Case Reports. Chemotherapy-Induced Late Acute Respiratory Distress Syndrome Following Right Pneumonectomy for Bronchogenic Carcinoma
|
|
|
- Derick Hardy
- 5 years ago
- Views:
Transcription
1 Case Reports Chemotherapy-Induced Late Acute Respiratory Distress Syndrome Following Right Pneumonectomy for Bronchogenic Carcinoma Mara Tosi MD and Guido Domenighetti MD We report 2 patients who suffered late postoperative acute respiratory distress syndrome (ARDS) that was probably chemotherapy-induced. Both patients underwent neoadjuvant combination chemotherapy prior to right pneumonectomy for primary bronchogenic carcinoma, and then suffered ARDS in the remaining lung a few weeks after surgery. No evidence of infection or other specific ARDS etiologies could be found, whereas the bronchoalveolar lavage fluid cell differentiation and protein content suggested the permeability form of lung edema. Both patients had rapid clinical, functional, and radiologic improvement with high-dose corticosteroids. In the first patient the course was complicated by the development of a critical illness polyneuropathy with complete tetraplegia, but the patient recovered. The second patient died from septic shock 4 weeks after starting mechanical ventilation. The incidence of a chemotherapy-related ARDS in the remaining lung, occurring more than 4 weeks after extensive operations or after a pneumonectomy, is unknown. This kind of acute lung injury calls for particularly delicate treatments, the most potentially life-threatening complications being mainly associated with difficulties in ventilatory support and the high doses of corticosteroids required to rescue the remaining lung. Key words: neoadjuvant, chemotherapy, pneumonectomy, acute respiratory distress syndrome, ARDS, mechanical ventilation, corticosteroids. [Respir Care 2003;48(6): Daedalus Enterprises] Introduction Acute lung injury (ALI) and acute respiratory distress syndrome (ARDS) are clinical syndromes characterized by acute and profound pulmonary inflammation, of different origin, with conclusive evidence of increasing permeability of the endothelial and epithelial barriers. 1 3 ALI/ ARDS can develop early after resection of primary bronchogenic carcinoma and is associated with a very high mortality rate, 4 6 particularly following right pneumonectomy and extended operations. 6 Several cancer drugs induce pulmonary damage, resulting in a variety of clinical and pathologic responses. 7 9 Chemotherapy-induced pulmonary parenchyma toxicity can include a noncardiogenic pulmonary edema compatible with ALI or ARDS. 9 Late Mara Tosi MD and Guido Domenighetti MD are affiliated with the Section of Intensive Care, Department of Medicine, Ospedale Regionale di Locarno La Carità, Locarno, Switzerland. Correspondence: Guido Domenighetti MD, Section of Intensive Care, Department of Medicine, Ospedale Regionale di Locarno La Carità, Locarno 6600, Switzerland. guido.domenighetti@eoc.ch. ( 30 d) ALI/ARDS after surgery and neoadjuvant therapy is a less well known impending severe complication after extensive resection of non-small-cell lung cancer. We report 2 cases of probable chemotherapy-induced late ARDS following right pneumonectomy for bronchogenic carcinoma. The first occurred in a patient treated with gemcitabine, the second in a patient receiving a combination of vinorelbine and mitomycin. Case Report 1 A 72-year-old man underwent right pneumonectomy with mediastinal lymphadenectomy for squamous cell lung cancer initially staged as pt3 pn1 Mx, G2, IIIA in March He had first undergone neoadjuvant chemotherapy with paclitaxel, carboplatin, and gemcitabine, from October 2000 to February Four weeks after surgery the patient had a dry cough and worsening of dyspnea. A few days later he developed progressive respiratory failure. On physical examination there was cyanosis, crackles were audible over the left lung, and he was afebrile. Respiratory rate was 35 breaths/min, heart rate was 130 beats/min, and arterial blood pressure was 150/80 mm Hg. The conven- 606 RESPIRATORY CARE JUNE 2003 VOL 48 NO 6
2 Fig. 1. Admission chest radiograph of patient 1, showing diffuse alveolar-interstitial infiltrates. The chest radiograph of patient 2 had a similar pattern of infiltrates. tional chest radiograph showed diffuse alveolar-interstitial infiltrates involving the whole left lung. The computed tomography (CT) scan demonstrated reticular opacities, thickened septal lines, and some areas of patchy consolidation (Fig. 1). Laboratory findings showed an inflammatory syndrome, with white blood cell count of 11 cells/ L, normal differential count, and C-reactive protein of 102 mg/l. While receiving 100% oxygen and continuous positive airway pressure of 6 cm H 2 O the patient had P ao2 38 mm Hg, P aco2 29 mm Hg, ph 7.40, and bicarbonate 20 meq/l. The ratio of P ao2 to fraction of inspired oxygen (P ao2 /F IO2 ) was 38. The patient was intubated and ventilated in supine position. To avoid ventilator-induced lung injury on the remaining lung we used a pressure-controlled mode (with a maximum plateau pressure titrated at 35 cm H 2 O), high positive end-expiratory pressure (PEEP) (15 cm H 2 O), and very low tidal volume (5 ml/kg of ideal body weight), as suggested by the recent results from the ARDS Network. 10 Inspiration-expiration ratio was 1:2 and respiratory rate was 18 breaths/min. While on those mechanical ventilation settings, arterial blood gas analysis revealed P ao2 46 mm Hg, P aco2 51 mm Hg, ph 7.31, bicarbonate 23 meq/l. F IO2 was 1.0 and the P ao2 /F IO2 was 46. Changes of the patient s position were not useful and even worsened gas exchange. The lung injury score was Blood cultures were negative for aerobic and anaerobic bacteria. Serologies for chlamydia, mycoplasma, and respiratory viruses were negative. The urine test for Legionella antigen was negative. Cardiac enzymes and the echocardiographically assessed left ventricular function were normal. Bronchoalveolar lavage fluid (BALF) was negative for Pneumocystis carinii, Mycobacterium tuberculosis, and pyogenic bacteria. No malignant cells were found. The cell differentiation showed moderately elevated polymorphonuclear leukocytes (10%) with rare lymphocytes (2%) and predominant macrophages (78%). The protein content was 5.1 g/dl and the ratio of edema fluid to plasma total protein was 0.9. Because of the high associated risks (severely disturbed gas exchange, right pneumonectomy, difficult mechanical ventilation with high PEEP, and unstable hemodynamics) a transbronchial biopsy was not carried out. High-dose corticosteroids were begun on day 3, with methylprednisolone 1 g/d during the first 3 days, followed by 2 mg/ kg/d. The antimicrobial spectrum consisted of imipenem and clarithromycin. During the first 3 days of mechanical ventilation, acceptable gas exchange was difficult to obtain, despite high PEEP (16 cm H 2 O), deep sedation, and pharmacologic paralysis (with pancuronium bromide). Turning the patient prone or on the left or right side worsened gas exchange. Acceptable oxygenation was achieved only with inhaled nitric oxide (5 15 ppm). After the third day the radiologic findings improved. Methylprednisolone was then maintained at 2 mg/kg over 20 days and thereafter progressively reduced to a maintenance dose of 20 mg/d prednisolone. The patient developed a critical illness polyneuropathy with complete tetraplegia. Weaning from mechanical ventilation was impossible, and after 81 days the patient was transferred to a paraplegic center for rehabilitation and long-term weaning. The patient is now living at home with a transtracheal oxygen device, breathing and walking spontaneously, with no evident clinical, bronchoscopic, or radiologic signs of tumor progression. Case Report 2 A 58-year-old man underwent right pneumonectomy for a large cell carcinoma of the lung, initially staged as pt3 pno MO, IIB, in October He had first undergone neoadjuvant chemotherapy with mitomycin, vinorelbine, and cisplatin, from August 2001 to September 2001, and radiotherapy with a total of 45 gray. On November 2001 (5 wk after surgery) the patient was readmitted to our hospital because of dyspnea and a dry cough. On physical examination he was subfebrile (37.8 C) and crackles were audible over the left lung. Respiratory rate was 30 breaths/min and heart rate was 114 beats/min. Chest radiography showed left diffuse alveolar-interstitial infiltrates. The CT scan demonstrated reticular opacities, thickened septal lines, and some areas of patchy consolidation (Fig. 2). Laboratory findings showed an inflammatory syndrome, with white blood cell count of 13 cells/ L, with normal differential count, and C-reactive protein of 178 mg/l. He was first treated with antibiotics (imipenem and clarithromycin), but his condition further deteriorated and he RESPIRATORY CARE JUNE 2003 VOL 48 NO 6 607
