Cerebellar infarcts may develop mass effect (CIMASS) in
|
|
|
- Dennis Booth
- 5 years ago
- Views:
Transcription
1 Neuroimaging in Deteriorating Patients With Cerebellar Infarcts and Mass Effect Merian G. Koh, MD, MBBS; Thanh G. Phan, MD, FRACP; John L.D. Atkinson, MD; Eelco F.M. Wijdicks, MD Background and Purpose The decision to proceed with surgery in cerebellar infarct with mass effect (CIMASS) in deteriorating patients is based on clinical features. The potential role of neuroimaging in predicting deterioration has not been systematically studied. In this study we determine the role of neuroimaging in predicting deterioration in CIMASS. Methods We retrospectively reviewed the clinical and neuroimaging features in 90 patients with cerebellar infarcts. We selected for detailed analysis CIMASS in 35 patients. Results Eighteen patients remained stable and 17 deteriorated. Of these 17 patients, 8 were treated conservatively and 9 had surgery. Radiological features indicative of progression were more common in deteriorating patients compared with stable patients: fourth ventricular shift (82.3% versus 50%, P 0.075, OR 4.67), hydrocephalus (76.5% versus 11.1%, P , OR 26), brain stem deformity (47% versus 5.6%, P , OR 15.1), and basal cistern compression (35.3% versus 0%, P , OR 20.91). Differences in upward displacement of the aqueduct and pontomesencephalic junction from Twining s line, tonsillar descent on sagittal MRI, and infarct volumes between stable and deteriorating patients were not statistically significant. Conclusions Hydrocephalus, brain stem deformity, and basal cistern compression may herald deterioration in CIMASS. Admission to a neurological-neurosurgical intensive care unit and consideration of preemptive surgery are warranted in these patients. Vertical displacement of tonsils or aqueduct, demonstrated by MR imaging, did not predict deterioration. (Stroke. 2000;31: ) Key Words: brain edema cerebellar infarction magnetic resonance imaging outcome tomography, x-ray computed Cerebellar infarcts may develop mass effect (CIMASS) in 10% to 25% of all cases. 1 3 When the infarcted tissue and surrounding edema become space occupying within the posterior fossa, brain stem compression and fourth ventricular collapse occur, resulting in obstructive hydrocephalus. Previous authors 4 6 have suggested that patients with CIMASS progress through 3 arbitrary clinical stages. The early clinical stage of CIMASS is characterized by signs from cerebellar dysfunction due to infarction, followed by a stage punctuated by brain stem compression in which the level of consciousness fluctuates, emerging into a final stage of coma. Both brain stem infarction and brain stem compression, caused by CIMASS, may have similar clinical presentation. 7,8 This distinction remains important in the decision to proceed with occipital craniotomy. It is not known whether correlation of the clinical stage of cerebellar infarct with neuroimaging offers any predictive value. Radiological features associated with CIMASS have been previously described; these include fourth ventricular shift or effacement, obstructive hydrocephalus, deformity of the brain stem, compression of the basal cisterns, aqueductal displacement, downward tonsillar herniation, and buckling of the quadrigeminal plate. 9,10 There has been no previous study establishing the sequence in which these changes occur over time, nor if such a sequence, correlated with clinical findings, would aid in the decision to proceed with neurosurgical intervention. Furthermore, the role of MR imaging in predicting deterioration, judged by the extent of horizontal and vertical tissue displacement, 9,11,12 is not known. We present a series of patients with CIMASS, propose the sequence of radiological features indicative of progression, and quantify the extent of vertical brain displacement. Subjects and Methods Subjects The medical records, investigations, management, and outcomes of patients who presented with acute cerebellar infarct from 1990 to April 1999 were reviewed. The patients had been diagnosed clinically and the diagnoses confirmed by CT, MRI, or both. Patients with indeterminate onset of symptoms (n 37) and those who were Received March 6, 2000; final revision received June 21, 2000; accepted June 21, From the Departments of Neurology (M.G.K., T.G.P., E.F.M.W.) and Neurologic Surgery (J.L.D.A.), Mayo Clinic and Mayo Foundation, Rochester, Minnesota. Correspondence to Eelco F.M. Wijdicks, MD, Department of Neurology, Mayo Clinic, 200 First St SW, Rochester, MN wijde@mayo.edu 2000 American Heart Association, Inc. Stroke is available at
2 Koh et al Cerebellar Infarct With Mass Effect 2063 originally admitted elsewhere for treatment and referred for rehabilitation only (n 30) were excluded, as were patients with prior cerebellar infarcts (n 40). Patients with clinical or radiological evidence of acute brain stem infarction (n 38) or concurrent cerebral infarction (n 38) were also excluded. In patients with previous strokes, the original territory of these strokes, together with their extent of recovery and baseline level of function, were noted. In total, 90 patients with cerebellar infarction were selected by using the above criteria. The clinical stage of CIMASS and the Glasgow Coma Score (GCS) at presentation and during the hospital stay were recorded. Deterioration was determined if there was decrease of 2 points in the GCS. This was attributed to the mass effect of the cerebellar infarct if there was radiological evidence of mass effect and in the absence of brain stem infarct. Patients with a GCS of 12 on admission were considered to have deteriorated. The progress of all patients was carefully abstracted from the records. The postoperative courses of all patients were recorded until their discharge from the hospital. The modified Rankin Scale score was used to assess each patient at discharge and at follow-up. A good outcome at discharge was defined as having a modified Rankin score of 0 to 2, a moderate outcome as having a modified Rankin score of 3 to 4, a poor outcome as having a score of 5, and death as a score of 6. Neuroimaging The CT imaging parameters were 10-mm contiguous slice thickness with additional contiguous fine cut of 3 to 5 mm through the posterior fossa. The field of view was 25 cm and the matrix 512. Patients underwent MR imaging on a 1.5-T scanner. The imaging parameters were 5-mm section thickness and 0- to 2.5-mm interslice gap, matrix, 20-cm field of view for conventional spinecho images, axial and sagittal T1-weighted (repetition time [TR] 500 ms/excitation time [TE] 20 ms), axial T2-weighted (TR 2200/TE 80), and proton density (TR 2200/TE 30). The location and vascular territory of each infarct was determined by comparing the hard copy films with illustrations from the anatomic map of the brain stem and cerebellum. 13 This was done by the authors, blinded to the clinical data, and the original radiological reports. All cases were then classified into 1 of 2 groups, CIMASS or non-cimass. Criteria for the diagnosis of CIMASS on CT and MRI were deformity or displacement of the fourth ventricle, obstructive hydrocephalus as evidenced by progressive dilatation of the lateral ventricles (with sulcal effacement of the frontal lobes and parieto-occipital lobes) and third ventricles on consecutive scans, effacement of the basal cisterns, and deformity or anterior bowing of the brain stem. Patients were diagnosed with CIMASS if 1 or more of the above criteria were met. When available, the remote effect of the CIMASS was further quantified by measuring vertical brain shifts in midsagittal MRI planes. 9,11,12 Technical Measurements The midsagittal MRI plane includes the corpus callosum, the straight sinus, cerebral aqueduct, and internal occipital protuberance. Within this plane, 3 MRI reference lines may be found: the Twining s line, the foramen magnum line, and the incisural line. Twining s line (T) extends from the anterior tuberculum sellae to the internal occipital protuberance (Figure 1). The foramen magnum line is drawn from the inferior tip of the clivus to the posterior lip of the foramen magnum. The incisural line extends from the anterior tuberculum sellae to the confluence of the straight sinus, the great cerebral vein of Galen, and the inferior sagittal sinus; the iter is normally contained within this plane. The perpendicular distance of the pontomesencephalic junction and aqueduct opening to T (T-PMJ and T-A, respectively) were measured to assess rostral displacement of the brain stem, as previously described. 