EARLY ONLINE RELEASE
|
|
|
- Tabitha Fox
- 5 years ago
- Views:
Transcription
1 EARLY ONLINE RELEASE Note: This article was posted on the Archives Web site as an Early Online Release. Early Online Release articles have been peer reviewed, copyedited, and reviewed by the authors. Additional changes or corrections may appear in these articles when they appear in a future print issue of the Archives. Early Online Release articles are citable by using the Digital Object Identifier (DOI), a unique number given to every article. The DOI will typically appear at the end of the abstract. The DOI for this manuscript is doi: /arpa OA The final published version of this manuscript will replace the Early Online Release version at the above DOI once it is available College of American Pathologists
2 Original Article Triaging Atypical Lobular Hyperplasia and Lobular Carcinoma In Situ on Percutaneous Core Biopsy to Surgery or Observation Assiduous Radiologic-Pathologic Correlation Works, Quantitating Extent of Disease Does Not Anna I. Holbrook, MD; Krisztina Hanley, MD; Caprichia Jeffers, MS; Jian Kang, PhD; Michael A. Cohen, MD Context. The management of lobular neoplasia (LN) found on core biopsy is controversial and ranges from obligatory surgical excision to clinical/imaging observation. Objective. To determine if in cases of core needle biopsy yielding LN, quantification of normal and diseased terminal ductal lobular units (TDLUs) can predict which cases require surgical excision and which can be safely followed. A secondary goal is to assess whether the concordance or discordance of core biopsy results, determined by rigorous radiologic-pathologic correlation, can predict for upgrade to malignancy at excision. Design. In this retrospective study, 79 specimens from 78 women who underwent image-guided core needle biopsies between 2005 and 2012 yielding LN were evaluated for total number of TDLUs and total number and percentage of TDLUs involved by LN. Additionally, radiologic-pathologic correlation was performed to assess concordance or discordance. All were correlated with the results of surgical excisional biopsy or imaging/clinical follow-up. Results. There were 5 upgrades to malignancy. There was no association between upgrade to malignancy and any of the 3 TDLU variables evaluated, including total TDLUs in the specimen (P ¼.42), total abnormal TDLUs (P ¼.56), and percent of TDLUs that are abnormal (P ¼.07). Kendall rank correlation demonstrated a correlation between discordance and upgrade to cancer at surgery that was statistically significant (sb ¼ 0.394, P,.001). Conclusions. Quantifying total TDLU and those involved by LN on core biopsy will not aid in triaging patients to surgery or observation. Assiduous radiologicpathologic correlation to determine lesion concordance/ discordance can predict those patients who would benefit from surgical excision. (Arch Pathol Lab Med. doi: /arpa OA) The management of atypical lobular hyperplasia (ALH) surgical excision ranging from 8% to 34%, 1 15 others have and lobular carcinoma in situ (LCIS), together known demonstrated significantly lower upgrade rates in the range as lobular neoplasia (LN), as the most significant lesion on of 0% to 3% As a result of the conflicting data, core biopsy remains controversial in spite of a relatively management at various institutions and practices ranges large number of publications dealing with the topic. from obligatory surgical excision of either ALH or LCIS Although many articles have detailed high upgrade rates to ductal carcinoma in situ (DCIS) or invasive carcinoma at obtained on core biopsy to surgical excision in only specific limited instances with clinical and imaging observation for the remaining majority. Several investigators have reported various features of the Accepted for publication July 10, From the Departments of Radiology and Imaging Sciences (Drs pathologic core biopsy specimens that might assist in Holbrook and Cohen), Pathology and Laboratory Medicine (Dr predicting for upgrade, but again with mixed results. Hanley), and Biostatistics and Bioinformatics (Ms Jeffers), Rollins 20,21,24 26,28,29 We defined 3 reproducible and quantifi- School of Public Health, Emory University, Atlanta, Georgia; and the able features inherent in the core samples that might predict Department of Biostatistics, University of Michigan, Ann Arbor (Dr for upgrade: total number of terminal ductal lobular units Kang). The authors have no relevant financial interest in the products or (TDLUs) in the core specimens as a predictor of overall companies described in this article. sampling adequacy, total number of TDLUs containing ALH Presented in part at the American Roentgen Ray Society annual or LCIS as a predictor of overall disease extent in the core meeting; April 20, 2016; Los Angeles, California. specimens, and ratio of ALH/LCIS cores to total overall Corresponding author: Anna Holbrook, MD, Department of Radiology and Imaging Sciences, Emory University, 1365C Clifton number of TDLUs as an estimate of disease density within Road NE, Building C, Suite C1104, Atlanta, GA ( the total sampled specimen. The purpose of this study is to aiholbr@emory.edu). determine if in cases of core needle biopsy yielding LN, Arch Pathol Lab Med Quantifying TDLU Holbrook et al 1
3 quantification of normal and diseased TDLUs might assist in predicting which cases require surgical excision and which can be safely followed. Additionally, Atkins et al 21 concluded that in cases of ALH/LCIS found at core needle biopsy, careful radiologicpathologic correlation could be used to determine which patients should undergo surgical excision. They found that in 43 cases considered concordant, there were no malignancies found at surgery or follow-up, whereas there were 2 upgrades to DCIS among the 7 discordant biopsy cases. 21 A secondary goal of our study is to validate their results using similar methodology to assess whether the concordance or discordance of core biopsy results, determined by rigorous radiologic-pathologic correlation, can predict for upgrade to malignancy at excision. MATERIALS AND METHODS This retrospective study was Institutional Review Board approved with waiver of informed consent and was compliant with the Health Insurance Portability and Accountability Act. The pathology database at our institution was searched for consecutive cases in which an image-guided core needle biopsy performed between 2005 and 2012 yielded LCIS and/or ALH. Those in which there was another finding that would prompt excision (atypical ductal hyperplasia, flat epithelial atypia, papilloma, radial scar, DCIS, invasive carcinoma) were excluded and only those with available surgical excision results or at least 2 years of clinical and/or imaging follow-up were included. Other exclusion criteria included incomplete imaging and/or pathologic material. The pathologist (K.H., with 9 years of experience) reviewed the original slides from each core needle biopsy blinded to the outcome at surgical excision or extended follow-up. All submitted cores were embedded in paraffin blocks. On each tissue block, 3 levels (L1, L3, and L5), each containing 5-lm tissue sections, were examined. Total TDLU and ALH/LCIS-containing TDLU counts were performed on the level with the greatest number of TDLUs. If multiple tissue blocks were necessary to embed all of the cores, then the number of total TDLUs and ALH/LCIS-containing TDLUs was the sum of the TDLUs from the salient levels from each block examined. In the final TDLU count, both lobules and lobules with an associated terminal duct were counted. The number of TDLUs involved by ALH/LCIS was then quantitated. In cases where ALH/ LCIS involved a fibroadenoma, an attempt was made to count the TDLUs within and outside of the fibroadenoma. The images pertinent to the case, including the diagnostic mammogram, ultrasound, and magnetic resonance imaging (MRI), and images from the biopsy, were reviewed by 2 radiologists (with 35 [M.A.C.] and 7 [A.I.H.] years of experience) also blinded to the results of any subsequent surgical excision or extended imaging/ clinical follow-up. Concordance or discordance of the biopsy results with the radiologic findings was then determined by consensus by the radiologists and pathologist. If the histologic results could fully account for the imaging features, then the results were considered concordant. Otherwise, the results were designated as discordant. For example, if a mass was seen on imaging but no mass-forming entity was found at histology, this would be considered discordant. We also included in this category cases in which sampling was considered inadequate for example, ones in which there were few calcifications in the specimen radiograph. Lastly, imaging findings that are highly suggestive of malignancy and given Breast Imaging Reporting and Data System (BI-RADS) 5 designation would be called discordant because a benign core biopsy result in these cases would not be acceptable. Only after all cases were fully analyzed were the authors unblinded to the result of surgical excision or follow-up as determined by review of the medical record. Upgrade of any case to DCIS or invasive carcinoma was recorded. We modeled the probability of upgrade as a function of total abnormal TDLUs, total TDLUs, and percent abnormal TDLUs using univariate and multivariate logistic regression models. Kendall rank correlation was run to determine the relationship between concordance status and upgrade to cancer at surgery (R Core Team (2016). R: A language and environment for statistical computing. R Foundation for Statistical Computing, Vienna, Austria. URL accessed July 2018). RESULTS There were 253 cases found in the pathology database in which an image-guided biopsy performed between 2005 and 2012 yielded LCIS and/or ALH. A total of 146 of these cases had a coexistent high-risk lesion or cancer in the specimen and were therefore excluded. Fifteen cases were lost to follow-up. Two patients were excluded because they received preoperative chemotherapy and radiation for treatment of synchronous cancer elsewhere in the breasts, and therefore upgrade at the biopsy site could not be assessed. There were 2 cases with missing images, and 9 cases were missing pathologic slides. One patient had 2 core needle biopsies in the left breast, 2 years apart, and