August 2018 Imaging Case of the Month: Dyspnea in a 55-Year-Old Smoker. Michael B. Gotway, MD
|
|
|
- Polly Bradford
- 5 years ago
- Views:
Transcription
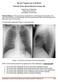
1 August 2018 Imaging Case of the Month: Dyspnea in a 55-Year-Old Smoker Michael B. Gotway, MD Department of Radiology Mayo Clinic Arizona Scottsdale, AZ USA Clinical History: A 55 year old woman presented to the emergency room with complaints of shortness of breath and lower extremity swelling. The patient noted her shortness of breath had been worsening over the previous 6 months, especially in the last 3 months. The patient denies cough, fever, chills, and night sweats. The patient admits to some fatigue but has not lost weight recently. The patient is a current smoker, averaging about 1 pack-per-day for the previous 40 years. Her allergies include penicillin and sulfa drugs, and her prior medical history was remarkable only for hypothyroidism and gastroesophageal reflux. Her only previous surgery was for an ectopic pregnancy. The patient s mediation list included use of opiates for pain related to a herniated disc in the lower cervical spine following an automobile accident two years earlier. Her physical examination was unremarkable aside from obesity and mild symmetric lower extremity edema. Her vital signs were within normal limits. Frontal and lateral chest radiography (Figure 1) was performed. Figure 1. Frontal (A) and lateral (B) chest radiography. Which of the following represents the most accurate assessment of the chest radiographic findings? 1. Chest radiography shows a mediastinal mass 2. Chest radiography shows cavitary pulmonary lesions 3. Chest radiography shows miliary nodules 4. Chest radiography shows an interstitial abnormality consisting of reticular and nodular opacities 5. Chest radiography shows basilar fibrotic opacities Southwest Journal of Pulmonary and Critical Care/2018/Volume 17 59
2 4. Chest radiography shows an interstitial abnormality consisting of reticular and nodular opacities The frontal and lateral chest radiograph show fairly symmetric, bilateral linear, reticular, and faintly nodular opacities without a clear zonal distribution. While some nodular elements are evident, the pattern is not that of miliary disease. Some linear opacities with some faint architectural distortion may be evident, the appearance is not the basilar, peripheral or frankly subpleural reticulation associated with low lung volumes that directly suggests basal fibrotic lung disease; note that the lung volumes in Figure 1 appear relatively normal. No mediastinal mass is evident. The heart size is upper normal, but the cardiomediastinal contour is otherwise unremarkable. No evidence of cavitary lung disease is present. At this point, which of the following represents the most appropriate step in this patient s management? FDG-PET scan 2. Bronchoscopy with transbronchial biopsy 3. High-resolution chest CT (HRCT) 4. Comparison to prior studies 5. More than one of the above Southwest Journal of Pulmonary and Critical Care/2018/Volume 17 60
3 5. More than one of the above The best answer may be comparison to prior studies, which is always the first step when evaluating an imaging abnormality. Nevertheless, high-resolution chest CT is also a reasonable choice, because the imaging findings is compelling and probably merit investigation in this symptomatic patient regardless of the chronicity as documented by comparison with prior chest radiographs. Even bronchoscopy with transbronchial biopsy is not wholly unreasonable as an interstitial abnormality associated with respiratory symptoms is present, but a tissue diagnosis is probably still premature at this point. 18 FDG-PET scanning in not appropriate, however. Typically, 18 FDG-PET scanning is used to investigate solitary pulmonary nodules or to stage patients with malignancies, and is not typically employed for the evaluation of interstitial lung abnormalities. Prior chest radiography from 5 years earlier (Figure 2) was located. Figure 2. A comparison frontal chest radiograph performed 5 years earlier. Which of the following represents the most accurate assessment of the current and prior chest radiographic findings? 1. Chest radiography shows that the findings seen at the presentation chest radiograph (Figure 1) are chronic and unchanged 2. Chest radiography shows that the findings seen at the presentation chest radiograph (Figure 1) are new 3. Chest radiography shows that the findings seen at the presentation chest radiograph (Figure 1) are chronic but have improved 4. Chest radiography shows that the findings seen at the presentation chest radiograph (Figure 1) have evolved from areas of consolidation previously 5. Chest radiography shows that the findings seen at the presentation chest radiograph (Figure 1) have progressed significantly Southwest Journal of Pulmonary and Critical Care/2018/Volume 17 61
4 2. Chest radiography shows that the findings seen at the presentation chest radiograph (Figure 1) are new The chest radiograph performed 5 years earlier (Figure 2) is essentially normal; therefore, the abnormalities noted at the presentation chest radiograph (Figure 1) are entirely new. The patient underwent pulmonary function testing, which showed slight reductions in the forced vital capacity and forced expiratory volume in one second, and she showed exercised-induced desaturation to 88% on room air with exercise. At this point, which of the following represents the most appropriate step in this patient s management? FDG-PET scan 2. Bronchoscopy with transbronchial biopsy 3. High-resolution chest CT (HRCT) 4. Thoracic MRI Ga-Dotatate scan Southwest Journal of Pulmonary and Critical Care/2018/Volume 17 62
5 3. High-resolution chest CT (HRCT) Thoracic MRI and 18 FDG-PET scanning typically do not play a role in the evaluation of interstitial lung abnormalities. As noted above, bronchoscopy with transbronchial biopsy is not unreasonable, but is probably premature when non-invasive imaging characterization of the pulmonary process with high-resolution chest CT (HRCT) has not yet been performed. 68 Ga-Dotatate scans are typically employed for the evaluation and staging of neuroendocrine malignancies. HRCT may provide information that allows a definitive diagnosis for the findings noted at chest radiography, or at least narrows the differential diagnostic considerations somewhat, and may be able to offer information regarding the best route for obtaining a tissue diagnosis. The patient underwent high-resolution chest CT (Figure 3). Figure 3. Representative views of axial enhanced thoracic CT displayed in lung windows. Which of the following represents the most accurate assessment of the highresolution chest CT findings? 1. HRCT shows numerous small, somewhat randomly scattered nodules 2. HRCT shows basilar reticular abnormalities with architectural distortion, suggesting fibrotic lung disease 3. HRCT shows multifocal bronchiectasis 4. HRCT shows multifocal cavitary consolidation 5. HRCT shows multifocal ground-glass opacity Southwest Journal of Pulmonary and Critical Care/2018/Volume 17 63
6 1. HRCT shows numerous small, somewhat randomly scattered nodules The HRCT study shows multiple small, somewhat randomly distributed nodules, all less than 1 cm in size. Areas if irregular, non-septal linear and reticular opacities are also present. No clear bronchiectasis or areas of ground-glass opacity are seen. There is no evidence of consolidation, although several faintly seen foci that appear somewhat cystic are evident, but these areas are unassociated with consolidation. Which of the following is the least appropriate consideration for the findings on this thoracic CT scan? 1. Hematogenous ( miliary ) infection 2. Viral bronchopneumonia 3. Sarcoidosis 4. Langerhans cell histiocytosis 5. Lymphocytic interstitial pneumonia Southwest Journal of Pulmonary and Critical Care/2018/Volume 17 64
