Morphometric evaluation of the uncinate process and its importance in surgical approaches to the cervical spine: a cadaveric study
|
|
|
- Gloria Eaton
- 5 years ago
- Views:
Transcription
1 Singapore Med J 2016; 57(10): doi: /smedj Morphometric evaluation of the uncinate process and its importance in surgical approaches to the cervical spine: a cadaveric study Mustafa Güvençer 1, MD, PhD, Sait Naderi 2, MD, Süleyman Men 3, MD, Salih Sayhan 4, MD, Süleyman Tetik 1, MD INTRODUCTION The uncinate process (UP) has an important role because of its relationship with the vertebral artery and spinal roots. Degenerative diseases cause osteophyte formation on the UP, leading to radiculopathy, myelopathy and vertebral vascular insufficiency, which may require surgical management. This study aimed to evaluate the morphometry of this region to shed light on the anatomy of the UP. METHODS Morphometric data was obtained from 13 male formaldehyde-fixed cadavers. Direct measurements were obtained using a metal caliper. Computed tomography (CT) morphometry was performed with the cadavers in the supine position. RESULTS Direct cadaveric measurements showed that the height of the UP increased from C3 (5.8 ± 1.0 mm) to C7 (6.6 ± 0.5 mm). On CT, the corresponding measurements were 5.9 ± 1.2 mm at C3 and 6.9 ± 0.6 mm at C7. The distance between the left and right apex of the UP from C3 to C7 also increased on both direct cadaveric and CT measurements (C3: 20.8 ± 1.0 mm and C7: 28.1 ± 2.4 mm vs. C3: 23.7 ± 3.4 mm and C7: 29.0 ± 3.0 mm, respectively). On CT, the distance between the UP and superior articular process at the C3 to C7 levels were 9.8 ± 1.7 mm, 7.9 ± 1.8 mm, 7.9 ± 1.6 mm, 7.8 ± 1.3 mm and 8.2 ± 1.7 mm, respectively. CONCLUSION Direct cadaveric and CT measurements of the UP are useful for preoperative evaluation of the cervical spine and may lead to better surgical outcomes. Keywords: cervical spine, cervical surgical approaches, morphometric study, surgical anatomy, uncinate process INTRODUCTION The uncinate process (UP) is located on the superior surfaces of the third to seventh cervical vertebral bodies (i.e. C3C7) and the first thoracic vertebra. According to Pait et al, (1) the UP was first identified in 1858 by Luschka, who named it eminentia costaria because it resembles the head of a rudimentary rib; Trolard introduced the current, widely used term, processus uncinatus (Latin for uncinate process) in The function of the UP is said to be protective, as it restricts lateral flexion. (1) The UP is located close to the vertebral artery, radicular artery and spinal nerve roots. The development of osteophytes on the UP, which may be due to some degenerative diseases, could result in increased pressure on neurovascular structures that are in close proximity to the UP. For instance, osteophytes arising from the UP vertebra may interfere with the transverse foramen, leading to compression of the vertebral artery. (2) Pathologies such as radiculopathy, myelopathy and vertebral vascular insufficiency may occur due to the formation of UP osteophytes. (2-4) To treat these conditions, uncoforaminectomy and corpectomy via the anterolateral or anteromedial approach may be necessary. (4-6) As the UP is a very important area in osteophyte resection, corpectomy and cervical surgery for decompression, knowledge of its morphometry is crucial to surgeons. Although several studies have been conducted on the UP based on the analysis of dry bone materials, (7-9) to the best of our knowledge, none used direct cadaveric measurements to evaluate the UP. The present study aimed to assess the anatomy of the UP and vertebral body via direct measurement of cadavers and angiographic computed tomography (CT). Using the aforementioned methods, the unity of vertebrae is not destroyed, thus ensuring that the bone materials measured are from the same cadaver. METHODS A total of 13 adult, male formaldehyde-fixed cadavers were obtained from the Department of Anatomy, School of Medicine, Dokuz Eylül University, Turkey. The vertebral arteries of the cadavers were washed with water and filled with barium and coloured silicone mixture. Angiographic CT of the vertebral arteries was conducted at the institution s angiography unit in the Department of Radiodiagnostics. A multislice CT scanner (Mx8000 Multislice System; Philips, Amsterdam, Netherland) was used. The cadavers were placed in the supine position and imaging was performed in the transverse plane. The following parameters were used during imaging: 1.3 mm slice thickness; 0.6 mm increment; pitch; 0.75 s rotating time; 120 kv power; 240 mas/slice; 180 scanning angle; and 512 acquisition matrix. The scanning area was between the upper level of the C2 vertebra and the lower level of the C7 vertebra. The mean scan time was 40 seconds. 1 Department of Anatomy, School of Medicine, Dokuz Eylül University, İzmir, 2 Department of Neurosurgery, Ümraniye Education and Research Hospital, Istanbul, 3 Department of Radiodiagnostics, School of Medicine, Dokuz Eylül University, İzmir, 4 Clinics of Neurosurgery, Denizli State Hospital, Denizli, Turkey Correspondence: A/Prof Mustafa Güvençer, Instructor, Department of Anatomy, School of Medicine, Dokuz Eylül University, Balçova, İzmir, Turkey. mustafa.guvencer@deu.edu.tr 570
2 1a VA UP 1b Fig. 1 (a) CT angiography image (reconstructed coronal slice view) shows the anterior view of the cervical spine and the vertebral artery. (b) Photograph shows the decapitated prevertebral and paravertebral tissues of a dissected cadaver, as well as the coloured silicon injected into the vertebral arteries. IVD: intervertebral disc; UP: uncinate process; VA: V2 segment of the vertebral artery; VB: vertebral body On completion, the imaging data was transferred to a picture archiving and communication system (PACS). Both the sagittal and coronal reformatted images (Fig. 1a) were also obtained using a postprocessing console connected to the PACS. Measurements were taken using the PACS viewing consoles. The prevertebral and paravertebral areas were dissected after two weeks (Fig. 1b). Direct measurements were made using a metal caliper (0.1 mm sensitivity) and a goniometer (1 sensitivity). Other parameters related to the UP (Figs. 2a & b) and vertebral body (Fig. 2c) were also measured using the direct cadaveric method and angiographic CT. The results of the measurements obtained via both methods were analysed using Student s t-test. RESULTS We observed that the height of the UP increased from the C3 to C7 level in both direct cadaveric and CT measurements (Table I). Based on direct measurement of the cadavers, the height of the UP at C3 and C7 was 5.8 ± 1.0 mm and 6.6 ± 0.5 mm, respectively. The corresponding measurements on CT were 5.9 ± 1.2 mm and 6.9 ± 0.6 mm. Both direct cadaveric and CT measurements showed that the width of the UP was at its minimum at C3 and maximum at C7 (C3: 5.7 ± 0.6 mm and C7: 6.2 ± 0.7 mm vs. C3: 6.1 ± 0.3 mm and C7: 6.2 ± 0.6 mm, respectively). The angle between the UP and vertebral body endplate also increased from C3 to C7 on both direct cadaveric and CT measurements (C3: ± 4.5 and C7: ± 3.5 vs. C3: ± 4.4 and C7: ± 3.9, respectively). The distance between the right and left apex of the UP using direct cadaveric measurements at C3 and C7 was 20.8 ± 1.0 mm and 28.1 ± 2.4 mm, respectively, while the corresponding measurements using CT were 23.7 ± 3.4 mm and 29.0 ± 3.0 mm, respectively. Again, the measurements showed an increase from the C3 to C7 level. The length of the medial border of the UP, and the distance between the UP and the superior articular process were measured using CT only. The maximum measurement for the length of the medial border of the UP was obtained at C6 and the minimum at C3 (C3: 12.1 ± 1.7 mm; C4: 12.8 ± 1.2 mm; C5: 12.8 ± 1.5 mm; C6: 13.0 ± 1.7 mm; and C7: 12.2 ± 1.5 mm), with no significant differences between the measurements on the right and left sides (p > 0.05). For the distance between the UP and superior articular process, the maximum distance was measured at C3 (9.8 ± 1.7 mm), while the minimum was measured at C6 (7.8 ± 1.3 mm). On CT, the anteroposterior diameter of the vertebral body was at its minimum at C3 (18.1 ± 1.9 mm) and maximum at C7 (19.3 ± 1.0 mm). The anterior height of the vertebral body was at its minimum at C4 and maximum at C7 on both direct cadaveric and CT measurements (C4: 10.5 ± 1.4 mm and C7: 12.1 ± 2.7 mm vs. C4: 10.7 ± 1.3 mm and C7: 12.7 ± 1.7 mm, respectively). Similarly, the width of the vertebral body increased from C3 to C7 on direct cadaveric and CT measurements (C3: 21.8 ± 2.7 mm and C7: 28.4 ± 2.8 mm vs. C3: 22.4 ± 2.8 mm and C7: 27.5 ± 2.4 mm, respectively). There were no significant differences between all measurements related to the UP from C3 to C7 on the right and left sides, for both direct cadaveric and CT measurements (p > 0.05; Table I). There were, likewise, no significant differences between the direct measurements and the measurements made on CT (p > 0.05; Table II). DISCUSSION Knowledge of the boundaries of the UP is important for good surgical outcomes. Patients with cervical radiculopathy require anterior or anterolateral decompression via the removal of the uncovertebral joints and bone spur. Researchers have shown that excessive decompression of the UP increases the risk of cervical instability. (8) Thus, in order for the surgery to be minimally invasive and to achieve sufficient decompression, surgeons should be aware of the morphology and morphometry of the UP; (9,10) it borders the lateral line of the intervertebral disc. Tubbs et al (3) did not regard uncovertebral joints as synovial joints; the UP was regarded as a product of the formation of fibrocartilage and new bone due to reactive osteogenesis and degeneration, i.e. new bone formation was seen as a response to ageing. (3) Compression of the posterolateral disc or UP is the most common cause of spinal nerve root compression. (7) Osteophytes can result in radiculopathy, myelopathy and vertebral vascular insufficiency due to their anatomical relationship with the spinal nerve roots, vertebral artery and spinal cord. (2,5) To treat these pathologies, uncoforaminectomy, decompressive surgery or osteophyte resection may be necessary. (2,6,8) However, foraminotomy and uncovertebral joint resection procedures may also cause vertebral artery injury, (11-16) possibly leading to ischaemic neurological pathologies. (17,18) Vertebral artery injury usually occurs following the use of a high-speed drill for lateral decompression, aggressive discectomy or decompression of bony tissues. Infection or tumour invasion of the lateral part of the spinal canal may also cause vertebral artery injury during surgery. 571
