The transverse process, intertransverse space, and vertebral artery in anterior approaches to the lower cervical spine
|
|
|
- Adele Cole
- 5 years ago
- Views:
Transcription
1 J Neurosurg (Spine 2) 98: , 2003 The transverse process, intertransverse space, and vertebral artery in anterior approaches to the lower cervical spine MASATOU KAWASHIMA, M.D., NECMETTIN TANRIOVER, M.D., ALBERT L. RHOTON, JR., M.D., AND TOSHIO MATSUSHIMA, M.D. Department of Neurological Surgery, University of Florida, Gainesville, Florida; and Department of Neurosurgery, Neurological Institute, Graduate School of Medical Sciences, Kyushu University, Fukuoka, Japan Object. The microsurgical anatomy of the C3 6 transverse processes and their relationship to the intertransverse space and vertebral artery (VA) were examined with special attention to the aspect exposed in the anterior surgical approach. Methods. Ten adult cadaveric spines were examined (magnification levels 3 40) after perfusion of the arteries and veins with colored silicone. The morphological detail of the transverse process and intertransverse space, the distances between selected surgical landmarks and the VA were measured, and the means and standard deviations were calculated. The osseous changes in the anterior root of the transverse process were classified according to their extent. The transverse processes became smaller, and the anterior intertransverse spaces and the width of the VA exposed in the space increased in size proceeding from caudal to rostral levels, thus exposing the VA to increased risk of injury during procedures at cephalad levels. The distance between the medial border of the longus colli muscle and the VA decreased when proceeding caudally from C2 3 to C4 5 interspaces but began to increase at the level of C5 6. The VA coursed closer to the lateral border of the vertebral body than to the medial border of the anterior tubercle of the transverse process. Osseous changes consisting of thinning or defects in the anterior root of the transverse process were observed from C-3 to C-5. The thinning was most prominent in the lower half of the anterior root just above where the VA ascends behind the lower edge of the anterior root. The osseous change may reflect the erosive effect of the VA on the anterior root of the transverse process. Conclusions. This study provides new information regarding the transverse process and especially the anterior root. An awareness of the thinness and defects in the anterior root of the transverse process and the relationships to the surrounding area will aid in reducing VA injury during anterior approaches to the cervical spine. KEY WORDS anterior root anterior tubercle microsurgery transverse process vertebral artery A N anterior surgical approach to the cervical spine is frequently selected in the treatment of patients with spondylotic, neoplastic, infectious, and posttraumatic lesions because it provides easy access to anteriorly or anterolaterally located cervical lesions. Although these approaches are associated with a lower incidence of neurological complications, 9 injury to the VA, occurring as an iatrogenic complication of extended lateral decompression during anterior cervical discectomy, has been reported. 2,3,8,12,14 The consequence of lacerating the artery is a challenging problem because of the difficulty in controlling the hemorrhage. Avoiding VA injury requires an understanding of the relationships between the VA and surrounding structures, including the transverse process and intertransverse space. The purposes of this study were threefold: to examine the microsurgical anatomy of the transverse process region, focusing on the anterior aspect; to define landmarks that would aid in avoiding VA injury; and to emphasize the importance of the osseous change in the anterior root of the transverse process. Abbreviations used in this paper: VA = vertebral artery; VB = vertebral body. 188 Materials and Methods Using a microscope (magnification levels 3 40), we examined the microsurgical anatomy of the transverse process and intertransverse space in the lower cervical vertebrae in 10 adult cadaveric cervical spines after perfusion of the arteries and veins with colored silicone. Measurements obtained at the C2 3 to C6 7 interspaces (Fig. 1) included minimum and maximum heights and width of the anterior root of the transverse process; the width of the groove on the upper surface of the transverse process for the spinal nerve (between the anterior and posterior tubercles); the height of the intertransverse space; the diameter of the VA in each intertransverse space; and the distances between the VA and adjacent landmarks, which included the medial border of the longus colli muscle, lateral border of the VB, and medial border of the anterior tubercle. The means and standard deviations of the measurements were calculated. The ratio of the minimum-to-maximum height of the anterior surface of each anterior root and the VA occupancy ratio, defined as the ratio of the diameter of the VA to the width of the anterior root of the transverse process in each intertransverse space, were also calculated. Anterior Root of the Transverse Process The normal anterior root is 1 to 2 mm thick. We found that the anterior root was frequently thin or was the site of osseous defects, thus exposing the VA as it ascended through the foramen transversarium. The anterior root was divided into three groups: in the first group, defined as thin anterior root, the width of the anterior root
2 Microsurgical anatomy of the transverse process region was thin, measuring less than 1 mm in thickness; in the second, or the fragile group, the bone was paper thin and the VA and venous plexus were seen through the thin bone; in the third, or defective group, the anterior root was the site of osseous defects that exposed the VA (Fig. 2). The site of the osseous change on the anterior root was also evaluated. Results Basic Anatomical Considerations Osseous Relationships. The cervical spine consists of three atypical and four typical cervical vertebrae. Typical cervical vertebrae, C-3 to C-6, include a VB, a vertebral arch, and several processes for muscular attachments and articulations. A typical cervical vertebra has a relatively small and transversely broad body. The spinal canal is large and triangular rather than round. The pedicles project from the posterolateral aspect of the VBs and, together with the lamina, form the vertebral arch covering the lateral and posterior aspects of the spinal cord. The pedicles project laterally as well as backward from the body (Fig. 3A). The laminae project posteromedially from the pedicles and join in the midline; they are relatively long with a thin upper border and a wider lower border. The short, bifid spinous processes project posteriorly from the junction of the laminae. There are often terminal tubercles of unequal size on the bifid tips. The superior articular process faces upward and posteriorly; the inferior articular facet faces downward and anteriorly. A superior process articulates with the corresponding inferior process of the adjacent cephalad VB to form the osseous elements of the zygapophyseal joints (Fig. 3B). The upper projection on the lateral edge of the superior surface of the caudal VB is called the uncus and is related to the lateral edge of the inferior surface of the cephalad vertebra, called the enchancure. These articulations also have been called the uncovertebral joints or joints of Luschka (Fig. 3C). The transverse process contains the transverse foramen, projects laterally, and is attached medially by anterior and posterior roots. The anterior root of the transverse process arises from the side of VB and ends in the roughened anterior tubercle to which are attached tendinous slips of the scalenus anterior, longus capitis, and longus colli muscles. The posterior root, which is thicker than the anterior counterpart, arises from the junction of the pedicle and lamina and ends in a rounded posterior tubercle, which is positioned lateral to the anterior tubercle. The two roots of the transverse process are connected laterally by the costotransverse bar that combines with the anterior and posterior roots and the pedicle to surround the transverse foramen. The costotransverse bar, which forms the lateral aspect of the intervertebral foramen, has a groove on its upper surface that is concave upward to accommodate the exiting spinal nerve (Fig. 3D). Musculature: Anterior Vertebral Muscles. The longus capitis muscle is attached below by tendinous slips to the anterior tubercles of the C3 6 transverse processes, and above to the inferior surface of the basilar part of the occipital bone (Fig. 4A). The longus colli, located on the anterior aspect of the cervical spine, is divided into three parts: 1) the superior oblique part originates below from the anterior tubercle of the C3 5 transverse processes and is attached above to the tubercle of the anterior arch of the FIG. 1. Anterior photograph of transverse process and adjacent structures. The measurement included the following. a c: Minimum (a) and maximum (b) heights, and width (c) of the anterior root of the transverse process. d: Width of the groove for the spinal nerve (between the anterior and posterior tubercles). e: Height of the intertransverse space. f: Diameter of the VA in each intertransverse space. g: Distance between the VA and medial border of the longus colli muscle. h: Distance between the VA and lateral border of the VB. i: Distance between the VA and medial border of the anterior tubercle. atlas; 2) the inferior oblique arises from the anterior surface of the VBs of the first two or three thoracic vertebrae and passes upward and laterally to the anterior tubercle of the C5 6 transverse process; and 3) the vertical part ascends from the bodies of the upper three thoracic and lower three cervical vertebrae to the anterior aspect of the C2 5 VBs (Fig. 4B). Reflecting or removing the longus capitis and longus colli muscles exposes the transverse process and VA (Fig. 4C). Musculature: Lateral Vertebral Muscles. The scalenus anterior muscle lies deep to the sternocleidomastoid muscle, arises from the anterior tubercles of the C3 6 transverse processes, and descends vertically to its attachment to the scalene tubercle on the upper aspect of the first rib (Fig. 4C). The scalenus medius originates from the lateral aspect of the posterior tubercles of the C2 7 transverse processes and attaches to the upper surface of the first rib behind the subclavian groove. The scalenus posterior passes from the posterior tubercles of the C4 6 transverse processes and attaches to the outer surface of the second rib just deep to the attachment of the scalene anterior. Intervertebral Foramen and Intertransverse Space. The intervertebral foramen is bound superiorly and inferiorly by the adjoining pedicles, posteriorly by the articular pro- 189