at 2 separate sites. A total of 79 cases in 78 patients met the inclusion criteria. The patients ranged in age from 36 to 87 years (mean age, 58 years). The imaging finding that prompted the biopsy included mass (n ¼ 17, including 7 masses seen at MRI), architectural distortion (n ¼ 2), asymmetry (n ¼ 1), focal asymmetry (n ¼ 7), focus of enhancement on MRI (n ¼ 1), non mass-like enhancement on MRI (n ¼ 6), and calcifications (n ¼ 45). Calcifications were classified as pleomorphic (n ¼ 21), amorphous (n ¼ 16), and punctate (n ¼ 8). Cases were classified as BI-RADS 4 (n ¼ 75) or BI-RADS 5 (n ¼ 4). Biopsies were performed under stereotactic guidance in 47 cases, of which 45 cases had reports specifying needle gauge (43 cases with 11-gauge needle and 2 cases with 9-gauge needle). Of the 47 cases, 32 had reports specifying number of cores obtained (average, 11.1 cores; range, 6 15 cores; median, 12 cores). Biopsies were performed under ultrasound guidance in 21 cases. Of these, 17 had reports that specified the needle gauge used (1 case with 16-gauge needle, 14 cases with 14-gauge needle, and 2 cases with 11- gauge needle). Of the 21 cases, 15 had reports specifying the number of cores obtained (average, 4.8 cores, range, 4 8 cores; median, 4 cores). A total of 11 cases were obtained under MRI guidance with a 9-gauge needle, and of these, 7 had reports specifying the number of cores obtained (average, 12.1 cores; range, cores; median, 12 cores). Core needle biopsy specimens demonstrated ALH (n ¼ 52), LCIS (n ¼ 17), ALH and LCIS (n ¼ 5), LCIS with necrosis (n ¼ 1), and pleomorphic LCIS (n ¼ 4). Of the 45 cases in which calcifications prompted the biopsy, 11 demonstrated calcium intrinsically associated with the LN. The total number of TDLUs counted in each specimen ranged from 2 to 180 (mean, 47.4). The total number of TDLUs involved by ALH/LCIS in each specimen ranged from 1 to 38 (mean, 6.1). The percent of TDLUs involved by ALH/LCIS in each specimen ranged from 0.6% (1 of 180) to 100% (2 of 2; mean, 21%; Table 1). Following radiologic-pathologic review, core biopsy results were considered discordant in 24 of 79 cases (30%). The most common reason for discordance was a mass seen on imaging but no mass-forming entity found at histology (14 cases). In 5 cases, there was non mass-like enhancement on MRI that prompted the biopsy, but no sufficient explanation for the enhancement was seen at pathology. In 3 cases, the target of the biopsy was suspicious calcifications; 2 Arch Pathol Lab Med Quantifying TDLU Holbrook et al
4 Table 1. Quantified Terminal Ductal Lobular Unit (TDLUs) Total, Total Involved by Lobular Neoplasia (LN), and % Involved by LN and Association With Upgrade to Malignancy at Surgery Upgrade to Malignancy at Surgery? Total Sample, No. Total TDLU Total Abnormal TDLU % Abnormal TDLU Mean SD Mean SD Mean SD Yes No Summary P (univariate) P (multivariate) however, few calcifications were seen in the specimen radiograph. Lastly, in 2 cases the findings were given a BI- RADS 5 designation and were so highly suggestive of malignancy that a benign core biopsy result could not be accepted. A total of 66 cases then underwent surgical excision. In the remaining 13 cases, the patients did not undergo excision of the LN but had at least 2 years of imaging and/or clinical follow-up (average follow-up, 5.5 years; range, 2 years to 10 years, 9 months). There were a total of 5 upgrades to malignancy at surgical excision (Table 2). There were no cases of malignancy found during clinical/imaging follow-up. In all of the upgraded cases, the imaging features were deemed discordant with the pathology findings on core biopsy (Figure 1). There were no concordant cases that were upgraded to malignancy (Figure 2). Statistical analysis demonstrates that there was no association between upgrade to cancer at surgical excision and any of the 3 TDLU variables evaluated, including total TDLUs in the specimen (P ¼.42), total abnormal TDLUs (P ¼.56), and percent of TDLUs that were abnormal (P ¼.07). Multivariate analysis also showed no significant association between the 3 TDLU variables, evaluated jointly, and upgrade to malignancy at excision (total TDLU P ¼.93; total abnormal TDLU P ¼.95; percent abnormal TDLU P ¼.23; Figure 3; Table 1). Kendall rank correlation demonstrated a correlation between discordance and upgrade to cancer at surgery that was statistically significant (sb ¼ 0.394, P,.001). DISCUSSION Atkins et al 21 found that in the setting of core biopsy yielding ALH/LCIS, careful radiologic-pathologic correlation could determine which patients could safely avoid undergoing surgical excision. Our results support their conclusions, because we also found no upgrades among our cases determined concordant at radiologic-pathologic review. All 5 upgrades occurred only among the cases determined discordant at radiologic-pathologic review. Our data would strongly support the hypothesis that assiduous radiologic-pathologic review of core biopsy cases yielding lobular neoplasia on core biopsy can triage those requiring surgery from those that can be managed safely with clinical and imaging follow-up. Beginning with observations by Ottesen et al 30 in the early 1990s, there has been an interest in quantification of ALH/LCIS at biopsy as a predictor of more serious adjacent invasive or in situ disease. Although their work predated widespread percutaneous core biopsy, these authors found that greater than 10 lobules containing LCIS on surgical excisional biopsy predicted for future development of invasive tumor. 30 Subsequently, several publications quantifying ALH and LCIS on core biopsy have produced conflicting data as to whether the extent of ALH or LCIS found at core needle biopsy predicts for upgrade to malignancy at excision (summarized in Table 3). Several authors suggested that quantity of LN on core biopsy did predict for upgrade to cancer at excision. Esserman and colleagues 13 found that in 2 cases of diffuse ALH/LCIS (defined as greater than 1 lobule per core involved by ALH/LCIS) diagnosed at core needle biopsy, invasive lobular carcinoma was found at excision in both cases. Both occurred in cases of LCIS and in both, the invasive lobular carcinomas were not associated with the targeted lesions. On the other hand, of their 24 cases of focal ALH/LCIS (1 involved lobule per core), there were no cases of infiltrating carcinoma and only 1 case of DCIS at a site remote from the sampled LN at excision. 13 They concluded that excision may not be necessary when a diagnosis of only focal LN is made on core biopsy. Similarly, Subhawong et al 27 found that when only minimal ALH, which they defined as 3 or fewer foci, was found at core needle biopsy, excision yielded no cancers. They defined a focus as ALH involvement of 1 to 3 adjacent lobules. Based on these results, they suggested that minimal incidental ALH on core biopsy does not require excision if there is radiologic-pathologic concordance and the means to follow up with imaging. Table 2. Characteristics of Cases in Which There Was an Upgrade to Malignancy at Surgical Excision Core Biopsy Pathology Imaging Finding Excision Pathology LCIS/ALH Architectural distortion IDC on mammography Irregular mass on US LCIS with necrosis Architectural distortion ILC and fibrocystic change on mammography Irregular mass on US Single focus of ALH Spiculated mass ILC and DCIS with fibrocystic change on MRI LCIS with fibrocystic Clumped, segmental ILC change enhancement on MRI Irregular mass on US ALH Irregular mass on MRI ILC Abbreviations: ALH, atypical lobular hyperplasia; DCIS, ductal carcinoma in situ; IDC, invasive ductal carcinoma; ILC, invasive lobular carcinoma; LCIS, lobular carcinoma in situ; MRI, magnetic resonance imaging; US, ultrasound. Arch Pathol Lab Med Quantifying TDLU Holbrook et al 3
5 Table 3. Source, y Calhoun et al, Chaudhary et al, Esserman et al, Karabakhtsian et al, Middleton et al, Rendi et al, Subhawong et al, Previous Publications Analyzing the Extent of Lobular Neoplasia (LN) on Core Biopsy as a Predictor of Upgrade to Malignancy at Surgical Excision No. of Biopsies With Surgical Follow-up Analysis Criteria Results Conclusions 76 LN % involvement by LN on core Greater % involvement correlated with increased chance of upgrade 87 pure ALH, LCIS,.4 total lobules involved 3 upgrades at surgery with or ALH þ LCIS.1 lobule per core no relationship to number of lobules involved 26 LN Diffuse LN:.1 lobule per Diffuse: 2 upgrades to ILC core Focal LN: 1 lobule per Focal: 1/24 upgraded to core DCIS at distant site from biopsy 92 pure ALH, LCIS, or ALH þ LCIS 20 cases of benign LN concordant selected for excision 73 ALH, 33 LCIS (including 25 with ADH) 42 ALH, 12 LCIS (benign, concordant) Total number of TDLUs involved on core biopsy Focal: 2 involved TDLUs Extensive: 3 involved TDLUs,4 TDLUs involved versus 4 TDLUs involved Minimal ALH: 3 foci (focus: ALH in 1 3 adjacent lobules) Extent of involvement may correlate with upgrade on excision No correlation between extent of LN and upgrade rate Excise diffuse LN 10/92 upstaged Number of TDLUs Upstaged: 1 4 TDLUs involved on core biopsy (mean, 2.3 TDLUs) does not predict for upgrade Not upstaged: 1 8 TDLUs (mean, 3.3 TDLUs) No upgrades for focal ALH, LCIS, LN 1/46 upgrades if,4 TDLUs 6/29 upgrades if 4 TDLUs Minimal ALH: 0 upgrades LCIS: 5/12 upgrades Surgical excision for,3 involved TDLUs is not necessary No surgery for calcium lesions in non high-risk patients with,4 TDLUs involved Minimal incidental ALH does not require excision Abbreviations: ADH, atypical ductal hyperplasia; ALH, atypical lobular hyperplasia; DCIS, ductal carcinoma in situ; ILC, invasive lobular carcinoma; LCIS, lobular carcinoma in situ; TDLU, terminal ductal lobular unit. Middleton and colleagues 31 found that if fewer than 3 TDLUs were involved by ALH/LCIS, the risk of upgrade to cancer was less than 2%, and they concluded that surgery was not necessary in these cases. Rendi et al 32 found no cases of upgrade to cancer at excision if fewer than 4 TDLUs were involved. Calhoun et al 33 found that cases averaging 30% involvement by LN on core needle biopsy were upgraded, whereas cases averaging 15% involvement were not. Finally, Aulmann et al 34 followed 88 patients with LCIS on biopsy for 10 years and found that 9 developed subsequent invasive cancer. Of these 9 patients, 4 had extensive LCIS, which they defined as greater than 10 affected lobules in their original biopsy. 