3 Because of high associated risks (pneumonectomy, high PEEP levels), a transbronchial biopsy was not carried out. Two days after intubation we initiated high doses of corticosteroids, with methylprednisolone 1 g/d over 3 days, followed by 2 mg/kg/d over 10 days. From then on the radiologic findings improved. Corticosteroids were thereafter progressively reduced to a maintenance dose of 20 mg/d prednisolone. Four weeks after starting mechanical ventilation the patient became highly febrile, gas exchange worsened, and new pulmonary infiltrates appeared on the conventional chest radiograph. Despite a new antimicrobial spectrum the patient developed septic shock and died. The recovered bronchial secretions showed a substantial growth of imipenem-resistant Pseudomonas aeruginosa. Fig. 2. Computed tomography scan of patient 2 (section above the carina), showing reticular opacities, thickened septal lines, and an area of patchy consolidation. The computed tomography scan of patient 1 had a similar pattern of infiltrates. developed progressive respiratory failure on the second day after admission. At that time P ao2 was 50 mm Hg, P aco2 was 28 mm Hg, ph was 7.40, and total bicarbonate was 26 meq/l. F IO2 was 1.0 and P ao2 /F IO2 was 50. After an unsuccessful attempt with noninvasive pressure-support ventilation (inspiratory pressure support of 14 cm H 2 O, PEEP of 6 cm H 2 O), he was intubated and mechanically ventilated in supine position. To avoid ventilator-induced lung injury to the remaining lung we used a pressure-controlled mode (maximum plateau pressure titrated at 35 cm H 2 O), high PEEP (12 cm H 2 O), and very low tidal volume (5 ml/kg of ideal body weight). 10 The inspiration-expiration ratio was 1:2 and the respiratory rate 18 breaths/min. At that time blood gas analysis showed P ao2 54 mm Hg, P aco mm Hg, ph 7.30, and bicarbonate 26 meq/l. F IO2 was 1.0 and P ao2 /F IO2 was 54. Changes of the patient s position were not useful and even worsened gas exchange. The lung injury score was 3. Blood cultures were negative for aerobic and anaerobic bacteria. Serologies for chlamydia, mycoplasma, and respiratory viruses were negative, as was the urine test for Legionella antigen. Cardiac enzymes and echocardiographically assessed left ventricular function were normal. BALF was negative for Pneumocystis carinii, Mycobacterium tuberculosis, and pyogenic bacteria. BALF cell differentiation showed elevated polymorphonuclear leukocytes (36%), a normal count of lymphocytes (6%), slightly increased eosinophils (4%), and the macrophages were 54%. No malignant cells were found. The protein content of the obtained fluid was 5.3 g/dl and the ratio of edema fluid to plasma total protein was 1:1. Discussion ALI and ARDS are considered the most unpredictable and serious early complications following lung resection of primary bronchogenic carcinoma, the highest mortality rate being observed following right pneumonectomy or extended operations. 4 6,12,13 A recent large study found the incidence of these major pulmonary events to be around 4% in a cohort of 1,139 cases undergoing pulmonary resection. 5 The etiology of these early postoperative complications remains mysterious, though animal experiments suggest that increased oxidative stress occurring with onelung anesthesia might trigger a chain of events leading to ALI/ARDS. 14 There is little knowledge about the incidence of late ( 30 d) ALI/ARDS in postoperative patients who were previously treated with neoadjuvant chemotherapy, including agents known to be associated with the development of noncardiogenic lung edema. The diagnosis of a late chemotherapy-induced ARDS relies first on the documented exclusion of other causes, such as infection, relapse of the underlying disease, and the effects of radiation. The usually observed time proximity to the administration of drugs known to be mainly associated with this syndrome and the early positive response to high doses of corticosteroids may further support the hypothesis that chemotherapy was the cause. 7 9,15 Both patients had CT scan features that suggested ARDS, 16 and these were corroborated by a CT imaging pattern suggestive of gemcitabine pulmonary toxicity in the first patient. 17 The history and diagnostic workup were inconsistent with left heart failure. Also ruled out were infection, a septic syndrome, or other cause such as pancreatitis, aspiration, or progression of the underlying tumoral disease. However, given their reported incidence, other possibilities, such as occult infection or idiopathic ARDS, cannot be excluded In cases of supposed chemotherapy-induced ALI, in vivo biopsy results have rarely been reported. 21 However, the 608 RESPIRATORY CARE JUNE 2003 VOL 48 NO 6
4 autopsy pathology findings in such patients are consistent with a pattern of diffuse alveolar damage. 7,8,21 Transbronchial biopsies were not carried out because significant associated risk factors were apparent on admission and during the acute ARDS stage. Yet the BALF cell differentiation and the protein content suggested the permeability form of lung edema. 22 Taken together, the clinical history, the BALF results, and most importantly, the probable exclusion of other common identifiable causes suggest the chemotherapy as the probable cause of the late ARDS in both patients. Gemcitabine, with or without paclitaxel, has been associated with ALI/ARDS in about 0.1% of clinical trials, 23 and a few case reports have supported that gemcitabine may be associated with a noncardiogenic pulmonary edema. 8,21,24 Combined vinorelbine-mitomycin treatment has also been considered risky for inducing lung injury, with an estimated 2% incidence of ALI/ARDS. 7,9,25 If started early in the course of the disease, intravenous corticosteroids have been reported to be a rescue therapy in a number of patients with this form of pulmonary injury. 7,8,15,21,26 However, no suggestion is offered concerning the initial dose or the treatment duration. The dramatic clinical presentation in both our patients resulted in the drastic choice of an initial treatment with high doses of methylprednisolone for 3 days, followed by a corticosteroid plan over 20 days (patient 1) or 10 days (patient 2), similar to the protocol proposed by Meduri et al for the unresolving form of ARDS. 27 Conclusions Though in these cases the connection between the chemotherapy and the ARDS could not be verified by biopsy results, these case reports remind us of the possibility of an association between chemotherapy and late ARDS following extended lung resection for primary bronchogenic carcinoma. In the illustrated clinical context prompt identification of new respiratory symptoms in such patients could lead to the early suspicion of ARDS, calling for immediate treatment with corticosteroids, after carefully excluding other more frequent causes of ARDS. REFERENCES 1. Bernard GR, Artigas A, Brigham KL, Carlet J, Falke K, Hudson L, et al. The American-European Consensus Conference on ARDS: definitions, mechanisms, relevant outcomes, and clinical trial coordination. Am J Respir Crit Care Med 1994;149(3 Pt 1): Bachofen M, Weibel ER. Structural alterations of lung parenchyma in the adult respiratory distress syndrome. Clin Chest Med 1982; 3(1): Ware LB, Matthay MA. The acute respiratory distress syndrome. N Engl J Med 2000;342(18): Stéphan F, Boucheseiche S, Hollande J, Flahault A, Cheffi A, Bazelly B, Bonnet F. Pulmonary complications following lung resection: a comprehensive analysis of incidence and possible risk factors.. Chest 2000;118(5): Kutlu CA, Williams EA, Evans TW, Pastorino U, Goldstraw P. Acute lung injury and acute respiratory distress syndrome after pulmonary resection. Ann Thorac Surg 2000;69(2): Ruffini E, Parola A, Papalia E, Filosso PL, Mancuso M, Oliaro A, et al. Frequency and mortality of acute lung injury and acute respiratory distress syndrome after pulmonary resection for bronchogenic carcinoma. Eur J Cardiothorac Surg 2001;20(1):30 36; discussion Briasoulis E, Pavlidis N. Noncardiogenic pulmonary edema: an unusual and serious complication of anticancer therapy. Oncologist 