3 M. Kawashima, et al. FIG. 2. Classification of osseous change in the anterior root of the transverse process. A and B: Thin anterior roots (arrows), left C-5 (A) and right C-3 (B) transverse processes; the lower parts of the anterior roots were less than 1 mm thick. C and D: Fragile bone (arrows), right C-3 (C) and left C-4 (D) transverse processes; lower parts of the anterior roots were paper thin. E and F: Bone defect (arrows), left C-4 (E) and right C-3 (F) transverse processes; the middle and lower edge of the anterior roots were eroded. cesses, and anteriorly by the intervertebral discs, uncovertebral joints, and VBs. The intertransverse space, located between the lower edge of the transverse process above and the upper edge of the transverse process below, contains the VA, a venous plexus, and a spinal nerve root, all encased by a fibroligamentous tissue. This tissue, attached to the lateral aspect of the uncovertebral joint, binds the VA, spinal nerve root, and uncovertebral joint together (Fig. 5A). The ventral and dorsal nerve roots join immediately beyond the spinal ganglion to form the spinal nerve that emerges through the intervertebral foramen and divides into posterior and anterior rami. The VA enters the transverse foramina of C-6 and ascends through the transverse foramina to the level of the atlas, passing ventral to the anterior rami of cervical nerves C2 6. The VA gives rise to the spinal and muscular branches in the intertransverse space (Fig. 5B and C). Measurement of Anatomical Structures The measurements of the transverse process, intertransverse space, diameter of the VA and VA occupancy ratio in each intertransverse space, and distances between anatomical landmarks and the VA are shown in Table 1. Parameters of the Transverse Process. The transverse processes gradually decreased in size at ascending levels from C-3 to C-6 (Table 1). The upper edge of the anterior root was concave rostrally, and the lower edge was concave caudally. It was tallest near the VB and shortest in the midportion in front of the VA. The ratio of the minimum to the maximum height of the anterior surface of the anterior root decreased from C-6 to C-3 (minimum/maximum ratio: 81.8% at C-6, 79.8% at C-5, 72.9% at C-4, and 68.7% at C-3) (Table 1). A lower ratio is associated with greater degrees of narrowing of the anterior root and greater exposure of the VA in the intertransverse space. Intertransverse Space, VA Diameter, and VA Occupancy Ratio. The height of the intertransverse space at C2 3 and C3 4 was greater than that at C4 5 and C5 6 ( mm at C2 3, mm at C3 4, mm at C4 5, and mm at C5 6). The diameter of the VA gradually decreased from C2 3 to C6 7 (from mm at C2 3 to mm at C6 7). The ratio of the diameter of the VA to the width of the lower edge of the anterior root of the transverse process in each intertransverse space (VA occupancy ratio) increased from C6 7 to C3 4 (from 44.8% at C6 7 to 50.8% at C3 4) (Table 1). Distances Between Anatomic Landmarks and the VA. The distance between the medial border of the longus colli and the medial edge of the VA at each intertransverse space decreased from C2 3 to C4 5; however, it began to increase at C5 6. The distance between the lateral border of the VB and the medial edge of the VA increased at each level from C3 4 to C6 7. The distance between the medial border of the anterior tubercle and the lateral edge of the VA was similar at each level except C6 7, where it was the shortest (Table 1). Anterior Root Changes Although the anterior root is normally 1 to 2 mm thick, more than 40% of specimens examined had thin or fragile anterior roots or anterior roots with defects. Twenty-four percent of the anterior roots were thin ( 1 mm) and 16% were fragile in that structures beneath the bone could be seen through the paper-thin bone. Areas in which part of the anterior root was absent were encountered in those with four transverse processes (5%) (Table 2). The number of thinning and osseous defect sites was greatest in the lower half of the anterior root of the transverse process (Table 3) just above where the VA ascended behind the anterior root (Fig. 6). Discussion In proceeding from the caudal to the rostral levels included in this study, the transverse processes became smaller, the upper and lower edges of the anterior roots became more concave, the intertransverse distance increased in height, and the VA occupied an increasing amount of the intertransverse space. All were associated with decrease in size of the anterior root protecting the VA and increased exposure of the VA at cephalad levels. There have been a limited number of studies of these vari- 190
4 Microsurgical anatomy of the transverse process region FIG. 3. Lower cervical vertebrae. A: Axial view. The typical cervical vertebrae, C3 6, include a VB, a vertebral arch, and several processes for muscular attachments and articulations. The spinal canal is large and triangular rather than round. The transverse foramen is located in the bottom of the transverse process, where the anteroposterior diameter of the transverse process is the shortest. B: Lateral view. The lamina is relatively long and narrow, with a thin upper border and a wider lower border. The spinous process projects posteriorly from the junction of the lamina. The spinous process is short and bifid, often with terminal tubercles of unequal size. The superior articular process faces upward and posteriorly; the inferior articular process faces downward and anteriorly. The groove for the spinal nerve is between the anterior and posterior tubercles. C: Anterior view. The upper projection on the lateral edge of the superior surface of the caudal VB is called the uncus and is related to the lateral edge of the inferior surface of the cephalad vertebra termed the enchancure. These articulations also have been called the uncovertebral joints or joints of Luschka. D: Enlarged view of the transverse process. The transverse process contains the transverse foramen, projects laterally, and is attached medially by anterior and posterior roots. The two roots of the transverse process are connected laterally by the costotransverse bar, which combines with the anterior and posterior roots and the pedicle to surround the transverse foramen. The costotransverse bar has a groove on its upper surface that is concave upward to accommodate the exiting spinal nerve. Ant = anterior; art = articular; costotrans = costotransverse; for = foramen; inf = inferior; intertrans = intertransverse; p = process; post = posterior; sup = superior; trans = transverse; transvers = transversarium. FIG. 4. Musculature of the cervical spine. A: The longus capitis is located lateral to the longus colli and attaches below to the anterior tubercles of the C3 6 transverse processes and above to the inferior surface of the basilar part of the occipital bone. B: The longus capitis has been removed. The longus colli is located on the anterior aspect of the cervical spine. The superior oblique part originates below from the anterior tubercle of the C3 5 transverse processes and is attached above to the tubercle of the atlantal anterior arch. C: The transverse process and VA have been exposed by removing the longus capitis and longus colli muscles. The scalenus anterior arises from the anterior tubercles of the C3 6 transverse processes and descends vertically to be attached to the scalene tubercle on the upper aspect of the first rib. Long = longitudinal. 191
5 M. Kawashima, et al. FIG. 5. Intertransverse space. A: The intertransverse space contains the VA, radicular arteries, venous plexus, and spinal nerve root, all of which are encased by a fibroligamentous tissue in the intertransverse space (C2 3 and C3 4). This tissue, which binds the VA, spinal nerve root, and uncovertebral joint together, is attached to the lateral aspect of the uncovertebral joint. B and C: The anterior and posterior nerve roots join immediately beyond the spinal ganglion to form the spinal nerve, which emerges through the intervertebral foramen and divides into posterior and anterior rami. The VA is located ventral to the anterior rami of cervical nerves C-6 to C-2. The VA gives rise to the spinal and muscular branches in the intertransverse space. FIG. 6. Anterior view of the cervical spine revealing the osseous changes in the anterior root of the transverse process. A and C: Before the dissection of the transverse process. B and D: After the dissection of the transverse process. A: The bone of the anterior root is thin (arrowheads) and the ventral venous plexus can be seen through the anterior root of C3 5. B: The osseous changes are just above where the VA ascends behind the anterior root of the transverse processes. C: The bone of the anterior root is absent (arrowheads) and the ventral venous plexus can be seen through the defect in the anterior root of left C-4. D: The osseous defect opens just above where the VA can be seen. 192