34 Other authors, however, have shown no correlation between extent of disease at core biopsy and likelihood of upgrade. For example, Karabakhtsian et al 8 counted TDLUs involved by ALH/LCIS in 92 cases and found that this number had no predictive value for the upgrade rate, with a mean of 2.3 TDLUs involved in upgraded cases, and 3.3 TDLUs involved in cases that were not upgraded. Their upgrade rate ranged from 8% (ALH) to 19% (LCIS). 8 Chaudhary and colleagues 19 also found no correlation between number of TDLUs involved by ALH/LCIS and risk of upgrade in 87 cases. Our results support this latter group in that we also found no correlation between the total number of TDLUs, the number of TDLUs involved by ALH/ LCIS, or the percentage of TLDUs involved by ALH/LCIS in the core biopsy specimen and upgrade to malignancy at surgical excision. In our opinion, quantifying morphologically normal and diseased TDLUs will not aid in triaging patients to surgery or not. However, there may well be specific histologically identifiable morphologic features of LN on core biopsy, including cellular and nuclear pleomorphism and comedonecrosis, that might suggest a higher likelihood of upgrade and the need for surgical excision. Pleomorphic LCIS and LCIS with necrosis are known to be associated with a worse prognosis than classic LCIS. 20,35 In our study, the only case of LCIS with necrosis was associated with an upgrade to malignancy at excision; however, the 4 cases of pleomorphic LCIS were not. Further, continued refinement in analyzing the genomic and immunohistochemical features of lobular neoplasia on core biopsy might also prove helpful in predicting those lesions more likely to presage or accompany frank malignancy. Our study is limited by the retrospective nature of the data collection. Not all patients included in this study had both core biopsy and surgical excision, introducing the possibility of selection bias with regard to which patients received surgery and which did not after a core biopsy diagnosis of ALH/LCIS. Additionally, of the 13 patients who did not have surgery, 5 (38.5%) received some type of chemoprevention. This may have prevented a malignancy from becoming apparent clinically or on imaging in the followup period. Lastly, this study is retrospective in nature. However, this limitation is mitigated somewhat by the blinded and thus prospective radiologic, pathologic, and radiologic-pathologic analysis that was the study design. Also, as in virtually all studies discussing the rare diagnosis of lobular neoplasia, our study involves a relatively small 4 Arch Pathol Lab Med Quantifying TDLU Holbrook et al
6 Figure 1. Radiologic-pathologic discordant mass in a 58-year-old woman undergoing high-risk screening magnetic resonance imaging (MRI). A, Axial T1 postcontrast MRI demonstrates a spiculated, enhancing mass in the left breast (arrow). B, MRI-guided biopsy yielded fibrocystic change with a single focus of atypical lobular hyperplasia. This result was felt to not sufficiently explain the mass, and therefore the case was considered discordant and excision performed (C), yielding invasive lobular carcinoma, Nottingham grade 1, and a focus of ductal carcinoma in situ (arrow) (hematoxylineosin, original magnifications 340 [B] and 3100 [C]). Figure 2. Radiologic-pathologic concordant lesion with no upgrade to malignancy in a 41-year-old woman with a mass noted at screening mammogram. A, Ultrasound of the left breast demonstrates a circumscribed, oval mass (calipers). B, Core needle biopsy reveals convex margin of a fibroadenoma (black arrows) with adjacent atypical lobular hyperplasia (ALH; white arrow). This was felt to be concordant. C, Excision yielded fibroadenoma completely involved by ALH (hematoxylin-eosin, original magnification 340). number of patients. This limits the study power, and thus its generalizability. In conclusion, we found no added value or utility in quantifying normal and abnormal TDLUs to aid in determining whether to recommend surgical excision or not. This study does validate the results of Atkins et al, 21 demonstrating again that assiduous radiologic-pathologic correlation to determine lesion concordance/discordance Arch Pathol Lab Med Quantifying TDLU Holbrook et al 5
7 Figure 3. A 48-year-old woman with extensive lobular carcinoma in situ (LCIS) without upgrade to malignancy. A, Craniocaudal magnification mammogram demonstrates amorphous calcifications (arrow). B, Core biopsy found extensive LCIS. This patient had the greatest total number of abnormal terminal ductal lobular units in our study (38 of 122; 31.1%). C, Despite this, at excision there was no upgrade to malignancy, with only LCIS found (hematoxylin-eosin, original magnification 3100). can predict those patients who would most likely benefit from surgical excision. Certainly, additional studies are required in order for definitive guidelines to be established. References 1. Arpino G, Allred DC, Mohsin SK, Weiss HL, Conrow D, Elledge RM. Lobular neoplasia on core-needle biopsy clinical significance. Cancer. 2004; 101(2): Brem RF, Lechner MC, Jackman RJ, et al. Lobular neoplasia at percutaneous breast biopsy: variables associated with carcinoma at surgical excision. AJR Am J Roentgenol. 2008;190(3): Destounis SV, Murphy PF, Seifert PJ, et al. Management of patients diagnosed with lobular carcinoma in situ at needle core biopsy at a communitybased outpatient facility. AJR Am J Roentgenol. 2012;198(2): Ibrahim N, Bessissow A, Lalonde L, et al. Surgical outcome of biopsyproven lobular neoplasia: is there any difference between lobular carcinoma in situ and atypical lobular hyperplasia? AJR Am J Roentgenol. 2012;198(2): Elsheikh TM, Silverman JF. Follow-up surgical excision is indicated when breast core needle biopsies show atypical lobular hyperplasia or lobular carcinoma in situ: a correlative study of 33 patients with review of the literature. Am J Surg Pathol. 2005;29(4): Polom K, Murawa D, Pawelska A, Murawa P. Atypical lobular hyperplasia and lobular carcinoma in situ without other high-risk lesions diagnosed on vacuum-assisted core needle biopsy: the problem of excisional biopsy. Tumori. 2009;95(1): Shin SJ, Rosen PP. Excisional biopsy should be performed if lobular carcinoma in situ is seen on needle core biopsy. Arch Pathol Lab Med. 2002; 126(6): Karabakhtsian RG, Johnson R, Sumkin J, Dabbs DJ. The clinical significance of lobular neoplasia on breast core biopsy. Am J Surg Pathol. 2007;31(5): Foster MC, Helvie MA, Gregory NE, Rebner M, Nees AV, Paramagul C. Lobular carcinoma in situ or atypical lobular hyperplasia at core-needle biopsy: is excisional biopsy necessary? Radiology. 2004;231(3): Lewis JL, Lee DY, Tartter PI. The significance of lobular carcinoma in situ and atypical lobular hyperplasia of the breast. Ann Surg Oncol. 2012;19(13): Cangiarella J, Guth A, Axelrod D, et al. Is surgical excision necessary for the management of atypical lobular hyperplasia and lobular carcinoma in situ diagnosed on core needle biopsy?: a report of 38 cases and review of the literature. Arch Pathol Lab Med. 2008;132(6): Crisi GM, Mandavilli S, Cronin E, Ricci A Jr. Invasive mammary carcinoma after immediate and short-term follow-up for lobular neoplasia on core biopsy. Am J Surg Pathol. 2003;27(3): Esserman LE, Lamea L, Tanev S, Poppiti R. Should the extent of lobular neoplasia on core biopsy influence the decision for excision? Breast J. 2007; 13(1): Hussain M, Cunnick GH. Management of lobular carcinoma in-situ and atypical lobular hyperplasia of the breast a review. Eur J Surg Oncol. 2011;37(4): Niell B, Specht M, Gerade B, Rafferty E. Is excisional biopsy required after a breast core biopsy yields lobular neoplasia? AJR Am J Roentgenol. 2012;199(4): Nagi CS, O Donnell JE, Tismenetsky M, Bleiweiss IJ, Jaffer SM. Lobular neoplasia on core needle biopsy does not require excision. Cancer. 2008; 112(10): Renshaw AA, Derhagopian RP, Martinez P, Gould EW. Lobular neoplasia in breast core needle biopsy specimens is associated with a low risk of ductal carcinoma in situ or invasive carcinoma on subsequent excision. Am J Clin Pathol. 2006;126(2): Renshaw AA, Cartagena N, Derhagopian RP, Gould EW. Lobular neoplasia in breast core needle biopsy specimens is not associated with an increased risk of ductal carcinoma in situ or invasive carcinoma. Am J Clin Pathol. 2002;117(5): Chaudhary S, Lawrence L, McGinty G, Kostroff K, Bhuiya T. Classic lobular neoplasia on core biopsy: a clinical and radio-pathologic correlation study with follow-up excision biopsy. Mod Pathol. 2013;26(6): Hwang H, Barke LD, Mendelson EB, Susnik B. Atypical lobular hyperplasia and classic lobular carcinoma in situ in core biopsy specimens: routine excision is not necessary. Mod Pathol. 2008;21(10): Atkins KA, Cohen MA, Nicholson B, Rao S. Atypical lobular hyperplasia and lobular carcinoma in situ at core breast biopsy: use of careful radiologicpathologic correlation to recommend excision or observation. Radiology. 2013; 269(2): Bauer VP, Ditkoff BA, Schnabel F, Brenin D, El-Tamer M, Smith S. The management of lobular neoplasia identified on percutaneous core breast biopsy. Breast J. 2003;9(1): Bowman K, Munoz A, Mahvi DM, Breslin TM. Lobular neoplasia diagnosed at core biopsy does not mandate surgical excision. J Surg Res. 2007;142(2): Middleton LP, Grant S, Stephens T, Stelling CB, Sneige N, Sahin AA. Lobular carcinoma in situ diagnosed by core needle biopsy: when should it be excised? Mod Pathol. 2003;16(2): Arch Pathol Lab Med Quantifying TDLU Holbrook et al
