Imaging of the knee in juvenile idiopathic arthritis
|
|
|
- Joy Evans
- 5 years ago
- Views:
Transcription
1 Pediatr Radiol (2018) 48: MINISYMPOSIUM: JUVENILE IDIOPATHIC ARTHRITIS Imaging of the knee in juvenile idiopathic arthritis Robert Hemke 1 & Nikolay Tzaribachev 2 & Anouk M. Barendregt 1,3 & J. Merlijn van den Berg 3 & Andrea S. Doria 4 & Mario Maas 1 Received: 29 August 2017 /Accepted: 11 October 2017 / Published online: 3 May 2018 # The Author(s) This article is an open access publication Abstract In juvenile idiopathic arthritis (JIA), imaging is increasingly used in clinical practice. In this paper we discuss imaging of the knee, the clinically most commonly affected joint in JIA. In the last decade, a number of important steps have been made in the development of imaging outcome measures in children with JIA knee involvement. Ultrasound is undergoing a fast validation process, which should be accomplished within the next few years. The validation processes of MRI as an imaging biomarker for clinical trials in the JIA knee are at an advanced stage, with important data available on the feasibility, reliability and validity of the Juvenile Arthritis MRI Scoring system. Moreover, both US and MRI data are emerging on the normal appearance of the growing knee joint. Keywords Children. Juvenile idiopathic arthritis. Knee. Magnetic resonance imaging. Radiography. Ultrasound * Robert Hemke r.hemke@amc.nl Department of Radiology and Nuclear Medicine Academic Medical Center, University of Amsterdam Meibergdreef 9, 1105AZ Amsterdam, The Netherlands Pediatric Rheumatology Research Institute Bad Bramstedt, Germany Department of Pediatric Hematology, Immunology, Rheumatology and Infectious Disease, Emma Children s Hospital AMC University of Amsterdam Amsterdam, The Netherlands Department of Diagnostic Imaging, The Hospital for Sick Children, University of Toronto Toronto, ON, Canada Introduction The knee joint is the most commonly affected joint in juvenile idiopathic arthritis (JIA) [1]. It can, therefore, be considered an index joint for evaluation of disease and for monitoring response to therapy. As in other joints, knee involvement in the scope of JIA is characterized by a swollen, painful, warm joint with loss of function. Conventional radiography has played an important role in the management of JIA, but imaging techniques such as ultrasonography (US) and MRI are now considered more helpful for several reasons. First, the trend towards early suppression of inflammation to prevent irreversible damage of cartilage and bone has shifted the emphasis from detecting damage (using radiography) to detecting early joint changes of JIA. This drives the need for imaging techniques that are more sensitive than radiography in the evaluation of inflammatory processes as well as early osteochondral changes. In this regard, MRI and US play an increasingly important role in evaluating and monitoring disease activity [2]. Second, the physical examination remains the reference standard for identifying disease activity in both daily practice and in clinical trials. However, physical examination has limited reliability, even if performed by an experienced observer [3], underpinning the potential of imaging in helping clinical decision-making. Moreover, advances in therapies have increased the number of children who reach clinically inactive disease. Further, knowledge about subclinical inflammation and its influence on the child s outcome is rising [2]. Conventional radiography In the clinical setting, conventional radiography still plays an important role, especially in narrowing the differential
2 Pediatr Radiol (2018) 48: diagnosis and in establishing a baseline for disease follow-up. Although radiography provides important information on growth disturbances and damage to cartilage and bone, it does not show early changes suggestive of active inflammation [4]. No validated scoring methods are available for evaluating JIA knee disease activity using radiography. There is little information on reliability and validity of scores for use in children or on the potential limitations of radiographic scoring systems for assessing growing joints because of the measurement properties of the scales [5]. Albeit nonspecific, the presence of joint fluid and synovial thickening can be seen as increased density in the infrapatellar fat pad and suprapatellar region. In the Western population, bone erosions in knee joints in children with JIA are relatively rare. Because of the availability of more effective treatment options and the relatively large amount of epiphyseal cartilage in knees in growing children, erosive damage is usually only seen as a late complication of JIA. When present, bone cysts and bone erosions can be seen. Moreover, loss of articular cartilage can cause gradual joint space narrowing. Joint malalignment and ankyloses in the knee are extremely rare. Radiography does have an advantage over ultrasound and MRI in the determination of growth disturbances. Due to hyperaemia, overgrowth of extremities and disturbance of epiphyseal bone formation can be observed. Moreover, it is easier to compare bilateral joints using radiography compared to, for instance, MRI. Ultrasound In paediatric rheumatology, ultrasound plays an important role in narrowing the differential diagnosis and can be useful for treatment monitoring as well as for guidance for joint injections [6]. It is superior to clinical examination in diagnosing disease activity and in detecting subclinical disease [7]. Because of its relatively low cost and wide accessibility, it allows for assessment of multiple joints within scanning times that vary according to the level of detail required for the examination. Limitations to the method include its inability to examine bone marrow or to reliably detect central erosive changes given the low penetration of the ultrasound beam to the central aspect of the joint with high-frequency transducers [8]. Acquisition techniques and ultrasound definitions For the application of US in paediatric rheumatology, both grey-scale B-mode and power/colour Doppler modes should be used in every examination. Also, standard scanning positions should be considered. For standard clinical paediatric ultrasound examination of the knee, the child is placed in supine position with a slightly flexed knee. The standard sagittal view includes the patella inferiorly, the quadriceps tendon, and the suprapatellar recess [9]. An axial view in the popliteal fossa can be considered to exclude a Baker cyst [9]. In the scope of research a more extensive ultrasound protocol of the knee can be considered (Table 1). The main US features characterizing pathology in JIA at this stage of the development of a US-based outcome measure are synovial thickening and synovial effusion [10]. Synovial thickening (Fig. 1) is defined as abnormal, intra-articular, hypoechoic material that is non-displaceable. Synovial effusion (Fig. 1) is defined as an abnormal, intra-articular, anechoic or hypoechoic material that is displaceable. When looking for a synovial effusion, one should be aware that a change of patient position can influence the level of effusion detected. Moreover, a scanning technique avoiding excessive pressure is warranted because joint fluid can shift to another synovial recess when too much pressure is used [11]. Power/colour Doppler is useful to acquire information about tissue perfusion. It is important to clarify that synovitis can be detected on the basis of B-mode findings (synovial thickening or synovial effusion) alone. Nevertheless power and colour Doppler have proved to be useful in differentiating active (hypervascular) from fibrotic (hypovascular) pannus [11]. In growing children, the sole detection of mildly increased vascularity does not allow for the diagnosis of synovitis because of the different levels of joint vascularity according to a child s age and level of physical activity of the joint [12]. It is important to recognize the presence of such normal vessels in paediatric joints from normal maturation and these should not be considered pathological [13]. In children with JIA, loss of cartilage thickness has been described. US has a strong correlation with MRI in the evaluation of cartilage thickness of the medial and lateral condyle and the intercondylar region, with a rho correlation of [14]. Scoring system We are currently developing a consensus-based US scoring system. The preliminary scoring system consists of three grades separated for synovitis and synovial perfusion (Table 2). Its reliability will be tested in a patient-based exercise. Normal values Age-related US findings have been described in healthy children [13, 15]. There are considerable age-related variations in children s joints, including the knee examined by US, where Doppler depicts vascularity, particularly within the epiphyseal cartilage of the children at a younger age. Also, age- and gender-related differences and standard reference values of the cartilage thickness of the knee in healthy children have
3 820 Pediatr Radiol (2018) 48: Table 1 Knee ultrasound technique Plane 1 (anterior suprapatellar recess)* Plane 2 (lateral parapatellar recess) Plane 3 (infrapatellar region) Plane 4 (condylar cartilage) Positioning knee joint 30 flexion Knee straightened, patella in 30 flexion 90 flexion a central position Positioning transducer Longitudinal to the suprapatellar recess/the quadriceps tendon 90 transversal to plane 1 Longitudinal to the infrapatellar tendon and Transversal to plane 1 Anatomical landmarks Features to assess Superior patellar edge, suprapatellar fat pad, quadriceps tendon, femur and pre-femoral fat pad Synovial effusion, synovial hypertrophy, synovial vascularity (hyperperfusion), erosive changes, morphology and structure of the tendons, vascularity of the tendon and the tendon sheet Superior patellar edge, femoral condyles, suprapatellar fat pad *Can alone be considered as a standard clinical paediatric ultrasound plane Synovial effusion, synovial hypertrophy, synovial vascularity (hyperperfusion), erosive changes the tibial tuberosity Inferior patellar edge, infrapatellar tendon, Hoffa fat pad, tibial tuberosity Synovial effusion, morphology and structure of the Hoffa fat pad, vascularity of the Hoffa fat pad, morphology and structure of the tendon, vascularity of the tendon, morphology and structure of the tibial tuberosity, vascularity of the tibial tuberosity Quadriceps tendon, suprapatellar fat pad, condylar cartilage Morphology and structure of the cartilage, erosive changes been elaborated [16]. However, the number of studies focusing on normal ultrasound values of the knee in children is limited. Therefore the normal appearance of the synovial membrane, for instance, should be interpreted with care. Magnetic resonance imaging Within the last decade, the use of MRI and advances in MRI techniques have substantially improved the evaluation of joint pathologies in children with JIA [4]. MRI is the preferred imaging modality for the assessment of inflammatory and destructive changes in JIA as compared to conventional radiography, ultrasonography and physical examination [3, 5]. Furthermore, MRI is the only imaging modality that is useful in visualizing bone marrow changes, a potential predictor of erosive joint damage in JIA, as previously demonstrated in adults [17]. Therefore despite practical limitations, MRI holds the potential to become an important outcome measure for assessing the knee joint in clinical trials of children with JIA. Main MRI features and imaging protocol In children with JIA and knee involvement, the main imaging features include synovial thickening, joint effusion and bone marrow oedema. Moreover cartilage loss and bone erosions Fig. 1 Ultrasound longitudinal to the suprapatellar recess in an 8- year-old girl with juvenile idiopathic arthritis. a There is evident synovial hypertrophy (arrow) and joint fluid in the suprapatellar recess (*). b After several months of treatment, the synovial hypertrophy and joint fluid have disappeared
