PARANASAL SINUS FRACTURES
|
|
|
- Cody Harrell
- 5 years ago
- Views:
Transcription
1 Paranasal Sinus Fractures Chapter 23 PARANASAL SINUS FRACTURES MARK GIBBONS, MD, FACS,* and NATHAN SALINAS, MD INTRODUCTION ANATOMY DIAGNOSIS: CLINICAL AND IMAGING STUDIES MANAGEMENT ISSUES AND ALGORITHM SUMMARY CASE PRESENTATIONS Case Study 23-1 Case Study 23-2 *Lieutenant Colonel (Retired), Medical Corps, US Army; formerly, Chief, Department of Otolaryngology, Carl R. Darnall Army Medical Center, Darnall Loop, Fort Hood, Texas Major, Medical Corps, US Army; Chief, Department of Otolaryngology, Fort Wainwright, 4076 Neely Road, Fort Wainwright, Alaska
2 Otolaryngology/Head and Neck Combat Casualty Care INTRODUCTION Frontal sinus trauma may be blunt or penetrating, with frontal sinus fractures representing 6% to 12% of craniofacial fractures. 1,2 Two-thirds of patients with frontal sinus trauma may have sustained concomitant injuries to other facial structures. 3 Contemporary algorithms for classification and management of frontal sinus trauma are largely based on civilian injury patterns, which carry a trend toward high-velocity blunt trauma. 1,2,4,5 War trauma yields a higher incidence of penetrating injuries due to the preponderance of blast and missile trauma. 6 8 Open craniomaxillofacial fractures may comprise up to 75% of injuries to the craniomaxillofacial skeleton. 6 Additionally, given the proximity of the frontal bone to the cranium and orbits, concomitant brain and/or eye injury is not uncommon with penetrating or blunt frontal trauma. In a recent review of concomitant cranial and ocular combat injuries, nearly half of all patients with both cranial and ocular combat injuries requiring surgical intervention also underwent frontal sinus repair, obliteration, or cranialization. 8 Another contemporary review of facial trauma following improvised explosive device blasts identified trauma to the forehead aesthetic subunit as a danger zone in massive facial trauma, which was defined as injury to three or more facial units. 9 Because massive facial trauma is associated with elevated Injury Severity Scores and an increased rate for blood transfusions in war trauma, early assessment of these patients may help identify patients who require rapid transport to higher levels of care. 9 Prompt evaluation by neurosurgery and ophthalmology is important to optimize the care of patients with significant frontal sinus and skull base trauma with potential or associated cranial or orbital injuries. ANATOMY Comprehensive knowledge of the surgical anatomy of the frontal sinus is important for appropriately managing frontal sinus fractures resulting from either blunt or penetrating injuries. Absent at birth, the frontal sinuses begin developing after age 2. Most patients develop a pair of frontal sinuses, which are not fully formed until ages 15 to However, 8% to 15% of patients may only develop one frontal sinus, and 5% have complete aplasia. 10,11 The frontal sinus is a three-dimensional structure composed of an anterior table, a posterior table, and a floor. The anterior table provides the skeletal contour of the forehead, brow, and glabella. The posterior table is the anterior portion of the anterior cranial fossa, separating the frontal sinus from the anterior cranial fossa. The medial portion of the orbital roof creates the floor of the frontal sinus. The frontal sinus outflow tract (FSOT), also known as the frontal recess, is the funnel-shaped space that connects the frontal sinus to the anterior ethmoid sinuses. 11 The frontal ostium is the apex of the FSOT. The frontal sinus is lined with mucosa, which provides mucociliary clearance from the frontal sinus via the FSOT. Frontal sinus fractures may be classified as nondisplaced or displaced fractures involving the anterior table, the posterior table, or both. Accurate classification also requires identification of FSOT involvement. DIAGNOSIS: CLINICAL AND IMAGING STUDIES Clinical diagnosis of a frontal sinus injury is based on physical examination findings. In the presence of blunt trauma, significant forehead edema may make clinical diagnosis difficult. Penetrating trauma is often more conspicuous. Pertinent clinical findings include supraorbital distribution anesthesia or paresthesia, forehead laceration, contour irregularity, and hematoma. Frontal sinus fractures may be suspected with bone fragments present in a laceration, cerebrospinal fluid (CSF) rhinorrhea, supraorbital/frontal bone stepoffs, or crepitus. Radiographic assessment with computed tomography (CT) scan in patients with head injuries is required to evaluate their intracranial status. Given the complex three-dimensional anatomy, frontal sinus fractures are best diagnosed with a thin-cut ( mm) CT scan in axial, coronal, and sagittal planes if available and if time allows. The axial images allow clear assessment of the anterior and posterior tables, whereas the coronal images define the sinus floor and anterior skull base. The sagittal images add the necessary dimension to fully assess the FSOT. Three-dimensional CT reconstructions are valuable in visualizing any external contour deformity that may not be appreciated on physical examination or on two-dimensional CT images. A radiographic finding of pneumocephalus suggests posterior table and/or skull base fracture. 282
3 Paranasal Sinus Fractures MANAGEMENT ISSUES AND ALGORITHM Frontal sinus fracture management strategies depend on clinical and radiographic assessments of the anterior table, the posterior table, the FSOT, and the dura. Assessment of these anatomical structures guides the head and neck surgeon in establishing the three key functions of the frontal sinus: 1. restoring the preoperative facial aesthetics; 2. avoiding long-term sinus complications (eg, mucocele), chronic rhinosinusitis, or osteomyelitis; and 3. isolating the neurocranium and preventing a CSF leak. Although these three elements are paramount, managing frontal sinus and skull base fractures in a deployed environment also requires an assessment of political factors and the military situation outside of the treatment facility. The head and neck surgeon must understand the nature and stage of the conflict, the general capabilities and limitations of the host nation medical system, and the patient s military occupation and primary duties. For example, a Marine who works in administration and sustains an anterior table frontal sinus fracture playing basketball during the nation-building phase of a conflict is treated differently than a soldier in an infantry unit who sustains the same injury during a firefight in the combat phase of a conflict. The former would benefit from an open reduction and external fixation and convalescence in theater, whereas the latter is best served by evacuation to a higher level of care for treatment. Wounded American and coalition service members often require different care than host nation patients and enemy combatants. American and coalition patients are often the most straightforward to manage in a deployed environment. In a fluid tactical setting, damage control surgery is performed. Neurosurgical and ophthalmological injuries are addressed; facial wounds are copiously irrigated, judiciously debrided, and closed primarily; and the patient is then transferred to a higher level treatment facility. In a more protracted conflict, less complex frontal sinus fractures may be treated in theater, thus allowing the patient to convalesce with his unit in a limited duty status and thereby minimizing disruption to unit personnel. Anterior skull base injuries with the exception of rare, nondisplaced fractures without a CSF leak require evacuation out of theater. Host nation patients are usually the most challenging to care for, especially when their medical system is overly stressed and inadequate. Because of the lim- ited time and resources at a Role 3 medical treatment facility, all necessary treatment is provided during one operation, if possible. These patients often have one operation and hospitalization for very complex, life-threatening injuries. Thoracic, abdominal, and orthopaedic injuries are treated based on priorities established by the trauma surgeon. The treatment priority for head and facial injuries is usually the brain, the globes, and then the maxillofacial region. Concurrent surgeries by different specialties occur when space allows and within the parameters of the patient s overall medical condition. Skull base reconstruction has significantly improved over the past 20 years, driven largely by advances in surgical treatment of skull base neoplasms. Large skull base defects following tumor extirpation are usually treated with microvascular free-tissue transfer that is the safest, most economical procedure. 12 However, this procedure has not been widely adopted in combat settings because of inadequate resources and time constraints. Regional flaps (eg, the pectoralis major flap) are an option, but are often impractical because of a concurrent chest or thoracic injury. Local flaps are usually the best option in a deployed environment. When available, a pericranial flap is an excellent means of isolating the intracranial contents. Unfortunately, penetrating head injuries often disrupt the pericranium, thus an alternative method (eg, temporalis fascia, tensor fasciae latae, or a dura substitute) is required. 12 For bone reconstruction, titanium mesh is malleable, is biocompatible with soft tissue and mucosa, undergoes osseointegration, and is readily available in the operating room. 13 A calvarial bone graft is also an option, but volume loss due to resorption is a potential longterm complication. Regardless of the materials used, a multilayer closure is essential. Definitive cranial reconstruction for decompressive craniectomy patients or patients with large frontoorbital bar defects may be delayed and surgically addressed at a later time using free flaps and bone grafts. 14 The algorithmic approach to frontal sinus fracture repair that is used in civilian trauma is also applicable to combat-related injuries, with some modifications. In general, the algorithm is simpler and shorter because observation with treatment as needed is not possible in host nation patients without a robust medical safety net. Although the inclination is to focus only on the anterior and posterior tables, the frontal recess is the key structure that requires evaluation and attention (Figure 23-1). Host nation patients with anything more than a very mild frontal recess injury are at high risk 283
