A Site-specific, Sustained-release Drug Delivery System for Aneurysmal Subarachnoid Hemorrhage
|
|
|
- Darcy Johnson
- 6 years ago
- Views:
Transcription
1 Neurotherapeutics (2016) 13: DOI /s ORIGINAL ARTICLE A Site-specific, Sustained-release Drug Delivery System for Aneurysmal Subarachnoid Hemorrhage Daniel Hänggi 1 & Nima Etminan 1 & Hans Jakob Steiger 2 & Mark Johnson 3 & M. Melissa Peet 3 & Tom Tice 4 & Kevin Burton 4 & Bruce Hudson 4 & Michele Turner 4 & Angela Stella 5 & Parissa Heshmati 6 & Cara Davis 4 & Herbert J. Faleck 7 & R. Loch Macdonald 7,8 Published online: 2 March 2016 # The American Society for Experimental NeuroTherapeutics, Inc Abstract Nimodipine is the only drug approved for use by the Food and Drug Administration for improving outcome after aneurysmal subarachnoid hemorrhage (SAH). It has less than optimal efficacy, causes dose-limiting hypotension in a substantial proportion of patients, and is administered enterally 6 times daily. We describe development of site-specific, sustainedrelease nimodipine microparticles that can be delivered once directly into the subarachnoid space or cerebral ventricles for potential improvement in outcome of patients with aneurysmal SAH. Eight injectable microparticle formulations of nimodipine in poly(dl-lactide-co-glycolide) (PLGA) polymers of varying composition were tested in vitro, and 1 was advanced into preclinical studies and clinical application. Intracisternal or intraventricular injection of nimodipine PLGA microparticles in * Daniel Hänggi daniel.haenggi@medma.uni-heidelberg.de rats and beagles demonstrated dose-dependent, sustained concentrations of nimodipine in plasma and cerebrospinal fluid for up to 29 days with minimal toxicity in the brain or systemic tissuesatdoses<2mginratsand51mginbeagles,which would be equivalent of up to mg in humans, based on scaling relative to cerebrospinal fluid volumes. Efficacy was tested in the double-hemorrhage dog model of SAH. Nimodipine PLGA microparticles significantly attenuated angiographic vasospasm. This therapeutic approach shows promise for improving outcome after SAH and may have broader applicability for similar diseases that are confined to body cavities or spaces, are self-limited, and lack effective treatments. Key Words Angiographic vasospasm. nimodipine. sustained release. subarachnoid hemorrhage. delayed cerebral ischemia. Introduction Department of Neurosurgery, University Medical Center Mannheim, Ruprecht-Karls-University Heidelberg, Germany, Mannheim, Germany Department of Neurosurgery, Medical Faculty, Heinrich-Heine-University, Düsseldorf, Germany MPI Research, Mattawan, MI, USA Evonik Industries, Birmingham, AL, USA Pharmaceutical Associates, LLC, Tampa, FL, USA Google, Mountain View, CA, USA Edge Therapeutics, Inc., Berkeley Heights, NJ, USA Division of Neurosurgery, St. Michael s Hospital, Labatt Family Centre of Excellence in Brain Injury and Trauma Research, Keenan Centre for Biomedical Science, Li Ka Shing Knowledge Institute, St. Michael s Hospital, Department of Surgery, University of Toronto, Toronto, ON, Canada Many drugs have been studied but have failed to improve outcome after serious brain diseases such as ischemic stroke, traumatic brain injury, subarachnoid hemorrhage (SAH), and malignant brain tumors [1]. For some drugs, adverse effects may limit the dose that can be administered systemically to achieve therapeutic concentrations in the brain or cerebrospinal fluid (CSF). Strategies that have been used to circumvent this and that have had limited success include blood brain barrier opening and use of transporters [2, 3]. Another is to deliver drugs directly into the brain or subarachnoid space by injection, surgical implantation, or endonasal route [2]. Only one such formulation has been developed to date [4]. Limitations of subarachnoid drug delivery are that injection into the CSF may not produce adequate drug concentrations in the brain. Another is that most diseases require sustained drug concentrations for
2 440 Hänggi et al. some time and there is limited ability to access the brain directly without invasive procedures that carry some risk. An ideal disease to develop intracranial drug delivery for would be a serious, self-limited, subarachnoid-based disease. One example is aneurysmal SAH, outcome from which remains poor with 35 % of patients dying and many having permanent neurological and neurocognitive morbidity [5, 6]. Furthermore, an important cause of morbidity after SAH is delayed cerebral ischemia (DCI), which does not occur until days after SAH and thus may permit some time to elapse before drug delivery [7]. Despite testing of >50 drugs, no pharmacologic treatment for improving outcome after SAH has been developed since nimodipine was approved for use in the USA in 1988 [8, 9]. Nimodipine, a dihydropyridine L-type calcium channel antagonist, has slight selective vasodilatory action on cerebral compared with systemic arteries, and is the only widely used drug for SAH [10]. Clinically, however, the dose that can be administered is limited because L-type calcium channels are located on arteries throughout the brain and body, and doses that dilate the cerebral arteries have some dilatory effect on systemic arteries, causing potentially deleterious adverse effects such as hypotension. Surgically placing pellets containing nicardipine, another dihydropyridine, into the subarachnoid space after aneurysmal SAH reduced DCI and cerebral infarction and improved outcome in experimental and clinical studies of aneurysmal SAH [11, 12]. However, the pellets can only be implanted during a craniotomy conducted for aneurysm repair and currently at least 50 % of aneurysms are repaired endovascularly. They are prepared with dichloromethane, a neurotoxin that may not be optimal for human use [11]. Given that nimodipine is effective at improving outcome, we sought to develop a formulation that could be administered either intracisternally after neurosurgical clipping of ruptured aneurysms, or intraventricularly to patients with a ventricular catheter who undergo endovascular aneurysm repair, or even neurosurgical clipping [13]. A sustained-release formulation was developed because intracranial access may be limited to the early phase after SAH, while nimodipine must be administered for days [14]. We report on our initial experiments in rodents, followed by characterization of a unique, programmable, sustained release, injectable formulation of nimodipine in a dog model of SAH, and toxicity studies in rats and beagles. Methods Detailed methods and results are available online (Supplementary methods and results). Formulation Development and Release In Vitro Nimodipine has an asymmetric carbon at position 4 of one of the pyridine rings. The synthesis results in a racemic mixture of the 2 enantiomers that, in solid form, has 2 polymorphs and an amorphous form. Form 1 was a yellow crystal with a melting point of 124 C. Form 2 was an almost white crystal with a melting point of 116 C and was a conglomerate when solid. The polymorphs were characterized by pycnometry, solubility measurements, differential scanning calorimetry, x-ray powder diffractometry, x-ray structure analysis, and infrared, Raman, and 1 H-nuclear magnetic resonance spectroscopy (Supplementary methods and results). Microparticles consisting mainly of form 1 were used. Microparticles were prepared by an oil/water emulsion microencapsulation technique using solvent extraction to precipitate the polymer, trap the drug, and harden the microparticles. This dispersion phase was combined with the continuous phase just prior to passing through the ceramic bead-filled column creating an emulsion that was then passed into an extraction bath containing deionized water. The extracted microparticles were collected on sieves, lyophilized, and stored at 20 C. The dried microparticles were sterilized using gamma irradiation (25 30 kilogray) from a cobalt 60 source (Sterix Isomedix, Libertyville, IL, USA). Release characteristics for 14 days in vitro were assessed for different formulations. Ten mg microparticles were weighed into a 50-ml polypropylene tube and 20 ml of sodium dodecyl sulfate/phosphate buffered saline (PBS) buffer was added. Tubes were incubated in a shaker water bath at 37 C. Buffer was sampled at 1, 3, 6, and 24 h, and then daily for 14 days. Nimodipine concentrations in sodium dodecyl sulfate/pbs buffer were measured by reverse-phase high-performance liquid chromatography and in plasma and CSF by liquid chromatography tandem mass spectroscopy using a United States Pharmacopea method (Agilent Technologies, Santa Clara, CA,USA,andPerkinElmer,Waltham,MA,USA). Nimodipine binding to plastic from CSF samples was prevented by adding octyl-d-glucopyranoside at approximately 1.5 % (weight/volume). Nimodipine Release In Vivo The low-viscosity hyaluronic acid used as a vehicle to prepare the nimodipine poly(dl-lactide-co-glycolide) (PLGA) microparticles suspension was obtained from Fidia (Hyalgan; Abano Terme, Italy). In 1 arm of the in vivo experiments, nimodipine PLGA microparticles injected into the cisterna magna were mixed with high-viscosity hyaluronic acid (Orthovisc, Bedford, MA, USA). Formulations and pure nimodipine were implanted subcutaneously in 44 male Wistar rats instrumented with jugular vein cannulas, approximately 9 weeks of age. Neat nimodipine was prepared in 1.87 % hydroxypropyl methylcellulose in PBS. The nimodipine reference solution and nimodipine PLGA microparticle formulations ,
3 Nimodipine Microparticles , , , , and were administered via a single subcutaneous injection in the left hindlimb of each animal at doses of 20 (in 0.15 ml) or 200 (0.7 ml) mg/kg. Blood samples were collected from2 alternating cohorts of 2 or 3 animals/cohort in the microparticle formulation-injected groups. Collection was immediately before injection and then 1, 12, and 24 h postdose, and on days 4, 8, 11, and 15. After the last blood sample collection interval, the surviving animals were euthanized via carbon dioxide inhalation. Animals were euthanized by cervical dislocation and the carcasses were discarded. Toxicity Studies We next tested whether nimodipine PLGA microparticles were toxic in rats and beagles. The primary objectives were to assess toxicity, determine a no observed adverse effect level (NOAEL), and measure pharmacokinetics. Rats [Crl:CD(SD),, g, 190 rats, CD; Charles River, Portage, MI, USA) were randomly allocated with equal numbers of each sex (n =7 13 per sex per group) to undergo intraventricular injection of equal volumes of 0.9 % NaCl, placebo microparticles, or nimodipine microparticles at doses 0.33, 1, or 2 mg nimodipine on day 1 and euthanasia on day 15 or 29 (Supplementary Table 1). These doses were selected based on preliminary maximum tolerated dose (MTD) studies showing that the MTD in rats was nimodipine PLGA, 2 mg. These doses correspond to human doses of 200, 600, and 1200 mg, scaled on relative CSF volumes, assuming a 300-g rat has a CSF volume of 150 μl and a 70-kg human has a CSF volume of 150 ml, with the maximum dose being the MTD [15]. Similar results are obtained scaling for body surface area [16]. Furthermore, we estimated a human dose of intracranial nimodipine PLGA might be in the vicinity of 760 mg because it is one-tenth of the human enteral dose over 21 days, given the approximately 10 % bioavailability of enteral nimodipine [17, 18]. Nimodipine and placebo microparticles were suspended in low-viscosity hyaluronic acid buffer prior to intraventricular injection. Animals were observed twice daily and examined on days 1 to 7, 14, 21, and 28. Functional observational battery, body weight, temperature, ophthalmoscopic examination, blood hematology, coagulation, clinical chemistry, urine samples, and plasma and CSF for nimodipine concentrations were assessed at various times (Supplementary methods and results). Seventy-eight beagles (8 12 kg, n = 3 per sex per group; Marshall BioResources, North Rose, NY, USA) were randomly allocated to receive intraventricular or intracisternal injection of 0.9 % NaCl, placebo microparticles, or nimodipine microparticles (Supplementary Table 2). For intraventricular injection, nimodipine or placebo microparticles were suspended in low-viscosity hyaluronic acid (Hyalgan) and for intracisternal injection they were suspended in highviscosity hyaluronic acid (Orthovisc). The injection volume was 1.15 ml and the dose of nimodipine was 17, 51, or 103 mg. These doses were selected based on preliminary MTD studies showing