A role for CCR4 in development of mature circulating cutaneous T helper memory cell populations
|
|
|
- Dwight Wiggins
- 5 years ago
- Views:
Transcription
1 A role for CCR4 in development of mature circulating cutaneous T helper memory cell populations Espen S. Baekkevold, 1,2,3 Marc-André Wurbel, 1,2 Pia Kivisäkk 1,2 Clare M. Wain, 1,2 Christine A. Power, 4 Guttorm Haraldsen, 3 and James J. Campbell 1,2 1 Children s Hospital, Joint Program in Transfusion Medicine and 2 Department of Pathology, Harvard Medical School, Boston, MA Institute of Pathology, University of Oslo, Rikshospitalet University Hospital, Oslo N-0027, Norway 4 Serono Pharmaceutical Research Institute, Geneva CH 1228, Switzerland The Journal of Experimental Medicine CORRESPONDENCE James J. Campbell: james.campbell@ childrens.harvard.edu Expression of the chemokine receptor CCR4 is strongly associated with trafficking of specialized cutaneous memory T helper (Th) lymphocytes to the skin. However, it is unknown whether CCR4 itself participates in the development of cutaneous Th populations. We have addressed this issue via competitive bone marrow (BM) reconstitution assays; equal numbers of BM cells from CCR4 / and CCR4 / donors were allowed to develop side-by-side within RAG-1 / hosts. Cells from both donor types developed equally well into B cells, naive CD8 T cells, naive CD4 T cells, interferon- Th1 cells, and interleukin-4 Th2 cells. In marked contrast, circulating cutaneous memory Th cells (i.e., E-selectin ligand [E-lig ]) were more than fourfold more likely to be derived from CCR4 / donors than from CCR4 / donors. Most of this effect resides within the CD103 subset of the E-lig Th population, in which donor CCR4 / cells can outnumber CCR4 / cells by 12-fold. No similar effect was observed for 4 7 intestinal memory Th cells or CD103 /E-lig Th cells. We conclude that CCR4 expression provides a competitive advantage to cutaneous Th cells, either by participating in their development from naive Th cells, or by preferentially maintaining them within the memory population over time. Each member of the Th lymphocyte population expresses only a subset of the total adhesion molecule and chemoattractant receptor repertoires. The specific fingerprint of these molecules on a given lymphocyte determines the tissues through which it can travel (1, 2). The two best understood tissue-specific memory Th subsets are distinguished by mutually exclusive expression of the carbohydrate ligand for E-selectin (E-lig; known as cutaneous lymphocyte-associated antigen in humans), which identifies cutaneous T cells, or the integrin 4 7, which identifies intestinal memory Th cells (1, 2). Interaction of E-lig with endothelial E-selectin plays an important role the skin-homing cascade (3, 4), whereas interaction of 4 7 with endothelial mucosal addressin cell adhesion molecule 1 plays a similar role in the gut E.S. Baekkevold and M.-A. Wurbel contributed equally to this work. The online version of this article contains supplemental material. (2, 5, 6). Memory lymphocytes with receptors for cutaneous antigens reside within the E-lig population (4), whereas those with receptors for intestinal antigens reside within the 4 7 population (6). Adoptive transfer models confirm that E-lig memory lymphocytes home specifically to cutaneous sites and 4 7 hi memory lymphocytes home to intestinal sites (2, 5, 6). The chemokine receptor CCR4 is expressed by essentially all cutaneous Th cells in human blood and skin, but is rarely found on intestinal Th cells (7 9). Equally important, one of the chemokine ligands for CCR4 (i.e., CCL17) is presented luminally by human cutaneous venules, but not by intestinal venules (7, 10). It is likely that CCR4 CCL17 interaction contributes to skin-specific homing by triggering adhesion to endothelium (7). CCR4 is also associated with cutaneous lymphocytes in the mouse, as murine E-lig but not E-lig memory Th cells respond to CCR4 ligands in chemo- JEM The Rockefeller University Press $8.00 Vol. 201, No. 7, April 4,
2 taxis assays (11). The evolutionary pressure implied by maintenance of this association since the time when humans and mice shared a common ancestor hints strongly at its biological relevance. Memory Th cells derive from naive Th cells that have recognized antigen (for review see reference 2). Naive Th cells express a limited, uniform fingerprint of trafficking molecules, contrasting sharply with the diverse repertoires of memory populations. The naive repertoire includes CD62L, CCR7, and LFA-1 (for review see references 1, 2) and restricts homing to lymphoid organs (1). Antigen is presented to naive T cells by dendritic cells within lymphoid organs, where dendritic cells orchestrate an imprinting process (12). This entails that dendritic cells convey information regarding the tissue-specific origins of the antigens they carry (12). Naive T cells receiving such information differentiate into memory cells capable of homing to the type of tissue from which the antigen originated (2). This scenario predicts that naive Th cells recognizing antigen on cutaneous-derived dendritic cells would differentiate into E-lig /CCR4 memory Th cells. In the present report, we explore the possibility that CCR4 might itself play a role in cutaneous Th development. This notion originates from the finding that Langerhans (cutaneous dendritic) cells, after acquiring cutaneous antigens in vivo, secrete functional CCR4 ligands upon entering the draining lymph node (13). However, initial studies suggested that CCR4 mice generate normal numbers of E-lig memory Th cells (11). Despite this finding, there are two hypotheses that might continue to support a role for CCR4 in this process. First, CCR4 might play a redundant role with other molecules compensating for its absence. Second, which we explore in this report, CCR4 mice may lack an important feature present in normal animals: developmental competition between cells lacking CCR4 and cells expressing CCR4. Cyster et al. proposed that competition between individual lymphocytes controls their access to limited microenvironments in vivo (14). Such competition is a matter of life or death if the microenvironment provides required signals for continued survival and development. By creating in vivo conditions where WT and CCR4 cells compete during memory Th differentiation, we ask whether the presence and/or function of CCR4 might play a role in the development of cutaneous memory Th populations. RESULTS AND DISCUSSION Competitive bone marrow reconstitution assay Equal numbers of mixed BM cells (10 6 each) from CCR4 and CCR4 donors were injected i.v. into lethally irradiated RAG-1 hosts to create experimental BM chimeras (BMCs). CCR4 (i.e., WT) donors expressed the CD45.1 congenic marker, whereas CCR4 donors expressed CD45.2. To control for potential differences in reconstitution efficiency between CD45.1 and CD45.2 donor stem cells, control BMCs were created in which both CD45.1 and 1046 CD45.2 donors were WT. Pairs of control and experimental BMCs were always created and harvested in parallel. Transferred BM cells were allowed to engraft the host for 6 12 wk before harvesting each BMC pair. To assess the engraftment efficiency of each donor type, we determined the CD45.1:CD45.2 ratio for a population of BM-derived cells that would not be affected by CCR4. B cells do not express CCR4 during their development (7), so the CD45.1:CD45.2 ratio was determined for splenic B cells in each BMC. This ratio ranged from 0.50 to 1.53 for 16 BMCs and was not significantly different between control and experimental BMCs. This confirms that CCR4 deficiency does not compromise donor cell engraftment, nor does it compromise B cell development. Thus, for each mouse, the CD45.1:CD45.2 ratio for each T cell population studied were corrected for engraftment efficiency to yield R by the formula: ( CD45.1:CD45.2) R = specific T cell pop ( CD24.1:CD45.2). B cell CCR4 deficiency does not influence development of naive, Th1, or Th2 T subsets R was next determined for naive CD4 and CD8 splenic T cells (Fig. 1 a). There were no significant differences in R between control (Fig. 1 b, white bars) and experimental BMCs (Fig. 1 b, black bars). The findings were identical for naive T cells from PLNs, MLNs, and PBLs (unpublished data). These results suggest that CCR4 function is not involved in the development of naive T cells. In addition, no significant differences were seen in R between experimental and control BMCs for neutrophils, NK cells, or any of the major thymic subsets (Fig. S1, available at org/cgi/content/full/jem /dc1). CCR4 has been proposed as a marker for cultured T cells polarized to produce Th2 cytokines (15). We used the competitive assay to assess the influence of CCR4 on Th1 and Th2 development in vivo. PLNs and spleen cells from BMCs were treated briefly with PMA, ionomycin, and brefeldin A to induce intracellular cytokine accumulation. Treated cells were stained for CD4 and congenic CD45 markers, plus intracellular IFN- and IL-4 (Fig. 1 c). There were no significant differences in R between control BMCs (Fig. 1 d, white bars) and experimental BMC (Fig. 1 d, black bars), suggesting that CCR4 function does not influence the development of Th1 or Th2 populations in vivo. A role for CCR4 in development of tissue-specific Th memory populations We found that memory Th cells expressing E-lig or 4 7 could be clearly identified in the PBLs of our BMCs (Fig. 2 a) as previously reported for humans (2). This suggests that normal tissue-specific memory Th development can occur in our BMCs. Interestingly, we found a dramatic (greater than fourfold) increase in R for E-lig memory Th cells between experimental and control BMCs (Fig. 2 b, top; P CCR4 AND THE DEVELOPMENT OF CUTANEOUS T CELL POPULATIONS Baekkevold et al.
