Intradural spinal tumours and their mimics: a review of radiographic features
|
|
|
- Wendy Blankenship
- 6 years ago
- Views:
Transcription
1 Department of Radiology, Royal Melbourne Hospital, Parkville, Victoria, Australia Correspondence to Dr Sara Wein, Radiology Department, Royal Melbourne Hospital, Grattan Street, Parkville, VIC 3050, Australia; Received 6 December 2012 Revised 5 May 2013 Accepted 14 May 2013 Published Online First 7 June 2013 Editor s choice Scan to access more free content To cite: Wein S, Gaillard F. Postgrad Med J 2013;89: Intradural spinal tumours and their mimics: a review of radiographic features Sara Wein, Francesco Gaillard ABSTRACT Intradural spinal tumours, although relatively uncommon, can be diagnostically challenging, and often result in significant morbidity. They can be subdivided according to their cell of origin and whether they are within the cord (intramedullary) or intradural but extramedullary in location. The differential diagnosis for masses of the cauda equina region is often considered separately. Additionally, some inflammatory processes, cysts, benign tumour-like masses and vascular malformations may mimic intradural tumours. Although in many instances, a precise preoperative diagnosis is not possible as many of the imaging findings overlap, some features may strongly suggest one diagnosis over others. This article reviews the range of intradural spinal tumours in the adult and paediatric populations, with an emphasis on pertinent imaging characteristics. An approach is provided for distinguishing tumours from lesions that mimic tumours and for narrowing the differential diagnosis according to imaging findings. INTRODUCTION Intradural spinal tumours can be diagnostically challenging and often result in significant morbidity. Although relatively uncommon compared with intracranial or extradural spinal masses, the need for a preoperative or non-operative diagnosis is in many ways greater, as biopsy of intradural lesions has the potential to cause devastating neurological impairment. Additionally, as the presentation of intradural spinal tumours is similar for all histologies, being dependent on tumour size and location, clinical features are often unhelpful in narrowing the differential. The most common presenting symptoms include back or neck pain, radicular pain, weakness, paraesthesia, gait disturbance and bowel and bladder dysfunction. Brown Sequard syndrome (ipsilateral paralysis and loss of proprioception, and contralateral loss of pain and temperature sensation) due to compression of one side of the spinal cord and acute headache due to subarachnoid haemorrhage are less common presenting features. 1 Intradural tumours can be subdivided according to their location into intramedullary and intradural extramedullary tumours. The cauda equina region is often considered separately to the remainder of the spinal cord as certain tumours are particular to it. Additionally, a number of non-neoplastic lesions may mimic intramedullary and intradural extramedullary tumours. This article reviews the range of intradural spinal tumours in the adult and paediatric populations, with an emphasis on pertinent imaging characteristics. An approach is provided for distinguishing tumours from lesions that mimic tumours and for narrowing the differential diagnosis according to imaging findings, thus allowing the formulation of an appropriate management plan. IMAGING OF INTRADURAL MASS LESIONS MRI is the modality of choice for the assessment of lesions within the spinal canal as it has exquisite contrast and structural resolution, is able to image all compartments, and is able to assess for the presence of enhancement, cystic change and blood product. Myelography, historically, was of prime importance, but is now routinely used only in patients for whom MRI is contraindicated, or occasionally as a problem-solving technique. It is usually combined with CT (ie, CT myelography). CT remains the best modality for assessing the osseous structures and is especially important in planning instrumentation. Angiography is useful in a select group of patients who have vascular tumours or vascular malformations, and may offer endovascular therapeutic options. Ultrasound has been shown to be valuable in the assessment of spinal tumours in newborns and young infants, however, does not have a role in older patients as it is unable to image the intradural compartment due to the overlying posterior spinal elements. 2 INTRAMEDULLARY TUMOURS Intramedullary spinal tumours represent 4 10% of all central nervous system (CNS) tumours. 3 4 They account for 20% of all intradural tumours in adults, and 35% of all intradural tumours in children (box 1). 1 The vast majority (95%) are glial tumours. 4 Three general characteristics of intramedullary neoplasms are recognised on MRI: they cause spinal cord expansion, they produce high signal intensity on T2 weighted images, and the majority show at least some contrast enhancement. Intramedullary tumours are also commonly Box 1 Intramedullary tumours (20% in adults, 35% in children) Ependymoma (60%) Astrocytoma (30%) Hemangioblastoma Ganglioglioma Intramedullary metastasis Primary intramedullary lymphoma Primitive neuroendocrine tumour Solitary fibrous tumour Review Wein S, et al. Postgrad Med J 2013;89: doi: /postgradmedj
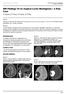
2 associated with cysts and syringohydromyelia, and may have evidence of prior haemorrhage. Ependymoma Ependymomas are the most common intramedullary neoplasm in adults and the most common intramedullary tumour overall, comprising approximately 60% of all glial spinal cord tumours, and occurring in approximately 0.21 per persons per year. 4 5 They represent 30% of paediatric intramedullary neoplasms, making them the second most common paediatric intramedullary neoplasm, after astrocytomas. 3 Although most are sporadic, there is an increased incidence in neurofibromatosis type 2 (NF2). The majority are WHO grade II lesions, however, anaplastic grade III lesions are encountered. They are generally slow growing and tend to compress adjacent spinal cord tissue rather than infiltrate it, almost always leaving a cleavage plane between tumour and spinal cord tissue. Ependymomas can occur anywhere along the spinal cord, however, the cervical cord is the most common site. 6 The myxopapillary variant almost exclusively appears as an extramedullary mass in the region of the cauda equina and is discussed separately. As ependymomas arise from ependymal cells lining the central canal, they tend to occupy the central portion of the spinal cord and cause symmetric cord expansion (figure 1). Although unencapsulated, they are well circumscribed, and are frequently associated with cysts (tumoral and non-tumoral) and syringohydromyelia. In contrast with intracranial ependymomas, calcification is uncommon. Most ependymomas are isointense to hypointense on T1, however, mixed signal may be seen if cyst formation, tumour necrosis or haemorrhage has occurred. Virtually all enhance strongly. They are typically hyperintense on T2, and most demonstrate peritumoural oedema. 4 Associated haemorrhage leads to a hypointense haemosiderin rim above and/or below the mass ( cap sign ) in approximately one-third of cases. 4 The cap sign is suggestive of but not pathognomonic of ependymoma, as it may also be seen in haemangioblastomas and paragangliomas. Scoliosis and bony remodelling may occur and are more commonly seen in association with ependymomas than astrocytomas (table 1). Astrocytoma Astrocytomas are the second most common intramedullary tumour overall, representing approximately 40% of such lesions and occurring in approximately 0.03 per persons per year. 5 6 They are associated with neurofibromatosis type 1 (NF1). 6 They generally have a lower histologic grade than Postgrad Med J: first published as /postgradmedj on 7 June Downloaded from Figure 1 Ependymoma. (A) and (B) T2 weighted images demonstrate a heterogeneous mass located centrally, displacing normal cord laterally (white arrow heads) with associated peritumoural cysts/syrinx (white arrow) and prominent inferior haemosiderin capping (black arrow) (C) T1 weighted. (D) T1 weighted with gadolinium demonstrating prominent tumoural enhancement. on 30 April 2018 by guest. Protected by copyright. 458 Wein S, et al. Postgrad Med J 2013;89: doi: /postgradmedj
3 Wein S, et al. Postgrad Med J 2013;89: doi: /postgradmedj Table 1 MRI features of intradural tumours Most common location T1 T2 Enhancement Morphology Special features Intramedullary tumours Ependymoma Cervical cord Isointense to hypointense Astrocytoma Thoracic cord Isointense to hypointense Hemangioblastoma Thoracic cord Isointense to hypointense hyperintense Strong Well-circumscribed. Central within cord Hyperintense Variable and patchy Poorly defined margins Eccentric within cord Isointense to hyperintense Cysts and syringohydromyelia common Haemosiderin cap sign May involve long cord segments Vivid Usually discrete nodules Cysts and syrinx common Flow voids Ganglioglioma Cervical cord Heterogeneous Hyperintense Patchy Eccentric within cord Calcification common Cysts common Intramedullary metastases Cervical cord Hypointense Hyperintense Vivid Well defined Prominent peritumoural oedema Primary intramedullary lymphoma Cervical cord isointense Hyperintense Homogeneous Poorly defined Primitive neuroendocrine tumour Solitary fibrous tumour Cauda equina/filum terminale Intradural extramedullary tumours Schwannoma Cervical cord Isointense to hypointense Meningioma Thoracic cord Isointense to hypointense Hypointense Hyperintense Heterogeneous Poorly defined Leptomeningeal metastases/enhancement common Isointense to Markedly hypointense Vivid Well circumscribed hypointense Hyperintense Isointense to hyperintense May be heterogeneous Round, sausage or dumbbell shaped Vivid diffuse Well circumscribed Dural tail May calcify Bony remodelling common Haemorrhage, cysts and fatty degeneration may occur Displace nerve roots Neurofibroma Cervical cord Hypointense Hyperintense Heterogeneous Fusiform Bony remodelling common Encase nerve roots Target sign Myxopapillary ependymoma Paraganglioma Cauda equina/ filum terminale Cauda equina/filum terminale Leptomeningeal metastases Lumbosacral spine Isointense Isointense to hyperinense Usually hypointense Hyperintense Usually homogeneous Well circumscribed Haemorrhage common Isointense Hyperintense Intense Well circumscribed Flow voids Cap sign Salt-and-pepper appearance Smooth or nodular Thickened nerve roots or nodular lesions Sugar coating Cord oedema may be present Review Postgrad Med J: first published as /postgradmedj on 7 June Downloaded from on 30 April 2018 by guest. Protected by copyright.
