Effect of prone positioning in patients with acute respiratory distress syndrome: A meta-analysis
|
|
|
- Branden James
- 5 years ago
- Views:
Transcription
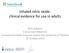
1 Review Articles Effect of prone positioning in patients with acute respiratory distress syndrome: A meta-analysis Abdullah H. Alsaghir, MD; Claudio M. Martin, MSc, MD, FRCPC Objective: To review the effectiveness of prone position as compared with supine position, with respect to mortality, improvement in oxygenation, number of days on mechanical ventilation, and ventilator-associated pneumonia. Data Source: PubMed, EMBASE, Cochrane database, and a manual review of article bibliographies. Study Selection: Randomized controlled trials comparing >6 hrs of prone position with supine position in adult patients with adult respiratory distress syndrome. Data Extraction: Two reviewers independently performed assessment of abstracts and study quality. Data were combined in a meta-analysis using random-effect models. Main Findings: Five studies were identified. We did not find any significant differences in intensive care unit mortality (three studies, 466 patients; odds ratio, 0.79; 95% confidence interval [CI], ), 28- to 30-day mortality (three studies, 1,231 patients; odds ratio, 0.95; 95% CI, ), and 90-day mortality (four studies, 1,271 patients; odds ratio, 0.99; 95% CI, ). However, prone position showed significant reduction in mortality in patients with higher illness severity (two studies, 113 patients; odds ratio, 0.29; 95% CI, ). Prone positioning also showed significant and persistent improvement in the PaO 2 /FIO 2 ratio in early (12 hrs to 2 days) (four studies, 866 patients; weighted mean difference, 51.5; 95% CI, ), intermediate (4 days) (three studies, 754 patients; weighted mean difference, 43.87; 95% CI, ), and late (10 days) period (four studies, 833 patients; weighted mean difference, 24.89; 95% CI, ). There were no significant differences in number of days on mechanical ventilation (two studies, 831 patients; weighted mean difference, 0.42 days; 95% CI, 1.56 to 0.72) or incidence of ventilator-associated pneumonia (three studies, 967 patients; weighted mean difference, 0.78%; 95% CI, ). Conclusion: Based on the results of this meta-analysis, prone position improves oxygenation in patients with adult respiratory distress syndrome, and in patients with higher illness severity, it also may reduce mortality. (Crit Care Med 2008; 36: ) KEY WORDS: mechanical ventilation; prone position; acute respiratory distress syndrome; meta-analysis; oxygenation; acute lung injury From the Division of Critical Care, Department of Medicine, Schulich School of Medicine and Dentistry, University of Western Ontario, London, Ontario, Canada (AHA, CMM); and London Health Sciences Centre, London, Ontario, Canada (CMM). The authors have not disclosed any potential conflicts of interest. For information regarding this article, cmartin1@uwo.ca Copyright 2007 by the Society of Critical Care Medicine and Lippincott Williams & Wilkins DOI: /01.CCM Acute respiratory distress syndrome (ARDS) is a diffuse heterogeneous lung disease that results in progressive hypoxemia because of ventilation/perfusion mismatching causing intrapulmonary shunt. It has diverse causes and is associated with high mortality and morbidity (1, 2). Application of high FIO 2 and positive end-expiratory pressure required to maintain oxygenation may induce more damage to the injured lungs, termed ventilator-induced lung injury, and contributes to increased morbidity and mortality (3). Mechanisms by which mechanical ventilation induces or augments lung injury include overstretching of the lung and repeated opening and closing of small airways (shear stress phenomena) (4 6). This ventilator-induced lung injury will manifest as diffuse alveolar damage (7 9), with release of cytokines and bacterial translocation (10). Patients with ARDS ventilated in the supine position develop atelectasis in the dependent regions of the lung (11). This may be due to lung edema, airway secretions, surfactant deficiency, and from cardiac and abdominal compression (12, 13). Perfusion to these regions is maintained, resulting in intrapulmonary shunt and severe hypoxemia. Since 1974, when Bryan (14) proposed prone position (PP) to improve oxygenation, many studies have demonstrated its effect on gas exchange (15 22). The mechanisms responsible for this improvement in oxygenation are not completely understood. It may recruit atelectatic regions and minimize ventilatorinduced lung injury when used early in the course of acute respiratory failure (23 25). Despite this improvement in oxygenation, studies with PP have not shown a clear survival benefit. Therefore, we performed a metaanalysis to compare the effectiveness of PP with supine position (SP) with respect to mortality, improvement in oxygenation, number of days on mechanical ventilation, and the incidence of ventilator-associated pneumonia (VAP). METHODS Design. A comprehensive literature search was performed in PubMed, EMBASE, Cochrane Library, by hand searching bibliographies of retrieved articles, and by contacting the authors of relevant articles. In the Cochrane Library, we searched both the Database of Systematic Reviews and the Cochrane Central Register of Controlled Trials. The following keywords were used: prone position combined with acute respiratory distress syndrome, acute lung injury, ARDS, ALI, or mechanical ventilation. 603
2 The search was confined to randomized controlled trials with human adults. The search was performed in November Two reviewers (AHA, CMM) independently selected the studies to be included in the review using the following inclusion criteria: adult mechanically ventilated intensive care unit (ICU) patients comparing PP and SP. PP had to be used for a minimum of 6 hrs. The study had to report at least one of the following outcomes: mortality, improvement in oxygenation, number of days receiving mechanical ventilation, and incidence of ventilatorassociated pneumonia. With respect to mortality, we extracted ICU mortality, mortality at 28 days, and mortality at 90 days. Because the earliest included study had reported a benefit in the subgroup with higher illness severity, we also extracted this information if possible. Oxygenation was assessed as the absolute change in the PaO 2 /FIO 2 ratio from baseline to early (12 hrs to 2 days), intermediate (day 4), and late (day 7 10) periods. If data were not available or could not be derived from the publication, we attempted to contact the corresponding author by . Both reviewers assessed the methodologic quality of each included trial based on the method described by Jadad et al (26). In particular, reviewers examined details of the randomization methods, using four ratings for quality of allocation concealment (27): 1) adequate concealment of the allocation; 2) uncertainty about adequate concealment of allocation; 3) allocation definitely not adequately concealed; 4) allocation concealment not used. Discrepancies in ratings were resolved through discussion between the reviewers. Data Analysis. All data were entered and analyzed using RevMan (Review Manager, version for Windows, Copenhagen, The Cochrane Collaboration, 2003). The synthesis of data were performed using a random effect model. For dichotomous outcomes, odds ratios (OR) were calculated. For continuous outcomes, weighted mean difference (WMD) was calculated. All effect measures are reported with 95% confidence intervals (CIs). To assess heterogeneity of treatment effects across studies, I 2 statistics were computed. I 2 measures the extent of inconsistency among the studies results, and the outcome is interpreted as a percentage of total variation across studies that are due to heterogeneity rather than chance (28). A value of 0% indicates that all variability in effect estimates is due to chance rather than to heterogeneity. Larger values show that most of the variability is due to heterogeneity rather than chance. Due to the small number of studies, we did not perform any analysis for possible publication bias. RESULTS From the literature search, 63 studies were identified. Five of these fulfilled the inclusion criteria and included a total of Figure 1. Literature search flow diagram. 1,316 patients (Gattinoni et al. [29], Guerin et al. [30], Mancebo et al. [31], Papazian et al. [32], Voggenreiter et al. [33]). The other studies were excluded for various reasons (Fig. 1). Four studies compared sessions of variable times of 6 hrs of PP with SP (29, 30, 31, 33). One study compared a single session of PP with SP in combination with high-frequency oscillation ventilation (32). The method of concealment for all included studies was ranked adequate (grade A) (Table 1). Two studies used central randomization (29, 33). Three studies performed concealment using sealed opaque envelopes (30 32). Treatment was not blinded due to the type of intervention. In one study (Guerin et al. [30]), 11 patients were excluded from the analysis (two participants were lost to followup, five patients due to secondary refusal to participate, three due to inclusion errors, and one had previously been enrolled in the study). Another study (Mancebo et al. [31]) excluded six patients (four patients lost to follow-up, and two patients had missing data). No patients were excluded from analysis in the other three studies (29, 32, 33). Guerin et al. (30) allowed patients randomized to SP to cross over to PP based on physiologic variables chosen at the time of study design. They analyzed these patients in the originally assigned group (intention to treat). Sample size varied from 39 to 780 patients in the included studies. Baseline characteristics of both groups in all the studies were not significantly different. Mortality. Three studies reported ICU mortality (29, 31, 32) (Table 1, Fig. 2). There was no significant difference in ICU mortality for those patients treated with PP vs. SP (pooled OR, 0.79; 95% CI, ). Three studies reported 28- to 30- day mortality (29, 30, 31). There were no significant differences in 28- to 30-day mortality (pooled OR, 0.95; 95% CI, ). Four studies examined 90-day mortality (29, 30, 31, 33). There were no significant differences in mortality between the groups (pooled OR, 0.99; 95% CI, ). In post hoc analysis, the studies by Gattinoni et al. (29) and Mancebo et al. 604
