulborn J., Atkinson A. and Olivier D. (1977). Primary vitrectomy as a preventive surgical procedure in the treatment of severely injured eyes. British Journal of Ophthalmology, 61, Fine B. S., and Zimmerman L. E. (1963). Light and electron microscopic observations on the ciliary epithelium in man and rhesus monkey with particular reference to the vitreous body. Investigative Ophthalmology, 2, Foos R. Y. (1977). Vitreoretinal juncture epiretinal membranes, and vitreous. Investigative Ophthalmology, 16, Freyer, W. C. (1966). Reactivity of the retinal pigment epithelium: an experimental and histopathologic study. Transactions of the American Ophthalmological Society, 64, Gabbiani, G., Hirschel, B. J., Ryan, G. B., Statkov, P. R., and Majno, G. (1972). Granulation tissue as a contractile organ. Journal of Experimental Medicine, 135, Gass, J. D. M. (1977). Stereoscopic Atlas ofmacular Diseases. Mosby: St Louis, Missouri. Grillo, H. C. (1964). Derivation of fibroblasts in the healing wound. Archives of Surgery, 88, Hogan, M. J., and Zimmerman, L. E. (1962). Ophthalmic Pathology: An Atlas and Textbook. Saunders: Philadelphia, Pennsylvania. Hutton, W. L., Snyder, W. B., and Vaiser, A. (1976). Vitrectomy in the treatment of ocular perforating injuries. American Journal of Ophthalmology, 81, Machemer, R., and Laqua, H. (1975). Pigment epithelium proliferation in retinal detachment (massive periretinal proliferation). American Journal of Ophthalmology, 80, Machemer, R., Van Horn, D., and Aaberg, T. M. (1978). Pigment epithelial proliferation in human retinal detachment with massive periretinal proliferation. American Journal of Ophthalmology, 85, Roth, A. M., and Foos, R. Y. (1971). Surface wrinkling retinopathy in eyes of enucleated at autopsy. Transactions of the American Academy of Ophthalmology and Otolaryngology, 75, Rudolph, R., Guber, S., Suzuki, M., and Woodward, M. (1977). The life cycle of the hyofibroblast. Surgery, Gynecology, and Obstetrics, 145, 1-6. Tso, M. (1973). Photic maculopathy in rhesus monkeys. Investigative Ophthalmology, 12, Wallow, I., and Tso, M. (1972). Proliferation of the retinal pigment epithelium over malignant choroidal tumors. American Journal of Ophthalmology, 73, Winthrop, S., Cleary, P. E., and Ryan, S. J. (1978). The histopathology of ocular trauma. In preparation. Wise, G. N. (1975). Clinical features of idiopathic preretinal macular fibrosis. American Journal of Ophthalmology, 79,
Experimental posterior penetrating eye injury in
 British Journal of Ophthalmology, 1980, 64, 801-808 Experimental posterior penetrating eye injury in the rhesus monkey: vitreous-lens admixture PHILIP E. CLEARY, GLEN JARUS, AND STEPHEN J. RYAN From the
British Journal of Ophthalmology, 1980, 64, 801-808 Experimental posterior penetrating eye injury in the rhesus monkey: vitreous-lens admixture PHILIP E. CLEARY, GLEN JARUS, AND STEPHEN J. RYAN From the
Ultrasonic examination in severe diabetic eye disease
 British Journal of Ophthalmology, 1979, 63, 533-538 Ultrasonic examination in severe diabetic eye disease DAVID McLEOD AND MARIE RESTORI From the Department of Ultrasound, Moorfields Eye Hospital, City
British Journal of Ophthalmology, 1979, 63, 533-538 Ultrasonic examination in severe diabetic eye disease DAVID McLEOD AND MARIE RESTORI From the Department of Ultrasound, Moorfields Eye Hospital, City
Vitreoretinal juncture; epiretinal membranes and vitreous. Robert Y. Foos
 Vitreoretinal juncture; epiretinal membranes and vitreous Robert Y. Foos This report reviews current knowledge of the ultrastructural features of the vitreoretinal juncture in its normal state, in eyes
Vitreoretinal juncture; epiretinal membranes and vitreous Robert Y. Foos This report reviews current knowledge of the ultrastructural features of the vitreoretinal juncture in its normal state, in eyes
Yasser R. Serag, MD Tamer Wasfi, MD El- Saied El-Dessoukey, MD Magdi S. Moussa, MD Anselm Kampik, MD
 Microperimetric Evaluation of Brilliant Blue G- assisted Internal Limiting Membrane Peeling By Yasser R. Serag, MD Tamer Wasfi, MD El- Saied El-Dessoukey, MD Magdi S. Moussa, MD Anselm Kampik, MD The internal
Microperimetric Evaluation of Brilliant Blue G- assisted Internal Limiting Membrane Peeling By Yasser R. Serag, MD Tamer Wasfi, MD El- Saied El-Dessoukey, MD Magdi S. Moussa, MD Anselm Kampik, MD The internal
Macular abnormalities in the reattached retina
 British Journal of Ophthalmology, 1978, 62, 595-603 Macular abnormalities in the reattached retina P. E. CLEARY AND P. K. LEAVER From Moorfields Eye Hospital and the Institute of Ophthalmology, London
British Journal of Ophthalmology, 1978, 62, 595-603 Macular abnormalities in the reattached retina P. E. CLEARY AND P. K. LEAVER From Moorfields Eye Hospital and the Institute of Ophthalmology, London
COMMUNICATIONS PHOTOCOAGULATION OF THE RETINA* OPHTHALMOSCOPIC AND HISTOLOGICAL FINDINGS. photocoagulation of the rabbit's retina.