6 Microsurgical anatomy of the transverse process region TABLE 1 Measurements of anatomical structures in 10 cadavers* Variable C-3 C-4 C-5 C-6 C2 3 C3 4 C4 5 C5 6 C6 7 transverse process anterior root min height max height min/max ratio (%) width of root groove width for spinal nerve intertransverse space, diameter of VA, & VA occupancy ratio height of intertransverse space diameter of VA width/diameter ratio (%) distance between anatomical landmarks & VA VA & medial border of longus colli VA & lat border of VB VA & medial border of anterior tubercle *All parameters and distances are in millimeters and are presented as the mean standard deviation. Abbreviations: max = maximum; min = minimum; = not applicable. Width/diameter = ratio of the intertransverse width of the anterior root to the diameter of the VA. TABLE 2 Positive percentage of the osseous change in the anterior root of the transverse process ables. Vaccaro, et al., 15 reported that the distance between the transverse foramen increased from C-3 to C-6. Ebraheim, et al., 4 found that the anteroposterior diameters of the transverse foramina and width of the VB decreased in the cephalad vertebrae. Based on our observation, and those of others, it is concluded that the risk of the VA laceration during the anterolateral decompressive surgery is greater at the cephalad vertebrae. Several structures in the region of the transverse process have been used as anatomical landmarks by which to avoid injuring the VA. Smith, et al., 14 recommended that the medial border of the longus colli muscle be used as the lateral limit of dissection. The distance between the medial edge of the paired longus colli muscles, however, increases in the caudal direction. 11 We found that the distance between the VA and the medial border of the longus colli decreased when proceeding caudally from C2 3 to C4 5, but it began to increase at C5 6. The medial border of the longus colli is nearest the VA at C4 5 and began to increase at C5 6 because the inferior oblique part of the longus colli below this level is directed downward and medially from the anterior tubercle of the C5 6 transverse processes to the anterior surface of the thoracic vertebrae. The lateral border of the VB or the uncinate process has been used as an anatomical landmark for the VA; however, no fixed pattern was found at the different levels in previous studies. 5,8,11 In our study, the distance between the lateral edge of the VB and the medial edge of the VA gradually increased when proceeding toward the caudal levels. The interval between the two structures, however, tended to be narrow and it was sometimes difficult to identify the lateral border of the VB or uncinate process because of degenerative changes such as osteophyte formation. Another landmark easily recognized intraoperatively is the anterior tubercle of the transverse process. Chassaignae 1 described the anterior tubercle of the C-6 transverse process as an important landmark for the identification of the VA. We observed that the distance between the VA and the anterior tubercle was similar from C-3 to C-6 and was greater than that between the VA and the lateral border of the VB. The separation at C6 7 is smaller because the anterior tubercle of the C-6 transverse process is larger and is referred to as the carotid tubercle. 17 The anterior tubercle is a more reliable landmark for estimating the position of the VA than either the longus colli muscle or lateral border of the VB. Finally, we found considerable variation in the thick- Osseous Posi- Changes tive Condition* C-3 C-4 C-5 C-6 (%) (%) + (thin) (76) (fragile) (76) (defective) (76) 5 osseous changes (no.) 16 (20) 12 (20) 6 (20) 0 (16) positive (%) *+ = thin; ++ = thinner (structures underneath the fragile bone can be observed); +++ = bone defect. 193
7 M. Kawashima, et al. TABLE 3 Location of the osseous change in the anterior root of the transverse process C-3 C-4 C-5 upper third middle third lower third upper half lower half whole total ness and configuration of the anterior root of the transverse process, which is considerably thinner than its posterior counterpart. The thinning was most striking in its lower half just above where the VA entered the foramen. This thickness has rarely been the subject of reports. No abnormalities in the transverse process have been described in the literature. The anterior root of the transverse process is important during anterior cervical approaches because it is the only bone protecting the anterior surface of the VA. In addition, should arterial injury occur, direct repair might only be achieved by removing the anterior root of the transverse process. In the lateral cervical approach, which provides access to the transverse process more directly in patients with spondylotic or neoplastic lesions, 6,7,10,13,16 mobilizing the VA by excision of the anterior root may aid in avoiding VA injury. Great care should be taken because the anterior root is sometimes so thin or defective that arterial injury can easily occur. The cause of the osseous change in the anterior root of the transverse process is probably due to the compression or pulsation of the VA. The change is most striking in its lower half just above where the VA ascends behind the anterior root. The occurrence of the osseous change in the lower part of the anterior root is probably caused by pulsation of the VA, which is tightly fixed in the lower part of the transverse foramen. The VA is loosely fixed in the upper part of the anterior root, which does not show the osseous changes. In addition, the osseous change at the cephalad vertebrae is explained by the smaller size of the transverse foramen 4,5,15 and its greater filling by the VA at cephalad levels. Conclusions The microsurgical anatomy of the transverse process region has been studied infrequently in the past despite its frequent exposure in approaches to the anterior cervical spine. This study provides new information regarding the transverse process and especially the anterior root. An awareness of the thinness and defects in anterior root of the transverse process and the relationships to the surrounding area will aid in reducing VA injury during anterior approaches to the cervical spine. Acknowledgments The authors thank Ronald Smith, M.S., Director, and David Peace, M.S., Medical Illustrator, of the Microneuroanatomy Laboratory, Department of Neurological Surgery, University of Florida, for constant support. They also thank Hidefuku Gi, M.D., Department of Neurosurgery, Baba Memorial Hospital, Osaka, Japan, for the valuable suggestions regarding the technical aspect of the anterior cervical surgery, and Laura Dickinson for preparation of the manuscript. References 1. Chassaignae E: Traité Clinique et Pratique des Opérations Chirurgicales, Vol. 1. Paris: Masson et Fil, 1861, pp Cosgrove GR, Theron J: Vertebral arteriovenous fistula following anterior cervical spine surgery. Report of two cases. J Neurosurg 66: , de los Reyes RA, Moser FG, Sachs DP, et al: Direct repair of an extracranial vertebral artery pseudoaneurysm: case report and review of the literature. Neurosurgery 26: , Ebraheim NA, Lu J, Brown JA, et al: Vulnerability of vertebral artery in anterolateral decompression for cervical spondylosis. Clin Orthop 322: , Ebraheim NA, Reader D, Xu R, et al: Location of the vertebral artery foramen on the anterior aspect of the lower cervical spine by computed tomography. J Spinal Disord 10: , George B, Gauthier N, Lot G: Multisegmental cervical spondylotic myelopathy and radiculopathy treated by multilevel oblique corpectomies without fusion. Neurosurgery 44:81 90, George B, Zerah M, Lot G, et al: Oblique transcorporeal approach to anteriorly located lesions in the cervical spinal canal. Acta Neurochir 121: , Golfinos JG, Dickman CA, Zabramski JM, et al: Repair of vertebral artery injury during anterior cervical decompression. Spine 19: , Graham JJ: Complications of cervical spine surgery. A fiveyear report on a survey of the membership of the Cervical Spine Research Society by the Morbidity and Mortality Committee. Spine 14: , Lot G, George B: Cervical neuromas with extradural components: surgical management in a series of 57 patients. Neurosurgery 41: , Pait TG, Killefer JA, Arnautovic KI: Surgical anatomy of the anterior cervical spine: the disc space, vertebral artery, and associated bony structures. Neurosurgery 39: , Pfeifer BA, Freidberg SR, Jewell ER: Repair of injured vertebral artery in anterior cervical procedures. Spine 19: , Sen C, Eisenberg M, Casden AM, et al: Management of the vertebral artery in excision of extradural tumors of the cervical spine. Neurosurgery 36: , Smith MD, Emery SE, Dudley A, et al: Vertebral artery injury during anterior decompression of the cervical spine. A retrospective review of ten patients. J Bone Joint Surg Br 75: , Vaccaro AR, Ring D, Scuderi G, et al: Vertebral artery location in relation to the vertebral body as determined by two-dimensional computed tomography evaluation. Spine 19: , Verbiest H: Chapter 24. The lateral approach to the cervical spine. Clin Neurosurg 20: , Warwick R, Williams PL: Osteology, in Gray s Anatomy, ed 35. Philadelphia: WB Saunders, 1973, pp 235 Manuscript received September 5, Accepted in final form November 1, Address reprint requests to: Albert L. Rhoton, Jr., M.D., Department of Neurological Surgery, University of Florida Brain Institute, PO Box , 100 South Newell Drive, Building 59, L2-100, Gainesville, Florida address: rhoton@neuro surgery.ufl.edu. 194
Any of the vertebra in the cervical (neck) region of the spinal column. The cervical vertebra are the smallest vertebra in the spine, reflective of th
 Any of the vertebra in the cervical (neck) region of the spinal column. The cervical vertebra are the smallest vertebra in the spine, reflective of the fact that they support the least load. In humans,
Any of the vertebra in the cervical (neck) region of the spinal column. The cervical vertebra are the smallest vertebra in the spine, reflective of the fact that they support the least load. In humans,
VERTEBRAL COLUMN VERTEBRAL COLUMN
 VERTEBRAL COLUMN FUNCTIONS: 1) Support weight - transmits weight to pelvis and lower limbs 2) Houses and protects spinal cord - spinal nerves leave cord between vertebrae 3) Permits movements - *clinical
VERTEBRAL COLUMN FUNCTIONS: 1) Support weight - transmits weight to pelvis and lower limbs 2) Houses and protects spinal cord - spinal nerves leave cord between vertebrae 3) Permits movements - *clinical
human anatomy 2015 lecture four Dr meethak ali ahmed neurosurgeon
 The Vertebral Column the vertebral columnis central pillar of the body.it serve to protect the spinal cord and support the weight of the head trunk, which it transmits to the hip bones & the lower limbs.
The Vertebral Column the vertebral columnis central pillar of the body.it serve to protect the spinal cord and support the weight of the head trunk, which it transmits to the hip bones & the lower limbs.
Cervical Spine Anatomy and Biomechanics. Typical Cervical Vertebra C3 6. Typical Cervical Vertebra Anterior 10/5/2017
 Cervical Spine Anatomy and Biomechanics Typical Cervical Vertebra C3 6 Small, relatively broad body Bifid SpinousProcess Long and narrow laminae Spinal Canal: large, triangular; remarkably consistent dimensions
Cervical Spine Anatomy and Biomechanics Typical Cervical Vertebra C3 6 Small, relatively broad body Bifid SpinousProcess Long and narrow laminae Spinal Canal: large, triangular; remarkably consistent dimensions
THE THORACIC WALL. Boundaries Posteriorly by the thoracic part of the vertebral column. Anteriorly by the sternum and costal cartilages
 THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces Superiorly by the suprapleural
THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces Superiorly by the suprapleural
THE VERTEBRAL COLUMN. Average adult length: In male: about 70 cms. In female: about 65 cms.