that the MTD in beagles was nimodipine PLGA, 103 mg. This corresponds to human doses of 200, 600, and 1200 mg, scaled on relative CSF volumes, assuming a CSF volume of 12.5 ml in a 12.5-kg beagle and a CSF volume of 150 ml in a 70-kg human, with the maximum dose being the maximum feasible dose [15]. These doses yield a similar human equivalent dose based on body surface area or CSF volume scaling as the doses used in the rat toxicity study [16]. All animals were observed twice daily. Clinical and behavior examinations were conducted on days 1 7, 15, 21, and 29 [19]. Body weight was measured weekly and ophthalmoscopy was conducted before injections and prior to euthanasia. Indirect blood pressure, heart rate, electrocardiography, blood samples, and urine data were collected; also, plasma and CSF for nimodipine concentrations were collected at intervals (Supplementary methods and results). Dog Efficacy Study Forty mongrel dogs (16 23 kg, n = 4 per sex per group; Marshall BioResources) were randomly allocated to undergo baseline cerebral angiography (day 1) and cisternal blood injection followed by treatment with placebo microparticles; placebo microparticles plus enteral nimodipine (5.2 mg/kg daily for 21 days, equivalent to a human dose of 30 mg every 4 h for a 60-kg human, based on body surface area) [16]; nimodipine PLGA microparticles, 40 mg intracisternal; nimodipine PLGA microparticles, 100 mg intracisternal; or nimodipine PLGA microparticles, 100 mg intraventricular. These doses were selected in mongrel dogs because they were gave similar human equivalent doses to the higher doses tested in the beagle toxicity study. Dogs were euthanized on day 28 or 49. Dogs were anesthetized as described above, blood was collected, and blood pressure, temperature, heart rate, and oxygen saturation were monitored continuously while animals were under anesthesia. Blood gases were obtained before and after the injections. Cerebral angiography was performed through a 4-F catheter inserted into the femoral artery and advanced under fluoroscopic guidance into the proximal portion of one vertebral artery using a guidewire. A single arterial-phase anteroposterior angiogram was obtained by injection of up to 8 ml contrast (diatrizoate meglumine 60 %; United States Pharmacopeia, Amersham Health, Princeton, NJ, USA). Images were captured digitally using identical exposure factors and magnification, and an internal magnification standard was included in every angiogram. After angiography, dogs were turned prone, tilted 30 head down and the cisterna magna was punctured percutaneously with a 14-gauge thin-walled spinal needle. CSF, 0.3 ml/kg,
4 442 Hänggi et al. was allowed to drain spontaneously, after which approximately ml/kg of fresh, autologous, arterial, nonheparinized blood was withdrawn from the femoral catheter and injected into the cisterna magna at a rate of 5 ml/min. Half of the blood was injected, followed by injection of nimodipine or placebo microparticles suspended in hyaluronic acid, followed by the remaining blood. The needle was withdrawn and the dogs were kept 30 head down for 15 min, after which the femoral catheter was removed, the artery ligated, and the incision closed. For intraventricular injection, the blood was injected into the cisterna magna and then the dog was placed prone in a stereotactic unit. Nimodipine microparticles were injected into the right lateral ventricle using the same procedure as described in the beagle toxicity study. On day 3, dogs were anesthetized as above and blood was injected into the cisterna magna using the same procedure as on day 1 except that microparticles were not injected. Angiography was repeated on days 8 and 15. The diameter of the basilar artery was measured at 5 equally spaced points by 2 blinded observers and the means averaged. Angiographic vasospasm was assessed by comparing the diameters of basilar arteries from days 1, 8, and 15, and the time course and severity of angiographic vasospasm was determined. In previous studies, as well as the current data, we found angiographic vasospasm was most severe in the basilar artery and was much less in the posterior communicating arteries and anterior circle of Willis [20]. Dogs were weighed weekly and examined daily for 14 days, including behavior examination (Supplementary methods and results)[19]. Indirect blood pressure was measured in awake dogs daily for the first 14 days and weekly thereafter. Plasma and CSF were collected for determination of nimodipine concentration. Dogs were euthanized by an intravenous overdose of sodium pentobarbital. They were perfused through the heart with PBS followed by 10 % neutral buffered formalin. The brain and spinal cord were excised and axial cross sections of the midbrain, pons, medulla, and cervical, thoracic, and lumbar spinal cord, and a coronal section of the cerebral hemispheres through the middle cerebral artery territory were taken, embedded in paraffin, and stained with hematoxylin and eosin. A section from each level was also stained with fluoro-jade B, activated caspase-3, or antithrombin III (Supplementary methods and results). Data Analysis and Statistics All data are mean ± SD. For the toxicity studies, we compared saline with placebo within each route of administration and time (15 or 29 day sacrifice), and placebo with nimodipine PLGA microparticles groups within each route of administration and time (Supplementary Tables 2 and 3). Leukocyte count and urinalysis results were transformed by log and rank transformation, respectively, prior to analysis. Groups were compared by ANOVA. If there was significant variance (p < 0.05), pair-wise comparisons were made after adjustment for multiple comparisons by the Holm Sidak or Tukey methods [21]. The functional observation battery was analyzed by the Cochran Mantel Haenszel test. All statistical analysis was done in Stata (version 9; Stata Corp., College Station, TX, USA). Results Formulation Development Eight nimodipine PLGA microparticle formulations were prepared considering a specific product profile target (Supplementary methods and results). Their chemical/ physical stability, sterilizability, and release characteristics in vitro were determined. PLGA was chosen as the microparticle excipient because it is a biocompatible, bioabsorbable polymer with a long safety record in humans, even when used intracranially, and it is one of few parenteral polymers that can release drug over weeks [22]. Parameters that were varied in the formulations were lactide to glycolide ratio, polymer end group chemistry, molecular weight, and co-solvents. The resulting microparticles varied from 25 % to 50 % glycolide, with % theoretical drug loading and mean particle sizes of approximately μm, all formulated with ethyl acetate solvent and > 99 % purity and > 91 % encapsulation efficiency (Table 1). Three selected formulations did not change in drug content, main peak purity, and mean particle size after sterilization with > 25 kgray gamma radiation (Supplementary Table 3). Sterilization did not change the microparticle release characteristics in vitro (Fig. 1; Supplementary Fig. 1). This result showed the ability to prepare formulations that released nimodipine with different initial bursts and cumulative release over 14 days. Formulations containing form 1 were the most stable and there was little-to-no impact when small amounts of form 2 were present (Fig. 2). Microparticles did not change significantly after storage for 1 month at 25 C, based on scanning electron microscopy and release characteristics in vitro (Table 2; Fig. 2). Release In Vivo Drug release from sustained-release formulations typically differs in vitro and in vivo. To characterize release profiles for nimodipine PLGA formulations, 6 nimodipine PLGA formulations (n = 6 per group) or pure nimodipine (n =4)were injected subcutaneously in Wistar rats at doses of 20 or 200 mg/kg. There was sustained release of nimodipine into plasma over time with all formulations, including with pure
5 Nimodipine Microparticles 443 Table 1 Characteristics of 6 nimodipine poly(dl-lactide-co-glycolide) formulations Number Polymer composition (lactide:glycolide ratio, end group) Theoretical drug content (weight %) Actual drug content (weight %) Encapsulation efficiency (%) Main peak purity (%) Particle size (μm) Residual solvent (weight %) Residual water (weight %) :35, ester :35, acid :25, acid :25, acid :50, acid :35, ester :35, ester Data are means ± SD (n = 3 per measurement) nimodipine, which was likely owing to its high lipid solubility and subsequent prolonged residence in subcutaneous fat (Fig. 3). There was a poor relationship between the time course of release in vitro and in vivo, although the order of release was similar. We reasoned that release in vitro might be more reflective of how the formulation would release in the aqueous subarachnoid space, rather than the fatty subcutaneous space. Based on this we selected for preclinical and clinical development a formulation that was stable and had predetermined release characteristics in vitro ( ). Injectability of microparticles was found to require at least an 18-gauge and, reliably, a 14-gauge needle and suspension in hyaluronic acid (Supplementary methods and results). Toxicity Studies All rats survived to sacrifice. There were no effects of nimodipine PLGA microparticles on clinical observations, Fig. 1 Cumulative release of nimodipine in vitro from 6 nimodipine poly(dl-lactide-co-glycolide) microparticle formulations under optimized sink conditions. Values are means ± SD (n =3 per measurement) neurobehavioral evaluations, body weight, food consumption, ophthalmoscopy, hematology, coagulation, clinical chemistry, urinalysis, organ weight, or macroscopic pathology. The only potential nimodipine PLGA microparticle-related microscopic finding consisted of more frequent and severe intracranial hemorrhage at day 15, usually at the injection site in the brain of rats injected with 2 mg nimodipine PLGA microparticles (Fig. 4). This finding was reversible as no differences were observed between groups by day 29. Histopathologic changes, including reactive gliosis, hydrocephalus, pigmented and foamy macrophages, focal mineralization and vacuolation, at or near the injection site at both times were observed in all groups (Fig. 4). The changes were thought to be related to the injection procedure, based on the lack of dose response and the similar incidence in all groups. Mean plasma nimodipine concentrations at 48 h increased with increasing dose, and ranged from 0.88 to 10.6 ng/ml at 48 h (Fig. 5). Plasma concentrations after administration of 2 mg nimodipine PLGA microparticles were measurable on day 15 but not on day 29. Mean plasma maximum observed concentration (C max ) and area under the curve from the time of dosing to the time of the last observation (AUC 0-t ) after injection of 2 mg nimodipine PLGA microparticles were, respectively, 40.5 ng/ml and 3902 ng*h/ml, 5.7 ng/ml and 901 ng*h/ ml after injection of 1 mg, and 1.9 ng/ml and 177 ng*hr/ml after injection of 0.33 mg nimodipine-plga microparticles. Nimodipine was only measureable in 2 CSF samples obtained on day 3, secondary to difficulty sampling CSF. The NOAEL was 2 mg. In the beagle toxicity study, there were 2 mortalities and otherwise no clinical findings, changes in body weight, heart rate or blood pressure, clinical pathology, electrocardiography, or macroscopic observations (Supplementary Fig. 2). Two males were euthanized in extremis prior to the completion of the study. Both received 103 mg nimodipine PLGA microparticles intracisternally. They were euthanized on days 10 and 15. The beagle euthanized on day 10 was found on microscopy to have the fourth ventricle of the brain expanded by granulomatous inflammation admixed with subacute/chronic