4 astrocytomas in the brain, with approximately 75% being either grade I or II lesions. 4 Spinal cord astrocytomas account for 60% of paediatric intramedullary tumours, making them the most common spinal cord tumour in children. 3 Pilocytic astrocytomas are a subtype of astrocytoma found predominantly in children and young adults. They are WHO grade I lesions and are associated with an excellent prognosis, as they behave much like grade I cerebellar pilocytic astrocytomas and displace neural tissue rather than infiltrate it. Diffuse astrocytomas are generally faster growing than ependymomas and typically have a worse prognosis. They are characterised by hypercellularity and the absence of a surrounding capsule and, in contrast with cord ependymomas, a cleavage plane is not present. Surgical excision is usually the treatment of choice, however, due to their infiltrative nature, resection is almost always histologically incomplete. The most common location of astrocytomas is the thoracic cord, followed by the cervical cord. Isolated involvement of the conus medullaris and filum terminale is rare. 4 Astrocytomas are typically long intramedullary masses that cause diffuse cord expansion. Involvement of the entire spinal cord (holocord presentation) may occur. It is more common in children than in adults, and is more frequent with pilocytic astrocytomas. As astrocytomas arise from cord parenchyma, they typically have an eccentric location (figure 2) and may be exophytic, sometimes even appearing largely extramedullary. They usually have poorly defined margins and, like ependymomas, are typically isointense to hypointense on T1 with variable and patchy contrast enhancement. They are hyperintense on T2. Haemorrhage is uncommon, and associated peritumoural oedema and cysts are less prominent than with ependymomas. Hemangioblastoma Hemangioblastomas are the third most common intramedullary spinal neoplasm, representing 2% of such tumours and occurring in approximately 0.02 per persons per year. 7 Two-thirds are sporadic, with a peak presentation in the fourth decade. One-third of patients have von Hippel Lindau syndrome. 8 These patients typically present earlier and with multiple tumours. Haemangioblastomas are vascular WHO grade I lesions and are usually treated by surgical resection, sometimes with preceding endovascular embolisation to reduce intraoperative blood loss. The most common location is the thoracic cord. Although they usually appear as discrete nodules, there can be diffuse cord expansion. They have a variable appearance on T1, however, the majority are isointense to hypointense and difficult to Postgrad Med J: first published as /postgradmedj on 7 June Downloaded from Figure 2 Astrocytoma. (A) T1 weighted. (B) T1 weighted image with gadolinium demonstrates an ill defined heterogeneously enhancing mass (white arrows) extending over four segments. It is of high T2 signal (C) and (D) and is located eccentrically within the cord, displacing the cord posteriorly and to the left. There is no definite evidence of haemorrhage. on 30 April 2018 by guest. Protected by copyright. 460 Wein S, et al. Postgrad Med J 2013;89: doi: /postgradmedj
5 differentiate from normal spinal cord. 8 They are isointense to hyperintense on T2 with associated tumour cyst or syrinx being common. 4 9 Contrast enhancement is vivid, haemosiderin capping may be present and focal flow voids are often seen. The characteristic angiographic finding is a densely enhancing nidus with associated dilated arteries and prominent draining veins. RARE INTRAMEDULLARY TUMOURS There are many other rare tumours which are found in the cord (figure 3). A detailed discussion of each is beyond the scope of this article, however, a number are worth discussing briefly. Ganglioglioma Spinal gangliogliomas are rare, comprising 1.1% of all spinal cord neoplasms. 6 They are most frequently encountered in children, representing 15% of paediatric intramedullary neoplasms. 3 They are WHO grade I or II neoplasms composed of both ganglion cells and glial elements, and are most frequently located eccentrically in the cervical region, although they often involve long segments of the cord. Their imaging features are non-specific with heterogenous T1 signal, patchy contrast Review enhancement and hyperintense T2 signal. 6 Calcification is common and approximately half contain tumoural cysts. 4 Intramedullary metastases Intramedullary metastases are less common than leptomeningeal metastases, occurring in approximately % of cancer patients. 10 They are most frequently found in the cervical cord. Lung cancer is the most common primary tumour, accounting for approximately 50% of cases. 10 One-third of patients have concomitant brain metastasis, and one-quarter have leptomeningeal metastases. 11 They are typically well defined, hypointense on T1, hyperintense on T2 and demonstrate avid homogeneous enhancement. Prominent oedema commonly surrounds the tumour nodule. In contrast with primary intramedullary neoplasms, associated cysts are rare. Intramedullary metastases generally occur in the setting of advanced disease and, as such, are rarely the presenting lesion. They are not surprisingly associated with a poor prognosis, mostly related to systemic disease. 4 Primary intramedullary lymphoma Lymphoma of the spinal cord is uncommon, accounting for 3.3% of all CNS lymphoma, which constitutes only 1% of all Postgrad Med J: first published as /postgradmedj on 7 June Downloaded from Figure 3 Rare intramedullary tumours. (A) Hemangioblastoma; T2 weighted image demonstrates peritumoural cysts (white arrow), posterior serpiginous flow void (black arrow) and cord oedema. (B) Ganglioglioma; T2 weighted image demonstrates an eccentrically located hyperintense mass (white arrow). Evidence of prior surgery for a biopsy is noted posteriorly (white arrow heads). (C) Intramedullary metastasis; a ring-enhancing lesion is demonstrated within the conus on postgadolinium T1 weighted image. Extensive cord oedema is seen as low signal on this image and confirmed on T2 weighted images (not shown). (D) Primary intramedullary lymphoma; postgadolinium T1 weighted image demonstrates a large enhancing mass with thickening and enhancement of the cauda equina (white arrows) and enhancing tissue in the thecal cul-de-sac (black arrow). on 30 April 2018 by guest. Protected by copyright. Wein S, et al. Postgrad Med J 2013;89: doi: /postgradmedj
6 lymphomas in the body. 4 Eighty-five per cent are non-hodgkin lymphomas. 1 Most are solitary lesions located within the cervical region, however, there may be multiple lesions throughout the cord. Cord expansion is usually present, and lesions are generally poorly defined, isointense on T1 with homogeneous contrast enhancement and, in contrast to the characteristic low T2 signal intensity seen in intracranial lesions, are hyperintense on T2. Haemorrhage, tumoural cysts and syringomyelia are generally not present. 12 The prognosis for patients with intramedullary spinal lymphoma is poor. 13 Primitive neuroendocrine tumour The majority of spinal primitive neuroendocrine tumours (PNETs) are secondary to metastatic spread through the subarachnoid space from a primary intracranial tumour, although cases of primary spinal PNETs have been reported. Unlike intracranial PNETs, those involving the spine are slightly more common in adults than in children. 14 The lesions are usually located in the region of the filum terminale and cauda equina, are hypointense on T1, hyperintense on T2 and demonstrate heterogeneous enhancement. CSF seeding may produce leptomeningeal enhancement. Spinal PNETs are associated with a poor prognosis. 4 Dissemination through the CSF may produce Box 2 Intradural extramedullary tumours (80% in adults, 65% in children) Schwannoma (30%) Meningioma (25%) Neurofibroma Paraganglioma Leptomeningeal metastasis secondary intracranial deposits; distant metastatic spread may occur to lungs, bone and lymph nodes. Solitary fibrous tumour Solitary fibrous tumours (SFTs) are rare spindle-cell neoplasms of probable mesenchymal origin. Although most intradural spinal SFTs are intramedullary, intradural extramedullary lesions may occur The majority of cases are considered benign, however, malignant CNS SFTs have also been reported. 16 The lesions are usually well circumscribed and encapsulated, isointense to hypointense on T1, and demonstrate avid homogeneous enhancement. 17 Marked hypointensity is demonstrated Postgrad Med J: first published as /postgradmedj on 7 June Downloaded from Figure 4 Dumbbell-shaped schwannoma. (A) and (B) Fat-saturated postgadolinium T1 weighted images demonstrate a vividly enhancing dumbbell shaped mass (black arrows) which passes out of the neural exit foramen. The cord is compressed and displaced towards the right (white arrow head). T2 weighted images demonstrate marked expansion of the neural exit foramen by the hyperintense mass (white arrow heads) (C) and faint increased signal within the cord substance (white arrow) (D). on 30 April 2018 by guest. Protected by copyright. 462 Wein S, et al. Postgrad Med J 2013;89: doi: /postgradmedj
7 Figure 5 Meningioma. (A) T1 weighted image demonstrates a well-circumscribed intradural extramedullary mass that is isointense to the spinal cord. (B) and (C) Fat-saturated postgadolinium T1 weighted images; the mass demonstrates homogenous enhancement and a broad dural base. Dural tails are seen extending above and below the mass (white arrows). The spinal cord is markedly compressed (white arrow head). (D) The mass is slightly hyperintense on T2 weighted image. on T2, a feature which helps distinguish SFTs from other spinal cord tumours, and which is thought to be due to the presence of abundant collagen fibres. 18 While surgical resection is curative in most cases, recurrence has been reported. INTRADURAL EXTRAMEDULLARY TUMOURS Intradural extramedullary tumours are far more common than intramedullary tumours, representing 80% of all intradural tumours in adults and 65% of all intradural tumours in children (box 2). 1 On MRI, intradural extramedullary lesions are characterised by displacement of the cord to the contralateral side and widening of the ipsilateral cerebrospinal fluid space immediately above and below the lesion. Schwannoma Schwannomas are the most common intradural extramedullary spinal tumours, representing 30% of such lesions and occurring at a rate of approximately cases per persons per year They are WHO grade I tumours and usually arise from the dorsal sensory roots. They are most frequently seen in the cervical cord but may also occur in the cauda equina region, where they are the second most commonly encountered tumour after myxopapillary ependymomas. The majority are solitary and sporadic, however, there is an association with NF2. Surgery is the treatment of choice and gross total resection is usually curative, although in patients with NF2 there is a high incidence of new tumour formation. In general, schwannomas appear as rounded lesions. When large, they may either align themselves with the long axis of the cord, forming a sausage-shaped mass which can extend over several levels, or may protrude out of the neural exit foramen, forming a dumbbell shaped mass (figure 4). Bone remodelling may be seen, with widening of the neural exit foramen, thinning of the pedicle and posterior vertebral body scalloping. They are isointense to hypointense on T1, and hyperintense on T2, often with mixed signal. Virtually all enhance. Although they are often indistinguishable from neurofibromas, schwannomas are more frequently associated with haemorrhage, cyst formation and fatty degeneration. These findings are rare in neurofibromas. 6 Meningioma Meningiomas are the second most common intradural extramedullary spinal tumours, representing 25% of such lesions and Wein S, et al. Postgrad Med J 2013;89: doi: /postgradmedj