4 Pediatr Radiol (2018) 48: Table 2 Suggested scoring system of ultrasound for the knee joint Feature Definition Locations Scale Synovitis B mode Synovitis power/colour Doppler mode Comprises synovial hypertrophy and synovial effusion Comprises synovial hypertrophy and hypervascularity* Suprapatellar recess, parapatellar recess Suprapatellar recess, parapatellar recess Grade 1 = mild Grade 2 = moderate Grade 3 = severe Grade 1 = mild Grade 2 = moderate Grade 3 = severe *Note that hypervascularity without synovial hypertrophy does not count for synovitis Synovitis = synovial hypertrophy and/or synovial effusion. Synovial hypertrophy is defined as abnormal, intraarticular, hypoechoic material that is non-displaceable. Synovial effusion is defined as abnormal, intra-articular, or hypoechoic material that is displaceable although relatively rare in paediatric patients can be observed. Tendinopathy, enthesopathy, inhomogeneity of the infra-patellar fat pad and bone cysts can be seen, as well, but these abnormalities are relatively uncommon in the knee joint. Moreover, the reliability of scoring these secondary features is unsatisfactory [18]. Table 3 shows an MRI protocol for evaluating the JIA knee joint. Synovial inflammation leading to synovial thickening is the principal pathological process in JIA, and the presence of synovial thickening on knee MRI is associated with the clinical onset of JIA [19]. On MRI, the inflamed synovial membrane is thickened and irregular, and its outline may be wavy. In the knee, a synovial thickness of >2 mm is considered pathological. The central locations in the knee (around the cruciate ligaments and retropatellar and suprapatellar areas, Fig. 2) are most commonly affected [20]. The signal intensity of this thickened synovial membrane is low to intermediate on T1-weighted images and high on T2-weighted images, similar to joint effusion. T1- weighted images after administration of gadolinium-based contrast agents provide better differentiation between joint effusion and synovial thickening [21]. Omitting intravenous gadolinium-based contrast agents in the MRI assessment of joints in JIA is therefore not advised. Although not specific for JIA, joint effusion (Fig. 2) can frequently be found in children with JIA [22]. On MRI, effusion demonstrates high signal intensity on fluid-sensitive images and low signal intensity on T1-weighted images. Joint effusions are predominantly located in the suprapatellar and central joint recesses. MRI is the state-of-the-art imaging technique to visualize changes in bone marrow suggestive of bone marrow oedema (Fig. 3). Bone marrow oedema can be seen as lesions with poorly defined margins within trabecular bone. It is marked by high signal intensity on T2-weighted fat-saturated images and low signal intensity on T1-weighted images. In rheumatoid arthritis, longitudinal studies have shown that the presence of bone marrow oedema is a key predictor of early erosive joint damage in adults with rheumatoid arthritis [17]. Therefore bone marrow oedema and synovial thickening are considered to be the most sensitive MRI features for monitoring disease activity in rheumatoid arthritis [23 25]. However to our knowledge there are a paucity of longitudinal studies, if any, focused on the prognostic value of bone marrow oedema in children with JIA. Cartilage loss may be seen as areas of increased water content (proton-density/t2 hyperintense) in the articular cartilage or contour abnormalities, defects or thinning of the Table 3 Knee MRI protocol Sequence Plane Goal Required or optional T2 FS or STIR (mdixon)* Sagittal Joint effusion, bone marrow oedema, bone erosions Required T2 FS or STIR (mdixon)* Coronal Bone marrow oedema, bone erosions Required T1 (mdixon)* Coronal Bone marrow oedema, bone erosions Required Gradient echo / PD Sagittal Cartilage loss Required T1 FS post-gd Axial Synovial thickening, joint effusion Required Gradient echo (3-D) Axial Cartilage loss Optional T1 FS pre-gd Axial Synovial thickening, joint effusion Optional T1 FS post-gd Sagittal Synovial thickening, joint effusion Optional *mdixon best option if available FS fat-suppressed, Gd gadolinium, PD proton density, STIR short tau inversion recovery, T1 T1-weighted spin echo, T2 T2-weighted
5 822 Pediatr Radiol (2018) 48: Fig. 2 Axial T1-weighted MRI of the knee with fat suppression after gadolinium-based contrast administration in three patients with juvenile idiopathic arthritis shows synovial hypertrophy in the central locations of the knee. a Enhancing synovial hypertrophy in the retropatellar region (arrow) in an 9-year old girl. b Enhancing synovial hypertrophy in the suprapatellar region (arrow) in an 11-year old boy. Notice the nonenhancing low-signal-intensity joint fluid in thesuprapatellar recess (*). c Enhancing synovial hypertrophy around the cruciate ligaments (arrow) in a 15-year old girl cartilage. Gradient-echo and proton-density-weighted sequences provide good contrast in the cartilage structure and can be used to evaluate the cartilage synovial fluid interface and the subchondral bone. MRI clearly shows the difference between changes in the articular cartilage and bone erosions. Bone erosions can be seen on T1-weighted images as loss of the normal low signal intensity of cortical bone and loss of the normal high signal intensity of trabecular bone (Fig. 3). Typically they have sharp margins. On T2-weighted images bone erosions appear as hypointense lesions, in contrast to subchondral cysts, which show as hyperintense signal on fluid-sensitive images. Scoring methods Although MRI is the preferred imaging modality for detecting both inflammatory as well as destructive changes in JIA, international experiences with the use of MRI as an outcome measure in JIA are limited. Subsequently, this technique is underused in both clinical practice and research. In order to further internationally validate MRI as an outcome measure in JIA, a special interest group on Outcome Measures in Rheumatology on MRI was created in 2011 [26]. Within this special interest group on MRI in JIA, three working groups were initiated for further assessment of MRI scoring systems: one group focuses on temporomandibular joints, another on small joints and the third on large joints (primarily the knee joint). Reliability In the last decade, two MRI scoring systems have been developed for the assessment of the paediatric knee joint: (1) the Juvenile Arthritis MRI Scoring system for use in JIA [27]and (2) the International Prophylaxis Study Group MRI Scoring system focusing on haemophilic arthropathy [28]. Fig. 3 Sagittal MR images of the knee in a 16-year-old girl with poly-articular juvenile idiopathic arthritis. a T2-weighted sagittal MRI with fat suppression shows bone marrow oedema in the femur (arrow) and tibial plateau. b T1-weighted sagittal MRI shows bone erosions in the tibial plateau (arrow), with irregular signal intensity of the cortical bone and loss of the normal high signal intensity of trabecular bone
6 Pediatr Radiol (2018) 48: Recently the Outcome Measures in Rheumatology (OMERACT) special interest group on MRI in JIA conducted a reliability study evaluating both scoring methods [18]. This study showed good inter-observer reliability for MRI scores focusing on active disease (e.g., synovial thickening, joint effusion and bone marrow changes) and moderate to substantial inter-observer reliability for scores focusing on damage (e.g., cartilage lesions, bone erosions). Finally, the group proposed a combined juvenile arthritis MRI scoring system (JAMRIS) shown in Table 4 including items from both the original Juvenile Arthritis MRI Scoring and the International Prophylaxis Study Group systems [18]. Besides this international reliability study, the intraobserver and inter-observer reliability of the original Juvenile Arthritis MRI Scoring system has been evaluated, and both proved to be reliable [27]. These data are trustworthy, especially regarding MRI features focusing on active disease. Caution is needed with regard to MRI characteristics focusing on damage because these features are relatively uncommonly observed in JIA patients. Feasibility Although MRI has some practical limitations such as limited availability in some regions/countries and the challenge of maintaining the same position for a prolonged period of time, it has proved feasible to perform contrast-enhanced knee MRI in children with JIA as young as 5 years old without the use of anaesthesia or sedation [29]. Moreover the use of the original Juvenile Arthritis MRI Scoring system proved feasible because the scoring takes an acceptable median of 6.6 min per patient [21]. Construct and clinical validity Within the last few years, two studies have focused on the sensitivity to changes in disease activity using the original Juvenile Arthritis MRI Scoring system [27, 30]. In both studies, with a follow-up period of 1 year, improvement of clinical JIA disease activity scores was associated with a significant decrease in MRI-based synovial thickening scores. These results represent good responsiveness of the Juvenile Arthritis MRI Scoring system, which is an important measure of validity. Moreover the Juvenile Arthritis MRI Scoring synovial thickening score proved useful in discriminating clinically active from clinically inactive JIA patients [31], indicating good discriminant validity. Next to the responsiveness and discriminant validity, the clinical validity has also been evaluated. In a study focusing on whether clinical, laboratory or MRI measures were able to differentiate JIA with active arthritis from other causes of non-infectious arthritis in a group of patients with clinical signs of early arthritis, multivariate analysis showed that MRI-based synovial thickening was independently associated with JIA (odds ratio [OR] 6.58, 95% confidence interval ) [19]. Normal values Because synovial inflammation is the hallmark of disease activity in JIA, it is important to determine the normal appearance and thickness of the synovial membrane in children. As stated, an intravenous injection of a gadolinium-based contrast agent is warranted for reliable evaluation of the synovial membrane. Therefore data on normal values for the synovial membrane in healthy children are sparse. Two studies that focused on the contrast-enhanced appearance of the synovial membraneinchildrenhavebeenperformed:(1)astudyby Nusman et al. [32] looked at the synovial membrane of the knee in children with inflammatory bowel disease who were clinically unaffected by arthritis; (2) Hemke et al. [33] determined the synovial membrane in knees of healthy children, using a standardized imaging protocol with post-contrast images obtained in the early phase (<5 min). The latter study showed that the normal synovial membrane thickness measures a maximum of 1.8 mm. The membrane was thickest around the cruciate ligaments, and retropatellar and suprapatellar recesses. The study by Nusman et al. showed a thickened synovial membrane (>2 mm) in more than half of patients with inflammatory bowel disease; however they did not observe any synovial thickness >4 mm. In all probability, the results from Hemke et al. are a more valid reflection of the true normal appearance of the synovial membrane because this study included healthy children (compared to patients with inflammatory bowel disease) and obtained post-contrast images in the early phase. Therefore, the Juvenile Arthritis MRI Scoring cut-off value of >2 mm for synovial thickening can be considered a valid measure. Some joint fluid in the knee can be seen in the majority of healthy children. The largest pockets of normal joint fluid in healthy children are located in the central locations of the knee around the cruciate ligaments and retropatellar region [33]. The mean diameter of the largest pocket of joint fluid in knees of healthy children is about 3 mm [15, 33]. Bone marrow changes suggestive of bone marrow oedema in knees of healthy children are relatively uncommon. In a study of 57 healthy children, bone marrow changes suggestive of bone marrow oedema were observed in 3 healthy children only. In all three children, the bone marrow changes were located in the apex patellae [33].The presence of bone marrow changes suggestive of bone marrow oedema in the apex patellae in children with JIA should, therefore, be interpreted with care. Moreover, zones of hematopoietic red bone marrow in the distal diaphysis and metaphysis of the femur might be seen as flame-like regions with signal characteristics fitting with bone
7 824 Pediatr Radiol (2018) 48: Table 4 Combined juvenile arthritis MRI scoring system Feature Definition Locations Scale Synovial thickening a An area of the synovial compartment that shows a thickened synovial membrane and which can show enhancement after intravenous gadolinium administration Six locations: patellofemoral area, suprapatellar recesses, infrapatellar fat pad, adjacent to the anterior and posterior cruciate ligaments, medial posterior condyle, and lateral posterior condyle The maximal diameter of the largest pocket of joint effusion is scored (0) normal, 2 mm (1) mild, >2 mm to 4 mm (2) moderate/severe, >4 mm Totals result in a minimum score of 0 and a maximum score of 12 (0) normal, 3 mm (1) mild, >3 mm to 5 mm (2) moderate/severe, >5 mm Totals result in a minimum score of 0 and a maximum score of 2 Presence of bone marrow edema is scored semi-quantitatively based on the subjectively estimated percentage of involved bone volume at each site as follows: (0) none (1) <10% of the whole bone volume (2) 10 25% of the whole bone volume (3) >25% of the whole bone volume Totals result in a minimum score of 0 and a maximum score of 24 (0) none (1) any loss (2) >50% volume loss (3) full-thickness loss (4) full-thickness loss >50% of surface Totals result in a minimum score of 0 and a maximum score of 4 (0) none (1) mild, any loss (2) moderate/severe, >50% surface involvement Totals result in a minimum score of 0 and a maximum score of 2 Joint effusion b An increased amount of fluid within the synovial compartment with high signal intensity on T2-weighted images and low signal intensity on T1-weighted images. Joint effusion has no post-gadolinium enhancement An abnormality within the trabecular bone of the epiphysis, with ill-defined margins and high signal intensity on T2-weighted fat-saturated images and low signal intensity on T1-weighted images Bone marrow oedema a Eight locations: lateral patella, medial patella, medial femur condyle, lateral femur condyle, medial weight-bearing region of the femur, lateral weight-bearing region of the femur, medial tibia plateau, lateral tibia plateau Cartilage loss b Loss of cartilaginous tissue either focally (superficial or deep) or diffusely Scored at the most severely affected location Bone erosions b A sharply marginated bone lesion with correct juxta-articular localization, typical signal characteristics and visible in two planes with a cortical break in at least one plane. On T1-weighted images there is a loss of the normal low signal intensity of cortical bone and loss of the normal high signal intensity of trabecular bone Scored at the most severely affected location a Original Juvenile Arthritis MRI Scoring item b Original International Prophylaxis Study Group item marrow oedema. Typically, these marrow flames originate from the physis and have straight vertical margins [34]. These hematopoietic bone marrow flames are a normal finding in growing children and should not be mistaken for bone marrow oedema. So-called speckled bone marrow is another normal variant that might be mistaken for pathology. Small spots with bone marrow oedema signal characteristics are predominantly located in the feet and ankles of children younger than 15 years, although the spots can be seen in the tibia plateau and the distal epiphysis of the femur as well [35]. The speckled appearance might be caused by focal regions of residual hematopoietic bone marrow or physiological stress, possibly related to weight-bearing or altered biomechanics during normal growth.