3 Table 1. Studies on prone positioning in acute respiratory distress syndrome Study Gattinoni et al. (29), 2001 Guerin et al. (30), 2004 Mancebo et al. (31), 2006 Papazian et al. (32), 2005 Voggenreiter et al. (33), 2005 Patients, n Quality a A A A A A Prone positioning Time after diagnosis Varied 24 hrs 24 hrs 24 hrs Varied Duration 7 hrs/day 8.6 hrs/day 20 hrs/day 12 hrs 11 hrs/day ICU mortality rate (%) SP 73/152 (48.0) 35/60 (58.3) 5/13 (38.5) PP 77/152 (50.7) 33/76 (43.4) 3/13 (23.1) 28- to 30-day mortality rate (%) SP 70/152 (46.1) 121/378 (32.0) 32/60 (53.3) PP 74/152 (48.7) 134/413 (32.4) 30/76 (39.5) 90-day mortality rate (%) SP 84/152 (55.3) 160/378 (42.3) 32/60 (53.3) 3/19 (15.8) PP 89/152 (58.6) 179/413 (43.3) 32/76 (42.1) 1/21 (4.8) Mortality rate in SAPS II 50 SP 16/33 (48.5) 9/11 (81.8) PP 9/47 (19.2) 15/22 (68.2) Early changes in oxygenation (SD) SP 27 (68.9) 10 (89.7) 4 (52.69) 37 (63.74) PP 38 (67.7) 86 (79.5) 101 (53.3) 65 (74.81) Intermediate changes in oxygenation (SD) SP 51 (71.38) 15 (84.5) 27.7 (78.9) PP 77 (71.79) 83 (73.54) 71 (75.5) Late changes in oxygenation (SD) SP 44.6 (68.2) 51 (66.98) 23 (90) 66.5 (89.1) PP 63 (66.8) 78 (72.86) 67 (76.64) 80.7 (77.3) Total ventilator days (SD) SP 14.1 (8.6) 33 (23) PP 13.7 (7.8) 30 (17) VAP rate (%) SP 91/378 (24.1) 9/60 (15) 17/19 (89.5) PP 85/413 (20.6) 14/76 (18.4) 13/21 (61.9) ICU, intensive care unit; SP, supine position; PP, prone position; SAPS II, Simplified Acute Physiology Score; VAP, ventilator-associated pneumonia. a Quality, allocation concealment was adequate (A), unclear (B), inadequate (C), or not used (D). (31) reported mortality for patients with SAPS II of 50. The study by Gattinoni et al. (29) showed a significant improvement in mortality at 10 days (19.4% for PP vs. 48.5% for SP [relative risk, 0.4; 95% CI, ]). The study by Mancebo et al. (31) found a nonsignificant improvement in ICU mortality in this subgroup, with 68% (15 of 22 patients) for PP vs. 82% (nine of 11 patients) for SP. The pooled results showed a significant decrease in mortality in this subgroup (OR, 0.29; 95% CI, ) (Fig. 3). Oxygenation. Four studies reported changes in oxygenation (PaO 2 /FIO 2 ratio) during the early period (30 33). The pooled results showed a statistically significant WMD of 51.5 (95% CI, ) favoring the PP group (Fig. 4). Three studies reported oxygenation changes in the intermediate period (30, 31, 33). There was a significant improvement in oxygenation favoring the PP group, with a pooled WMD of (95% CI, ) (Fig. 4). Four studies reported oxygenation changes in the late period (29, 30, 31, 33). The pooled results showed a significant improvement in oxygenation, with a WMD of (95% CI, ) favoring the PP group (Fig. 4, Table 1). Total Ventilator Days. Two studies reported the total number of days on ventilator (30, 33) (Table 1). There was no significant difference in length of ventilator days between PP and SP groups (pooled WMD, 0.42 days; 95% CI, 1.56 to 0.72) (Fig. 5). Incidence of VAP. Three studies reported VAP as a complication (30, 31, 33) (Table 1). There was no significant difference in the incidence of VAP in PP groups as compared with SP groups, with an overall WMD of 0.78% (95% CI, ) (Fig. 6). DISCUSSION In this systematic review and metaanalysis, we identified five randomized controlled studies that assessed the effect of PP as compared with SP on mortality and improvement in oxygenation in patients with ARDS. Overall, PP did not reduce mortality significantly, but it does improve oxygenation. Within this population, PP may have a positive effect on mortality in patients with higher illness severity. Individually, each of these studies had some limitations, primarily related to sample size and power. Two studies were stopped prematurely because the caregivers were unwilling to continue randomizing patients to PP (29) or due to decreased motivation of investigators and limited funding (31), and two studies had small sample sizes (32, 33). One study allowed crossover of patients from SP to PP (30), although they did use an intention-to-treat analysis. Two studies (29, 30) applied higher tidal volumes than is current practice because these studies were done before publication of the ARDSNet study (34). Although our review did not find an overall improvement in survival, we did find that the subgroup of patients with higher severity of illness had reduced mortality in the PP group as compared 605
4 Figure 2. Comparison of prone position (PP) and supine position (SP) for intensive care unit (ICU) (top), 28- to 30-day (middle), and 90-day (lower) mortality rates. Data are shown for each study for prone and supine groups as n (number of deaths) over N (number in group). ARDS, acute respiratory distress syndrome; OR, odds ratio; CI, confidence interval. Figure 3. Post hoc analysis of comparison of prone position (PP) and supine position (SP) regarding mortality of subgroup with Simplified Acute Physiology Score (SAPS) II of 50. ARDS, acute respiratory distress syndrome; Pts, patients; OR, odds ratio; CI, confidence interval. 606
5 Figure 4. Comparison of prone position (PP) and supine position (SP) for the oxygenation improvement in early (top), intermediate (middle), and late (back) periods. In contrast to the other figures with rates, the direction for an improvement in oxygenation with supine position favored is to the right (positive values). ARDS, acute respiratory distress syndrome; WMD, weighted mean difference; CI, confidence interval. Figure 5. Comparison of prone position (PP) and supine position (SP) regarding number of days on mechanical ventilation (MV). ARDS, acute respiratory distress syndrome; WMD, weighted mean difference; CI, confidence interval. with the SP group (OR, 0.29; 95% CI, ) (29, 31). Limitations of this observation are that it is a subgroup analysis, with incomplete data available to confirm similarity of the PP and SP subgroups at baseline. Also, mortality was reported at 10 days for one study and at ICU separation for the other study. Other issues related to the validity of this meta-analysis relate to the possible publication bias and heterogeneity between studies. Our literature review was 607
6 Figure 6. Comparison of prone position (PP) and supine position (SP) regarding incidence of ventilator-associated pneumonia (VAP). ARDS, acute respiratory distress syndrome; WMD, weighted mean difference; CI, confidence interval. extensive, but the number of studies included is too small to examine using funnel plots to detect publication bias. We used random-effects models to minimize the effect of study heterogeneity, which was not statistically significant in the analyses but may be present, as indicated by a high I 2 statistic for ICU mortality (40%) and by early (90%) and intermediate (72%) changes in oxygenation. There was clinical heterogeneity in the studies that might account for this statistical heterogeneity and could have affected the results. Three studies applied PP for short periods, ranging from 7 to 11 hrs/day and for up to 10 days (29, 30, 33), and another study used a single 12-hr period of prone ventilation (32). It has been shown in a nonrandomized study that PP applied for longer periods of about 20-hrs has persistent improvement in oxygenation (35), as compared with other studies that used PP for 6 12 hrs (36, 37). One study was limited to ARDS in trauma patients (33). The cause of ARDS may contribute to the results because the response to PP is probably better in secondary causes of ARDS because of diffuse distribution of densities and atelectasis that make it more responsive to recruitment (35, 38 40). Although, we did not examine the interval between onset of ARDS and use of PP, the optimal response and beneficial effect of PP may occur during the early edematous phase of ARDS, when atelectasis and lung edema predominate (41). All the studies in our review showed significant improvement in oxygenation during the early period of randomization but with variable persistence in individual studies. Our pooled results demonstrated a statistically significant improvement in oxygenation up to 10 days, although the clinical relevance is questionable because the WMD (the absolute change in PaO 2 /FIO 2 ) decreased from 51 at the early period to 25 at 10 days. VAP continues to be the most common nosocomial infection in the ICU (42 44). Patients who acquire VAP have worse outcomes and have longer ICU and hospital stays (42 46). Many of the human and experimental studies showed a reduced incidence of VAP with PP (47, 48). This could be due to better drainage of airway secretions, reopening atelectatic units in the dorsal region of the lungs, which decreases the favorable media for infection, and decreased bacterial translocation (49). However, this metaanalysis did not show any significant changes in the incidence of VAP with PP. CONCLUSION This systematic review and metaanalysis showed beneficial effects of PP on oxygenation in patients with ARDS. Despite the improvement in oxygenation, PP did not improve survival, except perhaps in the more severely ill patients. Because our review of these studies did not identify any major adverse effects of PP, and it is a relatively simple and inexpensive intervention, it should be considered early in the management of patients with ARDS and high illness severity. However, definitive recommendations require that this hypothesis be examined in a properly designed prospective trial. If the pooled OR of 0.29 in this subgroup, with a combined mortality of about 60%, were used to plan a randomized trial, the sample size required is 52 patients in each group. REFERENCES 1. Milberg JA, Davis DR, Steinberg KP, et al: Improved survival of patients with acute respiratory distress syndrome: JAMA 1995; 273: Lewandowski K, Metz J, Deutschmann C, et al: Incidence, severity, and mortality of acute respiratory distress syndrome. Am J Respir Crit Care Med 1995; 151: Mink SN, Light RB, Cooligan T: Effect of PEEP on gas exchange and pulmonary perfusion in canine lobar pneumonia. J Appl Physiol 1981; 50: Webb HH, Tierney DF: Experimental pulmonary edema due to intermittent positive pressure ventilation with high inflation pressures: Protection by positive end-expiratory pressure. Am Rev Respir Dis 1974; 110: Benito S, Lemaire F: Pulmonary pressurevolume relationship in acute respiratory distress syndrome in adults: Role of positive and expiratory pressure. J Crit Care 1990; 5: Gajic O, Lee J, Doerr CH, et al: Ventilatorinduced cell wounding and repair in the intact lung. Am J Respir Crit Care Med 2003; 167: Dreyfuss D, Saumon G: Ventilator induced lung injury: Lessons from experimental studies. Am J Respir Crit Care Med 1998; 157: Dreyfuss D, Soler P, Bassett G, et al: High inflation pressure pulmonary edema. Am Rev Respir Dis 1988; 137: Muscedere JG, Mullen JB, Gan K, et al: Tidal ventilation at low airway pressures can augment lung injury. Am J Respir Crit Care Med 1994; 149: Nahum A, Hoyt J, Schmitz L, et al: Effect of mechanical ventilation strategy on dissemination of intratracheally instilled Escherichia coli in dogs. Crit Care Med 1997; 25: Gattinoni L, Pelosi P, Vitale G, et al: Body position changes redistribute lung computedtomographic density in patients with acute respiratory failure. Anesthesiology 1991; 74: Rouby JJ, Constantin JM, Roberto de A Girardi C, et al: Mechanical ventilation in patients with acute respiratory distress syndrome. Anesthesiology 2004; 101:
7 13. Hubmayr RD: Perspective on lung injury and recruitment: A sceptical look at the opening and collapse story. Am J Respir Crit Care Med 2002; 165: Bryan A: Comments of a devil s advocate. Am Rev Respir Dis 1974; 110: Langer M, Mascheroni D, Marcolin R, et al: The prone position in ARDS patients: A clinical study. Chest 1988; 94: Chatte G, Sab JM, Dubois JM, et al: Prone position in mechanically ventilated patient with severe acute respiratory failure. Am J Respir Crit Care Med 1997; 155: Pappert D, Rossaint R, Slama K, et al: Influence of positioning on ventilation-perfusion relationship in severe adult respiratory distress syndrome. Chest 1994; 106: Blanch L, Mancebo J, Perez M, et al: Shortterm effects of prone position in critically ill patients with acute respiratory distress syndrome. Intensive Care Med 1997; 23: Mure M, Martling C, Lindahl S: Dramatic effect on oxygenation in patients with severe acute lung insufficiency treated in prone position. Crit Care Med 1997; 25: Servillo G, Roupie E, De Robetis E, et al: Effects of ventilation in ventral decubitus position on respiratory mechanics in adult respiratory distress syndrome. Intensive Care Med 1997; 23: Jolliet P, Bulpa P, Chevrolet J: Effects of the prone position on gas exchange and hemodynamics in severe acute respiratory distress syndrome. Crit Care Med 1998; 26: Nakos G, Tsangaris I, Kostanti E, et al: Effect of the prone position on patients with hydrostatic pulmonary edema compared with patients with acute respiratory distress syndrome and pulmonary fibrosis. Am J Respir Crit Care Med 2000; 161: Pelosi P, Brazzi L, Gattinoni L: Prone position in acute respiratory distress syndrome. Eur Respir J 2002; 20: Broccard A, Shapiro RS, Schmitz LL, et al: Prone positioning attenuates and redistributes ventilator-induced lung injury in dogs. Crit Care Med 2000; 28: Broccard A, Shapiro RS, Schmitz LL, et al: Influence of prone position on the extent and distribution of lung injury in a high tidal volume oleic acid model of acute respiratory distress syndrome. Crit Care Med 1997; 25: Jadad AR, Moore A, Carroll A, et al: Assessing the quality of reports of randomized clinical trials: Is blinding necessary? Control Clin Trials 1996; 17: Higgins JPT, Green S (Eds): Cochrane Handbook for Systematic Review of Interventions [updated March 2005]: The Cochrane Library. Chichester, UK, Willy, Higgins JPT, Thompson SG, Deeks JJ, et al: Measuring inconsistency in meta-analysis. BMJ 2003; 327: Gattinoni L, Tognoni G, Pesenti A, et al: Effects of prone positioning on the survival of patients with acute respiratory failure. N Engl J Med 2001; 345: Guerin C, Gaillard S, Lemasson S, et al: Effects of systematic prone positioning in hypoxemic acute respiratory failure: A randomized controlled trial. JAMA 2004; 292: Mancebo J, Fermandez R, Blanch L, et al: a Multicenter trial of prolonged prone ventilation in severe acute respiratory distress syndrome. Am J Respir Crit Care Med 2006; 173: Papazian L, Gainnier M, Marin V, et al: Comparison of prone positioning and high frequency oscillatory ventilation in patients with acute respiratory distress syndrome. Crit Care Med 2005; 33: Voggenreiter G, Aufmakolk M, Stiletto RJ, et al: Prone positioning improves oxygenation in post-traumatic lung injury: A prospective randomized trial. J Trauma 2005; 59: Ventilation with lower tidal volumes as compared with traditional tidal volumes for acute lung injury and the acute respiratory distress syndrome: The Acute Respiratory Distress Syndrome Network. N Engl J Med 2000; 342: Fridrich P, Krafft P, Hochlcuthner H, et al: The effects of long-term prone positioning in patients with trauma-induced adult respiratory distress syndrome. Anesth Analg 1996; 83: Papazian L, Paladini MH, Bergeon F, et al: Is a short trial of prone positioning sufficient to predict the improvement in oxygenation in patients with acute respiratory distress syndrome?. Intensive Care Med 2001; 27: Jolliet P, Bulpa P, Ritz M, et al: Additive beneficial effects of the prone position, nitric oxide, and almitrine bismesylate on gas exchange and oxygen transport in acute respiratory distress syndrome. Crit Care Med 1997; 25: Stocker R, Neff T, Stein S, et al: Prone positioning and low-volume pressure-limited ventilation improve survival in patients with severe ARDS. Chest 1997; 111: Guerin C, Badet M, Rosselli S, et al: Effects of prone position on alveolar recruitment and oxygenation in acute lung injury. Intensive Care Med 1999; 25: Goodman LR, Fumagalli R, Tagliabue P, et al: Adult respiratory distress syndrome due to pulmonary and extrapulmonary causes: CT, clinical and functional correlation. Radiology 1999; 213: Lamm WJE, Graham MM, Albert RK: Mechanism by which the prone position improves oxygenation in acute lung injury. Am J Respir Crit Care Med 1994; 150: Rello J, Ollendrof DA, Oster G, et al: Epidemiology and outcomes of ventilator-associated pneumonia in a large US database. Chest 2000; 122: Chastre J, Fagon JY: Ventilator-associated pneumonia. Am J Respir Crit Care Med 2002; 165: American Thoracic Society, Infectious Disease Society of America: Guidelines for the management of adults with hospital-acquired, ventilator-associated, and healthcareassociated pneumonia. Am J Respir Crit Care Med 2005; 171: Warren DK, Shukla SJ, Olsen MA, et al: Outcome and attributable cost of ventilatorassociated pneumonia among intensive care unit patients in a suburban medical center. Crit Care Med 2003; 31: Craven DE, De Rosa FG, Thornton D: Nosocomial pneumonia: Emerging concepts in diagnosis, management, and prophylaxis. Curr Opin Crit Care 2002; 8: Marquette CH, Wermert D, Wallet F, et al: Characterization of an animal model of ventilator-acquired pneumonia. Chest 1999; 115: Beuret P, Carton MJ, Nourdine K, et al: Prone position as a prevention of lung injury in comatose patients: A prospective, randomized, controlled study. Intensive Care Med 2002; 28: Van Kamm AH, Lachmann RA, Hertinge E, et al: Reducing atelectasis attenuates bacterial growth and translocation in experimental pneumonia. Am J Respir Crit Care Med 2004; 169:
The use of proning in the management of Acute Respiratory Distress Syndrome
 Case 3 The use of proning in the management of Acute Respiratory Distress Syndrome Clinical Problem This expanded case summary has been chosen to explore the rationale and evidence behind the use of proning
Case 3 The use of proning in the management of Acute Respiratory Distress Syndrome Clinical Problem This expanded case summary has been chosen to explore the rationale and evidence behind the use of proning
Prone positioning of patients with Acute Respiratory Distress Syndrome (ARDS)
 EVIDENCE CENTRE EVIDENCE REPORT Series 2002: Intervention Prone positioning of patients with Acute Respiratory Distress Syndrome (ARDS) Nicki Jackson May 2002 1 Centre for Clinical Effectiveness Monash
EVIDENCE CENTRE EVIDENCE REPORT Series 2002: Intervention Prone positioning of patients with Acute Respiratory Distress Syndrome (ARDS) Nicki Jackson May 2002 1 Centre for Clinical Effectiveness Monash
Management of refractory ARDS. Saurabh maji
 Management of refractory ARDS Saurabh maji Refractory hypoxemia as PaO2/FIO2 is less than 100 mm Hg, inability to keep plateau pressure below 30 cm H2O despite a VT of 4 ml/kg development of barotrauma
Management of refractory ARDS Saurabh maji Refractory hypoxemia as PaO2/FIO2 is less than 100 mm Hg, inability to keep plateau pressure below 30 cm H2O despite a VT of 4 ml/kg development of barotrauma
Landmark articles on ventilation
 Landmark articles on ventilation Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity ARDS AECC DEFINITION-1994 ALI Acute onset Bilateral chest infiltrates PCWP
Landmark articles on ventilation Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity ARDS AECC DEFINITION-1994 ALI Acute onset Bilateral chest infiltrates PCWP
The new ARDS definitions: what does it mean?
 The new ARDS definitions: what does it mean? Richard Beale 7 th September 2012 METHODS ESICM convened an international panel of experts, with representation of ATS and SCCM The objectives were to update
The new ARDS definitions: what does it mean? Richard Beale 7 th September 2012 METHODS ESICM convened an international panel of experts, with representation of ATS and SCCM The objectives were to update
Oxygenation improves during the first 8 h of extended-duration prone positioning in patients with respiratory failure: a retrospective study
 Miyamoto et al. Journal of Intensive Care 2014, 2:52 RESEARCH Open Access Oxygenation improves during the first 8 h of extended-duration prone positioning in patients with respiratory failure: a retrospective
Miyamoto et al. Journal of Intensive Care 2014, 2:52 RESEARCH Open Access Oxygenation improves during the first 8 h of extended-duration prone positioning in patients with respiratory failure: a retrospective
Sub-category: Intensive Care for Respiratory Distress
 Course n : Course 3 Title: RESPIRATORY PHYSIOLOGY, PHYSICS AND PATHOLOGY IN RELATION TO ANAESTHESIA AND INTENSIVE CARE Sub-category: Intensive Care for Respiratory Distress Topic: Acute Respiratory Distress
Course n : Course 3 Title: RESPIRATORY PHYSIOLOGY, PHYSICS AND PATHOLOGY IN RELATION TO ANAESTHESIA AND INTENSIVE CARE Sub-category: Intensive Care for Respiratory Distress Topic: Acute Respiratory Distress
What s New About Proning?