11 The perpendicular distance of the caudal poles of the cerebellar tonsils with respect to their positions above or below the foramen magnum line (F-ton) was measured as previously described 9 ; positions below the reference line were recorded as negative values. The distance of the iter to the incisural line (iter-i) was also measured. All distances were converted to true dimensions by using the scales accompanying the images. The vertical measurements on the mid-sagittal MRI were Figure 1. Sagittal T1-weighted MR image showing the reference lines in the midsagittal plane. A indicates foramen magnum line; B, Twining s line; C, Twining s line to pontomesencephalic junction; D, Twining s line to aqueduct; and E, incisural line. compared between the CIMASS and non-cimass group. A control group consisting of patients with no intracranial mass or stroke was selected at random and matched with the patients in the CIMASS group for sex and age. Infarct Volumes For calculating infarct volumes, a cursor was used to trace around the image of the infarct on each MR or CT slice as viewed on the computer screen, to obtain the area on each slice. This was multiplied with the slice thickness to calculate the volume for that level; the individual volumes of the slices and interslice gaps were then added to obtain an accurate infarct volume. Using these parameters, the volume of the infarct and the extent of vertical brain shift in the following groups were compared: age and sex-matched controls, patients with cerebellar infarcts without mass effect, patients with CIMASS who remained stable (group 1), and patients with CIMASS who deteriorated (group 2). Group 2 was further divided into 2 subgroups, patients who were treated conservatively (group 2A) and those who were treated surgically (group 2B). Controls were selected only for patients who had MRI to assess vertical shift. Statistical Analysis Categorical data, such as the presence or absence of hydrocephalus, were analyzed with Fisher s exact test for statistical significance. Continuous variables, such as the distance of the iter from the incisural line, were compared between the groups with Wilcoxon s rank sum test. Mechanism of Infarction The stroke mechanisms were categorized by using the results of cerebral angiography, transthoracic and transesophageal echocardiography, transcranial Doppler examination, and MR angiography. The TOAST classification was used to classify the mechanism of infarction. 14 Results Patient Characteristics We studied 90 patients with isolated cerebellar infarct. There was no difference in the risk factors or clinical features at presentation between those who subsequently developed CIMASS and those who did not. Thirteen had cerebral
3 2064 Stroke September 2000 Radiological Features of 90 Patients With Cerebellar Infarcts, by Group Deformity of Fourth Ventricle, n Shift of Fourth Ventricle From Midline, n Anterior Displacement or Deformity of Brain Stem, n Compression of Basal Cisterns, n Group Total CTs Reviewed, n Total MRIs Reviewed, n Hydrocephalus, n Non-CIMASS, n Group 1 (CIMASS with no deterioration, n 18) Group 2A (CIMASS with deterioration, conservative, n 8) Group 2B (CIMASS with deterioration and surgery, n 9) Groups 2A and 2B (CIMASS with deterioration, n 17) angiography, 19 had transthoracic echocardiography, 49 had transesophageal echocardiography, 12 had transcranial Doppler examination, and 35 had MR angiography. Of the 90 patients with cerebellar infarct, there were 35 patients (39%) who, on the basis of radiological criteria, had CIMASS. The brain stem signs associated with brain stem compression were: gaze palsy, cranial neuropathy and pupillary asymmetry, hemiplegia and quadriplegia, and decorticate and decerebrate posturing. The presence of brain stem signs (from brain stem compression) at presentation was associated with a higher risk of subsequent deterioration (P ). Neuroimaging Findings The radiological features are summarized in the Table and Figures 3 and 4. Twenty-one of 90 patients (23%) had a normal CT initially. In the CIMASS group, 9 of 35 patients (26%) had normal CT initially. The mean and median number of days that elapsed from ischemic stroke onset to the first appearance of radiological CIMASS features were 2.6 days and 2 days, respectively (range 1 to 6 days). Hemorrhagic cerebellar infarct was noted in 1 patient in the non-cimass group, 1 in group 1, 3 in group 2A, and 4 in group 2B. There was a statistically significant difference in the frequency of hemorrhagic transformation between non-cimass and CI- MASS (P 0.002). There was also a statistically significant difference between the CIMASS that remained stable and the CIMASS that deteriorated (groups 1 and 2), in the frequency of hemorrhagic transformation (P 0.01, OR 11.9[1.76 to ]). Fourth ventricular deformity was present in all patients. Ventricular shift was present in 9 of 18 patients with no deterioration and in 14 of 17 patients with deterioration. The sensitivity and specificity of ventricular shift for predicting clinical deterioration were 82% and 50%, respectively (P 0.08, OR 4.67 [1.07 to 25.63]). Hydrocephalus was present in 3 of the 18 patients with no deterioration and 13 of 17 patients with deterioration. The sensitivity and specificity of hydrocephalus for predicting clinical deterioration were 76% and 83%, respectively (P , OR 26 [4.87 to 219.9]). Brain stem deformity was present in 1 of 18 patients with no deterioration and 8 of 17 patients with deterioration. The sensitivity and specificity of brain stem deformity for predicting clinical deterioration were 47% and 94%, respectively (P 0.007, OR 15.1 [2.26 to ]). Basal cistern compression was not present in any patient with no deterioration and was present in 6 of 17 patients with deterioration. The sensitivity and specificity of basal cistern for predicting clinical deterioration were 35% and 100%, respectively (P 0.008, OR 20.9 [1.98 to ]). Vertical Brain Shift Parameters The median perpendicular distance from the most inferior portion of the tonsil to the foramen magnum line (F-ton) for the control group was 1.4 mm (range 5.7 to 8.6 mm); non-cimass patients, 1.4 mm (range 10.0 to 11.4 mm); group 1, 0.7 mm (range 8.6 to 5.7 mm); group 2A, 2 mm (range 4.3 to 0 mm); group 2B, 12.3 mm (range 17.1 to 0 mm); and combined groups 2A and 2B, 9.0 mm (range 17.1 to 0 mm). The median perpendicular distance from the iter of the aqueduct to the incisural line (Iter-I) for the control group was 0 mm (range 5.7 to 5.7 mm); non-cimass patients, 0 mm (range 2.8 to 5.7 mm); group 1, 2.9 mm (range 2.9 to 5.9 mm); group 2A, 2.7 mm (range 0 to 5 mm); group 2B, 2.9 mm (range 0 to 8.6 mm); and combined groups 2A and 2B, 2.9 mm (range 0 to 8.6 mm). The median perpendicular distance from the iter of the aqueduct to Twining s line (T-A) for the control group was 15.7 mm (range 11.4 to 20.0 mm); non-cimass patients, 17.1 mm (range 11.4 to 24.4 mm); group 1, 17.1 mm (range 11.7 to 22.9 mm); group 2A, 18.5 mm (range 16.0 to 20.0 mm); group 2B, 18.6 mm (range 10.0 to 22.9 mm); and combined groups 2A and 2B, 18.6 mm (range 10.0 to 22.9 mm). The median perpendicular distance from the pontomesencephalic junction to Twining s line (T-PMJ) for the control group was 5.4 mm (range 1.4 to 8.6 mm); non-cimass patients, 5.7 mm (range 0 to 8.6 mm); group 1, 6.5 mm (range 5.7 to 9.1 mm); group 2A, 8.0 mm (range 7.0 to 8.6 mm); group 2B, 7.1 mm (range 0 to 12.9 mm); and combined groups 2A and 2B, 7.3 mm (range 0 to 12.9 mm). There was no statistically significant difference in the F-ton,
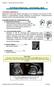
4 Koh et al Cerebellar Infarct With Mass Effect 2065 Figure 2. Summary of clinical progress and outcome at discharge. iter-i, T-A, or T-PMJ values between the control group and the non-cimass group. A larger extent of tonsillar descent was observed in CIMASS compared with non-cimass (P 0.001). Larger iter-i, T-A, and T-PMJ values were demonstrated in CIMASS compared with non-cimass (P 0.05, P 0.05, and P 0.001, respectively). Within the CIMASS group, there was no statistically significant difference in F-ton, iter-i, T-A, or T-PMJ values between those who deteriorated and those who remained stable. Infarct Volumes, Territories and Mechanisms The median infarct volumes were group 1, 24.2 cm 3 (range 6.6 to 49.0 cm 3 ); group 2A 23.4 cm 3 (range 17.5 to 37.4 cm 3 ); group 2B 42.0 cm 3 (range 15 to 55.7 cm 3 ); combined groups 2A and 2B 33.0 cm 3 (range 15 to 55.7 cm 3 ). Larger infarcts were demonstrated in CIMASS compared with non-cimass (P 0.001). There was no statistically significant difference in infarct volumes between groups 1 and 2 (Wilcoxon rank sum test). The arterial distributions of patients with CIMASS were posterior inferior cerebellar artery (PICA), 21 patients (60%); full PICA territory and contralateral medial PICA branch, 1 patient (3%); bilateral medial branch of PICA, 3 patients Figure 3. Axial CT scan showing shift and compression of the fourth with dilatation of the third ventricle and both temporal horns. Figure 4. Midsagittal T1-weighted MR in a patient with cerebellar infarct and mass effect showing vertical brain shift.