8 25. Murray MP, Luedtke C, Liberman L, Nehhozina T, Akram M, Brogi E. Classic lobular carcinoma in situ and atypical lobular hyperplasia at percutaneous breast core biopsy: outcomes of prospective excision. Cancer. 2013;119(5): Liberman L, Sama M, Susnik B, et al. Lobular carcinoma in situ at percutaneous breast biopsy: surgical biopsy findings. AJR Am J Roentgenol. 1999; 173(2): Subhawong AP, Subhawong TK, Khouri N, Tsangaris T, Nassar H. Incidental minimal atypical lobular hyperplasia on core needle biopsy: correlation with findings on follow-up excision. Am J Surg Pathol. 2010;34(6): Berg WA, Mrose HE, Ioffe OB. Atypical lobular hyperplasia or lobular carcinoma in situ at core-needle breast biopsy. Radiology. 2001;218(2): Philpotts LE, Shaheen NA, Jain KS, Carter D, Lee CH. Uncommon high-risk lesions of the breast diagnosed at stereotactic core-needle biopsy: clinical importance. Radiology. 2000;216(3): Ottesen GL, Graversen HP, Blichert-Toft M, Zedeler K, Andersen JA. Lobular carcinoma in situ of the female breast: short-term results of a prospective nationwide study: the Danish Breast Cancer Cooperative Group. Am J Surg Pathol. 1993;17(1): Middleton LP, Sneige N, Coyne R, et al. Most lobular carcinoma in situ and atypical lobular hyperplasia diagnosed on core needle biopsy can be managed clinically with radiologic follow-up in a multidisciplinary setting. Cancer Med. 2014;3(3): Rendi MH, Dintzis SM, Lehman CD, Calhoun KE, Allison KH. Lobular insitu neoplasia on breast core needle biopsy: imaging indication and pathologic extent can identify which patients require excisional biopsy. Ann Surg Oncol. 2012;19(3): Calhoun BC, Collie AM, Lott-Limbach AA, et al. Lobular neoplasia diagnosed on breast core biopsy: frequency of carcinoma on excision and implications for management. Ann Diagn Pathol. 2016;25: Aulmann S, Penzel R, Longerich T, Funke B, Schirmacher P, Sinn HP. Clonality of lobular carcinoma in situ (LCIS) and metachronous invasive breast cancer. Breast Cancer Res Treat. 2008;107(3): Eusebi V, Magalhaes F, Azzopardi JG. Pleomorphic lobular carcinoma of the breast: an aggressive tumor showing apocrine differentiation. Hum Pathol. 1992;23(6): Arch Pathol Lab Med Quantifying TDLU Holbrook et al 7
Classic lobular neoplasia on core biopsy: a clinical and radio-pathologic correlation study with follow-up excision biopsy
 762 & 2013 USCAP, Inc All rights reserved 0893-3952/13 $32.00 Classic lobular neoplasia on core biopsy: a clinical and radio-pathologic correlation study with follow-up excision biopsy Shweta Chaudhary
762 & 2013 USCAP, Inc All rights reserved 0893-3952/13 $32.00 Classic lobular neoplasia on core biopsy: a clinical and radio-pathologic correlation study with follow-up excision biopsy Shweta Chaudhary
Management of Patients Diagnosed With Lobular Carcinoma in Situ at Needle Core Biopsy at a Community-Based Outpatient Facility
 Women s Imaging Original Research Destounis et al. Management of LCIS Diagnosed at Core Needle Biopsy Women s Imaging Original Research FOCUS ON: Stamatia V. Destounis 1 Philip F. Murphy Posy J. Seifert
Women s Imaging Original Research Destounis et al. Management of LCIS Diagnosed at Core Needle Biopsy Women s Imaging Original Research FOCUS ON: Stamatia V. Destounis 1 Philip F. Murphy Posy J. Seifert
Atypical Ductal Hyperplasia and Papillomas: A Comparison of Ultrasound Guided Breast Biopsy and Stereotactic Guided Breast Biopsy
 Atypical Ductal Hyperplasia and Papillomas: A Comparison of Ultrasound Guided Breast Biopsy and Stereotactic Guided Breast Biopsy Breast Cancer is the most common cancer diagnosed in women in the United
Atypical Ductal Hyperplasia and Papillomas: A Comparison of Ultrasound Guided Breast Biopsy and Stereotactic Guided Breast Biopsy Breast Cancer is the most common cancer diagnosed in women in the United
CNB vs Surgical Excision
 Update on Core Needle Biopsy of Non-palpable Breast Lesions Nour Sneige, M.D. UT MD Anderson Cancer Center Houston, Tx Image-Guided CNB of Breast Lesions An alternative to surgical biospy CNB vs Surgical
Update on Core Needle Biopsy of Non-palpable Breast Lesions Nour Sneige, M.D. UT MD Anderson Cancer Center Houston, Tx Image-Guided CNB of Breast Lesions An alternative to surgical biospy CNB vs Surgical
Treatment options for the precancerous Atypical Breast lesions. Prof. YOUNG-JIN SUH The Catholic University of Korea
 Treatment options for the precancerous Atypical Breast lesions Prof. YOUNG-JIN SUH The Catholic University of Korea Not so benign lesions? Imaging abnormalities(10% recall) lead to diagnostic evaluation,
Treatment options for the precancerous Atypical Breast lesions Prof. YOUNG-JIN SUH The Catholic University of Korea Not so benign lesions? Imaging abnormalities(10% recall) lead to diagnostic evaluation,
Disclosures 5/27/2012. Outline of Talk. Outline of Talk. When Is LCIS Clinically Significant? Classic LCIS. Classic LCIS
 When Is LCIS Clinically Significant? Disclosures I have nothing to disclose Yunn-Yi Chen, MD, PhD Professor Outline of Talk Outline of Talk Classic LCIS Classic LCIS Definition of lobular differentiation
When Is LCIS Clinically Significant? Disclosures I have nothing to disclose Yunn-Yi Chen, MD, PhD Professor Outline of Talk Outline of Talk Classic LCIS Classic LCIS Definition of lobular differentiation
Atypical papillary lesions after core needle biopsy and subsequent breast carcinoma
 Asian Biomedicine Vol. 5 No. 2 April 2011; 243-248 DOI: 10.5372/1905-7415.0502.031 Original article Atypical papillary lesions after core needle biopsy and subsequent breast carcinoma Tuenchit Khamapirad
Asian Biomedicine Vol. 5 No. 2 April 2011; 243-248 DOI: 10.5372/1905-7415.0502.031 Original article Atypical papillary lesions after core needle biopsy and subsequent breast carcinoma Tuenchit Khamapirad
Advocating Nonsurgical Management of Patients With Small, Incidental Radial Scars at the Time of Needle Core Biopsy. A Study of 77 Cases
 Advocating Nonsurgical Management of Patients With Small, Incidental Radial Scars at the Time of Needle Core Biopsy A Study of 77 Cases Cathleen Matrai, MD; Timothy M. D Alfonso, MD; Lindsay Pharmer, MD;
Advocating Nonsurgical Management of Patients With Small, Incidental Radial Scars at the Time of Needle Core Biopsy A Study of 77 Cases Cathleen Matrai, MD; Timothy M. D Alfonso, MD; Lindsay Pharmer, MD;
Diagnostic benefits of ultrasound-guided. CNB) versus mammograph-guided biopsy for suspicious microcalcifications. without definite breast mass
 Volume 118 No. 19 2018, 531-543 ISSN: 1311-8080 (printed version); ISSN: 1314-3395 (on-line version) url: http://www.ijpam.eu ijpam.eu Diagnostic benefits of ultrasound-guided biopsy versus mammography-guided
Volume 118 No. 19 2018, 531-543 ISSN: 1311-8080 (printed version); ISSN: 1314-3395 (on-line version) url: http://www.ijpam.eu ijpam.eu Diagnostic benefits of ultrasound-guided biopsy versus mammography-guided
Stereotactic 11-Gauge Vacuum- Assisted Breast Biopsy: A Validation Study
 Georg Pfarl 1 Thomas H. Helbich 1 Christopher C. Riedl 1 Teresa Wagner 2 Michael Gnant 3 Margaretha Rudas 4 Laura Liberman 5 Received March 11, 2002; accepted after revision May 17, 2002. 1 Department
Georg Pfarl 1 Thomas H. Helbich 1 Christopher C. Riedl 1 Teresa Wagner 2 Michael Gnant 3 Margaretha Rudas 4 Laura Liberman 5 Received March 11, 2002; accepted after revision May 17, 2002. 1 Department
Flat Epithelial Atypia
 Flat Epithelial Atypia Richard Owings, M.D. University of Arkansas for Medical Sciences Department of Pathology Flat epithelial atypia can be a difficult lesion May be a subtle diagnosis Lots of changes
Flat Epithelial Atypia Richard Owings, M.D. University of Arkansas for Medical Sciences Department of Pathology Flat epithelial atypia can be a difficult lesion May be a subtle diagnosis Lots of changes
Columnar Cell Lesions
 Columnar Cell Lesions Laura C. Collins, M.D. Department of Pathology Beth Israel Deaconess Medical Center and Harvard Medical School Boston, MA Question? Columnar cell lesions are: a) Annoying lesions
Columnar Cell Lesions Laura C. Collins, M.D. Department of Pathology Beth Israel Deaconess Medical Center and Harvard Medical School Boston, MA Question? Columnar cell lesions are: a) Annoying lesions
3/27/2017. Disclosure of Relevant Financial Relationships. Papilloma???
 Management of Papillary Lesions Diagnosed at Rad Path Concordant Core Biopsy (CNB) Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position to
Management of Papillary Lesions Diagnosed at Rad Path Concordant Core Biopsy (CNB) Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position to
04/10/2018 HIGH RISK BREAST LESIONS. Pathology Perspectives of High Risk Breast Lesions ELEVATED RISK OF BREAST CANCER HISTORICAL PERSPECTIVES
 Pathology Perspectives of High Risk Breast Lesions Savitri Krishnamurthy MD Professor of Pathology Deputy Division Head Director of Clinical Trials, Research and Development The University of Texas MD
Pathology Perspectives of High Risk Breast Lesions Savitri Krishnamurthy MD Professor of Pathology Deputy Division Head Director of Clinical Trials, Research and Development The University of Texas MD
6/3/2010. Outline of Talk. Lobular Breast Cancer: Definition of lobular differentiation. Common Problems in Diagnosing LCIS in Core Biopsies
 Outline of Talk Lobular Breast Cancer: Common Problems in Diagnosing LCIS in Core Biopsies Definition of lobular differentiation Variants of LCIS that: carry risk for unsampled invasive cancer mimic DCIS
Outline of Talk Lobular Breast Cancer: Common Problems in Diagnosing LCIS in Core Biopsies Definition of lobular differentiation Variants of LCIS that: carry risk for unsampled invasive cancer mimic DCIS
Image guided core biopsies:
 Recommendations on the Surgical, Radiologic and Pathologic Approaches to Breast Disease: Using best practices based on multidisciplinary methodologies developed through the Allina Breast Committee. Image
Recommendations on the Surgical, Radiologic and Pathologic Approaches to Breast Disease: Using best practices based on multidisciplinary methodologies developed through the Allina Breast Committee. Image
Surgical Pathology Issues of Practical Importance
 Surgical Pathology Issues of Practical Importance Anne Moore, MD Medical Oncology Syed Hoda, MD Surgical Pathology The pathologist is central to the team approach needed to manage the patient with breast
Surgical Pathology Issues of Practical Importance Anne Moore, MD Medical Oncology Syed Hoda, MD Surgical Pathology The pathologist is central to the team approach needed to manage the patient with breast
The management of B3 lesions with emphasis on lobular neoplasia
 The management of B3 lesions with emphasis on lobular neoplasia Abeer Shaaban Queen Elizabeth Hospital Birmingham NHSBSP core biopsy categories B1 - Normal B2 - Benign B3 Uncertain malignant potential
The management of B3 lesions with emphasis on lobular neoplasia Abeer Shaaban Queen Elizabeth Hospital Birmingham NHSBSP core biopsy categories B1 - Normal B2 - Benign B3 Uncertain malignant potential
Interpretation of Breast Pathology in the Era of Minimally Invasive Procedures