3 Figure 1. CCR4 deficiency does not influence development of naive, Th1, or Th2 T cells. (a) Identification of naive CD4 (CD45RB hi / CD44 lo ) and naive CD8 (CD44 lo /PNA lo ) T cell populations. (b) Transplanted CCR4 bone marrow develops into naive T cells with the same efficiency as competing WT cells in BMCs, as there is no significant difference in the R for naive T splenocytes. Data from spleens of eight BMC pairs (mean SEM). (c) Intracellular staining for IL-4 and IFN- CD4 lymphocytes used for identification of IL-4 Th2 and IFN- Th1 cells in the BMCs. (d) CD4 cells in experimental BMCs show no significant difference in the R compared with control BMCs. Data from five BMC pairs (mean SEM) ). In contrast, we found only a small (but significant) 1.5-fold increase in R for 4 7 Th cells between experimental and control BMCs. The difference in R between E-lig and 4 7 Th cells from experimental, but not control, BMCs was highly significant (P 0.04). E-lig Th memory cells from PLNs, where 4 7 Th memory cells were too rare for analysis, showed a similarly dramatic difference in R between experimental and control BMCs (Fig. 2 b, bottom). These findings suggest a role for CCR4 function in development of the mature circulating cutaneous Th population. The CCR4 effect resides primarily within the E-lig /CD103 Th population A large percentage of intradermal T cells in humans (like intraepithelial T cells in many organs) express the integrin E (CD103), as a heterodimer with 7. The E 7 dimer is thought to participate in lymphocyte retention within epithelium via its ligand E-cadherin (16). Therefore, CD103 expression by E-lig mouse T cells may indicate their recent residence within the skin (17). We detected a large number of E-lig /CD103 Th cells within the PLNs of our BMCs (Fig. 2 c, bottom) as described previously (17). We also observed a significant population of E-lig /CD103 Th cells within the PBLs (Fig. 2 c, top). The difference in R between control and experimental BMCs was significantly larger for the E-lig /CD103 Th population than for the E-lig /CD103 Th population (Fig. 2 d), reaching a 5:1 ratio. There was no effect on the E-lig / CD103 population, showing this not to be a general effect on CD103 memory Th cells (Fig. 2 d). Results were similar for both PBLs Th cells (Fig. 2 d, top) and PLN Th cells (Fig. 2 d, bottom). Other subsets of E-lig Th cells Next, we examined E-lig Th subsets defined by markers other than CD103 (Fig. 3). We distinguished subsets by the Treg marker CD25 (Fig. 3, top center), or by the presence of intracellular IFN (i.e., cutaneous Th1 cells; Fig. 3, top right). E-lig cells producing IL-4 (i.e., cutaneous Th2) were not present in sufficient quantities to assess R (unpublished data). The Rs were significantly greater for experimental versus control chimeras in all E-lig populations, but not in any of the E-lig populations. CD103-defined subsets were included for comparison (Fig. 3, top left). The Rs for E-lig /CD103, E-lig /CD103, and E-lig /CD103 cells were similar to that seen previously in Fig. 2 d. In contrast, the R was not significantly different between E-lig /CD25 and E-lig /CD25 populations (Fig. 3, top middle), showing that absence of CCR4 affected both populations equally. The difference in R was also insignificant between E-lig /IFN and E-lig / IFN populations (Fig. 3, top right). Thus, the effect of CCR4 on cutaneous Th development resides mostly within JEM VOL. 201, April 4,
4 CD103 was dramatically greater for challenged versus unchallenged experimental BMCs (13 vs. 6; P 0.05; compare Fig. 3, left, top and bottom). There was no significant difference for subsets defined by CD25 or IFN. Thus, R was dramatically increased in the E-lig /CD103 population during cutaneous inflammatory responses, but unchanged in those populations defined by CD25 and IFN. This inflammatory model did not produce significant numbers of E-lig Th2 cells (unpublished data). Expression of functional CCR4 by Th subsets One testable explanation for the differences between E-lig / CD103 and E-lig /CD103 populations might be that CCR4 is only expressed by the CD103 cutaneous Th subset. Therefore, we assessed the ability of each population (from WT) to respond to a CCR4 ligand in chemotaxis assays (7, 11, 18). Naive Th cells from PBLs (Fig. 4 a, left) or PLN (right) had no appreciable increase in migration to CCL22 (black bars) over medium alone (gray bars). Both E-lig /CD103 and E-lig /CD103 Th cells responded robustly to CCL22, suggesting that both populations are likely to express high levels of CCR4. All three Th subsets responded equally well to the more universal chemoattractant CXCL12, a ligand for CXCR4 (Fig. 4 a, white bars). Figure 2. CCR4 participates in generation of cutaneous CD4 memory Th populations. (a) Identification of tissue-tropic PBL Th cell populations. CD4 T cells analyzed by FACS for E-lig (skin memory cells) or 4 7 integrin (intestinal memory cells) together with the naive Th marker CD45RB. (b) In PBLs, experimental chimeras show a highly increased R compared with control chimeras. This was significantly higher than that of 4 7 cells. Data from 6 and 10 BMC pairs are shown for PBLs and PLNs, respectively (mean SEM). (c) FACS analysis of PBLs and PLNs show that E-lig memory cells are separated into two subpopulations based CD103 expression. (d) Experimental chimeras show a significantly larger difference in R for the E-lig /CD103 Th population than for the E-lig /CD103 population. However, R within the E-lig /CD103 Th population shows no significant alteration between experimental and control chimeras. Data from 15 BMC pairs (mean SEM). the CD103 subset and is evenly distributed among CD25, CD25, IFN, and IFN Th subsets. E-lig Th subsets during cutaneous inflammation Next, we asked whether CCR4 influenced development of the aforementioned populations during cutaneous inflammation. We induced contact hypersensitivity by challenging the ears of presensitized mice with OVA peptide and harvesting the cervical PLNs on day 5. The R for E-lig / 1048 Expression of E-lig and CD103 by Th cells from unmanipulated WT and CCR4 / mice As reported previously, CCR4 mice possess normal proportions of E-lig memory Th cells (11). We have confirmed this finding for PLNs (Fig. 4 b, bottom left) and shown that it is also true for PBLs (Fig. 4 b, top left). Furthermore, we show that CCR4 mice have identical proportions of CD103 cells within their E-lig Th populations in both PLNs (Fig. 4 b, bottom right) and PBLs (top right). The fact that normal numbers of E-lig Th cells are found within unmanipulated CCR4 mice indicates that their naive cells are fully capable of differentiating into E-lig /CD103 and E-lig /CD103 Th cells. However, in the presence of competing WT cells, the CCR4 cells are less likely to be found within these populations. Thus, although clearly capable of differentiating into E-lig Th subsets, CCR4 cells are less efficient at doing so than WT cells. The effect is not observable in the unmanipulated CCR4 mice because we are seeing only a snapshot of a developmental process that has already reached a steady state; although less efficient at becoming E-lig Th cells than WT cells, CCR4 cells, when given enough time and protected from competition with normal cells, can form an E-lig Th pool that appears normal. Unlike the unmanipulated CCR4 mice, the chimeric mice provide an environment in which such competition can occur, mimicking the normal developmental environment of cutaneous Th cells. The role of CCR4 in generating cutaneous Th populations Tang and Cyster demonstrated that Langerhans cells that have recently acquired cutaneous antigen secrete functional CCR4 AND THE DEVELOPMENT OF CUTANEOUS T CELL POPULATIONS Baekkevold et al.
5 Figure 3. Comparison of E-lig Th subsets defined by CD103, CD25, and IFN before and after cutaneous inflammation. BMCs were sensitized to OVA PLNs were isolated from unchallenged mice (top row) or from challenged mice (bottom row) were harvested on day 5 after challenge. Data represent mean and SD from five unchallenged (top row) and four challenged BMC pairs (bottom row). CCR4 ligands upon entry into draining LNs (13). This could suggest that CCR4 ligands are part of the dendritic cell signaling event that imprints naive Th cells to become cutaneous memory Th cells. Although CCR4 is not observed on naive Th cells (Fig. 4 a and references 2, 7 9, 11), it is certainly possible that naive Th cells express CCR4 at levels below detectability that can nonetheless transduce an effective differentiation signal. Alternatively, CCR4 may influence proliferation or continued viability of E-lig cells after differentiation. Memory cell clonal lineages that repeatedly encounter antigen are likely to proliferate over time. In contrast, memory cells that never again encounter antigen after initial differentiation would remain only at low numbers, if maintained at all. If, as we have previously proposed (7), CCR4 plays a role in entry of Th cells into cutaneous sites from the blood, E-lig Th cells lacking CCR4 may have difficulty entering cutaneous sites, especially in the presence of competing WT cells. Thus, E-lig /CCR4 Th cells would be more likely to reencounter cutaneous antigens than E-lig /CCR4 Th cells. Memory Th cells recognizing cutaneous antigens but incapable of homing to skin would eventually be outnumbered by fully functional WT cutaneous Th cells. We feel that this latter interpretation is the most likely because the effects of CCR4 deficiency are most pronounced in the CD103 population and are greatly amplified during inflammation. As CD103 is a Figure 4. Comparison of memory Th populations from unmanipulated WT and CCR4 / mice. (a) Both E-lig /CD103 and E-lig /CD103 populations express functional CCR4. Lymphocytes were isolated from PBLs and PLNs, and migrated to medium alone (gray bars), the CCR4 ligand CCL22 (black bars), or the CXCR4 ligand CXCL12 (white bars) in transwells. The data (mean SEM) are from four independent experiments with four to eight transwells per data point per experiment. (b) Both WT and CCR4 / mice have similar numbers of E-lig cells in their PBL and PLN Th populations (left). Furthermore, there is no difference in the proportion of cutaneous Th cells expressing CD103 between the two genotypes (right). JEM VOL. 201, April 4,