5 2066 Stroke September 2000 (9%); superior cerebellar artery (SCA), 7 patients (20%); bilateral SCA infarcts, 2 patients (6%); and medial branch of SCA, 1 patient (3%). Of the 22 patients with full PICA territory infarction, 1 had infarction of the contralateral medial branch of PICA. Of the 9 patients with full SCA territory infarction, 1 had infarction of the contralateral medial branch of the SCA and another had contralateral full PICA territory infarction. There was no difference in the distribution of infarct territories between the CIMASS patients who deteriorated and those who did not. The mechanisms of infarction in the CIMASS group were large-artery disease (13 patients), cardioembolism (12 patients), ischemic stroke of undetermined etiology (2 patients), and incomplete workup (8 patients). There were 3 patients who had vertebral artery dissection; they were included under the large-artery disease group. There were no cases of small-vessel occlusion among the CIMASS patients. Twentyseven of 90 patients had incomplete workup as defined by TOAST criteria, 14 3 patients had 2 or more possible causes identified, and 1 patient had a negative evaluation. Outcome The clinical progress and outcome at discharge are summarized in Figure 2. The mean number of days that elapsed from the first onset of cerebellar stroke symptoms to the first onset of brain stem signs was 2 days (range 1 to 6 days). All patients who deteriorated were treated with mannitol, steroids, and/or hyperventilation. The 90 patients in this series were followed up for a median of 16 months (range 1 to 105 months). Most patients improved at follow-up. Seven of the patients without CIMASS (2 patients in group 1, 4 patients in group 2, and 3 patients in group 3) died of unrelated causes. Discussion In this study, downward displacement of tonsils or rostral displacement of the aqueduct/pontomesencephalic junction on midsagittal MRI did not predict deterioration. Mass effect from swelling of a cerebellar infarct occurred more commonly than previously reported, 1 3 but clinical deterioration occurred in less than half of the patients. Clinical deterioration coincided with the development of hydrocephalus, brain stem deformity, and basal cistern compression. Patients with CIMASS often have full territorial PICA or SCA infarcts, or the infarcts are confined to the medial vermian hemispheric branches of the PICA or SCA. Isolated lateral hemispheric branches of the PICA or SCA and any territorial infarct confined traditionally to AICA were not identified with CIMASS. Full territorial infarcts have been associated more frequently with the development of mass effect than small infarcts. 15,16 Between the groups of CI- MASS that deteriorated and the group that did not, there was no statistically significant difference in the distribution of the territories of the infarcts. These findings agree with the results of a recently published study. 17 Earlier definition of the involved territory would allow stratification of patients into those at risk and those at less risk, although the presence of an infarct in one of these territories does not always equate with deterioration. MR imaging with fluid-attenuated inversion recovery or diffusion-weighted imaging would improve early detection, but this technology was not applied uniformly through the study time frame and was therefore not included. Although other studies have not found a similar relationship, 18 our study found that the presence of hemorrhagic infarct was associated with deterioration. This may be a reflection of a larger volume of infarction. Of the CIMASS patients who deteriorated, obstructive hydrocephalus was linked to radiographic features of brain stem deformity and basal cistern compression. This observation can be explained by the cerebellar infarct exerting its mass effect in a posterior-to-anterior plane, leading to obliteration of the fourth ventricle and anterior displacement of the brain stem against the clivus. This is responsible for the dilatation of the third ventricle, temporal horns, and lateral ventricles. Based on the frequency of radiological signs found in patients with CIMASS, we propose that the order of progression of radiological signs was fourth ventricular deformity, fourth ventricular shift, obstructive hydrocephalus, brain stem deformity, and basal cistern compression. Ropper 19 reported that the vertical displacement of the PMJ on coronal films for patients with acute supratentorial masses did not differ from measurements in patients without masses. Our findings indicate statistically significant rostral displacement of the PMJ, aqueduct, and tonsillar descent in patients with CIMASS compared with non-cimass patients and controls. However, it was not possible to demonstrate a statistically significant difference between CIMASS patients who deteriorated and those who remained stable. These findings suggest that vertical brain displacement in CIMASS occurred, but they are not predictors of clinical deterioration. In addition, they support the hypothesis that the presence of hydrocephalus, brain stem compression, or both, but not vertical brain displacement, constitutes the main reason for neurological deterioration in patients with CIMASS. These findings are novel and should be taken into account when contemplating craniotomy. Development of hydrocephalus in the setting of impaired alertness coincided with deterioration in CIMASS. Admission to a neurological intensive care unit and consideration of preemptive surgery may be warranted in these patients. In patients with CIMASS, the presence of vertical displacement may not predict clinical deterioration, and decision to proceed with surgery should not be based solely on this MR finding. Our results should be interpreted with caution, because the number of patients with CIMASS in our study was small. Further MR studies are needed to extend these observations. References 1. Amarenco P. The spectrum of cerebellar infarctions. Neurology. 1991; 41: Kase CS, Norrving B, Levine SR, Babikian VL, Chodosh EH, Wolf PA, Welch KM. Cerebellar infarction: clinical and anatomic observations in 66 cases. Stroke. 1993;24: Macdonell RA, Kalnins RM, Donnan GA. Cerebellar infarction: natural history, prognosis, and pathology. Stroke. 1987;18: Heros RC. Cerebellar hemorrhage and infarction. Stroke. 1982;13:
6 Koh et al Cerebellar Infarct With Mass Effect Hornig CR, Rust DS, Busse O, Jauss M, Laun A. Space-occupying cerebellar infarction: clinical course and prognosis. Stroke. 1994;25: Heros RC. Surgical treatment of cerebellar infarction. Stroke. 1992;23: Kanis KB, Ropper AH, Adelman LS. Homolateral hemiparesis as an early sign of cerebellar mass effect. Neurology. 1994;44: Lehrich JR, Winkler GF, Ojemann RG. Cerebellar infarction with brain stem compression: diagnosis and surgical treatment. Arch Neurol. 1970; 22: Reich JB, Sierra J, Camp W, Zanzonico P, Deck MD, Plum F. Magnetic resonance imaging measurements and clinical changes accompanying transtentorial and foramen magnum brain herniation. Ann Neurol. 1993; 33: Tomaszek DE, Rosner MJ. Cerebellar infarction: analysis of twenty-one cases. Surg Neurol. 1985;24: Feldmann E, Gandy SE, Becker R, Zimmerman R, Thaler HT, Posner JB, Plum F. MRI demonstrates descending transtentorial herniation. Neurology. 1988;38: Ropper AH. A preliminary MRI study of the geometry of brain displacement and level of consciousness with acute intracranial masses. Neurology. 1989;39: Tatu L, Moulin T, Bogousslavsky J, Duvernoy H. Arterial territories of human brain: brainstem and cerebellum. Neurology. 1996;47: Adams HP Jr, Bendixen BH, Kappelle LJ, Biller J, Love BB, Gordon DL, Marsh EE III, and the TOAST Investigators. Classification of subtype of acute ischemic stroke: definitions for use in a multicenter clinical trial. Stroke. 1993;24: Sypert GW, Alvord EC Jr. Cerebellar infarction: a clinicopathological study. Arch Neurol. 1975;32: Amarenco P, Hauw JJ. Edematous cerebellar infarction: a clinicopathological study of 16 cases. Neurochirurgie. 1990;36: Jauss M, Krieger D, Hornig C, Schramm J, Busse O. Surgical and medical management of patients with massive cerebellar infarctions: results of the German-Austrian Cerebellar Infarction Study. J Neurol. 1999;246: Chaves CJ, Pessin MS, Caplan LR, Chung CS, Amarenco P, Breen J, Fine J, Kase C, Tapia J, Babikian V, Rosengart A, DeWitt LD. Cerebellar hemorrhagic infarction. Neurology. 1996;46: Ropper AH. Magnetic resonance imaging measurements and clinical changes accompanying transtentorial and foramen magnum brain herniation. Ann Neurol. 1993;34:
Neurological Features and Mechanisms of Acute Bilateral Cerebellar Infarction
 Neurological Features and Mechanisms of Acute Bilateral Cerebellar Infarction Ji-Man Hong, M.D., Sang Geon Shin, M.D., Jang-Sung Kim, M.D., Oh-Young Bang, M.D., In-Soo Joo, M.D., Kyoon-Huh, M.D. Department
Neurological Features and Mechanisms of Acute Bilateral Cerebellar Infarction Ji-Man Hong, M.D., Sang Geon Shin, M.D., Jang-Sung Kim, M.D., Oh-Young Bang, M.D., In-Soo Joo, M.D., Kyoon-Huh, M.D. Department
NEURO IMAGING 2. Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity
 NEURO IMAGING 2 Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity I. EPIDURAL HEMATOMA (EDH) LOCATION Seventy to seventy-five percent occur in temporoparietal region. CAUSE Most likely caused
NEURO IMAGING 2 Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity I. EPIDURAL HEMATOMA (EDH) LOCATION Seventy to seventy-five percent occur in temporoparietal region. CAUSE Most likely caused
Surgical Management of Stroke Brandon Evans, MD Department of Neurosurgery
 Surgical Management of Stroke Brandon Evans, MD Department of Neurosurgery 2 Stroke Stroke kills almost 130,000 Americans each year. - Third cause of all deaths in Arkansas. - Death Rate is highest in
Surgical Management of Stroke Brandon Evans, MD Department of Neurosurgery 2 Stroke Stroke kills almost 130,000 Americans each year. - Third cause of all deaths in Arkansas. - Death Rate is highest in
BRAIN HERNIATION S54 (1) Brain Herniation
 BRAIN HERNIATION S54 (1) Brain Herniation Last updated: September 5, 2017 PATHOPHYSIOLOGY... 1 TYPES OF HERNIATION... 2 SUPRATENTORIAL MASSES... 2 Central (s. downward transtentorial) herniation... 2 Uncal
BRAIN HERNIATION S54 (1) Brain Herniation Last updated: September 5, 2017 PATHOPHYSIOLOGY... 1 TYPES OF HERNIATION... 2 SUPRATENTORIAL MASSES... 2 Central (s. downward transtentorial) herniation... 2 Uncal
Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD
 Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD Boston Children s Hospital Harvard Medical School None Disclosures Conventional US Anterior fontanelle
Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD Boston Children s Hospital Harvard Medical School None Disclosures Conventional US Anterior fontanelle
Essentials of Clinical MR, 2 nd edition. 14. Ischemia and Infarction II
 14. Ischemia and Infarction II Lacunar infarcts are small deep parenchymal lesions involving the basal ganglia, internal capsule, thalamus, and brainstem. The vascular supply of these areas includes the
14. Ischemia and Infarction II Lacunar infarcts are small deep parenchymal lesions involving the basal ganglia, internal capsule, thalamus, and brainstem. The vascular supply of these areas includes the
Stroke - Intracranial hemorrhage. Dr. Amitesh Aggarwal Associate Professor Department of Medicine
 Stroke - Intracranial hemorrhage Dr. Amitesh Aggarwal Associate Professor Department of Medicine Etiology and pathogenesis ICH accounts for ~10% of all strokes 30 day mortality - 35 45% Incidence rates
Stroke - Intracranial hemorrhage Dr. Amitesh Aggarwal Associate Professor Department of Medicine Etiology and pathogenesis ICH accounts for ~10% of all strokes 30 day mortality - 35 45% Incidence rates
INCREASED INTRACRANIAL PRESSURE
 INCREASED INTRACRANIAL PRESSURE Sheba Medical Center, Acute Medicine Department Irene Frantzis P-Year student SGUL 2013 Normal Values Normal intracranial volume: 1700 ml Volume of brain: 1200-1400 ml CSF:
INCREASED INTRACRANIAL PRESSURE Sheba Medical Center, Acute Medicine Department Irene Frantzis P-Year student SGUL 2013 Normal Values Normal intracranial volume: 1700 ml Volume of brain: 1200-1400 ml CSF:
Principles Arteries & Veins of the CNS LO14
 Principles Arteries & Veins of the CNS LO14 14. Identify (on cadaver specimens, models and diagrams) and name the principal arteries and veins of the CNS: Why is it important to understand blood supply
Principles Arteries & Veins of the CNS LO14 14. Identify (on cadaver specimens, models and diagrams) and name the principal arteries and veins of the CNS: Why is it important to understand blood supply
CT and MR Imaging in Young Stroke Patients
 CT and MR Imaging in Young Stroke Patients Ashfaq A. Razzaq,Behram A. Khan,Shahid Baig ( Department of Neurology, Aga Khan University Hospital, Karachi. ) Abstract Pages with reference to book, From 66
CT and MR Imaging in Young Stroke Patients Ashfaq A. Razzaq,Behram A. Khan,Shahid Baig ( Department of Neurology, Aga Khan University Hospital, Karachi. ) Abstract Pages with reference to book, From 66
Stroke is the most prevalent disease involving the
 Treatment of Cerebellar Infarction by Decompressive Suboccipital Craniectomy Han-Jung Chen, MD; Tao-Chen Lee, MD; and Chi-Peng Wei, MD Background and Purpose: We present an anecdotal series of 11 patients
Treatment of Cerebellar Infarction by Decompressive Suboccipital Craniectomy Han-Jung Chen, MD; Tao-Chen Lee, MD; and Chi-Peng Wei, MD Background and Purpose: We present an anecdotal series of 11 patients
Attenuation value in HU From -500 To HU From -10 To HU From 60 To 90 HU. From 200 HU and above
 Brain Imaging Common CT attenuation values Structure Air Fat Water Brain tissue Recent hematoma Calcifications Bone Brain edema and infarction Normal liver parenchyma Attenuation value in HU From -500
Brain Imaging Common CT attenuation values Structure Air Fat Water Brain tissue Recent hematoma Calcifications Bone Brain edema and infarction Normal liver parenchyma Attenuation value in HU From -500
Head CT Scan Interpretation: A Five-Step Approach to Seeing Inside the Head Lawrence B. Stack, MD
 Head CT Scan Interpretation: A Five-Step Approach to Seeing Inside the Head Lawrence B. Stack, MD Five Step Approach 1. Adequate study 2. Bone windows 3. Ventricles 4. Quadrigeminal cistern 5. Parenchyma
Head CT Scan Interpretation: A Five-Step Approach to Seeing Inside the Head Lawrence B. Stack, MD Five Step Approach 1. Adequate study 2. Bone windows 3. Ventricles 4. Quadrigeminal cistern 5. Parenchyma
Acute cerebellar infarction or hemorrhage may initially manifest in a clinically indolent
 NEUROLOGICAL REVIEW SECTION EDITOR: DAVID E. PLEASURE, MD Management of Acute Cerebellar Stroke Matt B. Jensen, MD; Erik K. St. Louis, MD Acute cerebellar infarction or hemorrhage may initially manifest
NEUROLOGICAL REVIEW SECTION EDITOR: DAVID E. PLEASURE, MD Management of Acute Cerebellar Stroke Matt B. Jensen, MD; Erik K. St. Louis, MD Acute cerebellar infarction or hemorrhage may initially manifest
Cerebellar strokes: a clinical outcome review of 79 cases
 Singapore Med J 2015; 56(3): 145-149 doi: 10.11622/smedj.2014195 Cerebellar strokes: a clinical outcome review of 79 cases Zhi Xu Ng 1, MBBS, MRCSG, Wei Ren Eugene Yang 1, MRCSE, FRCS, Edwin Seet 2, MBBS,
Singapore Med J 2015; 56(3): 145-149 doi: 10.11622/smedj.2014195 Cerebellar strokes: a clinical outcome review of 79 cases Zhi Xu Ng 1, MBBS, MRCSG, Wei Ren Eugene Yang 1, MRCSE, FRCS, Edwin Seet 2, MBBS,
Microsurgery for ruptured cerebellar arteriovenous malformations
 European Review for Medical and Pharmacological Sciences Microsurgery for ruptured cerebellar arteriovenous malformations S.-F. GONG 1,2, X.-B. WANG 1,3, Y.-Q. LIAO 1,2, T.-P. JIANG 1,2, J.-B. HE 1,2,
European Review for Medical and Pharmacological Sciences Microsurgery for ruptured cerebellar arteriovenous malformations S.-F. GONG 1,2, X.-B. WANG 1,3, Y.-Q. LIAO 1,2, T.-P. JIANG 1,2, J.-B. HE 1,2,
CNS Imaging. Dr Amir Monir, MD. Lecturer of radiodiagnosis.
 CNS Imaging Dr Amir Monir, MD Lecturer of radiodiagnosis www.dramir.net Types of radiological examinations you know Plain X ray X ray with contrast GIT : barium (swallow, meal, follow through, enema) ERCP
CNS Imaging Dr Amir Monir, MD Lecturer of radiodiagnosis www.dramir.net Types of radiological examinations you know Plain X ray X ray with contrast GIT : barium (swallow, meal, follow through, enema) ERCP
MR Evaluation of Hydrocephalus
 591 MR Evaluation of Hydrocephalus Taher EI Gammal 1 Marshall B. Allen, Jr. 2 Betty Sue Brooks 1 Edward K. Mark2 An analysis of sagittal T1-weighted MR studies was performed in 23 patients with hydrocephalus,
591 MR Evaluation of Hydrocephalus Taher EI Gammal 1 Marshall B. Allen, Jr. 2 Betty Sue Brooks 1 Edward K. Mark2 An analysis of sagittal T1-weighted MR studies was performed in 23 patients with hydrocephalus,
Relation between brain displacement and local cerebral blood flow in patients with chronic subdural haematoma
 J Neurol Neurosurg Psychiatry 01;71:741 746 741 Department of Neurosurgery, Nagoya University School of Medicine, 65 Tsarumai Showa, Nagoya 466 8550, Japan S Inao TKawai R Kabeya T Sugimoto M Yamamoto
J Neurol Neurosurg Psychiatry 01;71:741 746 741 Department of Neurosurgery, Nagoya University School of Medicine, 65 Tsarumai Showa, Nagoya 466 8550, Japan S Inao TKawai R Kabeya T Sugimoto M Yamamoto
NEURO IMAGING OF ACUTE STROKE
 1 1 NEURO IMAGING OF ACUTE STROKE ALICIA RICHARDSON, MSN, RN, ACCNS-AG, ANVP-BC WENDY SMITH, MA, RN, MBA, SCRN, FAHA LYNN HUNDLEY, APRN, CNRN, CCNS, ANVP-BC 2 2 1 DISCLOSURES Alicia Richardson: Stryker
1 1 NEURO IMAGING OF ACUTE STROKE ALICIA RICHARDSON, MSN, RN, ACCNS-AG, ANVP-BC WENDY SMITH, MA, RN, MBA, SCRN, FAHA LYNN HUNDLEY, APRN, CNRN, CCNS, ANVP-BC 2 2 1 DISCLOSURES Alicia Richardson: Stryker
Corpus Callosal Signal Changes in Patients with Obstructive Hydrocephalus after Ventriculoperitoneal Shunting
 AJNR Am J Neuroradiol 22:158 162, January 2001 Corpus Callosal Signal Changes in Patients with Hydrocephalus after Ventriculoperitoneal Shunting John I. Lane, Patrick H. Luetmer, and John L. Atkinson BACKGROUND
AJNR Am J Neuroradiol 22:158 162, January 2001 Corpus Callosal Signal Changes in Patients with Hydrocephalus after Ventriculoperitoneal Shunting John I. Lane, Patrick H. Luetmer, and John L. Atkinson BACKGROUND
intracranial anomalies
 Chapter 5: Fetal Central Nervous System 84 intracranial anomalies Hydrocephaly Dilatation of ventricular system secondary to an increase in the amount of CSF. Effects of hydrocephalus include flattening
Chapter 5: Fetal Central Nervous System 84 intracranial anomalies Hydrocephaly Dilatation of ventricular system secondary to an increase in the amount of CSF. Effects of hydrocephalus include flattening
KEY WORDS: Brainstem compression, Cerebellar infarction, Treatment
 CLINICAL STUDIES MANAGEMENT OF ACUTE CEREBELLAR INFARCTION: ONE INSTITUTION S EXPERIENCE Antonino Raco, M.D. Emanuela Caroli, M.D. Alessandra Isidori, M.D. Tommaso Vangelista, M.D. Maurizio Salvati, M.D.
CLINICAL STUDIES MANAGEMENT OF ACUTE CEREBELLAR INFARCTION: ONE INSTITUTION S EXPERIENCE Antonino Raco, M.D. Emanuela Caroli, M.D. Alessandra Isidori, M.D. Tommaso Vangelista, M.D. Maurizio Salvati, M.D.
Stroke School for Internists Part 1
 Stroke School for Internists Part 1 November 4, 2017 Dr. Albert Jin Dr. Gurpreet Jaswal Disclosures I receive a stipend for my role as Medical Director of the Stroke Network of SEO I have no commercial
Stroke School for Internists Part 1 November 4, 2017 Dr. Albert Jin Dr. Gurpreet Jaswal Disclosures I receive a stipend for my role as Medical Director of the Stroke Network of SEO I have no commercial
Characteristic features of CNS pathology. By: Shifaa AlQa qa
 Characteristic features of CNS pathology By: Shifaa AlQa qa Normal brain: - The neocortex (gray matter): six layers: outer plexiform, outer granular, outer pyramidal, inner granular, inner pyramidal, polymorphous
Characteristic features of CNS pathology By: Shifaa AlQa qa Normal brain: - The neocortex (gray matter): six layers: outer plexiform, outer granular, outer pyramidal, inner granular, inner pyramidal, polymorphous
The choroid plexus of the fourth ventricle and its arteries
 O R I G I N A L A R T I C L E Folia Morphol. Vol. 64, No. 3, pp. 194 198 Copyright 2005 Via Medica ISSN 0015 5659 www.fm.viamedica.pl The choroid plexus of the fourth ventricle and its arteries Mansoor
O R I G I N A L A R T I C L E Folia Morphol. Vol. 64, No. 3, pp. 194 198 Copyright 2005 Via Medica ISSN 0015 5659 www.fm.viamedica.pl The choroid plexus of the fourth ventricle and its arteries Mansoor
CHAPTER 5. Symptomatic and Asymptomatic Retinal Embolism Have Different Mechanisms
 CHAPTER 5 Symptomatic and Asymptomatic Retinal Embolism Have Different Mechanisms Christine A.C. Wijman, Joao A. Gomes, Michael R. Winter, Behrooz Koleini, Ippolit C.A. Matjucha, Val E. Pochay, Viken L.