 THE VERTEBRAL COLUMN Average adult length: In male: about 70 cms. In female: about 65 cms. 1 Vertebral Column (Regions and Curvatures) Curvatures of the vertebral column: A. Primary curvature: C-shaped;
THE VERTEBRAL COLUMN Average adult length: In male: about 70 cms. In female: about 65 cms. 1 Vertebral Column (Regions and Curvatures) Curvatures of the vertebral column: A. Primary curvature: C-shaped;
THEME 2. VERTEBRAE (GENERAL DATA). CERVICAL, THORACIC AND LUMBAR VERTEBRAE. SACRUM. COCCYX. THE VERTEBRAL COLUMN AS A WHOLE
 THEME 2. VERTEBRAE (GENERAL DATA). CERVICAL, THORACIC AND LUMBAR VERTEBRAE. SACRUM. COCCYX. THE VERTEBRAL COLUMN AS A WHOLE Osteology of the Vertebral Column Bone Description vertebra Notes a vertebra
THEME 2. VERTEBRAE (GENERAL DATA). CERVICAL, THORACIC AND LUMBAR VERTEBRAE. SACRUM. COCCYX. THE VERTEBRAL COLUMN AS A WHOLE Osteology of the Vertebral Column Bone Description vertebra Notes a vertebra
2. The vertebral arch is composed of pedicles (projecting from the body) and laminae (uniting arch posteriorly).
 VERTEBRAL COLUMN 2018zillmusom I. VERTEBRAL COLUMN - functions to support weight of body and protect spinal cord while permitting movements of trunk and providing for muscle attachments. A. Typical vertebra
VERTEBRAL COLUMN 2018zillmusom I. VERTEBRAL COLUMN - functions to support weight of body and protect spinal cord while permitting movements of trunk and providing for muscle attachments. A. Typical vertebra
Cervical Cooled RF Training Presentation
 Cervical Cooled RF Training Presentation Agenda Patient Selection Considerations Diagnostic Block General Considerations COOLIEF* Cooled RF Technique Posterior Lateral Precautions Summary Appendix 2 Disclaimer
Cervical Cooled RF Training Presentation Agenda Patient Selection Considerations Diagnostic Block General Considerations COOLIEF* Cooled RF Technique Posterior Lateral Precautions Summary Appendix 2 Disclaimer
Anatomy and Physiology II. Spine
 Anatomy and Physiology II Spine Bones and Other Structures Vertibrae Contains Cervical, Thoracic, Lumbar, Sacral and Coccygeal regions We use Capital letters to refer to these (C, T, L, S, and Co) and
Anatomy and Physiology II Spine Bones and Other Structures Vertibrae Contains Cervical, Thoracic, Lumbar, Sacral and Coccygeal regions We use Capital letters to refer to these (C, T, L, S, and Co) and
Anatomy of the Thorax
 Anatomy of the Thorax A) THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces
Anatomy of the Thorax A) THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces
Copyright 2010 Pearson Education, Inc.
 E. VERTEBRAL COLUMN 1. The vertebral column extends from the skull to the pelvis and forms the vertical axis of the skeleton. 2. The vertebral column is composed of vertebrae that are separated by intervertebral
E. VERTEBRAL COLUMN 1. The vertebral column extends from the skull to the pelvis and forms the vertical axis of the skeleton. 2. The vertebral column is composed of vertebrae that are separated by intervertebral
OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function
 The root of the neck Jeff Dupree, Ph.D. e mail: jldupree@vcu.edu OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function READING ASSIGNMENT: Moore and
The root of the neck Jeff Dupree, Ph.D. e mail: jldupree@vcu.edu OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function READING ASSIGNMENT: Moore and
INDEPENDENT LEARNING: DISC HERNIATION IN THE NATIONAL FOOTBALL LEAGUE: ANATOMICAL FACTORS TO CONSIDER IN REVIEW
 INDEPENDENT LEARNING: DISC HERNIATION IN THE NATIONAL FOOTBALL LEAGUE: ANATOMICAL FACTORS TO CONSIDER IN REVIEW CDC REPORT - CAUSES OF DISABILITY, 2005 REVIEW QUESTIONS ABOUT DISC HERNIATION IN THE NATIONAL
INDEPENDENT LEARNING: DISC HERNIATION IN THE NATIONAL FOOTBALL LEAGUE: ANATOMICAL FACTORS TO CONSIDER IN REVIEW CDC REPORT - CAUSES OF DISABILITY, 2005 REVIEW QUESTIONS ABOUT DISC HERNIATION IN THE NATIONAL
Yara saddam & Dana Qatawneh. Razi kittaneh. Maher hadidi
 1 Yara saddam & Dana Qatawneh Razi kittaneh Maher hadidi LECTURE 10 THORAX The thorax extends from the root of the neck to the abdomen. The thorax has a Thoracic wall Thoracic cavity and it is divided
1 Yara saddam & Dana Qatawneh Razi kittaneh Maher hadidi LECTURE 10 THORAX The thorax extends from the root of the neck to the abdomen. The thorax has a Thoracic wall Thoracic cavity and it is divided
STERNUM. Lies in the midline of the anterior chest wall It is a flat bone Divides into three parts:
 STERNUM Lies in the midline of the anterior chest wall It is a flat bone Divides into three parts: 1-Manubrium sterni 2-Body of the sternum 3- Xiphoid process The body of the sternum articulates above
STERNUM Lies in the midline of the anterior chest wall It is a flat bone Divides into three parts: 1-Manubrium sterni 2-Body of the sternum 3- Xiphoid process The body of the sternum articulates above
Clarification of Terms
 Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Clarification of Terms
 Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Axial Skeleton: Vertebrae and Thorax
 Axial Skeleton: Vertebrae and Thorax Function of the vertebral column (spine or backbone): 1) 2) 3) Composition of Vertebral column The vertebral column is formed by 33 individual vertebrae (some of which
Axial Skeleton: Vertebrae and Thorax Function of the vertebral column (spine or backbone): 1) 2) 3) Composition of Vertebral column The vertebral column is formed by 33 individual vertebrae (some of which
The sacrum is a complex anatomical structure.
 A Review Paper Rongming Xu, MD, Nabil A. Ebraheim, MD, and Nicholas K. Gove, MD Abstract Treatment in spinal disorders, sacroiliac joint disruption, and sacral fractures may involve instrumentation of
A Review Paper Rongming Xu, MD, Nabil A. Ebraheim, MD, and Nicholas K. Gove, MD Abstract Treatment in spinal disorders, sacroiliac joint disruption, and sacral fractures may involve instrumentation of
The Thoracic wall including the diaphragm. Prof Oluwadiya KS
 The Thoracic wall including the diaphragm Prof Oluwadiya KS www.oluwadiya.com Components of the thoracic wall Skin Superficial fascia Chest wall muscles (see upper limb slides) Skeletal framework Intercostal
The Thoracic wall including the diaphragm Prof Oluwadiya KS www.oluwadiya.com Components of the thoracic wall Skin Superficial fascia Chest wall muscles (see upper limb slides) Skeletal framework Intercostal
Clarification of Terms
 Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Cervical Spine: Pearls and Pitfalls
 Cervical Spine: Pearls and Pitfalls Presenters Dr. Rob Donkin Functional Anatomy Current research Cervical Radiculopathy Dr. Gert Ferreira Red flags Case Study Kinesio Taping Chris Neethling Gonstead adjusting
Cervical Spine: Pearls and Pitfalls Presenters Dr. Rob Donkin Functional Anatomy Current research Cervical Radiculopathy Dr. Gert Ferreira Red flags Case Study Kinesio Taping Chris Neethling Gonstead adjusting
Anatomy Lecture #19 AN INTRODUCTION TO THE THORAX April 3, 2012
 Page 1 بسم الله الرحمن الرحيم The Thoracic Wall Firstly, when we talk about thorax, we should begin with the thorax wall which means not only bones that construct the thorax but also the muscles which
Page 1 بسم الله الرحمن الرحيم The Thoracic Wall Firstly, when we talk about thorax, we should begin with the thorax wall which means not only bones that construct the thorax but also the muscles which
Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi
 Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi For the purpose of anatomical description the neck is sub divided into two major triangles, the Anterior and the Posterior by muscle bellies
Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi For the purpose of anatomical description the neck is sub divided into two major triangles, the Anterior and the Posterior by muscle bellies
Inferior view of the skull showing foramina (Atlas of Human Anatomy, 5th edition, Plate 12)
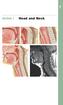 Section 1 Head and Neck Skull, Basal View Incisive foramen Choanae Foramen ovale Foramen lacerum Foramen spinosum Carotid canal Jugular fossa Mastoid process Inferior view of the skull showing foramina
Section 1 Head and Neck Skull, Basal View Incisive foramen Choanae Foramen ovale Foramen lacerum Foramen spinosum Carotid canal Jugular fossa Mastoid process Inferior view of the skull showing foramina
Ligaments of the vertebral column:
 In the last lecture we started talking about the joints in the vertebral column, and we said that there are two types of joints between adjacent vertebrae: 1. Between the bodies of the vertebrae; which
In the last lecture we started talking about the joints in the vertebral column, and we said that there are two types of joints between adjacent vertebrae: 1. Between the bodies of the vertebrae; which
Vertebral Column. Backbone consists of 26 vertebrae. Five vertebral regions. Cervical
 Vertebral Column Backbone consists of 26 vertebrae. Five vertebral regions Cervical vertebrae (7) in the neck. Thoracic vertebrae (12) in the thorax. Lumbar vertebrae (5) in the lower back. Sacrum (5,
Vertebral Column Backbone consists of 26 vertebrae. Five vertebral regions Cervical vertebrae (7) in the neck. Thoracic vertebrae (12) in the thorax. Lumbar vertebrae (5) in the lower back. Sacrum (5,
It consist of two components: the outer, laminar fibrous container (or annulus), and the inner, semifluid mass (the nucleus pulposus).