 Brit. J. Ophthal. (1963) 47, 577. COMMUNICATIONS PHOTOCOAGULATION OF THE RETINA* OPHTHALMOSCOPIC AND HISTOLOGICAL FINDINGS BY A. LAVYEL Haifa, Israel SINCE the introduction of the photocoagulator by Meyer-Schwickerath
Brit. J. Ophthal. (1963) 47, 577. COMMUNICATIONS PHOTOCOAGULATION OF THE RETINA* OPHTHALMOSCOPIC AND HISTOLOGICAL FINDINGS BY A. LAVYEL Haifa, Israel SINCE the introduction of the photocoagulator by Meyer-Schwickerath
Coagulative necrosis in a malignant melanoma of the choroid at the macula with extensive subretinal hemorrhage
 Coagulative necrosis in a malignant melanoma of the choroid at the macula with extensive subretinal hemorrhage Robert D. Yee, Robert Y. Foos, and Bradley R. Straatsma The authors present a case report
Coagulative necrosis in a malignant melanoma of the choroid at the macula with extensive subretinal hemorrhage Robert D. Yee, Robert Y. Foos, and Bradley R. Straatsma The authors present a case report
Cystoid macular edema associated with limbal melanoma*
 Graefe's Arch Clin Exp Ophthalmol (1983) 221:101-105 Graefe's Archive for CliniCal and Experimental Ophthalmology Springer-Verlag 1983 Cystoid macular edema associated with limbal melanoma* J. Reimer Wolter
Graefe's Arch Clin Exp Ophthalmol (1983) 221:101-105 Graefe's Archive for CliniCal and Experimental Ophthalmology Springer-Verlag 1983 Cystoid macular edema associated with limbal melanoma* J. Reimer Wolter
Diffuse infiltrating retinoblastoma
 Brit. 1. Ophthal. (I 971) 55, 6oo Diffuse infiltrating retinoblastoma GWYN MORGAN Department of Pathology, Institute of Ophthalmology, University of London The term "diffuse infiltrating retinoblastoma"
Brit. 1. Ophthal. (I 971) 55, 6oo Diffuse infiltrating retinoblastoma GWYN MORGAN Department of Pathology, Institute of Ophthalmology, University of London The term "diffuse infiltrating retinoblastoma"
Closed microsurgery for diabetic traction macular detachment
 British Journal of Ophthalmology, 198, 66, 754-758 Closed microsurgery for diabetic traction macular detachment TOM BARRIE,* ELIAS FERETIS,t PETER LEAVER, AND DAVID McLEOD From the Surgical Vitreoretinal
British Journal of Ophthalmology, 198, 66, 754-758 Closed microsurgery for diabetic traction macular detachment TOM BARRIE,* ELIAS FERETIS,t PETER LEAVER, AND DAVID McLEOD From the Surgical Vitreoretinal
Benign melanoma of the choroid
 Brit. J. Ophthal. (I969) 53, 621 Benign melanoma of the choroid Recognition of malignant change using clinical photographic techniques E. S. ROSEN* AND A. GARNERt Manchester Roval Eye Hospital* and the
Brit. J. Ophthal. (I969) 53, 621 Benign melanoma of the choroid Recognition of malignant change using clinical photographic techniques E. S. ROSEN* AND A. GARNERt Manchester Roval Eye Hospital* and the
Late retinal reattachment
 :British Journal of Ophthalmology, 1981, 65, 142-146 Late retinal reattachment S. N. KOKOLAKIS, L. BRAVO, AND A. H. CHIGNELL From the Ophthalmic Department, St Thomas's Hospital, London SEI SUMMARY Six
:British Journal of Ophthalmology, 1981, 65, 142-146 Late retinal reattachment S. N. KOKOLAKIS, L. BRAVO, AND A. H. CHIGNELL From the Ophthalmic Department, St Thomas's Hospital, London SEI SUMMARY Six
Retinal pigment epithelial detachments in the elderly:
 British Journal of Ophthalmology, 1985, 69, 397-403 Retinal pigment epithelial detachments in the elderly: classification and outcome A G CASSWELL, D KOHEN, AND A C BIRD From Moorfields Eye Hospital, City
British Journal of Ophthalmology, 1985, 69, 397-403 Retinal pigment epithelial detachments in the elderly: classification and outcome A G CASSWELL, D KOHEN, AND A C BIRD From Moorfields Eye Hospital, City
Photocoagulation of disciform macular lesions
 British Journal of Ophthalmology, 1979, 63, 669-673 Photocoagulation of disciform macular lesions with krypton laser A. C. BIRD AND R. H. B. GREY From the Institute of Ophthalmology, Moorfields Eye Hospital,
British Journal of Ophthalmology, 1979, 63, 669-673 Photocoagulation of disciform macular lesions with krypton laser A. C. BIRD AND R. H. B. GREY From the Institute of Ophthalmology, Moorfields Eye Hospital,
Scleral buckling. Surgical Treatment
 Dr. Ayman M. Khattab MD, FRCS professor of Ophthalmology Cairo University Surgical Treatment Pneumatic retinopexy. Primary pars plana vitrectomy. 1 Indications for scleral buckling. SB is used to treat
Dr. Ayman M. Khattab MD, FRCS professor of Ophthalmology Cairo University Surgical Treatment Pneumatic retinopexy. Primary pars plana vitrectomy. 1 Indications for scleral buckling. SB is used to treat
Vitreomacular interface disorders. Ghanbari MD 1393:10:25
 Vitreomacular interface disorders Ghanbari MD 1393:10:25 Human vitreous after dissection of the sclera, choroid, and retina. Lamellar structure of the posterior vitreous cortex (PVC) in the monkey. V =
Vitreomacular interface disorders Ghanbari MD 1393:10:25 Human vitreous after dissection of the sclera, choroid, and retina. Lamellar structure of the posterior vitreous cortex (PVC) in the monkey. V =
Infantile cystoid maculopathy
 British Journal of Ophthalmology, 1980, 64, 206-210 Infantile cystoid maculopathy MICHAEL T. TRESE AND ROBERT Y. FOOS From the Department of Ophthalmology and the Department of Pathology, Jules Stein Eye
British Journal of Ophthalmology, 1980, 64, 206-210 Infantile cystoid maculopathy MICHAEL T. TRESE AND ROBERT Y. FOOS From the Department of Ophthalmology and the Department of Pathology, Jules Stein Eye
Disease-Specific Fluorescein Angiography
 Ruth E. Picchiottino, CRA Disease-Specific Fluorescein Angiography 15 Disease-Specific Fluorescein Angiography Recommendations for tailoring retinal fluorescein angiography to diabetic retinopathy, macular
Ruth E. Picchiottino, CRA Disease-Specific Fluorescein Angiography 15 Disease-Specific Fluorescein Angiography Recommendations for tailoring retinal fluorescein angiography to diabetic retinopathy, macular
EPIRETINAL MEMBRANE & VITREOMACULAR TRACTION
 EPIRETINAL MEMBRANE & VITREOMACULAR TRACTION Management of ERM and VMT K.V.Chalam,MD,PhD,MBA,FACS Professor and Director of Retina Loma Linda Eye Institute Los Angeles, USA REVIEW ANATOMY The vitreous