6 marker of intradermal T cells, it is possible that its expression requires a further differentiation signal to cells that have already been committed to the cutaneous Th lineage. In light of our findings, it is possible that this further signal might require actual trafficking of E-lig Th cells to the skin. E-lig /CD103 Th cells are known to be greatly enriched in Treg activity when compared with E-lig /CD103 Th cells (17). However, we did not see a similar effect when assessing E-lig /CD25 Th cells in parallel. It is noteworthy that E-lig Th1 cells and other E-lig Th cells are similarly affected by CCR4 deficiency. In vitro studies of polarized Th cultures suggested that CCR4 was a marker of Th2 rather than Th1 cells (15). According to the data presented here, the influence of CCR4 on Th development depends more on the cutaneous homing profile of a given Th cell, rather than its Th1 or Th2 status. Conclusions We have tested the ability of CCR4 BM cells to differentiate in vivo into various lymphocyte subtypes when developing in the presence of equal numbers of WT BM cells. We found that CCR4 and WT donor cells develop equally well into B cells, naive CD4 T cells, naive CD8 T cells, Th1 cells, and Th2 cells. In contrast, CCR4 cells do not develop equally well into E-lig memory Th cells, with WT cells outnumbering CCR4 cells 13:1 within the CD103 /E-lig population during cutaneous inflammation. Our findings suggest that chemokine receptor function can strongly influence the development of mature tissue-specific memory lymphocyte populations. MATERIALS AND METHODS Mice. C57Bl/6N (Charles River Laboratories); RAG-1 and B6.SJLptprc(a)Pep3(b)BoyJ (WT, CD45.1 ; The Jackson Laboratory); CCR4 (11) maintained in our own facility on C57Bl/6N background. Chimeric mice. WT, CD45.1, WT, CD45.2, and CCR4, CD45.2 mice were killed at 4 7 wk, and BM was prepared as described previously (19) and mixed at a 1:1 ratio: WT, CD45.1 / WT, CD45.2 / control BMC ; and WT, CD45.1 CCR4, CD45.2 experimental BMCs BM cells were injected retro-orbitally to anesthesized RAG-1 recipients after rad X-irradiation. Drinking water contained antibiotics for the first 2 wk. Animals were killed 6 12 wk after reconstitution, and suspensions were prepared from PLNs, MLNs, and spleen by gentle disruption through nylon mesh. Blood was drawn by cardiac puncture, and PBLs were purified on Lympholyte Mammal (Cedar Lane). Animal experiments were approved by the Animal Care and Use Committee of Children s Hospital, Boston. Flow cytometry. The following conjugated MAbs were used: CD45.1- FITC or -PE, CD45RB-PE, CD19-PE, CD4-PECy7, CD8-PECy7, CD44-allophycocyanin, CD62L-allophycocyanin, CD103-PE, and CD25- PE (all obtained from BD Biosciences). 4 7 was detected with DATK32 (BD Biosciences), followed by biotinylated goat anti rat IgG (Caltag), and streptavidin-cy5 (Jackson ImmunoResearch Laboratories). Recombinant murine E-selectin IgG chimeric molecules (R&D Systems) was followed by Cy2 goat anti human IgG (Jackson ImmunoResearch Laboratories). Cytokine single cell analysis was performed as described previously (20). Cells were activated 5 h with 50 ng/ml PMA and 1 M ionomycin with 10 g/ml brefeldin-a (all obtained from Sigma-Aldrich). Cells were fixed and permeabilized with Fix & Perm kit (Caltag) and stained with anti IL4-PE and anti IFN -allophycocyanin together with anti-cd4 PECy7 and anti-cd45.1 FITC (all from BD Biosciences). Cells were analyzed on a dual-laser MoFlo cytometer (DakoCytomation) configured for six colors with Summit 3.1 software. Chemotaxis. PLNs and PBLs were obtained from ten 4 6 wk C57Bl/ 6N mice as described before. Migration was performed as described previously (7, 11, 18) with four to eight replicates for each chemokine or control. Optimal chemokine concentrations were used as determined previously: 100 nm for murine CCL22 (R&D Systems) and 30 nm for CXCL12 (Gryphon). Induction of contact hypersensitivity. Stratum corneum was gently stripped from mouse ears with adhesive tape, and cutaneous lipids were removed with acetone as described previously (21). Each prepared ear was painted with an aqueous mixture of 25 g cholera toxin (List Biologicals) and 200 g OVA (AnaSpec). This procedure was repeated three times at 10-d intervals for all mice presented in Fig. 3. PLNs from unchallenged mice were harvested d after the third topical immunization. Challenged mice were given a fourth topical immunization d after the third, and cervical LNs were harvested on day 5. Cervical LNs were appreciably larger in challenged versus unchallenged mice (unpublished data). Statistical analysis. For statistical comparison of two samples, a twotailed Student s t test was used when applicable. Online supplemental material. Additional experiments demonstrate that there are no significant differences in R between experimental and control BMCs for several more leukocyte populations. These include peripheral blood neutrophils, spleen NK cells, and each of the four major thymic subsets. Online supplemental material is available at cgi/content/full/jem /dc1. We thank Dr. J. Manis for critical reading of the manuscript. This work was supported by National Institute of Allergy and Infectious Diseases RO1 grant no. AI (to J.J. Campbell). E.S. Baekkevold was supported by a postdoctoral grant from the Norwegian Cancer Society. P. Kivisakk was supported by a postdoctoral fellowship from the National Multiple Sclerosis Society. The authors have no conflicting financial interests. Submitted: 28 May 2004 Accepted: 7 February 2005 REFERENCES 1. Butcher, E.C., M. Williams, K. Youngman, L. Rott, and M. Briskin Lymphocyte trafficking and regional immunity. Adv. Immunol. 72: Campbell, J.J., and E.C. Butcher Chemokines in tissue-specific and microenvironment-specific lymphocyte homing. Curr. Opin. Immunol. 12: Picker, L.J., S.A. Michie, L.S. Rott, and E.C. Butcher A unique phenotype of skin-associated lymphocytes in humans. Preferential expression of the HECA-452 epitope by benign and malignant T cells at cutaneous sites. Am. J. Pathol. 136: Santamaria Babi, L.F., L.J. Picker, M.T. Perez Soler, K. Drzimalla, P. Flohr, K. Blaser, and C. Hauser Circulating allergen-reactive T cells from patients with atopic dermatitis and allergic contact dermatitis express the skin-selective homing receptor, the cutaneous lymphocyteassociated antigen. J. Exp. Med. 181: Mackay, C.R., D.P. Andrew, M. Briskin, D.J. Ringler, and E.C. Butcher Phenotype, and migration properties of three major subsets of tissue homing T cells in sheep. Eur. J. Immunol. 26: Williams, M.B., and E.C. Butcher Homing of naive and memory T lymphocyte subsets to Peyer s patches, lymph nodes, and spleen. J. Immunol. 159: CCR4 AND THE DEVELOPMENT OF CUTANEOUS T CELL POPULATIONS Baekkevold et al.
7 7. Campbell, J.J., G. Haraldsen, J. Pan, J. Rottman, S. Qin, P. Ponath, D.P. Andrew, R. Warnke, N. Ruffing, N. Kassam, et al The chemokine receptor CCR4 in vascular recognition by cutaneous but not intestinal memory T cells. Nature. 400: Kunkel, E.J., J. Boisvert, K. Murphy, M.A. Vierra, M.C. Genovese, A.J. Wardlaw, H.B. Greenberg, M.R. Hodge, L. Wu, E.C. Butcher, and J.J. Campbell Expression of the chemokine receptors CCR4, CCR5, and CXCR3 by human tissue-infiltrating lymphocytes. Am. J. Pathol. 160: Soler, D., T.L. Humphreys, S.M. Spinola, and J.J. Campbell CCR4 versus CCR10 in human cutaneous TH lymphocyte trafficking. Blood. 101: Chong, B.F., J.E. Murphy, T.S. Kupper, and R.C. Fuhlbrigge E-selectin, thymus- and activation-regulated chemokine/ccl17, and intercellular adhesion molecule-1 are constitutively coexpressed in dermal microvessels: a foundation for a cutaneous immunosurveillance system. J. Immunol. 172: Reiss, Y., A.E. Proudfoot, C.A. Power, J.J. Campbell, and E.C. Butcher CC chemokine receptor (CCR)4 and the CCR10 ligand cutaneous T cell attracting chemokine (CTACK) in lymphocyte trafficking to inflamed skin. J. Exp. Med. 194: Mora, J.R., M.R. Bono, N. Manjunath, W. Weninger, L.L. Cavanagh, M. Rosemblatt, and U.H. Von Andrian Selective imprinting of gut-homing T cells by Peyer s patch dendritic cells. Nature. 424: Tang, H.L., and J.G. Cyster Chemokine up-regulation and activated T cell attraction by maturing dendritic cells. Science. 284: Cyster, J.G., S.B. Hartley, and C.C. Goodnow Competition for follicular niches excludes self-reactive cells from the recirculating B-cell repertoire. Nature. 371: Sallusto, F., D. Lenig, C.R. Mackay, and A. Lanzavecchia Flexible programs of chemokine receptor expression on human polarized T helper 1 and 2 lymphocytes. J. Exp. Med. 187: Pauls, K., M. Schon, R.C. Kubitza, B. Homey, A. Wiesenborn, P. Lehmann, T. Ruzicka, C.M. Parker, and M.P. Schon Role of integrin alphae(cd103)beta7 for tissue-specific epidermal localization of CD8 T lymphocytes. J. Invest. Dermatol. 117: Lehmann, J., J. Huehn, M. de la Rosa, F. Maszyna, U. Kretschmer, V. Krenn, M. Brunner, A. Scheffold, and A. Hamann Expression of the integrin alpha Ebeta 7 identifies unique subsets of CD25 as well as CD25 regulatory T cells. Proc. Natl. Acad. Sci. USA. 99: Campbell, J.J., S. Qin, K.B. Bacon, C.R. Mackay, and E.C. Butcher Biology of chemokine and classical chemoattractant receptors: differential requirements for adhesion-triggering versus chemotactic responses in lymphoid cells. J. Cell Biol. 134: Uehara, S., A. Grinberg, J.M. Farber, and P.E. Love A role for CCR9 in T lymphocyte development and migration. J. Immunol. 168: Kim, C.H., L. Rott, E.J. Kunkel, M.C. Genovese, D.P. Andrew, L. Wu, and E.C. Butcher Rules of chemokine receptor association with T cell polarization in vivo. J. Clin. Invest. 108: Kahlon, R., Y. Hu, C.H. Orteu, A. Kifayet, J.D. Trudeau, R. Tan, and J.P. Dutz Optimization of epicutaneous immunization for the induction of CTL. Vaccine. 21: JEM VOL. 201, April 4,
Innate immune cells---- one time migration preprogrammed homing properties
 Innate immune cells---- one time migration preprogrammed homing properties neutrophils---acute inflammation monocytes---subacute/chronic inflammation eosinophils---parasitic or allergic inflammation natural
Innate immune cells---- one time migration preprogrammed homing properties neutrophils---acute inflammation monocytes---subacute/chronic inflammation eosinophils---parasitic or allergic inflammation natural
Effector T Cells and
 1 Effector T Cells and Cytokines Andrew Lichtman, MD PhD Brigham and Women's Hospital Harvard Medical School 2 Lecture outline Cytokines Subsets of CD4+ T cells: definitions, functions, development New
1 Effector T Cells and Cytokines Andrew Lichtman, MD PhD Brigham and Women's Hospital Harvard Medical School 2 Lecture outline Cytokines Subsets of CD4+ T cells: definitions, functions, development New
The Immune Response in Time and Space
 The Immune Response in Time and Space Chapters 14 & 4 Sharon S. Evans, Ph.D. Department of Immunology 845-3421 sharon.evans@roswellpark.org September 18 & 23, 2014 Inflammation Inflammation Complex response
The Immune Response in Time and Space Chapters 14 & 4 Sharon S. Evans, Ph.D. Department of Immunology 845-3421 sharon.evans@roswellpark.org September 18 & 23, 2014 Inflammation Inflammation Complex response
Chapter 3, Part A (Pages 37-45): Leukocyte Migration into Tissues
 Allergy and Immunology Review Corner: Chapter 3, Part A (pages 37-45) of Cellular and Molecular Immunology (Seventh Edition), by Abul K. Abbas, Andrew H. Lichtman and Shiv Pillai. Chapter 3, Part A (Pages
Allergy and Immunology Review Corner: Chapter 3, Part A (pages 37-45) of Cellular and Molecular Immunology (Seventh Edition), by Abul K. Abbas, Andrew H. Lichtman and Shiv Pillai. Chapter 3, Part A (Pages
Question 1. Kupffer cells, microglial cells and osteoclasts are all examples of what type of immune system cell?