 Lumbar Spine The lumbar vertebrae are the last five vertebrae of the vertebral column. They are particularly large and heavy when compared with the vertebrae of the cervical or thoracicc spine. Their bodies
Lumbar Spine The lumbar vertebrae are the last five vertebrae of the vertebral column. They are particularly large and heavy when compared with the vertebrae of the cervical or thoracicc spine. Their bodies
Spinal nerves and cervical plexus Prof. Abdulameer Al Nuaimi. E mail: a.al E. mail:
 Spinal nerves and cervical plexus Prof. Abdulameer Al Nuaimi E mail: a.al nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Branches of ophthalmic artery Muscles of face A spinal nerve Spinal
Spinal nerves and cervical plexus Prof. Abdulameer Al Nuaimi E mail: a.al nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Branches of ophthalmic artery Muscles of face A spinal nerve Spinal
Posterior surgical procedures are those procedures
 9 Cervical Posterior surgical procedures are those procedures that have been in use for a long time with established efficacy in the treatment of radiculopathy and myelopathy caused by pathologies including
9 Cervical Posterior surgical procedures are those procedures that have been in use for a long time with established efficacy in the treatment of radiculopathy and myelopathy caused by pathologies including
Chapter 7 Part B The Skeleton
 Chapter 7 Part B The Skeleton 7.2 The Vertebral Column General Characteristics Extends from skull to pelvis Also called spine or spinal column Functions to transmit weight of trunk to lower limbs, surround
Chapter 7 Part B The Skeleton 7.2 The Vertebral Column General Characteristics Extends from skull to pelvis Also called spine or spinal column Functions to transmit weight of trunk to lower limbs, surround
Bony framework of the vertebral column Structure of the vertebral column
 5.1: Vertebral column & back. Overview. Bones o vertebral column. o typical vertebra. o vertebral canal. o spinal nerves. Joints o Intervertebral disc. o Zygapophyseal (facet) joint. Muscles o 2 compartments:
5.1: Vertebral column & back. Overview. Bones o vertebral column. o typical vertebra. o vertebral canal. o spinal nerves. Joints o Intervertebral disc. o Zygapophyseal (facet) joint. Muscles o 2 compartments:
Microsurgical anatomy of the transcondylar, supracondylar, and paracondylar extensions of the far-lateral approach
 J Neurosurg 87:555 585, 1997 Microsurgical anatomy of the transcondylar, supracondylar, and paracondylar extensions of the far-lateral approach HUNG T. WEN, M.D., ALBERT L. RHOTON, JR., M.D., TOSHIRO KATSUTA,
J Neurosurg 87:555 585, 1997 Microsurgical anatomy of the transcondylar, supracondylar, and paracondylar extensions of the far-lateral approach HUNG T. WEN, M.D., ALBERT L. RHOTON, JR., M.D., TOSHIRO KATSUTA,
Copyright 2010 Pearson Education, Inc. Copyright 2010 Pearson Education, Inc. Figure Sectioned spinous process. Interspinous.
 PowerPoint Lecture Slides prepared by Janice Meeking, Mount Royal College C H A P T E R 7 The Skeleton: Part B Vertebral Column Transmits weight of trunk to lower limbs Surrounds and protects spinal cord
PowerPoint Lecture Slides prepared by Janice Meeking, Mount Royal College C H A P T E R 7 The Skeleton: Part B Vertebral Column Transmits weight of trunk to lower limbs Surrounds and protects spinal cord
Multiple Neurovascular... Pit Baran Chakraborty, Santanu Bhattacharya, Sumita Dutta.
 Multiple Neurovascular... Pit Baran Chakraborty, Santanu Bhattacharya, Sumita Dutta. Fig-3: Showing high formation of Median nerve. Fig-1: Showing atypical formation of cords of Brachial plexus. 1 = Upper
Multiple Neurovascular... Pit Baran Chakraborty, Santanu Bhattacharya, Sumita Dutta. Fig-3: Showing high formation of Median nerve. Fig-1: Showing atypical formation of cords of Brachial plexus. 1 = Upper
Anatomy notes-thorax.
 Anatomy notes-thorax. Thorax: the part extending from the root of the neck to the abdomen. Parts of the thorax: - Thoracic cage (bones). - Thoracic wall. - Thoracic cavity. ** The thoracic cavity is covered
Anatomy notes-thorax. Thorax: the part extending from the root of the neck to the abdomen. Parts of the thorax: - Thoracic cage (bones). - Thoracic wall. - Thoracic cavity. ** The thoracic cavity is covered
1 Normal Anatomy and Variants
 1 Normal Anatomy and Variants 1.1 Normal Anatomy MR Technique. e standard MR protocol for a routine evaluation of the spine always comprises imaging in sagittal and axial planes, while coronal images are
1 Normal Anatomy and Variants 1.1 Normal Anatomy MR Technique. e standard MR protocol for a routine evaluation of the spine always comprises imaging in sagittal and axial planes, while coronal images are
INTERVERTEBRAL FORAMEN STUDIES
 INTERVERTEBRAL FORAMEN STUDIES I. FORAMEN ENCROACHMENT ASSOCIATED WITH DISC HERNIATION* LEE A. HADLEY, M.D. t Syracuse, New York (Received for publication November ] 8, 1949) T HESE studies are the outgrowth
INTERVERTEBRAL FORAMEN STUDIES I. FORAMEN ENCROACHMENT ASSOCIATED WITH DISC HERNIATION* LEE A. HADLEY, M.D. t Syracuse, New York (Received for publication November ] 8, 1949) T HESE studies are the outgrowth
Origins of the Segmental Arteries in the Aorta: An Anatomic Study for Selective Catheterization with Spinal Arteriography
 AJNR Am J Neuroradiol 26:922 928, April 2005 Origins of the Segmental Arteries in the Aorta: An Anatomic Study for Selective Catheterization with Spinal Arteriography Satoru Shimizu, Ryusui Tanaka, Shinichi
AJNR Am J Neuroradiol 26:922 928, April 2005 Origins of the Segmental Arteries in the Aorta: An Anatomic Study for Selective Catheterization with Spinal Arteriography Satoru Shimizu, Ryusui Tanaka, Shinichi
VERTEBRAL COLUMN ANATOMY IN CNS COURSE
 VERTEBRAL COLUMN ANATOMY IN CNS COURSE Vertebral body Sections of the spine Atlas (C1) Axis (C2) What type of joint is formed between atlas and axis? Pivot joint What name is given to a fracture of both
VERTEBRAL COLUMN ANATOMY IN CNS COURSE Vertebral body Sections of the spine Atlas (C1) Axis (C2) What type of joint is formed between atlas and axis? Pivot joint What name is given to a fracture of both
Surgical Anatomy of the Uncinate Process and Transverse Foramen Determined by Computed Tomography
 THIEME GLOBAL SPINE JOURNAL Original Article 383 Surgical Anatomy of the Uncinate Process and Transverse Foramen Determined by Computed Tomography Moon Soo Park 1 Seong-Hwan Moon 2 Tae-Hwan Kim 1 Jae Keun
THIEME GLOBAL SPINE JOURNAL Original Article 383 Surgical Anatomy of the Uncinate Process and Transverse Foramen Determined by Computed Tomography Moon Soo Park 1 Seong-Hwan Moon 2 Tae-Hwan Kim 1 Jae Keun
The posterior abdominal wall. Prof. Oluwadiya KS
 The posterior abdominal wall Prof. Oluwadiya KS www.oluwadiya.sitesled.com Posterior Abdominal Wall Lumbar vertebrae and discs. Muscles opsoas, quadratus lumborum, iliacus, transverse, abdominal wall
The posterior abdominal wall Prof. Oluwadiya KS www.oluwadiya.sitesled.com Posterior Abdominal Wall Lumbar vertebrae and discs. Muscles opsoas, quadratus lumborum, iliacus, transverse, abdominal wall
Skeletal System. Axial Division
 Skeletal System Axial Division The Axial Skeleton You will see that each bone has special features (overviewed in section I below) that provide Sites of Attachment (for muscles, ligaments, tendons, etc.)
Skeletal System Axial Division The Axial Skeleton You will see that each bone has special features (overviewed in section I below) that provide Sites of Attachment (for muscles, ligaments, tendons, etc.)