8 Pediatr Radiol (2018) 48: The thickness of the normal articular cartilage in knees of growing children differs with age. As expected, the cartilage is normally thicker in younger children compared to older children. A study performed by Keshava et al. [15] clearly demonstrates these differences among different age groups in healthy boys. Moreover they showed that the normal thickness of the articular cartilage differs per location within the knee joint [15]. In the distal femur, ossification usually starts in the centre of the cartilaginous epiphysis. Because the newly formed ossification centre contains hematopoietic bone marrow, its signal intensity is the same as that of red marrow in the adjacent distal femoral metaphysis [36]. The ossification centre enlarges from endochondral bone development. Adjacent cartilage cells undergo hypertrophy during endochondral ossification, which results in increased signal intensity on T2- weighted images [34]. This area of normal high signal intensity is most obvious in the posterior part of the distal femoral epiphysis and can be quite discrete [37]. Furthermore, it is important to be aware of the high prevalence of ossification variants of the femoral condyle among boys ages 2 12 years and girls ages 2 10 years; this should not be considered pathological [37]. Future work The validation process of US in children with JIA is moving forward. Despite the relatively easy applicability of US, until now there has been no specific US knee scoring system. Rather the US knee examination is part of a more global US score covering multiple joints with respect to disease activity. The Outcome Measures in Rheumatology paediatric ultrasound working sub-group has performed a number of steps towards the validation of US as an outcome measure in paediatric rheumatology. Next important steps of the work of the sub-group include multicentre reliability testing of the newly created score tested in a single-centre prospective study. In this case, sensitivity to change will also be tested. The sub-group has started its work in tendons and entheses and should follow the Outcome Measures in Rheumatology Filter 2.0 criteria for the validation process. Another important step will be to develop scores incorporating osteochondral changes, where US is expected to be beneficial in evaluating peripheral cartilage. Its utility in detecting erosive changes mightalsobetested,andcomparedtothatofmriand radiography. This underlines the importance of close collaboration between US and MRI working groups, which is planned to start in 2018 with a joint symposium. Although the first steps towards developing evidencebased guidelines for MRI data acquisition and interpretation have been made, further cooperation is necessary. The use of a juvenile arthritis MRI scoring system for the knee as an outcome measure in daily practice and clinical trials is promising. Thus far, juvenile arthritis MRI scoring has only been internationally tested in JIA patients visiting academic paediatric rheumatology centres in the Netherlands and Canada with full access to high-quality treatment. This has resulted in a population of studied JIA patients with only mild to moderate disease activity. Consequently, the presence of destructive changes of cartilage and bone has been relatively low in the studies performed until now. To evaluate the value of juvenile arthritis MRI scoring as a sensitive measure regarding destructive changes, further international collaboration is warranted, especially among research centres with access to more severely affected JIA patients. Furthermore, collaboration should focus on developing an MRI atlas of healthy joints in children, obtaining agreement on an optimal imaging protocol for the knee and further validating scoring methods. Interaction between researchers and health professionals in JIA imaging is essential to obtain international consensus and continuous improvement of MRI outcome measures. Such collaboration is expected to be very fruitful under the umbrella of an international, well-accepted collaborative international group such as the Outcome Measures in Rheumatology working group. According to the Quantification Imaging Biomarker Alliance of the Radiological Society of North America, quantitative imaging techniques covering the full spectrum of imaging have to be developed and validated to provide more objective tools to measure disease activity throughout all fields of medicine [38]. With respect to this, the Quantification Imaging Biomarker Alliance has formed the Contrast-enhanced Ultrasound Working Group to explore US contrast agent applications and use specific quantification software to evaluate disease activity and increase objectivity of the results of the US technique. Forthcoming research is expected to shed more light on the suitability of advanced quantitative MRI techniques for evaluating inflammatory and destructive changes in the JIA knee, including dynamic contrast-enhanced MRI, T2-mapping and diffusion-weighted imaging [39 44]. Currently these advanced imaging techniques are used particularly in the context of research and to a lesser extent in daily practice. The exact value of advanced MRI techniques in children with JIA has to be determined in larger prospective studies. To be viable in daily practice, these imaging techniques should be sensitive to change on which evidence is limited [45]. It is important to further develop and implement advanced imaging techniques in clinical practice. For example, the contrast-free approach of diffusion-weighted imaging is highly desirable in clinical practice because it could substantially improve patient care by optimizing MRI feasibility in paediatric JIA patients; moreover, establishing normal values for the MRI atlas of healthy joints is less ethically compromising if contrast-free imaging is available.
9 826 Pediatr Radiol (2018) 48: Conclusion In this paper, we discussed the status of imaging the JIA knee. In the last decade a number of important steps have been made in the development of imaging outcome measures in children with JIA knee involvement. Ultrasound is undergoing a fast validation process, which should be accomplished within the next few years. The validation processes of MRI as an imaging biomarker for clinical trials in the JIA knee are at an advanced stage, with important data forthcoming from both single-centre as well as international multi-centre studies on the feasibility, reliability and validity of the Juvenile Arthritis MRI Scoring system. Moreover, data are emerging in both US and MRI on the normal appearance of the growing knee joint. However, future research is clearly needed, especially within the scope of evaluating the value of Juvenile Arthritis MRI Scoring as a sensitive measure for assessing destructive changes. The ultrasound score needs further validation, as well. Moreover, further validation is needed for promising advanced quantitative US and MRI techniques for the evaluation of inflammatory and destructive changes in JIA. Compliance with ethical standards Conflicts of interest References None Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License ( creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. 1. Hemke R, Nusman CM, van der Heijde DM et al (2015) Frequency of joint involvement in juvenile idiopathic arthritis during a 5-year follow-up of newly diagnosed patients: implications for MR imaging as outcome measure. Rheumatol Int 35: Colebatch-Bourn AN, Edwards CJ, Collado P et al (2015) EULAR- PReS points to consider for the use of imaging in the diagnosis and management of juvenile idiopathic arthritis in clinical practice. Ann Rheum Dis 74: Guzman J, Burgos-Vargas R, Duarte-Salazar C et al (1995) Reliability of the articular examination in children with juvenile rheumatoid arthritis: interobserver agreement and sources of disagreement. J Rheumatol 22: Miller E, Uleryk E, Doria AS (2009) Evidence-based outcomes of studies addressing diagnostic accuracy of MRI of juvenile idiopathic arthritis. AJR Am J Roentgenol 192: Doria AS, Babyn PS, Feldman B (2006) A critical appraisal of radiographic scoring systems for assessment of juvenile idiopathic arthritis. Pediatr Radiol 36: Magni-Manzoni S, Collado P, Jousse-Joulin S et al (2014) Current state of musculoskeletal ultrasound in paediatric rheumatology: results of an international survey. Rheumatology 53: Rebollo-Polo M, Koujok K, Weisser C et al (2011) Ultrasound findings on patients with juvenile idiopathic arthritis in clinical remission. Arthritis Care Res 63: Malattia C, Damasio MB, Magnaguagno F et al (2008) Magnetic resonance imaging, ultrasonography, and conventional radiography in the assessment of bone erosions in juvenile idiopathic arthritis. Arthritis Rheum 59: Carmichael J, Rosendahl K (2016) Musculoskeletal imaging. In: Beek E, Rijn RR (eds) Diagnostic pediatric ultrasound. Georg Thieme Verlag, Stuttgart 10. Roth J, Jousse-Joulin S, Magni-Manzoni S et al (2015) Definitions for the sonographic features of joints in healthy children. Arthritis Care Res 67: Martinoli C, Bianchi S (2007) Knee. In: Bianchi S, Martinoli C (eds) Ultrasound of the musculoskeletal system. Springer, Berlin 12. Roth J, Ravagnani V, Backhaus M et al (2016) Preliminary definitions for the sonographic features of synovitis in children. Arthritis Care Res 69: Collado P, Vojinovic J, Nieto JC et al (2016) Toward standardized musculoskeletal ultrasound in pediatric rheumatology: normal agerelated ultrasound findings. Arthritis Care Res 68: Pradsgaard DO, Fiirgaard B, Spannow AH et al (2015) Cartilage thickness of the knee joint in juvenile idiopathic arthritis: comparative assessment by ultrasonography and magnetic resonance imaging. J Rheumatol 42: Keshava SN, Gibikote SV, Mohanta A et al (2015) Ultrasound and magnetic resonance imaging of healthy paediatric ankles and knees: a baseline for comparison with haemophilic joints. Haemophilia 21: e210 e Spannow AH, Pfeiffer-Jensen M, Andersen NT et al (2010) Ultrasonographic measurements of joint cartilage thickness in healthy children: age- and sex-related standard reference values. J Rheumatol 37: McQueen FM (2007) A vital clue to deciphering bone pathology: MRI bone oedema in rheumatoid arthritis and osteoarthritis. Ann Rheum Dis 66: Hemke R, Tzaribachev N, Nusman CM et al (2017) Magnetic resonance imaging (MRI) of the knee as an outcome measure in juvenile idiopathic arthritis: an OMERACT reliability study on MRI scales. J Rheumatol 44: Hemke R, Kuijpers TW, Nusman CM et al (2015) Contrastenhanced MRI features in the early diagnosis of juvenile idiopathic arthritis. Eur Radiol 25: Nusman CM, Hemke R, Schonenberg D et al (2014) Distribution pattern of MRI abnormalities within the knee and wrist of juvenile idiopathic arthritis patients: signature of disease activity. AJR Am J Roentgenol 202:W439 W Hemke R, Kuijpers TW, van den Berg JM et al (2013) The diagnostic accuracy of unenhanced MRI in the assessment of joint abnormalities in juvenile idiopathic arthritis. Eur Radiol 23: Gylys-Morin VM, Graham TB, Blebea JS et al (2001) Knee in early juvenile rheumatoid arthritis: MR imaging findings. Radiology 220: Haavardsholm EA, Bøyesen P, Østergaard M et al (2008) Magnetic resonance imaging findings in 84 patients with early rheumatoid arthritis: bone marrow oedema predicts erosive progression. Ann Rheum Dis 67: Conaghan PG, O'Connor P, McGonagle D et al (2003) Elucidation of the relationship between synovitis and bone damage: a randomized magnetic resonance imaging study of individual joints in patients with early rheumatoid arthritis. Arthritis Rheum 48:64 71