 1 What s New About Proning? J. Brady Scott, MSc, RRT-ACCS, AE-C, FAARC Director of Clinical Education and Assistant Professor Department of Cardiopulmonary Sciences Division of Respiratory Care Rush University
1 What s New About Proning? J. Brady Scott, MSc, RRT-ACCS, AE-C, FAARC Director of Clinical Education and Assistant Professor Department of Cardiopulmonary Sciences Division of Respiratory Care Rush University
Protective ventilation for ALL patients
 Protective ventilation for ALL patients PAOLO PELOSI, MD, FERS Department of Surgical Sciences and Integrated Diagnostics (DISC), San Martino Policlinico Hospital IRCCS for Oncology, University of Genoa,
Protective ventilation for ALL patients PAOLO PELOSI, MD, FERS Department of Surgical Sciences and Integrated Diagnostics (DISC), San Martino Policlinico Hospital IRCCS for Oncology, University of Genoa,
Clinical Commentary. The Pragmatics of Prone Positioning. Erica Messerole, Pam Peine, Sue Wittkopp, John J. Marini, and Richard K.
 Clinical Commentary The Pragmatics of Prone Positioning Erica Messerole, Pam Peine, Sue Wittkopp, John J. Marini, and Richard K. Albert Departments of Medicine and Nursing, Regions Hospital and University
Clinical Commentary The Pragmatics of Prone Positioning Erica Messerole, Pam Peine, Sue Wittkopp, John J. Marini, and Richard K. Albert Departments of Medicine and Nursing, Regions Hospital and University
Effect of peak inspiratory pressure on the development. of postoperative pulmonary complications.
 Effect of peak inspiratory pressure on the development of postoperative pulmonary complications in mechanically ventilated adult surgical patients: a systematic review protocol Chelsa Wamsley Donald Missel
Effect of peak inspiratory pressure on the development of postoperative pulmonary complications in mechanically ventilated adult surgical patients: a systematic review protocol Chelsa Wamsley Donald Missel
The Prone Position Eliminates Compression of the Lungs by the Heart
 The Prone Position Eliminates Compression of the Lungs by the Heart RICHARD K. ALBERT and ROLF D. HUBMAYR Medical Service, Denver Health Medical Center, and Department of Medicine, University of Colorado
The Prone Position Eliminates Compression of the Lungs by the Heart RICHARD K. ALBERT and ROLF D. HUBMAYR Medical Service, Denver Health Medical Center, and Department of Medicine, University of Colorado
Steroids in ARDS: if, when, how much? John Fowler, MD, FACEP Dept. of Emergency Medicine Kent Hospital, İzmir, Türkiye
 Steroids in ARDS: if, when, how much? John Fowler, MD, FACEP Dept. of Emergency Medicine Kent Hospital, İzmir, Türkiye Steroids in ARDS: conclusion Give low-dose steroids if indicated for another problem
Steroids in ARDS: if, when, how much? John Fowler, MD, FACEP Dept. of Emergency Medicine Kent Hospital, İzmir, Türkiye Steroids in ARDS: conclusion Give low-dose steroids if indicated for another problem
Lesson 11, Volume 14Which Developments in Mechanical Ventilation Will Outlast the Next Decade?
 Lesson 11, Volume 14Which Developments in Mechanical Ventilation Will Outlast the Next Decade? By Robert M. Kacmarek, PhD, RRT, FCCP Click to go to Poststudy Questions Information on Submitting Answers
Lesson 11, Volume 14Which Developments in Mechanical Ventilation Will Outlast the Next Decade? By Robert M. Kacmarek, PhD, RRT, FCCP Click to go to Poststudy Questions Information on Submitting Answers
Does proning patients with refractory hypoxaemia improve mortality?
 Does proning patients with refractory hypoxaemia improve mortality? Clinical problem and domain I selected this case because although this was the second patient we had proned in our unit within a week,
Does proning patients with refractory hypoxaemia improve mortality? Clinical problem and domain I selected this case because although this was the second patient we had proned in our unit within a week,
Back to the Future: Updated Guidelines for Evaluation and Management of Adrenal Insufficiency in the Critically Ill
 Back to the Future: Updated Guidelines for Evaluation and Management of Adrenal Insufficiency in the Critically Ill Joe Palumbo PGY-2 Critical Care Pharmacy Resident Buffalo General Medical Center Disclosures
Back to the Future: Updated Guidelines for Evaluation and Management of Adrenal Insufficiency in the Critically Ill Joe Palumbo PGY-2 Critical Care Pharmacy Resident Buffalo General Medical Center Disclosures
Short-term effects of prone positioning on oxygenation of pediatric patients submitted to mechanical ventilation
 0021-7557/01/77-05/361 Jornal de Pediatria Copyright 2001 by Sociedade Brasileira de Pediatria Jornal de Pediatria - Vol. 77, Nº5, 2001 361 ORIGINAL ARTICLE Short-term effects of prone positioning on oxygenation
0021-7557/01/77-05/361 Jornal de Pediatria Copyright 2001 by Sociedade Brasileira de Pediatria Jornal de Pediatria - Vol. 77, Nº5, 2001 361 ORIGINAL ARTICLE Short-term effects of prone positioning on oxygenation
Application of Lung Protective Ventilation MUST Begin Immediately After Intubation
 Conflict of Interest Disclosure Robert M Kacmarek Managing Severe Hypoxemia!" 9-28-17 FOCUS Bob Kacmarek PhD, RRT Massachusetts General Hospital, Harvard Medical School, Boston, Massachusetts I disclose
Conflict of Interest Disclosure Robert M Kacmarek Managing Severe Hypoxemia!" 9-28-17 FOCUS Bob Kacmarek PhD, RRT Massachusetts General Hospital, Harvard Medical School, Boston, Massachusetts I disclose
Prone positioning reduces mortality from acute respiratory distress syndrome in the low tidal volume era: a meta-analysis
 Intensive Care Med (2014) 40:332 341 DOI 10.1007/s00134-013-3194-3 SYSTEMATIC REVIEW Jeremy R. Beitler Shahzad Shaefi Sydney B. Montesi Amy Devlin Stephen H. Loring Daniel Talmor Atul Malhotra Prone positioning
Intensive Care Med (2014) 40:332 341 DOI 10.1007/s00134-013-3194-3 SYSTEMATIC REVIEW Jeremy R. Beitler Shahzad Shaefi Sydney B. Montesi Amy Devlin Stephen H. Loring Daniel Talmor Atul Malhotra Prone positioning
ARDS and Lung Protection
 ARDS and Lung Protection Kristina Sullivan, MD Associate Professor University of California, San Francisco Department of Anesthesia and Perioperative Care Division of Critical Care Medicine Overview Low
ARDS and Lung Protection Kristina Sullivan, MD Associate Professor University of California, San Francisco Department of Anesthesia and Perioperative Care Division of Critical Care Medicine Overview Low
Recruitment Maneuvers and Higher PEEP, the So-Called Open Lung Concept, in Patients with ARDS
 Zee and Gommers Critical Care (2019) 23:73 https://doi.org/10.1186/s13054-019-2365-1 REVIEW Recruitment Maneuvers and Higher PEEP, the So-Called Open Lung Concept, in Patients with ARDS Philip van der
Zee and Gommers Critical Care (2019) 23:73 https://doi.org/10.1186/s13054-019-2365-1 REVIEW Recruitment Maneuvers and Higher PEEP, the So-Called Open Lung Concept, in Patients with ARDS Philip van der
Prone Position in ARDS
 Prone Position in ARDS Rich Kallet MS RRT FAARC, FCCM Respiratory Care Services San Francisco General Hospital University of California, San Francisco, Case Study A 39 yo F admitted to SFGH TICU s/p hanging,
Prone Position in ARDS Rich Kallet MS RRT FAARC, FCCM Respiratory Care Services San Francisco General Hospital University of California, San Francisco, Case Study A 39 yo F admitted to SFGH TICU s/p hanging,
Lung Recruitment Strategies in Anesthesia
 Lung Recruitment Strategies in Anesthesia Intraoperative ventilatory management to prevent Post-operative Pulmonary Complications Kook-Hyun Lee, MD, PhD Department of Anesthesiology Seoul National University
Lung Recruitment Strategies in Anesthesia Intraoperative ventilatory management to prevent Post-operative Pulmonary Complications Kook-Hyun Lee, MD, PhD Department of Anesthesiology Seoul National University
Breathing life into new therapies: Updates on treatment for severe respiratory failure. Whitney Gannon, MSN ACNP-BC
 Breathing life into new therapies: Updates on treatment for severe respiratory failure Whitney Gannon, MSN ACNP-BC Overview Definition of ARDS Clinical signs and symptoms Causes Pathophysiology Management
Breathing life into new therapies: Updates on treatment for severe respiratory failure Whitney Gannon, MSN ACNP-BC Overview Definition of ARDS Clinical signs and symptoms Causes Pathophysiology Management
ECMO for Severe Hypoxemic Respiratory Failure: Pro-Con Debate. Carolyn Calfee, MD MAS Mark Eisner, MD MPH
 ECMO for Severe Hypoxemic Respiratory Failure: Pro-Con Debate Carolyn Calfee, MD MAS Mark Eisner, MD MPH June 3, 2010 Case Presentation Setting: Community hospital, November 2009 29 year old woman with
ECMO for Severe Hypoxemic Respiratory Failure: Pro-Con Debate Carolyn Calfee, MD MAS Mark Eisner, MD MPH June 3, 2010 Case Presentation Setting: Community hospital, November 2009 29 year old woman with
Difficult Ventilation in ARDS Patients
 Thank you for viewing this presentation. We would like to remind you that this material is the property of the author. It is provided to you by the ERS for your personal use only, as submitted by the author.
Thank you for viewing this presentation. We would like to remind you that this material is the property of the author. It is provided to you by the ERS for your personal use only, as submitted by the author.