 Shahla Masood, M.D. Professor and Chair Department of Pathology and Laboratory Medicine University of Florida College of Medicine Jacksonville Medical Director, UF Health Breast Center Chief of Pathology
Shahla Masood, M.D. Professor and Chair Department of Pathology and Laboratory Medicine University of Florida College of Medicine Jacksonville Medical Director, UF Health Breast Center Chief of Pathology
Pathology of Lobular & Ductal Preneoplasia. Syed A Hoda, MD Weill-Cornell, New York, NY
 Pathology of Lobular & Ductal Preneoplasia Syed A Hoda, MD Weill-Cornell, New York, NY Proliferative Epithelial Changes in Breast A wide range of proliferative epithelial changes occur in the breast There
Pathology of Lobular & Ductal Preneoplasia Syed A Hoda, MD Weill-Cornell, New York, NY Proliferative Epithelial Changes in Breast A wide range of proliferative epithelial changes occur in the breast There
Lobular Carcinoma In Situ Variants in Breast Cores
 Lobular Carcinoma In Situ Variants in Breast Cores Potential for Misdiagnosis, Upgrade Rates at Surgical Excision, and Practical Implications Megan E. Sullivan, MD; Seema A. Khan, MD; Yurdanur Sullu, MD;
Lobular Carcinoma In Situ Variants in Breast Cores Potential for Misdiagnosis, Upgrade Rates at Surgical Excision, and Practical Implications Megan E. Sullivan, MD; Seema A. Khan, MD; Yurdanur Sullu, MD;
Imaging in breast cancer. Mammography and Ultrasound Donya Farrokh.MD Radiologist Mashhad University of Medical Since
 Imaging in breast cancer Mammography and Ultrasound Donya Farrokh.MD Radiologist Mashhad University of Medical Since A mammogram report is a key component of the breast cancer diagnostic process. A mammogram
Imaging in breast cancer Mammography and Ultrasound Donya Farrokh.MD Radiologist Mashhad University of Medical Since A mammogram report is a key component of the breast cancer diagnostic process. A mammogram
Surgical Management of High- Risk Breast Lesions
 Surgical Management of High- Risk Breast Lesions Amy C. Degnim, MD a, Tari A. King, MD b, * KEYWORDS High-risk lesion Atypical hyperplasia Lobular carcinoma in situ Percutaneous breast biopsy Breast cancer
Surgical Management of High- Risk Breast Lesions Amy C. Degnim, MD a, Tari A. King, MD b, * KEYWORDS High-risk lesion Atypical hyperplasia Lobular carcinoma in situ Percutaneous breast biopsy Breast cancer
Ana Sofia Preto 19/06/2013
 Ana Sofia Preto 19/06/2013 Understanding the underlying pathophysiologic processes leading to the various types of calcifications Description and illustration of the several types of calcifications, according
Ana Sofia Preto 19/06/2013 Understanding the underlying pathophysiologic processes leading to the various types of calcifications Description and illustration of the several types of calcifications, according
Mammographic features and correlation with biopsy findings using 11-gauge stereotactic vacuum-assisted breast biopsy (SVABB)
 Original article Annals of Oncology 14: 450 454, 2003 DOI: 10.1093/annonc/mdh088 Mammographic features and correlation with biopsy findings using 11-gauge stereotactic vacuum-assisted breast biopsy (SVABB)
Original article Annals of Oncology 14: 450 454, 2003 DOI: 10.1093/annonc/mdh088 Mammographic features and correlation with biopsy findings using 11-gauge stereotactic vacuum-assisted breast biopsy (SVABB)
Atypical proliferative lesions diagnosed on core biopsy - 6 year review
 Atypical proliferative lesions diagnosed on core biopsy - 6 year review Dr Angela Harris, Dr Julie Weigner & Dr Ricardo Vilain NSW Health Pathology Pathology North, Hunter Anatomical Pathology & Cytology
Atypical proliferative lesions diagnosed on core biopsy - 6 year review Dr Angela Harris, Dr Julie Weigner & Dr Ricardo Vilain NSW Health Pathology Pathology North, Hunter Anatomical Pathology & Cytology
Controversies and Problematic Issues in Core Needle Biopsies (To excise or not to excise)
 Controversies and Problematic Issues in Core Needle Biopsies (To excise or not to excise) Laura C. Collins, M.D. Beth Israel Deaconess Medical Center and Harvard Medical School Boston, MA Schematic Representation
Controversies and Problematic Issues in Core Needle Biopsies (To excise or not to excise) Laura C. Collins, M.D. Beth Israel Deaconess Medical Center and Harvard Medical School Boston, MA Schematic Representation
Excisional biopsy or long term follow-up results in breast high-risk lesions diagnosed at core needle biopsy
 Excisional biopsy or long term follow-up results in breast high-risk lesions diagnosed at core needle biopsy Poster No.: C-2515 Congress: ECR 2015 Type: Authors: Scientific Exhibit Ö. S. Okcu 1, A. Oktay
Excisional biopsy or long term follow-up results in breast high-risk lesions diagnosed at core needle biopsy Poster No.: C-2515 Congress: ECR 2015 Type: Authors: Scientific Exhibit Ö. S. Okcu 1, A. Oktay
BI-RADS Categorization As a Predictor of Malignancy 1
 Susan G. Orel, MD Nicole Kay, BA Carol Reynolds, MD Daniel C. Sullivan, MD BI-RADS Categorization As a Predictor of Malignancy 1 Index terms: Breast, biopsy, 00.1261 Breast neoplasms, localization, 00.125,
Susan G. Orel, MD Nicole Kay, BA Carol Reynolds, MD Daniel C. Sullivan, MD BI-RADS Categorization As a Predictor of Malignancy 1 Index terms: Breast, biopsy, 00.1261 Breast neoplasms, localization, 00.125,
Imaging-Guided Core Needle Biopsy of Papillary Lesions of the Breast
 Eric L. Rosen 1 Rex C. Bentley 2 Jay A. Baker 1 Mary Scott Soo 1 Received January 30, 2002; accepted after revision April 12, 2002. 1 Department of Radiology, Breast Imaging Division, Duke University Medical
Eric L. Rosen 1 Rex C. Bentley 2 Jay A. Baker 1 Mary Scott Soo 1 Received January 30, 2002; accepted after revision April 12, 2002. 1 Department of Radiology, Breast Imaging Division, Duke University Medical
Anatomic Pathology / Mucocele-like Lesions on Breast Core Biopsy. Mucocele-like Lesions Diagnosed on Breast Core Biopsy
 Anatomic Pathology / Mucocele-like Lesions on Breast Core Biopsy Mucocele-like Lesions Diagnosed on Breast Core Biopsy Assessment of Upgrade Rate and Need for Surgical Excision Brian Sutton, MD, 1 Simone
Anatomic Pathology / Mucocele-like Lesions on Breast Core Biopsy Mucocele-like Lesions Diagnosed on Breast Core Biopsy Assessment of Upgrade Rate and Need for Surgical Excision Brian Sutton, MD, 1 Simone
LOBULAR CARCINOMA IN SITU: WHAT DOES IT MEAN? THE SURGEON'S PERSPECTIVE
 : WHAT DOES IT MEAN? THE SURGEON'S PERSPECTIVE Benjamin O. Anderson, M.D. Director, Breast Health Clinic Professor of Surgery and Global Health, University of Washington Joint Member, Fred Hutchinson Cancer
: WHAT DOES IT MEAN? THE SURGEON'S PERSPECTIVE Benjamin O. Anderson, M.D. Director, Breast Health Clinic Professor of Surgery and Global Health, University of Washington Joint Member, Fred Hutchinson Cancer
High risk lesions of the breast : Review of the current diagnostic and management strategies
 High risk lesions of the breast : Review of the current diagnostic and management strategies Poster No.: C-1204 Congress: ECR 2016 Type: Educational Exhibit Authors: P. Jagmohan, F. J. Pool, P. G. Pillay,
High risk lesions of the breast : Review of the current diagnostic and management strategies Poster No.: C-1204 Congress: ECR 2016 Type: Educational Exhibit Authors: P. Jagmohan, F. J. Pool, P. G. Pillay,
Pitfalls and Limitations of Breast MRI. Susan Orel Roth, MD Professor of Radiology University of Pennsylvania
 Pitfalls and Limitations of Breast MRI Susan Orel Roth, MD Professor of Radiology University of Pennsylvania Objectives Review the etiologies of false negative breast MRI examinations Discuss the limitations
Pitfalls and Limitations of Breast MRI Susan Orel Roth, MD Professor of Radiology University of Pennsylvania Objectives Review the etiologies of false negative breast MRI examinations Discuss the limitations
Columnar Cell Lesions and Flat Epithelial Atypia
 Columnar Cell Lesions and Flat Epithelial Atypia Laura C. Collins, M.D. Department of Pathology Beth Israel Deaconess Medical Center and Harvard Medical School, Boston, MA Terminology for Columnar Cell
Columnar Cell Lesions and Flat Epithelial Atypia Laura C. Collins, M.D. Department of Pathology Beth Israel Deaconess Medical Center and Harvard Medical School, Boston, MA Terminology for Columnar Cell
National Diagnostic Imaging Symposium 2013 SAM - Breast MRI 1
 National Diagnostic Imaging Symposium 2013 December 8-12, 2013 Disney s Yacht Club Resort Lake Buena Vista, Florida Self Assessment Module Questions, Answers and References Day SAM Title - Each SAM title
National Diagnostic Imaging Symposium 2013 December 8-12, 2013 Disney s Yacht Club Resort Lake Buena Vista, Florida Self Assessment Module Questions, Answers and References Day SAM Title - Each SAM title
Controversies on the Management of High Risk Breast Lesions on Core Biopsy: An Update on the Literature
 Controversies on the Management of High Risk Breast Lesions on Core Biopsy: An Update on the Literature Dianne Georgian- Smith MD Brigham and Women s Hospital Associate Professor of Radiology, Harvard
Controversies on the Management of High Risk Breast Lesions on Core Biopsy: An Update on the Literature Dianne Georgian- Smith MD Brigham and Women s Hospital Associate Professor of Radiology, Harvard
Proliferative Breast Disease: implications of core biopsy diagnosis. Proliferative Breast Disease
 Proliferative Breast Disease: implications of core biopsy diagnosis Jean F. Simpson, M.D. Breast Pathology Consultants, Inc. Nashville, TN Proliferative Breast Disease Must be interpreted in clinical and
Proliferative Breast Disease: implications of core biopsy diagnosis Jean F. Simpson, M.D. Breast Pathology Consultants, Inc. Nashville, TN Proliferative Breast Disease Must be interpreted in clinical and
Breast Cancer. Most common cancer among women in the US. 2nd leading cause of death in women. Mortality rates though have declined
 Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women Mortality rates though have declined 1 in 8 women will develop breast cancer Breast Cancer Breast cancer increases
Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women Mortality rates though have declined 1 in 8 women will develop breast cancer Breast Cancer Breast cancer increases
Breast Lesion Excision System-Intact (BLES): A Stereotactic Method of Biopsy of Suspicius Non-Palpable Mammographic Lesions.