8 Figure 6 Myxopapillary ependymoma. (A) and (B) T2 weighted images demonstrate a central intrathecal mass in the region of the cauda equina that is of heterogenous increased signal. The filum terminale is seen running in the midline behind the mass on the axial image (white arrow head). There is near-complete effacement of the CSF space. (C) The mass demonstrates intermediate signal on the T1 weighted image and homogeneously enhances on the postcontrast image (D). occurring in approximately 0.32 per persons per year. 59 The vast majority are WHO grade I lesions. In the adult population, women are approximately 10 times more commonly affected than men, although in children there does not appear to be a sex predilection. The female preponderance in the adult population is even stronger than that associated with intracranial meningiomas, and is thought to be due to the effect of oestrogen, although the exact mechanism remains unclear Except when seen in the setting of NF2, nearly all are solitary lesions. 1 Box 3 Tumours of the cauda equina region Myxopapillary ependymoma (90%) Schwannoma Paraganglioma Metastasis Hemangioblastoma Meningioma Astrocytoma Primitive neuroendocrine tumour Ganglioglioma Surgery is the treatment of choice, with complete tumour removal able to be achieved in most patients. Meningiomas are most frequently found in the thoracic region. They are often located posterolaterally in the thoracic region and anteriorly in the cervical region. 1 They are well circumscribed with a broad dural attachment, and share the imaging features of intracranial meningiomas; they are usually isointense to slightly hypointense on T1 with vivid homogenous enhancement. A dural tail sign is often present (figure 5). They are isointense to slightly hyperintense on T2. Occasionally, densely calcified meningiomas are hypointense on both T1 and T2, and show only minimal contrast enhancement. Neurofibroma Spinal neurofibromas are WHO grade I peripheral nerve sheath tumours. There is an association with NF1. Surgery is the treatment of choice for symptomatic lesions; however, as neurofibromas tend to encase the nerve roots, they usually cannot be dissected from the parent nerve. 9 Five per cent to 10% undergo malignant change, which may be indicated by rapid growth Wein S, et al. Postgrad Med J 2013;89: doi: /postgradmedj
9 Figure 7 Paraganglioma. (A) T2 weighted image demonstrates an intermediate signal intradural extramedullary mass which causes posterior vertebral body scalloping. A prominent flow void is seen anterior to the conus (white arrow). (B) The mass also of intermediate signal on the T1 weighted image; high T1 and T2 signal fluid inferior to the mass most likely represents proteinaceous material (black arrows). (C) and (D) The mass vividly enhances postgadolinium. Spinal paragangliomas occur almost exclusively in the cauda equina region. Spinal neurofibromas are often indistinguishable from schwannomas, although a number of features may help suggest the diagnosis. They are most commonly fusiform in shape, unlike schwannomas which are characteristically round. They tend to encase the nerve roots, in contrast with schwannomas which commonly displace the nerve root due to their asymmetric growth. They are generally hypointense on T1 and hyperintense on T2, although a T2 hyperintense rim and central area of low signal ( target sign ) may be seen. This sign is thought to be due to a dense central area of collagenous stroma, and although highly suggestive of neurofibroma, is occasionally also seen in schwannomas and malignant peripheral nerve sheath tumours. 23 Heterogenous enhancement with areas of low signal is more characteristic of a neurofibroma than a schwannoma. As with schwannomas, bone remodelling may be seen. Myxopapillary ependymoma Although, strictly speaking, myxopapillary ependymomas are intramedulary tumours, they appear radiologically as extramedullary masses in the region of the cauda equina (figure 6). They are WHO grade I lesions which arise from the ependymal cells lining the inferior continuation of the central canal within the filum terminale, and represent more than 90% of tumours in the cauda equina region (box 3). 21 They most commonly present in young adult men. They are usually hypointense on T1, although T1 hyperintensity is occasionally demonstrated due to a prominent mucinous component. 24 They are typically hyperintense on T2, however, are prone to haemorrhage and, thus, often demonstrate low intensity at the tumour margins. Enhancement is virtually always seen. Paraganglioma Spinal paragangliomas are rare WHO grade I neoplasms that occur almost exclusively in the cauda equina region. 25 Neuroendocrine symptoms are usually absent, with presentation most commonly being due to mass effect. Surgical resection is the treatment of choice, sometimes with preoperative embolisation to reduce intraoperative blood loss. Paragangliomas are usually well-circumscribed masses that are isointense on T1, hyperintense on T2 and intensely enhancing on postcontrast images. Flow voids are typically seen along the surface of and within the tumour nodule (figure 7). Haemorrhage is common, leading to a cap sign. Occasionally, Wein S, et al. Postgrad Med J 2013;89: doi: /postgradmedj
10 Figure 8 Leptomeningeal metastases. (A) and (B) Fat-saturated postgadolinium T1 weighted images demonstrate multiple enhancing nodules scattered along the cauda equina (black arrows) with extensive leptomeningeal enhancement of the conus (white arrows). (C) and (D) T2 weighted images; note liver (white stars) and widespread bony metastatic disease. the characteristic salt-and-pepper appearance of head and neck paragangliomas may also be demonstrated. Conventional angiography reveals an intense early blush that persists into the late arterial and early venous phases. Box 4 Lesions that mimic intradural tumours Intramedullary lesions Vascular lesions Cavernous malformation Dural arteriovenous fistula Spinal cord infarction Inflammatory lesions Demyelination Transverse myelitis Spinal cord abscess Spinal cord contusion Intradural extramedullary lesions Intradural spinal lipoma Epidermoid cyst Dermoid cyst Neurenteric cyst Arachnoid cyst Leptomeningeal metastases Although intradural extramedullary metastases are rare, overall, they are the most common intradural extramedullary neoplasm in children. In the paediatric population, leptomeningeal metastases usually result from primary brain tumours ( drop metastases ); in adults, non-cns tumours are more frequently encountered. The most commonly affected site is the lumbosacral spine, and multiple lesions are often seen. Prognosis depends on the primary tumour but is generally poor. T1 weighted images may demonstrate thickened nerve roots or nodular lesions that are isointense with the spinal cord. Cord oedema may be seen with more extensive disease, especially if there is an intramedullary component. Contrast-enhanced images reveal enhancing tumour nodules on the spinal cord, nerve roots or cauda equina. Innumerable small enhancing nodules may also be seen along the spinal cord and nerve roots ( sugar coating )(figure 8). LESIONS THAT MIMIC INTRADURAL TUMOURS Various lesions may mimic intradural tumours (box 4). The differential diagnosis of intramedullary tumours includes vascular lesions, such as cavernous malformations, dural arteriovenous fistulas and spinal cord infarction, inflammatory disorders, such as demyelination, transverse myelitis and spinal cord abscesses, and spinal cord contusions (figure 9). The differential diagnosis 466 Wein S, et al. Postgrad Med J 2013;89: doi: /postgradmedj
11 Figure 9 Lesions that mimic intramedullary tumours. (A) Cavernous malformation; gradient echo image demonstrates characteristic blooming of the haemosiderin ring (white arrow). Cavernous malformations typically demonstrate heterogenous signal on T1 and T2 weighted images due to blood products of varying ages. (B) Dural arteriovenous fistula; T2 weighted image demonstrates increased signal within the lower thoracic cord (white arrow heads) as well as numerous tortuous filling defects along the dorsal aspect of the cord (white arrows). The site of maximal MRI abnormality is not a reliable indicator of the location of the fistula; a complete spinal angiogram is therefore required. (C) Demyelination; T2 weighted image demonstrates a hyperintense lesion (white arrow) that does not cause significant spinal cord enlargement. The plaques are typically isointense to hypointense on T1 weighted images, and demonstrate variable enhancement depending on acute activity. In most patients, additional lesions of variable enhancement are present in the brain and spinal cord. (D) Transverse myelitis; T2 weighted image demonstrates increased signal and mild swelling involving most of the conus (white arrows). Lesions characteristically occupy greater than two-thirds of the cross-sectional area of the cord. An acute clinical course is typical, in contrast with that of most spinal cord tumours. for intradural extramedullary tumours includes intradural spinal lipomas, epidermoid cysts, dermoid cysts, neurenteric cysts and arachnoid cysts (figure 10). CONCLUSION The differential diagnosis of intradural spinal tumours depends upon their location as intramedullary, intradural extramedullary, or related to the cauda equina/filum terminale. Although the differential is wide and there is significant overlap of the imaging appearances, a few entities make up the majority of cases. Knowledge of certain characteristics may help differentiate between lesions, and aid in preoperative planning. MULTIPLE CHOICE QUESTIONS (TRUE (T)/FALSE (F): ANSWERS AFTER THE REFERENCES) 1. The following features are more characteristic of ependymoma than astrocytoma: A. Scoliosis and bony remodelling B. Eccentric location in spinal canal C. Haemosiderin capping D. Involvement of long cord segments E. Ill-defined margins 2. Regarding intramedullary tumours: A. Most patients with spinal haemangioblastomas have von Hippel Lindau syndrome B. Ganglioglioma typically demonstrate mixed signal intensity on T1 weighted images C. The vast majority of patients with intramedullary metastases will have visible CNS disease elsewhere D. Marked diffuse T2 hypointensity in an enhancing lesion is suggestive of a solitary fibrous tumour E. Ependymomas are the most common intramedullary neoplasm in children 3. Regarding spinal nerve sheath tumours: A. Most arise from the motor roots B. A T2 hyperintense rim and central area of low signal ( target sign ) is pathognomonic for neurofibroma C. On postcontrast images, heterogenous enhancement with areas of low signal is more characteristic of a neurofibroma than a schwannoma Wein S, et al. Postgrad Med J 2013;89: doi: /postgradmedj