4 Otolaryngology/Head and Neck Combat Casualty Care Anterior Table Fracture Obliterate Frontal Recess Injury > 1 table width or comminuted Cranialize Posterior Table Fracture <1 table width Obliterate Figure Treatment algorithm for frontal sinus fractures with a frontal recess injury. of chronic frontal sinus complications and should therefore undergo frontal sinus obliteration. Treatment of isolated posterior table fractures of the frontal sinus is controversial. Historically, if the posterior table has a fracture displaced more than one table width or is comminuted, the frontal sinus would be cranialized or obliterated. However, recent animal studies have shown that isolated, displaced (greater than one table width) posterior table fractures with an intact FSOT/nasofrontal duct rarely cause mucoceles. 15 Consequently, for those patients sustaining isolated displaced posterior table fractures with an intact FSOT and no CSF leak, observation should be considered. Furthermore, observation is indicated for the rare patient with a nondisplaced posterior table fracture and an intact anterior table (Figure 23-2). Anterior table fractures are treated to restore aesthetics and prevent long-term sinus complications. Nondisplaced anterior table fractures are not uncommon, especially with modern ballistic helmets. This type of facture can be safely observed because the forehead contour is not significantly affected, and the function of the frontal sinus is not jeopardized. Rigid fixation may be performed if the anterior table is displaced, but the FSOT is spared and the mucosa is minimally disrupted. Obliteration of the frontal sinus may be indicated for displaced anterior table fractures that are associated with significant mucosal disruption and compromise of the FSOT. Consultation and communication with a neurosurgeon and an ophthalmologist prior to repairing the maxillofacial fractures are critical to avoid further cranial or orbital injury and to coordinate care. The globes should be protected with either a tarsorrhaphy or corneal shields. Pressure on the brain, either from retraction or repair, is also avoided. Most combatrelated frontal sinus and anterior skull base fractures have associated lacerations that provide ready access for treatment. Occasionally, a bicoronal incision may be required for fractures because of blunt trauma. The wounds are copiously irrigated, and all foreign bodies and nonviable bone fragments are removed. The No Frontal Recess Injury Anterior Table Fracture Posterior Table Fracture Displaced Nondisplaced Displaced Nondisplaced ORIF Observe Observation versus Cranialization Observe Figure Treatment algorithm for frontal sinus fractures without a frontal recess injury. ORIF: open reduction internal fixation 284
5 Paranasal Sinus Fractures Figure Abdominal fat harvested for frontal sinus obliteration. frontal recess is then visually inspected to confirm the radiographic findings of patency or occlusion. Endoscopic approaches and techniques are not applicable in the deployed environment due to resource and time constraints. Both obliteration and cranialization require removal of all frontal sinus mucosa and occlusion of the frontal sinus ostia. A drill with both cutting and diamond burrs is the ideal tool for this task. However, because a drill is often unavailable in a Role 3 facility, periosteal elevators and curettes can be used. Meticulous removal of all mucosa is critical to avoid chronic infections and mucocele formation. The frontal recess is then occluded with a temporalis muscle plug or covered with bone fragments. Most anterior skull base injuries involve the frontal recess and posterior table. The frontal sinus is usually cranialized, and the frontal recess is occluded in the reconstruction. It is important to remove all posterior table bone during cranialization. Abdominal fat is the easiest and most available material for frontal sinus obliteration. Harvesting is done through a left lower quadrant incision or the laparotomy incision in patients with penetrating abdominal wounds. If possible, the fat is harvested in a single piece with minimal electrocautery (Figure 23-3). 4 The fat should fill the entire frontal sinus without placing undue tension on the anterior or posterior tables. Bone reconstruction is performed with a combination of miniplates and titanium mesh as needed. As in skull base reconstruction, titanium mesh is ideally suited for reconstructing the comminuted fractures associated with combat injuries. The final and often most timeconsuming step is soft-tissue closure, which is usually performed with a combination of primary closure and local advancement flaps. SUMMARY Treating combat-related frontal sinus and anterior skull base fractures is challenging because of their intimate relationship with the brain. The head and neck surgeon must always keep in mind the primary goals of protecting the brain, avoiding long-term complications, and restoring aesthetic contour. The medical challenge is usually compounded by the military and political situations, and the limited resources of a deployed environment. Fortunately, the complexity of these reconstructions and the opportunity to collaborate with both neurosurgeons and ophthalmologists make these cases very rewarding. CASE PRESENTATIONS Case Study 23-1 Presentation An Iraqi policeman was medically evacuated to the emergency department at the Air Force Theater Hospital on Balad Air Base, Iraq, with massive facial trauma from a vehicle-borne, improvised explosive device. The patient was intubated in the field, sedated, and his vital signs were stable. On examination, he had multiple facial injuries, primarily on the left, including a disrupted left globe (Figure 23-4). CT demonstrated a severely comminuted frontal recess and left anterior table frontal sinus fracture, including the superior orbital rim and orbital roof (Figure 23-5). The posterior table was intact, and there was no intracranial injury. There was a displaced nasal fracture. Operation The patient underwent an enucleation of the left globe by the ophthalmologist. The frontal sinus mucosa, along with multiple glass fragments, was removed. Titanium mesh was used to reconstruct the superior orbital rim and orbital roof, and the frontal sinus was obliterated with abdominal fat (Figure 23-6). Complex facial lacerations were then closed 285
6 Otolaryngology/Head and Neck Combat Casualty Care Figure Penetrating left facial injury from an improvised explosive device with a comminuted left frontal sinus fracture and a left globe injury. primarily. The patient was intubated, transferred to the intensive care unit, and his closed-head injury managed accordingly. Lessons Learned This case is typical of most frontal sinus fractures encountered in host nation patients in combat. Although the patient now has a large dead space in place of his left globe, he has an intact skin covering, a safe left frontal sinus, and his intracranial contents are isolated. Figure CT (computed tomography) maxillofacial demonstrating a comminuted left frontal sinus fracture with an intrasinus foreign body. Operation The neurosurgeon performed an anterior craniotomy and exploration of the frontal lobes, and the ophthalmologist then followed with a bilateral enucleation. There was no pericranium or dura remaining from the injury. A collagen matrix dura substitute was Case Study 23-2 Presentation An Iraqi male was dropped at the Balad Air Base gate after sustaining an isolated gunshot wound through both eyes, a common torture technique used by insurgents. There were no other injuries. The patient was disoriented and was intubated in the Air Force Theater Hospital emergency department. On examination, there was extensive soft-tissue loss involving the globes, the ocular adnexa, and the upper nose (Figure 23-7). A CT demonstrated complete loss of the anterior globes, the nasal bones, and the ascending process of the maxilla. The anterior and posterior tables of the frontal sinuses and the ethmoid sinuses sustained comminuted fractures. There were intracranial bone fragments in the frontal lobes. Figure Titanium mesh reconstruction of superior orbital rim and frontal sinus. 286