 Breast Lesion Excision System-Intact (BLES): A Stereotactic Method of Biopsy of Suspicius Non-Palpable Mammographic Lesions. Poster No.: C-1595 Congress: ECR 2014 Type: Authors: Scientific Exhibit I. Georgiou
Breast Lesion Excision System-Intact (BLES): A Stereotactic Method of Biopsy of Suspicius Non-Palpable Mammographic Lesions. Poster No.: C-1595 Congress: ECR 2014 Type: Authors: Scientific Exhibit I. Georgiou
Breast Cancer. Saima Saeed MD
 Breast Cancer Saima Saeed MD Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women 1 in 8 women will develop breast cancer Incidence/mortality rates have declined Breast
Breast Cancer Saima Saeed MD Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women 1 in 8 women will develop breast cancer Incidence/mortality rates have declined Breast
Case study 1. Rie Horii, M.D., Ph.D. Division of Pathology Cancer Institute Hospital, Japanese Foundation for Cancer Research
 NCCN/JCCNB Seminar in Japan April 15, 2012 Case study 1 Rie Horii, M.D., Ph.D. Division of Pathology Cancer Institute Hospital, Japanese Foundation for Cancer Research Present illness: A 50y.o.premenopausal
NCCN/JCCNB Seminar in Japan April 15, 2012 Case study 1 Rie Horii, M.D., Ph.D. Division of Pathology Cancer Institute Hospital, Japanese Foundation for Cancer Research Present illness: A 50y.o.premenopausal
Non-mass Enhancement on Breast MRI. Aditi A. Desai, MD Margaret Ann Mays, MD
 Non-mass Enhancement on Breast MRI Aditi A. Desai, MD Margaret Ann Mays, MD Breast MRI Important screening and diagnostic tool, given its high sensitivity for breast cancer detection Breast MRI - Indications
Non-mass Enhancement on Breast MRI Aditi A. Desai, MD Margaret Ann Mays, MD Breast MRI Important screening and diagnostic tool, given its high sensitivity for breast cancer detection Breast MRI - Indications
BI-RADS CATEGORIZATION AND BREAST BIOPSY categorization in the selection of appropriate breast biopsy technique is also discussed. Patients and method
 Original Article Positive Predictive Value of BI-RADS Categorization in an Asian Population Yah-Yuen Tan, Siew-Bock Wee, Mona P.C. Tan and Bee-Kiang Chong, 1 Departments of General Surgery and 1Diagnostic
Original Article Positive Predictive Value of BI-RADS Categorization in an Asian Population Yah-Yuen Tan, Siew-Bock Wee, Mona P.C. Tan and Bee-Kiang Chong, 1 Departments of General Surgery and 1Diagnostic
EARLY DETECTION: MAMMOGRAPHY AND SONOGRAPHY
 EARLY DETECTION: MAMMOGRAPHY AND SONOGRAPHY Elizabeth A. Rafferty, M.D. Avon Comprehensive Breast Center Massachusetts General Hospital Harvard Medical School Breast Cancer Screening Early detection of
EARLY DETECTION: MAMMOGRAPHY AND SONOGRAPHY Elizabeth A. Rafferty, M.D. Avon Comprehensive Breast Center Massachusetts General Hospital Harvard Medical School Breast Cancer Screening Early detection of
EARLY DETECTION: MAMMOGRAPHY AND SONOGRAPHY
 EARLY DETECTION: MAMMOGRAPHY AND SONOGRAPHY Elizabeth A. Rafferty, M.D. Avon Comprehensive Breast Center Massachusetts General Hospital Harvard Medical School Breast Cancer Screening Early detection of
EARLY DETECTION: MAMMOGRAPHY AND SONOGRAPHY Elizabeth A. Rafferty, M.D. Avon Comprehensive Breast Center Massachusetts General Hospital Harvard Medical School Breast Cancer Screening Early detection of
Breast Imaging Lexicon
 9//201 200 BI RADS th Edition 201 BI RADS th Edition Breast Imaging Lexicon Mammographic Pathology and Assessment Categories Deborah Thames, R.T.(R)(M)(QM) The Advanced Health Education Center Nonmember:
9//201 200 BI RADS th Edition 201 BI RADS th Edition Breast Imaging Lexicon Mammographic Pathology and Assessment Categories Deborah Thames, R.T.(R)(M)(QM) The Advanced Health Education Center Nonmember:
Incidence and Management of Complex Fibroadenomas
 Incidence and Management of Complex Fibroadenomas Women s Imaging Original Research 214.fm 11/29/07 WOMEN S IMAGING Miri Sklair-Levy 1 Tamar Sella 1 Tanir Alweiss 2 Ilia Craciun 1 Eugene Libson 1 Bella
Incidence and Management of Complex Fibroadenomas Women s Imaging Original Research 214.fm 11/29/07 WOMEN S IMAGING Miri Sklair-Levy 1 Tamar Sella 1 Tanir Alweiss 2 Ilia Craciun 1 Eugene Libson 1 Bella
Original Report. Mucocele-Like Tumors of the Breast: Mammographic and Sonographic Appearances. Katrina Glazebrook 1 Carol Reynolds 2
 Katrina Glazebrook 1 Carol Reynolds 2 Received January 2, 2002; accepted after revision August 28, 2002. 1 Department of Radiology, Mayo Clinic, 200 First St. S.W., Rochester, MN 55905. Address correspondence
Katrina Glazebrook 1 Carol Reynolds 2 Received January 2, 2002; accepted after revision August 28, 2002. 1 Department of Radiology, Mayo Clinic, 200 First St. S.W., Rochester, MN 55905. Address correspondence
DCIS of the Breast--MRI findings with mammographic correlation.
 DCIS of the Breast--MRI findings with mammographic correlation. Poster No.: C-1560 Congress: ECR 2013 Type: Educational Exhibit Authors: N. B. Ibrahim, P. Morris, S. ANANDAN; Burlington, MA/US Keywords:
DCIS of the Breast--MRI findings with mammographic correlation. Poster No.: C-1560 Congress: ECR 2013 Type: Educational Exhibit Authors: N. B. Ibrahim, P. Morris, S. ANANDAN; Burlington, MA/US Keywords:
IBCM 2, April 2009, Sarajevo, Bosnia and Herzegovina
 Preoperative diagnosis and treatment planning in breast cancer The pathologist s perspective L. Mazzucchelli Istituto Cantonale di Patologia Locarno, Switzerland IBCM 2, 23-25 April 2009, Sarajevo, Bosnia
Preoperative diagnosis and treatment planning in breast cancer The pathologist s perspective L. Mazzucchelli Istituto Cantonale di Patologia Locarno, Switzerland IBCM 2, 23-25 April 2009, Sarajevo, Bosnia
Radiologic and pathologic correlation of non-mass like breast lesions on US and MRI: Benign, high risk, versus malignant
 Radiologic and pathologic correlation of non-mass like breast lesions on US and MRI: Benign, high risk, versus malignant Poster No.: C-1161 Congress: ECR 2013 Type: Educational Exhibit Authors: J. Kwak,
Radiologic and pathologic correlation of non-mass like breast lesions on US and MRI: Benign, high risk, versus malignant Poster No.: C-1161 Congress: ECR 2013 Type: Educational Exhibit Authors: J. Kwak,
Radiologic and pathologic correlation of non-mass like breast lesions on US and MRI: Benign, high risk, versus malignant
 Radiologic and pathologic correlation of non-mass like breast lesions on US and MRI: Benign, high risk, versus malignant Poster No.: C-1161 Congress: ECR 2013 Type: Educational Exhibit Authors: J. Kwak,
Radiologic and pathologic correlation of non-mass like breast lesions on US and MRI: Benign, high risk, versus malignant Poster No.: C-1161 Congress: ECR 2013 Type: Educational Exhibit Authors: J. Kwak,
Cytyc Corporation - Case Presentation Archive - March 2002
 FirstCyte Ductal Lavage History: 68 Year Old Female Gail Index: Unknown Clinical History: Negative Mammogram in 1995 6 yrs. later presents with bloody nipple discharge Subsequent suspicious mammogram Suspicious
FirstCyte Ductal Lavage History: 68 Year Old Female Gail Index: Unknown Clinical History: Negative Mammogram in 1995 6 yrs. later presents with bloody nipple discharge Subsequent suspicious mammogram Suspicious
Women s Imaging Original Research
 Women s Imaging Original Research Villa et al. Biopsy of Atypical Ductal Hyperplasia Women s Imaging Original Research WOMEN S IMAGING Alessandro Villa 1 Alberto Tagliafico 2 Fabio Chiesa 1 Maurizio Chiaramondia
Women s Imaging Original Research Villa et al. Biopsy of Atypical Ductal Hyperplasia Women s Imaging Original Research WOMEN S IMAGING Alessandro Villa 1 Alberto Tagliafico 2 Fabio Chiesa 1 Maurizio Chiaramondia
Image-guided core needle biopsy has become a standard
 Pathologic Review of Atypical Hyperplasia Identified by Image-Guided Breast Needle Core Biopsy Correlation With Excision Specimen I-Tien Yeh, MD; Diana Dimitrov, MD; Pamela Otto, MD; Alexander R. Miller,
Pathologic Review of Atypical Hyperplasia Identified by Image-Guided Breast Needle Core Biopsy Correlation With Excision Specimen I-Tien Yeh, MD; Diana Dimitrov, MD; Pamela Otto, MD; Alexander R. Miller,
Tips and Tricks to performing Magnetic Resonance Imaging Guided Breast Interventional Procedures Habib Rahbar, MD, FSBI October 23, 2018, 7:00pm ET
 Tips and Tricks to performing Magnetic Resonance Imaging Guided Breast Interventional Procedures Habib Rahbar, MD, FSBI October 23, 2018, 7:00pm ET SAM Questions/Answers/Rationales/References 1. Below
Tips and Tricks to performing Magnetic Resonance Imaging Guided Breast Interventional Procedures Habib Rahbar, MD, FSBI October 23, 2018, 7:00pm ET SAM Questions/Answers/Rationales/References 1. Below
RSNA, /radiol Appendix E1. Methods
 RSNA, 2016 10.1148/radiol.2016151097 Appendix E1 Methods US and Near-infrared Data Acquisition Four optical wavelengths (740 nm, 780 nm, 808 nm, and 830 nm) were used to sequentially deliver the light
RSNA, 2016 10.1148/radiol.2016151097 Appendix E1 Methods US and Near-infrared Data Acquisition Four optical wavelengths (740 nm, 780 nm, 808 nm, and 830 nm) were used to sequentially deliver the light
Epithelial Columnar Breast Lesions: Histopathology and Molecular Markers
 29th Annual International Conference Advances in the Application of Monoclonal Antibodies in Clinical Oncology and Symposium on Cancer Stem Cells 25 th -27t h June, 2012, Mykonos, Greece Epithelial Columnar
29th Annual International Conference Advances in the Application of Monoclonal Antibodies in Clinical Oncology and Symposium on Cancer Stem Cells 25 th -27t h June, 2012, Mykonos, Greece Epithelial Columnar
Management of B3 lesions
 Management of B3 lesions Pathological view Abeer Shaaban Queen Elizabeth Hospital Birmingham FEA AIDP B3 lesions In situ Lobular neoplasia Papilloma Radial scar Fibroaepithelial lesion Mucocoele like lesion
Management of B3 lesions Pathological view Abeer Shaaban Queen Elizabeth Hospital Birmingham FEA AIDP B3 lesions In situ Lobular neoplasia Papilloma Radial scar Fibroaepithelial lesion Mucocoele like lesion
Vacuum-assisted breast biopsy using computer-aided 3.0 T- MRI guidance: diagnostic performance in 173 lesions
 Vacuum-assisted breast biopsy using computer-aided 3.0 T- MRI guidance: diagnostic performance in 173 lesions Poster No.: C-2870 Congress: ECR 2017 Type: Scientific Exhibit Authors: A. Pozzetto, L. Camera,
Vacuum-assisted breast biopsy using computer-aided 3.0 T- MRI guidance: diagnostic performance in 173 lesions Poster No.: C-2870 Congress: ECR 2017 Type: Scientific Exhibit Authors: A. Pozzetto, L. Camera,
Mammographic imaging of nonpalpable breast lesions. Malai Muttarak, MD Department of Radiology Chiang Mai University Chiang Mai, Thailand
 Mammographic imaging of nonpalpable breast lesions Malai Muttarak, MD Department of Radiology Chiang Mai University Chiang Mai, Thailand Introduction Contents Mammographic signs of nonpalpable breast cancer
Mammographic imaging of nonpalpable breast lesions Malai Muttarak, MD Department of Radiology Chiang Mai University Chiang Mai, Thailand Introduction Contents Mammographic signs of nonpalpable breast cancer
Malignant transformation of fibroadenomas
 Malignant transformation of fibroadenomas Poster No.: C-2503 Congress: ECR 2013 Type: Educational Exhibit Authors: L. N. Elias, M. A. Rudner, L. M. Yano, P. C. Moraes, Y. 1 1 1 1 1 1 2 1 2 Chang, M. B.