7 1. Hematogenous ( miliary ) infection The small nodules present are very non-specific, and, while their distribution is somewhat random, the nodules are not the typical size associated with hematogenous dissemination of infection, also often referred to as miliary disease. Miliary nodules are typically about 2 mm in size, far more profuse in number, and more widely distributed throughout the lungs (Figure 4), whereas the nodules in Figure 3 are far fewer in number and somewhat spare the bases. Figure 4. High-resolution chest CT (A-D) of hematogenously disseminated nodules, or miliary disease- numerous small nodules ranging in size from 1-3 mm equally distributed throughout the lungs (upper, mid, and lower lobes, centrally and peripherally) bilaterally. E, photograph of millet seeds. Some of the nodules are subpleural and the nodules are upper lobe predominant, and therefore sarcoidosis does merit some consideration. Viral bronchopneumonia may present in a wide variety of ways, often as a more clear-cut bronchopneumonia pattern, but occasionally as non-specific smaller nodules. Similarly, lymphocytic interstitial pneumonia (LIP) may present in a very non-specific fashion. Typically, the diagnosis of LIP is often associated with multiple, bilateral, thin-walled cysts, but LIP may present in numerous ways, including areas of ground-glass opacity, which may be centrilobular, as mild septal thickening, or small nodules that may be perifissural or peribronchovascular in distribution; these presentations are very non-specific. Langerhans cell histiocytosis often presents as upper lobe predominant bizarre-shaped cysts that evolve from nodules that cavitated, so, while non-specific, the nodules on the thoracic CT in Figure 3 could be consistent with that diagnosis. At this point, which of the following represents the most appropriate step in this patient s management? 1. Bronchoscopy with transbronchial biopsy 2. Follow-up thoracic CT 3. Upper endoscopy 4. Surgical lung biopsy 5. Pleuroscopy Southwest Journal of Pulmonary and Critical Care/2018/Volume 17 65
8 1. Bronchoscopy with transbronchial biopsy The HRCT findings are non-specific and suggest a small nodular and interstitial abnormality that may be diagnosable with bronchoscopy with transbronchial biopsy. Surgical lung biopsy could also provide a diagnosis, but is needlessly invasive when transbronchial biopsy has not yet been performed. Follow up thoracic is unlikely to yield useful information. If the abnormalities noted at the presentation thoracic CT progress, then the need for a tissue diagnosis is reaffirmed. In contrast, a conservative approach could be pursued if the abnormalities regress, but this possibility is unlikely. Upper endoscopy could be useful for sampling mediastinal abnormalities in a periesophageal location, but no such tissue intervention targets are present. Finally, as no pleural space abnormalities are evident, pleuroscopy is not indicated. The patient underwent bronchoscopy with transbronchial biopsy. The airways appeared normal, and no evidence of malignancy was noted on cytology review. No active inflammation was noted and no granulomas were seen. Cultures were negative, although 1+ Aspergillus species was noted, but thought to be a contaminant. The patient reported that she felt somewhat better, although her shortness of breath persisted. At this point, which of the following represents the most appropriate step in this patient s management? FDG PET 2. Repeat bronchoscopy with transbronchial biopsy and possibly lymph node biopsy with endobronchial ultrasound 3. Surgical lung biopsy 4. Serial follow up HRCT 5. CT pulmonary angiography Southwest Journal of Pulmonary and Critical Care/2018/Volume 17 66
9 3. Surgical lung biopsy The patient underwent bronchoscopy with transbronchial biopsy and that procedure was uneventful and without complication; repeating the exam is unlikely to provide new actionable information, particularly as no clear lymphadenopathy is present. As noted previously, 18 FDG-PET scanning is typically employed for staging malignancies and evaluating solitary pulmonary nodules, and not for the investigation of interstitial abnormalities. The absence of tracer utilization within the lung parenchymal abnormalities at 18 FDG-PET scanning in this patient would not obviate the need for a tissue diagnosis, whereas the presence of tracer uptake within the pulmonary abnormalities would merely reaffirm the need for such; therefore, 18 FDG-PET scanning is unlikely to provide management-altering information for this patient. Repeating the HRCT, or performing a repeat thoracic CT using pulmonary angiographic technique, would also probably not provide useful information in a patient with multifocal interstitial abnormalities and significant respiratory symptoms; indeed, the lung parenchymal findings are unlikely to be the result of thromboembolic disease. At this point, surgical lung biopsy is an indicated procedure. The patient underwent repeat chest CT (Figure 5). Figure 5. Axial enhanced thoracic CT displayed in lung windows performed 1 month after the presentation thoracic CT (Figure 3). Southwest Journal of Pulmonary and Critical Care/2018/Volume 17 67
10 Which of the following represents the most accurate assessment of the repeat highresolution chest CT findings? 1. The repeat HRCT shows numerous small, somewhat randomly scattered nodules unchanged from the previous thoracic CT (Figure 3) 2. The repeat HRCT shows worsening of the nodular and cystic abnormalities seen at the presentation thoracic CT (Figure 3) 3. The repeat HRCT shows improvement in the nodular and cystic abnormalities seen at the presentation thoracic CT (Figure 3) 4. The repeat HRCT shows new mediastinal and peribronchial lymph node enlargement 5. The repeat HRCT shows development of new multifocal ground-glass opacity and consolidation Southwest Journal of Pulmonary and Critical Care/2018/Volume 17 68
11 1. The repeat HRCT shows numerous small, somewhat randomly scattered nodules unchanged from the previous thoracic CT (Figure 3) The patient was referred to cardiothoracic surgery for surgical lung biopsy. Videoassisted thoracoscopic lung biopsy was attempted, but, owing to technical difficulties and inability to obtain adequate one-lung ventilation, was converted to an open thoracotomy for lung biopsy. Histopathological material obtained from lingular biopsy showed active smoking-related changes with cysts and stellate nodules consistent with both active and inactive Langerhans cell histiocytosis. Diagnosis: Pulmonary Langerhans Cell Histiocytosis References 1. Seaman DM, Meyer CA, Gilman MD, McCormack FX. Diffuse cystic lung disease at high-resolution CT. AJR Am J Roentgenol. 2011; 196(6): [CrossRef] [PubMed] 2. Seely JM, Salahudeen S Sr, Cadaval-Goncalves AT, Jamieson DH, Dennie CJ, Matzinger FR, Souza CA. Pulmonary Langerhans cell histiocytosis: a comparative study of computed tomography in children and adults. J Thorac Imaging. 2012;27(1): [CrossRef] [PubMed] 3. Sundar KM, Gosselin MV, Chung HL, Cahill BC. Pulmonary Langerhans cell histiocytosis: emerging concepts in pathobiology, radiology, and clinical evolution of disease. Chest. 2003;123(5): [CrossRef] [PubMed] 4. Vassallo R, Harari S, Tazi A. Current understanding and management of pulmonary Langerhans cell histiocytosis. Thorax. 2017;72(10): [CrossRef] [PubMed] 5. Gupta N, Vassallo R, Wikenheiser-Brokamp KA, McCormack FX. Diffuse cystic lung disease. part I. Am J Respir Crit Care Med. 2015;191(12): [CrossRef] [PubMed] 6. Gupta N, Vassallo R, Wikenheiser-Brokamp KA, McCormack FX. Diffuse cystic lung disease. part II. Am J Respir Crit Care Med. 2015;192(1): [CrossRef] [PubMed] 7. Vassallo R, Ryu JH. Pulmonary Langerhans' cell histiocytosis. Clin Chest Med. 2004; 25(3): [CrossRef] [PubMed] Southwest Journal of Pulmonary and Critical Care/2018/Volume 17 69