CHAPTER 5 Symptomatic and Asymptomatic Retinal Embolism Have Different Mechanisms Christine A.C. Wijman, Joao A. Gomes, Michael R. Winter, Behrooz Koleini, Ippolit C.A. Matjucha, Val E. Pochay, Viken L.
Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage
 Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Professor Dr.Muhammad Ajmal Dr.Tehmina Nazir. HOLY FAMILY HOSPITAL Rawalpindi
 Professor Dr.Muhammad Ajmal Dr.Tehmina Nazir HOLY FAMILY HOSPITAL Rawalpindi SCHEME OF PRESENTATION PLAIN X-RAYS CT SCAN MRI CONCLUSION IMAGING MODALITIES PLAIN X-RAYS CT SCAN MRI OCCIPITOMENTAL/WATER
Professor Dr.Muhammad Ajmal Dr.Tehmina Nazir HOLY FAMILY HOSPITAL Rawalpindi SCHEME OF PRESENTATION PLAIN X-RAYS CT SCAN MRI CONCLUSION IMAGING MODALITIES PLAIN X-RAYS CT SCAN MRI OCCIPITOMENTAL/WATER
Gross Organization I The Brain. Reading: BCP Chapter 7
 Gross Organization I The Brain Reading: BCP Chapter 7 Layout of the Nervous System Central Nervous System (CNS) Located inside of bone Includes the brain (in the skull) and the spinal cord (in the backbone)
Gross Organization I The Brain Reading: BCP Chapter 7 Layout of the Nervous System Central Nervous System (CNS) Located inside of bone Includes the brain (in the skull) and the spinal cord (in the backbone)
Pathological reaction to disease
 Chapter1 Pathological reaction to disease Normal anatomy Figures 1.1 1.6 2 4 Brain swelling and internal herniation Figures 1.7 1.15 5 9 Epilepsy Figures 1.16 1.18 9 10 Cerebellar atrophy Figures 1.19
Chapter1 Pathological reaction to disease Normal anatomy Figures 1.1 1.6 2 4 Brain swelling and internal herniation Figures 1.7 1.15 5 9 Epilepsy Figures 1.16 1.18 9 10 Cerebellar atrophy Figures 1.19
INTRACRANIAL PRESSURE -!!
 INTRACRANIAL PRESSURE - Significance raised ICP main cause of death in severe head injury main cause of morbidity in moderate and mild head injury main target and prognostic indicator in the ITU setting
INTRACRANIAL PRESSURE - Significance raised ICP main cause of death in severe head injury main cause of morbidity in moderate and mild head injury main target and prognostic indicator in the ITU setting
Regional and Lobe Parcellation Rhesus Monkey Brain Atlas. Manual Tracing for Parcellation Template
 Regional and Lobe Parcellation Rhesus Monkey Brain Atlas Manual Tracing for Parcellation Template Overview of Tracing Guidelines A) Traces are performed in a systematic order they, allowing the more easily
Regional and Lobe Parcellation Rhesus Monkey Brain Atlas Manual Tracing for Parcellation Template Overview of Tracing Guidelines A) Traces are performed in a systematic order they, allowing the more easily
Applicable Neuroradiology
 For the Clinical Neurology Clerkship LSU Medical School New Orleans Amy W Voigt, MD Clerkship Director Introduction The field of Radiology first developed following the discovery of X-Rays by Wilhelm Roentgen
For the Clinical Neurology Clerkship LSU Medical School New Orleans Amy W Voigt, MD Clerkship Director Introduction The field of Radiology first developed following the discovery of X-Rays by Wilhelm Roentgen
The central nervous system
 Sectc.qxd 29/06/99 09:42 Page 81 Section C The central nervous system CNS haemorrhage Subarachnoid haemorrhage Cerebral infarction Brain atrophy Ring enhancing lesions MRI of the pituitary Multiple sclerosis
Sectc.qxd 29/06/99 09:42 Page 81 Section C The central nervous system CNS haemorrhage Subarachnoid haemorrhage Cerebral infarction Brain atrophy Ring enhancing lesions MRI of the pituitary Multiple sclerosis
/ / / / / / Hospital Abstraction: Stroke/TIA. Participant ID: Hospital Code: Multi-Ethnic Study of Atherosclerosis
 Multi-Ethnic Study of Atherosclerosis Participant ID: Hospital Code: Hospital Abstraction: Stroke/TIA History and Hospital Record 1. Was the participant hospitalized as an immediate consequence of this
Multi-Ethnic Study of Atherosclerosis Participant ID: Hospital Code: Hospital Abstraction: Stroke/TIA History and Hospital Record 1. Was the participant hospitalized as an immediate consequence of this
Cerebro-vascular stroke
 Cerebro-vascular stroke CT Terminology Hypodense lesion = lesion of lower density than the normal brain tissue Hyperdense lesion = lesion of higher density than normal brain tissue Isodense lesion = lesion
Cerebro-vascular stroke CT Terminology Hypodense lesion = lesion of lower density than the normal brain tissue Hyperdense lesion = lesion of higher density than normal brain tissue Isodense lesion = lesion
For Emergency Doctors. Dr Suzanne Smallbane November 2011
 For Emergency Doctors Dr Suzanne Smallbane November 2011 A: Orbit B: Sphenoid Sinus C: Temporal Lobe D: EAC E: Mastoid air cells F: Cerebellar hemisphere A: Frontal lobe B: Frontal bone C: Dorsum sellae
For Emergency Doctors Dr Suzanne Smallbane November 2011 A: Orbit B: Sphenoid Sinus C: Temporal Lobe D: EAC E: Mastoid air cells F: Cerebellar hemisphere A: Frontal lobe B: Frontal bone C: Dorsum sellae
[(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD]
![[(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD] [(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD]](/thumbs/89/98619893.jpg) 2015 PHYSICIAN SIGN-OFF (1) STUDY NO (PHY-1) CASE, PER PHYSICIAN REVIEW 1=yes 2=no [strictly meets case definition] (PHY-1a) CASE, IN PHYSICIAN S OPINION 1=yes 2=no (PHY-2) (PHY-3) [based on all available
2015 PHYSICIAN SIGN-OFF (1) STUDY NO (PHY-1) CASE, PER PHYSICIAN REVIEW 1=yes 2=no [strictly meets case definition] (PHY-1a) CASE, IN PHYSICIAN S OPINION 1=yes 2=no (PHY-2) (PHY-3) [based on all available
HEAD AND NECK IMAGING. James Chen (MS IV)
 HEAD AND NECK IMAGING James Chen (MS IV) Anatomy Course Johns Hopkins School of Medicine Sept. 27, 2011 OBJECTIVES Introduce cross sectional imaging of head and neck Computed tomography (CT) Review head
HEAD AND NECK IMAGING James Chen (MS IV) Anatomy Course Johns Hopkins School of Medicine Sept. 27, 2011 OBJECTIVES Introduce cross sectional imaging of head and neck Computed tomography (CT) Review head
Morphometric Analysis of Left & Right Tonsils in Adult Symptomatic Type 1 Chiari Patients and Healthy Controls
 The University of Akron IdeaExchange@UAkron Honors Research Projects The Dr. Gary B. and Pamela S. Williams Honors College Spring 2015 Morphometric Analysis of Left & Right Tonsils in Adult Symptomatic
The University of Akron IdeaExchange@UAkron Honors Research Projects The Dr. Gary B. and Pamela S. Williams Honors College Spring 2015 Morphometric Analysis of Left & Right Tonsils in Adult Symptomatic
11/27/2017. Stroke Management in the Neurocritical Care Unit. Conflict of interest. Karel Fuentes MD Medical Director of Neurocritical Care
 Stroke Management in the Neurocritical Care Unit Karel Fuentes MD Medical Director of Neurocritical Care Conflict of interest None Introduction Reperfusion therapy remains the mainstay in the treatment
Stroke Management in the Neurocritical Care Unit Karel Fuentes MD Medical Director of Neurocritical Care Conflict of interest None Introduction Reperfusion therapy remains the mainstay in the treatment
CT - Brain Examination
 CT - Brain Examination Submitted by: Felemban 1 CT - Brain Examination The clinical indication of CT brain are: a) Chronic cases (e.g. headache - tumor - abscess) b) ER cases (e.g. trauma - RTA - child
CT - Brain Examination Submitted by: Felemban 1 CT - Brain Examination The clinical indication of CT brain are: a) Chronic cases (e.g. headache - tumor - abscess) b) ER cases (e.g. trauma - RTA - child
ISCHEMIC STROKE IMAGING
 ISCHEMIC STROKE IMAGING ผศ.พญ พญ.จ ร ร ตน ธรรมโรจน ภาคว ชาร งส ว ทยา คณะแพทยศาสตร มหาว ทยาล ยขอนแก น A case of acute hemiplegia Which side is the abnormality, right or left? Early Right MCA infarction
ISCHEMIC STROKE IMAGING ผศ.พญ พญ.จ ร ร ตน ธรรมโรจน ภาคว ชาร งส ว ทยา คณะแพทยศาสตร มหาว ทยาล ยขอนแก น A case of acute hemiplegia Which side is the abnormality, right or left? Early Right MCA infarction
Transient Bilateral Oculomotor Nerve. Palsy (TOP) Associated with Ruptured. Anterior Communicating Artery Aneurysm: A Case Report
 Case Report imedpub Journals http://www.imedpub.com Insights in Neurosurgery ISSN 2471-9633 DOI: 10.21767/2471-9633.100012 Abstract Transient Bilateral Oculomotor Nerve Palsy (TOP) Associated with Ruptured
Case Report imedpub Journals http://www.imedpub.com Insights in Neurosurgery ISSN 2471-9633 DOI: 10.21767/2471-9633.100012 Abstract Transient Bilateral Oculomotor Nerve Palsy (TOP) Associated with Ruptured
Meninges and Ventricles
 Meninges and Ventricles Irene Yu, class of 2019 LEARNING OBJECTIVES Describe the meningeal layers, the dural infolds, and the spaces they create. Name the contents of the subarachnoid space. Describe the
Meninges and Ventricles Irene Yu, class of 2019 LEARNING OBJECTIVES Describe the meningeal layers, the dural infolds, and the spaces they create. Name the contents of the subarachnoid space. Describe the
Pediatric MS MRI Study Methodology
 General Pediatric MS MRI Study Methodology SCAN PREPARATION axial T2-weighted scans and/or axial FLAIR scans were obtained for all subjects when available, both T2 and FLAIR scans were scored. In order
General Pediatric MS MRI Study Methodology SCAN PREPARATION axial T2-weighted scans and/or axial FLAIR scans were obtained for all subjects when available, both T2 and FLAIR scans were scored. In order
Classical CNS Disease Patterns
 Classical CNS Disease Patterns Inflammatory Traumatic In response to the trauma of having his head bashed in GM would have experienced some of these features. NOT TWO LITTLE PEENY WEENY I CM LACERATIONS.