10 Pediatr Radiol (2018) 48: Hetland ML, Ejbjerg B, Horslev-Petersen K et al (2009) MRI bone oedema is the strongest predictor of subsequent radiographic progression in early rheumatoid arthritis. Results from a 2-year randomised controlled trial (CIMESTRA). Ann Rheum Dis 68: Hemke R, Doria AS, Tzaribachev N et al (2014) Selecting magnetic resonance imaging (MRI) outcome measures for juvenile idiopathic arthritis (JIA) clinical trials: first report of the MRI in JIA special interest group. J Rheumatol 41: Hemke R, van Rossum MA, van Veenendaal M et al (2013) Reliability and responsiveness of the juvenile arthritis MRI scoring (JAMRIS) system for the knee. Eur Radiol 23: Feldman BM, Funk S, Lundin B et al (2008) Musculoskeletal measurement tools from the international prophylaxis study group (IPSG). Haemophilia 14: Hemke R, van Veenendaal M, Kuijpers TW et al (2012) Increasing feasibility and patient comfort of MRI in children with juvenile idiopathic arthritis. Pediatr Radiol 42: Hemke R, van Veenendaal M, van den Berg JM et al (2014) Oneyear followup study on clinical findings and changes in magnetic resonance imaging-based disease activity scores in juvenile idiopathic arthritis. J Rheumatol 41: Hemke R, Maas M, van Veenendaal M et al (2014) Contrastenhanced MRI compared with the physical examination in the evaluation of disease activity in juvenile idiopathic arthritis. Eur Radiol 24: Nusman CM, Hemke R, Benninga MA et al (2016) Contrastenhanced MRI of the knee in children unaffected by clinical arthritis compared to clinically active juvenile idiopathic arthritis patients. Eur Radiol 26: Hemke R, van den Berg JM, Nusman CM et al (2017) Contrast-enhanced MRI findings of the knee in healthy children; establishing normal values. Eur Radiol Laor T, Jaramillo D (2009) MR imaging insights into skeletal maturation: what is normal? Radiology 250: Shabshin N, Schweitzer ME, Morrison WB et al (2006) High-signal T2 changes of the bone marrow of the foot and ankle in children: red marrow or traumatic changes? Pediatr Radiol 36: Waitches G, Zawin JK, Poznanski AK (1994) Sequence and rate of bone marrow conversion in the femora of children as seen on MR imaging: are accepted standards accurate? AJR Am J Roentgenol 162: Jans L, Jaremko J, Ditchfield M et al (2012) Ossification variants of the femoral condyles are not associated with osteochondritis dissecans. Eur J Radiol 81: Radiological Society of North America (2017) Quantitative Imaging Biomarkers Alliance web page. QIBA/. Accessed 28 Sept Hilbert F, Holl-Wieden A, Sauer A et al (2017) Intravoxel incoherent motion magnetic resonance imaging of the knee joint in children with juvenile idiopathic arthritis. Pediatr Radiol 47: Barendregt AM, Nusman CM, Hemke R et al (2015) Feasibility of diffusion-weighted magnetic resonance imaging in patients with juvenile idiopathic arthritis on 1.0-T open-bore MRI. Skelet Radiol 44: Hemke R, Lavini C, Nusman CM et al (2014) Pixel-by-pixel analysis of DCE-MRI curve shape patterns in knees of active and inactive juvenile idiopathic arthritis patients. Eur Radiol 24: Nusman CM, Hemke R, Lavini C et al (2017) Dynamic contrastenhanced magnetic resonance imaging can play a role in predicting flare in juvenile idiopathic arthritis. Eur J Radiol 88: Nusman CM, Lavini C, Hemke R et al (2017) Dynamic contrastenhanced magnetic resonance imaging of the wrist in children with juvenile idiopathic arthritis. Pediatr Radiol 47: Barendregt AM, van Gulik EC, Lavini C et al (2017) Diffusionweighted imaging for assessment of synovial inflammation in juvenile idiopathic arthritis: a promising imaging biomarker as an alternative to gadolinium-based contrast agents. Eur Radiol. org/ /s y 45. Workie DW, Graham TB, Laor T et al (2007) Quantitative MR characterization of disease activity in the knee in children with juvenile idiopathic arthritis: a longitudinal pilot study. Pediatr Radiol 37:
Magnetic resonance imaging in juvenile idiopathic arthritis diagnosis and follow-up, beyond imagination Hemke, R.
 UvA-DARE (Digital Academic Repository) Magnetic resonance imaging in juvenile idiopathic arthritis diagnosis and follow-up, beyond imagination Hemke, R. Link to publication Citation for published version
UvA-DARE (Digital Academic Repository) Magnetic resonance imaging in juvenile idiopathic arthritis diagnosis and follow-up, beyond imagination Hemke, R. Link to publication Citation for published version
ELENI ANDIPA General Hospital of Athens G. Gennimatas
 ELENI ANDIPA General Hospital of Athens G. Gennimatas Technological advances over the last years have caused a dramatic improvement in ultrasound quality and resolution An established imaging modality
ELENI ANDIPA General Hospital of Athens G. Gennimatas Technological advances over the last years have caused a dramatic improvement in ultrasound quality and resolution An established imaging modality
MRI KNEE WHAT TO SEE. Dr. SHEKHAR SRIVASTAV. Sr.Consultant KNEE & SHOULDER ARTHROSCOPY
 MRI KNEE WHAT TO SEE Dr. SHEKHAR SRIVASTAV Sr.Consultant KNEE & SHOULDER ARTHROSCOPY MRI KNEE - WHAT TO SEE MRI is the most accurate and frequently used diagnostic tool for evaluation of internal derangement
MRI KNEE WHAT TO SEE Dr. SHEKHAR SRIVASTAV Sr.Consultant KNEE & SHOULDER ARTHROSCOPY MRI KNEE - WHAT TO SEE MRI is the most accurate and frequently used diagnostic tool for evaluation of internal derangement
Comparative study of high resolusion ultrasonography and magnetic resonance imaging in diagnosing traumatic knee injuries & pathologies
 Original article: Comparative study of high resolusion ultrasonography and magnetic resonance imaging in diagnosing traumatic knee injuries & pathologies Dr. Rakesh Gujjar*, Dr. R. P. Bansal, Dr. Sandeep
Original article: Comparative study of high resolusion ultrasonography and magnetic resonance imaging in diagnosing traumatic knee injuries & pathologies Dr. Rakesh Gujjar*, Dr. R. P. Bansal, Dr. Sandeep
Case Report: Knee MR Imaging of Haemarthrosis in a Case of Haemophilia A
 Clinical > Pediatric Imaging Case Report: Knee MR Imaging of Haemarthrosis in a Case of Haemophilia A M. A. Weber, J. K. Kloth University Hospital Heidelberg, Department of Diagnostic and Interventional
Clinical > Pediatric Imaging Case Report: Knee MR Imaging of Haemarthrosis in a Case of Haemophilia A M. A. Weber, J. K. Kloth University Hospital Heidelberg, Department of Diagnostic and Interventional
Scoring and Grading B-Mode Synovitis and Doppler findings in pediatric MSKUS. Johannes Roth MD PhD FRCPC RhMSUS
 Scoring and Grading B-Mode Synovitis and Doppler findings in pediatric MSKUS Johannes Roth MD PhD FRCPC RhMSUS Pathology - Definition Synovitis Synovitis on ultrasonography in children B-mode and Doppler
Scoring and Grading B-Mode Synovitis and Doppler findings in pediatric MSKUS Johannes Roth MD PhD FRCPC RhMSUS Pathology - Definition Synovitis Synovitis on ultrasonography in children B-mode and Doppler
Knee: Cruciate Ligaments
 72 Knee: Cruciate Ligaments R. Kent Sanders Sagittal oblique 2.5-mm sequences along the plane of the anterior cruciate ligament (ACL) typically yield three to four images of the ACL, with the first medial
72 Knee: Cruciate Ligaments R. Kent Sanders Sagittal oblique 2.5-mm sequences along the plane of the anterior cruciate ligament (ACL) typically yield three to four images of the ACL, with the first medial
Ultrasound in Rheumatology
 Arthritis Research UK Primary Care Centre Winner of a Queen s Anniversary Prize For Higher and Further Education 2009 Ultrasound in Rheumatology Alison Hall Consultant MSK Sonographer/Research Fellow Primary
Arthritis Research UK Primary Care Centre Winner of a Queen s Anniversary Prize For Higher and Further Education 2009 Ultrasound in Rheumatology Alison Hall Consultant MSK Sonographer/Research Fellow Primary
The EULAR OMERACT rheumatoid arthritis MRI reference image atlas: the wrist joint
 i23 The EULAR OMERACT rheumatoid arthritis MRI reference image atlas: the wrist joint B Ejbjerg, F McQueen, M Lassere, E Haavardsholm, P Conaghan, P O Connor, P Bird, C Peterfy, J Edmonds, M Szkudlarek,
i23 The EULAR OMERACT rheumatoid arthritis MRI reference image atlas: the wrist joint B Ejbjerg, F McQueen, M Lassere, E Haavardsholm, P Conaghan, P O Connor, P Bird, C Peterfy, J Edmonds, M Szkudlarek,
MR imaging of the knee in marathon runners before and after competition
 Skeletal Radiol (2001) 30:72 76 International Skeletal Society 2001 ARTICLE W. Krampla R. Mayrhofer J. Malcher K.H. Kristen M. Urban W. Hruby MR imaging of the knee in marathon runners before and after
Skeletal Radiol (2001) 30:72 76 International Skeletal Society 2001 ARTICLE W. Krampla R. Mayrhofer J. Malcher K.H. Kristen M. Urban W. Hruby MR imaging of the knee in marathon runners before and after
Imaging in juvenile idiopathic arthritis international initiatives and ongoing work
 Pediatric Radiology (2018) 48:828 834 https://doi.org/10.1007/s00247-017-4054-z MINISYMPOSIUM: JUVENILE IDIOPATHIC ARTHRITIS Imaging in juvenile idiopathic arthritis international initiatives and ongoing
Pediatric Radiology (2018) 48:828 834 https://doi.org/10.1007/s00247-017-4054-z MINISYMPOSIUM: JUVENILE IDIOPATHIC ARTHRITIS Imaging in juvenile idiopathic arthritis international initiatives and ongoing
8/29/2012. Outline Juvenile idiopathic arthritis. 1. Classification-ILAR. 1. Classification-clinical diagnosis. 1. JIA classification
 Outline Juvenile idiopathic arthritis 1. Classification and symptoms (ILAR-International league of Associations for Rheumatology) 2. Imaging J. Herman Kan, M.D. Section chief, musculoskeletal imaging Edward
Outline Juvenile idiopathic arthritis 1. Classification and symptoms (ILAR-International league of Associations for Rheumatology) 2. Imaging J. Herman Kan, M.D. Section chief, musculoskeletal imaging Edward
Knee Contusions and Stress Injuries. Laura W. Bancroft, M.D.