6 444 Hänggi et al. Fig. 2 (A, D, G, J) Scanning electron microscopy and (B, C, E, F, H, I, K, L) Raman spectroscopy of (A C, G I) fresh nimodipine microparticles or (D F, J L) the same formulations after storage at C for 30 days. Formulation showed no change in morphology or spectroscopy(top 2 rows, A F), whereas showed agglomeration of particles after storage and change in nimodipine from amorphous to form 2 (scale bar = 20 μm). (B, E, H, and K) Red is nimodipine, green is poly(dl-lactide-co-glycolide), and blue is epoxy in Raman spectroscopy. (C, F, I, and L) Red is nimodipine form 1, green is amorphous nimodipine and blue is nimodipine form 2 in Raman spectroscopy inflammation that infiltrated the lining of the fourth ventricle and choroid plexus. The inflammation surrounded moderate amounts of translucent, round, space-occupying foreign material. No foreign material or granulomatous inflammation was observed within the brain stem, midbrain, or cerebellum. Within the subjacent brain stem was an area of mild cavitation with rarefaction and edema of the neuropil, multifocal minimal hemorrhage, and minimal axonal/myelin degeneration with presence of spheroids, suggesting at some point an injection had penetrated the brainstem. In the beagle euthanized on day 15, the fourth ventricle of the brain contained minimal translucent foreign material surrounded by minimal granulomatous/subacute/chronic inflammation. No foreign material or granulomatous inflammation was observed within the brain stem, midbrain, or cerebellum. In general, microscopic findings were evident in the brain, spinal cord, and heart of some beagles (Fig. 6). Intraventricular or intracisternal injection caused a granulomatous foreign body type reaction in the cerebral ventricles and subarachnoid space. This inflammation and/or the injection procedure often lead to a disruption of the ependymal lining and subsequent extension of the inflammation and/or foreign material into the adjacent periventricular neuropil. The inflammatory reaction and presence of foreign material was observed after injection of any amount of PLGA microparticles, but the incidence and severity was related to dose. The periventricular extension of the inflammation was more prominent in animals receiving intraventricular injections. The foreign material and inflammatory reaction was incompletely resolved by day 29. Inflammation, fibrosis, cardiac myofiber Table 2 Characteristics and differential scanning calorimetry of 4 nimodipine poly(dl-lactide-co-glycolide) formulations after storage for 30 days Number Storage condition ( C) Average drug content (weight %) Encapsulation efficiency (%) Particle size (μm) Drug purity (%) T g ( C) Main melt ( C) Second melt ( C) No peak (tiny peak) (tiny peak) (tiny peak) No peak No peak No peak
7 Nimodipine Microparticles 445 Mean plasma nimodipine concentrations following intraventricular administration of nimodipine microparticles in beagles increased gradually during the first 48 h and then remained generally constant until 336 h (day 15; Fig. 7, Supplementary Table 4). Nimodipine was still detected at 672 h in all groups receiving nimodipine PLGA microparticles (day 29). Plasma C max and AUC 0-t increased with increasing dose. CSF nimodipine concentrations increased in a dosedependent fashion and were highest at the 48-h measurement (Fig. 7). Based upon the results of this study, a NOAEL of 51 mg nimodipine PLGA microparticles administered intraventricularly in the beagle was established. Fig. 3 Nimodipine plasma concentrations after subcutaneous injection of nimodipine (n = 4) or different nimodipine poly(dl-lactide-coglycolide) formulations in rats. Values are means ± SD (n =2 3 per measurement from groups of 6 rats) degeneration/necrosis, and/or hypertrophy/hyperplasia of the tunica media of small-to-medium-sized arteries of the left ventricle and interventricular septum of the heart were observed primarily in animals receiving nimodipine microparticles by intracisternal injection and 1 high dose (103 mg) male receiving intraventricular injection and euthanized on day 15. No abnormal findings were noted in the intraventricular injected animals on day 29. Minimal left ventricular cardiac inflammation and fibrosis was seen in only 1 high-dose intracisternal injected male, suggesting partial resolution of the microscopic findings in the heart by day 29. Mongrel Dog Efficacy Study One dog injected with nimodipine PLGA microparticles intraventricularly (100 mg) was euthanized on day 25, and 1 in the placebo microparticle plus enteral nimodipine group was euthanized on day 35. Both animals were well in the days leading up to CSF sampling after which they did not awaken. The cause of death was brainstem injury from aspiration of CSF from the cisterna magna. Clinical examination showed similar findings in all groups with decreased appetite and activity within the first 5 days of SAH, followed by recovery (Supplementary Fig. 3) [19]. Mean blood pressures varied over time within groups and between groups at different times (Fig. 8). The lack of relationship between plasma nimodipine concentration and blood pressure suggests that intracranial administration of nimodipine PLGA microparticles does not produce sufficient Fig. 4 Histologic (hematoxylin and eosin) effects of nimodipine microparticles in rats sacrificed 15 (top row) or 29 days (bottom row) after intraventricular injection of 0.9 % NaCl, placebo microparticles or nimodipine poly(dl-lactide-co-glycolide) (PLGA) microparticles (0.33, 1, or 2 mg nimodipine). There was reactive gliosis, hydrocephalus, pigmented and foamy macrophages, focal mineralization, and vacuolation after injection of microparticles that was not related to dose. More intracranial hemorrhage was observed 15 days after injection of nimodipine PLGA microparticles, 2 mg, that partly resolved by 29 days. Scale bar = 500 μm
8 446 Hänggi et al. Fig. 5 Plasma concentration of nimodipine in rats after intraventricular injection of 0.9 % NaCl, placebo microparticles or nimodipine poly(dllactide-co-glycolide) microparticles (0.33, 1, or 2 mg nimodipine). Values are means ± SD (n =7 32 per measurement) systemic exposure or fluctuations in plasma concentrations to produce substantial changes in blood pressure. Angiography showed significant reductions in basilar artery diameter 8 and 15 days after SAH in dogs treated with placebo microparticles with or without nimodipine (ANOVA, p = 0.001, days 8 and 15 significantly different from day 1; p < 0.05, Tukey test; Fig. 9, Supplementary Table 5). When comparing the percent reduction in basilar artery diameter between groups at day 8, the group treated with 100 mg nimodipine PLGA microparticles intraventricularly had significantly less arterial narrowing than the placebo microparticle groups with or without enteral nimodipine (p < 0.009, ANOVA, Holm Sidak). When comparing the percent reduction in basilar artery diameter between groups at day 15, the groups treated with 40 mg nimodipine PLGA microparticles intracisternal or 100 mg intraventricularly had significantly less arterial narrowing than the placebo microparticle groups with or without enteral nimodipine (p < 0.009, ANOVA, Holm Sidak). Plasma nimodipine concentrations increased in a dosedependent fashion to peak 36 h to 4 days after administration of nimodipine PLGA microparticles intracisternally or intraventricularly (Fig. 8). Nimodipine was detected in plasma 21 days after administration of nimodipine PLGA microparticles. The plasma concentration after administration of 100 mg nimodipine PLGA microparticles was qualitatively similar to that achieved with enteral nimodipine. Animals treated with enteral nimodipine had very low concentrations of nimodipine in CSF that were highest on day 3 ( ng/ml, n = 7). Nimodipine concentrations were approximately 1000-fold higher in animals treated with nimodipine PLGA microparticles. Dogs were euthanized on day 28 or 49 (n = 4 per group per day). Microscopic changes in the brains consisted of granulomatous inflammation (aggregates of giant cells engulfing foreign material), subacute/chronic inflammation (mixed inflammatory infiltrate), fibroplasia, hemorrhage, and pigmented macrophages. These findings were mostly located in the meninges of pons, medulla, and, to a lesser extent, the cervical subarachnoid space. They were more prominent at the 28 day time and had a lower incidence and severity at day 49. Fluoro-jade B staining did not reveal any degenerative/ necrotic neurons. Apoptotic neurons were not detected in Fig. 6 Histologic (hematoxylin and eosin) effects of nimodipine microparticles in beagles sacrificed 15 (top row) or 29 days (bottom row) after intraventricular injection of 0.9 % NaCl, intraventricular nimodipine poly(dl-lactide-coglycolide) (PLGA) microparticles (17, 51, or 103 mg nimodipine), or intracisternal nimodipine PLGA microparticles (103 mg nimodipine). Granulomatous foreign body type reaction was noted in the cerebral ventricles and subarachnoid space after injection of any of the microparticle formulations although the incidence and severity was related to dose. The presence of the foreign material and inflammatory reaction was incompletely resolved by day 29. Scale bar = 500 μm
9 Nimodipine Microparticles 447 Fig. 7 Plasma (top) and cerebrospinal fluid (bottom) concentration of nimodipine in beagles after intraventricular or intracisternal injection of nimodipine poly(dl-lactide-co-glycolide) microparticles (17, 51, or 103 mg nimodipine). Values are means ± SD any animals by immunoreactivity to activated caspase-3. Apoptosis was detected in glial cells evenly distributed throughout the brain. Microthrombi were noted in 2 dogs in the placebo microparticle, 1 in the placebo microparticle plus enteral nimodipine, 1 in the 40 mg intracisternally, 1 in the 100 mg intracisternally, and 2 in the 100 mg intraventricular nimodipine PLGA microparticle group. Microthrombi were limited to the cerebrum with too few microthrombi observed to conduct statistical analysis. Discussion We report the novel development of a sustained release formulation that releases nimodipine in high concentrations into the CSF for up to 21 days after intracisternal or intraventricular delivery. The concentrations of nimodipine in plasma remain below those associated with hypotension and the formulation is injectable and manufactured by standards acceptable for use in humans. The efficacy, assessed by angiographic vasospasm, was greater than enteral nimodipine in dogs. In rats, there was more intracranial hemorrhage in those injected with nimodipine PLGA microparticles, 2 mg, although this was reversible and had no observable effects. Importantly, this was not observed in beagles. Nimodipine has fibrinolytic activity that may contribute to its efficacy and could theoretically cause hemorrhage [7, 23]. However, there is no evidence that nimodipine is associated with hemorrhage in humans with SAH, even after intracisternal or intraventricular administration [9]. Dose-dependent and reversible granulomatous inflammation was observed after injection of nimodipine-plga microparticles, a known reaction to PLGA that was without any sequelae in toxicity studies and in decades of use in humans. Poor outcome after SAH is believed to result mainly from early brain injury and DCI. DCI is hypothesized to be due to a combination of angiographic vasospasm, microcirculatory dysfunction, cortical spreading ischemia, microthromboembolism, and delayed effects of early brain injury [7]. Nimodipine was noted to be a somewhat selective cerebral artery vasodilator that was studied in patients with SAH in order to reduce angiographic vasospasm. In the clinical trials, however, no or only a minimal decrease in angiographic vasospasm was observed in patients treated with nimodipine. Despite this and unlike other vasodilator drugs [24, 25], it improved clinical outcome. In addition to being a potent vasodilator, even of arteries with angiographic vasospasm [12, 26], it was later noted that nimodipine inhibited other delayed effects of SAH that maycontributetodci,suchascorticalspreadingischemia [27], and that it had fibrinolytic activity that could reduce microthromboemboli [23]. Other vasodilators may not have these pleiotrophic effects [28]. One hypothesis is that nimodipine improved outcome after SAH because it reduced these complications of SAH but that in the doses administered the effects were not measureable in clinical trials. There have been prior reports of sustained-release formulations of dihydropyridines and other drugs administered into the subarachnoid space for SAH [12, 13, 29, 30]. While there has been some evidence that these may be effective, these formulations have had limitations, including lack of characterization of pharmacokinetics, stability, and injectability, use of materials with known or unknown toxicity, and limited data on efficacy of the active drug. The current work allowed translation of a sustainedrelease nimodipine formulation from preclinical to clinical use by using materials with known brain biocompatibility, methods that allow programming of the polymers for desired release characteristics, stability, and commercial scalability, and a known active pharmacologic agent.
