Primary Intradural Conus and Cauda Equina Tumors: Long-time Outcome With 14 Years Follow- up
|
|
|
- Lorin Jefferson
- 5 years ago
- Views:
Transcription
1 Primary Intradural Conus and Cauda Equina Tumors: Long-time Outcome With 14 Years Follow- up Kadir KOT L Turgay B LGE Department of Neurosurgery, Haseki Educational and Research Hospital, Istanbul, Turkey ABSTRACT OBJECTIVE: This clinical study evaluated mixed tumor pathologies in the lumbar dural sac. Currently, there are few published clinical studies with longterm follow-up in the literature. METHODS: This is a retrospective review of the clinical presentation, diagnosis and management of 24 patients with primary intradural conus and cauda equina tumors (ICCET). We operated on 24 ICCET patients during the last 14 years. RESULTS: The largest pathology group of 9 (37.4%) cases was ependymomas. The rest were 5 (20.8%) neurinomas, 4 (16.6%) meningiomas, 1 (4.16%) epidermoid (with dermal sinus tract), 4 (16.6%) dermoids (one case with adult tethering cord and dermal sinus tract) and 1(4.16 %) hemangioblastoma. Two of the cases (ependymoma and neuironoma) had giant tumors, which extended from L1 to L5. Low back pain and urinary symptoms were the most common initial symptoms of the cases. The diagnosis was made with standart myelography (2 cases), computed tomographic myelography (4 cases) and magnetic resonance imaging (18 cases). All patients underwent tumor resection through a single posterior approach. The neurological conditions of 22 (91%) patients improved. Two patients did not improve and the postoperative Nurick Grade was grade 5. Postoperative radiotherapy was used in one case with malignant neurinoma. There was a rest tumor in one patient who had a dermoid tumor (4.6 %). The mean follow-up period was 75.5 months. CONCLUSION: We report the effect of surgical treatment for ICCET as excellent in nineteen out of 24 cases. ICCET are generally slow-growing, bening lesions. They are mostly surgically curable and radiotherapy is not usually necessary. The prognosis after surgical treatment depends not only on histology but also on the degree of neurological deficit before the surgery, and the importance of early diagnosis and subsequent treatment is well recognized. KEY WORDS: conus, cauda equina, intradural, primary, tumor. Received : Accepted : INTRODUCTION Primary tumors of the intradural conus and cauda equina (ICCET) region are uncommon and consist mainly of neurofibromas, ependymomas and neurinomas, and less commonly meningiomas, (7,10,14,16) dermoids, epidermoids, paragangliomas, high grade gliomas and hemangioblastomas (4,5,6). A high proportion of tumors in this region are benign (4). Intramedullary conus gliomas are rare and will not be discussed here. They have been considered to cause a progressive neurological deficit by compression of the surrounding intramedullary conus rather than infiltration into the surrounding neural tissues such as cauda equina nerves. In addition, they have been recognized as neoplasms that are amenable to complete surgical resection with Correspondence address Kadir KOT L Ba dat Cad. Hasan Ali Yücel Sk. Senil Apt Çiftehavuzlar, stanbul, Turkey Phone : Fax : kadirkotil@superonline.com Alternate kadirkotil@gmail.com 130
2 acceptable morbidity and mortality and a low incidence of recurrence. However, some cases associated with surgical morbidity have been reported.9 The functional results after microsurgical resection of ICCET are directly related to the preoperative neurological status. The emphasis of this paper is on the clinical presentation, indications, radiological and surgeryrelated findings and outcome of the tumors of this region. PATIENTS AND METHODS A total of 230 intradural spinal tumors were histologically diagnosed between 1990 and 2004 and 24 (11%) were ICCET. In the last fourteen years, 24 patients with ICCET were treated with the microsurgical posterior approach at our neurosurgery clinic. There were 16 males and 8 females with a mean age of 36.2 years (range 13 to 68 years). No correlation was found between tumor type and patient age. There was no significant relationship between neurogical abnormalities and tumor size. The localization of the tumor, patient's age at presentation, and duration of symptoms prior to admission are listed in (Table I). The main preoperative complaints included minor motor weakness in 12 out of the 24 patient (50%), paresthesia in 7 patients (29.4%) and pain in 20 patients (84.8%). The back pain became more severe at night or when the patient assumed a recumbent position for any length of time in most patients. The pain was only mitigated when the patient stood or sat up. The patients frequently reported sleeping in the sitting position. Bladder dysfunction was observed in 18 (75%) patients who had 100 cc of postvoiding residual urine. The duration of symptoms before the initial diagnosis ranged from 2 to 105 months (mean duration, 29 months). Outcome after operation was assesed from the clinical records, symptomatically in terms of pain, paresthesia, subjective lower limb weakness and sphincter disturbance, and by objective neurological examination. Preoperative evaluations All patients underwent both myelography and computed tomography between 1990 and We have only one case investigated by myelography (Figure 1) and this tumor was a myxopapillary ependymoma. Magnetic resonance imaging (MRI) was performed for the patients admitted after MRI showed well-demarcated ICCET in the 18 patients studied. Both solid (Figure 2) and cystic (Figure 3) components of the tumor were well represented in myelography pictures. The youngest patient was a 12-year-old girl with dermoid tumor (Figure 4). Most tumors were found to be extend for 1 or 2 vertebral segments, while the tumor extended over 5 vertebral segments in 2 cases. The long segmental spinal enrollment was demonstrated in (Figure 5) (ependymoma) and (Figure 6) (neurinoma). There was no dumbbell neurinoma in this location and all cases were single or solitary (Figure 7). One case had malignant neurinoma. One case who had hemangioblastoma was admitted with paraplegia, and was the only patient operated as an emergency. The location of the conus level was L1 except one patient who had a dermoid tumor with adult tethered cord syndrome (Figure 8). Meningiomas were the most recognized tumor in the preoperative period (Figure 9). Multisegmental spinal tumors were found in one case (4.6%). There were no cases with high-grade gliomas. All patients were evaluated preoperatively according to the grading system presented by Nurick (22): Table I. Data at presentation in 24 cases of conus and cauda equina tumors Tumor No of Age (yr) Duration of Symptoms (Year) Nurick grade type case (%) postoperative Mean Range Mean Range M:F Ependymoma 9 (37.4) :4 1 Neurinoma 5 (20.8) :2 1 Meningioma 4 (16.6) :1 1 Epidermoid 1 (4.16) M 1 Dermoid 4 (16.6) :3 5 Hemangioblastoma 1 (4.16) F 5 131
3 Figure 3: T1- and T2-weighted sagittal 3A and axial 3B images showing an intradural cystic ependymoma. Figure 1: Male, 33 years old, conus tumor is demonstrated by myelography. This lesion was caused a partial obstruction at the between L3 level. The histopathological diagnosis was myxopapillary ependymoma. Figure 4: Female, 13 years old, intradural conus dermoid tumor. Typical appearance of a dermoid tumor on a sagittal T1-weighted MR image. Figure 2: Male, 38 years old, T1- and T2-weighted sagittal image showing an intradural conus tumor (ependymoma). A B Figure 5 A: Female, 56 years old, sagittal T2-weighted image showing an intradural mass (ependymoma). B: T2- weighted enhanced sagittal imaging not showing postoperatively in the conus levels. 132
4 A C B Figure 6: Female, 66 years old, T1 and T2 weighted enhanced sagittal imaging showing an intradural giant tumor (neurinoma). The tumor was iso-hyperintense, the associated necrosis and cyst formation had low signal intensity on the T1-weighted image Figure 8: Female, 52 years old, sagittal T2-weighted MR image demonstrated tethered cord (arrow), dermal sinus tract (striped arrow) and dermoid tumor complex (small arrow). A B Figure 7: Male, 23 years old, T1-weighted sagittal (7A) and axial (7B) MR images after contrast: the tumor was remarkably enhanced, with tumor margin sharpened. The tumor was completely removed surgically and the histological diagnosis was neurinoma. Figure 9: Male, 45 years old, sagittal T1-weighted MR image post-contrast demonstrated an intradural conus meningioma (arrow). 133
5 Grade 1: Neurologically normal or normal walk Grade 2: Slight difficulty walking Grade 3: Disability limiting normal work or more severe neurological deficit Grade 4: Requires assistance with walk/gait or severe deficit Grade 5: Bedridden or wheelchair bound Surgical techniques and results A midline surgical approach was used for all our patients. After laminectomy and opening the dura, the tumors were resected under the microscope. In one case (13 years old) the tumor was resected by laminoplasty. Osteoblastic laminoplasty was preferred because of the age and the pathology (dermoid). In this case, we decided that laminectomy may cause delayed instability and myelopathy. This matter is very important at the thoracolumbar junction region and in this age. Myelotomy was performed after the midline dural incision if the tumor was intramedullary by gentle spreading of the posterior spinal cord column and cauda equina nerve roots using a microdissector and forceps. The tumors were always different in colour and softer than spinal cord tissue, and they were well-demarcated and encapsulated (such as neurinomas). The number of resected nerve roots was one root in 6 cases, two roots in 2, and three roots in one. Two dermal sinuses with dermoid tumor tracts were excised. Meningioma was the most easily resectable tumors in ICCET because of its extramedullary location. We did not observe prominent feeding vessels on the ventral surface of the tumors. A microsurgical approach was used in all cases and no blood or blood product transfusion was required. Complete removal of the tumor was achieved in 23 (95.4%) patients and subtotal removal was achieved in one case with a dermoid tumor. One