Effect of ST2825 on the proliferation and apoptosis of human hepatocellular carcinoma cells
|
|
|
- Dale Robbins
- 5 years ago
- Views:
Transcription
1 Effect of ST2825 on the proliferation and apoptosis of human hepatocellular carcinoma cells Y. Deng, J. Sun and L.D. Zhang Department of Hepatobiliary Surgery Institute, Southwest Hospital, Third Military Medical University, Chongqing, China Corresponding author: L.D. Zhang Genet. Mol. Res. 15 (1): gmr Received August 10, 2015 Accepted November 6, 2015 Published March 4, 2016 DOI ABSTRACT. The purpose of this study was to investigate the effect of ST2825, an inhibitor of myeloid differentiation factor 88 (MyD88), on the proliferation and apoptosis of human hepatocellular carcinoma (HCC) cells as well as the potential mechanism and clinical significance of ST2825 in the treatment of HCC. Immunohistochemical staining with an MyD88 antibody was performed on tissues from 80 human HCC patients and adjacent normal tissues. In the in vitro experiment, human HCC HepG- 2 cells cultured in vitro were divided into the following groups: blank, control (1% DMSO), low-dose (2 µm), medium-dose (10 µm), and highdose ST2825 (20 µm). Cell apoptosis was detected by the Annexin V-FITC assay, and HepG-2 cell proliferation was detected by the MTT assay. The expression of IκB, p65, cyclin D1, caspase-3, and bcl-2 in the cells after a 48-h treatment was assayed by western blot analysis. MyD88 expression in the HCC tissue was significantly higher than that in the adjacent normal tissue (P < 0.05). The proliferation and apoptosis rates of control HCC cells displayed no significant differences compared with those of the blank group (P > 0.05). Compared with the control, ST2825 significantly inhibited the proliferation of and promoted the apoptosis of HCC cells. Moreover,
2 Y. Deng et al. 2 ST2825 significantly decreased bcl-2 expression, increased cleaved caspase-3 expression (P < 0.05), and reduced p65 nuclear expression (P < 0.05) in a dose-dependent manner. ST2825 inhibits the proliferation of and promotes the apoptosis of HCC cells, thereby suggesting that ST2825 may be a new drug for HCC treatment. Key words: Hepatocellular carcinoma; ST2825; Apoptosis; Proliferation INTRODUCTION Hepatocellular carcinoma (HCC) is the fifth most common malignancy worldwide, with a high rate of mortality and poor prognosis. Currently, combined therapy with surgery, chemotherapy, radiation therapy, and biological therapy is used for the clinical treatment of HCC (Rasool et al., 2014). However, the majority of HCC patients are diagnosed with middle-advanced cancer, a stage in which the best opportunity for surgical treatment has passed. Additionally, owing to its insensitivity to conventional radiotherapy and chemotherapy regimens, HCC recurs easily after surgery (Bruix et al., 2014). Thus, the development of new chemotherapeutic drugs with high efficiency and few side effects is of great importance in the treatment of HCC. Myeloid differentiation factor 88 (MyD88) plays a key role in the development, progression, and invasion of HCC (Liang et al., 2013; Jia et al., 2014), and ST2825 is a specific inhibitor of MyD88 (Van Tassell et al., 2011). In this study, we investigated the effect of ST2825 on the proliferation and apoptosis of HCC cells to provide a new approach for the clinical treatment of HCC. MATERIAL AND METHODS General information We recruited 80 patients with HCC who received surgical treatment in our hospital from October 2010 to May Postoperative diagnosis was jointly made by three experienced pathologists. The study was approved by our hospital Ethics Committee, and all patients signed a written informed consent form prior to surgery. Immunohistochemical staining Tissue specimens were immersed in neutral formalin, embedded in paraffin, and cut into 4-µm sections for immunohistochemical staining. The tissue sections were dried in an oven at 70 C for 30 min followed by overnight incubation at 56 C. The dried sections were dewaxed in xylene twice (5 min each time) and dehydrated with a gradient of ethanol (75, 85, 95, and 100%). After being rinsed with tap water, the sections were washed with phosphate-buffered saline (PBS) on a shaker twice (10 min each time). Antigen retrieval was performed using antigen retrieval buffer, and the sections were blocked with normal goat serum blocking solution for 1 h at room temperature. After the blocking solution was discarded, MyD88 antibody dilution solution was immediately added, and the sections were incubated in a 37 C incubator for 2 h. The sections were then washed thoroughly with PBS and incubated with a secondary antibody for 1 h. The sections were washed again with PBS and incubated with horseradish peroxidase-conjugated streptavidin for 15 min. After washing with PBS, a color reaction was performed by adding dinitrobenzidine, and hematoxylin
3 Effect of ST2825 on HCC 3 was used to double-stain the nucleus for 1 min. The sections were subsequently dehydrated with an ethanol gradient, clarified with xylene, mounted with neutral resin, and then observed by microscopy. The negative control was prepared with PBS substituting for the primary antibodies. Interpretation of the immunohistochemical staining results and the scoring criteria were performed as previously described (Liang et al., 2013; Bruix et al., 2014): MyD88-positive cells were recognized upon the observation of brown-yellowish precipitate, and the results were independently interpreted by two experienced pathologists. Each section was examined in 15 fields of view at high magnification (400X) using a double-blind method. The average number of MyD88- positive cells in 100 cells was obtained as the percentage of positive cells. The positive immunohistochemical staining results (appearance of brown-yellowish particles in the nucleus or cytoplasm) were interpreted according to the literature (Jia et al., 2014) based on the following two aspects: 1) percentage of positive cells characterized as <1% for 0 points, 1-10% for 1 point, 10-30% for 2 points, 30-60% for 3 points, and >60% for 4 points; and 2) staining intensity of positive cells characterized as negative for 0 points, yellowish for 1 point, yellow for 2 points, and brown-yellowish for 3 points. The results were determined as follows: 0-2 points for negative and 3-7 points for positive. Cells and reagents The human HCC cell line (HepG-2) was provided by the Shanghai Institute of Biochemistry and Cell Biology at the Chinese Academy of Sciences. RPMI 1640 medium was purchased from Gibco (USA). MTT (M2128) was purchased from Sigma (USA). The Annexin V-FITC Apoptosis Detection Kit was purchased from BD Biosciences (USA). Total cellular protein (P0013), nuclear/plasma protein extraction reagent (P0028), and ECL reagent (P0018) were purchased from Beyotime (Shanghai, China). The bcl-2, H3, cyclin D1, p65 (sc-109), H3 (sc-8654) and β-actin (sc-7210) primary antibodies were purchased from Santa Cruz (USA). The cleaved caspase-3 antibody was purchased from Cell Signaling (USA). The horseradish peroxidase-conjugated rabbit anti-mouse IgG secondary antibody (sc-2020) was purchased from Bioworld. ST2825 was purchased from MedChem Express. HCC HepG-2 cell culture The HepG-2 HCC cell line was restored and seeded in culture flasks containing RPMI 1640 medium supplemented with 10% fetal bovine serum. The cells were incubated at 37 C in a humidified 5% CO 2 incubator. Cells were passaged once every 2 to 3 days, and logarithmic growth phase cells were collected for drug intervention. Drug treatment and grouping Cells were seeded on 96-well plates at 1 x 10 4 cells per well with 29 replicate wells for each group. Culture medium (100 µl) was added to each well. The experiment was performed with the following five groups: blank (no intervention), control (1% DMSO), low-dose ST2825 (2 µm), medium-dose ST2825 (10 µm), and high-dose ST2825 (20 µm). The final concentration of ST2825 was controlled at 1% for the three treatment groups. Annexin V-FITC apoptosis assay Cells were collected after 24, 48, and 72 h of treatment. HepG-2 cell apoptosis was assayed by flow cytometry following the manufacturer protocol.
4 Y. Deng et al. 4 MTT colorimetric assay of cell proliferation Plates added with drug were placed in a humidified 37 C, 5% CO 2 cell culture incubator for 24, 48, or 72 h of continuous culture. To each well, 20 µl MTT solution was added 4 h before termination of culture. After termination of culture, the supernatant was completely removed from each well by suction followed by the addition of 150 µl DMSO per well and oscillation for 10 min. The absorbance of the reaction solution in each well at 570 nm was measured using an ELISA reader. The results are reported as means of six replicate wells. The inhibition rate of cell proliferation in each group was calculated as follows: inhibition rate = (1 - OD treatment / OD blank ) x 100%; where OD is the absorbance at 570 nm. Western blot assay of p65, cyclin D1, bcl-2, and cleaved caspase-3 expression After 48 h of treatment, the HepG-2 cells in the ST2825 and control groups were washed twice with PBS and centrifuged at 12,000 g for 15 min. Total and nuclear proteins were extracted from cells using the corresponding extraction reagent in accordance with manufacturer protocol. Nuclear protein was used for the p65 assay with H3 as the internal control, and total protein was used for the cyclin D1, caspase-3, and bcl-2 expression assays. Protein quantification was performed using the bicinchoninic acid method. Protein samples (30 µg each) were electrophoresed, transferred to a membrane, and blocked with 5% nonfat milk for 1 h. H3, p65, cyclin D1, β-actin, cleaved caspase-3, and bcl-2 antibodies were diluted with 5% milk (1:200) and incubated with the membrane at 4 C overnight. After being washed with TBST, the membrane was incubated with horseradish peroxidase-conjugated rabbit anti-goat secondary antibody diluted in 5% milk. A 1:1 chemiluminescent working solution was prepared according to the ECL instructions. Gel images were acquired using a gel imaging system, and densitometry was performed using the Image J software. Statistical analysis Statistical analysis was performed using SPSS Version Quantitative data are reported as means ± SD. Comparison of the means between groups was performed using one-way ANOVA. The difference was considered significant at P < RESULTS MyD88 expression in HCC and adjacent normal tissues The number of MyD88-positive cells was higher in HCC tissues than that in adjacent normal tissues, showing a statistically significant difference between groups (P < 0.05; Figure 1 and Table 1). Effect of ST2825 on HepG-2 cell proliferation The inhibition rate of HepG-2 cell proliferation did not significantly differ between the control and blank groups (P > 0.05; Table 2). Compared with the control, ST2825 significantly inhibited HepG2 cell proliferation (P < 0.05; Table 2) in a time- and dose-dependent manner. The inhibition rate remained significantly higher in the high-dose ST2825 group than that in the low-dose group (P < 0.05; Table 2).