10 448 Hänggi et al. Fig. 8 Mean blood pressure (left), plasma (middle), and cerebrospinal fluid (right) nimodipine concentrations in mongrel dogs after subarachnoid hemorrhage treated with intracisternal placebo microparticles without (n = 8) or with enteral nimodipine (n = 8, 5.2 mg/kg daily for 21 days), intracisternal nimodipine-poly(dl-lactide-co-glycolide) (PLGA) microparticles (n = 8, 40 mg), intracisternal nimodipine PLGA microparticles (n = 6, 100 mg), or intraventricular nimodipine PLGA microparticles (n = 8, 100 mg). Mean blood pressure varied significantly in dogs treated with 40 mg intracisternal nimodipine PLGA microparticles (p <0.001, ANOVA, pairwise differences between day 21 and each of days 2, 3, 7, 9, 10, 12, and 28, and between day 28 and each of days 4, 5, and 14, Holm Sidak). There also was significant variance in mean blood pressure in the group treated with 100 mg intracisternal nimodipine PLGA microparticles (p < 0.019, no pairwise differences). When comparing between groups over time, there was significant variance in blood pressure on day 5 but no pairwise differences between groups (ANOVA, p = 0.033), on day 10, with pairwise differences between placebo and 100 mg intracisternal or intraventricular (ANOVA, p = 0.004; Holm Sidak, p < 0.05), and on day 21, with pairwise difference between 40 mg intracisternal and 100 mg intraventricular (ANOVA, p =0.029; Holm Sidak pairwise, p < 0.05). There were no significant differences in blood pressure within groups over time or between groups at each time (ANOVA). Values are means ± SD Fig. 9 Percent change in basilar artery diameter 8 and 15 days after subarachnoid hemorrhage in dogs treated with intracisternal placebo microparticles without (n = 7) or with enteral nimodipine (n = 8, 5.2 mg/ kg daily for 21 days), intracisternal nimodipine- poly(dl-lactide-coglycolide) (PLGA) microparticles (n = 8, 40 mg), intracisternal nimodipine PLGA microparticles (n = 6, 100 mg), or intraventricular nimodipine PLGA microparticles (n = 8, 100 mg). There was significantly less angiographic vasospasm at 8 days after treatment with 100 mg nimodipine PLGA microparticles intraventricularly, or at 15 days after treatment with 40 mg intracisternal or 100 mg intraventricular nimodipine PLGA microparticles (p < 0.05, ANOVA). Values are means ± SD Assessment of the nimodipine PLGA microparticles in humans with SAH is required and a dose-finding study is underway (NCT ). One question is what dose to use. An option would be to conduct detailed comparisons of the safety and efficacy of enteral nimodipine and nimodipine PLGA microparticles in animal models and then select the lowest efficacious and safe dose. The limitations of this approach include that animal models that reproduce brain injury and DCI similar to what occurs after human aneurysmal SAH are not well characterized or even nonexistent. The current dog efficacy study assessed angiographic vasospasm, but this is an imperfect surrogate measure of DCI [7]. No dose response may be detected, as was the case in the human nimodipine studies, in which the highest safe dose was approved for use. Finally, we have already conducted safety studies that demonstrate a dose-dependent, clinically undetectable, and resolving inflammatory reaction to nimodipine PLGA microparticles that is already a well-known effect of PLGA, a chemical already implanted intracranially as a dural substitute. Therefore, we adopted an approach is to conduct a dosefinding, safety, and pharmacokinetic study in humans starting with a dose well below the NOAEL, as recommended by regulatory agencies. It also may be warranted to use the current approach to study other drugs to treat other conditions that are self-limited and confined to preformed body cavities.
11 Nimodipine Microparticles 449 Acknowledgments Daniel Hänggi and Nima Etminan are scientific advisors for Edge Therapeutics, Inc.; Mark Johnson and M. Melissa Peet are employees of MPI Research. Tom Tice, Kevin Burton, Bruce Hudson, Michele Turner, Parissa Heshmati, and Cara Davis are employees of Evonik Degussa Corp. Angela Stella is an employee of Pharmaceutical Associates, LLC. R. Loch Macdonald is Chief Scientific Officer of Edge Therapeutics, Inc. and received grant support from the Physicians Services Incorporated Foundation, Brain Aneurysm Foundation, Canadian Institutes for Health Research, and the Heart and Stroke Foundation of Canada. H. Faleck is an employee of Edge Therapeutics, Inc. Required Author Forms Disclosure forms provided by the authors are available with the online version of this article. References 1. van der Worp HB, Howells DW, Sena ES, et al. Can animal models of disease reliably inform human studies? PLoS Med. 2010;7(3): e Begley DJ. Delivery of therapeutic agents to the central nervous system: the problems and the possibilities. Pharmacol Ther. 2004;104(1): Gabathuler R. Approaches to transport therapeutic drugs across the blood brain barrier to treat brain diseases. Neurobiol Dis. 2010;37(1): Brem H, Piantadosi S, Burger PC, et al. Placebo-controlled trial of safety and efficacy of intraoperative controlled delivery by biodegradable polymers of chemotherapy for recurrent gliomas. The Polymer-brain Tumor Treatment Group. Lancet. 1995;345(8956): Al-Khindi T, Macdonald RL, Schweizer TA. Cognitive and functional outcome after aneurysmal subarachnoid hemorrhage. Stroke. 2010;41(8):e519-e Nieuwkamp DJ, Setz LE, Algra A, Linn FH, de Rooij NK, Rinkel GJ. Changes in case fatality of aneurysmal subarachnoid haemorrhage over time, according to age, sex, and region: a meta-analysis. Lancet Neurol. 2009;8(7): Macdonald RL. Delayed neurological deterioration after subarachnoid haemorrhage. Nat Rev Neurol. 2014;10(1): Weyer GW, Nolan CP, Macdonald RL. Evidence-based cerebral vasospasm management. Neurosurg Focus. 2006;21(3):E8. 9. Dorhout Mees SM, Rinkel GJ, Feigin VL, et al. Calcium antagonists for aneurysmal subarachnoid haemorrhage. Cochrane Database Syst Rev. 2007(3):CD Towart R, Wehinger E, Meyer H, Kazda S. The effects of nimodipine, its optical isomers and metabolites on isolated vascular smooth muscle. Arzneimittelforschung. 1982;32(4): Kasuya H, Onda H, Sasahara A, Takeshita M, Hori T. Application of nicardipine prolonged-release implants: analysis of 97 consecutive patients with acute subarachnoid hemorrhage. Neurosurgery. 2005;56(5): Barth M, Capelle HH, Weidauer S, et al. Effect of nicardipine prolonged-release implants on cerebral vasospasm and clinical outcome after severe aneurysmal subarachnoid hemorrhage: a prospective, randomized, double-blind phase IIa study. Stroke. 2007;38(2): Bege N, Renette T, Endres T, Beck-Broichsitter M, Hanggi D, Kissel T. In situ forming nimodipine depot system based on microparticles for the treatment of posthemorrhagic cerebral vasospasm. Eur J Pharm Biopharm 2013;84: Toyota BD. The efficacy of an abbreviated course of nimodipine in patients with good-grade aneurysmal subarachnoid hemorrhage. J Neurosurg 1999;90: Davson H, Welch K, Segal MB. Secretion of the cerebrospinal fluid. The Physiology and Pathophysiology of the Cerebrospinal Fluid. London: Churchill-Livingstone; p Reagan-Shaw S, Nihal M, Ahmad N. Dose translation from animal to human studies revisited. FASEB J. 2008;22(3): Langley MS, Sorkin EM. Nimodipine. A review of its pharmacodynamic and pharmacokinetic properties, and therapeutic potential in cerebrovascular disease. Drugs. 1989;37(5): Scriabine A, Battye R, Hoffmeister F, et al. Nimodipine. New Drugs Annual: Cardiovasc Drugs. 1985;3: Zhou C, Yamaguchi M, Colohan AR, Zhang JH. Role of p53 and apoptosis in cerebral vasospasm after experimental subarachnoid hemorrhage. J Cereb Blood Flow Metab. 2005;25(5): Yarnitsky D, Lorian A, Shalev A, et al. Reversal of cerebral vasospasm by sphenopalatine ganglion stimulation in a dog model of subarachnoid hemorrhage. Surg Neurol 2005;64(1): Edwards D, Berry JJ. The efficiency of simulation-based multiple comparisons. Biometrics. 1987;43(4): Menei P, Montero-Menei C, Venier MC, Benoit JP. Drug delivery into the brain using poly(lactide-co-glycolide) microspheres. Expert Opin Drug Deliv. 2005;2(2): Vergouwen MD, Vermeulen M, de Haan RJ, Levi M, Roos YB. Dihydropyridine calcium antagonists increase fibrinolytic activity: a systematic review. J Cereb Blood Flow Metab. 2007;27(7): Macdonald RL, Kassell NF, Mayer S, et al. Clazosentan to overcome neurological ischemia and infarction occurring after subarachnoid hemorrhage (CONSCIOUS-1): randomized, doubleblind, placebo-controlled phase 2 dose-finding trial. Stroke. 2008;39(11): Etminan N, Vergouwen MD, Ilodigwe D, Macdonald RL. Effect of pharmaceutical treatment on vasospasm, delayed cerebral ischemia, and clinical outcome in patients with aneurysmal subarachnoid hemorrhage: a systematic review and meta-analysis. J Cereb Blood Flow Metab. 2011;31(6): Pierot L, Aggour M, Moret J. Vasospasm after aneurysmal subarachnoid hemorrhage: recent advances in endovascular management. Curr Opin Crit Care 2010;16: Dreier JP, Windmuller O, Petzold G, Lindauer U, Einhaupl KM, Dirnagl U. Ischemia triggered by red blood cell products in the subarachnoid space is inhibited by nimodipine administration or moderate volume expansion/hemodilution in rats. Neurosurgery. 2002;51(6): Sabri M, Ai J, Macdonald RL. Dissociation of vasospasm and secondary effects of experimental subarachnoid hemorrhage by clazosentan. Stroke. 2011;42(5): Omeis I, Jayson NA, Murali R, Abrahams JM. Treatment of cerebral vasospasm with biocompatible controlled-release systems for intracranial drug delivery. Neurosurgery. 2008;63(6): Zhang JH, Badaut J, Tang J, Obenaus A, Hartman R, Pearce WJ. The vascular neural network a new paradigm in stroke pathophysiology. Nat Rev Neurol. 2012;8(12):
N E W T O N. Hänggi D, Etminan N, Macdonald RL, Steiger HJ, Mayer SA, Aldrich F, Diringer MN, Hoh BJ, Mocco J, Strange P, Faleck HJ, Miller M
 N E W T O N Nimodipine microparticles to Enhance recovery While reducing TOxicity after subarachnoid hemorrhage Phase 1/2a Multicenter, Controlled, Randomized, Open Label, Dose Escalation, Safety, Tolerability,
N E W T O N Nimodipine microparticles to Enhance recovery While reducing TOxicity after subarachnoid hemorrhage Phase 1/2a Multicenter, Controlled, Randomized, Open Label, Dose Escalation, Safety, Tolerability,
WHITE PAPER: A GUIDE TO UNDERSTANDING SUBARACHNOID HEMORRHAGE
 WHITE PAPER: A GUIDE TO UNDERSTANDING SUBARACHNOID HEMORRHAGE Subarachnoid Hemorrhage is a serious, life-threatening type of hemorrhagic stroke caused by bleeding into the space surrounding the brain,
WHITE PAPER: A GUIDE TO UNDERSTANDING SUBARACHNOID HEMORRHAGE Subarachnoid Hemorrhage is a serious, life-threatening type of hemorrhagic stroke caused by bleeding into the space surrounding the brain,
Development of Nicardipine Prolonged-Release Implants After Clipping for Preventing Cerebral Vasospasm: From Laboratory to Clinical Trial
 178 The Open Conference Proceedings Journal, 2010, 1, 178-182 Open Access Development of Nicardipine Prolonged-Release Implants After Clipping for Preventing Cerebral Vasospasm: From Laboratory to Clinical
178 The Open Conference Proceedings Journal, 2010, 1, 178-182 Open Access Development of Nicardipine Prolonged-Release Implants After Clipping for Preventing Cerebral Vasospasm: From Laboratory to Clinical
7/18/2018. Cerebral Vasospasm: Current and Emerging Therapies. Disclosures. Objectives