case with dermoid tumor pathology was operated in two separate stages as residual tumor was identified after the first operation. The histological diagnoses were as follows: Ependymoma in 9 (37.4%) cases, Neurinoma in 5 (20.8%) cases (one case was malignant neurinoma) Meningiomas in 4 (16.64%) cases, Epidermoid in 1 (4.16 %) case, Dermoid in 4 (16.64 %) cases, Hemangioblastoma in 1 (4.16 %) case (Table II). No deaths occurred after a mean follow-up period of 54 months. One patient who had malignant neurinoma underwent radiation therapy after surgery. A syrinx was not detected in any of our cases. The myelotomy was not closed in any of the patients. After the surgical procedures, 2 (8.32 %) out of the 24 patients experienced a decrease of neurological function, and this persisted during the follow-up period (2 patients; grade 2). Except two cases with paraplegia, these neurological deficits included minor motor deficit, urinary dysfunction, and posterior column dysfunction. One patient had acute paraplegia due to intratumoral bleeding (hemangioblastoma) and emergency decompression was performed with subtotal tumor excision. The postoperative neurological function of this case (Nurick grade 5) was the same as the preoperative status. One patient experienced repeated growth or residue of a dermoid tumor in the conus causing partial cauda equina syndrome and did not show Table II: Clinical presentation (preoperative period) related to tumor histology Back pain Radiculopaty Motor Upper Sphincter Sensory Weakness motor involvement findings neuron N % sign Ependymomas 9 (100) 5 (55.5) 8 (88.8) 7 (77) 2 (22.2) 9 (100) Neurinomas 3 (60) 3 (60) 4 (80) 4 (80) 1 (20) 4 (80) Meningioma 4 (100) 2 (50) 2 (50) (75) Epidermoid 1 (100) Dermoid 4 (100) (100) - Hemangioblastoma - 1 (100) 1 (100) - 1(100) - 134
6 improvement months after the surgery (Nurick grade 5). However, neurological status improved thereafter. Twenty-two patients were neurologically intact at the time of the most recent follow-up examination (mean duration: 3 year). All the patients were given methylprednisolone and antibiotics in the preoperative period. DISCUSSION The ICCET are rare lesions, and a large clinical series with long follow-up has not been reported before in the neurosurgical literature. We have operated on 230 spinal intradural tumors in our clinic between 1990 and Twenty-four (10.5%) cases were localized to the conus. These tumors were further subdivided as extramedullary (5 cases; 20.8%) and intramedullary (19 cases; 79.4 %). The few population-based studies that have been published give annual incidence rates of 1 new tumor per 100,000 population.6 Attempts to distinguish conus from cauda equina lesions have been made clinically, but many authors believe the distinction is of little value. 10 The predominant symptoms and signs of these tumors are well documented. These tumors usually have benign histology. The prognosis after surgical treatment depends not only on histology but also on the degree of neurological deficit before the surgery, and the importance of early diagnosis and subsequent treatment is well recognized(4). The conus medullaris, which is the terminal segment of the adult spinal cord, lies at the inferior aspect of the L1 vertebra. The segment above the conus medullaris is termed the epiconus. Nerve roots travel caudally from the conus medullaris as the cauda equina. Clinical findings at the time of presentation to a specialist are documented in Table 2. Back pain was present in all patients and bilateral radiculopaty was also present in over half. Sensory findings were present in 18 (74.8%) patients. Bladder dysfunction was observed in 18 (74.8%) patients who had 100 cc of postmixture residual urine. Two patients had sphincter involvement (8.32 %) and did not improve postoperatively. Uchiyama26 et al. have reported that more than 83 % of the patients have urinary symptoms. Ependymomas of the conus and cauda equina almost exclusively have a myxopathic histology (8,16). Conus medullaris ependymomas originate from the ependymal cell cluster of the ventriculus terminalis in the filum (4,14,16,23). There are four histological types of ependymomas papillary, cellular, epithelial, or mixed. Myxopapillary ependymoma is most common ependymoma at the conus level. Cystic degeneration is observed in 40 %. Rostral and caudal cysts are seen in 90% of all patients; all cysts were are on T1-weighted images and hyperintense on T2-weighted images. This study included only one case of cystic ependymoma (Figure 3). Tumor-related cysts can be classified into three types (4,7,8). The first type is cystic tumors, most likely resulting from tumor necrosis or hemorrhage. The second type is syrinx formation, and the third type is the tumor-associated cyst, which is the most commonly seen. Ependymomas have a higher incidence of bleeding than other conus tumors. All ependymomas were slightly hyperintense on T2-weighted MR images and contrast enhanced. Precontrast, they were isointense on T1-weighted MR images. On histologic examination, these tumors contain rings of ependymal cells that surround cores of blood vessels and mucin (16). Histological examination revealed a benign ependymoma in all our patients. There is usually a plane of cleavage between tumor and spinal cord and complete excision can generally be achieved. Neurinomas or schwannomas can present with macroscopic cyst formation (7). We have 5 cases of neurinoma, one of which was a malignant neurinoma (20 %). Giant neurinomas of this region are very rare (4). This study included only one such a case (Figure 6). These patients usually have multiple cysts. Total excision could not be achieved. Despite incomplete removal of the tumor, the risk of recurrence is low (13). They must be distinguished from lumbar disc herniations. Neurinomas usually appear hypointense in comparison to the spinal cord on unenhanced T1-weighted images and hyperintense on T2-weighted images. Typically, meningiomas appear isointense on both T1- and T2- weighted images. Neurinomas often have smoother margins but more irregular enhancement in comparison to meningiomas, and neurinomas have cystic degeneration and internal necrosis.17 Two of our patients underwent myelography, three patients CT myelography, while 20 patients were investigated by MRI. Meningiomas arising in the lumbosacral region are uncommon, and represent only 2% of all spinal 135
7 cord meningiomas. Overall, spinal cord meningiomas occur more frequently in females, but the sex incidence is equal in the lumbosacral region (13). Meningiomas can be completely removed. All our meningiomas were the meningothelial subtype. For these tumors, it is important to remember that even patients who have a severe deficit preoperatively can have a dramatic improvement after removal of the intradural meningioma. These tumors have a classic appearance on MRI (Figure 9). Epidermoid and dermoid tumors are probably developmental in origin, and are lined by keratinizing squamous epithelium. Dermoid tumors also contain cutaneous adnexae, which accounts for their greasy contents, often admixed with hair. They can be microscopically totally excised in up to 40% of cases (13). This is reasonable, provided it is not associated with substantial morbidity, as partial removal can effectively relieve symptoms, often for many years and permanently in some cases. All of these tumors were intramedullary. They comprise approximately 10% of all intradural spinal cord tumors. They arise most frequently at the lumbar site. Two of the 5 patients with dermoid and epidermoid tumors had dermal sinus (Figure 8); one of these patients had an improvement in symptoms, while the other case had incomplete removal and no improvement. These tumors (midline congenital tumors) had a poor prognosis in this study. Spinal intradural hemangioblastomas make up between 2 and 6% all spinal cord tumors in most series (17). The origin of hemangioblastomas has not been clearly delineated. Hemangioblastomas may arise sporadically as single lesions or in the setting of Von Hippel-Lindau disease (VHL). Our case had VHL and was extramedullary. An association with VHL is found in only 30% of all spinal hemangioblastomas (17). We recommend complete excision because incomplete removal usually results in recurrence as in our case where regrwoth was seen 8 years later. We used irradiation for treatment in this case. On unenhanced T1-weighted and T2- weighted MR images, the tumors are usually isointense. They can also be hyperintense on T2- weighted MR images. In post-contrast study, the tumor nodules of hemangioblastoma often have stronger enhancement (17). Lumbar X-rays of our two patients whom has tumors of conus and cauda equina, occasionally demonstrates widening of the interpedicular distance, erosion of the posterior vertebral body, or enlargement of a neural foramen (scalloping). Because of their subarachnoidal location, these lesions are readily demonstrated by myelography or MRI (1,4,6-11,19,23,26). All clinically significant intradural-extramedullary tumors will be demonstrated by myelography, while small intramedullary conus tumors can be missed. When an intramedullary tumor produces complete obstruction, differential diagnosis from extramedullary tumors may be difficult. More frequently, the tumor produces a partial block, displacing the contrast column laterally; this appearance merely represents enlargement of the spinal cord and distinction from myelitis, intramedullary hematoma or syringomyelia may be impossible (2,21,25). In one of our cases, ICCET produced partial obstruction, displacing the contrast column laterally (fig1), not detected by other investigation methods as CT and MRI. More recent studies found MRI to be equal to or better than a CT myelogram. CT myelogram carries the risk of contrast dye which may induce nephrotoxicity, worsening neurologic function due to positioning for the procedure, and bleeding complications from the lumbar puncture. The advantages for MRI are multifold in the radiological evaluation for spinal cord tumors. In addition, MRI better identifies lesions for surgical interventions, and better differentiates extradural and intradural lesions. Contraindications to MRI include patients with pacemakers, non-compatible metallic implants, and severe claustrophobia (12,20). Contrast-enhanced MRI improves tumor characterisation and delineation. Almost all tumors enhance, and gadaolinium helps to separate the solid portion of tumors from adjacent edema and associated cysts (3). All of the tumors were totally excised except one case (96%). Sphincter dysfunction was present in four patients on admission and improved by following surgery in all except one. Back pain was the most important complain, present in 21(84%). There was bowel, bladder and sexual organ dysfunction in 6 cases, and only urodynamic dysfuntion in 19 (79 %) patients on admission and these were improved. In addition, spinal stability was rarely compromised. The surgical management of ICCET is a complex decision making process. The main determinants for surgical candidacy are tumor histobiology, 136