2001;6(2): Marruchella A, Fiorenzano G, Merizzi A, Rossi G, Chiodera PL. Diffuse alveolar damage in a patient treated with gemcitabine. Eur Respir J 1998;11(2): Rao SX, Ramaswamy G, Levin M, McCravey JW. Fatal acute respiratory failure after vinblastine-mitomycin therapy in lung carcinoma. Arch Intern Med 1985;145(10): Ventilation with lower tidal volumes as compared with traditional tidal volumes for acute lung injury and the acute respiratory distress syndrome. The Acute Respiratory Distress Syndrome Network. N Engl J Med 2000;342(18): Murray JF, Matthay MA, Luce JM, Flick MR. An expanded definition of the adult respiratory distress syndrome. Am Rev Respir Dis 1988;138(3): Erratum in: Am Rev Respir Dis 1989;139(4): Turnage WS, Lunn JJ. Postpneumonectomy pulmonary edema. A retrospective analysis of associated variables. Chest 1993;103(6): Mathisen DJ, Kuo EY, Hahn C, Moncure AC, Wain JC, Grillo HC, et al. Inhaled nitric oxide for adult respiratory distress syndrome after pulmonary resection. Ann Thorac Surg 1998;66(6): Williams EA, Quinlan GJ, Anning PB, Goldstraw P, Evans TW. Lung injury following pulmonary resection in the isolated, bloodperfused rat lung. Eur Respir J 1999;14(4): Vander Els NJ, Müller V. Successful treatment of gemcitabine toxicity with a brief course of oral corticosteroid therapy. Chest 1998; 114(6): Goodman LR, Fumagalli R, Tagliabue P, Tagliabue M, Ferrario M, Gattinoni L, Pesenti A. Adult respiratory distress syndrome due to pulmonary and extrapulmonary causes: CT, clinical, and functional correlations. Radiology 1999;213(2): Boiselle PM, Morrin MM, Huberman MS. Gemcitabine pulmonary toxicity: CT features. J Comput Assist Tomogr 2000;24(6): Nuckton TJ, Alonso JA, Kallet RH, Daniel BM, Pittet JF, Eisner MD, Matthay MA. Pulmonary dead-space fraction as a risk factor for death in the acute respiratory distress syndrome. N Engl J Med 2002;346(7): Zilberberg MD, Epstein SK. Acute lung injury in the medical ICU. Comorbid conditions, age, etiology, and hospital outcome. Am J Respir Crit Care Med 1998;157(4 Pt 1): Eisner MD, Thompson T, Hudson LD, Luce JM, Hayden D, Schoenfeld D, Matthay MA. Efficacy of low tidal volume ventilation in patients with different clinical risk factors for acute lung injury and the acute respiratory distress syndrome. Am J Respir Crit Care Med 2001;164(2): Pavlakis N, Bell DR, Millward MJ, Levi JA. Fatal pulmonary toxicity resulting from treatment with gemcitabine. Cancer 1997;80(2): Matthay MA, Wiener-Kronish JP. Intact epithelial barrier function is critical for the resolution of alveolar edema in humans. Am Rev Respir Dis 1990;142(6 Pt 1): RESPIRATORY CARE JUNE 2003 VOL 48 NO 6 609
5 23. Roychowdhury DF, Smith CA, Peterson P, et al. A report on serious pulmonary toxicity associated with gemcitabine-based therapy (abstract). Proc Am Soc Clin Oncol 2000;19:196a. 24. Dunsford ML, Mead GM, Bateman AC, Cook T, Tung K. Severe pulmonary toxicity in patients treated with a combination of docetaxel and gemcitabine for metastatic transitional cell carcinoma. Ann Oncol 1999;10(8): Hoelzer KL, Harrison BR, Luedke SW, Luedke DW. Vinblastineassociated pulmonary toxicity in patients receiving combination therapy with mitomycin and cisplatin. Drug Intell Clin Pharm 1986; 20(4): Linskens RK, Golding RP, van Groeningen CJ, Giaccone G. Severe acute lung injury induced by gemcitabine. Neth J Med 2000;56(6): Meduri GU, Headley AS, Golden E, Carson SJ, Umberger RA, Kelso T, Tolley EA. Effect of prolonged methylprednisolone therapy in unresolving acute respiratory distress syndrome: a randomized controlled trial. JAMA 1998;280(2): RESPIRATORY CARE JUNE 2003 VOL 48 NO 6
ACUTE RESPIRATORY DISTRESS SYNDROME
 ACUTE RESPIRATORY DISTRESS SYNDROME Angel Coz MD, FCCP, DCE Assistant Professor of Medicine UCSF Fresno November 4, 2017 No disclosures OBJECTIVES Identify current trends and risk factors of ARDS Describe
ACUTE RESPIRATORY DISTRESS SYNDROME Angel Coz MD, FCCP, DCE Assistant Professor of Medicine UCSF Fresno November 4, 2017 No disclosures OBJECTIVES Identify current trends and risk factors of ARDS Describe
clinical investigations in critical care The Role of Open-Lung Biopsy in ARDS*
 clinical investigations in critical care The Role of Open-Lung Biopsy in ARDS* Sanjay R. Patel, MD; Dimitri Karmpaliotis, MD; Najib T. Ayas, MD; Eugene J. Mark, MD; John Wain, MD, FCCP; B. Taylor Thompson,
clinical investigations in critical care The Role of Open-Lung Biopsy in ARDS* Sanjay R. Patel, MD; Dimitri Karmpaliotis, MD; Najib T. Ayas, MD; Eugene J. Mark, MD; John Wain, MD, FCCP; B. Taylor Thompson,
Acute Respiratory Distress Syndrome (ARDS) An Update
 Acute Respiratory Distress Syndrome (ARDS) An Update Prof. A.S.M. Areef Ahsan FCPS(Medicine) MD(Critical Care Medicine) MD ( Chest) Head, Dept. of Critical Care Medicine BIRDEM General Hospital INTRODUCTION
Acute Respiratory Distress Syndrome (ARDS) An Update Prof. A.S.M. Areef Ahsan FCPS(Medicine) MD(Critical Care Medicine) MD ( Chest) Head, Dept. of Critical Care Medicine BIRDEM General Hospital INTRODUCTION
Steroids in ARDS: if, when, how much? John Fowler, MD, FACEP Dept. of Emergency Medicine Kent Hospital, İzmir, Türkiye
 Steroids in ARDS: if, when, how much? John Fowler, MD, FACEP Dept. of Emergency Medicine Kent Hospital, İzmir, Türkiye Steroids in ARDS: conclusion Give low-dose steroids if indicated for another problem
Steroids in ARDS: if, when, how much? John Fowler, MD, FACEP Dept. of Emergency Medicine Kent Hospital, İzmir, Türkiye Steroids in ARDS: conclusion Give low-dose steroids if indicated for another problem
ARDS and Lung Protection
 ARDS and Lung Protection Kristina Sullivan, MD Associate Professor University of California, San Francisco Department of Anesthesia and Perioperative Care Division of Critical Care Medicine Overview Low
ARDS and Lung Protection Kristina Sullivan, MD Associate Professor University of California, San Francisco Department of Anesthesia and Perioperative Care Division of Critical Care Medicine Overview Low
Sub-category: Intensive Care for Respiratory Distress
 Course n : Course 3 Title: RESPIRATORY PHYSIOLOGY, PHYSICS AND PATHOLOGY IN RELATION TO ANAESTHESIA AND INTENSIVE CARE Sub-category: Intensive Care for Respiratory Distress Topic: Acute Respiratory Distress
Course n : Course 3 Title: RESPIRATORY PHYSIOLOGY, PHYSICS AND PATHOLOGY IN RELATION TO ANAESTHESIA AND INTENSIVE CARE Sub-category: Intensive Care for Respiratory Distress Topic: Acute Respiratory Distress
ERJ Express. Published on August 9, 2012 as doi: /
 ERJ Express. Published on August 9, 2012 as doi: 10.1183/09031936.00076912 Extracorporeal membrane oxygenation in a non intubated patient with acute respiratory distress syndrome (ARDS) Olaf Wiesner, *
ERJ Express. Published on August 9, 2012 as doi: 10.1183/09031936.00076912 Extracorporeal membrane oxygenation in a non intubated patient with acute respiratory distress syndrome (ARDS) Olaf Wiesner, *
7/4/2015. diffuse lung injury resulting in noncardiogenic pulmonary edema due to increase in capillary permeability
 Leanna R. Miller, RN, MN, CCRN-CMC, PCCN-CSC, CEN, CNRN, CMSRN, NP Education Specialist LRM Consulting Nashville, TN Objectives Identify the 5 criteria for the diagnosis of ARDS. Discuss the common etiologies
Leanna R. Miller, RN, MN, CCRN-CMC, PCCN-CSC, CEN, CNRN, CMSRN, NP Education Specialist LRM Consulting Nashville, TN Objectives Identify the 5 criteria for the diagnosis of ARDS. Discuss the common etiologies
New respiratory symptoms and lung imaging findings in a woman with polymyositis
 Maria Bolaki 1, Konstantinos Karagiannis 1, George Bertsias 2, Ioanna Mitrouska 1, Nikolaos Tzanakis 1, Katerina M. Antoniou 1 kantoniou@uoc.gr 1 Dept of Thoracic Medicine, Heraklion University Hospital,
Maria Bolaki 1, Konstantinos Karagiannis 1, George Bertsias 2, Ioanna Mitrouska 1, Nikolaos Tzanakis 1, Katerina M. Antoniou 1 kantoniou@uoc.gr 1 Dept of Thoracic Medicine, Heraklion University Hospital,
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv
 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv.8.18.18 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) SUDDEN PROGRESSIVE FORM OF ACUTE RESPIRATORY FAILURE ALVEOLAR CAPILLARY MEMBRANE BECOMES DAMAGED AND MORE
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv.8.18.18 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) SUDDEN PROGRESSIVE FORM OF ACUTE RESPIRATORY FAILURE ALVEOLAR CAPILLARY MEMBRANE BECOMES DAMAGED AND MORE
Pulmonary & Extra-pulmonary ARDS: FIZZ or FUSS?