September 2014 Imaging Case of the Month. Michael B. Gotway, MD. Department of Radiology Mayo Clinic Arizona Scottsdale, AZ
 September 2014 Imaging Case of the Month Michael B. Gotway, MD Department of Radiology Mayo Clinic Arizona Scottsdale, AZ Clinical History: A 57-year-old non-smoking woman presented to her physician as
September 2014 Imaging Case of the Month Michael B. Gotway, MD Department of Radiology Mayo Clinic Arizona Scottsdale, AZ Clinical History: A 57-year-old non-smoking woman presented to her physician as
October 2012 Imaging Case of the Month. Michael B. Gotway, MD Associate Editor Imaging. Department of Radiology Mayo Clinic Arizona Scottsdale, AZ
 October 2012 Imaging Case of the Month Michael B. Gotway, MD Associate Editor Imaging Department of Radiology Mayo Clinic Arizona Scottsdale, AZ Clinical History: A 65-year-old non-smoking woman presented
October 2012 Imaging Case of the Month Michael B. Gotway, MD Associate Editor Imaging Department of Radiology Mayo Clinic Arizona Scottsdale, AZ Clinical History: A 65-year-old non-smoking woman presented
HRCT in Diffuse Interstitial Lung Disease Steps in High Resolution CT Diagnosis. Where are the lymphatics? Anatomic distribution
 Steps in High Resolution CT Diagnosis Pattern of abnormality Distribution of disease Associated findings Clinical history Tomás Franquet MD What is the diagnosis? Hospital de Sant Pau. Barcelona Secondary
Steps in High Resolution CT Diagnosis Pattern of abnormality Distribution of disease Associated findings Clinical history Tomás Franquet MD What is the diagnosis? Hospital de Sant Pau. Barcelona Secondary
Financial disclosure COMMON DIAGNOSES IN HRCT. High Res Chest HRCT. HRCT Pre test. I have no financial relationships to disclose. Anatomy Nomenclature
 Financial disclosure I have no financial relationships to disclose. Douglas Johnson D.O. Cardiothoracic Imaging Gaston Radiology COMMON DIAGNOSES IN HRCT High Res Chest Anatomy Nomenclature HRCT Sampling
Financial disclosure I have no financial relationships to disclose. Douglas Johnson D.O. Cardiothoracic Imaging Gaston Radiology COMMON DIAGNOSES IN HRCT High Res Chest Anatomy Nomenclature HRCT Sampling
INTERSTITIAL LUNG DISEASE. Radhika Reddy MD Pulmonary/Critical Care Long Beach VA Medical Center January 5, 2018
 INTERSTITIAL LUNG DISEASE Radhika Reddy MD Pulmonary/Critical Care Long Beach VA Medical Center January 5, 2018 Interstitial Lung Disease Interstitial Lung Disease Prevalence by Diagnosis: Idiopathic Interstitial
INTERSTITIAL LUNG DISEASE Radhika Reddy MD Pulmonary/Critical Care Long Beach VA Medical Center January 5, 2018 Interstitial Lung Disease Interstitial Lung Disease Prevalence by Diagnosis: Idiopathic Interstitial
Acute and Chronic Lung Disease
 KATHOLIEKE UNIVERSITEIT LEUVEN Faculty of Medicine Acute and Chronic Lung Disease W De Wever, JA Verschakelen Department of Radiology, University Hospitals Leuven, Belgium Clinical utility of HRCT To detect
KATHOLIEKE UNIVERSITEIT LEUVEN Faculty of Medicine Acute and Chronic Lung Disease W De Wever, JA Verschakelen Department of Radiology, University Hospitals Leuven, Belgium Clinical utility of HRCT To detect
11/10/2014. Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective. Radiology
 Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective Radiology Pathology Clinical 1 Role of HRCT Diagnosis Fibrosis vs. inflammation Next step in management Response to treatment
Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective Radiology Pathology Clinical 1 Role of HRCT Diagnosis Fibrosis vs. inflammation Next step in management Response to treatment
Case 1: Question. 1.1 What is the main pattern of this HRCT? 1. Intralobular line 2. Groundglass opacity 3. Perilymphatic nodule
 HRCT WORK SHOP Case 1 Case 1: Question 1.1 What is the main pattern of this HRCT? 1. Intralobular line 2. Groundglass opacity 3. Perilymphatic nodule Case 1: Question 1.2 What is the diagnosis? 1. Hypersensitivity
HRCT WORK SHOP Case 1 Case 1: Question 1.1 What is the main pattern of this HRCT? 1. Intralobular line 2. Groundglass opacity 3. Perilymphatic nodule Case 1: Question 1.2 What is the diagnosis? 1. Hypersensitivity
Cryptogenic Organizing Pneumonia Diagnosis Approach Based on a Clinical-Radiologic-Pathologic Consensus
 Cryptogenic Organizing Pneumonia Diagnosis Approach Based on a Clinical-Radiologic-Pathologic Consensus Poster No.: C-1622 Congress: ECR 2012 Type: Scientific Exhibit Authors: C. Cordero Lares, E. Zorita
Cryptogenic Organizing Pneumonia Diagnosis Approach Based on a Clinical-Radiologic-Pathologic Consensus Poster No.: C-1622 Congress: ECR 2012 Type: Scientific Exhibit Authors: C. Cordero Lares, E. Zorita
T he diagnostic evaluation of a patient with
 546 REVIEW SERIES Challenges in pulmonary fibrosis? 1: Use of high resolution CT scanning of the lung for the evaluation of patients with idiopathic interstitial pneumonias Michael B Gotway, Michelle M
546 REVIEW SERIES Challenges in pulmonary fibrosis? 1: Use of high resolution CT scanning of the lung for the evaluation of patients with idiopathic interstitial pneumonias Michael B Gotway, Michelle M
May 2017 Imaging Case of the Month. Prasad M. Panse, MD and Michael B. Gotway, MD. Department of Radiology Mayo Clinic Arizona Scottsdale, Arizona USA
 May 2017 Imaging Case of the Month Prasad M. Panse, MD and Michael B. Gotway, MD Department of Radiology Mayo Clinic Arizona Scottsdale, Arizona USA Clinical History: A 32-year-old man presented for routine
May 2017 Imaging Case of the Month Prasad M. Panse, MD and Michael B. Gotway, MD Department of Radiology Mayo Clinic Arizona Scottsdale, Arizona USA Clinical History: A 32-year-old man presented for routine
10/17/2016. Nuts and Bolts of Thoracic Radiology. Objectives. Techniques
 Nuts and Bolts of Thoracic Radiology October 20, 2016 Carleen Risaliti Objectives Understand the basics of chest radiograph Develop a system for interpreting chest radiographs Correctly identify thoracic
Nuts and Bolts of Thoracic Radiology October 20, 2016 Carleen Risaliti Objectives Understand the basics of chest radiograph Develop a system for interpreting chest radiographs Correctly identify thoracic
Differential diagnosis
 Differential diagnosis Idiopathic pulmonary fibrosis (IPF) is part of a large family of idiopathic interstitial pneumonias (IIP), one of four subgroups of interstitial lung disease (ILD). Differential
Differential diagnosis Idiopathic pulmonary fibrosis (IPF) is part of a large family of idiopathic interstitial pneumonias (IIP), one of four subgroups of interstitial lung disease (ILD). Differential
Pulmonary Sarcoidosis - Radiological Evaluation
 Original Research Article Pulmonary Sarcoidosis - Radiological Evaluation Jayesh Shah 1, Darshan Shah 2*, C. Raychaudhuri 3 1 Associate Professor, 2 1 st Year Resident, 3 Professor and HOD Radiology Department,
Original Research Article Pulmonary Sarcoidosis - Radiological Evaluation Jayesh Shah 1, Darshan Shah 2*, C. Raychaudhuri 3 1 Associate Professor, 2 1 st Year Resident, 3 Professor and HOD Radiology Department,
PULMONARY TUBERCULOSIS RADIOLOGY
 PULMONARY TUBERCULOSIS RADIOLOGY RADIOLOGICAL MODALITIES Medical radiophotography Radiography Fluoroscopy Linear (conventional) tomography Computed tomography Pulmonary angiography, bronchography Ultrasonography,
PULMONARY TUBERCULOSIS RADIOLOGY RADIOLOGICAL MODALITIES Medical radiophotography Radiography Fluoroscopy Linear (conventional) tomography Computed tomography Pulmonary angiography, bronchography Ultrasonography,