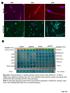
5 Effect of ST2825 on HCC 5 Figure 1. MyD88 expression in hepatocellular carcinoma and adjacent normal tissues. Table 1. MyD88 expression in hepatocellular carcinoma and adjacent normal tissues N MyD88 expression Group Positive cases (%) Negative cases (%) Hepatocellular carcinoma (62.5) 30 (37.5) Adjacent normal tissues (12.5) 70 (87.5) χ 2 P <0.05 Table 2. Effect of ST2825 on HepG-2 cell proliferation (means ± SD). Group N 0 h 24 h 48 h 72 h Blank Control ± ± ± ± 0.02 Low-dose ST ± ± 3.2 # * 10.1 ± 2.1 # * 24.6 ± 2.6 # * Medium-dose ST ± ± 3.9 # * 27.2 ± 3.1 # * 32.5 ± 3.5 # * High-dose ST ± ± 5.6 # * 58.3 ± 7.2 # * 63.2 ± 8.6 # * *P < 0.05, compared with the blank group; # P < 0.05, compared with the low- and medium-dose groups. Effect of ST2825 on HepG-2 cell apoptosis The apoptotic rate of HepG-2 cells did not change significantly between the blank and control groups (P > 0.05). Compared with the control, 24 and 48 h of ST2825 treatment significantly increased the rate of HepG-2 cell apoptosis (P < 0.05) in a dose-dependent manner. The apoptotic rate of HepG-2 cells in the high-dose ST2825 group was significantly higher than that in the lowdose group (P < 0.05; Table 3). Table 3. Effect of ST2825 on HepG-2 cell apoptotic rate (%). Group N 0 h 24 h 48 h 72 h Blank ± ± ± ± 0.15 Control ± ± ± ± 0.16 Low-dose ST ± ± ± ± 1.23 # * Medium-dose ST ± ± 1.01 # * 8.9 ± 1.35 # * 10.2 ± 1.79 # * High-dose ST ± # * 10.6 ± 1.42 # * ± 2.31 # * 16.9 ± 2.91 # * *P < 0.05, compared with the blank group; # P < 0.05, compared with the low- and medium-dose groups. Effect of ST2825 on IκB expression and p65 nuclear expression in HepG-2 cells Compared with the control, 24 h of ST2825 intervention significantly increased IκB (Figure 2) expression in HepG-2 cells in a dose-dependent manner (P > 0.05). Moreover, ST2825 signifi-
6 Y. Deng et al. 6 cantly inhibited p65 (Figure 3) expression in the nucleus in a dose-dependent manner (P < 0.05; Figures 2, 3 and Table 4). Figure 2. Effect of ST2825 on IκB, cyclin D1, cleaved caspase-3, and bcl-2 expression in HepG-2 cells as determined by western blot analysis (lane 1, blank; lane 2, control; and lane 3, high-dose ST2825). Figure 3. Effect of ST2825 on p65 expression in HepG-2 cells as determined by western blot analysis (lane 1, blank; lane 2, control; and lane 3, high-dose ST2825). Table 4. Densitometry of the western blot of IκB, p65, cyclin D1, bcl-2, and cleaved caspase-3 expression in HepG-2 cells. Group I B p65 Cyclin D1 Bcl-2 Cleaved caspase-3 Blank 0.92 ± ± ± ± ± 0.04 Control 0.09 ± ± ± ± ± 0.12 High-dose ST ± 0.26 # * 0.34 ± 0.11 # * 0.19 ± 0.09 # * 0.21 ± 0.09 # * 0.96 ± 0.29 # * *P < 0.05, compared with the blank group; # P < 0.05, compared with the control group. Effect of ST2825 on IκB, cyclin D1, cleaved caspase-3, and bcl-2 expression in HepG-2 cells Compared with the control, 24 h of ST2825 treatment significantly inhibited cyclin D1 and bcl-2 expression (P > 0.05; Figure 2 and Table 4), but 24-h treatment with ST2825 significantly increased cleaved caspase-3 expression (P < 0.05; Figure 2 and Table 4) in the high-dose group.
7 Effect of ST2825 on HCC 7 The solvent did not affect cyclin D1, cleaved caspase-3, and bcl-2 expression in control HepG-2 cells compared with that observed for the blank group (P < 0.05; Figure 2 and Table 4). DISCUSSION MyD88 is a member of the Toll/IL-1R family and death domain family, which has a pivotal role in regulating the transduction of the NF-κB signaling pathway (Wang et al., 2014). MyD88 is essentially a soluble cytoplasmic protein containing three functional domains: an N-terminal death domain of 90-amino acid residues that mainly mediates the interaction between death sequencecontaining proteins; an intermediate region; and a C-terminal Toll region of 130-amino acid residues that mainly transfers signals by recruiting connexin. The death domain of MyD88 can bind to the death domain of interleukin-1 receptor-associated kinase, causing the autophosphorylation of the kinase. Ultimately, this binding will induce IκB activation through a series of activation reactions leading to NF-κB activation and translocation. Previous studies have found that the NF-κB signaling pathway has a role in the development and progression of HCC. NF-κB activity is significantly increased in human HCC tissue (Qiao et al., 2006), and the inhibition of NF-κB expression substantially suppresses the proliferation and promotes the apoptosis of HCC cells (Wu et al., 2009). Moreover, many studies have indicated that MyD88 has an important role in the development, progression, invasion, and metastasis of a variety of tumors (Kfoury et al., 2014). The results obtained from the present study showed that the MyD88 expression level in HCC tissue was significantly higher than in adjacent normal tissue, which is consistent with the results of previous studies. Additionally, MyD88 is closely related to the clinical stage of HCC patients. The downregulation of MyD88 expression significantly inhibits the proliferation and promotes the apoptosis of HCC cells. (Liang et al., 2013). Together, these results suggest that MyD88 is an important component in the proliferation and apoptosis of HCC cells, and may therefore be an attractive new treatment target in HCC. ST2825 is a small-molecule compound consisting of a halogenated heptapeptide (Hinz et al., 1999; Loiarro et al., 2007), and it competitively binds to the Toll/IL-1 receptor domain of MyD88 to inhibit MyD88 dimerization. This mechanism prevents MyD88 from activation and TLR signal transduction, thereby blocking the transduction of the TLR signaling pathway. The present study found that ST2825, a selective inhibitor of MyD88, significantly inhibited cell proliferation and promoted apoptosis in the human HCC cell line HepG-2 in a dose-dependent manner. Thus, we used high-dose ST2825 to probe the underlying mechanism. The results showed that ST2825 significantly inhibited the translocation of p65 to the nucleus, thus inhibiting the transcription, translation and expression of the NF-κB-mediated downstream factor cyclin D1. Cyclin D1 is an important component in HCC cell proliferation (Deane et al., 2001), which may be the main reason why ST2825 can inhibit HCC cell proliferation. Additionally, ST2825 significantly increased cleaved caspase-3 protein expression but decreased the protein expression of bcl-2, an anti-apoptotic protein, in HCC cells, which may be one of the reasons why ST2825 can promote apoptosis in HCC cells. In summary, ST2825, a selective inhibitor of MyD88, significantly inhibits the proliferation and promotes the apoptosis of HCC cells. The possible mechanism is related to the inhibition of the NF-κB signaling pathway activity. The effect of ST2825 needs to be tested in animal models to provide evidence for its application in the clinical treatment of HCC. Conflicts of interest The authors declare no conflict of interest.