8 neurologic condition, and general medical condition. Surgery for ICCET is performed from the dorsal approach via Th11-12-L1 laminectomies. We generally resect ICCET tumors with the aid of the operating microscope and microneurosurgical techniques. Many surgeons do not utilize evoked potential monitoring for ICCET. We could not use peroperative spinal cord monitoring because it is unavailable. Peroperative frozen section must be used in conjunction with the clinical appearance and we used it for all of our patients. If a CSF leak is determined postoperatively, which usually occurs within the first week of surgery, a lumbar subarachnoidal drain may be placed at the time. If CSF diversion via a lumbar drain is not adequate, then surgical reexploration and closure of the dura may be necessary (15). CSF leak was determined in 2 of our cases postoperatively in Day 2 and a lumbar drain inserted was adequate for 3 days. There were no another surgical complications in this study. Spinal cord tumors account for 15% of all nervous system neoplasms, with 10% of these found in the conus and cauda equina (1). They do not metastasize except myxopapillary ependymomas that can rarely do so (9). The frequency of tumor type was different in our series. The predominant tumor was ependymoma, but neurofibromas are the most common tumor in the conus region in other series (4,18). We did not detect a neurofibroma in our cases. The roles for radiotherapy in the management of these benign tumors are limited. The correct diagnosis of ICCET and the definition of their subtype are always made postoperatively from the histological study of these tumors. Best functional outcome depends on duration of the symptoms and total removal of the tumor. The remaining 19 patients at long-term follow-up study (mean duration 75.5 months) were neurologically stabil, while remaining 4 cases minimal or moderate disability. CONCLUSION Long-term outcomes becomes more favourable by the development of new technologies for the diagnosis and treatment of ICCET. These developments have allowed more accurate preoperative diagnosis and safer, more effective operative interventions. Although follow-up surveillance may be needed, a majority of patients with solitary conus and cauda equina lesions can be cured, with gross total removal of the lesion. Probably the introduction of MRI will allow an early diagnosis of these lesions and the use of new surgical instruments. Early diagnosis gives excellent results and the prognosis is apparently directly related to the length of the preoperative clinical history. REFERENCES 1. Allen IM: Tumors of the cauda equina: A review of their clinical features and differential diagnosis. J Neurol Psychopathol 11: , Arseni C: Spinal cord dysembryoblastic tumors. Psychiat Neurol Neurochir 71: , Bronen RA, Size G: MR imaging control agents: Application to the CNS. J Neurosurg 3:820-39, Fearnside MR, Adams CBT: Tumours of the cauda-equina. J Neurol Neurosur Psychiatry 41:24-31, Greenberg MS. Handbook of Neurosurgery, Greenberg Graphics, Florida, 1994, 3rd Ed, pp Gudmundsson KR: A survey of tumours of ther central nervous system in the Iceland during the 10-years period Acta N eurol Scand 46: , Hanakita J, Suwa H, Nagayasu S, Nishi S, Lihara K, Sakaida H: Clinical features of intradural neurinomas in the cauda equina and around the conus medullaris. Neurochirurgia (stuttag). 35 (5): 145-9, Hoshimaru M, Koyama T, Hashimoto N, Kikuchi H: Results of microsurgical treatment for intramedullary spinal cord ependymomas: Analysis of 36 cases. Neurosurgery 44 2: , Kopelson G, Lingood R M, Kleiman G M: Management of intramedullary spinal cord tumors. Radiology 135:473-9, Levitt P, Ransohoff J: The differential diagnosis of tumours of the conus medullaris and cauda equina. In: Vinken PJ,bruyn GW, eds. Handbook of clinical neurology, Amsterdam:North- Holland 1975;19 pp Li MH, Holtas S, Larsson EM: MR imaging of intradural extramedullary tumors. Acta Radiol 33: , Li KC, Poon PY: Sensitivity and specifity of MRI in detecting malignant spinal cord compression and in distinguishing malignant from beningn compression fractures of vertebrae. Magn Reson Imaging 6: , Mathew P, Todd N V: Intradural conus and cauda equina tumors: a retrospective review of presentation, diagnosis and early outcome. J Neurol Neurosurg Psychiatry 56:69-74, McCormick PC, Torres R, Post KD, Stein BM: Intramedullary ependymoma of the spinal cord. J Neurosurg 72: , McCormick PC, Stein BM: Intramedullary Tumors in Adults. Neurosurgery Clin North Am 1: , Mozejatti A,Wayne TWS, Rauschning W, Ekholm SE: MR of the cauda equina. AJNR Am J Neuroradiol 8(5): , Murota T, Symon L. Surgical management of hemangioblastoma of the spinal cord: a report of 18 cases. Neurosurgery 25: , Nittner K: Spinal meningiomas, neurofibromas and neurinomas and hourglass tumor. In :Vinjken PJ, Bruyn BW. Tumor of the spine and spinal cord, part lll. Handbook of clinical neurology, Amsterdam, North Holland: 1976; 20 pp
9 19. Nurick S: The pathogenesis of the spinal cord disorder associated with cervical spondylosis. Brain 95:87-100, Osborn AG: Diagnostic Neuroradiology Mosby, New York, 1994, ed 2, pp Sharpio R: Myelography. London:Year Book Medical Publishers, 1975, ed 2, pp Solero CL, Fornari M, Giombini S, Lasio G, Oliveri G, Cimino C, Pluchino F. Spinal meningiomas: review of 174 operated cases. Neurosurgery 25(2):153-60, Sonneland PRL, Scheithauer BW,Onofrio BM: Myxopapillary ependymoma: a clinicopathologic and immunocytochemical study of 77 cases. Cancer 56-: , Souweidane MM, Benjamin V: Spinal cord meningiomas. Neurosurg Clin N Am 5: , Yoshii S, Shimizu K, Ido K, Nakamura T: Ependymoma of the spinal cord and cauda equina region. J Spinal Disord 12(2): , Uchiyama T, Sakakibara R, Hattori T, Yamanishi T: Lower urinary tract dysfunctions in patients with spinal cord tumors. Neurourology and Urodynamics 23:68-75,
Essentials of Clinical MR, 2 nd edition. 51. Primary Neoplasms
 51. Primary Neoplasms As with spinal central canal neoplasms in other regions, those of the lumbar spine may be classified as extradural, intradural extramedullary, and medullary. If an extradural lesion
51. Primary Neoplasms As with spinal central canal neoplasms in other regions, those of the lumbar spine may be classified as extradural, intradural extramedullary, and medullary. If an extradural lesion
Clinical Features of Cauda Equina Tumors Requiring Surgical Treatment
 Tohoku J. Exp. Med., 2006, 209, 1-6 Cauda Equina Tumors 1 Clinical Features of Cauda Equina Tumors Requiring Surgical Treatment YOICHI SHIMADA, NAOHISA MIYAKOSHI, 1 YUJI KASUKAWA, 1 MICHIO HONGO, 1 SHIGERU
Tohoku J. Exp. Med., 2006, 209, 1-6 Cauda Equina Tumors 1 Clinical Features of Cauda Equina Tumors Requiring Surgical Treatment YOICHI SHIMADA, NAOHISA MIYAKOSHI, 1 YUJI KASUKAWA, 1 MICHIO HONGO, 1 SHIGERU
ASJ. Myxopapillary Ependymoma of the Cauda Equina in a 5-Year-Old Boy. Asian Spine Journal. Introduction
 Asian Spine Journal 846 Masashi Case Uehara Report et al. Asian Spine J 2014;8(6):846-851 http://dx.doi.org/10.4184/asj.2014.8.6.846 Asian Spine J 2014;8(6):846-851 Myxopapillary Ependymoma of the Cauda
Asian Spine Journal 846 Masashi Case Uehara Report et al. Asian Spine J 2014;8(6):846-851 http://dx.doi.org/10.4184/asj.2014.8.6.846 Asian Spine J 2014;8(6):846-851 Myxopapillary Ependymoma of the Cauda
Clinico-pathological study of intradural extramedullary spinal tumors
 International Journal of Research in Medical Sciences Venugopal G et al. Int J Res Med Sci. 2015 Oct;3(10):2795-2799 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20150685
International Journal of Research in Medical Sciences Venugopal G et al. Int J Res Med Sci. 2015 Oct;3(10):2795-2799 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20150685
A Journey Down The Canal
 A Journey Down The Canal Radiological Assessment of Spinal Cord Masses John Berry-Candelario HMS III Gillian Lieberman, MD BIDMC Objectives Patient review Anatomy of the spine Imaging techniques Classification
A Journey Down The Canal Radiological Assessment of Spinal Cord Masses John Berry-Candelario HMS III Gillian Lieberman, MD BIDMC Objectives Patient review Anatomy of the spine Imaging techniques Classification
Spinal Cord Tumors of the Thoracolumbar Junction Requiring Surgery: A Retrospective Review of Clinical Features and Surgical Outcome
 Yonsei Med J 48(6):988-993, 2007 DOI 10.3349/ymj.2007.48.6.988 Spinal Cord Tumors of the Thoracolumbar Junction Requiring Surgery: A Retrospective Review of Clinical Features and Surgical Outcome Dong
Yonsei Med J 48(6):988-993, 2007 DOI 10.3349/ymj.2007.48.6.988 Spinal Cord Tumors of the Thoracolumbar Junction Requiring Surgery: A Retrospective Review of Clinical Features and Surgical Outcome Dong
IMAGING OF A CASE OF SPINAL MENINGIOMA- A CASE REPORT
 IMAGING OF A CASE OF SPINAL MENINGIOMA- A CASE REPORT Ramneet Wadi 1, Anil Kumar Shukla 2, Seetha Pramila V. V 3, Sabyasachi Basu 4, Sonam Sanjay 5 1Postgraduate Student, Department of Radiodiagnosis,
IMAGING OF A CASE OF SPINAL MENINGIOMA- A CASE REPORT Ramneet Wadi 1, Anil Kumar Shukla 2, Seetha Pramila V. V 3, Sabyasachi Basu 4, Sonam Sanjay 5 1Postgraduate Student, Department of Radiodiagnosis,
Spinal cord tumours Luc van den Hauwe et al.