 Cerebral : Current and Emerging Therapies Chad W. Washington MS, MD, MPHS Assistant Professor Department of Neurosurgery Disclosures None Objectives Brief Overview How we got here Review of Trials Meta-analysis
Cerebral : Current and Emerging Therapies Chad W. Washington MS, MD, MPHS Assistant Professor Department of Neurosurgery Disclosures None Objectives Brief Overview How we got here Review of Trials Meta-analysis
(aneurysmal subarachnoid hemorrhage, 17%~60% :SAH. ,asah , 22%~49% : Willis. :1927 Moniz ;(3) 2. ischemic neurological deficit,dind) SAH) SAH ;(6)
 ,, 2. : ;,, :(1), (delayed ;(2) ischemic neurological deficit,dind) ;(3) 2. :SAH ;(4) 5-10 10 HT -1-1 ;(5), 10 SAH ;(6) - - 27%~50%, ( cerebral vasospasm ) Glasgow (Glasgow Coma Scale,GCS), [1],, (aneurysmal
,, 2. : ;,, :(1), (delayed ;(2) ischemic neurological deficit,dind) ;(3) 2. :SAH ;(4) 5-10 10 HT -1-1 ;(5), 10 SAH ;(6) - - 27%~50%, ( cerebral vasospasm ) Glasgow (Glasgow Coma Scale,GCS), [1],, (aneurysmal
HEAD AND NECK IMAGING. James Chen (MS IV)
 HEAD AND NECK IMAGING James Chen (MS IV) Anatomy Course Johns Hopkins School of Medicine Sept. 27, 2011 OBJECTIVES Introduce cross sectional imaging of head and neck Computed tomography (CT) Review head
HEAD AND NECK IMAGING James Chen (MS IV) Anatomy Course Johns Hopkins School of Medicine Sept. 27, 2011 OBJECTIVES Introduce cross sectional imaging of head and neck Computed tomography (CT) Review head
Meninges and Ventricles
 Meninges and Ventricles Irene Yu, class of 2019 LEARNING OBJECTIVES Describe the meningeal layers, the dural infolds, and the spaces they create. Name the contents of the subarachnoid space. Describe the
Meninges and Ventricles Irene Yu, class of 2019 LEARNING OBJECTIVES Describe the meningeal layers, the dural infolds, and the spaces they create. Name the contents of the subarachnoid space. Describe the
CSF. Cerebrospinal Fluid(CSF) System
 Cerebrospinal Fluid(CSF) System By the end of the lecture, students must be able to describe Physiological Anatomy of CSF Compartments Composition Formation Circulation Reabsorption CSF Pressure Functions
Cerebrospinal Fluid(CSF) System By the end of the lecture, students must be able to describe Physiological Anatomy of CSF Compartments Composition Formation Circulation Reabsorption CSF Pressure Functions
Definition พ.ญ.ส ธ ดา เย นจ นทร. Epidemiology. Definition 5/25/2016. Seizures after stroke Can we predict? Poststroke seizure
 Seizures after stroke Can we predict? พ.ญ.ส ธ ดา เย นจ นทร PMK Epilepsy Annual Meeting 2016 Definition Poststroke seizure : single or multiple convulsive episode(s) after stroke and thought to be related
Seizures after stroke Can we predict? พ.ญ.ส ธ ดา เย นจ นทร PMK Epilepsy Annual Meeting 2016 Definition Poststroke seizure : single or multiple convulsive episode(s) after stroke and thought to be related
Characteristic features of CNS pathology. By: Shifaa AlQa qa
 Characteristic features of CNS pathology By: Shifaa AlQa qa Normal brain: - The neocortex (gray matter): six layers: outer plexiform, outer granular, outer pyramidal, inner granular, inner pyramidal, polymorphous
Characteristic features of CNS pathology By: Shifaa AlQa qa Normal brain: - The neocortex (gray matter): six layers: outer plexiform, outer granular, outer pyramidal, inner granular, inner pyramidal, polymorphous
Cerebral hemisphere. Parietal Frontal Occipital Temporal
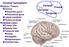 Cerebral hemisphere Sulcus / Fissure Central Precental gyrus Postcentral gyrus Lateral (cerebral) Parieto-occipital Cerebral cortex Frontal lobe Parietal lobe Temporal lobe Insula Amygdala Hippocampus
Cerebral hemisphere Sulcus / Fissure Central Precental gyrus Postcentral gyrus Lateral (cerebral) Parieto-occipital Cerebral cortex Frontal lobe Parietal lobe Temporal lobe Insula Amygdala Hippocampus
Observations on the effects of intrathecal papaverine in experimental vasospasm
 Observations on the effects of intrathecal papaverine in experimental vasospasm MASAHIRO OGATA:, M.D., B. M. MARSHALL:, M.D., ANn W. M. LOUGHEED, M.D. Division of Neurosurgery, Department o/ Surgery and
Observations on the effects of intrathecal papaverine in experimental vasospasm MASAHIRO OGATA:, M.D., B. M. MARSHALL:, M.D., ANn W. M. LOUGHEED, M.D. Division of Neurosurgery, Department o/ Surgery and
Intra-arterial nimodipine for the treatment of vasospasm due to aneurysmal subarachnoid hemorrhage
 Romanian Neurosurgery (2016) XXX 4: 461 466 461 DOI: 10.1515/romneu-2016-0074 Intra-arterial nimodipine for the treatment of vasospasm due to aneurysmal subarachnoid hemorrhage A. Chiriac, Georgiana Ion*,
Romanian Neurosurgery (2016) XXX 4: 461 466 461 DOI: 10.1515/romneu-2016-0074 Intra-arterial nimodipine for the treatment of vasospasm due to aneurysmal subarachnoid hemorrhage A. Chiriac, Georgiana Ion*,
NEURO IMAGING 2. Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity
 NEURO IMAGING 2 Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity I. EPIDURAL HEMATOMA (EDH) LOCATION Seventy to seventy-five percent occur in temporoparietal region. CAUSE Most likely caused
NEURO IMAGING 2 Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity I. EPIDURAL HEMATOMA (EDH) LOCATION Seventy to seventy-five percent occur in temporoparietal region. CAUSE Most likely caused
PTA 106 Unit 1 Lecture 3
 PTA 106 Unit 1 Lecture 3 The Basics Arteries: Carry blood away from the heart toward tissues. They typically have thicker vessels walls to handle increased pressure. Contain internal and external elastic
PTA 106 Unit 1 Lecture 3 The Basics Arteries: Carry blood away from the heart toward tissues. They typically have thicker vessels walls to handle increased pressure. Contain internal and external elastic
Treatment of Acute Hydrocephalus After Subarachnoid Hemorrhage With Serial Lumbar Puncture
 19 Treatment of Acute After Subarachnoid Hemorrhage With Serial Lumbar Puncture Djo Hasan, MD; Kenneth W. Lindsay, PhD, FRCS; and Marinus Vermeulen, MD Downloaded from http://ahajournals.org by on vember,
19 Treatment of Acute After Subarachnoid Hemorrhage With Serial Lumbar Puncture Djo Hasan, MD; Kenneth W. Lindsay, PhD, FRCS; and Marinus Vermeulen, MD Downloaded from http://ahajournals.org by on vember,
We previously studied the time course of the dependence
 Vasospasm in Monkeys Resolves Because of Loss of and Encasement of Subarachnoid Blood Clot Zhen-Du Zhang, MD, PhD; Baktair Yamini, MD; Taro Komuro, MD, PhD; Shigeki Ono, MD; Lydia Johns; Linda S. Marton,
Vasospasm in Monkeys Resolves Because of Loss of and Encasement of Subarachnoid Blood Clot Zhen-Du Zhang, MD, PhD; Baktair Yamini, MD; Taro Komuro, MD, PhD; Shigeki Ono, MD; Lydia Johns; Linda S. Marton,
ELUTING NOVEL BIODEGRADABLE VASCULAR STENTS FOR IMPLANTATION
 PREDNISOLONE ACETATE-ELUTING ELUTING NOVEL BIODEGRADABLE VASCULAR STENTS FOR IMPLANTATION Pharm. (M.Sc.) Can Sarisozen Assist. Prof. Dr. Betul Arica, Prof.Dr. Sema Calis, Prof.Dr. A.Atilla Hincal Hacettepe
PREDNISOLONE ACETATE-ELUTING ELUTING NOVEL BIODEGRADABLE VASCULAR STENTS FOR IMPLANTATION Pharm. (M.Sc.) Can Sarisozen Assist. Prof. Dr. Betul Arica, Prof.Dr. Sema Calis, Prof.Dr. A.Atilla Hincal Hacettepe
What Is an Arteriovenous malformation (AVM)?
 American Society of Neuroradiology What Is an Arteriovenous malformation (AVM)? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall
American Society of Neuroradiology What Is an Arteriovenous malformation (AVM)? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall
The dura is sensitive to stretching, which produces the sensation of headache.
 Dural Nerve Supply Branches of the trigeminal, vagus, and first three cervical nerves and branches from the sympathetic system pass to the dura. Numerous sensory endings are in the dura. The dura is sensitive
Dural Nerve Supply Branches of the trigeminal, vagus, and first three cervical nerves and branches from the sympathetic system pass to the dura. Numerous sensory endings are in the dura. The dura is sensitive
Central Nervous System (CNS) -> brain and spinal cord. Major Divisions of the nervous system:
 Central Nervous System (CNS) -> brain and spinal cord Major Divisions of the nervous system: Afferent (sensory input) -> cell bodies outside of the central nervous system (CNS), carry info into the CNS
Central Nervous System (CNS) -> brain and spinal cord Major Divisions of the nervous system: Afferent (sensory input) -> cell bodies outside of the central nervous system (CNS), carry info into the CNS
Applicable Neuroradiology
 For the Clinical Neurology Clerkship LSU Medical School New Orleans Amy W Voigt, MD Clerkship Director Introduction The field of Radiology first developed following the discovery of X-Rays by Wilhelm Roentgen
For the Clinical Neurology Clerkship LSU Medical School New Orleans Amy W Voigt, MD Clerkship Director Introduction The field of Radiology first developed following the discovery of X-Rays by Wilhelm Roentgen
Ventricles, CSF & Meninges. Steven McLoon Department of Neuroscience University of Minnesota
 Ventricles, CSF & Meninges Steven McLoon Department of Neuroscience University of Minnesota 1 Coffee Hour Thursday (Sept 14) 8:30-9:30am Surdyk s Café in Northrop Auditorium Stop by for a minute or an
Ventricles, CSF & Meninges Steven McLoon Department of Neuroscience University of Minnesota 1 Coffee Hour Thursday (Sept 14) 8:30-9:30am Surdyk s Café in Northrop Auditorium Stop by for a minute or an
BACKGROUND AND PURPOSE:
 Published August 12, 2010 as 10.3174/ajnr.A2215 ORIGINAL RESEARCH J.V. Sehy W.E. Holloway S.-P. Lin D.T. Cross III C.P. Derdeyn C.J. Moran Improvement in Angiographic Cerebral Vasospasm after Intra-Arterial
Published August 12, 2010 as 10.3174/ajnr.A2215 ORIGINAL RESEARCH J.V. Sehy W.E. Holloway S.-P. Lin D.T. Cross III C.P. Derdeyn C.J. Moran Improvement in Angiographic Cerebral Vasospasm after Intra-Arterial
The Nervous System. Functions of the Nervous System input gathering To monitor occurring inside and outside the body Changes =
 The Nervous System Functions of the Nervous System input gathering To monitor occurring inside and outside the body Changes = To process and sensory input and decide if is needed output A response to integrated
The Nervous System Functions of the Nervous System input gathering To monitor occurring inside and outside the body Changes = To process and sensory input and decide if is needed output A response to integrated
>>> Oral Formulation Optimization. Introduction. A Tiered Approach for Identifying Enabling Formulations
 Application Note #28-DMPK-3 >>> Oral Formulation Optimization Introduction Among the criteria required of compounds advancing from drug discovery programs, adequate systemic exposure (plasma concentrations
Application Note #28-DMPK-3 >>> Oral Formulation Optimization Introduction Among the criteria required of compounds advancing from drug discovery programs, adequate systemic exposure (plasma concentrations
CNS pathology Third year medical students. Dr Heyam Awad 2018 Lecture 5: disturbed fluid balance and increased intracranial pressure
 CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 5: disturbed fluid balance and increased intracranial pressure ILOs Understand causes and symptoms of increased intracranial pressure.
CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 5: disturbed fluid balance and increased intracranial pressure ILOs Understand causes and symptoms of increased intracranial pressure.