3 cranial cranial 2a 2b 2c cranial UP UP VB SAP UP TF VA VB Fig. 2 (ac) CT angiography images (reconstructed coronal slice view) show the parameters measured in the present study. A: uncinate process (UP) height, i.e. distance on the vertebra anterior between the endplate and the apex of the UP; B: width of the UP; C: angle between the UP and vertebral body (VB) endplate (the angle on the anterior vertebra between the endplate and medial side of the UP); D: anterior distance between the right and left apex of the UP; E: length of the medial border of the UP on the VB; F: distance between the UP apex and lateral side of the superior articular process (SAP); G: anteroposterior diameter of the VB (the distance between the front and back points in the middle of the superior VB); H: anterior height of the VB (the vertical distance between the midpoint of the VB on the superior and inferior side); I: width of the VB (the horizontal distance between the right and left attachment points of the transverse processes on the VB); TF: transverse foramen; VA: vertebral artery Although there is a very short distance between the UP and the medial border of the vertebral artery, the medial borders of the UP and the uncovertebral joints are referred to as safety zones for surgical procedures. (11,15) The vertebral artery and nerve roots are surrounded by a fibroligamentous band in the intertransverse area. The fibroligamentous tissue, which is laterally attached to the anterior border of both the vertebral artery and spinal nerve root, may stick to the high-speed drill and cause vertebral artery laceration. For this reason, this tissue must be dissected completely before resection. (11,16,19,20) Cervical spondylosis also narrows the foramen, making surgery more challenging in patients with this pathology. (11,19,21) Some authors refer to the line between the UP and the medial border of the uncovertebral joint as a safety line, although the short distance between the UP and vertebral artery reduces the safety of surgery. (1,22) Once an uncovertebral joint is encountered, there is less than 6 mm to the medial margin of the transverse foramen. (23) It is important to take note of this distance when drilling the UP, so as to prevent vertebral artery injury. The vertebral artery or spinal nerve root injury is a very serious complication of surgeries performed with an anterior cervical approach. (5,8,23) For patients who have spondylolisthesis, the distance between the UP and the medial border of the transverse foramen is narrower than that of a healthy person. (2,23) In a study conducted by Russo et al, (24) the distances between the medial border of the vertebral artery and the UP were as follows: C23 level left: 3.2 ± 1.0 mm, right: 3.5 ± 0.6 mm; C34 level left: 1.3 ± 0.6 mm, right: 1.1 ± 0.4 mm; C45 level left: 1.7 ± 0.9 mm, right: 1.6 ± 1.0 mm; C56 level left: 1.2 ± 0.8 mm, right: 1.1 ± 1.2 mm). (24) In our previous study, which was conducted on angiographic images of cadavers, the corresponding distances were as follows: C3: 1.8 ± 1.3 mm; C4: 2.4 ± 1.0 mm; C5: 2.5 ± 1.0 mm; and C6: 2.1 ± 1.2 mm. (12) In another study, we repeated the process using direct cadaveric and CT measurements, and found that the distance between the medial and lateral margin of the UP gradually increased from C3 to C7 (direct C3: 1.6 ± 0.2 mm, C4: 1.7 ± 0.2 mm, C5: 1.6 ± 0.4 mm, C6: 1.6 ± 0.4 mm vs. CT C3: 1.7 ± 0.3 mm, C4: 1.8 ± 0.3 mm, C5: 1.6 ± 0.4 mm, C6: 1.6 ± 0.5 mm), (13) as was found in the present study. The height and width of the UP may be considered as the entrance to the spinal nerve and vertebral artery for decompression of the intervertebral foramen anterolaterally. (2,25) The UP is an important bone landmark that becomes larger and flatter as individuals get older, losing its sharp and bony characteristics. (8) In the present study, we found that in both direct cadaveric and CT measurements, the height of the UP increased from C3 to C7 (i.e. C3: 5.8 ± 1.0 mm, C7: 6.6 ± 0.5 mm vs. C3: 5.9 ± 1.2 mm, C7: 6.9 ± 0.6 mm). There were no significant differences between the measurements made via the two methods (p > 0.05; Table I). Our results are similar to that of Lu et al. (15) However, Lee et al found no increasing pattern in the height of the UP from C3 to C7, and that the height of the UP at C5 was greater than at the other vertebral levels (men C3: 5.9 mm, C7: 5.1 mm; women C5: 6.0 mm, C7: 4.2 mm). (26) Pait et al (1) and Bozbuğa et al (7) found that the height of the UP increased from C3 to C7, with the greatest height noted at the C6 level (Table III). Saringer et al, on the other hand, reported that the height of the UP was greatest at the C5 level, with an increase in height from the C3 to C5 levels among 34 patients. (6) In Civelek et al s study on fresh cadavers, the height of the UP was noted to be 5.97 ± 0.72 mm at C3, 6.83 ± 0.79 mm at C4, 5.50 ± 0.63 mm at C5, 7.27 ± 0.58 mm at C6, and 5.90 ± 0.66 mm at C7. (27) In Russo et al s study, the height of the UP was 5.4 ± 1.5 mm on the left side and 5.6 ± 1.2 mm on the right side at the C23 level, 5.9 ± 1.3 mm on the left side and 6.0 ± 1.3 mm on the right side at the C34 level, 5.7 ± 1.2 mm on the left side and 6.1 ± 0.7 mm on the right side at the C45 level, 6.3 ± 2.2 mm on the left side and 6.2 ± 1.8 mm on the right side at the C56 level on cadavers. (24) The results of the present study support the findings of Uğur et al (8) and Yilmazlar et al, (20) in which the height of the UP increased from C3 to C7, with the maximum height recorded at C7 (Table III). Knowledge of the width of the UP is also important when decompressing nerve roots posterolaterally. Lee et al found that the mean values for the width of the UP in men ranged from 572
4 Table I. Measurements made at the uncovertebral region of 13 cadavers. Parameter Direct cadaveric measurement Computed tomography measurement C3 C4 C5 C6 C7 C3 C4 C5 C6 C7 UP height (mm) Right 5.8 ± ± ± ± ± ± ± ± ± ± 0.7 Left 5.7 ± ± ± ± ± ± ± ± ± ± 0.6 Total 5.8 ± ± ± ± ± ± ± ± ± ± 0.6 p value UP width (mm) Right 5.6 ± ± ± ± ± ± ± ± ± ± 0.6 Left 6.0 ± ± ± ± ± ± ± ± ± ± 0.5 Total 5.7 ± ± ± ± ± ± ± ± ± ± 0.6 p value Angle between UP and VB endplate ( ) Right ± ± ± ± ± ± ± ± ± ± 5.1 Left ± ± ± ± ± ± ± ± ± ± 1.6 Total ± ± ± ± ± ± ± ± ± ± 3.9 p value* Distance between right and left apex (mm) Medial border length of UP (mm) 20.8 ± ± ± ± ± ± ± ± ± ± 3.0 Right 12.2 ± ± ± ± ± 1.1 Left 12.0 ± ± ± ± ± 1.9 Total 12.1 ± ± ± ± ± 1.5 p value* Distance between UP and SAP (mm) Right 9.4 ± ± ± ± ± 1.3 Left 10.1 ± ± ± ± ± 1.9 Total 9.8 ± ± ± ± ± 1.7 p value* A P diameter of VB (mm) Anterior height of VB (mm) 18.1 ± ± ± ± ± ± ± ± ± ± ± ± ± ± ± 1.7 Width of VB (mm) 21.8 ± ± ± ± ± ± ± ± ± ± 2.4 All data presented as mean ± standard deviation, except for p-values. A P: anteroposterior; SAP: superior articular process; UP: uncinate process; VB: vertebral body 573
5 Table II. Results of paired samples t test comparing the measurements of the uncinate process (UP) using the direct cadaveric method and computed tomography. Parameter p value C3 C4 C5 C6 C7 UP height (mm) UP width (mm) Angle between UP and vertebral body endplate ( ) Distance between right and left apex of UP (mm) Anterior height of vertebral body (mm) Width of vertebral body (mm) Table III. Results of studies conducted on the anatomy of the uncinate process (UP). Parameter Pait et al (1) Bozbuğa et al (7) Study sample 6 cadavers 29 adults UP height (mm) C3 6.0 R: 5.1 ± 1.3 L: 5.2 ± 1.3 C4 7.5 R: 5.4 ± 0.9 L: 5.3 ± 1.0 C5 5.8 R: 5.4 ± 1.0 L: 5.6 ± 1.0 C6 8.1 R: 6.1 ± 1.7 L: 6.2 ± 1.4 C7 6.4 R: 5.9 ± 1.3 L: 5.9 ± 1.2 UP width (mm) C3 6.0 R: 4.5 ± 0.8 L: 4.8 ± 1.1 C4 6.1 R: 4.9 ± 1.1 L: 5.0 ± 1.2 C5 5.3 R: 5.2 ± 1.2 L: 5.3 ± 1.1 C6 5.8 R: 6.0 ± 1.4 L: 6.0 ± 1.5 C7 6.7 R: 6.1 ± 1.0 L: 6.2 ± 1.1 Medial border length of UP (mm) C3 R: 11.9 ± 1.0 L: 11.8 ± 1.2 C4 R: 12.1 ± 1.5 L: 12.0 ± 1.4 C5 R: 12.0 ± 1.3 L: 12.4 ± 1.5 C6 R: 6.0 ± 1.4 L: 6.0 ± 1.5 C7 R: 6.1 ± 1.0 L: 6.2 ± 1.1 Distance between right and left apex (mm) Russo et al (24) 10 adults R: 5.6 ± 1.2 L: 5.4 ± 1.5 R: 6.0 ± 1.3 L: 5.9 ± 1.3 R: 6.1 ± 0.7 L: 5.7 ± 1.2 R: 6.2 ± 1.8 L: 6.3 ± 2.2 Uğur et al (8) 49 adults Yilmazlar Civelek et al (27) Lee et al (26) Ebraheim et al (11) et al (9) 35 adults 30 fresh cadavers (23 M, 7 F) 4.9 ± ± 0.89 M: 5.97 ± 0.72 F: 5.80 ± ± ± 0.96 M: 6.83 ± 0.79 F: 6.88 ± ± ± 1.07 M: 5.50 ± 0.63 F: 5.45 ± ± ± 0.95 M: 7.27 ± 0.58 F: 7.29 ± ± ± 1.29 M: 5.90 ± 0.66 F: 5.76 ± ± ± 0.84 M: 5.17 ± 0.70 F: 5.21 ± ± ± 0.91 M: 6.20 ± 0.66 F: 6.18 ± ± ± 1.44 M: 4.97 ± 0.72 F: 4.98 ± ± ± 1.17 M: 6.70 ± 0.79 F: 6.65 ± ± ± 1.11 M: 7.40 ± 0.50 F: 7.39 ± ± ± 1.71 M: 9.37 ± 1.03 F: 9.26 ± ± ± 1.95 M: ± 1.20 F: ± ± ± 1.47 M: ± 1.00 F: ± ± ± 1.62 M: ± 1.17 F: ± ± ± 1.93 M: ± 0.98 F: ± adults M: 5.9 ± 1.1 F: 4.7 ± 0.8 M: 5.5 ± 1.2 F: 5.0 ± 0.8 M: 5.8 ± 1.1 F: 6.0 ± 1.6 M: 5.9 ± 1.0 F: 4.9 ± 0.8 M: 5.1 ± 1.3 F: 4.2 ± 0.6 M: 6.3 ± 0.8 F: 5.6 ± 0.8 M: 5.5 ± 0.7 F: 5.5 ± 0.6 M: 5.5 ± 0.7 F: 5.8 ± 0.8 M: 5.8 ± 1.0 F: 6.1 ± 1.1 M: 6.3 ± 0.9 F: 6.3 ± 0.5 M: 13.1 ± 1.1 F: 11.0 ± 0.6 M: 13.3 ± 1.1 F: 11.8 ± 1.3 M: 13.3 ± 1.2 F: 12.1 ± 1.4 M: 13.7 ± 1.7 F: 12.2 ± 1.3 M: 13.0 ± 1.5 F: 11.9 ± adults (31 M, 23 F) C ± ± ± 1.68 M: 19.4 ± 1.3 F: 18.9 ± 1.7 C ± ± ± 1.62 M: 20.5 ± 1.8 F: 20.5 ± 2.1 (Contd...) 574