 Abbas Chapter 2: Sarah Spriet February 8, 2015 Question 1. Kupffer cells, microglial cells and osteoclasts are all examples of what type of immune system cell? a. Dendritic cells b. Macrophages c. Monocytes
Abbas Chapter 2: Sarah Spriet February 8, 2015 Question 1. Kupffer cells, microglial cells and osteoclasts are all examples of what type of immune system cell? a. Dendritic cells b. Macrophages c. Monocytes
Adaptive immune responses: T cell-mediated immunity
 MICR2209 Adaptive immune responses: T cell-mediated immunity Dr Allison Imrie allison.imrie@uwa.edu.au 1 Synopsis: In this lecture we will discuss the T-cell mediated immune response, how it is activated,
MICR2209 Adaptive immune responses: T cell-mediated immunity Dr Allison Imrie allison.imrie@uwa.edu.au 1 Synopsis: In this lecture we will discuss the T-cell mediated immune response, how it is activated,
SUPPLEMENTARY INFORMATION
 Complete but curtailed T-cell response to very-low-affinity antigen Dietmar Zehn, Sarah Y. Lee & Michael J. Bevan Supp. Fig. 1: TCR chain usage among endogenous K b /Ova reactive T cells. C57BL/6 mice
Complete but curtailed T-cell response to very-low-affinity antigen Dietmar Zehn, Sarah Y. Lee & Michael J. Bevan Supp. Fig. 1: TCR chain usage among endogenous K b /Ova reactive T cells. C57BL/6 mice
Test Bank for Basic Immunology Functions and Disorders of the Immune System 4th Edition by Abbas
 Test Bank for Basic Immunology Functions and Disorders of the Immune System 4th Edition by Abbas Chapter 04: Antigen Recognition in the Adaptive Immune System Test Bank MULTIPLE CHOICE 1. Most T lymphocytes
Test Bank for Basic Immunology Functions and Disorders of the Immune System 4th Edition by Abbas Chapter 04: Antigen Recognition in the Adaptive Immune System Test Bank MULTIPLE CHOICE 1. Most T lymphocytes
The development of T cells in the thymus
 T cells rearrange their receptors in the thymus whereas B cells do so in the bone marrow. The development of T cells in the thymus The lobular/cellular organization of the thymus Immature cells are called
T cells rearrange their receptors in the thymus whereas B cells do so in the bone marrow. The development of T cells in the thymus The lobular/cellular organization of the thymus Immature cells are called
Interferon γ regulates idiopathic pneumonia syndrome, a. Th17 + CD4 + T-cell-mediated GvH disease
 Interferon γ regulates idiopathic pneumonia syndrome, a Th17 + CD4 + T-cell-mediated GvH disease Nora Mauermann, Julia Burian, Christophe von Garnier, Stefan Dirnhofer, Davide Germano, Christine Schuett,
Interferon γ regulates idiopathic pneumonia syndrome, a Th17 + CD4 + T-cell-mediated GvH disease Nora Mauermann, Julia Burian, Christophe von Garnier, Stefan Dirnhofer, Davide Germano, Christine Schuett,
Suppl Video: Tumor cells (green) and monocytes (white) are seeded on a confluent endothelial
 Supplementary Information Häuselmann et al. Monocyte induction of E-selectin-mediated endothelial activation releases VE-cadherin junctions to promote tumor cell extravasation in the metastasis cascade
Supplementary Information Häuselmann et al. Monocyte induction of E-selectin-mediated endothelial activation releases VE-cadherin junctions to promote tumor cell extravasation in the metastasis cascade
Supplementary Figure 1. Characterization of basophils after reconstitution of SCID mice
 Supplementary figure legends Supplementary Figure 1. Characterization of after reconstitution of SCID mice with CD4 + CD62L + T cells. (A-C) SCID mice (n = 6 / group) were reconstituted with 2 x 1 6 CD4
Supplementary figure legends Supplementary Figure 1. Characterization of after reconstitution of SCID mice with CD4 + CD62L + T cells. (A-C) SCID mice (n = 6 / group) were reconstituted with 2 x 1 6 CD4
Lecture 9: T-cell Mediated Immunity
 Lecture 9: T-cell Mediated Immunity Questions to Consider How do T cells know where to go? Questions to Consider How do T cells know where to go? How does antigen get targeted to a T cell expressing the
Lecture 9: T-cell Mediated Immunity Questions to Consider How do T cells know where to go? Questions to Consider How do T cells know where to go? How does antigen get targeted to a T cell expressing the
Review Questions: Janeway s Immunobiology 8th Edition by Kenneth Murphy
 Review Questions: Janeway s Immunobiology 8th Edition by Kenneth Murphy Chapter 11 (pages 429-460): Dynamics of Adaptive Immunity prepared by Kelly von Elten, Walter Reed National Military Medical Center,
Review Questions: Janeway s Immunobiology 8th Edition by Kenneth Murphy Chapter 11 (pages 429-460): Dynamics of Adaptive Immunity prepared by Kelly von Elten, Walter Reed National Military Medical Center,
Lymphoid architecture & Leukocyte recirculation. Thursday Jan 26th, 2017
 Lymphoid architecture & Leukocyte recirculation Thursday Jan 26th, 2017 Topics The life of immune cells Where are they born? Where are they educated? Where do they function? How do they get there? The
Lymphoid architecture & Leukocyte recirculation Thursday Jan 26th, 2017 Topics The life of immune cells Where are they born? Where are they educated? Where do they function? How do they get there? The
Lymphoid Organs and Lymphocyte Trafficking. Dr. Issa Abu-Dayyeh
 Lymphoid Organs and Lymphocyte Trafficking Dr. Issa Abu-Dayyeh Invader recognition Where does invader recognition take place?? Secondary lymphoid organs: Lymph nodes Spleen Mucosal-associated lymphoid
Lymphoid Organs and Lymphocyte Trafficking Dr. Issa Abu-Dayyeh Invader recognition Where does invader recognition take place?? Secondary lymphoid organs: Lymph nodes Spleen Mucosal-associated lymphoid
5/1/13. The proportion of thymus that produces T cells decreases with age. The cellular organization of the thymus
 T cell precursors migrate from the bone marrow via the blood to the thymus to mature 1 2 The cellular organization of the thymus The proportion of thymus that produces T cells decreases with age 3 4 1
T cell precursors migrate from the bone marrow via the blood to the thymus to mature 1 2 The cellular organization of the thymus The proportion of thymus that produces T cells decreases with age 3 4 1
LECTURE 12: MUCOSAL IMMUNITY GUT STRUCTURE
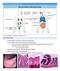 LECTURE 12: MUCOSAL IMMUNITY GUT STRUCTURE - Small intestine in humans is around 3-4 metres long - Internal surface of the small intestines are lined by villi o Villi are composed of absorptive cells (epithelial/enterocytes)
LECTURE 12: MUCOSAL IMMUNITY GUT STRUCTURE - Small intestine in humans is around 3-4 metres long - Internal surface of the small intestines are lined by villi o Villi are composed of absorptive cells (epithelial/enterocytes)
PBS Class #2 Introduction to the Immune System part II Suggested reading: Abbas, pgs , 27-30
 PBS 803 - Class #2 Introduction to the Immune System part II Suggested reading: Abbas, pgs. 15-25, 27-30 Learning Objectives Compare and contrast the maturation of B and T lymphocytes Compare and contrast
PBS 803 - Class #2 Introduction to the Immune System part II Suggested reading: Abbas, pgs. 15-25, 27-30 Learning Objectives Compare and contrast the maturation of B and T lymphocytes Compare and contrast
L-selectin Is Essential for Delivery of Activated CD8 + T Cells to Virus-Infected Organs for Protective Immunity
 Cell Reports Supplemental Information L-selectin Is Essential for Delivery of Activated CD8 + T Cells to Virus-Infected Organs for Protective Immunity Rebar N. Mohammed, H. Angharad Watson, Miriam Vigar,
Cell Reports Supplemental Information L-selectin Is Essential for Delivery of Activated CD8 + T Cells to Virus-Infected Organs for Protective Immunity Rebar N. Mohammed, H. Angharad Watson, Miriam Vigar,
activation with anti-cd3/cd28 beads and 3d following transduction. Supplemental Figure 2 shows
 Supplemental Data Supplemental Figure 1 compares CXCR4 expression in untreated CD8 + T cells, following activation with anti-cd3/cd28 beads and 3d following transduction. Supplemental Figure 2 shows the
Supplemental Data Supplemental Figure 1 compares CXCR4 expression in untreated CD8 + T cells, following activation with anti-cd3/cd28 beads and 3d following transduction. Supplemental Figure 2 shows the
Supplementary Figure 1 Lymphocytes can be tracked for at least 4 weeks after
 Supplementary Figure 1 Lymphocytes can be tracked for at least 4 weeks after photoconversion by using H2B-Dendra2. 4-5 PPs of H2B-Dendra2 BM chimeras were photoconverted and analyzed 7 days (upper panel)
Supplementary Figure 1 Lymphocytes can be tracked for at least 4 weeks after photoconversion by using H2B-Dendra2. 4-5 PPs of H2B-Dendra2 BM chimeras were photoconverted and analyzed 7 days (upper panel)
Sharon S. Evans, Ph.D. Dept. Immunology, RPCI Jan. 29 & Feb 3, 2015
 Adhesion Molecules And Lymphocyte Homing Sharon S. Evans, Ph.D. Dept. Immunology, RPCI Jan. 29 & Feb 3, 2015 Outline General introduction to lymphocyte trafficking homeostatic recirculation vs active recruitment.
Adhesion Molecules And Lymphocyte Homing Sharon S. Evans, Ph.D. Dept. Immunology, RPCI Jan. 29 & Feb 3, 2015 Outline General introduction to lymphocyte trafficking homeostatic recirculation vs active recruitment.