Assessment of Vasospasm and Delayed Cerebral Ischemia after Subarachnoid Hemorrhage: Current concepts and Value of CT Perfusion and CT Angiography
 Assessment of Vasospasm and Delayed Cerebral Ischemia after Subarachnoid Hemorrhage: Current concepts and Value of CT Perfusion and CT Angiography Poster No.: C-2563 Congress: ECR 2012 Type: Educational
Assessment of Vasospasm and Delayed Cerebral Ischemia after Subarachnoid Hemorrhage: Current concepts and Value of CT Perfusion and CT Angiography Poster No.: C-2563 Congress: ECR 2012 Type: Educational
SOME EFFECTS OF INJECTIONS OF HYALURONIDASE INTO THE SUBARACHNOID SPACE OF EXPERIMENTAL ANIMALS*
 SOME EFFECTS OF INJECTIONS OF HYALURONIDASE INTO THE SUBARACHNOID SPACE OF EXPERIMENTAL ANIMALS* GUY OWENS, M.D., AND SAM L. CLARK, M.D. Departments of Surgery and Anatomy, Vanderbilt University School
SOME EFFECTS OF INJECTIONS OF HYALURONIDASE INTO THE SUBARACHNOID SPACE OF EXPERIMENTAL ANIMALS* GUY OWENS, M.D., AND SAM L. CLARK, M.D. Departments of Surgery and Anatomy, Vanderbilt University School
Neurointensive Care of Aneurysmal Subarachnoid Hemorrhage. Alejandro A. Rabinstein Department of Neurology Mayo Clinic, Rochester, USA
 Neurointensive Care of Aneurysmal Subarachnoid Hemorrhage Alejandro A. Rabinstein Department of Neurology Mayo Clinic, Rochester, USA The traditional view: asah is a bad disease Pre-hospital mortality
Neurointensive Care of Aneurysmal Subarachnoid Hemorrhage Alejandro A. Rabinstein Department of Neurology Mayo Clinic, Rochester, USA The traditional view: asah is a bad disease Pre-hospital mortality
SAH READMISSIONS TO NCCU
 SAH READMISSIONS TO NCCU Are they preventable? João Amaral Rebecca Gorf Critical Care Outreach Team - NHNN 2015 Total admissions to NCCU =862 Total SAH admitted to NCCU= 104 (93e) (12.0%) Total SAH readmissions=
SAH READMISSIONS TO NCCU Are they preventable? João Amaral Rebecca Gorf Critical Care Outreach Team - NHNN 2015 Total admissions to NCCU =862 Total SAH admitted to NCCU= 104 (93e) (12.0%) Total SAH readmissions=
Section 5.2: Pharmacokinetic properties
 Section 5.2: Pharmacokinetic properties SmPC training presentation Note: for full information refer to the European Commission s Guideline on summary of product characteristics (SmPC) SmPC Advisory Group
Section 5.2: Pharmacokinetic properties SmPC training presentation Note: for full information refer to the European Commission s Guideline on summary of product characteristics (SmPC) SmPC Advisory Group
Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD
 Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD Boston Children s Hospital Harvard Medical School None Disclosures Conventional US Anterior fontanelle
Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD Boston Children s Hospital Harvard Medical School None Disclosures Conventional US Anterior fontanelle
Blood Supply. Allen Chung, class of 2013
 Blood Supply Allen Chung, class of 2013 Objectives Understand the importance of the cerebral circulation. Understand stroke and the types of vascular problems that cause it. Understand ischemic penumbra
Blood Supply Allen Chung, class of 2013 Objectives Understand the importance of the cerebral circulation. Understand stroke and the types of vascular problems that cause it. Understand ischemic penumbra
Cerebrovascular diseases-2
 Cerebrovascular diseases-2 Primary angiitis of CNS - Other causes of infarction i. Hypercoagulable states ii. Drug-abuse such as amphetamine, heroin and cocain Note - The venous side of the circulation
Cerebrovascular diseases-2 Primary angiitis of CNS - Other causes of infarction i. Hypercoagulable states ii. Drug-abuse such as amphetamine, heroin and cocain Note - The venous side of the circulation
Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage
 Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
ICP CSF Spinal Cord Anatomy Cord Transection. Alicia A C Waite March 2nd, 2017
 ICP CSF Spinal Cord Anatomy Cord Transection Alicia A C Waite March 2nd, 2017 Monro-Kellie doctrine Intracranial volume = brain volume (85%) + blood volume (10%) + CSF volume (5%) Brain parenchyma Skull
ICP CSF Spinal Cord Anatomy Cord Transection Alicia A C Waite March 2nd, 2017 Monro-Kellie doctrine Intracranial volume = brain volume (85%) + blood volume (10%) + CSF volume (5%) Brain parenchyma Skull
The central nervous system
 Sectc.qxd 29/06/99 09:42 Page 81 Section C The central nervous system CNS haemorrhage Subarachnoid haemorrhage Cerebral infarction Brain atrophy Ring enhancing lesions MRI of the pituitary Multiple sclerosis
Sectc.qxd 29/06/99 09:42 Page 81 Section C The central nervous system CNS haemorrhage Subarachnoid haemorrhage Cerebral infarction Brain atrophy Ring enhancing lesions MRI of the pituitary Multiple sclerosis
Cerebrovascular Disease
 Neuropathology lecture series Cerebrovascular Disease Physiology of cerebral blood flow Brain makes up only 2% of body weight Percentage of cardiac output: 15-20% Percentage of O 2 consumption (resting):
Neuropathology lecture series Cerebrovascular Disease Physiology of cerebral blood flow Brain makes up only 2% of body weight Percentage of cardiac output: 15-20% Percentage of O 2 consumption (resting):
CENTRAL NERVOUS SYSTEM TRAUMA and Subarachnoid Hemorrhage. By: Shifaa AlQa qa
 CENTRAL NERVOUS SYSTEM TRAUMA and Subarachnoid Hemorrhage By: Shifaa AlQa qa Subarachnoid Hemorrhage Causes: Rupture of a saccular (berry) aneurysm Vascular malformation Trauma Hematologic disturbances
CENTRAL NERVOUS SYSTEM TRAUMA and Subarachnoid Hemorrhage By: Shifaa AlQa qa Subarachnoid Hemorrhage Causes: Rupture of a saccular (berry) aneurysm Vascular malformation Trauma Hematologic disturbances
Ischemia cerebrale dopo emorragia subaracnoidea Vasospasmo e altri nemici
 Ischemia cerebrale dopo emorragia subaracnoidea Vasospasmo e altri nemici Nino Stocchetti Milan University Neuroscience ICU Ospedale Policlinico IRCCS Milano stocchet@policlinico.mi.it Macdonald RL et
Ischemia cerebrale dopo emorragia subaracnoidea Vasospasmo e altri nemici Nino Stocchetti Milan University Neuroscience ICU Ospedale Policlinico IRCCS Milano stocchet@policlinico.mi.it Macdonald RL et
Imaging of Moya Moya Disease
 Abstract Imaging of Moya Moya Disease Pages with reference to book, From 181 To 185 Rashid Ahmed, Hurnera Ahsan ( Liaquat National Hospital, Karachi. ) Moya Moya disease is a rare disease causing occlusion
Abstract Imaging of Moya Moya Disease Pages with reference to book, From 181 To 185 Rashid Ahmed, Hurnera Ahsan ( Liaquat National Hospital, Karachi. ) Moya Moya disease is a rare disease causing occlusion
Pharmaceutical Drug Development Consulting
 Dr. Julia Eva Diederichs Pharmaceutical Drug Development Consulting Preclinical investigations and animal studies: for comprehensive characterisation what is scientifically possible and meaningful A Case
Dr. Julia Eva Diederichs Pharmaceutical Drug Development Consulting Preclinical investigations and animal studies: for comprehensive characterisation what is scientifically possible and meaningful A Case
Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts
 Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts Exceptional healthcare, personally delivered Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts What is hydrocephalus? Hydrocephalus is the build up of an excess
Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts Exceptional healthcare, personally delivered Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts What is hydrocephalus? Hydrocephalus is the build up of an excess
Surgical Management of Stroke Brandon Evans, MD Department of Neurosurgery
 Surgical Management of Stroke Brandon Evans, MD Department of Neurosurgery 2 Stroke Stroke kills almost 130,000 Americans each year. - Third cause of all deaths in Arkansas. - Death Rate is highest in
Surgical Management of Stroke Brandon Evans, MD Department of Neurosurgery 2 Stroke Stroke kills almost 130,000 Americans each year. - Third cause of all deaths in Arkansas. - Death Rate is highest in
Neuropathology lecture series. III. Neuropathology of Cerebrovascular Disease. Physiology of cerebral blood flow
 Neuropathology lecture series III. Neuropathology of Cerebrovascular Disease Physiology of cerebral blood flow Brain makes up only 2% of body weight Percentage of cardiac output: 15-20% Percentage of O
Neuropathology lecture series III. Neuropathology of Cerebrovascular Disease Physiology of cerebral blood flow Brain makes up only 2% of body weight Percentage of cardiac output: 15-20% Percentage of O
The Nervous System PART C. PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College
 PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Nervous System 7 PART C Protection of the Central Nervous System Scalp and skin Skull and vertebral
PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Nervous System 7 PART C Protection of the Central Nervous System Scalp and skin Skull and vertebral
Department of Neurological Surgery
 Department of Neurological Surgery CAT 1 A Basic Privileges: Patient management, including H & Ps and diagnostic and therapeutic treatments, procedures and interventions, Requiring a level of training
Department of Neurological Surgery CAT 1 A Basic Privileges: Patient management, including H & Ps and diagnostic and therapeutic treatments, procedures and interventions, Requiring a level of training
MRI and CT of the CNS
 MRI and CT of the CNS Dr.Maha ELBeltagy Assistant Professor of Anatomy Faculty of Medicine The University of Jordan 2018 Computed Tomography CT is used for the detection of intracranial lesions. CT relies
MRI and CT of the CNS Dr.Maha ELBeltagy Assistant Professor of Anatomy Faculty of Medicine The University of Jordan 2018 Computed Tomography CT is used for the detection of intracranial lesions. CT relies
Biopharmaceutics Dosage form factors influencing bioavailability Lec:5
 Biopharmaceutics Dosage form factors influencing bioavailability Lec:5 Ali Y Ali BSc Pharmacy MSc Industrial Pharmaceutical Sciences Dept. of Pharmaceutics School of Pharmacy University of Sulaimani 09/01/2019
Biopharmaceutics Dosage form factors influencing bioavailability Lec:5 Ali Y Ali BSc Pharmacy MSc Industrial Pharmaceutical Sciences Dept. of Pharmaceutics School of Pharmacy University of Sulaimani 09/01/2019
Aneurysmal Subarachnoid Hemorrhage Presentation and Complications
 Aneurysmal Subarachnoid Hemorrhage Presentation and Complications Sherry H-Y. Chou MD MMSc FNCS Department of Critical Care Medicine, Neurology and Neurosurgery University of Pittsburgh School of Medicine
Aneurysmal Subarachnoid Hemorrhage Presentation and Complications Sherry H-Y. Chou MD MMSc FNCS Department of Critical Care Medicine, Neurology and Neurosurgery University of Pittsburgh School of Medicine
Quality Metrics. Stroke Related Procedure Outcomes
 Quality Metrics Stroke Related Procedure Outcomes Below is a description of some of the stroke-related procedures performed at St. Dominic Hospital in Jackson, with quality information on the complication
Quality Metrics Stroke Related Procedure Outcomes Below is a description of some of the stroke-related procedures performed at St. Dominic Hospital in Jackson, with quality information on the complication
Organization of The Nervous System PROF. SAEED ABUEL MAKAREM
 Organization of The Nervous System PROF. SAEED ABUEL MAKAREM Objectives By the end of the lecture, you should be able to: List the parts of the nervous system. List the function of the nervous system.
Organization of The Nervous System PROF. SAEED ABUEL MAKAREM Objectives By the end of the lecture, you should be able to: List the parts of the nervous system. List the function of the nervous system.
Sample page. Radiology. Cross Coder. Essential links from CPT codes to ICD-10-CM and HCPCS
 Cross Coder 2018 Radiology Essential links from CPT codes to ICD-10-CM and HCPCS POWER UP YOUR CODING with Optum360, your trusted coding partner for 32 years. Visit optum360coding.com. Contents Introduction...