8 Y. Deng et al. 8 ACKNOWLEDGMENTS We would like to acknowledge the reviewers for their helpful comments on this paper. REFERENCES Bruix J, Gores GJ and Mazzaferro V (2014). Hepatocellular carcinoma: clinical frontiers and perspectives. Gut 63: Deane NG, Parker MA, Aramandla R, Diehl L, et al. (2001). Hepatocellular carcinoma results from chronic cyclin D1 overexpression in transgenic mice. Cancer Res. 61: Hinz M, Krappmann D, Eichten A, Heder A, et al. (1999). NF-kappaB function in growth control: regulation of cyclin D1 expression and G0/G1-to-S-phase transition. Mol. Cell. Biol. 19: Jia RJ, Cao L, Zhang L, Jing W, et al. (2014). Enhanced myeloid differentiation factor 88 promotes tumor metastasis via induction of epithelial-mesenchymal transition in human hepatocellular carcinoma. Cell Death Dis. 5: e org/ /cddis Kfoury A, Virard F, Renno T and Coste I (2014). Dual function of MyD88 in inflammation and oncogenesis: implications for therapeutic intervention. Curr. Opin. Oncol. 26: Liang B, Chen R, Wang T, Cao L, et al. (2013). Myeloid differentiation factor 88 promotes growth and metastasis of human hepatocellular carcinoma. Clin. Cancer Res. 19: Loiarro M, Capolunghi F, Fantò N, Gallo G, et al. (2007). Pivotal Advance: Inhibition of MyD88 dimerization and recruitment of IRAK1 and IRAK4 by a novel peptidomimetic compound. J. Leukoc. Biol. 82: jlb Qiao L, Zhang H, Yu J, Francisco R, et al. (2006). Constitutive activation of NF-kappaB in human hepatocellular carcinoma: evidence of a cytoprotective role. Hum. Gene Ther. 17: Rasool M, Rashid S, Arooj M, Ansari SA, et al. (2014). New possibilities in hepatocellular carcinoma treatment. Anticancer Res. 34: Van Tassell BW, Seropian IM, Toldo S, Salloum FN, et al. (2011). Pharmacologic inhibition of myeloid differentiation factor 88 (MyD88) prevents left ventricular dilation and hypertrophy after experimental acute myocardial infarction in the mouse. J. Cardiovasc. Pharmacol. 57: PubMed Wang JQ, Jeelall YS, Ferguson LL and Horikawa K (2014). Toll-Like Receptors and Cancer: MYD88 Mutation and Inflammation. Front. Immunol. 5: Wu JM, Sheng H, Saxena R, Skill NJ, et al. (2009). NF-kappaB inhibition in human hepatocellular carcinoma and its potential as adjunct to sorafenib based therapy. Cancer Lett. 278:
Study on the expression of MMP-9 and NF-κB proteins in epithelial ovarian cancer tissue and their clinical value
 Study on the expression of MMP-9 and NF-κB proteins in epithelial ovarian cancer tissue and their clinical value Shen Wei 1,a, Chen Juan 2, Li Xiurong 1 and Yin Jie 1 1 Department of Obstetrics and Gynecology,
Study on the expression of MMP-9 and NF-κB proteins in epithelial ovarian cancer tissue and their clinical value Shen Wei 1,a, Chen Juan 2, Li Xiurong 1 and Yin Jie 1 1 Department of Obstetrics and Gynecology,
An analysis of the expression and function of myeloid differentiation factor 88 in human osteosarcoma
 ONCOLOGY LETTERS An analysis of the expression and function of myeloid differentiation factor 88 in human osteosarcoma JUN CHEN 1*, JIAN HE 1*, YUE YANG 2* and JIANNONG JIANG 1 1 Department of Orthopedics,
ONCOLOGY LETTERS An analysis of the expression and function of myeloid differentiation factor 88 in human osteosarcoma JUN CHEN 1*, JIAN HE 1*, YUE YANG 2* and JIANNONG JIANG 1 1 Department of Orthopedics,
EXOTESTTM. ELISA assay for exosome capture, quantification and characterization from cell culture supernatants and biological fluids
 DATA SHEET EXOTESTTM ELISA assay for exosome capture, quantification and characterization from cell culture supernatants and biological fluids INTRODUCTION Exosomes are small endosome-derived lipid nanoparticles
DATA SHEET EXOTESTTM ELISA assay for exosome capture, quantification and characterization from cell culture supernatants and biological fluids INTRODUCTION Exosomes are small endosome-derived lipid nanoparticles
Characterization and significance of MUC1 and c-myc expression in elderly patients with papillary thyroid carcinoma
 Characterization and significance of MUC1 and c-myc expression in elderly patients with papillary thyroid carcinoma Y.-J. Hu 1, X.-Y. Luo 2, Y. Yang 3, C.-Y. Chen 1, Z.-Y. Zhang 4 and X. Guo 1 1 Department
Characterization and significance of MUC1 and c-myc expression in elderly patients with papillary thyroid carcinoma Y.-J. Hu 1, X.-Y. Luo 2, Y. Yang 3, C.-Y. Chen 1, Z.-Y. Zhang 4 and X. Guo 1 1 Department
Chemical Chaperones Mitigate Experimental Asthma By Attenuating Endoplasmic
 Chemical Chaperones Mitigate Experimental Asthma By Attenuating Endoplasmic Reticulum Stress Lokesh Makhija, BE, Veda Krishnan, MSc, Rakhshinda Rehman, MTech, Samarpana Chakraborty, MSc, Shuvadeep Maity,
Chemical Chaperones Mitigate Experimental Asthma By Attenuating Endoplasmic Reticulum Stress Lokesh Makhija, BE, Veda Krishnan, MSc, Rakhshinda Rehman, MTech, Samarpana Chakraborty, MSc, Shuvadeep Maity,
Expression and clinical significance of Kelch-like epichlorohydrin-associated protein 1 in breast cancer
 Expression and clinical significance of Kelch-like epichlorohydrin-associated protein 1 in breast cancer L. Zhang*, W.P. Yang*, L.Y. Wu, X. Zhu and C.Y. Wei Department of Breast Surgery, Affiliated Tumor
Expression and clinical significance of Kelch-like epichlorohydrin-associated protein 1 in breast cancer L. Zhang*, W.P. Yang*, L.Y. Wu, X. Zhu and C.Y. Wei Department of Breast Surgery, Affiliated Tumor
Advances in Computer Science Research, volume 59 7th International Conference on Education, Management, Computer and Medicine (EMCM 2016)
 7th International Conference on Education, Management, Computer and Medicine (EMCM 2016) Expression of Beta-Adrenergic Receptor in Glioma LN229 Cells and Its Effect on Cell Proliferation Ping Wang1, Qingluan
7th International Conference on Education, Management, Computer and Medicine (EMCM 2016) Expression of Beta-Adrenergic Receptor in Glioma LN229 Cells and Its Effect on Cell Proliferation Ping Wang1, Qingluan
Cell Culture. The human thyroid follicular carcinoma cell lines FTC-238, FTC-236 and FTC-
 Supplemental material and methods Reagents. Hydralazine was purchased from Sigma-Aldrich. Cell Culture. The human thyroid follicular carcinoma cell lines FTC-238, FTC-236 and FTC- 133, human thyroid medullary
Supplemental material and methods Reagents. Hydralazine was purchased from Sigma-Aldrich. Cell Culture. The human thyroid follicular carcinoma cell lines FTC-238, FTC-236 and FTC- 133, human thyroid medullary
Lecithin Cholesterol Acyltransferase (LCAT) ELISA Kit
 Product Manual Lecithin Cholesterol Acyltransferase (LCAT) ELISA Kit Catalog Number STA-616 96 assays FOR RESEARCH USE ONLY Not for use in diagnostic procedures Introduction Cholesterol is a lipid sterol
Product Manual Lecithin Cholesterol Acyltransferase (LCAT) ELISA Kit Catalog Number STA-616 96 assays FOR RESEARCH USE ONLY Not for use in diagnostic procedures Introduction Cholesterol is a lipid sterol
HCC1937 is the HCC1937-pcDNA3 cell line, which was derived from a breast cancer with a mutation
 SUPPLEMENTARY INFORMATION Materials and Methods Human cell lines and culture conditions HCC1937 is the HCC1937-pcDNA3 cell line, which was derived from a breast cancer with a mutation in exon 20 of BRCA1
SUPPLEMENTARY INFORMATION Materials and Methods Human cell lines and culture conditions HCC1937 is the HCC1937-pcDNA3 cell line, which was derived from a breast cancer with a mutation in exon 20 of BRCA1
Supporting Information
 Supporting Information Pang et al. 10.1073/pnas.1322009111 SI Materials and Methods ELISAs. These assays were performed as previously described (1). ELISA plates (MaxiSorp Nunc; Thermo Fisher Scientific)
Supporting Information Pang et al. 10.1073/pnas.1322009111 SI Materials and Methods ELISAs. These assays were performed as previously described (1). ELISA plates (MaxiSorp Nunc; Thermo Fisher Scientific)
Annals of Oncology Advance Access published January 10, 2005
 Annals of Oncology Advance Access published January 10, 2005 Original article Annals of Oncology doi:10.1093/annonc/mdi077 Expression of survivin and bax/bcl-2 in peroxisome proliferator activated receptor-g
Annals of Oncology Advance Access published January 10, 2005 Original article Annals of Oncology doi:10.1093/annonc/mdi077 Expression of survivin and bax/bcl-2 in peroxisome proliferator activated receptor-g
B16-F10 (Mus musculus skin melanoma), NCI-H460 (human non-small cell lung cancer
 Electronic Supplementary Material (ESI) for ChemComm. This journal is The Royal Society of Chemistry 2017 Experimental Methods Cell culture B16-F10 (Mus musculus skin melanoma), NCI-H460 (human non-small
Electronic Supplementary Material (ESI) for ChemComm. This journal is The Royal Society of Chemistry 2017 Experimental Methods Cell culture B16-F10 (Mus musculus skin melanoma), NCI-H460 (human non-small
SUPPLEMENTARY INFORMATION
 SUPPLEMENTARY INFORMATION FOR Liver X Receptor α mediates hepatic triglyceride accumulation through upregulation of G0/G1 Switch Gene 2 (G0S2) expression I: SUPPLEMENTARY METHODS II: SUPPLEMENTARY FIGURES
SUPPLEMENTARY INFORMATION FOR Liver X Receptor α mediates hepatic triglyceride accumulation through upregulation of G0/G1 Switch Gene 2 (G0S2) expression I: SUPPLEMENTARY METHODS II: SUPPLEMENTARY FIGURES
Impact factor: Reporter:4A1H0019 Chen Zi Hao 4A1H0023 Huang Wan ting 4A1H0039 Sue Yi Zhu 4A1H0070 Lin Guan cheng 4A1H0077 Chen Bo xuan
 Curcumin Protects Neonatal Rat Cardiomyocytes against High Glucose-Induced Apoptosis via PI3K/Akt Signalling Pathway Wei Yu,1,2 Wenliang Zha,1 Zhiqiang Ke,1 Qing Min,2 Cairong Li,1 Huirong Sun,3 and Chao
Curcumin Protects Neonatal Rat Cardiomyocytes against High Glucose-Induced Apoptosis via PI3K/Akt Signalling Pathway Wei Yu,1,2 Wenliang Zha,1 Zhiqiang Ke,1 Qing Min,2 Cairong Li,1 Huirong Sun,3 and Chao
Supplementary Materials and Methods
 Supplementary Materials and Methods Immunoblotting Immunoblot analysis was performed as described previously (1). Due to high-molecular weight of MUC4 (~ 950 kda) and MUC1 (~ 250 kda) proteins, electrophoresis
Supplementary Materials and Methods Immunoblotting Immunoblot analysis was performed as described previously (1). Due to high-molecular weight of MUC4 (~ 950 kda) and MUC1 (~ 250 kda) proteins, electrophoresis
Protocol for Gene Transfection & Western Blotting
 The schedule and the manual of basic techniques for cell culture Advanced Protocol for Gene Transfection & Western Blotting Schedule Day 1 26/07/2008 Transfection Day 3 28/07/2008 Cell lysis Immunoprecipitation