EPIRETINAL MEMBRANE & VITREOMACULAR TRACTION Management of ERM and VMT K.V.Chalam,MD,PhD,MBA,FACS Professor and Director of Retina Loma Linda Eye Institute Los Angeles, USA REVIEW ANATOMY The vitreous
PART 1: GENERAL RETINAL ANATOMY
 PART 1: GENERAL RETINAL ANATOMY General Anatomy At Ora Serrata At Optic Nerve Head Fundoscopic View Of Normal Retina What Is So Special About Diabetic Retinopathy? The WHO definition of blindness is
PART 1: GENERAL RETINAL ANATOMY General Anatomy At Ora Serrata At Optic Nerve Head Fundoscopic View Of Normal Retina What Is So Special About Diabetic Retinopathy? The WHO definition of blindness is
Royal Berkshire Hospital Dunedin Hospital. Prince Charles Eye Unit Pi Princess Margaret Hospital
 Vitreoretinal Surgery Mr Vaughan Tanner www.tanner-eyes.co.uk eyes Reading Royal Berkshire Hospital Dunedin Hospital Windsor Prince Charles Eye Unit Pi Princess Margaret Hospital Success rates VR surgery
Vitreoretinal Surgery Mr Vaughan Tanner www.tanner-eyes.co.uk eyes Reading Royal Berkshire Hospital Dunedin Hospital Windsor Prince Charles Eye Unit Pi Princess Margaret Hospital Success rates VR surgery
Asadi-Amoli et al Adenocarcinoma of RPE Iranian Journal of Ophthalmology - Volume 19, Number 4, 2007
 Adenocarcinoma of Retinal Pigment Epithelium Clinically Diagnosed as Malignant Melanoma; A Case Report with Unsystematic Review of Literature Fahimeh Asadi-Amoli, MD, 1 Hedyeh Moradi, MD 2 Mohammad-Taher
Adenocarcinoma of Retinal Pigment Epithelium Clinically Diagnosed as Malignant Melanoma; A Case Report with Unsystematic Review of Literature Fahimeh Asadi-Amoli, MD, 1 Hedyeh Moradi, MD 2 Mohammad-Taher
elevations of the retina
 Brit. j. Ophthal. (I974) 58, 899 Patterns of non-rhegmatogenous elevations of the retina HARVEY LINCOFF New rork AND INGRID KREISSIG Bonn, Germany The purpose of this paper is to point out the differential
Brit. j. Ophthal. (I974) 58, 899 Patterns of non-rhegmatogenous elevations of the retina HARVEY LINCOFF New rork AND INGRID KREISSIG Bonn, Germany The purpose of this paper is to point out the differential
Medical School Histology Basics. VIBS 289 lab. Eye
 Medical School Histology Basics VIBS 289 lab Eye Larry Johnson Texas A&M University Aqueous humor OUTLINE OVERVIEW CELLULAR STRUCTURES THROUGH WHICH LIGHT PASSES A. CORNEA B. LENS C. RETINA STRUCTURES
Medical School Histology Basics VIBS 289 lab Eye Larry Johnson Texas A&M University Aqueous humor OUTLINE OVERVIEW CELLULAR STRUCTURES THROUGH WHICH LIGHT PASSES A. CORNEA B. LENS C. RETINA STRUCTURES
Experimental retinal detachment with a sulfated polysaccharide
 Experimental retinal detachment with a sulfated polysaccharide Wallace M. Landholm and Robert C. Watzke C, Research in the pathophysiology of retinal detachments would be aided if an experimental model
Experimental retinal detachment with a sulfated polysaccharide Wallace M. Landholm and Robert C. Watzke C, Research in the pathophysiology of retinal detachments would be aided if an experimental model
Encircling silicone rod without drainage
 Brit. J. Ophthal. (I 973) 57, 53 7 Encircling silicone rod without drainage for retinal detachment with giant breaks ABDEL-LATIF SIAM Ophthalmology Department, Ain Shams University, Cairo, Egypt Giant
Brit. J. Ophthal. (I 973) 57, 53 7 Encircling silicone rod without drainage for retinal detachment with giant breaks ABDEL-LATIF SIAM Ophthalmology Department, Ain Shams University, Cairo, Egypt Giant
Vitreo-retinal interface pathologies and fibrinolytic treatment approaches
 Vitreo-retinal interface pathologies and fibrinolytic treatment approaches Constantin J. Pournaras Memorial A. de Rothschild Clinical Research Group La Colline Ophthalmology Center Vitreoretinal Interface
Vitreo-retinal interface pathologies and fibrinolytic treatment approaches Constantin J. Pournaras Memorial A. de Rothschild Clinical Research Group La Colline Ophthalmology Center Vitreoretinal Interface
An A to Z guide on Epiretinal Membranes (ERMs) Paris Tranos PhD,ICO,FRCS OPHTHALMICA Vitreoretinal & Uveitis Department
 An A to Z guide on Epiretinal Membranes (ERMs) Paris Tranos PhD,ICO,FRCS OPHTHALMICA Vitreoretinal & Uveitis Department Types of ERM Natural history OCT prognostic factors ERM with co-existing pathology
An A to Z guide on Epiretinal Membranes (ERMs) Paris Tranos PhD,ICO,FRCS OPHTHALMICA Vitreoretinal & Uveitis Department Types of ERM Natural history OCT prognostic factors ERM with co-existing pathology
RETINAL DETACHMENT AT THE POSTERIOR POLE*
 Brit. J. Ophthal. (1958) 42, 749. RETINAL DETACHMENT AT THE POSTERIOR POLE* BY CALBERT I. PHILLIPSt Institute of Ophthalmology, University oflondon THE common feature of the cases to be described in this
Brit. J. Ophthal. (1958) 42, 749. RETINAL DETACHMENT AT THE POSTERIOR POLE* BY CALBERT I. PHILLIPSt Institute of Ophthalmology, University oflondon THE common feature of the cases to be described in this
optic disc neovascularisation
 British Journal of Ophthalmology, 1979, 63, 412-417 A comparative study of argon laser and krypton laser in the treatment of diabetic optic disc neovascularisation W. E. SCHULENBURG, A. M. HAMILTON, AND
British Journal of Ophthalmology, 1979, 63, 412-417 A comparative study of argon laser and krypton laser in the treatment of diabetic optic disc neovascularisation W. E. SCHULENBURG, A. M. HAMILTON, AND
Michael P. Blair, MD Retina Consultants, Ltd Libertyville/Des Plaines, Illinois Clinical Associate University of Chicago 17 October 2015
 Michael P. Blair, MD Retina Consultants, Ltd Libertyville/Des Plaines, Illinois Clinical Associate University of Chicago 17 October 2015 So What Parts of the Eye Retina are Affected by VHL Neural tissue
Michael P. Blair, MD Retina Consultants, Ltd Libertyville/Des Plaines, Illinois Clinical Associate University of Chicago 17 October 2015 So What Parts of the Eye Retina are Affected by VHL Neural tissue
OCT Angiography in Primary Eye Care