 Pulmonary & Extra-pulmonary ARDS: FIZZ or FUSS? Dr. Rajagopala Srinivas Senior Resident, Dept. Pulmonary Medicine, PGIMER, Chandigarh. The beginning.. "The etiology of this respiratory distress syndrome
Pulmonary & Extra-pulmonary ARDS: FIZZ or FUSS? Dr. Rajagopala Srinivas Senior Resident, Dept. Pulmonary Medicine, PGIMER, Chandigarh. The beginning.. "The etiology of this respiratory distress syndrome
Landmark articles on ventilation
 Landmark articles on ventilation Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity ARDS AECC DEFINITION-1994 ALI Acute onset Bilateral chest infiltrates PCWP
Landmark articles on ventilation Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity ARDS AECC DEFINITION-1994 ALI Acute onset Bilateral chest infiltrates PCWP
Surviving Sepsis Campaign. Guidelines for Management of Severe Sepsis/Septic Shock. An Overview
 Surviving Sepsis Campaign Guidelines for Management of Severe Sepsis/Septic Shock An Overview Mechanical Ventilation of Sepsis-Induced ALI/ARDS ARDSnet Mechanical Ventilation Protocol Results: Mortality
Surviving Sepsis Campaign Guidelines for Management of Severe Sepsis/Septic Shock An Overview Mechanical Ventilation of Sepsis-Induced ALI/ARDS ARDSnet Mechanical Ventilation Protocol Results: Mortality
Steroids for ARDS. Clinical Problem. Management
 Steroids for ARDS James Beck Clinical Problem A 60 year old lady re-presented to ICU with respiratory failure. She had previously been admitted for fluid management and electrolyte correction having presented
Steroids for ARDS James Beck Clinical Problem A 60 year old lady re-presented to ICU with respiratory failure. She had previously been admitted for fluid management and electrolyte correction having presented
Best of Pulmonary Jennifer R. Hucks, MD University of South Carolina School of Medicine
 Best of Pulmonary 2012-2013 Jennifer R. Hucks, MD University of South Carolina School of Medicine Topics ARDS- Berlin Definition Prone Positioning For ARDS Lung Protective Ventilation In Patients Without
Best of Pulmonary 2012-2013 Jennifer R. Hucks, MD University of South Carolina School of Medicine Topics ARDS- Berlin Definition Prone Positioning For ARDS Lung Protective Ventilation In Patients Without
Potential Effects of Corticosteroids on Physiological Dead-Space Fraction in Acute Respiratory Distress Syndrome
 Potential Effects of Corticosteroids on Physiological Dead-Space Fraction in Acute Respiratory Distress Syndrome Joan M Raurich MD PhD, Mireia Ferreruela MD, Juan A Llompart-Pou MD PhD, Margalida Vilar
Potential Effects of Corticosteroids on Physiological Dead-Space Fraction in Acute Respiratory Distress Syndrome Joan M Raurich MD PhD, Mireia Ferreruela MD, Juan A Llompart-Pou MD PhD, Margalida Vilar
The mortality from acute respiratory distress syndrome after pulmonary resection is reducing: a 10-year single institutional experience
 European Journal of Cardio-thoracic Surgery 34 (2008) 898 902 www.elsevier.com/locate/ejcts The mortality from acute respiratory distress syndrome after pulmonary resection is reducing: a 10-year single
European Journal of Cardio-thoracic Surgery 34 (2008) 898 902 www.elsevier.com/locate/ejcts The mortality from acute respiratory distress syndrome after pulmonary resection is reducing: a 10-year single
DAILY SCREENING FORM
 DAILY SCREENING FORM Patient s initials: Date of admission: Time of admission: Gender: M F Year of Birth: Type of admission: Medical/Surgical/Postoperative (elective) Days Date Mechanical ventilation Lung
DAILY SCREENING FORM Patient s initials: Date of admission: Time of admission: Gender: M F Year of Birth: Type of admission: Medical/Surgical/Postoperative (elective) Days Date Mechanical ventilation Lung
Fluid restriction is superior in acute lung injury and ARDS
 TAKE-HOME POINTS FROM LECTURES BY CLEVELAND CLINIC AND VISITING FACULTY MEDICAL GRAND ROUNDS CME CREDIT HERBERT P. WIEDEMANN, MD Chairman, Department of Pulmonary, Allergy, and Critical Care Medicine,
TAKE-HOME POINTS FROM LECTURES BY CLEVELAND CLINIC AND VISITING FACULTY MEDICAL GRAND ROUNDS CME CREDIT HERBERT P. WIEDEMANN, MD Chairman, Department of Pulmonary, Allergy, and Critical Care Medicine,
The ARDS is characterized by increased permeability. Incidence of ARDS in an Adult Population of Northeast Ohio*
 Incidence of ARDS in an Adult Population of Northeast Ohio* Alejandro C. Arroliga, MD, FCCP; Ziad W. Ghamra, MD; Alejandro Perez Trepichio, MD; Patricia Perez Trepichio, RRT; John J. Komara Jr., BA, RRT;
Incidence of ARDS in an Adult Population of Northeast Ohio* Alejandro C. Arroliga, MD, FCCP; Ziad W. Ghamra, MD; Alejandro Perez Trepichio, MD; Patricia Perez Trepichio, RRT; John J. Komara Jr., BA, RRT;
Effect of ARDS Severity and Etiology on Short-Term Outcomes
 Effect of ARDS Severity and Etiology on Short-Term Outcomes Haitham El-Haddad MD, Hyejeong Jang MSc, Wei Chen PhD, and Ayman O Soubani MD BACKGROUND: We evaluated the outcome of subjects with ARDS in relation
Effect of ARDS Severity and Etiology on Short-Term Outcomes Haitham El-Haddad MD, Hyejeong Jang MSc, Wei Chen PhD, and Ayman O Soubani MD BACKGROUND: We evaluated the outcome of subjects with ARDS in relation
Methods ROLE OF OPEN LUNG BIOPSY IN PATIENTS WITH DIFFUSE LUNG INFILTRATES AND ACUTE RESPIRATORY FAILURE
 ROLE OF OPEN LUNG BIOPSY IN PATIENTS WITH DIFFUSE LUNG INFILTRATES AND ACUTE RESPIRATORY FAILURE Li-Hui Soh, Chih-Feng Chian, Wen-Lin Su, Horng-Chin Yan, Wann-Cherng Perng, and Chin-Pyng Wu Background
ROLE OF OPEN LUNG BIOPSY IN PATIENTS WITH DIFFUSE LUNG INFILTRATES AND ACUTE RESPIRATORY FAILURE Li-Hui Soh, Chih-Feng Chian, Wen-Lin Su, Horng-Chin Yan, Wann-Cherng Perng, and Chin-Pyng Wu Background
Lecture Notes. Chapter 9: Smoke Inhalation Injury and Burns
 Lecture Notes Chapter 9: Smoke Inhalation Injury and Burns Objectives List the factors that influence mortality rate Describe the nature of smoke inhalation and the fire environment Recognize the pulmonary
Lecture Notes Chapter 9: Smoke Inhalation Injury and Burns Objectives List the factors that influence mortality rate Describe the nature of smoke inhalation and the fire environment Recognize the pulmonary
A Clinico-pharmacological Study on Effect of Methylprednisolone in Acute Respiratory Distress Syndrome Patients
 Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2018/135 A Clinico-pharmacological Study on Effect of Methylprednisolone in Acute Respiratory Distress Syndrome Patients
Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2018/135 A Clinico-pharmacological Study on Effect of Methylprednisolone in Acute Respiratory Distress Syndrome Patients
Keeping Patients Off the Vent: Bilevel, HFNC, Neither?
 Keeping Patients Off the Vent: Bilevel, HFNC, Neither? Robert Kempainen, MD Pulmonary and Critical Care Medicine Hennepin County Medical Center University of Minnesota School of Medicine Objectives Summarize
Keeping Patients Off the Vent: Bilevel, HFNC, Neither? Robert Kempainen, MD Pulmonary and Critical Care Medicine Hennepin County Medical Center University of Minnesota School of Medicine Objectives Summarize
Bronchoalveolar lavage (BAL) with surfactant in pediatric ARDS
 Bronchoalveolar lavage (BAL) with surfactant in pediatric ARDS M. Luchetti, E. M. Galassini, A. Galbiati, C. Pagani,, F. Silla and G. A. Marraro gmarraro@picu.it www.picu.it Anesthesia and Intensive Care
Bronchoalveolar lavage (BAL) with surfactant in pediatric ARDS M. Luchetti, E. M. Galassini, A. Galbiati, C. Pagani,, F. Silla and G. A. Marraro gmarraro@picu.it www.picu.it Anesthesia and Intensive Care
ARDS during Neutropenia. D Mokart DAR IPC GRRRRROH 2010
 ARDS during Neutropenia D Mokart DAR IPC GRRRRROH 2010 Definitions Neutropenia is a decrease in circulating neutrophil white cells in the peripheral blood. neutrophil count of 1,000 1,500 cells/ml = mild
ARDS during Neutropenia D Mokart DAR IPC GRRRRROH 2010 Definitions Neutropenia is a decrease in circulating neutrophil white cells in the peripheral blood. neutrophil count of 1,000 1,500 cells/ml = mild
Index. Note: Page numbers of article titles are in boldface type
 Index Note: Page numbers of article titles are in boldface type A Acute coronary syndrome, perioperative oxygen in, 599 600 Acute lung injury (ALI). See Lung injury and Acute respiratory distress syndrome.
Index Note: Page numbers of article titles are in boldface type A Acute coronary syndrome, perioperative oxygen in, 599 600 Acute lung injury (ALI). See Lung injury and Acute respiratory distress syndrome.
Trial protocol - NIVAS Study
 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 Trial protocol - NIVAS Study METHODS Study oversight The Non-Invasive Ventilation after Abdominal Surgery
1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 Trial protocol - NIVAS Study METHODS Study oversight The Non-Invasive Ventilation after Abdominal Surgery
Imaging Cancer Treatment Complications in the Chest
 Imaging Cancer Treatment Complications in the Chest Michelle S. Ginsberg, MD Objectives Imaging Cancer Treatment Complications in the Chest To understand the mechanisms of action of different classes of
Imaging Cancer Treatment Complications in the Chest Michelle S. Ginsberg, MD Objectives Imaging Cancer Treatment Complications in the Chest To understand the mechanisms of action of different classes of
Published Ahead of Print on July 9, 2008 as /theoncologist
 The Oncologist Gynecologic Oncology Gemcitabine Pulmonary Toxicity in Ovarian Cancer EMILY KO,SUSANNA LEE,ANNEKATHRYN GOODMAN Massachusetts General Hospital, Department of Gynecologic-Oncology, Boston,
The Oncologist Gynecologic Oncology Gemcitabine Pulmonary Toxicity in Ovarian Cancer EMILY KO,SUSANNA LEE,ANNEKATHRYN GOODMAN Massachusetts General Hospital, Department of Gynecologic-Oncology, Boston,
Inhaled Nitric Oxide for Adult Respiratory Distress Syndrome After Pulmonary Resection
 Inhaled Nitric Oxide for Adult Respiratory Distress Syndrome After Pulmonary Resection Douglas J. Mathisen, MD, Elbert Y. Kuo, MMS, Chiwon Hahn, MD, Ashby C. Moncure, MD, John C. Wain, MD, Hermes C. Grillo,
Inhaled Nitric Oxide for Adult Respiratory Distress Syndrome After Pulmonary Resection Douglas J. Mathisen, MD, Elbert Y. Kuo, MMS, Chiwon Hahn, MD, Ashby C. Moncure, MD, John C. Wain, MD, Hermes C. Grillo,
Acute Respiratory Distress Syndrome
 Acute Respiratory Distress Syndrome ARDS Lung complication resulting in dangerously low blood oxygen ARDS is often a result of other health complications Clinical Manifestations Related to systemic inflammatory
Acute Respiratory Distress Syndrome ARDS Lung complication resulting in dangerously low blood oxygen ARDS is often a result of other health complications Clinical Manifestations Related to systemic inflammatory
The new ARDS definitions: what does it mean?