Outline Definition of Terms: Lexicon. Traction Bronchiectasis
 HRCT OF IDIOPATHIC INTERSTITIAL PNEUMONIAS Disclosures Genentech, Inc. Speakers Bureau Tadashi Allen, MD University of Minnesota Assistant Professor Diagnostic Radiology 10/29/2016 Outline Definition of
HRCT OF IDIOPATHIC INTERSTITIAL PNEUMONIAS Disclosures Genentech, Inc. Speakers Bureau Tadashi Allen, MD University of Minnesota Assistant Professor Diagnostic Radiology 10/29/2016 Outline Definition of
Case 1 : Question. 1.1 What is the intralobular distribution? 1. Centrilobular 2. Perilymphatic 3. Random
 Interesting case Case 1 Case 1 : Question 1.1 What is the intralobular distribution? 1. Centrilobular 2. Perilymphatic 3. Random Case 1: Answer 1.1 What is the intralobular distribution? 1. Centrilobular
Interesting case Case 1 Case 1 : Question 1.1 What is the intralobular distribution? 1. Centrilobular 2. Perilymphatic 3. Random Case 1: Answer 1.1 What is the intralobular distribution? 1. Centrilobular
ARDS - a must know. Page 1 of 14
 ARDS - a must know Poster No.: C-1683 Congress: ECR 2016 Type: Authors: Keywords: DOI: Educational Exhibit M. Cristian; Turda/RO Education and training, Edema, Acute, Localisation, Education, Digital radiography,
ARDS - a must know Poster No.: C-1683 Congress: ECR 2016 Type: Authors: Keywords: DOI: Educational Exhibit M. Cristian; Turda/RO Education and training, Edema, Acute, Localisation, Education, Digital radiography,
Common things are common, but not always the answer
 Kevin Conroy, Joe Mackenzie, Stephen Cowie kevin.conroy@nhs.net Respiratory Dept, Darlington Memorial Hospital, Darlington, UK. Common things are common, but not always the answer Case report Cite as:
Kevin Conroy, Joe Mackenzie, Stephen Cowie kevin.conroy@nhs.net Respiratory Dept, Darlington Memorial Hospital, Darlington, UK. Common things are common, but not always the answer Case report Cite as:
June 2013 Pulmonary Case of the Month: Diagnosis Makes a Difference. Lewis J. Wesselius, MD 1 Henry D. Tazelaar, MD 2
 June 2013 Pulmonary Case of the Month: Diagnosis Makes a Difference Lewis J. Wesselius, MD 1 Henry D. Tazelaar, MD 2 Departments of Pulmonary Medicine 1 and Laboratory Medicine and Pathology 2 Mayo Clinic
June 2013 Pulmonary Case of the Month: Diagnosis Makes a Difference Lewis J. Wesselius, MD 1 Henry D. Tazelaar, MD 2 Departments of Pulmonary Medicine 1 and Laboratory Medicine and Pathology 2 Mayo Clinic
Idiopathic Pulmonary of Care
 Chapter 6.1 Living Medical etextbook A Digital Tool at the Point of Care From Projects In Knowledge Pulmonology Idiopathic Pulmonary Fibrosis @Point of Care IPF Case Study: Typical Presentation, Role of
Chapter 6.1 Living Medical etextbook A Digital Tool at the Point of Care From Projects In Knowledge Pulmonology Idiopathic Pulmonary Fibrosis @Point of Care IPF Case Study: Typical Presentation, Role of
Thoracic lung involvement in rheumatoid arthritis: Findings on HRCT
 Thoracic lung involvement in rheumatoid arthritis: Findings on HRCT Poster No.: C-2488 Congress: ECR 2015 Type: Educational Exhibit Authors: R. E. Correa Soto, M. J. Martín Sánchez, J. M. Fernandez 1 1
Thoracic lung involvement in rheumatoid arthritis: Findings on HRCT Poster No.: C-2488 Congress: ECR 2015 Type: Educational Exhibit Authors: R. E. Correa Soto, M. J. Martín Sánchez, J. M. Fernandez 1 1
Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations
 08/30/10 09/26/10 Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations Camila Downey S. Universidad de Chile, School of Medicine, Year VII Harvard University, School of Medicine Sept 17,
08/30/10 09/26/10 Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations Camila Downey S. Universidad de Chile, School of Medicine, Year VII Harvard University, School of Medicine Sept 17,
HYPERSENSITIVITY PNEUMONITIS
 HYPERSENSITIVITY PNEUMONITIS A preventable fibrosis MOSAVIR ANSARIE MB., FCCP INTERSTITIAL LUNG DISEASES A heterogeneous group of non infectious, non malignant diffuse parenchymal disorders of the lower
HYPERSENSITIVITY PNEUMONITIS A preventable fibrosis MOSAVIR ANSARIE MB., FCCP INTERSTITIAL LUNG DISEASES A heterogeneous group of non infectious, non malignant diffuse parenchymal disorders of the lower
Radiologic Approach to Smoking Related Interstitial Lung Disease
 Radiologic Approach to Smoking Related Interstitial Lung Disease Poster No.: C-1854 Congress: ECR 2013 Type: Educational Exhibit Authors: K.-N. Lee, J.-Y. Han, E.-J. Kang, J. Kang; Busan/KR Keywords: Toxicity,
Radiologic Approach to Smoking Related Interstitial Lung Disease Poster No.: C-1854 Congress: ECR 2013 Type: Educational Exhibit Authors: K.-N. Lee, J.-Y. Han, E.-J. Kang, J. Kang; Busan/KR Keywords: Toxicity,
An Introduction to Radiology for TB Nurses
 An Introduction to Radiology for TB Nurses Garold O. Minns, MD September 14, 2017 TB Nurse Case Management September 12 14, 2017 EXCELLENCE EXPERTISE INNOVATION Garold O. Minns, MD has the following disclosures
An Introduction to Radiology for TB Nurses Garold O. Minns, MD September 14, 2017 TB Nurse Case Management September 12 14, 2017 EXCELLENCE EXPERTISE INNOVATION Garold O. Minns, MD has the following disclosures
ARTICLE IN PRESS. Ahuva Grubstein a, Daniele Bendayan b, Ithak Schactman c, Maya Cohen a, David Shitrit b, Mordechai R. Kramer b,
 Respiratory Medicine (2005) 99, 948 954 Concomitant upper-lobe bullous emphysema, lower-lobe interstitial fibrosis and pulmonary hypertension in heavy smokers: report of eight cases and review of the literature
Respiratory Medicine (2005) 99, 948 954 Concomitant upper-lobe bullous emphysema, lower-lobe interstitial fibrosis and pulmonary hypertension in heavy smokers: report of eight cases and review of the literature
TB Radiology for Nurses Garold O. Minns, MD
 TB Nurse Case Management Salina, Kansas March 31-April 1, 2010 TB Radiology for Nurses Garold O. Minns, MD April 1, 2010 TB Radiology for Nurses Highway Patrol Training Center Salina, KS April 1, 2010
TB Nurse Case Management Salina, Kansas March 31-April 1, 2010 TB Radiology for Nurses Garold O. Minns, MD April 1, 2010 TB Radiology for Nurses Highway Patrol Training Center Salina, KS April 1, 2010
Spectrum of Cystic Lung Disease and its Mimics. Kathleen Jacobs MD and Elizabeth Weihe MD UC San Diego Medical Center, Department of Radiology
 Spectrum of Cystic Lung Disease and its Mimics Kathleen Jacobs MD and Elizabeth Weihe MD UC San Diego Medical Center, Department of Radiology No Financial Disclosures Learning Objectives 1. Review the
Spectrum of Cystic Lung Disease and its Mimics Kathleen Jacobs MD and Elizabeth Weihe MD UC San Diego Medical Center, Department of Radiology No Financial Disclosures Learning Objectives 1. Review the
Daria Manos RSNA 2016 RC 401. https://medicine.dal.ca/departments/depar tment-sites/radiology/contact/faculty/dariamanos.html
 Daria Manos RSNA 2016 RC 401 https://medicine.dal.ca/departments/depar tment-sites/radiology/contact/faculty/dariamanos.html STEP1: Is this fibrotic lung disease? STEP 2: Is this a UIP pattern? If yes:
Daria Manos RSNA 2016 RC 401 https://medicine.dal.ca/departments/depar tment-sites/radiology/contact/faculty/dariamanos.html STEP1: Is this fibrotic lung disease? STEP 2: Is this a UIP pattern? If yes:
Bronchioloalveolar Carcinoma Mimicking DILD:
 Bronchioloalveolar Carcinoma Mimicking DILD: A Case Report 1 Ju Young Lee, M.D., In Jae Lee, M.D., Dong Gyu Kim, M.D. 2, Soo Kee Min, M.D. 3, Min-Jeong Kim, M.D., Sung Il Hwang, M.D., Yul Lee, M.D., Sang
Bronchioloalveolar Carcinoma Mimicking DILD: A Case Report 1 Ju Young Lee, M.D., In Jae Lee, M.D., Dong Gyu Kim, M.D. 2, Soo Kee Min, M.D. 3, Min-Jeong Kim, M.D., Sung Il Hwang, M.D., Yul Lee, M.D., Sang
Usual Interstitial pneumonia and Nonspecific Interstitial Pneumonia. Nitra and the Gangs.