12 Figure 10 Lesions that mimic intradural extramedullary tumours. (A) Lipoma; T1 weighted sequence demonstrates a sharply circumscribed hyperintense mass (white arrow). The mass follows fat intensity on all sequences, does not enhance and may cause a chemical shift artefact. (B) Dermoid; T2 weighted image demonstrates a heterogenous mass posterior to the cord which contains fat and demonstrates prominent chemical shift artefact, seen as anterior dark and posterior white bounding lines (arrow heads). (C) Arachnoid cyst; T2 weighted image demonstrates anterior displacement of the thoracic cord by a mass that is isointense to CSF (black arrow). The mass follows CSF intensity on all sequences and may require myelography to distinguish it from ventral herniation of the cord. (D) Disc sequestrated fragment/extrusion; T2 weighted image demonstrates a large L5/S1 disc extrusion (white arrows). Although extradural in location, the appearance can mimic an intradural mass. Rarely calcified disc fragments can perforate the dura. D. Schwannomas are most commonly located in the thoracic cord E. Neurofibromas are frequently associated with haemorrhage, intrinsic vascular changes, cyst formation and fatty degeneration 4. Regarding intradural extramedullary tumours: A. Meningiomas are the most common intradural extramedullary tumours B. Paragangliomas usually present with neuroendocrine symptoms C. Spinal meningiomas are more frequent in women than men D. In the paediatric population, leptomeningeal metastases most commonly result from primary brain tumours E. There is an increased incidence of schwannomas and meningiomas in patients with neurofibromatosis type 2 5. Regarding tumours of the cauda equina region: A. Myxopapillary ependymomas are usually WHO grade II lesions B. Astrocytomas are frequently located in the cauda equina region C. Myxopapillary ependymomas most commonly present in young adult men D. Spinal paragangliomas occur almost exclusively in the cauda equina region E. Paragangliomas may demonstrate a cap sign Main messages The differential diagnosis of intradural spinal tumours depends upon their location as intramedullary, intradural extramedullary, or related to the cauda equina/filum terminale 95% of intramedullary tumours are glial tumours Spinal nerve sheath tumours and meningiomas comprise the vast majority of intradural extramedullary tumours Although many of the imaging characteristics of intradural tumours overlap, some features may strongly suggest one diagnosis over others Lesions that may mimic intradural spinal tumours include inflammatory processes, cysts, benign tumour-like masses and vascular malformations 468 Wein S, et al. Postgrad Med J 2013;89: doi: /postgradmedj
13 Directions for further research Adapting routine advanced imaging techniques used in the brain for the spinal cord (diffusion, perfusion, PET/CT) Using diffusion tensor imaging (DTI) tractography to identify the relationship of a mass to white matter tracts to enable safer and more complete surgery Key references Koeller KK, Rosenblum RS, Morrison AL. Neoplasms of the spinal cord and filum terminale: radiologic-pathologic correlation. Radiographics 20(6): Abul-kasim K, Thurnher MM, Mckeever P, et al. Intradural spinal tumours: current classification and MRI features. Neuroradiology 2008;50(4): Smith AB, Soderlund KA, Rushing EJ, et al. Radiologic-pathologic correlation of paediatric and adolescent spinal neoplasms: Part 1, Intramedullary spinal neoplasms. AJR Am J Roentgenol 2012;198(1): Soderlund KA, Smith AB, Rushing EJ, et al. Radiologic-pathologic correlation of paediatric and adolescent spinal neoplasms: Part 2, Intradural extramedullary spinal neoplasms. AJR Am J Roentgenol 2012;198(1): Wald JT, Imaging of spine neoplasm. Radiol Clin North Am 2012;50(4): Contributors SW and FG contributed to the writing of the article and share responsibility for the finished article. Competing interests None. Provenance and peer review Commissioned; externally peer reviewed. REFERENCES 1 Abul-kasim K, Thurnher MM, Mckeever P, et al. Intradural spinal tumours: current classification and MRI features. Neuroradiology 2008;50: American Institute of Ultrasound in Medicine. American College of Radiology; Society for Pediatric Radiology; Society of Radiologists in Ultrasound. J Ultrasound Med 2012;31: ( ). 3 Smith AB, Soderlund KA, Rushing EJ, et al. Radiologic-pathologic correlation of pediatric and adolescent spinal neoplasms: Part 1, Intramedullary spinal neoplasms. AJR Am J Roentgenol 2012;198: Koeller KK, Rosenblum RS, Morrison AL. Neoplasms of the spinal cord and filum terminale: radiologic-pathologic correlation. Radiographics 2000;20: Duong LM, Mccarthy BJ, Mclendon RE, et al. Descriptive epidemiology of malignant and nonmalignant primary spinal cord, spinal meninges, and cauda equina tumors, United States, Cancer 2012;118: Grossman RI, Yousem DM. Neuroradiology, the requisites. Philadelphia, USA: Mosby Inc., Brant WE, Helms CA. Fundamentals of diagnostic radiology. Philadelphia, USA: Lippincott Williams & Wilkins, Baker KB, Moran CJ, Wippold FJ, et al. MR imaging of spinal hemangioblastoma. AJR Am J Roentgenol 2000;174: Osborn AG. Diagnostic neuroradiology. St. Louis, USA: Mosby Inc., Schiff D, O neill BP. Intramedullary spinal cord metastases: clinical features and treatment outcome. Neurology 1996;47: Pellegrini D, Quezel MA, Bruetman JE. Intramedullary spinal cord metastasis. Arch Neurol 2009;66: Haque S, Law M, Abrey LE, et al. Imaging of lymphoma of the central nervous system, spine, and orbit. Radiol Clin North Am 2008;46: Caruso PA, Patel MR, Joseph J, et al. Primary intramedullary lymphoma of the spinal cord mimicking cervical spondylotic myelopathy. AJR Am J Roentgenol 1998;171: Deme S, Ang LC, Skaf G, et al. Primary intramedullary primitive neuroectodermal tumor of the spinal cord: case report and review of the literature. Neurosurgery 1997;41: Ogawa T, Moriyama E, Beck H, et al. Solitary fibrous tumor of the thoracic spinal cord. Neurol Med Chir (Tokyo) 2005;45: Metellus P, Bouvier C, Guyotat J, et al. Solitary fibrous tumours of the central nervous system: clinicopathological and therapeutic considerations of 18 cases. Neurosurgery 2007;60: Pakasa NM, Pasquier B, Chambonnière ML, et al. Atypical presentations of solitary fibrous tumours of the central nervous system: an analysis of unusual clinicopathological and outcome patterns in three new cases with a review of the literature. Virchows Arch 2005;447: Kawamura M, Izawa K, Hosono N, et al. Solitary fibrous tumor of the spinal cord: case report and review of the literature. Neurosurgery 2004;55: Seppala MT, Haltia MJ, Sankila RJ, et al. Long-term outcome after removal of spinal schwannoma: a clinicopathological study of 187 cases. JNeurosurg1995;83: Michaud DS, Gallo V, Schlehofer B, et al. Reproductive factors and exogenous hormone use in relation to risk of glioma and meningioma in a large European cohort study. Cancer Epidemiol Biomarkers Prev 2010;19: Wiemels J, Wrensch M, Claus EB. Epidemiology and etiology of meningioma. J Neurooncol 2010;99: Weissleder R, Wittenberg J MD MG, et al. Primer of diagnostic imaging. St. Louis: Mosby Inc., Soderlund KA, Smith AB, Rushing EJ, et al. Radiologic-pathologic correlation of pediatric and adolescent spinal neoplasms: Part 2, Intradural extramedullary spinal neoplasms. AJR Am J Roentgenol 2012;198: Kahan H, Sklar EM, Post MJ, et al. MR characteristics of histopathologic subtypes of spinal ependymoma. AJNR Am J Neuroradiol 1996;17: Wald JT. Imaging of spine neoplasm. Radiol Clin North Am 2012;50: ANSWERS 1. A. T B. F C. T D. F E. F 2. A. F B. T C. F D. T E. F 3. A. F B. F C. T D. F E. F 4. A. F B. F C. T D. T E. T 5. A. F B. F C. T D. T E. T Review Wein S, et al. Postgrad Med J 2013;89: doi: /postgradmedj
Essentials of Clinical MR, 2 nd edition. 51. Primary Neoplasms
 51. Primary Neoplasms As with spinal central canal neoplasms in other regions, those of the lumbar spine may be classified as extradural, intradural extramedullary, and medullary. If an extradural lesion
51. Primary Neoplasms As with spinal central canal neoplasms in other regions, those of the lumbar spine may be classified as extradural, intradural extramedullary, and medullary. If an extradural lesion
Spinal cord tumours Luc van den Hauwe et al.
 overview spinal cord tumours L. van den Hauwe 1,2, D. Balériaux 3, J.W. Van Goethem 2, C. Venstermans 2, F. De Belder 2, P.M. Parizel 2 introduction imaging spinal tumour classification spinal cord tumours
overview spinal cord tumours L. van den Hauwe 1,2, D. Balériaux 3, J.W. Van Goethem 2, C. Venstermans 2, F. De Belder 2, P.M. Parizel 2 introduction imaging spinal tumour classification spinal cord tumours
A Journey Down The Canal
 A Journey Down The Canal Radiological Assessment of Spinal Cord Masses John Berry-Candelario HMS III Gillian Lieberman, MD BIDMC Objectives Patient review Anatomy of the spine Imaging techniques Classification
A Journey Down The Canal Radiological Assessment of Spinal Cord Masses John Berry-Candelario HMS III Gillian Lieberman, MD BIDMC Objectives Patient review Anatomy of the spine Imaging techniques Classification
Imaging the Spinal Cord & Intradural Disease
 Department of Radiology University of California San Diego Imaging the Spinal Cord & Intradural Disease John R. Hesselink, M.D. Spinal Cord Diseases Tumors Syringohydromyelia Trauma Ischemia / Infarction
Department of Radiology University of California San Diego Imaging the Spinal Cord & Intradural Disease John R. Hesselink, M.D. Spinal Cord Diseases Tumors Syringohydromyelia Trauma Ischemia / Infarction
Pediatric Spine Tumors (and other masses)
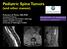 Pediatric Spine Tumors (and other masses) Francisco A Perez, MD, PhD Assistant Professor Neuroradiology and Pediatric Radiology Seattle Children s Hospital University of Washington, Seattle Commercial
Pediatric Spine Tumors (and other masses) Francisco A Perez, MD, PhD Assistant Professor Neuroradiology and Pediatric Radiology Seattle Children s Hospital University of Washington, Seattle Commercial
Spine. Neuroradiology. Spine. Spine Pathology. Distribution of fractures. Radiological algorithm. Role of radiology 18/11/2015
 Spine Neuroradiology Spine Prof.Dr.Nail Bulakbaşı X Ray: AP/L/Oblique Vertebra & disc spaces CT & CTA Vertebra, discs, vessels MRI & MRA Vertebra, disc, vessels, meninges Spinal cord & nerves Myelography
Spine Neuroradiology Spine Prof.Dr.Nail Bulakbaşı X Ray: AP/L/Oblique Vertebra & disc spaces CT & CTA Vertebra, discs, vessels MRI & MRA Vertebra, disc, vessels, meninges Spinal cord & nerves Myelography
Spinal Neoplasms. First Things First!! Localize the Lesion!! Ependymomas. Common Intramedullary Lesions
 Acta Radiológica Portuguesa, Vol.XXIII, nº 90, pág. 101-114, Abr.-Jun., 2011 Spinal Neoplasms Bruno A Policeni University of Iowa Hospitals and Clinics Assistant Professor of Radiology Disclosure of Commercial
Acta Radiológica Portuguesa, Vol.XXIII, nº 90, pág. 101-114, Abr.-Jun., 2011 Spinal Neoplasms Bruno A Policeni University of Iowa Hospitals and Clinics Assistant Professor of Radiology Disclosure of Commercial
IMAGING OF A CASE OF SPINAL MENINGIOMA- A CASE REPORT
 IMAGING OF A CASE OF SPINAL MENINGIOMA- A CASE REPORT Ramneet Wadi 1, Anil Kumar Shukla 2, Seetha Pramila V. V 3, Sabyasachi Basu 4, Sonam Sanjay 5 1Postgraduate Student, Department of Radiodiagnosis,
IMAGING OF A CASE OF SPINAL MENINGIOMA- A CASE REPORT Ramneet Wadi 1, Anil Kumar Shukla 2, Seetha Pramila V. V 3, Sabyasachi Basu 4, Sonam Sanjay 5 1Postgraduate Student, Department of Radiodiagnosis,
Ependymoma of the spine
 Ependymoma of the spine Tenny Zhang, MS-3 Harvard Medical School 1 Case presentation: history and exam HPI: A 30-year-old man with no significant past medical history presents with one week of bilateral
Ependymoma of the spine Tenny Zhang, MS-3 Harvard Medical School 1 Case presentation: history and exam HPI: A 30-year-old man with no significant past medical history presents with one week of bilateral
AMSER Rad-Path Case of the Month January 2019
 AMSER Rad-Path Case of the Month January 2019 Intradural Spinal Tumor Ashley Graziano OMS IV, Lake Erie College of Osteopathic Medicine Dr. Matthew Hartman M.D., Allegheny Health Network Dr. David Oliver-Smith
AMSER Rad-Path Case of the Month January 2019 Intradural Spinal Tumor Ashley Graziano OMS IV, Lake Erie College of Osteopathic Medicine Dr. Matthew Hartman M.D., Allegheny Health Network Dr. David Oliver-Smith
Introduction to Neuroimaging spine. John J. McCormick MD
 Introduction to Neuroimaging spine John J. McCormick MD Neuroanatomy Netter drawings Radiographic Anatomy Cervical Spine Cervical Spine Oblique View Cervical Spine Dens View Thoracic Spine Lumbar Spine