6 Parameter Pait et al (1) Bozbuğa et al (7) Russo et al (24) Uğur et al (8) Yilmazlar Civelek et al (27) Lee et al (26) Ebraheim et al (11) et al (9) C ± ± ± 1.87 M: 21.4 ± 1.7 F: 20.9 ± 1.5 C ± ± ± 2.26 M: 23.4 ± 1.9 F: 22.6 ± 1.8 C ± ± ± 2.53 M: 25.2 ± 2.0 F: 23.7 ± 1.9 Angle between UP and vertebral endplate ( ) C3 R: 112 ± 16 L: 108 ± 10 C4 R: 109 ± 21 L: 116 ± 15 C5 R: 114 ± 11 L: 110 ± 13 C6 R: 120 ± 18 L: 124 ± 15 C7 R: 124 ± 16 L: 118 ± ± ± ± ± ± 6.5 Measurements presented as either mean or mean ± standard deviation. F: female; L: left; M: male; R: right 5.5 mm (at C4 and C5) to 6.3 mm (at C3 and C7), and in women, from 5.8 mm (at C5) to 6.3 mm (at C7); the width of the UP was widest at C7 and narrowest at C5. (26) In the study by Civelek et al, (27) the measured width of the UP was 5.17 ± 0.70 mm at C3, 6.20 ± 0.66 mm at C4, 4.97 ± 0.72 mm at C5, 6.70 ± 0.79 mm at C6, and 7.40 ± 0.50 mm at C7 (Table III). As in the studies by Bozbuğa et al (7) and Uğur et al, (8) the width of the UP in the present study also increased gradually from C3 to C7. An increase in the width of the UP due to osteophyte formation in the UP may result in intervertebral foraminal stenosis and neural compression. (20) Resection of the UP or osteophyte is generally done mediolaterally, and the desired width of the UP is approximately 20%25% of the vertebral body. (25) The medial border length of the UP on CT was also noted in the present study. It was at its maximum at C6 and minimum at C3 (C3: 12.1 ± 1.7 mm, C4: 12.8 ± 1.2 mm, C5: 12.8 ± 1.5 mm, C6: 13.0 ± 1.7 mm and C7: 12.2 ± 1.5 mm). In studies on dry bone, the medial border length of the UP was found to increase gradually from C3 to C7; it was also found to have approximately the same values in different studies. (7-9) In posterior resection of the UP, while removing a third of the posterior UP is sufficient at upper cervical levels, removal of half of the UP is necessary at lower cervical levels. (9) The UP lies posterolaterally at C6 and C7 and laterally at C3 and C5. It has a course from lateral to medial obliquely and front to back anatomically. (7) The distance between the right and left apex of the UP increases from C3 to C7. At different cervical levels, the surgical method may be changed. (20) As the UP forms the lateral border of a corpectomy, knowledge of the distance between the right and left apex of the UP is important, so as to determine the width of the UP during corpectomy. The distance between the right and left apex of the UP decreases gradually from C6 to C3. (7,8,12,14,20) The width of the vertebral body is smaller in the vertebral endplate than the distance between the right and left apex of the UP at the same level, and accordingly, the angle between the UP medial side and vertebral body upper side is an obtuse angle. The distance between the right and left apex of the UP, vertebral body width and angle between the UP medial side and vertebral body upper side increases from C3 to C7. The results of the present study are supported by those of other studies found in the literature (Table III). (7,8) In the present study, the anteroposterior diameter of the vertebral body gradually increases from C3 to C7. It is approximately 6 mm longer than the medial border length of the UP at the same level. While the anteroposterior diameters of the vertebral body measured on dry bone vertebrae in the studies by Uğur et al (8) and Yilmazlar et al (9) were smaller than those in the present study, the corresponding diameters on CT measurement in studies by Bailey et al (28) and Kwon et al (29) were similar to the values found in the present study (Table IV). The vertebral artery travels closer to the UP at the mid-cervical region than at the lower cervical regions. (20) Vertebral artery compression due to osteophytes may occur anteriorly from the UP or posteriorly from the superior or inferior articular facet. In most cases, compression is likely to occur from the UP rather than the articular facets, as osteophytes are present in 48% of UPs and only 30% of articular facets. (30) In the present study, the distance between the UP and the lateral side of the superior articular process on CT measurements was the greatest at C3 (9.8 ± 1.7 mm) and the smallest at C6 (7.8 ± 1.3 mm). The distance between the lateral side of the superior articular process and the UP apex in the posterior and lateral aspects is important for orientation, in terms of defining the region where the vertebral artery and spinal nerve root exists. One study suggested the removal of the medial side of the superior articular process during UP localised osteophyte resection, especially at the C5, C6 and C7 levels. (8) Panjabi et al (10) made measurements directly on 12 adult cadavers and found the posterior height of the vertebral body to 575
7 Table IV. Results of studies conducted on the vertebral body (VB). Parameter Study sample A P diameter of vertebral body (mm) Panjabi et al (10) 12 adult cadavers Tan et al (31) 10 adult cadavers Yilmazlar et al (9) 35 adults Ugur Kwon et al (29) Bailey Civelek et al (27) Lee et al (26) et al (8) et al (28) 49 adults 50 adults; M Cadavers 30 fresh cadavers (23 M, 7 F) Dry bones (32 M, 19 F) C ± ± ± ± ± ± ± 1.0 C ± ± ± ± ± ± ± 1.5 C ± ± ± ± ± ± ± ± 1.6 C ± ± ± ± ± ± ± ± 1.5 C ± ± ± ± ± ± ± ± 1.8 Width of the (mm) C ± ± ± ± ± ± 2.2 C ± ± ± ± ± ± 1.6 C ± ± ± ± ± ± ± 1.9 C ± ± ± ± ± ± ± 2.1 C ± ± ± ± ± ± ± 1.8 Anterior height of VB (mm) C ± ± 1.0 C4 9.9 ± ± 1.6 C5 9.6 ± ± 1.5 C ± ± 1.5 C ± ± 1.3 Measurements presented as mean ± standard deviation. A P: anteroposterior; F: female; M: male be 11.6 ± 0.35 mm at C3, 11.4 ± 0.43 mm at C4, 11.4 ± 0.32 mm at C5, 10.9 ± 0.26 mm at C6 and 12.8 ± 0.46 mm at C7. In the study by Tan et al (31) conducted on ten cadavers of Singapore Chinese origin, the posterior height of the vertebral body was 11.2 ± 0.1 mm at C3, 11.3 ± 0.2 mm at C4, 11.3 ± 0.1 mm at C5, 11.3 ± 0.2 mm at C6 and 11.8 ± 0.3 mm at C7. The anterior height of the vertebral body was 10.0 ± 0.2 mm at C3, 9.9 ± 0.3 mm at C4, 9.6 ± 0.2 mm at C5, 10.4 ± 0.3 mm at C6 and 11.2 ± 0.2 mm at C7. In the study by Lee et al (26) on the dry bones of Korean origin, the anterior height of the vertebral body was 14.9 ± 1.0 mm at C3, 14.0 ± 1.6 mm at C4, 13.3 ± 1.5 mm at C5, 13.5 ± 1.5 mm at C6 and 15.2 ± 1.3 mm at C7. The measurements of the present study parallel those recorded in Tan et al s (31) study (Table IV). In conclusion, most published studies on the UP and vertebral body obtained measurements using dry bones. However, in the present study, morphometric measurements relating to the UP and vertebral body were taken directly and on CT of the same cadavers, with preservation of the complete vertebra of the cadaver in the vertebral series. This should result in more valid measurements of the anatomical structures that surgeons may encounter during surgical intervention. We hope that the measurements obtained in the present study will help spinal surgeons to achieve greater success in cervical operations. REFERENCES 1. Pait TG, Killefer JA, Arnautovic KI. Surgical anatomy of the anterior cervical spine: the disc space, vertebral artery, and associated bony structures. Neurosurgery 1996; 39: Klaassen Z, Tubbs RS, Apaydin N, et al. Vertebral spinal osteophytes. Anat Sci Int 2011; 86: Tubbs RS, Rompala OJ, Verma K, et al. Analysis of the uncinate processes of the cervical spine: an anatomical study. J Neurosurg Spine 2012; 16: Chibbaro S, Mirone G, Bresson D, George B. Cervical spine lateral approach for myeloradiculopathy: technique and pitfalls. Surg Neurol 2009; 72: Bruneau M, Cornelius JF, George B. Anterolateral approach to the V2 segment of the vertebral artery. Neurosurgery 2005; 57(4 Suppl): Saringer W, Nöbauer I, Reddy M, Tschabitscher M, Horaczek A. Microsurgical anterior cervical foraminotomy (uncoforaminotomy) for unilateral radiculopathy: clinical results of a new technique. Acta Neurochir (Wien) 2002; 144: Bozbuğa M, Öztürk A, Ari Z, et al. Surgical anatomic evaluation of cervical uncinate process for ventral and ventrolateral subaxial decompression. Okajimas Folia Anat Jpn 1999; 76: Uğur HC, Uz A, Attar A, et al. Anatomical projection of the cervical uncinate process in ventral, ventrolateral, and posterior decompressive surgery. J Neurosurg 2000; 93(2 Suppl): Yilmazlar S, Kocaeli H, Uz A, Tekdemir I. Clinical importance of ligamentous and osseous structures in the cervical uncovertebral foraminal region. Clin Anat 2003; 16: Panjabi MM, Duranceau J, Goel V, Oxland T, Takata K. Cervical human vertebra. Quantitative three-dimensional anatomy of the middle and lower regions. Spine (Phila Pa 1976) 1991; 16: Ebraheim N, Lu J, Haman SP, Yeasting RA. Anatomic basis of the anterior surgery on the cervical spine: relationships between uncus-artery-root complex and vertebral artery injury. Surg Radiol Anat 1998; 20: Güvençer M, Men S, Naderi S, Kirey S, Tetik S. The V2 segment of the vertebral artery in anterior and anterolateral cervical spinal surgery: a cadaver angiographic study. Clin Neurol Neurosurg 2006; 108: Güvençer M, Men S, Naderi S, Topçu I, Tetik S. Evaluating the V2 segment of the vertebral artery with computed tomography to assess risks during cervical spinal surgery: an anatomic study on cadaver. WSJ 2006; 1: Lu J, Ebraheim NA. The vertebral artery: surgical anatomy. Orthopedics 1999; 22: Lu J, Ebraheim NA, Georgiadis GM, Yang H, Yeasting RA. Anatomic considerations of the vertebral artery: implications for anterior 576
8 decompression of the cervical spine. J Spinal Disord 1998; 11: Smith MD, Emery SE, Dudley A, Murray KJ, Leventhal M. Vertebral artery injury during anterior decompression of the cervical spine. A retrospective review of ten patients. J Bone Joint Surg Br 1993; 75: Golueke P, Sclafani S, Phillips T, et al. Vertebral artery injury--diagnosis and management. J Trauma 1987; 27: Jenis LG, Leclair WJ. Late vascular complication with anterior cervical discectomy and fusion. Spine (Phila Pa 1976) 1994; 19: Nourbakhsh A, Yang J, Gallagher S, et al. A safe approach to explore/ identify the V(2) segment of the vertebral artery during anterior approaches to cervical spine and/or arterial repairs: anatomical study. J Neurosurg Spine 2010; 12: Yilmazlar S, Ikiz I, Kocaeli H, Tekdemir I, Adim SB. Details of fibroligamentous structures in the cervical unco-vertebral region: an obscure corner. Surg Radiol Anat 2003; 25: Brigham CD, Tsahakis PJ. Anterior cervical foraminotomy and fusion. Surgical technique and results. Spine (Phila Pa 1976) 1995; 20: Curylo LJ, Mason HC, Bohlman HH, Yoo JU. Tortuous course of the vertebral artery and anterior cervical decompression: a cadaveric and clinical case study. Spine (Phila Pa 1976) 2000; 25: Peng CW, Chou BT, Bendo JA, Spivak JM. Vertebral artery injury in cervical spine surgery: anatomical considerations, management, and preventive measures. Spine J 2009; 9: Russo VM, Graziano F, Peris-Celda M, Russo A, Ulm AJ. The V(2) segment of the vertebral artery: anatomical considerations and surgical implications. J Neurosurg Spine 2011; 15: Lu J, Ebraheim N, Yang H, Rollins J, Yeasting RA. Anatomic bases for anterior spinal surgery: surgical anatomy of the cervical vertebral body and disc space. Surg Radiol Anat 1999; 21: Lee TH, Kim SJ, Chung IH. Morphometrical study of uncinate processes and vertebral body of cervical spine. J Korean Neurosurg Soc 2012; 51: Civelek E, Kiris T, Hepgul K, et al. Anterolateral approach to the cervical spine: major anatomical structures and landmarks. Technical note. J Neurosurg Spine 2007; 7: Bailey AS, Stanescu S, Yeasting RA, Ebraheim NA, Jackson WT. Anatomic relationships of the cervicothoracic junction. Spine (Phila Pa 1976) 1995; 20: Kwon BK, Song F, Morrison WB, et al. Morphologic evaluation of cervical spine anatomy with computed tomography: anterior cervical plate fixation considerations. J Spinal Disord Tech 2004; 17: Cagnie B, Barbaix E, Vinck E, D Herde K, Cambier D. Extrinsic risk factors for compromised blood flow in the vertebral artery: anatomical observations of the transverse foramina from C3 to C7. Surg Radiol Anat 2005; 27: Tan SH, Teo EC, Chua HC. Quantitative three-dimensional anatomy of cervical, thoracic and lumbar vertebrae of Chinese Singaporeans. Eur Spine J 2004; 13:
Surgical Anatomy of the Uncinate Process and Transverse Foramen Determined by Computed Tomography
 THIEME GLOBAL SPINE JOURNAL Original Article 383 Surgical Anatomy of the Uncinate Process and Transverse Foramen Determined by Computed Tomography Moon Soo Park 1 Seong-Hwan Moon 2 Tae-Hwan Kim 1 Jae Keun
THIEME GLOBAL SPINE JOURNAL Original Article 383 Surgical Anatomy of the Uncinate Process and Transverse Foramen Determined by Computed Tomography Moon Soo Park 1 Seong-Hwan Moon 2 Tae-Hwan Kim 1 Jae Keun
A morphometric study of the Pedicles of dry human typical lumbar vertebrae
 Original article: A morphometric of the Pedicles of dry human typical lumbar vertebrae Dhaval K. Patil 1 *, Pritha S. Bhuiyan 2 1Resident, Department of Anatomy, Seth G S Medical College, Parel, Mumbai-400012,
Original article: A morphometric of the Pedicles of dry human typical lumbar vertebrae Dhaval K. Patil 1 *, Pritha S. Bhuiyan 2 1Resident, Department of Anatomy, Seth G S Medical College, Parel, Mumbai-400012,
The transverse process, intertransverse space, and vertebral artery in anterior approaches to the lower cervical spine
 J Neurosurg (Spine 2) 98:188 194, 2003 The transverse process, intertransverse space, and vertebral artery in anterior approaches to the lower cervical spine MASATOU KAWASHIMA, M.D., NECMETTIN TANRIOVER,
J Neurosurg (Spine 2) 98:188 194, 2003 The transverse process, intertransverse space, and vertebral artery in anterior approaches to the lower cervical spine MASATOU KAWASHIMA, M.D., NECMETTIN TANRIOVER,
The uncovertebral joints (Fig. 1) consist of the lateral. Analysis of the uncinate processes of the cervical spine: an anatomical study
 J Neurosurg Spine 16:402 407, 2012 Analysis of the uncinate processes of the cervical spine: an anatomical study Laboratory investigation R. Shane Tubbs, M.S., P.A.-C., Ph.D., 1 Olivia J. Rompala, B.S.,
J Neurosurg Spine 16:402 407, 2012 Analysis of the uncinate processes of the cervical spine: an anatomical study Laboratory investigation R. Shane Tubbs, M.S., P.A.-C., Ph.D., 1 Olivia J. Rompala, B.S.,
The Relationship amongst Intervertebral Disc Vertical Diameter, Lateral Foramen Diameter and Nerve Root Impingement in Lumbar Vertebra
 doi: http://dx.doi.org/10.5704/moj.1803.004 The Relationship amongst Intervertebral Disc Vertical Diameter, Lateral Foramen Diameter and Nerve Root Impingement in Lumbar Vertebra Yusof MI, MMed Orth, Hassan
doi: http://dx.doi.org/10.5704/moj.1803.004 The Relationship amongst Intervertebral Disc Vertical Diameter, Lateral Foramen Diameter and Nerve Root Impingement in Lumbar Vertebra Yusof MI, MMed Orth, Hassan
Posterior surgical procedures are those procedures
 9 Cervical Posterior surgical procedures are those procedures that have been in use for a long time with established efficacy in the treatment of radiculopathy and myelopathy caused by pathologies including
9 Cervical Posterior surgical procedures are those procedures that have been in use for a long time with established efficacy in the treatment of radiculopathy and myelopathy caused by pathologies including
Uncosectomy Facilitated Cervical Foraminotomy using a new high-speed shielded curved device
 Uncosectomy Facilitated Cervical Foraminotomy using a new high-speed shielded curved device Pierre Bernard, M.D. (1), Michal Tepper, Ph.D. (2), Ely Ashkenazi, M.D. (3) (1) Centre Aquitain du Dos, Hôpital
Uncosectomy Facilitated Cervical Foraminotomy using a new high-speed shielded curved device Pierre Bernard, M.D. (1), Michal Tepper, Ph.D. (2), Ely Ashkenazi, M.D. (3) (1) Centre Aquitain du Dos, Hôpital
Morphometric Anatomy of the Atlas and Axis Vertebrae
 Original Article Morphometric Anatomy of the Atlas and Axis Vertebrae Gökflin fiengül Hakan Hadi KADIO LU ABSTRACT OBJECTIVE: In this study, forty dried specimens of atlas and axis vertebrae were examined
Original Article Morphometric Anatomy of the Atlas and Axis Vertebrae Gökflin fiengül Hakan Hadi KADIO LU ABSTRACT OBJECTIVE: In this study, forty dried specimens of atlas and axis vertebrae were examined
The sacrum is a complex anatomical structure.
 A Review Paper Rongming Xu, MD, Nabil A. Ebraheim, MD, and Nicholas K. Gove, MD Abstract Treatment in spinal disorders, sacroiliac joint disruption, and sacral fractures may involve instrumentation of
A Review Paper Rongming Xu, MD, Nabil A. Ebraheim, MD, and Nicholas K. Gove, MD Abstract Treatment in spinal disorders, sacroiliac joint disruption, and sacral fractures may involve instrumentation of
Cervical Spine: Pearls and Pitfalls
 Cervical Spine: Pearls and Pitfalls Presenters Dr. Rob Donkin Functional Anatomy Current research Cervical Radiculopathy Dr. Gert Ferreira Red flags Case Study Kinesio Taping Chris Neethling Gonstead adjusting
Cervical Spine: Pearls and Pitfalls Presenters Dr. Rob Donkin Functional Anatomy Current research Cervical Radiculopathy Dr. Gert Ferreira Red flags Case Study Kinesio Taping Chris Neethling Gonstead adjusting
Study of Lumbar Vertebrae with respect to the dimensions of the pedicle in South Indian population
 Original article Study of Lumbar Vertebrae with respect to the dimensions of the pedicle in South Indian population 1 Dr.Sreevidya.J, 2 Dr.Dharani.V, 3 Dr.Savithri.K, 4 Dr.Sudha Seshayyan 1Senior Assistant
Original article Study of Lumbar Vertebrae with respect to the dimensions of the pedicle in South Indian population 1 Dr.Sreevidya.J, 2 Dr.Dharani.V, 3 Dr.Savithri.K, 4 Dr.Sudha Seshayyan 1Senior Assistant
SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT
 SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT 1 Anatomy 3 columns- Anterior, middle and Posterior Anterior- ALL, Anterior 2/3 rd body & disc. Middle- Posterior 1/3 rd of body & disc, PLL Posterior-
SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT 1 Anatomy 3 columns- Anterior, middle and Posterior Anterior- ALL, Anterior 2/3 rd body & disc. Middle- Posterior 1/3 rd of body & disc, PLL Posterior-
International J. of Healthcare & Biomedical Research, Volume: 1, Issue: 4, July 2013, Pages
 Original article: Morphometry of first pedicle of sacrum and its clinical relevance Sinha Manisha B, Rathore Mrithunjay, Trivedi Soumitra, Siddiqui A U Department of Anatomy, All India Institute of Medical
Original article: Morphometry of first pedicle of sacrum and its clinical relevance Sinha Manisha B, Rathore Mrithunjay, Trivedi Soumitra, Siddiqui A U Department of Anatomy, All India Institute of Medical
ANATOMIC REPORT. Surgical Anatomic Evaluation of the Cervical Pedicle and Adjacent Neural Structures
 ANATOMIC REPORT Surgical Anatomic Evaluation of the Cervical Pedicle and Adjacent Neural Structures Hasan Çağlar Uğur, M.D., Ayhan Attar, M.D., Aysun Uz, M.D., İbrahim Tekdemir, M.D., Nihat Egemen, M.D.,
ANATOMIC REPORT Surgical Anatomic Evaluation of the Cervical Pedicle and Adjacent Neural Structures Hasan Çağlar Uğur, M.D., Ayhan Attar, M.D., Aysun Uz, M.D., İbrahim Tekdemir, M.D., Nihat Egemen, M.D.,
VERTEBRAL COLUMN VERTEBRAL COLUMN
 VERTEBRAL COLUMN FUNCTIONS: 1) Support weight - transmits weight to pelvis and lower limbs 2) Houses and protects spinal cord - spinal nerves leave cord between vertebrae 3) Permits movements - *clinical
VERTEBRAL COLUMN FUNCTIONS: 1) Support weight - transmits weight to pelvis and lower limbs 2) Houses and protects spinal cord - spinal nerves leave cord between vertebrae 3) Permits movements - *clinical
1 Normal Anatomy and Variants
 1 Normal Anatomy and Variants 1.1 Normal Anatomy MR Technique. e standard MR protocol for a routine evaluation of the spine always comprises imaging in sagittal and axial planes, while coronal images are
1 Normal Anatomy and Variants 1.1 Normal Anatomy MR Technique. e standard MR protocol for a routine evaluation of the spine always comprises imaging in sagittal and axial planes, while coronal images are
A Morphometric study of lamina of lumbar vertebrae: A dry bone study conducted in RIMS, Imphal
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 11 Ver. 4 (November. 2018), PP 35-39 www.iosrjournals.org A Morphometric study of lamina of
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 11 Ver. 4 (November. 2018), PP 35-39 www.iosrjournals.org A Morphometric study of lamina of
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
Fractures of the thoracic and lumbar spine and thoracolumbar transition
 Most spinal column injuries occur in the thoracolumbar transition, the area between the lower thoracic spine and the upper lumbar spine; over half of all vertebral fractures involve the 12 th thoracic
Most spinal column injuries occur in the thoracolumbar transition, the area between the lower thoracic spine and the upper lumbar spine; over half of all vertebral fractures involve the 12 th thoracic
2. The vertebral arch is composed of pedicles (projecting from the body) and laminae (uniting arch posteriorly).
 VERTEBRAL COLUMN 2018zillmusom I. VERTEBRAL COLUMN - functions to support weight of body and protect spinal cord while permitting movements of trunk and providing for muscle attachments. A. Typical vertebra
VERTEBRAL COLUMN 2018zillmusom I. VERTEBRAL COLUMN - functions to support weight of body and protect spinal cord while permitting movements of trunk and providing for muscle attachments. A. Typical vertebra
Comprehension of the common spine disorder.