7 Paranasal Sinus Fractures Bilateral temporalis muscle flaps Frontal lobe Figure Anterior skull base, nose, and globe injury from gunshot wound. Figure Right lateral view of exposed brain and bilateral temporalis muscle flaps. placed over both frontal lobes and bilateral temporalis muscle flaps. They were rotated anteriorly to separate the dura from the nasal cavity and to provide bulk to the orbits (Figure 23-8). The frontal sinuses were cranialized. The anterior skull base was reconstructed with titanium mesh (Figure 23-9). Large, bilateral melolabial advancement flaps were used to cover the orbits and were sutured to the forehead skin. The patient was then then transferred to the intensive care unit for further management. drain into the nasal cavity. Division of the melolabial flaps at the reconstructed frontal bar and rotation onto the orbital floor would allow reconstruction of the orbits at a later date. Titanium mesh Lessons Learned Reconstruction of the skull base to separate the intracranial and extracranial contents is critical. A multilayered closure (to include fascia) is necessary to support the frontal lobes, prevent a spinal fluid leak, and protect the brain from outside pathogens. Although there are multiple reconstruction options for this case, the time and resource limitations inherent in a deployed environment generally mandate singlestage, expeditious surgical care. Although this reconstruction is not ideal from a cosmetic standpoint, the brain is supported and protected, there is an adequate skin barrier, and the remaining paranasal sinuses can Replaced calvarium Right orbit Figure Titanium mesh reconstruction of anterior skull base. REFERENCES 1. Ioannides C, Freihofer HP, Friens J. Fractures of the frontal sinus: a rationale of treatment. Br J Plast Surg. 1993;46: Luce EA. Frontal sinus fractures: guidelines to management. Plast Reconstr Surg. 1987;80: Wallis A, Donald PJ. Frontal sinus fractures: a review of 72 cases. Laryngoscope. 1988;98(6 Pt 1):
8 Otolaryngology/Head and Neck Combat Casualty Care 4. Strong EB. Frontal sinus fractures: current concepts. Craniomaxillofac Trauma Reconstr. 2009;2: Kalavrezos N. Current trends in the management of frontal sinus fractures. Injury. 2004;35: Chan RK, Siller-Jackson A, Verrett AJ, Wu J, Hale RG. Ten years of war: a characterization of craniomaxillofacial injuries incurred during Operations Enduring Freedom and Iraqi Freedom. J Trauma Acute Care Surg. 2012;73:S453 S Feldt BA, Salinas NL, Rasmussen TE, Brennan J. The joint facial and invasive neck trauma (J FAINT) project, Iraq and Afghanistan Otolaryngol Head Neck Surg. 2013;48: Cho RJ, Bakken HE, Reynolds ME, Schlifka BA, Powers D. Concomitant cranial and ocular combat injuries during Operation Iraqi Freedom. J Trauma. 2009;67: Salinas NL, Brennan J, Gibbons MD. Massive facial trauma following improvised explosive devices in Operation Iraqi Freedom. Otolaryngol Head Neck Surg. 2011;144: Bernstein L. Caldwell-Luc procedure. Otolaryngol Clin North Am. 1971;4: Lee WT, Kuhn FA, Citardi MJ. 3D computed tomographic analysis of frontal recess anatomy in patients without frontal sinusitis. Otolaryngol Head Neck Surg. 2004;131: Neligan PC, Mulholland S, Irish J, et al. Flap selection in cranial base reconstruction. Plast Reconstr Surg. 1996;98: Schubert W, Gear AJL, Lee C, et al. Incorporation of titanium mesh in orbital and midface reconstruction. Plast Reconstr Surg. 2002;110: Kumar AR, Tantawi D, Armonda R, Valerio I. Advanced cranial reconstruction using intracranial free flaps and cranial bone grafts: an algorithmic approach developed from the modern battlefield. Plast Reconstr Surg. 2012;130: Maturo S, Weitzel E, Cowhart J, Brennan J. Isolated posterior table frontal sinus fractures do not form mucoceles in goat model. Otolaryngol Head Neck Surg. 2008;139:
Fracture frontal bone and its management
 From the SelectedWorks of Balasubramanian Thiagarajan March 1, 2013 Fracture frontal bone and its management Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/14/ ISSN: 2250-0359
From the SelectedWorks of Balasubramanian Thiagarajan March 1, 2013 Fracture frontal bone and its management Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/14/ ISSN: 2250-0359
Management Strategies for Communited Fractures of Frontal Skull Base: An Institutional Experience
 80 Original Article THIEME Management Strategies for Communited Fractures of Frontal Skull Base: An Institutional Experience V. Velho 1 Hrushikesh U. Kharosekar 1 Jasmeet S. Thukral 1 Shonali Valsangkar
80 Original Article THIEME Management Strategies for Communited Fractures of Frontal Skull Base: An Institutional Experience V. Velho 1 Hrushikesh U. Kharosekar 1 Jasmeet S. Thukral 1 Shonali Valsangkar
FRONTAL SINUS FRACTURES February 1995
 TITLE: FRONTAL SINUS FRACTURES SOURCE: Dept. of Otolaryngology, UTMB, Grand Rounds DATE: February 22, 1995 RESIDENT PHYSICIAN: Kelly D. Sweeney, M.D. FACULTY: Brian P. Driscoll, M.D. SERIES EDITOR: Francis
TITLE: FRONTAL SINUS FRACTURES SOURCE: Dept. of Otolaryngology, UTMB, Grand Rounds DATE: February 22, 1995 RESIDENT PHYSICIAN: Kelly D. Sweeney, M.D. FACULTY: Brian P. Driscoll, M.D. SERIES EDITOR: Francis
Core Curriculum Syllabus Emergencies in Otolaryngology-Head and Neck Surgery FACIAL FRACTURES
 Core Curriculum Syllabus Emergencies in Otolaryngology-Head and Neck Surgery A. General Considerations FACIAL FRACTURES Look for other fractures like skull and/or cervical spine fractures Test function
Core Curriculum Syllabus Emergencies in Otolaryngology-Head and Neck Surgery A. General Considerations FACIAL FRACTURES Look for other fractures like skull and/or cervical spine fractures Test function
More than 43,000 US military personnel have been
 Original Research Facial Plastic and Reconstructive Surgery The Joint Facial and Invasive Neck Trauma (J-FAINT) Project, Iraq and Afghanistan 2003-2011 Otolaryngology Head and Neck Surgery 148(3) 403 408
Original Research Facial Plastic and Reconstructive Surgery The Joint Facial and Invasive Neck Trauma (J-FAINT) Project, Iraq and Afghanistan 2003-2011 Otolaryngology Head and Neck Surgery 148(3) 403 408
North Oaks Trauma Symposium Friday, November 3, 2017
 + Evaluation and Management of Facial Trauma D Antoni Dennis, MD North Oaks ENT an Allergy November 3, 2017 + Financial Disclosure I do not have any conflicts of interest or financial interest to disclose
+ Evaluation and Management of Facial Trauma D Antoni Dennis, MD North Oaks ENT an Allergy November 3, 2017 + Financial Disclosure I do not have any conflicts of interest or financial interest to disclose
CT of Maxillofacial Injuries
 CT of Maxillofacial Injuries Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Viking 1 1976 MGS 2001 Technology changes the diagnosis Technologic Evolution
CT of Maxillofacial Injuries Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Viking 1 1976 MGS 2001 Technology changes the diagnosis Technologic Evolution
Head and Neck Trauma in Iraq and Afghanistan: Different War, Different Surgery, Lessons Learned
 The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. TRIOLOGICAL SOCIETY CANDIDATE THESIS Head and Neck Trauma in Iraq and Afghanistan: Different War, Different
The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. TRIOLOGICAL SOCIETY CANDIDATE THESIS Head and Neck Trauma in Iraq and Afghanistan: Different War, Different
Maxillofacial and Ocular Injuries
 Maxillofacial and Ocular Injuries Objectives At the conclusion of this presentation the participant will be able to: Identify the key anatomical structures of the face and eye and the impact of force on
Maxillofacial and Ocular Injuries Objectives At the conclusion of this presentation the participant will be able to: Identify the key anatomical structures of the face and eye and the impact of force on
Imaging Orbit/Periorbital Injury
 Imaging Orbit/Periorbital Injury 9 th Nordic Trauma Radiology Course 2016 Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Fireworks Topics to Cover Struts
Imaging Orbit/Periorbital Injury 9 th Nordic Trauma Radiology Course 2016 Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Fireworks Topics to Cover Struts
FRONTAL SINUPLASTY P R E P A R E D A N D P R E S E N T E D B Y : D R. Y A H Y A F A G E E H R 4 16/ 12/ 2013
 FRONTAL SINUPLASTY P R E P A R E D A N D P R E S E N T E D B Y : D R. Y A H Y A F A G E E H R 4 16/ 12/ 2013 ANATOMY: FRONTAL SINUS Not present at birth Starts developing at 4 years Radiographically visualized
FRONTAL SINUPLASTY P R E P A R E D A N D P R E S E N T E D B Y : D R. Y A H Y A F A G E E H R 4 16/ 12/ 2013 ANATOMY: FRONTAL SINUS Not present at birth Starts developing at 4 years Radiographically visualized
Maxillofacial Injuries Practical Tips
 Saturday, October 29, 2016 Maxillofacial Injuries Practical Tips Suyash Mohan MD, PDCC THE ROOTS OF PENN RADIOLOGY RADIOLOGICAL Assistant Professor of Radiology Assistant Professor of Neurosurgery Neuroradiology
Saturday, October 29, 2016 Maxillofacial Injuries Practical Tips Suyash Mohan MD, PDCC THE ROOTS OF PENN RADIOLOGY RADIOLOGICAL Assistant Professor of Radiology Assistant Professor of Neurosurgery Neuroradiology
CT of Maxillofacial Fracture Patterns. CT of Maxillofacial Fracture Patterns
 CT of Maxillofacial Fracture Patterns CT of Maxillofacial Fracture Patterns Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Viking 1 1976 MGS 2001 Technology
CT of Maxillofacial Fracture Patterns CT of Maxillofacial Fracture Patterns Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Viking 1 1976 MGS 2001 Technology
ISPUB.COM. GSW To The Face: "Hunting Camp" C Perry, B Phillips CASE REPORT
 ISPUB.COM The Internet Journal of Rescue and Disaster Medicine Volume 2 Number 2 C Perry, B Phillips Citation C Perry, B Phillips.. The Internet Journal of Rescue and Disaster Medicine. 2000 Volume 2 Number
ISPUB.COM The Internet Journal of Rescue and Disaster Medicine Volume 2 Number 2 C Perry, B Phillips Citation C Perry, B Phillips.. The Internet Journal of Rescue and Disaster Medicine. 2000 Volume 2 Number
Tips and Tricks in Ventral Skull Base Dissection Narayanan Janakiram, Dharambir S. Sethi, Onkar K. Deshmukh, and Arvindh K.