 overview spinal cord tumours L. van den Hauwe 1,2, D. Balériaux 3, J.W. Van Goethem 2, C. Venstermans 2, F. De Belder 2, P.M. Parizel 2 introduction imaging spinal tumour classification spinal cord tumours
overview spinal cord tumours L. van den Hauwe 1,2, D. Balériaux 3, J.W. Van Goethem 2, C. Venstermans 2, F. De Belder 2, P.M. Parizel 2 introduction imaging spinal tumour classification spinal cord tumours
TUMOURS IN THE REGION OF FORAMEN MAGNUM
 TUMOURS IN THE REGION OF FORAMEN MAGNUM Abstract Pages with reference to book, From 119 To 122 Naim-ur-Rahman ( Department of Neurosurgery, Rawalpindi Medical College, Rawalpindi. ) A very unusual case
TUMOURS IN THE REGION OF FORAMEN MAGNUM Abstract Pages with reference to book, From 119 To 122 Naim-ur-Rahman ( Department of Neurosurgery, Rawalpindi Medical College, Rawalpindi. ) A very unusual case
Giant invasive spinal schwannomas: definition and surgical management
 J Neurosurg (Spine 2) 94:210 215, 2001 Giant invasive spinal schwannomas: definition and surgical management K. SRIDHAR, D.N.B. (NEUROSURG), RAVI RAMAMURTHI, M.S, F.R.C.S.ED. (SN), M. C. VASUDEVAN, M.D.,
J Neurosurg (Spine 2) 94:210 215, 2001 Giant invasive spinal schwannomas: definition and surgical management K. SRIDHAR, D.N.B. (NEUROSURG), RAVI RAMAMURTHI, M.S, F.R.C.S.ED. (SN), M. C. VASUDEVAN, M.D.,
SHORT OVERVIEW OF SPINAL CORD TUMORS
 SHORT OVERVIEW OF SPINAL CORD TUMORS 1 INTRODUCTION RARE HETEROGENEOUS GROUP OF TUMORS. 15%OFALLPRIMARYCNSNEOPLASMSARISEINTHESC. INCIDENCE HIGHER IN MALES THAN FEMALES AGE 10TO40YRS MOST PRIMARIES ARE
SHORT OVERVIEW OF SPINAL CORD TUMORS 1 INTRODUCTION RARE HETEROGENEOUS GROUP OF TUMORS. 15%OFALLPRIMARYCNSNEOPLASMSARISEINTHESC. INCIDENCE HIGHER IN MALES THAN FEMALES AGE 10TO40YRS MOST PRIMARIES ARE
MRI of chronic spinal cord injury
 The British Journal of Radiology, 76 (2003), 347 352 DOI: 10.1259/bjr/11881183 E 2003 The British Institute of Radiology Pictorial review MRI of chronic spinal cord injury 1 K POTTER, FRCR and 1 A SAIFUDDIN,
The British Journal of Radiology, 76 (2003), 347 352 DOI: 10.1259/bjr/11881183 E 2003 The British Institute of Radiology Pictorial review MRI of chronic spinal cord injury 1 K POTTER, FRCR and 1 A SAIFUDDIN,
AMSER Rad-Path Case of the Month January 2019
 AMSER Rad-Path Case of the Month January 2019 Intradural Spinal Tumor Ashley Graziano OMS IV, Lake Erie College of Osteopathic Medicine Dr. Matthew Hartman M.D., Allegheny Health Network Dr. David Oliver-Smith
AMSER Rad-Path Case of the Month January 2019 Intradural Spinal Tumor Ashley Graziano OMS IV, Lake Erie College of Osteopathic Medicine Dr. Matthew Hartman M.D., Allegheny Health Network Dr. David Oliver-Smith
Giant schwannoma with extensive scalloping of the lumbar vertebral body treated with one-stage posterior surgery: a case report
 Iizuka et al. Journal of Medical Case Reports 2014, 8:421 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Giant schwannoma with extensive scalloping of the lumbar vertebral body treated with one-stage
Iizuka et al. Journal of Medical Case Reports 2014, 8:421 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Giant schwannoma with extensive scalloping of the lumbar vertebral body treated with one-stage
Spinal Neoplasms. First Things First!! Localize the Lesion!! Ependymomas. Common Intramedullary Lesions
 Acta Radiológica Portuguesa, Vol.XXIII, nº 90, pág. 101-114, Abr.-Jun., 2011 Spinal Neoplasms Bruno A Policeni University of Iowa Hospitals and Clinics Assistant Professor of Radiology Disclosure of Commercial
Acta Radiológica Portuguesa, Vol.XXIII, nº 90, pág. 101-114, Abr.-Jun., 2011 Spinal Neoplasms Bruno A Policeni University of Iowa Hospitals and Clinics Assistant Professor of Radiology Disclosure of Commercial
NEURORADIOLOGY. Part III. Angela Csomor University of Szeged Department of Radiology
 NEURORADIOLOGY Part III Angela Csomor University of Szeged Department of Radiology DISEASES OF SPINE AND SPINAL CORD I. Non-tumourous diseases developmental anomalies vascular disorders inflammatory processes
NEURORADIOLOGY Part III Angela Csomor University of Szeged Department of Radiology DISEASES OF SPINE AND SPINAL CORD I. Non-tumourous diseases developmental anomalies vascular disorders inflammatory processes
Spine. Neuroradiology. Spine. Spine Pathology. Distribution of fractures. Radiological algorithm. Role of radiology 18/11/2015
 Spine Neuroradiology Spine Prof.Dr.Nail Bulakbaşı X Ray: AP/L/Oblique Vertebra & disc spaces CT & CTA Vertebra, discs, vessels MRI & MRA Vertebra, disc, vessels, meninges Spinal cord & nerves Myelography
Spine Neuroradiology Spine Prof.Dr.Nail Bulakbaşı X Ray: AP/L/Oblique Vertebra & disc spaces CT & CTA Vertebra, discs, vessels MRI & MRA Vertebra, disc, vessels, meninges Spinal cord & nerves Myelography
Ependymoma of the spine
 Ependymoma of the spine Tenny Zhang, MS-3 Harvard Medical School 1 Case presentation: history and exam HPI: A 30-year-old man with no significant past medical history presents with one week of bilateral
Ependymoma of the spine Tenny Zhang, MS-3 Harvard Medical School 1 Case presentation: history and exam HPI: A 30-year-old man with no significant past medical history presents with one week of bilateral
Giant cystic intradural extramedullary pilocytic astrocytoma of Cauda equina
 1 di 7 13/03/2014 09.02 J Neurosci Rural Pract. 2013 Oct-Dec; 4(4): 453 456. doi: 10.4103/0976-3147.120217 PMCID: PMC3858770 Giant cystic intradural extramedullary pilocytic astrocytoma of Cauda equina
1 di 7 13/03/2014 09.02 J Neurosci Rural Pract. 2013 Oct-Dec; 4(4): 453 456. doi: 10.4103/0976-3147.120217 PMCID: PMC3858770 Giant cystic intradural extramedullary pilocytic astrocytoma of Cauda equina
Cervical Intramedullary Epidermoid Cyst with Liquid Contents
 Asian Spine Journal Vol. 5, No. 1, pp 59~63, 2011 doi:10.4184/asj.2011.5.1.59 Cervical Intramedullary Epidermoid Cyst with Liquid Contents Amit Agarwal 1, Arvind Bhake 2, Anand Kakani 1 1 Department of
Asian Spine Journal Vol. 5, No. 1, pp 59~63, 2011 doi:10.4184/asj.2011.5.1.59 Cervical Intramedullary Epidermoid Cyst with Liquid Contents Amit Agarwal 1, Arvind Bhake 2, Anand Kakani 1 1 Department of
Treatment of cervicodorsalepidermiod cyst
 Treatment of cervicodorsalepidermiod cyst Ayied Motteb Turkey Department of Medicine, College of medicine, University of Tikret, Tekrit, Iraq Received 22 / 9/2011 Accepted 22/11/2011 Abstract Intramedullary
Treatment of cervicodorsalepidermiod cyst Ayied Motteb Turkey Department of Medicine, College of medicine, University of Tikret, Tekrit, Iraq Received 22 / 9/2011 Accepted 22/11/2011 Abstract Intramedullary
Extramedullary Spinal SOL Outcome of Surgery
 TAJ June 2009; Volume 22 Number 1 ISSN 1019-8555 The Journal of Teachers Association RMC, Rajshahi Original Article Extramedullary Spinal SOL Outcome of Surgery M Zahed Hossain 1, Monzurul Hoque 2 Abstract
TAJ June 2009; Volume 22 Number 1 ISSN 1019-8555 The Journal of Teachers Association RMC, Rajshahi Original Article Extramedullary Spinal SOL Outcome of Surgery M Zahed Hossain 1, Monzurul Hoque 2 Abstract
Dumbbell Shaped Thoracic Spine Cavernous Hemangioma: A Case Report and Review of the Literature
 ISPUB.COM The Internet Journal of Neurosurgery Volume 3 Number 1 Dumbbell Shaped Thoracic Spine Cavernous Hemangioma: A Case Report and Review of the Literature J Gonzalez-Cruz, A Nanda Citation J Gonzalez-Cruz,
ISPUB.COM The Internet Journal of Neurosurgery Volume 3 Number 1 Dumbbell Shaped Thoracic Spine Cavernous Hemangioma: A Case Report and Review of the Literature J Gonzalez-Cruz, A Nanda Citation J Gonzalez-Cruz,
Imaging the Spinal Cord & Intradural Disease
 Department of Radiology University of California San Diego Imaging the Spinal Cord & Intradural Disease John R. Hesselink, M.D. Spinal Cord Diseases Tumors Syringohydromyelia Trauma Ischemia / Infarction
Department of Radiology University of California San Diego Imaging the Spinal Cord & Intradural Disease John R. Hesselink, M.D. Spinal Cord Diseases Tumors Syringohydromyelia Trauma Ischemia / Infarction
Spinal schwannoma: Size has no correlation with presentation and outcome
 Spinal schwannoma: Size has no correlation with presentation and outcome Ravi Shankar Prasad*, Ruchi**, Kulwant Singh***, Ajit Singh**** *Assistant Professor, Department of Neurosurgery, Institute of Medical
Spinal schwannoma: Size has no correlation with presentation and outcome Ravi Shankar Prasad*, Ruchi**, Kulwant Singh***, Ajit Singh**** *Assistant Professor, Department of Neurosurgery, Institute of Medical
Chapter IV: Percutaneous Puncture of Spinal Cord Cysts
 Acta Radiologica: Diagnosis ISSN: 0567-8056 (Print) (Online) Journal homepage: http://www.tandfonline.com/loi/iard19 Chapter IV: Percutaneous Puncture of Spinal Cord Cysts To cite this article: (1966)
Acta Radiologica: Diagnosis ISSN: 0567-8056 (Print) (Online) Journal homepage: http://www.tandfonline.com/loi/iard19 Chapter IV: Percutaneous Puncture of Spinal Cord Cysts To cite this article: (1966)