 The new ARDS definitions: what does it mean? Richard Beale 7 th September 2012 METHODS ESICM convened an international panel of experts, with representation of ATS and SCCM The objectives were to update
The new ARDS definitions: what does it mean? Richard Beale 7 th September 2012 METHODS ESICM convened an international panel of experts, with representation of ATS and SCCM The objectives were to update
Differential diagnosis
 Differential diagnosis The onset of COPD is insidious. Pathological changes may begin years before symptoms appear. The major differential diagnosis is asthma, and in some cases, a clear distinction between
Differential diagnosis The onset of COPD is insidious. Pathological changes may begin years before symptoms appear. The major differential diagnosis is asthma, and in some cases, a clear distinction between
ECMO for Severe Hypoxemic Respiratory Failure: Pro-Con Debate. Carolyn Calfee, MD MAS Mark Eisner, MD MPH
 ECMO for Severe Hypoxemic Respiratory Failure: Pro-Con Debate Carolyn Calfee, MD MAS Mark Eisner, MD MPH June 3, 2010 Case Presentation Setting: Community hospital, November 2009 29 year old woman with
ECMO for Severe Hypoxemic Respiratory Failure: Pro-Con Debate Carolyn Calfee, MD MAS Mark Eisner, MD MPH June 3, 2010 Case Presentation Setting: Community hospital, November 2009 29 year old woman with
Bilateral Diffuse Radiation Pneumonitis Caused by Unilateral Thoracic Irradiation: A Case Report
 J Lung Cancer 2012;11(2):97-101 http://dx.doi.org/10.6058/jlc.2012.11.2.97 Bilateral Diffuse Radiation Pneumonitis Caused by Unilateral Thoracic Irradiation: A Case Report Radiation therapy is one of the
J Lung Cancer 2012;11(2):97-101 http://dx.doi.org/10.6058/jlc.2012.11.2.97 Bilateral Diffuse Radiation Pneumonitis Caused by Unilateral Thoracic Irradiation: A Case Report Radiation therapy is one of the
11/19/2012. The spectrum of pulmonary diseases in HIV-infected persons is broad.
 The spectrum of pulmonary diseases in HIV-infected persons is broad. HIV-associated Opportunistic infections Neoplasms Miscellaneous conditions Non HIV-associated Antiretroviral therapy (ART)-associated
The spectrum of pulmonary diseases in HIV-infected persons is broad. HIV-associated Opportunistic infections Neoplasms Miscellaneous conditions Non HIV-associated Antiretroviral therapy (ART)-associated
Oxygenation Failure. Increase FiO2. Titrate end-expiratory pressure. Adjust duty cycle to increase MAP. Patient Positioning. Inhaled Vasodilators
 Oxygenation Failure Increase FiO2 Titrate end-expiratory pressure Adjust duty cycle to increase MAP Patient Positioning Inhaled Vasodilators Extracorporeal Circulation ARDS Radiology Increasing Intensity
Oxygenation Failure Increase FiO2 Titrate end-expiratory pressure Adjust duty cycle to increase MAP Patient Positioning Inhaled Vasodilators Extracorporeal Circulation ARDS Radiology Increasing Intensity
What is the next best step?
 Noninvasive Ventilation William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center What is the next best step? 65 year old female
Noninvasive Ventilation William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center What is the next best step? 65 year old female
Part I Study Questions
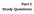 Part I Study Questions 1. A 59-year-old man with a history of pulmonary embolism diagnosed 2 years ago and treated with warfarin for 6 months is evaluated for progressive dyspnea and bilateral lower extremity
Part I Study Questions 1. A 59-year-old man with a history of pulmonary embolism diagnosed 2 years ago and treated with warfarin for 6 months is evaluated for progressive dyspnea and bilateral lower extremity
Gemcitabine-related pulmonary toxicity
 Short communication Peer reviewed article SWISS MED WKLY 2002;132:17 20 www.smw.ch 17 Gemcitabine-related pulmonary toxicity M. Joerger a, A. Gunz b, R. Speich b, B. C. Pestalozzi a a Division of Oncology
Short communication Peer reviewed article SWISS MED WKLY 2002;132:17 20 www.smw.ch 17 Gemcitabine-related pulmonary toxicity M. Joerger a, A. Gunz b, R. Speich b, B. C. Pestalozzi a a Division of Oncology
THE ACUTE RESPIRATORY DISTRESS SYNDROME. Daniel Brockman, DO
 THE ACUTE RESPIRATORY DISTRESS SYNDROME Daniel Brockman, DO Objectives Describe the history and evolution of the diagnosis of ARDS Review the diagnostic criteria for ARDS Discuss the primary interventions
THE ACUTE RESPIRATORY DISTRESS SYNDROME Daniel Brockman, DO Objectives Describe the history and evolution of the diagnosis of ARDS Review the diagnostic criteria for ARDS Discuss the primary interventions
Back to the Future: Updated Guidelines for Evaluation and Management of Adrenal Insufficiency in the Critically Ill
 Back to the Future: Updated Guidelines for Evaluation and Management of Adrenal Insufficiency in the Critically Ill Joe Palumbo PGY-2 Critical Care Pharmacy Resident Buffalo General Medical Center Disclosures
Back to the Future: Updated Guidelines for Evaluation and Management of Adrenal Insufficiency in the Critically Ill Joe Palumbo PGY-2 Critical Care Pharmacy Resident Buffalo General Medical Center Disclosures
Management of refractory ARDS. Saurabh maji
 Management of refractory ARDS Saurabh maji Refractory hypoxemia as PaO2/FIO2 is less than 100 mm Hg, inability to keep plateau pressure below 30 cm H2O despite a VT of 4 ml/kg development of barotrauma
Management of refractory ARDS Saurabh maji Refractory hypoxemia as PaO2/FIO2 is less than 100 mm Hg, inability to keep plateau pressure below 30 cm H2O despite a VT of 4 ml/kg development of barotrauma
ARDS: an update 6 th March A. Hakeem Al Hashim, MD, FRCP SQUH
 ARDS: an update 6 th March 2017 A. Hakeem Al Hashim, MD, FRCP SQUH 30M, previously healthy Hx: 1 week dry cough Gradually worsening SOB No travel Hx Case BP 130/70, HR 100/min ph 7.29 pco2 35 po2 50 HCO3
ARDS: an update 6 th March 2017 A. Hakeem Al Hashim, MD, FRCP SQUH 30M, previously healthy Hx: 1 week dry cough Gradually worsening SOB No travel Hx Case BP 130/70, HR 100/min ph 7.29 pco2 35 po2 50 HCO3
ARDS Management Protocol
 ARDS Management Protocol February 2018 ARDS Criteria Onset Within 1 week of a known clinical insult or new or worsening respiratory symptoms Bilateral opacities not fully explained by effusions, lobar/lung
ARDS Management Protocol February 2018 ARDS Criteria Onset Within 1 week of a known clinical insult or new or worsening respiratory symptoms Bilateral opacities not fully explained by effusions, lobar/lung
Sample Case Study. The patient was a 77-year-old female who arrived to the emergency room on
 Sample Case Study The patient was a 77-year-old female who arrived to the emergency room on February 25 th with a chief complaint of shortness of breath and a deteriorating pulmonary status along with
Sample Case Study The patient was a 77-year-old female who arrived to the emergency room on February 25 th with a chief complaint of shortness of breath and a deteriorating pulmonary status along with
Recognizing and Correcting Patient-Ventilator Dysynchrony
 2019 KRCS Annual State Education Seminar Recognizing and Correcting Patient-Ventilator Dysynchrony Eric Kriner BS,RRT Pulmonary Critical Care Clinical Specialist MedStar Washington Hospital Center Washington,
2019 KRCS Annual State Education Seminar Recognizing and Correcting Patient-Ventilator Dysynchrony Eric Kriner BS,RRT Pulmonary Critical Care Clinical Specialist MedStar Washington Hospital Center Washington,
Test Bank Pilbeam's Mechanical Ventilation Physiological and Clinical Applications 6th Edition Cairo
 Instant dowload and all chapters Test Bank Pilbeam's Mechanical Ventilation Physiological and Clinical Applications 6th Edition Cairo https://testbanklab.com/download/test-bank-pilbeams-mechanical-ventilation-physiologicalclinical-applications-6th-edition-cairo/
Instant dowload and all chapters Test Bank Pilbeam's Mechanical Ventilation Physiological and Clinical Applications 6th Edition Cairo https://testbanklab.com/download/test-bank-pilbeams-mechanical-ventilation-physiologicalclinical-applications-6th-edition-cairo/
PULMONARY MEDICINE BOARD REVIEW. Financial Conflicts of Interest. Question #1: Question #1 (Cont.): None. Christopher H. Fanta, M.D.