 05 Tips and Tricks in Ventral Skull Base Dissection Narayanan Janakiram, Dharambir S. Sethi, Onkar K. Deshmukh, and Arvindh K. Gananathan Introduction...75 General Principles...76 Tips and Tricks in Ventral
05 Tips and Tricks in Ventral Skull Base Dissection Narayanan Janakiram, Dharambir S. Sethi, Onkar K. Deshmukh, and Arvindh K. Gananathan Introduction...75 General Principles...76 Tips and Tricks in Ventral
TRAUMA TO THE FACE AND MOUTH
 Dr.Yahya A. Ali 3/10/2012 F.I.C.M.S TRAUMA TO THE FACE AND MOUTH Bailey & Love s 25 th edition Injuries to the orofacial region are common, but the majority are relatively minor in nature. A few are major
Dr.Yahya A. Ali 3/10/2012 F.I.C.M.S TRAUMA TO THE FACE AND MOUTH Bailey & Love s 25 th edition Injuries to the orofacial region are common, but the majority are relatively minor in nature. A few are major
ORIGINAL ARTICLE. Titanium Mesh Repair of the Severely Comminuted Frontal Sinus Fracture. relatively uncommon maxillofacial
 ORIGINAL ARTICLE Titanium Mesh Repair of the Severely Comminuted Frontal Sinus Fracture Raam S. Lakhani, MD; Terry Y. Shibuya, MD; Robert H. Mathog, MD; Steven C. Marks, MD; Don L. Burgio, MD; George H.
ORIGINAL ARTICLE Titanium Mesh Repair of the Severely Comminuted Frontal Sinus Fracture Raam S. Lakhani, MD; Terry Y. Shibuya, MD; Robert H. Mathog, MD; Steven C. Marks, MD; Don L. Burgio, MD; George H.
Chapter 7: Head & Neck
 Chapter 7: Head & Neck Osteology I. Overview A. Skull The cranium is composed of irregularly shaped bones that are fused together at unique joints called sutures The skull provides durable protection from
Chapter 7: Head & Neck Osteology I. Overview A. Skull The cranium is composed of irregularly shaped bones that are fused together at unique joints called sutures The skull provides durable protection from
Epidemiology 3002). Epidemiology and Pathophysiology
 Epidemiology Maxillofacial trauma or injuries are commonly encountered in the practice of emergency medicine and are presenting one of the most challenging problems to the attending surgeons or physicians
Epidemiology Maxillofacial trauma or injuries are commonly encountered in the practice of emergency medicine and are presenting one of the most challenging problems to the attending surgeons or physicians
Radiological anatomy of frontal sinus By drtbalu
 2009 Radiological anatomy of frontal sinus By drtbalu Anatomy of frontal sinus is highly variable. Precise understanding of these variables will help a surgeon to avoid unnecessary complications during
2009 Radiological anatomy of frontal sinus By drtbalu Anatomy of frontal sinus is highly variable. Precise understanding of these variables will help a surgeon to avoid unnecessary complications during
Hydroxyapatite Cement to Repair Skull Base Defects: Radiologic Appearance
 Hydroxyapatite Cement to Repair Skull Base Defects: Radiologic Appearance Jane L. Weissman, Carl H. Snyderman, and Barry E. Hirsch PURPOSE: To describe the radiologic appearance of hydroxyapatite cement
Hydroxyapatite Cement to Repair Skull Base Defects: Radiologic Appearance Jane L. Weissman, Carl H. Snyderman, and Barry E. Hirsch PURPOSE: To describe the radiologic appearance of hydroxyapatite cement
VARIABLES THAT AFFECT TREATMENT DECISIONS STABILIZING THE MANDIBLE INTERMAXILLARY FIXATION WITH ARCH BARS IMMEDIATE REPAIR VERSUS DELAYED REPAIR
 Mandible Fractures Chapter 26 MANDIBLE FRACTURES JEFFREY A. FAULKNER, MD, DDS* INTRODUCTION VARIABLES THAT AFFECT TREATMENT DECISIONS TREATMENT STABILIZING THE MANDIBLE INTERMAXILLARY FIXATION WITH ARCH
Mandible Fractures Chapter 26 MANDIBLE FRACTURES JEFFREY A. FAULKNER, MD, DDS* INTRODUCTION VARIABLES THAT AFFECT TREATMENT DECISIONS TREATMENT STABILIZING THE MANDIBLE INTERMAXILLARY FIXATION WITH ARCH
ORIGINAL ARTICLE TEMPORALIS MUSCLE FLAP FOR RECONSTRUCTION OF SKULL BASE DEFECTS
 ORIGINAL ARTICLE TEMPORALIS MUSCLE FLAP FOR RECONSTRUCTION OF SKULL BASE DEFECTS Jesse E. Smith, MD, 1,2 Yadranko Ducic, MD, FRCS(C), 1,2,3 Robert T. Adelson, MD 4 1 Department of Otolaryngology-Head and
ORIGINAL ARTICLE TEMPORALIS MUSCLE FLAP FOR RECONSTRUCTION OF SKULL BASE DEFECTS Jesse E. Smith, MD, 1,2 Yadranko Ducic, MD, FRCS(C), 1,2,3 Robert T. Adelson, MD 4 1 Department of Otolaryngology-Head and
DEMOGRAPHICS OF HEAD AND NECK INJURIES IN IRAQ AND AFGHANISTAN
 Demographics of Head and Neck Injuries in Iraq and Afghanistan Chapter 6 DEMOGRAPHICS OF HEAD AND NECK INJURIES IN IRAQ AND AFGHANISTAN JOSEPH A BRENNAN, MD, FACS* INTRODUCTION GENERAL DEMOGRAPHICS PRETREATMENT
Demographics of Head and Neck Injuries in Iraq and Afghanistan Chapter 6 DEMOGRAPHICS OF HEAD AND NECK INJURIES IN IRAQ AND AFGHANISTAN JOSEPH A BRENNAN, MD, FACS* INTRODUCTION GENERAL DEMOGRAPHICS PRETREATMENT
ORIGINAL ARTICLE. most commonly result. involving the paranasal sinuses, the overlying facial skin, or both. Such defects may result in substantial
 ORIGINAL ARTICLE Use of Precontoured Positioning Plates and Pericranial Flaps in Midfacial Reconstruction to Optimize Aesthetic and Functional Outcomes Yadranko Ducic, MD, FRCSC; Lance E. Oxford, MD Objectives:
ORIGINAL ARTICLE Use of Precontoured Positioning Plates and Pericranial Flaps in Midfacial Reconstruction to Optimize Aesthetic and Functional Outcomes Yadranko Ducic, MD, FRCSC; Lance E. Oxford, MD Objectives:
Reduction of Closed Frontal Sinus Fractures through Suprabrow Approach
 Archives of Craniofacial Surgery Arch Craniofac Surg Vol.18 No.4, 230-237 https://doi.org/10.7181/acfs.2017.18.4.230 Reduction of Closed Frontal Sinus Fractures through Suprabrow Approach Original Article
Archives of Craniofacial Surgery Arch Craniofac Surg Vol.18 No.4, 230-237 https://doi.org/10.7181/acfs.2017.18.4.230 Reduction of Closed Frontal Sinus Fractures through Suprabrow Approach Original Article
Oral and Maxillofacial Surgeons and the seriously injured patient. Barts and The London NHS Trust
 Oral and Maxillofacial Surgeons and the seriously injured patient Barts and The London NHS Trust How do you assess this? Primary Survey A B C D E Airway & Cervical Spine Breathing & Ventilation Circulation
Oral and Maxillofacial Surgeons and the seriously injured patient Barts and The London NHS Trust How do you assess this? Primary Survey A B C D E Airway & Cervical Spine Breathing & Ventilation Circulation
Endoscopic Management Of A Giant Ethmoid Mucocele
 ISPUB.COM The Internet Journal of Otorhinolaryngology Volume 6 Number 1 S Ceylan, F Bora Citation S Ceylan, F Bora.. The Internet Journal of Otorhinolaryngology. 2006 Volume 6 Number 1. Abstract We present
ISPUB.COM The Internet Journal of Otorhinolaryngology Volume 6 Number 1 S Ceylan, F Bora Citation S Ceylan, F Bora.. The Internet Journal of Otorhinolaryngology. 2006 Volume 6 Number 1. Abstract We present
ORIGINAL ARTICLE. Reconstruction of the Frontal Sinus and Frontofacial Skeleton With Hydroxyapatite Cement
 ORIGINAL ARTICLE Reconstruction of the Frontal Sinus and Frontofacial Skeleton With Hydroxyapatite Cement Craig D. Friedman, MD; Peter D. Costantino, MD; C. H. Snyderman, MD; Lawrence C. Chow, PhD; Shozo
ORIGINAL ARTICLE Reconstruction of the Frontal Sinus and Frontofacial Skeleton With Hydroxyapatite Cement Craig D. Friedman, MD; Peter D. Costantino, MD; C. H. Snyderman, MD; Lawrence C. Chow, PhD; Shozo
McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2019 #1 Facial Trauma
 McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2019 #1 Facial Trauma The face is vital to human appearance and function. Facial injuries can impair a patient
McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2019 #1 Facial Trauma The face is vital to human appearance and function. Facial injuries can impair a patient
T HERE is an unusual and interesting variety of craniosynostosis in
 SURGICAL TREATMENT OF CONGENITAL ANOMALIES OF THE CORONAL AND METOPIC SUTURES TECHNICAL NOTE DONALD D. MATSON, M.D. Neurosurgical Service, The Children's Medical Center, and Deparlment of Surgery, Itarvard
SURGICAL TREATMENT OF CONGENITAL ANOMALIES OF THE CORONAL AND METOPIC SUTURES TECHNICAL NOTE DONALD D. MATSON, M.D. Neurosurgical Service, The Children's Medical Center, and Deparlment of Surgery, Itarvard
Technique Guide. Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Prodecures.