 Knee Contusions and Stress Injuries Laura W. Bancroft, M.D. Objectives Review 5 types of contusion patterns Pivot shift Dashboard Hyperextension Clip Lateral patellar dislocation Demonstrate various stress
Knee Contusions and Stress Injuries Laura W. Bancroft, M.D. Objectives Review 5 types of contusion patterns Pivot shift Dashboard Hyperextension Clip Lateral patellar dislocation Demonstrate various stress
Standardised. knee. scanning of the. Basic pathology. Nemanja Damjanov. University of Belgrade Institute of Rheumatology
 Standardised scanning of the Nemanja Damjanov University of Belgrade Institute of Rheumatology knee Basic pathology Disclosure Lecturer: Pfizer, Abbvie, Roche, MSD, Boehringer-Ingelheim, Gedeon Richter,
Standardised scanning of the Nemanja Damjanov University of Belgrade Institute of Rheumatology knee Basic pathology Disclosure Lecturer: Pfizer, Abbvie, Roche, MSD, Boehringer-Ingelheim, Gedeon Richter,
Ultrasound of the Knee
 Ultrasound of the Knee Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures: Consultant: Bioclinica Book Royalties: Elsevier Advisory
Ultrasound of the Knee Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures: Consultant: Bioclinica Book Royalties: Elsevier Advisory
Ultrasound in Rheumatological Conditions:
 Ultrasound in Rheumatological Conditions: Status and Perspectives Nancy A. Chauvin, MD Assistant Professor of Radiology Director of Musculoskeletal Imaging The Children s Hospital of Philadelphia University
Ultrasound in Rheumatological Conditions: Status and Perspectives Nancy A. Chauvin, MD Assistant Professor of Radiology Director of Musculoskeletal Imaging The Children s Hospital of Philadelphia University
A Comparative Study of Ultrasonographic Findings with Clinical and Radiological Findings of Painful Osteoarthritis of the Knee Joint
 Med. J. Cairo Univ., Vol. 84, No. 3, December: 97-, www.medicaljournalofcairouniversity.net A Comparative Study of Ultrasonographic Findings with Clinical and Radiological Findings of Painful Osteoarthritis
Med. J. Cairo Univ., Vol. 84, No. 3, December: 97-, www.medicaljournalofcairouniversity.net A Comparative Study of Ultrasonographic Findings with Clinical and Radiological Findings of Painful Osteoarthritis
This presentation is the intellectual property of the author. Contact them for permission to reprint and/or distribute.
 MRI of the Knee Jennifer Swart, M.D. Musculoskeletal Radiology South Texas Radiology Group Outline Coils, Patient Positioning Acquisition Parameters, Planes and Pulse Sequences Knee Arthrography Normal
MRI of the Knee Jennifer Swart, M.D. Musculoskeletal Radiology South Texas Radiology Group Outline Coils, Patient Positioning Acquisition Parameters, Planes and Pulse Sequences Knee Arthrography Normal
This presentation is the intellectual property of the author. Contact them at for permission to reprint and/or distribute.
 MRI of the Knee Jennifer Swart, M.D. Musculoskeletal Radiology South Texas Radiology Group Financial Disclosure Dr. Jennifer Swart has no relevant financial relationships with commercial interests to disclose.
MRI of the Knee Jennifer Swart, M.D. Musculoskeletal Radiology South Texas Radiology Group Financial Disclosure Dr. Jennifer Swart has no relevant financial relationships with commercial interests to disclose.
Knee, Ankle, and Foot: Normal and Abnormal Features with MRI and Ultrasound Correlation. Disclosures. Outline. Joint Effusion. Suprapatellar recess
 Knee, Ankle, and Foot: Normal and Abnormal Features with MRI and Ultrasound Correlation Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan
Knee, Ankle, and Foot: Normal and Abnormal Features with MRI and Ultrasound Correlation Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan
Synovial hemangioma of the suprapatellar bursa
 Synovial hemangioma of the suprapatellar bursa Poster No.: P-0040 Congress: ESSR 2013 Type: Authors: Keywords: DOI: Scientific Exhibit A. YESILDAG, S. Keskin, H. Kalkan, S. Kucuksen, U. Kerimoglu; Konya/TR
Synovial hemangioma of the suprapatellar bursa Poster No.: P-0040 Congress: ESSR 2013 Type: Authors: Keywords: DOI: Scientific Exhibit A. YESILDAG, S. Keskin, H. Kalkan, S. Kucuksen, U. Kerimoglu; Konya/TR
BASELINE QUESTIONNAIRE (SURGEON)
 SECTION A: STUDY INFORMATION Subject ID: - - Study Visit: Baseline Site Number: Date: / / Surgeon ID: SECTION B: INITIAL SURGEON HISTORY B1. Previous Knee Surgery: Yes No Not recorded B2. Number of Previous
SECTION A: STUDY INFORMATION Subject ID: - - Study Visit: Baseline Site Number: Date: / / Surgeon ID: SECTION B: INITIAL SURGEON HISTORY B1. Previous Knee Surgery: Yes No Not recorded B2. Number of Previous
Sonographic assessment of adult and juvenile rheumatoid arthritis
 Sonographic assessment of adult and juvenile rheumatoid arthritis Poster No.: C-1485 Congress: ECR 2013 Type: Educational Exhibit Authors: C. A. S. Ruano, P. L. Pegado, J. M. G. Lourenco, P. Alves, L.
Sonographic assessment of adult and juvenile rheumatoid arthritis Poster No.: C-1485 Congress: ECR 2013 Type: Educational Exhibit Authors: C. A. S. Ruano, P. L. Pegado, J. M. G. Lourenco, P. Alves, L.
Running head: Radiological Modalities and Childhood Arthritis 1
 Running head: Radiological Modalities and Childhood Arthritis 1 Contemporary Radiological Modalities in the Diagnosis of Childhood Arthritis November 15 th, 2011 Radiological Modalities and Childhood Arthritis
Running head: Radiological Modalities and Childhood Arthritis 1 Contemporary Radiological Modalities in the Diagnosis of Childhood Arthritis November 15 th, 2011 Radiological Modalities and Childhood Arthritis
Why Talk About Technique? MRI of the Knee:
 Why Talk About Technique? MRI of the Knee: Part 1 - Imaging Techniques Mark Anderson, M.D. University of Virginia Health Sciences Center Charlottesville, Virginia Always had an interest teach our fellows
Why Talk About Technique? MRI of the Knee: Part 1 - Imaging Techniques Mark Anderson, M.D. University of Virginia Health Sciences Center Charlottesville, Virginia Always had an interest teach our fellows
Chronic knee pain in adults - a multimodality approach or which modality to choose and when?
 Chronic knee pain in adults - a multimodality approach or which modality to choose and when? Poster No.: P-0157 Congress: ESSR 2013 Type: Authors: Keywords: DOI: Scientific Exhibit E. Ilieva, V. Tasseva,
Chronic knee pain in adults - a multimodality approach or which modality to choose and when? Poster No.: P-0157 Congress: ESSR 2013 Type: Authors: Keywords: DOI: Scientific Exhibit E. Ilieva, V. Tasseva,
MRI of the Knee: Part 4 - normal variants that may simulate disease. Mark Anderson, M.D. University of Virginia
 MRI of the Knee: Part 4 - normal variants that may simulate disease Mark Anderson, M.D. University of Virginia discuss the most common normal variants in the pediatric knee that may simulate pathology
MRI of the Knee: Part 4 - normal variants that may simulate disease Mark Anderson, M.D. University of Virginia discuss the most common normal variants in the pediatric knee that may simulate pathology
Ultrasound in Rheumatology
 Ultrasound in Rheumatology Alison Hall Consultant MSK Sonographer Research Institute for Primary Care & Health Sciences, Keele University Department of Rheumatology, Cannock Hospital, Royal Wolverhampton
Ultrasound in Rheumatology Alison Hall Consultant MSK Sonographer Research Institute for Primary Care & Health Sciences, Keele University Department of Rheumatology, Cannock Hospital, Royal Wolverhampton
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 12/01/2012 Radiology Quiz of the Week # 101 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 12/01/2012 Radiology Quiz of the Week # 101 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Ultrasound of the Hip: Anatomy, Pathology, and Procedures
 Ultrasound of the Hip: Anatomy, Pathology, and Procedures Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Outline Hip Joint Native hip
Ultrasound of the Hip: Anatomy, Pathology, and Procedures Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Outline Hip Joint Native hip
and K n e e J o i n t Is the most complicated joint in the body!!!!
 K n e e J o i n t K n e e J o i n t Is the most complicated joint in the body!!!! 1-Consists of two condylar joints between: A-The medial and lateral condyles of the femur and The condyles of the tibia
K n e e J o i n t K n e e J o i n t Is the most complicated joint in the body!!!! 1-Consists of two condylar joints between: A-The medial and lateral condyles of the femur and The condyles of the tibia
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 11/24/2012 Radiology Quiz of the Week # 100 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 11/24/2012 Radiology Quiz of the Week # 100 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Magnetic resonance imaging of femoral head development in roentgenographically normal patients
 Skeletal Radiol (1985) 14:159-163 Skeletal Radiology Magnetic resonance imaging of femoral head development in roentgenographically normal patients Peter J. Littrup, M.D. 1, Alex M. Aisen, M.D. 2, Ethan
Skeletal Radiol (1985) 14:159-163 Skeletal Radiology Magnetic resonance imaging of femoral head development in roentgenographically normal patients Peter J. Littrup, M.D. 1, Alex M. Aisen, M.D. 2, Ethan
Numerous studies have demonstrated that magnetic resonance imaging (MRI) is more sensitive for detection of
 Reducing Invasiveness, Duration, and Cost of Magnetic Resonance Imaging in Rheumatoid Arthritis by Omitting Intravenous Contrast Injection Does It Change the Assessment of Inflammatory and Destructive
Reducing Invasiveness, Duration, and Cost of Magnetic Resonance Imaging in Rheumatoid Arthritis by Omitting Intravenous Contrast Injection Does It Change the Assessment of Inflammatory and Destructive
PEM GUIDE CHILDHOOD FRACTURES
 PEM GUIDE CHILDHOOD FRACTURES INTRODUCTION Skeletal injuries account for 10-15% of all injuries in children; 20% of those are fractures, 3 out of 4 fractures affect the physis or growth plate. Always consider
PEM GUIDE CHILDHOOD FRACTURES INTRODUCTION Skeletal injuries account for 10-15% of all injuries in children; 20% of those are fractures, 3 out of 4 fractures affect the physis or growth plate. Always consider
Knee ultrasound in pediatric patients - anatomy, diagnostic pitfalls, common pathologies.
 Knee ultrasound in pediatric patients - anatomy, diagnostic pitfalls, common pathologies. Poster No.: C-2434 Congress: ECR 2015 Type: Educational Exhibit Authors: C. M. Olchowy, M. Lasecki, M. Inglot,
Knee ultrasound in pediatric patients - anatomy, diagnostic pitfalls, common pathologies. Poster No.: C-2434 Congress: ECR 2015 Type: Educational Exhibit Authors: C. M. Olchowy, M. Lasecki, M. Inglot,
Introduction to Musculoskeletal Ultrasound. Disclosures. Evidence Based Medicine Key References 8/30/2017
 Introduction to Musculoskeletal Ultrasound Johannes Roth MD, PhD, FRCPC, RhMSUS Professor of Pediatrics University of Ottawa Gurjit S Kaeley MBBS, MRCP, RhMSUS Professor of Medicine Division Chief Director
Introduction to Musculoskeletal Ultrasound Johannes Roth MD, PhD, FRCPC, RhMSUS Professor of Pediatrics University of Ottawa Gurjit S Kaeley MBBS, MRCP, RhMSUS Professor of Medicine Division Chief Director
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/40654 holds various files of this Leiden University dissertation. Author: Stomp, W. Title: MR imaging in early rheumatoid arthritis : techniques and applications
Cover Page The handle http://hdl.handle.net/1887/40654 holds various files of this Leiden University dissertation. Author: Stomp, W. Title: MR imaging in early rheumatoid arthritis : techniques and applications
Oak foundation for donating the 3T Siemens Verio scanner. Board of directors BBH and Frh Hospitals for supporting the
 Knee pain and inflammation in the infrapatellar fat pad estimated by conventional and dynamic contrast-enhanced magnetic resonance imaging in obese patients with osteoarthritis: a crosssectional study
Knee pain and inflammation in the infrapatellar fat pad estimated by conventional and dynamic contrast-enhanced magnetic resonance imaging in obese patients with osteoarthritis: a crosssectional study
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/29578 holds various files of this Leiden University dissertation. Author: Krabben, Annemarie Title: Predictive factors for the development and disease course
Cover Page The handle http://hdl.handle.net/1887/29578 holds various files of this Leiden University dissertation. Author: Krabben, Annemarie Title: Predictive factors for the development and disease course
Acute Elbow Trauma in Children: Spectrum of Injury Revealed by MR Imaging Not Apparent on Radiographs
 James F. Griffith 1 Derek J. Roebuck 1,2 Jack C. Y. Cheng 3 Yu Leung Chan 1 Timothy H. Rainer 4 Bobby K. W. Ng 3 Constantine Metreweli 1 Received December 14, 1999; accepted after revision June 8, 2000.