 PULMONARY MEDICINE BOARD REVIEW Christopher H. Fanta, M.D. Pulmonary and Critical Care Division Brigham and Women s Hospital Partners Asthma Center Harvard Medical School Financial Conflicts of Interest
PULMONARY MEDICINE BOARD REVIEW Christopher H. Fanta, M.D. Pulmonary and Critical Care Division Brigham and Women s Hospital Partners Asthma Center Harvard Medical School Financial Conflicts of Interest
Cryptogenic Organizing Pneumonia Diagnosis Approach Based on a Clinical-Radiologic-Pathologic Consensus
 Cryptogenic Organizing Pneumonia Diagnosis Approach Based on a Clinical-Radiologic-Pathologic Consensus Poster No.: C-1622 Congress: ECR 2012 Type: Scientific Exhibit Authors: C. Cordero Lares, E. Zorita
Cryptogenic Organizing Pneumonia Diagnosis Approach Based on a Clinical-Radiologic-Pathologic Consensus Poster No.: C-1622 Congress: ECR 2012 Type: Scientific Exhibit Authors: C. Cordero Lares, E. Zorita
Invasive Pulmonary Aspergillosis in
 Infection & Sepsis Symposium Porto, April 1-3, 2009 Invasive Pulmonary Aspergillosis in Non-Immunocompromised Patients Stijn BLOT, PhD General Internal Medicine & Infectious Diseases Ghent University Hospital,
Infection & Sepsis Symposium Porto, April 1-3, 2009 Invasive Pulmonary Aspergillosis in Non-Immunocompromised Patients Stijn BLOT, PhD General Internal Medicine & Infectious Diseases Ghent University Hospital,
Original Contributions
 Original Contributions Utilization of Bronchodilators in Ventilated Patients Without Obstructive Airways Disease Lydia H Chang MD, Shyoko Honiden MD, John A Haithcock RRT, Aneesa M Das MD, Kathy A Short
Original Contributions Utilization of Bronchodilators in Ventilated Patients Without Obstructive Airways Disease Lydia H Chang MD, Shyoko Honiden MD, John A Haithcock RRT, Aneesa M Das MD, Kathy A Short
June 2013 Pulmonary Case of the Month: Diagnosis Makes a Difference. Lewis J. Wesselius, MD 1 Henry D. Tazelaar, MD 2
 June 2013 Pulmonary Case of the Month: Diagnosis Makes a Difference Lewis J. Wesselius, MD 1 Henry D. Tazelaar, MD 2 Departments of Pulmonary Medicine 1 and Laboratory Medicine and Pathology 2 Mayo Clinic
June 2013 Pulmonary Case of the Month: Diagnosis Makes a Difference Lewis J. Wesselius, MD 1 Henry D. Tazelaar, MD 2 Departments of Pulmonary Medicine 1 and Laboratory Medicine and Pathology 2 Mayo Clinic
Lecture Notes. Chapter 3: Asthma
 Lecture Notes Chapter 3: Asthma Objectives Define asthma and status asthmaticus List the potential causes of asthma attacks Describe the effect of asthma attacks on lung function List the clinical features
Lecture Notes Chapter 3: Asthma Objectives Define asthma and status asthmaticus List the potential causes of asthma attacks Describe the effect of asthma attacks on lung function List the clinical features
DIAGNOSTIC NOTE TEMPLATE
 DIAGNOSTIC NOTE TEMPLATE SOAP NOTE TEMPLATE WHEN CONSIDERING A DIAGNOSIS OF IDIOPATHIC PULMONARY FIBROSIS (IPF) CHIEF COMPLAINT HISTORY OF PRESENT ILLNESS Consider IPF as possible diagnosis if any of the
DIAGNOSTIC NOTE TEMPLATE SOAP NOTE TEMPLATE WHEN CONSIDERING A DIAGNOSIS OF IDIOPATHIC PULMONARY FIBROSIS (IPF) CHIEF COMPLAINT HISTORY OF PRESENT ILLNESS Consider IPF as possible diagnosis if any of the
Ventilation in Paediatric ARDS: extrapolate from adult studies?
 Ventilation in Paediatric ARDS: extrapolate from adult studies? ASMIC 2014 Dr Adrian Plunkett Consultant Paediatric Intensivist Birmingham Children s Hospital, UK Aims of the presentation Ventilation
Ventilation in Paediatric ARDS: extrapolate from adult studies? ASMIC 2014 Dr Adrian Plunkett Consultant Paediatric Intensivist Birmingham Children s Hospital, UK Aims of the presentation Ventilation
Outcomes From Severe ARDS Managed Without ECMO. Roy Brower, MD Johns Hopkins University Critical Care Canada Forum Toronto November 1, 2016
 Outcomes From Severe ARDS Managed Without ECMO Roy Brower, MD Johns Hopkins University Critical Care Canada Forum Toronto November 1, 2016 Severe ARDS Berlin Definition 2012 P:F ratio 100 mm Hg Prevalence:
Outcomes From Severe ARDS Managed Without ECMO Roy Brower, MD Johns Hopkins University Critical Care Canada Forum Toronto November 1, 2016 Severe ARDS Berlin Definition 2012 P:F ratio 100 mm Hg Prevalence:
11 th Annual Congress Turkish Thoracic Society. Mechanical Ventilation in Acute Hypoxemic Respiratory Failure
 11 th Annual Congress Turkish Thoracic Society Mechanical Ventilation in Acute Hypoxemic Respiratory Failure Lluis Blanch MD PhD Senior Critical Care Center Scientific Director Corporació Parc Taulí Universitat
11 th Annual Congress Turkish Thoracic Society Mechanical Ventilation in Acute Hypoxemic Respiratory Failure Lluis Blanch MD PhD Senior Critical Care Center Scientific Director Corporació Parc Taulí Universitat
Resident Case Review CHEST. Daria Manos CAR 2016
 Resident Case Review CHEST CAR 2016 Daria Manos Disclosure Speakers bureau, Roche CAR 2016 Daria Manos 1. Recognize common and critical chest radiograph and computed tomography signs and use these clues
Resident Case Review CHEST CAR 2016 Daria Manos Disclosure Speakers bureau, Roche CAR 2016 Daria Manos 1. Recognize common and critical chest radiograph and computed tomography signs and use these clues
Lecture Notes. Chapter 16: Bacterial Pneumonia
 Lecture Notes Chapter 16: Bacterial Pneumonia Objectives Explain the epidemiology Identify the common causes Explain the pathological changes in the lung Identify clinical features Explain the treatment
Lecture Notes Chapter 16: Bacterial Pneumonia Objectives Explain the epidemiology Identify the common causes Explain the pathological changes in the lung Identify clinical features Explain the treatment
Adjunct Therapies for Pediatric ARDS: Where are the Data?
 Adjunct Therapies for Pediatric ARDS: Where are the Data? Alexandre T. Rotta, MD, FCCM Professor of Pediatrics, Linsalata Family Endowed Chair in Pediatric Critical Care and Emergency Medicine Rainbow
Adjunct Therapies for Pediatric ARDS: Where are the Data? Alexandre T. Rotta, MD, FCCM Professor of Pediatrics, Linsalata Family Endowed Chair in Pediatric Critical Care and Emergency Medicine Rainbow
Breathing life into new therapies: Updates on treatment for severe respiratory failure. Whitney Gannon, MSN ACNP-BC
 Breathing life into new therapies: Updates on treatment for severe respiratory failure Whitney Gannon, MSN ACNP-BC Overview Definition of ARDS Clinical signs and symptoms Causes Pathophysiology Management
Breathing life into new therapies: Updates on treatment for severe respiratory failure Whitney Gannon, MSN ACNP-BC Overview Definition of ARDS Clinical signs and symptoms Causes Pathophysiology Management
Crit Care & Shock (2014) 1:3-7. Abstract. Introduction. Original Articles. Jun-ichi Hirata, Munehiko Ohya, Seishiro Marukawa, Keiji Kumon
 Original Articles Crit Care & Shock (2014) 1:3-7 Deep sedation contributes to high release of hypoxic pulmonary vasoconstriction in mechanically ventilated acute respiratory distress syndrome patients
Original Articles Crit Care & Shock (2014) 1:3-7 Deep sedation contributes to high release of hypoxic pulmonary vasoconstriction in mechanically ventilated acute respiratory distress syndrome patients
INTERSTITIAL LUNG DISEASE. Radhika Reddy MD Pulmonary/Critical Care Long Beach VA Medical Center January 5, 2018
 INTERSTITIAL LUNG DISEASE Radhika Reddy MD Pulmonary/Critical Care Long Beach VA Medical Center January 5, 2018 Interstitial Lung Disease Interstitial Lung Disease Prevalence by Diagnosis: Idiopathic Interstitial
INTERSTITIAL LUNG DISEASE Radhika Reddy MD Pulmonary/Critical Care Long Beach VA Medical Center January 5, 2018 Interstitial Lung Disease Interstitial Lung Disease Prevalence by Diagnosis: Idiopathic Interstitial
Clinical syndrome of severe dyspnea of rapid onset, hypoxemia, and diffuse pulmonary infiltrates leading to respiratory failure.