Case Report Uncommon Progression of an Extradural Spinal Meningioma
 , Article ID 630876, 4 pages http://dx.doi.org/10.1155/2014/630876 Case Report Uncommon Progression of an Extradural Spinal Meningioma Atef Ben Nsir, 1 Mohamed Boughamoura, 1 Houda Mahmoudi, 2 Mohamed
, Article ID 630876, 4 pages http://dx.doi.org/10.1155/2014/630876 Case Report Uncommon Progression of an Extradural Spinal Meningioma Atef Ben Nsir, 1 Mohamed Boughamoura, 1 Houda Mahmoudi, 2 Mohamed
Spectrum of Magnetic Resonance Imaging findings in infective intra spinal complications of dermal sinus and associated inclusion cysts
 Spectrum of Magnetic Resonance Imaging findings in infective intra spinal complications of dermal sinus and associated inclusion cysts Poster No.: C-1443 Congress: ECR 2015 Type: Educational Exhibit Authors:
Spectrum of Magnetic Resonance Imaging findings in infective intra spinal complications of dermal sinus and associated inclusion cysts Poster No.: C-1443 Congress: ECR 2015 Type: Educational Exhibit Authors:
102 Results RESULTS. Age Mean=S.D Range 42= years -84 years Number % <30 years years >50 years
 102 Results RESULTS A total of 50 cases were studied 39 males and 11females.Their age ranged between 16 years and 84 years (mean 42years). T1 and T2WI were acquired for all cases in sagittal and axial
102 Results RESULTS A total of 50 cases were studied 39 males and 11females.Their age ranged between 16 years and 84 years (mean 42years). T1 and T2WI were acquired for all cases in sagittal and axial
Sporadic hemangioblastoma of the filum terminale: Case report and review of literature
 DOI: 10.2478/romneu-2018-0064 Article Sporadic hemangioblastoma of the filum terminale: Case report and review of literature Prashant S. Gade, Vernon Velho, Harish Naik, Laxmikant Bhople INDIA Romanian
DOI: 10.2478/romneu-2018-0064 Article Sporadic hemangioblastoma of the filum terminale: Case report and review of literature Prashant S. Gade, Vernon Velho, Harish Naik, Laxmikant Bhople INDIA Romanian
Long segment composite split cord malformation with double bony spur
 Long segment composite split cord malformation with double bony spur Anand Sharma, Achal Sharma, R.S. Mittal SMS Medical College, Jaipur, India Abstract: A composite type of SCM is very rare and only a
Long segment composite split cord malformation with double bony spur Anand Sharma, Achal Sharma, R.S. Mittal SMS Medical College, Jaipur, India Abstract: A composite type of SCM is very rare and only a
Recommendations for cross-sectional imaging in cancer management, Second edition
 www.rcr.ac.uk Recommendations for cross-sectional imaging in cancer management, Second edition Tumours of the spinal cord Faculty of Clinical Radiology www.rcr.ac.uk Contents Primary spinal cord tumours
www.rcr.ac.uk Recommendations for cross-sectional imaging in cancer management, Second edition Tumours of the spinal cord Faculty of Clinical Radiology www.rcr.ac.uk Contents Primary spinal cord tumours
Management of intramedullary astrocytomas
 Romanian Neurosurgery (2013) XX 2 Daniel Serban, Florin Exergian, R.M. Gorgan Bagdasar-Arseni Clinical Emergency Hospital, Neurosurgery I, Spinal Surgery, Bucharest Abstract Primitive IMT represent 8-10%
Romanian Neurosurgery (2013) XX 2 Daniel Serban, Florin Exergian, R.M. Gorgan Bagdasar-Arseni Clinical Emergency Hospital, Neurosurgery I, Spinal Surgery, Bucharest Abstract Primitive IMT represent 8-10%
Sequestered High Lumbar Intradural Disc Herniation Mimicking A Spinal Tumor: Case Report And Review Of The Literature
 ISPUB.COM The Internet Journal of Neurosurgery Volume 3 Number 2 Sequestered High Lumbar Intradural Disc Herniation Mimicking A Spinal Tumor: Case Report And Review Of The Literature I Omeis, A Cutler,
ISPUB.COM The Internet Journal of Neurosurgery Volume 3 Number 2 Sequestered High Lumbar Intradural Disc Herniation Mimicking A Spinal Tumor: Case Report And Review Of The Literature I Omeis, A Cutler,
Adult intramedullary astrocytomas of the spinal cord
 J Neurosurg 77:355-359, 1992 Adult intramedullary astrocytomas of the spinal cord FRED J. EPSTEIN, M.D., JEAN-PIERRE FARMER, M.D., F.R.C.S., AND DIANA FREED Division of Pediatric Neurosurgery, Department
J Neurosurg 77:355-359, 1992 Adult intramedullary astrocytomas of the spinal cord FRED J. EPSTEIN, M.D., JEAN-PIERRE FARMER, M.D., F.R.C.S., AND DIANA FREED Division of Pediatric Neurosurgery, Department
SPINAL CORD DISEASE IN DOGS PART TWO: MOST LIKELY CAUSES
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk SPINAL CORD DISEASE IN DOGS PART TWO: MOST LIKELY CAUSES Author : RITA GONÇALVES Categories : Vets Date : April 7, 2014 RITA
Vet Times The website for the veterinary profession https://www.vettimes.co.uk SPINAL CORD DISEASE IN DOGS PART TWO: MOST LIKELY CAUSES Author : RITA GONÇALVES Categories : Vets Date : April 7, 2014 RITA
A rare case of cervical epidural extramedullary plasmacytoma presenting with monoparesis
 Romanian Neurosurgery Volume XXXI Number 1 2017 January - March Article A rare case of cervical epidural extramedullary plasmacytoma presenting with monoparesis Okan Turk, Ibrahim Burak Atci, Hakan Yilmaz,
Romanian Neurosurgery Volume XXXI Number 1 2017 January - March Article A rare case of cervical epidural extramedullary plasmacytoma presenting with monoparesis Okan Turk, Ibrahim Burak Atci, Hakan Yilmaz,
Introduction to Neuroimaging spine. John J. McCormick MD
 Introduction to Neuroimaging spine John J. McCormick MD Neuroanatomy Netter drawings Radiographic Anatomy Cervical Spine Cervical Spine Oblique View Cervical Spine Dens View Thoracic Spine Lumbar Spine
Introduction to Neuroimaging spine John J. McCormick MD Neuroanatomy Netter drawings Radiographic Anatomy Cervical Spine Cervical Spine Oblique View Cervical Spine Dens View Thoracic Spine Lumbar Spine
Value of Intravenous Contrast Enhancement in the CT Evaluation of Intraspinal Tumors
 939 Value of Intravenous Contrast Enhancement in the CT Evaluation of Intraspinal Tumors J. S. Lapointe 1 D.. Graeb R.. Nugent W. D. Robertson The usefulness of intravenous contrast-enhanced CT in delineating
939 Value of Intravenous Contrast Enhancement in the CT Evaluation of Intraspinal Tumors J. S. Lapointe 1 D.. Graeb R.. Nugent W. D. Robertson The usefulness of intravenous contrast-enhanced CT in delineating
Spine and spinal cord
 NEURORADIOLOGY Spine and spinal cord Erika Vörös University of Szeged Department of Radiology SZEGED DISEASES OF SPINE AND SPINAL CORD I. Non-tumourous diseases developmental anomalies vascular disorders
NEURORADIOLOGY Spine and spinal cord Erika Vörös University of Szeged Department of Radiology SZEGED DISEASES OF SPINE AND SPINAL CORD I. Non-tumourous diseases developmental anomalies vascular disorders
Pediatric Spine Tumors (and other masses)
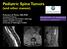 Pediatric Spine Tumors (and other masses) Francisco A Perez, MD, PhD Assistant Professor Neuroradiology and Pediatric Radiology Seattle Children s Hospital University of Washington, Seattle Commercial
Pediatric Spine Tumors (and other masses) Francisco A Perez, MD, PhD Assistant Professor Neuroradiology and Pediatric Radiology Seattle Children s Hospital University of Washington, Seattle Commercial
Neurosurgical Techniques
 Neurosurgical Techniques Neurosurgical Techniques Laminectomy for the Removal of Spinal Cord Tumors J. GRAFTON LOVE, M.D. Section of Neurologic Surgery, Mayo Clinic and Mayo Foundation, Rochester, Minnesota
Neurosurgical Techniques Neurosurgical Techniques Laminectomy for the Removal of Spinal Cord Tumors J. GRAFTON LOVE, M.D. Section of Neurologic Surgery, Mayo Clinic and Mayo Foundation, Rochester, Minnesota
Neuroimaging. spine / spinal cord
 Neuroimaging spine / spinal cord Spine & spinal cord imaging methodology Plain x-ray of spine Computed tomography CT - traditional ( normal CT) - reconstructions - myelo-ct Magnetic resonance MR - standard
Neuroimaging spine / spinal cord Spine & spinal cord imaging methodology Plain x-ray of spine Computed tomography CT - traditional ( normal CT) - reconstructions - myelo-ct Magnetic resonance MR - standard
Imaging in neurofibromatosis type 1: An original research article with focus on spinal lesions
 Original Research Article Imaging in neurofibromatosis type 1: An original research article with focus on spinal lesions Kalpesh Patel 1*, Siddharth Zala 2, C. Raychaudhuri 3 1 Assistant Professor, 2 1
Original Research Article Imaging in neurofibromatosis type 1: An original research article with focus on spinal lesions Kalpesh Patel 1*, Siddharth Zala 2, C. Raychaudhuri 3 1 Assistant Professor, 2 1
Tumors of the Nervous System
 Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they present? What do they look like? How do they behave? 1
Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they present? What do they look like? How do they behave? 1
Iatrogenic lumbar Pseudomeningocele: A case report and review of literature