 Objectives Comprehension of the common spine disorder. Disc degeneration/hernia. Spinal stenosis. Common spinal deformity (Spondylolisthesis, Scoliosis). Osteoporotic fracture. Anatomy Anatomy Anatomy
Objectives Comprehension of the common spine disorder. Disc degeneration/hernia. Spinal stenosis. Common spinal deformity (Spondylolisthesis, Scoliosis). Osteoporotic fracture. Anatomy Anatomy Anatomy
Quantitative Analysis of Vascular Canals in Vertebral Endplate
 Quantitative Analysis of Vascular Canals in Vertebral Endplate Kristine Tan 1, Won C. Bae, PhD 1, Tomonori Yamaguchi, MS 1,2, Kelli Xu, BS 1, Iris Shieh, BS 1, Jade He, BS 1, Robert L. Sah, MD, ScD 1,
Quantitative Analysis of Vascular Canals in Vertebral Endplate Kristine Tan 1, Won C. Bae, PhD 1, Tomonori Yamaguchi, MS 1,2, Kelli Xu, BS 1, Iris Shieh, BS 1, Jade He, BS 1, Robert L. Sah, MD, ScD 1,
SpineFAQs. Neck Pain Diagnosis and Treatment
 SpineFAQs Neck Pain Diagnosis and Treatment Neck pain is a common reason people visit their doctor. Neck pain typically doesn't start from a single injury. Instead, the problem usually develops over time
SpineFAQs Neck Pain Diagnosis and Treatment Neck pain is a common reason people visit their doctor. Neck pain typically doesn't start from a single injury. Instead, the problem usually develops over time
Innovative Techniques in Minimally Invasive Cervical Spine Surgery. Bruce McCormack, MD San Francisco California
 Innovative Techniques in Minimally Invasive Cervical Spine Surgery Bruce McCormack, MD San Francisco California PCF Posterior Cervical Fusion PCF not currently an ambulatory care procedure Pearl diver
Innovative Techniques in Minimally Invasive Cervical Spine Surgery Bruce McCormack, MD San Francisco California PCF Posterior Cervical Fusion PCF not currently an ambulatory care procedure Pearl diver
Cervical Spine Anatomy and Biomechanics. Typical Cervical Vertebra C3 6. Typical Cervical Vertebra Anterior 10/5/2017
 Cervical Spine Anatomy and Biomechanics Typical Cervical Vertebra C3 6 Small, relatively broad body Bifid SpinousProcess Long and narrow laminae Spinal Canal: large, triangular; remarkably consistent dimensions
Cervical Spine Anatomy and Biomechanics Typical Cervical Vertebra C3 6 Small, relatively broad body Bifid SpinousProcess Long and narrow laminae Spinal Canal: large, triangular; remarkably consistent dimensions
Thoracic Cooled-RF Training Presentation
 Thoracic Cooled-RF Training Presentation Patient Selection Anatomy Overview Neuroanatomy Lesion targets Technique Diagnostic Block Cooled-RF Precautions Summary Appendix AGENDA Patient Selection Thoracic
Thoracic Cooled-RF Training Presentation Patient Selection Anatomy Overview Neuroanatomy Lesion targets Technique Diagnostic Block Cooled-RF Precautions Summary Appendix AGENDA Patient Selection Thoracic
ASJ. Cervical Pedicle Screw Fixation: Anatomic Feasibility of Pedicle Morphology and Radiologic Evaluation of the Anatomical Measurements
 Asian Spine Journal Asian Spine Clinical Journal Study Asian Spine J 2014;8(3):273-280 Cervical http://dx.doi.org/10.4184/asj.2014.8.3.273 pedicle screw fixation 273 Cervical Pedicle Screw Fixation: Anatomic
Asian Spine Journal Asian Spine Clinical Journal Study Asian Spine J 2014;8(3):273-280 Cervical http://dx.doi.org/10.4184/asj.2014.8.3.273 pedicle screw fixation 273 Cervical Pedicle Screw Fixation: Anatomic
Original Article Clinics in Orthopedic Surgery 2013;5:
 Original Article Clinics in Orthopedic Surgery 2013;5:129-133 http://dx.doi.org/10.4055/cios.2013.5.2.129 The Efficacy of Carotid Tubercle as an Anatomical Landmark for Identification of Cervical Spinal
Original Article Clinics in Orthopedic Surgery 2013;5:129-133 http://dx.doi.org/10.4055/cios.2013.5.2.129 The Efficacy of Carotid Tubercle as an Anatomical Landmark for Identification of Cervical Spinal
LUMBAR SPINAL STENOSIS
 LUMBAR SPINAL STENOSIS Always occurs in the mobile segment. Factors play role in Stenosis Pre existing congenital or developmental narrowing of the lumbar spinal canal Translation of one anatomic segment
LUMBAR SPINAL STENOSIS Always occurs in the mobile segment. Factors play role in Stenosis Pre existing congenital or developmental narrowing of the lumbar spinal canal Translation of one anatomic segment
Facet orientation in patients with lumbar degenerative spondylolisthesis
 35 J. Tokyo Med. Univ., 71 1 35 0 Facet orientation in patients with lumbar degenerative spondylolisthesis Wuqikun ALIMASI, Kenji ENDO, Hidekazu SUZUKI, Yasunobu SAWAJI, Hirosuke NISHIMURA, Hidetoshi TANAKA,
35 J. Tokyo Med. Univ., 71 1 35 0 Facet orientation in patients with lumbar degenerative spondylolisthesis Wuqikun ALIMASI, Kenji ENDO, Hidekazu SUZUKI, Yasunobu SAWAJI, Hirosuke NISHIMURA, Hidetoshi TANAKA,
Module: #15 Lumbar Spine Fusion. Author(s): Jenni Buckley, PhD. Date Created: March 27 th, Last Updated:
 Module: #15 Lumbar Spine Fusion Author(s): Jenni Buckley, PhD Date Created: March 27 th, 2011 Last Updated: Summary: Students will perform a single level lumbar spine fusion to treat lumbar spinal stenosis.
Module: #15 Lumbar Spine Fusion Author(s): Jenni Buckley, PhD Date Created: March 27 th, 2011 Last Updated: Summary: Students will perform a single level lumbar spine fusion to treat lumbar spinal stenosis.
J Korean Soc Spine Surg 2011 Sep;18(3): Originally published online September 30, 2011;
 Journal of Korean Society of Spine Surgery The Changes in Neural Foramen Shown on Computed Tomography Depending on the Changes in the Height of Intervertebral Disc after Anterior Cervical Discectomy and
Journal of Korean Society of Spine Surgery The Changes in Neural Foramen Shown on Computed Tomography Depending on the Changes in the Height of Intervertebral Disc after Anterior Cervical Discectomy and
Range of motion of thoracic spine in sagittal plane
 DOI 10.1007/s00586-013-3088-7 ORIGINAL ARTICLE Range of motion of thoracic spine in sagittal plane Daigo Morita Yasutsugu Yukawa Hiroaki Nakashima Keigo Ito Go Yoshida Masaaki Machino Syunsuke Kanbara
DOI 10.1007/s00586-013-3088-7 ORIGINAL ARTICLE Range of motion of thoracic spine in sagittal plane Daigo Morita Yasutsugu Yukawa Hiroaki Nakashima Keigo Ito Go Yoshida Masaaki Machino Syunsuke Kanbara
The Back. Anatomy RHS 241 Lecture 9 Dr. Einas Al-Eisa
 The Back Anatomy RHS 241 Lecture 9 Dr. Einas Al-Eisa The spine has to meet 2 functions Strength Mobility Stability of the vertebral column is provided by: Deep intrinsic muscles of the back Ligaments
The Back Anatomy RHS 241 Lecture 9 Dr. Einas Al-Eisa The spine has to meet 2 functions Strength Mobility Stability of the vertebral column is provided by: Deep intrinsic muscles of the back Ligaments
3D titanium interbody fusion cages sharx. White Paper
 3D titanium interbody fusion cages sharx (SLM selective laser melted) Goal of the study: Does the sharx intervertebral cage due to innovative material, new design, and lordotic shape solve some problems
3D titanium interbody fusion cages sharx (SLM selective laser melted) Goal of the study: Does the sharx intervertebral cage due to innovative material, new design, and lordotic shape solve some problems
Imaging of Cervical Spine Trauma Tudor H Hughes, M.D.