The schedule and the manual of basic techniques for cell culture Advanced Protocol for Gene Transfection & Western Blotting Schedule Day 1 26/07/2008 Transfection Day 3 28/07/2008 Cell lysis Immunoprecipitation
The Schedule and the Manual of Basic Techniques for Cell Culture
 The Schedule and the Manual of Basic Techniques for Cell Culture 1 Materials Calcium Phosphate Transfection Kit: Invitrogen Cat.No.K2780-01 Falcon tube (Cat No.35-2054:12 x 75 mm, 5 ml tube) Cell: 293
The Schedule and the Manual of Basic Techniques for Cell Culture 1 Materials Calcium Phosphate Transfection Kit: Invitrogen Cat.No.K2780-01 Falcon tube (Cat No.35-2054:12 x 75 mm, 5 ml tube) Cell: 293
Caspase-3 Assay Cat. No. 8228, 100 tests. Introduction
 Introduction Caspase-3 Assay Cat. No. 8228, 100 tests Caspase-3 is a member of caspases that plays a key role in mediating apoptosis, or programmed cell death. Upon activation, it cleaves a variety of
Introduction Caspase-3 Assay Cat. No. 8228, 100 tests Caspase-3 is a member of caspases that plays a key role in mediating apoptosis, or programmed cell death. Upon activation, it cleaves a variety of
PUMA gene transfection can enhance the sensitivity of epirubicin-induced apoptosis of MCF-7 breast cancer cells
 PUMA gene transfection can enhance the sensitivity of epirubicin-induced apoptosis of MCF-7 breast cancer cells C.-G. Sun 1 *, J. Zhuang 1 *, W.-J. Teng 1, Z. Wang 2 and S.-S. Du 3 1 Department of Oncology,
PUMA gene transfection can enhance the sensitivity of epirubicin-induced apoptosis of MCF-7 breast cancer cells C.-G. Sun 1 *, J. Zhuang 1 *, W.-J. Teng 1, Z. Wang 2 and S.-S. Du 3 1 Department of Oncology,
Biodegradable Zwitterionic Nanogels with Long. Circulation for Antitumor Drug Delivery
 Supporting Information Biodegradable Zwitterionic Nanogels with Long Circulation for Antitumor Drug Delivery Yongzhi Men, Shaojun Peng, Peng Yang, Qin Jiang, Yanhui Zhang, Bin Shen, Pin Dong, *, Zhiqing
Supporting Information Biodegradable Zwitterionic Nanogels with Long Circulation for Antitumor Drug Delivery Yongzhi Men, Shaojun Peng, Peng Yang, Qin Jiang, Yanhui Zhang, Bin Shen, Pin Dong, *, Zhiqing
NF-κB p65 (Phospho-Thr254)
 Assay Biotechnology Company www.assaybiotech.com Tel: 1-877-883-7988 Fax: 1-877-610-9758 NF-κB p65 (Phospho-Thr254) Colorimetric Cell-Based ELISA Kit Catalog #: OKAG02015 Please read the provided manual
Assay Biotechnology Company www.assaybiotech.com Tel: 1-877-883-7988 Fax: 1-877-610-9758 NF-κB p65 (Phospho-Thr254) Colorimetric Cell-Based ELISA Kit Catalog #: OKAG02015 Please read the provided manual
Islet viability assay and Glucose Stimulated Insulin Secretion assay RT-PCR and Western Blot
 Islet viability assay and Glucose Stimulated Insulin Secretion assay Islet cell viability was determined by colorimetric (3-(4,5-dimethylthiazol-2-yl)-2,5- diphenyltetrazolium bromide assay using CellTiter
Islet viability assay and Glucose Stimulated Insulin Secretion assay Islet cell viability was determined by colorimetric (3-(4,5-dimethylthiazol-2-yl)-2,5- diphenyltetrazolium bromide assay using CellTiter
Supplementary data Supplementary Figure 1 Supplementary Figure 2
 Supplementary data Supplementary Figure 1 SPHK1 sirna increases RANKL-induced osteoclastogenesis in RAW264.7 cell culture. (A) RAW264.7 cells were transfected with oligocassettes containing SPHK1 sirna
Supplementary data Supplementary Figure 1 SPHK1 sirna increases RANKL-induced osteoclastogenesis in RAW264.7 cell culture. (A) RAW264.7 cells were transfected with oligocassettes containing SPHK1 sirna
Research on the inhibitory effect of metformin on human oral squamous cell carcinoma SCC-4 and CAL-27 cells and the relevant molecular mechanism.
 Biomedical Research 2017; 28 (14): 6350-6354 ISSN 0970-938X www.biomedres.info Research on the inhibitory effect of metformin on human oral squamous cell carcinoma SCC-4 and CAL-27 cells and the relevant
Biomedical Research 2017; 28 (14): 6350-6354 ISSN 0970-938X www.biomedres.info Research on the inhibitory effect of metformin on human oral squamous cell carcinoma SCC-4 and CAL-27 cells and the relevant
The expression and significance of tumor associated macrophages and CXCR4 in non-small cell lung cancer
 JBUON 2018; 23(2): 398-402 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE The expression and significance of tumor associated macrophages and
JBUON 2018; 23(2): 398-402 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE The expression and significance of tumor associated macrophages and
Exosome ELISA Complete Kits
 Exosome ELISA Complete Kits EXOEL-CD9A-1, EXOEL-CD63A-1, EXOEL-CD81A-1 User Manual See PAC for Storage Conditions for Individual Components Version 12 4/17/2017 A limited-use label license covers this
Exosome ELISA Complete Kits EXOEL-CD9A-1, EXOEL-CD63A-1, EXOEL-CD81A-1 User Manual See PAC for Storage Conditions for Individual Components Version 12 4/17/2017 A limited-use label license covers this
Correlation between expression and significance of δ-catenin, CD31, and VEGF of non-small cell lung cancer
 Correlation between expression and significance of δ-catenin, CD31, and VEGF of non-small cell lung cancer X.L. Liu 1, L.D. Liu 2, S.G. Zhang 1, S.D. Dai 3, W.Y. Li 1 and L. Zhang 1 1 Thoracic Surgery,
Correlation between expression and significance of δ-catenin, CD31, and VEGF of non-small cell lung cancer X.L. Liu 1, L.D. Liu 2, S.G. Zhang 1, S.D. Dai 3, W.Y. Li 1 and L. Zhang 1 1 Thoracic Surgery,
Expression and clinical significance of ADAM17 protein in esophageal squamous cell carcinoma
 Expression and clinical significance of ADAM17 protein in esophageal squamous cell carcinoma H.B. Liu, Y. Zhu, Q.C. Yang, Y. Shen, X.J. Zhang and H. Chen Department of Pathology First People s Hospital
Expression and clinical significance of ADAM17 protein in esophageal squamous cell carcinoma H.B. Liu, Y. Zhu, Q.C. Yang, Y. Shen, X.J. Zhang and H. Chen Department of Pathology First People s Hospital
Exosome ELISA Complete Kits
 Exosome ELISA Complete Kits EXOEL-CD9A-1, EXOEL-CD63A-1, EXOEL-CD81A-1 User Manual See PAC for Storage Conditions for Individual Components Version 12 4/17/2017 A limited-use label license covers this
Exosome ELISA Complete Kits EXOEL-CD9A-1, EXOEL-CD63A-1, EXOEL-CD81A-1 User Manual See PAC for Storage Conditions for Individual Components Version 12 4/17/2017 A limited-use label license covers this
The effect of insulin on chemotherapeutic drug sensitivity in human esophageal and lung cancer cells
 The effect of insulin on chemotherapeutic drug sensitivity in human esophageal and lung cancer cells Published in: Natl Med J China, February 10, 2003; Vol 83, No 3, Page 195-197. Authors: JIAO Shun-Chang,
The effect of insulin on chemotherapeutic drug sensitivity in human esophageal and lung cancer cells Published in: Natl Med J China, February 10, 2003; Vol 83, No 3, Page 195-197. Authors: JIAO Shun-Chang,
Comparison of Young and Old Cardiac Telocytes Using Atomic Force Microscopy
 Comparison of Young and Old Cardiac Telocytes Using Atomic Force Microscopy Jiali Luo 1, 2, 3, 4, a, Shanshan Feng 1, 2, 3, 4, b 1Key Laboratory of Regenerative Medicine, Ministry of Education, Jinan University,
Comparison of Young and Old Cardiac Telocytes Using Atomic Force Microscopy Jiali Luo 1, 2, 3, 4, a, Shanshan Feng 1, 2, 3, 4, b 1Key Laboratory of Regenerative Medicine, Ministry of Education, Jinan University,
EPIGENTEK. EpiQuik HDAC2 Assay Kit (Colorimetric) Base Catalog # P-4006 PLEASE READ THIS ENTIRE USER GUIDE BEFORE USE
 EpiQuik HDAC2 Assay Kit (Colorimetric) Base Catalog # PLEASE READ THIS ENTIRE USER GUIDE BEFORE USE The EpiQuik HDAC2 Assay Kit is very suitable for measuring HDAC2 levels from various fresh tissues and
EpiQuik HDAC2 Assay Kit (Colorimetric) Base Catalog # PLEASE READ THIS ENTIRE USER GUIDE BEFORE USE The EpiQuik HDAC2 Assay Kit is very suitable for measuring HDAC2 levels from various fresh tissues and
Effects of AFP gene silencing on Survivin mrna expression inhibition in HepG2 cells
 mrna expression inhibition in HepG2 cells Z.L. Fang 1, N. Fang 2, X.N. Han 3, G. Huang 2, X.J. Fu 2, G.S. Xie 2, N.R. Wang 2 and J.P. Xiong 1 1 Department of Medical Oncology, The First Affiliated Hospital
mrna expression inhibition in HepG2 cells Z.L. Fang 1, N. Fang 2, X.N. Han 3, G. Huang 2, X.J. Fu 2, G.S. Xie 2, N.R. Wang 2 and J.P. Xiong 1 1 Department of Medical Oncology, The First Affiliated Hospital
Human Urokinase / PLAU / UPA ELISA Pair Set
 Human Urokinase / PLAU / UPA ELISA Pair Set Catalog Number : SEK10815 To achieve the best assay results, this manual must be read carefully before using this product and the assay is run as summarized
Human Urokinase / PLAU / UPA ELISA Pair Set Catalog Number : SEK10815 To achieve the best assay results, this manual must be read carefully before using this product and the assay is run as summarized
Rat Leptin-HS ELISA FOR LABORATORY USE ONLY YANAIHARA INSTITUTE INC AWAKURA, FUJINOMIYA - SHI SHIZUOKA, JAPAN
 YK051 Rat Leptin-HS ELISA FOR LABORATORY USE ONLY YANAIHARA INSTITUTE INC. 2480-1 AWAKURA, FUJINOMIYA - SHI SHIZUOKA, JAPAN 418 0011 Contents Introduction 2 Characteristics 3 Composition 4 Method 5-6 Notes
YK051 Rat Leptin-HS ELISA FOR LABORATORY USE ONLY YANAIHARA INSTITUTE INC. 2480-1 AWAKURA, FUJINOMIYA - SHI SHIZUOKA, JAPAN 418 0011 Contents Introduction 2 Characteristics 3 Composition 4 Method 5-6 Notes
Data Sheet. PCSK9[Biotinylated]-LDLR Binding Assay Kit Catalog # 72002
![Data Sheet. PCSK9[Biotinylated]-LDLR Binding Assay Kit Catalog # 72002 Data Sheet. PCSK9[Biotinylated]-LDLR Binding Assay Kit Catalog # 72002](/thumbs/79/80181612.jpg) Data Sheet PCSK9[Biotinylated]-LDLR Binding Assay Kit Catalog # 72002 DESCRIPTION: The PCSK9[Biotinylated]-LDLR Binding Assay Kit is designed for screening and profiling purposes. PCSK9 is known to function
Data Sheet PCSK9[Biotinylated]-LDLR Binding Assay Kit Catalog # 72002 DESCRIPTION: The PCSK9[Biotinylated]-LDLR Binding Assay Kit is designed for screening and profiling purposes. PCSK9 is known to function
Supplementary Data 1. Alanine substitutions and position variants of APNCYGNIPL. Applied in
 Supplementary Data 1. Alanine substitutions and position variants of APNCYGNIPL. Applied in Supplementary Fig. 2 Substitution Sequence Position variant Sequence original APNCYGNIPL original APNCYGNIPL
Supplementary Data 1. Alanine substitutions and position variants of APNCYGNIPL. Applied in Supplementary Fig. 2 Substitution Sequence Position variant Sequence original APNCYGNIPL original APNCYGNIPL
[Abstract] Objective: Investigate the effect of KLT on the expression of Fas/Apo-1, FasL and PCNA genes in renal carcinoma cell line (GRC-1).