 Available online at Available online at: www.ijmrhs.com ISSN No: 2319-5886 International Journal of Medical Research & Health Sciences, 2016, 5, 1:153-157 Iatrogenic lumbar Pseudomeningocele: A case report
Available online at Available online at: www.ijmrhs.com ISSN No: 2319-5886 International Journal of Medical Research & Health Sciences, 2016, 5, 1:153-157 Iatrogenic lumbar Pseudomeningocele: A case report
CNS TUMORS. D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria)
 CNS TUMORS D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria) CNS TUMORS The annual incidence of intracranial tumors of the CNS ISmore than intraspinal tumors May be Primary or Secondary
CNS TUMORS D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria) CNS TUMORS The annual incidence of intracranial tumors of the CNS ISmore than intraspinal tumors May be Primary or Secondary
Case Report Adjacent Lumbar Disc Herniation after Lumbar Short Spinal Fusion
 Case Reports in Orthopedics, Article ID 456940, 4 pages http://dx.doi.org/10.1155/2014/456940 Case Report Adjacent Lumbar Disc Herniation after Lumbar Short Spinal Fusion Koshi Ninomiya, Koichi Iwatsuki,
Case Reports in Orthopedics, Article ID 456940, 4 pages http://dx.doi.org/10.1155/2014/456940 Case Report Adjacent Lumbar Disc Herniation after Lumbar Short Spinal Fusion Koshi Ninomiya, Koichi Iwatsuki,
Wound healing in trophic ulcers in spina bifida patients
 J Neurosurg 82:000 000, 1995 Wound healing in trophic ulcers in spina bifida patients VINOD KUMAR SRIVASTAVA, M.B.B.S, M.CH. Neurosurgical Unit, J. N. Medical College, Aligarh Muslim University, Aligarh,
J Neurosurg 82:000 000, 1995 Wound healing in trophic ulcers in spina bifida patients VINOD KUMAR SRIVASTAVA, M.B.B.S, M.CH. Neurosurgical Unit, J. N. Medical College, Aligarh Muslim University, Aligarh,
S YRINGOMYELIA and syringobulbia are
 Syringomyelia: A Look at Surgical Therapy J. GRAFTON LOVE, M.D. AND RICHARD A. OLAFSON, M.D. Mayo Clinic and Mayo Foundation, Section of Neurologic Surgery, and Mayo Graduate School of Medicine, University
Syringomyelia: A Look at Surgical Therapy J. GRAFTON LOVE, M.D. AND RICHARD A. OLAFSON, M.D. Mayo Clinic and Mayo Foundation, Section of Neurologic Surgery, and Mayo Graduate School of Medicine, University
Large Dumbbell-Shaped C1 Schwannoma Presenting as a Foramen Magnum Mass
 32 Large Dumbbell-Shaped C1 Schwannoma Presenting as a Foramen Magnum Mass Jody Helms, M.D. 1 Lattimore Madison Michael II, M.D., F.A.A.N.S., F.A.C.S. 1, 2 1 Department of Neurosurgery, University of Tennessee
32 Large Dumbbell-Shaped C1 Schwannoma Presenting as a Foramen Magnum Mass Jody Helms, M.D. 1 Lattimore Madison Michael II, M.D., F.A.A.N.S., F.A.C.S. 1, 2 1 Department of Neurosurgery, University of Tennessee
Surgery. Conus medullaris and Cauda Equina Syndromes. Anatomy. See online here
 Surgery Conus medullaris and Cauda Equina Syndromes See online here Conus medullaris and cauda equina syndromes are spinal cord injuries that involve injury to the lumbosacral segment of the spinal cord.
Surgery Conus medullaris and Cauda Equina Syndromes See online here Conus medullaris and cauda equina syndromes are spinal cord injuries that involve injury to the lumbosacral segment of the spinal cord.
Disclosure. Thoracolumbar Tumors. Intraspinal Tumor Removal Options 6/4/2011. Minimally Invasive Approaches for Spinal Tumors
 Minimally Invasive Approaches for Spinal Tumors Praveen V. Mummaneni, M.D. Disclosure Medtronic (Consultant, Grants) DePuy (Consultant, Other Financial Support) Associate Professor Dept. of Neurosurgery
Minimally Invasive Approaches for Spinal Tumors Praveen V. Mummaneni, M.D. Disclosure Medtronic (Consultant, Grants) DePuy (Consultant, Other Financial Support) Associate Professor Dept. of Neurosurgery
Astroblastoma: Radiologic-Pathologic Correlation and Distinction from Ependymoma
 AJNR Am J Neuroradiol 23:243 247, February 2002 Case Report Astroblastoma: Radiologic-Pathologic Correlation and Distinction from Ependymoma John D. Port, Daniel J. Brat, Peter C. Burger, and Martin G.
AJNR Am J Neuroradiol 23:243 247, February 2002 Case Report Astroblastoma: Radiologic-Pathologic Correlation and Distinction from Ependymoma John D. Port, Daniel J. Brat, Peter C. Burger, and Martin G.
1 Normal Anatomy and Variants
 1 Normal Anatomy and Variants 1.1 Normal Anatomy MR Technique. e standard MR protocol for a routine evaluation of the spine always comprises imaging in sagittal and axial planes, while coronal images are
1 Normal Anatomy and Variants 1.1 Normal Anatomy MR Technique. e standard MR protocol for a routine evaluation of the spine always comprises imaging in sagittal and axial planes, while coronal images are
The incidence of spinal schwannomas varies
 Intramedullary Schwannoma of Conus Medullaris: Case Report and Review of the Literature Rakesh Kumar, Radhey Shyam Mittal Department of Neurosurgery, Sawai Man Singh Medical Collage, Jaipur, Rajasthan,
Intramedullary Schwannoma of Conus Medullaris: Case Report and Review of the Literature Rakesh Kumar, Radhey Shyam Mittal Department of Neurosurgery, Sawai Man Singh Medical Collage, Jaipur, Rajasthan,
Synovial cyst of spinal facet
 Case report CHUN C. KAO, M.D., STEFAN S. WINKLER, M.D., AND J. H. TURNER, M.D. Sections of Neurosurgery, Radiology, and Pathology, Madison Veterans Administration Hospital, and University of Wisconsin,
Case report CHUN C. KAO, M.D., STEFAN S. WINKLER, M.D., AND J. H. TURNER, M.D. Sections of Neurosurgery, Radiology, and Pathology, Madison Veterans Administration Hospital, and University of Wisconsin,
Intradural spinal tumours and their mimics: a review of radiographic features
 Department of Radiology, Royal Melbourne Hospital, Parkville, Victoria, Australia Correspondence to Dr Sara Wein, Radiology Department, Royal Melbourne Hospital, Grattan Street, Parkville, VIC 3050, Australia;
Department of Radiology, Royal Melbourne Hospital, Parkville, Victoria, Australia Correspondence to Dr Sara Wein, Radiology Department, Royal Melbourne Hospital, Grattan Street, Parkville, VIC 3050, Australia;
The Natural History of Cerebellar Hemangioblastomas in von Hippel-Lindau Disease
 AJNR Am J Neuroradiol 24:1570 1574, September 2003 The Natural History of Cerebellar Hemangioblastomas in von Hippel-Lindau Disease Andrew Slater, Niall R. Moore, and Susan M. Huson BACKGROUND AND PURPOSE:
AJNR Am J Neuroradiol 24:1570 1574, September 2003 The Natural History of Cerebellar Hemangioblastomas in von Hippel-Lindau Disease Andrew Slater, Niall R. Moore, and Susan M. Huson BACKGROUND AND PURPOSE:
Cervical laminectomy for spinal cord compression. Information for patients Neurosurgery
 Cervical laminectomy for spinal cord compression Information for patients Neurosurgery What is a compression of the spinal cord and how has it been caused? The bones in our back are called vertebras and
Cervical laminectomy for spinal cord compression Information for patients Neurosurgery What is a compression of the spinal cord and how has it been caused? The bones in our back are called vertebras and
A NOVEL CAUSE FOR CAUDA- EQUINA SYNDROME WITH A NEW RADIOLOGICAL SIGN
 A NOVEL CAUSE FOR CAUDA- EQUINA SYNDROME WITH A NEW RADIOLOGICAL SIGN W Singleton, D Ramnarine, N Patel, C Wigfield Department of Neurological Surgery, Frenchay Hospital, Bristol, UK Introduction We present
A NOVEL CAUSE FOR CAUDA- EQUINA SYNDROME WITH A NEW RADIOLOGICAL SIGN W Singleton, D Ramnarine, N Patel, C Wigfield Department of Neurological Surgery, Frenchay Hospital, Bristol, UK Introduction We present
Spinal canal stenosis Degenerative diseases F 06
 What is spinal canal stenosis? The condition known as spinal canal stenosis is a narrowing (stenosis) of the spinal canal that in most cases develops due to the degenerative (wear-induced) deformation
What is spinal canal stenosis? The condition known as spinal canal stenosis is a narrowing (stenosis) of the spinal canal that in most cases develops due to the degenerative (wear-induced) deformation
Spinal meningioma imaging
 Spinal meningioma imaging Poster No.: C-0448 Congress: ECR 2018 Type: Educational Exhibit Authors: M. Smoljan, D. Zadravec ; Zagreb/HR, Zageb/HR Keywords: Neoplasia, Imaging sequences, Education, MR, CT,
Spinal meningioma imaging Poster No.: C-0448 Congress: ECR 2018 Type: Educational Exhibit Authors: M. Smoljan, D. Zadravec ; Zagreb/HR, Zageb/HR Keywords: Neoplasia, Imaging sequences, Education, MR, CT,
Symptomatic Multiple Level Lateral Meningoceles with Intraspinal Meningocele: A Case Study and Its Surgical Management
 THIEME Original Article 15 Symptomatic Multiple Level Lateral Meningoceles with Intraspinal Meningocele: A Case Study and Its Surgical Management Vernon Velho 1 Sachin Guthe 1 Pravin Survashe 1 Poonam
THIEME Original Article 15 Symptomatic Multiple Level Lateral Meningoceles with Intraspinal Meningocele: A Case Study and Its Surgical Management Vernon Velho 1 Sachin Guthe 1 Pravin Survashe 1 Poonam
Spinal schwannomas (SCHs), which are considered. How do spinal schwannomas progress? The natural progression of spinal schwannomas on MRI.