Molecular and Cellular Basis of Immune Protection of Mucosal Surfaces
 Molecular and Cellular Basis of Immune Protection of Mucosal Surfaces Department of Biologic & Materials Sciences School of Dentistry University of Michigan Ann Arbor, Michigan 48109-1078 1 Image quality
Molecular and Cellular Basis of Immune Protection of Mucosal Surfaces Department of Biologic & Materials Sciences School of Dentistry University of Michigan Ann Arbor, Michigan 48109-1078 1 Image quality
The recruitment of leukocytes and plasma proteins from the blood to sites of infection and tissue injury is called inflammation
 The migration of a particular type of leukocyte into a restricted type of tissue, or a tissue with an ongoing infection or injury, is often called leukocyte homing, and the general process of leukocyte
The migration of a particular type of leukocyte into a restricted type of tissue, or a tissue with an ongoing infection or injury, is often called leukocyte homing, and the general process of leukocyte
SUPPLEMENTARY FIGURE 1
 SUPPLEMENTARY FIGURE 1 A LN Cell count (1 ) 1 3 1 CD+ 1 1 CDL lo CD hi 1 CD+FoxP3+ 1 1 1 7 3 3 3 % of cells 9 7 7 % of cells CD+ 3 1 % of cells CDL lo CD hi 1 1 % of CD+ cells CD+FoxP3+ 3 1 % of CD+ T
SUPPLEMENTARY FIGURE 1 A LN Cell count (1 ) 1 3 1 CD+ 1 1 CDL lo CD hi 1 CD+FoxP3+ 1 1 1 7 3 3 3 % of cells 9 7 7 % of cells CD+ 3 1 % of cells CDL lo CD hi 1 1 % of CD+ cells CD+FoxP3+ 3 1 % of CD+ T
Chapter 2 (pages 22 33): Cells and Tissues of the Immune System. Prepared by Kristen Dazy, MD, Scripps Clinic Medical Group
 Allergy and Immunology Review Corner: Cellular and Molecular Immunology, 8th Edition By Abul K. Abbas, MBBS; Andrew H. H. Lichtman, MD, PhD; and Shiv Pillai, MBBS, PhD. Chapter 2 (pages 22 33): Cells and
Allergy and Immunology Review Corner: Cellular and Molecular Immunology, 8th Edition By Abul K. Abbas, MBBS; Andrew H. H. Lichtman, MD, PhD; and Shiv Pillai, MBBS, PhD. Chapter 2 (pages 22 33): Cells and
IMMUNOLOGICAL MEMORY. CD4 T Follicular Helper Cells. Memory CD8 T Cell Differentiation
 IMMUNOLOGICAL MEMORY CD4 T Follicular Helper Cells Memory CD8 T Cell Differentiation CD4 T Cell Differentiation Bcl-6 T-bet GATA-3 ROR t Foxp3 CD4 T follicular helper (Tfh) cells FUNCTION Provide essential
IMMUNOLOGICAL MEMORY CD4 T Follicular Helper Cells Memory CD8 T Cell Differentiation CD4 T Cell Differentiation Bcl-6 T-bet GATA-3 ROR t Foxp3 CD4 T follicular helper (Tfh) cells FUNCTION Provide essential
Cell isolation. Spleen and lymph nodes (axillary, inguinal) were removed from mice
 Supplementary Methods: Cell isolation. Spleen and lymph nodes (axillary, inguinal) were removed from mice and gently meshed in DMEM containing 10% FBS to prepare for single cell suspensions. CD4 + CD25
Supplementary Methods: Cell isolation. Spleen and lymph nodes (axillary, inguinal) were removed from mice and gently meshed in DMEM containing 10% FBS to prepare for single cell suspensions. CD4 + CD25
Antigen Presentation and T Lymphocyte Activation. Abul K. Abbas UCSF. FOCiS
 1 Antigen Presentation and T Lymphocyte Activation Abul K. Abbas UCSF FOCiS 2 Lecture outline Dendritic cells and antigen presentation The role of the MHC T cell activation Costimulation, the B7:CD28 family
1 Antigen Presentation and T Lymphocyte Activation Abul K. Abbas UCSF FOCiS 2 Lecture outline Dendritic cells and antigen presentation The role of the MHC T cell activation Costimulation, the B7:CD28 family
Effector mechanisms of cell-mediated immunity: Properties of effector, memory and regulatory T cells
 ICI Basic Immunology course Effector mechanisms of cell-mediated immunity: Properties of effector, memory and regulatory T cells Abul K. Abbas, MD UCSF Stages in the development of T cell responses: induction
ICI Basic Immunology course Effector mechanisms of cell-mediated immunity: Properties of effector, memory and regulatory T cells Abul K. Abbas, MD UCSF Stages in the development of T cell responses: induction
Optimizing Intracellular Flow Cytometry:
 Optimizing Intracellular Flow Cytometry: Simultaneous Detection of Cytokines and Transcription Factors An encore presentation by Jurg Rohrer, PhD, BD Biosciences 10.26.10 Outline Introduction Cytokines
Optimizing Intracellular Flow Cytometry: Simultaneous Detection of Cytokines and Transcription Factors An encore presentation by Jurg Rohrer, PhD, BD Biosciences 10.26.10 Outline Introduction Cytokines
Supplementary Information:
 Supplementary Information: Follicular regulatory T cells with Bcl6 expression suppress germinal center reactions by Yeonseok Chung, Shinya Tanaka, Fuliang Chu, Roza Nurieva, Gustavo J. Martinez, Seema
Supplementary Information: Follicular regulatory T cells with Bcl6 expression suppress germinal center reactions by Yeonseok Chung, Shinya Tanaka, Fuliang Chu, Roza Nurieva, Gustavo J. Martinez, Seema
ECM1 controls T H 2 cell egress from lymph nodes through re-expression of S1P 1
 ZH, Li et al, page 1 ECM1 controls T H 2 cell egress from lymph nodes through re-expression of S1P 1 Zhenhu Li 1,4,Yuan Zhang 1,4, Zhiduo Liu 1, Xiaodong Wu 1, Yuhan Zheng 1, Zhiyun Tao 1, Kairui Mao 1,
ZH, Li et al, page 1 ECM1 controls T H 2 cell egress from lymph nodes through re-expression of S1P 1 Zhenhu Li 1,4,Yuan Zhang 1,4, Zhiduo Liu 1, Xiaodong Wu 1, Yuhan Zheng 1, Zhiyun Tao 1, Kairui Mao 1,
Adaptive Immunity: Humoral Immune Responses
 MICR2209 Adaptive Immunity: Humoral Immune Responses Dr Allison Imrie 1 Synopsis: In this lecture we will review the different mechanisms which constitute the humoral immune response, and examine the antibody
MICR2209 Adaptive Immunity: Humoral Immune Responses Dr Allison Imrie 1 Synopsis: In this lecture we will review the different mechanisms which constitute the humoral immune response, and examine the antibody
Determinants of Immunogenicity and Tolerance. Abul K. Abbas, MD Department of Pathology University of California San Francisco
 Determinants of Immunogenicity and Tolerance Abul K. Abbas, MD Department of Pathology University of California San Francisco EIP Symposium Feb 2016 Why do some people respond to therapeutic proteins?
Determinants of Immunogenicity and Tolerance Abul K. Abbas, MD Department of Pathology University of California San Francisco EIP Symposium Feb 2016 Why do some people respond to therapeutic proteins?
T Cell Development. Xuefang Cao, MD, PhD. November 3, 2015
 T Cell Development Xuefang Cao, MD, PhD November 3, 2015 Thymocytes in the cortex of the thymus Early thymocytes development Positive and negative selection Lineage commitment Exit from the thymus and
T Cell Development Xuefang Cao, MD, PhD November 3, 2015 Thymocytes in the cortex of the thymus Early thymocytes development Positive and negative selection Lineage commitment Exit from the thymus and
Bonzo/CXCR6 expression defines type 1 polarized T-cell subsets with extralymphoid tissue homing potential
 Bonzo/CXCR6 expression defines type 1 polarized T-cell subsets with extralymphoid tissue homing potential Chang H. Kim, 1 Eric J. Kunkel, 1 Judie Boisvert, 2 Brent Johnston, 1 James J. Campbell, 1 Mark
Bonzo/CXCR6 expression defines type 1 polarized T-cell subsets with extralymphoid tissue homing potential Chang H. Kim, 1 Eric J. Kunkel, 1 Judie Boisvert, 2 Brent Johnston, 1 James J. Campbell, 1 Mark
CCR7 Plays No Appreciable Role in Trafficking of Central Memory CD4 T Cells to Lymph Nodes
 This information is current as of November 7, 2018. Supplementary Material References Subscription Permissions Email Alerts CCR7 Plays No Appreciable Role in Trafficking of Central Memory CD4 T Cells to
This information is current as of November 7, 2018. Supplementary Material References Subscription Permissions Email Alerts CCR7 Plays No Appreciable Role in Trafficking of Central Memory CD4 T Cells to
Immunology 2017: Lecture 12 handout. Secondary lymphoid organs. Dr H Awad
 Immunology 2017: Lecture 12 handout Secondary lymphoid organs Dr H Awad INTRODUCTION So far we discussed the cells of the immune system and how they recognize their antigens and get stimulated. The number
Immunology 2017: Lecture 12 handout Secondary lymphoid organs Dr H Awad INTRODUCTION So far we discussed the cells of the immune system and how they recognize their antigens and get stimulated. The number
ACTIVATION OF T LYMPHOCYTES AND CELL MEDIATED IMMUNITY
 ACTIVATION OF T LYMPHOCYTES AND CELL MEDIATED IMMUNITY The recognition of specific antigen by naïve T cell induces its own activation and effector phases. T helper cells recognize peptide antigens through
ACTIVATION OF T LYMPHOCYTES AND CELL MEDIATED IMMUNITY The recognition of specific antigen by naïve T cell induces its own activation and effector phases. T helper cells recognize peptide antigens through
B220 CD4 CD8. Figure 1. Confocal Image of Sensitized HLN. Representative image of a sensitized HLN
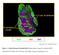 B220 CD4 CD8 Natarajan et al., unpublished data Figure 1. Confocal Image of Sensitized HLN. Representative image of a sensitized HLN showing B cell follicles and T cell areas. 20 µm thick. Image of magnification
B220 CD4 CD8 Natarajan et al., unpublished data Figure 1. Confocal Image of Sensitized HLN. Representative image of a sensitized HLN showing B cell follicles and T cell areas. 20 µm thick. Image of magnification
SUPPLEMENTARY INFORMATION
 Supplemental Figure 1. Furin is efficiently deleted in CD4 + and CD8 + T cells. a, Western blot for furin and actin proteins in CD4cre-fur f/f and fur f/f Th1 cells. Wild-type and furin-deficient CD4 +