James F. Griffith 1 Derek J. Roebuck 1,2 Jack C. Y. Cheng 3 Yu Leung Chan 1 Timothy H. Rainer 4 Bobby K. W. Ng 3 Constantine Metreweli 1 Received December 14, 1999; accepted after revision June 8, 2000.
Ultrasound Evaluation of Masses
 Ultrasound Evaluation of Masses Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures: Consultant: Bioclinica Advisory Panel: GE,
Ultrasound Evaluation of Masses Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures: Consultant: Bioclinica Advisory Panel: GE,
Osteochondritis Dissecans of the Knee. M Lucas Murnaghan MD, MEd, FRCSC
 Osteochondritis Dissecans of the Knee M Lucas Murnaghan MD, MEd, FRCSC Outline 1. Clinical Presentation 2. Investigations 3. Classification 4. Non-operative Treatment 5. Operative Treatment 6. Treatment
Osteochondritis Dissecans of the Knee M Lucas Murnaghan MD, MEd, FRCSC Outline 1. Clinical Presentation 2. Investigations 3. Classification 4. Non-operative Treatment 5. Operative Treatment 6. Treatment
S tructural joint damage, a major outcome in
 i3 An introduction to the EULAR OMERACT rheumatoid arthritis MRI reference image atlas M Østergaard, J Edmonds, F McQueen, C Peterfy, M Lassere, B Ejbjerg, P Bird, P Emery, H Genant, P Conaghan... This
i3 An introduction to the EULAR OMERACT rheumatoid arthritis MRI reference image atlas M Østergaard, J Edmonds, F McQueen, C Peterfy, M Lassere, B Ejbjerg, P Bird, P Emery, H Genant, P Conaghan... This
Sonographic appearance of chronic inflammatory rheumatism
 Sonographic appearance of chronic inflammatory rheumatism Poster No.: C-2237 Congress: ECR 2013 Type: Educational Exhibit Authors: H. Elfattach, F. Houari, O. Addou, M. Maaroufi, S. Tizniti ; 1 1 1 1 2
Sonographic appearance of chronic inflammatory rheumatism Poster No.: C-2237 Congress: ECR 2013 Type: Educational Exhibit Authors: H. Elfattach, F. Houari, O. Addou, M. Maaroufi, S. Tizniti ; 1 1 1 1 2
Publication for the Philips MRI Community
 FieldStrength Publication for the Philips MRI Community Issue 38 Summer 2009 Pediatric MSK imaging benefits from tailored scan protocols Vanderbilt University Children s Hospital builds dedicated scans
FieldStrength Publication for the Philips MRI Community Issue 38 Summer 2009 Pediatric MSK imaging benefits from tailored scan protocols Vanderbilt University Children s Hospital builds dedicated scans
Stability of Post Traumatic Osteochondritis Dissecans of the Knee: MR Imaging Findings
 Chin J Radiol 2005; 30: 199-204 199 Stability of Post Traumatic Osteochondritis Dissecans of the Knee: MR Imaging Findings YU-CHUNG HUNG 1 JON-KWAY HUANG 1,2 Department of Radiology 1, Mackay Memorial
Chin J Radiol 2005; 30: 199-204 199 Stability of Post Traumatic Osteochondritis Dissecans of the Knee: MR Imaging Findings YU-CHUNG HUNG 1 JON-KWAY HUANG 1,2 Department of Radiology 1, Mackay Memorial
Case Report Sequential MR Images and Radiographs of Epiphyseal Osteomyelitis in the Distal Femur of an Infant
 Case Reports in Radiology Volume 2013, Article ID 672815, 4 pages http://dx.doi.org/10.1155/2013/672815 Case Report Sequential MR Images and Radiographs of Epiphyseal Osteomyelitis in the Distal Femur
Case Reports in Radiology Volume 2013, Article ID 672815, 4 pages http://dx.doi.org/10.1155/2013/672815 Case Report Sequential MR Images and Radiographs of Epiphyseal Osteomyelitis in the Distal Femur
Ultrasound of the Knee Joint. Jun Sung Park,M.D. Bundang General Hospital Dept. of Rehabilitation Medicine
 Ultrasound of the Knee Joint Jun Sung Park,M.D. Bundang General Hospital Dept. of Rehabilitation Medicine Clinical History and P/E Chronic or Acute Symptoms Chronic Sx. : possible of systemic articular
Ultrasound of the Knee Joint Jun Sung Park,M.D. Bundang General Hospital Dept. of Rehabilitation Medicine Clinical History and P/E Chronic or Acute Symptoms Chronic Sx. : possible of systemic articular
Lipoma Arborescens of Subacromial-subdeltoid Bursa: Ultrasonographic Findings
 C A S E R E P O R T Lipoma Arborescens of Subacromial-subdeltoid Bursa: Ultrasonographic Findings Amelia Bargiela*, Esther Rodriguez, Rafaela Soler The present study describes the ultrasound findings of
C A S E R E P O R T Lipoma Arborescens of Subacromial-subdeltoid Bursa: Ultrasonographic Findings Amelia Bargiela*, Esther Rodriguez, Rafaela Soler The present study describes the ultrasound findings of
Knee Joint Anatomy 101
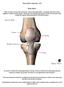 Knee Joint Anatomy 101 Bone Basics There are three bones at the knee joint femur, tibia and patella commonly referred to as the thighbone, shinbone and kneecap. The fibula is not typically associated with
Knee Joint Anatomy 101 Bone Basics There are three bones at the knee joint femur, tibia and patella commonly referred to as the thighbone, shinbone and kneecap. The fibula is not typically associated with
MRI of Cartilage. D. BENDAHAN (PhD)
 MRI of Cartilage D. BENDAHAN (PhD) Centre de Résonance Magnétique Biologique et Médicale UMR CNRS 7339 Faculté de Médecine de la Timone 27, Bd J. Moulin 13005 Marseille France david.bendahan@univ-amu.fr
MRI of Cartilage D. BENDAHAN (PhD) Centre de Résonance Magnétique Biologique et Médicale UMR CNRS 7339 Faculté de Médecine de la Timone 27, Bd J. Moulin 13005 Marseille France david.bendahan@univ-amu.fr
The Egyptian Journal of Hospital Medicine (October 2017) Vol. 69 (4), Page
 The Egyptian Journal of Hospital Medicine (October 2017) Vol. 69 (4), Page 2294-2300 Role of Magnetic Resonance Imaging and Ultrasonography in Diagnosis and Follow Up Rheumatoid Arthritis in Hand and Wrist
The Egyptian Journal of Hospital Medicine (October 2017) Vol. 69 (4), Page 2294-2300 Role of Magnetic Resonance Imaging and Ultrasonography in Diagnosis and Follow Up Rheumatoid Arthritis in Hand and Wrist
Brain Atrophy. Brain Atrophy
 Aging Central Nervous System Processes Age related brain atrophy Non-age related brain atrophy Cerebrovascular disease Cerebral infarction Hypertensive hemorrhage Carotid artery stenosis and occlusion
Aging Central Nervous System Processes Age related brain atrophy Non-age related brain atrophy Cerebrovascular disease Cerebral infarction Hypertensive hemorrhage Carotid artery stenosis and occlusion
ORIGINAL ARTICLE. ROLE OF MRI IN EVALUATION OF TRAUMATIC KNEE INJURIES Saurabh Chaudhuri, Priscilla Joshi, Mohit Goel
 ROLE OF MRI IN EVALUATION OF TRAUMATIC KNEE INJURIES Saurabh Chaudhuri, Priscilla Joshi, Mohit Goel 1. Associate Professor, Department of Radiodiagnosis & imaging, Bharati Vidyapeeth Medical College and
ROLE OF MRI IN EVALUATION OF TRAUMATIC KNEE INJURIES Saurabh Chaudhuri, Priscilla Joshi, Mohit Goel 1. Associate Professor, Department of Radiodiagnosis & imaging, Bharati Vidyapeeth Medical College and
Amendment of the OMERACT ultrasound definitions of joints features in healthy children when using the DOPPLER technique
 Collado et al. Pediatric Rheumatology (2018) 16:23 https://doi.org/10.1186/s12969-018-0240-2 RESEARCH ARTICLE Open Access Amendment of the OMERACT ultrasound definitions of joints features in healthy children
Collado et al. Pediatric Rheumatology (2018) 16:23 https://doi.org/10.1186/s12969-018-0240-2 RESEARCH ARTICLE Open Access Amendment of the OMERACT ultrasound definitions of joints features in healthy children
Rakesh Patel, MD 4/9/09
 Rakesh Patel, MD 4/9/09 Chondral Injuries Very common Present in 63-66% patients undergoing arthroscopy 11-19% full-thickness lesions Up to 79% patients with ACL deficient knee have some form of chondral
Rakesh Patel, MD 4/9/09 Chondral Injuries Very common Present in 63-66% patients undergoing arthroscopy 11-19% full-thickness lesions Up to 79% patients with ACL deficient knee have some form of chondral
MRI of Pediatric Ankle and Foot. Mahesh Thapa, MD Associate Professor Seattle Children s University of Washington School of Medicine
 MRI of Pediatric Ankle and Foot Mahesh Thapa, MD Associate Professor Seattle Children s University of Washington School of Medicine Disclosures Under contract with Lippincott Williams and Wilkins (LWW)
MRI of Pediatric Ankle and Foot Mahesh Thapa, MD Associate Professor Seattle Children s University of Washington School of Medicine Disclosures Under contract with Lippincott Williams and Wilkins (LWW)
Assessing synovitis based on dynamic gadolinium-enhanced MRI and EULAR-OMERACT scores of the wrist in patients with rheumatoid arthritis
 Assessing synovitis based on dynamic gadolinium-enhanced MRI and EULAR-OMERACT scores of the wrist in patients with rheumatoid arthritis W. Wojciechowski 1,2, Z. Tabor 3, A. Urbanik 2 1 Medical Centre
Assessing synovitis based on dynamic gadolinium-enhanced MRI and EULAR-OMERACT scores of the wrist in patients with rheumatoid arthritis W. Wojciechowski 1,2, Z. Tabor 3, A. Urbanik 2 1 Medical Centre
Citation Acta medica Nagasakiensia. 2000, 45
 NAOSITE: Nagasaki University's Ac Title Author(s) Pictorial Essay Magnetic Resonance Related Disorders Uetani, Masataka; Hashmi, Rashid; N Hayashi, Kuniaki Citation Acta medica Nagasakiensia. 2000, 45
NAOSITE: Nagasaki University's Ac Title Author(s) Pictorial Essay Magnetic Resonance Related Disorders Uetani, Masataka; Hashmi, Rashid; N Hayashi, Kuniaki Citation Acta medica Nagasakiensia. 2000, 45
Current Status in Pediatric Musculoskeletal Ultrasonography. Johannes Roth, MD PhD FRCPC RhMSUS
 1 Current Status in Pediatric Musculoskeletal Ultrasonography Johannes Roth, MD PhD FRCPC RhMSUS 2 Objectives Provide a rationale for the use of imaging and ultrasonography in particular in pediatric rheumatology
1 Current Status in Pediatric Musculoskeletal Ultrasonography Johannes Roth, MD PhD FRCPC RhMSUS 2 Objectives Provide a rationale for the use of imaging and ultrasonography in particular in pediatric rheumatology
The Knee. Prof. Oluwadiya Kehinde
 The Knee Prof. Oluwadiya Kehinde www.oluwadiya.sitesled.com The Knee: Introduction 3 bones: femur, tibia and patella 2 separate joints: tibiofemoral and patellofemoral. Function: i. Primarily a hinge joint,
The Knee Prof. Oluwadiya Kehinde www.oluwadiya.sitesled.com The Knee: Introduction 3 bones: femur, tibia and patella 2 separate joints: tibiofemoral and patellofemoral. Function: i. Primarily a hinge joint,
Focal Periphyseal Edema (FOPE) Zone on MRI of the Adolescent Knee: A Potentially Painful Manifestation of Physiologic Physeal Fusion?