 Yuanlin Song, M.D. Clinical syndrome of severe dyspnea of rapid onset, hypoxemia, and diffuse pulmonary infiltrates leading to respiratory failure. Pneumonia Trauma SARS PaO2/fiO2
Yuanlin Song, M.D. Clinical syndrome of severe dyspnea of rapid onset, hypoxemia, and diffuse pulmonary infiltrates leading to respiratory failure. Pneumonia Trauma SARS PaO2/fiO2
Acute Respiratory Distress Syndrome
 Colloquium series on Integrated Systems Physiology: from molecule to function to disease Series Editors: D. Neil Granger & Joey Granger Acute Respiratory Distress Syndrome Marie Carmelle Elie Donna Carden
Colloquium series on Integrated Systems Physiology: from molecule to function to disease Series Editors: D. Neil Granger & Joey Granger Acute Respiratory Distress Syndrome Marie Carmelle Elie Donna Carden
Chapter 16. Lung Abscess. Mosby items and derived items 2011, 2006 by Mosby, Inc., an affiliate of Elsevier Inc.
 Chapter 16 Lung Abscess 1 EDA PM C AFC RB A B Figure 16-1. Lung abscess. A, Cross-sectional view of lung abscess. B, Consolidation and (C) excessive bronchial secretions are common secondary anatomic alterations
Chapter 16 Lung Abscess 1 EDA PM C AFC RB A B Figure 16-1. Lung abscess. A, Cross-sectional view of lung abscess. B, Consolidation and (C) excessive bronchial secretions are common secondary anatomic alterations
October 2012 Imaging Case of the Month. Michael B. Gotway, MD Associate Editor Imaging. Department of Radiology Mayo Clinic Arizona Scottsdale, AZ
 October 2012 Imaging Case of the Month Michael B. Gotway, MD Associate Editor Imaging Department of Radiology Mayo Clinic Arizona Scottsdale, AZ Clinical History: A 65-year-old non-smoking woman presented
October 2012 Imaging Case of the Month Michael B. Gotway, MD Associate Editor Imaging Department of Radiology Mayo Clinic Arizona Scottsdale, AZ Clinical History: A 65-year-old non-smoking woman presented
Weaning and extubation in PICU An evidence-based approach
 Weaning and extubation in PICU An evidence-based approach Suchada Sritippayawan, MD. Div. Pulmonology & Crit Care Dept. Pediatrics Faculty of Medicine Chulalongkorn University Kanokporn Udomittipong, MD.
Weaning and extubation in PICU An evidence-based approach Suchada Sritippayawan, MD. Div. Pulmonology & Crit Care Dept. Pediatrics Faculty of Medicine Chulalongkorn University Kanokporn Udomittipong, MD.
SCLERODERMA LUNG DISEASE: WHAT THE PATIENT SHOULD KNOW
 SCLERODERMA LUNG DISEASE: WHAT THE PATIENT SHOULD KNOW Lung disease can be a serious complication of scleroderma. The two most common types of lung disease in patients with scleroderma are interstitial
SCLERODERMA LUNG DISEASE: WHAT THE PATIENT SHOULD KNOW Lung disease can be a serious complication of scleroderma. The two most common types of lung disease in patients with scleroderma are interstitial
ARDS and Ventilators PG26 Update in Surgical Critical Care October 9, 2013
 ARDS and Ventilators PG26 Update in Surgical Critical Care October 9, 2013 Pauline K. Park MD, FACS, FCCM University of Michigan School of Medicine Ann Arbor, MI OVERVIEW New Berlin definition of ARDS
ARDS and Ventilators PG26 Update in Surgical Critical Care October 9, 2013 Pauline K. Park MD, FACS, FCCM University of Michigan School of Medicine Ann Arbor, MI OVERVIEW New Berlin definition of ARDS
New Strategies in the Management of Patients with Severe Sepsis
 New Strategies in the Management of Patients with Severe Sepsis Michael Zgoda, MD, MBA President, Medical Staff Medical Director, ICU CMC-University, Charlotte, NC Factors of increases in the dx. of severe
New Strategies in the Management of Patients with Severe Sepsis Michael Zgoda, MD, MBA President, Medical Staff Medical Director, ICU CMC-University, Charlotte, NC Factors of increases in the dx. of severe
Treatment of Coccidioidomycosis-associated Eosinophilic Pneumonia with Corticosteroids
 Treatment of Coccidioidomycosis-associated Eosinophilic Pneumonia with Corticosteroids Joshua Malo, MD Yuval Raz, MD Linda Snyder, MD Kenneth Knox, MD University of Arizona Medical Center Department of
Treatment of Coccidioidomycosis-associated Eosinophilic Pneumonia with Corticosteroids Joshua Malo, MD Yuval Raz, MD Linda Snyder, MD Kenneth Knox, MD University of Arizona Medical Center Department of
Radiological syndroms. Alveolar syndrome Bronchial syndrome Interstitial syndrome Vascular syndrome Mediastinal Syndrome
 Radiological syndroms Alveolar syndrome Bronchial syndrome Interstitial syndrome Vascular syndrome Mediastinal Syndrome Alveolar syndrome Pulmonary architecture : Morphological unit is the lobule 15-25mm
Radiological syndroms Alveolar syndrome Bronchial syndrome Interstitial syndrome Vascular syndrome Mediastinal Syndrome Alveolar syndrome Pulmonary architecture : Morphological unit is the lobule 15-25mm
AECOPD: Management and Prevention
 Neil MacIntyre MD Duke University Medical Center Durham NC Professor P.J. Barnes, MD, National Heart and Lung Institute, London UK Professor Peter J. Barnes, MD National Heart and Lung Institute, London
Neil MacIntyre MD Duke University Medical Center Durham NC Professor P.J. Barnes, MD, National Heart and Lung Institute, London UK Professor Peter J. Barnes, MD National Heart and Lung Institute, London
Acute Respiratory Failure. Respiratory Failure. Respiratory Failure. Acute Respiratory Failure. Ventilatory Failure. Type 1 Respiratory Failure
 Acute Respiratory Failure Physiologic Classification Acute Respiratory Failure Type 1 Hypoxemic Type 2 Ventilatory Type 3 Post-op Type 4 Shock Mechanism Shunt Va Atelectasis Cardiac Output Phil Factor,
Acute Respiratory Failure Physiologic Classification Acute Respiratory Failure Type 1 Hypoxemic Type 2 Ventilatory Type 3 Post-op Type 4 Shock Mechanism Shunt Va Atelectasis Cardiac Output Phil Factor,
Molly Boyd, MD Glenn Mills, MD Syed Jafri, MD 1/1/2010
 LSU HEALTH SCIENCES CENTER NSCLC Guidelines Feist-Weiller Cancer Center Molly Boyd, MD Glenn Mills, MD Syed Jafri, MD 1/1/2010 Initial Evaluation/Intervention: 1. Pathology Review 2. History and Physical
LSU HEALTH SCIENCES CENTER NSCLC Guidelines Feist-Weiller Cancer Center Molly Boyd, MD Glenn Mills, MD Syed Jafri, MD 1/1/2010 Initial Evaluation/Intervention: 1. Pathology Review 2. History and Physical
ARDS and treatment strategies
 ARDS and treatment strategies Geoff Bellingan Medical Director University College Hospital ARDS: Definitions History of predisposing condition Refractory hypoxaemia of acute onset PaO 2 /FiO 2 ratio:
ARDS and treatment strategies Geoff Bellingan Medical Director University College Hospital ARDS: Definitions History of predisposing condition Refractory hypoxaemia of acute onset PaO 2 /FiO 2 ratio:
ECMO: a breakthrough in care for respiratory failure. PD Dr. Thomas Müller Regensburg no conflict of interest
 ECMO: a breakthrough in care for respiratory failure? PD Dr. Thomas Müller Regensburg no conflict of interest 1 Overview Mortality of severe ARDS Indication for ECMO PaO 2 /FiO 2 Efficiency of ECMO: gas
ECMO: a breakthrough in care for respiratory failure? PD Dr. Thomas Müller Regensburg no conflict of interest 1 Overview Mortality of severe ARDS Indication for ECMO PaO 2 /FiO 2 Efficiency of ECMO: gas
Is ARDS Important to Recognize?