Overview of the Skeleton: Bone Markings
 Name Overview of the Skeleton: Bone Markings Match the terms in column B with the appropriate description in column A. Column A 1. sharp, slender process* 2. small rounded projection* 3. narrow ridge of
Name Overview of the Skeleton: Bone Markings Match the terms in column B with the appropriate description in column A. Column A 1. sharp, slender process* 2. small rounded projection* 3. narrow ridge of
MEDICAL IMAGING OF THE VERTEBRAE
 MEDICAL IMAGING OF THE VERTEBRAE Vertebrae are your friends Matthew Harper MS-IV LECTURE OBJECTIVES INTRODUCE THE MOST COMMON MODALITIES OF MEDICAL IMAGING AND BASIC TECHNIQUES FOR READING THESE IMAGES
MEDICAL IMAGING OF THE VERTEBRAE Vertebrae are your friends Matthew Harper MS-IV LECTURE OBJECTIVES INTRODUCE THE MOST COMMON MODALITIES OF MEDICAL IMAGING AND BASIC TECHNIQUES FOR READING THESE IMAGES
_CH01redo.qxd 9/24/07 3:07 PM Page 1. [Half-Title to come]
![_CH01redo.qxd 9/24/07 3:07 PM Page 1. [Half-Title to come] _CH01redo.qxd 9/24/07 3:07 PM Page 1. [Half-Title to come]](/thumbs/81/84146690.jpg) 10752-01_CH01redo.qxd 9/24/07 3:07 PM Page 1 [Half-Title to come] 10752-01_CH01redo.qxd 9/24/07 3:07 PM Page 2 THE BACK Lippincott Williams & Wilkins atlas of ANATOMY CHAPTER 1 Plate 1-01 Palpable Structures
10752-01_CH01redo.qxd 9/24/07 3:07 PM Page 1 [Half-Title to come] 10752-01_CH01redo.qxd 9/24/07 3:07 PM Page 2 THE BACK Lippincott Williams & Wilkins atlas of ANATOMY CHAPTER 1 Plate 1-01 Palpable Structures
Thoracic Cooled-RF Training Presentation
 Thoracic Cooled-RF Training Presentation Patient Selection Anatomy Overview Neuroanatomy Lesion targets Technique Diagnostic Block Cooled-RF Precautions Summary Appendix AGENDA Patient Selection Thoracic
Thoracic Cooled-RF Training Presentation Patient Selection Anatomy Overview Neuroanatomy Lesion targets Technique Diagnostic Block Cooled-RF Precautions Summary Appendix AGENDA Patient Selection Thoracic
DESCRIPTION: This is the part of the trunk, which is located between the root of the neck and the superior border of the abdominal region.
 1 THE THORACIC REGION DESCRIPTION: This is the part of the trunk, which is located between the root of the neck and the superior border of the abdominal region. SHAPE : T It has the shape of a truncated
1 THE THORACIC REGION DESCRIPTION: This is the part of the trunk, which is located between the root of the neck and the superior border of the abdominal region. SHAPE : T It has the shape of a truncated
Main Menu. Trunk and Spinal Column click here. The Power is in Your Hands
 1 The Trunk and Spinal Column click here Main Menu K.9 http://www.handsonlineeducation.com/classes/k9/k9entry.htm[3/27/18, 2:00:55 PM] The Trunk and Spinal Column Vertebral column complex 24 intricate
1 The Trunk and Spinal Column click here Main Menu K.9 http://www.handsonlineeducation.com/classes/k9/k9entry.htm[3/27/18, 2:00:55 PM] The Trunk and Spinal Column Vertebral column complex 24 intricate
بسم الله الرحمن الرحيم
 بسم الله الرحمن الرحيم * Last lecture we talked about : thoracic wall sternum ribs (according to their features they are divided into typical and atypical) vertebral column ( which is made of 33 vertebrae
بسم الله الرحمن الرحيم * Last lecture we talked about : thoracic wall sternum ribs (according to their features they are divided into typical and atypical) vertebral column ( which is made of 33 vertebrae
1 Introduction. Scope of the problem. Chapter
 Chapter 1 Introduction Spine-related disease is, both literally and figuratively, a painful proposition. Pain in the neck, mid back, and low back is one of the most common medical conditions in adults.
Chapter 1 Introduction Spine-related disease is, both literally and figuratively, a painful proposition. Pain in the neck, mid back, and low back is one of the most common medical conditions in adults.
ABDOMINAL WALL & RECTUS SHEATH
 ABDOMINAL WALL & RECTUS SHEATH Learning Objectives Describe the anatomy, innervation and functions of the muscles of the anterior, lateral and posterior abdominal walls. Discuss their functional relations
ABDOMINAL WALL & RECTUS SHEATH Learning Objectives Describe the anatomy, innervation and functions of the muscles of the anterior, lateral and posterior abdominal walls. Discuss their functional relations
The Upper Limb III. The Brachial Plexus. Anatomy RHS 241 Lecture 12 Dr. Einas Al-Eisa
 The Upper Limb III The Brachial Plexus Anatomy RHS 241 Lecture 12 Dr. Einas Al-Eisa Brachial plexus Network of nerves supplying the upper limb Compression of the plexus results in motor & sensory changes
The Upper Limb III The Brachial Plexus Anatomy RHS 241 Lecture 12 Dr. Einas Al-Eisa Brachial plexus Network of nerves supplying the upper limb Compression of the plexus results in motor & sensory changes
The Back. Anatomy RHS 241 Lecture 9 Dr. Einas Al-Eisa
 The Back Anatomy RHS 241 Lecture 9 Dr. Einas Al-Eisa The spine has to meet 2 functions Strength Mobility Stability of the vertebral column is provided by: Deep intrinsic muscles of the back Ligaments
The Back Anatomy RHS 241 Lecture 9 Dr. Einas Al-Eisa The spine has to meet 2 functions Strength Mobility Stability of the vertebral column is provided by: Deep intrinsic muscles of the back Ligaments
Anatomy of the Nervous System. Brain Components
 Anatomy of the Nervous System Brain Components NERVOUS SYSTEM INTRODUCTION Is the master system of human body, controlling the functions of rest of the body systems Nervous System CLASSIFICATION A. Anatomical
Anatomy of the Nervous System Brain Components NERVOUS SYSTEM INTRODUCTION Is the master system of human body, controlling the functions of rest of the body systems Nervous System CLASSIFICATION A. Anatomical
AXIAL SKELETON FORM THE VERTICAL AXIS OF THE BODY CONSISTS OF 80 BONES INCLUDES BONES OF HEAD, VERTEBRAL COLUMN, RIBS,STERNUM
 AXIAL SKELETON FORM THE VERTICAL AXIS OF THE BODY CONSISTS OF 80 BONES INCLUDES BONES OF HEAD, VERTEBRAL COLUMN, RIBS,STERNUM APPENDICULAR SKELETON BONES OF THE FREE APPENDAGES & THEIR POINTS OF ATTACHMENTS
AXIAL SKELETON FORM THE VERTICAL AXIS OF THE BODY CONSISTS OF 80 BONES INCLUDES BONES OF HEAD, VERTEBRAL COLUMN, RIBS,STERNUM APPENDICULAR SKELETON BONES OF THE FREE APPENDAGES & THEIR POINTS OF ATTACHMENTS
You have 24 vertebrae in your spinal column. Two are special enough to be individually named.
 You have 24 vertebrae in your spinal column. Two are special enough to be individually named. Your atlas (C01) and axis (C02) are very important vertebrae. Without them, head and neck movement would be
You have 24 vertebrae in your spinal column. Two are special enough to be individually named. Your atlas (C01) and axis (C02) are very important vertebrae. Without them, head and neck movement would be
Diaphragm and intercostal muscles. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 Diaphragm and intercostal muscles Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Skeletal System Adult Human contains 206 Bones 2 parts: Axial skeleton (axis): Skull, Vertebral column,
Diaphragm and intercostal muscles Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Skeletal System Adult Human contains 206 Bones 2 parts: Axial skeleton (axis): Skull, Vertebral column,
Osteology of the Thorax. Prof Oluwadiya K S
 Osteology of the Thorax Prof Oluwadiya K S www.oluwadiya.com The thoracic skeleton consists of the following: 12 pairs of ribs and associated costal cartilages 12 thoracic vertebrae and their intervertebral
Osteology of the Thorax Prof Oluwadiya K S www.oluwadiya.com The thoracic skeleton consists of the following: 12 pairs of ribs and associated costal cartilages 12 thoracic vertebrae and their intervertebral
LECTURE -I. Intercostal Spaces & Its Content. BY Dr Farooq Khan Aurakzai. Date:
 LECTURE -I Intercostal Spaces & Its Content BY Dr Farooq Khan Aurakzai Date: 18.04.18 Layers of IC space: Following are the layers of the thoracic region: Skin Subcutaneous CT External IC muscle and membrane
LECTURE -I Intercostal Spaces & Its Content BY Dr Farooq Khan Aurakzai Date: 18.04.18 Layers of IC space: Following are the layers of the thoracic region: Skin Subcutaneous CT External IC muscle and membrane
Morphometric evaluation of the uncinate process and its importance in surgical approaches to the cervical spine: a cadaveric study
 Singapore Med J 2016; 57(10): 570-577 doi: 10.11622/smedj.2015193 Morphometric evaluation of the uncinate process and its importance in surgical approaches to the cervical spine: a cadaveric study Mustafa
Singapore Med J 2016; 57(10): 570-577 doi: 10.11622/smedj.2015193 Morphometric evaluation of the uncinate process and its importance in surgical approaches to the cervical spine: a cadaveric study Mustafa
Chest cavity, vertebral column and back muscles. Respiratory muscles. Sándor Katz M.D., Ph.D.