Introduction to Neuroimaging spine John J. McCormick MD Neuroanatomy Netter drawings Radiographic Anatomy Cervical Spine Cervical Spine Oblique View Cervical Spine Dens View Thoracic Spine Lumbar Spine
Spinal meningioma imaging
 Spinal meningioma imaging Poster No.: C-0448 Congress: ECR 2018 Type: Educational Exhibit Authors: M. Smoljan, D. Zadravec ; Zagreb/HR, Zageb/HR Keywords: Neoplasia, Imaging sequences, Education, MR, CT,
Spinal meningioma imaging Poster No.: C-0448 Congress: ECR 2018 Type: Educational Exhibit Authors: M. Smoljan, D. Zadravec ; Zagreb/HR, Zageb/HR Keywords: Neoplasia, Imaging sequences, Education, MR, CT,
Tumors of the Nervous System
 Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they present? What do they look like? How do they behave? 1
Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they present? What do they look like? How do they behave? 1
CNS TUMORS. D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria)
 CNS TUMORS D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria) CNS TUMORS The annual incidence of intracranial tumors of the CNS ISmore than intraspinal tumors May be Primary or Secondary
CNS TUMORS D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria) CNS TUMORS The annual incidence of intracranial tumors of the CNS ISmore than intraspinal tumors May be Primary or Secondary
1 Normal Anatomy and Variants
 1 Normal Anatomy and Variants 1.1 Normal Anatomy MR Technique. e standard MR protocol for a routine evaluation of the spine always comprises imaging in sagittal and axial planes, while coronal images are
1 Normal Anatomy and Variants 1.1 Normal Anatomy MR Technique. e standard MR protocol for a routine evaluation of the spine always comprises imaging in sagittal and axial planes, while coronal images are
Case 7391 Intraventricular Lesion
 Case 7391 Intraventricular Lesion Bastos Lima P1, Marques C1, Cabrita F2, Barbosa M2, Rebelo O3, Rio F1. 1Neuroradiology, 2Neurosurgery, 3Neuropathology, Coimbra University Hospitals, Portugal. University
Case 7391 Intraventricular Lesion Bastos Lima P1, Marques C1, Cabrita F2, Barbosa M2, Rebelo O3, Rio F1. 1Neuroradiology, 2Neurosurgery, 3Neuropathology, Coimbra University Hospitals, Portugal. University
SHORT OVERVIEW OF SPINAL CORD TUMORS
 SHORT OVERVIEW OF SPINAL CORD TUMORS 1 INTRODUCTION RARE HETEROGENEOUS GROUP OF TUMORS. 15%OFALLPRIMARYCNSNEOPLASMSARISEINTHESC. INCIDENCE HIGHER IN MALES THAN FEMALES AGE 10TO40YRS MOST PRIMARIES ARE
SHORT OVERVIEW OF SPINAL CORD TUMORS 1 INTRODUCTION RARE HETEROGENEOUS GROUP OF TUMORS. 15%OFALLPRIMARYCNSNEOPLASMSARISEINTHESC. INCIDENCE HIGHER IN MALES THAN FEMALES AGE 10TO40YRS MOST PRIMARIES ARE
Dr. T. Venkat Kishan Asst. Prof Department of Radiodiagnosis
 Dr. T. Venkat Kishan Asst. Prof Department of Radiodiagnosis Schwannomas (also called neurinomas or neurilemmomas) constitute the most common primary cranial nerve tumors. They are benign slow-growing
Dr. T. Venkat Kishan Asst. Prof Department of Radiodiagnosis Schwannomas (also called neurinomas or neurilemmomas) constitute the most common primary cranial nerve tumors. They are benign slow-growing
NEURORADIOLOGY. Part III. Angela Csomor University of Szeged Department of Radiology
 NEURORADIOLOGY Part III Angela Csomor University of Szeged Department of Radiology DISEASES OF SPINE AND SPINAL CORD I. Non-tumourous diseases developmental anomalies vascular disorders inflammatory processes
NEURORADIOLOGY Part III Angela Csomor University of Szeged Department of Radiology DISEASES OF SPINE AND SPINAL CORD I. Non-tumourous diseases developmental anomalies vascular disorders inflammatory processes
1/9/2013 EXTRAMEDULLARY TUMORS OF THE PEDIATRIC SPINE. Introduction. Classification for Extramedullary Tumors
 EXTRAMEDULLARY TUMORS OF THE PEDIATRIC SPINE Eugene Wang 1/20/12 Dent Neurologic Institute Introduction 2/3 of all intraspinal tumors of childhood are extramedullary 50% Extradural 10-15% Intradural Back
EXTRAMEDULLARY TUMORS OF THE PEDIATRIC SPINE Eugene Wang 1/20/12 Dent Neurologic Institute Introduction 2/3 of all intraspinal tumors of childhood are extramedullary 50% Extradural 10-15% Intradural Back
Giant cystic intradural extramedullary pilocytic astrocytoma of Cauda equina
 1 di 7 13/03/2014 09.02 J Neurosci Rural Pract. 2013 Oct-Dec; 4(4): 453 456. doi: 10.4103/0976-3147.120217 PMCID: PMC3858770 Giant cystic intradural extramedullary pilocytic astrocytoma of Cauda equina
1 di 7 13/03/2014 09.02 J Neurosci Rural Pract. 2013 Oct-Dec; 4(4): 453 456. doi: 10.4103/0976-3147.120217 PMCID: PMC3858770 Giant cystic intradural extramedullary pilocytic astrocytoma of Cauda equina
Recommendations for cross-sectional imaging in cancer management, Second edition
 www.rcr.ac.uk Recommendations for cross-sectional imaging in cancer management, Second edition Tumours of the spinal cord Faculty of Clinical Radiology www.rcr.ac.uk Contents Primary spinal cord tumours
www.rcr.ac.uk Recommendations for cross-sectional imaging in cancer management, Second edition Tumours of the spinal cord Faculty of Clinical Radiology www.rcr.ac.uk Contents Primary spinal cord tumours
Magnetic Resonance Imaging of Intrinsic Spinal Cord Lesions: A Pictorial Review
 Magnetic Resonance Imaging of Intrinsic Spinal Cord Lesions: A Pictorial Review Award: Guerbet Best Registrar Exhibit Prize Poster No.: R-0024 Congress: RANZCR ASM 2013 Type: Educational Exhibit Authors:
Magnetic Resonance Imaging of Intrinsic Spinal Cord Lesions: A Pictorial Review Award: Guerbet Best Registrar Exhibit Prize Poster No.: R-0024 Congress: RANZCR ASM 2013 Type: Educational Exhibit Authors:
General: Brain tumors are lesions that have mass effect distorting the normal tissue and often result in increased intracranial pressure.
 1 Lecture Objectives Know the histologic features of the most common tumors of the CNS. Know the differences in behavior of the different tumor types. Be aware of the treatment modalities in the various
1 Lecture Objectives Know the histologic features of the most common tumors of the CNS. Know the differences in behavior of the different tumor types. Be aware of the treatment modalities in the various
Peter Canoll MD. PhD.
 Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they ypresent? What do they look like? How do they behave?
Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they ypresent? What do they look like? How do they behave?
Kathleen R. Fink, MD Virginia Mason Medical Center. 6 th Nordic Emergency Radiology Course 2017
 Kathleen R. Fink, MD Virginia Mason Medical Center 6 th Nordic Emergency Radiology Course 2017 Disclosure My spouse receives research salary support from: Guerbet Outline Acute neck and back pain Acute
Kathleen R. Fink, MD Virginia Mason Medical Center 6 th Nordic Emergency Radiology Course 2017 Disclosure My spouse receives research salary support from: Guerbet Outline Acute neck and back pain Acute
CT & MRI Evaluation of Brain Tumour & Tumour like Conditions
 CT & MRI Evaluation of Brain Tumour & Tumour like Conditions Dr. Anjana Trivedi 1, Dr. Jay Thakkar 2, Dr. Maulik Jethva 3, Dr. Ishita Virda 4 1 M.D. Radiology, Professor and Head, P.D.U. Medical College
CT & MRI Evaluation of Brain Tumour & Tumour like Conditions Dr. Anjana Trivedi 1, Dr. Jay Thakkar 2, Dr. Maulik Jethva 3, Dr. Ishita Virda 4 1 M.D. Radiology, Professor and Head, P.D.U. Medical College
MRI of chronic spinal cord injury
 The British Journal of Radiology, 76 (2003), 347 352 DOI: 10.1259/bjr/11881183 E 2003 The British Institute of Radiology Pictorial review MRI of chronic spinal cord injury 1 K POTTER, FRCR and 1 A SAIFUDDIN,
The British Journal of Radiology, 76 (2003), 347 352 DOI: 10.1259/bjr/11881183 E 2003 The British Institute of Radiology Pictorial review MRI of chronic spinal cord injury 1 K POTTER, FRCR and 1 A SAIFUDDIN,
Pediatric Retroperitoneal Masses Radiologic-Pathologic Correlation
 Acta Radiológica Portuguesa, Vol.XVIII, nº 70, pág. 61-70, Abr.-Jun., 2006 Pediatric Retroperitoneal Masses Radiologic-Pathologic Correlation Marilyn J. Siegel Mallinckrodt Institute of Radiology, Washington
Acta Radiológica Portuguesa, Vol.XVIII, nº 70, pág. 61-70, Abr.-Jun., 2006 Pediatric Retroperitoneal Masses Radiologic-Pathologic Correlation Marilyn J. Siegel Mallinckrodt Institute of Radiology, Washington
Clinico-pathological study of intradural extramedullary spinal tumors
 International Journal of Research in Medical Sciences Venugopal G et al. Int J Res Med Sci. 2015 Oct;3(10):2795-2799 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20150685
International Journal of Research in Medical Sciences Venugopal G et al. Int J Res Med Sci. 2015 Oct;3(10):2795-2799 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20150685
Astroblastoma: Radiologic-Pathologic Correlation and Distinction from Ependymoma
 AJNR Am J Neuroradiol 23:243 247, February 2002 Case Report Astroblastoma: Radiologic-Pathologic Correlation and Distinction from Ependymoma John D. Port, Daniel J. Brat, Peter C. Burger, and Martin G.
AJNR Am J Neuroradiol 23:243 247, February 2002 Case Report Astroblastoma: Radiologic-Pathologic Correlation and Distinction from Ependymoma John D. Port, Daniel J. Brat, Peter C. Burger, and Martin G.
ORIGINAL ARTICLE. Abstract. Aim. Materials and methods. Introduction. Results
 Is anatomical distribution helpful for differentiating TB spondylitis from neoplastic causes of extradural spinal cord compression in children? A pilot study Reena George, MD, MMed Rad, FRCR (UK) Savvas
Is anatomical distribution helpful for differentiating TB spondylitis from neoplastic causes of extradural spinal cord compression in children? A pilot study Reena George, MD, MMed Rad, FRCR (UK) Savvas
Imaging in neurofibromatosis type 1: An original research article with focus on spinal lesions
 Original Research Article Imaging in neurofibromatosis type 1: An original research article with focus on spinal lesions Kalpesh Patel 1*, Siddharth Zala 2, C. Raychaudhuri 3 1 Assistant Professor, 2 1
Original Research Article Imaging in neurofibromatosis type 1: An original research article with focus on spinal lesions Kalpesh Patel 1*, Siddharth Zala 2, C. Raychaudhuri 3 1 Assistant Professor, 2 1
A Comprehensive Review of Intraspinal tumors: Diagnostic, classification and radio-pathologic correlation.
 A Comprehensive Review of Intraspinal tumors: Diagnostic, classification and radio-pathologic correlation. Award: Magna Cum Laude Poster No.: C-2112 Congress: ECR 2013 Type: Educational Exhibit Authors:
A Comprehensive Review of Intraspinal tumors: Diagnostic, classification and radio-pathologic correlation. Award: Magna Cum Laude Poster No.: C-2112 Congress: ECR 2013 Type: Educational Exhibit Authors:
Pathologic Analysis of CNS Surgical Specimens
 2015 Kenneth M. Earle Memorial Neuropathology Review Pathologic Analysis of CNS Surgical Specimens Peter C. Burger, MD Interdisciplinary Quality Control Familiarity with entities Use of diagnostic algorithm
2015 Kenneth M. Earle Memorial Neuropathology Review Pathologic Analysis of CNS Surgical Specimens Peter C. Burger, MD Interdisciplinary Quality Control Familiarity with entities Use of diagnostic algorithm
Optic Pathway Gliomas, Germinomas, Spinal Cord Tumours. Colin Kennedy March 2015
 Optic Pathway Gliomas, Germinomas, Spinal Cord Tumours Colin Kennedy March 2015 Glioma of the optic chiasm. T1-weighted MRI with gadolinium enhancement, showing intense irregular uptake of contrast. The
Optic Pathway Gliomas, Germinomas, Spinal Cord Tumours Colin Kennedy March 2015 Glioma of the optic chiasm. T1-weighted MRI with gadolinium enhancement, showing intense irregular uptake of contrast. The
A Comprehensive Review of Intraspinal tumors: Diagnostic, classification and radio-pathologic correlation.