 Imaging of Cervical Spine Trauma Tudor H Hughes, M.D. General Considerations Most spinal fractures are due to a single episode of major trauma. Fatigue fractures of the spine are unusual except in the
Imaging of Cervical Spine Trauma Tudor H Hughes, M.D. General Considerations Most spinal fractures are due to a single episode of major trauma. Fatigue fractures of the spine are unusual except in the
Variations in arterial supply to the lower lumbar spine
 Eur Spine J (2016) 25:4181 4187 DOI 10.1007/s00586-016-4427-2 ORIGINAL ARTICLE Variations in arterial supply to the lower lumbar spine Fumitake Tezuka 1 Toshinori Sakai 1 Toshihiko Nishisho 1 Yoichiro
Eur Spine J (2016) 25:4181 4187 DOI 10.1007/s00586-016-4427-2 ORIGINAL ARTICLE Variations in arterial supply to the lower lumbar spine Fumitake Tezuka 1 Toshinori Sakai 1 Toshihiko Nishisho 1 Yoichiro
Properties of Purdue. Anatomy. Positioning AXIAL SKELETAL RADIOLOGY FOR PRIVATE PRACTITIONERS 11/30/2018
 AXIAL SKELETAL RADIOLOGY FOR PRIVATE PRACTITIONERS Anatomy Complex Text book is needed Species Contrast Positioning Painful/ non cooperative Sedation General anesthesia Species Contrast 1 Slightly oblique
AXIAL SKELETAL RADIOLOGY FOR PRIVATE PRACTITIONERS Anatomy Complex Text book is needed Species Contrast Positioning Painful/ non cooperative Sedation General anesthesia Species Contrast 1 Slightly oblique
Changes in Spinal Canal Diameter and Vertebral Body Height with Age
 Original Article http://dx.doi.org/1.3349/ymj.213.54.6.1498 pissn: 513-5796, eissn: 1976-2437 Yonsei Med J 54(6):1498-154, 213 Changes in Spinal Canal Diameter and Vertebral Body Height with Age Kyung
Original Article http://dx.doi.org/1.3349/ymj.213.54.6.1498 pissn: 513-5796, eissn: 1976-2437 Yonsei Med J 54(6):1498-154, 213 Changes in Spinal Canal Diameter and Vertebral Body Height with Age Kyung
Lumbar radiculopathy caused by foraminal stenosis in rheumatoid arthritis
 Upsala Journal of Medical Sciences. 2011; 116: 133 137 ORIGINL RTICLE Lumbar radiculopathy caused by foraminal stenosis in rheumatoid arthritis TOMOKI KOKUTSU, NOKI MOROZUMI, YUTK KOIZUMI & YUSHIN ISHII
Upsala Journal of Medical Sciences. 2011; 116: 133 137 ORIGINL RTICLE Lumbar radiculopathy caused by foraminal stenosis in rheumatoid arthritis TOMOKI KOKUTSU, NOKI MOROZUMI, YUTK KOIZUMI & YUSHIN ISHII
Case Report: CASE REPORT OF FACET ARTHROPATHY INDUCED NERVE ROOT COMPRESSION RESULTING IN MOTOR WEAKNESS AND PAIN
 Cox Technic Case Report #100 published at www.coxtechnic.com (sent October 2011 on 10/11/11 ) 1 Case Report: CASE REPORT OF FACET ARTHROPATHY INDUCED NERVE ROOT COMPRESSION RESULTING IN MOTOR WEAKNESS
Cox Technic Case Report #100 published at www.coxtechnic.com (sent October 2011 on 10/11/11 ) 1 Case Report: CASE REPORT OF FACET ARTHROPATHY INDUCED NERVE ROOT COMPRESSION RESULTING IN MOTOR WEAKNESS
Ligaments of the vertebral column:
 In the last lecture we started talking about the joints in the vertebral column, and we said that there are two types of joints between adjacent vertebrae: 1. Between the bodies of the vertebrae; which
In the last lecture we started talking about the joints in the vertebral column, and we said that there are two types of joints between adjacent vertebrae: 1. Between the bodies of the vertebrae; which
Effect of Swallowing Function After ROI-C Anterior Cervical Interbody Fusion
 Journal of Surgery 2016; 4(6): 141-145 http://www.sciencepublishinggroup.com/j/js doi: 10.11648/j.js.20160406.14 ISSN: 2330-0914 (Print); ISSN: 2330-0930 (Online) Effect of Swallowing Function After ROI-C
Journal of Surgery 2016; 4(6): 141-145 http://www.sciencepublishinggroup.com/j/js doi: 10.11648/j.js.20160406.14 ISSN: 2330-0914 (Print); ISSN: 2330-0930 (Online) Effect of Swallowing Function After ROI-C
Pedicle screw placement accuracy in thoracic and lumbar spinal surgery with a patient-matched targeting guide: A cadaveric study
 Pedicle screw placement accuracy in thoracic and lumbar spinal surgery with a patient-matched targeting guide: A cadaveric study [ based on the homonymous paper from Prof.Lamartina et al. Anticipated publication
Pedicle screw placement accuracy in thoracic and lumbar spinal surgery with a patient-matched targeting guide: A cadaveric study [ based on the homonymous paper from Prof.Lamartina et al. Anticipated publication
Original article Morphometric analysis of the cervical spine of Indian population by using computerized tomography
 J M e d A l l i e d S c i 2 0 1 2 ; 2 ( 2 ) : 66-76 w w w. j m a s. i n P r i n t I S S N : 2 2 3 1 1 6 9 6 O n l i n e I S S N : 2 2 3 1 1 7 0 X Journal of Medical & Allied Sciences Original article Morphometric
J M e d A l l i e d S c i 2 0 1 2 ; 2 ( 2 ) : 66-76 w w w. j m a s. i n P r i n t I S S N : 2 2 3 1 1 6 9 6 O n l i n e I S S N : 2 2 3 1 1 7 0 X Journal of Medical & Allied Sciences Original article Morphometric
MRI Measurement of Neuroforaminal Dimension at the Index and Supradjacent Levels after Anterior Lumbar Interbody Fusion: A Prospective Study
 Original Article Clinics in Orthopedic Surgery 2013;5:49-54 http://dx.doi.org/10.4055/cios.2013.5.1.49 MRI Measurement of Neuroforaminal Dimension at the Index and Supradjacent Levels after Anterior Lumbar
Original Article Clinics in Orthopedic Surgery 2013;5:49-54 http://dx.doi.org/10.4055/cios.2013.5.1.49 MRI Measurement of Neuroforaminal Dimension at the Index and Supradjacent Levels after Anterior Lumbar
Computerized Tomographic Morphometric Analysis of the Cervical Spine
 250 The Open Orthopaedics Journal, 2012, 6, 250-254 Open Access Computerized Tomographic Morphometric Analysis of the Cervical Spine D.S. Evangelopoulos *,1,3, P. Kontovazenitis 1, S. Kouris 2, X. Zlatidou
250 The Open Orthopaedics Journal, 2012, 6, 250-254 Open Access Computerized Tomographic Morphometric Analysis of the Cervical Spine D.S. Evangelopoulos *,1,3, P. Kontovazenitis 1, S. Kouris 2, X. Zlatidou
human anatomy 2015 lecture four Dr meethak ali ahmed neurosurgeon
 The Vertebral Column the vertebral columnis central pillar of the body.it serve to protect the spinal cord and support the weight of the head trunk, which it transmits to the hip bones & the lower limbs.
The Vertebral Column the vertebral columnis central pillar of the body.it serve to protect the spinal cord and support the weight of the head trunk, which it transmits to the hip bones & the lower limbs.
EFSPINE CERVICAL COMBINED SET DISC PROTHESIS ORGANIZER BOX
 EFSPINE CERVICAL COMBINED SET INSTRUMENTS CERVICAL CAGE & DISC PROTHESIS ORGANIZER BOX Cervical Thoracic Thoraco - Lumbar Sacral EFSPINE CERVICAL COMBINED SET CERVICAL IMPLANTS INTRODUCTION Cervical Disc
EFSPINE CERVICAL COMBINED SET INSTRUMENTS CERVICAL CAGE & DISC PROTHESIS ORGANIZER BOX Cervical Thoracic Thoraco - Lumbar Sacral EFSPINE CERVICAL COMBINED SET CERVICAL IMPLANTS INTRODUCTION Cervical Disc
Quantitative Anatomic Evaluation of Cervical Lateral Mass Fixation With a Comparison of the Roy-Camille and the Magerl Screw Techniques
 Quantitative Anatomic Evaluation of Cervical Lateral Mass Fixation With a Comparison of the Roy-Camille and the Magerl Screw Techniques SPINE Volume 30, Number 6, pp E140 E147 2005, Lippincott Williams
Quantitative Anatomic Evaluation of Cervical Lateral Mass Fixation With a Comparison of the Roy-Camille and the Magerl Screw Techniques SPINE Volume 30, Number 6, pp E140 E147 2005, Lippincott Williams
Objectives. Comprehension of the common spine disorder
 Objectives Comprehension of the common spine disorder Disc degeneration/hernia Spinal stenosis Common spinal deformity (Spondylolisthesis, Scoliosis) Osteoporotic fracture Destructive spinal lesions Anatomy
Objectives Comprehension of the common spine disorder Disc degeneration/hernia Spinal stenosis Common spinal deformity (Spondylolisthesis, Scoliosis) Osteoporotic fracture Destructive spinal lesions Anatomy
Anatomy Lecture #19 AN INTRODUCTION TO THE THORAX April 3, 2012
 Page 1 بسم الله الرحمن الرحيم The Thoracic Wall Firstly, when we talk about thorax, we should begin with the thorax wall which means not only bones that construct the thorax but also the muscles which
Page 1 بسم الله الرحمن الرحيم The Thoracic Wall Firstly, when we talk about thorax, we should begin with the thorax wall which means not only bones that construct the thorax but also the muscles which
It consist of two components: the outer, laminar fibrous container (or annulus), and the inner, semifluid mass (the nucleus pulposus).
 Lumbar Spine The lumbar vertebrae are the last five vertebrae of the vertebral column. They are particularly large and heavy when compared with the vertebrae of the cervical or thoracicc spine. Their bodies
Lumbar Spine The lumbar vertebrae are the last five vertebrae of the vertebral column. They are particularly large and heavy when compared with the vertebrae of the cervical or thoracicc spine. Their bodies
MD Bones & Joints of the Back. A/Prof Chris Briggs Department of Anatomy & Neuroscience
 MD 2017 Bones & Joints of the Back A/Prof Chris Briggs Department of Anatomy & Neuroscience WARNING This material has been provided to you pursuant to section 49 of the Copyright Act 1968 (the Act) for
MD 2017 Bones & Joints of the Back A/Prof Chris Briggs Department of Anatomy & Neuroscience WARNING This material has been provided to you pursuant to section 49 of the Copyright Act 1968 (the Act) for
Morphometric study of the Axis vertebra
 ORIGINAL ARTICLE Eur J Anat, 16 (2): 98-103 (2012) Morphometric study of the Axis vertebra Shilpa Gosavi 1, Vatsala Swamy 2 1- Dept. of Anatomy, Padmashree Dr.Vitthalrao Vikhe Patil Foundation s Medical
ORIGINAL ARTICLE Eur J Anat, 16 (2): 98-103 (2012) Morphometric study of the Axis vertebra Shilpa Gosavi 1, Vatsala Swamy 2 1- Dept. of Anatomy, Padmashree Dr.Vitthalrao Vikhe Patil Foundation s Medical
Morphometric analysis of human occipital condyle
 Clinical Neurology and Neurosurgery 107 (2005) 191 199 Morphometric analysis of human occipital condyle Sait Naderi a,, Esin Korman b,güven Çıtak a, Mustafa Güvençer b, Candan Arman b, Mehmet Şenoğlu a,süleyman
Clinical Neurology and Neurosurgery 107 (2005) 191 199 Morphometric analysis of human occipital condyle Sait Naderi a,, Esin Korman b,güven Çıtak a, Mustafa Güvençer b, Candan Arman b, Mehmet Şenoğlu a,süleyman
THE VERTEBRAL COLUMN. Average adult length: In male: about 70 cms. In female: about 65 cms.