 Pediatric Imaging Original Research Zbojniewicz and Laor MRI of the Adolescent Knee Pediatric Imaging Original Research Andrew M. Zbojniewicz 1 Tal Laor Zbojniewicz AM, Laor T Keywords: children, knee,
Pediatric Imaging Original Research Zbojniewicz and Laor MRI of the Adolescent Knee Pediatric Imaging Original Research Andrew M. Zbojniewicz 1 Tal Laor Zbojniewicz AM, Laor T Keywords: children, knee,
Case 27 Clinical Presentation
 53 Case 27 Clinical Presentation 40-year-old man presents with acute shoulder pain and normal findings on radiographs. 54 RadCases Musculoskeletal Radiology Imaging Findings (,) Coronal images of the shoulder
53 Case 27 Clinical Presentation 40-year-old man presents with acute shoulder pain and normal findings on radiographs. 54 RadCases Musculoskeletal Radiology Imaging Findings (,) Coronal images of the shoulder
Screening for and Assessment of Osteonecrosis in Oncology Patients. Sue C. Kaste, DO SPR Postgraduate Course 2015
 Screening for and Assessment of Osteonecrosis in Oncology Patients Sue C. Kaste, DO SPR Postgraduate Course 2015 The author declares no potential conflicts of interest or financial disclosures Osteonecrosis
Screening for and Assessment of Osteonecrosis in Oncology Patients Sue C. Kaste, DO SPR Postgraduate Course 2015 The author declares no potential conflicts of interest or financial disclosures Osteonecrosis
Imaging the musculoskeletal system. An Introduction
 Imaging the musculoskeletal system An Introduction Objectives Discuss: commonly used imaging modalities in the musculoskeletal system normal imaging anatomy in the extremities fracture description Imaging
Imaging the musculoskeletal system An Introduction Objectives Discuss: commonly used imaging modalities in the musculoskeletal system normal imaging anatomy in the extremities fracture description Imaging
HOW DO WE DIAGNOSE LAMENESS IN YOUR HORSE?
 HOW DO WE DIAGNOSE LAMENESS IN YOUR HORSE? To help horse owners better understand the tools we routinely use at VetweRx to evaluate their horse s soundness, the following section of this website reviews
HOW DO WE DIAGNOSE LAMENESS IN YOUR HORSE? To help horse owners better understand the tools we routinely use at VetweRx to evaluate their horse s soundness, the following section of this website reviews
Benjamin E. Plotkin, M.D., Vishal K. Agarwal, M.D., and Rajeev Varma, M.D.
 Stump Entrapment of the Torn Anterior Cruciate Ligament Benjamin E. Plotkin, M.D., Vishal K. Agarwal, M.D., and Rajeev Varma, M.D. Citation: Plotkin BE, Agarwal VK, Varma R. Stump Entrapment of the Torn
Stump Entrapment of the Torn Anterior Cruciate Ligament Benjamin E. Plotkin, M.D., Vishal K. Agarwal, M.D., and Rajeev Varma, M.D. Citation: Plotkin BE, Agarwal VK, Varma R. Stump Entrapment of the Torn
Meniscal Tears with Fragments Displaced: What you need to know.
 Meniscal Tears with Fragments Displaced: What you need to know. Poster No.: C-1339 Congress: ECR 2015 Type: Authors: Keywords: DOI: Educational Exhibit M. V. Ferrufino, A. Stroe, E. Cordoba, A. Dehesa,
Meniscal Tears with Fragments Displaced: What you need to know. Poster No.: C-1339 Congress: ECR 2015 Type: Authors: Keywords: DOI: Educational Exhibit M. V. Ferrufino, A. Stroe, E. Cordoba, A. Dehesa,
When Pads of Fat are a Welcome Sight: Fat Pads in Acute Musculoskeletal Imaging
 When Pads of Fat are a Welcome Sight: Fat Pads in Acute Musculoskeletal Imaging Poster No.: C-2444 Congress: ECR 2013 Type: Authors: Keywords: DOI: Educational Exhibit M. Zakhary 1, M. Adix 2, C. Yablon
When Pads of Fat are a Welcome Sight: Fat Pads in Acute Musculoskeletal Imaging Poster No.: C-2444 Congress: ECR 2013 Type: Authors: Keywords: DOI: Educational Exhibit M. Zakhary 1, M. Adix 2, C. Yablon
MRI of LEFT KNEE. There is a fluid collection seen anterior to and inferior to the superiorly displaced patella.
 MRI of LEFT KNEE Protocol: Multiplanar MRI of the left knee joint performed in the sagittal, coronal and transverse planes using T1 weighted spin echo, T2 and proton-density weighted fast spin echo, fatsaturated
MRI of LEFT KNEE Protocol: Multiplanar MRI of the left knee joint performed in the sagittal, coronal and transverse planes using T1 weighted spin echo, T2 and proton-density weighted fast spin echo, fatsaturated
Sacroiliac Joint Imaging
 Sacroiliac Joint Imaging Jacob Jaremko, MD, PhD Edmonton, Canada SPR, May 2017 Longview, Alberta Overview SI joint anatomy Sacroiliitis pathophysiology Sacroiliitis imaging Disease features Imaging protocols
Sacroiliac Joint Imaging Jacob Jaremko, MD, PhD Edmonton, Canada SPR, May 2017 Longview, Alberta Overview SI joint anatomy Sacroiliitis pathophysiology Sacroiliitis imaging Disease features Imaging protocols
Available online at
 Original Research Article Evaluation of knee joint by MRI in 65 patients Gulamus sibtain asad *, Himanshu Singla, Ankit vasoya, P. J. Jhala 2 2 nd year Resident, 2 Professor Radiology Department, SBKS
Original Research Article Evaluation of knee joint by MRI in 65 patients Gulamus sibtain asad *, Himanshu Singla, Ankit vasoya, P. J. Jhala 2 2 nd year Resident, 2 Professor Radiology Department, SBKS
Granulocyte-Stimulating Factor-Induced Bone Marrow Reconversion Simulating Neuroblastoma Metastases on MRI: Case Report and Literature Review
 Radiology Case Reports Volume II, Issue 1, 2007 Granulocyte-Stimulating Factor-Induced Bone Marrow Reconversion Simulating Neuroblastoma Metastases on MRI: Case Report and Literature Review Jason C. Naples,
Radiology Case Reports Volume II, Issue 1, 2007 Granulocyte-Stimulating Factor-Induced Bone Marrow Reconversion Simulating Neuroblastoma Metastases on MRI: Case Report and Literature Review Jason C. Naples,
MY PATIENT HAS KNEE PAIN. David Levi, MD Chief, Division of Musculoskeletal l limaging Atlantic Medical Imaging
 MY PATIENT HAS KNEE PAIN David Levi, MD Chief, Division of Musculoskeletal l limaging Atlantic Medical Imaging Causes of knee pain Non traumatic Trauma Osteoarthritis Patellofemoral pain Menisci or ligaments
MY PATIENT HAS KNEE PAIN David Levi, MD Chief, Division of Musculoskeletal l limaging Atlantic Medical Imaging Causes of knee pain Non traumatic Trauma Osteoarthritis Patellofemoral pain Menisci or ligaments
Figuring out the "fronds"-synovial proliferative disorders of the knee.
 Figuring out the "fronds"-synovial proliferative disorders of the knee. Poster No.: C-1209 Congress: ECR 2014 Type: Educational Exhibit Authors: S. Sivasubramanian; Tamil Nadu/IN Keywords: Imaging sequences,
Figuring out the "fronds"-synovial proliferative disorders of the knee. Poster No.: C-1209 Congress: ECR 2014 Type: Educational Exhibit Authors: S. Sivasubramanian; Tamil Nadu/IN Keywords: Imaging sequences,
CLASSIFICATION OF JOINTS STRUCTURAL VS FUNCTIONAL
 CHAPTER 8 JOINTS CLASSIFICATION OF JOINTS STRUCTURAL VS FUNCTIONAL The most moveable type of joint is a 1) Synarthrosis 2) Amphiarthrosis 3) Diarthrosis FIBROUS JOINTS Figure 8.1 Fibrous joints. (a) Suture
CHAPTER 8 JOINTS CLASSIFICATION OF JOINTS STRUCTURAL VS FUNCTIONAL The most moveable type of joint is a 1) Synarthrosis 2) Amphiarthrosis 3) Diarthrosis FIBROUS JOINTS Figure 8.1 Fibrous joints. (a) Suture
Ultrasound in juvenile idiopathic arthritis
 Magni-Manzoni Pediatric Rheumatology (2016) 14:33 DOI 10.1186/s12969-016-0096-2 REVIEW Open Access Ultrasound in juvenile idiopathic arthritis Silvia Magni-Manzoni Abstract Background: In the recent years,
Magni-Manzoni Pediatric Rheumatology (2016) 14:33 DOI 10.1186/s12969-016-0096-2 REVIEW Open Access Ultrasound in juvenile idiopathic arthritis Silvia Magni-Manzoni Abstract Background: In the recent years,
1 st EULAR-PreS PAED MSUS Course Intermediate
 1 st EULAR-PreS PAED MSUS Course Intermediate Madrid, Spain Monday, 10 th June Wednesday, 12 th June 2019 The courses are a combination of lectures and hands-on scanning of models (Basic course) or patients
1 st EULAR-PreS PAED MSUS Course Intermediate Madrid, Spain Monday, 10 th June Wednesday, 12 th June 2019 The courses are a combination of lectures and hands-on scanning of models (Basic course) or patients
CONTRIBUTING SURGEON. Barry Waldman, MD Director, Center for Joint Preservation and Replacement Sinai Hospital of Baltimore Baltimore, MD
 CONTRIBUTING SURGEON Barry Waldman, MD Director, Center for Joint Preservation and Replacement Sinai Hospital of Baltimore Baltimore, MD System Overview The EPIK Uni is designed to ease the use of the
CONTRIBUTING SURGEON Barry Waldman, MD Director, Center for Joint Preservation and Replacement Sinai Hospital of Baltimore Baltimore, MD System Overview The EPIK Uni is designed to ease the use of the
OSTEOPHYTOSIS OF THE FEMORAL HEAD AND NECK
 908 RDIOLOGIC VIGNETTE OSTEOPHYTOSIS OF THE FEMORL HED ND NECK DONLD RESNICK Osteophytes are frequently considered the most characteristic abnormality of degenerative joint disease. In patients with osteoarthritis,
908 RDIOLOGIC VIGNETTE OSTEOPHYTOSIS OF THE FEMORL HED ND NECK DONLD RESNICK Osteophytes are frequently considered the most characteristic abnormality of degenerative joint disease. In patients with osteoarthritis,
Knee Ultrasonography step by step
 Knee Ultrasonography step by step Poster No.: C-2809 Congress: ECR 2018 Type: Educational Exhibit Authors: J. A. Torres de Abreu Macedo, N. Pereira da Silva, A. I. Aguiar, F. Alves, F. Caseiro Alves; Coimbra/PT
Knee Ultrasonography step by step Poster No.: C-2809 Congress: ECR 2018 Type: Educational Exhibit Authors: J. A. Torres de Abreu Macedo, N. Pereira da Silva, A. I. Aguiar, F. Alves, F. Caseiro Alves; Coimbra/PT
Ankle impingement syndromes - pictorial review.