 A Comprehensive Review of Intraspinal tumors: Diagnostic, classification and radio-pathologic correlation. Award: Magna Cum Laude Poster No.: C-2112 Congress: ECR 2013 Type: Educational Exhibit Authors:
A Comprehensive Review of Intraspinal tumors: Diagnostic, classification and radio-pathologic correlation. Award: Magna Cum Laude Poster No.: C-2112 Congress: ECR 2013 Type: Educational Exhibit Authors:
Spine and spinal cord
 NEURORADIOLOGY Spine and spinal cord Erika Vörös University of Szeged Department of Radiology SZEGED DISEASES OF SPINE AND SPINAL CORD I. Non-tumourous diseases developmental anomalies vascular disorders
NEURORADIOLOGY Spine and spinal cord Erika Vörös University of Szeged Department of Radiology SZEGED DISEASES OF SPINE AND SPINAL CORD I. Non-tumourous diseases developmental anomalies vascular disorders
Imaging Of Cystic Paravertebral Masses:
 Imaging Of Cystic Paravertebral Masses: Differential Diagnosis and Key Discriminators John P. Lichtenberger III, MD, Maj, USAF, MC Brent McCarragher, MD, CPT, USA John R. Dryden, MD, LT, USN P. Gabriel
Imaging Of Cystic Paravertebral Masses: Differential Diagnosis and Key Discriminators John P. Lichtenberger III, MD, Maj, USAF, MC Brent McCarragher, MD, CPT, USA John R. Dryden, MD, LT, USN P. Gabriel
ISSN X (Print) Original Research Article. DOI: /sjams
 DOI: 10.21276/sjams Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 27; 5(8A):32-31 Scholars Academic and Scientific Publisher (An International Publisher for Academic and
DOI: 10.21276/sjams Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 27; 5(8A):32-31 Scholars Academic and Scientific Publisher (An International Publisher for Academic and
Historical perspective
 SPINAL AVM Introduction Vascular malformations of spinal cord are a rare clinical entity, representing 5% of all primary spinal cord lesions, with arteriovenous malformations(avm) & cavernous malformations
SPINAL AVM Introduction Vascular malformations of spinal cord are a rare clinical entity, representing 5% of all primary spinal cord lesions, with arteriovenous malformations(avm) & cavernous malformations
CASE OF THE WEEK PROFESSOR YASSER METWALLY
 CLINICAL PICTURE CLINICAL PICTURE: A 22 years old male patient presented clinically with bilateral tinnitus, headache, bilateral diminution of hearing, bilateral papilledema, bilateral facial nerve palsy,
CLINICAL PICTURE CLINICAL PICTURE: A 22 years old male patient presented clinically with bilateral tinnitus, headache, bilateral diminution of hearing, bilateral papilledema, bilateral facial nerve palsy,
Tumors of the Central Nervous System
 Tumors of the Central Nervous System 1 Financial Disclosures I have NO SIGNIFICANT FINANCIAL, GENERAL, OR OBLIGATION INTERESTS TO REPORT Introduction General: Brain tumors are lesions that have mass effect
Tumors of the Central Nervous System 1 Financial Disclosures I have NO SIGNIFICANT FINANCIAL, GENERAL, OR OBLIGATION INTERESTS TO REPORT Introduction General: Brain tumors are lesions that have mass effect
Spinal Imaging. Bearbeitet von Herwig Imhof. 1. Auflage Taschenbuch. 312 S. Paperback ISBN Format (B x L): 12,5 x 19 cm
 Spinal Imaging Bearbeitet von Herwig Imhof 1. Auflage 2007. Taschenbuch. 312 S. Paperback ISBN 978 3 13 144071 6 Format (B x L): 12,5 x 19 cm Weitere Fachgebiete > Medizin > Sonstige Medizinische Fachgebiete
Spinal Imaging Bearbeitet von Herwig Imhof 1. Auflage 2007. Taschenbuch. 312 S. Paperback ISBN 978 3 13 144071 6 Format (B x L): 12,5 x 19 cm Weitere Fachgebiete > Medizin > Sonstige Medizinische Fachgebiete
Spinal Vascular Lesions
 Spinal Vascular Lesions Spinal Vascular Lesions Spinal cord infarction Hemangioblastoma Cavernous malformation Vascular malformations (Type 1-4) Spinal artery aneurysm Troy Hutchins, MD Assistant Professor
Spinal Vascular Lesions Spinal Vascular Lesions Spinal cord infarction Hemangioblastoma Cavernous malformation Vascular malformations (Type 1-4) Spinal artery aneurysm Troy Hutchins, MD Assistant Professor
Anatomy of the Nervous System. Brain Components
 Anatomy of the Nervous System Brain Components NERVOUS SYSTEM INTRODUCTION Is the master system of human body, controlling the functions of rest of the body systems Nervous System CLASSIFICATION A. Anatomical
Anatomy of the Nervous System Brain Components NERVOUS SYSTEM INTRODUCTION Is the master system of human body, controlling the functions of rest of the body systems Nervous System CLASSIFICATION A. Anatomical
Overview. Spinal Anatomy Spaces & Meninges Spinal Cord. Anatomy of the dura. Anatomy of the arachnoid. Anatomy of the spinal meninges
 European Course in Neuroradiology Module 1 - Anatomy and Embryology Dubrovnik, October 2018 Spinal Anatomy Spaces & Meninges Spinal Cord Johan Van Goethem Overview spinal meninges & spaces spinal cord
European Course in Neuroradiology Module 1 - Anatomy and Embryology Dubrovnik, October 2018 Spinal Anatomy Spaces & Meninges Spinal Cord Johan Van Goethem Overview spinal meninges & spaces spinal cord
Dumbbell Shaped Thoracic Spine Cavernous Hemangioma: A Case Report and Review of the Literature
 ISPUB.COM The Internet Journal of Neurosurgery Volume 3 Number 1 Dumbbell Shaped Thoracic Spine Cavernous Hemangioma: A Case Report and Review of the Literature J Gonzalez-Cruz, A Nanda Citation J Gonzalez-Cruz,
ISPUB.COM The Internet Journal of Neurosurgery Volume 3 Number 1 Dumbbell Shaped Thoracic Spine Cavernous Hemangioma: A Case Report and Review of the Literature J Gonzalez-Cruz, A Nanda Citation J Gonzalez-Cruz,
Masses of the Corpus Callosum
 Masses of the Corpus Callosum Kesav Raghavan, HMS Year III Dr. Agenda Corpus Callosum Development and Anatomy Our Patient: Clinical Presentation Differential Diagnosis of Masses in the Corpus Callosum
Masses of the Corpus Callosum Kesav Raghavan, HMS Year III Dr. Agenda Corpus Callosum Development and Anatomy Our Patient: Clinical Presentation Differential Diagnosis of Masses in the Corpus Callosum
Persistent Terminal Ventricle
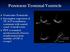 Persistent Terminal Ventricle Ventriculus Terminalis Incomplete regression of TV of 2 neurulation, continuity with central canal small cavity PTV vs terminal myelocystocele (?severe manifestation from
Persistent Terminal Ventricle Ventriculus Terminalis Incomplete regression of TV of 2 neurulation, continuity with central canal small cavity PTV vs terminal myelocystocele (?severe manifestation from
IMAGING OF SPINE TUMORS
 IMAGING OF SPINE TUMORS Laszlo Mechtler, MD, FAAN, FASN SUMMARY Historic classification of spine tumors based on computed tomography myelopgraphy. (A) Normal, (B) extradural extramedullary, (C) intradural
IMAGING OF SPINE TUMORS Laszlo Mechtler, MD, FAAN, FASN SUMMARY Historic classification of spine tumors based on computed tomography myelopgraphy. (A) Normal, (B) extradural extramedullary, (C) intradural
Detection of Leptomeningeal CNS Metastases in Children
 Detection of Leptomeningeal CNS Metastases in Children Noah D. Sabin, M.D. Julie H. Harreld M.D. Kathleen J. Helton M.D. Zoltan Patay M.D., Ph.D. St. Jude Children s Research Hospital Memphis, TN Leptomeningeal
Detection of Leptomeningeal CNS Metastases in Children Noah D. Sabin, M.D. Julie H. Harreld M.D. Kathleen J. Helton M.D. Zoltan Patay M.D., Ph.D. St. Jude Children s Research Hospital Memphis, TN Leptomeningeal
Pediatric Spinal Anomalies
 Department of Radiology University of California San Diego Pediatric Spinal Anomalies John R. Hesselink, M.D. Spine Embryogenesis 1. Primitive streak 2. Proliferation of cells at primitive pit (Hensen's
Department of Radiology University of California San Diego Pediatric Spinal Anomalies John R. Hesselink, M.D. Spine Embryogenesis 1. Primitive streak 2. Proliferation of cells at primitive pit (Hensen's
Intradural and extradural dorsal spinal pediatric lesions
 Intradural and extradural dorsal spinal pediatric lesions Poster No.: C-2520 Congress: ECR 2015 Type: Educational Exhibit Authors: L. Riaza, M. Pérez Rubiralta, C. Perez Balagueró, M. Rebollo, 1 2 4 3
Intradural and extradural dorsal spinal pediatric lesions Poster No.: C-2520 Congress: ECR 2015 Type: Educational Exhibit Authors: L. Riaza, M. Pérez Rubiralta, C. Perez Balagueró, M. Rebollo, 1 2 4 3
Year 2003 Paper two: Questions supplied by Tricia
 question 43 A 42-year-old man presents with a two-year history of increasing right facial numbness. He has a history of intermittent unsteadiness, mild hearing loss and vertigo but has otherwise been well.
question 43 A 42-year-old man presents with a two-year history of increasing right facial numbness. He has a history of intermittent unsteadiness, mild hearing loss and vertigo but has otherwise been well.
Spectrum of Magnetic Resonance Imaging findings in infective intra spinal complications of dermal sinus and associated inclusion cysts
 Spectrum of Magnetic Resonance Imaging findings in infective intra spinal complications of dermal sinus and associated inclusion cysts Poster No.: C-1443 Congress: ECR 2015 Type: Educational Exhibit Authors:
Spectrum of Magnetic Resonance Imaging findings in infective intra spinal complications of dermal sinus and associated inclusion cysts Poster No.: C-1443 Congress: ECR 2015 Type: Educational Exhibit Authors:
Pediatric CNS Tumors. Disclosures. Acknowledgements. Introduction. Introduction. Posterior Fossa Tumors. Whitney Finke, MD
 Pediatric CNS Tumors Disclosures Whitney Finke, MD Neuroradiology Fellow PGY-6 University of Utah Health Sciences Center Salt Lake City, Utah None Acknowledgements Introduction Nicholas A. Koontz, MD Luke
Pediatric CNS Tumors Disclosures Whitney Finke, MD Neuroradiology Fellow PGY-6 University of Utah Health Sciences Center Salt Lake City, Utah None Acknowledgements Introduction Nicholas A. Koontz, MD Luke
Retroperitoneal Sarcomas - A pictorial review
 Retroperitoneal Sarcomas - A pictorial review Poster No.: C-1409 Congress: ECR 2013 Type: Educational Exhibit Authors: D. Douraghi-Zadeh, K. L. Shahabuddin, R. H. Thomas, E. Moskovic; London/UK Keywords:
Retroperitoneal Sarcomas - A pictorial review Poster No.: C-1409 Congress: ECR 2013 Type: Educational Exhibit Authors: D. Douraghi-Zadeh, K. L. Shahabuddin, R. H. Thomas, E. Moskovic; London/UK Keywords:
4/14/2017. Unknown Case #1 Intramedullary Lesion
 4/14/2017 Intradural, Intramedullary Tumor or Mimic Intradural, Extramedullary Tumor or Mimic Extradural Tumor or Mimic Unknown Case #1 Intramedullary Lesion Unknown Case #1 -POST - MAG AXIAL Cranial Caudal
4/14/2017 Intradural, Intramedullary Tumor or Mimic Intradural, Extramedullary Tumor or Mimic Extradural Tumor or Mimic Unknown Case #1 Intramedullary Lesion Unknown Case #1 -POST - MAG AXIAL Cranial Caudal
Role of imaging in RCC. Ultrasonography. Solid lesion. Cystic RCC. Solid RCC 31/08/60. From Diagnosis to Treatment: the Radiologist Perspective
 Role of imaging in RCC From Diagnosis to Treatment: the Radiologist Perspective Diagnosis Staging Follow up Imaging modalities Limitations and pitfalls Duangkamon Prapruttam, MD Department of Therapeutic
Role of imaging in RCC From Diagnosis to Treatment: the Radiologist Perspective Diagnosis Staging Follow up Imaging modalities Limitations and pitfalls Duangkamon Prapruttam, MD Department of Therapeutic
TUMOURS IN THE REGION OF FORAMEN MAGNUM
 TUMOURS IN THE REGION OF FORAMEN MAGNUM Abstract Pages with reference to book, From 119 To 122 Naim-ur-Rahman ( Department of Neurosurgery, Rawalpindi Medical College, Rawalpindi. ) A very unusual case
TUMOURS IN THE REGION OF FORAMEN MAGNUM Abstract Pages with reference to book, From 119 To 122 Naim-ur-Rahman ( Department of Neurosurgery, Rawalpindi Medical College, Rawalpindi. ) A very unusual case
Cross sectional imaging of Intracranial cystic lesions Abdel Razek A
 Cross sectional imaging of Intracranial cystic lesions Abdel Razek A Department of Radiology. Mansoura Faculty of Medicine, Mansoura. Egypt. arazek@mans.edu.eg Introduction Intracranial cystic lesions
Cross sectional imaging of Intracranial cystic lesions Abdel Razek A Department of Radiology. Mansoura Faculty of Medicine, Mansoura. Egypt. arazek@mans.edu.eg Introduction Intracranial cystic lesions
Posterior fossa tumors: clues to differential diagnosis with case-based review
 Posterior fossa tumors: clues to differential diagnosis with case-based review Poster No.: C-0323 Congress: ECR 2017 Type: Educational Exhibit Authors: H. A. Aboughalia, M. Abdelhady; Doha/QA Keywords:
Posterior fossa tumors: clues to differential diagnosis with case-based review Poster No.: C-0323 Congress: ECR 2017 Type: Educational Exhibit Authors: H. A. Aboughalia, M. Abdelhady; Doha/QA Keywords:
MR imaging the post operative spine - What to expect!