 Chest cavity, vertebral column and back muscles. Respiratory muscles. Sándor Katz M.D., Ph.D. Chest cavity - bony structures Chest cavity- bony structures Sternum Ribs True ribs: first seven pairs connect
Chest cavity, vertebral column and back muscles. Respiratory muscles. Sándor Katz M.D., Ph.D. Chest cavity - bony structures Chest cavity- bony structures Sternum Ribs True ribs: first seven pairs connect
LUMBAR SPINAL STENOSIS
 LUMBAR SPINAL STENOSIS Always occurs in the mobile segment. Factors play role in Stenosis Pre existing congenital or developmental narrowing of the lumbar spinal canal Translation of one anatomic segment
LUMBAR SPINAL STENOSIS Always occurs in the mobile segment. Factors play role in Stenosis Pre existing congenital or developmental narrowing of the lumbar spinal canal Translation of one anatomic segment
Dr Ajit Singh Moderator Dr P S Chandra Dr Rajender Kumar
 BIOMECHANICS OF SPINE Dr Ajit Singh Moderator Dr P S Chandra Dr Rajender Kumar What is biomechanics? Biomechanics is the study of the consequences of application of external force on the spine Primary
BIOMECHANICS OF SPINE Dr Ajit Singh Moderator Dr P S Chandra Dr Rajender Kumar What is biomechanics? Biomechanics is the study of the consequences of application of external force on the spine Primary
Thoracic and Lumbar Spine Anatomy.
 Thoracic and Lumbar Spine Anatomy www.fisiokinesiterapia.biz Thoracic Vertebrae Bodies Pedicles Laminae Spinous Processes Transverse Processes Inferior & Superior Facets Distinguishing Feature Costal Fovea
Thoracic and Lumbar Spine Anatomy www.fisiokinesiterapia.biz Thoracic Vertebrae Bodies Pedicles Laminae Spinous Processes Transverse Processes Inferior & Superior Facets Distinguishing Feature Costal Fovea
The Far Lateral Approach to Skull Base: in the Context of Head and Neck Cancer
 Review article The Far Lateral Approach to Skull Base: in the Context of Head and Neck Cancer 1Dr. Jaspreet Singh Badwal, 2 Dr. Upkardeep Singh, 3 Dr. Neha Bharti, 4 Dr.Shivani Garg, 5 Dr.Simarpreet Singh
Review article The Far Lateral Approach to Skull Base: in the Context of Head and Neck Cancer 1Dr. Jaspreet Singh Badwal, 2 Dr. Upkardeep Singh, 3 Dr. Neha Bharti, 4 Dr.Shivani Garg, 5 Dr.Simarpreet Singh
Gross Anatomy Faculty: Gross Anatomy Faculty: Gross Anatomy Faculty: Dr. Melissa McGinn. Welcome to Gross and Developmental Anatomy
 Welcome to Gross and Developmental Anatomy M1 Anatomy Gross Anatomy Faculty: Dr. Richard Krieg Dr. Milton Sholley Dr. David Simpson 1 2 Gross Anatomy Faculty: Gross Anatomy Faculty: Dr. Steve Gudas Dr.
Welcome to Gross and Developmental Anatomy M1 Anatomy Gross Anatomy Faculty: Dr. Richard Krieg Dr. Milton Sholley Dr. David Simpson 1 2 Gross Anatomy Faculty: Gross Anatomy Faculty: Dr. Steve Gudas Dr.
The Neck the lower margin of the mandible above the suprasternal notch and the upper border of the clavicle
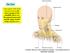 The Neck is the region of the body that lies between the lower margin of the mandible above and the suprasternal notch and the upper border of the clavicle below Nerves of the neck Cervical Plexus Is formed
The Neck is the region of the body that lies between the lower margin of the mandible above and the suprasternal notch and the upper border of the clavicle below Nerves of the neck Cervical Plexus Is formed
1TRUNK: BODY WALL AND SPINE
 TRUNK: BODY WALL AND SPINE SURFACE ANATOMY SKELETON JOINTS & LIGAMENTS MUSCLES VASCULATURE NERVES SPINAL CORD & VERTEBRAL CANAL ANTERIOR BODY WALL & MAMMARY GLAND LATERAL BODY WALL INGUINAL REGION SUPERFICIAL
TRUNK: BODY WALL AND SPINE SURFACE ANATOMY SKELETON JOINTS & LIGAMENTS MUSCLES VASCULATURE NERVES SPINAL CORD & VERTEBRAL CANAL ANTERIOR BODY WALL & MAMMARY GLAND LATERAL BODY WALL INGUINAL REGION SUPERFICIAL
Human Anatomy Biology 351
 nnnnn 1 Human Anatomy Biology 351 Exam #2 Please place your name on the back of the last page of this exam. You must answer all questions on this exam. Because statistics demonstrate that, on average,
nnnnn 1 Human Anatomy Biology 351 Exam #2 Please place your name on the back of the last page of this exam. You must answer all questions on this exam. Because statistics demonstrate that, on average,
Human Anatomy and Physiology - Problem Drill 07: The Skeletal System Axial Skeleton
 Human Anatomy and Physiology - Problem Drill 07: The Skeletal System Axial Skeleton Question No. 1 of 10 Which of the following statements about the axial skeleton is correct? Question #01 A. The axial
Human Anatomy and Physiology - Problem Drill 07: The Skeletal System Axial Skeleton Question No. 1 of 10 Which of the following statements about the axial skeleton is correct? Question #01 A. The axial
Structure and Function of the Vertebral Column
 Structure and Function of the Vertebral Column Posture Vertebral Alignment Does it really matter? Yes it does! Postural Curves The vertebral column has a series of counterbalancing curves posterior anterior
Structure and Function of the Vertebral Column Posture Vertebral Alignment Does it really matter? Yes it does! Postural Curves The vertebral column has a series of counterbalancing curves posterior anterior
The vault bones Frontal Parietals Occiput Temporals Sphenoid Ethmoid
 The Vertebral Column Head, Neck and Spine Bones of the head Some consider the bones of the head in terms of the vault bones and the facial bones hanging off the front of them The vault bones Frontal Parietals
The Vertebral Column Head, Neck and Spine Bones of the head Some consider the bones of the head in terms of the vault bones and the facial bones hanging off the front of them The vault bones Frontal Parietals
The Anatomy of the Atlantoaxial Complex
 The Anatomy of the Atlantoaxial Complex T. GLENN PAIT, M.D., KENAN 1. ARNAUTOVIC, M.D., and LUIS A.B. BORBA, M.D. Operating on the atlantoaxial complex has always posed a challenge to the surgeon because
The Anatomy of the Atlantoaxial Complex T. GLENN PAIT, M.D., KENAN 1. ARNAUTOVIC, M.D., and LUIS A.B. BORBA, M.D. Operating on the atlantoaxial complex has always posed a challenge to the surgeon because
Gateway to the upper limb. An area of transition between the neck and the arm.
 Gateway to the upper limb An area of transition between the neck and the arm. Pyramidal space inferior to shoulder @ junction of arm & thorax Distribution center for the neurovascular structures that serve
Gateway to the upper limb An area of transition between the neck and the arm. Pyramidal space inferior to shoulder @ junction of arm & thorax Distribution center for the neurovascular structures that serve
Morphometric Anatomy of the Atlas and Axis Vertebrae
 Original Article Morphometric Anatomy of the Atlas and Axis Vertebrae Gökflin fiengül Hakan Hadi KADIO LU ABSTRACT OBJECTIVE: In this study, forty dried specimens of atlas and axis vertebrae were examined
Original Article Morphometric Anatomy of the Atlas and Axis Vertebrae Gökflin fiengül Hakan Hadi KADIO LU ABSTRACT OBJECTIVE: In this study, forty dried specimens of atlas and axis vertebrae were examined
Dr.Noor Hashem Mohammad Lecture (5)
 Dr.Noor Hashem Mohammad Lecture (5) 2016-2017 If the mandible is discarded, the anterior part of this aspect of the skull is seen to be formed by the hard palate. The palatal processes of the maxillae
Dr.Noor Hashem Mohammad Lecture (5) 2016-2017 If the mandible is discarded, the anterior part of this aspect of the skull is seen to be formed by the hard palate. The palatal processes of the maxillae
Prevertebral Region, Pharynx and Soft Palate
 Unit 20: Prevertebral Region, Pharynx and Soft Palate Dissection Instructions: Step1 Step 2 Step 1: Insert your fingers posterior to the sternocleidomastoid muscle, vagus nerve, internal jugular vein,
Unit 20: Prevertebral Region, Pharynx and Soft Palate Dissection Instructions: Step1 Step 2 Step 1: Insert your fingers posterior to the sternocleidomastoid muscle, vagus nerve, internal jugular vein,
Anatomy of the Thyroid Gland
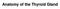 Anatomy of the Thyroid Gland Introduction Nomenclature G, thyreos= shield, eidos= like Location Root of the neck ventrally (C5-T1) Function endocrine gland that secretes: Thyroxine (T4) T3 Calcitonin LWW,
Anatomy of the Thyroid Gland Introduction Nomenclature G, thyreos= shield, eidos= like Location Root of the neck ventrally (C5-T1) Function endocrine gland that secretes: Thyroxine (T4) T3 Calcitonin LWW,
The Thoracic Cage. OpenStax College
 OpenStax-CNX module: m46350 1 The Thoracic Cage OpenStax College This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 3.0 By the end of this section, you will
OpenStax-CNX module: m46350 1 The Thoracic Cage OpenStax College This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 3.0 By the end of this section, you will
Surgical anatomy of the juxtadural ring area
 Surgical anatomy of the juxtadural ring area Susumu Oikawa, M.D., Kazuhiko Kyoshima, M.D., and Shigeaki Kobayashi, M.D. Department of Neurosurgery, Shinshu University School of Medicine, Matsumoto, Japan
Surgical anatomy of the juxtadural ring area Susumu Oikawa, M.D., Kazuhiko Kyoshima, M.D., and Shigeaki Kobayashi, M.D. Department of Neurosurgery, Shinshu University School of Medicine, Matsumoto, Japan
Lecture 4 The BRAINSTEM Medulla Oblongata
 Lecture 4 The BRAINSTEM Medulla Oblongata Introduction to brainstem 1- Medulla oblongata 2- Pons 3- Midbrain - - - occupies the posterior cranial fossa of the skull. connects the narrow spinal cord
Lecture 4 The BRAINSTEM Medulla Oblongata Introduction to brainstem 1- Medulla oblongata 2- Pons 3- Midbrain - - - occupies the posterior cranial fossa of the skull. connects the narrow spinal cord
International J. of Healthcare & Biomedical Research, Volume: 1, Issue: 4, July 2013, Pages
 Original article: Morphometry of first pedicle of sacrum and its clinical relevance Sinha Manisha B, Rathore Mrithunjay, Trivedi Soumitra, Siddiqui A U Department of Anatomy, All India Institute of Medical
Original article: Morphometry of first pedicle of sacrum and its clinical relevance Sinha Manisha B, Rathore Mrithunjay, Trivedi Soumitra, Siddiqui A U Department of Anatomy, All India Institute of Medical
Mediastinum and pericardium
 Mediastinum and pericardium Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com The mediastinum: is the central compartment of the thoracic cavity surrounded by
Mediastinum and pericardium Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com The mediastinum: is the central compartment of the thoracic cavity surrounded by
The Biomechanics of the Human Spine. Basic Biomechanics, 6 th edition By Susan J. Hall, Ph.D.