 OCT Angiography in Primary Eye Care An Image Interpretation Primer Julie Rodman, OD, MS, FAAO and Nadia Waheed, MD, MPH Table of Contents Diabetic Retinopathy 3-6 Choroidal Neovascularization 7-9 Central
OCT Angiography in Primary Eye Care An Image Interpretation Primer Julie Rodman, OD, MS, FAAO and Nadia Waheed, MD, MPH Table of Contents Diabetic Retinopathy 3-6 Choroidal Neovascularization 7-9 Central
AQUEOUS VEINS IN RABBITS*
 Brit. J. Ophthal., 35, 119. AQUEOUS VEINS IN RABBITS* BY D. P. GREAVES AND E. S. PERKINS Institute of Ophthalmology, London Director of Research, Sir Stewart Duke-Elder IN the course of investigations
Brit. J. Ophthal., 35, 119. AQUEOUS VEINS IN RABBITS* BY D. P. GREAVES AND E. S. PERKINS Institute of Ophthalmology, London Director of Research, Sir Stewart Duke-Elder IN the course of investigations
Abstract Aims To analyse the histopathology of classic and occult choroidal neovascular membrane surgical specimens in age
 Br J Ophthalmol 2000;84:239 243 239 ORIGINAL ARTICLES Clinical science Clinicopathological correlation in exudative age related macular degeneration: histological diverentiation between classic and occult
Br J Ophthalmol 2000;84:239 243 239 ORIGINAL ARTICLES Clinical science Clinicopathological correlation in exudative age related macular degeneration: histological diverentiation between classic and occult
Technique. 92i. M. M. J. McNicholas, 2 D. P. Brophy,1 W. J. Power,3 4 and J. F. Griffin1 3
 92i Ocular Sonography M. M. J. McNicholas, 2 D. P. Brophy,1 W. J. Power,3 4 and J. F. Griffin1 3 High-frequency ocular sonography is the ideal method for imaging the eye and intraocular structures. In
92i Ocular Sonography M. M. J. McNicholas, 2 D. P. Brophy,1 W. J. Power,3 4 and J. F. Griffin1 3 High-frequency ocular sonography is the ideal method for imaging the eye and intraocular structures. In
Corneal blood staining after hyphaema
 Brit. J_. Ophthal. (I 972) 56, 589 after hyphaema J. D. BRODRICK Sheffield has been described as a rare complication of contusion injury in which a hyphaema of relatively long duration and a raised intraocular
Brit. J_. Ophthal. (I 972) 56, 589 after hyphaema J. D. BRODRICK Sheffield has been described as a rare complication of contusion injury in which a hyphaema of relatively long duration and a raised intraocular
Outline. Brief history and principles of ophthalmic ultrasound. Types of ocular ultrasound. Examination techniques. Types of Ultrasound
 Ultrasound and Intraocular Tumors 2015 Ophthalmic Photographers' Society Mid-Year Program Cagri G. Besirli MD, PhD Kellogg Eye Center University of Michigan Outline Brief history and principles of ophthalmic
Ultrasound and Intraocular Tumors 2015 Ophthalmic Photographers' Society Mid-Year Program Cagri G. Besirli MD, PhD Kellogg Eye Center University of Michigan Outline Brief history and principles of ophthalmic
OPTIC DISC PIT Pathogenesis and Management OPTIC DISC PIT
 OPTIC DISC PIT Pathogenesis and Management Abdel-Latif Siam Ain Shams University Cairo Egypt OPTIC DISC PIT Congenital pit is an atypical coloboma usually located on the temporal edge of the disc, associated
OPTIC DISC PIT Pathogenesis and Management Abdel-Latif Siam Ain Shams University Cairo Egypt OPTIC DISC PIT Congenital pit is an atypical coloboma usually located on the temporal edge of the disc, associated
Histology of the Eye
 Histology of the Eye Objectives By the end of this lecture, the student should be able to describe: The general structure of the eye. The microscopic structure of:»cornea.»retina. EYE BULB Three coats
Histology of the Eye Objectives By the end of this lecture, the student should be able to describe: The general structure of the eye. The microscopic structure of:»cornea.»retina. EYE BULB Three coats
XUE HUI Department of Histology& Embryology, Basic Medicine College of Jilin University
 SENSE ORGAN XUE HUI Department of Histology& Embryology, Basic Medicine College of Jilin University EYE fibrous globe lens photosensitive cells a system of cells and nerves concentric layers the sclera
SENSE ORGAN XUE HUI Department of Histology& Embryology, Basic Medicine College of Jilin University EYE fibrous globe lens photosensitive cells a system of cells and nerves concentric layers the sclera
VITREOUS FLOATERS AND PHOTOPSIA AS PREDICTORS OF VITREORETINAL PATHOLOGY
 Basrah Journal Of Surgery VITREOUS FLOATERS AND PHOTOPSIA AS PREDICTORS OF VITREORETINAL PATHOLOGY Salah Zuhair Al-Asadi MB,ChB, FRCS, FIBMS, Lecturer of Ophthalmology, College of Medicine, University
Basrah Journal Of Surgery VITREOUS FLOATERS AND PHOTOPSIA AS PREDICTORS OF VITREORETINAL PATHOLOGY Salah Zuhair Al-Asadi MB,ChB, FRCS, FIBMS, Lecturer of Ophthalmology, College of Medicine, University
Histopathology: skin pathology
 Histopathology: skin pathology These presentations are to help you identify, and to test yourself on identifying, basic histopathological features. They do not contain the additional factual information
Histopathology: skin pathology These presentations are to help you identify, and to test yourself on identifying, basic histopathological features. They do not contain the additional factual information
evaluation of vitreoretinal adhesions in exudative AMD using optical coherence tomography
 evaluation of vitreoretinal adhesions in exudative AMD using optical coherence tomography Dr. Mahmoud Alaa Abouhusssein, FRCO Lecturer of ophthalmology, Alexandria university Dr. Amir Ramadan Gomaa, MD
evaluation of vitreoretinal adhesions in exudative AMD using optical coherence tomography Dr. Mahmoud Alaa Abouhusssein, FRCO Lecturer of ophthalmology, Alexandria university Dr. Amir Ramadan Gomaa, MD
Visual and Anatomical Outcomes of Vitreous Surgery for Large Macular Holes
 March 2009 Raju K.V. et al. - Closed Globe Injuries 31 ORIGINAL ARTICLE Visual and Anatomical Outcomes of Vitreous Surgery for Large Macular Holes Dr. Mahesh G. MS DO DNB FRCSEd, Dr. A. Giridhar MS, Dr.
March 2009 Raju K.V. et al. - Closed Globe Injuries 31 ORIGINAL ARTICLE Visual and Anatomical Outcomes of Vitreous Surgery for Large Macular Holes Dr. Mahesh G. MS DO DNB FRCSEd, Dr. A. Giridhar MS, Dr.