 Usual Interstitial pneumonia and Nonspecific Interstitial Pneumonia Nitra and the Gangs. บทน ำและบทท ๓, ๑๐, ๑๒, ๑๓, ๑๔, ๑๕, ๑๗ Usual Interstitial Pneumonia (UIP) Most common & basic pathologic pattern
Usual Interstitial pneumonia and Nonspecific Interstitial Pneumonia Nitra and the Gangs. บทน ำและบทท ๓, ๑๐, ๑๒, ๑๓, ๑๔, ๑๕, ๑๗ Usual Interstitial Pneumonia (UIP) Most common & basic pathologic pattern
Workshop Cyst & Lucency. How to Approach
 Workshop Cyst & Lucency How to Approach To Approach Cystic Lung Disease True cysts? Cavitary disease Cystic bronchiectasis Mosaic attenuation Subpleural cysts Bullae Paraseptal emphysema Honeycombing Birt
Workshop Cyst & Lucency How to Approach To Approach Cystic Lung Disease True cysts? Cavitary disease Cystic bronchiectasis Mosaic attenuation Subpleural cysts Bullae Paraseptal emphysema Honeycombing Birt
Thoracic Manifestations of Sarcoidosis Using Multi-Slice CT
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 9 Ver. II (Sep. 2015), PP 63-68 www.iosrjournals.org Thoracic Manifestations of Sarcoidosis
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 9 Ver. II (Sep. 2015), PP 63-68 www.iosrjournals.org Thoracic Manifestations of Sarcoidosis
Criteria for confident HRCT diagnosis of usual interstitial pneumonia (UIP)
 Criteria for confident HRCT diagnosis of usual interstitial pneumonia (UIP) Assem El Essawy (1) & Amr A. Nassef (٢) Abstract Identification of interstitial pneumonia (IP) was mainly based on histological
Criteria for confident HRCT diagnosis of usual interstitial pneumonia (UIP) Assem El Essawy (1) & Amr A. Nassef (٢) Abstract Identification of interstitial pneumonia (IP) was mainly based on histological
Manish Powari Regional Training Day 10/12/2014
 Manish Powari Regional Training Day 10/12/2014 Large number of different types of Interstitial Lung Disease (ILD). Most are very rare Most patients present with one of a smaller number of commoner diseases
Manish Powari Regional Training Day 10/12/2014 Large number of different types of Interstitial Lung Disease (ILD). Most are very rare Most patients present with one of a smaller number of commoner diseases
Imaging: how to recognise idiopathic pulmonary fibrosis
 REVIEW IDIOPATHIC PULMONARY FIBROSIS Imaging: how to recognise idiopathic pulmonary fibrosis Anand Devaraj Affiliations: Dept of Radiology, St George s Hospital, London, UK. Correspondence: Anand Devaraj,
REVIEW IDIOPATHIC PULMONARY FIBROSIS Imaging: how to recognise idiopathic pulmonary fibrosis Anand Devaraj Affiliations: Dept of Radiology, St George s Hospital, London, UK. Correspondence: Anand Devaraj,
The Imaging Analysis of Pulmonary Sarcodiosis
 www.cancercellresearch.org ISSN: 2161-2609 Article The Imaging Analysis of Pulmonary Sarcodiosis Xin He, Chuanyu Zhang* Department of Radiology, Affiliated Hospital of Qingdao University, Qingdao, China
www.cancercellresearch.org ISSN: 2161-2609 Article The Imaging Analysis of Pulmonary Sarcodiosis Xin He, Chuanyu Zhang* Department of Radiology, Affiliated Hospital of Qingdao University, Qingdao, China
Liebow and Carrington's original classification of IIP
 Liebow and Carrington's original classification of IIP-- 1969 Eric J. Stern MD University of Washington UIP Usual interstitial pneumonia DIP Desquamative interstitial pneumonia BIP Bronchiolitis obliterans
Liebow and Carrington's original classification of IIP-- 1969 Eric J. Stern MD University of Washington UIP Usual interstitial pneumonia DIP Desquamative interstitial pneumonia BIP Bronchiolitis obliterans
Interesting Cases. Pulmonary
 Interesting Cases Pulmonary 54M with prior history of COPD, hep B/C, and possible history of TB presented with acute on chronic dyspnea, and productive cough Hazy opacity overlying the left hemithorax
Interesting Cases Pulmonary 54M with prior history of COPD, hep B/C, and possible history of TB presented with acute on chronic dyspnea, and productive cough Hazy opacity overlying the left hemithorax
Idiopathic interstitial pneumonias (IIPs) are a group of
 SYMPOSIA C. Isabela S. Silva, MD, PhD and Nestor L. Müller, MD, PhD Abstract: The idiopathic interstitial pneumonias (IIPs) are a group of diffuse parenchymal lung diseases of unknown etiology characterized
SYMPOSIA C. Isabela S. Silva, MD, PhD and Nestor L. Müller, MD, PhD Abstract: The idiopathic interstitial pneumonias (IIPs) are a group of diffuse parenchymal lung diseases of unknown etiology characterized
Diagnosis of TB: Radiology David Finlay, MD
 TB Intensive Tyler, Texas June 2-4, 2010 Diagnosis of TB: Radiology David Finlay, MD June 3, 2010 2stages stages- Tuberculosis 1. primary infection 2. reactivation, or post primary disease 2 1 Primary
TB Intensive Tyler, Texas June 2-4, 2010 Diagnosis of TB: Radiology David Finlay, MD June 3, 2010 2stages stages- Tuberculosis 1. primary infection 2. reactivation, or post primary disease 2 1 Primary
Smoking-related Interstitial Lung Diseases: High-Resolution CT Findings
 Smoking-related Interstitial Lung Diseases: High-Resolution CT Findings Poster No.: C-2358 Congress: ECR 2013 Type: Educational Exhibit Authors: V. Cuartero Revilla, M. Nogueras Carrasco, P. Olmedilla
Smoking-related Interstitial Lung Diseases: High-Resolution CT Findings Poster No.: C-2358 Congress: ECR 2013 Type: Educational Exhibit Authors: V. Cuartero Revilla, M. Nogueras Carrasco, P. Olmedilla
The Egyptian Journal of Hospital Medicine (January 2014) Vol. 54, Page 31 35
 The Egyptian Journal of Hospital Medicine (January 2014) Vol. 54, Page 31 35 Pulmonary Langerhans Cell Histiocytosis X Presented with Bilateral Pneumothorax: A Case Report College of Medicine, Taif University,
The Egyptian Journal of Hospital Medicine (January 2014) Vol. 54, Page 31 35 Pulmonary Langerhans Cell Histiocytosis X Presented with Bilateral Pneumothorax: A Case Report College of Medicine, Taif University,
Thoracic Imaging: A Case of Metastatic Adenocarcinoma of Unknown Primary
 January 28, 2009 Thoracic Imaging: A Case of Metastatic Adenocarcinoma of Unknown Primary Kristina Mirabeau-Beale, Harvard Medical School Year III Gillian Lieberman, MD Agenda Introduce Patient RS Discuss
January 28, 2009 Thoracic Imaging: A Case of Metastatic Adenocarcinoma of Unknown Primary Kristina Mirabeau-Beale, Harvard Medical School Year III Gillian Lieberman, MD Agenda Introduce Patient RS Discuss
Chest Radiology Interpretation: Findings of Tuberculosis
 Chest Radiology Interpretation: Findings of Tuberculosis Get out your laptops, smart phones or other devices pollev.com/chestradiology Case #1 1 Plombage Pneumonia Cancer 2 Reading the TB CXR Be systematic!
Chest Radiology Interpretation: Findings of Tuberculosis Get out your laptops, smart phones or other devices pollev.com/chestradiology Case #1 1 Plombage Pneumonia Cancer 2 Reading the TB CXR Be systematic!
How to Analyse Difficult Chest CT
 How to Analyse Difficult Chest CT Complex diseases are:- - Large lesion - Unusual or atypical pattern - Multiple discordant findings Diffuse diseases are:- - Numerous findings in both sides 3 basic steps
How to Analyse Difficult Chest CT Complex diseases are:- - Large lesion - Unusual or atypical pattern - Multiple discordant findings Diffuse diseases are:- - Numerous findings in both sides 3 basic steps
4/17/2010 C ini n ca c l a Ev E a v l a ua u t a ion o n of o ILD U dat a e t e i n I LDs
 Update in ILDs Diagnosis 101: Clinical Evaluation April 17, 2010 Jay H. Ryu, MD Mayo Clinic, Rochester MN Clinical Evaluation of ILD Outline General aspects of ILDs Classification of ILDs Clinical evaluation
Update in ILDs Diagnosis 101: Clinical Evaluation April 17, 2010 Jay H. Ryu, MD Mayo Clinic, Rochester MN Clinical Evaluation of ILD Outline General aspects of ILDs Classification of ILDs Clinical evaluation
Lung Allograft Dysfunction
 Lung Allograft Dysfunction Carlos S. Restrepo M.D. Ameya Baxi M.D. Department of Radiology University of Texas Health San Antonio Disclaimer: We do not have any conflict of interest or financial gain to
Lung Allograft Dysfunction Carlos S. Restrepo M.D. Ameya Baxi M.D. Department of Radiology University of Texas Health San Antonio Disclaimer: We do not have any conflict of interest or financial gain to
5/9/2015. Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective. No, I am not a pulmonologist! Radiology
 Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective No, I am not a pulmonologist! Radiology Pathology Clinical 1 Everyone needs a CT Confidence in diagnosis Definitive HRCT +
Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective No, I am not a pulmonologist! Radiology Pathology Clinical 1 Everyone needs a CT Confidence in diagnosis Definitive HRCT +
Thoracic sarcoidosis: Pictoral review of typical and atypical findings