![[Abstract] Objective: Investigate the effect of KLT on the expression of Fas/Apo-1, FasL and PCNA genes in renal carcinoma cell line (GRC-1). [Abstract] Objective: Investigate the effect of KLT on the expression of Fas/Apo-1, FasL and PCNA genes in renal carcinoma cell line (GRC-1).](/thumbs/90/104150076.jpg) Study on Effect of Kanglaite Injection(KLT) on the Expression of Fas/Apo-1, FasL and PCNA in Renal Carcinoma Cell Lines Wang Junjie, Sun Xinchen, Sheng Wenjiang, Yu Lizhang [Abstract] Objective: Investigate
Study on Effect of Kanglaite Injection(KLT) on the Expression of Fas/Apo-1, FasL and PCNA in Renal Carcinoma Cell Lines Wang Junjie, Sun Xinchen, Sheng Wenjiang, Yu Lizhang [Abstract] Objective: Investigate
IMMP8-1. Different Mechanisms of Androg and IPAD on Apoptosis Induction in Cervical Cancer Cells
 IMMP8-1 Different Mechanisms of Androg and IPAD on Apoptosis Induction in Cervical Cancer Cells Assanan Dokmaikaew* Tipaya Ekalaksananan** Dr.Chamsai Pientong** ABSTRACT Androg and IPAD are recently known
IMMP8-1 Different Mechanisms of Androg and IPAD on Apoptosis Induction in Cervical Cancer Cells Assanan Dokmaikaew* Tipaya Ekalaksananan** Dr.Chamsai Pientong** ABSTRACT Androg and IPAD are recently known
Original Article Expression of RAGE and srage in adenoidal hypertrophy with secretory otitis media in children
 Int J Clin Exp Med 2016;9(5):8421-8425 www.ijcem.com /ISSN:1940-5901/IJCEM0016575 Original Article Expression of RAGE and srage in adenoidal hypertrophy with secretory otitis media in children Xi Chen,
Int J Clin Exp Med 2016;9(5):8421-8425 www.ijcem.com /ISSN:1940-5901/IJCEM0016575 Original Article Expression of RAGE and srage in adenoidal hypertrophy with secretory otitis media in children Xi Chen,
(A) PCR primers (arrows) designed to distinguish wild type (P1+P2), targeted (P1+P2) and excised (P1+P3)14-
 1 Supplemental Figure Legends Figure S1. Mammary tumors of ErbB2 KI mice with 14-3-3σ ablation have elevated ErbB2 transcript levels and cell proliferation (A) PCR primers (arrows) designed to distinguish
1 Supplemental Figure Legends Figure S1. Mammary tumors of ErbB2 KI mice with 14-3-3σ ablation have elevated ErbB2 transcript levels and cell proliferation (A) PCR primers (arrows) designed to distinguish
Supplementary Figure 1 Lymphocytes can be tracked for at least 4 weeks after
 Supplementary Figure 1 Lymphocytes can be tracked for at least 4 weeks after photoconversion by using H2B-Dendra2. 4-5 PPs of H2B-Dendra2 BM chimeras were photoconverted and analyzed 7 days (upper panel)
Supplementary Figure 1 Lymphocytes can be tracked for at least 4 weeks after photoconversion by using H2B-Dendra2. 4-5 PPs of H2B-Dendra2 BM chimeras were photoconverted and analyzed 7 days (upper panel)
Human Apolipoprotein A1 EIA Kit
 A helping hand for your research Product Manual Human Apolipoprotein A1 EIA Kit Catalog Number: 83901 96 assays 1 Table of Content Product Description 3 Assay Principle 3 Kit Components 3 Storage 4 Reagent
A helping hand for your research Product Manual Human Apolipoprotein A1 EIA Kit Catalog Number: 83901 96 assays 1 Table of Content Product Description 3 Assay Principle 3 Kit Components 3 Storage 4 Reagent
ab Hepatic Lipid Accumulation/ Steatosis Assay Kit
 ab133131 Hepatic Lipid Accumulation/ Steatosis Assay Kit Instructions for Use For evaluating steatosis risk of drug candidates using Oil Red O to stain neutral lipids in hepatocytes. This product is for
ab133131 Hepatic Lipid Accumulation/ Steatosis Assay Kit Instructions for Use For evaluating steatosis risk of drug candidates using Oil Red O to stain neutral lipids in hepatocytes. This product is for
Alcoholic hepatitis is a drug-induced disorder
 Alcoholic hepatitis is a drug-induced disorder Gyongyi Szabo, MD, PhD Professor of Medicine University of Massachusetts Medical School Source: 2 Sobernation.com Clinical Progression of ALD Mortality Acute
Alcoholic hepatitis is a drug-induced disorder Gyongyi Szabo, MD, PhD Professor of Medicine University of Massachusetts Medical School Source: 2 Sobernation.com Clinical Progression of ALD Mortality Acute
The effect of elemene reversing the multidurg resistance of A549/DDP lung cancer cells
 213 12 33 12 TUMOR Vol. 33, December 213 www.tumorsci.org 161 Basic Research DOI: 1.3781/j.issn.1-7431.213.12. 5 Copyright 213 by TUMOR A549/DDP 1, 2 2 1 3 4 1 1 1. 3619 2. 355 3. 3611 4. 361 elemene cisplatin
213 12 33 12 TUMOR Vol. 33, December 213 www.tumorsci.org 161 Basic Research DOI: 1.3781/j.issn.1-7431.213.12. 5 Copyright 213 by TUMOR A549/DDP 1, 2 2 1 3 4 1 1 1. 3619 2. 355 3. 3611 4. 361 elemene cisplatin
SensoLyte pnpp Alkaline Phosphatase Assay Kit *Colorimetric*
 SensoLyte pnpp Alkaline Phosphatase Assay Kit *Colorimetric* Catalog # 72146 Kit Size 500 Assays (96-well plate) Optimized Performance: This kit is optimized to detect alkaline phosphatase activity Enhanced
SensoLyte pnpp Alkaline Phosphatase Assay Kit *Colorimetric* Catalog # 72146 Kit Size 500 Assays (96-well plate) Optimized Performance: This kit is optimized to detect alkaline phosphatase activity Enhanced
Clinical significance of CD44 expression in children with hepatoblastoma
 Clinical significance of CD44 expression in children with hepatoblastoma H.-Y. Cai 1 *, B. Yu 1 *, Z.-C. Feng 2, X. Qi 1 and X.-J. Wei 1 1 Department of General Surgery, General Hospital of Beijing Military
Clinical significance of CD44 expression in children with hepatoblastoma H.-Y. Cai 1 *, B. Yu 1 *, Z.-C. Feng 2, X. Qi 1 and X.-J. Wei 1 1 Department of General Surgery, General Hospital of Beijing Military
Effect of starvation-induced autophagy on cell cycle of tumor cells
 [Chinese Journal of Cancer 27:8, 102-108; August 2008]; 2008 Sun Yat-Sen University Cancer Center Basic Research Paper Effect of starvation-induced autophagy on cell cycle of tumor cells Jun-Na Ge, 1 Dan
[Chinese Journal of Cancer 27:8, 102-108; August 2008]; 2008 Sun Yat-Sen University Cancer Center Basic Research Paper Effect of starvation-induced autophagy on cell cycle of tumor cells Jun-Na Ge, 1 Dan
RCD24, B7-H4 and PCNA expression and clinical significance in ovarian cancer
 JBUON 2019; 24(2): 715-719 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE RCD24, B7-H4 and PCNA expression and clinical significance in ovarian
JBUON 2019; 24(2): 715-719 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE RCD24, B7-H4 and PCNA expression and clinical significance in ovarian
Figure S1. PMVs from THP-1 cells expose phosphatidylserine and carry actin. A) Flow
 SUPPLEMENTARY DATA Supplementary Figure Legends Figure S1. PMVs from THP-1 cells expose phosphatidylserine and carry actin. A) Flow cytometry analysis of PMVs labelled with annexin-v-pe (Guava technologies)
SUPPLEMENTARY DATA Supplementary Figure Legends Figure S1. PMVs from THP-1 cells expose phosphatidylserine and carry actin. A) Flow cytometry analysis of PMVs labelled with annexin-v-pe (Guava technologies)
- 1 - Cell types Monocytes THP-1 cells Macrophages. LPS Treatment time (Hour) IL-6 level (pg/ml)
 Supplementary Table ST1: The dynamic effect of LPS on IL-6 production in monocytes and THP-1 cells after GdA treatment. Monocytes, THP-1 cells and macrophages (5x10 5 ) were incubated with 10 μg/ml of
Supplementary Table ST1: The dynamic effect of LPS on IL-6 production in monocytes and THP-1 cells after GdA treatment. Monocytes, THP-1 cells and macrophages (5x10 5 ) were incubated with 10 μg/ml of
Supplementary Information
 Supplementary Information Supplementary Figure 1. CD4 + T cell activation and lack of apoptosis after crosslinking with anti-cd3 + anti-cd28 + anti-cd160. (a) Flow cytometry of anti-cd160 (5D.10A11) binding
Supplementary Information Supplementary Figure 1. CD4 + T cell activation and lack of apoptosis after crosslinking with anti-cd3 + anti-cd28 + anti-cd160. (a) Flow cytometry of anti-cd160 (5D.10A11) binding
Instructions for Use. APO-AB Annexin V-Biotin Apoptosis Detection Kit 100 tests
 3URGXFW,QIRUPDWLRQ Sigma TACS Annexin V Apoptosis Detection Kits Instructions for Use APO-AB Annexin V-Biotin Apoptosis Detection Kit 100 tests For Research Use Only. Not for use in diagnostic procedures.