 MR imaging the post operative spine - What to expect! Poster No.: C-2334 Congress: ECR 2012 Type: Educational Exhibit Authors: A. Jain, M. Paravasthu, M. Bhojak, K. Das ; Warrington/UK, 1 1 1 2 1 2 Liverpool/UK
MR imaging the post operative spine - What to expect! Poster No.: C-2334 Congress: ECR 2012 Type: Educational Exhibit Authors: A. Jain, M. Paravasthu, M. Bhojak, K. Das ; Warrington/UK, 1 1 1 2 1 2 Liverpool/UK
Malignant melanoma and the central nervous system A guide for classification based on the clinical findings
 Journal ofneurology, Neurosurgery, and Psychiatry, 1976, 39, 526-530 Malignant melanoma and the central nervous system A guide for classification based on the clinical findings R. D. HAYWARD From the Department
Journal ofneurology, Neurosurgery, and Psychiatry, 1976, 39, 526-530 Malignant melanoma and the central nervous system A guide for classification based on the clinical findings R. D. HAYWARD From the Department
Magnetic resonance evaluation of intra dural spinal tumors with histopathology correlation
 International Journal of Research in Medical Sciences Rao UM et al. Int J Res Med Sci. 2015 Nov;3(11):3051-3057 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20151002
International Journal of Research in Medical Sciences Rao UM et al. Int J Res Med Sci. 2015 Nov;3(11):3051-3057 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20151002
Imaging in gastric cancer
 Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
SPINAL MAGNETIC RESONANCE IMAGING INTERPRETATION
 CLINICAL VIGNETTE 2017; 3:2 SPINAL MAGNETIC RESONANCE IMAGING INTERPRETATION Editor-in-Chief: Idowu, Olufemi E. Neurological surgery Division, Department of Surgery, LASUCOM/LASUTH, Ikeja, Lagos, Nigeria.
CLINICAL VIGNETTE 2017; 3:2 SPINAL MAGNETIC RESONANCE IMAGING INTERPRETATION Editor-in-Chief: Idowu, Olufemi E. Neurological surgery Division, Department of Surgery, LASUCOM/LASUTH, Ikeja, Lagos, Nigeria.
MR Imaging of Spinal Cord Arteriovenous Malformations at 0.5 T: Study of 34 Cases
 833 MR Imaging of Spinal Cord Arteriovenous Malformations at 0.5 T: Study of 34 Cases D. Dormont 1 F. Gelbert 2 E. Assouline 2 D. Reizine 2 A. Helias 2 M. C. Riche 2 J. Chiras 1 J. Sories 1 J. J. Merland
833 MR Imaging of Spinal Cord Arteriovenous Malformations at 0.5 T: Study of 34 Cases D. Dormont 1 F. Gelbert 2 E. Assouline 2 D. Reizine 2 A. Helias 2 M. C. Riche 2 J. Chiras 1 J. Sories 1 J. J. Merland
Neuroimaging. spine / spinal cord
 Neuroimaging spine / spinal cord Spine & spinal cord imaging methodology Plain x-ray of spine Computed tomography CT - traditional ( normal CT) - reconstructions - myelo-ct Magnetic resonance MR - standard
Neuroimaging spine / spinal cord Spine & spinal cord imaging methodology Plain x-ray of spine Computed tomography CT - traditional ( normal CT) - reconstructions - myelo-ct Magnetic resonance MR - standard
MRI Findings Of An Atypical Cystic Meningioma A Rare Case
 ISPUB.COM The Internet Journal of Radiology Volume 14 Number 1 MRI Findings Of An Atypical Cystic Meningioma A Rare Case D Saxena, P Rout, K Pavan, B Philip Citation D Saxena, P Rout, K Pavan, B Philip.
ISPUB.COM The Internet Journal of Radiology Volume 14 Number 1 MRI Findings Of An Atypical Cystic Meningioma A Rare Case D Saxena, P Rout, K Pavan, B Philip Citation D Saxena, P Rout, K Pavan, B Philip.
Vascular Pattern in Tumours
 Acta Radiologica ISSN: 0001-6926 (Print) (Online) Journal homepage: https://www.tandfonline.com/loi/iaro20 Vascular Pattern in Tumours To cite this article: (1957) Vascular Pattern in Tumours, Acta Radiologica,
Acta Radiologica ISSN: 0001-6926 (Print) (Online) Journal homepage: https://www.tandfonline.com/loi/iaro20 Vascular Pattern in Tumours To cite this article: (1957) Vascular Pattern in Tumours, Acta Radiologica,
Oligodendroglioma: imaging findings, radio-pathological correlation and evolution
 Oligodendroglioma: imaging findings, radio-pathological correlation and evolution Poster No.: C-2104 Congress: ECR 2013 Type: Authors: Keywords: DOI: Scientific Exhibit A. Hernandez Castro, M. D. Monedero
Oligodendroglioma: imaging findings, radio-pathological correlation and evolution Poster No.: C-2104 Congress: ECR 2013 Type: Authors: Keywords: DOI: Scientific Exhibit A. Hernandez Castro, M. D. Monedero
JMSCR Vol 04 Issue 04 Page April 2016
 www.jmscr.igmpublication.org Impact Factor 5.244 Index Copernicus Value: 5.88 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: http://dx.doi.org/10.18535/jmscr/v4i4.13 Malignant Nerve Sheath Tumor with Secondary
www.jmscr.igmpublication.org Impact Factor 5.244 Index Copernicus Value: 5.88 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: http://dx.doi.org/10.18535/jmscr/v4i4.13 Malignant Nerve Sheath Tumor with Secondary
Synovial cyst of spinal facet
 Case report CHUN C. KAO, M.D., STEFAN S. WINKLER, M.D., AND J. H. TURNER, M.D. Sections of Neurosurgery, Radiology, and Pathology, Madison Veterans Administration Hospital, and University of Wisconsin,
Case report CHUN C. KAO, M.D., STEFAN S. WINKLER, M.D., AND J. H. TURNER, M.D. Sections of Neurosurgery, Radiology, and Pathology, Madison Veterans Administration Hospital, and University of Wisconsin,
Value of Intravenous Contrast Enhancement in the CT Evaluation of Intraspinal Tumors
 939 Value of Intravenous Contrast Enhancement in the CT Evaluation of Intraspinal Tumors J. S. Lapointe 1 D.. Graeb R.. Nugent W. D. Robertson The usefulness of intravenous contrast-enhanced CT in delineating
939 Value of Intravenous Contrast Enhancement in the CT Evaluation of Intraspinal Tumors J. S. Lapointe 1 D.. Graeb R.. Nugent W. D. Robertson The usefulness of intravenous contrast-enhanced CT in delineating
Giant invasive spinal schwannomas: definition and surgical management
 J Neurosurg (Spine 2) 94:210 215, 2001 Giant invasive spinal schwannomas: definition and surgical management K. SRIDHAR, D.N.B. (NEUROSURG), RAVI RAMAMURTHI, M.S, F.R.C.S.ED. (SN), M. C. VASUDEVAN, M.D.,
J Neurosurg (Spine 2) 94:210 215, 2001 Giant invasive spinal schwannomas: definition and surgical management K. SRIDHAR, D.N.B. (NEUROSURG), RAVI RAMAMURTHI, M.S, F.R.C.S.ED. (SN), M. C. VASUDEVAN, M.D.,
ADRENAL MEDULLARY DISORDERS: PHAEOCHROMOCYTOMAS AND MORE
 ADRENAL MEDULLARY DISORDERS: PHAEOCHROMOCYTOMAS AND MORE DR ANJU SAHDEV READER AND CONSULTANT RADIOLOGIST QUEEN MARY UNIVERSITY AND ST BARTHOLOMEW S HOSPITAL BARTS HEALTH, LONDON, UK DISCLOSURE OF CONFLICT
ADRENAL MEDULLARY DISORDERS: PHAEOCHROMOCYTOMAS AND MORE DR ANJU SAHDEV READER AND CONSULTANT RADIOLOGIST QUEEN MARY UNIVERSITY AND ST BARTHOLOMEW S HOSPITAL BARTS HEALTH, LONDON, UK DISCLOSURE OF CONFLICT
Imaging in breast cancer. Mammography and Ultrasound Donya Farrokh.MD Radiologist Mashhad University of Medical Since
 Imaging in breast cancer Mammography and Ultrasound Donya Farrokh.MD Radiologist Mashhad University of Medical Since A mammogram report is a key component of the breast cancer diagnostic process. A mammogram
Imaging in breast cancer Mammography and Ultrasound Donya Farrokh.MD Radiologist Mashhad University of Medical Since A mammogram report is a key component of the breast cancer diagnostic process. A mammogram
Spinal tumour: primary cervical extradural meningioma at an unusual location
 Case Report Spinal tumour: primary cervical extradural meningioma at an unusual location Ishita Pant 1, Vinod Kumar Singh Gautam 2, Rima Kumari 3, Sujata Chaturvedi 1 1 Department of Pathology, 2 Department
Case Report Spinal tumour: primary cervical extradural meningioma at an unusual location Ishita Pant 1, Vinod Kumar Singh Gautam 2, Rima Kumari 3, Sujata Chaturvedi 1 1 Department of Pathology, 2 Department
Intracranial Lesions: MRI Signs for Localization
 Intracranial Lesions: MRI Signs for Localization Poster No.: C-1574 Congress: ECR 2017 Type: Educational Exhibit Authors: M. Cucos, A. Puiu, S. Manole ; Cluj-Napoca/RO, Cluj napoca/ RO Keywords: Cerebrospinal
Intracranial Lesions: MRI Signs for Localization Poster No.: C-1574 Congress: ECR 2017 Type: Educational Exhibit Authors: M. Cucos, A. Puiu, S. Manole ; Cluj-Napoca/RO, Cluj napoca/ RO Keywords: Cerebrospinal
Magnetic resonance imaging of intramedullary spinal cord lesions
 Magnetic resonance imaging of intramedullary spinal cord lesions Poster No.: C-1762 Congress: ECR 2014 Type: Educational Exhibit Authors: M. Abdelkafi, H. Derbel, H. Abid, S. Haddar, B. Souissi, N. 1 1
Magnetic resonance imaging of intramedullary spinal cord lesions Poster No.: C-1762 Congress: ECR 2014 Type: Educational Exhibit Authors: M. Abdelkafi, H. Derbel, H. Abid, S. Haddar, B. Souissi, N. 1 1