ACUTE RESPIRATORY DISTRESS SYNDROME
 ACUTE RESPIRATORY DISTRESS SYNDROME Angel Coz MD, FCCP, DCE Assistant Professor of Medicine UCSF Fresno November 4, 2017 No disclosures OBJECTIVES Identify current trends and risk factors of ARDS Describe
ACUTE RESPIRATORY DISTRESS SYNDROME Angel Coz MD, FCCP, DCE Assistant Professor of Medicine UCSF Fresno November 4, 2017 No disclosures OBJECTIVES Identify current trends and risk factors of ARDS Describe
Acute lung injury (ALI) and acute respiratory distress
 . 238. Prone positioning ventilation for treatment of acute lung injury and acute respiratory distress syndrome LAN Mei-juan 兰美娟 and 1 HE Xiao-di 何晓娣 Patients who are diagnosed with acute lung injury/acute
. 238. Prone positioning ventilation for treatment of acute lung injury and acute respiratory distress syndrome LAN Mei-juan 兰美娟 and 1 HE Xiao-di 何晓娣 Patients who are diagnosed with acute lung injury/acute
Inhaled nitric oxide: clinical evidence for use in adults
 Inhaled nitric oxide: clinical evidence for use in adults Neill Adhikari Critical Care Medicine Sunnybrook Health Sciences Centre and University of Toronto 31 October 2014 Conflict of interest Ikaria provided
Inhaled nitric oxide: clinical evidence for use in adults Neill Adhikari Critical Care Medicine Sunnybrook Health Sciences Centre and University of Toronto 31 October 2014 Conflict of interest Ikaria provided
Research. Sachin Sud MD, Maneesh Sud BSc, Jan O. Friedrich MD DPhil, Neill K.J. Adhikari MDCM MSc CMAJ 2008;178(9):
 Effect of mechanical ventilation in the prone position on clinical outcomes in patients with acute hypoxemic respiratory failure: a systematic review and meta-analysis Sachin Sud MD, Maneesh Sud BSc, Jan
Effect of mechanical ventilation in the prone position on clinical outcomes in patients with acute hypoxemic respiratory failure: a systematic review and meta-analysis Sachin Sud MD, Maneesh Sud BSc, Jan
New Surveillance Definitions for VAP
 New Surveillance Definitions for VAP 2012 Critical Care Canada Forum Toronto Dr. John Muscedere Associate Professor of Medicine, Queen s University Kingston, Ontario Presenter Disclosure Dr. J. G. Muscedere
New Surveillance Definitions for VAP 2012 Critical Care Canada Forum Toronto Dr. John Muscedere Associate Professor of Medicine, Queen s University Kingston, Ontario Presenter Disclosure Dr. J. G. Muscedere
Efficacy and safety of intrapulmonary percussive ventilation superimposed on conventional ventilation in obese patients with compression atelectasis
 Journal of Critical Care (2006) 21, 328 332 Efficacy and safety of intrapulmonary percussive ventilation superimposed on conventional ventilation in obese patients with compression atelectasis Ryosuke
Journal of Critical Care (2006) 21, 328 332 Efficacy and safety of intrapulmonary percussive ventilation superimposed on conventional ventilation in obese patients with compression atelectasis Ryosuke
Pulmonary & Extra-pulmonary ARDS: FIZZ or FUSS?
 Pulmonary & Extra-pulmonary ARDS: FIZZ or FUSS? Dr. Rajagopala Srinivas Senior Resident, Dept. Pulmonary Medicine, PGIMER, Chandigarh. The beginning.. "The etiology of this respiratory distress syndrome
Pulmonary & Extra-pulmonary ARDS: FIZZ or FUSS? Dr. Rajagopala Srinivas Senior Resident, Dept. Pulmonary Medicine, PGIMER, Chandigarh. The beginning.. "The etiology of this respiratory distress syndrome
11 th Annual Congress Turkish Thoracic Society. Mechanical Ventilation in Acute Hypoxemic Respiratory Failure
 11 th Annual Congress Turkish Thoracic Society Mechanical Ventilation in Acute Hypoxemic Respiratory Failure Lluis Blanch MD PhD Senior Critical Care Center Scientific Director Corporació Parc Taulí Universitat
11 th Annual Congress Turkish Thoracic Society Mechanical Ventilation in Acute Hypoxemic Respiratory Failure Lluis Blanch MD PhD Senior Critical Care Center Scientific Director Corporació Parc Taulí Universitat
Prone Positioning in Severe Acute Respiratory Distress Syndrome
 Prone Positioning in Severe Acute Respiratory Distress Syndrome Claude Guérin, M.D., Ph.D., Jean Reignier, M.D., Ph.D., Jean-Christophe Richard, M.D., Ph.D., Pascal Beuret, M.D., Arnaud Gacouin, M.D.,
Prone Positioning in Severe Acute Respiratory Distress Syndrome Claude Guérin, M.D., Ph.D., Jean Reignier, M.D., Ph.D., Jean-Christophe Richard, M.D., Ph.D., Pascal Beuret, M.D., Arnaud Gacouin, M.D.,
How the Knowledge Proceeds in Intensive Care: the ARDS Example
 How the Knowledge Proceeds in Intensive Care: the ARDS Example 2016, Antalya Luciano Gattinoni, MD, FRCP Georg-August-Universität Göttingen Germany INDUCTION: From particular (application) to general (law/theory)
How the Knowledge Proceeds in Intensive Care: the ARDS Example 2016, Antalya Luciano Gattinoni, MD, FRCP Georg-August-Universität Göttingen Germany INDUCTION: From particular (application) to general (law/theory)
Ventilatory Management of ARDS. Alexei Ortiz Milan; MD, MSc
 Ventilatory Management of ARDS Alexei Ortiz Milan; MD, MSc 2017 Outline Ventilatory management of ARDS Protected Ventilatory Strategy Use of NMB Selection of PEEP Driving pressure Lung Recruitment Prone
Ventilatory Management of ARDS Alexei Ortiz Milan; MD, MSc 2017 Outline Ventilatory management of ARDS Protected Ventilatory Strategy Use of NMB Selection of PEEP Driving pressure Lung Recruitment Prone
ARDS: an update 6 th March A. Hakeem Al Hashim, MD, FRCP SQUH
 ARDS: an update 6 th March 2017 A. Hakeem Al Hashim, MD, FRCP SQUH 30M, previously healthy Hx: 1 week dry cough Gradually worsening SOB No travel Hx Case BP 130/70, HR 100/min ph 7.29 pco2 35 po2 50 HCO3
ARDS: an update 6 th March 2017 A. Hakeem Al Hashim, MD, FRCP SQUH 30M, previously healthy Hx: 1 week dry cough Gradually worsening SOB No travel Hx Case BP 130/70, HR 100/min ph 7.29 pco2 35 po2 50 HCO3
7/4/2015. diffuse lung injury resulting in noncardiogenic pulmonary edema due to increase in capillary permeability
 Leanna R. Miller, RN, MN, CCRN-CMC, PCCN-CSC, CEN, CNRN, CMSRN, NP Education Specialist LRM Consulting Nashville, TN Objectives Identify the 5 criteria for the diagnosis of ARDS. Discuss the common etiologies
Leanna R. Miller, RN, MN, CCRN-CMC, PCCN-CSC, CEN, CNRN, CMSRN, NP Education Specialist LRM Consulting Nashville, TN Objectives Identify the 5 criteria for the diagnosis of ARDS. Discuss the common etiologies
The ARDS is characterized by increased permeability. Incidence of ARDS in an Adult Population of Northeast Ohio*
 Incidence of ARDS in an Adult Population of Northeast Ohio* Alejandro C. Arroliga, MD, FCCP; Ziad W. Ghamra, MD; Alejandro Perez Trepichio, MD; Patricia Perez Trepichio, RRT; John J. Komara Jr., BA, RRT;
Incidence of ARDS in an Adult Population of Northeast Ohio* Alejandro C. Arroliga, MD, FCCP; Ziad W. Ghamra, MD; Alejandro Perez Trepichio, MD; Patricia Perez Trepichio, RRT; John J. Komara Jr., BA, RRT;
Ventilator ECMO Interactions
 Ventilator ECMO Interactions Lorenzo Del Sorbo, MD CCCF Toronto, October 2 nd 2017 Disclosure Relevant relationships with commercial entities: none Potential for conflicts within this presentation: none
Ventilator ECMO Interactions Lorenzo Del Sorbo, MD CCCF Toronto, October 2 nd 2017 Disclosure Relevant relationships with commercial entities: none Potential for conflicts within this presentation: none
Noninvasive Ventilation: Non-COPD Applications
 Noninvasive Ventilation: Non-COPD Applications NONINVASIVE MECHANICAL VENTILATION Why Noninvasive Ventilation? Avoids upper A respiratory airway trauma system lacerations, protective hemorrhage strategy
Noninvasive Ventilation: Non-COPD Applications NONINVASIVE MECHANICAL VENTILATION Why Noninvasive Ventilation? Avoids upper A respiratory airway trauma system lacerations, protective hemorrhage strategy
How ARDS should be treated in 2017
 How ARDS should be treated in 2017 2017, Ostrava Luciano Gattinoni, MD, FRCP Georg-August-Universität Göttingen Germany ARDS 1. Keep the patient alive respiration circulation 2. Cure the disease leading
How ARDS should be treated in 2017 2017, Ostrava Luciano Gattinoni, MD, FRCP Georg-August-Universität Göttingen Germany ARDS 1. Keep the patient alive respiration circulation 2. Cure the disease leading
NIV in hypoxemic patients
 NIV in hypoxemic patients Massimo Antonelli, MD Dept. of Intensive Care & Anesthesiology Università Cattolica del Sacro Cuore Rome - Italy Conflict of interest (research grants and consultations): Maquet
NIV in hypoxemic patients Massimo Antonelli, MD Dept. of Intensive Care & Anesthesiology Università Cattolica del Sacro Cuore Rome - Italy Conflict of interest (research grants and consultations): Maquet
Respiratory insufficiency in bariatric patients
 Respiratory insufficiency in bariatric patients Special considerations or just more of the same? Weaning and rehabilation conference 6th November 2015 Definition of obesity Underweight BMI< 18 Normal weight
Respiratory insufficiency in bariatric patients Special considerations or just more of the same? Weaning and rehabilation conference 6th November 2015 Definition of obesity Underweight BMI< 18 Normal weight
ARDS Assisted ventilation and prone position. ICU Fellowship Training Radboudumc
 ARDS Assisted ventilation and prone position ICU Fellowship Training Radboudumc Fig. 1 Physiological mechanisms controlling respiratory drive and clinical consequences of inappropriate respiratory drive