Central serous chorioretinopathy (CSCR) was
 Case Report 777 Perfluorocarbon Liquid-Assisted External Drainage in the Management of Central Serous Chorioretinopathy with Bullous Serous Retinal Detachment Hung-Chiao Chen, MD; Jau-Der Ho, MD; San-Ni
Case Report 777 Perfluorocarbon Liquid-Assisted External Drainage in the Management of Central Serous Chorioretinopathy with Bullous Serous Retinal Detachment Hung-Chiao Chen, MD; Jau-Der Ho, MD; San-Ni
Macular Hole Associated with Vogt-Koyanagi-Harada Disease at the Acute Uveitic Stage
 Published online: September 15, 2015 2015 The Author(s) Published by S. Karger AG, Basel 1663 2699/15/0063 0328$39.50/0 This article is licensed under the Creative Commons Attribution-NonCommercial 4.0
Published online: September 15, 2015 2015 The Author(s) Published by S. Karger AG, Basel 1663 2699/15/0063 0328$39.50/0 This article is licensed under the Creative Commons Attribution-NonCommercial 4.0
The Foundation WHAT IS THE RETINA? continued next page. RETINA HEALTH SERIES Facts from the ASRS
 The Foundation American Society of Retina Specialists Committed to improving the quality of life of all people with retinal disease. Epiretinal Membranes (ERMs), also commonly known as cellophane maculopathy
The Foundation American Society of Retina Specialists Committed to improving the quality of life of all people with retinal disease. Epiretinal Membranes (ERMs), also commonly known as cellophane maculopathy
Pit-like changes of the optic nerve head
 Pit-like changes of the optic nerve head in open-angle glaucoma British Journal of Ophthalmology, 1978, 62, 389-393 RONALD L. RADIUS, A. EDWARD MAUMENEE, AND WILLIAM R. GREEN From the Wilmer Ophthalmologic
Pit-like changes of the optic nerve head in open-angle glaucoma British Journal of Ophthalmology, 1978, 62, 389-393 RONALD L. RADIUS, A. EDWARD MAUMENEE, AND WILLIAM R. GREEN From the Wilmer Ophthalmologic
Moncef Khairallah, MD
 Moncef Khairallah, MD Department of Ophthalmology, Fattouma Bourguiba University Hospital Faculty of Medicine, University of Monastir Monastir, Tunisia INTRODUCTION IU: anatomic form of uveitis involving
Moncef Khairallah, MD Department of Ophthalmology, Fattouma Bourguiba University Hospital Faculty of Medicine, University of Monastir Monastir, Tunisia INTRODUCTION IU: anatomic form of uveitis involving
Often asymptomatic but can cause a reduction in BCVA and distortion of vision.
 Christopher Wolfe, OD, FAAO, Dipl. ABO Epiretinal Membrane (ERM) and Vitreomacular Traction (VMT) Epiretinal membrane (macular pucker, cellophane maculopathy, premacular fibrosis) consists of a layer of
Christopher Wolfe, OD, FAAO, Dipl. ABO Epiretinal Membrane (ERM) and Vitreomacular Traction (VMT) Epiretinal membrane (macular pucker, cellophane maculopathy, premacular fibrosis) consists of a layer of
 measure of your overall performance. An isolated glucose test is helpful to let you know what your sugar level is at one moment, but it doesn t tell you whether or not your diabetes is under adequate control
measure of your overall performance. An isolated glucose test is helpful to let you know what your sugar level is at one moment, but it doesn t tell you whether or not your diabetes is under adequate control
Pathological Findings in Eyes with the Ganciclovir Implant
 Pathological Findings in Eyes with the Ganciclovir Implant Sunil K. Srivastava, MD, 1 Daniel F. Martin, MD, 1,2 Susan D. Mellow, RN, 1 David J. Parks, MD, 1 Kourosh Dastgheib, MD, 1 Chi-Chao Chan, MD 1
Pathological Findings in Eyes with the Ganciclovir Implant Sunil K. Srivastava, MD, 1 Daniel F. Martin, MD, 1,2 Susan D. Mellow, RN, 1 David J. Parks, MD, 1 Kourosh Dastgheib, MD, 1 Chi-Chao Chan, MD 1
A five-year survey of ocular shotgun injuries in Ireland
 British Journal of Ophthalmology, 1987, 71, 449-453 A five-year survey of ocular shotgun injuries in Ireland DERMOT RODEN,' PHILIP CLEARY,2 AND PETER EUSTACE From the 'Department of Ophthalmology, Mater
British Journal of Ophthalmology, 1987, 71, 449-453 A five-year survey of ocular shotgun injuries in Ireland DERMOT RODEN,' PHILIP CLEARY,2 AND PETER EUSTACE From the 'Department of Ophthalmology, Mater
It has previously been shown that pine
 The effects of cortisone on pine pollen-induced uveitis in guinea pigs Stan L. Coleman and Samuel Canaan Injection of pine pollen into the vitreous of guinea pigs previously sensitized with Freund's adjuvant
The effects of cortisone on pine pollen-induced uveitis in guinea pigs Stan L. Coleman and Samuel Canaan Injection of pine pollen into the vitreous of guinea pigs previously sensitized with Freund's adjuvant
Pediatric Ocular Sonography
 Pediatric Ocular Sonography Cicero J Torres A Silva, MD Associate Professor of Radiology 2016 SPR Pediatric Ultrasound Course Yale University School of Medicine None Disclosures Objectives of Presentation
Pediatric Ocular Sonography Cicero J Torres A Silva, MD Associate Professor of Radiology 2016 SPR Pediatric Ultrasound Course Yale University School of Medicine None Disclosures Objectives of Presentation
When optical coherence tomography (OCT)
 Macular Imaging: SD-OCT in nterior Segment Surgical Practice Many pathologic processes of the macula can be visualized or quantified only with this modality. y Steven G. Safran, MD When optical coherence
Macular Imaging: SD-OCT in nterior Segment Surgical Practice Many pathologic processes of the macula can be visualized or quantified only with this modality. y Steven G. Safran, MD When optical coherence
THE EYE: RETINA AND GLOBE
 Neuroanatomy Suzanne Stensaas February 24, 2011, 10:00-12:00 p.m. Reading: Waxman Ch. 15. Your histology and gross anatomy books should be useful. Reading: Histology of the Eye from any histology book
Neuroanatomy Suzanne Stensaas February 24, 2011, 10:00-12:00 p.m. Reading: Waxman Ch. 15. Your histology and gross anatomy books should be useful. Reading: Histology of the Eye from any histology book
Vitreoretinal surgical management In ocular oncology
 www.ophtalmique.ch Vitreoretinal surgical management In ocular oncology Pournaras Jean-Antoine C Vitreoretinal Surgery Unit 1. Surgical resection after proton beam therapy 2. Ocular Biopsy 3. RD in advanced
www.ophtalmique.ch Vitreoretinal surgical management In ocular oncology Pournaras Jean-Antoine C Vitreoretinal Surgery Unit 1. Surgical resection after proton beam therapy 2. Ocular Biopsy 3. RD in advanced
TYPES. Full thickness defect in the sensory retina (break) Secondary to Tumour, Inflammation or a Systemic disease