Cross Coder 2018 Radiology Essential links from CPT codes to ICD-10-CM and HCPCS POWER UP YOUR CODING with Optum360, your trusted coding partner for 32 years. Visit optum360coding.com. Contents Introduction...
Submitted to the University of Adelaide for the degree of. Doctor of Science. Robert Vink, BSc (Hons), PhD
 Submitted to the University of Adelaide for the degree of Doctor of Science Robert Vink, BSc (Hons), PhD TABLE OF CONTENTS DECLARATION STATEMENT SUPPORTING THE SUBMISSION... 1 Dot Point Summary 1 Detailed
Submitted to the University of Adelaide for the degree of Doctor of Science Robert Vink, BSc (Hons), PhD TABLE OF CONTENTS DECLARATION STATEMENT SUPPORTING THE SUBMISSION... 1 Dot Point Summary 1 Detailed
PARA210 SUMMARY Hyperglycaemia (DKA & HHS) Brain & Nervous System Anatomy & Physiology Degenerative Neurological Disorders
 PARA210 SUMMARY Page Topic 01-03 Diabetes Mellitus 04-05 Hyperglycaemia (DKA & HHS) 06-13 Toxicology 14-18 12 Lead ECG 19-21 Brain & Nervous System Anatomy & Physiology 22-24 Degenerative Neurological
PARA210 SUMMARY Page Topic 01-03 Diabetes Mellitus 04-05 Hyperglycaemia (DKA & HHS) 06-13 Toxicology 14-18 12 Lead ECG 19-21 Brain & Nervous System Anatomy & Physiology 22-24 Degenerative Neurological
CNS TUMORS. D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria)
 CNS TUMORS D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria) CNS TUMORS The annual incidence of intracranial tumors of the CNS ISmore than intraspinal tumors May be Primary or Secondary
CNS TUMORS D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria) CNS TUMORS The annual incidence of intracranial tumors of the CNS ISmore than intraspinal tumors May be Primary or Secondary
IN-SITU FORMING IMPLANT SYSTEM FOR LONG ACTING HIV PROPHYLAXIS
 IN-SITU FORMING IMPLANT SYSTEM FOR LONG ACTING HIV PROPHYLAXIS Shelby L. Hudson, MS PharmD Candidate UNC Eshelman School of Pharmacy November 17, 21 Research mentor: Soumya Rahima Benhabbour, PhD Date
IN-SITU FORMING IMPLANT SYSTEM FOR LONG ACTING HIV PROPHYLAXIS Shelby L. Hudson, MS PharmD Candidate UNC Eshelman School of Pharmacy November 17, 21 Research mentor: Soumya Rahima Benhabbour, PhD Date
From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council
 American Society of Neuroradiology What Is a Stroke? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall T. Higashida, M.D., Chair
American Society of Neuroradiology What Is a Stroke? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall T. Higashida, M.D., Chair
Hemodynamics in the Anterior Part of the Circle of Willis in Patients with Intracranial Aneurysms : A Study by Cerebral Angiography
 Tohoku J. exp. Med., 1980, 132, 69-73 Hemodynamics in the Anterior Part of the Circle of Willis in Patients with Intracranial Aneurysms : A Study by Cerebral Angiography RYUNGCHAN KWAK, HIROSHI NIIZUMA
Tohoku J. exp. Med., 1980, 132, 69-73 Hemodynamics in the Anterior Part of the Circle of Willis in Patients with Intracranial Aneurysms : A Study by Cerebral Angiography RYUNGCHAN KWAK, HIROSHI NIIZUMA
Case report: Intra-procedural aneurysm rupture during endovascular treatment causing immediate, transient angiographic vasospasm Zoe Zhang, MD
 Case report: Intra-procedural aneurysm rupture during endovascular treatment causing immediate, transient angiographic vasospasm Zoe Zhang, MD, Farhan Siddiq, MD, Wondwossen G Tekle, MD, Ameer E Hassan,
Case report: Intra-procedural aneurysm rupture during endovascular treatment causing immediate, transient angiographic vasospasm Zoe Zhang, MD, Farhan Siddiq, MD, Wondwossen G Tekle, MD, Ameer E Hassan,
Sciences, Sri Ramachandra Medical College and Research Institute, Chennai, India.
 IMAGES in PAEDIATRIC CARDIOLOGY Devara K V A, 1 Joseph S, 2 Uppu S C. 3 Spontaneous Subarachnoid Haemorrhage Due to Coarctation of Aorta and 1 Department of Radiology, Medall Healthcare Private Ltd, King
IMAGES in PAEDIATRIC CARDIOLOGY Devara K V A, 1 Joseph S, 2 Uppu S C. 3 Spontaneous Subarachnoid Haemorrhage Due to Coarctation of Aorta and 1 Department of Radiology, Medall Healthcare Private Ltd, King
Attenuation value in HU From -500 To HU From -10 To HU From 60 To 90 HU. From 200 HU and above
 Brain Imaging Common CT attenuation values Structure Air Fat Water Brain tissue Recent hematoma Calcifications Bone Brain edema and infarction Normal liver parenchyma Attenuation value in HU From -500
Brain Imaging Common CT attenuation values Structure Air Fat Water Brain tissue Recent hematoma Calcifications Bone Brain edema and infarction Normal liver parenchyma Attenuation value in HU From -500
Blood Supply. Steven McLoon Department of Neuroscience University of Minnesota
 Blood Supply Steven McLoon Department of Neuroscience University of Minnesota 1 Course News Review Sessions with Dr. Riedl Tuesdays 4-5pm in MCB 3-146 (the main lab room) The first exam is coming soon!
Blood Supply Steven McLoon Department of Neuroscience University of Minnesota 1 Course News Review Sessions with Dr. Riedl Tuesdays 4-5pm in MCB 3-146 (the main lab room) The first exam is coming soon!
Supplementary material 1. Definitions of study endpoints (extracted from the Endpoint Validation Committee Charter) 1.
 Rationale, design, and baseline characteristics of the SIGNIFY trial: a randomized, double-blind, placebo-controlled trial of ivabradine in patients with stable coronary artery disease without clinical
Rationale, design, and baseline characteristics of the SIGNIFY trial: a randomized, double-blind, placebo-controlled trial of ivabradine in patients with stable coronary artery disease without clinical
Monitoring of Regional Cerebral Blood Flow Using an Implanted Cerebral Thermal Perfusion Probe Archived Medical Policy
 Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Subarachnoid Hemorrhage and Brain Aneurysm
 Subarachnoid Hemorrhage and Brain Aneurysm DIN Department of Interventional Neurology What is SAH? Subarachnoid Haemorrhage is the sudden leaking (haemorrhage) of blood from the blood vessels of brain.
Subarachnoid Hemorrhage and Brain Aneurysm DIN Department of Interventional Neurology What is SAH? Subarachnoid Haemorrhage is the sudden leaking (haemorrhage) of blood from the blood vessels of brain.
Trigger factors for rupture of intracranial aneurysms in relation to patient and aneurysm characteristics
 J Neurol (2012) 259:1298 1302 DOI 10.1007/s00415-011-6341-1 ORIGINAL COMMUNICATION Trigger factors for rupture of intracranial aneurysms in relation to patient and aneurysm characteristics Monique H. M.
J Neurol (2012) 259:1298 1302 DOI 10.1007/s00415-011-6341-1 ORIGINAL COMMUNICATION Trigger factors for rupture of intracranial aneurysms in relation to patient and aneurysm characteristics Monique H. M.
[(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD]
![[(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD] [(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD]](/thumbs/89/98619893.jpg) 2015 PHYSICIAN SIGN-OFF (1) STUDY NO (PHY-1) CASE, PER PHYSICIAN REVIEW 1=yes 2=no [strictly meets case definition] (PHY-1a) CASE, IN PHYSICIAN S OPINION 1=yes 2=no (PHY-2) (PHY-3) [based on all available
2015 PHYSICIAN SIGN-OFF (1) STUDY NO (PHY-1) CASE, PER PHYSICIAN REVIEW 1=yes 2=no [strictly meets case definition] (PHY-1a) CASE, IN PHYSICIAN S OPINION 1=yes 2=no (PHY-2) (PHY-3) [based on all available
NANO 243/CENG 207 Course Use Only
 L6. Drug Administration & Transport by Fluid Motion April 19, 2018 Part I: Drug Administration Routes of Drug Administration Topical: local effect, substance is applied directly where its action is desired.
L6. Drug Administration & Transport by Fluid Motion April 19, 2018 Part I: Drug Administration Routes of Drug Administration Topical: local effect, substance is applied directly where its action is desired.