3URGXFW,QIRUPDWLRQ Sigma TACS Annexin V Apoptosis Detection Kits Instructions for Use APO-AB Annexin V-Biotin Apoptosis Detection Kit 100 tests For Research Use Only. Not for use in diagnostic procedures.
Sestrin2 and BNIP3 (Bcl-2/adenovirus E1B 19kDa-interacting. protein3) regulate autophagy and mitophagy in renal tubular cells in. acute kidney injury
 Sestrin2 and BNIP3 (Bcl-2/adenovirus E1B 19kDa-interacting protein3) regulate autophagy and mitophagy in renal tubular cells in acute kidney injury by Masayuki Ishihara 1, Madoka Urushido 2, Kazu Hamada
Sestrin2 and BNIP3 (Bcl-2/adenovirus E1B 19kDa-interacting protein3) regulate autophagy and mitophagy in renal tubular cells in acute kidney injury by Masayuki Ishihara 1, Madoka Urushido 2, Kazu Hamada
Original Article CREPT expression correlates with esophageal squamous cell carcinoma histological grade and clinical outcome
 Int J Clin Exp Pathol 2017;10(2):2030-2035 www.ijcep.com /ISSN:1936-2625/IJCEP0009456 Original Article CREPT expression correlates with esophageal squamous cell carcinoma histological grade and clinical
Int J Clin Exp Pathol 2017;10(2):2030-2035 www.ijcep.com /ISSN:1936-2625/IJCEP0009456 Original Article CREPT expression correlates with esophageal squamous cell carcinoma histological grade and clinical
TSH Receptor Monoclonal Antibody (49) Catalog Number MA3-218 Product data sheet
 Website: thermofisher.com Customer Service (US): 1 800 955 6288 ext. 1 Technical Support (US): 1 800 955 6288 ext. 441 TSH Receptor Monoclonal Antibody (49) Catalog Number MA3-218 Product data sheet Details
Website: thermofisher.com Customer Service (US): 1 800 955 6288 ext. 1 Technical Support (US): 1 800 955 6288 ext. 441 TSH Receptor Monoclonal Antibody (49) Catalog Number MA3-218 Product data sheet Details
SUPPLEMENTARY INFORMATION. Involvement of IL-21 in the epidermal hyperplasia of psoriasis
 SUPPLEMENTARY INFORMATION Involvement of IL-21 in the epidermal hyperplasia of psoriasis Roberta Caruso 1, Elisabetta Botti 2, Massimiliano Sarra 1, Maria Esposito 2, Carmine Stolfi 1, Laura Diluvio 2,
SUPPLEMENTARY INFORMATION Involvement of IL-21 in the epidermal hyperplasia of psoriasis Roberta Caruso 1, Elisabetta Botti 2, Massimiliano Sarra 1, Maria Esposito 2, Carmine Stolfi 1, Laura Diluvio 2,
Programmed necrosis, not apoptosis, is a key mediator of cell loss and DAMP-mediated inflammation in dsrna-induced retinal degeneration
 Programmed necrosis, not apoptosis, is a key mediator of cell loss and DAMP-mediated inflammation in dsrna-induced retinal degeneration The Harvard community has made this article openly available. Please
Programmed necrosis, not apoptosis, is a key mediator of cell loss and DAMP-mediated inflammation in dsrna-induced retinal degeneration The Harvard community has made this article openly available. Please
p47 negatively regulates IKK activation by inducing the lysosomal degradation of polyubiquitinated NEMO
 Supplementary Information p47 negatively regulates IKK activation by inducing the lysosomal degradation of polyubiquitinated NEMO Yuri Shibata, Masaaki Oyama, Hiroko Kozuka-Hata, Xiao Han, Yuetsu Tanaka,
Supplementary Information p47 negatively regulates IKK activation by inducing the lysosomal degradation of polyubiquitinated NEMO Yuri Shibata, Masaaki Oyama, Hiroko Kozuka-Hata, Xiao Han, Yuetsu Tanaka,
ab Adipogenesis Assay Kit (Cell-Based)
 ab133102 Adipogenesis Assay Kit (Cell-Based) Instructions for Use For the study of induction and inhibition of adipogenesis in adherent cells. This product is for research use only and is not intended
ab133102 Adipogenesis Assay Kit (Cell-Based) Instructions for Use For the study of induction and inhibition of adipogenesis in adherent cells. This product is for research use only and is not intended
Human Carbamylated LDL ELISA Kit (CBL-LDL Quantitation)
 Product Manual Human Carbamylated LDL ELISA Kit (CBL-LDL Quantitation) Catalog Number MET-5032 96 assays FOR RESEARCH USE ONLY Not for use in diagnostic procedures Introduction Lipoproteins are submicroscopic
Product Manual Human Carbamylated LDL ELISA Kit (CBL-LDL Quantitation) Catalog Number MET-5032 96 assays FOR RESEARCH USE ONLY Not for use in diagnostic procedures Introduction Lipoproteins are submicroscopic
NF-κB (p65) Transcription Factor Assay Kit
 NF-κB (p65) Transcription Factor Assay Kit Item No. 10007889 www.caymanchem.com Customer Service 800.364.9897 Technical Support 888.526.5351 1180 E. Ellsworth Rd Ann Arbor, MI USA TABLE OF CONTENTS GENERAL
NF-κB (p65) Transcription Factor Assay Kit Item No. 10007889 www.caymanchem.com Customer Service 800.364.9897 Technical Support 888.526.5351 1180 E. Ellsworth Rd Ann Arbor, MI USA TABLE OF CONTENTS GENERAL
RayBio Human PPAR-alpha Transcription Factor Activity Assay Kit
 RayBio Human PPAR-alpha Transcription Factor Activity Assay Kit Catalog #: TFEH-PPARa User Manual Jan 5, 2018 3607 Parkway Lane, Suite 200 Norcross, GA 30092 Tel: 1-888-494-8555 (Toll Free) or 770-729-2992,
RayBio Human PPAR-alpha Transcription Factor Activity Assay Kit Catalog #: TFEH-PPARa User Manual Jan 5, 2018 3607 Parkway Lane, Suite 200 Norcross, GA 30092 Tel: 1-888-494-8555 (Toll Free) or 770-729-2992,
Roles of transcriptional factor Snail and adhesion factor E-cadherin in clear cell renal cell carcinoma
 EXPERIMENTAL AND THERAPEUTIC MEDICINE 6: 1489-1493, 2013 Roles of transcriptional factor Snail and adhesion factor E-cadherin in clear cell renal cell carcinoma JINQUAN CAI Department of Urology, Fuzhou
EXPERIMENTAL AND THERAPEUTIC MEDICINE 6: 1489-1493, 2013 Roles of transcriptional factor Snail and adhesion factor E-cadherin in clear cell renal cell carcinoma JINQUAN CAI Department of Urology, Fuzhou
ab SREBP-2 Translocation Assay Kit (Cell-Based)
 ab133114 SREBP-2 Translocation Assay Kit (Cell-Based) Instructions for Use For analysis of translocation of SREBP-2 into nuclei. This product is for research use only and is not intended for diagnostic
ab133114 SREBP-2 Translocation Assay Kit (Cell-Based) Instructions for Use For analysis of translocation of SREBP-2 into nuclei. This product is for research use only and is not intended for diagnostic
TECHNICAL BULLETIN. Catalog Number RAB0447 Storage Temperature 20 C
 Phospho-Stat3 (ptyr 705 ) and pan-stat3 ELISA Kit for detection of human, mouse, or rat phospho-stat3 (ptyr 705 ) and pan-stat3 in cell and tissue lysates Catalog Number RAB0447 Storage Temperature 20
Phospho-Stat3 (ptyr 705 ) and pan-stat3 ELISA Kit for detection of human, mouse, or rat phospho-stat3 (ptyr 705 ) and pan-stat3 in cell and tissue lysates Catalog Number RAB0447 Storage Temperature 20
OxiSelect Human Oxidized LDL ELISA Kit (OxPL-LDL Quantitation)
 Product Manual OxiSelect Human Oxidized LDL ELISA Kit (OxPL-LDL Quantitation) Catalog Number STA-358 96 assays FOR RESEARCH USE ONLY Not for use in diagnostic procedures Introduction Lipoproteins are submicroscopic
Product Manual OxiSelect Human Oxidized LDL ELISA Kit (OxPL-LDL Quantitation) Catalog Number STA-358 96 assays FOR RESEARCH USE ONLY Not for use in diagnostic procedures Introduction Lipoproteins are submicroscopic
Sipper BK Experimental Animal Co. (Shanghai, China) and bred in a specific. pathogen-free environment. The animal study protocol was approved by the
 Supplementary information, Data S1 Materials and Methods Mice, Ad vectors and reagents Female C57BL/6 mice, 8-10 weeks of age, were purchased from Joint Ventures Sipper BK Experimental Animal Co. (Shanghai,
Supplementary information, Data S1 Materials and Methods Mice, Ad vectors and reagents Female C57BL/6 mice, 8-10 weeks of age, were purchased from Joint Ventures Sipper BK Experimental Animal Co. (Shanghai,
Total Histone H3 Acetylation Detection Fast Kit (Colorimetric)
 Total Histone H3 Acetylation Detection Fast Kit (Colorimetric) Catalog Number KA1538 48 assays Version: 02 Intended for research use only www.abnova.com Table of Contents Introduction... 3 Intended Use...