 Technique Guide Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Prodecures. Indications/Features Indications The Synthes Titanium Wire with Barb and straight Needle is
Technique Guide Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Prodecures. Indications/Features Indications The Synthes Titanium Wire with Barb and straight Needle is
COMPLICATIONS IN ENDOSCOPIC SINUS SURGERY
 COMPLICATIONS IN ENDOSCOPIC SINUS SURGERY John M. DelGaudio, MD Professor and Vice Chair Chief of Rhinology and Sinus Surgery Department of Otolaryngology-Head and Neck Surgery Emory University School
COMPLICATIONS IN ENDOSCOPIC SINUS SURGERY John M. DelGaudio, MD Professor and Vice Chair Chief of Rhinology and Sinus Surgery Department of Otolaryngology-Head and Neck Surgery Emory University School
MAXILLOFACIAL TRAUMA. The on-call maxillofacial surgeons can be contacted through the switchboard at the Southern General Hospital
 MAXILLOFACIAL TRAUMA The on-call maxillofacial surgeons can be contacted through the switchboard at the Southern General Hospital Mandibular Injuries Mechanism of injury Assault, falls, RTA-Direct trauma
MAXILLOFACIAL TRAUMA The on-call maxillofacial surgeons can be contacted through the switchboard at the Southern General Hospital Mandibular Injuries Mechanism of injury Assault, falls, RTA-Direct trauma
ENDOSCOPIC-ASSISTED CRANIONASAL RESECTION OF OLFACTORY NEUROBLASTOMA
 ENDOSCOPIC-ASSISTED CRANIONASAL RESECTION OF OLFACTORY NEUROBLASTOMA Anthony Po-Wing Yuen, FRCS, 1 Yiu Wah Fan, FRCS, 2 Ching Fai Fung, FRCS, 2 Kwan Ngai Hung, FRCS 2 1 Division of Otorhinolaryngology,
ENDOSCOPIC-ASSISTED CRANIONASAL RESECTION OF OLFACTORY NEUROBLASTOMA Anthony Po-Wing Yuen, FRCS, 1 Yiu Wah Fan, FRCS, 2 Ching Fai Fung, FRCS, 2 Kwan Ngai Hung, FRCS 2 1 Division of Otorhinolaryngology,
Lesson Plans and Objectives: Review material for article Prep work for article Picture recovery Review for placement on-line.
 Lesson Plans and Objectives: Review material for article Prep work for article Picture recovery Review for placement on-line. After reading the article, the staff will be able to: Define facial trauma
Lesson Plans and Objectives: Review material for article Prep work for article Picture recovery Review for placement on-line. After reading the article, the staff will be able to: Define facial trauma
HEAD AND NECK IMAGING. James Chen (MS IV)
 HEAD AND NECK IMAGING James Chen (MS IV) Anatomy Course Johns Hopkins School of Medicine Sept. 27, 2011 OBJECTIVES Introduce cross sectional imaging of head and neck Computed tomography (CT) Review head
HEAD AND NECK IMAGING James Chen (MS IV) Anatomy Course Johns Hopkins School of Medicine Sept. 27, 2011 OBJECTIVES Introduce cross sectional imaging of head and neck Computed tomography (CT) Review head
MEDPOR. Oral maxillofacial surgery
 MEDPOR Oral maxillofacial surgery MEDPOR biomaterial MEDPOR has been a trusted name in the industry since 1985, with hundreds of thousands of procedures performed, and hundreds of published clinical reports
MEDPOR Oral maxillofacial surgery MEDPOR biomaterial MEDPOR has been a trusted name in the industry since 1985, with hundreds of thousands of procedures performed, and hundreds of published clinical reports
Neurosurgical Techniques
 Neurosurgical Techniques EBEN ALEXANDER, JR., M.D., EDITOR Supratentorial Skull Flaps GuY L. ODOM, M.D., AND BARNES WOODHALL,!V[.D. Department of Surgery, Division of Neurosurgery, Duke University Medical
Neurosurgical Techniques EBEN ALEXANDER, JR., M.D., EDITOR Supratentorial Skull Flaps GuY L. ODOM, M.D., AND BARNES WOODHALL,!V[.D. Department of Surgery, Division of Neurosurgery, Duke University Medical
Mucocele of paranasal sinuses
 From the SelectedWorks of Balasubramanian Thiagarajan March 7, 2012 Mucocele of paranasal sinuses Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/57/ Mucoceles of paranasal
From the SelectedWorks of Balasubramanian Thiagarajan March 7, 2012 Mucocele of paranasal sinuses Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/57/ Mucoceles of paranasal
Pediatric Craniofacial Injuries: Concept of Treatment
 Med. J. Cairo Univ., Vol. 83, No. 1, March: 217-224, 201 5 www.medicaljournalofcairouniversity.net Pediatric Craniofacial Injuries: Concept of Treatment FAWZY T. AL-SAYED, Ph.D.* and MOHAMAD A. SHOEIB,
Med. J. Cairo Univ., Vol. 83, No. 1, March: 217-224, 201 5 www.medicaljournalofcairouniversity.net Pediatric Craniofacial Injuries: Concept of Treatment FAWZY T. AL-SAYED, Ph.D.* and MOHAMAD A. SHOEIB,
Bundeswehrkrankenhaus Ulm Abteilung HNO Kopf-Halschirurgie
 Kai Johannes Lorenz and Klaus Effinger Department of Otorhinolaryngology, Head and Neck Surgery Department of Radiology and interventional Radiology German Armed Forces Hospital Incidence of hemorrhage
Kai Johannes Lorenz and Klaus Effinger Department of Otorhinolaryngology, Head and Neck Surgery Department of Radiology and interventional Radiology German Armed Forces Hospital Incidence of hemorrhage
Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Procedures.
 Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Procedures. Technique Guide This publication is not intended for distribution in the USA. Instruments and implants approved
Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Procedures. Technique Guide This publication is not intended for distribution in the USA. Instruments and implants approved
Management of Cerebrospinal Fluid Leaks
 Management of Cerebrospinal Fluid Leaks J Trauma. 2001;51:S29 S33. I. RECOMMENDATIONS A. Standards The available data are not sufficient to support a treatment Standard for management of cerebrospinal
Management of Cerebrospinal Fluid Leaks J Trauma. 2001;51:S29 S33. I. RECOMMENDATIONS A. Standards The available data are not sufficient to support a treatment Standard for management of cerebrospinal
EVOS MINI with IM Nailing
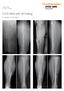 Case Series Dr. John A. Scolaro EVOS MINI with IM Nailing A series of studies Introduction Intramedullary nailing has become the standard for many long bone fractures. Fracture reduction prior to nail
Case Series Dr. John A. Scolaro EVOS MINI with IM Nailing A series of studies Introduction Intramedullary nailing has become the standard for many long bone fractures. Fracture reduction prior to nail
The diagnostic value of Computed Tomography in evaluation of maxillofacial Trauma
 The diagnostic value of Computed Tomography in evaluation of maxillofacial Trauma Qais H. Muassa FICMS College of Dentistry, Babylon University Ibrahim S. Gataa, BDS, FICMS College of Dentistry, Sulaimania
The diagnostic value of Computed Tomography in evaluation of maxillofacial Trauma Qais H. Muassa FICMS College of Dentistry, Babylon University Ibrahim S. Gataa, BDS, FICMS College of Dentistry, Sulaimania
Bones of the skull & face
 Bones of the skull & face Cranium= brain case or helmet Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. The cranium is composed of eight bones : frontal Occipital
Bones of the skull & face Cranium= brain case or helmet Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. The cranium is composed of eight bones : frontal Occipital
Rhinologic and Sleep Apnea Surgical Techniques
 Rhinologic and Sleep Apnea Surgical Techniques Bearbeitet von Stilianos E Kountakis, T. Metin Önerci 1. Auflage 2007. Buch. xviii, 433 S. ISBN 978 3 540 34019 5 Format (B x L): 20,3 x 27,6 cm Gewicht:
Rhinologic and Sleep Apnea Surgical Techniques Bearbeitet von Stilianos E Kountakis, T. Metin Önerci 1. Auflage 2007. Buch. xviii, 433 S. ISBN 978 3 540 34019 5 Format (B x L): 20,3 x 27,6 cm Gewicht:
Diagnosis of Midface Fractures with CT: What the Surgeon Needs to Know 1
 Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. EDUCATION EXHIBIT
Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. EDUCATION EXHIBIT
Three-Dimensional Alloplastic Orbital Reconstruction in Skull Base Surgery
 The Laryngoscope Lippincott Williams & Wilkins, Inc., Philadelphia 2001 The American Laryngological, Rhinological and Otological Society, Inc. HowIDoIt A Targeted Problem and Its Solution Three-Dimensional
The Laryngoscope Lippincott Williams & Wilkins, Inc., Philadelphia 2001 The American Laryngological, Rhinological and Otological Society, Inc. HowIDoIt A Targeted Problem and Its Solution Three-Dimensional
Dr. Esam Ahmad Z. Omar BDS, MSc-OMFS, FFDRCSI. Monitor the vital signs. Monitor the vital signs. Complications of Facial Traumas.