Supplemental Figure 1. Furin is efficiently deleted in CD4 + and CD8 + T cells. a, Western blot for furin and actin proteins in CD4cre-fur f/f and fur f/f Th1 cells. Wild-type and furin-deficient CD4 +
SUPPORTING INFORMATIONS
 SUPPORTING INFORMATIONS Mice MT/ret RetCD3ε KO α-cd25 treated MT/ret Age 1 month 3 mnths 6 months 1 month 3 months 6 months 1 month 3 months 6 months 2/87 Survival 87/87 incidence of 17/87 1 ary tumor
SUPPORTING INFORMATIONS Mice MT/ret RetCD3ε KO α-cd25 treated MT/ret Age 1 month 3 mnths 6 months 1 month 3 months 6 months 1 month 3 months 6 months 2/87 Survival 87/87 incidence of 17/87 1 ary tumor
Supplemental Materials
 Supplemental Materials Programmed death one homolog maintains the pool size of regulatory T cells by promoting their differentiation and stability Qi Wang 1, Jianwei He 1, Dallas B. Flies 2, Liqun Luo
Supplemental Materials Programmed death one homolog maintains the pool size of regulatory T cells by promoting their differentiation and stability Qi Wang 1, Jianwei He 1, Dallas B. Flies 2, Liqun Luo
ACTIVATION AND EFFECTOR FUNCTIONS OF CELL-MEDIATED IMMUNITY AND NK CELLS. Choompone Sakonwasun, MD (Hons), FRCPT
 ACTIVATION AND EFFECTOR FUNCTIONS OF CELL-MEDIATED IMMUNITY AND NK CELLS Choompone Sakonwasun, MD (Hons), FRCPT Types of Adaptive Immunity Types of T Cell-mediated Immune Reactions CTLs = cytotoxic T lymphocytes
ACTIVATION AND EFFECTOR FUNCTIONS OF CELL-MEDIATED IMMUNITY AND NK CELLS Choompone Sakonwasun, MD (Hons), FRCPT Types of Adaptive Immunity Types of T Cell-mediated Immune Reactions CTLs = cytotoxic T lymphocytes
Newly Recognized Components of the Innate Immune System
 Newly Recognized Components of the Innate Immune System NOD Proteins: Intracellular Peptidoglycan Sensors NOD-1 NOD-2 Nod Protein LRR; Ligand Recognition CARD RICK I-κB p50 p65 NF-κB Polymorphisms in Nod-2
Newly Recognized Components of the Innate Immune System NOD Proteins: Intracellular Peptidoglycan Sensors NOD-1 NOD-2 Nod Protein LRR; Ligand Recognition CARD RICK I-κB p50 p65 NF-κB Polymorphisms in Nod-2
Supplementary Figure S1. PTPN2 levels are not altered in proliferating CD8+ T cells. Lymph node (LN) CD8+ T cells from C57BL/6 mice were stained with
 Supplementary Figure S1. PTPN2 levels are not altered in proliferating CD8+ T cells. Lymph node (LN) CD8+ T cells from C57BL/6 mice were stained with CFSE and stimulated with plate-bound α-cd3ε (10µg/ml)
Supplementary Figure S1. PTPN2 levels are not altered in proliferating CD8+ T cells. Lymph node (LN) CD8+ T cells from C57BL/6 mice were stained with CFSE and stimulated with plate-bound α-cd3ε (10µg/ml)
A crucial role for HVEM and BTLA in preventing intestinal inflammation
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2008 A crucial role for HVEM and BTLA in preventing intestinal inflammation Marcos W. Steinberg La Jolla Institute
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2008 A crucial role for HVEM and BTLA in preventing intestinal inflammation Marcos W. Steinberg La Jolla Institute
1. Overview of Adaptive Immunity
 Chapter 17A: Adaptive Immunity Part I 1. Overview of Adaptive Immunity 2. T and B Cell Production 3. Antigens & Antigen Presentation 4. Helper T cells 1. Overview of Adaptive Immunity The Nature of Adaptive
Chapter 17A: Adaptive Immunity Part I 1. Overview of Adaptive Immunity 2. T and B Cell Production 3. Antigens & Antigen Presentation 4. Helper T cells 1. Overview of Adaptive Immunity The Nature of Adaptive
Supplementary Figure 1. Generation of knockin mice expressing L-selectinN138G. (a) Schematics of the Sellg allele (top), the targeting vector, the
 Supplementary Figure 1. Generation of knockin mice expressing L-selectinN138G. (a) Schematics of the Sellg allele (top), the targeting vector, the targeted allele in ES cells, and the mutant allele in
Supplementary Figure 1. Generation of knockin mice expressing L-selectinN138G. (a) Schematics of the Sellg allele (top), the targeting vector, the targeted allele in ES cells, and the mutant allele in
TITLE: MODULATION OF T CELL TOLERANCE IN A MURINE MODEL FOR IMMUNOTHERAPY OF PROSTATIC ADENOCARCINOMA
 AD Award Number: DAMD17-01-1-0085 TITLE: MODULATION OF T CELL TOLERANCE IN A MURINE MODEL FOR IMMUNOTHERAPY OF PROSTATIC ADENOCARCINOMA PRINCIPAL INVESTIGATOR: ARTHUR A HURWITZ, Ph.d. CONTRACTING ORGANIZATION:
AD Award Number: DAMD17-01-1-0085 TITLE: MODULATION OF T CELL TOLERANCE IN A MURINE MODEL FOR IMMUNOTHERAPY OF PROSTATIC ADENOCARCINOMA PRINCIPAL INVESTIGATOR: ARTHUR A HURWITZ, Ph.d. CONTRACTING ORGANIZATION:
Optimizing Intracellular Flow Cytometry:
 Optimizing Intracellular Flow Cytometry: Simultaneous Detection of Cytokines and Transcription Factors Presented by Jurg Rohrer, PhD, BD Biosciences 23-10780-00 Outline Introduction Cytokines Transcription
Optimizing Intracellular Flow Cytometry: Simultaneous Detection of Cytokines and Transcription Factors Presented by Jurg Rohrer, PhD, BD Biosciences 23-10780-00 Outline Introduction Cytokines Transcription
NK cell flow cytometric assay In vivo DC viability and migration assay
 NK cell flow cytometric assay 6 NK cells were purified, by negative selection with the NK Cell Isolation Kit (Miltenyi iotec), from spleen and lymph nodes of 6 RAG1KO mice, injected the day before with
NK cell flow cytometric assay 6 NK cells were purified, by negative selection with the NK Cell Isolation Kit (Miltenyi iotec), from spleen and lymph nodes of 6 RAG1KO mice, injected the day before with
Immune response. This overview figure summarizes simply how our body responds to foreign molecules that enter to it.
 Immune response This overview figure summarizes simply how our body responds to foreign molecules that enter to it. It s highly recommended to watch Dr Najeeb s lecture that s titled T Helper cells and
Immune response This overview figure summarizes simply how our body responds to foreign molecules that enter to it. It s highly recommended to watch Dr Najeeb s lecture that s titled T Helper cells and
SUPPLEMENTARY INFORMATION
 doi:1.138/nature1554 a TNF-α + in CD4 + cells [%] 1 GF SPF 6 b IL-1 + in CD4 + cells [%] 5 4 3 2 1 Supplementary Figure 1. Effect of microbiota on cytokine profiles of T cells in GALT. Frequencies of TNF-α
doi:1.138/nature1554 a TNF-α + in CD4 + cells [%] 1 GF SPF 6 b IL-1 + in CD4 + cells [%] 5 4 3 2 1 Supplementary Figure 1. Effect of microbiota on cytokine profiles of T cells in GALT. Frequencies of TNF-α
Supplemental Table I.
 Supplemental Table I Male / Mean ± SEM n Mean ± SEM n Body weight, g 29.2±0.4 17 29.7±0.5 17 Total cholesterol, mg/dl 534.0±30.8 17 561.6±26.1 17 HDL-cholesterol, mg/dl 9.6±0.8 17 10.1±0.7 17 Triglycerides,
Supplemental Table I Male / Mean ± SEM n Mean ± SEM n Body weight, g 29.2±0.4 17 29.7±0.5 17 Total cholesterol, mg/dl 534.0±30.8 17 561.6±26.1 17 HDL-cholesterol, mg/dl 9.6±0.8 17 10.1±0.7 17 Triglycerides,
MECHANISMS OF CELLULAR REJECTION IN ORGAN TRANSPLANTATION AN OVERVIEW
 MECHANISMS OF CELLULAR REJECTION IN ORGAN TRANSPLANTATION AN OVERVIEW YVON LEBRANCHU Service Néphrologie et Immunologie Clinique CHU TOURS ANTIGEN PRESENTING CELL CD4 + T CELL CYTOKINE PRODUCTION CLONAL
MECHANISMS OF CELLULAR REJECTION IN ORGAN TRANSPLANTATION AN OVERVIEW YVON LEBRANCHU Service Néphrologie et Immunologie Clinique CHU TOURS ANTIGEN PRESENTING CELL CD4 + T CELL CYTOKINE PRODUCTION CLONAL
General Overview of Immunology. Kimberly S. Schluns, Ph.D. Associate Professor Department of Immunology UT MD Anderson Cancer Center
 General Overview of Immunology Kimberly S. Schluns, Ph.D. Associate Professor Department of Immunology UT MD Anderson Cancer Center Objectives Describe differences between innate and adaptive immune responses
General Overview of Immunology Kimberly S. Schluns, Ph.D. Associate Professor Department of Immunology UT MD Anderson Cancer Center Objectives Describe differences between innate and adaptive immune responses
Supplemental Information. Gut Microbiota Promotes Hematopoiesis to Control Bacterial Infection. Cell Host & Microbe, Volume 15
 Cell Host & Microbe, Volume 15 Supplemental Information Gut Microbiota Promotes Hematopoiesis to Control Bacterial Infection Arya Khosravi, Alberto Yáñez, Jeremy G. Price, Andrew Chow, Miriam Merad, Helen
Cell Host & Microbe, Volume 15 Supplemental Information Gut Microbiota Promotes Hematopoiesis to Control Bacterial Infection Arya Khosravi, Alberto Yáñez, Jeremy G. Price, Andrew Chow, Miriam Merad, Helen
Identification of an alternative G q - dependent chemokine receptor signal transduction pathway in dendritic cells and granulocytes
 ARTICLE Identification of an alternative G q - dependent chemokine receptor signal transduction pathway in dendritic cells and granulocytes Guixiu Shi, 1 Santiago Partida-S á nchez, 1 Ravi S. Misra, 1
ARTICLE Identification of an alternative G q - dependent chemokine receptor signal transduction pathway in dendritic cells and granulocytes Guixiu Shi, 1 Santiago Partida-S á nchez, 1 Ravi S. Misra, 1
TCR, MHC and coreceptors
 Cooperation In Immune Responses Antigen processing how peptides get into MHC Antigen processing involves the intracellular proteolytic generation of MHC binding proteins Protein antigens may be processed
Cooperation In Immune Responses Antigen processing how peptides get into MHC Antigen processing involves the intracellular proteolytic generation of MHC binding proteins Protein antigens may be processed