ARDS Assisted ventilation and prone position ICU Fellowship Training Radboudumc Fig. 1 Physiological mechanisms controlling respiratory drive and clinical consequences of inappropriate respiratory drive
ARDS and Ventilators PG26 Update in Surgical Critical Care October 9, 2013
 ARDS and Ventilators PG26 Update in Surgical Critical Care October 9, 2013 Pauline K. Park MD, FACS, FCCM University of Michigan School of Medicine Ann Arbor, MI OVERVIEW New Berlin definition of ARDS
ARDS and Ventilators PG26 Update in Surgical Critical Care October 9, 2013 Pauline K. Park MD, FACS, FCCM University of Michigan School of Medicine Ann Arbor, MI OVERVIEW New Berlin definition of ARDS
ARDS: MANAGEMENT UPDATE
 ARDS: MANAGEMENT UPDATE Tanıl Kendirli, Assoc. Prof. Ankara University School of Medicine, Pediatric Critical Care Medicine The AECC Definition Timing Acute onset, within 48-72 hours Oxygenation ALI PaO2/FiO2
ARDS: MANAGEMENT UPDATE Tanıl Kendirli, Assoc. Prof. Ankara University School of Medicine, Pediatric Critical Care Medicine The AECC Definition Timing Acute onset, within 48-72 hours Oxygenation ALI PaO2/FiO2
INTRODUCTION The effect of CPAP works on lung mechanics to improve oxygenation (PaO 2
 2 Effects of CPAP INTRODUCTION The effect of CPAP works on lung mechanics to improve oxygenation (PaO 2 ). The effect on CO 2 is only secondary to the primary process of improvement in lung volume and
2 Effects of CPAP INTRODUCTION The effect of CPAP works on lung mechanics to improve oxygenation (PaO 2 ). The effect on CO 2 is only secondary to the primary process of improvement in lung volume and
Respiratory failure requiring mechanical ventilation
 Current Issues in Mechanical Ventilation for Respiratory Failure* Neil R. MacIntyre, MD The morbidity and mortality associated with respiratory failure is, to a certain extent, iatrogenic. Mechanical ventilation,
Current Issues in Mechanical Ventilation for Respiratory Failure* Neil R. MacIntyre, MD The morbidity and mortality associated with respiratory failure is, to a certain extent, iatrogenic. Mechanical ventilation,
Prone Position in ARDS
 Prone Position in ARDS Rich Kallet MS RRT FAARC, FCCM Respiratory Care Services Department of Anesthesia & Perioperative Care University of California, San Francisco, San Francisco General Hospital Case
Prone Position in ARDS Rich Kallet MS RRT FAARC, FCCM Respiratory Care Services Department of Anesthesia & Perioperative Care University of California, San Francisco, San Francisco General Hospital Case
Author: Thomas Sisson, MD, 2009
 Author: Thomas Sisson, MD, 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Non-commercial Share Alike 3.0 License: http://creativecommons.org/licenses/by-nc-sa/3.0/
Author: Thomas Sisson, MD, 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Non-commercial Share Alike 3.0 License: http://creativecommons.org/licenses/by-nc-sa/3.0/
Acute Lung Injury/ARDS. Disclosures. Overview. Acute Respiratory Failure 5/30/2014. Research funding: NIH, UCSF CTSI, Glaxo Smith Kline
 Disclosures Acute Respiratory Failure Carolyn S. Calfee, MD MAS UCSF Critical Care Medicine and Trauma CME May 30, 2014 Research funding: NIH, UCSF CTSI, Glaxo Smith Kline Medical advisory boards: Cerus
Disclosures Acute Respiratory Failure Carolyn S. Calfee, MD MAS UCSF Critical Care Medicine and Trauma CME May 30, 2014 Research funding: NIH, UCSF CTSI, Glaxo Smith Kline Medical advisory boards: Cerus
Long-Term Survival in Patients With Severe Acute Respiratory Distress Syndrome and Rescue Therapies for Refractory Hypoxemia*
 Long-Term Survival in Patients With Severe Acute Respiratory Distress Syndrome and Rescue Therapies for Refractory Hypoxemia* Nita Khandelwal, MD, MS 1 ; Catherine L. Hough, MD, MS 2 ; Aasthaa Bansal,
Long-Term Survival in Patients With Severe Acute Respiratory Distress Syndrome and Rescue Therapies for Refractory Hypoxemia* Nita Khandelwal, MD, MS 1 ; Catherine L. Hough, MD, MS 2 ; Aasthaa Bansal,
Original. Koichi ANDO 1 2, Akane ANDO 3 4, Ayako AKIZUKI 5, Takaaki KAMATANI 5, Kinuko GOTO 3, Tatsuo SHIROTA 5, Takehiko IIJIMA 3 and Shin INOUE 2
 Showa Univ J Med Sci 29 3, 263 272, September 2017 Original The Effects of Desflurane Versus Conventional Maintenance Anesthetics on the Incidence of Post-Operative Nausea and Vomiting in Patients Undergoing
Showa Univ J Med Sci 29 3, 263 272, September 2017 Original The Effects of Desflurane Versus Conventional Maintenance Anesthetics on the Incidence of Post-Operative Nausea and Vomiting in Patients Undergoing
Year in Review Intensive Care Training Program Radboud University Medical Centre Nijmegen
 Year in Review 2013 Intensive Care Training Program Radboud University Medical Centre Nijmegen Contents ARDS Ventilator associated pneumonia Tracheostomy and endotracheal intubation Enteral feeding Fluid
Year in Review 2013 Intensive Care Training Program Radboud University Medical Centre Nijmegen Contents ARDS Ventilator associated pneumonia Tracheostomy and endotracheal intubation Enteral feeding Fluid
Diagnosis of Ventilator- Associated Pneumonia: Where are we now?
 Diagnosis of Ventilator- Associated Pneumonia: Where are we now? Gary French Guy s & St. Thomas Hospital & King s College, London BSAC Guideline 2008 Masterton R, Galloway A, French G, Street M, Armstrong
Diagnosis of Ventilator- Associated Pneumonia: Where are we now? Gary French Guy s & St. Thomas Hospital & King s College, London BSAC Guideline 2008 Masterton R, Galloway A, French G, Street M, Armstrong
One Lung Ventilation in Obese patients
 One Lung Ventilation in Obese patients YUSNI PUSPITA DEPARTEMEN ANESTESIOLOGI DAN TERAPI INTENSIF FAKULTAS KEDOKTERAN UNIVERSITAS SRIWIJAYA/RSMH PALEMBANG One Lung Ventilation Lung isolation techniques
One Lung Ventilation in Obese patients YUSNI PUSPITA DEPARTEMEN ANESTESIOLOGI DAN TERAPI INTENSIF FAKULTAS KEDOKTERAN UNIVERSITAS SRIWIJAYA/RSMH PALEMBANG One Lung Ventilation Lung isolation techniques
Pro: Early use of VV ECMO for ARDS
 Pro: Early use of VV ECMO for ARDS Kyle J. Rehder, MD, FCCP Associate Professor Division of Pediatric Critical Care Medicine Department of Pediatrics Duke Children s Hospital The ventilator is slowly killing
Pro: Early use of VV ECMO for ARDS Kyle J. Rehder, MD, FCCP Associate Professor Division of Pediatric Critical Care Medicine Department of Pediatrics Duke Children s Hospital The ventilator is slowly killing
Meta Analysis. David R Urbach MD MSc Outcomes Research Course December 4, 2014
 Meta Analysis David R Urbach MD MSc Outcomes Research Course December 4, 2014 Overview Definitions Identifying studies Appraising studies Quantitative synthesis Presentation of results Examining heterogeneity
Meta Analysis David R Urbach MD MSc Outcomes Research Course December 4, 2014 Overview Definitions Identifying studies Appraising studies Quantitative synthesis Presentation of results Examining heterogeneity
The Role of the Lactate Dehydrogenase and the Effect of Prone Position during Ventilator-induced Lung Injury
 J Korean Med Sci 24; 19: 223-8 ISSN 111-8934 Copyright The Korean Academy of Medical Sciences The Role of the Lactate Dehydrogenase and the Effect of Prone Position during Ventilator-induced Lung Injury
J Korean Med Sci 24; 19: 223-8 ISSN 111-8934 Copyright The Korean Academy of Medical Sciences The Role of the Lactate Dehydrogenase and the Effect of Prone Position during Ventilator-induced Lung Injury
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv
 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv.8.18.18 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) SUDDEN PROGRESSIVE FORM OF ACUTE RESPIRATORY FAILURE ALVEOLAR CAPILLARY MEMBRANE BECOMES DAMAGED AND MORE
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv.8.18.18 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) SUDDEN PROGRESSIVE FORM OF ACUTE RESPIRATORY FAILURE ALVEOLAR CAPILLARY MEMBRANE BECOMES DAMAGED AND MORE
Steroids for ARDS. Clinical Problem. Management
 Steroids for ARDS James Beck Clinical Problem A 60 year old lady re-presented to ICU with respiratory failure. She had previously been admitted for fluid management and electrolyte correction having presented
Steroids for ARDS James Beck Clinical Problem A 60 year old lady re-presented to ICU with respiratory failure. She had previously been admitted for fluid management and electrolyte correction having presented
WE know that medicine cannot always be a provided
 Acta Anaesthesiol Scand 2004; 48: 267 271 Copyright # Acta Anaesthesiol Scand 2004 Printed in Denmark. All rights reserved ACTA ANAESTHESIOLOGICA SCANDINAVICA Review Article From ventilator-induced lung
Acta Anaesthesiol Scand 2004; 48: 267 271 Copyright # Acta Anaesthesiol Scand 2004 Printed in Denmark. All rights reserved ACTA ANAESTHESIOLOGICA SCANDINAVICA Review Article From ventilator-induced lung
PEEP nuove indicazioni, stesse problematiche
 PEEP nuove indicazioni, stesse problematiche Franco Valenza Department of Pathophysiology and Transplantation Fondazione IRCCS Ca' Granda - Ospedale Maggiore Policlinico Ossigenazione Clearance CO 2 Kats,
PEEP nuove indicazioni, stesse problematiche Franco Valenza Department of Pathophysiology and Transplantation Fondazione IRCCS Ca' Granda - Ospedale Maggiore Policlinico Ossigenazione Clearance CO 2 Kats,
What is the next best step?