Classical CNS Disease Patterns Inflammatory Traumatic In response to the trauma of having his head bashed in GM would have experienced some of these features. NOT TWO LITTLE PEENY WEENY I CM LACERATIONS.
QUADRIGEMINAL CISTERN
 J. Neurol. Neurosurg. Psychiat., 1961, 24, 374. RADIOLOGICAL AND CLINICAL FEATURES OF AN ARACHNOID CYST OF THE QUADRIGEMINAL CISTERN BY HERBERT LOURIE and ALFRED S. BERNE From the Division of Neurological
J. Neurol. Neurosurg. Psychiat., 1961, 24, 374. RADIOLOGICAL AND CLINICAL FEATURES OF AN ARACHNOID CYST OF THE QUADRIGEMINAL CISTERN BY HERBERT LOURIE and ALFRED S. BERNE From the Division of Neurological
Slide 1. Slide 2. Slide 3. Tomography vs Topography. Computed Tomography (CT): A simplified Topographical review of the Brain. Learning Objective
 Slide 1 Computed Tomography (CT): A simplified Topographical review of the Brain Jon Wheiler, ACNP-BC Slide 2 Tomography vs Topography Tomography: A technique for displaying a representation of a cross
Slide 1 Computed Tomography (CT): A simplified Topographical review of the Brain Jon Wheiler, ACNP-BC Slide 2 Tomography vs Topography Tomography: A technique for displaying a representation of a cross
Chapter XII: Temporal Expanding Processes, Including Those in the Sylvian Fissure and the Insula
 Acta Radiologica ISSN: 0001-6926 (Print) (Online) Journal homepage: https://www.tandfonline.com/loi/iaro20 Chapter XII: Temporal Expanding Processes, Including Those in the Sylvian Fissure and the Insula
Acta Radiologica ISSN: 0001-6926 (Print) (Online) Journal homepage: https://www.tandfonline.com/loi/iaro20 Chapter XII: Temporal Expanding Processes, Including Those in the Sylvian Fissure and the Insula
The significance of traumatic haematoma in the
 Journal of Neurology, Neurosurgery, and Psychiatry 1986;49:29-34 The significance of traumatic haematoma in the region of the basal ganglia P MACPHERSON, E TEASDALE, S DHAKER, G ALLERDYCE, S GALBRAITH
Journal of Neurology, Neurosurgery, and Psychiatry 1986;49:29-34 The significance of traumatic haematoma in the region of the basal ganglia P MACPHERSON, E TEASDALE, S DHAKER, G ALLERDYCE, S GALBRAITH
Ventriculostomy and Risk of Upward Herniation in Patients with Obstructive Hydrocephalus from Posterior Fossa Mass Lesions
 https://doi.org/10.1007/s12028-017-0487-3 ORIGINAL ARTICLE Ventriculostomy and Risk of Upward Herniation in Patients with Obstructive Hydrocephalus from Posterior Fossa Mass Lesions Sherri A. Braksick
https://doi.org/10.1007/s12028-017-0487-3 ORIGINAL ARTICLE Ventriculostomy and Risk of Upward Herniation in Patients with Obstructive Hydrocephalus from Posterior Fossa Mass Lesions Sherri A. Braksick
Complete Recovery of Perfusion Abnormalities in a Cardiac Arrest Patient Treated with Hypothermia: Results of Cerebral Perfusion MR Imaging
 pissn 2384-1095 eissn 2384-1109 imri 2018;22:56-60 https://doi.org/10.13104/imri.2018.22.1.56 Complete Recovery of Perfusion Abnormalities in a Cardiac Arrest Patient Treated with Hypothermia: Results
pissn 2384-1095 eissn 2384-1109 imri 2018;22:56-60 https://doi.org/10.13104/imri.2018.22.1.56 Complete Recovery of Perfusion Abnormalities in a Cardiac Arrest Patient Treated with Hypothermia: Results
CNS pathology Third year medical students. Dr Heyam Awad 2018 Lecture 5: disturbed fluid balance and increased intracranial pressure
 CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 5: disturbed fluid balance and increased intracranial pressure ILOs Understand causes and symptoms of increased intracranial pressure.
CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 5: disturbed fluid balance and increased intracranial pressure ILOs Understand causes and symptoms of increased intracranial pressure.
Department of Cognitive Science UCSD
 Department of Cognitive Science UCSD Verse 1: Neocortex, frontal lobe, Brain stem, brain stem, Hippocampus, neural node, Right hemisphere, Pons and cortex visual, Brain stem, brain stem, Sylvian fissure,
Department of Cognitive Science UCSD Verse 1: Neocortex, frontal lobe, Brain stem, brain stem, Hippocampus, neural node, Right hemisphere, Pons and cortex visual, Brain stem, brain stem, Sylvian fissure,
DIRECT SURGERY FOR INTRA-AXIAL
 Kitakanto Med. J. (S1) : 23 `28, 1998 23 DIRECT SURGERY FOR INTRA-AXIAL BRAINSTEM LESIONS Kazuhiko Kyoshima, Susumu Oikawa, Shigeaki Kobayashi Department of Neurosurgery, Shinshu University School of Medicine,
Kitakanto Med. J. (S1) : 23 `28, 1998 23 DIRECT SURGERY FOR INTRA-AXIAL BRAINSTEM LESIONS Kazuhiko Kyoshima, Susumu Oikawa, Shigeaki Kobayashi Department of Neurosurgery, Shinshu University School of Medicine,
Original Article CT grouping and microsurgical treatment strategies of hypertensive cerebellar hemorrhage
 Int J Clin Exp Med 2016;9(8):15921-15927 www.ijcem.com /ISSN:1940-5901/IJCEM0022273 Original Article CT grouping and microsurgical treatment strategies of hypertensive cerebellar hemorrhage Xielin Tang
Int J Clin Exp Med 2016;9(8):15921-15927 www.ijcem.com /ISSN:1940-5901/IJCEM0022273 Original Article CT grouping and microsurgical treatment strategies of hypertensive cerebellar hemorrhage Xielin Tang
Unit 18: Cranial Cavity and Contents
 Unit 18: Cranial Cavity and Contents Dissection Instructions: The calvaria is to be removed without damage to the dura mater which is attached to the inner surface of the calvaria. Cut through the outer
Unit 18: Cranial Cavity and Contents Dissection Instructions: The calvaria is to be removed without damage to the dura mater which is attached to the inner surface of the calvaria. Cut through the outer
Spartan Medical Research Journal
 Spartan Medical Research Journal Research at Michigan State University College of Osteopathic Medicine Volume 2 Number 2 Winter, 2017 Pages 38-49 Title: Posterior Inferior Cerebellar Infarct in a Younger
Spartan Medical Research Journal Research at Michigan State University College of Osteopathic Medicine Volume 2 Number 2 Winter, 2017 Pages 38-49 Title: Posterior Inferior Cerebellar Infarct in a Younger
Brainstem and Cerebellum
 Brainstem and Cerebellum Lecture two Objectives: 1. Identify radiological anatomy of brain stem and cerebellum. 2. Compares CT and MRI imaging of brain stem and cerebellum. 3. Recognize the imaging findings
Brainstem and Cerebellum Lecture two Objectives: 1. Identify radiological anatomy of brain stem and cerebellum. 2. Compares CT and MRI imaging of brain stem and cerebellum. 3. Recognize the imaging findings
 www.yassermetwally.com MANAGEMENT OF CEREBRAL HAEMORRHAGE (ICH): A QUICK GUIDE Overview 10% of strokes is caused by ICH. Main Causes: Less than 40 years old: vascular malformations and illicit drug use.
www.yassermetwally.com MANAGEMENT OF CEREBRAL HAEMORRHAGE (ICH): A QUICK GUIDE Overview 10% of strokes is caused by ICH. Main Causes: Less than 40 years old: vascular malformations and illicit drug use.