 THE VERTEBRAL COLUMN Average adult length: In male: about 70 cms. In female: about 65 cms. 1 Vertebral Column (Regions and Curvatures) Curvatures of the vertebral column: A. Primary curvature: C-shaped;
THE VERTEBRAL COLUMN Average adult length: In male: about 70 cms. In female: about 65 cms. 1 Vertebral Column (Regions and Curvatures) Curvatures of the vertebral column: A. Primary curvature: C-shaped;
THE THORACIC WALL. Boundaries Posteriorly by the thoracic part of the vertebral column. Anteriorly by the sternum and costal cartilages
 THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces Superiorly by the suprapleural
THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces Superiorly by the suprapleural
Surgical anatomy of the internal branch of the superior laryngeal nerve
 Eur Spine J (2005) DOI 10.1007/s00586-005-0006-7 ORIGINAL ARTICLE Amac Kiray Sait Naderi Ipek Ergur Esin Korman Surgical anatomy of the internal branch of the superior laryngeal nerve Received: 19 November
Eur Spine J (2005) DOI 10.1007/s00586-005-0006-7 ORIGINAL ARTICLE Amac Kiray Sait Naderi Ipek Ergur Esin Korman Surgical anatomy of the internal branch of the superior laryngeal nerve Received: 19 November
8/4/2012. Causes and Cures. Nucleus pulposus. Annulus fibrosis. Vertebral end plate % water. Deforms under pressure
 Causes and Cures Intervertebral discs Facet (zygopophyseal) joints Inter body joints Spinal nerve roots Nerve compression Pathological conditions Video Causes of back pain Nucleus pulposus Annulus fibrosis
Causes and Cures Intervertebral discs Facet (zygopophyseal) joints Inter body joints Spinal nerve roots Nerve compression Pathological conditions Video Causes of back pain Nucleus pulposus Annulus fibrosis
Western Orthopedics, PC Denver, CO Presbyterian/St. Luke s Medical Center
 Tim Birney, MD Western Orthopedics, PC Denver, CO Presbyterian/St. Luke s Medical Center Treating Neck & Low Back Pain The Fundamentals, and What s Old And What s New? Normal Anatomy Dual function of the
Tim Birney, MD Western Orthopedics, PC Denver, CO Presbyterian/St. Luke s Medical Center Treating Neck & Low Back Pain The Fundamentals, and What s Old And What s New? Normal Anatomy Dual function of the
Anatomy and Physiology II. Spine
 Anatomy and Physiology II Spine Bones and Other Structures Vertibrae Contains Cervical, Thoracic, Lumbar, Sacral and Coccygeal regions We use Capital letters to refer to these (C, T, L, S, and Co) and
Anatomy and Physiology II Spine Bones and Other Structures Vertibrae Contains Cervical, Thoracic, Lumbar, Sacral and Coccygeal regions We use Capital letters to refer to these (C, T, L, S, and Co) and
A Patient s Guide to Neck Pain. William T. Grant, MD
 A Patient s Guide to Neck Pain Dr. Grant is a talented orthopedic surgeon with more than 30 years of experience helping people return to their quality of life. He and GM Pugh, PA-C pride themselves in
A Patient s Guide to Neck Pain Dr. Grant is a talented orthopedic surgeon with more than 30 years of experience helping people return to their quality of life. He and GM Pugh, PA-C pride themselves in
Yara saddam & Dana Qatawneh. Razi kittaneh. Maher hadidi
 1 Yara saddam & Dana Qatawneh Razi kittaneh Maher hadidi LECTURE 10 THORAX The thorax extends from the root of the neck to the abdomen. The thorax has a Thoracic wall Thoracic cavity and it is divided
1 Yara saddam & Dana Qatawneh Razi kittaneh Maher hadidi LECTURE 10 THORAX The thorax extends from the root of the neck to the abdomen. The thorax has a Thoracic wall Thoracic cavity and it is divided
The Relationship between Increased Intervertebral Disc Height and Development of Postoperative Axial Neck Pain after Anterior Cervical Fusion
 online ML Comm www.jkns.or.kr http://dx.doi.org/10.3340/jkns.2014.55.6.343 J Korean Neurosurg Soc 55 (6) : 343-347, 2014 Print ISSN 2005-3711 On-line ISSN 1598-7876 Copyright 2014 The Korean Neurosurgical
online ML Comm www.jkns.or.kr http://dx.doi.org/10.3340/jkns.2014.55.6.343 J Korean Neurosurg Soc 55 (6) : 343-347, 2014 Print ISSN 2005-3711 On-line ISSN 1598-7876 Copyright 2014 The Korean Neurosurgical
Dorsal Cervical Surgeries and Techniques
 Dorsal Cervical Approaches Dorsal Cervical Surgeries and Techniques Gregory R. Trost, MD Professor and Vice Chair of Neurological Surgery University of Wisconsin-Madison Advantages Straightforward Easily
Dorsal Cervical Approaches Dorsal Cervical Surgeries and Techniques Gregory R. Trost, MD Professor and Vice Chair of Neurological Surgery University of Wisconsin-Madison Advantages Straightforward Easily
Lumbar Laminotomy DEFINING APPROPRIATE COVERAGE POSITIONS NASS COVERAGE POLICY RECOMMENDATIONS TASKFORCE
 NASS COVERAGE POLICY RECOMMENDATIONS Lumbar Laminotomy DEFINING APPROPRIATE COVERAGE POSITIONS North American Spine Society 7075 Veterans Blvd. Burr Ridge, IL 60527 TASKFORCE Introduction North American
NASS COVERAGE POLICY RECOMMENDATIONS Lumbar Laminotomy DEFINING APPROPRIATE COVERAGE POSITIONS North American Spine Society 7075 Veterans Blvd. Burr Ridge, IL 60527 TASKFORCE Introduction North American
Multidetector CT has enlarged our view of human vascular
 ORIGINAL RESEARCH D.H. Heo Y.J. Cho S.H. Sheen M.S. Hong S.M. Cho S.H. Park 3D Reconstructions of Spinal Using CT Angiography: Applications in Minimally Invasive Spinal Procedures BACKGROUND AND PURPOSE:
ORIGINAL RESEARCH D.H. Heo Y.J. Cho S.H. Sheen M.S. Hong S.M. Cho S.H. Park 3D Reconstructions of Spinal Using CT Angiography: Applications in Minimally Invasive Spinal Procedures BACKGROUND AND PURPOSE:
Copyright 2010 Pearson Education, Inc.
 E. VERTEBRAL COLUMN 1. The vertebral column extends from the skull to the pelvis and forms the vertical axis of the skeleton. 2. The vertebral column is composed of vertebrae that are separated by intervertebral
E. VERTEBRAL COLUMN 1. The vertebral column extends from the skull to the pelvis and forms the vertical axis of the skeleton. 2. The vertebral column is composed of vertebrae that are separated by intervertebral
Induction and Maintenance of Lordosis in MultiLevel ACDF Using Allograft. Saad Khairi, MD Jennifer Murphy Robert S. Pashman, MD
 Induction and Maintenance of Lordosis in MultiLevel ACDF Using Allograft Saad Khairi, MD Jennifer Murphy Robert S. Pashman, MD Purpose Is lordosis induced by multilevel cortical allograft ACDF placed on
Induction and Maintenance of Lordosis in MultiLevel ACDF Using Allograft Saad Khairi, MD Jennifer Murphy Robert S. Pashman, MD Purpose Is lordosis induced by multilevel cortical allograft ACDF placed on
2/5/2019. Facet Joint Pain. Biomechanics
 Facet Arthropathy as a Pain Source Evaluation and Management Shelby Spine Jan 31 st Feb 2 nd, 2019 Kushagra Verma MD, MS Adult and Pediatric Scoliosis And Spine Deformity Beach Orthopaedics Specialty Institute
Facet Arthropathy as a Pain Source Evaluation and Management Shelby Spine Jan 31 st Feb 2 nd, 2019 Kushagra Verma MD, MS Adult and Pediatric Scoliosis And Spine Deformity Beach Orthopaedics Specialty Institute
Bony framework of the vertebral column Structure of the vertebral column
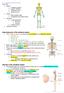 5.1: Vertebral column & back. Overview. Bones o vertebral column. o typical vertebra. o vertebral canal. o spinal nerves. Joints o Intervertebral disc. o Zygapophyseal (facet) joint. Muscles o 2 compartments:
5.1: Vertebral column & back. Overview. Bones o vertebral column. o typical vertebra. o vertebral canal. o spinal nerves. Joints o Intervertebral disc. o Zygapophyseal (facet) joint. Muscles o 2 compartments:
AO CLASSIFICATIONS THORACO-LUMBAR SPINAL INJURIES
 AO CLASSIFICATIONS THORACO-LUMBAR SPINAL INJURIES T H E A O / A S I F ( A R B E I T S G E M E I N S C H A F T F Ü R O S T E O S Y N T H E S E F R A G E N / A S S O C I A T I O N F O R T H E S T U D Y O
AO CLASSIFICATIONS THORACO-LUMBAR SPINAL INJURIES T H E A O / A S I F ( A R B E I T S G E M E I N S C H A F T F Ü R O S T E O S Y N T H E S E F R A G E N / A S S O C I A T I O N F O R T H E S T U D Y O
Vertebral Column. Backbone consists of 26 vertebrae. Five vertebral regions. Cervical
 Vertebral Column Backbone consists of 26 vertebrae. Five vertebral regions Cervical vertebrae (7) in the neck. Thoracic vertebrae (12) in the thorax. Lumbar vertebrae (5) in the lower back. Sacrum (5,
Vertebral Column Backbone consists of 26 vertebrae. Five vertebral regions Cervical vertebrae (7) in the neck. Thoracic vertebrae (12) in the thorax. Lumbar vertebrae (5) in the lower back. Sacrum (5,
CERVICAL SPINE EVALUATION MARK FIGUEROA PHYSICAL THERAPIST
 CERVICAL SPINE EVALUATION MARK FIGUEROA PHYSICAL THERAPIST OVERVIEW OF CLINICAL REASONING Stage of disorder Pathoanatomical diagnosis Signs and symptoms Consideration of the evidence gathered Common sense
CERVICAL SPINE EVALUATION MARK FIGUEROA PHYSICAL THERAPIST OVERVIEW OF CLINICAL REASONING Stage of disorder Pathoanatomical diagnosis Signs and symptoms Consideration of the evidence gathered Common sense
Repair of V2 vertebral artery injuries sustained during anterior cervical discectomy
 Accepted Manuscript Repair of V2 vertebral artery injuries sustained during anterior cervical discectomy Evgenii Belykh, MD, David S. Xu, MD, Kaan Yağmurlu, MD, Ting Lei, MD, Vadim A. Byvaltsev, MD, PhD,
Accepted Manuscript Repair of V2 vertebral artery injuries sustained during anterior cervical discectomy Evgenii Belykh, MD, David S. Xu, MD, Kaan Yağmurlu, MD, Ting Lei, MD, Vadim A. Byvaltsev, MD, PhD,
Morphological study of the foramen magnum and occipital condyle and its surgical implications in transcondylar approach
 Morphological study of the foramen magnum and occipital condyle and its surgical implications in transcondylar approach Joseph Naiem.S Aziz 1 and Ahmed Khaled Al-Hrabi2 1 Deparment of Anatomy, Faculty
Morphological study of the foramen magnum and occipital condyle and its surgical implications in transcondylar approach Joseph Naiem.S Aziz 1 and Ahmed Khaled Al-Hrabi2 1 Deparment of Anatomy, Faculty
MEDICAL IMAGING OF THE VERTEBRAE
 MEDICAL IMAGING OF THE VERTEBRAE Vertebrae are your friends Matthew Harper MS-IV LECTURE OBJECTIVES INTRODUCE THE MOST COMMON MODALITIES OF MEDICAL IMAGING AND BASIC TECHNIQUES FOR READING THESE IMAGES
MEDICAL IMAGING OF THE VERTEBRAE Vertebrae are your friends Matthew Harper MS-IV LECTURE OBJECTIVES INTRODUCE THE MOST COMMON MODALITIES OF MEDICAL IMAGING AND BASIC TECHNIQUES FOR READING THESE IMAGES
Accelerated spondylotic changes adjacent to the fused segment following central cervical corpectomy: magnetic resonance imaging study evidence