 Noninvasive Ventilation William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center What is the next best step? 65 year old female
Noninvasive Ventilation William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center What is the next best step? 65 year old female
Ventilation in Paediatric ARDS: extrapolate from adult studies?
 Ventilation in Paediatric ARDS: extrapolate from adult studies? ASMIC 2014 Dr Adrian Plunkett Consultant Paediatric Intensivist Birmingham Children s Hospital, UK Aims of the presentation Ventilation
Ventilation in Paediatric ARDS: extrapolate from adult studies? ASMIC 2014 Dr Adrian Plunkett Consultant Paediatric Intensivist Birmingham Children s Hospital, UK Aims of the presentation Ventilation
ARTICLE IN PRESS. Extended prone position ventilation in severe acute respiratory distress syndrome: A pilot feasibility study
 Journal of Critical Care (2008) xx, xxx xxx Extended prone position ventilation in severe acute respiratory distress syndrome: A pilot feasibility study Carlos M. Romero a,, Rodrigo A. Cornejo a, L. Ricardo
Journal of Critical Care (2008) xx, xxx xxx Extended prone position ventilation in severe acute respiratory distress syndrome: A pilot feasibility study Carlos M. Romero a,, Rodrigo A. Cornejo a, L. Ricardo
Adjunct Therapies for Pediatric ARDS: Where are the Data?
 Adjunct Therapies for Pediatric ARDS: Where are the Data? Alexandre T. Rotta, MD, FCCM Professor of Pediatrics, Linsalata Family Endowed Chair in Pediatric Critical Care and Emergency Medicine Rainbow
Adjunct Therapies for Pediatric ARDS: Where are the Data? Alexandre T. Rotta, MD, FCCM Professor of Pediatrics, Linsalata Family Endowed Chair in Pediatric Critical Care and Emergency Medicine Rainbow
Computed tomography in adult respiratory distress syndrome: what has it taught us?
 Eur Respir J, 1996, 9, 155 162 DOI: 1.1183/931936.96.95155 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1996 European Respiratory Journal ISSN 93-1936 SERIES 'CLINICAL PHYSIOLOGY IN RESPIRATORY
Eur Respir J, 1996, 9, 155 162 DOI: 1.1183/931936.96.95155 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1996 European Respiratory Journal ISSN 93-1936 SERIES 'CLINICAL PHYSIOLOGY IN RESPIRATORY
ARF. 8 8 (PaO 2 / FIO 2 ) NPPV NPPV ( P = 0.37) NPPV NPPV. (PaO 2 / FIO 2 > 200 PaO 2 / FIO 2 NPPV > 100) (P = 0.02) NPPV ( NPPV P = 0.
 Monica Rocco, MD; Donatella Dell'Utri, MD; Andrea Morelli, MD; Gustavo Spadetta, MD; Giorgio Conti, MD; Massimo Antonelli, MD; and Paolo Pietropaoli, MD (ARF) (NPPV) 19 ARF ( 8 8 3 ) NPPV 19 (PaO 2 / FIO
Monica Rocco, MD; Donatella Dell'Utri, MD; Andrea Morelli, MD; Gustavo Spadetta, MD; Giorgio Conti, MD; Massimo Antonelli, MD; and Paolo Pietropaoli, MD (ARF) (NPPV) 19 ARF ( 8 8 3 ) NPPV 19 (PaO 2 / FIO
High Flow Humidification Therapy, Updates.
 High Flow Humidification Therapy, Updates. Bernardo Selim, M.D. I have no relevant financial relationships to disclose. Assistant Professor, Pulmonary, Critical Care and Sleep Medicine, Mayo Clinic What
High Flow Humidification Therapy, Updates. Bernardo Selim, M.D. I have no relevant financial relationships to disclose. Assistant Professor, Pulmonary, Critical Care and Sleep Medicine, Mayo Clinic What
The Effect of Lateral Position on Oxygenation in ARDS Patients: A Pilot Study
 The Effect of Lateral Position on Oxygenation in ARDS Patients: A Pilot Study Surat Tongyoo MD*, Warakarn Vilaichone MD*, Ranistha Ratanarat MD*, Chairat Permpikul MD* * Critical Care Unit, Division of
The Effect of Lateral Position on Oxygenation in ARDS Patients: A Pilot Study Surat Tongyoo MD*, Warakarn Vilaichone MD*, Ranistha Ratanarat MD*, Chairat Permpikul MD* * Critical Care Unit, Division of
RESEARCH. High frequency oscillation in patients with acute lung injury andacuterespiratorydistresssyndrome(ards):systematic review and meta-analysis
 High frequency oscillation in patients with acute lung injury andacuterespiratorydistresssyndrome(ards):systematic review and meta-analysis Sachin Sud, fellow, 1 Maneesh Sud, medical student, 2 Jan O Friedrich,
High frequency oscillation in patients with acute lung injury andacuterespiratorydistresssyndrome(ards):systematic review and meta-analysis Sachin Sud, fellow, 1 Maneesh Sud, medical student, 2 Jan O Friedrich,
Does Prone Positioning Increase Intracranial Pressure? A Retrospective Analysis of Patients with Acute Brain Injury and Acute Respiratory Failure
 Neurocrit Care (2014) 21:186 191 DOI 10.1007/s12028-014-0004-x ORIGINAL ARTICLE Does Prone Positioning Increase Intracranial Pressure? A Retrospective Analysis of Patients with Acute Brain Injury and Acute
Neurocrit Care (2014) 21:186 191 DOI 10.1007/s12028-014-0004-x ORIGINAL ARTICLE Does Prone Positioning Increase Intracranial Pressure? A Retrospective Analysis of Patients with Acute Brain Injury and Acute
Conference Proceedings
 Conference Proceedings Patient Positioning and Ventilator-Associated Pneumonia Dean R Hess PhD RRT FAARC Introduction Rotational Therapy Review of the Evidence Observations Recommendations From Evidence-Based
Conference Proceedings Patient Positioning and Ventilator-Associated Pneumonia Dean R Hess PhD RRT FAARC Introduction Rotational Therapy Review of the Evidence Observations Recommendations From Evidence-Based
The effect of prone positioning on mortality in patients with acute respiratory distress syndrome: a meta-analysis of randomized controlled trials
 Hu et al. Critical Care 2014, 18:R109 RESEARCH Open Access The effect of prone positioning on mortality in patients with acute respiratory distress syndrome: a meta-analysis of randomized controlled trials
Hu et al. Critical Care 2014, 18:R109 RESEARCH Open Access The effect of prone positioning on mortality in patients with acute respiratory distress syndrome: a meta-analysis of randomized controlled trials
Effects of patient positioning on respiratory mechanics in mechanically ventilated ICU patients
 Review Article Page 1 of 9 Effects of patient positioning on respiratory mechanics in mechanically ventilated ICU patients Mehdi Mezidi 1,2, Claude Guérin 1,2,3 1 Service de réanimation médicale, Hôpital
Review Article Page 1 of 9 Effects of patient positioning on respiratory mechanics in mechanically ventilated ICU patients Mehdi Mezidi 1,2, Claude Guérin 1,2,3 1 Service de réanimation médicale, Hôpital
Effects of Prone Position on Inflammatory Markers in Patients with ARDS Due to Community-acquired Pneumonia
 ORIGINAL ARTICLE Effects of Prone Position on Inflammatory Markers in Patients with ARDS Due to Community-acquired Pneumonia Ming-Cheng Chan, 1,2 Jeng-Yuan Hsu, 1 Hsiu-Hwa Liu, 3 Yao-Ling Lee, 4 Su-Chen
ORIGINAL ARTICLE Effects of Prone Position on Inflammatory Markers in Patients with ARDS Due to Community-acquired Pneumonia Ming-Cheng Chan, 1,2 Jeng-Yuan Hsu, 1 Hsiu-Hwa Liu, 3 Yao-Ling Lee, 4 Su-Chen
Analyzing Lung protective ventilation F Javier Belda MD, PhD Sº de Anestesiología y Reanimación. Hospital Clinico Universitario Valencia (Spain)
 Analyzing Lung protective ventilation F Javier Belda MD, PhD Sº de Anestesiología y Reanimación Hospital Clinico Universitario Valencia (Spain) ALI/ARDS Report of the American-European consensus conference
Analyzing Lung protective ventilation F Javier Belda MD, PhD Sº de Anestesiología y Reanimación Hospital Clinico Universitario Valencia (Spain) ALI/ARDS Report of the American-European consensus conference
Higher PEEP improves outcomes in ARDS patients with clinically objective positive oxygenation response to PEEP: a systematic review and meta-analysis
 Guo et al. BMC Anesthesiology (2018) 18:172 https://doi.org/10.1186/s12871-018-0631-4 RESEARCH ARTICLE Open Access Higher PEEP improves outcomes in ARDS patients with clinically objective positive oxygenation
Guo et al. BMC Anesthesiology (2018) 18:172 https://doi.org/10.1186/s12871-018-0631-4 RESEARCH ARTICLE Open Access Higher PEEP improves outcomes in ARDS patients with clinically objective positive oxygenation
Gas Exchange in the Prone Posture
 Gas Exchange in the Prone Posture Nicholas J Johnson MD, Andrew M Luks MD, and Robb W Glenny MD Introduction Overview of Gas Exchange Lung Structure Normal Exchange of Oxygen and Carbon Dioxide Abnormal
Gas Exchange in the Prone Posture Nicholas J Johnson MD, Andrew M Luks MD, and Robb W Glenny MD Introduction Overview of Gas Exchange Lung Structure Normal Exchange of Oxygen and Carbon Dioxide Abnormal
NIV in acute hypoxic respiratory failure
 All course materials, including the original lecture, are available as webcasts/podcasts at www.ers-education. org/niv2009.htm NIV in acute hypoxic respiratory failure Educational aims This presentation