Large Dumbbell-Shaped C1 Schwannoma Presenting as a Foramen Magnum Mass
 32 Large Dumbbell-Shaped C1 Schwannoma Presenting as a Foramen Magnum Mass Jody Helms, M.D. 1 Lattimore Madison Michael II, M.D., F.A.A.N.S., F.A.C.S. 1, 2 1 Department of Neurosurgery, University of Tennessee
32 Large Dumbbell-Shaped C1 Schwannoma Presenting as a Foramen Magnum Mass Jody Helms, M.D. 1 Lattimore Madison Michael II, M.D., F.A.A.N.S., F.A.C.S. 1, 2 1 Department of Neurosurgery, University of Tennessee
Supra- and infratentorial brain tumors from childhood to maternity
 Supra- and infratentorial brain tumors from childhood to maternity What to expect? I am going to show you the characteristic imaging findings of following tumors: Thierry A.G.M. Huisman, MD, FICIS, EQNR
Supra- and infratentorial brain tumors from childhood to maternity What to expect? I am going to show you the characteristic imaging findings of following tumors: Thierry A.G.M. Huisman, MD, FICIS, EQNR
Tumors and tumorlike lesions of the craniovertebral junction
 Tumors and tumorlike lesions of the craniovertebral junction Poster No.: C-2632 Congress: ECR 2010 Type: Educational Exhibit Topic: Neuro Authors: S.-C. Hung, Y. L. Chen, W.-Y. Guo, G.-M. Yang ; Taoyuan/
Tumors and tumorlike lesions of the craniovertebral junction Poster No.: C-2632 Congress: ECR 2010 Type: Educational Exhibit Topic: Neuro Authors: S.-C. Hung, Y. L. Chen, W.-Y. Guo, G.-M. Yang ; Taoyuan/
Spinal schwannoma: Size has no correlation with presentation and outcome
 Spinal schwannoma: Size has no correlation with presentation and outcome Ravi Shankar Prasad*, Ruchi**, Kulwant Singh***, Ajit Singh**** *Assistant Professor, Department of Neurosurgery, Institute of Medical
Spinal schwannoma: Size has no correlation with presentation and outcome Ravi Shankar Prasad*, Ruchi**, Kulwant Singh***, Ajit Singh**** *Assistant Professor, Department of Neurosurgery, Institute of Medical
The central nervous system
 Sectc.qxd 29/06/99 09:42 Page 81 Section C The central nervous system CNS haemorrhage Subarachnoid haemorrhage Cerebral infarction Brain atrophy Ring enhancing lesions MRI of the pituitary Multiple sclerosis
Sectc.qxd 29/06/99 09:42 Page 81 Section C The central nervous system CNS haemorrhage Subarachnoid haemorrhage Cerebral infarction Brain atrophy Ring enhancing lesions MRI of the pituitary Multiple sclerosis
Chapter 13. The Spinal Cord & Spinal Nerves. Spinal Cord. Spinal Cord Protection. Meninges. Together with brain forms the CNS Functions
 Spinal Cord Chapter 13 The Spinal Cord & Spinal Nerves Together with brain forms the CNS Functions spinal cord reflexes integration (summation of inhibitory and excitatory) nerve impulses highway for upward
Spinal Cord Chapter 13 The Spinal Cord & Spinal Nerves Together with brain forms the CNS Functions spinal cord reflexes integration (summation of inhibitory and excitatory) nerve impulses highway for upward
Diplomate of the American Board of Pathology in Anatomic and Clinical Pathology
 A 33-year-old male with a left lower leg mass. Contributed by Shaoxiong Chen, MD, PhD Assistant Professor Indiana University School of Medicine/ IU Health Partners Department of Pathology and Laboratory
A 33-year-old male with a left lower leg mass. Contributed by Shaoxiong Chen, MD, PhD Assistant Professor Indiana University School of Medicine/ IU Health Partners Department of Pathology and Laboratory
Advances In Orbital Neuropathology
 Advances In Orbital Neuropathology Charles G. Eberhart, MD PhD Associate Professor of Pathology, Ophthalmology and Oncology Johns Hopkins University School of Medicine Overview Non-neoplastic lesions Microphthalmos/pseudoglioma
Advances In Orbital Neuropathology Charles G. Eberhart, MD PhD Associate Professor of Pathology, Ophthalmology and Oncology Johns Hopkins University School of Medicine Overview Non-neoplastic lesions Microphthalmos/pseudoglioma
Intraspinal Seeding from Intracranial Tumors in Children
 805 Intraspinal Seeding from Intracranial Tumors in Children Philip Stanley 1 Melvin O. Senac, Jr. Hervey D. Segall Cerebrospinal fluid-borne metastases were demonstrated by metrizamide myelography in
805 Intraspinal Seeding from Intracranial Tumors in Children Philip Stanley 1 Melvin O. Senac, Jr. Hervey D. Segall Cerebrospinal fluid-borne metastases were demonstrated by metrizamide myelography in
Malignant Peripheral Nerve Sheath Tumor
 C H A P T E R 120 Malignant Peripheral Nerve Sheath Tumor Currently, malignant peripheral nerve sheath tumor (MPNST) is the most commonly used generic name for the neoplasms known in the past as neurosarcoma,
C H A P T E R 120 Malignant Peripheral Nerve Sheath Tumor Currently, malignant peripheral nerve sheath tumor (MPNST) is the most commonly used generic name for the neoplasms known in the past as neurosarcoma,
RING ENCHANCING LESION BY M.S. HEMHNATH
 RING ENCHANCING LESION BY M.S. HEMHNATH A 21 YRS FEMALE CAME WITH H/O HEADACHE AND SEIZURE FOR THE PAST ONE MONTH. NO OTHER FOCAL NEUROLOGICAL DEFICIT. DIFFERENTIAL DIAGNOSIS For this case are Neurocysticerosis
RING ENCHANCING LESION BY M.S. HEMHNATH A 21 YRS FEMALE CAME WITH H/O HEADACHE AND SEIZURE FOR THE PAST ONE MONTH. NO OTHER FOCAL NEUROLOGICAL DEFICIT. DIFFERENTIAL DIAGNOSIS For this case are Neurocysticerosis
Sporadic hemangioblastoma of the filum terminale: Case report and review of literature
 DOI: 10.2478/romneu-2018-0064 Article Sporadic hemangioblastoma of the filum terminale: Case report and review of literature Prashant S. Gade, Vernon Velho, Harish Naik, Laxmikant Bhople INDIA Romanian
DOI: 10.2478/romneu-2018-0064 Article Sporadic hemangioblastoma of the filum terminale: Case report and review of literature Prashant S. Gade, Vernon Velho, Harish Naik, Laxmikant Bhople INDIA Romanian
Brainstem diffuse gliomas: radiologic findings.
 Brainstem diffuse gliomas: radiologic findings. Poster No.: C-2220 Congress: ECR 2013 Type: Educational Exhibit Authors: E. GARCIA MARTINEZ 1, D. H. Jiménez 1, L. Navarro Vilar 2, C. P. Fernandez Ruiz
Brainstem diffuse gliomas: radiologic findings. Poster No.: C-2220 Congress: ECR 2013 Type: Educational Exhibit Authors: E. GARCIA MARTINEZ 1, D. H. Jiménez 1, L. Navarro Vilar 2, C. P. Fernandez Ruiz
Unusual cauda equina syndrome due to multifocal ependymoma infiltrated by lymphoma
 Case Report Unusual cauda equina syndrome due to multifocal ependymoma infiltrated by lymphoma Nassim Bougaci 1, Stephane Litrico 1, Fanny Burel-Vandenbos 2, Philippe Paquis 1 1 Department of Neurosurgery,
Case Report Unusual cauda equina syndrome due to multifocal ependymoma infiltrated by lymphoma Nassim Bougaci 1, Stephane Litrico 1, Fanny Burel-Vandenbos 2, Philippe Paquis 1 1 Department of Neurosurgery,
PITUITARY PARASELLAR LESIONS. Kim Learned, MD
 PITUITARY PARASELLAR LESIONS Kim Learned, MD DIFFERENTIALS Pituitary Sella Clivus, Sphenoid Sinus Suprasellar Optic chiasm, Hypothalamus, Circle of Willis Parasellar Cavernous Sinus Case 1 17 YEAR-OLD
PITUITARY PARASELLAR LESIONS Kim Learned, MD DIFFERENTIALS Pituitary Sella Clivus, Sphenoid Sinus Suprasellar Optic chiasm, Hypothalamus, Circle of Willis Parasellar Cavernous Sinus Case 1 17 YEAR-OLD
Extramedullary Spinal SOL Outcome of Surgery
 TAJ June 2009; Volume 22 Number 1 ISSN 1019-8555 The Journal of Teachers Association RMC, Rajshahi Original Article Extramedullary Spinal SOL Outcome of Surgery M Zahed Hossain 1, Monzurul Hoque 2 Abstract
TAJ June 2009; Volume 22 Number 1 ISSN 1019-8555 The Journal of Teachers Association RMC, Rajshahi Original Article Extramedullary Spinal SOL Outcome of Surgery M Zahed Hossain 1, Monzurul Hoque 2 Abstract
NEURORADIOLOGY-NEUROPATHOLOGY CONFERENCE
 THE UNIVERSITY OF NORTH CAROLINA at CHAPEL HILL SEPTEMBER 2013 NEURORADIOLOGY-NEUROPATHOLOGY CONFERENCE Claudia da Costa Leite, MD, PhD Thomas Bouldin, MD CASE 1 6 y-o female with headaches and vomiting
THE UNIVERSITY OF NORTH CAROLINA at CHAPEL HILL SEPTEMBER 2013 NEURORADIOLOGY-NEUROPATHOLOGY CONFERENCE Claudia da Costa Leite, MD, PhD Thomas Bouldin, MD CASE 1 6 y-o female with headaches and vomiting
SPINAL CORD DISEASE IN DOGS PART TWO: MOST LIKELY CAUSES
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk SPINAL CORD DISEASE IN DOGS PART TWO: MOST LIKELY CAUSES Author : RITA GONÇALVES Categories : Vets Date : April 7, 2014 RITA
Vet Times The website for the veterinary profession https://www.vettimes.co.uk SPINAL CORD DISEASE IN DOGS PART TWO: MOST LIKELY CAUSES Author : RITA GONÇALVES Categories : Vets Date : April 7, 2014 RITA