 Dr.A.Divya Introduction Definition : Retinal deatchment is the separation of the neurosensory retina(nsr) from the retinal pigment epithelium(rpe) ; results in the accumulation of subretinal fluid(srf)
Dr.A.Divya Introduction Definition : Retinal deatchment is the separation of the neurosensory retina(nsr) from the retinal pigment epithelium(rpe) ; results in the accumulation of subretinal fluid(srf)
UNIQUE CHANGES IN THE RETINAL VEINS OF A DIABETIC PATIENT*
 Brit. J. Ophthal. (1962) 46, 737. UNIQUE CHANGES IN THE RETINAL VEINS OF A DIABETIC PATIENT* BY Nuffield Laboratory of Ophthalmology, Oxford, and Cape Town, Union of South Africa THis paper illustrates
Brit. J. Ophthal. (1962) 46, 737. UNIQUE CHANGES IN THE RETINAL VEINS OF A DIABETIC PATIENT* BY Nuffield Laboratory of Ophthalmology, Oxford, and Cape Town, Union of South Africa THis paper illustrates
Intraoperative Visualization of Peripheral Retina with Wide-Angle Viewing Systems
 Intraoperative Visualization of Peripheral Retina with Wide-Angle Viewing Systems Homayoun Tabandeh, M.D., MS, Francesco Boscia, M.D. 1. Retina -Vitreous Associates Medical Group, Los Angeles, California,
Intraoperative Visualization of Peripheral Retina with Wide-Angle Viewing Systems Homayoun Tabandeh, M.D., MS, Francesco Boscia, M.D. 1. Retina -Vitreous Associates Medical Group, Los Angeles, California,
Trauma. steve charles
 Trauma steve charles Pathobiology of Trauma Hypocellular Vitreous Collagen Contraction (formerly called gel contraction) Poor Names: Vitreous Bands & Vitreous Membranes (always along vitreous surface or
Trauma steve charles Pathobiology of Trauma Hypocellular Vitreous Collagen Contraction (formerly called gel contraction) Poor Names: Vitreous Bands & Vitreous Membranes (always along vitreous surface or
Adenocarcinorna of the Ciliary Body A Report of 2 Cases in Dogs
 Path. vet. 5: 122-126 (1968) From the Ophthalmic Pathology Laboratory, Department of Ophthalmology, New York University School of Medicine, New York Adenocarcinorna of the Ciliary Body A Report of 2 Cases
Path. vet. 5: 122-126 (1968) From the Ophthalmic Pathology Laboratory, Department of Ophthalmology, New York University School of Medicine, New York Adenocarcinorna of the Ciliary Body A Report of 2 Cases
The Foundation. RETINA HEALTH SERIES Facts from the ASRS
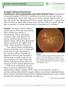 Complex Retinal Detachment: Proliferative Vitreoretinopathy and Giant Retinal Tears Proliferative vitreoretinopathy (PVR) is a condition in which retinal scar tissue, or membranes form; this may occur
Complex Retinal Detachment: Proliferative Vitreoretinopathy and Giant Retinal Tears Proliferative vitreoretinopathy (PVR) is a condition in which retinal scar tissue, or membranes form; this may occur
Choroidal Neovascularization in Sympathetic Ophthalmia
 Choroidal Neovascularization in Sympathetic Ophthalmia Lucia Sobrin, Miguel Cordero Coma, C. Stephen Foster Case Report A 49-year-old man presented after a ruptured globe repair of his left eye status
Choroidal Neovascularization in Sympathetic Ophthalmia Lucia Sobrin, Miguel Cordero Coma, C. Stephen Foster Case Report A 49-year-old man presented after a ruptured globe repair of his left eye status
SCLERAL BUCKLING OPERATION WITH ROLLED SCLERAL FLAP*
 Brit. J. Ophthal. (1959) 43, 361. SCLERAL BUCKLING OPERATION WITH ROLLED SCLERAL FLAP* BY V. CAVKA Belgrade, Yugoslavia AMONG the various operative procedures carried out for detachment of the retina,
Brit. J. Ophthal. (1959) 43, 361. SCLERAL BUCKLING OPERATION WITH ROLLED SCLERAL FLAP* BY V. CAVKA Belgrade, Yugoslavia AMONG the various operative procedures carried out for detachment of the retina,
Silicone Oil in the Treatment of Complicated Retinal Detachments
 Klaus Lucke Horst Laqua Silicone Oil in the Treatment of Complicated Retinal Detachments Techniques, Results, and Complications With 44 Figures (12 in color), and 15 Tables Springer-Verlag Berlin Heidelberg
Klaus Lucke Horst Laqua Silicone Oil in the Treatment of Complicated Retinal Detachments Techniques, Results, and Complications With 44 Figures (12 in color), and 15 Tables Springer-Verlag Berlin Heidelberg
Sorsby's pseudoinflammatory macular dystrophy
 British Journal of Ophthalmology, 1981, 65, 859-865 Sorsby's pseudoinflammatory macular dystrophy A. HOSKIN, K. SEHMI, AND A. C. BIRD From the Department of Clinical Ophthalmology, Institute of Ophthalmology,
British Journal of Ophthalmology, 1981, 65, 859-865 Sorsby's pseudoinflammatory macular dystrophy A. HOSKIN, K. SEHMI, AND A. C. BIRD From the Department of Clinical Ophthalmology, Institute of Ophthalmology,
Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome)
 Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome) John J. Chen MD, PhD; Young H. Kwon MD, PhD August 6, 2012 Chief complaint: Recurrent vitreous hemorrhage,
Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome) John J. Chen MD, PhD; Young H. Kwon MD, PhD August 6, 2012 Chief complaint: Recurrent vitreous hemorrhage,
Intraocular Radiation Therapy for Age-Related Macular Degeneration
 Medical Policy Manual Medicine, Policy No. 134 Intraocular Radiation Therapy for Age-Related Macular Degeneration Next Review: April 2019 Last Review: June 2018 Effective: August 1, 2018 IMPORTANT REMINDER
Medical Policy Manual Medicine, Policy No. 134 Intraocular Radiation Therapy for Age-Related Macular Degeneration Next Review: April 2019 Last Review: June 2018 Effective: August 1, 2018 IMPORTANT REMINDER
Pathology of the lens
 Pathology of the lens Carol Naranjo, LV, DACVP, DECVP, PhD IDEXX Laboratories Embryonal development Gelatt s Veterinary Ophthalmology, 5th Ed. Normal histology Lens capsule Anterior > posterior Lens cortex
Pathology of the lens Carol Naranjo, LV, DACVP, DECVP, PhD IDEXX Laboratories Embryonal development Gelatt s Veterinary Ophthalmology, 5th Ed. Normal histology Lens capsule Anterior > posterior Lens cortex
Fixing Retinal Detachments Simple and Complex. Avoiding a Dark Day in Surgery
 Fixing Retinal Detachments Simple and Complex Avoiding a Dark Day in Surgery Phakic inferior RD with hole in lattice degeneration and a demarcation line Management? Phakic macula-on RD with lattice degeneration
Fixing Retinal Detachments Simple and Complex Avoiding a Dark Day in Surgery Phakic inferior RD with hole in lattice degeneration and a demarcation line Management? Phakic macula-on RD with lattice degeneration
Dr/ Marwa Abdellah EOS /16/2018. Dr/ Marwa Abdellah EOS When do you ask Fluorescein angiography for optic disc diseases???