Malignant transformation of fibroadenomas Poster No.: C-2503 Congress: ECR 2013 Type: Educational Exhibit Authors: L. N. Elias, M. A. Rudner, L. M. Yano, P. C. Moraes, Y. 1 1 1 1 1 1 2 1 2 Chang, M. B.
Underestimation of cancer in case of diagnosis of atypical ductal hyperplasia (ADH) by vacuum assisted core needle biopsy
 reports of practical oncology and radiotherapy 1 7 (2 0 1 2) 129 133 Available online at www.sciencedirect.com journal homepage: http://www.elsevier.com/locate/rpor Original research article Underestimation
reports of practical oncology and radiotherapy 1 7 (2 0 1 2) 129 133 Available online at www.sciencedirect.com journal homepage: http://www.elsevier.com/locate/rpor Original research article Underestimation
Current Status of Supplementary Screening With Breast Ultrasound
 Current Status of Supplementary Screening With Breast Ultrasound Stephen A. Feig, M.D., FACR Fong and Jean Tsai Professor of Women s Imaging Department of Radiologic Sciences University of California,
Current Status of Supplementary Screening With Breast Ultrasound Stephen A. Feig, M.D., FACR Fong and Jean Tsai Professor of Women s Imaging Department of Radiologic Sciences University of California,
Breast Lesions of Uncertain Malignant Potential: A Challenge for Surgeons
 Breast Lesions of Uncertain Malignant Potential: A Challenge for Surgeons Deslauriers Nancy 1, Sidéris Lucas 1, Dufresne Michel-Pierre 2, Mitchell Andrew 3, Drolet Pierre 4, Dubé Pierre 1, Leclerc Yves
Breast Lesions of Uncertain Malignant Potential: A Challenge for Surgeons Deslauriers Nancy 1, Sidéris Lucas 1, Dufresne Michel-Pierre 2, Mitchell Andrew 3, Drolet Pierre 4, Dubé Pierre 1, Leclerc Yves
Sonographic Detection and Sonographically Guided Biopsy of Breast Microcalcifications
 Sonographic Detection and Sonographically Guided Biopsy of Breast Microcalcifications Mary Scott Soo 1 Jay A. Baker Eric L. Rosen OBJECTIVE. The purpose of this study was to evaluate the ability of sonography
Sonographic Detection and Sonographically Guided Biopsy of Breast Microcalcifications Mary Scott Soo 1 Jay A. Baker Eric L. Rosen OBJECTIVE. The purpose of this study was to evaluate the ability of sonography
Proliferative Epithelial lesions of the Breast. Sami Shousha, MD, FRCPath Charing Cross Hospital & Imperial College, London
 Proliferative Epithelial lesions of the Breast Sami Shousha, MD, FRCPath Charing Cross Hospital & Imperial College, London Amman, November2013 Proliferative Epithelial Lesions of the Breast Usual type
Proliferative Epithelial lesions of the Breast Sami Shousha, MD, FRCPath Charing Cross Hospital & Imperial College, London Amman, November2013 Proliferative Epithelial Lesions of the Breast Usual type
Lesion Imaging Characteristics Mass, Favoring Benign Circumscribed Margins Intramammary Lymph Node
 Lesion Imaging Characteristics Mass, Favoring Benign Circumscribed Margins Intramammary Lymph Node Oil Cyst Mass, Intermediate Concern Microlobulated Margins Obscured Margins Mass, Favoring Malignant Indistinct
Lesion Imaging Characteristics Mass, Favoring Benign Circumscribed Margins Intramammary Lymph Node Oil Cyst Mass, Intermediate Concern Microlobulated Margins Obscured Margins Mass, Favoring Malignant Indistinct
Amammography report is a key component of the breast
 Review Article Writing a Mammography Report Amammography report is a key component of the breast cancer diagnostic process. Although mammographic findings were not clearly differentiated between benign
Review Article Writing a Mammography Report Amammography report is a key component of the breast cancer diagnostic process. Although mammographic findings were not clearly differentiated between benign
Effective Health Care Program
 Comparative Effectiveness Review Number 19 Effective Health Care Program Comparative Effectiveness of Core-Needle and Open Surgical Biopsy for the Diagnosis of Breast Lesions Executive Summary Background
Comparative Effectiveness Review Number 19 Effective Health Care Program Comparative Effectiveness of Core-Needle and Open Surgical Biopsy for the Diagnosis of Breast Lesions Executive Summary Background
BI-RADS and Breast MRI. Kathy Borovicka, M.D. Thursday February 15, 2018
 BI-RADS and Breast MRI Kathy Borovicka, M.D. Thursday February 15, 2018 Learning Objectives Be familiar with the Breast Imaging Reporting and Data System (BI-RADS) Understand the components of a breast
BI-RADS and Breast MRI Kathy Borovicka, M.D. Thursday February 15, 2018 Learning Objectives Be familiar with the Breast Imaging Reporting and Data System (BI-RADS) Understand the components of a breast
Radiologic Findings of Mucocele-like Tumors of the breast: Can we differentiate pure benign from associated with high risk lesions?
 Radiologic Findings of Mucocele-like Tumors of the breast: Can we differentiate pure benign from associated with high risk lesions? Poster No.: C-0332 Congress: ECR 2014 Type: Educational Exhibit Authors:
Radiologic Findings of Mucocele-like Tumors of the breast: Can we differentiate pure benign from associated with high risk lesions? Poster No.: C-0332 Congress: ECR 2014 Type: Educational Exhibit Authors:
ACRIN 6666 IM Additional Evaluation: Additional Views/Targeted US
 Additional Evaluation: Additional Views/Targeted US For revised or corrected form check box and fax to 215-717-0936. Instructions: The form is completed based on recommendations (from ID form) for additional
Additional Evaluation: Additional Views/Targeted US For revised or corrected form check box and fax to 215-717-0936. Instructions: The form is completed based on recommendations (from ID form) for additional
Quality ID #263: Preoperative Diagnosis of Breast Cancer National Quality Strategy Domain: Effective Clinical Care
 Quality ID #263: Preoperative Diagnosis of Breast Cancer National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Process DESCRIPTION:
Quality ID #263: Preoperative Diagnosis of Breast Cancer National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Process DESCRIPTION:
Benign, Reactive and Inflammatory Lesions of the Breast
 Benign, Reactive and Inflammatory Lesions of the Breast Marilin Rosa, MD Associate Member Section Head of Breast Pathology Department of Anatomic Pathology Program Director, Breast Pathology Fellowship
Benign, Reactive and Inflammatory Lesions of the Breast Marilin Rosa, MD Associate Member Section Head of Breast Pathology Department of Anatomic Pathology Program Director, Breast Pathology Fellowship
Controversies on the Management of High-Risk Lesions at Core Biopsy from a Radiology/ Pathology Perspective
 Controversies on the Management of High-Risk Lesions at Core Biopsy from a Radiology/ Pathology Perspective Dianne Georgian-Smith, MD a, *, Thomas J. Lawton, MD b,c KEYWORDS Breast high-risk lesion Lobular
Controversies on the Management of High-Risk Lesions at Core Biopsy from a Radiology/ Pathology Perspective Dianne Georgian-Smith, MD a, *, Thomas J. Lawton, MD b,c KEYWORDS Breast high-risk lesion Lobular
The Ratio of Atypical Ductal Hyperplasia Foci to Core Numbers in Needle Biopsy: A Practical Index Predicting Breast Cancer in Subsequent Excision
 The Korean Journal of Pathology 2012; 46: 15-21 ORIGINAL ARTICLE The Ratio of Atypical Ductal Hyperplasia Foci to Core Numbers in Needle Biopsy: A Practical Index Predicting Breast Cancer in Subsequent
The Korean Journal of Pathology 2012; 46: 15-21 ORIGINAL ARTICLE The Ratio of Atypical Ductal Hyperplasia Foci to Core Numbers in Needle Biopsy: A Practical Index Predicting Breast Cancer in Subsequent
from Breast Biopsy: Are They Concordant? How Do I Manage the Results? 1
 Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. BREAST IMAGING Interactive
Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. BREAST IMAGING Interactive
During the last 20 years, magnetic resonance imaging
 Original Articles Pathologic Findings of Breast Lesions Detected on Magnetic Resonance Imaging Seema B. Jabbar, MD; Beverly Lynch, MD; Stephen Seiler, MD; Helena Hwang, MD; Sunati Sahoo, MD Context. Breast
Original Articles Pathologic Findings of Breast Lesions Detected on Magnetic Resonance Imaging Seema B. Jabbar, MD; Beverly Lynch, MD; Stephen Seiler, MD; Helena Hwang, MD; Sunati Sahoo, MD Context. Breast
Breast Screening in Singapore: Implications for Pathology
 Review Article 827 Breast Screening in Singapore: Implications for Pathology Puay-Hoon Tan, 1 FRCPA, MD, FRCPath Abstract The aim of this review is to discuss the impact of breast screening on pathology.
Review Article 827 Breast Screening in Singapore: Implications for Pathology Puay-Hoon Tan, 1 FRCPA, MD, FRCPath Abstract The aim of this review is to discuss the impact of breast screening on pathology.
Triple Negative Breast Cancer: Clinical Presentation and Multimodality Imaging Characteristics
 Triple Negative Breast Cancer: Clinical Presentation and Multimodality Imaging Characteristics Poster No.: R-0141 Congress: RANZCR-AOCR 2012 Type: Scientific Exhibit Authors: O. H. Woo, S. Jang, K. R.