 Complications of Facial Traumas 1) Immediate Complications 2) Late Complications Dr. Esam Ahmad Z. Omar BDS, MSc-OMFS, FFDRCSI Assistant Professor Oral & Maxillofacial Surgeon Taibah University Monitor
Complications of Facial Traumas 1) Immediate Complications 2) Late Complications Dr. Esam Ahmad Z. Omar BDS, MSc-OMFS, FFDRCSI Assistant Professor Oral & Maxillofacial Surgeon Taibah University Monitor
Transcranial resection of tumors of the paranasal sinuses and nasal cavity
 J Neurosurg 71:10-15, 1989 Transcranial resection of tumors of the paranasal sinuses and nasal cavity J. BoB BLACKLOCK, M.D., RANDAL S. WEBER, M.D., YA-YEN LEE, M.D., AND HELMUTH GOEPFERT~ M.D. Section
J Neurosurg 71:10-15, 1989 Transcranial resection of tumors of the paranasal sinuses and nasal cavity J. BoB BLACKLOCK, M.D., RANDAL S. WEBER, M.D., YA-YEN LEE, M.D., AND HELMUTH GOEPFERT~ M.D. Section
Pelvic Injuries. Chapter 21
 Chapter 21 Introduction Injuries of the pelvis are an uncommon, but potentially lethal, battlefield injury. Blunt injuries may be associated with major hemorrhage and early mortality. Death within the
Chapter 21 Introduction Injuries of the pelvis are an uncommon, but potentially lethal, battlefield injury. Blunt injuries may be associated with major hemorrhage and early mortality. Death within the
MRI masterfile Part 5 WM Heme Strokes.ppt 1
 Ocular and Orbital Trauma Eye Trauma: Incidence 1.3 million eye injuries in the US per year. 40,000 of these injuries lead to blindness in the US. Patrick Sibony, MD March 23, 2013 Ophthalmic Emergencies
Ocular and Orbital Trauma Eye Trauma: Incidence 1.3 million eye injuries in the US per year. 40,000 of these injuries lead to blindness in the US. Patrick Sibony, MD March 23, 2013 Ophthalmic Emergencies
By JOHN MARQUIS CONVERSE, M.D., and DAUBERT TELSEY, D.D.S.
 THE TRIPARTITE OSTEOTOMY OF THE MID-FACE FOR ORBITAL EXPANSION AND CORRECTION OF THE DEFORMITY IN CRANIOSTENOSIS By JOHN MARQUIS CONVERSE, M.D., and DAUBERT TELSEY, D.D.S. Center for Craniofacial Anomalies
THE TRIPARTITE OSTEOTOMY OF THE MID-FACE FOR ORBITAL EXPANSION AND CORRECTION OF THE DEFORMITY IN CRANIOSTENOSIS By JOHN MARQUIS CONVERSE, M.D., and DAUBERT TELSEY, D.D.S. Center for Craniofacial Anomalies
Craniomaxillofacial Battle Injuries: Injury Patterns, Conventional Treatment Limitations and Direction of Future Research
 Review Article Craniomaxillofacial Battle Injuries: Injury Patterns, Conventional Treatment Limitations and Direction of Future Research Robert G Hale, 1 Timothy Lew 2 and Joseph C Wenke 3 1 Craniomaxillofacial
Review Article Craniomaxillofacial Battle Injuries: Injury Patterns, Conventional Treatment Limitations and Direction of Future Research Robert G Hale, 1 Timothy Lew 2 and Joseph C Wenke 3 1 Craniomaxillofacial
MRI masterfile Part 5 WM Heme Strokes.ppt 2
 Imaging of Orbital Trauma Corneal Abrasion CT scan is preferable to MRI Bone, Rapid, Easy to monitor patient Foreign bodies, air, hemorrhage Fractures Cost Needed for an MRI MRI Globe and intraocular injuries
Imaging of Orbital Trauma Corneal Abrasion CT scan is preferable to MRI Bone, Rapid, Easy to monitor patient Foreign bodies, air, hemorrhage Fractures Cost Needed for an MRI MRI Globe and intraocular injuries
1. BRIEF DESCRIPTION OF TRAINING
 RHINOLOGY 1. BRIEF DESCRIPTION OF TRAINING Exposure to clinical rhinology is provided in each of the four ORL years over the course of several rotations in a graduated approach. MEE General Otolaryngology
RHINOLOGY 1. BRIEF DESCRIPTION OF TRAINING Exposure to clinical rhinology is provided in each of the four ORL years over the course of several rotations in a graduated approach. MEE General Otolaryngology
TITLE: CSF RHINORRHOEA SECONDARY TO MAYFIELD HEAD CLAMP
 TITLE: CSF RHINORRHOEA SECONDARY TO MAYFIELD HEAD CLAMP Authors Mr Ioannis Moumoulidis (MRCS), Miss Helen Fernandes (FRCS), Mr Ran De (FRCS) Institution Department of Neurosurgery / Otolaryngology University
TITLE: CSF RHINORRHOEA SECONDARY TO MAYFIELD HEAD CLAMP Authors Mr Ioannis Moumoulidis (MRCS), Miss Helen Fernandes (FRCS), Mr Ran De (FRCS) Institution Department of Neurosurgery / Otolaryngology University
SuFg W. The Use of Methyl Methacrylate Cranioplasty in Forehead Reconstruction
 Eur J Plast Surg (1986) 9:94-99 European Ill1 Joumal of I ~' l #~ll ~l'~lhr I SuFg W Springer-Verlag 1986 The Use of Methyl Methacrylate Cranioplasty in Forehead Reconstruction L.C. Argenta and M.H. Newman
Eur J Plast Surg (1986) 9:94-99 European Ill1 Joumal of I ~' l #~ll ~l'~lhr I SuFg W Springer-Verlag 1986 The Use of Methyl Methacrylate Cranioplasty in Forehead Reconstruction L.C. Argenta and M.H. Newman
cally, a distinct superior crease of the forehead marks this spot. The hairline and
 4 Forehead The anatomical boundaries of the forehead unit are the natural hairline (in patients without alopecia), the zygomatic arch, the lower border of the eyebrows, and the nasal root (Fig. 4.1). The
4 Forehead The anatomical boundaries of the forehead unit are the natural hairline (in patients without alopecia), the zygomatic arch, the lower border of the eyebrows, and the nasal root (Fig. 4.1). The
Occipital flattening in the infant skull
 Occipital flattening in the infant skull Kant Y. Lin, M.D., Richard S. Polin, M.D., Thomas Gampper, M.D., and John A. Jane, M.D., Ph.D. Departments of Plastic Surgery and Neurological Surgery, University
Occipital flattening in the infant skull Kant Y. Lin, M.D., Richard S. Polin, M.D., Thomas Gampper, M.D., and John A. Jane, M.D., Ph.D. Departments of Plastic Surgery and Neurological Surgery, University
Original Research THE USE OF REFORMATTED CONE BEAM CT IMAGES IN ASSESSING MID-FACE TRAUMA, WITH A FOCUS ON THE ORBITAL FLOOR FRACTURES
 DOI: 10.15386/cjmed-601 Original Research THE USE OF REFORMATTED CONE BEAM CT IMAGES IN ASSESSING MID-FACE TRAUMA, WITH A FOCUS ON THE ORBITAL FLOOR FRACTURES RALUCA ROMAN 1, MIHAELA HEDEȘIU 1, FLOAREA
DOI: 10.15386/cjmed-601 Original Research THE USE OF REFORMATTED CONE BEAM CT IMAGES IN ASSESSING MID-FACE TRAUMA, WITH A FOCUS ON THE ORBITAL FLOOR FRACTURES RALUCA ROMAN 1, MIHAELA HEDEȘIU 1, FLOAREA
ORIGINAL ARTICLE. Extended Endoscopic Frontal Sinus Surgery to Interrupted Nasofrontal Communication Caused by Scarring of the Anterior Ethmoid
 Extended Endoscopic Frontal Sinus Surgery to Interrupted Nasofrontal Communication Caused by Scarring of the nterior Ethmoid Long-term Results ORIGINL RTICLE Toru Kikawada, MD; Masao Fujigaki, MD; Mikino
Extended Endoscopic Frontal Sinus Surgery to Interrupted Nasofrontal Communication Caused by Scarring of the nterior Ethmoid Long-term Results ORIGINL RTICLE Toru Kikawada, MD; Masao Fujigaki, MD; Mikino