 Is ARDS Important to Recognize? Lorraine B. Ware MD Vanderbilt University Financial Disclosures: research funding from Boehringer Ingelheim, Global Blood Therapeutics Why diagnose ARDS? -initiate specific
Is ARDS Important to Recognize? Lorraine B. Ware MD Vanderbilt University Financial Disclosures: research funding from Boehringer Ingelheim, Global Blood Therapeutics Why diagnose ARDS? -initiate specific
Pulmonary Sarcoidosis - Radiological Evaluation
 Original Research Article Pulmonary Sarcoidosis - Radiological Evaluation Jayesh Shah 1, Darshan Shah 2*, C. Raychaudhuri 3 1 Associate Professor, 2 1 st Year Resident, 3 Professor and HOD Radiology Department,
Original Research Article Pulmonary Sarcoidosis - Radiological Evaluation Jayesh Shah 1, Darshan Shah 2*, C. Raychaudhuri 3 1 Associate Professor, 2 1 st Year Resident, 3 Professor and HOD Radiology Department,
SESSION IV: MECHANISMS OF HUMAN DISEASE: LABORATORY SESSIONS PULMONARY PATHOLOGY I. December 5, 2012
 SESSION IV: MECHANISMS OF HUMAN DISEASE: LABORATORY SESSIONS PULMONARY PATHOLOGY I December 5, 2012 FACULTY COPY GOAL: Describe the basic morphologic and pathophysiologic changes in various conditions
SESSION IV: MECHANISMS OF HUMAN DISEASE: LABORATORY SESSIONS PULMONARY PATHOLOGY I December 5, 2012 FACULTY COPY GOAL: Describe the basic morphologic and pathophysiologic changes in various conditions
Pneumonia in the Hospitalized
 Pneumonia in the Hospitalized Patient: Use of Steroids Nicolette Myers, MD Pulmonary/Sleep/Critical Care November 9, 2018 Park Nicollet Clinic Facts About Pneumonia CAP is the 8 th most common cause of
Pneumonia in the Hospitalized Patient: Use of Steroids Nicolette Myers, MD Pulmonary/Sleep/Critical Care November 9, 2018 Park Nicollet Clinic Facts About Pneumonia CAP is the 8 th most common cause of
Interpreting thoracic x-ray of the supine immobile patient: Syllabus
 Interpreting thoracic x-ray of the supine immobile patient: Syllabus Johannes Godt Dep. of Radiology and Nuclear Medicine Oslo University Hospital Ullevål NORDTER 2017, Helsinki Content - Why bedside chest
Interpreting thoracic x-ray of the supine immobile patient: Syllabus Johannes Godt Dep. of Radiology and Nuclear Medicine Oslo University Hospital Ullevål NORDTER 2017, Helsinki Content - Why bedside chest
The Effect of Tidal Volume on Pulmonary Complications following Minimally Invasive Esophagectomy: A Randomized and Controlled Study
 The Effect of Tidal Volume on Pulmonary Complications following Minimally Invasive Esophagectomy: A Randomized and Controlled Study Yaxing Shen, MD, Ming Zhong, MD, Lijie Tan, MD Zhongshan Hospital,Fudan
The Effect of Tidal Volume on Pulmonary Complications following Minimally Invasive Esophagectomy: A Randomized and Controlled Study Yaxing Shen, MD, Ming Zhong, MD, Lijie Tan, MD Zhongshan Hospital,Fudan
Case Presentations in ILD. Harold R. Collard, MD Department of Medicine University of California San Francisco
 Case Presentations in ILD Harold R. Collard, MD Department of Medicine University of California San Francisco Outline Overview of diagnosis in ILD Definition/Classification High-resolution CT scan Multidisciplinary
Case Presentations in ILD Harold R. Collard, MD Department of Medicine University of California San Francisco Outline Overview of diagnosis in ILD Definition/Classification High-resolution CT scan Multidisciplinary
Initial presentation of idiopathic pulmonary fibrosis as an acute exacerbation
 Respiratory Medicine CME (2008) 1, 43 47 respiratory MEDICINE CME CASE REPORT Initial presentation of idiopathic pulmonary fibrosis as an acute exacerbation Krishna M. Sundar a,b,, Dixie L. Harris a a
Respiratory Medicine CME (2008) 1, 43 47 respiratory MEDICINE CME CASE REPORT Initial presentation of idiopathic pulmonary fibrosis as an acute exacerbation Krishna M. Sundar a,b,, Dixie L. Harris a a
Bi-Level Therapy: Boosting Comfort & Compliance in Apnea Patients
 Bi-Level Therapy: Boosting Comfort & Compliance in Apnea Patients Objectives Describe nocturnal ventilation characteristics that may indicate underlying conditions and benefits of bilevel therapy for specific
Bi-Level Therapy: Boosting Comfort & Compliance in Apnea Patients Objectives Describe nocturnal ventilation characteristics that may indicate underlying conditions and benefits of bilevel therapy for specific
How ARDS should be treated in 2017
 How ARDS should be treated in 2017 2017, Ostrava Luciano Gattinoni, MD, FRCP Georg-August-Universität Göttingen Germany ARDS 1. Keep the patient alive respiration circulation 2. Cure the disease leading
How ARDS should be treated in 2017 2017, Ostrava Luciano Gattinoni, MD, FRCP Georg-August-Universität Göttingen Germany ARDS 1. Keep the patient alive respiration circulation 2. Cure the disease leading
4/17/2010 C ini n ca c l a Ev E a v l a ua u t a ion o n of o ILD U dat a e t e i n I LDs
 Update in ILDs Diagnosis 101: Clinical Evaluation April 17, 2010 Jay H. Ryu, MD Mayo Clinic, Rochester MN Clinical Evaluation of ILD Outline General aspects of ILDs Classification of ILDs Clinical evaluation
Update in ILDs Diagnosis 101: Clinical Evaluation April 17, 2010 Jay H. Ryu, MD Mayo Clinic, Rochester MN Clinical Evaluation of ILD Outline General aspects of ILDs Classification of ILDs Clinical evaluation
Wet Lungs Dry lungs Impact on Outcome in ARDS. Charlie Phillips MD Division of PCCM OHSU 2009
 Wet Lungs Dry lungs Impact on Outcome in ARDS Charlie Phillips MD Division of PCCM OHSU 2009 Today s talk Pathophysiology of ARDS The case for dry Targeting EVLW Disclosures Advisor for Pulsion Medical
Wet Lungs Dry lungs Impact on Outcome in ARDS Charlie Phillips MD Division of PCCM OHSU 2009 Today s talk Pathophysiology of ARDS The case for dry Targeting EVLW Disclosures Advisor for Pulsion Medical
Cardiorespiratory Interactions:
 Cardiorespiratory Interactions: The Heart - Lung Connection Jon N. Meliones, MD, MS, FCCM Professor of Pediatrics Duke University Medical Director PCVICU Optimizing CRI Cardiorespiratory Economics O2:
Cardiorespiratory Interactions: The Heart - Lung Connection Jon N. Meliones, MD, MS, FCCM Professor of Pediatrics Duke University Medical Director PCVICU Optimizing CRI Cardiorespiratory Economics O2:
Introduction and Overview of Acute Respiratory Failure
 Introduction and Overview of Acute Respiratory Failure Definition: Acute Respiratory Failure Failure to oxygenate Inadequate PaO 2 to saturate hemoglobin PaO 2 of 60 mm Hg ~ SaO 2 of 90% PaO 2 of 50 mm
Introduction and Overview of Acute Respiratory Failure Definition: Acute Respiratory Failure Failure to oxygenate Inadequate PaO 2 to saturate hemoglobin PaO 2 of 60 mm Hg ~ SaO 2 of 90% PaO 2 of 50 mm
Immunocompromised patients. Immunocompromised patients. Immunocompromised patients
 Value of CT in Early Pneumonia in Immunocompromised Patients Nantaka Kiranantawat, PSU Preventative Factors Phagocyts Cellular immunity Humoral immunity Predisposing Factors Infection, Stress, Poor nutrition,
Value of CT in Early Pneumonia in Immunocompromised Patients Nantaka Kiranantawat, PSU Preventative Factors Phagocyts Cellular immunity Humoral immunity Predisposing Factors Infection, Stress, Poor nutrition,
Prone ventilation revisited in H1N1 patients
 International Journal of Advanced Multidisciplinary Research ISSN: 2393-8870 www.ijarm.com DOI: 10.22192/ijamr Volume 5, Issue 10-2018 Case Report DOI: http://dx.doi.org/10.22192/ijamr.2018.05.10.005 Prone
International Journal of Advanced Multidisciplinary Research ISSN: 2393-8870 www.ijarm.com DOI: 10.22192/ijamr Volume 5, Issue 10-2018 Case Report DOI: http://dx.doi.org/10.22192/ijamr.2018.05.10.005 Prone
1. When a patient fails to ventilate or oxygenate adequately, the problem is caused by pathophysiological factors such as hyperventilation.
 Chapter 1: Principles of Mechanical Ventilation TRUE/FALSE 1. When a patient fails to ventilate or oxygenate adequately, the problem is caused by pathophysiological factors such as hyperventilation. F
Chapter 1: Principles of Mechanical Ventilation TRUE/FALSE 1. When a patient fails to ventilate or oxygenate adequately, the problem is caused by pathophysiological factors such as hyperventilation. F
Case Report Alveolar proteinosis in extremis: a critical case treated with whole lung lavage without extracorporeal membrane oxygenation
 Int J Clin Exp Med 2015;8(10):19556-19560 www.ijcem.com /ISSN:1940-5901/IJCEM0013532 Case Report Alveolar proteinosis in extremis: a critical case treated with whole lung lavage without extracorporeal
Int J Clin Exp Med 2015;8(10):19556-19560 www.ijcem.com /ISSN:1940-5901/IJCEM0013532 Case Report Alveolar proteinosis in extremis: a critical case treated with whole lung lavage without extracorporeal