 Thoracic sarcoidosis: Pictoral review of typical and atypical findings Poster No.: C-0804 Congress: ECR 2010 Type: Educational Exhibit Topic: Chest Authors: A. Ferreira, J. Calha; Lisbon/PT Keywords: Sarcoidosis,
Thoracic sarcoidosis: Pictoral review of typical and atypical findings Poster No.: C-0804 Congress: ECR 2010 Type: Educational Exhibit Topic: Chest Authors: A. Ferreira, J. Calha; Lisbon/PT Keywords: Sarcoidosis,
Thoracic Sarcoidosis Imaging Updated: Jul 19, 2013
 Thoracic Sarcoidosis Imaging Updated: Jul 19, 2013 Overview Radiography Computed Tomography Magnetic Resonance Imaging Nuclear Imaging Show All Multimedia Library References Overview For patients with
Thoracic Sarcoidosis Imaging Updated: Jul 19, 2013 Overview Radiography Computed Tomography Magnetic Resonance Imaging Nuclear Imaging Show All Multimedia Library References Overview For patients with
Tuberculosis: The Essentials
 Tuberculosis: The Essentials Kendra L. Fisher, MD, PhD THORACIC TUBERCULOSIS: THE BARE ESSENTIALS Kendra Fisher MD, FRCP (C) Department of Radiology Loma Linda University Medical Center TUBERCULOSIS ()
Tuberculosis: The Essentials Kendra L. Fisher, MD, PhD THORACIC TUBERCULOSIS: THE BARE ESSENTIALS Kendra Fisher MD, FRCP (C) Department of Radiology Loma Linda University Medical Center TUBERCULOSIS ()
Middle East Respiratory Syndrome-Coronavirus Infection: A Case Report of Serial Computed Tomographic Findings in a Young Male Patient
 Case Report Thoracic Imaging http://dx.doi.org/10.3348/kjr.2016.17.1.166 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2016;17(1):166-170 Middle East Respiratory Syndrome-Coronavirus Infection: A Case
Case Report Thoracic Imaging http://dx.doi.org/10.3348/kjr.2016.17.1.166 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2016;17(1):166-170 Middle East Respiratory Syndrome-Coronavirus Infection: A Case
A Review of Interstitial Lung Diseases. Paul J. Wolters, MD Associate Professor Department of Medicine University of California San Francisco
 A Review of Interstitial Lung Diseases Paul J. Wolters, MD Associate Professor Department of Medicine University of California San Francisco Outline Overview of diagnosis in ILD Why it is important Definition/Classification
A Review of Interstitial Lung Diseases Paul J. Wolters, MD Associate Professor Department of Medicine University of California San Francisco Outline Overview of diagnosis in ILD Why it is important Definition/Classification
An Image Repository for Chest CT
 An Image Repository for Chest CT Francesco Frajoli for the Chest CT in Antibody Deficiency Group An Image Repository for Chest CT he Chest CT in Antibody Deficiency Group is an international and interdisciplinary
An Image Repository for Chest CT Francesco Frajoli for the Chest CT in Antibody Deficiency Group An Image Repository for Chest CT he Chest CT in Antibody Deficiency Group is an international and interdisciplinary
42 yr old male with h/o Graves disease and prior I 131 treatment presents with hyperthyroidism and undetectable TSH. 2 hr uptake 20%, 24 hr uptake 50%
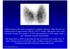 Pinhole images of the neck are acquired in multiple projections, 24hrs after the oral administration of approximately 200 µci of I123. Usually, 24hr uptake value if also calculated (normal 24 hr uptake
Pinhole images of the neck are acquired in multiple projections, 24hrs after the oral administration of approximately 200 µci of I123. Usually, 24hr uptake value if also calculated (normal 24 hr uptake
Pneumocystis jirovecci pneumonia: from mild disease to a real disaster. A pictorial review of the different radiologic patterns in acute settings
 Pneumocystis jirovecci pneumonia: from mild disease to a real disaster. A pictorial review of the different radiologic patterns in acute settings Poster No.: C-1425 Congress: ECR 2017 Type: Educational
Pneumocystis jirovecci pneumonia: from mild disease to a real disaster. A pictorial review of the different radiologic patterns in acute settings Poster No.: C-1425 Congress: ECR 2017 Type: Educational
Adam J. Hansen, MD UHC Thoracic Surgery
 Adam J. Hansen, MD UHC Thoracic Surgery Sometimes seen on Chest X-ray (CXR) Common incidental findings on computed tomography (CT) chest and abdomen done for other reasons Most lung cancers discovered
Adam J. Hansen, MD UHC Thoracic Surgery Sometimes seen on Chest X-ray (CXR) Common incidental findings on computed tomography (CT) chest and abdomen done for other reasons Most lung cancers discovered
Supplemental Figure 1. Gating strategies for flow cytometry and intracellular cytokinestaining
 Supplemental Figure 1. Gating strategies for flow cytometry and intracellular cytokinestaining of PBMCs. Forward scatter area (FSC-A) versus side scatter area (SSC-A) was used to select lymphocytes followed
Supplemental Figure 1. Gating strategies for flow cytometry and intracellular cytokinestaining of PBMCs. Forward scatter area (FSC-A) versus side scatter area (SSC-A) was used to select lymphocytes followed
Typical and atypical findings of pulmonary sarcoidosis at high resolution CT
 Typical and atypical findings of pulmonary sarcoidosis at high resolution CT Poster No.: C-0169 Congress: ECR 2013 Type: Educational Exhibit Authors: L. Raposo Rodríguez, C. Mejía, B. Escobar Mallada,
Typical and atypical findings of pulmonary sarcoidosis at high resolution CT Poster No.: C-0169 Congress: ECR 2013 Type: Educational Exhibit Authors: L. Raposo Rodríguez, C. Mejía, B. Escobar Mallada,
Chest radiograph of an. asymptomatic man. Case report. Case history
 Eleftheria Chaini 1, Niki Giannakou 2, Dimitra Haini 3, Anna Maria Athanassiadou 4, Angelos Tsipis 4, Nikolaos D. Hainis 5 elhaini@otenet.gr 1 Pulmonary Dept, Corfu General Hospital, Kontokali, Greece.
Eleftheria Chaini 1, Niki Giannakou 2, Dimitra Haini 3, Anna Maria Athanassiadou 4, Angelos Tsipis 4, Nikolaos D. Hainis 5 elhaini@otenet.gr 1 Pulmonary Dept, Corfu General Hospital, Kontokali, Greece.
Web Chapter 3. Image Gallery: Lesion detection on low dose chest CT
 Web Chapter 3 Image Gallery: Lesion detection on low dose chest CT Sarabjeet Singh, MD Mannudeep K. Kalra, MD *Eugene J. Mark, MD *James Stone, MD James H. Thrall, MD Department of Radiology and *Department
Web Chapter 3 Image Gallery: Lesion detection on low dose chest CT Sarabjeet Singh, MD Mannudeep K. Kalra, MD *Eugene J. Mark, MD *James Stone, MD James H. Thrall, MD Department of Radiology and *Department
Pulmonary changes induced by radiotherapy. HRCT findings
 Pulmonary changes induced by radiotherapy. HRCT findings Poster No.: C-2299 Congress: ECR 2015 Type: Educational Exhibit Authors: R. E. Correa Soto, M. Albert Antequera, K. Müller Campos, D. 1 2 4 3 1
Pulmonary changes induced by radiotherapy. HRCT findings Poster No.: C-2299 Congress: ECR 2015 Type: Educational Exhibit Authors: R. E. Correa Soto, M. Albert Antequera, K. Müller Campos, D. 1 2 4 3 1
Imaging findings in Hypersensitivity Pneumonitis - a pictorical review.
 Imaging findings in Hypersensitivity Pneumonitis - a pictorical review. Poster No.: C-1655 Congress: ECR 2014 Type: Educational Exhibit Authors: B. M. Araujo, A. F. S. Simões, M. S. C. Rodrigues, J. Pereira;
Imaging findings in Hypersensitivity Pneumonitis - a pictorical review. Poster No.: C-1655 Congress: ECR 2014 Type: Educational Exhibit Authors: B. M. Araujo, A. F. S. Simões, M. S. C. Rodrigues, J. Pereira;
Resident Case Review CHEST. Daria Manos CAR 2016
 Resident Case Review CHEST CAR 2016 Daria Manos Disclosure Speakers bureau, Roche CAR 2016 Daria Manos 1. Recognize common and critical chest radiograph and computed tomography signs and use these clues
Resident Case Review CHEST CAR 2016 Daria Manos Disclosure Speakers bureau, Roche CAR 2016 Daria Manos 1. Recognize common and critical chest radiograph and computed tomography signs and use these clues
A Rare Case of Lymphangioleiomyomatosis in Sri Lanka
 A Rare Case of Lymphangioleiomyomatosis in Sri Lanka Author s Details: (1) Dushantha Madegedara (2) Asela Rasika Bandara (3) Sachini Seneviratne (4) Samadara Nakandala (5) Rathnayake R.M.D.H.M - (1) (2)
A Rare Case of Lymphangioleiomyomatosis in Sri Lanka Author s Details: (1) Dushantha Madegedara (2) Asela Rasika Bandara (3) Sachini Seneviratne (4) Samadara Nakandala (5) Rathnayake R.M.D.H.M - (1) (2)
Atopic Pulmonary Disease: Findings on Thoracic Imaging
 July 2003 Atopic Pulmonary Disease: Findings on Thoracic Imaging Rebecca G. Breslow Harvard Medical School Year IV Churg-Strauss Syndrome Hypersensitivity Pneumonitis Asthma Atopic Pulmonary Disease Allergic
July 2003 Atopic Pulmonary Disease: Findings on Thoracic Imaging Rebecca G. Breslow Harvard Medical School Year IV Churg-Strauss Syndrome Hypersensitivity Pneumonitis Asthma Atopic Pulmonary Disease Allergic
Lung. 10/24/13 Chest X-ray: 2.9 cm mass like density in the inferior lingular segment worrisome for neoplasm. Malignancy cannot be excluded.