Measuring Dendritic Cells
 Measuring Dendritic Cells A.D. Donnenberg, V.S. Donnenberg UNIVERSITY of PITTSBURGH CANCER INSTITUTE CCS Longbeach 10_04 Measuring DC Rare event detection The basics of DC measurement Applications Cancer
Measuring Dendritic Cells A.D. Donnenberg, V.S. Donnenberg UNIVERSITY of PITTSBURGH CANCER INSTITUTE CCS Longbeach 10_04 Measuring DC Rare event detection The basics of DC measurement Applications Cancer
Adaptive Immunity. Jeffrey K. Actor, Ph.D. MSB 2.214,
 Adaptive Immunity Jeffrey K. Actor, Ph.D. MSB 2.214, 500-5344 Lecture Objectives: Understand role of various molecules including cytokines, chemokines, costimulatory and adhesion molecules in the development
Adaptive Immunity Jeffrey K. Actor, Ph.D. MSB 2.214, 500-5344 Lecture Objectives: Understand role of various molecules including cytokines, chemokines, costimulatory and adhesion molecules in the development
Supplemental Figure 1. Signature gene expression in in vitro differentiated Th0, Th1, Th2, Th17 and Treg cells. (A) Naïve CD4 + T cells were cultured
 Supplemental Figure 1. Signature gene expression in in vitro differentiated Th0, Th1, Th2, Th17 and Treg cells. (A) Naïve CD4 + T cells were cultured under Th0, Th1, Th2, Th17, and Treg conditions. mrna
Supplemental Figure 1. Signature gene expression in in vitro differentiated Th0, Th1, Th2, Th17 and Treg cells. (A) Naïve CD4 + T cells were cultured under Th0, Th1, Th2, Th17, and Treg conditions. mrna
How plasma cells develop. Deutsches Rheuma Forschungs Zentrum, Berlin Institut der Leibniz Gemeinschaft
 How plasma cells develop Deutsches Rheuma Forschungs Zentrum, Berlin Institut der Leibniz Gemeinschaft 1 Plasma cells develop from activated B cells Toll Like Receptor B Cell Receptor B cell B cell microbia
How plasma cells develop Deutsches Rheuma Forschungs Zentrum, Berlin Institut der Leibniz Gemeinschaft 1 Plasma cells develop from activated B cells Toll Like Receptor B Cell Receptor B cell B cell microbia
Medical Virology Immunology. Dr. Sameer Naji, MB, BCh, PhD (UK) Head of Basic Medical Sciences Dept. Faculty of Medicine The Hashemite University
 Medical Virology Immunology Dr. Sameer Naji, MB, BCh, PhD (UK) Head of Basic Medical Sciences Dept. Faculty of Medicine The Hashemite University Human blood cells Phases of immune responses Microbe Naïve
Medical Virology Immunology Dr. Sameer Naji, MB, BCh, PhD (UK) Head of Basic Medical Sciences Dept. Faculty of Medicine The Hashemite University Human blood cells Phases of immune responses Microbe Naïve
Darwinian selection and Newtonian physics wrapped up in systems biology
 Darwinian selection and Newtonian physics wrapped up in systems biology Concept published in 1957* by Macfarland Burnet (1960 Nobel Laureate for the theory of induced immune tolerance, leading to solid
Darwinian selection and Newtonian physics wrapped up in systems biology Concept published in 1957* by Macfarland Burnet (1960 Nobel Laureate for the theory of induced immune tolerance, leading to solid
Supporting Online Material for
 www.sciencemag.org/cgi/content/full/1175194/dc1 Supporting Online Material for A Vital Role for Interleukin-21 in the Control of a Chronic Viral Infection John S. Yi, Ming Du, Allan J. Zajac* *To whom
www.sciencemag.org/cgi/content/full/1175194/dc1 Supporting Online Material for A Vital Role for Interleukin-21 in the Control of a Chronic Viral Infection John S. Yi, Ming Du, Allan J. Zajac* *To whom
Chapter 1. Chapter 1 Concepts. MCMP422 Immunology and Biologics Immunology is important personally and professionally!
 MCMP422 Immunology and Biologics Immunology is important personally and professionally! Learn the language - use the glossary and index RNR - Reading, Note taking, Reviewing All materials in Chapters 1-3
MCMP422 Immunology and Biologics Immunology is important personally and professionally! Learn the language - use the glossary and index RNR - Reading, Note taking, Reviewing All materials in Chapters 1-3
Endogenous TNFα orchestrates the trafficking of neutrophils into and within lymphatic vessels during acute inflammation
 SUPPLEMENTARY INFORMATION Endogenous TNFα orchestrates the trafficking of neutrophils into and within lymphatic vessels during acute inflammation Samantha Arokiasamy 1,2, Christian Zakian 1, Jessica Dilliway
SUPPLEMENTARY INFORMATION Endogenous TNFα orchestrates the trafficking of neutrophils into and within lymphatic vessels during acute inflammation Samantha Arokiasamy 1,2, Christian Zakian 1, Jessica Dilliway
Control of intestinal inflammation by regulatory T cells
 Control of intestinal inflammation by regulatory T cells Fiona Powrie Sir William Dunn School of Pathology University of Oxford fiona.powrie@path.ox.ac.uk Regulatory T cells prevent immune pathology in
Control of intestinal inflammation by regulatory T cells Fiona Powrie Sir William Dunn School of Pathology University of Oxford fiona.powrie@path.ox.ac.uk Regulatory T cells prevent immune pathology in
Presented by Lucas Nemec. Nat. Med. 21, (2015)
 Presented by Lucas Nemec Nat. Med. 21, 647 53 (2015) 1 Introduction Sylvia S. Mader, Inquiry into Life, 8th Edition, 1997 2 Introduction Sylvia S. Mader, Inquiry into Life, 8th Edition, 1997 3 Introduction
Presented by Lucas Nemec Nat. Med. 21, 647 53 (2015) 1 Introduction Sylvia S. Mader, Inquiry into Life, 8th Edition, 1997 2 Introduction Sylvia S. Mader, Inquiry into Life, 8th Edition, 1997 3 Introduction
B6/COLODR/SPL/11C/83/LAP/#2.006 B6/COLODR/SPL/11C/86/LAP/#2.016 CD11C B6/COLODR/SPL/11C/80/LAP/#2.011 CD11C
 CD3-specific antibody-induced immune tolerance and suppression of autoimmune encephalomyelitis involves TGF-β production through phagocytes digesting apoptotic T cells Sylvain Perruche 1,3, Pin Zhang 1,
CD3-specific antibody-induced immune tolerance and suppression of autoimmune encephalomyelitis involves TGF-β production through phagocytes digesting apoptotic T cells Sylvain Perruche 1,3, Pin Zhang 1,
MATERIALS AND METHODS. Neutralizing antibodies specific to mouse Dll1, Dll4, J1 and J2 were prepared as described. 1,2 All
 MATERIALS AND METHODS Antibodies (Abs), flow cytometry analysis and cell lines Neutralizing antibodies specific to mouse Dll1, Dll4, J1 and J2 were prepared as described. 1,2 All other antibodies used
MATERIALS AND METHODS Antibodies (Abs), flow cytometry analysis and cell lines Neutralizing antibodies specific to mouse Dll1, Dll4, J1 and J2 were prepared as described. 1,2 All other antibodies used
Cytokines modulate the functional activities of individual cells and tissues both under normal and pathologic conditions Interleukins,
 Cytokines http://highered.mcgraw-hill.com/sites/0072507470/student_view0/chapter22/animation the_immune_response.html Cytokines modulate the functional activities of individual cells and tissues both under
Cytokines http://highered.mcgraw-hill.com/sites/0072507470/student_view0/chapter22/animation the_immune_response.html Cytokines modulate the functional activities of individual cells and tissues both under
Part III Innate and Adaptive Immune Cells: General Introduction
 Innate and Adaptive Immune Cells: General Introduction Iván López-Expósito As an organ specialized in food digestion and nutrient absorption, the intestinal mucosa presents a huge surface area (almost
Innate and Adaptive Immune Cells: General Introduction Iván López-Expósito As an organ specialized in food digestion and nutrient absorption, the intestinal mucosa presents a huge surface area (almost
SEVENTH EDITION CHAPTER
 Judy Owen Jenni Punt Sharon Stranford Kuby Immunology SEVENTH EDITION CHAPTER 16 Tolerance, Autoimmunity, and Transplantation Copyright 2013 by W. H. Freeman and Company Immune tolerance: history * Some
Judy Owen Jenni Punt Sharon Stranford Kuby Immunology SEVENTH EDITION CHAPTER 16 Tolerance, Autoimmunity, and Transplantation Copyright 2013 by W. H. Freeman and Company Immune tolerance: history * Some
The Journal of Experimental Medicine
 CXCL12 Mediates CCR7-independent Homing of Central Memory Cells, But Not Naive T Cells, in Peripheral Lymph Nodes M. Lucila Scimone, Thomas W. Felbinger, Irina B. Mazo, Jens V. Stein, Ulrich H. von Andrian,
CXCL12 Mediates CCR7-independent Homing of Central Memory Cells, But Not Naive T Cells, in Peripheral Lymph Nodes M. Lucila Scimone, Thomas W. Felbinger, Irina B. Mazo, Jens V. Stein, Ulrich H. von Andrian,
T cell-mediated immunity
 T cell-mediated immunity Overview For microbes within phagosomes in phagocytes.cd4+ T lymphocytes (TH1) Activate phagocyte by cytokines studies on Listeria monocytogenes For microbes infecting and replicating
T cell-mediated immunity Overview For microbes within phagosomes in phagocytes.cd4+ T lymphocytes (TH1) Activate phagocyte by cytokines studies on Listeria monocytogenes For microbes infecting and replicating
The Immune System. These are classified as the Innate and Adaptive Immune Responses. Innate Immunity
 The Immune System Biological mechanisms that defend an organism must be 1. triggered by a stimulus upon injury or pathogen attack 2. able to counteract the injury or invasion 3. able to recognise foreign
The Immune System Biological mechanisms that defend an organism must be 1. triggered by a stimulus upon injury or pathogen attack 2. able to counteract the injury or invasion 3. able to recognise foreign
Regulation of anti-tumor immunity through migration of immune cell subsets within the tumor microenvironment Thomas F. Gajewski, M.D., Ph.D.