Total Histone H3 Acetylation Detection Fast Kit (Colorimetric) Catalog Number KA1538 48 assays Version: 02 Intended for research use only www.abnova.com Table of Contents Introduction... 3 Intended Use...
TFEB-mediated increase in peripheral lysosomes regulates. Store Operated Calcium Entry
 TFEB-mediated increase in peripheral lysosomes regulates Store Operated Calcium Entry Luigi Sbano, Massimo Bonora, Saverio Marchi, Federica Baldassari, Diego L. Medina, Andrea Ballabio, Carlotta Giorgi
TFEB-mediated increase in peripheral lysosomes regulates Store Operated Calcium Entry Luigi Sbano, Massimo Bonora, Saverio Marchi, Federica Baldassari, Diego L. Medina, Andrea Ballabio, Carlotta Giorgi
Phospholipid Assay Kit
 Phospholipid Assay Kit Catalog Number KA1635 100 assays Version: 06 Intended for research use only www.abnova.com Table of Contents Introduction... 3 Intended Use... 3 Background... 3 General Information...
Phospholipid Assay Kit Catalog Number KA1635 100 assays Version: 06 Intended for research use only www.abnova.com Table of Contents Introduction... 3 Intended Use... 3 Background... 3 General Information...
IN VITRO HORMESIS EFFECTS OF SODIUM FLUORIDE ON KIDNEY CELLS OF THREE-DAY-OLD MALE RATS
 292 Tang, An, Du, Zhang, Zhou 292 IN VITRO HORMESIS EFFECTS OF SODIUM FLUORIDE ON KIDNEY CELLS OF THREE-DAY-OLD MALE RATS Qin-qing Tang, a Xiao-jing An, a Jun Du, a Zheng-xiang Zhang, a Xiao-jun Zhou a
292 Tang, An, Du, Zhang, Zhou 292 IN VITRO HORMESIS EFFECTS OF SODIUM FLUORIDE ON KIDNEY CELLS OF THREE-DAY-OLD MALE RATS Qin-qing Tang, a Xiao-jing An, a Jun Du, a Zheng-xiang Zhang, a Xiao-jun Zhou a
MyD88 expression is associated with paclitaxel resistance in lung cancer A549 cells
 ONCOLOGY REPORTS 32: 1837-1844, 2014 MyD88 expression is associated with paclitaxel resistance in lung cancer A549 cells Fenfen Xiang 1*, Rong Wu 1*, Zhenhua Ni 2, Chunying Pan 3, Yueping Zhan 2, Jian
ONCOLOGY REPORTS 32: 1837-1844, 2014 MyD88 expression is associated with paclitaxel resistance in lung cancer A549 cells Fenfen Xiang 1*, Rong Wu 1*, Zhenhua Ni 2, Chunying Pan 3, Yueping Zhan 2, Jian
EpiQuik Total Histone H3 Acetylation Detection Fast Kit (Colorimetric)
 EpiQuik Total Histone H3 Acetylation Detection Fast Kit (Colorimetric) Base Catalog # PLEASE READ THIS ENTIRE USER GUIDE BEFORE USE The EpiQuik Total Histone H3 Acetylation Detection Fast Kit (Colorimetric)
EpiQuik Total Histone H3 Acetylation Detection Fast Kit (Colorimetric) Base Catalog # PLEASE READ THIS ENTIRE USER GUIDE BEFORE USE The EpiQuik Total Histone H3 Acetylation Detection Fast Kit (Colorimetric)
GLP-2 ELISA. For the quantitative determination of GLP-2 in human serum and plasma samples.
 GLP-2 ELISA For the quantitative determination of GLP-2 in human serum and plasma samples. For Research Use Only. Not For Use In Diagnostic Procedures. Catalog Number: 48-GP2HU-E01.1 Size: 96 wells Version:
GLP-2 ELISA For the quantitative determination of GLP-2 in human serum and plasma samples. For Research Use Only. Not For Use In Diagnostic Procedures. Catalog Number: 48-GP2HU-E01.1 Size: 96 wells Version:
YK052 Mouse Leptin ELISA
 YK052 Mouse Leptin ELISA FOR LABORATORY USE ONLY YANAIHARA INSTITUTE INC. 2480-1 AWAKURA, FUJINOMIYA-SHI SHIZUOKA, JAPAN 418-0011 Contents Ⅰ. Introduction 2 Ⅱ. Characteristics 3 Ⅲ. Composition 4 Ⅳ. Method
YK052 Mouse Leptin ELISA FOR LABORATORY USE ONLY YANAIHARA INSTITUTE INC. 2480-1 AWAKURA, FUJINOMIYA-SHI SHIZUOKA, JAPAN 418-0011 Contents Ⅰ. Introduction 2 Ⅱ. Characteristics 3 Ⅲ. Composition 4 Ⅳ. Method
ab NF-kB p50/p65 Transcription Factor Assay Kit
 ab133128 NF-kB p50/p65 Transcription Factor Assay Kit Instructions for Use For the detection of specific transcription factor DNA binding activity in nuclear extracts. This product is for research use
ab133128 NF-kB p50/p65 Transcription Factor Assay Kit Instructions for Use For the detection of specific transcription factor DNA binding activity in nuclear extracts. This product is for research use
For the rapid, sensitive and accurate measurement of apoptosis in various samples.
 ab14082 500X Annexin V-FITC Apoptosis Detection Reagent Instructions for Use For the rapid, sensitive and accurate measurement of apoptosis in various samples. This product is for research use only and
ab14082 500X Annexin V-FITC Apoptosis Detection Reagent Instructions for Use For the rapid, sensitive and accurate measurement of apoptosis in various samples. This product is for research use only and
Supplementary Figure (OH) 22 nanoparticles did not affect cell viability and apoposis. MDA-MB-231, MCF-7, MCF-10A and BT549 cells were
 Supplementary Figure 1. Gd@C 82 (OH) 22 nanoparticles did not affect cell viability and apoposis. MDA-MB-231, MCF-7, MCF-10A and BT549 cells were treated with PBS, Gd@C 82 (OH) 22, C 60 (OH) 22 or GdCl
Supplementary Figure 1. Gd@C 82 (OH) 22 nanoparticles did not affect cell viability and apoposis. MDA-MB-231, MCF-7, MCF-10A and BT549 cells were treated with PBS, Gd@C 82 (OH) 22, C 60 (OH) 22 or GdCl
Data Sheet. PCSK9[Biotinylated]-LDLR Binding Assay Kit Catalog # 72002
![Data Sheet. PCSK9[Biotinylated]-LDLR Binding Assay Kit Catalog # 72002 Data Sheet. PCSK9[Biotinylated]-LDLR Binding Assay Kit Catalog # 72002](/thumbs/79/80181511.jpg) Data Sheet PCSK9[Biotinylated]-LDLR Binding Assay Kit Catalog # 72002 DESCRIPTION: The PCSK9[Biotinylated]-LDLR Binding Assay Kit is designed for screening and profiling purposes. PCSK9 is known to function
Data Sheet PCSK9[Biotinylated]-LDLR Binding Assay Kit Catalog # 72002 DESCRIPTION: The PCSK9[Biotinylated]-LDLR Binding Assay Kit is designed for screening and profiling purposes. PCSK9 is known to function
EPIGENTEK. EpiQuik HDAC Activity/Inhibition Assay Kit(Colorimetric) Base Catalog # P-4002 PLEASE READ THIS ENTIRE USER GUIDE BEFORE USE
 EpiQuik HDAC Activity/Inhibition Assay Kit(Colorimetric) Base Catalog # PLEASE READ THIS ENTIRE USER GUIDE BEFORE USE The EpiQuik HDAC Activity/Inhibition Assay Kit (Colorimetric) is very suitable for
EpiQuik HDAC Activity/Inhibition Assay Kit(Colorimetric) Base Catalog # PLEASE READ THIS ENTIRE USER GUIDE BEFORE USE The EpiQuik HDAC Activity/Inhibition Assay Kit (Colorimetric) is very suitable for
MOLECULAR MEDICINE REPORTS 14: , 2016
 MOLECULAR MEDICINE REPORTS 14: 2685-2690, 2016 Resveratrol inhibits phosphorylation within the signal transduction and activator of transcription 3 signaling pathway by activating sirtuin 1 in SW1353 chondrosarcoma
MOLECULAR MEDICINE REPORTS 14: 2685-2690, 2016 Resveratrol inhibits phosphorylation within the signal transduction and activator of transcription 3 signaling pathway by activating sirtuin 1 in SW1353 chondrosarcoma
SUPPLEMENTARY INFORMATION. Supplementary Figures S1-S9. Supplementary Methods
 SUPPLEMENTARY INFORMATION SUMO1 modification of PTEN regulates tumorigenesis by controlling its association with the plasma membrane Jian Huang 1,2#, Jie Yan 1,2#, Jian Zhang 3#, Shiguo Zhu 1, Yanli Wang
SUPPLEMENTARY INFORMATION SUMO1 modification of PTEN regulates tumorigenesis by controlling its association with the plasma membrane Jian Huang 1,2#, Jie Yan 1,2#, Jian Zhang 3#, Shiguo Zhu 1, Yanli Wang
RayBio Human, Mouse and Rat Phospho-NF-kB P65 (Ser536) and Total NF-kB P65 ELISA Kit
 RayBio Human, Mouse and Rat Phospho-NF-kB P65 (Ser536) and Total NF-kB P65 ELISA Kit Catalog #: PEL-NFKBP65-S536-T User Manual Last revised October 10, 2017 Caution: Extraordinarily useful information
RayBio Human, Mouse and Rat Phospho-NF-kB P65 (Ser536) and Total NF-kB P65 ELISA Kit Catalog #: PEL-NFKBP65-S536-T User Manual Last revised October 10, 2017 Caution: Extraordinarily useful information
EGFR (py1045)/ Pan EGFR (Human) ELISA Kit
 EGFR (py1045)/ Pan EGFR (Human) ELISA Kit Catalog Number KA2156 96 assays Version: 01 Intended for research use only www.abnova.com I. INTRODUCTION EGFR (py1045)/pan EGFR (Human) ELISA (Enzyme-Linked Immunosorbent
EGFR (py1045)/ Pan EGFR (Human) ELISA Kit Catalog Number KA2156 96 assays Version: 01 Intended for research use only www.abnova.com I. INTRODUCTION EGFR (py1045)/pan EGFR (Human) ELISA (Enzyme-Linked Immunosorbent
Annexin V-APC/7-AAD Apoptosis Kit
 Annexin V-APC/7-AAD Apoptosis Kit Catalog Number KA3808 100 assays Version: 04 Intended for research use only www.abnova.com Table of Contents Introduction... 3 Background... 3 General Information... 4
Annexin V-APC/7-AAD Apoptosis Kit Catalog Number KA3808 100 assays Version: 04 Intended for research use only www.abnova.com Table of Contents Introduction... 3 Background... 3 General Information... 4
A263 A352 A204. Pan CK. pstat STAT3 pstat3 STAT3 pstat3. Columns Columns 1-6 Positive control. Omentum. Rectosigmoid A195.