 clinical article J Neurosurg Spine 24:155 159, 2016 How do spinal schwannomas progress? The natural progression of spinal schwannomas on MRI Kei Ando, MD, PhD, Shiro Imagama, MD, PhD, Zenya Ito, MD, PhD,
clinical article J Neurosurg Spine 24:155 159, 2016 How do spinal schwannomas progress? The natural progression of spinal schwannomas on MRI Kei Ando, MD, PhD, Shiro Imagama, MD, PhD, Zenya Ito, MD, PhD,
SpineFAQs. Lumbar Spondylolisthesis
 SpineFAQs Lumbar Spondylolisthesis Normally, the bones of the spine (the vertebrae) stand neatly stacked on top of one another. The ligaments and joints support the spine. Spondylolisthesis alters the
SpineFAQs Lumbar Spondylolisthesis Normally, the bones of the spine (the vertebrae) stand neatly stacked on top of one another. The ligaments and joints support the spine. Spondylolisthesis alters the
Spinal Meningeal Melanocytoma with Benign Histology Showing Leptomeningeal Spread: Case Report
 Case Report Musculoskeletal Imaging A 37-year-old previously healthy man presented with a 2 months history of increasing posterior neck pain and radiating pain to the right upper extremity. Neurological
Case Report Musculoskeletal Imaging A 37-year-old previously healthy man presented with a 2 months history of increasing posterior neck pain and radiating pain to the right upper extremity. Neurological
ISSN X (Print) Original Research Article. DOI: /sjams
 DOI: 10.21276/sjams Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 27; 5(8A):32-31 Scholars Academic and Scientific Publisher (An International Publisher for Academic and
DOI: 10.21276/sjams Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 27; 5(8A):32-31 Scholars Academic and Scientific Publisher (An International Publisher for Academic and
Metastatic Lung Adenocarcinoma in the Spinal Cord with a Negative Positron Emission Tomography and Computed Tomography (PET/CT) scan
 C a s e R e p o r t J. of Advanced Spine Surgery Volume 5, Number 1, pp 28~32 Journal of Advanced Spine Surgery JASS Metastatic Lung Adenocarcinoma in the Spinal Cord with a Negative Positron Emission
C a s e R e p o r t J. of Advanced Spine Surgery Volume 5, Number 1, pp 28~32 Journal of Advanced Spine Surgery JASS Metastatic Lung Adenocarcinoma in the Spinal Cord with a Negative Positron Emission
Peter Canoll MD. PhD.
 Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they ypresent? What do they look like? How do they behave?
Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they ypresent? What do they look like? How do they behave?
SUPRAPUBIC PUNCTURE IN THE TREATMENT OF NEUROGENIC BLADDER
 SUPRAPUBIC PUNCTURE IN THE TREATMENT OF NEUROGENIC BLADDER CHARLES C. HIGGINS, M.D. W. JAMES GARDNER, M.D. WM. A. NOSIK, M.D. The treatment of "cord bladder", a disturbance of bladder function from disease
SUPRAPUBIC PUNCTURE IN THE TREATMENT OF NEUROGENIC BLADDER CHARLES C. HIGGINS, M.D. W. JAMES GARDNER, M.D. WM. A. NOSIK, M.D. The treatment of "cord bladder", a disturbance of bladder function from disease
The Surgical Treatment for Spinal Intradural Extramedullary Tumors
 Original Article Clinics in Orthopedic Surgery 2009;1:165-172 doi:10.4055/cios.2009.1.3.165 The Surgical Treatment for Spinal Intradural Extramedullary Tumors Dong-Ki Ahn, MD, Hoon-Seok Park, MD, Dae-Jung
Original Article Clinics in Orthopedic Surgery 2009;1:165-172 doi:10.4055/cios.2009.1.3.165 The Surgical Treatment for Spinal Intradural Extramedullary Tumors Dong-Ki Ahn, MD, Hoon-Seok Park, MD, Dae-Jung
Magnetic Resonance Imaging of Intramedullary Epidermoid Cyst of Low Thoracic Spinal Cord: a case report
 Chin J Radiol 2005; 30: 109-113 109 Magnetic Resonance Imaging of Intramedullary Epidermoid Cyst of Low Thoracic Spinal Cord: a case report MING-TSUNG WANG 1 TAI-CHING WU 2 JYH-CHING CHEN 1 TSUNG-CHIA
Chin J Radiol 2005; 30: 109-113 109 Magnetic Resonance Imaging of Intramedullary Epidermoid Cyst of Low Thoracic Spinal Cord: a case report MING-TSUNG WANG 1 TAI-CHING WU 2 JYH-CHING CHEN 1 TSUNG-CHIA
NEURORADIOLOGY-NEUROPATHOLOGY CONFERENCE
 THE UNIVERSITY OF NORTH CAROLINA at CHAPEL HILL SEPTEMBER 2013 NEURORADIOLOGY-NEUROPATHOLOGY CONFERENCE Claudia da Costa Leite, MD, PhD Thomas Bouldin, MD CASE 1 6 y-o female with headaches and vomiting
THE UNIVERSITY OF NORTH CAROLINA at CHAPEL HILL SEPTEMBER 2013 NEURORADIOLOGY-NEUROPATHOLOGY CONFERENCE Claudia da Costa Leite, MD, PhD Thomas Bouldin, MD CASE 1 6 y-o female with headaches and vomiting
Surgical Management of Solitary Nerve Sheath Tumors of the Cervical Spine: A Retrospective Case Analysis Based on Tumor Location and Extension
 ORIGINAL ARTICLE Neurol Med Chir (Tokyo) 54, 924 929, 2014 doi: 10.2176/nmc.oa.2014-0158 Online October 31, 2014 Surgical Management of Solitary Nerve Sheath Tumors of the Cervical Spine: A Retrospective
ORIGINAL ARTICLE Neurol Med Chir (Tokyo) 54, 924 929, 2014 doi: 10.2176/nmc.oa.2014-0158 Online October 31, 2014 Surgical Management of Solitary Nerve Sheath Tumors of the Cervical Spine: A Retrospective
MAGNETIC RESONANCE IMAGING OF SPINAL TUMORS
 MAGNETIC RESONANCE IMAGING OF SPINAL TUMORS A study using a 0.3 T vertical magnetic field MING HUA LI - HEXL- Lund 992 Organization LUND UNIVERSITY Department of Radiology University Hospital S-22 85 Lund,
MAGNETIC RESONANCE IMAGING OF SPINAL TUMORS A study using a 0.3 T vertical magnetic field MING HUA LI - HEXL- Lund 992 Organization LUND UNIVERSITY Department of Radiology University Hospital S-22 85 Lund,
Key Primary CPT Codes: Refer to pages: 7-9 Last Review Date: October 2016 Medical Coverage Guideline Number:
 National Imaging Associates, Inc. Clinical guidelines CERVICAL SPINE SURGERY: ANTERI CERVICAL DECOMPRESSION WITH FUSION CERVICAL POSTERI DECOMPRESSION WITH FUSION CERVICAL ARTIFICIAL DISC CERVICAL POSTERI
National Imaging Associates, Inc. Clinical guidelines CERVICAL SPINE SURGERY: ANTERI CERVICAL DECOMPRESSION WITH FUSION CERVICAL POSTERI DECOMPRESSION WITH FUSION CERVICAL ARTIFICIAL DISC CERVICAL POSTERI
Spinal tumour: primary cervical extradural meningioma at an unusual location
 Case Report Spinal tumour: primary cervical extradural meningioma at an unusual location Ishita Pant 1, Vinod Kumar Singh Gautam 2, Rima Kumari 3, Sujata Chaturvedi 1 1 Department of Pathology, 2 Department
Case Report Spinal tumour: primary cervical extradural meningioma at an unusual location Ishita Pant 1, Vinod Kumar Singh Gautam 2, Rima Kumari 3, Sujata Chaturvedi 1 1 Department of Pathology, 2 Department
Pediatric Spinal Anomalies
 Department of Radiology University of California San Diego Pediatric Spinal Anomalies John R. Hesselink, M.D. Spine Embryogenesis 1. Primitive streak 2. Proliferation of cells at primitive pit (Hensen's
Department of Radiology University of California San Diego Pediatric Spinal Anomalies John R. Hesselink, M.D. Spine Embryogenesis 1. Primitive streak 2. Proliferation of cells at primitive pit (Hensen's
Spinal Cord (2005) 43, & 2005 International Spinal Cord Society All rights reserved /05 $
 (2005) 43, 503 507 & 2005 International Society All rights reserved 1362-4393/05 $30.00 www.nature.com/sc Case Report Postmortem study of the spinal cord showing snake-eyes appearance due to damage by
(2005) 43, 503 507 & 2005 International Society All rights reserved 1362-4393/05 $30.00 www.nature.com/sc Case Report Postmortem study of the spinal cord showing snake-eyes appearance due to damage by
Spinal intradural arachnoid cyst with spinal dysraphism
 CASE REPORT Journal of Pediatric Neurology 2004; 2(4): 235-239 www.jpneurology.org with spinal dysraphism Kadir Kotil, Mustafa Ali Akçetin, Necmettin Güzel, Turgay Bilge Department of Neurosurgery, Haseki
CASE REPORT Journal of Pediatric Neurology 2004; 2(4): 235-239 www.jpneurology.org with spinal dysraphism Kadir Kotil, Mustafa Ali Akçetin, Necmettin Güzel, Turgay Bilge Department of Neurosurgery, Haseki
HIGH LEVEL - Science
 Learning Outcomes HIGH LEVEL - Science Describe the structure and function of the back and spine (8a) Outline the functional anatomy and physiology of the spinal cord and peripheral nerves (8a) Describe
Learning Outcomes HIGH LEVEL - Science Describe the structure and function of the back and spine (8a) Outline the functional anatomy and physiology of the spinal cord and peripheral nerves (8a) Describe
Department of Neurosurgery, Christliches Krankenhaus, Quakenbrück, Germany
 J Neurosurg Spine 19:12 26, 2013 AA, 2013 Treatment of intramedullary tumors: analysis of surgical morbidity and long-term results Clinical article Jörg Klekamp, M.D. Department of Neurosurgery, Christliches