 Lung Case Scenario 1 A 54 year white male presents with a recent abnormal CT of the chest. The patient has a history of melanoma, kidney, and prostate cancers. 10/24/13 Chest X-ray: 2.9 cm mass like density
Lung Case Scenario 1 A 54 year white male presents with a recent abnormal CT of the chest. The patient has a history of melanoma, kidney, and prostate cancers. 10/24/13 Chest X-ray: 2.9 cm mass like density
General History. 林陳 珠 Female 69 years old 住院期間 : ~ Chief Complaint : sudden loss of conscious 5 minutes in the morning.
 General History 林陳 珠 Female 69 years old 住院期間 : 93.5.8~93.5.15 Chief Complaint : sudden loss of conscious for 2-52 5 minutes in the morning. General History DM under regular medical control for 10 years.
General History 林陳 珠 Female 69 years old 住院期間 : 93.5.8~93.5.15 Chief Complaint : sudden loss of conscious for 2-52 5 minutes in the morning. General History DM under regular medical control for 10 years.
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Idiopathic Pulmonary Fibrosis Page 1 of 10 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Idiopathic Pulmonary Fibrosis (Esbriet /pirfenidone, Ofev /nintedanib)
Idiopathic Pulmonary Fibrosis Page 1 of 10 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Idiopathic Pulmonary Fibrosis (Esbriet /pirfenidone, Ofev /nintedanib)
A Review of Interstitial Lung Diseases
 Outline A Review of Interstitial Lung Diseases Paul J. Wolters, MD Associate Professor Department of Medicine University of California San Francisco Overview of diagnosis in ILD Why it is important Definition/Classification
Outline A Review of Interstitial Lung Diseases Paul J. Wolters, MD Associate Professor Department of Medicine University of California San Francisco Overview of diagnosis in ILD Why it is important Definition/Classification
CT Findings in the Elderly Lung
 CT Findings in the Elderly Lung Poster No.: C-2498 Congress: ECR 2015 Type: Educational Exhibit Authors: P. Ananias, R. Coelho, H. M. R. Marques, O. Fernandes, M. Simões, L. Figueiredo; Lisbon/PT Keywords:
CT Findings in the Elderly Lung Poster No.: C-2498 Congress: ECR 2015 Type: Educational Exhibit Authors: P. Ananias, R. Coelho, H. M. R. Marques, O. Fernandes, M. Simões, L. Figueiredo; Lisbon/PT Keywords:
Cystic Lung Disease. Cristopher A. Meyer, MD
 Cystic Lung Disease Cristopher A. Meyer, MD Air filled structure with definable wall typically less than 1 mm thick Cris A. Meyer, M.D. Professor of Radiology University of Wisconsin School of Medicine
Cystic Lung Disease Cristopher A. Meyer, MD Air filled structure with definable wall typically less than 1 mm thick Cris A. Meyer, M.D. Professor of Radiology University of Wisconsin School of Medicine
NONE OVERVIEW FINANCIAL DISCLOSURES UPDATE ON IDIOPATHIC PULMONARY FIBROSIS/IPF (UIP) FOR PATHOLOGISTS. IPF = Idiopathic UIP Radiologic UIP Path UIP
 UPDATE ON IDIOPATHIC PULMONARY FIBROSIS/IPF () FOR PATHOLOGISTS Thomas V. Colby, M.D. Professor of Pathology (Emeritus) Mayo Clinic Arizona FINANCIAL DISCLOSURES NONE OVERVIEW IPF Radiologic Dx Pathologic
UPDATE ON IDIOPATHIC PULMONARY FIBROSIS/IPF () FOR PATHOLOGISTS Thomas V. Colby, M.D. Professor of Pathology (Emeritus) Mayo Clinic Arizona FINANCIAL DISCLOSURES NONE OVERVIEW IPF Radiologic Dx Pathologic
Larry Tan, MD Thoracic Surgery, HSC. Community Cancer Care Educational Conference October 27, 2017
 Larry Tan, MD Thoracic Surgery, HSC Community Cancer Care Educational Conference October 27, 2017 To describe patient referral & triage for the patient with suspected lung cancer To describe the initial
Larry Tan, MD Thoracic Surgery, HSC Community Cancer Care Educational Conference October 27, 2017 To describe patient referral & triage for the patient with suspected lung cancer To describe the initial
Eosinophils and effusion: a clinical conundrum
 Ruth Sobala, Kevin Conroy, Hilary Tedd, Salem Elarbi kevin.peter.conroy@gmail.com Respiratory Dept, Queen Elizabeth Hospital, Gateshead, UK. Eosinophils and effusion: a clinical conundrum Case report A
Ruth Sobala, Kevin Conroy, Hilary Tedd, Salem Elarbi kevin.peter.conroy@gmail.com Respiratory Dept, Queen Elizabeth Hospital, Gateshead, UK. Eosinophils and effusion: a clinical conundrum Case report A
Diffuse Interstitial Lung Diseases: Is There Really Anything New?
 : Is There Really Anything New? Sujal R. Desai, MBBS, MD ESTI SPEAKER SUNDAY Society of Thoracic Radiology San Antonio, Texas March 2014 Diffuse Interstitial Lung Disease The State of Play DILDs Is There
: Is There Really Anything New? Sujal R. Desai, MBBS, MD ESTI SPEAKER SUNDAY Society of Thoracic Radiology San Antonio, Texas March 2014 Diffuse Interstitial Lung Disease The State of Play DILDs Is There
New respiratory symptoms and lung imaging findings in a woman with polymyositis
 Maria Bolaki 1, Konstantinos Karagiannis 1, George Bertsias 2, Ioanna Mitrouska 1, Nikolaos Tzanakis 1, Katerina M. Antoniou 1 kantoniou@uoc.gr 1 Dept of Thoracic Medicine, Heraklion University Hospital,
Maria Bolaki 1, Konstantinos Karagiannis 1, George Bertsias 2, Ioanna Mitrouska 1, Nikolaos Tzanakis 1, Katerina M. Antoniou 1 kantoniou@uoc.gr 1 Dept of Thoracic Medicine, Heraklion University Hospital,
Dilemma of Thoracic Tuberculosis Vs. Sarcoidosis in TB Endemic Areas: An Imaging Approach
 Dilemma of Thoracic Tuberculosis Vs. Sarcoidosis in TB Endemic Areas: An Imaging Approach A. S. Bhalla, A. Das, A. GOYAL, P. NARANJE, R. GULERIA, G. C. KHILNANI ALL INDIA INSTITUTE OF MEDICAL SCIENCES
Dilemma of Thoracic Tuberculosis Vs. Sarcoidosis in TB Endemic Areas: An Imaging Approach A. S. Bhalla, A. Das, A. GOYAL, P. NARANJE, R. GULERIA, G. C. KHILNANI ALL INDIA INSTITUTE OF MEDICAL SCIENCES
Progress in Idiopathic Pulmonary Fibrosis
 Progress in Idiopathic Pulmonary Fibrosis David A. Lynch, MB Disclosures Progress in Idiopathic Pulmonary Fibrosis David A Lynch, MB Consultant: t Research support: Perceptive Imaging Boehringer Ingelheim
Progress in Idiopathic Pulmonary Fibrosis David A. Lynch, MB Disclosures Progress in Idiopathic Pulmonary Fibrosis David A Lynch, MB Consultant: t Research support: Perceptive Imaging Boehringer Ingelheim
Pulmonary manifestations of Rheumatoid Arthritis: what is there waiting to be found?
 Pulmonary manifestations of Rheumatoid Arthritis: what is there waiting to be found? Poster No.: C-1795 Congress: ECR 2015 Type: Educational Exhibit Authors: M. S. C. Rodrigues, R. Correia, A. Carvalho,
Pulmonary manifestations of Rheumatoid Arthritis: what is there waiting to be found? Poster No.: C-1795 Congress: ECR 2015 Type: Educational Exhibit Authors: M. S. C. Rodrigues, R. Correia, A. Carvalho,
The Egyptian Journal of Hospital Medicine (July 2017) Vol.68 (2), Page
 The Egyptian Journal of Hospital Medicine (July 2017) Vol.68 (2), Page 1135-1140 Role of High Resolution Computed Tomography in Diagnosis of Interstitial Lung Diseases in Patients with Collagen Diseases
The Egyptian Journal of Hospital Medicine (July 2017) Vol.68 (2), Page 1135-1140 Role of High Resolution Computed Tomography in Diagnosis of Interstitial Lung Diseases in Patients with Collagen Diseases
CT findings of pulmonary nocardiosis: a report of 9 cases
 Original Article on Quantitative Imaging of Thoracic Diseases CT findings of pulmonary nocardiosis: a report of 9 cases Baoliang Liu 1, Yuanlong Zhang 1,2, Jingshan Gong 2, Shubing Jiang 1, Yunkai Huang
Original Article on Quantitative Imaging of Thoracic Diseases CT findings of pulmonary nocardiosis: a report of 9 cases Baoliang Liu 1, Yuanlong Zhang 1,2, Jingshan Gong 2, Shubing Jiang 1, Yunkai Huang
OBJECTIVES. Solitary Solid Spiculated Nodule. What would you do next? Case Based Discussion: State of the Art Management of Lung Nodules.