Brain tissue and white matter lesion volume analysis in diabetes mellitus type 2
 Brain tissue and white matter lesion volume analysis in diabetes mellitus type 2 C. Jongen J. van der Grond L.J. Kappelle G.J. Biessels M.A. Viergever J.P.W. Pluim On behalf of the Utrecht Diabetic Encephalopathy
Brain tissue and white matter lesion volume analysis in diabetes mellitus type 2 C. Jongen J. van der Grond L.J. Kappelle G.J. Biessels M.A. Viergever J.P.W. Pluim On behalf of the Utrecht Diabetic Encephalopathy
Skull-2. Norma Basalis Interna Norma Basalis Externa. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 Skull-2 Norma Basalis Interna Norma Basalis Externa Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Norma basalis interna Base of the skull- superior view The interior of the base of the
Skull-2 Norma Basalis Interna Norma Basalis Externa Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Norma basalis interna Base of the skull- superior view The interior of the base of the
External carotid blood supply to acoustic neurinomas
 External carotid blood supply to acoustic neurinomas Report of two cases HARVEY L. LEVINE, M.D., ERNEST J. FERmS, M.D., AND EDWARD L. SPATZ, M.D. Departments of Radiology, Neurology, and Neurosurgery,
External carotid blood supply to acoustic neurinomas Report of two cases HARVEY L. LEVINE, M.D., ERNEST J. FERmS, M.D., AND EDWARD L. SPATZ, M.D. Departments of Radiology, Neurology, and Neurosurgery,
What Are We Going to Do? Fourth Year Meds Clinical Neuroanatomy. Hydrocephalus and Effects of Interruption of CSF Flow. Tube Blockage Doctrine
 Fourth Year Meds Clinical Neuroanatomy Ventricles, CSF, Brain Swelling etc. David A. Ramsay, Neuropathologist, LHSC What Are We Going to Do? Hydrocephalus and some effects of the interruption of CSF flow
Fourth Year Meds Clinical Neuroanatomy Ventricles, CSF, Brain Swelling etc. David A. Ramsay, Neuropathologist, LHSC What Are We Going to Do? Hydrocephalus and some effects of the interruption of CSF flow
SOP: Cerebral Ultrasound
 SOP: Cerebral Ultrasound Version Author(s) Date Changes Approved by 1.0 Cornelia Hagmann Manon Benders 29.5.2012 Initial Version Gorm Greisen 1.1 Cornelia Hagmann 18.6.2012 Minor changes Gorm Greisen 1.2
SOP: Cerebral Ultrasound Version Author(s) Date Changes Approved by 1.0 Cornelia Hagmann Manon Benders 29.5.2012 Initial Version Gorm Greisen 1.1 Cornelia Hagmann 18.6.2012 Minor changes Gorm Greisen 1.2
Skull-2. Norma Basalis Interna. Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology
 Skull-2 Norma Basalis Interna Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology Norma basalis interna Base of the skull- superior view The interior of the base of the skull is divided into
Skull-2 Norma Basalis Interna Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology Norma basalis interna Base of the skull- superior view The interior of the base of the skull is divided into
BRAIN STEM AND CEREBELLUM..
 Lecture Title: BRAIN STEM AND CEREBELLUM.. (CNS Block, Radiology) Dr. Hamdy Hassan Ass.Prof. Consultant Radiology Department KKHU King Saud University Lecture Objectives.. Students at the end of the lecture
Lecture Title: BRAIN STEM AND CEREBELLUM.. (CNS Block, Radiology) Dr. Hamdy Hassan Ass.Prof. Consultant Radiology Department KKHU King Saud University Lecture Objectives.. Students at the end of the lecture
Angel J. Lacerda MD PhD, Daisy Abreu MD, Julio A. Díaz MD, Sandro Perez MD, Julio C Martin MD, Daiyan Martin MD.
 Angel J. Lacerda MD PhD, Daisy Abreu MD, Julio A. Díaz MD, Sandro Perez MD, Julio C Martin MD, Daiyan Martin MD. Introduction: Spontaneous intracerebral haemorrhage (SICH) represents one of the most severe
Angel J. Lacerda MD PhD, Daisy Abreu MD, Julio A. Díaz MD, Sandro Perez MD, Julio C Martin MD, Daiyan Martin MD. Introduction: Spontaneous intracerebral haemorrhage (SICH) represents one of the most severe
11/23/2015. Disclosures. Stroke Management in the Neurocritical Care Unit. Karel Fuentes MD Medical Director of Neurocritical Care.
 Stroke Management in the Neurocritical Care Unit Karel Fuentes MD Medical Director of Neurocritical Care Disclosures I have no relevant commercial relationships to disclose, and my presentations will not
Stroke Management in the Neurocritical Care Unit Karel Fuentes MD Medical Director of Neurocritical Care Disclosures I have no relevant commercial relationships to disclose, and my presentations will not
Acute stroke. Ischaemic stroke. Characteristics. Temporal classification. Clinical features. Interpretation of Emergency Head CT
 Ischaemic stroke Characteristics Stroke is the third most common cause of death in the UK, and the leading cause of disability. 80% of strokes are ischaemic Large vessel occlusive atheromatous disease
Ischaemic stroke Characteristics Stroke is the third most common cause of death in the UK, and the leading cause of disability. 80% of strokes are ischaemic Large vessel occlusive atheromatous disease
ORIGINAL CONTRIBUTION. Symptoms and Signs of Posterior Circulation Ischemia in the New England Medical Center Posterior Circulation Registry
 ONLINE FIRST ORIGINAL CONTRIBUTION Symptoms and of Posterior Circulation Ischemia in the New England Medical Center Posterior Circulation Registry D. Eric Searls, MD; Ladislav Pazdera, MD; Evzen Korbel,
ONLINE FIRST ORIGINAL CONTRIBUTION Symptoms and of Posterior Circulation Ischemia in the New England Medical Center Posterior Circulation Registry D. Eric Searls, MD; Ladislav Pazdera, MD; Evzen Korbel,
ANASTAMOSIS FOR BRAIN STEM ISCHEMIA/Khodadad et al.
 ANASTAMOSIS FOR BRAIN STEM ISCHEMIA/Khodadad et al. visualization of the posterior inferior cerebellar artery. The patient, now 11 months post-operative, has shown further neurological improvement since
ANASTAMOSIS FOR BRAIN STEM ISCHEMIA/Khodadad et al. visualization of the posterior inferior cerebellar artery. The patient, now 11 months post-operative, has shown further neurological improvement since
Causes and Mechanisms of Territorial and Nonterritorial Cerebellar Infarcts in 115 Consecutive Patients
 5 Causes and Mechanisms of Territorial and Nonterritorial Cerebellar Infarcts in 5 Consecutive Patients Pierre Amarenco, MD; Claude Levy, MD; Ariel Cohen, MD; Pierre-Jean Touboul, MD; Etienne Roullet,
5 Causes and Mechanisms of Territorial and Nonterritorial Cerebellar Infarcts in 5 Consecutive Patients Pierre Amarenco, MD; Claude Levy, MD; Ariel Cohen, MD; Pierre-Jean Touboul, MD; Etienne Roullet,
Medical Neuroscience Tutorial Notes
 Medical Neuroscience Tutorial Notes Blood Supply to the Brain MAP TO NEUROSCIENCE CORE CONCEPTS 1 NCC1. The brain is the body's most complex organ. LEARNING OBJECTIVES After study of the assigned learning
Medical Neuroscience Tutorial Notes Blood Supply to the Brain MAP TO NEUROSCIENCE CORE CONCEPTS 1 NCC1. The brain is the body's most complex organ. LEARNING OBJECTIVES After study of the assigned learning
Blood Supply. Allen Chung, class of 2013
 Blood Supply Allen Chung, class of 2013 Objectives Understand the importance of the cerebral circulation. Understand stroke and the types of vascular problems that cause it. Understand ischemic penumbra
Blood Supply Allen Chung, class of 2013 Objectives Understand the importance of the cerebral circulation. Understand stroke and the types of vascular problems that cause it. Understand ischemic penumbra
STROKE - IMAGING. Dr RAJASEKHAR REDDY 2nd Yr P.G. RADIODIAGNOSIS KIMS,Narkatpalli.
 STROKE - IMAGING Dr RAJASEKHAR REDDY 2nd Yr P.G. RADIODIAGNOSIS KIMS,Narkatpalli. STROKE Describes a clinical event that consists of sudden onset of neurological symptoms Types Infarction - occlusion of
STROKE - IMAGING Dr RAJASEKHAR REDDY 2nd Yr P.G. RADIODIAGNOSIS KIMS,Narkatpalli. STROKE Describes a clinical event that consists of sudden onset of neurological symptoms Types Infarction - occlusion of
NEURORADIOLOGY DIL part 4
 NEURORADIOLOGY DIL part 4 Strokes and infarcts K. Agyem MD, G. Hall MD, D. Palathinkal MD, Alexandre Menard March/April 2015 OVERVIEW Introduction to Neuroimaging - DIL part 1 Basic Brain Anatomy - DIL
NEURORADIOLOGY DIL part 4 Strokes and infarcts K. Agyem MD, G. Hall MD, D. Palathinkal MD, Alexandre Menard March/April 2015 OVERVIEW Introduction to Neuroimaging - DIL part 1 Basic Brain Anatomy - DIL
Clinical Study Circle of Willis Variants: Fetal PCA
 Stroke Research and Treatment Volume 2013, Article ID 105937, 6 pages http://dx.doi.org/10.1155/2013/105937 Clinical Study Circle of Willis Variants: Fetal PCA Amir Shaban, 1 Karen C. Albright, 2,3,4,5
Stroke Research and Treatment Volume 2013, Article ID 105937, 6 pages http://dx.doi.org/10.1155/2013/105937 Clinical Study Circle of Willis Variants: Fetal PCA Amir Shaban, 1 Karen C. Albright, 2,3,4,5
Fig.1: A, Sagittal 110x110 mm subimage close to the midline, passing through the cingulum. Note that the fibers of the corpus callosum run at a
 Fig.1 E Fig.1:, Sagittal 110x110 mm subimage close to the midline, passing through the cingulum. Note that the fibers of the corpus callosum run at a slight angle are through the plane (blue dots with
Fig.1 E Fig.1:, Sagittal 110x110 mm subimage close to the midline, passing through the cingulum. Note that the fibers of the corpus callosum run at a slight angle are through the plane (blue dots with
Moron General Hospital Ciego de Avila Cuba. Department of Neurological Surgery
 Moron General Hospital Ciego de Avila Cuba Department of Neurological Surgery Early decompressive craniectomy in severe head injury with intracranial hypertension Angel J. Lacerda MD PhD, Daisy Abreu MD,
Moron General Hospital Ciego de Avila Cuba Department of Neurological Surgery Early decompressive craniectomy in severe head injury with intracranial hypertension Angel J. Lacerda MD PhD, Daisy Abreu MD,
Correlation between Degree of Midline Shift at Computed Tomography Scan of Brain and Glasgow Coma Scale Score in Spontaneous Intracerebral Hemorrhage
 Correlation between Degree of Midline Shift at Computed Tomography Scan of Brain and Glasgow Coma Scale Score in Spontaneous Intracerebral Hemorrhage *Haque MZ, 1 Hossain A, 2 Mohammad QD, 3 Sarker S,
Correlation between Degree of Midline Shift at Computed Tomography Scan of Brain and Glasgow Coma Scale Score in Spontaneous Intracerebral Hemorrhage *Haque MZ, 1 Hossain A, 2 Mohammad QD, 3 Sarker S,
secondary effects and sequelae of head trauma.