 See the Editorial and the Response in this issue, p 1. J Neurosurg (Spine 1) 100:2 6, 2004 Accelerated spondylotic changes adjacent to the fused segment following central cervical corpectomy: magnetic
See the Editorial and the Response in this issue, p 1. J Neurosurg (Spine 1) 100:2 6, 2004 Accelerated spondylotic changes adjacent to the fused segment following central cervical corpectomy: magnetic
Akihito Minamide, MD, PhD Department of Orthopaedic Surgery Wakayama Medical University, Wakayama, JAPAN
 SURGICAL TECHNIQUES/DECISION -MAKING IN CERVICAL SPINE SURGERY: Cervico-Thoracic Junction Pathology Radiculopathy Akihito Minamide, MD, PhD Department of Orthopaedic Surgery Wakayama Medical University,
SURGICAL TECHNIQUES/DECISION -MAKING IN CERVICAL SPINE SURGERY: Cervico-Thoracic Junction Pathology Radiculopathy Akihito Minamide, MD, PhD Department of Orthopaedic Surgery Wakayama Medical University,
RETROLISTHESIS. Retrolisthesis. is found mainly in the cervical spine and lumbar region but can also be often seen in the thoracic spine
 RETROLISTHESIS A retrolisthesis is a posterior displacement of one vertebral body with respect to adjacent vertebrae Typically a vertebra is to be in retrolisthesis position when it translates backward
RETROLISTHESIS A retrolisthesis is a posterior displacement of one vertebral body with respect to adjacent vertebrae Typically a vertebra is to be in retrolisthesis position when it translates backward
Anterior Cervical Discectomy and Fusion Surgery
 Disclaimer This movie is an educational resource only and should not be used to manage orthopaedic health. All decisions about the management of orthopaedic conditions must be made in conjunction with
Disclaimer This movie is an educational resource only and should not be used to manage orthopaedic health. All decisions about the management of orthopaedic conditions must be made in conjunction with
Subaxial Cervical Spine Trauma. Introduction. Anatomic Considerations 7/23/2018
 Subaxial Cervical Spine Trauma Sheyan J. Armaghani, MD Florida Orthopedic Institute Assistant Professor USF Dept of Orthopedics Introduction Trauma to the cervical spine accounts for 5 of all spine injuries
Subaxial Cervical Spine Trauma Sheyan J. Armaghani, MD Florida Orthopedic Institute Assistant Professor USF Dept of Orthopedics Introduction Trauma to the cervical spine accounts for 5 of all spine injuries
Origin of lumbar spinal roots and their relationship to intervertebral discs
 Origin of lumbar spinal roots and their relationship to intervertebral discs A CADAVER AND RADIOLOGICAL STUDY S. W. Suh, V. U. Shingade, S. H. Lee, J. H. Bae, C. E. Park, J. Y. Song From the University
Origin of lumbar spinal roots and their relationship to intervertebral discs A CADAVER AND RADIOLOGICAL STUDY S. W. Suh, V. U. Shingade, S. H. Lee, J. H. Bae, C. E. Park, J. Y. Song From the University
INDEPENDENT LEARNING: DISC HERNIATION IN THE NATIONAL FOOTBALL LEAGUE: ANATOMICAL FACTORS TO CONSIDER IN REVIEW
 INDEPENDENT LEARNING: DISC HERNIATION IN THE NATIONAL FOOTBALL LEAGUE: ANATOMICAL FACTORS TO CONSIDER IN REVIEW CDC REPORT - CAUSES OF DISABILITY, 2005 REVIEW QUESTIONS ABOUT DISC HERNIATION IN THE NATIONAL
INDEPENDENT LEARNING: DISC HERNIATION IN THE NATIONAL FOOTBALL LEAGUE: ANATOMICAL FACTORS TO CONSIDER IN REVIEW CDC REPORT - CAUSES OF DISABILITY, 2005 REVIEW QUESTIONS ABOUT DISC HERNIATION IN THE NATIONAL
Ultimate Spinal Analysis PA USA-XRAY ( )
 Page: 1 Spine Atlas Angle 7.24 S Atlas Angle 21.67 S The Atlas Angle is a measurement of the stability of the Atlas. The Atlas Plane Line is compared to true horizontal. Any increase or decrease of this
Page: 1 Spine Atlas Angle 7.24 S Atlas Angle 21.67 S The Atlas Angle is a measurement of the stability of the Atlas. The Atlas Plane Line is compared to true horizontal. Any increase or decrease of this
Research article - Basic and applied anatomy Morphometric study of cervical vertebrae C3-C7 in South Indian population A clinico-anatomical approach
 IJAE Vol. 122, n. 1: 49-57, 2017 ITALIAN JOURNAL OF ANATOMY AND EMBRYOLOGY Research article - Basic and applied anatomy Morphometric study of cervical vertebrae C3-C7 in South Indian population A clinico-anatomical
IJAE Vol. 122, n. 1: 49-57, 2017 ITALIAN JOURNAL OF ANATOMY AND EMBRYOLOGY Research article - Basic and applied anatomy Morphometric study of cervical vertebrae C3-C7 in South Indian population A clinico-anatomical
Assessment of cervical spine morphology by computed tomography and its utility as a presurgical planning tool
 The University of Toledo The University of Toledo Digital Repository Theses and Dissertations 2004 Assessment of cervical spine morphology by computed tomography and its utility as a presurgical planning
The University of Toledo The University of Toledo Digital Repository Theses and Dissertations 2004 Assessment of cervical spine morphology by computed tomography and its utility as a presurgical planning
Corporate Medical Policy
 Corporate Medical Policy Image-Guided Minimally Invasive Decompression (IG-MLD) for File Name: Origination: Last CAP Review: Next CAP Review: Last Review: image-guided_minimally_invasive_decompression_for_spinal_stenosis
Corporate Medical Policy Image-Guided Minimally Invasive Decompression (IG-MLD) for File Name: Origination: Last CAP Review: Next CAP Review: Last Review: image-guided_minimally_invasive_decompression_for_spinal_stenosis
Research of thoracolumbar spine lateral vascular anatomy and imaging
 O R I G I N A L A R T I C L E Folia Morphol. Vol. 69, No. 3, pp. 128 133 Copyright 2010 Via Medica ISSN 0015 5659 www.fm.viamedica.pl Research of thoracolumbar spine lateral vascular anatomy and imaging
O R I G I N A L A R T I C L E Folia Morphol. Vol. 69, No. 3, pp. 128 133 Copyright 2010 Via Medica ISSN 0015 5659 www.fm.viamedica.pl Research of thoracolumbar spine lateral vascular anatomy and imaging
The Thoracic Cage ANATOMY 2: THORACIC CAGE AND VERTEBRAL COLUMN
 ANATOMY 2: THORACIC CAGE AND VERTEBRAL COLUMN PSK 4U Mr. S. Kelly North Grenville DHS The Thoracic Cage 7 true ribs 3 false ribs 2 floating ribs Clavicle = collarbone Manubrium Sternum Xiphoid Process
ANATOMY 2: THORACIC CAGE AND VERTEBRAL COLUMN PSK 4U Mr. S. Kelly North Grenville DHS The Thoracic Cage 7 true ribs 3 false ribs 2 floating ribs Clavicle = collarbone Manubrium Sternum Xiphoid Process
Pichayen Duangthongpon MD*, Chaiwit Thanapaisal MD*, Amnat Kitkhuandee MD*, Kowit Chaiciwamongkol MD**, Vilaiwan Morthong MD**
 The Relationships between Asterion, the Transverse-Sigmoid Junction, the Superior Nuchal Line and the Transverse Sinus in Thai Cadavers: Surgical Relevance Pichayen Duangthongpon MD*, Chaiwit Thanapaisal
The Relationships between Asterion, the Transverse-Sigmoid Junction, the Superior Nuchal Line and the Transverse Sinus in Thai Cadavers: Surgical Relevance Pichayen Duangthongpon MD*, Chaiwit Thanapaisal
MORPHOMETRIC ANALYSIS OF TYPICAL CERVICAL VERTEBRAE AND THEIR CLINICAL IMPLICATIONS: A CROSS SECTIONAL STUDY
 Original Research Article MORPHOMETRIC ANALYSIS OF TYPICAL CERVICAL VERTEBRAE AND THEIR CLINICAL IMPLICATIONS: A CROSS SECTIONAL STUDY Ephraim Vikram Rao. K * 1, B Sadananda Rao 2, B H Shiny Vinila 3.
Original Research Article MORPHOMETRIC ANALYSIS OF TYPICAL CERVICAL VERTEBRAE AND THEIR CLINICAL IMPLICATIONS: A CROSS SECTIONAL STUDY Ephraim Vikram Rao. K * 1, B Sadananda Rao 2, B H Shiny Vinila 3.
CERVICAL SPONDYLOSIS & CERVICAL DISC DISEASE
 CERVICAL SPONDYLOSIS & CERVICAL DISC DISEASE Cervical spondylosis l Cervical osteophytosis l Most common progressive disease in the aging cervical spine l Seen in 95% of the people by 65 years Pathophysiology
CERVICAL SPONDYLOSIS & CERVICAL DISC DISEASE Cervical spondylosis l Cervical osteophytosis l Most common progressive disease in the aging cervical spine l Seen in 95% of the people by 65 years Pathophysiology
Axial Skeleton: Vertebrae and Thorax
 Axial Skeleton: Vertebrae and Thorax Function of the vertebral column (spine or backbone): 1) 2) 3) Composition of Vertebral column The vertebral column is formed by 33 individual vertebrae (some of which
Axial Skeleton: Vertebrae and Thorax Function of the vertebral column (spine or backbone): 1) 2) 3) Composition of Vertebral column The vertebral column is formed by 33 individual vertebrae (some of which
Lumbar spinal canal stenosis Degenerative diseases F 08
 What is lumbar spinal canal stenosis? This condition involves the narrowing of the spinal canal, and of the lateral recesses (recesssus laterales) and exit openings (foramina intervertebralia) for the
What is lumbar spinal canal stenosis? This condition involves the narrowing of the spinal canal, and of the lateral recesses (recesssus laterales) and exit openings (foramina intervertebralia) for the
Radiculopathy Caused by Osteoporotic Vertebral Fractures in the Lumbar Spine
 Neurol Med Chir (Tokyo) 51, 484 489, 2011 Radiculopathy Caused by Osteoporotic Vertebral Fractures in the Lumbar Spine Manabu SASAKI, 1 Masanori AOKI, 2 Kazuya NISHIOKA, 3 and Toshiki YOSHIMINE 4 1 Department
Neurol Med Chir (Tokyo) 51, 484 489, 2011 Radiculopathy Caused by Osteoporotic Vertebral Fractures in the Lumbar Spine Manabu SASAKI, 1 Masanori AOKI, 2 Kazuya NISHIOKA, 3 and Toshiki YOSHIMINE 4 1 Department
Subaxial Cervical Spine Trauma Dr Hesarikia BUMS
 Subaxial Cervical Spine Trauma Dr. Hesarikia BUMS Subaxial Cervical Spine From C3-C7 ROM Majority of cervical flexion Lateral bending Approximately 50% rotation Ligamentous Anatomy Anterior ALL, PLL, intervertebral
Subaxial Cervical Spine Trauma Dr. Hesarikia BUMS Subaxial Cervical Spine From C3-C7 ROM Majority of cervical flexion Lateral bending Approximately 50% rotation Ligamentous Anatomy Anterior ALL, PLL, intervertebral
Anthem Blue Cross and Blue Shield Central Region Clinical Claim Edit
 Subject: Laminotomy (Hemilaminectomy) with Decompression of Nerve Root(s), Including Partial Facetectomy, Foraminotomy and/or Excision of Herniated Intervertebral Disc, Reexploration, Single Interspace-Lumbar
Subject: Laminotomy (Hemilaminectomy) with Decompression of Nerve Root(s), Including Partial Facetectomy, Foraminotomy and/or Excision of Herniated Intervertebral Disc, Reexploration, Single Interspace-Lumbar
Medical Policy Original Effective Date: Revised Date: Page 1 of 11
 Page 1 of 11 Content Disclaimer Description Coverage Determination Clinical Indications Lumbar Spine Surgery Lumbar Spine Surgery Description Indication Coding Lumbar Spinal Fusion (single level)surgery
Page 1 of 11 Content Disclaimer Description Coverage Determination Clinical Indications Lumbar Spine Surgery Lumbar Spine Surgery Description Indication Coding Lumbar Spinal Fusion (single level)surgery