 Organ Imaging : September 25 2015 OBJECTIVES Case Based Discussion: State of the Art Management of Lung Nodules Dr. Elsie T. Nguyen Dr. Kazuhiro Yasufuku 1. To review guidelines for follow up and management
Organ Imaging : September 25 2015 OBJECTIVES Case Based Discussion: State of the Art Management of Lung Nodules Dr. Elsie T. Nguyen Dr. Kazuhiro Yasufuku 1. To review guidelines for follow up and management
Interpretation of Chest Radiographs Paul Christensen, MD 10/21/09. Diagnostic Evaluation. Medical Evaluation & CXR Interpretation.
 Diagnostic Evaluation Medical Evaluation & CXR Interpretation University of Michigan TB Consultant Washtenaw County Medical history Physical examination Testing for TB exposure (previously covered) Radiologic
Diagnostic Evaluation Medical Evaluation & CXR Interpretation University of Michigan TB Consultant Washtenaw County Medical history Physical examination Testing for TB exposure (previously covered) Radiologic
Thoracic CT pattern in lung cancer: correlation of CT and pathologic diagnosis
 19 th Congress of APSR PG of Lung Cancer (ESAP): Update of Lung Cancer Thoracic CT pattern in lung cancer: correlation of CT and pathologic diagnosis Kazuma Kishi, M.D. Department of Respiratory Medicine,
19 th Congress of APSR PG of Lung Cancer (ESAP): Update of Lung Cancer Thoracic CT pattern in lung cancer: correlation of CT and pathologic diagnosis Kazuma Kishi, M.D. Department of Respiratory Medicine,
Lung Cancer Screening in the Midwest of the US: When Histoplasmosis Complicates the Picture
 Cronicon OPEN ACCESS EC PULMONOLOGY AND RESPIRATORY MEDICINE Case Report Lung Cancer Screening in the Midwest of the US: When Histoplasmosis Complicates the Picture Swan Lee 1 and Rolando Sanchez Sanchez
Cronicon OPEN ACCESS EC PULMONOLOGY AND RESPIRATORY MEDICINE Case Report Lung Cancer Screening in the Midwest of the US: When Histoplasmosis Complicates the Picture Swan Lee 1 and Rolando Sanchez Sanchez
Eun-Young Kang, M.D., Jae Wook Lee, M.D., Ji Yung Choo, M.D., Hwan Seok Yong, M.D., Ki Yeol Lee, M.D., Yu-Whan Oh, M.D.
 Eun-Young Kang, M.D., Jae Wook Lee, M.D., Ji Yung Choo, M.D., Hwan Seok Yong, M.D., Ki Yeol Lee, M.D., Yu-Whan Oh, M.D. Department of Radiology, Korea University Guro Hospital, College of Medicine, Korea
Eun-Young Kang, M.D., Jae Wook Lee, M.D., Ji Yung Choo, M.D., Hwan Seok Yong, M.D., Ki Yeol Lee, M.D., Yu-Whan Oh, M.D. Department of Radiology, Korea University Guro Hospital, College of Medicine, Korea
Diagnostic challenges in IPF
 Medicine, Nursing and Health Sciences Diagnostic challenges in IPF Dr Ian Glaspole Central and Eastern Clinical School, Alfred Hospital and Monash University March 2015 Disclosures Consultancy fees from
Medicine, Nursing and Health Sciences Diagnostic challenges in IPF Dr Ian Glaspole Central and Eastern Clinical School, Alfred Hospital and Monash University March 2015 Disclosures Consultancy fees from
Case Study #2. Case Study #1 cont 9/28/2011. CAPA 2011 Christy Wilson PA C. LH is 78 yowf with PMHx of metz breast CA presents
 Case Study #1 CAPA 2011 Christy Wilson PA C 46 yo female presents with community acquired PNA (CAP). Her condition worsened and she was transferred to the ICU and placed on mechanical ventilation. Describe
Case Study #1 CAPA 2011 Christy Wilson PA C 46 yo female presents with community acquired PNA (CAP). Her condition worsened and she was transferred to the ICU and placed on mechanical ventilation. Describe
Pulmonary Nodules & Masses
 Pulmonary Nodules & Masses A Diagnostic Approach Heber MacMahon The University of Chicago Department of Radiology Disclosure Information Consultant for Riverain Technology Minor equity in Hologic Royalties
Pulmonary Nodules & Masses A Diagnostic Approach Heber MacMahon The University of Chicago Department of Radiology Disclosure Information Consultant for Riverain Technology Minor equity in Hologic Royalties
Cryptogenic Organizing Pneumonia: Serial High-Resolution CT Findings in 22 Patients
 Cardiopulmonary Imaging Original Research Lee et al. High-Resolution CT of Cryptogenic Organizing Pneumonia Cardiopulmonary Imaging Original Research Ju Won Lee 1 Kyung Soo Lee 1 Ho Yun Lee 1 Man Pyo Chung
Cardiopulmonary Imaging Original Research Lee et al. High-Resolution CT of Cryptogenic Organizing Pneumonia Cardiopulmonary Imaging Original Research Ju Won Lee 1 Kyung Soo Lee 1 Ho Yun Lee 1 Man Pyo Chung
Bilateral Chest X-Ray Shadowing and Bilateral leg lesions - A case of Pulmonary Kaposi Sarcoma
 Article ID: WMC005047 ISSN 2046-1690 Bilateral Chest X-Ray Shadowing and Bilateral leg lesions - A case of Pulmonary Kaposi Sarcoma Peer review status: No Corresponding Author: Dr. Mohammad Fawad Khattak,
Article ID: WMC005047 ISSN 2046-1690 Bilateral Chest X-Ray Shadowing and Bilateral leg lesions - A case of Pulmonary Kaposi Sarcoma Peer review status: No Corresponding Author: Dr. Mohammad Fawad Khattak,
IPF: Epidemiologia e stato dell arte
 IPF: Epidemiologia e stato dell arte Clinical Classification Diffuse parenchimal lung diseases Exposure-related: - occupational - environmental - medication Desquamative interstitial pneumonia Idiopathic
IPF: Epidemiologia e stato dell arte Clinical Classification Diffuse parenchimal lung diseases Exposure-related: - occupational - environmental - medication Desquamative interstitial pneumonia Idiopathic
PULMONARY MEDICINE BOARD REVIEW. Financial Conflicts of Interest. Question #1: Question #1 (Cont.): None. Christopher H. Fanta, M.D.
 PULMONARY MEDICINE BOARD REVIEW Christopher H. Fanta, M.D. Pulmonary and Critical Care Division Brigham and Women s Hospital Partners Asthma Center Harvard Medical School Financial Conflicts of Interest
PULMONARY MEDICINE BOARD REVIEW Christopher H. Fanta, M.D. Pulmonary and Critical Care Division Brigham and Women s Hospital Partners Asthma Center Harvard Medical School Financial Conflicts of Interest
Pictorial essay of unusual radiologic manifestations of pulmonary and airway metastasis at initial presentation of lung cancer
 Pictorial essay of unusual radiologic manifestations of pulmonary and airway metastasis at initial presentation of lung cancer Poster No.: C-2297 Congress: ECR 2012 Type: Educational Exhibit Authors: Y.
Pictorial essay of unusual radiologic manifestations of pulmonary and airway metastasis at initial presentation of lung cancer Poster No.: C-2297 Congress: ECR 2012 Type: Educational Exhibit Authors: Y.
Pulmonary fibrosis on the lateral chest radiograph: Kerley D lines revisited
 Insights Imaging (2017) 8:483 489 DOI 10.1007/s13244-017-0565-2 PICTORIAL REVIEW Pulmonary fibrosis on the lateral chest radiograph: Kerley D lines revisited Daniel B. Green 1 & Alan C. Legasto 1 & Ian
Insights Imaging (2017) 8:483 489 DOI 10.1007/s13244-017-0565-2 PICTORIAL REVIEW Pulmonary fibrosis on the lateral chest radiograph: Kerley D lines revisited Daniel B. Green 1 & Alan C. Legasto 1 & Ian