 When do you ask Fluorescein angiography for optic disc diseases??? 1 NORMAL OPTIC DISC The normal optic disc on fluorescein angiography is fluorescent due to filling of vessels arising from the posterior
When do you ask Fluorescein angiography for optic disc diseases??? 1 NORMAL OPTIC DISC The normal optic disc on fluorescein angiography is fluorescent due to filling of vessels arising from the posterior
Natural history of retinopathy of prematurity
 British Journal of Ophthalmology, 1987, 71, 837-843 Natural history of retinopathy of prematurity W E SCHULENBURG, A PRENDIVILLE, AND R OHRI From the Departments of Surgery and Paediatrics, Hammersmith
British Journal of Ophthalmology, 1987, 71, 837-843 Natural history of retinopathy of prematurity W E SCHULENBURG, A PRENDIVILLE, AND R OHRI From the Departments of Surgery and Paediatrics, Hammersmith
generalized neurofibromatosis
 Brit. 7. Ophthal. (I972) 56, 487 Glial hamartoma of the retina in generalized neurofibromatosis von Recklinghausen's disease L. J. MNIARTYN AND D. L. KNOX From the li'ilmer Institute, the Johns Hopkins
Brit. 7. Ophthal. (I972) 56, 487 Glial hamartoma of the retina in generalized neurofibromatosis von Recklinghausen's disease L. J. MNIARTYN AND D. L. KNOX From the li'ilmer Institute, the Johns Hopkins
Retinal Tears and Detachments
 Retinal Tears and Detachments Understanding Retinal Problems When your eyes are working well, it s easy to take them for granted. But a tear or detachment of your eye s retina (the light-sensing lining
Retinal Tears and Detachments Understanding Retinal Problems When your eyes are working well, it s easy to take them for granted. But a tear or detachment of your eye s retina (the light-sensing lining
Case report 12/10/2014. Delphine Lam ; Dr Mayer Srour Service d ophtalmologie Professeur E.Souied Université Paris Est
 Case report 12/10/2014 Delphine Lam ; Dr Mayer Srour Service d ophtalmologie Professeur E.Souied Medical history Man, 75 years old Complaint: Vision loss in left eye in June 2014 Past ophthalmologic history:
Case report 12/10/2014 Delphine Lam ; Dr Mayer Srour Service d ophtalmologie Professeur E.Souied Medical history Man, 75 years old Complaint: Vision loss in left eye in June 2014 Past ophthalmologic history:
Epiretinal Membrane Formation in Terson Syndrome
 ESEVIER Epiretinal Membrane Formation in Terson Syndrome Masahiko Yokoi, Manabu Kase, Toshiki Hyodo, Midori Horimoto, Fumihiko Kitagawa and Renpei Nagata Department of Ophthalmology, Teine Keijinkai Hospital,
ESEVIER Epiretinal Membrane Formation in Terson Syndrome Masahiko Yokoi, Manabu Kase, Toshiki Hyodo, Midori Horimoto, Fumihiko Kitagawa and Renpei Nagata Department of Ophthalmology, Teine Keijinkai Hospital,
RETINITIS PIGMENTOSA* A NEW THERAPEUTIC APPROACH
 Brit. J. Ophthal. (1963) 47, 144. RETINITIS PIGMENTOSA* A NEW THERAPEUTIC APPROACH BY LALIT P. AGARWAL, S. R. K. MALIK, MADAN MOHAN, AND P. R. KARWAL From the Department of Ophthalmology, All-India Institute
Brit. J. Ophthal. (1963) 47, 144. RETINITIS PIGMENTOSA* A NEW THERAPEUTIC APPROACH BY LALIT P. AGARWAL, S. R. K. MALIK, MADAN MOHAN, AND P. R. KARWAL From the Department of Ophthalmology, All-India Institute
n Corneal epithelium is derived from surface ectoderm n Composed of stratified squamous epith. n 5% of total corneal thickness (50-90micro m thick)
 Cornea overview Dr. Sarita Tuladhar MD, Ophthalmology Gandaki Medical College Embryology CORNEA: n Corneal epithelium is derived from surface ectoderm n Corneal stroma, descement memb, bowman s layer,
Cornea overview Dr. Sarita Tuladhar MD, Ophthalmology Gandaki Medical College Embryology CORNEA: n Corneal epithelium is derived from surface ectoderm n Corneal stroma, descement memb, bowman s layer,
Fixing Retinal Detachments Simple and Complex. Avoiding a Dark Day in Surgery
 Fixing Retinal Detachments Simple and Complex Avoiding a Dark Day in Surgery Phakic inferior RD with hole in lattice degeneration and a demarcation line Management? Phakic macula-on RD with lattice degeneration
Fixing Retinal Detachments Simple and Complex Avoiding a Dark Day in Surgery Phakic inferior RD with hole in lattice degeneration and a demarcation line Management? Phakic macula-on RD with lattice degeneration
DOME SHAPED MACULOPATHY. Ιωάννης Ν. Βαγγελόπουλος Χειρ. Οφθαλμίατρος - Βόλος
 DOME SHAPED MACULOPATHY Ιωάννης Ν. Βαγγελόπουλος Χειρ. Οφθαλμίατρος - Βόλος DOME SHAPED MACULOPATHY-DEFINITIONS The entity Dome Shaped Macula ( DSM ) was first described by Gaucher and associates in 2008
DOME SHAPED MACULOPATHY Ιωάννης Ν. Βαγγελόπουλος Χειρ. Οφθαλμίατρος - Βόλος DOME SHAPED MACULOPATHY-DEFINITIONS The entity Dome Shaped Macula ( DSM ) was first described by Gaucher and associates in 2008
Shaken Baby Syndrome (SBS) Ocular Findings with Legal Implications
 United States and Canadian Academy of Pathology 2007 Annual Meeting Shaken Baby Syndrome (SBS) Ocular Findings with Legal Implications J. Douglas Cameron, MD Professor of Ophthalmology Mayo Clinic School
United States and Canadian Academy of Pathology 2007 Annual Meeting Shaken Baby Syndrome (SBS) Ocular Findings with Legal Implications J. Douglas Cameron, MD Professor of Ophthalmology Mayo Clinic School
surgery Macular puckers after retinal detachment and loss of the macular reflex with a greyish appearance of the macula
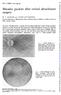 Brit. J. Ophthal. (97 ) 55, 451 Macular puckers after retinal detachment surgery W. S. HAGLER AND UPAL ATURALYA* From the Department of Ophthalmology, Emory University School of Medicine, and Emory University
Brit. J. Ophthal. (97 ) 55, 451 Macular puckers after retinal detachment surgery W. S. HAGLER AND UPAL ATURALYA* From the Department of Ophthalmology, Emory University School of Medicine, and Emory University
RED KRYPTON AND BLUE-GREEN ARGON PANRETINAL LASER PHOTOCOAGULATION FOR PROLIFERATIVE DIABETIC RETINOPATHY: A LABORATORY AND CLINICAL COMPARISON*
 967 RED KRYPTON AND BLUE-GREEN ARGON PANRETINAL LASER PHOTOCOAGULATION FOR PROLIFERATIVE DIABETIC RETINOPATHY: A LABORATORY AND CLINICAL COMPARISON* BY George W. Blankenship, MD INTRODUCTION SHORTLY AFrER