Anatomy and Physiology. Bones, Sutures, Teeth, Processes and Foramina of the Human Skull
 Anatomy and Physiology Chapter 6 DRO Bones, Sutures, Teeth, Processes and Foramina of the Human Skull Name: Period: Bones of the Human Skull Bones of the Cranium: Frontal bone: forms the forehead and the
Anatomy and Physiology Chapter 6 DRO Bones, Sutures, Teeth, Processes and Foramina of the Human Skull Name: Period: Bones of the Human Skull Bones of the Cranium: Frontal bone: forms the forehead and the
Titanium Wire With Barb and Needle
 For Canthal Tendon Procedures Titanium Wire With Barb and Needle Surgical Technique Table of Contents Introduction Titanium Wire With Barb and Needle 2 Indications 2 Surgical Technique Preoperative Planning
For Canthal Tendon Procedures Titanium Wire With Barb and Needle Surgical Technique Table of Contents Introduction Titanium Wire With Barb and Needle 2 Indications 2 Surgical Technique Preoperative Planning
Frontal sinus disease continues to be one of the great
 Unilateral transnasal endoscopic approach to frontal sinuses: Draf IIc Mohammed K. Al Komser, M.D., M.A.S. and Andrew N. Goldberg, M.D., M.S.C.E. ABSTRACT For chronic sinusitis surgery, the Draf III approach
Unilateral transnasal endoscopic approach to frontal sinuses: Draf IIc Mohammed K. Al Komser, M.D., M.A.S. and Andrew N. Goldberg, M.D., M.S.C.E. ABSTRACT For chronic sinusitis surgery, the Draf III approach
Thickened and thinner parts of the skull = important base for understanding of the functional structure of the skull - the transmission of masticatory
 Functional structure of the skull and Fractures of the skull Thickened and thinner parts of the skull = important base for understanding of the functional structure of the skull - the transmission of masticatory
Functional structure of the skull and Fractures of the skull Thickened and thinner parts of the skull = important base for understanding of the functional structure of the skull - the transmission of masticatory
Craniosynostosis. Diagnosis and Treatment
 Craniosynostosis Diagnosis and Treatment 2015 For more information about the Weill Cornell Craniofacial Program ABOUT The Weill Cornell Craniofacial Program takes a multidisciplinary approach to treating
Craniosynostosis Diagnosis and Treatment 2015 For more information about the Weill Cornell Craniofacial Program ABOUT The Weill Cornell Craniofacial Program takes a multidisciplinary approach to treating
SOFT TISSUE SUPPORT IS AN
 ORIGINAL ARTICLE Reconstructive Application of the Endotine Suspension Devices James H. Boehmler IV, MD; Benjamin L. Judson, MD; Steven P. Davison, MD, DDS Objective: To illustrate the potential reconstructive
ORIGINAL ARTICLE Reconstructive Application of the Endotine Suspension Devices James H. Boehmler IV, MD; Benjamin L. Judson, MD; Steven P. Davison, MD, DDS Objective: To illustrate the potential reconstructive
Citation Hong Kong Practitioner, 1996, v. 18 n. 12, p
 Title Radiological conference. Frontal sinus osteoma complicated by pneumocephalus Author(s) Fung, WT; Peh, WCG Citation Hong Kong Practitioner, 1996, v. 18 n. 12, p. 658-662 Issued Date 1996 URL http://hdl.handle.net/10722/44655
Title Radiological conference. Frontal sinus osteoma complicated by pneumocephalus Author(s) Fung, WT; Peh, WCG Citation Hong Kong Practitioner, 1996, v. 18 n. 12, p. 658-662 Issued Date 1996 URL http://hdl.handle.net/10722/44655
Learner Objectives. Overview. Minimally Invasive Sinus Surgery: What is the data for Balloon Catheter Dilation 7/31/2017
 Minimally Invasive Sinus Surgery: What is the data for Balloon Catheter Dilation David M. Poetker, MD Christopher M. Long, MD Rhinology and Sinus Surgery Medical College of Wisconsin Thank you to Susan
Minimally Invasive Sinus Surgery: What is the data for Balloon Catheter Dilation David M. Poetker, MD Christopher M. Long, MD Rhinology and Sinus Surgery Medical College of Wisconsin Thank you to Susan
Chapter Five. 1 of 8 11/3/2008 2:52 PM.
 1 of 8 11/3/2008 2:52 PM Email : myousefmian@hotmail.com Chapter Five FRONT COVER Introduction Acknowledgement CHAPTERS Chapter One Chapter Two Chapter Three Chapter Four Chapter Five Chapter Six Chapter
1 of 8 11/3/2008 2:52 PM Email : myousefmian@hotmail.com Chapter Five FRONT COVER Introduction Acknowledgement CHAPTERS Chapter One Chapter Two Chapter Three Chapter Four Chapter Five Chapter Six Chapter
Relationship of the Optic Nerve to the Posterior Paranasal Sinuses: A CT Anatomic Study
 Relationship of the Optic Nerve to the Posterior Paranasal Sinuses: A CT Anatomic Study Mark C. DeLano, F. Y. Fun, and S. James Zinreich PURPOSE: To delineate the relationship between the optic nerves
Relationship of the Optic Nerve to the Posterior Paranasal Sinuses: A CT Anatomic Study Mark C. DeLano, F. Y. Fun, and S. James Zinreich PURPOSE: To delineate the relationship between the optic nerves
Skeletal system. Prof. Abdulameer Al-Nuaimi. E. mail:
 Skeletal system Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Functions of Bone and The Skeletal System Support: The skeleton serves as the structural framework
Skeletal system Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Functions of Bone and The Skeletal System Support: The skeleton serves as the structural framework
Clinical Outcome of Endoscopic Surgery for Frontal Sinusitis
 Clinical Outcome of Endoscopic Surgery for Frontal Sinusitis Ralph Metson, MD; Richard E. Gliklich, MD ORIGINAL ARTICLE Objective: To determine the efficacy of endoscopic surgery for chronic frontal sinusitis.
Clinical Outcome of Endoscopic Surgery for Frontal Sinusitis Ralph Metson, MD; Richard E. Gliklich, MD ORIGINAL ARTICLE Objective: To determine the efficacy of endoscopic surgery for chronic frontal sinusitis.
Transnasal Endoscopic Medial Maxillary Sinus Wall Transposition With Preservation of Structures
 The Laryngoscope VC 2015 The American Laryngological, Rhinological and Otological Society, Inc. Transnasal Endoscopic Medial Maxillary Sinus Wall Transposition With Preservation of Structures Alice Z.
The Laryngoscope VC 2015 The American Laryngological, Rhinological and Otological Society, Inc. Transnasal Endoscopic Medial Maxillary Sinus Wall Transposition With Preservation of Structures Alice Z.
See the corresponding editorial in this issue, pp J Neurosurg 116: , 2012
 See the corresponding editorial in this issue, pp 529 530. J Neurosurg 116:531 535, 2012 Cranialization of the frontal sinus the final remedy for refractory chronic frontal sinusitis Clinical article J.
See the corresponding editorial in this issue, pp 529 530. J Neurosurg 116:531 535, 2012 Cranialization of the frontal sinus the final remedy for refractory chronic frontal sinusitis Clinical article J.