 Ankle impingement syndromes - pictorial review. Poster No.: P-0148 Congress: ESSR 2015 Type: Educational Poster Authors: R. D. T. Mesquita, J. Pinto, J. L. Rosas, A. Vieira ; Porto/PT, 1 2 2 3 1 1 3 Matosinhos/PT,
Ankle impingement syndromes - pictorial review. Poster No.: P-0148 Congress: ESSR 2015 Type: Educational Poster Authors: R. D. T. Mesquita, J. Pinto, J. L. Rosas, A. Vieira ; Porto/PT, 1 2 2 3 1 1 3 Matosinhos/PT,
Ankle impingement syndromes - pictorial review.
 Ankle impingement syndromes - pictorial review. Poster No.: P-0148 Congress: ESSR 2015 Type: Educational Poster Authors: R. D. T. Mesquita, J. Pinto, J. L. Rosas, A. Vieira ; Porto/PT, 1 2 2 3 1 1 3 Matosinhos/PT,
Ankle impingement syndromes - pictorial review. Poster No.: P-0148 Congress: ESSR 2015 Type: Educational Poster Authors: R. D. T. Mesquita, J. Pinto, J. L. Rosas, A. Vieira ; Porto/PT, 1 2 2 3 1 1 3 Matosinhos/PT,
Immanuel Krankenhaus Berlin, Medical Centre for Rheumatology Berlin - Buch; 2
 Low-field MRI versus ultrasound: which is more sensitive in detecting inflammation and bone damage in MCP and MTP joints in mild or moderate rheumatoid arthritis? W.A. Schmidt 1, B. Schicke 2, B. Ostendorf
Low-field MRI versus ultrasound: which is more sensitive in detecting inflammation and bone damage in MCP and MTP joints in mild or moderate rheumatoid arthritis? W.A. Schmidt 1, B. Schicke 2, B. Ostendorf
Paediatric rheumatology
 Paediatric rheumatology Ultrasonography vs. clinical examination in children with suspected arthritis. Does it make sense to use poliarticular ultrasonographic screening? G. Filippou, L. Cantarini, I.
Paediatric rheumatology Ultrasonography vs. clinical examination in children with suspected arthritis. Does it make sense to use poliarticular ultrasonographic screening? G. Filippou, L. Cantarini, I.
Suprapatellar fat-pad impingement:mri findings
 Suprapatellar fat-pad impingement:mri findings Poster No.: C-1672 Congress: ECR 2017 Type: Scientific Exhibit Authors: A. Arslan, S. Ulus, S. A. Kara, O. SAYG#L#; istanbul/tr Keywords: Trauma, Diagnostic
Suprapatellar fat-pad impingement:mri findings Poster No.: C-1672 Congress: ECR 2017 Type: Scientific Exhibit Authors: A. Arslan, S. Ulus, S. A. Kara, O. SAYG#L#; istanbul/tr Keywords: Trauma, Diagnostic
Pragmatic ultrasound in the diagnosis of soft tissue rheumatic pain. Plamen Todorov
 Pragmatic ultrasound in the diagnosis of soft tissue rheumatic pain Plamen Todorov INTRODUCTION Soft tissue rheumatism: nonsystemic, focal pathological syndromes involving the periarticular structures.
Pragmatic ultrasound in the diagnosis of soft tissue rheumatic pain Plamen Todorov INTRODUCTION Soft tissue rheumatism: nonsystemic, focal pathological syndromes involving the periarticular structures.
SSSR. 1. Nov Ankle. Postoperative Imaging of Cartilage Repair. and Lateral Ligament Reconstruction
 Ankle Postoperative Imaging of Cartilage Repair and Lateral Ligament Reconstruction Andrea B. Rosskopf, MD University Hospital Balgrist Imaging of Cartilage Repair Why? To assess the technical success
Ankle Postoperative Imaging of Cartilage Repair and Lateral Ligament Reconstruction Andrea B. Rosskopf, MD University Hospital Balgrist Imaging of Cartilage Repair Why? To assess the technical success
CASE REPORT GIANT OSTEOCHONDRAL LOOSE BODY OF THE KNEE JOINT
 Journal of Musculoskeletal Research, Vol. 4, No. 2 (2000) 145 149 World Scientific Publishing Company ORIGINAL CASE REPORT ARTICLES GIANT OSTEOCHONDRAL LOOSE BODY OF THE KNEE JOINT Mustafa Yel *,, Mustafa
Journal of Musculoskeletal Research, Vol. 4, No. 2 (2000) 145 149 World Scientific Publishing Company ORIGINAL CASE REPORT ARTICLES GIANT OSTEOCHONDRAL LOOSE BODY OF THE KNEE JOINT Mustafa Yel *,, Mustafa
FieldStrength. Achieva 3.0T enables cutting-edge applications, best-in-class MSK images
 FieldStrength Publication for the Philips MRI Community Issue 33 December 2007 Achieva 3.0T enables cutting-edge applications, best-in-class MSK images Palo Alto Medical Clinic Sports Medicine Center employs
FieldStrength Publication for the Philips MRI Community Issue 33 December 2007 Achieva 3.0T enables cutting-edge applications, best-in-class MSK images Palo Alto Medical Clinic Sports Medicine Center employs
Early diagnosis of Rheumatoid
 26 Original Article Diagnostic Accuracy of Ultrasonography in Detection of Destructive Changes in Small Joints of Hands in Patients of Rheumatoid Arthritis: A Comparison with Magnetic Resonance Imaging
26 Original Article Diagnostic Accuracy of Ultrasonography in Detection of Destructive Changes in Small Joints of Hands in Patients of Rheumatoid Arthritis: A Comparison with Magnetic Resonance Imaging
PRE & POST OPERATIVE RADIOLOGICAL ASSESSMENT IN TOTAL KNEE REPLACEMENT. Dr. Divya Rani K 2 nd Year Resident Dept. of Radiology
 PRE & POST OPERATIVE RADIOLOGICAL ASSESSMENT IN TOTAL KNEE REPLACEMENT Dr. Divya Rani K 2 nd Year Resident Dept. of Radiology PRE OPERATIVE ASSESSMENT RADIOGRAPHS Radiographs are used for assessment and
PRE & POST OPERATIVE RADIOLOGICAL ASSESSMENT IN TOTAL KNEE REPLACEMENT Dr. Divya Rani K 2 nd Year Resident Dept. of Radiology PRE OPERATIVE ASSESSMENT RADIOGRAPHS Radiographs are used for assessment and
Correspondence should be addressed to Thomas Kurien;
 Case Reports in Orthopedics Volume 2016, Article ID 6043497, 5 pages http://dx.doi.org/10.1155/2016/6043497 Case Report Resection and Resolution of Bone Marrow Lesions Associated with an Improvement of
Case Reports in Orthopedics Volume 2016, Article ID 6043497, 5 pages http://dx.doi.org/10.1155/2016/6043497 Case Report Resection and Resolution of Bone Marrow Lesions Associated with an Improvement of
Chapter 2 Pitfalls in Musculoskeletal Ultrasound
 Chapter 2 Pitfalls in Musculoskeletal Ultrasound Violeta Maria Vlad MD, PhD Introduction Taking a good ultrasound (US) picture is an art. Interpreting it is a science. This is in fact everything US is
Chapter 2 Pitfalls in Musculoskeletal Ultrasound Violeta Maria Vlad MD, PhD Introduction Taking a good ultrasound (US) picture is an art. Interpreting it is a science. This is in fact everything US is
Joints of the Lower Limb II
 Joints of the Lower Limb II Lecture Objectives Describe the components of the knee and ankle joint. List the ligaments associated with these joints and their attachments. List the muscles acting on these
Joints of the Lower Limb II Lecture Objectives Describe the components of the knee and ankle joint. List the ligaments associated with these joints and their attachments. List the muscles acting on these
Juvenile Idiopathic Arthritis of the Axial Joints: A Systematic Review of the Diagnostic Accuracy and Predictive Value of Conventional MRI
 Pediatric Imaging Review Munir et al. MRI for Diagnosis of JIA in the Axial Joints Pediatric Imaging Review Sohaib Munir 1 Kedar Patil 2 Elka Miller 3 Elizabeth Uleryk 3 Marinka Twilt 3 Lynn Spiegel 3
Pediatric Imaging Review Munir et al. MRI for Diagnosis of JIA in the Axial Joints Pediatric Imaging Review Sohaib Munir 1 Kedar Patil 2 Elka Miller 3 Elizabeth Uleryk 3 Marinka Twilt 3 Lynn Spiegel 3
MRI of Osteochondral Defects of the Lateral Femoral Condyle: Incidence and Pattern of Injury After Transient Lateral Dislocation of the Patella
 Sanders et al. MRI of Osteochond ral Defects of the Lateral Femoral Condyle Musculoskeletal Imaging Clinical Observations A C M E D E N T U R I C A L I M A G I N G AJR 2006; 187:1332 1337 0361 803X/06/1875
Sanders et al. MRI of Osteochond ral Defects of the Lateral Femoral Condyle Musculoskeletal Imaging Clinical Observations A C M E D E N T U R I C A L I M A G I N G AJR 2006; 187:1332 1337 0361 803X/06/1875
Note: This copy is for your personal, non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, cont
 Note: This copy is for your personal, non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. ORIGINAL RESEARCH
Note: This copy is for your personal, non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. ORIGINAL RESEARCH
Sonographic Findings of Adductor Insertion Avulsion Syndrome With Magnetic Resonance Imaging Correlation
 Case Report Sonographic Findings of Adductor Insertion Avulsion Syndrome With Magnetic Resonance Imaging Correlation Jennifer S. Weaver, MD, Jon A. Jacobson, MD, David A. Jamadar, MBBS, Curtis W. Hayes,
Case Report Sonographic Findings of Adductor Insertion Avulsion Syndrome With Magnetic Resonance Imaging Correlation Jennifer S. Weaver, MD, Jon A. Jacobson, MD, David A. Jamadar, MBBS, Curtis W. Hayes,