All course materials, including the original lecture, are available as webcasts/podcasts at www.ers-education. org/niv2009.htm NIV in acute hypoxic respiratory failure Educational aims This presentation
Disclosures. Learning Objectives. Mechanical Ventilation of Infants with Severe BPD: An Interdisciplinary Approach 3/10/2017
 Mechanical Ventilation of Infants with Severe BPD: An Interdisciplinary Approach Steven H. Abman, MD Professor, Department of Pediatrics Director, Pediatric Heart Lung Center University of Colorado School
Mechanical Ventilation of Infants with Severe BPD: An Interdisciplinary Approach Steven H. Abman, MD Professor, Department of Pediatrics Director, Pediatric Heart Lung Center University of Colorado School
INDEPENDENT LUNG VENTILATION
 INDEPENDENT LUNG VENTILATION Giuseppe A. Marraro, MD Director Anaesthesia and Intensive Care Department Paediatric Intensive Care Unit Fatebenefratelli and Ophthalmiatric Hospital Milan, Italy gmarraro@picu.it
INDEPENDENT LUNG VENTILATION Giuseppe A. Marraro, MD Director Anaesthesia and Intensive Care Department Paediatric Intensive Care Unit Fatebenefratelli and Ophthalmiatric Hospital Milan, Italy gmarraro@picu.it
5/15/2018. Background. Disclosure Statement
 5/15/218 Efficacy of Bronchoscopically-Administered in the Setting of Primary Graft Dysfunction after Lung Transplantation Primary Investigator: Sana Ahmed, PharmD Research Associates: Matthew Soto-Arenall,
5/15/218 Efficacy of Bronchoscopically-Administered in the Setting of Primary Graft Dysfunction after Lung Transplantation Primary Investigator: Sana Ahmed, PharmD Research Associates: Matthew Soto-Arenall,
Ventilation update Anaesthesia departmental PGME. Tuesday 10 th December Dr Alastair Glossop Consultant Anaesthesia and Critical Care
 Ventilation update Anaesthesia departmental PGME Tuesday 10 th December Dr Alastair Glossop Consultant Anaesthesia and Critical Care What s fashionable in ICU ventilation? Acute respiratory distress syndrome
Ventilation update Anaesthesia departmental PGME Tuesday 10 th December Dr Alastair Glossop Consultant Anaesthesia and Critical Care What s fashionable in ICU ventilation? Acute respiratory distress syndrome
Study protocol v. 1.0 Systematic review of the Sequential Organ Failure Assessment score as a surrogate endpoint in randomized controlled trials
 Study protocol v. 1.0 Systematic review of the Sequential Organ Failure Assessment score as a surrogate endpoint in randomized controlled trials Harm Jan de Grooth, Jean Jacques Parienti, [to be determined],
Study protocol v. 1.0 Systematic review of the Sequential Organ Failure Assessment score as a surrogate endpoint in randomized controlled trials Harm Jan de Grooth, Jean Jacques Parienti, [to be determined],
Use of corticosteroids in acute lung injury and acute respiratory distress syndrome: A systematic review and meta-analysis*
 Continuing Medical Education Article Use of corticosteroids in acute lung injury and acute respiratory distress syndrome: A systematic review and meta-analysis* Benjamin M. P. Tang, PhD; Jonathan C. Craig,
Continuing Medical Education Article Use of corticosteroids in acute lung injury and acute respiratory distress syndrome: A systematic review and meta-analysis* Benjamin M. P. Tang, PhD; Jonathan C. Craig,
«Best» PEEP? Physiologic? Therapeutic? Optimal? Super? Preferred? Minimal? Right? Protective? Prophylactic?
 1936-2005 «Best» PEEP? Physiologic? Therapeutic? Optimal? Super? Preferred? Minimal? Right? Protective? Prophylactic? 1990-2000 Post cardiac arrest First day of mechanical ventilation 1990-1991 No patient
1936-2005 «Best» PEEP? Physiologic? Therapeutic? Optimal? Super? Preferred? Minimal? Right? Protective? Prophylactic? 1990-2000 Post cardiac arrest First day of mechanical ventilation 1990-1991 No patient
Outcomes From Severe ARDS Managed Without ECMO. Roy Brower, MD Johns Hopkins University Critical Care Canada Forum Toronto November 1, 2016
 Outcomes From Severe ARDS Managed Without ECMO Roy Brower, MD Johns Hopkins University Critical Care Canada Forum Toronto November 1, 2016 Severe ARDS Berlin Definition 2012 P:F ratio 100 mm Hg Prevalence:
Outcomes From Severe ARDS Managed Without ECMO Roy Brower, MD Johns Hopkins University Critical Care Canada Forum Toronto November 1, 2016 Severe ARDS Berlin Definition 2012 P:F ratio 100 mm Hg Prevalence:
Noninvasive respiratory support:why is it working?
 Noninvasive respiratory support:why is it working? Paolo Pelosi Department of Surgical Sciences and Integrated Diagnostics (DISC) IRCCS San Martino IST University of Genoa, Genoa, Italy ppelosi@hotmail.com
Noninvasive respiratory support:why is it working? Paolo Pelosi Department of Surgical Sciences and Integrated Diagnostics (DISC) IRCCS San Martino IST University of Genoa, Genoa, Italy ppelosi@hotmail.com
Ventilator Associated
 Ventilator Associated Pneumonia: Key and Controversial Issues Christopher P. Michetti, MD, FACS Inova Fairfax Hospital, Falls Church, VA Forrest Dell Moore, MD, FACS Banner Healthcare System, Phoenix,
Ventilator Associated Pneumonia: Key and Controversial Issues Christopher P. Michetti, MD, FACS Inova Fairfax Hospital, Falls Church, VA Forrest Dell Moore, MD, FACS Banner Healthcare System, Phoenix,
The Effect of Tidal Volume on Pulmonary Complications following Minimally Invasive Esophagectomy: A Randomized and Controlled Study
 The Effect of Tidal Volume on Pulmonary Complications following Minimally Invasive Esophagectomy: A Randomized and Controlled Study Yaxing Shen, MD, Ming Zhong, MD, Lijie Tan, MD Zhongshan Hospital,Fudan
The Effect of Tidal Volume on Pulmonary Complications following Minimally Invasive Esophagectomy: A Randomized and Controlled Study Yaxing Shen, MD, Ming Zhong, MD, Lijie Tan, MD Zhongshan Hospital,Fudan
Review. Key words : asthma, benralizumab, interleukin-5, mepolizumab, reslizumab. Introduction
 Showa Univ J Med Sci 30 1, 11 25, March 2018 Review Comparative Efficacy and Safety of Anti-Interleukin-5 Therapies and Placebo in Patients with Uncontrolled Eosinophilic Asthma : A Systematic Review and
Showa Univ J Med Sci 30 1, 11 25, March 2018 Review Comparative Efficacy and Safety of Anti-Interleukin-5 Therapies and Placebo in Patients with Uncontrolled Eosinophilic Asthma : A Systematic Review and
Surgery Grand Rounds. Non-invasive Ventilation: A valuable tool. James Cromie, PGY 3 8/24/09
 Surgery Grand Rounds Non-invasive Ventilation: A valuable tool James Cromie, PGY 3 8/24/09 History of mechanical ventilation 1930 s: use of iron lung 1940 s: First NIV system (Bellevue Hospital) 1950 s:
Surgery Grand Rounds Non-invasive Ventilation: A valuable tool James Cromie, PGY 3 8/24/09 History of mechanical ventilation 1930 s: use of iron lung 1940 s: First NIV system (Bellevue Hospital) 1950 s:
Kansas City, MO 2 University of Missouri-Kansas City, MO 3 University of Kansas School of Pharmacy,
 in Acute Respiratory Distress Syndrome Joshua R. Howitt, Pharm.D. 1,2,3, John D. Hill, Pharm.D. Candidate 2, Trenton D. Nauser, M.D. 1,4 1 Department of Veterans Affairs, Kansas City, MO 2 University of
in Acute Respiratory Distress Syndrome Joshua R. Howitt, Pharm.D. 1,2,3, John D. Hill, Pharm.D. Candidate 2, Trenton D. Nauser, M.D. 1,4 1 Department of Veterans Affairs, Kansas City, MO 2 University of
Kaneyuki Kawamae, Ken Iseki ABSTRACT
 Yamagata Med J 2003 21 1) 37-46 Kaneyuki Kawamae, Ken Iseki Department of Emergency Medicine, Yamagata University School of Medicine, Yamagata 990-9585, Japan *Fukushima Medical University, 1 Hikariga-oka,
Yamagata Med J 2003 21 1) 37-46 Kaneyuki Kawamae, Ken Iseki Department of Emergency Medicine, Yamagata University School of Medicine, Yamagata 990-9585, Japan *Fukushima Medical University, 1 Hikariga-oka,
Fluid Treatments in Sepsis: Meta-Analyses
 Fluid Treatments in Sepsis: Recent Trials and Meta-Analyses Lauralyn McIntyre MD, FRCP(C), MSc Scientist, Ottawa Hospital Research Institute Assistant Professor, University of Ottawa Department of Epidemiology
Fluid Treatments in Sepsis: Recent Trials and Meta-Analyses Lauralyn McIntyre MD, FRCP(C), MSc Scientist, Ottawa Hospital Research Institute Assistant Professor, University of Ottawa Department of Epidemiology
Refresher Course MYTHS AND REALITY ABOUT LUNG MECHANICS 5 RC 2. European Society of Anaesthesiologists FIGURE 1 STATIC MEASUREMENTS
 European Society of Anaesthesiologists Refresher Course S AND ABOUT LUNG MECHANICS 5 RC 2 Anders LARSSON Gentofte University Hospital Copenhagen University Hellerup, Denmark Saturday May 31, 2003 Euroanaesthesia
European Society of Anaesthesiologists Refresher Course S AND ABOUT LUNG MECHANICS 5 RC 2 Anders LARSSON Gentofte University Hospital Copenhagen University Hellerup, Denmark Saturday May 31, 2003 Euroanaesthesia