 Chapter 9 The Biomechanics of the Human Spine Structure of the Spine The spine is a curved stack of 33 vertebrae structurally divided into five regions: cervical region - 7 vertebrae thoracic region -
Chapter 9 The Biomechanics of the Human Spine Structure of the Spine The spine is a curved stack of 33 vertebrae structurally divided into five regions: cervical region - 7 vertebrae thoracic region -
Lecturer: Ms DS Pillay ROOM 2P24 25 February 2013
 Lecturer: Ms DS Pillay ROOM 2P24 25 February 2013 Thoracic Wall Consists of thoracic cage Muscle Fascia Thoracic Cavity 3 Compartments of the Thorax (Great Vessels) (Heart) Superior thoracic aperture
Lecturer: Ms DS Pillay ROOM 2P24 25 February 2013 Thoracic Wall Consists of thoracic cage Muscle Fascia Thoracic Cavity 3 Compartments of the Thorax (Great Vessels) (Heart) Superior thoracic aperture
Chapter 3: Thorax. Thorax
 Chapter 3: Thorax Thorax Thoracic Cage I. Thoracic Cage Osteology A. Thoracic Vertebrae Basic structure: vertebral body, pedicles, laminae, spinous processes and transverse processes Natural kyphotic shape,
Chapter 3: Thorax Thorax Thoracic Cage I. Thoracic Cage Osteology A. Thoracic Vertebrae Basic structure: vertebral body, pedicles, laminae, spinous processes and transverse processes Natural kyphotic shape,
Surgical anatomy of the juxta dural ring area
 J Neurosurg 89:250 254, 1998 Surgical anatomy of the juxta dural ring area SUSUMU OIKAWA, M.D., KAZUHIKO KYOSHIMA, M.D., AND SHIGEAKI KOBAYASHI, M.D. Department of Neurosurgery, Shinshu University School
J Neurosurg 89:250 254, 1998 Surgical anatomy of the juxta dural ring area SUSUMU OIKAWA, M.D., KAZUHIKO KYOSHIMA, M.D., AND SHIGEAKI KOBAYASHI, M.D. Department of Neurosurgery, Shinshu University School
Gross Morphology of Spinal Cord
 Gross Morphology of Spinal Cord Lecture Objectives Describe the gross anatomical features of the spinal cord. Describe the level of the different spinal segments compared to the level of their respective
Gross Morphology of Spinal Cord Lecture Objectives Describe the gross anatomical features of the spinal cord. Describe the level of the different spinal segments compared to the level of their respective
Femoral Triangle and Adductor Canal. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 Femoral Triangle and Adductor Canal Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Femoral Triangle and Adductor Canal Femoral triangle Is a triangular depressed area located in the upper
Femoral Triangle and Adductor Canal Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Femoral Triangle and Adductor Canal Femoral triangle Is a triangular depressed area located in the upper
Bony Thorax. Anatomy and Procedures of the Bony Thorax Edited by M. Rhodes
 Bony Thorax Anatomy and Procedures of the Bony Thorax 10-526-191 Edited by M. Rhodes Anatomy Review Bony Thorax Formed by Sternum 12 pairs of ribs 12 thoracic vertebrae Conical in shape Narrow at top Posterior
Bony Thorax Anatomy and Procedures of the Bony Thorax 10-526-191 Edited by M. Rhodes Anatomy Review Bony Thorax Formed by Sternum 12 pairs of ribs 12 thoracic vertebrae Conical in shape Narrow at top Posterior
10/14/2018 Dr. Shatarat
 2018 Objectives To discuss mediastina and its boundaries To discuss and explain the contents of the superior mediastinum To describe the great veins of the superior mediastinum To describe the Arch of
2018 Objectives To discuss mediastina and its boundaries To discuss and explain the contents of the superior mediastinum To describe the great veins of the superior mediastinum To describe the Arch of
8/4/2012. Causes and Cures. Nucleus pulposus. Annulus fibrosis. Vertebral end plate % water. Deforms under pressure
 Causes and Cures Intervertebral discs Facet (zygopophyseal) joints Inter body joints Spinal nerve roots Nerve compression Pathological conditions Video Causes of back pain Nucleus pulposus Annulus fibrosis
Causes and Cures Intervertebral discs Facet (zygopophyseal) joints Inter body joints Spinal nerve roots Nerve compression Pathological conditions Video Causes of back pain Nucleus pulposus Annulus fibrosis
In the Last Three Lectures We Already Discussed the Importance of the Thoracic Cage.
 -This Lecture Will Revise what we took in the last three lectures and will introduce the concept of the chest cavity ( Thoracic Cavity ) In the Last Three Lectures We Already Discussed the Importance of
-This Lecture Will Revise what we took in the last three lectures and will introduce the concept of the chest cavity ( Thoracic Cavity ) In the Last Three Lectures We Already Discussed the Importance of
Gross Morphology of Spinal Cord
 Gross Morphology of Spinal Cord Done By : Rahmeh Alsukkar ** I did my best and sorry for any mistake ** the sheet does not contain pictures, tables and some slides so please be careful and go back to slides
Gross Morphology of Spinal Cord Done By : Rahmeh Alsukkar ** I did my best and sorry for any mistake ** the sheet does not contain pictures, tables and some slides so please be careful and go back to slides
Chapter 7. Skeletal System
 Chapter 7 Skeletal System 1 Skull A. The skull is made up of 22 bones: 8 cranial bones, 13 facial bones, and the mandible. B. The Cranium encloses and protects the brain, provides attachments for muscles,
Chapter 7 Skeletal System 1 Skull A. The skull is made up of 22 bones: 8 cranial bones, 13 facial bones, and the mandible. B. The Cranium encloses and protects the brain, provides attachments for muscles,
Alexander C Vlantis. Selective Neck Dissection 33
 05 Modified Radical Neck Dissection Type II Alexander C Vlantis Selective Neck Dissection 33 Modified Radical Neck Dissection Type II INCISION Various incisions can be used for a neck dissection. The incision
05 Modified Radical Neck Dissection Type II Alexander C Vlantis Selective Neck Dissection 33 Modified Radical Neck Dissection Type II INCISION Various incisions can be used for a neck dissection. The incision
Uncosectomy Facilitated Cervical Foraminotomy using a new high-speed shielded curved device
 Uncosectomy Facilitated Cervical Foraminotomy using a new high-speed shielded curved device Pierre Bernard, M.D. (1), Michal Tepper, Ph.D. (2), Ely Ashkenazi, M.D. (3) (1) Centre Aquitain du Dos, Hôpital
Uncosectomy Facilitated Cervical Foraminotomy using a new high-speed shielded curved device Pierre Bernard, M.D. (1), Michal Tepper, Ph.D. (2), Ely Ashkenazi, M.D. (3) (1) Centre Aquitain du Dos, Hôpital
Principles Arteries & Veins of the CNS LO14
 Principles Arteries & Veins of the CNS LO14 14. Identify (on cadaver specimens, models and diagrams) and name the principal arteries and veins of the CNS: Why is it important to understand blood supply
Principles Arteries & Veins of the CNS LO14 14. Identify (on cadaver specimens, models and diagrams) and name the principal arteries and veins of the CNS: Why is it important to understand blood supply