J Neurosurg Spine 19:12 26, 2013 AA, 2013 Treatment of intramedullary tumors: analysis of surgical morbidity and long-term results Clinical article Jörg Klekamp, M.D. Department of Neurosurgery, Christliches
Sir William Asher ANATOMY
 SPINAL CORD INJURY BASICS RELATED TO LIFE CARE PLANNING Lesson 1 Sir William Asher Picture the pathetic patient lying long abed, the urine leaking from his distended bladder, the lime draining from his
SPINAL CORD INJURY BASICS RELATED TO LIFE CARE PLANNING Lesson 1 Sir William Asher Picture the pathetic patient lying long abed, the urine leaking from his distended bladder, the lime draining from his
Stab wound of the neck: potential pitfalls in management
 Archives of Emergency Medicine, 1989, 6, 225-229 CASE REPORT Stab wound of the neck: potential pitfalls in management R.D. PAGE &R.H. LYE University Department of Neurosurgery, Manchester Royal Infirmary,
Archives of Emergency Medicine, 1989, 6, 225-229 CASE REPORT Stab wound of the neck: potential pitfalls in management R.D. PAGE &R.H. LYE University Department of Neurosurgery, Manchester Royal Infirmary,
1/9/2013 EXTRAMEDULLARY TUMORS OF THE PEDIATRIC SPINE. Introduction. Classification for Extramedullary Tumors
 EXTRAMEDULLARY TUMORS OF THE PEDIATRIC SPINE Eugene Wang 1/20/12 Dent Neurologic Institute Introduction 2/3 of all intraspinal tumors of childhood are extramedullary 50% Extradural 10-15% Intradural Back
EXTRAMEDULLARY TUMORS OF THE PEDIATRIC SPINE Eugene Wang 1/20/12 Dent Neurologic Institute Introduction 2/3 of all intraspinal tumors of childhood are extramedullary 50% Extradural 10-15% Intradural Back
Spinal myxopapillary ependymoma with interval drop metastasis presenting as cauda equina syndrome: case report and review of literature
 Case Report Spinal myxopapillary ependymoma with interval drop metastasis presenting as cauda equina syndrome: case report and review of literature Shrikant V. Rege, Sharadendu Narayan, Harshad Patil,
Case Report Spinal myxopapillary ependymoma with interval drop metastasis presenting as cauda equina syndrome: case report and review of literature Shrikant V. Rege, Sharadendu Narayan, Harshad Patil,
Spinal Imaging. Bearbeitet von Herwig Imhof. 1. Auflage Taschenbuch. 312 S. Paperback ISBN Format (B x L): 12,5 x 19 cm
 Spinal Imaging Bearbeitet von Herwig Imhof 1. Auflage 2007. Taschenbuch. 312 S. Paperback ISBN 978 3 13 144071 6 Format (B x L): 12,5 x 19 cm Weitere Fachgebiete > Medizin > Sonstige Medizinische Fachgebiete
Spinal Imaging Bearbeitet von Herwig Imhof 1. Auflage 2007. Taschenbuch. 312 S. Paperback ISBN 978 3 13 144071 6 Format (B x L): 12,5 x 19 cm Weitere Fachgebiete > Medizin > Sonstige Medizinische Fachgebiete
Posterior surgical procedures are those procedures
 9 Cervical Posterior surgical procedures are those procedures that have been in use for a long time with established efficacy in the treatment of radiculopathy and myelopathy caused by pathologies including
9 Cervical Posterior surgical procedures are those procedures that have been in use for a long time with established efficacy in the treatment of radiculopathy and myelopathy caused by pathologies including
Spine Pain Management Program
 Spine Pain Management Program Please complete the following information: Patient Name: Patient ID Number: Patient DOB: The procedure being requested is: Please check the indication (reason) for this procedure
Spine Pain Management Program Please complete the following information: Patient Name: Patient ID Number: Patient DOB: The procedure being requested is: Please check the indication (reason) for this procedure
Overview. Spinal Anatomy Spaces & Meninges Spinal Cord. Anatomy of the dura. Anatomy of the arachnoid. Anatomy of the spinal meninges
 European Course in Neuroradiology Module 1 - Anatomy and Embryology Dubrovnik, October 2018 Spinal Anatomy Spaces & Meninges Spinal Cord Johan Van Goethem Overview spinal meninges & spaces spinal cord
European Course in Neuroradiology Module 1 - Anatomy and Embryology Dubrovnik, October 2018 Spinal Anatomy Spaces & Meninges Spinal Cord Johan Van Goethem Overview spinal meninges & spaces spinal cord
Comprehension of the common spine disorder.
 Objectives Comprehension of the common spine disorder. Disc degeneration/hernia. Spinal stenosis. Common spinal deformity (Spondylolisthesis, Scoliosis). Osteoporotic fracture. Anatomy Anatomy Anatomy
Objectives Comprehension of the common spine disorder. Disc degeneration/hernia. Spinal stenosis. Common spinal deformity (Spondylolisthesis, Scoliosis). Osteoporotic fracture. Anatomy Anatomy Anatomy
Dorsal dermal sinus in children
 Dorsal dermal sinus in children Poster No.: C-2581 Congress: ECR 2015 Type: Educational Exhibit Authors: J. Marjanovic, A. Paterson, P. C. McSherry, A. Nixon, A. 1 1 2 1 2 1 1 2 TRIPALO BATOS, T. Grmoja
Dorsal dermal sinus in children Poster No.: C-2581 Congress: ECR 2015 Type: Educational Exhibit Authors: J. Marjanovic, A. Paterson, P. C. McSherry, A. Nixon, A. 1 1 2 1 2 1 1 2 TRIPALO BATOS, T. Grmoja
Management of Thoracal and Lumbar Schwannomas Using a Unilateral Approach without Instability: An Analysis of 15 Cases
 Asian Spine Journal Vol. 6, No. 1, pp 43~49, 2012 http://dx.doi.org/10.4184/asj.2012.6.1.43 Management of Thoracal and Lumbar Schwannomas Using a Unilateral Approach without Instability: An Analysis of
Asian Spine Journal Vol. 6, No. 1, pp 43~49, 2012 http://dx.doi.org/10.4184/asj.2012.6.1.43 Management of Thoracal and Lumbar Schwannomas Using a Unilateral Approach without Instability: An Analysis of
Focal Anterior Displacement of the Thoracic Spinal Cord without Evidence of Spinal Cord Herniation or an Intradural Mass
 Original Article Musculoskeletal Imaging http://dx.doi.org/10.3348/kjr.2014.15.6.733 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2014;15(6):733-738 Focal Anterior Displacement of the Thoracic Spinal
Original Article Musculoskeletal Imaging http://dx.doi.org/10.3348/kjr.2014.15.6.733 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2014;15(6):733-738 Focal Anterior Displacement of the Thoracic Spinal
JMSCR Vol 04 Issue 04 Page April 2016
 www.jmscr.igmpublication.org Impact Factor 5.244 Index Copernicus Value: 5.88 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: http://dx.doi.org/10.18535/jmscr/v4i4.13 Malignant Nerve Sheath Tumor with Secondary
www.jmscr.igmpublication.org Impact Factor 5.244 Index Copernicus Value: 5.88 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: http://dx.doi.org/10.18535/jmscr/v4i4.13 Malignant Nerve Sheath Tumor with Secondary
Intraoperative Spinal Sonography of Soft-Tissue Masses of the Spinal Cord and Spinal Canal
 507 Intraoperative Spinal Sonography of Soft-Tissue Masses of the Spinal Cord and Spinal Canal Robert M. Quencer' Berta M. Montalvo' Barth. Green 2 Frank J. Eismont 3 Intraoperative spinal sonography (loss)
507 Intraoperative Spinal Sonography of Soft-Tissue Masses of the Spinal Cord and Spinal Canal Robert M. Quencer' Berta M. Montalvo' Barth. Green 2 Frank J. Eismont 3 Intraoperative spinal sonography (loss)
APPROPRIATE USE GUIDELINES
 APPROPRIATE USE GUIDELINES Appropriateness of Advanced Imaging Procedures (MRI, CT, Bone Scan/PET) in Patients with Neck Pain CDI QUALITY INSTITUTE: PROVIDER LED ENTITY (PLE) Updated June, 2017 Contents
APPROPRIATE USE GUIDELINES Appropriateness of Advanced Imaging Procedures (MRI, CT, Bone Scan/PET) in Patients with Neck Pain CDI QUALITY INSTITUTE: PROVIDER LED ENTITY (PLE) Updated June, 2017 Contents
흉추척수증을유발한황색인대골화증의골절 - 증례보고 -
 대한척추외과학회지제 14 권제 1 호 Journal of Korean Spine Surg. Vol. 14, No. 1, pp 52~56, 2007 흉추척수증을유발한황색인대골화증의골절 - 증례보고 - 하기용 김영훈 # 지원희 $ 가톨릭대학교의과대학강남성모병원정형외과, 성모자애병원정형외과 #, 강남성모병원영상의학과 $ Fracture of Ossification
대한척추외과학회지제 14 권제 1 호 Journal of Korean Spine Surg. Vol. 14, No. 1, pp 52~56, 2007 흉추척수증을유발한황색인대골화증의골절 - 증례보고 - 하기용 김영훈 # 지원희 $ 가톨릭대학교의과대학강남성모병원정형외과, 성모자애병원정형외과 #, 강남성모병원영상의학과 $ Fracture of Ossification
Spine Pain Management Program
 Spine Pain Management Program Please complete the following information: Patient Name: Patient ID Number: Patient DOB: The procedure being requested: Epidural Injection Please check the indication (reason)
Spine Pain Management Program Please complete the following information: Patient Name: Patient ID Number: Patient DOB: The procedure being requested: Epidural Injection Please check the indication (reason)