 Neuroimaging of vascular/secondary secondary effects and sequelae of head trauma. Andrès Server Alonso Department of Neuroradiology Division of Radiology Ullevål University Hospital Oslo, Norway. Guidelines
Neuroimaging of vascular/secondary secondary effects and sequelae of head trauma. Andrès Server Alonso Department of Neuroradiology Division of Radiology Ullevål University Hospital Oslo, Norway. Guidelines
Imaging of Moya Moya Disease
 Abstract Imaging of Moya Moya Disease Pages with reference to book, From 181 To 185 Rashid Ahmed, Hurnera Ahsan ( Liaquat National Hospital, Karachi. ) Moya Moya disease is a rare disease causing occlusion
Abstract Imaging of Moya Moya Disease Pages with reference to book, From 181 To 185 Rashid Ahmed, Hurnera Ahsan ( Liaquat National Hospital, Karachi. ) Moya Moya disease is a rare disease causing occlusion
Introduction. Abstract. Michael Yannes 1, Jennifer V. Frabizzio, MD 1, and Qaisar A. Shah, MD 1 1
 Reversal of CT hypodensity after acute ischemic stroke Michael Yannes 1, Jennifer V. Frabizzio, MD 1, and Qaisar A. Shah, MD 1 1 Abington Memorial Hospital in Abington, Pennsylvania Abstract We report
Reversal of CT hypodensity after acute ischemic stroke Michael Yannes 1, Jennifer V. Frabizzio, MD 1, and Qaisar A. Shah, MD 1 1 Abington Memorial Hospital in Abington, Pennsylvania Abstract We report
MR imaging at 3.0 tesla of glossopharyngeal neuralgia by neurovascular compression
 MR imaging at 3.0 tesla of glossopharyngeal neuralgia by neurovascular compression Poster No.: C-1281 Congress: ECR 2011 Type: Scientific Exhibit Authors: M. Nishihara 1, T. Noguchi 1, H. Irie 1, K. Sasaguri
MR imaging at 3.0 tesla of glossopharyngeal neuralgia by neurovascular compression Poster No.: C-1281 Congress: ECR 2011 Type: Scientific Exhibit Authors: M. Nishihara 1, T. Noguchi 1, H. Irie 1, K. Sasaguri
Index. aneurysm, 92 carotid occlusion, 94 ICA stenosis, 95 intracranial, 92 MCA, 94
 A ADC. See Apparent diffusion coefficient (ADC) Aneurysm cerebral artery aneurysm, 93 CT scan, 93 gadolinium, 93 Angiography, 13 Anoxic brain injury, 25 Apparent diffusion coefficient (ADC), 7 Arachnoid
A ADC. See Apparent diffusion coefficient (ADC) Aneurysm cerebral artery aneurysm, 93 CT scan, 93 gadolinium, 93 Angiography, 13 Anoxic brain injury, 25 Apparent diffusion coefficient (ADC), 7 Arachnoid
JlntSocPlastination, Vol4:16-22,
 JlntSocPlastination, Vol4:16-22, 1990 16 SECTIONAL ANATOMY: STANDARDIZED METHODOLOGY Alexander Lane, Coordinator of Anatomy and Physiology, Triton College, Visiting Associate Professor, University of Illinois
JlntSocPlastination, Vol4:16-22, 1990 16 SECTIONAL ANATOMY: STANDARDIZED METHODOLOGY Alexander Lane, Coordinator of Anatomy and Physiology, Triton College, Visiting Associate Professor, University of Illinois
Neurosurgical management of cerebellar
 J7ournal ofneurology, Neurosurgery, and Psychiatry 1995;59:287-292 Department of Neurosurgery, Institute of Neurological Sciences, Southern General Hospital, Glasgow G51 4TF, Scotland, UK P Mathew G Teasdale
J7ournal ofneurology, Neurosurgery, and Psychiatry 1995;59:287-292 Department of Neurosurgery, Institute of Neurological Sciences, Southern General Hospital, Glasgow G51 4TF, Scotland, UK P Mathew G Teasdale
Pearls and Pitfalls in Neuroradiology of Cerebrovascular Disease The Essentials with MR and CT
 Pearls and Pitfalls in Neuroradiology of Cerebrovascular Disease The Essentials with MR and CT Val M. Runge, MD Wendy R. K. Smoker, MD Anton Valavanis, MD Control # 823 Purpose The focus of this educational
Pearls and Pitfalls in Neuroradiology of Cerebrovascular Disease The Essentials with MR and CT Val M. Runge, MD Wendy R. K. Smoker, MD Anton Valavanis, MD Control # 823 Purpose The focus of this educational
Magnetic resonance imaging (MRI) appears to
 297 Early Diagnosis of Basilar Artery Occlusion Using Magnetic Resonance Imaging Jos6 Biller, MD, William T.C. Yuh, MD, Galen W. Mitchell, MD, Askiel Bruno, MD, and Harold P. Adams Jr., MD Three patients
297 Early Diagnosis of Basilar Artery Occlusion Using Magnetic Resonance Imaging Jos6 Biller, MD, William T.C. Yuh, MD, Galen W. Mitchell, MD, Askiel Bruno, MD, and Harold P. Adams Jr., MD Three patients
Diagnostic and Therapeutic Consequences of Repeat Brain Imaging and Follow-up Vascular Imaging in Stroke Patients
 AJNR Am J Neuroradiol 0:7, January 999 Diagnostic and Therapeutic Consequences of Repeat Brain Imaging and Follow-up Vascular Imaging in Stroke Patients Birgit Ertl-Wagner, Tobias Brandt, Christina Seifart,
AJNR Am J Neuroradiol 0:7, January 999 Diagnostic and Therapeutic Consequences of Repeat Brain Imaging and Follow-up Vascular Imaging in Stroke Patients Birgit Ertl-Wagner, Tobias Brandt, Christina Seifart,
Typical idiopathic intracranial hypertension Optic nerve appearance and brain MRI findings. Jonathan A. Micieli, MD Valérie Biousse, MD
 Typical idiopathic intracranial hypertension Optic nerve appearance and brain MRI findings Jonathan A. Micieli, MD Valérie Biousse, MD A 24 year old African American woman is referred for bilateral optic
Typical idiopathic intracranial hypertension Optic nerve appearance and brain MRI findings Jonathan A. Micieli, MD Valérie Biousse, MD A 24 year old African American woman is referred for bilateral optic
Chiari Malformations. Google. Objectives Seventh Annual NKY TBI Conference 3/22/13. Kerry R. Crone, M.D.
 Chiari Malformations Kerry R. Crone, M.D. Professor of Neurosurgery and Pediatrics University of Cincinnati College of Medicine University of Cincinnati Medical Center Cincinnati Children s Hospital Medical
Chiari Malformations Kerry R. Crone, M.D. Professor of Neurosurgery and Pediatrics University of Cincinnati College of Medicine University of Cincinnati Medical Center Cincinnati Children s Hospital Medical
Distal anterior cerebral artery (DACA) aneurysms are. Case Report
 248 Formos J Surg 2010;43:248-252 Distal Anterior Cerebral Artery Aneurysm: an Infrequent Cause of Transient Ischemic Attack Followed by Diffuse Subarachnoid Hemorrhage: Report of a Case Che-Chuan Wang
248 Formos J Surg 2010;43:248-252 Distal Anterior Cerebral Artery Aneurysm: an Infrequent Cause of Transient Ischemic Attack Followed by Diffuse Subarachnoid Hemorrhage: Report of a Case Che-Chuan Wang
Chapter 3. Structure and Function of the Nervous System. Copyright (c) Allyn and Bacon 2004
 Chapter 3 Structure and Function of the Nervous System 1 Basic Features of the Nervous System Neuraxis: An imaginary line drawn through the center of the length of the central nervous system, from the
Chapter 3 Structure and Function of the Nervous System 1 Basic Features of the Nervous System Neuraxis: An imaginary line drawn through the center of the length of the central nervous system, from the
RECOGNIZING THE SIGNS OF A NEURO EMERGENCY
 RECOGNIZING THE SIGNS OF A NEURO EMERGENCY Noorin Darvesh BScN, RN, CNN (C) Clinical Nurse Educator, Unit 58 South Health Campus Department of Clinical Neurosciences None DISCLOSURES WHO AM I? WHO ARE
RECOGNIZING THE SIGNS OF A NEURO EMERGENCY Noorin Darvesh BScN, RN, CNN (C) Clinical Nurse Educator, Unit 58 South Health Campus Department of Clinical Neurosciences None DISCLOSURES WHO AM I? WHO ARE
IMAGING IN ACUTE ISCHEMIC STROKE
 IMAGING IN ACUTE ISCHEMIC STROKE Timo Krings MD, PhD, FRCP (C) Professor of Radiology & Surgery Braley Chair of Neuroradiology, Chief and Program Director of Diagnostic and Interventional Neuroradiology;
IMAGING IN ACUTE ISCHEMIC STROKE Timo Krings MD, PhD, FRCP (C) Professor of Radiology & Surgery Braley Chair of Neuroradiology, Chief and Program Director of Diagnostic and Interventional Neuroradiology;