967 RED KRYPTON AND BLUE-GREEN ARGON PANRETINAL LASER PHOTOCOAGULATION FOR PROLIFERATIVE DIABETIC RETINOPATHY: A LABORATORY AND CLINICAL COMPARISON* BY George W. Blankenship, MD INTRODUCTION SHORTLY AFrER
Repairing Macular Hole and Macular Pucker
 Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/revealing-retina/repairing-macular-hole-and-macular-pucker/3924/
Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/revealing-retina/repairing-macular-hole-and-macular-pucker/3924/
IN NICU OCT UTILIZES A CONCEPT KNOWN AS INTERFEROMETRY APPLICATIONS FOR OCT THE PRIMARY USE IN THE EYE - RETINA
 2016 25 YEARS OF OPTICAL COHERENCE TOMOGRAPHY OPTICAL COHERENCE TOMOGRAPHY IN NICU Marcin Stopa, MD, PhD, FEBO Department of Ophthalmology, Chair of Ophthalmology and Optometry. Poznan University of Medical
2016 25 YEARS OF OPTICAL COHERENCE TOMOGRAPHY OPTICAL COHERENCE TOMOGRAPHY IN NICU Marcin Stopa, MD, PhD, FEBO Department of Ophthalmology, Chair of Ophthalmology and Optometry. Poznan University of Medical
Pigmented lesions of the
 Pigmented lesions of the choroid and retina are commonly encountered by optometrists in everyday practice. The increasing use of retinal imaging and indirect ophthalmoscopy among community optometrists
Pigmented lesions of the choroid and retina are commonly encountered by optometrists in everyday practice. The increasing use of retinal imaging and indirect ophthalmoscopy among community optometrists
Infra-red transillumination stereophotography of the iris in Fuchs's heterochromic cyclitis
 British Journal of Ophthalmology, 1978, 62, 110-115 Infra-red transillumination stereophotography of the iris in Fuchs's heterochromic cyclitis M. SAARI, I. VUORRE, AND H. NIEMINEN From the University
British Journal of Ophthalmology, 1978, 62, 110-115 Infra-red transillumination stereophotography of the iris in Fuchs's heterochromic cyclitis M. SAARI, I. VUORRE, AND H. NIEMINEN From the University
Retina Center of Oklahoma Sam S. Dahr, M.D. Adult Intraocular Tumors
 Adult Intraocular Tumors Sam S. Dahr, M.D. Retina Center of Oklahoma www.retinacenteroklahoma.com www.rcoklahoma.com Table of Contents Posterior uveal malignant melanoma Uveal metastasis Uveal melanoma
Adult Intraocular Tumors Sam S. Dahr, M.D. Retina Center of Oklahoma www.retinacenteroklahoma.com www.rcoklahoma.com Table of Contents Posterior uveal malignant melanoma Uveal metastasis Uveal melanoma
Intraocular foreign bodies (IOFB) are a. Intraocular foreign bodies. Factors influencing final visual outcome. Patients and Methods
 Intraocular foreign bodies. Factors influencing final visual outcome Christophe Chiquet 1, Jean-Christophe Zech 1, Philippe Denis 1, Patrice Adeleine 2 and Christiane Trepsat 1 Department of Ophthalmology
Intraocular foreign bodies. Factors influencing final visual outcome Christophe Chiquet 1, Jean-Christophe Zech 1, Philippe Denis 1, Patrice Adeleine 2 and Christiane Trepsat 1 Department of Ophthalmology
Insertion of an epiretinal prosthesis for retinitis pigmentosa
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Insertion of an epiretinal prosthesis for retinitis pigmentosa Retinitis pigmentosa is a disease that affects
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Insertion of an epiretinal prosthesis for retinitis pigmentosa Retinitis pigmentosa is a disease that affects
Ocular imaging in acquired retinopathy with multiple myeloma
 Ocular imaging in acquired retinopathy with multiple myeloma ABDELRAHMAN GABER SALMAN MD- FRCS (GLASG)- MRCS (ED) ASSOCIATE PROFESSOR AIN SHAMS UNIVERSITY EVRS 2015 Immunogammopathies Immunogammopathies
Ocular imaging in acquired retinopathy with multiple myeloma ABDELRAHMAN GABER SALMAN MD- FRCS (GLASG)- MRCS (ED) ASSOCIATE PROFESSOR AIN SHAMS UNIVERSITY EVRS 2015 Immunogammopathies Immunogammopathies
RETINAL CONDITIONS RETINAL CONDITIONS
 GENERAL INFORMATION RETINAL CONDITIONS RETINAL CONDITIONS WHAT ARE RETINAL CONDITIONS? Retinal conditions affect the light-sensitive tissue at the back of eye known as the retina. They include diseases
GENERAL INFORMATION RETINAL CONDITIONS RETINAL CONDITIONS WHAT ARE RETINAL CONDITIONS? Retinal conditions affect the light-sensitive tissue at the back of eye known as the retina. They include diseases
Progressive Symptomatic Retinal Detachment Complicating Retinoschisis. Initial Reporting Questionnaire
 Progressive Symptomatic Retinal Detachment Complicating Retinoschisis In association with the British Ophthalmological Surveillance Unit Ethics ref: 13/NW/0037 Initial Reporting Questionnaire Case Definition:
Progressive Symptomatic Retinal Detachment Complicating Retinoschisis In association with the British Ophthalmological Surveillance Unit Ethics ref: 13/NW/0037 Initial Reporting Questionnaire Case Definition:
investigative ophthalmology & visual science
 MAY 1977 Vol. 16/5 investigative ophthalmology & visual science A Journal of Clinical and Basic Research National Eye Institute Symposium on Experimental Pathology Part II October 15, 1976 Bethesda, Maryland
MAY 1977 Vol. 16/5 investigative ophthalmology & visual science A Journal of Clinical and Basic Research National Eye Institute Symposium on Experimental Pathology Part II October 15, 1976 Bethesda, Maryland
Aphakic retinal detachment
 British Journal of Ophthalmology, 1985, 69, 737-741 R LE MESURIER, S VICKERS, S BOOTH-MASON, AND A H CHIGNELL From the Ophthalmic Department, St Thomas's Hospital, London SE] 7EH SUMMARY A study of 132
British Journal of Ophthalmology, 1985, 69, 737-741 R LE MESURIER, S VICKERS, S BOOTH-MASON, AND A H CHIGNELL From the Ophthalmic Department, St Thomas's Hospital, London SE] 7EH SUMMARY A study of 132
Uveal Melanoma. Protocol applies to malignant melanoma of the uvea.
 Uveal Melanoma Protocol applies to malignant melanoma of the uvea. Protocol revision date: January 2005 Based on AJCC/UICC TNM, 6 th edition Procedures Cytology (No Accompanying Checklist) Biopsy (No Accompanying
Uveal Melanoma Protocol applies to malignant melanoma of the uvea. Protocol revision date: January 2005 Based on AJCC/UICC TNM, 6 th edition Procedures Cytology (No Accompanying Checklist) Biopsy (No Accompanying