What Are We Going to Do? Fourth Year Meds Clinical Neuroanatomy. Hydrocephalus and Effects of Interruption of CSF Flow. Tube Blockage Doctrine
 Fourth Year Meds Clinical Neuroanatomy Ventricles, CSF, Brain Swelling etc. David A. Ramsay, Neuropathologist, LHSC What Are We Going to Do? Hydrocephalus and some effects of the interruption of CSF flow
Fourth Year Meds Clinical Neuroanatomy Ventricles, CSF, Brain Swelling etc. David A. Ramsay, Neuropathologist, LHSC What Are We Going to Do? Hydrocephalus and some effects of the interruption of CSF flow
Endosaccular aneurysm occlusion with Guglielmi detachable coils for obstructive hydrocephalus caused by a large basilar tip aneurysm Case report
 Neurosurg Focus 7 (4):Article 5, 1999 Endosaccular aneurysm occlusion with Guglielmi detachable coils for obstructive hydrocephalus caused by a large basilar tip aneurysm Case report Akira Watanabe, M.D.,
Neurosurg Focus 7 (4):Article 5, 1999 Endosaccular aneurysm occlusion with Guglielmi detachable coils for obstructive hydrocephalus caused by a large basilar tip aneurysm Case report Akira Watanabe, M.D.,
Head CT Scan Interpretation: A Five-Step Approach to Seeing Inside the Head Lawrence B. Stack, MD
 Head CT Scan Interpretation: A Five-Step Approach to Seeing Inside the Head Lawrence B. Stack, MD Five Step Approach 1. Adequate study 2. Bone windows 3. Ventricles 4. Quadrigeminal cistern 5. Parenchyma
Head CT Scan Interpretation: A Five-Step Approach to Seeing Inside the Head Lawrence B. Stack, MD Five Step Approach 1. Adequate study 2. Bone windows 3. Ventricles 4. Quadrigeminal cistern 5. Parenchyma
CNS pathology Third year medical students. Dr Heyam Awad 2018 Lecture 12: CNS tumours 2/3
 CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 12: CNS tumours 2/3 Pilocytic astrocytoma Relatively benign ( WHO grade 1) Occurs in children and young adults Mostly: in the cerebellum
CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 12: CNS tumours 2/3 Pilocytic astrocytoma Relatively benign ( WHO grade 1) Occurs in children and young adults Mostly: in the cerebellum
Spontaneous intracranial hypotension syndrome with extracranial vein dilatation
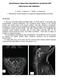 Spontaneous intracranial hypotension syndrome with extracranial vein dilatation C. Heine 1, H. Altinova 1, T. Pietilä 1, LC Stavrinou 1 1. Department of Neurosurgery, Evangelical Hospital Bielefeld, Germany
Spontaneous intracranial hypotension syndrome with extracranial vein dilatation C. Heine 1, H. Altinova 1, T. Pietilä 1, LC Stavrinou 1 1. Department of Neurosurgery, Evangelical Hospital Bielefeld, Germany
Supplementary Figure 1 Detailed description of the MDP fabrication procedures
 1 2 Supplementary Figure 1 Detailed description of the MDP fabrication procedures The MDP consists of two distinct units: a drug reservoir and an actuator. (a) To prepare the drug reservoir, a body cover
1 2 Supplementary Figure 1 Detailed description of the MDP fabrication procedures The MDP consists of two distinct units: a drug reservoir and an actuator. (a) To prepare the drug reservoir, a body cover
CEREBROSPINAL FLUID [CSF]
![CEREBROSPINAL FLUID [CSF] CEREBROSPINAL FLUID [CSF]](/thumbs/89/100552494.jpg) CEREBROSPINAL FLUID [CSF] All question is compulsory Minimum passing mark is 15. 1. Full form of a) CSF = b) LDH = c) ADA = 2. If patient serum glucose level is 300 mg%,than expected csf glucose level
CEREBROSPINAL FLUID [CSF] All question is compulsory Minimum passing mark is 15. 1. Full form of a) CSF = b) LDH = c) ADA = 2. If patient serum glucose level is 300 mg%,than expected csf glucose level
Current State of the Art
 SAH Current State of the Art Thomas C. Steineke, M.D., Ph.D. Director of Neurovascular Surgery NJ Neuroscience Institute JFK Medical Center Introduction Signs and symptoms of a problem What are aneurysms
SAH Current State of the Art Thomas C. Steineke, M.D., Ph.D. Director of Neurovascular Surgery NJ Neuroscience Institute JFK Medical Center Introduction Signs and symptoms of a problem What are aneurysms
Principles Arteries & Veins of the CNS LO14
 Principles Arteries & Veins of the CNS LO14 14. Identify (on cadaver specimens, models and diagrams) and name the principal arteries and veins of the CNS: Why is it important to understand blood supply
Principles Arteries & Veins of the CNS LO14 14. Identify (on cadaver specimens, models and diagrams) and name the principal arteries and veins of the CNS: Why is it important to understand blood supply
Cerebral aneurysms A case study
 August 2001 Cerebral aneurysms A case study Heather L. Hinds, Harvard Medical School Year III Our Patient 57yr old woman History of migraines Presents with persistent headache several months duration different
August 2001 Cerebral aneurysms A case study Heather L. Hinds, Harvard Medical School Year III Our Patient 57yr old woman History of migraines Presents with persistent headache several months duration different
B16-F10 (Mus musculus skin melanoma), NCI-H460 (human non-small cell lung cancer
 Electronic Supplementary Material (ESI) for ChemComm. This journal is The Royal Society of Chemistry 2017 Experimental Methods Cell culture B16-F10 (Mus musculus skin melanoma), NCI-H460 (human non-small
Electronic Supplementary Material (ESI) for ChemComm. This journal is The Royal Society of Chemistry 2017 Experimental Methods Cell culture B16-F10 (Mus musculus skin melanoma), NCI-H460 (human non-small
Guide to Draw It to Know It Neuroanatomy (relative to Medical Neuro, UI-COM Urbana)
 Guide to Draw It to Know It Neuroanatomy (relative to Medical Neuro, UI-COM Urbana) Note: Sometimes DITKI goes into far more detail than is necessary for the course, and in other cases not enough. As helpful
Guide to Draw It to Know It Neuroanatomy (relative to Medical Neuro, UI-COM Urbana) Note: Sometimes DITKI goes into far more detail than is necessary for the course, and in other cases not enough. As helpful
What You Should Know About Cerebral Aneurysms
 American Society of Neuroradiology American Society of Interventional & Therapeutic Neuroradiology What You Should Know About Cerebral Aneurysms From the Cerebrovascular Imaging and Intervention Committee
American Society of Neuroradiology American Society of Interventional & Therapeutic Neuroradiology What You Should Know About Cerebral Aneurysms From the Cerebrovascular Imaging and Intervention Committee
Management of Traumatic Brain Injury (and other neurosurgical emergencies)
 Management of Traumatic Brain Injury (and other neurosurgical emergencies) Laurel Moore, M.D. University of Michigan 22 nd Annual Review February 7, 2019 Greetings from Michigan! Objectives for Today s
Management of Traumatic Brain Injury (and other neurosurgical emergencies) Laurel Moore, M.D. University of Michigan 22 nd Annual Review February 7, 2019 Greetings from Michigan! Objectives for Today s
The role of the arachnoid villus in the removal of red blood cells from the subarachnoid space. An electron microscope study in the dog
 The role of the arachnoid villus in the removal of red blood cells from the subarachnoid space An electron microscope study in the dog JOHN 17. ALKSNE, M.D., AND ETHEL T. LOVlNGS Division of Neurological
The role of the arachnoid villus in the removal of red blood cells from the subarachnoid space An electron microscope study in the dog JOHN 17. ALKSNE, M.D., AND ETHEL T. LOVlNGS Division of Neurological
Thursday, January 24, 2019
 Thursday, January 24, 2019 6:45am 7:30am 7:30am 7:45am 7:45am 9:45am 9:45am 10:00am 10:00am- 12:00pm 12:00pm 12:30pm 12:30pm 1:30pm 1:30pm 3:30pm 3:30pm-3:45pm 3:45pm - 4:45pm 4:45pm 5:45pm Registrations:
Thursday, January 24, 2019 6:45am 7:30am 7:30am 7:45am 7:45am 9:45am 9:45am 10:00am 10:00am- 12:00pm 12:00pm 12:30pm 12:30pm 1:30pm 1:30pm 3:30pm 3:30pm-3:45pm 3:45pm - 4:45pm 4:45pm 5:45pm Registrations:
Cordis EXOSEAL Vascular Closure Device
 to receive our latest news and key activities. Cordis EXOSEAL Vascular Closure Device Polyglycolic Acid Plug (PGA) Material Absorption and Tissue Reaction Assessment 3 Days* 14 Days* 60 Days* LinkedIn
to receive our latest news and key activities. Cordis EXOSEAL Vascular Closure Device Polyglycolic Acid Plug (PGA) Material Absorption and Tissue Reaction Assessment 3 Days* 14 Days* 60 Days* LinkedIn
Subarachnoid Haemorrhage
 2011 Subarachnoid Haemorrhage Subarachnoid Haemorrhage This pamphlet will briefly describe what may happen to a person who has a subarachnoid haemorrhage (SAH). We would like to encourage you to read this
2011 Subarachnoid Haemorrhage Subarachnoid Haemorrhage This pamphlet will briefly describe what may happen to a person who has a subarachnoid haemorrhage (SAH). We would like to encourage you to read this
UPSTATE Comprehensive Stroke Center. Neurosurgical Interventions Satish Krishnamurthy MD, MCh
 UPSTATE Comprehensive Stroke Center Neurosurgical Interventions Satish Krishnamurthy MD, MCh Regional cerebral blood flow is important Some essential facts Neurons are obligatory glucose users Under anerobic
UPSTATE Comprehensive Stroke Center Neurosurgical Interventions Satish Krishnamurthy MD, MCh Regional cerebral blood flow is important Some essential facts Neurons are obligatory glucose users Under anerobic
Chapter 14. The Brain Meninges and Cerebral Spinal Fluid
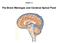 Chapter 14 The Brain Meninges and Cerebral Spinal Fluid Meninges of the Brain Skull Brain: Blood vessel Pia mater Gray matter White matter Dura mater: Periosteal layer Meningeal layer Arachnoid villus
Chapter 14 The Brain Meninges and Cerebral Spinal Fluid Meninges of the Brain Skull Brain: Blood vessel Pia mater Gray matter White matter Dura mater: Periosteal layer Meningeal layer Arachnoid villus
Essentials of Clinical MR, 2 nd edition. 14. Ischemia and Infarction II
 14. Ischemia and Infarction II Lacunar infarcts are small deep parenchymal lesions involving the basal ganglia, internal capsule, thalamus, and brainstem. The vascular supply of these areas includes the
14. Ischemia and Infarction II Lacunar infarcts are small deep parenchymal lesions involving the basal ganglia, internal capsule, thalamus, and brainstem. The vascular supply of these areas includes the
Treatment of Unruptured Vertebral Artery Dissecting Aneurysms
 33 Treatment of Unruptured Vertebral Artery Dissecting Aneurysms Isao NAITO, M.D., Shin TAKATAMA, M.D., Naoko MIYAMOTO, M.D., Hidetoshi SHIMAGUCHI, M.D., and Tomoyuki IWAI, M.D. Department of Neurosurgery,
33 Treatment of Unruptured Vertebral Artery Dissecting Aneurysms Isao NAITO, M.D., Shin TAKATAMA, M.D., Naoko MIYAMOTO, M.D., Hidetoshi SHIMAGUCHI, M.D., and Tomoyuki IWAI, M.D. Department of Neurosurgery,
CNS pathology Third year medical students. Dr Heyam Awad 2018 Lecture 7: Non traumatic brain haemorrhage
 CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 7: Non traumatic brain haemorrhage ILOS To list the causes of intracranial haemorrhage. To understand the pathogenesis of each cause.
CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 7: Non traumatic brain haemorrhage ILOS To list the causes of intracranial haemorrhage. To understand the pathogenesis of each cause.
Longitudinal anterior-to-posterior shift of collateral channels in patients with moyamoya disease: an implication for its hemorrhagic onset
 CLINICAL ARTICLE Longitudinal anterior-to-posterior shift of collateral channels in patients with moyamoya disease: an implication for its hemorrhagic onset Shusuke Yamamoto, MD, Satoshi Hori, MD, PhD,
CLINICAL ARTICLE Longitudinal anterior-to-posterior shift of collateral channels in patients with moyamoya disease: an implication for its hemorrhagic onset Shusuke Yamamoto, MD, Satoshi Hori, MD, PhD,
NACC Vascular Consortium. NACC Vascular Consortium. NACC Vascular Consortium
 NACC Vascular Consortium NACC Vascular Consortium Participating centers: Oregon Health and Science University ADC Rush University ADC Mount Sinai School of Medicine ADC Boston University ADC In consultation
NACC Vascular Consortium NACC Vascular Consortium Participating centers: Oregon Health and Science University ADC Rush University ADC Mount Sinai School of Medicine ADC Boston University ADC In consultation
SURGICAL MANAGEMENT OF BRAIN TUMORS
 SURGICAL MANAGEMENT OF BRAIN TUMORS LIGIA TATARANU, MD, Ph D NEUROSURGICAL CLINIC, BAGDASAR ARSENI CLINICAL HOSPITAL BUCHAREST, ROMANIA SURGICAL INDICATIONS CONFIRMING HISTOLOGIC DIAGNOSIS REDUCING TUMOR
SURGICAL MANAGEMENT OF BRAIN TUMORS LIGIA TATARANU, MD, Ph D NEUROSURGICAL CLINIC, BAGDASAR ARSENI CLINICAL HOSPITAL BUCHAREST, ROMANIA SURGICAL INDICATIONS CONFIRMING HISTOLOGIC DIAGNOSIS REDUCING TUMOR
Louisiana State University Health Sciences Center
 Louisiana State University Health Sciences Center Department of Neurosurgery Student Clerkship Guide 2017 2018 Introduction Welcome to LSUHSC New Orleans neurosurgery rotation. Our department is dedicated
Louisiana State University Health Sciences Center Department of Neurosurgery Student Clerkship Guide 2017 2018 Introduction Welcome to LSUHSC New Orleans neurosurgery rotation. Our department is dedicated
Brain Meninges, Ventricles and CSF
 Brain Meninges, Ventricles and CSF Lecture Objectives Describe the arrangement of the meninges and their relationship to brain and spinal cord. Explain the occurrence of epidural, subdural and subarachnoid
Brain Meninges, Ventricles and CSF Lecture Objectives Describe the arrangement of the meninges and their relationship to brain and spinal cord. Explain the occurrence of epidural, subdural and subarachnoid
Principles of Anatomy and Physiology
 Principles of Anatomy and Physiology 14 th Edition CHAPTER 14 The Brain and Cranial Nerves Introduction The purpose of the chapter is to: 1. Understand how the brain is organized, protected, and supplied
Principles of Anatomy and Physiology 14 th Edition CHAPTER 14 The Brain and Cranial Nerves Introduction The purpose of the chapter is to: 1. Understand how the brain is organized, protected, and supplied