Nasal Orbital Ethmoid (NOE) Fractures November, 2014
 TITLE: Nasal Orbital Ethmoid (NOE) Fractures SOURCE: Grand Rounds Presentation, The University of Texas Medical Branch at Galveston, Department of Otolaryngology DATE: November 19, 2014 RESIDENT PHYSICIAN:
TITLE: Nasal Orbital Ethmoid (NOE) Fractures SOURCE: Grand Rounds Presentation, The University of Texas Medical Branch at Galveston, Department of Otolaryngology DATE: November 19, 2014 RESIDENT PHYSICIAN:
ISOLATED ZYGOMATIC BONE FRACTURE; MANAGEMENT BY THREE POINT FIXATION
 The Professional Medical Journal 1. BDS, FCPS 2. BDS, FCPS 3. BDS, MSc Community Dentistry 4. BDS, MSc (Trainee) 5. MBBS, FRCS Associate Professor General Surgery LUMHS, Correspondence Address: Dr. Suneel
The Professional Medical Journal 1. BDS, FCPS 2. BDS, FCPS 3. BDS, MSc Community Dentistry 4. BDS, MSc (Trainee) 5. MBBS, FRCS Associate Professor General Surgery LUMHS, Correspondence Address: Dr. Suneel
Chapter 7 Part A The Skeleton
 Chapter 7 Part A The Skeleton Why This Matters Understanding the anatomy of the skeleton enables you to anticipate problems such as pelvic dimensions that may affect labor and delivery The Skeleton The
Chapter 7 Part A The Skeleton Why This Matters Understanding the anatomy of the skeleton enables you to anticipate problems such as pelvic dimensions that may affect labor and delivery The Skeleton The
The View through the Nose: ENT considerations for Pituitary/Skull Base Surgery
 The View through the Nose: ENT considerations for Pituitary/Skull Base Surgery Edsel Kim, M.D. Otolaryngology-Head and Neck Surgery The Oregon Clinic Providence Brain and Spine Institute Pituitary, Thyroid
The View through the Nose: ENT considerations for Pituitary/Skull Base Surgery Edsel Kim, M.D. Otolaryngology-Head and Neck Surgery The Oregon Clinic Providence Brain and Spine Institute Pituitary, Thyroid
Incisionless Brain Surgery
 Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/medical-breakthroughs-from-penn-medicine/incisionless-brainsurgery/3873/
Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/medical-breakthroughs-from-penn-medicine/incisionless-brainsurgery/3873/
Consumer summary. Endoscopic modified Lothrop procedure for the. treatment of chronic frontal sinusitis
 ASERNIP S Australian Safety and Efficacy Register of New Interventional Procedures Surgical Consumer summary Endoscopic modified Lothrop procedure for the treatment of chronic frontal sinusitis (The report
ASERNIP S Australian Safety and Efficacy Register of New Interventional Procedures Surgical Consumer summary Endoscopic modified Lothrop procedure for the treatment of chronic frontal sinusitis (The report
Interesting Case Series. Scalp Reconstruction With Free Latissimus Dorsi Muscle
 Interesting Case Series Scalp Reconstruction With Free Latissimus Dorsi Muscle Danielle H. Rochlin, BA, Justin M. Broyles, MD, and Justin M. Sacks, MD Department of Plastic and Reconstructive Surgery,
Interesting Case Series Scalp Reconstruction With Free Latissimus Dorsi Muscle Danielle H. Rochlin, BA, Justin M. Broyles, MD, and Justin M. Sacks, MD Department of Plastic and Reconstructive Surgery,
MEDPOR. Oculoplastic surgery
 MEDPOR Oculoplastic surgery MEDPOR biomaterial MEDPOR has been a trusted name in the industry since 1985, with hundreds of thousands of procedures performed, and hundreds of published clinical reports
MEDPOR Oculoplastic surgery MEDPOR biomaterial MEDPOR has been a trusted name in the industry since 1985, with hundreds of thousands of procedures performed, and hundreds of published clinical reports
Extended Bilaminar Forehead Flap With Cantilevered Bone Grafts for Reconstruction of Full-Thickness Nasal Defects
 J Oral Maxillofac Surg 63:566 570, 2005 Extended Bilaminar Forehead Flap With Cantilevered Bone Grafts for Reconstruction of Full-Thickness Nasal Defects Jason K. Potter, DDS, MD,* Yadranko Ducic, MD,
J Oral Maxillofac Surg 63:566 570, 2005 Extended Bilaminar Forehead Flap With Cantilevered Bone Grafts for Reconstruction of Full-Thickness Nasal Defects Jason K. Potter, DDS, MD,* Yadranko Ducic, MD,
CRANIAL RECONSTRUCTION SOLUTIONS
 CRANIAL RECONSTRUCTION SOLUTIONS CRANIAL RECONSTRUCTION SOLUTIONS Your partner of CHOiCE at depuy Synthes CMF, we are dedicated to providing solutions for your individual patient needs. We do this through
CRANIAL RECONSTRUCTION SOLUTIONS CRANIAL RECONSTRUCTION SOLUTIONS Your partner of CHOiCE at depuy Synthes CMF, we are dedicated to providing solutions for your individual patient needs. We do this through
Treatment Considerations in Management of Soft Tissues Injuries A Case Report. Key Words: Facial Injuries, Delayed Treatment, Antibiotics, Scar, etc.
 ISSN-0975-8437 INTERNATIONAL JOURNAL OF DENTAL CLINICS: 2 (1):22-27 CASE REPORT Treatment Considerations in Management of Soft Tissues Injuries A Case Report Siddqua Aaisha MDS 1 and Thakur Nitin MDS 2
ISSN-0975-8437 INTERNATIONAL JOURNAL OF DENTAL CLINICS: 2 (1):22-27 CASE REPORT Treatment Considerations in Management of Soft Tissues Injuries A Case Report Siddqua Aaisha MDS 1 and Thakur Nitin MDS 2
Open skull fractures with brain fungation: Simple principles for good outcome experience
 outcome Our experience. IAIM, 2015; 2(9): 65-69. Original Research Article Open skull fractures with brain fungation: Simple principles for good outcome Our experience M. V. Vijaya Sekhar 1, K.V. Ramprasad
outcome Our experience. IAIM, 2015; 2(9): 65-69. Original Research Article Open skull fractures with brain fungation: Simple principles for good outcome Our experience M. V. Vijaya Sekhar 1, K.V. Ramprasad
CT - Brain Examination
 CT - Brain Examination Submitted by: Felemban 1 CT - Brain Examination The clinical indication of CT brain are: a) Chronic cases (e.g. headache - tumor - abscess) b) ER cases (e.g. trauma - RTA - child
CT - Brain Examination Submitted by: Felemban 1 CT - Brain Examination The clinical indication of CT brain are: a) Chronic cases (e.g. headache - tumor - abscess) b) ER cases (e.g. trauma - RTA - child
Maxillary and Periorbital Fractures January 2004
 TITLE: Maxillary and Periorbital Fractures SOURCE: Grand Rounds Presentation, UTMB, Dept. of Otolaryngology DATE: January 7, 2004 RESIDENT PHYSICIAN: Gordon Shields, MD FACULTY ADVISOR: Francis B. Quinn,
TITLE: Maxillary and Periorbital Fractures SOURCE: Grand Rounds Presentation, UTMB, Dept. of Otolaryngology DATE: January 7, 2004 RESIDENT PHYSICIAN: Gordon Shields, MD FACULTY ADVISOR: Francis B. Quinn,
Chronic Frontal Rhinosinusitis: Diagnosis and Management
 Chapter Chronic Frontal Rhinosinusitis: Diagnosis and Management Core Messages Despite significant advances in surgical techniques, technology, and knowledge of pathophysiology, management of chronic frontal
Chapter Chronic Frontal Rhinosinusitis: Diagnosis and Management Core Messages Despite significant advances in surgical techniques, technology, and knowledge of pathophysiology, management of chronic frontal
30+ MEDPOR biomaterial. years of proven clinical history
 MEDPOR ENT surgery MEDPOR biomaterial MEDPOR has been a trusted name in the industry since 1985, with hundreds of thousands of procedures performed, and hundreds of published clinical reports in reconstructive,
MEDPOR ENT surgery MEDPOR biomaterial MEDPOR has been a trusted name in the industry since 1985, with hundreds of thousands of procedures performed, and hundreds of published clinical reports in reconstructive,
ANATOMY & PHYSIOLOGY I Laboratory Version B Name Section. REVIEW SHEET Exercise 10 Axial Skeleton
 ANATOMY & PHYSIOLOGY I Laboratory Version B Name Section REVIEW SHEET Exercise 10 Axial Skeleton 1 POINT EACH. THE SKULL MULTIPLE CHOICE 1. The major components of the axial skeleton include the 7. The
ANATOMY & PHYSIOLOGY I Laboratory Version B Name Section REVIEW SHEET Exercise 10 Axial Skeleton 1 POINT EACH. THE SKULL MULTIPLE CHOICE 1. The major components of the axial skeleton include the 7. The
The surgical approach to the sphenoid sinus continues to
 A comparison of two sphenoidotomy approaches using a novel computerized tomography grading system Heitham Gheriani, F.R.C.S.C., F.R.C.S.I., David Flamer, B.Sc., Trent Orton, M.D., Brad Mechor, F.R.C.S.C.,
A comparison of two sphenoidotomy approaches using a novel computerized tomography grading system Heitham Gheriani, F.R.C.S.C., F.R.C.S.I., David Flamer, B.Sc., Trent Orton, M.D., Brad Mechor, F.R.C.S.C.,
JPRAS Open 6 (2015) 5e10. Contents lists available at ScienceDirect. JPRAS Open. journal homepage:
 JPRAS Open 6 (2015) 5e10 Contents lists available at ScienceDirect JPRAS Open journal homepage: http://www.journals.elsevier.com/ jpras-open Case report Intraosseous hemangioma of the zygomatic bone Junji
JPRAS Open 6 (2015) 5e10 Contents lists available at ScienceDirect JPRAS Open journal homepage: http://www.journals.elsevier.com/ jpras-open Case report Intraosseous hemangioma of the zygomatic bone Junji
Independent italian ngo founded in EMERGENCY. Promotes a culture of peace, solidarity and respect for human rights.
 Independent italian ngo founded in 1994. EMERGENCY Promotes a culture of peace, solidarity and respect for human rights. 2 34% 26% 17% 16% 7% The victims War Victims WWI WWII after Combatants Civilians
Independent italian ngo founded in 1994. EMERGENCY Promotes a culture of peace, solidarity and respect for human rights. 2 34% 26% 17% 16% 7% The victims War Victims WWI WWII after Combatants Civilians