 Regulation of anti-tumor immunity through migration of immune cell subsets within the tumor microenvironment Thomas F. Gajewski, M.D., Ph.D. Professor, Departments of Pathology and Medicine Program Leader,
Regulation of anti-tumor immunity through migration of immune cell subsets within the tumor microenvironment Thomas F. Gajewski, M.D., Ph.D. Professor, Departments of Pathology and Medicine Program Leader,
Natural Killer Cells: Development, Diversity, and Applications to Human Disease Dr. Michael A. Caligiuri
 Natural Killer Cells: Development, Diversity, November 26, 2008 The Ohio State University Comprehensive Cancer Center The James Cancer Hospital and Solove Research Institute Columbus, Ohio, USA 1 Human
Natural Killer Cells: Development, Diversity, November 26, 2008 The Ohio State University Comprehensive Cancer Center The James Cancer Hospital and Solove Research Institute Columbus, Ohio, USA 1 Human
Homing and Inflammation!
 Homing and Inflammation! Micro 204. Molecular and Cellular Immunology! Lecturer: Jason Cyster! jason.cyster@ucsf.edu! How do cells migrate from blood into tissue?! the four step model! role of selectins,
Homing and Inflammation! Micro 204. Molecular and Cellular Immunology! Lecturer: Jason Cyster! jason.cyster@ucsf.edu! How do cells migrate from blood into tissue?! the four step model! role of selectins,
The Development of Lymphocytes: B Cell Development in the Bone Marrow & Peripheral Lymphoid Tissue Deborah A. Lebman, Ph.D.
 The Development of Lymphocytes: B Cell Development in the Bone Marrow & Peripheral Lymphoid Tissue Deborah A. Lebman, Ph.D. OBJECTIVES 1. To understand how ordered Ig gene rearrangements lead to the development
The Development of Lymphocytes: B Cell Development in the Bone Marrow & Peripheral Lymphoid Tissue Deborah A. Lebman, Ph.D. OBJECTIVES 1. To understand how ordered Ig gene rearrangements lead to the development
Putting it Together. Stephen Canfield Secondary Lymphoid System. Tonsil Anterior Cervical LN s
 Putting it Together Stephen Canfield smc12@columbia.edu Secondary Lymphoid System Tonsil Anterior Cervical LN s Axillary LN s Mediastinal/Retroperitoneal LN s Thoracic Duct Appendix Spleen Inguinal LN
Putting it Together Stephen Canfield smc12@columbia.edu Secondary Lymphoid System Tonsil Anterior Cervical LN s Axillary LN s Mediastinal/Retroperitoneal LN s Thoracic Duct Appendix Spleen Inguinal LN
The Skinny of the Immune System
 The Skinny of the Immune System Robert Hostoffer, DO, FACOP, FAAP Associate Professor of Pediatrics Case Western Reserve University, Cleveland, Ohio Overview 1. Immune system of the skin 2. Immune Players
The Skinny of the Immune System Robert Hostoffer, DO, FACOP, FAAP Associate Professor of Pediatrics Case Western Reserve University, Cleveland, Ohio Overview 1. Immune system of the skin 2. Immune Players
NIH Public Access Author Manuscript J Invest Dermatol. Author manuscript; available in PMC 2015 February 01.
 NIH Public Access Author Manuscript Published in final edited form as: J Invest Dermatol. 2014 August ; 134(8): 2071 2074. doi:10.1038/jid.2014.141. A possible role for IL-17A in establishing Th2 inflammation
NIH Public Access Author Manuscript Published in final edited form as: J Invest Dermatol. 2014 August ; 134(8): 2071 2074. doi:10.1038/jid.2014.141. A possible role for IL-17A in establishing Th2 inflammation
Homing and Inflammation!
 Homing and Inflammation! Micro 204. Molecular and Cellular Immunology! Lecturer: Jason Cyster! jason.cyster@ucsf.edu! How do cells migrate from blood into tissue?! the four step model! role of selectins,
Homing and Inflammation! Micro 204. Molecular and Cellular Immunology! Lecturer: Jason Cyster! jason.cyster@ucsf.edu! How do cells migrate from blood into tissue?! the four step model! role of selectins,
Dr. Yi-chi M. Kong August 8, 2001 Benjamini. Ch. 19, Pgs Page 1 of 10 TRANSPLANTATION
 Benjamini. Ch. 19, Pgs 379-399 Page 1 of 10 TRANSPLANTATION I. KINDS OF GRAFTS II. RELATIONSHIPS BETWEEN DONOR AND RECIPIENT Benjamini. Ch. 19, Pgs 379-399 Page 2 of 10 II.GRAFT REJECTION IS IMMUNOLOGIC
Benjamini. Ch. 19, Pgs 379-399 Page 1 of 10 TRANSPLANTATION I. KINDS OF GRAFTS II. RELATIONSHIPS BETWEEN DONOR AND RECIPIENT Benjamini. Ch. 19, Pgs 379-399 Page 2 of 10 II.GRAFT REJECTION IS IMMUNOLOGIC
7/6/2009. The study of the immune system and of diseases that occur as a result of inappropriate or inadequate actions of the immune system.
 Diseases of Immunity 2009 CL Davis General Pathology Paul W. Snyder, DVM, PhD Purdue University Acknowledgements Pathologic Basis of Veterinary Disease, 4 th Ed Veterinary Immunology, An Introduction 8
Diseases of Immunity 2009 CL Davis General Pathology Paul W. Snyder, DVM, PhD Purdue University Acknowledgements Pathologic Basis of Veterinary Disease, 4 th Ed Veterinary Immunology, An Introduction 8
There are 2 major lines of defense: Non-specific (Innate Immunity) and. Specific. (Adaptive Immunity) Photo of macrophage cell
 There are 2 major lines of defense: Non-specific (Innate Immunity) and Specific (Adaptive Immunity) Photo of macrophage cell Development of the Immune System ery pl neu mφ nk CD8 + CTL CD4 + thy TH1 mye
There are 2 major lines of defense: Non-specific (Innate Immunity) and Specific (Adaptive Immunity) Photo of macrophage cell Development of the Immune System ery pl neu mφ nk CD8 + CTL CD4 + thy TH1 mye
B and T lymphocyte attenuator regulates CD8 + T cell intrinsic homeostasis and memory cell generation
 27 Nature Publishing Group http://www.nature.com/natureimmunology B and T lymphocyte attenuator regulates CD8 + T cell intrinsic homeostasis and memory cell generation Carsten Krieg 1, Onur Boyman 1,2,
27 Nature Publishing Group http://www.nature.com/natureimmunology B and T lymphocyte attenuator regulates CD8 + T cell intrinsic homeostasis and memory cell generation Carsten Krieg 1, Onur Boyman 1,2,
Development of B and T lymphocytes
 Development of B and T lymphocytes What will we discuss today? B-cell development T-cell development B- cell development overview Stem cell In periphery Pro-B cell Pre-B cell Immature B cell Mature B cell
Development of B and T lymphocytes What will we discuss today? B-cell development T-cell development B- cell development overview Stem cell In periphery Pro-B cell Pre-B cell Immature B cell Mature B cell
Adaptive Immunity. PowerPoint Lecture Presentations prepared by Mindy Miller-Kittrell, North Carolina State University C H A P T E R
 PowerPoint Lecture Presentations prepared by Mindy Miller-Kittrell, North Carolina State University C H A P T E R 16 Adaptive Immunity The Body s Third Line of Defense Adaptive Immunity Adaptive immunity
PowerPoint Lecture Presentations prepared by Mindy Miller-Kittrell, North Carolina State University C H A P T E R 16 Adaptive Immunity The Body s Third Line of Defense Adaptive Immunity Adaptive immunity
Tbk1-TKO! DN cells (%)! 15! 10!
 a! T Cells! TKO! B Cells! TKO! b! CD4! 8.9 85.2 3.4 2.88 CD8! Tbk1-TKO! 1.1 84.8 2.51 2.54 c! DN cells (%)! 4 3 2 1 DP cells (%)! 9 8 7 6 CD4 + SP cells (%)! 5 4 3 2 1 5 TKO! TKO! TKO! TKO! 15 1 5 CD8
a! T Cells! TKO! B Cells! TKO! b! CD4! 8.9 85.2 3.4 2.88 CD8! Tbk1-TKO! 1.1 84.8 2.51 2.54 c! DN cells (%)! 4 3 2 1 DP cells (%)! 9 8 7 6 CD4 + SP cells (%)! 5 4 3 2 1 5 TKO! TKO! TKO! TKO! 15 1 5 CD8
Adaptive Immunity. PowerPoint Lecture Presentations prepared by Mindy Miller-Kittrell, North Carolina State University C H A P T E R
 CSLO7. Describe functions of host defenses and the immune system in combating infectious diseases and explain how immunizations protect against specific diseases. PowerPoint Lecture Presentations prepared
CSLO7. Describe functions of host defenses and the immune system in combating infectious diseases and explain how immunizations protect against specific diseases. PowerPoint Lecture Presentations prepared
CD8 T cell tumor infiltration following Tc1 or Tc2 therapy
 CD8 T cell tumor infiltration following Tc1 or Tc2 therapy Meredith L. Burgents A dissertation submitted to the faculty of the University of North Carolina at Chapel Hill in partial fulfillment of the
CD8 T cell tumor infiltration following Tc1 or Tc2 therapy Meredith L. Burgents A dissertation submitted to the faculty of the University of North Carolina at Chapel Hill in partial fulfillment of the
Immune response to infection
 Immune response to infection Dr. Sandra Nitsche (Sandra.Nitsche@rub.de ) 20.06.2018 1 Course of acute infection Typical acute infection that is cleared by an adaptive immune reaction 1. invasion of pathogen
Immune response to infection Dr. Sandra Nitsche (Sandra.Nitsche@rub.de ) 20.06.2018 1 Course of acute infection Typical acute infection that is cleared by an adaptive immune reaction 1. invasion of pathogen
Supplemental Figure 1
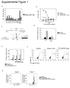 Supplemental Figure 1 1a 1c PD-1 MFI fold change 6 5 4 3 2 1 IL-1α IL-2 IL-4 IL-6 IL-1 IL-12 IL-13 IL-15 IL-17 IL-18 IL-21 IL-23 IFN-α Mut Human PD-1 promoter SBE-D 5 -GTCTG- -1.2kb SBE-P -CAGAC- -1.kb
Supplemental Figure 1 1a 1c PD-1 MFI fold change 6 5 4 3 2 1 IL-1α IL-2 IL-4 IL-6 IL-1 IL-12 IL-13 IL-15 IL-17 IL-18 IL-21 IL-23 IFN-α Mut Human PD-1 promoter SBE-D 5 -GTCTG- -1.2kb SBE-P -CAGAC- -1.kb