Triple Negative Breast Cancer: Clinical Presentation and Multimodality Imaging Characteristics Poster No.: R-0141 Congress: RANZCR-AOCR 2012 Type: Scientific Exhibit Authors: O. H. Woo, S. Jang, K. R.
Utility of Adequate Core Biopsy Samples from Ultrasound Biopsies Needed for Today s Breast Pathology
 Utility of Adequate Core Biopsy Samples from Ultrasound Biopsies Needed for Today s Breast Pathology Ugur Ozerdem, M.D. 1 Abstract Background: There is a paradigm shift in breast biopsy philosophy. In
Utility of Adequate Core Biopsy Samples from Ultrasound Biopsies Needed for Today s Breast Pathology Ugur Ozerdem, M.D. 1 Abstract Background: There is a paradigm shift in breast biopsy philosophy. In
Atypical ductal hyperplasia diagnosed at ultrasound guided biopsy of breast mass
 Atypical ductal hyperplasia diagnosed at ultrasound guided biopsy of breast mass Poster No.: C-1483 Congress: ECR 2014 Type: Authors: Keywords: DOI: Scientific Exhibit J. Cho, J. Chung, E. S. Cha, J. E.
Atypical ductal hyperplasia diagnosed at ultrasound guided biopsy of breast mass Poster No.: C-1483 Congress: ECR 2014 Type: Authors: Keywords: DOI: Scientific Exhibit J. Cho, J. Chung, E. S. Cha, J. E.
Guidance on the management of B3 lesions
 Guidance on the management of B3 lesions Lesion diagnosed on 14g or vacuumassisted biopsy (VAB) Risk of upgrade Recommended investigation Suggested approach for follow-up if no malignancy on VAE awaiting
Guidance on the management of B3 lesions Lesion diagnosed on 14g or vacuumassisted biopsy (VAB) Risk of upgrade Recommended investigation Suggested approach for follow-up if no malignancy on VAE awaiting
PURPOSE IMAGE-GUIDANCE MODALITIES IMAGE-GUIDED BREAST BIOPSY. US-Techniques. Ultrasound. US guided NLOBB. TH. Helbich
 IMAGE-GUIDED BREAST BIOPSY PURPOSE TH. Helbich Department of Radiology Division of Molecular & Gender Imaging Medical University of Vienna Imaging techniques Interventional procedures Quality management
IMAGE-GUIDED BREAST BIOPSY PURPOSE TH. Helbich Department of Radiology Division of Molecular & Gender Imaging Medical University of Vienna Imaging techniques Interventional procedures Quality management
OPTO-ACOUSTIC BREAST IMAGING
 OPTO-ACOUSTIC BREAST IMAGING A Novel Fusion of Functional and Morphologic Imaging Reni S. Butler, MD A. Thomas Stavros, MD F. Lee Tucker, MD Michael J. Ulissey, MD PURPOSE 1. Explain opto-acoustic (OA)
OPTO-ACOUSTIC BREAST IMAGING A Novel Fusion of Functional and Morphologic Imaging Reni S. Butler, MD A. Thomas Stavros, MD F. Lee Tucker, MD Michael J. Ulissey, MD PURPOSE 1. Explain opto-acoustic (OA)
Multicenter Evaluation of the Breast Lesion Excision System, a Percutaneous, Vacuum-Assisted, Intact-Specimen Breast Biopsy Device
 945 Multicenter Evaluation of the Breast Lesion Excision System, a Percutaneous, Vacuum-Assisted, Intact-Specimen Breast Biopsy Device Angela Sie, MD 1 David C. Bryan, MD 2 Victor Gaines, MD 3 Larry K.
945 Multicenter Evaluation of the Breast Lesion Excision System, a Percutaneous, Vacuum-Assisted, Intact-Specimen Breast Biopsy Device Angela Sie, MD 1 David C. Bryan, MD 2 Victor Gaines, MD 3 Larry K.
BI-RADS Update. Martha B. Mainiero, MD, FACR, FSBI Brown University Rhode Island Hospital
 BI-RADS Update Martha B. Mainiero, MD, FACR, FSBI Brown University Rhode Island Hospital No Disclosures BI-RADS History 1980s Quality Issues ACR Accreditation BI-RADS 1994 2003 4 th Edition MRI, US January
BI-RADS Update Martha B. Mainiero, MD, FACR, FSBI Brown University Rhode Island Hospital No Disclosures BI-RADS History 1980s Quality Issues ACR Accreditation BI-RADS 1994 2003 4 th Edition MRI, US January
CAP Laboratory Improvement Programs. Pathologic Diagnostic Correlation With Breast Imaging Findings
 CAP Laboratory Improvement Programs Pathologic Diagnostic Correlation With Breast Imaging Findings A College of American Pathologists Q-Probes Study of 48 Institutions Michael O. Idowu, MD, MPH; Linday
CAP Laboratory Improvement Programs Pathologic Diagnostic Correlation With Breast Imaging Findings A College of American Pathologists Q-Probes Study of 48 Institutions Michael O. Idowu, MD, MPH; Linday
Can magnetic resonance imaging obviate the need for biopsy for microcalcifications?
 Original Article Can magnetic resonance imaging obviate the need for biopsy for microcalcifications? Shinya Yamamoto, Takashi Chishima Department of Breast Surgery, Yokohama Rosai Hospital, Yokohama 222-0036,
Original Article Can magnetic resonance imaging obviate the need for biopsy for microcalcifications? Shinya Yamamoto, Takashi Chishima Department of Breast Surgery, Yokohama Rosai Hospital, Yokohama 222-0036,
Atypical Ductal Hyperplasia of the Breast:
 Atypical Ductal Hyperplasia of the Breast: Radiologic and Histopathologic Correlation 1 Ji Young Lee, M.D., Bo Kyoung Seo, M.D. 2, Jung Hyck Kim, M.D., Yu Whan Oh, M.D., Kyu Ran Cho, M.D., Eun Jeong Choi,
Atypical Ductal Hyperplasia of the Breast: Radiologic and Histopathologic Correlation 1 Ji Young Lee, M.D., Bo Kyoung Seo, M.D. 2, Jung Hyck Kim, M.D., Yu Whan Oh, M.D., Kyu Ran Cho, M.D., Eun Jeong Choi,
Macrobiopsy under X-Ray Guidance
 Macrobiopsy under X-Ray Guidance C. Balleyguier, B. Boyer Radiology Gustave Roussy, Villejuif, France Breast Intervention Imaging Major domain in breast imaging European guidelines recommend a pre surgical
Macrobiopsy under X-Ray Guidance C. Balleyguier, B. Boyer Radiology Gustave Roussy, Villejuif, France Breast Intervention Imaging Major domain in breast imaging European guidelines recommend a pre surgical
PAPER. Upstaging of Atypical Ductal Hyperplasia After Vacuum-Assisted 11-Gauge Stereotactic Core Needle Biopsy
 PAPER Upstaging of Atypical Ductal Hyperplasia After Vacuum-Assisted 11-Gauge Stereotactic Core Needle Biopsy David J. Winchester, MD; Joel R. Bernstein, MD; Jan M. Jeske, MD; Mary H. Nicholson, MD; Elizabeth
PAPER Upstaging of Atypical Ductal Hyperplasia After Vacuum-Assisted 11-Gauge Stereotactic Core Needle Biopsy David J. Winchester, MD; Joel R. Bernstein, MD; Jan M. Jeske, MD; Mary H. Nicholson, MD; Elizabeth
Columnar Cell Lesions. Columnar Cell Lesions and Flat Epithelial Atypia
 Columnar Cell Lesions and Stuart J. Schnitt, M.D. Beth Israel Deaconess Medical Center and Harvard Medical School Boston, MA, USA Columnar Cell Lesions Lesions characterized by columnar epithelial cells
Columnar Cell Lesions and Stuart J. Schnitt, M.D. Beth Israel Deaconess Medical Center and Harvard Medical School Boston, MA, USA Columnar Cell Lesions Lesions characterized by columnar epithelial cells
HHS Public Access Author manuscript Am J Surg Pathol. Author manuscript; available in PMC 2016 September 06.
 Radial Scar at Image-guided Needle Biopsy: Is Excision Necessary? Niamh Conlon, MB, FRCPath *, Clare D Arcy, MB, FRCPath *, Jennifer B. Kaplan, MD, Zenica L. Bowser, MS *, Anibal Cordero, BS *, Edi Brogi,
Radial Scar at Image-guided Needle Biopsy: Is Excision Necessary? Niamh Conlon, MB, FRCPath *, Clare D Arcy, MB, FRCPath *, Jennifer B. Kaplan, MD, Zenica L. Bowser, MS *, Anibal Cordero, BS *, Edi Brogi,
Breast: Difficulties in Core Biopsies
 Breast: Difficulties in Core Biopsies Anna Marie Mulligan, MB, MSc, FRCPath University Health Network and University of Toronto E-mail: annamarie.mulligan@uhn.ca No conflicts of interest Role of Core Needle
Breast: Difficulties in Core Biopsies Anna Marie Mulligan, MB, MSc, FRCPath University Health Network and University of Toronto E-mail: annamarie.mulligan@uhn.ca No conflicts of interest Role of Core Needle
CLINICAL SIGNIFICANCE OF BENIGN EPITHELIAL CHANGES
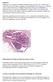 Papillomas. Papillomas are composed of multiple branching fibrovascular cores, each having a connective tissue axis lined by luminal and myoepithelial cells ( Fig. 23-11 ). Growth occurs within a dilated
Papillomas. Papillomas are composed of multiple branching fibrovascular cores, each having a connective tissue axis lined by luminal and myoepithelial cells ( Fig. 23-11 ). Growth occurs within a dilated
Is Probably Benign Really Just Benign? Peter R Eby, MD, FSBI Virginia Mason Medical Center Seattle, WA
 Is Probably Benign Really Just Benign? Peter R Eby, MD, FSBI Virginia Mason Medical Center Seattle, WA Disclosures: CONSULTANT FOR DEVICOR MEDICAL ARS Question 1 Is probably benign really just benign?
Is Probably Benign Really Just Benign? Peter R Eby, MD, FSBI Virginia Mason Medical Center Seattle, WA Disclosures: CONSULTANT FOR DEVICOR MEDICAL ARS Question 1 Is probably benign really just benign?
Breast pathology. 2nd Department of Pathology Semmelweis University
 Breast pathology 2nd Department of Pathology Semmelweis University Breast pathology - Summary - Benign lesions - Acute mastitis - Plasma cell mastitis / duct ectasia - Fat necrosis - Fibrocystic change/
Breast pathology 2nd Department of Pathology Semmelweis University Breast pathology - Summary - Benign lesions - Acute mastitis - Plasma cell mastitis / duct ectasia - Fat necrosis - Fibrocystic change/