 pstat3 75 Pan CK A A263 A352 A24 B Columns 1-6 Positive control A195 A22 A24 A183 Rectal Nodule STAT3 pstat3 STAT3 pstat3 Columns 7-12 Omentum Rectosigmoid Left Ovary Right Ovary Omentum Uterus Uterus
pstat3 75 Pan CK A A263 A352 A24 B Columns 1-6 Positive control A195 A22 A24 A183 Rectal Nodule STAT3 pstat3 STAT3 pstat3 Columns 7-12 Omentum Rectosigmoid Left Ovary Right Ovary Omentum Uterus Uterus
HIV-1 p24 ELISA Pair Set Cat#: orb54951 (ELISA Manual)
 HIV-1 p24 ELISA Pair Set Cat#: orb54951 (ELISA Manual) BACKGROUND Human Immunodeficiency Virus ( HIV ) can be divided into two major types, HIV type 1 (HIV-1) and HIV type 2 (HIV-2). HIV-1 is related to
HIV-1 p24 ELISA Pair Set Cat#: orb54951 (ELISA Manual) BACKGROUND Human Immunodeficiency Virus ( HIV ) can be divided into two major types, HIV type 1 (HIV-1) and HIV type 2 (HIV-2). HIV-1 is related to
(a) Significant biological processes (upper panel) and disease biomarkers (lower panel)
 Supplementary Figure 1. Functional enrichment analyses of secretomic proteins. (a) Significant biological processes (upper panel) and disease biomarkers (lower panel) 2 involved by hrab37-mediated secretory
Supplementary Figure 1. Functional enrichment analyses of secretomic proteins. (a) Significant biological processes (upper panel) and disease biomarkers (lower panel) 2 involved by hrab37-mediated secretory
Rat Leptin ELISA FOR LABORATORY USE ONLY YANAIHARA INSTITUTE INC AWAKURA, FUJINOMIYA - SHI SHIZUOKA, JAPAN
 YK050 Rat Leptin ELISA FOR LABORATORY USE ONLY YANAIHARA INSTITUTE INC. 2480-1 AWAKURA, FUJINOMIYA - SHI SHIZUOKA, JAPAN 418-0011 Contents Introduction 2 Characteristics 3 Composition 4 Method 5-6 Notes
YK050 Rat Leptin ELISA FOR LABORATORY USE ONLY YANAIHARA INSTITUTE INC. 2480-1 AWAKURA, FUJINOMIYA - SHI SHIZUOKA, JAPAN 418-0011 Contents Introduction 2 Characteristics 3 Composition 4 Method 5-6 Notes
Supplementary Figure 1. Normal T lymphocyte populations in Dapk -/- mice. (a) Normal thymic development in Dapk -/- mice. Thymocytes from WT and Dapk
 Supplementary Figure 1. Normal T lymphocyte populations in Dapk -/- mice. (a) Normal thymic development in Dapk -/- mice. Thymocytes from WT and Dapk -/- mice were stained for expression of CD4 and CD8.
Supplementary Figure 1. Normal T lymphocyte populations in Dapk -/- mice. (a) Normal thymic development in Dapk -/- mice. Thymocytes from WT and Dapk -/- mice were stained for expression of CD4 and CD8.
A Hepatocyte Growth Factor Receptor (Met) Insulin Receptor hybrid governs hepatic glucose metabolism SUPPLEMENTARY FIGURES, LEGENDS AND METHODS
 A Hepatocyte Growth Factor Receptor (Met) Insulin Receptor hybrid governs hepatic glucose metabolism Arlee Fafalios, Jihong Ma, Xinping Tan, John Stoops, Jianhua Luo, Marie C. DeFrances and Reza Zarnegar
A Hepatocyte Growth Factor Receptor (Met) Insulin Receptor hybrid governs hepatic glucose metabolism Arlee Fafalios, Jihong Ma, Xinping Tan, John Stoops, Jianhua Luo, Marie C. DeFrances and Reza Zarnegar
Oncolytic Adenovirus Complexes Coated with Lipids and Calcium Phosphate for Cancer Gene Therapy
 Oncolytic Adenovirus Complexes Coated with Lipids and Calcium Phosphate for Cancer Gene Therapy Jianhua Chen, Pei Gao, Sujing Yuan, Rongxin Li, Aimin Ni, Liang Chu, Li Ding, Ying Sun, Xin-Yuan Liu, Yourong
Oncolytic Adenovirus Complexes Coated with Lipids and Calcium Phosphate for Cancer Gene Therapy Jianhua Chen, Pei Gao, Sujing Yuan, Rongxin Li, Aimin Ni, Liang Chu, Li Ding, Ying Sun, Xin-Yuan Liu, Yourong
Effects of metallothionein-3 and metallothionein-1e gene transfection on proliferation, cell cycle, and apoptosis of esophageal cancer cells
 Effects of metallothionein-3 and metallothionein-1e gene transfection on proliferation, cell cycle, and apoptosis of esophageal cancer cells Z.Q. Tian 1, Y.Z. Xu 1, Y.F. Zhang 1, G.F. Ma 1, M. He 1 and
Effects of metallothionein-3 and metallothionein-1e gene transfection on proliferation, cell cycle, and apoptosis of esophageal cancer cells Z.Q. Tian 1, Y.Z. Xu 1, Y.F. Zhang 1, G.F. Ma 1, M. He 1 and
Fang et al. NMuMG. PyVmT unstained Anti-CCR2-PE MDA-MB MCF MCF10A
 A NMuMG PyVmT 16.5+.5 47.+7.2 Fang et al. unstained Anti-CCR2-PE 4T1 Control 37.6+6.3 56.1+.65 MCF1A 16.1+3. MCF-7 3.1+5.4 MDA-M-231 42.1+5.5 unstained Secondary antibody only Anti-CCR2 SUPPLEMENTAL FIGURE
A NMuMG PyVmT 16.5+.5 47.+7.2 Fang et al. unstained Anti-CCR2-PE 4T1 Control 37.6+6.3 56.1+.65 MCF1A 16.1+3. MCF-7 3.1+5.4 MDA-M-231 42.1+5.5 unstained Secondary antibody only Anti-CCR2 SUPPLEMENTAL FIGURE
Influenza A H7N9 (A/Anhui/1/2013) Hemagglutinin / HA ELISA Pair Set
 Influenza A H7N9 (A/Anhui/1/2013) Hemagglutinin / HA ELISA Pair Set Catalog Number : SEK40103 To achieve the best assay results, this manual must be read carefully before using this product and the assay
Influenza A H7N9 (A/Anhui/1/2013) Hemagglutinin / HA ELISA Pair Set Catalog Number : SEK40103 To achieve the best assay results, this manual must be read carefully before using this product and the assay
GLP-2 (Rat) ELISA. For the quantitative determination of glucagon-like peptide 2 (GLP-2) in rat serum and plasma
 GLP-2 (Rat) ELISA For the quantitative determination of glucagon-like peptide 2 (GLP-2) in rat serum and plasma For Research Use Only. Not For Use In Diagnostic Procedures. Catalog Number: 48-GP2RT-E01
GLP-2 (Rat) ELISA For the quantitative determination of glucagon-like peptide 2 (GLP-2) in rat serum and plasma For Research Use Only. Not For Use In Diagnostic Procedures. Catalog Number: 48-GP2RT-E01
RESEARCH ARTICLE. Ginsenoside-Rh2 Inhibits Proliferation and Induces Apoptosis of Human Gastric Cancer SGC-7901 Side Population Cells
 RESEARCH ARTICLE Ginsenoside-Rh2 Inhibits Proliferation and Induces Apoptosis of Human Gastric Cancer SGC-7901 Side Population Cells Jun Qian 1& *, Jing Li 1&, Jian-Guang Jia 1, Xin Jin 1, Da-Jun Yu 1,
RESEARCH ARTICLE Ginsenoside-Rh2 Inhibits Proliferation and Induces Apoptosis of Human Gastric Cancer SGC-7901 Side Population Cells Jun Qian 1& *, Jing Li 1&, Jian-Guang Jia 1, Xin Jin 1, Da-Jun Yu 1,
